These Highlights Do Not Include All The Information Needed To Use Lenalidomide Capsules Safely And Effectively. See Full Prescribing Information For Lenalidomide Capsules.
2166bbdf-eb12-4564-b9e4-b63ca21312bc
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
WARNING: EMBRYO-FETAL TOXICITY, HEMATOLOGIC TOXICITY, and VENOUS and ARTERIAL THROMBOEMBOLISM See full prescribing information for complete boxed warning. EMBRYO-FETAL TOXICITY Lenalidomide, a thalidomide analogue, caused limb abnormalities in a developmental monkey study similar to birth defects caused by thalidomide in humans. If lenalidomide is used during pregnancy, it may cause birth defects or embryo-fetal death. Pregnancy must be excluded before start of treatment. Prevent pregnancy during treatment by the use of two reliable methods of contraception ( 5.1 ). Lenalidomide capsules are available only through a restricted distribution program, called the Lenalidomide REMS program ( 5.2 , 17 ). HEMATOLOGIC TOXICITY . Lenalidomide can cause significant neutropenia and thrombocytopenia ( 5.3 ). VENOUS AND ARTERIAL THROMBOEMBOLISM Significantly increased risk of deep vein thrombosis (DVT) and pulmonary embolism (PE), as well as risk of myocardial infarction and stroke in patients with multiple myeloma receiving lenalidomide with dexamethasone. Anti-thrombotic prophylaxis is recommended ( 5.4 ).
Indications and Usage
Lenalidomide is a thalidomide analogue indicated for the treatment of adult patients with: Multiple myeloma (MM), in combination with dexamethasone ( 1.1 ). MM, as maintenance following autologous hematopoietic stem cell transplantation (auto-HSCT) ( 1.1 ). Transfusion-dependent anemia due to low- or intermediate-1-risk myelodysplastic syndromes (MDS) associated with a deletion 5q abnormality with or without additional cytogenetic abnormalities ( 1.2 ). Mantle cell lymphoma (MCL) whose disease has relapsed or progressed after two prior therapies, one of which included bortezomib ( 1.3 ). Previously treated follicular lymphoma (FL), in combination with a rituximab product ( 1.4 ). Previously treated marginal zone lymphoma (MZL), in combination with a rituximab product ( 1.5 ). Limitations of Use: Lenalidomide capsules are not indicated and are not recommended for the treatment of patients with chronic lymphocytic leukemia (CLL) outside of controlled clinical trials ( 1.6 ).
Dosage and Administration
MM combination therapy: 25 mg once daily orally on Days 1 to 21 of repeated 28-day cycles. ( 2.1 ). MM maintenance therapy following auto-HSCT: 10 mg once daily continuously on Days 1 to 28 of repeated 28-day cycles ( 2.1 ). MDS: 10 mg once daily ( 2.2 ). MCL: 25 mg once daily orally on Days 1 to 21 of repeated 28-day cycles ( 2.3 ). FL or MZL: 20 mg once daily orally on Days 1 to 21 of repeated 28-day cycles for up to 12 cycles ( 2.4 ). Renal impairment: Adjust starting dose based on the creatinine clearance value ( 2.6 ). For concomitant therapy doses, see Full Prescribing Information ( 2.1 , 2.4 , 14.1 , 14.4 ).
Warnings and Precautions
Increased Mortality: serious and fatal cardiac adverse reactions occurred in patients with CLL treated with lenalidomide ( 5.5 ). Second Primary Malignancies (SPM): Higher incidences of SPM were observed in controlled trials of patients with MM receiving lenalidomide ( 5.6 ). Increased Mortality: Observed in patients with MM when pembrolizumab was added to dexamethasone and a thalidomide analogue ( 5.7 ). Hepatotoxicity: Hepatic failure including fatalities; monitor liver function. Stop lenalidomide and evaluate if hepatotoxicity is suspected ( 5.8 ). Severe Cutaneous Reactions: Discontinue lenalidomide for severe reactions ( 5.9 ). Tumor lysis syndrome (TLS) including fatalities: Monitor patients at risk of TLS (i.e., those with high tumor burden) and take appropriate precautions ( 5.10 ). Tumor flare reaction: Serious tumor flare reactions, including fatal reactions, have occurred during investigational use of lenalidomide for chronic lymphocytic leukemia and lymphoma ( 5.11 ). Impaired Stem Cell mobilization: A decrease in the number of CD34+ cells collected after treatment (> 4 cycles) with lenalidomide has been reported. Consider early referral to transplant center ( 5.12 ). Early mortality in MCL: Higher rate of early deaths have occurred in patients with MCL ( 5.14 ). Hypersensitivity: Monitor patients for potential hypersensitivity. Discontinue lenalidomide for angioedema and anaphylaxis ( 5.15 ).
Contraindications
Pregnancy ( BOXED WARNING , 4.1 , 5.1 , 8.1 ). Demonstrated severe hypersensitivity to lenalidomide ( 4.2 , 5.9 , 5.15 ).
Adverse Reactions
The following clinically significant adverse reactions are described in detail in other sections of the prescribing information: Embryo-Fetal Toxicity [see Boxed Warning , Warnings and Precautions (5.1 , 5.2) ] Hematologic Toxicity [see Boxed Warning , Warnings and Precautions (5.3) ] Venous and Arterial Thromboembolism [see Boxed Warning , Warnings and Precautions (5.4) ] Increased Mortality in Patients with CLL [see Warnings and Precautions (5.5) ] Second Primary Malignancies [see Warnings and Precautions (5.6) ] Increased Mortality in Patients with MM When Pembrolizumab Is Added to a Thalidomide Analogue and Dexamethasone [see Warnings and Precautions (5.7) ] Hepatotoxicity [see Warnings and Precautions (5.8) ] Severe Cutaneous Reactions [see Warnings and Precautions (5.9) ] Tumor Lysis Syndrome [see Warnings and Precautions (5.10) ] Tumor Flare Reactions [see Warnings and Precautions (5.11) ] Impaired Stem Cell Mobilization [see Warnings and Precautions (5.12) ] Thyroid Disorders [see Warnings and Precautions (5.13) ] Early Mortality in Patients with MCL [see Warnings and Precautions (5.14) ] Hypersensitivity [see Warnings and Precautions (5.15) ]
Drug Interactions
Digoxin: Monitor digoxin plasma levels periodically due to increased C max and AUC with concomitant lenalidomide therapy ( 7.1 ). Concomitant use of erythropoietin stimulating agents or estrogen containing therapies with lenalidomide may increase the risk of thrombosis ( 7.2 ).
How Supplied
White to off-white powder filled in hard gelatin capsule size ‘4’ with blue-green opaque cap and white opaque body, imprinted with “LEN” on the cap and “2.5 mg” on the body with black ink: 2.5 mg bottles of 28 (NDC 82293-006-10) White to off-white powder filled in white opaque hard gelatin capsule size ‘4’, imprinted with “LEN” on the cap and “5 mg” on the body with black ink: 5 mg bottles of 28 (NDC 82293-007-10) White to off-white powder filled in hard gelatin capsule size ‘2’ with blue-green opaque cap and pale-yellow opaque body, imprinted with “LEN” on the cap and “10 mg” on the body with black ink: 10 mg bottles of 28 (NDC 82293-008-10) White to off-white powder filled in hard gelatin capsule size ‘1’ with pale blue opaque cap and white opaque body, imprinted with “LEN” on the cap and “15 mg” on the body with black ink: 15 mg bottles of 21 (NDC 82293-009-10) White to off-white powder filled in hard gelatin capsule size ‘0’ with blue-green opaque cap and pale blue opaque body, imprinted with “LEN” on the cap and “20 mg” on the body with black ink: 20 mg bottles of 21 (NDC 82293-010-10) White to off-white powder filled in white opaque hard gelatin capsule size ‘0EL’, imprinted with “LEN” on the cap and “25 mg” on the body with black ink: 25 mg bottles of 21 (NDC 82293-011-10)
Medication Information
Warnings and Precautions
Increased Mortality: serious and fatal cardiac adverse reactions occurred in patients with CLL treated with lenalidomide ( 5.5 ). Second Primary Malignancies (SPM): Higher incidences of SPM were observed in controlled trials of patients with MM receiving lenalidomide ( 5.6 ). Increased Mortality: Observed in patients with MM when pembrolizumab was added to dexamethasone and a thalidomide analogue ( 5.7 ). Hepatotoxicity: Hepatic failure including fatalities; monitor liver function. Stop lenalidomide and evaluate if hepatotoxicity is suspected ( 5.8 ). Severe Cutaneous Reactions: Discontinue lenalidomide for severe reactions ( 5.9 ). Tumor lysis syndrome (TLS) including fatalities: Monitor patients at risk of TLS (i.e., those with high tumor burden) and take appropriate precautions ( 5.10 ). Tumor flare reaction: Serious tumor flare reactions, including fatal reactions, have occurred during investigational use of lenalidomide for chronic lymphocytic leukemia and lymphoma ( 5.11 ). Impaired Stem Cell mobilization: A decrease in the number of CD34+ cells collected after treatment (> 4 cycles) with lenalidomide has been reported. Consider early referral to transplant center ( 5.12 ). Early mortality in MCL: Higher rate of early deaths have occurred in patients with MCL ( 5.14 ). Hypersensitivity: Monitor patients for potential hypersensitivity. Discontinue lenalidomide for angioedema and anaphylaxis ( 5.15 ).
Indications and Usage
Lenalidomide is a thalidomide analogue indicated for the treatment of adult patients with: Multiple myeloma (MM), in combination with dexamethasone ( 1.1 ). MM, as maintenance following autologous hematopoietic stem cell transplantation (auto-HSCT) ( 1.1 ). Transfusion-dependent anemia due to low- or intermediate-1-risk myelodysplastic syndromes (MDS) associated with a deletion 5q abnormality with or without additional cytogenetic abnormalities ( 1.2 ). Mantle cell lymphoma (MCL) whose disease has relapsed or progressed after two prior therapies, one of which included bortezomib ( 1.3 ). Previously treated follicular lymphoma (FL), in combination with a rituximab product ( 1.4 ). Previously treated marginal zone lymphoma (MZL), in combination with a rituximab product ( 1.5 ). Limitations of Use: Lenalidomide capsules are not indicated and are not recommended for the treatment of patients with chronic lymphocytic leukemia (CLL) outside of controlled clinical trials ( 1.6 ).
Dosage and Administration
MM combination therapy: 25 mg once daily orally on Days 1 to 21 of repeated 28-day cycles. ( 2.1 ). MM maintenance therapy following auto-HSCT: 10 mg once daily continuously on Days 1 to 28 of repeated 28-day cycles ( 2.1 ). MDS: 10 mg once daily ( 2.2 ). MCL: 25 mg once daily orally on Days 1 to 21 of repeated 28-day cycles ( 2.3 ). FL or MZL: 20 mg once daily orally on Days 1 to 21 of repeated 28-day cycles for up to 12 cycles ( 2.4 ). Renal impairment: Adjust starting dose based on the creatinine clearance value ( 2.6 ). For concomitant therapy doses, see Full Prescribing Information ( 2.1 , 2.4 , 14.1 , 14.4 ).
Contraindications
Pregnancy ( BOXED WARNING , 4.1 , 5.1 , 8.1 ). Demonstrated severe hypersensitivity to lenalidomide ( 4.2 , 5.9 , 5.15 ).
Adverse Reactions
The following clinically significant adverse reactions are described in detail in other sections of the prescribing information: Embryo-Fetal Toxicity [see Boxed Warning , Warnings and Precautions (5.1 , 5.2) ] Hematologic Toxicity [see Boxed Warning , Warnings and Precautions (5.3) ] Venous and Arterial Thromboembolism [see Boxed Warning , Warnings and Precautions (5.4) ] Increased Mortality in Patients with CLL [see Warnings and Precautions (5.5) ] Second Primary Malignancies [see Warnings and Precautions (5.6) ] Increased Mortality in Patients with MM When Pembrolizumab Is Added to a Thalidomide Analogue and Dexamethasone [see Warnings and Precautions (5.7) ] Hepatotoxicity [see Warnings and Precautions (5.8) ] Severe Cutaneous Reactions [see Warnings and Precautions (5.9) ] Tumor Lysis Syndrome [see Warnings and Precautions (5.10) ] Tumor Flare Reactions [see Warnings and Precautions (5.11) ] Impaired Stem Cell Mobilization [see Warnings and Precautions (5.12) ] Thyroid Disorders [see Warnings and Precautions (5.13) ] Early Mortality in Patients with MCL [see Warnings and Precautions (5.14) ] Hypersensitivity [see Warnings and Precautions (5.15) ]
Drug Interactions
Digoxin: Monitor digoxin plasma levels periodically due to increased C max and AUC with concomitant lenalidomide therapy ( 7.1 ). Concomitant use of erythropoietin stimulating agents or estrogen containing therapies with lenalidomide may increase the risk of thrombosis ( 7.2 ).
How Supplied
White to off-white powder filled in hard gelatin capsule size ‘4’ with blue-green opaque cap and white opaque body, imprinted with “LEN” on the cap and “2.5 mg” on the body with black ink: 2.5 mg bottles of 28 (NDC 82293-006-10) White to off-white powder filled in white opaque hard gelatin capsule size ‘4’, imprinted with “LEN” on the cap and “5 mg” on the body with black ink: 5 mg bottles of 28 (NDC 82293-007-10) White to off-white powder filled in hard gelatin capsule size ‘2’ with blue-green opaque cap and pale-yellow opaque body, imprinted with “LEN” on the cap and “10 mg” on the body with black ink: 10 mg bottles of 28 (NDC 82293-008-10) White to off-white powder filled in hard gelatin capsule size ‘1’ with pale blue opaque cap and white opaque body, imprinted with “LEN” on the cap and “15 mg” on the body with black ink: 15 mg bottles of 21 (NDC 82293-009-10) White to off-white powder filled in hard gelatin capsule size ‘0’ with blue-green opaque cap and pale blue opaque body, imprinted with “LEN” on the cap and “20 mg” on the body with black ink: 20 mg bottles of 21 (NDC 82293-010-10) White to off-white powder filled in white opaque hard gelatin capsule size ‘0EL’, imprinted with “LEN” on the cap and “25 mg” on the body with black ink: 25 mg bottles of 21 (NDC 82293-011-10)
Description
WARNING: EMBRYO-FETAL TOXICITY, HEMATOLOGIC TOXICITY, and VENOUS and ARTERIAL THROMBOEMBOLISM See full prescribing information for complete boxed warning. EMBRYO-FETAL TOXICITY Lenalidomide, a thalidomide analogue, caused limb abnormalities in a developmental monkey study similar to birth defects caused by thalidomide in humans. If lenalidomide is used during pregnancy, it may cause birth defects or embryo-fetal death. Pregnancy must be excluded before start of treatment. Prevent pregnancy during treatment by the use of two reliable methods of contraception ( 5.1 ). Lenalidomide capsules are available only through a restricted distribution program, called the Lenalidomide REMS program ( 5.2 , 17 ). HEMATOLOGIC TOXICITY . Lenalidomide can cause significant neutropenia and thrombocytopenia ( 5.3 ). VENOUS AND ARTERIAL THROMBOEMBOLISM Significantly increased risk of deep vein thrombosis (DVT) and pulmonary embolism (PE), as well as risk of myocardial infarction and stroke in patients with multiple myeloma receiving lenalidomide with dexamethasone. Anti-thrombotic prophylaxis is recommended ( 5.4 ).
Section 42229-5
Embryo-Fetal Toxicity
Do not use lenalidomide during pregnancy. Lenalidomide, a thalidomide analogue, caused limb abnormalities in a developmental monkey study. Thalidomide is a known human teratogen that causes severe life-threatening human birth defects. If lenalidomide is used during pregnancy, it may cause birth defects or embryo-fetal death. In females of reproductive potential, obtain 2 negative pregnancy tests before starting lenalidomide treatment. Females of reproductive potential must use 2 forms of contraception or continuously abstain from heterosexual sex during and for 4 weeks after lenalidomide treatment [see Warnings and Precautions (5.1), and Medication Guide (17)]. To avoid embryo-fetal exposure to lenalidomide, lenalidomide capsules are only available through a restricted distribution program, the Lenalidomide REMS program ( 5.2).
Information about the Lenalidomide REMS program is available at www.lenalidomiderems.com or by calling the REMS Call Center at 1-888-423-5436.
Hematologic Toxicity (Neutropenia and Thrombocytopenia)
Lenalidomide can cause significant neutropenia and thrombocytopenia.
Eighty percent of patients with del 5q myelodysplastic syndromes had to have a dose delay/reduction during the major study. Thirty-four percent of patients had to have a second dose delay/reduction. Grade 3 or 4 hematologic toxicity was seen in 80% of patients enrolled in the study. Patients on therapy for del 5q myelodysplastic syndromes should have their complete blood counts monitored weekly for the first 8 weeks of therapy and at least monthly thereafter. Patients may require dose interruption and/or reduction. Patients may require use of blood product support and/or growth factors [see Dosage and Administration (2.2) ] .
Venous and Arterial Thromboembolism
Lenalidomide has demonstrated a significantly increased risk of deep vein thrombosis (DVT) and pulmonary embolism (PE), as well as risk of myocardial infarction and stroke in patients with multiple myeloma who were treated with lenalidomide and dexamethasone therapy. Monitor for and advise patients about signs and symptoms of thromboembolism. Advise patients to seek immediate medical care if they develop symptoms such as shortness of breath, chest pain, or arm or leg swelling. Thromboprophylaxis is recommended and the choice of regimen should be based on an assessment of the patient’s underlying risks [see Warnings and Precautions (5.4)].
Section 42231-1
|
MEDICATION GUIDE Lenalidomide (len" a lid' oh mide) Capsules |
|
|
What is the most important information I should know about lenalidomide capsules? Before you begin taking lenalidomide capsules, you must read and agree to all of the instructions in the Lenalidomide REMS program. For more information, call 1-888-423-5436 or go to www.lenalidomiderems.com. Before prescribing lenalidomide capsules, your healthcare provider will explain the Lenalidomide REMS program to you and have you sign the Patient-Physician Agreement Form. Lenalidomide capsules may cause serious side effects including:
Lenalidomide capsules are similar to the medicine thalidomide.We know thalidomide can cause severe life-threatening birth defects. Lenalidomide capsules have not been tested in pregnant females. Lenalidomide capsules have harmed unborn animals in animal testing. Females must not get pregnant:
Females who can become pregnant:
If you become pregnant while taking lenalidomide capsules, stop taking it right away and call your healthcare provider. If your healthcare provider is not available, you can call the REMS Call Center at 1-888-423-5436. Healthcare providers and patients should report all cases of pregnancy to:
There is a pregnancy exposure registry that monitors the outcomes of females who take lenalidomide capsules during pregnancy, or if their male partner takes lenalidomide capsules and they are exposed during pregnancy. You can enroll in this registry by calling the REMS Call Center at the phone number listed above. Lenalidomide can pass into human semen:
Men, if your female partner becomes pregnant, you should call your healthcare provider right away.
Before taking lenalidomide capsules, tell your healthcare provider:
|
|
|
What are lenalidomide capsules?
Lenalidomide capsules are a prescription medicine, usedto treat adults with:
Lenalidomide capsules should not be usedto treat people who have chronic lymphocytic leukemia (CLL) unless they are participants in a controlled clinical trial. It is not known if lenalidomide capsules are safe and effective in children. |
|
|
Who should not take lenalidomide capsules? Do not take lenalidomide capsules if you:
|
|
|
What should I tell my healthcare provider before taking lenalidomide capsules? Before you take lenalidomide capsules, tell your healthcare provider about all of your medical conditions, including if you:
Tell your healthcare provider about all the medicines you take,including prescription and over-the-counter medicines, vitamins, and herbal supplements. Lenalidomide capsules and other medicines may affect each other, causing serious side effects. Talk with your healthcare provider before taking any new medicines. Know the medicines you take. Keep a list of them to show your healthcare provider and pharmacist. |
|
|
How should I take lenalidomide capsules?
|
|
|
What should I avoid while taking lenalidomide capsules?
|
|
|
What are the possible side effects of lenalidomide capsules? Lenalidomide capsules can cause serious side effects, including:
|
|
|
|
|
|
|
|
| Get emergency medical help right away if you develop any of the following signs or symptoms during treatment with lenalidomide capsules: | |
|
|
Your healthcare provider may tell you to decrease your dose, temporarily stop or permanently stop taking lenalidomide capsules if you develop certain serious side effects during treatment with lenalidomide capsules.
|
|
|
|
|
These are not all the possible side effects of lenalidomide capsules. Call your doctor for medical advice about side effects. You may report side effects to the FDA at 1-800-FDA-1088. |
|
|
How should I store lenalidomide capsules?
|
|
|
General information about the safe and effective use of lenalidomide capsules. Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not take lenalidomide capsules for conditions for which it was not prescribed. Do not give lenalidomide capsules to other people, even if they have the same symptoms you have. It may harm them and may cause birth defects. If you would like more information, talk with your healthcare provider. You can ask your healthcare provider or pharmacist for information about lenalidomide capsules that is written for health professionals. For more information, call 1-888-423-5436 or go to www.lenalidomiderems.com. |
|
|
What are the ingredients in lenalidomide capsules? Active ingredient:lenalidomide Inactive ingredients:croscarmellose sodium, magnesium stearate, mannitol, and microcrystalline cellulose. The 5 mg and 25 mg capsule shells contain gelatin, titanium dioxide, and black ink.
The capsules are printed with black ink composed of ammonia solution, black iron oxide, potassium hydroxide, propylene glycol, and shellac. Distributed by:
|
This Medication Guide has been approved by the U.S. Food and Drug Administration. Revised: November 2023
7.1 Digoxin
When digoxin was co-administered with multiple doses of lenalidomide (10 mg/day) the digoxin C maxand AUC infwere increased by 14%. Periodically monitor digoxin plasma levels, in accordance with clinical judgment and based on standard clinical practice in patients receiving this medication, during administration of lenalidomide.
16.2 Storage
Store at 20°C to 25°C (68°F to 77°F); excursions permitted to 15°C to 30°C (59°F to 86°F). [See USP Controlled Room Temperature].
7.3 Warfarin
Co-administration of multiple doses of lenalidomide (10 mg/day) with a single dose of warfarin (25 mg) had no effect on the pharmacokinetics of lenalidomide or R- and S-warfarin. Expected changes in laboratory assessments of PT and INR were observed after warfarin administration, but these changes were not affected by concomitant lenalidomide administration. It is not known whether there is an interaction between dexamethasone and warfarin. Close monitoring of PT and INR is recommended in patients with MM taking concomitant warfarin.
10 Overdosage
There is no specific experience in the management of lenalidomide overdose in patients with MM, MDS, MCL, FL, or MZL. In dose-ranging studies in healthy subjects, some were exposed to up to 200 mg (administered 100 mg BID) and in single-dose studies, some subjects were exposed to up to 400 mg. Pruritus, urticaria, rash, and elevated liver transaminases were the primary reported AEs. In clinical trials, the dose-limiting toxicity was neutropenia and thrombocytopenia.
15 References
1. OSHA Hazardous Drugs. OSHA[Accessed on 29 January 2013, from http://www.osha.gov/SLTC/hazardousdrugs/index.html]
4.1 Pregnancy
Lenalidomide can cause fetal harm when administered to a pregnant female. Limb abnormalities were seen in the offspring of monkeys that were dosed with lenalidomide during organogenesis. This effect was seen at all doses tested. Due to the results of this developmental monkey study, and lenalidomide's structural similarities to thalidomide, a known human teratogen, lenalidomide is contraindicated in females who are pregnant [see Boxed Warning] . If this drug is used during pregnancy or if the patient becomes pregnant while taking this drug, the patient should be apprised of the potential risk to a fetus [see Warnings and Precautions (5.1, 5.2), Use in Special Populations (8.1, 8.3)].
8.1 Pregnancy
Pregnancy Exposure Registry
There is a pregnancy exposure registry that monitors pregnancy outcomes in females exposed to lenalidomide during pregnancy as well as female partners of male patients who are exposed to lenalidomide. This registry is also used to understand the root cause for the pregnancy. Report any suspected fetal exposure to lenalidomide to the FDA via the MedWatch program at 1-800-FDA-1088 and also to the REMS Call Center at 1-888-423-5436.
Risk Summary
Based on the mechanism of action [see Clinical Pharmacology (12.1)] and findings from animal studies [see Data],lenalidomide can cause embryo-fetal harm when administered to a pregnant female and is contraindicated during pregnancy [see Boxed Warning, Contraindications (4.1), and Use in Specific Populations (5.1)] .
Lenalidomide is a thalidomide analogue. Thalidomide is a human teratogen, inducing a high frequency of severe and life-threatening birth defects such as amelia (absence of limbs), phocomelia (short limbs), hypoplasticity of the bones, absence of bones, external ear abnormalities (including anotia, micropinna, small or absent external auditory canals), facial palsy, eye abnormalities (anophthalmos, microphthalmos), and congenital heart defects. Alimentary tract, urinary tract, and genital malformations have also been documented and mortality at or shortly after birth has been reported in about 40% of infants.
Lenalidomide caused thalidomide-type limb defects in monkey offspring. Lenalidomide crossed the placenta after administration to pregnant rabbits and pregnant rats [see Data]. If this drug is used during pregnancy, or if the patient becomes pregnant while taking this drug, the patient should be apprised of the potential risk to a fetus.
If pregnancy does occur during treatment, immediately discontinue the drug. Under these conditions, refer patient to an obstetrician/gynecologist experienced in reproductive toxicity for further evaluation and counseling. Report any suspected fetal exposure to lenalidomide to the FDA via the MedWatch program at 1-800-FDA-1088 and also to the REMS Call Center at 1‑888-423-5436.
The estimated background risk of major birth defects and miscarriage for the indicated population is unknown. All pregnancies have a background risk of birth defect, loss, or other adverse outcomes. The estimated background risk in the U.S. general population of major birth defects is 2% to 4% and of miscarriage is 15% to 20% of clinically recognized pregnancies.
Data
Animal data
In an embryo-fetal developmental toxicity study in monkeys, teratogenicity, including thalidomide-like limb defects, occurred in offspring when pregnant monkeys received oral lenalidomide during organogenesis. Exposure (AUC) in monkeys at the lowest dose was 0.17 times the human exposure at the maximum recommended human dose (MRHD) of 25 mg. Similar studies in pregnant rabbits and rats at 20 times and 200 times the MRHD respectively, produced embryo lethality in rabbits and no adverse reproductive effects in rats.
In a pre- and post-natal development study in rats, animals received lenalidomide from organogenesis through lactation. The study revealed a few adverse effects on the offspring of female rats treated with lenalidomide at doses up to 500 mg/kg (approximately 200 times the human dose of 25 mg based on body surface area). The male offspring exhibited slightly delayed sexual maturation and the female offspring had slightly lower body weight gains during gestation when bred to male offspring. As with thalidomide, the rat model may not adequately address the full spectrum of potential human embryo-fetal developmental effects for lenalidomide.
Following daily oral administration of lenalidomide from Gestation Day 7 through Gestation Day 20 in pregnant rabbits, fetal plasma lenalidomide concentrations were approximately 20% to 40% of the maternal C max. Following a single oral dose to pregnant rats, lenalidomide was detected in fetal plasma and tissues; concentrations of radioactivity in fetal tissues were generally lower than those in maternal tissues. These data indicated that lenalidomide crossed the placenta.
8.2 Lactation
Risk Summary
There is no information regarding the presence of lenalidomide in human milk, the effects of lenalidomide on the breastfed child, or the effects of lenalidomide on milk production. Because many drugs are excreted in human milk and because of the potential for adverse reactions in breastfed children from lenalidomide, advise women not to breastfeed during treatment with lenalidomide.
11 Description
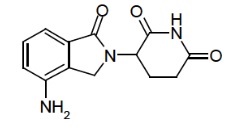
Lenalidomide, a thalidomide analogue, is an immunomodulatory agent with antiangiogenic and antineoplastic properties. The chemical name is 3-(7-amino-3-oxo-1H-isoindol-2-yl) piperidine-2,6-dione and it has the following chemical structure:
3-(7-amino-3-oxo-1H-isoindol-2-yl) piperidine-2,6-dione
The molecular formula for lenalidomide is C 13H 13N 3O 3,and the gram molecular weight is 259.26.
Lenalidomide is white to yellow crystalline powder. It is practically insoluble in isopropanol and ethanol. Very slightly soluble in water. Slightly soluble in acetonitrile and methanol. Lenalidomide has an asymmetric carbon atom and can exist as the optically active forms S(-) and R(+), and is produced as a racemic mixture with a net optical rotation of zero.
Lenalidomide is available in 2.5 mg, 5 mg, 10 mg, 15 mg, 20 mg, and 25 mg capsules for oral administration. Each capsule contains lenalidomide as the active ingredient and the following inactive ingredients: croscarmellose sodium, magnesium stearate, mannitol, and microcrystalline cellulose. The 5 mg and 25 mg capsule shells contain gelatin, titanium dioxide, and black ink. The 2.5 mg and 10 mg capsule shells contain FD&C blue #2, gelatin, titanium dioxide, yellow iron oxide, and black ink. The 15 mg capsule shells contain FD&C blue #2, gelatin, titanium dioxide, and black ink. The 20 mg capsule shells contain FD&C blue #2, gelatin, titanium dioxide, yellow iron oxide, and black ink. The capsules are printed with black ink composed of ammonia solution, black iron oxide, potassium hydroxide, propylene glycol, and shellac.
16.1 How Supplied
White to off-white powder filled in hard gelatin capsule size ‘4’ with blue-green opaque cap and white opaque body, imprinted with “LEN” on the cap and “2.5 mg” on the body with black ink:
2.5 mg bottles of 28 (NDC 82293-006-10)
White to off-white powder filled in white opaque hard gelatin capsule size ‘4’, imprinted with “LEN” on the cap and “5 mg” on the body with black ink:
5 mg bottles of 28 (NDC 82293-007-10)
White to off-white powder filled in hard gelatin capsule size ‘2’ with blue-green opaque cap and pale-yellow opaque body, imprinted with “LEN” on the cap and “10 mg” on the body with black ink:
10 mg bottles of 28 (NDC 82293-008-10)
White to off-white powder filled in hard gelatin capsule size ‘1’ with pale blue opaque cap and white opaque body, imprinted with “LEN” on the cap and “15 mg” on the body with black ink:
15 mg bottles of 21 (NDC 82293-009-10)
White to off-white powder filled in hard gelatin capsule size ‘0’ with blue-green opaque cap and pale blue opaque body, imprinted with “LEN” on the cap and “20 mg” on the body with black ink:
20 mg bottles of 21 (NDC 82293-010-10)
White to off-white powder filled in white opaque hard gelatin capsule size ‘0EL’, imprinted with “LEN” on the cap and “25 mg” on the body with black ink:
25 mg bottles of 21 (NDC 82293-011-10)
8.4 Pediatric Use
Safety and effectiveness have not been established in pediatric patients.
8.5 Geriatric Use
MM In Combination:Overall, of the 1,613 patients in the NDMM study who received study treatment, 94% (1,521 /1,613) were 65 years of age or older, while 35% (561/1,613) were over 75 years of age. The percentage of patients over age 75 was similar between study arms (Rd Continuous: 33%; Rd18: 34%; MPT: 33%). Overall, across all treatment arms, the frequency in most of the adverse reaction categories (eg, all adverse reactions, grade 3/4 adverse reactions, serious adverse reactions) was higher in older (>75 years of age) than in younger (≤75 years of age) subjects. Grade 3 or 4 adverse reactions in the General Disorders and Administration Site Conditions body system were consistently reported at a higher frequency (with a difference of at least 5%) in older subjects than in younger subjects across all treatment arms. Grade 3 or 4 adverse reactions in the Infections and Infestations, Cardiac Disorders (including cardiac failure and congestive cardiac failure), Skin and Subcutaneous Tissue Disorders, and Renal and Urinary Disorders (including renal failure) body systems were also reported slightly, but consistently, more frequently (<5% difference), in older subjects than in younger subjects across all treatment arms. For other body systems (e.g., Blood and Lymphatic System Disorders, Infections and Infestations, Cardiac Disorders, Vascular Disorders), there was a less consistent trend for increased frequency of grade 3/4 adverse reactions in older vs younger subjects across all treatment arms. Serious adverse reactions were generally reported at a higher frequency in the older subjects than in the younger subjects across all treatment arms.
MM Maintenance Therapy: Overall, 10% (106/1,018) of patients were 65 years of age or older, while no patients were over 75 years of age. Grade 3 or 4 adverse reactions were higher in the lenalidomide arm (more than 5% higher) in the patients 65 years of age or older versus younger patients. The frequency of Grade 3 or 4 adverse reactions in the Blood and Lymphatic System Disorders were higher in the lenalidomide arm (more than 5% higher) in the patients 65 years of age or older versus younger patients. There were not a sufficient number of patients 65 years of age or older in lenalidomide maintenance studies who experienced either a serious adverse reaction, or discontinued therapy due to an adverse reaction to determine whether elderly patients respond relative to safety differently from younger patients.
MM After At Least One Prior Therapy:Of the 703 MM patients who received study treatment in Studies 1 and 2, 45% were age 65 or over while 12% of patients were age 75 and over. The percentage of patients age 65 or over was not significantly different between the lenalidomide/dexamethasone and placebo/dexamethasone groups. Of the 353 patients who received lenalidomide/dexamethasone, 46% were age 65 and over. In both studies, patients >65 years of age were more likely than patients ≤65 years of age to experience DVT, pulmonary embolism, atrial fibrillation, and renal failure following use of lenalidomide. No differences in efficacy were observed between patients over 65 years of age and younger patients.
Of the 148 patients with del 5q MDS enrolled in the major study, 38% were age 65 and over, while 33% were age 75 and over. Although the overall frequency of adverse reactions (100%) was the same in patients over 65 years of age as in younger patients, the frequency of serious adverse reactions was higher in patients over 65 years of age than in younger patients (54% vs. 33%). A greater proportion of patients over 65 years of age discontinued from the clinical studies because of adverse reactions than the proportion of younger patients (27% vs. 16%). No differences in efficacy were observed between patients over 65 years of age and younger patients.
Of the 134 patients with MCL enrolled in the MCL trial, 63% were age 65 and over, while 22% of patients were age 75 and over. The overall frequency of adverse reactions was similar in patients over 65 years of age and in younger patients (98% vs. 100%). The overall incidence of grade 3 and 4 adverse reactions was also similar in these 2 patient groups (79% vs. 78%, respectively). The frequency of serious adverse reactions was higher in patients over 65 years of age than in younger patients (55% vs. 41%). No differences in efficacy were observed between patients over 65 years of age and younger patients.
FL or MZL in Combination:Overall, 48% (282/590) of patients were 65 years of age or older, while 14% (82/590) of patients were over 75 years of age. The overall frequency of adverse reactions was similar in patients 65 years of age or older and younger patients for both studies pooled (98%). Grade 3 or 4 adverse reactions were higher in the lenalidomide arm (more than 5% higher) in the patients 65 years of age or older versus younger patients (71% versus 59%). The frequency of Grade 3 or 4 adverse reactions were higher in the lenalidomide arm (more than 5% higher) in the patients 65 years of age or older versus younger patients in the Blood and Lymphatic System Disorders (47% versus 40%) and Infections and Infestations (16% versus 11%). Serious adverse reactions were higher in the lenalidomide arm (more than 5% higher) in the patients 65 years of age or older versus younger patients (37% versus 18%). The frequency of serious adverse reactions were higher in the lenalidomide arm (more than 5% higher) in the patients 65 years of age or older versus younger patients in Infections and Infestations (15% versus 6%).
Since elderly patients are more likely to have decreased renal function, care should be taken in dose selection. Monitor renal function.
2.7 Administration
Advise patients to take lenalidomide capsules orally at about the same time each day, either with or without food. Advise patients to swallow lenalidomide capsules whole with water and not to open, break, or chew them.
5.8 Hepatotoxicity
Hepatic failure, including fatal cases, has occurred in patients treated with lenalidomide in combination with dexamethasone. In clinical trials, 15% of patients experienced hepatotoxicity (with hepatocellular, cholestatic and mixed characteristics); 2% of patients with MM and 1% of patients with myelodysplasia had serious hepatotoxicity events. The mechanism of drug-induced hepatotoxicity is unknown. Pre-existing viral liver disease, elevated baseline liver enzymes, and concomitant medications may be risk factors. Monitor liver enzymes periodically. Stop lenalidomide upon elevation of liver enzymes. After return to baseline values, treatment at a lower dose may be considered.
4 Contraindications
6 Adverse Reactions
The following clinically significant adverse reactions are described in detail in other sections of the prescribing information:
- Embryo-Fetal Toxicity [see Boxed Warning, Warnings and Precautions (5.1, 5.2)]
- Hematologic Toxicity [see Boxed Warning, Warnings and Precautions (5.3)]
- Venous and Arterial Thromboembolism [see Boxed Warning, Warnings and Precautions (5.4)]
- Increased Mortality in Patients with CLL [see Warnings and Precautions (5.5)]
- Second Primary Malignancies [see Warnings and Precautions (5.6)]
- Increased Mortality in Patients with MM When Pembrolizumab Is Added to a Thalidomide Analogue and Dexamethasone [see Warnings and Precautions (5.7)]
- Hepatotoxicity [see Warnings and Precautions (5.8)]
- Severe Cutaneous Reactions [see Warnings and Precautions (5.9)]
- Tumor Lysis Syndrome [see Warnings and Precautions (5.10)]
- Tumor Flare Reactions [see Warnings and Precautions (5.11)]
- Impaired Stem Cell Mobilization [see Warnings and Precautions (5.12)]
- Thyroid Disorders [see Warnings and Precautions (5.13)]
- Early Mortality in Patients with MCL [see Warnings and Precautions (5.14)]
- Hypersensitivity [see Warnings and Precautions (5.15)]
7 Drug Interactions
1.1 Multiple Myeloma
Lenalidomide capsules in combination with dexamethasone is indicated for the treatment of adult patients with multiple myeloma (MM).
Lenalidomide capsules are indicated as maintenance therapy in adult patients with MM following autologous hematopoietic stem cell transplantation (auto-HSCT).
8.6 Renal Impairment
Adjust the starting dose of lenalidomide based on the creatinine clearance value and for patients on dialysis [see Dosage and Administration (2.6)].
5.15 Hypersensitivity
Hypersensitivity, including angioedema, anaphylaxis, and anaphylactic reactions to lenalidomide has been reported. Permanently discontinue lenalidomide for angioedema and anaphylaxis [see Dosage and Administration (2.2)] .
1.6 Limitations of Use
Lenalidomide capsules are not indicated and are not recommended for the treatment of patients with CLL outside of controlled clinical trials [see Warnings and Precautions (5.5)] .
5.13 Thyroid Disorders
Both hypothyroidism and hyperthyroidism have been reported [see Adverse Reactions (6.2)] . Measure thyroid function before start of lenalidomide treatment and during therapy.
1 Indications and Usage
Lenalidomide is a thalidomide analogue indicated for the treatment of adult patients with:
- Multiple myeloma (MM), in combination with dexamethasone ( 1.1).
- MM, as maintenance following autologous hematopoietic stem cell transplantation (auto-HSCT) ( 1.1).
- Transfusion-dependent anemia due to low- or intermediate-1-risk myelodysplastic syndromes (MDS) associated with a deletion 5q abnormality with or without additional cytogenetic abnormalities ( 1.2).
- Mantle cell lymphoma (MCL) whose disease has relapsed or progressed after two prior therapies, one of which included bortezomib ( 1.3).
- Previously treated follicular lymphoma (FL), in combination with a rituximab product ( 1.4).
- Previously treated marginal zone lymphoma (MZL), in combination with a rituximab product ( 1.5).
Limitations of Use:
- Lenalidomide capsules are not indicated and are not recommended for the treatment of patients with chronic lymphocytic leukemia (CLL) outside of controlled clinical trials ( 1.6).
1.4 Follicular Lymphoma
Lenalidomide capsules in combination with a rituximab product, is indicated for the treatment of adult patients with previously treated follicular lymphoma (FL).
1.3 Mantle Cell Lymphoma
Lenalidomide capsules are indicated for the treatment of adult patients with mantle cell lymphoma (MCL) whose disease has relapsed or progressed after two prior therapies, one of which included bortezomib.
12.1 Mechanism of Action
Lenalidomide is an analogue of thalidomide with immunomodulatory, antiangiogenic, and antineoplastic properties. Cellular activities of lenalidomide are mediated through its target cereblon, a component of a cullin ring E3 ubiquitin ligase enzyme complex. In vitro, in the presence of drug, substrate proteins (including Aiolos, Ikaros, and CK1α) are targeted for ubiquitination and subsequent degradation leading to direct cytotoxic and immunomodulatory effects. Lenalidomide inhibits proliferation and induces apoptosis of certain hematopoietic tumor cells including MM, mantle cell lymphoma, and del (5q) myelodysplastic syndromes, follicular lymphoma and marginal zone lymphoma in vitro. Lenalidomide causes a delay in tumor growth in some in vivononclinical hematopoietic tumor models including MM. Immunomodulatory properties of lenalidomide include increased number and activation of T cells and natural killer (NK) cells leading to direct and enhanced antibody-dependent cell-mediated cytotoxicity (ADCC) via increased secretion of interleukin-2 and interferon-gamma, increased numbers of NKT cells, and inhibition of pro-inflammatory cytokines (e.g., TNF-α and IL-6) by monocytes. In MM cells, the combination of lenalidomide and dexamethasone synergizes the inhibition of cell proliferation and the induction of apoptosis. The combination of lenalidomide and rituximab increases ADCC and direct tumor apoptosis in follicular lymphoma cells and increases ADCC in marginal zone lymphoma cells compared to rituximab alone in vitro.
5.3 Hematologic Toxicity
Lenalidomide can cause significant neutropenia and thrombocytopenia. Monitor patients with neutropenia for signs of infection. Advise patients to observe for bleeding or bruising, especially with use of concomitant medication that may increase risk of bleeding. Patients taking lenalidomide should have their complete blood counts assessed periodically as described below [see Dosage and Administration (2.1, 2.2, 2.3)] .
Monitor complete blood counts (CBC) in patients taking lenalidomide capsules in combination with dexamethasone or as lenalidomide maintenance therapy for MM every 7 days (weekly) for the first 2 cycles, on Days 1 and 15 of Cycle 3, and every 28 days (4 weeks) thereafter. A dose interruption and/or dose reduction may be required [see Dosage and Administration (2.1)] . In the MM maintenance therapy trials, Grade 3 or 4 neutropenia was reported in up to 59% of lenalidomide-treated patients and Grade 3 or 4 thrombocytopenia in up to 38% of lenalidomide-treated patients [see Adverse Reactions (6.1)] .
Monitor complete blood counts (CBC) in patients taking lenalidomide for MDS weekly for the first 8 weeks and at least monthly thereafter. Grade 3 or 4 hematologic toxicity was seen in 80% of patients enrolled in the MDS study. In the 48% of patients who developed Grade 3 or 4 neutropenia, the median time to onset was 42 days (range, 14 days to 411 days), and the median time to documented recovery was 17 days (range, 2 days to 170 days). In the 54% of patients who developed Grade 3 or 4 thrombocytopenia, the median time to onset was 28 days (range, 8 days to 290 days), and the median time to documented recovery was 22 days (range, 5 days to 224 days) [see Boxed Warningand Dosage and Administration (2.2)] .
Monitor complete blood counts (CBC) in patients taking lenalidomide for MCL weekly for the first cycle (28 days), every 2 weeks during cycles 2 to 4, and then monthly thereafter. Patients may require dose interruption and/or dose reduction. In the MCL trial, Grade 3 or 4 neutropenia was reported in 43% of the patients. Grade 3 or 4 thrombocytopenia was reported in 28% of the patients.
Monitor complete blood counts (CBC) in patients taking lenalidomide for FL or MZL weekly for the first 3 weeks of Cycle 1 (28 days), every 2 weeks during Cycles 2 to 4, and then monthly thereafter. Patients may require dose interruption and/or dose reduction. In the AUGMENT and MAGNIFY trials, Grade 3 or 4 neutropenia was reported in 50% and 33%, respectively, of patients in the lenalidomide/rituximab arm. Grade 3 or 4 thrombocytopenia was reported in 2% and 8%, respectively, of patients in the lenalidomide/rituximab arm [see Adverse Reactions (6.1) ].
14.3 Mantle Cell Lymphoma
A multicenter, single-arm, open-label trial of single-agent lenalidomide was conducted to evaluate the safety and efficacy of lenalidomide in patients with mantle cell lymphoma who have relapsed after or were refractory to bortezomib or a bortezomib-containing regimen. Patients with a creatinine clearance ≥60 mL/min were given lenalidomide at a dose of 25 mg once daily for 21 days every 28 days. Patients with a creatinine clearance ≥30 mL/min and <60 mL/min were given lenalidomide at a dose of 10 mg once daily for 21 days every 28 days. Treatment was continued until disease progression, unacceptable toxicity, or withdrawal of consent.
The trial included patients who were at least 18 years of age with biopsy-proven MCL with measurable disease by CT scan. Patients were required to have received prior treatment with an anthracycline or mitoxantrone, cyclophosphamide, rituximab, and bortezomib, alone or in combination. Patients were required to have documented refractory disease (defined as without any response of PR or better during treatment with bortezomib or a bortezomib-containing regimen), or relapsed disease (defined as progression within one year after treatment with bortezomib or a bortezomib-containing regimen). At enrollment patients were to have an absolute neutrophil counts (ANC) ≥1,500/ mm
3, platelet counts ≥60,000/mm
3, serum SGOT/AST or SGPT/ALT ≤3x upper limit of normal (ULN) unless there was documented evidence of liver involvement by lymphoma, serum total bilirubin ≤1.5 x ULN except in cases of Gilbert’s syndrome or documented liver involvement by lymphoma, and calculated creatinine clearance (Cockcroft-Gault formula) ≥30 mL/min.
The median age was 67 years (43 to 83), 81% were male and 96% were Caucasian. The table below summarizes the baseline disease-related characteristics and prior anti-lymphoma therapy in the Mantle Cell Lymphoma trial.
| Baseline Disease Characteristics and Prior Anti- Lymphoma Treatment |
Total Patients
(N = 134) |
|
ECOG Performance Status
ECOG = Eastern Cooperative Oncology Group. n (%)
|
|
| 0 | 43 (32)) |
| 1 | 73 (54) |
| 2 | 17 (13) |
| 3 | 1 (< 1) |
| Advanced MCL Stage, n (%) | |
| III | 27 (20) |
| IV | 97 (72) |
|
High or Intermediate MIPI Score
MIPI = MCL International Prognostic Index. , n (%)
|
90 (67) |
|
High Tumor Burden
High tumor burden is defined as at least one lesion that is ≥5 cm in diameter or 3 lesions that are ≥3 cm in diameter. , n (%)
|
77 (57) |
|
Bulky Disease
Bulky disease is defined as at least one lesion that is ≥7cm in the longest diameter. , n (%)
|
44 (33) |
| Extranodal Disease, n (%) | 101 (75) |
| Number of Prior Systemic Anti-Lymphoma Therapies, n (%) | |
| Median (range) | 4 (2, 10) |
| 1 | 0 (0) |
| 2 | 29 (22) |
| 3 | 34 (25) |
| ≥4 | 71 (53) |
| Number of Subjects Who Received Prior Regimen Containing, n (%): | |
| Anthracycline/mitoxantrone | 133 (99) |
| Cyclophosphamide | 133 (99) |
| Rituximab | 134 (100) |
| Bortezomib | 134 (100) |
| Refractory to Prior Bortezomib, n (%) | 81 (60) |
| Refractory to Last Prior Therapy, n (%) | 74 (55) |
| Prior Autologous Bone Marrow or Stem Cell Transplant, n (%) | 39 (29) |
The efficacy endpoints in the MCL trial were overall response rate (ORR) and duration of response (DOR). Response was determined based on review of radiographic scans by an independent review committee according to a modified version of the International Workshop Lymphoma Response Criteria (Cheson, 1999). The DOR is defined as the time from the initial response (at least PR) to documented disease progression. The efficacy results for the MCL population were based on all evaluable patients who received at least one dose of study drug and are presented in Table 20. The median time to response was 2.2 months (range 1.8 months to 13 months).
| Response Analyses (N = 133) | N (%) | 95% CI | |
| Overall Response Rate (IWRC) (CR + CRu +PR) | 34 (26) | (18.4, 33.9) | |
| Complete Response (CR + CRu) | 9 (7) | (3.1, 12.5) | |
| CR | 1 (1) | ||
| CRu | 8 (6) | ||
| Partial Response (PR) | 25 (19) | ||
| Duration of Response (months) | Median | 95% CI | |
| Duration of Overall Response (CR + CRu + PR) | (N = 34) | 16.6 | (7.7, 26.7) |
5.1 Embryo Fetal Toxicity
Lenalidomide is a thalidomide analogue and is contraindicated for use during pregnancy. Thalidomide is a known human teratogen that causes life-threatening human birth defects or embryo-fetal death [see Use in Specific Populations (8.1)]. An embryo-fetal development study in monkeys indicates that lenalidomide produced malformations in the offspring of female monkeys who received the drug during pregnancy, similar to birth defects observed in humans following exposure to thalidomide during pregnancy.
Lenalidomide capsules are only available through the Lenalidomide REMS program [see Warnings and Precautions (5.2)].
5.10 Tumor Lysis Syndrome
Fatal instances of tumor lysis syndrome (TLS) have been reported during treatment with lenalidomide. The patients at risk of TLS are those with high tumor burden prior to treatment. Monitor patients at risk closely and take appropriate preventive approaches. In the AUGMENT trial in FL or MZL patients, TLS occurred in 2 patients (1.1%) in the lenalidomide/rituximab arm. TLS occurred in 1 patient (0.5%) in the MAGNIFY trial during the lenalidomide/rituximab induction period; the event was a serious, Grade 3 adverse reaction.
5.11 Tumor Flare Reaction
Tumor flare reaction (TFR), including fatal reactions, have occurred during investigational use of lenalidomide for CLL and lymphoma, and is characterized by tender lymph node swelling, low grade fever, pain and rash. Lenalidomide is not indicated and not recommended for use in CLL outside of controlled clinical trials.
Monitoring and evaluation for TFR is recommended in patients with MCL, FL, or MZL. Tumor flare reaction may mimic progression of disease (PD).
In the MCL trial, 13/134 (10%) of subjects experienced TFR; all reports were Grade 1 or 2 in severity. All of the events occurred in Cycle 1 and one patient developed TFR again in Cycle 11. In the AUGMENT trial in FL or MZL patients, TFR was reported in 19/176 (10.8%) of patients in lenalidomide with rituximab arm; one patient in the lenalidomide/rituximab arm experienced a Grade 3 TFR. In the MAGNIFY trial, 9/222 (4.1%) of patients experienced TFR; all reports were Grade 1 or 2 in severity and 1 event was considered as serious. In a separate MCL phase 2 trial, one case of TFR resulted in a fatal outcome.
Lenalidomide may be continued in patients with Grade 1 and 2 TFR without interruption or modification, at the physician's discretion. Patients with Grade 1 and 2 TFR may also be treated with corticosteroids, non-steroidal anti-inflammatory drugs (NSAIDs) and/or narcotic analgesics for management of TFR symptoms. In patients with Grade 3 or 4 TFR, it is recommended to withhold treatment with lenalidomide until TFR resolves to ≤Grade 1. Patients with Grade 3 or 4 TFR may be treated for management of symptoms per the guidance for treatment of Grade 1 and 2 TFR.
1.5 Marginal Zone Lymphoma
Lenalidomide capsules in combination with a rituximab product, is indicated for the treatment of adult patients with previously treated marginal zone lymphoma (MZL).
16.3 Handling and Disposal
Care should be exercised in the handling of lenalidomide capsules. Lenalidomide capsules should not be opened or broken. If powder from lenalidomide capsules contacts the skin, wash the skin immediately and thoroughly with soap and water. If lenalidomide capsules contacts the mucous membranes, flush thoroughly with water.
Procedures for the proper handling and disposal of anticancer drugs should be considered. Several guidelines on the subject have been published. 1
Dispense no more than a 28-day supply.
5 Warnings and Precautions
- Increased Mortality: serious and fatal cardiac adverse reactions occurred in patients with CLL treated with lenalidomide ( 5.5).
- Second Primary Malignancies (SPM): Higher incidences of SPM were observed in controlled trials of patients with MM receiving lenalidomide ( 5.6).
- Increased Mortality: Observed in patients with MM when pembrolizumab was added to dexamethasone and a thalidomide analogue ( 5.7).
- Hepatotoxicity: Hepatic failure including fatalities; monitor liver function. Stop lenalidomide and evaluate if hepatotoxicity is suspected ( 5.8).
- Severe Cutaneous Reactions: Discontinue lenalidomide for severe reactions ( 5.9).
- Tumor lysis syndrome (TLS) including fatalities: Monitor patients at risk of TLS (i.e., those with high tumor burden) and take appropriate precautions ( 5.10).
- Tumor flare reaction: Serious tumor flare reactions, including fatal reactions, have occurred during investigational use of lenalidomide for chronic lymphocytic leukemia and lymphoma ( 5.11).
- Impaired Stem Cell mobilization: A decrease in the number of CD34+ cells collected after treatment (> 4 cycles) with lenalidomide has been reported. Consider early referral to transplant center ( 5.12).
- Early mortality in MCL: Higher rate of early deaths have occurred in patients with MCL ( 5.14).
- Hypersensitivity: Monitor patients for potential hypersensitivity. Discontinue lenalidomide for angioedema and anaphylaxis ( 5.15).
2 Dosage and Administration
- MM combination therapy: 25 mg once daily orally on Days 1 to 21 of repeated 28-day cycles. ( 2.1).
- MM maintenance therapy following auto-HSCT: 10 mg once daily continuously on Days 1 to 28 of repeated 28-day cycles ( 2.1).
- MDS: 10 mg once daily ( 2.2).
- MCL: 25 mg once daily orally on Days 1 to 21 of repeated 28-day cycles ( 2.3).
- FL or MZL: 20 mg once daily orally on Days 1 to 21 of repeated 28-day cycles for up to 12 cycles ( 2.4).
- Renal impairment: Adjust starting dose based on the creatinine clearance value ( 2.6).
- For concomitant therapy doses, see Full Prescribing Information ( 2.1, 2.4, 14.1, 14.4).
3 Dosage Forms and Strengths
Capsules:
- 2.5 mg, white to off-white powder filled in hard gelatin capsule size ‘4’ with blue-green opaque cap and white opaque body, imprinted with “LEN” on the cap and “2.5 mg” on the body with black ink
- 5 mg, white to off-white powder filled in white opaque hard gelatin capsule size ‘4’, imprinted with “LEN” on the cap and “5 mg” on the body with black ink
- 10 mg, white to off-white powder filled in hard gelatin capsule size ‘2’ with blue-green opaque cap and pale-yellow opaque body, imprinted with “LEN” on the cap and “10 mg” on the body with black ink
- 15 mg, white to off-white powder filled in hard gelatin capsule size ‘1’ with pale blue opaque cap and white opaque body, imprinted with “LEN” on the cap and “15 mg” on the body with black ink
- 20 mg, white to off-white powder filled in hard gelatin capsule size ‘0’ with blue-green opaque cap and pale blue opaque body, imprinted with “LEN” on the cap and “20 mg” on the body with black ink
- 25 mg, white to off-white powder filled in white opaque hard gelatin capsule size ‘0EL’, imprinted with “LEN” on the cap and “25 mg” on the body with black ink
6.2 Postmarketing Experience
The following adverse drug reactions have been identified from the worldwide post-marketing experience with lenalidomide. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure [see Warnings and Precautions Section (5.8to 5.11, and 5.13)]
Endocrine disorders:Hypothyroidism, hyperthyroidism
Hepatobiliary disorders:Hepatic failure (including fatality), toxic hepatitis, cytolytic hepatitis, cholestatic hepatitis, mixed cytolytic/cholestatic hepatitis, transient abnormal liver laboratory tests
Immune system disorders:Angioedema, anaphylaxis, acute graft-versus-host disease (following allogeneic hematopoietic transplant), solid organ transplant rejection
Infections and infestations:Viral reactivation (such as hepatitis B virus and herpes zoster), progressive multifocal leukoencephalopathy (PML)
Neoplasms benign, malignant and unspecified (including cysts and polyps):Tumor lysis syndrome, tumor flare reaction
Respiratory, thoracic and mediastinal disorders:Pneumonitis
Skin and subcutaneous tissue disorders:Stevens-Johnson Syndrome, toxic epidermal necrolysis, drug reaction with eosinophilia and systemic symptoms (DRESS)
1.2 Myelodysplastic Syndromes
Lenalidomide capsules are indicated for the treatment of adult patients with transfusion-dependent anemia due to low- or intermediate-1-risk myelodysplastic syndromes (MDS) associated with a deletion 5q cytogenetic abnormality with or without additional cytogenetic abnormalities.
5.2 Lenalidomide Rems Program
Because of the embryo-fetal risk [see Warnings and Precautions (5.1)], lenalidomide capsules are available only through a restricted program under a Risk Evaluation and Mitigation Strategy (REMS), the Lenalidomide REMSprogram.
Required components of the Lenalidomide REMSprogram include the following:
- Prescribers must be certified with the Lenalidomide REMSprogram by enrolling and complying with the REMS requirements.
- Patients must sign a Patient-Physician agreement form and comply with the REMS requirements. In particular, female patients of reproductive potential who are not pregnant must comply with the pregnancy testing and contraception requirements [see Use in Specific Populations (8.3)] and males must comply with contraception requirements [see Use in Specific Populations (8.3)] .
- Pharmacies must be certified with the Lenalidomide REMSprogram, must only dispense to patients who are authorized to receive lenalidomide capsules and comply with REMS requirements.
Further information about the Lenalidomide REMSprogram is available at www.lenalidomiderems.comor by telephone at 1-888-423-5436.
8 Use in Specific Populations
- Lactation: Advise not to breastfeed ( 8.2).
5.9 Severe Cutaneous Reactions
Severe cutaneous reactions including Stevens-Johnson syndrome (SJS), toxic epidermal necrolysis (TEN), and drug reaction with eosinophilia and systemic symptoms (DRESS) have been reported. DRESS may present with a cutaneous reaction (such as rash or exfoliative dermatitis), eosinophilia, fever, and/or lymphadenopathy with systemic complications such as hepatitis, nephritis, pneumonitis, myocarditis, and/or pericarditis. These events can be fatal. Patients with a prior history of Grade 4 rash associated with thalidomide treatment should not receive lenalidomide. Consider lenalidomide interruption or discontinuation for Grade 2 to 3 skin rash. Permanently discontinue lenalidomide for Grade 4 rash, exfoliative or bullous rash, or for other severe cutaneous reactions such as SJS, TEN or DRESS [see Dosage and Administration (2.5)] .
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
5.6 Second Primary Malignancies
In clinical trials in patients with MM receiving lenalidomide, an increase of hematologic plus solid tumor second primary malignancies (SPM) notably AML and MDS have been observed. An increase in hematologic SPM including AML and MDS occurred in 5.3% of patients with NDMM receiving lenalidomide in combination with oral melphalan compared with 1.3% of patients receiving melphalan without lenalidomide. The frequency of AML and MDS cases in patients with NDMM treated with lenalidomide in combination with dexamethasone without melphalan was 0.4%.
In patients receiving lenalidomide maintenance therapy following high dose intravenous melphalan and auto-HSCT, hematologic SPM occurred in 7.5% of patients compared to 3.3% in patients receiving placebo. The incidence of hematologic plus solid tumor (excluding squamous cell carcinoma and basal cell carcinoma) SPM was 14.9%, compared to 8.8% in patients receiving placebo with a median follow-up of 91.5 months. Non-melanoma skin cancer SPM, including squamous cell carcinoma and basal cell carcinoma, occurred in 3.9% of patients receiving lenalidomide maintenance, compared to 2.6% in the placebo arm.
In patients with relapsed or refractory MM treated with lenalidomide/dexamethasone, the incidence of hematologic plus solid tumor (excluding squamous cell carcinoma and basal cell carcinoma) SPM was 2.3% versus 0.6% in the dexamethasone alone arm. Non-melanoma skin cancer SPM, including squamous cell carcinoma and basal cell carcinoma, occurred in 3.1% of patients receiving lenalidomide/dexamethasone, compared to 0.6% in the dexamethasone alone arm.
Patients who received lenalidomide-containing therapy until disease progression did not show a higher incidence of invasive SPM than patients treated in the fixed duration lenalidomide-containing arms. Monitor patients for the development of second primary malignancies. Take into account both the potential benefit of lenalidomide and the risk of second primary malignancies when considering treatment with lenalidomide.
In the AUGMENT trial with FL or MZL patients receiving lenalidomide/rituximab therapy, hematologic plus solid tumor SPMs, notably AML, have been observed. In the AUGMENT trial, hematologic SPM of AML occurred in 0.6% of patients with FL or MZL receiving lenalidomide/rituximab therapy. The incidence of hematologic plus solid tumor SPMs (excluding nonmelanoma skin cancers) was 1.7% in the lenalidomide/rituximab arm with a median follow-up of 29.8 months (range 0.5 month to 51.3 months) [see Adverse Reactions (6.1)] . Monitor patients for the development of second primary malignancies. Take into account both the potential benefit of lenalidomide and the risk of second primary malignancies when considering treatment with lenalidomide.
Principal Display Panel – 5 Mg
NDC 82293-007-10
Lenalidomide Capsules
5 mg
WARNING: POTENTIAL FOR HUMAN BIRTH DEFECTS.
PHARMACIST: Dispense the accompanying Medication Guide to each patient.
28 Capsules
Rx only
17 Patient Counseling Information
Advise the patient to read the FDA-approved Patient labeling (Medication Guide)
Embryo-Fetal Toxicity
Advise patients that lenalidomide capsules are contraindicated in pregnancy [see Boxed Warningand Contraindications (4.1)]. Lenalidomide capsules are a thalidomide analogue and can cause serious birth defects or death to a developing baby [see Warnings and Precautions (5.1)and Use in Specific Populations (8.1)] .
- Advise females of reproductive potential that they must avoid pregnancy while taking lenalidomide capsules and for at least 4 weeks after completing therapy.
- Initiate lenalidomide capsules treatment in females of reproductive potential only following a negative pregnancy test.
- Advise females of reproductive potential of the importance of monthly pregnancy tests and the need to use 2 different forms of contraception including at least 1 highly effective form, simultaneously during lenalidomide capsules therapy, during dose interruption and for 4 weeks after she has completely finished taking lenalidomide capsules. Highly effective forms of contraception other than tubal ligation include IUD and hormonal (birth control pills, injections, patch or implants) and a partner’s vasectomy. Additional effective contraceptive methods include latex or synthetic condom, diaphragm and cervical cap.
- Instruct patient to immediately stop taking lenalidomide capsules and contact her healthcare provider if she becomes pregnant while taking this drug, if she misses her menstrual period, or experiences unusual menstrual bleeding, if she stops taking birth control, or if she thinks FOR ANY REASON that she may be pregnant.
- Advise patient that if her healthcare provider is not available, she should call the REMS Call Center at 1-888-423-5436 [see Warnings and Precautions (5.1)and Use in Specific Populations (8.3)].
- Advise males to always use a latex or synthetic condom during any sexual contact with females of reproductive potential while taking lenalidomide capsules and for up to 4 weeks after discontinuing lenalidomide capsules, even if they have undergone a successful vasectomy.
- Advise male patients taking lenalidomide capsules that they must not donate sperm and for up to 4 weeks after discontinuation of lenalidomide capsules [see Warnings and Precautions (5.1)and Use in Specific Populations (8.3)] .
- All patients must be instructed to not donate blood while taking lenalidomide capsules, during dose interruptions and for 4 weeks following discontinuation of lenalidomide capsules [see Warnings and Precautions (5.1)] .
Lenalidomide REMS program
Because of the risk of embryo-fetal toxicity, lenalidomide capsules are only available through a restricted program called the Lenalidomide REMS program [see Warnings and Precautions (5.2)] .
- Patients must sign a Patient-Physician agreement form and comply with the requirements to receive lenalidomide capsules. In particular, females of reproductive potential must comply with the pregnancy testing, contraception requirements and participate in monthly telephone surveys. Males must comply with the contraception requirements [see Use in Specific Populations (8.3)] .
- Lenalidomide capsules are available only from pharmacies that are certified in the Lenalidomide REMS program. Provide patients with the telephone number and website for information on how to obtain the product.
Pregnancy Exposure Registry
Inform females there is a Pregnancy Exposure Registry that monitors pregnancy outcomes in females exposed to lenalidomide capsules during pregnancy and that they can contact the Pregnancy Exposure Registry by calling 1-888-423-5436 [see Use in Specific Populations (8.1) ] .
Hematologic Toxicity
Inform patients that lenalidomide capsules are associated with significant neutropenia and thrombocytopenia [see Boxed Warningand Warnings and Precautions (5.3)] .
Venous and Arterial Thromboembolism
Inform patients of the risk of thrombosis including DVT, PE, MI, and stroke and to report immediately any signs and symptoms suggestive of these events for evaluation [see Boxed Warningand Warnings and Precautions (5.4)] .
Increased Mortality in Patients with CLL
Inform patients that lenalidomide capsules had increased mortality in patients with CLL and serious adverse cardiovascular reactions, including atrial fibrillation, myocardial infarction, and cardiac failure [see Warnings and Precautions (5.5)] .
Second Primary Malignancies
Inform patients of the potential risk of developing second primary malignancies during treatment with lenalidomide capsules [see Warnings and Precautions (5.6)] .
Hepatotoxicity
Inform patients of the risk of hepatotoxicity, including hepatic failure and death, and to report any signs and symptoms associated with this event to their healthcare provider for evaluation [see Warnings and Precautions (5.8)] .
Severe Cutaneous Reactions
Inform patients of the potential risk for severe skin reactions such as SJS, TEN, and DRESS and report any signs and symptoms associated with these reactions to their healthcare provider for evaluation. Patients with a prior history of Grade 4 rash associated with thalidomide treatment should not receive lenalidomide capsules [see Warnings and Precautions (5.9)].
Tumor Lysis Syndrome
Inform patients of the potential risk of tumor lysis syndrome and to report any signs and symptoms associated with this event to their healthcare provider for evaluation [see Warnings and Precautions (5.10)] .
Tumor Flare Reaction
Inform patients of the potential risk of tumor flare reaction and to report any signs and symptoms associated with this event to their healthcare provider for evaluation [see Warnings and Precautions (5.11)] .
Early Mortality in Patients with MCL
Inform patients with MCL of the potential for early death
[see
Warnings and Precautions (5.14)].
Hypersensitivity
Inform patients of the potential for severe hypersensitivity reactions such as angioedema and anaphylaxis to lenalidomide capsules. Instruct patients to contact their healthcare provider right away for signs and symptoms of these reactions. Advise patients to seek emergency medical attention for signs or symptoms of severe hypersensitivity reactions [see Warnings and Precautions (5.15)] .
Dosing Instructions
Inform patients how to take lenalidomide capsules [see Dosage and Administration (2)]
- Lenalidomide capsules should be taken once daily at about the same time each day,
- Lenalidomide capsules may be taken either with or without food.
- The capsules should not be opened, broken, or chewed. Lenalidomide capsules should be swallowed whole with water.
- Instruct patients that if they miss a dose of lenalidomide capsules, they may still take it up to 12 hours after the time they would normally take it. If more than 12 hours have elapsed, they should be instructed to skip the dose for that day. The next day, they should take lenalidomide capsules at the usual time. Warn patients to not take 2 doses to make up for the one that they missed.
Distributed by:
Novugen Pharma (USA) LLC
100 Overlook Center
Princeton, NJ 08540, USA
MADE IN INDIA
Revised: 11/2023
Principal Display Panel – 10 Mg
NDC 82293-008-10
Lenalidomide Capsules
10 mg
WARNING: POTENTIAL FOR HUMAN BIRTH DEFECTS.
PHARMACIST: Dispense the accompanying Medication Guide to each patient.
28 Capsules
Rx only
Principal Display Panel – 15 Mg
NDC 82293-009-10
Lenalidomide Capsules
15 mg
WARNING: POTENTIAL FOR HUMAN BIRTH DEFECTS.
PHARMACIST: Dispense the accompanying Medication Guide to each patient.
21 Capsules
Rx only
Principal Display Panel – 20 Mg
NDC 82293-010-10
Lenalidomide Capsules
20 mg
WARNING: POTENTIAL FOR HUMAN BIRTH DEFECTS.
PHARMACIST: Dispense the accompanying Medication Guide to each patient.
21 Capsules
Rx only
Principal Display Panel – 25 Mg
NDC 82293-011-10
Lenalidomide Capsules
25 mg
WARNING: POTENTIAL FOR HUMAN BIRTH DEFECTS.
PHARMACIST: Dispense the accompanying Medication Guide to each patient.
21 Capsules
Rx only
Principal Display Panel – 2.5 Mg
NDC 82293-006-10
Lenalidomide Capsules
2.5 mg
WARNING: POTENTIAL FOR HUMAN BIRTH DEFECTS.
PHARMACIST: Dispense the accompanying Medication Guide to each patient.
28 Capsules
Rx only
5.12 Impaired Stem Cell Mobilization
A decrease in the number of CD34+ cells collected after treatment (>4 cycles) with lenalidomide has been reported. In patients who are auto-HSCT candidates, referral to a transplant center should occur early in treatment to optimize the timing of the stem cell collection. In patients who received more than 4 cycles of a lenalidomide-containing treatment or for whom inadequate numbers of CD 34+ cells have been collected with G-CSF alone, G-CSF with cyclophosphamide or the combination of G-CSF with a CXCR4 inhibitor may be considered.
4.2 Severe Hypersensitivity Reactions
Lenalidomide is contraindicated in patients who have demonstrated severe hypersensitivity (e.g., angioedema, Stevens-Johnson syndrome, toxic epidermal necrolysis) to lenalidomide [see Warnings and Precautions (5.9, 5.15)].
5.4 Venous and Arterial Thromboembolism
Venous thromboembolic events (VTE [DVT and PE]) and arterial thromboembolic events (ATE, myocardial infarction and stroke) are increased in patients treated with lenalidomide.
A significantly increased risk of DVT (7.4%) and of PE (3.7%) occurred in patients with MM after at least one prior therapy who were treated with lenalidomide and dexamethasone therapy compared to patients treated in the placebo and dexamethasone group (3.1% and 0.9%) in clinical trials with varying use of anticoagulant therapies. In the newly diagnosed multiple myeloma (NDMM) study in which nearly all patients received antithrombotic prophylaxis, DVT was reported as a serious adverse reaction (3.6%, 2.0%, and 1.7%) in the Rd Continuous, Rd18, and MPT Arms, respectively. The frequency of serious adverse reactions of PE was similar between the Rd Continuous, Rd18, and MPT Arms (3.8%, 2.8%, and 3.7%, respectively) [see Boxed Warningand Adverse Reactions (6.1)] .
Myocardial infarction (1.7%) and stroke (CVA) (2.3%) are increased in patients with MM after at least one prior therapy who were treated with lenalidomide and dexamethasone therapy compared to patients treated with placebo and dexamethasone (0.6%, and 0.9%) in clinical trials. In the NDMM study, myocardial infarction (including acute) was reported as a serious adverse reaction (2.3%, 0.6%, and 1.1%) in the Rd Continuous, Rd18, and MPT Arms, respectively. The frequency of serious adverse reactions of CVA was similar between the Rd Continuous, Rd18, and MPT Arms (0.8%, 0.6 %, and 0.6%, respectively) [see Adverse Reactions (6.1)].
Patients with known risk factors, including prior thrombosis, may be at greater risk and actions should be taken to try to minimize all modifiable factors (e.g., hyperlipidemia, hypertension, smoking).
In controlled clinical trials that did not use concomitant thromboprophylaxis, 21.5% overall thrombotic events (Standardized MedDRA Query Embolic and Thrombotic events) occurred in patients with refractory and relapsed MM who were treated with lenalidomide and dexamethasone compared to 8.3% thrombosis in patients treated with placebo and dexamethasone. The median time to first thrombosis event was 2.8 months. In the NDMM study in which nearly all patients received antithrombotic prophylaxis, the overall frequency of thrombotic events was 17.4% in patients in the combined Rd Continuous and Rd18 Arms, and was 11.6% in the MPT Arm. The median time to first thrombosis event was 4.3 months in the combined Rd Continuous and Rd18 Arms.
In the AUGMENT trial, the incidence of VTE (including DVT and PE) in FL or MZL patients was 3.4% in the lenalidomide/rituximab arm [see Adverse Reactions (6.1)] . In the AUGMENT trial, the incidence of ATE (including MI) in FL or MZL patients was 0.6% in the lenalidomide/rituximab arm [see Adverse Reactions (6.1)] .
Thromboprophylaxis is recommended. The regimen of thromboprophylaxis should be based on an assessment of the patient's underlying risks. Instruct patients to report immediately any signs and symptoms suggestive of thrombotic events. ESAs and estrogens may further increase the risk of thrombosis and their use should be based on a benefit-risk decision in patients receiving lenalidomide [see Drug Interactions (7.2)].
5.14 Early Mortality in Patients With Mcl
In another MCL study, there was an increase in early deaths (within 20 weeks), 12.9% in the lenalidomide arm versus 7.1% in the control arm. On exploratory multivariate analysis, risk factors for early deaths include high tumor burden, MIPI score at diagnosis, and high WBC at baseline (≥10 x 10 9/L).
14.4 Follicular and Marginal Zone Lymphoma
The efficacy of lenalidomide with rituximab in patients with relapsed or refractory follicular and marginal zone lymphoma was evaluated in the AUGMENT ( NCT01938001) and MAGNIFY ( NCT01996865) trials.
AUGMENT is a randomized, double-blind, multicenter trial (n = 358) in which patients with relapsed or refractory follicular or marginal zone lymphoma were randomized 1:1 to receive lenalidomide and rituximab or rituximab and placebo. AUGMENT included patients diagnosed with Grade 1, 2, or 3a follicular lymphoma, who received at least 1 prior systemic therapy, were refractory or relapsed, not rituximab-refractory, had at least one measurable nodal or extranodal lesion by CT or MRI scan, and had adequate bone marrow, liver, and renal function. Randomization was stratified by follicular versus marginal zone lymphoma, previous rituximab therapy, and time since other anti-lymphoma therapy. In AUGMENT, lenalidomide was administered orally 20 mg once daily for Days 1 to 21 of repeating 28-day cycles for a maximum of 12 cycles or until unacceptable toxicity. The dose of rituximab was 375 mg/m 2every week in Cycle 1 (Days 1, 8, 15, and 22) and on Day 1 of every 28-day cycle from Cycles 2 through 5. All dosage calculations for rituximab were based on the patient's body surface area (BSA), using actual patient weight. Dose adjustments for lenalidomide were allowed based on clinical and laboratory findings. A patient with moderate renal insufficiency (≥30 mL/minute to <60 mL/minute) received a lower lenalidomide starting dose of 10 mg daily on the same schedule. After 2 cycles, the lenalidomide dose could be increased to 15 mg once daily on Days 1 to 21 of each 28-day cycle if the patient tolerated the medication.
MAGNIFY is an open-label, multicenter trial (n = 232) in which patients with relapsed or refractory follicular, marginal zone, or mantle cell lymphoma received 12 induction cycles of lenalidomide and rituximab. MAGNIFY included patients diagnosed with Grade 1, 2, 3a, 3b follicular (including transformed), marginal zone, or mantle cell lymphoma Stage I to IV who were previously treated for their lymphoma, had been refractory or had a relapse after their last treatment, had at least one measurable nodal or extranodal lesion by CT or MRI scan, and had adequate bone marrow, liver, and renal function. Patients refractory to rituximab were also included. The information from the subjects who received at least 1 dose of initial therapy in the first 12 induction cycles (n = 222) in the MAGNIFY trial was included in the evaluation of the efficacy of lenalidomide/rituximab in patients with relapsed or refractory follicular and marginal zone lymphoma. In MAGNIFY, lenalidomide 20 mg was given on Days 1 to 21 of repeated 28-day cycles for up to 12 cycles or until unacceptable toxicity, progression, or withdrawal of consent. The dose of rituximab was 375 mg/m 2every week in Cycle 1 (Days 1, 8, 15, and 22) and on Day 1 of every other 28-day cycle (Cycles 3, 5, 7, 9, and 11) up to 12 cycles therapy. All dosage calculations for rituximab were based on the patient BSA and actual weight. Dose adjustments were allowed based on clinical and laboratory findings.
The demographic and disease-related baseline characteristics in the AUGMENT and MAGNIFY trials are shown in the following table.
| Parameter | AUGMENT Trial | MAGNIFY Trial | |
|
Lenalidomide + Rituximab
(N = 178) |
Rituximab + Placebo
(Control Arm) (N = 180) |
Lenalidomide + Rituximab
(N = 222) |
|
| Age (years) | |||
| Median (Max, Min) | 64 (26, 86) | 62 (35, 88) | 65 (35, 91) |
| Age distribution, n (%) | |||
| <65 years | 96 (54) | 107 (59) | 103 (46) |
| ≥65 years | 82 (46) | 73 (41) | 119 (54) |
| Sex, n (%) | |||
| Male | 75 (42) | 97 (54) | 122 (55) |
| Female | 103 (58) | 83 (46) | 100 (45) |
| Race | |||
| White | 118 (66) | 115 (64) | 206 (93) |
| Other races | 54 (30) | 64 (36) | 14 (6) |
| Not collected or reported | 6 (3) | 1 (0.6) | 2 (1) |
| Body Surface Area (BSA, m 2) | |||
| Median (Max, Min) | 1.8 (1.4, 3.1) | 1.8 (1.3, 2.7) | 2 (1.3, 2.6) |
| Disease Type FL or MZL | |||
| Follicular lymphoma | 147 (83) | 148 (82) | 177 (80) |
| Marginal zone lymphoma | 31 (17) | 32 (18) | 45 (20) |
| MZL subtype at diagnosis (investigator), n (%) | |||
| MALT | 14 (45) | 16 (50) | 10 (22) |
| Nodal | 8 (26) | 10 (31) | 25 (56) |
| Splenic | 9 (29) | 6 (19) | 10 (22) |
| FL stage at diagnosis (investigator), n (%) | |||
| FL Grade 1 to 2 | 125 (85) | 123 (83) | 149 (84) |
| FL Grade 3a | 22 (15) | 25 (17) | 28 (16) |
| FLIPI score at baseline (calculated), n (%) | |||
| Low risk (0,1) | 52 (29) | 67 (37) | Not Collected |
| Intermediate risk (2) | 55 (31) | 58 (32) | |
| High risk (≥3) | 69 (39) | 54 (30) | |
| Missing | 2 (1) | 1 (0.6) | |
| ECOG score at baseline, n (%) | |||
| 0 | 116 (65) | 128 (71) | 102 (46) |
| 1 | 60 (34) | 50 (28) | 113 (51) |
| 2 | 2 (1) | 2 (1) | 7 (3) |
| High tumor burden
Defined by GELF criteria. at baseline, n (%)
|
|||
| Yes | 97 (54) | 86 (48) | 148 (67) |
| No | 81 (46) | 94 (52) | 74 (33) |
| Number of prior systemic antilymphoma therapies | |||
| 1 | 102 (57) | 97 (54) | 94 (42)
Patient had either 0 (n = 2) or 1 prior systemic therapy.
|
| >1 | 76 (43) | 83 (46) | 128 (58) |
Data Cutoff: 22 June 2018 (AUGMENT) and 1 May 2017 (MAGNIFY).
ECOG = Eastern Cooperative Oncology Group; FLIPI = follicular lymphoma international prognostic index
In AUGMENT, efficacy was established in the intent-to-treat (ITT) population based on progression-free survival by Independent Review Committee using modified 2007 International Working Group response criteria. Efficacy results are summarized in Table 22.
| Parameter |
Lenalidomide + Rituximab
(N = 178) |
Rituximab + Placebo
(N = 180) |
| PFS | ||
| Patients with event, n (%) | 68 (38.2) | 115 (63.9) |
| Death | 6 (8.8) | 2 (1.7) |
| Progression of disease | 62 (91.2) | 113 (98.3) |
| PFS, median
Median estimate is from Kaplan-Meier analysis. [95% CI] (months)
|
39.4 [ 22.9, NE] | 14.1 [11.4, 16.7] |
| HR
hazard ratio and its CI were estimated from Cox proportional hazard model adjusting for the stratification 3: previous rituximab treatment (yes, no), time since last antilymphoma therapy (≤2, >2 years), and disease histology (FL, MZL). [95% CI]
|
0.46 [ 0.34, 0.62] | |
| p-value
p-value from log-rank test stratified by 3 factors noted above: previous rituximab treatment (yes, no), time since last antilymphoma therapy (≤2, >2 years), and disease histology (FL, MZL).
|
<0.0001 | |
| Objective response (CR+PR), n(%)
[95% CI] Exact confidence interval for binomial distribution.
|
138 (77.5) [70.7, 83.4] | 96 (53.3) [45.8, 60.8] |
Kaplan-Meier Curves of Progression-free Survival by IRC Assessment Between Arms in AUGMENT Trial (ITT FL and MZL Population)
a = Stratification factors included: previous rituximab treatment (y/n), time since last anti-lymphoma therapy (≤2 years, >2 years), and disease histology (FL or MZL).
CI = confidence interval; HR = hazard ratio; KM = Kaplan-Meier; PFS = progression-free survival
Follicular Lymphoma
In AUGMENT, the objective response by IRC assessment for patients with follicular lymphoma was 80% (118/147) [95% CI: 73%, 86%]) in Lenalidomide with rituximab arm compared to 55% (82/148) [95% CI: 47, 64] in control arm.
In MAGNIFY, the overall response by investigator assessment was 59% (104/177) [95% CI: 51, 66] for patients with follicular lymphoma. Median duration of response was not reached with a median follow‑up time of 7.9 months [95% CI: 4.6, 9.2].
Marginal Zone Lymphoma
In AUGMENT, the objective response by IRC assessment for patients with marginal zone lymphoma was 65% (20/31) [95% CI: 45%, 81%] in Lenalidomide with rituximab arm compared to 44% (14/32) [95% CI: 26%, 62%] in control arm.
In MAGNIFY, the overall response by investigator assessment was 51% (23/45) [95% CI: 36, 66] for patients with marginal zone lymphoma. Median duration of response was not reached with a median follow‑up time of 11.5 months [95% CI: 8.0, 18.9].
5.5 Increased Mortality in Patients With Cll
In a prospective randomized (1:1) clinical trial in the first line treatment of patients with chronic lymphocytic leukemia, single agent lenalidomide therapy increased the risk of death as compared to single agent chlorambucil. In an interim analysis, there were 34 deaths among 210 patients on the lenalidomide treatment arm compared to 18 deaths among 211 patients in the chlorambucil treatment arm, and hazard ratio for overall survival was 1.92 [95% CI: 1.08 to 3.41], consistent with a 92% increase in the risk of death. The trial was halted for safety in July 2013.
Serious adverse cardiovascular reactions, including atrial fibrillation, myocardial infarction, and cardiac failure occurred more frequently in the lenalidomide treatment arm. Lenalidomide is not indicated and not recommended for use in CLL outside of controlled clinical trials.
2.3 Recommended Dosage for Mantle Cell Lymphoma
The recommended starting dose of lenalidomide capsules is 25 mg/day orally on Days 1 to 21 of repeated 28-day cycles for relapsed or refractory mantle cell lymphoma. Treatment should be continued until disease progression or unacceptable toxicity.
Treatment is continued, modified or discontinued based upon clinical and laboratory findings.
Dose Adjustments for Hematologic Toxicities During MCL Treatment
Dose modification guidelines as summarized below are recommended to manage Grade 3 or 4 neutropenia or thrombocytopenia or other Grade 3 or 4 toxicities considered to be related to lenalidomide capsules.
Platelet counts
Thrombocytopenia during treatment in MCL
| When Platelets | Recommended Course |
| Fall below 50,000/mcL | Interrupt lenalidomide capsules treatment and follow CBC weekly |
| Return to at least 50,000/mcL | Resume lenalidomide capsules at 5 mg less than the previous dose. Do not dose below 5 mg daily |
Absolute Neutrophil counts (ANC)
Neutropenia during treatment in MCL
| When Neutrophils | Recommended Course |
| Fall below 1,000/mcL for at least 7 days
OR Falls below 1,000/mcL with an associated temperature at least 38.5°C OR Falls below 500/mcL |
Interrupt lenalidomide capsules treatment and follow CBC weekly |
| Return to at least 1,000/mcL | Resume lenalidomide capsules at 5 mg less than the previous dose. Do not dose below 5 mg daily |
8.3 Females and Males of Reproductive Potential
Pregnancy Testing
Lenalidomide can cause fetal harm when administered during pregnancy [see Use in Specific Populations (8.1)] . Verify the pregnancy status of females of reproductive potential prior to initiating lenalidomide therapy and during therapy. Advise females of reproductive potential that they must avoid pregnancy 4 weeks before therapy, while taking lenalidomide, during dose interruptions and for at least 4 weeks after completing therapy.
Females of reproductive potential must have 2 negative pregnancy tests before initiating lenalidomide. The first test should be performed within 10 days to 14 days, and the second test within 24 hours prior to prescribing lenalidomide. Once treatment has started and during dose interruptions, pregnancy testing for females of reproductive potential should occur weekly during the first 4 weeks of use, then pregnancy testing should be repeated every 4 weeks in females with regular menstrual cycles. If menstrual cycles are irregular, the pregnancy testing should occur every 2 weeks. Pregnancy testing and counseling should be performed if a patient misses her period or if there is any abnormality in her menstrual bleeding. Lenalidomide treatment must be discontinued during this evaluation.
Contraception
Females
Females of reproductive potential must commit either to abstain continuously from heterosexual sexual intercourse or to use 2 methods of reliable birth control simultaneously: one highly effective form of contraception – tubal ligation, IUD, hormonal (birth control pills, injections, hormonal patches, vaginal rings, or implants), or partner’s vasectomy, and 1 additional effective contraceptive method – male latex or synthetic condom, diaphragm, or cervical cap. Contraception must begin 4 weeks prior to initiating treatment with lenalidomide, during therapy, during dose interruptions, and continuing for 4 weeks following discontinuation of lenalidomide therapy. Reliable contraception is indicated even where there has been a history of infertility, unless due to hysterectomy. Females of reproductive potential should be referred to a qualified provider of contraceptive methods, if needed.
Males
Lenalidomide is present in the semen of males who take lenalidomide. Therefore, males must always use a latex or synthetic condom during any sexual contact with females of reproductive potential while taking lenalidomide and for up to 4 weeks after discontinuing lenalidomide, even if they have undergone a successful vasectomy. Male patients taking lenalidomide must not donate sperm and for up to 4 weeks after discontinuing lenalidomide.
2.2 Recommended Dosage for Myelodysplastic Syndromes
The recommended starting dose of lenalidomide capsules is 10 mg daily. Treatment is continued or modified based upon clinical and laboratory findings. Continue treatment until disease progression or unacceptable toxicity.
Dose Adjustments for Hematologic Toxicities During MDS Treatment
Patients who are dosed initially at 10 mg and who experience thrombocytopenia should have their dosage adjusted as follows:
Platelet counts
If thrombocytopenia develops WITHIN 4 weeks of starting treatment at 10 mg daily in MDS
| If baseline is at least 100,000/mcL | |
| When Platelets | Recommended Course |
| Fall below 50,000/mcL | Interrupt lenalidomide capsules treatment |
| Return to at least 50,000/mcL | Resume lenalidomide capsules at 5 mg daily |
| If baseline is below 100,000/mcL | |
| When Platelets | Recommended Course |
| Fall to 50% of the baseline value | Interrupt lenalidomide capsules treatment |
| If baseline is at least 60,000/mcL and returns to at least 50,000/mcL | Resume lenalidomide capsules at 5 mg daily |
| If baseline is below 60,000/mcL and returns to at least 30,000/mcL | Resume lenalidomide capsules at 5 mg daily |
If thrombocytopenia develops AFTER 4 weeks of starting treatment at 10 mg daily in MDS
| When Platelets | Recommended Course |
| Fall below 30,000/mcL or below 50,000/mcL with platelet transfusions | Interrupt lenalidomide capsules treatment |
| Return to at least 30,000/mcL (without hemostatic failure) | Resume lenalidomide capsules at 5 mg daily |
Patients who experience thrombocytopenia at 5 mg daily should have their dosage adjusted as follows:
If thrombocytopenia develops during treatment at 5 mg daily in MDS
| When Platelets | Recommended Course |
| Fall below 30,000/mcL or below 50,000/mcL with platelet transfusions | Interrupt lenalidomide capsules treatment |
| Return to at least 30,000/mcL (without hemostatic failure) | Resume lenalidomide capsules at 2.5 mg daily |
Patients who are dosed initially at 10 mg and experience neutropenia should have their dosage adjusted as follows:
Absolute Neutrophil counts (ANC)
If neutropenia develops WITHIN 4 weeks of starting treatment at 10 mg daily in MDS
| If baseline ANC is at least 1,000/mcL | |
| When Neutrophils | Recommended Course |
| Fall below 750/mcL | Interrupt lenalidomide capsules treatment |
| Return to at least 1,000/mcL | Resume lenalidomide capsules at 5 mg daily |
| If baseline ANC is below 1,000/mcL | |
| When Neutrophils | Recommended Course |
| Fall below 500/mcL | Interrupt lenalidomide capsules treatment |
| Return to at least 500/mcL | Resume lenalidomide capsules at 5 mg daily |
If neutropenia develops AFTER 4 weeks of starting treatment at 10 mg daily in MDS
| When Neutrophils | Recommended Course |
| Fall below 500/mcL for at least 7 days or below 500/mcL associated with fever (at least 38.5°C) | Interrupt lenalidomide capsules treatment |
| Return to at least 500/mcL | Resume lenalidomide capsules at 5 mg daily |
Patients who experience neutropenia at 5 mg daily should have their dosage adjusted as follows:
If neutropenia develops during treatment at 5 mg daily in MDS
| When Neutrophils | Recommended Course |
| Fall below 500/mcL for at least 7 days or below 500/mcL associated with fever (at least 38.5°C) | Interrupt lenalidomide capsules treatment |
| Return to at least 500/mcL | Resume lenalidomide capsules at 2.5 mg daily |
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenicity studies with lenalidomide have not been conducted.
Lenalidomide was not mutagenic in the bacterial reverse mutation assay (Ames test) and did not induce chromosome aberrations in cultured human peripheral blood lymphocytes, or mutations at the thymidine kinase (tk) locus of mouse lymphoma L5178Y cells. Lenalidomide did not increase morphological transformation in Syrian Hamster Embryo assay or induce micronuclei in the polychromatic erythrocytes of the bone marrow of male rats.
A fertility and early embryonic development study in rats, with administration of lenalidomide up to 500 mg/kg (approximately 200 times the human dose of 25 mg, based on body surface area) produced no parental toxicity and no adverse effects on fertility.
2.6 Recommended Dosage for Patients With Renal Impairment
The recommendations for dosing patients with renal impairment are shown in the following table [see Clinical Pharmacology (12.3)] .
|
Renal Function
(Cockcroft-Gault) |
Dose in Lenalidomide Capsules Combination Therapy for MM and MCL | Dose in Lenalidomide Capsules Combination Therapy for FL and MZL | Dose in Lenalidomide Capsules Maintenance Therapy Following Auto-HSCT for MM and for MDS |
| CLcr 30 mL/min to 60 mL/min | 10 mg once daily | 10 mg once daily | 5 mg once daily |
| CLcr below 30 mL/min (not requiring dialysis) | 15 mg every other day | 5 mg once daily | 2.5 mg once daily |
| CLcr below 30 mL/min (requiring dialysis) | 5 mg once daily. On dialysis days, administer the dose following dialysis. | 5 mg once daily. On dialysis days, administer the dose following dialysis. | 2.5 mg once daily. On dialysis days, administer the dose following dialysis. |
2.5 Dosage Modifications for Non Hematologic Adverse Reactions
For non-hematologic Grade 3/4 toxicities judged to be related to lenalidomide capsules, hold treatment and restart at the physician's discretion at next lower dose level when toxicity has resolved to Grade 2 or below.
Permanently discontinue lenalidomide capsules for angioedema, anaphylaxis, Grade 4 rash, skin exfoliation, bullae, or any other severe dermatologic reactions [see Warnings and Precautions (5.9, 5.15)] .
7.2 Concomitant Therapies That May Increase the Risk of Thrombosis
Erythropoietic agents, or other agents that may increase the risk of thrombosis, such as estrogen containing therapies, should be used with caution after making a benefit-risk assessment in patients receiving lenalidomide [see Warnings and Precautions (5.4)] .
2.4 Recommended Dosage for Follicular Lymphoma Or Marginal Zone Lymphoma
The recommended starting dose of lenalidomide capsules is 20 mg orally once daily on Days 1 to 21 of repeated 28-day cycles for up to 12 cycles of treatment in combination with a rituximab-product. Refer to Section 14.4 for specific rituximab dosing from the AUGMENT trial. For dose adjustments due to toxicity with rituximab, refer to the product prescribing information.
Dose Adjustments for Hematologic Toxicities during FL or MZL Treatment
Dose modification guidelines, as summarized below, are recommended to manage Grade 3 or 4 neutropenia or thrombocytopenia or other Grade 3 or 4 toxicity judged to be related to lenalidomide capsules.
Platelet counts
Thrombocytopenia during treatment in FL or MZL
| When Platelets | Recommended Course |
| Fall below 50,000/mcL | Interrupt lenalidomide capsules treatment and follow CBC weekly. |
|
Return to at least 50,000/mcL |
If patient starting dose was 20 mg daily, resume lenalidomide capsules at 5 mg less than the previous dose. Do not dose below 5 mg daily. If patient starting dose was 10 mg daily, resume at 5 mg less than previous dose. Do not dose below 2.5 mg daily. |
Absolute Neutrophil counts (ANC)
Neutropenia during treatment in FL or MZL
| When Neutrophils | Recommended Course |
|
Fall below 1,000/mcL for at least 7 days
OR
|
Interrupt lenalidomide capsules treatment and follow CBC weekly. |
| Return to at least 1,000/mcL |
If patient starting dose was 20 mg daily, resume lenalidomide capsules at 5 mg less than the previous dose. Do not dose below 5 mg daily.
|
14.2 Myelodysplastic Syndromes (mds) With A Deletion 5q Cytogenetic Abnormality
The efficacy and safety of lenalidomide were evaluated in patients with transfusion-dependent anemia in low- or intermediate-1- risk MDS with a 5q (q31 to 33) cytogenetic abnormality in isolation or with additional cytogenetic abnormalities, at a dose of 10 mg once daily or 10 mg once daily for 21 days every 28 days in an open-label, single-arm, multi-center study. The major study was not designed nor powered to prospectively compare the efficacy of the 2 dosing regimens. Sequential dose reductions to 5 mg daily and 5 mg every other day, as well as dose delays, were allowed for toxicity [ Dosage and Administration (2.2)] .
This major study enrolled 148 patients who had RBC transfusion dependent anemia. RBC transfusion dependence was defined as having received ≥2 units of RBCs within 8 weeks prior to study treatment. The study enrolled patients with absolute neutrophil counts (ANC) ≥500/mm 3, platelet counts ≥50,000/mm 3, serum creatinine ≤2.5 mg/dL, serum SGOT/AST or SGPT/ALT ≤3x upper limit of normal (ULN), and serum direct bilirubin ≤2 mg/dL. Granulocyte colony-stimulating factor was permitted for patients who developed neutropenia or fever in association with neutropenia. Baseline patient and disease-related characteristics are summarized in Table 18.
|
Overall
(N = 148) |
||
| Age (years) | ||
| Median | 71 | |
| Min, Max | 37, 95 | |
| Gender | n | (%) |
| Male | 51 | (34.5) |
| Female | 97 | (65.5) |
| Race | n | (%) |
| White | 143 | (96.6) |
| Other | 5 | (3.4) |
| Duration of MDS (years) | ||
| Median | 2.5 | |
| Min, Max | 0.1, 20.7 | |
| Del 5 (q31 to 33) Cytogenetic Abnormality | n | (%) |
| Yes | 148 | (100) |
| Other cytogenetic abnormalities | 37 | (25.2) |
|
IPSS Score
IPSS Risk Category: Low (combined score = 0), Intermediate-1 (combined score = 0.5 to 1), Intermediate-2 (combined score = 1.5 to 2.0), High (combined score ≥ 2.5); Combined score = (Marrow blast score + Karyotype score + Cytopenia score).
|
n | (%) |
| Low (0) | 55 | (37.2) |
| Intermediate-1 (0.5 to 1.0) | 65 | (43.9) |
| Intermediate-2 (1.5 to 2.0) | 6 | (4.1) |
| High (≥2.5) | 2 | (1.4) |
| Missing | 20 | (13.5) |
|
FAB Classification
French-American-British (FAB) classification of MDS. from central review
|
n | (%) |
| RA | 77 | (52) |
| RARS | 16 | (10.8) |
| RAEB | 30 | (20.3) |
| CMML | 3 | (2) |
The frequency of RBC transfusion independence was assessed using criteria modified from the International Working Group (IWG) response criteria for MDS. RBC transfusion independence was defined as the absence of any RBC transfusion during any consecutive rolling 56 days (8 weeks) during the treatment period.
Transfusion independence was seen in 99/148 (67%) patients (95% CI [59, 74]). The median duration from the date when RBC transfusion independence was first declared (i.e., the last day of the 56-day RBC transfusion-free period) to the date when an additional transfusion was received after the 56-day transfusion-free period among the 99 responders was 44 weeks (range of 0 week to >67 weeks). Ninety percent of patients who achieved a transfusion benefit did so by completion of three months in the study.
RBC transfusion independence rates were unaffected by age or gender.
The dose of lenalidomide was reduced or interrupted at least once due to an adverse event in 118 (79.7%) of the 148 patients; the median time to the first dose reduction or interruption was 21 days (mean, 35.1 days; range, 2 days to 253 days), and the median duration of the first dose interruption was 22 days (mean, 28.5 days; range, 2 days to 265 days). A second dose reduction or interruption due to adverse events was required in 50 (33.8%) of the 148 patients. The median interval between the first and second dose reduction or interruption was 51 days (mean, 59.7 days; range, 15 days to 205 days) and the median duration of the second dose interruption was 21 days (mean, 26 days; range, 2 days to 148 days).
Warning: Embryo Fetal Toxicity, Hematologic Toxicity, and Venous and Arterial Thromboembolism
WARNING: EMBRYO-FETAL TOXICITY, HEMATOLOGIC TOXICITY, and VENOUS and ARTERIAL THROMBOEMBOLISM
See full prescribing information for complete boxed warning.
EMBRYO-FETAL TOXICITY
- Lenalidomide, a thalidomide analogue, caused limb abnormalities in a developmental monkey study similar to birth defects caused by thalidomide in humans. If lenalidomide is used during pregnancy, it may cause birth defects or embryo-fetal death.
- Pregnancy must be excluded before start of treatment. Prevent pregnancy during treatment by the use of two reliable methods of contraception ( 5.1).
Lenalidomide capsules are available only through a restricted distribution program, called the Lenalidomide REMS program ( 5.2, 17).
HEMATOLOGIC TOXICITY. Lenalidomide can cause significant neutropenia and thrombocytopenia ( 5.3).
VENOUS AND ARTERIAL THROMBOEMBOLISM
- Significantly increased risk of deep vein thrombosis (DVT) and pulmonary embolism (PE), as well as risk of myocardial infarction and stroke in patients with multiple myeloma receiving lenalidomide with dexamethasone. Anti-thrombotic prophylaxis is recommended ( 5.4).
5.7 Increased Mortality in Patients With Mm When Pembrolizumab Is Added to A Thalidomide Analogue and Dexamethasone
In two randomized clinical trials in patients with MM, the addition of pembrolizumab to a thalidomide analogue plus dexamethasone, a use for which no PD-1 or PD-L1 blocking antibody is indicated, resulted in increased mortality. Treatment of patients with MM with a PD-1 or PD-L1 blocking antibody in combination with a thalidomide analogue plus dexamethasone is not recommended outside of controlled clinical trials.
Structured Label Content
Section 42229-5 (42229-5)
Embryo-Fetal Toxicity
Do not use lenalidomide during pregnancy. Lenalidomide, a thalidomide analogue, caused limb abnormalities in a developmental monkey study. Thalidomide is a known human teratogen that causes severe life-threatening human birth defects. If lenalidomide is used during pregnancy, it may cause birth defects or embryo-fetal death. In females of reproductive potential, obtain 2 negative pregnancy tests before starting lenalidomide treatment. Females of reproductive potential must use 2 forms of contraception or continuously abstain from heterosexual sex during and for 4 weeks after lenalidomide treatment [see Warnings and Precautions (5.1), and Medication Guide (17)]. To avoid embryo-fetal exposure to lenalidomide, lenalidomide capsules are only available through a restricted distribution program, the Lenalidomide REMS program ( 5.2).
Information about the Lenalidomide REMS program is available at www.lenalidomiderems.com or by calling the REMS Call Center at 1-888-423-5436.
Hematologic Toxicity (Neutropenia and Thrombocytopenia)
Lenalidomide can cause significant neutropenia and thrombocytopenia.
Eighty percent of patients with del 5q myelodysplastic syndromes had to have a dose delay/reduction during the major study. Thirty-four percent of patients had to have a second dose delay/reduction. Grade 3 or 4 hematologic toxicity was seen in 80% of patients enrolled in the study. Patients on therapy for del 5q myelodysplastic syndromes should have their complete blood counts monitored weekly for the first 8 weeks of therapy and at least monthly thereafter. Patients may require dose interruption and/or reduction. Patients may require use of blood product support and/or growth factors [see Dosage and Administration (2.2) ] .
Venous and Arterial Thromboembolism
Lenalidomide has demonstrated a significantly increased risk of deep vein thrombosis (DVT) and pulmonary embolism (PE), as well as risk of myocardial infarction and stroke in patients with multiple myeloma who were treated with lenalidomide and dexamethasone therapy. Monitor for and advise patients about signs and symptoms of thromboembolism. Advise patients to seek immediate medical care if they develop symptoms such as shortness of breath, chest pain, or arm or leg swelling. Thromboprophylaxis is recommended and the choice of regimen should be based on an assessment of the patient’s underlying risks [see Warnings and Precautions (5.4)].
Section 42231-1 (42231-1)
|
MEDICATION GUIDE Lenalidomide (len" a lid' oh mide) Capsules |
|
|
What is the most important information I should know about lenalidomide capsules? Before you begin taking lenalidomide capsules, you must read and agree to all of the instructions in the Lenalidomide REMS program. For more information, call 1-888-423-5436 or go to www.lenalidomiderems.com. Before prescribing lenalidomide capsules, your healthcare provider will explain the Lenalidomide REMS program to you and have you sign the Patient-Physician Agreement Form. Lenalidomide capsules may cause serious side effects including:
Lenalidomide capsules are similar to the medicine thalidomide.We know thalidomide can cause severe life-threatening birth defects. Lenalidomide capsules have not been tested in pregnant females. Lenalidomide capsules have harmed unborn animals in animal testing. Females must not get pregnant:
Females who can become pregnant:
If you become pregnant while taking lenalidomide capsules, stop taking it right away and call your healthcare provider. If your healthcare provider is not available, you can call the REMS Call Center at 1-888-423-5436. Healthcare providers and patients should report all cases of pregnancy to:
There is a pregnancy exposure registry that monitors the outcomes of females who take lenalidomide capsules during pregnancy, or if their male partner takes lenalidomide capsules and they are exposed during pregnancy. You can enroll in this registry by calling the REMS Call Center at the phone number listed above. Lenalidomide can pass into human semen:
Men, if your female partner becomes pregnant, you should call your healthcare provider right away.
Before taking lenalidomide capsules, tell your healthcare provider:
|
|
|
What are lenalidomide capsules?
Lenalidomide capsules are a prescription medicine, usedto treat adults with:
Lenalidomide capsules should not be usedto treat people who have chronic lymphocytic leukemia (CLL) unless they are participants in a controlled clinical trial. It is not known if lenalidomide capsules are safe and effective in children. |
|
|
Who should not take lenalidomide capsules? Do not take lenalidomide capsules if you:
|
|
|
What should I tell my healthcare provider before taking lenalidomide capsules? Before you take lenalidomide capsules, tell your healthcare provider about all of your medical conditions, including if you:
Tell your healthcare provider about all the medicines you take,including prescription and over-the-counter medicines, vitamins, and herbal supplements. Lenalidomide capsules and other medicines may affect each other, causing serious side effects. Talk with your healthcare provider before taking any new medicines. Know the medicines you take. Keep a list of them to show your healthcare provider and pharmacist. |
|
|
How should I take lenalidomide capsules?
|
|
|
What should I avoid while taking lenalidomide capsules?
|
|
|
What are the possible side effects of lenalidomide capsules? Lenalidomide capsules can cause serious side effects, including:
|
|
|
|
|
|
|
|
| Get emergency medical help right away if you develop any of the following signs or symptoms during treatment with lenalidomide capsules: | |
|
|
Your healthcare provider may tell you to decrease your dose, temporarily stop or permanently stop taking lenalidomide capsules if you develop certain serious side effects during treatment with lenalidomide capsules.
|
|
|
|
|
These are not all the possible side effects of lenalidomide capsules. Call your doctor for medical advice about side effects. You may report side effects to the FDA at 1-800-FDA-1088. |
|
|
How should I store lenalidomide capsules?
|
|
|
General information about the safe and effective use of lenalidomide capsules. Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not take lenalidomide capsules for conditions for which it was not prescribed. Do not give lenalidomide capsules to other people, even if they have the same symptoms you have. It may harm them and may cause birth defects. If you would like more information, talk with your healthcare provider. You can ask your healthcare provider or pharmacist for information about lenalidomide capsules that is written for health professionals. For more information, call 1-888-423-5436 or go to www.lenalidomiderems.com. |
|
|
What are the ingredients in lenalidomide capsules? Active ingredient:lenalidomide Inactive ingredients:croscarmellose sodium, magnesium stearate, mannitol, and microcrystalline cellulose. The 5 mg and 25 mg capsule shells contain gelatin, titanium dioxide, and black ink.
The capsules are printed with black ink composed of ammonia solution, black iron oxide, potassium hydroxide, propylene glycol, and shellac. Distributed by:
|
This Medication Guide has been approved by the U.S. Food and Drug Administration. Revised: November 2023
7.1 Digoxin
When digoxin was co-administered with multiple doses of lenalidomide (10 mg/day) the digoxin C maxand AUC infwere increased by 14%. Periodically monitor digoxin plasma levels, in accordance with clinical judgment and based on standard clinical practice in patients receiving this medication, during administration of lenalidomide.
16.2 Storage
Store at 20°C to 25°C (68°F to 77°F); excursions permitted to 15°C to 30°C (59°F to 86°F). [See USP Controlled Room Temperature].
7.3 Warfarin
Co-administration of multiple doses of lenalidomide (10 mg/day) with a single dose of warfarin (25 mg) had no effect on the pharmacokinetics of lenalidomide or R- and S-warfarin. Expected changes in laboratory assessments of PT and INR were observed after warfarin administration, but these changes were not affected by concomitant lenalidomide administration. It is not known whether there is an interaction between dexamethasone and warfarin. Close monitoring of PT and INR is recommended in patients with MM taking concomitant warfarin.
10 Overdosage (10 OVERDOSAGE)
There is no specific experience in the management of lenalidomide overdose in patients with MM, MDS, MCL, FL, or MZL. In dose-ranging studies in healthy subjects, some were exposed to up to 200 mg (administered 100 mg BID) and in single-dose studies, some subjects were exposed to up to 400 mg. Pruritus, urticaria, rash, and elevated liver transaminases were the primary reported AEs. In clinical trials, the dose-limiting toxicity was neutropenia and thrombocytopenia.
15 References (15 REFERENCES)
1. OSHA Hazardous Drugs. OSHA[Accessed on 29 January 2013, from http://www.osha.gov/SLTC/hazardousdrugs/index.html]
4.1 Pregnancy
Lenalidomide can cause fetal harm when administered to a pregnant female. Limb abnormalities were seen in the offspring of monkeys that were dosed with lenalidomide during organogenesis. This effect was seen at all doses tested. Due to the results of this developmental monkey study, and lenalidomide's structural similarities to thalidomide, a known human teratogen, lenalidomide is contraindicated in females who are pregnant [see Boxed Warning] . If this drug is used during pregnancy or if the patient becomes pregnant while taking this drug, the patient should be apprised of the potential risk to a fetus [see Warnings and Precautions (5.1, 5.2), Use in Special Populations (8.1, 8.3)].
8.1 Pregnancy
Pregnancy Exposure Registry
There is a pregnancy exposure registry that monitors pregnancy outcomes in females exposed to lenalidomide during pregnancy as well as female partners of male patients who are exposed to lenalidomide. This registry is also used to understand the root cause for the pregnancy. Report any suspected fetal exposure to lenalidomide to the FDA via the MedWatch program at 1-800-FDA-1088 and also to the REMS Call Center at 1-888-423-5436.
Risk Summary
Based on the mechanism of action [see Clinical Pharmacology (12.1)] and findings from animal studies [see Data],lenalidomide can cause embryo-fetal harm when administered to a pregnant female and is contraindicated during pregnancy [see Boxed Warning, Contraindications (4.1), and Use in Specific Populations (5.1)] .
Lenalidomide is a thalidomide analogue. Thalidomide is a human teratogen, inducing a high frequency of severe and life-threatening birth defects such as amelia (absence of limbs), phocomelia (short limbs), hypoplasticity of the bones, absence of bones, external ear abnormalities (including anotia, micropinna, small or absent external auditory canals), facial palsy, eye abnormalities (anophthalmos, microphthalmos), and congenital heart defects. Alimentary tract, urinary tract, and genital malformations have also been documented and mortality at or shortly after birth has been reported in about 40% of infants.
Lenalidomide caused thalidomide-type limb defects in monkey offspring. Lenalidomide crossed the placenta after administration to pregnant rabbits and pregnant rats [see Data]. If this drug is used during pregnancy, or if the patient becomes pregnant while taking this drug, the patient should be apprised of the potential risk to a fetus.
If pregnancy does occur during treatment, immediately discontinue the drug. Under these conditions, refer patient to an obstetrician/gynecologist experienced in reproductive toxicity for further evaluation and counseling. Report any suspected fetal exposure to lenalidomide to the FDA via the MedWatch program at 1-800-FDA-1088 and also to the REMS Call Center at 1‑888-423-5436.
The estimated background risk of major birth defects and miscarriage for the indicated population is unknown. All pregnancies have a background risk of birth defect, loss, or other adverse outcomes. The estimated background risk in the U.S. general population of major birth defects is 2% to 4% and of miscarriage is 15% to 20% of clinically recognized pregnancies.
Data
Animal data
In an embryo-fetal developmental toxicity study in monkeys, teratogenicity, including thalidomide-like limb defects, occurred in offspring when pregnant monkeys received oral lenalidomide during organogenesis. Exposure (AUC) in monkeys at the lowest dose was 0.17 times the human exposure at the maximum recommended human dose (MRHD) of 25 mg. Similar studies in pregnant rabbits and rats at 20 times and 200 times the MRHD respectively, produced embryo lethality in rabbits and no adverse reproductive effects in rats.
In a pre- and post-natal development study in rats, animals received lenalidomide from organogenesis through lactation. The study revealed a few adverse effects on the offspring of female rats treated with lenalidomide at doses up to 500 mg/kg (approximately 200 times the human dose of 25 mg based on body surface area). The male offspring exhibited slightly delayed sexual maturation and the female offspring had slightly lower body weight gains during gestation when bred to male offspring. As with thalidomide, the rat model may not adequately address the full spectrum of potential human embryo-fetal developmental effects for lenalidomide.
Following daily oral administration of lenalidomide from Gestation Day 7 through Gestation Day 20 in pregnant rabbits, fetal plasma lenalidomide concentrations were approximately 20% to 40% of the maternal C max. Following a single oral dose to pregnant rats, lenalidomide was detected in fetal plasma and tissues; concentrations of radioactivity in fetal tissues were generally lower than those in maternal tissues. These data indicated that lenalidomide crossed the placenta.
8.2 Lactation
Risk Summary
There is no information regarding the presence of lenalidomide in human milk, the effects of lenalidomide on the breastfed child, or the effects of lenalidomide on milk production. Because many drugs are excreted in human milk and because of the potential for adverse reactions in breastfed children from lenalidomide, advise women not to breastfeed during treatment with lenalidomide.
11 Description (11 DESCRIPTION)
Lenalidomide, a thalidomide analogue, is an immunomodulatory agent with antiangiogenic and antineoplastic properties. The chemical name is 3-(7-amino-3-oxo-1H-isoindol-2-yl) piperidine-2,6-dione and it has the following chemical structure:
3-(7-amino-3-oxo-1H-isoindol-2-yl) piperidine-2,6-dione
The molecular formula for lenalidomide is C 13H 13N 3O 3,and the gram molecular weight is 259.26.
Lenalidomide is white to yellow crystalline powder. It is practically insoluble in isopropanol and ethanol. Very slightly soluble in water. Slightly soluble in acetonitrile and methanol. Lenalidomide has an asymmetric carbon atom and can exist as the optically active forms S(-) and R(+), and is produced as a racemic mixture with a net optical rotation of zero.
Lenalidomide is available in 2.5 mg, 5 mg, 10 mg, 15 mg, 20 mg, and 25 mg capsules for oral administration. Each capsule contains lenalidomide as the active ingredient and the following inactive ingredients: croscarmellose sodium, magnesium stearate, mannitol, and microcrystalline cellulose. The 5 mg and 25 mg capsule shells contain gelatin, titanium dioxide, and black ink. The 2.5 mg and 10 mg capsule shells contain FD&C blue #2, gelatin, titanium dioxide, yellow iron oxide, and black ink. The 15 mg capsule shells contain FD&C blue #2, gelatin, titanium dioxide, and black ink. The 20 mg capsule shells contain FD&C blue #2, gelatin, titanium dioxide, yellow iron oxide, and black ink. The capsules are printed with black ink composed of ammonia solution, black iron oxide, potassium hydroxide, propylene glycol, and shellac.
16.1 How Supplied
White to off-white powder filled in hard gelatin capsule size ‘4’ with blue-green opaque cap and white opaque body, imprinted with “LEN” on the cap and “2.5 mg” on the body with black ink:
2.5 mg bottles of 28 (NDC 82293-006-10)
White to off-white powder filled in white opaque hard gelatin capsule size ‘4’, imprinted with “LEN” on the cap and “5 mg” on the body with black ink:
5 mg bottles of 28 (NDC 82293-007-10)
White to off-white powder filled in hard gelatin capsule size ‘2’ with blue-green opaque cap and pale-yellow opaque body, imprinted with “LEN” on the cap and “10 mg” on the body with black ink:
10 mg bottles of 28 (NDC 82293-008-10)
White to off-white powder filled in hard gelatin capsule size ‘1’ with pale blue opaque cap and white opaque body, imprinted with “LEN” on the cap and “15 mg” on the body with black ink:
15 mg bottles of 21 (NDC 82293-009-10)
White to off-white powder filled in hard gelatin capsule size ‘0’ with blue-green opaque cap and pale blue opaque body, imprinted with “LEN” on the cap and “20 mg” on the body with black ink:
20 mg bottles of 21 (NDC 82293-010-10)
White to off-white powder filled in white opaque hard gelatin capsule size ‘0EL’, imprinted with “LEN” on the cap and “25 mg” on the body with black ink:
25 mg bottles of 21 (NDC 82293-011-10)
8.4 Pediatric Use
Safety and effectiveness have not been established in pediatric patients.
8.5 Geriatric Use
MM In Combination:Overall, of the 1,613 patients in the NDMM study who received study treatment, 94% (1,521 /1,613) were 65 years of age or older, while 35% (561/1,613) were over 75 years of age. The percentage of patients over age 75 was similar between study arms (Rd Continuous: 33%; Rd18: 34%; MPT: 33%). Overall, across all treatment arms, the frequency in most of the adverse reaction categories (eg, all adverse reactions, grade 3/4 adverse reactions, serious adverse reactions) was higher in older (>75 years of age) than in younger (≤75 years of age) subjects. Grade 3 or 4 adverse reactions in the General Disorders and Administration Site Conditions body system were consistently reported at a higher frequency (with a difference of at least 5%) in older subjects than in younger subjects across all treatment arms. Grade 3 or 4 adverse reactions in the Infections and Infestations, Cardiac Disorders (including cardiac failure and congestive cardiac failure), Skin and Subcutaneous Tissue Disorders, and Renal and Urinary Disorders (including renal failure) body systems were also reported slightly, but consistently, more frequently (<5% difference), in older subjects than in younger subjects across all treatment arms. For other body systems (e.g., Blood and Lymphatic System Disorders, Infections and Infestations, Cardiac Disorders, Vascular Disorders), there was a less consistent trend for increased frequency of grade 3/4 adverse reactions in older vs younger subjects across all treatment arms. Serious adverse reactions were generally reported at a higher frequency in the older subjects than in the younger subjects across all treatment arms.
MM Maintenance Therapy: Overall, 10% (106/1,018) of patients were 65 years of age or older, while no patients were over 75 years of age. Grade 3 or 4 adverse reactions were higher in the lenalidomide arm (more than 5% higher) in the patients 65 years of age or older versus younger patients. The frequency of Grade 3 or 4 adverse reactions in the Blood and Lymphatic System Disorders were higher in the lenalidomide arm (more than 5% higher) in the patients 65 years of age or older versus younger patients. There were not a sufficient number of patients 65 years of age or older in lenalidomide maintenance studies who experienced either a serious adverse reaction, or discontinued therapy due to an adverse reaction to determine whether elderly patients respond relative to safety differently from younger patients.
MM After At Least One Prior Therapy:Of the 703 MM patients who received study treatment in Studies 1 and 2, 45% were age 65 or over while 12% of patients were age 75 and over. The percentage of patients age 65 or over was not significantly different between the lenalidomide/dexamethasone and placebo/dexamethasone groups. Of the 353 patients who received lenalidomide/dexamethasone, 46% were age 65 and over. In both studies, patients >65 years of age were more likely than patients ≤65 years of age to experience DVT, pulmonary embolism, atrial fibrillation, and renal failure following use of lenalidomide. No differences in efficacy were observed between patients over 65 years of age and younger patients.
Of the 148 patients with del 5q MDS enrolled in the major study, 38% were age 65 and over, while 33% were age 75 and over. Although the overall frequency of adverse reactions (100%) was the same in patients over 65 years of age as in younger patients, the frequency of serious adverse reactions was higher in patients over 65 years of age than in younger patients (54% vs. 33%). A greater proportion of patients over 65 years of age discontinued from the clinical studies because of adverse reactions than the proportion of younger patients (27% vs. 16%). No differences in efficacy were observed between patients over 65 years of age and younger patients.
Of the 134 patients with MCL enrolled in the MCL trial, 63% were age 65 and over, while 22% of patients were age 75 and over. The overall frequency of adverse reactions was similar in patients over 65 years of age and in younger patients (98% vs. 100%). The overall incidence of grade 3 and 4 adverse reactions was also similar in these 2 patient groups (79% vs. 78%, respectively). The frequency of serious adverse reactions was higher in patients over 65 years of age than in younger patients (55% vs. 41%). No differences in efficacy were observed between patients over 65 years of age and younger patients.
FL or MZL in Combination:Overall, 48% (282/590) of patients were 65 years of age or older, while 14% (82/590) of patients were over 75 years of age. The overall frequency of adverse reactions was similar in patients 65 years of age or older and younger patients for both studies pooled (98%). Grade 3 or 4 adverse reactions were higher in the lenalidomide arm (more than 5% higher) in the patients 65 years of age or older versus younger patients (71% versus 59%). The frequency of Grade 3 or 4 adverse reactions were higher in the lenalidomide arm (more than 5% higher) in the patients 65 years of age or older versus younger patients in the Blood and Lymphatic System Disorders (47% versus 40%) and Infections and Infestations (16% versus 11%). Serious adverse reactions were higher in the lenalidomide arm (more than 5% higher) in the patients 65 years of age or older versus younger patients (37% versus 18%). The frequency of serious adverse reactions were higher in the lenalidomide arm (more than 5% higher) in the patients 65 years of age or older versus younger patients in Infections and Infestations (15% versus 6%).
Since elderly patients are more likely to have decreased renal function, care should be taken in dose selection. Monitor renal function.
2.7 Administration
Advise patients to take lenalidomide capsules orally at about the same time each day, either with or without food. Advise patients to swallow lenalidomide capsules whole with water and not to open, break, or chew them.
5.8 Hepatotoxicity
Hepatic failure, including fatal cases, has occurred in patients treated with lenalidomide in combination with dexamethasone. In clinical trials, 15% of patients experienced hepatotoxicity (with hepatocellular, cholestatic and mixed characteristics); 2% of patients with MM and 1% of patients with myelodysplasia had serious hepatotoxicity events. The mechanism of drug-induced hepatotoxicity is unknown. Pre-existing viral liver disease, elevated baseline liver enzymes, and concomitant medications may be risk factors. Monitor liver enzymes periodically. Stop lenalidomide upon elevation of liver enzymes. After return to baseline values, treatment at a lower dose may be considered.
4 Contraindications (4 CONTRAINDICATIONS)
6 Adverse Reactions (6 ADVERSE REACTIONS)
The following clinically significant adverse reactions are described in detail in other sections of the prescribing information:
- Embryo-Fetal Toxicity [see Boxed Warning, Warnings and Precautions (5.1, 5.2)]
- Hematologic Toxicity [see Boxed Warning, Warnings and Precautions (5.3)]
- Venous and Arterial Thromboembolism [see Boxed Warning, Warnings and Precautions (5.4)]
- Increased Mortality in Patients with CLL [see Warnings and Precautions (5.5)]
- Second Primary Malignancies [see Warnings and Precautions (5.6)]
- Increased Mortality in Patients with MM When Pembrolizumab Is Added to a Thalidomide Analogue and Dexamethasone [see Warnings and Precautions (5.7)]
- Hepatotoxicity [see Warnings and Precautions (5.8)]
- Severe Cutaneous Reactions [see Warnings and Precautions (5.9)]
- Tumor Lysis Syndrome [see Warnings and Precautions (5.10)]
- Tumor Flare Reactions [see Warnings and Precautions (5.11)]
- Impaired Stem Cell Mobilization [see Warnings and Precautions (5.12)]
- Thyroid Disorders [see Warnings and Precautions (5.13)]
- Early Mortality in Patients with MCL [see Warnings and Precautions (5.14)]
- Hypersensitivity [see Warnings and Precautions (5.15)]
7 Drug Interactions (7 DRUG INTERACTIONS)
1.1 Multiple Myeloma
Lenalidomide capsules in combination with dexamethasone is indicated for the treatment of adult patients with multiple myeloma (MM).
Lenalidomide capsules are indicated as maintenance therapy in adult patients with MM following autologous hematopoietic stem cell transplantation (auto-HSCT).
8.6 Renal Impairment
Adjust the starting dose of lenalidomide based on the creatinine clearance value and for patients on dialysis [see Dosage and Administration (2.6)].
5.15 Hypersensitivity
Hypersensitivity, including angioedema, anaphylaxis, and anaphylactic reactions to lenalidomide has been reported. Permanently discontinue lenalidomide for angioedema and anaphylaxis [see Dosage and Administration (2.2)] .
1.6 Limitations of Use
Lenalidomide capsules are not indicated and are not recommended for the treatment of patients with CLL outside of controlled clinical trials [see Warnings and Precautions (5.5)] .
5.13 Thyroid Disorders
Both hypothyroidism and hyperthyroidism have been reported [see Adverse Reactions (6.2)] . Measure thyroid function before start of lenalidomide treatment and during therapy.
1 Indications and Usage (1 INDICATIONS AND USAGE)
Lenalidomide is a thalidomide analogue indicated for the treatment of adult patients with:
- Multiple myeloma (MM), in combination with dexamethasone ( 1.1).
- MM, as maintenance following autologous hematopoietic stem cell transplantation (auto-HSCT) ( 1.1).
- Transfusion-dependent anemia due to low- or intermediate-1-risk myelodysplastic syndromes (MDS) associated with a deletion 5q abnormality with or without additional cytogenetic abnormalities ( 1.2).
- Mantle cell lymphoma (MCL) whose disease has relapsed or progressed after two prior therapies, one of which included bortezomib ( 1.3).
- Previously treated follicular lymphoma (FL), in combination with a rituximab product ( 1.4).
- Previously treated marginal zone lymphoma (MZL), in combination with a rituximab product ( 1.5).
Limitations of Use:
- Lenalidomide capsules are not indicated and are not recommended for the treatment of patients with chronic lymphocytic leukemia (CLL) outside of controlled clinical trials ( 1.6).
1.4 Follicular Lymphoma
Lenalidomide capsules in combination with a rituximab product, is indicated for the treatment of adult patients with previously treated follicular lymphoma (FL).
1.3 Mantle Cell Lymphoma
Lenalidomide capsules are indicated for the treatment of adult patients with mantle cell lymphoma (MCL) whose disease has relapsed or progressed after two prior therapies, one of which included bortezomib.
12.1 Mechanism of Action
Lenalidomide is an analogue of thalidomide with immunomodulatory, antiangiogenic, and antineoplastic properties. Cellular activities of lenalidomide are mediated through its target cereblon, a component of a cullin ring E3 ubiquitin ligase enzyme complex. In vitro, in the presence of drug, substrate proteins (including Aiolos, Ikaros, and CK1α) are targeted for ubiquitination and subsequent degradation leading to direct cytotoxic and immunomodulatory effects. Lenalidomide inhibits proliferation and induces apoptosis of certain hematopoietic tumor cells including MM, mantle cell lymphoma, and del (5q) myelodysplastic syndromes, follicular lymphoma and marginal zone lymphoma in vitro. Lenalidomide causes a delay in tumor growth in some in vivononclinical hematopoietic tumor models including MM. Immunomodulatory properties of lenalidomide include increased number and activation of T cells and natural killer (NK) cells leading to direct and enhanced antibody-dependent cell-mediated cytotoxicity (ADCC) via increased secretion of interleukin-2 and interferon-gamma, increased numbers of NKT cells, and inhibition of pro-inflammatory cytokines (e.g., TNF-α and IL-6) by monocytes. In MM cells, the combination of lenalidomide and dexamethasone synergizes the inhibition of cell proliferation and the induction of apoptosis. The combination of lenalidomide and rituximab increases ADCC and direct tumor apoptosis in follicular lymphoma cells and increases ADCC in marginal zone lymphoma cells compared to rituximab alone in vitro.
5.3 Hematologic Toxicity
Lenalidomide can cause significant neutropenia and thrombocytopenia. Monitor patients with neutropenia for signs of infection. Advise patients to observe for bleeding or bruising, especially with use of concomitant medication that may increase risk of bleeding. Patients taking lenalidomide should have their complete blood counts assessed periodically as described below [see Dosage and Administration (2.1, 2.2, 2.3)] .
Monitor complete blood counts (CBC) in patients taking lenalidomide capsules in combination with dexamethasone or as lenalidomide maintenance therapy for MM every 7 days (weekly) for the first 2 cycles, on Days 1 and 15 of Cycle 3, and every 28 days (4 weeks) thereafter. A dose interruption and/or dose reduction may be required [see Dosage and Administration (2.1)] . In the MM maintenance therapy trials, Grade 3 or 4 neutropenia was reported in up to 59% of lenalidomide-treated patients and Grade 3 or 4 thrombocytopenia in up to 38% of lenalidomide-treated patients [see Adverse Reactions (6.1)] .
Monitor complete blood counts (CBC) in patients taking lenalidomide for MDS weekly for the first 8 weeks and at least monthly thereafter. Grade 3 or 4 hematologic toxicity was seen in 80% of patients enrolled in the MDS study. In the 48% of patients who developed Grade 3 or 4 neutropenia, the median time to onset was 42 days (range, 14 days to 411 days), and the median time to documented recovery was 17 days (range, 2 days to 170 days). In the 54% of patients who developed Grade 3 or 4 thrombocytopenia, the median time to onset was 28 days (range, 8 days to 290 days), and the median time to documented recovery was 22 days (range, 5 days to 224 days) [see Boxed Warningand Dosage and Administration (2.2)] .
Monitor complete blood counts (CBC) in patients taking lenalidomide for MCL weekly for the first cycle (28 days), every 2 weeks during cycles 2 to 4, and then monthly thereafter. Patients may require dose interruption and/or dose reduction. In the MCL trial, Grade 3 or 4 neutropenia was reported in 43% of the patients. Grade 3 or 4 thrombocytopenia was reported in 28% of the patients.
Monitor complete blood counts (CBC) in patients taking lenalidomide for FL or MZL weekly for the first 3 weeks of Cycle 1 (28 days), every 2 weeks during Cycles 2 to 4, and then monthly thereafter. Patients may require dose interruption and/or dose reduction. In the AUGMENT and MAGNIFY trials, Grade 3 or 4 neutropenia was reported in 50% and 33%, respectively, of patients in the lenalidomide/rituximab arm. Grade 3 or 4 thrombocytopenia was reported in 2% and 8%, respectively, of patients in the lenalidomide/rituximab arm [see Adverse Reactions (6.1) ].
14.3 Mantle Cell Lymphoma
A multicenter, single-arm, open-label trial of single-agent lenalidomide was conducted to evaluate the safety and efficacy of lenalidomide in patients with mantle cell lymphoma who have relapsed after or were refractory to bortezomib or a bortezomib-containing regimen. Patients with a creatinine clearance ≥60 mL/min were given lenalidomide at a dose of 25 mg once daily for 21 days every 28 days. Patients with a creatinine clearance ≥30 mL/min and <60 mL/min were given lenalidomide at a dose of 10 mg once daily for 21 days every 28 days. Treatment was continued until disease progression, unacceptable toxicity, or withdrawal of consent.
The trial included patients who were at least 18 years of age with biopsy-proven MCL with measurable disease by CT scan. Patients were required to have received prior treatment with an anthracycline or mitoxantrone, cyclophosphamide, rituximab, and bortezomib, alone or in combination. Patients were required to have documented refractory disease (defined as without any response of PR or better during treatment with bortezomib or a bortezomib-containing regimen), or relapsed disease (defined as progression within one year after treatment with bortezomib or a bortezomib-containing regimen). At enrollment patients were to have an absolute neutrophil counts (ANC) ≥1,500/ mm
3, platelet counts ≥60,000/mm
3, serum SGOT/AST or SGPT/ALT ≤3x upper limit of normal (ULN) unless there was documented evidence of liver involvement by lymphoma, serum total bilirubin ≤1.5 x ULN except in cases of Gilbert’s syndrome or documented liver involvement by lymphoma, and calculated creatinine clearance (Cockcroft-Gault formula) ≥30 mL/min.
The median age was 67 years (43 to 83), 81% were male and 96% were Caucasian. The table below summarizes the baseline disease-related characteristics and prior anti-lymphoma therapy in the Mantle Cell Lymphoma trial.
| Baseline Disease Characteristics and Prior Anti- Lymphoma Treatment |
Total Patients
(N = 134) |
|
ECOG Performance Status
ECOG = Eastern Cooperative Oncology Group. n (%)
|
|
| 0 | 43 (32)) |
| 1 | 73 (54) |
| 2 | 17 (13) |
| 3 | 1 (< 1) |
| Advanced MCL Stage, n (%) | |
| III | 27 (20) |
| IV | 97 (72) |
|
High or Intermediate MIPI Score
MIPI = MCL International Prognostic Index. , n (%)
|
90 (67) |
|
High Tumor Burden
High tumor burden is defined as at least one lesion that is ≥5 cm in diameter or 3 lesions that are ≥3 cm in diameter. , n (%)
|
77 (57) |
|
Bulky Disease
Bulky disease is defined as at least one lesion that is ≥7cm in the longest diameter. , n (%)
|
44 (33) |
| Extranodal Disease, n (%) | 101 (75) |
| Number of Prior Systemic Anti-Lymphoma Therapies, n (%) | |
| Median (range) | 4 (2, 10) |
| 1 | 0 (0) |
| 2 | 29 (22) |
| 3 | 34 (25) |
| ≥4 | 71 (53) |
| Number of Subjects Who Received Prior Regimen Containing, n (%): | |
| Anthracycline/mitoxantrone | 133 (99) |
| Cyclophosphamide | 133 (99) |
| Rituximab | 134 (100) |
| Bortezomib | 134 (100) |
| Refractory to Prior Bortezomib, n (%) | 81 (60) |
| Refractory to Last Prior Therapy, n (%) | 74 (55) |
| Prior Autologous Bone Marrow or Stem Cell Transplant, n (%) | 39 (29) |
The efficacy endpoints in the MCL trial were overall response rate (ORR) and duration of response (DOR). Response was determined based on review of radiographic scans by an independent review committee according to a modified version of the International Workshop Lymphoma Response Criteria (Cheson, 1999). The DOR is defined as the time from the initial response (at least PR) to documented disease progression. The efficacy results for the MCL population were based on all evaluable patients who received at least one dose of study drug and are presented in Table 20. The median time to response was 2.2 months (range 1.8 months to 13 months).
| Response Analyses (N = 133) | N (%) | 95% CI | |
| Overall Response Rate (IWRC) (CR + CRu +PR) | 34 (26) | (18.4, 33.9) | |
| Complete Response (CR + CRu) | 9 (7) | (3.1, 12.5) | |
| CR | 1 (1) | ||
| CRu | 8 (6) | ||
| Partial Response (PR) | 25 (19) | ||
| Duration of Response (months) | Median | 95% CI | |
| Duration of Overall Response (CR + CRu + PR) | (N = 34) | 16.6 | (7.7, 26.7) |
5.1 Embryo Fetal Toxicity (5.1 Embryo-Fetal Toxicity)
Lenalidomide is a thalidomide analogue and is contraindicated for use during pregnancy. Thalidomide is a known human teratogen that causes life-threatening human birth defects or embryo-fetal death [see Use in Specific Populations (8.1)]. An embryo-fetal development study in monkeys indicates that lenalidomide produced malformations in the offspring of female monkeys who received the drug during pregnancy, similar to birth defects observed in humans following exposure to thalidomide during pregnancy.
Lenalidomide capsules are only available through the Lenalidomide REMS program [see Warnings and Precautions (5.2)].
5.10 Tumor Lysis Syndrome
Fatal instances of tumor lysis syndrome (TLS) have been reported during treatment with lenalidomide. The patients at risk of TLS are those with high tumor burden prior to treatment. Monitor patients at risk closely and take appropriate preventive approaches. In the AUGMENT trial in FL or MZL patients, TLS occurred in 2 patients (1.1%) in the lenalidomide/rituximab arm. TLS occurred in 1 patient (0.5%) in the MAGNIFY trial during the lenalidomide/rituximab induction period; the event was a serious, Grade 3 adverse reaction.
5.11 Tumor Flare Reaction
Tumor flare reaction (TFR), including fatal reactions, have occurred during investigational use of lenalidomide for CLL and lymphoma, and is characterized by tender lymph node swelling, low grade fever, pain and rash. Lenalidomide is not indicated and not recommended for use in CLL outside of controlled clinical trials.
Monitoring and evaluation for TFR is recommended in patients with MCL, FL, or MZL. Tumor flare reaction may mimic progression of disease (PD).
In the MCL trial, 13/134 (10%) of subjects experienced TFR; all reports were Grade 1 or 2 in severity. All of the events occurred in Cycle 1 and one patient developed TFR again in Cycle 11. In the AUGMENT trial in FL or MZL patients, TFR was reported in 19/176 (10.8%) of patients in lenalidomide with rituximab arm; one patient in the lenalidomide/rituximab arm experienced a Grade 3 TFR. In the MAGNIFY trial, 9/222 (4.1%) of patients experienced TFR; all reports were Grade 1 or 2 in severity and 1 event was considered as serious. In a separate MCL phase 2 trial, one case of TFR resulted in a fatal outcome.
Lenalidomide may be continued in patients with Grade 1 and 2 TFR without interruption or modification, at the physician's discretion. Patients with Grade 1 and 2 TFR may also be treated with corticosteroids, non-steroidal anti-inflammatory drugs (NSAIDs) and/or narcotic analgesics for management of TFR symptoms. In patients with Grade 3 or 4 TFR, it is recommended to withhold treatment with lenalidomide until TFR resolves to ≤Grade 1. Patients with Grade 3 or 4 TFR may be treated for management of symptoms per the guidance for treatment of Grade 1 and 2 TFR.
1.5 Marginal Zone Lymphoma
Lenalidomide capsules in combination with a rituximab product, is indicated for the treatment of adult patients with previously treated marginal zone lymphoma (MZL).
16.3 Handling and Disposal
Care should be exercised in the handling of lenalidomide capsules. Lenalidomide capsules should not be opened or broken. If powder from lenalidomide capsules contacts the skin, wash the skin immediately and thoroughly with soap and water. If lenalidomide capsules contacts the mucous membranes, flush thoroughly with water.
Procedures for the proper handling and disposal of anticancer drugs should be considered. Several guidelines on the subject have been published. 1
Dispense no more than a 28-day supply.
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
- Increased Mortality: serious and fatal cardiac adverse reactions occurred in patients with CLL treated with lenalidomide ( 5.5).
- Second Primary Malignancies (SPM): Higher incidences of SPM were observed in controlled trials of patients with MM receiving lenalidomide ( 5.6).
- Increased Mortality: Observed in patients with MM when pembrolizumab was added to dexamethasone and a thalidomide analogue ( 5.7).
- Hepatotoxicity: Hepatic failure including fatalities; monitor liver function. Stop lenalidomide and evaluate if hepatotoxicity is suspected ( 5.8).
- Severe Cutaneous Reactions: Discontinue lenalidomide for severe reactions ( 5.9).
- Tumor lysis syndrome (TLS) including fatalities: Monitor patients at risk of TLS (i.e., those with high tumor burden) and take appropriate precautions ( 5.10).
- Tumor flare reaction: Serious tumor flare reactions, including fatal reactions, have occurred during investigational use of lenalidomide for chronic lymphocytic leukemia and lymphoma ( 5.11).
- Impaired Stem Cell mobilization: A decrease in the number of CD34+ cells collected after treatment (> 4 cycles) with lenalidomide has been reported. Consider early referral to transplant center ( 5.12).
- Early mortality in MCL: Higher rate of early deaths have occurred in patients with MCL ( 5.14).
- Hypersensitivity: Monitor patients for potential hypersensitivity. Discontinue lenalidomide for angioedema and anaphylaxis ( 5.15).
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
- MM combination therapy: 25 mg once daily orally on Days 1 to 21 of repeated 28-day cycles. ( 2.1).
- MM maintenance therapy following auto-HSCT: 10 mg once daily continuously on Days 1 to 28 of repeated 28-day cycles ( 2.1).
- MDS: 10 mg once daily ( 2.2).
- MCL: 25 mg once daily orally on Days 1 to 21 of repeated 28-day cycles ( 2.3).
- FL or MZL: 20 mg once daily orally on Days 1 to 21 of repeated 28-day cycles for up to 12 cycles ( 2.4).
- Renal impairment: Adjust starting dose based on the creatinine clearance value ( 2.6).
- For concomitant therapy doses, see Full Prescribing Information ( 2.1, 2.4, 14.1, 14.4).
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
Capsules:
- 2.5 mg, white to off-white powder filled in hard gelatin capsule size ‘4’ with blue-green opaque cap and white opaque body, imprinted with “LEN” on the cap and “2.5 mg” on the body with black ink
- 5 mg, white to off-white powder filled in white opaque hard gelatin capsule size ‘4’, imprinted with “LEN” on the cap and “5 mg” on the body with black ink
- 10 mg, white to off-white powder filled in hard gelatin capsule size ‘2’ with blue-green opaque cap and pale-yellow opaque body, imprinted with “LEN” on the cap and “10 mg” on the body with black ink
- 15 mg, white to off-white powder filled in hard gelatin capsule size ‘1’ with pale blue opaque cap and white opaque body, imprinted with “LEN” on the cap and “15 mg” on the body with black ink
- 20 mg, white to off-white powder filled in hard gelatin capsule size ‘0’ with blue-green opaque cap and pale blue opaque body, imprinted with “LEN” on the cap and “20 mg” on the body with black ink
- 25 mg, white to off-white powder filled in white opaque hard gelatin capsule size ‘0EL’, imprinted with “LEN” on the cap and “25 mg” on the body with black ink
6.2 Postmarketing Experience
The following adverse drug reactions have been identified from the worldwide post-marketing experience with lenalidomide. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure [see Warnings and Precautions Section (5.8to 5.11, and 5.13)]
Endocrine disorders:Hypothyroidism, hyperthyroidism
Hepatobiliary disorders:Hepatic failure (including fatality), toxic hepatitis, cytolytic hepatitis, cholestatic hepatitis, mixed cytolytic/cholestatic hepatitis, transient abnormal liver laboratory tests
Immune system disorders:Angioedema, anaphylaxis, acute graft-versus-host disease (following allogeneic hematopoietic transplant), solid organ transplant rejection
Infections and infestations:Viral reactivation (such as hepatitis B virus and herpes zoster), progressive multifocal leukoencephalopathy (PML)
Neoplasms benign, malignant and unspecified (including cysts and polyps):Tumor lysis syndrome, tumor flare reaction
Respiratory, thoracic and mediastinal disorders:Pneumonitis
Skin and subcutaneous tissue disorders:Stevens-Johnson Syndrome, toxic epidermal necrolysis, drug reaction with eosinophilia and systemic symptoms (DRESS)
1.2 Myelodysplastic Syndromes
Lenalidomide capsules are indicated for the treatment of adult patients with transfusion-dependent anemia due to low- or intermediate-1-risk myelodysplastic syndromes (MDS) associated with a deletion 5q cytogenetic abnormality with or without additional cytogenetic abnormalities.
5.2 Lenalidomide Rems Program (5.2 Lenalidomide REMS Program)
Because of the embryo-fetal risk [see Warnings and Precautions (5.1)], lenalidomide capsules are available only through a restricted program under a Risk Evaluation and Mitigation Strategy (REMS), the Lenalidomide REMSprogram.
Required components of the Lenalidomide REMSprogram include the following:
- Prescribers must be certified with the Lenalidomide REMSprogram by enrolling and complying with the REMS requirements.
- Patients must sign a Patient-Physician agreement form and comply with the REMS requirements. In particular, female patients of reproductive potential who are not pregnant must comply with the pregnancy testing and contraception requirements [see Use in Specific Populations (8.3)] and males must comply with contraception requirements [see Use in Specific Populations (8.3)] .
- Pharmacies must be certified with the Lenalidomide REMSprogram, must only dispense to patients who are authorized to receive lenalidomide capsules and comply with REMS requirements.
Further information about the Lenalidomide REMSprogram is available at www.lenalidomiderems.comor by telephone at 1-888-423-5436.
8 Use in Specific Populations (8 USE IN SPECIFIC POPULATIONS)
- Lactation: Advise not to breastfeed ( 8.2).
5.9 Severe Cutaneous Reactions
Severe cutaneous reactions including Stevens-Johnson syndrome (SJS), toxic epidermal necrolysis (TEN), and drug reaction with eosinophilia and systemic symptoms (DRESS) have been reported. DRESS may present with a cutaneous reaction (such as rash or exfoliative dermatitis), eosinophilia, fever, and/or lymphadenopathy with systemic complications such as hepatitis, nephritis, pneumonitis, myocarditis, and/or pericarditis. These events can be fatal. Patients with a prior history of Grade 4 rash associated with thalidomide treatment should not receive lenalidomide. Consider lenalidomide interruption or discontinuation for Grade 2 to 3 skin rash. Permanently discontinue lenalidomide for Grade 4 rash, exfoliative or bullous rash, or for other severe cutaneous reactions such as SJS, TEN or DRESS [see Dosage and Administration (2.5)] .
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
5.6 Second Primary Malignancies
In clinical trials in patients with MM receiving lenalidomide, an increase of hematologic plus solid tumor second primary malignancies (SPM) notably AML and MDS have been observed. An increase in hematologic SPM including AML and MDS occurred in 5.3% of patients with NDMM receiving lenalidomide in combination with oral melphalan compared with 1.3% of patients receiving melphalan without lenalidomide. The frequency of AML and MDS cases in patients with NDMM treated with lenalidomide in combination with dexamethasone without melphalan was 0.4%.
In patients receiving lenalidomide maintenance therapy following high dose intravenous melphalan and auto-HSCT, hematologic SPM occurred in 7.5% of patients compared to 3.3% in patients receiving placebo. The incidence of hematologic plus solid tumor (excluding squamous cell carcinoma and basal cell carcinoma) SPM was 14.9%, compared to 8.8% in patients receiving placebo with a median follow-up of 91.5 months. Non-melanoma skin cancer SPM, including squamous cell carcinoma and basal cell carcinoma, occurred in 3.9% of patients receiving lenalidomide maintenance, compared to 2.6% in the placebo arm.
In patients with relapsed or refractory MM treated with lenalidomide/dexamethasone, the incidence of hematologic plus solid tumor (excluding squamous cell carcinoma and basal cell carcinoma) SPM was 2.3% versus 0.6% in the dexamethasone alone arm. Non-melanoma skin cancer SPM, including squamous cell carcinoma and basal cell carcinoma, occurred in 3.1% of patients receiving lenalidomide/dexamethasone, compared to 0.6% in the dexamethasone alone arm.
Patients who received lenalidomide-containing therapy until disease progression did not show a higher incidence of invasive SPM than patients treated in the fixed duration lenalidomide-containing arms. Monitor patients for the development of second primary malignancies. Take into account both the potential benefit of lenalidomide and the risk of second primary malignancies when considering treatment with lenalidomide.
In the AUGMENT trial with FL or MZL patients receiving lenalidomide/rituximab therapy, hematologic plus solid tumor SPMs, notably AML, have been observed. In the AUGMENT trial, hematologic SPM of AML occurred in 0.6% of patients with FL or MZL receiving lenalidomide/rituximab therapy. The incidence of hematologic plus solid tumor SPMs (excluding nonmelanoma skin cancers) was 1.7% in the lenalidomide/rituximab arm with a median follow-up of 29.8 months (range 0.5 month to 51.3 months) [see Adverse Reactions (6.1)] . Monitor patients for the development of second primary malignancies. Take into account both the potential benefit of lenalidomide and the risk of second primary malignancies when considering treatment with lenalidomide.
Principal Display Panel – 5 Mg (Principal Display Panel – 5 mg)
NDC 82293-007-10
Lenalidomide Capsules
5 mg
WARNING: POTENTIAL FOR HUMAN BIRTH DEFECTS.
PHARMACIST: Dispense the accompanying Medication Guide to each patient.
28 Capsules
Rx only
17 Patient Counseling Information (17 PATIENT COUNSELING INFORMATION)
Advise the patient to read the FDA-approved Patient labeling (Medication Guide)
Embryo-Fetal Toxicity
Advise patients that lenalidomide capsules are contraindicated in pregnancy [see Boxed Warningand Contraindications (4.1)]. Lenalidomide capsules are a thalidomide analogue and can cause serious birth defects or death to a developing baby [see Warnings and Precautions (5.1)and Use in Specific Populations (8.1)] .
- Advise females of reproductive potential that they must avoid pregnancy while taking lenalidomide capsules and for at least 4 weeks after completing therapy.
- Initiate lenalidomide capsules treatment in females of reproductive potential only following a negative pregnancy test.
- Advise females of reproductive potential of the importance of monthly pregnancy tests and the need to use 2 different forms of contraception including at least 1 highly effective form, simultaneously during lenalidomide capsules therapy, during dose interruption and for 4 weeks after she has completely finished taking lenalidomide capsules. Highly effective forms of contraception other than tubal ligation include IUD and hormonal (birth control pills, injections, patch or implants) and a partner’s vasectomy. Additional effective contraceptive methods include latex or synthetic condom, diaphragm and cervical cap.
- Instruct patient to immediately stop taking lenalidomide capsules and contact her healthcare provider if she becomes pregnant while taking this drug, if she misses her menstrual period, or experiences unusual menstrual bleeding, if she stops taking birth control, or if she thinks FOR ANY REASON that she may be pregnant.
- Advise patient that if her healthcare provider is not available, she should call the REMS Call Center at 1-888-423-5436 [see Warnings and Precautions (5.1)and Use in Specific Populations (8.3)].
- Advise males to always use a latex or synthetic condom during any sexual contact with females of reproductive potential while taking lenalidomide capsules and for up to 4 weeks after discontinuing lenalidomide capsules, even if they have undergone a successful vasectomy.
- Advise male patients taking lenalidomide capsules that they must not donate sperm and for up to 4 weeks after discontinuation of lenalidomide capsules [see Warnings and Precautions (5.1)and Use in Specific Populations (8.3)] .
- All patients must be instructed to not donate blood while taking lenalidomide capsules, during dose interruptions and for 4 weeks following discontinuation of lenalidomide capsules [see Warnings and Precautions (5.1)] .
Lenalidomide REMS program
Because of the risk of embryo-fetal toxicity, lenalidomide capsules are only available through a restricted program called the Lenalidomide REMS program [see Warnings and Precautions (5.2)] .
- Patients must sign a Patient-Physician agreement form and comply with the requirements to receive lenalidomide capsules. In particular, females of reproductive potential must comply with the pregnancy testing, contraception requirements and participate in monthly telephone surveys. Males must comply with the contraception requirements [see Use in Specific Populations (8.3)] .
- Lenalidomide capsules are available only from pharmacies that are certified in the Lenalidomide REMS program. Provide patients with the telephone number and website for information on how to obtain the product.
Pregnancy Exposure Registry
Inform females there is a Pregnancy Exposure Registry that monitors pregnancy outcomes in females exposed to lenalidomide capsules during pregnancy and that they can contact the Pregnancy Exposure Registry by calling 1-888-423-5436 [see Use in Specific Populations (8.1) ] .
Hematologic Toxicity
Inform patients that lenalidomide capsules are associated with significant neutropenia and thrombocytopenia [see Boxed Warningand Warnings and Precautions (5.3)] .
Venous and Arterial Thromboembolism
Inform patients of the risk of thrombosis including DVT, PE, MI, and stroke and to report immediately any signs and symptoms suggestive of these events for evaluation [see Boxed Warningand Warnings and Precautions (5.4)] .
Increased Mortality in Patients with CLL
Inform patients that lenalidomide capsules had increased mortality in patients with CLL and serious adverse cardiovascular reactions, including atrial fibrillation, myocardial infarction, and cardiac failure [see Warnings and Precautions (5.5)] .
Second Primary Malignancies
Inform patients of the potential risk of developing second primary malignancies during treatment with lenalidomide capsules [see Warnings and Precautions (5.6)] .
Hepatotoxicity
Inform patients of the risk of hepatotoxicity, including hepatic failure and death, and to report any signs and symptoms associated with this event to their healthcare provider for evaluation [see Warnings and Precautions (5.8)] .
Severe Cutaneous Reactions
Inform patients of the potential risk for severe skin reactions such as SJS, TEN, and DRESS and report any signs and symptoms associated with these reactions to their healthcare provider for evaluation. Patients with a prior history of Grade 4 rash associated with thalidomide treatment should not receive lenalidomide capsules [see Warnings and Precautions (5.9)].
Tumor Lysis Syndrome
Inform patients of the potential risk of tumor lysis syndrome and to report any signs and symptoms associated with this event to their healthcare provider for evaluation [see Warnings and Precautions (5.10)] .
Tumor Flare Reaction
Inform patients of the potential risk of tumor flare reaction and to report any signs and symptoms associated with this event to their healthcare provider for evaluation [see Warnings and Precautions (5.11)] .
Early Mortality in Patients with MCL
Inform patients with MCL of the potential for early death
[see
Warnings and Precautions (5.14)].
Hypersensitivity
Inform patients of the potential for severe hypersensitivity reactions such as angioedema and anaphylaxis to lenalidomide capsules. Instruct patients to contact their healthcare provider right away for signs and symptoms of these reactions. Advise patients to seek emergency medical attention for signs or symptoms of severe hypersensitivity reactions [see Warnings and Precautions (5.15)] .
Dosing Instructions
Inform patients how to take lenalidomide capsules [see Dosage and Administration (2)]
- Lenalidomide capsules should be taken once daily at about the same time each day,
- Lenalidomide capsules may be taken either with or without food.
- The capsules should not be opened, broken, or chewed. Lenalidomide capsules should be swallowed whole with water.
- Instruct patients that if they miss a dose of lenalidomide capsules, they may still take it up to 12 hours after the time they would normally take it. If more than 12 hours have elapsed, they should be instructed to skip the dose for that day. The next day, they should take lenalidomide capsules at the usual time. Warn patients to not take 2 doses to make up for the one that they missed.
Distributed by:
Novugen Pharma (USA) LLC
100 Overlook Center
Princeton, NJ 08540, USA
MADE IN INDIA
Revised: 11/2023
Principal Display Panel – 10 Mg (Principal Display Panel – 10 mg)
NDC 82293-008-10
Lenalidomide Capsules
10 mg
WARNING: POTENTIAL FOR HUMAN BIRTH DEFECTS.
PHARMACIST: Dispense the accompanying Medication Guide to each patient.
28 Capsules
Rx only
Principal Display Panel – 15 Mg (Principal Display Panel – 15 mg)
NDC 82293-009-10
Lenalidomide Capsules
15 mg
WARNING: POTENTIAL FOR HUMAN BIRTH DEFECTS.
PHARMACIST: Dispense the accompanying Medication Guide to each patient.
21 Capsules
Rx only
Principal Display Panel – 20 Mg (Principal Display Panel – 20 mg)
NDC 82293-010-10
Lenalidomide Capsules
20 mg
WARNING: POTENTIAL FOR HUMAN BIRTH DEFECTS.
PHARMACIST: Dispense the accompanying Medication Guide to each patient.
21 Capsules
Rx only
Principal Display Panel – 25 Mg (Principal Display Panel – 25 mg)
NDC 82293-011-10
Lenalidomide Capsules
25 mg
WARNING: POTENTIAL FOR HUMAN BIRTH DEFECTS.
PHARMACIST: Dispense the accompanying Medication Guide to each patient.
21 Capsules
Rx only
Principal Display Panel – 2.5 Mg (Principal Display Panel – 2.5 mg)
NDC 82293-006-10
Lenalidomide Capsules
2.5 mg
WARNING: POTENTIAL FOR HUMAN BIRTH DEFECTS.
PHARMACIST: Dispense the accompanying Medication Guide to each patient.
28 Capsules
Rx only
5.12 Impaired Stem Cell Mobilization
A decrease in the number of CD34+ cells collected after treatment (>4 cycles) with lenalidomide has been reported. In patients who are auto-HSCT candidates, referral to a transplant center should occur early in treatment to optimize the timing of the stem cell collection. In patients who received more than 4 cycles of a lenalidomide-containing treatment or for whom inadequate numbers of CD 34+ cells have been collected with G-CSF alone, G-CSF with cyclophosphamide or the combination of G-CSF with a CXCR4 inhibitor may be considered.
4.2 Severe Hypersensitivity Reactions
Lenalidomide is contraindicated in patients who have demonstrated severe hypersensitivity (e.g., angioedema, Stevens-Johnson syndrome, toxic epidermal necrolysis) to lenalidomide [see Warnings and Precautions (5.9, 5.15)].
5.4 Venous and Arterial Thromboembolism
Venous thromboembolic events (VTE [DVT and PE]) and arterial thromboembolic events (ATE, myocardial infarction and stroke) are increased in patients treated with lenalidomide.
A significantly increased risk of DVT (7.4%) and of PE (3.7%) occurred in patients with MM after at least one prior therapy who were treated with lenalidomide and dexamethasone therapy compared to patients treated in the placebo and dexamethasone group (3.1% and 0.9%) in clinical trials with varying use of anticoagulant therapies. In the newly diagnosed multiple myeloma (NDMM) study in which nearly all patients received antithrombotic prophylaxis, DVT was reported as a serious adverse reaction (3.6%, 2.0%, and 1.7%) in the Rd Continuous, Rd18, and MPT Arms, respectively. The frequency of serious adverse reactions of PE was similar between the Rd Continuous, Rd18, and MPT Arms (3.8%, 2.8%, and 3.7%, respectively) [see Boxed Warningand Adverse Reactions (6.1)] .
Myocardial infarction (1.7%) and stroke (CVA) (2.3%) are increased in patients with MM after at least one prior therapy who were treated with lenalidomide and dexamethasone therapy compared to patients treated with placebo and dexamethasone (0.6%, and 0.9%) in clinical trials. In the NDMM study, myocardial infarction (including acute) was reported as a serious adverse reaction (2.3%, 0.6%, and 1.1%) in the Rd Continuous, Rd18, and MPT Arms, respectively. The frequency of serious adverse reactions of CVA was similar between the Rd Continuous, Rd18, and MPT Arms (0.8%, 0.6 %, and 0.6%, respectively) [see Adverse Reactions (6.1)].
Patients with known risk factors, including prior thrombosis, may be at greater risk and actions should be taken to try to minimize all modifiable factors (e.g., hyperlipidemia, hypertension, smoking).
In controlled clinical trials that did not use concomitant thromboprophylaxis, 21.5% overall thrombotic events (Standardized MedDRA Query Embolic and Thrombotic events) occurred in patients with refractory and relapsed MM who were treated with lenalidomide and dexamethasone compared to 8.3% thrombosis in patients treated with placebo and dexamethasone. The median time to first thrombosis event was 2.8 months. In the NDMM study in which nearly all patients received antithrombotic prophylaxis, the overall frequency of thrombotic events was 17.4% in patients in the combined Rd Continuous and Rd18 Arms, and was 11.6% in the MPT Arm. The median time to first thrombosis event was 4.3 months in the combined Rd Continuous and Rd18 Arms.
In the AUGMENT trial, the incidence of VTE (including DVT and PE) in FL or MZL patients was 3.4% in the lenalidomide/rituximab arm [see Adverse Reactions (6.1)] . In the AUGMENT trial, the incidence of ATE (including MI) in FL or MZL patients was 0.6% in the lenalidomide/rituximab arm [see Adverse Reactions (6.1)] .
Thromboprophylaxis is recommended. The regimen of thromboprophylaxis should be based on an assessment of the patient's underlying risks. Instruct patients to report immediately any signs and symptoms suggestive of thrombotic events. ESAs and estrogens may further increase the risk of thrombosis and their use should be based on a benefit-risk decision in patients receiving lenalidomide [see Drug Interactions (7.2)].
5.14 Early Mortality in Patients With Mcl (5.14 Early Mortality in Patients with MCL)
In another MCL study, there was an increase in early deaths (within 20 weeks), 12.9% in the lenalidomide arm versus 7.1% in the control arm. On exploratory multivariate analysis, risk factors for early deaths include high tumor burden, MIPI score at diagnosis, and high WBC at baseline (≥10 x 10 9/L).
14.4 Follicular and Marginal Zone Lymphoma
The efficacy of lenalidomide with rituximab in patients with relapsed or refractory follicular and marginal zone lymphoma was evaluated in the AUGMENT ( NCT01938001) and MAGNIFY ( NCT01996865) trials.
AUGMENT is a randomized, double-blind, multicenter trial (n = 358) in which patients with relapsed or refractory follicular or marginal zone lymphoma were randomized 1:1 to receive lenalidomide and rituximab or rituximab and placebo. AUGMENT included patients diagnosed with Grade 1, 2, or 3a follicular lymphoma, who received at least 1 prior systemic therapy, were refractory or relapsed, not rituximab-refractory, had at least one measurable nodal or extranodal lesion by CT or MRI scan, and had adequate bone marrow, liver, and renal function. Randomization was stratified by follicular versus marginal zone lymphoma, previous rituximab therapy, and time since other anti-lymphoma therapy. In AUGMENT, lenalidomide was administered orally 20 mg once daily for Days 1 to 21 of repeating 28-day cycles for a maximum of 12 cycles or until unacceptable toxicity. The dose of rituximab was 375 mg/m 2every week in Cycle 1 (Days 1, 8, 15, and 22) and on Day 1 of every 28-day cycle from Cycles 2 through 5. All dosage calculations for rituximab were based on the patient's body surface area (BSA), using actual patient weight. Dose adjustments for lenalidomide were allowed based on clinical and laboratory findings. A patient with moderate renal insufficiency (≥30 mL/minute to <60 mL/minute) received a lower lenalidomide starting dose of 10 mg daily on the same schedule. After 2 cycles, the lenalidomide dose could be increased to 15 mg once daily on Days 1 to 21 of each 28-day cycle if the patient tolerated the medication.
MAGNIFY is an open-label, multicenter trial (n = 232) in which patients with relapsed or refractory follicular, marginal zone, or mantle cell lymphoma received 12 induction cycles of lenalidomide and rituximab. MAGNIFY included patients diagnosed with Grade 1, 2, 3a, 3b follicular (including transformed), marginal zone, or mantle cell lymphoma Stage I to IV who were previously treated for their lymphoma, had been refractory or had a relapse after their last treatment, had at least one measurable nodal or extranodal lesion by CT or MRI scan, and had adequate bone marrow, liver, and renal function. Patients refractory to rituximab were also included. The information from the subjects who received at least 1 dose of initial therapy in the first 12 induction cycles (n = 222) in the MAGNIFY trial was included in the evaluation of the efficacy of lenalidomide/rituximab in patients with relapsed or refractory follicular and marginal zone lymphoma. In MAGNIFY, lenalidomide 20 mg was given on Days 1 to 21 of repeated 28-day cycles for up to 12 cycles or until unacceptable toxicity, progression, or withdrawal of consent. The dose of rituximab was 375 mg/m 2every week in Cycle 1 (Days 1, 8, 15, and 22) and on Day 1 of every other 28-day cycle (Cycles 3, 5, 7, 9, and 11) up to 12 cycles therapy. All dosage calculations for rituximab were based on the patient BSA and actual weight. Dose adjustments were allowed based on clinical and laboratory findings.
The demographic and disease-related baseline characteristics in the AUGMENT and MAGNIFY trials are shown in the following table.
| Parameter | AUGMENT Trial | MAGNIFY Trial | |
|
Lenalidomide + Rituximab
(N = 178) |
Rituximab + Placebo
(Control Arm) (N = 180) |
Lenalidomide + Rituximab
(N = 222) |
|
| Age (years) | |||
| Median (Max, Min) | 64 (26, 86) | 62 (35, 88) | 65 (35, 91) |
| Age distribution, n (%) | |||
| <65 years | 96 (54) | 107 (59) | 103 (46) |
| ≥65 years | 82 (46) | 73 (41) | 119 (54) |
| Sex, n (%) | |||
| Male | 75 (42) | 97 (54) | 122 (55) |
| Female | 103 (58) | 83 (46) | 100 (45) |
| Race | |||
| White | 118 (66) | 115 (64) | 206 (93) |
| Other races | 54 (30) | 64 (36) | 14 (6) |
| Not collected or reported | 6 (3) | 1 (0.6) | 2 (1) |
| Body Surface Area (BSA, m 2) | |||
| Median (Max, Min) | 1.8 (1.4, 3.1) | 1.8 (1.3, 2.7) | 2 (1.3, 2.6) |
| Disease Type FL or MZL | |||
| Follicular lymphoma | 147 (83) | 148 (82) | 177 (80) |
| Marginal zone lymphoma | 31 (17) | 32 (18) | 45 (20) |
| MZL subtype at diagnosis (investigator), n (%) | |||
| MALT | 14 (45) | 16 (50) | 10 (22) |
| Nodal | 8 (26) | 10 (31) | 25 (56) |
| Splenic | 9 (29) | 6 (19) | 10 (22) |
| FL stage at diagnosis (investigator), n (%) | |||
| FL Grade 1 to 2 | 125 (85) | 123 (83) | 149 (84) |
| FL Grade 3a | 22 (15) | 25 (17) | 28 (16) |
| FLIPI score at baseline (calculated), n (%) | |||
| Low risk (0,1) | 52 (29) | 67 (37) | Not Collected |
| Intermediate risk (2) | 55 (31) | 58 (32) | |
| High risk (≥3) | 69 (39) | 54 (30) | |
| Missing | 2 (1) | 1 (0.6) | |
| ECOG score at baseline, n (%) | |||
| 0 | 116 (65) | 128 (71) | 102 (46) |
| 1 | 60 (34) | 50 (28) | 113 (51) |
| 2 | 2 (1) | 2 (1) | 7 (3) |
| High tumor burden
Defined by GELF criteria. at baseline, n (%)
|
|||
| Yes | 97 (54) | 86 (48) | 148 (67) |
| No | 81 (46) | 94 (52) | 74 (33) |
| Number of prior systemic antilymphoma therapies | |||
| 1 | 102 (57) | 97 (54) | 94 (42)
Patient had either 0 (n = 2) or 1 prior systemic therapy.
|
| >1 | 76 (43) | 83 (46) | 128 (58) |
Data Cutoff: 22 June 2018 (AUGMENT) and 1 May 2017 (MAGNIFY).
ECOG = Eastern Cooperative Oncology Group; FLIPI = follicular lymphoma international prognostic index
In AUGMENT, efficacy was established in the intent-to-treat (ITT) population based on progression-free survival by Independent Review Committee using modified 2007 International Working Group response criteria. Efficacy results are summarized in Table 22.
| Parameter |
Lenalidomide + Rituximab
(N = 178) |
Rituximab + Placebo
(N = 180) |
| PFS | ||
| Patients with event, n (%) | 68 (38.2) | 115 (63.9) |
| Death | 6 (8.8) | 2 (1.7) |
| Progression of disease | 62 (91.2) | 113 (98.3) |
| PFS, median
Median estimate is from Kaplan-Meier analysis. [95% CI] (months)
|
39.4 [ 22.9, NE] | 14.1 [11.4, 16.7] |
| HR
hazard ratio and its CI were estimated from Cox proportional hazard model adjusting for the stratification 3: previous rituximab treatment (yes, no), time since last antilymphoma therapy (≤2, >2 years), and disease histology (FL, MZL). [95% CI]
|
0.46 [ 0.34, 0.62] | |
| p-value
p-value from log-rank test stratified by 3 factors noted above: previous rituximab treatment (yes, no), time since last antilymphoma therapy (≤2, >2 years), and disease histology (FL, MZL).
|
<0.0001 | |
| Objective response (CR+PR), n(%)
[95% CI] Exact confidence interval for binomial distribution.
|
138 (77.5) [70.7, 83.4] | 96 (53.3) [45.8, 60.8] |
Kaplan-Meier Curves of Progression-free Survival by IRC Assessment Between Arms in AUGMENT Trial (ITT FL and MZL Population)
a = Stratification factors included: previous rituximab treatment (y/n), time since last anti-lymphoma therapy (≤2 years, >2 years), and disease histology (FL or MZL).
CI = confidence interval; HR = hazard ratio; KM = Kaplan-Meier; PFS = progression-free survival
Follicular Lymphoma
In AUGMENT, the objective response by IRC assessment for patients with follicular lymphoma was 80% (118/147) [95% CI: 73%, 86%]) in Lenalidomide with rituximab arm compared to 55% (82/148) [95% CI: 47, 64] in control arm.
In MAGNIFY, the overall response by investigator assessment was 59% (104/177) [95% CI: 51, 66] for patients with follicular lymphoma. Median duration of response was not reached with a median follow‑up time of 7.9 months [95% CI: 4.6, 9.2].
Marginal Zone Lymphoma
In AUGMENT, the objective response by IRC assessment for patients with marginal zone lymphoma was 65% (20/31) [95% CI: 45%, 81%] in Lenalidomide with rituximab arm compared to 44% (14/32) [95% CI: 26%, 62%] in control arm.
In MAGNIFY, the overall response by investigator assessment was 51% (23/45) [95% CI: 36, 66] for patients with marginal zone lymphoma. Median duration of response was not reached with a median follow‑up time of 11.5 months [95% CI: 8.0, 18.9].
5.5 Increased Mortality in Patients With Cll (5.5 Increased Mortality in Patients with CLL)
In a prospective randomized (1:1) clinical trial in the first line treatment of patients with chronic lymphocytic leukemia, single agent lenalidomide therapy increased the risk of death as compared to single agent chlorambucil. In an interim analysis, there were 34 deaths among 210 patients on the lenalidomide treatment arm compared to 18 deaths among 211 patients in the chlorambucil treatment arm, and hazard ratio for overall survival was 1.92 [95% CI: 1.08 to 3.41], consistent with a 92% increase in the risk of death. The trial was halted for safety in July 2013.
Serious adverse cardiovascular reactions, including atrial fibrillation, myocardial infarction, and cardiac failure occurred more frequently in the lenalidomide treatment arm. Lenalidomide is not indicated and not recommended for use in CLL outside of controlled clinical trials.
2.3 Recommended Dosage for Mantle Cell Lymphoma
The recommended starting dose of lenalidomide capsules is 25 mg/day orally on Days 1 to 21 of repeated 28-day cycles for relapsed or refractory mantle cell lymphoma. Treatment should be continued until disease progression or unacceptable toxicity.
Treatment is continued, modified or discontinued based upon clinical and laboratory findings.
Dose Adjustments for Hematologic Toxicities During MCL Treatment
Dose modification guidelines as summarized below are recommended to manage Grade 3 or 4 neutropenia or thrombocytopenia or other Grade 3 or 4 toxicities considered to be related to lenalidomide capsules.
Platelet counts
Thrombocytopenia during treatment in MCL
| When Platelets | Recommended Course |
| Fall below 50,000/mcL | Interrupt lenalidomide capsules treatment and follow CBC weekly |
| Return to at least 50,000/mcL | Resume lenalidomide capsules at 5 mg less than the previous dose. Do not dose below 5 mg daily |
Absolute Neutrophil counts (ANC)
Neutropenia during treatment in MCL
| When Neutrophils | Recommended Course |
| Fall below 1,000/mcL for at least 7 days
OR Falls below 1,000/mcL with an associated temperature at least 38.5°C OR Falls below 500/mcL |
Interrupt lenalidomide capsules treatment and follow CBC weekly |
| Return to at least 1,000/mcL | Resume lenalidomide capsules at 5 mg less than the previous dose. Do not dose below 5 mg daily |
8.3 Females and Males of Reproductive Potential
Pregnancy Testing
Lenalidomide can cause fetal harm when administered during pregnancy [see Use in Specific Populations (8.1)] . Verify the pregnancy status of females of reproductive potential prior to initiating lenalidomide therapy and during therapy. Advise females of reproductive potential that they must avoid pregnancy 4 weeks before therapy, while taking lenalidomide, during dose interruptions and for at least 4 weeks after completing therapy.
Females of reproductive potential must have 2 negative pregnancy tests before initiating lenalidomide. The first test should be performed within 10 days to 14 days, and the second test within 24 hours prior to prescribing lenalidomide. Once treatment has started and during dose interruptions, pregnancy testing for females of reproductive potential should occur weekly during the first 4 weeks of use, then pregnancy testing should be repeated every 4 weeks in females with regular menstrual cycles. If menstrual cycles are irregular, the pregnancy testing should occur every 2 weeks. Pregnancy testing and counseling should be performed if a patient misses her period or if there is any abnormality in her menstrual bleeding. Lenalidomide treatment must be discontinued during this evaluation.
Contraception
Females
Females of reproductive potential must commit either to abstain continuously from heterosexual sexual intercourse or to use 2 methods of reliable birth control simultaneously: one highly effective form of contraception – tubal ligation, IUD, hormonal (birth control pills, injections, hormonal patches, vaginal rings, or implants), or partner’s vasectomy, and 1 additional effective contraceptive method – male latex or synthetic condom, diaphragm, or cervical cap. Contraception must begin 4 weeks prior to initiating treatment with lenalidomide, during therapy, during dose interruptions, and continuing for 4 weeks following discontinuation of lenalidomide therapy. Reliable contraception is indicated even where there has been a history of infertility, unless due to hysterectomy. Females of reproductive potential should be referred to a qualified provider of contraceptive methods, if needed.
Males
Lenalidomide is present in the semen of males who take lenalidomide. Therefore, males must always use a latex or synthetic condom during any sexual contact with females of reproductive potential while taking lenalidomide and for up to 4 weeks after discontinuing lenalidomide, even if they have undergone a successful vasectomy. Male patients taking lenalidomide must not donate sperm and for up to 4 weeks after discontinuing lenalidomide.
2.2 Recommended Dosage for Myelodysplastic Syndromes
The recommended starting dose of lenalidomide capsules is 10 mg daily. Treatment is continued or modified based upon clinical and laboratory findings. Continue treatment until disease progression or unacceptable toxicity.
Dose Adjustments for Hematologic Toxicities During MDS Treatment
Patients who are dosed initially at 10 mg and who experience thrombocytopenia should have their dosage adjusted as follows:
Platelet counts
If thrombocytopenia develops WITHIN 4 weeks of starting treatment at 10 mg daily in MDS
| If baseline is at least 100,000/mcL | |
| When Platelets | Recommended Course |
| Fall below 50,000/mcL | Interrupt lenalidomide capsules treatment |
| Return to at least 50,000/mcL | Resume lenalidomide capsules at 5 mg daily |
| If baseline is below 100,000/mcL | |
| When Platelets | Recommended Course |
| Fall to 50% of the baseline value | Interrupt lenalidomide capsules treatment |
| If baseline is at least 60,000/mcL and returns to at least 50,000/mcL | Resume lenalidomide capsules at 5 mg daily |
| If baseline is below 60,000/mcL and returns to at least 30,000/mcL | Resume lenalidomide capsules at 5 mg daily |
If thrombocytopenia develops AFTER 4 weeks of starting treatment at 10 mg daily in MDS
| When Platelets | Recommended Course |
| Fall below 30,000/mcL or below 50,000/mcL with platelet transfusions | Interrupt lenalidomide capsules treatment |
| Return to at least 30,000/mcL (without hemostatic failure) | Resume lenalidomide capsules at 5 mg daily |
Patients who experience thrombocytopenia at 5 mg daily should have their dosage adjusted as follows:
If thrombocytopenia develops during treatment at 5 mg daily in MDS
| When Platelets | Recommended Course |
| Fall below 30,000/mcL or below 50,000/mcL with platelet transfusions | Interrupt lenalidomide capsules treatment |
| Return to at least 30,000/mcL (without hemostatic failure) | Resume lenalidomide capsules at 2.5 mg daily |
Patients who are dosed initially at 10 mg and experience neutropenia should have their dosage adjusted as follows:
Absolute Neutrophil counts (ANC)
If neutropenia develops WITHIN 4 weeks of starting treatment at 10 mg daily in MDS
| If baseline ANC is at least 1,000/mcL | |
| When Neutrophils | Recommended Course |
| Fall below 750/mcL | Interrupt lenalidomide capsules treatment |
| Return to at least 1,000/mcL | Resume lenalidomide capsules at 5 mg daily |
| If baseline ANC is below 1,000/mcL | |
| When Neutrophils | Recommended Course |
| Fall below 500/mcL | Interrupt lenalidomide capsules treatment |
| Return to at least 500/mcL | Resume lenalidomide capsules at 5 mg daily |
If neutropenia develops AFTER 4 weeks of starting treatment at 10 mg daily in MDS
| When Neutrophils | Recommended Course |
| Fall below 500/mcL for at least 7 days or below 500/mcL associated with fever (at least 38.5°C) | Interrupt lenalidomide capsules treatment |
| Return to at least 500/mcL | Resume lenalidomide capsules at 5 mg daily |
Patients who experience neutropenia at 5 mg daily should have their dosage adjusted as follows:
If neutropenia develops during treatment at 5 mg daily in MDS
| When Neutrophils | Recommended Course |
| Fall below 500/mcL for at least 7 days or below 500/mcL associated with fever (at least 38.5°C) | Interrupt lenalidomide capsules treatment |
| Return to at least 500/mcL | Resume lenalidomide capsules at 2.5 mg daily |
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenicity studies with lenalidomide have not been conducted.
Lenalidomide was not mutagenic in the bacterial reverse mutation assay (Ames test) and did not induce chromosome aberrations in cultured human peripheral blood lymphocytes, or mutations at the thymidine kinase (tk) locus of mouse lymphoma L5178Y cells. Lenalidomide did not increase morphological transformation in Syrian Hamster Embryo assay or induce micronuclei in the polychromatic erythrocytes of the bone marrow of male rats.
A fertility and early embryonic development study in rats, with administration of lenalidomide up to 500 mg/kg (approximately 200 times the human dose of 25 mg, based on body surface area) produced no parental toxicity and no adverse effects on fertility.
2.6 Recommended Dosage for Patients With Renal Impairment (2.6 Recommended Dosage for Patients with Renal Impairment)
The recommendations for dosing patients with renal impairment are shown in the following table [see Clinical Pharmacology (12.3)] .
|
Renal Function
(Cockcroft-Gault) |
Dose in Lenalidomide Capsules Combination Therapy for MM and MCL | Dose in Lenalidomide Capsules Combination Therapy for FL and MZL | Dose in Lenalidomide Capsules Maintenance Therapy Following Auto-HSCT for MM and for MDS |
| CLcr 30 mL/min to 60 mL/min | 10 mg once daily | 10 mg once daily | 5 mg once daily |
| CLcr below 30 mL/min (not requiring dialysis) | 15 mg every other day | 5 mg once daily | 2.5 mg once daily |
| CLcr below 30 mL/min (requiring dialysis) | 5 mg once daily. On dialysis days, administer the dose following dialysis. | 5 mg once daily. On dialysis days, administer the dose following dialysis. | 2.5 mg once daily. On dialysis days, administer the dose following dialysis. |
2.5 Dosage Modifications for Non Hematologic Adverse Reactions (2.5 Dosage Modifications for Non-Hematologic Adverse Reactions)
For non-hematologic Grade 3/4 toxicities judged to be related to lenalidomide capsules, hold treatment and restart at the physician's discretion at next lower dose level when toxicity has resolved to Grade 2 or below.
Permanently discontinue lenalidomide capsules for angioedema, anaphylaxis, Grade 4 rash, skin exfoliation, bullae, or any other severe dermatologic reactions [see Warnings and Precautions (5.9, 5.15)] .
7.2 Concomitant Therapies That May Increase the Risk of Thrombosis
Erythropoietic agents, or other agents that may increase the risk of thrombosis, such as estrogen containing therapies, should be used with caution after making a benefit-risk assessment in patients receiving lenalidomide [see Warnings and Precautions (5.4)] .
2.4 Recommended Dosage for Follicular Lymphoma Or Marginal Zone Lymphoma (2.4 Recommended Dosage for Follicular Lymphoma or Marginal Zone Lymphoma)
The recommended starting dose of lenalidomide capsules is 20 mg orally once daily on Days 1 to 21 of repeated 28-day cycles for up to 12 cycles of treatment in combination with a rituximab-product. Refer to Section 14.4 for specific rituximab dosing from the AUGMENT trial. For dose adjustments due to toxicity with rituximab, refer to the product prescribing information.
Dose Adjustments for Hematologic Toxicities during FL or MZL Treatment
Dose modification guidelines, as summarized below, are recommended to manage Grade 3 or 4 neutropenia or thrombocytopenia or other Grade 3 or 4 toxicity judged to be related to lenalidomide capsules.
Platelet counts
Thrombocytopenia during treatment in FL or MZL
| When Platelets | Recommended Course |
| Fall below 50,000/mcL | Interrupt lenalidomide capsules treatment and follow CBC weekly. |
|
Return to at least 50,000/mcL |
If patient starting dose was 20 mg daily, resume lenalidomide capsules at 5 mg less than the previous dose. Do not dose below 5 mg daily. If patient starting dose was 10 mg daily, resume at 5 mg less than previous dose. Do not dose below 2.5 mg daily. |
Absolute Neutrophil counts (ANC)
Neutropenia during treatment in FL or MZL
| When Neutrophils | Recommended Course |
|
Fall below 1,000/mcL for at least 7 days
OR
|
Interrupt lenalidomide capsules treatment and follow CBC weekly. |
| Return to at least 1,000/mcL |
If patient starting dose was 20 mg daily, resume lenalidomide capsules at 5 mg less than the previous dose. Do not dose below 5 mg daily.
|
14.2 Myelodysplastic Syndromes (mds) With A Deletion 5q Cytogenetic Abnormality (14.2 Myelodysplastic Syndromes (MDS) with a Deletion 5q Cytogenetic Abnormality)
The efficacy and safety of lenalidomide were evaluated in patients with transfusion-dependent anemia in low- or intermediate-1- risk MDS with a 5q (q31 to 33) cytogenetic abnormality in isolation or with additional cytogenetic abnormalities, at a dose of 10 mg once daily or 10 mg once daily for 21 days every 28 days in an open-label, single-arm, multi-center study. The major study was not designed nor powered to prospectively compare the efficacy of the 2 dosing regimens. Sequential dose reductions to 5 mg daily and 5 mg every other day, as well as dose delays, were allowed for toxicity [ Dosage and Administration (2.2)] .
This major study enrolled 148 patients who had RBC transfusion dependent anemia. RBC transfusion dependence was defined as having received ≥2 units of RBCs within 8 weeks prior to study treatment. The study enrolled patients with absolute neutrophil counts (ANC) ≥500/mm 3, platelet counts ≥50,000/mm 3, serum creatinine ≤2.5 mg/dL, serum SGOT/AST or SGPT/ALT ≤3x upper limit of normal (ULN), and serum direct bilirubin ≤2 mg/dL. Granulocyte colony-stimulating factor was permitted for patients who developed neutropenia or fever in association with neutropenia. Baseline patient and disease-related characteristics are summarized in Table 18.
|
Overall
(N = 148) |
||
| Age (years) | ||
| Median | 71 | |
| Min, Max | 37, 95 | |
| Gender | n | (%) |
| Male | 51 | (34.5) |
| Female | 97 | (65.5) |
| Race | n | (%) |
| White | 143 | (96.6) |
| Other | 5 | (3.4) |
| Duration of MDS (years) | ||
| Median | 2.5 | |
| Min, Max | 0.1, 20.7 | |
| Del 5 (q31 to 33) Cytogenetic Abnormality | n | (%) |
| Yes | 148 | (100) |
| Other cytogenetic abnormalities | 37 | (25.2) |
|
IPSS Score
IPSS Risk Category: Low (combined score = 0), Intermediate-1 (combined score = 0.5 to 1), Intermediate-2 (combined score = 1.5 to 2.0), High (combined score ≥ 2.5); Combined score = (Marrow blast score + Karyotype score + Cytopenia score).
|
n | (%) |
| Low (0) | 55 | (37.2) |
| Intermediate-1 (0.5 to 1.0) | 65 | (43.9) |
| Intermediate-2 (1.5 to 2.0) | 6 | (4.1) |
| High (≥2.5) | 2 | (1.4) |
| Missing | 20 | (13.5) |
|
FAB Classification
French-American-British (FAB) classification of MDS. from central review
|
n | (%) |
| RA | 77 | (52) |
| RARS | 16 | (10.8) |
| RAEB | 30 | (20.3) |
| CMML | 3 | (2) |
The frequency of RBC transfusion independence was assessed using criteria modified from the International Working Group (IWG) response criteria for MDS. RBC transfusion independence was defined as the absence of any RBC transfusion during any consecutive rolling 56 days (8 weeks) during the treatment period.
Transfusion independence was seen in 99/148 (67%) patients (95% CI [59, 74]). The median duration from the date when RBC transfusion independence was first declared (i.e., the last day of the 56-day RBC transfusion-free period) to the date when an additional transfusion was received after the 56-day transfusion-free period among the 99 responders was 44 weeks (range of 0 week to >67 weeks). Ninety percent of patients who achieved a transfusion benefit did so by completion of three months in the study.
RBC transfusion independence rates were unaffected by age or gender.
The dose of lenalidomide was reduced or interrupted at least once due to an adverse event in 118 (79.7%) of the 148 patients; the median time to the first dose reduction or interruption was 21 days (mean, 35.1 days; range, 2 days to 253 days), and the median duration of the first dose interruption was 22 days (mean, 28.5 days; range, 2 days to 265 days). A second dose reduction or interruption due to adverse events was required in 50 (33.8%) of the 148 patients. The median interval between the first and second dose reduction or interruption was 51 days (mean, 59.7 days; range, 15 days to 205 days) and the median duration of the second dose interruption was 21 days (mean, 26 days; range, 2 days to 148 days).
Warning: Embryo Fetal Toxicity, Hematologic Toxicity, and Venous and Arterial Thromboembolism (WARNING: EMBRYO-FETAL TOXICITY, HEMATOLOGIC TOXICITY, and VENOUS and ARTERIAL THROMBOEMBOLISM)
WARNING: EMBRYO-FETAL TOXICITY, HEMATOLOGIC TOXICITY, and VENOUS and ARTERIAL THROMBOEMBOLISM
See full prescribing information for complete boxed warning.
EMBRYO-FETAL TOXICITY
- Lenalidomide, a thalidomide analogue, caused limb abnormalities in a developmental monkey study similar to birth defects caused by thalidomide in humans. If lenalidomide is used during pregnancy, it may cause birth defects or embryo-fetal death.
- Pregnancy must be excluded before start of treatment. Prevent pregnancy during treatment by the use of two reliable methods of contraception ( 5.1).
Lenalidomide capsules are available only through a restricted distribution program, called the Lenalidomide REMS program ( 5.2, 17).
HEMATOLOGIC TOXICITY. Lenalidomide can cause significant neutropenia and thrombocytopenia ( 5.3).
VENOUS AND ARTERIAL THROMBOEMBOLISM
- Significantly increased risk of deep vein thrombosis (DVT) and pulmonary embolism (PE), as well as risk of myocardial infarction and stroke in patients with multiple myeloma receiving lenalidomide with dexamethasone. Anti-thrombotic prophylaxis is recommended ( 5.4).
5.7 Increased Mortality in Patients With Mm When Pembrolizumab Is Added to A Thalidomide Analogue and Dexamethasone (5.7 Increased Mortality in Patients with MM When Pembrolizumab Is Added to a Thalidomide Analogue and Dexamethasone)
In two randomized clinical trials in patients with MM, the addition of pembrolizumab to a thalidomide analogue plus dexamethasone, a use for which no PD-1 or PD-L1 blocking antibody is indicated, resulted in increased mortality. Treatment of patients with MM with a PD-1 or PD-L1 blocking antibody in combination with a thalidomide analogue plus dexamethasone is not recommended outside of controlled clinical trials.
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:51:55.266390 · Updated: 2026-03-14T22:42:19.657154