Etodolac Tablets, Usp
f86d2b22-d3f7-49cd-98f6-cdb2bd855192
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
Cardiovascular Thrombotic Events Nonsteroidal anti-inflammatory drugs (NSAIDs) cause an increased risk of serious cardiovascular thrombotic events, including myocardial infarction and stroke, which can be fatal. This risk may occur early in treatment and may increase with duration of use [see WARNINGS and PRECAUTIONS ]. Etodolac Tablets, 400 mg and 500 mg are contraindicated in the setting of coronary artery bypass graft (CABG) surgery [see CONTRAINDICATIONS and WARNINGS ]. Gastrointestinal Risk NSAIDs cause an increased risk of serious gastrointestinal adverse events including bleeding, ulceration, and perforation of the stomach or intestines, which can be fatal. These events can occur at any time during use and without warning symptoms. Elderly patients are at greater risk for serious gastrointestinal (GI) events. (See WARNINGS ).
Boxed Warning
Cardiovascular Thrombotic Events Nonsteroidal anti-inflammatory drugs (NSAIDs) cause an increased risk of serious cardiovascular thrombotic events, including myocardial infarction and stroke, which can be fatal. This risk may occur early in treatment and may increase with duration of use [see WARNINGS and PRECAUTIONS ]. Etodolac Tablets, 400 mg and 500 mg are contraindicated in the setting of coronary artery bypass graft (CABG) surgery [see CONTRAINDICATIONS and WARNINGS ]. Gastrointestinal Risk NSAIDs cause an increased risk of serious gastrointestinal adverse events including bleeding, ulceration, and perforation of the stomach or intestines, which can be fatal. These events can occur at any time during use and without warning symptoms. Elderly patients are at greater risk for serious gastrointestinal (GI) events. (See WARNINGS ).
Contraindications
Etodolac Tablets are contraindicated in patients with known hypersensitivity to etodolac or other ingredients in etodolac. Etodolac Tablets should not be given to patients who have experienced asthma, urticaria, or other allergic-type reactions after taking aspirin or other NSAIDs. Severe, rarely fatal, anaphylactic‑like reactions to NSAIDs have been reported in such patients (see WARNINGS, Anaphylactoid Reactions and PRECAUTIONS, Pre-existing Asthma ) In the setting of coronary artery bypass graft (CABG) surgery [see WARNINGS ]
Adverse Reactions
In patients taking Etodolac Tablets or other NSAIDs, the most frequently reported adverse experiences occurring in approximately 1 to 10% of patients are: Gastrointestinal experiences including : abdominal pain, constipation, diarrhea, dyspepsia, flatulence, gross bleeding/perforation, heartburn, nausea, GI ulcers (gastric/duodenal), vomiting. Other events including: abnormal renal function, anemia, dizziness, edema, elevated liver enzymes, headaches, increased bleeding time, pruritis, rashes, tinnitus. Adverse-reaction information for etodolac was derived from 2,629 arthritic patients treated with Etodolac Tablets in double-blind and open-label clinical trials of 4 to 320 weeks in duration and worldwide postmarketing surveillance studies. In clinical trials, most adverse reactions were mild and transient. The discontinuation rate in controlled clinical trials, because of adverse events, was up to 10% for patients treated with etodolac. New patient complaints (with an incidence greater than or equal to 1%) are listed below by body system. The incidences were determined from clinical trials involving 465 patients with osteoarthritis treated with 300 to 500 mg of etodolac b.i.d. (i.e., 600 to 1000 mg/day). Incidence Greater Than Or Equal To 1% - Probably Causally Related Body as a whole - Chills and fever. Digestive system - Dyspepsia (10%), abdominal pain 1 , diarrhea 1 , flatulence 1 , nausea 1 , abdominal distension, epigastric pain, abnormal stools, constipation, gastritis, melena, vomiting. Nervous system - Asthenia/malaise 1 , dizziness 1 , depression, nervousness, fatigue. Skin and appendages - Pruritus, rash. Special senses - Blurred vision, tinnitus. Urogenital system - Dysuria, urinary frequency. Musculoskeletal—Arthralgia. 1 Drug-related patient complaints occurring in 3 to 9% of patients treated with etodolac. Drug-related patient complaints occurring in fewer than 3%, but more than 1%, are unmarked. Incidence Less Than 1% - Probably Causally Related (Adverse reactions reported only in worldwide postmarketing experience, not seen in clinical trials, are considered rarer and are italicized.) Body as a whole - Allergic reaction, anaphylactic/anaphylactoid reactions (including shock). Cardiovascular system - Hypertension, congestive heart failure, flushing, palpitations, syncope, vasculitis (including necrotizing and allergic) . Digestive system - Thirst, dry mouth, ulcerative stomatitis, anorexia, eructation, elevated liver enzymes, cholestatic hepatitis , hepatitis, cholestatic jaundice , duodenitis , jaundice , hepatic failure , liver necrosis , peptic ulcer with or without bleeding and/or perforation, intestinal ulceration , pancreatitis . Hemic and lymphatic system - Ecchymosis, anemia, thrombocytopenia, bleeding time increased, agranulocytosis , hemolytic anemia , aplastic anemia , leukopenia , neutropenia , pancytopenia . Metabolic and nutritional - Edema, serum creatinine increase, hyperglycemia in previously controlled diabetic patients . Nervous system - Insomnia, somnolence. Respiratory system - Asthma, pulmonary infiltration with eosinophilia. Skin and appendages - Angioedema, sweating, urticaria, exfoliative dermatitis, vesiculobullous rash, cutaneous vasculitis with purpura , Stevens-Johnson Syndrome , toxic epidermal necrolysis , leukocytoclastic vasculitis , hyperpigmentation, erythema multiforme . Special senses - Photophobia, transient visual disturbances. Urogenital system - Elevated BUN, renal failure, renal insufficiency, renal papillary necrosis. Incidence Less Than 1% - Causal Relationship Unknown (Medical events occurring under circumstances where causal relationship to etodolac is uncertain. These reactions are listed as alerting information for physicians.) Body as a whole - Infection, headache. Cardiovascular system - Arrhythmias, myocardial infarction, cerebrovascular accident. Digestive system - Esophagitis with or without stricture or cardiospasm, colitis, GI discomfort, burning sensation, blood in stools, gastralgia, upper abdominal discomfort. Metabolic and nutritional - Change in weight. Nervous system - Paresthesia, confusion, irritability. Respiratory system - Bronchitis, bronchospasm, dyspnea, pharyngitis, rhinitis, sinusitis. Skin and appendages - Alopecia, maculopapular rash, photosensitivity, skin peeling. Special senses - Conjunctivitis, deafness, taste perversion, loss of taste. Urogenital system - Cystitis, hematuria, leukorrhea, renal calculus, interstitial nephritis, uterine bleeding irregularities, renal impairment. Musculoskeletal - Muscle pain. Additional Adverse Reactions Reported with NSAIDs Body as a whole - Sepsis, death Cardiovascular system - Tachycardia Digestive system - Gastric ulcers, gastritis, gastrointestinal bleeding, glossitis, hematemesis Hemic and lymphatic system - Lymphadenopathy Nervous system - Anxiety, dream abnormalities, convulsions, coma, hallucinations, meningitis, tremors, vertigo Respiratory system - Respiratory depression, pneumonia Urogenital system - Oliguria/polyuria, proteinuria
How Supplied
Etodolac Tablets, USP are available as: 400 mg tablets: Pink, oval shaped, film-coated tablet debossed with on one side and plain on the other side. - in bottles of 60, NDC 62135-910-60 500 mg tablets: Blue, oval shaped, film-coated tablet debossed with on one side and plain on the other side. - in bottles of 60, NDC 62135-911-60 Store at 20° to 25°C (68° to 77°F) [see USP Controlled Room Temperature]. Store tablets in original container until ready to use. Dispense in light-resistant container. Manufactured for: Chartwell RX, LLC Congers, NY 10920 L72316 Revised: 08/2024 Print Medication Guides at: www.chartwellpharma.com/medguides.
Medication Information
Boxed Warning
Cardiovascular Thrombotic Events
- Nonsteroidal anti-inflammatory drugs (NSAIDs) cause an increased risk of serious cardiovascular thrombotic events, including myocardial infarction and stroke, which can be fatal. This risk may occur early in treatment and may increase with duration of use [see WARNINGSand PRECAUTIONS].
- Etodolac Tablets, 400 mg and 500 mg are contraindicated in the setting of coronary artery bypass graft (CABG) surgery [see CONTRAINDICATIONSand WARNINGS].
Gastrointestinal Risk
- NSAIDs cause an increased risk of serious gastrointestinal adverse events including bleeding, ulceration, and perforation of the stomach or intestines, which can be fatal. These events can occur at any time during use and without warning symptoms. Elderly patients are at greater risk for serious gastrointestinal (GI) events. (See WARNINGS).
Contraindications
Etodolac Tablets are contraindicated in patients with known hypersensitivity to etodolac or other ingredients in etodolac.
Etodolac Tablets should not be given to patients who have experienced asthma, urticaria, or other allergic-type reactions after taking aspirin or other NSAIDs. Severe, rarely fatal, anaphylactic‑like reactions to NSAIDs have been reported in such patients (see WARNINGS, Anaphylactoid Reactions and PRECAUTIONS, Pre-existing Asthma)
- In the setting of coronary artery bypass graft (CABG) surgery [see WARNINGS ]
Adverse Reactions
In patients taking Etodolac Tablets or other NSAIDs, the most frequently reported adverse experiences occurring in approximately 1 to 10% of patients are:
Gastrointestinal experiences including: abdominal pain, constipation, diarrhea, dyspepsia, flatulence, gross bleeding/perforation, heartburn, nausea, GI ulcers (gastric/duodenal), vomiting.
Other events including:abnormal renal function, anemia, dizziness, edema, elevated liver enzymes, headaches, increased bleeding time, pruritis, rashes, tinnitus.
Adverse-reaction information for etodolac was derived from 2,629 arthritic patients treated with Etodolac Tablets in double-blind and open-label clinical trials of 4 to 320 weeks in duration and worldwide postmarketing surveillance studies. In clinical trials, most adverse reactions were mild and transient. The discontinuation rate in controlled clinical trials, because of adverse events, was up to 10% for patients treated with etodolac.
New patient complaints (with an incidence greater than or equal to 1%) are listed below by body system. The incidences were determined from clinical trials involving 465 patients with osteoarthritis treated with 300 to 500 mg of etodolac b.i.d. (i.e., 600 to 1000 mg/day).
Incidence Greater Than Or Equal To 1% - Probably Causally Related
Body as a whole - Chills and fever.
Digestive system - Dyspepsia (10%), abdominal pain 1, diarrhea 1, flatulence 1, nausea 1, abdominal distension, epigastric pain, abnormal stools, constipation, gastritis, melena, vomiting.
Nervous system - Asthenia/malaise 1, dizziness 1, depression, nervousness, fatigue.
Skin and appendages - Pruritus, rash.
Special senses - Blurred vision, tinnitus.
Urogenital system - Dysuria, urinary frequency.
Musculoskeletal—Arthralgia.
1Drug-related patient complaints occurring in 3 to 9% of patients treated with etodolac. Drug-related patient complaints occurring in fewer than 3%, but more than 1%, are unmarked.
Incidence Less Than 1% - Probably Causally Related
(Adverse reactions reported only in worldwide postmarketing experience, not seen in clinical trials, are considered rarer and are italicized.)
Body as a whole - Allergic reaction, anaphylactic/anaphylactoid reactions (including shock).
Cardiovascular system - Hypertension, congestive heart failure, flushing, palpitations, syncope, vasculitis (including necrotizing and allergic).
Digestive system - Thirst, dry mouth, ulcerative stomatitis, anorexia, eructation, elevated liver enzymes, cholestatic hepatitis, hepatitis, cholestatic jaundice, duodenitis, jaundice, hepatic failure, liver necrosis, peptic ulcer with or without bleeding and/or perforation, intestinal ulceration, pancreatitis.
Hemic and lymphatic system - Ecchymosis, anemia, thrombocytopenia, bleeding time increased, agranulocytosis, hemolytic anemia, aplastic anemia, leukopenia, neutropenia, pancytopenia.
Metabolic and nutritional - Edema, serum creatinine increase, hyperglycemia in previously controlled diabetic patients.
Nervous system - Insomnia, somnolence.
Respiratory system - Asthma, pulmonary infiltration with eosinophilia.
Skin and appendages - Angioedema, sweating, urticaria, exfoliative dermatitis, vesiculobullous rash, cutaneous vasculitis with purpura, Stevens-Johnson Syndrome, toxic epidermal necrolysis, leukocytoclastic vasculitis, hyperpigmentation, erythema multiforme.
Special senses - Photophobia, transient visual disturbances.
Urogenital system - Elevated BUN, renal failure, renal insufficiency, renal papillary necrosis.
Incidence Less Than 1% - Causal Relationship Unknown
(Medical events occurring under circumstances where causal relationship to etodolac is uncertain. These reactions are listed as alerting information for physicians.)
Body as a whole - Infection, headache.
Cardiovascular system - Arrhythmias, myocardial infarction, cerebrovascular accident.
Digestive system - Esophagitis with or without stricture or cardiospasm, colitis, GI discomfort, burning sensation, blood in stools, gastralgia, upper abdominal discomfort.
Metabolic and nutritional - Change in weight.
Nervous system - Paresthesia, confusion, irritability.
Respiratory system - Bronchitis, bronchospasm, dyspnea, pharyngitis, rhinitis, sinusitis.
Skin and appendages - Alopecia, maculopapular rash, photosensitivity, skin peeling.
Special senses - Conjunctivitis, deafness, taste perversion, loss of taste.
Urogenital system - Cystitis, hematuria, leukorrhea, renal calculus, interstitial nephritis, uterine bleeding irregularities, renal impairment.
Musculoskeletal - Muscle pain.
Additional Adverse Reactions Reported with NSAIDs
Body as a whole - Sepsis, death
Cardiovascular system - Tachycardia
Digestive system - Gastric ulcers, gastritis, gastrointestinal bleeding, glossitis, hematemesis
Hemic and lymphatic system - Lymphadenopathy
Nervous system - Anxiety, dream abnormalities, convulsions, coma, hallucinations, meningitis, tremors, vertigo
Respiratory system - Respiratory depression, pneumonia
Urogenital system - Oliguria/polyuria, proteinuria
How Supplied
Etodolac Tablets, USP are available as:
400 mg tablets: Pink, oval shaped, film-coated tablet debossed with
on one side and plain on the other side.- in bottles of 60, NDC 62135-910-60
500 mg tablets: Blue, oval shaped, film-coated tablet debossed with
on one side and plain on the other side.- in bottles of 60, NDC 62135-911-60
Store at 20° to 25°C (68° to 77°F) [see USP Controlled Room Temperature]. Store tablets in original container until ready to use. Dispense in light-resistant container.
Manufactured for:
Chartwell RX, LLC
Congers, NY 10920
L72316
Revised: 08/2024
Print Medication Guides at: www.chartwellpharma.com/medguides.
Description
Etodolac Tablets USP are members of the pyranocarboxylic acid group of nonsteroidal anti-inflammatory drugs (NSAIDs). Each tablet contains etodolac for oral administration. Etodolac is a racemic mixture of [+]S and [-]R-enantiomers. Etodolac is a white crystalline compound, insoluble in water but soluble in alcohols, chloroform, dimethyl sulfoxide, and aqueous polyethylene glycol.
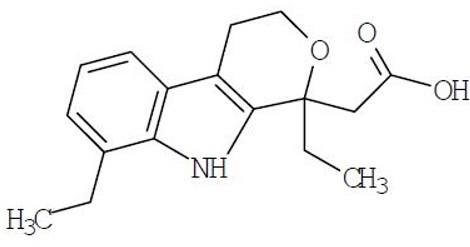
The chemical name is (±) 1,8-diethyl-1,3,4,9-tetrahydropyrano-[3,4-b]indole-1-acetic acid. The molecular weight of the base is 287.37. It has a pKa of 4.65 and an n-octanol: water partition coefficient of 11.4 at pH 7.4. The molecular formula for etodolac is C 17H 21NO 3, and it has the following structural formula:
Each tablet, for oral administration, contains 400 mg or 500 mg of etodolac. In addition, each tablet contains the following inactive ingredients: Hydroxypropyl Methylcellulose USP, Lactose Monohydrate NF, Magnesium Stearate, Microcrystalline Cellulose NF, Polyethylene Glycol, Povidone USP, Sodium Starch Glycolate NF and Titanium Dioxide. Also, each 400 mg tablet contains Iron Oxide Yellow and Iron Oxide Red. Each 500 mg tablet contains FD&C Indigo Carmine Aluminum Lake, Polysorbate 80 and Iron Oxide Red.
Section 42229-5
Distribution
The mean apparent volume of distribution (Vd/F) of etodolac is approximately 390 mL/kg. Etodolac is more than 99% bound to plasma proteins, primarily to albumin. The free fraction is less than 1% and is independent of etodolac total concentration over the dose range studied. It is not known whether etodolac is excreted in human milk; however, based on its physical-chemical properties, excretion into breast milk is expected. Data from in vitrostudies, using peak serum concentrations at reported therapeutic doses in humans, show that the etodolac free fraction is not significantly altered by acetaminophen, ibuprofen, indomethacin, naproxen, piroxicam, chlorpropamide, glipizide, glyburide, phenytoin, and probenecid.
Section 42231-1
Print Medication Guides at: www.chartwellpharma.com/medguides.
Medication Guide
What is the most important information I should know about medicines called Nonsteroidal Anti-inflammatory Drugs (NSAIDs)?
NSAIDs can cause serious side effects, including:
- Increased risk of a heart attack or stroke that can lead to death. This risk may happen early in treatment and may increase:
- with increasing doses of NSAIDs
- with longer use of NSAIDs
Do not take NSAIDs right before or after a heart surgery called a "coronary artery bypass graft (CABG)."
Avoid taking NSAIDs after a recent heart attack, unless your healthcare provider tells you to. You may have an increased risk of another heart attack if you take NSAIDs after a recent heart attack.
- Increased risk of bleeding, ulcers, and tears (perforation) of the esophagus (tube leading from the mouth to the stomach), stomach and intestines:
- anytime during use
- without warning symptoms
- that may cause death
The risk of getting an ulcer or bleeding increases with:
- past history of stomach ulcers, or stomach or intestinal bleeding with use of NSAIDs
- taking medicines called "corticosteroids", "anticoagulants", "SSRIs", or "SNRIs"
- increasing doses of NSAIDs
- longer use of NSAIDs
- smoking
- drinking alcohol
- older age
- poor health
- advanced liver disease
- bleeding problems
NSAIDs should only be used:
- exactly as prescribed
- at the lowest dose possible for your treatment
- for the shortest time needed
What are NSAIDs?
NSAIDs are used to treat pain and redness, swelling, and heat (inflammation) from medical conditions such as different types of arthritis, menstrual cramps, and other types of short-term pain.
Who should not take NSAIDs?
Do not take NSAIDs:
- if you have had an asthma attack, hives, or other allergic reaction with aspirin or any other NSAIDs.
- right before or after heart bypass surgery.
Before taking NSAIDs, tell your healthcare provider about all of your medical conditions, including if you:
- have liver or kidney problems
- have high blood pressure
- have asthma
- are pregnant or plan to become pregnant. Taking NSAIDs at about 20 weeks of pregnancy or later may harm your unborn baby. If you need to take NSAIDs for more than 2 days when you are between 20 and 30 weeks of pregnancy, your healthcare provider may need to monitor the amount of fluid in your womb around your baby. You should not take NSAIDs after about 30 weeks of pregnancy.
- are breastfeeding or plan to breast feed.
Tell your healthcare provider about all of the medicines you take, including prescription or over-the-counter medicines, vitamins or herbal supplements.NSAIDs and some other medicines can interact with each other and cause serious side effects. Do not start taking any new medicine without talking to your healthcare provider first.
What are the possible side effects of NSAIDs?
NSAIDs can cause serious side effects, including:
See "What is the most important information I should know about medicines called Nonsteroidal Anti-inflammatory Drugs (NSAIDs)?
- new or worse high blood pressure
- heart failure
- liver problems including liver failure
- kidney problems including kidney failure
- low red blood cells (anemia)
- life-threatening skin reactions
- life-threatening allergic reactions
- Other side effects of NSAIDs include:stomach pain, constipation, diarrhea, gas, heartburn, nausea, vomiting, and dizziness.
Get emergency help right away if you get any of the following symptoms:
- shortness of breath or trouble breathing
- chest pain
- weakness in one part or side of your body
- slurred speech
- swelling of the face or throat
Stop taking your NSAID and call your healthcare provider right away if you get any of the following symptoms:
- nausea
- more tired or weaker than usual
- diarrhea
- itching
- your skin or eyes look yellow
- indigestion or stomach pain
- flu-like symptoms
- vomit blood
- there is blood in your bowel movement or it is black and sticky like tar
- unusual weight gain
- skin rash or blisters with fever
- swelling of the arms, legs, hands and feet
If you take too much of your NSAID, call your healthcare provider or get medical help right away.
These are not all the possible side effects of NSAIDs. For more information, ask your healthcare provider or pharmacist about NSAIDs.
Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.
Other information about NSAIDs
- Aspirin is an NSAID but it does not increase the chance of a heart attack. Aspirin can cause bleeding in the brain, stomach, and intestines. Aspirin can also cause ulcers in the stomach and intestines.
- Some NSAIDs are sold in lower doses without a prescription (over-the-counter). Talk to your healthcare provider before using over-the-counter NSAIDs for more than 10 days.
General information about the safe and effective use of NSAIDs
Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide.
Do not use NSAIDs for a condition for which it was not prescribed. Do not give NSAIDs to other people, even if they have the same symptoms that you have. It may harm them.
If you would like more information about NSAIDs, talk with your healthcare provider. You can ask your pharmacist or healthcare provider for information about NSAIDs that is written for health professionals.
Manufactured for:
Chartwell RX, LLC.
Congers, NY 10920
This Medication Guide has been approved by the U.S. Food and Drug Administration.
L72317
Revised: 08/2024
Pregnancy
Risk Summary
Use of NSAIDs, including Etodolac Tablets, can cause premature closure of the fetal ductus arteriosus and fetal renal dysfunction leading to oligohydramnios and, in some cases, neonatal renal impairment. Because of these risks, limit dose and duration of Etodolac Tablets use between about 20 and 30 weeks of gestation, and avoid Etodolac Tablets use at about 30 weeks of gestation and later in pregnancy [see WARNINGS; Fetal Toxicity].
Premature Closure of Fetal Ductus Arteriosus
Use of NSAIDs, including Etodolac Tablets, at about 30 weeks gestation or later in pregnancy increases the risk of premature closure of the fetal ductus arteriosus.
Oligohydramnios/Neonatal Renal Impairment
Use of NSAIDs at about 20 weeks gestation or later in pregnancy has been associated with cases of fetal renal dysfunction leading to oligohydramnios, and in some cases, neonatal renal impairment.
Data from observational studies regarding other potential embryofetal risks of NSAID use in women in the first or second trimesters of pregnancy are inconclusive. In animal reproduction studies, isolated occurrences of alterations in limb development were found and included polydactly, oligodactyly, syndactyly, and unossified phalanges in rats and oligodactyly and synostosis of metatarsals in rabbits. These were observed at dose levels (2 to 14 mg/kg/day) close to human clinical doses. However, the frequency and the dosage group distribution of these findings in initial or repeated studies did not establish a clear drug or dose-response relationship. Animal reproduction studies are not always predictive of human response Based on animal data, prostaglandins have been shown to have an important role in endometrial vascular permeability, blastocyst implantation, and decidualization. In animal studies, administration of prostaglandin synthesis inhibitors such as Etodolac, resulted in increased pre- and post-implantation loss. Prostaglandins also have been shown to have an important role in fetal kidney development. In published animal studies, prostaglandin synthesis inhibitors have been reported to impair kidney development when administered at clinically relevant doses. The estimated background risk of major birth defects and miscarriage for the indicated population(s) is unknown. All pregnancies have a background risk of birth defect, loss, or other adverse outcomes. In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2-4% and 15-20%, respectively.
Clinical Considerations
Fetal/Neonatal Adverse Reactions
Premature Closure of Fetal Ductus Arteriosus:
Avoid use of NSAIDs in women at about 30 weeks gestation and later in pregnancy, because NSAIDs, including Etodolac Tablets, can cause premature closure of the fetal ductus arteriosus (see WARNINGS; Fetal Toxicity).
Oligohydramnios Neonatal Renal Impairment
If an NASAID is necessary at about 20 weeks gestation or later in pregnancy, limit the use to the lowest effective dose and shortest duration possible. If Etodolac Tablets treatment extends beyond 48 hours, consider monitoring with ultrasounds for oligohydramnios. If oligohyramnios occurs, discontinue Etodolac Tablets and follow up according to clinical practice (see WARNINGS; Fetal Toxicity).
Data
Human Data
There are no adequate, well-controlled studies in pregnant women. Etodolac tablets should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus.
Premature Closure of fetal Ductus Arteriosus:
Published literature reports that the use of NSAIDs at about 30 weeks of gestation and later in pregnancy may cause premature closure of the fetal ductus arteriosus.
Oligohydramnios Neonatal Renal Impairment:
Published studies and postmarketing reports describe maternal NSAID use at about 20 weeks gestation or later in pregnancy associated with fetal renal dysfunction leading to oligohydramnios, and in some cases, neonatal renal impairment. These adverse outcomes are seen, on average, after days to weeks of treatment, although oligohydramnios has been infrequently reported as soon as 48 hours after NSAID initiation. In many cases, but not all, the decrease in amniotic fluid was transient and reversible with cessation of the drug. There have been a limited number of case reports of maternal NSAID use and neonatal renal dysfunction without oligohydramnios, some of which were irreversible. Some cases of neonatal renal dysfunction required treatment with invasive procedures, such as exchange transfusion or dialysis.
Methodological limitations of these postmarketing studies and reports include lack of a control group; limited information regarding dose, duration, and timing of drug exposure; and concomitant use of other medications. These limitations preclude establishing a reliable estimate of the risk of adverse fetal and neonatal outcomes with maternal NSAID use. Because the published safety data on neonatal outcomes involved mostly preterm infants, the generalizability of certain reported risks to the full-term infant exposed to NSAIDs through maternal use is uncertain.
Absorption
The systemic bioavailability of etodolac from etodolac tablets is 100% as compared to solution and at least 80% as determined from mass balance studies. Etodolac is well absorbed and had a relative bioavailability of 100% when 200 mg capsules were compared with a solution of etodolac. Based on mass balance studies, the systemic availability of etodolac from the tablet formulation is at least 80%. Etodolac does not undergo significant first-pass metabolism following oral administration. Mean (± 1 SD) peak plasma concentrations (C max) range from approximately 14 ± 4 to 37 ± 9 µg/mL after 200 to 600 mg single doses and are reached in 80 ± 30 minutes (see Table 1 for summary of pharmacokinetic parameters). The dose-proportionality based on the area under the plasma concentration-time curve (AUC) is linear following doses up to 600 mg every 12 hours. Peak concentrations are dose proportional for both total and free etodolac following doses up to 400 mg every 12 hours, but following a 600 mg dose, the peak is about 20% higher than predicted on the basis of lower doses. The extent of absorption of etodolac is not affected when etodolac tablets are administered after a meal. Food intake, however, reduces the peak concentration reached by approximately one-half and increases the time to peak concentration by 1.4 to 3.8 hours.
|
Table 1: Mean (CV%) Pharmacokinetic Parameters of etodolac in Normal Healthy Adults and Various Special Populations |
||||||||
|
PK
|
Normal Healthy Adults (18-65)†
|
Healthy Males (18‑65)
|
Healthy Females (27-65)
|
Elderly (> 65)
|
Hemodialysis (24-65)
|
Renal Impairment
|
Hepatic Impairment
|
|
|
Dialysis On |
Dialysis
|
|||||||
|
T max, h |
1.4
|
1.4
|
1.7
|
1.2
|
1.7
|
0.9
|
2.1
|
1.1
|
|
Oral Clearance, mL/h/kg (CL/F) |
49.1
|
49.4
|
35.7
|
45.7
|
NA |
NA |
58.3
|
42.0
|
|
Apparent Volume of Distribution, mL/kg (Vd/F) |
393
|
394
|
300
|
414
|
NA |
NA |
NA |
NA |
|
Terminal Half-Life, h |
6.4
|
6.4
|
7.9
|
6.5
|
5.1
|
7.5
|
NA |
5.7
|
|
NA = not available
|
Overdosage
Symptoms following acute NSAID overdose are usually limited to lethargy, drowsiness, nausea, vomiting, and epigastric pain, which are generally reversible with supportive care. Gastrointestinal bleeding can occur and coma has occurred following massive ibuprofen or mefenamic-acid overdose. Hypertension, acute renal failure, and respiratory depression may occur but are rare. Anaphylactoid reactions have been reported with therapeutic ingestion of NSAIDs, and may occur following overdose. Patients should be managed by symptomatic and supportive care following an NSAID overdose.
There are no specific antidotes. Emesis and/or activated charcoal (60 to 100 g in adults, 1 to 2 g/kg in children) and/or osmotic cathartic may be indicated in patients seen within 4 hours of ingestion with symptoms or following a large overdose (5 to 10 times the usual dose). Forced diuresis, alkalinization of the urine, hemodialysis, or hemoperfusion would probably not be useful due to etodolac's high protein binding.
Geriatric Use
As with any NSAID, caution should be exercised in treating the elderly (65 years and older) and when increasing the dose (see WARNINGS ).
In Etodolac Tablets clinical studies, no overall differences in safety or effectiveness were observed between these patients and younger patients. In pharmacokinetic studies, age was shown not to have any effect on etodolac half-life or protein binding, and there was no change in expected drug accumulation. Therefore, no dosage adjustment is generally necessary in the elderly on the basis of pharmacokinetics (see CLINICAL PHARMACOLOGY, Special Populations).
Elderly patients may be more sensitive to the antiprostaglandin effects of NSAIDs (on the gastrointestinal tract and kidneys) than younger patients (see WARNINGS ). In particular, elderly or debilitated patients who receive NSAID therapy seem to tolerate gastrointestinal ulceration or bleeding less well than other individuals, and most spontaneous reports of fatal GI events are in this population.
Etodolac is eliminated primarily by the kidney. Because elderly patients are more likely to have decreased renal function, care should be taken in dose selection, and it may be useful to monitor renal function (see WARNINGS, Renal Effects).
Pediatric Use
Safety and effectiveness in pediatric patients below the age of 18 have not been established.
Clinical Trials
Nursing Mothers
Trace amounts of some NSAIDs have been reported in human milk. It is not known whether etodalac is excreted in human milk. Because many drugs are excreted in human milk and because of the potential for serious adverse reactions in nursing infants from Etodolac Tablets, a decision should be made whether to discontinue nursing or to discontinue the drug taking into account the importance of the drug to the mother.
Labor & Delivery
In rat studies with NSAIDs, as with other drugs known to inhibit prostaglandin synthesis, an increased incidence of dystocia, delayed parturition, and decreased pup survival occurred. The effects of Etodolac Tablets on labor and delivery in pregnant women are unknown.
Laboratory Tests
Because serious GI tract ulcerations and bleeding can occur without warning symptoms, physicians should monitor for signs or symptoms of GI bleeding. Patients on long-term treatment with NSAIDs should have their CBC and a chemistry profile checked periodically for signs or symptoms of anemia. Appropriate measures should be taken in case such signs of anemia occur. If clinical signs and symptoms consistent with liver or renal disease develop, systemic manifestations occur (e.g., eosinophilia, rash, etc.) or if abnormal liver tests persist or worsen, Etodolac Tablets should be discontinued.
Pharmacodynamics
Etodolac is a nonsteroidal anti-inflammatory drug (NSAID) that exhibits anti-inflammatory, analgesic, and antipyretic activities in animal models. The mechanism of action of etodolac, like that of other NSAIDs, is not completely understood, but may be related to the prostaglandin synthetase inhibition.
Etodolac is a racemic mixture of [-]R- and [+]S-etodolac. As with other NSAIDs, it has been demonstrated in animals that the [+]S-form is biologically active. Both enantiomers are stable and there is no [-]R to [+]S conversion in vivo.
General Precautions
Etodolac Tablets cannot be expected to substitute for corticosteroids or to treat corticosteroid insufficiency. Abrupt discontinuation of corticosteroids may lead to disease exacerbation. Patients on prolonged corticosteroid therapy should have their therapy tapered solely if a decision is made to discontinue corticosteroids.
The pharmacological activity of Etodolac Tablets in reducing fever and inflammation may diminish the utility of these diagnostic signs in detecting complications of presumed noninfectious, painful conditions.
Indications & Usage
Carefully consider the potential benefits and risks of Etodolac Tablets and other treatment options before deciding to use Etodolac Tablets. Use the lowest effective dose for the shortest duration consistent with individual patient treatment goals (see WARNINGS ).
Etodolac Tablets are indicated:
For acute and long-term use in the management of signs and symptoms of the following:
- Osteoarthritis
- Rheumatoid arthritis
- For the management of acute pain
Clinical Pharmacology
Dosage & Administration
Carefully consider the potential benefits and risks of Etodolac Tablets and other treatment options before deciding to use Etodolac Tablets. Use the lowest effective dose for the shortest duration consistent with individual patient treatment goals (see WARNINGS ).
After observing the response to initial therapy with Etodolac Tablets, the dose and frequency should be adjusted to suit an individual patient's needs.
Dosage adjustment of Etodolac Tablets is generally not required in patients with mild to moderate renal impairment. Etodolac should be used with caution in such patients, because, as with other NSAIDs, it may further decrease renal function in some patients with impaired renal function (see WARNINGS, Renal Effects ).
Analgesia
The recommended total daily dose of etodolac for acute pain is up to 1000 mg, given as 200 to 400 mg every 6 to 8 hours. Doses of etodolac greater than 1000 mg/day have not been adequately evaluated in well-controlled trials.
Osteoarthritis and Rheumatoid Arthritis
The recommended starting dose of etodolac for the management of the signs and symptoms of osteoarthritis or rheumatoid arthritis is: 300 mg b.i.d., t.i.d., 400 mg b.i.d., or 500 mg b.i.d. A lower dose of 600 mg/day may suffice for long-term administration. Physicians should be aware that doses above 1000 mg/day have not been adequately evaluated in well-controlled clinical trials.
In chronic conditions, a therapeutic response to therapy with etodolac is sometimes seen within one week of therapy, but most often is observed by two weeks. After a satisfactory response has been achieved, the patient's dose should be reviewed and adjusted as required.
Principal Display Panel
Etodolac Tablets, USP 400 mg - NDC 62135-910-60 - 60s Bottle Label
Etodolac Tablets, USP 500 mg - NDC 62135-911-60 - 60s Bottle Label
Information for Patients
Patients should be informed of the following information before initiating therapy with an NSAID and periodically during the course of ongoing therapy. Patients should also be encouraged to read the NSAID Medication Guide that accompanies each prescription dispensed.
-
Cardiovascular Thrombotic Events
Advise patients to be alert for the symptoms of cardiovascular thrombotic events, including chest pain, shortness of breath, weakness, or slurring of speech, and to report any of these symptoms to their health care provider immediately [see WARNINGS ]. - Etodolac Tablets, like other NSAIDs, can cause GI discomfort and, rarely, serious GI side effects, such as ulcers and bleeding, which may result in hospitalization and even death. Although serious GI tract ulcerations and bleeding can occur without warning symptoms, patients should be alert for the signs and symptoms of ulcerations and bleeding, and should ask for medical advice when observing any indicative sign or symptoms including epigastric pain, dyspepsia, melena, and hematemesis. Patients should be apprised of the importance of this follow-up (see WARNINGS, Gastrointestinal Effects - Risk of Ulceration, Bleeding, and Perforation).
- Serious Skin Reactions, including DRESS
Advise patients to stop taking Etodolac Tablets immediately if they develop any type of rash or fever and to contact their healthcare provider as soon as possible [see Warnings]. -
Heart Failure and Edema
Advise patients to be alert for the symptoms of congestive heart failure including shortness of breath, unexplained weight gain, or edema and to contact their healthcare provider if such symptoms occur [see WARNINGS ]. - Patients should be informed of the warning signs and symptoms of hepatotoxicity (e.g., nausea, fatigue, lethargy, pruritus, jaundice, right upper quadrant tenderness, and "flu-like" symptoms). If these occur, patients should be instructed to stop therapy and seek immediate medical therapy.
- Patients should be informed of the signs of an anaphylactoid reaction (e.g. difficulty breathing, swelling of the face or throat). If these occur, patients should be instructed to seek immediate emergency help (see WARNINGS ).
-
Fetal Toxicity
Inform pregnant women to avoid use of Etodolac Tablets and other NSAIDs starting at 30 weeks gestation because of the risk of the premature closing of the fetal ductus asteriosus. If treatment with Etodolac Tablets is needed for a pregnant woman between about 20 to 30 weeks gestation, advise her that she may need to be monitored for oligohydramnios, if treatment continues for longer than 48 hours [see WARNINGS; Fetal Toxicity, PRECAUTIONS; Pregnancy].
Drug & Or Laboratory Test Interactions
The urine of patients who take etodolac can give a false-positive reaction for urinary bilirubin (urobilin) due to the presence of phenolic metabolites of etodolac. Diagnostic dip-stick methodology, used to detect ketone bodies in urine, has resulted in false-positive findings in some patients treated with etodolac. Generally, this phenomenon has not been associated with other clinically significant events. No dose relationship has been observed.
Etodolac treatment is associated with a small decrease in serum uric acid levels. In clinical trials, mean decreases of 1 to 2 mg/dL were observed in arthritic patients receiving etodolac (600 to 1000 mg/day) after 4 weeks of therapy. These levels then remained stable for up to 1 year of therapy.
Carcinogenesis & Mutagenesis & Impairment of Fertility
No carcinogenic effect of etodolac was observed in mice or rats receiving oral doses of 15 mg/kg/day (45 to 89 mg/m 2, respectively) or less for periods of 2 years or 18 months, respectively. Etodolac was not mutagenic in in vitrotests performed with S. typhimuriumand mouse lymphoma cells as well as in an in vivomouse micronucleus test. However, data from the in vitrohuman peripheral lymphocyte test showed an increase in the number of gaps (3.0 to 5.3% unstained regions in the chromatid without dislocation) among the etodolac-treated cultures (50 to 200 µg/mL) compared to negative controls (2.0%); no other difference was noted between the controls and drug-treated groups. Etodolac showed no impairment of fertility in male and female rats up to oral doses of 16 mg/kg (94 mg/m 2). However, reduced implantation of fertilized eggs occurred in the 8 mg/kg group.
Structured Label Content
Section 42229-5 (42229-5)
Distribution
The mean apparent volume of distribution (Vd/F) of etodolac is approximately 390 mL/kg. Etodolac is more than 99% bound to plasma proteins, primarily to albumin. The free fraction is less than 1% and is independent of etodolac total concentration over the dose range studied. It is not known whether etodolac is excreted in human milk; however, based on its physical-chemical properties, excretion into breast milk is expected. Data from in vitrostudies, using peak serum concentrations at reported therapeutic doses in humans, show that the etodolac free fraction is not significantly altered by acetaminophen, ibuprofen, indomethacin, naproxen, piroxicam, chlorpropamide, glipizide, glyburide, phenytoin, and probenecid.
Section 42231-1 (42231-1)
Print Medication Guides at: www.chartwellpharma.com/medguides.
Medication Guide
What is the most important information I should know about medicines called Nonsteroidal Anti-inflammatory Drugs (NSAIDs)?
NSAIDs can cause serious side effects, including:
- Increased risk of a heart attack or stroke that can lead to death. This risk may happen early in treatment and may increase:
- with increasing doses of NSAIDs
- with longer use of NSAIDs
Do not take NSAIDs right before or after a heart surgery called a "coronary artery bypass graft (CABG)."
Avoid taking NSAIDs after a recent heart attack, unless your healthcare provider tells you to. You may have an increased risk of another heart attack if you take NSAIDs after a recent heart attack.
- Increased risk of bleeding, ulcers, and tears (perforation) of the esophagus (tube leading from the mouth to the stomach), stomach and intestines:
- anytime during use
- without warning symptoms
- that may cause death
The risk of getting an ulcer or bleeding increases with:
- past history of stomach ulcers, or stomach or intestinal bleeding with use of NSAIDs
- taking medicines called "corticosteroids", "anticoagulants", "SSRIs", or "SNRIs"
- increasing doses of NSAIDs
- longer use of NSAIDs
- smoking
- drinking alcohol
- older age
- poor health
- advanced liver disease
- bleeding problems
NSAIDs should only be used:
- exactly as prescribed
- at the lowest dose possible for your treatment
- for the shortest time needed
What are NSAIDs?
NSAIDs are used to treat pain and redness, swelling, and heat (inflammation) from medical conditions such as different types of arthritis, menstrual cramps, and other types of short-term pain.
Who should not take NSAIDs?
Do not take NSAIDs:
- if you have had an asthma attack, hives, or other allergic reaction with aspirin or any other NSAIDs.
- right before or after heart bypass surgery.
Before taking NSAIDs, tell your healthcare provider about all of your medical conditions, including if you:
- have liver or kidney problems
- have high blood pressure
- have asthma
- are pregnant or plan to become pregnant. Taking NSAIDs at about 20 weeks of pregnancy or later may harm your unborn baby. If you need to take NSAIDs for more than 2 days when you are between 20 and 30 weeks of pregnancy, your healthcare provider may need to monitor the amount of fluid in your womb around your baby. You should not take NSAIDs after about 30 weeks of pregnancy.
- are breastfeeding or plan to breast feed.
Tell your healthcare provider about all of the medicines you take, including prescription or over-the-counter medicines, vitamins or herbal supplements.NSAIDs and some other medicines can interact with each other and cause serious side effects. Do not start taking any new medicine without talking to your healthcare provider first.
What are the possible side effects of NSAIDs?
NSAIDs can cause serious side effects, including:
See "What is the most important information I should know about medicines called Nonsteroidal Anti-inflammatory Drugs (NSAIDs)?
- new or worse high blood pressure
- heart failure
- liver problems including liver failure
- kidney problems including kidney failure
- low red blood cells (anemia)
- life-threatening skin reactions
- life-threatening allergic reactions
- Other side effects of NSAIDs include:stomach pain, constipation, diarrhea, gas, heartburn, nausea, vomiting, and dizziness.
Get emergency help right away if you get any of the following symptoms:
- shortness of breath or trouble breathing
- chest pain
- weakness in one part or side of your body
- slurred speech
- swelling of the face or throat
Stop taking your NSAID and call your healthcare provider right away if you get any of the following symptoms:
- nausea
- more tired or weaker than usual
- diarrhea
- itching
- your skin or eyes look yellow
- indigestion or stomach pain
- flu-like symptoms
- vomit blood
- there is blood in your bowel movement or it is black and sticky like tar
- unusual weight gain
- skin rash or blisters with fever
- swelling of the arms, legs, hands and feet
If you take too much of your NSAID, call your healthcare provider or get medical help right away.
These are not all the possible side effects of NSAIDs. For more information, ask your healthcare provider or pharmacist about NSAIDs.
Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.
Other information about NSAIDs
- Aspirin is an NSAID but it does not increase the chance of a heart attack. Aspirin can cause bleeding in the brain, stomach, and intestines. Aspirin can also cause ulcers in the stomach and intestines.
- Some NSAIDs are sold in lower doses without a prescription (over-the-counter). Talk to your healthcare provider before using over-the-counter NSAIDs for more than 10 days.
General information about the safe and effective use of NSAIDs
Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide.
Do not use NSAIDs for a condition for which it was not prescribed. Do not give NSAIDs to other people, even if they have the same symptoms that you have. It may harm them.
If you would like more information about NSAIDs, talk with your healthcare provider. You can ask your pharmacist or healthcare provider for information about NSAIDs that is written for health professionals.
Manufactured for:
Chartwell RX, LLC.
Congers, NY 10920
This Medication Guide has been approved by the U.S. Food and Drug Administration.
L72317
Revised: 08/2024
Pregnancy (PREGNANCY)
Risk Summary
Use of NSAIDs, including Etodolac Tablets, can cause premature closure of the fetal ductus arteriosus and fetal renal dysfunction leading to oligohydramnios and, in some cases, neonatal renal impairment. Because of these risks, limit dose and duration of Etodolac Tablets use between about 20 and 30 weeks of gestation, and avoid Etodolac Tablets use at about 30 weeks of gestation and later in pregnancy [see WARNINGS; Fetal Toxicity].
Premature Closure of Fetal Ductus Arteriosus
Use of NSAIDs, including Etodolac Tablets, at about 30 weeks gestation or later in pregnancy increases the risk of premature closure of the fetal ductus arteriosus.
Oligohydramnios/Neonatal Renal Impairment
Use of NSAIDs at about 20 weeks gestation or later in pregnancy has been associated with cases of fetal renal dysfunction leading to oligohydramnios, and in some cases, neonatal renal impairment.
Data from observational studies regarding other potential embryofetal risks of NSAID use in women in the first or second trimesters of pregnancy are inconclusive. In animal reproduction studies, isolated occurrences of alterations in limb development were found and included polydactly, oligodactyly, syndactyly, and unossified phalanges in rats and oligodactyly and synostosis of metatarsals in rabbits. These were observed at dose levels (2 to 14 mg/kg/day) close to human clinical doses. However, the frequency and the dosage group distribution of these findings in initial or repeated studies did not establish a clear drug or dose-response relationship. Animal reproduction studies are not always predictive of human response Based on animal data, prostaglandins have been shown to have an important role in endometrial vascular permeability, blastocyst implantation, and decidualization. In animal studies, administration of prostaglandin synthesis inhibitors such as Etodolac, resulted in increased pre- and post-implantation loss. Prostaglandins also have been shown to have an important role in fetal kidney development. In published animal studies, prostaglandin synthesis inhibitors have been reported to impair kidney development when administered at clinically relevant doses. The estimated background risk of major birth defects and miscarriage for the indicated population(s) is unknown. All pregnancies have a background risk of birth defect, loss, or other adverse outcomes. In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2-4% and 15-20%, respectively.
Clinical Considerations
Fetal/Neonatal Adverse Reactions
Premature Closure of Fetal Ductus Arteriosus:
Avoid use of NSAIDs in women at about 30 weeks gestation and later in pregnancy, because NSAIDs, including Etodolac Tablets, can cause premature closure of the fetal ductus arteriosus (see WARNINGS; Fetal Toxicity).
Oligohydramnios Neonatal Renal Impairment
If an NASAID is necessary at about 20 weeks gestation or later in pregnancy, limit the use to the lowest effective dose and shortest duration possible. If Etodolac Tablets treatment extends beyond 48 hours, consider monitoring with ultrasounds for oligohydramnios. If oligohyramnios occurs, discontinue Etodolac Tablets and follow up according to clinical practice (see WARNINGS; Fetal Toxicity).
Data
Human Data
There are no adequate, well-controlled studies in pregnant women. Etodolac tablets should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus.
Premature Closure of fetal Ductus Arteriosus:
Published literature reports that the use of NSAIDs at about 30 weeks of gestation and later in pregnancy may cause premature closure of the fetal ductus arteriosus.
Oligohydramnios Neonatal Renal Impairment:
Published studies and postmarketing reports describe maternal NSAID use at about 20 weeks gestation or later in pregnancy associated with fetal renal dysfunction leading to oligohydramnios, and in some cases, neonatal renal impairment. These adverse outcomes are seen, on average, after days to weeks of treatment, although oligohydramnios has been infrequently reported as soon as 48 hours after NSAID initiation. In many cases, but not all, the decrease in amniotic fluid was transient and reversible with cessation of the drug. There have been a limited number of case reports of maternal NSAID use and neonatal renal dysfunction without oligohydramnios, some of which were irreversible. Some cases of neonatal renal dysfunction required treatment with invasive procedures, such as exchange transfusion or dialysis.
Methodological limitations of these postmarketing studies and reports include lack of a control group; limited information regarding dose, duration, and timing of drug exposure; and concomitant use of other medications. These limitations preclude establishing a reliable estimate of the risk of adverse fetal and neonatal outcomes with maternal NSAID use. Because the published safety data on neonatal outcomes involved mostly preterm infants, the generalizability of certain reported risks to the full-term infant exposed to NSAIDs through maternal use is uncertain.
Absorption
The systemic bioavailability of etodolac from etodolac tablets is 100% as compared to solution and at least 80% as determined from mass balance studies. Etodolac is well absorbed and had a relative bioavailability of 100% when 200 mg capsules were compared with a solution of etodolac. Based on mass balance studies, the systemic availability of etodolac from the tablet formulation is at least 80%. Etodolac does not undergo significant first-pass metabolism following oral administration. Mean (± 1 SD) peak plasma concentrations (C max) range from approximately 14 ± 4 to 37 ± 9 µg/mL after 200 to 600 mg single doses and are reached in 80 ± 30 minutes (see Table 1 for summary of pharmacokinetic parameters). The dose-proportionality based on the area under the plasma concentration-time curve (AUC) is linear following doses up to 600 mg every 12 hours. Peak concentrations are dose proportional for both total and free etodolac following doses up to 400 mg every 12 hours, but following a 600 mg dose, the peak is about 20% higher than predicted on the basis of lower doses. The extent of absorption of etodolac is not affected when etodolac tablets are administered after a meal. Food intake, however, reduces the peak concentration reached by approximately one-half and increases the time to peak concentration by 1.4 to 3.8 hours.
|
Table 1: Mean (CV%) Pharmacokinetic Parameters of etodolac in Normal Healthy Adults and Various Special Populations |
||||||||
|
PK
|
Normal Healthy Adults (18-65)†
|
Healthy Males (18‑65)
|
Healthy Females (27-65)
|
Elderly (> 65)
|
Hemodialysis (24-65)
|
Renal Impairment
|
Hepatic Impairment
|
|
|
Dialysis On |
Dialysis
|
|||||||
|
T max, h |
1.4
|
1.4
|
1.7
|
1.2
|
1.7
|
0.9
|
2.1
|
1.1
|
|
Oral Clearance, mL/h/kg (CL/F) |
49.1
|
49.4
|
35.7
|
45.7
|
NA |
NA |
58.3
|
42.0
|
|
Apparent Volume of Distribution, mL/kg (Vd/F) |
393
|
394
|
300
|
414
|
NA |
NA |
NA |
NA |
|
Terminal Half-Life, h |
6.4
|
6.4
|
7.9
|
6.5
|
5.1
|
7.5
|
NA |
5.7
|
|
NA = not available
|
Overdosage (OVERDOSAGE)
Symptoms following acute NSAID overdose are usually limited to lethargy, drowsiness, nausea, vomiting, and epigastric pain, which are generally reversible with supportive care. Gastrointestinal bleeding can occur and coma has occurred following massive ibuprofen or mefenamic-acid overdose. Hypertension, acute renal failure, and respiratory depression may occur but are rare. Anaphylactoid reactions have been reported with therapeutic ingestion of NSAIDs, and may occur following overdose. Patients should be managed by symptomatic and supportive care following an NSAID overdose.
There are no specific antidotes. Emesis and/or activated charcoal (60 to 100 g in adults, 1 to 2 g/kg in children) and/or osmotic cathartic may be indicated in patients seen within 4 hours of ingestion with symptoms or following a large overdose (5 to 10 times the usual dose). Forced diuresis, alkalinization of the urine, hemodialysis, or hemoperfusion would probably not be useful due to etodolac's high protein binding.
Description (DESCRIPTION)
Etodolac Tablets USP are members of the pyranocarboxylic acid group of nonsteroidal anti-inflammatory drugs (NSAIDs). Each tablet contains etodolac for oral administration. Etodolac is a racemic mixture of [+]S and [-]R-enantiomers. Etodolac is a white crystalline compound, insoluble in water but soluble in alcohols, chloroform, dimethyl sulfoxide, and aqueous polyethylene glycol.
The chemical name is (±) 1,8-diethyl-1,3,4,9-tetrahydropyrano-[3,4-b]indole-1-acetic acid. The molecular weight of the base is 287.37. It has a pKa of 4.65 and an n-octanol: water partition coefficient of 11.4 at pH 7.4. The molecular formula for etodolac is C 17H 21NO 3, and it has the following structural formula:
Each tablet, for oral administration, contains 400 mg or 500 mg of etodolac. In addition, each tablet contains the following inactive ingredients: Hydroxypropyl Methylcellulose USP, Lactose Monohydrate NF, Magnesium Stearate, Microcrystalline Cellulose NF, Polyethylene Glycol, Povidone USP, Sodium Starch Glycolate NF and Titanium Dioxide. Also, each 400 mg tablet contains Iron Oxide Yellow and Iron Oxide Red. Each 500 mg tablet contains FD&C Indigo Carmine Aluminum Lake, Polysorbate 80 and Iron Oxide Red.
How Supplied (HOW SUPPLIED)
Etodolac Tablets, USP are available as:
400 mg tablets: Pink, oval shaped, film-coated tablet debossed with
on one side and plain on the other side.- in bottles of 60, NDC 62135-910-60
500 mg tablets: Blue, oval shaped, film-coated tablet debossed with
on one side and plain on the other side.- in bottles of 60, NDC 62135-911-60
Store at 20° to 25°C (68° to 77°F) [see USP Controlled Room Temperature]. Store tablets in original container until ready to use. Dispense in light-resistant container.
Manufactured for:
Chartwell RX, LLC
Congers, NY 10920
L72316
Revised: 08/2024
Print Medication Guides at: www.chartwellpharma.com/medguides.
Boxed Warning (BOXED WARNING)
Cardiovascular Thrombotic Events
- Nonsteroidal anti-inflammatory drugs (NSAIDs) cause an increased risk of serious cardiovascular thrombotic events, including myocardial infarction and stroke, which can be fatal. This risk may occur early in treatment and may increase with duration of use [see WARNINGSand PRECAUTIONS].
- Etodolac Tablets, 400 mg and 500 mg are contraindicated in the setting of coronary artery bypass graft (CABG) surgery [see CONTRAINDICATIONSand WARNINGS].
Gastrointestinal Risk
- NSAIDs cause an increased risk of serious gastrointestinal adverse events including bleeding, ulceration, and perforation of the stomach or intestines, which can be fatal. These events can occur at any time during use and without warning symptoms. Elderly patients are at greater risk for serious gastrointestinal (GI) events. (See WARNINGS).
Geriatric Use (GERIATRIC USE)
As with any NSAID, caution should be exercised in treating the elderly (65 years and older) and when increasing the dose (see WARNINGS ).
In Etodolac Tablets clinical studies, no overall differences in safety or effectiveness were observed between these patients and younger patients. In pharmacokinetic studies, age was shown not to have any effect on etodolac half-life or protein binding, and there was no change in expected drug accumulation. Therefore, no dosage adjustment is generally necessary in the elderly on the basis of pharmacokinetics (see CLINICAL PHARMACOLOGY, Special Populations).
Elderly patients may be more sensitive to the antiprostaglandin effects of NSAIDs (on the gastrointestinal tract and kidneys) than younger patients (see WARNINGS ). In particular, elderly or debilitated patients who receive NSAID therapy seem to tolerate gastrointestinal ulceration or bleeding less well than other individuals, and most spontaneous reports of fatal GI events are in this population.
Etodolac is eliminated primarily by the kidney. Because elderly patients are more likely to have decreased renal function, care should be taken in dose selection, and it may be useful to monitor renal function (see WARNINGS, Renal Effects).
Pediatric Use (PEDIATRIC USE)
Safety and effectiveness in pediatric patients below the age of 18 have not been established.
Clinical Trials (CLINICAL TRIALS)
Nursing Mothers (NURSING MOTHERS)
Trace amounts of some NSAIDs have been reported in human milk. It is not known whether etodalac is excreted in human milk. Because many drugs are excreted in human milk and because of the potential for serious adverse reactions in nursing infants from Etodolac Tablets, a decision should be made whether to discontinue nursing or to discontinue the drug taking into account the importance of the drug to the mother.
Labor & Delivery (LABOR & DELIVERY)
In rat studies with NSAIDs, as with other drugs known to inhibit prostaglandin synthesis, an increased incidence of dystocia, delayed parturition, and decreased pup survival occurred. The effects of Etodolac Tablets on labor and delivery in pregnant women are unknown.
Laboratory Tests (LABORATORY TESTS)
Because serious GI tract ulcerations and bleeding can occur without warning symptoms, physicians should monitor for signs or symptoms of GI bleeding. Patients on long-term treatment with NSAIDs should have their CBC and a chemistry profile checked periodically for signs or symptoms of anemia. Appropriate measures should be taken in case such signs of anemia occur. If clinical signs and symptoms consistent with liver or renal disease develop, systemic manifestations occur (e.g., eosinophilia, rash, etc.) or if abnormal liver tests persist or worsen, Etodolac Tablets should be discontinued.
Pharmacodynamics
Etodolac is a nonsteroidal anti-inflammatory drug (NSAID) that exhibits anti-inflammatory, analgesic, and antipyretic activities in animal models. The mechanism of action of etodolac, like that of other NSAIDs, is not completely understood, but may be related to the prostaglandin synthetase inhibition.
Etodolac is a racemic mixture of [-]R- and [+]S-etodolac. As with other NSAIDs, it has been demonstrated in animals that the [+]S-form is biologically active. Both enantiomers are stable and there is no [-]R to [+]S conversion in vivo.
Adverse Reactions (ADVERSE REACTIONS)
In patients taking Etodolac Tablets or other NSAIDs, the most frequently reported adverse experiences occurring in approximately 1 to 10% of patients are:
Gastrointestinal experiences including: abdominal pain, constipation, diarrhea, dyspepsia, flatulence, gross bleeding/perforation, heartburn, nausea, GI ulcers (gastric/duodenal), vomiting.
Other events including:abnormal renal function, anemia, dizziness, edema, elevated liver enzymes, headaches, increased bleeding time, pruritis, rashes, tinnitus.
Adverse-reaction information for etodolac was derived from 2,629 arthritic patients treated with Etodolac Tablets in double-blind and open-label clinical trials of 4 to 320 weeks in duration and worldwide postmarketing surveillance studies. In clinical trials, most adverse reactions were mild and transient. The discontinuation rate in controlled clinical trials, because of adverse events, was up to 10% for patients treated with etodolac.
New patient complaints (with an incidence greater than or equal to 1%) are listed below by body system. The incidences were determined from clinical trials involving 465 patients with osteoarthritis treated with 300 to 500 mg of etodolac b.i.d. (i.e., 600 to 1000 mg/day).
Incidence Greater Than Or Equal To 1% - Probably Causally Related
Body as a whole - Chills and fever.
Digestive system - Dyspepsia (10%), abdominal pain 1, diarrhea 1, flatulence 1, nausea 1, abdominal distension, epigastric pain, abnormal stools, constipation, gastritis, melena, vomiting.
Nervous system - Asthenia/malaise 1, dizziness 1, depression, nervousness, fatigue.
Skin and appendages - Pruritus, rash.
Special senses - Blurred vision, tinnitus.
Urogenital system - Dysuria, urinary frequency.
Musculoskeletal—Arthralgia.
1Drug-related patient complaints occurring in 3 to 9% of patients treated with etodolac. Drug-related patient complaints occurring in fewer than 3%, but more than 1%, are unmarked.
Incidence Less Than 1% - Probably Causally Related
(Adverse reactions reported only in worldwide postmarketing experience, not seen in clinical trials, are considered rarer and are italicized.)
Body as a whole - Allergic reaction, anaphylactic/anaphylactoid reactions (including shock).
Cardiovascular system - Hypertension, congestive heart failure, flushing, palpitations, syncope, vasculitis (including necrotizing and allergic).
Digestive system - Thirst, dry mouth, ulcerative stomatitis, anorexia, eructation, elevated liver enzymes, cholestatic hepatitis, hepatitis, cholestatic jaundice, duodenitis, jaundice, hepatic failure, liver necrosis, peptic ulcer with or without bleeding and/or perforation, intestinal ulceration, pancreatitis.
Hemic and lymphatic system - Ecchymosis, anemia, thrombocytopenia, bleeding time increased, agranulocytosis, hemolytic anemia, aplastic anemia, leukopenia, neutropenia, pancytopenia.
Metabolic and nutritional - Edema, serum creatinine increase, hyperglycemia in previously controlled diabetic patients.
Nervous system - Insomnia, somnolence.
Respiratory system - Asthma, pulmonary infiltration with eosinophilia.
Skin and appendages - Angioedema, sweating, urticaria, exfoliative dermatitis, vesiculobullous rash, cutaneous vasculitis with purpura, Stevens-Johnson Syndrome, toxic epidermal necrolysis, leukocytoclastic vasculitis, hyperpigmentation, erythema multiforme.
Special senses - Photophobia, transient visual disturbances.
Urogenital system - Elevated BUN, renal failure, renal insufficiency, renal papillary necrosis.
Incidence Less Than 1% - Causal Relationship Unknown
(Medical events occurring under circumstances where causal relationship to etodolac is uncertain. These reactions are listed as alerting information for physicians.)
Body as a whole - Infection, headache.
Cardiovascular system - Arrhythmias, myocardial infarction, cerebrovascular accident.
Digestive system - Esophagitis with or without stricture or cardiospasm, colitis, GI discomfort, burning sensation, blood in stools, gastralgia, upper abdominal discomfort.
Metabolic and nutritional - Change in weight.
Nervous system - Paresthesia, confusion, irritability.
Respiratory system - Bronchitis, bronchospasm, dyspnea, pharyngitis, rhinitis, sinusitis.
Skin and appendages - Alopecia, maculopapular rash, photosensitivity, skin peeling.
Special senses - Conjunctivitis, deafness, taste perversion, loss of taste.
Urogenital system - Cystitis, hematuria, leukorrhea, renal calculus, interstitial nephritis, uterine bleeding irregularities, renal impairment.
Musculoskeletal - Muscle pain.
Additional Adverse Reactions Reported with NSAIDs
Body as a whole - Sepsis, death
Cardiovascular system - Tachycardia
Digestive system - Gastric ulcers, gastritis, gastrointestinal bleeding, glossitis, hematemesis
Hemic and lymphatic system - Lymphadenopathy
Nervous system - Anxiety, dream abnormalities, convulsions, coma, hallucinations, meningitis, tremors, vertigo
Respiratory system - Respiratory depression, pneumonia
Urogenital system - Oliguria/polyuria, proteinuria
Contraindications (CONTRAINDICATIONS)
Etodolac Tablets are contraindicated in patients with known hypersensitivity to etodolac or other ingredients in etodolac.
Etodolac Tablets should not be given to patients who have experienced asthma, urticaria, or other allergic-type reactions after taking aspirin or other NSAIDs. Severe, rarely fatal, anaphylactic‑like reactions to NSAIDs have been reported in such patients (see WARNINGS, Anaphylactoid Reactions and PRECAUTIONS, Pre-existing Asthma)
- In the setting of coronary artery bypass graft (CABG) surgery [see WARNINGS ]
General Precautions (GENERAL PRECAUTIONS)
Etodolac Tablets cannot be expected to substitute for corticosteroids or to treat corticosteroid insufficiency. Abrupt discontinuation of corticosteroids may lead to disease exacerbation. Patients on prolonged corticosteroid therapy should have their therapy tapered solely if a decision is made to discontinue corticosteroids.
The pharmacological activity of Etodolac Tablets in reducing fever and inflammation may diminish the utility of these diagnostic signs in detecting complications of presumed noninfectious, painful conditions.
Indications & Usage (INDICATIONS & USAGE)
Carefully consider the potential benefits and risks of Etodolac Tablets and other treatment options before deciding to use Etodolac Tablets. Use the lowest effective dose for the shortest duration consistent with individual patient treatment goals (see WARNINGS ).
Etodolac Tablets are indicated:
For acute and long-term use in the management of signs and symptoms of the following:
- Osteoarthritis
- Rheumatoid arthritis
- For the management of acute pain
Clinical Pharmacology (CLINICAL PHARMACOLOGY)
Dosage & Administration (DOSAGE & ADMINISTRATION)
Carefully consider the potential benefits and risks of Etodolac Tablets and other treatment options before deciding to use Etodolac Tablets. Use the lowest effective dose for the shortest duration consistent with individual patient treatment goals (see WARNINGS ).
After observing the response to initial therapy with Etodolac Tablets, the dose and frequency should be adjusted to suit an individual patient's needs.
Dosage adjustment of Etodolac Tablets is generally not required in patients with mild to moderate renal impairment. Etodolac should be used with caution in such patients, because, as with other NSAIDs, it may further decrease renal function in some patients with impaired renal function (see WARNINGS, Renal Effects ).
Analgesia
The recommended total daily dose of etodolac for acute pain is up to 1000 mg, given as 200 to 400 mg every 6 to 8 hours. Doses of etodolac greater than 1000 mg/day have not been adequately evaluated in well-controlled trials.
Osteoarthritis and Rheumatoid Arthritis
The recommended starting dose of etodolac for the management of the signs and symptoms of osteoarthritis or rheumatoid arthritis is: 300 mg b.i.d., t.i.d., 400 mg b.i.d., or 500 mg b.i.d. A lower dose of 600 mg/day may suffice for long-term administration. Physicians should be aware that doses above 1000 mg/day have not been adequately evaluated in well-controlled clinical trials.
In chronic conditions, a therapeutic response to therapy with etodolac is sometimes seen within one week of therapy, but most often is observed by two weeks. After a satisfactory response has been achieved, the patient's dose should be reviewed and adjusted as required.
Principal Display Panel (PRINCIPAL DISPLAY PANEL)
Etodolac Tablets, USP 400 mg - NDC 62135-910-60 - 60s Bottle Label
Etodolac Tablets, USP 500 mg - NDC 62135-911-60 - 60s Bottle Label
Information for Patients (INFORMATION FOR PATIENTS)
Patients should be informed of the following information before initiating therapy with an NSAID and periodically during the course of ongoing therapy. Patients should also be encouraged to read the NSAID Medication Guide that accompanies each prescription dispensed.
-
Cardiovascular Thrombotic Events
Advise patients to be alert for the symptoms of cardiovascular thrombotic events, including chest pain, shortness of breath, weakness, or slurring of speech, and to report any of these symptoms to their health care provider immediately [see WARNINGS ]. - Etodolac Tablets, like other NSAIDs, can cause GI discomfort and, rarely, serious GI side effects, such as ulcers and bleeding, which may result in hospitalization and even death. Although serious GI tract ulcerations and bleeding can occur without warning symptoms, patients should be alert for the signs and symptoms of ulcerations and bleeding, and should ask for medical advice when observing any indicative sign or symptoms including epigastric pain, dyspepsia, melena, and hematemesis. Patients should be apprised of the importance of this follow-up (see WARNINGS, Gastrointestinal Effects - Risk of Ulceration, Bleeding, and Perforation).
- Serious Skin Reactions, including DRESS
Advise patients to stop taking Etodolac Tablets immediately if they develop any type of rash or fever and to contact their healthcare provider as soon as possible [see Warnings]. -
Heart Failure and Edema
Advise patients to be alert for the symptoms of congestive heart failure including shortness of breath, unexplained weight gain, or edema and to contact their healthcare provider if such symptoms occur [see WARNINGS ]. - Patients should be informed of the warning signs and symptoms of hepatotoxicity (e.g., nausea, fatigue, lethargy, pruritus, jaundice, right upper quadrant tenderness, and "flu-like" symptoms). If these occur, patients should be instructed to stop therapy and seek immediate medical therapy.
- Patients should be informed of the signs of an anaphylactoid reaction (e.g. difficulty breathing, swelling of the face or throat). If these occur, patients should be instructed to seek immediate emergency help (see WARNINGS ).
-
Fetal Toxicity
Inform pregnant women to avoid use of Etodolac Tablets and other NSAIDs starting at 30 weeks gestation because of the risk of the premature closing of the fetal ductus asteriosus. If treatment with Etodolac Tablets is needed for a pregnant woman between about 20 to 30 weeks gestation, advise her that she may need to be monitored for oligohydramnios, if treatment continues for longer than 48 hours [see WARNINGS; Fetal Toxicity, PRECAUTIONS; Pregnancy].
Drug & Or Laboratory Test Interactions (DRUG & OR LABORATORY TEST INTERACTIONS)
The urine of patients who take etodolac can give a false-positive reaction for urinary bilirubin (urobilin) due to the presence of phenolic metabolites of etodolac. Diagnostic dip-stick methodology, used to detect ketone bodies in urine, has resulted in false-positive findings in some patients treated with etodolac. Generally, this phenomenon has not been associated with other clinically significant events. No dose relationship has been observed.
Etodolac treatment is associated with a small decrease in serum uric acid levels. In clinical trials, mean decreases of 1 to 2 mg/dL were observed in arthritic patients receiving etodolac (600 to 1000 mg/day) after 4 weeks of therapy. These levels then remained stable for up to 1 year of therapy.
Carcinogenesis & Mutagenesis & Impairment of Fertility (CARCINOGENESIS & MUTAGENESIS & IMPAIRMENT OF FERTILITY)
No carcinogenic effect of etodolac was observed in mice or rats receiving oral doses of 15 mg/kg/day (45 to 89 mg/m 2, respectively) or less for periods of 2 years or 18 months, respectively. Etodolac was not mutagenic in in vitrotests performed with S. typhimuriumand mouse lymphoma cells as well as in an in vivomouse micronucleus test. However, data from the in vitrohuman peripheral lymphocyte test showed an increase in the number of gaps (3.0 to 5.3% unstained regions in the chromatid without dislocation) among the etodolac-treated cultures (50 to 200 µg/mL) compared to negative controls (2.0%); no other difference was noted between the controls and drug-treated groups. Etodolac showed no impairment of fertility in male and female rats up to oral doses of 16 mg/kg (94 mg/m 2). However, reduced implantation of fertilized eggs occurred in the 8 mg/kg group.
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:51:02.104947 · Updated: 2026-03-14T22:39:05.457483