f1a10203-f027-4f9c-8dd6-907c6db24d47
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
Rx only
Indications and Usage
Severe essential hypertension when the drug cannot be given orally or when there is an urgent need to lower blood pressure.
Dosage and Administration
When there is urgent need, therapy in the hospitalized patient may be initiated intramuscularly or as a rapid intravenous bolus injection directly into the vein. Hydralazine Hydrochloride Injection should be used only when the drug cannot be given orally. The usual dose is 20 mg to 40 mg, repeated as necessary. Certain patients (especially those with marked renal damage) may require a lower dose. Blood pressure should be checked frequently. It may begin to fall within a few minutes after injection, with the average maximal decrease occurring in 10 minutes to 80 minutes. In cases where there has been increased intracranial pressure, lowering the blood pressure may increase cerebral ischemia. Most patients can be transferred to oral hydralazine hydrochloride within 24 hours to 48 hours. The product should be used immediately after the vial is opened. It should not be added to infusion solution. Hydralazine hydrochloride injection may discolor upon contact with metal; discolored solutions should be discarded. Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration, whenever solution and container permit. Discard unused portion.
Contraindications
Hypersensitivity to hydralazine, coronary artery disease; mitral valvular rheumatic heart disease.
Adverse Reactions
Adverse reactions with hydralazine hydrochloride injection are usually reversible when dosage is reduced. However, in some cases it may be necessary to discontinue the drug. The following adverse reactions have been observed, but there has not been enough systematic collection of data to support an estimate of their frequency. Common: Headache, anorexia, nausea, vomiting, diarrhea, palpitations, tachycardia, angina pectoris. Less Frequent: Digestive: constipation, paralytic ileus Cardiovascular : hypotension, paradoxical pressor response, edema Respiratory: dyspnea Neurologic: peripheral neuritis, evidenced by paresthesia, numbness, and tingling; dizziness; tremors; muscle cramps; psychotic reactions characterized by depression, disorientation, or anxiety Genitourinary: difficulty in urination Hematologic: blood dyscrasias, consisting of reduction in hemoglobin and red cell count, leukopenia, agranulocytosis, purpura; lymphadenopathy; splenomegaly Hypersensitive Reactions: rash, urticaria, pruritus, fever, chills, arthralgia, eosinophilia, and, rarely, hepatitis Other: nasal congestion, flushing, lacrimation, conjunctivitis To report SUSPECTED ADVERSE REACTIONS, contact Baxter Healthcare Corporation at 1-877-725-2747 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
Drug Interactions
MAO inhibitors should be used with caution in patients receiving hydralazine. When other potent parenteral antihypertensive drugs, such as diazoxide, are used in combination with hydralazine, patients should be continuously observed for several hours for any excessive fall in blood pressure. Profound hypotensive episodes may occur when diazoxide injection and hydralazine hydrochloride injection are used concomitantly.
How Supplied
1 ml single-dose vial containing 20 mg of hydralazine hydrochloride, USP and it is available as follows: 1 ml single-dose vial: NDC 43066-041-01 25 single-dose vials in a Carton: NDC 43066-041-25 Store at 20°C to 25°C (68°F to 77°F) [see USP Controlled Room Temperature]. Manufactured for: Baxter Healthcare Corporation Deerfield, IL 60015 USA Manufactured by: Immacule Lifesciences Private Limited, Village Thanthewal, Ropar Road, Nalagarh, Solan, Himachal Pradesh 174101, India (IND) Baxter is a registered trademark of Baxter International Inc. Rev. 2025-03-10 07-19-00-8443 10575 LEIA-312.00
Medication Information
Indications and Usage
Severe essential hypertension when the drug cannot be given orally or when there is an urgent need to lower blood pressure.
Dosage and Administration
When there is urgent need, therapy in the hospitalized patient may be initiated intramuscularly or as a rapid intravenous bolus injection directly into the vein. Hydralazine Hydrochloride Injection should be used only when the drug cannot be given orally. The usual dose is 20 mg to 40 mg, repeated as necessary. Certain patients (especially those with marked renal damage) may require a lower dose. Blood pressure should be checked frequently. It may begin to fall within a few minutes after injection, with the average maximal decrease occurring in 10 minutes to 80 minutes. In cases where there has been increased intracranial pressure, lowering the blood pressure may increase cerebral ischemia. Most patients can be transferred to oral hydralazine hydrochloride within 24 hours to 48 hours.
The product should be used immediately after the vial is opened. It should not be added to infusion solution.
Hydralazine hydrochloride injection may discolor upon contact with metal; discolored solutions should be discarded.
Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration, whenever solution and container permit.
Discard unused portion.
Contraindications
Hypersensitivity to hydralazine, coronary artery disease; mitral valvular rheumatic heart disease.
Adverse Reactions
Adverse reactions with hydralazine hydrochloride injection are usually reversible when dosage is reduced. However, in some cases it may be necessary to discontinue the drug.
The following adverse reactions have been observed, but there has not been enough systematic collection of data to support an estimate of their frequency.
Common: Headache, anorexia, nausea, vomiting, diarrhea, palpitations, tachycardia, angina pectoris.
Less Frequent: Digestive: constipation, paralytic ileus
Cardiovascular: hypotension, paradoxical pressor response, edema
Respiratory: dyspnea
Neurologic: peripheral neuritis, evidenced by paresthesia, numbness, and tingling; dizziness; tremors; muscle cramps; psychotic reactions characterized by depression, disorientation, or anxiety
Genitourinary: difficulty in urination
Hematologic: blood dyscrasias, consisting of reduction in hemoglobin and red cell count, leukopenia, agranulocytosis, purpura; lymphadenopathy; splenomegaly
Hypersensitive Reactions: rash, urticaria, pruritus, fever, chills, arthralgia, eosinophilia, and, rarely, hepatitis
Other: nasal congestion, flushing, lacrimation, conjunctivitis
To report SUSPECTED ADVERSE REACTIONS, contact Baxter Healthcare Corporation at 1-877-725-2747 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
Drug Interactions
MAO inhibitors should be used with caution in patients receiving hydralazine.
When other potent parenteral antihypertensive drugs, such as diazoxide, are used in combination with hydralazine, patients should be continuously observed for several hours for any excessive fall in blood pressure. Profound hypotensive episodes may occur when diazoxide injection and hydralazine hydrochloride injection are used concomitantly.
How Supplied
1 ml single-dose vial containing 20 mg of hydralazine hydrochloride, USP and it is available as follows:
1 ml single-dose vial: NDC 43066-041-01
25 single-dose vials in a Carton: NDC 43066-041-25
Store at 20°C to 25°C (68°F to 77°F) [see USP Controlled Room Temperature].
Manufactured for:
Baxter Healthcare Corporation
Deerfield, IL 60015 USA
Manufactured by:
Immacule Lifesciences Private Limited,
Village Thanthewal, Ropar Road, Nalagarh, Solan,
Himachal Pradesh 174101, India (IND)
Baxter is a registered trademark of Baxter International Inc.
Rev. 2025-03-10
07-19-00-8443
10575
LEIA-312.00
Description
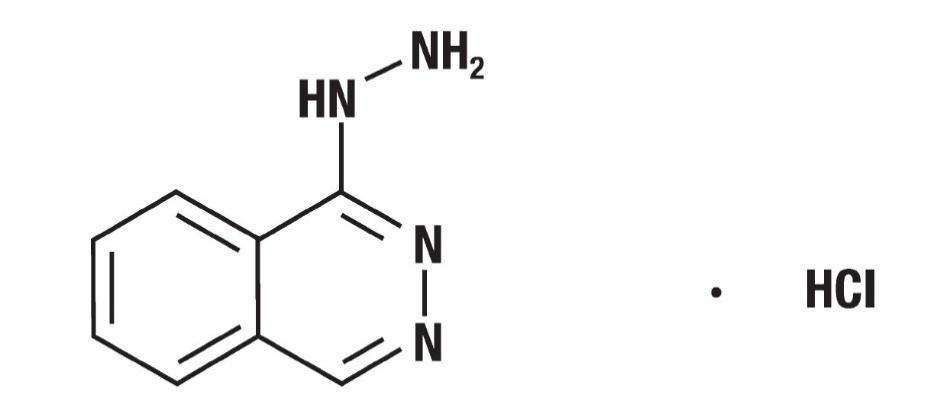
Hydralazine hydrochloride injection, USP is an antihypertensive available in 1 ml vial for intravenous and intramuscular administration. Each milliliter of the sterile, clear, and colorless solution contains hydralazine hydrochloride USP, 20 mg; methylparaben NF, 0.65 mg; propylparaben NF, 0.35 mg; propylene glycol USP, 103.6 mg. The pH of the solution is 3.4 to 4.0. Hydralazine hydrochloride, USP is 1-hydrazinophthalazine monohydrochloride, and its structural formula is:
Molecular formula – C8H8N4 · HCl
Hydralazine hydrochloride, USP is a white to off-white, crystalline powder. It is soluble in water, slightly soluble in alcohol, and very slightly soluble in ether. It melts at about 275°C, with decomposition, and has a molecular weight of 196.64 g/mol.
General
Myocardial stimulation produced by hydralazine hydrochloride injection can cause anginal attacks and ECG changes of myocardial ischemia. The drug has been implicated in the production of myocardial infarction. It must, therefore, be used with caution in patients with suspected coronary artery disease.
The “hyperdynamic” circulation caused by hydralazine hydrochloride injection may accentuate specific cardiovascular inadequacies. For example, hydralazine hydrochloride injection may increase pulmonary artery pressure in patients with mitral valvular disease. The drug may reduce the pressor responses to epinephrine. Postural hypotension may result from hydralazine hydrochloride injection but is less common than with ganglionic blocking agents. It should be used with caution in patients with cerebral vascular accidents.
In hypertensive patients with normal kidneys who are treated with hydralazine hydrochloride injection, there is evidence of increased renal blood flow and a maintenance of glomerular filtration rate. In some instances where control values were below normal, improved renal function has been noted after administration of hydralazine hydrochloride injection. However, as with any antihypertensive agent, hydralazine hydrochloride injection should be used with caution in patients with advanced renal damage.
Peripheral neuritis, evidenced by paresthesia, numbness, and tingling, has been observed. Published evidence suggests an antipyridoxine effect, and that pyridoxine should be added to the regimen if symptoms develop.
Warnings
In a few patients hydralazine may produce a clinical picture simulating systemic lupus erythematosus including glomerulonephritis. In such patients hydralazine should be discontinued unless the benefit-to-risk determination requires continued antihypertensive therapy with this drug. Symptoms and signs usually regress when the drug is discontinued but residua have been detected many years later. Long-term treatment with steroids may be necessary (see PRECAUTIONS, Laboratory Tests ).
Pregnancy
Teratogenic effects Animal studies indicate that hydralazine is teratogenic in mice at 20 times to 30 times the maximum daily human dose of 200 mg to 300 mg and possibly in rabbits at 10 times to 15 times the maximum daily human dose, but that it is nonteratogenic in rats. Teratogenic effects observed were cleft palate and malformations of facial and cranial bones.
There are no adequate and well-controlled studies in pregnant women. Although clinical experience does not include any positive evidence of adverse effects on the human fetus, hydralazine should be used during pregnancy only if the expected benefit justifies the potential risk to the fetus.
Overdosage
Acute Toxicity: No deaths due to acute poisoning have been reported.
Highest known dose survived: adults, 10 g orally.
Oral LD50 in rats: 173 mg/kg and 187 mg/kg.
Signs and Symptoms: Signs and symptoms of overdosage include hypotension, tachycardia, headache, and generalized skin flushing.
Complications can include myocardial ischemia and subsequent myocardial infarction, cardiac arrhythmia, and profound shock.
Treatment: There is no specific antidote.
Support of the cardiovascular system is of primary importance. Shock should be treated with plasma expanders. If possible, vasopressors should not be given, but if a vasopressor is required, care should be taken not to precipitate or aggravate cardiac arrhythmia. Tachycardia responds to beta blockers. Digitalization may be necessary, and renal function should be monitored and supported as required.
No experience has been reported with extracorporeal or peritoneal dialysis.
Pediatric Use
Safety and effectiveness in pediatric patients have not been established in controlled clinical trials, although there is experience with the use of hydralazine hydrochloride injection in children. The usual recommended parenteral dosage, administered intramuscularly or intravenously, is 1.7 mg/kg to 3.5 mg/kg of body weight daily, divided into four to six doses.
Nursing Mothers
Hydralazine has been shown to be excreted in breast milk.
Laboratory Tests
Complete blood counts and antinuclear antibody titer determinations are indicated before and periodically during prolonged therapy with hydralazine even though the patient is asymptomatic. These studies are also indicated if the patient develops arthralgia, fever, chest pain, continued malaise, or other unexplained signs or symptoms.
A positive antinuclear antibody titer requires that the physician carefully weigh the implications of the test results against the benefits to be derived from antihypertensive therapy with hydralazine.
Blood dyscrasias, consisting of reduction in hemoglobin and red cell count, leukopenia, agranulocytosis, and purpura, have been reported. If such abnormalities develop, therapy should be discontinued.
Clinical Pharmacology
Although the precise mechanism of action of hydralazine is not fully understood, the major effects are on the cardiovascular system. Hydralazine apparently lowers blood pressure by exerting a peripheral vasodilating effect through a direct relaxation of vascular smooth muscle. Hydralazine, by altering cellular calcium metabolism, interferes with the calcium movements within the vascular smooth muscle that are responsible for initiating or maintaining the contractile state.
The peripheral vasodilating effect of hydralazine results in decreased arterial blood pressure (diastolic more than systolic), decreased peripheral vascular resistance, and an increased heart rate, stroke volume, and cardiac output. The preferential dilatation of arterioles, as compared to veins, minimizes postural hypotension and promotes the increase in cardiac output. Hydralazine usually increases renin activity in plasma, presumably as a result of increased secretion of renin by the renal juxtaglomerular cells in response to reflex sympathetic discharge. This increase in renin activity leads to the production of angiotensin II, which then causes stimulation of aldosterone and consequent sodium reabsorption. Hydralazine also maintains or increases renal and cerebral blood flow.
The average maximal decrease in blood pressure usually occurs 10 to 80 minutes after administration of hydralazine hydrochloride injection. No other pharmacokinetic data on hydralazine hydrochloride injection are available.
Package/label Principal Display Panel
NDC 43066-041-01
Rx only
hydrALAZINE
Hydrochloride
Injection, USP
20 mg/mL
For Intramuscular or
Intravenous Use
1 mL Single-Dose Vial
NDC 43066-041-25
Rx only
hydrALAZINE
Hydrochloride Injection, USP
20 mg/mL
For Intramuscular or Intravenous Use
25 x 1 mL Single-Dose Vials
Baxter
Hydralazine Hydrochloride Injection, Usp
Rx only
Carcinogenesis, Mutagenesis, Impairment of Fertility
In a lifetime study in Swiss albino mice, there was a statistically significant increase in the incidence of lung tumors (adenomas and adenocarcinomas) of both male and female mice given hydralazine continuously in their drinking water at a dosage of about 250 mg/kg per day (about 80 times the maximum recommended human dose). In a 2-year carcinogenicity study of rats given hydralazine by gavage at dose levels of 15 mg/kg/day, 30 mg/kg/day, and 60 mg/kg/day (approximately 5 to 20 times the recommended human daily dosage), microscopic examination of the liver revealed a small, but statistically significant, increase in benign neoplastic nodules in male and female rats from the high-dose group and in female rats from the intermediate-dose group. Benign interstitial cell tumors of the testes were also significantly increased in male rats from the high-dose group. The tumors observed are common in aged rats and a significantly increased incidence was not observed until 18 months of treatment. Hydralazine was shown to be mutagenic in bacterial systems (Gene Mutation and DNA Repair) and in one of two rats and one rabbit hepatocyte in vitro DNA repair studies. Additional in vivo and in vitro studies using lymphoma cells, germinal cells, and fibroblasts from mice, bone marrow cells from chinese hamsters and fibroblasts from human cell lines did not demonstrate any mutagenic potential for hydralazine.
The extent to which these findings indicate a risk to man is uncertain. While long-term clinical observation has not suggested that human cancer is associated with hydralazine use, epidemiologic studies have so far been insufficient to arrive at any conclusions.
Structured Label Content
General
Myocardial stimulation produced by hydralazine hydrochloride injection can cause anginal attacks and ECG changes of myocardial ischemia. The drug has been implicated in the production of myocardial infarction. It must, therefore, be used with caution in patients with suspected coronary artery disease.
The “hyperdynamic” circulation caused by hydralazine hydrochloride injection may accentuate specific cardiovascular inadequacies. For example, hydralazine hydrochloride injection may increase pulmonary artery pressure in patients with mitral valvular disease. The drug may reduce the pressor responses to epinephrine. Postural hypotension may result from hydralazine hydrochloride injection but is less common than with ganglionic blocking agents. It should be used with caution in patients with cerebral vascular accidents.
In hypertensive patients with normal kidneys who are treated with hydralazine hydrochloride injection, there is evidence of increased renal blood flow and a maintenance of glomerular filtration rate. In some instances where control values were below normal, improved renal function has been noted after administration of hydralazine hydrochloride injection. However, as with any antihypertensive agent, hydralazine hydrochloride injection should be used with caution in patients with advanced renal damage.
Peripheral neuritis, evidenced by paresthesia, numbness, and tingling, has been observed. Published evidence suggests an antipyridoxine effect, and that pyridoxine should be added to the regimen if symptoms develop.
Warnings (WARNINGS)
In a few patients hydralazine may produce a clinical picture simulating systemic lupus erythematosus including glomerulonephritis. In such patients hydralazine should be discontinued unless the benefit-to-risk determination requires continued antihypertensive therapy with this drug. Symptoms and signs usually regress when the drug is discontinued but residua have been detected many years later. Long-term treatment with steroids may be necessary (see PRECAUTIONS, Laboratory Tests ).
Pregnancy
Teratogenic effects Animal studies indicate that hydralazine is teratogenic in mice at 20 times to 30 times the maximum daily human dose of 200 mg to 300 mg and possibly in rabbits at 10 times to 15 times the maximum daily human dose, but that it is nonteratogenic in rats. Teratogenic effects observed were cleft palate and malformations of facial and cranial bones.
There are no adequate and well-controlled studies in pregnant women. Although clinical experience does not include any positive evidence of adverse effects on the human fetus, hydralazine should be used during pregnancy only if the expected benefit justifies the potential risk to the fetus.
Overdosage (OVERDOSAGE)
Acute Toxicity: No deaths due to acute poisoning have been reported.
Highest known dose survived: adults, 10 g orally.
Oral LD50 in rats: 173 mg/kg and 187 mg/kg.
Signs and Symptoms: Signs and symptoms of overdosage include hypotension, tachycardia, headache, and generalized skin flushing.
Complications can include myocardial ischemia and subsequent myocardial infarction, cardiac arrhythmia, and profound shock.
Treatment: There is no specific antidote.
Support of the cardiovascular system is of primary importance. Shock should be treated with plasma expanders. If possible, vasopressors should not be given, but if a vasopressor is required, care should be taken not to precipitate or aggravate cardiac arrhythmia. Tachycardia responds to beta blockers. Digitalization may be necessary, and renal function should be monitored and supported as required.
No experience has been reported with extracorporeal or peritoneal dialysis.
Description (DESCRIPTION)
Hydralazine hydrochloride injection, USP is an antihypertensive available in 1 ml vial for intravenous and intramuscular administration. Each milliliter of the sterile, clear, and colorless solution contains hydralazine hydrochloride USP, 20 mg; methylparaben NF, 0.65 mg; propylparaben NF, 0.35 mg; propylene glycol USP, 103.6 mg. The pH of the solution is 3.4 to 4.0. Hydralazine hydrochloride, USP is 1-hydrazinophthalazine monohydrochloride, and its structural formula is:
Molecular formula – C8H8N4 · HCl
Hydralazine hydrochloride, USP is a white to off-white, crystalline powder. It is soluble in water, slightly soluble in alcohol, and very slightly soluble in ether. It melts at about 275°C, with decomposition, and has a molecular weight of 196.64 g/mol.
How Supplied (HOW SUPPLIED)
1 ml single-dose vial containing 20 mg of hydralazine hydrochloride, USP and it is available as follows:
1 ml single-dose vial: NDC 43066-041-01
25 single-dose vials in a Carton: NDC 43066-041-25
Store at 20°C to 25°C (68°F to 77°F) [see USP Controlled Room Temperature].
Manufactured for:
Baxter Healthcare Corporation
Deerfield, IL 60015 USA
Manufactured by:
Immacule Lifesciences Private Limited,
Village Thanthewal, Ropar Road, Nalagarh, Solan,
Himachal Pradesh 174101, India (IND)
Baxter is a registered trademark of Baxter International Inc.
Rev. 2025-03-10
07-19-00-8443
10575
LEIA-312.00
Pediatric Use
Safety and effectiveness in pediatric patients have not been established in controlled clinical trials, although there is experience with the use of hydralazine hydrochloride injection in children. The usual recommended parenteral dosage, administered intramuscularly or intravenously, is 1.7 mg/kg to 3.5 mg/kg of body weight daily, divided into four to six doses.
Nursing Mothers
Hydralazine has been shown to be excreted in breast milk.
Laboratory Tests
Complete blood counts and antinuclear antibody titer determinations are indicated before and periodically during prolonged therapy with hydralazine even though the patient is asymptomatic. These studies are also indicated if the patient develops arthralgia, fever, chest pain, continued malaise, or other unexplained signs or symptoms.
A positive antinuclear antibody titer requires that the physician carefully weigh the implications of the test results against the benefits to be derived from antihypertensive therapy with hydralazine.
Blood dyscrasias, consisting of reduction in hemoglobin and red cell count, leukopenia, agranulocytosis, and purpura, have been reported. If such abnormalities develop, therapy should be discontinued.
Adverse Reactions (ADVERSE REACTIONS)
Adverse reactions with hydralazine hydrochloride injection are usually reversible when dosage is reduced. However, in some cases it may be necessary to discontinue the drug.
The following adverse reactions have been observed, but there has not been enough systematic collection of data to support an estimate of their frequency.
Common: Headache, anorexia, nausea, vomiting, diarrhea, palpitations, tachycardia, angina pectoris.
Less Frequent: Digestive: constipation, paralytic ileus
Cardiovascular: hypotension, paradoxical pressor response, edema
Respiratory: dyspnea
Neurologic: peripheral neuritis, evidenced by paresthesia, numbness, and tingling; dizziness; tremors; muscle cramps; psychotic reactions characterized by depression, disorientation, or anxiety
Genitourinary: difficulty in urination
Hematologic: blood dyscrasias, consisting of reduction in hemoglobin and red cell count, leukopenia, agranulocytosis, purpura; lymphadenopathy; splenomegaly
Hypersensitive Reactions: rash, urticaria, pruritus, fever, chills, arthralgia, eosinophilia, and, rarely, hepatitis
Other: nasal congestion, flushing, lacrimation, conjunctivitis
To report SUSPECTED ADVERSE REACTIONS, contact Baxter Healthcare Corporation at 1-877-725-2747 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
Contraindications (CONTRAINDICATIONS)
Hypersensitivity to hydralazine, coronary artery disease; mitral valvular rheumatic heart disease.
Drug Interactions
MAO inhibitors should be used with caution in patients receiving hydralazine.
When other potent parenteral antihypertensive drugs, such as diazoxide, are used in combination with hydralazine, patients should be continuously observed for several hours for any excessive fall in blood pressure. Profound hypotensive episodes may occur when diazoxide injection and hydralazine hydrochloride injection are used concomitantly.
Clinical Pharmacology (CLINICAL PHARMACOLOGY)
Although the precise mechanism of action of hydralazine is not fully understood, the major effects are on the cardiovascular system. Hydralazine apparently lowers blood pressure by exerting a peripheral vasodilating effect through a direct relaxation of vascular smooth muscle. Hydralazine, by altering cellular calcium metabolism, interferes with the calcium movements within the vascular smooth muscle that are responsible for initiating or maintaining the contractile state.
The peripheral vasodilating effect of hydralazine results in decreased arterial blood pressure (diastolic more than systolic), decreased peripheral vascular resistance, and an increased heart rate, stroke volume, and cardiac output. The preferential dilatation of arterioles, as compared to veins, minimizes postural hypotension and promotes the increase in cardiac output. Hydralazine usually increases renin activity in plasma, presumably as a result of increased secretion of renin by the renal juxtaglomerular cells in response to reflex sympathetic discharge. This increase in renin activity leads to the production of angiotensin II, which then causes stimulation of aldosterone and consequent sodium reabsorption. Hydralazine also maintains or increases renal and cerebral blood flow.
The average maximal decrease in blood pressure usually occurs 10 to 80 minutes after administration of hydralazine hydrochloride injection. No other pharmacokinetic data on hydralazine hydrochloride injection are available.
Indications and Usage (INDICATIONS AND USAGE)
Severe essential hypertension when the drug cannot be given orally or when there is an urgent need to lower blood pressure.
Dosage and Administration (DOSAGE AND ADMINISTRATION)
When there is urgent need, therapy in the hospitalized patient may be initiated intramuscularly or as a rapid intravenous bolus injection directly into the vein. Hydralazine Hydrochloride Injection should be used only when the drug cannot be given orally. The usual dose is 20 mg to 40 mg, repeated as necessary. Certain patients (especially those with marked renal damage) may require a lower dose. Blood pressure should be checked frequently. It may begin to fall within a few minutes after injection, with the average maximal decrease occurring in 10 minutes to 80 minutes. In cases where there has been increased intracranial pressure, lowering the blood pressure may increase cerebral ischemia. Most patients can be transferred to oral hydralazine hydrochloride within 24 hours to 48 hours.
The product should be used immediately after the vial is opened. It should not be added to infusion solution.
Hydralazine hydrochloride injection may discolor upon contact with metal; discolored solutions should be discarded.
Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration, whenever solution and container permit.
Discard unused portion.
Package/label Principal Display Panel (PACKAGE/LABEL PRINCIPAL DISPLAY PANEL)
NDC 43066-041-01
Rx only
hydrALAZINE
Hydrochloride
Injection, USP
20 mg/mL
For Intramuscular or
Intravenous Use
1 mL Single-Dose Vial
NDC 43066-041-25
Rx only
hydrALAZINE
Hydrochloride Injection, USP
20 mg/mL
For Intramuscular or Intravenous Use
25 x 1 mL Single-Dose Vials
Baxter
Hydralazine Hydrochloride Injection, Usp (Hydralazine Hydrochloride Injection, USP)
Rx only
Carcinogenesis, Mutagenesis, Impairment of Fertility
In a lifetime study in Swiss albino mice, there was a statistically significant increase in the incidence of lung tumors (adenomas and adenocarcinomas) of both male and female mice given hydralazine continuously in their drinking water at a dosage of about 250 mg/kg per day (about 80 times the maximum recommended human dose). In a 2-year carcinogenicity study of rats given hydralazine by gavage at dose levels of 15 mg/kg/day, 30 mg/kg/day, and 60 mg/kg/day (approximately 5 to 20 times the recommended human daily dosage), microscopic examination of the liver revealed a small, but statistically significant, increase in benign neoplastic nodules in male and female rats from the high-dose group and in female rats from the intermediate-dose group. Benign interstitial cell tumors of the testes were also significantly increased in male rats from the high-dose group. The tumors observed are common in aged rats and a significantly increased incidence was not observed until 18 months of treatment. Hydralazine was shown to be mutagenic in bacterial systems (Gene Mutation and DNA Repair) and in one of two rats and one rabbit hepatocyte in vitro DNA repair studies. Additional in vivo and in vitro studies using lymphoma cells, germinal cells, and fibroblasts from mice, bone marrow cells from chinese hamsters and fibroblasts from human cell lines did not demonstrate any mutagenic potential for hydralazine.
The extent to which these findings indicate a risk to man is uncertain. While long-term clinical observation has not suggested that human cancer is associated with hydralazine use, epidemiologic studies have so far been insufficient to arrive at any conclusions.
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:48:22.000846 · Updated: 2026-03-14T22:29:41.730396