These Highlights Do Not Include All The Information Needed To Use Apidra Safely And Effectively. See Full Prescribing Information For Apidra.
e7af6a7a-8046-4fb4-9979-4ec4230b23aa
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
APIDRA is indicated to improve glycemic control in adult and pediatric patients with diabetes mellitus.
Indications and Usage
APIDRA is indicated to improve glycemic control in adult and pediatric patients with diabetes mellitus.
Dosage and Administration
See Full Prescribing Information for important administration instructions. ( 2.1 , 2.2 ) Individualize and adjust the dosage of APIDRA based on route of administration, individual's metabolic needs, blood glucose monitoring results, and glycemic control goal. ( 2.3 ) Dosage adjustments may be needed when switching from another insulin, with changes in physical activity, changes in concomitant medications, changes in meal patterns, changes in renal or hepatic function or during acute illness. ( 2.3 ) Subcutaneous Injection: ( 2.2 ) Inject within 15 minutes before a meal or within 20 minutes after starting a meal into the abdomen, thigh, or upper arm. Rotate injection sites within the same region to reduce the risk of lipodystrophy and localized cutaneous amyloidosis. Should generally be used in regimens with an intermediate or long-acting insulin. Continuous Subcutaneous Infusion (Insulin Pump): ( 2.2 ) Refer to the insulin infusion pump user manual to see if APIDRA can be used. Use in accordance with the insulin pump instructions for use. Administer by continuous subcutaneous infusion using an insulin pump in a region recommended in the instructions from the pump manufacturer. Rotate infusion sites within the same region to reduce the risk of lipodystrophy and localized cutaneous amyloidosis. Do not mix with other insulins or diluents in the pump. Intravenous Administration: Administer only under medical supervision after diluting to concentrations from 0.05 to 1 unit/mL APIDRA in 0.9% sodium chloride injection, USP using polyvinyl chloride infusion bags. ( 2.2 )
Warnings and Precautions
Never share an APIDRA SoloStar pen between patients, even if the needle is changed. ( 5.1 ) Hyperglycemia or Hypoglycemia with Changes in Insulin Regimen: Make changes to a patient's insulin regimen (e.g., insulin strength, manufacturer, type, injection site or method of administration) under close medical supervision with increased frequency of blood glucose monitoring. ( 5.2 ) Hypoglycemia: May be life-threatening. Increase frequency of glucose monitoring with changes to: insulin dosage, coadministered glucose lowering medications, meal pattern, physical activity; and in patients with renal impairment or hepatic impairment or hypoglycemia unawareness. ( 5.3 ) Hypoglycemia Due to Medication Errors: Accidental mix-ups between insulin products can occur. Instruct patients to check insulin labels before injection. ( 5.4 ) Hypokalemia: May be life-threatening. Monitor potassium levels in patients at risk for hypokalemia and treat if indicated. ( 5.5 ) Hypersensitivity Reactions: Severe, life-threatening, generalized allergy, including anaphylaxis, can occur. Discontinue APIDRA, monitor and treat if indicated. ( 5.6 ) Fluid Retention and Heart Failure Can Occur with Concomitant Use of Thiazolidinediones (TZDs): Observe for signs and symptoms of heart failure; consider dosage reduction or discontinuation of TZD if heart failure occurs. ( 5.7 ) Hyperglycemia and Ketoacidosis Due to Insulin Pump Device Malfunction: Monitor glucose and administer APIDRA by subcutaneous injection if pump malfunction occurs. ( 5.8 )
Contraindications
APIDRA is contraindicated: during episodes of hypoglycemia in patients with known hypersensitivity to insulin glulisine or to any of the excipients in APIDRA; systemic allergic reactions have occurred with APIDRA [see Adverse Reactions (6.1) ] .
Adverse Reactions
The following adverse reactions are discussed elsewhere: Hypoglycemia [see Warnings and Precautions (5.3) ] Hypoglycemia Due to Medication Errors [see Warnings and Precautions (5.4) ] Hypokalemia [see Warnings and Precautions (5.5) ] Hypersensitivity Reactions [see Warnings and Precautions (5.6) ]
Drug Interactions
Table 6: Clinically Significant Drug Interactions with APIDRA Drugs that May Increase the Risk of Hypoglycemia Drugs: Antidiabetic agents, ACE inhibitors, angiotensin II receptor blocking agents, disopyramide, fibrates, fluoxetine, monoamine oxidase inhibitors, pentoxifylline, pramlintide, salicylates, somatostatin analog (e.g., octreotide), and sulfonamide antibiotics. Intervention: Dose adjustment and increased frequency of glucose monitoring may be required when APIDRA is coadministered with these drugs. Drugs that May Decrease the Blood Glucose Lowering Effect of APIDRA Drugs: Atypical antipsychotics, corticosteroids, danazol, diuretics, estrogens, glucagon, isoniazid, niacin, phenothiazine derivatives, progestogens (e.g., in oral contraceptives), protease inhibitors, somatropin, sympathomimetic agents (e.g., albuterol, epinephrine, terbutaline), and thyroid hormones. Intervention: Dose adjustment and increased frequency of glucose monitoring may be required when APIDRA is coadministered with these drugs. Drugs that May Increase or Decrease the Blood Glucose Lowering Effect of APIDRA Drugs: Alcohol, beta-blockers, clonidine, and lithium salts. Pentamidine may cause hypoglycemia, which may sometimes be followed by hyperglycemia. Intervention: Dose adjustment and increased frequency of glucose monitoring may be required when APIDRA is coadministered with these drugs. Drugs that May Blunt Signs and Symptoms of Hypoglycemia Drugs: Beta-blockers, clonidine, guanethidine, and reserpine. Intervention: Increased frequency of glucose monitoring may be required when APIDRA is coadministered with these drugs.
How Supplied
APIDRA injection, 100 units/mL (U-100), is a clear and colorless solution available as: APIDRA NDC number Package size 10 mL multiple-dose vial 0088-2500-33 1 vial per carton 3 mL single-patient-use APIDRA SoloStar prefilled pen 0088-2502-05 5 pens per carton Pen needles are not included in the packs. SoloStar is compatible with all pen needles from Becton Dickinson and Company, Ypsomed, and Owen Mumford. The APIDRA SoloStar prefilled pen dials in 1-unit increments.
Medication Information
Warnings and Precautions
Never share an APIDRA SoloStar pen between patients, even if the needle is changed. ( 5.1 ) Hyperglycemia or Hypoglycemia with Changes in Insulin Regimen: Make changes to a patient's insulin regimen (e.g., insulin strength, manufacturer, type, injection site or method of administration) under close medical supervision with increased frequency of blood glucose monitoring. ( 5.2 ) Hypoglycemia: May be life-threatening. Increase frequency of glucose monitoring with changes to: insulin dosage, coadministered glucose lowering medications, meal pattern, physical activity; and in patients with renal impairment or hepatic impairment or hypoglycemia unawareness. ( 5.3 ) Hypoglycemia Due to Medication Errors: Accidental mix-ups between insulin products can occur. Instruct patients to check insulin labels before injection. ( 5.4 ) Hypokalemia: May be life-threatening. Monitor potassium levels in patients at risk for hypokalemia and treat if indicated. ( 5.5 ) Hypersensitivity Reactions: Severe, life-threatening, generalized allergy, including anaphylaxis, can occur. Discontinue APIDRA, monitor and treat if indicated. ( 5.6 ) Fluid Retention and Heart Failure Can Occur with Concomitant Use of Thiazolidinediones (TZDs): Observe for signs and symptoms of heart failure; consider dosage reduction or discontinuation of TZD if heart failure occurs. ( 5.7 ) Hyperglycemia and Ketoacidosis Due to Insulin Pump Device Malfunction: Monitor glucose and administer APIDRA by subcutaneous injection if pump malfunction occurs. ( 5.8 )
Indications and Usage
APIDRA is indicated to improve glycemic control in adult and pediatric patients with diabetes mellitus.
Dosage and Administration
See Full Prescribing Information for important administration instructions. ( 2.1 , 2.2 ) Individualize and adjust the dosage of APIDRA based on route of administration, individual's metabolic needs, blood glucose monitoring results, and glycemic control goal. ( 2.3 ) Dosage adjustments may be needed when switching from another insulin, with changes in physical activity, changes in concomitant medications, changes in meal patterns, changes in renal or hepatic function or during acute illness. ( 2.3 ) Subcutaneous Injection: ( 2.2 ) Inject within 15 minutes before a meal or within 20 minutes after starting a meal into the abdomen, thigh, or upper arm. Rotate injection sites within the same region to reduce the risk of lipodystrophy and localized cutaneous amyloidosis. Should generally be used in regimens with an intermediate or long-acting insulin. Continuous Subcutaneous Infusion (Insulin Pump): ( 2.2 ) Refer to the insulin infusion pump user manual to see if APIDRA can be used. Use in accordance with the insulin pump instructions for use. Administer by continuous subcutaneous infusion using an insulin pump in a region recommended in the instructions from the pump manufacturer. Rotate infusion sites within the same region to reduce the risk of lipodystrophy and localized cutaneous amyloidosis. Do not mix with other insulins or diluents in the pump. Intravenous Administration: Administer only under medical supervision after diluting to concentrations from 0.05 to 1 unit/mL APIDRA in 0.9% sodium chloride injection, USP using polyvinyl chloride infusion bags. ( 2.2 )
Contraindications
APIDRA is contraindicated: during episodes of hypoglycemia in patients with known hypersensitivity to insulin glulisine or to any of the excipients in APIDRA; systemic allergic reactions have occurred with APIDRA [see Adverse Reactions (6.1) ] .
Adverse Reactions
The following adverse reactions are discussed elsewhere: Hypoglycemia [see Warnings and Precautions (5.3) ] Hypoglycemia Due to Medication Errors [see Warnings and Precautions (5.4) ] Hypokalemia [see Warnings and Precautions (5.5) ] Hypersensitivity Reactions [see Warnings and Precautions (5.6) ]
Drug Interactions
Table 6: Clinically Significant Drug Interactions with APIDRA Drugs that May Increase the Risk of Hypoglycemia Drugs: Antidiabetic agents, ACE inhibitors, angiotensin II receptor blocking agents, disopyramide, fibrates, fluoxetine, monoamine oxidase inhibitors, pentoxifylline, pramlintide, salicylates, somatostatin analog (e.g., octreotide), and sulfonamide antibiotics. Intervention: Dose adjustment and increased frequency of glucose monitoring may be required when APIDRA is coadministered with these drugs. Drugs that May Decrease the Blood Glucose Lowering Effect of APIDRA Drugs: Atypical antipsychotics, corticosteroids, danazol, diuretics, estrogens, glucagon, isoniazid, niacin, phenothiazine derivatives, progestogens (e.g., in oral contraceptives), protease inhibitors, somatropin, sympathomimetic agents (e.g., albuterol, epinephrine, terbutaline), and thyroid hormones. Intervention: Dose adjustment and increased frequency of glucose monitoring may be required when APIDRA is coadministered with these drugs. Drugs that May Increase or Decrease the Blood Glucose Lowering Effect of APIDRA Drugs: Alcohol, beta-blockers, clonidine, and lithium salts. Pentamidine may cause hypoglycemia, which may sometimes be followed by hyperglycemia. Intervention: Dose adjustment and increased frequency of glucose monitoring may be required when APIDRA is coadministered with these drugs. Drugs that May Blunt Signs and Symptoms of Hypoglycemia Drugs: Beta-blockers, clonidine, guanethidine, and reserpine. Intervention: Increased frequency of glucose monitoring may be required when APIDRA is coadministered with these drugs.
How Supplied
APIDRA injection, 100 units/mL (U-100), is a clear and colorless solution available as: APIDRA NDC number Package size 10 mL multiple-dose vial 0088-2500-33 1 vial per carton 3 mL single-patient-use APIDRA SoloStar prefilled pen 0088-2502-05 5 pens per carton Pen needles are not included in the packs. SoloStar is compatible with all pen needles from Becton Dickinson and Company, Ypsomed, and Owen Mumford. The APIDRA SoloStar prefilled pen dials in 1-unit increments.
Description
APIDRA is indicated to improve glycemic control in adult and pediatric patients with diabetes mellitus.
Section 42229-5
Subcutaneous Injection
- Inject APIDRA subcutaneously within 15 minutes before a meal or within 20 minutes after starting a meal into the abdominal wall, thigh, or upper arm.
- Rotate injection sites within the same region from one injection to the next to reduce the risk of lipodystrophy and localized cutaneous amyloidosis. Do not inject into areas of lipodystrophy or localized cutaneous amyloidosis [see Warnings and Precautions (5.2), Adverse Reactions (6)].
- APIDRA given by subcutaneous injection should generally be used in regimens with an intermediate or long-acting insulin.
- The APIDRA SoloStar prefilled pen dials in 1-unit increments.
- Do not mix APIDRA for subcutaneous injection with insulins other than NPH insulin. If APIDRA is mixed with NPH insulin, draw APIDRA into the syringe first and inject immediately after mixing.
Section 42230-3
| PATIENT INFORMATION APIDRA® (uh PEE druh) (insulin glulisine) injection for subcutaneous use 100 units/mL (U-100) |
|
|---|---|
| This Patient Information has been approved by the U.S. Food and Drug Administration. | Revised: May 2025 |
| Do not share your APIDRA SoloStar® pen or syringes with other people, even if the needle has been changed. You may give other people a serious infection, or get a serious infection from them. | |
|
What is APIDRA?
APIDRA is a fast (rapid) acting man-made insulin used to control high blood sugar in adults and children with diabetes mellitus. |
|
|
Who should not use APIDRA? Do not use APIDRA if you:
|
|
|
What should I tell my healthcare provider before using APIDRA? Before using APIDRA, tell your healthcare provider about all your medical conditions including if you:
Before you start using APIDRA, talk to your healthcare provider about low blood sugar and how to manage it. |
|
How should I use APIDRA?
|
|
Your dose of APIDRA may need to change because of:
|
|
|
What should I avoid while using APIDRA? While using APIDRA do not:
|
|
|
What are the possible side effects of APIDRA? APIDRA may cause serious side effects that can lead to death, including:
|
|
|
General information about the safe and effective use of APIDRA.
Medicines are sometimes prescribed for purposes other than those listed in a Patient Information leaflet. Do not use APIDRA for a condition for which it was not prescribed. Do not give APIDRA to other people, even if they have the same symptoms that you have. It may harm them. This Patient Information leaflet summarizes the most important information about APIDRA. If you would like more information, talk with your healthcare provider. You can ask your healthcare provider or pharmacist for information about APIDRA that is written for health professionals. |
|
What are the ingredients in APIDRA?
|
|
| Manufactured by: sanofi-aventis U.S. LLC, Morristown, NJ 07960, A SANOFI COMPANY. U.S. License No. 1752 For more information, go to www.APIDRA.com or call 1-800-633-1610. |
Section 59845-8
Instructions for Use
APIDRA® 10 mL vial (100 Units/mL)
(insulin glulisine) injection
for subcutaneous use
These Instructions for Use contain information on how to inject APIDRA using the vial. Read these Instructions for Use before you start taking APIDRA and each time you get a new APIDRA vial. There may be new information. This information does not take the place of talking to your healthcare provider about your medical condition or your treatment.
Do not share your APIDRA syringes with other people, even if the needle has been changed. You may give other people a serious infection, or get a serious infection from them.
Supplies needed to give your injection
- an APIDRA 10 mL vial
- a U-100 insulin syringe and needle
- 2 alcohol swabs
- 1 sharps container for throwing away used needles and syringes. See "Disposing of used needles and syringes" at the end of these instructions.
Preparing your APIDRA dose
- Wash your hands with soap and water or clean your hands with alcohol.
- Check the APIDRA label to make sure that you are taking the right type of insulin. This is especially important if you use more than 1 type of insulin.
- Look at the APIDRA in the vial. It should look clear and colorless. Do not use this vial of APIDRA if the solution is colored, or cloudy, or if you see particles in it.
- Do not use APIDRA after the expiration date stamped on the label or 28 days after you first use it.
- Always use a syringe that is marked for U-100 insulin. If you use a syringe other than a U-100 insulin syringe, you may get the wrong dose of insulin.
- Always use a new syringe or needle for each injection to help prevent infections and prevent blocked needles. Do not reuse or share your syringes or needles with other people. You may give other people a serious infection or get a serious infection from them.
Step 1:
If you are using a new vial, remove the protective cap. Do not remove the stopper.
Step 2:
Wipe the rubber stopper with an alcohol swab. You do not have to shake the vial of APIDRA before use.
Step 3:
Draw air into the syringe equal to the insulin dose. Put the needle through the rubber top of the vial and push the plunger to inject the air into the vial.
Step 4:
Leave the syringe in the vial and turn both upside down. Hold the syringe and vial firmly in one hand. Make sure the tip of the needle is in the insulin. With your free hand, pull the plunger to withdraw the correct dose into the syringe.
Step 5:
Before you take the needle out of the vial, check the syringe for air bubbles. If you see bubbles in the syringe, hold the syringe straight up and tap the side of the syringe with your finger a few times to make any air bubbles float to the top. Gently push the air bubbles out with the plunger and draw insulin back into the syringe until you have the correct dose. If you are mixing APIDRA with NPH insulin, check with your healthcare provider on how to mix it the right way.
Step 6:
Remove the needle from the vial. Do not let the needle touch anything. You are now ready to inject.
Giving your APIDRA injection with a syringe
- Inject your insulin exactly as your healthcare provider has shown you.
- APIDRA starts acting fast, so give your injection within 15 minutes before or right after you eat a meal.
Step 7:
- Choose your injection site: APIDRA is injected under the skin (subcutaneously) of your upper arms, thighs, or stomach area (abdomen).
- Change (rotate) your injection sites within the area you choose for each dose to reduce your risk of getting lipodystrophy (pits in the skin or thickened skin) and localized cutaneous amyloidosis (skin with lumps) at the injection sites.
- Do not inject where the skin has pits, is thickened, or has lumps.
- Do not inject where the skin is tender, bruised, scaly or hard, or into scars or damaged skin.
- Wipe the skin with an alcohol swab to clean the injection site. Let the injection site dry before you inject.
Step 8:
- Pinch the skin.
- Insert the needle in the way your healthcare provider showed you.
- Release the skin.
- Slowly push in the plunger of the syringe all the way, making sure you have injected all the insulin.
- Leave the needle in the skin for about 10 seconds.
Step 9:
- Pull the needle straight out of your skin.
- Gently press the injection site for several seconds. Do not rub the area.
- Do not recap the used needle. Recapping the needle can lead to a needle-stick injury.
Giving your APIDRA using an insulin pump
- If you have been prescribed an insulin pump, check the pump manufacturer's user manual to see if APIDRA can be used with the pump.
- APIDRA should be given into an area of your body recommended in the instructions that come with your insulin pump.
- Change (rotate) your injection sites within the area you choose for each insertion to reduce your risk of getting lipodystrophy (pits in skin or thickened skin) and localized cutaneous amyloidosis (skin with lumps) at the injection sites. Do not inject into the exact same spot for each injection. Do not inject where the skin has pits, is thickened, or has lumps. Do not inject where the skin is tender, bruised, scaly or hard, or into scars or damaged skin.
- Call your healthcare provider and choose a new infusion site if the skin at the infusion site becomes red, itchy, or thickened.
- Change the insulin in the reservoir at least every 2 days or according to the pump user manual, whichever is shorter, even if you have not used all of the insulin.
- Do not dilute or mix APIDRA with other insulins in your insulin pump.
- You should be trained on how to give insulin by injection and have an alternative insulin delivery system in case of pump failure.
- When you start using APIDRA by infusion pump, your insulin dose may need to be adjusted. Check with your healthcare provider before making any changes to your insulin dose.
- Your healthcare provider should provide recommendations for appropriate pump basal and meal-time infusion rates. Call your healthcare provider if you have any questions about using the insulin pump.
Disposing of used needles and syringes
- Put your used needles and syringes in a FDA-cleared sharps disposal container right away after use. Do not throw away (dispose of) loose needles and syringes in your household trash.
- If you do not have a FDA-cleared sharps container, you may use a household container that is:
- made of a heavy-duty plastic,
- can be closed with a tight-fitting, puncture-resistant lid, without sharps being able to come out,
- upright and stable during use,
- leak resistant, and
- properly labeled to warn of hazardous waste inside the container.
- When your sharps disposal container is almost full, you will need to follow your community guidelines for the right way to dispose of your sharps disposal container. There may be state or local laws about how you should throw away used needles and syringes. For more information about safe sharps disposal, and for specific information about sharps disposal in the state that you live in, go to the FDA's website at: http://www.fda.gov/safesharpsdisposal.
- Do not dispose of your used sharps disposal container in your household trash unless your community guidelines permit this. Do not recycle your used sharps disposal container.
How should I store APIDRA 10 mL vial?
Unopened (not in-use) APIDRA vials
- Store unused APIDRA vials in the refrigerator from 36°F to 46°F (2°C to 8°C).
- Do not freeze APIDRA.
- Keep APIDRA away from direct heat and light.
- If a vial has been frozen or overheated, throw it away.
- Unopened vials can be used until the expiration date on the carton and label if they have been stored in the refrigerator.
- Unopened vials should be thrown away after 28 days if they are stored at room temperature.
After APIDRA vials have been opened (in-use)
- Store in-use (opened) APIDRA vials in a refrigerator from 36°F to 46°F (2°C to 8°C) or at room temperature below 77°F (25°C) for up to 28 days.
- Do not freeze APIDRA.
- Keep APIDRA out of direct heat and light.
- If a vial has been frozen, throw it away.
- The APIDRA vial you are using should be thrown away after 28 days, even if it still has insulin left in it.
APIDRA in an insulin pump
- Throw away APIDRA in the pump reservoir if it has been exposed to temperatures higher than 98.6°F (37°C). This may occur if the pump housing, cover, tubing, or sport case is exposed to sunlight or direct heat.
This Instructions for Use has been approved by the U.S. Food and Drug Administration.
Revised: May 2025
Manufactured by:
sanofi-aventis U.S. LLC
Morristown, NJ 07960
A SANOFI COMPANY
U.S. License No. 1752
©2025 sanofi-aventis U.S. LLC
16.2 Storage
Dispense in the original sealed carton with the enclosed Instructions for Use. Do not freeze.
Do not use after the expiration date (see carton and container).
Storage conditions are summarized in the following table:
| Not in-use (unopened) Refrigerated (36°F-46°F [2°C-8°C]). Protect from light |
Not in-use (unopened) Room Temperature (up to 77°F [25°C]) |
In-use (opened) (See temperature below) |
|
|---|---|---|---|
| 10 mL multiple-dose vial | Until expiration date | 28 days | 28 days The in-use time for multiple-dose vial is either 28 days at room temperature up to 77°F (25°C) or 48 hours in insulin pump up to 98.6°F (37°C). , Refrigerated or room temperature |
| 3 mL single-patient-use APIDRA SoloStar prefilled pen | Until expiration date | 28 days | 28 days, Room temperature (Do not refrigerate) |
10 Overdosage
Excess insulin may cause hypoglycemia and, particularly when given intravenously, hypokalemia. Mild episodes of hypoglycemia usually can be treated with oral glucose. Adjustments in drug dosage, meal patterns, or exercise may be needed. More severe episodes of hypoglycemia with coma, seizure, or neurologic impairment may be treated with a glucagon product for emergency use or concentrated intravenous glucose. Sustained carbohydrate intake and observation may be necessary because hypoglycemia may recur after apparent clinical recovery. Hypokalemia must be corrected appropriately.
11 Description
Insulin glulisine is a rapid-acting human insulin analog used to lower blood glucose. Insulin glulisine is produced by recombinant DNA technology utilizing a non-pathogenic laboratory strain of Escherichia coli (K12). Insulin glulisine differs from human insulin in that the amino acid asparagine at position B3 is replaced by lysine and the lysine in position B29 is replaced by glutamic acid. Insulin glulisine has a molecular weight of 5.823 kDa.
APIDRA (insulin glulisine) injection is a sterile, aqueous, clear, and colorless solution for subcutaneous or intravenous use. Each milliliter of APIDRA contains 100 units insulin glulisine, metacresol (3.15 mg), polysorbate 20 (0.01 mg), sodium chloride (5 mg), tromethamine (6 mg), and water for injection. APIDRA has a pH of approximately 7.3. The pH is adjusted by addition of aqueous solutions of hydrochloric acid and/or sodium hydroxide.
5.5 Hypokalemia
All insulins, including APIDRA, cause a shift in potassium from the extracellular to intracellular space, possibly leading to hypokalemia. Untreated hypokalemia may cause respiratory paralysis, ventricular arrhythmia, and death. Use caution in patients who may be at risk for hypokalemia (e.g., patients using potassium-lowering medications, patients taking medications sensitive to serum potassium concentrations).
5.3 Hypoglycemia
Hypoglycemia is the most common adverse reaction of all insulins, including APIDRA [see Adverse Reactions (6.1)]. Severe hypoglycemia can cause seizures, may lead to unconsciousness, may be life-threatening, or cause death. Hypoglycemia can impair concentration ability and reaction time; this may place the patient and others at risk in situations where these abilities are important (e.g., driving or operating other machinery). APIDRA, or any insulin, should not be used during episodes of hypoglycemia [see Contraindications (4)].
Hypoglycemia can happen suddenly, and symptoms may differ in each patient and change over time in the same patient. Symptomatic awareness of hypoglycemia may be less pronounced in patients with longstanding diabetes, in patients with diabetic neuropathy, in patients using medications that block the sympathetic nervous system (e.g., beta-blockers) [see Drug Interactions (7)], or in patients who experience recurrent hypoglycemia.
16.1 How Supplied
APIDRA injection, 100 units/mL (U-100), is a clear and colorless solution available as:
| APIDRA | NDC number | Package size |
|---|---|---|
| 10 mL multiple-dose vial | 0088-2500-33 | 1 vial per carton |
| 3 mL single-patient-use APIDRA SoloStar prefilled pen | 0088-2502-05 | 5 pens per carton |
Pen needles are not included in the packs.
SoloStar is compatible with all pen needles from Becton Dickinson and Company, Ypsomed, and Owen Mumford.
The APIDRA SoloStar prefilled pen dials in 1-unit increments.
8.4 Pediatric Use
The safety and effectiveness of APIDRA to improve glycemic control have been established in pediatric patients. Use of APIDRA for this indication is supported by evidence from an active-controlled non-inferiority study in pediatric patients 4 years of age and older with type 1 diabetes mellitus treated with APIDRA (n=271) and from studies in adults with diabetes mellitus [see Clinical Pharmacology (12.3), and Clinical Studies (14)].
In the clinical trials, pediatric patients with type 1 diabetes mellitus had a higher incidence of severe symptomatic hypoglycemia in the two treatment groups compared to adults with type 1 diabetes mellitus [see Adverse Reactions (6.1)].
8.5 Geriatric Use
In clinical trials, APIDRA was administered to 147 patients ≥65 years of age and 27 patients ≥75 years of age. The majority of this small subset of geriatric patients had type 2 diabetes. The change in HbA1c values and hypoglycemia frequencies did not differ by age.
Nevertheless, caution should be exercised when APIDRA is administered to geriatric patients. In geriatric patients with diabetes, the initial dosing, dose increments, and maintenance dosage should be conservative to reduce the risk of hypoglycemia [see Warnings and Precautions (5.3)].
6.2 Immunogenicity
As with all therapeutic proteins, there is potential for immunogenicity. The detection of antibody formation is highly dependent on the sensitivity and specificity of the assay. Additionally, the observed incidence of antibody (including neutralizing antibody) positivity in an assay may be influenced by several factors including assay methodology, sample handling, timing of sample collection, concomitant medication, and underlying disease. For these reasons, comparison of the incidence of antibodies to APIDRA in the studies described below with the incidence of antibodies in other studies or to other insulin products may be misleading.
In a study in patients with type 1 diabetes (n=333), the concentrations of insulin antibodies that react with both human insulin and insulin glulisine (cross-reactive insulin antibodies) remained near baseline during the first 6 months of the study in the patients treated with APIDRA. A decrease in antibody concentration was observed during the following 6 months of the study. In a study in patients with type 2 diabetes (n=411), a similar increase in cross-reactive insulin antibody concentration was observed in the patients treated with APIDRA and in the patients treated with human insulin during the first 9 months of the study. Thereafter the concentration of antibodies decreased in the APIDRA patients and remained stable in the human insulin patients. There was no correlation between cross-reactive insulin antibody concentration and changes in HbA1c, insulin doses, or incidence of hypoglycemia. APIDRA did not elicit a significant antibody response in a study of pediatric patients with type 1 diabetes.
14 Clinical Studies
The safety and efficacy of APIDRA were studied in adult patients with type 1 and type 2 diabetes (n=1833) and in pediatric patients (4 to 17 years) with type 1 diabetes (n=572). The primary efficacy parameter in these trials was glycemic control, assessed using glycated hemoglobin (GHb reported as HbA1c equivalent).
4 Contraindications
APIDRA is contraindicated:
- during episodes of hypoglycemia
- in patients with known hypersensitivity to insulin glulisine or to any of the excipients in APIDRA; systemic allergic reactions have occurred with APIDRA [see Adverse Reactions (6.1)].
6 Adverse Reactions
The following adverse reactions are discussed elsewhere:
- Hypoglycemia [see Warnings and Precautions (5.3)]
- Hypoglycemia Due to Medication Errors [see Warnings and Precautions (5.4)]
- Hypokalemia [see Warnings and Precautions (5.5)]
- Hypersensitivity Reactions [see Warnings and Precautions (5.6)]
7 Drug Interactions
| Drugs that May Increase the Risk of Hypoglycemia | |
| Drugs: | Antidiabetic agents, ACE inhibitors, angiotensin II receptor blocking agents, disopyramide, fibrates, fluoxetine, monoamine oxidase inhibitors, pentoxifylline, pramlintide, salicylates, somatostatin analog (e.g., octreotide), and sulfonamide antibiotics. |
| Intervention: | Dose adjustment and increased frequency of glucose monitoring may be required when APIDRA is coadministered with these drugs. |
| Drugs that May Decrease the Blood Glucose Lowering Effect of APIDRA | |
| Drugs: | Atypical antipsychotics, corticosteroids, danazol, diuretics, estrogens, glucagon, isoniazid, niacin, phenothiazine derivatives, progestogens (e.g., in oral contraceptives), protease inhibitors, somatropin, sympathomimetic agents (e.g., albuterol, epinephrine, terbutaline), and thyroid hormones. |
| Intervention: | Dose adjustment and increased frequency of glucose monitoring may be required when APIDRA is coadministered with these drugs. |
| Drugs that May Increase or Decrease the Blood Glucose Lowering Effect of APIDRA | |
| Drugs: | Alcohol, beta-blockers, clonidine, and lithium salts. Pentamidine may cause hypoglycemia, which may sometimes be followed by hyperglycemia. |
| Intervention: | Dose adjustment and increased frequency of glucose monitoring may be required when APIDRA is coadministered with these drugs. |
| Drugs that May Blunt Signs and Symptoms of Hypoglycemia | |
| Drugs: | Beta-blockers, clonidine, guanethidine, and reserpine. |
| Intervention: | Increased frequency of glucose monitoring may be required when APIDRA is coadministered with these drugs. |
8.6 Renal Impairment
Patients with renal impairment may be at increased risk of hypoglycemia and may require more frequent APIDRA dose adjustment and more frequent blood glucose monitoring [see Warnings and Precautions (5.3) and Clinical Pharmacology (12.3)].
12.2 Pharmacodynamics
Studies in healthy volunteers and patients with diabetes demonstrated that APIDRA has a more rapid onset of action and a shorter duration of activity than regular human insulin when given subcutaneously.
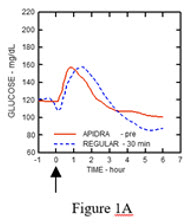
In a study in patients with type 1 diabetes (n=20), the glucose-lowering profiles of APIDRA and regular human insulin were assessed at various times in relation to a standard meal at a dose of 0.15 units/kg (see Figure 1).
The maximum blood glucose excursion (ΔGLUmax; baseline subtracted glucose concentration) for APIDRA injected 2 minutes before a meal was 65 mg/dL compared to 64 mg/dL for regular human insulin injected 30 minutes before a meal (see Figure 1A), and 84 mg/dL for regular human insulin injected 2 minutes before a meal (see Figure 1B). The maximum blood glucose excursion for APIDRA injected 15 minutes after the start of a meal was 85 mg/dL compared to 84 mg/dL for regular human insulin injected 2 minutes before a meal (see Figure 1C).
Figure 1: Serial mean blood glucose collected up to 6 hours following a single dose of APIDRA and regular human insulin. APIDRA given 2 minutes (APIDRA - pre) before the start of a meal compared to regular human insulin given 30 minutes (Regular - 30 min) before start of the meal (see Figure 1A) and compared to regular human insulin (Regular - pre) given 2 minutes before a meal (see Figure 1B). APIDRA given 15 minutes (APIDRA - post) after start of a meal compared to regular human insulin (Regular - pre) given 2 minutes before a meal (see Figure 1C). On the x-axis, zero (0) is the start of a 15-minute meal.
In a randomized, open-label, two-way crossover study, 16 healthy male subjects received an intravenous infusion of APIDRA or regular human insulin with saline diluent at a rate of 0.8 milliunits/kg/min for two hours. Infusion of the same dose of APIDRA or regular human insulin produced equivalent glucose disposal at steady state.
2.3 Dosage Information
- Individualize and adjust the dosage of APIDRA based on the patient's metabolic needs, blood glucose monitoring results, and glycemic control goal.
- Dose adjustments may be needed when switching from another insulin, with changes in physical activity, changes in concomitant medications, changes in meal patterns (i.e., macronutrient content or timing of food intake), changes in renal or hepatic function, or during acute illness to minimize the risk of hypoglycemia or hyperglycemia [see Warnings and Precautions (5.2, 5.3), Drug Interactions (7), Use in Specific Populations (8.6, 8.7)].
8.7 Hepatic Impairment
Patients with hepatic impairment may be at increased risk of hypoglycemia and may require more frequent APIDRA dose adjustment and more frequent blood glucose monitoring [see Warnings and Precautions (5.3) and Clinical Pharmacology (12.3)].
1 Indications and Usage
APIDRA is indicated to improve glycemic control in adult and pediatric patients with diabetes mellitus.
12.1 Mechanism of Action
Regulation of glucose metabolism is the primary activity of insulins and insulin analogs, including insulin glulisine. Insulins lower blood glucose by stimulating peripheral glucose uptake by skeletal muscle and fat, and by inhibiting hepatic glucose production. Insulins inhibit lipolysis and proteolysis and enhance protein synthesis.
5 Warnings and Precautions
- Never share an APIDRA SoloStar pen between patients, even if the needle is changed. (5.1)
- Hyperglycemia or Hypoglycemia with Changes in Insulin Regimen: Make changes to a patient's insulin regimen (e.g., insulin strength, manufacturer, type, injection site or method of administration) under close medical supervision with increased frequency of blood glucose monitoring. (5.2)
- Hypoglycemia: May be life-threatening. Increase frequency of glucose monitoring with changes to: insulin dosage, coadministered glucose lowering medications, meal pattern, physical activity; and in patients with renal impairment or hepatic impairment or hypoglycemia unawareness. (5.3)
- Hypoglycemia Due to Medication Errors: Accidental mix-ups between insulin products can occur. Instruct patients to check insulin labels before injection. (5.4)
- Hypokalemia: May be life-threatening. Monitor potassium levels in patients at risk for hypokalemia and treat if indicated. (5.5)
- Hypersensitivity Reactions: Severe, life-threatening, generalized allergy, including anaphylaxis, can occur. Discontinue APIDRA, monitor and treat if indicated. (5.6)
- Fluid Retention and Heart Failure Can Occur with Concomitant Use of Thiazolidinediones (TZDs): Observe for signs and symptoms of heart failure; consider dosage reduction or discontinuation of TZD if heart failure occurs. (5.7)
- Hyperglycemia and Ketoacidosis Due to Insulin Pump Device Malfunction: Monitor glucose and administer APIDRA by subcutaneous injection if pump malfunction occurs. (5.8)
14.1 Type 1 Diabetes Adults
A 26-week, randomized, open-label, active-controlled, non-inferiority study was conducted in patients with type 1 diabetes to assess the safety and efficacy of APIDRA (n=339) compared to insulin lispro (n=333) when administered subcutaneously within 15 minutes before a meal. Insulin glargine was administered once daily in the evening as the basal insulin. There was a 4-week run-in period with insulin lispro and insulin glargine prior to randomization. Most patients were Caucasian (97%). Fifty-eight percent of the patients were men. The mean age was 39 years (range 18 to 74 years). Glycemic control, the number of daily short-acting insulin injections and the total daily doses of APIDRA and insulin lispro were similar in the two treatment groups (see Table 7).
| Treatment duration Treatment in combination with: |
26 weeks Insulin glargine |
|
|---|---|---|
| APIDRA | Insulin Lispro | |
| Glycated hemoglobin (GHb) GHb reported as HbA1c equivalent (%)Number of patients |
331 |
322 |
| Baseline mean | 7.6 | 7.6 |
| Adjusted mean change from baseline | -0.1 | -0.1 |
| Treatment difference: APIDRA – Insulin Lispro | 0.0 | |
| 95% CI for treatment difference | (-0.1; 0.1) | |
| Basal insulin dose (Units/day) | ||
| Baseline mean | 24 | 24 |
| Adjusted mean change from baseline | 0 | 2 |
| Short-acting insulin dose (Units/day) | ||
| Baseline mean | 30 | 31 |
| Adjusted mean change from baseline | -1 | -1 |
| Mean number of short-acting insulin injections per day | 3 | 3 |
| Body weight (kg) | ||
| Baseline mean | 73.9 | 74.1 |
| Mean change from baseline | 0.6 | 0.3 |
14.2 Type 2 Diabetes Adults
A 26-week, randomized, open-label, active-controlled, non-inferiority study was conducted in insulin-treated patients with type 2 diabetes to assess the safety and efficacy of APIDRA (n=435) given within 15 minutes before a meal compared to regular human insulin (n=441) administered 30 to 45 minutes prior to a meal. NPH human insulin was given twice a day as the basal insulin. All patients participated in a 4-week run-in period with regular human insulin and NPH human insulin. Eighty-five percent of patients were Caucasian and 11% were Black. The mean age was 58 years (range 26 to 84 years). The average body mass index (BMI) was 34.6 kg/m2. At randomization, 58% of the patients were taking an oral antidiabetic agent. These patients were instructed to continue use of their oral antidiabetic agent at the same dose throughout the trial. The majority of patients (79%) mixed their short-acting insulin with NPH human insulin immediately prior to injection. The reductions from baseline in GHb were similar between the 2 treatment groups (see Table 8). No differences between APIDRA and regular human insulin groups were seen in the number of daily short-acting insulin injections or basal or short-acting insulin doses (see Table 8).
| Treatment duration Treatment in combination with: |
26 weeks NPH human insulin |
|
|---|---|---|
| APIDRA | Regular Human Insulin | |
| Glycated hemoglobin (GHb) GHb reported as HbA1c equivalent (%)Number of patients |
404 |
403 |
| Baseline mean | 7.6 | 7.5 |
| Adjusted mean change from baseline | -0.5 | -0.3 |
| Treatment difference: APIDRA – Regular Human Insulin | -0.2 | |
| 95% CI for treatment difference | (-0.3; -0.1) | |
| Basal insulin dose (Units/day) | ||
| Baseline mean | 59 | 57 |
| Adjusted mean change from baseline | 6 | 6 |
| Short-acting insulin dose (Units/day) | ||
| Baseline mean | 32 | 31 |
| Adjusted mean change from baseline | 4 | 5 |
| Mean number of short-acting insulin injections per day | 2 | 2 |
| Body weight (kg) | ||
| Baseline mean | 100.5 | 99.2 |
| Mean change from baseline | 1.8 | 2.0 |
2 Dosage and Administration
- See Full Prescribing Information for important administration instructions. (2.1, 2.2)
- Individualize and adjust the dosage of APIDRA based on route of administration, individual's metabolic needs, blood glucose monitoring results, and glycemic control goal. (2.3)
- Dosage adjustments may be needed when switching from another insulin, with changes in physical activity, changes in concomitant medications, changes in meal patterns, changes in renal or hepatic function or during acute illness. (2.3)
-
Subcutaneous Injection: (2.2)
- Inject within 15 minutes before a meal or within 20 minutes after starting a meal into the abdomen, thigh, or upper arm.
- Rotate injection sites within the same region to reduce the risk of lipodystrophy and localized cutaneous amyloidosis.
- Should generally be used in regimens with an intermediate or long-acting insulin.
-
Continuous Subcutaneous Infusion (Insulin Pump): (2.2)
- Refer to the insulin infusion pump user manual to see if APIDRA can be used. Use in accordance with the insulin pump instructions for use.
- Administer by continuous subcutaneous infusion using an insulin pump in a region recommended in the instructions from the pump manufacturer.
- Rotate infusion sites within the same region to reduce the risk of lipodystrophy and localized cutaneous amyloidosis.
- Do not mix with other insulins or diluents in the pump.
- Intravenous Administration: Administer only under medical supervision after diluting to concentrations from 0.05 to 1 unit/mL APIDRA in 0.9% sodium chloride injection, USP using polyvinyl chloride infusion bags. (2.2)
3 Dosage Forms and Strengths
Injection: 100 units per mL (U-100), a clear and colorless solution available as:
- 10 mL multiple-dose vial
- 3 mL single-patient-use APIDRA SoloStar prefilled pen
6.3 Postmarketing Experience
The following adverse reactions have been identified during postapproval use of APIDRA. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to estimate reliably their frequency or establish a causal relationship to drug exposure.
Medication errors have been reported in which other insulins, particularly long-acting insulins, have been accidentally administered instead of APIDRA.
Localized cutaneous amyloidosis at the injection site has occurred. Hyperglycemia has been reported with repeated insulin injections into areas of localized cutaneous amyloidosis; hypoglycemia has been reported with a sudden change to an unaffected injection site.
5.6 Hypersensitivity Reactions
Severe, life-threatening, generalized allergy, including anaphylaxis, can occur with insulins, including APIDRA [see Adverse Reactions (6.1)]. If hypersensitivity reactions occur, discontinue APIDRA; treat per standard of care and monitor until symptoms and signs resolve. APIDRA is contraindicated in patients who have had a hypersensitivity reaction to insulin glulisine or any of its excipients.
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying designs, the adverse reaction rates reported in one clinical trial may not be easily compared to those rates reported in another clinical trial and may not reflect the rates actually observed in clinical practice.
The data in Table 1 reflect the exposure of 1591 patients with type 1 diabetes to APIDRA or comparators [see Clinical Studies (14.1)]. The type 1 diabetes population had the following characteristics: Mean age was 39.74 years. 54.5 % were male, 95.5% were Caucasian, 1.5% were Black or African American.
The data in Table 2 reflect the exposure of 1766 patients with type 2 diabetes to APIDRA or comparators [see Clinical Studies (14.2)]. The type 2 diabetes population had the following characteristics: Mean age was 59.08 years. 51.2% were male, 88.5% were Caucasian, 7.2% were Black or African American.
The frequencies of adverse drug reactions during APIDRA clinical trials in patients with type 1 diabetes mellitus and type 2 diabetes mellitus are listed in the tables below.
| APIDRA, % (n=950) |
All Comparators Insulin lispro, regular human insulin, insulin aspart , %(n=641) |
|
|---|---|---|
| Nasopharyngitis | 10.6 | 12.9 |
| Hypoglycemia Only severe symptomatic hypoglycemia
|
6.8 | 6.7 |
| Upper respiratory tract infection | 6.6 | 5.6 |
| Influenza | 4.0 | 5.0 |
| APIDRA, % (n=883) |
Regular Human Insulin, % (n=883) |
|
|---|---|---|
| Upper respiratory tract infection | 10.5 | 7.7 |
| Nasopharyngitis | 7.6 | 8.2 |
| Edema peripheral | 7.5 | 7.8 |
| Influenza | 6.2 | 4.2 |
| Arthralgia | 5.9 | 6.3 |
| Hypertension | 3.9 | 5.3 |
17 Patient Counseling Information
Advise the patient to read the FDA-approved patient labeling (Patient Information and Instructions for Use).
14.4 Type 1 Diabetes Pediatric Patients
A 26-week, randomized, open-label, active-controlled, non-inferiority study was conducted in children and adolescents older than 4 years of age with type 1 diabetes mellitus to assess the safety and efficacy of APIDRA (n=277) compared to insulin lispro (n=295) when administered subcutaneously within 15 minutes before a meal. Patients also received insulin glargine (administered once daily in the evening) or NPH insulin (administered once in the morning and once in the evening). There was a 4-week run-in period with insulin lispro and insulin glargine or NPH prior to randomization. Most patients were Caucasian (91%). Fifty percent of the patients were male. The mean age was 12.5 years (range 4 to 17 years). Mean BMI was 20.6 kg/m2. Glycemic control (see Table 10) was comparable for the two treatment regimens.
| APIDRA | Insulin Lispro | |
|---|---|---|
| Number of patients | 271 | 291 |
| Basal Insulin | NPH or insulin glargine | NPH or insulin glargine |
| Glycated hemoglobin (GHb) GHb reported as HbA1c equivalent (%) |
||
| Baseline mean | 8.2 | 8.2 |
| Adjusted mean change from baseline | 0.1 | 0.2 |
| Treatment Difference: Mean (95% confidence interval) | -0.1 (-0.2, 0.1) | |
| Basal insulin dose (Units/kg/day) | ||
| Baseline mean | 0.5 | 0.5 |
| Mean change from baseline | 0.0 | 0.0 |
| Short-acting insulin dose (Units/kg/day) | ||
| Baseline mean | 0.5 | 0.5 |
| Mean change from baseline | 0.0 | 0.0 |
| Mean number of short-acting insulin injections per day | 3 | 3 |
| Baseline mean body weight (kg) Mean weight change from baseline (kg) |
51.5 2.2 |
50.8 2.2 |
2.1 Important Administration Instructions
- Always check insulin label before administration [see Warnings and Precautions (5.4)].
- Inspect visually for particulate matter and discoloration. Only use APIDRA if the solution appears clear and colorless.
- Use APIDRA SoloStar prefilled pen with caution in patients with visual impairment who may rely on audible clicks to dial their dose.
5.4 Hypoglycemia Due to Medication Errors
Accidental mix-ups between insulin products have been reported. To avoid medication errors between APIDRA and other insulins, instruct patients to always check the insulin label before each injection [see Adverse Reactions (6.3)].
Principal Display Panel 3 Ml Pen Carton
NDC 0088-2502-05
Rx only
Apidra® SoloStar®
(insulin glulisine) injection
For Single Patient Use Only
100 units/mL (U-100)
For subcutaneous use
Five 3 mL prefilled pens – Dispense in this sealed carton
Solution for injection in a disposable insulin delivery device
Use only if solution is clear and colorless with no particles visible
Use within 28 days after initial use
*Needles not included (see back panel)
sanofi
Principal Display Panel 10 Ml Vial Carton
NDC 0088-2500-33
Rx only
Apidra®
(insulin glulisine)
injection
100 units/mL
(U-100)
For subcutaneous use
For intravenous infusion
after further dilution
ONLY under direct
medical supervision
Use only if solution is
clear and colorless
with no particles visible
One 10 mL
multiple-dose vial
sanofi
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Long-term carcinogenicity studies in animals have not been performed. In Sprague Dawley rats, a 12-month study was conducted with insulin glulisine at subcutaneous doses of 2.5, 5, 20 or 50 units/kg administered twice daily, resulting in an exposure 1, 2, 8, and 20 times the average human dose, based on body surface area.
There was a non-dose dependent higher incidence of mammary gland tumors in female rats administered insulin glulisine compared to untreated controls. The incidence of mammary tumors for insulin glulisine and regular human insulin was similar. Insulin glulisine was not mutagenic in the following tests: Ames test, in vitro mammalian chromosome aberration test in V79 Chinese hamster cells, and in vivo mammalian erythrocyte micronucleus test in rats.
In fertility studies in male and female rats at subcutaneous doses up to 10 units/kg/day (2 times the average human dose, based on body surface area comparison), no clear adverse effects on male and female fertility, or general reproductive performance of animals were observed.
14.3 Type 1 Diabetes Adults: Pre and Postmeal Administration
A 12-week, randomized, open-label, active-controlled, non-inferiority study was conducted in patients with type 1 diabetes to assess the safety and efficacy of APIDRA administered at different times with respect to a meal. APIDRA was administered subcutaneously either within 15 minutes before a meal (n=286) or immediately after a meal (n=296) and regular human insulin (n=278) was administered subcutaneously 30 to 45 minutes prior to a meal. Insulin glargine was administered once daily at bedtime as the basal insulin. There was a 4-week run-in period with regular human insulin and insulin glargine followed by randomization. Most patients were Caucasian (94%). The mean age was 40 years (range 18 to 73 years). Glycemic control (see Table 9) was comparable for the 3 treatment regimens. No changes from baseline between the treatments were seen in the total daily number of short-acting insulin injections (see Table 9).
| Treatment duration Treatment in combination with: |
12 weeks insulin glargine |
12 weeks insulin glargine |
12 weeks insulin glargine |
|---|---|---|---|
|
APIDRA pre meal |
APIDRA post meal |
Regular Human Insulin | |
| Glycated hemoglobin (GHb) GHb reported as HbA1c equivalent (%)Number of patients |
268 |
276 |
257 |
| Baseline mean | 7.7 | 7.7 | 7.6 |
| Adjusted mean change from baseline Adjusted mean change from baseline treatment difference (98.33% CI for treatment difference):
APIDRA pre meal vs Regular Human Insulin -0.1 (-0.3; 0.0) APIDRA post meal vs Regular Human Insulin 0.0 (-0.1; 0.2) APIDRA post meal vs pre meal 0.2 (0.0; 0.3) |
-0.3 | -0.1 | -0.1 |
| Basal insulin dose (Units/day) | |||
| Baseline mean | 29 | 29 | 28 |
| Adjusted mean change from baseline | 1 | 0 | 1 |
| Short-acting insulin dose (Units/day) | |||
| Baseline mean | 29 | 29 | 27 |
| Adjusted mean change from baseline | -1 | -1 | 2 |
| Mean number of short-acting insulin injections per day | 3 | 3 | 3 |
| Body weight (kg) | |||
| Baseline mean | 79.2 | 80.3 | 78.9 |
| Mean change from baseline | 0.3 | -0.3 | 0.3 |
5.2 Hyperglycemia Or Hypoglycemia With Changes in Insulin Regimen
Changes in an insulin regimen (e.g., insulin, insulin strength, manufacturer, type, injection site or method of administration) may affect glycemic control and predispose to hypoglycemia [see Warnings and Precautions (5.3)] or hyperglycemia. Repeated insulin injections into areas of lipodystrophy or localized cutaneous amyloidosis have been reported to result in hyperglycemia; a sudden change in the injection site (to unaffected area) has been reported to result in hypoglycemia [see Adverse Reactions (6)].
Make any changes to a patient's insulin regimen under close medical supervision with increased frequency of blood glucose monitoring. Advise patients who have repeatedly injected into areas of lipodystrophy or localized cutaneous amyloidosis to change the injection site to unaffected areas and closely monitor for hypoglycemia. For patients with type 2 diabetes, dosage adjustments in concomitant oral antidiabetic treatment may be needed.
14.5 Type 1 Diabetes Adults: Continuous Subcutaneous Insulin Infusion
A 12-week randomized, active control study (APIDRA versus insulin aspart) conducted in adults with type 1 diabetes (APIDRA n=29, insulin aspart n=30) evaluated the use of APIDRA in an external continuous subcutaneous insulin pump. All patients were Caucasian. The mean age was 46 years (range 21 to 73 years). The mean GHb increased from baseline to endpoint in both treatment groups (from 6.8% to 7.0% for APIDRA; from 7.1% to 7.2% for insulin aspart).
5.8 Hyperglycemia and Ketoacidosis Due to Insulin Pump Device Malfunction
Malfunction of the insulin pump or insulin infusion set or insulin degradation can rapidly lead to hyperglycemia and ketoacidosis. Prompt identification and correction of the cause of hyperglycemia or ketosis is necessary. Interim subcutaneous injections with APIDRA may be required. Patients using continuous subcutaneous insulin infusion pump therapy must be trained to administer insulin by injection and have alternate insulin therapy available in case of pump failure [see How Supplied/Storage and Handling (16.2)].
5.1 Never Share An Apidra Solostar Pen Or Syringe Or Needle Between Patients
APIDRA SoloStar pens must never be shared between patients, even if the needle is changed. Patients using APIDRA vials must never reuse or share needles or syringes with another person. Sharing poses a risk for transmission of blood-borne pathogens.
5.7 Fluid Retention and Heart Failure With Concomitant Use of Ppar Gamma Agonists
Thiazolidinediones (TZDs), which are peroxisome proliferator-activated receptor (PPAR) gamma agonists, can cause dose-related fluid retention, when used in combination with insulin. Fluid retention may lead to or exacerbate heart failure. Patients treated with insulin, including APIDRA and a PPAR-gamma agonist should be observed for signs and symptoms of heart failure. If heart failure develops, it should be managed according to current standards of care, and discontinuation or dose reduction of the PPAR-gamma agonist must be considered.
Structured Label Content
Section 42229-5 (42229-5)
Subcutaneous Injection
- Inject APIDRA subcutaneously within 15 minutes before a meal or within 20 minutes after starting a meal into the abdominal wall, thigh, or upper arm.
- Rotate injection sites within the same region from one injection to the next to reduce the risk of lipodystrophy and localized cutaneous amyloidosis. Do not inject into areas of lipodystrophy or localized cutaneous amyloidosis [see Warnings and Precautions (5.2), Adverse Reactions (6)].
- APIDRA given by subcutaneous injection should generally be used in regimens with an intermediate or long-acting insulin.
- The APIDRA SoloStar prefilled pen dials in 1-unit increments.
- Do not mix APIDRA for subcutaneous injection with insulins other than NPH insulin. If APIDRA is mixed with NPH insulin, draw APIDRA into the syringe first and inject immediately after mixing.
Section 42230-3 (42230-3)
| PATIENT INFORMATION APIDRA® (uh PEE druh) (insulin glulisine) injection for subcutaneous use 100 units/mL (U-100) |
|
|---|---|
| This Patient Information has been approved by the U.S. Food and Drug Administration. | Revised: May 2025 |
| Do not share your APIDRA SoloStar® pen or syringes with other people, even if the needle has been changed. You may give other people a serious infection, or get a serious infection from them. | |
|
What is APIDRA?
APIDRA is a fast (rapid) acting man-made insulin used to control high blood sugar in adults and children with diabetes mellitus. |
|
|
Who should not use APIDRA? Do not use APIDRA if you:
|
|
|
What should I tell my healthcare provider before using APIDRA? Before using APIDRA, tell your healthcare provider about all your medical conditions including if you:
Before you start using APIDRA, talk to your healthcare provider about low blood sugar and how to manage it. |
|
How should I use APIDRA?
|
|
Your dose of APIDRA may need to change because of:
|
|
|
What should I avoid while using APIDRA? While using APIDRA do not:
|
|
|
What are the possible side effects of APIDRA? APIDRA may cause serious side effects that can lead to death, including:
|
|
|
General information about the safe and effective use of APIDRA.
Medicines are sometimes prescribed for purposes other than those listed in a Patient Information leaflet. Do not use APIDRA for a condition for which it was not prescribed. Do not give APIDRA to other people, even if they have the same symptoms that you have. It may harm them. This Patient Information leaflet summarizes the most important information about APIDRA. If you would like more information, talk with your healthcare provider. You can ask your healthcare provider or pharmacist for information about APIDRA that is written for health professionals. |
|
What are the ingredients in APIDRA?
|
|
| Manufactured by: sanofi-aventis U.S. LLC, Morristown, NJ 07960, A SANOFI COMPANY. U.S. License No. 1752 For more information, go to www.APIDRA.com or call 1-800-633-1610. |
Section 59845-8 (59845-8)
Instructions for Use
APIDRA® 10 mL vial (100 Units/mL)
(insulin glulisine) injection
for subcutaneous use
These Instructions for Use contain information on how to inject APIDRA using the vial. Read these Instructions for Use before you start taking APIDRA and each time you get a new APIDRA vial. There may be new information. This information does not take the place of talking to your healthcare provider about your medical condition or your treatment.
Do not share your APIDRA syringes with other people, even if the needle has been changed. You may give other people a serious infection, or get a serious infection from them.
Supplies needed to give your injection
- an APIDRA 10 mL vial
- a U-100 insulin syringe and needle
- 2 alcohol swabs
- 1 sharps container for throwing away used needles and syringes. See "Disposing of used needles and syringes" at the end of these instructions.
Preparing your APIDRA dose
- Wash your hands with soap and water or clean your hands with alcohol.
- Check the APIDRA label to make sure that you are taking the right type of insulin. This is especially important if you use more than 1 type of insulin.
- Look at the APIDRA in the vial. It should look clear and colorless. Do not use this vial of APIDRA if the solution is colored, or cloudy, or if you see particles in it.
- Do not use APIDRA after the expiration date stamped on the label or 28 days after you first use it.
- Always use a syringe that is marked for U-100 insulin. If you use a syringe other than a U-100 insulin syringe, you may get the wrong dose of insulin.
- Always use a new syringe or needle for each injection to help prevent infections and prevent blocked needles. Do not reuse or share your syringes or needles with other people. You may give other people a serious infection or get a serious infection from them.
Step 1:
If you are using a new vial, remove the protective cap. Do not remove the stopper.
Step 2:
Wipe the rubber stopper with an alcohol swab. You do not have to shake the vial of APIDRA before use.
Step 3:
Draw air into the syringe equal to the insulin dose. Put the needle through the rubber top of the vial and push the plunger to inject the air into the vial.
Step 4:
Leave the syringe in the vial and turn both upside down. Hold the syringe and vial firmly in one hand. Make sure the tip of the needle is in the insulin. With your free hand, pull the plunger to withdraw the correct dose into the syringe.
Step 5:
Before you take the needle out of the vial, check the syringe for air bubbles. If you see bubbles in the syringe, hold the syringe straight up and tap the side of the syringe with your finger a few times to make any air bubbles float to the top. Gently push the air bubbles out with the plunger and draw insulin back into the syringe until you have the correct dose. If you are mixing APIDRA with NPH insulin, check with your healthcare provider on how to mix it the right way.
Step 6:
Remove the needle from the vial. Do not let the needle touch anything. You are now ready to inject.
Giving your APIDRA injection with a syringe
- Inject your insulin exactly as your healthcare provider has shown you.
- APIDRA starts acting fast, so give your injection within 15 minutes before or right after you eat a meal.
Step 7:
- Choose your injection site: APIDRA is injected under the skin (subcutaneously) of your upper arms, thighs, or stomach area (abdomen).
- Change (rotate) your injection sites within the area you choose for each dose to reduce your risk of getting lipodystrophy (pits in the skin or thickened skin) and localized cutaneous amyloidosis (skin with lumps) at the injection sites.
- Do not inject where the skin has pits, is thickened, or has lumps.
- Do not inject where the skin is tender, bruised, scaly or hard, or into scars or damaged skin.
- Wipe the skin with an alcohol swab to clean the injection site. Let the injection site dry before you inject.
Step 8:
- Pinch the skin.
- Insert the needle in the way your healthcare provider showed you.
- Release the skin.
- Slowly push in the plunger of the syringe all the way, making sure you have injected all the insulin.
- Leave the needle in the skin for about 10 seconds.
Step 9:
- Pull the needle straight out of your skin.
- Gently press the injection site for several seconds. Do not rub the area.
- Do not recap the used needle. Recapping the needle can lead to a needle-stick injury.
Giving your APIDRA using an insulin pump
- If you have been prescribed an insulin pump, check the pump manufacturer's user manual to see if APIDRA can be used with the pump.
- APIDRA should be given into an area of your body recommended in the instructions that come with your insulin pump.
- Change (rotate) your injection sites within the area you choose for each insertion to reduce your risk of getting lipodystrophy (pits in skin or thickened skin) and localized cutaneous amyloidosis (skin with lumps) at the injection sites. Do not inject into the exact same spot for each injection. Do not inject where the skin has pits, is thickened, or has lumps. Do not inject where the skin is tender, bruised, scaly or hard, or into scars or damaged skin.
- Call your healthcare provider and choose a new infusion site if the skin at the infusion site becomes red, itchy, or thickened.
- Change the insulin in the reservoir at least every 2 days or according to the pump user manual, whichever is shorter, even if you have not used all of the insulin.
- Do not dilute or mix APIDRA with other insulins in your insulin pump.
- You should be trained on how to give insulin by injection and have an alternative insulin delivery system in case of pump failure.
- When you start using APIDRA by infusion pump, your insulin dose may need to be adjusted. Check with your healthcare provider before making any changes to your insulin dose.
- Your healthcare provider should provide recommendations for appropriate pump basal and meal-time infusion rates. Call your healthcare provider if you have any questions about using the insulin pump.
Disposing of used needles and syringes
- Put your used needles and syringes in a FDA-cleared sharps disposal container right away after use. Do not throw away (dispose of) loose needles and syringes in your household trash.
- If you do not have a FDA-cleared sharps container, you may use a household container that is:
- made of a heavy-duty plastic,
- can be closed with a tight-fitting, puncture-resistant lid, without sharps being able to come out,
- upright and stable during use,
- leak resistant, and
- properly labeled to warn of hazardous waste inside the container.
- When your sharps disposal container is almost full, you will need to follow your community guidelines for the right way to dispose of your sharps disposal container. There may be state or local laws about how you should throw away used needles and syringes. For more information about safe sharps disposal, and for specific information about sharps disposal in the state that you live in, go to the FDA's website at: http://www.fda.gov/safesharpsdisposal.
- Do not dispose of your used sharps disposal container in your household trash unless your community guidelines permit this. Do not recycle your used sharps disposal container.
How should I store APIDRA 10 mL vial?
Unopened (not in-use) APIDRA vials
- Store unused APIDRA vials in the refrigerator from 36°F to 46°F (2°C to 8°C).
- Do not freeze APIDRA.
- Keep APIDRA away from direct heat and light.
- If a vial has been frozen or overheated, throw it away.
- Unopened vials can be used until the expiration date on the carton and label if they have been stored in the refrigerator.
- Unopened vials should be thrown away after 28 days if they are stored at room temperature.
After APIDRA vials have been opened (in-use)
- Store in-use (opened) APIDRA vials in a refrigerator from 36°F to 46°F (2°C to 8°C) or at room temperature below 77°F (25°C) for up to 28 days.
- Do not freeze APIDRA.
- Keep APIDRA out of direct heat and light.
- If a vial has been frozen, throw it away.
- The APIDRA vial you are using should be thrown away after 28 days, even if it still has insulin left in it.
APIDRA in an insulin pump
- Throw away APIDRA in the pump reservoir if it has been exposed to temperatures higher than 98.6°F (37°C). This may occur if the pump housing, cover, tubing, or sport case is exposed to sunlight or direct heat.
This Instructions for Use has been approved by the U.S. Food and Drug Administration.
Revised: May 2025
Manufactured by:
sanofi-aventis U.S. LLC
Morristown, NJ 07960
A SANOFI COMPANY
U.S. License No. 1752
©2025 sanofi-aventis U.S. LLC
16.2 Storage
Dispense in the original sealed carton with the enclosed Instructions for Use. Do not freeze.
Do not use after the expiration date (see carton and container).
Storage conditions are summarized in the following table:
| Not in-use (unopened) Refrigerated (36°F-46°F [2°C-8°C]). Protect from light |
Not in-use (unopened) Room Temperature (up to 77°F [25°C]) |
In-use (opened) (See temperature below) |
|
|---|---|---|---|
| 10 mL multiple-dose vial | Until expiration date | 28 days | 28 days The in-use time for multiple-dose vial is either 28 days at room temperature up to 77°F (25°C) or 48 hours in insulin pump up to 98.6°F (37°C). , Refrigerated or room temperature |
| 3 mL single-patient-use APIDRA SoloStar prefilled pen | Until expiration date | 28 days | 28 days, Room temperature (Do not refrigerate) |
10 Overdosage (10 OVERDOSAGE)
Excess insulin may cause hypoglycemia and, particularly when given intravenously, hypokalemia. Mild episodes of hypoglycemia usually can be treated with oral glucose. Adjustments in drug dosage, meal patterns, or exercise may be needed. More severe episodes of hypoglycemia with coma, seizure, or neurologic impairment may be treated with a glucagon product for emergency use or concentrated intravenous glucose. Sustained carbohydrate intake and observation may be necessary because hypoglycemia may recur after apparent clinical recovery. Hypokalemia must be corrected appropriately.
11 Description (11 DESCRIPTION)
Insulin glulisine is a rapid-acting human insulin analog used to lower blood glucose. Insulin glulisine is produced by recombinant DNA technology utilizing a non-pathogenic laboratory strain of Escherichia coli (K12). Insulin glulisine differs from human insulin in that the amino acid asparagine at position B3 is replaced by lysine and the lysine in position B29 is replaced by glutamic acid. Insulin glulisine has a molecular weight of 5.823 kDa.
APIDRA (insulin glulisine) injection is a sterile, aqueous, clear, and colorless solution for subcutaneous or intravenous use. Each milliliter of APIDRA contains 100 units insulin glulisine, metacresol (3.15 mg), polysorbate 20 (0.01 mg), sodium chloride (5 mg), tromethamine (6 mg), and water for injection. APIDRA has a pH of approximately 7.3. The pH is adjusted by addition of aqueous solutions of hydrochloric acid and/or sodium hydroxide.
5.5 Hypokalemia
All insulins, including APIDRA, cause a shift in potassium from the extracellular to intracellular space, possibly leading to hypokalemia. Untreated hypokalemia may cause respiratory paralysis, ventricular arrhythmia, and death. Use caution in patients who may be at risk for hypokalemia (e.g., patients using potassium-lowering medications, patients taking medications sensitive to serum potassium concentrations).
5.3 Hypoglycemia
Hypoglycemia is the most common adverse reaction of all insulins, including APIDRA [see Adverse Reactions (6.1)]. Severe hypoglycemia can cause seizures, may lead to unconsciousness, may be life-threatening, or cause death. Hypoglycemia can impair concentration ability and reaction time; this may place the patient and others at risk in situations where these abilities are important (e.g., driving or operating other machinery). APIDRA, or any insulin, should not be used during episodes of hypoglycemia [see Contraindications (4)].
Hypoglycemia can happen suddenly, and symptoms may differ in each patient and change over time in the same patient. Symptomatic awareness of hypoglycemia may be less pronounced in patients with longstanding diabetes, in patients with diabetic neuropathy, in patients using medications that block the sympathetic nervous system (e.g., beta-blockers) [see Drug Interactions (7)], or in patients who experience recurrent hypoglycemia.
16.1 How Supplied
APIDRA injection, 100 units/mL (U-100), is a clear and colorless solution available as:
| APIDRA | NDC number | Package size |
|---|---|---|
| 10 mL multiple-dose vial | 0088-2500-33 | 1 vial per carton |
| 3 mL single-patient-use APIDRA SoloStar prefilled pen | 0088-2502-05 | 5 pens per carton |
Pen needles are not included in the packs.
SoloStar is compatible with all pen needles from Becton Dickinson and Company, Ypsomed, and Owen Mumford.
The APIDRA SoloStar prefilled pen dials in 1-unit increments.
8.4 Pediatric Use
The safety and effectiveness of APIDRA to improve glycemic control have been established in pediatric patients. Use of APIDRA for this indication is supported by evidence from an active-controlled non-inferiority study in pediatric patients 4 years of age and older with type 1 diabetes mellitus treated with APIDRA (n=271) and from studies in adults with diabetes mellitus [see Clinical Pharmacology (12.3), and Clinical Studies (14)].
In the clinical trials, pediatric patients with type 1 diabetes mellitus had a higher incidence of severe symptomatic hypoglycemia in the two treatment groups compared to adults with type 1 diabetes mellitus [see Adverse Reactions (6.1)].
8.5 Geriatric Use
In clinical trials, APIDRA was administered to 147 patients ≥65 years of age and 27 patients ≥75 years of age. The majority of this small subset of geriatric patients had type 2 diabetes. The change in HbA1c values and hypoglycemia frequencies did not differ by age.
Nevertheless, caution should be exercised when APIDRA is administered to geriatric patients. In geriatric patients with diabetes, the initial dosing, dose increments, and maintenance dosage should be conservative to reduce the risk of hypoglycemia [see Warnings and Precautions (5.3)].
6.2 Immunogenicity
As with all therapeutic proteins, there is potential for immunogenicity. The detection of antibody formation is highly dependent on the sensitivity and specificity of the assay. Additionally, the observed incidence of antibody (including neutralizing antibody) positivity in an assay may be influenced by several factors including assay methodology, sample handling, timing of sample collection, concomitant medication, and underlying disease. For these reasons, comparison of the incidence of antibodies to APIDRA in the studies described below with the incidence of antibodies in other studies or to other insulin products may be misleading.
In a study in patients with type 1 diabetes (n=333), the concentrations of insulin antibodies that react with both human insulin and insulin glulisine (cross-reactive insulin antibodies) remained near baseline during the first 6 months of the study in the patients treated with APIDRA. A decrease in antibody concentration was observed during the following 6 months of the study. In a study in patients with type 2 diabetes (n=411), a similar increase in cross-reactive insulin antibody concentration was observed in the patients treated with APIDRA and in the patients treated with human insulin during the first 9 months of the study. Thereafter the concentration of antibodies decreased in the APIDRA patients and remained stable in the human insulin patients. There was no correlation between cross-reactive insulin antibody concentration and changes in HbA1c, insulin doses, or incidence of hypoglycemia. APIDRA did not elicit a significant antibody response in a study of pediatric patients with type 1 diabetes.
14 Clinical Studies (14 CLINICAL STUDIES)
The safety and efficacy of APIDRA were studied in adult patients with type 1 and type 2 diabetes (n=1833) and in pediatric patients (4 to 17 years) with type 1 diabetes (n=572). The primary efficacy parameter in these trials was glycemic control, assessed using glycated hemoglobin (GHb reported as HbA1c equivalent).
4 Contraindications (4 CONTRAINDICATIONS)
APIDRA is contraindicated:
- during episodes of hypoglycemia
- in patients with known hypersensitivity to insulin glulisine or to any of the excipients in APIDRA; systemic allergic reactions have occurred with APIDRA [see Adverse Reactions (6.1)].
6 Adverse Reactions (6 ADVERSE REACTIONS)
The following adverse reactions are discussed elsewhere:
- Hypoglycemia [see Warnings and Precautions (5.3)]
- Hypoglycemia Due to Medication Errors [see Warnings and Precautions (5.4)]
- Hypokalemia [see Warnings and Precautions (5.5)]
- Hypersensitivity Reactions [see Warnings and Precautions (5.6)]
7 Drug Interactions (7 DRUG INTERACTIONS)
| Drugs that May Increase the Risk of Hypoglycemia | |
| Drugs: | Antidiabetic agents, ACE inhibitors, angiotensin II receptor blocking agents, disopyramide, fibrates, fluoxetine, monoamine oxidase inhibitors, pentoxifylline, pramlintide, salicylates, somatostatin analog (e.g., octreotide), and sulfonamide antibiotics. |
| Intervention: | Dose adjustment and increased frequency of glucose monitoring may be required when APIDRA is coadministered with these drugs. |
| Drugs that May Decrease the Blood Glucose Lowering Effect of APIDRA | |
| Drugs: | Atypical antipsychotics, corticosteroids, danazol, diuretics, estrogens, glucagon, isoniazid, niacin, phenothiazine derivatives, progestogens (e.g., in oral contraceptives), protease inhibitors, somatropin, sympathomimetic agents (e.g., albuterol, epinephrine, terbutaline), and thyroid hormones. |
| Intervention: | Dose adjustment and increased frequency of glucose monitoring may be required when APIDRA is coadministered with these drugs. |
| Drugs that May Increase or Decrease the Blood Glucose Lowering Effect of APIDRA | |
| Drugs: | Alcohol, beta-blockers, clonidine, and lithium salts. Pentamidine may cause hypoglycemia, which may sometimes be followed by hyperglycemia. |
| Intervention: | Dose adjustment and increased frequency of glucose monitoring may be required when APIDRA is coadministered with these drugs. |
| Drugs that May Blunt Signs and Symptoms of Hypoglycemia | |
| Drugs: | Beta-blockers, clonidine, guanethidine, and reserpine. |
| Intervention: | Increased frequency of glucose monitoring may be required when APIDRA is coadministered with these drugs. |
8.6 Renal Impairment
Patients with renal impairment may be at increased risk of hypoglycemia and may require more frequent APIDRA dose adjustment and more frequent blood glucose monitoring [see Warnings and Precautions (5.3) and Clinical Pharmacology (12.3)].
12.2 Pharmacodynamics
Studies in healthy volunteers and patients with diabetes demonstrated that APIDRA has a more rapid onset of action and a shorter duration of activity than regular human insulin when given subcutaneously.
In a study in patients with type 1 diabetes (n=20), the glucose-lowering profiles of APIDRA and regular human insulin were assessed at various times in relation to a standard meal at a dose of 0.15 units/kg (see Figure 1).
The maximum blood glucose excursion (ΔGLUmax; baseline subtracted glucose concentration) for APIDRA injected 2 minutes before a meal was 65 mg/dL compared to 64 mg/dL for regular human insulin injected 30 minutes before a meal (see Figure 1A), and 84 mg/dL for regular human insulin injected 2 minutes before a meal (see Figure 1B). The maximum blood glucose excursion for APIDRA injected 15 minutes after the start of a meal was 85 mg/dL compared to 84 mg/dL for regular human insulin injected 2 minutes before a meal (see Figure 1C).
Figure 1: Serial mean blood glucose collected up to 6 hours following a single dose of APIDRA and regular human insulin. APIDRA given 2 minutes (APIDRA - pre) before the start of a meal compared to regular human insulin given 30 minutes (Regular - 30 min) before start of the meal (see Figure 1A) and compared to regular human insulin (Regular - pre) given 2 minutes before a meal (see Figure 1B). APIDRA given 15 minutes (APIDRA - post) after start of a meal compared to regular human insulin (Regular - pre) given 2 minutes before a meal (see Figure 1C). On the x-axis, zero (0) is the start of a 15-minute meal.
In a randomized, open-label, two-way crossover study, 16 healthy male subjects received an intravenous infusion of APIDRA or regular human insulin with saline diluent at a rate of 0.8 milliunits/kg/min for two hours. Infusion of the same dose of APIDRA or regular human insulin produced equivalent glucose disposal at steady state.
2.3 Dosage Information
- Individualize and adjust the dosage of APIDRA based on the patient's metabolic needs, blood glucose monitoring results, and glycemic control goal.
- Dose adjustments may be needed when switching from another insulin, with changes in physical activity, changes in concomitant medications, changes in meal patterns (i.e., macronutrient content or timing of food intake), changes in renal or hepatic function, or during acute illness to minimize the risk of hypoglycemia or hyperglycemia [see Warnings and Precautions (5.2, 5.3), Drug Interactions (7), Use in Specific Populations (8.6, 8.7)].
8.7 Hepatic Impairment
Patients with hepatic impairment may be at increased risk of hypoglycemia and may require more frequent APIDRA dose adjustment and more frequent blood glucose monitoring [see Warnings and Precautions (5.3) and Clinical Pharmacology (12.3)].
1 Indications and Usage (1 INDICATIONS AND USAGE)
APIDRA is indicated to improve glycemic control in adult and pediatric patients with diabetes mellitus.
12.1 Mechanism of Action
Regulation of glucose metabolism is the primary activity of insulins and insulin analogs, including insulin glulisine. Insulins lower blood glucose by stimulating peripheral glucose uptake by skeletal muscle and fat, and by inhibiting hepatic glucose production. Insulins inhibit lipolysis and proteolysis and enhance protein synthesis.
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
- Never share an APIDRA SoloStar pen between patients, even if the needle is changed. (5.1)
- Hyperglycemia or Hypoglycemia with Changes in Insulin Regimen: Make changes to a patient's insulin regimen (e.g., insulin strength, manufacturer, type, injection site or method of administration) under close medical supervision with increased frequency of blood glucose monitoring. (5.2)
- Hypoglycemia: May be life-threatening. Increase frequency of glucose monitoring with changes to: insulin dosage, coadministered glucose lowering medications, meal pattern, physical activity; and in patients with renal impairment or hepatic impairment or hypoglycemia unawareness. (5.3)
- Hypoglycemia Due to Medication Errors: Accidental mix-ups between insulin products can occur. Instruct patients to check insulin labels before injection. (5.4)
- Hypokalemia: May be life-threatening. Monitor potassium levels in patients at risk for hypokalemia and treat if indicated. (5.5)
- Hypersensitivity Reactions: Severe, life-threatening, generalized allergy, including anaphylaxis, can occur. Discontinue APIDRA, monitor and treat if indicated. (5.6)
- Fluid Retention and Heart Failure Can Occur with Concomitant Use of Thiazolidinediones (TZDs): Observe for signs and symptoms of heart failure; consider dosage reduction or discontinuation of TZD if heart failure occurs. (5.7)
- Hyperglycemia and Ketoacidosis Due to Insulin Pump Device Malfunction: Monitor glucose and administer APIDRA by subcutaneous injection if pump malfunction occurs. (5.8)
14.1 Type 1 Diabetes Adults (14.1 Type 1 Diabetes-Adults)
A 26-week, randomized, open-label, active-controlled, non-inferiority study was conducted in patients with type 1 diabetes to assess the safety and efficacy of APIDRA (n=339) compared to insulin lispro (n=333) when administered subcutaneously within 15 minutes before a meal. Insulin glargine was administered once daily in the evening as the basal insulin. There was a 4-week run-in period with insulin lispro and insulin glargine prior to randomization. Most patients were Caucasian (97%). Fifty-eight percent of the patients were men. The mean age was 39 years (range 18 to 74 years). Glycemic control, the number of daily short-acting insulin injections and the total daily doses of APIDRA and insulin lispro were similar in the two treatment groups (see Table 7).
| Treatment duration Treatment in combination with: |
26 weeks Insulin glargine |
|
|---|---|---|
| APIDRA | Insulin Lispro | |
| Glycated hemoglobin (GHb) GHb reported as HbA1c equivalent (%)Number of patients |
331 |
322 |
| Baseline mean | 7.6 | 7.6 |
| Adjusted mean change from baseline | -0.1 | -0.1 |
| Treatment difference: APIDRA – Insulin Lispro | 0.0 | |
| 95% CI for treatment difference | (-0.1; 0.1) | |
| Basal insulin dose (Units/day) | ||
| Baseline mean | 24 | 24 |
| Adjusted mean change from baseline | 0 | 2 |
| Short-acting insulin dose (Units/day) | ||
| Baseline mean | 30 | 31 |
| Adjusted mean change from baseline | -1 | -1 |
| Mean number of short-acting insulin injections per day | 3 | 3 |
| Body weight (kg) | ||
| Baseline mean | 73.9 | 74.1 |
| Mean change from baseline | 0.6 | 0.3 |
14.2 Type 2 Diabetes Adults (14.2 Type 2 Diabetes-Adults)
A 26-week, randomized, open-label, active-controlled, non-inferiority study was conducted in insulin-treated patients with type 2 diabetes to assess the safety and efficacy of APIDRA (n=435) given within 15 minutes before a meal compared to regular human insulin (n=441) administered 30 to 45 minutes prior to a meal. NPH human insulin was given twice a day as the basal insulin. All patients participated in a 4-week run-in period with regular human insulin and NPH human insulin. Eighty-five percent of patients were Caucasian and 11% were Black. The mean age was 58 years (range 26 to 84 years). The average body mass index (BMI) was 34.6 kg/m2. At randomization, 58% of the patients were taking an oral antidiabetic agent. These patients were instructed to continue use of their oral antidiabetic agent at the same dose throughout the trial. The majority of patients (79%) mixed their short-acting insulin with NPH human insulin immediately prior to injection. The reductions from baseline in GHb were similar between the 2 treatment groups (see Table 8). No differences between APIDRA and regular human insulin groups were seen in the number of daily short-acting insulin injections or basal or short-acting insulin doses (see Table 8).
| Treatment duration Treatment in combination with: |
26 weeks NPH human insulin |
|
|---|---|---|
| APIDRA | Regular Human Insulin | |
| Glycated hemoglobin (GHb) GHb reported as HbA1c equivalent (%)Number of patients |
404 |
403 |
| Baseline mean | 7.6 | 7.5 |
| Adjusted mean change from baseline | -0.5 | -0.3 |
| Treatment difference: APIDRA – Regular Human Insulin | -0.2 | |
| 95% CI for treatment difference | (-0.3; -0.1) | |
| Basal insulin dose (Units/day) | ||
| Baseline mean | 59 | 57 |
| Adjusted mean change from baseline | 6 | 6 |
| Short-acting insulin dose (Units/day) | ||
| Baseline mean | 32 | 31 |
| Adjusted mean change from baseline | 4 | 5 |
| Mean number of short-acting insulin injections per day | 2 | 2 |
| Body weight (kg) | ||
| Baseline mean | 100.5 | 99.2 |
| Mean change from baseline | 1.8 | 2.0 |
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
- See Full Prescribing Information for important administration instructions. (2.1, 2.2)
- Individualize and adjust the dosage of APIDRA based on route of administration, individual's metabolic needs, blood glucose monitoring results, and glycemic control goal. (2.3)
- Dosage adjustments may be needed when switching from another insulin, with changes in physical activity, changes in concomitant medications, changes in meal patterns, changes in renal or hepatic function or during acute illness. (2.3)
-
Subcutaneous Injection: (2.2)
- Inject within 15 minutes before a meal or within 20 minutes after starting a meal into the abdomen, thigh, or upper arm.
- Rotate injection sites within the same region to reduce the risk of lipodystrophy and localized cutaneous amyloidosis.
- Should generally be used in regimens with an intermediate or long-acting insulin.
-
Continuous Subcutaneous Infusion (Insulin Pump): (2.2)
- Refer to the insulin infusion pump user manual to see if APIDRA can be used. Use in accordance with the insulin pump instructions for use.
- Administer by continuous subcutaneous infusion using an insulin pump in a region recommended in the instructions from the pump manufacturer.
- Rotate infusion sites within the same region to reduce the risk of lipodystrophy and localized cutaneous amyloidosis.
- Do not mix with other insulins or diluents in the pump.
- Intravenous Administration: Administer only under medical supervision after diluting to concentrations from 0.05 to 1 unit/mL APIDRA in 0.9% sodium chloride injection, USP using polyvinyl chloride infusion bags. (2.2)
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
Injection: 100 units per mL (U-100), a clear and colorless solution available as:
- 10 mL multiple-dose vial
- 3 mL single-patient-use APIDRA SoloStar prefilled pen
6.3 Postmarketing Experience
The following adverse reactions have been identified during postapproval use of APIDRA. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to estimate reliably their frequency or establish a causal relationship to drug exposure.
Medication errors have been reported in which other insulins, particularly long-acting insulins, have been accidentally administered instead of APIDRA.
Localized cutaneous amyloidosis at the injection site has occurred. Hyperglycemia has been reported with repeated insulin injections into areas of localized cutaneous amyloidosis; hypoglycemia has been reported with a sudden change to an unaffected injection site.
5.6 Hypersensitivity Reactions
Severe, life-threatening, generalized allergy, including anaphylaxis, can occur with insulins, including APIDRA [see Adverse Reactions (6.1)]. If hypersensitivity reactions occur, discontinue APIDRA; treat per standard of care and monitor until symptoms and signs resolve. APIDRA is contraindicated in patients who have had a hypersensitivity reaction to insulin glulisine or any of its excipients.
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying designs, the adverse reaction rates reported in one clinical trial may not be easily compared to those rates reported in another clinical trial and may not reflect the rates actually observed in clinical practice.
The data in Table 1 reflect the exposure of 1591 patients with type 1 diabetes to APIDRA or comparators [see Clinical Studies (14.1)]. The type 1 diabetes population had the following characteristics: Mean age was 39.74 years. 54.5 % were male, 95.5% were Caucasian, 1.5% were Black or African American.
The data in Table 2 reflect the exposure of 1766 patients with type 2 diabetes to APIDRA or comparators [see Clinical Studies (14.2)]. The type 2 diabetes population had the following characteristics: Mean age was 59.08 years. 51.2% were male, 88.5% were Caucasian, 7.2% were Black or African American.
The frequencies of adverse drug reactions during APIDRA clinical trials in patients with type 1 diabetes mellitus and type 2 diabetes mellitus are listed in the tables below.
| APIDRA, % (n=950) |
All Comparators Insulin lispro, regular human insulin, insulin aspart , %(n=641) |
|
|---|---|---|
| Nasopharyngitis | 10.6 | 12.9 |
| Hypoglycemia Only severe symptomatic hypoglycemia
|
6.8 | 6.7 |
| Upper respiratory tract infection | 6.6 | 5.6 |
| Influenza | 4.0 | 5.0 |
| APIDRA, % (n=883) |
Regular Human Insulin, % (n=883) |
|
|---|---|---|
| Upper respiratory tract infection | 10.5 | 7.7 |
| Nasopharyngitis | 7.6 | 8.2 |
| Edema peripheral | 7.5 | 7.8 |
| Influenza | 6.2 | 4.2 |
| Arthralgia | 5.9 | 6.3 |
| Hypertension | 3.9 | 5.3 |
17 Patient Counseling Information (17 PATIENT COUNSELING INFORMATION)
Advise the patient to read the FDA-approved patient labeling (Patient Information and Instructions for Use).
14.4 Type 1 Diabetes Pediatric Patients (14.4 Type 1 Diabetes-Pediatric Patients)
A 26-week, randomized, open-label, active-controlled, non-inferiority study was conducted in children and adolescents older than 4 years of age with type 1 diabetes mellitus to assess the safety and efficacy of APIDRA (n=277) compared to insulin lispro (n=295) when administered subcutaneously within 15 minutes before a meal. Patients also received insulin glargine (administered once daily in the evening) or NPH insulin (administered once in the morning and once in the evening). There was a 4-week run-in period with insulin lispro and insulin glargine or NPH prior to randomization. Most patients were Caucasian (91%). Fifty percent of the patients were male. The mean age was 12.5 years (range 4 to 17 years). Mean BMI was 20.6 kg/m2. Glycemic control (see Table 10) was comparable for the two treatment regimens.
| APIDRA | Insulin Lispro | |
|---|---|---|
| Number of patients | 271 | 291 |
| Basal Insulin | NPH or insulin glargine | NPH or insulin glargine |
| Glycated hemoglobin (GHb) GHb reported as HbA1c equivalent (%) |
||
| Baseline mean | 8.2 | 8.2 |
| Adjusted mean change from baseline | 0.1 | 0.2 |
| Treatment Difference: Mean (95% confidence interval) | -0.1 (-0.2, 0.1) | |
| Basal insulin dose (Units/kg/day) | ||
| Baseline mean | 0.5 | 0.5 |
| Mean change from baseline | 0.0 | 0.0 |
| Short-acting insulin dose (Units/kg/day) | ||
| Baseline mean | 0.5 | 0.5 |
| Mean change from baseline | 0.0 | 0.0 |
| Mean number of short-acting insulin injections per day | 3 | 3 |
| Baseline mean body weight (kg) Mean weight change from baseline (kg) |
51.5 2.2 |
50.8 2.2 |
2.1 Important Administration Instructions
- Always check insulin label before administration [see Warnings and Precautions (5.4)].
- Inspect visually for particulate matter and discoloration. Only use APIDRA if the solution appears clear and colorless.
- Use APIDRA SoloStar prefilled pen with caution in patients with visual impairment who may rely on audible clicks to dial their dose.
5.4 Hypoglycemia Due to Medication Errors
Accidental mix-ups between insulin products have been reported. To avoid medication errors between APIDRA and other insulins, instruct patients to always check the insulin label before each injection [see Adverse Reactions (6.3)].
Principal Display Panel 3 Ml Pen Carton (PRINCIPAL DISPLAY PANEL - 3 mL Pen Carton)
NDC 0088-2502-05
Rx only
Apidra® SoloStar®
(insulin glulisine) injection
For Single Patient Use Only
100 units/mL (U-100)
For subcutaneous use
Five 3 mL prefilled pens – Dispense in this sealed carton
Solution for injection in a disposable insulin delivery device
Use only if solution is clear and colorless with no particles visible
Use within 28 days after initial use
*Needles not included (see back panel)
sanofi
Principal Display Panel 10 Ml Vial Carton (PRINCIPAL DISPLAY PANEL - 10 mL Vial Carton)
NDC 0088-2500-33
Rx only
Apidra®
(insulin glulisine)
injection
100 units/mL
(U-100)
For subcutaneous use
For intravenous infusion
after further dilution
ONLY under direct
medical supervision
Use only if solution is
clear and colorless
with no particles visible
One 10 mL
multiple-dose vial
sanofi
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Long-term carcinogenicity studies in animals have not been performed. In Sprague Dawley rats, a 12-month study was conducted with insulin glulisine at subcutaneous doses of 2.5, 5, 20 or 50 units/kg administered twice daily, resulting in an exposure 1, 2, 8, and 20 times the average human dose, based on body surface area.
There was a non-dose dependent higher incidence of mammary gland tumors in female rats administered insulin glulisine compared to untreated controls. The incidence of mammary tumors for insulin glulisine and regular human insulin was similar. Insulin glulisine was not mutagenic in the following tests: Ames test, in vitro mammalian chromosome aberration test in V79 Chinese hamster cells, and in vivo mammalian erythrocyte micronucleus test in rats.
In fertility studies in male and female rats at subcutaneous doses up to 10 units/kg/day (2 times the average human dose, based on body surface area comparison), no clear adverse effects on male and female fertility, or general reproductive performance of animals were observed.
14.3 Type 1 Diabetes Adults: Pre and Postmeal Administration (14.3 Type 1 Diabetes-Adults: Pre and Postmeal Administration)
A 12-week, randomized, open-label, active-controlled, non-inferiority study was conducted in patients with type 1 diabetes to assess the safety and efficacy of APIDRA administered at different times with respect to a meal. APIDRA was administered subcutaneously either within 15 minutes before a meal (n=286) or immediately after a meal (n=296) and regular human insulin (n=278) was administered subcutaneously 30 to 45 minutes prior to a meal. Insulin glargine was administered once daily at bedtime as the basal insulin. There was a 4-week run-in period with regular human insulin and insulin glargine followed by randomization. Most patients were Caucasian (94%). The mean age was 40 years (range 18 to 73 years). Glycemic control (see Table 9) was comparable for the 3 treatment regimens. No changes from baseline between the treatments were seen in the total daily number of short-acting insulin injections (see Table 9).
| Treatment duration Treatment in combination with: |
12 weeks insulin glargine |
12 weeks insulin glargine |
12 weeks insulin glargine |
|---|---|---|---|
|
APIDRA pre meal |
APIDRA post meal |
Regular Human Insulin | |
| Glycated hemoglobin (GHb) GHb reported as HbA1c equivalent (%)Number of patients |
268 |
276 |
257 |
| Baseline mean | 7.7 | 7.7 | 7.6 |
| Adjusted mean change from baseline Adjusted mean change from baseline treatment difference (98.33% CI for treatment difference):
APIDRA pre meal vs Regular Human Insulin -0.1 (-0.3; 0.0) APIDRA post meal vs Regular Human Insulin 0.0 (-0.1; 0.2) APIDRA post meal vs pre meal 0.2 (0.0; 0.3) |
-0.3 | -0.1 | -0.1 |
| Basal insulin dose (Units/day) | |||
| Baseline mean | 29 | 29 | 28 |
| Adjusted mean change from baseline | 1 | 0 | 1 |
| Short-acting insulin dose (Units/day) | |||
| Baseline mean | 29 | 29 | 27 |
| Adjusted mean change from baseline | -1 | -1 | 2 |
| Mean number of short-acting insulin injections per day | 3 | 3 | 3 |
| Body weight (kg) | |||
| Baseline mean | 79.2 | 80.3 | 78.9 |
| Mean change from baseline | 0.3 | -0.3 | 0.3 |
5.2 Hyperglycemia Or Hypoglycemia With Changes in Insulin Regimen (5.2 Hyperglycemia or Hypoglycemia with Changes in Insulin Regimen)
Changes in an insulin regimen (e.g., insulin, insulin strength, manufacturer, type, injection site or method of administration) may affect glycemic control and predispose to hypoglycemia [see Warnings and Precautions (5.3)] or hyperglycemia. Repeated insulin injections into areas of lipodystrophy or localized cutaneous amyloidosis have been reported to result in hyperglycemia; a sudden change in the injection site (to unaffected area) has been reported to result in hypoglycemia [see Adverse Reactions (6)].
Make any changes to a patient's insulin regimen under close medical supervision with increased frequency of blood glucose monitoring. Advise patients who have repeatedly injected into areas of lipodystrophy or localized cutaneous amyloidosis to change the injection site to unaffected areas and closely monitor for hypoglycemia. For patients with type 2 diabetes, dosage adjustments in concomitant oral antidiabetic treatment may be needed.
14.5 Type 1 Diabetes Adults: Continuous Subcutaneous Insulin Infusion (14.5 Type 1 Diabetes-Adults: Continuous Subcutaneous Insulin Infusion)
A 12-week randomized, active control study (APIDRA versus insulin aspart) conducted in adults with type 1 diabetes (APIDRA n=29, insulin aspart n=30) evaluated the use of APIDRA in an external continuous subcutaneous insulin pump. All patients were Caucasian. The mean age was 46 years (range 21 to 73 years). The mean GHb increased from baseline to endpoint in both treatment groups (from 6.8% to 7.0% for APIDRA; from 7.1% to 7.2% for insulin aspart).
5.8 Hyperglycemia and Ketoacidosis Due to Insulin Pump Device Malfunction
Malfunction of the insulin pump or insulin infusion set or insulin degradation can rapidly lead to hyperglycemia and ketoacidosis. Prompt identification and correction of the cause of hyperglycemia or ketosis is necessary. Interim subcutaneous injections with APIDRA may be required. Patients using continuous subcutaneous insulin infusion pump therapy must be trained to administer insulin by injection and have alternate insulin therapy available in case of pump failure [see How Supplied/Storage and Handling (16.2)].
5.1 Never Share An Apidra Solostar Pen Or Syringe Or Needle Between Patients (5.1 Never Share an APIDRA SoloStar Pen or Syringe or Needle between Patients)
APIDRA SoloStar pens must never be shared between patients, even if the needle is changed. Patients using APIDRA vials must never reuse or share needles or syringes with another person. Sharing poses a risk for transmission of blood-borne pathogens.
5.7 Fluid Retention and Heart Failure With Concomitant Use of Ppar Gamma Agonists (5.7 Fluid Retention and Heart Failure with Concomitant Use of PPAR-Gamma Agonists)
Thiazolidinediones (TZDs), which are peroxisome proliferator-activated receptor (PPAR) gamma agonists, can cause dose-related fluid retention, when used in combination with insulin. Fluid retention may lead to or exacerbate heart failure. Patients treated with insulin, including APIDRA and a PPAR-gamma agonist should be observed for signs and symptoms of heart failure. If heart failure develops, it should be managed according to current standards of care, and discontinuation or dose reduction of the PPAR-gamma agonist must be considered.
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:50:35.354314 · Updated: 2026-03-14T22:37:58.050044