These Highlights Do Not Include All The Information Needed To Use Posaconazole Safely And Effectively. See Full Prescribing Information For Posaconazole.
e2b69c68-8696-4f81-8e2f-e4798116d055
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
Posaconazole is an azole antifungal indicated as follows: Posaconazole delayed-release tablets are indicated for the treatment of invasive aspergillosis in adults and pediatric patients 13 years of age and older. ( 1.1 ) Posaconazole is indicated for the prophylaxis of invasive Aspergillus and Candida infections in patients who are at high risk of developing these infections due to being severely immunocompromised, such as hematopoietic stem cell transplant (HSCT) recipients with graft-versus-host disease (GVHD) or those with hematologic malignancies with prolonged neutropenia from chemotherapy as follows: ( 1.2 ) Posaconazole delayed-release tablets: adults and pediatric patients 2 years of age and older who weigh greater than 40 kg Posaconazole oral suspension: adults and pediatric patients 13 years of age and older Posaconazole oral suspension is indicated for the treatment of oropharyngeal candidiasis (OPC), including OPC refractory (rOPC) to itraconazole and/or fluconazole in adult and pediatric patients aged 13 years and older. ( 1.3 )
Indications and Usage
Posaconazole is an azole antifungal indicated as follows: Posaconazole delayed-release tablets are indicated for the treatment of invasive aspergillosis in adults and pediatric patients 13 years of age and older. ( 1.1 ) Posaconazole is indicated for the prophylaxis of invasive Aspergillus and Candida infections in patients who are at high risk of developing these infections due to being severely immunocompromised, such as hematopoietic stem cell transplant (HSCT) recipients with graft-versus-host disease (GVHD) or those with hematologic malignancies with prolonged neutropenia from chemotherapy as follows: ( 1.2 ) Posaconazole delayed-release tablets: adults and pediatric patients 2 years of age and older who weigh greater than 40 kg Posaconazole oral suspension: adults and pediatric patients 13 years of age and older Posaconazole oral suspension is indicated for the treatment of oropharyngeal candidiasis (OPC), including OPC refractory (rOPC) to itraconazole and/or fluconazole in adult and pediatric patients aged 13 years and older. ( 1.3 )
Dosage and Administration
Posaconazole oral suspension is not substitutable with Posaconazole delayed-release tablets or Noxafil PowderMix for delayed-release oral suspension due to the differences in the dosing of each formulation. Therefore, follow the specific dosage recommendations for each of the formulations. ( 2.1 , 2.2 , 2.3 ) Administer Posaconazole delayed-release tablets with or without food. ( 2.1 ) Administer Posaconazole oral suspension with a full meal. ( 2.1 ) Table 1: Recommended Dosage in Adult Patients Indication Dosage Form, Dose, and Duration of Therapy Treatment of invasive Aspergillosis Posaconazole Delayed-Release Tablets: Loading dose: 300 mg (three 100 mg delayed-release tablets) twice a day on the first day. Maintenance dose : 300 mg (three 100 mg delayed-release tablets) once a day thereafter. Recommended total duration of therapy is 6 to 12 weeks. ( 2.2 ) Switching between the intravenous and delayed-release tablets is acceptable. A loading dose is not required when switching between formulations. ( 2.2 ) Prophylaxis of invasive Aspergillus and Candida infections Posaconazole Delayed-Release Tablets : Loading dose : 300 mg (three 100 mg delayed-release tablets) twice a day on the first day. Maintenance dose : 300 mg (three 100 mg delayed-release tablets) once a day, starting on the second day. Duration of therapy is based on recovery from neutropenia or immunosuppression. ( 2.2 , 2.3 ) Posaconazole Oral Suspension: 200 mg (5 mL) three times a day. Duration of therapy is based on recovery from neutropenia or immunosuppression. ( 2.2 , 2.3 ) Oropharyngeal Candidiasis (OPC) Posaconazole Oral Suspension: Loading dose : 100 mg (2.5 mL) twice a day on the first day. Maintenance dose : 100 mg (2.5 mL) once a day for 13 days. ( 2.2 , 2.3 ) OPC Refractory (rOPC) to Itraconazole and/or Fluconazole Posaconazole Oral Suspension: 400 mg (10 mL) twice a day. Duration of therapy is based on the severity of the patient’s underlying disease and clinical response. ( 2.2 , 2.3 ) For pediatric patients, see the Full Prescribing Information for dosing recommendations for Posaconazole delayed-release tablets and Posaconazole oral suspension based on the age and indication associated with the dosage form. ( 1.1 , 1.2 , 1.3 , 2.1 , 2.3 )
Warnings and Precautions
Calcineurin-Inhibitor Toxicity: Posaconazole increases concentrations of cyclosporine or tacrolimus; reduce dose of cyclosporine and tacrolimus and monitor concentrations frequently. ( 5.1 ) Arrhythmias and QTc Prolongation: Posaconazole has been shown to prolong the QTc interval and cause cases of TdP. Administer with caution to patients with potentially proarrhythmic conditions. Do not administer with drugs known to prolong QTc interval and metabolized through CYP3A4. ( 5.2 ) Electrolyte Disturbances: Monitor and correct, especially those involving potassium (K + ), magnesium (Mg ++ ), and calcium (Ca ++ ), before and during posaconazole therapy. ( 5.3 ) Hepatic Toxicity: Elevations in liver tests may occur. Discontinuation should be considered in patients who develop abnormal liver tests or monitor liver tests during treatment. ( 5.4 ) Concomitant Use with Midazolam: Posaconazole can prolong hypnotic/sedative effects. Monitor patients and benzodiazepine receptor antagonists should be available. ( 5.6 , 7.5 ) Vincristine Toxicity: Concomitant administration of azole antifungals, including posaconazole, with vincristine has been associated with neurotoxicity and other serious adverse reactions; reserve azole antifungals, including posaconazole, for patients receiving a vinca alkaloid, including vincristine, who have no alternative antifungal treatment options. ( 5.7 , 7.10 ) Breakthrough Fungal Infections : Monitor patients with severe diarrhea or vomiting when receiving Posaconazole delayed-release tablets and Posaconazole oral suspension. ( 5.8 ) Venetoclax Toxicity: Concomitant administration of posaconazole with venetoclax may increase venetoclax toxicities, including the risk of tumor lysis syndrome, neutropenia, and serious infections; monitor for toxicity and reduce venetoclax dose. ( 4.6 , 5.9 , 7.15 )
Contraindications
Known hypersensitivity to posaconazole or other azole antifungal agents. ( 4.1 ) Coadministration of posaconazole with the following drugs is contraindicated: posaconazole increases concentrations and toxicities of: Sirolimus ( 4.2 , 5.1 , 7.1 ) CYP3A4 substrates (pimozide, quinidine): can result in QTc interval prolongation and cases of torsades de pointes (TdP) ( 4.3 , 5.2 , 7.2 ) HMG-CoA Reductase Inhibitors Primarily Metabolized through CYP3A4 ( 4.4 , 7.3 ) Ergot alkaloids ( 4.5 , 7.4 ) Venetoclax: In patients with chronic lymphocytic leukemia (CLL) or small lymphocytic lymphoma (SLL) at initiation and during the ramp-up phase ( 4.6 , 5.9 , 7.15 )
Adverse Reactions
The following serious and otherwise important adverse reactions are discussed in detail in another section of the labeling: Hypersensitivity [see Contraindications (4.1) ] Arrhythmias and QT Prolongation [see Warnings and Precautions (5.2) ] Hepatic Toxicity [see Warnings and Precautions (5.4) ]
Drug Interactions
Posaconazole is primarily metabolized via UDP glucuronosyltransferase and is a substrate of p-glycoprotein (P-gp) efflux. Therefore, inhibitors or inducers of these clearance pathways may affect posaconazole plasma concentrations. Coadministration of drugs that can decrease the plasma concentrations of posaconazole should generally be avoided unless the benefit outweighs the risk. If such drugs are necessary, patients should be monitored closely for breakthrough fungal infections. Posaconazole is also a strong inhibitor of CYP3A4. Therefore, plasma concentrations of drugs predominantly metabolized by CYP3A4 may be increased by posaconazole [see Clinical Pharmacology (12.3) ] . The following information was derived from data with Noxafil oral suspension or early tablet formulation unless otherwise noted. All drug interactions with Posaconazole oral suspension, except for those that affect the absorption of posaconazole (via gastric pH and motility), are considered relevant to Posaconazole injection, Posaconazole delayed-release tablet, and Posaconazole PowderMix for delayed-release oral suspension as well [see Drug Interactions (7.9) and (7.13) ] .
Storage and Handling
16.1 How Supplied Delayed-Release Tablets Posaconazole delayed-release tablets are available as yellow, coated, oblong, debossed with "100" on one side containing 100 mg of posaconazole. Bottles with child-resistant closures of 60 delayed-release tablets (NDC 63629-2236-1). 16.2 Storage and Handling Posaconazole Delayed-Release Tablets Store at 20°C to 25°C (68°F to 77°F), excursions permitted to 15°C to 30°C (59°F to 86°F) [see USP Controlled Room Temperature]. Repackaged/Relabeled by: Bryant Ranch Prepack, Inc. Burbank, CA 91504
How Supplied
16.1 How Supplied Delayed-Release Tablets Posaconazole delayed-release tablets are available as yellow, coated, oblong, debossed with "100" on one side containing 100 mg of posaconazole. Bottles with child-resistant closures of 60 delayed-release tablets (NDC 63629-2236-1). 16.2 Storage and Handling Posaconazole Delayed-Release Tablets Store at 20°C to 25°C (68°F to 77°F), excursions permitted to 15°C to 30°C (59°F to 86°F) [see USP Controlled Room Temperature]. Repackaged/Relabeled by: Bryant Ranch Prepack, Inc. Burbank, CA 91504
Medication Information
Warnings and Precautions
Calcineurin-Inhibitor Toxicity: Posaconazole increases concentrations of cyclosporine or tacrolimus; reduce dose of cyclosporine and tacrolimus and monitor concentrations frequently. ( 5.1 ) Arrhythmias and QTc Prolongation: Posaconazole has been shown to prolong the QTc interval and cause cases of TdP. Administer with caution to patients with potentially proarrhythmic conditions. Do not administer with drugs known to prolong QTc interval and metabolized through CYP3A4. ( 5.2 ) Electrolyte Disturbances: Monitor and correct, especially those involving potassium (K + ), magnesium (Mg ++ ), and calcium (Ca ++ ), before and during posaconazole therapy. ( 5.3 ) Hepatic Toxicity: Elevations in liver tests may occur. Discontinuation should be considered in patients who develop abnormal liver tests or monitor liver tests during treatment. ( 5.4 ) Concomitant Use with Midazolam: Posaconazole can prolong hypnotic/sedative effects. Monitor patients and benzodiazepine receptor antagonists should be available. ( 5.6 , 7.5 ) Vincristine Toxicity: Concomitant administration of azole antifungals, including posaconazole, with vincristine has been associated with neurotoxicity and other serious adverse reactions; reserve azole antifungals, including posaconazole, for patients receiving a vinca alkaloid, including vincristine, who have no alternative antifungal treatment options. ( 5.7 , 7.10 ) Breakthrough Fungal Infections : Monitor patients with severe diarrhea or vomiting when receiving Posaconazole delayed-release tablets and Posaconazole oral suspension. ( 5.8 ) Venetoclax Toxicity: Concomitant administration of posaconazole with venetoclax may increase venetoclax toxicities, including the risk of tumor lysis syndrome, neutropenia, and serious infections; monitor for toxicity and reduce venetoclax dose. ( 4.6 , 5.9 , 7.15 )
Indications and Usage
Posaconazole is an azole antifungal indicated as follows: Posaconazole delayed-release tablets are indicated for the treatment of invasive aspergillosis in adults and pediatric patients 13 years of age and older. ( 1.1 ) Posaconazole is indicated for the prophylaxis of invasive Aspergillus and Candida infections in patients who are at high risk of developing these infections due to being severely immunocompromised, such as hematopoietic stem cell transplant (HSCT) recipients with graft-versus-host disease (GVHD) or those with hematologic malignancies with prolonged neutropenia from chemotherapy as follows: ( 1.2 ) Posaconazole delayed-release tablets: adults and pediatric patients 2 years of age and older who weigh greater than 40 kg Posaconazole oral suspension: adults and pediatric patients 13 years of age and older Posaconazole oral suspension is indicated for the treatment of oropharyngeal candidiasis (OPC), including OPC refractory (rOPC) to itraconazole and/or fluconazole in adult and pediatric patients aged 13 years and older. ( 1.3 )
Dosage and Administration
Posaconazole oral suspension is not substitutable with Posaconazole delayed-release tablets or Noxafil PowderMix for delayed-release oral suspension due to the differences in the dosing of each formulation. Therefore, follow the specific dosage recommendations for each of the formulations. ( 2.1 , 2.2 , 2.3 ) Administer Posaconazole delayed-release tablets with or without food. ( 2.1 ) Administer Posaconazole oral suspension with a full meal. ( 2.1 ) Table 1: Recommended Dosage in Adult Patients Indication Dosage Form, Dose, and Duration of Therapy Treatment of invasive Aspergillosis Posaconazole Delayed-Release Tablets: Loading dose: 300 mg (three 100 mg delayed-release tablets) twice a day on the first day. Maintenance dose : 300 mg (three 100 mg delayed-release tablets) once a day thereafter. Recommended total duration of therapy is 6 to 12 weeks. ( 2.2 ) Switching between the intravenous and delayed-release tablets is acceptable. A loading dose is not required when switching between formulations. ( 2.2 ) Prophylaxis of invasive Aspergillus and Candida infections Posaconazole Delayed-Release Tablets : Loading dose : 300 mg (three 100 mg delayed-release tablets) twice a day on the first day. Maintenance dose : 300 mg (three 100 mg delayed-release tablets) once a day, starting on the second day. Duration of therapy is based on recovery from neutropenia or immunosuppression. ( 2.2 , 2.3 ) Posaconazole Oral Suspension: 200 mg (5 mL) three times a day. Duration of therapy is based on recovery from neutropenia or immunosuppression. ( 2.2 , 2.3 ) Oropharyngeal Candidiasis (OPC) Posaconazole Oral Suspension: Loading dose : 100 mg (2.5 mL) twice a day on the first day. Maintenance dose : 100 mg (2.5 mL) once a day for 13 days. ( 2.2 , 2.3 ) OPC Refractory (rOPC) to Itraconazole and/or Fluconazole Posaconazole Oral Suspension: 400 mg (10 mL) twice a day. Duration of therapy is based on the severity of the patient’s underlying disease and clinical response. ( 2.2 , 2.3 ) For pediatric patients, see the Full Prescribing Information for dosing recommendations for Posaconazole delayed-release tablets and Posaconazole oral suspension based on the age and indication associated with the dosage form. ( 1.1 , 1.2 , 1.3 , 2.1 , 2.3 )
Contraindications
Known hypersensitivity to posaconazole or other azole antifungal agents. ( 4.1 ) Coadministration of posaconazole with the following drugs is contraindicated: posaconazole increases concentrations and toxicities of: Sirolimus ( 4.2 , 5.1 , 7.1 ) CYP3A4 substrates (pimozide, quinidine): can result in QTc interval prolongation and cases of torsades de pointes (TdP) ( 4.3 , 5.2 , 7.2 ) HMG-CoA Reductase Inhibitors Primarily Metabolized through CYP3A4 ( 4.4 , 7.3 ) Ergot alkaloids ( 4.5 , 7.4 ) Venetoclax: In patients with chronic lymphocytic leukemia (CLL) or small lymphocytic lymphoma (SLL) at initiation and during the ramp-up phase ( 4.6 , 5.9 , 7.15 )
Adverse Reactions
The following serious and otherwise important adverse reactions are discussed in detail in another section of the labeling: Hypersensitivity [see Contraindications (4.1) ] Arrhythmias and QT Prolongation [see Warnings and Precautions (5.2) ] Hepatic Toxicity [see Warnings and Precautions (5.4) ]
Drug Interactions
Posaconazole is primarily metabolized via UDP glucuronosyltransferase and is a substrate of p-glycoprotein (P-gp) efflux. Therefore, inhibitors or inducers of these clearance pathways may affect posaconazole plasma concentrations. Coadministration of drugs that can decrease the plasma concentrations of posaconazole should generally be avoided unless the benefit outweighs the risk. If such drugs are necessary, patients should be monitored closely for breakthrough fungal infections. Posaconazole is also a strong inhibitor of CYP3A4. Therefore, plasma concentrations of drugs predominantly metabolized by CYP3A4 may be increased by posaconazole [see Clinical Pharmacology (12.3) ] . The following information was derived from data with Noxafil oral suspension or early tablet formulation unless otherwise noted. All drug interactions with Posaconazole oral suspension, except for those that affect the absorption of posaconazole (via gastric pH and motility), are considered relevant to Posaconazole injection, Posaconazole delayed-release tablet, and Posaconazole PowderMix for delayed-release oral suspension as well [see Drug Interactions (7.9) and (7.13) ] .
Storage and Handling
16.1 How Supplied Delayed-Release Tablets Posaconazole delayed-release tablets are available as yellow, coated, oblong, debossed with "100" on one side containing 100 mg of posaconazole. Bottles with child-resistant closures of 60 delayed-release tablets (NDC 63629-2236-1). 16.2 Storage and Handling Posaconazole Delayed-Release Tablets Store at 20°C to 25°C (68°F to 77°F), excursions permitted to 15°C to 30°C (59°F to 86°F) [see USP Controlled Room Temperature]. Repackaged/Relabeled by: Bryant Ranch Prepack, Inc. Burbank, CA 91504
How Supplied
16.1 How Supplied Delayed-Release Tablets Posaconazole delayed-release tablets are available as yellow, coated, oblong, debossed with "100" on one side containing 100 mg of posaconazole. Bottles with child-resistant closures of 60 delayed-release tablets (NDC 63629-2236-1). 16.2 Storage and Handling Posaconazole Delayed-Release Tablets Store at 20°C to 25°C (68°F to 77°F), excursions permitted to 15°C to 30°C (59°F to 86°F) [see USP Controlled Room Temperature]. Repackaged/Relabeled by: Bryant Ranch Prepack, Inc. Burbank, CA 91504
Description
Posaconazole is an azole antifungal indicated as follows: Posaconazole delayed-release tablets are indicated for the treatment of invasive aspergillosis in adults and pediatric patients 13 years of age and older. ( 1.1 ) Posaconazole is indicated for the prophylaxis of invasive Aspergillus and Candida infections in patients who are at high risk of developing these infections due to being severely immunocompromised, such as hematopoietic stem cell transplant (HSCT) recipients with graft-versus-host disease (GVHD) or those with hematologic malignancies with prolonged neutropenia from chemotherapy as follows: ( 1.2 ) Posaconazole delayed-release tablets: adults and pediatric patients 2 years of age and older who weigh greater than 40 kg Posaconazole oral suspension: adults and pediatric patients 13 years of age and older Posaconazole oral suspension is indicated for the treatment of oropharyngeal candidiasis (OPC), including OPC refractory (rOPC) to itraconazole and/or fluconazole in adult and pediatric patients aged 13 years and older. ( 1.3 )
Section 42229-5
Posaconazole delayed-release tablets
- Swallow tablets whole. Do not divide, crush, or chew.
- Administer with or without food [see Dosage and Administration (2.2) and Clinical Pharmacology (12.3)].
- For patients who cannot eat a full meal, Posaconazole delayed-release tablets should be used instead of Posaconazole oral suspension for the prophylaxis indication. Posaconazole delayed-release tablets generally provide higher plasma drug exposures than Posaconazole oral suspension under both fed and fasted conditions [see Dosage and Administration (2.5)].
Posaconazole oral suspension
- Administer with a full meal or with a liquid nutritional supplement or an acidic carbonated beverage (e.g., ginger ale) in patients who cannot eat a full meal [see Dosage and Administration (2.5)].
- Co-administration of drugs that can decrease the plasma concentrations of posaconazole should generally be avoided unless the benefit outweighs the risk. If such drugs are necessary, patients should be monitored closely for breakthrough fungal infections [see Drug Interactions (7.6, 7.7, 7.8, 7.9, 7.13)].
Section 42230-3
| This Patient Information has been approved by the U.S. Food and Drug Administration. | Revised: 06/2024 | ||
|
Patient Information
Posaconazole delayed-release tablets Posaconazole oral suspension |
|||
|
What is posaconazole?
Posaconazole (which refers to delayed-release tablets and oral suspension) is a prescription medicine used in adults and children to help prevent or treat fungal infections that can spread throughout your body (invasive fungal infections). These infections are caused by fungi called Aspergillus or Candida. Posaconazole is used in people who have an increased chance of getting these infections due to a weak immune system. These include people who have had a hematopoietic stem cell transplantation (bone marrow transplant) with graft versus host disease or those with a low white blood cell count due to chemotherapy for blood cancers (hematologic malignancies). Posaconazole delayed-release tablets are used for:
Posaconazole oral suspension is for adults and children 13 years of age and older. It is not known if posaconazole is safe and effective in children under 2 years of age. |
|||
|
Who should not take posaconazole? Do not take posaconazole if you:
Do not start taking a new medicine without talking to your healthcare provider or pharmacist. |
|||
|
What should I tell my healthcare provider before taking posaconazole? Before you take posaconazole, tell your healthcare provider if you:
Especially tell your healthcare provider if you take:
Know the medicines you take. Keep a list of them with you to show your healthcare provider or pharmacist when you get a new medicine. |
|||
How will I take posaconazole?
|
|||
|
What are the possible side effects of posaconazole? Posaconazole may cause serious side effects, including:
|
|||
|
|
||
|
|||
|
|
||
| If you take Posaconazole delayed-release tablets or Posaconazole oral suspension, tell your healthcare provider right away if you have diarrhea or vomiting. Tell your healthcare provider if you have any side effect that bothers you or that does not go away. These are not all the possible side effects of posaconazole. For more information, ask your healthcare provider or pharmacist. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. |
|||
|
How should I store posaconazole?
Posaconazole delayed-release tablets
Keep posaconazole and all medicines out of the reach of children. |
|||
|
General information about the safe and effective use of posaconazole.
Medicines are sometimes prescribed for purposes other than those listed in a Patient Information leaflet. Do not use posaconazole for a condition for which it was not prescribed. Do not give posaconazole to other people, even if they have the same symptoms that you have. It may harm them. You can ask your pharmacist or healthcare provider for information about posaconazole that is written for health professionals. |
|||
|
What are the ingredients in posaconazole? Active ingredient: posaconazole Inactive ingredients: Posaconazole delayed-release tablets: croscarmellose sodium, hydroxypropylcellulose, hypromellose acetate succinate, iron oxide yellow, Macrogol/PEG 3350, magnesium stearate, microcrystalline cellulose, polyvinyl alcohol partially hydrolyzed, silicon dioxide, talc, and titanium dioxide. Posaconazole oral suspension: artificial cherry flavor, citric acid monohydrate, glycerin, liquid glucose, polysorbate 80, purified water, simethicone, sodium benzoate, sodium citrate dihydrate, titanium dioxide, and xanthan gum. Manufactured for: Endo USA, Malvern, PA 19355 Delayed-Release Tablets: Manuf. by: N. V. Organon, Kloosterstraat 6, 5349 AB Oss, Netherlands Oral Suspension: Manuf. by: Patheon Inc., Whitby, Ontario, Canada L1N5Z5 usppi-gmk5592-mf-2406r005 PI1016-01-78-03 |
Section 51945-4
Posaconazole 100 mg Tablets
8.9 Race
The pharmacokinetic profile of posaconazole is not significantly affected by race. No adjustment in the dosage of posaconazole is necessary based on race.
8.8 Gender
The pharmacokinetics of posaconazole are comparable in males and females. No adjustment in the dosage of posaconazole is necessary based on gender.
8.10 Weight
Pharmacokinetic modeling suggests that patients weighing greater than 120 kg may have lower posaconazole plasma drug exposure. It is, therefore, suggested to closely monitor for breakthrough fungal infections particularly when using Posaconazole oral suspension [see Clinical Pharmacology (12.3)].
7.12 Digoxin
Increased plasma concentrations of digoxin have been reported in patients receiving digoxin and posaconazole. Therefore, monitoring of digoxin plasma concentrations is recommended during coadministration.
10 Overdosage
There is no experience with overdosage of Posaconazole delayed-release tablets.
During the clinical trials, some patients received Noxafil oral suspension up to 1600 mg/day with no adverse reactions noted that were different from the lower doses. In addition, accidental overdose was noted in one patient who took 1200 mg twice daily Noxafil oral suspension for 3 days. No related adverse reactions were noted by the investigator.
Posaconazole is not removed by hemodialysis.
7.7 Rifabutin
Rifabutin induces UDP-glucuronidase and decreases posaconazole plasma concentrations. Rifabutin is also metabolized by CYP3A4. Therefore, coadministration of rifabutin with posaconazole increases rifabutin plasma concentrations [see Clinical Pharmacology (12.3)]. Concomitant use of posaconazole and rifabutin should be avoided unless the benefit to the patient outweighs the risk. However, if concomitant administration is required, close monitoring for breakthrough fungal infections as well as frequent monitoring of full blood counts and adverse reactions due to increased rifabutin plasma concentrations (e.g., uveitis, leukopenia) are recommended.
7.8 Phenytoin
Phenytoin induces UDP-glucuronidase and decreases posaconazole plasma concentrations. Phenytoin is also metabolized by CYP3A4. Therefore, coadministration of phenytoin with posaconazole increases phenytoin plasma concentrations [see Clinical Pharmacology (12.3)]. Concomitant use of posaconazole and phenytoin should be avoided unless the benefit to the patient outweighs the risk. However, if concomitant administration is required, close monitoring for breakthrough fungal infections is recommended and frequent monitoring of phenytoin concentrations should be performed while coadministered with posaconazole and dose reduction of phenytoin should be considered.
11 Description
Posaconazole is an azole antifungal agent available as delayed-release tablet or suspension for oral administration.
Posaconazole is designated chemically as 4-[4-[4-[4-[[ (3R,5R)-5- (2,4-difluorophenyl)tetrahydro-5- (1H-1,2,4-triazol-1-ylmethyl)-3-furanyl]methoxy]phenyl]-1-piperazinyl]phenyl]-2-[(1S,2S)-1-ethyl-2-hydroxypropyl]-2,4-dihydro-3H-1,2,4-triazol-3-one with an empirical formula of C37H42F2N8O4 and a molecular weight of 700.8. The chemical structure is:
Posaconazole Delayed-Release Tablets
Posaconazole is a white powder with a low aqueous solubility.
Posaconazole delayed-release tablet is a yellow, coated, oblong tablet containing 100 mg of posaconazole. Each delayed-release tablet contains the inactive ingredients: croscarmellose sodium, hydroxypropylcellulose, hypromellose acetate succinate, iron oxide yellow, Macrogol/PEG 3350, magnesium stearate, microcrystalline cellulose, polyvinyl alcohol partially hydrolyzed, silicon dioxide, talc, and titanium dioxide.
Posaconazole Oral Suspension
Posaconazole oral suspension is a white, cherry-flavored immediate-release suspension containing 40 mg of posaconazole per mL and the following inactive ingredients: artificial cherry flavor, citric acid monohydrate, glycerin, liquid glucose, polysorbate 80, purified water, simethicone, sodium benzoate, sodium citrate dihydrate, titanium dioxide, and xanthan gum.
7.14 Glipizide
Although no dosage adjustment of glipizide is required, it is recommended to monitor glucose concentrations when posaconazole and glipizide are concomitantly used.
7.15 Venetoclax
Concomitant use of venetoclax (a CYP3A4 substrate) with posaconazole increases venetoclax Cmax and AUC0-INF, which may increase venetoclax toxicities [see Contraindications (4.6), Warnings and Precautions (5.9)]. Refer to the venetoclax prescribing information for more information on the dosing instructions and the extent of increase in venetoclax exposure.
8.4 Pediatric Use
The safety and effectiveness of Posaconazole oral suspension and Posaconazole delayed-release tablets for the prophylaxis of invasive Aspergillus and Candida infections have been established in pediatric patients aged 2 and older who are at high risk of developing these infections due to being severely immunocompromised, such as HSCT recipients with GVHD or those with hematologic malignancies with prolonged neutropenia from chemotherapy.
The safety and effectiveness of Posaconazole injection and Posaconazole delayed-release tablets for the treatment of invasive aspergillosis have been established in pediatric patients aged 13 years and older.
The safety and effectiveness of Posaconazole oral suspension have been established for the treatment of oropharyngeal candidiasis (OPC), including OPC refractory (rOPC) to itraconazole and/or fluconazole in pediatric patients aged 13 years and older.
Use of posaconazole in these age groups is supported by evidence from adequate and well-controlled studies of Noxafil in adult and pediatric patients and additional pharmacokinetic and safety data in pediatric patients 2 years of age and older [see Adverse Reactions (6.1), Clinical Pharmacology (12.3), and Clinical Studies (14)]. The safety and effectiveness of posaconazole have not been established in pediatric patients younger than 2 years of age.
8.5 Geriatric Use
No overall differences in the safety of Noxafil delayed-release tablets and Noxafil oral suspension were observed between geriatric patients and younger adult patients in the clinical trials; therefore, no dosage adjustment is recommended for any formulation of posaconazole in geriatric patients. No clinically meaningful differences in the pharmacokinetics of Noxafil were observed in geriatric patients compared to younger adult patients during clinical trials [see Clinical Pharmacology (12.3)].
Of the 230 patients treated with Noxafil delayed-release tablets, 38 (17%) were greater than 65 years of age.
Of the 605 patients randomized to Noxafil oral suspension in Noxafil Oral Suspension Study 1 and Study 2, 63 (10%) were ≥65 years of age. In addition, 48 patients treated with greater than or equal to 800-mg/day Noxafil oral suspension in another indication were ≥65 years of age. Of the 288 patients randomized to Noxafil injection/Noxafil delayed-release tablets in the Aspergillosis Treatment Study, 85 (29%) were ≥65 years of age.
No overall differences in the pharmacokinetics and safety were observed between elderly and young subjects during clinical trials, but greater sensitivity of some older individuals cannot be ruled out.
4 Contraindications
- Known hypersensitivity to posaconazole or other azole antifungal agents. (4.1)
- Coadministration of posaconazole with the following drugs is contraindicated: posaconazole increases concentrations and toxicities of:
- Sirolimus (4.2, 5.1, 7.1)
- CYP3A4 substrates (pimozide, quinidine): can result in QTc interval prolongation and cases of torsades de pointes (TdP) (4.3, 5.2, 7.2)
- HMG-CoA Reductase Inhibitors Primarily Metabolized through CYP3A4 (4.4, 7.3)
- Ergot alkaloids (4.5, 7.4)
- Venetoclax: In patients with chronic lymphocytic leukemia (CLL) or small lymphocytic lymphoma (SLL) at initiation and during the ramp-up phase (4.6, 5.9, 7.15)
6 Adverse Reactions
The following serious and otherwise important adverse reactions are discussed in detail in another section of the labeling:
- Hypersensitivity [see Contraindications (4.1)]
- Arrhythmias and QT Prolongation [see Warnings and Precautions (5.2)]
- Hepatic Toxicity [see Warnings and Precautions (5.4)]
7 Drug Interactions
Posaconazole is primarily metabolized via UDP glucuronosyltransferase and is a substrate of p-glycoprotein (P-gp) efflux. Therefore, inhibitors or inducers of these clearance pathways may affect posaconazole plasma concentrations. Coadministration of drugs that can decrease the plasma concentrations of posaconazole should generally be avoided unless the benefit outweighs the risk. If such drugs are necessary, patients should be monitored closely for breakthrough fungal infections.
Posaconazole is also a strong inhibitor of CYP3A4. Therefore, plasma concentrations of drugs predominantly metabolized by CYP3A4 may be increased by posaconazole [see Clinical Pharmacology (12.3)].
The following information was derived from data with Noxafil oral suspension or early tablet formulation unless otherwise noted. All drug interactions with Posaconazole oral suspension, except for those that affect the absorption of posaconazole (via gastric pH and motility), are considered relevant to Posaconazole injection, Posaconazole delayed-release tablet, and Posaconazole PowderMix for delayed-release oral suspension as well [see Drug Interactions (7.9) and (7.13)].
7.4 Ergot Alkaloids
Most of the ergot alkaloids are substrates of CYP3A4. Posaconazole may increase the plasma concentrations of ergot alkaloids (ergotamine and dihydroergotamine) which may lead to ergotism. Therefore, posaconazole is contraindicated with ergot alkaloids [see Contraindications (4.5)].
4.1 Hypersensitivity
Posaconazole is contraindicated in persons with known hypersensitivity to posaconazole or other azole antifungal agents.
5.4 Hepatic Toxicity
Hepatic reactions (e.g., mild to moderate elevations in alanine aminotransferase (ALT), aspartate aminotransferase (AST), alkaline phosphatase, total bilirubin, and/or clinical hepatitis) have been reported in clinical trials. The elevations in liver tests were generally reversible on discontinuation of therapy, and in some instances these tests normalized without drug interruption. Cases of more severe hepatic reactions including cholestasis or hepatic failure including deaths have been reported in patients with serious underlying medical conditions (e.g., hematologic malignancy) during treatment with posaconazole. These severe hepatic reactions were seen primarily in subjects receiving the Posaconazole oral suspension 800 mg daily (400 mg twice daily or 200 mg four times a day) in clinical trials.
Liver tests should be evaluated at the start of and during the course of posaconazole therapy. Patients who develop abnormal liver tests during posaconazole therapy should be monitored for the development of more severe hepatic injury. Patient management should include laboratory evaluation of hepatic function (particularly liver tests and bilirubin). Discontinuation of posaconazole must be considered if clinical signs and symptoms consistent with liver disease develop that may be attributable to posaconazole.
5.5 Renal Impairment
Due to the variability in exposure with Posaconazole delayed-release tablets and Posaconazole oral suspension, patients with severe renal impairment should be monitored closely for breakthrough fungal infections [see Dosage and Administration (2.4) and Use in Specific Populations (8.6)].
7.10 Vinca Alkaloids
Most of the vinca alkaloids (e.g., vincristine and vinblastine) are substrates of CYP3A4. Concomitant administration of azole antifungals, including posaconazole, with vincristine has been associated with serious adverse reactions [see Warnings and Precautions (5.7)]. Posaconazole may increase the plasma concentrations of vinca alkaloids which may lead to neurotoxicity and other serious adverse reactions. Therefore, reserve azole antifungals, including posaconazole, for patients receiving a vinca alkaloid, including vincristine, who have no alternative antifungal treatment options.
8.6 Renal Impairment
Following single-dose administration of 400 mg of the Noxafil oral suspension, there was no significant effect of mild (eGFR: 50-80 mL/min/1.73 m2, n=6) or moderate (eGFR: 20-49 mL/min/1.73 m2, n=6) renal impairment on posaconazole pharmacokinetics; therefore, no dose adjustment is required in patients with mild to moderate renal impairment. In subjects with severe renal impairment (eGFR: <20 mL/min/1.73 m2), the mean plasma exposure (AUC) was similar to that in patients with normal renal function (eGFR: >80 mL/min/1.73 m2); however, the range of the AUC estimates was highly variable (CV=96%) in these subjects with severe renal impairment as compared to that in the other renal impairment groups (CV<40%). Due to the variability in exposure, patients with severe renal impairment should be monitored closely for breakthrough fungal infections [see Dosage and Administration (2)]. Similar recommendations apply to Posaconazole delayed-release tablets; however, a specific study has not been conducted with the Posaconazole delayed-release tablets.
7.2 Cyp3a4 Substrates
Concomitant administration of posaconazole with CYP3A4 substrates such as pimozide and quinidine may result in increased plasma concentrations of these drugs, leading to QTc prolongation and cases of torsades de pointes. Therefore, posaconazole is contraindicated with these drugs [see Contraindications (4.3) and Warnings and Precautions (5.2)].
4.2 Use With Sirolimus
Posaconazole is contraindicated with sirolimus. Concomitant administration of posaconazole with sirolimus increases the sirolimus blood concentrations by approximately 9-fold and can result in sirolimus toxicity [see Drug Interactions (7.1) and Clinical Pharmacology (12.3)].
5.6 Midazolam Toxicity
Concomitant administration of posaconazole with midazolam increases the midazolam plasma concentrations by approximately 5-fold. Increased plasma midazolam concentrations could potentiate and prolong hypnotic and sedative effects. Patients must be monitored closely for adverse effects associated with high plasma concentrations of midazolam and benzodiazepine receptor antagonists must be available to reverse these effects [see Drug Interactions (7.5) and Clinical Pharmacology (12.3)].
8.7 Hepatic Impairment
After a single oral dose of Noxafil oral suspension 400 mg, the mean AUC was 43%, 27%, and 21% higher in subjects with mild (Child-Pugh Class A, N=6), moderate (Child-Pugh Class B, N=6), or severe (Child-Pugh Class C, N=6) hepatic impairment, respectively, compared to subjects with normal hepatic function (N=18). Compared to subjects with normal hepatic function, the mean Cmax was 1% higher, 40% higher, and 34% lower in subjects with mild, moderate, or severe hepatic impairment, respectively. The mean apparent oral clearance (CL/F) was reduced by 18%, 36%, and 28% in subjects with mild, moderate, or severe hepatic impairment, respectively, compared to subjects with normal hepatic function. The elimination half-life (t½) was 27 hours, 39 hours, 27 hours, and 43 hours in subjects with normal hepatic function and mild, moderate, or severe hepatic impairment, respectively.
It is recommended that no dose adjustment of posaconazole is needed in patients with mild to severe hepatic impairment (Child-Pugh Class A, B, or C) [see Dosage and Administration (2) and Warnings and Precautions (5.4)]. Similar recommendations apply to Posaconazole delayed-release tablets; however, a specific study has not been conducted with the Posaconazole delayed-release tablets.
1 Indications and Usage
Posaconazole is an azole antifungal indicated as follows:
- Posaconazole delayed-release tablets are indicated for the treatment of invasive aspergillosis in adults and pediatric patients 13 years of age and older. (1.1)
-
Posaconazole is indicated for the prophylaxis of invasive Aspergillus and Candida infections in patients who are at high risk of developing these infections due to being severely immunocompromised, such as hematopoietic stem cell transplant (HSCT) recipients with graft-versus-host disease (GVHD) or those with hematologic malignancies with prolonged neutropenia from chemotherapy as follows: (1.2)
- Posaconazole delayed-release tablets: adults and pediatric patients 2 years of age and older who weigh greater than 40 kg
- Posaconazole oral suspension: adults and pediatric patients 13 years of age and older
- Posaconazole oral suspension is indicated for the treatment of oropharyngeal candidiasis (OPC), including OPC refractory (rOPC) to itraconazole and/or fluconazole in adult and pediatric patients aged 13 years and older. (1.3)
4.6 Use With Venetoclax
Coadministration of posaconazole with venetoclax at initiation and during the ramp-up phase is contraindicated in patients with chronic lymphocytic leukemia (CLL) or small lymphocytic lymphoma (SLL) due to the potential for increased risk of tumor lysis syndrome [see Warnings and Precautions (5.9) and Drug Interactions (7.15)].
5.9 Venetoclax Toxicity
Concomitant administration of posaconazole, a strong CYP3A4 inhibitor, with venetoclax may increase venetoclax toxicities, including the risk of tumor lysis syndrome (TLS), neutropenia, and serious infections. In patients with CLL/SLL, administration of posaconazole during initiation and the ramp-up phase of venetoclax is contraindicated [see Contraindications (4.6)]. Refer to the venetoclax labeling for safety monitoring and dose reduction in the steady daily dosing phase in CLL/SLL patients.
For patients with acute myeloid leukemia (AML), dose reduction and safety monitoring are recommended across all dosing phases when coadministering posaconazole with venetoclax [see Drug Interactions (7.15)]. Refer to the venetoclax prescribing information for dosing instructions.
12.1 Mechanism of Action
Posaconazole is an azole antifungal agent [see Clinical Pharmacology (12.4)].
5.7 Vincristine Toxicity
Concomitant administration of azole antifungals, including posaconazole, with vincristine has been associated with neurotoxicity and other serious adverse reactions, including seizures, peripheral neuropathy, syndrome of inappropriate antidiuretic hormone secretion, and paralytic ileus. Reserve azole antifungals, including posaconazole, for patients receiving a vinca alkaloid, including vincristine, who have no alternative antifungal treatment options [see Drug Interactions (7.10)].
5 Warnings and Precautions
- Calcineurin-Inhibitor Toxicity: Posaconazole increases concentrations of cyclosporine or tacrolimus; reduce dose of cyclosporine and tacrolimus and monitor concentrations frequently. (5.1)
- Arrhythmias and QTc Prolongation: Posaconazole has been shown to prolong the QTc interval and cause cases of TdP. Administer with caution to patients with potentially proarrhythmic conditions. Do not administer with drugs known to prolong QTc interval and metabolized through CYP3A4. (5.2)
- Electrolyte Disturbances: Monitor and correct, especially those involving potassium (K+), magnesium (Mg++), and calcium (Ca++), before and during posaconazole therapy. (5.3)
- Hepatic Toxicity: Elevations in liver tests may occur. Discontinuation should be considered in patients who develop abnormal liver tests or monitor liver tests during treatment. (5.4)
- Concomitant Use with Midazolam: Posaconazole can prolong hypnotic/sedative effects. Monitor patients and benzodiazepine receptor antagonists should be available. (5.6, 7.5)
- Vincristine Toxicity: Concomitant administration of azole antifungals, including posaconazole, with vincristine has been associated with neurotoxicity and other serious adverse reactions; reserve azole antifungals, including posaconazole, for patients receiving a vinca alkaloid, including vincristine, who have no alternative antifungal treatment options. (5.7, 7.10)
- Breakthrough Fungal Infections: Monitor patients with severe diarrhea or vomiting when receiving Posaconazole delayed-release tablets and Posaconazole oral suspension. (5.8)
- Venetoclax Toxicity: Concomitant administration of posaconazole with venetoclax may increase venetoclax toxicities, including the risk of tumor lysis syndrome, neutropenia, and serious infections; monitor for toxicity and reduce venetoclax dose. (4.6, 5.9, 7.15)
2 Dosage and Administration
- Posaconazole oral suspension is not substitutable with Posaconazole delayed-release tablets or Noxafil PowderMix for delayed-release oral suspension due to the differences in the dosing of each formulation. Therefore, follow the specific dosage recommendations for each of the formulations. (2.1, 2.2, 2.3)
- Administer Posaconazole delayed-release tablets with or without food. (2.1)
- Administer Posaconazole oral suspension with a full meal. (2.1)
| Table 1: Recommended Dosage in Adult Patients | |
|---|---|
| Indication | Dosage Form, Dose, and Duration of Therapy |
| Treatment of invasive Aspergillosis |
Posaconazole Delayed-Release Tablets:
Loading dose: 300 mg (three 100 mg delayed-release tablets) twice a day on the first day. Maintenance dose: 300 mg (three 100 mg delayed-release tablets) once a day thereafter. Recommended total duration of therapy is 6 to 12 weeks. (2.2) Switching between the intravenous and delayed-release tablets is acceptable. A loading dose is not required when switching between formulations. (2.2) |
| Prophylaxis of invasive Aspergillus and Candida infections |
Posaconazole Delayed-Release Tablets
:
Loading dose: 300 mg (three 100 mg delayed-release tablets) twice a day on the first day. Maintenance dose: 300 mg (three 100 mg delayed-release tablets) once a day, starting on the second day. Duration of therapy is based on recovery from neutropenia or immunosuppression. (2.2, 2.3) Posaconazole Oral Suspension: 200 mg (5 mL) three times a day. Duration of therapy is based on recovery from neutropenia or immunosuppression. (2.2, 2.3) |
| Oropharyngeal Candidiasis (OPC) |
Posaconazole Oral Suspension:
Loading dose: 100 mg (2.5 mL) twice a day on the first day. Maintenance dose: 100 mg (2.5 mL) once a day for 13 days. (2.2, 2.3) |
| OPC Refractory (rOPC) to Itraconazole and/or Fluconazole | Posaconazole Oral Suspension: 400 mg (10 mL) twice a day. Duration of therapy is based on the severity of the patient’s underlying disease and clinical response. (2.2, 2.3) |
3 Dosage Forms and Strengths
Posaconazole Delayed-Release Tablets
Posaconazole delayed-release tablets are available as yellow, coated, oblong tablets, debossed with "100" on one side containing 100 mg of posaconazole.
Posaconazole Oral Suspension
Posaconazole oral suspension is available as a white, cherry-flavored suspension in 4-ounce (123 mL) amber glass bottles with child-resistant closures containing 105 mL of suspension (40 mg of posaconazole per mL).
4.5 Use With Ergot Alkaloids
Posaconazole may increase the plasma concentrations of ergot alkaloids (ergotamine and dihydroergotamine) which may lead to ergotism [see Drug Interactions (7.4)].
5.3 Electrolyte Disturbances
Electrolyte disturbances, especially those involving potassium, magnesium or calcium levels, should be monitored and corrected as necessary before and during posaconazole therapy.
6.2 Postmarketing Experience
The following adverse reaction has been identified during the post-approval use of posaconazole. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency.
Endocrine Disorders: Pseudoaldosteronism
8 Use in Specific Populations
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in clinical trials of Noxafil cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
14.2 Prophylaxis of Aspergillus
Two randomized, controlled studies were conducted using Noxafil as prophylaxis for the prevention of invasive fungal infections (IFIs) among patients at high risk due to severely compromised immune systems.
The first study (Noxafil Oral Suspension Study 1) was a randomized, double-blind trial that compared Noxafil oral suspension (200 mg three times a day) with fluconazole capsules (400 mg once daily) as prophylaxis against invasive fungal infections in allogeneic hematopoietic stem cell transplant (HSCT) recipients with Graft versus Host Disease (GVHD). Efficacy of prophylaxis was evaluated using a composite endpoint of proven/probable IFIs, death, or treatment with systemic antifungal therapy (patients may have met more than one of these criteria). This assessed all patients while on study therapy plus 7 days and at 16 weeks post-randomization. The mean duration of therapy was comparable between the 2 treatment groups (80 days, Noxafil oral suspension; 77 days, fluconazole). Table 23 contains the results from Noxafil Oral Suspension Study 1.
| Posaconazole n=301 |
Fluconazole n=299 |
|
|---|---|---|
| On therapy plus 7 days | ||
|
Clinical Failure Patients may have met more than one criterion defining failure.
|
50 (17%) | 55 (18%) |
| Failure due to: | ||
| Proven/Probable IFI | 7 (2%) | 22 (7%) |
| (Aspergillus) | 3 (1%) | 17 (6%) |
| (Candida) | 1 (<1%) | 3 (1%) |
| (Other) | 3 (1%) | 2 (1%) |
| All Deaths | 22 (7%) | 24 (8%) |
| Proven/probable fungal infection prior to death | 2 (<1%) | 6 (2%) |
| SAF Use of systemic antifungal therapy (SAF) criterion is based on protocol definitions (empiric/IFI usage >4 consecutive days).
|
27 (9%) | 25 (8%) |
| Through 16 weeks | ||
|
Clinical Failure
,
95% confidence interval (posaconazole-fluconazole) = (-11.5%, +3.7%).
|
99 (33%) | 110 (37%) |
| Failure due to: | ||
| Proven/Probable IFI | 16 (5%) | 27 (9%) |
| (Aspergillus) | 7 (2%) | 21 (7%) |
| (Candida) | 4 (1%) | 4 (1%) |
| (Other) | 5 (2%) | 2 (1%) |
| All Deaths | 58 (19%) | 59 (20%) |
| Proven/probable fungal infection prior to death | 10 (3%) | 16 (5%) |
| SAF | 26 (9%) | 30 (10%) |
| Event free lost to follow-up Patients who are lost to follow-up (not observed for 112 days), and who did not meet another clinical failure endpoint. These patients were considered failures.
|
24 (8%) | 30 (10%) |
The second study (Noxafil Oral Suspension Study 2) was a randomized, open-label study that compared Noxafil oral suspension (200 mg 3 times a day) with fluconazole suspension (400 mg once daily) or itraconazole oral solution (200 mg twice a day) as prophylaxis against IFIs in neutropenic patients who were receiving cytotoxic chemotherapy for AML or MDS. As in Noxafil Oral Suspension Study 1, efficacy of prophylaxis was evaluated using a composite endpoint of proven/probable IFIs, death, or treatment with systemic antifungal therapy (Patients might have met more than one of these criteria). This study assessed patients while on treatment plus 7 days and 100 days postrandomization. The mean duration of therapy was comparable between the 2 treatment groups (29 days, posaconazole; 25 days, fluconazole or itraconazole). Table 24 contains the results from Noxafil Oral Suspension Study 2.
| Posaconazole n=304 |
Fluconazole/Itraconazole n=298 |
|
|---|---|---|
| On therapy plus 7 days | ||
|
Clinical Failure 95% confidence interval (posaconazole-fluconazole/itraconazole) = (-22.9%, -7.8%).
,
Patients may have met more than one criterion defining failure.
|
82 (27%) | 126 (42%) |
| Failure due to: | ||
| Proven/Probable IFI | 7 (2%) | 25 (8%) |
| (Aspergillus) | 2 (1%) | 20 (7%) |
| (Candida) | 3 (1%) | 2 (1%) |
| (Other) | 2 (1%) | 3 (1%) |
| All Deaths | 17 (6%) | 25 (8%) |
| Proven/probable fungal infection prior to death | 1 (<1%) | 2 (1%) |
| SAF Use of systemic antifungal therapy (SAF) criterion is based on protocol definitions (empiric/IFI usage >3 consecutive days).
|
67 (22%) | 98 (33%) |
| Through 100 days postrandomization | ||
| Clinical Failure | 158 (52%) | 191 (64%) |
| Failure due to: | ||
| Proven/Probable IFI | 14 (5%) | 33 (11%) |
| (Aspergillus) | 2 (1%) | 26 (9%) |
| (Candida) | 10 (3%) | 4 (1%) |
| (Other) | 2 (1%) | 3 (1%) |
| All Deaths | 44 (14%) | 64 (21%) |
| Proven/probable fungal infection prior to death | 2 (1%) | 16 (5%) |
| SAF | 98 (32%) | 125 (42%) |
| Event free lost to follow-up Patients who are lost to follow-up (not observed for 100 days), and who did not meet another clinical failure endpoint. These patients were considered failures.
|
34 (11%) | 24 (8%) |
In summary, 2 clinical studies of prophylaxis were conducted with the Noxafil oral suspension. As seen in the accompanying tables (Tables 23 and 24), clinical failure represented a composite endpoint of breakthrough IFI, mortality and use of systemic antifungal therapy. In Noxafil Oral Suspension Study 1 (Table 23), the clinical failure rate of posaconazole (33%) was similar to fluconazole (37%), (95% CI for the difference posaconazole–comparator -11.5% to 3.7%) while in Noxafil Oral Suspension Study 2 (Table 24) clinical failure was lower for patients treated with posaconazole (27%) when compared to patients treated with fluconazole or itraconazole (42%), (95% CI for the difference posaconazole–comparator -22.9% to -7.8%).
All-cause mortality was similar at 16 weeks for both treatment arms in Noxafil Oral Suspension Study 1 [POS 58/301 (19%) vs. FLU 59/299 (20%)]; all-cause mortality was lower at 100 days for Noxafil-treated patients in Noxafil Oral Suspension Study 2 [POS 44/304 (14%) vs. FLU/ITZ 64/298 (21%)]. Both studies demonstrated fewer breakthrough infections caused by Aspergillus species in patients receiving Noxafil prophylaxis when compared to patients receiving fluconazole or itraconazole.
17 Patient Counseling Information
Advise the patient to read the FDA-approved patient labeling (Patient Information).
Important Administration Instructions
Posaconazole Delayed-Release Tablets
Advise patients that Posaconazole delayed-release tablets must be swallowed whole and not divided, crushed, or chewed.
Instruct patients that if they miss a dose, they should take it as soon as they remember. If they do not remember until it is within 12 hours of the next dose, they should be instructed to skip the missed dose and go back to the regular schedule. Patients should not double their next dose or take more than the prescribed dose.
Posaconazole Oral Suspension
Advise patients to take each dose of Posaconazole oral suspension during or immediately (i.e., within 20 minutes) following a full meal. In patients who cannot eat a full meal, each dose of Posaconazole oral suspension should be administered with a liquid nutritional supplement or an acidic carbonated beverage (e.g., ginger ale) in order to enhance absorption.
Instruct patients that if they miss a dose, they should take it as soon as they remember. However, if it is almost time for the next dose, they should be instructed to skip the missed dose and go back to the regular schedule. Patients should not double their next dose or take more than the prescribed dose.
Drug Interactions
Advise patients to inform their physician immediately if they:
- develop severe diarrhea or vomiting.
- are currently taking drugs that are known to prolong the QTc interval and are metabolized through CYP3A4.
- are currently taking a cyclosporine or tacrolimus, or they notice swelling in an arm or leg or shortness of breath.
- are taking other drugs or before they begin taking other drugs as certain drugs can decrease or increase the plasma concentrations of posaconazole.
Serious and Potentially Serious Adverse Reactions
Advise patients to inform their physician immediately if they:
- notice a change in heart rate or heart rhythm or have a heart condition or circulatory disease. Posaconazole can be administered with caution to patients with potentially proarrhythmic conditions.
- are pregnant, plan to become pregnant, or are nursing.
- have liver disease or develop itching, nausea or vomiting, their eyes or skin turn yellow, they feel more tired than usual or feel like they have the flu.
- have ever had an allergic reaction to other antifungal medicines such as ketoconazole, fluconazole, itraconazole, or voriconazole.
5.1 Calcineurin Inhibitor Toxicity
Concomitant administration of posaconazole with cyclosporine or tacrolimus increases the whole blood trough concentrations of these calcineurin-inhibitors [see Drug Interactions (7.1) and Clinical Pharmacology (12.3)]. Nephrotoxicity and leukoencephalopathy (including deaths) have been reported in clinical efficacy studies in patients with elevated cyclosporine or tacrolimus concentrations. Frequent monitoring of tacrolimus or cyclosporine whole blood trough concentrations should be performed during and at discontinuation of posaconazole treatment and the tacrolimus or cyclosporine dose adjusted accordingly.
5.8 Breakthrough Fungal Infections
Patients who have severe diarrhea or vomiting should be monitored closely for breakthrough fungal infections when receiving Posaconazole delayed-release tablets or Posaconazole oral suspension.
5.2 Arrhythmias and Qt Prolongation
Some azoles, including posaconazole, have been associated with prolongation of the QT interval on the electrocardiogram. In addition, cases of torsades de pointes have been reported in patients taking posaconazole.
Results from a multiple time-matched ECG analysis in healthy volunteers did not show any increase in the mean of the QTc interval. Multiple, time-matched ECGs collected over a 12-hour period were recorded at baseline and steady-state from 173 healthy male and female volunteers (18-85 years of age) administered Noxafil oral suspension 400 mg twice daily with a high-fat meal. In this pooled analysis, the mean QTc (Fridericia) interval change from baseline was –5 msec following administration of the recommended clinical dose. A decrease in the QTc(F) interval (–3 msec) was also observed in a small number of subjects (n=16) administered placebo. The placebo-adjusted mean maximum QTc(F) interval change from baseline was <0 msec (–8 msec). No healthy subject administered Noxafil had a QTc(F) interval ≥500 msec or an increase ≥60 msec in their QTc(F) interval from baseline.
Posaconazole should be administered with caution to patients with potentially proarrhythmic conditions. Do not administer with drugs that are known to prolong the QTc interval and are metabolized through CYP3A4 [see Contraindications (4.3) and Drug Interactions (7.2)].
16 How Supplied/storage and Handling
16.1 How Supplied
Delayed-Release Tablets
Posaconazole delayed-release tablets are available as yellow, coated, oblong, debossed with "100" on one side containing 100 mg of posaconazole. Bottles with child-resistant closures of 60 delayed-release tablets (NDC 63629-2236-1).
16.2 Storage and Handling
Posaconazole Delayed-Release Tablets
Store at 20°C to 25°C (68°F to 77°F), excursions permitted to 15°C to 30°C (59°F to 86°F) [see USP Controlled Room Temperature].
Repackaged/Relabeled by:
Bryant Ranch Prepack, Inc.
Burbank, CA 91504
1.1 Treatment of Invasive Aspergillosis
Posaconazole delayed-release tablets are indicated for the treatment of invasive aspergillosis in adults and pediatric patients 13 years of age and older.
1.2 Prophylaxis of Invasive Aspergillus
Posaconazole is indicated for the prophylaxis of invasive Aspergillus and Candida infections in patients who are at high risk of developing these infections due to being severely immunocompromised, such as hematopoietic stem cell transplant (HSCT) recipients with graft-versus-host disease (GVHD) or those with hematologic malignancies with prolonged neutropenia from chemotherapy [see Clinical Studies (14.1)] as follows:
- Posaconazole delayed-release tablets: adults and pediatric patients 2 years of age and older who weigh greater than 40 kg
- Posaconazole oral suspension: adults and pediatric patients 13 years of age and older
2.1 Important Administration Instructions
Non-substitutable
Posaconazole oral suspension is not substitutable with Posaconazole delayed-release tablets or Noxafil PowderMix for delayed-release oral suspension due to the differences in the dosing of each formulation. Therefore, follow the specific dosage recommendations for each of the formulations [see Dosage and Administration (2.2, 2.3)].
7.5 Benzodiazepines Metabolized By Cyp3a4
Concomitant administration of posaconazole with midazolam increases the midazolam plasma concentrations by approximately 5-fold. Increased plasma midazolam concentrations could potentiate and prolong hypnotic and sedative effects. Concomitant use of posaconazole and other benzodiazepines metabolized by CYP3A4 (e.g., alprazolam, triazolam) could result in increased plasma concentrations of these benzodiazepines. Patients must be monitored closely for adverse effects associated with high plasma concentrations of benzodiazepines metabolized by CYP3A4 and benzodiazepine receptor antagonists must be available to reverse these effects [see Warnings and Precautions (5.6) and Clinical Pharmacology (12.3)].
13.2 Animal Toxicology And/or Pharmacology
In a nonclinical study using intravenous administration of posaconazole in very young dogs (dosed from 2 to 8 weeks of age), an increase in the incidence of brain ventricle enlargement was observed in treated animals as compared with concurrent control animals. No difference in the incidence of brain ventricle enlargement between control and treated animals was observed following the subsequent 5-month treatment-free period. There were no neurologic, behavioral or developmental abnormalities in the dogs with this finding, and a similar brain finding was not seen with oral posaconazole administration to juvenile dogs (4 days to 9 months of age). There were no drug-related increases in the incidence of brain ventricle enlargement when treated, and control animals were compared in a separate study of 10-week old dogs dosed with intravenous posaconazole for 13 weeks with a 9-week recovery period or a follow-up study of 31-week old dogs dosed for 3 months.
7.11 Calcium Channel Blockers Metabolized By Cyp3a4
Posaconazole may increase the plasma concentrations of calcium channel blockers metabolized by CYP3A4 (e.g., verapamil, diltiazem, nifedipine, nicardipine, felodipine). Frequent monitoring for adverse reactions and toxicity related to calcium channel blockers is recommended during coadministration. Dose reduction of calcium channel blockers may be needed.
2.7 Dosage Adjustments in Patients With Renal Impairment
The pharmacokinetics of Posaconazole oral suspension and Posaconazole delayed-release tablets are not significantly affected by renal impairment. Therefore, no adjustment is necessary for oral dosing in patients with mild to severe renal impairment.
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenesis
No drug-related neoplasms were recorded in rats or mice treated with posaconazole for 2 years at doses higher than the clinical dose. In a 2-year carcinogenicity study, rats were given posaconazole orally at doses up to 20 mg/kg (females), or 30 mg/kg (males). These doses are equivalent to 3.9- or 3.5-times the exposure achieved with a 400-mg twice daily oral suspension regimen, respectively, based on steady-state AUC in healthy volunteers administered a high-fat meal (400-mg twice daily oral suspension regimen). In the mouse study, mice were treated at oral doses up to 60 mg/kg/day or 4.8-times the exposure achieved with a 400-mg twice daily oral suspension regimen.
Mutagenesis
Posaconazole was not genotoxic or clastogenic when evaluated in bacterial mutagenicity (Ames), a chromosome aberration study in human peripheral blood lymphocytes, a Chinese hamster ovary cell mutagenicity study, and a mouse bone marrow micronucleus study.
Impairment of Fertility
Posaconazole had no effect on fertility of male rats at a dose up to 180 mg/kg (1.7 x the 400-mg twice daily oral suspension regimen based on steady-state plasma concentrations in healthy volunteers) or female rats at a dose up to 45 mg/kg (2.2 x the 400-mg twice daily oral suspension regimen).
4.3 Qt Prolongation With Concomitant Use With Cyp3a4 Substrates
Posaconazole is contraindicated with CYP3A4 substrates that prolong the QT interval. Concomitant administration of posaconazole with the CYP3A4 substrates, pimozide and quinidine may result in increased plasma concentrations of these drugs, leading to QTc prolongation and cases of torsades de pointes [see Warnings and Precautions (5.2) and Drug Interactions (7.2)].
2.5 Administration Instructions for Posaconazole Oral Suspension
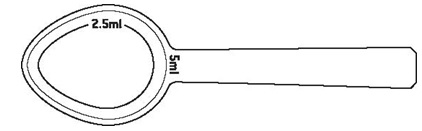
- Shake Posaconazole oral suspension well before use. Administer with measured dosing spoon (see Figure 1) provided.
| Figure 1: A measured dosing spoon is provided, marked for doses of 2.5 mL and 5 mL. |
- Rinse the spoon with water after each administration and before storage.
- Administer each dose of Posaconazole oral suspension during or immediately (i.e., within 20 minutes) following a full meal [see Clinical Pharmacology (12.3)].
- For patients who cannot eat a full meal, Posaconazole delayed-release tablets should be used instead of Posaconazole oral suspension for the prophylaxis indication. Posaconazole delayed-release tablets provide higher plasma drug exposures than Posaconazole oral suspension under fasted conditions [see Dosage and Administration (2.1)].
- In patients who cannot eat a full meal and for whom Posaconazole delayed-release tablets or Noxafil injection are not options, administer each dose of Posaconazole oral suspension with a liquid nutritional supplement or an acidic carbonated beverage (e.g., ginger ale).
- For patients who cannot eat a full meal or tolerate an oral nutritional supplement or an acidic carbonated beverage and who do not have the option of taking Posaconazole delayed-release tablets or Noxafil injection, an alternative antifungal therapy should be considered or patients should be monitored closely for breakthrough fungal infections.
4.4 Hmg Coa Reductase Inhibitors Primarily Metabolized Through Cyp3a4
Coadministration with the HMG-CoA reductase inhibitors that are primarily metabolized through CYP3A4 (e.g., atorvastatin, lovastatin, and simvastatin) is contraindicated since increased plasma concentration of these drugs can lead to rhabdomyolysis [see Drug Interactions (7.3) and Clinical Pharmacology (12.3)].
14.3 Treatment of Oropharyngeal Candidiasis With Noxafil Oral Suspension
Noxafil Oral Suspension Study 3 was a randomized, controlled, evaluator-blinded study in HIV-infected patients with oropharyngeal candidiasis. Patients were treated with Noxafil or fluconazole oral suspension (both Noxafil and fluconazole were given as follows: 100 mg twice a day for 1 day followed by 100 mg once a day for 13 days).
Clinical and mycological outcomes were assessed after 14 days of treatment and at 4 weeks after the end of treatment. Patients who received at least 1 dose of study medication and had a positive oral swish culture of Candida species at baseline were included in the analyses (see Table 25 ). The majority of the subjects had C. albicans as the baseline pathogen.
Clinical success at Day 14 (complete or partial resolution of all ulcers and/or plaques and symptoms) and clinical relapse rates (recurrence of signs or symptoms after initial cure or improvement) 4 weeks after the end of treatment were similar between the treatment arms (see Table 25 ).
Mycologic eradication rates (absence of colony forming units in quantitative culture at the end of therapy, Day 14), as well as mycologic relapse rates (4 weeks after the end of treatment) were also similar between the treatment arms (see Table 25 ).
| Noxafil | Fluconazole | |
|---|---|---|
| Clinical Success at End of Therapy (Day 14) | 155/169 (91.7%) | 148/160 (92.5%) |
| Clinical Relapse (4 Weeks after End of Therapy) | 45/155 (29.0%) | 52/148 (35.1%) |
| Mycological Eradication (absence of CFU) at End of Therapy (Day 14) | 88/169 (52.1%) | 80/160 (50.0%) |
| Mycological Relapse (4 Weeks after End of Treatment) | 49/88 (55.6%) | 51/80 (63.7%) |
Mycologic response rates, using a criterion for success as a posttreatment quantitative culture with ≤20 colony forming units (CFU/mL) were also similar between the two groups (Noxafil 68.0%, fluconazole 68.1%). The clinical significance of this finding is unknown.
2.4 Administration Instructions for Posaconazole Delayed Release Tablets
- Swallow tablets whole. Do not divide, crush, or chew.
- Administer Posaconazole delayed-release tablets with or without food [see Clinical Pharmacology (12.3)].
2.3 Dosing Regimen in Pediatric Patients (ages 2 to Less Than 18 Years of Age)
- The recommended dosing regimen of posaconazole for pediatric patients 2 to less than 18 years of age is shown in Tables 2 and 3 [see Dosage and Administration (2.4, 2.5) and Clinical Pharmacology (12.3)].
| Recommended Pediatric Dosage and Formulation | |||
|---|---|---|---|
| Indication | Weight/Age | Delayed-Release Tablet | Duration of therapy |
| Prophylaxis of invasive Aspergillus and Candida infections | Less than or equal to 40 kg (2 to less than 18 years of age) | Not Applicable | Duration of therapy is based on recovery from neutropenia or immunosuppression. |
| Greater than 40 kg (2 to less than 18 years of age) |
Loading dose:
300 mg twice daily on the first day Maintenance dose: 300 mg once daily |
||
| Treatment of invasive Aspergillosis | 13 to less than 18 years of age regardless of weight. |
Loading dose:
300 mg (three 100 mg delayed-release tablets) twice a day on the first day. Maintenance dose: 300 mg (three 100 mg delayed-release tablets) once a day, starting on the second day. Switching between the intravenous and delayed-release tablets is acceptable. A loading dose is not required when switching between formulations. |
Loading dose:
1 day Maintenance dose: Recommended total duration of therapy is 6 to 12 weeks. |
| Indication |
Loading Dose (volume) and frequency |
Maintenance Dose (volume) and frequency |
Duration of therapy |
|---|---|---|---|
| Prophylaxis of invasive Aspergillus and Candida infections | 200 mg (5 mL) three times a day | 200 mg (5 mL) three times a day | Duration of therapy is based on recovery from neutropenia or immunosuppression. |
| Oropharyngeal Candidiasis (OPC) | 100 mg (2.5 mL) twice daily on the first day | 100 mg (2.5 mL) once daily | 13 days |
| OPC Refractory (rOPC) to Itraconazole and/or Fluconazole | 400 mg (10 mL) twice daily | 400 mg (10 mL) twice daily | Duration of therapy is based on the severity of the patient’s underlying disease and clinical response. |
7.3 Hmg Coa Reductase Inhibitors (statins) Primarily Metabolized Through Cyp3a4
Concomitant administration of posaconazole with simvastatin increases the simvastatin plasma concentrations by approximately 10-fold. Therefore, posaconazole is contraindicated with HMG-CoA reductase inhibitors primarily metabolized through CYP3A4 [see Contraindications (4.4) and Clinical Pharmacology (12.3)].
2.6 Non Substitutability Between Posaconazole Oral Suspension and Other Formulations
Posaconazole oral suspension is not substitutable with Posaconazole delayed-release tablets or Noxafil PowderMix for delayed-release oral suspension due to the differences in the dosing of each formulation. Therefore, follow the specific dosage recommendations for each of the formulations [see Dosage and Administration (2.2, 2.3)].
14.1 Treatment of Invasive Aspergillosis With Noxafil Injection and Noxafil Delayed Release Tablets
Aspergillosis Treatment Study (NCT01782131) was a randomized, double-blind, controlled trial which evaluated the safety and efficacy of Noxafil injection and Noxafil delayed-release tablets versus voriconazole for primary treatment of invasive fungal disease caused by Aspergillus species. Eligible patients had proven, probable, or possible invasive fungal infections per the European Organization for Research and Treatment of Cancer/Mycoses Study Group, EORTC/MSG criteria. Patients were stratified by risk for mortality or poor outcome where high risk included a history of allogeneic bone marrow transplant, liver transplant, or relapsed leukemia undergoing salvage chemotherapy. The median age of patients was 57 years (range 14-91 years), with 27.8% of patients aged ≥65 years; 5 patients were pediatric patients 14-16 years of age, of whom 3 were treated with Noxafil and 2 with voriconazole. The majority of patients were male (59.8%) and white (67.1%). With regard to risk factors for invasive aspergillosis, approximately two-thirds of the patients in the study had a recent history of neutropenia, while approximately 20% with a history of an allogeneic stem cell transplant. Over 80% of subjects in each treatment group had infection limited to the lower respiratory tract (primarily lung), while approximately 11% to 13% also had infection in another organ. Invasive aspergillosis was proven or probable in 58.1% of patients as classified by independent adjudicators blinded to study treatment assignment. At least one Aspergillus species was identified in 21% of the patients; A. fumigatus and A. flavus were the most common pathogens identified.
Patients randomized to receive Noxafil were given a dose of 300 mg once daily (twice daily on Day 1) IV or tablet. Patients randomized to receive voriconazole were given a dose of 6 mg/kg twice daily Day 1 followed by 4 mg/kg twice daily IV, or oral 300 mg twice daily Day 1 followed by 200 mg twice daily. The recommended initial route of administration was IV; however, patients could begin oral therapy if clinically stable and able to tolerate oral dosing. The transition from IV to oral therapy occurred when the patient was clinically stable. The protocol recommended duration of therapy was 84 days with a maximum allowed duration of 98 days. Median treatment duration was 67 days for Noxafil patients and 64 days for voriconazole patients. Overall, 55% to 60% of patients began treatment with the IV formulation with a median duration of 9 days for the initial IV dosing.
The Intent to Treat (ITT) population included all patients randomized and receiving at least one dose of study treatment. All-cause mortality through Day 42 in the overall population (ITT) was 15.3% for Noxafil patients compared to 20.6% for voriconazole patients for an adjusted treatment difference of -5.3% with a 95% confidence interval of -11.6 to 1.0%. Consistent results were seen in patients with proven or probable invasive aspergillosis per EORTC criteria (see Table 21 ).
| Noxafil Injection and Delayed-Release Tablets | Voriconazole | ||||
|---|---|---|---|---|---|
| Population | N | n (%) | N | n (%) | Difference Adjusted treatment difference based on Miettinen and Nurminen’s method stratified by randomization factor (risk for mortality/poor outcome), using Cochran-Mantel-Haenszel weighting scheme. (95% CI) |
| Intent to Treat | 288 | 44 (15.3) | 287 | 59 (20.6) | -5.3 (-11.6, 1.0) |
| Proven/Probable Invasive Aspergillosis | 163 | 31 (19.0) | 171 | 32 (18.7) | 0.3 (-8.2, 8.8) |
Global clinical response at Week 6 was assessed by a blinded, independent adjudication committee based upon prespecified clinical, radiologic, and mycologic criteria. In the subgroup of patients with proven or probable invasive aspergillosis per EORTC criteria, the global clinical response of success (complete or partial response) at Week 6 was seen in 44.8% for Noxafil-treated patients compared to 45.6% for voriconazole-treated patients (see Table 22 ).
| Posaconazole | Voriconazole | ||||
|---|---|---|---|---|---|
| Population | N | Success | N | Success | Difference Adjusted treatment difference based on Miettinen and Nurminen’s method stratified by randomization factor (risk for mortality/poor outcome), using Cochran-Mantel-Haenszel weighting scheme. (95% CI) |
| Proven/Probable Invasive Aspergillosis | 163 | 73 (44.8) | 171 | 78 (45.6) | -0.6 (-11.2, 10.1) |
1.3 Treatment of Oropharyngeal Candidiasis Including Oropharyngeal Candidiasis Refractory to Itraconazole And/or Fluconazole
Posaconazole oral suspension is indicated for the treatment of oropharyngeal candidiasis, including oropharyngeal candidiasis refractory to itraconazole and/or fluconazole in adults and pediatric patients 13 years of age and older.
14.4 Noxafil Oral Suspension Treatment of Oropharyngeal Candidiasis Refractory to Treatment With Fluconazole Or Itraconazole
Noxafil Oral Suspension Study 4 was a noncomparative study of Noxafil oral suspension in HIV-infected subjects with OPC that was refractory to treatment with fluconazole or itraconazole. An episode of OPC was considered refractory if there was failure to improve or worsening of OPC after a standard course of therapy with fluconazole greater than or equal to 100 mg/day for at least 10 consecutive days or itraconazole 200 mg/day for at least 10 consecutive days and treatment with either fluconazole or itraconazole had not been discontinued for more than 14 days prior to treatment with Noxafil. Of the 199 subjects enrolled in this study, 89 subjects met these strict criteria for refractory infection.
Forty-five subjects with refractory OPC were treated with Noxafil oral suspension 400 mg twice daily for 3 days, followed by 400 mg once daily for 25 days with an option for further treatment during a 3-month maintenance period. Following a dosing amendment, a further 44 subjects were treated with Noxafil 400 mg twice daily for 28 days. The efficacy of Noxafil was assessed by the clinical success (cure or improvement) rate after 4 weeks of treatment. The clinical success rate was 74.2% (66/89). The clinical success rates for both the original and the amended dosing regimens were similar (73.3% and 75.0%, respectively).
Structured Label Content
Section 42229-5 (42229-5)
Posaconazole delayed-release tablets
- Swallow tablets whole. Do not divide, crush, or chew.
- Administer with or without food [see Dosage and Administration (2.2) and Clinical Pharmacology (12.3)].
- For patients who cannot eat a full meal, Posaconazole delayed-release tablets should be used instead of Posaconazole oral suspension for the prophylaxis indication. Posaconazole delayed-release tablets generally provide higher plasma drug exposures than Posaconazole oral suspension under both fed and fasted conditions [see Dosage and Administration (2.5)].
Posaconazole oral suspension
- Administer with a full meal or with a liquid nutritional supplement or an acidic carbonated beverage (e.g., ginger ale) in patients who cannot eat a full meal [see Dosage and Administration (2.5)].
- Co-administration of drugs that can decrease the plasma concentrations of posaconazole should generally be avoided unless the benefit outweighs the risk. If such drugs are necessary, patients should be monitored closely for breakthrough fungal infections [see Drug Interactions (7.6, 7.7, 7.8, 7.9, 7.13)].
Section 42230-3 (42230-3)
| This Patient Information has been approved by the U.S. Food and Drug Administration. | Revised: 06/2024 | ||
|
Patient Information
Posaconazole delayed-release tablets Posaconazole oral suspension |
|||
|
What is posaconazole?
Posaconazole (which refers to delayed-release tablets and oral suspension) is a prescription medicine used in adults and children to help prevent or treat fungal infections that can spread throughout your body (invasive fungal infections). These infections are caused by fungi called Aspergillus or Candida. Posaconazole is used in people who have an increased chance of getting these infections due to a weak immune system. These include people who have had a hematopoietic stem cell transplantation (bone marrow transplant) with graft versus host disease or those with a low white blood cell count due to chemotherapy for blood cancers (hematologic malignancies). Posaconazole delayed-release tablets are used for:
Posaconazole oral suspension is for adults and children 13 years of age and older. It is not known if posaconazole is safe and effective in children under 2 years of age. |
|||
|
Who should not take posaconazole? Do not take posaconazole if you:
Do not start taking a new medicine without talking to your healthcare provider or pharmacist. |
|||
|
What should I tell my healthcare provider before taking posaconazole? Before you take posaconazole, tell your healthcare provider if you:
Especially tell your healthcare provider if you take:
Know the medicines you take. Keep a list of them with you to show your healthcare provider or pharmacist when you get a new medicine. |
|||
How will I take posaconazole?
|
|||
|
What are the possible side effects of posaconazole? Posaconazole may cause serious side effects, including:
|
|||
|
|
||
|
|||
|
|
||
| If you take Posaconazole delayed-release tablets or Posaconazole oral suspension, tell your healthcare provider right away if you have diarrhea or vomiting. Tell your healthcare provider if you have any side effect that bothers you or that does not go away. These are not all the possible side effects of posaconazole. For more information, ask your healthcare provider or pharmacist. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. |
|||
|
How should I store posaconazole?
Posaconazole delayed-release tablets
Keep posaconazole and all medicines out of the reach of children. |
|||
|
General information about the safe and effective use of posaconazole.
Medicines are sometimes prescribed for purposes other than those listed in a Patient Information leaflet. Do not use posaconazole for a condition for which it was not prescribed. Do not give posaconazole to other people, even if they have the same symptoms that you have. It may harm them. You can ask your pharmacist or healthcare provider for information about posaconazole that is written for health professionals. |
|||
|
What are the ingredients in posaconazole? Active ingredient: posaconazole Inactive ingredients: Posaconazole delayed-release tablets: croscarmellose sodium, hydroxypropylcellulose, hypromellose acetate succinate, iron oxide yellow, Macrogol/PEG 3350, magnesium stearate, microcrystalline cellulose, polyvinyl alcohol partially hydrolyzed, silicon dioxide, talc, and titanium dioxide. Posaconazole oral suspension: artificial cherry flavor, citric acid monohydrate, glycerin, liquid glucose, polysorbate 80, purified water, simethicone, sodium benzoate, sodium citrate dihydrate, titanium dioxide, and xanthan gum. Manufactured for: Endo USA, Malvern, PA 19355 Delayed-Release Tablets: Manuf. by: N. V. Organon, Kloosterstraat 6, 5349 AB Oss, Netherlands Oral Suspension: Manuf. by: Patheon Inc., Whitby, Ontario, Canada L1N5Z5 usppi-gmk5592-mf-2406r005 PI1016-01-78-03 |
Section 51945-4 (51945-4)
Posaconazole 100 mg Tablets
8.9 Race
The pharmacokinetic profile of posaconazole is not significantly affected by race. No adjustment in the dosage of posaconazole is necessary based on race.
8.8 Gender
The pharmacokinetics of posaconazole are comparable in males and females. No adjustment in the dosage of posaconazole is necessary based on gender.
8.10 Weight
Pharmacokinetic modeling suggests that patients weighing greater than 120 kg may have lower posaconazole plasma drug exposure. It is, therefore, suggested to closely monitor for breakthrough fungal infections particularly when using Posaconazole oral suspension [see Clinical Pharmacology (12.3)].
7.12 Digoxin
Increased plasma concentrations of digoxin have been reported in patients receiving digoxin and posaconazole. Therefore, monitoring of digoxin plasma concentrations is recommended during coadministration.
10 Overdosage (10 OVERDOSAGE)
There is no experience with overdosage of Posaconazole delayed-release tablets.
During the clinical trials, some patients received Noxafil oral suspension up to 1600 mg/day with no adverse reactions noted that were different from the lower doses. In addition, accidental overdose was noted in one patient who took 1200 mg twice daily Noxafil oral suspension for 3 days. No related adverse reactions were noted by the investigator.
Posaconazole is not removed by hemodialysis.
7.7 Rifabutin
Rifabutin induces UDP-glucuronidase and decreases posaconazole plasma concentrations. Rifabutin is also metabolized by CYP3A4. Therefore, coadministration of rifabutin with posaconazole increases rifabutin plasma concentrations [see Clinical Pharmacology (12.3)]. Concomitant use of posaconazole and rifabutin should be avoided unless the benefit to the patient outweighs the risk. However, if concomitant administration is required, close monitoring for breakthrough fungal infections as well as frequent monitoring of full blood counts and adverse reactions due to increased rifabutin plasma concentrations (e.g., uveitis, leukopenia) are recommended.
7.8 Phenytoin
Phenytoin induces UDP-glucuronidase and decreases posaconazole plasma concentrations. Phenytoin is also metabolized by CYP3A4. Therefore, coadministration of phenytoin with posaconazole increases phenytoin plasma concentrations [see Clinical Pharmacology (12.3)]. Concomitant use of posaconazole and phenytoin should be avoided unless the benefit to the patient outweighs the risk. However, if concomitant administration is required, close monitoring for breakthrough fungal infections is recommended and frequent monitoring of phenytoin concentrations should be performed while coadministered with posaconazole and dose reduction of phenytoin should be considered.
11 Description (11 DESCRIPTION)
Posaconazole is an azole antifungal agent available as delayed-release tablet or suspension for oral administration.
Posaconazole is designated chemically as 4-[4-[4-[4-[[ (3R,5R)-5- (2,4-difluorophenyl)tetrahydro-5- (1H-1,2,4-triazol-1-ylmethyl)-3-furanyl]methoxy]phenyl]-1-piperazinyl]phenyl]-2-[(1S,2S)-1-ethyl-2-hydroxypropyl]-2,4-dihydro-3H-1,2,4-triazol-3-one with an empirical formula of C37H42F2N8O4 and a molecular weight of 700.8. The chemical structure is:
Posaconazole Delayed-Release Tablets
Posaconazole is a white powder with a low aqueous solubility.
Posaconazole delayed-release tablet is a yellow, coated, oblong tablet containing 100 mg of posaconazole. Each delayed-release tablet contains the inactive ingredients: croscarmellose sodium, hydroxypropylcellulose, hypromellose acetate succinate, iron oxide yellow, Macrogol/PEG 3350, magnesium stearate, microcrystalline cellulose, polyvinyl alcohol partially hydrolyzed, silicon dioxide, talc, and titanium dioxide.
Posaconazole Oral Suspension
Posaconazole oral suspension is a white, cherry-flavored immediate-release suspension containing 40 mg of posaconazole per mL and the following inactive ingredients: artificial cherry flavor, citric acid monohydrate, glycerin, liquid glucose, polysorbate 80, purified water, simethicone, sodium benzoate, sodium citrate dihydrate, titanium dioxide, and xanthan gum.
7.14 Glipizide
Although no dosage adjustment of glipizide is required, it is recommended to monitor glucose concentrations when posaconazole and glipizide are concomitantly used.
7.15 Venetoclax
Concomitant use of venetoclax (a CYP3A4 substrate) with posaconazole increases venetoclax Cmax and AUC0-INF, which may increase venetoclax toxicities [see Contraindications (4.6), Warnings and Precautions (5.9)]. Refer to the venetoclax prescribing information for more information on the dosing instructions and the extent of increase in venetoclax exposure.
8.4 Pediatric Use
The safety and effectiveness of Posaconazole oral suspension and Posaconazole delayed-release tablets for the prophylaxis of invasive Aspergillus and Candida infections have been established in pediatric patients aged 2 and older who are at high risk of developing these infections due to being severely immunocompromised, such as HSCT recipients with GVHD or those with hematologic malignancies with prolonged neutropenia from chemotherapy.
The safety and effectiveness of Posaconazole injection and Posaconazole delayed-release tablets for the treatment of invasive aspergillosis have been established in pediatric patients aged 13 years and older.
The safety and effectiveness of Posaconazole oral suspension have been established for the treatment of oropharyngeal candidiasis (OPC), including OPC refractory (rOPC) to itraconazole and/or fluconazole in pediatric patients aged 13 years and older.
Use of posaconazole in these age groups is supported by evidence from adequate and well-controlled studies of Noxafil in adult and pediatric patients and additional pharmacokinetic and safety data in pediatric patients 2 years of age and older [see Adverse Reactions (6.1), Clinical Pharmacology (12.3), and Clinical Studies (14)]. The safety and effectiveness of posaconazole have not been established in pediatric patients younger than 2 years of age.
8.5 Geriatric Use
No overall differences in the safety of Noxafil delayed-release tablets and Noxafil oral suspension were observed between geriatric patients and younger adult patients in the clinical trials; therefore, no dosage adjustment is recommended for any formulation of posaconazole in geriatric patients. No clinically meaningful differences in the pharmacokinetics of Noxafil were observed in geriatric patients compared to younger adult patients during clinical trials [see Clinical Pharmacology (12.3)].
Of the 230 patients treated with Noxafil delayed-release tablets, 38 (17%) were greater than 65 years of age.
Of the 605 patients randomized to Noxafil oral suspension in Noxafil Oral Suspension Study 1 and Study 2, 63 (10%) were ≥65 years of age. In addition, 48 patients treated with greater than or equal to 800-mg/day Noxafil oral suspension in another indication were ≥65 years of age. Of the 288 patients randomized to Noxafil injection/Noxafil delayed-release tablets in the Aspergillosis Treatment Study, 85 (29%) were ≥65 years of age.
No overall differences in the pharmacokinetics and safety were observed between elderly and young subjects during clinical trials, but greater sensitivity of some older individuals cannot be ruled out.
4 Contraindications (4 CONTRAINDICATIONS)
- Known hypersensitivity to posaconazole or other azole antifungal agents. (4.1)
- Coadministration of posaconazole with the following drugs is contraindicated: posaconazole increases concentrations and toxicities of:
- Sirolimus (4.2, 5.1, 7.1)
- CYP3A4 substrates (pimozide, quinidine): can result in QTc interval prolongation and cases of torsades de pointes (TdP) (4.3, 5.2, 7.2)
- HMG-CoA Reductase Inhibitors Primarily Metabolized through CYP3A4 (4.4, 7.3)
- Ergot alkaloids (4.5, 7.4)
- Venetoclax: In patients with chronic lymphocytic leukemia (CLL) or small lymphocytic lymphoma (SLL) at initiation and during the ramp-up phase (4.6, 5.9, 7.15)
6 Adverse Reactions (6 ADVERSE REACTIONS)
The following serious and otherwise important adverse reactions are discussed in detail in another section of the labeling:
- Hypersensitivity [see Contraindications (4.1)]
- Arrhythmias and QT Prolongation [see Warnings and Precautions (5.2)]
- Hepatic Toxicity [see Warnings and Precautions (5.4)]
7 Drug Interactions (7 DRUG INTERACTIONS)
Posaconazole is primarily metabolized via UDP glucuronosyltransferase and is a substrate of p-glycoprotein (P-gp) efflux. Therefore, inhibitors or inducers of these clearance pathways may affect posaconazole plasma concentrations. Coadministration of drugs that can decrease the plasma concentrations of posaconazole should generally be avoided unless the benefit outweighs the risk. If such drugs are necessary, patients should be monitored closely for breakthrough fungal infections.
Posaconazole is also a strong inhibitor of CYP3A4. Therefore, plasma concentrations of drugs predominantly metabolized by CYP3A4 may be increased by posaconazole [see Clinical Pharmacology (12.3)].
The following information was derived from data with Noxafil oral suspension or early tablet formulation unless otherwise noted. All drug interactions with Posaconazole oral suspension, except for those that affect the absorption of posaconazole (via gastric pH and motility), are considered relevant to Posaconazole injection, Posaconazole delayed-release tablet, and Posaconazole PowderMix for delayed-release oral suspension as well [see Drug Interactions (7.9) and (7.13)].
7.4 Ergot Alkaloids
Most of the ergot alkaloids are substrates of CYP3A4. Posaconazole may increase the plasma concentrations of ergot alkaloids (ergotamine and dihydroergotamine) which may lead to ergotism. Therefore, posaconazole is contraindicated with ergot alkaloids [see Contraindications (4.5)].
4.1 Hypersensitivity
Posaconazole is contraindicated in persons with known hypersensitivity to posaconazole or other azole antifungal agents.
5.4 Hepatic Toxicity
Hepatic reactions (e.g., mild to moderate elevations in alanine aminotransferase (ALT), aspartate aminotransferase (AST), alkaline phosphatase, total bilirubin, and/or clinical hepatitis) have been reported in clinical trials. The elevations in liver tests were generally reversible on discontinuation of therapy, and in some instances these tests normalized without drug interruption. Cases of more severe hepatic reactions including cholestasis or hepatic failure including deaths have been reported in patients with serious underlying medical conditions (e.g., hematologic malignancy) during treatment with posaconazole. These severe hepatic reactions were seen primarily in subjects receiving the Posaconazole oral suspension 800 mg daily (400 mg twice daily or 200 mg four times a day) in clinical trials.
Liver tests should be evaluated at the start of and during the course of posaconazole therapy. Patients who develop abnormal liver tests during posaconazole therapy should be monitored for the development of more severe hepatic injury. Patient management should include laboratory evaluation of hepatic function (particularly liver tests and bilirubin). Discontinuation of posaconazole must be considered if clinical signs and symptoms consistent with liver disease develop that may be attributable to posaconazole.
5.5 Renal Impairment
Due to the variability in exposure with Posaconazole delayed-release tablets and Posaconazole oral suspension, patients with severe renal impairment should be monitored closely for breakthrough fungal infections [see Dosage and Administration (2.4) and Use in Specific Populations (8.6)].
7.10 Vinca Alkaloids
Most of the vinca alkaloids (e.g., vincristine and vinblastine) are substrates of CYP3A4. Concomitant administration of azole antifungals, including posaconazole, with vincristine has been associated with serious adverse reactions [see Warnings and Precautions (5.7)]. Posaconazole may increase the plasma concentrations of vinca alkaloids which may lead to neurotoxicity and other serious adverse reactions. Therefore, reserve azole antifungals, including posaconazole, for patients receiving a vinca alkaloid, including vincristine, who have no alternative antifungal treatment options.
8.6 Renal Impairment
Following single-dose administration of 400 mg of the Noxafil oral suspension, there was no significant effect of mild (eGFR: 50-80 mL/min/1.73 m2, n=6) or moderate (eGFR: 20-49 mL/min/1.73 m2, n=6) renal impairment on posaconazole pharmacokinetics; therefore, no dose adjustment is required in patients with mild to moderate renal impairment. In subjects with severe renal impairment (eGFR: <20 mL/min/1.73 m2), the mean plasma exposure (AUC) was similar to that in patients with normal renal function (eGFR: >80 mL/min/1.73 m2); however, the range of the AUC estimates was highly variable (CV=96%) in these subjects with severe renal impairment as compared to that in the other renal impairment groups (CV<40%). Due to the variability in exposure, patients with severe renal impairment should be monitored closely for breakthrough fungal infections [see Dosage and Administration (2)]. Similar recommendations apply to Posaconazole delayed-release tablets; however, a specific study has not been conducted with the Posaconazole delayed-release tablets.
7.2 Cyp3a4 Substrates (7.2 CYP3A4 Substrates)
Concomitant administration of posaconazole with CYP3A4 substrates such as pimozide and quinidine may result in increased plasma concentrations of these drugs, leading to QTc prolongation and cases of torsades de pointes. Therefore, posaconazole is contraindicated with these drugs [see Contraindications (4.3) and Warnings and Precautions (5.2)].
4.2 Use With Sirolimus (4.2 Use with Sirolimus)
Posaconazole is contraindicated with sirolimus. Concomitant administration of posaconazole with sirolimus increases the sirolimus blood concentrations by approximately 9-fold and can result in sirolimus toxicity [see Drug Interactions (7.1) and Clinical Pharmacology (12.3)].
5.6 Midazolam Toxicity
Concomitant administration of posaconazole with midazolam increases the midazolam plasma concentrations by approximately 5-fold. Increased plasma midazolam concentrations could potentiate and prolong hypnotic and sedative effects. Patients must be monitored closely for adverse effects associated with high plasma concentrations of midazolam and benzodiazepine receptor antagonists must be available to reverse these effects [see Drug Interactions (7.5) and Clinical Pharmacology (12.3)].
8.7 Hepatic Impairment
After a single oral dose of Noxafil oral suspension 400 mg, the mean AUC was 43%, 27%, and 21% higher in subjects with mild (Child-Pugh Class A, N=6), moderate (Child-Pugh Class B, N=6), or severe (Child-Pugh Class C, N=6) hepatic impairment, respectively, compared to subjects with normal hepatic function (N=18). Compared to subjects with normal hepatic function, the mean Cmax was 1% higher, 40% higher, and 34% lower in subjects with mild, moderate, or severe hepatic impairment, respectively. The mean apparent oral clearance (CL/F) was reduced by 18%, 36%, and 28% in subjects with mild, moderate, or severe hepatic impairment, respectively, compared to subjects with normal hepatic function. The elimination half-life (t½) was 27 hours, 39 hours, 27 hours, and 43 hours in subjects with normal hepatic function and mild, moderate, or severe hepatic impairment, respectively.
It is recommended that no dose adjustment of posaconazole is needed in patients with mild to severe hepatic impairment (Child-Pugh Class A, B, or C) [see Dosage and Administration (2) and Warnings and Precautions (5.4)]. Similar recommendations apply to Posaconazole delayed-release tablets; however, a specific study has not been conducted with the Posaconazole delayed-release tablets.
1 Indications and Usage (1 INDICATIONS AND USAGE)
Posaconazole is an azole antifungal indicated as follows:
- Posaconazole delayed-release tablets are indicated for the treatment of invasive aspergillosis in adults and pediatric patients 13 years of age and older. (1.1)
-
Posaconazole is indicated for the prophylaxis of invasive Aspergillus and Candida infections in patients who are at high risk of developing these infections due to being severely immunocompromised, such as hematopoietic stem cell transplant (HSCT) recipients with graft-versus-host disease (GVHD) or those with hematologic malignancies with prolonged neutropenia from chemotherapy as follows: (1.2)
- Posaconazole delayed-release tablets: adults and pediatric patients 2 years of age and older who weigh greater than 40 kg
- Posaconazole oral suspension: adults and pediatric patients 13 years of age and older
- Posaconazole oral suspension is indicated for the treatment of oropharyngeal candidiasis (OPC), including OPC refractory (rOPC) to itraconazole and/or fluconazole in adult and pediatric patients aged 13 years and older. (1.3)
4.6 Use With Venetoclax (4.6 Use with Venetoclax)
Coadministration of posaconazole with venetoclax at initiation and during the ramp-up phase is contraindicated in patients with chronic lymphocytic leukemia (CLL) or small lymphocytic lymphoma (SLL) due to the potential for increased risk of tumor lysis syndrome [see Warnings and Precautions (5.9) and Drug Interactions (7.15)].
5.9 Venetoclax Toxicity
Concomitant administration of posaconazole, a strong CYP3A4 inhibitor, with venetoclax may increase venetoclax toxicities, including the risk of tumor lysis syndrome (TLS), neutropenia, and serious infections. In patients with CLL/SLL, administration of posaconazole during initiation and the ramp-up phase of venetoclax is contraindicated [see Contraindications (4.6)]. Refer to the venetoclax labeling for safety monitoring and dose reduction in the steady daily dosing phase in CLL/SLL patients.
For patients with acute myeloid leukemia (AML), dose reduction and safety monitoring are recommended across all dosing phases when coadministering posaconazole with venetoclax [see Drug Interactions (7.15)]. Refer to the venetoclax prescribing information for dosing instructions.
12.1 Mechanism of Action
Posaconazole is an azole antifungal agent [see Clinical Pharmacology (12.4)].
5.7 Vincristine Toxicity
Concomitant administration of azole antifungals, including posaconazole, with vincristine has been associated with neurotoxicity and other serious adverse reactions, including seizures, peripheral neuropathy, syndrome of inappropriate antidiuretic hormone secretion, and paralytic ileus. Reserve azole antifungals, including posaconazole, for patients receiving a vinca alkaloid, including vincristine, who have no alternative antifungal treatment options [see Drug Interactions (7.10)].
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
- Calcineurin-Inhibitor Toxicity: Posaconazole increases concentrations of cyclosporine or tacrolimus; reduce dose of cyclosporine and tacrolimus and monitor concentrations frequently. (5.1)
- Arrhythmias and QTc Prolongation: Posaconazole has been shown to prolong the QTc interval and cause cases of TdP. Administer with caution to patients with potentially proarrhythmic conditions. Do not administer with drugs known to prolong QTc interval and metabolized through CYP3A4. (5.2)
- Electrolyte Disturbances: Monitor and correct, especially those involving potassium (K+), magnesium (Mg++), and calcium (Ca++), before and during posaconazole therapy. (5.3)
- Hepatic Toxicity: Elevations in liver tests may occur. Discontinuation should be considered in patients who develop abnormal liver tests or monitor liver tests during treatment. (5.4)
- Concomitant Use with Midazolam: Posaconazole can prolong hypnotic/sedative effects. Monitor patients and benzodiazepine receptor antagonists should be available. (5.6, 7.5)
- Vincristine Toxicity: Concomitant administration of azole antifungals, including posaconazole, with vincristine has been associated with neurotoxicity and other serious adverse reactions; reserve azole antifungals, including posaconazole, for patients receiving a vinca alkaloid, including vincristine, who have no alternative antifungal treatment options. (5.7, 7.10)
- Breakthrough Fungal Infections: Monitor patients with severe diarrhea or vomiting when receiving Posaconazole delayed-release tablets and Posaconazole oral suspension. (5.8)
- Venetoclax Toxicity: Concomitant administration of posaconazole with venetoclax may increase venetoclax toxicities, including the risk of tumor lysis syndrome, neutropenia, and serious infections; monitor for toxicity and reduce venetoclax dose. (4.6, 5.9, 7.15)
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
- Posaconazole oral suspension is not substitutable with Posaconazole delayed-release tablets or Noxafil PowderMix for delayed-release oral suspension due to the differences in the dosing of each formulation. Therefore, follow the specific dosage recommendations for each of the formulations. (2.1, 2.2, 2.3)
- Administer Posaconazole delayed-release tablets with or without food. (2.1)
- Administer Posaconazole oral suspension with a full meal. (2.1)
| Table 1: Recommended Dosage in Adult Patients | |
|---|---|
| Indication | Dosage Form, Dose, and Duration of Therapy |
| Treatment of invasive Aspergillosis |
Posaconazole Delayed-Release Tablets:
Loading dose: 300 mg (three 100 mg delayed-release tablets) twice a day on the first day. Maintenance dose: 300 mg (three 100 mg delayed-release tablets) once a day thereafter. Recommended total duration of therapy is 6 to 12 weeks. (2.2) Switching between the intravenous and delayed-release tablets is acceptable. A loading dose is not required when switching between formulations. (2.2) |
| Prophylaxis of invasive Aspergillus and Candida infections |
Posaconazole Delayed-Release Tablets
:
Loading dose: 300 mg (three 100 mg delayed-release tablets) twice a day on the first day. Maintenance dose: 300 mg (three 100 mg delayed-release tablets) once a day, starting on the second day. Duration of therapy is based on recovery from neutropenia or immunosuppression. (2.2, 2.3) Posaconazole Oral Suspension: 200 mg (5 mL) three times a day. Duration of therapy is based on recovery from neutropenia or immunosuppression. (2.2, 2.3) |
| Oropharyngeal Candidiasis (OPC) |
Posaconazole Oral Suspension:
Loading dose: 100 mg (2.5 mL) twice a day on the first day. Maintenance dose: 100 mg (2.5 mL) once a day for 13 days. (2.2, 2.3) |
| OPC Refractory (rOPC) to Itraconazole and/or Fluconazole | Posaconazole Oral Suspension: 400 mg (10 mL) twice a day. Duration of therapy is based on the severity of the patient’s underlying disease and clinical response. (2.2, 2.3) |
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
Posaconazole Delayed-Release Tablets
Posaconazole delayed-release tablets are available as yellow, coated, oblong tablets, debossed with "100" on one side containing 100 mg of posaconazole.
Posaconazole Oral Suspension
Posaconazole oral suspension is available as a white, cherry-flavored suspension in 4-ounce (123 mL) amber glass bottles with child-resistant closures containing 105 mL of suspension (40 mg of posaconazole per mL).
4.5 Use With Ergot Alkaloids (4.5 Use with Ergot Alkaloids)
Posaconazole may increase the plasma concentrations of ergot alkaloids (ergotamine and dihydroergotamine) which may lead to ergotism [see Drug Interactions (7.4)].
5.3 Electrolyte Disturbances
Electrolyte disturbances, especially those involving potassium, magnesium or calcium levels, should be monitored and corrected as necessary before and during posaconazole therapy.
6.2 Postmarketing Experience
The following adverse reaction has been identified during the post-approval use of posaconazole. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency.
Endocrine Disorders: Pseudoaldosteronism
8 Use in Specific Populations (8 USE IN SPECIFIC POPULATIONS)
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in clinical trials of Noxafil cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
14.2 Prophylaxis of Aspergillus
Two randomized, controlled studies were conducted using Noxafil as prophylaxis for the prevention of invasive fungal infections (IFIs) among patients at high risk due to severely compromised immune systems.
The first study (Noxafil Oral Suspension Study 1) was a randomized, double-blind trial that compared Noxafil oral suspension (200 mg three times a day) with fluconazole capsules (400 mg once daily) as prophylaxis against invasive fungal infections in allogeneic hematopoietic stem cell transplant (HSCT) recipients with Graft versus Host Disease (GVHD). Efficacy of prophylaxis was evaluated using a composite endpoint of proven/probable IFIs, death, or treatment with systemic antifungal therapy (patients may have met more than one of these criteria). This assessed all patients while on study therapy plus 7 days and at 16 weeks post-randomization. The mean duration of therapy was comparable between the 2 treatment groups (80 days, Noxafil oral suspension; 77 days, fluconazole). Table 23 contains the results from Noxafil Oral Suspension Study 1.
| Posaconazole n=301 |
Fluconazole n=299 |
|
|---|---|---|
| On therapy plus 7 days | ||
|
Clinical Failure Patients may have met more than one criterion defining failure.
|
50 (17%) | 55 (18%) |
| Failure due to: | ||
| Proven/Probable IFI | 7 (2%) | 22 (7%) |
| (Aspergillus) | 3 (1%) | 17 (6%) |
| (Candida) | 1 (<1%) | 3 (1%) |
| (Other) | 3 (1%) | 2 (1%) |
| All Deaths | 22 (7%) | 24 (8%) |
| Proven/probable fungal infection prior to death | 2 (<1%) | 6 (2%) |
| SAF Use of systemic antifungal therapy (SAF) criterion is based on protocol definitions (empiric/IFI usage >4 consecutive days).
|
27 (9%) | 25 (8%) |
| Through 16 weeks | ||
|
Clinical Failure
,
95% confidence interval (posaconazole-fluconazole) = (-11.5%, +3.7%).
|
99 (33%) | 110 (37%) |
| Failure due to: | ||
| Proven/Probable IFI | 16 (5%) | 27 (9%) |
| (Aspergillus) | 7 (2%) | 21 (7%) |
| (Candida) | 4 (1%) | 4 (1%) |
| (Other) | 5 (2%) | 2 (1%) |
| All Deaths | 58 (19%) | 59 (20%) |
| Proven/probable fungal infection prior to death | 10 (3%) | 16 (5%) |
| SAF | 26 (9%) | 30 (10%) |
| Event free lost to follow-up Patients who are lost to follow-up (not observed for 112 days), and who did not meet another clinical failure endpoint. These patients were considered failures.
|
24 (8%) | 30 (10%) |
The second study (Noxafil Oral Suspension Study 2) was a randomized, open-label study that compared Noxafil oral suspension (200 mg 3 times a day) with fluconazole suspension (400 mg once daily) or itraconazole oral solution (200 mg twice a day) as prophylaxis against IFIs in neutropenic patients who were receiving cytotoxic chemotherapy for AML or MDS. As in Noxafil Oral Suspension Study 1, efficacy of prophylaxis was evaluated using a composite endpoint of proven/probable IFIs, death, or treatment with systemic antifungal therapy (Patients might have met more than one of these criteria). This study assessed patients while on treatment plus 7 days and 100 days postrandomization. The mean duration of therapy was comparable between the 2 treatment groups (29 days, posaconazole; 25 days, fluconazole or itraconazole). Table 24 contains the results from Noxafil Oral Suspension Study 2.
| Posaconazole n=304 |
Fluconazole/Itraconazole n=298 |
|
|---|---|---|
| On therapy plus 7 days | ||
|
Clinical Failure 95% confidence interval (posaconazole-fluconazole/itraconazole) = (-22.9%, -7.8%).
,
Patients may have met more than one criterion defining failure.
|
82 (27%) | 126 (42%) |
| Failure due to: | ||
| Proven/Probable IFI | 7 (2%) | 25 (8%) |
| (Aspergillus) | 2 (1%) | 20 (7%) |
| (Candida) | 3 (1%) | 2 (1%) |
| (Other) | 2 (1%) | 3 (1%) |
| All Deaths | 17 (6%) | 25 (8%) |
| Proven/probable fungal infection prior to death | 1 (<1%) | 2 (1%) |
| SAF Use of systemic antifungal therapy (SAF) criterion is based on protocol definitions (empiric/IFI usage >3 consecutive days).
|
67 (22%) | 98 (33%) |
| Through 100 days postrandomization | ||
| Clinical Failure | 158 (52%) | 191 (64%) |
| Failure due to: | ||
| Proven/Probable IFI | 14 (5%) | 33 (11%) |
| (Aspergillus) | 2 (1%) | 26 (9%) |
| (Candida) | 10 (3%) | 4 (1%) |
| (Other) | 2 (1%) | 3 (1%) |
| All Deaths | 44 (14%) | 64 (21%) |
| Proven/probable fungal infection prior to death | 2 (1%) | 16 (5%) |
| SAF | 98 (32%) | 125 (42%) |
| Event free lost to follow-up Patients who are lost to follow-up (not observed for 100 days), and who did not meet another clinical failure endpoint. These patients were considered failures.
|
34 (11%) | 24 (8%) |
In summary, 2 clinical studies of prophylaxis were conducted with the Noxafil oral suspension. As seen in the accompanying tables (Tables 23 and 24), clinical failure represented a composite endpoint of breakthrough IFI, mortality and use of systemic antifungal therapy. In Noxafil Oral Suspension Study 1 (Table 23), the clinical failure rate of posaconazole (33%) was similar to fluconazole (37%), (95% CI for the difference posaconazole–comparator -11.5% to 3.7%) while in Noxafil Oral Suspension Study 2 (Table 24) clinical failure was lower for patients treated with posaconazole (27%) when compared to patients treated with fluconazole or itraconazole (42%), (95% CI for the difference posaconazole–comparator -22.9% to -7.8%).
All-cause mortality was similar at 16 weeks for both treatment arms in Noxafil Oral Suspension Study 1 [POS 58/301 (19%) vs. FLU 59/299 (20%)]; all-cause mortality was lower at 100 days for Noxafil-treated patients in Noxafil Oral Suspension Study 2 [POS 44/304 (14%) vs. FLU/ITZ 64/298 (21%)]. Both studies demonstrated fewer breakthrough infections caused by Aspergillus species in patients receiving Noxafil prophylaxis when compared to patients receiving fluconazole or itraconazole.
17 Patient Counseling Information (17 PATIENT COUNSELING INFORMATION)
Advise the patient to read the FDA-approved patient labeling (Patient Information).
Important Administration Instructions
Posaconazole Delayed-Release Tablets
Advise patients that Posaconazole delayed-release tablets must be swallowed whole and not divided, crushed, or chewed.
Instruct patients that if they miss a dose, they should take it as soon as they remember. If they do not remember until it is within 12 hours of the next dose, they should be instructed to skip the missed dose and go back to the regular schedule. Patients should not double their next dose or take more than the prescribed dose.
Posaconazole Oral Suspension
Advise patients to take each dose of Posaconazole oral suspension during or immediately (i.e., within 20 minutes) following a full meal. In patients who cannot eat a full meal, each dose of Posaconazole oral suspension should be administered with a liquid nutritional supplement or an acidic carbonated beverage (e.g., ginger ale) in order to enhance absorption.
Instruct patients that if they miss a dose, they should take it as soon as they remember. However, if it is almost time for the next dose, they should be instructed to skip the missed dose and go back to the regular schedule. Patients should not double their next dose or take more than the prescribed dose.
Drug Interactions
Advise patients to inform their physician immediately if they:
- develop severe diarrhea or vomiting.
- are currently taking drugs that are known to prolong the QTc interval and are metabolized through CYP3A4.
- are currently taking a cyclosporine or tacrolimus, or they notice swelling in an arm or leg or shortness of breath.
- are taking other drugs or before they begin taking other drugs as certain drugs can decrease or increase the plasma concentrations of posaconazole.
Serious and Potentially Serious Adverse Reactions
Advise patients to inform their physician immediately if they:
- notice a change in heart rate or heart rhythm or have a heart condition or circulatory disease. Posaconazole can be administered with caution to patients with potentially proarrhythmic conditions.
- are pregnant, plan to become pregnant, or are nursing.
- have liver disease or develop itching, nausea or vomiting, their eyes or skin turn yellow, they feel more tired than usual or feel like they have the flu.
- have ever had an allergic reaction to other antifungal medicines such as ketoconazole, fluconazole, itraconazole, or voriconazole.
5.1 Calcineurin Inhibitor Toxicity (5.1 Calcineurin-Inhibitor Toxicity)
Concomitant administration of posaconazole with cyclosporine or tacrolimus increases the whole blood trough concentrations of these calcineurin-inhibitors [see Drug Interactions (7.1) and Clinical Pharmacology (12.3)]. Nephrotoxicity and leukoencephalopathy (including deaths) have been reported in clinical efficacy studies in patients with elevated cyclosporine or tacrolimus concentrations. Frequent monitoring of tacrolimus or cyclosporine whole blood trough concentrations should be performed during and at discontinuation of posaconazole treatment and the tacrolimus or cyclosporine dose adjusted accordingly.
5.8 Breakthrough Fungal Infections
Patients who have severe diarrhea or vomiting should be monitored closely for breakthrough fungal infections when receiving Posaconazole delayed-release tablets or Posaconazole oral suspension.
5.2 Arrhythmias and Qt Prolongation (5.2 Arrhythmias and QT Prolongation)
Some azoles, including posaconazole, have been associated with prolongation of the QT interval on the electrocardiogram. In addition, cases of torsades de pointes have been reported in patients taking posaconazole.
Results from a multiple time-matched ECG analysis in healthy volunteers did not show any increase in the mean of the QTc interval. Multiple, time-matched ECGs collected over a 12-hour period were recorded at baseline and steady-state from 173 healthy male and female volunteers (18-85 years of age) administered Noxafil oral suspension 400 mg twice daily with a high-fat meal. In this pooled analysis, the mean QTc (Fridericia) interval change from baseline was –5 msec following administration of the recommended clinical dose. A decrease in the QTc(F) interval (–3 msec) was also observed in a small number of subjects (n=16) administered placebo. The placebo-adjusted mean maximum QTc(F) interval change from baseline was <0 msec (–8 msec). No healthy subject administered Noxafil had a QTc(F) interval ≥500 msec or an increase ≥60 msec in their QTc(F) interval from baseline.
Posaconazole should be administered with caution to patients with potentially proarrhythmic conditions. Do not administer with drugs that are known to prolong the QTc interval and are metabolized through CYP3A4 [see Contraindications (4.3) and Drug Interactions (7.2)].
16 How Supplied/storage and Handling (16 HOW SUPPLIED/STORAGE AND HANDLING)
16.1 How Supplied
Delayed-Release Tablets
Posaconazole delayed-release tablets are available as yellow, coated, oblong, debossed with "100" on one side containing 100 mg of posaconazole. Bottles with child-resistant closures of 60 delayed-release tablets (NDC 63629-2236-1).
16.2 Storage and Handling
Posaconazole Delayed-Release Tablets
Store at 20°C to 25°C (68°F to 77°F), excursions permitted to 15°C to 30°C (59°F to 86°F) [see USP Controlled Room Temperature].
Repackaged/Relabeled by:
Bryant Ranch Prepack, Inc.
Burbank, CA 91504
1.1 Treatment of Invasive Aspergillosis
Posaconazole delayed-release tablets are indicated for the treatment of invasive aspergillosis in adults and pediatric patients 13 years of age and older.
1.2 Prophylaxis of Invasive Aspergillus
Posaconazole is indicated for the prophylaxis of invasive Aspergillus and Candida infections in patients who are at high risk of developing these infections due to being severely immunocompromised, such as hematopoietic stem cell transplant (HSCT) recipients with graft-versus-host disease (GVHD) or those with hematologic malignancies with prolonged neutropenia from chemotherapy [see Clinical Studies (14.1)] as follows:
- Posaconazole delayed-release tablets: adults and pediatric patients 2 years of age and older who weigh greater than 40 kg
- Posaconazole oral suspension: adults and pediatric patients 13 years of age and older
2.1 Important Administration Instructions
Non-substitutable
Posaconazole oral suspension is not substitutable with Posaconazole delayed-release tablets or Noxafil PowderMix for delayed-release oral suspension due to the differences in the dosing of each formulation. Therefore, follow the specific dosage recommendations for each of the formulations [see Dosage and Administration (2.2, 2.3)].
7.5 Benzodiazepines Metabolized By Cyp3a4 (7.5 Benzodiazepines Metabolized by CYP3A4)
Concomitant administration of posaconazole with midazolam increases the midazolam plasma concentrations by approximately 5-fold. Increased plasma midazolam concentrations could potentiate and prolong hypnotic and sedative effects. Concomitant use of posaconazole and other benzodiazepines metabolized by CYP3A4 (e.g., alprazolam, triazolam) could result in increased plasma concentrations of these benzodiazepines. Patients must be monitored closely for adverse effects associated with high plasma concentrations of benzodiazepines metabolized by CYP3A4 and benzodiazepine receptor antagonists must be available to reverse these effects [see Warnings and Precautions (5.6) and Clinical Pharmacology (12.3)].
13.2 Animal Toxicology And/or Pharmacology (13.2 Animal Toxicology and/or Pharmacology)
In a nonclinical study using intravenous administration of posaconazole in very young dogs (dosed from 2 to 8 weeks of age), an increase in the incidence of brain ventricle enlargement was observed in treated animals as compared with concurrent control animals. No difference in the incidence of brain ventricle enlargement between control and treated animals was observed following the subsequent 5-month treatment-free period. There were no neurologic, behavioral or developmental abnormalities in the dogs with this finding, and a similar brain finding was not seen with oral posaconazole administration to juvenile dogs (4 days to 9 months of age). There were no drug-related increases in the incidence of brain ventricle enlargement when treated, and control animals were compared in a separate study of 10-week old dogs dosed with intravenous posaconazole for 13 weeks with a 9-week recovery period or a follow-up study of 31-week old dogs dosed for 3 months.
7.11 Calcium Channel Blockers Metabolized By Cyp3a4 (7.11 Calcium Channel Blockers Metabolized by CYP3A4)
Posaconazole may increase the plasma concentrations of calcium channel blockers metabolized by CYP3A4 (e.g., verapamil, diltiazem, nifedipine, nicardipine, felodipine). Frequent monitoring for adverse reactions and toxicity related to calcium channel blockers is recommended during coadministration. Dose reduction of calcium channel blockers may be needed.
2.7 Dosage Adjustments in Patients With Renal Impairment (2.7 Dosage Adjustments in Patients with Renal Impairment)
The pharmacokinetics of Posaconazole oral suspension and Posaconazole delayed-release tablets are not significantly affected by renal impairment. Therefore, no adjustment is necessary for oral dosing in patients with mild to severe renal impairment.
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenesis
No drug-related neoplasms were recorded in rats or mice treated with posaconazole for 2 years at doses higher than the clinical dose. In a 2-year carcinogenicity study, rats were given posaconazole orally at doses up to 20 mg/kg (females), or 30 mg/kg (males). These doses are equivalent to 3.9- or 3.5-times the exposure achieved with a 400-mg twice daily oral suspension regimen, respectively, based on steady-state AUC in healthy volunteers administered a high-fat meal (400-mg twice daily oral suspension regimen). In the mouse study, mice were treated at oral doses up to 60 mg/kg/day or 4.8-times the exposure achieved with a 400-mg twice daily oral suspension regimen.
Mutagenesis
Posaconazole was not genotoxic or clastogenic when evaluated in bacterial mutagenicity (Ames), a chromosome aberration study in human peripheral blood lymphocytes, a Chinese hamster ovary cell mutagenicity study, and a mouse bone marrow micronucleus study.
Impairment of Fertility
Posaconazole had no effect on fertility of male rats at a dose up to 180 mg/kg (1.7 x the 400-mg twice daily oral suspension regimen based on steady-state plasma concentrations in healthy volunteers) or female rats at a dose up to 45 mg/kg (2.2 x the 400-mg twice daily oral suspension regimen).
4.3 Qt Prolongation With Concomitant Use With Cyp3a4 Substrates (4.3 QT Prolongation with Concomitant Use with CYP3A4 Substrates)
Posaconazole is contraindicated with CYP3A4 substrates that prolong the QT interval. Concomitant administration of posaconazole with the CYP3A4 substrates, pimozide and quinidine may result in increased plasma concentrations of these drugs, leading to QTc prolongation and cases of torsades de pointes [see Warnings and Precautions (5.2) and Drug Interactions (7.2)].
2.5 Administration Instructions for Posaconazole Oral Suspension
- Shake Posaconazole oral suspension well before use. Administer with measured dosing spoon (see Figure 1) provided.
| Figure 1: A measured dosing spoon is provided, marked for doses of 2.5 mL and 5 mL. |
- Rinse the spoon with water after each administration and before storage.
- Administer each dose of Posaconazole oral suspension during or immediately (i.e., within 20 minutes) following a full meal [see Clinical Pharmacology (12.3)].
- For patients who cannot eat a full meal, Posaconazole delayed-release tablets should be used instead of Posaconazole oral suspension for the prophylaxis indication. Posaconazole delayed-release tablets provide higher plasma drug exposures than Posaconazole oral suspension under fasted conditions [see Dosage and Administration (2.1)].
- In patients who cannot eat a full meal and for whom Posaconazole delayed-release tablets or Noxafil injection are not options, administer each dose of Posaconazole oral suspension with a liquid nutritional supplement or an acidic carbonated beverage (e.g., ginger ale).
- For patients who cannot eat a full meal or tolerate an oral nutritional supplement or an acidic carbonated beverage and who do not have the option of taking Posaconazole delayed-release tablets or Noxafil injection, an alternative antifungal therapy should be considered or patients should be monitored closely for breakthrough fungal infections.
4.4 Hmg Coa Reductase Inhibitors Primarily Metabolized Through Cyp3a4 (4.4 HMG-CoA Reductase Inhibitors Primarily Metabolized Through CYP3A4)
Coadministration with the HMG-CoA reductase inhibitors that are primarily metabolized through CYP3A4 (e.g., atorvastatin, lovastatin, and simvastatin) is contraindicated since increased plasma concentration of these drugs can lead to rhabdomyolysis [see Drug Interactions (7.3) and Clinical Pharmacology (12.3)].
14.3 Treatment of Oropharyngeal Candidiasis With Noxafil Oral Suspension (14.3 Treatment of Oropharyngeal Candidiasis with Noxafil Oral Suspension)
Noxafil Oral Suspension Study 3 was a randomized, controlled, evaluator-blinded study in HIV-infected patients with oropharyngeal candidiasis. Patients were treated with Noxafil or fluconazole oral suspension (both Noxafil and fluconazole were given as follows: 100 mg twice a day for 1 day followed by 100 mg once a day for 13 days).
Clinical and mycological outcomes were assessed after 14 days of treatment and at 4 weeks after the end of treatment. Patients who received at least 1 dose of study medication and had a positive oral swish culture of Candida species at baseline were included in the analyses (see Table 25 ). The majority of the subjects had C. albicans as the baseline pathogen.
Clinical success at Day 14 (complete or partial resolution of all ulcers and/or plaques and symptoms) and clinical relapse rates (recurrence of signs or symptoms after initial cure or improvement) 4 weeks after the end of treatment were similar between the treatment arms (see Table 25 ).
Mycologic eradication rates (absence of colony forming units in quantitative culture at the end of therapy, Day 14), as well as mycologic relapse rates (4 weeks after the end of treatment) were also similar between the treatment arms (see Table 25 ).
| Noxafil | Fluconazole | |
|---|---|---|
| Clinical Success at End of Therapy (Day 14) | 155/169 (91.7%) | 148/160 (92.5%) |
| Clinical Relapse (4 Weeks after End of Therapy) | 45/155 (29.0%) | 52/148 (35.1%) |
| Mycological Eradication (absence of CFU) at End of Therapy (Day 14) | 88/169 (52.1%) | 80/160 (50.0%) |
| Mycological Relapse (4 Weeks after End of Treatment) | 49/88 (55.6%) | 51/80 (63.7%) |
Mycologic response rates, using a criterion for success as a posttreatment quantitative culture with ≤20 colony forming units (CFU/mL) were also similar between the two groups (Noxafil 68.0%, fluconazole 68.1%). The clinical significance of this finding is unknown.
2.4 Administration Instructions for Posaconazole Delayed Release Tablets (2.4 Administration Instructions for Posaconazole Delayed-Release Tablets)
- Swallow tablets whole. Do not divide, crush, or chew.
- Administer Posaconazole delayed-release tablets with or without food [see Clinical Pharmacology (12.3)].
2.3 Dosing Regimen in Pediatric Patients (ages 2 to Less Than 18 Years of Age) (2.3 Dosing Regimen in Pediatric Patients (ages 2 to less than 18 years of age))
- The recommended dosing regimen of posaconazole for pediatric patients 2 to less than 18 years of age is shown in Tables 2 and 3 [see Dosage and Administration (2.4, 2.5) and Clinical Pharmacology (12.3)].
| Recommended Pediatric Dosage and Formulation | |||
|---|---|---|---|
| Indication | Weight/Age | Delayed-Release Tablet | Duration of therapy |
| Prophylaxis of invasive Aspergillus and Candida infections | Less than or equal to 40 kg (2 to less than 18 years of age) | Not Applicable | Duration of therapy is based on recovery from neutropenia or immunosuppression. |
| Greater than 40 kg (2 to less than 18 years of age) |
Loading dose:
300 mg twice daily on the first day Maintenance dose: 300 mg once daily |
||
| Treatment of invasive Aspergillosis | 13 to less than 18 years of age regardless of weight. |
Loading dose:
300 mg (three 100 mg delayed-release tablets) twice a day on the first day. Maintenance dose: 300 mg (three 100 mg delayed-release tablets) once a day, starting on the second day. Switching between the intravenous and delayed-release tablets is acceptable. A loading dose is not required when switching between formulations. |
Loading dose:
1 day Maintenance dose: Recommended total duration of therapy is 6 to 12 weeks. |
| Indication |
Loading Dose (volume) and frequency |
Maintenance Dose (volume) and frequency |
Duration of therapy |
|---|---|---|---|
| Prophylaxis of invasive Aspergillus and Candida infections | 200 mg (5 mL) three times a day | 200 mg (5 mL) three times a day | Duration of therapy is based on recovery from neutropenia or immunosuppression. |
| Oropharyngeal Candidiasis (OPC) | 100 mg (2.5 mL) twice daily on the first day | 100 mg (2.5 mL) once daily | 13 days |
| OPC Refractory (rOPC) to Itraconazole and/or Fluconazole | 400 mg (10 mL) twice daily | 400 mg (10 mL) twice daily | Duration of therapy is based on the severity of the patient’s underlying disease and clinical response. |
7.3 Hmg Coa Reductase Inhibitors (statins) Primarily Metabolized Through Cyp3a4 (7.3 HMG-CoA Reductase Inhibitors (Statins) Primarily Metabolized Through CYP3A4)
Concomitant administration of posaconazole with simvastatin increases the simvastatin plasma concentrations by approximately 10-fold. Therefore, posaconazole is contraindicated with HMG-CoA reductase inhibitors primarily metabolized through CYP3A4 [see Contraindications (4.4) and Clinical Pharmacology (12.3)].
2.6 Non Substitutability Between Posaconazole Oral Suspension and Other Formulations (2.6 Non-substitutability between Posaconazole Oral Suspension and Other Formulations)
Posaconazole oral suspension is not substitutable with Posaconazole delayed-release tablets or Noxafil PowderMix for delayed-release oral suspension due to the differences in the dosing of each formulation. Therefore, follow the specific dosage recommendations for each of the formulations [see Dosage and Administration (2.2, 2.3)].
14.1 Treatment of Invasive Aspergillosis With Noxafil Injection and Noxafil Delayed Release Tablets (14.1 Treatment of Invasive Aspergillosis with Noxafil Injection and Noxafil Delayed-Release Tablets)
Aspergillosis Treatment Study (NCT01782131) was a randomized, double-blind, controlled trial which evaluated the safety and efficacy of Noxafil injection and Noxafil delayed-release tablets versus voriconazole for primary treatment of invasive fungal disease caused by Aspergillus species. Eligible patients had proven, probable, or possible invasive fungal infections per the European Organization for Research and Treatment of Cancer/Mycoses Study Group, EORTC/MSG criteria. Patients were stratified by risk for mortality or poor outcome where high risk included a history of allogeneic bone marrow transplant, liver transplant, or relapsed leukemia undergoing salvage chemotherapy. The median age of patients was 57 years (range 14-91 years), with 27.8% of patients aged ≥65 years; 5 patients were pediatric patients 14-16 years of age, of whom 3 were treated with Noxafil and 2 with voriconazole. The majority of patients were male (59.8%) and white (67.1%). With regard to risk factors for invasive aspergillosis, approximately two-thirds of the patients in the study had a recent history of neutropenia, while approximately 20% with a history of an allogeneic stem cell transplant. Over 80% of subjects in each treatment group had infection limited to the lower respiratory tract (primarily lung), while approximately 11% to 13% also had infection in another organ. Invasive aspergillosis was proven or probable in 58.1% of patients as classified by independent adjudicators blinded to study treatment assignment. At least one Aspergillus species was identified in 21% of the patients; A. fumigatus and A. flavus were the most common pathogens identified.
Patients randomized to receive Noxafil were given a dose of 300 mg once daily (twice daily on Day 1) IV or tablet. Patients randomized to receive voriconazole were given a dose of 6 mg/kg twice daily Day 1 followed by 4 mg/kg twice daily IV, or oral 300 mg twice daily Day 1 followed by 200 mg twice daily. The recommended initial route of administration was IV; however, patients could begin oral therapy if clinically stable and able to tolerate oral dosing. The transition from IV to oral therapy occurred when the patient was clinically stable. The protocol recommended duration of therapy was 84 days with a maximum allowed duration of 98 days. Median treatment duration was 67 days for Noxafil patients and 64 days for voriconazole patients. Overall, 55% to 60% of patients began treatment with the IV formulation with a median duration of 9 days for the initial IV dosing.
The Intent to Treat (ITT) population included all patients randomized and receiving at least one dose of study treatment. All-cause mortality through Day 42 in the overall population (ITT) was 15.3% for Noxafil patients compared to 20.6% for voriconazole patients for an adjusted treatment difference of -5.3% with a 95% confidence interval of -11.6 to 1.0%. Consistent results were seen in patients with proven or probable invasive aspergillosis per EORTC criteria (see Table 21 ).
| Noxafil Injection and Delayed-Release Tablets | Voriconazole | ||||
|---|---|---|---|---|---|
| Population | N | n (%) | N | n (%) | Difference Adjusted treatment difference based on Miettinen and Nurminen’s method stratified by randomization factor (risk for mortality/poor outcome), using Cochran-Mantel-Haenszel weighting scheme. (95% CI) |
| Intent to Treat | 288 | 44 (15.3) | 287 | 59 (20.6) | -5.3 (-11.6, 1.0) |
| Proven/Probable Invasive Aspergillosis | 163 | 31 (19.0) | 171 | 32 (18.7) | 0.3 (-8.2, 8.8) |
Global clinical response at Week 6 was assessed by a blinded, independent adjudication committee based upon prespecified clinical, radiologic, and mycologic criteria. In the subgroup of patients with proven or probable invasive aspergillosis per EORTC criteria, the global clinical response of success (complete or partial response) at Week 6 was seen in 44.8% for Noxafil-treated patients compared to 45.6% for voriconazole-treated patients (see Table 22 ).
| Posaconazole | Voriconazole | ||||
|---|---|---|---|---|---|
| Population | N | Success | N | Success | Difference Adjusted treatment difference based on Miettinen and Nurminen’s method stratified by randomization factor (risk for mortality/poor outcome), using Cochran-Mantel-Haenszel weighting scheme. (95% CI) |
| Proven/Probable Invasive Aspergillosis | 163 | 73 (44.8) | 171 | 78 (45.6) | -0.6 (-11.2, 10.1) |
1.3 Treatment of Oropharyngeal Candidiasis Including Oropharyngeal Candidiasis Refractory to Itraconazole And/or Fluconazole (1.3 Treatment of Oropharyngeal Candidiasis Including Oropharyngeal Candidiasis Refractory to Itraconazole and/or Fluconazole)
Posaconazole oral suspension is indicated for the treatment of oropharyngeal candidiasis, including oropharyngeal candidiasis refractory to itraconazole and/or fluconazole in adults and pediatric patients 13 years of age and older.
14.4 Noxafil Oral Suspension Treatment of Oropharyngeal Candidiasis Refractory to Treatment With Fluconazole Or Itraconazole (14.4 Noxafil Oral Suspension Treatment of Oropharyngeal Candidiasis Refractory to Treatment with Fluconazole or Itraconazole)
Noxafil Oral Suspension Study 4 was a noncomparative study of Noxafil oral suspension in HIV-infected subjects with OPC that was refractory to treatment with fluconazole or itraconazole. An episode of OPC was considered refractory if there was failure to improve or worsening of OPC after a standard course of therapy with fluconazole greater than or equal to 100 mg/day for at least 10 consecutive days or itraconazole 200 mg/day for at least 10 consecutive days and treatment with either fluconazole or itraconazole had not been discontinued for more than 14 days prior to treatment with Noxafil. Of the 199 subjects enrolled in this study, 89 subjects met these strict criteria for refractory infection.
Forty-five subjects with refractory OPC were treated with Noxafil oral suspension 400 mg twice daily for 3 days, followed by 400 mg once daily for 25 days with an option for further treatment during a 3-month maintenance period. Following a dosing amendment, a further 44 subjects were treated with Noxafil 400 mg twice daily for 28 days. The efficacy of Noxafil was assessed by the clinical success (cure or improvement) rate after 4 weeks of treatment. The clinical success rate was 74.2% (66/89). The clinical success rates for both the original and the amended dosing regimens were similar (73.3% and 75.0%, respectively).
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:42:50.888910 · Updated: 2026-03-14T22:11:10.971269