These Highlights Do Not Include All The Information Needed To Use Baclofen Injection Safely And Effectively. See Full Prescribing Information For Baclofen Injection.
d4bfba33-9f4d-4c43-ae6c-bcf67ef8fe51
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
Abrupt discontinuation of intrathecal baclofen, regardless of the cause, has resulted in sequelae that include high fever, altered mental status, exaggerated rebound spasticity, and muscle rigidity, that in rare cases has advanced to rhabdomyolysis, multiple organ-system failure and death. Prevention of abrupt discontinuation of intrathecal baclofen requires careful attention to programming and monitoring of the infusion system, refill scheduling and procedures, and pump alarms. Patients and caregivers should be advised of the importance of keeping scheduled refill visits and should be educated on the early symptoms of baclofen withdrawal. Special attention should be given to patients at apparent risk (e.g., spinal cord injuries at T-6 or above, communication difficulties, history of withdrawal symptoms from oral or intrathecal baclofen). Consult the technical manual of the implantable infusion system for additional post-implant clinician and patient information [see Warnings and Precautions ( 5.4 )] .
Indications and Usage
Baclofen injection is indicated for use in the management of severe spasticity in adult and pediatric patients age 4 years and above. Patients should first respond to a screening dose of intrathecal baclofen prior to consideration for long term infusion via an implantable pump. For spasticity of spinal cord origin, chronic infusion of baclofen injection via an implantable pump should be reserved for patients unresponsive to oral baclofen therapy, or those who experience intolerable CNS side effects at effective doses. Patients with spasticity due to traumatic brain injury should wait at least one year after the injury before consideration of long term intrathecal baclofen therapy. Baclofen injection is intended for use by the intrathecal route in single bolus test doses (via spinal catheter or lumbar puncture) and, for chronic use, only with the Medtronic SynchroMed ® II Programmable Pump or other pumps labeled for intrathecal administration of baclofen injection [see Clinical Studies ( 14 )] . Prior to implantation of a device for chronic intrathecal infusion of baclofen injection, patients must show a response to baclofen injection in a screening trial [see Dosage and Administration ( 2.2 )] .
Dosage and Administration
Baclofen injection is intended for use by the intrathecal route in single bolus test doses (via spinal catheter or lumbar puncture) and, for chronic use in the Medtronic SynchroMed ® II Programmable Pump or other pumps labeled for intrathecal administration of baclofen injection; Refer to the pump manufacturer's manual and follow the specific instructions and precautions for programming the pump and/or refilling the reservoir ( 2.1 ) Screening : Patients who do not respond to a 100 mcg intrathecal bolus should not be considered for an implanted pump for chronic infusion ( 2.2 ) Dose Titration : Spasticity may be necessary to sustain upright posture and balance in locomotion or may be useful to obtain optimal function and care ( 2.5 ) Maintenance Therapy : Titrate patients individually; Lowest dose with an optimal response should be used, generally 300 mcg/day to 800 mcg/day for spasticity of spinal cord origin and 90 mcg/day to 700 mcg/day for spasticity of cerebral origin; Titrate baclofen injection to maintain some degree of muscle tone and allow occasional spasms. ( 2.6 )
Warnings and Precautions
Do not directly inject baclofen injection into the pump catheter access port, as this may cause a life-threatening overdose ( 5.1 ) Potential for contamination due to non-sterile external surface of prefilled syringe ( 5.2 ) Potentially life-threatening CNS depression, cardiovascular collapse, and/or respiratory failure; Resuscitative equipment and trained staff must be available during screening, dose titration, and refills ( 5.3 ) Overdose may cause drowsiness, lightheadedness, dizziness, somnolence, respiratory depression, seizures, rostral progression of hypotonia and loss of consciousness progressing to coma ( 5.4 ) Possible exacerbation of psychotic disorders, schizophrenia or confusional states ( 5.6 )
Contraindications
Baclofen injection is contraindicated in patients with a hypersensitivity to baclofen. Do not use baclofen injection for intravenous, intramuscular, subcutaneous or epidural administration.
Adverse Reactions
The most common adverse reactions in patients with spasticity of spinal origin were somnolence, dizziness, nausea, hypotension, headache, convulsions and hypotonia ( 6.1 ) The most common adverse reactions in patients with spasticity of cerebral origin were agitation, constipation, somnolence, leukocytosis, chills, urinary retention and hypotonia ( 6.2 ) To report SUSPECTED ADVERSE REACTIONS, contact Sagent Pharmaceuticals, Inc. at 1-866-625-1618 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch .
Drug Interactions
There is inadequate systematic experience with the use of intrathecal baclofen in combination with other medications to predict specific drug-drug interactions. Interactions attributed to the combined use of baclofen injection and epidural morphine include hypotension and dyspnea.
Storage and Handling
Baclofen injection, USP* is a clear, colorless, isotonic solution consisting of the active ingredient, Baclofen USP, and the excipients Sodium Chloride USP and Water for Injection USP and is supplied in single-dose clear glass vials as follows: NDC Baclofen Injection, USP* (1,000 mcg per mL) Package Factor 25021-680-20 20,000 mcg per 20 mL Single-Dose Vial 1 vial per carton Sterile, Nonpyrogenic, Preservative-free. The container closure is not made with natural rubber latex.
How Supplied
Baclofen injection, USP* is a clear, colorless, isotonic solution consisting of the active ingredient, Baclofen USP, and the excipients Sodium Chloride USP and Water for Injection USP and is supplied in single-dose clear glass vials as follows: NDC Baclofen Injection, USP* (1,000 mcg per mL) Package Factor 25021-680-20 20,000 mcg per 20 mL Single-Dose Vial 1 vial per carton Sterile, Nonpyrogenic, Preservative-free. The container closure is not made with natural rubber latex.
Medication Information
Warnings and Precautions
Do not directly inject baclofen injection into the pump catheter access port, as this may cause a life-threatening overdose ( 5.1 ) Potential for contamination due to non-sterile external surface of prefilled syringe ( 5.2 ) Potentially life-threatening CNS depression, cardiovascular collapse, and/or respiratory failure; Resuscitative equipment and trained staff must be available during screening, dose titration, and refills ( 5.3 ) Overdose may cause drowsiness, lightheadedness, dizziness, somnolence, respiratory depression, seizures, rostral progression of hypotonia and loss of consciousness progressing to coma ( 5.4 ) Possible exacerbation of psychotic disorders, schizophrenia or confusional states ( 5.6 )
Indications and Usage
Baclofen injection is indicated for use in the management of severe spasticity in adult and pediatric patients age 4 years and above. Patients should first respond to a screening dose of intrathecal baclofen prior to consideration for long term infusion via an implantable pump. For spasticity of spinal cord origin, chronic infusion of baclofen injection via an implantable pump should be reserved for patients unresponsive to oral baclofen therapy, or those who experience intolerable CNS side effects at effective doses. Patients with spasticity due to traumatic brain injury should wait at least one year after the injury before consideration of long term intrathecal baclofen therapy. Baclofen injection is intended for use by the intrathecal route in single bolus test doses (via spinal catheter or lumbar puncture) and, for chronic use, only with the Medtronic SynchroMed ® II Programmable Pump or other pumps labeled for intrathecal administration of baclofen injection [see Clinical Studies ( 14 )] . Prior to implantation of a device for chronic intrathecal infusion of baclofen injection, patients must show a response to baclofen injection in a screening trial [see Dosage and Administration ( 2.2 )] .
Dosage and Administration
Baclofen injection is intended for use by the intrathecal route in single bolus test doses (via spinal catheter or lumbar puncture) and, for chronic use in the Medtronic SynchroMed ® II Programmable Pump or other pumps labeled for intrathecal administration of baclofen injection; Refer to the pump manufacturer's manual and follow the specific instructions and precautions for programming the pump and/or refilling the reservoir ( 2.1 ) Screening : Patients who do not respond to a 100 mcg intrathecal bolus should not be considered for an implanted pump for chronic infusion ( 2.2 ) Dose Titration : Spasticity may be necessary to sustain upright posture and balance in locomotion or may be useful to obtain optimal function and care ( 2.5 ) Maintenance Therapy : Titrate patients individually; Lowest dose with an optimal response should be used, generally 300 mcg/day to 800 mcg/day for spasticity of spinal cord origin and 90 mcg/day to 700 mcg/day for spasticity of cerebral origin; Titrate baclofen injection to maintain some degree of muscle tone and allow occasional spasms. ( 2.6 )
Contraindications
Baclofen injection is contraindicated in patients with a hypersensitivity to baclofen. Do not use baclofen injection for intravenous, intramuscular, subcutaneous or epidural administration.
Adverse Reactions
The most common adverse reactions in patients with spasticity of spinal origin were somnolence, dizziness, nausea, hypotension, headache, convulsions and hypotonia ( 6.1 ) The most common adverse reactions in patients with spasticity of cerebral origin were agitation, constipation, somnolence, leukocytosis, chills, urinary retention and hypotonia ( 6.2 ) To report SUSPECTED ADVERSE REACTIONS, contact Sagent Pharmaceuticals, Inc. at 1-866-625-1618 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch .
Drug Interactions
There is inadequate systematic experience with the use of intrathecal baclofen in combination with other medications to predict specific drug-drug interactions. Interactions attributed to the combined use of baclofen injection and epidural morphine include hypotension and dyspnea.
Storage and Handling
Baclofen injection, USP* is a clear, colorless, isotonic solution consisting of the active ingredient, Baclofen USP, and the excipients Sodium Chloride USP and Water for Injection USP and is supplied in single-dose clear glass vials as follows: NDC Baclofen Injection, USP* (1,000 mcg per mL) Package Factor 25021-680-20 20,000 mcg per 20 mL Single-Dose Vial 1 vial per carton Sterile, Nonpyrogenic, Preservative-free. The container closure is not made with natural rubber latex.
How Supplied
Baclofen injection, USP* is a clear, colorless, isotonic solution consisting of the active ingredient, Baclofen USP, and the excipients Sodium Chloride USP and Water for Injection USP and is supplied in single-dose clear glass vials as follows: NDC Baclofen Injection, USP* (1,000 mcg per mL) Package Factor 25021-680-20 20,000 mcg per 20 mL Single-Dose Vial 1 vial per carton Sterile, Nonpyrogenic, Preservative-free. The container closure is not made with natural rubber latex.
Description
Abrupt discontinuation of intrathecal baclofen, regardless of the cause, has resulted in sequelae that include high fever, altered mental status, exaggerated rebound spasticity, and muscle rigidity, that in rare cases has advanced to rhabdomyolysis, multiple organ-system failure and death. Prevention of abrupt discontinuation of intrathecal baclofen requires careful attention to programming and monitoring of the infusion system, refill scheduling and procedures, and pump alarms. Patients and caregivers should be advised of the importance of keeping scheduled refill visits and should be educated on the early symptoms of baclofen withdrawal. Special attention should be given to patients at apparent risk (e.g., spinal cord injuries at T-6 or above, communication difficulties, history of withdrawal symptoms from oral or intrathecal baclofen). Consult the technical manual of the implantable infusion system for additional post-implant clinician and patient information [see Warnings and Precautions ( 5.4 )] .
Section 42229-5
Pediatric Patients
The starting screening dose for pediatric patients is the same as in adult patients, i.e., 50 mcg. However, for very small patients, a screening dose of 25 mcg may be tried first.
Patients who do not respond to a 100 mcg intrathecal bolus should not be considered candidates for an implanted pump for chronic infusion.
Section 44425-7
Storage Conditions
Does not require refrigeration.
Store at 20° to 25°C (68° to 77°F); excursions permitted between 15° to 30°C (59° to 86°F). [See USP Controlled Room Temperature.]
Do not freeze.
Do not heat sterilize.
*The USP osmolality specification is pending
Section 51945-4
PACKAGE LABEL – PRINCIPAL DISPLAY PANEL – Vial Label
NDC 25021-680-20
Rx only
Baclofen Injection, USP
20,000 mcg per 20 mL
(1,000 mcg per mL)
For Intrathecal Use Only
20 mL Single-Dose Vial
Discard unused portion
5.4 Overdose
Signs of overdose may appear suddenly or insidiously. Acute massive overdose may present as coma. Less sudden and/or less severe forms of overdose may present with signs of drowsiness, lightheadedness, dizziness, somnolence, respiratory depression, seizures, rostral progression of hypotonia and loss of consciousness progressing to coma. Should overdose appear likely, the patient should be taken immediately to a hospital for assessment and emptying of the pump reservoir. In cases reported to date, overdose has generally been related to pump malfunction or dosing error [see Overdosage (10)].
Extreme caution must be used when filling the implantable pump.
Medtronic SynchroMed® II Programmable Pump should only be refilled through the reservoir refill septum. The Medtronic SynchroMed® II Programmable Pump is also equipped with a catheter access port that allows direct access to the intrathecal catheter. Direct injection into this catheter access port may cause a life-threatening overdose.
10 Overdosage
Special attention must be given to recognizing the signs and symptoms of overdosage, especially during the initial screening and dose-titration phase of treatment, but also during re-introduction of baclofen injection after a period of interruption in therapy.
11 Description
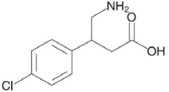
Baclofen injection, USP* is a muscle relaxant and antispastic. Baclofen's pharmacological class is a gamma-aminobutyric acid (GABA) ergic agonist. Baclofen's chemical name is 4-amino- 3-(4- chlorophenyl) butanoic acid, and its structural formula is:
Baclofen
Baclofen is a white to off-white, odorless or practically odorless crystalline powder, with a molecular weight of 213.66. It is slightly soluble in water, very slightly soluble in methanol, and insoluble in chloroform.
5.5 Withdrawal
Abrupt withdrawal of intrathecal baclofen, regardless of the cause, has resulted in sequelae that included high fever, altered mental status, exaggerated rebound spasticity and muscle rigidity that in rare cases progressed to rhabdomyolysis, multiple organ-system failure, and death. In the first 9 years of post-marketing experience, 27 cases of withdrawal temporally related to the cessation of baclofen therapy were reported; six patients died. In most cases, symptoms of withdrawal appeared within hours to a few days following interruption of baclofen therapy. Common reasons for abrupt interruption of intrathecal baclofen therapy included malfunction of the catheter (especially disconnection), low volume in the pump reservoir, and end of pump battery life; human error may have played a causal or contributing role in some cases. Cases of intrathecal mass at the tip of the implanted catheter leading to withdrawal symptoms have also been reported, most of them involving pharmacy compounded analgesic admixtures [see Warnings and Precautions (5.10)].
Prevention of abrupt discontinuation of intrathecal baclofen requires careful attention to programming and monitoring of the infusion system, refill scheduling and procedures, and pump alarms. Patients and caregivers should be advised of the importance of keeping scheduled refill visits and should be educated on the early symptoms of baclofen withdrawal.
All patients receiving intrathecal baclofen therapy are potentially at risk for withdrawal. Early symptoms of baclofen withdrawal may include return of baseline spasticity, pruritus, hypotension, and paresthesias. Some clinical characteristics of the advanced intrathecal baclofen withdrawal syndrome may resemble autonomic dysreflexia, infection (sepsis), malignant hyperthermia, neuroleptic-malignant syndrome, or other conditions associated with a hypermetabolic state or widespread rhabdomyolysis.
Rapid, accurate diagnosis and treatment in an emergency-room or intensive-care setting are important in order to prevent the potentially life-threatening central nervous system and systemic effects of intrathecal baclofen withdrawal. The suggested treatment for intrathecal baclofen withdrawal is the restoration of intrathecal baclofen at or near the same dosage as before therapy was interrupted. However, if restoration of intrathecal delivery is delayed, treatment with GABA-ergic agonist drugs such as oral or enteral baclofen, or oral, enteral, or intravenous benzodiazepines may prevent potentially fatal sequelae. Oral or enteral baclofen alone should not be relied upon to halt the progression of intrathecal baclofen withdrawal.
Seizures have been reported during overdose and with withdrawal from intrathecal baclofen as well as in patients maintained on therapeutic doses of intrathecal baclofen.
5.9 Infections
Patients should be infection-free prior to the screening trial with baclofen injection because the presence of a systemic infection may interfere with an assessment of the patient's response to bolus baclofen injection. Patients should be infection-free prior to implantation of the pump because the presence of infection may increase the risk of surgical complications. Moreover, a systemic infection may complicate dosing.
5.10 Drowsiness
Drowsiness has been reported in patients on intrathecal baclofen. Patients should be cautioned regarding the operation of automobiles or other dangerous machinery, and activities made hazardous by decreased alertness. Patients should also be cautioned that the central nervous system depressant effects of intrathecal baclofen may be additive to those of alcohol and other CNS depressants.
8.4 Pediatric Use
Children should be of sufficient body mass to accommodate the implantable pump for chronic infusion. Please consult pump manufacturer's manual for specific recommendations.
Safety and effectiveness in pediatric patients below the age of 4 have not been established.
5.12 Ovarian Cysts
A dose-related increase in incidence of ovarian cysts was observed in female rats treated chronically with oral baclofen. Ovarian cysts have been found by palpation in about 4% of the multiple sclerosis patients who were treated with oral baclofen for up to one year. In most cases these cysts disappeared spontaneously while patients continued to receive the drug. Ovarian cysts are estimated to occur spontaneously in approximately 1% to 5% of the normal female population.
2.2 Screening Phase
Prior to pump implantation and initiation of chronic infusion of baclofen injection, patients must demonstrate a positive clinical response to a baclofen injection bolus dose administered intrathecally in a screening trial. The screening trial employs baclofen injection at a concentration of 50 mcg per mL. A 1 mL syringe (50 mcg per mL) is available for use in the screening trial. The screening procedure is as follows. An initial bolus containing 50 micrograms in a volume of 1 milliliter is administered into the intrathecal space by barbotage over a period of not less than one minute. The patient is observed over the ensuing 4 to 8 hours. A positive response consists of a significant decrease in muscle tone and/or frequency and/or severity of spasms. If the initial response is less than desired, a second bolus injection may be administered 24 hours after the first. The second screening bolus dose consists of 75 micrograms in 1.5 milliliters. Again, the patient should be observed for an interval of 4 to 8 hours. If the response is still inadequate, a final bolus screening dose of 100 micrograms in 2 milliliters may be administered 24 hours later.
4 Contraindications
Baclofen injection is contraindicated in patients with a hypersensitivity to baclofen. Do not use baclofen injection for intravenous, intramuscular, subcutaneous or epidural administration.
6 Adverse Reactions
- The most common adverse reactions in patients with spasticity of spinal origin were somnolence, dizziness, nausea, hypotension, headache, convulsions and hypotonia (6.1)
- The most common adverse reactions in patients with spasticity of cerebral origin were agitation, constipation, somnolence, leukocytosis, chills, urinary retention and hypotonia (6.2)
To report SUSPECTED ADVERSE REACTIONS, contact Sagent Pharmaceuticals, Inc. at 1-866-625-1618 or FDA at 1-800-FDA-1088 or
www.fda.gov/medwatch
.
7 Drug Interactions
There is inadequate systematic experience with the use of intrathecal baclofen in combination with other medications to predict specific drug-drug interactions. Interactions attributed to the combined use of baclofen injection and epidural morphine include hypotension and dyspnea.
12.3 Pharmacokinetics
The pharmacokinetics of cerebrospinal fluid (CSF) clearance of intrathecal baclofen calculated from intrathecal bolus or continuous infusion studies approximates CSF turnover, suggesting elimination is by bulk-flow removal of CSF.
1 Indications and Usage
Baclofen injection is indicated for use in the management of severe spasticity in adult and pediatric patients age 4 years and above. Patients should first respond to a screening dose of intrathecal baclofen prior to consideration for long term infusion via an implantable pump. For spasticity of spinal cord origin, chronic infusion of baclofen injection via an implantable pump should be reserved for patients unresponsive to oral baclofen therapy, or those who experience intolerable CNS side effects at effective doses. Patients with spasticity due to traumatic brain injury should wait at least one year after the injury before consideration of long term intrathecal baclofen therapy. Baclofen injection is intended for use by the intrathecal route in single bolus test doses (via spinal catheter or lumbar puncture) and, for chronic use, only with the Medtronic SynchroMed® II Programmable Pump or other pumps labeled for intrathecal administration of baclofen injection [see Clinical Studies (14)].
Prior to implantation of a device for chronic intrathecal infusion of baclofen injection, patients must show a response to baclofen injection in a screening trial [see Dosage and Administration (2.2)].
12.1 Mechanism of Action
The precise mechanism of action of baclofen as a muscle relaxant and antispasticity agent is not fully understood. Baclofen inhibits both monosynaptic and polysynaptic reflexes at the spinal level, possibly by decreasing excitatory neurotransmitter release from primary afferent terminals, although actions at supraspinal sites may also occur and contribute to its clinical effect. Baclofen is a structural analog of the inhibitory neurotransmitter gamma-aminobutyric acid (GABA), and may exert its effects by stimulation of the GABAB receptor subtype.
Baclofen when introduced directly into the intrathecal space permits effective CSF concentrations to be achieved with resultant plasma concentrations 100 times less than those occurring with oral administration. In people, as well as in animals, baclofen has been shown to have general CNS depressant properties as indicated by the production of sedation with tolerance, somnolence, ataxia, and respiratory and cardiovascular depression.
5 Warnings and Precautions
- Do not directly inject baclofen injection into the pump catheter access port, as this may cause a life-threatening overdose (5.1)
- Potential for contamination due to non-sterile external surface of prefilled syringe (5.2)
- Potentially life-threatening CNS depression, cardiovascular collapse, and/or respiratory failure; Resuscitative equipment and trained staff must be available during screening, dose titration, and refills (5.3)
- Overdose may cause drowsiness, lightheadedness, dizziness, somnolence, respiratory depression, seizures, rostral progression of hypotonia and loss of consciousness progressing to coma (5.4)
- Possible exacerbation of psychotic disorders, schizophrenia or confusional states (5.6)
2 Dosage and Administration
- Baclofen injection is intended for use by the intrathecal route in single bolus test doses (via spinal catheter or lumbar puncture) and, for chronic use in the Medtronic SynchroMed® II Programmable Pump or other pumps labeled for intrathecal administration of baclofen injection; Refer to the pump manufacturer's manual and follow the specific instructions and precautions for programming the pump and/or refilling the reservoir (2.1)
- Screening: Patients who do not respond to a 100 mcg intrathecal bolus should not be considered for an implanted pump for chronic infusion (2.2)
- Dose Titration: Spasticity may be necessary to sustain upright posture and balance in locomotion or may be useful to obtain optimal function and care (2.5)
- Maintenance Therapy: Titrate patients individually; Lowest dose with an optimal response should be used, generally 300 mcg/day to 800 mcg/day for spasticity of spinal cord origin and 90 mcg/day to 700 mcg/day for spasticity of cerebral origin; Titrate baclofen injection to maintain some degree of muscle tone and allow occasional spasms. (2.6)
3 Dosage Forms and Strengths
Baclofen injection, USP is a sterile, nonpyrogenic, isotonic solution free of antioxidants, preservatives or other potentially neurotoxic additives indicated only for intrathecal administration. The drug is stable in solution at 37°C and compatible with CSF. Each milliliter of baclofen injection contains baclofen USP 1,000 mcg and sodium chloride 9 mg in Water for Injection; pH range is 5.5 to 7.5. Each vial is intended for single use only. Discard any unused portion. Do not autoclave.
8 Use in Specific Populations
2.4 Administration Information
Parenteral drug products should be inspected for particulate matter and discoloration prior to administration, whenever solution and container permit.
The external surface of baclofen injection prefilled syringes (all strengths, including the 50 mcg per mL strength) are non-sterile. The use of baclofen injection prefilled syringe in an aseptic setting (i.e., operating room) to fill sterile intrathecal pumps prior to implantation in patients is not recommended. For outpatient use, modify aseptic procedures to avoid contamination of sterile surfaces through contact with the non-sterile exterior of the baclofen injection prefilled syringe when filling the pump reservoir [see Warnings and Precautions (5.2)].
5.11 Intrathecal Mass Formation
Cases of intrathecal mass at the tip of the implanted catheter have been reported, most of them involving pharmacy compounded analgesic admixtures. The most frequent symptoms associated with intrathecal mass are: 1) decreased therapeutic response (worsening spasticity, return of spasticity when previously well controlled, withdrawal symptoms, poor response to escalating doses, or frequent or large dosage increases), 2) pain, 3) neurological deficit/dysfunction. Clinicians should monitor patients on intraspinal therapy carefully for any new neurological signs or symptoms. In patients with new neurological signs or symptoms suggestive of an intrathecal mass, consider a neurosurgical consultation, since many of the symptoms of inflammatory mass are not unlike the symptoms experienced by patients with severe spasticity from their disease. In some cases, performance of an imaging procedure may be appropriate to confirm or rule-out the diagnosis of an intrathecal mass.
16 How Supplied/storage and Handling
Baclofen injection, USP* is a clear, colorless, isotonic solution consisting of the active ingredient, Baclofen USP, and the excipients Sodium Chloride USP and Water for Injection USP and is supplied in single-dose clear glass vials as follows:
| NDC | Baclofen Injection, USP* (1,000 mcg per mL) | Package Factor |
| 25021-680-20 | 20,000 mcg per 20 mL Single-Dose Vial | 1 vial per carton |
Sterile, Nonpyrogenic, Preservative-free.
The container closure is not made with natural rubber latex.
Warning: Do Not Discontinue Abruptly
Abrupt discontinuation of intrathecal baclofen, regardless of the cause, has resulted in sequelae that include high fever, altered mental status, exaggerated rebound spasticity, and muscle rigidity, that in rare cases has advanced to rhabdomyolysis, multiple organ-system failure and death.
Prevention of abrupt discontinuation of intrathecal baclofen requires careful attention to programming and monitoring of the infusion system, refill scheduling and procedures, and pump alarms. Patients and caregivers should be advised of the importance of keeping scheduled refill visits and should be educated on the early symptoms of baclofen withdrawal. Special attention should be given to patients at apparent risk (e.g., spinal cord injuries at T-6 or above, communication difficulties, history of withdrawal symptoms from oral or intrathecal baclofen). Consult the technical manual of the implantable infusion system for additional post-implant clinician and patient information [see Warnings and Precautions (5.4)] .
2.1 Use Only in Medtronic Synchromed®
Baclofen injection is approved only for use with the Medtronic SynchroMed® II Programmable Pump or other pumps labeled for intrathecal administration of baclofen injection. Refer to the manufacturer's manual for specific instructions and precautions for programming the pump and/or refilling the reservoir. It is important to select the appropriate refill kit for the pump used to administer baclofen injection. Baclofen injection is not to be compounded with other medications.
5.1 Risk of Life Threatening Overdose During Pump Refills
Use extreme caution when filling the Medtronic SynchroMed® II Programmable Pump which is equipped with an injection port that allows direct access to the intrathecal catheter. Direct injection into the catheter through the catheter access port may cause a life-threatening overdose.
Reservoir refilling must be performed by fully trained and qualified personnel following the directions provided by the pump manufacturer. Carefully calculate refill intervals to prevent depletion of the reservoir, as this would result in the return of severe spasticity and possibly symptoms of withdrawal.
Strict aseptic technique in filling is required to avoid bacterial contamination and serious infection. A period of observation appropriate to the clinical situation should follow each refill or manipulation of the drug reservoir.
5.8 Use With Caution in Patients With A History of Autonomic Dysreflexia
Baclofen injection should be used with caution in patients with a history of autonomic dysreflexia. The presence of nociceptive stimuli or abrupt withdrawal of baclofen injection may cause an autonomic dysreflexic episode.
5.6 Possible Exacerbation of Psychotic Disorders, Schizophrenia, Or Confusional States
Patients suffering from psychotic disorders, schizophrenia, or confusional states should be treated cautiously with baclofen injection and kept under careful surveillance, because exacerbations of these conditions have been observed with oral administration.
5.2 Potential for Contamination Due to Non Sterile External Surface of Prefilled Syringe
Although the drug solution and pathway in the baclofen injection prefilled syringes are sterile, the external surface of the prefilled syringes (all strengths, including the 50 mcg/mL strength) are non-sterile. This has the potential to lead to contamination and consequent adverse reactions. The use of baclofen injection prefilled syringe in an aseptic setting (e.g., operating room) to fill sterile intrathecal pumps prior to implantation in patients is not recommended, unless the external surface of the prefilled syringe is treated to ensure sterility. Baclofen injection supplied in vials may be used with conventional aseptic technique to fill intrathecal pumps prior to implantation. Procedures should also be put in place while refilling implantable intrathecal pumps in an outpatient setting to avoid contamination of sterile surfaces through contact with the non-sterile exterior of the baclofen injection prefilled syringe.
5.3 Prescriber, Caregiver and Patient Training and Screening Procedure/post Implantation Environment
Baclofen injection is for use in single bolus intrathecal injections (via a catheter placed in the lumbar intrathecal space or injection by lumbar puncture) and in the implantable Medtronic SynchroMed® II Programmable Pump or other pumps labeled for intrathecal administration of baclofen injection. Because of the possibility of potentially life-threatening CNS depression, cardiovascular collapse, and/or respiratory failure, physicians must be adequately trained and educated in chronic intrathecal infusion therapy.
The pump system should not be implanted until the patient's response to bolus baclofen injection is adequately evaluated. Evaluation (consisting of a screening procedure) requires that baclofen injection be administered into the intrathecal space via a catheter or lumbar puncture [see Dosage and Administration (2.2)]. Because of the risks associated with the screening procedure and the adjustment of dosage following pump implantation, these phases must be conducted in a medically supervised and adequately equipped environment following the instructions outlined in the Dosage and Administration section [see Dosage and Administration (2.2 and 2.5)].
Resuscitative equipment should be available.
Following surgical implantation of the pump, particularly during the initial phases of pump use, the patient should be monitored closely until it is certain that the patient's response to the infusion is acceptable and reasonably stable.
On each occasion that the dosing rate of the pump and/or the concentration of baclofen injection in the reservoir is adjusted, close medical monitoring is required until it is certain that the patient's response to the infusion is acceptable and reasonably stable.
It is mandatory that the patient, all patient caregivers, and the physicians responsible for the patient receive adequate information regarding the risks of this mode of treatment. All medical personnel and caregivers should be instructed in 1) the signs and symptoms of overdose, 2) procedures to be followed in the event of overdose and 3) proper home care of the pump and insertion site.
Structured Label Content
Section 42229-5 (42229-5)
Pediatric Patients
The starting screening dose for pediatric patients is the same as in adult patients, i.e., 50 mcg. However, for very small patients, a screening dose of 25 mcg may be tried first.
Patients who do not respond to a 100 mcg intrathecal bolus should not be considered candidates for an implanted pump for chronic infusion.
Section 44425-7 (44425-7)
Storage Conditions
Does not require refrigeration.
Store at 20° to 25°C (68° to 77°F); excursions permitted between 15° to 30°C (59° to 86°F). [See USP Controlled Room Temperature.]
Do not freeze.
Do not heat sterilize.
*The USP osmolality specification is pending
Section 51945-4 (51945-4)
PACKAGE LABEL – PRINCIPAL DISPLAY PANEL – Vial Label
NDC 25021-680-20
Rx only
Baclofen Injection, USP
20,000 mcg per 20 mL
(1,000 mcg per mL)
For Intrathecal Use Only
20 mL Single-Dose Vial
Discard unused portion
5.4 Overdose
Signs of overdose may appear suddenly or insidiously. Acute massive overdose may present as coma. Less sudden and/or less severe forms of overdose may present with signs of drowsiness, lightheadedness, dizziness, somnolence, respiratory depression, seizures, rostral progression of hypotonia and loss of consciousness progressing to coma. Should overdose appear likely, the patient should be taken immediately to a hospital for assessment and emptying of the pump reservoir. In cases reported to date, overdose has generally been related to pump malfunction or dosing error [see Overdosage (10)].
Extreme caution must be used when filling the implantable pump.
Medtronic SynchroMed® II Programmable Pump should only be refilled through the reservoir refill septum. The Medtronic SynchroMed® II Programmable Pump is also equipped with a catheter access port that allows direct access to the intrathecal catheter. Direct injection into this catheter access port may cause a life-threatening overdose.
10 Overdosage (10 OVERDOSAGE)
Special attention must be given to recognizing the signs and symptoms of overdosage, especially during the initial screening and dose-titration phase of treatment, but also during re-introduction of baclofen injection after a period of interruption in therapy.
11 Description (11 DESCRIPTION)
Baclofen injection, USP* is a muscle relaxant and antispastic. Baclofen's pharmacological class is a gamma-aminobutyric acid (GABA) ergic agonist. Baclofen's chemical name is 4-amino- 3-(4- chlorophenyl) butanoic acid, and its structural formula is:
Baclofen
Baclofen is a white to off-white, odorless or practically odorless crystalline powder, with a molecular weight of 213.66. It is slightly soluble in water, very slightly soluble in methanol, and insoluble in chloroform.
5.5 Withdrawal
Abrupt withdrawal of intrathecal baclofen, regardless of the cause, has resulted in sequelae that included high fever, altered mental status, exaggerated rebound spasticity and muscle rigidity that in rare cases progressed to rhabdomyolysis, multiple organ-system failure, and death. In the first 9 years of post-marketing experience, 27 cases of withdrawal temporally related to the cessation of baclofen therapy were reported; six patients died. In most cases, symptoms of withdrawal appeared within hours to a few days following interruption of baclofen therapy. Common reasons for abrupt interruption of intrathecal baclofen therapy included malfunction of the catheter (especially disconnection), low volume in the pump reservoir, and end of pump battery life; human error may have played a causal or contributing role in some cases. Cases of intrathecal mass at the tip of the implanted catheter leading to withdrawal symptoms have also been reported, most of them involving pharmacy compounded analgesic admixtures [see Warnings and Precautions (5.10)].
Prevention of abrupt discontinuation of intrathecal baclofen requires careful attention to programming and monitoring of the infusion system, refill scheduling and procedures, and pump alarms. Patients and caregivers should be advised of the importance of keeping scheduled refill visits and should be educated on the early symptoms of baclofen withdrawal.
All patients receiving intrathecal baclofen therapy are potentially at risk for withdrawal. Early symptoms of baclofen withdrawal may include return of baseline spasticity, pruritus, hypotension, and paresthesias. Some clinical characteristics of the advanced intrathecal baclofen withdrawal syndrome may resemble autonomic dysreflexia, infection (sepsis), malignant hyperthermia, neuroleptic-malignant syndrome, or other conditions associated with a hypermetabolic state or widespread rhabdomyolysis.
Rapid, accurate diagnosis and treatment in an emergency-room or intensive-care setting are important in order to prevent the potentially life-threatening central nervous system and systemic effects of intrathecal baclofen withdrawal. The suggested treatment for intrathecal baclofen withdrawal is the restoration of intrathecal baclofen at or near the same dosage as before therapy was interrupted. However, if restoration of intrathecal delivery is delayed, treatment with GABA-ergic agonist drugs such as oral or enteral baclofen, or oral, enteral, or intravenous benzodiazepines may prevent potentially fatal sequelae. Oral or enteral baclofen alone should not be relied upon to halt the progression of intrathecal baclofen withdrawal.
Seizures have been reported during overdose and with withdrawal from intrathecal baclofen as well as in patients maintained on therapeutic doses of intrathecal baclofen.
5.9 Infections
Patients should be infection-free prior to the screening trial with baclofen injection because the presence of a systemic infection may interfere with an assessment of the patient's response to bolus baclofen injection. Patients should be infection-free prior to implantation of the pump because the presence of infection may increase the risk of surgical complications. Moreover, a systemic infection may complicate dosing.
5.10 Drowsiness
Drowsiness has been reported in patients on intrathecal baclofen. Patients should be cautioned regarding the operation of automobiles or other dangerous machinery, and activities made hazardous by decreased alertness. Patients should also be cautioned that the central nervous system depressant effects of intrathecal baclofen may be additive to those of alcohol and other CNS depressants.
8.4 Pediatric Use
Children should be of sufficient body mass to accommodate the implantable pump for chronic infusion. Please consult pump manufacturer's manual for specific recommendations.
Safety and effectiveness in pediatric patients below the age of 4 have not been established.
5.12 Ovarian Cysts
A dose-related increase in incidence of ovarian cysts was observed in female rats treated chronically with oral baclofen. Ovarian cysts have been found by palpation in about 4% of the multiple sclerosis patients who were treated with oral baclofen for up to one year. In most cases these cysts disappeared spontaneously while patients continued to receive the drug. Ovarian cysts are estimated to occur spontaneously in approximately 1% to 5% of the normal female population.
2.2 Screening Phase
Prior to pump implantation and initiation of chronic infusion of baclofen injection, patients must demonstrate a positive clinical response to a baclofen injection bolus dose administered intrathecally in a screening trial. The screening trial employs baclofen injection at a concentration of 50 mcg per mL. A 1 mL syringe (50 mcg per mL) is available for use in the screening trial. The screening procedure is as follows. An initial bolus containing 50 micrograms in a volume of 1 milliliter is administered into the intrathecal space by barbotage over a period of not less than one minute. The patient is observed over the ensuing 4 to 8 hours. A positive response consists of a significant decrease in muscle tone and/or frequency and/or severity of spasms. If the initial response is less than desired, a second bolus injection may be administered 24 hours after the first. The second screening bolus dose consists of 75 micrograms in 1.5 milliliters. Again, the patient should be observed for an interval of 4 to 8 hours. If the response is still inadequate, a final bolus screening dose of 100 micrograms in 2 milliliters may be administered 24 hours later.
4 Contraindications (4 CONTRAINDICATIONS)
Baclofen injection is contraindicated in patients with a hypersensitivity to baclofen. Do not use baclofen injection for intravenous, intramuscular, subcutaneous or epidural administration.
6 Adverse Reactions (6 ADVERSE REACTIONS)
- The most common adverse reactions in patients with spasticity of spinal origin were somnolence, dizziness, nausea, hypotension, headache, convulsions and hypotonia (6.1)
- The most common adverse reactions in patients with spasticity of cerebral origin were agitation, constipation, somnolence, leukocytosis, chills, urinary retention and hypotonia (6.2)
To report SUSPECTED ADVERSE REACTIONS, contact Sagent Pharmaceuticals, Inc. at 1-866-625-1618 or FDA at 1-800-FDA-1088 or
www.fda.gov/medwatch
.
7 Drug Interactions (7 DRUG INTERACTIONS)
There is inadequate systematic experience with the use of intrathecal baclofen in combination with other medications to predict specific drug-drug interactions. Interactions attributed to the combined use of baclofen injection and epidural morphine include hypotension and dyspnea.
12.3 Pharmacokinetics
The pharmacokinetics of cerebrospinal fluid (CSF) clearance of intrathecal baclofen calculated from intrathecal bolus or continuous infusion studies approximates CSF turnover, suggesting elimination is by bulk-flow removal of CSF.
1 Indications and Usage (1 INDICATIONS AND USAGE)
Baclofen injection is indicated for use in the management of severe spasticity in adult and pediatric patients age 4 years and above. Patients should first respond to a screening dose of intrathecal baclofen prior to consideration for long term infusion via an implantable pump. For spasticity of spinal cord origin, chronic infusion of baclofen injection via an implantable pump should be reserved for patients unresponsive to oral baclofen therapy, or those who experience intolerable CNS side effects at effective doses. Patients with spasticity due to traumatic brain injury should wait at least one year after the injury before consideration of long term intrathecal baclofen therapy. Baclofen injection is intended for use by the intrathecal route in single bolus test doses (via spinal catheter or lumbar puncture) and, for chronic use, only with the Medtronic SynchroMed® II Programmable Pump or other pumps labeled for intrathecal administration of baclofen injection [see Clinical Studies (14)].
Prior to implantation of a device for chronic intrathecal infusion of baclofen injection, patients must show a response to baclofen injection in a screening trial [see Dosage and Administration (2.2)].
12.1 Mechanism of Action
The precise mechanism of action of baclofen as a muscle relaxant and antispasticity agent is not fully understood. Baclofen inhibits both monosynaptic and polysynaptic reflexes at the spinal level, possibly by decreasing excitatory neurotransmitter release from primary afferent terminals, although actions at supraspinal sites may also occur and contribute to its clinical effect. Baclofen is a structural analog of the inhibitory neurotransmitter gamma-aminobutyric acid (GABA), and may exert its effects by stimulation of the GABAB receptor subtype.
Baclofen when introduced directly into the intrathecal space permits effective CSF concentrations to be achieved with resultant plasma concentrations 100 times less than those occurring with oral administration. In people, as well as in animals, baclofen has been shown to have general CNS depressant properties as indicated by the production of sedation with tolerance, somnolence, ataxia, and respiratory and cardiovascular depression.
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
- Do not directly inject baclofen injection into the pump catheter access port, as this may cause a life-threatening overdose (5.1)
- Potential for contamination due to non-sterile external surface of prefilled syringe (5.2)
- Potentially life-threatening CNS depression, cardiovascular collapse, and/or respiratory failure; Resuscitative equipment and trained staff must be available during screening, dose titration, and refills (5.3)
- Overdose may cause drowsiness, lightheadedness, dizziness, somnolence, respiratory depression, seizures, rostral progression of hypotonia and loss of consciousness progressing to coma (5.4)
- Possible exacerbation of psychotic disorders, schizophrenia or confusional states (5.6)
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
- Baclofen injection is intended for use by the intrathecal route in single bolus test doses (via spinal catheter or lumbar puncture) and, for chronic use in the Medtronic SynchroMed® II Programmable Pump or other pumps labeled for intrathecal administration of baclofen injection; Refer to the pump manufacturer's manual and follow the specific instructions and precautions for programming the pump and/or refilling the reservoir (2.1)
- Screening: Patients who do not respond to a 100 mcg intrathecal bolus should not be considered for an implanted pump for chronic infusion (2.2)
- Dose Titration: Spasticity may be necessary to sustain upright posture and balance in locomotion or may be useful to obtain optimal function and care (2.5)
- Maintenance Therapy: Titrate patients individually; Lowest dose with an optimal response should be used, generally 300 mcg/day to 800 mcg/day for spasticity of spinal cord origin and 90 mcg/day to 700 mcg/day for spasticity of cerebral origin; Titrate baclofen injection to maintain some degree of muscle tone and allow occasional spasms. (2.6)
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
Baclofen injection, USP is a sterile, nonpyrogenic, isotonic solution free of antioxidants, preservatives or other potentially neurotoxic additives indicated only for intrathecal administration. The drug is stable in solution at 37°C and compatible with CSF. Each milliliter of baclofen injection contains baclofen USP 1,000 mcg and sodium chloride 9 mg in Water for Injection; pH range is 5.5 to 7.5. Each vial is intended for single use only. Discard any unused portion. Do not autoclave.
8 Use in Specific Populations (8 USE IN SPECIFIC POPULATIONS)
2.4 Administration Information
Parenteral drug products should be inspected for particulate matter and discoloration prior to administration, whenever solution and container permit.
The external surface of baclofen injection prefilled syringes (all strengths, including the 50 mcg per mL strength) are non-sterile. The use of baclofen injection prefilled syringe in an aseptic setting (i.e., operating room) to fill sterile intrathecal pumps prior to implantation in patients is not recommended. For outpatient use, modify aseptic procedures to avoid contamination of sterile surfaces through contact with the non-sterile exterior of the baclofen injection prefilled syringe when filling the pump reservoir [see Warnings and Precautions (5.2)].
5.11 Intrathecal Mass Formation
Cases of intrathecal mass at the tip of the implanted catheter have been reported, most of them involving pharmacy compounded analgesic admixtures. The most frequent symptoms associated with intrathecal mass are: 1) decreased therapeutic response (worsening spasticity, return of spasticity when previously well controlled, withdrawal symptoms, poor response to escalating doses, or frequent or large dosage increases), 2) pain, 3) neurological deficit/dysfunction. Clinicians should monitor patients on intraspinal therapy carefully for any new neurological signs or symptoms. In patients with new neurological signs or symptoms suggestive of an intrathecal mass, consider a neurosurgical consultation, since many of the symptoms of inflammatory mass are not unlike the symptoms experienced by patients with severe spasticity from their disease. In some cases, performance of an imaging procedure may be appropriate to confirm or rule-out the diagnosis of an intrathecal mass.
16 How Supplied/storage and Handling (16 HOW SUPPLIED/STORAGE AND HANDLING)
Baclofen injection, USP* is a clear, colorless, isotonic solution consisting of the active ingredient, Baclofen USP, and the excipients Sodium Chloride USP and Water for Injection USP and is supplied in single-dose clear glass vials as follows:
| NDC | Baclofen Injection, USP* (1,000 mcg per mL) | Package Factor |
| 25021-680-20 | 20,000 mcg per 20 mL Single-Dose Vial | 1 vial per carton |
Sterile, Nonpyrogenic, Preservative-free.
The container closure is not made with natural rubber latex.
Warning: Do Not Discontinue Abruptly (WARNING: DO NOT DISCONTINUE ABRUPTLY)
Abrupt discontinuation of intrathecal baclofen, regardless of the cause, has resulted in sequelae that include high fever, altered mental status, exaggerated rebound spasticity, and muscle rigidity, that in rare cases has advanced to rhabdomyolysis, multiple organ-system failure and death.
Prevention of abrupt discontinuation of intrathecal baclofen requires careful attention to programming and monitoring of the infusion system, refill scheduling and procedures, and pump alarms. Patients and caregivers should be advised of the importance of keeping scheduled refill visits and should be educated on the early symptoms of baclofen withdrawal. Special attention should be given to patients at apparent risk (e.g., spinal cord injuries at T-6 or above, communication difficulties, history of withdrawal symptoms from oral or intrathecal baclofen). Consult the technical manual of the implantable infusion system for additional post-implant clinician and patient information [see Warnings and Precautions (5.4)] .
2.1 Use Only in Medtronic Synchromed® (2.1 Use Only in Medtronic SynchroMed®)
Baclofen injection is approved only for use with the Medtronic SynchroMed® II Programmable Pump or other pumps labeled for intrathecal administration of baclofen injection. Refer to the manufacturer's manual for specific instructions and precautions for programming the pump and/or refilling the reservoir. It is important to select the appropriate refill kit for the pump used to administer baclofen injection. Baclofen injection is not to be compounded with other medications.
5.1 Risk of Life Threatening Overdose During Pump Refills (5.1 Risk of Life-Threatening Overdose During Pump Refills)
Use extreme caution when filling the Medtronic SynchroMed® II Programmable Pump which is equipped with an injection port that allows direct access to the intrathecal catheter. Direct injection into the catheter through the catheter access port may cause a life-threatening overdose.
Reservoir refilling must be performed by fully trained and qualified personnel following the directions provided by the pump manufacturer. Carefully calculate refill intervals to prevent depletion of the reservoir, as this would result in the return of severe spasticity and possibly symptoms of withdrawal.
Strict aseptic technique in filling is required to avoid bacterial contamination and serious infection. A period of observation appropriate to the clinical situation should follow each refill or manipulation of the drug reservoir.
5.8 Use With Caution in Patients With A History of Autonomic Dysreflexia (5.8 Use with Caution in Patients with a History of Autonomic Dysreflexia)
Baclofen injection should be used with caution in patients with a history of autonomic dysreflexia. The presence of nociceptive stimuli or abrupt withdrawal of baclofen injection may cause an autonomic dysreflexic episode.
5.6 Possible Exacerbation of Psychotic Disorders, Schizophrenia, Or Confusional States (5.6 Possible Exacerbation of Psychotic Disorders, Schizophrenia, or Confusional States)
Patients suffering from psychotic disorders, schizophrenia, or confusional states should be treated cautiously with baclofen injection and kept under careful surveillance, because exacerbations of these conditions have been observed with oral administration.
5.2 Potential for Contamination Due to Non Sterile External Surface of Prefilled Syringe (5.2 Potential for Contamination due to Non-sterile External Surface of Prefilled Syringe)
Although the drug solution and pathway in the baclofen injection prefilled syringes are sterile, the external surface of the prefilled syringes (all strengths, including the 50 mcg/mL strength) are non-sterile. This has the potential to lead to contamination and consequent adverse reactions. The use of baclofen injection prefilled syringe in an aseptic setting (e.g., operating room) to fill sterile intrathecal pumps prior to implantation in patients is not recommended, unless the external surface of the prefilled syringe is treated to ensure sterility. Baclofen injection supplied in vials may be used with conventional aseptic technique to fill intrathecal pumps prior to implantation. Procedures should also be put in place while refilling implantable intrathecal pumps in an outpatient setting to avoid contamination of sterile surfaces through contact with the non-sterile exterior of the baclofen injection prefilled syringe.
5.3 Prescriber, Caregiver and Patient Training and Screening Procedure/post Implantation Environment (5.3 Prescriber, Caregiver and Patient Training and Screening Procedure/Post-Implantation Environment)
Baclofen injection is for use in single bolus intrathecal injections (via a catheter placed in the lumbar intrathecal space or injection by lumbar puncture) and in the implantable Medtronic SynchroMed® II Programmable Pump or other pumps labeled for intrathecal administration of baclofen injection. Because of the possibility of potentially life-threatening CNS depression, cardiovascular collapse, and/or respiratory failure, physicians must be adequately trained and educated in chronic intrathecal infusion therapy.
The pump system should not be implanted until the patient's response to bolus baclofen injection is adequately evaluated. Evaluation (consisting of a screening procedure) requires that baclofen injection be administered into the intrathecal space via a catheter or lumbar puncture [see Dosage and Administration (2.2)]. Because of the risks associated with the screening procedure and the adjustment of dosage following pump implantation, these phases must be conducted in a medically supervised and adequately equipped environment following the instructions outlined in the Dosage and Administration section [see Dosage and Administration (2.2 and 2.5)].
Resuscitative equipment should be available.
Following surgical implantation of the pump, particularly during the initial phases of pump use, the patient should be monitored closely until it is certain that the patient's response to the infusion is acceptable and reasonably stable.
On each occasion that the dosing rate of the pump and/or the concentration of baclofen injection in the reservoir is adjusted, close medical monitoring is required until it is certain that the patient's response to the infusion is acceptable and reasonably stable.
It is mandatory that the patient, all patient caregivers, and the physicians responsible for the patient receive adequate information regarding the risks of this mode of treatment. All medical personnel and caregivers should be instructed in 1) the signs and symptoms of overdose, 2) procedures to be followed in the event of overdose and 3) proper home care of the pump and insertion site.
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:36:13.320533 · Updated: 2026-03-14T22:26:24.564180