Metronidazole Cream
cdf2e251-4bbc-4434-9b00-bef6284491e4
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
FOR TOPICAL USE ONLY NOT FOR OPHTHALMIC USE
Indications and Usage
METRONIDAZOLE CREAM is indicated for the topical treatment of inflammatory lesions and erythema of rosacea.
Dosage and Administration
Areas to be treated should be cleansed before application of METRONIDAZOLE CREAM . Apply and rub in a thin film of METRONIDAZOLE CREAM once daily to entire affected area(s). Patients may use cosmetics after application of METRONIDAZOLE CREAM .
Contraindications
METRONIDAZOLE CREAM is contraindicated in those patients with a history of hypersensitivity to metronidazole or to any other ingredient in this formulation.
Adverse Reactions
Safety data from 302 patients who used METRONIDAZOLE CREAM (n=200) or vehicle control (n=102) once daily in clinical trials and experienced an adverse event considered to be treatment related include: application site reaction ( METRONIDAZOLE CREAM 1, vehicle 1), condition aggravated ( METRONIDAZOLE CREAM 1, vehicle 0), paresthesia ( METRONIDAZOLE CREAM 0, vehicle 1), acne ( METRONIDAZOLE CREAM 1, vehicle 0), dry skin ( METRONIDAZOLE CREAM 0, vehicle 2). The majority of adverse reactions were mild to moderate in severity. Two patients treated with METRONIDAZOLE CREAM once daily discontinued treatment because of adverse events: one for a severe flare of comedonal acne and one for rosacea aggravated. Additional clinical adverse effects reported spontaneously since the drug was marketed are uncommon and include tingling or numbness of extremities, allergic reactions, skin and eye irritation, rash, headache, nausea and dry mouth. To report SUSPECTED ADVERSE REACTIONS, contact Oceanside Pharmaceuticals at 1-800-321-4576 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch .
Drug Interactions
Oral metronidazole has been reported to potentiate the anticoagulant effect of coumarin and warfarin resulting in a prolongation of prothrombin time. Drug interactions should be kept in mind when METRONIDAZOLE CREAM is prescribed for patients who are receiving anticoagulant treatment, although they are less likely to occur with topical metronidazole administration because of low absorption. (See CLINICAL PHARMACOLOGY , Pharmacokinetics . )
How Supplied
Cream - 60 g aluminum tube - NDC 68682-202-60. Keep out of reach of children.
Medication Information
Indications and Usage
METRONIDAZOLE CREAM is indicated for the topical treatment of inflammatory lesions and erythema of rosacea.
Dosage and Administration
Areas to be treated should be cleansed before application of METRONIDAZOLE CREAM. Apply and rub in a thin film of METRONIDAZOLE CREAM once daily to entire affected area(s). Patients may use cosmetics after application of METRONIDAZOLE CREAM.
Contraindications
METRONIDAZOLE CREAM is contraindicated in those patients with a history of hypersensitivity to metronidazole or to any other ingredient in this formulation.
Adverse Reactions
Safety data from 302 patients who used METRONIDAZOLE CREAM (n=200) or vehicle control (n=102) once daily in clinical trials and experienced an adverse event considered to be treatment related include: application site reaction (METRONIDAZOLE CREAM 1, vehicle 1), condition aggravated (METRONIDAZOLE CREAM 1, vehicle 0), paresthesia (METRONIDAZOLE CREAM 0, vehicle 1), acne (METRONIDAZOLE CREAM 1, vehicle 0), dry skin (METRONIDAZOLE CREAM 0, vehicle 2). The majority of adverse reactions were mild to moderate in severity.
Two patients treated with METRONIDAZOLE CREAM once daily discontinued treatment because of adverse events: one for a severe flare of comedonal acne and one for rosacea aggravated.
Additional clinical adverse effects reported spontaneously since the drug was marketed are uncommon and include tingling or numbness of extremities, allergic reactions, skin and eye irritation, rash, headache, nausea and dry mouth.
To report SUSPECTED ADVERSE REACTIONS, contact Oceanside Pharmaceuticals at 1-800-321-4576 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
Drug Interactions
Oral metronidazole has been reported to potentiate the anticoagulant effect of coumarin and warfarin resulting in a prolongation of prothrombin time. Drug interactions should be kept in mind when METRONIDAZOLE CREAM is prescribed for patients who are receiving anticoagulant treatment, although they are less likely to occur with topical metronidazole administration because of low absorption. (See CLINICAL PHARMACOLOGY , Pharmacokinetics . )
How Supplied
Cream - 60 g aluminum tube - NDC 68682-202-60.
Keep out of reach of children.
Description
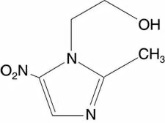
METRONIDAZOLE CREAM, 1%, contains metronidazole USP. Chemically, metronidazole is 2-methyl-5-nitro-1H-imidazole-1-ethanol. The molecular formula for metronidazole is C6H9N3O3. It has the following structural formula:
Metronidazole has a molecular weight of 171.16. It is a white to pale yellow crystalline powder. It is slightly soluble in alcohol and has a solubility in water of 10 mg/mL at 20°C. Metronidazole is a member of the imidazole class of antibacterial agents and is classified as an antiprotozoal and antibacterial agent.
METRONIDAZOLE CREAM is an emollient cream; each gram contains 10 mg micronized metronidazole USP, in a base of glycerin USP, glyceryl monostearate NF, methylparaben NF, propylparaben NF, purified water USP, stearic acid NF and trolamine NF.
Section 42229-5
FOR TOPICAL USE ONLY
NOT FOR OPHTHALMIC USE
General:
If a reaction suggesting local skin irritation occurs, patients should be directed to discontinue use of the medication. Conjunctivitis associated with topical use of metronidazole on the face has been reported. Contact with the eyes should be avoided. Metronidazole is a nitroimidazole and should be used with care in patients with evidence of, or history of, blood dyscrasia.
Storage:
Store at controlled room temperature 20° to 25°C (68° to 77°F).
Pediatric Use:
Safety and effectiveness in pediatric patients have not been established.
Safety Studies:
Studies of contact sensitization (n=258), phototoxicity (n=21), and photocontact sensitization (n=29) of METRONIDAZOLE CREAM were conducted. No evidence of sensitization or phototoxicity was seen in these studies.
Nursing Mothers:
After oral administration, metronidazole is secreted in breast milk in concentrations similar to those found in the plasma. Even though blood levels taken after topical metronidazole application are significantly lower than those achieved after oral metronidazole, a decision should be made whether to discontinue nursing or to discontinue the drug, taking into account the importance of the drug to the mother and the risk to the infant.
Clinical Studies:
Safety and efficacy of METRONIDAZOLE CREAM were evaluated in two randomized vehicle-controlled clinical studies for the treatment of rosacea, which excluded patients who had nodules, moderate or severe rhinophyma, dense telangiectases, plaque-like facial edema or ocular involvement and those who had a history of not responding to metronidazole therapy for rosacea. Of the patients included in the efficacy database (n=416), there were 142 men and 274 women. Endpoint efficacy data comparisons for patients treated with daily METRONIDAZOLE CREAM or vehicle applications are listed below.
| METRONIDAZOLE CREAM | Vehicle | |||||||
|---|---|---|---|---|---|---|---|---|
| Study 1 | Study 2 | Study 1 | Study 2 | |||||
| N | Result | N | Result | N | Result | N | Result | |
|
Papules + Pustules Count |
||||||||
|
Baseline |
89 |
15 |
92 |
19 |
50 |
18 |
49 |
17 |
|
Week 10 |
80 |
7* |
82 |
8 |
45 |
15 |
41 |
12 |
|
Reduction |
49%* |
58%* |
17% |
30% |
||||
|
Papules Count |
||||||||
|
Baseline |
89 |
13 |
92 |
17 |
50 |
15 |
49 |
15 |
|
Week 10 |
80 |
7* |
82 |
7 |
45 |
12 |
41 |
11 |
|
Reduction |
41%* |
55%* |
14% |
28% |
||||
|
Erythema Score |
||||||||
|
Baseline |
89 |
2.2 |
92 |
2.3 |
50 |
2.2 |
49 |
2.2 |
|
Week 10 |
80 |
1.3* |
82 |
1.4* |
45 |
1.7 |
40 |
1.8 |
|
Reduction |
42%* |
40%* |
25% |
19% |
*Statistically significant differences between METRONIDAZOLE CREAM and vehicle groups with p≤0.05. Erythema scores: 0=none, 1=mild, 2=moderate and 3=severe.
Pharmacodynamics:
The mechanisms by which metronidazole acts in reducing inflammatory lesions of rosacea are unknown.
Pharmacokinetics:
When a one gram dose of METRONIDAZOLE CREAM, 1%, was applied in a single application to the face of 16 healthy volunteers, low concentrations of metronidazole were detected in the plasma of 7 of the volunteers. The mean±SD Cmax of metronidazole was 27.6±7.3 ng/mL, which is about 1% of the value reported for a single 250 mg oral dose of metronidazole. The time to maximum plasma concentration (Tmax) in the volunteers with detectable metronidazole was 8-12 hours after topical application.
Drug Interactions:
Oral metronidazole has been reported to potentiate the anticoagulant effect of coumarin and warfarin resulting in a prolongation of prothrombin time. Drug interactions should be kept in mind when METRONIDAZOLE CREAM is prescribed for patients who are receiving anticoagulant treatment, although they are less likely to occur with topical metronidazole administration because of low absorption. (See CLINICAL PHARMACOLOGY , Pharmacokinetics.)
Teratogenic Effects:
There are no adequate and well-controlled studies with the use of METRONIDAZOLE CREAM in pregnant women. Metronidazole crosses the placental barrier and enters the fetal circulation rapidly. No fetotoxicity was observed after oral administration of metronidazole to rats or mice at 200 and 20 times, respectively, the expected clinical dose. However, oral metronidazole has shown carcinogenic activity in rodents. Because animal reproduction studies are not always predictive of human response, METRONIDAZOLE CREAM should be used during pregnancy only if clearly needed.
Information for Patients:
Patients using METRONIDAZOLE CREAM should receive the following information and instructions:
-
1.This medication is to be used as directed.
-
2.It is for external use only.
-
3.Avoid contact with the eyes.
-
4.Cleanse affected area(s) before applying METRONIDAZOLE CREAM.
-
5.This medication should not be used for any disorder other than that for which it is prescribed.
-
6.Patients should report any adverse reaction to their physician.
Principal Display Panel 60 G Tube
NDC 68682-202-60
Rx only
METRONIDAZOLE
CREAM
1%
Net Wt. 60 g
ONCE-A-DAY
FOR TOPICAL USE ONLY
OCEANSIDE
PHARMACEUTICALS
Carcinogenesis, Mutagenesis, Impairment of Fertility:
Metronidazole has shown evidence of carcinogenic activity in a number of studies involving chronic, oral administration in mice and rats but not in studies involving hamsters.
In several long-term studies in mice, oral doses of approximately 225 mg/m2/day or greater (approximately 37 times the human topical dose on a mg/m2 basis) were associated with an increase in pulmonary tumors and lymphomas. Several long-term oral studies in the rat have shown statistically significant increases in mammary and hepatic tumors at doses >885 mg/m2/day (144 times the topical human dose).
Metronidazole has shown evidence of mutagenic activity in several in vitro bacterial assay systems. In addition, a dose-related increase in the frequency of micronuclei was observed in mice after intraperitoneal injections. An increase in chromosomal aberrations in peripheral blood lymphocytes was reported in patients with Crohn’s disease who were treated with 200 to 1200 mg/day of metronidazole for 1 to 24 months. However, in another study, no increase in chromosomal aberrations in circulating lymphocytes was observed in patients with Crohn’s disease treated with the drug for 8 months.
In one published study, using albino hairless mice, intraperitoneal administration of metronidazole at a dose of 45 mg/m2/day (approximately 7 times the human topical dose on a mg/m2 basis) was associated with an increase in ultraviolet radiation-induced skin carcinogenesis. Neither dermal carcinogenicity nor photocarcinogenicity studies have been performed with METRONIDAZOLE CREAM or any marketed metronidazole formulations.
Structured Label Content
Section 42229-5 (42229-5)
FOR TOPICAL USE ONLY
NOT FOR OPHTHALMIC USE
General:
If a reaction suggesting local skin irritation occurs, patients should be directed to discontinue use of the medication. Conjunctivitis associated with topical use of metronidazole on the face has been reported. Contact with the eyes should be avoided. Metronidazole is a nitroimidazole and should be used with care in patients with evidence of, or history of, blood dyscrasia.
Storage:
Store at controlled room temperature 20° to 25°C (68° to 77°F).
Description (DESCRIPTION)
METRONIDAZOLE CREAM, 1%, contains metronidazole USP. Chemically, metronidazole is 2-methyl-5-nitro-1H-imidazole-1-ethanol. The molecular formula for metronidazole is C6H9N3O3. It has the following structural formula:
Metronidazole has a molecular weight of 171.16. It is a white to pale yellow crystalline powder. It is slightly soluble in alcohol and has a solubility in water of 10 mg/mL at 20°C. Metronidazole is a member of the imidazole class of antibacterial agents and is classified as an antiprotozoal and antibacterial agent.
METRONIDAZOLE CREAM is an emollient cream; each gram contains 10 mg micronized metronidazole USP, in a base of glycerin USP, glyceryl monostearate NF, methylparaben NF, propylparaben NF, purified water USP, stearic acid NF and trolamine NF.
How Supplied (HOW SUPPLIED)
Cream - 60 g aluminum tube - NDC 68682-202-60.
Keep out of reach of children.
Pediatric Use:
Safety and effectiveness in pediatric patients have not been established.
Safety Studies:
Studies of contact sensitization (n=258), phototoxicity (n=21), and photocontact sensitization (n=29) of METRONIDAZOLE CREAM were conducted. No evidence of sensitization or phototoxicity was seen in these studies.
Nursing Mothers:
After oral administration, metronidazole is secreted in breast milk in concentrations similar to those found in the plasma. Even though blood levels taken after topical metronidazole application are significantly lower than those achieved after oral metronidazole, a decision should be made whether to discontinue nursing or to discontinue the drug, taking into account the importance of the drug to the mother and the risk to the infant.
Adverse Reactions (ADVERSE REACTIONS)
Safety data from 302 patients who used METRONIDAZOLE CREAM (n=200) or vehicle control (n=102) once daily in clinical trials and experienced an adverse event considered to be treatment related include: application site reaction (METRONIDAZOLE CREAM 1, vehicle 1), condition aggravated (METRONIDAZOLE CREAM 1, vehicle 0), paresthesia (METRONIDAZOLE CREAM 0, vehicle 1), acne (METRONIDAZOLE CREAM 1, vehicle 0), dry skin (METRONIDAZOLE CREAM 0, vehicle 2). The majority of adverse reactions were mild to moderate in severity.
Two patients treated with METRONIDAZOLE CREAM once daily discontinued treatment because of adverse events: one for a severe flare of comedonal acne and one for rosacea aggravated.
Additional clinical adverse effects reported spontaneously since the drug was marketed are uncommon and include tingling or numbness of extremities, allergic reactions, skin and eye irritation, rash, headache, nausea and dry mouth.
To report SUSPECTED ADVERSE REACTIONS, contact Oceanside Pharmaceuticals at 1-800-321-4576 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
Contraindications (CONTRAINDICATIONS)
METRONIDAZOLE CREAM is contraindicated in those patients with a history of hypersensitivity to metronidazole or to any other ingredient in this formulation.
Clinical Studies:
Safety and efficacy of METRONIDAZOLE CREAM were evaluated in two randomized vehicle-controlled clinical studies for the treatment of rosacea, which excluded patients who had nodules, moderate or severe rhinophyma, dense telangiectases, plaque-like facial edema or ocular involvement and those who had a history of not responding to metronidazole therapy for rosacea. Of the patients included in the efficacy database (n=416), there were 142 men and 274 women. Endpoint efficacy data comparisons for patients treated with daily METRONIDAZOLE CREAM or vehicle applications are listed below.
| METRONIDAZOLE CREAM | Vehicle | |||||||
|---|---|---|---|---|---|---|---|---|
| Study 1 | Study 2 | Study 1 | Study 2 | |||||
| N | Result | N | Result | N | Result | N | Result | |
|
Papules + Pustules Count |
||||||||
|
Baseline |
89 |
15 |
92 |
19 |
50 |
18 |
49 |
17 |
|
Week 10 |
80 |
7* |
82 |
8 |
45 |
15 |
41 |
12 |
|
Reduction |
49%* |
58%* |
17% |
30% |
||||
|
Papules Count |
||||||||
|
Baseline |
89 |
13 |
92 |
17 |
50 |
15 |
49 |
15 |
|
Week 10 |
80 |
7* |
82 |
7 |
45 |
12 |
41 |
11 |
|
Reduction |
41%* |
55%* |
14% |
28% |
||||
|
Erythema Score |
||||||||
|
Baseline |
89 |
2.2 |
92 |
2.3 |
50 |
2.2 |
49 |
2.2 |
|
Week 10 |
80 |
1.3* |
82 |
1.4* |
45 |
1.7 |
40 |
1.8 |
|
Reduction |
42%* |
40%* |
25% |
19% |
*Statistically significant differences between METRONIDAZOLE CREAM and vehicle groups with p≤0.05. Erythema scores: 0=none, 1=mild, 2=moderate and 3=severe.
Pharmacodynamics:
The mechanisms by which metronidazole acts in reducing inflammatory lesions of rosacea are unknown.
Pharmacokinetics:
When a one gram dose of METRONIDAZOLE CREAM, 1%, was applied in a single application to the face of 16 healthy volunteers, low concentrations of metronidazole were detected in the plasma of 7 of the volunteers. The mean±SD Cmax of metronidazole was 27.6±7.3 ng/mL, which is about 1% of the value reported for a single 250 mg oral dose of metronidazole. The time to maximum plasma concentration (Tmax) in the volunteers with detectable metronidazole was 8-12 hours after topical application.
Drug Interactions:
Oral metronidazole has been reported to potentiate the anticoagulant effect of coumarin and warfarin resulting in a prolongation of prothrombin time. Drug interactions should be kept in mind when METRONIDAZOLE CREAM is prescribed for patients who are receiving anticoagulant treatment, although they are less likely to occur with topical metronidazole administration because of low absorption. (See CLINICAL PHARMACOLOGY , Pharmacokinetics.)
Teratogenic Effects:
There are no adequate and well-controlled studies with the use of METRONIDAZOLE CREAM in pregnant women. Metronidazole crosses the placental barrier and enters the fetal circulation rapidly. No fetotoxicity was observed after oral administration of metronidazole to rats or mice at 200 and 20 times, respectively, the expected clinical dose. However, oral metronidazole has shown carcinogenic activity in rodents. Because animal reproduction studies are not always predictive of human response, METRONIDAZOLE CREAM should be used during pregnancy only if clearly needed.
Indications and Usage (INDICATIONS AND USAGE)
METRONIDAZOLE CREAM is indicated for the topical treatment of inflammatory lesions and erythema of rosacea.
Dosage and Administration (DOSAGE AND ADMINISTRATION)
Areas to be treated should be cleansed before application of METRONIDAZOLE CREAM. Apply and rub in a thin film of METRONIDAZOLE CREAM once daily to entire affected area(s). Patients may use cosmetics after application of METRONIDAZOLE CREAM.
Information for Patients:
Patients using METRONIDAZOLE CREAM should receive the following information and instructions:
-
1.This medication is to be used as directed.
-
2.It is for external use only.
-
3.Avoid contact with the eyes.
-
4.Cleanse affected area(s) before applying METRONIDAZOLE CREAM.
-
5.This medication should not be used for any disorder other than that for which it is prescribed.
-
6.Patients should report any adverse reaction to their physician.
Principal Display Panel 60 G Tube (PRINCIPAL DISPLAY PANEL - 60 g Tube)
NDC 68682-202-60
Rx only
METRONIDAZOLE
CREAM
1%
Net Wt. 60 g
ONCE-A-DAY
FOR TOPICAL USE ONLY
OCEANSIDE
PHARMACEUTICALS
Carcinogenesis, Mutagenesis, Impairment of Fertility:
Metronidazole has shown evidence of carcinogenic activity in a number of studies involving chronic, oral administration in mice and rats but not in studies involving hamsters.
In several long-term studies in mice, oral doses of approximately 225 mg/m2/day or greater (approximately 37 times the human topical dose on a mg/m2 basis) were associated with an increase in pulmonary tumors and lymphomas. Several long-term oral studies in the rat have shown statistically significant increases in mammary and hepatic tumors at doses >885 mg/m2/day (144 times the topical human dose).
Metronidazole has shown evidence of mutagenic activity in several in vitro bacterial assay systems. In addition, a dose-related increase in the frequency of micronuclei was observed in mice after intraperitoneal injections. An increase in chromosomal aberrations in peripheral blood lymphocytes was reported in patients with Crohn’s disease who were treated with 200 to 1200 mg/day of metronidazole for 1 to 24 months. However, in another study, no increase in chromosomal aberrations in circulating lymphocytes was observed in patients with Crohn’s disease treated with the drug for 8 months.
In one published study, using albino hairless mice, intraperitoneal administration of metronidazole at a dose of 45 mg/m2/day (approximately 7 times the human topical dose on a mg/m2 basis) was associated with an increase in ultraviolet radiation-induced skin carcinogenesis. Neither dermal carcinogenicity nor photocarcinogenicity studies have been performed with METRONIDAZOLE CREAM or any marketed metronidazole formulations.
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:38:42.332214 · Updated: 2026-03-14T21:55:28.640025