Tri-sprintec®
c1fc22e5-e02d-4dda-a9ac-c592e922c467
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
9018 Rx only
Indications and Usage
Tri-Sprintec ® (norgestimate and ethinyl estradiol tablets USP) is indicated for the prevention of pregnancy in women who elect to use oral contraceptives as a method of contraception. Tri-Sprintec (norgestimate and ethinyl estradiol tablets USP) is indicated for the treatment of moderate acne vulgaris in females at least 15 years of age, who have no known contraindications to oral contraceptive therapy and have achieved menarche. Tri-Sprintec (norgestimate and ethinyl estradiol tablets USP) should be used for the treatment of acne only if the patient desires an oral contraceptive for birth control. Oral contraceptives are highly effective for pregnancy prevention. Table 2 lists the typical accidental pregnancy rates for users of combination oral contraceptives and other methods of contraception. The efficacy of these contraceptive methods, except sterilization, the IUD, and the Norplant ® System, depends upon the reliability with which they are used. Correct and consistent use of methods can result in lower failure rates. Table 2: Percentage of Women Experiencing an Unintended Pregnancy During the First Year of Typical Use and the First Year of Perfect Use of Contraception and the Percentage Continuing Use at the End of the First Year. United States. % of Women Experiencing an Unintended Pregnancy within the First Year of Use % of Women Continuing Use at One Year Among couples attempting to avoid pregnancy, the percentage who continue to use a method for one year. Method Typical Use Among typical couples who initiate use of a method (not necessarily for the first time), the percentage who experience an accidental pregnancy during the first year if they do not stop use for any other reason. Perfect Use Among couples who initiate use of a method (not necessarily for the first time) and who use it perfectly (both consistently and correctly), the percentage who experience an accidental pregnancy during the first year if they do not stop use for any other reason. (1) (2) (3) (4) Chance The percents becoming pregnant in columns (2) and (3) are based on data from populations where contraception is not used and from women who cease using contraception in order to become pregnant. Among such populations, about 89% become pregnant within one year. This estimate was lowered slightly (to 85%) to represent the percent who would become pregnant within one year among women now relying on reversible methods of contraception if they abandoned contraception altogether. 85 85 Spermicides Foams, creams, gels, vaginal suppositories, and vaginal film. 26 6 40 Periodic abstinence 25 63 Calendar 9 Ovulation Method 3 Sympto-Thermal Cervical mucus (ovulation) method supplemented by calendar in the pre-ovulatory and basal body temperature in the post-ovulatory phases. 2 Post-Ovulation 1 Cap With spermicidal cream or jelly. Parous Women 40 26 42 Nulliparous Women 20 9 56 Sponge Parous Women 40 20 42 Nulliparous Women 20 9 56 Diaphragm 20 6 56 Withdrawal 19 4 Condom Without spermicides. Female (Reality ® ) 21 5 56 Male 14 3 61 Pill 5 71 Progestin Only 0.5 Combined 0.1 IUD Progesterone T 2 1.5 81 Copper T380A 0.8 0.6 78 LNg 20 0.1 0.1 81 Depo-Provera ® 0.3 0.3 70 Norplant ® and Norplant-2 ® 0.05 0.05 88 Female Sterilization 0.5 0.5 100 Male Sterilization 0.15 0.10 100 Hatcher et al., 1998 Ref. #1. Emergency Contraceptive Pills: Treatment initiated within 72 hours after unprotected intercourse reduces the risk of pregnancy by at least 75%. The treatment schedule is one dose within 72 hours after unprotected intercourse, and a second dose 12 hours after the first dose. The Food and Drug Administration has declared the following brands of oral contraceptives to be safe and effective for emergency contraception: Ovral ® (1 dose is 2 white pills), Alesse ® (1 dose is 5 pink pills), Nordette ® or Levlen ® (1 dose is 2 light-orange pills), Lo/Ovral ® (1 dose is 4 white pills), Triphasil ® or Tri-Levlen ® (1 dose is 4 yellow pills). Lactational Amenorrhea Method: LAM is a highly effective, temporary method of contraception. However, to maintain effective protection against pregnancy, another method of contraception must be used as soon as menstruation resumes, the frequency or duration of breastfeeds is reduced, bottle feeds are introduced, or the baby reaches six months of age. Source: Trussell J, Contraceptive efficacy. In Hatcher RA, Trussell J, Stewart F, Cates W, Stewart GK, Kowal D, Guest F, Contraceptive Technology: Seventeenth Revised Edition. New York NY: Irvington Publishers, 1998. Tri-Sprintec (norgestimate and ethinyl estradiol tablets USP) has not been studied for and is not indicated for use in emergency contraception. In four clinical trials with Tri-Sprintec (norgestimate and ethinyl estradiol tablets USP), a total of 4,756 subjects completed 45,244 cycles, and the use-efficacy pregnancy rate was approximately 1 pregnancy per 100 women-years. Tri-Sprintec (norgestimate and ethinyl estradiol tablets USP) was evaluated for the treatment of acne vulgaris in two randomized, double-blind, placebo-controlled, multicenter, Phase 3, six (28 day) cycle studies. 221 patients received Tri-Sprintec (norgestimate and ethinyl estradiol tablets USP) and 234 patients received placebo. Mean age at enrollment for both groups was 28 years. At the end of 6 months, the mean total lesion count changes from 55 to 31 (42% reduction) in patients treated with Tri-Sprintec (norgestimate and ethinyl estradiol tablets USP) and from 54 to 38 (27% reduction) in patients similarly treated with placebo. Table 3 summarizes the changes in lesion count for each type of lesion in the ITT population. Based on the investigator’s global assessment conducted at the final visit, patients treated with Tri-Sprintec (norgestimate and ethinyl estradiol tablets USP) showed a statistically significant improvement in total lesions compared to those treated with placebo. Table 3: Acne Vulgaris Indication. Combined Results: Two Multicenter, Placebo-Controlled Trials. Observed Means at Six Months (LOCF) LOCF: Last Observation Carried Forward and at Baseline. Intent to Treat Population. Tri-Sprintec (N = 221) Placebo (N = 234) Difference in Counts Between Tri-Sprintec and Placebo at 6 Months # of Lesions Counts % Reduction Counts % Reduction INFLAMMATORY LESIONS Baseline Mean 19 19 Sixth Month Mean 10 48% 13 30% 3 (95% CI: -1.2, 5.1) NON-INFLAMMATORY LESIONS Baseline Mean 36 35 Sixth Month Mean 22 34% 25 21% 3 (95% CI: -0.2, 7.8) TOTAL LESIONS Baseline Mean 55 54 Sixth Month Mean 31 42% 38 27% 7 (95% CI: 2, 11.9)
Dosage and Administration
Oral Contraception To achieve maximum contraceptive effectiveness, Tri-Sprintec ® tablets must be taken exactly as directed and at intervals not exceeding 24 hours. The possibility of ovulation and conception prior to initiation of medication should be considered. Tri-Sprintec tablets are available in the Blister Pack Tablet Dispenser which is preset for a Sunday Start. Day 1 Start is also provided. Sunday Start When taking Tri-Sprintec ® the first tablet should be taken on the first Sunday after menstruation begins. If the period begins on Sunday, the first tablet should be taken that day. Take one active tablet daily for 21 days followed by one white inactive tablet daily for 7 days. After 28 tablets have been taken, a new course is started the next day (Sunday). For the first cycle of a Sunday Start regimen, another method of contraception should be used until after the first seven consecutive days of administration. If the patient misses one (1) active tablet in Weeks 1, 2, or 3, the tablet should be taken as soon as she remembers. If the patient misses two (2) active tablets in Week 1 or Week 2, the patient should take two (2) tablets the day she remembers and two (2) tablets the next day; and then continue taking one (1) tablet a day until she finishes the pack. The patient should be instructed to use a back-up method of birth control such as a condom or spermicide if she has sex in the seven (7) days after missing pills. If the patient misses two (2) active tablets in the third week or misses three (3) or more active tablets in a row, the patient should continue taking one tablet every day until Sunday. On Sunday the patient should throw out the rest of the pack and start a new pack that same day. The patient should be instructed to use a back-up method of birth control if she has sex in the seven (7) days after missing pills. Complete instructions to facilitate patient counseling on proper pill usage may be found in the Detailed Patient Labeling (“ How to Take the Pill ” section). Day 1 Start The dosage of Tri-Sprintec ® tablets, for the initial cycle of therapy, is one active tablet administered daily from the 1st day through the 21st day of the menstrual cycle, counting the first day of menstrual flow as “Day 1” followed by one white inactive tablet daily for 7 days. Tablets are taken without interruption for 28 days. After 28 tablets have been taken, a new course is started the next day. If the patient misses one (1) active tablet in Weeks 1, 2, or 3, the tablet should be taken as soon as she remembers. If the patient misses two (2) active tablets in Week 1 or Week 2, the patient should take two (2) tablets the day she remembers and two (2) tablets the next day; and then continue taking one (1) tablet a day until she finishes the pack. The patient should be instructed to use a back-up method of birth control such as a condom or spermicide if she has sex in the seven (7) days after missing pills. If the patient misses two (2) active tablets in the third week or misses three (3) or more active tablets in a row, the patient should throw out the rest of the pack and start a new pack that same day. The patient should be instructed to use a back-up method of birth control if she has sex in the seven (7) days after missing pills. Complete instructions to facilitate patient counseling on proper pill usage may be found in the Detailed Patient Labeling (“ How to Take the Pill ” section). The use of Tri-Sprintec ® tablets for contraception may be initiated 4 weeks postpartum in women who elect not to breastfeed. When the tablets are administered during the postpartum period, the increased risk of thromboembolic disease associated with the postpartum period must be considered. (See CONTRAINDICATIONS and WARNINGS concerning thromboembolic disease. See also PRECAUTIONS , Nursing Mothers .) The possibility of ovulation and conception prior to initiation of medication should be considered. (See Discussion of Dose-Related Risk of Vascular Disease from Oral Contraceptives .)
Contraindications
Oral contraceptives should not be used in women who currently have the following conditions: • Thrombophlebitis or thromboembolic disorders • A past history of deep vein thrombophlebitis or thromboembolic disorders • Known thrombophilic conditions • Cerebral vascular or coronary artery disease (current or past history) • Valvular heart disease with complications • Persistent blood pressure values of ≥ 160 mm Hg systolic or ≥ 100 mg Hg diastolic 102 • Diabetes with vascular involvement • Headaches with focal neurological symptoms • Major surgery with prolonged immobilization • Known or suspected carcinoma of the breast or personal history of breast cancer • Carcinoma of the endometrium or other known or suspected estrogen-dependent neoplasia • Undiagnosed abnormal genital bleeding • Cholestatic jaundice of pregnancy or jaundice with prior pill use • Acute or chronic hepatocellular disease with abnormal liver function • Hepatic adenomas or carcinomas • Known or suspected pregnancy • Hypersensitivity to any component of this product
Adverse Reactions
An increased risk of the following serious adverse reactions has been associated with the use of oral contraceptives (see WARNINGS ). • Thrombophlebitis and venous thrombosis with or without embolism • Arterial thromboembolism • Pulmonary embolism • Myocardial infarction • Cerebral hemorrhage • Cerebral thrombosis • Hypertension • Gallbladder disease • Hepatic adenomas or benign liver tumors There is evidence of an association between the following conditions and the use of oral contraceptives: • Mesenteric thrombosis • Retinal thrombosis The following adverse reactions have been reported in patients receiving oral contraceptives and are believed to be drug-related: • Nausea • Vomiting • Gastrointestinal symptoms (such as abdominal cramps and bloating) • Breakthrough bleeding • Spotting • Change in menstrual flow • Amenorrhea • Temporary infertility after discontinuation of treatment • Edema • Melasma which may persist • Breast changes: tenderness, enlargement, secretion • Change in weight (increase or decrease) • Change in cervical erosion and secretion • Diminution in lactation when given immediately postpartum • Cholestatic jaundice • Migraine • Allergic reaction, including rash, urticaria, angioedema • Mental depression • Reduced tolerance to carbohydrates • Vaginal candidiasis • Change in corneal curvature (steepening) • Intolerance to contact lenses The following adverse reactions have been reported in users of oral contraceptives and a causal association has been neither confirmed nor refuted: • Pre-menstrual syndrome • Cataracts • Changes in appetite • Cystitis-like syndrome • Headache • Nervousness • Dizziness • Hirsutism • Loss of scalp hair • Erythema multiforme • Erythema nodosum • Hemorrhagic eruption • Vaginitis • Porphyria • Impaired renal function • Hemolytic uremic syndrome • Acne • Changes in libido • Colitis • Budd-Chiari Syndrome The following adverse reactions were also reported in clinical trials or during post-marketing experience: Infections and Infestations: vaginal infection, urinary tract infection; Psychiatric Disorders: mood altered, anxiety, insomnia; Gastrointestinal Disorders: flatulence, pancreatitis, diarrhea, constipation; Reproductive System and Breast Disorders: dysmenorrhea; ovarian cyst, vulvovaginal dryness; Neoplasms Benign, Malignant and Unspecified (Including Cysts and Polyps): benign breast neoplasm, fibroadenoma of breast, breast cyst; Nervous System Disorders: syncope, convulsion, paraesthesia; Eye Disorders: visual impairment, dry eye; Ear and Labyrinth Disorders: vertigo; Cardiac Disorders: tachycardia, palpitations; Vascular Disorders : hot flush; Respiratory, Thoracic and Mediastinal Disorders: dyspnoea; Hepatobiliary Disorders: hepatitis; Skin and Subcutaneous Tissue Disorders: night sweats, hyperhidrosis, photosensitivity reaction, pruritus; Musculoskeletal, Connective Tissue, and Bone Disorders: muscle spasms, pain in extremity, myalgia, back pain; General Disorders and Administration Site Conditions: chest pain, asthenic conditions.
Drug Interactions
Consult the labeling of concurrently-used drugs to obtain further information about interactions with hormonal contraceptives or the potential for enzyme alterations. Effects of Other Drugs on Combined Hormonal Contraceptives Substances Decreasing the Plasma Concentrations of COCs and Potentially Diminishing the Efficacy of COCs Drugs or herbal products that induce certain enzymes, including cytochrome P450 3A4 (CYP3A4), may decrease the plasma concentrations of COCs and potentially diminish the effectiveness of CHCs or increase breakthrough bleeding. Some drugs or herbal products that may decrease the effectiveness of hormonal contraceptives include phenytoin, barbiturates, carbamazepine, bosentan, felbamate, griseofulvin, oxcarbazepine, rifampicin, topiramate, rifabutin, rufinamide, aprepitant, and products containing St. John’s wort. Interactions between hormonal contraceptives and other drugs may lead to breakthrough bleeding and/or contraceptive failure. Counsel women to use an alternative method of contraception or a back-up method when enzyme inducers are used with CHCs, and to continue back-up contraception for 28 days after discontinuing the enzyme inducer to ensure contraceptive reliability. Substances Increasing the Plasma Concentrations of COCs Coadministration of atorvastatin or rosuvastatin and certain COCs containing EE increase AUC values for EE by approximately 20 to 25%. Ascorbic acid and acetaminophen may increase plasma EE concentrations, possibly by inhibition of conjugation. CYP3A4 inhibitors such as itraconazole, voriconazole, fluconazole, grapefruit juice, or ketoconazole may increase plasma hormone concentrations. Human Immunodeficiency Virus (HIV)/Hepatitis C virus (HCV) Protease Inhibitors and Non-Nucleoside Reverse Transcriptase Inhibitors Significant changes (increase or decrease) in the plasma concentrations of estrogen and/or progestin have been noted in some cases of coadministration with HIV protease inhibitors (decrease [e.g., nelfinavir, ritonavir, darunavir/ritonavir, (fos)amprenavir/ritonavir, lopinavir/ritonavir, and tipranavir/ritonavir] or increase [e.g., indinavir and atazanavir/ritonavir]) /HCV protease inhibitors (decrease [e.g., boceprevir and telaprevir]) or with nonnucleoside reverse transcriptase inhibitors (decrease [e.g., nevirapine] or increase [e.g., etravirine]). Colesevelam Colesevelam, a bile acid sequestrant, given together with a combination oral hormonal contraceptive, has been shown to significantly decrease the AUC of EE. A drug interaction between the contraceptive and colesevelam was decreased when the two drug products were given 4 hours apart. Effects of Combined Hormonal Contraceptives on Other Drugs COCs containing EE may inhibit the metabolism of other compounds (e.g., cyclosporine, prednisolone, theophylline, tizanidine, and voriconazole) and increase their plasma concentrations. COCs have been shown to decrease plasma concentrations of acetaminophen, clofibric acid, morphine, salicylic acid, temazepam and lamotrigine. Significant decrease in plasma concentration of lamotrigine has been shown, likely due to induction of lamotrigine glucuronidation. This may reduce seizure control; therefore, dosage adjustments of lamotrigine may be necessary. Women on thyroid hormone replacement therapy may need increased doses of thyroid hormone because serum concentrations of thyroid-binding globulin increases with use of COCs. 9. Interactions with Laboratory Tests Certain endocrine and liver function tests and blood components may be affected by oral contraceptives: a. Increased prothrombin and factors VII, VIII, IX, and X; decreased antithrombin 3; increased norepinephrine-induced platelet aggregability. b. Increased thyroid binding globulin (TBG) leading to increased circulating total thyroid hormone, as measured by protein-bound iodine (PBI), T4 by column or by radioimmunoassay. Free T3 resin uptake is decreased, reflecting the elevated TBG, free T4 concentration is unaltered. c. Other binding proteins may be elevated in serum. d. Sex hormone binding globulins are increased and result in elevated levels of total circulating sex steroids; however, free or biologically active levels either decrease or remain unchanged. e. Triglycerides may be increased and levels of various other lipids and lipoproteins may be affected. f. Glucose tolerance may be decreased. g. Serum folate levels may be depressed by oral contraceptive therapy. This may be of clinical significance if a woman becomes pregnant shortly after discontinuing oral contraceptives.
How Supplied
Tri-Sprintec ® (norgestimate and ethinyl estradiol tablets USP) 0.18 mg/0.035 mg are gray, round, flat-faced, beveled-edge, unscored tablets debossed with stylized b on one side and 985 on the other side; 0.215 mg/0.035 mg are light blue, round, flat-faced, beveled-edge, unscored tablets debossed with stylized b on one side and 986 on the other side; 0.25 mg/0.035 mg are blue, round, flat-faced, beveled-edge, unscored tablets debossed with stylized b on one side and 987 on the other side; placebo tablets are white, round, flat-faced, beveled-edge, unscored tablets, debossed with stylized b on one side and 143 on the other side. Tri-Sprintec ® (norgestimate and ethinyl estradiol tablets USP) are packaged in cartons of six blister cards. Each card contains 28 tablets as follows: Each gray tablet contains 0.18 mg of the progestational compound, norgestimate, USP, together with 0.035 mg of the estrogenic compound, ethinyl estradiol, USP. Each light blue tablet contains 0.215 mg of the progestational compound, norgestimate, USP, together with 0.035 mg of the estrogenic compound, ethinyl estradiol, USP. Each blue tablet contains 0.25 mg of the progestational compound, norgestimate, USP, together with 0.035 mg of the estrogenic compound, ethinyl estradiol, USP, and the 7 white placebo tablets contain inert ingredients. Store at 20° to 25°C (68° to 77°F) [See USP Controlled Room Temperature]. PROTECT FROM LIGHT. KEEP THIS AND ALL MEDICATIONS OUT OF THE REACH OF CHILDREN.
Medication Information
Recent Major Changes
WARNINGS: CARDIOVASCULAR RISK ASSOCIATED WITH SMOKING
Cigarette smoking increases the risk of serious cardiovascular events from combination oral contraceptive use. This risk increases with age, particularly in women over 35 years of age, and with the number of cigarettes smoked. For this reason, combination oral contraceptives, including Tri-Sprintec®, should not be used by women who are over 35 years of age and smoke.
Indications and Usage
Tri-Sprintec® (norgestimate and ethinyl estradiol tablets USP) is indicated for the prevention of pregnancy in women who elect to use oral contraceptives as a method of contraception.
Tri-Sprintec (norgestimate and ethinyl estradiol tablets USP) is indicated for the treatment of moderate acne vulgaris in females at least 15 years of age, who have no known contraindications to oral contraceptive therapy and have achieved menarche. Tri-Sprintec (norgestimate and ethinyl estradiol tablets USP) should be used for the treatment of acne only if the patient desires an oral contraceptive for birth control.
Oral contraceptives are highly effective for pregnancy prevention. Table 2 lists the typical accidental pregnancy rates for users of combination oral contraceptives and other methods of contraception. The efficacy of these contraceptive methods, except sterilization, the IUD, and the Norplant® System, depends upon the reliability with which they are used. Correct and consistent use of methods can result in lower failure rates.
|
% of Women Experiencing an Unintended Pregnancy within the First Year of Use |
% of Women Continuing Use at One Year Among couples attempting to avoid pregnancy, the percentage who continue to use a method for one year.
|
||
|
Method |
Typical Use Among typical couples who initiate use of a method (not necessarily for the first time), the percentage who experience an accidental pregnancy during the first year if they do not stop use for any other reason.
|
Perfect Use Among couples who initiate use of a method (not necessarily for the first time) and who use it perfectly (both consistently and correctly), the percentage who experience an accidental pregnancy during the first year if they do not stop use for any other reason.
|
|
|
(1) |
(2) |
(3) |
(4) |
|
Chance The percents becoming pregnant in columns (2) and (3) are based on data from populations where contraception is not used and from women who cease using contraception in order to become pregnant. Among such populations, about 89% become pregnant within one year. This estimate was lowered slightly (to 85%) to represent the percent who would become pregnant within one year among women now relying on reversible methods of contraception if they abandoned contraception altogether.
|
85 |
85 |
|
|
Spermicides Foams, creams, gels, vaginal suppositories, and vaginal film.
|
26 |
6 |
40 |
|
Periodic abstinence |
25 |
63 |
|
|
Calendar |
9 |
||
|
Ovulation Method |
3 |
||
|
Sympto-Thermal Cervical mucus (ovulation) method supplemented by calendar in the pre-ovulatory and basal body temperature in the post-ovulatory phases.
|
2 |
||
|
Post-Ovulation |
1 |
||
|
Cap With spermicidal cream or jelly.
|
|||
|
Parous Women |
40 |
26 |
42 |
|
Nulliparous Women |
20 |
9 |
56 |
|
Sponge |
|||
|
Parous Women |
40 |
20 |
42 |
|
Nulliparous Women |
20 |
9 |
56 |
|
Diaphragm |
20 |
6 |
56 |
|
Withdrawal |
19 |
4 |
|
|
Condom Without spermicides.
|
|||
|
Female (Reality®) |
21 |
5 |
56 |
|
Male |
14 |
3 |
61 |
|
Pill |
5 |
71 |
|
|
Progestin Only |
0.5 |
||
|
Combined |
0.1 |
||
|
IUD |
|||
|
Progesterone T |
2 |
1.5 |
81 |
|
Copper T380A |
0.8 |
0.6 |
78 |
|
LNg 20 |
0.1 |
0.1 |
81 |
|
Depo-Provera® |
0.3 |
0.3 |
70 |
|
Norplant® and Norplant-2® |
0.05 |
0.05 |
88 |
|
Female Sterilization |
0.5 |
0.5 |
100 |
|
Male Sterilization |
0.15 |
0.10 |
100 |
|
Hatcher et al., 1998 Ref. #1. Emergency Contraceptive Pills: Treatment initiated within 72 hours after unprotected intercourse reduces the risk of pregnancy by at least 75%. The treatment schedule is one dose within 72 hours after unprotected intercourse, and a second dose 12 hours after the first dose. The Food and Drug Administration has declared the following brands of oral contraceptives to be safe and effective for emergency contraception: Ovral® (1 dose is 2 white pills), Alesse® (1 dose is 5 pink pills), Nordette® or Levlen® (1 dose is 2 light-orange pills), Lo/Ovral® (1 dose is 4 white pills), Triphasil® or Tri-Levlen® (1 dose is 4 yellow pills).
Lactational Amenorrhea Method: LAM is a highly effective, temporary method of contraception. However, to maintain effective protection against pregnancy, another method of contraception must be used as soon as menstruation resumes, the frequency or duration of breastfeeds is reduced, bottle feeds are introduced, or the baby reaches six months of age.
Source: Trussell J, Contraceptive efficacy. In Hatcher RA, Trussell J, Stewart F, Cates W, Stewart GK, Kowal D, Guest F, Contraceptive Technology: Seventeenth Revised Edition. New York NY: Irvington Publishers, 1998. |
Tri-Sprintec (norgestimate and ethinyl estradiol tablets USP) has not been studied for and is not indicated for use in emergency contraception.
In four clinical trials with Tri-Sprintec (norgestimate and ethinyl estradiol tablets USP), a total of 4,756 subjects completed 45,244 cycles, and the use-efficacy pregnancy rate was approximately 1 pregnancy per 100 women-years.
Tri-Sprintec (norgestimate and ethinyl estradiol tablets USP) was evaluated for the treatment of acne vulgaris in two randomized, double-blind, placebo-controlled, multicenter, Phase 3, six (28 day) cycle studies. 221 patients received Tri-Sprintec (norgestimate and ethinyl estradiol tablets USP) and 234 patients received placebo. Mean age at enrollment for both groups was 28 years. At the end of 6 months, the mean total lesion count changes from 55 to 31 (42% reduction) in patients treated with Tri-Sprintec (norgestimate and ethinyl estradiol tablets USP) and from 54 to 38 (27% reduction) in patients similarly treated with placebo. Table 3 summarizes the changes in lesion count for each type of lesion in the ITT population. Based on the investigator’s global assessment conducted at the final visit, patients treated with Tri-Sprintec (norgestimate and ethinyl estradiol tablets USP) showed a statistically significant improvement in total lesions compared to those treated with placebo.
|
Tri-Sprintec (N = 221) |
Placebo (N = 234) |
Difference in Counts Between |
|||
|
# of Lesions |
Counts |
% Reduction |
Counts |
% Reduction |
|
|
INFLAMMATORY LESIONS |
|||||
|
Baseline Mean |
19 |
19 |
|||
|
Sixth Month Mean |
10 |
48% |
13 |
30% |
3 (95% CI: -1.2, 5.1) |
|
NON-INFLAMMATORY LESIONS |
|||||
|
Baseline Mean |
36 |
35 |
|||
|
Sixth Month Mean |
22 |
34% |
25 |
21% |
3 (95% CI: -0.2, 7.8) |
|
TOTAL LESIONS |
|||||
|
Baseline Mean |
55 |
54 |
|||
|
Sixth Month Mean |
31 |
42% |
38 |
27% |
7 (95% CI: 2, 11.9) |
Dosage and Administration
Oral Contraception
To achieve maximum contraceptive effectiveness, Tri-Sprintec® tablets must be taken exactly as directed and at intervals not exceeding 24 hours. The possibility of ovulation and conception prior to initiation of medication should be considered. Tri-Sprintec tablets are available in the Blister Pack Tablet Dispenser which is preset for a Sunday Start. Day 1 Start is also provided.
Sunday Start
When taking Tri-Sprintec® the first tablet should be taken on the first Sunday after menstruation begins. If the period begins on Sunday, the first tablet should be taken that day. Take one active tablet daily for 21 days followed by one white inactive tablet daily for 7 days. After 28 tablets have been taken, a new course is started the next day (Sunday). For the first cycle of a Sunday Start regimen, another method of contraception should be used until after the first seven consecutive days of administration.
If the patient misses one (1) active tablet in Weeks 1, 2, or 3, the tablet should be taken as soon as she remembers. If the patient misses two (2) active tablets in Week 1 or Week 2, the patient should take two (2) tablets the day she remembers and two (2) tablets the next day; and then continue taking one (1) tablet a day until she finishes the pack. The patient should be instructed to use a back-up method of birth control such as a condom or spermicide if she has sex in the seven (7) days after missing pills. If the patient misses two (2) active tablets in the third week or misses three (3) or more active tablets in a row, the patient should continue taking one tablet every day until Sunday. On Sunday the patient should throw out the rest of the pack and start a new pack that same day. The patient should be instructed to use a back-up method of birth control if she has sex in the seven (7) days after missing pills.
Complete instructions to facilitate patient counseling on proper pill usage may be found in the Detailed Patient Labeling (“How to Take the Pill” section).
Day 1 Start
The dosage of Tri-Sprintec® tablets, for the initial cycle of therapy, is one active tablet administered daily from the 1st day through the 21st day of the menstrual cycle, counting the first day of menstrual flow as “Day 1” followed by one white inactive tablet daily for 7 days. Tablets are taken without interruption for 28 days. After 28 tablets have been taken, a new course is started the next day.
If the patient misses one (1) active tablet in Weeks 1, 2, or 3, the tablet should be taken as soon as she remembers. If the patient misses two (2) active tablets in Week 1 or Week 2, the patient should take two (2) tablets the day she remembers and two (2) tablets the next day; and then continue taking one (1) tablet a day until she finishes the pack. The patient should be instructed to use a back-up method of birth control such as a condom or spermicide if she has sex in the seven (7) days after missing pills. If the patient misses two (2) active tablets in the third week or misses three (3) or more active tablets in a row, the patient should throw out the rest of the pack and start a new pack that same day. The patient should be instructed to use a back-up method of birth control if she has sex in the seven (7) days after missing pills.
Complete instructions to facilitate patient counseling on proper pill usage may be found in the Detailed Patient Labeling (“How to Take the Pill” section).
The use of Tri-Sprintec® tablets for contraception may be initiated 4 weeks postpartum in women who elect not to breastfeed. When the tablets are administered during the postpartum period, the increased risk of thromboembolic disease associated with the postpartum period must be considered. (See CONTRAINDICATIONS and WARNINGS concerning thromboembolic disease. See also PRECAUTIONS, Nursing Mothers.) The possibility of ovulation and conception prior to initiation of medication should be considered.
(See Discussion of Dose-Related Risk of Vascular Disease from Oral Contraceptives.)
Contraindications
Oral contraceptives should not be used in women who currently have the following conditions:
-
•Thrombophlebitis or thromboembolic disorders
-
•A past history of deep vein thrombophlebitis or thromboembolic disorders
-
•Known thrombophilic conditions
-
•Cerebral vascular or coronary artery disease (current or past history)
-
•Valvular heart disease with complications
-
•Persistent blood pressure values of ≥ 160 mm Hg systolic or ≥ 100 mg Hg diastolic 102
-
•Diabetes with vascular involvement
-
•Headaches with focal neurological symptoms
-
•Major surgery with prolonged immobilization
-
•Known or suspected carcinoma of the breast or personal history of breast cancer
-
•Carcinoma of the endometrium or other known or suspected estrogen-dependent neoplasia
-
•Undiagnosed abnormal genital bleeding
-
•Cholestatic jaundice of pregnancy or jaundice with prior pill use
-
•Acute or chronic hepatocellular disease with abnormal liver function
-
•Hepatic adenomas or carcinomas
-
•Known or suspected pregnancy
-
•Hypersensitivity to any component of this product
Adverse Reactions
An increased risk of the following serious adverse reactions has been associated with the use of oral contraceptives (see WARNINGS).
-
•Thrombophlebitis and venous thrombosis with or without embolism
-
•Arterial thromboembolism
-
•Pulmonary embolism
-
•Myocardial infarction
-
•Cerebral hemorrhage
-
•Cerebral thrombosis
-
•Hypertension
-
•Gallbladder disease
-
•Hepatic adenomas or benign liver tumors
There is evidence of an association between the following conditions and the use of oral contraceptives:
• Mesenteric thrombosis
• Retinal thrombosis
The following adverse reactions have been reported in patients receiving oral contraceptives and are believed to be drug-related:
-
•Nausea
-
•Vomiting
-
•Gastrointestinal symptoms (such as abdominal cramps and bloating)
-
•Breakthrough bleeding
-
•Spotting
-
•Change in menstrual flow
-
•Amenorrhea
-
•Temporary infertility after discontinuation of treatment
-
•Edema
-
•Melasma which may persist
-
•Breast changes: tenderness, enlargement, secretion
-
•Change in weight (increase or decrease)
-
•Change in cervical erosion and secretion
-
•Diminution in lactation when given immediately postpartum
-
•Cholestatic jaundice
-
•Migraine
-
•Allergic reaction, including rash, urticaria, angioedema
-
•Mental depression
-
•Reduced tolerance to carbohydrates
-
•Vaginal candidiasis
-
•Change in corneal curvature (steepening)
-
•Intolerance to contact lenses
The following adverse reactions have been reported in users of oral contraceptives and a causal association has been neither confirmed nor refuted:
-
•Pre-menstrual syndrome
-
•Cataracts
-
•Changes in appetite
-
•Cystitis-like syndrome
-
•Headache
-
•Nervousness
-
•Dizziness
-
•Hirsutism
-
•Loss of scalp hair
-
•Erythema multiforme
-
•Erythema nodosum
-
•Hemorrhagic eruption
-
•Vaginitis
-
•Porphyria
-
•Impaired renal function
-
•Hemolytic uremic syndrome
-
•Acne
-
•Changes in libido
-
•Colitis
-
•Budd-Chiari Syndrome
The following adverse reactions were also reported in clinical trials or during post-marketing experience: Infections and Infestations: vaginal infection, urinary tract infection; Psychiatric Disorders: mood altered, anxiety, insomnia; Gastrointestinal Disorders: flatulence, pancreatitis, diarrhea, constipation; Reproductive System and Breast Disorders: dysmenorrhea; ovarian cyst, vulvovaginal dryness; Neoplasms Benign, Malignant and Unspecified (Including Cysts and Polyps): benign breast neoplasm, fibroadenoma of breast, breast cyst; Nervous System Disorders: syncope, convulsion, paraesthesia; Eye Disorders: visual impairment, dry eye; Ear and Labyrinth Disorders: vertigo; Cardiac Disorders: tachycardia, palpitations; Vascular Disorders: hot flush; Respiratory, Thoracic and Mediastinal Disorders: dyspnoea; Hepatobiliary Disorders: hepatitis; Skin and Subcutaneous Tissue Disorders: night sweats, hyperhidrosis, photosensitivity reaction, pruritus; Musculoskeletal, Connective Tissue, and Bone Disorders: muscle spasms, pain in extremity, myalgia, back pain; General Disorders and Administration Site Conditions: chest pain, asthenic conditions.
Drug Interactions
Consult the labeling of concurrently-used drugs to obtain further information about interactions with hormonal contraceptives or the potential for enzyme alterations. Effects of Other Drugs on Combined Hormonal Contraceptives Substances Decreasing the Plasma Concentrations of COCs and Potentially Diminishing the Efficacy of COCs Drugs or herbal products that induce certain enzymes, including cytochrome P450 3A4 (CYP3A4), may decrease the plasma concentrations of COCs and potentially diminish the effectiveness of CHCs or increase breakthrough bleeding. Some drugs or herbal products that may decrease the effectiveness of hormonal contraceptives include phenytoin, barbiturates, carbamazepine, bosentan, felbamate, griseofulvin, oxcarbazepine, rifampicin, topiramate, rifabutin, rufinamide, aprepitant, and products containing St. John’s wort. Interactions between hormonal contraceptives and other drugs may lead to breakthrough bleeding and/or contraceptive failure. Counsel women to use an alternative method of contraception or a back-up method when enzyme inducers are used with CHCs, and to continue back-up contraception for 28 days after discontinuing the enzyme inducer to ensure contraceptive reliability. Substances Increasing the Plasma Concentrations of COCs Coadministration of atorvastatin or rosuvastatin and certain COCs containing EE increase AUC values for EE by approximately 20 to 25%. Ascorbic acid and acetaminophen may increase plasma EE concentrations, possibly by inhibition of conjugation. CYP3A4 inhibitors such as itraconazole, voriconazole, fluconazole, grapefruit juice, or ketoconazole may increase plasma hormone concentrations. Human Immunodeficiency Virus (HIV)/Hepatitis C virus (HCV) Protease Inhibitors and Non-Nucleoside Reverse Transcriptase Inhibitors Significant changes (increase or decrease) in the plasma concentrations of estrogen and/or progestin have been noted in some cases of coadministration with HIV protease inhibitors (decrease [e.g., nelfinavir, ritonavir, darunavir/ritonavir, (fos)amprenavir/ritonavir, lopinavir/ritonavir, and tipranavir/ritonavir] or increase [e.g., indinavir and atazanavir/ritonavir]) /HCV protease inhibitors (decrease [e.g., boceprevir and telaprevir]) or with nonnucleoside reverse transcriptase inhibitors (decrease [e.g., nevirapine] or increase [e.g., etravirine]). Colesevelam Colesevelam, a bile acid sequestrant, given together with a combination oral hormonal contraceptive, has been shown to significantly decrease the AUC of EE. A drug interaction between the contraceptive and colesevelam was decreased when the two drug products were given 4 hours apart. Effects of Combined Hormonal Contraceptives on Other Drugs COCs containing EE may inhibit the metabolism of other compounds (e.g., cyclosporine, prednisolone, theophylline, tizanidine, and voriconazole) and increase their plasma concentrations. COCs have been shown to decrease plasma concentrations of acetaminophen, clofibric acid, morphine, salicylic acid, temazepam and lamotrigine. Significant decrease in plasma concentration of lamotrigine has been shown, likely due to induction of lamotrigine glucuronidation. This may reduce seizure control; therefore, dosage adjustments of lamotrigine may be necessary. Women on thyroid hormone replacement therapy may need increased doses of thyroid hormone because serum concentrations of thyroid-binding globulin increases with use of COCs. 9. Interactions with Laboratory Tests Certain endocrine and liver function tests and blood components may be affected by oral contraceptives: a. Increased prothrombin and factors VII, VIII, IX, and X; decreased antithrombin 3; increased norepinephrine-induced platelet aggregability. b. Increased thyroid binding globulin (TBG) leading to increased circulating total thyroid hormone, as measured by protein-bound iodine (PBI), T4 by column or by radioimmunoassay. Free T3 resin uptake is decreased, reflecting the elevated TBG, free T4 concentration is unaltered. c. Other binding proteins may be elevated in serum. d. Sex hormone binding globulins are increased and result in elevated levels of total circulating sex steroids; however, free or biologically active levels either decrease or remain unchanged. e. Triglycerides may be increased and levels of various other lipids and lipoproteins may be affected. f. Glucose tolerance may be decreased. g. Serum folate levels may be depressed by oral contraceptive therapy. This may be of clinical significance if a woman becomes pregnant shortly after discontinuing oral contraceptives.
How Supplied
Tri-Sprintec® (norgestimate and ethinyl estradiol tablets USP) 0.18 mg/0.035 mg are gray, round, flat-faced, beveled-edge, unscored tablets debossed with stylized b on one side and 985 on the other side; 0.215 mg/0.035 mg are light blue, round, flat-faced, beveled-edge, unscored tablets debossed with stylized b on one side and 986 on the other side; 0.25 mg/0.035 mg are blue, round, flat-faced, beveled-edge, unscored tablets debossed with stylized b on one side and 987 on the other side; placebo tablets are white, round, flat-faced, beveled-edge, unscored tablets, debossed with stylized b on one side and 143 on the other side.
Tri-Sprintec® (norgestimate and ethinyl estradiol tablets USP) are packaged in cartons of six blister cards. Each card contains 28 tablets as follows: Each gray tablet contains 0.18 mg of the progestational compound, norgestimate, USP, together with 0.035 mg of the estrogenic compound, ethinyl estradiol, USP. Each light blue tablet contains 0.215 mg of the progestational compound, norgestimate, USP, together with 0.035 mg of the estrogenic compound, ethinyl estradiol, USP. Each blue tablet contains 0.25 mg of the progestational compound, norgestimate, USP, together with 0.035 mg of the estrogenic compound, ethinyl estradiol, USP, and the 7 white placebo tablets contain inert ingredients.
Store at 20° to 25°C (68° to 77°F) [See USP Controlled Room Temperature].
PROTECT FROM LIGHT.
KEEP THIS AND ALL MEDICATIONS OUT OF THE REACH OF CHILDREN.
Description
Tri-Sprintec® (norgestimate and ethinyl estradiol tablets USP) is a combination oral contraceptive containing the progestational compound norgestimate, USP and the estrogenic compound ethinyl estradiol, USP.
Each gray tablet contains 0.18 mg of the progestational compound, norgestimate, USP (18,19-Dinor-17-pregn-4-en-20-yn-3-one, 17-(acetyloxy)-13-ethyl-, oxime, (17α)-(+)-) and 0.035 mg of the estrogenic compound, ethinyl estradiol, USP (19-Nor-17α-pregna,1,3,5(10)-trien-20-yne-3, 17-diol), and the inactive ingredients include anhydrous lactose, lactose monohydrate, lake blend black LB 636 (ingredients include aluminum sulfate solution, aluminum-chloride solution, FD&C blue no. 2, FD&C red no. 40, FD&C yellow no. 6, sodium bicarbonate and sodium carbonate), magnesium stearate, and pregelatinized corn starch.
Each light blue tablet contains 0.215 mg of the progestational compound norgestimate, USP (18,19-Dinor-17-pregn-4-en-20-yn-3-one,17-(acetyloxy)-13-ethyl-, oxime, (17α)-(+)-) and 0.035 mg of the estrogenic compound, ethinyl estradiol, USP (19-Nor-17α-pregna,1,3,5(10)-trien-20-yne-3, 17-diol), and the inactive ingredients include anhydrous lactose, FD&C blue no. 2 aluminum lake (ingredients include aluminum sulfate solution, aluminum-chloride solution, FD&C blue no. 2, sodium bicarbonate and sodium carbonate), lactose monohydrate, magnesium stearate, and pregelatinized corn starch.
Each blue tablet contains 0.25 mg of the progestational compound norgestimate, USP (18,19-Dinor-17-pregn-4-en-20-yn-3-one, 17-(acetyloxy)-13-ethyl-, oxime, (17α)-(+)-) and 0.035 mg of the estrogenic compound, ethinyl estradiol, USP (19-Nor-17α-pregna,1,3,5(10)-trien-20-yne-3, 17-diol), and the inactive ingredients include anhydrous lactose, FD&C blue no. 2 aluminum lake (ingredients include aluminum sulfate solution, aluminum-chloride solution, FD&C blue no. 2, sodium bicarbonate and sodium carbonate), lactose monohydrate, magnesium stearate, and pregelatinized corn starch.
Each white tablet contains only inert ingredients as follows: anhydrous lactose, hypromellose, magnesium stearate, and microcrystalline cellulose.
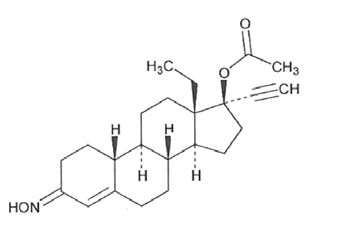
The structural formulas are as follows:
Norgestimate
C23H31NO3 M.W. 369.50
Ethinyl Estradiol
C20H24O2 M.W. 296.40
Section 42229-5
9018
Rx only
Excretion
The metabolites of norelgestromin and ethinyl estradiol are eliminated by renal and fecal pathways. Following administration of 14C-norgestimate, 47% (45 to 49%) and 37% (16 to 49%) of the administered radioactivity was eliminated in the urine and feces, respectively. Unchanged norgestimate was not detected in the urine. In addition to 17-deacetyl norgestimate, a number of metabolites of norgestimate have been identified in human urine following administration of radiolabeled norgestimate. These include 18, 19-Dinor-17-pregn-4-en-20-yn-3-one,17-hydroxy-13-ethyl,(17α)-(-);18,19-Dinor-5β-17-pregnan-20-yn,3α,17β-dihydroxy-13-ethyl,(17α), various hydroxylated metabolites and conjugates of these metabolites.
Absorption
Norgestimate (NGM) and ethinyl estradiol (EE) are rapidly absorbed following oral administration. Norgestimate is rapidly and completely metabolized by first pass (intestinal and/or hepatic) mechanisms to norelgestromin (NGMN) and norgestrel (NG), which are the major active metabolites of norgestimate.
Peak serum concentrations of NGMN and EE are generally reached by 2 hours after administration of Tri-Sprintec . Accumulation following multiple dosing of the 250 mcg NGM / 35 mcg dose is approximately 2-fold for NGMN and EE compared with single dose administration. The pharmacokinetics of NGMN is dose proportional following NGM doses of 180 mcg to 250 mcg. Steady-state concentration of EE is achieved by Day 7 of each dosing cycle. Steady-state concentrations of NGMN and NG are achieved by Day 21. Non-linear accumulation (approximately 8 fold) of norgestrel is observed as a result of high affinity binding to SHBG (sex hormone-binding globulin), which limits its biological activity.
|
Mean (SD) Pharmacokinetic Parameters of Tri-Sprintec During a Three Cycle Study |
||||||
|
Analyte |
Cycle |
Day |
Cmax |
tmax (h) |
AUC0-24h |
t1/2 (h) |
|
NGMN |
3 |
7 |
1.80 (0.46) |
1.42 (0.73) |
15 (3.88) |
NC |
|
14 |
2.12 (0.56) |
1.21 (0.26) |
16.1 (4.97) |
NC |
||
|
21 |
2.66 (0.47) |
1.29 (0.26) |
21.4 (3.46) |
22.3 (6.54) |
||
|
NG |
3 |
7 |
1.94 (0.82) |
3.15 (4.05) |
34.8 (16.5) |
NC |
|
14 |
3 (1.04) |
2.21 (2.03) |
55.2 (23.5) |
NC |
||
|
21 |
3.66 (1.15) |
2.58 (2.97) |
69.3 (23.8) |
40.2 (15.4) |
||
|
EE |
3 |
7 |
124 (39.5) |
1.27 (0.26) |
1130 (420) |
NC |
|
14 |
128 (38.4) |
1.32 (0.25) |
1130 (324) |
NC |
||
|
21 |
126 (34.7) |
1.31 (0.56) |
1090 (359) |
15.9 (4.39) |
Cmax= peak serum concentration, tmax= time to reach peak serum concentration,
AUC0-24h= area under serum concentration vs time curve from 0 to 24 hours,
t1/2= elimination half-life, NC = not calculated.
NGMN and NG: Cmax= ng/mL, AUC0-24h=h•ng/mL
EE: Cmax=pg/mL, AUC0-24h=h•pg/mL
The effect of food on the pharmacokinetics of Tri-Sprintec has not been studied.
Metabolism
Norgestimate is extensively metabolized by first-pass mechanisms in the gastrointestinal tract and/or liver. Norgestimate’s primary active metabolite is norelgestromin. Subsequent hepatic metabolism of norelgestromin occurs and metabolites include norgestrel, which is also active, and various hydroxylated and conjugated metabolites. Ethinyl estradiol is also metabolized to various hydroxylated products and their glucuronide and sulfate conjugates.
Overdosage
Serious ill effects have not been reported following acute ingestion of large doses of oral contraceptives by young children. Overdosage may cause nausea and withdrawal bleeding may occur in females.
References
1. Trussell J. Contraceptive efficacy. In Hatcher RA, Trussell J, Stewart F, Cates W, Stewart GK, Kowal D, Guest F, Contraceptive Technology: Seventeenth Revised Edition. New York, NY: Irvington Publishers, 1998. 2. Stadel BV, Oral contraceptives and cardiovascular disease. (Pt.1). N Engl J Med 1981; 305:612-618. 3. Stadel BV, Oral contraceptives and cardiovascular disease. (Pt.2). N Engl J Med 1981; 305:672-677. 4. Adam SA, Thorogood M. Oral contraception and myocardial infarction revisited: the effects of new preparations and prescribing patterns. Br J Obstet Gynaecol 1981; 88:838-845. 5. Mann Jl, Inman WH. Oral contraceptives and death from myocardial infarction. Br Med J 1975; 2(5965):245-248. 6. Mann Jl, Vessey MP, Thorogood M, Doll R. Myocardial infarction in young women with special reference to oral contraceptive practice. Br Med J 1975; 2(5956):241-245. 7. Royal College of General Practitioners' Oral Contraception Study: Further analyses of mortality in oral contraceptive users. Lancet 1981; 1:541-546. 8. Slone D, Shapiro S, Kaufman DW, Rosenberg L, Miettinen OS, Stolley PD. Risk of myocardial infarction in relation to current and discontinued use of oral contraceptives. N Engl J Med 1981:305:420-424. 9. Vessey MP. Female hormones and vascular disease - an epidemiological overview. Br J Fam Plann 1980; 6(Supplement): 1-12. 10. Russell-Briefel RG, Ezzati TM, Fulwood R, Perlman JA, Murphy RS. Cardiovascular risk status and oral contraceptive use, United States, 1976-80. Prevent Med 1986; 15:352-362. 11. Goldbaum GM, Kendrick JS, Hogelin GC, Gentry EM. The relative impact of smoking and oral contraceptive use on women in the United States. JAMA 1987; 258:1339-1342. 12. Layde PM, Beral V. Further analyses of mortality in oral contraceptive users; Royal College of General Practitioners' Oral Contraception Study. (Table 5) Lancet 1981; 1:541-546. 13. Knopp RH. Arteriosclerosis risk: the roles of oral contraceptives and postmenopausal estrogens. J Reprod Med 1986; 31(9) (Supplement):913-921. 14. Krauss RM, Roy S, Mishell DR, Casagrande J, Pike MC. Effects of two low-dose oral contraceptives on serum lipids and lipoproteins: Differential changes in high-density lipoproteins subclasses. Am J Obstet 1983; 145:446-452. 15. Wahl P, Walden C, Knopp R, Hoover J, Wallace R, Heiss G, Rifkind B. Effect of estrogen/progestin potency on lipid/lipoprotein cholesterol. N Engl J Med 1983; 308:862-867. 16. Wynn V, Niththyananthan R. The effect of progestin in combined oral contraceptives on serum lipids with special reference to high density lipoproteins. Am J Obstet Gynecol 1982;142:766-771. 17. Wynn V, Godsland I. Effects of oral contraceptives on carbohydrate metabolism. J Reprod Med 1986;31(9)(Supplement):892-897. 18. LaRosa JC. Atherosclerotic risk factors in cardiovascular disease. J Reprod Med 1986;31(9)(Supplement):906-912. 19. Inman WH, Vessey MP. Investigation of death from pulmonary, coronary, and cerebral thrombosis and embolism in women of child-bearing age. Br Med J 1968;2(5599):193-199. 20. Maguire MG, Tonascia J, Sartwell PE, Stolley PD, Tockman MS. Increased risk of thrombosis due to oral contraceptives: a further report. Am J Epidemiol 1979;110(2):188-195. 21. Petitti DB, Wingerd J, Pellegrin F, Ramacharan S. Risk of vascular disease in women: smoking, oral contraceptives, noncontraceptive estrogens, and other factors. JAMA 1979; 242:1150-1154. 22. Vessey MP, Doll R. Investigation of relation between use of oral contraceptives and thromboembolic disease. Br Med J 1968;2(5599):199-205. 23. Vessey MP, Doll R. Investigation of relation between use of oral contraceptives and thromboembolic disease. A further report. Br Med J 1969; 2(5658):651-657. 24. Porter JB, Hunter JR, Danielson DA, Jick H, Stergachis A. Oral contraceptives and non-fatal vascular disease-recent experience. Obstet Gynecol 1982;59(3):299-302. 25. Vessey M, Doll R, Peto R, Johnson B, Wiggins P. A long-term follow-up study of women using different methods of contraception: an interim report. J Biosocial Sci 1976;8:375-427. 26. Royal College of General Practitioners: Oral Contraceptives, venous thrombosis, and varicose veins. J Royal Coll Gen Pract 1978; 28:393-399. 27. Collaborative Group for the Study of Stroke in Young Women: Oral contraception and increased risk of cerebral ischemia or thrombosis. N Engl J Med 1973;288:871-878. 28. Petitti DB, Wingerd J. Use of oral contraceptives, cigarette smoking, and risk of subarachnoid hemorrhage. Lancet 1978;2:234-236. 29. Inman WH. Oral contraceptives and fatal subarachnoid hemorrhage. Br Med J 1979;2(6203):1468-1470. 30. Collaborative Group for the Study of Stroke in Young Women: Oral Contraceptives and stroke in young women: associated risk factors. JAMA 1975; 231:718-722. 31. Inman WH, Vessey MP, Westerholm B, Engelund A. Thromboembolic disease and the steroidal content of oral contraceptives. A report to the Committee on Safety of Drugs. Br Med J 1970;2:203-209. 32. Meade TW, Greenberg G, Thompson SG. Progestogens and cardiovascular reactions associated with oral contraceptives and a comparison of the safety of 50- and 35-mcg oestrogen preparations. Br Med J 1980;280(6224):1157-1161. 33. Kay CR. Progestogens and arterial disease-evidence from the Royal College of General Practitioners' Study. Am J Obstet Gynecol 1982;142:762-765. 34. Royal College of General Practitioners: Incidence of arterial disease among oral contraceptive users. J Royal Coll Gen Pract 1983;33:75-82. 35. Ory HW. Mortality associated with fertility and fertility control: 1983. Family Planning Perspectives 1983;15:50-56. 36. The Cancer and Steroid Hormone Study of the Centers for Disease Control and the National Institute of Child Health and Human Development: Oral contraceptive use and the risk of breast cancer. N Engl J Med 1986;315:405-411. 37. Pike MC, Henderson BE, Krailo MD, Duke A, Roy S. Breast cancer in young women and use of oral contraceptives: possible modifying effect of formulation and age at use. Lancet 1983;2:926-929. 38. Paul C, Skegg DG, Spears GFS, Kaldor JM. Oral contraceptives and breast cancer: A national study. Br Med J 1986; 293:723-725. 39. Miller DR, Rosenberg L, Kaufman DW, Schottenfeld D, Stolley PD, Shapiro S. Breast cancer risk in relation to early oral contraceptive use. Obstet Gynecol 1986;68:863-868. 40. Olsson H, Olsson ML, Moller TR, Ranstam J, Holm P. Oral contraceptive use and breast cancer in young women in Sweden (letter). Lancet 1985; 1(8431):748-749. 41. McPherson K, Vessey M, Neil A, Doll R, Jones L, Roberts M. Early contraceptive use and breast cancer: Results of another case-control study. Br J Cancer 1987; 56:653-660. 42. Huggins GR, Zucker PF. Oral contraceptives and neoplasia; 1987 update. Fertil Steril 1987; 47:733-761. 43. McPherson K, Drife JO. The pill and breast cancer: why the uncertainty? Br Med J 1986; 293:709-710. 44. Shapiro S. Oral contraceptives-time to take stock. N Engl J Med 1987; 315:450-451. 45. Ory H, Naib Z, Conger SB, Hatcher RA, Tyler CW. Contraceptive choice and prevalence of cervical dysplasia and carcinoma in situ. Am J Obstet Gynecol 1976; 124:573-577. 46. Vessey MP, Lawless M, McPherson K, Yeates D. Neoplasia of the cervix uteri and contraception: a possible adverse effect of the pill. Lancet 1983; 2:930. 47. Brinton LA, Huggins GR, Lehman HF, Malli K, Savitz DA, Trapido E, Rosenthal J, Hoover R. Long term use of oral contraceptives and risk of invasive cervical cancer. Int J Cancer 1986; 38:339-344. 48. WHO Collaborative Study of Neoplasia and Steroid Contraceptives: Invasive cervical cancer and combined oral contraceptives. Br Med J 1985; 290:961-965. 49. Rooks JB, Ory HW, Ishak KG, Strauss LT, Greenspan JR, Hill AP, Tyler CW. Epidemiology of hepatocellular adenoma: the role of oral contraceptive use. JAMA 1979; 242:644-648. 50. Bein NN, Goldsmith HS. Recurrent massive hemorrhage from benign hepatic tumors secondary to oral contraceptives. Br J Surg 1977; 64:433-435. 51. Klatskin G. Hepatic tumors: possible relationship to use of oral contraceptives. Gastroenterology 1977; 73:386-394. 52. Henderson BE, Preston-Martin S, Edmondson HA, Peters RL, Pike MC. Hepatocellular carcinoma and oral contraceptives. Br J Cancer 1983;48:437-440. 53. Neuberger J, Forman D, Doll R, Williams R. Oral contraceptives and hepatocellular carcinoma. Br Med J 1986; 292:1355-1357. 54. Forman D, Vincent TJ, Doll R. Cancer of the liver and oral contraceptives. Br Med J 1986; 292:1357-1361. 55. Harlap S, Eldor J. Births following oral contraceptive failures. Obstet Gynecol 1980; 55:447-452. 56. Savolainen E, Saksela E, Saxen L. Teratogenic hazards of oral contraceptives analyzed in a national malformation register. Am J Obstet Gynecol 1981: 140:521-524. 57. Janerich DT, Piper JM, Glebatis DM. Oral contraceptives and birth defects. Am J Epidemiol 1980; 112:73-79. 58. Ferencz C, Matanoski GM, Wilson PD, Rubin JD, Neill CA, Gutberlet R. Maternal hormone therapy and congenital heart disease. Teratology 1980; 21:225-239. 59. Rothman KJ, Fyler DC, Goldblatt A, Kreidberg MB. Exogenous hormones and other drug exposures of children with congenital heart disease. Am J Epidemiol 1979; 109:433-439. 60. Boston Collaborative Drug Surveillance Program: Oral contraceptives and venous thromboembolic disease, surgically confirmed gallbladder disease, and breast tumors. Lancet 1973; 1:1399-1404. 61. Royal College of General Practitioners: Oral contraceptives and health. New York, Pittman 1974. 62. Layde PM, Vessey MP, Yeates D. Risk of gallbladder disease: a cohort study of young women attending family planning clinics. J Epidemiol Community Health 1982; 36:274-278. 63. Rome Group for Epidemiology and Prevention of Cholelithiasis (GREPCO): Prevalence of gallstone disease in an Italian adult female population. Am J Epidemiol 1984; 119:796-805. 64. Storm BL, Tamragouri RT, Morse ML, Lazar EL, West SL, Stolley PD, Jones JK. Oral contraceptives and other risk factors for gallbladder disease. Clin Pharmacol Ther 1986; 39:335-341. 65. Wynn V, Adams PW, Godsland IF, Melrose J, Niththyananthan R, Oakley NW, Seedj A. Comparison of effects of different combined oral contraceptive formulations on carbohydrate and lipid metabolism. Lancet 1979; 1:1045-1049. 66. Wynn V. Effect of progesterone and progestins on carbohydrate metabolism. In: Progesterone and Progestin. Bardin CW, Milgrom E, Mauvis-Jarvis P. eds. New York, Raven Press 1983; pp. 395-410. 67. Perlman JA, Roussell-Briefel RG, Ezzati TM, Lieberknecht G. Oral glucose tolerance and the potency of oral contraceptive progestogens. J Chronic Dis 1985;38:857-864. 68. Royal College of General Practitioners' Oral Contraception Study: Effect on hypertension and benign breast disease of progestogen component in combined oral contraceptives. Lancet 1977; 1:624. 69. Fisch IR, Frank J. Oral contraceptives and blood pressure. JAMA 1977; 237:2499-2503. 70. Laragh AJ. Oral contraceptive induced hypertension-nine years later. Am J Obstet Gynecol 1976; 126:141-147. 71. Ramcharan S, Peritz E, Pellegrin FA, Williams WT. Incidence of hypertension in the Walnut Creek Contraceptive Drug Study cohort: In: Pharmacology of steroid contraceptive drugs. Garattini S, Berendes HW. Eds. New York, Raven Press, 1977; pp. 277-288, (Monographs of the Mario Negri Institute for Pharmacological Research Milan.) 72. Stockley I. Interactions with oral contraceptives. J Pharm 1976;216:140-143. 73. The Cancer and Steroid Hormone Study of the Centers for Disease Control and the National Institute of Child Health and Human Development: Oral contraceptive use and the risk of ovarian cancer. JAMA 1983; 249:1596-1599. 74. The Cancer and Steroid Hormone Study of the Centers for Disease Control and the National Institute of Child Health and Human Development: Combination oral contraceptive use and the risk of endometrial cancer. JAMA 1987; 257:796-800. 75. Ory HW. Functional ovarian cysts and oral contraceptives: negative association confirmed surgically. JAMA 1974; 228:68-69. 76. Ory HW, Cole P, MacMahon B, Hoover R. Oral contraceptives and reduced risk of benign breast disease. N Engl J Med 1976; 294:419-422. 77. Ory HW. The noncontraceptive health benefits from oral contraceptive use. Fam Plann Perspect 1982; 14:182-184. 78. Ory HW, Forrest JD, Lincoln R. Making choices: Evaluating the health risks and benefits of birth control methods. New York, The Alan Guttmacher Institute, 1983; p.1. 79. Schlesselman J, Stadel BV, Murray P, Lai S. Breast cancer in relation to early use of oral contraceptives. JAMA 1988; 259:1828-1833. 80. Hennekens CH, Speizer FE, Lipnick RJ, Rosner B, Bain C, Belanger C, Stampfer MJ, Willett W, Peto R. A case-control study of oral contraceptive use and breast cancer. JNCI 1984; 72:39-42. 81. LaVecchia C, Decarli A, Fasoli M, Franceschi S, Gentile A, Negri E, Parazzini F, Tognoni G. Oral contraceptives and cancers of the breast and of the female genital tract. Interim results from a case-control study. Br J Cancer 1986; 54:311-317. 82. Meirik O, Lund E, Adami H, Bergstrom R, Christoffersen T, Bergsjo P. Oral contraceptive use and breast cancer in young women. A Joint National Case-control study in Sweden and Norway. Lancet 1986; 11:650-654. 83. Kay CR, Hannaford PC. Breast cancer and the pill-A further report from the Royal College of General Practitioners' oral contraception study. Br J Cancer 1988;58:675-680. 84. Stadel BV, Lai S, Schlesselman JJ, Murray P. Oral contraceptives and premenopausal breast cancer in nulliparous women. Contraception 1988; 38:287-299. 85. Miller DR, Rosenberg L, Kaufman DW, Stolley P, Warshauer ME, Shapiro S. Breast cancer before age 45 and oral contraceptive use: New Findings. Am J Epidemiol 1989; 129:269-280. 86. The UK National Case-Control Study Group, Oral contraceptive use and breast cancer risk in young women. Lancet 1989; 1:973-982. 87. Schlesselman JJ. Cancer of the breast and reproductive tract in relation to use of oral contraceptives. Contraception 1989; 40:1-38. 88. Vessey MP, McPherson K, Villard-Mackintosh L, Yeates D. Oral contraceptives and breast cancer: latest findings in a large cohort study. Br J Cancer 1989; 59:613-617. 89. Jick SS, Walker AM, Stergachis A, Jick H. Oral contraceptives and breast cancer. Br J Cancer 1989; 59:618-621. 90. Anderson FD. Selectivity and minimal androgenicity of norgestimate in monophasic and triphasic oral contraceptives. Acta Obstet Gynecol Scand 1992; 156 (Supplement):15-21. 91. Chapdelaine A, Desmaris J-L, Derman RJ. Clinical evidence of minimal androgenic activity of norgestimate. Int J Fertil 1989; 34(51):347-352. 92. Phillips A, Demarest K, Hahn DW, Wong F, McGuire JL. Progestational and androgenic receptor binding affinities and in vivo activities of norgestimate and other progestins. Contraception 1989; 41(4):399-409. 93. Phillips A, Hahn DW, Klimek S, McGuire JL. A comparison of the potencies and activities of progestogens used in contraceptives. Contraception 1987; 36(2):181-192. 94. Janaud A, Rouffy J, Upmalis D, Dain M-P. A comparison study of lipid and androgen metabolism with triphasic oral contraceptive formulations containing norgestimate or levonorgestrel. Acta Obstet Gynecol Scand 1992; 156 (Supplement):34-38. 95. Collaborative Group on Hormonal Factors in Breast Cancer. Breast cancer and hormonal contraceptives: collaborative reanalysis of individual data on 53 297 women with breast cancer and 100 239 women without breast cancer from 54 epidemiological studies. Lancet 1996; 347:1713-1727. 96. Palmer JR, Rosenberg L, Kaufman DW, Warshauer ME, Stolley P, Shapiro S. Oral Contraceptive Use and Liver Cancer. Am J Epidemiol 1989;130:878-882. 97. Lewis M, Spitzer WO, Heinemann LAJ, MacRae KD, Bruppacher R, Thorogood M on behalf of Transnational Research Group on Oral Contraceptives and Health of Young Women. Third generation oral contraceptives and risk of myocardial infarction: an international case-control study. Br Med J, 1996; 312:88-90. 98. Improving access to quality care in family planning: Medical eligibility criteria for contraceptive use. Geneva, WHO, Family and Reproductive Health, 1996. 99. Bork K, Fischer B, DeWald G. Recurrent episodes of skin angioedema and severe attacks of abdominal pain induced by oral contraceptives or hormone replacement therapy. Am J Med 2003;114:294-298. 100. Van Giersbergen PLM, Halabi A, Dingemanse J. Pharmacokinetic interaction between bosentan and the oral contraceptives norethisterone and ethinyl estradiol. Int J Clin Pharmacol Ther 2006;44(3):113-118. 101. Christensen J, Petrenaite V, Atterman J, et al. Oral contraceptives induce lamotrigine metabolism: evidence from a double-blind, placebo-controlled trial. Epilepsia
2007;48(3):484-489. 102. Chobanian et al. Seventh report of the joint national committee on prevention, detection, evaluation, and treatment of high blood pressure. Hypertension 2003;42;1206-1252. 103. Brown KS, Armstrong IC, Wang A, Walker JR, Noveck RJ, Swearingen D, Allison M, Kissling JC, Kisicki J, Salazar D. Effect of the bile acid sequestrant colesevelam on the pharmacokinetics of pioglitazone, repaglinide, estrogen estradiol, norethindrone, levothyroxine, and glyburide. J Clin Pharmacol 2010;50:554-565.
Precautions
1. General
Patients should be counseled that this product does not protect against HIV infection (AIDS) and other sexually transmitted diseases.
2. Physical Examination and Follow-Up
It is good medical practice for all women to have annual history and physical examinations, including women using oral contraceptives. The physical examination, however, may be deferred until after initiation of oral contraceptives if requested by the woman and judged appropriate by the clinician. The physical examination should include special reference to blood pressure, breasts, abdomen and pelvic organs, including cervical cytology, and relevant laboratory tests. In case of undiagnosed, persistent or recurrent abnormal vaginal bleeding, appropriate measures should be conducted to rule out malignancy. Women with a strong family history of breast cancer or who have breast nodules should be monitored with particular care.
3. Lipid Disorders
Women who are being treated for hyperlipidemias should be followed closely if they elect to use oral contraceptives. Some progestogens may elevate LDL levels and may render the control of hyperlipidemias more difficult.
4. Liver Function
If jaundice develops in any woman receiving such drugs, the medication should be discontinued. Steroid hormones may be poorly metabolized in patients with impaired liver function.
5. Fluid Retention
Oral contraceptives may cause some degree of fluid retention. They should be prescribed with caution, and only with careful monitoring, in patients with conditions which might be aggravated by fluid retention.
6. Emotional Disorders
Women with a history of depression should be carefully observed and the drug discontinued if depression recurs to a serious degree.
7. Contact Lenses
Contact lens wearers who develop visual changes or changes in lens tolerance should be assessed by an ophthalmologist.
Distribution
Norelgestromin and norgestrel are highly bound (> 97%) to serum proteins. Norelgestromin is bound to albumin and not to SHBG, while norgestrel is bound primarily to SHBG. Ethinyl estradiol is extensively bound (> 97%) to serum albumin and induces an increase in the serum concentrations of SHBG.
Renal Impairment
The effects of renal impairment on the pharmacokinetics of Tri-Sprintec have not been studied.
13. Pediatric Use
Safety and efficacy of Tri-Sprintec® tablets have been established in women of reproductive age. Safety and efficacy are expected to be the same for postpubertal adolescents under the age of 16 and for users 16 years and older. There was no significant difference between Tri-Sprintec tablets and placebo in mean change in total lumbar spine (L1 to L4) and total hip bone mineral density between baseline and Cycle 13 in 123 adolescent females with anorexia nervosa in a double-blind, placebo-controlled, multicenter, one-year treatment duration clinical trial for the Intent To Treat (ITT) population. Use of this product before menarche is not indicated.
14. Geriatric Use
This product has not been studied in women over 65 years of age and is not indicated in this population.
10. Carcinogenesis
See WARNINGS.
Hepatic Impairment
The effects of hepatic impairment on the pharmacokinetics of Tri-Sprintec have not been studied. However, steroid hormones may be poorly metabolized in women with impaired liver function (see PRECAUTIONS).
12. Nursing Mothers
Small amounts of oral contraceptive steroids have been identified in the milk of nursing mothers and a few adverse effects on the child have been reported, including jaundice and breast enlargement. In addition, combination oral contraceptives given in the postpartum period may interfere with lactation by decreasing the quantity and quality of breast milk. If possible, the nursing mother should be advised not to use combination oral contraceptives but to use other forms of contraception until she has completely weaned her child.
Special Populations
The effects of body weight, body surface area or age on the pharmacokinetics of Tri-Sprintec have not been studied.
8. Drug Interactions
Consult the labeling of concurrently-used drugs to obtain further information about interactions with hormonal contraceptives or the potential for enzyme alterations.
Effects of Other Drugs on Combined Hormonal Contraceptives
Substances Decreasing the Plasma Concentrations of COCs and Potentially Diminishing the Efficacy of COCs
Drugs or herbal products that induce certain enzymes, including cytochrome P450 3A4 (CYP3A4), may decrease the plasma concentrations of COCs and potentially diminish the effectiveness of CHCs or increase breakthrough bleeding. Some drugs or herbal products that may decrease the effectiveness of hormonal contraceptives include phenytoin, barbiturates, carbamazepine, bosentan, felbamate, griseofulvin, oxcarbazepine, rifampicin, topiramate, rifabutin, rufinamide, aprepitant, and products containing St. John’s wort. Interactions between hormonal contraceptives and other drugs may lead to breakthrough bleeding and/or contraceptive failure. Counsel women to use an alternative method of contraception or a back-up method when enzyme inducers are used with CHCs, and to continue back-up contraception for 28 days after discontinuing the enzyme inducer to ensure contraceptive reliability.
Substances Increasing the Plasma Concentrations of COCs
Coadministration of atorvastatin or rosuvastatin and certain COCs containing EE increase AUC values for EE by approximately 20 to 25%. Ascorbic acid and acetaminophen may increase plasma EE concentrations, possibly by inhibition of conjugation. CYP3A4 inhibitors such as itraconazole, voriconazole, fluconazole, grapefruit juice, or ketoconazole may increase plasma hormone concentrations.
Human Immunodeficiency Virus (HIV)/Hepatitis C virus (HCV) Protease Inhibitors and Non-Nucleoside Reverse Transcriptase Inhibitors
Significant changes (increase or decrease) in the plasma concentrations of estrogen and/or progestin have been noted in some cases of coadministration with HIV protease inhibitors (decrease [e.g., nelfinavir, ritonavir, darunavir/ritonavir, (fos)amprenavir/ritonavir, lopinavir/ritonavir, and tipranavir/ritonavir] or increase [e.g., indinavir and atazanavir/ritonavir]) /HCV protease inhibitors (decrease [e.g., boceprevir and telaprevir]) or with nonnucleoside reverse transcriptase inhibitors (decrease [e.g., nevirapine] or increase [e.g., etravirine]).
Colesevelam
Colesevelam, a bile acid sequestrant, given together with a combination oral hormonal contraceptive, has been shown to significantly decrease the AUC of EE. A drug interaction between the contraceptive and colesevelam was decreased when the two drug products were given 4 hours apart.
Effects of Combined Hormonal Contraceptives on Other Drugs
COCs containing EE may inhibit the metabolism of other compounds (e.g., cyclosporine, prednisolone, theophylline, tizanidine, and voriconazole) and increase their plasma concentrations. COCs have been shown to decrease plasma concentrations of acetaminophen, clofibric acid, morphine, salicylic acid, temazepam and lamotrigine. Significant decrease in plasma concentration of lamotrigine has been shown, likely due to induction of lamotrigine glucuronidation. This may reduce seizure control; therefore, dosage adjustments of lamotrigine may be necessary.
Women on thyroid hormone replacement therapy may need increased doses of thyroid hormone because serum concentrations of thyroid-binding globulin increases with use of COCs.
9. Interactions with Laboratory Tests
Certain endocrine and liver function tests and blood components may be affected by oral contraceptives:
a. Increased prothrombin and factors VII, VIII, IX, and X; decreased antithrombin 3; increased norepinephrine-induced platelet aggregability.
b. Increased thyroid binding globulin (TBG) leading to increased circulating total thyroid hormone, as measured by protein-bound iodine (PBI), T4 by column or by radioimmunoassay. Free T3 resin uptake is decreased, reflecting the elevated TBG, free T4 concentration is unaltered.
c. Other binding proteins may be elevated in serum.
d. Sex hormone binding globulins are increased and result in elevated levels of total circulating sex steroids; however, free or biologically active levels either decrease or remain unchanged.
e. Triglycerides may be increased and levels of various other lipids and lipoproteins may be affected.
f. Glucose tolerance may be decreased.
g. Serum folate levels may be depressed by oral contraceptive therapy. This may be of clinical significance if a woman becomes pregnant shortly after discontinuing oral contraceptives.
Pregnancy Category X
See CONTRAINDICATIONS and WARNINGS.
Clinical Pharmacology
Oral Contraception
Combination oral contraceptives act by suppression of gonadotropins. Although the primary mechanism of this action is inhibition of ovulation, other alterations include changes in the cervical mucus (which increase the difficulty of sperm entry into the uterus) and the endometrium (which reduce the likelihood of implantation).
Receptor binding studies, as well as studies in animals and humans, have shown that norgestimate and 17-deacetyl norgestimate, the major serum metabolite, combine high progestational activity with minimal intrinsic androgenicity.90-93
Norgestimate, in combination with ethinyl estradiol, does not counteract the estrogen-induced increases in sex hormone binding globulin (SHBG), resulting in lower serum testosterone.90,91,94
Acne
Acne is a skin condition with a multifactorial etiology, including androgen stimulation of sebum production. While the combination of ethinyl estradiol and norgestimate increases sex hormone binding globulin (SHBG) and decreases free testosterone, the relationship between these changes and a decrease in the severity of facial acne in otherwise healthy women with this skin condition has not been established.
Drug Drug Interactions
No formal drug-drug interaction studies were conducted with Tri-Sprintec. Interactions between contraceptive steroids and other drugs have been reported in the literature (see PRECAUTIONS).
Although norelgestromin and its metabolites inhibit a variety of P450 enzymes in human liver microsomes, under the recommended dosing regimen, the in vivo concentrations of norelgestromin and its metabolites, even at the peak serum levels, are relatively low compared to the inhibitory constant (Ki).
Additional Instructions
Breakthrough bleeding, spotting, and amenorrhea are frequent reasons for patients discontinuing oral contraceptives. In breakthrough bleeding, as in all cases of irregular bleeding from the vagina, nonfunctional causes should be borne in mind. In undiagnosed persistent or recurrent abnormal bleeding from the vagina, adequate diagnostic measures are indicated to rule out pregnancy or malignancy. If pathology has been excluded, time or a change to another formulation may solve the problem. Changing to an oral contraceptive with a higher estrogen content, while potentially useful in minimizing menstrual irregularity, should be done only if necessary since this may increase the risk of thromboembolic disease.
Use of oral contraceptives in the event of a missed menstrual period:
-
•If the patient has not adhered to the prescribed schedule, the possibility of pregnancy should be considered at the time of the first missed period and oral contraceptive use should be discontinued if pregnancy is confirmed.
-
•If the patient has adhered to the prescribed regimen and misses two consecutive periods, pregnancy should be ruled out.
Acne
The timing of initiation of dosing with Tri-Sprintec® for acne should follow the guidelines for use of Tri-Sprintec as an oral contraceptive. Consult the DOSAGE AND ADMINISTRATION section for oral contraceptives. The dosage regimen for Tri-Sprintec for treatment of facial acne, as available in a Blister Pack Tablet Dispenser, utilizes a 21-day active and a 7-day placebo schedule. Take one active tablet daily for 21 days followed by one white inactive tablet for 7 days. After 28 tablets have been taken, a new course is started the next day.
Principal Display Panel
Detailed Patient Labeling
PLEASE NOTE: This labeling is revised from time to time as important new medical information becomesavailable. Therefore, please review this labeling carefully.
This product (like all oral contraceptives) does not protect against HIV infection (AIDS) and other sexually transmitted diseases.
Tri-Sprintec® (norgestimate and ethinyl estradiol tablets USP)
Each gray tablet contains 0.18 mg norgestimate and 0.035 mg ethinyl estradiol. Each light blue tablet contains 0.215 mg norgestimate and 0.035 mg ethinyl estradiol. Each blue tablet contains 0.25 mg norgestimate and 0.035 mg ethinyl estradiol. Each white tablet contains inert ingredients.
INTRODUCTION
Any woman who considers using oral contraceptives (the birth control pill or the pill) should understand the benefits and risks of using this form of birth control. This patient labeling will give you much of the information you will need to make this decision and will also help you determine if you are at risk of developing any of the serious side effects of the pill. It will tell you how to use the pill properly so that it will be as effective as possible. However, this labeling is not a replacement for a careful discussion between you and your healthcare professional. You should discuss the information provided in this labeling with him or her, both when you first start taking the pill and during your revisits. You should also follow your healthcare professional’s advice with regard to regular check-ups while you are on the pill.
EFFECTIVENESS OF ORAL CONTRACEPTIVES FOR CONTRACEPTION
Oral contraceptives or “birth control pills” or “the pill” are used to prevent pregnancy and are more effective than most other nonsurgical methods of birth control. When they are taken correctly without missing any pills, the chance of becoming pregnant is approximately 1% per year (1 pregnancy per 100 women per year of use). Typical failure rates, including women who do not always take the pill correctly, are approximately 5% per year (5 pregnancies per 100 women per year of use). The chance of becoming pregnant increases with each missed pill during a menstrual cycle.
In comparison, typical failure rates for other nonsurgical methods of birth control during the first year of use are as follows:
Implant: < 1%
Injection: < 1%
IUD: 1 to 2%
Diaphragm with spermicides: 20%
Spermicides alone: 26%
Vaginal sponge: 20 to 40%
Female sterilization: < 1%
Male sterilization: < 1%
Cervical Cap with spermicides: 20 to 40%
Condom alone (male): 14%
Condom alone (female): 21%
Periodic abstinence: 25%
Withdrawal: 19%
No methods: 85%
Tri-Sprintec may also be taken to treat moderate acne if all of the following are true:
• You have started having menstrual cycles
• You are at least 15 years old
• Your healthcare professional says it is safe for you to use the pill
• You want to use the pill for birth control
WHO SHOULD NOT TAKE ORAL CONTRACEPTIVES
Information for the Patient
See Patient Labeling printed below.
Package/label Display Panel
Pregnancy Due to Pill Failure
The incidence of pill failure resulting in pregnancy is approximately 5%, including women who do not always take the pills exactly as directed. If failure does occur, the risk to the fetus is minimal.
PREGNANCY AFTER STOPPING THE PILL
There may be some delay in becoming pregnant after you stop using oral contraceptives, especially if you had irregular menstrual cycles before you used oral contraceptives. It may be advisable to postpone conception until you begin menstruating regularly once you have stopped taking the pill and desire pregnancy.
There does not appear to be any increase in birth defects in newborn babies when pregnancy occurs soon after stopping the pill.
OVERDOSAGE
Serious ill effects have not been reported following ingestion of large doses of oral contraceptives by young children. Overdosage may cause nausea and withdrawal bleeding in females. In case of overdosage, contact your healthcare professional or pharmacist.
OTHER INFORMATION
Your healthcare professional will take a medical and family history before prescribing oral contraceptives and will examine you. The physical examination may be delayed to another time if you request it and the healthcare professional believes that it is a good medical practice to postpone it. You should be reexamined at least once a year. Be sure to inform your healthcare professional if there is a family history of any of the conditions listed previously in this leaflet. Be sure to keep all appointments with your healthcare professional, because this is a time to determine if there are early signs of side effects of oral contraceptive use.
Do not use the drug for any condition other than the one for which it was prescribed. This drug has been prescribed specifically for you; do not give it to others who may want birth control pills.
HEALTH BENEFITS FROM ORAL CONTRACEPTIVES
In addition to preventing pregnancy, use of combination oral contraceptives may provide certain benefits. They are:
-
•menstrual cycles may become more regular
-
•blood flow during menstruation may be lighter and less iron may be lost. Therefore, anemia due to iron deficiency is less likely to occur.
-
•pain or other symptoms during menstruation may be encountered less frequently
-
•ectopic (tubal) pregnancy may occur less frequently
-
•noncancerous cysts or lumps in the breast may occur less frequently
-
•acute pelvic inflammatory disease may occur less frequently
-
•oral contraceptive use may provide some protection against developing two forms of cancer: cancer of the ovaries and cancer of the lining of the uterus.
If you want more information about birth control pills, ask your healthcare professional or pharmacist. They have a more technical leaflet called the Professional Labeling, which you may wish to read.
Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.
Store at 20° to 25°C (68° to 77°F) [See USP Controlled Room Temperature].
PROTECT FROM LIGHT.
KEEP THIS AND ALL MEDICATIONS OUT OF THE REACH OF CHILDREN.
All brand names listed are the registered trademarks of their respective owners and are not trademarks of Teva Pharmaceuticals USA.
TEVA PHARMACEUTICALS USA
Sellersville, PA 18960
Rev. A 10/2013
Relabeled By:
Proficient Rx LP
Thousand Oaks, CA 91320
Noncontraceptive Health Benefits
The following noncontraceptive health benefits related to the use of combination oral contraceptives are supported by epidemiological studies which largely utilized oral contraceptive formulations containing estrogen doses exceeding 0.035 mg of ethinyl estradiol or 0.05 mg mestranol.73-78
Effects on menses:
-
•increased menstrual cycle regularity
-
•decreased blood loss and decreased incidence of iron deficiency anemia
-
•decreased incidence of dysmenorrhea
Effects related to inhibition of ovulation:
-
•decreased incidence of functional ovarian cysts
-
•decreased incidence of ectopic pregnancies
Other effects:
-
•decreased incidence of fibroadenomas and fibrocystic disease of the breast
-
•decreased incidence of acute pelvic inflammatory disease
-
•decreased incidence of endometrial cancer
-
•decreased incidence of ovarian cancer
Brief Summary Patient Package Insert
This product (like all oral contraceptives) does not protect against HIV infection (AIDS) and other sexually transmitted diseases.
Tri-Sprintec® (norgestimate and ethinyl estradiol tablets USP)
Each gray tablet contains 0.18 mg norgestimate and 0.035 mg ethinyl estradiol. Each light blue tablet contains 0.215 mg norgestimate and 0.035 mg ethinyl estradiol. Each blue tablet contains 0.25 mg norgestimate and 0.035 mg ethinyl estradiol. Each white tablet contains inert ingredients.
Oral contraceptives, also known as “birth control pills” or “the pill,” are taken to prevent pregnancy. When taken correctly to prevent pregnancy, oral contraceptives have a failure rate of approximately 1% per year (1 pregnancy per 100 women per year of use) when used without missing any pills. The typical failure rate is approximately 5% per year (5 pregnancies per 100 women per year of use) when women who miss pills are included. For most women oral contraceptives are also free of serious or unpleasant side effects. However, forgetting to take pills considerably increases the chances of pregnancy.
Tri-Sprintec may also be taken to treat moderate acne in females at least 15 years of age, who have started having menstrual periods, are able to take the pill and want to use the pill for birth control.
For the majority of women, oral contraceptives can be taken safely. But there are some women who are at high risk of developing certain serious diseases that can be fatal or may cause temporary or permanent disability. The risks associated with taking oral contraceptives increase significantly if you:
-
•smoke
-
•have high blood pressure, diabetes, high cholesterol
-
•have or have had clotting disorders, heart attack, stroke, angina pectoris, cancer of the breast or sex organs, jaundice, or malignant or benign liver tumors
Although cardiovascular disease risks may be increased with oral contraceptive use after age 40 in healthy, nonsmoking women (even with the newer low-dose formulations), there are also greater potential health risks associated with pregnancy in older women.
You should not take the pill if you suspect you are pregnant or have unexplained vaginal bleeding.
Tri Sprintec® 28 Day Regimen Carton Text
NDC 0555-9018-58
6 Blister Cards, 28 Tablets Each 28 Day
Tri-Sprintec®
(norgestimate and
ethinyl estradiol tablets USP)
Contains 6 blister cards, each containing 28 tablets. Each gray tablet
contains 0.18 mg norgestimate, USP and 0.035 mg ethinyl estradiol,
USP. Each light blue tablet contains 0.215 mg norgestimate, USP and
0.035 mg ethinyl estradiol, USP. Each blue tablet contains 0.25 mg
norgestimate, USP and 0.035 mg ethinyl estradiol, USP. Each white
tablet contains inert ingredients.
Rx only
Shaping
Women's Health®
TEVA
Structured Label Content
Recent Major Changes (34066-1)
WARNINGS: CARDIOVASCULAR RISK ASSOCIATED WITH SMOKING
Cigarette smoking increases the risk of serious cardiovascular events from combination oral contraceptive use. This risk increases with age, particularly in women over 35 years of age, and with the number of cigarettes smoked. For this reason, combination oral contraceptives, including Tri-Sprintec®, should not be used by women who are over 35 years of age and smoke.
Section 42229-5 (42229-5)
9018
Rx only
Excretion
The metabolites of norelgestromin and ethinyl estradiol are eliminated by renal and fecal pathways. Following administration of 14C-norgestimate, 47% (45 to 49%) and 37% (16 to 49%) of the administered radioactivity was eliminated in the urine and feces, respectively. Unchanged norgestimate was not detected in the urine. In addition to 17-deacetyl norgestimate, a number of metabolites of norgestimate have been identified in human urine following administration of radiolabeled norgestimate. These include 18, 19-Dinor-17-pregn-4-en-20-yn-3-one,17-hydroxy-13-ethyl,(17α)-(-);18,19-Dinor-5β-17-pregnan-20-yn,3α,17β-dihydroxy-13-ethyl,(17α), various hydroxylated metabolites and conjugates of these metabolites.
Absorption
Norgestimate (NGM) and ethinyl estradiol (EE) are rapidly absorbed following oral administration. Norgestimate is rapidly and completely metabolized by first pass (intestinal and/or hepatic) mechanisms to norelgestromin (NGMN) and norgestrel (NG), which are the major active metabolites of norgestimate.
Peak serum concentrations of NGMN and EE are generally reached by 2 hours after administration of Tri-Sprintec . Accumulation following multiple dosing of the 250 mcg NGM / 35 mcg dose is approximately 2-fold for NGMN and EE compared with single dose administration. The pharmacokinetics of NGMN is dose proportional following NGM doses of 180 mcg to 250 mcg. Steady-state concentration of EE is achieved by Day 7 of each dosing cycle. Steady-state concentrations of NGMN and NG are achieved by Day 21. Non-linear accumulation (approximately 8 fold) of norgestrel is observed as a result of high affinity binding to SHBG (sex hormone-binding globulin), which limits its biological activity.
|
Mean (SD) Pharmacokinetic Parameters of Tri-Sprintec During a Three Cycle Study |
||||||
|
Analyte |
Cycle |
Day |
Cmax |
tmax (h) |
AUC0-24h |
t1/2 (h) |
|
NGMN |
3 |
7 |
1.80 (0.46) |
1.42 (0.73) |
15 (3.88) |
NC |
|
14 |
2.12 (0.56) |
1.21 (0.26) |
16.1 (4.97) |
NC |
||
|
21 |
2.66 (0.47) |
1.29 (0.26) |
21.4 (3.46) |
22.3 (6.54) |
||
|
NG |
3 |
7 |
1.94 (0.82) |
3.15 (4.05) |
34.8 (16.5) |
NC |
|
14 |
3 (1.04) |
2.21 (2.03) |
55.2 (23.5) |
NC |
||
|
21 |
3.66 (1.15) |
2.58 (2.97) |
69.3 (23.8) |
40.2 (15.4) |
||
|
EE |
3 |
7 |
124 (39.5) |
1.27 (0.26) |
1130 (420) |
NC |
|
14 |
128 (38.4) |
1.32 (0.25) |
1130 (324) |
NC |
||
|
21 |
126 (34.7) |
1.31 (0.56) |
1090 (359) |
15.9 (4.39) |
Cmax= peak serum concentration, tmax= time to reach peak serum concentration,
AUC0-24h= area under serum concentration vs time curve from 0 to 24 hours,
t1/2= elimination half-life, NC = not calculated.
NGMN and NG: Cmax= ng/mL, AUC0-24h=h•ng/mL
EE: Cmax=pg/mL, AUC0-24h=h•pg/mL
The effect of food on the pharmacokinetics of Tri-Sprintec has not been studied.
Metabolism
Norgestimate is extensively metabolized by first-pass mechanisms in the gastrointestinal tract and/or liver. Norgestimate’s primary active metabolite is norelgestromin. Subsequent hepatic metabolism of norelgestromin occurs and metabolites include norgestrel, which is also active, and various hydroxylated and conjugated metabolites. Ethinyl estradiol is also metabolized to various hydroxylated products and their glucuronide and sulfate conjugates.
Overdosage (OVERDOSAGE)
Serious ill effects have not been reported following acute ingestion of large doses of oral contraceptives by young children. Overdosage may cause nausea and withdrawal bleeding may occur in females.
References (REFERENCES)
1. Trussell J. Contraceptive efficacy. In Hatcher RA, Trussell J, Stewart F, Cates W, Stewart GK, Kowal D, Guest F, Contraceptive Technology: Seventeenth Revised Edition. New York, NY: Irvington Publishers, 1998. 2. Stadel BV, Oral contraceptives and cardiovascular disease. (Pt.1). N Engl J Med 1981; 305:612-618. 3. Stadel BV, Oral contraceptives and cardiovascular disease. (Pt.2). N Engl J Med 1981; 305:672-677. 4. Adam SA, Thorogood M. Oral contraception and myocardial infarction revisited: the effects of new preparations and prescribing patterns. Br J Obstet Gynaecol 1981; 88:838-845. 5. Mann Jl, Inman WH. Oral contraceptives and death from myocardial infarction. Br Med J 1975; 2(5965):245-248. 6. Mann Jl, Vessey MP, Thorogood M, Doll R. Myocardial infarction in young women with special reference to oral contraceptive practice. Br Med J 1975; 2(5956):241-245. 7. Royal College of General Practitioners' Oral Contraception Study: Further analyses of mortality in oral contraceptive users. Lancet 1981; 1:541-546. 8. Slone D, Shapiro S, Kaufman DW, Rosenberg L, Miettinen OS, Stolley PD. Risk of myocardial infarction in relation to current and discontinued use of oral contraceptives. N Engl J Med 1981:305:420-424. 9. Vessey MP. Female hormones and vascular disease - an epidemiological overview. Br J Fam Plann 1980; 6(Supplement): 1-12. 10. Russell-Briefel RG, Ezzati TM, Fulwood R, Perlman JA, Murphy RS. Cardiovascular risk status and oral contraceptive use, United States, 1976-80. Prevent Med 1986; 15:352-362. 11. Goldbaum GM, Kendrick JS, Hogelin GC, Gentry EM. The relative impact of smoking and oral contraceptive use on women in the United States. JAMA 1987; 258:1339-1342. 12. Layde PM, Beral V. Further analyses of mortality in oral contraceptive users; Royal College of General Practitioners' Oral Contraception Study. (Table 5) Lancet 1981; 1:541-546. 13. Knopp RH. Arteriosclerosis risk: the roles of oral contraceptives and postmenopausal estrogens. J Reprod Med 1986; 31(9) (Supplement):913-921. 14. Krauss RM, Roy S, Mishell DR, Casagrande J, Pike MC. Effects of two low-dose oral contraceptives on serum lipids and lipoproteins: Differential changes in high-density lipoproteins subclasses. Am J Obstet 1983; 145:446-452. 15. Wahl P, Walden C, Knopp R, Hoover J, Wallace R, Heiss G, Rifkind B. Effect of estrogen/progestin potency on lipid/lipoprotein cholesterol. N Engl J Med 1983; 308:862-867. 16. Wynn V, Niththyananthan R. The effect of progestin in combined oral contraceptives on serum lipids with special reference to high density lipoproteins. Am J Obstet Gynecol 1982;142:766-771. 17. Wynn V, Godsland I. Effects of oral contraceptives on carbohydrate metabolism. J Reprod Med 1986;31(9)(Supplement):892-897. 18. LaRosa JC. Atherosclerotic risk factors in cardiovascular disease. J Reprod Med 1986;31(9)(Supplement):906-912. 19. Inman WH, Vessey MP. Investigation of death from pulmonary, coronary, and cerebral thrombosis and embolism in women of child-bearing age. Br Med J 1968;2(5599):193-199. 20. Maguire MG, Tonascia J, Sartwell PE, Stolley PD, Tockman MS. Increased risk of thrombosis due to oral contraceptives: a further report. Am J Epidemiol 1979;110(2):188-195. 21. Petitti DB, Wingerd J, Pellegrin F, Ramacharan S. Risk of vascular disease in women: smoking, oral contraceptives, noncontraceptive estrogens, and other factors. JAMA 1979; 242:1150-1154. 22. Vessey MP, Doll R. Investigation of relation between use of oral contraceptives and thromboembolic disease. Br Med J 1968;2(5599):199-205. 23. Vessey MP, Doll R. Investigation of relation between use of oral contraceptives and thromboembolic disease. A further report. Br Med J 1969; 2(5658):651-657. 24. Porter JB, Hunter JR, Danielson DA, Jick H, Stergachis A. Oral contraceptives and non-fatal vascular disease-recent experience. Obstet Gynecol 1982;59(3):299-302. 25. Vessey M, Doll R, Peto R, Johnson B, Wiggins P. A long-term follow-up study of women using different methods of contraception: an interim report. J Biosocial Sci 1976;8:375-427. 26. Royal College of General Practitioners: Oral Contraceptives, venous thrombosis, and varicose veins. J Royal Coll Gen Pract 1978; 28:393-399. 27. Collaborative Group for the Study of Stroke in Young Women: Oral contraception and increased risk of cerebral ischemia or thrombosis. N Engl J Med 1973;288:871-878. 28. Petitti DB, Wingerd J. Use of oral contraceptives, cigarette smoking, and risk of subarachnoid hemorrhage. Lancet 1978;2:234-236. 29. Inman WH. Oral contraceptives and fatal subarachnoid hemorrhage. Br Med J 1979;2(6203):1468-1470. 30. Collaborative Group for the Study of Stroke in Young Women: Oral Contraceptives and stroke in young women: associated risk factors. JAMA 1975; 231:718-722. 31. Inman WH, Vessey MP, Westerholm B, Engelund A. Thromboembolic disease and the steroidal content of oral contraceptives. A report to the Committee on Safety of Drugs. Br Med J 1970;2:203-209. 32. Meade TW, Greenberg G, Thompson SG. Progestogens and cardiovascular reactions associated with oral contraceptives and a comparison of the safety of 50- and 35-mcg oestrogen preparations. Br Med J 1980;280(6224):1157-1161. 33. Kay CR. Progestogens and arterial disease-evidence from the Royal College of General Practitioners' Study. Am J Obstet Gynecol 1982;142:762-765. 34. Royal College of General Practitioners: Incidence of arterial disease among oral contraceptive users. J Royal Coll Gen Pract 1983;33:75-82. 35. Ory HW. Mortality associated with fertility and fertility control: 1983. Family Planning Perspectives 1983;15:50-56. 36. The Cancer and Steroid Hormone Study of the Centers for Disease Control and the National Institute of Child Health and Human Development: Oral contraceptive use and the risk of breast cancer. N Engl J Med 1986;315:405-411. 37. Pike MC, Henderson BE, Krailo MD, Duke A, Roy S. Breast cancer in young women and use of oral contraceptives: possible modifying effect of formulation and age at use. Lancet 1983;2:926-929. 38. Paul C, Skegg DG, Spears GFS, Kaldor JM. Oral contraceptives and breast cancer: A national study. Br Med J 1986; 293:723-725. 39. Miller DR, Rosenberg L, Kaufman DW, Schottenfeld D, Stolley PD, Shapiro S. Breast cancer risk in relation to early oral contraceptive use. Obstet Gynecol 1986;68:863-868. 40. Olsson H, Olsson ML, Moller TR, Ranstam J, Holm P. Oral contraceptive use and breast cancer in young women in Sweden (letter). Lancet 1985; 1(8431):748-749. 41. McPherson K, Vessey M, Neil A, Doll R, Jones L, Roberts M. Early contraceptive use and breast cancer: Results of another case-control study. Br J Cancer 1987; 56:653-660. 42. Huggins GR, Zucker PF. Oral contraceptives and neoplasia; 1987 update. Fertil Steril 1987; 47:733-761. 43. McPherson K, Drife JO. The pill and breast cancer: why the uncertainty? Br Med J 1986; 293:709-710. 44. Shapiro S. Oral contraceptives-time to take stock. N Engl J Med 1987; 315:450-451. 45. Ory H, Naib Z, Conger SB, Hatcher RA, Tyler CW. Contraceptive choice and prevalence of cervical dysplasia and carcinoma in situ. Am J Obstet Gynecol 1976; 124:573-577. 46. Vessey MP, Lawless M, McPherson K, Yeates D. Neoplasia of the cervix uteri and contraception: a possible adverse effect of the pill. Lancet 1983; 2:930. 47. Brinton LA, Huggins GR, Lehman HF, Malli K, Savitz DA, Trapido E, Rosenthal J, Hoover R. Long term use of oral contraceptives and risk of invasive cervical cancer. Int J Cancer 1986; 38:339-344. 48. WHO Collaborative Study of Neoplasia and Steroid Contraceptives: Invasive cervical cancer and combined oral contraceptives. Br Med J 1985; 290:961-965. 49. Rooks JB, Ory HW, Ishak KG, Strauss LT, Greenspan JR, Hill AP, Tyler CW. Epidemiology of hepatocellular adenoma: the role of oral contraceptive use. JAMA 1979; 242:644-648. 50. Bein NN, Goldsmith HS. Recurrent massive hemorrhage from benign hepatic tumors secondary to oral contraceptives. Br J Surg 1977; 64:433-435. 51. Klatskin G. Hepatic tumors: possible relationship to use of oral contraceptives. Gastroenterology 1977; 73:386-394. 52. Henderson BE, Preston-Martin S, Edmondson HA, Peters RL, Pike MC. Hepatocellular carcinoma and oral contraceptives. Br J Cancer 1983;48:437-440. 53. Neuberger J, Forman D, Doll R, Williams R. Oral contraceptives and hepatocellular carcinoma. Br Med J 1986; 292:1355-1357. 54. Forman D, Vincent TJ, Doll R. Cancer of the liver and oral contraceptives. Br Med J 1986; 292:1357-1361. 55. Harlap S, Eldor J. Births following oral contraceptive failures. Obstet Gynecol 1980; 55:447-452. 56. Savolainen E, Saksela E, Saxen L. Teratogenic hazards of oral contraceptives analyzed in a national malformation register. Am J Obstet Gynecol 1981: 140:521-524. 57. Janerich DT, Piper JM, Glebatis DM. Oral contraceptives and birth defects. Am J Epidemiol 1980; 112:73-79. 58. Ferencz C, Matanoski GM, Wilson PD, Rubin JD, Neill CA, Gutberlet R. Maternal hormone therapy and congenital heart disease. Teratology 1980; 21:225-239. 59. Rothman KJ, Fyler DC, Goldblatt A, Kreidberg MB. Exogenous hormones and other drug exposures of children with congenital heart disease. Am J Epidemiol 1979; 109:433-439. 60. Boston Collaborative Drug Surveillance Program: Oral contraceptives and venous thromboembolic disease, surgically confirmed gallbladder disease, and breast tumors. Lancet 1973; 1:1399-1404. 61. Royal College of General Practitioners: Oral contraceptives and health. New York, Pittman 1974. 62. Layde PM, Vessey MP, Yeates D. Risk of gallbladder disease: a cohort study of young women attending family planning clinics. J Epidemiol Community Health 1982; 36:274-278. 63. Rome Group for Epidemiology and Prevention of Cholelithiasis (GREPCO): Prevalence of gallstone disease in an Italian adult female population. Am J Epidemiol 1984; 119:796-805. 64. Storm BL, Tamragouri RT, Morse ML, Lazar EL, West SL, Stolley PD, Jones JK. Oral contraceptives and other risk factors for gallbladder disease. Clin Pharmacol Ther 1986; 39:335-341. 65. Wynn V, Adams PW, Godsland IF, Melrose J, Niththyananthan R, Oakley NW, Seedj A. Comparison of effects of different combined oral contraceptive formulations on carbohydrate and lipid metabolism. Lancet 1979; 1:1045-1049. 66. Wynn V. Effect of progesterone and progestins on carbohydrate metabolism. In: Progesterone and Progestin. Bardin CW, Milgrom E, Mauvis-Jarvis P. eds. New York, Raven Press 1983; pp. 395-410. 67. Perlman JA, Roussell-Briefel RG, Ezzati TM, Lieberknecht G. Oral glucose tolerance and the potency of oral contraceptive progestogens. J Chronic Dis 1985;38:857-864. 68. Royal College of General Practitioners' Oral Contraception Study: Effect on hypertension and benign breast disease of progestogen component in combined oral contraceptives. Lancet 1977; 1:624. 69. Fisch IR, Frank J. Oral contraceptives and blood pressure. JAMA 1977; 237:2499-2503. 70. Laragh AJ. Oral contraceptive induced hypertension-nine years later. Am J Obstet Gynecol 1976; 126:141-147. 71. Ramcharan S, Peritz E, Pellegrin FA, Williams WT. Incidence of hypertension in the Walnut Creek Contraceptive Drug Study cohort: In: Pharmacology of steroid contraceptive drugs. Garattini S, Berendes HW. Eds. New York, Raven Press, 1977; pp. 277-288, (Monographs of the Mario Negri Institute for Pharmacological Research Milan.) 72. Stockley I. Interactions with oral contraceptives. J Pharm 1976;216:140-143. 73. The Cancer and Steroid Hormone Study of the Centers for Disease Control and the National Institute of Child Health and Human Development: Oral contraceptive use and the risk of ovarian cancer. JAMA 1983; 249:1596-1599. 74. The Cancer and Steroid Hormone Study of the Centers for Disease Control and the National Institute of Child Health and Human Development: Combination oral contraceptive use and the risk of endometrial cancer. JAMA 1987; 257:796-800. 75. Ory HW. Functional ovarian cysts and oral contraceptives: negative association confirmed surgically. JAMA 1974; 228:68-69. 76. Ory HW, Cole P, MacMahon B, Hoover R. Oral contraceptives and reduced risk of benign breast disease. N Engl J Med 1976; 294:419-422. 77. Ory HW. The noncontraceptive health benefits from oral contraceptive use. Fam Plann Perspect 1982; 14:182-184. 78. Ory HW, Forrest JD, Lincoln R. Making choices: Evaluating the health risks and benefits of birth control methods. New York, The Alan Guttmacher Institute, 1983; p.1. 79. Schlesselman J, Stadel BV, Murray P, Lai S. Breast cancer in relation to early use of oral contraceptives. JAMA 1988; 259:1828-1833. 80. Hennekens CH, Speizer FE, Lipnick RJ, Rosner B, Bain C, Belanger C, Stampfer MJ, Willett W, Peto R. A case-control study of oral contraceptive use and breast cancer. JNCI 1984; 72:39-42. 81. LaVecchia C, Decarli A, Fasoli M, Franceschi S, Gentile A, Negri E, Parazzini F, Tognoni G. Oral contraceptives and cancers of the breast and of the female genital tract. Interim results from a case-control study. Br J Cancer 1986; 54:311-317. 82. Meirik O, Lund E, Adami H, Bergstrom R, Christoffersen T, Bergsjo P. Oral contraceptive use and breast cancer in young women. A Joint National Case-control study in Sweden and Norway. Lancet 1986; 11:650-654. 83. Kay CR, Hannaford PC. Breast cancer and the pill-A further report from the Royal College of General Practitioners' oral contraception study. Br J Cancer 1988;58:675-680. 84. Stadel BV, Lai S, Schlesselman JJ, Murray P. Oral contraceptives and premenopausal breast cancer in nulliparous women. Contraception 1988; 38:287-299. 85. Miller DR, Rosenberg L, Kaufman DW, Stolley P, Warshauer ME, Shapiro S. Breast cancer before age 45 and oral contraceptive use: New Findings. Am J Epidemiol 1989; 129:269-280. 86. The UK National Case-Control Study Group, Oral contraceptive use and breast cancer risk in young women. Lancet 1989; 1:973-982. 87. Schlesselman JJ. Cancer of the breast and reproductive tract in relation to use of oral contraceptives. Contraception 1989; 40:1-38. 88. Vessey MP, McPherson K, Villard-Mackintosh L, Yeates D. Oral contraceptives and breast cancer: latest findings in a large cohort study. Br J Cancer 1989; 59:613-617. 89. Jick SS, Walker AM, Stergachis A, Jick H. Oral contraceptives and breast cancer. Br J Cancer 1989; 59:618-621. 90. Anderson FD. Selectivity and minimal androgenicity of norgestimate in monophasic and triphasic oral contraceptives. Acta Obstet Gynecol Scand 1992; 156 (Supplement):15-21. 91. Chapdelaine A, Desmaris J-L, Derman RJ. Clinical evidence of minimal androgenic activity of norgestimate. Int J Fertil 1989; 34(51):347-352. 92. Phillips A, Demarest K, Hahn DW, Wong F, McGuire JL. Progestational and androgenic receptor binding affinities and in vivo activities of norgestimate and other progestins. Contraception 1989; 41(4):399-409. 93. Phillips A, Hahn DW, Klimek S, McGuire JL. A comparison of the potencies and activities of progestogens used in contraceptives. Contraception 1987; 36(2):181-192. 94. Janaud A, Rouffy J, Upmalis D, Dain M-P. A comparison study of lipid and androgen metabolism with triphasic oral contraceptive formulations containing norgestimate or levonorgestrel. Acta Obstet Gynecol Scand 1992; 156 (Supplement):34-38. 95. Collaborative Group on Hormonal Factors in Breast Cancer. Breast cancer and hormonal contraceptives: collaborative reanalysis of individual data on 53 297 women with breast cancer and 100 239 women without breast cancer from 54 epidemiological studies. Lancet 1996; 347:1713-1727. 96. Palmer JR, Rosenberg L, Kaufman DW, Warshauer ME, Stolley P, Shapiro S. Oral Contraceptive Use and Liver Cancer. Am J Epidemiol 1989;130:878-882. 97. Lewis M, Spitzer WO, Heinemann LAJ, MacRae KD, Bruppacher R, Thorogood M on behalf of Transnational Research Group on Oral Contraceptives and Health of Young Women. Third generation oral contraceptives and risk of myocardial infarction: an international case-control study. Br Med J, 1996; 312:88-90. 98. Improving access to quality care in family planning: Medical eligibility criteria for contraceptive use. Geneva, WHO, Family and Reproductive Health, 1996. 99. Bork K, Fischer B, DeWald G. Recurrent episodes of skin angioedema and severe attacks of abdominal pain induced by oral contraceptives or hormone replacement therapy. Am J Med 2003;114:294-298. 100. Van Giersbergen PLM, Halabi A, Dingemanse J. Pharmacokinetic interaction between bosentan and the oral contraceptives norethisterone and ethinyl estradiol. Int J Clin Pharmacol Ther 2006;44(3):113-118. 101. Christensen J, Petrenaite V, Atterman J, et al. Oral contraceptives induce lamotrigine metabolism: evidence from a double-blind, placebo-controlled trial. Epilepsia
2007;48(3):484-489. 102. Chobanian et al. Seventh report of the joint national committee on prevention, detection, evaluation, and treatment of high blood pressure. Hypertension 2003;42;1206-1252. 103. Brown KS, Armstrong IC, Wang A, Walker JR, Noveck RJ, Swearingen D, Allison M, Kissling JC, Kisicki J, Salazar D. Effect of the bile acid sequestrant colesevelam on the pharmacokinetics of pioglitazone, repaglinide, estrogen estradiol, norethindrone, levothyroxine, and glyburide. J Clin Pharmacol 2010;50:554-565.
Description (DESCRIPTION)
Tri-Sprintec® (norgestimate and ethinyl estradiol tablets USP) is a combination oral contraceptive containing the progestational compound norgestimate, USP and the estrogenic compound ethinyl estradiol, USP.
Each gray tablet contains 0.18 mg of the progestational compound, norgestimate, USP (18,19-Dinor-17-pregn-4-en-20-yn-3-one, 17-(acetyloxy)-13-ethyl-, oxime, (17α)-(+)-) and 0.035 mg of the estrogenic compound, ethinyl estradiol, USP (19-Nor-17α-pregna,1,3,5(10)-trien-20-yne-3, 17-diol), and the inactive ingredients include anhydrous lactose, lactose monohydrate, lake blend black LB 636 (ingredients include aluminum sulfate solution, aluminum-chloride solution, FD&C blue no. 2, FD&C red no. 40, FD&C yellow no. 6, sodium bicarbonate and sodium carbonate), magnesium stearate, and pregelatinized corn starch.
Each light blue tablet contains 0.215 mg of the progestational compound norgestimate, USP (18,19-Dinor-17-pregn-4-en-20-yn-3-one,17-(acetyloxy)-13-ethyl-, oxime, (17α)-(+)-) and 0.035 mg of the estrogenic compound, ethinyl estradiol, USP (19-Nor-17α-pregna,1,3,5(10)-trien-20-yne-3, 17-diol), and the inactive ingredients include anhydrous lactose, FD&C blue no. 2 aluminum lake (ingredients include aluminum sulfate solution, aluminum-chloride solution, FD&C blue no. 2, sodium bicarbonate and sodium carbonate), lactose monohydrate, magnesium stearate, and pregelatinized corn starch.
Each blue tablet contains 0.25 mg of the progestational compound norgestimate, USP (18,19-Dinor-17-pregn-4-en-20-yn-3-one, 17-(acetyloxy)-13-ethyl-, oxime, (17α)-(+)-) and 0.035 mg of the estrogenic compound, ethinyl estradiol, USP (19-Nor-17α-pregna,1,3,5(10)-trien-20-yne-3, 17-diol), and the inactive ingredients include anhydrous lactose, FD&C blue no. 2 aluminum lake (ingredients include aluminum sulfate solution, aluminum-chloride solution, FD&C blue no. 2, sodium bicarbonate and sodium carbonate), lactose monohydrate, magnesium stearate, and pregelatinized corn starch.
Each white tablet contains only inert ingredients as follows: anhydrous lactose, hypromellose, magnesium stearate, and microcrystalline cellulose.
The structural formulas are as follows:
Norgestimate
C23H31NO3 M.W. 369.50
Ethinyl Estradiol
C20H24O2 M.W. 296.40
Precautions (PRECAUTIONS)
1. General
Patients should be counseled that this product does not protect against HIV infection (AIDS) and other sexually transmitted diseases.
2. Physical Examination and Follow-Up
It is good medical practice for all women to have annual history and physical examinations, including women using oral contraceptives. The physical examination, however, may be deferred until after initiation of oral contraceptives if requested by the woman and judged appropriate by the clinician. The physical examination should include special reference to blood pressure, breasts, abdomen and pelvic organs, including cervical cytology, and relevant laboratory tests. In case of undiagnosed, persistent or recurrent abnormal vaginal bleeding, appropriate measures should be conducted to rule out malignancy. Women with a strong family history of breast cancer or who have breast nodules should be monitored with particular care.
3. Lipid Disorders
Women who are being treated for hyperlipidemias should be followed closely if they elect to use oral contraceptives. Some progestogens may elevate LDL levels and may render the control of hyperlipidemias more difficult.
4. Liver Function
If jaundice develops in any woman receiving such drugs, the medication should be discontinued. Steroid hormones may be poorly metabolized in patients with impaired liver function.
5. Fluid Retention
Oral contraceptives may cause some degree of fluid retention. They should be prescribed with caution, and only with careful monitoring, in patients with conditions which might be aggravated by fluid retention.
6. Emotional Disorders
Women with a history of depression should be carefully observed and the drug discontinued if depression recurs to a serious degree.
7. Contact Lenses
Contact lens wearers who develop visual changes or changes in lens tolerance should be assessed by an ophthalmologist.
Distribution
Norelgestromin and norgestrel are highly bound (> 97%) to serum proteins. Norelgestromin is bound to albumin and not to SHBG, while norgestrel is bound primarily to SHBG. Ethinyl estradiol is extensively bound (> 97%) to serum albumin and induces an increase in the serum concentrations of SHBG.
How Supplied (HOW SUPPLIED)
Tri-Sprintec® (norgestimate and ethinyl estradiol tablets USP) 0.18 mg/0.035 mg are gray, round, flat-faced, beveled-edge, unscored tablets debossed with stylized b on one side and 985 on the other side; 0.215 mg/0.035 mg are light blue, round, flat-faced, beveled-edge, unscored tablets debossed with stylized b on one side and 986 on the other side; 0.25 mg/0.035 mg are blue, round, flat-faced, beveled-edge, unscored tablets debossed with stylized b on one side and 987 on the other side; placebo tablets are white, round, flat-faced, beveled-edge, unscored tablets, debossed with stylized b on one side and 143 on the other side.
Tri-Sprintec® (norgestimate and ethinyl estradiol tablets USP) are packaged in cartons of six blister cards. Each card contains 28 tablets as follows: Each gray tablet contains 0.18 mg of the progestational compound, norgestimate, USP, together with 0.035 mg of the estrogenic compound, ethinyl estradiol, USP. Each light blue tablet contains 0.215 mg of the progestational compound, norgestimate, USP, together with 0.035 mg of the estrogenic compound, ethinyl estradiol, USP. Each blue tablet contains 0.25 mg of the progestational compound, norgestimate, USP, together with 0.035 mg of the estrogenic compound, ethinyl estradiol, USP, and the 7 white placebo tablets contain inert ingredients.
Store at 20° to 25°C (68° to 77°F) [See USP Controlled Room Temperature].
PROTECT FROM LIGHT.
KEEP THIS AND ALL MEDICATIONS OUT OF THE REACH OF CHILDREN.
Renal Impairment
The effects of renal impairment on the pharmacokinetics of Tri-Sprintec have not been studied.
13. Pediatric Use
Safety and efficacy of Tri-Sprintec® tablets have been established in women of reproductive age. Safety and efficacy are expected to be the same for postpubertal adolescents under the age of 16 and for users 16 years and older. There was no significant difference between Tri-Sprintec tablets and placebo in mean change in total lumbar spine (L1 to L4) and total hip bone mineral density between baseline and Cycle 13 in 123 adolescent females with anorexia nervosa in a double-blind, placebo-controlled, multicenter, one-year treatment duration clinical trial for the Intent To Treat (ITT) population. Use of this product before menarche is not indicated.
14. Geriatric Use
This product has not been studied in women over 65 years of age and is not indicated in this population.
Adverse Reactions (ADVERSE REACTIONS)
An increased risk of the following serious adverse reactions has been associated with the use of oral contraceptives (see WARNINGS).
-
•Thrombophlebitis and venous thrombosis with or without embolism
-
•Arterial thromboembolism
-
•Pulmonary embolism
-
•Myocardial infarction
-
•Cerebral hemorrhage
-
•Cerebral thrombosis
-
•Hypertension
-
•Gallbladder disease
-
•Hepatic adenomas or benign liver tumors
There is evidence of an association between the following conditions and the use of oral contraceptives:
• Mesenteric thrombosis
• Retinal thrombosis
The following adverse reactions have been reported in patients receiving oral contraceptives and are believed to be drug-related:
-
•Nausea
-
•Vomiting
-
•Gastrointestinal symptoms (such as abdominal cramps and bloating)
-
•Breakthrough bleeding
-
•Spotting
-
•Change in menstrual flow
-
•Amenorrhea
-
•Temporary infertility after discontinuation of treatment
-
•Edema
-
•Melasma which may persist
-
•Breast changes: tenderness, enlargement, secretion
-
•Change in weight (increase or decrease)
-
•Change in cervical erosion and secretion
-
•Diminution in lactation when given immediately postpartum
-
•Cholestatic jaundice
-
•Migraine
-
•Allergic reaction, including rash, urticaria, angioedema
-
•Mental depression
-
•Reduced tolerance to carbohydrates
-
•Vaginal candidiasis
-
•Change in corneal curvature (steepening)
-
•Intolerance to contact lenses
The following adverse reactions have been reported in users of oral contraceptives and a causal association has been neither confirmed nor refuted:
-
•Pre-menstrual syndrome
-
•Cataracts
-
•Changes in appetite
-
•Cystitis-like syndrome
-
•Headache
-
•Nervousness
-
•Dizziness
-
•Hirsutism
-
•Loss of scalp hair
-
•Erythema multiforme
-
•Erythema nodosum
-
•Hemorrhagic eruption
-
•Vaginitis
-
•Porphyria
-
•Impaired renal function
-
•Hemolytic uremic syndrome
-
•Acne
-
•Changes in libido
-
•Colitis
-
•Budd-Chiari Syndrome
The following adverse reactions were also reported in clinical trials or during post-marketing experience: Infections and Infestations: vaginal infection, urinary tract infection; Psychiatric Disorders: mood altered, anxiety, insomnia; Gastrointestinal Disorders: flatulence, pancreatitis, diarrhea, constipation; Reproductive System and Breast Disorders: dysmenorrhea; ovarian cyst, vulvovaginal dryness; Neoplasms Benign, Malignant and Unspecified (Including Cysts and Polyps): benign breast neoplasm, fibroadenoma of breast, breast cyst; Nervous System Disorders: syncope, convulsion, paraesthesia; Eye Disorders: visual impairment, dry eye; Ear and Labyrinth Disorders: vertigo; Cardiac Disorders: tachycardia, palpitations; Vascular Disorders: hot flush; Respiratory, Thoracic and Mediastinal Disorders: dyspnoea; Hepatobiliary Disorders: hepatitis; Skin and Subcutaneous Tissue Disorders: night sweats, hyperhidrosis, photosensitivity reaction, pruritus; Musculoskeletal, Connective Tissue, and Bone Disorders: muscle spasms, pain in extremity, myalgia, back pain; General Disorders and Administration Site Conditions: chest pain, asthenic conditions.
Contraindications (CONTRAINDICATIONS)
Oral contraceptives should not be used in women who currently have the following conditions:
-
•Thrombophlebitis or thromboembolic disorders
-
•A past history of deep vein thrombophlebitis or thromboembolic disorders
-
•Known thrombophilic conditions
-
•Cerebral vascular or coronary artery disease (current or past history)
-
•Valvular heart disease with complications
-
•Persistent blood pressure values of ≥ 160 mm Hg systolic or ≥ 100 mg Hg diastolic 102
-
•Diabetes with vascular involvement
-
•Headaches with focal neurological symptoms
-
•Major surgery with prolonged immobilization
-
•Known or suspected carcinoma of the breast or personal history of breast cancer
-
•Carcinoma of the endometrium or other known or suspected estrogen-dependent neoplasia
-
•Undiagnosed abnormal genital bleeding
-
•Cholestatic jaundice of pregnancy or jaundice with prior pill use
-
•Acute or chronic hepatocellular disease with abnormal liver function
-
•Hepatic adenomas or carcinomas
-
•Known or suspected pregnancy
-
•Hypersensitivity to any component of this product
10. Carcinogenesis
See WARNINGS.
Hepatic Impairment
The effects of hepatic impairment on the pharmacokinetics of Tri-Sprintec have not been studied. However, steroid hormones may be poorly metabolized in women with impaired liver function (see PRECAUTIONS).
12. Nursing Mothers
Small amounts of oral contraceptive steroids have been identified in the milk of nursing mothers and a few adverse effects on the child have been reported, including jaundice and breast enlargement. In addition, combination oral contraceptives given in the postpartum period may interfere with lactation by decreasing the quantity and quality of breast milk. If possible, the nursing mother should be advised not to use combination oral contraceptives but to use other forms of contraception until she has completely weaned her child.
Special Populations
The effects of body weight, body surface area or age on the pharmacokinetics of Tri-Sprintec have not been studied.
8. Drug Interactions
Consult the labeling of concurrently-used drugs to obtain further information about interactions with hormonal contraceptives or the potential for enzyme alterations.
Effects of Other Drugs on Combined Hormonal Contraceptives
Substances Decreasing the Plasma Concentrations of COCs and Potentially Diminishing the Efficacy of COCs
Drugs or herbal products that induce certain enzymes, including cytochrome P450 3A4 (CYP3A4), may decrease the plasma concentrations of COCs and potentially diminish the effectiveness of CHCs or increase breakthrough bleeding. Some drugs or herbal products that may decrease the effectiveness of hormonal contraceptives include phenytoin, barbiturates, carbamazepine, bosentan, felbamate, griseofulvin, oxcarbazepine, rifampicin, topiramate, rifabutin, rufinamide, aprepitant, and products containing St. John’s wort. Interactions between hormonal contraceptives and other drugs may lead to breakthrough bleeding and/or contraceptive failure. Counsel women to use an alternative method of contraception or a back-up method when enzyme inducers are used with CHCs, and to continue back-up contraception for 28 days after discontinuing the enzyme inducer to ensure contraceptive reliability.
Substances Increasing the Plasma Concentrations of COCs
Coadministration of atorvastatin or rosuvastatin and certain COCs containing EE increase AUC values for EE by approximately 20 to 25%. Ascorbic acid and acetaminophen may increase plasma EE concentrations, possibly by inhibition of conjugation. CYP3A4 inhibitors such as itraconazole, voriconazole, fluconazole, grapefruit juice, or ketoconazole may increase plasma hormone concentrations.
Human Immunodeficiency Virus (HIV)/Hepatitis C virus (HCV) Protease Inhibitors and Non-Nucleoside Reverse Transcriptase Inhibitors
Significant changes (increase or decrease) in the plasma concentrations of estrogen and/or progestin have been noted in some cases of coadministration with HIV protease inhibitors (decrease [e.g., nelfinavir, ritonavir, darunavir/ritonavir, (fos)amprenavir/ritonavir, lopinavir/ritonavir, and tipranavir/ritonavir] or increase [e.g., indinavir and atazanavir/ritonavir]) /HCV protease inhibitors (decrease [e.g., boceprevir and telaprevir]) or with nonnucleoside reverse transcriptase inhibitors (decrease [e.g., nevirapine] or increase [e.g., etravirine]).
Colesevelam
Colesevelam, a bile acid sequestrant, given together with a combination oral hormonal contraceptive, has been shown to significantly decrease the AUC of EE. A drug interaction between the contraceptive and colesevelam was decreased when the two drug products were given 4 hours apart.
Effects of Combined Hormonal Contraceptives on Other Drugs
COCs containing EE may inhibit the metabolism of other compounds (e.g., cyclosporine, prednisolone, theophylline, tizanidine, and voriconazole) and increase their plasma concentrations. COCs have been shown to decrease plasma concentrations of acetaminophen, clofibric acid, morphine, salicylic acid, temazepam and lamotrigine. Significant decrease in plasma concentration of lamotrigine has been shown, likely due to induction of lamotrigine glucuronidation. This may reduce seizure control; therefore, dosage adjustments of lamotrigine may be necessary.
Women on thyroid hormone replacement therapy may need increased doses of thyroid hormone because serum concentrations of thyroid-binding globulin increases with use of COCs.
9. Interactions with Laboratory Tests
Certain endocrine and liver function tests and blood components may be affected by oral contraceptives:
a. Increased prothrombin and factors VII, VIII, IX, and X; decreased antithrombin 3; increased norepinephrine-induced platelet aggregability.
b. Increased thyroid binding globulin (TBG) leading to increased circulating total thyroid hormone, as measured by protein-bound iodine (PBI), T4 by column or by radioimmunoassay. Free T3 resin uptake is decreased, reflecting the elevated TBG, free T4 concentration is unaltered.
c. Other binding proteins may be elevated in serum.
d. Sex hormone binding globulins are increased and result in elevated levels of total circulating sex steroids; however, free or biologically active levels either decrease or remain unchanged.
e. Triglycerides may be increased and levels of various other lipids and lipoproteins may be affected.
f. Glucose tolerance may be decreased.
g. Serum folate levels may be depressed by oral contraceptive therapy. This may be of clinical significance if a woman becomes pregnant shortly after discontinuing oral contraceptives.
Pregnancy Category X
See CONTRAINDICATIONS and WARNINGS.
Clinical Pharmacology (CLINICAL PHARMACOLOGY)
Oral Contraception
Combination oral contraceptives act by suppression of gonadotropins. Although the primary mechanism of this action is inhibition of ovulation, other alterations include changes in the cervical mucus (which increase the difficulty of sperm entry into the uterus) and the endometrium (which reduce the likelihood of implantation).
Receptor binding studies, as well as studies in animals and humans, have shown that norgestimate and 17-deacetyl norgestimate, the major serum metabolite, combine high progestational activity with minimal intrinsic androgenicity.90-93
Norgestimate, in combination with ethinyl estradiol, does not counteract the estrogen-induced increases in sex hormone binding globulin (SHBG), resulting in lower serum testosterone.90,91,94
Acne
Acne is a skin condition with a multifactorial etiology, including androgen stimulation of sebum production. While the combination of ethinyl estradiol and norgestimate increases sex hormone binding globulin (SHBG) and decreases free testosterone, the relationship between these changes and a decrease in the severity of facial acne in otherwise healthy women with this skin condition has not been established.
Indications and Usage (INDICATIONS AND USAGE)
Tri-Sprintec® (norgestimate and ethinyl estradiol tablets USP) is indicated for the prevention of pregnancy in women who elect to use oral contraceptives as a method of contraception.
Tri-Sprintec (norgestimate and ethinyl estradiol tablets USP) is indicated for the treatment of moderate acne vulgaris in females at least 15 years of age, who have no known contraindications to oral contraceptive therapy and have achieved menarche. Tri-Sprintec (norgestimate and ethinyl estradiol tablets USP) should be used for the treatment of acne only if the patient desires an oral contraceptive for birth control.
Oral contraceptives are highly effective for pregnancy prevention. Table 2 lists the typical accidental pregnancy rates for users of combination oral contraceptives and other methods of contraception. The efficacy of these contraceptive methods, except sterilization, the IUD, and the Norplant® System, depends upon the reliability with which they are used. Correct and consistent use of methods can result in lower failure rates.
|
% of Women Experiencing an Unintended Pregnancy within the First Year of Use |
% of Women Continuing Use at One Year Among couples attempting to avoid pregnancy, the percentage who continue to use a method for one year.
|
||
|
Method |
Typical Use Among typical couples who initiate use of a method (not necessarily for the first time), the percentage who experience an accidental pregnancy during the first year if they do not stop use for any other reason.
|
Perfect Use Among couples who initiate use of a method (not necessarily for the first time) and who use it perfectly (both consistently and correctly), the percentage who experience an accidental pregnancy during the first year if they do not stop use for any other reason.
|
|
|
(1) |
(2) |
(3) |
(4) |
|
Chance The percents becoming pregnant in columns (2) and (3) are based on data from populations where contraception is not used and from women who cease using contraception in order to become pregnant. Among such populations, about 89% become pregnant within one year. This estimate was lowered slightly (to 85%) to represent the percent who would become pregnant within one year among women now relying on reversible methods of contraception if they abandoned contraception altogether.
|
85 |
85 |
|
|
Spermicides Foams, creams, gels, vaginal suppositories, and vaginal film.
|
26 |
6 |
40 |
|
Periodic abstinence |
25 |
63 |
|
|
Calendar |
9 |
||
|
Ovulation Method |
3 |
||
|
Sympto-Thermal Cervical mucus (ovulation) method supplemented by calendar in the pre-ovulatory and basal body temperature in the post-ovulatory phases.
|
2 |
||
|
Post-Ovulation |
1 |
||
|
Cap With spermicidal cream or jelly.
|
|||
|
Parous Women |
40 |
26 |
42 |
|
Nulliparous Women |
20 |
9 |
56 |
|
Sponge |
|||
|
Parous Women |
40 |
20 |
42 |
|
Nulliparous Women |
20 |
9 |
56 |
|
Diaphragm |
20 |
6 |
56 |
|
Withdrawal |
19 |
4 |
|
|
Condom Without spermicides.
|
|||
|
Female (Reality®) |
21 |
5 |
56 |
|
Male |
14 |
3 |
61 |
|
Pill |
5 |
71 |
|
|
Progestin Only |
0.5 |
||
|
Combined |
0.1 |
||
|
IUD |
|||
|
Progesterone T |
2 |
1.5 |
81 |
|
Copper T380A |
0.8 |
0.6 |
78 |
|
LNg 20 |
0.1 |
0.1 |
81 |
|
Depo-Provera® |
0.3 |
0.3 |
70 |
|
Norplant® and Norplant-2® |
0.05 |
0.05 |
88 |
|
Female Sterilization |
0.5 |
0.5 |
100 |
|
Male Sterilization |
0.15 |
0.10 |
100 |
|
Hatcher et al., 1998 Ref. #1. Emergency Contraceptive Pills: Treatment initiated within 72 hours after unprotected intercourse reduces the risk of pregnancy by at least 75%. The treatment schedule is one dose within 72 hours after unprotected intercourse, and a second dose 12 hours after the first dose. The Food and Drug Administration has declared the following brands of oral contraceptives to be safe and effective for emergency contraception: Ovral® (1 dose is 2 white pills), Alesse® (1 dose is 5 pink pills), Nordette® or Levlen® (1 dose is 2 light-orange pills), Lo/Ovral® (1 dose is 4 white pills), Triphasil® or Tri-Levlen® (1 dose is 4 yellow pills).
Lactational Amenorrhea Method: LAM is a highly effective, temporary method of contraception. However, to maintain effective protection against pregnancy, another method of contraception must be used as soon as menstruation resumes, the frequency or duration of breastfeeds is reduced, bottle feeds are introduced, or the baby reaches six months of age.
Source: Trussell J, Contraceptive efficacy. In Hatcher RA, Trussell J, Stewart F, Cates W, Stewart GK, Kowal D, Guest F, Contraceptive Technology: Seventeenth Revised Edition. New York NY: Irvington Publishers, 1998. |
Tri-Sprintec (norgestimate and ethinyl estradiol tablets USP) has not been studied for and is not indicated for use in emergency contraception.
In four clinical trials with Tri-Sprintec (norgestimate and ethinyl estradiol tablets USP), a total of 4,756 subjects completed 45,244 cycles, and the use-efficacy pregnancy rate was approximately 1 pregnancy per 100 women-years.
Tri-Sprintec (norgestimate and ethinyl estradiol tablets USP) was evaluated for the treatment of acne vulgaris in two randomized, double-blind, placebo-controlled, multicenter, Phase 3, six (28 day) cycle studies. 221 patients received Tri-Sprintec (norgestimate and ethinyl estradiol tablets USP) and 234 patients received placebo. Mean age at enrollment for both groups was 28 years. At the end of 6 months, the mean total lesion count changes from 55 to 31 (42% reduction) in patients treated with Tri-Sprintec (norgestimate and ethinyl estradiol tablets USP) and from 54 to 38 (27% reduction) in patients similarly treated with placebo. Table 3 summarizes the changes in lesion count for each type of lesion in the ITT population. Based on the investigator’s global assessment conducted at the final visit, patients treated with Tri-Sprintec (norgestimate and ethinyl estradiol tablets USP) showed a statistically significant improvement in total lesions compared to those treated with placebo.
|
Tri-Sprintec (N = 221) |
Placebo (N = 234) |
Difference in Counts Between |
|||
|
# of Lesions |
Counts |
% Reduction |
Counts |
% Reduction |
|
|
INFLAMMATORY LESIONS |
|||||
|
Baseline Mean |
19 |
19 |
|||
|
Sixth Month Mean |
10 |
48% |
13 |
30% |
3 (95% CI: -1.2, 5.1) |
|
NON-INFLAMMATORY LESIONS |
|||||
|
Baseline Mean |
36 |
35 |
|||
|
Sixth Month Mean |
22 |
34% |
25 |
21% |
3 (95% CI: -0.2, 7.8) |
|
TOTAL LESIONS |
|||||
|
Baseline Mean |
55 |
54 |
|||
|
Sixth Month Mean |
31 |
42% |
38 |
27% |
7 (95% CI: 2, 11.9) |
Drug Drug Interactions (Drug-Drug Interactions)
No formal drug-drug interaction studies were conducted with Tri-Sprintec. Interactions between contraceptive steroids and other drugs have been reported in the literature (see PRECAUTIONS).
Although norelgestromin and its metabolites inhibit a variety of P450 enzymes in human liver microsomes, under the recommended dosing regimen, the in vivo concentrations of norelgestromin and its metabolites, even at the peak serum levels, are relatively low compared to the inhibitory constant (Ki).
Additional Instructions (ADDITIONAL INSTRUCTIONS)
Breakthrough bleeding, spotting, and amenorrhea are frequent reasons for patients discontinuing oral contraceptives. In breakthrough bleeding, as in all cases of irregular bleeding from the vagina, nonfunctional causes should be borne in mind. In undiagnosed persistent or recurrent abnormal bleeding from the vagina, adequate diagnostic measures are indicated to rule out pregnancy or malignancy. If pathology has been excluded, time or a change to another formulation may solve the problem. Changing to an oral contraceptive with a higher estrogen content, while potentially useful in minimizing menstrual irregularity, should be done only if necessary since this may increase the risk of thromboembolic disease.
Use of oral contraceptives in the event of a missed menstrual period:
-
•If the patient has not adhered to the prescribed schedule, the possibility of pregnancy should be considered at the time of the first missed period and oral contraceptive use should be discontinued if pregnancy is confirmed.
-
•If the patient has adhered to the prescribed regimen and misses two consecutive periods, pregnancy should be ruled out.
Acne
The timing of initiation of dosing with Tri-Sprintec® for acne should follow the guidelines for use of Tri-Sprintec as an oral contraceptive. Consult the DOSAGE AND ADMINISTRATION section for oral contraceptives. The dosage regimen for Tri-Sprintec for treatment of facial acne, as available in a Blister Pack Tablet Dispenser, utilizes a 21-day active and a 7-day placebo schedule. Take one active tablet daily for 21 days followed by one white inactive tablet for 7 days. After 28 tablets have been taken, a new course is started the next day.
Principal Display Panel (PRINCIPAL DISPLAY PANEL)
Detailed Patient Labeling (DETAILED PATIENT LABELING)
PLEASE NOTE: This labeling is revised from time to time as important new medical information becomesavailable. Therefore, please review this labeling carefully.
This product (like all oral contraceptives) does not protect against HIV infection (AIDS) and other sexually transmitted diseases.
Tri-Sprintec® (norgestimate and ethinyl estradiol tablets USP)
Each gray tablet contains 0.18 mg norgestimate and 0.035 mg ethinyl estradiol. Each light blue tablet contains 0.215 mg norgestimate and 0.035 mg ethinyl estradiol. Each blue tablet contains 0.25 mg norgestimate and 0.035 mg ethinyl estradiol. Each white tablet contains inert ingredients.
INTRODUCTION
Any woman who considers using oral contraceptives (the birth control pill or the pill) should understand the benefits and risks of using this form of birth control. This patient labeling will give you much of the information you will need to make this decision and will also help you determine if you are at risk of developing any of the serious side effects of the pill. It will tell you how to use the pill properly so that it will be as effective as possible. However, this labeling is not a replacement for a careful discussion between you and your healthcare professional. You should discuss the information provided in this labeling with him or her, both when you first start taking the pill and during your revisits. You should also follow your healthcare professional’s advice with regard to regular check-ups while you are on the pill.
EFFECTIVENESS OF ORAL CONTRACEPTIVES FOR CONTRACEPTION
Oral contraceptives or “birth control pills” or “the pill” are used to prevent pregnancy and are more effective than most other nonsurgical methods of birth control. When they are taken correctly without missing any pills, the chance of becoming pregnant is approximately 1% per year (1 pregnancy per 100 women per year of use). Typical failure rates, including women who do not always take the pill correctly, are approximately 5% per year (5 pregnancies per 100 women per year of use). The chance of becoming pregnant increases with each missed pill during a menstrual cycle.
In comparison, typical failure rates for other nonsurgical methods of birth control during the first year of use are as follows:
Implant: < 1%
Injection: < 1%
IUD: 1 to 2%
Diaphragm with spermicides: 20%
Spermicides alone: 26%
Vaginal sponge: 20 to 40%
Female sterilization: < 1%
Male sterilization: < 1%
Cervical Cap with spermicides: 20 to 40%
Condom alone (male): 14%
Condom alone (female): 21%
Periodic abstinence: 25%
Withdrawal: 19%
No methods: 85%
Tri-Sprintec may also be taken to treat moderate acne if all of the following are true:
• You have started having menstrual cycles
• You are at least 15 years old
• Your healthcare professional says it is safe for you to use the pill
• You want to use the pill for birth control
WHO SHOULD NOT TAKE ORAL CONTRACEPTIVES
Dosage and Administration (DOSAGE AND ADMINISTRATION)
Oral Contraception
To achieve maximum contraceptive effectiveness, Tri-Sprintec® tablets must be taken exactly as directed and at intervals not exceeding 24 hours. The possibility of ovulation and conception prior to initiation of medication should be considered. Tri-Sprintec tablets are available in the Blister Pack Tablet Dispenser which is preset for a Sunday Start. Day 1 Start is also provided.
Sunday Start
When taking Tri-Sprintec® the first tablet should be taken on the first Sunday after menstruation begins. If the period begins on Sunday, the first tablet should be taken that day. Take one active tablet daily for 21 days followed by one white inactive tablet daily for 7 days. After 28 tablets have been taken, a new course is started the next day (Sunday). For the first cycle of a Sunday Start regimen, another method of contraception should be used until after the first seven consecutive days of administration.
If the patient misses one (1) active tablet in Weeks 1, 2, or 3, the tablet should be taken as soon as she remembers. If the patient misses two (2) active tablets in Week 1 or Week 2, the patient should take two (2) tablets the day she remembers and two (2) tablets the next day; and then continue taking one (1) tablet a day until she finishes the pack. The patient should be instructed to use a back-up method of birth control such as a condom or spermicide if she has sex in the seven (7) days after missing pills. If the patient misses two (2) active tablets in the third week or misses three (3) or more active tablets in a row, the patient should continue taking one tablet every day until Sunday. On Sunday the patient should throw out the rest of the pack and start a new pack that same day. The patient should be instructed to use a back-up method of birth control if she has sex in the seven (7) days after missing pills.
Complete instructions to facilitate patient counseling on proper pill usage may be found in the Detailed Patient Labeling (“How to Take the Pill” section).
Day 1 Start
The dosage of Tri-Sprintec® tablets, for the initial cycle of therapy, is one active tablet administered daily from the 1st day through the 21st day of the menstrual cycle, counting the first day of menstrual flow as “Day 1” followed by one white inactive tablet daily for 7 days. Tablets are taken without interruption for 28 days. After 28 tablets have been taken, a new course is started the next day.
If the patient misses one (1) active tablet in Weeks 1, 2, or 3, the tablet should be taken as soon as she remembers. If the patient misses two (2) active tablets in Week 1 or Week 2, the patient should take two (2) tablets the day she remembers and two (2) tablets the next day; and then continue taking one (1) tablet a day until she finishes the pack. The patient should be instructed to use a back-up method of birth control such as a condom or spermicide if she has sex in the seven (7) days after missing pills. If the patient misses two (2) active tablets in the third week or misses three (3) or more active tablets in a row, the patient should throw out the rest of the pack and start a new pack that same day. The patient should be instructed to use a back-up method of birth control if she has sex in the seven (7) days after missing pills.
Complete instructions to facilitate patient counseling on proper pill usage may be found in the Detailed Patient Labeling (“How to Take the Pill” section).
The use of Tri-Sprintec® tablets for contraception may be initiated 4 weeks postpartum in women who elect not to breastfeed. When the tablets are administered during the postpartum period, the increased risk of thromboembolic disease associated with the postpartum period must be considered. (See CONTRAINDICATIONS and WARNINGS concerning thromboembolic disease. See also PRECAUTIONS, Nursing Mothers.) The possibility of ovulation and conception prior to initiation of medication should be considered.
(See Discussion of Dose-Related Risk of Vascular Disease from Oral Contraceptives.)
Information for the Patient (INFORMATION FOR THE PATIENT)
See Patient Labeling printed below.
Package/label Display Panel (Package/Label Display Panel)
Pregnancy Due to Pill Failure (PREGNANCY DUE TO PILL FAILURE)
The incidence of pill failure resulting in pregnancy is approximately 5%, including women who do not always take the pills exactly as directed. If failure does occur, the risk to the fetus is minimal.
PREGNANCY AFTER STOPPING THE PILL
There may be some delay in becoming pregnant after you stop using oral contraceptives, especially if you had irregular menstrual cycles before you used oral contraceptives. It may be advisable to postpone conception until you begin menstruating regularly once you have stopped taking the pill and desire pregnancy.
There does not appear to be any increase in birth defects in newborn babies when pregnancy occurs soon after stopping the pill.
OVERDOSAGE
Serious ill effects have not been reported following ingestion of large doses of oral contraceptives by young children. Overdosage may cause nausea and withdrawal bleeding in females. In case of overdosage, contact your healthcare professional or pharmacist.
OTHER INFORMATION
Your healthcare professional will take a medical and family history before prescribing oral contraceptives and will examine you. The physical examination may be delayed to another time if you request it and the healthcare professional believes that it is a good medical practice to postpone it. You should be reexamined at least once a year. Be sure to inform your healthcare professional if there is a family history of any of the conditions listed previously in this leaflet. Be sure to keep all appointments with your healthcare professional, because this is a time to determine if there are early signs of side effects of oral contraceptive use.
Do not use the drug for any condition other than the one for which it was prescribed. This drug has been prescribed specifically for you; do not give it to others who may want birth control pills.
HEALTH BENEFITS FROM ORAL CONTRACEPTIVES
In addition to preventing pregnancy, use of combination oral contraceptives may provide certain benefits. They are:
-
•menstrual cycles may become more regular
-
•blood flow during menstruation may be lighter and less iron may be lost. Therefore, anemia due to iron deficiency is less likely to occur.
-
•pain or other symptoms during menstruation may be encountered less frequently
-
•ectopic (tubal) pregnancy may occur less frequently
-
•noncancerous cysts or lumps in the breast may occur less frequently
-
•acute pelvic inflammatory disease may occur less frequently
-
•oral contraceptive use may provide some protection against developing two forms of cancer: cancer of the ovaries and cancer of the lining of the uterus.
If you want more information about birth control pills, ask your healthcare professional or pharmacist. They have a more technical leaflet called the Professional Labeling, which you may wish to read.
Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.
Store at 20° to 25°C (68° to 77°F) [See USP Controlled Room Temperature].
PROTECT FROM LIGHT.
KEEP THIS AND ALL MEDICATIONS OUT OF THE REACH OF CHILDREN.
All brand names listed are the registered trademarks of their respective owners and are not trademarks of Teva Pharmaceuticals USA.
TEVA PHARMACEUTICALS USA
Sellersville, PA 18960
Rev. A 10/2013
Relabeled By:
Proficient Rx LP
Thousand Oaks, CA 91320
Noncontraceptive Health Benefits (NONCONTRACEPTIVE HEALTH BENEFITS)
The following noncontraceptive health benefits related to the use of combination oral contraceptives are supported by epidemiological studies which largely utilized oral contraceptive formulations containing estrogen doses exceeding 0.035 mg of ethinyl estradiol or 0.05 mg mestranol.73-78
Effects on menses:
-
•increased menstrual cycle regularity
-
•decreased blood loss and decreased incidence of iron deficiency anemia
-
•decreased incidence of dysmenorrhea
Effects related to inhibition of ovulation:
-
•decreased incidence of functional ovarian cysts
-
•decreased incidence of ectopic pregnancies
Other effects:
-
•decreased incidence of fibroadenomas and fibrocystic disease of the breast
-
•decreased incidence of acute pelvic inflammatory disease
-
•decreased incidence of endometrial cancer
-
•decreased incidence of ovarian cancer
Brief Summary Patient Package Insert (BRIEF SUMMARY PATIENT PACKAGE INSERT)
This product (like all oral contraceptives) does not protect against HIV infection (AIDS) and other sexually transmitted diseases.
Tri-Sprintec® (norgestimate and ethinyl estradiol tablets USP)
Each gray tablet contains 0.18 mg norgestimate and 0.035 mg ethinyl estradiol. Each light blue tablet contains 0.215 mg norgestimate and 0.035 mg ethinyl estradiol. Each blue tablet contains 0.25 mg norgestimate and 0.035 mg ethinyl estradiol. Each white tablet contains inert ingredients.
Oral contraceptives, also known as “birth control pills” or “the pill,” are taken to prevent pregnancy. When taken correctly to prevent pregnancy, oral contraceptives have a failure rate of approximately 1% per year (1 pregnancy per 100 women per year of use) when used without missing any pills. The typical failure rate is approximately 5% per year (5 pregnancies per 100 women per year of use) when women who miss pills are included. For most women oral contraceptives are also free of serious or unpleasant side effects. However, forgetting to take pills considerably increases the chances of pregnancy.
Tri-Sprintec may also be taken to treat moderate acne in females at least 15 years of age, who have started having menstrual periods, are able to take the pill and want to use the pill for birth control.
For the majority of women, oral contraceptives can be taken safely. But there are some women who are at high risk of developing certain serious diseases that can be fatal or may cause temporary or permanent disability. The risks associated with taking oral contraceptives increase significantly if you:
-
•smoke
-
•have high blood pressure, diabetes, high cholesterol
-
•have or have had clotting disorders, heart attack, stroke, angina pectoris, cancer of the breast or sex organs, jaundice, or malignant or benign liver tumors
Although cardiovascular disease risks may be increased with oral contraceptive use after age 40 in healthy, nonsmoking women (even with the newer low-dose formulations), there are also greater potential health risks associated with pregnancy in older women.
You should not take the pill if you suspect you are pregnant or have unexplained vaginal bleeding.
Tri Sprintec® 28 Day Regimen Carton Text (Tri-Sprintec® 28 Day Regimen Carton Text)
NDC 0555-9018-58
6 Blister Cards, 28 Tablets Each 28 Day
Tri-Sprintec®
(norgestimate and
ethinyl estradiol tablets USP)
Contains 6 blister cards, each containing 28 tablets. Each gray tablet
contains 0.18 mg norgestimate, USP and 0.035 mg ethinyl estradiol,
USP. Each light blue tablet contains 0.215 mg norgestimate, USP and
0.035 mg ethinyl estradiol, USP. Each blue tablet contains 0.25 mg
norgestimate, USP and 0.035 mg ethinyl estradiol, USP. Each white
tablet contains inert ingredients.
Rx only
Shaping
Women's Health®
TEVA
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:35:11.837857 · Updated: 2026-03-14T21:42:54.187107