These Highlights Do Not Include All The Information Needed To Use Abecma Safely And Effectively. See Full Prescribing Information For Abecma.
b90c1fe7-f5cc-464e-958a-af36e9c26d7c
60684-8
CELLULAR THERAPY
Drug Facts
Composition & Product
Identifiers & Packaging
Description
Boxed Warning 6/2025 Dosage and Administration ( 2.2 ) 11/2025 Dosage and Administration ( 2.2 , 2.3 ) 6/2025 Warnings and Precautions ( 5.2 , 5.3 ) 6/2025 Warnings and Precautions ( 5.2 , 5.3 ) 11/2025 Warnings and Precautions, ABECMA REMS ( 5.5 ) Removed 6/2025 Warnings and Precautions, Effects on Ability to Drive and Use Machines (5.11) Removed 6/2025
Indications and Usage
ABECMA is indicated for the treatment of adult patients with relapsed or refractory multiple myeloma after two or more prior lines of therapy including an immunomodulatory agent, a proteasome inhibitor, and an anti-CD38 monoclonal antibody.
Dosage and Administration
For autologous use only. For intravenous use only. • Do NOT use a leukodepleting filter. ( 2.2 ) • Administer a lymphodepleting chemotherapy regimen of cyclophosphamide and fludarabine before infusion of ABECMA. ( 2.2 ) • Confirm the patient's identity prior to infusion. ( 2.2 ) • Premedicate with acetaminophen and an H 1 -antihistamine. ( 2.2 ) • Avoid prophylactic use of dexamethasone or other systemic corticosteroids. ( 2.2 ) • Confirm availability of tocilizumab prior to infusion. ( 2.2 , 5.2 ) • Dosing of ABECMA is based on the number of chimeric antigen receptor (CAR)-positive T cells. ( 2.1 ) • The recommended dose range is 300 to 510 × 10 6 CAR-positive T cells. ( 2.1 )
Warnings and Precautions
• Hypersensitivity Reactions : Monitor for hypersensitivity reactions during infusion. ( 5.5 ) • Infections : Monitor patients for signs and symptoms of infection; treat appropriately. ( 5.6 ) • Prolonged Cytopenias : Patients may exhibit prolonged Grade 3 or higher cytopenias following ABECMA infusion. Monitor blood counts prior to and after ABECMA infusion. ( 5.7 ) • Hypogammaglobulinemia : Monitor and consider immunoglobulin replacement therapy. ( 5.8 ) • Secondary Malignancies : T cell malignancies have occurred following treatment of hematologic malignancies with BCMA- and CD19-directed genetically modified autologous T cell immunotherapies, including ABECMA. In the event that a secondary malignancy occurs after treatment with ABECMA, contact Bristol-Myers Squibb at 1-888-805-4555. ( 5.9 )
Contraindications
None.
Adverse Reactions
The following adverse reactions are described elsewhere in the labeling: • Early Death [see Warnings and Precautions (5.1) , Clinical Studies (14) ] • Cytokine Release Syndrome [see Warnings and Precautions (5.2) ] • Neurologic Toxicities [see Warnings and Precautions (5.3) ] • Hemophagocytic Lymphohistiocytosis (HLH)/Macrophage Activation Syndrome (MAS) [see Warnings and Precautions (5.4) ] • Hypersensitivity Reactions [see Warnings and Precautions (5.5) ] • Infections [see Warnings and Precautions (5.6) ] • Prolonged Cytopenias [see Warnings and Precautions (5.7) ] • Hypogammaglobulinemia [see Warnings and Precautions (5.8) ]
Drug Interactions
Drug/Laboratory Test Interactions HIV and the lentivirus used to make ABECMA have limited, short spans of identical genetic material (RNA). Therefore, some commercial HIV nucleic acid tests may yield false-positive results in patients who have received ABECMA.
Storage and Handling
ABECMA is supplied in one or more infusion bag(s) (see below) containing a frozen suspension of genetically modified autologous T cells in 5% DMSO. Each infusion bag of ABECMA is overwrapped with a transparent plastic sleeve that is folded to the back of the infusion bag and individually packed in a metal cassette. ABECMA is stored in the vapor phase of liquid nitrogen and supplied in a liquid nitrogen dry vapor shipper. An RFI Certificate is affixed inside the shipper. • 50 mL infusion bag and metal cassette (NDC 59572-515-01) • 250 mL infusion bag and metal cassette (NDC 59572-515-02) • 500 mL infusion bag and metal cassette (NDC 59572-515-03) Match the identity of the patient with the patient identifiers on the cassette(s) and infusion bag(s) upon receipt.
How Supplied
ABECMA is supplied in one or more infusion bag(s) (see below) containing a frozen suspension of genetically modified autologous T cells in 5% DMSO. Each infusion bag of ABECMA is overwrapped with a transparent plastic sleeve that is folded to the back of the infusion bag and individually packed in a metal cassette. ABECMA is stored in the vapor phase of liquid nitrogen and supplied in a liquid nitrogen dry vapor shipper. An RFI Certificate is affixed inside the shipper. • 50 mL infusion bag and metal cassette (NDC 59572-515-01) • 250 mL infusion bag and metal cassette (NDC 59572-515-02) • 500 mL infusion bag and metal cassette (NDC 59572-515-03) Match the identity of the patient with the patient identifiers on the cassette(s) and infusion bag(s) upon receipt.
Medication Information
Warnings and Precautions
• Hypersensitivity Reactions : Monitor for hypersensitivity reactions during infusion. ( 5.5 ) • Infections : Monitor patients for signs and symptoms of infection; treat appropriately. ( 5.6 ) • Prolonged Cytopenias : Patients may exhibit prolonged Grade 3 or higher cytopenias following ABECMA infusion. Monitor blood counts prior to and after ABECMA infusion. ( 5.7 ) • Hypogammaglobulinemia : Monitor and consider immunoglobulin replacement therapy. ( 5.8 ) • Secondary Malignancies : T cell malignancies have occurred following treatment of hematologic malignancies with BCMA- and CD19-directed genetically modified autologous T cell immunotherapies, including ABECMA. In the event that a secondary malignancy occurs after treatment with ABECMA, contact Bristol-Myers Squibb at 1-888-805-4555. ( 5.9 )
Indications and Usage
ABECMA is indicated for the treatment of adult patients with relapsed or refractory multiple myeloma after two or more prior lines of therapy including an immunomodulatory agent, a proteasome inhibitor, and an anti-CD38 monoclonal antibody.
Dosage and Administration
For autologous use only. For intravenous use only. • Do NOT use a leukodepleting filter. ( 2.2 ) • Administer a lymphodepleting chemotherapy regimen of cyclophosphamide and fludarabine before infusion of ABECMA. ( 2.2 ) • Confirm the patient's identity prior to infusion. ( 2.2 ) • Premedicate with acetaminophen and an H 1 -antihistamine. ( 2.2 ) • Avoid prophylactic use of dexamethasone or other systemic corticosteroids. ( 2.2 ) • Confirm availability of tocilizumab prior to infusion. ( 2.2 , 5.2 ) • Dosing of ABECMA is based on the number of chimeric antigen receptor (CAR)-positive T cells. ( 2.1 ) • The recommended dose range is 300 to 510 × 10 6 CAR-positive T cells. ( 2.1 )
Contraindications
None.
Adverse Reactions
The following adverse reactions are described elsewhere in the labeling: • Early Death [see Warnings and Precautions (5.1) , Clinical Studies (14) ] • Cytokine Release Syndrome [see Warnings and Precautions (5.2) ] • Neurologic Toxicities [see Warnings and Precautions (5.3) ] • Hemophagocytic Lymphohistiocytosis (HLH)/Macrophage Activation Syndrome (MAS) [see Warnings and Precautions (5.4) ] • Hypersensitivity Reactions [see Warnings and Precautions (5.5) ] • Infections [see Warnings and Precautions (5.6) ] • Prolonged Cytopenias [see Warnings and Precautions (5.7) ] • Hypogammaglobulinemia [see Warnings and Precautions (5.8) ]
Drug Interactions
Drug/Laboratory Test Interactions HIV and the lentivirus used to make ABECMA have limited, short spans of identical genetic material (RNA). Therefore, some commercial HIV nucleic acid tests may yield false-positive results in patients who have received ABECMA.
Storage and Handling
ABECMA is supplied in one or more infusion bag(s) (see below) containing a frozen suspension of genetically modified autologous T cells in 5% DMSO. Each infusion bag of ABECMA is overwrapped with a transparent plastic sleeve that is folded to the back of the infusion bag and individually packed in a metal cassette. ABECMA is stored in the vapor phase of liquid nitrogen and supplied in a liquid nitrogen dry vapor shipper. An RFI Certificate is affixed inside the shipper. • 50 mL infusion bag and metal cassette (NDC 59572-515-01) • 250 mL infusion bag and metal cassette (NDC 59572-515-02) • 500 mL infusion bag and metal cassette (NDC 59572-515-03) Match the identity of the patient with the patient identifiers on the cassette(s) and infusion bag(s) upon receipt.
How Supplied
ABECMA is supplied in one or more infusion bag(s) (see below) containing a frozen suspension of genetically modified autologous T cells in 5% DMSO. Each infusion bag of ABECMA is overwrapped with a transparent plastic sleeve that is folded to the back of the infusion bag and individually packed in a metal cassette. ABECMA is stored in the vapor phase of liquid nitrogen and supplied in a liquid nitrogen dry vapor shipper. An RFI Certificate is affixed inside the shipper. • 50 mL infusion bag and metal cassette (NDC 59572-515-01) • 250 mL infusion bag and metal cassette (NDC 59572-515-02) • 500 mL infusion bag and metal cassette (NDC 59572-515-03) Match the identity of the patient with the patient identifiers on the cassette(s) and infusion bag(s) upon receipt.
Description
Boxed Warning 6/2025 Dosage and Administration ( 2.2 ) 11/2025 Dosage and Administration ( 2.2 , 2.3 ) 6/2025 Warnings and Precautions ( 5.2 , 5.3 ) 6/2025 Warnings and Precautions ( 5.2 , 5.3 ) 11/2025 Warnings and Precautions, ABECMA REMS ( 5.5 ) Removed 6/2025 Warnings and Precautions, Effects on Ability to Drive and Use Machines (5.11) Removed 6/2025
Section 42229-5
Preparing Patient for ABECMA Infusion
Confirm the availability of ABECMA prior to starting the lymphodepleting chemotherapy regimen.
Section 42231-1
|
MEDICATION GUIDE
ABECMA® (uh-BEK-muh) (idecabtagene vicleucel) |
|---|
| This Medication Guide has been approved by the U.S. Food and Drug Administration. Revised: November 2025 |
|
Read this Medication Guide before you start your ABECMA treatment. The more you know about your treatment, the more active you can be in your care. Talk with your healthcare provider if you have questions about your health condition or treatment. Reading this Medication Guide does not take the place of talking with your healthcare provider about your treatment. |
|
What is the most important information I should know about ABECMA?
It is important that you tell your healthcare providers that you have received ABECMA and to show them your ABECMA Patient Wallet Card. Your healthcare provider may give you other medicines to treat your side effects. |
|
What is ABECMA?
|
|
How will I receive ABECMA?
|
|
What should I avoid after receiving ABECMA?
|
|
What are the possible or reasonably likely side effects of ABECMA?
In a study comparing ABECMA to standard regimen, a higher proportion of patients experienced death within the first nine months from randomization in the ABECMA arm compared to the standard regimens arm. This higher rate of early death was mainly observed before receiving ABECMA with the main reason being progression of multiple myeloma. There was also an increase in the rate of death from adverse events after ABECMA. ABECMA can cause a very common side effect called cytokine release syndrome or CRS, which can be severe or fatal. Symptoms of CRS include fever, difficulty breathing, dizziness or light-headedness, nausea, headache, fast heartbeat, low blood pressure, or fatigue. Tell your healthcare provider right away if you develop fever or any of these other symptoms after receiving ABECMA. ABECMA can increase the risk of life-threatening infections that may lead to death. Tell your healthcare provider right away if you develop fever, chills, or any signs or symptoms of an infection. ABECMA can lower one or more types of your blood cells (red blood cells, white blood cells, or platelets), which may make you feel weak or tired or increase your risk of severe infection or bleeding. After treatment, your healthcare provider will test your blood to check for this. Tell your healthcare provider right away if you get a fever, are feeling tired, or have bruising or bleeding. ABECMA may increase your risk of getting cancers including certain types of blood cancers. Your healthcare provider should monitor you for this. Having ABECMA in your blood may cause a false-positive human immunodeficiency virus (HIV) test result by some commercial tests. These are not all the possible side effects of ABECMA. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. |
|
General information about the safe and effective use of ABECMA
|
Section 43683-2
Section 44425-7
Store ABECMA frozen in the vapor phase of liquid nitrogen (less than or equal to minus 130°C).
Thaw ABECMA prior to infusion [see Dosage and Administration (2.2)].
2.1 Dose
For autologous use only. For intravenous use only.
ABECMA is provided as a single dose for infusion containing a suspension of chimeric antigen receptor (CAR)-positive T cells in one or more infusion bags. The recommended dose range is 300 to 510 × 106 CAR-positive T cells.
See the accompanying Release for Infusion Certificate (RFI Certificate) for additional information pertaining to dose [see How Supplied/Storage and Handling (16)].
15 References
-
1.Lee DW, Gardner R, Porter DL, et al. Current concepts in the diagnosis and management of cytokine release syndrome. Blood 2014; 124(2): 188-95. Errata in Blood: 2015;126(8):1048. and 2016;128(11):1533.
-
2.Kumar S, Paiva B, Anderson KC, et al. International Myeloma Working Group consensus criteria for response and minimal residual disease assessment in multiple myeloma. Lancet Oncol 2016; 17(8): e328-46.
8.1 Pregnancy
Risk Summary
There are no available data with ABECMA use in pregnant women. No animal reproductive and developmental toxicity studies have been conducted with ABECMA to assess whether it can cause fetal harm when administered to a pregnant woman.
It is not known if ABECMA has the potential to be transferred to the fetus. Based on the mechanism of action, if the transduced cells cross the placenta, they may cause fetal toxicity, including plasma cell aplasia or hypogammaglobulinemia. Therefore, ABECMA is not recommended for women who are pregnant, and pregnancy after ABECMA infusion should be discussed with the treating physician. Assess immunoglobulin levels in newborns of mothers treated with ABECMA.
The estimated background risk of major birth defects and miscarriage for the indicated population is unknown. The estimated background risk in the U.S. general population of major birth defects is 2% to 4% and of miscarriage is 15% to 20% of clinically recognized pregnancies.
8.2 Lactation
Risk Summary
There is no information regarding the presence of ABECMA in human milk, the effect on the breastfed infant, and the effects on milk production. The developmental and health benefits of breastfeeding should be considered along with the mother's clinical need for ABECMA and any potential adverse effects on the breastfed infant from ABECMA or from the underlying maternal condition.
11 Description
ABECMA is a BCMA-directed genetically modified autologous T cell immunotherapy product consisting of a patient's own T cells that are harvested and genetically modified ex vivo through transduction with an anti-BCMA02 chimeric antigen receptor (CAR) lentiviral vector (LVV). Autologous T cells transduced with the anti-BCMA02 CAR LVV express the anti-BCMA CAR on the T cell surface. The CAR is comprised of a murine extracellular single-chain variable fragment (scFv) specific for recognizing B cell maturation antigen (BCMA) followed by a human CD8α hinge and transmembrane domain fused to the T cell cytoplasmic signaling domains of CD137 (4-1BB) and CD3ζ chain, in tandem. Binding of ABECMA to BCMA-expressing target cells leads to signaling initiated by CD3ζ and 4-1BB domains, and subsequent CAR-positive T cell activation. Antigen-specific activation of ABECMA results in CAR-positive T cell proliferation, cytokine secretion, and subsequent cytolytic killing of BCMA-expressing cells.
ABECMA is prepared from the patient's peripheral blood mononuclear cells (PBMCs), which are obtained via a standard leukapheresis procedure. The mononuclear cells are enriched for T cells, through activation with anti-CD3 and anti-CD28 antibodies in the presence of IL-2, which are then transduced with the replication-incompetent lentiviral vector containing the anti-BCMA CAR transgene. The transduced T cells are expanded in cell culture, washed, formulated into a suspension, and cryopreserved. The product must pass a sterility test before release for shipping as a frozen suspension in one or more patient-specific infusion bag(s). The product is thawed prior to infusion back into the patient [see Dosage and Administration (2.3) and How Supplied/Storage and Handling (16)].
The ABECMA formulation contains 50% Plasma-Lyte A and 50% CryoStor® CS10, resulting in a final DMSO concentration of 5%.
5.6 Infections
ABECMA should not be administered to patients with active infections or inflammatory disorders. Severe, life‑threatening, or fatal infections occurred in patients after ABECMA infusion.
In all patients receiving ABECMA in Study 1 and Study 2, infections (all grades) occurred in 61% of patients. Grade 3 or 4 infections occurred in 21% of patients. Grade 3 or 4 infections with an unspecified pathogen occurred in 12%, viral infections in 7%, bacterial infections in 4.3%, and fungal infections in 1.4% of patients. Overall, 15 patients had Grade 5 infections (4.3%); 8 patients (2.3%) with infections of pathogen unspecified, 3 patients (0.9%) with fungal infections, 3 patients (0.9%) with viral infections, and 1 patient (0.3%) with bacterial infection.
Monitor patients for signs and symptoms of infection before and after ABECMA infusion and treat appropriately. Administer prophylactic, pre-emptive, and/or therapeutic antimicrobials according to standard institutional guidelines.
Febrile neutropenia was observed in 38% (133/349) of patients after ABECMA infusion and may be concurrent with CRS. In the event of febrile neutropenia, evaluate for infection and manage with broad-spectrum antibiotics, fluids, and other supportive care as medically indicated.
5.1 Early Death
In Study 1, a randomized (2:1), controlled trial, a higher proportion of patients experienced death within nine months after randomization in the ABECMA arm (45/254; 18%) compared to the standard regimens arm (15/132; 11%) [see Clinical Studies (14)]. Early deaths occurred in 8% (20/254) and 0% prior to ABECMA infusion and standard regimen administration, respectively, and 10% (25/254) and 11% (15/132) after ABECMA infusion and standard regimen administration, respectively. Out of the 20 deaths that occurred prior to ABECMA infusion, 15 occurred from disease progression, 3 occurred from adverse events and 2 occurred from unknown causes. Out of the 25 deaths that occurred after ABECMA infusion, 10 occurred from disease progression, 11 occurred from adverse events, and 4 occurred from unknown causes.
8.4 Pediatric Use
The safety and efficacy of ABECMA in pediatric patients have not been established.
8.5 Geriatric Use
In the clinical trials of ABECMA, 141 (40%) of the 349 patients were 65 years of age or older and 16/349 (4.6%) patients were 75 years of age or older. In Study 2, all five cases of Grade 3 neurotoxicity occurred in patients ≥65 years of age (66 to 74 years). No clinically important differences in effectiveness of ABECMA were observed between these patients and patients younger than 65 years of age.
2.2 Administration
ABECMA is for autologous use only. The patient's identity must match the patient identifiers on the ABECMA cassette(s) and infusion bag(s). Do not infuse ABECMA if the information on the patient-specific label(s) does not match the intended patient.
12.6 Immunogenicity
The observed incidence of anti-drug antibodies is highly dependent on the sensitivity and specificity of the assay. Differences in assay methods preclude meaningful comparisons of the incidence of anti-drug antibodies in the studies described below with the incidence of anti-drug antibodies in other studies, including those of ABECMA or of other similar products.
In Study 1 and Study 2, humoral immunogenicity of ABECMA was measured by determination of anti-CAR antibody in serum pre- and post-administration. In the clinical studies, 2.6% of patients (9/349) tested positive for pre-infusion anti-CAR antibodies and treatment-induced anti-CAR antibodies were detected in 53% (186/349) of the patients. There is no identified clinically significant impact of pre-existing or post-infusion anti-CAR antibodies on the cellular expansion, safety, or effectiveness of ABECMA.
4 Contraindications
None.
6 Adverse Reactions
The following adverse reactions are described elsewhere in the labeling:
-
•Early Death [see Warnings and Precautions (5.1), Clinical Studies (14)]
-
•Cytokine Release Syndrome [see Warnings and Precautions (5.2) ]
-
•Neurologic Toxicities [see Warnings and Precautions (5.3) ]
-
•Hemophagocytic Lymphohistiocytosis (HLH)/Macrophage Activation Syndrome (MAS) [see Warnings and Precautions (5.4) ]
-
•Hypersensitivity Reactions [see Warnings and Precautions (5.5) ]
-
•Infections [see Warnings and Precautions (5.6) ]
-
•Prolonged Cytopenias [see Warnings and Precautions (5.7) ]
-
•Hypogammaglobulinemia [see Warnings and Precautions (5.8) ]
7 Drug Interactions
Drug/Laboratory Test Interactions
HIV and the lentivirus used to make ABECMA have limited, short spans of identical genetic material (RNA). Therefore, some commercial HIV nucleic acid tests may yield false-positive results in patients who have received ABECMA.
12.2 Pharmacodynamics
Following ABECMA infusion, pharmacodynamic responses of CAR activation and anti-tumor efficacy were evaluated. Peak elevation of plasma cytokines, chemokines, and soluble immune mediators occurred within 14 days of ABECMA infusion and returned to baseline levels within one month.
Rapid decreases in tumor markers associated with clinical response, including serum levels of soluble BCMA, and bone marrow CD138+ cells, as well as minimal residual disease (MRD) negative responses, were observed within the first month following ABECMA infusion.
12.3 Pharmacokinetics
Following ABECMA infusion, the CAR-positive T cells proliferate and undergo rapid multi-log expansion followed by a bi-exponential decline. The median time of maximal expansion in peripheral blood (Tmax) occurred 11 days after infusion.
ABECMA can persist in peripheral blood for up to 1 year post-infusion. A summary of Tmax, AUC0-28days, and Cmax from Study 1 and Study 2 is provided in Table 7.
| AUC0-28days=area under the curve of the transgene level from time of dose to 28 days post-infusion; Cmax=the maximum transgene level; ddPCR=droplet digital polymerase chain reaction; qPCR=quantitative polymerase chain reaction; PK=pharmacokinetics; Tmax=time of maximum observed transgene level. a The PK parameters of Study 1 were determined by time course of transgene copies per microgram of DNA extracted from whole blood as quantified by droplet digital PCR (ddPCR). b The PK parameters of Study 2 were determined by time course of transgene copies per microgram of DNA extracted from CD3+ sorted cells as quantified by quantitative polymerase chain reaction (qPCR). |
|||
| Note: The PK parameters should not be directly compared between Study 1 and Study 2 due to different primary PK assays used in these two studies. | |||
|
Pharmacokinetic Parameter |
Summary Statistic |
Study 1
Total CAR-Positive T Cells (Quantified by ddPCR)a |
Study 2 Total [300 to 460 × 106] CAR-Positive T Cells (Quantified by qPCR)b |
|
Tmax (days) |
Median (Range) |
11 (4-31) |
11 (7-28) N=99 |
|
Cmax (copies/mcg) |
Geometric mean (geometric CV%) |
117,557 (215) N=207 |
256,333 (165) N=99 |
|
AUC0-28days
|
Geometric mean (geometric CV%) |
1,098,862 (228) |
3,088,455 (190) N=98 |
ABECMA transgene levels were positively associated with objective tumor response (partial response or better). Among patients who received ABECMA in Study 1, the median Cmax levels in responders (N=172) were approximately 6.5-fold higher compared to the corresponding levels in non-responders (N=35). Median AUC0-28days in responders (N=172) was approximately 6.1-fold higher than non-responders (N=33). Among patients who received ABECMA in Study 2, the median Cmax levels in responders (N=72) were approximately 4.6-fold higher than the corresponding levels in non-responders (N=27). Median AUC0-28days in responders (N=72) was approximately 5.6-fold higher than non-responders (N=26).
Tocilizumab or Siltuximab and Corticosteroid Use
Some patients required tocilizumab or siltuximab and/or corticosteroid for the management of CRS. ABECMA can continue to expand and persist following tocilizumab or siltuximab or corticosteroid administration [see Warnings and Precautions (5.2)].
In Study 2, patients with CRS treated with tocilizumab had higher ABECMA cellular expansion levels, as measured by 1.3‑fold and 1.6-fold higher median Cmax (N=67) and AUC0‑28days (N=66), respectively, compared to patients who did not receive tocilizumab (N=59 for Cmax and N=58 for AUC0‑28days).
Patients with CRS treated with corticosteroids had higher ABECMA cellular expansion levels, as measured by 1.7-fold and 2.2-fold higher median Cmax (N=18) and AUC0‑28days (N=18), respectively, compared to patients who did not receive corticosteroids (N=108 for Cmax and N=106 for AUC0‑28days).
Similar trend was observed in Study 1.
Specific Populations
Geriatric
Age (range: 30 to 81 years) had no significant impact on expansion parameters [see Use in Special Populations (8.5)].
Pediatric
The pharmacokinetics of ABECMA in patients less than 18 years of age have not been evaluated.
Patients with Hepatic/Renal Impairment
Hepatic and renal impairment studies of ABECMA were not conducted.
Patients with Other Intrinsic Factors
Gender, race, and ethnicity had no significant impact on ABECMA expansion parameters. Patients with lower body weight had higher expansion. Due to high variability in pharmacokinetic cellular expansion, the overall effect of weight on the pharmacokinetics of ABECMA is considered to be not clinically relevant.
1 Indications and Usage
ABECMA is indicated for the treatment of adult patients with relapsed or refractory multiple myeloma after two or more prior lines of therapy including an immunomodulatory agent, a proteasome inhibitor, and an anti-CD38 monoclonal antibody.
12.1 Mechanism of Action
ABECMA is a chimeric antigen receptor (CAR)-positive T cell therapy targeting B-cell maturation antigen (BCMA), which is expressed on the surface of normal and malignant plasma cells. The CAR construct includes an anti-BCMA scFv-targeting domain for antigen specificity, a transmembrane domain, a CD3-zeta T cell activation domain, and a 4-1BB costimulatory domain. Antigen-specific activation of ABECMA results in CAR-positive T cell proliferation, cytokine secretion, and subsequent cytolytic killing of BCMA-expressing cells.
5.7 Prolonged Cytopenias
Patients may exhibit prolonged cytopenias following lymphodepleting chemotherapy and ABECMA infusion.
In patients receiving ABECMA in Study 1 and Study 2, 40% of patients (139/349) experienced prolonged Grade 3 or 4 neutropenia and 42% (145/349) experienced prolonged Grade 3 or 4 thrombocytopenia that had not resolved by Month 1 following ABECMA infusion. In 89% (123/139) of patients who recovered from Grade 3 or 4 neutropenia after Month 1, the median time to recovery from ABECMA infusion was 1.9 months. In 76% (110/145) of patients who recovered from Grade 3 or 4 thrombocytopenia, the median time to recovery was 1.9 months. Five patients underwent stem cell therapy for hematopoietic reconstitution due to prolonged cytopenia. The rate of Grade 3 or 4 thrombocytopenia was 62% (44/71) and 56% (135/241) for patients treated in dose range of 460 to 510 × 106 CAR-positive T cells and 300 to 460 × 106 CAR-positive T cells, respectively.
Monitor blood counts prior to and after ABECMA infusion. Manage cytopenia with myeloid growth factor and blood product transfusion support according to local institutional guidelines.
5.3 Neurologic Toxicities
Neurologic toxicities, including immune-effector cell-associated neurotoxicity (ICANS), which may be severe or life-threatening, occurred concurrently with CRS, after CRS resolution, or in the absence of CRS following treatment with ABECMA.
In patients receiving ABECMA in Study 1 and Study 2, CAR T cell-associated neurotoxicity occurred in 40% (139/349), including Grade 3 in 4% (14/349) and Grade 4 in 0.6% (2/349) of patients. The median time to onset of neurotoxicity was 2 days (range: 1 to 148 days). The median duration of CAR T cell-associated neurotoxicity was 8 days (range: 1 to 720 days) in all patients including those with ongoing neurologic events at the time of death or data cut off. CAR T cell-associated neurotoxicity resolved in 123 of 139 (88%) patients and median time to resolution was 5 days (range: 1 to 245 days). One-hundred and thirty four out of 349 (38%) patients with neurotoxicity had CRS. The onset of neurotoxicity during CRS was observed in 93 patients, before the onset of CRS in 12 patients, and after the CRS event in 29 patients. The rate of Grade 3 or 4 CAR T cell-associated neurotoxicity was 5.6% (4/71) and 3.7% (9/241) for patients treated in dose range of 460 to 510 × 106 CAR-positive T cells and 300 to 460 × 106 CAR-positive T cells, respectively. The most frequent (≥5%) manifestations of CAR T cell-associated neurotoxicity include encephalopathy (21%), headache (15%), dizziness (8%), delirium (6%), and tremor (6%).
At the safety update for Study 1, one patient developed fatal neurotoxicity 43 days after ABECMA. In Study 2, one patient had ongoing Grade 2 neurotoxicity at the time of death. Two patients had ongoing Grade 1 tremor at the time of data cutoff.
Cerebral edema has been associated with ABECMA in a patient in another study in multiple myeloma. Grade 3 myelitis and Grade 3 parkinsonism have occurred after treatment with ABECMA in another study in multiple myeloma.
Monitor patients at least daily for seven days following ABECMA infusion for signs and symptoms of neurologic toxicities. Rule out other causes of neurologic symptoms. Continue to monitor patients for signs or symptoms of neurologic toxicities for at least one week after infusion and treat promptly. Neurologic toxicity should be managed with supportive care and/or corticosteroids as needed [see Dosage and Administration (2.2) , (2.3)]. Advise patients to avoid driving for at least one week following infusion.
Counsel patients to seek immediate medical attention should signs or symptoms of neurologic toxicity occur at any time [see Patient Counseling Information (17)].
5.8 Hypogammaglobulinemia
Plasma cell aplasia and hypogammaglobulinemia can occur in patients receiving treatment with ABECMA.
In all patients receiving ABECMA in Study 1 and Study 2, hypogammaglobulinemia was reported as an adverse event in 13% (46/349) of patients; laboratory IgG levels fell below 500 mg/dL after infusion in 37% (130/349) of patients treated with ABECMA.
Hypogammaglobulinemia either as an adverse reaction or laboratory IgG level below 500 mg/dL after infusion occurred in 45% (158/349) of patients treated with ABECMA. Forty-one percent of patients received intravenous immunoglobulin (IVIG) post-ABECMA for serum IgG <400 mg/dL.
Monitor immunoglobulin levels after treatment with ABECMA and administer IVIG for IgG <400 mg/dL. Manage per local institutional guidelines, including infection precautions and antibiotic or antiviral prophylaxis.
Use of Live Vaccines
The safety of immunization with live viral vaccines during or following ABECMA treatment has not been studied. Vaccination with live virus vaccines is not recommended for at least six weeks prior to the start of lymphodepleting chemotherapy, during ABECMA treatment, and until immune recovery following treatment with ABECMA.
5 Warnings and Precautions
-
•Hypersensitivity Reactions: Monitor for hypersensitivity reactions during infusion. (5.5)
-
•Infections: Monitor patients for signs and symptoms of infection; treat appropriately. (5.6)
-
•Prolonged Cytopenias: Patients may exhibit prolonged Grade 3 or higher cytopenias following ABECMA infusion. Monitor blood counts prior to and after ABECMA infusion. (5.7)
-
•Hypogammaglobulinemia: Monitor and consider immunoglobulin replacement therapy. (5.8)
-
•Secondary Malignancies: T cell malignancies have occurred following treatment of hematologic malignancies with BCMA- and CD19-directed genetically modified autologous T cell immunotherapies, including ABECMA. In the event that a secondary malignancy occurs after treatment with ABECMA, contact Bristol-Myers Squibb at 1-888-805-4555. (5.9)
5.9 Secondary Malignancies
Patients treated with ABECMA may develop secondary malignancies. In Study 1, myeloid neoplasms (four cases of myelodysplastic syndrome and one case of acute myeloid leukemia) occurred in 2.2% (5/222) of patients following treatment with ABECMA compared to none in the standard regimens arm at the time of the safety update. The median time to onset of myeloid neoplasm from ABECMA infusion was 338 days (Range: 277 to 794 days). Three of these five patients have died following the development of myeloid neoplasm. One out of the five cases of myeloid neoplasm occurred after initiation of subsequent antimyeloma therapy.
T cell malignancies have occurred following treatment of hematologic malignancies with BCMA- and CD19‑directed genetically modified autologous T cell immunotherapies, including ABECMA. Mature T cell malignancies, including CAR-positive tumors, may present as soon as weeks following infusion, and may include fatal outcomes [see Boxed Warning, Adverse Reactions (6.3), Patient Counseling Information (17)].
Monitor life-long for secondary malignancies. In the event that a secondary malignancy occurs, contact
Bristol-Myers Squibb at 1‑888‑805‑4555 for reporting and to obtain instructions on collection of patient samples for testing of secondary malignancy.
2 Dosage and Administration
For autologous use only. For intravenous use only.
-
•Do NOT use a leukodepleting filter. (2.2)
-
•Administer a lymphodepleting chemotherapy regimen of cyclophosphamide and fludarabine before infusion of ABECMA. (2.2)
-
•Confirm the patient's identity prior to infusion. (2.2)
-
•Premedicate with acetaminophen and an H1-antihistamine. (2.2)
-
•Avoid prophylactic use of dexamethasone or other systemic corticosteroids. (2.2)
-
•Confirm availability of tocilizumab prior to infusion. (2.2, 5.2)
-
•Dosing of ABECMA is based on the number of chimeric antigen receptor (CAR)-positive T cells. (2.1)
-
•The recommended dose range is 300 to 510 × 106 CAR-positive T cells. (2.1)
3 Dosage Forms and Strengths
A single dose of ABECMA contains a cell suspension of 300 to 510 × 106 chimeric antigen receptor (CAR)-positive T cells in one or more infusion bags [see How Supplied/Storage and Handling (16)].
6.2 Postmarketing Experience
Because adverse events to marketed products are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to product exposure.
The following adverse event has been identified during postmarketing use of ABECMA:
Nervous system disorders: Immune effector cell-associated neurotoxicity syndrome (ICANS).
The following adverse event has been identified during postmarketing use of BCMA- or CD19-directed genetically modified autologous T cell immunotherapies:
Neoplasms: T cell malignancies.
5.5 Hypersensitivity Reactions
Allergic reactions may occur with the infusion of ABECMA. Serious hypersensitivity reactions, including anaphylaxis, may be due to dimethyl sulfoxide (DMSO) in ABECMA.
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in clinical practice.
The safety data described in the WARNINGS and PRECAUTIONS section reflect exposure to ABECMA in 349 patients with relapsed or refractory multiple myeloma: one randomized, open-label study with 222 patients in Study 1 and one single-arm, open-label study with 127 patients in Study 2.
Study 1
The safety data described in this section reflect the exposure to ABECMA in Study 1, in which 222 patients with relapsed or refractory multiple myeloma received ABECMA across a dose range of 175 to 529 × 106 CAR-positive T cells (median dose: 445 × 106 CAR-positive T cells) [see Clinical Studies (14)]. Patients with a history of CNS disease or requiring ongoing treatment with chronic immunosuppression were excluded. The median age of the safety population was 63 years (range: 30 to 81 years); 43% were 65 years or older, and 63% were men. The Eastern Cooperative Oncology Group (ECOG) performance status at baseline was 0 in 47%, 1 in 51%, 2 in 1.4% and 3 in 0.5% of patients. Four (1.8%) patients treated with ABECMA had creatinine clearance <45 mL/min. For details about the study population, [see Clinical Studies (14)].
The most common (≥10%) Grade 3 or 4 nonlaboratory adverse reactions was febrile neutropenia (51%) and any infections (16%).
The most common nonlaboratory adverse reactions (incidence ≥20%) included CRS, pyrexia, any infection, febrile neutropenia, hypogammaglobulinemia, musculoskeletal pain, hypotension, infections–pathogen unspecified, fatigue, tachycardia, diarrhea, nausea, headache, encephalopathy, dyspnea and edema.
Serious adverse reactions occurred in 43% of patients. The most common nonlaboratory (≥5%) serious adverse reactions included infections–pathogen unspecified (10%), pneumonia (9%), viral infections (8%), encephalopathy (6%), pyrexia (6%) and sepsis (5%). Fatal adverse reactions occurred in 9%.
Table 3 summarizes the adverse reactions that occurred in at least 10% of patients treated with ABECMA. Table 4 describes the most common Grade 3 or 4 laboratory abnormalities.
| CAR=chimeric antigen receptor. | ||||
| * Represents multiple related terms. | ||||
| a Coagulopathy includes activated partial thromboplastin time prolonged, blood fibrinogen decreased, coagulopathy, disseminated intravascular coagulation, hypofibrinogenemia, international normalized ratio increased, prothrombin time prolonged. | ||||
| b Encephalopathy includes amnesia, cognitive disorder, confusional state, depressed level of consciousness, disturbance in attention, dysgraphia, encephalopathy, Immune effector cell-associated neurotoxicity syndrome incoherent, lethargy, memory impairment, mental status changes, metabolic encephalopathy, somnolence, stupor, toxic encephalopathy. | ||||
| c Neuropathy includes carpal tunnel syndrome, dysesthesia, hyperesthesia, hypoesthesia, hypoesthesia oral, mononeuropathy, neuralgia, neuritis, neuropathy peripheral, paresthesia, paresthesia oral, peripheral motor neuropathy, peripheral sensorimotor neuropathy, peripheral sensory neuropathy, peroneal nerve palsy, radicular pain, radiculopathy, sacral radiculopathy, sciatica, sensory loss, toxic neuropathy. | ||||
|
ABECMA (N=222) |
Standard Regimens (N=126) |
|||
|
Any Grade (%) |
Grade 3 or 4 (%) |
Any Grade (%) |
Grade 3 or 4 (%) |
|
|
Blood and lymphatic system disorders |
||||
|
Febrile neutropenia |
51 |
51 |
28 |
28 |
|
Coagulopathya |
14 |
2.7 |
4.8 |
0.8 |
|
Cardiac disorders |
||||
|
Tachycardia* |
32 |
0 |
21 |
0 |
|
Gastrointestinal disorders |
||||
|
Diarrhea* |
31 |
2.3 |
35 |
3.2 |
|
Nausea |
27 |
0.9 |
48 |
0 |
|
Constipation |
17 |
0 |
15 |
0 |
|
Vomiting* |
14 |
0 |
17 |
0 |
|
Abdominal pain* |
10 |
0.5 |
14 |
0 |
|
General disorders and administration site conditions |
||||
|
Pyrexia |
91 |
9 |
53 |
6 |
|
Fatigue* |
33 |
1.4 |
48 |
4 |
|
Edema* |
20 |
0.5 |
28 |
2.4 |
|
Chills |
19 |
0.5 |
13 |
0 |
|
Immune system disorders |
||||
|
Cytokine release syndrome |
91 |
4.1 |
40 |
0.8 |
|
Hypogammaglobulinemia |
48 |
0.9 |
25 |
0 |
|
Infections and infestations |
||||
|
Any infection |
56 |
16 |
64 |
18 |
|
Infections–pathogen unspecified* |
35 |
9 |
40 |
11 |
|
Upper respiratory tract infection* |
19 |
1.8 |
17 |
0.8 |
|
Infections–viral* |
18 |
5 |
28 |
6 |
|
Infections–bacterial* |
15 |
4.5 |
19 |
8 |
|
Pneumonia* |
13 |
8 |
13 |
11 |
|
Metabolism and nutrition disorders |
||||
|
Decreased appetite |
17 |
1.8 |
21 |
0 |
|
Musculoskeletal and connective tissue disorders |
||||
|
Musculoskeletal pain* |
36 |
1.8 |
49 |
8 |
|
Nervous system disorders |
||||
|
Headache* |
24 |
0 |
29 |
1.6 |
|
Encephalopathyb |
22 |
3.6 |
21 |
4.8 |
|
Dizziness* |
14 |
1.8 |
18 |
3.2 |
|
Neuropathyc |
10 |
0 |
21 |
0.8 |
|
Psychiatric disorders |
||||
|
Sleep disorder* |
11 |
0 |
22 |
2.4 |
|
Renal and urinary disorders |
||||
|
Renal failure* |
13 |
5 |
15 |
4 |
|
Respiratory, thoracic, and mediastinal disorders |
||||
|
Dyspnea* |
21 |
1.8 |
31 |
2.4 |
|
Cough* |
14 |
0 |
21 |
0 |
|
Hypoxia* |
18 |
6 |
8 |
1.6 |
|
Vascular disorders |
||||
|
Hypotension* |
36 |
2.3 |
19 |
1.6 |
|
Hypertension |
14 |
7 |
21 |
11 |
|
Skin disorders |
||||
|
Rash* |
10 |
0 |
19 |
0.8 |
Other clinically important adverse reactions that occurred in less than 10% of patients treated with ABECMA include the following:
-
•Cardiac disorders: cardiac arrhythmia (7%)
-
•Gastrointestinal disorders: gastrointestinal hemorrhage (0.5%)
-
•Immune system disorders: hemophagocytic lymphohistiocytosis (2.3%)
-
•Infections and infestations: infections-fungal (5%), sepsis (6%)
-
•Musculoskeletal and connective tissue disorders: motor dysfunction (9%)
-
•Nervous system disorders: tremor (4.1%), aphasia (3.2%), ataxia (2.3%), seizure (0.5%)
-
•Psychiatric disorders: anxiety (4.1%), delirium (7%)
-
•Respiratory, thoracic, and mediastinal disorders: pulmonary edema (1.4%)
-
•Vascular disorders: thrombosis (3.2%)
Laboratory Abnormalities
Table 4 presents the most common Grade 3 or 4 laboratory abnormalities, based on laboratory data, occurring in at least 10% of patients.
| CAR=chimeric antigen receptor; CTCAE=Common Terminology Criteria for Adverse Events; NCI=National Cancer Institute. | ||
| a Laboratory tests were graded according to NCI CTCAE Version 4.03. | ||
|
Laboratory Abnormality |
ABECMA N=222 (%) |
Standard Regimens N=126 (%) |
|
Grade 3 or 4 (%) |
Grade 3 or 4 (%) |
|
|
Lymphocyte decreased |
98 |
78 |
|
Leukocyte decreased |
96 |
64 |
|
Neutrophil decreased |
96 |
72 |
|
Platelet decreased |
59 |
46 |
|
Hemoglobin decreased |
52 |
45 |
|
Phosphate decreased |
45 |
30 |
|
Triglyceride increased |
21 |
10 |
|
Alanine aminotransferase increased |
13 |
8 |
|
Sodium decreased |
11 |
7 |
|
Gamma-glutamyltransferase increased |
10 |
6 |
Other clinically important Grade 3 or 4 laboratory abnormalities (based on laboratory data) that occurred in less than 10% of patients treated with ABECMA include the following: aspartate aminotransferase increased, potassium decreased, albumin decreased, alkaline phosphatase increased, calcium decreased, glucose increased, activated partial thromboplastin time increased (seconds), fibrinogen decreased, bilirubin increased and hypomagnesemia.
Study 2
The safety data described in this section reflect the exposure to ABECMA in Study 2, in which 127 patients with relapsed/refractory multiple myeloma received ABECMA across a dose range of 150 to 518 × 106 CAR-positive T cells [see Clinical Studies (14)]. Patients with a history of CNS disease (such as seizure or cerebrovascular ischemia) or requiring ongoing treatment with chronic immunosuppression were excluded. The median duration of follow-up was 11.4 months. The median age of the study population was 61 years (range: 33 to 78 years); 35% were 65 years or older, and 60% were men. The Eastern Cooperative Oncology Group (ECOG) performance status at baseline was 0 in 45%, 1 in 53%, and 2 in 2% of patients. Seven percent of the patients treated with ABECMA had creatinine clearance <45 mL/min. For details about the study population, [see Clinical Studies (14)].
The most common (≥10%) Grade 3 or 4 nonlaboratory adverse reactions were febrile neutropenia (16%) and infections–pathogen unspecified (15%).
The most common nonlaboratory adverse reactions (incidence ≥20%) included CRS, infections–pathogen unspecified, fatigue, musculoskeletal pain, hypogammaglobulinemia, diarrhea, upper respiratory tract infection, nausea, viral infections, encephalopathy, edema, pyrexia, cough, headache, and decreased appetite.
Serious adverse reactions occurred in 67% of patients. The most common nonlaboratory (≥5%) serious adverse reactions included CRS (18%), general physical health deterioration (10%), pneumonia (12%), infections–pathogen unspecified (19%), viral infections (9%), sepsis (7%), and febrile neutropenia (6%). Fatal adverse reactions occurred in 6%.
Table 5 summarizes the adverse reactions that occurred in at least 10% of patients treated with ABECMA. Table 6 describes the most common Grade 3 or 4 laboratory abnormalities.
| CAR=chimeric antigen receptor. * Represents multiple related terms. |
||
| a Encephalopathy includes amnesia, bradyphrenia, cognitive disorder, confusional state, depressed level of consciousness, disturbance in attention, dyscalculia, dysgraphia, encephalopathy, lethargy, memory impairment, mental status changes, metabolic encephalopathy, somnolence, toxic encephalopathy. | ||
| b Neuropathy peripheral includes carpal tunnel syndrome, hypoesthesia, hypoesthesia oral, neuralgia, neuropathy peripheral, paresthesia, peripheral sensorimotor neuropathy, peripheral sensory neuropathy, sciatica. | ||
|
System Organ Class
|
Target Dose of ABECMA (CAR-Positive T Cells) |
|
|
Any Grade |
Grade 3 or Higher |
|
|
[150 to 450 × 106]
|
[150 to 450 × 106]
|
|
|
Blood and lymphatic system disorders |
||
|
Febrile neutropenia |
16 |
16 |
|
Cardiac disorders |
||
|
Tachycardia* |
19 |
0 |
|
Gastrointestinal disorders |
||
|
Diarrhea |
35 |
1.6 |
|
Nausea |
29 |
0 |
|
Constipation |
16 |
0 |
|
Vomiting |
15 |
0 |
|
Oral pain* |
12 |
0 |
|
General disorders and administration site conditions |
||
|
Fatigue* |
45 |
3.1 |
|
Pyrexia |
25 |
1.6 |
|
General physical health deterioration |
11 |
10 |
|
Edema* |
25 |
0 |
|
Chills |
11 |
0 |
|
Immune system disorders |
||
|
Cytokine release syndrome |
85 |
9 |
|
Hypogammaglobulinemia* |
41 |
0.8 |
|
Infections and infestations * |
||
|
Infections–Pathogen unspecified |
51 |
15 |
|
Viral infections |
27 |
9 |
|
Bacterial infections |
15 |
3.9 |
|
Pneumonia* |
17 |
9 |
|
Upper respiratory tract infection* |
34 |
1.6 |
|
Investigations |
||
|
Weight decreased |
13 |
1.6 |
|
Metabolism and nutrition disorders |
||
|
Decreased appetite* |
22 |
0.8 |
|
Musculoskeletal and connective tissue disorders |
||
|
Musculoskeletal pain* |
45 |
3.1 |
|
Motor dysfunction* |
11 |
0 |
|
Nervous system disorders |
||
|
Encephalopathya |
26 |
6 |
|
Headache* |
23 |
0 |
|
Dizziness* |
17 |
0.8 |
|
Neuropathy peripheralb |
17 |
0.8 |
|
Tremor* |
10 |
0 |
|
Psychiatric disorders |
||
|
Insomnia* |
13 |
0 |
|
Anxiety* |
12 |
0.8 |
|
Renal and urinary disorders |
||
|
Renal failure* |
10 |
2.4 |
|
Respiratory, thoracic, and mediastinal disorders |
||
|
Cough* |
23 |
0 |
|
Dyspnea* |
13 |
2.4 |
|
Skin and subcutaneous tissue disorder |
||
|
Rash* |
14 |
0.8 |
|
Xerosis* |
11 |
0 |
|
Vascular disorders |
||
|
Hypotension* |
17 |
0 |
|
Hypertension |
11 |
3.1 |
Other clinically important adverse reactions that occurred in less than 10% of patients treated with ABECMA include the following:
-
•Blood and lymphatic system disorders: coagulopathy (9%)
-
•Cardiac disorders: atrial fibrillation (4.7%), cardiomyopathy (1.6%)
-
•Gastrointestinal disorders: gastrointestinal hemorrhage (3.1%)
-
•Immune system disorders: hemophagocytic lymphohistiocytosis (3.1%)
-
•Infections and infestations: fungal infections (8%), sepsis (9%)
-
•Nervous system disorders: aphasia (7%), ataxia (3.1%), paresis (2.4%), seizure (1.6%)
-
•Psychiatric disorders: delirium (6%)
-
•Respiratory, thoracic, and mediastinal disorders: hypoxia (2.4%), pulmonary edema (2.4%)
-
•Vascular disorders: thrombosis (3.1%)
17 Patient Counseling Information
Advise the patient to read the FDA-approved patient labeling (Medication Guide).
Advise patients that the risk of manufacturing failure is 2.1% [8/384 in the clinical studies]. In case of a manufacturing failure, a second manufacturing of ABECMA may be attempted. In addition, while the patient awaits the product, additional anticancer treatment (not the lymphodepletion) may be necessary and may increase the risk of adverse events during the pre-infusion period, which could delay or prevent the administration of ABECMA.
Inform patients of the risk of early death: In a clinical study, a higher proportion of patients experienced death within the first nine months from randomization in the ABECMA arm compared to the standard regimens arm. This higher rate of early death was mainly observed before receiving ABECMA with the main reason being progression of multiple myeloma. There was also an increase in the rate of death from adverse events after ABECMA.
Advise patients to seek immediate attention for any of the following:
-
•Cytokine Release Syndrome (CRS): Signs or symptoms associated with CRS, including fever, hypotension, tachycardia, chills, hypoxia, headache, and fatigue [see Dosage and Administration (2.3), Warnings and Precautions (5.2) , and Adverse Reactions (6.1)].
-
•Neurologic Toxicities: Signs or symptoms associated with neurologic events, including encephalopathy, confusion, seizures, tremor, aphasia, delirium, and somnolence [see Dosage and Administration (2.3), Warnings and Precautions (5.3) , and Adverse Reactions (6.1)].
-
•Infections: Signs or symptoms associated with infection [see Warnings and Precautions (5.6) and Adverse Reactions (6.1)].
-
•Prolonged Cytopenias: Signs or symptoms associated with bone marrow suppression, including neutropenia, anemia, thrombocytopenia, or febrile neutropenia [see Warnings and Precautions (5.7) and Adverse Reactions (6.1)].
-
•Secondary malignancies: Secondary malignancies, including T cell malignancies, have occurred [see Boxed Warning, Warnings and Precautions (5.9) , Adverse Reactions (6.3)].
Advise patients for the need to:
-
•Contact Bristol-Myers Squibb at 1-888-805-4555 if they are diagnosed with a secondary malignancy [see Warnings and Precautions (5.9) ].
-
•Have periodic monitoring of blood counts before and after ABECMA infusion [see Warnings and Precautions (5.7) ].
-
•Avoid driving for at least one week.
5.2 Cytokine Release Syndrome (crs)
CRS, including fatal or life-threatening reactions, occurred following treatment with ABECMA. Among patients receiving ABECMA for relapsed or refractory multiple myeloma in Study 1 and Study 2 (N=349), CRS occurred in 89% (310/349), including ≥ Grade 3 CRS (Lee grading system) in 7% (23/349) of patients and Grade 5 CRS in 0.9% (3/349) of patients. The median time-to-onset of CRS, any grade, was 1 day (range: 1 to 27 days), and the median duration of CRS was 5 days (range: 1 to 63 days). In the pooled studies, the rate of ≥ Grade 3 CRS was 10% (7/71) for patients treated in dose range of 460 to 510 × 106 CAR-positive T cells and 5.4% (13/241) for patients treated in dose range of 300 to 460 × 106 CAR-positive T cells.
The most common manifestations of CRS (≥10%) included pyrexia (87%), hypotension (30%), tachycardia (26%), chills (19%), and hypoxia (16%). Grade 3 or higher events that may be associated with CRS include hypotension, hypoxia, hyperbilirubinemia, hypofibrinogenemia, ARDS, atrial fibrillation, hepatocellular injury, metabolic acidosis, pulmonary edema, coagulopathy, renal failure, multiple organ dysfunction syndrome and hemophagocytic lymphohistiocytosis/macrophage activation syndrome (HLH/MAS) [see Adverse Reactions (6.1)].
Identify CRS based on clinical presentation. Evaluate for and treat other causes of fever, hypoxia, and hypotension. CRS has been reported to be associated with findings of HLH/MAS, and the physiology of the syndromes may overlap. HLH/MAS is a potentially life-threatening condition. In patients with progressive symptoms of CRS or refractory CRS despite treatment, evaluate for evidence of HLH/MAS. Please see Section 5.4 ; Hemophagocytic Lymphohistiocytosis/Macrophage Activation Syndrome.
Of the 349 patients who received ABECMA in clinical trials, 226 (65%) patients received tocilizumab; 39% (135/349) received a single dose, while 26% (91/349) received more than 1 dose of tocilizumab. Overall, 24% (82/349) of patients received at least 1 dose of corticosteroids for treatment of CRS. Almost all patients who received corticosteroids for CRS also received tocilizumab. For patients treated in dose range of 460 to 510 × 106 CAR-positive T cells, 76% (54/71) of patients received tocilizumab and 35% (25/71) received at least 1 dose of corticosteroids for treatment of CRS. For patients treated in dose range of 300 to 460 × 106 CAR-positive T cells, 63% (152/241) of patients received tocilizumab and 20% (49/241) received at least 1 dose of corticosteroid for treatment of CRS.
Ensure that a minimum of two doses of tocilizumab are available prior to infusion of ABECMA.
Monitor patients at least daily for seven days following ABECMA infusion for signs and symptoms of CRS. Continue to monitor patients for signs or symptoms of CRS for at least one week after infusion. At the first sign of CRS, institute treatment with supportive care, tocilizumab and/or corticosteroids as indicated [see Dosage and Administration (2.2) , (2.3) ].
Counsel patients to seek immediate medical attention should signs or symptoms of CRS occur at any time [see Patient Counseling Information (17)].
16 How Supplied/storage and Handling
ABECMA is supplied in one or more infusion bag(s) (see below) containing a frozen suspension of genetically modified autologous T cells in 5% DMSO.
Each infusion bag of ABECMA is overwrapped with a transparent plastic sleeve that is folded to the back of the infusion bag and individually packed in a metal cassette. ABECMA is stored in the vapor phase of liquid nitrogen and supplied in a liquid nitrogen dry vapor shipper. An RFI Certificate is affixed inside the shipper.
-
•50 mL infusion bag and metal cassette (NDC 59572-515-01)
-
•250 mL infusion bag and metal cassette (NDC 59572-515-02)
-
•500 mL infusion bag and metal cassette (NDC 59572-515-03)
Match the identity of the patient with the patient identifiers on the cassette(s) and infusion bag(s) upon receipt.
Principal Display Panel 30 Ml Bag Label
idecabtagene vicleucel
Abecma™
NDC 59572-515-01
Genetically modified autologous T cells
FOR AUTOLOGOUS AND INTRAVENOUS USE ONLY
Suspension for IV Infusion
Rx Only
Acceptable Volume 10mL - 30mL per bag
Dosage: See prescribing information and
Release for Infusion Certificate (inside shipper).
Contains: 300 to 510 x 106 anti-BCMA02
CAR-positive T cells in cryopreservative
solution containing 5% DMSO USP.
Dose may be suspended in 1 or more
infusion bag(s).
Do not use a leukodepleting filter
or irradiate.
Not evaluated for infectious substances.
Preservative free.
Store in vapor phase of liquid nitrogen
(≤ -130°C).
Mfd by: Celgene Corporation,
a Bristol-Myers Squibb Company
Summit, NJ 07901 USA
Phone: 1-888-805-4555
US License No. 2252
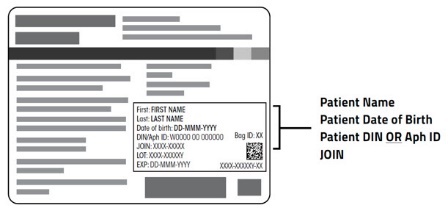
First: FIRST NAME
Last: LAST NAME
Date of birth: DD-MMM-YYYY
DIN/Aph ID: W0000 00 000000
JOIN: XXXX-XXXXX
LOT: XXXX-XXXXXY
EXP: DD-MMM-YYYY
Bag ID: XX
XXXX-XXXXXY-XX
304492
Principal Display Panel 70 Ml Bag Label
idecabtagene vicleucel
Abecma™
NDC 59572-515-02
Genetically modified autologous T cells
FOR AUTOLOGOUS AND INTRAVENOUS USE ONLY
Suspension for IV Infusion
Rx Only
Acceptable Volume 30mL - 70mL per bag
Dosage: See prescribing information and
Release for Infusion Certificate (inside shipper).
Contains: 300 to 510 x 106 anti-BCMA02
CAR-positive T cells in cryopreservative
solution containing 5% DMSO USP.
Dose may be suspended in 1 or more
infusion bag(s).
Do not use a leukodepleting filter
or irradiate.
Not evaluated for infectious substances.
Preservative free.
Store in vapor phase of liquid nitrogen
(≤ -130°C).
Mfd by: Celgene Corporation,
a Bristol-Myers Squibb Company
Summit, NJ 07901 USA
Phone: 1-888-805-4555
US License No. 2252
First: FIRST NAME
Last: LAST NAME
Date of birth: DD-MMM-YYYY
DIN/Aph ID: W0000 00 000000
JOIN: XXXX-XXXXX
LOT: XXXX-XXXXXY
EXP: DD-MMM-YYYY
Bag ID: XX
XXXX-XXXXXY-XX
304492
Principal Display Panel 100 Ml Bag Label
idecabtagene vicleucel
Abecma™
NDC 59572-515-03
Genetically modified autologous T cells
FOR AUTOLOGOUS AND INTRAVENOUS USE ONLY
Suspension for IV Infusion
Rx Only
Acceptable Volume 55mL - 100mL per bag
Dosage: See prescribing information and
Release for Infusion Certificate (inside shipper).
Contains: 300 to 510 x 106 anti-BCMA02
CAR-positive T cells in cryopreservative
solution containing 5% DMSO USP.
Dose may be suspended in 1 or more
infusion bag(s).
Do not use a leukodepleting filter
or irradiate.
Not evaluated for infectious substances.
Preservative free.
Store in vapor phase of liquid nitrogen
(≤ -130°C).
Mfd by: Celgene Corporation,
a Bristol-Myers Squibb Company
Summit, NJ 07901 USA
Phone: 1-888-805-4555
US License No. 2252
First: FIRST NAME
Last: LAST NAME
Date of birth: DD-MMM-YYYY
DIN/Aph ID: W0000 00 000000
JOIN: XXXX-XXXXX
LOT: XXXX-XXXXXY
EXP: DD-MMM-YYYY
Bag ID: XX
XXXX-XXXXXY-XX
304492
Principal Display Panel 30 Ml Cassette Label
idecabtagene vicleucel
Abecma™
NDC 59572-515-01
Genetically modified autologous T cells
FOR AUTOLOGOUS AND INTRAVENOUS USE ONLY
Suspension for IV Infusion
Rx Only
Acceptable Volume 10mL - 30mL per bag
Dosage: See prescribing information and Release for
Infusion Certificate (inside shipper).
Contains: 300 to 510 x 106 anti-BCMA02 CAR-positive T cells
in cryopreservative solution containing 5% DMSO USP.
Dose may be suspended in 1 or more infusion bag(s).
Do not use a leukodepleting filter or irradiate.
Not evaluated for infectious substances. Preservative free.
Store in vapor phase of liquid nitrogen (≤ -130°C).
Mfd by: Celgene Corporation, a Bristol-Myers Squibb Company
Summit, NJ 07901 USA
Phone: 1-888-805-4555
US License No. 2252
First: FIRST NAME
Last: LAST NAME
Date of birth: DD-MMM-YYYY
DIN/Aph ID: W0000 00 000000
JOIN: XXXX-XXXXX
LOT: XXXX-XXXXXY
EXP: DD-MMM-YYYY
Bag ID: XX
XXXX-XXXXXY-XX
304493
Principal Display Panel 70 Ml Cassette Label
idecabtagene vicleucel
Abecma™
NDC 59572-515-02
Genetically modified autologous T cells
FOR AUTOLOGOUS AND INTRAVENOUS USE ONLY
Suspension for IV Infusion
Rx Only
Acceptable Volume 30mL - 70mL per bag
Dosage: See prescribing information and Release for
Infusion Certificate (inside shipper).
Contains: 300 to 510 x 106 anti-BCMA02 CAR-positive T cells
in cryopreservative solution containing 5% DMSO USP.
Dose may be suspended in 1 or more infusion bag(s).
Do not use a leukodepleting filter or irradiate.
Not evaluated for infectious substances. Preservative free.
Store in vapor phase of liquid nitrogen (≤ -130°C).
Mfd by: Celgene Corporation, a Bristol-Myers Squibb Company
Summit, NJ 07901 USA
Phone: 1-888-805-4555
US License No. 2252
First: FIRST NAME
Last: LAST NAME
Date of birth: DD-MMM-YYYY
DIN/Aph ID: W0000 00 000000
JOIN: XXXX-XXXXX
LOT: XXXX-XXXXXY
EXP: DD-MMM-YYYY
Bag ID: XX
XXXX-XXXXXY-XX
304493
Principal Display Panel 100 Ml Cassette Label
idecabtagene vicleucel
Abecma™
NDC 59572-515-03
Genetically modified autologous T cells
FOR AUTOLOGOUS AND INTRAVENOUS USE ONLY
Suspension for IV Infusion
Rx Only
Acceptable Volume 55mL - 100mL per bag
Dosage: See prescribing information and Release for
Infusion Certificate (inside shipper).
Contains: 300 to 510 x 106 anti-BCMA02 CAR-positive T cells
in cryopreservative solution containing 5% DMSO USP.
Dose may be suspended in 1 or more infusion bag(s).
Do not use a leukodepleting filter or irradiate.
Not evaluated for infectious substances. Preservative free.
Store in vapor phase of liquid nitrogen (≤ -130°C).
Mfd by: Celgene Corporation, a Bristol-Myers Squibb Company
Summit, NJ 07901 USA
Phone: 1-888-805-4555
US License No. 2252
First: FIRST NAME
Last: LAST NAME
Date of birth: DD-MMM-YYYY
DIN/Aph ID: W0000 00 000000
JOIN: XXXX-XXXXX
LOT: XXXX-XXXXXY
EXP: DD-MMM-YYYY
Bag ID: XX
XXXX-XXXXXY-XX
304493
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Genotoxicity assays and carcinogenicity studies in rodents were not performed for ABECMA.
In vitro expansion studies with CAR-positive T cells (ABECMA) from five patients and two healthy donor drug product lots showed no evidence for transformation and/or immortalization of T cells. A genomic insertion site analysis of the lentiviral vector was performed on ABECMA samples from twenty (20) individual patient donors. There was no evidence for preferential integration near genes of concern or preferential outgrowth of cells harboring integration sites of concern.
No studies on the effects of ABECMA on fertility have been conducted.
5.4 Hemophagocytic Lymphohistiocytosis (hlh)/macrophage Activation Syndrome (mas)
In patients receiving ABECMA in Study 1 and Study 2, HLH/MAS occurred in 2.9% (10/349) of patients. All events of HLH/MAS had onset within 10 days of receiving ABECMA, with a median onset of 6.5 days (range: 4 to 10 days) and occurred in the setting of ongoing or worsening CRS. Five patients with HLH/MAS had overlapping neurotoxicity. The manifestations of HLH/MAS include hypotension, hypoxia, multiple organ dysfunction, renal dysfunction, and cytopenia.
In Study 1, one patient had Grade 5, two patients had Grade 4 and two patients had Grade 3 HLH/MAS. The patient with Grade 5 HLH/MAS also had Grade 5 candida sepsis and Grade 5 CRS. In another patient who died due to stroke, the Grade 4 HLH/MAS had resolved prior to death. Two cases of Grade 3 and one case of Grade 4 HLH/MAS had resolved.
In Study 2, one patient treated in the 300 × 106 CAR-positive T cells dose cohort developed fatal multi-organ HLH/MAS with CRS. In another patient with fatal bronchopulmonary aspergillosis, HLH/MAS was contributory to the fatal outcome. Three cases of Grade 2 HLH/MAS resolved.
HLH/MAS is a potentially life-threatening condition with a high mortality rate if not recognized early and treated. Treatment of HLH/MAS should be administered per institutional standards.
Warning: Cytokine Release Syndrome, Neurologic Toxicities, Hlh/mas, Prolonged Cytopenia, and Secondary Hematological Malignancies
-
•Cytokine Release Syndrome (CRS), including fatal or life-threatening reactions, occurred in patients following treatment with ABECMA. Do not administer ABECMA to patients with active infection or inflammatory disorders. Treat severe or life-threatening CRS with tocilizumab or tocilizumab and corticosteroids [see Dosage and Administration (2.2, 2.3), Warnings and Precautions (5.2) ].
-
•Neurologic toxicities, which may be severe or life-threatening, occurred following treatment with ABECMA, including concurrently with CRS, after CRS resolution, or in the absence of CRS. Monitor for neurologic events after treatment with ABECMA. Provide supportive care and/or corticosteroids as needed [see Dosage and Administration (2.2, 2.3) and Warnings and Precautions (5.3) ].
-
•Hemophagocytic Lymphohistiocytosis/Macrophage Activation Syndrome (HLH/MAS) including fatal and life-threatening reactions, occurred in patients following treatment with ABECMA. HLH/MAS can occur with CRS or neurologic toxicities [see Warnings and Precautions (5.4) ].
-
•Prolonged Cytopenia with bleeding and infection, including fatal outcomes following stem cell transplantation for hematopoietic recovery, occurred following treatment with ABECMA [see Warnings and Precautions (5.7) ].
-
•T cell malignancies have occurred following treatment of hematologic malignancies with BCMA- and CD19-directed genetically modified autologous T cell immunotherapies, including ABECMA [see Warnings and Precautions (5.9) ].
Structured Label Content
Section 42229-5 (42229-5)
Preparing Patient for ABECMA Infusion
Confirm the availability of ABECMA prior to starting the lymphodepleting chemotherapy regimen.
Section 42231-1 (42231-1)
|
MEDICATION GUIDE
ABECMA® (uh-BEK-muh) (idecabtagene vicleucel) |
|---|
| This Medication Guide has been approved by the U.S. Food and Drug Administration. Revised: November 2025 |
|
Read this Medication Guide before you start your ABECMA treatment. The more you know about your treatment, the more active you can be in your care. Talk with your healthcare provider if you have questions about your health condition or treatment. Reading this Medication Guide does not take the place of talking with your healthcare provider about your treatment. |
|
What is the most important information I should know about ABECMA?
It is important that you tell your healthcare providers that you have received ABECMA and to show them your ABECMA Patient Wallet Card. Your healthcare provider may give you other medicines to treat your side effects. |
|
What is ABECMA?
|
|
How will I receive ABECMA?
|
|
What should I avoid after receiving ABECMA?
|
|
What are the possible or reasonably likely side effects of ABECMA?
In a study comparing ABECMA to standard regimen, a higher proportion of patients experienced death within the first nine months from randomization in the ABECMA arm compared to the standard regimens arm. This higher rate of early death was mainly observed before receiving ABECMA with the main reason being progression of multiple myeloma. There was also an increase in the rate of death from adverse events after ABECMA. ABECMA can cause a very common side effect called cytokine release syndrome or CRS, which can be severe or fatal. Symptoms of CRS include fever, difficulty breathing, dizziness or light-headedness, nausea, headache, fast heartbeat, low blood pressure, or fatigue. Tell your healthcare provider right away if you develop fever or any of these other symptoms after receiving ABECMA. ABECMA can increase the risk of life-threatening infections that may lead to death. Tell your healthcare provider right away if you develop fever, chills, or any signs or symptoms of an infection. ABECMA can lower one or more types of your blood cells (red blood cells, white blood cells, or platelets), which may make you feel weak or tired or increase your risk of severe infection or bleeding. After treatment, your healthcare provider will test your blood to check for this. Tell your healthcare provider right away if you get a fever, are feeling tired, or have bruising or bleeding. ABECMA may increase your risk of getting cancers including certain types of blood cancers. Your healthcare provider should monitor you for this. Having ABECMA in your blood may cause a false-positive human immunodeficiency virus (HIV) test result by some commercial tests. These are not all the possible side effects of ABECMA. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. |
|
General information about the safe and effective use of ABECMA
|
Section 43683-2 (43683-2)
Section 44425-7 (44425-7)
Store ABECMA frozen in the vapor phase of liquid nitrogen (less than or equal to minus 130°C).
Thaw ABECMA prior to infusion [see Dosage and Administration (2.2)].
2.1 Dose
For autologous use only. For intravenous use only.
ABECMA is provided as a single dose for infusion containing a suspension of chimeric antigen receptor (CAR)-positive T cells in one or more infusion bags. The recommended dose range is 300 to 510 × 106 CAR-positive T cells.
See the accompanying Release for Infusion Certificate (RFI Certificate) for additional information pertaining to dose [see How Supplied/Storage and Handling (16)].
15 References (15 REFERENCES)
-
1.Lee DW, Gardner R, Porter DL, et al. Current concepts in the diagnosis and management of cytokine release syndrome. Blood 2014; 124(2): 188-95. Errata in Blood: 2015;126(8):1048. and 2016;128(11):1533.
-
2.Kumar S, Paiva B, Anderson KC, et al. International Myeloma Working Group consensus criteria for response and minimal residual disease assessment in multiple myeloma. Lancet Oncol 2016; 17(8): e328-46.
8.1 Pregnancy
Risk Summary
There are no available data with ABECMA use in pregnant women. No animal reproductive and developmental toxicity studies have been conducted with ABECMA to assess whether it can cause fetal harm when administered to a pregnant woman.
It is not known if ABECMA has the potential to be transferred to the fetus. Based on the mechanism of action, if the transduced cells cross the placenta, they may cause fetal toxicity, including plasma cell aplasia or hypogammaglobulinemia. Therefore, ABECMA is not recommended for women who are pregnant, and pregnancy after ABECMA infusion should be discussed with the treating physician. Assess immunoglobulin levels in newborns of mothers treated with ABECMA.
The estimated background risk of major birth defects and miscarriage for the indicated population is unknown. The estimated background risk in the U.S. general population of major birth defects is 2% to 4% and of miscarriage is 15% to 20% of clinically recognized pregnancies.
8.2 Lactation
Risk Summary
There is no information regarding the presence of ABECMA in human milk, the effect on the breastfed infant, and the effects on milk production. The developmental and health benefits of breastfeeding should be considered along with the mother's clinical need for ABECMA and any potential adverse effects on the breastfed infant from ABECMA or from the underlying maternal condition.
11 Description (11 DESCRIPTION)
ABECMA is a BCMA-directed genetically modified autologous T cell immunotherapy product consisting of a patient's own T cells that are harvested and genetically modified ex vivo through transduction with an anti-BCMA02 chimeric antigen receptor (CAR) lentiviral vector (LVV). Autologous T cells transduced with the anti-BCMA02 CAR LVV express the anti-BCMA CAR on the T cell surface. The CAR is comprised of a murine extracellular single-chain variable fragment (scFv) specific for recognizing B cell maturation antigen (BCMA) followed by a human CD8α hinge and transmembrane domain fused to the T cell cytoplasmic signaling domains of CD137 (4-1BB) and CD3ζ chain, in tandem. Binding of ABECMA to BCMA-expressing target cells leads to signaling initiated by CD3ζ and 4-1BB domains, and subsequent CAR-positive T cell activation. Antigen-specific activation of ABECMA results in CAR-positive T cell proliferation, cytokine secretion, and subsequent cytolytic killing of BCMA-expressing cells.
ABECMA is prepared from the patient's peripheral blood mononuclear cells (PBMCs), which are obtained via a standard leukapheresis procedure. The mononuclear cells are enriched for T cells, through activation with anti-CD3 and anti-CD28 antibodies in the presence of IL-2, which are then transduced with the replication-incompetent lentiviral vector containing the anti-BCMA CAR transgene. The transduced T cells are expanded in cell culture, washed, formulated into a suspension, and cryopreserved. The product must pass a sterility test before release for shipping as a frozen suspension in one or more patient-specific infusion bag(s). The product is thawed prior to infusion back into the patient [see Dosage and Administration (2.3) and How Supplied/Storage and Handling (16)].
The ABECMA formulation contains 50% Plasma-Lyte A and 50% CryoStor® CS10, resulting in a final DMSO concentration of 5%.
5.6 Infections
ABECMA should not be administered to patients with active infections or inflammatory disorders. Severe, life‑threatening, or fatal infections occurred in patients after ABECMA infusion.
In all patients receiving ABECMA in Study 1 and Study 2, infections (all grades) occurred in 61% of patients. Grade 3 or 4 infections occurred in 21% of patients. Grade 3 or 4 infections with an unspecified pathogen occurred in 12%, viral infections in 7%, bacterial infections in 4.3%, and fungal infections in 1.4% of patients. Overall, 15 patients had Grade 5 infections (4.3%); 8 patients (2.3%) with infections of pathogen unspecified, 3 patients (0.9%) with fungal infections, 3 patients (0.9%) with viral infections, and 1 patient (0.3%) with bacterial infection.
Monitor patients for signs and symptoms of infection before and after ABECMA infusion and treat appropriately. Administer prophylactic, pre-emptive, and/or therapeutic antimicrobials according to standard institutional guidelines.
Febrile neutropenia was observed in 38% (133/349) of patients after ABECMA infusion and may be concurrent with CRS. In the event of febrile neutropenia, evaluate for infection and manage with broad-spectrum antibiotics, fluids, and other supportive care as medically indicated.
5.1 Early Death
In Study 1, a randomized (2:1), controlled trial, a higher proportion of patients experienced death within nine months after randomization in the ABECMA arm (45/254; 18%) compared to the standard regimens arm (15/132; 11%) [see Clinical Studies (14)]. Early deaths occurred in 8% (20/254) and 0% prior to ABECMA infusion and standard regimen administration, respectively, and 10% (25/254) and 11% (15/132) after ABECMA infusion and standard regimen administration, respectively. Out of the 20 deaths that occurred prior to ABECMA infusion, 15 occurred from disease progression, 3 occurred from adverse events and 2 occurred from unknown causes. Out of the 25 deaths that occurred after ABECMA infusion, 10 occurred from disease progression, 11 occurred from adverse events, and 4 occurred from unknown causes.
8.4 Pediatric Use
The safety and efficacy of ABECMA in pediatric patients have not been established.
8.5 Geriatric Use
In the clinical trials of ABECMA, 141 (40%) of the 349 patients were 65 years of age or older and 16/349 (4.6%) patients were 75 years of age or older. In Study 2, all five cases of Grade 3 neurotoxicity occurred in patients ≥65 years of age (66 to 74 years). No clinically important differences in effectiveness of ABECMA were observed between these patients and patients younger than 65 years of age.
2.2 Administration
ABECMA is for autologous use only. The patient's identity must match the patient identifiers on the ABECMA cassette(s) and infusion bag(s). Do not infuse ABECMA if the information on the patient-specific label(s) does not match the intended patient.
12.6 Immunogenicity
The observed incidence of anti-drug antibodies is highly dependent on the sensitivity and specificity of the assay. Differences in assay methods preclude meaningful comparisons of the incidence of anti-drug antibodies in the studies described below with the incidence of anti-drug antibodies in other studies, including those of ABECMA or of other similar products.
In Study 1 and Study 2, humoral immunogenicity of ABECMA was measured by determination of anti-CAR antibody in serum pre- and post-administration. In the clinical studies, 2.6% of patients (9/349) tested positive for pre-infusion anti-CAR antibodies and treatment-induced anti-CAR antibodies were detected in 53% (186/349) of the patients. There is no identified clinically significant impact of pre-existing or post-infusion anti-CAR antibodies on the cellular expansion, safety, or effectiveness of ABECMA.
4 Contraindications (4 CONTRAINDICATIONS)
None.
6 Adverse Reactions (6 ADVERSE REACTIONS)
The following adverse reactions are described elsewhere in the labeling:
-
•Early Death [see Warnings and Precautions (5.1), Clinical Studies (14)]
-
•Cytokine Release Syndrome [see Warnings and Precautions (5.2) ]
-
•Neurologic Toxicities [see Warnings and Precautions (5.3) ]
-
•Hemophagocytic Lymphohistiocytosis (HLH)/Macrophage Activation Syndrome (MAS) [see Warnings and Precautions (5.4) ]
-
•Hypersensitivity Reactions [see Warnings and Precautions (5.5) ]
-
•Infections [see Warnings and Precautions (5.6) ]
-
•Prolonged Cytopenias [see Warnings and Precautions (5.7) ]
-
•Hypogammaglobulinemia [see Warnings and Precautions (5.8) ]
7 Drug Interactions (7 DRUG INTERACTIONS)
Drug/Laboratory Test Interactions
HIV and the lentivirus used to make ABECMA have limited, short spans of identical genetic material (RNA). Therefore, some commercial HIV nucleic acid tests may yield false-positive results in patients who have received ABECMA.
12.2 Pharmacodynamics
Following ABECMA infusion, pharmacodynamic responses of CAR activation and anti-tumor efficacy were evaluated. Peak elevation of plasma cytokines, chemokines, and soluble immune mediators occurred within 14 days of ABECMA infusion and returned to baseline levels within one month.
Rapid decreases in tumor markers associated with clinical response, including serum levels of soluble BCMA, and bone marrow CD138+ cells, as well as minimal residual disease (MRD) negative responses, were observed within the first month following ABECMA infusion.
12.3 Pharmacokinetics
Following ABECMA infusion, the CAR-positive T cells proliferate and undergo rapid multi-log expansion followed by a bi-exponential decline. The median time of maximal expansion in peripheral blood (Tmax) occurred 11 days after infusion.
ABECMA can persist in peripheral blood for up to 1 year post-infusion. A summary of Tmax, AUC0-28days, and Cmax from Study 1 and Study 2 is provided in Table 7.
| AUC0-28days=area under the curve of the transgene level from time of dose to 28 days post-infusion; Cmax=the maximum transgene level; ddPCR=droplet digital polymerase chain reaction; qPCR=quantitative polymerase chain reaction; PK=pharmacokinetics; Tmax=time of maximum observed transgene level. a The PK parameters of Study 1 were determined by time course of transgene copies per microgram of DNA extracted from whole blood as quantified by droplet digital PCR (ddPCR). b The PK parameters of Study 2 were determined by time course of transgene copies per microgram of DNA extracted from CD3+ sorted cells as quantified by quantitative polymerase chain reaction (qPCR). |
|||
| Note: The PK parameters should not be directly compared between Study 1 and Study 2 due to different primary PK assays used in these two studies. | |||
|
Pharmacokinetic Parameter |
Summary Statistic |
Study 1
Total CAR-Positive T Cells (Quantified by ddPCR)a |
Study 2 Total [300 to 460 × 106] CAR-Positive T Cells (Quantified by qPCR)b |
|
Tmax (days) |
Median (Range) |
11 (4-31) |
11 (7-28) N=99 |
|
Cmax (copies/mcg) |
Geometric mean (geometric CV%) |
117,557 (215) N=207 |
256,333 (165) N=99 |
|
AUC0-28days
|
Geometric mean (geometric CV%) |
1,098,862 (228) |
3,088,455 (190) N=98 |
ABECMA transgene levels were positively associated with objective tumor response (partial response or better). Among patients who received ABECMA in Study 1, the median Cmax levels in responders (N=172) were approximately 6.5-fold higher compared to the corresponding levels in non-responders (N=35). Median AUC0-28days in responders (N=172) was approximately 6.1-fold higher than non-responders (N=33). Among patients who received ABECMA in Study 2, the median Cmax levels in responders (N=72) were approximately 4.6-fold higher than the corresponding levels in non-responders (N=27). Median AUC0-28days in responders (N=72) was approximately 5.6-fold higher than non-responders (N=26).
Tocilizumab or Siltuximab and Corticosteroid Use
Some patients required tocilizumab or siltuximab and/or corticosteroid for the management of CRS. ABECMA can continue to expand and persist following tocilizumab or siltuximab or corticosteroid administration [see Warnings and Precautions (5.2)].
In Study 2, patients with CRS treated with tocilizumab had higher ABECMA cellular expansion levels, as measured by 1.3‑fold and 1.6-fold higher median Cmax (N=67) and AUC0‑28days (N=66), respectively, compared to patients who did not receive tocilizumab (N=59 for Cmax and N=58 for AUC0‑28days).
Patients with CRS treated with corticosteroids had higher ABECMA cellular expansion levels, as measured by 1.7-fold and 2.2-fold higher median Cmax (N=18) and AUC0‑28days (N=18), respectively, compared to patients who did not receive corticosteroids (N=108 for Cmax and N=106 for AUC0‑28days).
Similar trend was observed in Study 1.
Specific Populations
Geriatric
Age (range: 30 to 81 years) had no significant impact on expansion parameters [see Use in Special Populations (8.5)].
Pediatric
The pharmacokinetics of ABECMA in patients less than 18 years of age have not been evaluated.
Patients with Hepatic/Renal Impairment
Hepatic and renal impairment studies of ABECMA were not conducted.
Patients with Other Intrinsic Factors
Gender, race, and ethnicity had no significant impact on ABECMA expansion parameters. Patients with lower body weight had higher expansion. Due to high variability in pharmacokinetic cellular expansion, the overall effect of weight on the pharmacokinetics of ABECMA is considered to be not clinically relevant.
1 Indications and Usage (1 INDICATIONS AND USAGE)
ABECMA is indicated for the treatment of adult patients with relapsed or refractory multiple myeloma after two or more prior lines of therapy including an immunomodulatory agent, a proteasome inhibitor, and an anti-CD38 monoclonal antibody.
12.1 Mechanism of Action
ABECMA is a chimeric antigen receptor (CAR)-positive T cell therapy targeting B-cell maturation antigen (BCMA), which is expressed on the surface of normal and malignant plasma cells. The CAR construct includes an anti-BCMA scFv-targeting domain for antigen specificity, a transmembrane domain, a CD3-zeta T cell activation domain, and a 4-1BB costimulatory domain. Antigen-specific activation of ABECMA results in CAR-positive T cell proliferation, cytokine secretion, and subsequent cytolytic killing of BCMA-expressing cells.
5.7 Prolonged Cytopenias
Patients may exhibit prolonged cytopenias following lymphodepleting chemotherapy and ABECMA infusion.
In patients receiving ABECMA in Study 1 and Study 2, 40% of patients (139/349) experienced prolonged Grade 3 or 4 neutropenia and 42% (145/349) experienced prolonged Grade 3 or 4 thrombocytopenia that had not resolved by Month 1 following ABECMA infusion. In 89% (123/139) of patients who recovered from Grade 3 or 4 neutropenia after Month 1, the median time to recovery from ABECMA infusion was 1.9 months. In 76% (110/145) of patients who recovered from Grade 3 or 4 thrombocytopenia, the median time to recovery was 1.9 months. Five patients underwent stem cell therapy for hematopoietic reconstitution due to prolonged cytopenia. The rate of Grade 3 or 4 thrombocytopenia was 62% (44/71) and 56% (135/241) for patients treated in dose range of 460 to 510 × 106 CAR-positive T cells and 300 to 460 × 106 CAR-positive T cells, respectively.
Monitor blood counts prior to and after ABECMA infusion. Manage cytopenia with myeloid growth factor and blood product transfusion support according to local institutional guidelines.
5.3 Neurologic Toxicities
Neurologic toxicities, including immune-effector cell-associated neurotoxicity (ICANS), which may be severe or life-threatening, occurred concurrently with CRS, after CRS resolution, or in the absence of CRS following treatment with ABECMA.
In patients receiving ABECMA in Study 1 and Study 2, CAR T cell-associated neurotoxicity occurred in 40% (139/349), including Grade 3 in 4% (14/349) and Grade 4 in 0.6% (2/349) of patients. The median time to onset of neurotoxicity was 2 days (range: 1 to 148 days). The median duration of CAR T cell-associated neurotoxicity was 8 days (range: 1 to 720 days) in all patients including those with ongoing neurologic events at the time of death or data cut off. CAR T cell-associated neurotoxicity resolved in 123 of 139 (88%) patients and median time to resolution was 5 days (range: 1 to 245 days). One-hundred and thirty four out of 349 (38%) patients with neurotoxicity had CRS. The onset of neurotoxicity during CRS was observed in 93 patients, before the onset of CRS in 12 patients, and after the CRS event in 29 patients. The rate of Grade 3 or 4 CAR T cell-associated neurotoxicity was 5.6% (4/71) and 3.7% (9/241) for patients treated in dose range of 460 to 510 × 106 CAR-positive T cells and 300 to 460 × 106 CAR-positive T cells, respectively. The most frequent (≥5%) manifestations of CAR T cell-associated neurotoxicity include encephalopathy (21%), headache (15%), dizziness (8%), delirium (6%), and tremor (6%).
At the safety update for Study 1, one patient developed fatal neurotoxicity 43 days after ABECMA. In Study 2, one patient had ongoing Grade 2 neurotoxicity at the time of death. Two patients had ongoing Grade 1 tremor at the time of data cutoff.
Cerebral edema has been associated with ABECMA in a patient in another study in multiple myeloma. Grade 3 myelitis and Grade 3 parkinsonism have occurred after treatment with ABECMA in another study in multiple myeloma.
Monitor patients at least daily for seven days following ABECMA infusion for signs and symptoms of neurologic toxicities. Rule out other causes of neurologic symptoms. Continue to monitor patients for signs or symptoms of neurologic toxicities for at least one week after infusion and treat promptly. Neurologic toxicity should be managed with supportive care and/or corticosteroids as needed [see Dosage and Administration (2.2) , (2.3)]. Advise patients to avoid driving for at least one week following infusion.
Counsel patients to seek immediate medical attention should signs or symptoms of neurologic toxicity occur at any time [see Patient Counseling Information (17)].
5.8 Hypogammaglobulinemia
Plasma cell aplasia and hypogammaglobulinemia can occur in patients receiving treatment with ABECMA.
In all patients receiving ABECMA in Study 1 and Study 2, hypogammaglobulinemia was reported as an adverse event in 13% (46/349) of patients; laboratory IgG levels fell below 500 mg/dL after infusion in 37% (130/349) of patients treated with ABECMA.
Hypogammaglobulinemia either as an adverse reaction or laboratory IgG level below 500 mg/dL after infusion occurred in 45% (158/349) of patients treated with ABECMA. Forty-one percent of patients received intravenous immunoglobulin (IVIG) post-ABECMA for serum IgG <400 mg/dL.
Monitor immunoglobulin levels after treatment with ABECMA and administer IVIG for IgG <400 mg/dL. Manage per local institutional guidelines, including infection precautions and antibiotic or antiviral prophylaxis.
Use of Live Vaccines
The safety of immunization with live viral vaccines during or following ABECMA treatment has not been studied. Vaccination with live virus vaccines is not recommended for at least six weeks prior to the start of lymphodepleting chemotherapy, during ABECMA treatment, and until immune recovery following treatment with ABECMA.
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
-
•Hypersensitivity Reactions: Monitor for hypersensitivity reactions during infusion. (5.5)
-
•Infections: Monitor patients for signs and symptoms of infection; treat appropriately. (5.6)
-
•Prolonged Cytopenias: Patients may exhibit prolonged Grade 3 or higher cytopenias following ABECMA infusion. Monitor blood counts prior to and after ABECMA infusion. (5.7)
-
•Hypogammaglobulinemia: Monitor and consider immunoglobulin replacement therapy. (5.8)
-
•Secondary Malignancies: T cell malignancies have occurred following treatment of hematologic malignancies with BCMA- and CD19-directed genetically modified autologous T cell immunotherapies, including ABECMA. In the event that a secondary malignancy occurs after treatment with ABECMA, contact Bristol-Myers Squibb at 1-888-805-4555. (5.9)
5.9 Secondary Malignancies
Patients treated with ABECMA may develop secondary malignancies. In Study 1, myeloid neoplasms (four cases of myelodysplastic syndrome and one case of acute myeloid leukemia) occurred in 2.2% (5/222) of patients following treatment with ABECMA compared to none in the standard regimens arm at the time of the safety update. The median time to onset of myeloid neoplasm from ABECMA infusion was 338 days (Range: 277 to 794 days). Three of these five patients have died following the development of myeloid neoplasm. One out of the five cases of myeloid neoplasm occurred after initiation of subsequent antimyeloma therapy.
T cell malignancies have occurred following treatment of hematologic malignancies with BCMA- and CD19‑directed genetically modified autologous T cell immunotherapies, including ABECMA. Mature T cell malignancies, including CAR-positive tumors, may present as soon as weeks following infusion, and may include fatal outcomes [see Boxed Warning, Adverse Reactions (6.3), Patient Counseling Information (17)].
Monitor life-long for secondary malignancies. In the event that a secondary malignancy occurs, contact
Bristol-Myers Squibb at 1‑888‑805‑4555 for reporting and to obtain instructions on collection of patient samples for testing of secondary malignancy.
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
For autologous use only. For intravenous use only.
-
•Do NOT use a leukodepleting filter. (2.2)
-
•Administer a lymphodepleting chemotherapy regimen of cyclophosphamide and fludarabine before infusion of ABECMA. (2.2)
-
•Confirm the patient's identity prior to infusion. (2.2)
-
•Premedicate with acetaminophen and an H1-antihistamine. (2.2)
-
•Avoid prophylactic use of dexamethasone or other systemic corticosteroids. (2.2)
-
•Confirm availability of tocilizumab prior to infusion. (2.2, 5.2)
-
•Dosing of ABECMA is based on the number of chimeric antigen receptor (CAR)-positive T cells. (2.1)
-
•The recommended dose range is 300 to 510 × 106 CAR-positive T cells. (2.1)
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
A single dose of ABECMA contains a cell suspension of 300 to 510 × 106 chimeric antigen receptor (CAR)-positive T cells in one or more infusion bags [see How Supplied/Storage and Handling (16)].
6.2 Postmarketing Experience
Because adverse events to marketed products are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to product exposure.
The following adverse event has been identified during postmarketing use of ABECMA:
Nervous system disorders: Immune effector cell-associated neurotoxicity syndrome (ICANS).
The following adverse event has been identified during postmarketing use of BCMA- or CD19-directed genetically modified autologous T cell immunotherapies:
Neoplasms: T cell malignancies.
5.5 Hypersensitivity Reactions
Allergic reactions may occur with the infusion of ABECMA. Serious hypersensitivity reactions, including anaphylaxis, may be due to dimethyl sulfoxide (DMSO) in ABECMA.
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in clinical practice.
The safety data described in the WARNINGS and PRECAUTIONS section reflect exposure to ABECMA in 349 patients with relapsed or refractory multiple myeloma: one randomized, open-label study with 222 patients in Study 1 and one single-arm, open-label study with 127 patients in Study 2.
Study 1
The safety data described in this section reflect the exposure to ABECMA in Study 1, in which 222 patients with relapsed or refractory multiple myeloma received ABECMA across a dose range of 175 to 529 × 106 CAR-positive T cells (median dose: 445 × 106 CAR-positive T cells) [see Clinical Studies (14)]. Patients with a history of CNS disease or requiring ongoing treatment with chronic immunosuppression were excluded. The median age of the safety population was 63 years (range: 30 to 81 years); 43% were 65 years or older, and 63% were men. The Eastern Cooperative Oncology Group (ECOG) performance status at baseline was 0 in 47%, 1 in 51%, 2 in 1.4% and 3 in 0.5% of patients. Four (1.8%) patients treated with ABECMA had creatinine clearance <45 mL/min. For details about the study population, [see Clinical Studies (14)].
The most common (≥10%) Grade 3 or 4 nonlaboratory adverse reactions was febrile neutropenia (51%) and any infections (16%).
The most common nonlaboratory adverse reactions (incidence ≥20%) included CRS, pyrexia, any infection, febrile neutropenia, hypogammaglobulinemia, musculoskeletal pain, hypotension, infections–pathogen unspecified, fatigue, tachycardia, diarrhea, nausea, headache, encephalopathy, dyspnea and edema.
Serious adverse reactions occurred in 43% of patients. The most common nonlaboratory (≥5%) serious adverse reactions included infections–pathogen unspecified (10%), pneumonia (9%), viral infections (8%), encephalopathy (6%), pyrexia (6%) and sepsis (5%). Fatal adverse reactions occurred in 9%.
Table 3 summarizes the adverse reactions that occurred in at least 10% of patients treated with ABECMA. Table 4 describes the most common Grade 3 or 4 laboratory abnormalities.
| CAR=chimeric antigen receptor. | ||||
| * Represents multiple related terms. | ||||
| a Coagulopathy includes activated partial thromboplastin time prolonged, blood fibrinogen decreased, coagulopathy, disseminated intravascular coagulation, hypofibrinogenemia, international normalized ratio increased, prothrombin time prolonged. | ||||
| b Encephalopathy includes amnesia, cognitive disorder, confusional state, depressed level of consciousness, disturbance in attention, dysgraphia, encephalopathy, Immune effector cell-associated neurotoxicity syndrome incoherent, lethargy, memory impairment, mental status changes, metabolic encephalopathy, somnolence, stupor, toxic encephalopathy. | ||||
| c Neuropathy includes carpal tunnel syndrome, dysesthesia, hyperesthesia, hypoesthesia, hypoesthesia oral, mononeuropathy, neuralgia, neuritis, neuropathy peripheral, paresthesia, paresthesia oral, peripheral motor neuropathy, peripheral sensorimotor neuropathy, peripheral sensory neuropathy, peroneal nerve palsy, radicular pain, radiculopathy, sacral radiculopathy, sciatica, sensory loss, toxic neuropathy. | ||||
|
ABECMA (N=222) |
Standard Regimens (N=126) |
|||
|
Any Grade (%) |
Grade 3 or 4 (%) |
Any Grade (%) |
Grade 3 or 4 (%) |
|
|
Blood and lymphatic system disorders |
||||
|
Febrile neutropenia |
51 |
51 |
28 |
28 |
|
Coagulopathya |
14 |
2.7 |
4.8 |
0.8 |
|
Cardiac disorders |
||||
|
Tachycardia* |
32 |
0 |
21 |
0 |
|
Gastrointestinal disorders |
||||
|
Diarrhea* |
31 |
2.3 |
35 |
3.2 |
|
Nausea |
27 |
0.9 |
48 |
0 |
|
Constipation |
17 |
0 |
15 |
0 |
|
Vomiting* |
14 |
0 |
17 |
0 |
|
Abdominal pain* |
10 |
0.5 |
14 |
0 |
|
General disorders and administration site conditions |
||||
|
Pyrexia |
91 |
9 |
53 |
6 |
|
Fatigue* |
33 |
1.4 |
48 |
4 |
|
Edema* |
20 |
0.5 |
28 |
2.4 |
|
Chills |
19 |
0.5 |
13 |
0 |
|
Immune system disorders |
||||
|
Cytokine release syndrome |
91 |
4.1 |
40 |
0.8 |
|
Hypogammaglobulinemia |
48 |
0.9 |
25 |
0 |
|
Infections and infestations |
||||
|
Any infection |
56 |
16 |
64 |
18 |
|
Infections–pathogen unspecified* |
35 |
9 |
40 |
11 |
|
Upper respiratory tract infection* |
19 |
1.8 |
17 |
0.8 |
|
Infections–viral* |
18 |
5 |
28 |
6 |
|
Infections–bacterial* |
15 |
4.5 |
19 |
8 |
|
Pneumonia* |
13 |
8 |
13 |
11 |
|
Metabolism and nutrition disorders |
||||
|
Decreased appetite |
17 |
1.8 |
21 |
0 |
|
Musculoskeletal and connective tissue disorders |
||||
|
Musculoskeletal pain* |
36 |
1.8 |
49 |
8 |
|
Nervous system disorders |
||||
|
Headache* |
24 |
0 |
29 |
1.6 |
|
Encephalopathyb |
22 |
3.6 |
21 |
4.8 |
|
Dizziness* |
14 |
1.8 |
18 |
3.2 |
|
Neuropathyc |
10 |
0 |
21 |
0.8 |
|
Psychiatric disorders |
||||
|
Sleep disorder* |
11 |
0 |
22 |
2.4 |
|
Renal and urinary disorders |
||||
|
Renal failure* |
13 |
5 |
15 |
4 |
|
Respiratory, thoracic, and mediastinal disorders |
||||
|
Dyspnea* |
21 |
1.8 |
31 |
2.4 |
|
Cough* |
14 |
0 |
21 |
0 |
|
Hypoxia* |
18 |
6 |
8 |
1.6 |
|
Vascular disorders |
||||
|
Hypotension* |
36 |
2.3 |
19 |
1.6 |
|
Hypertension |
14 |
7 |
21 |
11 |
|
Skin disorders |
||||
|
Rash* |
10 |
0 |
19 |
0.8 |
Other clinically important adverse reactions that occurred in less than 10% of patients treated with ABECMA include the following:
-
•Cardiac disorders: cardiac arrhythmia (7%)
-
•Gastrointestinal disorders: gastrointestinal hemorrhage (0.5%)
-
•Immune system disorders: hemophagocytic lymphohistiocytosis (2.3%)
-
•Infections and infestations: infections-fungal (5%), sepsis (6%)
-
•Musculoskeletal and connective tissue disorders: motor dysfunction (9%)
-
•Nervous system disorders: tremor (4.1%), aphasia (3.2%), ataxia (2.3%), seizure (0.5%)
-
•Psychiatric disorders: anxiety (4.1%), delirium (7%)
-
•Respiratory, thoracic, and mediastinal disorders: pulmonary edema (1.4%)
-
•Vascular disorders: thrombosis (3.2%)
Laboratory Abnormalities
Table 4 presents the most common Grade 3 or 4 laboratory abnormalities, based on laboratory data, occurring in at least 10% of patients.
| CAR=chimeric antigen receptor; CTCAE=Common Terminology Criteria for Adverse Events; NCI=National Cancer Institute. | ||
| a Laboratory tests were graded according to NCI CTCAE Version 4.03. | ||
|
Laboratory Abnormality |
ABECMA N=222 (%) |
Standard Regimens N=126 (%) |
|
Grade 3 or 4 (%) |
Grade 3 or 4 (%) |
|
|
Lymphocyte decreased |
98 |
78 |
|
Leukocyte decreased |
96 |
64 |
|
Neutrophil decreased |
96 |
72 |
|
Platelet decreased |
59 |
46 |
|
Hemoglobin decreased |
52 |
45 |
|
Phosphate decreased |
45 |
30 |
|
Triglyceride increased |
21 |
10 |
|
Alanine aminotransferase increased |
13 |
8 |
|
Sodium decreased |
11 |
7 |
|
Gamma-glutamyltransferase increased |
10 |
6 |
Other clinically important Grade 3 or 4 laboratory abnormalities (based on laboratory data) that occurred in less than 10% of patients treated with ABECMA include the following: aspartate aminotransferase increased, potassium decreased, albumin decreased, alkaline phosphatase increased, calcium decreased, glucose increased, activated partial thromboplastin time increased (seconds), fibrinogen decreased, bilirubin increased and hypomagnesemia.
Study 2
The safety data described in this section reflect the exposure to ABECMA in Study 2, in which 127 patients with relapsed/refractory multiple myeloma received ABECMA across a dose range of 150 to 518 × 106 CAR-positive T cells [see Clinical Studies (14)]. Patients with a history of CNS disease (such as seizure or cerebrovascular ischemia) or requiring ongoing treatment with chronic immunosuppression were excluded. The median duration of follow-up was 11.4 months. The median age of the study population was 61 years (range: 33 to 78 years); 35% were 65 years or older, and 60% were men. The Eastern Cooperative Oncology Group (ECOG) performance status at baseline was 0 in 45%, 1 in 53%, and 2 in 2% of patients. Seven percent of the patients treated with ABECMA had creatinine clearance <45 mL/min. For details about the study population, [see Clinical Studies (14)].
The most common (≥10%) Grade 3 or 4 nonlaboratory adverse reactions were febrile neutropenia (16%) and infections–pathogen unspecified (15%).
The most common nonlaboratory adverse reactions (incidence ≥20%) included CRS, infections–pathogen unspecified, fatigue, musculoskeletal pain, hypogammaglobulinemia, diarrhea, upper respiratory tract infection, nausea, viral infections, encephalopathy, edema, pyrexia, cough, headache, and decreased appetite.
Serious adverse reactions occurred in 67% of patients. The most common nonlaboratory (≥5%) serious adverse reactions included CRS (18%), general physical health deterioration (10%), pneumonia (12%), infections–pathogen unspecified (19%), viral infections (9%), sepsis (7%), and febrile neutropenia (6%). Fatal adverse reactions occurred in 6%.
Table 5 summarizes the adverse reactions that occurred in at least 10% of patients treated with ABECMA. Table 6 describes the most common Grade 3 or 4 laboratory abnormalities.
| CAR=chimeric antigen receptor. * Represents multiple related terms. |
||
| a Encephalopathy includes amnesia, bradyphrenia, cognitive disorder, confusional state, depressed level of consciousness, disturbance in attention, dyscalculia, dysgraphia, encephalopathy, lethargy, memory impairment, mental status changes, metabolic encephalopathy, somnolence, toxic encephalopathy. | ||
| b Neuropathy peripheral includes carpal tunnel syndrome, hypoesthesia, hypoesthesia oral, neuralgia, neuropathy peripheral, paresthesia, peripheral sensorimotor neuropathy, peripheral sensory neuropathy, sciatica. | ||
|
System Organ Class
|
Target Dose of ABECMA (CAR-Positive T Cells) |
|
|
Any Grade |
Grade 3 or Higher |
|
|
[150 to 450 × 106]
|
[150 to 450 × 106]
|
|
|
Blood and lymphatic system disorders |
||
|
Febrile neutropenia |
16 |
16 |
|
Cardiac disorders |
||
|
Tachycardia* |
19 |
0 |
|
Gastrointestinal disorders |
||
|
Diarrhea |
35 |
1.6 |
|
Nausea |
29 |
0 |
|
Constipation |
16 |
0 |
|
Vomiting |
15 |
0 |
|
Oral pain* |
12 |
0 |
|
General disorders and administration site conditions |
||
|
Fatigue* |
45 |
3.1 |
|
Pyrexia |
25 |
1.6 |
|
General physical health deterioration |
11 |
10 |
|
Edema* |
25 |
0 |
|
Chills |
11 |
0 |
|
Immune system disorders |
||
|
Cytokine release syndrome |
85 |
9 |
|
Hypogammaglobulinemia* |
41 |
0.8 |
|
Infections and infestations * |
||
|
Infections–Pathogen unspecified |
51 |
15 |
|
Viral infections |
27 |
9 |
|
Bacterial infections |
15 |
3.9 |
|
Pneumonia* |
17 |
9 |
|
Upper respiratory tract infection* |
34 |
1.6 |
|
Investigations |
||
|
Weight decreased |
13 |
1.6 |
|
Metabolism and nutrition disorders |
||
|
Decreased appetite* |
22 |
0.8 |
|
Musculoskeletal and connective tissue disorders |
||
|
Musculoskeletal pain* |
45 |
3.1 |
|
Motor dysfunction* |
11 |
0 |
|
Nervous system disorders |
||
|
Encephalopathya |
26 |
6 |
|
Headache* |
23 |
0 |
|
Dizziness* |
17 |
0.8 |
|
Neuropathy peripheralb |
17 |
0.8 |
|
Tremor* |
10 |
0 |
|
Psychiatric disorders |
||
|
Insomnia* |
13 |
0 |
|
Anxiety* |
12 |
0.8 |
|
Renal and urinary disorders |
||
|
Renal failure* |
10 |
2.4 |
|
Respiratory, thoracic, and mediastinal disorders |
||
|
Cough* |
23 |
0 |
|
Dyspnea* |
13 |
2.4 |
|
Skin and subcutaneous tissue disorder |
||
|
Rash* |
14 |
0.8 |
|
Xerosis* |
11 |
0 |
|
Vascular disorders |
||
|
Hypotension* |
17 |
0 |
|
Hypertension |
11 |
3.1 |
Other clinically important adverse reactions that occurred in less than 10% of patients treated with ABECMA include the following:
-
•Blood and lymphatic system disorders: coagulopathy (9%)
-
•Cardiac disorders: atrial fibrillation (4.7%), cardiomyopathy (1.6%)
-
•Gastrointestinal disorders: gastrointestinal hemorrhage (3.1%)
-
•Immune system disorders: hemophagocytic lymphohistiocytosis (3.1%)
-
•Infections and infestations: fungal infections (8%), sepsis (9%)
-
•Nervous system disorders: aphasia (7%), ataxia (3.1%), paresis (2.4%), seizure (1.6%)
-
•Psychiatric disorders: delirium (6%)
-
•Respiratory, thoracic, and mediastinal disorders: hypoxia (2.4%), pulmonary edema (2.4%)
-
•Vascular disorders: thrombosis (3.1%)
17 Patient Counseling Information (17 PATIENT COUNSELING INFORMATION)
Advise the patient to read the FDA-approved patient labeling (Medication Guide).
Advise patients that the risk of manufacturing failure is 2.1% [8/384 in the clinical studies]. In case of a manufacturing failure, a second manufacturing of ABECMA may be attempted. In addition, while the patient awaits the product, additional anticancer treatment (not the lymphodepletion) may be necessary and may increase the risk of adverse events during the pre-infusion period, which could delay or prevent the administration of ABECMA.
Inform patients of the risk of early death: In a clinical study, a higher proportion of patients experienced death within the first nine months from randomization in the ABECMA arm compared to the standard regimens arm. This higher rate of early death was mainly observed before receiving ABECMA with the main reason being progression of multiple myeloma. There was also an increase in the rate of death from adverse events after ABECMA.
Advise patients to seek immediate attention for any of the following:
-
•Cytokine Release Syndrome (CRS): Signs or symptoms associated with CRS, including fever, hypotension, tachycardia, chills, hypoxia, headache, and fatigue [see Dosage and Administration (2.3), Warnings and Precautions (5.2) , and Adverse Reactions (6.1)].
-
•Neurologic Toxicities: Signs or symptoms associated with neurologic events, including encephalopathy, confusion, seizures, tremor, aphasia, delirium, and somnolence [see Dosage and Administration (2.3), Warnings and Precautions (5.3) , and Adverse Reactions (6.1)].
-
•Infections: Signs or symptoms associated with infection [see Warnings and Precautions (5.6) and Adverse Reactions (6.1)].
-
•Prolonged Cytopenias: Signs or symptoms associated with bone marrow suppression, including neutropenia, anemia, thrombocytopenia, or febrile neutropenia [see Warnings and Precautions (5.7) and Adverse Reactions (6.1)].
-
•Secondary malignancies: Secondary malignancies, including T cell malignancies, have occurred [see Boxed Warning, Warnings and Precautions (5.9) , Adverse Reactions (6.3)].
Advise patients for the need to:
-
•Contact Bristol-Myers Squibb at 1-888-805-4555 if they are diagnosed with a secondary malignancy [see Warnings and Precautions (5.9) ].
-
•Have periodic monitoring of blood counts before and after ABECMA infusion [see Warnings and Precautions (5.7) ].
-
•Avoid driving for at least one week.
5.2 Cytokine Release Syndrome (crs) (5.2 Cytokine Release Syndrome (CRS))
CRS, including fatal or life-threatening reactions, occurred following treatment with ABECMA. Among patients receiving ABECMA for relapsed or refractory multiple myeloma in Study 1 and Study 2 (N=349), CRS occurred in 89% (310/349), including ≥ Grade 3 CRS (Lee grading system) in 7% (23/349) of patients and Grade 5 CRS in 0.9% (3/349) of patients. The median time-to-onset of CRS, any grade, was 1 day (range: 1 to 27 days), and the median duration of CRS was 5 days (range: 1 to 63 days). In the pooled studies, the rate of ≥ Grade 3 CRS was 10% (7/71) for patients treated in dose range of 460 to 510 × 106 CAR-positive T cells and 5.4% (13/241) for patients treated in dose range of 300 to 460 × 106 CAR-positive T cells.
The most common manifestations of CRS (≥10%) included pyrexia (87%), hypotension (30%), tachycardia (26%), chills (19%), and hypoxia (16%). Grade 3 or higher events that may be associated with CRS include hypotension, hypoxia, hyperbilirubinemia, hypofibrinogenemia, ARDS, atrial fibrillation, hepatocellular injury, metabolic acidosis, pulmonary edema, coagulopathy, renal failure, multiple organ dysfunction syndrome and hemophagocytic lymphohistiocytosis/macrophage activation syndrome (HLH/MAS) [see Adverse Reactions (6.1)].
Identify CRS based on clinical presentation. Evaluate for and treat other causes of fever, hypoxia, and hypotension. CRS has been reported to be associated with findings of HLH/MAS, and the physiology of the syndromes may overlap. HLH/MAS is a potentially life-threatening condition. In patients with progressive symptoms of CRS or refractory CRS despite treatment, evaluate for evidence of HLH/MAS. Please see Section 5.4 ; Hemophagocytic Lymphohistiocytosis/Macrophage Activation Syndrome.
Of the 349 patients who received ABECMA in clinical trials, 226 (65%) patients received tocilizumab; 39% (135/349) received a single dose, while 26% (91/349) received more than 1 dose of tocilizumab. Overall, 24% (82/349) of patients received at least 1 dose of corticosteroids for treatment of CRS. Almost all patients who received corticosteroids for CRS also received tocilizumab. For patients treated in dose range of 460 to 510 × 106 CAR-positive T cells, 76% (54/71) of patients received tocilizumab and 35% (25/71) received at least 1 dose of corticosteroids for treatment of CRS. For patients treated in dose range of 300 to 460 × 106 CAR-positive T cells, 63% (152/241) of patients received tocilizumab and 20% (49/241) received at least 1 dose of corticosteroid for treatment of CRS.
Ensure that a minimum of two doses of tocilizumab are available prior to infusion of ABECMA.
Monitor patients at least daily for seven days following ABECMA infusion for signs and symptoms of CRS. Continue to monitor patients for signs or symptoms of CRS for at least one week after infusion. At the first sign of CRS, institute treatment with supportive care, tocilizumab and/or corticosteroids as indicated [see Dosage and Administration (2.2) , (2.3) ].
Counsel patients to seek immediate medical attention should signs or symptoms of CRS occur at any time [see Patient Counseling Information (17)].
16 How Supplied/storage and Handling (16 HOW SUPPLIED/STORAGE AND HANDLING)
ABECMA is supplied in one or more infusion bag(s) (see below) containing a frozen suspension of genetically modified autologous T cells in 5% DMSO.
Each infusion bag of ABECMA is overwrapped with a transparent plastic sleeve that is folded to the back of the infusion bag and individually packed in a metal cassette. ABECMA is stored in the vapor phase of liquid nitrogen and supplied in a liquid nitrogen dry vapor shipper. An RFI Certificate is affixed inside the shipper.
-
•50 mL infusion bag and metal cassette (NDC 59572-515-01)
-
•250 mL infusion bag and metal cassette (NDC 59572-515-02)
-
•500 mL infusion bag and metal cassette (NDC 59572-515-03)
Match the identity of the patient with the patient identifiers on the cassette(s) and infusion bag(s) upon receipt.
Principal Display Panel 30 Ml Bag Label (PRINCIPAL DISPLAY PANEL - 30 mL Bag Label)
idecabtagene vicleucel
Abecma™
NDC 59572-515-01
Genetically modified autologous T cells
FOR AUTOLOGOUS AND INTRAVENOUS USE ONLY
Suspension for IV Infusion
Rx Only
Acceptable Volume 10mL - 30mL per bag
Dosage: See prescribing information and
Release for Infusion Certificate (inside shipper).
Contains: 300 to 510 x 106 anti-BCMA02
CAR-positive T cells in cryopreservative
solution containing 5% DMSO USP.
Dose may be suspended in 1 or more
infusion bag(s).
Do not use a leukodepleting filter
or irradiate.
Not evaluated for infectious substances.
Preservative free.
Store in vapor phase of liquid nitrogen
(≤ -130°C).
Mfd by: Celgene Corporation,
a Bristol-Myers Squibb Company
Summit, NJ 07901 USA
Phone: 1-888-805-4555
US License No. 2252
First: FIRST NAME
Last: LAST NAME
Date of birth: DD-MMM-YYYY
DIN/Aph ID: W0000 00 000000
JOIN: XXXX-XXXXX
LOT: XXXX-XXXXXY
EXP: DD-MMM-YYYY
Bag ID: XX
XXXX-XXXXXY-XX
304492
Principal Display Panel 70 Ml Bag Label (PRINCIPAL DISPLAY PANEL - 70 mL Bag Label)
idecabtagene vicleucel
Abecma™
NDC 59572-515-02
Genetically modified autologous T cells
FOR AUTOLOGOUS AND INTRAVENOUS USE ONLY
Suspension for IV Infusion
Rx Only
Acceptable Volume 30mL - 70mL per bag
Dosage: See prescribing information and
Release for Infusion Certificate (inside shipper).
Contains: 300 to 510 x 106 anti-BCMA02
CAR-positive T cells in cryopreservative
solution containing 5% DMSO USP.
Dose may be suspended in 1 or more
infusion bag(s).
Do not use a leukodepleting filter
or irradiate.
Not evaluated for infectious substances.
Preservative free.
Store in vapor phase of liquid nitrogen
(≤ -130°C).
Mfd by: Celgene Corporation,
a Bristol-Myers Squibb Company
Summit, NJ 07901 USA
Phone: 1-888-805-4555
US License No. 2252
First: FIRST NAME
Last: LAST NAME
Date of birth: DD-MMM-YYYY
DIN/Aph ID: W0000 00 000000
JOIN: XXXX-XXXXX
LOT: XXXX-XXXXXY
EXP: DD-MMM-YYYY
Bag ID: XX
XXXX-XXXXXY-XX
304492
Principal Display Panel 100 Ml Bag Label (PRINCIPAL DISPLAY PANEL - 100 mL Bag Label)
idecabtagene vicleucel
Abecma™
NDC 59572-515-03
Genetically modified autologous T cells
FOR AUTOLOGOUS AND INTRAVENOUS USE ONLY
Suspension for IV Infusion
Rx Only
Acceptable Volume 55mL - 100mL per bag
Dosage: See prescribing information and
Release for Infusion Certificate (inside shipper).
Contains: 300 to 510 x 106 anti-BCMA02
CAR-positive T cells in cryopreservative
solution containing 5% DMSO USP.
Dose may be suspended in 1 or more
infusion bag(s).
Do not use a leukodepleting filter
or irradiate.
Not evaluated for infectious substances.
Preservative free.
Store in vapor phase of liquid nitrogen
(≤ -130°C).
Mfd by: Celgene Corporation,
a Bristol-Myers Squibb Company
Summit, NJ 07901 USA
Phone: 1-888-805-4555
US License No. 2252
First: FIRST NAME
Last: LAST NAME
Date of birth: DD-MMM-YYYY
DIN/Aph ID: W0000 00 000000
JOIN: XXXX-XXXXX
LOT: XXXX-XXXXXY
EXP: DD-MMM-YYYY
Bag ID: XX
XXXX-XXXXXY-XX
304492
Principal Display Panel 30 Ml Cassette Label (PRINCIPAL DISPLAY PANEL - 30 mL Cassette Label)
idecabtagene vicleucel
Abecma™
NDC 59572-515-01
Genetically modified autologous T cells
FOR AUTOLOGOUS AND INTRAVENOUS USE ONLY
Suspension for IV Infusion
Rx Only
Acceptable Volume 10mL - 30mL per bag
Dosage: See prescribing information and Release for
Infusion Certificate (inside shipper).
Contains: 300 to 510 x 106 anti-BCMA02 CAR-positive T cells
in cryopreservative solution containing 5% DMSO USP.
Dose may be suspended in 1 or more infusion bag(s).
Do not use a leukodepleting filter or irradiate.
Not evaluated for infectious substances. Preservative free.
Store in vapor phase of liquid nitrogen (≤ -130°C).
Mfd by: Celgene Corporation, a Bristol-Myers Squibb Company
Summit, NJ 07901 USA
Phone: 1-888-805-4555
US License No. 2252
First: FIRST NAME
Last: LAST NAME
Date of birth: DD-MMM-YYYY
DIN/Aph ID: W0000 00 000000
JOIN: XXXX-XXXXX
LOT: XXXX-XXXXXY
EXP: DD-MMM-YYYY
Bag ID: XX
XXXX-XXXXXY-XX
304493
Principal Display Panel 70 Ml Cassette Label (PRINCIPAL DISPLAY PANEL - 70 mL Cassette Label)
idecabtagene vicleucel
Abecma™
NDC 59572-515-02
Genetically modified autologous T cells
FOR AUTOLOGOUS AND INTRAVENOUS USE ONLY
Suspension for IV Infusion
Rx Only
Acceptable Volume 30mL - 70mL per bag
Dosage: See prescribing information and Release for
Infusion Certificate (inside shipper).
Contains: 300 to 510 x 106 anti-BCMA02 CAR-positive T cells
in cryopreservative solution containing 5% DMSO USP.
Dose may be suspended in 1 or more infusion bag(s).
Do not use a leukodepleting filter or irradiate.
Not evaluated for infectious substances. Preservative free.
Store in vapor phase of liquid nitrogen (≤ -130°C).
Mfd by: Celgene Corporation, a Bristol-Myers Squibb Company
Summit, NJ 07901 USA
Phone: 1-888-805-4555
US License No. 2252
First: FIRST NAME
Last: LAST NAME
Date of birth: DD-MMM-YYYY
DIN/Aph ID: W0000 00 000000
JOIN: XXXX-XXXXX
LOT: XXXX-XXXXXY
EXP: DD-MMM-YYYY
Bag ID: XX
XXXX-XXXXXY-XX
304493
Principal Display Panel 100 Ml Cassette Label (PRINCIPAL DISPLAY PANEL - 100 mL Cassette Label)
idecabtagene vicleucel
Abecma™
NDC 59572-515-03
Genetically modified autologous T cells
FOR AUTOLOGOUS AND INTRAVENOUS USE ONLY
Suspension for IV Infusion
Rx Only
Acceptable Volume 55mL - 100mL per bag
Dosage: See prescribing information and Release for
Infusion Certificate (inside shipper).
Contains: 300 to 510 x 106 anti-BCMA02 CAR-positive T cells
in cryopreservative solution containing 5% DMSO USP.
Dose may be suspended in 1 or more infusion bag(s).
Do not use a leukodepleting filter or irradiate.
Not evaluated for infectious substances. Preservative free.
Store in vapor phase of liquid nitrogen (≤ -130°C).
Mfd by: Celgene Corporation, a Bristol-Myers Squibb Company
Summit, NJ 07901 USA
Phone: 1-888-805-4555
US License No. 2252
First: FIRST NAME
Last: LAST NAME
Date of birth: DD-MMM-YYYY
DIN/Aph ID: W0000 00 000000
JOIN: XXXX-XXXXX
LOT: XXXX-XXXXXY
EXP: DD-MMM-YYYY
Bag ID: XX
XXXX-XXXXXY-XX
304493
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Genotoxicity assays and carcinogenicity studies in rodents were not performed for ABECMA.
In vitro expansion studies with CAR-positive T cells (ABECMA) from five patients and two healthy donor drug product lots showed no evidence for transformation and/or immortalization of T cells. A genomic insertion site analysis of the lentiviral vector was performed on ABECMA samples from twenty (20) individual patient donors. There was no evidence for preferential integration near genes of concern or preferential outgrowth of cells harboring integration sites of concern.
No studies on the effects of ABECMA on fertility have been conducted.
5.4 Hemophagocytic Lymphohistiocytosis (hlh)/macrophage Activation Syndrome (mas) (5.4 Hemophagocytic Lymphohistiocytosis (HLH)/Macrophage Activation Syndrome (MAS))
In patients receiving ABECMA in Study 1 and Study 2, HLH/MAS occurred in 2.9% (10/349) of patients. All events of HLH/MAS had onset within 10 days of receiving ABECMA, with a median onset of 6.5 days (range: 4 to 10 days) and occurred in the setting of ongoing or worsening CRS. Five patients with HLH/MAS had overlapping neurotoxicity. The manifestations of HLH/MAS include hypotension, hypoxia, multiple organ dysfunction, renal dysfunction, and cytopenia.
In Study 1, one patient had Grade 5, two patients had Grade 4 and two patients had Grade 3 HLH/MAS. The patient with Grade 5 HLH/MAS also had Grade 5 candida sepsis and Grade 5 CRS. In another patient who died due to stroke, the Grade 4 HLH/MAS had resolved prior to death. Two cases of Grade 3 and one case of Grade 4 HLH/MAS had resolved.
In Study 2, one patient treated in the 300 × 106 CAR-positive T cells dose cohort developed fatal multi-organ HLH/MAS with CRS. In another patient with fatal bronchopulmonary aspergillosis, HLH/MAS was contributory to the fatal outcome. Three cases of Grade 2 HLH/MAS resolved.
HLH/MAS is a potentially life-threatening condition with a high mortality rate if not recognized early and treated. Treatment of HLH/MAS should be administered per institutional standards.
Warning: Cytokine Release Syndrome, Neurologic Toxicities, Hlh/mas, Prolonged Cytopenia, and Secondary Hematological Malignancies (WARNING: CYTOKINE RELEASE SYNDROME, NEUROLOGIC TOXICITIES, HLH/MAS, PROLONGED CYTOPENIA, AND SECONDARY HEMATOLOGICAL MALIGNANCIES)
-
•Cytokine Release Syndrome (CRS), including fatal or life-threatening reactions, occurred in patients following treatment with ABECMA. Do not administer ABECMA to patients with active infection or inflammatory disorders. Treat severe or life-threatening CRS with tocilizumab or tocilizumab and corticosteroids [see Dosage and Administration (2.2, 2.3), Warnings and Precautions (5.2) ].
-
•Neurologic toxicities, which may be severe or life-threatening, occurred following treatment with ABECMA, including concurrently with CRS, after CRS resolution, or in the absence of CRS. Monitor for neurologic events after treatment with ABECMA. Provide supportive care and/or corticosteroids as needed [see Dosage and Administration (2.2, 2.3) and Warnings and Precautions (5.3) ].
-
•Hemophagocytic Lymphohistiocytosis/Macrophage Activation Syndrome (HLH/MAS) including fatal and life-threatening reactions, occurred in patients following treatment with ABECMA. HLH/MAS can occur with CRS or neurologic toxicities [see Warnings and Precautions (5.4) ].
-
•Prolonged Cytopenia with bleeding and infection, including fatal outcomes following stem cell transplantation for hematopoietic recovery, occurred following treatment with ABECMA [see Warnings and Precautions (5.7) ].
-
•T cell malignancies have occurred following treatment of hematologic malignancies with BCMA- and CD19-directed genetically modified autologous T cell immunotherapies, including ABECMA [see Warnings and Precautions (5.9) ].
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T12:13:06.079634 · Updated: 2026-03-14T23:19:37.925742