These Highlights Do Not Include All The Information Needed To Use Symproic Safely And Effectively. See Full Prescribing Information For Symproic.
b1a1256c-a1eb-4abe-ab1e-30e4711afd16
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
Warnings and Precautions, Gastrointestinal Perforation ( 5.1 ) 07/2025
Indications and Usage
SYMPROIC is indicated for the treatment of opioid-induced constipation (OIC) in adult patients with chronic non-cancer pain, including patients with chronic pain related to prior cancer or its treatment who do not require frequent (e.g., weekly) opioid dosage escalation.
Dosage and Administration
Administration ( 2.1 ) : Alteration of analgesic dosing regimen prior to initiating SYMPROIC is not required Patients receiving opioids for less than 4 weeks may be less responsive to SYMPROIC Discontinue SYMPROIC if treatment with the opioid pain medication is also discontinued Dosage ( 2.2 ) : In adults, the recommended dosage is 0.2 mg once daily with or without food
Warnings and Precautions
Gastrointestinal perforation : Consider the overall risk benefit in patients with known or suspected lesions of the GI tract. Monitor for severe, persistent, or worsening abdominal pain; discontinue if development of symptoms ( 5.1 ) Opioid withdrawal : Consider the overall risk benefit in patients with disruptions to the blood-brain barrier. Monitor symptoms of opioid withdrawal ( 5.2 )
Contraindications
SYMPROIC is contraindicated in: Patients with known or suspected gastrointestinal obstruction and patients at increased risk of recurrent obstruction, due to the potential for gastrointestinal perforation [see Warnings and Precautions (5.1) ]. Patients with a history of a hypersensitivity reaction to naldemedine. Reactions have included bronchospasm and rash [see Adverse Reactions (6.1) ] .
Adverse Reactions
Serious and important adverse reactions described elsewhere in labeling include: Gastrointestinal perforation [see Warnings and Precautions (5.1) ] Opioid withdrawal [see Warnings and Precautions (5.2) ]
Drug Interactions
Table 3 includes drugs with clinically important drug interactions with SYMPROIC and instructions for preventing or managing the interaction. Table 3: Clinically Relevant Interactions Affecting Naldemedine When Co-Administered with Other Drugs Strong CYP3A Inducers (e.g., rifampin, carbamazepine, phenytoin, St. John's Wort) Clinical Impact Significant decrease in plasma naldemedine concentrations, which may reduce efficacy [see Clinical Pharmacology (12.3) ] Intervention Avoid use of SYMPROIC with strong CYP3A inducers. Other Opioid Antagonists Clinical Impact Potential for additive effect of opioid receptor antagonism and increased risk of opioid withdrawal. Intervention Avoid use of SYMPROIC with another opioid antagonist. Moderate (e.g., fluconazole, atazanavir, aprepitant, diltiazem, erythromycin) and Strong (e.g., itraconazole, ketoconazole, clarithromycin, ritonavir, saquinavir) CYP3A Inhibitors Clinical Impact Increase in plasma naldemedine concentrations [see Clinical Pharmacology (12.3) ] Intervention Monitor for potential naldemedine-related adverse reactions [see Adverse Reactions (6.1) ] . P-glycoprotein (P-gp) Inhibitors (e.g., amiodarone, captopril, cyclosporine, quercetin, quinidine, verapamil) Clinical Impact Increase in plasma naldemedine concentrations [see Clinical Pharmacology (12.3) ] Intervention Monitor for potential naldemedine-related adverse reactions [see Adverse Reactions (6.1) ] .
Storage and Handling
SYMPROIC is supplied as 0.2 mg naldemedine tablets as follows: bottle of 30 tablets - NDC 59385-041-30
How Supplied
SYMPROIC is supplied as 0.2 mg naldemedine tablets as follows: bottle of 30 tablets - NDC 59385-041-30
Medication Information
Warnings and Precautions
Gastrointestinal perforation : Consider the overall risk benefit in patients with known or suspected lesions of the GI tract. Monitor for severe, persistent, or worsening abdominal pain; discontinue if development of symptoms ( 5.1 ) Opioid withdrawal : Consider the overall risk benefit in patients with disruptions to the blood-brain barrier. Monitor symptoms of opioid withdrawal ( 5.2 )
Indications and Usage
SYMPROIC is indicated for the treatment of opioid-induced constipation (OIC) in adult patients with chronic non-cancer pain, including patients with chronic pain related to prior cancer or its treatment who do not require frequent (e.g., weekly) opioid dosage escalation.
Dosage and Administration
Administration ( 2.1 ) : Alteration of analgesic dosing regimen prior to initiating SYMPROIC is not required Patients receiving opioids for less than 4 weeks may be less responsive to SYMPROIC Discontinue SYMPROIC if treatment with the opioid pain medication is also discontinued Dosage ( 2.2 ) : In adults, the recommended dosage is 0.2 mg once daily with or without food
Contraindications
SYMPROIC is contraindicated in: Patients with known or suspected gastrointestinal obstruction and patients at increased risk of recurrent obstruction, due to the potential for gastrointestinal perforation [see Warnings and Precautions (5.1) ]. Patients with a history of a hypersensitivity reaction to naldemedine. Reactions have included bronchospasm and rash [see Adverse Reactions (6.1) ] .
Adverse Reactions
Serious and important adverse reactions described elsewhere in labeling include: Gastrointestinal perforation [see Warnings and Precautions (5.1) ] Opioid withdrawal [see Warnings and Precautions (5.2) ]
Drug Interactions
Table 3 includes drugs with clinically important drug interactions with SYMPROIC and instructions for preventing or managing the interaction. Table 3: Clinically Relevant Interactions Affecting Naldemedine When Co-Administered with Other Drugs Strong CYP3A Inducers (e.g., rifampin, carbamazepine, phenytoin, St. John's Wort) Clinical Impact Significant decrease in plasma naldemedine concentrations, which may reduce efficacy [see Clinical Pharmacology (12.3) ] Intervention Avoid use of SYMPROIC with strong CYP3A inducers. Other Opioid Antagonists Clinical Impact Potential for additive effect of opioid receptor antagonism and increased risk of opioid withdrawal. Intervention Avoid use of SYMPROIC with another opioid antagonist. Moderate (e.g., fluconazole, atazanavir, aprepitant, diltiazem, erythromycin) and Strong (e.g., itraconazole, ketoconazole, clarithromycin, ritonavir, saquinavir) CYP3A Inhibitors Clinical Impact Increase in plasma naldemedine concentrations [see Clinical Pharmacology (12.3) ] Intervention Monitor for potential naldemedine-related adverse reactions [see Adverse Reactions (6.1) ] . P-glycoprotein (P-gp) Inhibitors (e.g., amiodarone, captopril, cyclosporine, quercetin, quinidine, verapamil) Clinical Impact Increase in plasma naldemedine concentrations [see Clinical Pharmacology (12.3) ] Intervention Monitor for potential naldemedine-related adverse reactions [see Adverse Reactions (6.1) ] .
Storage and Handling
SYMPROIC is supplied as 0.2 mg naldemedine tablets as follows: bottle of 30 tablets - NDC 59385-041-30
How Supplied
SYMPROIC is supplied as 0.2 mg naldemedine tablets as follows: bottle of 30 tablets - NDC 59385-041-30
Description
Warnings and Precautions, Gastrointestinal Perforation ( 5.1 ) 07/2025
Section 42229-5
Opioid Withdrawal
In Studies 1, 2 and 3, adverse reactions consistent with opioid withdrawal were based on investigator assessment and adjudicated based upon the occurrence of at least 3 adverse reactions potentially related to opioid withdrawal with onset of a constellation of those symptoms occurring on the same day or within one day of each other.
Adverse reactions of possible opioid withdrawal could include non-gastrointestinal (GI) symptoms (e.g., hyperhidrosis, hot flush or flushing, chills, tremor, tachycardia, anxiety, agitation, yawning, rhinorrhea, increased lacrimation, sneezing, feeling cold, and pyrexia), GI symptoms (e.g., vomiting, diarrhea, or abdominal pain), or both GI and non-GI symptoms.
In pooled Studies 1 and 2, the incidence of adverse reactions of opioid withdrawal was 1% (8/542) for SYMPROIC and 1% (3/546) for placebo. In Study 3 (52-week data), the incidence was 3% (20/621) for SYMPROIC and 1% (9/619) for placebo. Most SYMPROIC treated subjects experienced nearly equal incidence of GI only or both GI and non-GI symptoms.
Section 42231-1
| This Medication Guide has been approved by the U.S. Food and Drug Administration. | Revised: 07/2025 |
|
MEDICATION GUIDE SYMPROIC® (sim proe' ik) (naldemedine) tablets, for oral use |
|
|
What is the most important information I should know about SYMPROIC? |
|
SYMPROIC may cause serious side effects, including:
|
|
| What is SYMPROIC? | |
| SYMPROIC is a prescription medicine used to treat constipation that is caused by prescription pain medicines called opioids in adults with long-lasting (chronic) pain that is not caused by active cancer. It is not known if SYMPROIC is safe and effective in children. |
|
Do not take SYMPROIC if you:
|
|
Before you take SYMPROIC, tell your healthcare provider about all of your medical conditions, including if you:
|
|
| Tell your healthcare provider about all the medicines you take, including prescription and over-the-counter medicines, vitamins, and herbal supplements. Other medicines may affect the way SYMPROIC works. | |
How should I take SYMPROIC?
|
|
| What are the possible side effects of SYMPROIC? | |
| See "What is the most important information I should know about SYMPROIC?" | |
|
The most common side effects of SYMPROIC include stomach (abdomen) pain, diarrhea, nausea and vomiting (gastroenteritis). Tell your healthcare provider if you have any side effect that bothers you or that does not go away. These are not all the possible side effects of SYMPROIC. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. |
|
How should I store SYMPROIC?
|
|
| Keep SYMPROIC and all medicines out of the reach of children. | |
| General information about the safe and effective use of SYMPROIC. | |
| Medicines are sometimes prescribed for purposes other than those in a Medication Guide. Do not take SYMPROIC for a condition for which it was not prescribed. Do not give SYMPROIC to other people, even if they have the same symptoms that you have. It may harm them. You can ask your pharmacist or healthcare provider for information about SYMPROIC that is written for health professionals. | |
| What are the ingredients in SYMPROIC? | |
| Active Ingredient: naldemedine tosylate | |
|
Inactive ingredients: D-mannitol, croscarmellose sodium, magnesium stearate, hypromellose, talc, and yellow ferric oxide. Manufactured for: Collegium Pharmaceutical, Inc. Stoughton, MA 02072 |
|
| SYM-001-MG-JULY2025 SYMPROIC is a registered trademark of Shionogi & Co., Ltd. For more information, go to www.symproic.com or call 1-800-469-0261. |
Section 43683-2
| Warnings and Precautions, Gastrointestinal Perforation (5.1) | 07/2025 |
Section 44425-7
Store SYMPROIC in a light resistant container at 20°C to 25°C (68°F to 77°F); excursions permitted between 15°C and 30°C (59°F and 86°F) [see USP Controlled Room Temperature].
10 Overdosage
Single doses of naldemedine up to 100 mg (500 times the recommended dose) and multiple doses of up to 30 mg (150 times the recommended dose) for 10 days have been administered to healthy subjects in clinical studies. Dose-dependent increases in gastrointestinal-related adverse reactions, including abdominal pain, diarrhea, and nausea, were observed.
Single doses of naldemedine up to 3 mg (15 times the recommended dose) and multiple doses of 0.4 mg (twice the recommended dose) for 28 days have been administered to patients with OIC in clinical studies. Dose-dependent increases in gastrointestinal-related adverse reactions, including abdominal pain, diarrhea, nausea, and vomiting, were observed. Also, chills, hyperhidrosis, and dizziness were reported more frequently at 1 and 3 mg doses and hyperhidrosis at the 0.4 mg dose.
No antidote for naldemedine is known. Hemodialysis is not an effective means to remove naldemedine from the blood [see Clinical Pharmacology (12.3)].
11 Description
SYMPROIC (naldemedine), an opioid antagonist, contains naldemedine tosylate as the active ingredient.
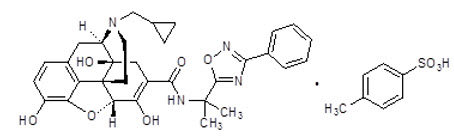
The chemical name for naldemedine tosylate is: 17-(cyclopropylmethyl)-6,7-didehydro-4,5α-epoxy-3,6,14-trihydroxy-N-[2-(3-phenyl-1,2,4-oxadiazol-5-yl)propan-2-yl]morphinan-7-carboxamide 4-methylbenzenesulfonic acid.
The structural formula is:
The empirical formula for naldemedine tosylate is C32H34N4O6∙C7H8O3S and the molecular weight is 742.84.
Naldemedine tosylate is a white to light tan powder, soluble in dimethylsulfoxide and methanol, slightly soluble in alcohol and water, and independent of pH.
SYMPROIC (naldemedine) tablets for oral use contain 0.2 mg naldemedine (equivalent to 0.26 mg of naldemedine tosylate).
Excipients are: D-mannitol, croscarmellose sodium, magnesium stearate, hypromellose, talc, and yellow ferric oxide.
2.2 Adult Dosage
The recommended dosage of SYMPROIC is 0.2 mg orally once daily with or without food.
8.4 Pediatric Use
The safety and effectiveness of SYMPROIC have not been established in pediatric patients.
8.5 Geriatric Use
Of the 1163 patients exposed to SYMPROIC in clinical studies, 183 (16%) were 65 years of age and over, while 37 (3%) were 75 years and over. No overall differences in safety or effectiveness between these and younger patients were observed, but greater sensitivity of some older individuals cannot be ruled out. In a population pharmacokinetic analysis, no age-related alterations in the pharmacokinetics of naldemedine were observed [see Clinical Pharmacology (12.3)].
2.1 Administration
- Alteration of analgesic dosing regimen prior to initiating SYMPROIC is not required.
- Patients receiving opioids for less than 4 weeks may be less responsive to SYMPROIC [see Clinical Studies (14)].
- Discontinue SYMPROIC if treatment with the opioid pain medication is also discontinued.
14 Clinical Studies
SYMPROIC was evaluated in two replicate, 12-week, randomized, double-blind, placebo-controlled trials (Study 1 and Study 2) in which SYMPROIC was used without laxatives in patients with OIC and chronic non-cancer pain.
Patients receiving a stable opioid morphine equivalent daily dose of at least 30 mg for at least 4 weeks before enrollment and self-reported OIC were eligible for clinical trial participation.
Patients with evidence of significant structural abnormalities of the GI tract were not enrolled in these trials.
In Studies 1 and 2, patients had to either be not using laxatives or willing to discontinue laxative use at the time of screening and willing to use only the provided rescue laxatives during the screening and treatment periods.
In Studies 1 and 2, OIC was confirmed through a two-week run in period and was defined as no more than 4 spontaneous bowel movements (SBMs) total over 14 consecutive days and less than 3 SBMs in a given week with at least 25% of the SBMs associated with one or more of the following conditions: (1) straining; (2) hard or lumpy stools; (3) having a sensation of incomplete evacuation; and (4) having a sensation of anorectal obstruction/blockage.
An SBM was defined as a bowel movement (BM) without rescue laxative taken within the past 24 hours. Patients with no BMs over the 7 consecutive days prior to and during the 2-week screening period or patients who had never taken laxatives were excluded.
In the screening and treatment periods, bisacodyl was used as rescue laxative if patients had not had a BM for 72 hours and were allowed one-time use of an enema, if after 24 hours of taking bisacodyl they still had not had a BM.
A total of 547 patients in Study 1 and 553 patients in Study 2 were randomized in a 1:1 ratio to receive SYMPROIC 0.2 mg once daily or placebo for 12 weeks. Study medication was administered without regard to meals.
The mean age of subjects in Studies 1 and 2 was 54 years; 59% were women; and 80% were white. The most common types of pain in Studies 1 and 2 were back or neck pain (61%). The mean baseline number of SBMs was 1.3 and 1.2 per week for Studies 1 and 2, respectively.
Prior to enrollment, patients were using their current opioid for a mean duration of approximately 5 years. A wide range of types of opioids were used. The mean baseline opioid morphine equivalent daily dosage was 132 mg and 121 mg per day for Studies 1 and 2, respectively.
The efficacy of SYMPROIC was assessed in Studies 1 and 2 using a responder analysis. A responder was defined as a patient who had at least 3 SBMs per week and a change from baseline of at least 1 SBM per week for at least 9 out of the 12 weeks and 3 out of the last 4 weeks in Studies 1 and 2.
The responder rates in Studies 1 and 2 are shown in Table 4.
| Study 1 | Study 2 | |||||
|---|---|---|---|---|---|---|
| SYMPROIC 0.2 mg once daily (N=273) |
Placebo (N=272) |
Treatment Difference [95% CI] |
SYMPROIC 0.2 mg once daily (N=276) |
Placebo (N=274) |
Treatment Difference [95% CI] |
|
| CI=Confidence Interval | ||||||
| Responder The primary endpoint was defined as a patient who had at least 3 SBMs per week and a change from baseline of at least 1 SBM per week for at least 9 out of the 12 study weeks and 3 out of the last 4 weeks.
|
130 (48%) | 94 (35%) | 13% [5%, 21%] |
145 (53%) | 92 (34%) | 19% [11%, 27%] |
| p value Cochran-Mantel-Haenszel test adjusted for opioid dose strata (30 to 100 mg; greater than 100 mg)
|
0.0020 | <0.0001 |
In Studies 1 and 2, the mean increase in frequency of SBMs per week from baseline to the last 2 weeks of the 12-week treatment period was 3.1 for SYMPROIC vs. 2.0 for placebo (difference 1.0, 95% CI 0.6, 1.5), and 3.3 for SYMPROIC vs. 2.1 for placebo (difference 1.2, 95% CI 0.8, 1.7), respectively.
During week 1 of the treatment period, the mean increase in frequency of SBMs per week from baseline was 3.3 for SYMPROIC vs. 1.3 for placebo (difference 2.0, 95% CI 1.5, 2.5) in Study 1 and 3.7 for SYMPROIC vs. 1.6 for placebo (difference 2.1, 95% CI 1.5, 2.6) in Study 2.
The mean increase in the frequency of complete SBM (CSBM) per week from baseline to the last 2 weeks of 12-week treatment period was 2.3 for SYMPROIC vs. 1.5 for placebo (difference 0.8, 95% CI 0.4, 1.2) in Study 1 and 2.6 for SYMPROIC vs. 1.6 for placebo (difference 1.1, 95% CI 0.6, 1.5) in Study 2. A CSBM was defined as a SBM that was associated with a sense of complete evacuation.
The change in the frequency of SBMs without straining per week from baseline to the last 2 weeks of the treatment period was 1.3 for SYMPROIC vs. 0.7 for placebo (difference 0.6, 95% CI 0.2, 0.9) in Study 1 and 1.8 for SYMPROIC vs. 1.1 for placebo (difference 0.7, 95% CI 0.3, 1.2) in Study 2.
4 Contraindications
SYMPROIC is contraindicated in:
- Patients with known or suspected gastrointestinal obstruction and patients at increased risk of recurrent obstruction, due to the potential for gastrointestinal perforation [see Warnings and Precautions (5.1)].
- Patients with a history of a hypersensitivity reaction to naldemedine. Reactions have included bronchospasm and rash [see Adverse Reactions (6.1)].
6 Adverse Reactions
Serious and important adverse reactions described elsewhere in labeling include:
- Gastrointestinal perforation [see Warnings and Precautions (5.1)]
- Opioid withdrawal [see Warnings and Precautions (5.2)]
7 Drug Interactions
Table 3 includes drugs with clinically important drug interactions with SYMPROIC and instructions for preventing or managing the interaction.
| Strong CYP3A Inducers (e.g., rifampin, carbamazepine, phenytoin, St. John's Wort) | |
| Clinical Impact | Significant decrease in plasma naldemedine concentrations, which may reduce efficacy [see Clinical Pharmacology (12.3)] |
| Intervention | Avoid use of SYMPROIC with strong CYP3A inducers. |
| Other Opioid Antagonists | |
| Clinical Impact | Potential for additive effect of opioid receptor antagonism and increased risk of opioid withdrawal. |
| Intervention | Avoid use of SYMPROIC with another opioid antagonist. |
| Moderate (e.g., fluconazole, atazanavir, aprepitant, diltiazem, erythromycin) and Strong (e.g., itraconazole, ketoconazole, clarithromycin, ritonavir, saquinavir) CYP3A Inhibitors | |
| Clinical Impact | Increase in plasma naldemedine concentrations [see Clinical Pharmacology (12.3)] |
| Intervention | Monitor for potential naldemedine-related adverse reactions [see Adverse Reactions (6.1)]. |
| P-glycoprotein (P-gp) Inhibitors (e.g., amiodarone, captopril, cyclosporine, quercetin, quinidine, verapamil) | |
| Clinical Impact | Increase in plasma naldemedine concentrations [see Clinical Pharmacology (12.3)] |
| Intervention | Monitor for potential naldemedine-related adverse reactions [see Adverse Reactions (6.1)]. |
12.2 Pharmacodynamics
Use of opioids induces slowing of gastrointestinal motility and transit. Antagonism of gastrointestinal mu-opioid receptors by naldemedine inhibits opioid-induced delay of gastrointestinal transit time.
5.2 Opioid Withdrawal
Clusters of symptoms consistent with opioid withdrawal, including hyperhidrosis, chills, increased lacrimation, hot flush/flushing, pyrexia, sneezing, feeling cold, abdominal pain, diarrhea, nausea, and vomiting have occurred in patients treated with SYMPROIC [see Adverse Reactions (6.1)].
Patients having disruptions to the blood-brain barrier may be at increased risk for opioid withdrawal or reduced analgesia. Take into account the overall risk-benefit profile when using SYMPROIC in such patients. Monitor for symptoms of opioid withdrawal in such patients.
8.6 Hepatic Impairment
The effect of severe hepatic impairment (Child-Pugh Class C) on the pharmacokinetics of naldemedine has not been evaluated. Avoid use of SYMPROIC in patients with severe hepatic impairment. No dose adjustment of SYMPROIC is required in patients with mild or moderate hepatic impairment [see Clinical Pharmacology (12.3)].
1 Indications and Usage
SYMPROIC is indicated for the treatment of opioid-induced constipation (OIC) in adult patients with chronic non-cancer pain, including patients with chronic pain related to prior cancer or its treatment who do not require frequent (e.g., weekly) opioid dosage escalation.
12.1 Mechanism of Action
Naldemedine is an opioid antagonist with binding affinities for mu-, delta-, and kappa-opioid receptors. Naldemedine functions as a peripherally-acting mu-opioid receptor antagonist in tissues such as the gastrointestinal tract, thereby decreasing the constipating effects of opioids.
Naldemedine is a derivative of naltrexone to which a side chain has been added that increases the molecular weight and the polar surface area, thereby reducing its ability to cross the blood-brain barrier (BBB). Naldemedine is also a substrate of the P-glycoprotein (P-gp) efflux transporter. Based on these properties, the CNS penetration of naldemedine is expected to be negligible at the recommended dose levels, limiting the potential for interference with centrally-mediated opioid analgesia.
5 Warnings and Precautions
- Gastrointestinal perforation: Consider the overall risk benefit in patients with known or suspected lesions of the GI tract. Monitor for severe, persistent, or worsening abdominal pain; discontinue if development of symptoms (5.1)
- Opioid withdrawal: Consider the overall risk benefit in patients with disruptions to the blood-brain barrier. Monitor symptoms of opioid withdrawal (5.2)
2 Dosage and Administration
Administration ( 2.1 ):
- Alteration of analgesic dosing regimen prior to initiating SYMPROIC is not required
- Patients receiving opioids for less than 4 weeks may be less responsive to SYMPROIC
- Discontinue SYMPROIC if treatment with the opioid pain medication is also discontinued
Dosage ( 2.2 ):
- In adults, the recommended dosage is 0.2 mg once daily with or without food
3 Dosage Forms and Strengths
Tablets: 0.2 mg naldemedine; supplied as yellow, round, film-coated, debossed with Shionogi marking above the identifier code 222 on one side and 0.2 on the other side.
6.2 Postmarketing Experience
The following adverse reactions have been identified during post-approval use of SYMPROIC. Because reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate the frequency or establish a causal relationship to drug exposure.
Gastrointestinal disorders: Gastrointestinal perforation [see Warnings and Precautions (5.1) ].
8 Use in Specific Populations
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
The data described below reflect exposure to SYMPROIC in 1163 patients in clinical trials, including 487 patients with exposures greater than six months and 203 patients with exposures of 12 months.
The following safety data are derived from three double-blind, placebo-controlled trials in patients with OIC and chronic non-cancer pain: two 12-week studies (Studies 1 and 2) and one 52-week study (Study 3) [see Clinical Studies (14)].
In Studies 1 and 2, patients on laxatives were required to discontinue their use prior to study enrollment. All patients were restricted to bisacodyl rescue treatment during the study. In Study 3, approximately 60% of patients in both treatment groups were on a laxative regimen at baseline; patients were allowed to continue using their laxative regimen throughout the study duration. The safety profile of SYMPROIC relative to placebo was similar regardless of laxative use.
Tables 1 and 2 list common adverse reactions occurring in at least 2% of patients receiving SYMPROIC and at an incidence greater than placebo. Table 1 shows pooled 12-week data from Studies 1 and 2. Table 2 shows 12-week data from Study 3.
| Adverse Reaction | SYMPROIC 0.2 mg once daily N=542 |
Placebo N=546 |
|---|---|---|
| Abdominal pain Abdominal pain includes abdominal discomfort, abdominal pain, abdominal pain lower, abdominal pain upper, gastrointestinal pain.
|
8% | 2% |
| Diarrhea | 7% | 2% |
| Nausea | 4% | 2% |
| Gastroenteritis | 2% | 1% |
| Adverse Reaction | SYMPROIC 0.2 mg once daily N=621 |
Placebo N=619 |
|---|---|---|
| Abdominal pain Abdominal pain includes abdominal discomfort, abdominal pain, abdominal pain lower, abdominal pain upper.
|
11% | 5% |
| Diarrhea | 7% | 3% |
| Nausea | 6% | 5% |
| Vomiting | 3% | 2% |
| Gastroenteritis | 3% | 1% |
Adverse reactions up to 12 months in Study 3 are similar to those listed in Tables 1 and 2 (diarrhea: 11% vs. 5%, abdominal pain: 8% vs. 3%, and nausea: 8% vs. 6% for SYMPROIC and placebo, respectively).
5.1 Gastrointestinal Perforation
Cases of gastrointestinal (GI) perforation have been reported with use of another peripherally acting opioid antagonist, including SYMPROIC. Postmarketing cases of GI perforation, including fatal cases, were reported when SYMPROIC was used in patients at risk of GI perforation (e.g., GI cancer, past GI surgery, diverticulitis, chemotherapy/radiation). SYMPROIC is contraindicated in patients with known or suspected gastrointestinal obstruction or in patients at risk of recurrent obstruction. Take into account the overall risk-benefit profile when using SYMPROIC in patients with these conditions or other conditions which might result in impaired integrity of the gastrointestinal tract wall (e.g., Crohn's disease). Monitor for the development of severe, persistent, or worsening abdominal pain; discontinue SYMPROIC in patients who develop this symptom.
17 Patient Counseling Information
Advise the patient to read the FDA-approved patient labeling (Medication Guide).
16 How Supplied/storage and Handling
SYMPROIC is supplied as 0.2 mg naldemedine tablets as follows:
- bottle of 30 tablets - NDC 59385-041-30
Principal Display Panel 0.2 Mg Tablet Blister Pack
7 Tablets
Each tablet contains 0.2 mg of naldemedine
(equivalent to 0.26 mg of naldemedine tosylate).
Usual adult dosage: See package insert.
Store at 20°C to 25°C (68°F to 77°F).
Mfd. for BioDelivery Sciences International, Inc.
Raleigh, NC 27612
Symproic®
(naldemedine) tablets
0.2 mg
NDC 59385-041-07 Rx ONLY
Keep out of reach of children.
PHYSICIAN SAMPLES NOT FOR SALE
319623 04/19 SYM-0001.1b
DAY 1
DAY 2
DAY 3
DAY 4
DAY 5
DAY 6
DAY 7
LOT:
EXP:
Principal Display Panel 0.2 Mg Tablet Blister Pack Carton
NDC 59385-041-07
7 Tablets
Dosage: Take 1 tablet
once daily
Each tablet contains 0.2 mg of
naldemedine (equivalent to
0.26 mg of naldemedine tosylate).
Please see the included
Prescribing Information.
Keep out of reach of children.
Dispense the enclosed Medication Guide
to each patient.
Symproic®
(naldemedine) tablets
0.2 mg
PHYSICIAN SAMPLES NOT FOR SALE
FOR ORAL USE ONLY
Rx ONLY
Principal Display Panel 0.2 Mg Tablet Bottle Label 30 Tablets
NDC 59385-041-30
Rx ONLY
30 Tablets
Symproic®
(naldemedine) tablets
0.2 mg
Dispense the enclosed Medication Guide
to each patient.
Collegium®
PHARMACEUTICAL
© 2023 Collegium Pharmaceutical, Inc.
Stoughton, MA 02072
Structured Label Content
Section 42229-5 (42229-5)
Opioid Withdrawal
In Studies 1, 2 and 3, adverse reactions consistent with opioid withdrawal were based on investigator assessment and adjudicated based upon the occurrence of at least 3 adverse reactions potentially related to opioid withdrawal with onset of a constellation of those symptoms occurring on the same day or within one day of each other.
Adverse reactions of possible opioid withdrawal could include non-gastrointestinal (GI) symptoms (e.g., hyperhidrosis, hot flush or flushing, chills, tremor, tachycardia, anxiety, agitation, yawning, rhinorrhea, increased lacrimation, sneezing, feeling cold, and pyrexia), GI symptoms (e.g., vomiting, diarrhea, or abdominal pain), or both GI and non-GI symptoms.
In pooled Studies 1 and 2, the incidence of adverse reactions of opioid withdrawal was 1% (8/542) for SYMPROIC and 1% (3/546) for placebo. In Study 3 (52-week data), the incidence was 3% (20/621) for SYMPROIC and 1% (9/619) for placebo. Most SYMPROIC treated subjects experienced nearly equal incidence of GI only or both GI and non-GI symptoms.
Section 42231-1 (42231-1)
| This Medication Guide has been approved by the U.S. Food and Drug Administration. | Revised: 07/2025 |
|
MEDICATION GUIDE SYMPROIC® (sim proe' ik) (naldemedine) tablets, for oral use |
|
|
What is the most important information I should know about SYMPROIC? |
|
SYMPROIC may cause serious side effects, including:
|
|
| What is SYMPROIC? | |
| SYMPROIC is a prescription medicine used to treat constipation that is caused by prescription pain medicines called opioids in adults with long-lasting (chronic) pain that is not caused by active cancer. It is not known if SYMPROIC is safe and effective in children. |
|
Do not take SYMPROIC if you:
|
|
Before you take SYMPROIC, tell your healthcare provider about all of your medical conditions, including if you:
|
|
| Tell your healthcare provider about all the medicines you take, including prescription and over-the-counter medicines, vitamins, and herbal supplements. Other medicines may affect the way SYMPROIC works. | |
How should I take SYMPROIC?
|
|
| What are the possible side effects of SYMPROIC? | |
| See "What is the most important information I should know about SYMPROIC?" | |
|
The most common side effects of SYMPROIC include stomach (abdomen) pain, diarrhea, nausea and vomiting (gastroenteritis). Tell your healthcare provider if you have any side effect that bothers you or that does not go away. These are not all the possible side effects of SYMPROIC. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. |
|
How should I store SYMPROIC?
|
|
| Keep SYMPROIC and all medicines out of the reach of children. | |
| General information about the safe and effective use of SYMPROIC. | |
| Medicines are sometimes prescribed for purposes other than those in a Medication Guide. Do not take SYMPROIC for a condition for which it was not prescribed. Do not give SYMPROIC to other people, even if they have the same symptoms that you have. It may harm them. You can ask your pharmacist or healthcare provider for information about SYMPROIC that is written for health professionals. | |
| What are the ingredients in SYMPROIC? | |
| Active Ingredient: naldemedine tosylate | |
|
Inactive ingredients: D-mannitol, croscarmellose sodium, magnesium stearate, hypromellose, talc, and yellow ferric oxide. Manufactured for: Collegium Pharmaceutical, Inc. Stoughton, MA 02072 |
|
| SYM-001-MG-JULY2025 SYMPROIC is a registered trademark of Shionogi & Co., Ltd. For more information, go to www.symproic.com or call 1-800-469-0261. |
Section 43683-2 (43683-2)
| Warnings and Precautions, Gastrointestinal Perforation (5.1) | 07/2025 |
Section 44425-7 (44425-7)
Store SYMPROIC in a light resistant container at 20°C to 25°C (68°F to 77°F); excursions permitted between 15°C and 30°C (59°F and 86°F) [see USP Controlled Room Temperature].
10 Overdosage (10 OVERDOSAGE)
Single doses of naldemedine up to 100 mg (500 times the recommended dose) and multiple doses of up to 30 mg (150 times the recommended dose) for 10 days have been administered to healthy subjects in clinical studies. Dose-dependent increases in gastrointestinal-related adverse reactions, including abdominal pain, diarrhea, and nausea, were observed.
Single doses of naldemedine up to 3 mg (15 times the recommended dose) and multiple doses of 0.4 mg (twice the recommended dose) for 28 days have been administered to patients with OIC in clinical studies. Dose-dependent increases in gastrointestinal-related adverse reactions, including abdominal pain, diarrhea, nausea, and vomiting, were observed. Also, chills, hyperhidrosis, and dizziness were reported more frequently at 1 and 3 mg doses and hyperhidrosis at the 0.4 mg dose.
No antidote for naldemedine is known. Hemodialysis is not an effective means to remove naldemedine from the blood [see Clinical Pharmacology (12.3)].
11 Description (11 DESCRIPTION)
SYMPROIC (naldemedine), an opioid antagonist, contains naldemedine tosylate as the active ingredient.
The chemical name for naldemedine tosylate is: 17-(cyclopropylmethyl)-6,7-didehydro-4,5α-epoxy-3,6,14-trihydroxy-N-[2-(3-phenyl-1,2,4-oxadiazol-5-yl)propan-2-yl]morphinan-7-carboxamide 4-methylbenzenesulfonic acid.
The structural formula is:
The empirical formula for naldemedine tosylate is C32H34N4O6∙C7H8O3S and the molecular weight is 742.84.
Naldemedine tosylate is a white to light tan powder, soluble in dimethylsulfoxide and methanol, slightly soluble in alcohol and water, and independent of pH.
SYMPROIC (naldemedine) tablets for oral use contain 0.2 mg naldemedine (equivalent to 0.26 mg of naldemedine tosylate).
Excipients are: D-mannitol, croscarmellose sodium, magnesium stearate, hypromellose, talc, and yellow ferric oxide.
2.2 Adult Dosage
The recommended dosage of SYMPROIC is 0.2 mg orally once daily with or without food.
8.4 Pediatric Use
The safety and effectiveness of SYMPROIC have not been established in pediatric patients.
8.5 Geriatric Use
Of the 1163 patients exposed to SYMPROIC in clinical studies, 183 (16%) were 65 years of age and over, while 37 (3%) were 75 years and over. No overall differences in safety or effectiveness between these and younger patients were observed, but greater sensitivity of some older individuals cannot be ruled out. In a population pharmacokinetic analysis, no age-related alterations in the pharmacokinetics of naldemedine were observed [see Clinical Pharmacology (12.3)].
2.1 Administration
- Alteration of analgesic dosing regimen prior to initiating SYMPROIC is not required.
- Patients receiving opioids for less than 4 weeks may be less responsive to SYMPROIC [see Clinical Studies (14)].
- Discontinue SYMPROIC if treatment with the opioid pain medication is also discontinued.
14 Clinical Studies (14 CLINICAL STUDIES)
SYMPROIC was evaluated in two replicate, 12-week, randomized, double-blind, placebo-controlled trials (Study 1 and Study 2) in which SYMPROIC was used without laxatives in patients with OIC and chronic non-cancer pain.
Patients receiving a stable opioid morphine equivalent daily dose of at least 30 mg for at least 4 weeks before enrollment and self-reported OIC were eligible for clinical trial participation.
Patients with evidence of significant structural abnormalities of the GI tract were not enrolled in these trials.
In Studies 1 and 2, patients had to either be not using laxatives or willing to discontinue laxative use at the time of screening and willing to use only the provided rescue laxatives during the screening and treatment periods.
In Studies 1 and 2, OIC was confirmed through a two-week run in period and was defined as no more than 4 spontaneous bowel movements (SBMs) total over 14 consecutive days and less than 3 SBMs in a given week with at least 25% of the SBMs associated with one or more of the following conditions: (1) straining; (2) hard or lumpy stools; (3) having a sensation of incomplete evacuation; and (4) having a sensation of anorectal obstruction/blockage.
An SBM was defined as a bowel movement (BM) without rescue laxative taken within the past 24 hours. Patients with no BMs over the 7 consecutive days prior to and during the 2-week screening period or patients who had never taken laxatives were excluded.
In the screening and treatment periods, bisacodyl was used as rescue laxative if patients had not had a BM for 72 hours and were allowed one-time use of an enema, if after 24 hours of taking bisacodyl they still had not had a BM.
A total of 547 patients in Study 1 and 553 patients in Study 2 were randomized in a 1:1 ratio to receive SYMPROIC 0.2 mg once daily or placebo for 12 weeks. Study medication was administered without regard to meals.
The mean age of subjects in Studies 1 and 2 was 54 years; 59% were women; and 80% were white. The most common types of pain in Studies 1 and 2 were back or neck pain (61%). The mean baseline number of SBMs was 1.3 and 1.2 per week for Studies 1 and 2, respectively.
Prior to enrollment, patients were using their current opioid for a mean duration of approximately 5 years. A wide range of types of opioids were used. The mean baseline opioid morphine equivalent daily dosage was 132 mg and 121 mg per day for Studies 1 and 2, respectively.
The efficacy of SYMPROIC was assessed in Studies 1 and 2 using a responder analysis. A responder was defined as a patient who had at least 3 SBMs per week and a change from baseline of at least 1 SBM per week for at least 9 out of the 12 weeks and 3 out of the last 4 weeks in Studies 1 and 2.
The responder rates in Studies 1 and 2 are shown in Table 4.
| Study 1 | Study 2 | |||||
|---|---|---|---|---|---|---|
| SYMPROIC 0.2 mg once daily (N=273) |
Placebo (N=272) |
Treatment Difference [95% CI] |
SYMPROIC 0.2 mg once daily (N=276) |
Placebo (N=274) |
Treatment Difference [95% CI] |
|
| CI=Confidence Interval | ||||||
| Responder The primary endpoint was defined as a patient who had at least 3 SBMs per week and a change from baseline of at least 1 SBM per week for at least 9 out of the 12 study weeks and 3 out of the last 4 weeks.
|
130 (48%) | 94 (35%) | 13% [5%, 21%] |
145 (53%) | 92 (34%) | 19% [11%, 27%] |
| p value Cochran-Mantel-Haenszel test adjusted for opioid dose strata (30 to 100 mg; greater than 100 mg)
|
0.0020 | <0.0001 |
In Studies 1 and 2, the mean increase in frequency of SBMs per week from baseline to the last 2 weeks of the 12-week treatment period was 3.1 for SYMPROIC vs. 2.0 for placebo (difference 1.0, 95% CI 0.6, 1.5), and 3.3 for SYMPROIC vs. 2.1 for placebo (difference 1.2, 95% CI 0.8, 1.7), respectively.
During week 1 of the treatment period, the mean increase in frequency of SBMs per week from baseline was 3.3 for SYMPROIC vs. 1.3 for placebo (difference 2.0, 95% CI 1.5, 2.5) in Study 1 and 3.7 for SYMPROIC vs. 1.6 for placebo (difference 2.1, 95% CI 1.5, 2.6) in Study 2.
The mean increase in the frequency of complete SBM (CSBM) per week from baseline to the last 2 weeks of 12-week treatment period was 2.3 for SYMPROIC vs. 1.5 for placebo (difference 0.8, 95% CI 0.4, 1.2) in Study 1 and 2.6 for SYMPROIC vs. 1.6 for placebo (difference 1.1, 95% CI 0.6, 1.5) in Study 2. A CSBM was defined as a SBM that was associated with a sense of complete evacuation.
The change in the frequency of SBMs without straining per week from baseline to the last 2 weeks of the treatment period was 1.3 for SYMPROIC vs. 0.7 for placebo (difference 0.6, 95% CI 0.2, 0.9) in Study 1 and 1.8 for SYMPROIC vs. 1.1 for placebo (difference 0.7, 95% CI 0.3, 1.2) in Study 2.
4 Contraindications (4 CONTRAINDICATIONS)
SYMPROIC is contraindicated in:
- Patients with known or suspected gastrointestinal obstruction and patients at increased risk of recurrent obstruction, due to the potential for gastrointestinal perforation [see Warnings and Precautions (5.1)].
- Patients with a history of a hypersensitivity reaction to naldemedine. Reactions have included bronchospasm and rash [see Adverse Reactions (6.1)].
6 Adverse Reactions (6 ADVERSE REACTIONS)
Serious and important adverse reactions described elsewhere in labeling include:
- Gastrointestinal perforation [see Warnings and Precautions (5.1)]
- Opioid withdrawal [see Warnings and Precautions (5.2)]
7 Drug Interactions (7 DRUG INTERACTIONS)
Table 3 includes drugs with clinically important drug interactions with SYMPROIC and instructions for preventing or managing the interaction.
| Strong CYP3A Inducers (e.g., rifampin, carbamazepine, phenytoin, St. John's Wort) | |
| Clinical Impact | Significant decrease in plasma naldemedine concentrations, which may reduce efficacy [see Clinical Pharmacology (12.3)] |
| Intervention | Avoid use of SYMPROIC with strong CYP3A inducers. |
| Other Opioid Antagonists | |
| Clinical Impact | Potential for additive effect of opioid receptor antagonism and increased risk of opioid withdrawal. |
| Intervention | Avoid use of SYMPROIC with another opioid antagonist. |
| Moderate (e.g., fluconazole, atazanavir, aprepitant, diltiazem, erythromycin) and Strong (e.g., itraconazole, ketoconazole, clarithromycin, ritonavir, saquinavir) CYP3A Inhibitors | |
| Clinical Impact | Increase in plasma naldemedine concentrations [see Clinical Pharmacology (12.3)] |
| Intervention | Monitor for potential naldemedine-related adverse reactions [see Adverse Reactions (6.1)]. |
| P-glycoprotein (P-gp) Inhibitors (e.g., amiodarone, captopril, cyclosporine, quercetin, quinidine, verapamil) | |
| Clinical Impact | Increase in plasma naldemedine concentrations [see Clinical Pharmacology (12.3)] |
| Intervention | Monitor for potential naldemedine-related adverse reactions [see Adverse Reactions (6.1)]. |
12.2 Pharmacodynamics
Use of opioids induces slowing of gastrointestinal motility and transit. Antagonism of gastrointestinal mu-opioid receptors by naldemedine inhibits opioid-induced delay of gastrointestinal transit time.
5.2 Opioid Withdrawal
Clusters of symptoms consistent with opioid withdrawal, including hyperhidrosis, chills, increased lacrimation, hot flush/flushing, pyrexia, sneezing, feeling cold, abdominal pain, diarrhea, nausea, and vomiting have occurred in patients treated with SYMPROIC [see Adverse Reactions (6.1)].
Patients having disruptions to the blood-brain barrier may be at increased risk for opioid withdrawal or reduced analgesia. Take into account the overall risk-benefit profile when using SYMPROIC in such patients. Monitor for symptoms of opioid withdrawal in such patients.
8.6 Hepatic Impairment
The effect of severe hepatic impairment (Child-Pugh Class C) on the pharmacokinetics of naldemedine has not been evaluated. Avoid use of SYMPROIC in patients with severe hepatic impairment. No dose adjustment of SYMPROIC is required in patients with mild or moderate hepatic impairment [see Clinical Pharmacology (12.3)].
1 Indications and Usage (1 INDICATIONS AND USAGE)
SYMPROIC is indicated for the treatment of opioid-induced constipation (OIC) in adult patients with chronic non-cancer pain, including patients with chronic pain related to prior cancer or its treatment who do not require frequent (e.g., weekly) opioid dosage escalation.
12.1 Mechanism of Action
Naldemedine is an opioid antagonist with binding affinities for mu-, delta-, and kappa-opioid receptors. Naldemedine functions as a peripherally-acting mu-opioid receptor antagonist in tissues such as the gastrointestinal tract, thereby decreasing the constipating effects of opioids.
Naldemedine is a derivative of naltrexone to which a side chain has been added that increases the molecular weight and the polar surface area, thereby reducing its ability to cross the blood-brain barrier (BBB). Naldemedine is also a substrate of the P-glycoprotein (P-gp) efflux transporter. Based on these properties, the CNS penetration of naldemedine is expected to be negligible at the recommended dose levels, limiting the potential for interference with centrally-mediated opioid analgesia.
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
- Gastrointestinal perforation: Consider the overall risk benefit in patients with known or suspected lesions of the GI tract. Monitor for severe, persistent, or worsening abdominal pain; discontinue if development of symptoms (5.1)
- Opioid withdrawal: Consider the overall risk benefit in patients with disruptions to the blood-brain barrier. Monitor symptoms of opioid withdrawal (5.2)
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
Administration ( 2.1 ):
- Alteration of analgesic dosing regimen prior to initiating SYMPROIC is not required
- Patients receiving opioids for less than 4 weeks may be less responsive to SYMPROIC
- Discontinue SYMPROIC if treatment with the opioid pain medication is also discontinued
Dosage ( 2.2 ):
- In adults, the recommended dosage is 0.2 mg once daily with or without food
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
Tablets: 0.2 mg naldemedine; supplied as yellow, round, film-coated, debossed with Shionogi marking above the identifier code 222 on one side and 0.2 on the other side.
6.2 Postmarketing Experience
The following adverse reactions have been identified during post-approval use of SYMPROIC. Because reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate the frequency or establish a causal relationship to drug exposure.
Gastrointestinal disorders: Gastrointestinal perforation [see Warnings and Precautions (5.1) ].
8 Use in Specific Populations (8 USE IN SPECIFIC POPULATIONS)
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
The data described below reflect exposure to SYMPROIC in 1163 patients in clinical trials, including 487 patients with exposures greater than six months and 203 patients with exposures of 12 months.
The following safety data are derived from three double-blind, placebo-controlled trials in patients with OIC and chronic non-cancer pain: two 12-week studies (Studies 1 and 2) and one 52-week study (Study 3) [see Clinical Studies (14)].
In Studies 1 and 2, patients on laxatives were required to discontinue their use prior to study enrollment. All patients were restricted to bisacodyl rescue treatment during the study. In Study 3, approximately 60% of patients in both treatment groups were on a laxative regimen at baseline; patients were allowed to continue using their laxative regimen throughout the study duration. The safety profile of SYMPROIC relative to placebo was similar regardless of laxative use.
Tables 1 and 2 list common adverse reactions occurring in at least 2% of patients receiving SYMPROIC and at an incidence greater than placebo. Table 1 shows pooled 12-week data from Studies 1 and 2. Table 2 shows 12-week data from Study 3.
| Adverse Reaction | SYMPROIC 0.2 mg once daily N=542 |
Placebo N=546 |
|---|---|---|
| Abdominal pain Abdominal pain includes abdominal discomfort, abdominal pain, abdominal pain lower, abdominal pain upper, gastrointestinal pain.
|
8% | 2% |
| Diarrhea | 7% | 2% |
| Nausea | 4% | 2% |
| Gastroenteritis | 2% | 1% |
| Adverse Reaction | SYMPROIC 0.2 mg once daily N=621 |
Placebo N=619 |
|---|---|---|
| Abdominal pain Abdominal pain includes abdominal discomfort, abdominal pain, abdominal pain lower, abdominal pain upper.
|
11% | 5% |
| Diarrhea | 7% | 3% |
| Nausea | 6% | 5% |
| Vomiting | 3% | 2% |
| Gastroenteritis | 3% | 1% |
Adverse reactions up to 12 months in Study 3 are similar to those listed in Tables 1 and 2 (diarrhea: 11% vs. 5%, abdominal pain: 8% vs. 3%, and nausea: 8% vs. 6% for SYMPROIC and placebo, respectively).
5.1 Gastrointestinal Perforation
Cases of gastrointestinal (GI) perforation have been reported with use of another peripherally acting opioid antagonist, including SYMPROIC. Postmarketing cases of GI perforation, including fatal cases, were reported when SYMPROIC was used in patients at risk of GI perforation (e.g., GI cancer, past GI surgery, diverticulitis, chemotherapy/radiation). SYMPROIC is contraindicated in patients with known or suspected gastrointestinal obstruction or in patients at risk of recurrent obstruction. Take into account the overall risk-benefit profile when using SYMPROIC in patients with these conditions or other conditions which might result in impaired integrity of the gastrointestinal tract wall (e.g., Crohn's disease). Monitor for the development of severe, persistent, or worsening abdominal pain; discontinue SYMPROIC in patients who develop this symptom.
17 Patient Counseling Information (17 PATIENT COUNSELING INFORMATION)
Advise the patient to read the FDA-approved patient labeling (Medication Guide).
16 How Supplied/storage and Handling (16 HOW SUPPLIED/STORAGE AND HANDLING)
SYMPROIC is supplied as 0.2 mg naldemedine tablets as follows:
- bottle of 30 tablets - NDC 59385-041-30
Principal Display Panel 0.2 Mg Tablet Blister Pack (PRINCIPAL DISPLAY PANEL - 0.2 mg Tablet Blister Pack)
7 Tablets
Each tablet contains 0.2 mg of naldemedine
(equivalent to 0.26 mg of naldemedine tosylate).
Usual adult dosage: See package insert.
Store at 20°C to 25°C (68°F to 77°F).
Mfd. for BioDelivery Sciences International, Inc.
Raleigh, NC 27612
Symproic®
(naldemedine) tablets
0.2 mg
NDC 59385-041-07 Rx ONLY
Keep out of reach of children.
PHYSICIAN SAMPLES NOT FOR SALE
319623 04/19 SYM-0001.1b
DAY 1
DAY 2
DAY 3
DAY 4
DAY 5
DAY 6
DAY 7
LOT:
EXP:
Principal Display Panel 0.2 Mg Tablet Blister Pack Carton (PRINCIPAL DISPLAY PANEL - 0.2 mg Tablet Blister Pack Carton)
NDC 59385-041-07
7 Tablets
Dosage: Take 1 tablet
once daily
Each tablet contains 0.2 mg of
naldemedine (equivalent to
0.26 mg of naldemedine tosylate).
Please see the included
Prescribing Information.
Keep out of reach of children.
Dispense the enclosed Medication Guide
to each patient.
Symproic®
(naldemedine) tablets
0.2 mg
PHYSICIAN SAMPLES NOT FOR SALE
FOR ORAL USE ONLY
Rx ONLY
Principal Display Panel 0.2 Mg Tablet Bottle Label 30 Tablets (PRINCIPAL DISPLAY PANEL - 0.2 mg Tablet Bottle Label - 30 Tablets)
NDC 59385-041-30
Rx ONLY
30 Tablets
Symproic®
(naldemedine) tablets
0.2 mg
Dispense the enclosed Medication Guide
to each patient.
Collegium®
PHARMACEUTICAL
© 2023 Collegium Pharmaceutical, Inc.
Stoughton, MA 02072
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:48:33.018347 · Updated: 2026-03-14T22:30:10.662825