These Highlights Do Not Include All The Information Needed To Use Xtampza®
b0a5ded2-8ee2-49ca-a86c-2b28ae40f60c
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
WARNING: SERIOUS AND LIFE-THREATENING RISKS FROM USE OF XTAMPZA ER See full prescribing information for complete boxed warning . XTAMPZA ER exposes users to risks of addiction, abuse, and misuse, which can lead to overdose and death. Assess each patient's risk before prescribing and reassess regularly for these behaviors and conditions. ( 5.1 ) Serious, life-threatening, or fatal respiratory depression may occur especially during initiation or following a dosage increase. To reduce the risk of respiratory depression, proper dosing and titration of XTAMPZA ER are essential. ( 5.2 ) Accidental ingestion of XTAMPZA ER, especially by children, can result in fatal overdose of oxycodone. ( 5.2 ) Concomitant use of opioids with benzodiazepines or other central nervous system (CNS) depressants, including alcohol, may result in profound sedation, respiratory depression, coma, and death. Reserve concomitant prescribing for use in patients for whom alternative treatment options are inadequate. ( 5.3 , 7 ) Advise pregnant using opioids for an extended period of time of the risk of Neonatal Opioid Withdrawal Syndrome, which may be life-threatening if not recognized and treated. Ensure that management by neonatology experts will be available at delivery. ( 5.4 ) Healthcare providers are strongly encouraged to complete a REMS-compliant education program and to counsel patients and caregivers on serious risks, safe use, and the importance of reading the Medication Guide with each prescription. ( 5.5 ) Concomitant use with CYP3A4 inhibitors (or discontinuation of CYP3A4 inducers) can result in a fatal overdose of oxycodone from XTAMPZA ER. ( 5.6 , 12.3 )
Indications and Usage
XTAMPZA ER is indicated for the management of severe and persistent pain that requires an opioid analgesic and that cannot be adequately treated with alternative options, including immediate-release opioids.
Dosage and Administration
XTAMPZA ER should be prescribed only by healthcare professionals who are knowledgeable about the use of extended-release/long-acting opioids and how to mitigate the associated risks. XTAMPZA ER single doses greater than 36 mg (equivalent to 40 mg oxycodone hydrochloride [HCl]) or a total daily dose greater than 72 mg (equivalent to 80 mg oxycodone HCl) are to be administered only to patients in whom tolerance to an opioid of comparable potency has been established. Patients who are opioid-tolerant are those receiving, for one week or longer, at least 60 mg oral morphine per day, 25 mcg transdermal fentanyl per hour, 30 mg oral oxycodone HCl per day, 8 mg oral hydromorphone per day, 25 mg oral oxymorphone per day, 60 mg oral hydrocodone per day, or an equianalgesic dose of another opioid. Use the lowest effective dosage for the shortest duration of time consistent with individual patient treatment goals [see Warnings and Precautions (5) ]. Because the risk of overdose increases as opioid doses increase, reserve titration to higher doses of XTAMPZA ER for patients in whom lower doses are insufficiently effective and in whom the expected benefits of using a higher dose opioid clearly outweigh the substantial risks. Initiate the dosing regimen for each patient individually, taking into account the patient's underlying cause and severity of pain, prior analgesic treatment and response, and risk factors for addiction, abuse, and misuse [see Warnings and Precautions (5.1) ] . Respiratory depression can occur at any time during opioid therapy, especially when initiating and following dosage increases with XTAMPZA ER. Consider this risk when selecting an initial dose and when making dose adjustments [see Warnings and Precautions (5.2) ]. XTAMPZA ER is administered, twice daily, every 12 hours, and must be taken with food. Instruct patients to take XTAMPZA ER capsules with approximately the same amount of food for every dose in order to ensure consistent plasma levels are achieved [see Clinical Pharmacology (12.3) ] . Patients who are unable to swallow XTAMPZA ER should be instructed to sprinkle the capsule contents on soft foods or into a cup and then administer directly into the mouth and immediately swallow. XTAMPZA ER may also be administered through a gastrostomy or nasogastric feeding tube [see Dosage and Administration (2.7) ]. The maximum daily dose of XTAMPZA ER is 288 mg per day (eight 36 mg capsules, equivalent to 320 mg oxycodone HCl per day) as the safety of the excipients in XTAMPZA ER for doses over 288 mg/day has not been established.
Warnings and Precautions
Opioid-Induced Hyperalgesia and Allodynia : Opioid-Induced Hyperalgesia (OIH) occurs when an opioid analgesic paradoxically causes an increase in pain, or an increase in sensitivity to pain. If OIH is suspected, carefully consider appropriately decreasing the dose of the current opioid analgesic or opioid rotation. ( 5.7 ) Risk of life-threatening respiratory depression in patients with chronic pulmonary disease or in elderly, cachectic, or debilitated patients : Regularly evaluate. ( 5.8 ) Adrenal Insufficiency : If diagnosed, treat with physiologic replacement of corticosteroids, and wean patient off of the opioid. ( 5.9 ) Severe hypotension : Regularly evaluate. Avoid use of XTAMPZA ER in patients with circulatory shock. ( 5.10 ) Risks of use in patients with increased intracranial pressure, brain tumors, head injury, or impaired consciousness : Monitor for sedation and respiratory depression. Avoid use of XTAMPZA ER in patients with impaired consciousness or coma. ( 5.11 )
Contraindications
XTAMPZA ER is contraindicated in patients with: Significant respiratory depression [see Warnings and Precautions (5.2) ] Acute or severe bronchial asthma in an unmonitored setting or in the absence of resuscitative equipment [see Warnings and Precautions (5.8) ] Known or suspected gastrointestinal obstruction, including paralytic ileus [see Warnings and Precautions (5.12) ] Hypersensitivity (e.g., anaphylaxis) to oxycodone.
Adverse Reactions
The following serious adverse reactions are described elsewhere in the labeling: Addiction, Abuse, and Misuse [see Warnings and Precautions (5.1) ] Life-Threatening Respiratory Depression [see Warnings and Precautions (5.2) ] Interactions with Benzodiazepines or Other CNS Depressants [see Warnings and Precautions (5.3) ] Neonatal Opioid Withdrawal Syndrome [see Warnings and Precautions (5.4) ] Opioid-Induced Hyperalgesia and Allodynia [see Warnings and Precautions (5.7) ] Adrenal Insufficiency [see Warnings and Precautions (5.9) ] Severe Hypotension [see Warnings and Precautions (5.10) ] Gastrointestinal Adverse Reactions [see Warnings and Precautions (5.12) ] Seizures [see Warnings and Precautions (5.13) ] Withdrawal [see Warnings and Precautions (5.14) ]
Drug Interactions
Table includes clinically significant drug interactions with XTAMPZA ER. Table 3: Clinically Significant Drug Interactions with XTAMPZA ER Inhibitors of CYP3A4 and CYP2D6 Clinical Impact: The concomitant use of XTAMPZA ER and CYP3A4 inhibitors can increase the plasma concentration of oxycodone, resulting in increased or prolonged opioid effects. These effects could be more pronounced with concomitant use of XTAMPZA ER and CYP2D6 and CYP3A4 inhibitors , particularly when an inhibitor is added after a stable dose of XTAMPZA ER is achieved [see Warnings and Precautions (5.6) ]. After stopping a CYP3A4 inhibitor, as the effects of the inhibitor decline, the oxycodone plasma concentration will decrease [see Clinical Pharmacology (12.3) ] , resulting in decreased opioid efficacy or a withdrawal syndrome in patients who had developed physical dependence to oxycodone. Intervention: If concomitant use is necessary, consider dosage reduction of XTAMPZA ER until stable drug effects are achieved. Evaluate patients at frequent intervals for respiratory depression and sedation. If a CYP3A4 inhibitor is discontinued, consider increasing the XTAMPZA ER dosage until stable drug effects are achieved. Assess for signs of opioid withdrawal. Examples: Macrolide antibiotics (e.g., erythromycin), azole-antifungal agents (e.g., ketoconazole), protease inhibitors (e.g., ritonavir) CYP3A4 Inducers Clinical Impact: The concomitant use of XTAMPZA ER and CYP3A4 inducers can decrease the plasma concentration of oxycodone [see Clinical Pharmacology (12.3) ] , resulting in decreased efficacy or onset of a withdrawal syndrome in patients who have developed physical dependence to oxycodone [see Warnings and Precautions (5.6) ] . After stopping a CYP3A4 inducer, as the effects of the inducer decline, the oxycodone plasma concentration will increase [see Clinical Pharmacology (12.3) ] , which could increase or prolong both the therapeutic effects and adverse reactions and may cause serious respiratory depression. Intervention: If concomitant use is necessary, consider increasing the XTAMPZA ER dosage until stable drug effects are achieved [see Dosage and Administration (2.5) ] . Evaluate patients for signs of opioid withdrawal. If a CYP3A4 inducer is discontinued, consider XTAMPZA ER dosage reduction and evaluate patients at frequent intervals for signs of respiratory depression and sedation. Examples: Rifampin, carbamazepine, phenytoin Benzodiazepines and other Central Nervous System (CNS) Depressants Clinical Impact: Due to additive pharmacological effect, the concomitant use of benzodiazepines or other CNS depressants including alcohol, increases the risk of respiratory depression, profound sedation, coma, and death [see Warnings and Precautions (5.3) ] . Intervention: Reserve concomitant prescribing of these drugs for use in patients for whom alternative treatment options are inadequate. Limit dosages and durations to the minimum required. Inform patients and caregivers of this potential interaction and educate them on the signs and symptoms of respiratory depression (including sedation). If concomitant use is warranted, consider recommending or prescribing an opioid overdose reversal agent [see Dosage and Administration (2.2) , Warnings and Precautions (5.1 , 5.2 , 5.3) ] . Examples Benzodiazepines and other sedatives/hypnotics, anxiolytics, tranquilizers, muscle relaxants, general anesthetics, antipsychotics, gabapentinoids (gabapentin or pregabalin), other opioids, alcohol Serotonergic Drugs Clinical Impact: The concomitant use of opioids with other drugs that affect the serotonergic neurotransmitter system has resulted in serotonin syndrome . Intervention: If concomitant use is warranted, frequently evaluate the patient, particularly during treatment initiation and dose adjustment. Discontinue XTAMPZA ER if serotonin syndrome is suspected. Examples: Selective serotonin reuptake inhibitors (SSRIs), serotonin and norepinephrine reuptake inhibitors (SNRIs), tricyclic antidepressants (TCAs), triptans, 5-HT3 receptor antagonists, drugs that effect the serotonin neurotransmitter system (e.g., mirtazapine, trazodone, tramadol), certain muscle relaxants (i.e., cyclobenzaprine, metaxalone), monoamine oxidase inhibitors (those intended to treat psychiatric disorders and also others, such as linezolid and intravenous methylene blue) Monoamine Oxidase Inhibitors (MAOIs) Clinical Impact: MAOI interactions with opioids may manifest as serotonin syndrome or opioid toxicity (e.g., respiratory depression, coma) [see Warnings and Precautions (5.2) ]. Intervention: The use of XTAMPZA ER is not recommended for patients taking MAOIs or within 14 days of stopping such treatment. Examples: phenelzine, tranylcypromine, linezolid Mixed Agonist/Antagonist and Partial Agonist Opioid Analgesics Clinical Impact: May reduce the analgesic effect of XTAMPZA ER and/or precipitate withdrawal symptoms. Intervention: Avoid concomitant use. Examples: Butorphanol, nalbuphine, pentazocine, buprenorphine Muscle Relaxants Clinical Impact: Oxycodone may enhance the neuromuscular blocking action of skeletal muscle relaxants and produce an increased degree of respiratory depression. Intervention: Because respiratory depression may be greater than otherwise expected, decrease the dosage of XTAMPZA ER and/or the muscle relaxant as necessary. Due to the risk of respiratory depression with concomitant use of skeletal muscle relaxants and opioids, consider recommending or prescribing an opioid overdose reversal agent [ see Dosage and Administration (2.2) , Warnings and Precautions (5.2 , 5.3) ]. Examples: Cyclobenzaprine, metaxalone Diuretics Clinical Impact: Opioids can reduce the efficacy of diuretics by inducing the release of antidiuretic hormone. Intervention: Evaluate patients for signs of diminished diuresis and/or effects on blood pressure and increase the dosage of the diuretic as needed. Anticholinergic Drugs Clinical Impact: The concomitant use of anticholinergic drugs may increase risk of urinary retention and/or severe constipation, which may lead to paralytic ileus. Intervention: Evaluate patients for signs of urinary retention or reduced gastric motility when XTAMPZA ER is used concomitantly with anticholinergic drugs.
Storage and Handling
XTAMPZA ER capsules are supplied in 100-count bottles with a child-resistant closure and as a hospital unit dose package with 10 individually blistered capsules per card; two cards per carton as follows: Table 9: Summary of XTAMPZA ER Capsule Strengths and Packaging Configurations Strength Capsule Description NDC Number (100-count Bottles with a child-resistant closure) NDC Number (20-count Hospital Unit Dose Blister Cartons) 9 mg (equivalent to 10 mg oxycodone HCl) Size 3, ivory cap printed with "XTAMPZA ER" and white body printed with "9 mg" NDC 24510-110-10 NDC 24510-110-20 13.5 mg (equivalent to 15 mg oxycodone HCl) Size 2, Swedish orange cap printed with "XTAMPZA ER" and white body printed with "13.5 mg" NDC 24510-115-10 NDC 24510-115-20 18 mg (equivalent to 20 mg oxycodone HCl) Size 1, rich yellow cap printed with "XTAMPZA ER" and white body printed with "18 mg" NDC 24510-120-10 NDC 24510-120-20 27 mg (equivalent to 30 mg oxycodone HCl) Size 0, light gray cap printed with "XTAMPZA ER" and white body printed with "27 mg" NDC 24510-130-10 NDC 24510-130-20 36 mg (equivalent to 40 mg oxycodone HCl) Size 00, flesh color cap printed with "XTAMPZA ER" and white body printed with "36 mg" NDC 24510-140-10 NDC 24510-140-20
How Supplied
XTAMPZA ER capsules are supplied in 100-count bottles with a child-resistant closure and as a hospital unit dose package with 10 individually blistered capsules per card; two cards per carton as follows: Table 9: Summary of XTAMPZA ER Capsule Strengths and Packaging Configurations Strength Capsule Description NDC Number (100-count Bottles with a child-resistant closure) NDC Number (20-count Hospital Unit Dose Blister Cartons) 9 mg (equivalent to 10 mg oxycodone HCl) Size 3, ivory cap printed with "XTAMPZA ER" and white body printed with "9 mg" NDC 24510-110-10 NDC 24510-110-20 13.5 mg (equivalent to 15 mg oxycodone HCl) Size 2, Swedish orange cap printed with "XTAMPZA ER" and white body printed with "13.5 mg" NDC 24510-115-10 NDC 24510-115-20 18 mg (equivalent to 20 mg oxycodone HCl) Size 1, rich yellow cap printed with "XTAMPZA ER" and white body printed with "18 mg" NDC 24510-120-10 NDC 24510-120-20 27 mg (equivalent to 30 mg oxycodone HCl) Size 0, light gray cap printed with "XTAMPZA ER" and white body printed with "27 mg" NDC 24510-130-10 NDC 24510-130-20 36 mg (equivalent to 40 mg oxycodone HCl) Size 00, flesh color cap printed with "XTAMPZA ER" and white body printed with "36 mg" NDC 24510-140-10 NDC 24510-140-20
Medication Information
Warnings and Precautions
Opioid-Induced Hyperalgesia and Allodynia : Opioid-Induced Hyperalgesia (OIH) occurs when an opioid analgesic paradoxically causes an increase in pain, or an increase in sensitivity to pain. If OIH is suspected, carefully consider appropriately decreasing the dose of the current opioid analgesic or opioid rotation. ( 5.7 ) Risk of life-threatening respiratory depression in patients with chronic pulmonary disease or in elderly, cachectic, or debilitated patients : Regularly evaluate. ( 5.8 ) Adrenal Insufficiency : If diagnosed, treat with physiologic replacement of corticosteroids, and wean patient off of the opioid. ( 5.9 ) Severe hypotension : Regularly evaluate. Avoid use of XTAMPZA ER in patients with circulatory shock. ( 5.10 ) Risks of use in patients with increased intracranial pressure, brain tumors, head injury, or impaired consciousness : Monitor for sedation and respiratory depression. Avoid use of XTAMPZA ER in patients with impaired consciousness or coma. ( 5.11 )
Indications and Usage
XTAMPZA ER is indicated for the management of severe and persistent pain that requires an opioid analgesic and that cannot be adequately treated with alternative options, including immediate-release opioids.
Dosage and Administration
XTAMPZA ER should be prescribed only by healthcare professionals who are knowledgeable about the use of extended-release/long-acting opioids and how to mitigate the associated risks. XTAMPZA ER single doses greater than 36 mg (equivalent to 40 mg oxycodone hydrochloride [HCl]) or a total daily dose greater than 72 mg (equivalent to 80 mg oxycodone HCl) are to be administered only to patients in whom tolerance to an opioid of comparable potency has been established. Patients who are opioid-tolerant are those receiving, for one week or longer, at least 60 mg oral morphine per day, 25 mcg transdermal fentanyl per hour, 30 mg oral oxycodone HCl per day, 8 mg oral hydromorphone per day, 25 mg oral oxymorphone per day, 60 mg oral hydrocodone per day, or an equianalgesic dose of another opioid. Use the lowest effective dosage for the shortest duration of time consistent with individual patient treatment goals [see Warnings and Precautions (5) ]. Because the risk of overdose increases as opioid doses increase, reserve titration to higher doses of XTAMPZA ER for patients in whom lower doses are insufficiently effective and in whom the expected benefits of using a higher dose opioid clearly outweigh the substantial risks. Initiate the dosing regimen for each patient individually, taking into account the patient's underlying cause and severity of pain, prior analgesic treatment and response, and risk factors for addiction, abuse, and misuse [see Warnings and Precautions (5.1) ] . Respiratory depression can occur at any time during opioid therapy, especially when initiating and following dosage increases with XTAMPZA ER. Consider this risk when selecting an initial dose and when making dose adjustments [see Warnings and Precautions (5.2) ]. XTAMPZA ER is administered, twice daily, every 12 hours, and must be taken with food. Instruct patients to take XTAMPZA ER capsules with approximately the same amount of food for every dose in order to ensure consistent plasma levels are achieved [see Clinical Pharmacology (12.3) ] . Patients who are unable to swallow XTAMPZA ER should be instructed to sprinkle the capsule contents on soft foods or into a cup and then administer directly into the mouth and immediately swallow. XTAMPZA ER may also be administered through a gastrostomy or nasogastric feeding tube [see Dosage and Administration (2.7) ]. The maximum daily dose of XTAMPZA ER is 288 mg per day (eight 36 mg capsules, equivalent to 320 mg oxycodone HCl per day) as the safety of the excipients in XTAMPZA ER for doses over 288 mg/day has not been established.
Contraindications
XTAMPZA ER is contraindicated in patients with: Significant respiratory depression [see Warnings and Precautions (5.2) ] Acute or severe bronchial asthma in an unmonitored setting or in the absence of resuscitative equipment [see Warnings and Precautions (5.8) ] Known or suspected gastrointestinal obstruction, including paralytic ileus [see Warnings and Precautions (5.12) ] Hypersensitivity (e.g., anaphylaxis) to oxycodone.
Adverse Reactions
The following serious adverse reactions are described elsewhere in the labeling: Addiction, Abuse, and Misuse [see Warnings and Precautions (5.1) ] Life-Threatening Respiratory Depression [see Warnings and Precautions (5.2) ] Interactions with Benzodiazepines or Other CNS Depressants [see Warnings and Precautions (5.3) ] Neonatal Opioid Withdrawal Syndrome [see Warnings and Precautions (5.4) ] Opioid-Induced Hyperalgesia and Allodynia [see Warnings and Precautions (5.7) ] Adrenal Insufficiency [see Warnings and Precautions (5.9) ] Severe Hypotension [see Warnings and Precautions (5.10) ] Gastrointestinal Adverse Reactions [see Warnings and Precautions (5.12) ] Seizures [see Warnings and Precautions (5.13) ] Withdrawal [see Warnings and Precautions (5.14) ]
Drug Interactions
Table includes clinically significant drug interactions with XTAMPZA ER. Table 3: Clinically Significant Drug Interactions with XTAMPZA ER Inhibitors of CYP3A4 and CYP2D6 Clinical Impact: The concomitant use of XTAMPZA ER and CYP3A4 inhibitors can increase the plasma concentration of oxycodone, resulting in increased or prolonged opioid effects. These effects could be more pronounced with concomitant use of XTAMPZA ER and CYP2D6 and CYP3A4 inhibitors , particularly when an inhibitor is added after a stable dose of XTAMPZA ER is achieved [see Warnings and Precautions (5.6) ]. After stopping a CYP3A4 inhibitor, as the effects of the inhibitor decline, the oxycodone plasma concentration will decrease [see Clinical Pharmacology (12.3) ] , resulting in decreased opioid efficacy or a withdrawal syndrome in patients who had developed physical dependence to oxycodone. Intervention: If concomitant use is necessary, consider dosage reduction of XTAMPZA ER until stable drug effects are achieved. Evaluate patients at frequent intervals for respiratory depression and sedation. If a CYP3A4 inhibitor is discontinued, consider increasing the XTAMPZA ER dosage until stable drug effects are achieved. Assess for signs of opioid withdrawal. Examples: Macrolide antibiotics (e.g., erythromycin), azole-antifungal agents (e.g., ketoconazole), protease inhibitors (e.g., ritonavir) CYP3A4 Inducers Clinical Impact: The concomitant use of XTAMPZA ER and CYP3A4 inducers can decrease the plasma concentration of oxycodone [see Clinical Pharmacology (12.3) ] , resulting in decreased efficacy or onset of a withdrawal syndrome in patients who have developed physical dependence to oxycodone [see Warnings and Precautions (5.6) ] . After stopping a CYP3A4 inducer, as the effects of the inducer decline, the oxycodone plasma concentration will increase [see Clinical Pharmacology (12.3) ] , which could increase or prolong both the therapeutic effects and adverse reactions and may cause serious respiratory depression. Intervention: If concomitant use is necessary, consider increasing the XTAMPZA ER dosage until stable drug effects are achieved [see Dosage and Administration (2.5) ] . Evaluate patients for signs of opioid withdrawal. If a CYP3A4 inducer is discontinued, consider XTAMPZA ER dosage reduction and evaluate patients at frequent intervals for signs of respiratory depression and sedation. Examples: Rifampin, carbamazepine, phenytoin Benzodiazepines and other Central Nervous System (CNS) Depressants Clinical Impact: Due to additive pharmacological effect, the concomitant use of benzodiazepines or other CNS depressants including alcohol, increases the risk of respiratory depression, profound sedation, coma, and death [see Warnings and Precautions (5.3) ] . Intervention: Reserve concomitant prescribing of these drugs for use in patients for whom alternative treatment options are inadequate. Limit dosages and durations to the minimum required. Inform patients and caregivers of this potential interaction and educate them on the signs and symptoms of respiratory depression (including sedation). If concomitant use is warranted, consider recommending or prescribing an opioid overdose reversal agent [see Dosage and Administration (2.2) , Warnings and Precautions (5.1 , 5.2 , 5.3) ] . Examples Benzodiazepines and other sedatives/hypnotics, anxiolytics, tranquilizers, muscle relaxants, general anesthetics, antipsychotics, gabapentinoids (gabapentin or pregabalin), other opioids, alcohol Serotonergic Drugs Clinical Impact: The concomitant use of opioids with other drugs that affect the serotonergic neurotransmitter system has resulted in serotonin syndrome . Intervention: If concomitant use is warranted, frequently evaluate the patient, particularly during treatment initiation and dose adjustment. Discontinue XTAMPZA ER if serotonin syndrome is suspected. Examples: Selective serotonin reuptake inhibitors (SSRIs), serotonin and norepinephrine reuptake inhibitors (SNRIs), tricyclic antidepressants (TCAs), triptans, 5-HT3 receptor antagonists, drugs that effect the serotonin neurotransmitter system (e.g., mirtazapine, trazodone, tramadol), certain muscle relaxants (i.e., cyclobenzaprine, metaxalone), monoamine oxidase inhibitors (those intended to treat psychiatric disorders and also others, such as linezolid and intravenous methylene blue) Monoamine Oxidase Inhibitors (MAOIs) Clinical Impact: MAOI interactions with opioids may manifest as serotonin syndrome or opioid toxicity (e.g., respiratory depression, coma) [see Warnings and Precautions (5.2) ]. Intervention: The use of XTAMPZA ER is not recommended for patients taking MAOIs or within 14 days of stopping such treatment. Examples: phenelzine, tranylcypromine, linezolid Mixed Agonist/Antagonist and Partial Agonist Opioid Analgesics Clinical Impact: May reduce the analgesic effect of XTAMPZA ER and/or precipitate withdrawal symptoms. Intervention: Avoid concomitant use. Examples: Butorphanol, nalbuphine, pentazocine, buprenorphine Muscle Relaxants Clinical Impact: Oxycodone may enhance the neuromuscular blocking action of skeletal muscle relaxants and produce an increased degree of respiratory depression. Intervention: Because respiratory depression may be greater than otherwise expected, decrease the dosage of XTAMPZA ER and/or the muscle relaxant as necessary. Due to the risk of respiratory depression with concomitant use of skeletal muscle relaxants and opioids, consider recommending or prescribing an opioid overdose reversal agent [ see Dosage and Administration (2.2) , Warnings and Precautions (5.2 , 5.3) ]. Examples: Cyclobenzaprine, metaxalone Diuretics Clinical Impact: Opioids can reduce the efficacy of diuretics by inducing the release of antidiuretic hormone. Intervention: Evaluate patients for signs of diminished diuresis and/or effects on blood pressure and increase the dosage of the diuretic as needed. Anticholinergic Drugs Clinical Impact: The concomitant use of anticholinergic drugs may increase risk of urinary retention and/or severe constipation, which may lead to paralytic ileus. Intervention: Evaluate patients for signs of urinary retention or reduced gastric motility when XTAMPZA ER is used concomitantly with anticholinergic drugs.
Storage and Handling
XTAMPZA ER capsules are supplied in 100-count bottles with a child-resistant closure and as a hospital unit dose package with 10 individually blistered capsules per card; two cards per carton as follows: Table 9: Summary of XTAMPZA ER Capsule Strengths and Packaging Configurations Strength Capsule Description NDC Number (100-count Bottles with a child-resistant closure) NDC Number (20-count Hospital Unit Dose Blister Cartons) 9 mg (equivalent to 10 mg oxycodone HCl) Size 3, ivory cap printed with "XTAMPZA ER" and white body printed with "9 mg" NDC 24510-110-10 NDC 24510-110-20 13.5 mg (equivalent to 15 mg oxycodone HCl) Size 2, Swedish orange cap printed with "XTAMPZA ER" and white body printed with "13.5 mg" NDC 24510-115-10 NDC 24510-115-20 18 mg (equivalent to 20 mg oxycodone HCl) Size 1, rich yellow cap printed with "XTAMPZA ER" and white body printed with "18 mg" NDC 24510-120-10 NDC 24510-120-20 27 mg (equivalent to 30 mg oxycodone HCl) Size 0, light gray cap printed with "XTAMPZA ER" and white body printed with "27 mg" NDC 24510-130-10 NDC 24510-130-20 36 mg (equivalent to 40 mg oxycodone HCl) Size 00, flesh color cap printed with "XTAMPZA ER" and white body printed with "36 mg" NDC 24510-140-10 NDC 24510-140-20
How Supplied
XTAMPZA ER capsules are supplied in 100-count bottles with a child-resistant closure and as a hospital unit dose package with 10 individually blistered capsules per card; two cards per carton as follows: Table 9: Summary of XTAMPZA ER Capsule Strengths and Packaging Configurations Strength Capsule Description NDC Number (100-count Bottles with a child-resistant closure) NDC Number (20-count Hospital Unit Dose Blister Cartons) 9 mg (equivalent to 10 mg oxycodone HCl) Size 3, ivory cap printed with "XTAMPZA ER" and white body printed with "9 mg" NDC 24510-110-10 NDC 24510-110-20 13.5 mg (equivalent to 15 mg oxycodone HCl) Size 2, Swedish orange cap printed with "XTAMPZA ER" and white body printed with "13.5 mg" NDC 24510-115-10 NDC 24510-115-20 18 mg (equivalent to 20 mg oxycodone HCl) Size 1, rich yellow cap printed with "XTAMPZA ER" and white body printed with "18 mg" NDC 24510-120-10 NDC 24510-120-20 27 mg (equivalent to 30 mg oxycodone HCl) Size 0, light gray cap printed with "XTAMPZA ER" and white body printed with "27 mg" NDC 24510-130-10 NDC 24510-130-20 36 mg (equivalent to 40 mg oxycodone HCl) Size 00, flesh color cap printed with "XTAMPZA ER" and white body printed with "36 mg" NDC 24510-140-10 NDC 24510-140-20
Description
WARNING: SERIOUS AND LIFE-THREATENING RISKS FROM USE OF XTAMPZA ER See full prescribing information for complete boxed warning . XTAMPZA ER exposes users to risks of addiction, abuse, and misuse, which can lead to overdose and death. Assess each patient's risk before prescribing and reassess regularly for these behaviors and conditions. ( 5.1 ) Serious, life-threatening, or fatal respiratory depression may occur especially during initiation or following a dosage increase. To reduce the risk of respiratory depression, proper dosing and titration of XTAMPZA ER are essential. ( 5.2 ) Accidental ingestion of XTAMPZA ER, especially by children, can result in fatal overdose of oxycodone. ( 5.2 ) Concomitant use of opioids with benzodiazepines or other central nervous system (CNS) depressants, including alcohol, may result in profound sedation, respiratory depression, coma, and death. Reserve concomitant prescribing for use in patients for whom alternative treatment options are inadequate. ( 5.3 , 7 ) Advise pregnant using opioids for an extended period of time of the risk of Neonatal Opioid Withdrawal Syndrome, which may be life-threatening if not recognized and treated. Ensure that management by neonatology experts will be available at delivery. ( 5.4 ) Healthcare providers are strongly encouraged to complete a REMS-compliant education program and to counsel patients and caregivers on serious risks, safe use, and the importance of reading the Medication Guide with each prescription. ( 5.5 ) Concomitant use with CYP3A4 inhibitors (or discontinuation of CYP3A4 inducers) can result in a fatal overdose of oxycodone from XTAMPZA ER. ( 5.6 , 12.3 )
Section 42229-5
Addiction, Abuse, and Misuse
Because the use of XTAMPZA ER exposes patients and other users to the risks of opioid addiction, abuse, and misuse, which can lead to overdose and death, assess each patient's risk prior to prescribing and reassess all patients regularly for the development of these behaviors and conditions [see Warnings and Precautions (5.1)].
Section 42231-1
| Medication Guide XTAMPZA® ER (ex tamp' zah ee ar) (oxycodone) extended-release capsules, CII |
|
|---|---|
| This Medication Guide has been approved by the U.S. Food and Drug Administration. | Issued: December 2025 |
XTAMPZA ER is:
|
|
Important information about XTAMPZA ER:
|
|
Do not take XTAMPZA ER if you have:
|
|
| Before taking XTAMPZA ER, tell your healthcare provider if you have a history of: | |
|
|
|
|
Tell your healthcare provider if you are:
|
|
When taking XTAMPZA ER:
|
|
While taking XTAMPZA ER DO NOT:
|
|
The possible side effects of XTAMPZA ER are:
Manufactured by: Patheon Pharmaceuticals, 2110 Galbraith Road, Cincinnati, OH 45237, www.collegiumpharma.com or call 855-331-5615 |
Section 43683-2
Section 44425-7
Store at 25°C (77°F); excursions permitted between 15°-30°C (59°-86°F) [see USP Controlled Room Temperature].
Dispense in tight, light-resistant container, with child-resistant closure.
Store XTAMPZA ER securely and dispose of properly [see Patient Counseling Information (17)].
9.2 Abuse
XTAMPZA ER contains oxycodone, a substance with high potential for misuse and abuse, which can lead to the development of substance use disorder, including addiction [see Warnings and Precautions (5.1)].
Misuse is the intentional use, for therapeutic purposes, of a drug by an individual in a way other than prescribed by a healthcare provider or for whom it was not prescribed.
Abuse is the intentional, non-therapeutic use of a drug, even once, for its desirable psychological or physiological effects.
Drug addiction is a cluster of behavioral, cognitive, and physiological phenomena that may include a strong desire to take the drug, difficulties in controlling drug use (e.g., continuing drug use despite harmful consequences, giving a higher priority to drug use than other activities and obligations), and possible tolerance or physical dependence.
Misuse and abuse of XTAMPZA ER increases risk of overdose, which may lead to central nervous system and respiratory depression, hypotension, seizures, and death. The risk is increased with concurrent abuse of XTAMPZA ER with alcohol and/or other CNS depressants. Abuse of and addiction to opioids in some individuals may not be accompanied by concurrent tolerance and symptoms of physical dependence. In addition, abuse of opioids can occur in the absence of addiction.
All patients treated with opioids require careful and frequent reevaluation for signs of misuse, abuse, and addiction, because use of opioid analgesic products carries the risk of addiction even under appropriate medical use. Patients at high risk of XTAMPZA ER abuse include those with a history of prolonged use of any opioid, including products containing buprenorphine, those with a history of drug or alcohol abuse, or those who use XTAMPZA ER in combination with other abused drugs.
"Drug-seeking" behavior is very common in persons with substance use disorders. Drug-seeking tactics include emergency calls or visits near the end of office hours, refusal to undergo appropriate examination, testing, or referral, repeated "loss" of prescriptions, tampering with prescriptions, and reluctance to provide prior medical records or contact information for other treating healthcare provider(s). "Doctor shopping" (visiting multiple prescribers to obtain additional prescriptions) is common among people who abuse drugs and people with substance use disorder. Preoccupation with achieving adequate pain relief can be appropriate behavior in a patient with inadequate pain control.
XTAMPZA ER, like other opioids, can be diverted for nonmedical use into illicit channels of distribution. Careful record-keeping of prescribing information, including quantity, frequency, and renewal requests, as required by state and federal law, is strongly advised.
Proper assessment of the patient, proper prescribing practices, periodic reevaluation of therapy, and proper dispensing and storage are appropriate measures that help to limit abuse of opioid drugs.
11 Description
XTAMPZA ER (oxycodone) extended-release capsules are an opioid agonist for oral use. The capsules contain microspheres formulated with oxycodone base and are supplied in strengths of 9 mg (equivalent to 10 mg oxycodone HCl), 13.5 mg (equivalent to 15 mg oxycodone HCl), 18 mg (equivalent to 20 mg oxycodone HCl), 27 mg (equivalent to 30 mg oxycodone HCl), and 36 mg (equivalent to 40 mg oxycodone HCl) capsules. The capsule strengths describe the amount of oxycodone base per capsule. The structural formula for oxycodone is as follows:
The chemical name is 4,5 α-Epoxy-14-hydroxy-3-methoxy-17-methylmorphinan-6-one.
Oxycodone base is a white, odorless crystalline powder derived from the opium alkaloid, thebaine. Oxycodone is present as myristate salt in the XTAMPZA ER formulation.
Each XTAMPZA ER capsule contains either 9, 13.5, 18, 27, or 36 mg of oxycodone (equivalent to 10, 15, 20, 30, or 40 mg of oxycodone HCl, respectively) and the following inactive ingredients: myristic acid, yellow beeswax, carnauba wax, stearoyl polyoxyl-32 glycerides, magnesium stearate, and colloidal silicon dioxide. The capsule shells collectively contain titanium dioxide, hypromellose, and water. Additionally, the 9 mg and 18 mg strength capsule shells contain yellow iron oxide, the 13.5 and 36 mg strength capsule shells contain red iron oxide, and the 27 mg strength capsule shells contain black iron oxide.
9.3 Dependence
Both tolerance and physical dependence can develop during use of opioid therapy.
Tolerance is a physiological state characterized by a reduced response to a drug after repeated administration (i.e., a higher dose of a drug is required to produce the same effect that was once obtained at a lower dose).
Physical dependence is a state that develops as a result of a physiological adaptation in response to repeated drug use, manifested by withdrawal signs and symptoms after abrupt discontinuation or a significant dose reduction of a drug.
Withdrawal may be precipitated through the administration of drugs with opioid antagonist activity (e.g., naloxone, nalmefene), mixed agonist/antagonist analgesics (e.g., pentazocine, butorphanol, nalbuphine), or partial agonists (e.g., buprenorphine). Physical dependence may not occur to a clinically significant degree until after several days to weeks of continued use.
Do not rapidly reduce or abruptly discontinue XTAMPZA ER in a patient physically dependent on opioids. Rapid tapering of XTAMPZA ER in a patient physically dependent on opioids may lead to serious withdrawal symptoms, uncontrolled pain, and suicide. Rapid discontinuation has also been associated with attempts to find other sources of opioid analgesics, which may be confused with drug-seeking for abuse.
When discontinuing XTAMPZA ER, gradually taper the dosage using a patient-specific plan that considers the following: the dose of XTAMPZA ER the patient has been taking, the duration of treatment, and the physical and psychological attributes of the patient. To improve the likelihood of a successful taper and minimize withdrawal symptoms, it is important that the opioid tapering schedule is agreed upon by the patient. In patients taking opioids for an extended period of time at high doses, ensure that a multimodal approach to pain management, including mental health support (if needed), is in place prior to initiating an opioid analgesic taper [see Dosage and Administration (2.6), Warnings and Precautions (5.14) ].
Infants born to mothers physically dependent on opioids will also be physically dependent and may exhibit respiratory difficulties and withdrawal signs [see Use in Specific Populations (8.1) ].
5.14 Withdrawal
Do not rapidly reduce or abruptly discontinue XTAMPZA ER in a patient physically dependent on opioids. When discontinuing XTAMPZA ER in a physically dependent patient, gradually taper the dosage. Rapid tapering of oxycodone in a patient physically dependent on opioids may lead to a withdrawal syndrome and return of pain [see Dosage and Administration (2.6), Drug Abuse and Dependence (9.3)].
Additionally, avoid the use of mixed agonist/antagonist (e.g., pentazocine, nalbuphine, and butorphanol) or partial agonist (e.g., buprenorphine) analgesics in patients who have received or are receiving a course of therapy with a full opioid agonist analgesic, including XTAMPZA ER. In these patients, mixed agonist/antagonist and partial agonist analgesics may reduce the analgesic effect and/or may precipitate withdrawal symptoms [see Dosage and Administration (2.6), Drug Interactions (7)].
8.4 Pediatric Use
Safety and effectiveness of XTAMPZA ER in pediatric patients below the age of 18 years have not been established.
8.5 Geriatric Use
In controlled pharmacokinetic studies in elderly subjects (greater than 65 years) the clearance of oxycodone was slightly reduced. Compared to young adults, the plasma concentrations of oxycodone were increased approximately 15% [see Clinical Pharmacology (12.3)]. Of the total number of subjects entered into the titration phase of the Phase 3 study for XTAMPZA ER (740), 88 (12%) were age 65 and older. In this clinical trial with appropriate initiation of therapy and dose titration, no untoward or unexpected adverse reactions were seen in the elderly patients who received XTAMPZA ER. Thus, the usual doses and dosing intervals may be appropriate for elderly patients. Use caution when selecting a dosage for an elderly patient, usually starting at the low end of the dosing range, reflecting the greater frequency of decreased hepatic, renal, or cardiac function, concomitant disease, and use of other drug therapy.
Respiratory depression is the chief risk in elderly patients treated with opioids and has occurred after large initial doses were administered to patients who were not opioid-tolerant or when opioids were co-administered with other agents that depress respiration. Titrate the dosage of XTAMPZA ER slowly in geriatric patients and frequently reevaluate the patient for signs of central nervous system and respiratory depression [see Warnings and Precautions (5.8)].
2.3 Initial Dosage
It is safer to underestimate a patient's 24-hour oral oxycodone dosage and provide rescue medication (e.g., immediate-release opioid) than to overestimate the 24-hour oral oxycodone dosage and manage adverse reactions due to an overdose. While useful tables of opioid equivalents are readily available, there is substantial inter-patient variability in the relative potency of different opioid drugs and products. Frequently reevaluate patients for signs and symptoms of opioid withdrawal and for signs of oversedation/toxicity after converting patients to XTAMPZA ER.
14 Clinical Studies
An enriched-enrollment, randomized-withdrawal, double-blind, placebo-controlled, parallel group, study was conducted in 740 patients with persistent, moderate-to-severe chronic lower back pain, with inadequate pain control from their prior therapy. During screening, patients stopped their prior opioid analgesics and/or non-opioid analgesics prior to starting XTAMPZA ER treatment. Patients were titrated to a stable and tolerated dose between 18 mg (equivalent to 20 mg oxycodone HCl) twice daily and 72 mg (equivalent to 80 mg oxycodone HCl) twice daily of XTAMPZA ER in an open-label fashion during the first six weeks of the trial. Optional use of rescue medication (acetaminophen 500 mg tablets) up to 2 tablets every 4-6 hours was permitted during the dose titration phase, up to 2000 mg per day. XTAMPZA ER was titrated once every three to seven days until a stable and tolerable dose was identified (maximum dose of 72 mg [equivalent to 80 mg oxycodone HCl] twice daily).
Following the titration phase, 389 subjects (53%) met the study randomization criteria of adequate analgesia (pain reduction of at least 2 points from screening baseline to a score of 4 or less on a 0-10 numerical rating scale) and acceptable tolerability of XTAMPZA ER and entered the randomized, double-blind maintenance phase. Subjects discontinued from the dose-titration phase for the following reasons: failure to meet entrance criteria (18%), adverse events (13%), subject request (7%) and lack of efficacy (5%). Patients were randomized at a ratio of 1:1 into a 12-week double-blind maintenance phase with their fixed stable dose of XTAMPZA ER (or matching placebo). Patients randomized to placebo were given a blinded taper of XTAMPZA ER according to a prespecified tapering schedule; XTAMPZA ER was decreased by 25% to 35% every 5 days for the higher doses of XTAMPZA ER and up to 50% every 5 days for the mid-to-lower doses of XTAMPZA ER over the first 20 days of the double-blind maintenance phase. Patients were allowed to use rescue medication (acetaminophen 500 mg tablets) up to a maximum dose of 2000 mg per day. During the double-blind maintenance phase, 122 patients (63%) completed the 12-week treatment with XTAMPZA ER and 100 (51%) completed with placebo. Overall, 11% of patients discontinued due to lack of efficacy (4% of XTAMPZA ER patients and 17% of placebo patients), and 7% discontinued due to adverse events (7% of XTAMPZA ER patients and 7% of placebo patients).
In this study, there was a significant difference in pain reduction, favoring XTAMPZA ER, between XTAMPZA ER (doses of 36-144 mg per day, equivalent to 40-160 mg of oxycodone HCl) and placebo, based on the primary endpoint of change in average pain intensity from randomization baseline to Week 12 of the double-blind maintenance phase.
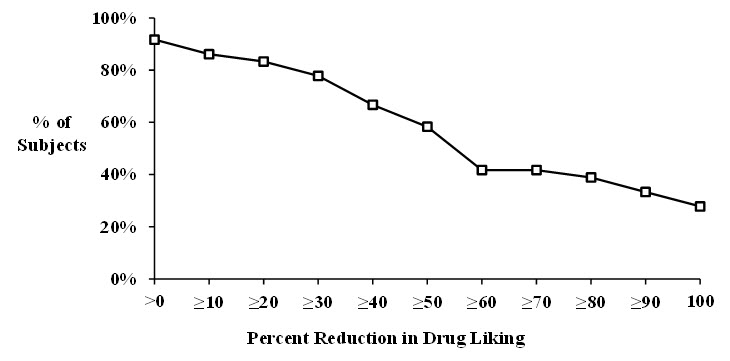
The proportion of patients (responders) in each group who demonstrated improvement in their weekly average pain scores from screening baseline to Week 12, is shown in Figure 2. The figure is cumulative, so that patients whose change from screening is, for example, 30%, are also included at every level of improvement below 30%. Patients who did not complete the study were classified as non-responders. Treatment with XTAMPZA ER resulted in a higher proportion of responders, defined as patients with at least a 30% and 50% improvement as compared to placebo.
Figure 2: Responder Analysis for Pain Intensity: Percent Reduction/Improvement (Intent-to-Treat Population)
4 Contraindications
XTAMPZA ER is contraindicated in patients with:
- Significant respiratory depression [see Warnings and Precautions (5.2)]
- Acute or severe bronchial asthma in an unmonitored setting or in the absence of resuscitative equipment [see Warnings and Precautions (5.8)]
- Known or suspected gastrointestinal obstruction, including paralytic ileus [see Warnings and Precautions (5.12)]
- Hypersensitivity (e.g., anaphylaxis) to oxycodone.
6 Adverse Reactions
The following serious adverse reactions are described elsewhere in the labeling:
- Addiction, Abuse, and Misuse [see Warnings and Precautions (5.1)]
- Life-Threatening Respiratory Depression [see Warnings and Precautions (5.2)]
- Interactions with Benzodiazepines or Other CNS Depressants [see Warnings and Precautions (5.3)]
- Neonatal Opioid Withdrawal Syndrome [see Warnings and Precautions (5.4)]
- Opioid-Induced Hyperalgesia and Allodynia [see Warnings and Precautions (5.7)]
- Adrenal Insufficiency [see Warnings and Precautions (5.9)]
- Severe Hypotension [see Warnings and Precautions (5.10)]
- Gastrointestinal Adverse Reactions [see Warnings and Precautions (5.12)]
- Seizures [see Warnings and Precautions (5.13)]
- Withdrawal [see Warnings and Precautions (5.14)]
7 Drug Interactions
Table includes clinically significant drug interactions with XTAMPZA ER.
| Inhibitors of CYP3A4 and CYP2D6 | |
|---|---|
| Clinical Impact: | The concomitant use of XTAMPZA ER and CYP3A4 inhibitors can increase the plasma concentration of oxycodone, resulting in increased or prolonged opioid effects. These effects could be more pronounced with concomitant use of XTAMPZA ER and CYP2D6 and CYP3A4 inhibitors, particularly when an inhibitor is added after a stable dose of XTAMPZA ER is achieved [see Warnings and Precautions (5.6)].
After stopping a CYP3A4 inhibitor, as the effects of the inhibitor decline, the oxycodone plasma concentration will decrease [see Clinical Pharmacology (12.3)], resulting in decreased opioid efficacy or a withdrawal syndrome in patients who had developed physical dependence to oxycodone. |
| Intervention: | If concomitant use is necessary, consider dosage reduction of XTAMPZA ER until stable drug effects are achieved. Evaluate patients at frequent intervals for respiratory depression and sedation. If a CYP3A4 inhibitor is discontinued, consider increasing the XTAMPZA ER dosage until stable drug effects are achieved. Assess for signs of opioid withdrawal. |
| Examples: | Macrolide antibiotics (e.g., erythromycin), azole-antifungal agents (e.g., ketoconazole), protease inhibitors (e.g., ritonavir) |
| CYP3A4 Inducers | |
| Clinical Impact: | The concomitant use of XTAMPZA ER and CYP3A4 inducers can decrease the plasma concentration of oxycodone [see Clinical Pharmacology (12.3)], resulting in decreased efficacy or onset of a withdrawal syndrome in patients who have developed physical dependence to oxycodone [see Warnings and Precautions (5.6)]. After stopping a CYP3A4 inducer, as the effects of the inducer decline, the oxycodone plasma concentration will increase [see Clinical Pharmacology (12.3)], which could increase or prolong both the therapeutic effects and adverse reactions and may cause serious respiratory depression. |
| Intervention: | If concomitant use is necessary, consider increasing the XTAMPZA ER dosage until stable drug effects are achieved [see Dosage and Administration (2.5)]. Evaluate patients for signs of opioid withdrawal. If a CYP3A4 inducer is discontinued, consider XTAMPZA ER dosage reduction and evaluate patients at frequent intervals for signs of respiratory depression and sedation. |
| Examples: | Rifampin, carbamazepine, phenytoin |
| Benzodiazepines and other Central Nervous System (CNS) Depressants | |
| Clinical Impact: | Due to additive pharmacological effect, the concomitant use of benzodiazepines or other CNS depressants including alcohol, increases the risk of respiratory depression, profound sedation, coma, and death [see Warnings and Precautions (5.3)]. |
| Intervention: | Reserve concomitant prescribing of these drugs for use in patients for whom alternative treatment options are inadequate. Limit dosages and durations to the minimum required. Inform patients and caregivers of this potential interaction and educate them on the signs and symptoms of respiratory depression (including sedation). If concomitant use is warranted, consider recommending or prescribing an opioid overdose reversal agent [see Dosage and Administration (2.2), Warnings and Precautions (5.1, 5.2, 5.3)]. |
| Examples | Benzodiazepines and other sedatives/hypnotics, anxiolytics, tranquilizers, muscle relaxants, general anesthetics, antipsychotics, gabapentinoids (gabapentin or pregabalin), other opioids, alcohol |
| Serotonergic Drugs | |
| Clinical Impact: | The concomitant use of opioids with other drugs that affect the serotonergic neurotransmitter system has resulted in serotonin syndrome. |
| Intervention: | If concomitant use is warranted, frequently evaluate the patient, particularly during treatment initiation and dose adjustment. Discontinue XTAMPZA ER if serotonin syndrome is suspected. |
| Examples: | Selective serotonin reuptake inhibitors (SSRIs), serotonin and norepinephrine reuptake inhibitors (SNRIs), tricyclic antidepressants (TCAs), triptans, 5-HT3 receptor antagonists, drugs that effect the serotonin neurotransmitter system (e.g., mirtazapine, trazodone, tramadol), certain muscle relaxants (i.e., cyclobenzaprine, metaxalone), monoamine oxidase inhibitors (those intended to treat psychiatric disorders and also others, such as linezolid and intravenous methylene blue) |
| Monoamine Oxidase Inhibitors (MAOIs) | |
| Clinical Impact: | MAOI interactions with opioids may manifest as serotonin syndrome or opioid toxicity (e.g., respiratory depression, coma) [see Warnings and Precautions (5.2)]. |
| Intervention: | The use of XTAMPZA ER is not recommended for patients taking MAOIs or within 14 days of stopping such treatment. |
| Examples: | phenelzine, tranylcypromine, linezolid |
| Mixed Agonist/Antagonist and Partial Agonist Opioid Analgesics | |
| Clinical Impact: | May reduce the analgesic effect of XTAMPZA ER and/or precipitate withdrawal symptoms. |
| Intervention: | Avoid concomitant use. |
| Examples: | Butorphanol, nalbuphine, pentazocine, buprenorphine |
| Muscle Relaxants | |
| Clinical Impact: | Oxycodone may enhance the neuromuscular blocking action of skeletal muscle relaxants and produce an increased degree of respiratory depression. |
| Intervention: | Because respiratory depression may be greater than otherwise expected, decrease the dosage of XTAMPZA ER and/or the muscle relaxant as necessary. Due to the risk of respiratory depression with concomitant use of skeletal muscle relaxants and opioids, consider recommending or prescribing an opioid overdose reversal agent [see Dosage and Administration (2.2), Warnings and Precautions (5.2, 5.3)]. |
| Examples: | Cyclobenzaprine, metaxalone |
| Diuretics | |
| Clinical Impact: | Opioids can reduce the efficacy of diuretics by inducing the release of antidiuretic hormone. |
| Intervention: | Evaluate patients for signs of diminished diuresis and/or effects on blood pressure and increase the dosage of the diuretic as needed. |
| Anticholinergic Drugs | |
| Clinical Impact: | The concomitant use of anticholinergic drugs may increase risk of urinary retention and/or severe constipation, which may lead to paralytic ileus. |
| Intervention: | Evaluate patients for signs of urinary retention or reduced gastric motility when XTAMPZA ER is used concomitantly with anticholinergic drugs. |
8.8 Sex Differences
In pharmacokinetic studies with XTAMPZA ER, healthy female subjects demonstrate up to 20% higher oxycodone plasma exposures than males, even after considering differences in body weight or BMI. The clinical relevance of a difference of this magnitude is low for a drug intended for chronic usage at individualized dosages. In the Phase 3 clinical trial there was a greater frequency of typical opioid adverse events for females than males; there was no male/female difference detected for efficacy.
8.7 Renal Impairment
In patients with renal impairment, as evidenced by decreased creatinine clearance (<60 mL/min), the concentrations of oxycodone in the plasma are approximately 50% higher than in subjects with normal renal function. Follow a conservative approach to dose initiation and adjust according to the clinical situation. Use of alternative analgesics is recommended for patients who require a dose of XTAMPZA ER less than 9 mg [see Clinical Pharmacology (12.3)].
Instructions for Use
Always take XTAMPZA ER with approximately the same amount of food. If you cannot swallow XTAMPZA ER capsules, tell your healthcare provider. If your healthcare provider tells you that you can take XTAMPZA ER by sprinkling the capsule contents, follow these steps:
XTAMPZA ER can be opened and the contents inside the capsule can be sprinkled onto soft foods (such as, applesauce, pudding, yogurt, ice cream, or jam) as follows:
|
Figure 1 |
|
|
Figure 2 |
|
|
Figure 3 |
|
|
Figure 4 |
|
XTAMPZA ER capsule contents can also be sprinkled into a cup and then put directly into the mouth.
Giving XTAMPZA ER through a nasogastric or gastrostomy tube:
Use water, milk, or a liquid nutritional supplement to flush the tube when giving XTAMPZA ER.
| Step 1: | Flush the nasogastric or gastrostomy tube with liquid. |
| Step 2: | Open an XTAMPZA ER capsule and carefully pour the contents of the capsule directly into the tube. Do not pre-mix the capsule contents with the liquid used to flush the capsule contents through the tube. |
| Step 3: | Draw up 15 mL of liquid into a syringe, insert the syringe into the tube, and flush the contents of the capsule through the tube to give the dose. |
| Step 4: | Flush the tube two more times, each time with 10 mL of liquid, to ensure that none of the contents of the capsule are left in the tube. |
This Instruction for Use has been approved by the U.S. Food and Drug Administration. Issued: December 2025
Collegium®
PHARMACEUTICAL
12.3 Pharmacokinetics
The activity of XTAMPZA ER is primarily due to the parent drug oxycodone. XTAMPZA ER is designed to provide delivery of oxycodone over 12 hours.
13.2 Animal Toxicology
The safety of beeswax, carnauba wax, and myristic acid in XTAMPZA ER in doses exceeding a total daily dose of 288 mg oxycodone per day (equivalent to 320 mg oxycodone HCl per day) has not been studied.
8.6 Hepatic Impairment
A study in patients with hepatic impairment demonstrated greater plasma oxycodone concentrations than those seen at equivalent doses in persons with normal hepatic function. A similar effect on plasma oxycodone concentrations can be expected for patients with hepatic impairment taking XTAMPZA ER. Therefore, in the setting of hepatic impairment, start dosing patients at 1/3 to 1/2 the usual starting dose followed by careful dose titration. Use of alternative analgesics is recommended for patients who require a dose of XTAMPZA ER less than 9 mg [see Dosage and Administration (2.4), Clinical Pharmacology (12.3)].
1 Indications and Usage
XTAMPZA ER is indicated for the management of severe and persistent pain that requires an opioid analgesic and that cannot be adequately treated with alternative options, including immediate-release opioids.
5.10 Severe Hypotension
XTAMPZA ER may cause severe hypotension including orthostatic hypotension and syncope in ambulatory patients. There is an increased risk in patients whose ability to maintain blood pressure has already been compromised by a reduced blood volume or concurrent administration of certain CNS depressant drugs (e.g., phenothiazines or general anesthetics) [see Drug Interactions (7)]. Regularly evaluate these patients for signs of hypotension after initiating or titrating the dosage of XTAMPZA ER. In patients with circulatory shock, XTAMPZA ER may cause vasodilation that can further reduce cardiac output and blood pressure. Avoid the use of XTAMPZA ER in patients with circulatory shock.
12.1 Mechanism of Action
Oxycodone is a full opioid agonist and is relatively selective for the mu receptor, although it can bind to other opioid receptors at higher doses. The principal therapeutic action of oxycodone is analgesia. Like all full opioid agonists, there is no ceiling effect to analgesia for oxycodone. Clinically, dosage is titrated to provide adequate analgesia and may be limited by adverse reactions, including respiratory and CNS depression.
The precise mechanism of the analgesic action is unknown. However, specific CNS opioid receptors for endogenous compounds with opioid-like activity have been identified throughout the brain and spinal cord and are thought to play a role in the analgesic effects of this drug. In addition, when oxycodone binds to mu-opioid receptors, it results in positive subjective effects, such as drug liking, euphoria, and high.
9.1 Controlled Substance
XTAMPZA ER contains oxycodone, a Schedule II controlled substance.
5.9 Adrenal Insufficiency
Cases of adrenal insufficiency have been reported with opioid use, more often following greater than one month of use. Presentation of adrenal insufficiency may include non-specific symptoms and signs including nausea, vomiting, anorexia, fatigue, weakness, dizziness, and low blood pressure. If adrenal insufficiency is suspected, confirm the diagnosis with diagnostic testing as soon as possible. If adrenal insufficiency is diagnosed, treat with physiologic replacement doses of corticosteroids. Wean the patient off of the opioid to allow adrenal function to recover and continue corticosteroid treatment until adrenal function recovers. Other opioids may be tried as some cases reported use of a different opioid without recurrence of adrenal insufficiency. The information available does not identify any particular opioids as being more likely to be associated with adrenal insufficiency.
5 Warnings and Precautions
- Opioid-Induced Hyperalgesia and Allodynia: Opioid-Induced Hyperalgesia (OIH) occurs when an opioid analgesic paradoxically causes an increase in pain, or an increase in sensitivity to pain. If OIH is suspected, carefully consider appropriately decreasing the dose of the current opioid analgesic or opioid rotation. (5.7)
- Risk of life-threatening respiratory depression in patients with chronic pulmonary disease or in elderly, cachectic, or debilitated patients: Regularly evaluate. (5.8)
- Adrenal Insufficiency: If diagnosed, treat with physiologic replacement of corticosteroids, and wean patient off of the opioid. (5.9)
- Severe hypotension: Regularly evaluate. Avoid use of XTAMPZA ER in patients with circulatory shock. (5.10)
- Risks of use in patients with increased intracranial pressure, brain tumors, head injury, or impaired consciousness: Monitor for sedation and respiratory depression. Avoid use of XTAMPZA ER in patients with impaired consciousness or coma. (5.11)
5.16 Laboratory Monitoring
Not every urine drug test for "opioids" or "opiates" detects oxycodone reliably, especially those designed for in-office use. Further, many laboratories will report urine drug concentrations below a specified "cut-off" value as "negative". Therefore, if urine testing for oxycodone is considered in the clinical management of an individual patient, ensure that the sensitivity and specificity of the assay is appropriate, and consider the limitations of the testing used when interpreting results.
2 Dosage and Administration
- XTAMPZA ER should be prescribed only by healthcare professionals who are knowledgeable about the use of extended-release/long-acting opioids and how to mitigate the associated risks. (2.1)
- XTAMPZA ER at a total daily dose greater than 72 mg (equivalent to 80 mg oxycodone hydrochloride [HCl]) or a single dose greater than 36 mg (equivalent to 40 mg oxycodone HCl) is only for use in patients in whom tolerance to an opioid of comparable potency has been established. (2.1)
- Patients considered opioid-tolerant are those receiving, for one week or longer, at least 60 mg oral morphine per day, 25 mcg transdermal fentanyl per hour, 30 mg oral oxycodone HCl per day, 8 mg oral hydromorphone per day, 25 mg oral oxymorphone per day, 60 mg oral hydrocodone per day, or an equianalgesic dose of another opioid. (2.1)
- Use the lowest effective dose for the shortest duration of time consistent with individual patient treatment goals. Reserve titration to higher doses of XTAMPZA ER for patients in whom lower doses are insufficiently effective and in whom the expected benefits of using a higher dose opioid clearly outweigh the substantial risks. (2, 5)
- Initiate the dosing regimen for each patient individually, taking into account the patient's underlying cause and severity of pain, prior analgesic treatment and response, and risk factors for addiction, abuse, and misuse. (2.1, 5.1).
- Respiratory depression can occur at any time during opioid therapy, especially when initiating and following dosage increases with XTAMPZA ER. Consider this risk when selecting an initial dose and when making dose adjustments. (2.1, 5.2)
- Discuss opioid overdose reversal agents and options for acquiring them with the patient and/or caregiver, both when initiating and renewing treatment with XTAMPZA ER, especially if the patient has additional risk factors for overdose, or close contacts at risk for exposure and overdose. (2.2, 5.1, 5.2, 5.3)
- XTAMPZA ER is administered, twice daily, every 12 hours, and must be taken with food. Instruct patients to take XTAMPZA ER capsules with approximately the same amount of food for every dose to ensure consistent plasma levels are achieved. (2.1, 2.3)
- For patients who are not opioid tolerant, initiate with 9 mg (equivalent to 10 mg oxycodone HCl per day). (2.3)
- The daily dose of XTAMPZA ER must be limited to a maximum of 288 mg per day (equivalent to 320 mg oxycodone HCl per day). (2.1)
- Hepatic impairment: Initiate therapy at 1/3 to 1/2 the usual dosage and titrate carefully. Regularly evaluate. Use alternate analgesia for patients requiring less than 9 mg. (2.4, 8.6)
- Periodically reassess patients receiving XTAMPZA ER to evaluate the continued need for opioid analgesics to maintain pain control, for the signs or symptoms of adverse reactions, and for the development of addiction, abuse, or misuse. (2.5)
- Do not rapidly reduce or abruptly discontinue XTAMPZA ER in a physically-dependent patient because rapid reduction or abrupt discontinuation of opioid analgesics has resulted in serious withdrawal symptoms, uncontrolled pain, and suicide. (2.6 , 5.14)
- Instruct patients to take XTAMPZA ER capsules with food in order to ensure consistent plasma levels are achieved. For patients who have difficulty swallowing, XTAMPZA ER can also be taken by sprinkling the capsule contents on soft foods or into a cup and then administering directly into the mouth, or through a gastrostomy or nasogastric feeding tube. (2.7)
3 Dosage Forms and Strengths
XTAMPZA ER capsules contain yellow to light brown microspheres, and each available strength has an outer opaque capsule with colors as identified below.
| Strength | Capsule Description |
|---|---|
| 9 mg (equivalent to 10 mg oxycodone HCl) |
Size 3, ivory cap printed with "XTAMPZA ER" and white body printed with "9 mg" |
| 13.5 mg (equivalent to 15 mg oxycodone HCl) |
Size 2, Swedish orange cap printed with "XTAMPZA ER" and white body printed with "13.5 mg" |
| 18 mg (equivalent to 20 mg oxycodone HCl) |
Size 1, rich yellow cap printed with "XTAMPZA ER" and white body printed with "18 mg" |
| 27 mg (equivalent to 30 mg oxycodone HCl) |
Size 0, light gray cap printed with "XTAMPZA ER" and white body printed with "27 mg" |
| 36 mg (equivalent to 40 mg oxycodone HCl) |
Size 00, flesh color cap printed with "XTAMPZA ER" and white body printed with "36 mg" |
6.2 Postmarketing Experience
The following adverse reactions have been identified during post approval use of oxycodone. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Serotonin syndrome: Cases of serotonin syndrome, a potentially life-threatening condition, have been reported during concomitant use of opioids with serotonergic drugs.
Adrenal insufficiency: Cases of adrenal insufficiency have been reported with opioid use, more often following greater than one month of use.
Anaphylaxis: Anaphylaxis has been reported with ingredients contained in XTAMPZA ER.
Androgen deficiency: Cases of androgen deficiency have occurred with use of opioids for an extended period of time [see Clinical Pharmacology (12.2)].
Hyperalgesia and Allodynia: Cases of hyperalgesia and allodynia have been reported with opioid therapy of any duration [see Warnings and Precautions (5.7)].
Hypoglycemia: Cases of hypoglycemia have been reported in patients taking opioids. Most reports were in patients with at least one predisposing risk factor (e.g., diabetes).
Opioid-induced esophageal dysfunction (OIED): Cases of OIED have been reported in patients taking opioids and may occur more frequently in patients taking higher doses of opioids, and/or in patients taking opioids longer term [see Warnings and Precautions (5.12) ].
6.1 Clinical Trial Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
The safety of XTAMPZA ER was evaluated in a Phase 3, randomized-withdrawal, double-blind clinical trial involving 740 patients with moderate-to-severe chronic lower back pain. In the double-blind maintenance phase, 389 patients were randomized and 193 patients were assigned to the XTAMPZA ER treatment group.
The most common AEs (>5%) reported by patients in the Phase 3 clinical trial during the titration phase were: nausea (16.6%), headache (13.9%), constipation (13.0%), somnolence (8.8%), pruritus (7.4%), vomiting (6.4%), and dizziness (5.7%).
The most common adverse reactions (>5%) reported by patients in the Phase 3 clinical trial comparing XTAMPZA ER with placebo are shown in Table below:
| Titration | Maintenance | ||
|---|---|---|---|
| Adverse Reaction | XTAMPZA ER (n = 740) (%) |
XTAMPZA ER (n = 193) (%) |
Placebo (n = 196) (%) |
| Nausea | 16.6 | 10.9 | 4.6 |
| Headache | 13.9 | 6.2 | 11.7 |
| Constipation | 13.0 | 5.2 | 0.5 |
| Somnolence | 8.8 | <1 | <1 |
| Pruritus | 7.4 | 2.6 | 1.5 |
| Vomiting | 6.4 | 4.1 | 1.5 |
| Dizziness | 5.7 | 1.6 | 0 |
In the Phase 3 clinical trial, the following adverse reactions were reported in patients treated with XTAMPZA ER with incidences of 1% to 5%:
Eye disorders: vision blurred
Gastrointestinal disorders: abdominal pain, upper abdominal pain, diarrhea, gastroesophageal reflux disease
General disorders and administration site conditions: chills, drug withdrawal syndrome, fatigue, irritability, edema, pyrexia
Injury, poisoning and procedural complications: excoriation
Metabolism and nutrition disorders: decreased appetite, hyperglycemia
Musculoskeletal and connective tissue disorders: arthralgia, back pain, musculoskeletal pain, myalgia
Nervous system disorders: migraine, tremor
Psychiatric disorders: anxiety, insomnia, withdrawal syndrome
Respiratory, thoracic and mediastinal disorders: cough, oropharyngeal pain
Skin and subcutaneous tissue disorders: hyperhidrosis, rash
Vascular disorders: hot flush, hypertension
In the Phase 3 clinical trial, the following treatment-related adverse reactions were reported in patients treated with XTAMPZA ER with incidences of less than 1% of patients.
Investigations: increased gamma-glutamyl transferase, increased heart rate
Nervous system disorders: lethargy, memory impairment, poor-quality sleep
Psychiatric disorders: abnormal dreams, euphoric mood, restlessness
Respiratory, thoracic and mediastinal disorders: dyspnea
Skin and subcutaneous tissue disorders: night sweats
8 Use in Specific Populations
2.7 Administration of Xtampza Er
Instruct patients to always take XTAMPZA ER capsules with food and with approximately the same amount of food in order to ensure consistent plasma levels are achieved [see Dosage and Administration (2.1), Clinical Pharmacology (12.3)].
For patients who have difficulty swallowing, XTAMPZA ER can also be taken by sprinkling the capsule contents on soft foods or sprinkling the contents into a cup and then administering directly into the mouth or through a gastrostomy or nasogastric feeding tube. Patients who are unable to swallow a capsule should be instructed to:
- Open the capsule.
- Sprinkle the capsule contents (microspheres) onto a small amount of soft food (e.g., applesauce, pudding, yogurt, ice cream, or jam) or into a cup and then administer directly into the mouth and swallow immediately.
- Rinse the mouth to ensure all capsule contents (microspheres) have been swallowed.
- Discard the XTAMPZA ER capsule shells after the contents have been sprinkled on soft food or into a cup and then administered directly into the mouth.
The contents of the XTAMPZA ER capsules (microspheres) may be administered through a nasogastric tube or gastrostomy tube. When administering XTAMPZA ER through a nasogastric or gastrostomy tube:
- Flush the tube with water.
- Open an XTAMPZA ER capsule and carefully pour the microspheres directly into the tube. Do not pre-mix the capsule contents with the liquid that you will be using to flush them through the tube.
- Draw up 15 mL of water into a syringe, insert the syringe into the tube, and flush the microspheres through the tube.
- Repeat the flushing two more times, each with 10 mL of water, to ensure no microspheres remain in the tube.
Alternatively, milk or liquid nutritional supplement may be used as vehicles for flush and administration through feeding tubes.
5.1 Addiction, Abuse, and Misuse
XTAMPZA ER contains oxycodone, a Schedule II controlled substance. As an opioid, XTAMPZA ER exposes users to the risks of addiction, abuse, and misuse [see Drug Abuse and Dependence (9)].
Although the risk of addiction in any individual is unknown, it can occur in patients appropriately prescribed XTAMPZA ER. Addiction can occur at recommended dosages and if the drug is misused or abused. The risk of opioid-related overdose or overdose-related death is increased with higher opioid doses, and this risk persists over the course of therapy. In postmarketing studies, addiction, abuse, misuse, and fatal and non-fatal opioid overdose were observed in patients with long-term opioid use [see Adverse Reactions (6.2) ].
Assess each patient's risk for opioid addiction, abuse, or misuse prior to prescribing XTAMPZA ER, and reassess all patients receiving XTAMPZA ER for the development of these behaviors or conditions. Risks are increased in patients with a personal or family history of substance abuse (including drug or alcohol abuse or addiction) or mental illness (e.g., major depression). The potential for these risks should not, however, prevent the proper management of pain in any given patient. Patients at increased risk may be prescribed opioids such as XTAMPZA ER but use in such patients necessitates intensive counseling about the risks and proper use of XTAMPZA ER along with frequent evaluation for signs of addiction, abuse, and misuse. Consider recommending or prescribing an opioid overdose reversal agent [see Dosage and Administration (2.2), Warnings and Precautions (5.2)].
Abuse or misuse of XTAMPZA ER by snorting or by injecting the dissolved product can result in overdose and death [see Overdosage (10)].
Opioids are sought for nonmedical use and are subject to diversion from legitimate prescribed use. Consider these risks when prescribing or dispensing XTAMPZA ER. Strategies to reduce these risks include prescribing the drug in the smallest appropriate quantity and advising the patient on careful storage of the drug during the course of treatment and the proper disposal of unused drug. Contact local state professional licensing board or state-controlled substances authority for information on how to prevent and detect abuse or diversion of this product.
17 Patient Counseling Information
Advise the patient to read the FDA-approved patient labeling (Medication Guide).
16 How Supplied/storage and Handling
XTAMPZA ER capsules are supplied in 100-count bottles with a child-resistant closure and as a hospital unit dose package with 10 individually blistered capsules per card; two cards per carton as follows:
| Strength | Capsule Description | NDC Number (100-count Bottles with a child-resistant closure) |
NDC Number (20-count Hospital Unit Dose Blister Cartons) |
|---|---|---|---|
| 9 mg (equivalent to 10 mg oxycodone HCl) |
Size 3, ivory cap printed with "XTAMPZA ER" and white body printed with "9 mg" | NDC 24510-110-10 | NDC 24510-110-20 |
| 13.5 mg (equivalent to 15 mg oxycodone HCl) |
Size 2, Swedish orange cap printed with "XTAMPZA ER" and white body printed with "13.5 mg" | NDC 24510-115-10 | NDC 24510-115-20 |
| 18 mg (equivalent to 20 mg oxycodone HCl) |
Size 1, rich yellow cap printed with "XTAMPZA ER" and white body printed with "18 mg" | NDC 24510-120-10 | NDC 24510-120-20 |
| 27 mg (equivalent to 30 mg oxycodone HCl) |
Size 0, light gray cap printed with "XTAMPZA ER" and white body printed with "27 mg" | NDC 24510-130-10 | NDC 24510-130-20 |
| 36 mg (equivalent to 40 mg oxycodone HCl) |
Size 00, flesh color cap printed with "XTAMPZA ER" and white body printed with "36 mg" | NDC 24510-140-10 | NDC 24510-140-20 |
5.4 Neonatal Opioid Withdrawal Syndrome
Use of XTAMPZA ER for an extended period of time during pregnancy can result in withdrawal in the neonate. Neonatal opioid withdrawal syndrome, unlike opioid withdrawal syndrome in adults, may be life-threatening if not recognized and treated, and requires management according to protocols developed by neonatology experts. Observe newborns for signs of neonatal opioid withdrawal syndrome and manage accordingly. Advise pregnant women using opioids for an extended period of time of the risk of neonatal opioid withdrawal syndrome and ensure that appropriate treatment will be available [see Use in Specific Populations (8.1)].
2.5 Titration and Maintenance of Therapy
Individually titrate XTAMPZA ER to a dose that provides adequate analgesia and minimizes adverse reactions. Continually reevaluate patients receiving XTAMPZA ER to assess the maintenance of pain control and the relative incidence of adverse reactions, as well as to reassess for the development of addiction, abuse, and misuse. Frequent communication is important among the prescriber, other members of the healthcare team, the patient, and the caregiver/family during periods of changing analgesic requirements, including initial titration. During use of opioid therapy for an extended period of time, periodically reassess the continued need for the use of opioid analgesics.
Patients who experience breakthrough pain may require a dose increase of XTAMPZA ER or may need rescue medication with an appropriate dose of an immediate-release analgesic. If the level of pain increases after dose stabilization, attempt to identify the source of increased pain before increasing the XTAMPZA ER dose. If after increasing the dosage, unacceptable opioid-related adverse reactions are observed (including an increase in pain after a dosage increase), consider reducing the dosage [see Warnings and Precautions (5)]. Adjust the dosage to obtain an appropriate balance between management of pain and opioid-related adverse reactions.
Because steady-state plasma concentrations are approximated in 1 to 2 days, XTAMPZA ER dosage may be adjusted every 1 to 2 days. If unacceptable opioid-related adverse reactions are observed, the subsequent dose may be reduced. Adjust the dose to obtain an appropriate balance between management of pain and opioid-related adverse reactions.
There are no well-controlled clinical studies evaluating the safety and efficacy with dosing more frequently than every 12 hours. As a guideline, the total daily oxycodone dose usually can be increased by 25% to 50% of the current dose, each time an increase is clinically indicated.
5.2 Life Threatening Respiratory Depression
Serious, life-threatening, or fatal respiratory depression has been reported with the use of opioids, even when used as recommended. Respiratory depression, if not immediately recognized and treated, may lead to respiratory arrest and death. Management of respiratory depression may include close observation, supportive measures, and use of opioid overdose reversal agents, depending on the patient's clinical status [see Overdosage (10)]. Carbon dioxide (CO2) retention from opioid-induced respiratory depression can exacerbate the sedating effects of opioids.
While serious, life-threatening, or fatal respiratory depression can occur at any time during the use of XTAMPZA ER, the risk is greatest during the initiation of therapy or following a dosage increase.
To reduce the risk of respiratory depression, proper dosing and titration of XTAMPZA ER are essential [see Dosage and Administration (2)]. Overestimating the XTAMPZA ER dose when converting patients from another opioid product can result in a fatal overdose with the first dose.
Accidental ingestion of even one dose of XTAMPZA ER, especially by children, can result in respiratory depression and death due to an overdose of oxycodone.
Educate patients and caregivers on how to recognize respiratory depression and emphasize the importance of calling 911 or getting emergency medical help right away in the event of a known or suspected overdose.
Opioids can cause sleep-related breathing disorders including central sleep apnea (CSA) and sleep-related hypoxemia. Opioid use increases the risk of CSA in a dose-dependent fashion. In patients who present with CSA, consider decreasing the opioid dosage using best practices for opioid taper [see Dosage and Administration (2.6) ].
5.12 Risks of Gastrointestinal Complications
XTAMPZA ER is contraindicated in patients with gastrointestinal obstruction, including paralytic ileus.
The oxycodone in XTAMPZA ER may cause spasm of the sphincter of Oddi. Opioids may cause increases in the serum amylase. Regularly evaluate with biliary tract disease, including acute pancreatitis, for worsening symptoms.
Cases of opioid-induced esophageal dysfunction (OIED) have been reported in patients taking opioids. The risk of OIED may increase as the dose and/or duration of opioids increases. Regularly evaluate patients for signs and symptoms of OIED (e.g., dysphagia, regurgitation, non-cardiac chest pain) and, if necessary, adjust opioid therapy as clinically appropriate [see Clinical Pharmacology (12.2)]. .
5.15 Risks of Driving and Operating Machinery
XTAMPZA ER may impair the mental or physical abilities needed to perform potentially hazardous activities such as driving a car or operating machinery. Warn patients not to drive or operate dangerous machinery unless they are tolerant to the effects of XTAMPZA ER and know how they will react to the medication.
5.7 Opioid Induced Hyperalgesia and Allodynia
Opioid-Induced Hyperalgesia (OIH) occurs when an opioid analgesic paradoxically causes an increase in pain, or an increase in sensitivity to pain. This condition differs from tolerance, which is the need for increasing doses of opioids to maintain a defined effect [see Dependence (9.3)]. Symptoms of OIH include (but may not be limited to) increased levels of pain upon opioid dosage increase, decreased levels of pain upon opioid dosage decrease, or pain from ordinarily non-painful stimuli (allodynia). These symptoms may suggest OIH only if there is no evidence of underlying disease progression, opioid tolerance, opioid withdrawal, or addictive behavior.
Cases of OIH have been reported, both with short-term and longer-term use of opioid analgesics. Though the mechanism of OIH is not fully understood, multiple biochemical pathways have been implicated. Medical literature suggests a strong biologic plausibility between opioid analgesics and OIH and allodynia. If a patient is suspected to be experiencing OIH, carefully consider appropriately decreasing the dose of the current opioid analgesic or opioid rotation (safely switching the patient to a different opioid moiety) [see Dosage and Administration (2.6), Warnings and Precautions (5.14)].
2.6 Safe Reduction Or Discontinuation of Xtampza Er
Do not rapidly reduce or abruptly discontinue XTAMPZA ER in patients who may be physically dependent on opioids. Rapid reduction or abrupt discontinuation of opioid analgesics in patients who are physically dependent on opioids has resulted in serious withdrawal symptoms, uncontrolled pain, and suicide. Rapid reduction or abrupt discontinuation has also been associated with attempts to find other sources of opioid analgesics, which may be confused with drug-seeking for abuse. Patients may also attempt to treat their pain or withdrawal symptoms with illicit opioids, such as heroin, and other substances.
When a decision has been made to decrease the dose or discontinue therapy in an opioid-dependent patient taking XTAMPZA ER, there are a variety of factors that should be considered, including the total daily dose of opioid (including XTAMPZA ER) the patient has been taking, the duration of treatment, the type of pain being treated, and the physical and psychological attributes of the patient. It is important to ensure ongoing care of the patient and to agree on an appropriate tapering schedule and follow-up plan so that patient and provider goals and expectations are clear and realistic. When opioid analgesics are being discontinued due to a suspected substance use disorder, evaluate and treat the patient, or refer for evaluation and treatment of the substance use disorder. Treatment should include evidence-based approaches, such as medication assisted treatment of opioid use disorder. Complex patients with co-morbid pain and substance use disorders may benefit from referral to a specialist.
There are no standard opioid tapering schedules that are suitable for all patients. Good clinical practice dictates a patient-specific plan to taper the dose of the opioid gradually. For patients on XTAMPZA ER who are physically opioid-dependent, initiate the taper by a small enough increment (e.g., no greater than 10% to 25% of the total daily dose) to avoid withdrawal symptoms, and proceed with dose-lowering at an interval of every 2 to 4 weeks. Patients who have been taking opioids for briefer periods of time may tolerate a more rapid taper.
It may be necessary to provide the patient with lower dosage strengths to accomplish a successful taper. Reassess the patient frequently to manage pain and withdrawal symptoms, should they emerge. Common withdrawal symptoms include restlessness, lacrimation, rhinorrhea, yawning, perspiration, chills, myalgia, and mydriasis. Other signs and symptoms also may develop, including irritability, anxiety, backache, joint pain, weakness, abdominal cramps, insomnia, nausea, anorexia, vomiting, diarrhea, or increased blood pressure, respiratory rate, or heart rate. If withdrawal symptoms arise, it may be necessary to pause the taper for a period of time or raise the dose of the opioid analgesic to the previous dose, and then proceed with a slower taper. In addition, evaluate patients for any changes in mood, emergence of suicidal thoughts, or use of other substances.
When managing patients taking opioid analgesics, particularly those who have been treated for an extended period of time, and/or with high doses for chronic pain, ensure that a multimodal approach to pain management, including mental health support (if needed), is in place prior to initiating an opioid analgesic taper. A multimodal approach to pain management may optimize the treatment of chronic pain, as well as assist with the successful tapering of the opioid analgesic [see Warnings and Precautions (5.14), Drug Abuse and Dependence (9.3)].
Principal Display Panel 9 Mg Capsule Bottle Label
NDC 24510-110-10
Xtampza® ER
(oxycodone)
EXTENDED-RELEASE
CAPSULES
CII
9 mg
Each capsule contains Oxycodone 9 mg
(Equivalent to 10 mg Oxycodone Hydrochloride)
100 Capsules
Rx Only
Always take with food. Taking on an empty
stomach can decrease drug absorption.
Attention Dispenser: Accompanying Medication
Guide must be provided to the patient upon dispensing.
2.1 Important Dosage and Administration Instructions
- XTAMPZA ER should be prescribed only by healthcare professionals who are knowledgeable about the use of extended-release/long-acting opioids and how to mitigate the associated risks.
- XTAMPZA ER single doses greater than 36 mg (equivalent to 40 mg oxycodone hydrochloride [HCl]) or a total daily dose greater than 72 mg (equivalent to 80 mg oxycodone HCl) are to be administered only to patients in whom tolerance to an opioid of comparable potency has been established. Patients who are opioid-tolerant are those receiving, for one week or longer, at least 60 mg oral morphine per day, 25 mcg transdermal fentanyl per hour, 30 mg oral oxycodone HCl per day, 8 mg oral hydromorphone per day, 25 mg oral oxymorphone per day, 60 mg oral hydrocodone per day, or an equianalgesic dose of another opioid.
- Use the lowest effective dosage for the shortest duration of time consistent with individual patient treatment goals [see Warnings and Precautions (5)]. Because the risk of overdose increases as opioid doses increase, reserve titration to higher doses of XTAMPZA ER for patients in whom lower doses are insufficiently effective and in whom the expected benefits of using a higher dose opioid clearly outweigh the substantial risks.
- Initiate the dosing regimen for each patient individually, taking into account the patient's underlying cause and severity of pain, prior analgesic treatment and response, and risk factors for addiction, abuse, and misuse [see Warnings and Precautions (5.1)].
- Respiratory depression can occur at any time during opioid therapy, especially when initiating and following dosage increases with XTAMPZA ER. Consider this risk when selecting an initial dose and when making dose adjustments [see Warnings and Precautions (5.2)].
- XTAMPZA ER is administered, twice daily, every 12 hours, and must be taken with food. Instruct patients to take XTAMPZA ER capsules with approximately the same amount of food for every dose in order to ensure consistent plasma levels are achieved [see Clinical Pharmacology (12.3)].
- Patients who are unable to swallow XTAMPZA ER should be instructed to sprinkle the capsule contents on soft foods or into a cup and then administer directly into the mouth and immediately swallow. XTAMPZA ER may also be administered through a gastrostomy or nasogastric feeding tube [see Dosage and Administration (2.7)].
- The maximum daily dose of XTAMPZA ER is 288 mg per day (eight 36 mg capsules, equivalent to 320 mg oxycodone HCl per day) as the safety of the excipients in XTAMPZA ER for doses over 288 mg/day has not been established.
Principal Display Panel 18 Mg Capsule Bottle Label
NDC 24510-120-10
Xtampza® ER
(oxycodone)
EXTENDED-RELEASE
CAPSULES
CII
18 mg
Each capsule contains Oxycodone 18 mg
(Equivalent to 20 mg Oxycodone Hydrochloride)
100 Capsules
Rx Only
Always take with food. Taking on an empty
stomach can decrease drug absorption.
Attention Dispenser: Accompanying
Medication Guide must be provided to
the patient upon dispensing.
Principal Display Panel 27 Mg Capsule Bottle Label
NDC 24510-130-10
Xtampza® ER
(oxycodone)
EXTENDED-RELEASE
CAPSULES
CII
27 mg
Each capsule contains Oxycodone 27 mg
(Equivalent to 30 mg Oxycodone Hydrochloride)
100 Capsules
Rx Only
Always take with food. Taking on an empty
stomach can decrease drug absorption.
Attention Dispenser: Accompanying
Medication Guide must be provided to
the patient upon dispensing.
Principal Display Panel 36 Mg Capsule Bottle Label
NDC 24510-140-10
Xtampza® ER
(oxycodone)
EXTENDED-RELEASE
CAPSULES
CII
36 mg
Each capsule contains Oxycodone 36 mg
(Equivalent to 40 mg Oxycodone Hydrochloride)
100 Capsules
Rx Only
Always take with food. Taking on an empty
stomach can decrease drug absorption.
Attention Dispenser: Accompanying
Medication Guide must be provided to
the patient upon dispensing.
Principal Display Panel 13.5 Mg Capsule Bottle Label
NDC 24510-115-10
Xtampza® ER
(oxycodone)
EXTENDED-RELEASE
CAPSULES
CII
13.5 mg
Each capsule contains Oxycodone 13.5 mg
(Equivalent to 15 mg Oxycodone Hydrochloride)
100 Capsules
Rx Only
Always take with food. Taking on an empty
stomach can decrease drug absorption.
Attention Dispenser: Accompanying
Medication Guide must be provided to
the patient upon dispensing.
2.4 Dosage Modifications in Patients With Hepatic Impairment
For patients with hepatic impairment, start dosing patients at 1/3 to 1/2 the usual starting dose followed by careful dose titration. Regularly evaluate for adverse events such as respiratory depression. Use of alternate analgesics is recommended for patients who require an XTAMPZA ER dose of less than 9 mg [see Use in Specific Populations (8.5), Clinical Pharmacology (12.3)].
5.13 Increased Risk of Seizures in Patients With Seizure Disorders
The oxycodone in XTAMPZA ER may increase the frequency of seizures in patients with seizure disorders and may increase the risk of seizures in other clinical settings associated with seizures. Regularly evaluate patients with a history of seizure disorders for worsened seizure control during XTAMPZA ER therapy.
Warning: Serious and Life Threatening Risks From Use of Xtampza Er
WARNING: SERIOUS AND LIFE-THREATENING RISKS FROM USE OF XTAMPZA ER
See full prescribing information for complete boxed warning.
- XTAMPZA ER exposes users to risks of addiction, abuse, and misuse, which can lead to overdose and death. Assess each patient's risk before prescribing and reassess regularly for these behaviors and conditions. (5.1)
- Serious, life-threatening, or fatal respiratory depression may occur especially during initiation or following a dosage increase. To reduce the risk of respiratory depression, proper dosing and titration of XTAMPZA ER are essential. (5.2)
- Accidental ingestion of XTAMPZA ER, especially by children, can result in fatal overdose of oxycodone. (5.2)
- Concomitant use of opioids with benzodiazepines or other central nervous system (CNS) depressants, including alcohol, may result in profound sedation, respiratory depression, coma, and death. Reserve concomitant prescribing for use in patients for whom alternative treatment options are inadequate. (5.3, 7)
- Advise pregnant using opioids for an extended period of time of the risk of Neonatal Opioid Withdrawal Syndrome, which may be life-threatening if not recognized and treated. Ensure that management by neonatology experts will be available at delivery. (5.4)
- Healthcare providers are strongly encouraged to complete a REMS-compliant education program and to counsel patients and caregivers on serious risks, safe use, and the importance of reading the Medication Guide with each prescription. (5.5)
- Concomitant use with CYP3A4 inhibitors (or discontinuation of CYP3A4 inducers) can result in a fatal overdose of oxycodone from XTAMPZA ER. (5.6, 12.3)
5.5 Opioid Analgesic Risk Evaluation and Mitigation Strategy (rems)
To ensure that the benefits of opioid analgesics outweigh the risks of addiction, abuse, and misuse, the Food and Drug Administration (FDA) has required a Risk Evaluation and Mitigation Strategy (REMS) for these products. Under the requirements of the REMS, drug companies with approved opioid analgesic products must make REMS-compliant education programs available to healthcare providers. Healthcare providers are strongly encouraged to do all of the following:
- Complete a REMS-compliant education program offered by an accredited provider of continuing education (CE) or another education program that includes all the elements of the FDA Education Blueprint for Health Care Providers Involved in the Management or Support of Patients with Pain.
- Discuss the safe use, serious risks, and proper storage and disposal of opioid analgesics with patients and/or their caregivers every time these medicines are prescribed. The Patient Counseling Guide (PCG) can be obtained at this link: www.fda.gov/OpioidAnalgesicREMSPCG.
- Emphasize to patients and their caregivers the importance of reading the Medication Guide that they will receive from their pharmacist every time an opioid analgesic is dispensed to them.
- Consider using other tools to improve patient, household, and community safety, such as patient-prescriber agreements that reinforce patient-prescriber responsibilities.
To obtain further information on the opioid analgesic REMS and for a list of accredited REMS CME/CE, call 1-800-503-0784, or log on to www.opioidanalgesicrems.com. The FDA Blueprint can be found at www.fda.gov/OpioidAnalgesicREMSBlueprint.
5.3 Risks From Concomitant Use With Benzodiazepines Or Other Cns Depressants
Profound sedation, respiratory depression, coma, and death may result from the concomitant use of XTAMPZA ER with benzodiazepines and/or other CNS depressants, including alcohol (e.g., non-benzodiazepine sedatives/hypnotics, anxiolytics, tranquilizers, muscle relaxants, general anesthetics, antipsychotics, gabapentinoids [gabapentin or pregabalin], and other opioids). Because of these risks, reserve concomitant prescribing of these drugs for use in patients for whom alternative treatment options are inadequate.
Observational studies have demonstrated that concomitant use of opioid analgesics and benzodiazepines increases the risk of drug-related mortality compared to use of opioid analgesics alone. Because of similar pharmacological properties, it is reasonable to expect similar risk with the concomitant use of other CNS depressant drugs with opioid analgesics [see Drug Interactions (7)].
If the decision is made to prescribe a benzodiazepine or other CNS depressant concomitantly with an opioid analgesic, prescribe the lowest effective dosages and minimum durations of concomitant use. In patients already receiving an opioid analgesic, prescribe a lower initial dose of the benzodiazepine or other CNS depressants than indicated in the absence of an opioid, and titrate based on clinical response. If an opioid analgesic is initiated in a patient already taking a benzodiazepine or other CNS depressant, prescribe a lower initial dose of the opioid analgesic, and titrate based on clinical response. Inform patients and caregivers of this potential interaction and educate them on the signs and symptoms of respiratory depression (including sedation).
If concomitant use is warranted, consider recommending or prescribing an opioid overdose reversal agent for the emergency treatment of opioid overdose [see Dosage and Administration (2.2), Warnings and Precautions (5.2), Overdosage (10)].
Advise both patients and caregivers about the risks of respiratory depression and sedation when XTAMPZA ER is used with benzodiazepines or other CNS depressants (including alcohol and illicit drugs). Advise patients not to drive or operate heavy machinery until the effects of concomitant use of the benzodiazepine or other CNS depressant have been determined. Screen patients for risk of substance use disorders, including opioid abuse and misuse, and warn them of the risk for overdose and death associated with the use of additional CNS depressants including alcohol and illicit drugs [see Drug Interactions (7)].
5.6 Risks of Concomitant Use Or Discontinuation of Cytochrome P450 3a4 Inhibitors and Inducers
Concomitant use of XTAMPZA ER with a CYP3A4 inhibitor, such as macrolide antibiotics (e.g., erythromycin), azole-antifungal agents (e.g., ketoconazole), and protease inhibitors (e.g., ritonavir), may increase plasma concentrations of oxycodone and prolong opioid adverse reactions, which may cause potentially fatal respiratory depression [see Warnings and Precautions (5.2)], particularly when an inhibitor is added after a stable dose of XTAMPZA ER is achieved. Similarly, discontinuation of a CYP3A4 inducer, such as rifampin, carbamazepine, and phenytoin, in XTAMPZA ER-treated patients may increase oxycodone plasma concentrations and prolong opioid adverse reactions. When using XTAMPZA ER with CYP3A4 inhibitors or discontinuing CYP3A4 inducers in XTAMPZA ER-treated patients, evaluate patients at frequent intervals and consider dosage reduction of XTAMPZA ER until stable drug effects are achieved [see Drug Interactions (7)].
Concomitant use of XTAMPZA ER with CYP3A4 inducers or discontinuation of a CYP3A4 inhibitor could decrease oxycodone plasma concentrations, decrease opioid efficacy or, possibly, lead to a withdrawal syndrome in a patient who had developed physical dependence to oxycodone. When using XTAMPZA ER with CYP3A4 inducers or discontinuing CYP3A4 inhibitors, evaluate patients at frequent intervals and consider increasing the opioid dosage if needed to maintain adequate analgesia or if symptoms of opioid withdrawal occur [see Drug Interactions (7)].
2.2 Patient Access to An Opioid Overdose Reversal Agent for the Emergency Treatment of Opioid Overdose
Inform patients and caregivers about opioid overdose reversal agents (e.g., naloxone, nalmefene). Discuss the importance of having access to an opioid overdose reversal agent, especially if the patient has risk factors for overdose (e.g., concomitant use of CNS depressants, a history of opioid use disorder, or prior opioid overdose) or if there are household members (including children) or other close contacts at risk for accidental ingestion or opioid overdose. The presence of risk factors for overdose should not prevent the management of pain in any patient [see Warnings and Precautions (5.1, 5.2, 5.3) ].
Discuss the options for obtaining an opioid overdose reversal agent (e.g., prescription, over-the-counter, or as part of a community-based program) [see Warnings and Precautions (5.2) ].
There are important differences among the opioid overdose reversal agents, such as route of administration, product strength, approved patient age range, and pharmacokinetics. Be familiar with these differences, as outlined in the approved labeling for those products, prior to recommending or prescribing such an agent.
5.11 Risks of Use in Patients With Increased Intracranial Pressure, Brain Tumors, Head Injury, Or Impaired Consciousness
In patients who may be susceptible to the intracranial effects of CO2 retention (e.g., those with evidence of increased intracranial pressure or brain tumors), XTAMPZA ER may reduce respiratory drive, and the resultant CO2 retention can further increase intracranial pressure. Monitor such patients for signs of sedation and respiratory depression, particularly when initiating therapy with XTAMPZA ER.
Opioids may also obscure the clinical course in a patient with a head injury. Avoid the use of XTAMPZA ER in patients with impaired consciousness or coma.
5.8 Risk of Life Threatening Respiratory Depression in Patients With Chronic Pulmonary Disease Or in Elderly, Cachectic, Or Debilitated Patients
The use of XTAMPZA ER in patients with acute or severe bronchial asthma in an unmonitored setting or in the absence of resuscitative equipment is contraindicated.
Structured Label Content
Section 42229-5 (42229-5)
Addiction, Abuse, and Misuse
Because the use of XTAMPZA ER exposes patients and other users to the risks of opioid addiction, abuse, and misuse, which can lead to overdose and death, assess each patient's risk prior to prescribing and reassess all patients regularly for the development of these behaviors and conditions [see Warnings and Precautions (5.1)].
Section 42231-1 (42231-1)
| Medication Guide XTAMPZA® ER (ex tamp' zah ee ar) (oxycodone) extended-release capsules, CII |
|
|---|---|
| This Medication Guide has been approved by the U.S. Food and Drug Administration. | Issued: December 2025 |
XTAMPZA ER is:
|
|
Important information about XTAMPZA ER:
|
|
Do not take XTAMPZA ER if you have:
|
|
| Before taking XTAMPZA ER, tell your healthcare provider if you have a history of: | |
|
|
|
|
Tell your healthcare provider if you are:
|
|
When taking XTAMPZA ER:
|
|
While taking XTAMPZA ER DO NOT:
|
|
The possible side effects of XTAMPZA ER are:
Manufactured by: Patheon Pharmaceuticals, 2110 Galbraith Road, Cincinnati, OH 45237, www.collegiumpharma.com or call 855-331-5615 |
Section 43683-2 (43683-2)
Section 44425-7 (44425-7)
Store at 25°C (77°F); excursions permitted between 15°-30°C (59°-86°F) [see USP Controlled Room Temperature].
Dispense in tight, light-resistant container, with child-resistant closure.
Store XTAMPZA ER securely and dispose of properly [see Patient Counseling Information (17)].
9.2 Abuse
XTAMPZA ER contains oxycodone, a substance with high potential for misuse and abuse, which can lead to the development of substance use disorder, including addiction [see Warnings and Precautions (5.1)].
Misuse is the intentional use, for therapeutic purposes, of a drug by an individual in a way other than prescribed by a healthcare provider or for whom it was not prescribed.
Abuse is the intentional, non-therapeutic use of a drug, even once, for its desirable psychological or physiological effects.
Drug addiction is a cluster of behavioral, cognitive, and physiological phenomena that may include a strong desire to take the drug, difficulties in controlling drug use (e.g., continuing drug use despite harmful consequences, giving a higher priority to drug use than other activities and obligations), and possible tolerance or physical dependence.
Misuse and abuse of XTAMPZA ER increases risk of overdose, which may lead to central nervous system and respiratory depression, hypotension, seizures, and death. The risk is increased with concurrent abuse of XTAMPZA ER with alcohol and/or other CNS depressants. Abuse of and addiction to opioids in some individuals may not be accompanied by concurrent tolerance and symptoms of physical dependence. In addition, abuse of opioids can occur in the absence of addiction.
All patients treated with opioids require careful and frequent reevaluation for signs of misuse, abuse, and addiction, because use of opioid analgesic products carries the risk of addiction even under appropriate medical use. Patients at high risk of XTAMPZA ER abuse include those with a history of prolonged use of any opioid, including products containing buprenorphine, those with a history of drug or alcohol abuse, or those who use XTAMPZA ER in combination with other abused drugs.
"Drug-seeking" behavior is very common in persons with substance use disorders. Drug-seeking tactics include emergency calls or visits near the end of office hours, refusal to undergo appropriate examination, testing, or referral, repeated "loss" of prescriptions, tampering with prescriptions, and reluctance to provide prior medical records or contact information for other treating healthcare provider(s). "Doctor shopping" (visiting multiple prescribers to obtain additional prescriptions) is common among people who abuse drugs and people with substance use disorder. Preoccupation with achieving adequate pain relief can be appropriate behavior in a patient with inadequate pain control.
XTAMPZA ER, like other opioids, can be diverted for nonmedical use into illicit channels of distribution. Careful record-keeping of prescribing information, including quantity, frequency, and renewal requests, as required by state and federal law, is strongly advised.
Proper assessment of the patient, proper prescribing practices, periodic reevaluation of therapy, and proper dispensing and storage are appropriate measures that help to limit abuse of opioid drugs.
11 Description (11 DESCRIPTION)
XTAMPZA ER (oxycodone) extended-release capsules are an opioid agonist for oral use. The capsules contain microspheres formulated with oxycodone base and are supplied in strengths of 9 mg (equivalent to 10 mg oxycodone HCl), 13.5 mg (equivalent to 15 mg oxycodone HCl), 18 mg (equivalent to 20 mg oxycodone HCl), 27 mg (equivalent to 30 mg oxycodone HCl), and 36 mg (equivalent to 40 mg oxycodone HCl) capsules. The capsule strengths describe the amount of oxycodone base per capsule. The structural formula for oxycodone is as follows:
The chemical name is 4,5 α-Epoxy-14-hydroxy-3-methoxy-17-methylmorphinan-6-one.
Oxycodone base is a white, odorless crystalline powder derived from the opium alkaloid, thebaine. Oxycodone is present as myristate salt in the XTAMPZA ER formulation.
Each XTAMPZA ER capsule contains either 9, 13.5, 18, 27, or 36 mg of oxycodone (equivalent to 10, 15, 20, 30, or 40 mg of oxycodone HCl, respectively) and the following inactive ingredients: myristic acid, yellow beeswax, carnauba wax, stearoyl polyoxyl-32 glycerides, magnesium stearate, and colloidal silicon dioxide. The capsule shells collectively contain titanium dioxide, hypromellose, and water. Additionally, the 9 mg and 18 mg strength capsule shells contain yellow iron oxide, the 13.5 and 36 mg strength capsule shells contain red iron oxide, and the 27 mg strength capsule shells contain black iron oxide.
9.3 Dependence
Both tolerance and physical dependence can develop during use of opioid therapy.
Tolerance is a physiological state characterized by a reduced response to a drug after repeated administration (i.e., a higher dose of a drug is required to produce the same effect that was once obtained at a lower dose).
Physical dependence is a state that develops as a result of a physiological adaptation in response to repeated drug use, manifested by withdrawal signs and symptoms after abrupt discontinuation or a significant dose reduction of a drug.
Withdrawal may be precipitated through the administration of drugs with opioid antagonist activity (e.g., naloxone, nalmefene), mixed agonist/antagonist analgesics (e.g., pentazocine, butorphanol, nalbuphine), or partial agonists (e.g., buprenorphine). Physical dependence may not occur to a clinically significant degree until after several days to weeks of continued use.
Do not rapidly reduce or abruptly discontinue XTAMPZA ER in a patient physically dependent on opioids. Rapid tapering of XTAMPZA ER in a patient physically dependent on opioids may lead to serious withdrawal symptoms, uncontrolled pain, and suicide. Rapid discontinuation has also been associated with attempts to find other sources of opioid analgesics, which may be confused with drug-seeking for abuse.
When discontinuing XTAMPZA ER, gradually taper the dosage using a patient-specific plan that considers the following: the dose of XTAMPZA ER the patient has been taking, the duration of treatment, and the physical and psychological attributes of the patient. To improve the likelihood of a successful taper and minimize withdrawal symptoms, it is important that the opioid tapering schedule is agreed upon by the patient. In patients taking opioids for an extended period of time at high doses, ensure that a multimodal approach to pain management, including mental health support (if needed), is in place prior to initiating an opioid analgesic taper [see Dosage and Administration (2.6), Warnings and Precautions (5.14) ].
Infants born to mothers physically dependent on opioids will also be physically dependent and may exhibit respiratory difficulties and withdrawal signs [see Use in Specific Populations (8.1) ].
5.14 Withdrawal
Do not rapidly reduce or abruptly discontinue XTAMPZA ER in a patient physically dependent on opioids. When discontinuing XTAMPZA ER in a physically dependent patient, gradually taper the dosage. Rapid tapering of oxycodone in a patient physically dependent on opioids may lead to a withdrawal syndrome and return of pain [see Dosage and Administration (2.6), Drug Abuse and Dependence (9.3)].
Additionally, avoid the use of mixed agonist/antagonist (e.g., pentazocine, nalbuphine, and butorphanol) or partial agonist (e.g., buprenorphine) analgesics in patients who have received or are receiving a course of therapy with a full opioid agonist analgesic, including XTAMPZA ER. In these patients, mixed agonist/antagonist and partial agonist analgesics may reduce the analgesic effect and/or may precipitate withdrawal symptoms [see Dosage and Administration (2.6), Drug Interactions (7)].
8.4 Pediatric Use
Safety and effectiveness of XTAMPZA ER in pediatric patients below the age of 18 years have not been established.
8.5 Geriatric Use
In controlled pharmacokinetic studies in elderly subjects (greater than 65 years) the clearance of oxycodone was slightly reduced. Compared to young adults, the plasma concentrations of oxycodone were increased approximately 15% [see Clinical Pharmacology (12.3)]. Of the total number of subjects entered into the titration phase of the Phase 3 study for XTAMPZA ER (740), 88 (12%) were age 65 and older. In this clinical trial with appropriate initiation of therapy and dose titration, no untoward or unexpected adverse reactions were seen in the elderly patients who received XTAMPZA ER. Thus, the usual doses and dosing intervals may be appropriate for elderly patients. Use caution when selecting a dosage for an elderly patient, usually starting at the low end of the dosing range, reflecting the greater frequency of decreased hepatic, renal, or cardiac function, concomitant disease, and use of other drug therapy.
Respiratory depression is the chief risk in elderly patients treated with opioids and has occurred after large initial doses were administered to patients who were not opioid-tolerant or when opioids were co-administered with other agents that depress respiration. Titrate the dosage of XTAMPZA ER slowly in geriatric patients and frequently reevaluate the patient for signs of central nervous system and respiratory depression [see Warnings and Precautions (5.8)].
2.3 Initial Dosage
It is safer to underestimate a patient's 24-hour oral oxycodone dosage and provide rescue medication (e.g., immediate-release opioid) than to overestimate the 24-hour oral oxycodone dosage and manage adverse reactions due to an overdose. While useful tables of opioid equivalents are readily available, there is substantial inter-patient variability in the relative potency of different opioid drugs and products. Frequently reevaluate patients for signs and symptoms of opioid withdrawal and for signs of oversedation/toxicity after converting patients to XTAMPZA ER.
14 Clinical Studies (14 CLINICAL STUDIES)
An enriched-enrollment, randomized-withdrawal, double-blind, placebo-controlled, parallel group, study was conducted in 740 patients with persistent, moderate-to-severe chronic lower back pain, with inadequate pain control from their prior therapy. During screening, patients stopped their prior opioid analgesics and/or non-opioid analgesics prior to starting XTAMPZA ER treatment. Patients were titrated to a stable and tolerated dose between 18 mg (equivalent to 20 mg oxycodone HCl) twice daily and 72 mg (equivalent to 80 mg oxycodone HCl) twice daily of XTAMPZA ER in an open-label fashion during the first six weeks of the trial. Optional use of rescue medication (acetaminophen 500 mg tablets) up to 2 tablets every 4-6 hours was permitted during the dose titration phase, up to 2000 mg per day. XTAMPZA ER was titrated once every three to seven days until a stable and tolerable dose was identified (maximum dose of 72 mg [equivalent to 80 mg oxycodone HCl] twice daily).
Following the titration phase, 389 subjects (53%) met the study randomization criteria of adequate analgesia (pain reduction of at least 2 points from screening baseline to a score of 4 or less on a 0-10 numerical rating scale) and acceptable tolerability of XTAMPZA ER and entered the randomized, double-blind maintenance phase. Subjects discontinued from the dose-titration phase for the following reasons: failure to meet entrance criteria (18%), adverse events (13%), subject request (7%) and lack of efficacy (5%). Patients were randomized at a ratio of 1:1 into a 12-week double-blind maintenance phase with their fixed stable dose of XTAMPZA ER (or matching placebo). Patients randomized to placebo were given a blinded taper of XTAMPZA ER according to a prespecified tapering schedule; XTAMPZA ER was decreased by 25% to 35% every 5 days for the higher doses of XTAMPZA ER and up to 50% every 5 days for the mid-to-lower doses of XTAMPZA ER over the first 20 days of the double-blind maintenance phase. Patients were allowed to use rescue medication (acetaminophen 500 mg tablets) up to a maximum dose of 2000 mg per day. During the double-blind maintenance phase, 122 patients (63%) completed the 12-week treatment with XTAMPZA ER and 100 (51%) completed with placebo. Overall, 11% of patients discontinued due to lack of efficacy (4% of XTAMPZA ER patients and 17% of placebo patients), and 7% discontinued due to adverse events (7% of XTAMPZA ER patients and 7% of placebo patients).
In this study, there was a significant difference in pain reduction, favoring XTAMPZA ER, between XTAMPZA ER (doses of 36-144 mg per day, equivalent to 40-160 mg of oxycodone HCl) and placebo, based on the primary endpoint of change in average pain intensity from randomization baseline to Week 12 of the double-blind maintenance phase.
The proportion of patients (responders) in each group who demonstrated improvement in their weekly average pain scores from screening baseline to Week 12, is shown in Figure 2. The figure is cumulative, so that patients whose change from screening is, for example, 30%, are also included at every level of improvement below 30%. Patients who did not complete the study were classified as non-responders. Treatment with XTAMPZA ER resulted in a higher proportion of responders, defined as patients with at least a 30% and 50% improvement as compared to placebo.
Figure 2: Responder Analysis for Pain Intensity: Percent Reduction/Improvement (Intent-to-Treat Population)
4 Contraindications (4 CONTRAINDICATIONS)
XTAMPZA ER is contraindicated in patients with:
- Significant respiratory depression [see Warnings and Precautions (5.2)]
- Acute or severe bronchial asthma in an unmonitored setting or in the absence of resuscitative equipment [see Warnings and Precautions (5.8)]
- Known or suspected gastrointestinal obstruction, including paralytic ileus [see Warnings and Precautions (5.12)]
- Hypersensitivity (e.g., anaphylaxis) to oxycodone.
6 Adverse Reactions (6 ADVERSE REACTIONS)
The following serious adverse reactions are described elsewhere in the labeling:
- Addiction, Abuse, and Misuse [see Warnings and Precautions (5.1)]
- Life-Threatening Respiratory Depression [see Warnings and Precautions (5.2)]
- Interactions with Benzodiazepines or Other CNS Depressants [see Warnings and Precautions (5.3)]
- Neonatal Opioid Withdrawal Syndrome [see Warnings and Precautions (5.4)]
- Opioid-Induced Hyperalgesia and Allodynia [see Warnings and Precautions (5.7)]
- Adrenal Insufficiency [see Warnings and Precautions (5.9)]
- Severe Hypotension [see Warnings and Precautions (5.10)]
- Gastrointestinal Adverse Reactions [see Warnings and Precautions (5.12)]
- Seizures [see Warnings and Precautions (5.13)]
- Withdrawal [see Warnings and Precautions (5.14)]
7 Drug Interactions (7 DRUG INTERACTIONS)
Table includes clinically significant drug interactions with XTAMPZA ER.
| Inhibitors of CYP3A4 and CYP2D6 | |
|---|---|
| Clinical Impact: | The concomitant use of XTAMPZA ER and CYP3A4 inhibitors can increase the plasma concentration of oxycodone, resulting in increased or prolonged opioid effects. These effects could be more pronounced with concomitant use of XTAMPZA ER and CYP2D6 and CYP3A4 inhibitors, particularly when an inhibitor is added after a stable dose of XTAMPZA ER is achieved [see Warnings and Precautions (5.6)].
After stopping a CYP3A4 inhibitor, as the effects of the inhibitor decline, the oxycodone plasma concentration will decrease [see Clinical Pharmacology (12.3)], resulting in decreased opioid efficacy or a withdrawal syndrome in patients who had developed physical dependence to oxycodone. |
| Intervention: | If concomitant use is necessary, consider dosage reduction of XTAMPZA ER until stable drug effects are achieved. Evaluate patients at frequent intervals for respiratory depression and sedation. If a CYP3A4 inhibitor is discontinued, consider increasing the XTAMPZA ER dosage until stable drug effects are achieved. Assess for signs of opioid withdrawal. |
| Examples: | Macrolide antibiotics (e.g., erythromycin), azole-antifungal agents (e.g., ketoconazole), protease inhibitors (e.g., ritonavir) |
| CYP3A4 Inducers | |
| Clinical Impact: | The concomitant use of XTAMPZA ER and CYP3A4 inducers can decrease the plasma concentration of oxycodone [see Clinical Pharmacology (12.3)], resulting in decreased efficacy or onset of a withdrawal syndrome in patients who have developed physical dependence to oxycodone [see Warnings and Precautions (5.6)]. After stopping a CYP3A4 inducer, as the effects of the inducer decline, the oxycodone plasma concentration will increase [see Clinical Pharmacology (12.3)], which could increase or prolong both the therapeutic effects and adverse reactions and may cause serious respiratory depression. |
| Intervention: | If concomitant use is necessary, consider increasing the XTAMPZA ER dosage until stable drug effects are achieved [see Dosage and Administration (2.5)]. Evaluate patients for signs of opioid withdrawal. If a CYP3A4 inducer is discontinued, consider XTAMPZA ER dosage reduction and evaluate patients at frequent intervals for signs of respiratory depression and sedation. |
| Examples: | Rifampin, carbamazepine, phenytoin |
| Benzodiazepines and other Central Nervous System (CNS) Depressants | |
| Clinical Impact: | Due to additive pharmacological effect, the concomitant use of benzodiazepines or other CNS depressants including alcohol, increases the risk of respiratory depression, profound sedation, coma, and death [see Warnings and Precautions (5.3)]. |
| Intervention: | Reserve concomitant prescribing of these drugs for use in patients for whom alternative treatment options are inadequate. Limit dosages and durations to the minimum required. Inform patients and caregivers of this potential interaction and educate them on the signs and symptoms of respiratory depression (including sedation). If concomitant use is warranted, consider recommending or prescribing an opioid overdose reversal agent [see Dosage and Administration (2.2), Warnings and Precautions (5.1, 5.2, 5.3)]. |
| Examples | Benzodiazepines and other sedatives/hypnotics, anxiolytics, tranquilizers, muscle relaxants, general anesthetics, antipsychotics, gabapentinoids (gabapentin or pregabalin), other opioids, alcohol |
| Serotonergic Drugs | |
| Clinical Impact: | The concomitant use of opioids with other drugs that affect the serotonergic neurotransmitter system has resulted in serotonin syndrome. |
| Intervention: | If concomitant use is warranted, frequently evaluate the patient, particularly during treatment initiation and dose adjustment. Discontinue XTAMPZA ER if serotonin syndrome is suspected. |
| Examples: | Selective serotonin reuptake inhibitors (SSRIs), serotonin and norepinephrine reuptake inhibitors (SNRIs), tricyclic antidepressants (TCAs), triptans, 5-HT3 receptor antagonists, drugs that effect the serotonin neurotransmitter system (e.g., mirtazapine, trazodone, tramadol), certain muscle relaxants (i.e., cyclobenzaprine, metaxalone), monoamine oxidase inhibitors (those intended to treat psychiatric disorders and also others, such as linezolid and intravenous methylene blue) |
| Monoamine Oxidase Inhibitors (MAOIs) | |
| Clinical Impact: | MAOI interactions with opioids may manifest as serotonin syndrome or opioid toxicity (e.g., respiratory depression, coma) [see Warnings and Precautions (5.2)]. |
| Intervention: | The use of XTAMPZA ER is not recommended for patients taking MAOIs or within 14 days of stopping such treatment. |
| Examples: | phenelzine, tranylcypromine, linezolid |
| Mixed Agonist/Antagonist and Partial Agonist Opioid Analgesics | |
| Clinical Impact: | May reduce the analgesic effect of XTAMPZA ER and/or precipitate withdrawal symptoms. |
| Intervention: | Avoid concomitant use. |
| Examples: | Butorphanol, nalbuphine, pentazocine, buprenorphine |
| Muscle Relaxants | |
| Clinical Impact: | Oxycodone may enhance the neuromuscular blocking action of skeletal muscle relaxants and produce an increased degree of respiratory depression. |
| Intervention: | Because respiratory depression may be greater than otherwise expected, decrease the dosage of XTAMPZA ER and/or the muscle relaxant as necessary. Due to the risk of respiratory depression with concomitant use of skeletal muscle relaxants and opioids, consider recommending or prescribing an opioid overdose reversal agent [see Dosage and Administration (2.2), Warnings and Precautions (5.2, 5.3)]. |
| Examples: | Cyclobenzaprine, metaxalone |
| Diuretics | |
| Clinical Impact: | Opioids can reduce the efficacy of diuretics by inducing the release of antidiuretic hormone. |
| Intervention: | Evaluate patients for signs of diminished diuresis and/or effects on blood pressure and increase the dosage of the diuretic as needed. |
| Anticholinergic Drugs | |
| Clinical Impact: | The concomitant use of anticholinergic drugs may increase risk of urinary retention and/or severe constipation, which may lead to paralytic ileus. |
| Intervention: | Evaluate patients for signs of urinary retention or reduced gastric motility when XTAMPZA ER is used concomitantly with anticholinergic drugs. |
8.8 Sex Differences
In pharmacokinetic studies with XTAMPZA ER, healthy female subjects demonstrate up to 20% higher oxycodone plasma exposures than males, even after considering differences in body weight or BMI. The clinical relevance of a difference of this magnitude is low for a drug intended for chronic usage at individualized dosages. In the Phase 3 clinical trial there was a greater frequency of typical opioid adverse events for females than males; there was no male/female difference detected for efficacy.
8.7 Renal Impairment
In patients with renal impairment, as evidenced by decreased creatinine clearance (<60 mL/min), the concentrations of oxycodone in the plasma are approximately 50% higher than in subjects with normal renal function. Follow a conservative approach to dose initiation and adjust according to the clinical situation. Use of alternative analgesics is recommended for patients who require a dose of XTAMPZA ER less than 9 mg [see Clinical Pharmacology (12.3)].
Instructions for Use
Always take XTAMPZA ER with approximately the same amount of food. If you cannot swallow XTAMPZA ER capsules, tell your healthcare provider. If your healthcare provider tells you that you can take XTAMPZA ER by sprinkling the capsule contents, follow these steps:
XTAMPZA ER can be opened and the contents inside the capsule can be sprinkled onto soft foods (such as, applesauce, pudding, yogurt, ice cream, or jam) as follows:
|
Figure 1 |
|
|
Figure 2 |
|
|
Figure 3 |
|
|
Figure 4 |
|
XTAMPZA ER capsule contents can also be sprinkled into a cup and then put directly into the mouth.
Giving XTAMPZA ER through a nasogastric or gastrostomy tube:
Use water, milk, or a liquid nutritional supplement to flush the tube when giving XTAMPZA ER.
| Step 1: | Flush the nasogastric or gastrostomy tube with liquid. |
| Step 2: | Open an XTAMPZA ER capsule and carefully pour the contents of the capsule directly into the tube. Do not pre-mix the capsule contents with the liquid used to flush the capsule contents through the tube. |
| Step 3: | Draw up 15 mL of liquid into a syringe, insert the syringe into the tube, and flush the contents of the capsule through the tube to give the dose. |
| Step 4: | Flush the tube two more times, each time with 10 mL of liquid, to ensure that none of the contents of the capsule are left in the tube. |
This Instruction for Use has been approved by the U.S. Food and Drug Administration. Issued: December 2025
Collegium®
PHARMACEUTICAL
12.3 Pharmacokinetics
The activity of XTAMPZA ER is primarily due to the parent drug oxycodone. XTAMPZA ER is designed to provide delivery of oxycodone over 12 hours.
13.2 Animal Toxicology
The safety of beeswax, carnauba wax, and myristic acid in XTAMPZA ER in doses exceeding a total daily dose of 288 mg oxycodone per day (equivalent to 320 mg oxycodone HCl per day) has not been studied.
8.6 Hepatic Impairment
A study in patients with hepatic impairment demonstrated greater plasma oxycodone concentrations than those seen at equivalent doses in persons with normal hepatic function. A similar effect on plasma oxycodone concentrations can be expected for patients with hepatic impairment taking XTAMPZA ER. Therefore, in the setting of hepatic impairment, start dosing patients at 1/3 to 1/2 the usual starting dose followed by careful dose titration. Use of alternative analgesics is recommended for patients who require a dose of XTAMPZA ER less than 9 mg [see Dosage and Administration (2.4), Clinical Pharmacology (12.3)].
1 Indications and Usage (1 INDICATIONS AND USAGE)
XTAMPZA ER is indicated for the management of severe and persistent pain that requires an opioid analgesic and that cannot be adequately treated with alternative options, including immediate-release opioids.
5.10 Severe Hypotension
XTAMPZA ER may cause severe hypotension including orthostatic hypotension and syncope in ambulatory patients. There is an increased risk in patients whose ability to maintain blood pressure has already been compromised by a reduced blood volume or concurrent administration of certain CNS depressant drugs (e.g., phenothiazines or general anesthetics) [see Drug Interactions (7)]. Regularly evaluate these patients for signs of hypotension after initiating or titrating the dosage of XTAMPZA ER. In patients with circulatory shock, XTAMPZA ER may cause vasodilation that can further reduce cardiac output and blood pressure. Avoid the use of XTAMPZA ER in patients with circulatory shock.
12.1 Mechanism of Action
Oxycodone is a full opioid agonist and is relatively selective for the mu receptor, although it can bind to other opioid receptors at higher doses. The principal therapeutic action of oxycodone is analgesia. Like all full opioid agonists, there is no ceiling effect to analgesia for oxycodone. Clinically, dosage is titrated to provide adequate analgesia and may be limited by adverse reactions, including respiratory and CNS depression.
The precise mechanism of the analgesic action is unknown. However, specific CNS opioid receptors for endogenous compounds with opioid-like activity have been identified throughout the brain and spinal cord and are thought to play a role in the analgesic effects of this drug. In addition, when oxycodone binds to mu-opioid receptors, it results in positive subjective effects, such as drug liking, euphoria, and high.
9.1 Controlled Substance
XTAMPZA ER contains oxycodone, a Schedule II controlled substance.
5.9 Adrenal Insufficiency
Cases of adrenal insufficiency have been reported with opioid use, more often following greater than one month of use. Presentation of adrenal insufficiency may include non-specific symptoms and signs including nausea, vomiting, anorexia, fatigue, weakness, dizziness, and low blood pressure. If adrenal insufficiency is suspected, confirm the diagnosis with diagnostic testing as soon as possible. If adrenal insufficiency is diagnosed, treat with physiologic replacement doses of corticosteroids. Wean the patient off of the opioid to allow adrenal function to recover and continue corticosteroid treatment until adrenal function recovers. Other opioids may be tried as some cases reported use of a different opioid without recurrence of adrenal insufficiency. The information available does not identify any particular opioids as being more likely to be associated with adrenal insufficiency.
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
- Opioid-Induced Hyperalgesia and Allodynia: Opioid-Induced Hyperalgesia (OIH) occurs when an opioid analgesic paradoxically causes an increase in pain, or an increase in sensitivity to pain. If OIH is suspected, carefully consider appropriately decreasing the dose of the current opioid analgesic or opioid rotation. (5.7)
- Risk of life-threatening respiratory depression in patients with chronic pulmonary disease or in elderly, cachectic, or debilitated patients: Regularly evaluate. (5.8)
- Adrenal Insufficiency: If diagnosed, treat with physiologic replacement of corticosteroids, and wean patient off of the opioid. (5.9)
- Severe hypotension: Regularly evaluate. Avoid use of XTAMPZA ER in patients with circulatory shock. (5.10)
- Risks of use in patients with increased intracranial pressure, brain tumors, head injury, or impaired consciousness: Monitor for sedation and respiratory depression. Avoid use of XTAMPZA ER in patients with impaired consciousness or coma. (5.11)
5.16 Laboratory Monitoring
Not every urine drug test for "opioids" or "opiates" detects oxycodone reliably, especially those designed for in-office use. Further, many laboratories will report urine drug concentrations below a specified "cut-off" value as "negative". Therefore, if urine testing for oxycodone is considered in the clinical management of an individual patient, ensure that the sensitivity and specificity of the assay is appropriate, and consider the limitations of the testing used when interpreting results.
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
- XTAMPZA ER should be prescribed only by healthcare professionals who are knowledgeable about the use of extended-release/long-acting opioids and how to mitigate the associated risks. (2.1)
- XTAMPZA ER at a total daily dose greater than 72 mg (equivalent to 80 mg oxycodone hydrochloride [HCl]) or a single dose greater than 36 mg (equivalent to 40 mg oxycodone HCl) is only for use in patients in whom tolerance to an opioid of comparable potency has been established. (2.1)
- Patients considered opioid-tolerant are those receiving, for one week or longer, at least 60 mg oral morphine per day, 25 mcg transdermal fentanyl per hour, 30 mg oral oxycodone HCl per day, 8 mg oral hydromorphone per day, 25 mg oral oxymorphone per day, 60 mg oral hydrocodone per day, or an equianalgesic dose of another opioid. (2.1)
- Use the lowest effective dose for the shortest duration of time consistent with individual patient treatment goals. Reserve titration to higher doses of XTAMPZA ER for patients in whom lower doses are insufficiently effective and in whom the expected benefits of using a higher dose opioid clearly outweigh the substantial risks. (2, 5)
- Initiate the dosing regimen for each patient individually, taking into account the patient's underlying cause and severity of pain, prior analgesic treatment and response, and risk factors for addiction, abuse, and misuse. (2.1, 5.1).
- Respiratory depression can occur at any time during opioid therapy, especially when initiating and following dosage increases with XTAMPZA ER. Consider this risk when selecting an initial dose and when making dose adjustments. (2.1, 5.2)
- Discuss opioid overdose reversal agents and options for acquiring them with the patient and/or caregiver, both when initiating and renewing treatment with XTAMPZA ER, especially if the patient has additional risk factors for overdose, or close contacts at risk for exposure and overdose. (2.2, 5.1, 5.2, 5.3)
- XTAMPZA ER is administered, twice daily, every 12 hours, and must be taken with food. Instruct patients to take XTAMPZA ER capsules with approximately the same amount of food for every dose to ensure consistent plasma levels are achieved. (2.1, 2.3)
- For patients who are not opioid tolerant, initiate with 9 mg (equivalent to 10 mg oxycodone HCl per day). (2.3)
- The daily dose of XTAMPZA ER must be limited to a maximum of 288 mg per day (equivalent to 320 mg oxycodone HCl per day). (2.1)
- Hepatic impairment: Initiate therapy at 1/3 to 1/2 the usual dosage and titrate carefully. Regularly evaluate. Use alternate analgesia for patients requiring less than 9 mg. (2.4, 8.6)
- Periodically reassess patients receiving XTAMPZA ER to evaluate the continued need for opioid analgesics to maintain pain control, for the signs or symptoms of adverse reactions, and for the development of addiction, abuse, or misuse. (2.5)
- Do not rapidly reduce or abruptly discontinue XTAMPZA ER in a physically-dependent patient because rapid reduction or abrupt discontinuation of opioid analgesics has resulted in serious withdrawal symptoms, uncontrolled pain, and suicide. (2.6 , 5.14)
- Instruct patients to take XTAMPZA ER capsules with food in order to ensure consistent plasma levels are achieved. For patients who have difficulty swallowing, XTAMPZA ER can also be taken by sprinkling the capsule contents on soft foods or into a cup and then administering directly into the mouth, or through a gastrostomy or nasogastric feeding tube. (2.7)
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
XTAMPZA ER capsules contain yellow to light brown microspheres, and each available strength has an outer opaque capsule with colors as identified below.
| Strength | Capsule Description |
|---|---|
| 9 mg (equivalent to 10 mg oxycodone HCl) |
Size 3, ivory cap printed with "XTAMPZA ER" and white body printed with "9 mg" |
| 13.5 mg (equivalent to 15 mg oxycodone HCl) |
Size 2, Swedish orange cap printed with "XTAMPZA ER" and white body printed with "13.5 mg" |
| 18 mg (equivalent to 20 mg oxycodone HCl) |
Size 1, rich yellow cap printed with "XTAMPZA ER" and white body printed with "18 mg" |
| 27 mg (equivalent to 30 mg oxycodone HCl) |
Size 0, light gray cap printed with "XTAMPZA ER" and white body printed with "27 mg" |
| 36 mg (equivalent to 40 mg oxycodone HCl) |
Size 00, flesh color cap printed with "XTAMPZA ER" and white body printed with "36 mg" |
6.2 Postmarketing Experience
The following adverse reactions have been identified during post approval use of oxycodone. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Serotonin syndrome: Cases of serotonin syndrome, a potentially life-threatening condition, have been reported during concomitant use of opioids with serotonergic drugs.
Adrenal insufficiency: Cases of adrenal insufficiency have been reported with opioid use, more often following greater than one month of use.
Anaphylaxis: Anaphylaxis has been reported with ingredients contained in XTAMPZA ER.
Androgen deficiency: Cases of androgen deficiency have occurred with use of opioids for an extended period of time [see Clinical Pharmacology (12.2)].
Hyperalgesia and Allodynia: Cases of hyperalgesia and allodynia have been reported with opioid therapy of any duration [see Warnings and Precautions (5.7)].
Hypoglycemia: Cases of hypoglycemia have been reported in patients taking opioids. Most reports were in patients with at least one predisposing risk factor (e.g., diabetes).
Opioid-induced esophageal dysfunction (OIED): Cases of OIED have been reported in patients taking opioids and may occur more frequently in patients taking higher doses of opioids, and/or in patients taking opioids longer term [see Warnings and Precautions (5.12) ].
6.1 Clinical Trial Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
The safety of XTAMPZA ER was evaluated in a Phase 3, randomized-withdrawal, double-blind clinical trial involving 740 patients with moderate-to-severe chronic lower back pain. In the double-blind maintenance phase, 389 patients were randomized and 193 patients were assigned to the XTAMPZA ER treatment group.
The most common AEs (>5%) reported by patients in the Phase 3 clinical trial during the titration phase were: nausea (16.6%), headache (13.9%), constipation (13.0%), somnolence (8.8%), pruritus (7.4%), vomiting (6.4%), and dizziness (5.7%).
The most common adverse reactions (>5%) reported by patients in the Phase 3 clinical trial comparing XTAMPZA ER with placebo are shown in Table below:
| Titration | Maintenance | ||
|---|---|---|---|
| Adverse Reaction | XTAMPZA ER (n = 740) (%) |
XTAMPZA ER (n = 193) (%) |
Placebo (n = 196) (%) |
| Nausea | 16.6 | 10.9 | 4.6 |
| Headache | 13.9 | 6.2 | 11.7 |
| Constipation | 13.0 | 5.2 | 0.5 |
| Somnolence | 8.8 | <1 | <1 |
| Pruritus | 7.4 | 2.6 | 1.5 |
| Vomiting | 6.4 | 4.1 | 1.5 |
| Dizziness | 5.7 | 1.6 | 0 |
In the Phase 3 clinical trial, the following adverse reactions were reported in patients treated with XTAMPZA ER with incidences of 1% to 5%:
Eye disorders: vision blurred
Gastrointestinal disorders: abdominal pain, upper abdominal pain, diarrhea, gastroesophageal reflux disease
General disorders and administration site conditions: chills, drug withdrawal syndrome, fatigue, irritability, edema, pyrexia
Injury, poisoning and procedural complications: excoriation
Metabolism and nutrition disorders: decreased appetite, hyperglycemia
Musculoskeletal and connective tissue disorders: arthralgia, back pain, musculoskeletal pain, myalgia
Nervous system disorders: migraine, tremor
Psychiatric disorders: anxiety, insomnia, withdrawal syndrome
Respiratory, thoracic and mediastinal disorders: cough, oropharyngeal pain
Skin and subcutaneous tissue disorders: hyperhidrosis, rash
Vascular disorders: hot flush, hypertension
In the Phase 3 clinical trial, the following treatment-related adverse reactions were reported in patients treated with XTAMPZA ER with incidences of less than 1% of patients.
Investigations: increased gamma-glutamyl transferase, increased heart rate
Nervous system disorders: lethargy, memory impairment, poor-quality sleep
Psychiatric disorders: abnormal dreams, euphoric mood, restlessness
Respiratory, thoracic and mediastinal disorders: dyspnea
Skin and subcutaneous tissue disorders: night sweats
8 Use in Specific Populations (8 USE IN SPECIFIC POPULATIONS)
2.7 Administration of Xtampza Er (2.7 Administration of XTAMPZA ER)
Instruct patients to always take XTAMPZA ER capsules with food and with approximately the same amount of food in order to ensure consistent plasma levels are achieved [see Dosage and Administration (2.1), Clinical Pharmacology (12.3)].
For patients who have difficulty swallowing, XTAMPZA ER can also be taken by sprinkling the capsule contents on soft foods or sprinkling the contents into a cup and then administering directly into the mouth or through a gastrostomy or nasogastric feeding tube. Patients who are unable to swallow a capsule should be instructed to:
- Open the capsule.
- Sprinkle the capsule contents (microspheres) onto a small amount of soft food (e.g., applesauce, pudding, yogurt, ice cream, or jam) or into a cup and then administer directly into the mouth and swallow immediately.
- Rinse the mouth to ensure all capsule contents (microspheres) have been swallowed.
- Discard the XTAMPZA ER capsule shells after the contents have been sprinkled on soft food or into a cup and then administered directly into the mouth.
The contents of the XTAMPZA ER capsules (microspheres) may be administered through a nasogastric tube or gastrostomy tube. When administering XTAMPZA ER through a nasogastric or gastrostomy tube:
- Flush the tube with water.
- Open an XTAMPZA ER capsule and carefully pour the microspheres directly into the tube. Do not pre-mix the capsule contents with the liquid that you will be using to flush them through the tube.
- Draw up 15 mL of water into a syringe, insert the syringe into the tube, and flush the microspheres through the tube.
- Repeat the flushing two more times, each with 10 mL of water, to ensure no microspheres remain in the tube.
Alternatively, milk or liquid nutritional supplement may be used as vehicles for flush and administration through feeding tubes.
5.1 Addiction, Abuse, and Misuse
XTAMPZA ER contains oxycodone, a Schedule II controlled substance. As an opioid, XTAMPZA ER exposes users to the risks of addiction, abuse, and misuse [see Drug Abuse and Dependence (9)].
Although the risk of addiction in any individual is unknown, it can occur in patients appropriately prescribed XTAMPZA ER. Addiction can occur at recommended dosages and if the drug is misused or abused. The risk of opioid-related overdose or overdose-related death is increased with higher opioid doses, and this risk persists over the course of therapy. In postmarketing studies, addiction, abuse, misuse, and fatal and non-fatal opioid overdose were observed in patients with long-term opioid use [see Adverse Reactions (6.2) ].
Assess each patient's risk for opioid addiction, abuse, or misuse prior to prescribing XTAMPZA ER, and reassess all patients receiving XTAMPZA ER for the development of these behaviors or conditions. Risks are increased in patients with a personal or family history of substance abuse (including drug or alcohol abuse or addiction) or mental illness (e.g., major depression). The potential for these risks should not, however, prevent the proper management of pain in any given patient. Patients at increased risk may be prescribed opioids such as XTAMPZA ER but use in such patients necessitates intensive counseling about the risks and proper use of XTAMPZA ER along with frequent evaluation for signs of addiction, abuse, and misuse. Consider recommending or prescribing an opioid overdose reversal agent [see Dosage and Administration (2.2), Warnings and Precautions (5.2)].
Abuse or misuse of XTAMPZA ER by snorting or by injecting the dissolved product can result in overdose and death [see Overdosage (10)].
Opioids are sought for nonmedical use and are subject to diversion from legitimate prescribed use. Consider these risks when prescribing or dispensing XTAMPZA ER. Strategies to reduce these risks include prescribing the drug in the smallest appropriate quantity and advising the patient on careful storage of the drug during the course of treatment and the proper disposal of unused drug. Contact local state professional licensing board or state-controlled substances authority for information on how to prevent and detect abuse or diversion of this product.
17 Patient Counseling Information (17 PATIENT COUNSELING INFORMATION)
Advise the patient to read the FDA-approved patient labeling (Medication Guide).
16 How Supplied/storage and Handling (16 HOW SUPPLIED/STORAGE AND HANDLING)
XTAMPZA ER capsules are supplied in 100-count bottles with a child-resistant closure and as a hospital unit dose package with 10 individually blistered capsules per card; two cards per carton as follows:
| Strength | Capsule Description | NDC Number (100-count Bottles with a child-resistant closure) |
NDC Number (20-count Hospital Unit Dose Blister Cartons) |
|---|---|---|---|
| 9 mg (equivalent to 10 mg oxycodone HCl) |
Size 3, ivory cap printed with "XTAMPZA ER" and white body printed with "9 mg" | NDC 24510-110-10 | NDC 24510-110-20 |
| 13.5 mg (equivalent to 15 mg oxycodone HCl) |
Size 2, Swedish orange cap printed with "XTAMPZA ER" and white body printed with "13.5 mg" | NDC 24510-115-10 | NDC 24510-115-20 |
| 18 mg (equivalent to 20 mg oxycodone HCl) |
Size 1, rich yellow cap printed with "XTAMPZA ER" and white body printed with "18 mg" | NDC 24510-120-10 | NDC 24510-120-20 |
| 27 mg (equivalent to 30 mg oxycodone HCl) |
Size 0, light gray cap printed with "XTAMPZA ER" and white body printed with "27 mg" | NDC 24510-130-10 | NDC 24510-130-20 |
| 36 mg (equivalent to 40 mg oxycodone HCl) |
Size 00, flesh color cap printed with "XTAMPZA ER" and white body printed with "36 mg" | NDC 24510-140-10 | NDC 24510-140-20 |
5.4 Neonatal Opioid Withdrawal Syndrome
Use of XTAMPZA ER for an extended period of time during pregnancy can result in withdrawal in the neonate. Neonatal opioid withdrawal syndrome, unlike opioid withdrawal syndrome in adults, may be life-threatening if not recognized and treated, and requires management according to protocols developed by neonatology experts. Observe newborns for signs of neonatal opioid withdrawal syndrome and manage accordingly. Advise pregnant women using opioids for an extended period of time of the risk of neonatal opioid withdrawal syndrome and ensure that appropriate treatment will be available [see Use in Specific Populations (8.1)].
2.5 Titration and Maintenance of Therapy
Individually titrate XTAMPZA ER to a dose that provides adequate analgesia and minimizes adverse reactions. Continually reevaluate patients receiving XTAMPZA ER to assess the maintenance of pain control and the relative incidence of adverse reactions, as well as to reassess for the development of addiction, abuse, and misuse. Frequent communication is important among the prescriber, other members of the healthcare team, the patient, and the caregiver/family during periods of changing analgesic requirements, including initial titration. During use of opioid therapy for an extended period of time, periodically reassess the continued need for the use of opioid analgesics.
Patients who experience breakthrough pain may require a dose increase of XTAMPZA ER or may need rescue medication with an appropriate dose of an immediate-release analgesic. If the level of pain increases after dose stabilization, attempt to identify the source of increased pain before increasing the XTAMPZA ER dose. If after increasing the dosage, unacceptable opioid-related adverse reactions are observed (including an increase in pain after a dosage increase), consider reducing the dosage [see Warnings and Precautions (5)]. Adjust the dosage to obtain an appropriate balance between management of pain and opioid-related adverse reactions.
Because steady-state plasma concentrations are approximated in 1 to 2 days, XTAMPZA ER dosage may be adjusted every 1 to 2 days. If unacceptable opioid-related adverse reactions are observed, the subsequent dose may be reduced. Adjust the dose to obtain an appropriate balance between management of pain and opioid-related adverse reactions.
There are no well-controlled clinical studies evaluating the safety and efficacy with dosing more frequently than every 12 hours. As a guideline, the total daily oxycodone dose usually can be increased by 25% to 50% of the current dose, each time an increase is clinically indicated.
5.2 Life Threatening Respiratory Depression (5.2 Life-Threatening Respiratory Depression)
Serious, life-threatening, or fatal respiratory depression has been reported with the use of opioids, even when used as recommended. Respiratory depression, if not immediately recognized and treated, may lead to respiratory arrest and death. Management of respiratory depression may include close observation, supportive measures, and use of opioid overdose reversal agents, depending on the patient's clinical status [see Overdosage (10)]. Carbon dioxide (CO2) retention from opioid-induced respiratory depression can exacerbate the sedating effects of opioids.
While serious, life-threatening, or fatal respiratory depression can occur at any time during the use of XTAMPZA ER, the risk is greatest during the initiation of therapy or following a dosage increase.
To reduce the risk of respiratory depression, proper dosing and titration of XTAMPZA ER are essential [see Dosage and Administration (2)]. Overestimating the XTAMPZA ER dose when converting patients from another opioid product can result in a fatal overdose with the first dose.
Accidental ingestion of even one dose of XTAMPZA ER, especially by children, can result in respiratory depression and death due to an overdose of oxycodone.
Educate patients and caregivers on how to recognize respiratory depression and emphasize the importance of calling 911 or getting emergency medical help right away in the event of a known or suspected overdose.
Opioids can cause sleep-related breathing disorders including central sleep apnea (CSA) and sleep-related hypoxemia. Opioid use increases the risk of CSA in a dose-dependent fashion. In patients who present with CSA, consider decreasing the opioid dosage using best practices for opioid taper [see Dosage and Administration (2.6) ].
5.12 Risks of Gastrointestinal Complications
XTAMPZA ER is contraindicated in patients with gastrointestinal obstruction, including paralytic ileus.
The oxycodone in XTAMPZA ER may cause spasm of the sphincter of Oddi. Opioids may cause increases in the serum amylase. Regularly evaluate with biliary tract disease, including acute pancreatitis, for worsening symptoms.
Cases of opioid-induced esophageal dysfunction (OIED) have been reported in patients taking opioids. The risk of OIED may increase as the dose and/or duration of opioids increases. Regularly evaluate patients for signs and symptoms of OIED (e.g., dysphagia, regurgitation, non-cardiac chest pain) and, if necessary, adjust opioid therapy as clinically appropriate [see Clinical Pharmacology (12.2)]. .
5.15 Risks of Driving and Operating Machinery
XTAMPZA ER may impair the mental or physical abilities needed to perform potentially hazardous activities such as driving a car or operating machinery. Warn patients not to drive or operate dangerous machinery unless they are tolerant to the effects of XTAMPZA ER and know how they will react to the medication.
5.7 Opioid Induced Hyperalgesia and Allodynia (5.7 Opioid-Induced Hyperalgesia and Allodynia)
Opioid-Induced Hyperalgesia (OIH) occurs when an opioid analgesic paradoxically causes an increase in pain, or an increase in sensitivity to pain. This condition differs from tolerance, which is the need for increasing doses of opioids to maintain a defined effect [see Dependence (9.3)]. Symptoms of OIH include (but may not be limited to) increased levels of pain upon opioid dosage increase, decreased levels of pain upon opioid dosage decrease, or pain from ordinarily non-painful stimuli (allodynia). These symptoms may suggest OIH only if there is no evidence of underlying disease progression, opioid tolerance, opioid withdrawal, or addictive behavior.
Cases of OIH have been reported, both with short-term and longer-term use of opioid analgesics. Though the mechanism of OIH is not fully understood, multiple biochemical pathways have been implicated. Medical literature suggests a strong biologic plausibility between opioid analgesics and OIH and allodynia. If a patient is suspected to be experiencing OIH, carefully consider appropriately decreasing the dose of the current opioid analgesic or opioid rotation (safely switching the patient to a different opioid moiety) [see Dosage and Administration (2.6), Warnings and Precautions (5.14)].
2.6 Safe Reduction Or Discontinuation of Xtampza Er (2.6 Safe Reduction or Discontinuation of XTAMPZA ER)
Do not rapidly reduce or abruptly discontinue XTAMPZA ER in patients who may be physically dependent on opioids. Rapid reduction or abrupt discontinuation of opioid analgesics in patients who are physically dependent on opioids has resulted in serious withdrawal symptoms, uncontrolled pain, and suicide. Rapid reduction or abrupt discontinuation has also been associated with attempts to find other sources of opioid analgesics, which may be confused with drug-seeking for abuse. Patients may also attempt to treat their pain or withdrawal symptoms with illicit opioids, such as heroin, and other substances.
When a decision has been made to decrease the dose or discontinue therapy in an opioid-dependent patient taking XTAMPZA ER, there are a variety of factors that should be considered, including the total daily dose of opioid (including XTAMPZA ER) the patient has been taking, the duration of treatment, the type of pain being treated, and the physical and psychological attributes of the patient. It is important to ensure ongoing care of the patient and to agree on an appropriate tapering schedule and follow-up plan so that patient and provider goals and expectations are clear and realistic. When opioid analgesics are being discontinued due to a suspected substance use disorder, evaluate and treat the patient, or refer for evaluation and treatment of the substance use disorder. Treatment should include evidence-based approaches, such as medication assisted treatment of opioid use disorder. Complex patients with co-morbid pain and substance use disorders may benefit from referral to a specialist.
There are no standard opioid tapering schedules that are suitable for all patients. Good clinical practice dictates a patient-specific plan to taper the dose of the opioid gradually. For patients on XTAMPZA ER who are physically opioid-dependent, initiate the taper by a small enough increment (e.g., no greater than 10% to 25% of the total daily dose) to avoid withdrawal symptoms, and proceed with dose-lowering at an interval of every 2 to 4 weeks. Patients who have been taking opioids for briefer periods of time may tolerate a more rapid taper.
It may be necessary to provide the patient with lower dosage strengths to accomplish a successful taper. Reassess the patient frequently to manage pain and withdrawal symptoms, should they emerge. Common withdrawal symptoms include restlessness, lacrimation, rhinorrhea, yawning, perspiration, chills, myalgia, and mydriasis. Other signs and symptoms also may develop, including irritability, anxiety, backache, joint pain, weakness, abdominal cramps, insomnia, nausea, anorexia, vomiting, diarrhea, or increased blood pressure, respiratory rate, or heart rate. If withdrawal symptoms arise, it may be necessary to pause the taper for a period of time or raise the dose of the opioid analgesic to the previous dose, and then proceed with a slower taper. In addition, evaluate patients for any changes in mood, emergence of suicidal thoughts, or use of other substances.
When managing patients taking opioid analgesics, particularly those who have been treated for an extended period of time, and/or with high doses for chronic pain, ensure that a multimodal approach to pain management, including mental health support (if needed), is in place prior to initiating an opioid analgesic taper. A multimodal approach to pain management may optimize the treatment of chronic pain, as well as assist with the successful tapering of the opioid analgesic [see Warnings and Precautions (5.14), Drug Abuse and Dependence (9.3)].
Principal Display Panel 9 Mg Capsule Bottle Label (PRINCIPAL DISPLAY PANEL - 9 mg Capsule Bottle Label)
NDC 24510-110-10
Xtampza® ER
(oxycodone)
EXTENDED-RELEASE
CAPSULES
CII
9 mg
Each capsule contains Oxycodone 9 mg
(Equivalent to 10 mg Oxycodone Hydrochloride)
100 Capsules
Rx Only
Always take with food. Taking on an empty
stomach can decrease drug absorption.
Attention Dispenser: Accompanying Medication
Guide must be provided to the patient upon dispensing.
2.1 Important Dosage and Administration Instructions
- XTAMPZA ER should be prescribed only by healthcare professionals who are knowledgeable about the use of extended-release/long-acting opioids and how to mitigate the associated risks.
- XTAMPZA ER single doses greater than 36 mg (equivalent to 40 mg oxycodone hydrochloride [HCl]) or a total daily dose greater than 72 mg (equivalent to 80 mg oxycodone HCl) are to be administered only to patients in whom tolerance to an opioid of comparable potency has been established. Patients who are opioid-tolerant are those receiving, for one week or longer, at least 60 mg oral morphine per day, 25 mcg transdermal fentanyl per hour, 30 mg oral oxycodone HCl per day, 8 mg oral hydromorphone per day, 25 mg oral oxymorphone per day, 60 mg oral hydrocodone per day, or an equianalgesic dose of another opioid.
- Use the lowest effective dosage for the shortest duration of time consistent with individual patient treatment goals [see Warnings and Precautions (5)]. Because the risk of overdose increases as opioid doses increase, reserve titration to higher doses of XTAMPZA ER for patients in whom lower doses are insufficiently effective and in whom the expected benefits of using a higher dose opioid clearly outweigh the substantial risks.
- Initiate the dosing regimen for each patient individually, taking into account the patient's underlying cause and severity of pain, prior analgesic treatment and response, and risk factors for addiction, abuse, and misuse [see Warnings and Precautions (5.1)].
- Respiratory depression can occur at any time during opioid therapy, especially when initiating and following dosage increases with XTAMPZA ER. Consider this risk when selecting an initial dose and when making dose adjustments [see Warnings and Precautions (5.2)].
- XTAMPZA ER is administered, twice daily, every 12 hours, and must be taken with food. Instruct patients to take XTAMPZA ER capsules with approximately the same amount of food for every dose in order to ensure consistent plasma levels are achieved [see Clinical Pharmacology (12.3)].
- Patients who are unable to swallow XTAMPZA ER should be instructed to sprinkle the capsule contents on soft foods or into a cup and then administer directly into the mouth and immediately swallow. XTAMPZA ER may also be administered through a gastrostomy or nasogastric feeding tube [see Dosage and Administration (2.7)].
- The maximum daily dose of XTAMPZA ER is 288 mg per day (eight 36 mg capsules, equivalent to 320 mg oxycodone HCl per day) as the safety of the excipients in XTAMPZA ER for doses over 288 mg/day has not been established.
Principal Display Panel 18 Mg Capsule Bottle Label (PRINCIPAL DISPLAY PANEL - 18 mg Capsule Bottle Label)
NDC 24510-120-10
Xtampza® ER
(oxycodone)
EXTENDED-RELEASE
CAPSULES
CII
18 mg
Each capsule contains Oxycodone 18 mg
(Equivalent to 20 mg Oxycodone Hydrochloride)
100 Capsules
Rx Only
Always take with food. Taking on an empty
stomach can decrease drug absorption.
Attention Dispenser: Accompanying
Medication Guide must be provided to
the patient upon dispensing.
Principal Display Panel 27 Mg Capsule Bottle Label (PRINCIPAL DISPLAY PANEL - 27 mg Capsule Bottle Label)
NDC 24510-130-10
Xtampza® ER
(oxycodone)
EXTENDED-RELEASE
CAPSULES
CII
27 mg
Each capsule contains Oxycodone 27 mg
(Equivalent to 30 mg Oxycodone Hydrochloride)
100 Capsules
Rx Only
Always take with food. Taking on an empty
stomach can decrease drug absorption.
Attention Dispenser: Accompanying
Medication Guide must be provided to
the patient upon dispensing.
Principal Display Panel 36 Mg Capsule Bottle Label (PRINCIPAL DISPLAY PANEL - 36 mg Capsule Bottle Label)
NDC 24510-140-10
Xtampza® ER
(oxycodone)
EXTENDED-RELEASE
CAPSULES
CII
36 mg
Each capsule contains Oxycodone 36 mg
(Equivalent to 40 mg Oxycodone Hydrochloride)
100 Capsules
Rx Only
Always take with food. Taking on an empty
stomach can decrease drug absorption.
Attention Dispenser: Accompanying
Medication Guide must be provided to
the patient upon dispensing.
Principal Display Panel 13.5 Mg Capsule Bottle Label (PRINCIPAL DISPLAY PANEL - 13.5 mg Capsule Bottle Label)
NDC 24510-115-10
Xtampza® ER
(oxycodone)
EXTENDED-RELEASE
CAPSULES
CII
13.5 mg
Each capsule contains Oxycodone 13.5 mg
(Equivalent to 15 mg Oxycodone Hydrochloride)
100 Capsules
Rx Only
Always take with food. Taking on an empty
stomach can decrease drug absorption.
Attention Dispenser: Accompanying
Medication Guide must be provided to
the patient upon dispensing.
2.4 Dosage Modifications in Patients With Hepatic Impairment (2.4 Dosage Modifications in Patients with Hepatic Impairment)
For patients with hepatic impairment, start dosing patients at 1/3 to 1/2 the usual starting dose followed by careful dose titration. Regularly evaluate for adverse events such as respiratory depression. Use of alternate analgesics is recommended for patients who require an XTAMPZA ER dose of less than 9 mg [see Use in Specific Populations (8.5), Clinical Pharmacology (12.3)].
5.13 Increased Risk of Seizures in Patients With Seizure Disorders (5.13 Increased Risk of Seizures in Patients with Seizure Disorders)
The oxycodone in XTAMPZA ER may increase the frequency of seizures in patients with seizure disorders and may increase the risk of seizures in other clinical settings associated with seizures. Regularly evaluate patients with a history of seizure disorders for worsened seizure control during XTAMPZA ER therapy.
Warning: Serious and Life Threatening Risks From Use of Xtampza Er (WARNING: SERIOUS AND LIFE-THREATENING RISKS FROM USE OF XTAMPZA ER)
WARNING: SERIOUS AND LIFE-THREATENING RISKS FROM USE OF XTAMPZA ER
See full prescribing information for complete boxed warning.
- XTAMPZA ER exposes users to risks of addiction, abuse, and misuse, which can lead to overdose and death. Assess each patient's risk before prescribing and reassess regularly for these behaviors and conditions. (5.1)
- Serious, life-threatening, or fatal respiratory depression may occur especially during initiation or following a dosage increase. To reduce the risk of respiratory depression, proper dosing and titration of XTAMPZA ER are essential. (5.2)
- Accidental ingestion of XTAMPZA ER, especially by children, can result in fatal overdose of oxycodone. (5.2)
- Concomitant use of opioids with benzodiazepines or other central nervous system (CNS) depressants, including alcohol, may result in profound sedation, respiratory depression, coma, and death. Reserve concomitant prescribing for use in patients for whom alternative treatment options are inadequate. (5.3, 7)
- Advise pregnant using opioids for an extended period of time of the risk of Neonatal Opioid Withdrawal Syndrome, which may be life-threatening if not recognized and treated. Ensure that management by neonatology experts will be available at delivery. (5.4)
- Healthcare providers are strongly encouraged to complete a REMS-compliant education program and to counsel patients and caregivers on serious risks, safe use, and the importance of reading the Medication Guide with each prescription. (5.5)
- Concomitant use with CYP3A4 inhibitors (or discontinuation of CYP3A4 inducers) can result in a fatal overdose of oxycodone from XTAMPZA ER. (5.6, 12.3)
5.5 Opioid Analgesic Risk Evaluation and Mitigation Strategy (rems) (5.5 Opioid Analgesic Risk Evaluation and Mitigation Strategy (REMS))
To ensure that the benefits of opioid analgesics outweigh the risks of addiction, abuse, and misuse, the Food and Drug Administration (FDA) has required a Risk Evaluation and Mitigation Strategy (REMS) for these products. Under the requirements of the REMS, drug companies with approved opioid analgesic products must make REMS-compliant education programs available to healthcare providers. Healthcare providers are strongly encouraged to do all of the following:
- Complete a REMS-compliant education program offered by an accredited provider of continuing education (CE) or another education program that includes all the elements of the FDA Education Blueprint for Health Care Providers Involved in the Management or Support of Patients with Pain.
- Discuss the safe use, serious risks, and proper storage and disposal of opioid analgesics with patients and/or their caregivers every time these medicines are prescribed. The Patient Counseling Guide (PCG) can be obtained at this link: www.fda.gov/OpioidAnalgesicREMSPCG.
- Emphasize to patients and their caregivers the importance of reading the Medication Guide that they will receive from their pharmacist every time an opioid analgesic is dispensed to them.
- Consider using other tools to improve patient, household, and community safety, such as patient-prescriber agreements that reinforce patient-prescriber responsibilities.
To obtain further information on the opioid analgesic REMS and for a list of accredited REMS CME/CE, call 1-800-503-0784, or log on to www.opioidanalgesicrems.com. The FDA Blueprint can be found at www.fda.gov/OpioidAnalgesicREMSBlueprint.
5.3 Risks From Concomitant Use With Benzodiazepines Or Other Cns Depressants (5.3 Risks from Concomitant Use with Benzodiazepines or Other CNS Depressants)
Profound sedation, respiratory depression, coma, and death may result from the concomitant use of XTAMPZA ER with benzodiazepines and/or other CNS depressants, including alcohol (e.g., non-benzodiazepine sedatives/hypnotics, anxiolytics, tranquilizers, muscle relaxants, general anesthetics, antipsychotics, gabapentinoids [gabapentin or pregabalin], and other opioids). Because of these risks, reserve concomitant prescribing of these drugs for use in patients for whom alternative treatment options are inadequate.
Observational studies have demonstrated that concomitant use of opioid analgesics and benzodiazepines increases the risk of drug-related mortality compared to use of opioid analgesics alone. Because of similar pharmacological properties, it is reasonable to expect similar risk with the concomitant use of other CNS depressant drugs with opioid analgesics [see Drug Interactions (7)].
If the decision is made to prescribe a benzodiazepine or other CNS depressant concomitantly with an opioid analgesic, prescribe the lowest effective dosages and minimum durations of concomitant use. In patients already receiving an opioid analgesic, prescribe a lower initial dose of the benzodiazepine or other CNS depressants than indicated in the absence of an opioid, and titrate based on clinical response. If an opioid analgesic is initiated in a patient already taking a benzodiazepine or other CNS depressant, prescribe a lower initial dose of the opioid analgesic, and titrate based on clinical response. Inform patients and caregivers of this potential interaction and educate them on the signs and symptoms of respiratory depression (including sedation).
If concomitant use is warranted, consider recommending or prescribing an opioid overdose reversal agent for the emergency treatment of opioid overdose [see Dosage and Administration (2.2), Warnings and Precautions (5.2), Overdosage (10)].
Advise both patients and caregivers about the risks of respiratory depression and sedation when XTAMPZA ER is used with benzodiazepines or other CNS depressants (including alcohol and illicit drugs). Advise patients not to drive or operate heavy machinery until the effects of concomitant use of the benzodiazepine or other CNS depressant have been determined. Screen patients for risk of substance use disorders, including opioid abuse and misuse, and warn them of the risk for overdose and death associated with the use of additional CNS depressants including alcohol and illicit drugs [see Drug Interactions (7)].
5.6 Risks of Concomitant Use Or Discontinuation of Cytochrome P450 3a4 Inhibitors and Inducers (5.6 Risks of Concomitant Use or Discontinuation of Cytochrome P450 3A4 Inhibitors and Inducers)
Concomitant use of XTAMPZA ER with a CYP3A4 inhibitor, such as macrolide antibiotics (e.g., erythromycin), azole-antifungal agents (e.g., ketoconazole), and protease inhibitors (e.g., ritonavir), may increase plasma concentrations of oxycodone and prolong opioid adverse reactions, which may cause potentially fatal respiratory depression [see Warnings and Precautions (5.2)], particularly when an inhibitor is added after a stable dose of XTAMPZA ER is achieved. Similarly, discontinuation of a CYP3A4 inducer, such as rifampin, carbamazepine, and phenytoin, in XTAMPZA ER-treated patients may increase oxycodone plasma concentrations and prolong opioid adverse reactions. When using XTAMPZA ER with CYP3A4 inhibitors or discontinuing CYP3A4 inducers in XTAMPZA ER-treated patients, evaluate patients at frequent intervals and consider dosage reduction of XTAMPZA ER until stable drug effects are achieved [see Drug Interactions (7)].
Concomitant use of XTAMPZA ER with CYP3A4 inducers or discontinuation of a CYP3A4 inhibitor could decrease oxycodone plasma concentrations, decrease opioid efficacy or, possibly, lead to a withdrawal syndrome in a patient who had developed physical dependence to oxycodone. When using XTAMPZA ER with CYP3A4 inducers or discontinuing CYP3A4 inhibitors, evaluate patients at frequent intervals and consider increasing the opioid dosage if needed to maintain adequate analgesia or if symptoms of opioid withdrawal occur [see Drug Interactions (7)].
2.2 Patient Access to An Opioid Overdose Reversal Agent for the Emergency Treatment of Opioid Overdose (2.2 Patient Access to an Opioid Overdose Reversal Agent for the Emergency Treatment of Opioid Overdose)
Inform patients and caregivers about opioid overdose reversal agents (e.g., naloxone, nalmefene). Discuss the importance of having access to an opioid overdose reversal agent, especially if the patient has risk factors for overdose (e.g., concomitant use of CNS depressants, a history of opioid use disorder, or prior opioid overdose) or if there are household members (including children) or other close contacts at risk for accidental ingestion or opioid overdose. The presence of risk factors for overdose should not prevent the management of pain in any patient [see Warnings and Precautions (5.1, 5.2, 5.3) ].
Discuss the options for obtaining an opioid overdose reversal agent (e.g., prescription, over-the-counter, or as part of a community-based program) [see Warnings and Precautions (5.2) ].
There are important differences among the opioid overdose reversal agents, such as route of administration, product strength, approved patient age range, and pharmacokinetics. Be familiar with these differences, as outlined in the approved labeling for those products, prior to recommending or prescribing such an agent.
5.11 Risks of Use in Patients With Increased Intracranial Pressure, Brain Tumors, Head Injury, Or Impaired Consciousness (5.11 Risks of Use in Patients with Increased Intracranial Pressure, Brain Tumors, Head Injury, or Impaired Consciousness)
In patients who may be susceptible to the intracranial effects of CO2 retention (e.g., those with evidence of increased intracranial pressure or brain tumors), XTAMPZA ER may reduce respiratory drive, and the resultant CO2 retention can further increase intracranial pressure. Monitor such patients for signs of sedation and respiratory depression, particularly when initiating therapy with XTAMPZA ER.
Opioids may also obscure the clinical course in a patient with a head injury. Avoid the use of XTAMPZA ER in patients with impaired consciousness or coma.
5.8 Risk of Life Threatening Respiratory Depression in Patients With Chronic Pulmonary Disease Or in Elderly, Cachectic, Or Debilitated Patients (5.8 Risk of Life-Threatening Respiratory Depression in Patients with Chronic Pulmonary Disease or in Elderly, Cachectic, or Debilitated Patients)
The use of XTAMPZA ER in patients with acute or severe bronchial asthma in an unmonitored setting or in the absence of resuscitative equipment is contraindicated.
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:51:57.752619 · Updated: 2026-03-14T22:42:19.657154