These Highlights Do Not Include All The Information Needed To Use Herzuma Safely And Effectively. See Full Prescribing Information For Herzuma.
ae71c003-883a-4cd8-ad50-e8cc9a54e971
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
WARNING: CARDIOMYOPATHY, INFUSION REACTIONS, EMBRYO-FETAL TOXICITY, and PULMONARY TOXICITY See full prescribing information for complete boxed warning Cardiomyopathy: Trastuzumab products can result in subclinical and clinical cardiac failure manifesting as CHF, and decreased LVEF, with greatest risk when administered concurrently with anthracyclines. Evaluate cardiac function prior to and during treatment. Discontinue HERZUMA for cardiomyopathy. ( 2.5 , 5.1 ) Infusion Reactions, Pulmonary Toxicity: Discontinue HERZUMA for anaphylaxis, angioedema, interstitial pneumonitis, or acute respiratory distress syndrome. ( 5.2 , 5.4 ) Embryo-Fetal Toxicity: Exposure to trastuzumab products during pregnancy can result in oligohydramnios, in some cases complicated by pulmonary hypoplasia and neonatal death. Advise patients of these risks and the need for effective contraception. ( 5.3 , 8.1 , 8.3 )
Indications and Usage
HERZUMA is a HER2/neu receptor antagonist indicated in adults for: the treatment of HER2-overexpressing breast cancer. ( 1.1 , 1.2 ) the treatment of HER2-overexpressing metastatic gastric or gastroesophageal junction adenocarcinoma. ( 1.3 ) Select patients for therapy based on an FDA-approved companion diagnostic for a trastuzumab product. ( 1 , 2.2 )
Dosage and Administration
For intravenous (IV) infusion only. Do not administer as an IV push or bolus. HERZUMA has different dosage and administration instructions than subcutaneous trastuzumab products. ( 2.3 ) Do not substitute HERZUMA (trastuzumab-pkrb) for or with ado-trastuzumab emtansine or fam-trastuzumab deruxtecan. ( 2.3 ) Perform HER2 testing using FDA-approved tests by laboratories with demonstrated proficiency. ( 1 , 2.2 ) Adjuvant Treatment of HER2-Overexpressing Breast Cancer ( 2.2 ) Administer at either: Initial dose of 4 mg/kg over 90 minutes IV infusion, then 2 mg/kg over 30 minutes IV infusion weekly for 12 weeks (with paclitaxel or docetaxel) or 18 weeks (with docetaxel and carboplatin). One week after the last weekly dose of HERZUMA, administer 6 mg/kg as an IV infusion over 30 to 90 minutes every three weeks to complete a total of 52 weeks of therapy, or Initial dose of 8 mg/kg over 90 minutes IV infusion, then 6 mg/kg over 30 to 90 minutes IV infusion every three weeks for 52 weeks. Metastatic HER2-Overexpressing Breast Cancer ( 2.3 ) Initial dose of 4 mg/kg as a 90 minutes IV infusion followed by subsequent weekly doses of 2 mg/kg as 30 minutes IV infusions. Metastatic HER2-Overexpressing Gastric Cancer ( 2.3 ) Initial dose of 8 mg/kg over 90 minutes IV infusion, followed by 6 mg/kg over 30 to 90 minutes IV infusion every 3 weeks.
Warnings and Precautions
Exacerbation of Chemotherapy-Induced Neutropenia. ( 5.5 , 6.1 )
Contraindications
None.
Adverse Reactions
The following adverse reactions are discussed in greater detail in other sections of the label: Cardiomyopathy [see Warnings and Precautions (5.1) ] Infusion Reactions [see Warnings and Precautions (5.2) ] Embryo-Fetal Toxicity [see Warnings and Precautions (5.3) ] Pulmonary Toxicity [see Warnings and Precautions (5.4) ] Exacerbation of Chemotherapy-induced Neutropenia [see Warnings and Precautions (5.5) ]
Drug Interactions
Anthracyclines Patients who receive anthracycline after stopping trastuzumab products may be at increased risk of cardiac dysfunction because of trastuzumab products' estimated long washout period [see Clinical Pharmacology (12.3) ] . If possible, avoid anthracycline-based therapy for up to 7 months after stopping trastuzumab products. If anthracyclines are used, closely monitor the patient's cardiac function.
Medication Information
Warnings and Precautions
Exacerbation of Chemotherapy-Induced Neutropenia. ( 5.5 , 6.1 )
Indications and Usage
HERZUMA is a HER2/neu receptor antagonist indicated in adults for: the treatment of HER2-overexpressing breast cancer. ( 1.1 , 1.2 ) the treatment of HER2-overexpressing metastatic gastric or gastroesophageal junction adenocarcinoma. ( 1.3 ) Select patients for therapy based on an FDA-approved companion diagnostic for a trastuzumab product. ( 1 , 2.2 )
Dosage and Administration
For intravenous (IV) infusion only. Do not administer as an IV push or bolus. HERZUMA has different dosage and administration instructions than subcutaneous trastuzumab products. ( 2.3 ) Do not substitute HERZUMA (trastuzumab-pkrb) for or with ado-trastuzumab emtansine or fam-trastuzumab deruxtecan. ( 2.3 ) Perform HER2 testing using FDA-approved tests by laboratories with demonstrated proficiency. ( 1 , 2.2 ) Adjuvant Treatment of HER2-Overexpressing Breast Cancer ( 2.2 ) Administer at either: Initial dose of 4 mg/kg over 90 minutes IV infusion, then 2 mg/kg over 30 minutes IV infusion weekly for 12 weeks (with paclitaxel or docetaxel) or 18 weeks (with docetaxel and carboplatin). One week after the last weekly dose of HERZUMA, administer 6 mg/kg as an IV infusion over 30 to 90 minutes every three weeks to complete a total of 52 weeks of therapy, or Initial dose of 8 mg/kg over 90 minutes IV infusion, then 6 mg/kg over 30 to 90 minutes IV infusion every three weeks for 52 weeks. Metastatic HER2-Overexpressing Breast Cancer ( 2.3 ) Initial dose of 4 mg/kg as a 90 minutes IV infusion followed by subsequent weekly doses of 2 mg/kg as 30 minutes IV infusions. Metastatic HER2-Overexpressing Gastric Cancer ( 2.3 ) Initial dose of 8 mg/kg over 90 minutes IV infusion, followed by 6 mg/kg over 30 to 90 minutes IV infusion every 3 weeks.
Contraindications
None.
Adverse Reactions
The following adverse reactions are discussed in greater detail in other sections of the label: Cardiomyopathy [see Warnings and Precautions (5.1) ] Infusion Reactions [see Warnings and Precautions (5.2) ] Embryo-Fetal Toxicity [see Warnings and Precautions (5.3) ] Pulmonary Toxicity [see Warnings and Precautions (5.4) ] Exacerbation of Chemotherapy-induced Neutropenia [see Warnings and Precautions (5.5) ]
Drug Interactions
Anthracyclines Patients who receive anthracycline after stopping trastuzumab products may be at increased risk of cardiac dysfunction because of trastuzumab products' estimated long washout period [see Clinical Pharmacology (12.3) ] . If possible, avoid anthracycline-based therapy for up to 7 months after stopping trastuzumab products. If anthracyclines are used, closely monitor the patient's cardiac function.
Description
WARNING: CARDIOMYOPATHY, INFUSION REACTIONS, EMBRYO-FETAL TOXICITY, and PULMONARY TOXICITY See full prescribing information for complete boxed warning Cardiomyopathy: Trastuzumab products can result in subclinical and clinical cardiac failure manifesting as CHF, and decreased LVEF, with greatest risk when administered concurrently with anthracyclines. Evaluate cardiac function prior to and during treatment. Discontinue HERZUMA for cardiomyopathy. ( 2.5 , 5.1 ) Infusion Reactions, Pulmonary Toxicity: Discontinue HERZUMA for anaphylaxis, angioedema, interstitial pneumonitis, or acute respiratory distress syndrome. ( 5.2 , 5.4 ) Embryo-Fetal Toxicity: Exposure to trastuzumab products during pregnancy can result in oligohydramnios, in some cases complicated by pulmonary hypoplasia and neonatal death. Advise patients of these risks and the need for effective contraception. ( 5.3 , 8.1 , 8.3 )
Section 42229-5
Cardiomyopathy
Administration of trastuzumab products can result in sub-clinical and clinical cardiac failure. The incidence and severity was highest in patients receiving trastuzumab with anthracycline-containing chemotherapy regimens.
Evaluate left ventricular function in all patients prior to and during treatment with HERZUMA. Discontinue HERZUMA treatment in patients receiving adjuvant therapy and withhold HERZUMA in patients with metastatic disease for clinically significant decrease in left ventricular function [see Dosage and Administration ( 2.5 ) and Warnings and Precautions (5.1)] .
Section 43683-2
| Dosage and Administration, Evaluation and Testing Before Initiating HERZUMA (2.1) | 11/2024 |
11 Description
Trastuzumab-pkrb is a humanized IgG1 kappa monoclonal antibody that selectively binds with high affinity to the extracellular domain of the human epidermal growth factor receptor 2 protein, HER2. Trastuzumab-pkrb is produced by recombinant DNA technology in a mammalian cell (Chinese Hamster Ovary) culture.
HERZUMA (trastuzumab-pkrb) for injection is a sterile, white to pale yellow, preservative-free lyophilized powder with a cake-like appearance, for intravenous administration.
Each multiple-dose vial of HERZUMA delivers 420 mg trastuzumab-pkrb, 839 mg α,α-trehalose dihydrate, 9.5 mg L-histidine HCl, 6.1 mg L-histidine, and 1.7 mg polysorbate 20. Reconstitution with 20 mL of the appropriate diluent (BWFI or SWFI) yields a solution containing 21 mg/mL trastuzumab-pkrb that delivers 20 mL (420 mg trastuzumab-pkrb), at a pH of approximately 6. If HERZUMA is reconstituted with SWFI without preservative, the reconstituted solution is considered single-dose.
Each single-dose vial of HERZUMA delivers 150 mg trastuzumab-pkrb, 299.6 mg α,α-trehalose dihydrate, 3.4 mg L-histidine HCl, 2.2 mg L-histidine, and 0.6 mg polysorbate 20. Reconstitution with 7.4 mL of sterile water for injection (SWFI) yields a solution containing 21 mg/mL trastuzumab-pkrb that delivers 7.15 mL (150 mg trastuzumab-pkrb), at a pH of approximately 6.
8.4 Pediatric Use
The safety and effectiveness of HERZUMA in pediatric patients have not been established.
8.5 Geriatric Use
Trastuzumab has been administered to 386 patients who were 65 years of age or over (253 in the adjuvant treatment and 133 in metastatic breast cancer treatment settings). The risk of cardiac dysfunction was increased in geriatric patients as compared to younger patients in both those receiving treatment for metastatic disease in H0648g and H0649g, or adjuvant therapy in NSABP B31 and NCCTG N9831. Limitations in data collection and differences in study design of the 4 studies of trastuzumab in adjuvant treatment of breast cancer preclude a determination of whether the toxicity profile of trastuzumab in older patients is different from younger patients. The reported clinical experience is not adequate to determine whether the efficacy improvements (ORR, TTP, OS, DFS) of trastuzumab treatment in older patients is different from that observed in patients < 65 years of age for metastatic disease and adjuvant treatment.
In ToGA (metastatic gastric cancer), of the 294 patients treated with trastuzumab, 108 (37%) were 65 years of age or older, while 13 (4.4%) were 75 and over. No overall differences in safety or effectiveness were observed.
5.1 Cardiomyopathy
Trastuzumab products can cause left ventricular cardiac dysfunction, arrhythmias, hypertension, disabling cardiac failure, cardiomyopathy, and cardiac death [see Boxed Warning: Cardiomyopathy]. Trastuzumab products can also cause asymptomatic decline in left ventricular ejection fraction (LVEF).
There is a 4 to 6 fold increase in the incidence of symptomatic myocardial dysfunction among patients receiving trastuzumab products as a single agent or in combination therapy compared with those not receiving trastuzumab products. The highest absolute incidence occurs when a trastuzumab product is administered with an anthracycline.
Withhold HERZUMA for ≥ 16% absolute decrease in LVEF from pre-treatment values or an LVEF value below institutional limits of normal and ≥ 10% absolute decrease in LVEF from pretreatment values [see Dosage and Administration (2.5)]. The safety of continuation or resumption of trastuzumab products in patients with trastuzumab product-induced left ventricular cardiac dysfunction has not been studied.
Patients who receive anthracycline after stopping trastuzumab products may also be at increased risk of cardiac dysfunction [see Drug Interactions (7) and Clinical Pharmacology (12.3)].
12.6 Immunogenicity
The observed incidence of anti-drug antibodies is highly dependent on the sensitivity and specificity of the assay. Differences in assay methods preclude meaningful comparisons of the incidence of anti-drug antibodies in the studies described below with the incidence of anti-drug antibodies in other studies, including those of trastuzumab or of other trastuzumab products.
Among 903 women with metastatic breast cancer, human anti human antibody (HAHA) to trastuzumab was detected in one patient using an enzyme linked immunosorbent assay (ELISA). This patient did not experience an allergic reaction. Samples for assessment of HAHA were not collected in studies of adjuvant breast cancer.
The clinical relevance of the development of anti-trastuzumab antibodies after treatment with trastuzumab is not known.
4 Contraindications
None.
6 Adverse Reactions
The following adverse reactions are discussed in greater detail in other sections of the label:
- Cardiomyopathy [see Warnings and Precautions (5.1)]
- Infusion Reactions [see Warnings and Precautions (5.2)]
- Embryo-Fetal Toxicity [see Warnings and Precautions (5.3)]
- Pulmonary Toxicity [see Warnings and Precautions (5.4)]
- Exacerbation of Chemotherapy-induced Neutropenia [see Warnings and Precautions (5.5)]
7 Drug Interactions
Anthracyclines
Patients who receive anthracycline after stopping trastuzumab products may be at increased risk of cardiac dysfunction because of trastuzumab products' estimated long washout period [see Clinical Pharmacology (12.3)]. If possible, avoid anthracycline-based therapy for up to 7 months after stopping trastuzumab products. If anthracyclines are used, closely monitor the patient's cardiac function.
12.3 Pharmacokinetics
The pharmacokinetics of trastuzumab were evaluated in a pooled population pharmacokinetic (PK) model analysis of 1,582 subjects with primarily breast cancer and metastatic gastric cancer (MGC) receiving intravenous trastuzumab. Total trastuzumab clearance increases with decreasing concentrations due to parallel linear and non-linear elimination pathways.
Although the average trastuzumab exposure was higher following the first cycle in breast cancer patients receiving the once every three week schedule compared to the weekly schedule of trastuzumab, the average steady-state exposure was essentially the same at both dosages. The average trastuzumab exposure following the first cycle and at steady state as well as the time to steady state was higher in breast cancer patients compared to MGC patients at the same dosage; however, the reason for this exposure difference is unknown. Additional predicted trastuzumab exposure and PK parameters following the first trastuzumab cycle and at steady state exposure are described in Tables 7 and 8, respectively.
Population PK based simulations indicate that following discontinuation of trastuzumab, concentrations in at least 95% of breast cancer patients and MGC patients will decrease to approximately 3% of the population predicted steady-state trough serum concentration (approximately 97% washout) by 7 months [see Warnings and Precautions (5.1) and Use in Specific Populations (8.1, 8.3)].
| Schedule | Primary tumor type | N | Cmin
(mcg/mL) |
Cmax
(mcg/mL) |
AUC0-21 days
(mcg.day/mL) |
|---|---|---|---|---|---|
| 8 mg/kg + 6 mg/kg q3w | Breast cancer | 1195 | 29.4 (5.8 to 59.5) |
178 (117 to 291) |
1373 (736 to 2245) |
| MGC | 274 | 23.1 (6.1 to 50.3) |
132 (84.2 to 225) |
1109 (588 to 1938) |
|
| 4 mg/kg + 2 mg/kg qw | Breast cancer | 1195 | 37.7 (12.3 to 70.9) |
88.3 (58 to 144) |
1066 (586 to 1754) |
| Schedule | Primary tumor type | N | Cmin,ss
Steady-state trough serum concentration of trastuzumab
(mcg/mL) |
Cmax,ss
Maximum steady-state serum concentration of trastuzumab
(mcg/mL) |
AUCss, 0-21 days
(mcg.day/mL) |
Time to steady-state (week) | Total CL range at steady-state (L/day) |
|---|---|---|---|---|---|---|---|
| 8 mg/kg + 6 mg/kg q3w | Breast cancer | 1195 | 47.4 (5 to 115) |
179 (107 to 309) |
1794 (673 to 3618) |
12 | 0.173 to 0.283 |
| MGC | 274 | 32.9 (6.1 to 88.9) |
131 (72.5 to 251) |
1338 (557 to 2875) |
9 | 0.189 to 0.337 | |
| 4 mg/kg + 2 mg/kg qw | Breast cancer | 1195 | 66.1 (14.9 to 142) |
109 (51.0 to 209) |
1765 (647 to 3578) |
12 | 0.201 to 0.244 |
2.2 Patient Selection
Select patients based on HER2 protein overexpression or HER2 gene amplification in tumor specimens [see Indications and Usage (1) and Clinical Studies (14)]. Assessment of HER2 protein overexpression and HER2 gene amplification should be performed using FDA-approved tests specific for breast or gastric cancers by laboratories with demonstrated proficiency. Information on the FDA-approved tests for the detection of HER2 protein overexpression and HER2 gene amplification is available at: http://www.fda.gov/CompanionDiagnostics.
Assessment of HER2 protein overexpression and HER2 gene amplification in metastatic gastric cancer should be performed using FDA-approved tests specifically for gastric cancers due to differences in gastric vs. breast histopathology, including incomplete membrane staining and more frequent heterogeneous expression of HER2 seen in gastric cancers.
Improper assay performance, including use of suboptimally fixed tissue, failure to utilize specified reagents, deviation from specific assay instructions, and failure to include appropriate controls for assay validation, can lead to unreliable results.
2.3 Recommended Dosage
- HERZUMA is for intravenous infusion only. Do not administer as an intravenous push or bolus.
- HERZUMA has different dosage and administration instructions than subcutaneous trastuzumab products.
- Do not mix HERZUMA with other drugs.
- Do not substitute HERZUMA (trastuzumab-pkrb) for or with ado-trastuzumab emtansine or fam-trastuzumab deruxtecan.
5.2 Infusion Reactions
Infusion reactions consist of a symptom complex characterized by fever and chills, and on occasion included nausea, vomiting, pain (in some cases at tumor sites), headache, dizziness, dyspnea, hypotension, rash, and asthenia [see Adverse Reactions (6.1)].
In post-marketing reports, serious and fatal infusion reactions have been reported. Severe reactions, which include bronchospasm, anaphylaxis, angioedema, hypoxia, and severe hypotension, were usually reported during or immediately following the initial infusion. However, the onset and clinical course were variable, including progressive worsening, initial improvement followed by clinical deterioration, or delayed post-infusion events with rapid clinical deterioration. For fatal events, death occurred within hours to days following a serious infusion reaction.
Interrupt HERZUMA infusion in all patients experiencing dyspnea, clinically significant hypotension, and intervention of medical therapy administered (which may include epinephrine, corticosteroids, diphenhydramine, bronchodilators, and oxygen). Patients should be evaluated and carefully monitored until complete resolution of signs and symptoms. Permanent discontinuation should be strongly considered in all patients with severe infusion reactions.
There are no data regarding the most appropriate method of identification of patients who may safely be retreated with trastuzumab products after experiencing a severe infusion reaction. Prior to resumption of trastuzumab infusion, the majority of patients who experienced a severe infusion reaction were pre-medicated with antihistamines and/or corticosteroids. While some patients tolerated trastuzumab infusions, others had recurrent severe infusion reactions despite pre-medications.
5.4 Pulmonary Toxicity
Trastuzumab product use can result in serious and fatal pulmonary toxicity. Pulmonary toxicity includes dyspnea, interstitial pneumonitis, pulmonary infiltrates, pleural effusions, non-cardiogenic pulmonary edema, pulmonary insufficiency and hypoxia, acute respiratory distress syndrome, and pulmonary fibrosis. Such events can occur as sequelae of infusion reactions [see Warnings and Precautions (5.2)]. Patients with symptomatic intrinsic lung disease or with extensive tumor involvement of the lungs, resulting in dyspnea at rest, appear to have more severe toxicity.
1 Indications and Usage
HERZUMA is a HER2/neu receptor antagonist indicated in adults for:
- the treatment of HER2-overexpressing breast cancer. (1.1, 1.2)
- the treatment of HER2-overexpressing metastatic gastric or gastroesophageal junction adenocarcinoma. (1.3)
Select patients for therapy based on an FDA-approved companion diagnostic for a trastuzumab product. (1, 2.2)
12.1 Mechanism of Action
The HER2 (or c-erbB2) proto-oncogene encodes a transmembrane receptor protein of 185 kDa, which is structurally related to the epidermal growth factor receptor. Trastuzumab products have been shown, in both in vitro assays and in animals, to inhibit the proliferation of human tumor cells that overexpress HER2.
Trastuzumab products are mediators of antibody-dependent cellular cytotoxicity (ADCC). In vitro, trastuzumab product-mediated ADCC has been shown to be preferentially exerted on HER2 overexpressing cancer cells compared with cancer cells that do not overexpress HER2.
5.3 Embryo Fetal Toxicity
Trastuzumab products can cause fetal harm when administered to a pregnant woman. In post marketing reports, use of trastuzumab during pregnancy resulted in cases of oligohydramnios and oligohydramnios sequence manifesting as pulmonary hypoplasia, skeletal abnormalities, and neonatal death.
Verify the pregnancy status of females of reproductive potential prior to the initiation of HERZUMA. Advise pregnant women and females of reproductive potential that exposure to HERZUMA during pregnancy or within 7 months prior to conception can result in fetal harm. Advise females of reproductive potential to use effective contraception during treatment and for 7 months following the last dose of HERZUMA [see Use in Specific Populations (8.1, 8.3) and Clinical Pharmacology (12.3)].
1.1 Adjuvant Breast Cancer
HERZUMA is indicated in adults for adjuvant treatment of HER2 overexpressing node positive or node negative (ER/PR negative or with one high risk feature [see Clinical Studies (14.1)]) breast cancer
- as part of a treatment regimen consisting of doxorubicin, cyclophosphamide, and either paclitaxel or docetaxel
- as part of a treatment regimen with docetaxel and carboplatin
- as a single agent following multi-modality anthracycline based therapy
Select patients for therapy based on an FDA-approved companion diagnostic for a trastuzumab product [see Dosage and Administration (2.2)].
14.1 Adjuvant Breast Cancer
The safety and efficacy of trastuzumab in women receiving adjuvant chemotherapy for HER2 overexpressing breast cancer were evaluated in an integrated analysis of two randomized, open-label, clinical trials (NSABP B31 and NCCTG N9831) with a total of 4063 women at the protocol-specified final overall survival analysis, a third randomized, open-label, clinical trial (HERA) with a total of 3386 women at definitive Disease-Free Survival analysis for one-year trastuzumab treatment versus observation, and a fourth randomized, open-label clinical trial with a total of 3222 patients (BCIRG006).
2 Dosage and Administration
For intravenous (IV) infusion only. Do not administer as an IV push or bolus. HERZUMA has different dosage and administration instructions than subcutaneous trastuzumab products. (2.3)
Do not substitute HERZUMA (trastuzumab-pkrb) for or with ado-trastuzumab emtansine or fam-trastuzumab deruxtecan. (2.3)
Perform HER2 testing using FDA-approved tests by laboratories with demonstrated proficiency. (1, 2.2)
Adjuvant Treatment of HER2-Overexpressing Breast Cancer (2.2)
Administer at either:
- Initial dose of 4 mg/kg over 90 minutes IV infusion, then 2 mg/kg over 30 minutes IV infusion weekly for 12 weeks (with paclitaxel or docetaxel) or 18 weeks (with docetaxel and carboplatin). One week after the last weekly dose of HERZUMA, administer 6 mg/kg as an IV infusion over 30 to 90 minutes every three weeks to complete a total of 52 weeks of therapy, or
- Initial dose of 8 mg/kg over 90 minutes IV infusion, then 6 mg/kg over 30 to 90 minutes IV infusion every three weeks for 52 weeks.
Metastatic HER2-Overexpressing Breast Cancer (2.3)
- Initial dose of 4 mg/kg as a 90 minutes IV infusion followed by subsequent weekly doses of 2 mg/kg as 30 minutes IV infusions.
Metastatic HER2-Overexpressing Gastric Cancer (2.3)
- Initial dose of 8 mg/kg over 90 minutes IV infusion, followed by 6 mg/kg over 30 to 90 minutes IV infusion every 3 weeks.
1.2 Metastatic Breast Cancer
HERZUMA is indicated in adults:
- In combination with paclitaxel for first-line treatment of HER2-overexpressing metastatic breast cancer
- As a single agent for treatment of HER2-overexpressing breast cancer in patients who have received one or more chemotherapy regimens for metastatic disease.
Select patients for therapy based on an FDA-approved companion diagnostic for a trastuzumab product [see Dosage and Administration (2.2)].
2.6 Preparation Instructions
To prevent medication errors, it is important to check the vial labels to ensure that the drug being prepared and administered is HERZUMA (trastuzumab-pkrb) and not ado-trastuzumab emtansine or fam-trastuzumab deruxtecan.
420 mg Multiple-dose vial
Reconstitution
Reconstitute each 420 mg vial of HERZUMA with 20 mL of Bacteriostatic Water for Injection (BWFI), USP, containing 1.1% benzyl alcohol as a preservative to yield a multiple-dose solution containing 21 mg/mL trastuzumab-pkrb that delivers 20 mL (420 mg trastuzumab-pkrb). In patients with known hypersensitivity to benzyl alcohol, reconstitute with 20 mL of Sterile Water for Injection (SWFI) without preservative to yield a one-time use solution.
Use appropriate aseptic technique when performing the following reconstitution steps:
- Using a sterile syringe, slowly inject the 20 mL of diluent into the vial containing the lyophilized powder of HERZUMA, which has a cake-like appearance. The stream of diluent should be directed into the cake. The reconstituted vial yields a solution for multiple-dose use, containing 21 mg/mL trastuzumab-pkrb.
- Swirl the vial gently to aid reconstitution. DO NOT SHAKE.
- Slight foaming of the product may be present upon reconstitution. Allow the vial to stand undisturbed for approximately 5 minutes.
- Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration, whenever solution and container permit. Inspect visually for particulates and discoloration. The solution should be free of visible particulates, clear to slightly opalescent and colorless to pale yellow.
- Store reconstituted HERZUMA in the refrigerator at 2°C to 8°C (36°F to 46°F); discard unused HERZUMA after 28 days. If HERZUMA is reconstituted with SWFI without preservative, use immediately and discard any unused portion. Do not freeze.
Dilution
- Determine the dose (mg) of HERZUMA [see Dosage and Administration (2.3)]. Calculate the volume of the 21 mg/mL reconstituted HERZUMA solution needed, withdraw this amount from the vial using a sterile needle and syringe and add it to an infusion bag containing 250 mL of 0.9% Sodium Chloride Injection, USP. DO NOT USE DEXTROSE (5%) SOLUTION.
- Gently invert the bag to mix the solution.
- The solution of HERZUMA for infusion diluted in polyvinylchloride or polyethylene bags containing 0.9% Sodium Chloride Injection, USP, should be stored at 2°C to 8°C (36°F to 46°F) for no more than 24 hours prior to use. This storage time is additional to the time allowed for the reconstituted vials. Do not freeze.
150 mg Single-dose vial
Reconstitution
Reconstitute each 150 mg vial of HERZUMA with 7.4 mL of Sterile Water for Injection (SWFI) (not supplied) to yield a single-dose solution containing 21 mg/mL trastuzumab-pkrb that delivers 7.15 mL (150 mg trastuzumab-pkrb).
Use appropriate aseptic technique when performing the following reconstitution steps:
- Using a sterile syringe, slowly inject 7.4 mL of SWFI (not supplied) into the vial containing the lyophilized powder of HERZUMA, which has a cake-like appearance. The stream of diluent should be directed into the cake. The reconstituted vial yields a solution containing 21 mg/mL trastuzumab-pkrb.
- Swirl the vial gently to aid reconstitution. DO NOT SHAKE.
- Slight foaming of the product may be present upon reconstitution. Allow the vial to stand undisturbed for approximately 5 minutes.
- Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration, whenever solution and container permit. Inspect visually for particulates and discoloration. The solution should be free of visible particulates, clear to slightly opalescent and colorless to pale yellow.
- Use the HERZUMA solution immediately following reconstitution with SWFI, as it contains no preservative and is intended for one-time use only. If not used immediately, store the reconstituted HERZUMA solution for up to 24 hours at 2°C to 8°C (36°F to 46°F); discard any unused HERZUMA after 24 hours. Do not freeze.
Dilution
- Determine the dose (mg) of HERZUMA [see Dosage and Administration (2.3)].
- Calculate the volume of the 21 mg/mL reconstituted HERZUMA solution needed.
- Withdraw this amount from the vial using a sterile needle and syringe and add it to an infusion bag containing 250 mL of 0.9% Sodium Chloride Injection, USP. DO NOT USE DEXTROSE (5%) SOLUTION.
- Gently invert the bag to mix the solution.
- The solution of HERZUMA for infusion diluted in polyvinylchloride or polyethylene bags containing 0.9% Sodium Chloride Injection, USP, should be stored at 2°C to 8°C (36°F to 46°F) for no more than 24 hours prior to use. Discard after 24 hours. This storage time is additional to the time allowed for the reconstituted vials. Do not freeze.
3 Dosage Forms and Strengths
- For injection: 150 mg of HERZUMA as a white to pale yellow lyophilized powder in a single-dose vial
- For injection: 420 mg of HERZUMA as a white to pale yellow lyophilized powder in a multiple-dose vial.
1.3 Metastatic Gastric Cancer
HERZUMA is indicated in adults, in combination with cisplatin and capecitabine or 5-fluorouracil, for the treatment of patients with HER2 overexpressing metastatic gastric or gastroesophageal junction adenocarcinoma who have not received prior treatment for metastatic disease.
Select patients for therapy based on an FDA-approved companion diagnostic for a trastuzumab product [see Dosage and Administration (2.2)].
14.2 Metastatic Breast Cancer
The safety and efficacy of trastuzumab in treatment of women with metastatic breast cancer were studied in a randomized, controlled clinical trial in combination with chemotherapy (H0648g, n = 469 patients) and an open-label, single agent clinical trial (H0649g, n = 222 patients). Both trials studied patients with metastatic breast cancer whose tumors overexpress the HER2 protein. Patients were eligible if they had 2 or 3 levels of overexpression (based on a 0 to 3 scale) by immunohistochemical assessment of tumor tissue performed by a central testing lab.
8 Use in Specific Populations
Females and Males of Reproductive Potential: Verify the pregnancy status of females prior to initiation of HERZUMA. (8.3)
14.3 Metastatic Gastric Cancer
The safety and efficacy of trastuzumab in combination with cisplatin and a fluoropyrimidine (capecitabine or 5-fluorouracil) were studied in patients previously untreated for metastatic gastric or gastroesophageal junction adenocarcinoma (ToGA). In this open-label, multi-center trial, 594 patients were randomized 1:1 to trastuzumab in combination with cisplatin and a fluoropyrimidine (FC+H) or chemotherapy alone (FC). Randomization was stratified by extent of disease (metastatic vs. locally advanced), primary site (gastric vs. gastroesophageal junction), tumor measurability (yes vs. no), ECOG performance status (0, 1 vs. 2), and fluoropyrimidine (capecitabine vs. 5-fluorouracil). All patients were either HER2 gene amplified (FISH+) or HER2 overexpressing (IHC 3+). Patients were also required to have adequate cardiac function (e.g., LVEF > 50%).
On the trastuzumab-containing arm, trastuzumab was administered as an IV infusion at an initial dose of 8 mg/kg followed by 6 mg/kg every 3 weeks until disease progression. On both study arms, cisplatin was administered at a dose of 80 mg/m2 Day 1 every 3 weeks for 6 cycles as a 2 hour IV infusion. On both study arms, capecitabine was administered at 1000 mg/m2 dose orally twice daily (total daily dose 2000 mg/m2) for 14 days of each 21 day cycle for 6 cycles. Alternatively, continuous intravenous infusion (CIV) 5-fluorouracil was administered at a dose of 800 mg/m2/day from Day 1 through Day 5 every three weeks for 6 cycles.
The median age of the study population was 60 years (range: 21 to 83); 76% were male; 53% were Asian, 38% Caucasian, 5% Hispanic, 5% other racial/ethnic groups; 91% had ECOG PS of 0 or 1; 82% had primary gastric cancer and 18% had primary gastroesophageal adenocarcinoma. Of these patients, 23% had undergone prior gastrectomy, 7% had received prior neoadjuvant and/or adjuvant therapy, and 2% had received prior radiotherapy.
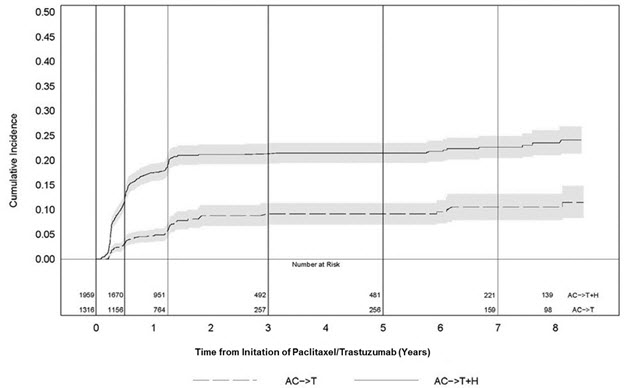
The main outcome measure of ToGA was overall survival (OS), analyzed by the unstratified log-rank test. The final OS analysis based on 351 deaths was statistically significant (nominal significance level of 0.0193). An updated OS analysis was conducted at one year after the final analysis. The efficacy results of both the final and the updated analyses are summarized in Table 13 and Figure 7.
| FC + Trastuzumab Arm N = 298 |
FC FC = capecitabine vs. 5-fluorouracil ArmN = 296 |
|
|---|---|---|
| Overall Survival (interim analysis) | ||
| N (%) | 167 (56.0%) | 184 (62.2%) |
| Median (months) | 13.5 | 11.0 |
| 95% CI | (11.7, 15.7) | (9.4, 12.5) |
| Hazard Ratio | 0.73 | |
| 95% CI | (0.60, 0.91) | |
| p value Two sided p-value comparing with the nominal significance level of 0.0193
|
0.0038 | |
| Overall Survival (updated) | ||
| N (%) | 221 (74.2%) | 227 (76.7%) |
| Median (months) | 13.1 | 11.7 |
| 95% CI | (11.9, 15.1) | (10.3, 13.0) |
| Hazard Ratio | 0.80 | |
| 95% CI | (0.67, 0.97) |
Figure 7: Updated Overall Survival in Patients with Metastatic Gastric Cancer (ToGA)
An exploratory analysis of OS in patients based on HER2 gene amplification (FISH) and protein overexpression (IHC) testing is summarized in Table 14.
| FC (N = 296) Two patients on the FC arm who were FISH+ but IHC status unknown were excluded from the exploratory subgroup analyses.
|
FC + H (N = 298) Five patients on the trastuzumab-containing arm who were FISH+, but IHC status unknown were excluded from the exploratory subgroup analyses.
|
|
|---|---|---|
| FISH+ / IHC 0, 1+ subgroup (N=133) | ||
| No. Deaths / n (%) | 57/71 (80%) | 56/62 (90%) |
| Median OS Duration (mos.) | 8.8 | 8.3 |
| 95% CI (mos.) | (6.4, 11.7) | (6.2, 10.7) |
| Hazard ratio (95% CI) | 1.33 (0.92, 1.92) | |
| FISH+ / IHC2+ subgroup (N=160) | ||
| No. Deaths / n (%) | 65/80 (81%) | 64/80 (80%) |
| Median OS Duration (mos.) | 10.8 | 12.3 |
| 95% CI (mos.) | (6.8, 12.8) | (9.5, 15.7) |
| Hazard ratio (95% CI) | 0.78 (0.55, 1.10) | |
|
FISH+ or FISH- / IHC3+ Includes 6 patients on chemotherapy arm, 10 patients on trastuzumab arm with FISH–, IHC3+ and 8 patients on chemotherapy arm, 8 patients on trastuzumab arm with FISH status unknown, IHC 3+. subgroup (N=294)
|
||
| No. Deaths / n (%) | 104/143 (73%) | 96/151 (64%) |
| Median OS Duration (mos.) | 13.2 | 18.0 |
| 95% CI (mos.) | (11.5, 15.2) | (15.5, 21.2) |
| Hazard ratio (95% CI) | 0.66 (0.50, 0.87) |
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
The most common adverse reactions in patients receiving trastuzumab products in the adjuvant and metastatic breast cancer setting are fever, nausea, vomiting, infusion reactions, diarrhea, infections, increased cough, headache, fatigue, dyspnea, rash, neutropenia, anemia, and myalgia. Adverse reactions requiring interruption or discontinuation of trastuzumab product treatment include CHF, significant decline in left ventricular cardiac function, severe infusion reactions, and pulmonary toxicity [see Dosage and Administration (2.5)].
In the metastatic gastric cancer setting, the most common adverse reactions (≥ 10%) that were increased (≥ 5% difference) in the trastuzumab arm as compared to the chemotherapy alone arm were neutropenia, diarrhea, fatigue, anemia, stomatitis, weight loss, upper respiratory tract infections, fever, thrombocytopenia, mucosal inflammation, nasopharyngitis, and dysgeusia.
The most common adverse reactions which resulted in discontinuation of treatment on the trastuzumab-containing arm in the absence of disease progression were infection, diarrhea, and febrile neutropenia.
6.2 Post Marketing Experience
The following adverse reactions have been identified during post-approval use of trastuzumab products. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
- Infusion reaction [see Warnings and Precautions (5.2)]
- Oligohydramnios or oligohydramnios sequence, including pulmonary hypoplasia, skeletal abnormalities, and neonatal death [see Warnings and Precautions (5.3)]
- Glomerulopathy [see Adverse Reactions (6.1)]
- Immune thrombocytopenia
- Tumor lysis syndrome (TLS): Cases of possible TLS have been reported in patients treated with trastuzumab products. Patients with significant tumor burden (e.g. bulky metastases) may be at a higher risk. Patients could present with hyperuricemia, hyperphosphatemia, and acute renal failure which may represent possible TLS. Providers should consider additional monitoring and/or treatment as clinically indicated.
2.4 Important Dosing Considerations
Missed Dose
If the patient has missed a dose of HERZUMA by one week or less, then the usual maintenance dose (weekly schedule: 2 mg/kg; once every three week schedule: 6 mg/kg) should be administered as soon as possible. Do not wait until the next planned cycle. Subsequent HERZUMA maintenance doses should be administered 7 days or 21 days later according to the weekly or once every three week schedules, respectively.
If the patient has missed a dose of HERZUMA by more than one week, a re-loading dose of HERZUMA should be administered over approximately 90 minutes (weekly schedule: 4 mg/kg; once every three week schedule: 8 mg/kg) as soon as possible. Subsequent HERZUMA maintenance doses (weekly schedule: 2 mg/kg; once every three week schedule 6 mg/kg) should be administered 7 days or 21 days later according to the weekly or once every three week schedules, respectively.
Principal Display Panel Kit Carton Label
NDC 63459-305-47
Rx only
Multiple-dose vial
Herzuma®
(trastuzumab-pkrb)
For Injection
420 mg/vial
For Intravenous Infusion Only.
Reconstitution and dilution required (see insert).
No preservative
KEEP REFRIGERATED
teva
Principal Display Panel 150 Mg Vial Label
NDC 63459-303-43
Rx only
Single-dose vial
Herzuma®
(trastuzumab-pkrb)
For Injection
150 mg/vial
For Intravenous Infusion Only.
Reconstitution and dilution required (see insert).
No preservative
KEEP REFRIGERATED
teva
2.5 Dosage Modifications for Adverse Reactions
Infusion Reactions
[see Boxed Warning, Warnings and Precautions (5.2)]
- Decrease the rate of infusion for mild or moderate infusion reactions
- Interrupt the infusion in patients with dyspnea or clinically significant hypotension
- Discontinue HERZUMA for severe or life-threatening infusion reactions.
Cardiomyopathy
[see Boxed Warning, Warnings and Precautions (5.1)]
Assess left ventricular ejection fraction (LVEF) prior to initiation of HERZUMA and at regular intervals during treatment. Withhold HERZUMA dosing for at least 4 weeks for either of the following:
- ≥ 16% absolute decrease in LVEF from pre-treatment values
- LVEF below institutional limits of normal and ≥ 10% absolute decrease in LVEF from pretreatment values.
HERZUMA may be resumed if, within 4 to 8 weeks, the LVEF returns to normal limits and the absolute decrease from baseline is ≤ 15%.
Permanently discontinue HERZUMA for a persistent (> 8 weeks) LVEF decline or for suspension of HERZUMA dosing on more than 3 occasions for cardiomyopathy.
5.5 Exacerbation of Chemotherapy Induced Neutropenia
In randomized, controlled clinical trials, the per-patient incidences of NCI-CTC Grade 3 to 4 neutropenia and of febrile neutropenia were higher in patients receiving trastuzumab in combination with myelosuppressive chemotherapy as compared to those who received chemotherapy alone. The incidence of septic death was similar among patients who received trastuzumab and those who did not [see Adverse Reactions (6.1)].
2.1 evaluation and Testing Before Initiating Herzuma
Assess left ventricular ejection fraction (LVEF) prior to initiation of HERZUMA and at regular intervals during treatment. [see Boxed Warning, Dosage and Administration (2.5), Warnings and Precautions (5.1)].
Verify the pregnancy status of females of reproductive potential prior to the initiation of HERZUMA [see Warnings and Precautions (5.3), Use in Specific Populations (8.1, 8.3)].
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Trastuzumab products have not been tested for carcinogenic potential.
No evidence of mutagenic activity was observed when trastuzumab was tested in the standard Ames bacterial and human peripheral blood lymphocyte mutagenicity assays, at concentrations of up to 5000 mcg/mL. In an in vivo micronucleus assay, no evidence of chromosomal damage to mouse bone marrow cells was observed following bolus intravenous doses of up to 118 mg/kg of trastuzumab.
A fertility study was conducted in female Cynomolgus monkeys at doses up to 25 times the weekly recommended human dose of 2 mg/kg of trastuzumab and has revealed no evidence of impaired fertility, as measured by menstrual cycle duration and female sex hormone levels.
Warning: Cardiomyopathy, Infusion Reactions, Embryo Fetal Toxicity, and Pulmonary Toxicity
WARNING: CARDIOMYOPATHY, INFUSION REACTIONS, EMBRYO-FETAL TOXICITY, and PULMONARY TOXICITY
See full prescribing information for complete boxed warning
Cardiomyopathy: Trastuzumab products can result in subclinical and clinical cardiac failure manifesting as CHF, and decreased LVEF, with greatest risk when administered concurrently with anthracyclines. Evaluate cardiac function prior to and during treatment. Discontinue HERZUMA for cardiomyopathy. (2.5, 5.1)
Infusion Reactions, Pulmonary Toxicity: Discontinue HERZUMA for anaphylaxis, angioedema, interstitial pneumonitis, or acute respiratory distress syndrome. (5.2, 5.4)
Embryo-Fetal Toxicity: Exposure to trastuzumab products during pregnancy can result in oligohydramnios, in some cases complicated by pulmonary hypoplasia and neonatal death. Advise patients of these risks and the need for effective contraception. (5.3, 8.1, 8.3)
Structured Label Content
Section 42229-5 (42229-5)
Cardiomyopathy
Administration of trastuzumab products can result in sub-clinical and clinical cardiac failure. The incidence and severity was highest in patients receiving trastuzumab with anthracycline-containing chemotherapy regimens.
Evaluate left ventricular function in all patients prior to and during treatment with HERZUMA. Discontinue HERZUMA treatment in patients receiving adjuvant therapy and withhold HERZUMA in patients with metastatic disease for clinically significant decrease in left ventricular function [see Dosage and Administration ( 2.5 ) and Warnings and Precautions (5.1)] .
Section 43683-2 (43683-2)
| Dosage and Administration, Evaluation and Testing Before Initiating HERZUMA (2.1) | 11/2024 |
11 Description (11 DESCRIPTION)
Trastuzumab-pkrb is a humanized IgG1 kappa monoclonal antibody that selectively binds with high affinity to the extracellular domain of the human epidermal growth factor receptor 2 protein, HER2. Trastuzumab-pkrb is produced by recombinant DNA technology in a mammalian cell (Chinese Hamster Ovary) culture.
HERZUMA (trastuzumab-pkrb) for injection is a sterile, white to pale yellow, preservative-free lyophilized powder with a cake-like appearance, for intravenous administration.
Each multiple-dose vial of HERZUMA delivers 420 mg trastuzumab-pkrb, 839 mg α,α-trehalose dihydrate, 9.5 mg L-histidine HCl, 6.1 mg L-histidine, and 1.7 mg polysorbate 20. Reconstitution with 20 mL of the appropriate diluent (BWFI or SWFI) yields a solution containing 21 mg/mL trastuzumab-pkrb that delivers 20 mL (420 mg trastuzumab-pkrb), at a pH of approximately 6. If HERZUMA is reconstituted with SWFI without preservative, the reconstituted solution is considered single-dose.
Each single-dose vial of HERZUMA delivers 150 mg trastuzumab-pkrb, 299.6 mg α,α-trehalose dihydrate, 3.4 mg L-histidine HCl, 2.2 mg L-histidine, and 0.6 mg polysorbate 20. Reconstitution with 7.4 mL of sterile water for injection (SWFI) yields a solution containing 21 mg/mL trastuzumab-pkrb that delivers 7.15 mL (150 mg trastuzumab-pkrb), at a pH of approximately 6.
8.4 Pediatric Use
The safety and effectiveness of HERZUMA in pediatric patients have not been established.
8.5 Geriatric Use
Trastuzumab has been administered to 386 patients who were 65 years of age or over (253 in the adjuvant treatment and 133 in metastatic breast cancer treatment settings). The risk of cardiac dysfunction was increased in geriatric patients as compared to younger patients in both those receiving treatment for metastatic disease in H0648g and H0649g, or adjuvant therapy in NSABP B31 and NCCTG N9831. Limitations in data collection and differences in study design of the 4 studies of trastuzumab in adjuvant treatment of breast cancer preclude a determination of whether the toxicity profile of trastuzumab in older patients is different from younger patients. The reported clinical experience is not adequate to determine whether the efficacy improvements (ORR, TTP, OS, DFS) of trastuzumab treatment in older patients is different from that observed in patients < 65 years of age for metastatic disease and adjuvant treatment.
In ToGA (metastatic gastric cancer), of the 294 patients treated with trastuzumab, 108 (37%) were 65 years of age or older, while 13 (4.4%) were 75 and over. No overall differences in safety or effectiveness were observed.
5.1 Cardiomyopathy
Trastuzumab products can cause left ventricular cardiac dysfunction, arrhythmias, hypertension, disabling cardiac failure, cardiomyopathy, and cardiac death [see Boxed Warning: Cardiomyopathy]. Trastuzumab products can also cause asymptomatic decline in left ventricular ejection fraction (LVEF).
There is a 4 to 6 fold increase in the incidence of symptomatic myocardial dysfunction among patients receiving trastuzumab products as a single agent or in combination therapy compared with those not receiving trastuzumab products. The highest absolute incidence occurs when a trastuzumab product is administered with an anthracycline.
Withhold HERZUMA for ≥ 16% absolute decrease in LVEF from pre-treatment values or an LVEF value below institutional limits of normal and ≥ 10% absolute decrease in LVEF from pretreatment values [see Dosage and Administration (2.5)]. The safety of continuation or resumption of trastuzumab products in patients with trastuzumab product-induced left ventricular cardiac dysfunction has not been studied.
Patients who receive anthracycline after stopping trastuzumab products may also be at increased risk of cardiac dysfunction [see Drug Interactions (7) and Clinical Pharmacology (12.3)].
12.6 Immunogenicity
The observed incidence of anti-drug antibodies is highly dependent on the sensitivity and specificity of the assay. Differences in assay methods preclude meaningful comparisons of the incidence of anti-drug antibodies in the studies described below with the incidence of anti-drug antibodies in other studies, including those of trastuzumab or of other trastuzumab products.
Among 903 women with metastatic breast cancer, human anti human antibody (HAHA) to trastuzumab was detected in one patient using an enzyme linked immunosorbent assay (ELISA). This patient did not experience an allergic reaction. Samples for assessment of HAHA were not collected in studies of adjuvant breast cancer.
The clinical relevance of the development of anti-trastuzumab antibodies after treatment with trastuzumab is not known.
4 Contraindications (4 CONTRAINDICATIONS)
None.
6 Adverse Reactions (6 ADVERSE REACTIONS)
The following adverse reactions are discussed in greater detail in other sections of the label:
- Cardiomyopathy [see Warnings and Precautions (5.1)]
- Infusion Reactions [see Warnings and Precautions (5.2)]
- Embryo-Fetal Toxicity [see Warnings and Precautions (5.3)]
- Pulmonary Toxicity [see Warnings and Precautions (5.4)]
- Exacerbation of Chemotherapy-induced Neutropenia [see Warnings and Precautions (5.5)]
7 Drug Interactions (7 DRUG INTERACTIONS)
Anthracyclines
Patients who receive anthracycline after stopping trastuzumab products may be at increased risk of cardiac dysfunction because of trastuzumab products' estimated long washout period [see Clinical Pharmacology (12.3)]. If possible, avoid anthracycline-based therapy for up to 7 months after stopping trastuzumab products. If anthracyclines are used, closely monitor the patient's cardiac function.
12.3 Pharmacokinetics
The pharmacokinetics of trastuzumab were evaluated in a pooled population pharmacokinetic (PK) model analysis of 1,582 subjects with primarily breast cancer and metastatic gastric cancer (MGC) receiving intravenous trastuzumab. Total trastuzumab clearance increases with decreasing concentrations due to parallel linear and non-linear elimination pathways.
Although the average trastuzumab exposure was higher following the first cycle in breast cancer patients receiving the once every three week schedule compared to the weekly schedule of trastuzumab, the average steady-state exposure was essentially the same at both dosages. The average trastuzumab exposure following the first cycle and at steady state as well as the time to steady state was higher in breast cancer patients compared to MGC patients at the same dosage; however, the reason for this exposure difference is unknown. Additional predicted trastuzumab exposure and PK parameters following the first trastuzumab cycle and at steady state exposure are described in Tables 7 and 8, respectively.
Population PK based simulations indicate that following discontinuation of trastuzumab, concentrations in at least 95% of breast cancer patients and MGC patients will decrease to approximately 3% of the population predicted steady-state trough serum concentration (approximately 97% washout) by 7 months [see Warnings and Precautions (5.1) and Use in Specific Populations (8.1, 8.3)].
| Schedule | Primary tumor type | N | Cmin
(mcg/mL) |
Cmax
(mcg/mL) |
AUC0-21 days
(mcg.day/mL) |
|---|---|---|---|---|---|
| 8 mg/kg + 6 mg/kg q3w | Breast cancer | 1195 | 29.4 (5.8 to 59.5) |
178 (117 to 291) |
1373 (736 to 2245) |
| MGC | 274 | 23.1 (6.1 to 50.3) |
132 (84.2 to 225) |
1109 (588 to 1938) |
|
| 4 mg/kg + 2 mg/kg qw | Breast cancer | 1195 | 37.7 (12.3 to 70.9) |
88.3 (58 to 144) |
1066 (586 to 1754) |
| Schedule | Primary tumor type | N | Cmin,ss
Steady-state trough serum concentration of trastuzumab
(mcg/mL) |
Cmax,ss
Maximum steady-state serum concentration of trastuzumab
(mcg/mL) |
AUCss, 0-21 days
(mcg.day/mL) |
Time to steady-state (week) | Total CL range at steady-state (L/day) |
|---|---|---|---|---|---|---|---|
| 8 mg/kg + 6 mg/kg q3w | Breast cancer | 1195 | 47.4 (5 to 115) |
179 (107 to 309) |
1794 (673 to 3618) |
12 | 0.173 to 0.283 |
| MGC | 274 | 32.9 (6.1 to 88.9) |
131 (72.5 to 251) |
1338 (557 to 2875) |
9 | 0.189 to 0.337 | |
| 4 mg/kg + 2 mg/kg qw | Breast cancer | 1195 | 66.1 (14.9 to 142) |
109 (51.0 to 209) |
1765 (647 to 3578) |
12 | 0.201 to 0.244 |
2.2 Patient Selection
Select patients based on HER2 protein overexpression or HER2 gene amplification in tumor specimens [see Indications and Usage (1) and Clinical Studies (14)]. Assessment of HER2 protein overexpression and HER2 gene amplification should be performed using FDA-approved tests specific for breast or gastric cancers by laboratories with demonstrated proficiency. Information on the FDA-approved tests for the detection of HER2 protein overexpression and HER2 gene amplification is available at: http://www.fda.gov/CompanionDiagnostics.
Assessment of HER2 protein overexpression and HER2 gene amplification in metastatic gastric cancer should be performed using FDA-approved tests specifically for gastric cancers due to differences in gastric vs. breast histopathology, including incomplete membrane staining and more frequent heterogeneous expression of HER2 seen in gastric cancers.
Improper assay performance, including use of suboptimally fixed tissue, failure to utilize specified reagents, deviation from specific assay instructions, and failure to include appropriate controls for assay validation, can lead to unreliable results.
2.3 Recommended Dosage
- HERZUMA is for intravenous infusion only. Do not administer as an intravenous push or bolus.
- HERZUMA has different dosage and administration instructions than subcutaneous trastuzumab products.
- Do not mix HERZUMA with other drugs.
- Do not substitute HERZUMA (trastuzumab-pkrb) for or with ado-trastuzumab emtansine or fam-trastuzumab deruxtecan.
5.2 Infusion Reactions
Infusion reactions consist of a symptom complex characterized by fever and chills, and on occasion included nausea, vomiting, pain (in some cases at tumor sites), headache, dizziness, dyspnea, hypotension, rash, and asthenia [see Adverse Reactions (6.1)].
In post-marketing reports, serious and fatal infusion reactions have been reported. Severe reactions, which include bronchospasm, anaphylaxis, angioedema, hypoxia, and severe hypotension, were usually reported during or immediately following the initial infusion. However, the onset and clinical course were variable, including progressive worsening, initial improvement followed by clinical deterioration, or delayed post-infusion events with rapid clinical deterioration. For fatal events, death occurred within hours to days following a serious infusion reaction.
Interrupt HERZUMA infusion in all patients experiencing dyspnea, clinically significant hypotension, and intervention of medical therapy administered (which may include epinephrine, corticosteroids, diphenhydramine, bronchodilators, and oxygen). Patients should be evaluated and carefully monitored until complete resolution of signs and symptoms. Permanent discontinuation should be strongly considered in all patients with severe infusion reactions.
There are no data regarding the most appropriate method of identification of patients who may safely be retreated with trastuzumab products after experiencing a severe infusion reaction. Prior to resumption of trastuzumab infusion, the majority of patients who experienced a severe infusion reaction were pre-medicated with antihistamines and/or corticosteroids. While some patients tolerated trastuzumab infusions, others had recurrent severe infusion reactions despite pre-medications.
5.4 Pulmonary Toxicity
Trastuzumab product use can result in serious and fatal pulmonary toxicity. Pulmonary toxicity includes dyspnea, interstitial pneumonitis, pulmonary infiltrates, pleural effusions, non-cardiogenic pulmonary edema, pulmonary insufficiency and hypoxia, acute respiratory distress syndrome, and pulmonary fibrosis. Such events can occur as sequelae of infusion reactions [see Warnings and Precautions (5.2)]. Patients with symptomatic intrinsic lung disease or with extensive tumor involvement of the lungs, resulting in dyspnea at rest, appear to have more severe toxicity.
1 Indications and Usage (1 INDICATIONS AND USAGE)
HERZUMA is a HER2/neu receptor antagonist indicated in adults for:
- the treatment of HER2-overexpressing breast cancer. (1.1, 1.2)
- the treatment of HER2-overexpressing metastatic gastric or gastroesophageal junction adenocarcinoma. (1.3)
Select patients for therapy based on an FDA-approved companion diagnostic for a trastuzumab product. (1, 2.2)
12.1 Mechanism of Action
The HER2 (or c-erbB2) proto-oncogene encodes a transmembrane receptor protein of 185 kDa, which is structurally related to the epidermal growth factor receptor. Trastuzumab products have been shown, in both in vitro assays and in animals, to inhibit the proliferation of human tumor cells that overexpress HER2.
Trastuzumab products are mediators of antibody-dependent cellular cytotoxicity (ADCC). In vitro, trastuzumab product-mediated ADCC has been shown to be preferentially exerted on HER2 overexpressing cancer cells compared with cancer cells that do not overexpress HER2.
5.3 Embryo Fetal Toxicity (5.3 Embryo-Fetal Toxicity)
Trastuzumab products can cause fetal harm when administered to a pregnant woman. In post marketing reports, use of trastuzumab during pregnancy resulted in cases of oligohydramnios and oligohydramnios sequence manifesting as pulmonary hypoplasia, skeletal abnormalities, and neonatal death.
Verify the pregnancy status of females of reproductive potential prior to the initiation of HERZUMA. Advise pregnant women and females of reproductive potential that exposure to HERZUMA during pregnancy or within 7 months prior to conception can result in fetal harm. Advise females of reproductive potential to use effective contraception during treatment and for 7 months following the last dose of HERZUMA [see Use in Specific Populations (8.1, 8.3) and Clinical Pharmacology (12.3)].
1.1 Adjuvant Breast Cancer
HERZUMA is indicated in adults for adjuvant treatment of HER2 overexpressing node positive or node negative (ER/PR negative or with one high risk feature [see Clinical Studies (14.1)]) breast cancer
- as part of a treatment regimen consisting of doxorubicin, cyclophosphamide, and either paclitaxel or docetaxel
- as part of a treatment regimen with docetaxel and carboplatin
- as a single agent following multi-modality anthracycline based therapy
Select patients for therapy based on an FDA-approved companion diagnostic for a trastuzumab product [see Dosage and Administration (2.2)].
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
14.1 Adjuvant Breast Cancer
The safety and efficacy of trastuzumab in women receiving adjuvant chemotherapy for HER2 overexpressing breast cancer were evaluated in an integrated analysis of two randomized, open-label, clinical trials (NSABP B31 and NCCTG N9831) with a total of 4063 women at the protocol-specified final overall survival analysis, a third randomized, open-label, clinical trial (HERA) with a total of 3386 women at definitive Disease-Free Survival analysis for one-year trastuzumab treatment versus observation, and a fourth randomized, open-label clinical trial with a total of 3222 patients (BCIRG006).
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
For intravenous (IV) infusion only. Do not administer as an IV push or bolus. HERZUMA has different dosage and administration instructions than subcutaneous trastuzumab products. (2.3)
Do not substitute HERZUMA (trastuzumab-pkrb) for or with ado-trastuzumab emtansine or fam-trastuzumab deruxtecan. (2.3)
Perform HER2 testing using FDA-approved tests by laboratories with demonstrated proficiency. (1, 2.2)
Adjuvant Treatment of HER2-Overexpressing Breast Cancer (2.2)
Administer at either:
- Initial dose of 4 mg/kg over 90 minutes IV infusion, then 2 mg/kg over 30 minutes IV infusion weekly for 12 weeks (with paclitaxel or docetaxel) or 18 weeks (with docetaxel and carboplatin). One week after the last weekly dose of HERZUMA, administer 6 mg/kg as an IV infusion over 30 to 90 minutes every three weeks to complete a total of 52 weeks of therapy, or
- Initial dose of 8 mg/kg over 90 minutes IV infusion, then 6 mg/kg over 30 to 90 minutes IV infusion every three weeks for 52 weeks.
Metastatic HER2-Overexpressing Breast Cancer (2.3)
- Initial dose of 4 mg/kg as a 90 minutes IV infusion followed by subsequent weekly doses of 2 mg/kg as 30 minutes IV infusions.
Metastatic HER2-Overexpressing Gastric Cancer (2.3)
- Initial dose of 8 mg/kg over 90 minutes IV infusion, followed by 6 mg/kg over 30 to 90 minutes IV infusion every 3 weeks.
1.2 Metastatic Breast Cancer
HERZUMA is indicated in adults:
- In combination with paclitaxel for first-line treatment of HER2-overexpressing metastatic breast cancer
- As a single agent for treatment of HER2-overexpressing breast cancer in patients who have received one or more chemotherapy regimens for metastatic disease.
Select patients for therapy based on an FDA-approved companion diagnostic for a trastuzumab product [see Dosage and Administration (2.2)].
2.6 Preparation Instructions
To prevent medication errors, it is important to check the vial labels to ensure that the drug being prepared and administered is HERZUMA (trastuzumab-pkrb) and not ado-trastuzumab emtansine or fam-trastuzumab deruxtecan.
420 mg Multiple-dose vial
Reconstitution
Reconstitute each 420 mg vial of HERZUMA with 20 mL of Bacteriostatic Water for Injection (BWFI), USP, containing 1.1% benzyl alcohol as a preservative to yield a multiple-dose solution containing 21 mg/mL trastuzumab-pkrb that delivers 20 mL (420 mg trastuzumab-pkrb). In patients with known hypersensitivity to benzyl alcohol, reconstitute with 20 mL of Sterile Water for Injection (SWFI) without preservative to yield a one-time use solution.
Use appropriate aseptic technique when performing the following reconstitution steps:
- Using a sterile syringe, slowly inject the 20 mL of diluent into the vial containing the lyophilized powder of HERZUMA, which has a cake-like appearance. The stream of diluent should be directed into the cake. The reconstituted vial yields a solution for multiple-dose use, containing 21 mg/mL trastuzumab-pkrb.
- Swirl the vial gently to aid reconstitution. DO NOT SHAKE.
- Slight foaming of the product may be present upon reconstitution. Allow the vial to stand undisturbed for approximately 5 minutes.
- Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration, whenever solution and container permit. Inspect visually for particulates and discoloration. The solution should be free of visible particulates, clear to slightly opalescent and colorless to pale yellow.
- Store reconstituted HERZUMA in the refrigerator at 2°C to 8°C (36°F to 46°F); discard unused HERZUMA after 28 days. If HERZUMA is reconstituted with SWFI without preservative, use immediately and discard any unused portion. Do not freeze.
Dilution
- Determine the dose (mg) of HERZUMA [see Dosage and Administration (2.3)]. Calculate the volume of the 21 mg/mL reconstituted HERZUMA solution needed, withdraw this amount from the vial using a sterile needle and syringe and add it to an infusion bag containing 250 mL of 0.9% Sodium Chloride Injection, USP. DO NOT USE DEXTROSE (5%) SOLUTION.
- Gently invert the bag to mix the solution.
- The solution of HERZUMA for infusion diluted in polyvinylchloride or polyethylene bags containing 0.9% Sodium Chloride Injection, USP, should be stored at 2°C to 8°C (36°F to 46°F) for no more than 24 hours prior to use. This storage time is additional to the time allowed for the reconstituted vials. Do not freeze.
150 mg Single-dose vial
Reconstitution
Reconstitute each 150 mg vial of HERZUMA with 7.4 mL of Sterile Water for Injection (SWFI) (not supplied) to yield a single-dose solution containing 21 mg/mL trastuzumab-pkrb that delivers 7.15 mL (150 mg trastuzumab-pkrb).
Use appropriate aseptic technique when performing the following reconstitution steps:
- Using a sterile syringe, slowly inject 7.4 mL of SWFI (not supplied) into the vial containing the lyophilized powder of HERZUMA, which has a cake-like appearance. The stream of diluent should be directed into the cake. The reconstituted vial yields a solution containing 21 mg/mL trastuzumab-pkrb.
- Swirl the vial gently to aid reconstitution. DO NOT SHAKE.
- Slight foaming of the product may be present upon reconstitution. Allow the vial to stand undisturbed for approximately 5 minutes.
- Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration, whenever solution and container permit. Inspect visually for particulates and discoloration. The solution should be free of visible particulates, clear to slightly opalescent and colorless to pale yellow.
- Use the HERZUMA solution immediately following reconstitution with SWFI, as it contains no preservative and is intended for one-time use only. If not used immediately, store the reconstituted HERZUMA solution for up to 24 hours at 2°C to 8°C (36°F to 46°F); discard any unused HERZUMA after 24 hours. Do not freeze.
Dilution
- Determine the dose (mg) of HERZUMA [see Dosage and Administration (2.3)].
- Calculate the volume of the 21 mg/mL reconstituted HERZUMA solution needed.
- Withdraw this amount from the vial using a sterile needle and syringe and add it to an infusion bag containing 250 mL of 0.9% Sodium Chloride Injection, USP. DO NOT USE DEXTROSE (5%) SOLUTION.
- Gently invert the bag to mix the solution.
- The solution of HERZUMA for infusion diluted in polyvinylchloride or polyethylene bags containing 0.9% Sodium Chloride Injection, USP, should be stored at 2°C to 8°C (36°F to 46°F) for no more than 24 hours prior to use. Discard after 24 hours. This storage time is additional to the time allowed for the reconstituted vials. Do not freeze.
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
- For injection: 150 mg of HERZUMA as a white to pale yellow lyophilized powder in a single-dose vial
- For injection: 420 mg of HERZUMA as a white to pale yellow lyophilized powder in a multiple-dose vial.
1.3 Metastatic Gastric Cancer
HERZUMA is indicated in adults, in combination with cisplatin and capecitabine or 5-fluorouracil, for the treatment of patients with HER2 overexpressing metastatic gastric or gastroesophageal junction adenocarcinoma who have not received prior treatment for metastatic disease.
Select patients for therapy based on an FDA-approved companion diagnostic for a trastuzumab product [see Dosage and Administration (2.2)].
14.2 Metastatic Breast Cancer
The safety and efficacy of trastuzumab in treatment of women with metastatic breast cancer were studied in a randomized, controlled clinical trial in combination with chemotherapy (H0648g, n = 469 patients) and an open-label, single agent clinical trial (H0649g, n = 222 patients). Both trials studied patients with metastatic breast cancer whose tumors overexpress the HER2 protein. Patients were eligible if they had 2 or 3 levels of overexpression (based on a 0 to 3 scale) by immunohistochemical assessment of tumor tissue performed by a central testing lab.
8 Use in Specific Populations (8 USE IN SPECIFIC POPULATIONS)
Females and Males of Reproductive Potential: Verify the pregnancy status of females prior to initiation of HERZUMA. (8.3)
14.3 Metastatic Gastric Cancer
The safety and efficacy of trastuzumab in combination with cisplatin and a fluoropyrimidine (capecitabine or 5-fluorouracil) were studied in patients previously untreated for metastatic gastric or gastroesophageal junction adenocarcinoma (ToGA). In this open-label, multi-center trial, 594 patients were randomized 1:1 to trastuzumab in combination with cisplatin and a fluoropyrimidine (FC+H) or chemotherapy alone (FC). Randomization was stratified by extent of disease (metastatic vs. locally advanced), primary site (gastric vs. gastroesophageal junction), tumor measurability (yes vs. no), ECOG performance status (0, 1 vs. 2), and fluoropyrimidine (capecitabine vs. 5-fluorouracil). All patients were either HER2 gene amplified (FISH+) or HER2 overexpressing (IHC 3+). Patients were also required to have adequate cardiac function (e.g., LVEF > 50%).
On the trastuzumab-containing arm, trastuzumab was administered as an IV infusion at an initial dose of 8 mg/kg followed by 6 mg/kg every 3 weeks until disease progression. On both study arms, cisplatin was administered at a dose of 80 mg/m2 Day 1 every 3 weeks for 6 cycles as a 2 hour IV infusion. On both study arms, capecitabine was administered at 1000 mg/m2 dose orally twice daily (total daily dose 2000 mg/m2) for 14 days of each 21 day cycle for 6 cycles. Alternatively, continuous intravenous infusion (CIV) 5-fluorouracil was administered at a dose of 800 mg/m2/day from Day 1 through Day 5 every three weeks for 6 cycles.
The median age of the study population was 60 years (range: 21 to 83); 76% were male; 53% were Asian, 38% Caucasian, 5% Hispanic, 5% other racial/ethnic groups; 91% had ECOG PS of 0 or 1; 82% had primary gastric cancer and 18% had primary gastroesophageal adenocarcinoma. Of these patients, 23% had undergone prior gastrectomy, 7% had received prior neoadjuvant and/or adjuvant therapy, and 2% had received prior radiotherapy.
The main outcome measure of ToGA was overall survival (OS), analyzed by the unstratified log-rank test. The final OS analysis based on 351 deaths was statistically significant (nominal significance level of 0.0193). An updated OS analysis was conducted at one year after the final analysis. The efficacy results of both the final and the updated analyses are summarized in Table 13 and Figure 7.
| FC + Trastuzumab Arm N = 298 |
FC FC = capecitabine vs. 5-fluorouracil ArmN = 296 |
|
|---|---|---|
| Overall Survival (interim analysis) | ||
| N (%) | 167 (56.0%) | 184 (62.2%) |
| Median (months) | 13.5 | 11.0 |
| 95% CI | (11.7, 15.7) | (9.4, 12.5) |
| Hazard Ratio | 0.73 | |
| 95% CI | (0.60, 0.91) | |
| p value Two sided p-value comparing with the nominal significance level of 0.0193
|
0.0038 | |
| Overall Survival (updated) | ||
| N (%) | 221 (74.2%) | 227 (76.7%) |
| Median (months) | 13.1 | 11.7 |
| 95% CI | (11.9, 15.1) | (10.3, 13.0) |
| Hazard Ratio | 0.80 | |
| 95% CI | (0.67, 0.97) |
Figure 7: Updated Overall Survival in Patients with Metastatic Gastric Cancer (ToGA)
An exploratory analysis of OS in patients based on HER2 gene amplification (FISH) and protein overexpression (IHC) testing is summarized in Table 14.
| FC (N = 296) Two patients on the FC arm who were FISH+ but IHC status unknown were excluded from the exploratory subgroup analyses.
|
FC + H (N = 298) Five patients on the trastuzumab-containing arm who were FISH+, but IHC status unknown were excluded from the exploratory subgroup analyses.
|
|
|---|---|---|
| FISH+ / IHC 0, 1+ subgroup (N=133) | ||
| No. Deaths / n (%) | 57/71 (80%) | 56/62 (90%) |
| Median OS Duration (mos.) | 8.8 | 8.3 |
| 95% CI (mos.) | (6.4, 11.7) | (6.2, 10.7) |
| Hazard ratio (95% CI) | 1.33 (0.92, 1.92) | |
| FISH+ / IHC2+ subgroup (N=160) | ||
| No. Deaths / n (%) | 65/80 (81%) | 64/80 (80%) |
| Median OS Duration (mos.) | 10.8 | 12.3 |
| 95% CI (mos.) | (6.8, 12.8) | (9.5, 15.7) |
| Hazard ratio (95% CI) | 0.78 (0.55, 1.10) | |
|
FISH+ or FISH- / IHC3+ Includes 6 patients on chemotherapy arm, 10 patients on trastuzumab arm with FISH–, IHC3+ and 8 patients on chemotherapy arm, 8 patients on trastuzumab arm with FISH status unknown, IHC 3+. subgroup (N=294)
|
||
| No. Deaths / n (%) | 104/143 (73%) | 96/151 (64%) |
| Median OS Duration (mos.) | 13.2 | 18.0 |
| 95% CI (mos.) | (11.5, 15.2) | (15.5, 21.2) |
| Hazard ratio (95% CI) | 0.66 (0.50, 0.87) |
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
The most common adverse reactions in patients receiving trastuzumab products in the adjuvant and metastatic breast cancer setting are fever, nausea, vomiting, infusion reactions, diarrhea, infections, increased cough, headache, fatigue, dyspnea, rash, neutropenia, anemia, and myalgia. Adverse reactions requiring interruption or discontinuation of trastuzumab product treatment include CHF, significant decline in left ventricular cardiac function, severe infusion reactions, and pulmonary toxicity [see Dosage and Administration (2.5)].
In the metastatic gastric cancer setting, the most common adverse reactions (≥ 10%) that were increased (≥ 5% difference) in the trastuzumab arm as compared to the chemotherapy alone arm were neutropenia, diarrhea, fatigue, anemia, stomatitis, weight loss, upper respiratory tract infections, fever, thrombocytopenia, mucosal inflammation, nasopharyngitis, and dysgeusia.
The most common adverse reactions which resulted in discontinuation of treatment on the trastuzumab-containing arm in the absence of disease progression were infection, diarrhea, and febrile neutropenia.
6.2 Post Marketing Experience (6.2 Post-Marketing Experience)
The following adverse reactions have been identified during post-approval use of trastuzumab products. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
- Infusion reaction [see Warnings and Precautions (5.2)]
- Oligohydramnios or oligohydramnios sequence, including pulmonary hypoplasia, skeletal abnormalities, and neonatal death [see Warnings and Precautions (5.3)]
- Glomerulopathy [see Adverse Reactions (6.1)]
- Immune thrombocytopenia
- Tumor lysis syndrome (TLS): Cases of possible TLS have been reported in patients treated with trastuzumab products. Patients with significant tumor burden (e.g. bulky metastases) may be at a higher risk. Patients could present with hyperuricemia, hyperphosphatemia, and acute renal failure which may represent possible TLS. Providers should consider additional monitoring and/or treatment as clinically indicated.
2.4 Important Dosing Considerations
Missed Dose
If the patient has missed a dose of HERZUMA by one week or less, then the usual maintenance dose (weekly schedule: 2 mg/kg; once every three week schedule: 6 mg/kg) should be administered as soon as possible. Do not wait until the next planned cycle. Subsequent HERZUMA maintenance doses should be administered 7 days or 21 days later according to the weekly or once every three week schedules, respectively.
If the patient has missed a dose of HERZUMA by more than one week, a re-loading dose of HERZUMA should be administered over approximately 90 minutes (weekly schedule: 4 mg/kg; once every three week schedule: 8 mg/kg) as soon as possible. Subsequent HERZUMA maintenance doses (weekly schedule: 2 mg/kg; once every three week schedule 6 mg/kg) should be administered 7 days or 21 days later according to the weekly or once every three week schedules, respectively.
Principal Display Panel Kit Carton Label (PRINCIPAL DISPLAY PANEL - Kit Carton Label)
NDC 63459-305-47
Rx only
Multiple-dose vial
Herzuma®
(trastuzumab-pkrb)
For Injection
420 mg/vial
For Intravenous Infusion Only.
Reconstitution and dilution required (see insert).
No preservative
KEEP REFRIGERATED
teva
Principal Display Panel 150 Mg Vial Label (PRINCIPAL DISPLAY PANEL - 150 mg Vial Label)
NDC 63459-303-43
Rx only
Single-dose vial
Herzuma®
(trastuzumab-pkrb)
For Injection
150 mg/vial
For Intravenous Infusion Only.
Reconstitution and dilution required (see insert).
No preservative
KEEP REFRIGERATED
teva
2.5 Dosage Modifications for Adverse Reactions
Infusion Reactions
[see Boxed Warning, Warnings and Precautions (5.2)]
- Decrease the rate of infusion for mild or moderate infusion reactions
- Interrupt the infusion in patients with dyspnea or clinically significant hypotension
- Discontinue HERZUMA for severe or life-threatening infusion reactions.
Cardiomyopathy
[see Boxed Warning, Warnings and Precautions (5.1)]
Assess left ventricular ejection fraction (LVEF) prior to initiation of HERZUMA and at regular intervals during treatment. Withhold HERZUMA dosing for at least 4 weeks for either of the following:
- ≥ 16% absolute decrease in LVEF from pre-treatment values
- LVEF below institutional limits of normal and ≥ 10% absolute decrease in LVEF from pretreatment values.
HERZUMA may be resumed if, within 4 to 8 weeks, the LVEF returns to normal limits and the absolute decrease from baseline is ≤ 15%.
Permanently discontinue HERZUMA for a persistent (> 8 weeks) LVEF decline or for suspension of HERZUMA dosing on more than 3 occasions for cardiomyopathy.
5.5 Exacerbation of Chemotherapy Induced Neutropenia (5.5 Exacerbation of Chemotherapy-Induced Neutropenia)
In randomized, controlled clinical trials, the per-patient incidences of NCI-CTC Grade 3 to 4 neutropenia and of febrile neutropenia were higher in patients receiving trastuzumab in combination with myelosuppressive chemotherapy as compared to those who received chemotherapy alone. The incidence of septic death was similar among patients who received trastuzumab and those who did not [see Adverse Reactions (6.1)].
2.1 evaluation and Testing Before Initiating Herzuma (2.1 Evaluation and Testing Before Initiating HERZUMA)
Assess left ventricular ejection fraction (LVEF) prior to initiation of HERZUMA and at regular intervals during treatment. [see Boxed Warning, Dosage and Administration (2.5), Warnings and Precautions (5.1)].
Verify the pregnancy status of females of reproductive potential prior to the initiation of HERZUMA [see Warnings and Precautions (5.3), Use in Specific Populations (8.1, 8.3)].
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Trastuzumab products have not been tested for carcinogenic potential.
No evidence of mutagenic activity was observed when trastuzumab was tested in the standard Ames bacterial and human peripheral blood lymphocyte mutagenicity assays, at concentrations of up to 5000 mcg/mL. In an in vivo micronucleus assay, no evidence of chromosomal damage to mouse bone marrow cells was observed following bolus intravenous doses of up to 118 mg/kg of trastuzumab.
A fertility study was conducted in female Cynomolgus monkeys at doses up to 25 times the weekly recommended human dose of 2 mg/kg of trastuzumab and has revealed no evidence of impaired fertility, as measured by menstrual cycle duration and female sex hormone levels.
Warning: Cardiomyopathy, Infusion Reactions, Embryo Fetal Toxicity, and Pulmonary Toxicity (WARNING: CARDIOMYOPATHY, INFUSION REACTIONS, EMBRYO-FETAL TOXICITY, and PULMONARY TOXICITY)
WARNING: CARDIOMYOPATHY, INFUSION REACTIONS, EMBRYO-FETAL TOXICITY, and PULMONARY TOXICITY
See full prescribing information for complete boxed warning
Cardiomyopathy: Trastuzumab products can result in subclinical and clinical cardiac failure manifesting as CHF, and decreased LVEF, with greatest risk when administered concurrently with anthracyclines. Evaluate cardiac function prior to and during treatment. Discontinue HERZUMA for cardiomyopathy. (2.5, 5.1)
Infusion Reactions, Pulmonary Toxicity: Discontinue HERZUMA for anaphylaxis, angioedema, interstitial pneumonitis, or acute respiratory distress syndrome. (5.2, 5.4)
Embryo-Fetal Toxicity: Exposure to trastuzumab products during pregnancy can result in oligohydramnios, in some cases complicated by pulmonary hypoplasia and neonatal death. Advise patients of these risks and the need for effective contraception. (5.3, 8.1, 8.3)
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:51:31.728277 · Updated: 2026-03-14T22:40:41.023270