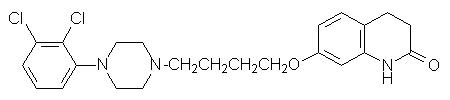Aripiprazole Tablets
aaf7dc7e-04f3-442b-86d7-5f54d17d102c
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Indications and Usage
Aripiprazole tablets are indicated for the treatment of: Schizophrenia [see Clinical Studies (14.1) ] Additional pediatric use information is approved for Otsuka America Pharmaceutical, Inc.’s ABILIFY ® (aripiprazole) product. However, due to Otsuka America Pharmaceutical, Inc.’s marketing exclusivity rights, this drug product is not labeled with that information.
Dosage and Administration
Initial Dose Recommended Dose Maximum Dose Schizophrenia – adults (2.1) 10 to 15 mg/day 10 to 15 mg/day 30 mg/day Schizophrenia – adolescents (2.1) 2 mg/day 10 mg/day 30 mg/day Oral formulations: Administer once daily without regard to meals (2) Known CYP2D6 poor metabolizers: Half of the usual dose (2.7)
Contraindications
Aripiprazole tablets are contraindicated in patients with a history of a hypersensitivity reaction to aripiprazole. Reactions have ranged from pruritus/urticaria to anaphylaxis [see Adverse Reactions (6.2) ].
Warnings and Precautions
Cerebrovascular Adverse Reactions in Elderly Patients with Dementia- Related Psychosis: Increased incidence of cerebrovascular adverse reactions (e.g., stroke, transient ischemic attack, including fatalities) (5.2) Neuroleptic Malignant Syndrome: Manage with immediate discontinuation and close monitoring (5.4) Tardive Dyskinesia: Discontinue if clinically appropriate (5.5) Metabolic Changes: Atypical antipsychotic drugs have been associated with metabolic changes that include hyperglycemia/diabetes mellitus, dyslipidemia, and body weight gain (5.6) Hyperglycemia/Diabetes Mellitus: Monitor glucose regularly in patients with and at risk for diabetes (5.6) Dyslipidemia: Undesirable alterations in lipid levels have been observed in patients treated with atypical antipsychotics (5.6) Weight Gain: Weight gain has been observed with atypical antipsychotic use. Monitor weight (5.6) Pathological Gambling and Other Compulsive Behaviors: Consider dose reduction or discontinuation (5.7) Orthostatic Hypotension: Monitor heart rate and blood pressure and warn patients with known cardiovascular or cerebrovascular disease, and risk of dehydration or syncope (5.8) Leukopenia, Neutropenia, and Agranulocytosis: have been reported with antipsychotics including aripiprazole. Patients with a history of a clinically significant low white blood cell count (WBC) or a drug-induced leukopenia/neutropenia should have their complete blood count (CBC) monitored frequently during the first few months of therapy and discontinuation of aripiprazole should be considered at the first sign of a clinically significant decline in WBC in the absence of other causative factors (5.10) Seizures/Convulsions: Use cautiously in patients with a history of seizures or with conditions that lower the seizure threshold (5.11) Potential for Cognitive and Motor Impairment: Use caution when operating machinery (5.12) Suicide: The possibility of a suicide attempt is inherent in schizophrenia and bipolar disorder. Closely supervise high-risk patients (5.14)
Adverse Reactions
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice. The following adverse reactions are discussed in more detail in other sections of the labeling: Increased Mortality in Elderly Patients with Dementia-Related Psychosis [see Boxed Warning and Warnings and Precautions (5.1) ] Cerebrovascular Adverse Events, Including Stroke [see Warnings and Precautions (5.2) ] Suicidal Thoughts and Behaviors in Children, Adolescents, and Young Adults [see Boxed Warning and Warnings and Precautions (5.3) ] Neuroleptic Malignant Syndrome (NMS) [see Warnings and Precautions (5.4) ] Tardive Dyskinesia [see Warnings and Precautions (5.5) ] Metabolic Changes [see Warnings and Precautions (5.6) ] Pathological Gambling and Other Compulsive Behaviors [see Warnings and Precautions (5.7) ] Orthostatic Hypotension [see Warnings and Precautions (5.8) ] Falls [see Warnings and Precautions (5.9) ] Leukopenia, Neutropenia, and Agranulocytosis [see Warnings and Precautions (5.10) ] Seizures/Convulsions [see Warnings and Precautions (5.11) ] Potential for Cognitive and Motor Impairment [see Warnings and Precautions (5.12) ] Body Temperature Regulation [see Warnings and Precautions (5.13) ] Suicide [see Warnings and Precautions (5.14) ] Dysphagia [see Warnings and Precautions (5.15) ] The most common adverse reactions in adult patients in clinical trials (≥10%) were nausea, vomiting, constipation, headache, dizziness, akathisia, anxiety, insomnia, and restlessness. The most common adverse reactions in the pediatric clinical trials (≥10%) were somnolence, headache, vomiting, extrapyramidal disorder, fatigue, increased appetite, insomnia, nausea, nasopharyngitis, and weight increased. Aripiprazole has been evaluated for safety in 13,543 adult patients who participated in multiple-dose, clinical trials in schizophrenia, other indications, Dementia of the Alzheimer’s type, Parkinson’s disease, and alcoholism, and who had approximately 7619 patient-years of exposure to oral aripiprazole. A total of 3390 patients were treated with oral aripiprazole for at least 180 days and 1933 patients treated with oral aripiprazole had at least 1 year of exposure. Aripiprazole has been evaluated for safety in 1,686 patients (6 to 18 years) who participated in multiple-dose, clinical trials in schizophrenia, or other indications and who had approximately 1,342 patient-years of exposure to oral aripiprazole. A total of 959 pediatric patients were treated with oral aripiprazole for at least 180 days and 556 pediatric patients treated with oral aripiprazole had at least 1 year of exposure. The conditions and duration of treatment with aripiprazole included (in overlapping categories) double-blind, comparative and noncomparative open-label studies, inpatient and outpatient studies, fixed-and flexible-dose studies, and short-and longer-term exposure. Additional pediatric use information is approved for Otsuka America Pharmaceutical, Inc.’s ABILIFY ® (aripiprazole) product. However, due to Otsuka America Pharmaceutical, Inc.’s marketing exclusivity rights, this drug product is not labeled with that information.
Drug Interactions
Dosage adjustment due to drug interactions (7.1) : Factors Dosage Adjustments for Aripiprazole Known CYP2D6 Poor Metabolizers Administer half of usual dose Known CYP2D6 Poor Metabolizers and strong CYP3A4 inhibitors Administer a quarter of usual dose Strong CYP2D6 or CYP3A4 inhibitors Administer half of usual dose Strong CYP2D6 and CYP3A4 inhibitors Administer a quarter of usual dose Strong CYP3A4 inducers Double usual dose over 1 to 2 weeks
How Supplied
Product: 50090-6063 NDC: 50090-6063-0 30 TABLET in a BOTTLE
Storage and Handling
Product: 50090-6063 NDC: 50090-6063-0 30 TABLET in a BOTTLE
Description
Elderly patients with dementia-related psychosis treated with antipsychotic drugs are at an increased risk of death. Aripiprazole is not approved for the treatment of patients with dementia-related psychosis [see Warnings and Precautions (5.1) ] . Antidepressants increased the risk of suicidal thoughts and behavior in children, adolescents, and young adults in short-term studies. These studies did not show an increase in the risk of suicidal thoughts and behavior with antidepressant use in patients over age 24; there was a reduction in risk with antidepressant use in patients aged 65 and older [see Warnings and Precautions (5.3) ] . In patients of all ages who are started on antidepressant therapy, monitor closely for worsening, and for emergence of suicidal thoughts and behaviors. Advise families and caregivers of the need for close observation and communication with the prescriber [see Warnings and Precautions (5.3) ] .
Medication Information
Warnings and Precautions
Cerebrovascular Adverse Reactions in Elderly Patients with Dementia- Related Psychosis: Increased incidence of cerebrovascular adverse reactions (e.g., stroke, transient ischemic attack, including fatalities) (5.2) Neuroleptic Malignant Syndrome: Manage with immediate discontinuation and close monitoring (5.4) Tardive Dyskinesia: Discontinue if clinically appropriate (5.5) Metabolic Changes: Atypical antipsychotic drugs have been associated with metabolic changes that include hyperglycemia/diabetes mellitus, dyslipidemia, and body weight gain (5.6) Hyperglycemia/Diabetes Mellitus: Monitor glucose regularly in patients with and at risk for diabetes (5.6) Dyslipidemia: Undesirable alterations in lipid levels have been observed in patients treated with atypical antipsychotics (5.6) Weight Gain: Weight gain has been observed with atypical antipsychotic use. Monitor weight (5.6) Pathological Gambling and Other Compulsive Behaviors: Consider dose reduction or discontinuation (5.7) Orthostatic Hypotension: Monitor heart rate and blood pressure and warn patients with known cardiovascular or cerebrovascular disease, and risk of dehydration or syncope (5.8) Leukopenia, Neutropenia, and Agranulocytosis: have been reported with antipsychotics including aripiprazole. Patients with a history of a clinically significant low white blood cell count (WBC) or a drug-induced leukopenia/neutropenia should have their complete blood count (CBC) monitored frequently during the first few months of therapy and discontinuation of aripiprazole should be considered at the first sign of a clinically significant decline in WBC in the absence of other causative factors (5.10) Seizures/Convulsions: Use cautiously in patients with a history of seizures or with conditions that lower the seizure threshold (5.11) Potential for Cognitive and Motor Impairment: Use caution when operating machinery (5.12) Suicide: The possibility of a suicide attempt is inherent in schizophrenia and bipolar disorder. Closely supervise high-risk patients (5.14)
Indications and Usage
Aripiprazole tablets are indicated for the treatment of: Schizophrenia [see Clinical Studies (14.1) ] Additional pediatric use information is approved for Otsuka America Pharmaceutical, Inc.’s ABILIFY ® (aripiprazole) product. However, due to Otsuka America Pharmaceutical, Inc.’s marketing exclusivity rights, this drug product is not labeled with that information.
Dosage and Administration
Adults
The recommended starting and target dose for aripiprazole tablets is 10 or 15 mg/day administered on a once-a-day schedule without regard to meals. Aripiprazole has been systematically evaluated and shown to be effective in a dose range of 10 to 30 mg/day, when administered as the tablet formulation; however, doses higher than 10 or 15 mg/day were not more effective than 10 or 15 mg/day. Dosage increases should generally not be made before 2 weeks, the time needed to achieve steady-state [see Clinical Studies (14.1)] .
Maintenance Treatment: Maintenance of efficacy in schizophrenia was demonstrated in a trial involving patients with schizophrenia who had been symptomatically stable on other antipsychotic medications for periods of 3 months or longer. These patients were discontinued from those medications and randomized to either aripiprazole 15 mg/day or placebo, and observed for relapse [see Clinical Studies (14.1)] . Patients should be periodically reassessed to determine the continued need for maintenance treatment.
Contraindications
Aripiprazole tablets are contraindicated in patients with a history of a hypersensitivity reaction to aripiprazole. Reactions have ranged from pruritus/urticaria to anaphylaxis [see Adverse Reactions (6.2) ].
Adverse Reactions
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice. The following adverse reactions are discussed in more detail in other sections of the labeling: Increased Mortality in Elderly Patients with Dementia-Related Psychosis [see Boxed Warning and Warnings and Precautions (5.1) ] Cerebrovascular Adverse Events, Including Stroke [see Warnings and Precautions (5.2) ] Suicidal Thoughts and Behaviors in Children, Adolescents, and Young Adults [see Boxed Warning and Warnings and Precautions (5.3) ] Neuroleptic Malignant Syndrome (NMS) [see Warnings and Precautions (5.4) ] Tardive Dyskinesia [see Warnings and Precautions (5.5) ] Metabolic Changes [see Warnings and Precautions (5.6) ] Pathological Gambling and Other Compulsive Behaviors [see Warnings and Precautions (5.7) ] Orthostatic Hypotension [see Warnings and Precautions (5.8) ] Falls [see Warnings and Precautions (5.9) ] Leukopenia, Neutropenia, and Agranulocytosis [see Warnings and Precautions (5.10) ] Seizures/Convulsions [see Warnings and Precautions (5.11) ] Potential for Cognitive and Motor Impairment [see Warnings and Precautions (5.12) ] Body Temperature Regulation [see Warnings and Precautions (5.13) ] Suicide [see Warnings and Precautions (5.14) ] Dysphagia [see Warnings and Precautions (5.15) ] The most common adverse reactions in adult patients in clinical trials (≥10%) were nausea, vomiting, constipation, headache, dizziness, akathisia, anxiety, insomnia, and restlessness. The most common adverse reactions in the pediatric clinical trials (≥10%) were somnolence, headache, vomiting, extrapyramidal disorder, fatigue, increased appetite, insomnia, nausea, nasopharyngitis, and weight increased. Aripiprazole has been evaluated for safety in 13,543 adult patients who participated in multiple-dose, clinical trials in schizophrenia, other indications, Dementia of the Alzheimer’s type, Parkinson’s disease, and alcoholism, and who had approximately 7619 patient-years of exposure to oral aripiprazole. A total of 3390 patients were treated with oral aripiprazole for at least 180 days and 1933 patients treated with oral aripiprazole had at least 1 year of exposure. Aripiprazole has been evaluated for safety in 1,686 patients (6 to 18 years) who participated in multiple-dose, clinical trials in schizophrenia, or other indications and who had approximately 1,342 patient-years of exposure to oral aripiprazole. A total of 959 pediatric patients were treated with oral aripiprazole for at least 180 days and 556 pediatric patients treated with oral aripiprazole had at least 1 year of exposure. The conditions and duration of treatment with aripiprazole included (in overlapping categories) double-blind, comparative and noncomparative open-label studies, inpatient and outpatient studies, fixed-and flexible-dose studies, and short-and longer-term exposure. Additional pediatric use information is approved for Otsuka America Pharmaceutical, Inc.’s ABILIFY ® (aripiprazole) product. However, due to Otsuka America Pharmaceutical, Inc.’s marketing exclusivity rights, this drug product is not labeled with that information.
Drug Interactions
Dosage adjustment due to drug interactions (7.1) : Factors Dosage Adjustments for Aripiprazole Known CYP2D6 Poor Metabolizers Administer half of usual dose Known CYP2D6 Poor Metabolizers and strong CYP3A4 inhibitors Administer a quarter of usual dose Strong CYP2D6 or CYP3A4 inhibitors Administer half of usual dose Strong CYP2D6 and CYP3A4 inhibitors Administer a quarter of usual dose Strong CYP3A4 inducers Double usual dose over 1 to 2 weeks
Storage and Handling
Product: 50090-6063 NDC: 50090-6063-0 30 TABLET in a BOTTLE
How Supplied
Product: 50090-6063 NDC: 50090-6063-0 30 TABLET in a BOTTLE
Description
Elderly patients with dementia-related psychosis treated with antipsychotic drugs are at an increased risk of death. Aripiprazole is not approved for the treatment of patients with dementia-related psychosis [see Warnings and Precautions (5.1) ] . Antidepressants increased the risk of suicidal thoughts and behavior in children, adolescents, and young adults in short-term studies. These studies did not show an increase in the risk of suicidal thoughts and behavior with antidepressant use in patients over age 24; there was a reduction in risk with antidepressant use in patients aged 65 and older [see Warnings and Precautions (5.3) ] . In patients of all ages who are started on antidepressant therapy, monitor closely for worsening, and for emergence of suicidal thoughts and behaviors. Advise families and caregivers of the need for close observation and communication with the prescriber [see Warnings and Precautions (5.3) ] .
Section 34083-6
Carcinogenesis
Lifetime carcinogenicity studies were conducted in ICR mice, F344 rats, and Sprague-Dawley (SD) rats. Aripiprazole was administered for 2 years in the diet at doses of 1, 3, 10, and 30 mg/kg/day to ICR mice and 1, 3, and 10 mg/kg/day to F344 rats (0.2, 0.5, 2 and 5 times and 0.3, 1 and 3 times the MRHD of 30 mg/day based on mg/m 2 body surface area, respectively). In addition, SD rats were dosed orally for 2 years at 10, 20, 40, and 60 mg/kg/day, which are 3, 6, 13 and 19 times the MRHD based on mg/m 2 body surface area. Aripiprazole did not induce tumors in male mice or male rats. In female mice, the incidences of pituitary gland adenomas and mammary gland adenocarcinomas and adenoacanthomas were increased at dietary doses of 3 to 30 mg/kg/day (0.5 to 5 times the MRHD). In female rats, the incidence of mammary gland fibroadenomas was increased at a dietary dose of 10 mg/kg/day (3 times the MRHD); and the incidences of adrenocortical carcinomas and combined adrenocortical adenomas/carcinomas were increased at an oral dose of 60 mg/kg/day (19 times the MRHD).
An increase in mammary, pituitary, and endocrine pancreas neoplasms has been found in rodents after chronic administration of other antipsychotic drugs and is considered to be mediated by prolonged dopamine D2-receptor antagonism and hyperprolactinemia. Serum prolactin was not measured in the aripiprazole carcinogenicity studies. However, increases in serum prolactin levels were observed in female mice in a 13-week dietary study at the doses associated with mammary gland and pituitary tumors. Serum prolactin was not increased in female rats in 4-week and 13-week dietary studies at the dose associated with mammary gland tumors. The relevance for human risk of the findings of prolactin-mediated endocrine tumors in rodents is unclear.
Section 34084-4
Less Common Adverse Reactions in Adults
Table 17 enumerates the pooled incidence, rounded to the nearest percent, of adverse reactions that occurred during acute therapy (up to 6 weeks in schizophrenia and upto 3 weeks in another indication), including only those reactions that occurred in 2% or more of patients treated with aripiprazole (doses ≥2 mg/day) and for which the incidence in patients treated with aripiprazole was greater than the incidence in patients treated with placebo in the combined dataset.
| System Organ Class
Preferred Term |
||
|---|---|---|
| Percentage of Patients Reporting Reaction
Adverse reactions reported by at least 2% of patients treated with oral aripiprazole, except adverse reactions which had an incidence equal to or less than placebo.
|
||
| Aripiprazole | Placebo | |
| (n=1843) | (n=1166) | |
| Eye Disorders | ||
| Blurred Vision | 3 | 1 |
| Gastrointestinal Disorders | ||
| Nausea | 15 | 11 |
| Constipation | 11 | 7 |
| Vomiting | 11 | 6 |
| Dyspepsia | 9 | 7 |
| Dry Mouth | 5 | 4 |
| Toothache | 4 | 3 |
| Abdominal Discomfort | 3 | 2 |
| Stomach Discomfort | 3 | 2 |
| General Disorders and Administration Site Conditions | ||
| Fatigue | 6 | 4 |
| Pain | 3 | 2 |
| Musculoskeletal and Connective Tissue Disorders | ||
| Musculoskeletal Stiffness | 4 | 3 |
| Pain in Extremity | 4 | 2 |
| Myalgia | 2 | 1 |
| Muscle Spasms | 2 | 1 |
| Nervous System Disorders | ||
| Headache | 27 | 23 |
| Dizziness | 10 | 7 |
| Akathisia | 10 | 4 |
| Sedation | 7 | 4 |
| Extrapyramidal Disorder | 5 | 3 |
| Tremor | 5 | 3 |
| Somnolence | 5 | 3 |
| Psychiatric Disorders | ||
| Agitation | 19 | 17 |
| Insomnia | 18 | 13 |
| Anxiety | 17 | 13 |
| Restlessness | 5 | 3 |
| Respiratory, Thoracic, and Mediastinal Disorders | ||
| Pharyngolaryngeal Pain | 3 | 2 |
| Cough | 3 | 2 |
An examination of population subgroups did not reveal any clear evidence of differential adverse reaction incidence on the basis of age, gender, or race.
Section 34092-7
Adults
The efficacy of aripiprazole in the treatment of schizophrenia was evaluated in five short-term (4-week and 6-week), placebo-controlled trials of acutely relapsed inpatients who predominantly met DSM-III/IV criteria for schizophrenia. Four of the five trials were able to distinguish aripiprazole from placebo, but one study, the smallest, did not. Three of these studies also included an active control group consisting of either risperidone (one trial) or haloperidol (two trials), but they were not designed to allow for a comparison of aripiprazole and the active comparators.
In the four positive trials for aripiprazole, four primary measures were used for assessing psychiatric signs and symptoms. Efficacy was evaluated using the total score on the Positive and Negative Syndrome Scale (PANSS). The PANSS is a 30 item scale that measures positive symptoms of schizophrenia (7 items), negative symptoms of schizophrenia (7 items), and general psychopathology (16 items), each rated on a scale of 1 (absent) to 7 (extreme); total PANSS scores range from 30 to 210. The Clinical Global Impression (CGI) assessment reflects the impression of a skilled observer, fully familiar with the manifestations of schizophrenia, about the overall clinical state of the patient.
- In a 4-week trial (n=414) comparing two fixed doses of aripiprazole (15 or 30 mg/day) to placebo, both doses of aripiprazole were superior to placebo in the PANSS total score (Study 1 in
Table 26), PANSS positive subscale, and CGI- severity score. In addition, the 15 mg dose was superior to placebo in the PANSS negative subscale.
- In a 4-week trial (n=404) comparing two fixed doses of aripiprazole (20 or 30 mg/day) to placebo, both doses of aripiprazole were superior to placebo in the PANSS total score (Study 2 in
Table 26), PANSS positive subscale, PANSS negative subscale, and CGI-severity score.
- In a 6-week trial (n=420) comparing three fixed doses of aripiprazole (10, 15, or 20 mg/day) to placebo, all three doses of aripiprazole were superior to placebo in the PANSS total score (Study 3 in
Table 26), PANSS positive subscale, and the PANSS negative subscale.
- In a 6-week trial (n=367) comparing three fixed doses of aripiprazole (2, 5, or 10 mg/day) to placebo, the 10 mg dose of aripiprazole was superior to placebo in the PANSS total score (Study 4 in
Table 26), the primary outcome measure of the study. The 2 and 5 mg doses did not demonstrate superiority to placebo on the primary outcome measure.
Thus, the efficacy of 10, 15, 20, and 30 mg daily doses was established in two studies for each dose. Among these doses, there was no evidence that the higher dose groups offered any advantage over the lowest dose group of these studies.
An examination of population subgroups did not reveal any clear evidence of differential responsiveness on the basis of age, gender, or race.
A longer-term trial enrolled 310 inpatients or outpatients meeting DSM-IV criteria for schizophrenia who were, by history, symptomatically stable on other antipsychotic medications for periods of 3 months or longer. These patients were discontinued from their antipsychotic medications and randomized to aripiprazole 15 mg/day or placebo for up to 26 weeks of observation for relapse. Relapse during the double-blind phase was defined as CGI-Improvement score of ≥5 (minimally worse), scores ≥5 (moderately severe) on the hostility or uncooperativeness items of the PANSS, or ≥20% increase in the PANSS total score. Patients receiving aripiprazole 15 mg/day experienced a significantly longer time to relapse over the subsequent 26 weeks compared to those receiving placebo (Study 5 in Figure 6).
Section 42231-1
MEDICATION GUIDE
Aripiprazole Tablets
(AR-i-PIP-ra-zole)
What is the most important information I should know about aripiprazole tablets?
(For other side effects, also see “What are the possible side effects of aripiprazole tablets?”).
Serious side effects may happen when you take aripiprazole tablets, including:
- Increased risk of death in elderly patients with dementia-related psychosis: Medicines like aripiprazole tablets can raise the risk of death in elderly people who have lost touch with reality (psychosis) due to confusion and memory loss (dementia). Aripiprazole tablets are not approved for the treatment of patients with dementia-related psychosis.
-
Risk of suicidal thoughts or actions: Antidepressant medicines, depression and other serious mental illnesses, and suicidal thoughts or actions:
- Antidepressant medicines may increase suicidal thoughts or actions in some children, teenagers, and young adults within the first few months of treatment.
- Depression and other serious mental illnesses are the most important causes of suicidal thoughts and actions. Some people may have a particularly high risk of having suicidal thoughts or actions. These include people who have (or have a family history of) bipolar illness (also called manic-depressive illness) or suicidal thoughts or actions.
-
How can I watch for and try to prevent suicidal thoughts and actions in myself or a family member?
- Pay close attention to any changes, especially sudden changes, in mood, behaviors, thoughts, or feelings. This is very important when an antidepressant medicine is started or when the dose is changed.
- Call the healthcare provider right away to report new or sudden changes in mood, behavior, thoughts, or feelings.
- Keep all follow-up visits with the healthcare provider as scheduled. Call the healthcare provider between visits as needed, especially if you have concerns about symptoms.
Call a healthcare provider right away if you or your family member has any of the following symptoms, especially if they are new, worse, or worry you:
- thoughts about suicide or dying
- attempts to commit suicide
- new or worse depression
- new or worse anxiety
- feeling very agitated or restless
- panic attacks
- trouble sleeping (insomnia)
- new or worse irritability
- acting aggressive, being angry, or violent
- acting on dangerous impulses
- an extreme increase in activity and talking (mania)
- other unusual changes in behavior or mood
What else do I need to know about antidepressant medicines?
- Never stop an antidepressant medicine without first talking to a healthcare provider. Stopping an antidepressant medicine suddenly can cause other symptoms.
- Antidepressants are medicines used to treat depression and other illnesses. It is important to discuss all the risks of treating depression and also the risks of not treating it. Patients and their families or other caregivers should discuss all treatment choices with the healthcare provider, not just the use of antidepressants.
- Antidepressant medicines have other side effects. Talk to the healthcare provider about the side effects of the medicine prescribed for you or your family member.
- Antidepressant medicines can interact with other medicines. Know all of the medicines that you or your family member takes. Keep a list of all medicines to show the healthcare provider. Do not start new medicines without first checking with your healthcare provider.
- Not all antidepressant medicines prescribed for children are FDA approved for use in children. Talk to your child’s healthcare provider for more information.
What are aripiprazole tablets?
Aripiprazole tablets are prescription medicines used to treat:
- Schizophrenia
It is not known if aripiprazole is safe or effective in children:
- under 13 years of age with schizophrenia
- under 10 years of age with bipolar I disorder
Do not take aripiprazole tablets if you are allergic to aripiprazole or any ingredients in aripiprazole tablets. See the end of this Medication Guide for a complete list of ingredients in aripiprazole tablets.
Before taking aripiprazole tablets, tell your healthcare provider about all your medical conditions, including if you have or had:
- diabetes or high blood sugar in you or your family; your healthcare provider should check your blood sugar before you start aripiprazole tablets and also during therapy.
- seizures (convulsions).
- low or high blood pressure.
- heart problems or stroke.
- pregnancy or plans to become pregnant. It is not known if aripiprazole tablets will harm your unborn baby.
- If you become pregnant while receiving aripiprazole, talk to your healthcare provider about registering with the National Pregnancy Registry for Atypical Antipsychotics. You can register by calling 1-866-961-2388 or go to http://womensmentalhealth.org/clinical-and-research-programs/pregnancyregistry/
- breast-feeding or plans to breast-feed. Aripiprazole passes into your breast milk. Talk to your healthcare provider about the best way to feed your baby if you receive aripiprazole tablets.
- low white blood cell count.
Tell your healthcare provider about all the medicines that you take, including prescription and over-the-counter medicines, vitamins, and herbal supplements.
Aripiprazole tablets and other medicines may affect each other causing possible serious side effects. Aripiprazole tablets may affect the way other medicines work, and other medicines may affect how aripiprazole works.
Your healthcare provider can tell you if it is safe to take aripiprazole tablets with your other medicines. Do not start or stop any medicines while taking aripiprazole tablets without talking to your healthcare provider first. Know the medicines you take. Keep a list of your medicines to show your healthcare provider and pharmacist when you get a new medicine.
How should I take aripiprazole tablets?
- Take aripiprazole tablets exactly as your healthcare provider tells you to take it. Do not change the dose or stop taking aripiprazole tablets yourself.
- Aripiprazole tablets can be taken with or without food.
- Aripiprazole tablets should be swallowed whole.
- If you miss a dose of aripiprazole tablets, take the missed dose as soon as you remember. If it is almost time for the next dose, just skip the missed dose and take your next dose at the regular time. Do not take two doses of aripiprazole tablets at the same time.
- If you take too much aripiprazole tablets, call your healthcare provider or poison control center at 1-800-222-1222 right away, or go to the nearest hospital emergency room.
What should I avoid while taking aripiprazole tablets?
- Do not drive, operate heavy machinery, or do other dangerous activities until you know how aripiprazole tablets affect you. Aripiprazole tablets may make you drowsy.
- Avoid getting over-heated or dehydrated.
- Do not over-exercise.
- In hot weather, stay inside in a cool place if possible.
- Stay out of the sun. Do not wear too much or heavy clothing.
- Drink plenty of water.
What are the possible side effects of aripiprazole tablets?
Aripiprazole tablets may cause serious side effects, including:
- See “What is the most important information I should know about aripiprazole tablets?”
- Stroke in elderly people (cerebrovascular problems) that can lead to death
- Neuroleptic malignant syndrome (NMS). Tell your healthcare provider right away if you have some or all of the following symptoms: high fever, stiff muscles, confusion, sweating, changes in pulse, heart rate, and blood pressure. These may be symptoms of a rare and serious condition that can lead to death. Call your healthcare provider right away if you have any of these symptoms.
- Uncontrolled body movements (tardive dyskinesia). Aripiprazole tablets may cause movements that you cannot control in your face, tongue, or other body parts. Tardive dyskinesia may not go away, even if you stop receiving aripiprazole tablets. Tardive dyskinesia may also start after you stop receiving aripiprazole tablets.
-
Problems with your metabolism such as:
- High blood sugar (hyperglycemia) and diabetes. Increases in blood sugar can happen in some people who take aripiprazole tablets. Extremely high blood sugar can lead to coma or death. If you have diabetes or risk factors for diabetes (such as being overweight or a family history of diabetes), your healthcare provider should check your blood sugar before you start aripiprazole tablets and during your treatment.
Call your healthcare provider if you have any of these symptoms of high blood sugar while receiving aripiprazole tablets:
►feel very thirsty
►need to urinate more than usual
►feel very hungry
►feel weak or tired
►feel sick to your stomach
►feel confused, or your breath smells fruity
- Increased fat levels (cholesterol and triglycerides) in your blood.
- Weight gain. You and your healthcare provider should check your weight regularly.
-
Unusual urges. Some people taking aripiprazole tablets have had unusual urges, such as gambling, binge eating or eating that you cannot control (compulsive), compulsive shopping and sexual urges.
If you or your family members notice that you are having unusual urges or behaviors, talk to your healthcare provider. - Orthostatic hypotension (decreased blood pressure). Lightheadedness or fainting may happen when rising too quickly from a sitting or lying position.
- Falls. Aripiprazole tablets may make you sleepy or dizzy, may cause a decrease in your blood pressure when changing position and can slow your thinking and motor skills which may lead to falls that can cause fractures or other injuries.
- Low white blood cell count
- Seizures (convulsions)
- Problems with control of your body temperature especially when you exercise a lot or are in an area that is very hot. It is important for you to drink water to avoid dehydration. See “What should I avoid while receiving aripiprazole tablets?”
- Difficulty swallowing that can cause food or liquid to get into your lungs.
The most common side effects of aripiprazole tablets in adults include:
| • Nausea | • dizziness |
| • vomiting | • anxiety |
| • constipation | • insomnia |
| • headache | • restlessness |
| • blurred vision | • inner sense of restlessness/need to move (akathisia) |
| • upper respiratory illness |
The most common side effects of aripiprazole tablets in children include:
| • feeling sleepy | • insomnia |
| • headache | • nausea |
| • vomiting | • stuffy nose |
| • fatigue | • weight gain |
| • increased or decreased appetite | • uncontrolled movement such as restlessness, tremor |
| • increased saliva or drooling | • muscle stiffness |
These are not all the possible side effects of aripiprazole tablets.
Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.
How should I store aripiprazole tablets?
- Store aripiprazole tablets at room temperature, between 68°F to 77°F (20°C to 25°C).
- Bottles of 30’s & 100’s count comes with a child-resistant package.
Keep aripiprazole tablets and all medicines out of the reach of children.
General information about the safe and effective use of aripiprazole tablets
Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not use aripiprazole for a condition for which it was not prescribed. Do not give aripiprazole to other people, even if they have the same symptoms you have. It may harm them.
You can ask your healthcare provider or pharmacist for information about aripiprazole tablets that was written for healthcare professionals.
What are the ingredients in aripiprazole tablets?
Active ingredient: aripiprazole
Inactive ingredients: hydroxypropyl cellulose, lactose monohydrate, magnesium stearate, maize starch and microcrystalline cellulose. Colorants include ferric oxide red (10 mg and 30 mg), ferric oxide yellow (2 mg and 15 mg), and FD&C Blue No. 2 aluminum lake (2 mg and 5 mg).
Additional pediatric use information is approved for Otsuka America Pharmaceutical, Inc.’s ABILIFY ® (aripiprazole) product. However, due to Otsuka America Pharmaceutical, Inc.’s marketing exclusivity rights, this drug product is not labeled with that information.
For more information about aripiprazole tablets, visit www.accordhealthcare.us or call Accord Healthcare Inc. at 1-866-941-7875.
This Medication Guide has been approved by the U.S. Food and Drug Administration.
ABILIFY ® is a trademark of Otsuka Pharmaceutical Company.
Medication guide available at www.accordhealthcare.us/medication-guides.
Manufactured For:
Accord Healthcare, Inc.,
1009 Slater Road,
Suite 210-B,
Durham, NC 27703,
USA
Manufactured By:
Intas Pharmaceuticals Limited.
Plot No. 5 to 12, Pharmez,
Sarkhej-Bavla, National Highway No 8-A,
Near Village Matoda, Tal Sanand,
Ahmedabad - 382213, Gujarat, India
51 1878 2 722646
Issued March 2020
Section 43682-4
ORAL ADMINISTRATION
Section 43683-2
Warnings and Precautions( 5.5) 08/2019
Section 43685-7
Hyperglycemia/Diabetes Mellitus
Hyperglycemia, in some cases extreme and associated with ketoacidosis or hyperosmolar coma or death, has been reported in patients treated with atypical antipsychotics. There have been reports of hyperglycemia in patients treated with aripiprazole [see Adverse Reactions (6.1, 6.2)] . Assessment of the relationship between atypical antipsychotic use and glucose abnormalities is complicated by the possibility of an increased background risk of diabetes mellitus in patients with schizophrenia and the increasing incidence of diabetes mellitus in the general population. Given these confounders, the relationship between atypical antipsychotic use and hyperglycemia-related adverse events is not completely understood. However, epidemiological studies suggest an increased risk of hyperglycemia-related adverse reactions in patients treated with the atypical antipsychotics. Because aripiprazole was not marketed at the time these studies were performed, it is not known if aripiprazole is associated with this increased risk. Precise risk estimates for hyperglycemia-related adverse reactions in patients treated with atypical antipsychotics are not available.
Patients with an established diagnosis of diabetes mellitus who are started on atypical antipsychotics should be monitored regularly for worsening of glucose control. Patients with risk factors for diabetes mellitus (e.g., obesity, family history of diabetes) who are starting treatment with atypical antipsychotics should undergo fasting blood glucose testing at the beginning of treatment and periodically during treatment. Any patient treated with atypical antipsychotics should be monitored for symptoms of hyperglycemia including polydipsia, polyuria, polyphagia, and weakness. Patients who develop symptoms of hyperglycemia during treatment with atypical antipsychotics should undergo fasting blood glucose testing. In some cases, hyperglycemia has resolved when the atypical antipsychotic was discontinued; however, some patients required continuation of anti-diabetic treatment despite discontinuation of the suspect drug.
Adults
In an analysis of 13 placebo-controlled monotherapy trials in adults, primarily with schizophrenia or another disorder, the mean change in fasting glucose in aripiprazole-treated patients (+4.4 mg/dL; median exposure 25 days; N=1057) was not significantly different than in placebo-treated patients (+2.5 mg/dL; median exposure 22 days; N=799). Table 6 shows the proportion of aripiprazole-treated patients with normal and borderline fasting glucose at baseline (median exposure 25 days) that had treatment-emergent high fasting glucose measurements compared to placebo-treated patients (median exposure 22 days).
| Category Change (at least once) from Baseline | Treatment Arm | n/N | % | |
|---|---|---|---|---|
| Fasting Glucose | Normal to High (<100 mg/dL to ≥126 mg/dL) |
Aripiprazole | 31/822 | 3.8 |
| Placebo | 22/605 | 3.6 | ||
| Borderline to High (≥100 mg/dL and <126 mg/dL to ≥126 mg/dL) |
Aripiprazole | 31/176 | 17.6 | |
| Placebo | 13/142 | 9.2 |
At 24 weeks, the mean change in fasting glucose in aripiprazole-treated patients was not significantly different than in placebo-treated patients [+2.2 mg/dL (n=42) and +9.6 mg/dL (n=28), respectively].
Pediatric Patients and Adolescents
In an analysis of two placebo-controlled trials in adolescents with schizophrenia (13 to 17 years) and pediatric patients with another disorder (10 to 17 years), the mean change in fasting glucose in aripiprazole-treated patients (+4.8 mg/dL; with a median exposure of 43 days; N=259) was not significantly different than in placebo-treated patients (+1.7 mg/dL; with a median exposure of 42 days; N=123).
Table 8 shows the proportion of patients with changes in fasting glucose levels from the pooled adolescent schizophrenia and other pediatric patients (median exposure of 42 to 43 days).
| Category Change (at least once) from Baseline | Indication | Treatment Arm | n/N | % |
|---|---|---|---|---|
|
Fasting Glucose
Normal to High (<100 mg/dL to ≥126 mg/dL) |
||||
| Pooled Schizophrenia and Another Disorder | Aripiprazole | 2/236 | 0.8 | |
| Placebo | 2/110 | 1.8 | ||
|
Fasting Glucose
Borderline to High (≥100 mg/dL and <126 mg/dL to ≥126 mg/dL) |
||||
| Pooled Schizophrenia and Another Disorder | Aripiprazole | 1/22 | 4.5 | |
| Placebo | 0/12 | 0 |
At 12 weeks in the pooled adolescent schizophrenia and other pediatric disorder trials, the mean change in fasting glucose in aripiprazole-treated patients was not significantly different than in placebo-treated patients [+2.4 mg/dL (n=81) and +0.1 mg/dL (n=15), respectively].
5.9 Falls
Antipsychotics, including aripiprazole, may cause somnolence, postural hypotension, motor and sensory instability, which may lead to falls and, consequently, fractures or other injuries. For patients with diseases, conditions, or medications that could exacerbate these effects, complete fall risk assessments when initiating antipsychotic treatment and recurrently for patients on long-term antipsychotic therapy.
9.2 Abuse
Aripiprazole has not been systematically studied in humans for its potential for abuse, tolerance, or physical dependence. Consequently, patients should be evaluated carefully for a history of drug abuse, and such patients should be observed closely for signs of aripiprazole misuse or abuse (e.g., development of tolerance, increases in dose, drug-seeking behavior).
5.14 Suicide
The possibility of a suicide attempt is inherent in psychotic illnesses and bipolar disorder, and close supervision of high-risk patients should accompany drug therapy. Prescriptions for aripiprazole should be written for the smallest quantity consistent with good patient management in order to reduce the risk of overdose [see Adverse Reactions (6.1, 6.2)] .
Aripiprazole
10 Overdosage
MedDRA terminology has been used to classify the adverse reactions.
8.1 Pregnancy
Pregnancy Exposure Registry
There is a pregnancy exposure registry that monitors pregnancy outcomes in women exposed to atypical antipsychotics, including aripiprazole, during pregnancy. Healthcare providers are encouraged to register patients by contacting the National Pregnancy Registry for Atypical Antipsychotics at 1-866-961-2388 or visit http://womensmentalhealth.org/clinical-and-research-programs/pregnancyregistry/.
Risk Summary
Neonates exposed to antipsychotic drugs, including aripiprazole, during the third trimester of pregnancy are at risk for extrapyramidal and/or withdrawal symptoms following delivery (see Clinical Considerations). Overall available data from published epidemiologic studies of pregnant women exposed to aripiprazole have not established a drug-associated risk of major birth defects, miscarriage, or adverse maternal or fetal outcomes (see Data). There are risks to the mother associated with untreated schizophrenia, bipolar I disorder, or major depressive disorder, and with exposure to antipsychotics, including aripiprazole, during pregnancy (see Clinical Considerations).
In animal reproduction studies, oral and intravenous aripiprazole administration during organogenesis in rats and/or rabbits at doses 10 and 19 times, respectively, the maximum recommended human dose (MRHD) of 30 mg/day based on mg/m 2 body surface area, produced fetal death, decreased fetal weight, undescended testicles, delayed skeletal ossification, skeletal abnormalities, and diaphragmatic hernia. Oral and intravenous aripiprazole administration during the pre- and post-natal period in rats at doses 10 times the MRHD based on mg/m 2 body surface area, produced prolonged gestation, stillbirths, decreased pup weight, and decreased pup survival (see Data).
The estimated background risk of major birth defects and miscarriage for the indicated population is unknown. All pregnancies have a background risk of birth defect, loss, or other adverse outcomes. In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2 to 4% and 15 to 20%, respectively..
Clinical Considerations
Disease-associated maternal and/or embryo/fetal risk
There is a risk to the mother from untreated schizophrenia or bipolar I disorder, including increased risk of relapse, hospitalization, and suicide. Schizophrenia and bipolar I disorder are associated with increased adverse perinatal outcomes, including preterm birth. It is not known if this is a direct result of the illness or other comorbid factors.
A prospective, longitudinal study followed 201 pregnant women with a history of major depressive disorder who were euthymic and taking antidepressants at the beginning of pregnancy. The women who discontinued antidepressants during pregnancy were more likely to experience a relapse of major depression than women who continued antidepressants. Consider the risk of untreated depression when discontinuing or changing treatment with antidepressant medication during pregnancy and postpartum.
Fetal/Neonatal Adverse Reactions
Extrapyramidal and/or withdrawal symptoms, including agitation, hypertonia, hypotonia, tremor, somnolence, respiratory distress, and feeding disorder have been reported in neonates who were exposed to antipsychotic drugs (including aripiprazole) during the third trimester of pregnancy. These symptoms have varied in severity. Monitor neonates for extrapyramidal and/or withdrawal symptoms, and manage symptoms appropriately. Some neonates recovered within hours or days without specific treatment; others required prolonged hospitalization.
Data
Human Data
Published data from observational studies, birth registries, and case reports on the use of atypical antipsychotics during pregnancy do not report a clear association with antipsychotics and major birth defects. A retrospective study from a Medicaid database of 9258 women exposed to antipsychotics during pregnancy did not indicate an overall increased risk for major birth defects.
Animal Data
In animal studies, aripiprazole demonstrated developmental toxicity, including possible teratogenic effects in rats and rabbits.
In pregnant rats treated orally with aripiprazole during organogenesis at doses of 3, 10, and 30 mg/kg/day, which are approximately 1, 3 and 10 times the MRHD of 30 mg/day based on mg/m 2 body surface area, a slight prolongation of gestation and delay in fetal development, as evidenced by decreased fetal weight and undescended testes, were observed at 10 times the MRHD. Delayed skeletal ossification was observed at 3 and 10 times the MRHD. Delivered offspring had increased incidences of hepatodiaphragmatic nodules and diaphragmatic hernia were observed at 10 times the MRHD (the other dose groups were not examined for these findings). Postnatally, delayed vaginal opening was seen at 3 and 10 times the MRHD. Impaired reproductive performance (decreased fertility rate, corpora lutea, implants, live fetuses, and increased post-implantation loss, likely mediated through effects on female offspring) were observed at 10 times the MRHD; however, there was no evidence to suggest that these developmental effects were secondary to maternal toxicity.
In pregnant rats injected intravenously with aripiprazole during organogenesis at doses of 3, 9, and 27 mg/kg/day, which are 1, 3, and 9 times the MRHD of 30 mg/day based on mg/m 2 body surface area, decreased fetal weight and delayed skeletal ossification were observed at 9 times the MRHD; this dose also caused maternal toxicity.
In pregnant rabbits treated orally with aripiprazole during organogenesis at doses of 10, 30, and 100 mg/kg/day which are 6, 19, and 65 times the MRHD of 30 mg/day based on mg/m 2 body surface area, decreased maternal food consumption, and increased abortions as well as increased fetal mortality were observed at 65 times the MHRD. Decreased fetal weight and increased incidence of fused sternebrae were observed at 19 and 65 times the MRHD.
In pregnant rabbits injected intravenously with aripiprazole during organogenesis at doses of 3, 10, and 30 mg/kg/day, which are 2, 6, and 19 times the MRHD of 30 mg/day based on mg/m 2 body surface area, decreased fetal weight, increased fetal abnormalities (primarily skeletal), and decreased fetal skeletal ossification were observed at 19 times the MRHD; this dose also caused maternal toxicity. The fetal no-effect dose was 10 mg/kg/day, which is 6 times the MRHD.
In rats treated orally with aripiprazole peri- and post-natally from gestation day 17 through postpartum day 21 at doses of 3, 10, and 30 mg/kg/day which are 1, 3, and 10 times the MRHD of 30 mg/day based on mg/m 2 body surface area slight maternal toxicity and slightly prolonged gestation were observed at 10 times the MHRD. An increase in stillbirths and, decreases in pup weight (persisting into adulthood) and survival were also seen at this dose.
In rats injected intravenously with aripiprazole from gestation day 6 through lactation day 20 at doses of 3, 8, and 20 mg/kg/day, which are 1, 3, and 6 times the MRHD of 30 mg/day based on mg/m 2 body surface area, increased stillbirths were observed at 3 and 6 times the MRHD; and decreases in early postnatal pup weight and survival were observed at 6 times the MRHD; these doses also caused some maternal toxicity. There were no effects on postnatal behavioral and reproductive development.
8.2 Lactation
Risk Summary
Limited data from published literature report the presence of aripiprazole in human breast milk, at relative infant doses ranging between 0.7% to 8.3% of the maternal weight-adjusted dosage. There are reports of poor weight gain in breastfed infants exposed to aripiprazole and reports of inadequate milk supply in lactating women taking aripiprazole.
The development and health benefits of breastfeeding should be considered along with the mother’s clinical need for aripiprazole and any potential adverse effects on the breastfed infant from aripiprazole or from the underlying maternal condition.
11 Description
Aripiprazole is an atypical antipsychotic drug that is available as aripiprazole tablets, USP. Aripiprazole is 7-[4-[4-(2,3-dichlorophenyl)-1-piperazinyl]butoxy]-3,4-dihydrocarbostyril. The empirical formula is C 23H 27Cl 2N 3O 2 and its molecular weight is 448.38. The chemical structure is:
Aripiprazole tablets, USP are available in 2 mg, 5 mg, 10 mg, 15 mg, 20 mg, and 30 mg strengths. Inactive ingredients include hydroxypropyl cellulose, lactose monohydrate, magnesium stearate, maize starch and microcrystalline cellulose. Colorants include ferric oxide red (10 mg and 30 mg), ferric oxide yellow (2 mg and 15 mg), and FD&C Blue No. 2 aluminum lake (2 mg and 5 mg).
5.15 Dysphagia
Esophageal dysmotility and aspiration have been associated with antipsychotic drug use, including aripiprazole. Aspiration pneumonia is a common cause of morbidity and mortality in elderly patients, in particular those with advanced Alzheimer’s dementia. Aripiprazole and other antipsychotic drugs should be used cautiously in patients at risk for aspiration pneumonia [see Warnings and Precautions (5.1) and Adverse Reactions (6.2)] .
9.3 Dependence
In physical dependence studies in monkeys, withdrawal symptoms were observed upon abrupt cessation of dosing. While the clinical trials did not reveal any tendency for any drug-seeking behavior, these observations were not systematic and it is not possible to predict on the basis of this limited experience the extent to which a CNS-active drug will be misused, diverted, and/or abused once marketed.
Unmapped Section
Adult Patients with Schizophrenia
The following findings are based on a pool of five placebo-controlled trials (four 4-week and one 6-week) in which oral aripiprazole was administered in doses ranging from 2 to 30 mg/day.
Commonly Observed Adverse Reactions
The only commonly observed adverse reaction associated with the use of aripiprazole in patients with schizophrenia (incidence of 5% or greater and aripiprazole incidence at least twice that for placebo) was akathisia (aripiprazole 8%; placebo 4%).
8.4 Pediatric Use
The pharmacokinetics of aripiprazole and dehydro-aripiprazole in pediatric patients, 10 to 17 years of age, were similar to those in adults after correcting for the differences in body weight [see Clinical Pharmacology (12.3)] .
Schizophrenia
Safety and effectiveness in pediatric patients with schizophrenia were established in a 6-week, placebo-controlled clinical trial in 202 pediatric patients aged 13 to 17 years [see Dosage and Administration (2.1), Adverse Reactions (6.1), and Clinical Studies (14.1)] . Although maintenance efficacy in pediatric patients has not been systematically evaluated, maintenance efficacy can be extrapolated from adult data along with comparisons of aripiprazole pharmacokinetic parameters in adult and pediatric patients.
Bipolar I Disorder
Although maintenance efficacy in pediatric patients has not been systematically evaluated, maintenance efficacy can be extrapolated from adult data along with comparisons of aripiprazole pharmacokinetic parameters in adult and pediatric patients.
The efficacy of adjunctive aripiprazole with concomitant lithium or valproate in the treatment of manic or mixed episodes in pediatric patients has not been systematically evaluated. However, such efficacy and lack of pharmacokinetic interaction between aripiprazole and lithium or valproate can be extrapolated from adult data, along with comparisons of aripiprazole pharmacokinetic parameters in adult and pediatric patients.
Information describing a clinical study in which efficacy was not demonstrated in patients ages 6 to 17 years is approved for Otsuka America Pharmaceutical, Inc.’s ABILIFY ® (aripiprazole). Additional pediatric use information in patients ages 6 to 18 years is approved for Otsuka America Pharmaceutical, Inc.’s ABILIFY ® (aripiprazole) product. However, due to Otsuka America Pharmaceutical, Inc.’s marketing exclusivity rights, this drug product is not labeled with that pediatric information.
Juvenile Animal Studies
Aripiprazole in juvenile rats caused mortality, CNS clinical signs, impaired memory and learning, and delayed sexual maturation when administered at oral doses of 10, 20, 40 mg/kg/day from weaning (21 days old) through maturity (80 days old). At 40 mg/kg/day, mortality, decreased activity, splayed hind limbs, hunched posture, ataxia, tremors and other CNS signs were observed in both genders. In addition, delayed sexual maturation was observed in males. At all doses and in a dose-dependent manner, impaired memory and learning, increased motor activity, and histopathology changes in the pituitary (atrophy), adrenals (adrenocortical hypertrophy), mammary glands (hyperplasia and increased secretion), and female reproductive organs (vaginal mucification, endometrial atrophy, decrease in ovarian corpora lutea) were observed. The changes in female reproductive organs were considered secondary to the increase in prolactin serum levels. A No Observed Adverse Effect Level (NOAEL) could not be determined and, at the lowest tested dose of 10 mg/kg/day, there is no safety margin relative to the systemic exposures (AUC 0-24) for aripiprazole or its major active metabolite in adolescents at the maximum recommended pediatric dose of 15 mg/day. All drug-related effects were reversible after a 2-month recovery period, and most of the drug effects in juvenile rats were also observed in adult rats from previously conducted studies.
Aripiprazole in juvenile dogs (2 months old) caused CNS clinical signs of tremors, hypoactivity, ataxia, recumbency and limited use of hind limbs when administered orally for 6 months at 3, 10, 30 mg/kg/day. Mean body weight and weight gain were decreased up to 18% in females in all drug groups relative to control values. A NOAEL could not be determined and, at the lowest tested dose of 3 mg/kg/day, there is no safety margin relative to the systemic exposures (AUC 0-24) for aripiprazole or its major active metabolite in adolescents at the maximum recommended pediatric dose of 15 mg/day. All drug-related effects were reversible after a 2-month recovery period.
8.5 Geriatric Use
No dosage adjustment is recommended for elderly patients [see Boxed Warning, Warnings and Precautions (5.1), and Clinical Pharmacology (12.3)] .
Of the 13,543 patients treated with oral aripiprazole in clinical trials, 1073 (8%) were ≥65 years old and 799 (6%) were ≥75 years old. Placebo-controlled studies of oral aripiprazole in schizophrenia or other indications did not include sufficient numbers of subjects aged 65 and over to determine whether they respond differently from younger subjects.
Aripiprazole is not approved for the treatment of patients with psychosis associated with Alzheimer’s disease [see Boxed Warning and Warnings and Precautions (5.1)].
14 Clinical Studies
Efficacy of the oral formulations of aripiprazole was established in the following adequate and well-controlled trials:
- Four short-term trials and one maintenance trial in adult patients and one short-term trial in adolescents (ages 13 to 17) with schizophrenia [see Clinical Studies (14.1)]
- One maintenance monotherapy trial and in one maintenance adjunctive trial in adult patients with bipolar I disorder [see Clinical Studies (14.2)]
Additional pediatric use information is approved for Otsuka America Pharmaceutical, Inc.’s ABILIFY ® (aripiprazole) product. However, due to Otsuka America Pharmaceutical, Inc.’s marketing exclusivity rights, this drug product is not labeled with that information.
4 Contraindications
Aripiprazole tablets are contraindicated in patients with a history of a hypersensitivity reaction to aripiprazole. Reactions have ranged from pruritus/urticaria to anaphylaxis [see Adverse Reactions (6.2)].
6 Adverse Reactions
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
The following adverse reactions are discussed in more detail in other sections of the labeling:
- Increased Mortality in Elderly Patients with Dementia-Related Psychosis [see Boxed Warning and Warnings and Precautions (5.1)]
- Cerebrovascular Adverse Events, Including Stroke [see Warnings and Precautions (5.2)]
- Suicidal Thoughts and Behaviors in Children, Adolescents, and Young Adults [see Boxed Warning and Warnings and Precautions (5.3)]
- Neuroleptic Malignant Syndrome (NMS) [see Warnings and Precautions (5.4)]
- Tardive Dyskinesia [see Warnings and Precautions (5.5)]
- Metabolic Changes [see Warnings and Precautions (5.6)]
- Pathological Gambling and Other Compulsive Behaviors [see Warnings and Precautions (5.7)]
- Orthostatic Hypotension [see Warnings and Precautions (5.8)]
- Falls [see Warnings and Precautions (5.9)]
- Leukopenia, Neutropenia, and Agranulocytosis [see Warnings and Precautions (5.10)]
- Seizures/Convulsions [see Warnings and Precautions (5.11)]
- Potential for Cognitive and Motor Impairment [see Warnings and Precautions (5.12)]
- Body Temperature Regulation [see Warnings and Precautions (5.13)]
- Suicide [see Warnings and Precautions (5.14)]
- Dysphagia [see Warnings and Precautions (5.15)]
The most common adverse reactions in adult patients in clinical trials (≥10%) were nausea, vomiting, constipation, headache, dizziness, akathisia, anxiety, insomnia, and restlessness.
The most common adverse reactions in the pediatric clinical trials (≥10%) were somnolence, headache, vomiting, extrapyramidal disorder, fatigue, increased appetite, insomnia, nausea, nasopharyngitis, and weight increased.
Aripiprazole has been evaluated for safety in 13,543 adult patients who participated in multiple-dose, clinical trials in schizophrenia, other indications, Dementia of the Alzheimer’s type, Parkinson’s disease, and alcoholism, and who had approximately 7619 patient-years of exposure to oral aripiprazole. A total of 3390 patients were treated with oral aripiprazole for at least 180 days and 1933 patients treated with oral aripiprazole had at least 1 year of exposure.
Aripiprazole has been evaluated for safety in 1,686 patients (6 to 18 years) who participated in multiple-dose, clinical trials in schizophrenia, or other indications and who had approximately 1,342 patient-years of exposure to oral aripiprazole. A total of 959 pediatric patients were treated with oral aripiprazole for at least 180 days and 556 pediatric patients treated with oral aripiprazole had at least 1 year of exposure.
The conditions and duration of treatment with aripiprazole included (in overlapping categories) double-blind, comparative and noncomparative open-label studies, inpatient and outpatient studies, fixed-and flexible-dose studies, and short-and longer-term exposure.
Additional pediatric use information is approved for Otsuka America Pharmaceutical, Inc.’s ABILIFY ® (aripiprazole) product. However, due to Otsuka America Pharmaceutical, Inc.’s marketing exclusivity rights, this drug product is not labeled with that information.
7 Drug Interactions
Dosage adjustment due to drug interactions (7.1) :
| Factors | Dosage Adjustments for Aripiprazole |
| Known CYP2D6 Poor Metabolizers | Administer half of usual dose |
| Known CYP2D6 Poor Metabolizers and strong CYP3A4 inhibitors | Administer a quarter of usual dose |
| Strong CYP2D6 or CYP3A4 inhibitors | Administer half of usual dose |
| Strong CYP2D6 and CYP3A4 inhibitors | Administer a quarter of usual dose |
| Strong CYP3A4 inducers | Double usual dose over 1 to 2 weeks |
10.1 Human Experience
In clinical trials and in postmarketing experience, adverse reactions of deliberate or accidental overdosage with oral aripiprazole have been reported worldwide. These include overdoses with oral aripiprazole alone and in combination with other substances. No fatality was reported with aripiprazole alone. The largest known dose with a known outcome involved acute ingestion of 1260 mg of oral aripiprazole (42 times the maximum recommended daily dose) by a patient who fully recovered. Deliberate or accidental overdosage was also reported in children (age 12 and younger) involving oral aripiprazole ingestions up to 195 mg with no fatalities.
Common adverse reactions (reported in at least 5% of all overdose cases) reported with oral aripiprazole overdosage (alone or in combination with other substances) include vomiting, somnolence, and tremor. Other clinically important signs and symptoms observed in one or more patients with aripiprazole overdoses (alone or with other substances) include acidosis, aggression, aspartate aminotransferase increased, atrial fibrillation, bradycardia, coma, confusional state, convulsion, blood creatine phosphokinase increased, depressed level of consciousness, hypertension, hypokalemia, hypotension, lethargy, loss of consciousness, QRS complex prolonged, QT prolonged, pneumonia aspiration, respiratory arrest, status epilepticus, and tachycardia.
12.2 Pharmacodynamics
Aripiprazole exhibits high affinity for dopamine D 2 and D 3, serotonin 5-HT 1A and 5-HT 2A receptors (K i values of 0.34 nM, 0.8 nM, 1.7 nM, and 3.4 nM, respectively), moderate affinity for dopamine D 4, serotonin 5-HT 2C and 5-HT 7, alpha1-adrenergic and histamine H 1 receptors (K i values of 44 nM, 15 nM, 39 nM, 57 nM, and 61 nM, respectively), and moderate affinity for the serotonin reuptake site (K i=98 nM). Aripiprazole has no appreciable affinity for cholinergic muscarinic receptors (IC 50>1000 nM).
12.3 Pharmacokinetics
Aripiprazole activity is presumably primarily due to the parent drug, aripiprazole, and to a lesser extent, to its major metabolite, dehydro-aripiprazole, which has been shown to have affinities for D 2 receptors similar to the parent drug and represents 40% of the parent drug exposure in plasma. The mean elimination half-lives are about 75 hours and 94 hours for aripiprazole and dehydro-aripiprazole, respectively. Steady-state concentrations are attained within 14 days of dosing for both active moieties. Aripiprazole accumulation is predictable from single-dose pharmacokinetics. At steady-state, the pharmacokinetics of aripiprazole is dose-proportional. Elimination of aripiprazole is mainly through hepatic metabolism involving two P450 isozymes, CYP2D6 and CYP3A4. For CYP2D6 poor metabolizers, the mean elimination half-life for aripiprazole is about 146 hours.
Pharmacokinetic studies showed that aripiprazole orally disintegrating tablets are bioequivalent to aripiprazole tablets.
5.6 Metabolic Changes
Atypical antipsychotic drugs have been associated with metabolic changes that include hyperglycemia/diabetes mellitus, dyslipidemia, and body weight gain. While all drugs in the class have been shown to produce some metabolic changes, each drug has its own specific risk profile.
5.5 Tardive Dyskinesia
A syndrome of potentially irreversible, involuntary, dyskinetic movements may develop in patients treated with antipsychotic drugs. Although the prevalence of the syndrome appears to be highest among the elderly, especially elderly women, it is impossible to rely upon prevalence estimates to predict, at the inception of antipsychotic treatment, which patients are likely to develop the syndrome. Whether antipsychotic drug products differ in their potential to cause tardive dyskinesia is unknown.A syndrome of potentially irreversible, involuntary, dyskinetic movements may develop in patients treated with antipsychotic drugs. Although the prevalence of the syndrome appears to be highest among the elderly, especially elderly women, it is impossible to rely upon prevalence estimates to predict, at the inception of antipsychotic treatment, which patients are likely to develop the syndrome. Whether antipsychotic drug products differ in their potential to cause tardive dyskinesia is unknown.
The risk of developing tardive dyskinesia and the likelihood that it will become irreversible are believed to increase as the duration of treatment and the total cumulative dose of antipsychotic drugs administered to the patient increase. However, the syndrome can develop, although much less commonly, after relatively brief treatment periods at low doses. The risk of developing tardive dyskinesia and the likelihood that it will become irreversible are believed to increase as the duration of treatment and the total cumulative dose of antipsychotic drugs administered to the patient increase. However, the syndrome can develop, although much less commonly, after relatively brief treatment periods at low doses.
Tardive dyskinesia may remit, partially or completely, if antipsychotic treatment is withdrawn. Antipsychotic treatment, itself, however, may suppress (or partially suppress) the signs and symptoms of the syndrome and, thereby, may possibly mask the underlying process. The effect that symptomatic suppression has upon the long-term course of the syndrome is unknown.
Given these considerations, aripiprazole should be prescribed in a manner that is most likely to minimize the occurrence of tardive dyskinesia. Chronic antipsychotic treatment should generally be reserved for patients who suffer from a chronic illness that (1) is known to respond to antipsychotic drugs and (2) for whom alternative, equally effective, but potentially less harmful treatments are not available or appropriate. In patients who do require chronic treatment, the smallest dose and the shortest duration of treatment producing a satisfactory clinical response should be sought. The need for continued treatment should be reassessed periodically.Given these considerations, aripiprazole should be prescribed in a manner that is most likely to minimize the occurrence of tardive dyskinesia. Chronic antipsychotic treatment should generally be reserved for patients who suffer from a chronic illness that (1) is known to respond to antipsychotic drugs and (2) for whom alternative, equally effective, but potentially less harmful treatments are not available or appropriate. In patients who do require chronic treatment, the smallest dose and the shortest duration of treatment producing a satisfactory clinical response should be sought. The need for continued treatment should be reassessed periodically.
If signs and symptoms of tardive dyskinesia appear in a patient on aripiprazole, drug discontinuation should be considered. However, some patients may require treatment with aripiprazole despite the presence of the syndrome.If signs and symptoms of tardive dyskinesia appear in a patient on aripiprazole, drug discontinuation should be considered. However, some patients may require treatment with aripiprazole despite the presence of the syndrome.
1 Indications and Usage
Aripiprazole tablets are indicated for the treatment of:
- Schizophrenia [see Clinical Studies (14.1)]
Additional pediatric use information is approved for Otsuka America Pharmaceutical, Inc.’s ABILIFY ® (aripiprazole) product. However, due to Otsuka America Pharmaceutical, Inc.’s marketing exclusivity rights, this drug product is not labeled with that information.
12.1 Mechanism of Action
The mechanism of action of aripiprazole in schizophrenia is unclear. However, the efficacy of aripiprazole in the listed indications could be mediated through a combination of partial agonist activity at D 2 and 5-HT 1A receptors and antagonist activity at 5-HT 2A receptors.
9.1 Controlled Substance
Aripiprazole is not a controlled substance.
5.11 Seizures/convulsions
In short-term, placebo-controlled trials, patients with a history of seizures excluded seizures/convulsions occurred in 0.1% (3/2467) of undiagnosed adult patients treated with oral aripiprazole, and in 0.1% (1/732) of pediatric patients (6 to 18 years).
As with other antipsychotic drugs, aripiprazole should be used cautiously in patients with a history of seizures or with conditions that lower the seizure threshold. Conditions that lower the seizure threshold may be more prevalent in a population of 65 years or older.
5 Warnings and Precautions
- Cerebrovascular Adverse Reactions in Elderly Patients with Dementia- Related Psychosis: Increased incidence of cerebrovascular adverse reactions (e.g., stroke, transient ischemic attack, including fatalities) (5.2)
- Neuroleptic Malignant Syndrome: Manage with immediate discontinuation and close monitoring (5.4)
- Tardive Dyskinesia: Discontinue if clinically appropriate (5.5)
-
Metabolic Changes: Atypical antipsychotic drugs have been associated with metabolic changes that include hyperglycemia/diabetes mellitus, dyslipidemia, and body weight gain
(5.6)
- Hyperglycemia/Diabetes Mellitus: Monitor glucose regularly in patients with and at risk for diabetes (5.6)
- Dyslipidemia: Undesirable alterations in lipid levels have been observed in patients treated with atypical antipsychotics (5.6)
- Weight Gain: Weight gain has been observed with atypical antipsychotic use. Monitor weight (5.6)
- Pathological Gambling and Other Compulsive Behaviors: Consider dose reduction or discontinuation (5.7)
- Orthostatic Hypotension: Monitor heart rate and blood pressure and warn patients with known cardiovascular or cerebrovascular disease, and risk of dehydration or syncope (5.8)
- Leukopenia, Neutropenia, and Agranulocytosis: have been reported with antipsychotics including aripiprazole. Patients with a history of a clinically significant low white blood cell count (WBC) or a drug-induced leukopenia/neutropenia should have their complete blood count (CBC) monitored frequently during the first few months of therapy and discontinuation of aripiprazole should be considered at the first sign of a clinically significant decline in WBC in the absence of other causative factors (5.10)
- Seizures/Convulsions: Use cautiously in patients with a history of seizures or with conditions that lower the seizure threshold (5.11)
- Potential for Cognitive and Motor Impairment: Use caution when operating machinery (5.12)
- Suicide: The possibility of a suicide attempt is inherent in schizophrenia and bipolar disorder. Closely supervise high-risk patients (5.14)
2 Dosage and Administration
5.8 Orthostatic Hypotension
Aripiprazole may cause orthostatic hypotension, perhaps due to its α1-adrenergic receptor antagonism. The incidence of orthostatic hypotension-associated events from short-term, placebo-controlled trials of adult patients on oral aripiprazole (n=2467) included (aripiprazole incidence, placebo incidence) orthostatic hypotension (1%, 0.3%), postural dizziness (0.5%, 0.3%), and syncope (0.5%, 0.4%); of pediatric patients 6 to 18 years of age (n=732) on oral aripiprazole included orthostatic hypotension (0.5%, 0%), postural dizziness (0.4%, 0 %), and syncope (0.2%, 0%). [see Adverse Reactions (6.1)] .
The incidence of a significant orthostatic change in blood pressure (defined as a decrease in systolic blood pressure ≥20 mmHg accompanied by an increase in heart rate ≥25 bpm when comparing standing to supine values) for aripiprazole was not meaningfully different from placebo (aripiprazole incidence, placebo incidence): in adult oral aripiprazole -treated patients (4%, 2%), or in pediatric oral aripiprazole -treated patients aged 6 to 18 years (0.4%, 1%).
Aripiprazole should be used with caution in patients with known cardiovascular disease (history of myocardial infarction or ischemic heart disease, heart failure or conduction abnormalities), cerebrovascular disease, or conditions which would predispose patients to hypotension (dehydration, hypovolemia, and treatment with antihypertensive medications) [see Drug Interactions (7.1)] .
3 Dosage Forms and Strengths
Aripiprazole tablets, USP are available as described in Table 3.
|
Tablet
Strength |
Tablet
Color/Shape |
Tablet
Markings |
| 2 mg | green
modified rectangle |
“A2” on one side
and another side is plain |
| 5 mg | blue
modified rectangle |
“A5” on one side
and another side is plain |
| 10 mg | pink
modified rectangle |
“A10” on one side
and another side is plain |
| 15 mg | yellow
round |
“A15” on one side
and another side is plain |
| 20 mg | white to off white
round |
“A20” on one side
and another side is plain |
| 30 mg | pink
round |
“A30” on one side
and another side is plain |
6.2 Postmarketing Experience
The following adverse reactions have been identified during post-approval use of aripiprazole. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to establish a causal relationship to drug exposure: occurrences of allergic reaction (anaphylactic reaction, angioedema, laryngospasm, pruritus/urticaria, or oropharyngeal spasm), pathological gambling, hiccups, blood glucose fluctuation, oculogyric crisis, and drug reaction with eosinophilia and systemic symptoms (DRESS).
8.6 Cyp2d6 Poor Metabolizers
Dosage adjustment is recommended in known CYP2D6 poor metabolizers due to high aripiprazole concentrations. Approximately 8% of Caucasians and 3 to 8% of Black/African Americans cannot metabolize CYP2D6 substrates and are classified as poor metabolizers (PM) [see Dosage and Administration (2.7) and Clinical Pharmacology (12.3)] .
10.2 Management of Overdosage
No specific information is available on the treatment of overdose with aripiprazole. An electrocardiogram should be obtained in case of overdosage and if QT interval prolongation is present, cardiac monitoring should be instituted. Otherwise, management of overdose should concentrate on supportive therapy, maintaining an adequate airway, oxygenation and ventilation, and management of symptoms. Close medical supervision and monitoring should continue until the patient recovers.
Charcoal: In the event of an overdose of aripiprazole, an early charcoal administration may be useful in partially preventing the absorption of aripiprazole. Administration of 50 g of activated charcoal, one hour after a single 15 mg oral dose of aripiprazole, decreased the mean AUC and C max of aripiprazole by 50%.
Hemodialysis: Although there is no information on the effect of hemodialysis in treating an overdose with aripiprazole, hemodialysis is unlikely to be useful in overdose management since aripiprazole is highly bound to plasma proteins.
8 Use in Specific Populations
Pregnancy: May cause extrapyramidal and/or withdrawal symptoms in neonates with third trimester exposure (8.1)
Additional pediatric use information is approved for Otsuka America Pharmaceutical, Inc.’s ABILIFY ® (aripiprazole) product. However, due to Otsuka America Pharmaceutical, Inc.’s marketing exclusivity rights, this drug product is not labeled with that information.
8.8 Other Specific Populations
No dosage adjustment for aripiprazole is required on the basis of a patient’s sex, race, or smoking status [see Clinical Pharmacology (12.3) ].
5.13 Body Temperature Regulation
Disruption of the body’s ability to reduce core body temperature has been attributed to antipsychotic agents. Appropriate care is advised when prescribing aripiprazole for patients who will be experiencing conditions which may contribute to an elevation in core body temperature, (e.g., exercising strenuously, exposure to extreme heat, receiving concomitant medication with anticholinergic activity, or being subject to dehydration) [see Adverse Reactions (6.2)] .
8.7 Hepatic and Renal Impairment
No dosage adjustment for aripiprazole is required on the basis of a patient’s hepatic function (mild to severe hepatic impairment, Child-Pugh score between 5 and 15), or renal function (mild to severe renal impairment, glomerular filtration rate between 15 and 90 mL/minute) [see Clinical Pharmacology (12.3) ].
17 Patient Counseling Information
Advise the patient to read the FDA-approved patient labeling ( Medication Guide).
Discuss the following issues with patients prescribed aripiprazole:
Clinical Worsening of Depression and Suicide Risk
Patients, their families, and their caregivers should be encouraged to be alert to the emergence of anxiety, agitation, panic attacks, insomnia, irritability, hostility, aggressiveness, impulsivity, akathisia (psychomotor restlessness), hypomania, mania, other unusual changes in behavior, worsening of depression, and suicidal ideation, especially early during antidepressant treatment and when the dose is adjusted up or down. Families and caregivers of patients should be advised to look for the emergence of such symptoms on a day-to-day basis, since changes may be abrupt. Such symptoms should be reported to the patient’s prescriber or health professional, especially if they are severe, abrupt in onset, or were not part of the patient’s presenting symptoms. Symptoms such as these may be associated with an increased risk for suicidal thinking and behavior and indicate a need for very close monitoring and possibly changes in the medication [see Warnings and Precautions (5.3)] .
Prescribers or other health professionals should inform patients, their families, and their caregivers about the benefits and risks associated with treatment with aripiprazole and should counsel them in its appropriate use. A patient Medication Guide including information about “Antidepressant Medicines, Depression and other Serious Mental Illness, and Suicidal Thoughts or Actions” is available for aripiprazole. The prescriber or health professional should instruct patients, their families, and their caregivers to read the Medication Guide and should assist them in understanding its contents. Patients should be given the opportunity to discuss the contents of the Medication Guide and to obtain answers to any questions they may have. It should be noted that aripiprazole is not approved as a single agent for treatment of depression and has not been evaluated in pediatric major depressive disorder.
Pathological Gambling and Other Compulsive Behaviors
Advise patients and their caregivers of the possibility that they may experience compulsive urges to shop, intense urges to gamble, compulsive sexual urges, binge eating and/or other compulsive urges and the inability to control these urges while taking aripiprazole. In some cases, but not all, the urges were reported to have stopped when the dose was reduced or stopped [see Warnings and Precautions (5.7)] .
Interference with Cognitive and Motor Performance
Because aripiprazole may have the potential to impair judgment, thinking, or motor skills, patients should be cautioned about operating hazardous machinery, including automobiles, until they are reasonably certain that aripiprazole therapy does not affect them adversely [see Warnings and Precautions (5.12)] .
Concomitant Medication
Patients should be advised to inform their physicians if they are taking, or plan to take, any prescription or over-the-counter drugs, since there is a potential for interactions [see Drug Interactions (7)] .
Heat Exposure and Dehydration
Patients should be advised regarding appropriate care in avoiding overheating and dehydration [see Warnings and Precautions (5.13)] .
Pregnancy
Advise patients to notify their healthcare provider if they become pregnant or intend to become pregnant during treatment with aripiprazole. Advise patients that aripiprazole may cause extrapyramidal and/or withdrawal symptoms (agitation, hypertonia, hypotonia, tremor, somnolence, respiratory distress, and feeding disorder) in a neonate. Advise patients that there is a pregnancy registry that monitors pregnancy outcomes in women exposed to aripiprazole during pregnancy [see Use in Specific Populations (8.1)] .
ABILIFY ® is a trademark of Otsuka Pharmaceutical Company.
Manufactured For:
Accord Healthcare, Inc.,
1009 Slater Road,
Suite 210-B,
Durham, NC 27703,
USA
Manufactured By:
Intas Pharmaceuticals Limited.
Plot No. 5 to 12, Pharmez,
Sarkhej-Bavla, National Highway No 8-A,
Near Village Matoda, Tal Sanand,
Ahmedabad - 382213, Gujarat, India
51 1878 2 722646
Issued March 2020
16 How Supplied/storage and Handling
Product: 50090-6063
NDC: 50090-6063-0 30 TABLET in a BOTTLE
5.4 Neuroleptic Malignant Syndrome (nms)
A potentially fatal symptom complex sometimes referred to as Neuroleptic Malignant Syndrome (NMS) may occur with administration of antipsychotic drugs, including aripiprazole. Rare cases of NMS occurred during aripiprazole treatment in the worldwide clinical database. Clinical manifestations of NMS are hyperpyrexia, muscle rigidity, altered mental status, and evidence of autonomic instability (irregular pulse or blood pressure, tachycardia, diaphoresis, and cardiac dysrhythmia). Additional signs may include elevated creatine phosphokinase, myoglobinuria (rhabdomyolysis), and acute renal failure.
The diagnostic evaluation of patients with this syndrome is complicated. In arriving at a diagnosis, it is important to exclude cases where the clinical presentation includes both serious medical illness (e.g., pneumonia, systemic infection) and untreated or inadequately treated extrapyramidal signs and symptoms (EPS). Other important considerations in the differential diagnosis include central anticholinergic toxicity, heat stroke, drug fever, and primary central nervous system pathology.
The management of NMS should include: 1) immediate discontinuation of antipsychotic drugs and other drugs not essential to concurrent therapy; 2) intensive symptomatic treatment and medical monitoring; and 3) treatment of any concomitant serious medical problems for which specific treatments are available. There is no general agreement about specific pharmacological treatment regimens for uncomplicated NMS.
If a patient requires antipsychotic drug treatment after recovery from NMS, the potential reintroduction of drug therapy should be carefully considered. The patient should be carefully monitored, since recurrences of NMS have been reported.
13.2 Animal Toxicology And/or Pharmacology
Aripiprazole produced retinal degeneration in albino rats in a 26-week chronic toxicity study at a dose of 60 mg/kg/day and in a 2-year carcinogenicity study at doses of 40 and 60 mg/kg/day which are 13 and 19 times the MRHD of 30 mg/day based on mg/m 2 body surface area. Evaluation of the retinas of albino mice and of monkeys did not reveal evidence of retinal degeneration. Additional studies to further evaluate the mechanism have not been performed. The relevance of this finding to human risk is unknown.
5.10 Leukopenia, Neutropenia, and Agranulocytosis
In clinical trials and/or postmarketing experience, events of leukopenia and neutropenia have been reported temporally related to antipsychotic agents, including aripiprazole. Agranulocytosis has also been reported.
Possible risk factors for leukopenia/neutropenia include pre-existing low white blood cell count (WBC)/absolute neutrophil count (ANC) and history of drug-induced leukopenia/neutropenia. In patients with a history of a clinically significant low WBC/ANC or drug-induced leukopenia/neutropenia, perform a complete blood count (CBC) frequently during the first few months of therapy. In such patients, consider discontinuation of aripiprazole at the first sign of a clinically significant decline in WBC in the absence of other causative factors.
Monitor patients with clinically significant neutropenia for fever or other symptoms or signs of infection and treat promptly if such symptoms or signs occur. Discontinue aripiprazole in patients with severe neutropenia (absolute neutrophil count <1000/mm 3) and follow their WBC counts until recovery.
5.12 Potential for Cognitive and Motor Impairment
Aripiprazole, like other antipsychotics, may have the potential to impair judgment, thinking, or motor skills. For example, in short-term, placebo-controlled trials, somnolence (including sedation) was reported as follows (aripiprazole incidence, placebo incidence): in adult patients (n=2467) treated with oral aripiprazole (11%, 6%), and in pediatric patients ages 6 to 17 (n=611) (24%, 6%). Somnolence (including sedation) led to discontinuation in 0.3% (8/2467) of adult patients and 3% (20/732) of pediatric patients (6 to 18 years) on oral aripiprazole in short-term, placebo-controlled trials.
Despite the relatively modest increased incidence of these events compared to placebo, patients should be cautioned about operating hazardous machinery, including automobiles, until they are reasonably certain that therapy with aripiprazole does not affect them adversely.
5.2 Cerebrovascular Adverse Events, Including Stroke
In placebo-controlled clinical studies (two flexible dose and one fixed dose study) of dementia-related psychosis, there was an increased incidence of cerebrovascular adverse events (e.g., stroke, transient ischemic attack), including fatalities, in aripiprazole-treated patients (mean age: 84 years; range: 78 to 88 years). In the fixed-dose study, there was a statistically significant dose response relationship for cerebrovascular adverse events in patients treated with aripiprazole. Aripiprazole is not approved for the treatment of patients with dementia-related psychosis [see Boxed Warning] .
5.7 Pathological Gambling and Other Compulsive Behaviors
Post-marketing case reports suggest that patients can experience intense urges, particularly for gambling, and the inability to control these urges while taking aripiprazole. Other compulsive urges, reported less frequently include: sexual urges, shopping, eating or binge eating, and other impulsive or compulsive behaviors. Because patients may not recognize these behaviors as abnormal, it is important for prescribers to ask patients or their caregivers specifically about the development of new or intense gambling urges, compulsive sexual urges, compulsive shopping, binge or compulsive eating, or other urges while being treated with aripiprazole. It should be noted that impulse-control symptoms can be associated with the underlying disorder. In some cases, although not all, urges were reported to have stopped when the dose was reduced or the medication was discontinued. Compulsive behaviors may result in harm to the patient and others if not recognized. Consider dose reduction or stopping the medication if a patient develops such urges.
7.1 Drugs Having Clinically Important Interactions With Aripiprazole
| Concomitant Drug Name or Drug Class | Clinical Rationale | Clinical Recommendation |
|---|---|---|
| Strong CYP3A4 Inhibitors (e.g., itraconazole, clarithromycin) or strong CYP2D6 inhibitors (e.g., quinidine, fluoxetine, paroxetine) | The concomitant use of aripiprazole with strong CYP 3A4 or CYP2D6 inhibitors increased the exposure of aripiprazole compared to the use of aripiprazole alone [see Clinical Pharmacology (12.3)] . | With concomitant use of aripiprazole with a strong CYP3A4 inhibitor or CYP2D6 inhibitor, reduce the aripiprazole dosage [see Dosage and Administration (2.7)] . |
| Strong CYP3A4 Inducers (e.g., carbamazepine, rifampin) | The concomitant use of aripiprazole and carbamazepine decreased the exposure of aripiprazole compared to the use of aripiprazole alone [see Clinical Pharmacology (12.3)] . | With concomitant use of aripiprazole with a strong CYP3A4 inducer, consider increasing the aripiprazole dosage [see Dosage and Administration (2.7)] . |
| Antihypertensive Drugs | Due to its alpha adrenergic antagonism, aripiprazole has the potential to enhance the effect of certain antihypertensive agents. | Monitor blood pressure and adjust dose accordingly [see Warnings and Precautions (5.8)] . |
| Benzodiazepines (e.g., lorazepam) | The intensity of sedation was greater with the combination of oral aripiprazole and lorazepam as compared to that observed with aripiprazole alone. The orthostatic hypotension observed was greater with the combination as compared to that observed with lorazepam alone [see Warnings and Precautions (5.8)] . | Monitor sedation and blood pressure. Adjust dose accordingly. |
7.2 Drugs Having No Clinically Important Interactions With Aripiprazole
Based on pharmacokinetic studies, no dosage adjustment of aripiprazole is required when administered concomitantly with famotidine, valproate, lithium, lorazepam.
In addition, no dosage adjustment is necessary for substrates of CYP2D6 (e.g., dextromethorphan, fluoxetine, paroxetine, or venlafaxine), CYP2C9 (e.g., warfarin), CYP2C19 (e.g., omeprazole, warfarin, escitalopram), or CYP3A4 (e.g., dextromethorphan) when co-administered with aripiprazole. Additionally, no dosage adjustment is necessary for valproate, lithium, lamotrigine, lorazepam, or sertraline when co-administered with aripiprazole [see Clinical Pharmacology (12.3)] .
5.1 Increased Mortality in Elderly Patients With Dementia Related Psychosis
Increased Mortality
Elderly patients with dementia-related psychosis treated with antipsychotic drugs are at an increased risk of death. Aripiprazole is not approved for the treatment of patients with dementia-related psychosis [see Boxed Warning] .
Safety Experience in Elderly Patients with Psychosis Associated with Alzheimer’s Disease
In three, 10-week, placebo-controlled studies of aripiprazole in elderly patients with psychosis associated with Alzheimer’s disease (n=938; mean age: 82.4 years; range: 56 to 99 years), the adverse reactions that were reported at an incidence of ≥3% and aripiprazole incidence at least twice that for placebo were lethargy [placebo 2%, aripiprazole 5%], somnolence (including sedation) [placebo 3%, aripiprazole 8%], and incontinence (primarily, urinary incontinence) [placebo 1%, aripiprazole 5%], excessive salivation [placebo 0%, aripiprazole 4%], and lightheadedness [placebo 1%, aripiprazole 4%].
The safety and efficacy of aripiprazole in the treatment of patients with psychosis associated with dementia have not been established. If the prescriber elects to treat such patients with aripiprazole, assess for the emergence of difficulty swallowing or excessive somnolence, which could predispose to accidental injury or aspiration [see Boxed Warning] .
5.3 Suicidal Thoughts and Behaviors in Children, Adolescents, and Young Adults
Patients with major depressive disorder (MDD), both adult and pediatric, may experience worsening of their depression and/or the emergence of suicidal ideation and behavior (suicidality) or unusual changes in behavior, whether or not they are taking antidepressant medications, and this risk may persist until significant remission occurs. Suicide is a known risk of depression and certain other psychiatric disorders, and these disorders themselves are the strongest predictors of suicide. There has been a long-standing concern, however, that antidepressants may have a role in inducing worsening of depression and the emergence of suicidality in certain patients during the early phases of treatment. Pooled analyses of short-term, placebo-controlled trials of antidepressant drugs (SSRIs and others) showed that these drugs increase the risk of suicidal thinking and behavior (suicidality) in children, adolescents, and young adults (ages 18 to 24) with MDD and other psychiatric disorders. Short-term studies did not show an increase in the risk of suicidality with antidepressants compared to placebo in adults beyond age 24; there was a reduction with antidepressants compared to placebo in adults aged 65 and older.
The pooled analyses of placebo-controlled trials in children and adolescents with MDD, Obsessive Compulsive Disorder (OCD), or other psychiatric disorders included a total of 24 short-term trials of 9 antidepressant drugs in over 4400 patients. The pooled analyses of placebo-controlled trials in adults with MDD or other psychiatric disorders included a total of 295 short-term trials (median duration of 2 months) of 11 antidepressant drugs in over 77,000 patients. There was considerable variation in risk of suicidality among drugs, but a tendency toward an increase in the younger patients for almost all drugs studied. There were differences in absolute risk of suicidality across the different indications, with the highest incidence in MDD. The risk differences (drug vs. placebo), however, were relatively stable within age strata and across indications. These risk differences (drug-placebo difference in the number of cases of suicidality per 1000 patients treated) are provided in Table 5.
| Age Range |
Drug-Placebo Difference in Number of
Cases of Suicidality per 1000 Patients Treated |
| Increases Compared to Placebo | |
| <18 | 14 additional cases |
| 18 to 24 | 5 additional cases |
| Decreases Compared to Placebo | |
| 25 to 64 | 1 fewer case |
| ≥65 | 6 fewer cases |
No suicides occurred in any of the pediatric trials. There were suicides in the adult trials, but the number was not sufficient to reach any conclusion about drug effect on suicide.
It is unknown whether the suicidality risk extends to longer-term use, i.e., beyond several months. However, there is substantial evidence from placebo-controlled maintenance trials in adults with depression that the use of antidepressants can delay the recurrence of depression.
All patients being treated with antidepressants for any indication should be monitored appropriately and observed closely for clinical worsening, suicidality, and unusual changes in behavior, especially during the initial few months of a course of drug therapy, or at times of dose changes, either increases or decreases.
The following symptoms, anxiety, agitation, panic attacks, insomnia, irritability, hostility, aggressiveness, impulsivity, akathisia (psychomotor restlessness), hypomania, and mania, have been reported in adult and pediatric patients being treated with antidepressants for MDD as well as for other indications, both psychiatric and nonpsychiatric. Although a causal link between the emergence of such symptoms and either the worsening of depression and/or the emergence of suicidal impulses has not been established, there is concern that such symptoms may represent precursors to emerging suicidality.
Consideration should be given to changing the therapeutic regimen, including possibly discontinuing the medication, in patients whose depression is persistently worse, or who are experiencing emergent suicidality or symptoms that might be precursors to worsening depression or suicidality, especially if these symptoms are severe, abrupt in onset, or were not part of the patient’s presenting symptoms.
Families and caregivers of patients being treated with antidepressants for major depressive disorder or other indications, both psychiatric and nonpsychiatric, should be alerted about the need to monitor patients for the emergence of agitation, irritability, unusual changes in behavior, and the other symptoms described above, as well as the emergence of suicidality, and to report such symptoms immediately to healthcare providers. Such monitoring should include daily observation by families and caregivers. Prescriptions for aripiprazole should be written for the smallest quantity of tablets consistent with good patient management, in order to reduce the risk of overdose.
Screening Patients for Bipolar Disorder: A major depressive episode may be the initial presentation of bipolar disorder. It is generally believed (though not established in controlled trials) that treating such an episode with an antidepressant alone may increase the likelihood of precipitation of a mixed/manic episode in patients at risk for bipolar disorder. Whether any of the symptoms described above represent such a conversion is unknown. However, prior to initiating treatment with an antidepressant, patients with depressive symptoms should be adequately screened to determine if they are at risk for bipolar disorder; such screening should include a detailed psychiatric history, including a family history of suicide, bipolar disorder, and depression.
It should be noted that aripiprazole is not approved for use in treating depression in the pediatric population.
Warning: Increased Mortality in Elderly Patients With Dementia Related Psychosis; and Suicidal Thoughts and Behaviors With Antidepressant Drugs
Elderly patients with dementia-related psychosis treated with antipsychotic drugs are at an increased risk of death. Aripiprazole is not approved for the treatment of patients with dementia-related psychosis [see Warnings and Precautions (5.1)] .
Antidepressants increased the risk of suicidal thoughts and behavior in children, adolescents, and young adults in short-term studies. These studies did not show an increase in the risk of suicidal thoughts and behavior with antidepressant use in patients over age 24; there was a reduction in risk with antidepressant use in patients aged 65 and older [see Warnings and Precautions (5.3)] .
In patients of all ages who are started on antidepressant therapy, monitor closely for worsening, and for emergence of suicidal thoughts and behaviors. Advise families and caregivers of the need for close observation and communication with the prescriber [see Warnings and Precautions (5.3)] .
Structured Label Content
Dosage and Administration (34068-7)
Adults
The recommended starting and target dose for aripiprazole tablets is 10 or 15 mg/day administered on a once-a-day schedule without regard to meals. Aripiprazole has been systematically evaluated and shown to be effective in a dose range of 10 to 30 mg/day, when administered as the tablet formulation; however, doses higher than 10 or 15 mg/day were not more effective than 10 or 15 mg/day. Dosage increases should generally not be made before 2 weeks, the time needed to achieve steady-state [see Clinical Studies (14.1)] .
Maintenance Treatment: Maintenance of efficacy in schizophrenia was demonstrated in a trial involving patients with schizophrenia who had been symptomatically stable on other antipsychotic medications for periods of 3 months or longer. These patients were discontinued from those medications and randomized to either aripiprazole 15 mg/day or placebo, and observed for relapse [see Clinical Studies (14.1)] . Patients should be periodically reassessed to determine the continued need for maintenance treatment.
Section 34083-6 (34083-6)
Carcinogenesis
Lifetime carcinogenicity studies were conducted in ICR mice, F344 rats, and Sprague-Dawley (SD) rats. Aripiprazole was administered for 2 years in the diet at doses of 1, 3, 10, and 30 mg/kg/day to ICR mice and 1, 3, and 10 mg/kg/day to F344 rats (0.2, 0.5, 2 and 5 times and 0.3, 1 and 3 times the MRHD of 30 mg/day based on mg/m 2 body surface area, respectively). In addition, SD rats were dosed orally for 2 years at 10, 20, 40, and 60 mg/kg/day, which are 3, 6, 13 and 19 times the MRHD based on mg/m 2 body surface area. Aripiprazole did not induce tumors in male mice or male rats. In female mice, the incidences of pituitary gland adenomas and mammary gland adenocarcinomas and adenoacanthomas were increased at dietary doses of 3 to 30 mg/kg/day (0.5 to 5 times the MRHD). In female rats, the incidence of mammary gland fibroadenomas was increased at a dietary dose of 10 mg/kg/day (3 times the MRHD); and the incidences of adrenocortical carcinomas and combined adrenocortical adenomas/carcinomas were increased at an oral dose of 60 mg/kg/day (19 times the MRHD).
An increase in mammary, pituitary, and endocrine pancreas neoplasms has been found in rodents after chronic administration of other antipsychotic drugs and is considered to be mediated by prolonged dopamine D2-receptor antagonism and hyperprolactinemia. Serum prolactin was not measured in the aripiprazole carcinogenicity studies. However, increases in serum prolactin levels were observed in female mice in a 13-week dietary study at the doses associated with mammary gland and pituitary tumors. Serum prolactin was not increased in female rats in 4-week and 13-week dietary studies at the dose associated with mammary gland tumors. The relevance for human risk of the findings of prolactin-mediated endocrine tumors in rodents is unclear.
Section 34084-4 (34084-4)
Less Common Adverse Reactions in Adults
Table 17 enumerates the pooled incidence, rounded to the nearest percent, of adverse reactions that occurred during acute therapy (up to 6 weeks in schizophrenia and upto 3 weeks in another indication), including only those reactions that occurred in 2% or more of patients treated with aripiprazole (doses ≥2 mg/day) and for which the incidence in patients treated with aripiprazole was greater than the incidence in patients treated with placebo in the combined dataset.
| System Organ Class
Preferred Term |
||
|---|---|---|
| Percentage of Patients Reporting Reaction
Adverse reactions reported by at least 2% of patients treated with oral aripiprazole, except adverse reactions which had an incidence equal to or less than placebo.
|
||
| Aripiprazole | Placebo | |
| (n=1843) | (n=1166) | |
| Eye Disorders | ||
| Blurred Vision | 3 | 1 |
| Gastrointestinal Disorders | ||
| Nausea | 15 | 11 |
| Constipation | 11 | 7 |
| Vomiting | 11 | 6 |
| Dyspepsia | 9 | 7 |
| Dry Mouth | 5 | 4 |
| Toothache | 4 | 3 |
| Abdominal Discomfort | 3 | 2 |
| Stomach Discomfort | 3 | 2 |
| General Disorders and Administration Site Conditions | ||
| Fatigue | 6 | 4 |
| Pain | 3 | 2 |
| Musculoskeletal and Connective Tissue Disorders | ||
| Musculoskeletal Stiffness | 4 | 3 |
| Pain in Extremity | 4 | 2 |
| Myalgia | 2 | 1 |
| Muscle Spasms | 2 | 1 |
| Nervous System Disorders | ||
| Headache | 27 | 23 |
| Dizziness | 10 | 7 |
| Akathisia | 10 | 4 |
| Sedation | 7 | 4 |
| Extrapyramidal Disorder | 5 | 3 |
| Tremor | 5 | 3 |
| Somnolence | 5 | 3 |
| Psychiatric Disorders | ||
| Agitation | 19 | 17 |
| Insomnia | 18 | 13 |
| Anxiety | 17 | 13 |
| Restlessness | 5 | 3 |
| Respiratory, Thoracic, and Mediastinal Disorders | ||
| Pharyngolaryngeal Pain | 3 | 2 |
| Cough | 3 | 2 |
An examination of population subgroups did not reveal any clear evidence of differential adverse reaction incidence on the basis of age, gender, or race.
Section 34092-7 (34092-7)
Adults
The efficacy of aripiprazole in the treatment of schizophrenia was evaluated in five short-term (4-week and 6-week), placebo-controlled trials of acutely relapsed inpatients who predominantly met DSM-III/IV criteria for schizophrenia. Four of the five trials were able to distinguish aripiprazole from placebo, but one study, the smallest, did not. Three of these studies also included an active control group consisting of either risperidone (one trial) or haloperidol (two trials), but they were not designed to allow for a comparison of aripiprazole and the active comparators.
In the four positive trials for aripiprazole, four primary measures were used for assessing psychiatric signs and symptoms. Efficacy was evaluated using the total score on the Positive and Negative Syndrome Scale (PANSS). The PANSS is a 30 item scale that measures positive symptoms of schizophrenia (7 items), negative symptoms of schizophrenia (7 items), and general psychopathology (16 items), each rated on a scale of 1 (absent) to 7 (extreme); total PANSS scores range from 30 to 210. The Clinical Global Impression (CGI) assessment reflects the impression of a skilled observer, fully familiar with the manifestations of schizophrenia, about the overall clinical state of the patient.
- In a 4-week trial (n=414) comparing two fixed doses of aripiprazole (15 or 30 mg/day) to placebo, both doses of aripiprazole were superior to placebo in the PANSS total score (Study 1 in
Table 26), PANSS positive subscale, and CGI- severity score. In addition, the 15 mg dose was superior to placebo in the PANSS negative subscale.
- In a 4-week trial (n=404) comparing two fixed doses of aripiprazole (20 or 30 mg/day) to placebo, both doses of aripiprazole were superior to placebo in the PANSS total score (Study 2 in
Table 26), PANSS positive subscale, PANSS negative subscale, and CGI-severity score.
- In a 6-week trial (n=420) comparing three fixed doses of aripiprazole (10, 15, or 20 mg/day) to placebo, all three doses of aripiprazole were superior to placebo in the PANSS total score (Study 3 in
Table 26), PANSS positive subscale, and the PANSS negative subscale.
- In a 6-week trial (n=367) comparing three fixed doses of aripiprazole (2, 5, or 10 mg/day) to placebo, the 10 mg dose of aripiprazole was superior to placebo in the PANSS total score (Study 4 in
Table 26), the primary outcome measure of the study. The 2 and 5 mg doses did not demonstrate superiority to placebo on the primary outcome measure.
Thus, the efficacy of 10, 15, 20, and 30 mg daily doses was established in two studies for each dose. Among these doses, there was no evidence that the higher dose groups offered any advantage over the lowest dose group of these studies.
An examination of population subgroups did not reveal any clear evidence of differential responsiveness on the basis of age, gender, or race.
A longer-term trial enrolled 310 inpatients or outpatients meeting DSM-IV criteria for schizophrenia who were, by history, symptomatically stable on other antipsychotic medications for periods of 3 months or longer. These patients were discontinued from their antipsychotic medications and randomized to aripiprazole 15 mg/day or placebo for up to 26 weeks of observation for relapse. Relapse during the double-blind phase was defined as CGI-Improvement score of ≥5 (minimally worse), scores ≥5 (moderately severe) on the hostility or uncooperativeness items of the PANSS, or ≥20% increase in the PANSS total score. Patients receiving aripiprazole 15 mg/day experienced a significantly longer time to relapse over the subsequent 26 weeks compared to those receiving placebo (Study 5 in Figure 6).
Section 42231-1 (42231-1)
MEDICATION GUIDE
Aripiprazole Tablets
(AR-i-PIP-ra-zole)
What is the most important information I should know about aripiprazole tablets?
(For other side effects, also see “What are the possible side effects of aripiprazole tablets?”).
Serious side effects may happen when you take aripiprazole tablets, including:
- Increased risk of death in elderly patients with dementia-related psychosis: Medicines like aripiprazole tablets can raise the risk of death in elderly people who have lost touch with reality (psychosis) due to confusion and memory loss (dementia). Aripiprazole tablets are not approved for the treatment of patients with dementia-related psychosis.
-
Risk of suicidal thoughts or actions: Antidepressant medicines, depression and other serious mental illnesses, and suicidal thoughts or actions:
- Antidepressant medicines may increase suicidal thoughts or actions in some children, teenagers, and young adults within the first few months of treatment.
- Depression and other serious mental illnesses are the most important causes of suicidal thoughts and actions. Some people may have a particularly high risk of having suicidal thoughts or actions. These include people who have (or have a family history of) bipolar illness (also called manic-depressive illness) or suicidal thoughts or actions.
-
How can I watch for and try to prevent suicidal thoughts and actions in myself or a family member?
- Pay close attention to any changes, especially sudden changes, in mood, behaviors, thoughts, or feelings. This is very important when an antidepressant medicine is started or when the dose is changed.
- Call the healthcare provider right away to report new or sudden changes in mood, behavior, thoughts, or feelings.
- Keep all follow-up visits with the healthcare provider as scheduled. Call the healthcare provider between visits as needed, especially if you have concerns about symptoms.
Call a healthcare provider right away if you or your family member has any of the following symptoms, especially if they are new, worse, or worry you:
- thoughts about suicide or dying
- attempts to commit suicide
- new or worse depression
- new or worse anxiety
- feeling very agitated or restless
- panic attacks
- trouble sleeping (insomnia)
- new or worse irritability
- acting aggressive, being angry, or violent
- acting on dangerous impulses
- an extreme increase in activity and talking (mania)
- other unusual changes in behavior or mood
What else do I need to know about antidepressant medicines?
- Never stop an antidepressant medicine without first talking to a healthcare provider. Stopping an antidepressant medicine suddenly can cause other symptoms.
- Antidepressants are medicines used to treat depression and other illnesses. It is important to discuss all the risks of treating depression and also the risks of not treating it. Patients and their families or other caregivers should discuss all treatment choices with the healthcare provider, not just the use of antidepressants.
- Antidepressant medicines have other side effects. Talk to the healthcare provider about the side effects of the medicine prescribed for you or your family member.
- Antidepressant medicines can interact with other medicines. Know all of the medicines that you or your family member takes. Keep a list of all medicines to show the healthcare provider. Do not start new medicines without first checking with your healthcare provider.
- Not all antidepressant medicines prescribed for children are FDA approved for use in children. Talk to your child’s healthcare provider for more information.
What are aripiprazole tablets?
Aripiprazole tablets are prescription medicines used to treat:
- Schizophrenia
It is not known if aripiprazole is safe or effective in children:
- under 13 years of age with schizophrenia
- under 10 years of age with bipolar I disorder
Do not take aripiprazole tablets if you are allergic to aripiprazole or any ingredients in aripiprazole tablets. See the end of this Medication Guide for a complete list of ingredients in aripiprazole tablets.
Before taking aripiprazole tablets, tell your healthcare provider about all your medical conditions, including if you have or had:
- diabetes or high blood sugar in you or your family; your healthcare provider should check your blood sugar before you start aripiprazole tablets and also during therapy.
- seizures (convulsions).
- low or high blood pressure.
- heart problems or stroke.
- pregnancy or plans to become pregnant. It is not known if aripiprazole tablets will harm your unborn baby.
- If you become pregnant while receiving aripiprazole, talk to your healthcare provider about registering with the National Pregnancy Registry for Atypical Antipsychotics. You can register by calling 1-866-961-2388 or go to http://womensmentalhealth.org/clinical-and-research-programs/pregnancyregistry/
- breast-feeding or plans to breast-feed. Aripiprazole passes into your breast milk. Talk to your healthcare provider about the best way to feed your baby if you receive aripiprazole tablets.
- low white blood cell count.
Tell your healthcare provider about all the medicines that you take, including prescription and over-the-counter medicines, vitamins, and herbal supplements.
Aripiprazole tablets and other medicines may affect each other causing possible serious side effects. Aripiprazole tablets may affect the way other medicines work, and other medicines may affect how aripiprazole works.
Your healthcare provider can tell you if it is safe to take aripiprazole tablets with your other medicines. Do not start or stop any medicines while taking aripiprazole tablets without talking to your healthcare provider first. Know the medicines you take. Keep a list of your medicines to show your healthcare provider and pharmacist when you get a new medicine.
How should I take aripiprazole tablets?
- Take aripiprazole tablets exactly as your healthcare provider tells you to take it. Do not change the dose or stop taking aripiprazole tablets yourself.
- Aripiprazole tablets can be taken with or without food.
- Aripiprazole tablets should be swallowed whole.
- If you miss a dose of aripiprazole tablets, take the missed dose as soon as you remember. If it is almost time for the next dose, just skip the missed dose and take your next dose at the regular time. Do not take two doses of aripiprazole tablets at the same time.
- If you take too much aripiprazole tablets, call your healthcare provider or poison control center at 1-800-222-1222 right away, or go to the nearest hospital emergency room.
What should I avoid while taking aripiprazole tablets?
- Do not drive, operate heavy machinery, or do other dangerous activities until you know how aripiprazole tablets affect you. Aripiprazole tablets may make you drowsy.
- Avoid getting over-heated or dehydrated.
- Do not over-exercise.
- In hot weather, stay inside in a cool place if possible.
- Stay out of the sun. Do not wear too much or heavy clothing.
- Drink plenty of water.
What are the possible side effects of aripiprazole tablets?
Aripiprazole tablets may cause serious side effects, including:
- See “What is the most important information I should know about aripiprazole tablets?”
- Stroke in elderly people (cerebrovascular problems) that can lead to death
- Neuroleptic malignant syndrome (NMS). Tell your healthcare provider right away if you have some or all of the following symptoms: high fever, stiff muscles, confusion, sweating, changes in pulse, heart rate, and blood pressure. These may be symptoms of a rare and serious condition that can lead to death. Call your healthcare provider right away if you have any of these symptoms.
- Uncontrolled body movements (tardive dyskinesia). Aripiprazole tablets may cause movements that you cannot control in your face, tongue, or other body parts. Tardive dyskinesia may not go away, even if you stop receiving aripiprazole tablets. Tardive dyskinesia may also start after you stop receiving aripiprazole tablets.
-
Problems with your metabolism such as:
- High blood sugar (hyperglycemia) and diabetes. Increases in blood sugar can happen in some people who take aripiprazole tablets. Extremely high blood sugar can lead to coma or death. If you have diabetes or risk factors for diabetes (such as being overweight or a family history of diabetes), your healthcare provider should check your blood sugar before you start aripiprazole tablets and during your treatment.
Call your healthcare provider if you have any of these symptoms of high blood sugar while receiving aripiprazole tablets:
►feel very thirsty
►need to urinate more than usual
►feel very hungry
►feel weak or tired
►feel sick to your stomach
►feel confused, or your breath smells fruity
- Increased fat levels (cholesterol and triglycerides) in your blood.
- Weight gain. You and your healthcare provider should check your weight regularly.
-
Unusual urges. Some people taking aripiprazole tablets have had unusual urges, such as gambling, binge eating or eating that you cannot control (compulsive), compulsive shopping and sexual urges.
If you or your family members notice that you are having unusual urges or behaviors, talk to your healthcare provider. - Orthostatic hypotension (decreased blood pressure). Lightheadedness or fainting may happen when rising too quickly from a sitting or lying position.
- Falls. Aripiprazole tablets may make you sleepy or dizzy, may cause a decrease in your blood pressure when changing position and can slow your thinking and motor skills which may lead to falls that can cause fractures or other injuries.
- Low white blood cell count
- Seizures (convulsions)
- Problems with control of your body temperature especially when you exercise a lot or are in an area that is very hot. It is important for you to drink water to avoid dehydration. See “What should I avoid while receiving aripiprazole tablets?”
- Difficulty swallowing that can cause food or liquid to get into your lungs.
The most common side effects of aripiprazole tablets in adults include:
| • Nausea | • dizziness |
| • vomiting | • anxiety |
| • constipation | • insomnia |
| • headache | • restlessness |
| • blurred vision | • inner sense of restlessness/need to move (akathisia) |
| • upper respiratory illness |
The most common side effects of aripiprazole tablets in children include:
| • feeling sleepy | • insomnia |
| • headache | • nausea |
| • vomiting | • stuffy nose |
| • fatigue | • weight gain |
| • increased or decreased appetite | • uncontrolled movement such as restlessness, tremor |
| • increased saliva or drooling | • muscle stiffness |
These are not all the possible side effects of aripiprazole tablets.
Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.
How should I store aripiprazole tablets?
- Store aripiprazole tablets at room temperature, between 68°F to 77°F (20°C to 25°C).
- Bottles of 30’s & 100’s count comes with a child-resistant package.
Keep aripiprazole tablets and all medicines out of the reach of children.
General information about the safe and effective use of aripiprazole tablets
Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not use aripiprazole for a condition for which it was not prescribed. Do not give aripiprazole to other people, even if they have the same symptoms you have. It may harm them.
You can ask your healthcare provider or pharmacist for information about aripiprazole tablets that was written for healthcare professionals.
What are the ingredients in aripiprazole tablets?
Active ingredient: aripiprazole
Inactive ingredients: hydroxypropyl cellulose, lactose monohydrate, magnesium stearate, maize starch and microcrystalline cellulose. Colorants include ferric oxide red (10 mg and 30 mg), ferric oxide yellow (2 mg and 15 mg), and FD&C Blue No. 2 aluminum lake (2 mg and 5 mg).
Additional pediatric use information is approved for Otsuka America Pharmaceutical, Inc.’s ABILIFY ® (aripiprazole) product. However, due to Otsuka America Pharmaceutical, Inc.’s marketing exclusivity rights, this drug product is not labeled with that information.
For more information about aripiprazole tablets, visit www.accordhealthcare.us or call Accord Healthcare Inc. at 1-866-941-7875.
This Medication Guide has been approved by the U.S. Food and Drug Administration.
ABILIFY ® is a trademark of Otsuka Pharmaceutical Company.
Medication guide available at www.accordhealthcare.us/medication-guides.
Manufactured For:
Accord Healthcare, Inc.,
1009 Slater Road,
Suite 210-B,
Durham, NC 27703,
USA
Manufactured By:
Intas Pharmaceuticals Limited.
Plot No. 5 to 12, Pharmez,
Sarkhej-Bavla, National Highway No 8-A,
Near Village Matoda, Tal Sanand,
Ahmedabad - 382213, Gujarat, India
51 1878 2 722646
Issued March 2020
Section 43682-4 (43682-4)
ORAL ADMINISTRATION
Section 43683-2 (43683-2)
Warnings and Precautions( 5.5) 08/2019
Section 43685-7 (43685-7)
Hyperglycemia/Diabetes Mellitus
Hyperglycemia, in some cases extreme and associated with ketoacidosis or hyperosmolar coma or death, has been reported in patients treated with atypical antipsychotics. There have been reports of hyperglycemia in patients treated with aripiprazole [see Adverse Reactions (6.1, 6.2)] . Assessment of the relationship between atypical antipsychotic use and glucose abnormalities is complicated by the possibility of an increased background risk of diabetes mellitus in patients with schizophrenia and the increasing incidence of diabetes mellitus in the general population. Given these confounders, the relationship between atypical antipsychotic use and hyperglycemia-related adverse events is not completely understood. However, epidemiological studies suggest an increased risk of hyperglycemia-related adverse reactions in patients treated with the atypical antipsychotics. Because aripiprazole was not marketed at the time these studies were performed, it is not known if aripiprazole is associated with this increased risk. Precise risk estimates for hyperglycemia-related adverse reactions in patients treated with atypical antipsychotics are not available.
Patients with an established diagnosis of diabetes mellitus who are started on atypical antipsychotics should be monitored regularly for worsening of glucose control. Patients with risk factors for diabetes mellitus (e.g., obesity, family history of diabetes) who are starting treatment with atypical antipsychotics should undergo fasting blood glucose testing at the beginning of treatment and periodically during treatment. Any patient treated with atypical antipsychotics should be monitored for symptoms of hyperglycemia including polydipsia, polyuria, polyphagia, and weakness. Patients who develop symptoms of hyperglycemia during treatment with atypical antipsychotics should undergo fasting blood glucose testing. In some cases, hyperglycemia has resolved when the atypical antipsychotic was discontinued; however, some patients required continuation of anti-diabetic treatment despite discontinuation of the suspect drug.
Adults
In an analysis of 13 placebo-controlled monotherapy trials in adults, primarily with schizophrenia or another disorder, the mean change in fasting glucose in aripiprazole-treated patients (+4.4 mg/dL; median exposure 25 days; N=1057) was not significantly different than in placebo-treated patients (+2.5 mg/dL; median exposure 22 days; N=799). Table 6 shows the proportion of aripiprazole-treated patients with normal and borderline fasting glucose at baseline (median exposure 25 days) that had treatment-emergent high fasting glucose measurements compared to placebo-treated patients (median exposure 22 days).
| Category Change (at least once) from Baseline | Treatment Arm | n/N | % | |
|---|---|---|---|---|
| Fasting Glucose | Normal to High (<100 mg/dL to ≥126 mg/dL) |
Aripiprazole | 31/822 | 3.8 |
| Placebo | 22/605 | 3.6 | ||
| Borderline to High (≥100 mg/dL and <126 mg/dL to ≥126 mg/dL) |
Aripiprazole | 31/176 | 17.6 | |
| Placebo | 13/142 | 9.2 |
At 24 weeks, the mean change in fasting glucose in aripiprazole-treated patients was not significantly different than in placebo-treated patients [+2.2 mg/dL (n=42) and +9.6 mg/dL (n=28), respectively].
Pediatric Patients and Adolescents
In an analysis of two placebo-controlled trials in adolescents with schizophrenia (13 to 17 years) and pediatric patients with another disorder (10 to 17 years), the mean change in fasting glucose in aripiprazole-treated patients (+4.8 mg/dL; with a median exposure of 43 days; N=259) was not significantly different than in placebo-treated patients (+1.7 mg/dL; with a median exposure of 42 days; N=123).
Table 8 shows the proportion of patients with changes in fasting glucose levels from the pooled adolescent schizophrenia and other pediatric patients (median exposure of 42 to 43 days).
| Category Change (at least once) from Baseline | Indication | Treatment Arm | n/N | % |
|---|---|---|---|---|
|
Fasting Glucose
Normal to High (<100 mg/dL to ≥126 mg/dL) |
||||
| Pooled Schizophrenia and Another Disorder | Aripiprazole | 2/236 | 0.8 | |
| Placebo | 2/110 | 1.8 | ||
|
Fasting Glucose
Borderline to High (≥100 mg/dL and <126 mg/dL to ≥126 mg/dL) |
||||
| Pooled Schizophrenia and Another Disorder | Aripiprazole | 1/22 | 4.5 | |
| Placebo | 0/12 | 0 |
At 12 weeks in the pooled adolescent schizophrenia and other pediatric disorder trials, the mean change in fasting glucose in aripiprazole-treated patients was not significantly different than in placebo-treated patients [+2.4 mg/dL (n=81) and +0.1 mg/dL (n=15), respectively].
5.9 Falls
Antipsychotics, including aripiprazole, may cause somnolence, postural hypotension, motor and sensory instability, which may lead to falls and, consequently, fractures or other injuries. For patients with diseases, conditions, or medications that could exacerbate these effects, complete fall risk assessments when initiating antipsychotic treatment and recurrently for patients on long-term antipsychotic therapy.
9.2 Abuse
Aripiprazole has not been systematically studied in humans for its potential for abuse, tolerance, or physical dependence. Consequently, patients should be evaluated carefully for a history of drug abuse, and such patients should be observed closely for signs of aripiprazole misuse or abuse (e.g., development of tolerance, increases in dose, drug-seeking behavior).
5.14 Suicide
The possibility of a suicide attempt is inherent in psychotic illnesses and bipolar disorder, and close supervision of high-risk patients should accompany drug therapy. Prescriptions for aripiprazole should be written for the smallest quantity consistent with good patient management in order to reduce the risk of overdose [see Adverse Reactions (6.1, 6.2)] .
Aripiprazole (ARIPIPRAZOLE)
10 Overdosage (10 OVERDOSAGE)
MedDRA terminology has been used to classify the adverse reactions.
8.1 Pregnancy
Pregnancy Exposure Registry
There is a pregnancy exposure registry that monitors pregnancy outcomes in women exposed to atypical antipsychotics, including aripiprazole, during pregnancy. Healthcare providers are encouraged to register patients by contacting the National Pregnancy Registry for Atypical Antipsychotics at 1-866-961-2388 or visit http://womensmentalhealth.org/clinical-and-research-programs/pregnancyregistry/.
Risk Summary
Neonates exposed to antipsychotic drugs, including aripiprazole, during the third trimester of pregnancy are at risk for extrapyramidal and/or withdrawal symptoms following delivery (see Clinical Considerations). Overall available data from published epidemiologic studies of pregnant women exposed to aripiprazole have not established a drug-associated risk of major birth defects, miscarriage, or adverse maternal or fetal outcomes (see Data). There are risks to the mother associated with untreated schizophrenia, bipolar I disorder, or major depressive disorder, and with exposure to antipsychotics, including aripiprazole, during pregnancy (see Clinical Considerations).
In animal reproduction studies, oral and intravenous aripiprazole administration during organogenesis in rats and/or rabbits at doses 10 and 19 times, respectively, the maximum recommended human dose (MRHD) of 30 mg/day based on mg/m 2 body surface area, produced fetal death, decreased fetal weight, undescended testicles, delayed skeletal ossification, skeletal abnormalities, and diaphragmatic hernia. Oral and intravenous aripiprazole administration during the pre- and post-natal period in rats at doses 10 times the MRHD based on mg/m 2 body surface area, produced prolonged gestation, stillbirths, decreased pup weight, and decreased pup survival (see Data).
The estimated background risk of major birth defects and miscarriage for the indicated population is unknown. All pregnancies have a background risk of birth defect, loss, or other adverse outcomes. In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2 to 4% and 15 to 20%, respectively..
Clinical Considerations
Disease-associated maternal and/or embryo/fetal risk
There is a risk to the mother from untreated schizophrenia or bipolar I disorder, including increased risk of relapse, hospitalization, and suicide. Schizophrenia and bipolar I disorder are associated with increased adverse perinatal outcomes, including preterm birth. It is not known if this is a direct result of the illness or other comorbid factors.
A prospective, longitudinal study followed 201 pregnant women with a history of major depressive disorder who were euthymic and taking antidepressants at the beginning of pregnancy. The women who discontinued antidepressants during pregnancy were more likely to experience a relapse of major depression than women who continued antidepressants. Consider the risk of untreated depression when discontinuing or changing treatment with antidepressant medication during pregnancy and postpartum.
Fetal/Neonatal Adverse Reactions
Extrapyramidal and/or withdrawal symptoms, including agitation, hypertonia, hypotonia, tremor, somnolence, respiratory distress, and feeding disorder have been reported in neonates who were exposed to antipsychotic drugs (including aripiprazole) during the third trimester of pregnancy. These symptoms have varied in severity. Monitor neonates for extrapyramidal and/or withdrawal symptoms, and manage symptoms appropriately. Some neonates recovered within hours or days without specific treatment; others required prolonged hospitalization.
Data
Human Data
Published data from observational studies, birth registries, and case reports on the use of atypical antipsychotics during pregnancy do not report a clear association with antipsychotics and major birth defects. A retrospective study from a Medicaid database of 9258 women exposed to antipsychotics during pregnancy did not indicate an overall increased risk for major birth defects.
Animal Data
In animal studies, aripiprazole demonstrated developmental toxicity, including possible teratogenic effects in rats and rabbits.
In pregnant rats treated orally with aripiprazole during organogenesis at doses of 3, 10, and 30 mg/kg/day, which are approximately 1, 3 and 10 times the MRHD of 30 mg/day based on mg/m 2 body surface area, a slight prolongation of gestation and delay in fetal development, as evidenced by decreased fetal weight and undescended testes, were observed at 10 times the MRHD. Delayed skeletal ossification was observed at 3 and 10 times the MRHD. Delivered offspring had increased incidences of hepatodiaphragmatic nodules and diaphragmatic hernia were observed at 10 times the MRHD (the other dose groups were not examined for these findings). Postnatally, delayed vaginal opening was seen at 3 and 10 times the MRHD. Impaired reproductive performance (decreased fertility rate, corpora lutea, implants, live fetuses, and increased post-implantation loss, likely mediated through effects on female offspring) were observed at 10 times the MRHD; however, there was no evidence to suggest that these developmental effects were secondary to maternal toxicity.
In pregnant rats injected intravenously with aripiprazole during organogenesis at doses of 3, 9, and 27 mg/kg/day, which are 1, 3, and 9 times the MRHD of 30 mg/day based on mg/m 2 body surface area, decreased fetal weight and delayed skeletal ossification were observed at 9 times the MRHD; this dose also caused maternal toxicity.
In pregnant rabbits treated orally with aripiprazole during organogenesis at doses of 10, 30, and 100 mg/kg/day which are 6, 19, and 65 times the MRHD of 30 mg/day based on mg/m 2 body surface area, decreased maternal food consumption, and increased abortions as well as increased fetal mortality were observed at 65 times the MHRD. Decreased fetal weight and increased incidence of fused sternebrae were observed at 19 and 65 times the MRHD.
In pregnant rabbits injected intravenously with aripiprazole during organogenesis at doses of 3, 10, and 30 mg/kg/day, which are 2, 6, and 19 times the MRHD of 30 mg/day based on mg/m 2 body surface area, decreased fetal weight, increased fetal abnormalities (primarily skeletal), and decreased fetal skeletal ossification were observed at 19 times the MRHD; this dose also caused maternal toxicity. The fetal no-effect dose was 10 mg/kg/day, which is 6 times the MRHD.
In rats treated orally with aripiprazole peri- and post-natally from gestation day 17 through postpartum day 21 at doses of 3, 10, and 30 mg/kg/day which are 1, 3, and 10 times the MRHD of 30 mg/day based on mg/m 2 body surface area slight maternal toxicity and slightly prolonged gestation were observed at 10 times the MHRD. An increase in stillbirths and, decreases in pup weight (persisting into adulthood) and survival were also seen at this dose.
In rats injected intravenously with aripiprazole from gestation day 6 through lactation day 20 at doses of 3, 8, and 20 mg/kg/day, which are 1, 3, and 6 times the MRHD of 30 mg/day based on mg/m 2 body surface area, increased stillbirths were observed at 3 and 6 times the MRHD; and decreases in early postnatal pup weight and survival were observed at 6 times the MRHD; these doses also caused some maternal toxicity. There were no effects on postnatal behavioral and reproductive development.
8.2 Lactation
Risk Summary
Limited data from published literature report the presence of aripiprazole in human breast milk, at relative infant doses ranging between 0.7% to 8.3% of the maternal weight-adjusted dosage. There are reports of poor weight gain in breastfed infants exposed to aripiprazole and reports of inadequate milk supply in lactating women taking aripiprazole.
The development and health benefits of breastfeeding should be considered along with the mother’s clinical need for aripiprazole and any potential adverse effects on the breastfed infant from aripiprazole or from the underlying maternal condition.
11 Description (11 DESCRIPTION)
Aripiprazole is an atypical antipsychotic drug that is available as aripiprazole tablets, USP. Aripiprazole is 7-[4-[4-(2,3-dichlorophenyl)-1-piperazinyl]butoxy]-3,4-dihydrocarbostyril. The empirical formula is C 23H 27Cl 2N 3O 2 and its molecular weight is 448.38. The chemical structure is:
Aripiprazole tablets, USP are available in 2 mg, 5 mg, 10 mg, 15 mg, 20 mg, and 30 mg strengths. Inactive ingredients include hydroxypropyl cellulose, lactose monohydrate, magnesium stearate, maize starch and microcrystalline cellulose. Colorants include ferric oxide red (10 mg and 30 mg), ferric oxide yellow (2 mg and 15 mg), and FD&C Blue No. 2 aluminum lake (2 mg and 5 mg).
5.15 Dysphagia
Esophageal dysmotility and aspiration have been associated with antipsychotic drug use, including aripiprazole. Aspiration pneumonia is a common cause of morbidity and mortality in elderly patients, in particular those with advanced Alzheimer’s dementia. Aripiprazole and other antipsychotic drugs should be used cautiously in patients at risk for aspiration pneumonia [see Warnings and Precautions (5.1) and Adverse Reactions (6.2)] .
9.3 Dependence
In physical dependence studies in monkeys, withdrawal symptoms were observed upon abrupt cessation of dosing. While the clinical trials did not reveal any tendency for any drug-seeking behavior, these observations were not systematic and it is not possible to predict on the basis of this limited experience the extent to which a CNS-active drug will be misused, diverted, and/or abused once marketed.
Unmapped Section (UNMAPPED_SECTION)
Adult Patients with Schizophrenia
The following findings are based on a pool of five placebo-controlled trials (four 4-week and one 6-week) in which oral aripiprazole was administered in doses ranging from 2 to 30 mg/day.
Commonly Observed Adverse Reactions
The only commonly observed adverse reaction associated with the use of aripiprazole in patients with schizophrenia (incidence of 5% or greater and aripiprazole incidence at least twice that for placebo) was akathisia (aripiprazole 8%; placebo 4%).
8.4 Pediatric Use
The pharmacokinetics of aripiprazole and dehydro-aripiprazole in pediatric patients, 10 to 17 years of age, were similar to those in adults after correcting for the differences in body weight [see Clinical Pharmacology (12.3)] .
Schizophrenia
Safety and effectiveness in pediatric patients with schizophrenia were established in a 6-week, placebo-controlled clinical trial in 202 pediatric patients aged 13 to 17 years [see Dosage and Administration (2.1), Adverse Reactions (6.1), and Clinical Studies (14.1)] . Although maintenance efficacy in pediatric patients has not been systematically evaluated, maintenance efficacy can be extrapolated from adult data along with comparisons of aripiprazole pharmacokinetic parameters in adult and pediatric patients.
Bipolar I Disorder
Although maintenance efficacy in pediatric patients has not been systematically evaluated, maintenance efficacy can be extrapolated from adult data along with comparisons of aripiprazole pharmacokinetic parameters in adult and pediatric patients.
The efficacy of adjunctive aripiprazole with concomitant lithium or valproate in the treatment of manic or mixed episodes in pediatric patients has not been systematically evaluated. However, such efficacy and lack of pharmacokinetic interaction between aripiprazole and lithium or valproate can be extrapolated from adult data, along with comparisons of aripiprazole pharmacokinetic parameters in adult and pediatric patients.
Information describing a clinical study in which efficacy was not demonstrated in patients ages 6 to 17 years is approved for Otsuka America Pharmaceutical, Inc.’s ABILIFY ® (aripiprazole). Additional pediatric use information in patients ages 6 to 18 years is approved for Otsuka America Pharmaceutical, Inc.’s ABILIFY ® (aripiprazole) product. However, due to Otsuka America Pharmaceutical, Inc.’s marketing exclusivity rights, this drug product is not labeled with that pediatric information.
Juvenile Animal Studies
Aripiprazole in juvenile rats caused mortality, CNS clinical signs, impaired memory and learning, and delayed sexual maturation when administered at oral doses of 10, 20, 40 mg/kg/day from weaning (21 days old) through maturity (80 days old). At 40 mg/kg/day, mortality, decreased activity, splayed hind limbs, hunched posture, ataxia, tremors and other CNS signs were observed in both genders. In addition, delayed sexual maturation was observed in males. At all doses and in a dose-dependent manner, impaired memory and learning, increased motor activity, and histopathology changes in the pituitary (atrophy), adrenals (adrenocortical hypertrophy), mammary glands (hyperplasia and increased secretion), and female reproductive organs (vaginal mucification, endometrial atrophy, decrease in ovarian corpora lutea) were observed. The changes in female reproductive organs were considered secondary to the increase in prolactin serum levels. A No Observed Adverse Effect Level (NOAEL) could not be determined and, at the lowest tested dose of 10 mg/kg/day, there is no safety margin relative to the systemic exposures (AUC 0-24) for aripiprazole or its major active metabolite in adolescents at the maximum recommended pediatric dose of 15 mg/day. All drug-related effects were reversible after a 2-month recovery period, and most of the drug effects in juvenile rats were also observed in adult rats from previously conducted studies.
Aripiprazole in juvenile dogs (2 months old) caused CNS clinical signs of tremors, hypoactivity, ataxia, recumbency and limited use of hind limbs when administered orally for 6 months at 3, 10, 30 mg/kg/day. Mean body weight and weight gain were decreased up to 18% in females in all drug groups relative to control values. A NOAEL could not be determined and, at the lowest tested dose of 3 mg/kg/day, there is no safety margin relative to the systemic exposures (AUC 0-24) for aripiprazole or its major active metabolite in adolescents at the maximum recommended pediatric dose of 15 mg/day. All drug-related effects were reversible after a 2-month recovery period.
8.5 Geriatric Use
No dosage adjustment is recommended for elderly patients [see Boxed Warning, Warnings and Precautions (5.1), and Clinical Pharmacology (12.3)] .
Of the 13,543 patients treated with oral aripiprazole in clinical trials, 1073 (8%) were ≥65 years old and 799 (6%) were ≥75 years old. Placebo-controlled studies of oral aripiprazole in schizophrenia or other indications did not include sufficient numbers of subjects aged 65 and over to determine whether they respond differently from younger subjects.
Aripiprazole is not approved for the treatment of patients with psychosis associated with Alzheimer’s disease [see Boxed Warning and Warnings and Precautions (5.1)].
14 Clinical Studies (14 CLINICAL STUDIES)
Efficacy of the oral formulations of aripiprazole was established in the following adequate and well-controlled trials:
- Four short-term trials and one maintenance trial in adult patients and one short-term trial in adolescents (ages 13 to 17) with schizophrenia [see Clinical Studies (14.1)]
- One maintenance monotherapy trial and in one maintenance adjunctive trial in adult patients with bipolar I disorder [see Clinical Studies (14.2)]
Additional pediatric use information is approved for Otsuka America Pharmaceutical, Inc.’s ABILIFY ® (aripiprazole) product. However, due to Otsuka America Pharmaceutical, Inc.’s marketing exclusivity rights, this drug product is not labeled with that information.
4 Contraindications (4 CONTRAINDICATIONS)
Aripiprazole tablets are contraindicated in patients with a history of a hypersensitivity reaction to aripiprazole. Reactions have ranged from pruritus/urticaria to anaphylaxis [see Adverse Reactions (6.2)].
6 Adverse Reactions (6 ADVERSE REACTIONS)
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
The following adverse reactions are discussed in more detail in other sections of the labeling:
- Increased Mortality in Elderly Patients with Dementia-Related Psychosis [see Boxed Warning and Warnings and Precautions (5.1)]
- Cerebrovascular Adverse Events, Including Stroke [see Warnings and Precautions (5.2)]
- Suicidal Thoughts and Behaviors in Children, Adolescents, and Young Adults [see Boxed Warning and Warnings and Precautions (5.3)]
- Neuroleptic Malignant Syndrome (NMS) [see Warnings and Precautions (5.4)]
- Tardive Dyskinesia [see Warnings and Precautions (5.5)]
- Metabolic Changes [see Warnings and Precautions (5.6)]
- Pathological Gambling and Other Compulsive Behaviors [see Warnings and Precautions (5.7)]
- Orthostatic Hypotension [see Warnings and Precautions (5.8)]
- Falls [see Warnings and Precautions (5.9)]
- Leukopenia, Neutropenia, and Agranulocytosis [see Warnings and Precautions (5.10)]
- Seizures/Convulsions [see Warnings and Precautions (5.11)]
- Potential for Cognitive and Motor Impairment [see Warnings and Precautions (5.12)]
- Body Temperature Regulation [see Warnings and Precautions (5.13)]
- Suicide [see Warnings and Precautions (5.14)]
- Dysphagia [see Warnings and Precautions (5.15)]
The most common adverse reactions in adult patients in clinical trials (≥10%) were nausea, vomiting, constipation, headache, dizziness, akathisia, anxiety, insomnia, and restlessness.
The most common adverse reactions in the pediatric clinical trials (≥10%) were somnolence, headache, vomiting, extrapyramidal disorder, fatigue, increased appetite, insomnia, nausea, nasopharyngitis, and weight increased.
Aripiprazole has been evaluated for safety in 13,543 adult patients who participated in multiple-dose, clinical trials in schizophrenia, other indications, Dementia of the Alzheimer’s type, Parkinson’s disease, and alcoholism, and who had approximately 7619 patient-years of exposure to oral aripiprazole. A total of 3390 patients were treated with oral aripiprazole for at least 180 days and 1933 patients treated with oral aripiprazole had at least 1 year of exposure.
Aripiprazole has been evaluated for safety in 1,686 patients (6 to 18 years) who participated in multiple-dose, clinical trials in schizophrenia, or other indications and who had approximately 1,342 patient-years of exposure to oral aripiprazole. A total of 959 pediatric patients were treated with oral aripiprazole for at least 180 days and 556 pediatric patients treated with oral aripiprazole had at least 1 year of exposure.
The conditions and duration of treatment with aripiprazole included (in overlapping categories) double-blind, comparative and noncomparative open-label studies, inpatient and outpatient studies, fixed-and flexible-dose studies, and short-and longer-term exposure.
Additional pediatric use information is approved for Otsuka America Pharmaceutical, Inc.’s ABILIFY ® (aripiprazole) product. However, due to Otsuka America Pharmaceutical, Inc.’s marketing exclusivity rights, this drug product is not labeled with that information.
7 Drug Interactions (7 DRUG INTERACTIONS)
Dosage adjustment due to drug interactions (7.1) :
| Factors | Dosage Adjustments for Aripiprazole |
| Known CYP2D6 Poor Metabolizers | Administer half of usual dose |
| Known CYP2D6 Poor Metabolizers and strong CYP3A4 inhibitors | Administer a quarter of usual dose |
| Strong CYP2D6 or CYP3A4 inhibitors | Administer half of usual dose |
| Strong CYP2D6 and CYP3A4 inhibitors | Administer a quarter of usual dose |
| Strong CYP3A4 inducers | Double usual dose over 1 to 2 weeks |
10.1 Human Experience
In clinical trials and in postmarketing experience, adverse reactions of deliberate or accidental overdosage with oral aripiprazole have been reported worldwide. These include overdoses with oral aripiprazole alone and in combination with other substances. No fatality was reported with aripiprazole alone. The largest known dose with a known outcome involved acute ingestion of 1260 mg of oral aripiprazole (42 times the maximum recommended daily dose) by a patient who fully recovered. Deliberate or accidental overdosage was also reported in children (age 12 and younger) involving oral aripiprazole ingestions up to 195 mg with no fatalities.
Common adverse reactions (reported in at least 5% of all overdose cases) reported with oral aripiprazole overdosage (alone or in combination with other substances) include vomiting, somnolence, and tremor. Other clinically important signs and symptoms observed in one or more patients with aripiprazole overdoses (alone or with other substances) include acidosis, aggression, aspartate aminotransferase increased, atrial fibrillation, bradycardia, coma, confusional state, convulsion, blood creatine phosphokinase increased, depressed level of consciousness, hypertension, hypokalemia, hypotension, lethargy, loss of consciousness, QRS complex prolonged, QT prolonged, pneumonia aspiration, respiratory arrest, status epilepticus, and tachycardia.
12.2 Pharmacodynamics
Aripiprazole exhibits high affinity for dopamine D 2 and D 3, serotonin 5-HT 1A and 5-HT 2A receptors (K i values of 0.34 nM, 0.8 nM, 1.7 nM, and 3.4 nM, respectively), moderate affinity for dopamine D 4, serotonin 5-HT 2C and 5-HT 7, alpha1-adrenergic and histamine H 1 receptors (K i values of 44 nM, 15 nM, 39 nM, 57 nM, and 61 nM, respectively), and moderate affinity for the serotonin reuptake site (K i=98 nM). Aripiprazole has no appreciable affinity for cholinergic muscarinic receptors (IC 50>1000 nM).
12.3 Pharmacokinetics
Aripiprazole activity is presumably primarily due to the parent drug, aripiprazole, and to a lesser extent, to its major metabolite, dehydro-aripiprazole, which has been shown to have affinities for D 2 receptors similar to the parent drug and represents 40% of the parent drug exposure in plasma. The mean elimination half-lives are about 75 hours and 94 hours for aripiprazole and dehydro-aripiprazole, respectively. Steady-state concentrations are attained within 14 days of dosing for both active moieties. Aripiprazole accumulation is predictable from single-dose pharmacokinetics. At steady-state, the pharmacokinetics of aripiprazole is dose-proportional. Elimination of aripiprazole is mainly through hepatic metabolism involving two P450 isozymes, CYP2D6 and CYP3A4. For CYP2D6 poor metabolizers, the mean elimination half-life for aripiprazole is about 146 hours.
Pharmacokinetic studies showed that aripiprazole orally disintegrating tablets are bioequivalent to aripiprazole tablets.
5.6 Metabolic Changes
Atypical antipsychotic drugs have been associated with metabolic changes that include hyperglycemia/diabetes mellitus, dyslipidemia, and body weight gain. While all drugs in the class have been shown to produce some metabolic changes, each drug has its own specific risk profile.
5.5 Tardive Dyskinesia
A syndrome of potentially irreversible, involuntary, dyskinetic movements may develop in patients treated with antipsychotic drugs. Although the prevalence of the syndrome appears to be highest among the elderly, especially elderly women, it is impossible to rely upon prevalence estimates to predict, at the inception of antipsychotic treatment, which patients are likely to develop the syndrome. Whether antipsychotic drug products differ in their potential to cause tardive dyskinesia is unknown.A syndrome of potentially irreversible, involuntary, dyskinetic movements may develop in patients treated with antipsychotic drugs. Although the prevalence of the syndrome appears to be highest among the elderly, especially elderly women, it is impossible to rely upon prevalence estimates to predict, at the inception of antipsychotic treatment, which patients are likely to develop the syndrome. Whether antipsychotic drug products differ in their potential to cause tardive dyskinesia is unknown.
The risk of developing tardive dyskinesia and the likelihood that it will become irreversible are believed to increase as the duration of treatment and the total cumulative dose of antipsychotic drugs administered to the patient increase. However, the syndrome can develop, although much less commonly, after relatively brief treatment periods at low doses. The risk of developing tardive dyskinesia and the likelihood that it will become irreversible are believed to increase as the duration of treatment and the total cumulative dose of antipsychotic drugs administered to the patient increase. However, the syndrome can develop, although much less commonly, after relatively brief treatment periods at low doses.
Tardive dyskinesia may remit, partially or completely, if antipsychotic treatment is withdrawn. Antipsychotic treatment, itself, however, may suppress (or partially suppress) the signs and symptoms of the syndrome and, thereby, may possibly mask the underlying process. The effect that symptomatic suppression has upon the long-term course of the syndrome is unknown.
Given these considerations, aripiprazole should be prescribed in a manner that is most likely to minimize the occurrence of tardive dyskinesia. Chronic antipsychotic treatment should generally be reserved for patients who suffer from a chronic illness that (1) is known to respond to antipsychotic drugs and (2) for whom alternative, equally effective, but potentially less harmful treatments are not available or appropriate. In patients who do require chronic treatment, the smallest dose and the shortest duration of treatment producing a satisfactory clinical response should be sought. The need for continued treatment should be reassessed periodically.Given these considerations, aripiprazole should be prescribed in a manner that is most likely to minimize the occurrence of tardive dyskinesia. Chronic antipsychotic treatment should generally be reserved for patients who suffer from a chronic illness that (1) is known to respond to antipsychotic drugs and (2) for whom alternative, equally effective, but potentially less harmful treatments are not available or appropriate. In patients who do require chronic treatment, the smallest dose and the shortest duration of treatment producing a satisfactory clinical response should be sought. The need for continued treatment should be reassessed periodically.
If signs and symptoms of tardive dyskinesia appear in a patient on aripiprazole, drug discontinuation should be considered. However, some patients may require treatment with aripiprazole despite the presence of the syndrome.If signs and symptoms of tardive dyskinesia appear in a patient on aripiprazole, drug discontinuation should be considered. However, some patients may require treatment with aripiprazole despite the presence of the syndrome.
1 Indications and Usage (1 INDICATIONS AND USAGE)
Aripiprazole tablets are indicated for the treatment of:
- Schizophrenia [see Clinical Studies (14.1)]
Additional pediatric use information is approved for Otsuka America Pharmaceutical, Inc.’s ABILIFY ® (aripiprazole) product. However, due to Otsuka America Pharmaceutical, Inc.’s marketing exclusivity rights, this drug product is not labeled with that information.
12.1 Mechanism of Action
The mechanism of action of aripiprazole in schizophrenia is unclear. However, the efficacy of aripiprazole in the listed indications could be mediated through a combination of partial agonist activity at D 2 and 5-HT 1A receptors and antagonist activity at 5-HT 2A receptors.
9.1 Controlled Substance
Aripiprazole is not a controlled substance.
5.11 Seizures/convulsions (5.11 Seizures/Convulsions)
In short-term, placebo-controlled trials, patients with a history of seizures excluded seizures/convulsions occurred in 0.1% (3/2467) of undiagnosed adult patients treated with oral aripiprazole, and in 0.1% (1/732) of pediatric patients (6 to 18 years).
As with other antipsychotic drugs, aripiprazole should be used cautiously in patients with a history of seizures or with conditions that lower the seizure threshold. Conditions that lower the seizure threshold may be more prevalent in a population of 65 years or older.
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
- Cerebrovascular Adverse Reactions in Elderly Patients with Dementia- Related Psychosis: Increased incidence of cerebrovascular adverse reactions (e.g., stroke, transient ischemic attack, including fatalities) (5.2)
- Neuroleptic Malignant Syndrome: Manage with immediate discontinuation and close monitoring (5.4)
- Tardive Dyskinesia: Discontinue if clinically appropriate (5.5)
-
Metabolic Changes: Atypical antipsychotic drugs have been associated with metabolic changes that include hyperglycemia/diabetes mellitus, dyslipidemia, and body weight gain
(5.6)
- Hyperglycemia/Diabetes Mellitus: Monitor glucose regularly in patients with and at risk for diabetes (5.6)
- Dyslipidemia: Undesirable alterations in lipid levels have been observed in patients treated with atypical antipsychotics (5.6)
- Weight Gain: Weight gain has been observed with atypical antipsychotic use. Monitor weight (5.6)
- Pathological Gambling and Other Compulsive Behaviors: Consider dose reduction or discontinuation (5.7)
- Orthostatic Hypotension: Monitor heart rate and blood pressure and warn patients with known cardiovascular or cerebrovascular disease, and risk of dehydration or syncope (5.8)
- Leukopenia, Neutropenia, and Agranulocytosis: have been reported with antipsychotics including aripiprazole. Patients with a history of a clinically significant low white blood cell count (WBC) or a drug-induced leukopenia/neutropenia should have their complete blood count (CBC) monitored frequently during the first few months of therapy and discontinuation of aripiprazole should be considered at the first sign of a clinically significant decline in WBC in the absence of other causative factors (5.10)
- Seizures/Convulsions: Use cautiously in patients with a history of seizures or with conditions that lower the seizure threshold (5.11)
- Potential for Cognitive and Motor Impairment: Use caution when operating machinery (5.12)
- Suicide: The possibility of a suicide attempt is inherent in schizophrenia and bipolar disorder. Closely supervise high-risk patients (5.14)
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
5.8 Orthostatic Hypotension
Aripiprazole may cause orthostatic hypotension, perhaps due to its α1-adrenergic receptor antagonism. The incidence of orthostatic hypotension-associated events from short-term, placebo-controlled trials of adult patients on oral aripiprazole (n=2467) included (aripiprazole incidence, placebo incidence) orthostatic hypotension (1%, 0.3%), postural dizziness (0.5%, 0.3%), and syncope (0.5%, 0.4%); of pediatric patients 6 to 18 years of age (n=732) on oral aripiprazole included orthostatic hypotension (0.5%, 0%), postural dizziness (0.4%, 0 %), and syncope (0.2%, 0%). [see Adverse Reactions (6.1)] .
The incidence of a significant orthostatic change in blood pressure (defined as a decrease in systolic blood pressure ≥20 mmHg accompanied by an increase in heart rate ≥25 bpm when comparing standing to supine values) for aripiprazole was not meaningfully different from placebo (aripiprazole incidence, placebo incidence): in adult oral aripiprazole -treated patients (4%, 2%), or in pediatric oral aripiprazole -treated patients aged 6 to 18 years (0.4%, 1%).
Aripiprazole should be used with caution in patients with known cardiovascular disease (history of myocardial infarction or ischemic heart disease, heart failure or conduction abnormalities), cerebrovascular disease, or conditions which would predispose patients to hypotension (dehydration, hypovolemia, and treatment with antihypertensive medications) [see Drug Interactions (7.1)] .
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
Aripiprazole tablets, USP are available as described in Table 3.
|
Tablet
Strength |
Tablet
Color/Shape |
Tablet
Markings |
| 2 mg | green
modified rectangle |
“A2” on one side
and another side is plain |
| 5 mg | blue
modified rectangle |
“A5” on one side
and another side is plain |
| 10 mg | pink
modified rectangle |
“A10” on one side
and another side is plain |
| 15 mg | yellow
round |
“A15” on one side
and another side is plain |
| 20 mg | white to off white
round |
“A20” on one side
and another side is plain |
| 30 mg | pink
round |
“A30” on one side
and another side is plain |
6.2 Postmarketing Experience
The following adverse reactions have been identified during post-approval use of aripiprazole. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to establish a causal relationship to drug exposure: occurrences of allergic reaction (anaphylactic reaction, angioedema, laryngospasm, pruritus/urticaria, or oropharyngeal spasm), pathological gambling, hiccups, blood glucose fluctuation, oculogyric crisis, and drug reaction with eosinophilia and systemic symptoms (DRESS).
8.6 Cyp2d6 Poor Metabolizers (8.6 CYP2D6 Poor Metabolizers)
Dosage adjustment is recommended in known CYP2D6 poor metabolizers due to high aripiprazole concentrations. Approximately 8% of Caucasians and 3 to 8% of Black/African Americans cannot metabolize CYP2D6 substrates and are classified as poor metabolizers (PM) [see Dosage and Administration (2.7) and Clinical Pharmacology (12.3)] .
10.2 Management of Overdosage
No specific information is available on the treatment of overdose with aripiprazole. An electrocardiogram should be obtained in case of overdosage and if QT interval prolongation is present, cardiac monitoring should be instituted. Otherwise, management of overdose should concentrate on supportive therapy, maintaining an adequate airway, oxygenation and ventilation, and management of symptoms. Close medical supervision and monitoring should continue until the patient recovers.
Charcoal: In the event of an overdose of aripiprazole, an early charcoal administration may be useful in partially preventing the absorption of aripiprazole. Administration of 50 g of activated charcoal, one hour after a single 15 mg oral dose of aripiprazole, decreased the mean AUC and C max of aripiprazole by 50%.
Hemodialysis: Although there is no information on the effect of hemodialysis in treating an overdose with aripiprazole, hemodialysis is unlikely to be useful in overdose management since aripiprazole is highly bound to plasma proteins.
8 Use in Specific Populations (8 USE IN SPECIFIC POPULATIONS)
Pregnancy: May cause extrapyramidal and/or withdrawal symptoms in neonates with third trimester exposure (8.1)
Additional pediatric use information is approved for Otsuka America Pharmaceutical, Inc.’s ABILIFY ® (aripiprazole) product. However, due to Otsuka America Pharmaceutical, Inc.’s marketing exclusivity rights, this drug product is not labeled with that information.
8.8 Other Specific Populations
No dosage adjustment for aripiprazole is required on the basis of a patient’s sex, race, or smoking status [see Clinical Pharmacology (12.3) ].
5.13 Body Temperature Regulation
Disruption of the body’s ability to reduce core body temperature has been attributed to antipsychotic agents. Appropriate care is advised when prescribing aripiprazole for patients who will be experiencing conditions which may contribute to an elevation in core body temperature, (e.g., exercising strenuously, exposure to extreme heat, receiving concomitant medication with anticholinergic activity, or being subject to dehydration) [see Adverse Reactions (6.2)] .
8.7 Hepatic and Renal Impairment
No dosage adjustment for aripiprazole is required on the basis of a patient’s hepatic function (mild to severe hepatic impairment, Child-Pugh score between 5 and 15), or renal function (mild to severe renal impairment, glomerular filtration rate between 15 and 90 mL/minute) [see Clinical Pharmacology (12.3) ].
17 Patient Counseling Information (17 PATIENT COUNSELING INFORMATION)
Advise the patient to read the FDA-approved patient labeling ( Medication Guide).
Discuss the following issues with patients prescribed aripiprazole:
Clinical Worsening of Depression and Suicide Risk
Patients, their families, and their caregivers should be encouraged to be alert to the emergence of anxiety, agitation, panic attacks, insomnia, irritability, hostility, aggressiveness, impulsivity, akathisia (psychomotor restlessness), hypomania, mania, other unusual changes in behavior, worsening of depression, and suicidal ideation, especially early during antidepressant treatment and when the dose is adjusted up or down. Families and caregivers of patients should be advised to look for the emergence of such symptoms on a day-to-day basis, since changes may be abrupt. Such symptoms should be reported to the patient’s prescriber or health professional, especially if they are severe, abrupt in onset, or were not part of the patient’s presenting symptoms. Symptoms such as these may be associated with an increased risk for suicidal thinking and behavior and indicate a need for very close monitoring and possibly changes in the medication [see Warnings and Precautions (5.3)] .
Prescribers or other health professionals should inform patients, their families, and their caregivers about the benefits and risks associated with treatment with aripiprazole and should counsel them in its appropriate use. A patient Medication Guide including information about “Antidepressant Medicines, Depression and other Serious Mental Illness, and Suicidal Thoughts or Actions” is available for aripiprazole. The prescriber or health professional should instruct patients, their families, and their caregivers to read the Medication Guide and should assist them in understanding its contents. Patients should be given the opportunity to discuss the contents of the Medication Guide and to obtain answers to any questions they may have. It should be noted that aripiprazole is not approved as a single agent for treatment of depression and has not been evaluated in pediatric major depressive disorder.
Pathological Gambling and Other Compulsive Behaviors
Advise patients and their caregivers of the possibility that they may experience compulsive urges to shop, intense urges to gamble, compulsive sexual urges, binge eating and/or other compulsive urges and the inability to control these urges while taking aripiprazole. In some cases, but not all, the urges were reported to have stopped when the dose was reduced or stopped [see Warnings and Precautions (5.7)] .
Interference with Cognitive and Motor Performance
Because aripiprazole may have the potential to impair judgment, thinking, or motor skills, patients should be cautioned about operating hazardous machinery, including automobiles, until they are reasonably certain that aripiprazole therapy does not affect them adversely [see Warnings and Precautions (5.12)] .
Concomitant Medication
Patients should be advised to inform their physicians if they are taking, or plan to take, any prescription or over-the-counter drugs, since there is a potential for interactions [see Drug Interactions (7)] .
Heat Exposure and Dehydration
Patients should be advised regarding appropriate care in avoiding overheating and dehydration [see Warnings and Precautions (5.13)] .
Pregnancy
Advise patients to notify their healthcare provider if they become pregnant or intend to become pregnant during treatment with aripiprazole. Advise patients that aripiprazole may cause extrapyramidal and/or withdrawal symptoms (agitation, hypertonia, hypotonia, tremor, somnolence, respiratory distress, and feeding disorder) in a neonate. Advise patients that there is a pregnancy registry that monitors pregnancy outcomes in women exposed to aripiprazole during pregnancy [see Use in Specific Populations (8.1)] .
ABILIFY ® is a trademark of Otsuka Pharmaceutical Company.
Manufactured For:
Accord Healthcare, Inc.,
1009 Slater Road,
Suite 210-B,
Durham, NC 27703,
USA
Manufactured By:
Intas Pharmaceuticals Limited.
Plot No. 5 to 12, Pharmez,
Sarkhej-Bavla, National Highway No 8-A,
Near Village Matoda, Tal Sanand,
Ahmedabad - 382213, Gujarat, India
51 1878 2 722646
Issued March 2020
16 How Supplied/storage and Handling (16 HOW SUPPLIED/STORAGE AND HANDLING)
Product: 50090-6063
NDC: 50090-6063-0 30 TABLET in a BOTTLE
5.4 Neuroleptic Malignant Syndrome (nms) (5.4 Neuroleptic Malignant Syndrome (NMS))
A potentially fatal symptom complex sometimes referred to as Neuroleptic Malignant Syndrome (NMS) may occur with administration of antipsychotic drugs, including aripiprazole. Rare cases of NMS occurred during aripiprazole treatment in the worldwide clinical database. Clinical manifestations of NMS are hyperpyrexia, muscle rigidity, altered mental status, and evidence of autonomic instability (irregular pulse or blood pressure, tachycardia, diaphoresis, and cardiac dysrhythmia). Additional signs may include elevated creatine phosphokinase, myoglobinuria (rhabdomyolysis), and acute renal failure.
The diagnostic evaluation of patients with this syndrome is complicated. In arriving at a diagnosis, it is important to exclude cases where the clinical presentation includes both serious medical illness (e.g., pneumonia, systemic infection) and untreated or inadequately treated extrapyramidal signs and symptoms (EPS). Other important considerations in the differential diagnosis include central anticholinergic toxicity, heat stroke, drug fever, and primary central nervous system pathology.
The management of NMS should include: 1) immediate discontinuation of antipsychotic drugs and other drugs not essential to concurrent therapy; 2) intensive symptomatic treatment and medical monitoring; and 3) treatment of any concomitant serious medical problems for which specific treatments are available. There is no general agreement about specific pharmacological treatment regimens for uncomplicated NMS.
If a patient requires antipsychotic drug treatment after recovery from NMS, the potential reintroduction of drug therapy should be carefully considered. The patient should be carefully monitored, since recurrences of NMS have been reported.
13.2 Animal Toxicology And/or Pharmacology (13.2 Animal Toxicology and/or Pharmacology)
Aripiprazole produced retinal degeneration in albino rats in a 26-week chronic toxicity study at a dose of 60 mg/kg/day and in a 2-year carcinogenicity study at doses of 40 and 60 mg/kg/day which are 13 and 19 times the MRHD of 30 mg/day based on mg/m 2 body surface area. Evaluation of the retinas of albino mice and of monkeys did not reveal evidence of retinal degeneration. Additional studies to further evaluate the mechanism have not been performed. The relevance of this finding to human risk is unknown.
5.10 Leukopenia, Neutropenia, and Agranulocytosis
In clinical trials and/or postmarketing experience, events of leukopenia and neutropenia have been reported temporally related to antipsychotic agents, including aripiprazole. Agranulocytosis has also been reported.
Possible risk factors for leukopenia/neutropenia include pre-existing low white blood cell count (WBC)/absolute neutrophil count (ANC) and history of drug-induced leukopenia/neutropenia. In patients with a history of a clinically significant low WBC/ANC or drug-induced leukopenia/neutropenia, perform a complete blood count (CBC) frequently during the first few months of therapy. In such patients, consider discontinuation of aripiprazole at the first sign of a clinically significant decline in WBC in the absence of other causative factors.
Monitor patients with clinically significant neutropenia for fever or other symptoms or signs of infection and treat promptly if such symptoms or signs occur. Discontinue aripiprazole in patients with severe neutropenia (absolute neutrophil count <1000/mm 3) and follow their WBC counts until recovery.
5.12 Potential for Cognitive and Motor Impairment
Aripiprazole, like other antipsychotics, may have the potential to impair judgment, thinking, or motor skills. For example, in short-term, placebo-controlled trials, somnolence (including sedation) was reported as follows (aripiprazole incidence, placebo incidence): in adult patients (n=2467) treated with oral aripiprazole (11%, 6%), and in pediatric patients ages 6 to 17 (n=611) (24%, 6%). Somnolence (including sedation) led to discontinuation in 0.3% (8/2467) of adult patients and 3% (20/732) of pediatric patients (6 to 18 years) on oral aripiprazole in short-term, placebo-controlled trials.
Despite the relatively modest increased incidence of these events compared to placebo, patients should be cautioned about operating hazardous machinery, including automobiles, until they are reasonably certain that therapy with aripiprazole does not affect them adversely.
5.2 Cerebrovascular Adverse Events, Including Stroke
In placebo-controlled clinical studies (two flexible dose and one fixed dose study) of dementia-related psychosis, there was an increased incidence of cerebrovascular adverse events (e.g., stroke, transient ischemic attack), including fatalities, in aripiprazole-treated patients (mean age: 84 years; range: 78 to 88 years). In the fixed-dose study, there was a statistically significant dose response relationship for cerebrovascular adverse events in patients treated with aripiprazole. Aripiprazole is not approved for the treatment of patients with dementia-related psychosis [see Boxed Warning] .
5.7 Pathological Gambling and Other Compulsive Behaviors
Post-marketing case reports suggest that patients can experience intense urges, particularly for gambling, and the inability to control these urges while taking aripiprazole. Other compulsive urges, reported less frequently include: sexual urges, shopping, eating or binge eating, and other impulsive or compulsive behaviors. Because patients may not recognize these behaviors as abnormal, it is important for prescribers to ask patients or their caregivers specifically about the development of new or intense gambling urges, compulsive sexual urges, compulsive shopping, binge or compulsive eating, or other urges while being treated with aripiprazole. It should be noted that impulse-control symptoms can be associated with the underlying disorder. In some cases, although not all, urges were reported to have stopped when the dose was reduced or the medication was discontinued. Compulsive behaviors may result in harm to the patient and others if not recognized. Consider dose reduction or stopping the medication if a patient develops such urges.
7.1 Drugs Having Clinically Important Interactions With Aripiprazole (7.1 Drugs Having Clinically Important Interactions with Aripiprazole)
| Concomitant Drug Name or Drug Class | Clinical Rationale | Clinical Recommendation |
|---|---|---|
| Strong CYP3A4 Inhibitors (e.g., itraconazole, clarithromycin) or strong CYP2D6 inhibitors (e.g., quinidine, fluoxetine, paroxetine) | The concomitant use of aripiprazole with strong CYP 3A4 or CYP2D6 inhibitors increased the exposure of aripiprazole compared to the use of aripiprazole alone [see Clinical Pharmacology (12.3)] . | With concomitant use of aripiprazole with a strong CYP3A4 inhibitor or CYP2D6 inhibitor, reduce the aripiprazole dosage [see Dosage and Administration (2.7)] . |
| Strong CYP3A4 Inducers (e.g., carbamazepine, rifampin) | The concomitant use of aripiprazole and carbamazepine decreased the exposure of aripiprazole compared to the use of aripiprazole alone [see Clinical Pharmacology (12.3)] . | With concomitant use of aripiprazole with a strong CYP3A4 inducer, consider increasing the aripiprazole dosage [see Dosage and Administration (2.7)] . |
| Antihypertensive Drugs | Due to its alpha adrenergic antagonism, aripiprazole has the potential to enhance the effect of certain antihypertensive agents. | Monitor blood pressure and adjust dose accordingly [see Warnings and Precautions (5.8)] . |
| Benzodiazepines (e.g., lorazepam) | The intensity of sedation was greater with the combination of oral aripiprazole and lorazepam as compared to that observed with aripiprazole alone. The orthostatic hypotension observed was greater with the combination as compared to that observed with lorazepam alone [see Warnings and Precautions (5.8)] . | Monitor sedation and blood pressure. Adjust dose accordingly. |
7.2 Drugs Having No Clinically Important Interactions With Aripiprazole (7.2 Drugs Having No Clinically Important Interactions with Aripiprazole)
Based on pharmacokinetic studies, no dosage adjustment of aripiprazole is required when administered concomitantly with famotidine, valproate, lithium, lorazepam.
In addition, no dosage adjustment is necessary for substrates of CYP2D6 (e.g., dextromethorphan, fluoxetine, paroxetine, or venlafaxine), CYP2C9 (e.g., warfarin), CYP2C19 (e.g., omeprazole, warfarin, escitalopram), or CYP3A4 (e.g., dextromethorphan) when co-administered with aripiprazole. Additionally, no dosage adjustment is necessary for valproate, lithium, lamotrigine, lorazepam, or sertraline when co-administered with aripiprazole [see Clinical Pharmacology (12.3)] .
5.1 Increased Mortality in Elderly Patients With Dementia Related Psychosis (5.1 Increased Mortality in Elderly Patients with Dementia-Related Psychosis)
Increased Mortality
Elderly patients with dementia-related psychosis treated with antipsychotic drugs are at an increased risk of death. Aripiprazole is not approved for the treatment of patients with dementia-related psychosis [see Boxed Warning] .
Safety Experience in Elderly Patients with Psychosis Associated with Alzheimer’s Disease
In three, 10-week, placebo-controlled studies of aripiprazole in elderly patients with psychosis associated with Alzheimer’s disease (n=938; mean age: 82.4 years; range: 56 to 99 years), the adverse reactions that were reported at an incidence of ≥3% and aripiprazole incidence at least twice that for placebo were lethargy [placebo 2%, aripiprazole 5%], somnolence (including sedation) [placebo 3%, aripiprazole 8%], and incontinence (primarily, urinary incontinence) [placebo 1%, aripiprazole 5%], excessive salivation [placebo 0%, aripiprazole 4%], and lightheadedness [placebo 1%, aripiprazole 4%].
The safety and efficacy of aripiprazole in the treatment of patients with psychosis associated with dementia have not been established. If the prescriber elects to treat such patients with aripiprazole, assess for the emergence of difficulty swallowing or excessive somnolence, which could predispose to accidental injury or aspiration [see Boxed Warning] .
5.3 Suicidal Thoughts and Behaviors in Children, Adolescents, and Young Adults
Patients with major depressive disorder (MDD), both adult and pediatric, may experience worsening of their depression and/or the emergence of suicidal ideation and behavior (suicidality) or unusual changes in behavior, whether or not they are taking antidepressant medications, and this risk may persist until significant remission occurs. Suicide is a known risk of depression and certain other psychiatric disorders, and these disorders themselves are the strongest predictors of suicide. There has been a long-standing concern, however, that antidepressants may have a role in inducing worsening of depression and the emergence of suicidality in certain patients during the early phases of treatment. Pooled analyses of short-term, placebo-controlled trials of antidepressant drugs (SSRIs and others) showed that these drugs increase the risk of suicidal thinking and behavior (suicidality) in children, adolescents, and young adults (ages 18 to 24) with MDD and other psychiatric disorders. Short-term studies did not show an increase in the risk of suicidality with antidepressants compared to placebo in adults beyond age 24; there was a reduction with antidepressants compared to placebo in adults aged 65 and older.
The pooled analyses of placebo-controlled trials in children and adolescents with MDD, Obsessive Compulsive Disorder (OCD), or other psychiatric disorders included a total of 24 short-term trials of 9 antidepressant drugs in over 4400 patients. The pooled analyses of placebo-controlled trials in adults with MDD or other psychiatric disorders included a total of 295 short-term trials (median duration of 2 months) of 11 antidepressant drugs in over 77,000 patients. There was considerable variation in risk of suicidality among drugs, but a tendency toward an increase in the younger patients for almost all drugs studied. There were differences in absolute risk of suicidality across the different indications, with the highest incidence in MDD. The risk differences (drug vs. placebo), however, were relatively stable within age strata and across indications. These risk differences (drug-placebo difference in the number of cases of suicidality per 1000 patients treated) are provided in Table 5.
| Age Range |
Drug-Placebo Difference in Number of
Cases of Suicidality per 1000 Patients Treated |
| Increases Compared to Placebo | |
| <18 | 14 additional cases |
| 18 to 24 | 5 additional cases |
| Decreases Compared to Placebo | |
| 25 to 64 | 1 fewer case |
| ≥65 | 6 fewer cases |
No suicides occurred in any of the pediatric trials. There were suicides in the adult trials, but the number was not sufficient to reach any conclusion about drug effect on suicide.
It is unknown whether the suicidality risk extends to longer-term use, i.e., beyond several months. However, there is substantial evidence from placebo-controlled maintenance trials in adults with depression that the use of antidepressants can delay the recurrence of depression.
All patients being treated with antidepressants for any indication should be monitored appropriately and observed closely for clinical worsening, suicidality, and unusual changes in behavior, especially during the initial few months of a course of drug therapy, or at times of dose changes, either increases or decreases.
The following symptoms, anxiety, agitation, panic attacks, insomnia, irritability, hostility, aggressiveness, impulsivity, akathisia (psychomotor restlessness), hypomania, and mania, have been reported in adult and pediatric patients being treated with antidepressants for MDD as well as for other indications, both psychiatric and nonpsychiatric. Although a causal link between the emergence of such symptoms and either the worsening of depression and/or the emergence of suicidal impulses has not been established, there is concern that such symptoms may represent precursors to emerging suicidality.
Consideration should be given to changing the therapeutic regimen, including possibly discontinuing the medication, in patients whose depression is persistently worse, or who are experiencing emergent suicidality or symptoms that might be precursors to worsening depression or suicidality, especially if these symptoms are severe, abrupt in onset, or were not part of the patient’s presenting symptoms.
Families and caregivers of patients being treated with antidepressants for major depressive disorder or other indications, both psychiatric and nonpsychiatric, should be alerted about the need to monitor patients for the emergence of agitation, irritability, unusual changes in behavior, and the other symptoms described above, as well as the emergence of suicidality, and to report such symptoms immediately to healthcare providers. Such monitoring should include daily observation by families and caregivers. Prescriptions for aripiprazole should be written for the smallest quantity of tablets consistent with good patient management, in order to reduce the risk of overdose.
Screening Patients for Bipolar Disorder: A major depressive episode may be the initial presentation of bipolar disorder. It is generally believed (though not established in controlled trials) that treating such an episode with an antidepressant alone may increase the likelihood of precipitation of a mixed/manic episode in patients at risk for bipolar disorder. Whether any of the symptoms described above represent such a conversion is unknown. However, prior to initiating treatment with an antidepressant, patients with depressive symptoms should be adequately screened to determine if they are at risk for bipolar disorder; such screening should include a detailed psychiatric history, including a family history of suicide, bipolar disorder, and depression.
It should be noted that aripiprazole is not approved for use in treating depression in the pediatric population.
Warning: Increased Mortality in Elderly Patients With Dementia Related Psychosis; and Suicidal Thoughts and Behaviors With Antidepressant Drugs (WARNING: INCREASED MORTALITY IN ELDERLY PATIENTS WITH DEMENTIA-RELATED PSYCHOSIS; AND SUICIDAL THOUGHTS AND BEHAVIORS WITH ANTIDEPRESSANT DRUGS)
Elderly patients with dementia-related psychosis treated with antipsychotic drugs are at an increased risk of death. Aripiprazole is not approved for the treatment of patients with dementia-related psychosis [see Warnings and Precautions (5.1)] .
Antidepressants increased the risk of suicidal thoughts and behavior in children, adolescents, and young adults in short-term studies. These studies did not show an increase in the risk of suicidal thoughts and behavior with antidepressant use in patients over age 24; there was a reduction in risk with antidepressant use in patients aged 65 and older [see Warnings and Precautions (5.3)] .
In patients of all ages who are started on antidepressant therapy, monitor closely for worsening, and for emergence of suicidal thoughts and behaviors. Advise families and caregivers of the need for close observation and communication with the prescriber [see Warnings and Precautions (5.3)] .
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:37:57.351518 · Updated: 2026-03-14T21:52:52.492895