These Highlights Do Not Include All The Information Needed To Use Tuxarin Er™ Safely And Effectively. See Full Prescribing Information For Tuxarin Er.
a7cfab67-6087-4ab4-b7cd-4f9295413180
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
WARNING: ADDICTION, ABUSE, AND MISUSE; LIFE-THREATENING RESPIRATORY DEPRESSION; ACCIDENTIAL INGESTION; ULTRA-RAPID METABOLISM OF CODEINE AND OTHER RISK FACTORS FOR LIFE-THREATENING RESPIRATORY DEPRESSION IN CHILDREN; MEDICATION ERRORS; INTERACTIONS WITH DRUGS AFFECTING CYTOCHROME P450 ISOENZYMES; CONCOMITANT USE WITH BENZODIAZEPINES OR OTHER CNS DEPRESSANTS; NEONATAL OPOID WITHDRAWAL SYNDROME See full prescribing information for complete boxed warning. TUXARIN ER exposes users to risks of addiction, abuse, and misuse, which can lead to overdose and death. Assess patient's risk before prescribing and monitor closely for these behaviors and conditions. ( 5.1 ) Serious, life-threatening, or fatal respiratory depression may occur. Monitor closely, especially upon initiation or when used in patients at higher risk. ( 5.2 ) Accidental ingestion of TUXARIN ER, especially by children, can result in a fatal overdose of codeine. ( 5.2 ) Life-threatening respiratory depression and death have occurred in children who received codeine; most cases followed tonsillectomy and/or adenoidectomy, and many of the children had evidence of being an ultra-rapid metabolizer of codeine due to a CYP2D6 polymorphism. ( 5.3 ) TUXARIN ER is contraindicated in children younger than 12 years of age and in children younger than 18 years of age following tonsillectomy and/or adenoidectomy. ( 4 ) Avoid the use of TUXARIN ER in adolescents 12 to 18 years of age who have other risk factors that may increase their sensitivity to the respiratory depressant effects of codeine. Ensure accuracy when prescribing, dispensing, and administering TUXARIN ER. Dosing errors can result in accidental overdose and death. ( 2.1 , 5.6 ) The effects of concomitant use or discontinuation of cytochrome P450 3A4 inducers, 3A4 inhibitors, or 2D6 inhibitors with codeine are complex, requiring careful consideration of the effects on the parent drug, codeine, and the active metabolite, morphine. Avoid the use of TUXARIN ER in these patients. ( 5.4 , 7.1 , 7.2 , 7.4 ) Concomitant use of opioids with benzodiazepines or other central nervous system (CNS) depressants, including alcohol, may result in profound sedation, respiratory depression, coma, and death. Avoid the use of TUXARIN ER in patients taking benzodiazepines, other CNS depressants, or alcohol. ( 5.9 , 7.5 ) TUXARIN ER is not recommended for use in pregnant women. Prolonged use of TUXARIN ER during pregnancy can result in neonatal opioid withdrawal syndrome, which may be life-threatening if not recognized and treated. If TUXARIN ER is used for a prolonged period in a pregnant woman, advise the patient of the risk of neonatal opioid withdrawal syndrome and ensure that appropriate treatment will be available. ( 5.15 , 8.1 )
Indications and Usage
TUXARIN ER is indicated for the temporary relief of cough and upper respiratory symptoms associated with allergy or the common cold in patients 18 years of age and older.
Dosage and Administration
Administer TUXARIN ER by the oral route only. Advise patients not to increase the dose or dosing frequency of TUXARIN ER because serious adverse events such as respiratory depression may occur with overdosage [ see Warnings and Precautions (5.2) , Overdosage (10) ]. The dosage of TUXARIN ER should not be increased if cough fails to respond; an unresponsive cough should be reevaluated for possible underlying pathology [ see Dosage and Administration (2.3) , Warnings and Precautions (5.5) ].
Warnings and Precautions
See Boxed WARNINGS Life-threatening respiratory depression in patients with chronic pulmonary disease or in elderly, cachectic, or debilitated patients: Monitor closely, particularly during initiation of therapy. ( 5.5 ) Activities requiring mental alertness: Avoid engaging in hazardous tasks requiring mental alertness such as driving or operating machinery. ( 5.7 ) Risks of use in patients with head injury, impaired consciousness, increased intracranial pressure, or brain tumors: Avoid use. May increase intracranial pressure and obscure the clinical course of head injuries. ( 5.11 ) Seizures in patients with seizure disorders: Monitor during therapy. ( 5.12 ) Severe hypotension: Monitor during initiation of therapy. Avoid use in patients with circulatory shock. ( 5.14 ) Adrenal insufficiency: If diagnosed, treat with physiologic replacement of corticosteroids, and wean patient off of the opioid. ( 5.16 )
Contraindications
TUXARIN ER is contraindicated for: All children younger than 12 years of age [ see Warnings and Precautions (5.2 , 5.3 , 5.4) , Use in Specific Populations (8.4) ]. Postoperative management in children younger than 18 years of age following tonsillectomy and/or adenoidectomy [ see Warnings and Precautions (5.2 , 5.3) ]. TUXARIN ER is also contraindicated in patients with: Significant respiratory depression [see Warnings and Precautions (5.2) ] Acute or severe bronchial asthma in an unmonitored setting or in the absence of resuscitative equipment [ see Warnings and Precautions (5.5) ]. Known or suspected gastrointestinal obstruction, including paralytic ileus [ see Warnings and Precautions (5.10) ]. Concurrent use of monoamine oxidase inhibitors (MAOIs) or use of MAOIs within 14 days [ see Warnings and Precautions (5.13) , Drug Interactions (7.7) ]. Hypersensitivity to codeine, chlorpheniramine, or any of the inactive ingredients in TUXARIN ER [ see Adverse Reactions (6) ]. Persons known to be hypersensitive to certain other opioids may exhibit cross-reactivity to codeine.
Adverse Reactions
The following serious adverse reactions are described, or described in greater detail, in other sections: Addiction, abuse, and misuse [ see Warnings and Precautions (5.1) , Drug Abuse and Dependence (9.3) ] Life-threatening respiratory depression [ see Warnings and Precautions (5.2 , 5.3 , 5.4 , 5.5 , 5.9) , Overdosage (10) ] Ultra-rapid metabolism of codeine and other risk factors for life-threatening respiratory depression in children [ see Warnings and Precautions (5.3) ] Accidental overdose and death due to medication errors [ see Warnings and Precautions (5.6) ] Decreased mental alertness with impaired mental and/or physical abilities [ see Warnings and Precautions (5.7) ] Interactions with benzodiazepines and other CNS depressants [ see Warnings and Precautions (5.9) ] Paralytic ileus, gastrointestinal adverse reactions [ see Warnings and Precautions (5.10) ] Increased intracranial pressure [ see Warnings and Precautions (5.11) ] Obscured clinical course in patients with head injuries [ see Warnings and Precautions (5.11) ] Seizures [ see Warnings and Precautions (5.12) ] Interactions with MAOI [ see Warnings and Precautions (5.13) ] Severe hypotension [ see Warnings and Precautions (5.14) ] Neonatal Opioid Withdrawal Syndrome [ see Warnings and Precautions (5.15) ] Adrenal insufficiency [ see Warnings and Precautions (5.16) ] The following adverse reactions have been identified during clinical studies, or during post-approval use of codeine and/or chlorpheniramine. Because these reactions may be reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure. The most common adverse reactions to TUXARIN ER include: Sedation (somnolence, mental clouding, lethargy), impaired mental and physical performance, lightheadedness, dizziness, headache, dry mouth, nausea, vomiting, constipation, shortness of breath, and sweating. Other reactions include: Anaphylaxis : Anaphylaxis has been reported with codeine, one of the ingredients in TUXARIN ER. Body as a whole : Coma, death, fatigue, falling injuries, lethargy. Cardiovascular : Peripheral edema, increased blood pressure, decreased blood pressure, tachycardia, chest pain, palpitation, syncope, orthostatic hypotension, prolonged QT interval, hot flush. Central Nervous System : Ataxia, facial dyskinesia, insomnia, increased intracranial pressure, migraine, seizure, tremor, tinnitus, vertigo. Dermatologic : Flushing, hyperhidrosis, pruritus, rash. Endocrine/Metabolic : Cases of serotonin syndrome, a potentially life-threatening condition, have been reported during concomitant use of opioids with serotonergic drugs. Cases of adrenal insufficiency have been reported with opioid use, more often following greater than one month of use. Cases of androgen deficiency have occurred with chronic use of opioids [ see Clinical Pharmacology (12.2) ]. Gastrointestinal : Abdominal pain, bowel obstruction, decreased appetite, diarrhea, difficulty swallowing, GERD, indigestion, pancreatitis, paralytic ileus, biliary tract spasm (spasm of the sphincter of Oddi). Genitourinary : Urinary tract infection, ureteral spasm, spasm of vesicle sphincters, urinary retention. Hematologic : Agranulocytosis, aplastic anemia, and thrombocytopenia have been reported. Laboratory: Increases in serum amylase. Musculoskeletal : Arthralgia, backache, muscle spasm. Ophthalmic : Blurred vision, diplopia, miosis (constricted pupils), visual disturbances. Psychiatric : Agitation, anxiety, confusion, fear, dysphoria, depression, hallucinations. Reproductive : Hypogonadism, infertility. Respiratory : Bronchitis, cough, dry nose, dry throat, dyspnea, nasal congestion, nasopharyngitis, respiratory depression, sinusitis, thickening of bronchial secretions, tightness of chest and wheezing, upper respiratory tract infection. Other : Drug abuse, drug dependence, opioid withdrawal syndrome. Hypoglycemia: Cases of hypoglycemia have been reported in patients taking opioids. Most reports were in patients with at least one predisposing risk factor (e.g., diabetes).
Drug Interactions
No specific drug interaction studies have been conducted with TUXARIN ER.
Storage and Handling
TUXARIN ER (codeine phosphate and chlorpheniramine maleate) 54.3 mg/ 8 mg extended-release tablets, are white to off-white, uncoated, standard round tablets, debossed with MP on one side and CC on the other side. Supplied in bottles of 30 tablets (NDC 71269-040-30) and 100 tablets (NDC 71269-040-10).
How Supplied
TUXARIN ER (codeine phosphate and chlorpheniramine maleate) 54.3 mg/ 8 mg extended-release tablets, are white to off-white, uncoated, standard round tablets, debossed with MP on one side and CC on the other side. Supplied in bottles of 30 tablets (NDC 71269-040-30) and 100 tablets (NDC 71269-040-10).
Medication Information
Warnings and Precautions
See Boxed WARNINGS Life-threatening respiratory depression in patients with chronic pulmonary disease or in elderly, cachectic, or debilitated patients: Monitor closely, particularly during initiation of therapy. ( 5.5 ) Activities requiring mental alertness: Avoid engaging in hazardous tasks requiring mental alertness such as driving or operating machinery. ( 5.7 ) Risks of use in patients with head injury, impaired consciousness, increased intracranial pressure, or brain tumors: Avoid use. May increase intracranial pressure and obscure the clinical course of head injuries. ( 5.11 ) Seizures in patients with seizure disorders: Monitor during therapy. ( 5.12 ) Severe hypotension: Monitor during initiation of therapy. Avoid use in patients with circulatory shock. ( 5.14 ) Adrenal insufficiency: If diagnosed, treat with physiologic replacement of corticosteroids, and wean patient off of the opioid. ( 5.16 )
Indications and Usage
TUXARIN ER is indicated for the temporary relief of cough and upper respiratory symptoms associated with allergy or the common cold in patients 18 years of age and older.
Dosage and Administration
Administer TUXARIN ER by the oral route only. Advise patients not to increase the dose or dosing frequency of TUXARIN ER because serious adverse events such as respiratory depression may occur with overdosage [ see Warnings and Precautions (5.2) , Overdosage (10) ]. The dosage of TUXARIN ER should not be increased if cough fails to respond; an unresponsive cough should be reevaluated for possible underlying pathology [ see Dosage and Administration (2.3) , Warnings and Precautions (5.5) ].
Contraindications
TUXARIN ER is contraindicated for: All children younger than 12 years of age [ see Warnings and Precautions (5.2 , 5.3 , 5.4) , Use in Specific Populations (8.4) ]. Postoperative management in children younger than 18 years of age following tonsillectomy and/or adenoidectomy [ see Warnings and Precautions (5.2 , 5.3) ]. TUXARIN ER is also contraindicated in patients with: Significant respiratory depression [see Warnings and Precautions (5.2) ] Acute or severe bronchial asthma in an unmonitored setting or in the absence of resuscitative equipment [ see Warnings and Precautions (5.5) ]. Known or suspected gastrointestinal obstruction, including paralytic ileus [ see Warnings and Precautions (5.10) ]. Concurrent use of monoamine oxidase inhibitors (MAOIs) or use of MAOIs within 14 days [ see Warnings and Precautions (5.13) , Drug Interactions (7.7) ]. Hypersensitivity to codeine, chlorpheniramine, or any of the inactive ingredients in TUXARIN ER [ see Adverse Reactions (6) ]. Persons known to be hypersensitive to certain other opioids may exhibit cross-reactivity to codeine.
Adverse Reactions
The following serious adverse reactions are described, or described in greater detail, in other sections: Addiction, abuse, and misuse [ see Warnings and Precautions (5.1) , Drug Abuse and Dependence (9.3) ] Life-threatening respiratory depression [ see Warnings and Precautions (5.2 , 5.3 , 5.4 , 5.5 , 5.9) , Overdosage (10) ] Ultra-rapid metabolism of codeine and other risk factors for life-threatening respiratory depression in children [ see Warnings and Precautions (5.3) ] Accidental overdose and death due to medication errors [ see Warnings and Precautions (5.6) ] Decreased mental alertness with impaired mental and/or physical abilities [ see Warnings and Precautions (5.7) ] Interactions with benzodiazepines and other CNS depressants [ see Warnings and Precautions (5.9) ] Paralytic ileus, gastrointestinal adverse reactions [ see Warnings and Precautions (5.10) ] Increased intracranial pressure [ see Warnings and Precautions (5.11) ] Obscured clinical course in patients with head injuries [ see Warnings and Precautions (5.11) ] Seizures [ see Warnings and Precautions (5.12) ] Interactions with MAOI [ see Warnings and Precautions (5.13) ] Severe hypotension [ see Warnings and Precautions (5.14) ] Neonatal Opioid Withdrawal Syndrome [ see Warnings and Precautions (5.15) ] Adrenal insufficiency [ see Warnings and Precautions (5.16) ] The following adverse reactions have been identified during clinical studies, or during post-approval use of codeine and/or chlorpheniramine. Because these reactions may be reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure. The most common adverse reactions to TUXARIN ER include: Sedation (somnolence, mental clouding, lethargy), impaired mental and physical performance, lightheadedness, dizziness, headache, dry mouth, nausea, vomiting, constipation, shortness of breath, and sweating. Other reactions include: Anaphylaxis : Anaphylaxis has been reported with codeine, one of the ingredients in TUXARIN ER. Body as a whole : Coma, death, fatigue, falling injuries, lethargy. Cardiovascular : Peripheral edema, increased blood pressure, decreased blood pressure, tachycardia, chest pain, palpitation, syncope, orthostatic hypotension, prolonged QT interval, hot flush. Central Nervous System : Ataxia, facial dyskinesia, insomnia, increased intracranial pressure, migraine, seizure, tremor, tinnitus, vertigo. Dermatologic : Flushing, hyperhidrosis, pruritus, rash. Endocrine/Metabolic : Cases of serotonin syndrome, a potentially life-threatening condition, have been reported during concomitant use of opioids with serotonergic drugs. Cases of adrenal insufficiency have been reported with opioid use, more often following greater than one month of use. Cases of androgen deficiency have occurred with chronic use of opioids [ see Clinical Pharmacology (12.2) ]. Gastrointestinal : Abdominal pain, bowel obstruction, decreased appetite, diarrhea, difficulty swallowing, GERD, indigestion, pancreatitis, paralytic ileus, biliary tract spasm (spasm of the sphincter of Oddi). Genitourinary : Urinary tract infection, ureteral spasm, spasm of vesicle sphincters, urinary retention. Hematologic : Agranulocytosis, aplastic anemia, and thrombocytopenia have been reported. Laboratory: Increases in serum amylase. Musculoskeletal : Arthralgia, backache, muscle spasm. Ophthalmic : Blurred vision, diplopia, miosis (constricted pupils), visual disturbances. Psychiatric : Agitation, anxiety, confusion, fear, dysphoria, depression, hallucinations. Reproductive : Hypogonadism, infertility. Respiratory : Bronchitis, cough, dry nose, dry throat, dyspnea, nasal congestion, nasopharyngitis, respiratory depression, sinusitis, thickening of bronchial secretions, tightness of chest and wheezing, upper respiratory tract infection. Other : Drug abuse, drug dependence, opioid withdrawal syndrome. Hypoglycemia: Cases of hypoglycemia have been reported in patients taking opioids. Most reports were in patients with at least one predisposing risk factor (e.g., diabetes).
Drug Interactions
No specific drug interaction studies have been conducted with TUXARIN ER.
Storage and Handling
TUXARIN ER (codeine phosphate and chlorpheniramine maleate) 54.3 mg/ 8 mg extended-release tablets, are white to off-white, uncoated, standard round tablets, debossed with MP on one side and CC on the other side. Supplied in bottles of 30 tablets (NDC 71269-040-30) and 100 tablets (NDC 71269-040-10).
How Supplied
TUXARIN ER (codeine phosphate and chlorpheniramine maleate) 54.3 mg/ 8 mg extended-release tablets, are white to off-white, uncoated, standard round tablets, debossed with MP on one side and CC on the other side. Supplied in bottles of 30 tablets (NDC 71269-040-30) and 100 tablets (NDC 71269-040-10).
Description
WARNING: ADDICTION, ABUSE, AND MISUSE; LIFE-THREATENING RESPIRATORY DEPRESSION; ACCIDENTIAL INGESTION; ULTRA-RAPID METABOLISM OF CODEINE AND OTHER RISK FACTORS FOR LIFE-THREATENING RESPIRATORY DEPRESSION IN CHILDREN; MEDICATION ERRORS; INTERACTIONS WITH DRUGS AFFECTING CYTOCHROME P450 ISOENZYMES; CONCOMITANT USE WITH BENZODIAZEPINES OR OTHER CNS DEPRESSANTS; NEONATAL OPOID WITHDRAWAL SYNDROME See full prescribing information for complete boxed warning. TUXARIN ER exposes users to risks of addiction, abuse, and misuse, which can lead to overdose and death. Assess patient's risk before prescribing and monitor closely for these behaviors and conditions. ( 5.1 ) Serious, life-threatening, or fatal respiratory depression may occur. Monitor closely, especially upon initiation or when used in patients at higher risk. ( 5.2 ) Accidental ingestion of TUXARIN ER, especially by children, can result in a fatal overdose of codeine. ( 5.2 ) Life-threatening respiratory depression and death have occurred in children who received codeine; most cases followed tonsillectomy and/or adenoidectomy, and many of the children had evidence of being an ultra-rapid metabolizer of codeine due to a CYP2D6 polymorphism. ( 5.3 ) TUXARIN ER is contraindicated in children younger than 12 years of age and in children younger than 18 years of age following tonsillectomy and/or adenoidectomy. ( 4 ) Avoid the use of TUXARIN ER in adolescents 12 to 18 years of age who have other risk factors that may increase their sensitivity to the respiratory depressant effects of codeine. Ensure accuracy when prescribing, dispensing, and administering TUXARIN ER. Dosing errors can result in accidental overdose and death. ( 2.1 , 5.6 ) The effects of concomitant use or discontinuation of cytochrome P450 3A4 inducers, 3A4 inhibitors, or 2D6 inhibitors with codeine are complex, requiring careful consideration of the effects on the parent drug, codeine, and the active metabolite, morphine. Avoid the use of TUXARIN ER in these patients. ( 5.4 , 7.1 , 7.2 , 7.4 ) Concomitant use of opioids with benzodiazepines or other central nervous system (CNS) depressants, including alcohol, may result in profound sedation, respiratory depression, coma, and death. Avoid the use of TUXARIN ER in patients taking benzodiazepines, other CNS depressants, or alcohol. ( 5.9 , 7.5 ) TUXARIN ER is not recommended for use in pregnant women. Prolonged use of TUXARIN ER during pregnancy can result in neonatal opioid withdrawal syndrome, which may be life-threatening if not recognized and treated. If TUXARIN ER is used for a prolonged period in a pregnant woman, advise the patient of the risk of neonatal opioid withdrawal syndrome and ensure that appropriate treatment will be available. ( 5.15 , 8.1 )
Section 42229-5
Addiction, Abuse, and Misuse
TUXARIN ER exposes patients and other users to the risks of opioid addiction, abuse, and misuse, which can lead to overdose and death. Reserve TUXARIN ER for use in adult patients for whom the benefits of cough suppression are expected to outweigh the risks, and in whom an adequate assessment of the etiology of the cough has been made. Assess each patient's risk prior to prescribing TUXARIN ER, prescribe TUXARIN ER for the shortest duration that is consistent with individual patient treatment goals, monitor all patients regularly for the development of addition or abuse, and refill only after reevaluation of the need for continued treatment. [see Warnings and Precautions (5.1) ]
Section 42231-1
| Medication Guide TUXARIN® ER (Tuks-a-ren) (codeine phosphate and chlorpheniramine maleate) extended-release tablets, C-III |
|||
|---|---|---|---|
| This Medication Guide has been approved by the U.S. Food and Drug Administration | Revised: June 2018 | ||
|
What is the most important information I should know about TUXARIN ER? TUXARIN ER is not for children under 18 years of age.TUXARIN ER can cause serious side effects, including:
|
|||
|
|
||
| Keep TUXARIN ER in a safe place away from children. Accidental use of even 1 dose of TUXARIN ER, especially by a child, is a medical emergency and can cause breathing problems (respiratory depression) which can lead to death. If a child accidentally takes TUXARIN ER, get emergency help right away. | |||
|
|||
What is TUXARIN ER?
|
|||
|
Who should not take TUXARIN ER? TUXARIN ER is not for children under 18 years of age. See "What is the most important information I should know about TUXARIN ER?"Do not take TUXARIN ER if you:
|
|||
| Before taking TUXARIN ER, tell your healthcare provider about all of your medical conditions, including if you: | |||
|
|
||
Taking TUXARIN ER with certain other medicines can cause side effects or affect how well TUXARIN ER or the other medicines work. Do not start or stop taking other medicines without talking to your healthcare provider. Especially tell your healthcare provider if you:
|
|||
|
How should I take TUXARIN ER?
|
|||
|
What should I avoid doing while taking TUXARIN ER?
|
|||
|
What are the possible side effects of TUXARIN ER? TUXARIN ER can cause serious side effects, including:
|
|||
|
|
||
| The most common side effects of TUXARIN ER include: | |||
|
|
||
| These are not all the possible side effects of TUXARIN ER. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. |
|||
How should I store TUXARIN ER?
|
|||
|
How should I dispose of TUXARIN ER?
Remove unused TUXARIN ER from the container and mix it with an undesirable, non-toxic substance such as cat litter or used coffee grounds to make it less appealing to children and pets. Place the mixture in a container such as a sealed plastic bag and throw it away in the household trash. You can also follow your state or local guidelines on how to safely throw away TUXARIN ER. |
|||
|
General information about the safe and effective use of TUXARIN ER.
Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not use TUXARIN ER for a condition for which it was not prescribed. Do not give TUXARIN ER to other people, even if they have the same symptoms that you have. It may harm them. You can ask your pharmacist or healthcare provider for information about TUXARIN ER that is written for health professionals. |
|||
|
What are the ingredients in TUXARIN ER? Active ingredients: codeine phosphate and chlorpheniramine maleate Inactive ingredients: Hypromellose, lactose monohydrate, cellulose microcrystalline, polysorbate 80, magnesium stearate, and colloidal silicon dioxide. Distributed By: MainPointe Pharmaceuticals, LLC Louisville, KY, 40206 For more information go to mainpointepharmaceuticals.com or call 502-709-7544 |
Section 44425-7
Store at 20 to 25°C (68 to 77°F) [see USP Controlled Room Temperature].
Dispense in a tight, light-resistant container, as defined in the USP, with a child-resistant closure.
Keep this and all medicine out of reach of children.
7.3 Phenytoin
Adverse event reports in the literature suggest a possible drug interaction involving increased serum phenytoin levels and phenytoin toxicity when chlorpheniramine and phenytoin are co-administered. The exact mechanism for this interaction is not known, however it is believed that chlorpheniramine may inhibit the hepatic metabolism of phenytoin. Avoid the use of TUXARIN ER while taking phenytoin.
7.9 Diuretics
Opioids can reduce the efficacy of diuretics by inducing the release of antidiuretic hormone. Monitor patients for signs of diminished diuresis and/or effects on blood pressure and increase the dosage of the diuretic as needed.
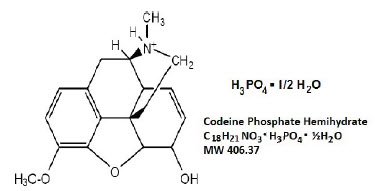
11 Description
TUXARIN ER (codeine phosphate and chlorpheniramine maleate) extended-release tablets, contains codeine, an opioid agonist; and chlorpheniramine, a histamine-1 (H1) receptor antagonist.
Each tablet of TUXARIN ER contains 54.3 mg of codeine phosphate and 8 mg of chlorpheniramine maleate for oral administration.
TUXARIN ER are white to off-white, uncoated, standard round extended-release matrix tablets.
TUXARIN ER also contains the following inactive ingredients: hypromellose, lactose monohydrate, cellulose microcrystalline, polysorbate 80, magnesium stearate, and colloidal silicon dioxide.
9.3 Dependence
Psychological dependence, physical dependence, and tolerance may develop upon repeated administration of opioids; therefore, TUXARIN ER should be prescribed and administered for the shortest duration that is consistent with individual patient treatment goals and patients should be reevaluated prior to refills [see Dosage and Administration (2.3), Warnings and Precautions (5.1) ].
Physical dependence, the condition in which continued administration of the drug is required to prevent the appearance of a withdrawal syndrome, assumes clinically significant proportions only after several weeks of continued oral opioid use, although some mild degree of physical dependence may develop after a few days of opioid therapy.
If TUXARIN ER is abruptly discontinued in a physically-dependent patient, a withdrawal syndrome may occur. Withdrawal also may be precipitated through the administration of drugs with opioid antagonist activity (e.g., naloxone, nalmefene), mixed agonist/antagonist analgesics (e.g., pentazocine, butorphanol, nalbuphine), or partial agonists (e.g., buprenorphine). Some or all of the following can characterize this syndrome: restlessness, lacrimation, rhinorrhea, yawning, perspiration, chills, myalgia, and mydriasis. Other signs and symptoms also may develop, including irritability, anxiety, backache, joint pain, weakness, abdominal cramps, insomnia, nausea, anorexia, vomiting, diarrhea, or increased blood pressure, respiratory rate, or heart rate.
Infants born to mothers physically dependent on opioids will also be physically dependent and may exhibit respiratory difficulties and withdrawal signs [see Use in Specific Populations (8.1) ].
8.4 Pediatric Use
TUXARIN ER is not indicated for use in patients younger than 18 years of age because the benefits of symptomatic treatment of cough associated with allergies or the common cold do not outweigh the risks for use of codeine in these patients [see Indications (1), Warnings and Precautions (5.4) ].
Life-threatening respiratory depression and death have occurred in children who received codeine [see Warnings and Precautions (5.2) ]. In most of the reported cases, these events followed tonsillectomy and/or adenoidectomy, and many of the children had evidence of being ultra-rapid metabolizers of codeine (i.e., multiple copies of the gene for cytochrome P450 isoenzyme 2D6 or high morphine concentrations). Children with sleep apnea may be particularly sensitive to the respiratory depressant effects of codeine.
Because of the risk of life-threatening respiratory depression and death:
- TUXARIN ER is contraindicated in all children younger than 12 years of age [see Contraindications (4)].
- TUXARIN ER is contraindicated for post-operative management in pediatric patients younger than 18 years of age following tonsillectomy and/or adenoidectomy [see Contraindications (4)].
- Avoid the use of TUXARIN ER in adolescents 12 to 18 years of age who have other risk factors that may increase their sensitivity to the respiratory depressant effects of codeine unless the benefits outweigh the risks. Risk factors include conditions associated with hypoventilation, such as postoperative status, obstructive sleep apnea, obesity, severe pulmonary disease, neuromuscular disease, and concomitant use of other medications that cause respiratory depression. [see Warnings and Precautions (5.3)].
8.5 Geriatric Use
Clinical studies have not been conducted with TUXARIN ER in geriatric populations.
Use caution when considering the use of TUXARIN ER in patients 65 years of age or older. Elderly patients may have increased sensitivity to codeine; greater frequency of decreased hepatic, renal, or cardiac function; or concomitant disease or other drug therapy [see Warnings and Precautions (5.5) ].
Respiratory depression is the chief risk for elderly patients treated with opioids, including TUXARIN ER. Respiratory depression has occurred after large initial doses of opioids were administered to patients who were not opioid-tolerant or when opioids were co-administered with other agents that depress respiration [see Warnings and Precautions (5.5, 5.9) ].
Codeine is known to be substantially excreted by the kidney, and the risk of adverse reactions to this drug may be greater in patients with impaired renal function. Because elderly patients are more likely to have decreased renal function, monitor these patients closely for respiratory depression, sedation, and hypotension.
4 Contraindications
TUXARIN ER is contraindicated for:
- All children younger than 12 years of age [see Warnings and Precautions (5.2, 5.3, 5.4), Use in Specific Populations (8.4) ].
- Postoperative management in children younger than 18 years of age following tonsillectomy and/or adenoidectomy [see Warnings and Precautions (5.2, 5.3)].
TUXARIN ER is also contraindicated in patients with:
- Significant respiratory depression [see Warnings and Precautions (5.2)]
- Acute or severe bronchial asthma in an unmonitored setting or in the absence of resuscitative equipment [see Warnings and Precautions (5.5) ].
- Known or suspected gastrointestinal obstruction, including paralytic ileus [see Warnings and Precautions (5.10) ].
- Concurrent use of monoamine oxidase inhibitors (MAOIs) or use of MAOIs within 14 days [see Warnings and Precautions (5.13), Drug Interactions (7.7) ].
- Hypersensitivity to codeine, chlorpheniramine, or any of the inactive ingredients in TUXARIN ER [see Adverse Reactions (6) ]. Persons known to be hypersensitive to certain other opioids may exhibit cross-reactivity to codeine.
6 Adverse Reactions
The following serious adverse reactions are described, or described in greater detail, in other sections:
- Addiction, abuse, and misuse [see Warnings and Precautions (5.1), Drug Abuse and Dependence (9.3) ]
- Life-threatening respiratory depression [see Warnings and Precautions (5.2, 5.3, 5.4, 5.5, 5.9), Overdosage (10) ]
- Ultra-rapid metabolism of codeine and other risk factors for life-threatening respiratory depression in children [see Warnings and Precautions (5.3) ]
- Accidental overdose and death due to medication errors [see Warnings and Precautions (5.6) ]
- Decreased mental alertness with impaired mental and/or physical abilities [see Warnings and Precautions (5.7) ]
- Interactions with benzodiazepines and other CNS depressants [see Warnings and Precautions (5.9) ]
- Paralytic ileus, gastrointestinal adverse reactions [see Warnings and Precautions (5.10) ]
- Increased intracranial pressure [see Warnings and Precautions (5.11) ]
- Obscured clinical course in patients with head injuries [see Warnings and Precautions (5.11) ]
- Seizures [see Warnings and Precautions (5.12) ]
- Interactions with MAOI [see Warnings and Precautions (5.13) ]
- Severe hypotension [see Warnings and Precautions (5.14) ]
- Neonatal Opioid Withdrawal Syndrome [see Warnings and Precautions (5.15) ]
- Adrenal insufficiency [see Warnings and Precautions (5.16) ]
The following adverse reactions have been identified during clinical studies, or during post-approval use of codeine and/or chlorpheniramine. Because these reactions may be reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
The most common adverse reactions to TUXARIN ER include: Sedation (somnolence, mental clouding, lethargy), impaired mental and physical performance, lightheadedness, dizziness, headache, dry mouth, nausea, vomiting, constipation, shortness of breath, and sweating.
Other reactions include:
Anaphylaxis: Anaphylaxis has been reported with codeine, one of the ingredients in TUXARIN ER.
Body as a whole: Coma, death, fatigue, falling injuries, lethargy.
Cardiovascular: Peripheral edema, increased blood pressure, decreased blood pressure, tachycardia, chest pain, palpitation, syncope, orthostatic hypotension, prolonged QT interval, hot flush.
Central Nervous System: Ataxia, facial dyskinesia, insomnia, increased intracranial pressure, migraine, seizure, tremor, tinnitus, vertigo.
Dermatologic: Flushing, hyperhidrosis, pruritus, rash.
Endocrine/Metabolic: Cases of serotonin syndrome, a potentially life-threatening condition, have been reported during concomitant use of opioids with serotonergic drugs. Cases of adrenal insufficiency have been reported with opioid use, more often following greater than one month of use. Cases of androgen deficiency have occurred with chronic use of opioids [see Clinical Pharmacology (12.2) ].
Gastrointestinal: Abdominal pain, bowel obstruction, decreased appetite, diarrhea, difficulty swallowing, GERD, indigestion, pancreatitis, paralytic ileus, biliary tract spasm (spasm of the sphincter of Oddi).
Genitourinary: Urinary tract infection, ureteral spasm, spasm of vesicle sphincters, urinary retention.
Hematologic: Agranulocytosis, aplastic anemia, and thrombocytopenia have been reported.
Laboratory: Increases in serum amylase.
Musculoskeletal: Arthralgia, backache, muscle spasm.
Ophthalmic: Blurred vision, diplopia, miosis (constricted pupils), visual disturbances.
Psychiatric: Agitation, anxiety, confusion, fear, dysphoria, depression, hallucinations.
Reproductive: Hypogonadism, infertility.
Respiratory: Bronchitis, cough, dry nose, dry throat, dyspnea, nasal congestion, nasopharyngitis, respiratory depression, sinusitis, thickening of bronchial secretions, tightness of chest and wheezing, upper respiratory tract infection.
Other: Drug abuse, drug dependence, opioid withdrawal syndrome.
Hypoglycemia: Cases of hypoglycemia have been reported in patients taking opioids. Most reports were in patients with at least one predisposing risk factor (e.g., diabetes).
7 Drug Interactions
No specific drug interaction studies have been conducted with TUXARIN ER.
7.2 Cyp3a4 Inducers
The concomitant use of TUXARIN ER and CYP3A4 inducers, such as rifampin, carbamazepine, or phenytoin, can result in lower codeine levels, greater norcodeine levels, and less metabolism via 2D6 with resultant lower morphine levels [see Clinical Pharmacology (12.3) ], resulting in decreased efficacy or onset of a withdrawal syndrome in patients who have developed physical dependence [see Warnings and Precautions (5.8) ]. After stopping a CYP3A4 inducer, as the effects of the inducer decline, codeine plasma concentrations may increase with subsequently greater metabolism by cytochrome CYP2D6, resulting in greater morphine levels [see Clinical Pharmacology (12.3) ], which could increase or prolong both the therapeutic effects and adverse reactions, and may cause serious respiratory depression.
Avoid the use of TUXARIN ER in patients who are taking CYP3A4 inducers. If concomitant use of a CYP3A4 inducer is necessary, follow the patient for reduced efficacy.
7.8 Muscle Relaxants
Codeine may enhance the neuromuscular blocking action of skeletal muscle relaxants and produce an increased degree of respiratory depression. Avoid the use of TUXARIN ER in patients taking muscle relaxants. If concomitant use is necessary, monitor patients for signs of respiratory depression that may be greater than otherwise expected.
8.6 Renal Impairment
The pharmacokinetics of TUXARIN ER has not been characterized in patients with renal impairment. Codeine pharmacokinetics may be altered in patients with renal failure. Clearance may be decreased and the metabolites may accumulate to much higher plasma levels in patients with renal failure as compared to patients with normal renal function. Chlorpheniramine is cleared substantially by the kidney. As such, impaired renal function could potentially lead to the risk of decreased clearance and thereby increased retention or systemic levels of chlorpheniramine. Therefore, TUXARIN ER should be used with caution in patients with severe impairment of renal function, and patients should be monitored closely for signs of hydrocodone toxicity (respiratory depression, sedation, and hypotension) and chlorpheniramine toxicity.
7.6 Serotonergic Drugs
The concomitant use of opioids with other drugs that affect the serotonergic neurotransmitter system has resulted in serotonin syndrome. If concomitant use is warranted, carefully observe the patient, particularly during treatment initiation. Discontinue TUXARIN ER if serotonin syndrome is suspected.
8.7 Hepatic Impairment
No formal studies have been conducted in patients with hepatic impairment so the pharmacokinetics of TUXARIN ER in this patient population are unknown. Chlorpheniramine is extensively metabolized by liver before elimination from the body. As such, impaired hepatic function could potentially lead to the risk of decreased metabolism and thereby increased systemic levels of chlorpheniramine. Therefore, TUXARIN ER should be used with caution in patients with severe impairment of hepatic function, and patients should be monitored closely for signs of hydrocodone toxicity (respiratory depression, sedation, and hypotension) and chlorpheniramine toxicity.
1 Indications and Usage
TUXARIN ER is indicated for the temporary relief of cough and upper respiratory symptoms associated with allergy or the common cold in patients 18 years of age and older.
5.14 Severe Hypotension
TUXARIN ER may cause severe hypotension including orthostatic hypotension and syncope in ambulatory patients. There is increased risk in patients whose ability to maintain blood pressure has already been compromised by a reduced blood volume or concurrent administration of certain CNS depressant drugs (e.g., phenothiazines or general anesthetics) [see Drug Interactions (7.5) ]. Monitor these patients for signs of hypotension after initiating TUXARIN ER.
In patients with circulatory shock, TUXARIN ER may cause vasodilation that can further reduce cardiac output and blood pressure. Avoid the use of TUXARIN ER in patients with circulatory shock.
7.1 Inhibitors of Cyp3a4
The concomitant use of TUXARIN ER with CYP3A4 inhibitors, such as macrolide antibiotics (e.g., erythromycin), azole-antifungal agents (e.g. ketoconazole), or protease inhibitors (e.g., ritonavir), may result in an increase in codeine plasma concentrations with subsequently greater metabolism by cytochrome CYP2D6, resulting in greater morphine levels, which could increase or prolong adverse reactions and may cause potentially fatal respiratory depression, particularly when an inhibitor is added after a stable dose of TUXARIN ER is achieved [see Warnings and Precautions (5.8) ]. After stopping a CYP3A4 inhibitor, as the effects of the inhibitor decline, it may result in lower codeine levels, greater norcodeine levels, and less metabolism via CYP2D6 with resultant lower morphine levels [see Clinical Pharmacology (12.3) ], resulting in decreased opioid efficacy or a withdrawal syndrome in patients who had developed physical dependence to codeine.
Avoid the use of TUXARIN ER while taking a CYP3A4 inhibitor. If concomitant use is necessary, monitor patients for respiratory depression and sedation at frequent intervals.
7.4 Inhibitors of Cyp2d6
Codeine is metabolized by CYP2D6 to form morphine. The concomitant use of TUXARIN ER and CYP2D6 inhibitors, such as paroxetine, fluoxetine, bupropion, or quinidine, can increase the plasma concentration of codeine, but can decrease the plasma concentration of active metabolite morphine, which could result in reduced efficacy [see Clinical Pharmacology (12.3) ]. After stopping a CYP2D6 inhibitor, as the effects of the inhibitor decline, the codeine plasma concentration will decrease but the active metabolite morphine plasma concentration will increase, which could increase or prolong adverse reactions and may cause potentially fatal respiratory depression [see Clinical Pharmacology (12.3) ].
Avoid the use of TUXARIN ER in patients who are taking inhibitors of CYP2D6.
9.1 Controlled Substance
TUXARIN ER contains codeine, a Schedule III controlled substance.
5 Warnings and Precautions
See Boxed WARNINGS
- Life-threatening respiratory depression in patients with chronic pulmonary disease or in elderly, cachectic, or debilitated patients: Monitor closely, particularly during initiation of therapy. (5.5)
- Activities requiring mental alertness: Avoid engaging in hazardous tasks requiring mental alertness such as driving or operating machinery. (5.7)
- Risks of use in patients with head injury, impaired consciousness, increased intracranial pressure, or brain tumors: Avoid use. May increase intracranial pressure and obscure the clinical course of head injuries. (5.11)
- Seizures in patients with seizure disorders: Monitor during therapy. (5.12)
- Severe hypotension: Monitor during initiation of therapy. Avoid use in patients with circulatory shock. (5.14)
- Adrenal insufficiency: If diagnosed, treat with physiologic replacement of corticosteroids, and wean patient off of the opioid. (5.16)
5.16 Adrenal Insufficiency
Cases of adrenal insufficiency have been reported with opioid use, more often following greater than one month of use. Presentation of adrenal insufficiency may include non-specific symptoms and signs including nausea, vomiting, anorexia, fatigue, weakness, dizziness, and low blood pressure. If adrenal insufficiency is suspected, confirm the diagnosis with diagnostic testing as soon as possible. If adrenal insufficiency is diagnosed, treat with physiologic replacement doses of corticosteroids. Wean the patient off of the opioid to allow adrenal function to recover and continue corticosteroid treatment until adrenal function recovers. Other opioids may be tried as some cases reported use of a different opioid without recurrence of adrenal insufficiency. The information available does not identify any particular opioids as being more likely to be associated with adrenal insufficiency.
7.10 Anticholinergic Drugs
The concomitant use of anticholinergic drugs with TUXARIN ER may increase risk of urinary retention and/or severe constipation, which may lead to paralytic ileus [see Warnings and Precautions (5.10) ]. Monitor patients for signs of urinary retention or reduced gastric motility when TUXARIN ER is used concomitantly with anticholinergic drugs.
Additive adverse effects resulting from cholinergic blockade (e.g., xerostomia, blurred vision, or constipation) may occur when anticholinergic drugs are administered with chlorpheniramine.
2 Dosage and Administration
- Adults 18 years of age and older: 1 tablet every 12 hours as needed, not to exceed 2 tablets in 24 hours. (2.2)
- Do not increase the dose or dosing frequency. (2.1)
- Prescribe for the shortest duration consistent with treatment goals. (2.3)
- Reevaluate patients with unresponsive cough in 5 days or sooner for possible underlying pathology. (2.3)
- Reevaluate patient prior to refilling. (2.3)
3 Dosage Forms and Strengths
Extended-release tablets: Each tablet contains 54.3 mg of codeine phosphate (equivalent to 40 mg of codeine); and 8 mg of chlorpheniramine maleate (equivalent to 5.6 mg of chlorpheniramine). Each tablet is white to off-white, uncoated, round, debossed with MP on one side and CC on the other side [see Description (11) ].
8 Use in Specific Populations
5.1 Addiction, Abuse, and Misuse
TUXARIN ER contains codeine, a Schedule III controlled substance. As an opioid, TUXARIN ER exposes users to the risks of addiction, abuse, and misuse [see Drug Abuse and Dependence (9) ], which can lead to overdose and death [see Overdosage (10) ]. Reserve TUXARIN ER for use in adult patients for whom the benefits of cough suppression are expected to outweigh the risks, and in whom an adequate assessment of the etiology of the cough has been made. Assess each patient's risk prior to prescribing TUXARIN ER, prescribe TUXARIN ER for the shortest duration that is consistent with individual patient treatment goals, monitor all patients regularly for the development of addiction or abuse, and refill only after reevaluation of the need for continued treatment.
Although the risk of addiction in any individual is unknown, it can occur in patients appropriately prescribed TUXARIN ER. Addiction can occur at recommended dosages and if the drug is misused or abused. Risks are increased in patients with a personal or family history of substance abuse (including drug or alcohol abuse or addiction) or mental illness (e.g., major depression).
Opioids are sought by drug abusers and people with addiction disorders and are subject to criminal diversion. Consider these risks when prescribing or dispensing TUXARIN ER. Strategies to reduce these risks include prescribing the drug in the smallest appropriate quantity and advising the patient on the proper disposal of unused drug [see Patient Counseling Information (17) ]. Contact local state professional licensing board or state controlled substances authority for information on how to prevent and detect abuse or diversion of this product.
17 Patient Counseling Information
Advise the patient to read the FDA-approved patient labeling (Medication Guide).
16 How Supplied/storage and Handling
TUXARIN ER (codeine phosphate and chlorpheniramine maleate) 54.3 mg/ 8 mg extended-release tablets, are white to off-white, uncoated, standard round tablets, debossed with MP on one side and CC on the other side. Supplied in bottles of 30 tablets (NDC 71269-040-30) and 100 tablets (NDC 71269-040-10).
5.17 Drug/laboratory Test Interactions
Because opioid agonists may increase biliary tract pressure, with resultant increase in plasma amylase or lipase levels, determination of these enzyme levels may be unreliable for 24 hours after administration of a dose of TUXARIN ER.
5.15 Neonatal Opioid Withdrawal Syndrome
TUXARIN ER is not recommended for use in pregnant women. Prolonged use of TUXARIN ER during pregnancy can result in withdrawal in the neonate. Neonatal opioid withdrawal syndrome, unlike opioid withdrawal syndrome in adults, may be life-threatening if not recognized and treated, and requires management according to protocols developed by neonatology experts. Observe newborns for signs of neonatal opioid withdrawal syndrome and manage accordingly. Advise pregnant women using opioids for a prolonged period of the risk of neonatal opioid withdrawal syndrome and ensure that appropriate treatment will be available. [see Use in Specific Populations (8.1), Patient Counseling Information (17) ]
7.7 Monoamine Oxidase Inhibitors (maois)
TUXARIN ER is contraindicated in patients who are taking MAOIs (i.e., certain drugs used for depression, psychiatric or emotional conditions, or Parkinson's disease) or have taken MAOIs within 14 days [see Contraindications (4) ].
MAOI interactions with opioids may manifest as serotonin syndrome or opioid toxicity (e.g., respiratory depression, coma) [see Warnings and Precautions (5.13) ].
5.2 Life Threatening Respiratory Depression
Serious, life-threatening, or fatal respiratory depression has been reported with the use of opioids, including codeine, one of the active ingredients in TUXARIN ER. Codeine produces dose-related respiratory depression by directly acting on the brain stem respiratory center that controls respiratory rhythm and may produce irregular and periodic breathing. Codeine is subject to variability in metabolism based upon CYP2D6 genotype, which can lead to an increased exposure to the active metabolite morphine [see Warnings and Precautions (5.3) ]. Respiratory depression, if not immediately recognized and treated, may lead to respiratory arrest and death. Management of respiratory depression includes discontinuation of TUXARIN ER, close observation, supportive measures, and use of opioid antagonists (e.g. naloxone), depending on the patient's clinical status [see Overdosage (10) ]. Carbon dioxide (CO2) retention from opioid-induced respiratory depression can exacerbate the sedating effects of opioids.
While serious, life-threatening, or fatal respiratory depression can occur at any time during the use of TUXARIN ER, the risk is greatest during the initiation of therapy, when TUXARIN ER is used concomitantly with other drugs that may cause respiratory depression [see Warnings and Precautions (5.9) ], in patients with chronic pulmonary disease or decreased respiratory reserve, and in patients with altered pharmacokinetics or altered clearance (e.g. elderly, cachectic, or debilitated patients) [see Warnings and Precautions (5.5) ].
To reduce the risk of respiratory depression, proper dosing of TUXARIN ER is essential [see Dosage and Administration (2.1), Warnings and Precautions (5.6)]. Monitor patients closely, especially within the first 24- 72 hours of initiating therapy or when used in patients at higher risk.
Overdose of codeine in adults has been associated with fatal respiratory depression, and the use of codeine in children younger than 12 years of age has been associated with fatal respiratory depression when used as recommended [see Warnings and Precautions (5.3) ]. Accidental ingestion of even one dose of TUXARIN ER, especially by children, can result in respiratory depression and death.
5.4 Risks With Use in Pediatric Populations
Children are particularly sensitive to the respiratory depressant effects of codeine [see Warnings and Precautions (5.2, 5.3) ]. Because of the risk of life-threatening respiratory depression and death, TUXARIN ER is contraindicated in children less than 12 years of age, and in pediatric patients younger than 18 years of age following tonsillectomy and/or adenoidectomy [see Contraindications (4) ].
Use of TUXARIN ER in children also exposes them to the risks of addiction, abuse, and misuse [see Drug Abuse and Dependence (9) ], which can lead to overdose and death [see Warnings and Precautions (5.1), Overdosage (10) ]. Because the benefits of symptomatic treatment of cough associated with allergies or the common cold do not outweigh the risks of use of codeine in pediatric patients, TUXARIN ER is not indicated for use in patients younger than 18 years of age [see Indications (1), Use in Specific Populations (8.4) ].
7.5 Benzodiazepines and Other Cns Depressants
Due to additive pharmacologic effect, the concomitant use of benzodiazepines or other CNS depressants, including alcohol, other sedatives/hypnotics, anxiolytics, tranquilizers, muscle relaxants, general anesthetics, antipsychotics, and other opioids, can increase the risk of hypotension, respiratory depression, profound sedation, coma, and death. Avoid the use of TUXARIN ER in patients who are taking benzodiazepines or other CNS depressants. [see Warnings and Precautions (5.9) ].
Principal Display Panel 100 Tablet Bottle Label
NDC 71269-040-10
CIII
Tuxarin ER™
(codeine phosphate and
chlorpheniramine maleate
extended-release tablets)
54.3 mg/ 8 mg
Each Tablet Contains:
Codeine Phosphate, USP 54.3 mg
(Equivalent to 40 mg of Codeine)
Chlorpheniramine Maleate, USP 8 mg
(Equivalent to 5.6 mg of Chlorpheniramine)
PHARMACIST: PLEASE DISPENSE WITH
MEDICATION GUIDE
Rx only
100 Tablets
2.1 Important Dosage and Administration Instructions
Administer TUXARIN ER by the oral route only.
Advise patients not to increase the dose or dosing frequency of TUXARIN ER because serious adverse events such as respiratory depression may occur with overdosage [see Warnings and Precautions (5.2), Overdosage (10) ]. The dosage of TUXARIN ER should not be increased if cough fails to respond; an unresponsive cough should be reevaluated for possible underlying pathology [see Dosage and Administration (2.3), Warnings and Precautions (5.5) ].
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenicity, mutagenicity, and fertility studies have not been conducted with TUXARIN ER; however, published information is available for the active ingredients.
2.3 Monitoring, Maintenance, and Discontinuation of Therapy
Prescribe TUXARIN ER for the shortest duration that is consistent with individual patient treatment goals [see Warnings and Precautions (5.1) ]
Monitor patients closely for respiratory depression, especially within the first 24-72 hours of initiating therapy [see Warnings and Precautions (5.2) ].
Reevaluate patients with unresponsive cough in 5 days or sooner for possible underlying pathology, such as foreign body or lower respiratory tract disease [see Warnings and Precautions (5.5) ]. If a patient requires a refill, reevaluate the cause of the cough and assess the need for continued treatment with TUXARIN ER, the relative incidence of adverse reactions, and the development of addiction, abuse, or misuse [see Warnings and Precautions (5.1) ].
Do not abruptly discontinue TUXARIN ER in a physically-dependent patient [see Drug Abuse and Dependence (9.3) ]. When a patient who has been taking TUXARIN ER regularly and may be physically dependent no longer requires therapy with TUXARIN ER, taper the dose gradually, by 25% to 50% every 2 to 4 days, while monitoring carefully for signs and symptoms of withdrawal. If the patient develops these signs or symptoms, raise the dose to the previous level and taper more slowly, either by increasing the interval between decreases, decreasing the amount of change in dose, or both.
5.10 Risks of Use in Patients With Gastrointestinal Conditions
TUXARIN ER is contraindicated in patients with known or suspected gastrointestinal obstruction, including paralytic ileus [see Contraindications (4) ]. The use of codeine in TUXARIN ER may obscure the diagnosis or clinical course of patients with acute abdominal conditions.
The concurrent use of anticholinergics with TUXARIN ER may produce paralytic ileus [see Drug Interactions (7.10) ].
The codeine in TUXARIN ER may result in constipation or obstructive bowel disease, especially in patients with underlying intestinal motility disorders. Use with caution in patients with underlying intestinal motility disorders.
The codeine in TUXARIN ER may cause spasm of the sphincter of Oddi, resulting in an increase in biliary tract pressure. Opioids may cause increases in serum amylase [see Warnings and Precautions (5.17) ]. Monitor patients with biliary tract disease, including acute pancreatitis for worsening symptoms.
5.13 Co Administration With Monoamine Oxidase Inhibitors (maois)
Concurrent use of TUXARIN ER is contraindicated in patients receiving monoamine oxidase inhibitors (MAOIs) or within 14 days of stopping such therapy [see Contraindications (4) ]. MAOIs may potentiate the effects of morphine, codeine's active metabolite, including respiratory depression, coma, and confusion MAOIs [see Drug Interactions (7.7) ].
5.12 Increased Risk of Seizures in Patients With Seizure Disorders
The codeine and chlorpheniramine in TUXARIN ER may increase the frequency of seizures in patients with seizure disorders, and may increase the risk of seizures occurring in other clinical settings associated with seizures. Monitor patients with a history of seizure disorders for worsened seizure control during TUXARIN ER therapy.
5.6 Risk of Accidental Overdose and Death Due to Medication Errors
Dosing errors can result in accidental overdose and death. To reduce the risk of overdose and respiratory depression, ensure that the dose of TUXARIN ER is communicated clearly and dispensed accurately [see Dosage and Administration (2.1) ].
5.8 Risks of Interactions With Drugs Affecting Cytochrome P450 Isoenzymes
The effects of concomitant use or discontinuation of cytochrome P450 3A4 inducers, 3A4 inhibitors, or 2D6 inhibitors with codeine are complex. Use of cytochrome P450 3A4 inducers, 3A4 inhibitors, or 2D6 inhibitors with TUXARIN ER requires careful consideration of the effects on the parent drug, codeine, and the active metabolite, morphine.
5.9 Risks From Concomitant Use With Benzodiazepines Or Other Cns Depressants
Concomitant use of opioids, including TUXARIN ER, with benzodiazepines, or other CNS depressants, including alcohol, may result in profound sedation, respiratory depression, coma, and death. Because of these risks, avoid use of opioid cough medications in patients taking benzodiazepines, other CNS depressants, or alcohol [see Drug Interactions (7.5) ].
Observational studies have demonstrated that concomitant use of opioid analgesics and benzodiazepines increases the risk of drug-related mortality compared to use of opioids alone. Because of similar pharmacologic properties, it is reasonable to expect similar risk with concomitant use of opioid cough medications and benzodiazepines, other CNS depressants, or alcohol.
Advise both patients and caregivers about the risks of respiratory depression and sedation if TUXARIN ER is used with benzodiazepines, alcohol, or other CNS depressants [see Patient Counseling Information (17) ].
5.7 Activities Requiring Mental Alertness: Risks of Driving and Operating Machinery
Codeine and chlorpheniramine, the active ingredients in TUXARIN ER, may produce marked drowsiness and impair the mental and/or physical abilities required for the performance of potentially hazardous tasks such as driving a car or operating machinery. Advise patients to avoid engaging in hazardous tasks requiring mental alertness and motor coordination after ingestion of TUXARIN ER. Avoid concurrent use of TUXARIN ER with alcohol or other central nervous system depressants because additional impairment of central nervous system performance may occur [See Warnings and Precautions (5.9) ].
5.3 Ultra Rapid Metabolism of Codeine and Other Risk Factors for Life Threatening Respiratory Depression in Children
Life-threatening respiratory depression and death have occurred in children who received codeine. Codeine is subject to variability in metabolism based upon CYP2D6 genotype (described below), which can lead to an increased exposure to the active metabolite morphine. Based upon post-marketing reports, children younger than 12 years old appear to be more susceptible to the respiratory depressant effects of codeine, particularly if there are risk factors for respiratory depression. For example, many reported cases of death occurred in the post-operative period following tonsillectomy and/or adenoidectomy, and many of the children had evidence of being ultra-rapid metabolizers of codeine. Furthermore, children with obstructive sleep apnea who are treated with codeine for post-tonsillectomy and/or adenoidectomy pain may be particularly sensitive to its respiratory depressant effect. Because of the risk of life-threatening respiratory depression and death:
- TUXARIN ER is contraindicated in all children younger than 12 years of age [see Contraindications (4) ].
- TUXARIN ER is contraindicated for post-operative management in pediatric patients younger than 18 years of age following tonsillectomy and/or adenoidectomy [see Contraindications (4) ].
- Avoid the use of TUXARIN ER in adolescents 12 to 18 years of age who have other risk factors that may increase their sensitivity to the respiratory depressant effects of codeine. Risk factors include conditions associated with hypoventilation, such as postoperative status, obstructive sleep apnea, obesity, severe pulmonary disease, neuromuscular disease, and concomitant use of other medications that cause respiratory depression. [see Warnings and Precautions (5.9), Use in Specific Populations (8.4) ]
- Healthcare providers should choose the lowest effective dose for the shortest period of time and inform patients and caregivers about these risks and the signs of morphine overdose [see Warnings and Precautions (5.1), Overdosage (10) ].
5.11 Risks of Use in Patients With Head Injury, Impaired Consciousness, Increased Intracranial Pressure, Or Brain Tumors
Avoid the use of TUXARIN ER in patients with head injury, intracranial lesions, or a pre-existing increase in intracranial pressure. In patients who may be susceptible to the intracranial effects of CO2 retention (e.g., those with evidence of increased intracranial pressure or brain tumors), TUXARIN ER may reduce respiratory drive, and the resultant CO2 retention can further increase intracranial pressure. Furthermore, opioids produce adverse reactions that may obscure the clinical course of patients with head injuries.
Warning: Addiction, Abuse, and Misuse; Life Threatening Respiratory Depression; Accidential Ingestion; Ultra Rapid Metabolism of Codeine and Other Risk Factors for Life Threatening Respiratory Depression in Children; Medication Errors; Interactions With Drugs Affecting Cytochrome P450 Isoenzymes; Concomitant Use With Benzodiazepines Or Other Cns Depressants; Neonatal Opoid Withdrawal Syndrome
WARNING: ADDICTION, ABUSE, AND MISUSE; LIFE-THREATENING RESPIRATORY DEPRESSION; ACCIDENTIAL INGESTION; ULTRA-RAPID METABOLISM OF CODEINE AND OTHER RISK FACTORS FOR LIFE-THREATENING RESPIRATORY DEPRESSION IN CHILDREN; MEDICATION ERRORS; INTERACTIONS WITH DRUGS AFFECTING CYTOCHROME P450 ISOENZYMES; CONCOMITANT USE WITH BENZODIAZEPINES OR OTHER CNS DEPRESSANTS; NEONATAL OPOID WITHDRAWAL SYNDROME
See full prescribing information for complete boxed warning.
- TUXARIN ER exposes users to risks of addiction, abuse, and misuse, which can lead to overdose and death. Assess patient's risk before prescribing and monitor closely for these behaviors and conditions. (5.1)
- Serious, life-threatening, or fatal respiratory depression may occur. Monitor closely, especially upon initiation or when used in patients at higher risk. (5.2)
- Accidental ingestion of TUXARIN ER, especially by children, can result in a fatal overdose of codeine. (5.2)
- Life-threatening respiratory depression and death have occurred in children who received codeine; most cases followed tonsillectomy and/or adenoidectomy, and many of the children had evidence of being an ultra-rapid metabolizer of codeine due to a CYP2D6 polymorphism. (5.3) TUXARIN ER is contraindicated in children younger than 12 years of age and in children younger than 18 years of age following tonsillectomy and/or adenoidectomy. (4) Avoid the use of TUXARIN ER in adolescents 12 to 18 years of age who have other risk factors that may increase their sensitivity to the respiratory depressant effects of codeine.
- Ensure accuracy when prescribing, dispensing, and administering TUXARIN ER. Dosing errors can result in accidental overdose and death. (2.1, 5.6)
- The effects of concomitant use or discontinuation of cytochrome P450 3A4 inducers, 3A4 inhibitors, or 2D6 inhibitors with codeine are complex, requiring careful consideration of the effects on the parent drug, codeine, and the active metabolite, morphine. Avoid the use of TUXARIN ER in these patients. (5.4, 7.1, 7.2, 7.4)
- Concomitant use of opioids with benzodiazepines or other central nervous system (CNS) depressants, including alcohol, may result in profound sedation, respiratory depression, coma, and death. Avoid the use of TUXARIN ER in patients taking benzodiazepines, other CNS depressants, or alcohol. (5.9, 7.5)
- TUXARIN ER is not recommended for use in pregnant women. Prolonged use of TUXARIN ER during pregnancy can result in neonatal opioid withdrawal syndrome, which may be life-threatening if not recognized and treated. If TUXARIN ER is used for a prolonged period in a pregnant woman, advise the patient of the risk of neonatal opioid withdrawal syndrome and ensure that appropriate treatment will be available. (5.15, 8.1)
Structured Label Content
Section 42229-5 (42229-5)
Addiction, Abuse, and Misuse
TUXARIN ER exposes patients and other users to the risks of opioid addiction, abuse, and misuse, which can lead to overdose and death. Reserve TUXARIN ER for use in adult patients for whom the benefits of cough suppression are expected to outweigh the risks, and in whom an adequate assessment of the etiology of the cough has been made. Assess each patient's risk prior to prescribing TUXARIN ER, prescribe TUXARIN ER for the shortest duration that is consistent with individual patient treatment goals, monitor all patients regularly for the development of addition or abuse, and refill only after reevaluation of the need for continued treatment. [see Warnings and Precautions (5.1) ]
Section 42231-1 (42231-1)
| Medication Guide TUXARIN® ER (Tuks-a-ren) (codeine phosphate and chlorpheniramine maleate) extended-release tablets, C-III |
|||
|---|---|---|---|
| This Medication Guide has been approved by the U.S. Food and Drug Administration | Revised: June 2018 | ||
|
What is the most important information I should know about TUXARIN ER? TUXARIN ER is not for children under 18 years of age.TUXARIN ER can cause serious side effects, including:
|
|||
|
|
||
| Keep TUXARIN ER in a safe place away from children. Accidental use of even 1 dose of TUXARIN ER, especially by a child, is a medical emergency and can cause breathing problems (respiratory depression) which can lead to death. If a child accidentally takes TUXARIN ER, get emergency help right away. | |||
|
|||
What is TUXARIN ER?
|
|||
|
Who should not take TUXARIN ER? TUXARIN ER is not for children under 18 years of age. See "What is the most important information I should know about TUXARIN ER?"Do not take TUXARIN ER if you:
|
|||
| Before taking TUXARIN ER, tell your healthcare provider about all of your medical conditions, including if you: | |||
|
|
||
Taking TUXARIN ER with certain other medicines can cause side effects or affect how well TUXARIN ER or the other medicines work. Do not start or stop taking other medicines without talking to your healthcare provider. Especially tell your healthcare provider if you:
|
|||
|
How should I take TUXARIN ER?
|
|||
|
What should I avoid doing while taking TUXARIN ER?
|
|||
|
What are the possible side effects of TUXARIN ER? TUXARIN ER can cause serious side effects, including:
|
|||
|
|
||
| The most common side effects of TUXARIN ER include: | |||
|
|
||
| These are not all the possible side effects of TUXARIN ER. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. |
|||
How should I store TUXARIN ER?
|
|||
|
How should I dispose of TUXARIN ER?
Remove unused TUXARIN ER from the container and mix it with an undesirable, non-toxic substance such as cat litter or used coffee grounds to make it less appealing to children and pets. Place the mixture in a container such as a sealed plastic bag and throw it away in the household trash. You can also follow your state or local guidelines on how to safely throw away TUXARIN ER. |
|||
|
General information about the safe and effective use of TUXARIN ER.
Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not use TUXARIN ER for a condition for which it was not prescribed. Do not give TUXARIN ER to other people, even if they have the same symptoms that you have. It may harm them. You can ask your pharmacist or healthcare provider for information about TUXARIN ER that is written for health professionals. |
|||
|
What are the ingredients in TUXARIN ER? Active ingredients: codeine phosphate and chlorpheniramine maleate Inactive ingredients: Hypromellose, lactose monohydrate, cellulose microcrystalline, polysorbate 80, magnesium stearate, and colloidal silicon dioxide. Distributed By: MainPointe Pharmaceuticals, LLC Louisville, KY, 40206 For more information go to mainpointepharmaceuticals.com or call 502-709-7544 |
Section 44425-7 (44425-7)
Store at 20 to 25°C (68 to 77°F) [see USP Controlled Room Temperature].
Dispense in a tight, light-resistant container, as defined in the USP, with a child-resistant closure.
Keep this and all medicine out of reach of children.
7.3 Phenytoin
Adverse event reports in the literature suggest a possible drug interaction involving increased serum phenytoin levels and phenytoin toxicity when chlorpheniramine and phenytoin are co-administered. The exact mechanism for this interaction is not known, however it is believed that chlorpheniramine may inhibit the hepatic metabolism of phenytoin. Avoid the use of TUXARIN ER while taking phenytoin.
7.9 Diuretics
Opioids can reduce the efficacy of diuretics by inducing the release of antidiuretic hormone. Monitor patients for signs of diminished diuresis and/or effects on blood pressure and increase the dosage of the diuretic as needed.
11 Description (11 DESCRIPTION)
TUXARIN ER (codeine phosphate and chlorpheniramine maleate) extended-release tablets, contains codeine, an opioid agonist; and chlorpheniramine, a histamine-1 (H1) receptor antagonist.
Each tablet of TUXARIN ER contains 54.3 mg of codeine phosphate and 8 mg of chlorpheniramine maleate for oral administration.
TUXARIN ER are white to off-white, uncoated, standard round extended-release matrix tablets.
TUXARIN ER also contains the following inactive ingredients: hypromellose, lactose monohydrate, cellulose microcrystalline, polysorbate 80, magnesium stearate, and colloidal silicon dioxide.
9.3 Dependence
Psychological dependence, physical dependence, and tolerance may develop upon repeated administration of opioids; therefore, TUXARIN ER should be prescribed and administered for the shortest duration that is consistent with individual patient treatment goals and patients should be reevaluated prior to refills [see Dosage and Administration (2.3), Warnings and Precautions (5.1) ].
Physical dependence, the condition in which continued administration of the drug is required to prevent the appearance of a withdrawal syndrome, assumes clinically significant proportions only after several weeks of continued oral opioid use, although some mild degree of physical dependence may develop after a few days of opioid therapy.
If TUXARIN ER is abruptly discontinued in a physically-dependent patient, a withdrawal syndrome may occur. Withdrawal also may be precipitated through the administration of drugs with opioid antagonist activity (e.g., naloxone, nalmefene), mixed agonist/antagonist analgesics (e.g., pentazocine, butorphanol, nalbuphine), or partial agonists (e.g., buprenorphine). Some or all of the following can characterize this syndrome: restlessness, lacrimation, rhinorrhea, yawning, perspiration, chills, myalgia, and mydriasis. Other signs and symptoms also may develop, including irritability, anxiety, backache, joint pain, weakness, abdominal cramps, insomnia, nausea, anorexia, vomiting, diarrhea, or increased blood pressure, respiratory rate, or heart rate.
Infants born to mothers physically dependent on opioids will also be physically dependent and may exhibit respiratory difficulties and withdrawal signs [see Use in Specific Populations (8.1) ].
8.4 Pediatric Use
TUXARIN ER is not indicated for use in patients younger than 18 years of age because the benefits of symptomatic treatment of cough associated with allergies or the common cold do not outweigh the risks for use of codeine in these patients [see Indications (1), Warnings and Precautions (5.4) ].
Life-threatening respiratory depression and death have occurred in children who received codeine [see Warnings and Precautions (5.2) ]. In most of the reported cases, these events followed tonsillectomy and/or adenoidectomy, and many of the children had evidence of being ultra-rapid metabolizers of codeine (i.e., multiple copies of the gene for cytochrome P450 isoenzyme 2D6 or high morphine concentrations). Children with sleep apnea may be particularly sensitive to the respiratory depressant effects of codeine.
Because of the risk of life-threatening respiratory depression and death:
- TUXARIN ER is contraindicated in all children younger than 12 years of age [see Contraindications (4)].
- TUXARIN ER is contraindicated for post-operative management in pediatric patients younger than 18 years of age following tonsillectomy and/or adenoidectomy [see Contraindications (4)].
- Avoid the use of TUXARIN ER in adolescents 12 to 18 years of age who have other risk factors that may increase their sensitivity to the respiratory depressant effects of codeine unless the benefits outweigh the risks. Risk factors include conditions associated with hypoventilation, such as postoperative status, obstructive sleep apnea, obesity, severe pulmonary disease, neuromuscular disease, and concomitant use of other medications that cause respiratory depression. [see Warnings and Precautions (5.3)].
8.5 Geriatric Use
Clinical studies have not been conducted with TUXARIN ER in geriatric populations.
Use caution when considering the use of TUXARIN ER in patients 65 years of age or older. Elderly patients may have increased sensitivity to codeine; greater frequency of decreased hepatic, renal, or cardiac function; or concomitant disease or other drug therapy [see Warnings and Precautions (5.5) ].
Respiratory depression is the chief risk for elderly patients treated with opioids, including TUXARIN ER. Respiratory depression has occurred after large initial doses of opioids were administered to patients who were not opioid-tolerant or when opioids were co-administered with other agents that depress respiration [see Warnings and Precautions (5.5, 5.9) ].
Codeine is known to be substantially excreted by the kidney, and the risk of adverse reactions to this drug may be greater in patients with impaired renal function. Because elderly patients are more likely to have decreased renal function, monitor these patients closely for respiratory depression, sedation, and hypotension.
4 Contraindications (4 CONTRAINDICATIONS)
TUXARIN ER is contraindicated for:
- All children younger than 12 years of age [see Warnings and Precautions (5.2, 5.3, 5.4), Use in Specific Populations (8.4) ].
- Postoperative management in children younger than 18 years of age following tonsillectomy and/or adenoidectomy [see Warnings and Precautions (5.2, 5.3)].
TUXARIN ER is also contraindicated in patients with:
- Significant respiratory depression [see Warnings and Precautions (5.2)]
- Acute or severe bronchial asthma in an unmonitored setting or in the absence of resuscitative equipment [see Warnings and Precautions (5.5) ].
- Known or suspected gastrointestinal obstruction, including paralytic ileus [see Warnings and Precautions (5.10) ].
- Concurrent use of monoamine oxidase inhibitors (MAOIs) or use of MAOIs within 14 days [see Warnings and Precautions (5.13), Drug Interactions (7.7) ].
- Hypersensitivity to codeine, chlorpheniramine, or any of the inactive ingredients in TUXARIN ER [see Adverse Reactions (6) ]. Persons known to be hypersensitive to certain other opioids may exhibit cross-reactivity to codeine.
6 Adverse Reactions (6 ADVERSE REACTIONS)
The following serious adverse reactions are described, or described in greater detail, in other sections:
- Addiction, abuse, and misuse [see Warnings and Precautions (5.1), Drug Abuse and Dependence (9.3) ]
- Life-threatening respiratory depression [see Warnings and Precautions (5.2, 5.3, 5.4, 5.5, 5.9), Overdosage (10) ]
- Ultra-rapid metabolism of codeine and other risk factors for life-threatening respiratory depression in children [see Warnings and Precautions (5.3) ]
- Accidental overdose and death due to medication errors [see Warnings and Precautions (5.6) ]
- Decreased mental alertness with impaired mental and/or physical abilities [see Warnings and Precautions (5.7) ]
- Interactions with benzodiazepines and other CNS depressants [see Warnings and Precautions (5.9) ]
- Paralytic ileus, gastrointestinal adverse reactions [see Warnings and Precautions (5.10) ]
- Increased intracranial pressure [see Warnings and Precautions (5.11) ]
- Obscured clinical course in patients with head injuries [see Warnings and Precautions (5.11) ]
- Seizures [see Warnings and Precautions (5.12) ]
- Interactions with MAOI [see Warnings and Precautions (5.13) ]
- Severe hypotension [see Warnings and Precautions (5.14) ]
- Neonatal Opioid Withdrawal Syndrome [see Warnings and Precautions (5.15) ]
- Adrenal insufficiency [see Warnings and Precautions (5.16) ]
The following adverse reactions have been identified during clinical studies, or during post-approval use of codeine and/or chlorpheniramine. Because these reactions may be reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
The most common adverse reactions to TUXARIN ER include: Sedation (somnolence, mental clouding, lethargy), impaired mental and physical performance, lightheadedness, dizziness, headache, dry mouth, nausea, vomiting, constipation, shortness of breath, and sweating.
Other reactions include:
Anaphylaxis: Anaphylaxis has been reported with codeine, one of the ingredients in TUXARIN ER.
Body as a whole: Coma, death, fatigue, falling injuries, lethargy.
Cardiovascular: Peripheral edema, increased blood pressure, decreased blood pressure, tachycardia, chest pain, palpitation, syncope, orthostatic hypotension, prolonged QT interval, hot flush.
Central Nervous System: Ataxia, facial dyskinesia, insomnia, increased intracranial pressure, migraine, seizure, tremor, tinnitus, vertigo.
Dermatologic: Flushing, hyperhidrosis, pruritus, rash.
Endocrine/Metabolic: Cases of serotonin syndrome, a potentially life-threatening condition, have been reported during concomitant use of opioids with serotonergic drugs. Cases of adrenal insufficiency have been reported with opioid use, more often following greater than one month of use. Cases of androgen deficiency have occurred with chronic use of opioids [see Clinical Pharmacology (12.2) ].
Gastrointestinal: Abdominal pain, bowel obstruction, decreased appetite, diarrhea, difficulty swallowing, GERD, indigestion, pancreatitis, paralytic ileus, biliary tract spasm (spasm of the sphincter of Oddi).
Genitourinary: Urinary tract infection, ureteral spasm, spasm of vesicle sphincters, urinary retention.
Hematologic: Agranulocytosis, aplastic anemia, and thrombocytopenia have been reported.
Laboratory: Increases in serum amylase.
Musculoskeletal: Arthralgia, backache, muscle spasm.
Ophthalmic: Blurred vision, diplopia, miosis (constricted pupils), visual disturbances.
Psychiatric: Agitation, anxiety, confusion, fear, dysphoria, depression, hallucinations.
Reproductive: Hypogonadism, infertility.
Respiratory: Bronchitis, cough, dry nose, dry throat, dyspnea, nasal congestion, nasopharyngitis, respiratory depression, sinusitis, thickening of bronchial secretions, tightness of chest and wheezing, upper respiratory tract infection.
Other: Drug abuse, drug dependence, opioid withdrawal syndrome.
Hypoglycemia: Cases of hypoglycemia have been reported in patients taking opioids. Most reports were in patients with at least one predisposing risk factor (e.g., diabetes).
7 Drug Interactions (7 DRUG INTERACTIONS)
No specific drug interaction studies have been conducted with TUXARIN ER.
7.2 Cyp3a4 Inducers (7.2 CYP3A4 Inducers)
The concomitant use of TUXARIN ER and CYP3A4 inducers, such as rifampin, carbamazepine, or phenytoin, can result in lower codeine levels, greater norcodeine levels, and less metabolism via 2D6 with resultant lower morphine levels [see Clinical Pharmacology (12.3) ], resulting in decreased efficacy or onset of a withdrawal syndrome in patients who have developed physical dependence [see Warnings and Precautions (5.8) ]. After stopping a CYP3A4 inducer, as the effects of the inducer decline, codeine plasma concentrations may increase with subsequently greater metabolism by cytochrome CYP2D6, resulting in greater morphine levels [see Clinical Pharmacology (12.3) ], which could increase or prolong both the therapeutic effects and adverse reactions, and may cause serious respiratory depression.
Avoid the use of TUXARIN ER in patients who are taking CYP3A4 inducers. If concomitant use of a CYP3A4 inducer is necessary, follow the patient for reduced efficacy.
7.8 Muscle Relaxants
Codeine may enhance the neuromuscular blocking action of skeletal muscle relaxants and produce an increased degree of respiratory depression. Avoid the use of TUXARIN ER in patients taking muscle relaxants. If concomitant use is necessary, monitor patients for signs of respiratory depression that may be greater than otherwise expected.
8.6 Renal Impairment
The pharmacokinetics of TUXARIN ER has not been characterized in patients with renal impairment. Codeine pharmacokinetics may be altered in patients with renal failure. Clearance may be decreased and the metabolites may accumulate to much higher plasma levels in patients with renal failure as compared to patients with normal renal function. Chlorpheniramine is cleared substantially by the kidney. As such, impaired renal function could potentially lead to the risk of decreased clearance and thereby increased retention or systemic levels of chlorpheniramine. Therefore, TUXARIN ER should be used with caution in patients with severe impairment of renal function, and patients should be monitored closely for signs of hydrocodone toxicity (respiratory depression, sedation, and hypotension) and chlorpheniramine toxicity.
7.6 Serotonergic Drugs
The concomitant use of opioids with other drugs that affect the serotonergic neurotransmitter system has resulted in serotonin syndrome. If concomitant use is warranted, carefully observe the patient, particularly during treatment initiation. Discontinue TUXARIN ER if serotonin syndrome is suspected.
8.7 Hepatic Impairment
No formal studies have been conducted in patients with hepatic impairment so the pharmacokinetics of TUXARIN ER in this patient population are unknown. Chlorpheniramine is extensively metabolized by liver before elimination from the body. As such, impaired hepatic function could potentially lead to the risk of decreased metabolism and thereby increased systemic levels of chlorpheniramine. Therefore, TUXARIN ER should be used with caution in patients with severe impairment of hepatic function, and patients should be monitored closely for signs of hydrocodone toxicity (respiratory depression, sedation, and hypotension) and chlorpheniramine toxicity.
1 Indications and Usage (1 INDICATIONS AND USAGE)
TUXARIN ER is indicated for the temporary relief of cough and upper respiratory symptoms associated with allergy or the common cold in patients 18 years of age and older.
5.14 Severe Hypotension
TUXARIN ER may cause severe hypotension including orthostatic hypotension and syncope in ambulatory patients. There is increased risk in patients whose ability to maintain blood pressure has already been compromised by a reduced blood volume or concurrent administration of certain CNS depressant drugs (e.g., phenothiazines or general anesthetics) [see Drug Interactions (7.5) ]. Monitor these patients for signs of hypotension after initiating TUXARIN ER.
In patients with circulatory shock, TUXARIN ER may cause vasodilation that can further reduce cardiac output and blood pressure. Avoid the use of TUXARIN ER in patients with circulatory shock.
7.1 Inhibitors of Cyp3a4 (7.1 Inhibitors of CYP3A4)
The concomitant use of TUXARIN ER with CYP3A4 inhibitors, such as macrolide antibiotics (e.g., erythromycin), azole-antifungal agents (e.g. ketoconazole), or protease inhibitors (e.g., ritonavir), may result in an increase in codeine plasma concentrations with subsequently greater metabolism by cytochrome CYP2D6, resulting in greater morphine levels, which could increase or prolong adverse reactions and may cause potentially fatal respiratory depression, particularly when an inhibitor is added after a stable dose of TUXARIN ER is achieved [see Warnings and Precautions (5.8) ]. After stopping a CYP3A4 inhibitor, as the effects of the inhibitor decline, it may result in lower codeine levels, greater norcodeine levels, and less metabolism via CYP2D6 with resultant lower morphine levels [see Clinical Pharmacology (12.3) ], resulting in decreased opioid efficacy or a withdrawal syndrome in patients who had developed physical dependence to codeine.
Avoid the use of TUXARIN ER while taking a CYP3A4 inhibitor. If concomitant use is necessary, monitor patients for respiratory depression and sedation at frequent intervals.
7.4 Inhibitors of Cyp2d6 (7.4 Inhibitors of CYP2D6)
Codeine is metabolized by CYP2D6 to form morphine. The concomitant use of TUXARIN ER and CYP2D6 inhibitors, such as paroxetine, fluoxetine, bupropion, or quinidine, can increase the plasma concentration of codeine, but can decrease the plasma concentration of active metabolite morphine, which could result in reduced efficacy [see Clinical Pharmacology (12.3) ]. After stopping a CYP2D6 inhibitor, as the effects of the inhibitor decline, the codeine plasma concentration will decrease but the active metabolite morphine plasma concentration will increase, which could increase or prolong adverse reactions and may cause potentially fatal respiratory depression [see Clinical Pharmacology (12.3) ].
Avoid the use of TUXARIN ER in patients who are taking inhibitors of CYP2D6.
9.1 Controlled Substance
TUXARIN ER contains codeine, a Schedule III controlled substance.
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
See Boxed WARNINGS
- Life-threatening respiratory depression in patients with chronic pulmonary disease or in elderly, cachectic, or debilitated patients: Monitor closely, particularly during initiation of therapy. (5.5)
- Activities requiring mental alertness: Avoid engaging in hazardous tasks requiring mental alertness such as driving or operating machinery. (5.7)
- Risks of use in patients with head injury, impaired consciousness, increased intracranial pressure, or brain tumors: Avoid use. May increase intracranial pressure and obscure the clinical course of head injuries. (5.11)
- Seizures in patients with seizure disorders: Monitor during therapy. (5.12)
- Severe hypotension: Monitor during initiation of therapy. Avoid use in patients with circulatory shock. (5.14)
- Adrenal insufficiency: If diagnosed, treat with physiologic replacement of corticosteroids, and wean patient off of the opioid. (5.16)
5.16 Adrenal Insufficiency
Cases of adrenal insufficiency have been reported with opioid use, more often following greater than one month of use. Presentation of adrenal insufficiency may include non-specific symptoms and signs including nausea, vomiting, anorexia, fatigue, weakness, dizziness, and low blood pressure. If adrenal insufficiency is suspected, confirm the diagnosis with diagnostic testing as soon as possible. If adrenal insufficiency is diagnosed, treat with physiologic replacement doses of corticosteroids. Wean the patient off of the opioid to allow adrenal function to recover and continue corticosteroid treatment until adrenal function recovers. Other opioids may be tried as some cases reported use of a different opioid without recurrence of adrenal insufficiency. The information available does not identify any particular opioids as being more likely to be associated with adrenal insufficiency.
7.10 Anticholinergic Drugs
The concomitant use of anticholinergic drugs with TUXARIN ER may increase risk of urinary retention and/or severe constipation, which may lead to paralytic ileus [see Warnings and Precautions (5.10) ]. Monitor patients for signs of urinary retention or reduced gastric motility when TUXARIN ER is used concomitantly with anticholinergic drugs.
Additive adverse effects resulting from cholinergic blockade (e.g., xerostomia, blurred vision, or constipation) may occur when anticholinergic drugs are administered with chlorpheniramine.
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
- Adults 18 years of age and older: 1 tablet every 12 hours as needed, not to exceed 2 tablets in 24 hours. (2.2)
- Do not increase the dose or dosing frequency. (2.1)
- Prescribe for the shortest duration consistent with treatment goals. (2.3)
- Reevaluate patients with unresponsive cough in 5 days or sooner for possible underlying pathology. (2.3)
- Reevaluate patient prior to refilling. (2.3)
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
Extended-release tablets: Each tablet contains 54.3 mg of codeine phosphate (equivalent to 40 mg of codeine); and 8 mg of chlorpheniramine maleate (equivalent to 5.6 mg of chlorpheniramine). Each tablet is white to off-white, uncoated, round, debossed with MP on one side and CC on the other side [see Description (11) ].
8 Use in Specific Populations (8 USE IN SPECIFIC POPULATIONS)
5.1 Addiction, Abuse, and Misuse
TUXARIN ER contains codeine, a Schedule III controlled substance. As an opioid, TUXARIN ER exposes users to the risks of addiction, abuse, and misuse [see Drug Abuse and Dependence (9) ], which can lead to overdose and death [see Overdosage (10) ]. Reserve TUXARIN ER for use in adult patients for whom the benefits of cough suppression are expected to outweigh the risks, and in whom an adequate assessment of the etiology of the cough has been made. Assess each patient's risk prior to prescribing TUXARIN ER, prescribe TUXARIN ER for the shortest duration that is consistent with individual patient treatment goals, monitor all patients regularly for the development of addiction or abuse, and refill only after reevaluation of the need for continued treatment.
Although the risk of addiction in any individual is unknown, it can occur in patients appropriately prescribed TUXARIN ER. Addiction can occur at recommended dosages and if the drug is misused or abused. Risks are increased in patients with a personal or family history of substance abuse (including drug or alcohol abuse or addiction) or mental illness (e.g., major depression).
Opioids are sought by drug abusers and people with addiction disorders and are subject to criminal diversion. Consider these risks when prescribing or dispensing TUXARIN ER. Strategies to reduce these risks include prescribing the drug in the smallest appropriate quantity and advising the patient on the proper disposal of unused drug [see Patient Counseling Information (17) ]. Contact local state professional licensing board or state controlled substances authority for information on how to prevent and detect abuse or diversion of this product.
17 Patient Counseling Information (17 PATIENT COUNSELING INFORMATION)
Advise the patient to read the FDA-approved patient labeling (Medication Guide).
16 How Supplied/storage and Handling (16 HOW SUPPLIED/STORAGE AND HANDLING)
TUXARIN ER (codeine phosphate and chlorpheniramine maleate) 54.3 mg/ 8 mg extended-release tablets, are white to off-white, uncoated, standard round tablets, debossed with MP on one side and CC on the other side. Supplied in bottles of 30 tablets (NDC 71269-040-30) and 100 tablets (NDC 71269-040-10).
5.17 Drug/laboratory Test Interactions (5.17 Drug/Laboratory Test Interactions)
Because opioid agonists may increase biliary tract pressure, with resultant increase in plasma amylase or lipase levels, determination of these enzyme levels may be unreliable for 24 hours after administration of a dose of TUXARIN ER.
5.15 Neonatal Opioid Withdrawal Syndrome
TUXARIN ER is not recommended for use in pregnant women. Prolonged use of TUXARIN ER during pregnancy can result in withdrawal in the neonate. Neonatal opioid withdrawal syndrome, unlike opioid withdrawal syndrome in adults, may be life-threatening if not recognized and treated, and requires management according to protocols developed by neonatology experts. Observe newborns for signs of neonatal opioid withdrawal syndrome and manage accordingly. Advise pregnant women using opioids for a prolonged period of the risk of neonatal opioid withdrawal syndrome and ensure that appropriate treatment will be available. [see Use in Specific Populations (8.1), Patient Counseling Information (17) ]
7.7 Monoamine Oxidase Inhibitors (maois) (7.7 Monoamine Oxidase Inhibitors (MAOIs))
TUXARIN ER is contraindicated in patients who are taking MAOIs (i.e., certain drugs used for depression, psychiatric or emotional conditions, or Parkinson's disease) or have taken MAOIs within 14 days [see Contraindications (4) ].
MAOI interactions with opioids may manifest as serotonin syndrome or opioid toxicity (e.g., respiratory depression, coma) [see Warnings and Precautions (5.13) ].
5.2 Life Threatening Respiratory Depression (5.2 Life-Threatening Respiratory Depression)
Serious, life-threatening, or fatal respiratory depression has been reported with the use of opioids, including codeine, one of the active ingredients in TUXARIN ER. Codeine produces dose-related respiratory depression by directly acting on the brain stem respiratory center that controls respiratory rhythm and may produce irregular and periodic breathing. Codeine is subject to variability in metabolism based upon CYP2D6 genotype, which can lead to an increased exposure to the active metabolite morphine [see Warnings and Precautions (5.3) ]. Respiratory depression, if not immediately recognized and treated, may lead to respiratory arrest and death. Management of respiratory depression includes discontinuation of TUXARIN ER, close observation, supportive measures, and use of opioid antagonists (e.g. naloxone), depending on the patient's clinical status [see Overdosage (10) ]. Carbon dioxide (CO2) retention from opioid-induced respiratory depression can exacerbate the sedating effects of opioids.
While serious, life-threatening, or fatal respiratory depression can occur at any time during the use of TUXARIN ER, the risk is greatest during the initiation of therapy, when TUXARIN ER is used concomitantly with other drugs that may cause respiratory depression [see Warnings and Precautions (5.9) ], in patients with chronic pulmonary disease or decreased respiratory reserve, and in patients with altered pharmacokinetics or altered clearance (e.g. elderly, cachectic, or debilitated patients) [see Warnings and Precautions (5.5) ].
To reduce the risk of respiratory depression, proper dosing of TUXARIN ER is essential [see Dosage and Administration (2.1), Warnings and Precautions (5.6)]. Monitor patients closely, especially within the first 24- 72 hours of initiating therapy or when used in patients at higher risk.
Overdose of codeine in adults has been associated with fatal respiratory depression, and the use of codeine in children younger than 12 years of age has been associated with fatal respiratory depression when used as recommended [see Warnings and Precautions (5.3) ]. Accidental ingestion of even one dose of TUXARIN ER, especially by children, can result in respiratory depression and death.
5.4 Risks With Use in Pediatric Populations (5.4 Risks with Use in Pediatric Populations)
Children are particularly sensitive to the respiratory depressant effects of codeine [see Warnings and Precautions (5.2, 5.3) ]. Because of the risk of life-threatening respiratory depression and death, TUXARIN ER is contraindicated in children less than 12 years of age, and in pediatric patients younger than 18 years of age following tonsillectomy and/or adenoidectomy [see Contraindications (4) ].
Use of TUXARIN ER in children also exposes them to the risks of addiction, abuse, and misuse [see Drug Abuse and Dependence (9) ], which can lead to overdose and death [see Warnings and Precautions (5.1), Overdosage (10) ]. Because the benefits of symptomatic treatment of cough associated with allergies or the common cold do not outweigh the risks of use of codeine in pediatric patients, TUXARIN ER is not indicated for use in patients younger than 18 years of age [see Indications (1), Use in Specific Populations (8.4) ].
7.5 Benzodiazepines and Other Cns Depressants (7.5 Benzodiazepines and Other CNS Depressants)
Due to additive pharmacologic effect, the concomitant use of benzodiazepines or other CNS depressants, including alcohol, other sedatives/hypnotics, anxiolytics, tranquilizers, muscle relaxants, general anesthetics, antipsychotics, and other opioids, can increase the risk of hypotension, respiratory depression, profound sedation, coma, and death. Avoid the use of TUXARIN ER in patients who are taking benzodiazepines or other CNS depressants. [see Warnings and Precautions (5.9) ].
Principal Display Panel 100 Tablet Bottle Label (PRINCIPAL DISPLAY PANEL - 100 Tablet Bottle Label)
NDC 71269-040-10
CIII
Tuxarin ER™
(codeine phosphate and
chlorpheniramine maleate
extended-release tablets)
54.3 mg/ 8 mg
Each Tablet Contains:
Codeine Phosphate, USP 54.3 mg
(Equivalent to 40 mg of Codeine)
Chlorpheniramine Maleate, USP 8 mg
(Equivalent to 5.6 mg of Chlorpheniramine)
PHARMACIST: PLEASE DISPENSE WITH
MEDICATION GUIDE
Rx only
100 Tablets
2.1 Important Dosage and Administration Instructions
Administer TUXARIN ER by the oral route only.
Advise patients not to increase the dose or dosing frequency of TUXARIN ER because serious adverse events such as respiratory depression may occur with overdosage [see Warnings and Precautions (5.2), Overdosage (10) ]. The dosage of TUXARIN ER should not be increased if cough fails to respond; an unresponsive cough should be reevaluated for possible underlying pathology [see Dosage and Administration (2.3), Warnings and Precautions (5.5) ].
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenicity, mutagenicity, and fertility studies have not been conducted with TUXARIN ER; however, published information is available for the active ingredients.
2.3 Monitoring, Maintenance, and Discontinuation of Therapy
Prescribe TUXARIN ER for the shortest duration that is consistent with individual patient treatment goals [see Warnings and Precautions (5.1) ]
Monitor patients closely for respiratory depression, especially within the first 24-72 hours of initiating therapy [see Warnings and Precautions (5.2) ].
Reevaluate patients with unresponsive cough in 5 days or sooner for possible underlying pathology, such as foreign body or lower respiratory tract disease [see Warnings and Precautions (5.5) ]. If a patient requires a refill, reevaluate the cause of the cough and assess the need for continued treatment with TUXARIN ER, the relative incidence of adverse reactions, and the development of addiction, abuse, or misuse [see Warnings and Precautions (5.1) ].
Do not abruptly discontinue TUXARIN ER in a physically-dependent patient [see Drug Abuse and Dependence (9.3) ]. When a patient who has been taking TUXARIN ER regularly and may be physically dependent no longer requires therapy with TUXARIN ER, taper the dose gradually, by 25% to 50% every 2 to 4 days, while monitoring carefully for signs and symptoms of withdrawal. If the patient develops these signs or symptoms, raise the dose to the previous level and taper more slowly, either by increasing the interval between decreases, decreasing the amount of change in dose, or both.
5.10 Risks of Use in Patients With Gastrointestinal Conditions (5.10 Risks of Use in Patients with Gastrointestinal Conditions)
TUXARIN ER is contraindicated in patients with known or suspected gastrointestinal obstruction, including paralytic ileus [see Contraindications (4) ]. The use of codeine in TUXARIN ER may obscure the diagnosis or clinical course of patients with acute abdominal conditions.
The concurrent use of anticholinergics with TUXARIN ER may produce paralytic ileus [see Drug Interactions (7.10) ].
The codeine in TUXARIN ER may result in constipation or obstructive bowel disease, especially in patients with underlying intestinal motility disorders. Use with caution in patients with underlying intestinal motility disorders.
The codeine in TUXARIN ER may cause spasm of the sphincter of Oddi, resulting in an increase in biliary tract pressure. Opioids may cause increases in serum amylase [see Warnings and Precautions (5.17) ]. Monitor patients with biliary tract disease, including acute pancreatitis for worsening symptoms.
5.13 Co Administration With Monoamine Oxidase Inhibitors (maois) (5.13 Co-administration with Monoamine Oxidase Inhibitors (MAOIs))
Concurrent use of TUXARIN ER is contraindicated in patients receiving monoamine oxidase inhibitors (MAOIs) or within 14 days of stopping such therapy [see Contraindications (4) ]. MAOIs may potentiate the effects of morphine, codeine's active metabolite, including respiratory depression, coma, and confusion MAOIs [see Drug Interactions (7.7) ].
5.12 Increased Risk of Seizures in Patients With Seizure Disorders (5.12 Increased Risk of Seizures in Patients with Seizure Disorders)
The codeine and chlorpheniramine in TUXARIN ER may increase the frequency of seizures in patients with seizure disorders, and may increase the risk of seizures occurring in other clinical settings associated with seizures. Monitor patients with a history of seizure disorders for worsened seizure control during TUXARIN ER therapy.
5.6 Risk of Accidental Overdose and Death Due to Medication Errors (5.6 Risk of Accidental Overdose and Death due to Medication Errors)
Dosing errors can result in accidental overdose and death. To reduce the risk of overdose and respiratory depression, ensure that the dose of TUXARIN ER is communicated clearly and dispensed accurately [see Dosage and Administration (2.1) ].
5.8 Risks of Interactions With Drugs Affecting Cytochrome P450 Isoenzymes (5.8 Risks of Interactions with Drugs Affecting Cytochrome P450 Isoenzymes)
The effects of concomitant use or discontinuation of cytochrome P450 3A4 inducers, 3A4 inhibitors, or 2D6 inhibitors with codeine are complex. Use of cytochrome P450 3A4 inducers, 3A4 inhibitors, or 2D6 inhibitors with TUXARIN ER requires careful consideration of the effects on the parent drug, codeine, and the active metabolite, morphine.
5.9 Risks From Concomitant Use With Benzodiazepines Or Other Cns Depressants (5.9 Risks from Concomitant Use with Benzodiazepines or other CNS Depressants)
Concomitant use of opioids, including TUXARIN ER, with benzodiazepines, or other CNS depressants, including alcohol, may result in profound sedation, respiratory depression, coma, and death. Because of these risks, avoid use of opioid cough medications in patients taking benzodiazepines, other CNS depressants, or alcohol [see Drug Interactions (7.5) ].
Observational studies have demonstrated that concomitant use of opioid analgesics and benzodiazepines increases the risk of drug-related mortality compared to use of opioids alone. Because of similar pharmacologic properties, it is reasonable to expect similar risk with concomitant use of opioid cough medications and benzodiazepines, other CNS depressants, or alcohol.
Advise both patients and caregivers about the risks of respiratory depression and sedation if TUXARIN ER is used with benzodiazepines, alcohol, or other CNS depressants [see Patient Counseling Information (17) ].
5.7 Activities Requiring Mental Alertness: Risks of Driving and Operating Machinery
Codeine and chlorpheniramine, the active ingredients in TUXARIN ER, may produce marked drowsiness and impair the mental and/or physical abilities required for the performance of potentially hazardous tasks such as driving a car or operating machinery. Advise patients to avoid engaging in hazardous tasks requiring mental alertness and motor coordination after ingestion of TUXARIN ER. Avoid concurrent use of TUXARIN ER with alcohol or other central nervous system depressants because additional impairment of central nervous system performance may occur [See Warnings and Precautions (5.9) ].
5.3 Ultra Rapid Metabolism of Codeine and Other Risk Factors for Life Threatening Respiratory Depression in Children (5.3 Ultra-Rapid Metabolism of Codeine and Other Risk Factors for Life-Threatening Respiratory Depression in Children)
Life-threatening respiratory depression and death have occurred in children who received codeine. Codeine is subject to variability in metabolism based upon CYP2D6 genotype (described below), which can lead to an increased exposure to the active metabolite morphine. Based upon post-marketing reports, children younger than 12 years old appear to be more susceptible to the respiratory depressant effects of codeine, particularly if there are risk factors for respiratory depression. For example, many reported cases of death occurred in the post-operative period following tonsillectomy and/or adenoidectomy, and many of the children had evidence of being ultra-rapid metabolizers of codeine. Furthermore, children with obstructive sleep apnea who are treated with codeine for post-tonsillectomy and/or adenoidectomy pain may be particularly sensitive to its respiratory depressant effect. Because of the risk of life-threatening respiratory depression and death:
- TUXARIN ER is contraindicated in all children younger than 12 years of age [see Contraindications (4) ].
- TUXARIN ER is contraindicated for post-operative management in pediatric patients younger than 18 years of age following tonsillectomy and/or adenoidectomy [see Contraindications (4) ].
- Avoid the use of TUXARIN ER in adolescents 12 to 18 years of age who have other risk factors that may increase their sensitivity to the respiratory depressant effects of codeine. Risk factors include conditions associated with hypoventilation, such as postoperative status, obstructive sleep apnea, obesity, severe pulmonary disease, neuromuscular disease, and concomitant use of other medications that cause respiratory depression. [see Warnings and Precautions (5.9), Use in Specific Populations (8.4) ]
- Healthcare providers should choose the lowest effective dose for the shortest period of time and inform patients and caregivers about these risks and the signs of morphine overdose [see Warnings and Precautions (5.1), Overdosage (10) ].
5.11 Risks of Use in Patients With Head Injury, Impaired Consciousness, Increased Intracranial Pressure, Or Brain Tumors (5.11 Risks of Use in Patients with Head Injury, Impaired Consciousness, Increased Intracranial Pressure, or Brain Tumors)
Avoid the use of TUXARIN ER in patients with head injury, intracranial lesions, or a pre-existing increase in intracranial pressure. In patients who may be susceptible to the intracranial effects of CO2 retention (e.g., those with evidence of increased intracranial pressure or brain tumors), TUXARIN ER may reduce respiratory drive, and the resultant CO2 retention can further increase intracranial pressure. Furthermore, opioids produce adverse reactions that may obscure the clinical course of patients with head injuries.
Warning: Addiction, Abuse, and Misuse; Life Threatening Respiratory Depression; Accidential Ingestion; Ultra Rapid Metabolism of Codeine and Other Risk Factors for Life Threatening Respiratory Depression in Children; Medication Errors; Interactions With Drugs Affecting Cytochrome P450 Isoenzymes; Concomitant Use With Benzodiazepines Or Other Cns Depressants; Neonatal Opoid Withdrawal Syndrome (WARNING: ADDICTION, ABUSE, AND MISUSE; LIFE-THREATENING RESPIRATORY DEPRESSION; ACCIDENTIAL INGESTION; ULTRA-RAPID METABOLISM OF CODEINE AND OTHER RISK FACTORS FOR LIFE-THREATENING RESPIRATORY DEPRESSION IN CHILDREN; MEDICATION ERRORS; INTERACTIONS WITH DRUGS AFFECTING CYTOCHROME P450 ISOENZYMES; CONCOMITANT USE WITH BENZODIAZEPINES OR OTHER CNS DEPRESSANTS; NEONATAL OPOID WITHDRAWAL SYNDROME)
WARNING: ADDICTION, ABUSE, AND MISUSE; LIFE-THREATENING RESPIRATORY DEPRESSION; ACCIDENTIAL INGESTION; ULTRA-RAPID METABOLISM OF CODEINE AND OTHER RISK FACTORS FOR LIFE-THREATENING RESPIRATORY DEPRESSION IN CHILDREN; MEDICATION ERRORS; INTERACTIONS WITH DRUGS AFFECTING CYTOCHROME P450 ISOENZYMES; CONCOMITANT USE WITH BENZODIAZEPINES OR OTHER CNS DEPRESSANTS; NEONATAL OPOID WITHDRAWAL SYNDROME
See full prescribing information for complete boxed warning.
- TUXARIN ER exposes users to risks of addiction, abuse, and misuse, which can lead to overdose and death. Assess patient's risk before prescribing and monitor closely for these behaviors and conditions. (5.1)
- Serious, life-threatening, or fatal respiratory depression may occur. Monitor closely, especially upon initiation or when used in patients at higher risk. (5.2)
- Accidental ingestion of TUXARIN ER, especially by children, can result in a fatal overdose of codeine. (5.2)
- Life-threatening respiratory depression and death have occurred in children who received codeine; most cases followed tonsillectomy and/or adenoidectomy, and many of the children had evidence of being an ultra-rapid metabolizer of codeine due to a CYP2D6 polymorphism. (5.3) TUXARIN ER is contraindicated in children younger than 12 years of age and in children younger than 18 years of age following tonsillectomy and/or adenoidectomy. (4) Avoid the use of TUXARIN ER in adolescents 12 to 18 years of age who have other risk factors that may increase their sensitivity to the respiratory depressant effects of codeine.
- Ensure accuracy when prescribing, dispensing, and administering TUXARIN ER. Dosing errors can result in accidental overdose and death. (2.1, 5.6)
- The effects of concomitant use or discontinuation of cytochrome P450 3A4 inducers, 3A4 inhibitors, or 2D6 inhibitors with codeine are complex, requiring careful consideration of the effects on the parent drug, codeine, and the active metabolite, morphine. Avoid the use of TUXARIN ER in these patients. (5.4, 7.1, 7.2, 7.4)
- Concomitant use of opioids with benzodiazepines or other central nervous system (CNS) depressants, including alcohol, may result in profound sedation, respiratory depression, coma, and death. Avoid the use of TUXARIN ER in patients taking benzodiazepines, other CNS depressants, or alcohol. (5.9, 7.5)
- TUXARIN ER is not recommended for use in pregnant women. Prolonged use of TUXARIN ER during pregnancy can result in neonatal opioid withdrawal syndrome, which may be life-threatening if not recognized and treated. If TUXARIN ER is used for a prolonged period in a pregnant woman, advise the patient of the risk of neonatal opioid withdrawal syndrome and ensure that appropriate treatment will be available. (5.15, 8.1)
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:39:58.755053 · Updated: 2026-03-14T22:00:22.611975