These Highlights Do Not Include All The Information Needed To Use Segluromet Safely And Effectively. See Full Prescribing Information For Segluromet.
a6aeb99a-ce49-4125-90ce-642df3f1ebad
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
Dosage and Administration ( 2.4 ) 12/2024 Warnings and Precautions ( 5.3 , 5.6 ) 12/2024
Indications and Usage
SEGLUROMET ® is indicated as an adjunct to diet and exercise to improve glycemic control in adults with type 2 diabetes mellitus.
Dosage and Administration
Assess renal function prior to initiation and as clinically indicated. ( 2.1 ) Correct volume depletion before initiation. ( 2.1 ) Individualize the starting dosage based on the patient's current regimen. ( 2.2 ) Maximum recommended dosage is 7.5 mg ertugliflozin/1,000 mg metformin orally twice daily. ( 2.2 ) Take orally twice daily with meals, with gradual dose escalation. ( 2.2 ) Do not use in patients with an estimated glomerular filtration rate (eGFR) below 30 mL/minute/1.73 m 2 . Use is not recommended in patients with an eGFR less than 45 mL/min/1.73 m 2 . ( 2.2 ) Use is contraindicated in patients with severe renal impairment (eGFR less than 30 mL/min/1.73 m 2 ), end stage-renal disease (ESRD), or on dialysis. ( 2.2 ) SEGLUROMET may need to be discontinued at time of, or prior to, iodinated contrast imaging procedures. ( 2.3 ) Withhold SEGLUROMET for at least 4 days, if possible, prior to surgery or procedures associated with prolonged fasting. ( 2.4 )
Warnings and Precautions
Lactic Acidosis: See boxed warning . ( 5.1 ) Diabetic Ketoacidosis in Patients with Type 1 Diabetes Mellitus and Other Ketoacidosis: Consider ketone monitoring in patients at risk for ketoacidosis, as indicated. Assess for ketoacidosis regardless of presenting blood glucose levels and discontinue SEGLUROMET if ketoacidosis is suspected. Monitor patients for resolution of ketoacidosis before restarting. ( 5.2 ) Lower Limb Amputation: Monitor patients for infections or ulcers of lower limbs, and discontinue if these occur. ( 5.3 ) Volume Depletion: May result in acute kidney injury. Before initiating, assess and correct volume status in patients with renal impairment, low systolic blood pressure, elderly patients, or patients on diuretics. Monitor for signs and symptoms during therapy. ( 5.4 ) Urosepsis and Pyelonephritis: Evaluate patients for signs and symptoms of urinary tract infections and treat promptly, if indicated. ( 5.5 ) Hypoglycemia: Consider a lower dose of insulin or insulin secretagogue to reduce risk of hypoglycemia when used in combination. ( 5.6 ) Necrotizing Fasciitis of the Perineum (Fournier's Gangrene): Serious, life-threatening cases have occurred in both females and males. Assess patients presenting with pain or tenderness, erythema, or swelling in the genital or perineal area, along with fever or malaise. If suspected, institute prompt treatment. ( 5.7 ) Genital Mycotic Infections: Monitor and treat if indicated. ( 5.8 ) Vitamin B 12 Deficiency: Metformin may lower vitamin B 12 levels. Measure hematological parameters annually. ( 5.9 )
Contraindications
SEGLUROMET is contraindicated in patients with: Hypersensitivity to ertugliflozin, metformin, or any excipient in SEGLUROMET. Reactions such as angioedema or anaphylaxis have occurred [see Adverse Reactions (6.2) ]. Severe renal impairment (eGFR less than 30 mL/min/1.73 m 2 ), end stage-renal disease (ESRD), or on dialysis [see Use in Specific Populations (8.6) ] . Acute or chronic metabolic acidosis, including diabetic ketoacidosis, with or without coma.
Adverse Reactions
The following important adverse reactions are described elsewhere in the labeling: Lactic Acidosis [see Boxed Warning and Warnings and Precautions (5.1) ] Diabetic Ketoacidosis in Patients with Type 1 Diabetes and Other Ketoacidosis [see Warnings and Precautions (5.2) ] Lower Limb Amputation [see Warnings and Precautions (5.3) ] Volume Depletion [see Warnings and Precautions (5.4) ] Urosepsis and Pyelonephritis [see Warnings and Precautions (5.5) ] Hypoglycemia with Concomitant Use with Insulin or Insulin Secretagogues [see Warnings and Precautions (5.6) ] Necrotizing Fasciitis of the Perineum (Fournier's Gangrene) [see Warnings and Precautions (5.7) ] Genital Mycotic Infections [see Warnings and Precautions (5.8) ] Vitamin B 12 Deficiency [see Warnings and Precautions (5.9) ]
Drug Interactions
Table 3: Clinically Significant Drug Interactions with SEGLUROMET Carbonic Anhydrase Inhibitors Clinical Impact: The risk of lactic acidosis may increase due to concomitant use of Topiramate or other carbonic anhydrase inhibitors (e.g., zonisamide, acetazolamide or dichlorphenamide) with metformin. These drugs frequently cause a decrease in serum bicarbonate and induce non-anion gap, hyperchloremic metabolic acidosis. Intervention: more frequent monitoring of these patients. Drugs that Reduce Metformin Clearance Clinical Impact: The risk of lactic acidosis may increase due to concomitant use of drugs that interfere with common renal tubular transport systems involved in the renal elimination of metformin (e.g., organic cationic transporter-2 [OCT2] / multidrug and toxin extrusion [MATE] inhibitors such as ranolazine, vandetanib, dolutegravir, and cimetidine) which increase systemic exposure to metformin Intervention Consider the benefits and risks of concomitant use. Alcohol Clinical Impact: Potentiate the effect of metformin on lactate metabolism. Intervention: Warn patients against excessive alcohol intake while receiving SEGLUROMET. Insulin or Insulin Secretagogues Clinical Impact: The risk of hypoglycemia is increased when ertugliflozin is used in combination with insulin or an insulin secretagogue. Intervention: A lower dose of insulin or insulin secretagogue may be required to minimize the risk of hypoglycemia when used in combination with SEGLUROMET. Drugs that Affect Glycemic Control Clinical Impact: Certain drugs tend to produce hyperglycemia and may lead to loss of glycemic control. These drugs include the thiazides and other diuretics, corticosteroids, phenothiazines, thyroid products, estrogens, oral contraceptives, phenytoin, nicotinic acid, sympathomimetics, calcium channel blocking drugs, and isoniazid. Intervention: When a patient is receiving SEGLUROMET along with such drugs, the patient should be closely observed to maintain adequate glycemic control. Lithium Clinical Impact: Concomitant use of an SGLT2 inhibitor with lithium may decrease serum lithium concentrations. Intervention: Monitor serum lithium concentration more frequently during SEGLUROMET initiation and dosage changes. Positive Urine Glucose Test Clinical Impact: SGLT2 inhibitors increase urinary glucose excretion and will lead to positive urine glucose tests. Intervention: Monitoring glycemic control with urine glucose tests is not recommended in patients taking SEGLUROMET. Use alternative methods to monitor glycemic control. Interference with 1,5-anhydroglucitol (1,5-AG) Assay Clinical Impact: Measurements of 1,5-AG are unreliable in assessing glycemic control in patients taking SGLT2 inhibitors. Intervention: Monitoring glycemic control with 1,5-AG assay is not recommended. Use alternative methods to monitor glycemic control.
Storage and Handling
SEGLUROMET (ertugliflozin and metformin hydrochloride) tablets are available as follows: Strength Description How Supplied NDC ertugliflozin 2.5 mg and metformin hydrochloride 500 mg tablets pink, oval, debossed with “2.5/500” on one side and plain on the other side unit-of-use bottles of 60 0006-5369-03 unit-of-use bottles of 180 0006-5369-06 ertugliflozin 2.5 mg and metformin hydrochloride 1,000 mg tablets pink, oval, debossed with “2.5/1000” on one side and plain on the other side unit-of-use bottles of 60 0006-5373-03 unit-of-use bottles of 180 0006-5373-06 ertugliflozin 7.5 mg and metformin hydrochloride 500 mg tablets red, oval, debossed with “7.5/500” on one side and plain on the other side unit-of-use bottles of 60 0006-5370-03 unit-of-use bottles of 180 0006-5370-06 ertugliflozin 7.5 mg and metformin hydrochloride 1,000 mg tablets red, oval, debossed with “7.5/1000” on one side and plain on the other side unit-of-use bottles of 60 0006-5374-03 unit-of-use bottles of 180 0006-5374-06
How Supplied
SEGLUROMET (ertugliflozin and metformin hydrochloride) tablets are available as follows: Strength Description How Supplied NDC ertugliflozin 2.5 mg and metformin hydrochloride 500 mg tablets pink, oval, debossed with “2.5/500” on one side and plain on the other side unit-of-use bottles of 60 0006-5369-03 unit-of-use bottles of 180 0006-5369-06 ertugliflozin 2.5 mg and metformin hydrochloride 1,000 mg tablets pink, oval, debossed with “2.5/1000” on one side and plain on the other side unit-of-use bottles of 60 0006-5373-03 unit-of-use bottles of 180 0006-5373-06 ertugliflozin 7.5 mg and metformin hydrochloride 500 mg tablets red, oval, debossed with “7.5/500” on one side and plain on the other side unit-of-use bottles of 60 0006-5370-03 unit-of-use bottles of 180 0006-5370-06 ertugliflozin 7.5 mg and metformin hydrochloride 1,000 mg tablets red, oval, debossed with “7.5/1000” on one side and plain on the other side unit-of-use bottles of 60 0006-5374-03 unit-of-use bottles of 180 0006-5374-06
Medication Information
Warnings and Precautions
Lactic Acidosis: See boxed warning . ( 5.1 ) Diabetic Ketoacidosis in Patients with Type 1 Diabetes Mellitus and Other Ketoacidosis: Consider ketone monitoring in patients at risk for ketoacidosis, as indicated. Assess for ketoacidosis regardless of presenting blood glucose levels and discontinue SEGLUROMET if ketoacidosis is suspected. Monitor patients for resolution of ketoacidosis before restarting. ( 5.2 ) Lower Limb Amputation: Monitor patients for infections or ulcers of lower limbs, and discontinue if these occur. ( 5.3 ) Volume Depletion: May result in acute kidney injury. Before initiating, assess and correct volume status in patients with renal impairment, low systolic blood pressure, elderly patients, or patients on diuretics. Monitor for signs and symptoms during therapy. ( 5.4 ) Urosepsis and Pyelonephritis: Evaluate patients for signs and symptoms of urinary tract infections and treat promptly, if indicated. ( 5.5 ) Hypoglycemia: Consider a lower dose of insulin or insulin secretagogue to reduce risk of hypoglycemia when used in combination. ( 5.6 ) Necrotizing Fasciitis of the Perineum (Fournier's Gangrene): Serious, life-threatening cases have occurred in both females and males. Assess patients presenting with pain or tenderness, erythema, or swelling in the genital or perineal area, along with fever or malaise. If suspected, institute prompt treatment. ( 5.7 ) Genital Mycotic Infections: Monitor and treat if indicated. ( 5.8 ) Vitamin B 12 Deficiency: Metformin may lower vitamin B 12 levels. Measure hematological parameters annually. ( 5.9 )
Indications and Usage
SEGLUROMET ® is indicated as an adjunct to diet and exercise to improve glycemic control in adults with type 2 diabetes mellitus.
Dosage and Administration
Assess renal function prior to initiation and as clinically indicated. ( 2.1 ) Correct volume depletion before initiation. ( 2.1 ) Individualize the starting dosage based on the patient's current regimen. ( 2.2 ) Maximum recommended dosage is 7.5 mg ertugliflozin/1,000 mg metformin orally twice daily. ( 2.2 ) Take orally twice daily with meals, with gradual dose escalation. ( 2.2 ) Do not use in patients with an estimated glomerular filtration rate (eGFR) below 30 mL/minute/1.73 m 2 . Use is not recommended in patients with an eGFR less than 45 mL/min/1.73 m 2 . ( 2.2 ) Use is contraindicated in patients with severe renal impairment (eGFR less than 30 mL/min/1.73 m 2 ), end stage-renal disease (ESRD), or on dialysis. ( 2.2 ) SEGLUROMET may need to be discontinued at time of, or prior to, iodinated contrast imaging procedures. ( 2.3 ) Withhold SEGLUROMET for at least 4 days, if possible, prior to surgery or procedures associated with prolonged fasting. ( 2.4 )
Contraindications
SEGLUROMET is contraindicated in patients with: Hypersensitivity to ertugliflozin, metformin, or any excipient in SEGLUROMET. Reactions such as angioedema or anaphylaxis have occurred [see Adverse Reactions (6.2) ]. Severe renal impairment (eGFR less than 30 mL/min/1.73 m 2 ), end stage-renal disease (ESRD), or on dialysis [see Use in Specific Populations (8.6) ] . Acute or chronic metabolic acidosis, including diabetic ketoacidosis, with or without coma.
Adverse Reactions
The following important adverse reactions are described elsewhere in the labeling: Lactic Acidosis [see Boxed Warning and Warnings and Precautions (5.1) ] Diabetic Ketoacidosis in Patients with Type 1 Diabetes and Other Ketoacidosis [see Warnings and Precautions (5.2) ] Lower Limb Amputation [see Warnings and Precautions (5.3) ] Volume Depletion [see Warnings and Precautions (5.4) ] Urosepsis and Pyelonephritis [see Warnings and Precautions (5.5) ] Hypoglycemia with Concomitant Use with Insulin or Insulin Secretagogues [see Warnings and Precautions (5.6) ] Necrotizing Fasciitis of the Perineum (Fournier's Gangrene) [see Warnings and Precautions (5.7) ] Genital Mycotic Infections [see Warnings and Precautions (5.8) ] Vitamin B 12 Deficiency [see Warnings and Precautions (5.9) ]
Drug Interactions
Table 3: Clinically Significant Drug Interactions with SEGLUROMET Carbonic Anhydrase Inhibitors Clinical Impact: The risk of lactic acidosis may increase due to concomitant use of Topiramate or other carbonic anhydrase inhibitors (e.g., zonisamide, acetazolamide or dichlorphenamide) with metformin. These drugs frequently cause a decrease in serum bicarbonate and induce non-anion gap, hyperchloremic metabolic acidosis. Intervention: more frequent monitoring of these patients. Drugs that Reduce Metformin Clearance Clinical Impact: The risk of lactic acidosis may increase due to concomitant use of drugs that interfere with common renal tubular transport systems involved in the renal elimination of metformin (e.g., organic cationic transporter-2 [OCT2] / multidrug and toxin extrusion [MATE] inhibitors such as ranolazine, vandetanib, dolutegravir, and cimetidine) which increase systemic exposure to metformin Intervention Consider the benefits and risks of concomitant use. Alcohol Clinical Impact: Potentiate the effect of metformin on lactate metabolism. Intervention: Warn patients against excessive alcohol intake while receiving SEGLUROMET. Insulin or Insulin Secretagogues Clinical Impact: The risk of hypoglycemia is increased when ertugliflozin is used in combination with insulin or an insulin secretagogue. Intervention: A lower dose of insulin or insulin secretagogue may be required to minimize the risk of hypoglycemia when used in combination with SEGLUROMET. Drugs that Affect Glycemic Control Clinical Impact: Certain drugs tend to produce hyperglycemia and may lead to loss of glycemic control. These drugs include the thiazides and other diuretics, corticosteroids, phenothiazines, thyroid products, estrogens, oral contraceptives, phenytoin, nicotinic acid, sympathomimetics, calcium channel blocking drugs, and isoniazid. Intervention: When a patient is receiving SEGLUROMET along with such drugs, the patient should be closely observed to maintain adequate glycemic control. Lithium Clinical Impact: Concomitant use of an SGLT2 inhibitor with lithium may decrease serum lithium concentrations. Intervention: Monitor serum lithium concentration more frequently during SEGLUROMET initiation and dosage changes. Positive Urine Glucose Test Clinical Impact: SGLT2 inhibitors increase urinary glucose excretion and will lead to positive urine glucose tests. Intervention: Monitoring glycemic control with urine glucose tests is not recommended in patients taking SEGLUROMET. Use alternative methods to monitor glycemic control. Interference with 1,5-anhydroglucitol (1,5-AG) Assay Clinical Impact: Measurements of 1,5-AG are unreliable in assessing glycemic control in patients taking SGLT2 inhibitors. Intervention: Monitoring glycemic control with 1,5-AG assay is not recommended. Use alternative methods to monitor glycemic control.
Storage and Handling
SEGLUROMET (ertugliflozin and metformin hydrochloride) tablets are available as follows: Strength Description How Supplied NDC ertugliflozin 2.5 mg and metformin hydrochloride 500 mg tablets pink, oval, debossed with “2.5/500” on one side and plain on the other side unit-of-use bottles of 60 0006-5369-03 unit-of-use bottles of 180 0006-5369-06 ertugliflozin 2.5 mg and metformin hydrochloride 1,000 mg tablets pink, oval, debossed with “2.5/1000” on one side and plain on the other side unit-of-use bottles of 60 0006-5373-03 unit-of-use bottles of 180 0006-5373-06 ertugliflozin 7.5 mg and metformin hydrochloride 500 mg tablets red, oval, debossed with “7.5/500” on one side and plain on the other side unit-of-use bottles of 60 0006-5370-03 unit-of-use bottles of 180 0006-5370-06 ertugliflozin 7.5 mg and metformin hydrochloride 1,000 mg tablets red, oval, debossed with “7.5/1000” on one side and plain on the other side unit-of-use bottles of 60 0006-5374-03 unit-of-use bottles of 180 0006-5374-06
How Supplied
SEGLUROMET (ertugliflozin and metformin hydrochloride) tablets are available as follows: Strength Description How Supplied NDC ertugliflozin 2.5 mg and metformin hydrochloride 500 mg tablets pink, oval, debossed with “2.5/500” on one side and plain on the other side unit-of-use bottles of 60 0006-5369-03 unit-of-use bottles of 180 0006-5369-06 ertugliflozin 2.5 mg and metformin hydrochloride 1,000 mg tablets pink, oval, debossed with “2.5/1000” on one side and plain on the other side unit-of-use bottles of 60 0006-5373-03 unit-of-use bottles of 180 0006-5373-06 ertugliflozin 7.5 mg and metformin hydrochloride 500 mg tablets red, oval, debossed with “7.5/500” on one side and plain on the other side unit-of-use bottles of 60 0006-5370-03 unit-of-use bottles of 180 0006-5370-06 ertugliflozin 7.5 mg and metformin hydrochloride 1,000 mg tablets red, oval, debossed with “7.5/1000” on one side and plain on the other side unit-of-use bottles of 60 0006-5374-03 unit-of-use bottles of 180 0006-5374-06
Description
Dosage and Administration ( 2.4 ) 12/2024 Warnings and Precautions ( 5.3 , 5.6 ) 12/2024
Section 42229-5
Limitations of Use
Not recommended for use to improve glycemic control in patients with type 1 diabetes mellitus [see Warnings and Precautions (5.2)].
Section 42231-1
| Medication Guide SEGLUROMET® [seg-LUR-oh-met] (ertugliflozin and metformin hydrochloride) tablets, for oral use |
|||
|---|---|---|---|
| This Medication Guide has been approved by the U.S. Food and Drug Administration. | Revised: 09/2023 | ||
| Read this Medication Guide carefully before you start taking SEGLUROMET and each time you get a refill. There may be new information. This information does not take the place of talking with your healthcare provider about your medical condition or your treatment. | |||
|
What is the most important information I should know about SEGLUROMET?
SEGLUROMET may cause serious side effects, including: Lactic Acidosis. Metformin, one of the medicines in SEGLUROMET, can cause a rare but serious condition called lactic acidosis (a buildup of an acid in the blood) that can cause death. Lactic acidosis is a medical emergency and must be treated in the hospital. Call your healthcare provider right away if you have any of the following symptoms, which could be signs of lactic acidosis: |
|||
|
|
||
Most people who have had lactic acidosis had other conditions that, in combination with metformin use, led to the lactic acidosis. Tell your healthcare provider if you have any of the following, because you have a higher chance for getting lactic acidosis with SEGLUROMET if you:
|
|||
|
|
||
| SEGLUROMET can have other serious side effects. See "What are the possible side effects of SEGLUROMET?" | |||
What is SEGLUROMET?
|
|||
|
Who should not take SEGLUROMET?
|
|||
Before you take SEGLUROMET, tell your healthcare provider about all of your medical conditions, including if you:
SEGLUROMET may affect the way other medicines work, and other medicines may affect how SEGLUROMET works. Know the medicines you take. Keep a list of them to show your healthcare provider and pharmacist when you get a new medicine. |
|||
How should I take SEGLUROMET?
|
|||
What should I avoid while taking SEGLUROMET?
|
|||
|
What are the possible side effects of SEGLUROMET? SEGLUROMET may cause serious side effects, including: See " What is the most important information I should know about SEGLUROMET? " |
|||
Call your healthcare provider right away if you have new pain or tenderness, any sores, ulcers, or infections in your leg or foot. Your healthcare provider may decide to stop your SEGLUROMET for a while if you have any of these signs or symptoms. Talk to your healthcare provider about proper foot care.
|
|||
|
|
|
|
|
|||
|
|
|
|
|
|||
|
|
||
Talk to your healthcare provider about what to do if you get symptoms of a yeast infection of the vagina or penis. Your healthcare provider may suggest you use an over-the-counter antifungal medicine. Talk to your healthcare provider right away if you use an over-the-counter antifungal medicine and your symptoms do not go away.
|
|||
|
|
|
|
| These are not all the possible side effects of SEGLUROMET. Call your healthcare provider for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. |
|||
How should I store SEGLUROMET?
|
|||
|
General information about the safe and effective use of SEGLUROMET.
Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not use SEGLUROMET for a condition for which it was not prescribed. Do not give SEGLUROMET to other people, even if they have the same symptoms that you have. It may harm them. You can ask your pharmacist or healthcare provider for information about SEGLUROMET that is written for health professionals. For more information about SEGLUROMET, go to www.segluromet.com or call 1-800-622-4477. |
|||
|
What are the ingredients in SEGLUROMET?
Active ingredients: ertugliflozin and metformin hydrochloride. Inactive ingredients: povidone, microcrystalline cellulose, crospovidone, sodium lauryl sulfate, and magnesium stearate. The tablet film coating contains the following inactive ingredients: hydroxypropyl methylcellulose, hydroxypropyl cellulose, titanium dioxide, iron oxide red, and carnauba wax. |
|||
| Manufactured for: Merck Sharp & Dohme LLC Rahway, NJ 07065, USA For patent information, go to: www.msd.com/research/patent Copyright © 2017-2023 Merck & Co., Inc., Rahway, NJ, USA, and its affiliates. All rights reserved. usmg-mk8835b-t-2309r007 |
Section 44425-7
Store at 20°C-25°C (68°F-77°F), excursions permitted between 15°C-30°C (between 59°F-86°F) [see USP Controlled Room Temperature]. Protect from moisture. Store in a dry place.
11 Description
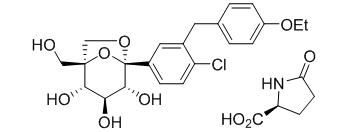
SEGLUROMET (ertugliflozin and metformin hydrochloride) tablet for oral use contains ertugliflozin L-pyroglutamic acid, a SGLT2 inhibitor, and metformin HCl, a member of the biguanide class.
5.9 Vitamin B12
In metformin clinical trials of 29-week duration, a decrease to subnormal levels of previously normal serum vitamin B12 levels was observed in approximately 7% of patients. Such decrease, possibly due to interference with B12 absorption from the B12-intrinsic factor complex, may be associated with anemia but appears to be rapidly reversible with discontinuation of metformin or vitamin B12 supplementation. Certain individuals (those with inadequate vitamin B12 or calcium intake or absorption) appear to be predisposed to developing subnormal vitamin B12 levels. Measure hematologic parameters on an annual basis and vitamin B12 at 2 to 3 year intervals in patients on metformin and manage any abnormalities [see Adverse Reactions (6.1)].
8.4 Pediatric Use
Safety and effectiveness of SEGLUROMET in pediatric patients under 18 years of age have not been established.
4 Contraindications
SEGLUROMET is contraindicated in patients with:
- Hypersensitivity to ertugliflozin, metformin, or any excipient in SEGLUROMET. Reactions such as angioedema or anaphylaxis have occurred [see Adverse Reactions (6.2)].
- Severe renal impairment (eGFR less than 30 mL/min/1.73 m2), end stage-renal disease (ESRD), or on dialysis [see Use in Specific Populations (8.6)].
- Acute or chronic metabolic acidosis, including diabetic ketoacidosis, with or without coma.
5.1 Lactic Acidosis
There have been postmarketing cases of metformin-associated lactic acidosis, including fatal cases. These cases had a subtle onset and were accompanied by nonspecific symptoms such as malaise, myalgias, abdominal pain, respiratory distress, or increased somnolence; however, hypothermia, hypotension and resistant bradyarrhythmias have occurred with severe acidosis. Metformin-associated lactic acidosis was characterized by elevated blood lactate concentrations (>5 mmol/Liter), anion gap acidosis (without evidence of ketonuria or ketonemia), and an increased lactate: pyruvate ratio; metformin plasma levels were generally >5 mcg/mL. Metformin decreases liver uptake of lactate increasing lactate blood levels which may increase the risk of lactic acidosis, especially in patients at risk.
If metformin-associated lactic acidosis is suspected, general supportive measures should be instituted promptly in a hospital setting, along with immediate discontinuation of SEGLUROMET. In SEGLUROMET-treated patients with a diagnosis or strong suspicion of lactic acidosis, prompt hemodialysis is recommended to correct the acidosis and remove accumulated metformin (metformin hydrochloride is dialyzable, with a clearance of up to 170 mL/minute under good hemodynamic conditions). Hemodialysis has often resulted in reversal of symptoms and recovery.
Educate patients and their families about the symptoms of lactic acidosis and if these symptoms occur instruct them to discontinue SEGLUROMET and report these symptoms to their healthcare provider.
For each of the known and possible risk factors for metformin-associated lactic acidosis, recommendations to reduce the risk of and manage metformin-associated lactic acidosis are provided below:
6 Adverse Reactions
The following important adverse reactions are described elsewhere in the labeling:
- Lactic Acidosis [see Boxed Warning and Warnings and Precautions (5.1)]
- Diabetic Ketoacidosis in Patients with Type 1 Diabetes and Other Ketoacidosis [see Warnings and Precautions (5.2)]
- Lower Limb Amputation [see Warnings and Precautions (5.3)]
- Volume Depletion [see Warnings and Precautions (5.4)]
- Urosepsis and Pyelonephritis [see Warnings and Precautions (5.5)]
- Hypoglycemia with Concomitant Use with Insulin or Insulin Secretagogues [see Warnings and Precautions (5.6)]
- Necrotizing Fasciitis of the Perineum (Fournier's Gangrene) [see Warnings and Precautions (5.7)]
- Genital Mycotic Infections [see Warnings and Precautions (5.8)]
- Vitamin B12 Deficiency [see Warnings and Precautions (5.9)]
7 Drug Interactions
| Carbonic Anhydrase Inhibitors | |
|---|---|
| Clinical Impact: | The risk of lactic acidosis may increase due to concomitant use of Topiramate or other carbonic anhydrase inhibitors (e.g., zonisamide, acetazolamide or dichlorphenamide) with metformin. These drugs frequently cause a decrease in serum bicarbonate and induce non-anion gap, hyperchloremic metabolic acidosis. |
| Intervention: | more frequent monitoring of these patients. |
| Drugs that Reduce Metformin Clearance | |
| Clinical Impact: | The risk of lactic acidosis may increase due to concomitant use of drugs that interfere with common renal tubular transport systems involved in the renal elimination of metformin (e.g., organic cationic transporter-2 [OCT2] / multidrug and toxin extrusion [MATE] inhibitors such as ranolazine, vandetanib, dolutegravir, and cimetidine) which increase systemic exposure to metformin |
| Intervention | Consider the benefits and risks of concomitant use. |
| Alcohol | |
| Clinical Impact: | Potentiate the effect of metformin on lactate metabolism. |
| Intervention: | Warn patients against excessive alcohol intake while receiving SEGLUROMET. |
| Insulin or Insulin Secretagogues | |
| Clinical Impact: | The risk of hypoglycemia is increased when ertugliflozin is used in combination with insulin or an insulin secretagogue. |
| Intervention: | A lower dose of insulin or insulin secretagogue may be required to minimize the risk of hypoglycemia when used in combination with SEGLUROMET. |
| Drugs that Affect Glycemic Control | |
| Clinical Impact: | Certain drugs tend to produce hyperglycemia and may lead to loss of glycemic control. These drugs include the thiazides and other diuretics, corticosteroids, phenothiazines, thyroid products, estrogens, oral contraceptives, phenytoin, nicotinic acid, sympathomimetics, calcium channel blocking drugs, and isoniazid. |
| Intervention: | When a patient is receiving SEGLUROMET along with such drugs, the patient should be closely observed to maintain adequate glycemic control. |
| Lithium | |
| Clinical Impact: | Concomitant use of an SGLT2 inhibitor with lithium may decrease serum lithium concentrations. |
| Intervention: | Monitor serum lithium concentration more frequently during SEGLUROMET initiation and dosage changes. |
| Positive Urine Glucose Test | |
| Clinical Impact: | SGLT2 inhibitors increase urinary glucose excretion and will lead to positive urine glucose tests. |
| Intervention: | Monitoring glycemic control with urine glucose tests is not recommended in patients taking SEGLUROMET. Use alternative methods to monitor glycemic control. |
| Interference with 1,5-anhydroglucitol (1,5-AG) Assay | |
| Clinical Impact: | Measurements of 1,5-AG are unreliable in assessing glycemic control in patients taking SGLT2 inhibitors. |
| Intervention: | Monitoring glycemic control with 1,5-AG assay is not recommended. Use alternative methods to monitor glycemic control. |
5.4 Volume Depletion
SEGLUROMET can cause intravascular volume contraction which may sometimes manifest as symptomatic hypotension or acute transient changes in creatinine [see Adverse Reactions (6.1)]. There have been postmarketing reports of acute kidney injury, some requiring hospitalization and dialysis, in patients with type 2 diabetes mellitus receiving SGLT2 inhibitors, including SEGLUROMET. Patients with impaired renal function (eGFR less than 60 mL/min/1.73 m2) [see Use in Specific Populations (8.6)], elderly patients, patients with low systolic blood pressure, or patients on loop diuretics may be at increased risk for volume depletion or hypotension. Before initiating SEGLUROMET in patients with one or more of these characteristics, assess volume status and renal function. In patients with volume depletion, correct this condition before initiating SEGLUROMET. Monitor for signs and symptoms of volume depletion, and renal function after initiating therapy.
8.6 Renal Impairment
A 26-week placebo-controlled study of 313 patients with Stage 3 Chronic Kidney Disease (eGFR ≥30 to less than 60 mL/min/1.73 m2) treated with ertugliflozin did not have improvement in glycemic control.
In the VERTIS CV study, there were 1370 patients (25%) with an eGFR ≥90 mL/min/1.73 m2, 2929 patients (53%) with an eGFR of ≥60 to less than 90 mL/min/1.73 m2, 879 patients (16%) with an eGFR of ≥45 to less than 60 mL/min/1.73 m2, and 299 patients (5%) with eGFR of 30 to <45 mL/min/1.73 m2 treated with ertugliflozin. Similar effects on glycemic control at Week 18 were observed in patients treated with ertugliflozin in each eGFR subgroup and also in the overall patient population.
SEGLUROMET is contraindicated in patients with severe renal impairment (eGFR less than 30 mL/min/1.73 m2), ESRD, or on dialysis [see Contraindications (4)].
No dosage adjustment is needed in patients with eGFR ≥45 mL/min/1.73 m2.
Metformin is substantially excreted by the kidney, and the risk of metformin accumulation and lactic acidosis increases with the degree of renal impairment.
2.2 Recommended Dosage
- Individualize the starting dosage of SEGLUROMET, ertugliflozin and metformin hydrochloride (HCI), based on the patient’s current regimen, while not exceeding the maximum recommended oral daily dosage of 15 mg ertugliflozin and 2,000 mg metformin HCl:
- In patients on metformin HCI, switch to SEGLUROMET tablets containing 2.5 mg ertugliflozin, with a similar total oral daily dosage of metformin HCl.
- In patients on ertugliflozin, switch to SEGLUROMET tablets containing 500 mg metformin HCl, with a similar total oral daily dosage of ertugliflozin.
- In patients already treated with ertugliflozin and metformin HCl, switch to SEGLUROMET tablets containing the same total oral daily dosage of ertugliflozin and a similar daily dosage of metformin HCI.
- Take SEGLUROMET orally twice daily with meals, with gradual dosage escalation for those initiating metformin HCl to reduce the gastrointestinal side effects due to metformin [see Adverse Reactions (6.1)].
- Dosing may be adjusted based on effectiveness and tolerability.
- Use of SEGLUROMET is not recommended in patients with an estimated glomerular filtration rate (eGFR) less than 45 mL/min/1.73 m2.
- Use of SEGLUROMET is contraindicated in patients with severe renal impairment (eGFR less than 30 mL/min/1.73 m2), end stage-renal disease (ESRD), or on dialysis [see Contraindications (4)].
8.7 Hepatic Impairment
Use of metformin in patients with hepatic impairment has been associated with some cases of lactic acidosis. SEGLUROMET is not recommended in patients with hepatic impairment [see Warnings and Precautions (5.1)].
1 Indications and Usage
SEGLUROMET® is indicated as an adjunct to diet and exercise to improve glycemic control in adults with type 2 diabetes mellitus.
Warning: Lactic Acidosis
Postmarketing cases of metformin-associated lactic acidosis have resulted in death, hypothermia, hypotension, and resistant bradyarrhythmias. The onset of metformin-associated lactic acidosis is often subtle, accompanied only by nonspecific symptoms such as malaise, myalgias, respiratory distress, somnolence, and abdominal pain. Metformin-associated lactic acidosis was characterized by elevated blood lactate levels (>5 mmol/Liter), anion gap acidosis (without evidence of ketonuria or ketonemia), an increased lactate/pyruvate ratio, and metformin plasma levels generally >5 mcg/mL [see Warnings and Precautions (5.1)].
Risk factors for metformin-associated lactic acidosis include renal impairment, concomitant use of certain drugs (e.g., carbonic anhydrase inhibitors such as topiramate), age 65 years old or greater, having a radiological study with contrast, surgery and other procedures, hypoxic states (e.g., acute congestive heart failure), excessive alcohol intake, and hepatic impairment.
Steps to reduce the risk of and manage metformin-associated lactic acidosis in these high risk groups are provided in the Full Prescribing Information [see Dosage and Administration (2.2), Contraindications (4), Warnings and Precautions (5.1), Drug Interactions (7), and Use in Specific Populations (8.6, 8.7)].
If metformin-associated lactic acidosis is suspected, immediately discontinue SEGLUROMET and institute general supportive measures in a hospital setting. Prompt hemodialysis is recommended [see Warnings and Precautions (5.1)].
5.3 Lower Limb Amputation
In a long-term cardiovascular outcomes study [see Clinical Studies (14.2)], in patients with type 2 diabetes mellitus and established cardiovascular disease, the occurrence of non-traumatic lower limb amputations was reported with event rates of 4.7, 5.7, and 6.0 events per 1,000 patient-years in the placebo, ertugliflozin 5 mg, and ertugliflozin 15 mg treatment arms, respectively.
Amputation of the toe and foot were most frequent (81 out of 109 patients with lower limb amputations). Some patients had multiple amputations, some involving both lower limbs.
Lower limb infections, gangrene, and diabetic foot ulcers were the most common precipitating medical events leading to the need for an amputation. Patients with amputations were more likely to be male, have higher A1C (%) at baseline, have a history of peripheral arterial disease, amputation or peripheral revascularization procedure, diabetic foot, and to have been taking diuretics or insulin.
Across seven ertugliflozin clinical trials, non-traumatic lower limb amputations were reported in 1 (0.1%) patient in the comparator group, 3 (0.2%) patients in the ertugliflozin 5 mg group, and 8 (0.5%) patients in the ertugliflozin 15 mg group.
Monitor patients receiving SEGLUROMET for signs and symptoms of infection (including osteomyelitis), new pain or tenderness, sores or ulcers involving the lower limbs, and discontinue SEGLUROMET if these complications occur.
5 Warnings and Precautions
- Lactic Acidosis: See boxed warning. (5.1)
- Diabetic Ketoacidosis in Patients with Type 1 Diabetes Mellitus and Other Ketoacidosis: Consider ketone monitoring in patients at risk for ketoacidosis, as indicated. Assess for ketoacidosis regardless of presenting blood glucose levels and discontinue SEGLUROMET if ketoacidosis is suspected. Monitor patients for resolution of ketoacidosis before restarting. (5.2)
- Lower Limb Amputation: Monitor patients for infections or ulcers of lower limbs, and discontinue if these occur. (5.3)
- Volume Depletion: May result in acute kidney injury. Before initiating, assess and correct volume status in patients with renal impairment, low systolic blood pressure, elderly patients, or patients on diuretics. Monitor for signs and symptoms during therapy. (5.4)
- Urosepsis and Pyelonephritis: Evaluate patients for signs and symptoms of urinary tract infections and treat promptly, if indicated. (5.5)
- Hypoglycemia: Consider a lower dose of insulin or insulin secretagogue to reduce risk of hypoglycemia when used in combination. (5.6)
- Necrotizing Fasciitis of the Perineum (Fournier's Gangrene): Serious, life-threatening cases have occurred in both females and males. Assess patients presenting with pain or tenderness, erythema, or swelling in the genital or perineal area, along with fever or malaise. If suspected, institute prompt treatment. (5.7)
- Genital Mycotic Infections: Monitor and treat if indicated. (5.8)
- Vitamin B12 Deficiency: Metformin may lower vitamin B12 levels. Measure hematological parameters annually. (5.9)
2 Dosage and Administration
- Assess renal function prior to initiation and as clinically indicated. (2.1)
- Correct volume depletion before initiation. (2.1)
- Individualize the starting dosage based on the patient's current regimen. (2.2)
- Maximum recommended dosage is 7.5 mg ertugliflozin/1,000 mg metformin orally twice daily. (2.2)
- Take orally twice daily with meals, with gradual dose escalation. (2.2)
- Do not use in patients with an estimated glomerular filtration rate (eGFR) below 30 mL/minute/1.73 m2.
- Use is not recommended in patients with an eGFR less than 45 mL/min/1.73 m2. (2.2)
- Use is contraindicated in patients with severe renal impairment (eGFR less than 30 mL/min/1.73 m2), end stage-renal disease (ESRD), or on dialysis. (2.2)
- SEGLUROMET may need to be discontinued at time of, or prior to, iodinated contrast imaging procedures. (2.3)
- Withhold SEGLUROMET for at least 4 days, if possible, prior to surgery or procedures associated with prolonged fasting. (2.4)
3 Dosage Forms and Strengths
- Tablets: ertugliflozin 2.5 mg and metformin HCl 500 mg, pink, oval, debossed with "2.5/500" on one side and plain on the other side.
- Tablets: ertugliflozin 2.5 mg and metformin HCl 1,000 mg, pink, oval, debossed with "2.5/1000" on one side and plain on the other side.
- Tablets: ertugliflozin 7.5 mg and metformin HCl 500 mg, red, oval, debossed with "7.5/500" on one side and plain on the other side.
- Tablets: ertugliflozin 7.5 mg and metformin HCl 1,000 mg, red, oval, debossed with "7.5/1000" on one side and plain on the other side.
6.2 Postmarketing Experience
Additional adverse reactions have been identified during post approval use of ertugliflozin, metformin HCl, both components of SEGLUROMET. Because these reactions are reported voluntarily from a population of uncertain size, it is generally not possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Ertugliflozin
- Infections: necrotizing fasciitis of the perineum (Fournier’s Gangrene)
- Skin and Subcutaneous Tissue Disorders: angioedema, rash
Metformin HCl
- Hepatobiliary Disorders: cholestatic, hepatocellular, and mixed hepatocellular liver injury
8 Use in Specific Populations
- Pregnancy: Advise females of the potential risk to a fetus, especially during the second and third trimesters. (8.1)
- Lactation: Breastfeeding not recommended. (8.2)
- Females and Males of Reproductive Potential: Advise premenopausal females of the potential for an unintended pregnancy. (8.3)
- Geriatrics: Higher incidence of adverse reactions related to reduced intravascular volume. (8.5)
- Renal impairment: Higher incidence of adverse reactions related to reduced intravascular volume and renal function. (8.6)
- Hepatic impairment : Avoid use in patients with hepatic impairment. (8.7)
5.8 Genital Mycotic Infections
Ertugliflozin increases the risk of genital mycotic infections. Patients who have a history of genital mycotic infections or who are uncircumcised are more likely to develop genital mycotic infections [see Adverse Reactions (6.1)]. Monitor and treat appropriately.
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
5.5 Urosepsis and Pyelonephritis
There have been postmarketing reports of serious urinary tract infections, including urosepsis and pyelonephritis, requiring hospitalization in patients receiving medicines containing SGLT2 inhibitors. Treatment with medicines containing SGLT2 inhibitors increases the risk for urinary tract infections. Evaluate patients for signs and symptoms of urinary tract infections and treat promptly, if indicated [see Adverse Reactions (6)].
17 Patient Counseling Information
Advise the patient to read the FDA-approved patient labeling (Medication Guide).
16 How Supplied/storage and Handling
SEGLUROMET (ertugliflozin and metformin hydrochloride) tablets are available as follows:
| Strength | Description | How Supplied | NDC |
|---|---|---|---|
| ertugliflozin 2.5 mg and metformin hydrochloride 500 mg tablets | pink, oval, debossed with “2.5/500” on one side and plain on the other side | unit-of-use bottles of 60 | 0006-5369-03 |
| unit-of-use bottles of 180 | 0006-5369-06 | ||
| ertugliflozin 2.5 mg and metformin hydrochloride 1,000 mg tablets | pink, oval, debossed with “2.5/1000” on one side and plain on the other side | unit-of-use bottles of 60 | 0006-5373-03 |
| unit-of-use bottles of 180 | 0006-5373-06 | ||
| ertugliflozin 7.5 mg and metformin hydrochloride 500 mg tablets | red, oval, debossed with “7.5/500” on one side and plain on the other side | unit-of-use bottles of 60 | 0006-5370-03 |
| unit-of-use bottles of 180 | 0006-5370-06 | ||
| ertugliflozin 7.5 mg and metformin hydrochloride 1,000 mg tablets | red, oval, debossed with “7.5/1000” on one side and plain on the other side | unit-of-use bottles of 60 | 0006-5374-03 |
| unit-of-use bottles of 180 | 0006-5374-06 |
2.1 Prior to Initiation of Segluromet
- Assess renal function before initiating SEGLUROMET and as clinically indicated [see Warnings and Precautions (5.2)].
- Assess volume status. In patients with volume depletion, correct this condition before initiating SEGLUROMET [see Warnings and Precautions (5.4) and Use in Specific Populations (8.5, 8.6)].
2.4 Temporary Interruption for Surgery
Withhold SEGLUROMET for at least 4 days, if possible, prior to surgery or procedures associated with prolonged fasting. Resume SEGLUROMET when the patient is clinically stable and has resumed oral intake [see Warnings and Precautions (5.2) and Clinical Pharmacology (12.2)].
8.3 Females and Males of Reproductive Potential
Discuss the potential for unintended pregnancy with premenopausal women as therapy with metformin may result in ovulation in some anovulatory women.
Principal Display Panel 2.5 Mg/500 Mg Tablet Bottle Label
NDC 0006-5369-03
Segluromet®
(ertugliflozin and
metformin HCl) tablets
2.5 mg / 500 mg
Dispense the accompanying Medication Guide
to each patient.
Each tablet contains 3.24 mg ertugliflozin L-pyroglutamic
acid (equivalent to 2.5 mg ertugliflozin) and
500 mg of metformin hydrochloride.
Rx only
60 Tablets
Principal Display Panel 7.5 Mg/500 Mg Tablet Bottle Label
NDC 0006-5370-03
Segluromet®
(ertugliflozin and
metformin HCl) tablets
7.5 mg / 500 mg
Dispense the accompanying Medication Guide
to each patient.
Each tablet contains 9.71 mg ertugliflozin L-pyroglutamic
acid (equivalent to 7.5 mg ertugliflozin)
and 500 mg of metformin
hydrochloride.
Rx only
60 Tablets
2.3 Discontinuation for Iodinated Contrast Imaging Procedures
Discontinue SEGLUROMET at the time of, or prior to, an iodinated contrast imaging procedure in patients with an eGFR less than 60 mL/min/1.73 m2; in patients with a history of liver disease, alcoholism or heart failure; or in patients who will be administered intra-arterial iodinated contrast. Re-evaluate eGFR 48 hours after the imaging procedure; restart SEGLUROMET if renal function is stable [see Warnings and Precautions (5.1)].
Principal Display Panel 2.5 Mg/1,000 Mg Tablet Bottle Label
NDC 0006-5373-03
Segluromet®
(ertugliflozin and
metformin HCl) tablets
2.5 mg / 1,000 mg
Dispense the accompanying Medication Guide
to each patient.
Each tablet contains 3.24 mg ertugliflozin
L-pyroglutamic acid (equivalent
to 2.5 mg ertugliflozin) and
1,000 mg of metformin
hydrochloride.
60 Tablets
Rx only
Principal Display Panel 7.5 Mg/1,000 Mg Tablet Bottle Label
NDC 0006-5374-03
Segluromet®
(ertugliflozin and
metformin HCl) tablets
7.5 mg / 1,000 mg
Dispense the accompanying Medication Guide
to each patient.
Each tablet contains 9.71 mg ertugliflozin L-pyroglutamic
acid (equivalent to 7.5 mg
ertugliflozin) and 1,000 mg
of metformin hydrochloride.
Rx only
60 Tablets
5.7 Necrotizing Fasciitis of the Perineum (fournier's Gangrene)
Reports of necrotizing fasciitis of the perineum (Fournier’s Gangrene), a rare but serious and life-threatening necrotizing infection requiring urgent surgical intervention, have been identified in postmarketing surveillance in patients with diabetes mellitus receiving SGLT2 inhibitors, including ertugliflozin. Cases have been reported in females and males. Serious outcomes have included hospitalization, multiple surgeries, and death.
Patients treated with SEGLUROMET presenting with pain or tenderness, erythema, or swelling in the genital or perineal area, along with fever or malaise, should be assessed for necrotizing fasciitis. If suspected, start treatment immediately with broad-spectrum antibiotics and, if necessary, surgical debridement. Discontinue SEGLUROMET, closely monitor blood glucose levels, and provide appropriate alternative therapy for glycemic control.
14.1 Glycemic Control Trials in Patients With Type 2 Diabetes Mellitus
The efficacy and safety of ertugliflozin in combination with metformin HCl have been studied in 4 multicenter, randomized, double-blind, placebo- and active comparator-controlled, clinical studies involving 3,643 patients with type 2 diabetes mellitus. These studies included White, Hispanic or Latino, Black or African American, Asian, and other racial and ethnic groups, and patients with an age range of 21 to 86 years.
In VERTIS CV, ertugliflozin has been studied as add on to insulin (with or without metformin HCl) and as add on to metformin HCl plus a sulfonylurea in substudies.
In patients with type 2 diabetes mellitus, treatment with ertugliflozin in combination with metformin HCl reduced hemoglobin A1c (HbA1c) compared to placebo.
In patients with type 2 diabetes mellitus treated with ertugliflozin in combination with metformin HCl, the reduction in HbA1c was generally similar across subgroups defined by age, sex, race, geographic region, baseline body mass index (BMI), and duration of type 2 diabetes mellitus.
Ertugliflozin as Add-on Combination Therapy with Metformin HCl
A total of 621 patients with type 2 diabetes mellitus inadequately controlled (HbA1c between 7% and 10.5%) on metformin HCl monotherapy (≥1,500 mg/day for ≥8 weeks) participated in a randomized, double-blind, multi-center, 26-week, placebo-controlled study (NCT02033889) to evaluate the efficacy and safety of ertugliflozin in combination with metformin HCl. Patients entered a 2-week, single-blind, placebo run-in, and were randomized to placebo, ertugliflozin 5 mg, or ertugliflozin 15 mg administered orally once daily in addition to continuation of background metformin HCl therapy.
At Week 26, statistically significant reductions in HbA1c were observed in the ertugliflozin 5 mg and 15 mg groups compared to placebo. Ertugliflozin also resulted in a greater proportion of patients achieving an HbA1c <7% compared to placebo (see Table 6 and Figure 3).
| Placebo | Ertugliflozin 5 mg | Ertugliflozin 15 mg | |
|---|---|---|---|
| HbA1c (%) | N = 207 | N = 205 | N = 201 |
| Baseline (mean) | 8.2 | 8.1 | 8.1 |
| Change from baseline (LS mean Intent-to-treat analysis using ANCOVA adjusted for baseline value, prior antihyperglycemic medication, menopausal status and baseline eGFR. ) |
-0.2 | -0.7 | -0.9 |
| Difference from placebo (LS mean, 95% CI) | -0.5 p<0.001 compared to placebo. (-0.7, -0.4) |
-0.7 (-0.9, -0.5) | |
| Patients [N (%)] with HbA1c <7% | 38 (18.4) | 74 (36.3) | 87 (43.3) |
| FPG (mg/dL) | N = 202 | N = 199 | N = 201 |
| Baseline (mean) | 169.1 | 168.1 | 167.9 |
| Change from baseline (LS mean) | -8.7 | -30.3 | -40.9 |
| Difference from placebo (LS mean, 95% CI) | -21.6 (-27.8, -15.5) | -32.3 (-38.5, -26.0) |
The mean baseline body weight was 84.5 kg, 84.9 kg, and 85.3 kg in the placebo, ertugliflozin 5 mg, and ertugliflozin 15 mg groups, respectively. The mean changes from baseline to Week 26 were -1.4 kg, -3.2 kg, and -3.0 kg in the placebo, ertugliflozin 5 mg, and ertugliflozin 15 mg groups, respectively. The difference from placebo (95% CI) for ertugliflozin 5 mg was -1.8 kg (-2.4, -1.2) and for ertugliflozin 15 mg was -1.7 kg (-2.2, -1.1).
The mean baseline systolic blood pressure was 129.3 mmHg, 130.5 mmHg, and 130.2 mmHg in the placebo, ertugliflozin 5 mg, and ertugliflozin 15 mg groups, respectively. The mean changes from baseline to Week 26 were -1.8 mmHg, -5.1 mmHg, and -5.7 mmHg in the placebo, ertugliflozin 5 mg, and ertugliflozin 15 mg groups, respectively. The difference from placebo (95% CI) for ertugliflozin 5 mg was -3.3 mmHg (-5.6, -1.1) and for ertugliflozin 15 mg was -3.8 mmHg (-6.1, -1.5).
|
Figure 3: HbA1c (%) Change over Time in a 26-Week Placebo-Controlled Study for Ertugliflozin Used in Combination with Metformin HCl in Patients with Type 2 Diabetes Mellitus Data to the left of the vertical line are observed means (non-model-based) excluding values occurring post glycemic rescue. Data to the right of the vertical line represent the final Week 26 data, including all values regardless of use of glycemic rescue medication and use of study drug, with missing Week 26 values imputed using multiple imputation (26-MI) with a mean equal to the baseline value of the patient (see Table 6).
|
In Combination with Sitagliptin versus Ertugliflozin Alone and Sitagliptin Alone, as Add-on to Metformin HCl
A total of 1,233 patients with type 2 diabetes mellitus with inadequate glycemic control (HbA1c between 7.5% and 11%) on metformin HCl monotherapy (≥1,500 mg/day for ≥8 weeks) participated in a randomized, double-blind, 26-week, active controlled study (NCT02099110) to evaluate the efficacy and safety of ertugliflozin 5 mg or 15 mg administered orally in combination with sitagliptin 100 mg compared to the individual components. Patients were randomized to one of five treatment arms: ertugliflozin 5 mg, ertugliflozin 15 mg, sitagliptin 100 mg, ertugliflozin 5 mg + sitagliptin 100 mg, or ertugliflozin 15 mg + sitagliptin 100 mg.
At Week 26, ertugliflozin 5 mg or 15 mg + sitagliptin 100 mg provided statistically significantly greater reductions in HbA1c compared to ertugliflozin (5 mg or 15 mg) alone or sitagliptin 100 mg alone. The mean change from baseline in HbA1c was -1.4% for ertugliflozin 5 mg or 15 mg + sitagliptin 100 mg versus -1.0%, for ertugliflozin 5 mg, ertugliflozin 15 mg, or sitagliptin 100 mg, respectively. More patients receiving ertugliflozin 5 mg or 15 mg + sitagliptin 100 mg achieved an HbA1c <7% (53.3% and 50.9%, for ertugliflozin 5 mg or 15 mg, respectively, + sitagliptin 100 mg) compared to the individual components (29.3%, 33.7%, and 38.5% for ertugliflozin 5 mg, ertugliflozin 15 mg, or sitagliptin 100 mg, respectively).
Ertugliflozin as Add-on Combination Therapy with Metformin HCl and Sitagliptin
A total of 463 patients with type 2 diabetes mellitus inadequately controlled (HbA1c between 7% and 10.5%) on metformin HCl (≥1,500 mg/day for ≥8 weeks) and sitagliptin 100 mg orally once daily participated in a randomized, double-blind, multi-center, 26-week, placebo-controlled study (NCT02036515) to evaluate the efficacy and safety of ertugliflozin. Patients entered a 2-week, single-blind, placebo run-in period and were randomized to placebo, ertugliflozin 5 mg, or ertugliflozin 15 mg.
At Week 26, treatment with ertugliflozin at 5 mg or 15 mg daily provided statistically significant reductions in HbA1c. Ertugliflozin also resulted in a higher proportion of patients achieving an HbA1c <7% compared to placebo (see Table 7).
| Placebo | Ertugliflozin 5 mg | Ertugliflozin 15 mg | |
|---|---|---|---|
| HbA1c (%) | N = 152 | N = 155 | N = 152 |
| Baseline (mean) | 8.0 | 8.1 | 8.0 |
| Change from baseline (LS mean Intent-to-treat analysis using ANCOVA adjusted for baseline value, prior antihyperglycemic medication and baseline eGFR. ) |
-0.2 | -0.7 | -0.8 |
| Difference from placebo (LS mean, 95% CI) | -0.5 p<0.001 compared to placebo. (-0.7, -0.3) |
-0.6 (-0.8, -0.4) | |
| Patients [N (%)] with HbA1c <7% | 31 (20.2) | 54 (34.6) | 64 (42.3) |
| FPG (mg/dL) | N = 152 | N = 156 | N = 152 |
| Baseline (mean) | 169.6 | 167.7 | 171.7 |
| Change from baseline (LS mean) | -6.5 | -25.7 | -32.1 |
| Difference from placebo (LS mean, 95% CI) | -19.2 (-26.8, -11.6) | -25.6 (-33.2, -18.0) |
The mean baseline body weight was 86.5 kg, 87.6 kg, and 86.6 kg in the placebo, ertugliflozin 5 mg, and ertugliflozin 15 mg groups, respectively. The mean changes from baseline to Week 26 were -1.0 kg, -3.0 kg, and -2.8 kg in the placebo, ertugliflozin 5 mg, and ertugliflozin 15 mg groups, respectively. The difference from placebo (95% CI) for ertugliflozin 5 mg was -1.9 kg (-2.6, -1.3) and for ertugliflozin 15 mg was -1.8 kg (-2.4, -1.2).
The mean baseline systolic blood pressure was 130.2 mmHg, 132.1 mmHg, and 131.6 mmHg in the placebo, ertugliflozin 5 mg, and ertugliflozin 15 mg groups, respectively. The mean changes from baseline to Week 26 were -0.2 mmHg, -3.8 mmHg, and -4.5 mmHg in the placebo, ertugliflozin 5 mg, and ertugliflozin 15 mg groups, respectively. The difference from placebo (95% CI) for ertugliflozin 5 mg was -3.7 mmHg (-6.1, -1.2) and for ertugliflozin 15 mg was -4.3 mmHg (-6.7, -1.9).
Active Controlled Study of Ertugliflozin Versus Glimepiride as Add-on Combination Therapy with Metformin HCl
A total of 1,326 patients with type 2 diabetes mellitus inadequately controlled (HbA1c between 7% and 9%) on metformin HCl monotherapy participated in a randomized, double-blind, multi-center, 52-week, active comparator-controlled study (NCT01999218) to evaluate the efficacy and safety of ertugliflozin in combination with metformin HCl. These patients, who were receiving metformin HCl monotherapy (≥1,500 mg/day for ≥8 weeks), entered a 2-week, single-blind, placebo run-in period and were randomized to glimepiride, ertugliflozin 5 mg, or ertugliflozin 15 mg, administered orally once daily in addition to continuation of background metformin HCl therapy. Glimepiride was initiated at 1 mg/day and titrated up to a maximum dose of 6 or 8 mg/day (depending on maximum approved dose in each country) or a maximum tolerated dose or down-titrated to avoid or manage hypoglycemia. The mean daily dose of glimepiride was 3.0 mg.
Ertugliflozin 15 mg was non-inferior to glimepiride after 52 weeks of treatment. (See Table 8.)
| Glimepiride | Ertugliflozin 5 mg | Ertugliflozin 15 mg | |
|---|---|---|---|
| HbA1c (%) | N = 437 | N = 447 | N = 440 |
| Baseline (mean) | 7.8 | 7.8 | 7.8 |
| Change from baseline (LS mean Intent-to-treat analysis using ANCOVA adjusted for baseline value, prior antihyperglycemic medication and baseline eGFR. ) |
-0.6 | -0.5 | -0.5 |
| Difference from glimepiride (LS mean, 95% CI) | 0.2 Non-inferiority is declared when the upper bound of the two-sided 95% confidence interval (CI) for the mean difference is less than 0.3%. (0.0, 0.3) |
0.1 (-0.0, 0.2) | |
| Patients [N (%)] with HbA1c <7% | 208 (47.7) | 177 (39.5) | 186 (42.2) |
The mean baseline body weight was 86.8 kg, 87.9 kg, and 85.6 kg in the glimepiride, ertugliflozin 5 mg, and ertugliflozin 15 mg groups, respectively. The mean changes from baseline to Week 52 were 0.6 kg, -2.6 kg, and -3.0 kg in the glimepiride, ertugliflozin 5 mg, and ertugliflozin 15 mg groups, respectively. The difference from glimepiride (95% CI) for ertugliflozin 5 mg was -3.2 kg (-3.7, -2.7) and for ertugliflozin 15 mg was -3.6 kg (-4.1, -3.1).
Ertugliflozin as Add-on Combination Therapy with Insulin (With or Without Metformin HCl)
In an 18-week randomized, double-blind, multi-center, placebo-controlled, glycemic sub-study of VERTIS CV (NCT01986881, study details see 14.2), a total of 1,065 patients with type 2 diabetes mellitus and established atherosclerotic cardiovascular disease with inadequate glycemic control (HbA1c between 7% and 10.5%) on background therapy of insulin ≥20 units/day (59% also on metformin HCl ≥1,500 mg/day) were randomized to placebo, ertugliflozin 5 mg or ertugliflozin 15 mg oral once daily treatment.
At Week 18, treatment with ertugliflozin at 5 mg or 15 mg daily provided statistically significant reductions in HbA1c compared to placebo (see Table 9).
| Placebo | Ertugliflozin 5 mg | Ertugliflozin 15 mg | |
|---|---|---|---|
| SE: standard error. | |||
| HbA1c (%) | N = 346 | N = 346 | N = 367 |
| Baseline (mean) | 8.4 | 8.4 | 8.4 |
| Change from baseline (LS mean Intent-to-treat analysis using ANCOVA adjusted for baseline value, insulin stratum, and baseline eGFR. , SE) |
-0.2 (0.05) | -0.7 (0.05) | -0.7 (0.05) |
| Difference from placebo (LS mean, 95% CI) | -0.5 p<0.001 compared to placebo. (-0.6, -0.4) |
-0.5 (-0.7, -0.4) | |
|
Patients [N (%)] with HbA1c <7%
Missing values imputed as not meeting the <7% criterion.
|
37 (10.7) | 79 (22.8) | 81 (22.1) |
| FPG (mg/dL) | N = 343 | N = 346 | N = 368 |
| Baseline (mean) | 167.4 | 173.8 | 175.4 |
| Change from baseline (LS mean, SE) | -6.3 (2.91) | -25.6 (2.90) | -29.8 (2.86) |
| Difference from placebo (LS mean, 95% CI) | -19.2 (-26.8, -11.6) | -23.4 (-30.9, -16.0) |
The mean baseline body weights were 93.3 kg, 93.8 kg, and 92.1 kg in the placebo, ertugliflozin 5 mg, and ertugliflozin 15 mg groups, respectively. The mean changes from baseline to Week 18 were -0.2 kg, - 1.6 kg, and -1.9 kg in the placebo, ertugliflozin 5 mg, and ertugliflozin 15 mg groups, respectively. The differences from placebo (95% CI) for ertugliflozin 5 mg were - 1.4 kg (- 1.9, - 0.9) and for ertugliflozin 15 mg was -1.6 kg (-2.1, -1.1).
The mean baseline systolic blood pressures were 134.0 mmHg, 135.6 mmHg, and 133.7 mmHg in the placebo, ertugliflozin 5 mg, and ertugliflozin 15 mg groups, respectively. The mean changes from baseline to Week 18 were 0.7 mmHg, -2.2 mmHg, and -1.7 mmHg in the placebo, ertugliflozin 5 mg, and ertugliflozin 15 mg groups, respectively. The differences from placebo (95% CI) for ertugliflozin 5 mg was – 2.9 mmHg (-4.9, -1.0) and for ertugliflozin 15 mg were -2.5 mmHg (- 4.4, - 0.5).
Add-on Combination Therapy with Metformin HCl and Sulfonylurea
In an 18-week randomized, double-blind, multi-center, placebo-controlled, glycemic sub-study of VERTIS CV (NCT01986881, study details see 14.2), a total of 330 patients with type 2 diabetes mellitus and established atherosclerotic cardiovascular disease with inadequate glycemic control (HbA1c between 7% and 10.5%) with background therapy of metformin HCl ≥1,500 mg/day and a sulfonylurea (SU) were randomized to placebo, ertugliflozin 5 mg or ertugliflozin 15 mg oral once daily treatment.
At Week 18, treatment with ertugliflozin at 5 mg or 15 mg daily provided statistically significant reductions in HbA1c compared to placebo (see Table 10).
| Placebo | Ertugliflozin 5 mg | Ertugliflozin 15 mg | |
|---|---|---|---|
| SE: standard error | |||
| HbA1c (%) | N = 116 | N = 99 | N = 113 |
| Baseline (mean) | 8.3 | 8.4 | 8.3 |
| Change from baseline (LS mean Intent-to-treat analysis using ANCOVA adjusted for baseline value and baseline eGFR. , SE) |
-0.3 (0.08) | -0.8 (0.09) | -0.9 (0.08) |
| Difference from placebo (LS mean, 95% CI) | -0.6 p<0.001 compared to placebo. (-0.8, -0.3) |
-0.7 (-0.9, -0.4) | |
|
Patients [N (%)] with HbA1c <7% Missing values imputed as not meeting the <7% criterion.
|
17 (14.7) | 39 (39.4) | 38 (33.6) |
| FPG (mg/dL) | N = 117 | N = 99 | N = 113 |
| Baseline (mean) | 177.3 | 183.5 | 174.0 |
| Change from baseline (LS mean, SE) | -3.5 (3.65) | -31.3 (3.87) | -33.0 (3.67) |
| Difference from placebo (LS mean, 95% CI) | -27.9 (-37.8, -17.9) | -29.5 (-39.0, -19.9) |
The mean baseline body weights were 90.5 kg, 92.1 kg, and 92.9 kg in the placebo, ertugliflozin 5 mg, and ertugliflozin 15 mg groups, respectively. The mean changes from baseline to Week 18 were - 0.6 kg, -2.0 kg, and - 2.2 kg in the placebo, ertugliflozin 5 mg, and ertugliflozin 15 mg groups, respectively. The differences from placebo (95% CI) for ertugliflozin 5 mg were - 1.4 kg (- 2.2, - 0.7) and for ertugliflozin 15 mg was - 1.6 kg (- 2.3, - 0.9).
5.6 Hypoglycemia With Concomitant Use With Insulin Or Insulin Secretagogues
Insulin and insulin secretagogues (e.g., sulfonylurea) are known to cause hypoglycemia. SEGLUROMET may increase the risk of hypoglycemia when used in combination with insulin or an insulin secretagogue [see Adverse Reactions (6.1)]. The risk of hypoglycemia may be lowered by a reduction in the dose of insulin or sulfonylurea (or other concomitantly administered insulin secretagogues). Inform patients using these medications concomitantly of this risk and educate them on the signs and symptoms of hypoglycemia.
5.2 Diabetic Ketoacidosis in Patients With Type 1 Diabetes Mellitus and Other Ketoacidosis
In patients with type 1 diabetes mellitus, SEGLUROMET significantly increases the risk of diabetic ketoacidosis, a life-threatening event, beyond the background rate. In placebo-controlled trials of patients with type 1 diabetes mellitus, the risk of ketoacidosis was markedly increased in patients who received sodium glucose transporter 2 (SGLT2) inhibitors compared to patients who received placebo; this risk may be greater with higher doses. SEGLUROMET is not indicated for glycemic control in patients with type 1 diabetes mellitus.
Type 2 diabetes mellitus and pancreatic disorders (e.g., history of pancreatitis or pancreatic surgery) are also risk factors for ketoacidosis. There have been postmarketing reports of fatal events of ketoacidosis in patients with type 2 diabetes mellitus using SGLT2 inhibitors.
Precipitating conditions for diabetic ketoacidosis or other ketoacidosis include under-insulinization due to insulin dose reduction or missed insulin doses, acute febrile illness, reduced caloric intake, ketogenic diet, surgery, volume depletion, and alcohol abuse.
Signs and symptoms are consistent with dehydration and severe metabolic acidosis and include nausea, vomiting, abdominal pain, generalized malaise, and shortness of breath. Blood glucose levels at presentation may be below those typically expected for diabetic ketoacidosis (e.g., less than 250 mg/dL). Ketoacidosis and glucosuria may persist longer than typically expected. Urinary glucose excretion persists for 4 days after discontinuing SEGLUROMET [see Clinical Pharmacology (12.2)]; however, there have been postmarketing reports of ketoacidosis and/or glucosuria lasting greater than 6 days and some up to 2 weeks after discontinuation of SGLT2 inhibitors.
Consider ketone monitoring in patients at risk for ketoacidosis if indicated by the clinical situation. Assess for ketoacidosis regardless of presenting blood glucose levels in patients who present with signs and symptoms consistent with severe metabolic acidosis. If ketoacidosis is suspected, discontinue SEGLUROMET, promptly evaluate, and treat ketoacidosis, if confirmed. Monitor patients for resolution of ketoacidosis before restarting SEGLUROMET.
Withhold SEGLUROMET, if possible, in temporary clinical situations that could predispose patients to ketoacidosis. Resume SEGLUROMET when the patient is clinically stable and has resumed oral intake [see Dosage and Administration (2.4)].
Educate all patients on the signs and symptoms of ketoacidosis and instruct patients to discontinue SEGLUROMET and seek medical attention immediately if signs and symptoms occur.
14.2 Ertugliflozin Cardiovascular Outcomes in Patients With Type 2 Diabetes and Established Cardiovascular Disease
The effect of ertugliflozin on cardiovascular risk in adult patients with type 2 diabetes and established atherosclerotic cardiovascular disease was evaluated in the VERTIS CV study (NCT 01986881), a multicenter, multi-national, randomized, double-blind, placebo-controlled, event-driven trial. The study compared the risk of experiencing a major adverse cardiovascular event (MACE) between ertugliflozin and placebo when these were added to and used concomitantly with standard of care treatments for diabetes and atherosclerotic cardiovascular disease.
A total of 8,246 patients were randomized to placebo (N=2,747), oral once daily ertugliflozin 5 mg (N=2,752), or oral once daily ertugliflozin 15 mg (N=2,747) and followed for a median of 3 years. Approximately 88% of the study population was White, 6% Asian, and 3% Black or African American. The mean age was 64 years and approximately 70% were male.
All patients in the study had inadequately controlled type 2 diabetes mellitus at baseline (HbA1c greater than or equal to 7%). The mean duration of type 2 diabetes mellitus was 13 years, the mean HbA1c at baseline was 8.2% and the mean eGFR was 76 mL/min/1.73 m2. At baseline, patients were treated with one (32%) or more (67%) antidiabetic medications including biguanides (metformin HCl) (76%), insulin (47%), sulfonylureas (41%), DPP-4 inhibitors (11%) and GLP-1 receptor agonists (3%).
Almost all patients (99%) had established atherosclerotic cardiovascular disease at baseline including: a documented history of coronary artery disease (76%), cerebrovascular disease (23%) or peripheral artery disease (19%). Approximately 24% patients had a history of heart failure (HF). At baseline, the mean systolic blood pressure was 133 mmHg, the mean diastolic blood pressure was 77 mmHg, the mean LDL was 89 mg/dL, and the mean HDL was 44 mg/dL. At baseline, approximately 81% of patients were treated with renin angiotensin system inhibitors, 69% with beta-blockers, 43% with diuretics, 82% with statins, 4% ezetimibe, and 89% with antiplatelet agents.
The primary endpoint in VERTIS CV was the time to first occurrence of a Major Adverse Cardiac Event (MACE). A major adverse cardiovascular event was defined as occurrence of either a cardiovascular death or a nonfatal myocardial infarction (MI) or a nonfatal stroke. The statistical analysis plan pre-specified that the 5 and 15 mg doses would be combined for the analysis. A Cox proportional hazards model was used to test for non-inferiority against the pre-specified risk margin of 1.3 for the hazard ratio of MACE. Type-1 error was controlled across multiple tests using a hierarchical testing strategy.
The incidence rate of MACE was similar between the ertugliflozin-treated and placebo-treated patients. The estimated hazard ratio of MACE associated with ertugliflozin relative to placebo was 0.97 with 95.6% confidence interval (0.85, 1.11). The upper bound of this confidence interval excluded a risk larger than 1.3 (Table 11). Results for the 5 mg and 15 mg doses were consistent with results for the combined dose group.
| Endpoint MACE was evaluated in subjects who took at least one dose of study medication and, for subjects who discontinued study medication prior to the end of the study, censored events that occurred more than 365 days after the last dose of study medication. Other endpoints were evaluated using all randomized subjects and events that occurred any time after the first dose of study medication until the last contact date. The total number of first events was analyzed for each endpoint.
|
Placebo (N=2747) | ertugliflozin (N=5499) | Hazard Ratio vs Placebo (CI) HR and CI are based on Cox proportional hazards regression model, stratified by cohorts. For MACE a 95.6% CI is presented, for other endpoints a 95% CI is presented.
|
||
|---|---|---|---|---|---|
| N (%) | Event Rate (per 100 person-years) | N (%) | Event Rate (per 100 person-years) | ||
| N=Number of patients, CI=Confidence interval, CV=Cardiovascular, MI=Myocardial infarction. | |||||
| MACE (CV death, non-fatal MI, or non-fatal stroke) Composite | 327 (11.9) | 4.0 | 653 (11.9) | 3.9 | 0.97 (0.85, 1.11) |
| Components of Composite Endpoint | |||||
| Non-fatal MI | 148 (5.4) | 1.6 | 310 (5.6) | 1.7 | 1.04 (0.86, 1.27) |
| Non-fatal Stroke | 78 (2.8) | 0.8 | 157 (2.9) | 0.8 | 1.00 (0.76, 1.32) |
| CV death | 184 (6.7) | 1.9 | 341 (6.2) | 1.8 | 0.92 (0.77, 1.11) |
Structured Label Content
Section 42229-5 (42229-5)
Limitations of Use
Not recommended for use to improve glycemic control in patients with type 1 diabetes mellitus [see Warnings and Precautions (5.2)].
Section 42231-1 (42231-1)
| Medication Guide SEGLUROMET® [seg-LUR-oh-met] (ertugliflozin and metformin hydrochloride) tablets, for oral use |
|||
|---|---|---|---|
| This Medication Guide has been approved by the U.S. Food and Drug Administration. | Revised: 09/2023 | ||
| Read this Medication Guide carefully before you start taking SEGLUROMET and each time you get a refill. There may be new information. This information does not take the place of talking with your healthcare provider about your medical condition or your treatment. | |||
|
What is the most important information I should know about SEGLUROMET?
SEGLUROMET may cause serious side effects, including: Lactic Acidosis. Metformin, one of the medicines in SEGLUROMET, can cause a rare but serious condition called lactic acidosis (a buildup of an acid in the blood) that can cause death. Lactic acidosis is a medical emergency and must be treated in the hospital. Call your healthcare provider right away if you have any of the following symptoms, which could be signs of lactic acidosis: |
|||
|
|
||
Most people who have had lactic acidosis had other conditions that, in combination with metformin use, led to the lactic acidosis. Tell your healthcare provider if you have any of the following, because you have a higher chance for getting lactic acidosis with SEGLUROMET if you:
|
|||
|
|
||
| SEGLUROMET can have other serious side effects. See "What are the possible side effects of SEGLUROMET?" | |||
What is SEGLUROMET?
|
|||
|
Who should not take SEGLUROMET?
|
|||
Before you take SEGLUROMET, tell your healthcare provider about all of your medical conditions, including if you:
SEGLUROMET may affect the way other medicines work, and other medicines may affect how SEGLUROMET works. Know the medicines you take. Keep a list of them to show your healthcare provider and pharmacist when you get a new medicine. |
|||
How should I take SEGLUROMET?
|
|||
What should I avoid while taking SEGLUROMET?
|
|||
|
What are the possible side effects of SEGLUROMET? SEGLUROMET may cause serious side effects, including: See " What is the most important information I should know about SEGLUROMET? " |
|||
Call your healthcare provider right away if you have new pain or tenderness, any sores, ulcers, or infections in your leg or foot. Your healthcare provider may decide to stop your SEGLUROMET for a while if you have any of these signs or symptoms. Talk to your healthcare provider about proper foot care.
|
|||
|
|
|
|
|
|||
|
|
|
|
|
|||
|
|
||
Talk to your healthcare provider about what to do if you get symptoms of a yeast infection of the vagina or penis. Your healthcare provider may suggest you use an over-the-counter antifungal medicine. Talk to your healthcare provider right away if you use an over-the-counter antifungal medicine and your symptoms do not go away.
|
|||
|
|
|
|
| These are not all the possible side effects of SEGLUROMET. Call your healthcare provider for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. |
|||
How should I store SEGLUROMET?
|
|||
|
General information about the safe and effective use of SEGLUROMET.
Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not use SEGLUROMET for a condition for which it was not prescribed. Do not give SEGLUROMET to other people, even if they have the same symptoms that you have. It may harm them. You can ask your pharmacist or healthcare provider for information about SEGLUROMET that is written for health professionals. For more information about SEGLUROMET, go to www.segluromet.com or call 1-800-622-4477. |
|||
|
What are the ingredients in SEGLUROMET?
Active ingredients: ertugliflozin and metformin hydrochloride. Inactive ingredients: povidone, microcrystalline cellulose, crospovidone, sodium lauryl sulfate, and magnesium stearate. The tablet film coating contains the following inactive ingredients: hydroxypropyl methylcellulose, hydroxypropyl cellulose, titanium dioxide, iron oxide red, and carnauba wax. |
|||
| Manufactured for: Merck Sharp & Dohme LLC Rahway, NJ 07065, USA For patent information, go to: www.msd.com/research/patent Copyright © 2017-2023 Merck & Co., Inc., Rahway, NJ, USA, and its affiliates. All rights reserved. usmg-mk8835b-t-2309r007 |
Section 43683-2 (43683-2)
Section 44425-7 (44425-7)
Store at 20°C-25°C (68°F-77°F), excursions permitted between 15°C-30°C (between 59°F-86°F) [see USP Controlled Room Temperature]. Protect from moisture. Store in a dry place.
11 Description (11 DESCRIPTION)
SEGLUROMET (ertugliflozin and metformin hydrochloride) tablet for oral use contains ertugliflozin L-pyroglutamic acid, a SGLT2 inhibitor, and metformin HCl, a member of the biguanide class.
5.9 Vitamin B12
In metformin clinical trials of 29-week duration, a decrease to subnormal levels of previously normal serum vitamin B12 levels was observed in approximately 7% of patients. Such decrease, possibly due to interference with B12 absorption from the B12-intrinsic factor complex, may be associated with anemia but appears to be rapidly reversible with discontinuation of metformin or vitamin B12 supplementation. Certain individuals (those with inadequate vitamin B12 or calcium intake or absorption) appear to be predisposed to developing subnormal vitamin B12 levels. Measure hematologic parameters on an annual basis and vitamin B12 at 2 to 3 year intervals in patients on metformin and manage any abnormalities [see Adverse Reactions (6.1)].
8.4 Pediatric Use
Safety and effectiveness of SEGLUROMET in pediatric patients under 18 years of age have not been established.
4 Contraindications (4 CONTRAINDICATIONS)
SEGLUROMET is contraindicated in patients with:
- Hypersensitivity to ertugliflozin, metformin, or any excipient in SEGLUROMET. Reactions such as angioedema or anaphylaxis have occurred [see Adverse Reactions (6.2)].
- Severe renal impairment (eGFR less than 30 mL/min/1.73 m2), end stage-renal disease (ESRD), or on dialysis [see Use in Specific Populations (8.6)].
- Acute or chronic metabolic acidosis, including diabetic ketoacidosis, with or without coma.
5.1 Lactic Acidosis
There have been postmarketing cases of metformin-associated lactic acidosis, including fatal cases. These cases had a subtle onset and were accompanied by nonspecific symptoms such as malaise, myalgias, abdominal pain, respiratory distress, or increased somnolence; however, hypothermia, hypotension and resistant bradyarrhythmias have occurred with severe acidosis. Metformin-associated lactic acidosis was characterized by elevated blood lactate concentrations (>5 mmol/Liter), anion gap acidosis (without evidence of ketonuria or ketonemia), and an increased lactate: pyruvate ratio; metformin plasma levels were generally >5 mcg/mL. Metformin decreases liver uptake of lactate increasing lactate blood levels which may increase the risk of lactic acidosis, especially in patients at risk.
If metformin-associated lactic acidosis is suspected, general supportive measures should be instituted promptly in a hospital setting, along with immediate discontinuation of SEGLUROMET. In SEGLUROMET-treated patients with a diagnosis or strong suspicion of lactic acidosis, prompt hemodialysis is recommended to correct the acidosis and remove accumulated metformin (metformin hydrochloride is dialyzable, with a clearance of up to 170 mL/minute under good hemodynamic conditions). Hemodialysis has often resulted in reversal of symptoms and recovery.
Educate patients and their families about the symptoms of lactic acidosis and if these symptoms occur instruct them to discontinue SEGLUROMET and report these symptoms to their healthcare provider.
For each of the known and possible risk factors for metformin-associated lactic acidosis, recommendations to reduce the risk of and manage metformin-associated lactic acidosis are provided below:
6 Adverse Reactions (6 ADVERSE REACTIONS)
The following important adverse reactions are described elsewhere in the labeling:
- Lactic Acidosis [see Boxed Warning and Warnings and Precautions (5.1)]
- Diabetic Ketoacidosis in Patients with Type 1 Diabetes and Other Ketoacidosis [see Warnings and Precautions (5.2)]
- Lower Limb Amputation [see Warnings and Precautions (5.3)]
- Volume Depletion [see Warnings and Precautions (5.4)]
- Urosepsis and Pyelonephritis [see Warnings and Precautions (5.5)]
- Hypoglycemia with Concomitant Use with Insulin or Insulin Secretagogues [see Warnings and Precautions (5.6)]
- Necrotizing Fasciitis of the Perineum (Fournier's Gangrene) [see Warnings and Precautions (5.7)]
- Genital Mycotic Infections [see Warnings and Precautions (5.8)]
- Vitamin B12 Deficiency [see Warnings and Precautions (5.9)]
7 Drug Interactions (7 DRUG INTERACTIONS)
| Carbonic Anhydrase Inhibitors | |
|---|---|
| Clinical Impact: | The risk of lactic acidosis may increase due to concomitant use of Topiramate or other carbonic anhydrase inhibitors (e.g., zonisamide, acetazolamide or dichlorphenamide) with metformin. These drugs frequently cause a decrease in serum bicarbonate and induce non-anion gap, hyperchloremic metabolic acidosis. |
| Intervention: | more frequent monitoring of these patients. |
| Drugs that Reduce Metformin Clearance | |
| Clinical Impact: | The risk of lactic acidosis may increase due to concomitant use of drugs that interfere with common renal tubular transport systems involved in the renal elimination of metformin (e.g., organic cationic transporter-2 [OCT2] / multidrug and toxin extrusion [MATE] inhibitors such as ranolazine, vandetanib, dolutegravir, and cimetidine) which increase systemic exposure to metformin |
| Intervention | Consider the benefits and risks of concomitant use. |
| Alcohol | |
| Clinical Impact: | Potentiate the effect of metformin on lactate metabolism. |
| Intervention: | Warn patients against excessive alcohol intake while receiving SEGLUROMET. |
| Insulin or Insulin Secretagogues | |
| Clinical Impact: | The risk of hypoglycemia is increased when ertugliflozin is used in combination with insulin or an insulin secretagogue. |
| Intervention: | A lower dose of insulin or insulin secretagogue may be required to minimize the risk of hypoglycemia when used in combination with SEGLUROMET. |
| Drugs that Affect Glycemic Control | |
| Clinical Impact: | Certain drugs tend to produce hyperglycemia and may lead to loss of glycemic control. These drugs include the thiazides and other diuretics, corticosteroids, phenothiazines, thyroid products, estrogens, oral contraceptives, phenytoin, nicotinic acid, sympathomimetics, calcium channel blocking drugs, and isoniazid. |
| Intervention: | When a patient is receiving SEGLUROMET along with such drugs, the patient should be closely observed to maintain adequate glycemic control. |
| Lithium | |
| Clinical Impact: | Concomitant use of an SGLT2 inhibitor with lithium may decrease serum lithium concentrations. |
| Intervention: | Monitor serum lithium concentration more frequently during SEGLUROMET initiation and dosage changes. |
| Positive Urine Glucose Test | |
| Clinical Impact: | SGLT2 inhibitors increase urinary glucose excretion and will lead to positive urine glucose tests. |
| Intervention: | Monitoring glycemic control with urine glucose tests is not recommended in patients taking SEGLUROMET. Use alternative methods to monitor glycemic control. |
| Interference with 1,5-anhydroglucitol (1,5-AG) Assay | |
| Clinical Impact: | Measurements of 1,5-AG are unreliable in assessing glycemic control in patients taking SGLT2 inhibitors. |
| Intervention: | Monitoring glycemic control with 1,5-AG assay is not recommended. Use alternative methods to monitor glycemic control. |
5.4 Volume Depletion
SEGLUROMET can cause intravascular volume contraction which may sometimes manifest as symptomatic hypotension or acute transient changes in creatinine [see Adverse Reactions (6.1)]. There have been postmarketing reports of acute kidney injury, some requiring hospitalization and dialysis, in patients with type 2 diabetes mellitus receiving SGLT2 inhibitors, including SEGLUROMET. Patients with impaired renal function (eGFR less than 60 mL/min/1.73 m2) [see Use in Specific Populations (8.6)], elderly patients, patients with low systolic blood pressure, or patients on loop diuretics may be at increased risk for volume depletion or hypotension. Before initiating SEGLUROMET in patients with one or more of these characteristics, assess volume status and renal function. In patients with volume depletion, correct this condition before initiating SEGLUROMET. Monitor for signs and symptoms of volume depletion, and renal function after initiating therapy.
8.6 Renal Impairment
A 26-week placebo-controlled study of 313 patients with Stage 3 Chronic Kidney Disease (eGFR ≥30 to less than 60 mL/min/1.73 m2) treated with ertugliflozin did not have improvement in glycemic control.
In the VERTIS CV study, there were 1370 patients (25%) with an eGFR ≥90 mL/min/1.73 m2, 2929 patients (53%) with an eGFR of ≥60 to less than 90 mL/min/1.73 m2, 879 patients (16%) with an eGFR of ≥45 to less than 60 mL/min/1.73 m2, and 299 patients (5%) with eGFR of 30 to <45 mL/min/1.73 m2 treated with ertugliflozin. Similar effects on glycemic control at Week 18 were observed in patients treated with ertugliflozin in each eGFR subgroup and also in the overall patient population.
SEGLUROMET is contraindicated in patients with severe renal impairment (eGFR less than 30 mL/min/1.73 m2), ESRD, or on dialysis [see Contraindications (4)].
No dosage adjustment is needed in patients with eGFR ≥45 mL/min/1.73 m2.
Metformin is substantially excreted by the kidney, and the risk of metformin accumulation and lactic acidosis increases with the degree of renal impairment.
2.2 Recommended Dosage
- Individualize the starting dosage of SEGLUROMET, ertugliflozin and metformin hydrochloride (HCI), based on the patient’s current regimen, while not exceeding the maximum recommended oral daily dosage of 15 mg ertugliflozin and 2,000 mg metformin HCl:
- In patients on metformin HCI, switch to SEGLUROMET tablets containing 2.5 mg ertugliflozin, with a similar total oral daily dosage of metformin HCl.
- In patients on ertugliflozin, switch to SEGLUROMET tablets containing 500 mg metformin HCl, with a similar total oral daily dosage of ertugliflozin.
- In patients already treated with ertugliflozin and metformin HCl, switch to SEGLUROMET tablets containing the same total oral daily dosage of ertugliflozin and a similar daily dosage of metformin HCI.
- Take SEGLUROMET orally twice daily with meals, with gradual dosage escalation for those initiating metformin HCl to reduce the gastrointestinal side effects due to metformin [see Adverse Reactions (6.1)].
- Dosing may be adjusted based on effectiveness and tolerability.
- Use of SEGLUROMET is not recommended in patients with an estimated glomerular filtration rate (eGFR) less than 45 mL/min/1.73 m2.
- Use of SEGLUROMET is contraindicated in patients with severe renal impairment (eGFR less than 30 mL/min/1.73 m2), end stage-renal disease (ESRD), or on dialysis [see Contraindications (4)].
8.7 Hepatic Impairment
Use of metformin in patients with hepatic impairment has been associated with some cases of lactic acidosis. SEGLUROMET is not recommended in patients with hepatic impairment [see Warnings and Precautions (5.1)].
1 Indications and Usage (1 INDICATIONS AND USAGE)
SEGLUROMET® is indicated as an adjunct to diet and exercise to improve glycemic control in adults with type 2 diabetes mellitus.
Warning: Lactic Acidosis (WARNING: LACTIC ACIDOSIS)
Postmarketing cases of metformin-associated lactic acidosis have resulted in death, hypothermia, hypotension, and resistant bradyarrhythmias. The onset of metformin-associated lactic acidosis is often subtle, accompanied only by nonspecific symptoms such as malaise, myalgias, respiratory distress, somnolence, and abdominal pain. Metformin-associated lactic acidosis was characterized by elevated blood lactate levels (>5 mmol/Liter), anion gap acidosis (without evidence of ketonuria or ketonemia), an increased lactate/pyruvate ratio, and metformin plasma levels generally >5 mcg/mL [see Warnings and Precautions (5.1)].
Risk factors for metformin-associated lactic acidosis include renal impairment, concomitant use of certain drugs (e.g., carbonic anhydrase inhibitors such as topiramate), age 65 years old or greater, having a radiological study with contrast, surgery and other procedures, hypoxic states (e.g., acute congestive heart failure), excessive alcohol intake, and hepatic impairment.
Steps to reduce the risk of and manage metformin-associated lactic acidosis in these high risk groups are provided in the Full Prescribing Information [see Dosage and Administration (2.2), Contraindications (4), Warnings and Precautions (5.1), Drug Interactions (7), and Use in Specific Populations (8.6, 8.7)].
If metformin-associated lactic acidosis is suspected, immediately discontinue SEGLUROMET and institute general supportive measures in a hospital setting. Prompt hemodialysis is recommended [see Warnings and Precautions (5.1)].
5.3 Lower Limb Amputation
In a long-term cardiovascular outcomes study [see Clinical Studies (14.2)], in patients with type 2 diabetes mellitus and established cardiovascular disease, the occurrence of non-traumatic lower limb amputations was reported with event rates of 4.7, 5.7, and 6.0 events per 1,000 patient-years in the placebo, ertugliflozin 5 mg, and ertugliflozin 15 mg treatment arms, respectively.
Amputation of the toe and foot were most frequent (81 out of 109 patients with lower limb amputations). Some patients had multiple amputations, some involving both lower limbs.
Lower limb infections, gangrene, and diabetic foot ulcers were the most common precipitating medical events leading to the need for an amputation. Patients with amputations were more likely to be male, have higher A1C (%) at baseline, have a history of peripheral arterial disease, amputation or peripheral revascularization procedure, diabetic foot, and to have been taking diuretics or insulin.
Across seven ertugliflozin clinical trials, non-traumatic lower limb amputations were reported in 1 (0.1%) patient in the comparator group, 3 (0.2%) patients in the ertugliflozin 5 mg group, and 8 (0.5%) patients in the ertugliflozin 15 mg group.
Monitor patients receiving SEGLUROMET for signs and symptoms of infection (including osteomyelitis), new pain or tenderness, sores or ulcers involving the lower limbs, and discontinue SEGLUROMET if these complications occur.
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
- Lactic Acidosis: See boxed warning. (5.1)
- Diabetic Ketoacidosis in Patients with Type 1 Diabetes Mellitus and Other Ketoacidosis: Consider ketone monitoring in patients at risk for ketoacidosis, as indicated. Assess for ketoacidosis regardless of presenting blood glucose levels and discontinue SEGLUROMET if ketoacidosis is suspected. Monitor patients for resolution of ketoacidosis before restarting. (5.2)
- Lower Limb Amputation: Monitor patients for infections or ulcers of lower limbs, and discontinue if these occur. (5.3)
- Volume Depletion: May result in acute kidney injury. Before initiating, assess and correct volume status in patients with renal impairment, low systolic blood pressure, elderly patients, or patients on diuretics. Monitor for signs and symptoms during therapy. (5.4)
- Urosepsis and Pyelonephritis: Evaluate patients for signs and symptoms of urinary tract infections and treat promptly, if indicated. (5.5)
- Hypoglycemia: Consider a lower dose of insulin or insulin secretagogue to reduce risk of hypoglycemia when used in combination. (5.6)
- Necrotizing Fasciitis of the Perineum (Fournier's Gangrene): Serious, life-threatening cases have occurred in both females and males. Assess patients presenting with pain or tenderness, erythema, or swelling in the genital or perineal area, along with fever or malaise. If suspected, institute prompt treatment. (5.7)
- Genital Mycotic Infections: Monitor and treat if indicated. (5.8)
- Vitamin B12 Deficiency: Metformin may lower vitamin B12 levels. Measure hematological parameters annually. (5.9)
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
- Assess renal function prior to initiation and as clinically indicated. (2.1)
- Correct volume depletion before initiation. (2.1)
- Individualize the starting dosage based on the patient's current regimen. (2.2)
- Maximum recommended dosage is 7.5 mg ertugliflozin/1,000 mg metformin orally twice daily. (2.2)
- Take orally twice daily with meals, with gradual dose escalation. (2.2)
- Do not use in patients with an estimated glomerular filtration rate (eGFR) below 30 mL/minute/1.73 m2.
- Use is not recommended in patients with an eGFR less than 45 mL/min/1.73 m2. (2.2)
- Use is contraindicated in patients with severe renal impairment (eGFR less than 30 mL/min/1.73 m2), end stage-renal disease (ESRD), or on dialysis. (2.2)
- SEGLUROMET may need to be discontinued at time of, or prior to, iodinated contrast imaging procedures. (2.3)
- Withhold SEGLUROMET for at least 4 days, if possible, prior to surgery or procedures associated with prolonged fasting. (2.4)
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
- Tablets: ertugliflozin 2.5 mg and metformin HCl 500 mg, pink, oval, debossed with "2.5/500" on one side and plain on the other side.
- Tablets: ertugliflozin 2.5 mg and metformin HCl 1,000 mg, pink, oval, debossed with "2.5/1000" on one side and plain on the other side.
- Tablets: ertugliflozin 7.5 mg and metformin HCl 500 mg, red, oval, debossed with "7.5/500" on one side and plain on the other side.
- Tablets: ertugliflozin 7.5 mg and metformin HCl 1,000 mg, red, oval, debossed with "7.5/1000" on one side and plain on the other side.
6.2 Postmarketing Experience
Additional adverse reactions have been identified during post approval use of ertugliflozin, metformin HCl, both components of SEGLUROMET. Because these reactions are reported voluntarily from a population of uncertain size, it is generally not possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Ertugliflozin
- Infections: necrotizing fasciitis of the perineum (Fournier’s Gangrene)
- Skin and Subcutaneous Tissue Disorders: angioedema, rash
Metformin HCl
- Hepatobiliary Disorders: cholestatic, hepatocellular, and mixed hepatocellular liver injury
8 Use in Specific Populations (8 USE IN SPECIFIC POPULATIONS)
- Pregnancy: Advise females of the potential risk to a fetus, especially during the second and third trimesters. (8.1)
- Lactation: Breastfeeding not recommended. (8.2)
- Females and Males of Reproductive Potential: Advise premenopausal females of the potential for an unintended pregnancy. (8.3)
- Geriatrics: Higher incidence of adverse reactions related to reduced intravascular volume. (8.5)
- Renal impairment: Higher incidence of adverse reactions related to reduced intravascular volume and renal function. (8.6)
- Hepatic impairment : Avoid use in patients with hepatic impairment. (8.7)
5.8 Genital Mycotic Infections
Ertugliflozin increases the risk of genital mycotic infections. Patients who have a history of genital mycotic infections or who are uncircumcised are more likely to develop genital mycotic infections [see Adverse Reactions (6.1)]. Monitor and treat appropriately.
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
5.5 Urosepsis and Pyelonephritis
There have been postmarketing reports of serious urinary tract infections, including urosepsis and pyelonephritis, requiring hospitalization in patients receiving medicines containing SGLT2 inhibitors. Treatment with medicines containing SGLT2 inhibitors increases the risk for urinary tract infections. Evaluate patients for signs and symptoms of urinary tract infections and treat promptly, if indicated [see Adverse Reactions (6)].
17 Patient Counseling Information (17 PATIENT COUNSELING INFORMATION)
Advise the patient to read the FDA-approved patient labeling (Medication Guide).
16 How Supplied/storage and Handling (16 HOW SUPPLIED/STORAGE AND HANDLING)
SEGLUROMET (ertugliflozin and metformin hydrochloride) tablets are available as follows:
| Strength | Description | How Supplied | NDC |
|---|---|---|---|
| ertugliflozin 2.5 mg and metformin hydrochloride 500 mg tablets | pink, oval, debossed with “2.5/500” on one side and plain on the other side | unit-of-use bottles of 60 | 0006-5369-03 |
| unit-of-use bottles of 180 | 0006-5369-06 | ||
| ertugliflozin 2.5 mg and metformin hydrochloride 1,000 mg tablets | pink, oval, debossed with “2.5/1000” on one side and plain on the other side | unit-of-use bottles of 60 | 0006-5373-03 |
| unit-of-use bottles of 180 | 0006-5373-06 | ||
| ertugliflozin 7.5 mg and metformin hydrochloride 500 mg tablets | red, oval, debossed with “7.5/500” on one side and plain on the other side | unit-of-use bottles of 60 | 0006-5370-03 |
| unit-of-use bottles of 180 | 0006-5370-06 | ||
| ertugliflozin 7.5 mg and metformin hydrochloride 1,000 mg tablets | red, oval, debossed with “7.5/1000” on one side and plain on the other side | unit-of-use bottles of 60 | 0006-5374-03 |
| unit-of-use bottles of 180 | 0006-5374-06 |
2.1 Prior to Initiation of Segluromet (2.1 Prior to Initiation of SEGLUROMET)
- Assess renal function before initiating SEGLUROMET and as clinically indicated [see Warnings and Precautions (5.2)].
- Assess volume status. In patients with volume depletion, correct this condition before initiating SEGLUROMET [see Warnings and Precautions (5.4) and Use in Specific Populations (8.5, 8.6)].
2.4 Temporary Interruption for Surgery
Withhold SEGLUROMET for at least 4 days, if possible, prior to surgery or procedures associated with prolonged fasting. Resume SEGLUROMET when the patient is clinically stable and has resumed oral intake [see Warnings and Precautions (5.2) and Clinical Pharmacology (12.2)].
8.3 Females and Males of Reproductive Potential
Discuss the potential for unintended pregnancy with premenopausal women as therapy with metformin may result in ovulation in some anovulatory women.
Principal Display Panel 2.5 Mg/500 Mg Tablet Bottle Label (PRINCIPAL DISPLAY PANEL - 2.5 mg/500 mg Tablet Bottle Label)
NDC 0006-5369-03
Segluromet®
(ertugliflozin and
metformin HCl) tablets
2.5 mg / 500 mg
Dispense the accompanying Medication Guide
to each patient.
Each tablet contains 3.24 mg ertugliflozin L-pyroglutamic
acid (equivalent to 2.5 mg ertugliflozin) and
500 mg of metformin hydrochloride.
Rx only
60 Tablets
Principal Display Panel 7.5 Mg/500 Mg Tablet Bottle Label (PRINCIPAL DISPLAY PANEL - 7.5 mg/500 mg Tablet Bottle Label)
NDC 0006-5370-03
Segluromet®
(ertugliflozin and
metformin HCl) tablets
7.5 mg / 500 mg
Dispense the accompanying Medication Guide
to each patient.
Each tablet contains 9.71 mg ertugliflozin L-pyroglutamic
acid (equivalent to 7.5 mg ertugliflozin)
and 500 mg of metformin
hydrochloride.
Rx only
60 Tablets
2.3 Discontinuation for Iodinated Contrast Imaging Procedures
Discontinue SEGLUROMET at the time of, or prior to, an iodinated contrast imaging procedure in patients with an eGFR less than 60 mL/min/1.73 m2; in patients with a history of liver disease, alcoholism or heart failure; or in patients who will be administered intra-arterial iodinated contrast. Re-evaluate eGFR 48 hours after the imaging procedure; restart SEGLUROMET if renal function is stable [see Warnings and Precautions (5.1)].
Principal Display Panel 2.5 Mg/1,000 Mg Tablet Bottle Label (PRINCIPAL DISPLAY PANEL - 2.5 mg/1,000 mg Tablet Bottle Label)
NDC 0006-5373-03
Segluromet®
(ertugliflozin and
metformin HCl) tablets
2.5 mg / 1,000 mg
Dispense the accompanying Medication Guide
to each patient.
Each tablet contains 3.24 mg ertugliflozin
L-pyroglutamic acid (equivalent
to 2.5 mg ertugliflozin) and
1,000 mg of metformin
hydrochloride.
60 Tablets
Rx only
Principal Display Panel 7.5 Mg/1,000 Mg Tablet Bottle Label (PRINCIPAL DISPLAY PANEL - 7.5 mg/1,000 mg Tablet Bottle Label)
NDC 0006-5374-03
Segluromet®
(ertugliflozin and
metformin HCl) tablets
7.5 mg / 1,000 mg
Dispense the accompanying Medication Guide
to each patient.
Each tablet contains 9.71 mg ertugliflozin L-pyroglutamic
acid (equivalent to 7.5 mg
ertugliflozin) and 1,000 mg
of metformin hydrochloride.
Rx only
60 Tablets
5.7 Necrotizing Fasciitis of the Perineum (fournier's Gangrene) (5.7 Necrotizing Fasciitis of the Perineum (Fournier's Gangrene))
Reports of necrotizing fasciitis of the perineum (Fournier’s Gangrene), a rare but serious and life-threatening necrotizing infection requiring urgent surgical intervention, have been identified in postmarketing surveillance in patients with diabetes mellitus receiving SGLT2 inhibitors, including ertugliflozin. Cases have been reported in females and males. Serious outcomes have included hospitalization, multiple surgeries, and death.
Patients treated with SEGLUROMET presenting with pain or tenderness, erythema, or swelling in the genital or perineal area, along with fever or malaise, should be assessed for necrotizing fasciitis. If suspected, start treatment immediately with broad-spectrum antibiotics and, if necessary, surgical debridement. Discontinue SEGLUROMET, closely monitor blood glucose levels, and provide appropriate alternative therapy for glycemic control.
14.1 Glycemic Control Trials in Patients With Type 2 Diabetes Mellitus (14.1 Glycemic Control Trials in Patients with Type 2 Diabetes Mellitus)
The efficacy and safety of ertugliflozin in combination with metformin HCl have been studied in 4 multicenter, randomized, double-blind, placebo- and active comparator-controlled, clinical studies involving 3,643 patients with type 2 diabetes mellitus. These studies included White, Hispanic or Latino, Black or African American, Asian, and other racial and ethnic groups, and patients with an age range of 21 to 86 years.
In VERTIS CV, ertugliflozin has been studied as add on to insulin (with or without metformin HCl) and as add on to metformin HCl plus a sulfonylurea in substudies.
In patients with type 2 diabetes mellitus, treatment with ertugliflozin in combination with metformin HCl reduced hemoglobin A1c (HbA1c) compared to placebo.
In patients with type 2 diabetes mellitus treated with ertugliflozin in combination with metformin HCl, the reduction in HbA1c was generally similar across subgroups defined by age, sex, race, geographic region, baseline body mass index (BMI), and duration of type 2 diabetes mellitus.
Ertugliflozin as Add-on Combination Therapy with Metformin HCl
A total of 621 patients with type 2 diabetes mellitus inadequately controlled (HbA1c between 7% and 10.5%) on metformin HCl monotherapy (≥1,500 mg/day for ≥8 weeks) participated in a randomized, double-blind, multi-center, 26-week, placebo-controlled study (NCT02033889) to evaluate the efficacy and safety of ertugliflozin in combination with metformin HCl. Patients entered a 2-week, single-blind, placebo run-in, and were randomized to placebo, ertugliflozin 5 mg, or ertugliflozin 15 mg administered orally once daily in addition to continuation of background metformin HCl therapy.
At Week 26, statistically significant reductions in HbA1c were observed in the ertugliflozin 5 mg and 15 mg groups compared to placebo. Ertugliflozin also resulted in a greater proportion of patients achieving an HbA1c <7% compared to placebo (see Table 6 and Figure 3).
| Placebo | Ertugliflozin 5 mg | Ertugliflozin 15 mg | |
|---|---|---|---|
| HbA1c (%) | N = 207 | N = 205 | N = 201 |
| Baseline (mean) | 8.2 | 8.1 | 8.1 |
| Change from baseline (LS mean Intent-to-treat analysis using ANCOVA adjusted for baseline value, prior antihyperglycemic medication, menopausal status and baseline eGFR. ) |
-0.2 | -0.7 | -0.9 |
| Difference from placebo (LS mean, 95% CI) | -0.5 p<0.001 compared to placebo. (-0.7, -0.4) |
-0.7 (-0.9, -0.5) | |
| Patients [N (%)] with HbA1c <7% | 38 (18.4) | 74 (36.3) | 87 (43.3) |
| FPG (mg/dL) | N = 202 | N = 199 | N = 201 |
| Baseline (mean) | 169.1 | 168.1 | 167.9 |
| Change from baseline (LS mean) | -8.7 | -30.3 | -40.9 |
| Difference from placebo (LS mean, 95% CI) | -21.6 (-27.8, -15.5) | -32.3 (-38.5, -26.0) |
The mean baseline body weight was 84.5 kg, 84.9 kg, and 85.3 kg in the placebo, ertugliflozin 5 mg, and ertugliflozin 15 mg groups, respectively. The mean changes from baseline to Week 26 were -1.4 kg, -3.2 kg, and -3.0 kg in the placebo, ertugliflozin 5 mg, and ertugliflozin 15 mg groups, respectively. The difference from placebo (95% CI) for ertugliflozin 5 mg was -1.8 kg (-2.4, -1.2) and for ertugliflozin 15 mg was -1.7 kg (-2.2, -1.1).
The mean baseline systolic blood pressure was 129.3 mmHg, 130.5 mmHg, and 130.2 mmHg in the placebo, ertugliflozin 5 mg, and ertugliflozin 15 mg groups, respectively. The mean changes from baseline to Week 26 were -1.8 mmHg, -5.1 mmHg, and -5.7 mmHg in the placebo, ertugliflozin 5 mg, and ertugliflozin 15 mg groups, respectively. The difference from placebo (95% CI) for ertugliflozin 5 mg was -3.3 mmHg (-5.6, -1.1) and for ertugliflozin 15 mg was -3.8 mmHg (-6.1, -1.5).
|
Figure 3: HbA1c (%) Change over Time in a 26-Week Placebo-Controlled Study for Ertugliflozin Used in Combination with Metformin HCl in Patients with Type 2 Diabetes Mellitus Data to the left of the vertical line are observed means (non-model-based) excluding values occurring post glycemic rescue. Data to the right of the vertical line represent the final Week 26 data, including all values regardless of use of glycemic rescue medication and use of study drug, with missing Week 26 values imputed using multiple imputation (26-MI) with a mean equal to the baseline value of the patient (see Table 6).
|
In Combination with Sitagliptin versus Ertugliflozin Alone and Sitagliptin Alone, as Add-on to Metformin HCl
A total of 1,233 patients with type 2 diabetes mellitus with inadequate glycemic control (HbA1c between 7.5% and 11%) on metformin HCl monotherapy (≥1,500 mg/day for ≥8 weeks) participated in a randomized, double-blind, 26-week, active controlled study (NCT02099110) to evaluate the efficacy and safety of ertugliflozin 5 mg or 15 mg administered orally in combination with sitagliptin 100 mg compared to the individual components. Patients were randomized to one of five treatment arms: ertugliflozin 5 mg, ertugliflozin 15 mg, sitagliptin 100 mg, ertugliflozin 5 mg + sitagliptin 100 mg, or ertugliflozin 15 mg + sitagliptin 100 mg.
At Week 26, ertugliflozin 5 mg or 15 mg + sitagliptin 100 mg provided statistically significantly greater reductions in HbA1c compared to ertugliflozin (5 mg or 15 mg) alone or sitagliptin 100 mg alone. The mean change from baseline in HbA1c was -1.4% for ertugliflozin 5 mg or 15 mg + sitagliptin 100 mg versus -1.0%, for ertugliflozin 5 mg, ertugliflozin 15 mg, or sitagliptin 100 mg, respectively. More patients receiving ertugliflozin 5 mg or 15 mg + sitagliptin 100 mg achieved an HbA1c <7% (53.3% and 50.9%, for ertugliflozin 5 mg or 15 mg, respectively, + sitagliptin 100 mg) compared to the individual components (29.3%, 33.7%, and 38.5% for ertugliflozin 5 mg, ertugliflozin 15 mg, or sitagliptin 100 mg, respectively).
Ertugliflozin as Add-on Combination Therapy with Metformin HCl and Sitagliptin
A total of 463 patients with type 2 diabetes mellitus inadequately controlled (HbA1c between 7% and 10.5%) on metformin HCl (≥1,500 mg/day for ≥8 weeks) and sitagliptin 100 mg orally once daily participated in a randomized, double-blind, multi-center, 26-week, placebo-controlled study (NCT02036515) to evaluate the efficacy and safety of ertugliflozin. Patients entered a 2-week, single-blind, placebo run-in period and were randomized to placebo, ertugliflozin 5 mg, or ertugliflozin 15 mg.
At Week 26, treatment with ertugliflozin at 5 mg or 15 mg daily provided statistically significant reductions in HbA1c. Ertugliflozin also resulted in a higher proportion of patients achieving an HbA1c <7% compared to placebo (see Table 7).
| Placebo | Ertugliflozin 5 mg | Ertugliflozin 15 mg | |
|---|---|---|---|
| HbA1c (%) | N = 152 | N = 155 | N = 152 |
| Baseline (mean) | 8.0 | 8.1 | 8.0 |
| Change from baseline (LS mean Intent-to-treat analysis using ANCOVA adjusted for baseline value, prior antihyperglycemic medication and baseline eGFR. ) |
-0.2 | -0.7 | -0.8 |
| Difference from placebo (LS mean, 95% CI) | -0.5 p<0.001 compared to placebo. (-0.7, -0.3) |
-0.6 (-0.8, -0.4) | |
| Patients [N (%)] with HbA1c <7% | 31 (20.2) | 54 (34.6) | 64 (42.3) |
| FPG (mg/dL) | N = 152 | N = 156 | N = 152 |
| Baseline (mean) | 169.6 | 167.7 | 171.7 |
| Change from baseline (LS mean) | -6.5 | -25.7 | -32.1 |
| Difference from placebo (LS mean, 95% CI) | -19.2 (-26.8, -11.6) | -25.6 (-33.2, -18.0) |
The mean baseline body weight was 86.5 kg, 87.6 kg, and 86.6 kg in the placebo, ertugliflozin 5 mg, and ertugliflozin 15 mg groups, respectively. The mean changes from baseline to Week 26 were -1.0 kg, -3.0 kg, and -2.8 kg in the placebo, ertugliflozin 5 mg, and ertugliflozin 15 mg groups, respectively. The difference from placebo (95% CI) for ertugliflozin 5 mg was -1.9 kg (-2.6, -1.3) and for ertugliflozin 15 mg was -1.8 kg (-2.4, -1.2).
The mean baseline systolic blood pressure was 130.2 mmHg, 132.1 mmHg, and 131.6 mmHg in the placebo, ertugliflozin 5 mg, and ertugliflozin 15 mg groups, respectively. The mean changes from baseline to Week 26 were -0.2 mmHg, -3.8 mmHg, and -4.5 mmHg in the placebo, ertugliflozin 5 mg, and ertugliflozin 15 mg groups, respectively. The difference from placebo (95% CI) for ertugliflozin 5 mg was -3.7 mmHg (-6.1, -1.2) and for ertugliflozin 15 mg was -4.3 mmHg (-6.7, -1.9).
Active Controlled Study of Ertugliflozin Versus Glimepiride as Add-on Combination Therapy with Metformin HCl
A total of 1,326 patients with type 2 diabetes mellitus inadequately controlled (HbA1c between 7% and 9%) on metformin HCl monotherapy participated in a randomized, double-blind, multi-center, 52-week, active comparator-controlled study (NCT01999218) to evaluate the efficacy and safety of ertugliflozin in combination with metformin HCl. These patients, who were receiving metformin HCl monotherapy (≥1,500 mg/day for ≥8 weeks), entered a 2-week, single-blind, placebo run-in period and were randomized to glimepiride, ertugliflozin 5 mg, or ertugliflozin 15 mg, administered orally once daily in addition to continuation of background metformin HCl therapy. Glimepiride was initiated at 1 mg/day and titrated up to a maximum dose of 6 or 8 mg/day (depending on maximum approved dose in each country) or a maximum tolerated dose or down-titrated to avoid or manage hypoglycemia. The mean daily dose of glimepiride was 3.0 mg.
Ertugliflozin 15 mg was non-inferior to glimepiride after 52 weeks of treatment. (See Table 8.)
| Glimepiride | Ertugliflozin 5 mg | Ertugliflozin 15 mg | |
|---|---|---|---|
| HbA1c (%) | N = 437 | N = 447 | N = 440 |
| Baseline (mean) | 7.8 | 7.8 | 7.8 |
| Change from baseline (LS mean Intent-to-treat analysis using ANCOVA adjusted for baseline value, prior antihyperglycemic medication and baseline eGFR. ) |
-0.6 | -0.5 | -0.5 |
| Difference from glimepiride (LS mean, 95% CI) | 0.2 Non-inferiority is declared when the upper bound of the two-sided 95% confidence interval (CI) for the mean difference is less than 0.3%. (0.0, 0.3) |
0.1 (-0.0, 0.2) | |
| Patients [N (%)] with HbA1c <7% | 208 (47.7) | 177 (39.5) | 186 (42.2) |
The mean baseline body weight was 86.8 kg, 87.9 kg, and 85.6 kg in the glimepiride, ertugliflozin 5 mg, and ertugliflozin 15 mg groups, respectively. The mean changes from baseline to Week 52 were 0.6 kg, -2.6 kg, and -3.0 kg in the glimepiride, ertugliflozin 5 mg, and ertugliflozin 15 mg groups, respectively. The difference from glimepiride (95% CI) for ertugliflozin 5 mg was -3.2 kg (-3.7, -2.7) and for ertugliflozin 15 mg was -3.6 kg (-4.1, -3.1).
Ertugliflozin as Add-on Combination Therapy with Insulin (With or Without Metformin HCl)
In an 18-week randomized, double-blind, multi-center, placebo-controlled, glycemic sub-study of VERTIS CV (NCT01986881, study details see 14.2), a total of 1,065 patients with type 2 diabetes mellitus and established atherosclerotic cardiovascular disease with inadequate glycemic control (HbA1c between 7% and 10.5%) on background therapy of insulin ≥20 units/day (59% also on metformin HCl ≥1,500 mg/day) were randomized to placebo, ertugliflozin 5 mg or ertugliflozin 15 mg oral once daily treatment.
At Week 18, treatment with ertugliflozin at 5 mg or 15 mg daily provided statistically significant reductions in HbA1c compared to placebo (see Table 9).
| Placebo | Ertugliflozin 5 mg | Ertugliflozin 15 mg | |
|---|---|---|---|
| SE: standard error. | |||
| HbA1c (%) | N = 346 | N = 346 | N = 367 |
| Baseline (mean) | 8.4 | 8.4 | 8.4 |
| Change from baseline (LS mean Intent-to-treat analysis using ANCOVA adjusted for baseline value, insulin stratum, and baseline eGFR. , SE) |
-0.2 (0.05) | -0.7 (0.05) | -0.7 (0.05) |
| Difference from placebo (LS mean, 95% CI) | -0.5 p<0.001 compared to placebo. (-0.6, -0.4) |
-0.5 (-0.7, -0.4) | |
|
Patients [N (%)] with HbA1c <7%
Missing values imputed as not meeting the <7% criterion.
|
37 (10.7) | 79 (22.8) | 81 (22.1) |
| FPG (mg/dL) | N = 343 | N = 346 | N = 368 |
| Baseline (mean) | 167.4 | 173.8 | 175.4 |
| Change from baseline (LS mean, SE) | -6.3 (2.91) | -25.6 (2.90) | -29.8 (2.86) |
| Difference from placebo (LS mean, 95% CI) | -19.2 (-26.8, -11.6) | -23.4 (-30.9, -16.0) |
The mean baseline body weights were 93.3 kg, 93.8 kg, and 92.1 kg in the placebo, ertugliflozin 5 mg, and ertugliflozin 15 mg groups, respectively. The mean changes from baseline to Week 18 were -0.2 kg, - 1.6 kg, and -1.9 kg in the placebo, ertugliflozin 5 mg, and ertugliflozin 15 mg groups, respectively. The differences from placebo (95% CI) for ertugliflozin 5 mg were - 1.4 kg (- 1.9, - 0.9) and for ertugliflozin 15 mg was -1.6 kg (-2.1, -1.1).
The mean baseline systolic blood pressures were 134.0 mmHg, 135.6 mmHg, and 133.7 mmHg in the placebo, ertugliflozin 5 mg, and ertugliflozin 15 mg groups, respectively. The mean changes from baseline to Week 18 were 0.7 mmHg, -2.2 mmHg, and -1.7 mmHg in the placebo, ertugliflozin 5 mg, and ertugliflozin 15 mg groups, respectively. The differences from placebo (95% CI) for ertugliflozin 5 mg was – 2.9 mmHg (-4.9, -1.0) and for ertugliflozin 15 mg were -2.5 mmHg (- 4.4, - 0.5).
Add-on Combination Therapy with Metformin HCl and Sulfonylurea
In an 18-week randomized, double-blind, multi-center, placebo-controlled, glycemic sub-study of VERTIS CV (NCT01986881, study details see 14.2), a total of 330 patients with type 2 diabetes mellitus and established atherosclerotic cardiovascular disease with inadequate glycemic control (HbA1c between 7% and 10.5%) with background therapy of metformin HCl ≥1,500 mg/day and a sulfonylurea (SU) were randomized to placebo, ertugliflozin 5 mg or ertugliflozin 15 mg oral once daily treatment.
At Week 18, treatment with ertugliflozin at 5 mg or 15 mg daily provided statistically significant reductions in HbA1c compared to placebo (see Table 10).
| Placebo | Ertugliflozin 5 mg | Ertugliflozin 15 mg | |
|---|---|---|---|
| SE: standard error | |||
| HbA1c (%) | N = 116 | N = 99 | N = 113 |
| Baseline (mean) | 8.3 | 8.4 | 8.3 |
| Change from baseline (LS mean Intent-to-treat analysis using ANCOVA adjusted for baseline value and baseline eGFR. , SE) |
-0.3 (0.08) | -0.8 (0.09) | -0.9 (0.08) |
| Difference from placebo (LS mean, 95% CI) | -0.6 p<0.001 compared to placebo. (-0.8, -0.3) |
-0.7 (-0.9, -0.4) | |
|
Patients [N (%)] with HbA1c <7% Missing values imputed as not meeting the <7% criterion.
|
17 (14.7) | 39 (39.4) | 38 (33.6) |
| FPG (mg/dL) | N = 117 | N = 99 | N = 113 |
| Baseline (mean) | 177.3 | 183.5 | 174.0 |
| Change from baseline (LS mean, SE) | -3.5 (3.65) | -31.3 (3.87) | -33.0 (3.67) |
| Difference from placebo (LS mean, 95% CI) | -27.9 (-37.8, -17.9) | -29.5 (-39.0, -19.9) |
The mean baseline body weights were 90.5 kg, 92.1 kg, and 92.9 kg in the placebo, ertugliflozin 5 mg, and ertugliflozin 15 mg groups, respectively. The mean changes from baseline to Week 18 were - 0.6 kg, -2.0 kg, and - 2.2 kg in the placebo, ertugliflozin 5 mg, and ertugliflozin 15 mg groups, respectively. The differences from placebo (95% CI) for ertugliflozin 5 mg were - 1.4 kg (- 2.2, - 0.7) and for ertugliflozin 15 mg was - 1.6 kg (- 2.3, - 0.9).
5.6 Hypoglycemia With Concomitant Use With Insulin Or Insulin Secretagogues (5.6 Hypoglycemia with Concomitant Use with Insulin or Insulin Secretagogues)
Insulin and insulin secretagogues (e.g., sulfonylurea) are known to cause hypoglycemia. SEGLUROMET may increase the risk of hypoglycemia when used in combination with insulin or an insulin secretagogue [see Adverse Reactions (6.1)]. The risk of hypoglycemia may be lowered by a reduction in the dose of insulin or sulfonylurea (or other concomitantly administered insulin secretagogues). Inform patients using these medications concomitantly of this risk and educate them on the signs and symptoms of hypoglycemia.
5.2 Diabetic Ketoacidosis in Patients With Type 1 Diabetes Mellitus and Other Ketoacidosis (5.2 Diabetic Ketoacidosis in Patients with Type 1 Diabetes Mellitus and Other Ketoacidosis)
In patients with type 1 diabetes mellitus, SEGLUROMET significantly increases the risk of diabetic ketoacidosis, a life-threatening event, beyond the background rate. In placebo-controlled trials of patients with type 1 diabetes mellitus, the risk of ketoacidosis was markedly increased in patients who received sodium glucose transporter 2 (SGLT2) inhibitors compared to patients who received placebo; this risk may be greater with higher doses. SEGLUROMET is not indicated for glycemic control in patients with type 1 diabetes mellitus.
Type 2 diabetes mellitus and pancreatic disorders (e.g., history of pancreatitis or pancreatic surgery) are also risk factors for ketoacidosis. There have been postmarketing reports of fatal events of ketoacidosis in patients with type 2 diabetes mellitus using SGLT2 inhibitors.
Precipitating conditions for diabetic ketoacidosis or other ketoacidosis include under-insulinization due to insulin dose reduction or missed insulin doses, acute febrile illness, reduced caloric intake, ketogenic diet, surgery, volume depletion, and alcohol abuse.
Signs and symptoms are consistent with dehydration and severe metabolic acidosis and include nausea, vomiting, abdominal pain, generalized malaise, and shortness of breath. Blood glucose levels at presentation may be below those typically expected for diabetic ketoacidosis (e.g., less than 250 mg/dL). Ketoacidosis and glucosuria may persist longer than typically expected. Urinary glucose excretion persists for 4 days after discontinuing SEGLUROMET [see Clinical Pharmacology (12.2)]; however, there have been postmarketing reports of ketoacidosis and/or glucosuria lasting greater than 6 days and some up to 2 weeks after discontinuation of SGLT2 inhibitors.
Consider ketone monitoring in patients at risk for ketoacidosis if indicated by the clinical situation. Assess for ketoacidosis regardless of presenting blood glucose levels in patients who present with signs and symptoms consistent with severe metabolic acidosis. If ketoacidosis is suspected, discontinue SEGLUROMET, promptly evaluate, and treat ketoacidosis, if confirmed. Monitor patients for resolution of ketoacidosis before restarting SEGLUROMET.
Withhold SEGLUROMET, if possible, in temporary clinical situations that could predispose patients to ketoacidosis. Resume SEGLUROMET when the patient is clinically stable and has resumed oral intake [see Dosage and Administration (2.4)].
Educate all patients on the signs and symptoms of ketoacidosis and instruct patients to discontinue SEGLUROMET and seek medical attention immediately if signs and symptoms occur.
14.2 Ertugliflozin Cardiovascular Outcomes in Patients With Type 2 Diabetes and Established Cardiovascular Disease (14.2 Ertugliflozin Cardiovascular Outcomes in Patients with Type 2 Diabetes and Established Cardiovascular Disease)
The effect of ertugliflozin on cardiovascular risk in adult patients with type 2 diabetes and established atherosclerotic cardiovascular disease was evaluated in the VERTIS CV study (NCT 01986881), a multicenter, multi-national, randomized, double-blind, placebo-controlled, event-driven trial. The study compared the risk of experiencing a major adverse cardiovascular event (MACE) between ertugliflozin and placebo when these were added to and used concomitantly with standard of care treatments for diabetes and atherosclerotic cardiovascular disease.
A total of 8,246 patients were randomized to placebo (N=2,747), oral once daily ertugliflozin 5 mg (N=2,752), or oral once daily ertugliflozin 15 mg (N=2,747) and followed for a median of 3 years. Approximately 88% of the study population was White, 6% Asian, and 3% Black or African American. The mean age was 64 years and approximately 70% were male.
All patients in the study had inadequately controlled type 2 diabetes mellitus at baseline (HbA1c greater than or equal to 7%). The mean duration of type 2 diabetes mellitus was 13 years, the mean HbA1c at baseline was 8.2% and the mean eGFR was 76 mL/min/1.73 m2. At baseline, patients were treated with one (32%) or more (67%) antidiabetic medications including biguanides (metformin HCl) (76%), insulin (47%), sulfonylureas (41%), DPP-4 inhibitors (11%) and GLP-1 receptor agonists (3%).
Almost all patients (99%) had established atherosclerotic cardiovascular disease at baseline including: a documented history of coronary artery disease (76%), cerebrovascular disease (23%) or peripheral artery disease (19%). Approximately 24% patients had a history of heart failure (HF). At baseline, the mean systolic blood pressure was 133 mmHg, the mean diastolic blood pressure was 77 mmHg, the mean LDL was 89 mg/dL, and the mean HDL was 44 mg/dL. At baseline, approximately 81% of patients were treated with renin angiotensin system inhibitors, 69% with beta-blockers, 43% with diuretics, 82% with statins, 4% ezetimibe, and 89% with antiplatelet agents.
The primary endpoint in VERTIS CV was the time to first occurrence of a Major Adverse Cardiac Event (MACE). A major adverse cardiovascular event was defined as occurrence of either a cardiovascular death or a nonfatal myocardial infarction (MI) or a nonfatal stroke. The statistical analysis plan pre-specified that the 5 and 15 mg doses would be combined for the analysis. A Cox proportional hazards model was used to test for non-inferiority against the pre-specified risk margin of 1.3 for the hazard ratio of MACE. Type-1 error was controlled across multiple tests using a hierarchical testing strategy.
The incidence rate of MACE was similar between the ertugliflozin-treated and placebo-treated patients. The estimated hazard ratio of MACE associated with ertugliflozin relative to placebo was 0.97 with 95.6% confidence interval (0.85, 1.11). The upper bound of this confidence interval excluded a risk larger than 1.3 (Table 11). Results for the 5 mg and 15 mg doses were consistent with results for the combined dose group.
| Endpoint MACE was evaluated in subjects who took at least one dose of study medication and, for subjects who discontinued study medication prior to the end of the study, censored events that occurred more than 365 days after the last dose of study medication. Other endpoints were evaluated using all randomized subjects and events that occurred any time after the first dose of study medication until the last contact date. The total number of first events was analyzed for each endpoint.
|
Placebo (N=2747) | ertugliflozin (N=5499) | Hazard Ratio vs Placebo (CI) HR and CI are based on Cox proportional hazards regression model, stratified by cohorts. For MACE a 95.6% CI is presented, for other endpoints a 95% CI is presented.
|
||
|---|---|---|---|---|---|
| N (%) | Event Rate (per 100 person-years) | N (%) | Event Rate (per 100 person-years) | ||
| N=Number of patients, CI=Confidence interval, CV=Cardiovascular, MI=Myocardial infarction. | |||||
| MACE (CV death, non-fatal MI, or non-fatal stroke) Composite | 327 (11.9) | 4.0 | 653 (11.9) | 3.9 | 0.97 (0.85, 1.11) |
| Components of Composite Endpoint | |||||
| Non-fatal MI | 148 (5.4) | 1.6 | 310 (5.6) | 1.7 | 1.04 (0.86, 1.27) |
| Non-fatal Stroke | 78 (2.8) | 0.8 | 157 (2.9) | 0.8 | 1.00 (0.76, 1.32) |
| CV death | 184 (6.7) | 1.9 | 341 (6.2) | 1.8 | 0.92 (0.77, 1.11) |
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:44:53.310731 · Updated: 2026-03-14T22:21:24.209091