These Highlights Do Not Include All The Information Needed To Use Olanzapine For Injection Safely And Effectively. See Full Prescribing Information For Olanzapine For Injection.
9d9f25d5-4513-434a-a37a-392a0c978f2e
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
Warnings and Precautions ( 5.11 ) 1/2025
Indications and Usage
Olanzapine is an atypical antipsychotic indicated: As Olanzapine for Injection for the: Treatment of acute agitation associated with schizophrenia and bipolar I mania. ( 1.4 ) Efficacy was established in three 1-day trials in adults. ( 14.3 )
Dosage and Administration
Agitation associated with Schizophrenia and Bipolar I Mania in adults ( 2.4 ) IM: 10 mg (5 mg or 7.5 mg when clinically warranted) Assess for orthostatic hypotension prior to subsequent dosing (max. 3 doses 2-4 hrs apart) Lower starting dose recommended in debilitated or pharmacodynamically sensitive patients or patients with predisposition to hypotensive reactions, or with potential for slowed metabolism. ( 2.4 )
Warnings and Precautions
Elderly Patients with Dementia-Related Psychosis: Increased risk of death and increased incidence of cerebrovascular adverse events (e.g., stroke, transient ischemic attack). ( 5.1 ) Suicide: The possibility of a suicide attempt is inherent in schizophrenia and in bipolar I disorder, and close supervision of high-risk patients should accompany drug therapy. ( 5.2 ) Neuroleptic Malignant Syndrome: Manage with immediate discontinuation and close monitoring. ( 5.3 ) Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS): Discontinue if DRESS is suspected. ( 5.4 ) Metabolic Changes: Atypical antipsychotic drugs have been associated with metabolic changes including hyperglycemia, dyslipidemia, and weight gain. ( 5.5 ) Hyperglycemia and Diabetes Mellitus: In some cases extreme and associated with ketoacidosis or hyperosmolar coma or death, has been reported in patients taking olanzapine. Patients taking olanzapine should be monitored for symptoms of hyperglycemia and undergo fasting blood glucose testing at the beginning of, and periodically during, treatment. ( 5.5 ) Dyslipidemia: Undesirable alterations in lipids have been observed. Appropriate clinical monitoring is recommended, including fasting blood lipid testing at the beginning of, and periodically during, treatment. ( 5.5 ) Weight Gain: Potential consequences of weight gain should be considered. Patients should receive regular monitoring of weight. ( 5.5 ) Tardive Dyskinesia: Discontinue if clinically appropriate. ( 5.6 ) Orthostatic Hypotension: Orthostatic hypotension associated with dizziness, tachycardia, bradycardia and, in some patients, syncope, may occur especially during initial dose titration. Use caution in patients with cardiovascular disease, cerebrovascular disease, and those conditions that could affect hemodynamic responses. ( 5.7 ) Leukopenia, Neutropenia, and Agranulocytosis: Has been reported with antipsychotics, including Olanzapine. Patients with a history of a clinically significant low white blood cell count (WBC) or drug induced leukopenia/neutropenia should have their complete blood count (CBC) monitored frequently during the first few months of therapy and discontinuation of Olanzapine should be considered at the first sign of a clinically significant decline in WBC in the absence of other causative factors. ( 5.9 ) Seizures: Use cautiously in patients with a history of seizures or with conditions that potentially lower the seizure threshold. ( 5.11 ) Potential for Cognitive and Motor Impairment: Has potential to impair judgment, thinking, and motor skills. Use caution when operating machinery. ( 5.12 ) Anticholinergic (antimuscarinic) Effects: Use with caution with other anticholinergic drugs and in patients with urinary retention, prostatic hypertrophy, constipation, paralytic ileus or related conditions. ( 5.14 ) Hyperprolactinemia: May elevate prolactin levels. ( 5.15 ) Use in Combination with Lithium or Valproate: Also refer to the package inserts for lithium or valproate. ( 5.16 ) Laboratory Tests: Monitor fasting blood glucose and lipid profiles at the beginning of, and periodically during, treatment. ( 5.17 )
Contraindications
None with Olanzapine monotherapy. For specific information about the contraindications of lithium or valproate, refer to the Contraindications section of the package inserts for these other products.
Adverse Reactions
Most common adverse reactions (≥5% and at least twice that for placebo) associated with: Combination of Olanzapine and Lithium or Valproate: Manic or Mixed Episodes, Bipolar I Disorder (Adults) – dry mouth, weight gain, increased appetite, dizziness, back pain, constipation, speech disorder, increased salivation, amnesia, paresthesia ( 6.1 ) Olanzapine for Injection: Agitation with Schizophrenia and Bipolar I Mania (Adults) – somnolence ( 6.1 ) To report SUSPECTED ADVERSE REACTIONS, contact PAI Pharma at 1-800-845-8210 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch
Drug Interactions
The risks of using olanzapine in combination with other drugs have not been extensively evaluated in systematic studies.
Storage and Handling
Store Olanzapine for Injection vials (before reconstitution) at controlled room temperature, 20° to 25°C (68° to 77°F) [ see USP]. Reconstituted Olanzapine for Injection may be stored at controlled room temperature, 20° to 25°C (68° to 77°F) [ see USP] for up to 1 hour if necessary. Discard any unused portion of reconstituted Olanzapine for Injection. The USP defines controlled room temperature as a temperature maintained thermostatically that encompasses the usual and customary working environment of 20° to 25°C (68° to 77°F); that results in a mean kinetic temperature calculated to be not more than 25°C; and that allows for excursions between 15° and 30°C (59° and 86°F) that are experienced in pharmacies, hospitals, and warehouses. Protect Olanzapine for Injection from light, do not freeze.
How Supplied
Olanzapine for Injection is available in: NDC 0121-1072-55 – 10 mg single-dose vial (1s)
Medication Information
Warnings and Precautions
Elderly Patients with Dementia-Related Psychosis: Increased risk of death and increased incidence of cerebrovascular adverse events (e.g., stroke, transient ischemic attack). ( 5.1 ) Suicide: The possibility of a suicide attempt is inherent in schizophrenia and in bipolar I disorder, and close supervision of high-risk patients should accompany drug therapy. ( 5.2 ) Neuroleptic Malignant Syndrome: Manage with immediate discontinuation and close monitoring. ( 5.3 ) Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS): Discontinue if DRESS is suspected. ( 5.4 ) Metabolic Changes: Atypical antipsychotic drugs have been associated with metabolic changes including hyperglycemia, dyslipidemia, and weight gain. ( 5.5 ) Hyperglycemia and Diabetes Mellitus: In some cases extreme and associated with ketoacidosis or hyperosmolar coma or death, has been reported in patients taking olanzapine. Patients taking olanzapine should be monitored for symptoms of hyperglycemia and undergo fasting blood glucose testing at the beginning of, and periodically during, treatment. ( 5.5 ) Dyslipidemia: Undesirable alterations in lipids have been observed. Appropriate clinical monitoring is recommended, including fasting blood lipid testing at the beginning of, and periodically during, treatment. ( 5.5 ) Weight Gain: Potential consequences of weight gain should be considered. Patients should receive regular monitoring of weight. ( 5.5 ) Tardive Dyskinesia: Discontinue if clinically appropriate. ( 5.6 ) Orthostatic Hypotension: Orthostatic hypotension associated with dizziness, tachycardia, bradycardia and, in some patients, syncope, may occur especially during initial dose titration. Use caution in patients with cardiovascular disease, cerebrovascular disease, and those conditions that could affect hemodynamic responses. ( 5.7 ) Leukopenia, Neutropenia, and Agranulocytosis: Has been reported with antipsychotics, including Olanzapine. Patients with a history of a clinically significant low white blood cell count (WBC) or drug induced leukopenia/neutropenia should have their complete blood count (CBC) monitored frequently during the first few months of therapy and discontinuation of Olanzapine should be considered at the first sign of a clinically significant decline in WBC in the absence of other causative factors. ( 5.9 ) Seizures: Use cautiously in patients with a history of seizures or with conditions that potentially lower the seizure threshold. ( 5.11 ) Potential for Cognitive and Motor Impairment: Has potential to impair judgment, thinking, and motor skills. Use caution when operating machinery. ( 5.12 ) Anticholinergic (antimuscarinic) Effects: Use with caution with other anticholinergic drugs and in patients with urinary retention, prostatic hypertrophy, constipation, paralytic ileus or related conditions. ( 5.14 ) Hyperprolactinemia: May elevate prolactin levels. ( 5.15 ) Use in Combination with Lithium or Valproate: Also refer to the package inserts for lithium or valproate. ( 5.16 ) Laboratory Tests: Monitor fasting blood glucose and lipid profiles at the beginning of, and periodically during, treatment. ( 5.17 )
Indications and Usage
Olanzapine is an atypical antipsychotic indicated: As Olanzapine for Injection for the: Treatment of acute agitation associated with schizophrenia and bipolar I mania. ( 1.4 ) Efficacy was established in three 1-day trials in adults. ( 14.3 )
Dosage and Administration
Agitation associated with Schizophrenia and Bipolar I Mania in adults ( 2.4 ) IM: 10 mg (5 mg or 7.5 mg when clinically warranted) Assess for orthostatic hypotension prior to subsequent dosing (max. 3 doses 2-4 hrs apart) Lower starting dose recommended in debilitated or pharmacodynamically sensitive patients or patients with predisposition to hypotensive reactions, or with potential for slowed metabolism. ( 2.4 )
Contraindications
None with Olanzapine monotherapy. For specific information about the contraindications of lithium or valproate, refer to the Contraindications section of the package inserts for these other products.
Adverse Reactions
Most common adverse reactions (≥5% and at least twice that for placebo) associated with: Combination of Olanzapine and Lithium or Valproate: Manic or Mixed Episodes, Bipolar I Disorder (Adults) – dry mouth, weight gain, increased appetite, dizziness, back pain, constipation, speech disorder, increased salivation, amnesia, paresthesia ( 6.1 ) Olanzapine for Injection: Agitation with Schizophrenia and Bipolar I Mania (Adults) – somnolence ( 6.1 ) To report SUSPECTED ADVERSE REACTIONS, contact PAI Pharma at 1-800-845-8210 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch
Drug Interactions
The risks of using olanzapine in combination with other drugs have not been extensively evaluated in systematic studies.
Storage and Handling
Store Olanzapine for Injection vials (before reconstitution) at controlled room temperature, 20° to 25°C (68° to 77°F) [ see USP]. Reconstituted Olanzapine for Injection may be stored at controlled room temperature, 20° to 25°C (68° to 77°F) [ see USP] for up to 1 hour if necessary. Discard any unused portion of reconstituted Olanzapine for Injection. The USP defines controlled room temperature as a temperature maintained thermostatically that encompasses the usual and customary working environment of 20° to 25°C (68° to 77°F); that results in a mean kinetic temperature calculated to be not more than 25°C; and that allows for excursions between 15° and 30°C (59° and 86°F) that are experienced in pharmacies, hospitals, and warehouses. Protect Olanzapine for Injection from light, do not freeze.
How Supplied
Olanzapine for Injection is available in: NDC 0121-1072-55 – 10 mg single-dose vial (1s)
Description
Warnings and Precautions ( 5.11 ) 1/2025
Section 34077-8
Pregnancy Exposure Registry
There is a pregnancy exposure registry that monitors pregnancy outcomes in women exposed to atypical antipsychotics, including Olanzapine, during pregnancy. Healthcare providers are encouraged to register patients by contacting the National Pregnancy Registry for Atypical Antipsychotics at 1-866-961-2388 or visit http://womensmentalhealth.org/clinical-and-research-programs/pregnancyregistry/.
Risk Summary
Neonates exposed to antipsychotic drugs, including Olanzapine, during the third trimester are at risk for extrapyramidal and/or withdrawal symptoms following delivery (see
Clinical Considerations). Overall available data from published epidemiologic studies of pregnant women exposed to olanzapine have not established a drug-associated risk of major birth defects, miscarriage, or adverse maternal or fetal outcomes (see
Data). There are risks to the mother associated with untreated schizophrenia or bipolar I disorder and with exposure to antipsychotics, including Olanzapine, during pregnancy (see
Clinical Considerations).
Olanzapine was not teratogenic when administered orally to pregnant rats and rabbits at doses that are 9- and 30-times the daily oral maximum recommended human dose (MRHD), based on mg/m
2body surface area; some fetal toxicities were observed at these doses (see
Data).
The estimated background risk of major birth defects and miscarriage for the indicated populations is unknown. All pregnancies have a background risk of birth defects, loss, or other adverse outcomes. In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2% to 4% and 15% to 20%, respectively.
Clinical Considerations
Disease-associated maternal and embryo/fetal risk
There is a risk to the mother from untreated schizophrenia or bipolar I disorder, including increased risk of relapse, hospitalization, and suicide. Schizophrenia and bipolar I disorder are associated with increased adverse perinatal outcomes, including preterm birth. It is not known if this is a direct result of the illness or other comorbid factors.
Fetal/Neonatal adverse reactions
Extrapyramidal and/or withdrawal symptoms, including agitation, hypertonia, hypotonia, tremor, somnolence, respiratory distress, and feeding disorder have been reported in neonates who were exposed to antipsychotic drugs, including Olanzapine, during the third trimester of pregnancy. These symptoms have varied in severity. Monitor neonates for extrapyramidal and/or withdrawal symptoms and manage symptoms appropriately. Some neonates recovered within hours or days without specific treatment; others required prolonged hospitalization.
Section 34078-6
Data
Human Data
Placental passage has been reported in published study reports; however, the placental passage ratio was highly variable ranging between 7% to 167% at birth following exposure during pregnancy. The clinical relevance of this finding is unknown.
Published data from observational studies, birth registries, and case reports that have evaluated the use of atypical antipsychotics during pregnancy do not establish an increased risk of major birth defects. A retrospective cohort study from a Medicaid database of 9258 women exposed to antipsychotics during pregnancy did not indicate an overall increased risk for major birth defects.
Animal Data
In oral reproduction studies in rats at doses up to 18 mg/kg/day and in rabbits at doses up to 30 mg/kg/day (9 and 30 times the daily oral MRHD based on mg/m
2body surface area, respectively), no evidence of teratogenicity was observed. In an oral rat teratology study, early resorptions and increased numbers of nonviable fetuses were observed at a dose of 18 mg/kg/day (9 times the daily oral MRHD based on mg/m
2body surface area), and gestation was prolonged at 10 mg/kg/day (5 times the daily oral MRHD based on mg/m
2body surface area). In an oral rabbit teratology study, fetal toxicity manifested as increased resorptions and decreased fetal weight, occurred at a maternally toxic dose of 30 mg/kg/day (30 times the daily oral MRHD based on mg/m
2body surface area).
Section 42229-5
Dose Selection for Agitated Adult Patients with Schizophrenia and Bipolar I Mania — The efficacy of intramuscular olanzapine for injection in controlling agitation in these disorders was demonstrated in a dose range of 2.5 mg to 10 mg. The recommended dose in these patients is 10 mg. A lower dose of 5 or 7.5 mg may be considered when clinical factors warrant [see Clinical Studies (14.3)] . If agitation warranting additional intramuscular doses persists following the initial dose, subsequent doses up to 10 mg may be given. However, the efficacy of repeated doses of intramuscular olanzapine for injection in agitated patients has not been systematically evaluated in controlled clinical trials. Also, the safety of total daily doses greater than 30 mg, or 10 mg injections given more frequently than 2 hours after the initial dose, and 4 hours after the second dose have not been evaluated in clinical trials. Maximal dosing of intramuscular olanzapine (e.g., 3 doses of 10 mg administered 2-4 hours apart) may be associated with a substantial occurrence of significant orthostatic hypotension [see Warnings and Precautions (5.7)] . Thus, it is recommended that patients requiring subsequent intramuscular injections be assessed for orthostatic hypotension prior to the administration of any subsequent doses of intramuscular olanzapine for injection. The administration of an additional dose to a patient with a clinically significant postural change in systolic blood pressure is not recommended.
If ongoing olanzapine therapy is clinically indicated, oral olanzapine may be initiated in a range of 5-20 mg/day as soon as clinically appropriate.
Section 43683-2
| Warnings and Precautions (5.11) | 1/2025 |
5.8 Falls
Olanzapine may cause somnolence, postural hypotension, motor and sensory instability, which may lead to falls and, consequently, fractures or other injuries. For patients with diseases, conditions, or medications that could exacerbate these effects, complete fall risk assessments when initiating antipsychotic treatment and recurrently for patients on long-term antipsychotic therapy.
5.2 Suicide
The possibility of a suicide attempt is inherent in schizophrenia and in bipolar I disorder, and close supervision of high-risk patients should accompany drug therapy. Prescriptions for olanzapine should be written for the smallest quantity of tablets consistent with good patient management, in order to reduce the risk of overdose.
5.11 Seizures
During premarketing testing, seizures occurred in 0.9% (22/2500) of olanzapine-treated patients. There were confounding factors that may have contributed to the occurrence of seizures in many of these cases. Olanzapine should be used cautiously in patients with a history of seizures or with conditions that potentially lower the seizure threshold, e.g., Alzheimer's dementia. Olanzapine is not approved for the treatment of patients with Alzheimer's disease. Conditions that lower the seizure threshold may be more prevalent in a population of 65 years or older.
11 Description
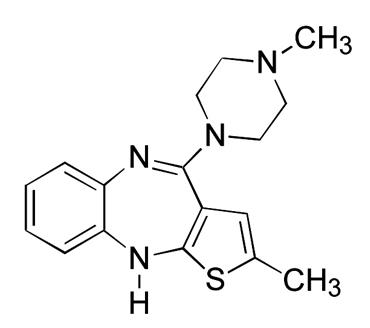
Olanzapine is an atypical antipsychotic that belongs to the thienobenzodiazepine class. The chemical designation is 2-methyl-4-(4-methyl-1-piperazinyl)-10 H-thieno[2,3- b] [1,5]benzodiazepine. The molecular formula is C 17H 20N 4S, which corresponds to a molecular weight of 312.44. The chemical structure is:
Olanzapine is a yellow crystalline solid, which is practically insoluble in water.
Olanzapine for injection is intended for intramuscular use only.
Each single-dose vial provides for the administration of 10 mg (32 μmol) olanzapine with inactive ingredients 50 mg lactose monohydrate and 3.5 mg tartaric acid. Hydrochloric acid and/or sodium hydroxide may have been added during manufacturing to adjust pH.
5.10 Dysphagia
Esophageal dysmotility and aspiration have been associated with antipsychotic drug use. Aspiration pneumonia is a common cause of morbidity and mortality in patients with advanced Alzheimer's disease. Olanzapine is not approved for the treatment of patients with Alzheimer's disease.
8.2 lactation
Risk Summary
Olanzapine is present in human milk. There are reports of excess sedation, irritability, poor feeding and extrapyramidal symptoms (tremors and abnormal muscle movements) in infants exposed to olanzapine through breast milk (see
Clinical Considerations). There is no information on the effects of olanzapine on milk production.
The developmental and health benefits of breastfeeding should be considered along with the mother’s clinical need for Olanzapine and any potential adverse effects on the breastfed child from Olanzapine or from the mother’s underlying condition.
Clinical Considerations
Infants exposed to Olanzapine should be monitored for excess sedation, irritability, poor feeding, and extrapyramidal symptoms (tremors and abnormal muscle movements).
9.3 Dependence
In studies prospectively designed to assess abuse and dependence potential, olanzapine was shown to have acute depressive CNS effects but little or no potential of abuse or physical dependence in rats administered oral doses up to 15 times the daily oral MRHD (20 mg) and rhesus monkeys administered oral doses up to 8 times the daily oral MRHD based on mg/m 2body surface area.
Olanzapine has not been systematically studied in humans for its potential for abuse, tolerance, or physical dependence. While the clinical trials did not reveal any tendency for any drug-seeking behavior, these observations were not systematic, and it is not possible to predict on the basis of this limited experience the extent to which a CNS-active drug will be misused, diverted, and/or abused once marketed. Consequently, patients should be evaluated carefully for a history of drug abuse, and such patients should be observed closely for signs of misuse or abuse of olanzapine (e.g., development of tolerance, increases in dose, drug-seeking behavior).
16.1 How Supplied
Olanzapine for Injection is available in:
NDC 0121-1072-55 – 10 mg single-dose vial (1s)
8.4 Pediatric Use
Compared to patients from adult clinical trials, adolescents were likely to gain more weight, experience increased sedation, and have greater increases in total cholesterol, triglycerides, LDL cholesterol, prolactin and hepatic aminotransferase levels [see Warnings and Precautions (5.5, 5.15, 5.17) and Adverse Reactions (6.1)] . When deciding among the alternative treatments available for adolescents, clinicians should consider the increased potential (in adolescents as compared with adults) for weight gain and dyslipidemia. Clinicians should consider the potential long-term risks when prescribing to adolescents, and in many cases this may lead them to consider prescribing other drugs first in adolescents.
Safety and effectiveness of olanzapine in children <13 years of age have not been established [see Patient Counseling Information (17)] .
8.5 Geriatric Use
Of the 2500 patients in premarketing clinical studies with oral olanzapine, 11% (263) were 65 years of age or over. In patients with schizophrenia, there was no indication of any different tolerability of olanzapine in the elderly compared to younger patients. Studies in elderly patients with dementia-related psychosis have suggested that there may be a different tolerability profile in this population compared to younger patients with schizophrenia. Elderly patients with dementia-related psychosis treated with olanzapine are at an increased risk of death compared to placebo. In placebo-controlled studies of olanzapine in elderly patients with dementia-related psychosis, there was a higher incidence of cerebrovascular adverse events (e.g., stroke, transient ischemic attack) in patients treated with olanzapine compared to patients treated with placebo. In 5 placebo-controlled studies of olanzapine in elderly patients with dementia-related psychosis (n=1184), the following adverse reactions were reported in olanzapine-treated patients at an incidence of at least 2% and significantly greater than placebo-treated patients: falls, somnolence, peripheral edema, abnormal gait, urinary incontinence, lethargy, increased weight, asthenia, pyrexia, pneumonia, dry mouth and visual hallucinations. The rate of discontinuation due to adverse reactions was greater with olanzapine than placebo (13% vs 7%). Elderly patients with dementia-related psychosis treated with olanzapine are at an increased risk of death compared to placebo. Olanzapine is not approved for the treatment of patients with dementia-related psychosis [see Boxed Warning, Warnings and Precautions (5.1), and Patient Counseling Information (17)] . Olanzapine is not approved for the treatment of patients with dementia-related psychosis. Also, the presence of factors that might decrease pharmacokinetic clearance or increase the pharmacodynamic response to olanzapine should lead to consideration of a lower starting dose for any geriatric patient [see Boxed Warning and Warnings and Precautions (5.1)] .
4 Contraindications
- None with Olanzapine monotherapy.
- For specific information about the contraindications of lithium or valproate, refer to the Contraindications section of the package inserts for these other products.
6 Adverse Reactions
Most common adverse reactions (≥5% and at least twice that for placebo) associated with:
Combination of Olanzapine and Lithium or Valproate:
- Manic or Mixed Episodes, Bipolar I Disorder (Adults) – dry mouth, weight gain, increased appetite, dizziness, back pain, constipation, speech disorder, increased salivation, amnesia, paresthesia (6.1)
Olanzapine for Injection:
- Agitation with Schizophrenia and Bipolar I Mania (Adults) – somnolence (6.1)
To report SUSPECTED ADVERSE REACTIONS, contact PAI Pharma at 1-800-845-8210 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch
7 Drug Interactions
The risks of using olanzapine in combination with other drugs have not been extensively evaluated in systematic studies.
10.1 Human Experience
In premarketing trials involving more than 3100 patients and/or normal subjects, accidental or intentional acute overdosage of olanzapine was identified in 67 patients. In the patient taking the largest identified amount, 300 mg, the only symptoms reported were drowsiness and slurred speech. In the limited number of patients who were evaluated in hospitals, including the patient taking 300 mg, there were no observations indicating an adverse change in laboratory analytes or ECG. Vital signs were usually within normal limits following overdoses.
In postmarketing reports of overdose with olanzapine alone, symptoms have been reported in the majority of cases. In symptomatic patients, symptoms with ≥10% incidence included agitation/aggressiveness, dysarthria, tachycardia, various extrapyramidal symptoms, and reduced level of consciousness ranging from sedation to coma. Among less commonly reported symptoms were the following potentially medically serious reactions: aspiration, cardiopulmonary arrest, cardiac arrhythmias (such as supraventricular tachycardia and 1 patient experiencing sinus pause with spontaneous resumption of normal rhythm), delirium, possible neuroleptic malignant syndrome, respiratory depression/arrest, convulsion, hypertension, and hypotension. Eli Lilly and Company has received reports of fatality in association with overdose of olanzapine alone. In 1 case of death, the amount of acutely ingested olanzapine was reported to be possibly as low as 450 mg of oral olanzapine; however, in another case, a patient was reported to survive an acute olanzapine ingestion of approximately 2 g of oral olanzapine.
12.2 Pharmacodynamics
Olanzapine binds with high affinity to the following receptors: serotonin 5HT 2A/2C, 5HT 6(K i=4, 11, and 5 nM, respectively), dopamine D 1-4(K i=11-31 nM), histamine H 1(K i=7 nM), and adrenergic α 1receptors (K i=19 nM). Olanzapine is an antagonist with moderate affinity binding for serotonin 5HT 3(K i=57 nM) and muscarinic M 1-5(K i=73, 96, 132, 32, and 48 nM, respectively). Olanzapine binds with low affinity to GABA A, BZD, and β-adrenergic receptors (K i>10 μM).
5.17 Laboratory Tests
5.5 Metabolic Changes
Atypical antipsychotic drugs have been associated with metabolic changes including hyperglycemia, dyslipidemia, and weight gain. Metabolic changes may be associated with increased cardiovascular/cerebrovascular risk. Olanzapine's specific metabolic profile is presented below.
5.6 Tardive Dyskinesia
A syndrome of potentially irreversible, involuntary, dyskinetic movements may develop in patients treated with antipsychotic drugs. Although the prevalence of the syndrome appears to be highest among the elderly, especially elderly women, it is impossible to rely upon prevalence estimates to predict, at the inception of antipsychotic treatment, which patients are likely to develop the syndrome. Whether antipsychotic drug products differ in their potential to cause tardive dyskinesia is unknown.
The risk of developing tardive dyskinesia and the likelihood that it will become irreversible are believed to increase as the duration of treatment and the total cumulative dose of antipsychotic drugs administered to the patient increase. However, the syndrome can develop, although much less commonly, after relatively brief treatment periods at low doses or may even arise after discontinuation of treatment.
Tardive dyskinesia may remit, partially or completely, if antipsychotic treatment is withdrawn. Antipsychotic treatment, itself, however, may suppress (or partially suppress) the signs and symptoms of the syndrome and thereby may possibly mask the underlying process. The effect that symptomatic suppression has upon the long-term course of the syndrome is unknown.
Given these considerations, olanzapine should be prescribed in a manner that is most likely to minimize the occurrence of tardive dyskinesia. Chronic antipsychotic treatment should generally be reserved for patients (1) who suffer from a chronic illness that is known to respond to antipsychotic drugs, and (2) for whom alternative, equally effective, but potentially less harmful treatments are not available or appropriate. In patients who do require chronic treatment, the smallest dose and the shortest duration of treatment producing a satisfactory clinical response should be sought. The need for continued treatment should be reassessed periodically.
If signs and symptoms of tardive dyskinesia appear in a patient on olanzapine, drug discontinuation should be considered. However, some patients may require treatment with olanzapine despite the presence of the syndrome.
For specific information about the warnings of lithium or valproate, refer to the Warnings section of the package inserts for these other products.
1 Indications and Usage
5.15 Hyperprolactinemia
As with other drugs that antagonize dopamine D 2receptors, olanzapine elevates prolactin levels, and the elevation persists during chronic administration. Hyperprolactinemia may suppress hypothalamic GnRH, resulting in reduced pituitary gonadotropin secretion. This, in turn, may inhibit reproductive function by impairing gonadal steroidogenesis in both female and male patients. Galactorrhea, amenorrhea, gynecomastia, and impotence have been reported in patients receiving prolactin-elevating compounds. Long-standing hyperprolactinemia when associated with hypogonadism may lead to decreased bone density in both female and male subjects.
Tissue culture experiments indicate that approximately one-third of human breast cancers are prolactin dependent in vitro, a factor of potential importance if the prescription of these drugs is contemplated in a patient with previously detected breast cancer. As is common with compounds which increase prolactin release, an increase in mammary gland neoplasia was observed in the olanzapine carcinogenicity studies conducted in mice and rats [see Nonclinical Toxicology (13.1)] . Published epidemiologic studies have shown inconsistent results when exploring the potential association between hyperprolactinemia and breast cancer.
In placebo-controlled olanzapine clinical studies (up to 12 weeks), changes from normal to high in prolactin concentrations were observed in 30% of adults treated with olanzapine as compared to 10.5% of adults treated with placebo. In a pooled analysis from clinical studies including 8136 adults treated with olanzapine, potentially associated clinical manifestations included menstrual-related events 1(2% [49/3240] of females), sexual function-related events 2(2% [150/8136] of females and males), and breast-related events 3(0.7% [23/3240] of females, 0.2% [9/4896] of males).
In placebo-controlled olanzapine monotherapy studies in adolescent patients (up to 6 weeks) with schizophrenia or bipolar I disorder (manic or mixed episodes), changes from normal to high in prolactin concentrations were observed in 47% of olanzapine-treated patients compared to 7% of placebo-treated patients. In a pooled analysis from clinical trials including 454 adolescents treated with olanzapine, potentially associated clinical manifestations included menstrual-related events 1(1% [2/168] of females), sexual function-related events 2(0.7% [3/454] of females and males), and breast-related events 3(2% [3/168] of females, 2% [7/286] of males) [see Use in Specific Populations (8.4)] .
1 Based on a search of the following terms: amenorrhea, hypomenorrhea, menstruation delayed, and oligomenorrhea.
2 Based on a search of the following terms: anorgasmia, delayed ejaculation, erectile dysfunction, decreased libido, loss of libido, abnormal orgasm, and sexual dysfunction.
3 Based on a search of the following terms: breast discharge, enlargement or swelling, galactorrhea, gynecomastia, and lactation disorder.
Dose group differences with respect to prolactin elevation have been observed. In a single 8-week randomized, double-blind, fixed-dose study comparing 10 (N=199), 20 (N=200) and 40 (N=200) mg/day of oral olanzapine in adult patients with schizophrenia or schizoaffective disorder, incidence of prolactin elevation >24.2 ng/mL (female) or >18.77 ng/mL (male) at any time during the trial (10 mg/day: 31.2%; 20 mg/day: 42.7%; 40 mg/day: 61.1%) indicated significant differences between 10 vs 40 mg/day and 20 vs 40 mg/day.
12.1 Mechanism of Action
The mechanism of action of olanzapine, in the listed indications is unclear. However, the efficacy of olanzapine in schizophrenia could be mediated through a combination of dopamine and serotonin type 2 (5HT2) antagonism.
16.2 Storage and Handling
Store Olanzapine for Injection vials (before reconstitution) at controlled room temperature, 20° to 25°C (68° to 77°F) [ seeUSP]. Reconstituted Olanzapine for Injection may be stored at controlled room temperature, 20° to 25°C (68° to 77°F) [ seeUSP] for up to 1 hour if necessary. Discard any unused portion of reconstituted Olanzapine for Injection.The USP defines controlled room temperature as a temperature maintained thermostatically that encompasses the usual and customary working environment of 20° to 25°C (68° to 77°F); that results in a mean kinetic temperature calculated to be not more than 25°C; and that allows for excursions between 15° and 30°C (59° and 86°F) that are experienced in pharmacies, hospitals, and warehouses.
Protect Olanzapine for Injection from light, do not freeze.
5 Warnings and Precautions
- Elderly Patients with Dementia-Related Psychosis:Increased risk of death and increased incidence of cerebrovascular adverse events (e.g., stroke, transient ischemic attack). (5.1)
- Suicide:The possibility of a suicide attempt is inherent in schizophrenia and in bipolar I disorder, and close supervision of high-risk patients should accompany drug therapy. (5.2)
- Neuroleptic Malignant Syndrome:Manage with immediate discontinuation and close monitoring. (5.3)
- Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS):Discontinue if DRESS is suspected. (5.4)
-
Metabolic Changes:Atypical antipsychotic drugs have been associated with metabolic changes including hyperglycemia, dyslipidemia, and weight gain. (5.5)
- Hyperglycemia and Diabetes Mellitus:In some cases extreme and associated with ketoacidosis or hyperosmolar coma or death, has been reported in patients taking olanzapine. Patients taking olanzapine should be monitored for symptoms of hyperglycemia and undergo fasting blood glucose testing at the beginning of, and periodically during, treatment. (5.5)
- Dyslipidemia:Undesirable alterations in lipids have been observed. Appropriate clinical monitoring is recommended, including fasting blood lipid testing at the beginning of, and periodically during, treatment. (5.5)
- Weight Gain:Potential consequences of weight gain should be considered. Patients should receive regular monitoring of weight. (5.5)
- Tardive Dyskinesia:Discontinue if clinically appropriate. (5.6)
- Orthostatic Hypotension:Orthostatic hypotension associated with dizziness, tachycardia, bradycardia and, in some patients, syncope, may occur especially during initial dose titration. Use caution in patients with cardiovascular disease, cerebrovascular disease, and those conditions that could affect hemodynamic responses. (5.7)
- Leukopenia, Neutropenia, and Agranulocytosis:Has been reported with antipsychotics, including Olanzapine. Patients with a history of a clinically significant low white blood cell count (WBC) or drug induced leukopenia/neutropenia should have their complete blood count (CBC) monitored frequently during the first few months of therapy and discontinuation of Olanzapine should be considered at the first sign of a clinically significant decline in WBC in the absence of other causative factors. (5.9)
- Seizures:Use cautiously in patients with a history of seizures or with conditions that potentially lower the seizure threshold. (5.11)
- Potential for Cognitive and Motor Impairment:Has potential to impair judgment, thinking, and motor skills. Use caution when operating machinery. (5.12)
- Anticholinergic (antimuscarinic) Effects:Use with caution with other anticholinergic drugs and in patients with urinary retention, prostatic hypertrophy, constipation, paralytic ileus or related conditions. (5.14)
- Hyperprolactinemia:May elevate prolactin levels. (5.15)
- Use in Combination with Lithium or Valproate:Also refer to the package inserts for lithium or valproate. (5.16)
- Laboratory Tests:Monitor fasting blood glucose and lipid profiles at the beginning of, and periodically during, treatment. (5.17)
10.2 Management of Overdose
There is no specific antidote to an overdose of Olanzapine. The possibility of multiple drug involvement should be considered. Establish and maintain an airway and ensure adequate oxygenation and ventilation. Cardiovascular monitoring should commence immediately and should include continuous electrocardiographic monitoring to detect possible arrhythmias.
Contact a Certified Poison Control Center for the most up to date information on the management of overdosage (1-800-222-1222).
For specific information about overdosage with lithium or valproate, refer to the Overdosage section of the prescribing information for these products.
2 Dosage and Administration
| Agitation associated with Schizophrenia and Bipolar I Mania in adults (2.4) | IM: 10 mg (5 mg or 7.5 mg when clinically warranted)
Assess for orthostatic hypotension prior to subsequent dosing (max. 3 doses 2-4 hrs apart) |
- Lower starting dose recommended in debilitated or pharmacodynamically sensitive patients or patients with predisposition to hypotensive reactions, or with potential for slowed metabolism. (2.4)
5.7 Orthostatic Hypotension
Olanzapine may induce orthostatic hypotension associated with dizziness, tachycardia, bradycardia and, in some patients, syncope, especially during the initial dose-titration period, probably reflecting its α 1-adrenergic antagonistic properties [see Patient Counseling Information (17)] .
From an analysis of the vital sign data in an integrated database of 41 completed clinical studies in adult patients treated with oral olanzapine, orthostatic hypotension was recorded in ≥20% (1277/6030) of patients.
For oral olanzapine therapy, the risk of orthostatic hypotension and syncope may be minimized by initiating therapy with 5 mg QD [see Dosage and Administration (2)] . A more gradual titration to the target dose should be considered if hypotension occurs.
Hypotension, bradycardia with or without hypotension, tachycardia, and syncope were also reported during the clinical trials with intramuscular olanzapine for injection. In an open-label clinical pharmacology study in nonagitated patients with schizophrenia in which the safety and tolerability of intramuscular olanzapine were evaluated under a maximal dosing regimen (three 10 mg doses administered 4 hours apart), approximately one-third of these patients experienced a significant orthostatic decrease in systolic blood pressure (i.e., decrease ≥30 mmHg) [see Dosage and Administration (2.4)] . Syncope was reported in 0.6% (15/2500) of olanzapine-treated patients in phase 2-3 oral olanzapine studies and in 0.3% (2/722) of olanzapine-treated patients with agitation in the intramuscular olanzapine for injection studies. Three normal volunteers in phase 1 studies with intramuscular olanzapine experienced hypotension, bradycardia, and sinus pauses of up to 6 seconds that spontaneously resolved (in 2 cases the reactions occurred on intramuscular olanzapine, and in 1 case, on oral olanzapine). The risk for this sequence of hypotension, bradycardia, and sinus pause may be greater in nonpsychiatric patients compared to psychiatric patients who are possibly more adapted to certain effects of psychotropic drugs. For intramuscular olanzapine for injection therapy, patients should remain recumbent if drowsy or dizzy after injection until examination has indicated that they are not experiencing postural hypotension, bradycardia, and/or hypoventilation.
Olanzapine should be used with particular caution in patients with known cardiovascular disease (history of myocardial infarction or ischemia, heart failure, or conduction abnormalities), cerebrovascular disease, and conditions which would predispose patients to hypotension (dehydration, hypovolemia, and treatment with antihypertensive medications) where the occurrence of syncope, or hypotension and/or bradycardia might put the patient at increased medical risk.
Caution is necessary in patients who receive treatment with other drugs having effects that can induce hypotension, bradycardia, respiratory or central nervous system depression [see Drug Interactions (7)] . Concomitant administration of intramuscular olanzapine and parenteral benzodiazepine is not recommended due to the potential for excessive sedation and cardiorespiratory depression.
3 Dosage Forms and Strengths
Olanzapine for Injection is available as single-dose 10 mg vial (1s).
6.2 Postmarketing Experience
The following adverse reactions have been identified during post-approval use of Olanzapine. Because these reactions are reported voluntarily from a population of uncertain size, it is difficult to reliably estimate their frequency or evaluate a causal relationship to drug exposure.
Adverse reactions reported since market introduction that were temporally (but not necessarily causally) related to Olanzapine therapy include the following: allergic reaction (e.g., anaphylactoid reaction, angioedema, pruritus or urticaria), cholestatic or mixed liver injury, diabetic coma, diabetic ketoacidosis, discontinuation reaction (diaphoresis, nausea or vomiting), Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS), hepatitis, jaundice, neutropenia, pancreatitis, priapism, rash, restless legs syndrome, rhabdomyolysis, salivary hypersecretion, stuttering 1, venous thromboembolic events (including pulmonary embolism and deep venous thrombosis), fecal incontinence, and somnambulism. Random cholesterol levels of ≥240 mg/dL and random triglyceride levels of ≥1000 mg/dL have been reported.
1Stuttering was only studied in oral and long acting injection (LAI) formulations.
8 Use in Specific Populations
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect or predict the rates observed in practice.
5.13 Body Temperature Regulation
Disruption of the body’s ability to reduce core body temperature has been attributed to antipsychotic agents. Appropriate care is advised when prescribing olanzapine for patients who will be experiencing conditions which may contribute to an elevation in core body temperature, e.g., exercising strenuously, exposure to extreme heat, receiving concomitant medication with anticholinergic activity, or being subject to dehydration [see Patient Counseling Information (17)] .
17 Patient Counseling Information
Patients should be advised of the following issues and asked to alert their prescriber if these occur while taking Olanzapine as monotherapy. If you do not think you are getting better or have any concerns about your condition while taking Olanzapine, call your doctor.
5.3 Neuroleptic Malignant Syndrome (nms)
A potentially fatal symptom complex sometimes referred to as Neuroleptic Malignant Syndrome (NMS) has been reported in association with administration of antipsychotic drugs, including olanzapine. Clinical manifestations of NMS are hyperpyrexia, muscle rigidity, altered mental status and evidence of autonomic instability (irregular pulse or blood pressure, tachycardia, diaphoresis and cardiac dysrhythmia). Additional signs may include elevated creatinine phosphokinase, myoglobinuria (rhabdomyolysis), and acute renal failure.
The diagnostic evaluation of patients with this syndrome is complicated. In arriving at a diagnosis, it is important to exclude cases where the clinical presentation includes both serious medical illness (e.g., pneumonia, systemic infection, etc.) and untreated or inadequately treated extrapyramidal signs and symptoms (EPS). Other important considerations in the differential diagnosis include central anticholinergic toxicity, heat stroke, drug fever, and primary central nervous system pathology.
The management of NMS should include: 1) immediate discontinuation of antipsychotic drugs and other drugs not essential to concurrent therapy; 2) intensive symptomatic treatment and medical monitoring; and 3) treatment of any concomitant serious medical problems for which specific treatments are available. There is no general agreement about specific pharmacological treatment regimens for NMS.
If a patient requires antipsychotic drug treatment after recovery from NMS, the potential reintroduction of drug therapy should be carefully considered. The patient should be carefully monitored, since recurrences of NMS have been reported [see Patient Counseling Information (17)] .
13.2 Animal Toxicology And/or Pharmacology
In animal studies with olanzapine, the principal hematologic findings were reversible peripheral cytopenias in individual dogs dosed at 10 mg/kg (17 times the daily oral MRHD based on mg/m 2body surface area), dose-related decreases in lymphocytes and neutrophils in mice, and lymphopenia in rats. A few dogs treated with 10 mg/kg developed reversible neutropenia and/or reversible hemolytic anemia between 1 and 10 months of treatment. Dose-related decreases in lymphocytes and neutrophils were seen in mice given doses of 10 mg/kg (equal to 2 times the daily oral MRHD based on mg/m 2body surface area) in studies of 3 months' duration. Nonspecific lymphopenia, consistent with decreased body weight gain, occurred in rats receiving 22.5 mg/kg (11 times the daily oral MRHD based on mg/m 2body surface area) for 3 months or 16 mg/kg (8 times the daily oral MRHD based on mg/m 2body surface area) for 6 or 12 months. No evidence of bone marrow cytotoxicity was found in any of the species examined. Bone marrows were normocellular or hypercellular, indicating that the reductions in circulating blood cells were probably due to peripheral (non-marrow) factors.
5.14 anticholinergic (antimuscarinic) Effects
Olanzapine exhibits in vitro muscarinic receptor affinity [see Clinical Pharmacology 12.2] . In premarketing clinical trials, Olanzapine was associated with constipation, dry mouth, and tachycardia, all adverse reactions possibly related to cholinergic antagonism. Such adverse reactions were not often the basis for discontinuations, but Olanzapine should be used with caution in patients with a current diagnosis or prior history of urinary retention, clinically significant prostatic hypertrophy, constipation, or a history of paralytic ileus or related conditions. In post marketing experience, the risk for severe adverse reactions (including fatalities) was increased with concomitant use of anticholinergic medications [see Drug Interactions (7.1)] .
Package Label Vial Principal Display Panel
NDC 0121-1072-55
Olanzapine
for Injection
10 mg/ vial
For Intramuscular Use Only
Single-Dose Vial
PAI Pharma Rx Only
5.9 Leukopenia, Neutropenia, and Agranulocytosis
Class Effect— In clinical trial and/or postmarketing experience, events of leukopenia/neutropenia have been reported temporally related to antipsychotic agents, including Olanzapine. Agranulocytosis has also been reported.
Possible risk factors for leukopenia/neutropenia include pre-existing low white blood cell count (WBC) and history of drug induced leukopenia/neutropenia. Patients with a history of a clinically significant low WBC or drug induced leukopenia/neutropenia should have their complete blood count (CBC) monitored frequently during the first few months of therapy and discontinuation of Olanzapine should be considered at the first sign of a clinically significant decline in WBC in the absence of other causative factors.
Patients with clinically significant neutropenia should be carefully monitored for fever or other symptoms or signs of infection and treated promptly if such symptoms or signs occur. Patients with severe neutropenia (absolute neutrophil count <1000/mm 3) should discontinue Olanzapine and have their WBC followed until recovery.
8.3 females and Males of Reproductive Potential
Infertility
Females
Based on the pharmacologic action of olanzapine (D
2receptor antagonism), treatment with Olanzapine may result in an increase in serum prolactin levels, which may lead to a reversible reduction in fertility in females of reproductive potential
[see Warnings and Precautions (5.15)]
.
Package Label Carton Principal Display Panel
NDC 0121-1072-55
Olanzapine
for Injection
10 mg/ vial
Single-Dose Vial
For Intramuscular
Use Only
Rx Only
P AI Pharma
5.12 Potential for Cognitive and Motor Impairment
Somnolence was a commonly reported adverse reaction associated with olanzapine treatment, occurring at an incidence of 26% in olanzapine patients compared to 15% in placebo patients. This adverse reaction was also dose related. Somnolence led to discontinuation in 0.4% (9/2500) of patients in the premarketing database.
Since olanzapine has the potential to impair judgment, thinking, or motor skills, patients should be cautioned about operating hazardous machinery, including automobiles, until they are reasonably certain that olanzapine therapy does not affect them adversely [see Patient Counseling Information (17)] .
5.16 Use in Combination With Lithium Or Valproate
When using Olanzapine in combination with lithium or valproate, the prescriber should refer to the Warnings and Precautions sections of the package inserts for lithium or valproate [see Drug Interactions (7)] .
14.3 Agitation Associated With Schizophrenia and Bipolar I Mania
The efficacy of intramuscular olanzapine for injection for the treatment of agitation was established in 3 short-term (24 hours of IM treatment) placebo-controlled trials in agitated adult inpatients from 2 diagnostic groups: schizophrenia and bipolar I disorder (manic or mixed episodes). Each of the trials included a single active comparator treatment arm of either haloperidol injection (schizophrenia studies) or lorazepam injection (bipolar I mania study). Patients enrolled in the trials needed to be: (1) judged by the clinical investigators as clinically agitated and clinically appropriate candidates for treatment with intramuscular medication, and (2) exhibiting a level of agitation that met or exceeded a threshold score of ≥14 on the 5 items comprising the Positive and Negative Syndrome Scale (PANSS) Excited Component (i.e., poor impulse control, tension, hostility, uncooperativeness and excitement items) with at least 1 individual item score ≥4 using a 1-7 scoring system (1=absent, 4=moderate, 7=extreme). In the studies, the mean baseline PANSS Excited Component score was 18.4, with scores ranging from 13 to 32 (out of a maximum score of 35), thus suggesting predominantly moderate levels of agitation with some patients experiencing mild or severe levels of agitation. The primary efficacy measure used for assessing agitation signs and symptoms in these trials was the change from baseline in the PANSS Excited Component at 2 hours post-injection. Patients could receive up to 3 injections during the 24 hour IM treatment periods; however, patients could not receive the second injection until after the initial 2 hour period when the primary efficacy measure was assessed. The results of the trials follow:
(1) In a placebo-controlled trial in agitated inpatients meeting DSM-IV criteria for schizophrenia (n=270), 4 fixed intramuscular olanzapine for injection doses of 2.5 mg, 5 mg, 7.5 mg and 10 mg were evaluated. All doses were statistically superior to placebo on the PANSS Excited Component at 2 hours post-injection. However, the effect was larger and more consistent for the 3 highest doses. There were no significant pairwise differences for the 7.5 and 10 mg doses over the 5 mg dose.
(2) In a second placebo-controlled trial in agitated inpatients meeting DSM-IV criteria for schizophrenia (n=311), 1 fixed intramuscular olanzapine for injection dose of 10 mg was evaluated. Olanzapine for injection was statistically superior to placebo on the PANSS Excited Component at 2 hours post-injection.
(3) In a placebo-controlled trial in agitated inpatients meeting DSM-IV criteria for bipolar I disorder (and currently displaying an acute manic or mixed episode with or without psychotic features) (n=201), 1 fixed intramuscular olanzapine for injection dose of 10 mg was evaluated. Olanzapine for injection was statistically superior to placebo on the PANSS Excited Component at 2 hours post-injection.
Examination of population subsets (age, race, and gender) did not reveal any differential responsiveness on the basis of these subgroupings.
5.4 Drug Reaction With Eosinophilia and Systemic Symptoms (dress)
Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS) has been reported with olanzapine exposure. DRESS may present with a cutaneous reaction (such as rash or exfoliative dermatitis), eosinophilia, fever, and/or lymphadenopathy with systemic complications such as hepatitis, nephritis, pneumonitis, myocarditis, and/or pericarditis. DRESS is sometimes fatal. Discontinue olanzapine if DRESS is suspected [see Patient Counseling Information (17)] .
Warning: Increased Mortality in Elderly Patients With Dementia Related Psychosis
Elderly patients with dementia-related psychosis treated with antipsychotic drugs are at an increased risk of death. Analyses of seventeen placebo-controlled trials (modal duration of 10 weeks), largely in patients taking atypical antipsychotic drugs, revealed a risk of death in drug-treated patients of between 1.6 to 1.7 times the risk of death in placebo-treated patients. Over the course of a typical 10-week controlled trial, the rate of death in drug-treated patients was about 4.5%, compared to a rate of about 2.6% in the placebo group. Although the causes of death were varied, most of the deaths appeared to be either cardiovascular (e.g., heart failure, sudden death) or infectious (e.g., pneumonia) in nature. Observational studies suggest that, similar to atypical antipsychotic drugs, treatment with conventional antipsychotic drugs may increase mortality. The extent to which the findings of increased mortality in observational studies may be attributed to the antipsychotic drug as opposed to some characteristic(s) of the patients is not clear. Olanzapine is not approved for the treatment of patients with dementia-related psychosis [see Warnings and Precautions (5.1), Use in Specific Populations (8.5), and Patient Counseling Information (17)] .
1.4 olanzapine for Injection: Agitation Associated With Schizophrenia and Bipolar I Mania
Olanzapine for Injection is indicated for the treatment of acute agitation associated with schizophrenia and bipolar I mania.
Efficacy was demonstrated in 3 short-term (24 hours of IM treatment) placebo-controlled trials in agitated adult inpatients with: schizophrenia or bipolar I disorder (manic or mixed episodes) [see Clinical Studies (14.3)] .
“Psychomotor agitation” is defined in DSM-IV as “excessive motor activity associated with a feeling of inner tension.” Patients experiencing agitation often manifest behaviors that interfere with their diagnosis and care, e.g., threatening behaviors, escalating or urgently distressing behavior, or self-exhausting behavior, leading clinicians to the use of intramuscular antipsychotic medications to achieve immediate control of the agitation.
Structured Label Content
Section 34077-8 (34077-8)
Pregnancy Exposure Registry
There is a pregnancy exposure registry that monitors pregnancy outcomes in women exposed to atypical antipsychotics, including Olanzapine, during pregnancy. Healthcare providers are encouraged to register patients by contacting the National Pregnancy Registry for Atypical Antipsychotics at 1-866-961-2388 or visit http://womensmentalhealth.org/clinical-and-research-programs/pregnancyregistry/.
Risk Summary
Neonates exposed to antipsychotic drugs, including Olanzapine, during the third trimester are at risk for extrapyramidal and/or withdrawal symptoms following delivery (see
Clinical Considerations). Overall available data from published epidemiologic studies of pregnant women exposed to olanzapine have not established a drug-associated risk of major birth defects, miscarriage, or adverse maternal or fetal outcomes (see
Data). There are risks to the mother associated with untreated schizophrenia or bipolar I disorder and with exposure to antipsychotics, including Olanzapine, during pregnancy (see
Clinical Considerations).
Olanzapine was not teratogenic when administered orally to pregnant rats and rabbits at doses that are 9- and 30-times the daily oral maximum recommended human dose (MRHD), based on mg/m
2body surface area; some fetal toxicities were observed at these doses (see
Data).
The estimated background risk of major birth defects and miscarriage for the indicated populations is unknown. All pregnancies have a background risk of birth defects, loss, or other adverse outcomes. In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2% to 4% and 15% to 20%, respectively.
Clinical Considerations
Disease-associated maternal and embryo/fetal risk
There is a risk to the mother from untreated schizophrenia or bipolar I disorder, including increased risk of relapse, hospitalization, and suicide. Schizophrenia and bipolar I disorder are associated with increased adverse perinatal outcomes, including preterm birth. It is not known if this is a direct result of the illness or other comorbid factors.
Fetal/Neonatal adverse reactions
Extrapyramidal and/or withdrawal symptoms, including agitation, hypertonia, hypotonia, tremor, somnolence, respiratory distress, and feeding disorder have been reported in neonates who were exposed to antipsychotic drugs, including Olanzapine, during the third trimester of pregnancy. These symptoms have varied in severity. Monitor neonates for extrapyramidal and/or withdrawal symptoms and manage symptoms appropriately. Some neonates recovered within hours or days without specific treatment; others required prolonged hospitalization.
Section 34078-6 (34078-6)
Data
Human Data
Placental passage has been reported in published study reports; however, the placental passage ratio was highly variable ranging between 7% to 167% at birth following exposure during pregnancy. The clinical relevance of this finding is unknown.
Published data from observational studies, birth registries, and case reports that have evaluated the use of atypical antipsychotics during pregnancy do not establish an increased risk of major birth defects. A retrospective cohort study from a Medicaid database of 9258 women exposed to antipsychotics during pregnancy did not indicate an overall increased risk for major birth defects.
Animal Data
In oral reproduction studies in rats at doses up to 18 mg/kg/day and in rabbits at doses up to 30 mg/kg/day (9 and 30 times the daily oral MRHD based on mg/m
2body surface area, respectively), no evidence of teratogenicity was observed. In an oral rat teratology study, early resorptions and increased numbers of nonviable fetuses were observed at a dose of 18 mg/kg/day (9 times the daily oral MRHD based on mg/m
2body surface area), and gestation was prolonged at 10 mg/kg/day (5 times the daily oral MRHD based on mg/m
2body surface area). In an oral rabbit teratology study, fetal toxicity manifested as increased resorptions and decreased fetal weight, occurred at a maternally toxic dose of 30 mg/kg/day (30 times the daily oral MRHD based on mg/m
2body surface area).
Section 42229-5 (42229-5)
Dose Selection for Agitated Adult Patients with Schizophrenia and Bipolar I Mania — The efficacy of intramuscular olanzapine for injection in controlling agitation in these disorders was demonstrated in a dose range of 2.5 mg to 10 mg. The recommended dose in these patients is 10 mg. A lower dose of 5 or 7.5 mg may be considered when clinical factors warrant [see Clinical Studies (14.3)] . If agitation warranting additional intramuscular doses persists following the initial dose, subsequent doses up to 10 mg may be given. However, the efficacy of repeated doses of intramuscular olanzapine for injection in agitated patients has not been systematically evaluated in controlled clinical trials. Also, the safety of total daily doses greater than 30 mg, or 10 mg injections given more frequently than 2 hours after the initial dose, and 4 hours after the second dose have not been evaluated in clinical trials. Maximal dosing of intramuscular olanzapine (e.g., 3 doses of 10 mg administered 2-4 hours apart) may be associated with a substantial occurrence of significant orthostatic hypotension [see Warnings and Precautions (5.7)] . Thus, it is recommended that patients requiring subsequent intramuscular injections be assessed for orthostatic hypotension prior to the administration of any subsequent doses of intramuscular olanzapine for injection. The administration of an additional dose to a patient with a clinically significant postural change in systolic blood pressure is not recommended.
If ongoing olanzapine therapy is clinically indicated, oral olanzapine may be initiated in a range of 5-20 mg/day as soon as clinically appropriate.
Section 43683-2 (43683-2)
| Warnings and Precautions (5.11) | 1/2025 |
5.8 Falls
Olanzapine may cause somnolence, postural hypotension, motor and sensory instability, which may lead to falls and, consequently, fractures or other injuries. For patients with diseases, conditions, or medications that could exacerbate these effects, complete fall risk assessments when initiating antipsychotic treatment and recurrently for patients on long-term antipsychotic therapy.
5.2 Suicide
The possibility of a suicide attempt is inherent in schizophrenia and in bipolar I disorder, and close supervision of high-risk patients should accompany drug therapy. Prescriptions for olanzapine should be written for the smallest quantity of tablets consistent with good patient management, in order to reduce the risk of overdose.
5.11 Seizures
During premarketing testing, seizures occurred in 0.9% (22/2500) of olanzapine-treated patients. There were confounding factors that may have contributed to the occurrence of seizures in many of these cases. Olanzapine should be used cautiously in patients with a history of seizures or with conditions that potentially lower the seizure threshold, e.g., Alzheimer's dementia. Olanzapine is not approved for the treatment of patients with Alzheimer's disease. Conditions that lower the seizure threshold may be more prevalent in a population of 65 years or older.
11 Description (11 DESCRIPTION)
Olanzapine is an atypical antipsychotic that belongs to the thienobenzodiazepine class. The chemical designation is 2-methyl-4-(4-methyl-1-piperazinyl)-10 H-thieno[2,3- b] [1,5]benzodiazepine. The molecular formula is C 17H 20N 4S, which corresponds to a molecular weight of 312.44. The chemical structure is:
Olanzapine is a yellow crystalline solid, which is practically insoluble in water.
Olanzapine for injection is intended for intramuscular use only.
Each single-dose vial provides for the administration of 10 mg (32 μmol) olanzapine with inactive ingredients 50 mg lactose monohydrate and 3.5 mg tartaric acid. Hydrochloric acid and/or sodium hydroxide may have been added during manufacturing to adjust pH.
5.10 Dysphagia
Esophageal dysmotility and aspiration have been associated with antipsychotic drug use. Aspiration pneumonia is a common cause of morbidity and mortality in patients with advanced Alzheimer's disease. Olanzapine is not approved for the treatment of patients with Alzheimer's disease.
8.2 lactation (8.2 Lactation)
Risk Summary
Olanzapine is present in human milk. There are reports of excess sedation, irritability, poor feeding and extrapyramidal symptoms (tremors and abnormal muscle movements) in infants exposed to olanzapine through breast milk (see
Clinical Considerations). There is no information on the effects of olanzapine on milk production.
The developmental and health benefits of breastfeeding should be considered along with the mother’s clinical need for Olanzapine and any potential adverse effects on the breastfed child from Olanzapine or from the mother’s underlying condition.
Clinical Considerations
Infants exposed to Olanzapine should be monitored for excess sedation, irritability, poor feeding, and extrapyramidal symptoms (tremors and abnormal muscle movements).
9.3 Dependence
In studies prospectively designed to assess abuse and dependence potential, olanzapine was shown to have acute depressive CNS effects but little or no potential of abuse or physical dependence in rats administered oral doses up to 15 times the daily oral MRHD (20 mg) and rhesus monkeys administered oral doses up to 8 times the daily oral MRHD based on mg/m 2body surface area.
Olanzapine has not been systematically studied in humans for its potential for abuse, tolerance, or physical dependence. While the clinical trials did not reveal any tendency for any drug-seeking behavior, these observations were not systematic, and it is not possible to predict on the basis of this limited experience the extent to which a CNS-active drug will be misused, diverted, and/or abused once marketed. Consequently, patients should be evaluated carefully for a history of drug abuse, and such patients should be observed closely for signs of misuse or abuse of olanzapine (e.g., development of tolerance, increases in dose, drug-seeking behavior).
16.1 How Supplied
Olanzapine for Injection is available in:
NDC 0121-1072-55 – 10 mg single-dose vial (1s)
8.4 Pediatric Use
Compared to patients from adult clinical trials, adolescents were likely to gain more weight, experience increased sedation, and have greater increases in total cholesterol, triglycerides, LDL cholesterol, prolactin and hepatic aminotransferase levels [see Warnings and Precautions (5.5, 5.15, 5.17) and Adverse Reactions (6.1)] . When deciding among the alternative treatments available for adolescents, clinicians should consider the increased potential (in adolescents as compared with adults) for weight gain and dyslipidemia. Clinicians should consider the potential long-term risks when prescribing to adolescents, and in many cases this may lead them to consider prescribing other drugs first in adolescents.
Safety and effectiveness of olanzapine in children <13 years of age have not been established [see Patient Counseling Information (17)] .
8.5 Geriatric Use
Of the 2500 patients in premarketing clinical studies with oral olanzapine, 11% (263) were 65 years of age or over. In patients with schizophrenia, there was no indication of any different tolerability of olanzapine in the elderly compared to younger patients. Studies in elderly patients with dementia-related psychosis have suggested that there may be a different tolerability profile in this population compared to younger patients with schizophrenia. Elderly patients with dementia-related psychosis treated with olanzapine are at an increased risk of death compared to placebo. In placebo-controlled studies of olanzapine in elderly patients with dementia-related psychosis, there was a higher incidence of cerebrovascular adverse events (e.g., stroke, transient ischemic attack) in patients treated with olanzapine compared to patients treated with placebo. In 5 placebo-controlled studies of olanzapine in elderly patients with dementia-related psychosis (n=1184), the following adverse reactions were reported in olanzapine-treated patients at an incidence of at least 2% and significantly greater than placebo-treated patients: falls, somnolence, peripheral edema, abnormal gait, urinary incontinence, lethargy, increased weight, asthenia, pyrexia, pneumonia, dry mouth and visual hallucinations. The rate of discontinuation due to adverse reactions was greater with olanzapine than placebo (13% vs 7%). Elderly patients with dementia-related psychosis treated with olanzapine are at an increased risk of death compared to placebo. Olanzapine is not approved for the treatment of patients with dementia-related psychosis [see Boxed Warning, Warnings and Precautions (5.1), and Patient Counseling Information (17)] . Olanzapine is not approved for the treatment of patients with dementia-related psychosis. Also, the presence of factors that might decrease pharmacokinetic clearance or increase the pharmacodynamic response to olanzapine should lead to consideration of a lower starting dose for any geriatric patient [see Boxed Warning and Warnings and Precautions (5.1)] .
4 Contraindications (4 CONTRAINDICATIONS)
- None with Olanzapine monotherapy.
- For specific information about the contraindications of lithium or valproate, refer to the Contraindications section of the package inserts for these other products.
6 Adverse Reactions (6 ADVERSE REACTIONS)
Most common adverse reactions (≥5% and at least twice that for placebo) associated with:
Combination of Olanzapine and Lithium or Valproate:
- Manic or Mixed Episodes, Bipolar I Disorder (Adults) – dry mouth, weight gain, increased appetite, dizziness, back pain, constipation, speech disorder, increased salivation, amnesia, paresthesia (6.1)
Olanzapine for Injection:
- Agitation with Schizophrenia and Bipolar I Mania (Adults) – somnolence (6.1)
To report SUSPECTED ADVERSE REACTIONS, contact PAI Pharma at 1-800-845-8210 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch
7 Drug Interactions (7 DRUG INTERACTIONS)
The risks of using olanzapine in combination with other drugs have not been extensively evaluated in systematic studies.
10.1 Human Experience
In premarketing trials involving more than 3100 patients and/or normal subjects, accidental or intentional acute overdosage of olanzapine was identified in 67 patients. In the patient taking the largest identified amount, 300 mg, the only symptoms reported were drowsiness and slurred speech. In the limited number of patients who were evaluated in hospitals, including the patient taking 300 mg, there were no observations indicating an adverse change in laboratory analytes or ECG. Vital signs were usually within normal limits following overdoses.
In postmarketing reports of overdose with olanzapine alone, symptoms have been reported in the majority of cases. In symptomatic patients, symptoms with ≥10% incidence included agitation/aggressiveness, dysarthria, tachycardia, various extrapyramidal symptoms, and reduced level of consciousness ranging from sedation to coma. Among less commonly reported symptoms were the following potentially medically serious reactions: aspiration, cardiopulmonary arrest, cardiac arrhythmias (such as supraventricular tachycardia and 1 patient experiencing sinus pause with spontaneous resumption of normal rhythm), delirium, possible neuroleptic malignant syndrome, respiratory depression/arrest, convulsion, hypertension, and hypotension. Eli Lilly and Company has received reports of fatality in association with overdose of olanzapine alone. In 1 case of death, the amount of acutely ingested olanzapine was reported to be possibly as low as 450 mg of oral olanzapine; however, in another case, a patient was reported to survive an acute olanzapine ingestion of approximately 2 g of oral olanzapine.
12.2 Pharmacodynamics
Olanzapine binds with high affinity to the following receptors: serotonin 5HT 2A/2C, 5HT 6(K i=4, 11, and 5 nM, respectively), dopamine D 1-4(K i=11-31 nM), histamine H 1(K i=7 nM), and adrenergic α 1receptors (K i=19 nM). Olanzapine is an antagonist with moderate affinity binding for serotonin 5HT 3(K i=57 nM) and muscarinic M 1-5(K i=73, 96, 132, 32, and 48 nM, respectively). Olanzapine binds with low affinity to GABA A, BZD, and β-adrenergic receptors (K i>10 μM).
5.17 Laboratory Tests
5.5 Metabolic Changes
Atypical antipsychotic drugs have been associated with metabolic changes including hyperglycemia, dyslipidemia, and weight gain. Metabolic changes may be associated with increased cardiovascular/cerebrovascular risk. Olanzapine's specific metabolic profile is presented below.
5.6 Tardive Dyskinesia
A syndrome of potentially irreversible, involuntary, dyskinetic movements may develop in patients treated with antipsychotic drugs. Although the prevalence of the syndrome appears to be highest among the elderly, especially elderly women, it is impossible to rely upon prevalence estimates to predict, at the inception of antipsychotic treatment, which patients are likely to develop the syndrome. Whether antipsychotic drug products differ in their potential to cause tardive dyskinesia is unknown.
The risk of developing tardive dyskinesia and the likelihood that it will become irreversible are believed to increase as the duration of treatment and the total cumulative dose of antipsychotic drugs administered to the patient increase. However, the syndrome can develop, although much less commonly, after relatively brief treatment periods at low doses or may even arise after discontinuation of treatment.
Tardive dyskinesia may remit, partially or completely, if antipsychotic treatment is withdrawn. Antipsychotic treatment, itself, however, may suppress (or partially suppress) the signs and symptoms of the syndrome and thereby may possibly mask the underlying process. The effect that symptomatic suppression has upon the long-term course of the syndrome is unknown.
Given these considerations, olanzapine should be prescribed in a manner that is most likely to minimize the occurrence of tardive dyskinesia. Chronic antipsychotic treatment should generally be reserved for patients (1) who suffer from a chronic illness that is known to respond to antipsychotic drugs, and (2) for whom alternative, equally effective, but potentially less harmful treatments are not available or appropriate. In patients who do require chronic treatment, the smallest dose and the shortest duration of treatment producing a satisfactory clinical response should be sought. The need for continued treatment should be reassessed periodically.
If signs and symptoms of tardive dyskinesia appear in a patient on olanzapine, drug discontinuation should be considered. However, some patients may require treatment with olanzapine despite the presence of the syndrome.
For specific information about the warnings of lithium or valproate, refer to the Warnings section of the package inserts for these other products.
1 Indications and Usage (1 INDICATIONS AND USAGE)
5.15 Hyperprolactinemia
As with other drugs that antagonize dopamine D 2receptors, olanzapine elevates prolactin levels, and the elevation persists during chronic administration. Hyperprolactinemia may suppress hypothalamic GnRH, resulting in reduced pituitary gonadotropin secretion. This, in turn, may inhibit reproductive function by impairing gonadal steroidogenesis in both female and male patients. Galactorrhea, amenorrhea, gynecomastia, and impotence have been reported in patients receiving prolactin-elevating compounds. Long-standing hyperprolactinemia when associated with hypogonadism may lead to decreased bone density in both female and male subjects.
Tissue culture experiments indicate that approximately one-third of human breast cancers are prolactin dependent in vitro, a factor of potential importance if the prescription of these drugs is contemplated in a patient with previously detected breast cancer. As is common with compounds which increase prolactin release, an increase in mammary gland neoplasia was observed in the olanzapine carcinogenicity studies conducted in mice and rats [see Nonclinical Toxicology (13.1)] . Published epidemiologic studies have shown inconsistent results when exploring the potential association between hyperprolactinemia and breast cancer.
In placebo-controlled olanzapine clinical studies (up to 12 weeks), changes from normal to high in prolactin concentrations were observed in 30% of adults treated with olanzapine as compared to 10.5% of adults treated with placebo. In a pooled analysis from clinical studies including 8136 adults treated with olanzapine, potentially associated clinical manifestations included menstrual-related events 1(2% [49/3240] of females), sexual function-related events 2(2% [150/8136] of females and males), and breast-related events 3(0.7% [23/3240] of females, 0.2% [9/4896] of males).
In placebo-controlled olanzapine monotherapy studies in adolescent patients (up to 6 weeks) with schizophrenia or bipolar I disorder (manic or mixed episodes), changes from normal to high in prolactin concentrations were observed in 47% of olanzapine-treated patients compared to 7% of placebo-treated patients. In a pooled analysis from clinical trials including 454 adolescents treated with olanzapine, potentially associated clinical manifestations included menstrual-related events 1(1% [2/168] of females), sexual function-related events 2(0.7% [3/454] of females and males), and breast-related events 3(2% [3/168] of females, 2% [7/286] of males) [see Use in Specific Populations (8.4)] .
1 Based on a search of the following terms: amenorrhea, hypomenorrhea, menstruation delayed, and oligomenorrhea.
2 Based on a search of the following terms: anorgasmia, delayed ejaculation, erectile dysfunction, decreased libido, loss of libido, abnormal orgasm, and sexual dysfunction.
3 Based on a search of the following terms: breast discharge, enlargement or swelling, galactorrhea, gynecomastia, and lactation disorder.
Dose group differences with respect to prolactin elevation have been observed. In a single 8-week randomized, double-blind, fixed-dose study comparing 10 (N=199), 20 (N=200) and 40 (N=200) mg/day of oral olanzapine in adult patients with schizophrenia or schizoaffective disorder, incidence of prolactin elevation >24.2 ng/mL (female) or >18.77 ng/mL (male) at any time during the trial (10 mg/day: 31.2%; 20 mg/day: 42.7%; 40 mg/day: 61.1%) indicated significant differences between 10 vs 40 mg/day and 20 vs 40 mg/day.
12.1 Mechanism of Action
The mechanism of action of olanzapine, in the listed indications is unclear. However, the efficacy of olanzapine in schizophrenia could be mediated through a combination of dopamine and serotonin type 2 (5HT2) antagonism.
16.2 Storage and Handling
Store Olanzapine for Injection vials (before reconstitution) at controlled room temperature, 20° to 25°C (68° to 77°F) [ seeUSP]. Reconstituted Olanzapine for Injection may be stored at controlled room temperature, 20° to 25°C (68° to 77°F) [ seeUSP] for up to 1 hour if necessary. Discard any unused portion of reconstituted Olanzapine for Injection.The USP defines controlled room temperature as a temperature maintained thermostatically that encompasses the usual and customary working environment of 20° to 25°C (68° to 77°F); that results in a mean kinetic temperature calculated to be not more than 25°C; and that allows for excursions between 15° and 30°C (59° and 86°F) that are experienced in pharmacies, hospitals, and warehouses.
Protect Olanzapine for Injection from light, do not freeze.
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
- Elderly Patients with Dementia-Related Psychosis:Increased risk of death and increased incidence of cerebrovascular adverse events (e.g., stroke, transient ischemic attack). (5.1)
- Suicide:The possibility of a suicide attempt is inherent in schizophrenia and in bipolar I disorder, and close supervision of high-risk patients should accompany drug therapy. (5.2)
- Neuroleptic Malignant Syndrome:Manage with immediate discontinuation and close monitoring. (5.3)
- Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS):Discontinue if DRESS is suspected. (5.4)
-
Metabolic Changes:Atypical antipsychotic drugs have been associated with metabolic changes including hyperglycemia, dyslipidemia, and weight gain. (5.5)
- Hyperglycemia and Diabetes Mellitus:In some cases extreme and associated with ketoacidosis or hyperosmolar coma or death, has been reported in patients taking olanzapine. Patients taking olanzapine should be monitored for symptoms of hyperglycemia and undergo fasting blood glucose testing at the beginning of, and periodically during, treatment. (5.5)
- Dyslipidemia:Undesirable alterations in lipids have been observed. Appropriate clinical monitoring is recommended, including fasting blood lipid testing at the beginning of, and periodically during, treatment. (5.5)
- Weight Gain:Potential consequences of weight gain should be considered. Patients should receive regular monitoring of weight. (5.5)
- Tardive Dyskinesia:Discontinue if clinically appropriate. (5.6)
- Orthostatic Hypotension:Orthostatic hypotension associated with dizziness, tachycardia, bradycardia and, in some patients, syncope, may occur especially during initial dose titration. Use caution in patients with cardiovascular disease, cerebrovascular disease, and those conditions that could affect hemodynamic responses. (5.7)
- Leukopenia, Neutropenia, and Agranulocytosis:Has been reported with antipsychotics, including Olanzapine. Patients with a history of a clinically significant low white blood cell count (WBC) or drug induced leukopenia/neutropenia should have their complete blood count (CBC) monitored frequently during the first few months of therapy and discontinuation of Olanzapine should be considered at the first sign of a clinically significant decline in WBC in the absence of other causative factors. (5.9)
- Seizures:Use cautiously in patients with a history of seizures or with conditions that potentially lower the seizure threshold. (5.11)
- Potential for Cognitive and Motor Impairment:Has potential to impair judgment, thinking, and motor skills. Use caution when operating machinery. (5.12)
- Anticholinergic (antimuscarinic) Effects:Use with caution with other anticholinergic drugs and in patients with urinary retention, prostatic hypertrophy, constipation, paralytic ileus or related conditions. (5.14)
- Hyperprolactinemia:May elevate prolactin levels. (5.15)
- Use in Combination with Lithium or Valproate:Also refer to the package inserts for lithium or valproate. (5.16)
- Laboratory Tests:Monitor fasting blood glucose and lipid profiles at the beginning of, and periodically during, treatment. (5.17)
10.2 Management of Overdose
There is no specific antidote to an overdose of Olanzapine. The possibility of multiple drug involvement should be considered. Establish and maintain an airway and ensure adequate oxygenation and ventilation. Cardiovascular monitoring should commence immediately and should include continuous electrocardiographic monitoring to detect possible arrhythmias.
Contact a Certified Poison Control Center for the most up to date information on the management of overdosage (1-800-222-1222).
For specific information about overdosage with lithium or valproate, refer to the Overdosage section of the prescribing information for these products.
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
| Agitation associated with Schizophrenia and Bipolar I Mania in adults (2.4) | IM: 10 mg (5 mg or 7.5 mg when clinically warranted)
Assess for orthostatic hypotension prior to subsequent dosing (max. 3 doses 2-4 hrs apart) |
- Lower starting dose recommended in debilitated or pharmacodynamically sensitive patients or patients with predisposition to hypotensive reactions, or with potential for slowed metabolism. (2.4)
5.7 Orthostatic Hypotension
Olanzapine may induce orthostatic hypotension associated with dizziness, tachycardia, bradycardia and, in some patients, syncope, especially during the initial dose-titration period, probably reflecting its α 1-adrenergic antagonistic properties [see Patient Counseling Information (17)] .
From an analysis of the vital sign data in an integrated database of 41 completed clinical studies in adult patients treated with oral olanzapine, orthostatic hypotension was recorded in ≥20% (1277/6030) of patients.
For oral olanzapine therapy, the risk of orthostatic hypotension and syncope may be minimized by initiating therapy with 5 mg QD [see Dosage and Administration (2)] . A more gradual titration to the target dose should be considered if hypotension occurs.
Hypotension, bradycardia with or without hypotension, tachycardia, and syncope were also reported during the clinical trials with intramuscular olanzapine for injection. In an open-label clinical pharmacology study in nonagitated patients with schizophrenia in which the safety and tolerability of intramuscular olanzapine were evaluated under a maximal dosing regimen (three 10 mg doses administered 4 hours apart), approximately one-third of these patients experienced a significant orthostatic decrease in systolic blood pressure (i.e., decrease ≥30 mmHg) [see Dosage and Administration (2.4)] . Syncope was reported in 0.6% (15/2500) of olanzapine-treated patients in phase 2-3 oral olanzapine studies and in 0.3% (2/722) of olanzapine-treated patients with agitation in the intramuscular olanzapine for injection studies. Three normal volunteers in phase 1 studies with intramuscular olanzapine experienced hypotension, bradycardia, and sinus pauses of up to 6 seconds that spontaneously resolved (in 2 cases the reactions occurred on intramuscular olanzapine, and in 1 case, on oral olanzapine). The risk for this sequence of hypotension, bradycardia, and sinus pause may be greater in nonpsychiatric patients compared to psychiatric patients who are possibly more adapted to certain effects of psychotropic drugs. For intramuscular olanzapine for injection therapy, patients should remain recumbent if drowsy or dizzy after injection until examination has indicated that they are not experiencing postural hypotension, bradycardia, and/or hypoventilation.
Olanzapine should be used with particular caution in patients with known cardiovascular disease (history of myocardial infarction or ischemia, heart failure, or conduction abnormalities), cerebrovascular disease, and conditions which would predispose patients to hypotension (dehydration, hypovolemia, and treatment with antihypertensive medications) where the occurrence of syncope, or hypotension and/or bradycardia might put the patient at increased medical risk.
Caution is necessary in patients who receive treatment with other drugs having effects that can induce hypotension, bradycardia, respiratory or central nervous system depression [see Drug Interactions (7)] . Concomitant administration of intramuscular olanzapine and parenteral benzodiazepine is not recommended due to the potential for excessive sedation and cardiorespiratory depression.
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
Olanzapine for Injection is available as single-dose 10 mg vial (1s).
6.2 Postmarketing Experience
The following adverse reactions have been identified during post-approval use of Olanzapine. Because these reactions are reported voluntarily from a population of uncertain size, it is difficult to reliably estimate their frequency or evaluate a causal relationship to drug exposure.
Adverse reactions reported since market introduction that were temporally (but not necessarily causally) related to Olanzapine therapy include the following: allergic reaction (e.g., anaphylactoid reaction, angioedema, pruritus or urticaria), cholestatic or mixed liver injury, diabetic coma, diabetic ketoacidosis, discontinuation reaction (diaphoresis, nausea or vomiting), Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS), hepatitis, jaundice, neutropenia, pancreatitis, priapism, rash, restless legs syndrome, rhabdomyolysis, salivary hypersecretion, stuttering 1, venous thromboembolic events (including pulmonary embolism and deep venous thrombosis), fecal incontinence, and somnambulism. Random cholesterol levels of ≥240 mg/dL and random triglyceride levels of ≥1000 mg/dL have been reported.
1Stuttering was only studied in oral and long acting injection (LAI) formulations.
8 Use in Specific Populations (8 USE IN SPECIFIC POPULATIONS)
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect or predict the rates observed in practice.
5.13 Body Temperature Regulation
Disruption of the body’s ability to reduce core body temperature has been attributed to antipsychotic agents. Appropriate care is advised when prescribing olanzapine for patients who will be experiencing conditions which may contribute to an elevation in core body temperature, e.g., exercising strenuously, exposure to extreme heat, receiving concomitant medication with anticholinergic activity, or being subject to dehydration [see Patient Counseling Information (17)] .
17 Patient Counseling Information (17 PATIENT COUNSELING INFORMATION)
Patients should be advised of the following issues and asked to alert their prescriber if these occur while taking Olanzapine as monotherapy. If you do not think you are getting better or have any concerns about your condition while taking Olanzapine, call your doctor.
5.3 Neuroleptic Malignant Syndrome (nms) (5.3 Neuroleptic Malignant Syndrome (NMS))
A potentially fatal symptom complex sometimes referred to as Neuroleptic Malignant Syndrome (NMS) has been reported in association with administration of antipsychotic drugs, including olanzapine. Clinical manifestations of NMS are hyperpyrexia, muscle rigidity, altered mental status and evidence of autonomic instability (irregular pulse or blood pressure, tachycardia, diaphoresis and cardiac dysrhythmia). Additional signs may include elevated creatinine phosphokinase, myoglobinuria (rhabdomyolysis), and acute renal failure.
The diagnostic evaluation of patients with this syndrome is complicated. In arriving at a diagnosis, it is important to exclude cases where the clinical presentation includes both serious medical illness (e.g., pneumonia, systemic infection, etc.) and untreated or inadequately treated extrapyramidal signs and symptoms (EPS). Other important considerations in the differential diagnosis include central anticholinergic toxicity, heat stroke, drug fever, and primary central nervous system pathology.
The management of NMS should include: 1) immediate discontinuation of antipsychotic drugs and other drugs not essential to concurrent therapy; 2) intensive symptomatic treatment and medical monitoring; and 3) treatment of any concomitant serious medical problems for which specific treatments are available. There is no general agreement about specific pharmacological treatment regimens for NMS.
If a patient requires antipsychotic drug treatment after recovery from NMS, the potential reintroduction of drug therapy should be carefully considered. The patient should be carefully monitored, since recurrences of NMS have been reported [see Patient Counseling Information (17)] .
13.2 Animal Toxicology And/or Pharmacology (13.2 Animal Toxicology and/or Pharmacology)
In animal studies with olanzapine, the principal hematologic findings were reversible peripheral cytopenias in individual dogs dosed at 10 mg/kg (17 times the daily oral MRHD based on mg/m 2body surface area), dose-related decreases in lymphocytes and neutrophils in mice, and lymphopenia in rats. A few dogs treated with 10 mg/kg developed reversible neutropenia and/or reversible hemolytic anemia between 1 and 10 months of treatment. Dose-related decreases in lymphocytes and neutrophils were seen in mice given doses of 10 mg/kg (equal to 2 times the daily oral MRHD based on mg/m 2body surface area) in studies of 3 months' duration. Nonspecific lymphopenia, consistent with decreased body weight gain, occurred in rats receiving 22.5 mg/kg (11 times the daily oral MRHD based on mg/m 2body surface area) for 3 months or 16 mg/kg (8 times the daily oral MRHD based on mg/m 2body surface area) for 6 or 12 months. No evidence of bone marrow cytotoxicity was found in any of the species examined. Bone marrows were normocellular or hypercellular, indicating that the reductions in circulating blood cells were probably due to peripheral (non-marrow) factors.
5.14 anticholinergic (antimuscarinic) Effects (5.14 Anticholinergic (antimuscarinic) Effects)
Olanzapine exhibits in vitro muscarinic receptor affinity [see Clinical Pharmacology 12.2] . In premarketing clinical trials, Olanzapine was associated with constipation, dry mouth, and tachycardia, all adverse reactions possibly related to cholinergic antagonism. Such adverse reactions were not often the basis for discontinuations, but Olanzapine should be used with caution in patients with a current diagnosis or prior history of urinary retention, clinically significant prostatic hypertrophy, constipation, or a history of paralytic ileus or related conditions. In post marketing experience, the risk for severe adverse reactions (including fatalities) was increased with concomitant use of anticholinergic medications [see Drug Interactions (7.1)] .
Package Label Vial Principal Display Panel (PACKAGE LABEL - VIAL - PRINCIPAL DISPLAY PANEL)
NDC 0121-1072-55
Olanzapine
for Injection
10 mg/ vial
For Intramuscular Use Only
Single-Dose Vial
PAI Pharma Rx Only
5.9 Leukopenia, Neutropenia, and Agranulocytosis
Class Effect— In clinical trial and/or postmarketing experience, events of leukopenia/neutropenia have been reported temporally related to antipsychotic agents, including Olanzapine. Agranulocytosis has also been reported.
Possible risk factors for leukopenia/neutropenia include pre-existing low white blood cell count (WBC) and history of drug induced leukopenia/neutropenia. Patients with a history of a clinically significant low WBC or drug induced leukopenia/neutropenia should have their complete blood count (CBC) monitored frequently during the first few months of therapy and discontinuation of Olanzapine should be considered at the first sign of a clinically significant decline in WBC in the absence of other causative factors.
Patients with clinically significant neutropenia should be carefully monitored for fever or other symptoms or signs of infection and treated promptly if such symptoms or signs occur. Patients with severe neutropenia (absolute neutrophil count <1000/mm 3) should discontinue Olanzapine and have their WBC followed until recovery.
8.3 females and Males of Reproductive Potential (8.3 Females and Males of Reproductive Potential)
Infertility
Females
Based on the pharmacologic action of olanzapine (D
2receptor antagonism), treatment with Olanzapine may result in an increase in serum prolactin levels, which may lead to a reversible reduction in fertility in females of reproductive potential
[see Warnings and Precautions (5.15)]
.
Package Label Carton Principal Display Panel (PACKAGE LABEL - CARTON - PRINCIPAL DISPLAY PANEL)
NDC 0121-1072-55
Olanzapine
for Injection
10 mg/ vial
Single-Dose Vial
For Intramuscular
Use Only
Rx Only
P AI Pharma
5.12 Potential for Cognitive and Motor Impairment
Somnolence was a commonly reported adverse reaction associated with olanzapine treatment, occurring at an incidence of 26% in olanzapine patients compared to 15% in placebo patients. This adverse reaction was also dose related. Somnolence led to discontinuation in 0.4% (9/2500) of patients in the premarketing database.
Since olanzapine has the potential to impair judgment, thinking, or motor skills, patients should be cautioned about operating hazardous machinery, including automobiles, until they are reasonably certain that olanzapine therapy does not affect them adversely [see Patient Counseling Information (17)] .
5.16 Use in Combination With Lithium Or Valproate (5.16 Use in Combination with Lithium or Valproate)
When using Olanzapine in combination with lithium or valproate, the prescriber should refer to the Warnings and Precautions sections of the package inserts for lithium or valproate [see Drug Interactions (7)] .
14.3 Agitation Associated With Schizophrenia and Bipolar I Mania (14.3 Agitation Associated with Schizophrenia and Bipolar I Mania)
The efficacy of intramuscular olanzapine for injection for the treatment of agitation was established in 3 short-term (24 hours of IM treatment) placebo-controlled trials in agitated adult inpatients from 2 diagnostic groups: schizophrenia and bipolar I disorder (manic or mixed episodes). Each of the trials included a single active comparator treatment arm of either haloperidol injection (schizophrenia studies) or lorazepam injection (bipolar I mania study). Patients enrolled in the trials needed to be: (1) judged by the clinical investigators as clinically agitated and clinically appropriate candidates for treatment with intramuscular medication, and (2) exhibiting a level of agitation that met or exceeded a threshold score of ≥14 on the 5 items comprising the Positive and Negative Syndrome Scale (PANSS) Excited Component (i.e., poor impulse control, tension, hostility, uncooperativeness and excitement items) with at least 1 individual item score ≥4 using a 1-7 scoring system (1=absent, 4=moderate, 7=extreme). In the studies, the mean baseline PANSS Excited Component score was 18.4, with scores ranging from 13 to 32 (out of a maximum score of 35), thus suggesting predominantly moderate levels of agitation with some patients experiencing mild or severe levels of agitation. The primary efficacy measure used for assessing agitation signs and symptoms in these trials was the change from baseline in the PANSS Excited Component at 2 hours post-injection. Patients could receive up to 3 injections during the 24 hour IM treatment periods; however, patients could not receive the second injection until after the initial 2 hour period when the primary efficacy measure was assessed. The results of the trials follow:
(1) In a placebo-controlled trial in agitated inpatients meeting DSM-IV criteria for schizophrenia (n=270), 4 fixed intramuscular olanzapine for injection doses of 2.5 mg, 5 mg, 7.5 mg and 10 mg were evaluated. All doses were statistically superior to placebo on the PANSS Excited Component at 2 hours post-injection. However, the effect was larger and more consistent for the 3 highest doses. There were no significant pairwise differences for the 7.5 and 10 mg doses over the 5 mg dose.
(2) In a second placebo-controlled trial in agitated inpatients meeting DSM-IV criteria for schizophrenia (n=311), 1 fixed intramuscular olanzapine for injection dose of 10 mg was evaluated. Olanzapine for injection was statistically superior to placebo on the PANSS Excited Component at 2 hours post-injection.
(3) In a placebo-controlled trial in agitated inpatients meeting DSM-IV criteria for bipolar I disorder (and currently displaying an acute manic or mixed episode with or without psychotic features) (n=201), 1 fixed intramuscular olanzapine for injection dose of 10 mg was evaluated. Olanzapine for injection was statistically superior to placebo on the PANSS Excited Component at 2 hours post-injection.
Examination of population subsets (age, race, and gender) did not reveal any differential responsiveness on the basis of these subgroupings.
5.4 Drug Reaction With Eosinophilia and Systemic Symptoms (dress) (5.4 Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS))
Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS) has been reported with olanzapine exposure. DRESS may present with a cutaneous reaction (such as rash or exfoliative dermatitis), eosinophilia, fever, and/or lymphadenopathy with systemic complications such as hepatitis, nephritis, pneumonitis, myocarditis, and/or pericarditis. DRESS is sometimes fatal. Discontinue olanzapine if DRESS is suspected [see Patient Counseling Information (17)] .
Warning: Increased Mortality in Elderly Patients With Dementia Related Psychosis (WARNING: INCREASED MORTALITY IN ELDERLY PATIENTS WITH DEMENTIA-RELATED PSYCHOSIS)
Elderly patients with dementia-related psychosis treated with antipsychotic drugs are at an increased risk of death. Analyses of seventeen placebo-controlled trials (modal duration of 10 weeks), largely in patients taking atypical antipsychotic drugs, revealed a risk of death in drug-treated patients of between 1.6 to 1.7 times the risk of death in placebo-treated patients. Over the course of a typical 10-week controlled trial, the rate of death in drug-treated patients was about 4.5%, compared to a rate of about 2.6% in the placebo group. Although the causes of death were varied, most of the deaths appeared to be either cardiovascular (e.g., heart failure, sudden death) or infectious (e.g., pneumonia) in nature. Observational studies suggest that, similar to atypical antipsychotic drugs, treatment with conventional antipsychotic drugs may increase mortality. The extent to which the findings of increased mortality in observational studies may be attributed to the antipsychotic drug as opposed to some characteristic(s) of the patients is not clear. Olanzapine is not approved for the treatment of patients with dementia-related psychosis [see Warnings and Precautions (5.1), Use in Specific Populations (8.5), and Patient Counseling Information (17)] .
1.4 olanzapine for Injection: Agitation Associated With Schizophrenia and Bipolar I Mania (1.4 Olanzapine for Injection: Agitation Associated with Schizophrenia and Bipolar I Mania)
Olanzapine for Injection is indicated for the treatment of acute agitation associated with schizophrenia and bipolar I mania.
Efficacy was demonstrated in 3 short-term (24 hours of IM treatment) placebo-controlled trials in agitated adult inpatients with: schizophrenia or bipolar I disorder (manic or mixed episodes) [see Clinical Studies (14.3)] .
“Psychomotor agitation” is defined in DSM-IV as “excessive motor activity associated with a feeling of inner tension.” Patients experiencing agitation often manifest behaviors that interfere with their diagnosis and care, e.g., threatening behaviors, escalating or urgently distressing behavior, or self-exhausting behavior, leading clinicians to the use of intramuscular antipsychotic medications to achieve immediate control of the agitation.
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:48:30.271282 · Updated: 2026-03-14T22:29:58.342833