These Highlights Do Not Include All The Information Needed To Use Jardiance Safely And Effectively. See Full Prescribing Information For Jardiance.
942a82a4-cbbd-4e44-9965-8d03f767912b
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
Indications and Usage ( 1 ) 6/2023 Dosage and Administration ( 2.2 , 2.3 ) 6/2023 Warnings and Precautions ( 5.4 ) 6/2023
Indications and Usage
JARDIANCE is indicated: to reduce the risk of cardiovascular death and hospitalization for heart failure in adults with heart failure. to reduce the risk of cardiovascular death in adults with type 2 diabetes mellitus and established cardiovascular disease. as an adjunct to diet and exercise to improve glycemic control in adults and pediatric patients aged 10 years and older with type 2 diabetes mellitus.
Dosage and Administration
Assess renal function before initiating and as clinically indicated. Correct volume depletion before initiating ( 2.1 ) Recommended dosage is 10 mg once daily in the morning, taken with or without food ( 2.2 ) For additional glycemic control, dosage may be increased to 25 mg in patients tolerating JARDIANCE ( 2.2 )
Warnings and Precautions
Ketoacidosis: Assess patients who present with signs and symptoms of metabolic acidosis for ketoacidosis, regardless of blood glucose level. If suspected, discontinue JARDIANCE, evaluate and treat promptly. Before initiating JARDIANCE, consider risk factors for ketoacidosis. Patients on JARDIANCE may require monitoring and temporary discontinuation of therapy in clinical situations known to predispose to ketoacidosis. ( 5.1 ) Volume Depletion: Before initiating JARDIANCE, assess volume status and renal function in patients with impaired renal function, elderly patients, or patients on loop diuretics. Monitor for signs and symptoms during therapy. ( 5.2 ) Urosepsis and Pyelonephritis: Evaluate patients for signs and symptoms of urinary tract infections and treat promptly, if indicated ( 5.3 ) Hypoglycemia: Adult patients taking an insulin secretagogue or insulin may have an increased risk of hypoglycemia. In pediatric patients 10 years of age and older, the risk of hypoglycemia was higher regardless of insulin use. Consider lowering the dosage of insulin secretagogue or insulin to reduce the risk of hypoglycemia when initiating JARDIANCE. ( 5.4 ) Necrotizing Fasciitis of the Perineum (Fournier's Gangrene): Serious, life-threatening cases have occurred in both females and males. Assess patients presenting with pain or tenderness, erythema, or swelling in the genital or perineal area, along with fever or malaise. If suspected, institute prompt treatment. ( 5.5 ) Genital Mycotic Infections: Monitor and treat as appropriate ( 5.6 ) Hypersensitivity Reactions: Serious hypersensitivity reactions (e.g., angioedema) have occurred with JARDIANCE. If hypersensitivity reactions occur, discontinue JARDIANCE, treat promptly, and monitor until signs and symptoms resolve. ( 5.7 )
Contraindications
JARDIANCE is contraindicated in patients: with a hypersensitivity to empagliflozin or any of the excipients in JARDIANCE, reactions such as angioedema have occurred [see Warnings and Precautions (5.7) ] . on dialysis [see Use in Specific Populations (8.6) ] .
Adverse Reactions
The following important adverse reactions are described below and elsewhere in the labeling: Ketoacidosis [see Warnings and Precautions (5.1) ] Volume Depletion [see Warnings and Precautions (5.2) ] Urosepsis and Pyelonephritis [see Warnings and Precautions (5.3) ] Hypoglycemia [see Warnings and Precautions (5.4) ] Necrotizing Fasciitis of the Perineum (Fournier's Gangrene) [see Warnings and Precautions (5.5) ] Genital Mycotic Infections [see Warnings and Precautions (5.6) ] Hypersensitivity Reactions [see Warnings and Precautions (5.7) ]
Drug Interactions
See Table 4 for clinically relevant interactions with JARDIANCE. Table 4 Clinically Relevant Interactions with JARDIANCE Diuretics Clinical Impact Coadministration of empagliflozin with diuretics resulted in increased urine volume and frequency of voids, which might enhance the potential for volume depletion. Intervention Before initiating JARDIANCE, assess volume status and renal function. In patients with volume depletion, correct this condition before initiating JARDIANCE. Monitor for signs and symptoms of volume depletion, and renal function after initiating therapy. Insulin or Insulin Secretagogues Clinical Impact The risk of hypoglycemia is increased when JARDIANCE is used in combination with insulin secretagogues (e.g., sulfonylurea) or insulin. Intervention Coadministration of JARDIANCE with an insulin secretagogue (e.g., sulfonylurea) or insulin may require lower dosages of the insulin secretagogue or insulin to reduce the risk of hypoglycemia. Lithium Clinical Impact Concomitant use of an SGLT2 inhibitor with lithium may decrease serum lithium concentrations. Intervention Monitor serum lithium concentration more frequently during JARDIANCE initiation and dosage changes. Positive Urine Glucose Test Clinical Impact SGLT2 inhibitors increase urinary glucose excretion and will lead to positive urine glucose tests. Intervention Monitoring glycemic control with urine glucose tests is not recommended in patients taking SGLT2 inhibitors. Use alternative methods to monitor glycemic control. Interference with 1,5-anhydroglucitol (1,5-AG) Assay Clinical Impact Measurements of 1,5-AG are unreliable in assessing glycemic control in patients taking SGLT2 inhibitors. Intervention Monitoring glycemic control with 1,5-AG assay is not recommended. Use alternative methods to monitor glycemic control.
Storage and Handling
Product: 50090-4492 NDC: 50090-4492-0 90 TABLET, FILM COATED in a BOTTLE NDC: 50090-4492-1 30 TABLET, FILM COATED in a BOTTLE
How Supplied
Product: 50090-4492 NDC: 50090-4492-0 90 TABLET, FILM COATED in a BOTTLE NDC: 50090-4492-1 30 TABLET, FILM COATED in a BOTTLE
Medication Information
Warnings and Precautions
Ketoacidosis: Assess patients who present with signs and symptoms of metabolic acidosis for ketoacidosis, regardless of blood glucose level. If suspected, discontinue JARDIANCE, evaluate and treat promptly. Before initiating JARDIANCE, consider risk factors for ketoacidosis. Patients on JARDIANCE may require monitoring and temporary discontinuation of therapy in clinical situations known to predispose to ketoacidosis. ( 5.1 ) Volume Depletion: Before initiating JARDIANCE, assess volume status and renal function in patients with impaired renal function, elderly patients, or patients on loop diuretics. Monitor for signs and symptoms during therapy. ( 5.2 ) Urosepsis and Pyelonephritis: Evaluate patients for signs and symptoms of urinary tract infections and treat promptly, if indicated ( 5.3 ) Hypoglycemia: Adult patients taking an insulin secretagogue or insulin may have an increased risk of hypoglycemia. In pediatric patients 10 years of age and older, the risk of hypoglycemia was higher regardless of insulin use. Consider lowering the dosage of insulin secretagogue or insulin to reduce the risk of hypoglycemia when initiating JARDIANCE. ( 5.4 ) Necrotizing Fasciitis of the Perineum (Fournier's Gangrene): Serious, life-threatening cases have occurred in both females and males. Assess patients presenting with pain or tenderness, erythema, or swelling in the genital or perineal area, along with fever or malaise. If suspected, institute prompt treatment. ( 5.5 ) Genital Mycotic Infections: Monitor and treat as appropriate ( 5.6 ) Hypersensitivity Reactions: Serious hypersensitivity reactions (e.g., angioedema) have occurred with JARDIANCE. If hypersensitivity reactions occur, discontinue JARDIANCE, treat promptly, and monitor until signs and symptoms resolve. ( 5.7 )
Indications and Usage
JARDIANCE is indicated: to reduce the risk of cardiovascular death and hospitalization for heart failure in adults with heart failure. to reduce the risk of cardiovascular death in adults with type 2 diabetes mellitus and established cardiovascular disease. as an adjunct to diet and exercise to improve glycemic control in adults and pediatric patients aged 10 years and older with type 2 diabetes mellitus.
Dosage and Administration
Assess renal function before initiating and as clinically indicated. Correct volume depletion before initiating ( 2.1 ) Recommended dosage is 10 mg once daily in the morning, taken with or without food ( 2.2 ) For additional glycemic control, dosage may be increased to 25 mg in patients tolerating JARDIANCE ( 2.2 )
Contraindications
JARDIANCE is contraindicated in patients: with a hypersensitivity to empagliflozin or any of the excipients in JARDIANCE, reactions such as angioedema have occurred [see Warnings and Precautions (5.7) ] . on dialysis [see Use in Specific Populations (8.6) ] .
Adverse Reactions
The following important adverse reactions are described below and elsewhere in the labeling: Ketoacidosis [see Warnings and Precautions (5.1) ] Volume Depletion [see Warnings and Precautions (5.2) ] Urosepsis and Pyelonephritis [see Warnings and Precautions (5.3) ] Hypoglycemia [see Warnings and Precautions (5.4) ] Necrotizing Fasciitis of the Perineum (Fournier's Gangrene) [see Warnings and Precautions (5.5) ] Genital Mycotic Infections [see Warnings and Precautions (5.6) ] Hypersensitivity Reactions [see Warnings and Precautions (5.7) ]
Drug Interactions
See Table 4 for clinically relevant interactions with JARDIANCE. Table 4 Clinically Relevant Interactions with JARDIANCE Diuretics Clinical Impact Coadministration of empagliflozin with diuretics resulted in increased urine volume and frequency of voids, which might enhance the potential for volume depletion. Intervention Before initiating JARDIANCE, assess volume status and renal function. In patients with volume depletion, correct this condition before initiating JARDIANCE. Monitor for signs and symptoms of volume depletion, and renal function after initiating therapy. Insulin or Insulin Secretagogues Clinical Impact The risk of hypoglycemia is increased when JARDIANCE is used in combination with insulin secretagogues (e.g., sulfonylurea) or insulin. Intervention Coadministration of JARDIANCE with an insulin secretagogue (e.g., sulfonylurea) or insulin may require lower dosages of the insulin secretagogue or insulin to reduce the risk of hypoglycemia. Lithium Clinical Impact Concomitant use of an SGLT2 inhibitor with lithium may decrease serum lithium concentrations. Intervention Monitor serum lithium concentration more frequently during JARDIANCE initiation and dosage changes. Positive Urine Glucose Test Clinical Impact SGLT2 inhibitors increase urinary glucose excretion and will lead to positive urine glucose tests. Intervention Monitoring glycemic control with urine glucose tests is not recommended in patients taking SGLT2 inhibitors. Use alternative methods to monitor glycemic control. Interference with 1,5-anhydroglucitol (1,5-AG) Assay Clinical Impact Measurements of 1,5-AG are unreliable in assessing glycemic control in patients taking SGLT2 inhibitors. Intervention Monitoring glycemic control with 1,5-AG assay is not recommended. Use alternative methods to monitor glycemic control.
Storage and Handling
Product: 50090-4492 NDC: 50090-4492-0 90 TABLET, FILM COATED in a BOTTLE NDC: 50090-4492-1 30 TABLET, FILM COATED in a BOTTLE
How Supplied
Product: 50090-4492 NDC: 50090-4492-0 90 TABLET, FILM COATED in a BOTTLE NDC: 50090-4492-1 30 TABLET, FILM COATED in a BOTTLE
Description
Indications and Usage ( 1 ) 6/2023 Dosage and Administration ( 2.2 , 2.3 ) 6/2023 Warnings and Precautions ( 5.4 ) 6/2023
Section 42229-5
Limitations of Use
JARDIANCE is not recommended in patients with type 1 diabetes mellitus. It may increase the risk of diabetic ketoacidosis in these patients [see Warnings and Precautions (5.1)].
JARDIANCE is not recommended for use to improve glycemic control in patients with type 2 diabetes mellitus with an eGFR less than 30 mL/min/1.73 m2. JARDIANCE is likely to be ineffective in this setting based upon its mechanism of action.
Section 42231-1
| This MEDICATION GUIDE has been approved by the U.S. Food and Drug Administration. | Revised: June 2023 | |||
|
MEDICATION GUIDE JARDIANCE® (jar DEE ans) (empagliflozin tablets) for oral use |
||||
|
What is the most important information I should know about JARDIANCE?
JARDIANCE can cause serious side effects, including: |
||||
|
||||
|
|
|||
| If you get any of these symptoms during treatment with JARDIANCE, if possible, check for ketones in your urine, even if your blood sugar is less than 250 mg/dL. | ||||
Talk to your healthcare provider right away if you reduce the amount of food or liquid you drink, for example if you are sick or cannot eat, or start to lose liquids from your body, for example from vomiting, diarrhea or being in the sun too long. |
||||
| What is JARDIANCE? | ||||
| JARDIANCE is a prescription medicine used to: | ||||
JARDIANCE is not for use to lower blood sugar in adults with type 2 diabetes who have severe kidney problems, because it may not work. It is not known if JARDIANCE is safe and effective in children under 10 years of age. |
||||
|
Who should not take JARDIANCE? Do not take JARDIANCE if you: |
||||
|
||||
|
What should I tell my healthcare provider before taking JARDIANCE? Before taking JARDIANCE, tell your healthcare provider about all of your medical conditions, including if you: |
||||
|
||||
|
Tell your healthcare provider about all the medicines you take, including prescription and over-the-counter medicines, vitamins, and herbal supplements. JARDIANCE may affect the way other medicines work, and other medicines may affect how JARDIANCE works. Know the medicines you take. Keep a list of them to show your healthcare provider and pharmacist when you get a new medicine. |
||||
| How should I take JARDIANCE? | ||||
|
||||
| What are the possible side effects of JARDIANCE? | ||||
| JARDIANCE may cause serious side effects, including: | ||||
|
||||
|
||||
|
|
|
|
|
|
||||
|
|
|
||
|
||||
|
||||
| These are not all the possible side effects of JARDIANCE. For more information, ask your healthcare provider or pharmacist. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. |
||||
How should I store JARDIANCE?
|
||||
|
General information about the safe and effective use of JARDIANCE.
Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not use JARDIANCE for a condition for which it is not prescribed. Do not give JARDIANCE to other people, even if they have the same symptoms you have. It may harm them. You can ask your pharmacist or healthcare provider for information about JARDIANCE that is written for health professionals. |
||||
| What are the ingredients in JARDIANCE? | ||||
| Active Ingredient: empagliflozin | ||||
| Inactive Ingredients: colloidal silicon dioxide, croscarmellose sodium, hydroxypropyl cellulose, lactose monohydrate, magnesium stearate, and microcrystalline cellulose. In addition, the film coating contains the following inactive ingredients: hypromellose, polyethylene glycol, talc, titanium dioxide, and yellow ferric oxide. | ||||
| Distributed by: Boehringer Ingelheim Pharmaceuticals, Inc.; Ridgefield, CT 06877 USA Marketed by: Boehringer Ingelheim Pharmaceuticals, Inc.; Ridgefield, CT 06877 USA and Eli Lilly and Company, Indianapolis, IN 46285 USA |
||||
| Licensed from: Boehringer Ingelheim International GmbH, Ingelheim, Germany JARDIANCE is a registered trademark of and used under license from Boehringer Ingelheim International GmbH. |
||||
| Boehringer Ingelheim Pharmaceuticals, Inc. either owns or uses the EMPA-REG OUTCOME®, EMPEROR-Reduced®, and EMPEROR-Preserved® trademarks under license. | ||||
| The other brands listed are trademarks of their respective owners and are not trademarks of Boehringer Ingelheim Pharmaceuticals, Inc. | ||||
| Copyright © 2023 Boehringer Ingelheim International GmbH ALL RIGHTS RESERVED |
||||
| COL8914JF202023 | ||||
| For more information about JARDIANCE, including current prescribing information and Medication Guide, go to www.jardiance.com, scan the code, or call Boehringer Ingelheim Pharmaceuticals, Inc. at 1-800-542-6257.
|
Section 43683-2
Storage
Store at 25°C (77°F); excursions permitted to 15°-30°C (59°-86°F) [see USP Controlled Room Temperature].
10 Overdosage
In the event of an overdose with JARDIANCE, consider contacting the Poison Help line (1-800-222-1222) or a medical toxicologist for additional overdosage management recommendations. Removal of empagliflozin by hemodialysis has not been studied.
Empagliflozin
11 Description
JARDIANCE tablets for oral use contain empagliflozin, an inhibitor of the SGLT2.
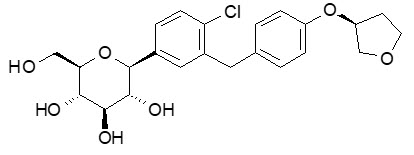
The chemical name of empagliflozin is D-Glucitol,1,5-anhydro-1-C-[4-chloro-3-[[4-[[(3S)-tetrahydro-3-furanyl]oxy]phenyl]methyl]phenyl]-, (1S).
Its molecular formula is C23H27ClO7 and the molecular weight is 450.91. The structural formula is:
Empagliflozin is a white to yellowish, non-hygroscopic powder. It is very slightly soluble in water, sparingly soluble in methanol, slightly soluble in ethanol and acetonitrile, soluble in 50% acetonitrile/water, and practically insoluble in toluene.
Each film-coated tablet of JARDIANCE contains 10 mg or 25 mg of empagliflozin (free base) and the following inactive ingredients: colloidal silicon dioxide, croscarmellose sodium, hydroxypropyl cellulose, lactose monohydrate, magnesium stearate, and microcrystalline cellulose. In addition, the film coating contains the following inactive ingredients: hypromellose, polyethylene glycol, talc, titanium dioxide, and yellow ferric oxide.
5.1 Ketoacidosis
Reports of ketoacidosis, a serious life-threatening condition requiring urgent hospitalization have been identified in clinical trials and postmarketing surveillance in patients with type 1 and type 2 diabetes mellitus receiving sodium glucose co-transporter-2 (SGLT2) inhibitors, including JARDIANCE. Fatal cases of ketoacidosis have been reported in patients taking JARDIANCE. In placebo-controlled trials of patients with type 1 diabetes, the risk of ketoacidosis was increased in patients who received SGLT2 inhibitors compared to patients who received placebo. JARDIANCE is not indicated for the treatment of patients with type 1 diabetes mellitus [see Indications and Usage (1)].
Patients treated with JARDIANCE who present with signs and symptoms consistent with severe metabolic acidosis should be assessed for ketoacidosis regardless of presenting blood glucose levels, as ketoacidosis associated with JARDIANCE may be present even if blood glucose levels are less than 250 mg/dL. If ketoacidosis is suspected, JARDIANCE should be discontinued, patient should be evaluated, and prompt treatment should be instituted. Treatment of ketoacidosis may require insulin, fluid and carbohydrate replacement.
In many of the postmarketing reports, and particularly in patients with type 1 diabetes, the presence of ketoacidosis was not immediately recognized and institution of treatment was delayed because presenting blood glucose levels were below those typically expected for diabetic ketoacidosis (often less than 250 mg/dL). Signs and symptoms at presentation were consistent with dehydration and severe metabolic acidosis and included nausea, vomiting, abdominal pain, generalized malaise, and shortness of breath. In some but not all cases, factors predisposing to ketoacidosis such as insulin dose reduction, acute febrile illness, reduced caloric intake, surgery, pancreatic disorders suggesting insulin deficiency (e.g., type 1 diabetes, history of pancreatitis or pancreatic surgery), and alcohol abuse were identified.
Before initiating JARDIANCE, consider factors in the patient history that may predispose to ketoacidosis including pancreatic insulin deficiency from any cause, caloric restriction, and alcohol abuse.
For patients who undergo scheduled surgery, consider temporarily discontinuing JARDIANCE for at least 3 days prior to surgery [see Clinical Pharmacology (12.2, 12.3)].
Consider monitoring for ketoacidosis and temporarily discontinuing JARDIANCE in other clinical situations known to predispose to ketoacidosis (e.g., prolonged fasting due to acute illness or post-surgery). Ensure risk factors for ketoacidosis are resolved prior to restarting JARDIANCE.
Educate patients on the signs and symptoms of ketoacidosis and instruct patients to discontinue JARDIANCE and seek medical attention immediately if signs and symptoms occur.
5.4 Hypoglycemia
Insulin and insulin secretagogues are known to cause hypoglycemia. In adult patients, the risk of hypoglycemia may be increased when JARDIANCE is used in combination with insulin secretagogues (e.g., sulfonylurea) or insulin. In pediatric patients aged 10 years and older, the risk of hypoglycemia was higher with JARDIANCE regardless of insulin use [see Adverse Reactions (6.1)].
The risk of hypoglycemia may be lowered by a reduction in the dose of sulfonylurea (or other concomitantly administered insulin secretagogues) or insulin. Inform patients using these concomitant medications and pediatric patients of the risk of hypoglycemia and educate them on the signs and symptoms of hypoglycemia.
8.4 Pediatric Use
The safety and effectiveness of JARDIANCE as an adjunct to diet and exercise to improve glycemic control in type 2 diabetes mellitus have been established in pediatric patients aged 10 years and older. Use of JARDIANCE for this indication is supported by evidence from a 26-week double-blind, placebo-controlled clinical trial, with a double-blind active treatment safety extension period of up to 52 weeks in 157 pediatric patients aged 10 to 17 years with type 2 diabetes mellitus and a pediatric pharmacokinetic study [see Clinical Pharmacology (12.3) and Clinical Studies (14.2)]. The safety profile of pediatric patients treated with JARDIANCE was similar to that observed in adults with type 2 diabetes mellitus, with the exception of hypoglycemia risk which was higher in pediatric patients treated with JARDIANCE regardless of concomitant insulin use [see Warnings and Precautions (5.4) and Adverse Reactions (6.1)].
The safety and effectiveness of JARDIANCE have not been established in pediatric patients less than 10 years of age.
8.5 Geriatric Use
In glycemic control trials in patients with type 2 diabetes mellitus, a total of 2,721 (32%) patients treated with JARDIANCE were 65 years of age and older, and 491 (6%) were 75 years of age and older. JARDIANCE is expected to have diminished glycemic efficacy in elderly patients with renal impairment [see Use in Specific Populations (8.6)]. The risk of volume depletion-related adverse reactions increased in patients who were 75 years of age and older to 2.1%, 2.3%, and 4.4% for placebo, JARDIANCE 10 mg, and JARDIANCE 25 mg. The risk of urinary tract infections increased in patients who were 75 years of age and older to 10.5%, 15.7%, and 15.1% in patients randomized to placebo, JARDIANCE 10 mg, and JARDIANCE 25 mg, respectively [see Warnings and Precautions (5.2) and Adverse Reactions (6.1)].
In heart failure trials, EMPEROR-Reduced included 1,188 (64%) patients treated with JARDIANCE 65 years of age and older, and 503 (27%) patients 75 years of age and older. EMPEROR-Preserved included 2,402 (80%) patients treated with JARDIANCE 65 years of age and older, and 1,281 (43%) patients 75 years of age and older. No overall differences in safety and effectiveness have been observed between patients 65 years of age and older and younger adult patients.
4 Contraindications
JARDIANCE is contraindicated in patients:
- with a hypersensitivity to empagliflozin or any of the excipients in JARDIANCE, reactions such as angioedema have occurred [see Warnings and Precautions (5.7)].
- on dialysis [see Use in Specific Populations (8.6)].
6 Adverse Reactions
The following important adverse reactions are described below and elsewhere in the labeling:
- Ketoacidosis [see Warnings and Precautions (5.1)]
- Volume Depletion [see Warnings and Precautions (5.2)]
- Urosepsis and Pyelonephritis [see Warnings and Precautions (5.3)]
- Hypoglycemia [see Warnings and Precautions (5.4)]
- Necrotizing Fasciitis of the Perineum (Fournier's Gangrene) [see Warnings and Precautions (5.5)]
- Genital Mycotic Infections [see Warnings and Precautions (5.6)]
- Hypersensitivity Reactions [see Warnings and Precautions (5.7)]
7 Drug Interactions
See Table 4 for clinically relevant interactions with JARDIANCE.
| Diuretics | |
|---|---|
| Clinical Impact | Coadministration of empagliflozin with diuretics resulted in increased urine volume and frequency of voids, which might enhance the potential for volume depletion. |
| Intervention | Before initiating JARDIANCE, assess volume status and renal function. In patients with volume depletion, correct this condition before initiating JARDIANCE. Monitor for signs and symptoms of volume depletion, and renal function after initiating therapy. |
| Insulin or Insulin Secretagogues | |
| Clinical Impact | The risk of hypoglycemia is increased when JARDIANCE is used in combination with insulin secretagogues (e.g., sulfonylurea) or insulin. |
| Intervention | Coadministration of JARDIANCE with an insulin secretagogue (e.g., sulfonylurea) or insulin may require lower dosages of the insulin secretagogue or insulin to reduce the risk of hypoglycemia. |
| Lithium | |
| Clinical Impact | Concomitant use of an SGLT2 inhibitor with lithium may decrease serum lithium concentrations. |
| Intervention | Monitor serum lithium concentration more frequently during JARDIANCE initiation and dosage changes. |
| Positive Urine Glucose Test | |
| Clinical Impact | SGLT2 inhibitors increase urinary glucose excretion and will lead to positive urine glucose tests. |
| Intervention | Monitoring glycemic control with urine glucose tests is not recommended in patients taking SGLT2 inhibitors. Use alternative methods to monitor glycemic control. |
| Interference with 1,5-anhydroglucitol (1,5-AG) Assay | |
| Clinical Impact | Measurements of 1,5-AG are unreliable in assessing glycemic control in patients taking SGLT2 inhibitors. |
| Intervention | Monitoring glycemic control with 1,5-AG assay is not recommended. Use alternative methods to monitor glycemic control. |
5.2 Volume Depletion
JARDIANCE can cause intravascular volume depletion which may sometimes manifest as symptomatic hypotension or acute transient changes in creatinine [see Adverse Reactions (6.1)]. There have been post-marketing reports of acute kidney injury, some requiring hospitalization and dialysis, in patients with type 2 diabetes mellitus receiving SGLT2 inhibitors, including JARDIANCE. Patients with impaired renal function (eGFR less than 60 mL/min/1.73 m2), elderly patients, or patients on loop diuretics may be at increased risk for volume depletion or hypotension. Before initiating JARDIANCE in patients with one or more of these characteristics, assess volume status and renal function. In patients with volume depletion, correct this condition before initiating JARDIANCE. Monitor for signs and symptoms of volume depletion, and renal function after initiating therapy.
8.6 Renal Impairment
The efficacy and safety of JARDIANCE for glycemic control were evaluated in a study of adult patients with type 2 diabetes mellitus with mild and moderate renal impairment (eGFR 30 to less than 90 mL/min/1.73 m2) [see Clinical Studies (14)]. In this study, 195 adult patients exposed to JARDIANCE had an eGFR between 60 and 90 mL/min/1.73 m2, 91 adult patients exposed to JARDIANCE had an eGFR between 45 and 60 mL/min/1.73 m2, and 97 patients exposed to JARDIANCE had an eGFR between 30 and 45 mL/min/1.73 m2. The glucose lowering benefit of JARDIANCE 25 mg decreased in adult patients with worsening renal function. The risks of renal impairment, volume depletion adverse reactions and urinary tract infection-related adverse reactions increased with worsening renal function [see Warnings and Precautions (5.2)]. Use of JARDIANCE for glycemic control in patients without established cardiovascular disease or cardiovascular risk factors is not recommended when eGFR is less than 30 mL/min/1.73 m2.
In a large cardiovascular outcomes study of adult patients with type 2 diabetes mellitus and established cardiovascular disease, there were 1,819 patients with eGFR below 60 mL/min/1.73 m2. The cardiovascular death findings in this subgroup were consistent with the overall findings [see Clinical Studies (14)].
Studies of adult patients with heart failure [see Clinical Studies (14)] enrolled patients with eGFR equal to or above 20 mL/min/1.73 m2. No dosage adjustment is recommended for these patients. There are insufficient data to support a dosing recommendation in patients with eGFR below 20 mL/min/1.73 m2.
Efficacy and safety trials with JARDIANCE did not enroll adult patients with an eGFR less than 20 mL/min/1.73 m2. JARDIANCE is contraindicated in patients on dialysis [see Contraindications (4)].
In the trial of pediatric patients aged 10 to 17 years with type 2 diabetes mellitus, patients with an eGFR less than 60 mL/min/1.73 m2 were not enrolled.
12.3 Pharmacokinetics
The pharmacokinetics of empagliflozin has been characterized in healthy volunteers and patients with type 2 diabetes mellitus and no clinically relevant differences were noted between the two populations. The steady-state mean plasma AUC and Cmax were 1,870 nmol∙h/L and 259 nmol/L, respectively, with 10 mg empagliflozin once daily treatment, and 4,740 nmol∙h/L and 687 nmol/L, respectively, with 25 mg empagliflozin once daily treatment. Systemic exposure of empagliflozin increased in a dose-proportional manner in the therapeutic dose range. Empagliflozin does not appear to have time-dependent pharmacokinetic characteristics. Following once-daily dosing, up to 22% accumulation, with respect to plasma AUC, was observed at steady-state.
2.2 Recommended Dosage
Table 1 presents the recommended dosage of JARDIANCE in adult and pediatric patients aged 10 years and older.
| Population | Indication | Recommended Dosage |
|---|---|---|
| Adults | Reduce the risk of cardiovascular death and hospitalization in patients with heart failure |
|
| Reduce the risk of cardiovascular death in patients with type 2 diabetes mellitus with established cardiovascular disease | ||
| Glycemic control in type 2 diabetes mellitus |
|
|
| Pediatric patients aged 10 years and older | Glycemic control in type 2 diabetes mellitus |
|
8.7 Hepatic Impairment
JARDIANCE may be used in patients with hepatic impairment [see Clinical Pharmacology (12.3)].
1 Indications and Usage
JARDIANCE is indicated:
- to reduce the risk of cardiovascular death and hospitalization for heart failure in adults with heart failure.
- to reduce the risk of cardiovascular death in adults with type 2 diabetes mellitus and established cardiovascular disease.
- as an adjunct to diet and exercise to improve glycemic control in adults and pediatric patients aged 10 years and older with type 2 diabetes mellitus.
12.1 Mechanism of Action
Empagliflozin is an inhibitor of SGLT2, the predominant transporter responsible for reabsorption of glucose from the glomerular filtrate back into the circulation. By inhibiting SGLT2, empagliflozin reduces renal reabsorption of filtered glucose and lowers the renal threshold for glucose, and thereby increases urinary glucose excretion.
Empagliflozin also reduces sodium reabsorption and increases the delivery of sodium to the distal tubule. This may influence several physiological functions such as lowering both pre- and afterload of the heart and downregulating sympathetic activity.
5 Warnings and Precautions
- Ketoacidosis: Assess patients who present with signs and symptoms of metabolic acidosis for ketoacidosis, regardless of blood glucose level. If suspected, discontinue JARDIANCE, evaluate and treat promptly. Before initiating JARDIANCE, consider risk factors for ketoacidosis. Patients on JARDIANCE may require monitoring and temporary discontinuation of therapy in clinical situations known to predispose to ketoacidosis. (5.1)
- Volume Depletion: Before initiating JARDIANCE, assess volume status and renal function in patients with impaired renal function, elderly patients, or patients on loop diuretics. Monitor for signs and symptoms during therapy. (5.2)
- Urosepsis and Pyelonephritis: Evaluate patients for signs and symptoms of urinary tract infections and treat promptly, if indicated (5.3)
- Hypoglycemia: Adult patients taking an insulin secretagogue or insulin may have an increased risk of hypoglycemia. In pediatric patients 10 years of age and older, the risk of hypoglycemia was higher regardless of insulin use. Consider lowering the dosage of insulin secretagogue or insulin to reduce the risk of hypoglycemia when initiating JARDIANCE. (5.4)
- Necrotizing Fasciitis of the Perineum (Fournier's Gangrene): Serious, life-threatening cases have occurred in both females and males. Assess patients presenting with pain or tenderness, erythema, or swelling in the genital or perineal area, along with fever or malaise. If suspected, institute prompt treatment. (5.5)
- Genital Mycotic Infections: Monitor and treat as appropriate (5.6)
- Hypersensitivity Reactions: Serious hypersensitivity reactions (e.g., angioedema) have occurred with JARDIANCE. If hypersensitivity reactions occur, discontinue JARDIANCE, treat promptly, and monitor until signs and symptoms resolve. (5.7)
2 Dosage and Administration
- Assess renal function before initiating and as clinically indicated. Correct volume depletion before initiating (2.1)
- Recommended dosage is 10 mg once daily in the morning, taken with or without food (2.2)
- For additional glycemic control, dosage may be increased to 25 mg in patients tolerating JARDIANCE (2.2)
3 Dosage Forms and Strengths
JARDIANCE tablets available as:
- 10 mg pale yellow, round, biconvex and bevel-edged, film-coated tablets debossed with "S 10" on one side and the Boehringer Ingelheim company symbol on the other side.
- 25 mg pale yellow, oval, biconvex, film-coated tablets debossed with "S 25" on one side and the Boehringer Ingelheim company symbol on the other side.
6.2 Postmarketing Experience
Additional adverse reactions have been identified during postapproval use of JARDIANCE. Because these reactions are reported voluntarily from a population of uncertain size, it is generally not possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Gastrointestinal Disorders: Constipation
Infections: Necrotizing fasciitis of the perineum (Fournier's gangrene), urosepsis and pyelonephritis
Metabolism and Nutrition Disorders: Ketoacidosis
Renal and Urinary Disorders: Acute kidney injury
Skin and Subcutaneous Tissue Disorders: Angioedema, skin reactions (e.g., rash, urticaria)
8 Use in Specific Populations
- Pregnancy: Advise females of the potential risk to a fetus especially during the second and third trimesters (8.1)
- Lactation: Not recommended when breastfeeding (8.2)
- Geriatric Patients: Higher incidence of adverse reactions related to volume depletion and reduced renal function (8.5, 8.6)
- Renal Impairment: Higher incidence of adverse reactions related to reduced renal function (8.6)
5.6 Genital Mycotic Infections
JARDIANCE increases the risk for genital mycotic infections [see Adverse Reactions (6.1)]. Patients with a history of chronic or recurrent genital mycotic infections were more likely to develop genital mycotic infections. Monitor and treat as appropriate.
5.7 Hypersensitivity Reactions
There have been postmarketing reports of serious hypersensitivity reactions (e.g., angioedema) in patients treated with JARDIANCE. If a hypersensitivity reaction occurs, discontinue JARDIANCE; treat promptly per standard of care, and monitor until signs and symptoms resolve. JARDIANCE is contraindicated in patients with hypersensitivity to empagliflozin or any of the excipients in JARDIANCE [see Contraindications (4)].
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
JARDIANCE has been evaluated in clinical trials in adult and pediatric patients aged 10 to 17 years with type 2 diabetes mellitus and in adults with heart failure. The overall safety profile of JARDIANCE was generally consistent across the studied indications.
5.3 Urosepsis and Pyelonephritis
There have been reports of serious urinary tract infections including urosepsis and pyelonephritis requiring hospitalization in patients receiving JARDIANCE. Treatment with JARDIANCE increases the risk for urinary tract infections. Evaluate patients for signs and symptoms of urinary tract infections and treat promptly, if indicated [see Adverse Reactions (6)].
17 Patient Counseling Information
Advise the patient to read the FDA-approved patient labeling (Medication Guide).
14.4 Heart Failure Trials in Adults
EMPEROR-Reduced (NCT03057977) was a double-blind trial conducted in adults with chronic heart failure (New York Heart Association [NYHA] functional class II-IV) with left ventricular ejection fraction (LVEF) ≤40% to evaluate the efficacy of JARDIANCE as adjunct to standard of care heart failure therapy.
Of 3,730 patients, 1,863 were randomized to JARDIANCE 10 mg and 1,867 to placebo and were followed for a median of 16 months. The mean age of the trial population was 67 years (range: 25 to 94 years) and 76% were men, 24% were women, and 27% were 75 years of age or older. Approximately 71% of the trial population were White, 18% Asian and 7% Black or African American. At baseline, 50% of the patients had type 2 diabetes mellitus.
At randomization, 75% of patients were NYHA class II, 24% were class III and 0.5% were class IV. The mean LVEF was 28%. At baseline, the mean eGFR was 62 mL/min/1.73 m2 and the median urinary albumin to creatinine ratio (UACR) was 22 mg/g. Approximately half of the patients (52%) had eGFR equal to or above 60 mL/min/1.73 m2, 24% had eGFR 45 to less than 60 mL/min/1.73 m2, 19% had eGFR 30 to less than 45 mL/min/1.73 m2 and 5% had eGFR 20 to less than 30 mL/min/1.73 m2.
At baseline, 88% of patients were treated with angiotensin-converting enzyme (ACE) inhibitors, angiotensin receptor blockers (ARB), or angiotensin receptor-neprilysin inhibitors (ARNI), 95% with beta-blockers, 71% with mineralocorticoid receptor antagonists (MRA), and 95% with diuretics.
The primary endpoint was the time to first event of either cardiovascular (CV) death or hospitalization for heart failure (HHF). First and recurrent HHF was assessed as a key secondary endpoint.
JARDIANCE was superior in reducing the risk of the primary composite endpoint of cardiovascular death or hospitalization for heart failure compared with placebo, mostly through a reduction in hospitalization for heart failure. JARDIANCE reduced the risk of first and recurrent HHF (see Table 16 and Figures 7 and 8).
| Placebo N=1,867 |
JARDIANCE 10 mg N=1,863 |
Hazard ratio vs placebo (95% CI) |
p-value | |
|---|---|---|---|---|
| Number of Patients (%) | ||||
|
aTime to first event bIncludes deaths following hospitalization cJoint frailty model accounting for CV death |
||||
| CV death or HHFa | 462 (24.7%) | 361 (19.4%) | 0.75 (0.65, 0.86) | <0.0001 |
| CV deatha,b | 202 (10.8%) | 187 (10.0%) | 0.92 (0.75, 1.12) | |
| HHFa | 342 (18.3%) | 246 (13.2%) | 0.69 (0.59, 0.81) | |
| Number of Events | ||||
| First and recurrent HHFc | 553 | 388 | 0.70 (0.58, 0.85) | 0.0003 |
Figure 7 Time to First Occurrence of the Primary Composite Endpoint of CV Death or Hospitalization for Heart Failure
Figure 8 Time to Event of Hospitalization for Heart Failure (First and Recurrent)
The results of the primary composite were generally consistent across the pre-specified subgroups (see Figure 9).
Figure 9 Treatment Effects for the Primary Composite Endpoint (CV Death and Hospitalization for Heart Failure) Subgroup Analysis (EMPEROR-Reduced)
LVEF >30%: Includes both above and below the median NT-proBNP. To be eligible for inclusion, patients with an LVEF >30% were required to meet a higher NT-proBNP threshold than those with LVEF ≤30%, unless they additionally had a history of HHF within the past 12 months.
EMPEROR-Preserved (NCT03057951) was a double-blind trial conducted in patients with chronic heart failure NYHA Class II-IV with LVEF >40% to evaluate the efficacy of JARDIANCE as adjunct to standard of care therapy.
Of 5,988 patients, 2,997 were randomized to JARDIANCE 10 mg and 2,991 to placebo and were followed for a median of 26 months. The mean age of the trial population was 72 years (range: 22 to 100 years) and 55% were men, 45% were women, and 43% were 75 years of age or older. Approximately 76% of the trial population were White, 14% Asian and 4% Black or African American.
At randomization, 82% of patients were NYHA class II, 18% were class III and 0.3% were class IV. The EMPEROR-Preserved trial population included patients with a LVEF <50% (33.1%), with a LVEF 50 to <60% (34.4%) and a LVEF ≥60% (32.5%). At baseline, the mean eGFR was 61 mL/min/1.73 m2 and the median urinary albumin to creatinine ratio (UACR) was 21 mg/g. Approximately half of the patients (50%) had eGFR equal to or above 60 mL/min/1.73 m2, 26% had eGFR 45 to less than 60 mL/min/1.73 m2, 19% had eGFR 30 to less than 45 mL/min/1.73 m2, and 5% had eGFR 20 to less than 30 mL/min/1.73 m2.
At baseline, 81% of patients were treated with ACE inhibitors, ARBs, or ARNI, 86% with beta-blockers, 38% with MRAs, and 86% with diuretics.
The primary endpoint was the time to first event of either CV death or HHF. First and recurrent HHF was assessed as a key secondary endpoint.
JARDIANCE was superior in reducing the risk of the primary composite endpoint compared with placebo, mostly through a reduction in hospitalization for heart failure. JARDIANCE reduced the risk of first and recurrent HHF (see Table 17 and Figures 10 and 11).
| Placebo N=2,991 |
JARDIANCE 10 mg N=2,997 |
Hazard ratio vs placebo (95% CI) |
p-value | |
|---|---|---|---|---|
| Number of Patients (%) | ||||
|
aTime to first event bIncludes deaths following hospitalization cJoint frailty model accounting for CV death |
||||
| CV death or HHFa | 511 (17.1%) | 415 (13.8%) | 0.79 (0.69, 0.90) | 0.0003 |
| CV deatha,b | 244 (8.2%) | 219 (7.3%) | 0.91 (0.76, 1.09) | |
| HHFa | 352 (11.8%) | 259 (8.6%) | 0.71 (0.60, 0.83) | |
| Number of Events | ||||
| First and recurrent HHFc | 541 | 407 | 0.73 (0.61, 0.88) | 0.0009 |
Figure 10 Time to First Occurrence of the Primary Composite Endpoint of CV Death or Hospitalization for Heart Failure
Figure 11 Time to Event of Hospitalization for Heart Failure (First and Recurrent)
The results of the primary composite endpoint were consistent across the pre-specified subgroups (see Figure 12).
Figure 12 Treatment Effects for the Primary Composite Endpoint (CV Death or Hospitalization for Heart Failure) Subgroup Analysis (EMPEROR-Preserved)
16 How Supplied/storage and Handling
Product: 50090-4492
NDC: 50090-4492-0 90 TABLET, FILM COATED in a BOTTLE
NDC: 50090-4492-1 30 TABLET, FILM COATED in a BOTTLE
2.3 Recommendations Regarding Missed Dose
- If a dose is missed, instruct patients to take the dose as soon as possible.
- Do not double up the next dose.
2.1 Testing Prior to Initiation of Jardiance
- Assess renal function before initiating JARDIANCE and as clinically indicated [see Warnings and Precautions (5.2)].
- Use for glycemic control is not recommended in patients with an eGFR less than 30 mL/min/1.73 m2 [see Use in Specific Populations (8.6)].
- JARDIANCE is contraindicated in patients on dialysis [see Use in Specific Populations (8.6)].
- Assess volume status in patients with volume depletion and correct this condition before initiating JARDIANCE [see Warnings and Precautions (5.2) and Use in Specific Populations (8.5, 8.6)].
5.5 Necrotizing Fasciitis of the Perineum (fournier's Gangrene)
Reports of necrotizing fasciitis of the perineum (Fournier's gangrene), a rare but serious and life-threatening necrotizing infection requiring urgent surgical intervention, have been identified in patients with diabetes mellitus receiving SGLT2 inhibitors, including JARDIANCE. Cases have been reported in both females and males. Serious outcomes have included hospitalization, multiple surgeries, and death.
Patients treated with JARDIANCE presenting with pain or tenderness, erythema, or swelling in the genital or perineal area, along with fever or malaise, should be assessed for necrotizing fasciitis. If suspected, start treatment immediately with broad-spectrum antibiotics and, if necessary, surgical debridement. Discontinue JARDIANCE, closely monitor blood glucose levels, and provide appropriate alternative therapy for glycemic control.
14.1 Glycemic Control Trials in Adults With Type 2 Diabetes Mellitus
JARDIANCE has been studied as monotherapy and in combination with metformin, sulfonylurea, pioglitazone, linagliptin, and insulin. JARDIANCE has also been studied in patients with type 2 diabetes mellitus with mild or moderate renal impairment.
In adult patients with type 2 diabetes mellitus, treatment with JARDIANCE reduced hemoglobin A1c (HbA1c), compared to placebo. The reduction in HbA1c for JARDIANCE compared with placebo was observed across subgroups including sex, race, geographic region, baseline BMI and duration of disease.
14.2 Glycemic Control Trial in Pediatric Patients Aged 10 to 17 Years With Type 2 Diabetes Mellitus
DINAMO (NCT03429543) was a 26-week, double-blind, randomized, placebo-controlled, parallel group trial, with a double-blind active treatment safety extension period up to 52 weeks to assess the efficacy of JARDIANCE. The trial enrolled pediatric patients aged 10 to 17 years with inadequately controlled type 2 diabetes mellitus (HbA1c 6.5 to 10.5%). Patients treated with metformin (at least 1,000 mg daily or maximally tolerated dose), with or without insulin therapy, and those with a history of intolerance to metformin therapy were enrolled. Patients were randomized to 3 treatment arms (JARDIANCE 10 mg, a dipeptidyl peptidase-4 (DPP-4) inhibitor or placebo), over 26 weeks. Patients in the JARDIANCE 10 mg group who failed to achieve HbA1c <7.0% at Week 12 underwent a second randomization at Week 14 to remain on the 10 mg dose or increase to 25 mg. Patients on placebo were re-randomized at Week 26 to one of the JARDIANCE doses (10 mg or 25 mg) or a DPP-4 inhibitor.
A total of 157 patients were treated with either JARDIANCE (10 mg or 25 mg; N=52), a DPP-4 inhibitor (N=52), or placebo (N=53). Background therapies as adjunct to diet and exercise included metformin (51%), a combination of metformin and insulin (40.1%), insulin (3.2%), or none (5.7%). The mean HbA1c at baseline was 8.0% and the mean duration of type 2 diabetes mellitus was 2.1 years. The mean age was 14.5 years (range: 10-17 years) and 51.6% were aged 15 years and older. Approximately, 50% were White, 6% were Asian, 31% were Black or African American, and 38% were of Hispanic or Latino ethnicity. The mean BMI was 36.0 kg/m2 and mean BMI Z-score was 3.0. Patients with an eGFR less than 60 mL/min/1.73 m2 were not enrolled in the trial. Approximately 25% of the study population had microalbuminuria or macroalbuminuria.
At Week 26, treatment with JARDIANCE was superior in reducing HbA1c from baseline versus placebo (see Table 14).
| JARDIANCE 10 mg and 25 mg |
Placebo | |
|---|---|---|
|
aModified intent-to-treat set (All randomized and treated patients with baseline measurement). bMultiple imputations using placebo wash-out approach with 500 iterations for missing data. Imputed for HbA1c (Jardiance N=5 (9.6 %), Placebo N=3 (5.7%)), for FPG (Jardiance N=4 (8.3%), Placebo N=2 (3.8%)). cLeast-Square Mean from Analysis of Covariance (ANCOVA) adjusted for baseline value and baseline age stratum (< 15 years vs 15 to < 18 years). dNot evaluated for statistical significance, not part of sequential testing procedure. ep-value=0.0116 (two-sided) |
||
| HbA1c (%)b | ||
| Number of patients | n=52 | n=53 |
| Baseline (mean) | 8.0 | 8.1 |
| Change from baselinec | -0.2 | 0.7 |
| Difference from placeboc (95% CI) | -0.8e (-1.5, -0.2) | -- |
| FPG (mg/dL)b,d | ||
| Number of patients | n=48 | n=52 |
| Baseline (mean) | 154 | 159 |
| Change from baselinec | -19 | 17 |
| Difference from placeboc (95% CI) | -36 (-60.7, -10.7) | -- |
14.3 Cardiovascular Outcomes in Adults With Type 2 Diabetes Mellitus and Atherosclerotic Cardiovascular Disease
The effect of JARDIANCE on cardiovascular (CV) risk in adult patients with type 2 diabetes mellitus and established, stable, atherosclerotic CV disease was evaluated in the EMPA-REG OUTCOME trial, a multicenter, multinational, randomized, double-blind parallel group trial. The trial compared the risk of experiencing a major adverse cardiovascular event (MACE) between JARDIANCE and placebo when these were added to and used concomitantly with standard of care treatments for diabetes mellitus and atherosclerotic CV disease. Concomitant antidiabetic medications were to be kept stable for the first 12 weeks of the trial. Thereafter, antidiabetic and atherosclerotic therapies could be adjusted, at the discretion of investigators, to ensure participants were treated according to the standard care for these diseases.
A total of 7,020 patients were treated (JARDIANCE 10 mg = 2,345; JARDIANCE 25 mg = 2,342; placebo = 2,333) and followed for a median of 3.1 years. Approximately 72% of the trial population was White, 22% was Asian, and 5% was Black. The mean age was 63 years and approximately 72% were male.
All patients in the trial had inadequately controlled type 2 diabetes mellitus at baseline (HbA1c greater than or equal to 7%). The mean HbA1c at baseline was 8.1% and 57% of participants had diabetes mellitus for more than 10 years. Approximately 31%, 22% and 20% reported a past history of neuropathy, retinopathy and nephropathy to investigators, respectively and the mean eGFR was 74 mL/min/1.73 m2. At baseline, patients were treated with one (~30%) or more (~70%) antidiabetic medications including metformin (74%), insulin (48%), and sulfonylurea (43%).
All patients had established atherosclerotic CV disease at baseline including one (82%) or more (18%) of the following: a documented history of coronary artery disease (76%), stroke (23%) or peripheral artery disease (21%). At baseline, the mean systolic blood pressure was 136 mmHg, the mean diastolic blood pressure was 76 mmHg, the mean LDL was 86 mg/dL, the mean HDL was 44 mg/dL, and the mean urinary albumin to creatinine ratio (UACR) was 175 mg/g. At baseline, approximately 81% of patients were treated with renin angiotensin system inhibitors, 65% with beta-blockers, 43% with diuretics, 77% with statins, and 86% with antiplatelet agents (mostly aspirin).
The primary endpoint in EMPA-REG OUTCOME was the time to first occurrence of a Major Adverse Cardiac Event (MACE). A major adverse cardiac event was defined as occurrence of either a CV death or a non-fatal myocardial infarction (MI) or a non-fatal stroke. The statistical analysis plan had pre-specified that the 10 and 25 mg doses would be combined. A Cox proportional hazards model was used to test for non-inferiority against the pre-specified risk margin of 1.3 for the hazard ratio of MACE and superiority on MACE if non-inferiority was demonstrated. Type-1 error was controlled across multiples tests using a hierarchical testing strategy.
JARDIANCE significantly reduced the risk of first occurrence of primary composite endpoint of CV death, non-fatal myocardial infarction, or non-fatal stroke (HR: 0.86; 95% CI: 0.74, 0.99). The treatment effect was due to a significant reduction in the risk of CV death in subjects randomized to empagliflozin (HR: 0.62; 95% CI: 0.49, 0.77), with no change in the risk of non-fatal myocardial infarction or non-fatal stroke (see Table 15 and Figures 5 and 6). Results for the 10 mg and 25 mg empagliflozin dosages were consistent with results for the combined dosage groups.
| Placebo N=2,333 |
JARDIANCE N=4,687 |
Hazard ratio vs placebo (95% CI) |
|
|---|---|---|---|
|
aTreated set (patients who had received at least one dose of trial drug) bp-value for superiority (2-sided) 0.04 cTotal number of events |
|||
| Composite of CV death, non-fatal myocardial infarction, non-fatal stroke (time to first occurrence)b | 282 (12.1%) | 490 (10.5%) | 0.86 (0.74, 0.99) |
| Non-fatal myocardial infarctionc | 121 (5.2%) | 213 (4.5%) | 0.87 (0.70, 1.09) |
| Non-fatal strokec | 60 (2.6%) | 150 (3.2%) | 1.24 (0.92, 1.67) |
| CV deathc | 137 (5.9%) | 172 (3.7%) | 0.62 (0.49, 0.77) |
The efficacy of JARDIANCE on CV death was generally consistent across major demographic and disease subgroups.
Vital status was obtained for 99.2% of subjects in the trial. A total of 463 deaths were recorded during the EMPA-REG OUTCOME trial. Most of these deaths were categorized as CV deaths. The non-CV deaths were only a small proportion of deaths and were balanced between the treatment groups (2.1% in patients treated with JARDIANCE, and 2.4% of patients treated with placebo).
Structured Label Content
Section 42229-5 (42229-5)
Limitations of Use
JARDIANCE is not recommended in patients with type 1 diabetes mellitus. It may increase the risk of diabetic ketoacidosis in these patients [see Warnings and Precautions (5.1)].
JARDIANCE is not recommended for use to improve glycemic control in patients with type 2 diabetes mellitus with an eGFR less than 30 mL/min/1.73 m2. JARDIANCE is likely to be ineffective in this setting based upon its mechanism of action.
Section 42231-1 (42231-1)
| This MEDICATION GUIDE has been approved by the U.S. Food and Drug Administration. | Revised: June 2023 | |||
|
MEDICATION GUIDE JARDIANCE® (jar DEE ans) (empagliflozin tablets) for oral use |
||||
|
What is the most important information I should know about JARDIANCE?
JARDIANCE can cause serious side effects, including: |
||||
|
||||
|
|
|||
| If you get any of these symptoms during treatment with JARDIANCE, if possible, check for ketones in your urine, even if your blood sugar is less than 250 mg/dL. | ||||
Talk to your healthcare provider right away if you reduce the amount of food or liquid you drink, for example if you are sick or cannot eat, or start to lose liquids from your body, for example from vomiting, diarrhea or being in the sun too long. |
||||
| What is JARDIANCE? | ||||
| JARDIANCE is a prescription medicine used to: | ||||
JARDIANCE is not for use to lower blood sugar in adults with type 2 diabetes who have severe kidney problems, because it may not work. It is not known if JARDIANCE is safe and effective in children under 10 years of age. |
||||
|
Who should not take JARDIANCE? Do not take JARDIANCE if you: |
||||
|
||||
|
What should I tell my healthcare provider before taking JARDIANCE? Before taking JARDIANCE, tell your healthcare provider about all of your medical conditions, including if you: |
||||
|
||||
|
Tell your healthcare provider about all the medicines you take, including prescription and over-the-counter medicines, vitamins, and herbal supplements. JARDIANCE may affect the way other medicines work, and other medicines may affect how JARDIANCE works. Know the medicines you take. Keep a list of them to show your healthcare provider and pharmacist when you get a new medicine. |
||||
| How should I take JARDIANCE? | ||||
|
||||
| What are the possible side effects of JARDIANCE? | ||||
| JARDIANCE may cause serious side effects, including: | ||||
|
||||
|
||||
|
|
|
|
|
|
||||
|
|
|
||
|
||||
|
||||
| These are not all the possible side effects of JARDIANCE. For more information, ask your healthcare provider or pharmacist. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. |
||||
How should I store JARDIANCE?
|
||||
|
General information about the safe and effective use of JARDIANCE.
Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not use JARDIANCE for a condition for which it is not prescribed. Do not give JARDIANCE to other people, even if they have the same symptoms you have. It may harm them. You can ask your pharmacist or healthcare provider for information about JARDIANCE that is written for health professionals. |
||||
| What are the ingredients in JARDIANCE? | ||||
| Active Ingredient: empagliflozin | ||||
| Inactive Ingredients: colloidal silicon dioxide, croscarmellose sodium, hydroxypropyl cellulose, lactose monohydrate, magnesium stearate, and microcrystalline cellulose. In addition, the film coating contains the following inactive ingredients: hypromellose, polyethylene glycol, talc, titanium dioxide, and yellow ferric oxide. | ||||
| Distributed by: Boehringer Ingelheim Pharmaceuticals, Inc.; Ridgefield, CT 06877 USA Marketed by: Boehringer Ingelheim Pharmaceuticals, Inc.; Ridgefield, CT 06877 USA and Eli Lilly and Company, Indianapolis, IN 46285 USA |
||||
| Licensed from: Boehringer Ingelheim International GmbH, Ingelheim, Germany JARDIANCE is a registered trademark of and used under license from Boehringer Ingelheim International GmbH. |
||||
| Boehringer Ingelheim Pharmaceuticals, Inc. either owns or uses the EMPA-REG OUTCOME®, EMPEROR-Reduced®, and EMPEROR-Preserved® trademarks under license. | ||||
| The other brands listed are trademarks of their respective owners and are not trademarks of Boehringer Ingelheim Pharmaceuticals, Inc. | ||||
| Copyright © 2023 Boehringer Ingelheim International GmbH ALL RIGHTS RESERVED |
||||
| COL8914JF202023 | ||||
| For more information about JARDIANCE, including current prescribing information and Medication Guide, go to www.jardiance.com, scan the code, or call Boehringer Ingelheim Pharmaceuticals, Inc. at 1-800-542-6257.
|
Section 43683-2 (43683-2)
Storage
Store at 25°C (77°F); excursions permitted to 15°-30°C (59°-86°F) [see USP Controlled Room Temperature].
10 Overdosage (10 OVERDOSAGE)
In the event of an overdose with JARDIANCE, consider contacting the Poison Help line (1-800-222-1222) or a medical toxicologist for additional overdosage management recommendations. Removal of empagliflozin by hemodialysis has not been studied.
Empagliflozin
11 Description (11 DESCRIPTION)
JARDIANCE tablets for oral use contain empagliflozin, an inhibitor of the SGLT2.
The chemical name of empagliflozin is D-Glucitol,1,5-anhydro-1-C-[4-chloro-3-[[4-[[(3S)-tetrahydro-3-furanyl]oxy]phenyl]methyl]phenyl]-, (1S).
Its molecular formula is C23H27ClO7 and the molecular weight is 450.91. The structural formula is:
Empagliflozin is a white to yellowish, non-hygroscopic powder. It is very slightly soluble in water, sparingly soluble in methanol, slightly soluble in ethanol and acetonitrile, soluble in 50% acetonitrile/water, and practically insoluble in toluene.
Each film-coated tablet of JARDIANCE contains 10 mg or 25 mg of empagliflozin (free base) and the following inactive ingredients: colloidal silicon dioxide, croscarmellose sodium, hydroxypropyl cellulose, lactose monohydrate, magnesium stearate, and microcrystalline cellulose. In addition, the film coating contains the following inactive ingredients: hypromellose, polyethylene glycol, talc, titanium dioxide, and yellow ferric oxide.
5.1 Ketoacidosis
Reports of ketoacidosis, a serious life-threatening condition requiring urgent hospitalization have been identified in clinical trials and postmarketing surveillance in patients with type 1 and type 2 diabetes mellitus receiving sodium glucose co-transporter-2 (SGLT2) inhibitors, including JARDIANCE. Fatal cases of ketoacidosis have been reported in patients taking JARDIANCE. In placebo-controlled trials of patients with type 1 diabetes, the risk of ketoacidosis was increased in patients who received SGLT2 inhibitors compared to patients who received placebo. JARDIANCE is not indicated for the treatment of patients with type 1 diabetes mellitus [see Indications and Usage (1)].
Patients treated with JARDIANCE who present with signs and symptoms consistent with severe metabolic acidosis should be assessed for ketoacidosis regardless of presenting blood glucose levels, as ketoacidosis associated with JARDIANCE may be present even if blood glucose levels are less than 250 mg/dL. If ketoacidosis is suspected, JARDIANCE should be discontinued, patient should be evaluated, and prompt treatment should be instituted. Treatment of ketoacidosis may require insulin, fluid and carbohydrate replacement.
In many of the postmarketing reports, and particularly in patients with type 1 diabetes, the presence of ketoacidosis was not immediately recognized and institution of treatment was delayed because presenting blood glucose levels were below those typically expected for diabetic ketoacidosis (often less than 250 mg/dL). Signs and symptoms at presentation were consistent with dehydration and severe metabolic acidosis and included nausea, vomiting, abdominal pain, generalized malaise, and shortness of breath. In some but not all cases, factors predisposing to ketoacidosis such as insulin dose reduction, acute febrile illness, reduced caloric intake, surgery, pancreatic disorders suggesting insulin deficiency (e.g., type 1 diabetes, history of pancreatitis or pancreatic surgery), and alcohol abuse were identified.
Before initiating JARDIANCE, consider factors in the patient history that may predispose to ketoacidosis including pancreatic insulin deficiency from any cause, caloric restriction, and alcohol abuse.
For patients who undergo scheduled surgery, consider temporarily discontinuing JARDIANCE for at least 3 days prior to surgery [see Clinical Pharmacology (12.2, 12.3)].
Consider monitoring for ketoacidosis and temporarily discontinuing JARDIANCE in other clinical situations known to predispose to ketoacidosis (e.g., prolonged fasting due to acute illness or post-surgery). Ensure risk factors for ketoacidosis are resolved prior to restarting JARDIANCE.
Educate patients on the signs and symptoms of ketoacidosis and instruct patients to discontinue JARDIANCE and seek medical attention immediately if signs and symptoms occur.
5.4 Hypoglycemia
Insulin and insulin secretagogues are known to cause hypoglycemia. In adult patients, the risk of hypoglycemia may be increased when JARDIANCE is used in combination with insulin secretagogues (e.g., sulfonylurea) or insulin. In pediatric patients aged 10 years and older, the risk of hypoglycemia was higher with JARDIANCE regardless of insulin use [see Adverse Reactions (6.1)].
The risk of hypoglycemia may be lowered by a reduction in the dose of sulfonylurea (or other concomitantly administered insulin secretagogues) or insulin. Inform patients using these concomitant medications and pediatric patients of the risk of hypoglycemia and educate them on the signs and symptoms of hypoglycemia.
8.4 Pediatric Use
The safety and effectiveness of JARDIANCE as an adjunct to diet and exercise to improve glycemic control in type 2 diabetes mellitus have been established in pediatric patients aged 10 years and older. Use of JARDIANCE for this indication is supported by evidence from a 26-week double-blind, placebo-controlled clinical trial, with a double-blind active treatment safety extension period of up to 52 weeks in 157 pediatric patients aged 10 to 17 years with type 2 diabetes mellitus and a pediatric pharmacokinetic study [see Clinical Pharmacology (12.3) and Clinical Studies (14.2)]. The safety profile of pediatric patients treated with JARDIANCE was similar to that observed in adults with type 2 diabetes mellitus, with the exception of hypoglycemia risk which was higher in pediatric patients treated with JARDIANCE regardless of concomitant insulin use [see Warnings and Precautions (5.4) and Adverse Reactions (6.1)].
The safety and effectiveness of JARDIANCE have not been established in pediatric patients less than 10 years of age.
8.5 Geriatric Use
In glycemic control trials in patients with type 2 diabetes mellitus, a total of 2,721 (32%) patients treated with JARDIANCE were 65 years of age and older, and 491 (6%) were 75 years of age and older. JARDIANCE is expected to have diminished glycemic efficacy in elderly patients with renal impairment [see Use in Specific Populations (8.6)]. The risk of volume depletion-related adverse reactions increased in patients who were 75 years of age and older to 2.1%, 2.3%, and 4.4% for placebo, JARDIANCE 10 mg, and JARDIANCE 25 mg. The risk of urinary tract infections increased in patients who were 75 years of age and older to 10.5%, 15.7%, and 15.1% in patients randomized to placebo, JARDIANCE 10 mg, and JARDIANCE 25 mg, respectively [see Warnings and Precautions (5.2) and Adverse Reactions (6.1)].
In heart failure trials, EMPEROR-Reduced included 1,188 (64%) patients treated with JARDIANCE 65 years of age and older, and 503 (27%) patients 75 years of age and older. EMPEROR-Preserved included 2,402 (80%) patients treated with JARDIANCE 65 years of age and older, and 1,281 (43%) patients 75 years of age and older. No overall differences in safety and effectiveness have been observed between patients 65 years of age and older and younger adult patients.
4 Contraindications (4 CONTRAINDICATIONS)
JARDIANCE is contraindicated in patients:
- with a hypersensitivity to empagliflozin or any of the excipients in JARDIANCE, reactions such as angioedema have occurred [see Warnings and Precautions (5.7)].
- on dialysis [see Use in Specific Populations (8.6)].
6 Adverse Reactions (6 ADVERSE REACTIONS)
The following important adverse reactions are described below and elsewhere in the labeling:
- Ketoacidosis [see Warnings and Precautions (5.1)]
- Volume Depletion [see Warnings and Precautions (5.2)]
- Urosepsis and Pyelonephritis [see Warnings and Precautions (5.3)]
- Hypoglycemia [see Warnings and Precautions (5.4)]
- Necrotizing Fasciitis of the Perineum (Fournier's Gangrene) [see Warnings and Precautions (5.5)]
- Genital Mycotic Infections [see Warnings and Precautions (5.6)]
- Hypersensitivity Reactions [see Warnings and Precautions (5.7)]
7 Drug Interactions (7 DRUG INTERACTIONS)
See Table 4 for clinically relevant interactions with JARDIANCE.
| Diuretics | |
|---|---|
| Clinical Impact | Coadministration of empagliflozin with diuretics resulted in increased urine volume and frequency of voids, which might enhance the potential for volume depletion. |
| Intervention | Before initiating JARDIANCE, assess volume status and renal function. In patients with volume depletion, correct this condition before initiating JARDIANCE. Monitor for signs and symptoms of volume depletion, and renal function after initiating therapy. |
| Insulin or Insulin Secretagogues | |
| Clinical Impact | The risk of hypoglycemia is increased when JARDIANCE is used in combination with insulin secretagogues (e.g., sulfonylurea) or insulin. |
| Intervention | Coadministration of JARDIANCE with an insulin secretagogue (e.g., sulfonylurea) or insulin may require lower dosages of the insulin secretagogue or insulin to reduce the risk of hypoglycemia. |
| Lithium | |
| Clinical Impact | Concomitant use of an SGLT2 inhibitor with lithium may decrease serum lithium concentrations. |
| Intervention | Monitor serum lithium concentration more frequently during JARDIANCE initiation and dosage changes. |
| Positive Urine Glucose Test | |
| Clinical Impact | SGLT2 inhibitors increase urinary glucose excretion and will lead to positive urine glucose tests. |
| Intervention | Monitoring glycemic control with urine glucose tests is not recommended in patients taking SGLT2 inhibitors. Use alternative methods to monitor glycemic control. |
| Interference with 1,5-anhydroglucitol (1,5-AG) Assay | |
| Clinical Impact | Measurements of 1,5-AG are unreliable in assessing glycemic control in patients taking SGLT2 inhibitors. |
| Intervention | Monitoring glycemic control with 1,5-AG assay is not recommended. Use alternative methods to monitor glycemic control. |
5.2 Volume Depletion
JARDIANCE can cause intravascular volume depletion which may sometimes manifest as symptomatic hypotension or acute transient changes in creatinine [see Adverse Reactions (6.1)]. There have been post-marketing reports of acute kidney injury, some requiring hospitalization and dialysis, in patients with type 2 diabetes mellitus receiving SGLT2 inhibitors, including JARDIANCE. Patients with impaired renal function (eGFR less than 60 mL/min/1.73 m2), elderly patients, or patients on loop diuretics may be at increased risk for volume depletion or hypotension. Before initiating JARDIANCE in patients with one or more of these characteristics, assess volume status and renal function. In patients with volume depletion, correct this condition before initiating JARDIANCE. Monitor for signs and symptoms of volume depletion, and renal function after initiating therapy.
8.6 Renal Impairment
The efficacy and safety of JARDIANCE for glycemic control were evaluated in a study of adult patients with type 2 diabetes mellitus with mild and moderate renal impairment (eGFR 30 to less than 90 mL/min/1.73 m2) [see Clinical Studies (14)]. In this study, 195 adult patients exposed to JARDIANCE had an eGFR between 60 and 90 mL/min/1.73 m2, 91 adult patients exposed to JARDIANCE had an eGFR between 45 and 60 mL/min/1.73 m2, and 97 patients exposed to JARDIANCE had an eGFR between 30 and 45 mL/min/1.73 m2. The glucose lowering benefit of JARDIANCE 25 mg decreased in adult patients with worsening renal function. The risks of renal impairment, volume depletion adverse reactions and urinary tract infection-related adverse reactions increased with worsening renal function [see Warnings and Precautions (5.2)]. Use of JARDIANCE for glycemic control in patients without established cardiovascular disease or cardiovascular risk factors is not recommended when eGFR is less than 30 mL/min/1.73 m2.
In a large cardiovascular outcomes study of adult patients with type 2 diabetes mellitus and established cardiovascular disease, there were 1,819 patients with eGFR below 60 mL/min/1.73 m2. The cardiovascular death findings in this subgroup were consistent with the overall findings [see Clinical Studies (14)].
Studies of adult patients with heart failure [see Clinical Studies (14)] enrolled patients with eGFR equal to or above 20 mL/min/1.73 m2. No dosage adjustment is recommended for these patients. There are insufficient data to support a dosing recommendation in patients with eGFR below 20 mL/min/1.73 m2.
Efficacy and safety trials with JARDIANCE did not enroll adult patients with an eGFR less than 20 mL/min/1.73 m2. JARDIANCE is contraindicated in patients on dialysis [see Contraindications (4)].
In the trial of pediatric patients aged 10 to 17 years with type 2 diabetes mellitus, patients with an eGFR less than 60 mL/min/1.73 m2 were not enrolled.
12.3 Pharmacokinetics
The pharmacokinetics of empagliflozin has been characterized in healthy volunteers and patients with type 2 diabetes mellitus and no clinically relevant differences were noted between the two populations. The steady-state mean plasma AUC and Cmax were 1,870 nmol∙h/L and 259 nmol/L, respectively, with 10 mg empagliflozin once daily treatment, and 4,740 nmol∙h/L and 687 nmol/L, respectively, with 25 mg empagliflozin once daily treatment. Systemic exposure of empagliflozin increased in a dose-proportional manner in the therapeutic dose range. Empagliflozin does not appear to have time-dependent pharmacokinetic characteristics. Following once-daily dosing, up to 22% accumulation, with respect to plasma AUC, was observed at steady-state.
2.2 Recommended Dosage
Table 1 presents the recommended dosage of JARDIANCE in adult and pediatric patients aged 10 years and older.
| Population | Indication | Recommended Dosage |
|---|---|---|
| Adults | Reduce the risk of cardiovascular death and hospitalization in patients with heart failure |
|
| Reduce the risk of cardiovascular death in patients with type 2 diabetes mellitus with established cardiovascular disease | ||
| Glycemic control in type 2 diabetes mellitus |
|
|
| Pediatric patients aged 10 years and older | Glycemic control in type 2 diabetes mellitus |
|
8.7 Hepatic Impairment
JARDIANCE may be used in patients with hepatic impairment [see Clinical Pharmacology (12.3)].
1 Indications and Usage (1 INDICATIONS AND USAGE)
JARDIANCE is indicated:
- to reduce the risk of cardiovascular death and hospitalization for heart failure in adults with heart failure.
- to reduce the risk of cardiovascular death in adults with type 2 diabetes mellitus and established cardiovascular disease.
- as an adjunct to diet and exercise to improve glycemic control in adults and pediatric patients aged 10 years and older with type 2 diabetes mellitus.
12.1 Mechanism of Action
Empagliflozin is an inhibitor of SGLT2, the predominant transporter responsible for reabsorption of glucose from the glomerular filtrate back into the circulation. By inhibiting SGLT2, empagliflozin reduces renal reabsorption of filtered glucose and lowers the renal threshold for glucose, and thereby increases urinary glucose excretion.
Empagliflozin also reduces sodium reabsorption and increases the delivery of sodium to the distal tubule. This may influence several physiological functions such as lowering both pre- and afterload of the heart and downregulating sympathetic activity.
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
- Ketoacidosis: Assess patients who present with signs and symptoms of metabolic acidosis for ketoacidosis, regardless of blood glucose level. If suspected, discontinue JARDIANCE, evaluate and treat promptly. Before initiating JARDIANCE, consider risk factors for ketoacidosis. Patients on JARDIANCE may require monitoring and temporary discontinuation of therapy in clinical situations known to predispose to ketoacidosis. (5.1)
- Volume Depletion: Before initiating JARDIANCE, assess volume status and renal function in patients with impaired renal function, elderly patients, or patients on loop diuretics. Monitor for signs and symptoms during therapy. (5.2)
- Urosepsis and Pyelonephritis: Evaluate patients for signs and symptoms of urinary tract infections and treat promptly, if indicated (5.3)
- Hypoglycemia: Adult patients taking an insulin secretagogue or insulin may have an increased risk of hypoglycemia. In pediatric patients 10 years of age and older, the risk of hypoglycemia was higher regardless of insulin use. Consider lowering the dosage of insulin secretagogue or insulin to reduce the risk of hypoglycemia when initiating JARDIANCE. (5.4)
- Necrotizing Fasciitis of the Perineum (Fournier's Gangrene): Serious, life-threatening cases have occurred in both females and males. Assess patients presenting with pain or tenderness, erythema, or swelling in the genital or perineal area, along with fever or malaise. If suspected, institute prompt treatment. (5.5)
- Genital Mycotic Infections: Monitor and treat as appropriate (5.6)
- Hypersensitivity Reactions: Serious hypersensitivity reactions (e.g., angioedema) have occurred with JARDIANCE. If hypersensitivity reactions occur, discontinue JARDIANCE, treat promptly, and monitor until signs and symptoms resolve. (5.7)
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
- Assess renal function before initiating and as clinically indicated. Correct volume depletion before initiating (2.1)
- Recommended dosage is 10 mg once daily in the morning, taken with or without food (2.2)
- For additional glycemic control, dosage may be increased to 25 mg in patients tolerating JARDIANCE (2.2)
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
JARDIANCE tablets available as:
- 10 mg pale yellow, round, biconvex and bevel-edged, film-coated tablets debossed with "S 10" on one side and the Boehringer Ingelheim company symbol on the other side.
- 25 mg pale yellow, oval, biconvex, film-coated tablets debossed with "S 25" on one side and the Boehringer Ingelheim company symbol on the other side.
6.2 Postmarketing Experience
Additional adverse reactions have been identified during postapproval use of JARDIANCE. Because these reactions are reported voluntarily from a population of uncertain size, it is generally not possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Gastrointestinal Disorders: Constipation
Infections: Necrotizing fasciitis of the perineum (Fournier's gangrene), urosepsis and pyelonephritis
Metabolism and Nutrition Disorders: Ketoacidosis
Renal and Urinary Disorders: Acute kidney injury
Skin and Subcutaneous Tissue Disorders: Angioedema, skin reactions (e.g., rash, urticaria)
8 Use in Specific Populations (8 USE IN SPECIFIC POPULATIONS)
- Pregnancy: Advise females of the potential risk to a fetus especially during the second and third trimesters (8.1)
- Lactation: Not recommended when breastfeeding (8.2)
- Geriatric Patients: Higher incidence of adverse reactions related to volume depletion and reduced renal function (8.5, 8.6)
- Renal Impairment: Higher incidence of adverse reactions related to reduced renal function (8.6)
5.6 Genital Mycotic Infections
JARDIANCE increases the risk for genital mycotic infections [see Adverse Reactions (6.1)]. Patients with a history of chronic or recurrent genital mycotic infections were more likely to develop genital mycotic infections. Monitor and treat as appropriate.
5.7 Hypersensitivity Reactions
There have been postmarketing reports of serious hypersensitivity reactions (e.g., angioedema) in patients treated with JARDIANCE. If a hypersensitivity reaction occurs, discontinue JARDIANCE; treat promptly per standard of care, and monitor until signs and symptoms resolve. JARDIANCE is contraindicated in patients with hypersensitivity to empagliflozin or any of the excipients in JARDIANCE [see Contraindications (4)].
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
JARDIANCE has been evaluated in clinical trials in adult and pediatric patients aged 10 to 17 years with type 2 diabetes mellitus and in adults with heart failure. The overall safety profile of JARDIANCE was generally consistent across the studied indications.
5.3 Urosepsis and Pyelonephritis
There have been reports of serious urinary tract infections including urosepsis and pyelonephritis requiring hospitalization in patients receiving JARDIANCE. Treatment with JARDIANCE increases the risk for urinary tract infections. Evaluate patients for signs and symptoms of urinary tract infections and treat promptly, if indicated [see Adverse Reactions (6)].
17 Patient Counseling Information (17 PATIENT COUNSELING INFORMATION)
Advise the patient to read the FDA-approved patient labeling (Medication Guide).
14.4 Heart Failure Trials in Adults
EMPEROR-Reduced (NCT03057977) was a double-blind trial conducted in adults with chronic heart failure (New York Heart Association [NYHA] functional class II-IV) with left ventricular ejection fraction (LVEF) ≤40% to evaluate the efficacy of JARDIANCE as adjunct to standard of care heart failure therapy.
Of 3,730 patients, 1,863 were randomized to JARDIANCE 10 mg and 1,867 to placebo and were followed for a median of 16 months. The mean age of the trial population was 67 years (range: 25 to 94 years) and 76% were men, 24% were women, and 27% were 75 years of age or older. Approximately 71% of the trial population were White, 18% Asian and 7% Black or African American. At baseline, 50% of the patients had type 2 diabetes mellitus.
At randomization, 75% of patients were NYHA class II, 24% were class III and 0.5% were class IV. The mean LVEF was 28%. At baseline, the mean eGFR was 62 mL/min/1.73 m2 and the median urinary albumin to creatinine ratio (UACR) was 22 mg/g. Approximately half of the patients (52%) had eGFR equal to or above 60 mL/min/1.73 m2, 24% had eGFR 45 to less than 60 mL/min/1.73 m2, 19% had eGFR 30 to less than 45 mL/min/1.73 m2 and 5% had eGFR 20 to less than 30 mL/min/1.73 m2.
At baseline, 88% of patients were treated with angiotensin-converting enzyme (ACE) inhibitors, angiotensin receptor blockers (ARB), or angiotensin receptor-neprilysin inhibitors (ARNI), 95% with beta-blockers, 71% with mineralocorticoid receptor antagonists (MRA), and 95% with diuretics.
The primary endpoint was the time to first event of either cardiovascular (CV) death or hospitalization for heart failure (HHF). First and recurrent HHF was assessed as a key secondary endpoint.
JARDIANCE was superior in reducing the risk of the primary composite endpoint of cardiovascular death or hospitalization for heart failure compared with placebo, mostly through a reduction in hospitalization for heart failure. JARDIANCE reduced the risk of first and recurrent HHF (see Table 16 and Figures 7 and 8).
| Placebo N=1,867 |
JARDIANCE 10 mg N=1,863 |
Hazard ratio vs placebo (95% CI) |
p-value | |
|---|---|---|---|---|
| Number of Patients (%) | ||||
|
aTime to first event bIncludes deaths following hospitalization cJoint frailty model accounting for CV death |
||||
| CV death or HHFa | 462 (24.7%) | 361 (19.4%) | 0.75 (0.65, 0.86) | <0.0001 |
| CV deatha,b | 202 (10.8%) | 187 (10.0%) | 0.92 (0.75, 1.12) | |
| HHFa | 342 (18.3%) | 246 (13.2%) | 0.69 (0.59, 0.81) | |
| Number of Events | ||||
| First and recurrent HHFc | 553 | 388 | 0.70 (0.58, 0.85) | 0.0003 |
Figure 7 Time to First Occurrence of the Primary Composite Endpoint of CV Death or Hospitalization for Heart Failure
Figure 8 Time to Event of Hospitalization for Heart Failure (First and Recurrent)
The results of the primary composite were generally consistent across the pre-specified subgroups (see Figure 9).
Figure 9 Treatment Effects for the Primary Composite Endpoint (CV Death and Hospitalization for Heart Failure) Subgroup Analysis (EMPEROR-Reduced)
LVEF >30%: Includes both above and below the median NT-proBNP. To be eligible for inclusion, patients with an LVEF >30% were required to meet a higher NT-proBNP threshold than those with LVEF ≤30%, unless they additionally had a history of HHF within the past 12 months.
EMPEROR-Preserved (NCT03057951) was a double-blind trial conducted in patients with chronic heart failure NYHA Class II-IV with LVEF >40% to evaluate the efficacy of JARDIANCE as adjunct to standard of care therapy.
Of 5,988 patients, 2,997 were randomized to JARDIANCE 10 mg and 2,991 to placebo and were followed for a median of 26 months. The mean age of the trial population was 72 years (range: 22 to 100 years) and 55% were men, 45% were women, and 43% were 75 years of age or older. Approximately 76% of the trial population were White, 14% Asian and 4% Black or African American.
At randomization, 82% of patients were NYHA class II, 18% were class III and 0.3% were class IV. The EMPEROR-Preserved trial population included patients with a LVEF <50% (33.1%), with a LVEF 50 to <60% (34.4%) and a LVEF ≥60% (32.5%). At baseline, the mean eGFR was 61 mL/min/1.73 m2 and the median urinary albumin to creatinine ratio (UACR) was 21 mg/g. Approximately half of the patients (50%) had eGFR equal to or above 60 mL/min/1.73 m2, 26% had eGFR 45 to less than 60 mL/min/1.73 m2, 19% had eGFR 30 to less than 45 mL/min/1.73 m2, and 5% had eGFR 20 to less than 30 mL/min/1.73 m2.
At baseline, 81% of patients were treated with ACE inhibitors, ARBs, or ARNI, 86% with beta-blockers, 38% with MRAs, and 86% with diuretics.
The primary endpoint was the time to first event of either CV death or HHF. First and recurrent HHF was assessed as a key secondary endpoint.
JARDIANCE was superior in reducing the risk of the primary composite endpoint compared with placebo, mostly through a reduction in hospitalization for heart failure. JARDIANCE reduced the risk of first and recurrent HHF (see Table 17 and Figures 10 and 11).
| Placebo N=2,991 |
JARDIANCE 10 mg N=2,997 |
Hazard ratio vs placebo (95% CI) |
p-value | |
|---|---|---|---|---|
| Number of Patients (%) | ||||
|
aTime to first event bIncludes deaths following hospitalization cJoint frailty model accounting for CV death |
||||
| CV death or HHFa | 511 (17.1%) | 415 (13.8%) | 0.79 (0.69, 0.90) | 0.0003 |
| CV deatha,b | 244 (8.2%) | 219 (7.3%) | 0.91 (0.76, 1.09) | |
| HHFa | 352 (11.8%) | 259 (8.6%) | 0.71 (0.60, 0.83) | |
| Number of Events | ||||
| First and recurrent HHFc | 541 | 407 | 0.73 (0.61, 0.88) | 0.0009 |
Figure 10 Time to First Occurrence of the Primary Composite Endpoint of CV Death or Hospitalization for Heart Failure
Figure 11 Time to Event of Hospitalization for Heart Failure (First and Recurrent)
The results of the primary composite endpoint were consistent across the pre-specified subgroups (see Figure 12).
Figure 12 Treatment Effects for the Primary Composite Endpoint (CV Death or Hospitalization for Heart Failure) Subgroup Analysis (EMPEROR-Preserved)
16 How Supplied/storage and Handling (16 HOW SUPPLIED/STORAGE AND HANDLING)
Product: 50090-4492
NDC: 50090-4492-0 90 TABLET, FILM COATED in a BOTTLE
NDC: 50090-4492-1 30 TABLET, FILM COATED in a BOTTLE
2.3 Recommendations Regarding Missed Dose
- If a dose is missed, instruct patients to take the dose as soon as possible.
- Do not double up the next dose.
2.1 Testing Prior to Initiation of Jardiance (2.1 Testing Prior to Initiation of JARDIANCE)
- Assess renal function before initiating JARDIANCE and as clinically indicated [see Warnings and Precautions (5.2)].
- Use for glycemic control is not recommended in patients with an eGFR less than 30 mL/min/1.73 m2 [see Use in Specific Populations (8.6)].
- JARDIANCE is contraindicated in patients on dialysis [see Use in Specific Populations (8.6)].
- Assess volume status in patients with volume depletion and correct this condition before initiating JARDIANCE [see Warnings and Precautions (5.2) and Use in Specific Populations (8.5, 8.6)].
5.5 Necrotizing Fasciitis of the Perineum (fournier's Gangrene) (5.5 Necrotizing Fasciitis of the Perineum (Fournier's Gangrene))
Reports of necrotizing fasciitis of the perineum (Fournier's gangrene), a rare but serious and life-threatening necrotizing infection requiring urgent surgical intervention, have been identified in patients with diabetes mellitus receiving SGLT2 inhibitors, including JARDIANCE. Cases have been reported in both females and males. Serious outcomes have included hospitalization, multiple surgeries, and death.
Patients treated with JARDIANCE presenting with pain or tenderness, erythema, or swelling in the genital or perineal area, along with fever or malaise, should be assessed for necrotizing fasciitis. If suspected, start treatment immediately with broad-spectrum antibiotics and, if necessary, surgical debridement. Discontinue JARDIANCE, closely monitor blood glucose levels, and provide appropriate alternative therapy for glycemic control.
14.1 Glycemic Control Trials in Adults With Type 2 Diabetes Mellitus (14.1 Glycemic Control Trials in Adults with Type 2 Diabetes Mellitus)
JARDIANCE has been studied as monotherapy and in combination with metformin, sulfonylurea, pioglitazone, linagliptin, and insulin. JARDIANCE has also been studied in patients with type 2 diabetes mellitus with mild or moderate renal impairment.
In adult patients with type 2 diabetes mellitus, treatment with JARDIANCE reduced hemoglobin A1c (HbA1c), compared to placebo. The reduction in HbA1c for JARDIANCE compared with placebo was observed across subgroups including sex, race, geographic region, baseline BMI and duration of disease.
14.2 Glycemic Control Trial in Pediatric Patients Aged 10 to 17 Years With Type 2 Diabetes Mellitus (14.2 Glycemic Control Trial in Pediatric Patients Aged 10 to 17 Years with Type 2 Diabetes Mellitus)
DINAMO (NCT03429543) was a 26-week, double-blind, randomized, placebo-controlled, parallel group trial, with a double-blind active treatment safety extension period up to 52 weeks to assess the efficacy of JARDIANCE. The trial enrolled pediatric patients aged 10 to 17 years with inadequately controlled type 2 diabetes mellitus (HbA1c 6.5 to 10.5%). Patients treated with metformin (at least 1,000 mg daily or maximally tolerated dose), with or without insulin therapy, and those with a history of intolerance to metformin therapy were enrolled. Patients were randomized to 3 treatment arms (JARDIANCE 10 mg, a dipeptidyl peptidase-4 (DPP-4) inhibitor or placebo), over 26 weeks. Patients in the JARDIANCE 10 mg group who failed to achieve HbA1c <7.0% at Week 12 underwent a second randomization at Week 14 to remain on the 10 mg dose or increase to 25 mg. Patients on placebo were re-randomized at Week 26 to one of the JARDIANCE doses (10 mg or 25 mg) or a DPP-4 inhibitor.
A total of 157 patients were treated with either JARDIANCE (10 mg or 25 mg; N=52), a DPP-4 inhibitor (N=52), or placebo (N=53). Background therapies as adjunct to diet and exercise included metformin (51%), a combination of metformin and insulin (40.1%), insulin (3.2%), or none (5.7%). The mean HbA1c at baseline was 8.0% and the mean duration of type 2 diabetes mellitus was 2.1 years. The mean age was 14.5 years (range: 10-17 years) and 51.6% were aged 15 years and older. Approximately, 50% were White, 6% were Asian, 31% were Black or African American, and 38% were of Hispanic or Latino ethnicity. The mean BMI was 36.0 kg/m2 and mean BMI Z-score was 3.0. Patients with an eGFR less than 60 mL/min/1.73 m2 were not enrolled in the trial. Approximately 25% of the study population had microalbuminuria or macroalbuminuria.
At Week 26, treatment with JARDIANCE was superior in reducing HbA1c from baseline versus placebo (see Table 14).
| JARDIANCE 10 mg and 25 mg |
Placebo | |
|---|---|---|
|
aModified intent-to-treat set (All randomized and treated patients with baseline measurement). bMultiple imputations using placebo wash-out approach with 500 iterations for missing data. Imputed for HbA1c (Jardiance N=5 (9.6 %), Placebo N=3 (5.7%)), for FPG (Jardiance N=4 (8.3%), Placebo N=2 (3.8%)). cLeast-Square Mean from Analysis of Covariance (ANCOVA) adjusted for baseline value and baseline age stratum (< 15 years vs 15 to < 18 years). dNot evaluated for statistical significance, not part of sequential testing procedure. ep-value=0.0116 (two-sided) |
||
| HbA1c (%)b | ||
| Number of patients | n=52 | n=53 |
| Baseline (mean) | 8.0 | 8.1 |
| Change from baselinec | -0.2 | 0.7 |
| Difference from placeboc (95% CI) | -0.8e (-1.5, -0.2) | -- |
| FPG (mg/dL)b,d | ||
| Number of patients | n=48 | n=52 |
| Baseline (mean) | 154 | 159 |
| Change from baselinec | -19 | 17 |
| Difference from placeboc (95% CI) | -36 (-60.7, -10.7) | -- |
14.3 Cardiovascular Outcomes in Adults With Type 2 Diabetes Mellitus and Atherosclerotic Cardiovascular Disease (14.3 Cardiovascular Outcomes in Adults with Type 2 Diabetes Mellitus and Atherosclerotic Cardiovascular Disease)
The effect of JARDIANCE on cardiovascular (CV) risk in adult patients with type 2 diabetes mellitus and established, stable, atherosclerotic CV disease was evaluated in the EMPA-REG OUTCOME trial, a multicenter, multinational, randomized, double-blind parallel group trial. The trial compared the risk of experiencing a major adverse cardiovascular event (MACE) between JARDIANCE and placebo when these were added to and used concomitantly with standard of care treatments for diabetes mellitus and atherosclerotic CV disease. Concomitant antidiabetic medications were to be kept stable for the first 12 weeks of the trial. Thereafter, antidiabetic and atherosclerotic therapies could be adjusted, at the discretion of investigators, to ensure participants were treated according to the standard care for these diseases.
A total of 7,020 patients were treated (JARDIANCE 10 mg = 2,345; JARDIANCE 25 mg = 2,342; placebo = 2,333) and followed for a median of 3.1 years. Approximately 72% of the trial population was White, 22% was Asian, and 5% was Black. The mean age was 63 years and approximately 72% were male.
All patients in the trial had inadequately controlled type 2 diabetes mellitus at baseline (HbA1c greater than or equal to 7%). The mean HbA1c at baseline was 8.1% and 57% of participants had diabetes mellitus for more than 10 years. Approximately 31%, 22% and 20% reported a past history of neuropathy, retinopathy and nephropathy to investigators, respectively and the mean eGFR was 74 mL/min/1.73 m2. At baseline, patients were treated with one (~30%) or more (~70%) antidiabetic medications including metformin (74%), insulin (48%), and sulfonylurea (43%).
All patients had established atherosclerotic CV disease at baseline including one (82%) or more (18%) of the following: a documented history of coronary artery disease (76%), stroke (23%) or peripheral artery disease (21%). At baseline, the mean systolic blood pressure was 136 mmHg, the mean diastolic blood pressure was 76 mmHg, the mean LDL was 86 mg/dL, the mean HDL was 44 mg/dL, and the mean urinary albumin to creatinine ratio (UACR) was 175 mg/g. At baseline, approximately 81% of patients were treated with renin angiotensin system inhibitors, 65% with beta-blockers, 43% with diuretics, 77% with statins, and 86% with antiplatelet agents (mostly aspirin).
The primary endpoint in EMPA-REG OUTCOME was the time to first occurrence of a Major Adverse Cardiac Event (MACE). A major adverse cardiac event was defined as occurrence of either a CV death or a non-fatal myocardial infarction (MI) or a non-fatal stroke. The statistical analysis plan had pre-specified that the 10 and 25 mg doses would be combined. A Cox proportional hazards model was used to test for non-inferiority against the pre-specified risk margin of 1.3 for the hazard ratio of MACE and superiority on MACE if non-inferiority was demonstrated. Type-1 error was controlled across multiples tests using a hierarchical testing strategy.
JARDIANCE significantly reduced the risk of first occurrence of primary composite endpoint of CV death, non-fatal myocardial infarction, or non-fatal stroke (HR: 0.86; 95% CI: 0.74, 0.99). The treatment effect was due to a significant reduction in the risk of CV death in subjects randomized to empagliflozin (HR: 0.62; 95% CI: 0.49, 0.77), with no change in the risk of non-fatal myocardial infarction or non-fatal stroke (see Table 15 and Figures 5 and 6). Results for the 10 mg and 25 mg empagliflozin dosages were consistent with results for the combined dosage groups.
| Placebo N=2,333 |
JARDIANCE N=4,687 |
Hazard ratio vs placebo (95% CI) |
|
|---|---|---|---|
|
aTreated set (patients who had received at least one dose of trial drug) bp-value for superiority (2-sided) 0.04 cTotal number of events |
|||
| Composite of CV death, non-fatal myocardial infarction, non-fatal stroke (time to first occurrence)b | 282 (12.1%) | 490 (10.5%) | 0.86 (0.74, 0.99) |
| Non-fatal myocardial infarctionc | 121 (5.2%) | 213 (4.5%) | 0.87 (0.70, 1.09) |
| Non-fatal strokec | 60 (2.6%) | 150 (3.2%) | 1.24 (0.92, 1.67) |
| CV deathc | 137 (5.9%) | 172 (3.7%) | 0.62 (0.49, 0.77) |
The efficacy of JARDIANCE on CV death was generally consistent across major demographic and disease subgroups.
Vital status was obtained for 99.2% of subjects in the trial. A total of 463 deaths were recorded during the EMPA-REG OUTCOME trial. Most of these deaths were categorized as CV deaths. The non-CV deaths were only a small proportion of deaths and were balanced between the treatment groups (2.1% in patients treated with JARDIANCE, and 2.4% of patients treated with placebo).
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:38:41.343160 · Updated: 2026-03-14T21:55:28.640025