These Highlights Do Not Include All The Information Needed To Use Lomustine Capsules Safely And Effectively. See Full Prescribing Information For Lomustine Capsules.
916dfac8-da11-40e4-9e44-a909e29a6b5f
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
DELAYED MYELOSUPPRESSION Lomustine Capsules cause myelosuppression including fatal myelosuppression. Myelosuppression is delayed, dose-related, and cumulative; occurring 4 to 6 weeks after drug administration and persisting for 1 to 2 weeks. Thrombocytopenia is generally more severe than leukopenia. Cumulative myelosuppression from Lomustine Capsules is manifested by greater severity and longer duration of cytopenias. Monitor blood counts for at least 6 weeks after each dose. Do not give Lomustine Capsules more frequently than every 6 weeks [see Warnings and Precautions (5.1) , Dosage and Administration (2.2 , 2.3) ]. RISK OF OVERDOSAGE PRESCRIBE, DISPENSE, AND ADMINISTER ONLY ENOUGH CAPSULES FOR ONE DOSE. Fatal toxicity occurs with overdosage of Lomustine Capsules. Both physician and pharmacist should emphasize to the patient that only one dose of Lomustine Capsules is taken every 6 weeks [see Dosage and Administration (2.1) , Warnings and Precautions (5.2) , Overdosage (10) ].
Indications and Usage
Lomustine Capsules are an alkylating drug indicated for the treatment of patients with: Brain tumors, primary and metastatic, following appropriate surgical and/or radiotherapeutic procedures. (1) Hodgkin’s lymphoma in combination with other chemotherapies, following disease progression with initial chemotherapy. (1)
Dosage and Administration
Recommended dose in adult and pediatric patients is 130 mg/m 2 orally every 6 weeks. (2.1) Round dose to nearest 5 mg. Give as a single oral dose and do not repeat for at least 6 weeks.
Warnings and Precautions
Pulmonary toxicity : Pulmonary infiltrates and/or fibrosis occurs with Lomustine Capsules. Perform pulmonary function tests prior to treatment and repeat frequently. Permanently discontinue Lomustine Capsules in patients diagnosed with pulmonary fibrosis. (5.3) Secondary malignancies : Acute leukemia and myelodysplasia can occur with long-term use. (5.4) Hepatotoxicity : Increased levels of transaminases, alkaline phosphatase and bilirubin can occur with Lomustine Capsules. Monitor liver function. (5.5) Nephrotoxicity : Can cause renal failure. Monitor renal function. (5.6) Embryo-fetal toxicity : Can cause fetal harm. Advise males and females of reproductive potential of the potential risk to a fetus and to use effective contraception. (5.7 , 8.1 , 8.3)
Contraindications
None.
Adverse Reactions
The following serious adverse reactions are discussed in greater detail in other sections of the labeling: Delayed myelosuppression [see Warnings and Precautions (5.1) ] Risks of overdosage [see Warnings and Precautions (5.2) ] Pulmonary toxicity [see Warnings and Precautions (5.3) ] Secondary malignancies [see Warnings and Precautions (5.4) ] Hepatotoxicity [see Warnings and Precautions (5.5) ] Nephrotoxicity [see Warnings and Precautions (5.6) ] The following adverse reactions associated with the use of Lomustine Capsules were identified in clinical trials or postmarketing reports. Because these reactions were reported from a population of uncertain size, it is not possible to estimate their frequency, reliability, or establish a causal relationship to drug exposure. Gastrointestinal disorders: nausea, vomiting, and stomatitis Ocular disorders: optic atrophy, visual disturbances, and blindness Neurologic disorders: disorientation, lethargy, ataxia, and dysarthria Other: alopecia
Storage and Handling
Store at 20º to 25ºC (68º to 77ºF); excursions permitted to 15° to 30°C (59° to 86°F) [See USP Controlled Room Temperature]. Avoid temperatures over 40°C (104°F). Lomustine Capsules, USP is a cytotoxic drug. Follow applicable special handling and disposal procedures. 1 To minimize the risk of dermal exposure, always wear impervious gloves when handling bottles containing Lomustine Capsules, USP. Do not break Lomustine Capsules, USP; avoid exposure to broken capsules. If dermal contact occurs, wash areas of skin contact immediately and thoroughly.
How Supplied
Lomustine Capsules, USP are available in three strengths, distinguishable by the color of the capsules, in individual bottles of 5 capsules each: Strength Capsule Description NDC Code 100 mg Hard gelatin capsule shell with light green opaque body and light green opaque cap, imprinted with black ink “CP116” on cap, containing white powder. 80005-116-02 40 mg Hard gelatin capsule shell with light green opaque body and bright white opaque cap, imprinted with black ink “CP115” on cap, containing white powder. 80005-115-02 10 mg Hard gelatin capsule shell with bright white opaque body and bright white opaque cap, imprinted with black ink “CP114” on cap, containing white powder. 80005-114-02
Medication Information
Warnings and Precautions
Pulmonary toxicity : Pulmonary infiltrates and/or fibrosis occurs with Lomustine Capsules. Perform pulmonary function tests prior to treatment and repeat frequently. Permanently discontinue Lomustine Capsules in patients diagnosed with pulmonary fibrosis. (5.3) Secondary malignancies : Acute leukemia and myelodysplasia can occur with long-term use. (5.4) Hepatotoxicity : Increased levels of transaminases, alkaline phosphatase and bilirubin can occur with Lomustine Capsules. Monitor liver function. (5.5) Nephrotoxicity : Can cause renal failure. Monitor renal function. (5.6) Embryo-fetal toxicity : Can cause fetal harm. Advise males and females of reproductive potential of the potential risk to a fetus and to use effective contraception. (5.7 , 8.1 , 8.3)
Indications and Usage
Lomustine Capsules are an alkylating drug indicated for the treatment of patients with: Brain tumors, primary and metastatic, following appropriate surgical and/or radiotherapeutic procedures. (1) Hodgkin’s lymphoma in combination with other chemotherapies, following disease progression with initial chemotherapy. (1)
Dosage and Administration
Recommended dose in adult and pediatric patients is 130 mg/m 2 orally every 6 weeks. (2.1) Round dose to nearest 5 mg. Give as a single oral dose and do not repeat for at least 6 weeks.
Contraindications
None.
Adverse Reactions
The following serious adverse reactions are discussed in greater detail in other sections of the labeling: Delayed myelosuppression [see Warnings and Precautions (5.1) ] Risks of overdosage [see Warnings and Precautions (5.2) ] Pulmonary toxicity [see Warnings and Precautions (5.3) ] Secondary malignancies [see Warnings and Precautions (5.4) ] Hepatotoxicity [see Warnings and Precautions (5.5) ] Nephrotoxicity [see Warnings and Precautions (5.6) ] The following adverse reactions associated with the use of Lomustine Capsules were identified in clinical trials or postmarketing reports. Because these reactions were reported from a population of uncertain size, it is not possible to estimate their frequency, reliability, or establish a causal relationship to drug exposure. Gastrointestinal disorders: nausea, vomiting, and stomatitis Ocular disorders: optic atrophy, visual disturbances, and blindness Neurologic disorders: disorientation, lethargy, ataxia, and dysarthria Other: alopecia
Storage and Handling
Store at 20º to 25ºC (68º to 77ºF); excursions permitted to 15° to 30°C (59° to 86°F) [See USP Controlled Room Temperature]. Avoid temperatures over 40°C (104°F). Lomustine Capsules, USP is a cytotoxic drug. Follow applicable special handling and disposal procedures. 1 To minimize the risk of dermal exposure, always wear impervious gloves when handling bottles containing Lomustine Capsules, USP. Do not break Lomustine Capsules, USP; avoid exposure to broken capsules. If dermal contact occurs, wash areas of skin contact immediately and thoroughly.
How Supplied
Lomustine Capsules, USP are available in three strengths, distinguishable by the color of the capsules, in individual bottles of 5 capsules each: Strength Capsule Description NDC Code 100 mg Hard gelatin capsule shell with light green opaque body and light green opaque cap, imprinted with black ink “CP116” on cap, containing white powder. 80005-116-02 40 mg Hard gelatin capsule shell with light green opaque body and bright white opaque cap, imprinted with black ink “CP115” on cap, containing white powder. 80005-115-02 10 mg Hard gelatin capsule shell with bright white opaque body and bright white opaque cap, imprinted with black ink “CP114” on cap, containing white powder. 80005-114-02
Description
DELAYED MYELOSUPPRESSION Lomustine Capsules cause myelosuppression including fatal myelosuppression. Myelosuppression is delayed, dose-related, and cumulative; occurring 4 to 6 weeks after drug administration and persisting for 1 to 2 weeks. Thrombocytopenia is generally more severe than leukopenia. Cumulative myelosuppression from Lomustine Capsules is manifested by greater severity and longer duration of cytopenias. Monitor blood counts for at least 6 weeks after each dose. Do not give Lomustine Capsules more frequently than every 6 weeks [see Warnings and Precautions (5.1) , Dosage and Administration (2.2 , 2.3) ]. RISK OF OVERDOSAGE PRESCRIBE, DISPENSE, AND ADMINISTER ONLY ENOUGH CAPSULES FOR ONE DOSE. Fatal toxicity occurs with overdosage of Lomustine Capsules. Both physician and pharmacist should emphasize to the patient that only one dose of Lomustine Capsules is taken every 6 weeks [see Dosage and Administration (2.1) , Warnings and Precautions (5.2) , Overdosage (10) ].
10 Overdosage
Overdosage with Lomustine Capsules has occurred, including fatal cases [see Dosage and Administration (2.1), Warnings and Precautions (5.2) ]. Overdosage causes severe myelosuppression, as well as abdominal pain, diarrhea, vomiting, anorexia, lethargy, dizziness, abnormal hepatic function, cough, and shortness of breath.
No antidotes exist for Lomustine Capsules overdosage.
15 References
OSHA. http://www.osha.gov/SLTC/hazardousdrugs/index.html.
8.1 Pregnancy
Risk Summary
Based on animal data and its mechanism of action, Lomustine Capsules can cause fetal harm when administered to a pregnant woman [see Clinical Pharmacology (12.1) ]. There are no available data on Lomustine Capsules exposure in pregnant women. Lomustine was teratogenic in rats and embryotoxic in rabbits at total dose levels approximately two to four times the total human dose of 130 mg/m2 over 6 weeks (0.18 to 0.27 times the single human dose of 130 mg/m2) based on BSA [see Data]. Advise pregnant women of the potential risk to a fetus.
In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2-4% and 15-20%, respectively.
Data
Animal Data
Lomustine was administered by intraperitoneal injection daily to pregnant rats during the period of organogenesis at dose levels of 0, 2, 4, 6, and 8 mg/kg. Resorption rates and post-implantation loss occurred at doses greater than or equal to 4 mg/kg (approximately 0.18 times the clinical dose of 130 mg/m2 based on BSA or approximately twice the total clinical dose of lomustine over 6 weeks). Malformations (omphalocele, ectopia cordis, scoliosis, syndactyly, hydrocephalus, microphthalmia, anophthalmia, anomalies of aortic arch, dextrocardia, malpositioning of the ovaries and testes, sternoschisis, and shortened/misshapen bone of the fore or hind limbs) and decreased fetal body weight occurred at all dose levels. In pregnant rabbits treated with lomustine at 3 mg/kg (approximately 0.27 times the 130 mg/m2 clinical dose based on BSA or approximately four times the total clinical dose of lomustine over 6 weeks) during organogenesis, there were increases in abortions and decreases in surviving pup weight that persisted postnatally.
11 Description
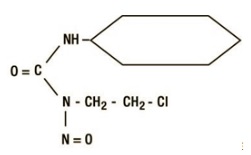
Lomustine Capsules, USP (lomustine) is an alkylating drug for oral administration. The chemical name for lomustine is 1-(2-chloro-ethyl)-3-cyclohexyl-1-nitrosourea and the molecular formula is C9H16ClN3O2. The molecular weight is 233.71. Lomustine is a yellow powder, which is soluble in 10% ethanol (0.05 mg per mL) and in absolute alcohol (70 mg per mL). Lomustine is insoluble in water (<0.05 mg per mL).
The chemical structure is:
Lomustine Capsules, USP are supplied as 10 mg, 40 mg, and 100 mg capsules and contain the following inactive ingredients: magnesium stearate NF and mannitol USP. The 10 mg capsule shells are composed of gelatin and titanium dioxide. The 40 mg and 100 mg capsule shells are composed of FD&C blue #1, gelatin, iron oxide black, iron oxide yellow, and titanium dioxide. The capsules are printed with black ink composed of iron oxide black, potassium hydroxide, propylene glycol, shellac, and strong ammonia solution.
FDA approved dissolution method is not listed in the USP Monograph for Lomustine Capsules, USP, 10 mg, 40 mg, and 100 mg.
8.2 lactation
Risk Summary
There is no information on the presence of lomustine or its metabolites in human milk, its effects on the breastfed infant, or its effects on milk production. Because of the potential for serious adverse reactions in breastfed infants from Lomustine Capsules, advise women not to breastfeed during treatment with Lomustine Capsules and for 2 weeks after the final dose.
1.1 Brain Tumors
Lomustine Capsules are indicated for the treatment of patients with primary and metastatic brain tumors following appropriate surgical and/or radiotherapeutic procedures.
16.1 How Supplied
Lomustine Capsules, USP are available in three strengths, distinguishable by the color of the capsules, in individual bottles of 5 capsules each:
|
Strength |
Capsule Description |
NDC Code |
|
100 mg |
Hard gelatin capsule shell with light green opaque body and light green opaque cap, imprinted with black ink “CP116” on cap, containing white powder. |
80005-116-02 |
|
40 mg |
Hard gelatin capsule shell with light green opaque body and bright white opaque cap, imprinted with black ink “CP115” on cap, containing white powder. |
80005-115-02 |
|
10 mg |
Hard gelatin capsule shell with bright white opaque body and bright white opaque cap, imprinted with black ink “CP114” on cap, containing white powder. |
80005-114-02 |
8.4 Pediatric Use
Pediatric use, including dose, is not based on adequate and well-controlled clinical studies.
8.5 Geriatric Use
No data in the clinical studies of Lomustine Capsules are available for patients 65 years of age and over to determine whether they respond differently than younger patients. Other reported clinical experience has not identified differences in responses between elderly and younger patients. In general, dose selection for an elderly patient should be cautious, reflecting the greater frequency of decreased hepatic, renal, or cardiac function and of concomitant disease or other drug therapy.
Lomustine and its metabolites are known to be substantially excreted by the kidney, and the risk of toxic reactions to this drug may be greater in patients with impaired renal function. Because elderly patients are more likely to have decreased renal function, care should be taken in dose selection, and renal function should be monitored.
5.5 Hepatotoxicity
Hepatic toxicity, manifested by increased levels of transaminases, alkaline phosphatase, and bilirubin occurs with Lomustine Capsules.
Monitor liver function.
5.6 Nephrotoxicity
Progressive renal failure with a decrease in kidney size occurs with Lomustine Capsules.
Monitor renal function.
4 Contraindications
None.
6 Adverse Reactions
The following serious adverse reactions are discussed in greater detail in other sections of the labeling:
- Delayed myelosuppression [see Warnings and Precautions (5.1) ]
- Risks of overdosage [see Warnings and Precautions (5.2) ]
- Pulmonary toxicity [see Warnings and Precautions (5.3) ]
- Secondary malignancies [see Warnings and Precautions (5.4) ]
- Hepatotoxicity [see Warnings and Precautions (5.5) ]
- Nephrotoxicity [see Warnings and Precautions (5.6) ]
The following adverse reactions associated with the use of Lomustine Capsules were identified in clinical trials or postmarketing reports. Because these reactions were reported from a population of uncertain size, it is not possible to estimate their frequency, reliability, or establish a causal relationship to drug exposure.
Gastrointestinal disorders: nausea, vomiting, and stomatitis
Ocular disorders: optic atrophy, visual disturbances, and blindness
Neurologic disorders: disorientation, lethargy, ataxia, and dysarthria
Other: alopecia
2.2 Recommended Dose
The recommended dose of Lomustine Capsules in adult and pediatric patients is 130 mg/m2 taken as a single oral dose every 6 weeks. Round doses to the nearest 5 mg. Give as a single oral dose and do not repeat for at least 6 weeks. Reduce dose to 100 mg/m2 every 6 weeks in patients with compromised bone marrow function. Also reduce dose accordingly when using with other myelosuppressive drugs.
12.2 Pharmacodynamics
The pharmacodynamics of lomustine are unknown.
12.3 Pharmacokinetics
Distribution
Lomustine crosses the blood-brain barrier.
Elimination
The serum half-life of lomustine metabolites ranges from 16 hours to 48 hours.
Metabolism
Metabolic pathways involved in the elimination of lomustine have not been characterized.
Excretion
Following oral administration of radioactive lomustine at doses ranging from 30 mg/m2 to 100 mg/m2, approximately half of the radioactivity administered was excreted in the urine in the form of degradation products within 24 hours.
Specific Populations
The impact of patient specific (e.g., age, sex, and race) or disease (e.g., renal or hepatic impairment) characteristics on the pharmacokinetics of lomustine is unknown.
2.3 Dose Modifications
Perform weekly complete blood counts and withhold each subsequent dose for more than 6 weeks if needed until platelet counts recover to 100,000/mm3 or greater and leukocytes recover to 4000/mm3 or greater [see Warnings and Precautions (5.1) ].
Modify each dose of Lomustine Capsules according to the hematologic response of the preceding dose as described in Table 1:
Table 1. Dose Modifications for Lomustine Capsules
|
Nadir After Prior Dose |
Dose Adjustment |
|
|
Leukocytes (/mm3) |
Platelets (/mm3) |
|
|
≥ 4000 |
≥ 100,000 |
None |
|
3000 – 3999 |
75,000 – 99,999 |
None |
|
2000 – 2999 |
25,000 – 74,999 |
Reduce dose by 30% |
|
< 2000 |
< 25,000 |
Reduce dose by 50% |
5.2 Risk of Overdosage
Fatal toxicity occurs with overdosage of Lomustine Capsules. Dispensing or administering more than one dose can lead to fatal toxicity.
Prescribe only one dose at a time. Dispense only enough capsules for one dose. Both physician and pharmacist should emphasize to the patient that only one dose of Lomustine Capsules is taken every 6 weeks [see Dosage and Administration (2.1) and Overdosage (10)].
5.3 Pulmonary Toxicity
Pulmonary toxicity characterized by pulmonary infiltrates and/or fibrosis occurs with Lomustine Capsules. Patients with a baseline below 70% of the predicted Forced Vital Capacity (FVC) or Carbon Monoxide Diffusing Capacity (DLCO) are at increased risk. The onset of pulmonary toxicity occurs after an interval of 6 months or longer from the start of therapy, with cumulative doses of Lomustine Capsules usually greater than 1100 mg/m2.
Obtain baseline pulmonary function tests prior to initiating treatment and repeat frequently during treatment. Permanently discontinue Lomustine Capsules in patients diagnosed with pulmonary fibrosis.
1 Indications and Usage
1.2 Hodgkin’s Lymphoma
Lomustine Capsules are indicated as a component of combination chemotherapy for the treatment of patients with Hodgkin’s lymphoma whose disease has progressed following initial chemotherapy.
12 Clinical Pharmacology
12.1 Mechanism of Action
Lomustine alkylates DNA and RNA. As with other nitrosoureas, it may also inhibit several key enzymatic processes by carbamoylation of amino acids in proteins.
13 Nonclinical Toxicology
16.2 Storage and Handling
Store at 20º to 25ºC (68º to 77ºF); excursions permitted to 15° to 30°C (59° to 86°F) [See USP Controlled Room Temperature]. Avoid temperatures over 40°C (104°F).
Lomustine Capsules, USP is a cytotoxic drug. Follow applicable special handling and disposal procedures.1
To minimize the risk of dermal exposure, always wear impervious gloves when handling bottles containing Lomustine Capsules, USP. Do not break Lomustine Capsules, USP; avoid exposure to broken capsules. If dermal contact occurs, wash areas of skin contact immediately and thoroughly.
5.7 Embryo Fetal Toxicity
Based on animal data and its mechanism of action, Lomustine Capsules can cause fetal harm when administered to a pregnant woman. Embryo-fetal toxicity and teratogenicity occurred in rats and rabbits receiving lomustine daily during organogenesis at doses approximately two to four times the total human dose of 130 mg/m2 over 6 weeks (0.18 to 0.27 times the single human dose of 130 mg/m2) based on body surface area (BSA). Advise pregnant women of the potential risk to a fetus. Advise females of reproductive potential to use effective contraception during treatment with Lomustine Capsules and for 2 weeks after the final dose. Advise males with female partners of reproductive potential to use effective contraception during treatment with Lomustine Capsules and for 3.5 months after the final dose [see Use in Specific Populations (8.1, 8.3) ].
5 Warnings and Precautions
5.4 Secondary Malignancies
Secondary malignancies, including acute leukemia and myelodysplasia, occur with long term use.
2 Dosage and Administration
3 Dosage Forms and Strengths
Lomustine Capsules, USP are available in three strengths, distinguishable by the color of the capsules:
- 100 mg capsules (light green/light green)
- 40 mg capsules (light green/bright white)
- 10 mg capsules (bright white/bright white)
5.1 Delayed Myelosuppression
Lomustine Capsules cause myelosuppression that can result in fatal infections and bleeding. Myelosuppression from Lomustine Capsules is delayed, dose-related, and cumulative. It usually occurs 4 to 6 weeks after drug administration and persists for 1 to 2 weeks. Thrombocytopenia is generally more severe than leukopenia. Cumulative myelosuppression from Lomustine Capsules is manifested by greater severity and longer duration of cytopenias.
Monitor blood counts for at least 6 weeks after each dose. Do not give Lomustine Capsules more frequently than every 6 weeks. Adjust dose based on nadir blood counts from prior dose [see Dosage and Administration (2.3) ].
8 Use in Specific Populations
17 Patient Counseling Information
Myelosuppression
Advise patients that periodic assessment of their blood counts are required. Advise patients to contact their healthcare provider for new onset of bleeding or fever or symptoms of infection [see Warnings and Precautions (5.1) ].
Overdosage
Advise patients that toxicity including fatal toxicity occurs with Lomustine Capsules overdosage [see Warnings and Precautions (5.2), Overdosage (10), Dosage and Administration (2.1) ].
Advise patients to take Lomustine Capsules as directed:
- Lomustine Capsules are taken as a single oral dose that will not be repeated for at least 6 weeks.
- Use of the recommended dose at less than 6 week intervals leads to toxicities including fatal toxicities.
- Each dose may consist of 2 or more different strengths and colors of capsules.
Pulmonary Fibrosis
Advise patients to contact their healthcare provider for new or worsening cough, chest pain, or shortness of breath [see Warnings and Precautions (5.3)].
Hepatotoxicity
Inform patients that Lomustine Capsules can cause hepatotoxicity and that liver function monitoring during treatment is necessary [see Warnings and Precautions (5.5) ].
Nephrotoxicity
Inform patients that Lomustine Capsules can cause nephrotoxicity and that renal function and electrolyte monitoring during treatment is necessary [see Warnings and Precautions (5.6) ].
Embryo-Fetal Toxicity
Advise females of reproductive potential of the potential risk to a fetus and to inform their healthcare provider of a known or suspected pregnancy [see Warnings and Precautions (5.7), Use in Specific Populations (8.1) ].
Advise females of reproductive potential to use effective contraception during treatment with Lomustine Capsules and for at least 2 weeks after the final dose [see Use in Specific Populations (8.3) ].
Advise male patients with female partners of reproductive potential to use condoms during treatment with Lomustine Capsules and for 4 months after the final dose [see Use in Specific Populations (8.3) ].
Lactation
Advise women not to breastfeed during treatment with Lomustine Capsules and for 2 weeks after the final dose [see Use in Specific Populations (8.2) ].
Infertility
Advise females and males of reproductive potential of the potential for reduced fertility from Lomustine Capsules [see Use in Specific Populations (8.3) and Nonclinical Toxicology (13.1) ].
Distributed by:
Carnegie Pharmaceuticals LLC
Delran, NJ 08075, USA
Revised: 07/2025
16 How Supplied/storage and Handling
Package Label Principal Display Panel
NDC 80005-114-02
Lomustine Capsules, USP
10 mg per capsule
Caution: DO NOT DISPENSE ENTIRE CONTAINER. Dispense only enough capsules for one dose.
Rx only
5 capsules
Label
Carton
NDC 80005-115-02
Lomustine Capsules, USP
40 mg per capsule
Caution: DO NOT DISPENSE ENTIRE CONTAINER. Dispense only enough capsules for one dose.
Rx only
5 capsules
Label
Carton
NDC 80005-116-02
Lomustine Capsules, USP
100 mg per capsule
Caution: DO NOT DISPENSE ENTIRE CONTAINER. Dispense only enough capsules for one dose.
Rx only
5 capsules
Label
Carton
8.3 Females and Males of Reproductive Potential
Contraception
Females
Based on animal data and its mechanism of action, Lomustine Capsules can cause fetal harm [see Use in Specific Populations (8.1) ]. Advise females of reproductive potential to use effective contraception during treatment and for 2 weeks after the final dose.
Males
Based on Lomustine Capsules's mechanism of action, advise males with female partners of reproductive potential to use effective contraception during treatment with Lomustine Capsules and for 3.5 months after the final dose [see Clinical Pharmacology (12.1) ].
Infertility
Based on animal findings and its mechanism of action, Lomustine Capsules may result in reduced fertility in males and females of reproductive potential [see Nonclinical Toxicology (13.1) ].
2.1 Important Prescribing and Dispensing Information
PRESCRIBE ONLY ONE DOSE FOR EACH TREATMENT CYCLE. DO NOT DISPENSE ENTIRE CONTAINER. Dispense only a sufficient number of capsules for one dose.
Confirm the total dose prescribed by the physician and the appropriate combination of capsule strengths.
Dispense only the appropriate number of Lomustine Capsules required for the administration of a single dose.
The prescribed dose may consist of two or more different strengths and colors of capsules.
Instruct patients that Lomustine Capsules are taken as a single oral dose and will not be repeated for at least 6 weeks. Taking more than the recommended dose causes toxicities, including fatal outcomes [see Warnings and Precautions (5.2) and Overdosage (10) ].
Lomustine Capsules is a cytotoxic drug. Follow applicable special handling and disposal procedures.1
To minimize the risk of dermal exposure, always wear impervious gloves when handling bottles containing Lomustine Capsules. Do not break Lomustine Capsules; avoid exposure to broken capsules. If dermal contact occurs, wash areas of skin contact immediately and thoroughly.
Warning: Delayed Myelosuppression and Risk of Overdosage
DELAYED MYELOSUPPRESSION
Lomustine Capsules cause myelosuppression including fatal myelosuppression. Myelosuppression is delayed, dose-related, and cumulative; occurring 4 to 6 weeks after drug administration and persisting for 1 to 2 weeks. Thrombocytopenia is generally more severe than leukopenia. Cumulative myelosuppression from Lomustine Capsules is manifested by greater severity and longer duration of cytopenias. Monitor blood counts for at least 6 weeks after each dose. Do not give Lomustine Capsules more frequently than every 6 weeks [see Warnings and Precautions (5.1), Dosage and Administration (2.2, 2.3) ].
RISK OF OVERDOSAGE
PRESCRIBE, DISPENSE, AND ADMINISTER ONLY ENOUGH CAPSULES FOR ONE DOSE. Fatal toxicity occurs with overdosage of Lomustine Capsules. Both physician and pharmacist should emphasize to the patient that only one dose of Lomustine Capsules is taken every 6 weeks [see Dosage and Administration (2.1), Warnings and Precautions (5.2), Overdosage (10) ].
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Lomustine is carcinogenic in rats and mice, producing a marked increase in tumor incidence in doses lower than those employed clinically.
In female rats, daily intraperitoneal treatment with lomustine for 2 weeks prior to mating with untreated males resulted in dose dependent decreases in number of corpora lutea and resorption rates with no live births at a dose of 3 mg/kg (approximately 0.14 times the recommended clinical dose of 130 mg/m2 based on body surface area (BSA), or approximately twice the total clinical dose of lomustine over 6 weeks) and decreased pup survival during the first 4 postnatal days at doses greater than or equal to 1.5 mg/kg (a daily dose of approximately 0.06 times the recommended clinical dose of 130 mg/m2 based on BSA or approximately equal to the total clinical dose of lomustine over 6 weeks). Lomustine Capsules may also result in decreased male fertility. Intraperitoneal injection of lomustine resulted in decreased fertility in male rats mated to untreated females based on decreased implantations and decreased fetal body weight at weekly doses greater than or equal to 5 mg/kg (approximately 0.23 times the single clinical dose of 130 mg/m2 based on BSA, or approximately equal to the total clinical dose of lomustine over 6 weeks), and increased resorptions at doses greater than or equal to 2.5 mg/kg/week.
Structured Label Content
10 Overdosage (10 OVERDOSAGE)
Overdosage with Lomustine Capsules has occurred, including fatal cases [see Dosage and Administration (2.1), Warnings and Precautions (5.2) ]. Overdosage causes severe myelosuppression, as well as abdominal pain, diarrhea, vomiting, anorexia, lethargy, dizziness, abnormal hepatic function, cough, and shortness of breath.
No antidotes exist for Lomustine Capsules overdosage.
15 References (15 REFERENCES)
OSHA. http://www.osha.gov/SLTC/hazardousdrugs/index.html.
8.1 Pregnancy
Risk Summary
Based on animal data and its mechanism of action, Lomustine Capsules can cause fetal harm when administered to a pregnant woman [see Clinical Pharmacology (12.1) ]. There are no available data on Lomustine Capsules exposure in pregnant women. Lomustine was teratogenic in rats and embryotoxic in rabbits at total dose levels approximately two to four times the total human dose of 130 mg/m2 over 6 weeks (0.18 to 0.27 times the single human dose of 130 mg/m2) based on BSA [see Data]. Advise pregnant women of the potential risk to a fetus.
In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2-4% and 15-20%, respectively.
Data
Animal Data
Lomustine was administered by intraperitoneal injection daily to pregnant rats during the period of organogenesis at dose levels of 0, 2, 4, 6, and 8 mg/kg. Resorption rates and post-implantation loss occurred at doses greater than or equal to 4 mg/kg (approximately 0.18 times the clinical dose of 130 mg/m2 based on BSA or approximately twice the total clinical dose of lomustine over 6 weeks). Malformations (omphalocele, ectopia cordis, scoliosis, syndactyly, hydrocephalus, microphthalmia, anophthalmia, anomalies of aortic arch, dextrocardia, malpositioning of the ovaries and testes, sternoschisis, and shortened/misshapen bone of the fore or hind limbs) and decreased fetal body weight occurred at all dose levels. In pregnant rabbits treated with lomustine at 3 mg/kg (approximately 0.27 times the 130 mg/m2 clinical dose based on BSA or approximately four times the total clinical dose of lomustine over 6 weeks) during organogenesis, there were increases in abortions and decreases in surviving pup weight that persisted postnatally.
11 Description (11 DESCRIPTION)
Lomustine Capsules, USP (lomustine) is an alkylating drug for oral administration. The chemical name for lomustine is 1-(2-chloro-ethyl)-3-cyclohexyl-1-nitrosourea and the molecular formula is C9H16ClN3O2. The molecular weight is 233.71. Lomustine is a yellow powder, which is soluble in 10% ethanol (0.05 mg per mL) and in absolute alcohol (70 mg per mL). Lomustine is insoluble in water (<0.05 mg per mL).
The chemical structure is:
Lomustine Capsules, USP are supplied as 10 mg, 40 mg, and 100 mg capsules and contain the following inactive ingredients: magnesium stearate NF and mannitol USP. The 10 mg capsule shells are composed of gelatin and titanium dioxide. The 40 mg and 100 mg capsule shells are composed of FD&C blue #1, gelatin, iron oxide black, iron oxide yellow, and titanium dioxide. The capsules are printed with black ink composed of iron oxide black, potassium hydroxide, propylene glycol, shellac, and strong ammonia solution.
FDA approved dissolution method is not listed in the USP Monograph for Lomustine Capsules, USP, 10 mg, 40 mg, and 100 mg.
8.2 lactation (8.2 Lactation)
Risk Summary
There is no information on the presence of lomustine or its metabolites in human milk, its effects on the breastfed infant, or its effects on milk production. Because of the potential for serious adverse reactions in breastfed infants from Lomustine Capsules, advise women not to breastfeed during treatment with Lomustine Capsules and for 2 weeks after the final dose.
1.1 Brain Tumors
Lomustine Capsules are indicated for the treatment of patients with primary and metastatic brain tumors following appropriate surgical and/or radiotherapeutic procedures.
16.1 How Supplied
Lomustine Capsules, USP are available in three strengths, distinguishable by the color of the capsules, in individual bottles of 5 capsules each:
|
Strength |
Capsule Description |
NDC Code |
|
100 mg |
Hard gelatin capsule shell with light green opaque body and light green opaque cap, imprinted with black ink “CP116” on cap, containing white powder. |
80005-116-02 |
|
40 mg |
Hard gelatin capsule shell with light green opaque body and bright white opaque cap, imprinted with black ink “CP115” on cap, containing white powder. |
80005-115-02 |
|
10 mg |
Hard gelatin capsule shell with bright white opaque body and bright white opaque cap, imprinted with black ink “CP114” on cap, containing white powder. |
80005-114-02 |
8.4 Pediatric Use
Pediatric use, including dose, is not based on adequate and well-controlled clinical studies.
8.5 Geriatric Use
No data in the clinical studies of Lomustine Capsules are available for patients 65 years of age and over to determine whether they respond differently than younger patients. Other reported clinical experience has not identified differences in responses between elderly and younger patients. In general, dose selection for an elderly patient should be cautious, reflecting the greater frequency of decreased hepatic, renal, or cardiac function and of concomitant disease or other drug therapy.
Lomustine and its metabolites are known to be substantially excreted by the kidney, and the risk of toxic reactions to this drug may be greater in patients with impaired renal function. Because elderly patients are more likely to have decreased renal function, care should be taken in dose selection, and renal function should be monitored.
5.5 Hepatotoxicity
Hepatic toxicity, manifested by increased levels of transaminases, alkaline phosphatase, and bilirubin occurs with Lomustine Capsules.
Monitor liver function.
5.6 Nephrotoxicity
Progressive renal failure with a decrease in kidney size occurs with Lomustine Capsules.
Monitor renal function.
4 Contraindications (4 CONTRAINDICATIONS)
None.
6 Adverse Reactions (6 ADVERSE REACTIONS)
The following serious adverse reactions are discussed in greater detail in other sections of the labeling:
- Delayed myelosuppression [see Warnings and Precautions (5.1) ]
- Risks of overdosage [see Warnings and Precautions (5.2) ]
- Pulmonary toxicity [see Warnings and Precautions (5.3) ]
- Secondary malignancies [see Warnings and Precautions (5.4) ]
- Hepatotoxicity [see Warnings and Precautions (5.5) ]
- Nephrotoxicity [see Warnings and Precautions (5.6) ]
The following adverse reactions associated with the use of Lomustine Capsules were identified in clinical trials or postmarketing reports. Because these reactions were reported from a population of uncertain size, it is not possible to estimate their frequency, reliability, or establish a causal relationship to drug exposure.
Gastrointestinal disorders: nausea, vomiting, and stomatitis
Ocular disorders: optic atrophy, visual disturbances, and blindness
Neurologic disorders: disorientation, lethargy, ataxia, and dysarthria
Other: alopecia
2.2 Recommended Dose
The recommended dose of Lomustine Capsules in adult and pediatric patients is 130 mg/m2 taken as a single oral dose every 6 weeks. Round doses to the nearest 5 mg. Give as a single oral dose and do not repeat for at least 6 weeks. Reduce dose to 100 mg/m2 every 6 weeks in patients with compromised bone marrow function. Also reduce dose accordingly when using with other myelosuppressive drugs.
12.2 Pharmacodynamics
The pharmacodynamics of lomustine are unknown.
12.3 Pharmacokinetics
Distribution
Lomustine crosses the blood-brain barrier.
Elimination
The serum half-life of lomustine metabolites ranges from 16 hours to 48 hours.
Metabolism
Metabolic pathways involved in the elimination of lomustine have not been characterized.
Excretion
Following oral administration of radioactive lomustine at doses ranging from 30 mg/m2 to 100 mg/m2, approximately half of the radioactivity administered was excreted in the urine in the form of degradation products within 24 hours.
Specific Populations
The impact of patient specific (e.g., age, sex, and race) or disease (e.g., renal or hepatic impairment) characteristics on the pharmacokinetics of lomustine is unknown.
2.3 Dose Modifications
Perform weekly complete blood counts and withhold each subsequent dose for more than 6 weeks if needed until platelet counts recover to 100,000/mm3 or greater and leukocytes recover to 4000/mm3 or greater [see Warnings and Precautions (5.1) ].
Modify each dose of Lomustine Capsules according to the hematologic response of the preceding dose as described in Table 1:
Table 1. Dose Modifications for Lomustine Capsules
|
Nadir After Prior Dose |
Dose Adjustment |
|
|
Leukocytes (/mm3) |
Platelets (/mm3) |
|
|
≥ 4000 |
≥ 100,000 |
None |
|
3000 – 3999 |
75,000 – 99,999 |
None |
|
2000 – 2999 |
25,000 – 74,999 |
Reduce dose by 30% |
|
< 2000 |
< 25,000 |
Reduce dose by 50% |
5.2 Risk of Overdosage
Fatal toxicity occurs with overdosage of Lomustine Capsules. Dispensing or administering more than one dose can lead to fatal toxicity.
Prescribe only one dose at a time. Dispense only enough capsules for one dose. Both physician and pharmacist should emphasize to the patient that only one dose of Lomustine Capsules is taken every 6 weeks [see Dosage and Administration (2.1) and Overdosage (10)].
5.3 Pulmonary Toxicity
Pulmonary toxicity characterized by pulmonary infiltrates and/or fibrosis occurs with Lomustine Capsules. Patients with a baseline below 70% of the predicted Forced Vital Capacity (FVC) or Carbon Monoxide Diffusing Capacity (DLCO) are at increased risk. The onset of pulmonary toxicity occurs after an interval of 6 months or longer from the start of therapy, with cumulative doses of Lomustine Capsules usually greater than 1100 mg/m2.
Obtain baseline pulmonary function tests prior to initiating treatment and repeat frequently during treatment. Permanently discontinue Lomustine Capsules in patients diagnosed with pulmonary fibrosis.
1 Indications and Usage (1 INDICATIONS AND USAGE)
1.2 Hodgkin’s Lymphoma
Lomustine Capsules are indicated as a component of combination chemotherapy for the treatment of patients with Hodgkin’s lymphoma whose disease has progressed following initial chemotherapy.
12 Clinical Pharmacology (12 CLINICAL PHARMACOLOGY)
12.1 Mechanism of Action
Lomustine alkylates DNA and RNA. As with other nitrosoureas, it may also inhibit several key enzymatic processes by carbamoylation of amino acids in proteins.
13 Nonclinical Toxicology (13 NONCLINICAL TOXICOLOGY)
16.2 Storage and Handling
Store at 20º to 25ºC (68º to 77ºF); excursions permitted to 15° to 30°C (59° to 86°F) [See USP Controlled Room Temperature]. Avoid temperatures over 40°C (104°F).
Lomustine Capsules, USP is a cytotoxic drug. Follow applicable special handling and disposal procedures.1
To minimize the risk of dermal exposure, always wear impervious gloves when handling bottles containing Lomustine Capsules, USP. Do not break Lomustine Capsules, USP; avoid exposure to broken capsules. If dermal contact occurs, wash areas of skin contact immediately and thoroughly.
5.7 Embryo Fetal Toxicity (5.7 Embryo-Fetal Toxicity)
Based on animal data and its mechanism of action, Lomustine Capsules can cause fetal harm when administered to a pregnant woman. Embryo-fetal toxicity and teratogenicity occurred in rats and rabbits receiving lomustine daily during organogenesis at doses approximately two to four times the total human dose of 130 mg/m2 over 6 weeks (0.18 to 0.27 times the single human dose of 130 mg/m2) based on body surface area (BSA). Advise pregnant women of the potential risk to a fetus. Advise females of reproductive potential to use effective contraception during treatment with Lomustine Capsules and for 2 weeks after the final dose. Advise males with female partners of reproductive potential to use effective contraception during treatment with Lomustine Capsules and for 3.5 months after the final dose [see Use in Specific Populations (8.1, 8.3) ].
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
5.4 Secondary Malignancies
Secondary malignancies, including acute leukemia and myelodysplasia, occur with long term use.
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
Lomustine Capsules, USP are available in three strengths, distinguishable by the color of the capsules:
- 100 mg capsules (light green/light green)
- 40 mg capsules (light green/bright white)
- 10 mg capsules (bright white/bright white)
5.1 Delayed Myelosuppression
Lomustine Capsules cause myelosuppression that can result in fatal infections and bleeding. Myelosuppression from Lomustine Capsules is delayed, dose-related, and cumulative. It usually occurs 4 to 6 weeks after drug administration and persists for 1 to 2 weeks. Thrombocytopenia is generally more severe than leukopenia. Cumulative myelosuppression from Lomustine Capsules is manifested by greater severity and longer duration of cytopenias.
Monitor blood counts for at least 6 weeks after each dose. Do not give Lomustine Capsules more frequently than every 6 weeks. Adjust dose based on nadir blood counts from prior dose [see Dosage and Administration (2.3) ].
8 Use in Specific Populations (8 USE IN SPECIFIC POPULATIONS)
17 Patient Counseling Information (17 PATIENT COUNSELING INFORMATION)
Myelosuppression
Advise patients that periodic assessment of their blood counts are required. Advise patients to contact their healthcare provider for new onset of bleeding or fever or symptoms of infection [see Warnings and Precautions (5.1) ].
Overdosage
Advise patients that toxicity including fatal toxicity occurs with Lomustine Capsules overdosage [see Warnings and Precautions (5.2), Overdosage (10), Dosage and Administration (2.1) ].
Advise patients to take Lomustine Capsules as directed:
- Lomustine Capsules are taken as a single oral dose that will not be repeated for at least 6 weeks.
- Use of the recommended dose at less than 6 week intervals leads to toxicities including fatal toxicities.
- Each dose may consist of 2 or more different strengths and colors of capsules.
Pulmonary Fibrosis
Advise patients to contact their healthcare provider for new or worsening cough, chest pain, or shortness of breath [see Warnings and Precautions (5.3)].
Hepatotoxicity
Inform patients that Lomustine Capsules can cause hepatotoxicity and that liver function monitoring during treatment is necessary [see Warnings and Precautions (5.5) ].
Nephrotoxicity
Inform patients that Lomustine Capsules can cause nephrotoxicity and that renal function and electrolyte monitoring during treatment is necessary [see Warnings and Precautions (5.6) ].
Embryo-Fetal Toxicity
Advise females of reproductive potential of the potential risk to a fetus and to inform their healthcare provider of a known or suspected pregnancy [see Warnings and Precautions (5.7), Use in Specific Populations (8.1) ].
Advise females of reproductive potential to use effective contraception during treatment with Lomustine Capsules and for at least 2 weeks after the final dose [see Use in Specific Populations (8.3) ].
Advise male patients with female partners of reproductive potential to use condoms during treatment with Lomustine Capsules and for 4 months after the final dose [see Use in Specific Populations (8.3) ].
Lactation
Advise women not to breastfeed during treatment with Lomustine Capsules and for 2 weeks after the final dose [see Use in Specific Populations (8.2) ].
Infertility
Advise females and males of reproductive potential of the potential for reduced fertility from Lomustine Capsules [see Use in Specific Populations (8.3) and Nonclinical Toxicology (13.1) ].
Distributed by:
Carnegie Pharmaceuticals LLC
Delran, NJ 08075, USA
Revised: 07/2025
16 How Supplied/storage and Handling (16 HOW SUPPLIED/STORAGE AND HANDLING)
Package Label Principal Display Panel (PACKAGE LABEL PRINCIPAL DISPLAY PANEL )
NDC 80005-114-02
Lomustine Capsules, USP
10 mg per capsule
Caution: DO NOT DISPENSE ENTIRE CONTAINER. Dispense only enough capsules for one dose.
Rx only
5 capsules
Label
Carton
NDC 80005-115-02
Lomustine Capsules, USP
40 mg per capsule
Caution: DO NOT DISPENSE ENTIRE CONTAINER. Dispense only enough capsules for one dose.
Rx only
5 capsules
Label
Carton
NDC 80005-116-02
Lomustine Capsules, USP
100 mg per capsule
Caution: DO NOT DISPENSE ENTIRE CONTAINER. Dispense only enough capsules for one dose.
Rx only
5 capsules
Label
Carton
8.3 Females and Males of Reproductive Potential
Contraception
Females
Based on animal data and its mechanism of action, Lomustine Capsules can cause fetal harm [see Use in Specific Populations (8.1) ]. Advise females of reproductive potential to use effective contraception during treatment and for 2 weeks after the final dose.
Males
Based on Lomustine Capsules's mechanism of action, advise males with female partners of reproductive potential to use effective contraception during treatment with Lomustine Capsules and for 3.5 months after the final dose [see Clinical Pharmacology (12.1) ].
Infertility
Based on animal findings and its mechanism of action, Lomustine Capsules may result in reduced fertility in males and females of reproductive potential [see Nonclinical Toxicology (13.1) ].
2.1 Important Prescribing and Dispensing Information
PRESCRIBE ONLY ONE DOSE FOR EACH TREATMENT CYCLE. DO NOT DISPENSE ENTIRE CONTAINER. Dispense only a sufficient number of capsules for one dose.
Confirm the total dose prescribed by the physician and the appropriate combination of capsule strengths.
Dispense only the appropriate number of Lomustine Capsules required for the administration of a single dose.
The prescribed dose may consist of two or more different strengths and colors of capsules.
Instruct patients that Lomustine Capsules are taken as a single oral dose and will not be repeated for at least 6 weeks. Taking more than the recommended dose causes toxicities, including fatal outcomes [see Warnings and Precautions (5.2) and Overdosage (10) ].
Lomustine Capsules is a cytotoxic drug. Follow applicable special handling and disposal procedures.1
To minimize the risk of dermal exposure, always wear impervious gloves when handling bottles containing Lomustine Capsules. Do not break Lomustine Capsules; avoid exposure to broken capsules. If dermal contact occurs, wash areas of skin contact immediately and thoroughly.
Warning: Delayed Myelosuppression and Risk of Overdosage (WARNING: DELAYED MYELOSUPPRESSION and RISK OF OVERDOSAGE)
DELAYED MYELOSUPPRESSION
Lomustine Capsules cause myelosuppression including fatal myelosuppression. Myelosuppression is delayed, dose-related, and cumulative; occurring 4 to 6 weeks after drug administration and persisting for 1 to 2 weeks. Thrombocytopenia is generally more severe than leukopenia. Cumulative myelosuppression from Lomustine Capsules is manifested by greater severity and longer duration of cytopenias. Monitor blood counts for at least 6 weeks after each dose. Do not give Lomustine Capsules more frequently than every 6 weeks [see Warnings and Precautions (5.1), Dosage and Administration (2.2, 2.3) ].
RISK OF OVERDOSAGE
PRESCRIBE, DISPENSE, AND ADMINISTER ONLY ENOUGH CAPSULES FOR ONE DOSE. Fatal toxicity occurs with overdosage of Lomustine Capsules. Both physician and pharmacist should emphasize to the patient that only one dose of Lomustine Capsules is taken every 6 weeks [see Dosage and Administration (2.1), Warnings and Precautions (5.2), Overdosage (10) ].
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Lomustine is carcinogenic in rats and mice, producing a marked increase in tumor incidence in doses lower than those employed clinically.
In female rats, daily intraperitoneal treatment with lomustine for 2 weeks prior to mating with untreated males resulted in dose dependent decreases in number of corpora lutea and resorption rates with no live births at a dose of 3 mg/kg (approximately 0.14 times the recommended clinical dose of 130 mg/m2 based on body surface area (BSA), or approximately twice the total clinical dose of lomustine over 6 weeks) and decreased pup survival during the first 4 postnatal days at doses greater than or equal to 1.5 mg/kg (a daily dose of approximately 0.06 times the recommended clinical dose of 130 mg/m2 based on BSA or approximately equal to the total clinical dose of lomustine over 6 weeks). Lomustine Capsules may also result in decreased male fertility. Intraperitoneal injection of lomustine resulted in decreased fertility in male rats mated to untreated females based on decreased implantations and decreased fetal body weight at weekly doses greater than or equal to 5 mg/kg (approximately 0.23 times the single clinical dose of 130 mg/m2 based on BSA, or approximately equal to the total clinical dose of lomustine over 6 weeks), and increased resorptions at doses greater than or equal to 2.5 mg/kg/week.
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:54:40.414556 · Updated: 2026-03-14T22:49:26.517746