These Highlights Do Not Include All The Information Needed To Use Propafenone Hydrochloride Extended-release Capsules Safely And Effectively. See Full Prescribing Information For Propafenone Hydrochloride Extended-release Capsules.
8aa6f58a-2980-4caa-9c54-d55d69d5d132
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
In the National Heart, Lung, and Blood Institute's Cardiac Arrhythmia Suppression Trial (CAST), a long-term, multicenter, randomized, double-blind trial in patients with asymptomatic non-life-threatening ventricular arrhythmias who had a myocardial infarction more than 6 days but less than 2 years previously, an increased rate of death or reversed cardiac arrest rate (7.7%; 56/730) was seen in patients treated with encainide or flecainide (Class IC antiarrhythmics) compared with that seen in patients assigned to placebo (3.0%; 22/725). The average duration of treatment with encainide or flecainide in this trial was 10 months. The applicability of the CAST results to other populations (e.g., those without recent myocardial infarction) or other antiarrhythmic drugs is uncertain, but at present, it is prudent to consider any IC antiarrhythmic to have a significant proarrhythmic risk in patients with structural heart disease. Given the lack of any evidence that these drugs improve survival, antiarrhythmic agents should generally be avoided in patients with non-life-threatening ventricular arrhythmias, even if the patients are experiencing unpleasant, but not life-threatening, symptoms or signs.
Indications and Usage
Propafenone hydrochloride extended-release capsules are indicated to prolong the time to recurrence of symptomatic atrial fibrillation (AF) in patients with episodic (most likely paroxysmal or persistent) AF who do not have structural heart disease.
Dosage and Administration
Propafenone hydrochloride extended-release capsules can be taken with or without food. Do not crush or further divide the contents of the capsule. The dose of propafenone hydrochloride extended-release capsules must be individually titrated on the basis of response and tolerance. Initiate therapy with propafenone hydrochloride extended-release capsules, USP 225 mg given every 12 hours. Dosage may be increased at a minimum of 5-day intervals to 325 mg given every 12 hours. If additional therapeutic effect is needed, the dose of propafenone hydrochloride extended-release capsules may be increased to 425 mg given every 12 hours. In patients with hepatic impairment or those with significant widening of the QRS complex or second- or third-degree AV block, consider reducing the dose. The combination of cytochrome P450 3A4 (CYP3A4) inhibition and either cytochrome P450 2D6 (CYP2D6) deficiency or CYP2D6 inhibition with the simultaneous administration of propafenone may significantly increase the concentration of propafenone and thereby increase the risk of proarrhythmia and other adverse events. Therefore, avoid simultaneous use of propafenone hydrochloride extended-release capsules, USP with both a CYP2D6 inhibitor and a CYP3A4 inhibitor [see Warnings and Precautions (5.4) , Drug Interactions (7.1) ] .
Warnings and Precautions
May cause new or worsened arrhythmias. Evaluate patients via ECG prior to and during therapy. ( 5.1 ) Propafenone hydrochloride extended-release capsules may unmask Brugada or Brugada-like Syndrome. Evaluate patients via ECG after initiation of therapy. ( 4 , 5.2 ) Avoid use with other antiarrhythmic agents or drugs that prolong the QT interval. ( 5.3 ) Avoid simultaneous use of propafenone with both a cytochrome P450 2D6 (CYP2D6) inhibitor and a 3A4 inhibitor (CYP3A4). ( 5.4 ) May provoke overt heart failure. ( 5.5 ) May cause dose-related first-degree AV block or other conduction disturbances. Should not be given to patients with conduction defects in absence of a pacemaker. ( 5.6 ) May affect artificial pacemakers. Pacemakers should be monitored during therapy. ( 5.7 ) Agranulocytosis: Patients should report signs of infection. ( 5.8 ) Administer cautiously to patients with impaired hepatic and renal function. ( 5.9 , 5.10 ) Exacerbation of myasthenia gravis has been reported. ( 5.11 )
Contraindications
Propafenone hydrochloride extended-release capsules are contraindicated in the following circumstances: Heart failure Cardiogenic shock Sinoatrial, atrioventricular, and intraventricular disorders of impulse generation or conduction (e.g., sick sinus node syndrome, AV block) in the absence of an artificial pacemaker Known Brugada Syndrome Bradycardia Marked hypotension Bronchospastic disorders or severe obstructive pulmonary disease Marked electrolyte imbalance
Adverse Reactions
The most commonly reported adverse events with propafenone (greater than 5% and greater than placebo) excluding those not reasonably associated with the use of the drug included the following: dizziness, palpitations, chest pain, dyspnea, taste disturbance, nausea, fatigue, anxiety, constipation, upper respiratory tract infection, edema, and influenza. ( 6.1 ) To report SUSPECTED ADVERSE REACTIONS, contact Upsher-Smith Laboratories, LLC at 1-855-899-9180 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch .
Drug Interactions
Propafenone is metabolized by CYP2D6, CYP3A4, and CYP1A2 isoenzymes. Approximately 6% of Caucasians in the U.S. population are naturally deficient in CYP2D6 activity and other demographic groups are deficient to a somewhat lesser extent. Drugs that inhibit these CYP pathways (such as desipramine, paroxetine, ritonavir, sertraline for CYP2D6; ketoconazole, erythromycin, saquinavir, and grapefruit juice for CYP3A4; and amiodarone and tobacco smoke for CYP1A2) can be expected to cause increased plasma levels of propafenone. Increased exposure to propafenone may lead to cardiac arrhythmias and exaggerated beta-adrenergic blocking activity. Because of its metabolism, the combination of CYP3A4 inhibition and either CYP2D6 deficiency or CYP2D6 inhibition in users of propafenone is potentially hazardous. Therefore, avoid simultaneous use of propafenone hydrochloride extended-release with both a CYP2D6 inhibitor and a CYP3A4 inhibitor.
Storage and Handling
Propafenone hydrochloride extended-release capsules, USP are supplied as white, opaque, hard gelatin capsules containing either 225 mg, 325 mg, or 425 mg of propafenone hydrochloride. The 225 mg capsule is printed with "UPSHER-SMITH" over "0740" and "225mg" in black ink. Supplied as follows: Bottles of 60 capsules NDC 0832-0740-60 The 325 mg capsule is printed with "UPSHER-SMITH" over "0741" and "325mg" in black ink. Supplied as follows: Bottles of 60 capsules NDC 0832-0741-60 The 425 mg capsule is printed with "UPSHER-SMITH" over "0742" and "425mg" in black ink. Supplied as follows: Bottles of 60 capsules NDC 0832-0742-60
How Supplied
Propafenone hydrochloride extended-release capsules, USP are supplied as white, opaque, hard gelatin capsules containing either 225 mg, 325 mg, or 425 mg of propafenone hydrochloride. The 225 mg capsule is printed with "UPSHER-SMITH" over "0740" and "225mg" in black ink. Supplied as follows: Bottles of 60 capsules NDC 0832-0740-60 The 325 mg capsule is printed with "UPSHER-SMITH" over "0741" and "325mg" in black ink. Supplied as follows: Bottles of 60 capsules NDC 0832-0741-60 The 425 mg capsule is printed with "UPSHER-SMITH" over "0742" and "425mg" in black ink. Supplied as follows: Bottles of 60 capsules NDC 0832-0742-60
Patient Information
What are propafenone hydrochloride extended-release capsules? Propafenone hydrochloride extended-release capsules are a prescription medicine that is used: in certain people who have a heart rhythm disorder called atrial fibrillation (AF) to increase the amount of time between having symptoms of AF It is not known if propafenone hydrochloride extended-release capsules are safe and effective in children. Who should not take propafenone hydrochloride extended-release capsules? Do not take propafenone hydrochloride extended-release capsules if you have: heart failure (weak heart) had a recent heart attack a heart condition called Brugada Syndrome a heart rate that is too slow, and you do not have a pacemaker very low blood pressure certain breathing problems that make you short of breath or wheeze certain abnormal body salt (electrolyte) levels in your blood Talk to your doctor before taking propafenone hydrochloride extended-release capsules if you think you have any of the conditions listed above. What should I tell my doctor before taking propafenone hydrochloride extended-release capsules? Before you take propafenone hydrochloride extended-release capsules, tell your doctor if you: have liver or kidney problems have breathing problems have symptoms including diarrhea, sweating, vomiting, or loss of appetite or thirst that are severe. These symptoms may be a sign of abnormal electrolyte levels in your blood. have myasthenia gravis have lupus erythematosus have been told you have or had an abnormal blood test called Antinuclear Antibody Test or ANA Test are pregnant or plan to become pregnant are breastfeeding or plan to breastfeed. Propafenone hydrochloride extended-release capsules can pass into your milk. You and your doctor should discuss the best way to feed your baby during this time. have any other medical conditions Tell your doctor about all the medicines you take , including prescription and over-the-counter medicines, vitamins, and herbal supplements. Propafenone hydrochloride extended-release capsules and certain other medicines can affect each other and cause serious side effects. Propafenone hydrochloride extended-release capsules may affect the way other medicines work, and other medicines may affect how propafenone hydrochloride extended-release capsules work. Especially tell your doctor if you take: amiodarone or other medicines for your abnormal heart beats an antidepressant medicine a medicine to treat anxiety ritonavir (for example, KALETRA, NORVIR) or saquinavir (for example, INVIRASE) an antibiotic medicine ketoconazole (for example, NIZORAL) digoxin (LANOXIN) warfarin sodium (for example, COUMADIN, JANTOVEN) Know the medicines you take. Keep a list of them to show your doctor and pharmacist when you get a new medicine. How should I take propafenone hydrochloride extended-release capsules? Take propafenone hydrochloride extended-release capsules exactly as prescribed. Your doctor will tell you how many capsules to take and how often to take them. To help reduce the chance of certain side effects, your doctor may start you with a low dose of propafenone hydrochloride extended-release capsules, and then slowly increase the dose. Do not open or crush the capsule. You may take propafenone hydrochloride extended-release capsules with or without food. You should not drink grapefruit juice during treatment with propafenone hydrochloride extended-release capsules. If you miss a dose of propafenone hydrochloride extended-release capsules, take your next dose at the usual time. Do not take 2 doses at the same time. If you take too much propafenone hydrochloride extended-release capsules, call your doctor or go to the nearest hospital emergency room right away. Call your doctor if your heart problems get worse. What are possible side effects of propafenone hydrochloride extended-release capsules? Propafenone hydrochloride extended-release capsules can cause serious side effects including: New or worsened abnormal heart beats, that can cause sudden death or be life-threatening. Your doctor may do an electrocardiogram (ECG or EKG) before and during treatment to check your heart for these problems. New or worsened heart failure. Tell your doctor about any changes in your heart symptoms, including: any new or increased swelling in your arms or legs trouble breathing sudden weight gain Effects on pacemaker function. Propafenone hydrochloride extended-release capsules may affect how an implanted pacemaker or defibrillator works. Your doctor should check how your pacemaker or defibrillator is working during and after treatment with propafenone hydrochloride extended-release capsules. They may need to be re-programmed. Very low white blood cell levels in your blood (agranulocytosis). Your bone marrow may not produce enough of a certain type of white blood cells called neutrophils. If this happens, you are more likely to get infections. Tell your doctor right away if you have any of these symptoms, especially during the first 3 months of treatment: fever sore throat chills Worsening of myasthenia gravis in people who already have this condition. Tell your doctor about any change in your symptoms. Propafenone hydrochloride extended-release capsules may cause lower sperm counts in men. This could affect the ability to father a child. Talk to your doctor if this is a concern for you. Common side effects of propafenone hydrochloride extended-release capsules include: dizziness fast or irregular heart beats chest pain trouble breathing taste changes nausea tiredness feeling anxious constipation upper respiratory infection or flu swelling Tell your doctor if you have any side effect that bothers you or that does not go away. These are not all the possible side effects of propafenone hydrochloride extended-release capsules. For more information, ask your doctor or pharmacist. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. How should I store propafenone hydrochloride extended-release capsules? Store propafenone hydrochloride extended-release capsules at room temperature between 15° to 30°C (59° to 86°F). Keep the bottle tightly closed. Keep propafenone hydrochloride extended-release capsules and all medicines out of the reach of children. General information about propafenone hydrochloride extended-release capsules Medicines are sometimes prescribed for conditions other than those described in patient information leaflets. Do not use propafenone hydrochloride extended-release capsules for a condition for which it was not prescribed by your doctor. Do not give propafenone hydrochloride extended-release capsules to other people, even if they have the same symptoms you have. It may harm them. This leaflet summarizes the most important information about propafenone hydrochloride extended-release capsules. If you would like more information, talk with your doctor. You can ask your doctor or pharmacist for information about propafenone hydrochloride extended-release capsules that is written for healthcare professionals. For more information about propafenone hydrochloride extended-release capsules, call 1-888-650-3789. What are the ingredients in propafenone hydrochloride extended-release capsules? Active Ingredient: Propafenone hydrochloride Inactive Ingredients: gelatin, hypromellose, magnesium stearate, and titanium dioxide. Black ink ingredients: D&C Yellow #10, FD&C Blue #2, FD&C Blue #1 and FD&C Red #40. All other marks are property of their respective owners. Manufactured by UPSHER-SMITH LABORATORIES, LLC Maple Grove, MN 55369 Revised: 5/2023
Medication Information
Warnings and Precautions
May cause new or worsened arrhythmias. Evaluate patients via ECG prior to and during therapy. ( 5.1 ) Propafenone hydrochloride extended-release capsules may unmask Brugada or Brugada-like Syndrome. Evaluate patients via ECG after initiation of therapy. ( 4 , 5.2 ) Avoid use with other antiarrhythmic agents or drugs that prolong the QT interval. ( 5.3 ) Avoid simultaneous use of propafenone with both a cytochrome P450 2D6 (CYP2D6) inhibitor and a 3A4 inhibitor (CYP3A4). ( 5.4 ) May provoke overt heart failure. ( 5.5 ) May cause dose-related first-degree AV block or other conduction disturbances. Should not be given to patients with conduction defects in absence of a pacemaker. ( 5.6 ) May affect artificial pacemakers. Pacemakers should be monitored during therapy. ( 5.7 ) Agranulocytosis: Patients should report signs of infection. ( 5.8 ) Administer cautiously to patients with impaired hepatic and renal function. ( 5.9 , 5.10 ) Exacerbation of myasthenia gravis has been reported. ( 5.11 )
Indications and Usage
Propafenone hydrochloride extended-release capsules are indicated to prolong the time to recurrence of symptomatic atrial fibrillation (AF) in patients with episodic (most likely paroxysmal or persistent) AF who do not have structural heart disease.
Dosage and Administration
Propafenone hydrochloride extended-release capsules can be taken with or without food. Do not crush or further divide the contents of the capsule. The dose of propafenone hydrochloride extended-release capsules must be individually titrated on the basis of response and tolerance. Initiate therapy with propafenone hydrochloride extended-release capsules, USP 225 mg given every 12 hours. Dosage may be increased at a minimum of 5-day intervals to 325 mg given every 12 hours. If additional therapeutic effect is needed, the dose of propafenone hydrochloride extended-release capsules may be increased to 425 mg given every 12 hours. In patients with hepatic impairment or those with significant widening of the QRS complex or second- or third-degree AV block, consider reducing the dose. The combination of cytochrome P450 3A4 (CYP3A4) inhibition and either cytochrome P450 2D6 (CYP2D6) deficiency or CYP2D6 inhibition with the simultaneous administration of propafenone may significantly increase the concentration of propafenone and thereby increase the risk of proarrhythmia and other adverse events. Therefore, avoid simultaneous use of propafenone hydrochloride extended-release capsules, USP with both a CYP2D6 inhibitor and a CYP3A4 inhibitor [see Warnings and Precautions (5.4) , Drug Interactions (7.1) ] .
Contraindications
Propafenone hydrochloride extended-release capsules are contraindicated in the following circumstances: Heart failure Cardiogenic shock Sinoatrial, atrioventricular, and intraventricular disorders of impulse generation or conduction (e.g., sick sinus node syndrome, AV block) in the absence of an artificial pacemaker Known Brugada Syndrome Bradycardia Marked hypotension Bronchospastic disorders or severe obstructive pulmonary disease Marked electrolyte imbalance
Adverse Reactions
The most commonly reported adverse events with propafenone (greater than 5% and greater than placebo) excluding those not reasonably associated with the use of the drug included the following: dizziness, palpitations, chest pain, dyspnea, taste disturbance, nausea, fatigue, anxiety, constipation, upper respiratory tract infection, edema, and influenza. ( 6.1 ) To report SUSPECTED ADVERSE REACTIONS, contact Upsher-Smith Laboratories, LLC at 1-855-899-9180 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch .
Drug Interactions
Propafenone is metabolized by CYP2D6, CYP3A4, and CYP1A2 isoenzymes. Approximately 6% of Caucasians in the U.S. population are naturally deficient in CYP2D6 activity and other demographic groups are deficient to a somewhat lesser extent. Drugs that inhibit these CYP pathways (such as desipramine, paroxetine, ritonavir, sertraline for CYP2D6; ketoconazole, erythromycin, saquinavir, and grapefruit juice for CYP3A4; and amiodarone and tobacco smoke for CYP1A2) can be expected to cause increased plasma levels of propafenone. Increased exposure to propafenone may lead to cardiac arrhythmias and exaggerated beta-adrenergic blocking activity. Because of its metabolism, the combination of CYP3A4 inhibition and either CYP2D6 deficiency or CYP2D6 inhibition in users of propafenone is potentially hazardous. Therefore, avoid simultaneous use of propafenone hydrochloride extended-release with both a CYP2D6 inhibitor and a CYP3A4 inhibitor.
Storage and Handling
Propafenone hydrochloride extended-release capsules, USP are supplied as white, opaque, hard gelatin capsules containing either 225 mg, 325 mg, or 425 mg of propafenone hydrochloride. The 225 mg capsule is printed with "UPSHER-SMITH" over "0740" and "225mg" in black ink. Supplied as follows: Bottles of 60 capsules NDC 0832-0740-60 The 325 mg capsule is printed with "UPSHER-SMITH" over "0741" and "325mg" in black ink. Supplied as follows: Bottles of 60 capsules NDC 0832-0741-60 The 425 mg capsule is printed with "UPSHER-SMITH" over "0742" and "425mg" in black ink. Supplied as follows: Bottles of 60 capsules NDC 0832-0742-60
How Supplied
Propafenone hydrochloride extended-release capsules, USP are supplied as white, opaque, hard gelatin capsules containing either 225 mg, 325 mg, or 425 mg of propafenone hydrochloride. The 225 mg capsule is printed with "UPSHER-SMITH" over "0740" and "225mg" in black ink. Supplied as follows: Bottles of 60 capsules NDC 0832-0740-60 The 325 mg capsule is printed with "UPSHER-SMITH" over "0741" and "325mg" in black ink. Supplied as follows: Bottles of 60 capsules NDC 0832-0741-60 The 425 mg capsule is printed with "UPSHER-SMITH" over "0742" and "425mg" in black ink. Supplied as follows: Bottles of 60 capsules NDC 0832-0742-60
Patient Information
What are propafenone hydrochloride extended-release capsules?
Propafenone hydrochloride extended-release capsules are a prescription medicine that is used:
- in certain people who have a heart rhythm disorder called atrial fibrillation (AF)
- to increase the amount of time between having symptoms of AF
It is not known if propafenone hydrochloride extended-release capsules are safe and effective in children.
Who should not take propafenone hydrochloride extended-release capsules?
Do not take propafenone hydrochloride extended-release capsules if you have:
- heart failure (weak heart)
- had a recent heart attack
- a heart condition called Brugada Syndrome
- a heart rate that is too slow, and you do not have a pacemaker
- very low blood pressure
- certain breathing problems that make you short of breath or wheeze
- certain abnormal body salt (electrolyte) levels in your blood
Talk to your doctor before taking propafenone hydrochloride extended-release capsules if you think you have any of the conditions listed above.
What should I tell my doctor before taking propafenone hydrochloride extended-release capsules?
Before you take propafenone hydrochloride extended-release capsules, tell your doctor if you:
- have liver or kidney problems
- have breathing problems
- have symptoms including diarrhea, sweating, vomiting, or loss of appetite or thirst that are severe. These symptoms may be a sign of abnormal electrolyte levels in your blood.
- have myasthenia gravis
- have lupus erythematosus
- have been told you have or had an abnormal blood test called Antinuclear Antibody Test or ANA Test
- are pregnant or plan to become pregnant
- are breastfeeding or plan to breastfeed. Propafenone hydrochloride extended-release capsules can pass into your milk. You and your doctor should discuss the best way to feed your baby during this time.
- have any other medical conditions
Tell your doctor about all the medicines you take, including prescription and over-the-counter medicines, vitamins, and herbal supplements. Propafenone hydrochloride extended-release capsules and certain other medicines can affect each other and cause serious side effects. Propafenone hydrochloride extended-release capsules may affect the way other medicines work, and other medicines may affect how propafenone hydrochloride extended-release capsules work.
Especially tell your doctor if you take:
- amiodarone or other medicines for your abnormal heart beats
- an antidepressant medicine
- a medicine to treat anxiety
- ritonavir (for example, KALETRA, NORVIR) or saquinavir (for example, INVIRASE)
- an antibiotic medicine
- ketoconazole (for example, NIZORAL)
- digoxin (LANOXIN)
- warfarin sodium (for example, COUMADIN, JANTOVEN)
Know the medicines you take. Keep a list of them to show your doctor and pharmacist when you get a new medicine.
How should I take propafenone hydrochloride extended-release capsules?
- Take propafenone hydrochloride extended-release capsules exactly as prescribed. Your doctor will tell you how many capsules to take and how often to take them.
- To help reduce the chance of certain side effects, your doctor may start you with a low dose of propafenone hydrochloride extended-release capsules, and then slowly increase the dose.
- Do not open or crush the capsule.
- You may take propafenone hydrochloride extended-release capsules with or without food.
- You should not drink grapefruit juice during treatment with propafenone hydrochloride extended-release capsules.
- If you miss a dose of propafenone hydrochloride extended-release capsules, take your next dose at the usual time. Do not take 2 doses at the same time.
- If you take too much propafenone hydrochloride extended-release capsules, call your doctor or go to the nearest hospital emergency room right away.
- Call your doctor if your heart problems get worse.
What are possible side effects of propafenone hydrochloride extended-release capsules?
Propafenone hydrochloride extended-release capsules can cause serious side effects including:
- New or worsened abnormal heart beats, that can cause sudden death or be life-threatening.Your doctor may do an electrocardiogram (ECG or EKG) before and during treatment to check your heart for these problems.
-
New or worsened heart failure. Tell your doctor about any changes in your heart symptoms, including:
- any new or increased swelling in your arms or legs
- trouble breathing
- sudden weight gain
- Effects on pacemaker function.Propafenone hydrochloride extended-release capsules may affect how an implanted pacemaker or defibrillator works. Your doctor should check how your pacemaker or defibrillator is working during and after treatment with propafenone hydrochloride extended-release capsules. They may need to be re-programmed.
-
Very low white blood cell levels in your blood (agranulocytosis).Your bone marrow may not produce enough of a certain type of white blood cells called neutrophils. If this happens, you are more likely to get infections. Tell your doctor right away if you have any of these symptoms, especially during the first 3 months of treatment:
- fever
- sore throat
- chills
- Worsening of myasthenia gravis in people who already have this condition.Tell your doctor about any change in your symptoms.
- Propafenone hydrochloride extended-release capsules may cause lower sperm counts in men.This could affect the ability to father a child. Talk to your doctor if this is a concern for you.
Common side effects of propafenone hydrochloride extended-release capsules include:
- dizziness
- fast or irregular heart beats
- chest pain
- trouble breathing
- taste changes
- nausea
- tiredness
- feeling anxious
- constipation
- upper respiratory infection or flu
- swelling
Tell your doctor if you have any side effect that bothers you or that does not go away.
These are not all the possible side effects of propafenone hydrochloride extended-release capsules. For more information, ask your doctor or pharmacist.
Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.
How should I store propafenone hydrochloride extended-release capsules?
- Store propafenone hydrochloride extended-release capsules at room temperature between 15° to 30°C (59° to 86°F).
- Keep the bottle tightly closed.
Keep propafenone hydrochloride extended-release capsules and all medicines out of the reach of children.
General information about propafenone hydrochloride extended-release capsules
Medicines are sometimes prescribed for conditions other than those described in patient information leaflets. Do not use propafenone hydrochloride extended-release capsules for a condition for which it was not prescribed by your doctor. Do not give propafenone hydrochloride extended-release capsules to other people, even if they have the same symptoms you have. It may harm them.
This leaflet summarizes the most important information about propafenone hydrochloride extended-release capsules. If you would like more information, talk with your doctor. You can ask your doctor or pharmacist for information about propafenone hydrochloride extended-release capsules that is written for healthcare professionals. For more information about propafenone hydrochloride extended-release capsules, call 1-888-650-3789.
What are the ingredients in propafenone hydrochloride extended-release capsules?
Active Ingredient: Propafenone hydrochloride
Inactive Ingredients: gelatin, hypromellose, magnesium stearate, and titanium dioxide. Black ink ingredients: D&C Yellow #10, FD&C Blue #2, FD&C Blue #1 and FD&C Red #40.
All other marks are property of their respective owners.
Manufactured by
UPSHER-SMITH LABORATORIES, LLC
Maple Grove, MN 55369
Revised: 5/2023
Description
In the National Heart, Lung, and Blood Institute's Cardiac Arrhythmia Suppression Trial (CAST), a long-term, multicenter, randomized, double-blind trial in patients with asymptomatic non-life-threatening ventricular arrhythmias who had a myocardial infarction more than 6 days but less than 2 years previously, an increased rate of death or reversed cardiac arrest rate (7.7%; 56/730) was seen in patients treated with encainide or flecainide (Class IC antiarrhythmics) compared with that seen in patients assigned to placebo (3.0%; 22/725). The average duration of treatment with encainide or flecainide in this trial was 10 months. The applicability of the CAST results to other populations (e.g., those without recent myocardial infarction) or other antiarrhythmic drugs is uncertain, but at present, it is prudent to consider any IC antiarrhythmic to have a significant proarrhythmic risk in patients with structural heart disease. Given the lack of any evidence that these drugs improve survival, antiarrhythmic agents should generally be avoided in patients with non-life-threatening ventricular arrhythmias, even if the patients are experiencing unpleasant, but not life-threatening, symptoms or signs.
Section 42229-5
Usage Considerations:
- The use of propafenone hydrochloride extended-release capsules in patients with permanent AF or in patients exclusively with atrial flutter or paroxysmal supraventricular tachycardia (PSVT) has not been evaluated. Do not use propafenone hydrochloride extended-release capsules to control ventricular rate during AF.
- Some patients with atrial flutter treated with propafenone have developed 1:1 conduction, producing an increase in ventricular rate. Concomitant treatment with drugs that increase the functional atrioventricular (AV) nodal refractory period is recommended.
- The effect of propafenone on mortality has not been determined [see Boxed Warning] .
Section 44425-7
Storage:Store at 20° to 25°C (68° to 77°F); excursions permitted to 15° to 30°C (59° to 86°F) [See USP Controlled Room Temperature]. Dispense in a tight, light-resistant container as defined in the USP using a child-resistant closure.
7.2 Digoxin
Concomitant use of propafenone and digoxin increased steady-state serum digoxin exposure (AUC) in patients by 60% to 270% and decreased the clearance of digoxin by 31% to 67%. Monitor plasma digoxin levels of patients receiving propafenone and adjust digoxin dosage as needed.
7.3 Warfarin
The concomitant administration of propafenone and warfarin increased warfarin plasma concentrations at steady state by 39% in healthy volunteers and prolonged the prothrombin time (PT) in patients taking warfarin. Adjust the warfarin dose as needed by monitoring INR (international normalized ratio).
7.4 Orlistat
Orlistat may limit the fraction of propafenone available for absorption. In postmarketing reports, abrupt cessation of orlistat in patients stabilized on propafenone has resulted in severe adverse events including convulsions, atrioventricular block, and acute circulatory failure.
10 Overdosage
The symptoms of overdosage may include hypotension, somnolence, bradycardia, intra-atrial and intraventricular conduction disturbances, and rarely, convulsions and high-grade ventricular arrhythmias. Defibrillation, as well as infusion of dopamine and isoproterenol, has been effective in controlling abnormal rhythm and blood pressure. Convulsions have been alleviated with intravenous diazepam. General supportive measures such as mechanical respiratory assistance and external cardiac massage may be necessary.
The hemodialysis of propafenone in patients with an overdose is expected to be of limited value in the removal of propafenone as a result of both its high protein binding (greater than 95%) and large volume of distribution.
7.6 Lidocaine
No significant effects on the pharmacokinetics of propafenone or lidocaine have been seen following their concomitant use in patients. However, concomitant use of propafenone and lidocaine has been reported to increase the risks of central nervous system side effects of lidocaine.
11 Description
Propafenone hydrochloride, USP is an antiarrhythmic drug supplied in extended-release capsules of 225 mg, 325 mg and 425 mg for oral administration.
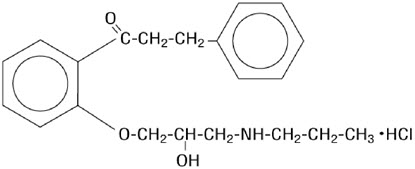
Chemically, propafenone hydrochloride is 2'-[2-hydroxy-3-(propylamino)-propoxy]-3-phenylpropiophenone hydrochloride, with a molecular weight of 377.92. The molecular formula is C 21H 27NO 3∙HCl.
Propafenone hydrochloride has some structural similarities to beta-blocking agents. The structural formula of propafenone hydrochloride is given below:
Propafenone hydrochloride occurs as colorless crystals or white crystalline powder with a very bitter taste. It is slightly soluble in water (20°C), chloroform and ethanol. Propafenone hydrochloride extended-release capsules, USP are filled with cylindrical-shaped 2 × 2 mm microtablets containing propafenone and the following inactive ingredients: gelatin, hypromellose, magnesium stearate, and titanium dioxide. Black ink ingredients: D&C Yellow #10, FD&C Blue #2, FD&C Blue #1 and FD&C Red #40.
Meets USP Dissolution Test 5.
8.4 Pediatric Use
The safety and effectiveness of propafenone in pediatric patients have not been established.
8.5 Geriatric Use
Of the total number of subjects in Phase 3 clinical trials of propafenone hydrochloride 46% were 65 and older, while 16% were 75 and older. No overall differences in safety or effectiveness were observed between these subjects and younger subjects, but greater sensitivity of some older individuals at higher doses cannot be ruled out. The effect of age on the pharmacokinetics and pharmacodynamics of propafenone has not been studied.
Warning: Mortality
- In the National Heart, Lung, and Blood Institute's Cardiac Arrhythmia Suppression Trial (CAST), a long-term, multicenter, randomized, double-blind trial in patients with asymptomatic non-life-threatening ventricular arrhythmias who had a myocardial infarction more than 6 days but less than 2 years previously, an increased rate of death or reversed cardiac arrest rate (7.7%; 56/730) was seen in patients treated with encainide or flecainide (Class IC antiarrhythmics) compared with that seen in patients assigned to placebo (3.0%; 22/725). The average duration of treatment with encainide or flecainide in this trial was 10 months.
- The applicability of the CAST results to other populations (e.g., those without recent myocardial infarction) or other antiarrhythmic drugs is uncertain, but at present, it is prudent to consider any IC antiarrhythmic to have a significant proarrhythmic risk in patients with structural heart disease. Given the lack of any evidence that these drugs improve survival, antiarrhythmic agents should generally be avoided in patients with non-life-threatening ventricular arrhythmias, even if the patients are experiencing unpleasant, but not life-threatening, symptoms or signs.
14 Clinical Studies
Propafenone hydrochloride extended-release has been evaluated in patients with a history of electrocardiographically documented recurrent episodes of symptomatic AF in 2 randomized, double-blind, placebo-controlled trials.
4 Contraindications
Propafenone hydrochloride extended-release capsules are contraindicated in the following circumstances:
- Heart failure
- Cardiogenic shock
- Sinoatrial, atrioventricular, and intraventricular disorders of impulse generation or conduction (e.g., sick sinus node syndrome, AV block) in the absence of an artificial pacemaker
- Known Brugada Syndrome
- Bradycardia
- Marked hypotension
- Bronchospastic disorders or severe obstructive pulmonary disease
- Marked electrolyte imbalance
5.8 Agranulocytosis
Agranulocytosis has been reported in patients receiving propafenone. Generally, the agranulocytosis occurred within the first 2 months of propafenone therapy, and upon discontinuation of therapy the white count usually normalized by 14 days. Unexplained fever or decrease in white cell count, particularly during the initial 3 months of therapy, warrant consideration of possible agranulocytosis or granulocytopenia. Instruct patients to report promptly any signs of infection such as fever, sore throat, or chills.
6 Adverse Reactions
The most commonly reported adverse events with propafenone (greater than 5% and greater than placebo) excluding those not reasonably associated with the use of the drug included the following: dizziness, palpitations, chest pain, dyspnea, taste disturbance, nausea, fatigue, anxiety, constipation, upper respiratory tract infection, edema, and influenza. ( 6.1)
To report SUSPECTED ADVERSE REACTIONS, contact Upsher-Smith Laboratories, LLC at 1-855-899-9180 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
7 Drug Interactions
- Inhibitors of CYP2D6, 1A2, and 3A4 may increase propafenone levels which may lead to cardiac arrhythmias. Simultaneous use with both a CYP3A4 and CYP2D6 inhibitor (or in patients with CYP2D6 deficiency) should be avoided. ( 7.1)
- Propafenone may increase digoxin or warfarin levels. ( 7.2, 7.3)
- Orlistat may reduce propafenone concentrations. Abrupt cessation of orlistat in patients stable on propafenone hydrochloride extended-release capsules has resulted in convulsions, atrioventricular block, and circulatory failure. ( 7.4)
- Concomitant use of lidocaine may increase central nervous system side effects. ( 7.6)
7.5 Beta Antagonists
Concomitant use of propafenone and propranolol in healthy subjects increased propranolol plasma concentrations at steady state by 113%. In 4 patients, administration of metoprolol with propafenone increased the metoprolol plasma concentrations at steady state by 100% to 400%. The pharmacokinetics of propafenone was not affected by the coadministration of either propranolol or metoprolol. In clinical trials using propafenone immediate-release tablets, patients who were receiving beta-blockers concurrently did not experience an increased incidence of side effects.
1 Indications and Usage
Propafenone hydrochloride extended-release capsules are indicated to prolong the time to recurrence of symptomatic atrial fibrillation (AF) in patients with episodic (most likely paroxysmal or persistent) AF who do not have structural heart disease.
12.1 Mechanism of Action
Propafenone is a Class 1C antiarrhythmic drug with local anesthetic effects and a direct stabilizing action on myocardial membranes. The electrophysiological effect of propafenone manifests itself in a reduction of upstroke velocity (Phase 0) of the monophasic action potential. In Purkinje fibers, and, to a lesser extent, myocardial fibers, propafenone reduces the fast-inward current carried by sodium ions. Diastolic excitability threshold is increased and effective refractory period prolonged. Propafenone reduces spontaneous automaticity and depresses triggered activity.
Studies in anesthetized dogs and isolated organ preparations show that propafenone has beta-sympatholytic activity at about 1/ 50the potency of propranolol. Clinical studies employing isoproterenol challenge and exercise testing after single doses of propafenone indicate a beta-adrenergic blocking potency (per mg) about 1/ 40that of propranolol in man. In clinical trials with the immediate-release formulation, resting heart rate decreases of about 8% were noted at the higher end of the therapeutic plasma concentration range. At very high concentrations in vitro, propafenone can inhibit the slow inward current carried by calcium, but this calcium antagonist effect probably does not contribute to antiarrhythmic efficacy. Moreover, propafenone inhibits a variety of cardiac potassium currents in in vitrostudies (i.e., the transient outward, the delayed rectifier, and the inward rectifier current). Propafenone has local anesthetic activity approximately equal to procaine. Compared with propafenone, the main metabolite, 5-hydroxypropafenone, has similar sodium and calcium channel activity, but about 10 times less beta-blocking activity (N-depropylpropafenone has weaker sodium channel activity but equivalent affinity for beta-receptors).
5.12 Elevated Ana Titers
Positive ANA titers have been reported in patients receiving propafenone. They have been reversible upon cessation of treatment and may disappear even in the face of continued propafenone therapy. These laboratory findings were usually not associated with clinical symptoms, but there is one published case of drug-induced lupus erythematosis (positive rechallenge); it resolved completely upon discontinuation of therapy. Carefully evaluate patients who develop an abnormal ANA test and, if persistent or worsening elevation of ANA titers is detected, consider discontinuing therapy.
5.1 Proarrhythmic Effects
Propafenone has caused new or worsened arrhythmias. Such proarrhythmic effects include sudden death and life-threatening ventricular arrhythmias such as ventricular fibrillation, ventricular tachycardia, asystole, and torsade de pointes. It may also worsen premature ventricular contractions or supraventricular arrhythmias, and it may prolong the QT interval. It is therefore essential that each patient given propafenone hydrochloride extended-release be evaluated electrocardiographically prior to and during therapy to determine whether the response to propafenone hydrochloride extended-release supports continued treatment. Because propafenone prolongs the QRS interval in the electrocardiogram, changes in the QT interval are difficult to interpret [see Clinical Pharmacology (12.2)] .
In the RAFT trial [see Clinical Studies (14)] , there were too few deaths to assess the long-term risk to patients. There were 5 deaths, 3 in the pooled group for propafenone hydrochloride extended-release (0.8%), and 2 in the placebo group (1.6%). In the overall database of 8 trials of propafenone hydrochloride extended-release and propafenone hydrochloride immediate-release, the mortality rate was 2.5% per year on propafenone and 4.0% per year on placebo. Concurrent use of propafenone with other antiarrhythmic agents has not been well studied.
In a U.S. uncontrolled, open-label, multicenter trial using the immediate-release formulation in patients with symptomatic supraventricular tachycardia (SVT), 1.9% (9/474) of these patients experienced ventricular tachycardia (VT) or ventricular fibrillation (VF) during the trial. However, in 4 of the 9 patients, the ventricular tachycardia was of atrial origin. Six of the 9 patients that developed ventricular arrhythmias did so within 14 days of onset of therapy. About 2.3% (11/474) of all patients had recurrence of SVT during the trial which could have been a change in the patients' arrhythmia behavior or could represent a proarrhythmic event. Case reports in patients treated with propafenone for atrial fibrillation/flutter have included increased premature ventricular contractions (PVCs), VT, VF, torsades de pointes, asystole, and death.
Overall in clinical trials with propafenone hydrochloride immediate-release (which included patients treated for ventricular arrhythmias, atrial fibrillation/flutter, and PSVT), 4.7% of all patients had new or worsened ventricular arrhythmia possibly representing a proarrhythmic event (0.7% was an increase in PVCs; 4.0% a worsening or new appearance of VT or VF). Of the patients who had worsening of VT (4%), 92% had a history of VT and/or VT/VF, 71% had coronary artery disease, and 68% had a prior myocardial infarction. The incidence of proarrhythmia in patients with less serious or benign arrhythmias, which include patients with an increase in frequency of PVCs, was 1.6%. Although most proarrhythmic events occurred during the first week of therapy, late events also were seen and the CAST trial [see Boxed Warning: Mortality] suggests that an increased risk of proarrythmia is present throughout treatment.
5 Warnings and Precautions
- May cause new or worsened arrhythmias. Evaluate patients via ECG prior to and during therapy. ( 5.1)
- Propafenone hydrochloride extended-release capsules may unmask Brugada or Brugada-like Syndrome. Evaluate patients via ECG after initiation of therapy. ( 4, 5.2)
- Avoid use with other antiarrhythmic agents or drugs that prolong the QT interval. ( 5.3)
- Avoid simultaneous use of propafenone with both a cytochrome P450 2D6 (CYP2D6) inhibitor and a 3A4 inhibitor (CYP3A4). ( 5.4)
- May provoke overt heart failure. ( 5.5)
- May cause dose-related first-degree AV block or other conduction disturbances. Should not be given to patients with conduction defects in absence of a pacemaker. ( 5.6)
- May affect artificial pacemakers. Pacemakers should be monitored during therapy. ( 5.7)
- Agranulocytosis: Patients should report signs of infection. ( 5.8)
- Administer cautiously to patients with impaired hepatic and renal function. ( 5.9, 5.10)
- Exacerbation of myasthenia gravis has been reported. ( 5.11)
2 Dosage and Administration
Propafenone hydrochloride extended-release capsules can be taken with or without food. Do not crush or further divide the contents of the capsule.
The dose of propafenone hydrochloride extended-release capsules must be individually titrated on the basis of response and tolerance. Initiate therapy with propafenone hydrochloride extended-release capsules, USP 225 mg given every 12 hours. Dosage may be increased at a minimum of 5-day intervals to 325 mg given every 12 hours. If additional therapeutic effect is needed, the dose of propafenone hydrochloride extended-release capsules may be increased to 425 mg given every 12 hours.
In patients with hepatic impairment or those with significant widening of the QRS complex or second- or third-degree AV block, consider reducing the dose.
The combination of cytochrome P450 3A4 (CYP3A4) inhibition and either cytochrome P450 2D6 (CYP2D6) deficiency or CYP2D6 inhibition with the simultaneous administration of propafenone may significantly increase the concentration of propafenone and thereby increase the risk of proarrhythmia and other adverse events. Therefore, avoid simultaneous use of propafenone hydrochloride extended-release capsules, USP with both a CYP2D6 inhibitor and a CYP3A4 inhibitor [see Warnings and Precautions (5.4), Drug Interactions (7.1)] .
5.6 Conduction Disturbances
Propafenone slows atrioventricular conduction and may also cause dose-related first-degree AV block. Average PR interval prolongation and increases in QRS duration are also dose-related. Do not give propafenone to patients with atrioventricular and intraventricular conduction defects in the absence of a pacemaker [see Contraindications (4), Clinical Pharmacology (12.2)] .
In a U.S. trial (RAFT) in 523 patients with a history of symptomatic AF treated with propafenone hydrochloride extended-release, sinus bradycardia (rate less than 50 beats/min) was reported with the same frequency with propafenone hydrochloride extended-release and placebo.
3 Dosage Forms and Strengths
Propafenone hydrochloride extended-release capsules, USP is supplied as white, opaque, hard gelatin capsules containing either 225 mg, 325 mg, or 425 mg of propafenone hydrochloride.
The 225 mg capsule is printed with "UPSHER-SMITH" over "0740" and "225mg" in black ink.
The 325 mg capsule is printed with "UPSHER-SMITH" over "0741" and "325mg" in black ink.
The 425 mg capsule is printed with "UPSHER-SMITH" over "0742" and "425mg" in black ink.
5.2 Unmasking Brugada Syndrome
Brugada Syndrome may be unmasked after exposure to propafenone hydrochloride extended-release. Perform an ECG after initiation of propafenone hydrochloride extended-release and discontinue the drug if changes are suggestive of Brugada Syndrome [see Contraindications (4)] .
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared with rates in the clinical trials of another drug and may not reflect the rates observed in practice.
The data described below reflect exposure to propafenone hydrochloride extended-release 225 mg twice daily in 126 patients, to propafenone hydrochloride extended-release 325 mg twice daily in 135 patients, to propafenone hydrochloride extended-release 425 mg twice daily in 136 patients, and to placebo in 126 patients for up to 39 weeks (mean: 20 weeks) in a placebo-controlled trial (RAFT) conducted in the U.S. The most commonly reported adverse events with propafenone (greater than 5% and greater than placebo) excluding those not reasonably associated with the use of the drug or because they were associated with the condition being treated, were dizziness, palpitations, chest pain, dyspnea, taste disturbance, nausea, fatigue, anxiety, constipation, upper respiratory tract infection, edema, and influenza. The frequency of discontinuation due to adverse events was 17%, and the rate was highest during the first 14 days of treatment.
Cardiac-related adverse events occurring in greater than or equal to 2% of the patients in any of the RAFT propafenone extended-release treatment groups and more common with propafenone than with placebo, excluding those that are common in the population and those not plausibly related to drug therapy, included the following: angina pectoris, atrial flutter, AV block first- degree, bradycardia, congestive cardiac failure, cardiac murmur, edema, dyspnea, rales, wheezing, and cardioactive drug level above therapeutic.
Propafenone prolongs the PR and QRS intervals in patients with atrial and ventricular arrhythmias. Prolongation of the QRS interval makes it difficult to interpret the effect of propafenone on the QT interval [see Clinical Pharmacology (12.2)] .
Non-cardiac related adverse events occurring in greater than or equal to 2% of the patients in any of the RAFT propafenone extended-release treatment groups and more common with propafenone than with placebo, excluding those that are common in the population and those not plausibly related to drug therapy, included the following: blurred vision, constipation, diarrhea, dry mouth, flatulence, nausea, vomiting, fatigue, weakness, upper respiratory tract infection, blood alkaline phosphatase increased, hematuria, muscle weakness, dizziness (excluding vertigo), headache, taste disturbance, tremor, somnolence, anxiety, depression, ecchymosis.
No clinically important differences in incidence of adverse reactions were noted by age or gender. Too few non-Caucasian patients were enrolled to assess adverse events according to race.
Adverse events occurring in 2% or more of the patients in any of the ERAFT [see Clinical Studies (14)] propafenone extended-release treatment groups and not listed above include the following: bundle branch block left, bundle branch block right, conduction disorders, sinus bradycardia, and hypotension.
Other adverse events reported with propafenone clinical trials not already listed elsewhere in the prescribing information include the following adverse events by body system and preferred term.
Blood and Lymphatic System
Anemia, lymphadenopathy, spleen disorder, thrombocytopenia.
Cardiac
Unstable angina, atrial hypertrophy, cardiac arrest, coronary artery disease, extrasystoles, myocardial infarction, nodal arrhythmia, palpitations, pericarditis, sinoatrial block, sinus arrest, sinus arrhythmia, supraventricular extrasystoles, ventricular extrasystoles, ventricular hypertrophy.
Ear and Labyrinth
Hearing impaired, tinnitus, vertigo.
Eye
Eye hemorrhage, eye inflammation, eyelid ptosis, miosis, retinal disorder, visual acuity reduced.
Gastrointestinal
Abdominal distension, abdominal pain, duodenitis, dyspepsia, dysphagia, eructation, gastritis, gastroesophageal reflux disease, gingival bleeding, glossitis, glossodynia, gum pain, halitosis, intestinal obstruction, melena, mouth ulceration, pancreatitis, peptic ulcer, rectal bleeding, sore throat.
General Disorders and Administration Site Conditions
Chest pain, feeling hot, hemorrhage, malaise, pain, pyrexia.
Hepatobiliary
Hepatomegaly.
Investigations
Abnormal heart sounds, abnormal pulse, carotid bruit, decreased blood chloride, decreased blood pressure, decreased blood sodium, decreased hemoglobin, decreased neutrophil count, decreased platelet count, decreased prothrombin level, decreased red blood cell count, decreased weight, glycosuria present, increased alanine aminotransferase, increased aspartate aminotransferase, increased blood bilirubin, increased blood cholesterol, increased blood creatinine, increased blood glucose, increased blood lactate dehydrogenase, increased blood pressure, increased blood prolactin, increased blood triglycerides, increased blood urea, increased blood uric acid, increased eosinophil count, increased gamma-glutamyltransferase, increased monocyte count, increased prostatic specific antigen, increased prothrombin level, increased weight, increased white blood cell count, ketonuria present, proteinuria present.
Metabolism and Nutrition
Anorexia, dehydration, diabetes mellitus, gout, hypercholesterolemia, hyperglycemia, hyperlipidemia, hypokalemia.
Musculoskeletal, Connective Tissue, and Bone
Arthritis, bursitis, collagen-vascular disease, costochondritis, joint disorder, muscle cramps, muscle spasms, myalgia, neck pain, pain in jaw, sciatica, tendonitis.
Nervous System
Amnesia, ataxia, balance impaired, brain damage, cerebrovascular accident, dementia, gait abnormal, hypertonia, hypothesia, insomnia, paralysis, paresthesia, peripheral neuropathy, speech disorder, syncope, tongue hypoesthesia.
Psychiatric
Decreased libido, emotional disturbance, mental disorder, neurosis, nightmare, sleep disorder.
Renal and Urinary
Dysuria, nocturia, oliguria, pyuria, renal failure, urinary casts, urinary frequency, urinary incontinence, urinary retention, urine abnormal.
Reproductive System and Breast
Breast pain, impotence, prostatism.
Respiratory, Thoracic, and Mediastinal
Atelectasis, breath sounds decreased, chronic obstructive airways disease, cough, epistaxis, hemoptysis, lung disorder, pleural effusion, pulmonary congestion, rales, respiratory failure, rhinitis, throat tightness.
Skin and Subcutaneous Tissue
Alopecia, dermatitis, dry skin, erythema, nail abnormality, petechiae, pruritus, sweating increased, urticaria.
Vascular
Arterial embolism limb, deep limb venous thrombosis, flushing, hematoma, hypertension, hypertensive crisis, hypotension, labile blood pressure, pallor, peripheral coldness, peripheral vascular disease, thrombosis.
7.1 Cyp2d6 and Cyp3a4 Inhibitors
Drugs that inhibit CYP2D6 (such as desipramine, paroxetine, ritonavir, sertraline) and CYP3A4 (such as ketoconazole, ritonavir, saquinavir, erythromycin, and grapefruit juice) can be expected to cause increased plasma levels of propafenone. The combination of CYP3A4 inhibition and either CYP2D6 deficiency or CYP2D6 inhibition with administration of propafenone may increase the risk of adverse reactions, including proarrhythmia. Therefore, simultaneous use of propafenone hydrochloride extended-release with both a CYP2D6 inhibitor and a CYP3A4 inhibitor should be avoided [see Warnings and Precautions (5.4), Dosage and Administration (2)] .
Amiodarone
Concomitant administration of propafenone and amiodarone can affect conduction and repolarization and is not recommended.
Cimetidine
Concomitant administration of propafenone immediate-release tablets and cimetidine in 12 healthy subjects resulted in a 20% increase in steady-state plasma concentrations of propafenone.
Fluoxetine
Concomitant administration of propafenone and fluoxetine in extensive metabolizers increased the S-propafenone C maxand AUC by 39% and 50%, respectively, and the R-propafenone C maxand AUC by 71% and 50%, respectively.
Quinidine
Small doses of quinidine completely inhibit the CYP2D6 hydroxylation metabolic pathway, making all patients, in effect, slow metabolizers [see Clinical Pharmacology (12.3)] . Concomitant administration of quinidine (50 mg 3 times daily) with 150-mg immediate-release propafenone 3 times daily decreased the clearance of propafenone by 60% in extensive metabolizers, making them poor metabolizers. Steady-state plasma concentrations increased by more than 2-fold for propafenone and decreased 50% for 5-OH-propafenone. A 100-mg dose of quinidine increased steady-state concentrations of propafenone 3-fold. Avoid concomitant use of propafenone and quinidine.
Rifampin
Concomitant administration of rifampin and propafenone in extensive metabolizers decreased the plasma concentrations of propafenone by 67% with a corresponding decrease of 5-OH-propafenone by 65%. The concentrations of norpropafenone increased by 30%. In poor metabolizers, there was a 50% decrease in propafenone plasma concentrations and an increase in the AUC and C maxof norpropafenone by 74% and 20%, respectively. Urinary excretion of propafenone and its metabolites decreased significantly. Similar results were noted in elderly patients: Both the AUC and C maxof propafenone decreased by 84%, with a corresponding decrease in AUC and C maxof 5-OH-propafenone by 69% and 57%, respectively.
17 Patient Counseling Information
Advise the patient to read the FDA-approved patient labeling (Patient Information).
- Instruct patients to notify their healthcare providers of any change in over-the-counter, prescription, and supplement use.
- Instruct patients to report symptoms that may be associated with altered electrolyte balance, such as excessive or prolonged diarrhea, sweating, vomiting, or loss of appetite or thirst.
- Instruct patients not to double the next dose if a dose is missed. The next dose should be taken at the usual time.
5.7 Effects On Pacemaker Threshold
Propafenone may alter both pacing and sensing thresholds of implanted pacemakers and defibrillators. During and after therapy, monitor and re-program these devices accordingly.
16 How Supplied/storage and Handling
Propafenone hydrochloride extended-release capsules, USP are supplied as white, opaque, hard gelatin capsules containing either 225 mg, 325 mg, or 425 mg of propafenone hydrochloride.
The 225 mg capsule is printed with "UPSHER-SMITH" over "0740" and "225mg" in black ink. Supplied as follows:
| Bottles of 60 capsules | NDC 0832-0740-60 |
The 325 mg capsule is printed with "UPSHER-SMITH" over "0741" and "325mg" in black ink. Supplied as follows:
| Bottles of 60 capsules | NDC 0832-0741-60 |
The 425 mg capsule is printed with "UPSHER-SMITH" over "0742" and "425mg" in black ink. Supplied as follows:
| Bottles of 60 capsules | NDC 0832-0742-60 |
13.2 Animal Toxicology And/or Pharmacology
Renal changes have been observed in the rat following 6 months of oral administration of propafenone hydrochloride at doses of 180 and 360 mg/kg/day (about 2 and 4 times, respectively, the MRHD on a mg/m 2basis). Both inflammatory and non-inflammatory changes in the renal tubules, with accompanying interstitial nephritis, were observed. These changes were reversible, as they were not found in rats allowed to recover for 6 weeks. Fatty degenerative changes of the liver were found in rats following longer durations of administration of propafenone hydrochloride at a dose of 270 mg/kg/day (about 3 times the MRHD on a mg/m 2basis). There were no renal or hepatic changes at 90 mg/kg/day equivalent to the MRHD on a mg/m 2basis).
5.10 Use in Patients With Renal Dysfunction
Approximately 50% of propafenone metabolites are excreted in the urine following administration of propafenone hydrochloride immediate-release tablets. No trials have been performed to assess the percentage of metabolites eliminated in the urine following the administration of propafenone hydrochloride extended-release capsules.
In patients with impaired renal function, monitor for signs of overdosage [see Overdosage (10)] .
5.11 Use in Patients With Myasthenia Gravis
Exacerbation of myasthenia gravis has been reported during propafenone therapy.
5.9 Use in Patients With Hepatic Dysfunction
Propafenone is highly metabolized by the liver. Severe liver dysfunction increases the bioavailability of propafenone to approximately 70% compared with 3% to 40% in patients with normal liver function when given propafenone hydrochloride immediate-release tablets. In 8 patients with moderate to severe liver disease administered propafenone hydrochloride immediate-release tablets, the mean half-life was approximately 9 hours. No trials have compared bioavailability of propafenone from propafenone hydrochloride extended-release capsules in patients with normal and impaired hepatic function. Increased bioavailability of propafenone in these patients may result in excessive accumulation. Carefully monitor patients with impaired hepatic function for excessive pharmacological effects [see Overdosage (10)] .
5.5 Use in Patients With A History of Heart Failure
Propafenone exerts a negative inotropic activity on the myocardium as well as beta-blockade effects and may provoke overt heart failure. In the U.S. trial (RAFT) in patients with symptomatic AF, heart failure was reported in 4 (1.0%) patients receiving propafenone hydrochloride extended-release (all doses) compared with 1 (0.8%) patient receiving placebo. Proarrhythmic effects more likely occur when propafenone is administered to patients with heart failure (NYHA III and IV) or severe myocardial ischemia [see Contraindications (4)] .
In clinical trial experience with propafenone hydrochloride immediate-release, new or worsened congestive heart failure has been reported in 3.7% of patients with ventricular arrhythmia. These events were more likely in subjects with pre-existing heart failure and coronary artery disease. New onset of heart failure attributable to propafenone developed in less than 0.2% of patients with ventricular arrhythmia and in 1.9% of patients with paroxysmal AF or PSVT.
Principal Display Panel 225 Mg Capsule Bottle Label
NDC 0832-0740-60
Propafenone
Hydrochloride
Extended-Release
Capsules, USP
225 mg
60 Capsules
Rx only
UPSHER-SMITH
Principal Display Panel 325 Mg Capsule Bottle Label
NDC 0832-0741-60
Propafenone
Hydrochloride
Extended-Release
Capsules, USP
325 mg
60 Capsules
Rx only
UPSHER-SMITH
Principal Display Panel 425 Mg Capsule Bottle Label
NDC 0832-0742-60
Propafenone
Hydrochloride
Extended-Release
Capsules, USP
425 mg
60 Capsules
Rx only
UPSHER-SMITH
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Lifetime maximally tolerated oral dose studies in mice (up to 360 mg/kg/day, approximately twice the MRHD on a mg/m 2basis) and rats (up to 270 mg/kg/day, approximately 3 times the MRHD on a mg/m 2basis) provided no evidence of a carcinogenic potential for propafenone.
Propafenone was not mutagenic in the Ames (salmonella) test and the in vivomouse dominant lethal test. Propafenone was not clastogenic in the human lymphocyte chromosome aberration assay in vitro, the rat and Chinese hamster micronucleus tests, and other in vivotests for chromosomal aberrations in rat bone marrow and Chinese hamster bone marrow and spermatogonia.
Propafenone, administered intravenously, has been shown to decrease spermatogenesis at lethal doses in rabbits (≥3.5 mg/kg/day) or at near-lethal dose levels in monkeys and dogs (≤5 mg/kg/day); doses were less than the MRHD on a mg/m 2basis. These effects were reversible and did not impair fertility in rabbits at an intravenous dose of 3.5 mg/kg/day (a spermatogenesis-impairing dose). Effects on spermatogenesis were not found when propafenone was administered to rats either orally or intravenously up to 360 mg/kg/day or 6 mg/kg/day, respectively, or in dogs at oral doses up to 240 mg/kg/day (up to approximately 4 or 9 times the MRHD on a mg/m2 basis in rats and dogs, respectively). Treatment of male rabbits for 10 weeks prior to mating at an oral dose of 120 mg/kg/day (approximately 2 times the MRHD on a mg/m 2basis) did not result in evidence of impaired fertility. Nor was there evidence of impaired fertility when propafenone was administered orally to male and female rats at dose levels up to 270 mg/kg/day (approximately 3 times the MRHD on a mg/m 2basis) for 10 weeks (males) or 2 weeks (females) prior to mating through mating.
5.3 Use With Drugs That Prolong the Qt Interval and Antiarrhythmic Agents
The use of propafenone hydrochloride extended-release in conjunction with other drugs that prolong the QT interval has not been extensively studied. Such drugs may include many antiarrhythmics, some phenothiazines, tricyclic antidepressants, and oral macrolides. Withhold Class IA and III antiarrhythmic agents for at least 5 half-lives prior to dosing with propafenone hydrochloride extended-release. Avoid the use of propafenone with Class IA and III antiarrhythmic agents (including quinidine and amiodarone). There is only limited experience with the concomitant use of Class IB or IC antiarrhythmics.
5.4 Drug Interactions: Simultaneous Use With Inhibitors of Cytochrome P450 Isoenzymes 2d6 and 3a4
Propafenone is metabolized by CYP2D6, CYP3A4, and CYP1A2 isoenzymes. Approximately 6% of Caucasians in the U.S. population are naturally deficient in CYP2D6 activity and other demographic groups are deficient to a somewhat lesser extent. Drugs that inhibit these CYP pathways (such as desipramine, paroxetine, ritonavir, sertraline for CYP2D6; ketoconazole, erythromycin, saquinavir, and grapefruit juice for CYP3A4; and amiodarone and tobacco smoke for CYP1A2) can be expected to cause increased plasma levels of propafenone.
Increased exposure to propafenone may lead to cardiac arrhythmias and exaggerated beta-adrenergic blocking activity. Because of its metabolism, the combination of CYP3A4 inhibition and either CYP2D6 deficiency or CYP2D6 inhibition in users of propafenone is potentially hazardous. Therefore, avoid simultaneous use of propafenone hydrochloride extended-release with both a CYP2D6 inhibitor and a CYP3A4 inhibitor.
Structured Label Content
Section 42229-5 (42229-5)
Usage Considerations:
- The use of propafenone hydrochloride extended-release capsules in patients with permanent AF or in patients exclusively with atrial flutter or paroxysmal supraventricular tachycardia (PSVT) has not been evaluated. Do not use propafenone hydrochloride extended-release capsules to control ventricular rate during AF.
- Some patients with atrial flutter treated with propafenone have developed 1:1 conduction, producing an increase in ventricular rate. Concomitant treatment with drugs that increase the functional atrioventricular (AV) nodal refractory period is recommended.
- The effect of propafenone on mortality has not been determined [see Boxed Warning] .
Section 44425-7 (44425-7)
Storage:Store at 20° to 25°C (68° to 77°F); excursions permitted to 15° to 30°C (59° to 86°F) [See USP Controlled Room Temperature]. Dispense in a tight, light-resistant container as defined in the USP using a child-resistant closure.
7.2 Digoxin
Concomitant use of propafenone and digoxin increased steady-state serum digoxin exposure (AUC) in patients by 60% to 270% and decreased the clearance of digoxin by 31% to 67%. Monitor plasma digoxin levels of patients receiving propafenone and adjust digoxin dosage as needed.
7.3 Warfarin
The concomitant administration of propafenone and warfarin increased warfarin plasma concentrations at steady state by 39% in healthy volunteers and prolonged the prothrombin time (PT) in patients taking warfarin. Adjust the warfarin dose as needed by monitoring INR (international normalized ratio).
7.4 Orlistat
Orlistat may limit the fraction of propafenone available for absorption. In postmarketing reports, abrupt cessation of orlistat in patients stabilized on propafenone has resulted in severe adverse events including convulsions, atrioventricular block, and acute circulatory failure.
10 Overdosage (10 OVERDOSAGE)
The symptoms of overdosage may include hypotension, somnolence, bradycardia, intra-atrial and intraventricular conduction disturbances, and rarely, convulsions and high-grade ventricular arrhythmias. Defibrillation, as well as infusion of dopamine and isoproterenol, has been effective in controlling abnormal rhythm and blood pressure. Convulsions have been alleviated with intravenous diazepam. General supportive measures such as mechanical respiratory assistance and external cardiac massage may be necessary.
The hemodialysis of propafenone in patients with an overdose is expected to be of limited value in the removal of propafenone as a result of both its high protein binding (greater than 95%) and large volume of distribution.
7.6 Lidocaine
No significant effects on the pharmacokinetics of propafenone or lidocaine have been seen following their concomitant use in patients. However, concomitant use of propafenone and lidocaine has been reported to increase the risks of central nervous system side effects of lidocaine.
11 Description (11 DESCRIPTION)
Propafenone hydrochloride, USP is an antiarrhythmic drug supplied in extended-release capsules of 225 mg, 325 mg and 425 mg for oral administration.
Chemically, propafenone hydrochloride is 2'-[2-hydroxy-3-(propylamino)-propoxy]-3-phenylpropiophenone hydrochloride, with a molecular weight of 377.92. The molecular formula is C 21H 27NO 3∙HCl.
Propafenone hydrochloride has some structural similarities to beta-blocking agents. The structural formula of propafenone hydrochloride is given below:
Propafenone hydrochloride occurs as colorless crystals or white crystalline powder with a very bitter taste. It is slightly soluble in water (20°C), chloroform and ethanol. Propafenone hydrochloride extended-release capsules, USP are filled with cylindrical-shaped 2 × 2 mm microtablets containing propafenone and the following inactive ingredients: gelatin, hypromellose, magnesium stearate, and titanium dioxide. Black ink ingredients: D&C Yellow #10, FD&C Blue #2, FD&C Blue #1 and FD&C Red #40.
Meets USP Dissolution Test 5.
8.4 Pediatric Use
The safety and effectiveness of propafenone in pediatric patients have not been established.
8.5 Geriatric Use
Of the total number of subjects in Phase 3 clinical trials of propafenone hydrochloride 46% were 65 and older, while 16% were 75 and older. No overall differences in safety or effectiveness were observed between these subjects and younger subjects, but greater sensitivity of some older individuals at higher doses cannot be ruled out. The effect of age on the pharmacokinetics and pharmacodynamics of propafenone has not been studied.
Warning: Mortality (WARNING: MORTALITY)
- In the National Heart, Lung, and Blood Institute's Cardiac Arrhythmia Suppression Trial (CAST), a long-term, multicenter, randomized, double-blind trial in patients with asymptomatic non-life-threatening ventricular arrhythmias who had a myocardial infarction more than 6 days but less than 2 years previously, an increased rate of death or reversed cardiac arrest rate (7.7%; 56/730) was seen in patients treated with encainide or flecainide (Class IC antiarrhythmics) compared with that seen in patients assigned to placebo (3.0%; 22/725). The average duration of treatment with encainide or flecainide in this trial was 10 months.
- The applicability of the CAST results to other populations (e.g., those without recent myocardial infarction) or other antiarrhythmic drugs is uncertain, but at present, it is prudent to consider any IC antiarrhythmic to have a significant proarrhythmic risk in patients with structural heart disease. Given the lack of any evidence that these drugs improve survival, antiarrhythmic agents should generally be avoided in patients with non-life-threatening ventricular arrhythmias, even if the patients are experiencing unpleasant, but not life-threatening, symptoms or signs.
14 Clinical Studies (14 CLINICAL STUDIES)
Propafenone hydrochloride extended-release has been evaluated in patients with a history of electrocardiographically documented recurrent episodes of symptomatic AF in 2 randomized, double-blind, placebo-controlled trials.
4 Contraindications (4 CONTRAINDICATIONS)
Propafenone hydrochloride extended-release capsules are contraindicated in the following circumstances:
- Heart failure
- Cardiogenic shock
- Sinoatrial, atrioventricular, and intraventricular disorders of impulse generation or conduction (e.g., sick sinus node syndrome, AV block) in the absence of an artificial pacemaker
- Known Brugada Syndrome
- Bradycardia
- Marked hypotension
- Bronchospastic disorders or severe obstructive pulmonary disease
- Marked electrolyte imbalance
5.8 Agranulocytosis
Agranulocytosis has been reported in patients receiving propafenone. Generally, the agranulocytosis occurred within the first 2 months of propafenone therapy, and upon discontinuation of therapy the white count usually normalized by 14 days. Unexplained fever or decrease in white cell count, particularly during the initial 3 months of therapy, warrant consideration of possible agranulocytosis or granulocytopenia. Instruct patients to report promptly any signs of infection such as fever, sore throat, or chills.
6 Adverse Reactions (6 ADVERSE REACTIONS)
The most commonly reported adverse events with propafenone (greater than 5% and greater than placebo) excluding those not reasonably associated with the use of the drug included the following: dizziness, palpitations, chest pain, dyspnea, taste disturbance, nausea, fatigue, anxiety, constipation, upper respiratory tract infection, edema, and influenza. ( 6.1)
To report SUSPECTED ADVERSE REACTIONS, contact Upsher-Smith Laboratories, LLC at 1-855-899-9180 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
7 Drug Interactions (7 DRUG INTERACTIONS)
- Inhibitors of CYP2D6, 1A2, and 3A4 may increase propafenone levels which may lead to cardiac arrhythmias. Simultaneous use with both a CYP3A4 and CYP2D6 inhibitor (or in patients with CYP2D6 deficiency) should be avoided. ( 7.1)
- Propafenone may increase digoxin or warfarin levels. ( 7.2, 7.3)
- Orlistat may reduce propafenone concentrations. Abrupt cessation of orlistat in patients stable on propafenone hydrochloride extended-release capsules has resulted in convulsions, atrioventricular block, and circulatory failure. ( 7.4)
- Concomitant use of lidocaine may increase central nervous system side effects. ( 7.6)
Patient Information (PATIENT INFORMATION)
What are propafenone hydrochloride extended-release capsules?
Propafenone hydrochloride extended-release capsules are a prescription medicine that is used:
- in certain people who have a heart rhythm disorder called atrial fibrillation (AF)
- to increase the amount of time between having symptoms of AF
It is not known if propafenone hydrochloride extended-release capsules are safe and effective in children.
Who should not take propafenone hydrochloride extended-release capsules?
Do not take propafenone hydrochloride extended-release capsules if you have:
- heart failure (weak heart)
- had a recent heart attack
- a heart condition called Brugada Syndrome
- a heart rate that is too slow, and you do not have a pacemaker
- very low blood pressure
- certain breathing problems that make you short of breath or wheeze
- certain abnormal body salt (electrolyte) levels in your blood
Talk to your doctor before taking propafenone hydrochloride extended-release capsules if you think you have any of the conditions listed above.
What should I tell my doctor before taking propafenone hydrochloride extended-release capsules?
Before you take propafenone hydrochloride extended-release capsules, tell your doctor if you:
- have liver or kidney problems
- have breathing problems
- have symptoms including diarrhea, sweating, vomiting, or loss of appetite or thirst that are severe. These symptoms may be a sign of abnormal electrolyte levels in your blood.
- have myasthenia gravis
- have lupus erythematosus
- have been told you have or had an abnormal blood test called Antinuclear Antibody Test or ANA Test
- are pregnant or plan to become pregnant
- are breastfeeding or plan to breastfeed. Propafenone hydrochloride extended-release capsules can pass into your milk. You and your doctor should discuss the best way to feed your baby during this time.
- have any other medical conditions
Tell your doctor about all the medicines you take, including prescription and over-the-counter medicines, vitamins, and herbal supplements. Propafenone hydrochloride extended-release capsules and certain other medicines can affect each other and cause serious side effects. Propafenone hydrochloride extended-release capsules may affect the way other medicines work, and other medicines may affect how propafenone hydrochloride extended-release capsules work.
Especially tell your doctor if you take:
- amiodarone or other medicines for your abnormal heart beats
- an antidepressant medicine
- a medicine to treat anxiety
- ritonavir (for example, KALETRA, NORVIR) or saquinavir (for example, INVIRASE)
- an antibiotic medicine
- ketoconazole (for example, NIZORAL)
- digoxin (LANOXIN)
- warfarin sodium (for example, COUMADIN, JANTOVEN)
Know the medicines you take. Keep a list of them to show your doctor and pharmacist when you get a new medicine.
How should I take propafenone hydrochloride extended-release capsules?
- Take propafenone hydrochloride extended-release capsules exactly as prescribed. Your doctor will tell you how many capsules to take and how often to take them.
- To help reduce the chance of certain side effects, your doctor may start you with a low dose of propafenone hydrochloride extended-release capsules, and then slowly increase the dose.
- Do not open or crush the capsule.
- You may take propafenone hydrochloride extended-release capsules with or without food.
- You should not drink grapefruit juice during treatment with propafenone hydrochloride extended-release capsules.
- If you miss a dose of propafenone hydrochloride extended-release capsules, take your next dose at the usual time. Do not take 2 doses at the same time.
- If you take too much propafenone hydrochloride extended-release capsules, call your doctor or go to the nearest hospital emergency room right away.
- Call your doctor if your heart problems get worse.
What are possible side effects of propafenone hydrochloride extended-release capsules?
Propafenone hydrochloride extended-release capsules can cause serious side effects including:
- New or worsened abnormal heart beats, that can cause sudden death or be life-threatening.Your doctor may do an electrocardiogram (ECG or EKG) before and during treatment to check your heart for these problems.
-
New or worsened heart failure. Tell your doctor about any changes in your heart symptoms, including:
- any new or increased swelling in your arms or legs
- trouble breathing
- sudden weight gain
- Effects on pacemaker function.Propafenone hydrochloride extended-release capsules may affect how an implanted pacemaker or defibrillator works. Your doctor should check how your pacemaker or defibrillator is working during and after treatment with propafenone hydrochloride extended-release capsules. They may need to be re-programmed.
-
Very low white blood cell levels in your blood (agranulocytosis).Your bone marrow may not produce enough of a certain type of white blood cells called neutrophils. If this happens, you are more likely to get infections. Tell your doctor right away if you have any of these symptoms, especially during the first 3 months of treatment:
- fever
- sore throat
- chills
- Worsening of myasthenia gravis in people who already have this condition.Tell your doctor about any change in your symptoms.
- Propafenone hydrochloride extended-release capsules may cause lower sperm counts in men.This could affect the ability to father a child. Talk to your doctor if this is a concern for you.
Common side effects of propafenone hydrochloride extended-release capsules include:
- dizziness
- fast or irregular heart beats
- chest pain
- trouble breathing
- taste changes
- nausea
- tiredness
- feeling anxious
- constipation
- upper respiratory infection or flu
- swelling
Tell your doctor if you have any side effect that bothers you or that does not go away.
These are not all the possible side effects of propafenone hydrochloride extended-release capsules. For more information, ask your doctor or pharmacist.
Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.
How should I store propafenone hydrochloride extended-release capsules?
- Store propafenone hydrochloride extended-release capsules at room temperature between 15° to 30°C (59° to 86°F).
- Keep the bottle tightly closed.
Keep propafenone hydrochloride extended-release capsules and all medicines out of the reach of children.
General information about propafenone hydrochloride extended-release capsules
Medicines are sometimes prescribed for conditions other than those described in patient information leaflets. Do not use propafenone hydrochloride extended-release capsules for a condition for which it was not prescribed by your doctor. Do not give propafenone hydrochloride extended-release capsules to other people, even if they have the same symptoms you have. It may harm them.
This leaflet summarizes the most important information about propafenone hydrochloride extended-release capsules. If you would like more information, talk with your doctor. You can ask your doctor or pharmacist for information about propafenone hydrochloride extended-release capsules that is written for healthcare professionals. For more information about propafenone hydrochloride extended-release capsules, call 1-888-650-3789.
What are the ingredients in propafenone hydrochloride extended-release capsules?
Active Ingredient: Propafenone hydrochloride
Inactive Ingredients: gelatin, hypromellose, magnesium stearate, and titanium dioxide. Black ink ingredients: D&C Yellow #10, FD&C Blue #2, FD&C Blue #1 and FD&C Red #40.
All other marks are property of their respective owners.
Manufactured by
UPSHER-SMITH LABORATORIES, LLC
Maple Grove, MN 55369
Revised: 5/2023
7.5 Beta Antagonists (7.5 Beta-Antagonists)
Concomitant use of propafenone and propranolol in healthy subjects increased propranolol plasma concentrations at steady state by 113%. In 4 patients, administration of metoprolol with propafenone increased the metoprolol plasma concentrations at steady state by 100% to 400%. The pharmacokinetics of propafenone was not affected by the coadministration of either propranolol or metoprolol. In clinical trials using propafenone immediate-release tablets, patients who were receiving beta-blockers concurrently did not experience an increased incidence of side effects.
1 Indications and Usage (1 INDICATIONS AND USAGE)
Propafenone hydrochloride extended-release capsules are indicated to prolong the time to recurrence of symptomatic atrial fibrillation (AF) in patients with episodic (most likely paroxysmal or persistent) AF who do not have structural heart disease.
12.1 Mechanism of Action
Propafenone is a Class 1C antiarrhythmic drug with local anesthetic effects and a direct stabilizing action on myocardial membranes. The electrophysiological effect of propafenone manifests itself in a reduction of upstroke velocity (Phase 0) of the monophasic action potential. In Purkinje fibers, and, to a lesser extent, myocardial fibers, propafenone reduces the fast-inward current carried by sodium ions. Diastolic excitability threshold is increased and effective refractory period prolonged. Propafenone reduces spontaneous automaticity and depresses triggered activity.
Studies in anesthetized dogs and isolated organ preparations show that propafenone has beta-sympatholytic activity at about 1/ 50the potency of propranolol. Clinical studies employing isoproterenol challenge and exercise testing after single doses of propafenone indicate a beta-adrenergic blocking potency (per mg) about 1/ 40that of propranolol in man. In clinical trials with the immediate-release formulation, resting heart rate decreases of about 8% were noted at the higher end of the therapeutic plasma concentration range. At very high concentrations in vitro, propafenone can inhibit the slow inward current carried by calcium, but this calcium antagonist effect probably does not contribute to antiarrhythmic efficacy. Moreover, propafenone inhibits a variety of cardiac potassium currents in in vitrostudies (i.e., the transient outward, the delayed rectifier, and the inward rectifier current). Propafenone has local anesthetic activity approximately equal to procaine. Compared with propafenone, the main metabolite, 5-hydroxypropafenone, has similar sodium and calcium channel activity, but about 10 times less beta-blocking activity (N-depropylpropafenone has weaker sodium channel activity but equivalent affinity for beta-receptors).
5.12 Elevated Ana Titers (5.12 Elevated ANA Titers)
Positive ANA titers have been reported in patients receiving propafenone. They have been reversible upon cessation of treatment and may disappear even in the face of continued propafenone therapy. These laboratory findings were usually not associated with clinical symptoms, but there is one published case of drug-induced lupus erythematosis (positive rechallenge); it resolved completely upon discontinuation of therapy. Carefully evaluate patients who develop an abnormal ANA test and, if persistent or worsening elevation of ANA titers is detected, consider discontinuing therapy.
5.1 Proarrhythmic Effects
Propafenone has caused new or worsened arrhythmias. Such proarrhythmic effects include sudden death and life-threatening ventricular arrhythmias such as ventricular fibrillation, ventricular tachycardia, asystole, and torsade de pointes. It may also worsen premature ventricular contractions or supraventricular arrhythmias, and it may prolong the QT interval. It is therefore essential that each patient given propafenone hydrochloride extended-release be evaluated electrocardiographically prior to and during therapy to determine whether the response to propafenone hydrochloride extended-release supports continued treatment. Because propafenone prolongs the QRS interval in the electrocardiogram, changes in the QT interval are difficult to interpret [see Clinical Pharmacology (12.2)] .
In the RAFT trial [see Clinical Studies (14)] , there were too few deaths to assess the long-term risk to patients. There were 5 deaths, 3 in the pooled group for propafenone hydrochloride extended-release (0.8%), and 2 in the placebo group (1.6%). In the overall database of 8 trials of propafenone hydrochloride extended-release and propafenone hydrochloride immediate-release, the mortality rate was 2.5% per year on propafenone and 4.0% per year on placebo. Concurrent use of propafenone with other antiarrhythmic agents has not been well studied.
In a U.S. uncontrolled, open-label, multicenter trial using the immediate-release formulation in patients with symptomatic supraventricular tachycardia (SVT), 1.9% (9/474) of these patients experienced ventricular tachycardia (VT) or ventricular fibrillation (VF) during the trial. However, in 4 of the 9 patients, the ventricular tachycardia was of atrial origin. Six of the 9 patients that developed ventricular arrhythmias did so within 14 days of onset of therapy. About 2.3% (11/474) of all patients had recurrence of SVT during the trial which could have been a change in the patients' arrhythmia behavior or could represent a proarrhythmic event. Case reports in patients treated with propafenone for atrial fibrillation/flutter have included increased premature ventricular contractions (PVCs), VT, VF, torsades de pointes, asystole, and death.
Overall in clinical trials with propafenone hydrochloride immediate-release (which included patients treated for ventricular arrhythmias, atrial fibrillation/flutter, and PSVT), 4.7% of all patients had new or worsened ventricular arrhythmia possibly representing a proarrhythmic event (0.7% was an increase in PVCs; 4.0% a worsening or new appearance of VT or VF). Of the patients who had worsening of VT (4%), 92% had a history of VT and/or VT/VF, 71% had coronary artery disease, and 68% had a prior myocardial infarction. The incidence of proarrhythmia in patients with less serious or benign arrhythmias, which include patients with an increase in frequency of PVCs, was 1.6%. Although most proarrhythmic events occurred during the first week of therapy, late events also were seen and the CAST trial [see Boxed Warning: Mortality] suggests that an increased risk of proarrythmia is present throughout treatment.
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
- May cause new or worsened arrhythmias. Evaluate patients via ECG prior to and during therapy. ( 5.1)
- Propafenone hydrochloride extended-release capsules may unmask Brugada or Brugada-like Syndrome. Evaluate patients via ECG after initiation of therapy. ( 4, 5.2)
- Avoid use with other antiarrhythmic agents or drugs that prolong the QT interval. ( 5.3)
- Avoid simultaneous use of propafenone with both a cytochrome P450 2D6 (CYP2D6) inhibitor and a 3A4 inhibitor (CYP3A4). ( 5.4)
- May provoke overt heart failure. ( 5.5)
- May cause dose-related first-degree AV block or other conduction disturbances. Should not be given to patients with conduction defects in absence of a pacemaker. ( 5.6)
- May affect artificial pacemakers. Pacemakers should be monitored during therapy. ( 5.7)
- Agranulocytosis: Patients should report signs of infection. ( 5.8)
- Administer cautiously to patients with impaired hepatic and renal function. ( 5.9, 5.10)
- Exacerbation of myasthenia gravis has been reported. ( 5.11)
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
Propafenone hydrochloride extended-release capsules can be taken with or without food. Do not crush or further divide the contents of the capsule.
The dose of propafenone hydrochloride extended-release capsules must be individually titrated on the basis of response and tolerance. Initiate therapy with propafenone hydrochloride extended-release capsules, USP 225 mg given every 12 hours. Dosage may be increased at a minimum of 5-day intervals to 325 mg given every 12 hours. If additional therapeutic effect is needed, the dose of propafenone hydrochloride extended-release capsules may be increased to 425 mg given every 12 hours.
In patients with hepatic impairment or those with significant widening of the QRS complex or second- or third-degree AV block, consider reducing the dose.
The combination of cytochrome P450 3A4 (CYP3A4) inhibition and either cytochrome P450 2D6 (CYP2D6) deficiency or CYP2D6 inhibition with the simultaneous administration of propafenone may significantly increase the concentration of propafenone and thereby increase the risk of proarrhythmia and other adverse events. Therefore, avoid simultaneous use of propafenone hydrochloride extended-release capsules, USP with both a CYP2D6 inhibitor and a CYP3A4 inhibitor [see Warnings and Precautions (5.4), Drug Interactions (7.1)] .
5.6 Conduction Disturbances
Propafenone slows atrioventricular conduction and may also cause dose-related first-degree AV block. Average PR interval prolongation and increases in QRS duration are also dose-related. Do not give propafenone to patients with atrioventricular and intraventricular conduction defects in the absence of a pacemaker [see Contraindications (4), Clinical Pharmacology (12.2)] .
In a U.S. trial (RAFT) in 523 patients with a history of symptomatic AF treated with propafenone hydrochloride extended-release, sinus bradycardia (rate less than 50 beats/min) was reported with the same frequency with propafenone hydrochloride extended-release and placebo.
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
Propafenone hydrochloride extended-release capsules, USP is supplied as white, opaque, hard gelatin capsules containing either 225 mg, 325 mg, or 425 mg of propafenone hydrochloride.
The 225 mg capsule is printed with "UPSHER-SMITH" over "0740" and "225mg" in black ink.
The 325 mg capsule is printed with "UPSHER-SMITH" over "0741" and "325mg" in black ink.
The 425 mg capsule is printed with "UPSHER-SMITH" over "0742" and "425mg" in black ink.
5.2 Unmasking Brugada Syndrome
Brugada Syndrome may be unmasked after exposure to propafenone hydrochloride extended-release. Perform an ECG after initiation of propafenone hydrochloride extended-release and discontinue the drug if changes are suggestive of Brugada Syndrome [see Contraindications (4)] .
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared with rates in the clinical trials of another drug and may not reflect the rates observed in practice.
The data described below reflect exposure to propafenone hydrochloride extended-release 225 mg twice daily in 126 patients, to propafenone hydrochloride extended-release 325 mg twice daily in 135 patients, to propafenone hydrochloride extended-release 425 mg twice daily in 136 patients, and to placebo in 126 patients for up to 39 weeks (mean: 20 weeks) in a placebo-controlled trial (RAFT) conducted in the U.S. The most commonly reported adverse events with propafenone (greater than 5% and greater than placebo) excluding those not reasonably associated with the use of the drug or because they were associated with the condition being treated, were dizziness, palpitations, chest pain, dyspnea, taste disturbance, nausea, fatigue, anxiety, constipation, upper respiratory tract infection, edema, and influenza. The frequency of discontinuation due to adverse events was 17%, and the rate was highest during the first 14 days of treatment.
Cardiac-related adverse events occurring in greater than or equal to 2% of the patients in any of the RAFT propafenone extended-release treatment groups and more common with propafenone than with placebo, excluding those that are common in the population and those not plausibly related to drug therapy, included the following: angina pectoris, atrial flutter, AV block first- degree, bradycardia, congestive cardiac failure, cardiac murmur, edema, dyspnea, rales, wheezing, and cardioactive drug level above therapeutic.
Propafenone prolongs the PR and QRS intervals in patients with atrial and ventricular arrhythmias. Prolongation of the QRS interval makes it difficult to interpret the effect of propafenone on the QT interval [see Clinical Pharmacology (12.2)] .
Non-cardiac related adverse events occurring in greater than or equal to 2% of the patients in any of the RAFT propafenone extended-release treatment groups and more common with propafenone than with placebo, excluding those that are common in the population and those not plausibly related to drug therapy, included the following: blurred vision, constipation, diarrhea, dry mouth, flatulence, nausea, vomiting, fatigue, weakness, upper respiratory tract infection, blood alkaline phosphatase increased, hematuria, muscle weakness, dizziness (excluding vertigo), headache, taste disturbance, tremor, somnolence, anxiety, depression, ecchymosis.
No clinically important differences in incidence of adverse reactions were noted by age or gender. Too few non-Caucasian patients were enrolled to assess adverse events according to race.
Adverse events occurring in 2% or more of the patients in any of the ERAFT [see Clinical Studies (14)] propafenone extended-release treatment groups and not listed above include the following: bundle branch block left, bundle branch block right, conduction disorders, sinus bradycardia, and hypotension.
Other adverse events reported with propafenone clinical trials not already listed elsewhere in the prescribing information include the following adverse events by body system and preferred term.
Blood and Lymphatic System
Anemia, lymphadenopathy, spleen disorder, thrombocytopenia.
Cardiac
Unstable angina, atrial hypertrophy, cardiac arrest, coronary artery disease, extrasystoles, myocardial infarction, nodal arrhythmia, palpitations, pericarditis, sinoatrial block, sinus arrest, sinus arrhythmia, supraventricular extrasystoles, ventricular extrasystoles, ventricular hypertrophy.
Ear and Labyrinth
Hearing impaired, tinnitus, vertigo.
Eye
Eye hemorrhage, eye inflammation, eyelid ptosis, miosis, retinal disorder, visual acuity reduced.
Gastrointestinal
Abdominal distension, abdominal pain, duodenitis, dyspepsia, dysphagia, eructation, gastritis, gastroesophageal reflux disease, gingival bleeding, glossitis, glossodynia, gum pain, halitosis, intestinal obstruction, melena, mouth ulceration, pancreatitis, peptic ulcer, rectal bleeding, sore throat.
General Disorders and Administration Site Conditions
Chest pain, feeling hot, hemorrhage, malaise, pain, pyrexia.
Hepatobiliary
Hepatomegaly.
Investigations
Abnormal heart sounds, abnormal pulse, carotid bruit, decreased blood chloride, decreased blood pressure, decreased blood sodium, decreased hemoglobin, decreased neutrophil count, decreased platelet count, decreased prothrombin level, decreased red blood cell count, decreased weight, glycosuria present, increased alanine aminotransferase, increased aspartate aminotransferase, increased blood bilirubin, increased blood cholesterol, increased blood creatinine, increased blood glucose, increased blood lactate dehydrogenase, increased blood pressure, increased blood prolactin, increased blood triglycerides, increased blood urea, increased blood uric acid, increased eosinophil count, increased gamma-glutamyltransferase, increased monocyte count, increased prostatic specific antigen, increased prothrombin level, increased weight, increased white blood cell count, ketonuria present, proteinuria present.
Metabolism and Nutrition
Anorexia, dehydration, diabetes mellitus, gout, hypercholesterolemia, hyperglycemia, hyperlipidemia, hypokalemia.
Musculoskeletal, Connective Tissue, and Bone
Arthritis, bursitis, collagen-vascular disease, costochondritis, joint disorder, muscle cramps, muscle spasms, myalgia, neck pain, pain in jaw, sciatica, tendonitis.
Nervous System
Amnesia, ataxia, balance impaired, brain damage, cerebrovascular accident, dementia, gait abnormal, hypertonia, hypothesia, insomnia, paralysis, paresthesia, peripheral neuropathy, speech disorder, syncope, tongue hypoesthesia.
Psychiatric
Decreased libido, emotional disturbance, mental disorder, neurosis, nightmare, sleep disorder.
Renal and Urinary
Dysuria, nocturia, oliguria, pyuria, renal failure, urinary casts, urinary frequency, urinary incontinence, urinary retention, urine abnormal.
Reproductive System and Breast
Breast pain, impotence, prostatism.
Respiratory, Thoracic, and Mediastinal
Atelectasis, breath sounds decreased, chronic obstructive airways disease, cough, epistaxis, hemoptysis, lung disorder, pleural effusion, pulmonary congestion, rales, respiratory failure, rhinitis, throat tightness.
Skin and Subcutaneous Tissue
Alopecia, dermatitis, dry skin, erythema, nail abnormality, petechiae, pruritus, sweating increased, urticaria.
Vascular
Arterial embolism limb, deep limb venous thrombosis, flushing, hematoma, hypertension, hypertensive crisis, hypotension, labile blood pressure, pallor, peripheral coldness, peripheral vascular disease, thrombosis.
7.1 Cyp2d6 and Cyp3a4 Inhibitors (7.1 CYP2D6 and CYP3A4 Inhibitors)
Drugs that inhibit CYP2D6 (such as desipramine, paroxetine, ritonavir, sertraline) and CYP3A4 (such as ketoconazole, ritonavir, saquinavir, erythromycin, and grapefruit juice) can be expected to cause increased plasma levels of propafenone. The combination of CYP3A4 inhibition and either CYP2D6 deficiency or CYP2D6 inhibition with administration of propafenone may increase the risk of adverse reactions, including proarrhythmia. Therefore, simultaneous use of propafenone hydrochloride extended-release with both a CYP2D6 inhibitor and a CYP3A4 inhibitor should be avoided [see Warnings and Precautions (5.4), Dosage and Administration (2)] .
Amiodarone
Concomitant administration of propafenone and amiodarone can affect conduction and repolarization and is not recommended.
Cimetidine
Concomitant administration of propafenone immediate-release tablets and cimetidine in 12 healthy subjects resulted in a 20% increase in steady-state plasma concentrations of propafenone.
Fluoxetine
Concomitant administration of propafenone and fluoxetine in extensive metabolizers increased the S-propafenone C maxand AUC by 39% and 50%, respectively, and the R-propafenone C maxand AUC by 71% and 50%, respectively.
Quinidine
Small doses of quinidine completely inhibit the CYP2D6 hydroxylation metabolic pathway, making all patients, in effect, slow metabolizers [see Clinical Pharmacology (12.3)] . Concomitant administration of quinidine (50 mg 3 times daily) with 150-mg immediate-release propafenone 3 times daily decreased the clearance of propafenone by 60% in extensive metabolizers, making them poor metabolizers. Steady-state plasma concentrations increased by more than 2-fold for propafenone and decreased 50% for 5-OH-propafenone. A 100-mg dose of quinidine increased steady-state concentrations of propafenone 3-fold. Avoid concomitant use of propafenone and quinidine.
Rifampin
Concomitant administration of rifampin and propafenone in extensive metabolizers decreased the plasma concentrations of propafenone by 67% with a corresponding decrease of 5-OH-propafenone by 65%. The concentrations of norpropafenone increased by 30%. In poor metabolizers, there was a 50% decrease in propafenone plasma concentrations and an increase in the AUC and C maxof norpropafenone by 74% and 20%, respectively. Urinary excretion of propafenone and its metabolites decreased significantly. Similar results were noted in elderly patients: Both the AUC and C maxof propafenone decreased by 84%, with a corresponding decrease in AUC and C maxof 5-OH-propafenone by 69% and 57%, respectively.
17 Patient Counseling Information (17 PATIENT COUNSELING INFORMATION)
Advise the patient to read the FDA-approved patient labeling (Patient Information).
- Instruct patients to notify their healthcare providers of any change in over-the-counter, prescription, and supplement use.
- Instruct patients to report symptoms that may be associated with altered electrolyte balance, such as excessive or prolonged diarrhea, sweating, vomiting, or loss of appetite or thirst.
- Instruct patients not to double the next dose if a dose is missed. The next dose should be taken at the usual time.
5.7 Effects On Pacemaker Threshold (5.7 Effects on Pacemaker Threshold)
Propafenone may alter both pacing and sensing thresholds of implanted pacemakers and defibrillators. During and after therapy, monitor and re-program these devices accordingly.
16 How Supplied/storage and Handling (16 HOW SUPPLIED/STORAGE AND HANDLING)
Propafenone hydrochloride extended-release capsules, USP are supplied as white, opaque, hard gelatin capsules containing either 225 mg, 325 mg, or 425 mg of propafenone hydrochloride.
The 225 mg capsule is printed with "UPSHER-SMITH" over "0740" and "225mg" in black ink. Supplied as follows:
| Bottles of 60 capsules | NDC 0832-0740-60 |
The 325 mg capsule is printed with "UPSHER-SMITH" over "0741" and "325mg" in black ink. Supplied as follows:
| Bottles of 60 capsules | NDC 0832-0741-60 |
The 425 mg capsule is printed with "UPSHER-SMITH" over "0742" and "425mg" in black ink. Supplied as follows:
| Bottles of 60 capsules | NDC 0832-0742-60 |
13.2 Animal Toxicology And/or Pharmacology (13.2 Animal Toxicology and/or Pharmacology)
Renal changes have been observed in the rat following 6 months of oral administration of propafenone hydrochloride at doses of 180 and 360 mg/kg/day (about 2 and 4 times, respectively, the MRHD on a mg/m 2basis). Both inflammatory and non-inflammatory changes in the renal tubules, with accompanying interstitial nephritis, were observed. These changes were reversible, as they were not found in rats allowed to recover for 6 weeks. Fatty degenerative changes of the liver were found in rats following longer durations of administration of propafenone hydrochloride at a dose of 270 mg/kg/day (about 3 times the MRHD on a mg/m 2basis). There were no renal or hepatic changes at 90 mg/kg/day equivalent to the MRHD on a mg/m 2basis).
5.10 Use in Patients With Renal Dysfunction (5.10 Use in Patients with Renal Dysfunction)
Approximately 50% of propafenone metabolites are excreted in the urine following administration of propafenone hydrochloride immediate-release tablets. No trials have been performed to assess the percentage of metabolites eliminated in the urine following the administration of propafenone hydrochloride extended-release capsules.
In patients with impaired renal function, monitor for signs of overdosage [see Overdosage (10)] .
5.11 Use in Patients With Myasthenia Gravis (5.11 Use in Patients with Myasthenia Gravis)
Exacerbation of myasthenia gravis has been reported during propafenone therapy.
5.9 Use in Patients With Hepatic Dysfunction (5.9 Use in Patients with Hepatic Dysfunction)
Propafenone is highly metabolized by the liver. Severe liver dysfunction increases the bioavailability of propafenone to approximately 70% compared with 3% to 40% in patients with normal liver function when given propafenone hydrochloride immediate-release tablets. In 8 patients with moderate to severe liver disease administered propafenone hydrochloride immediate-release tablets, the mean half-life was approximately 9 hours. No trials have compared bioavailability of propafenone from propafenone hydrochloride extended-release capsules in patients with normal and impaired hepatic function. Increased bioavailability of propafenone in these patients may result in excessive accumulation. Carefully monitor patients with impaired hepatic function for excessive pharmacological effects [see Overdosage (10)] .
5.5 Use in Patients With A History of Heart Failure (5.5 Use in Patients with a History of Heart Failure)
Propafenone exerts a negative inotropic activity on the myocardium as well as beta-blockade effects and may provoke overt heart failure. In the U.S. trial (RAFT) in patients with symptomatic AF, heart failure was reported in 4 (1.0%) patients receiving propafenone hydrochloride extended-release (all doses) compared with 1 (0.8%) patient receiving placebo. Proarrhythmic effects more likely occur when propafenone is administered to patients with heart failure (NYHA III and IV) or severe myocardial ischemia [see Contraindications (4)] .
In clinical trial experience with propafenone hydrochloride immediate-release, new or worsened congestive heart failure has been reported in 3.7% of patients with ventricular arrhythmia. These events were more likely in subjects with pre-existing heart failure and coronary artery disease. New onset of heart failure attributable to propafenone developed in less than 0.2% of patients with ventricular arrhythmia and in 1.9% of patients with paroxysmal AF or PSVT.
Principal Display Panel 225 Mg Capsule Bottle Label (PRINCIPAL DISPLAY PANEL - 225 mg Capsule Bottle Label)
NDC 0832-0740-60
Propafenone
Hydrochloride
Extended-Release
Capsules, USP
225 mg
60 Capsules
Rx only
UPSHER-SMITH
Principal Display Panel 325 Mg Capsule Bottle Label (PRINCIPAL DISPLAY PANEL - 325 mg Capsule Bottle Label)
NDC 0832-0741-60
Propafenone
Hydrochloride
Extended-Release
Capsules, USP
325 mg
60 Capsules
Rx only
UPSHER-SMITH
Principal Display Panel 425 Mg Capsule Bottle Label (PRINCIPAL DISPLAY PANEL - 425 mg Capsule Bottle Label)
NDC 0832-0742-60
Propafenone
Hydrochloride
Extended-Release
Capsules, USP
425 mg
60 Capsules
Rx only
UPSHER-SMITH
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Lifetime maximally tolerated oral dose studies in mice (up to 360 mg/kg/day, approximately twice the MRHD on a mg/m 2basis) and rats (up to 270 mg/kg/day, approximately 3 times the MRHD on a mg/m 2basis) provided no evidence of a carcinogenic potential for propafenone.
Propafenone was not mutagenic in the Ames (salmonella) test and the in vivomouse dominant lethal test. Propafenone was not clastogenic in the human lymphocyte chromosome aberration assay in vitro, the rat and Chinese hamster micronucleus tests, and other in vivotests for chromosomal aberrations in rat bone marrow and Chinese hamster bone marrow and spermatogonia.
Propafenone, administered intravenously, has been shown to decrease spermatogenesis at lethal doses in rabbits (≥3.5 mg/kg/day) or at near-lethal dose levels in monkeys and dogs (≤5 mg/kg/day); doses were less than the MRHD on a mg/m 2basis. These effects were reversible and did not impair fertility in rabbits at an intravenous dose of 3.5 mg/kg/day (a spermatogenesis-impairing dose). Effects on spermatogenesis were not found when propafenone was administered to rats either orally or intravenously up to 360 mg/kg/day or 6 mg/kg/day, respectively, or in dogs at oral doses up to 240 mg/kg/day (up to approximately 4 or 9 times the MRHD on a mg/m2 basis in rats and dogs, respectively). Treatment of male rabbits for 10 weeks prior to mating at an oral dose of 120 mg/kg/day (approximately 2 times the MRHD on a mg/m 2basis) did not result in evidence of impaired fertility. Nor was there evidence of impaired fertility when propafenone was administered orally to male and female rats at dose levels up to 270 mg/kg/day (approximately 3 times the MRHD on a mg/m 2basis) for 10 weeks (males) or 2 weeks (females) prior to mating through mating.
5.3 Use With Drugs That Prolong the Qt Interval and Antiarrhythmic Agents (5.3 Use with Drugs that Prolong the QT Interval and Antiarrhythmic Agents)
The use of propafenone hydrochloride extended-release in conjunction with other drugs that prolong the QT interval has not been extensively studied. Such drugs may include many antiarrhythmics, some phenothiazines, tricyclic antidepressants, and oral macrolides. Withhold Class IA and III antiarrhythmic agents for at least 5 half-lives prior to dosing with propafenone hydrochloride extended-release. Avoid the use of propafenone with Class IA and III antiarrhythmic agents (including quinidine and amiodarone). There is only limited experience with the concomitant use of Class IB or IC antiarrhythmics.
5.4 Drug Interactions: Simultaneous Use With Inhibitors of Cytochrome P450 Isoenzymes 2d6 and 3a4 (5.4 Drug Interactions: Simultaneous Use with Inhibitors of Cytochrome P450 Isoenzymes 2D6 and 3A4)
Propafenone is metabolized by CYP2D6, CYP3A4, and CYP1A2 isoenzymes. Approximately 6% of Caucasians in the U.S. population are naturally deficient in CYP2D6 activity and other demographic groups are deficient to a somewhat lesser extent. Drugs that inhibit these CYP pathways (such as desipramine, paroxetine, ritonavir, sertraline for CYP2D6; ketoconazole, erythromycin, saquinavir, and grapefruit juice for CYP3A4; and amiodarone and tobacco smoke for CYP1A2) can be expected to cause increased plasma levels of propafenone.
Increased exposure to propafenone may lead to cardiac arrhythmias and exaggerated beta-adrenergic blocking activity. Because of its metabolism, the combination of CYP3A4 inhibition and either CYP2D6 deficiency or CYP2D6 inhibition in users of propafenone is potentially hazardous. Therefore, avoid simultaneous use of propafenone hydrochloride extended-release with both a CYP2D6 inhibitor and a CYP3A4 inhibitor.
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:51:06.661007 · Updated: 2026-03-14T22:39:21.707817