Vytorin
89b860d2-de83-468e-b7e8-76aeec2edca2
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Indications and Usage
VYTORIN VYTORIN ® is a combination of simvastatin and ezetimibe indicated: As an adjunct to diet to reduce elevated low density lipoprotein cholesterol (LDL-C): In adults with primary hyperlipidemia. In adults and pediatric patients aged 10 years and older with heterozygous familial hypercholesterolemia (HeFH). As an adjunct to other LDL-C-lowering therapies to reduce elevated LDL-C in adults with homozygous familial hypercholesterolemia (HoFH). Simvastatin Simvastatin, when used as a component of VYTORIN, is indicated to reduce the risk of total mortality by reducing risk of coronary heart disease death, non-fatal myocardial infarction and stroke, and the need for coronary and non-coronary revascularization procedures in adults with established coronary heart disease, cerebrovascular disease, peripheral vascular disease, and/or diabetes, who are at high risk of coronary heart disease events.
Dosage and Administration
Important Dosage and Administration Information: ( 2.1 ) Take VYTORIN orally once daily in the evening with or without food. Maximum recommended dosage is VYTORIN 10/40 mg once daily. VYTORIN 10/80 mg daily dosage is restricted to patients who have been taking VYTORIN 10/80 mg daily chronically (e.g., for 12 months or more) without evidence of muscle toxicity. For patients that require a high-intensity statin or are unable to achieve their LDL-C goal receiving VYTORIN 10/40 mg daily, prescribe alternative LDL-C-lowering treatment. If as dose is missed, take the missed dose as soon as possible. Do not double the next dose. Assess LDL-C when clinically appropriate, as early as 2 weeks after initiating VYTORIN, and adjust the dosage if necessary. Adults: Recommended dosage range of 10/10 mg to 10/40 mg once daily. ( 2.2 ) See full prescribing information for VYTORIN dosage modifications due to drug interactions. ( 2.3 ) Patients with Renal Impairment: Doses exceeding 10/20 mg should be used with caution and close monitoring in patients with moderate to severe renal impairment. ( 2.4 )
Contraindications
VYTORIN is contraindicated in the following conditions: Concomitant use of strong CYP3A4 inhibitors (select azole anti-fungals, macrolide antibiotics, anti-viral medications, and nefazodone) [see Drug Interactions (7.1) ] . Concomitant use of cyclosporine, danazol, or danazol [see Drug Interactions (7.1) ] . Acute liver failure or decompensated cirrhosis [see Warnings and Precautions (5.3) ] . Hypersensitivity to simvastatin, ezetimibe, or any excipients in VYTORIN. Hypersensitivity reactions, including anaphylaxis, angioedema, and Stevens-Johnson syndrome, have been reported [see Adverse Reactions (6.2) ] .
Warnings and Precautions
Myopathy and Rhabdomyolysis: Risk factors include age 65 years or greater, uncontrolled hypothyroidism, renal impairment, concomitant use with certain other drugs, and higher VYTORIN dosage. Chinese patients may be at higher risk for myopathy. Discontinue VYTORIN if markedly elevated CK levels occur or myopathy is diagnosed or suspected. Temporarily discontinue VYTORIN in patients experiencing an acute or serious condition at high risk of developing renal failure secondary to rhabdomyolysis. Inform patients of the risk of myopathy and rhabdomyolysis when starting or increasing VYTORIN dosage. Instruct patients to promptly report unexplained muscle pain, tenderness, or weakness, particularly if accompanied by malaise or fever. ( 5.1 ) Immune-Mediated Necrotizing Myopathy (IMNM): Rare reports of IMNM, an autoimmune myopathy, have been reported. Discontinue VYTORIN if IMNM is suspected. ( 5.2 ) Hepatic Dysfunction: Increases in serum transaminases have occurred, some persistent. Rare reports of fatal and non-fatal hepatic failure have occurred. Consider testing liver enzyme before initiating therapy and as clinically indicated thereafter. If serious hepatic injury with clinical symptoms and/or hyperbilirubinemia or jaundice occurs, promptly discontinue VYTORIN. ( 5.3 )
Adverse Reactions
The following serious adverse reactions are discussed in greater detail in other sections of the label: Myopathy and Rhabdomyolysis [see Warnings and Precautions (5.1) ] Immune-Mediated Necrotizing Myopathy [see Warnings and Precautions (5.2) ] Hepatic Dysfunction [see Warnings and Precautions (5.3) ] Increases in HbA1c and Fasting Serum Glucose Levels [see Warnings and Precautions (5.4) ]
Drug Interactions
VYTORIN is a substrate of CYP3A4 and of the transport protein OATP1B1. VYTORIN plasma levels can be significantly increased with concomitant administration of inhibitors of CYP3A4 and OATP1B1. Table 2 includes a list of drugs that increase the risk of myopathy and rhabdomyolysis when used concomitantly with VYTORIN and instructions for preventing or managing them [see Warnings and Precautions (5.1) and Clinical Pharmacology (12.3) ] . Table 2: Drug Interactions that Increase the Risk of Myopathy and Rhabdomyolysis with VYTORIN Strong CYP3A4 inhibitors Clinical Impact: Simvastatin is a substrate of CYP3A4. Concomitant use of strong CYP3A4 inhibitors with VYTORIN increases simvastatin exposure and increases the risk of myopathy and rhabdomyolysis, particularly with higher VYTORIN dosages. Intervention: Concomitant use of strong CYP3A4 inhibitors with VYTORIN is contraindicated [see Contraindications (4) ] . If treatment with a CYP3A4 inhibitor is unavoidable, suspend VYTORIN during the course of strong CYP3A4 inhibitor treatment. Examples: Select azole anti-fungals (e.g., itraconazole, ketoconazole, posaconazole, and voriconazole), select macrolide antibiotics (e.g., erythromycin and clarithromycin, telithromycin), select HIV protease inhibitors (e.g., nelfinavir, ritonavir, and darunavir/ritonavir), select HCV protease inhibitors (e.g., boceprevir and telaprevir), cobicistat-containing products, and nefazodone. Cyclosporine, Danazol, or Gemfibrozil Clinical Impact: The risk of myopathy and rhabdomyolysis is increased with concomitant use of cyclosporine, danazol, or gemfibrozil with VYTORIN. Gemfibrozil may cause myopathy when given alone. Intervention: Concomitant use of cyclosporine, danazol, or gemfibrozil with VYTORIN is contraindicated [see Contraindications (4) ] . Amiodarone, Dronedarone, Ranolazine, or Calcium Channel Blockers Clinical Impact: The risk of myopathy and rhabdomyolysis is increased by concomitant use of amiodarone, dronedarone, ranolazine, or calcium channel blockers with VYTORIN. Intervention: For patients taking verapamil, diltiazem, or dronedarone, do not exceed VYTORIN 10/10 mg daily. For patients taking amiodarone, amlodipine, or ranolazine, do not exceed VYTORIN 10/20 mg daily [see Dosage and Administration (2.3) ] . Lomitapide Clinical Impact: Simvastatin exposure is approximately doubled with concomitant use of lomitapide and the risk of myopathy and rhabdomyolysis is increased. Intervention: Reduce the dose of VYTORIN by 50% if initiating lomitapide. Do not exceed VYTORIN 10/20 mg daily (or VYTORIN 10/40 mg daily for patients who have previously taken VYTORIN 10/80 mg daily chronically) while taking lomitapide [see Dosage and Administration (2.1 , 2.3) ] . Daptomycin Clinical Impact: Cases of rhabdomyolysis have been reported with simvastatin administered with daptomycin. Both VYTORIN and daptomycin can cause myopathy and rhabdomyolysis when given alone and the risk of myopathy and rhabdomyolysis may be increased by coadministration. Intervention: If treatment with daptomycin is required, consider temporarily suspending VYTORIN during the course of daptomycin treatment. Niacin Clinical Impact: Cases of myopathy and rhabdomyolysis have been observed with concomitant use of lipid modifying dosages of niacin-containing products (≥1 gram/day niacin) with VYTORIN. The risk of myopathy is greater in Chinese patients. In a clinical trial (median follow-up 3.9 years) of patients at high risk of CVD and with well-controlled LDL-C levels on simvastatin 40 mg/day with or without ezetimibe 10 mg/day, there was no incremental benefit on cardiovascular outcomes with the addition of lipid-modifying doses of niacin Intervention: Concomitant use of VYTORIN with lipid-modifying dosages of niacin is not recommended in Chinese patients [see Use in Specific Populations (8.8) ] . For non-Chinese patients, consider if the benefit of using lipid-modifying doses of niacin concomitantly with VYTORIN outweighs the increased risk of myopathy and rhabdomyolysis. If concomitant use is decided, monitor patients for signs and symptoms of myopathy, particularly during initiation of therapy and during upward dose titration of either drug. Fibrates (other than Gemfibrozil) Clinical Impact: Fibrates may cause myopathy when given alone. The risk of myopathy and rhabdomyolysis is increased with concomitant use of fibrates with VYTORIN. Intervention: Consider if the benefit of using fibrates concomitantly with VYTORIN outweighs the increased risk of myopathy and rhabdomyolysis. If concomitant use is decided, monitor patients for signs and symptoms of myopathy, particularly during initiation of therapy and during upward dose titration of either drug. Colchicine Clinical Impact: Cases of myopathy and rhabdomyolysis have been reported with concomitant use of colchicine with VYTORIN. Intervention: Consider if the benefit of using colchicine concomitantly with VYTORIN outweighs the increased risk of myopathy and rhabdomyolysis. If concomitant use is decided, monitor patients for signs and symptoms of myopathy, particularly during initiation of therapy and during upward dose titration of either drug. Grapefruit Juice Clinical Impact: Grapefruit juice can raise the plasma levels of simvastatin and may increase the risk of myopathy and rhabdomyolysis. Intervention: Avoid grapefruit juice when taking VYTORIN.
How Supplied
VYTORIN tablets are supplied as follows: Strength How Supplied NDC Tablet Description 10/10 mg unit of use bottles of 30 78206-174-01 white to off-white capsule-shaped tablets with code “311” on one side unit of use bottles of 90 78206-174-02 10/20 mg unit of use bottles of 30 78206-175-01 white to off-white capsule-shaped tablets with code “312” on one side unit of use bottles of 90 78206-175-02 10/40 mg unit of use bottles of 30 78206-176-01 white to off-white capsule-shaped tablets with code “313” on one side unit of use bottles of 90 78206-176-02 10/80 mg unit of use bottles of 30 78206-177-01 white to off-white capsule-shaped tablets with code “315” on one side unit of use bottles of 90 78206-177-02
Storage and Handling
VYTORIN tablets are supplied as follows: Strength How Supplied NDC Tablet Description 10/10 mg unit of use bottles of 30 78206-174-01 white to off-white capsule-shaped tablets with code “311” on one side unit of use bottles of 90 78206-174-02 10/20 mg unit of use bottles of 30 78206-175-01 white to off-white capsule-shaped tablets with code “312” on one side unit of use bottles of 90 78206-175-02 10/40 mg unit of use bottles of 30 78206-176-01 white to off-white capsule-shaped tablets with code “313” on one side unit of use bottles of 90 78206-176-02 10/80 mg unit of use bottles of 30 78206-177-01 white to off-white capsule-shaped tablets with code “315” on one side unit of use bottles of 90 78206-177-02
Description
Indications and Usage ( 1 ) 2/2024 Dosage and Administration ( 2.1 , 2.2 , 2.3 , 2.4 , 2.5 ) 2/2024 Contraindications, Pregnancy and Lactation ( 4 ) Removed 2/2024 Warnings and Precautions ( 5.1 , 5.2 , 5.3 ) 2/2024
Medication Information
Warnings and Precautions
Myopathy and Rhabdomyolysis: Risk factors include age 65 years or greater, uncontrolled hypothyroidism, renal impairment, concomitant use with certain other drugs, and higher VYTORIN dosage. Chinese patients may be at higher risk for myopathy. Discontinue VYTORIN if markedly elevated CK levels occur or myopathy is diagnosed or suspected. Temporarily discontinue VYTORIN in patients experiencing an acute or serious condition at high risk of developing renal failure secondary to rhabdomyolysis. Inform patients of the risk of myopathy and rhabdomyolysis when starting or increasing VYTORIN dosage. Instruct patients to promptly report unexplained muscle pain, tenderness, or weakness, particularly if accompanied by malaise or fever. ( 5.1 ) Immune-Mediated Necrotizing Myopathy (IMNM): Rare reports of IMNM, an autoimmune myopathy, have been reported. Discontinue VYTORIN if IMNM is suspected. ( 5.2 ) Hepatic Dysfunction: Increases in serum transaminases have occurred, some persistent. Rare reports of fatal and non-fatal hepatic failure have occurred. Consider testing liver enzyme before initiating therapy and as clinically indicated thereafter. If serious hepatic injury with clinical symptoms and/or hyperbilirubinemia or jaundice occurs, promptly discontinue VYTORIN. ( 5.3 )
Indications and Usage
VYTORIN VYTORIN ® is a combination of simvastatin and ezetimibe indicated: As an adjunct to diet to reduce elevated low density lipoprotein cholesterol (LDL-C): In adults with primary hyperlipidemia. In adults and pediatric patients aged 10 years and older with heterozygous familial hypercholesterolemia (HeFH). As an adjunct to other LDL-C-lowering therapies to reduce elevated LDL-C in adults with homozygous familial hypercholesterolemia (HoFH). Simvastatin Simvastatin, when used as a component of VYTORIN, is indicated to reduce the risk of total mortality by reducing risk of coronary heart disease death, non-fatal myocardial infarction and stroke, and the need for coronary and non-coronary revascularization procedures in adults with established coronary heart disease, cerebrovascular disease, peripheral vascular disease, and/or diabetes, who are at high risk of coronary heart disease events.
Dosage and Administration
Important Dosage and Administration Information: ( 2.1 ) Take VYTORIN orally once daily in the evening with or without food. Maximum recommended dosage is VYTORIN 10/40 mg once daily. VYTORIN 10/80 mg daily dosage is restricted to patients who have been taking VYTORIN 10/80 mg daily chronically (e.g., for 12 months or more) without evidence of muscle toxicity. For patients that require a high-intensity statin or are unable to achieve their LDL-C goal receiving VYTORIN 10/40 mg daily, prescribe alternative LDL-C-lowering treatment. If as dose is missed, take the missed dose as soon as possible. Do not double the next dose. Assess LDL-C when clinically appropriate, as early as 2 weeks after initiating VYTORIN, and adjust the dosage if necessary. Adults: Recommended dosage range of 10/10 mg to 10/40 mg once daily. ( 2.2 ) See full prescribing information for VYTORIN dosage modifications due to drug interactions. ( 2.3 ) Patients with Renal Impairment: Doses exceeding 10/20 mg should be used with caution and close monitoring in patients with moderate to severe renal impairment. ( 2.4 )
Contraindications
VYTORIN is contraindicated in the following conditions: Concomitant use of strong CYP3A4 inhibitors (select azole anti-fungals, macrolide antibiotics, anti-viral medications, and nefazodone) [see Drug Interactions (7.1) ] . Concomitant use of cyclosporine, danazol, or danazol [see Drug Interactions (7.1) ] . Acute liver failure or decompensated cirrhosis [see Warnings and Precautions (5.3) ] . Hypersensitivity to simvastatin, ezetimibe, or any excipients in VYTORIN. Hypersensitivity reactions, including anaphylaxis, angioedema, and Stevens-Johnson syndrome, have been reported [see Adverse Reactions (6.2) ] .
Adverse Reactions
The following serious adverse reactions are discussed in greater detail in other sections of the label: Myopathy and Rhabdomyolysis [see Warnings and Precautions (5.1) ] Immune-Mediated Necrotizing Myopathy [see Warnings and Precautions (5.2) ] Hepatic Dysfunction [see Warnings and Precautions (5.3) ] Increases in HbA1c and Fasting Serum Glucose Levels [see Warnings and Precautions (5.4) ]
Drug Interactions
VYTORIN is a substrate of CYP3A4 and of the transport protein OATP1B1. VYTORIN plasma levels can be significantly increased with concomitant administration of inhibitors of CYP3A4 and OATP1B1. Table 2 includes a list of drugs that increase the risk of myopathy and rhabdomyolysis when used concomitantly with VYTORIN and instructions for preventing or managing them [see Warnings and Precautions (5.1) and Clinical Pharmacology (12.3) ] . Table 2: Drug Interactions that Increase the Risk of Myopathy and Rhabdomyolysis with VYTORIN Strong CYP3A4 inhibitors Clinical Impact: Simvastatin is a substrate of CYP3A4. Concomitant use of strong CYP3A4 inhibitors with VYTORIN increases simvastatin exposure and increases the risk of myopathy and rhabdomyolysis, particularly with higher VYTORIN dosages. Intervention: Concomitant use of strong CYP3A4 inhibitors with VYTORIN is contraindicated [see Contraindications (4) ] . If treatment with a CYP3A4 inhibitor is unavoidable, suspend VYTORIN during the course of strong CYP3A4 inhibitor treatment. Examples: Select azole anti-fungals (e.g., itraconazole, ketoconazole, posaconazole, and voriconazole), select macrolide antibiotics (e.g., erythromycin and clarithromycin, telithromycin), select HIV protease inhibitors (e.g., nelfinavir, ritonavir, and darunavir/ritonavir), select HCV protease inhibitors (e.g., boceprevir and telaprevir), cobicistat-containing products, and nefazodone. Cyclosporine, Danazol, or Gemfibrozil Clinical Impact: The risk of myopathy and rhabdomyolysis is increased with concomitant use of cyclosporine, danazol, or gemfibrozil with VYTORIN. Gemfibrozil may cause myopathy when given alone. Intervention: Concomitant use of cyclosporine, danazol, or gemfibrozil with VYTORIN is contraindicated [see Contraindications (4) ] . Amiodarone, Dronedarone, Ranolazine, or Calcium Channel Blockers Clinical Impact: The risk of myopathy and rhabdomyolysis is increased by concomitant use of amiodarone, dronedarone, ranolazine, or calcium channel blockers with VYTORIN. Intervention: For patients taking verapamil, diltiazem, or dronedarone, do not exceed VYTORIN 10/10 mg daily. For patients taking amiodarone, amlodipine, or ranolazine, do not exceed VYTORIN 10/20 mg daily [see Dosage and Administration (2.3) ] . Lomitapide Clinical Impact: Simvastatin exposure is approximately doubled with concomitant use of lomitapide and the risk of myopathy and rhabdomyolysis is increased. Intervention: Reduce the dose of VYTORIN by 50% if initiating lomitapide. Do not exceed VYTORIN 10/20 mg daily (or VYTORIN 10/40 mg daily for patients who have previously taken VYTORIN 10/80 mg daily chronically) while taking lomitapide [see Dosage and Administration (2.1 , 2.3) ] . Daptomycin Clinical Impact: Cases of rhabdomyolysis have been reported with simvastatin administered with daptomycin. Both VYTORIN and daptomycin can cause myopathy and rhabdomyolysis when given alone and the risk of myopathy and rhabdomyolysis may be increased by coadministration. Intervention: If treatment with daptomycin is required, consider temporarily suspending VYTORIN during the course of daptomycin treatment. Niacin Clinical Impact: Cases of myopathy and rhabdomyolysis have been observed with concomitant use of lipid modifying dosages of niacin-containing products (≥1 gram/day niacin) with VYTORIN. The risk of myopathy is greater in Chinese patients. In a clinical trial (median follow-up 3.9 years) of patients at high risk of CVD and with well-controlled LDL-C levels on simvastatin 40 mg/day with or without ezetimibe 10 mg/day, there was no incremental benefit on cardiovascular outcomes with the addition of lipid-modifying doses of niacin Intervention: Concomitant use of VYTORIN with lipid-modifying dosages of niacin is not recommended in Chinese patients [see Use in Specific Populations (8.8) ] . For non-Chinese patients, consider if the benefit of using lipid-modifying doses of niacin concomitantly with VYTORIN outweighs the increased risk of myopathy and rhabdomyolysis. If concomitant use is decided, monitor patients for signs and symptoms of myopathy, particularly during initiation of therapy and during upward dose titration of either drug. Fibrates (other than Gemfibrozil) Clinical Impact: Fibrates may cause myopathy when given alone. The risk of myopathy and rhabdomyolysis is increased with concomitant use of fibrates with VYTORIN. Intervention: Consider if the benefit of using fibrates concomitantly with VYTORIN outweighs the increased risk of myopathy and rhabdomyolysis. If concomitant use is decided, monitor patients for signs and symptoms of myopathy, particularly during initiation of therapy and during upward dose titration of either drug. Colchicine Clinical Impact: Cases of myopathy and rhabdomyolysis have been reported with concomitant use of colchicine with VYTORIN. Intervention: Consider if the benefit of using colchicine concomitantly with VYTORIN outweighs the increased risk of myopathy and rhabdomyolysis. If concomitant use is decided, monitor patients for signs and symptoms of myopathy, particularly during initiation of therapy and during upward dose titration of either drug. Grapefruit Juice Clinical Impact: Grapefruit juice can raise the plasma levels of simvastatin and may increase the risk of myopathy and rhabdomyolysis. Intervention: Avoid grapefruit juice when taking VYTORIN.
Storage and Handling
VYTORIN tablets are supplied as follows: Strength How Supplied NDC Tablet Description 10/10 mg unit of use bottles of 30 78206-174-01 white to off-white capsule-shaped tablets with code “311” on one side unit of use bottles of 90 78206-174-02 10/20 mg unit of use bottles of 30 78206-175-01 white to off-white capsule-shaped tablets with code “312” on one side unit of use bottles of 90 78206-175-02 10/40 mg unit of use bottles of 30 78206-176-01 white to off-white capsule-shaped tablets with code “313” on one side unit of use bottles of 90 78206-176-02 10/80 mg unit of use bottles of 30 78206-177-01 white to off-white capsule-shaped tablets with code “315” on one side unit of use bottles of 90 78206-177-02
How Supplied
VYTORIN tablets are supplied as follows: Strength How Supplied NDC Tablet Description 10/10 mg unit of use bottles of 30 78206-174-01 white to off-white capsule-shaped tablets with code “311” on one side unit of use bottles of 90 78206-174-02 10/20 mg unit of use bottles of 30 78206-175-01 white to off-white capsule-shaped tablets with code “312” on one side unit of use bottles of 90 78206-175-02 10/40 mg unit of use bottles of 30 78206-176-01 white to off-white capsule-shaped tablets with code “313” on one side unit of use bottles of 90 78206-176-02 10/80 mg unit of use bottles of 30 78206-177-01 white to off-white capsule-shaped tablets with code “315” on one side unit of use bottles of 90 78206-177-02
Description
Indications and Usage ( 1 ) 2/2024 Dosage and Administration ( 2.1 , 2.2 , 2.3 , 2.4 , 2.5 ) 2/2024 Contraindications, Pregnancy and Lactation ( 4 ) Removed 2/2024 Warnings and Precautions ( 5.1 , 5.2 , 5.3 ) 2/2024
Section 42229-5
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
VYTORIN
In the VYTORIN (ezetimibe and simvastatin) placebo-controlled clinical trials database of 1420 patients (age range 20-83 years, 52% female, 87% White, 3% Black or African American, 3% Asians, 5% other races identified as Hispanic or Latino ethnicity) with a median treatment duration of 27 weeks, 5% of patients on VYTORIN and 2.2% of patients on placebo discontinued due to adverse reactions.
The most commonly reported adverse reactions (incidence ≥2% and greater than placebo) in controlled clinical trials were: headache (5.8%), increased ALT (3.7%), myalgia (3.6%), upper respiratory tract infection (3.6%), and diarrhea (2.8%). The most common adverse reactions in the group treated with VYTORIN that led to treatment discontinuation and occurred at a rate greater than placebo were: increased ALT (0.9%), myalgia (0.6%), increased AST (0.4%), and back pain (0.4%).
VYTORIN has been evaluated for safety in more than 10,189 patients in clinical trials.
Table 1 summarizes the frequency of clinical adverse reactions reported in ≥2% of patients treated with VYTORIN (n=1420) and at an incidence greater than placebo from four placebo-controlled trials.
| % Placebo N = 371 |
% Ezetimibe 10 mg N = 302 |
% Simvastatin All doses.
N = 1234 |
% VYTORIN
N = 1420 |
|
|---|---|---|---|---|
| Headache | 5.4 | 6.0 | 5.9 | 5.8 |
| Upper respiratory tract infection | 2.7 | 5.0 | 5.0 | 3.6 |
| Myalgia | 2.4 | 2.3 | 2.6 | 3.6 |
| Diarrhea | 2.2 | 5.0 | 3.7 | 2.8 |
| Pain in extremity | 1.3 | 3.0 | 2.0 | 2.3 |
| Influenza | 0.8 | 1.0 | 1.9 | 2.3 |
Section 42230-3
| This Patient Information has been approved by the U.S. Food and Drug Administration. | Revised: 2/2024 |
|
PATIENT INFORMATION VYTORIN® [VI-tor-in] (ezetimibe and simvastatin) tablets, for oral use |
|
| Read this Information carefully before you start taking VYTORIN® and each time you get a VYTORIN. There may be new information. This information does not take the place of talking with your healthcare provider about your medical condition or your treatment. If you have any questions about VYTORIN, ask your healthcare provider. Only your healthcare provider can determine if VYTORIN is right for you. | |
|
What is VYTORIN? VYTORIN is a prescription medicine that contains the cholesterol lowering medicines, simvastatin and ezetimibe:
The safety and effectiveness of VYTORIN has not been established in children younger than 10 years of age with inherited heterozygous familial hypercholesterolemia (HeFH) or other types of hyperlipidemia. |
|
Do not take VYTORIN if you:
Ask your healthcare provider or pharmacist if you are not sure if your medicine is listed above. |
|
Before you take VYTORIN, tell your healthcare provider about all of your medical conditions, including if you:
|
|
|
Tell your healthcare provider about all the medicines you take, including prescription and over-the-counter medicines, vitamins, and herbal supplements. Talk to your healthcare provider before you start taking any new medicines. Tell your healthcare provider who prescribes VYTORIN if another healthcare provider increases the dose of another medicine you are taking. VYTORIN may affect the way other medicines work, and other medicines may affect how VYTORIN works. Especially tell your healthcare provider if you take:
Taking VYTORIN with certain substances can also increase the risk of muscle problems. Especially tell your healthcare provider if you take:
Ask your healthcare provider or pharmacist for a list of medicines if you are not sure. Know the medicines you take. Keep a list of them to show your healthcare provider and pharmacist when you get a new medicine. |
|
How should I take VYTORIN?
If you take too much VYTORIN, call your healthcare provider or Poison Help Line at 1-800-222-1222 or go to the nearest hospital emergency room right away. |
|
|
What are the possible side effects of VYTORIN? VYTORIN may cause serious side effects including: |
|
The most common side effects of VYTORIN include:
Tell your healthcare provider if you have any side effect that bothers you or does not go away. These are not all the possible side effects of VYTORIN. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. |
|
How should I store VYTORIN?
Keep VYTORIN and all medicines out of the reach of children. |
|
| General information about safe and effective use of VYTORIN. | |
| Medicines are sometimes prescribed for purposes other than those listed in a Patient Information leaflet. Do not use VYTORIN for a condition for which it was not prescribed. Do not give VYTORIN to other people, even if they have the same symptoms that you have. It may harm them. | |
| You can ask your pharmacist or healthcare provider for information about VYTORIN that is written for health professionals. | |
| What are the ingredients in VYTORIN? | |
| Active Ingredients: ezetimibe and simvastatin. | |
| Inactive Ingredients: butylated hydroxyanisole, citric acid monohydrate, croscarmellose sodium, hypromellose, lactose monohydrate, magnesium stearate, microcrystalline cellulose, and propyl gallate. | |
|
Distributed by: Organon LLC, a subsidiary of For patent information: www.organon.com/our-solutions/patent/ © 2024 Organon group of companies. All rights reserved. For more information, go to www.organon.com/our-focus/products-list/ or call 1-844-674-3200. usppi-og0653a-t-2402r001 |
Section 43683-2
Section 44425-7
Storage
Store at 68°F to 77°F (20°C to 25°C). [See USP Controlled Room Temperature.] Keep container tightly closed.
10 Overdosage
No specific antidotes for VYTORIN are known. In the event of an overdose with VYTORIN, consider contacting the Poison Help Line (1-800-222-1222) or a medical toxicologist for overdosage management recommendations.
8.2 Lactation
Risk Summary
There is no information about the presence of ezetimibe or simvastatin in human breast milk, the effects of the drug on the breastfed infant or the effect of the drug on milk production. However, it has been shown that other statins pass into human milk. Statins, including VYTORIN, decrease cholesterol synthesis and possibly the synthesis of other biologically active substances derived from cholesterol and may cause harm to the breast fed infant.
Because of the potential for serious adverse reactions in a breastfed infant, based on the mechanism of action, advise patients that breastfeeding is not recommended during treatment with VYTORIN [see Use in Specific Populations (8.2) and Clinical Pharmacology (12.1)].
Data
Animal Data
Ezetimibe was present in the milk of lactating rats. The pup to maternal plasma ratio for total ezetimibe was 0.5 on lactation day 12.
11 Description
VYTORIN contains ezetimibe, a dietary cholesterol absorption inhibitor, and simvastatin, an HMG CoA reductase inhibitor.
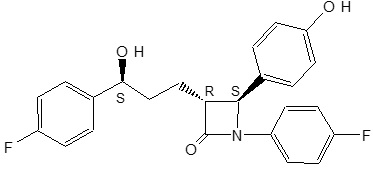
The chemical name of ezetimibe is 1-(4-fluorophenyl)-3(R)-[3-(4-fluorophenyl)-3(S)-hydroxypropyl]-4(S)-(4-hydroxyphenyl)-2-azetidinone. The empirical formula is C24H21F2NO3 and its molecular weight is 409.4.
Ezetimibe is a white, crystalline powder that is freely to very soluble in ethanol, methanol, and acetone and practically insoluble in water. Its structural formula is:
Simvastatin, an inactive lactone, is hydrolyzed to the corresponding β-hydroxyacid form, which is an inhibitor of HMG-CoA reductase. Simvastatin is butanoic acid, 2,2-dimethyl-,1,2,3,7,8,8a-hexahydro-3,7-dimethyl-8-[2-(tetrahydro-4-hydroxy-6-oxo-2H-pyran-2-yl)-ethyl]-1-naphthalenyl ester, [1S-[1α,3α,7β,8β(2S*,4S*),-8aβ]]. The empirical formula of simvastatin is C25H38O5 and its molecular weight is 418.57.
Simvastatin is a white to off-white, nonhygroscopic, crystalline powder that is practically insoluble in water and freely soluble in chloroform, methanol and ethanol. Its structural formula is:
VYTORIN is available for oral use as tablets containing 10 mg of ezetimibe, and 10 mg of simvastatin (VYTORIN 10/10), 20 mg of simvastatin (VYTORIN 10/20), 40 mg of simvastatin (VYTORIN 10/40), or 80 mg of simvastatin (VYTORIN 10/80). Each tablet contains the following inactive ingredients: butylated hydroxyanisole NF, citric acid monohydrate USP, croscarmellose sodium NF, hypromellose USP, lactose monohydrate NF, magnesium stearate NF, microcrystalline cellulose NF, and propyl gallate NF.
8.4 Pediatric Use
The safety and effectiveness of ezetimibe in combination with a statin as an adjunct to diet to reduce LDL-C have been established in pediatric patients 10 years of age and older with HeFH. Use of VYTORIN for this indication is based on a double-blind, placebo-controlled clinical trial in 248 pediatric patients (142 males and 106 postmenarchal females) 10 years of age and older with HeFH [see Clinical Studies (14)]. In this limited controlled trial, there was no significant effect on growth or sexual maturation in the adolescent males or females, or on menstrual cycle length in females.
The safety and effectiveness of VYTORIN have not been established in pediatric patients younger than 10 years of age with HeFH, or in pediatric patients with other types of hyperlipidemia.
8.5 Geriatric Use
Advanced age (≥65 years) is a risk factor for VYTORIN-associated myopathy and rhabdomyolysis. Dose selection for an elderly patient should be cautious, recognizing the greater frequency of decreased hepatic, renal, or cardiac function, and of concomitant disease or other drug therapy and the higher risk of myopathy. Monitor geriatric patients receiving VYTORIN for the increased risk of myopathy [see Warnings and Precautions (5.1)].
Of the 10,189 patients who received VYTORIN in clinical studies, 3242 (32%) were 65 and older (this included 844 (8%) who were 75 and older). No overall differences in safety or effectiveness were observed between these subjects and younger subjects, and other reported clinical experience has not identified differences in responses between the elderly and younger patients but greater sensitivity of some older individuals cannot be ruled out.
14 Clinical Studies
Primary Hyperlipidemia in Adults
VYTORIN
VYTORIN reduces LDL-C in adult patients with primary hyperlipidemia. Maximal to near maximal response is generally achieved within 2 weeks and maintained during chronic therapy.
VYTORIN is effective in males and females with primary hyperlipidemia. There were insufficient numbers of patients who self-identified as Black or African American, Asian, or other races to determine if these patients responded differently than White patients.
Five multicenter, double-blind trials conducted with either VYTORIN or coadministered ezetimibe and simvastatin equivalent to VYTORIN in patients with primary hyperlipidemia are reported: two were comparisons with simvastatin, two were comparisons with atorvastatin, and one was a comparison with rosuvastatin.
In a multicenter, double-blind, placebo-controlled, 12-week trial, 1528 patients with primary hyperlipidemia were randomized to one of ten treatment groups: placebo, ezetimibe (10 mg), simvastatin (10 mg, 20 mg, 40 mg, or 80 mg), or VYTORIN (10/10, 10/20, 10/40, or 10/80).
When patients receiving VYTORIN were compared to those receiving all doses of simvastatin, VYTORIN significantly lowered total-C, LDL-C, Apo B, TG, and non-HDL-C. The effects of VYTORIN on HDL-C were similar to the effects seen with simvastatin. Further analysis showed VYTORIN significantly increased HDL-C compared with placebo. (See Table 8.) The lipid response to VYTORIN was similar in patients with TG levels greater than or less than 200 mg/dL.
| Treatment | |||||||
|---|---|---|---|---|---|---|---|
| (Daily Dose) | N | Total-C | LDL-C | Apo B | HDL-C | TG | Non-HDL-C |
| Pooled data (All VYTORIN doses) VYTORIN doses pooled (10/10-10/80) significantly reduced total-C, LDL-C, Apo B, TG, and non-HDL-C compared to simvastatin and significantly increased HDL-C compared to placebo.
|
609 | -38 | -53 | -42 | +7 | -24 | -49 |
| Pooled data (All simvastatin doses) | 622 | -28 | -39 | -32 | +7 | -21 | -36 |
| Ezetimibe 10 mg | 149 | -13 | -19 | -15 | +5 | -11 | -18 |
| Placebo | 148 | -1 | -2 | 0 | 0 | -2 | -2 |
| VYTORIN by dose | |||||||
| 10/10 | 152 | -31 | -45 | -35 | +8 | -23 | -41 |
| 10/20 | 156 | -36 | -52 | -41 | +10 | -24 | -47 |
| 10/40 | 147 | -39 | -55 | -44 | +6 | -23 | -51 |
| 10/80 | 154 | -43 | -60 | -49 | +6 | -31 | -56 |
| Simvastatin by dose | |||||||
| 10 mg | 158 | -23 | -33 | -26 | +5 | -17 | -30 |
| 20 mg | 150 | -24 | -34 | -28 | +7 | -18 | -32 |
| 40 mg | 156 | -29 | -41 | -33 | +8 | -21 | -38 |
| 80 mg | 158 | -35 | -49 | -39 | +7 | -27 | -45 |
In a multicenter, double-blind, controlled, 23-week trial, 710 patients with known CHD or CHD risk equivalents, as defined by the NCEP ATP III guidelines, and an LDL-C ≥130 mg/dL were randomized to one of four treatment groups: coadministered ezetimibe and simvastatin equivalent to VYTORIN (10/10, 10/20, and 10/40) or simvastatin 20 mg. Patients not reaching an LDL-C <100 mg/dL had their simvastatin dose titrated at 6-week intervals to a maximal dose of 80 mg. At Week 5, the LDL-C reductions with VYTORIN 10/10, 10/20, or 10/40 were significantly larger than with simvastatin 20 mg (see Table 9).
| Simvastatin 20 mg |
VYTORIN 10/10 |
VYTORIN 10/20 |
VYTORIN 10/40 |
|
|---|---|---|---|---|
| N | 253 | 251 | 109 | 97 |
| Mean baseline LDL-C | 174 | 165 | 167 | 171 |
| Percent change LDL-C | -38 | -47 | -53 | -59 |
In a multicenter, double-blind, 6-week trial, 1902 patients with primary hyperlipidemia were randomized to one of eight treatment groups: VYTORIN (10/10, 10/20, 10/40, or 10/80) or atorvastatin (10 mg, 20 mg, 40 mg, or 80 mg).
Across the dosage range, when patients receiving VYTORIN were compared to those receiving milligram-equivalent statin doses of atorvastatin, VYTORIN lowered total-C, LDL-C, Apo B, and non-HDL-C significantly more than atorvastatin. Only the 10/40 mg and 10/80 mg VYTORIN doses increased HDL-C significantly more than the corresponding milligram-equivalent statin dose of atorvastatin. The effects of VYTORIN on TG were similar to the effects seen with atorvastatin. (See Table 10.)
| Treatment | |||||||
|---|---|---|---|---|---|---|---|
| (Daily Dose) | N | Total-C VYTORIN doses pooled (10/10-10/80) provided significantly greater reductions in total-C, LDL-C, Apo B, and non-HDL-C compared to atorvastatin doses pooled (10-80).
|
LDL-C | Apo B | HDL-C | TG | Non-HDL-C |
| VYTORIN by dose | |||||||
| 10/10 | 230 | -34 p<0.05 for difference with atorvastatin at equal mg doses of the simvastatin component.
|
-47 | -37 | +8 | -26 | -43 |
| 10/20 | 233 | -37 | -51 | -40 | +7 | -25 | -46 |
| 10/40 | 236 | -41 | -57 | -46 | +9 | -27 | -52 |
| 10/80 | 224 | -43 | -59 | -48 | +8 | -31 | -54 |
| Atorvastatin by dose | |||||||
| 10 mg | 235 | -27 | -36 | -31 | +7 | -21 | -34 |
| 20 mg | 230 | -32 | -44 | -37 | +5 | -25 | -41 |
| 40 mg | 232 | -36 | -48 | -40 | +4 | -24 | -45 |
| 80 mg | 230 | -40 | -53 | -44 | +1 | -32 | -50 |
In a multicenter, double-blind, 24-week, forced-titration trial, 788 patients with primary hyperlipidemia were randomized to receive coadministered ezetimibe and simvastatin equivalent to VYTORIN (10/10 and 10/20) or atorvastatin 10 mg. For all three treatment groups, the dose of the statin was titrated at 6-week intervals to 80 mg. At each pre-specified dose comparison, VYTORIN lowered LDL-C to a greater degree than atorvastatin (see Table 11).
| Treatment | N | Total-C | LDL-C | Apo B | HDL-C | TG | Non-HDL-C |
|---|---|---|---|---|---|---|---|
| Week 6 | |||||||
| Atorvastatin 10 mg Atorvastatin: 10 mg start dose titrated to 20 mg, 40 mg, and 80 mg through Weeks 6, 12, 18, and 24.
|
262 | -28 | -37 | -32 | +5 | -23 | -35 |
| VYTORIN 10/10 VYTORIN: 10/10 start dose titrated to 10/20, 10/40, and 10/80 through Weeks 6, 12, 18, and 24.
|
263 | -34 p≤0.05 for difference with atorvastatin in the specified week.
|
-46 | -38 | +8 | -26 | -43 |
| VYTORIN 10/20 VYTORIN: 10/20 start dose titrated to 10/40, 10/40, and 10/80 through Weeks 6, 12, 18, and 24.
|
263 | -36 | -50 | -41 | +10 | -25 | -46 |
| Week 12 | |||||||
| Atorvastatin 20 mg | 246 | -33 | -44 | -38 | +7 | -28 | -42 |
| VYTORIN 10/20 | 250 | -37 | -50 | -41 | +9 | -28 | -46 |
| VYTORIN 10/40 | 252 | -39 | -54 | -45 | +12 | -31 | -50 |
| Week 18 | |||||||
| Atorvastatin 40 mg | 237 | -37 | -49 | -42 | +8 | -31 | -47 |
| VYTORIN 10/40 Data pooled for common doses of VYTORIN at Weeks 18 and 24.
|
482 | -40 | -56 | -45 | +11 | -32 | -52 |
| Week 24 | |||||||
| Atorvastatin 80 mg | 228 | -40 | -53 | -45 | +6 | -35 | -50 |
| VYTORIN 10/80 | 459 | -43 | -59 | -49 | +12 | -35 | -55 |
In a multicenter, double-blind, 6-week trial, 2959 patients with primary hyperlipidemia, were randomized to one of six treatment groups: VYTORIN (10/20, 10/40, or 10/80) or rosuvastatin (10 mg, 20 mg, or 40 mg).
The effects of VYTORIN and rosuvastatin on total-C, LDL-C, Apo B, TG, non-HDL-C and HDL-C are shown in Table 12.
| Treatment | |||||||
|---|---|---|---|---|---|---|---|
| (Daily Dose) | N | Total-C VYTORIN doses pooled (10/20-10/80) provided significantly greater reductions in total-C, LDL-C, Apo B, and non-HDL-C compared to rosuvastatin doses pooled (10-40 mg).
|
LDL-C | Apo B | HDL-C | TG | Non-HDL-C |
| VYTORIN by dose | |||||||
| 10/20 | 476 | -37 p<0.05 vs. rosuvastatin 10 mg.
|
-52 | -42 | +7 | -23 | -47 |
| 10/40 | 477 | -39 p<0.05 vs. rosuvastatin 20 mg.
|
-55 | -44 | +8 | -27 | -50 |
| 10/80 | 474 | -44 p<0.05 vs. rosuvastatin 40 mg.
|
-61 | -50 | +8 | -30 | -56 |
| Rosuvastatin by dose | |||||||
| 10 mg | 475 | -32 | -46 | -37 | +7 | -20 | -42 |
| 20 mg | 478 | -37 | -52 | -43 | +8 | -26 | -48 |
| 40 mg | 475 | -41 | -57 | -47 | +8 | -28 | -52 |
In a multicenter, double-blind, 24-week trial, 214 patients with type 2 diabetes mellitus treated with thiazolidinediones (rosiglitazone or pioglitazone) for a minimum of 3 months and simvastatin 20 mg for a minimum of 6 weeks were randomized to receive either simvastatin 40 mg or the coadministered active ingredients equivalent to VYTORIN 10/20. The median LDL-C and HbA1c levels at baseline were 89 mg/dL and 7.1%, respectively.
VYTORIN 10/20 was significantly more effective than doubling the dose of simvastatin to 40 mg. The median percent changes from baseline for VYTORIN vs. simvastatin were: LDL-C -25% and -5%; total-C -16% and -5%; Apo B -19% and -5%; and non-HDL-C -23% and -5%. Results for HDL-C and TG between the two treatment groups were not significantly different.
Ezetimibe
In two multicenter, double-blind, placebo-controlled, 12-week trials in 1719 patients with primary hyperlipidemia, ezetimibe significantly lowered total-C (-13%), LDL-C (-19%), Apo B (-14%), and TG (-8%), and increased HDL-C (+3%) compared to placebo. Reduction in LDL-C was consistent across age, sex, and baseline LDL-C.
Simvastatin
In two large, placebo-controlled clinical trials, the Scandinavian Simvastatin Survival Trial (N=4,444 patients) and the Heart Protection Trial (N=20,536 patients), the effects of treatment with simvastatin were assessed in patients at high risk of coronary events because of existing coronary heart disease, diabetes, peripheral vessel disease, history of stroke or other cerebrovascular disease. Simvastatin was proven to reduce: the risk of total mortality by reducing CHD deaths; the risk of non-fatal myocardial infarction and stroke; and the need for coronary and non-coronary revascularization procedures.
No incremental benefit of VYTORIN on cardiovascular morbidity and mortality over and above that demonstrated for simvastatin has been established.
Heterozygous Familial Hypercholesterolemia (HeFH) in Pediatric Patients
The effects of ezetimibe coadministered with simvastatin (n=126) compared to simvastatin monotherapy (n=122) have been evaluated in males and females with HeFH. In a multicenter, double-blind, controlled trial followed by an open-label phase, 142 males and 106 postmenarchal females, 10 to 17 years of age (mean age 14.2 years, 43% females, 82% White, 4% Asian, 2% Black or African American, 13% multi- racial; 14% identified as Hispanic or Latino ethnicity) with HeFH were randomized to receive either ezetimibe coadministered with simvastatin or simvastatin monotherapy. Inclusion in the trial required 1) a baseline LDL-C level between 160 and 400 mg/dL and 2) a medical history and clinical presentation consistent with HeFH. The mean baseline LDL-C value was 225 mg/dL (range: 161 to 351 mg/dL) in the ezetimibe coadministered with simvastatin group compared to 219 mg/dL (range: 149 to 336 mg/dL) in the simvastatin monotherapy group. The patients received coadministered ezetimibe and simvastatin (10 mg, 20 mg, or 40 mg) or simvastatin monotherapy (10 mg, 20 mg, or 40 mg) for 6 weeks, coadministered ezetimibe and 40- mg simvastatin or 40-mg simvastatin monotherapy for the next 27 weeks, and open-label coadministered ezetimibe and simvastatin (10 mg, 20 mg, or 40 mg) for 20 weeks thereafter.
The results of the trial at Week 6 are summarized in Table 13. Results at Week 33 were consistent with those at Week 6.
| Total-C | LDL-C | Apo B | Non-HDL-C | |
|---|---|---|---|---|
| Mean percent difference between treatment groups | -12% | -15% | -12% | -14% |
| 95% Confidence Interval | (-15%,-9%) | (-18%,-12%) | (-15%,-9%) | (-17%,-11%) |
Homozygous Familial Hypercholesterolemia (HoFH) in Adults
A double-blind, randomized, 12-week trial was performed in patients with a clinical and/or genotypic diagnosis of HoFH. Data were analyzed from a subgroup of patients (n=14) receiving simvastatin 40 mg at baseline. Increasing the dose of simvastatin from 40 to 80 mg (n=5) produced a reduction of LDL-C of 13% from baseline on simvastatin 40 mg. Coadministered ezetimibe and simvastatin equivalent to VYTORIN (10/40 and 10/80 pooled, n=9), produced a reduction of LDL-C of 23% from baseline on simvastatin 40 mg. In those patients coadministered ezetimibe and simvastatin equivalent to VYTORIN (10/80, n=5), a reduction of LDL-C of 29% from baseline on simvastatin 40 mg was produced.
Chronic Kidney Disease (CKD) in Adults
The Trial of Heart and Renal Protection (SHARP) was a multinational, randomized, placebo-controlled, double-blind trial that investigated the effect of VYTORIN on the time to a first major vascular event (MVE) among 9438 patients with moderate to severe chronic kidney disease (approximately one-third on dialysis at baseline) who did not have a history of myocardial infarction or coronary revascularization. An MVE was defined as nonfatal MI, cardiac death, stroke, or any revascularization procedure. Patients were allocated to treatment using a method that took into account the distribution of 8 important baseline characteristics of patients already enrolled and minimized the imbalance of those characteristics across the groups.
For the first year, 9438 patients were allocated 4:4:1, to VYTORIN 10/20, placebo, or simvastatin 20 mg daily, respectively. The 1-year simvastatin arm enabled the comparison of VYTORIN to simvastatin with regard to safety and effect on lipid levels. At 1 year the simvastatin-only arm was re-allocated 1:1 to VYTORIN 10/20 or placebo. A total of 9270 patients were ever allocated to VYTORIN 10/20 (n=4650) or placebo (n=4620) during the trial. The median follow-up duration was 4.9 years. Patients had a mean age of 61 years; 63% were male, 72% were White, and 23% were diabetic; and, for those not on dialysis at baseline, the median serum creatinine was 2.5 mg/dL and the median estimated glomerular filtration rate (eGFR) was 25.6 mL/min/1.73 m2, with 94% of patients having an eGFR < 45 mL/min/1.73m2. Eligibility did not depend on lipid levels. Mean LDL-C at baseline was 108 mg/dL. At 1 year, the mean LDL-C was 26% lower in the simvastatin arm and 38% lower in the VYTORIN arm relative to placebo. At the midpoint of the trial (2.5 years), the mean LDL-C was 32% lower for VYTORIN relative to placebo. Patients no longer taking trial medication were included in all lipid measurements.
In the primary intent-to-treat analysis, 639 (15.2%) of 4193 patients initially allocated to VYTORIN and 749 (17.9%) of 4191 patients initially allocated to placebo experienced an MVE. This corresponded to a relative risk reduction of 16% (p=0.001) (see Figure 1). Similarly, 526 (11.3%) of 4650 patients ever allocated to VYTORIN and 619 (13.4%) of 4620 patients ever allocated to placebo experienced a major atherosclerotic event (MAE; a subset of the MVE composite that excluded non-coronary cardiac deaths and hemorrhagic stroke), corresponding to a relative risk reduction of 17% (p=0.002). The trial demonstrated that treatment with VYTORIN 10/20 mg versus placebo reduced the risk for MVE and MAE in this CKD population. The trial design precluded drawing conclusions regarding the independent contribution of either ezetimibe or simvastatin to the observed effect.
The treatment effect of VYTORIN on MVE was attenuated among patients on dialysis at baseline compared with those not on dialysis at baseline. Among 3023 patients on dialysis at baseline, VYTORIN reduced the risk of MVE by 6% (RR 0.94: 95% CI 0.80-1.09) compared with 22% (RR 0.78: 95% CI 0.69-0.89) among 6247 patients not on dialysis at baseline (interaction P=0.08).
| Figure 1: Effect of VYTORIN on the Primary Endpoint of Risk of Major Vascular Events |
The individual components of MVE in all patients ever allocated to VYTORIN or placebo are presented in Table 14.
| Outcome | VYTORIN 10/20 (N=4650) |
Placebo (N=4620) |
Risk Ratio (95% CI) |
P-value |
|---|---|---|---|---|
| Major Vascular Events | 701 (15.1%) | 814 (17.6%) | 0.85 (0.77-0.94) | 0.001 |
| Nonfatal MI | 134 (2.9%) | 159 (3.4%) | 0.84 (0.66-1.05) | 0.12 |
| Cardiac Death | 253 (5.4%) | 272 (5.9%) | 0.93 (0.78-1.10) | 0.38 |
| Any Stroke | 171 (3.7%) | 210 (4.5%) | 0.81 (0.66-0.99) | 0.038 |
| Non-hemorrhagic Stroke | 131 (2.8%) | 174 (3.8%) | 0.75 (0.60-0.94) | 0.011 |
| Hemorrhagic Stroke | 45 (1.0%) | 37 (0.8%) | 1.21 (0.78-1.86) | 0.40 |
| Any Revascularization | 284 (6.1%) | 352 (7.6%) | 0.79 (0.68-0.93) | 0.004 |
Among patients not on dialysis at baseline, VYTORIN did not reduce the risk of progressing to end-stage renal disease compared with placebo (RR 0.97: 95% CI 0.89-1.05).
Simvastatin Cardiovascular Outcome Trials in Adults at High Risk of Coronary Heart Disease Events
In a randomized, double-blind, placebo-controlled, multi-centered trial [the Scandinavian Simvastatin Survival Trial (Trial 4S)], the effect of therapy with simvastatin on total mortality was assessed in 4,444 adult patients with CHD (history of angina and/or a previous myocardial infarction) and baseline total cholesterol (total-C) between 212 and 309 mg/dL who were on a lipid-lowering diet. In Trial 4S, patients were treated with standard care, including lipid-lowering diet, and randomized to either simvastatin 20-40 mg/day (n=2,221) or placebo (n=2,223) for a median duration of 5.4 years.
- Simvastatin significantly reduced the risk of mortality by 30% (p=0.0003, 182 deaths in the simvastatin group vs 256 deaths in the placebo group). The risk of CHD mortality was significantly reduced by 42% (p=0.00001, 111 deaths in the simvastatin group vs 189 deaths in the placebo group). There was no statistically significant difference between groups in non-cardiovascular mortality.
- Simvastatin significantly reduced the risk for the secondary composite endpoint (time to first occurrence of CHD death, definite or probable hospital verified non-fatal MI, silent MI verified by ECG, or resuscitated cardiac arrest) by 34% (p<0.00001, 431 vs 622 patients with one or more events). Simvastatin reduced the risk of major coronary events to a similar extent across the range of baseline total and LDL cholesterol levels. The risk of having a hospital-verified non-fatal MI was reduced by 37%.
- Simvastatin significantly reduced the risk for undergoing myocardial revascularization procedures (coronary artery bypass grafting or percutaneous transluminal coronary angioplasty) by 37% (p<0.00001, 252 vs 383 patients).
- Simvastatin significantly reduced the risk of fatal plus non-fatal cerebrovascular events (combined stroke and transient ischemic attacks) by 28% (p=0.033, 75 vs 102 patients).
- Over the course of the trial, treatment with simvastatin led to mean reductions in total-C, LDL-C and triglycerides (TG) of 25%, 35%, and 10%, respectively, and a mean increase in high-density lipoprotein cholesterol (HDL-C) of 8%. In contrast, treatment with placebo led to increases in total- C, LDL-C and TG of 1%, 1%, and 7%, respectively.
- Because there were only 53 female deaths (approximately 18% of the trial population was female), the effect of simvastatin on mortality in females could not be adequately assessed. However, simvastatin significantly reduced the risk of having major coronary events in females by 34% (60 vs 91 women with one or more event).
- Simvastatin resulted in similar decreases in relative risk for total mortality, CHD mortality, and major coronary events in geriatric patients (≥65 years) compared with younger adults.
The Heart Protection Trial (Trial HPS) was a randomized, placebo-controlled, double-blind, multi- centered trial with a mean duration of 5 years conducted in 10,269 patients on simvastatin 40 mg and 10,267 on placebo. Patients had a mean age of 64 years (range 40-80 years old), 97% were White, and were at high risk of developing a major coronary event because of existing CHD (65%), diabetes (Type 2, 26%; Type 1, 3%), history of stroke or other cerebrovascular disease (16%), peripheral vascular disease (33%), or they were males ≥65 years with hypertension in (6%). At baseline:
- 3,421 patients (17%) had LDL-C levels below 100 mg/dL, including 953 (5%) below 80 mg/dL; and
- 10,047 patients (49%) had levels greater than 130 mg/dL.
Patients were randomized to simvastatin or placebo using a covariate adaptive method which considered the distribution of 10 important baseline characteristics of patients already enrolled.
The Trial HPS results showed that simvastatin 40 mg/day significantly reduced: total and CHD mortality; and non-fatal MI, stroke, and revascularization procedures (coronary and non-coronary) (see Table 15).
| Endpoint | Simvastatin (N=10,269) n (%) n = number of patients with indicated event
|
Placebo (N=10,267) n (%) |
Risk Reduction (%) (95% CI) |
p-Value |
|---|---|---|---|---|
| Primary | ||||
| Mortality | 1,328 (12.9%) |
1,507 (14.7%) |
13% (6-19%) | p=0.0003 |
| CHD mortality | 587 (5.7%) | 707 (6.9%) | 18% (8-26%) | p=0.0005 |
| Secondary | ||||
| Non-fatal MI | 357 (3.5%) | 574 (5.6%) | 38% (30-46%) | p<0.0001 |
| Stroke | 444 (4.3%) | 585 (5.7%) | 25% (15-34%) | p<0.0001 |
| Tertiary | ||||
| Coronary revascularization | 513 (5%) | 725 (7.1%) | 30% (22-38%) | p<0.0001 |
| Peripheral and other non-coronary revascularization | 450 (4.4%) | 532 (5.2%) | 16% (5-26%) | p=0.006 |
Two composite endpoints were defined to have enough events to assess relative risk reductions across a range of baseline characteristics:
- Major coronary events (MCE) was comprised of CHD mortality and non-fatal MI. Analyzed by time-to-first event; 898 patients (8.7%) treated with simvastatin had events and 1,212 patients (11.8%) treated with placebo had events.
- Major vascular events (MVE) was comprised of MCE, stroke, and revascularization procedures including coronary, peripheral and other non-coronary procedures. Analyzed by time-to-first event; 2,033 patients (19.8%) treated with simvastatin had events and 2,585 patients (25.2%) on placebo had events.
Simvastatin use led to significant relative risk reductions for both composite endpoints (27% for MCE and 24% for MVE, p<0.0001) and for all components of the composite endpoints. The risk reductions produced by simvastatin in both MCE and MVE were evident and consistent regardless of cardiovascular disease related medical history at trial entry (i.e., CHD alone; or peripheral vascular disease, cerebrovascular disease, diabetes or treated hypertension, with or without CHD), gender, age, baseline levels of LDL-C, baseline concomitant cardiovascular medications (i.e., aspirin, beta blockers, or calcium channel blockers), smoking status, or obesity. Patients with diabetes showed risk reductions for MCE and MVE due to simvastatin treatment regardless of baseline HbA1c levels or obesity.
4 Contraindications
VYTORIN is contraindicated in the following conditions:
- Concomitant use of strong CYP3A4 inhibitors (select azole anti-fungals, macrolide antibiotics, anti-viral medications, and nefazodone) [see Drug Interactions (7.1)].
- Concomitant use of cyclosporine, danazol, or danazol [see Drug Interactions (7.1)].
- Acute liver failure or decompensated cirrhosis [see Warnings and Precautions (5.3)].
- Hypersensitivity to simvastatin, ezetimibe, or any excipients in VYTORIN. Hypersensitivity reactions, including anaphylaxis, angioedema, and Stevens-Johnson syndrome, have been reported [see Adverse Reactions (6.2)].
6 Adverse Reactions
The following serious adverse reactions are discussed in greater detail in other sections of the label:
- Myopathy and Rhabdomyolysis [see Warnings and Precautions (5.1)]
- Immune-Mediated Necrotizing Myopathy [see Warnings and Precautions (5.2)]
- Hepatic Dysfunction [see Warnings and Precautions (5.3)]
- Increases in HbA1c and Fasting Serum Glucose Levels [see Warnings and Precautions (5.4)]
7 Drug Interactions
VYTORIN
8.6 Renal Impairment
Renal impairment is a risk factor for myopathy and rhabdomyolysis. Monitor all patients with renal impairment for development of myopathy. Doses of VYTORIN exceeding 10/20 mg should be used with caution and close monitoring in patients with moderate to severe renal impairment [see Dosage and Administration (2.4) and Warnings and Precautions (5.1)].
In the SHARP trial of 9270 patients with moderate to severe renal impairment (6247 non-dialysis patients with median serum creatinine 2.5 mg/dL and median estimated glomerular filtration rate 25.6 mL/min/1.73 m2, and 3023 dialysis patients), the incidence of serious adverse events, adverse events leading to discontinuation of trial treatment, or adverse events of special interest (musculoskeletal adverse events, liver enzyme abnormalities, incident cancer) was similar between patients ever assigned to VYTORIN 10/20 mg (n=4650) or placebo (n=4620) during a median follow-up of 4.9 years.
8.8 Chinese Patients
In a clinical trial in which patients at high risk of CVD were treated with simvastatin 40 mg/day (median follow-up 3.9 years), the incidence of myopathy was approximately 0.05% for non-Chinese patients (n=7367) compared with 0.24% for Chinese patients (n=5468). In this trial the incidence of myopathy for Chinese patients on simvastatin 40 mg/day or ezetimibe and simvastatin 10/40 mg/day coadministered with extended-release niacin 2 g/day was 1.24%.
Chinese patients may be at higher risk for myopathy, monitor these patients appropriately. Coadministration of VYTORIN with lipid-modifying doses of niacin-containing products (≥1 g/day niacin) is not recommended in Chinese patients [see Warnings and Precautions (5.1) and Drug Interactions (7.1)].
12.2 Pharmacodynamics
VYTORIN reduces total cholesterol (total-C), LDL-C, apolipoprotein (Apo) B, and non-high-density lipoprotein cholesterol (non-HDL-C) in patients with hyperlipidemia.
Ezetimibe
In a 2-week clinical trial in 18 hypercholesterolemic patients, ezetimibe inhibited intestinal cholesterol absorption by 54%, compared with placebo. Ezetimibe had no clinically meaningful effect on the plasma concentrations of the fat-soluble vitamins A, D, and E and did not impair adrenocortical steroid hormone production.
Simvastatin
Inhibition of HMG-CoA reductase by simvastatin acid accelerates the expression of LDL-receptors, followed by the uptake of LDL-C from blood to the liver, leading to a decrease in plasma LDL-C and total cholesterol. Sustained inhibition of cholesterol synthesis in the liver also decreases levels of very-low density lipoproteins. The maximum LDL-C reduction of ZOCOR is usually achieved by 4 weeks and is maintained after that.
12.3 Pharmacokinetics
The results of a bioequivalence trial in healthy subjects demonstrated that the VYTORIN (ezetimibe and simvastatin) 10 mg/10 mg to 10 mg/80 mg combination tablets are bioequivalent to coadministration of corresponding doses of ezetimibe (ZETIA®) and simvastatin (ZOCOR®) as individual tablets.
8.7 Hepatic Impairment
VYTORIN is contraindicated in patients with acute liver failure or decompensated cirrhosis. [See Contraindications (4) and Warnings and Precautions (5.3).]
1 Indications and Usage
VYTORIN
VYTORIN® is a combination of simvastatin and ezetimibe indicated:
-
As an adjunct to diet to reduce elevated low density lipoprotein cholesterol (LDL-C):
- In adults with primary hyperlipidemia.
- In adults and pediatric patients aged 10 years and older with heterozygous familial hypercholesterolemia (HeFH).
- As an adjunct to other LDL-C-lowering therapies to reduce elevated LDL-C in adults with homozygous familial hypercholesterolemia (HoFH).
Simvastatin
Simvastatin, when used as a component of VYTORIN, is indicated to reduce the risk of total mortality by reducing risk of coronary heart disease death, non-fatal myocardial infarction and stroke, and the need for coronary and non-coronary revascularization procedures in adults with established coronary heart disease, cerebrovascular disease, peripheral vascular disease, and/or diabetes, who are at high risk of coronary heart disease events.
5.3 Hepatic Dysfunction
Increases in serum transaminases have been reported with use of VYTORIN [see Adverse Reactions (6.1)]. In most cases, these changes appeared soon after initiation, were transient, were not accompanied by symptoms, and resolved or improved on continued therapy or after a brief interruption in therapy. Marked persistent increases of hepatic transaminases have also occurred with VYTORIN. There have been rare postmarketing reports of fatal and non-fatal hepatic failure in patients taking statins, including VYTORIN.
In three placebo-controlled, 12-week trials, the incidence of consecutive elevations (≥3 X ULN) in serum transaminases was 1.7% overall for patients treated with VYTORIN and appeared to be dose-related with an incidence of 2.6% for patients treated with VYTORIN 10/80. In controlled long-term (48-week) extensions, which included both newly-treated and previously-treated patients, the incidence of consecutive elevations (≥3 X ULN) in serum transaminases was 1.8% overall and 3.6% for patients treated with VYTORIN 10/80. These elevations in transaminases were generally asymptomatic, not associated with cholestasis, and returned to baseline after discontinuation of therapy or with continued treatment.
In SHARP, 9270 patients with chronic kidney disease were allocated to receive VYTORIN 10/20 mg daily (n=4650), or placebo (n=4620). During a median follow-up period of 4.9 years, the incidence of consecutive elevations of transaminases (>3 X ULN) was 0.7% for VYTORIN and 0.6% for placebo.
Patients who consume substantial quantities of alcohol and/or have a history of liver disease may be at increased risk for hepatic injury.
Consider liver enzyme testing before VYTORIN initiation and when clinically indicated thereafter. VYTORIN is contraindicated in patients with acute liver failure or decompensated cirrhosis [see Contraindications (4)]. If serious hepatic injury with clinical symptoms and/or hyperbilirubinemia or jaundice occurs, promptly discontinue VYTORIN.
5 Warnings and Precautions
- Myopathy and Rhabdomyolysis: Risk factors include age 65 years or greater, uncontrolled hypothyroidism, renal impairment, concomitant use with certain other drugs, and higher VYTORIN dosage. Chinese patients may be at higher risk for myopathy. Discontinue VYTORIN if markedly elevated CK levels occur or myopathy is diagnosed or suspected. Temporarily discontinue VYTORIN in patients experiencing an acute or serious condition at high risk of developing renal failure secondary to rhabdomyolysis. Inform patients of the risk of myopathy and rhabdomyolysis when starting or increasing VYTORIN dosage. Instruct patients to promptly report unexplained muscle pain, tenderness, or weakness, particularly if accompanied by malaise or fever. (5.1)
- Immune-Mediated Necrotizing Myopathy (IMNM): Rare reports of IMNM, an autoimmune myopathy, have been reported. Discontinue VYTORIN if IMNM is suspected. (5.2)
- Hepatic Dysfunction: Increases in serum transaminases have occurred, some persistent. Rare reports of fatal and non-fatal hepatic failure have occurred. Consider testing liver enzyme before initiating therapy and as clinically indicated thereafter. If serious hepatic injury with clinical symptoms and/or hyperbilirubinemia or jaundice occurs, promptly discontinue VYTORIN. (5.3)
2 Dosage and Administration
-
Important Dosage and Administration Information: (2.1)
- Take VYTORIN orally once daily in the evening with or without food.
- Maximum recommended dosage is VYTORIN 10/40 mg once daily. VYTORIN 10/80 mg daily dosage is restricted to patients who have been taking VYTORIN 10/80 mg daily chronically (e.g., for 12 months or more) without evidence of muscle toxicity.
- For patients that require a high-intensity statin or are unable to achieve their LDL-C goal receiving VYTORIN 10/40 mg daily, prescribe alternative LDL-C-lowering treatment.
- If as dose is missed, take the missed dose as soon as possible. Do not double the next dose.
- Assess LDL-C when clinically appropriate, as early as 2 weeks after initiating VYTORIN, and adjust the dosage if necessary.
- Adults: Recommended dosage range of 10/10 mg to 10/40 mg once daily. (2.2)
- See full prescribing information for VYTORIN dosage modifications due to drug interactions. (2.3)
- Patients with Renal Impairment: Doses exceeding 10/20 mg should be used with caution and close monitoring in patients with moderate to severe renal impairment. (2.4)
3 Dosage Forms and Strengths
VYTORIN tablets:
- 10/10, (ezetimibe 10 mg and simvastatin 10 mg tablets) are white to off-white capsule-shaped and debossed with “311” on one side.
- 10/20, (ezetimibe 10 mg and simvastatin 20 mg tablets) are white to off-white capsule-shaped and debossed with “312” on one side.
- 10/40, (ezetimibe 10 mg and simvastatin 40 mg tablets) are white to off-white capsule-shaped and debossed with “313” on one side.
- 10/80, (ezetimibe 10 mg and simvastatin 80 mg tablets) are white to off-white capsule-shaped and debossed with “315” on one side.
6.2 Postmarketing Experience
The following adverse reactions have been identified during post-approval use of VYTORIN. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Body as Whole: fever, chills, malaise, asthenia
Blood and Lymphatic System Disorders: anemia, thrombocytopenia, leukopenia, hemolytic anemia, positive ANA, ESR increase, eosinophilia
Gastrointestinal Disorders: pancreatitis, nausea, vomiting
Hepatobiliary Disorders: cholelithiasis, cholecystitis, elevations in liver transaminases including elevations more than 5 X ULN, hepatitis/jaundice, fatal and non-fatal hepatic failure
Immune System Disorders: hypersensitivity syndrome including: anaphylaxis, angioedema, lupus erythematous-like syndrome, dermatomyositis, vasculitis
Musculoskeletal and Connective Tissue Disorders: muscle cramps, immune-mediated necrotizing myopathy, rhabdomyolysis, myalgia, arthralgia, polymyalgia rheumatica, arthritis, elevated creatine phosphokinase
Nervous System Disorders: dizziness, depression, paresthesia, peripheral neuropathy, rare reports of cognitive impairment (e.g., memory loss, forgetfulness, amnesia, memory impairment, confusion) associated with statin use. Cognitive impairment was generally nonserious, and reversible upon statin discontinuation, with variable times to symptom onset (1 day to years) and symptom resolution (median of 3 weeks). There have been rare reports of new-onset or exacerbation of myasthenia gravis, including ocular myasthenia, and reports of recurrence when the same or a different statin was administered.
Skin and Subcutaneous Tissue Disorders: rash, pruritus, alopecia, a variety of skin changes (e.g., nodules, discoloration, dryness of skin/mucous membranes, changes to hair/nails), purpura, lichen planus, urticaria, photosensitivity, flushing, toxic epidermal necrolysis, erythema multiforme, including Stevens-Johnson syndrome.
Respiratory and Thoracic: interstitial lung disease, dyspnea
Reproductive System Disorders: erectile dysfunction
8 Use in Specific Populations
5.1 Myopathy and Rhabdomyolysis
VYTORIN may cause myopathy and rhabdomyolysis. Acute kidney injury secondary to myoglobinuria and rare fatalities have occurred as a result of rhabdomyolysis in patients treated with statins, including VYTORIN.
In clinical trials of 24,747 simvastatin-treated patients with a median follow-up of 4 years, the incidence of myopathy, defined as unexplained muscle weakness, pain, or tenderness accompanied by creatinine kinase (CK) increases greater than ten times the upper limit of normal (10 X ULN), were approximately 0.03%, 0.08%, and 0.61% in patients treated with simvastatin 20 mg, 40 mg, and 80 mg daily, respectively. In another clinical trial of 12,064 simvastatin-treated patients (with a history of myocardial infarction) with a mean follow-up of 6.7 years, the incidences of myopathy in patients taking simvastatin 20 mg and 80 mg daily were approximately 0.02% and 0.9%, respectively. The incidences of rhabdomyolysis (defined as myopathy with a CK >40 X ULN) in patients taking simvastatin 20 mg and 80 mg daily were approximately 0% and 0.4%, respectively [see Adverse Reactions (6.1)].
In the Trial of Heart and Renal Protection (SHARP), 9270 patients with chronic kidney disease were allocated to receive VYTORIN 10/20 mg daily (n=4650) or placebo (n=4620). During a median follow-up period of 4.9 years, the incidence of myopathy (defined as unexplained muscle weakness or pain with a serum creatine kinase [CK] >10 times upper limit of normal [ULN]) was 0.2% for VYTORIN and 0.1% for placebo: the incidence of rhabdomyolysis (defined as myopathy with a CK > 40 times ULN) was 0.09% for VYTORIN and 0.02% for placebo.
In postmarketing experience with ezetimibe, cases of myopathy and rhabdomyolysis have been reported. Most patients who developed rhabdomyolysis were taking a statin prior to initiating ezetimibe. However, rhabdomyolysis has been reported with ezetimibe monotherapy and with the addition of ezetimibe to agents known to be associated with increased risk of rhabdomyolysis, such as fibric acid derivatives. VYTORIN and a fenofibrate, if taking concomitantly, should both be immediately discontinued if myopathy is diagnosed or suspected.
Risk Factors for Myopathy
Risk factors for myopathy include age 65 years or greater, uncontrolled hypothyroidism, renal impairment, concomitant use with certain other drugs (including other lipid-lowering therapies), and higher VYTORIN dosage; Chinese patients on VYTORIN may be at higher risk for myopathy [see Contraindications (4), Drug Interactions (7.1), and Use in Specific Populations (8.8)]. The risk of myopathy is increased by elevated plasma levels of simvastatin and simvastatin acid. The risk is also greater in patients taking VYTORIN 80 mg daily compared with patients taking lower VYTORIN dosages and compared with patients using other statins with similar or greater LDL-C-lowering efficacy [see Adverse Reactions (6.1)].
Steps to Prevent or Reduce the Risk of Myopathy and Rhabdomyolysis
The concomitant use of strong CYP3A4 inhibitors with VYTORIN is contraindicated. If short-term treatment with strong CYP3A4 inhibitors is required, temporarily suspend VYTORIN during the duration of strong CYP3A4 inhibitor treatment. The concomitant use of VYTORIN with gemfibrozil, cyclosporine, or danazol is also contraindicated [see Contraindications (4) and Drug Interactions (7.1)].
VYTORIN dosage modifications are recommended for patients taking lomitapide, verapamil, diltiazem, dronedarone, amiodarone, amlodipine or ranolazine [see Dosage and Administration (2.5)]. VYTORIN use should be temporarily suspended in patients taking daptomycin. Lipid modifying doses (≥1 gram/day) of niacin, fibrates, colchicine, and grapefruit juice may also increase the risk of myopathy and rhabdomyolysis [see Drug Interactions (7.1)].
Use the 80 mg daily dosage of VYTORIN only in patients who have been taking simvastatin 80 mg daily chronically without evidence of muscle toxicity [see Dosage and Administration (2.1)]. If patients treated with VYTORIN 80 mg are prescribed an interacting drug that increases the risk for myopathy and rhabdomyolysis, switch to an alternate statin [see Drug Interactions (7.1)].
Discontinue VYTORIN if markedly elevated CK levels occur or if myopathy is either diagnosed or suspected. Muscle symptoms and CK increases may resolve if VYTORIN is discontinued. Temporarily discontinue VYTORIN in patients experiencing an acute or serious condition at high risk of developing renal failure secondary to rhabdomyolysis, e.g., sepsis; shock; severe hypovolemia; major surgery; trauma; severe metabolic, endocrine, or electrolyte disorders; or uncontrolled epilepsy.
Inform patients of the risk of myopathy and rhabdomyolysis when starting or increasing the VYTORIN dosage and advise patients receiving VYTORIN 80 mg of the increased risk of myopathy and rhabdomyolysis. Instruct patients to promptly report any unexplained muscle pain, tenderness or weakness, particularly if accompanied by malaise or fever.
17 Patient Counseling Information
Advise the patient to read the FDA-approved patient labeling (Patient Information).
Myopathy and Rhabdomyolysis
Advise patients that VYTORIN may cause myopathy and rhabdomyolysis. Inform patients taking the 80 mg daily dose of simvastatin that they are at an increased risk. Inform patients that the risk is also increased when taking certain types of medication or consuming grapefruit juice and they should discuss all medication, both prescription and over the counter, with their healthcare provider. Instruct patients to inform other healthcare providers prescribing a new medication or increasing the dose of an existing medication that they are taking VYTORIN. Instruct patients to promptly report any unexplained muscle pain, tenderness or weakness particularly if accompanied by malaise or fever [see Contraindications (4), Warnings and Precautions (5.1), and Drug Interactions (7.1)].
Hepatic Dysfunction
Inform patients that VYTORIN may cause liver enzyme elevations and possibly liver failure. Advise patients to promptly report fatigue, anorexia, right upper abdominal discomfort, dark urine or jaundice [see Warnings and Precautions (5.3)].
Increases in HbA1c and Fasting Serum Glucose Levels
Inform patients that increases in HbA1c and fasting serum glucose levels may occur with VYTORIN. Encourage patients to optimize lifestyle measures, including regular exercise, maintaining a healthy body weight, and making healthy food choices [see Warnings and Precautions (5.4)].
Pregnancy
Advise pregnant patients and patients who can become pregnant of the potential risk to a fetus. Advise patients to inform their healthcare provider of a known or suspected pregnancy to discuss if VYTORIN should be discontinued [see Use in Specific Populations (8.1)].
Lactation
Advise patients that breastfeeding is not recommended during treatment with VYTORIN [see Use in Specific Populations (8.2)].
Missed Dose
Instruct patients to take VYTORIN only as prescribed. If a dose is missed, it should be taken as soon as possible. Advise patients not to double their next dose.
16 How Supplied/storage and Handling
VYTORIN tablets are supplied as follows:
| Strength | How Supplied | NDC | Tablet Description |
|---|---|---|---|
| 10/10 mg | unit of use bottles of 30 | 78206-174-01 | white to off-white capsule-shaped tablets with code “311” on one side |
| unit of use bottles of 90 | 78206-174-02 | ||
| 10/20 mg | unit of use bottles of 30 | 78206-175-01 | white to off-white capsule-shaped tablets with code “312” on one side |
| unit of use bottles of 90 | 78206-175-02 | ||
| 10/40 mg | unit of use bottles of 30 | 78206-176-01 | white to off-white capsule-shaped tablets with code “313” on one side |
| unit of use bottles of 90 | 78206-176-02 | ||
| 10/80 mg | unit of use bottles of 30 | 78206-177-01 | white to off-white capsule-shaped tablets with code “315” on one side |
| unit of use bottles of 90 | 78206-177-02 |
7.3 Vytorin’s Effect On Other Drugs
Table 4 presents VYTORIN’s effect on other drugs and instructions for preventing or managing them.
| Coumarin Anticoagulants | |
|---|---|
| Clinical Impact: | VYTORIN may potentiate the effect of coumarin anticoagulants and increase the INR. The concomitant use of simvastatin (20 to 40 mg) and coumarin anticoagulants increased the INR from a baseline of 1.7 to 1.8 in healthy subjects and from 2.6 to 3.4 in patients with hyperlipidemia. There are postmarketing reports of clinically evident bleeding and/or increased INR in patients taking concomitant statins (with or without ezetimibe) and coumarin anticoagulants. |
| Intervention: | In patients taking coumarin anticoagulants, obtain an INR before starting VYTORIN and frequently enough after initiation, dose titration, or discontinuation to ensure that no significant alteration in INR occurs. Once the INR is stable, monitor INR at regularly recommended intervals. |
| Digoxin | |
| Clinical Impact: | Concomitant use of digoxin with VYTORIN may result in elevated plasma digoxin concentrations [see Clinical Pharmacology (12.3)]. |
| Intervention: | Monitor digoxin levels in patients taking digoxin when VYTORIN is initiated. |
| Fenofibrates | |
| Clinical Impact: | Both ezetimibe and fenofibrates may increase cholesterol excretion into the bile, leading to cholelithiasis. |
| Intervention: | If cholelithiasis is suspected in a patient receiving VYTORIN and a fenofibrate, gallbladder studies are indicated and alternative lipid-lowering therapy should be considered [see the product labeling for fenofibrate and fenofibric acid]. |
2.2 Recommended Dosage in Adult Patients
The recommended dosage range of VYTORIN 10/10 mg to 10/40 mg once a day.
5.2 Immune Mediated Necrotizing Myopathy
There have been rare reports of immune-mediated necrotizing myopathy (IMNM), an autoimmune myopathy, associated with statin use, including reports of recurrence when the same or a different statin was administered. IMNM is characterized by proximal muscle weakness and elevated serum creatine kinase that persist despite discontinuation of statin treatment; positive anti-HMG CoA reductase antibody; muscle biopsy showing necrotizing myopathy without significant inflammation; and improvement with immunosuppressive agents. Additional neuromuscular and serologic testing may be necessary. Treatment with immunosuppressive agents may be required. Discontinue VYTORIN if IMNM is suspected.
2.5 Dosage Modifications Due to Drug Interactions
Concomitant use of VYTORIN with the following drugs requires dosage modification of VYTORIN [see Warnings and Precautions (5.1) and Drug Interactions (7.1)].
Patients taking Lomitapide
Reduce the dosage of VYTORIN by 50%. Do not exceed VYTORIN 10/20 mg once daily (or 10/40 mg once daily for patients who have previously taken VYTORIN 10/80 mg daily chronically while taking lomitapide) [see Dosage and Administration (2.1)].
Patients taking Verapamil, Diltiazem, or Dronedarone
Do not exceed VYTORIN 10/10 mg once daily.
Patients taking Amiodarone, Amlodipine, or Ranolazine
Do not exceed VYTORIN 10/20 mg once daily.
Patients taking Bile Acid Sequestrants
In patients taking a bile acid sequestrant, administer VYTORIN at least 2 hours before or 4 hours after the bile acid sequestrant.
2.1 Important Dosage and Administration Information
- Take VYTORIN orally once daily in the evening with or without food.
- The maximum recommended dosage is VYTORIN 10/40 mg once daily. The VYTORIN 10/80 mg daily dosage is restricted to adult patients who have been taking VYTORIN 10/80 mg daily chronically (e.g., for 12 months or more) without evidence of muscle toxicity [see Warnings and Precautions (5.1)].
- For patients that require a high-intensity statin or are unable to achieve their LDL-C goal receiving VYTORIN 10/40 mg daily, prescribe alternative LDL-C-lowering treatment.
- If as dose is missed, take the missed dose as soon as possible. Do not double the next dose.
- Assess LDL-C when clinically appropriate, as early as 4 weeks after initiating VYTORIN, and adjust the dosage if necessary.
5.4 Increases in Hba1c and Fasting Serum Glucose Levels
Increases in HbA1c and fasting serum glucose levels have been reported with statins, including VYTORIN. Optimize lifestyle measures, including regular exercise, maintaining a healthy body weight, and making healthy food choices.
2.4 Recommended Dosage in Patients With Renal Impairment
Renal impairment is a risk factor for statin-associated myopathy. Doses of VYTORIN exceeding 10/20 mg should be used with caution and close monitoring in patients with moderate to severe renal impairment [see Warnings and Precautions (5.1) and Use in Specific Populations (8.6)].
There are no dosage adjustment recommendations for patients with mild renal impairment.
Principal Display Panel 10 Mg /10 Mg Tablet Bottle Label
NDC 78206-174-01
Vytorin
®
(ezetimibe and
simvastatin) tablets
10 mg /10 mg
Each tablet contains 10 mg ezetimibe and
10 mg simvastatin.
Rx only
30 Tablets
Principal Display Panel 10 Mg /20 Mg Tablet Bottle Label
NDC 78206-175-01
Vytorin
®
(ezetimibe and
simvastatin) tablets
10 mg /20 mg
Each tablet contains 10 mg ezetimibe and
20 mg simvastatin.
Rx only
30 Tablets
Principal Display Panel 10 Mg /40 Mg Tablet Bottle Label
NDC 78206-176-01
Vytorin
®
(ezetimibe and
simvastatin) tablets
10 mg /40 mg
Each tablet contains 10 mg ezetimibe and
40 mg simvastatin.
Rx only
30 Tablets
Principal Display Panel 10 Mg /80 Mg Tablet Bottle Label
NDC 78206-177-01
Vytorin
®
(ezetimibe and
simvastatin) tablets
10 mg /80 mg
Each tablet contains 10 mg ezetimibe and
80 mg simvastatin.
Rx only
30 Tablets
7.2 Drug Interactions That Decrease the Efficacy of Vytorin
Table 3 presents drug interactions that may decrease the efficacy of VYTORIN and instructions for preventing or managing them.
| Bile Acid Sequestrants | |
|---|---|
| Clinical Impact: | Concomitant cholestyramine administration decreased the mean exposure of total ezetimibe approximately 55%. The incremental LDL-C reduction due to adding VYTORIN to cholestyramine may be reduced by this interaction [see Clinical Pharmacology (12.3)]. |
| Intervention: | In patients taking a bile acid sequestrant, administer VYTORIN at least 2 hours before or at least 4 hours after cholestyramine [see Dosage and Administration (2.3)]. |
2.3 Recommended Dosage in Pediatric Patients 10 Years of Age and Older With Hefh
The recommended dosage range of VYTORIN 10/10 mg to 10/40 mg once a day.
7.1 Drug Interactions That Increase the Risk of Myopathy and Rhabdomyolysis With Vytorin
VYTORIN is a substrate of CYP3A4 and of the transport protein OATP1B1. VYTORIN plasma levels can be significantly increased with concomitant administration of inhibitors of CYP3A4 and OATP1B1.
Table 2 includes a list of drugs that increase the risk of myopathy and rhabdomyolysis when used concomitantly with VYTORIN and instructions for preventing or managing them [see Warnings and Precautions (5.1) and Clinical Pharmacology (12.3)].
| Strong CYP3A4 inhibitors | |
|---|---|
| Clinical Impact: | Simvastatin is a substrate of CYP3A4. Concomitant use of strong CYP3A4 inhibitors with VYTORIN increases simvastatin exposure and increases the risk of myopathy and rhabdomyolysis, particularly with higher VYTORIN dosages. |
| Intervention: | Concomitant use of strong CYP3A4 inhibitors with VYTORIN is contraindicated [see Contraindications (4)]. If treatment with a CYP3A4 inhibitor is unavoidable, suspend VYTORIN during the course of strong CYP3A4 inhibitor treatment. |
| Examples: | Select azole anti-fungals (e.g., itraconazole, ketoconazole, posaconazole, and voriconazole), select macrolide antibiotics (e.g., erythromycin and clarithromycin, telithromycin), select HIV protease inhibitors (e.g., nelfinavir, ritonavir, and darunavir/ritonavir), select HCV protease inhibitors (e.g., boceprevir and telaprevir), cobicistat-containing products, and nefazodone. |
| Cyclosporine, Danazol, or Gemfibrozil | |
| Clinical Impact: | The risk of myopathy and rhabdomyolysis is increased with concomitant use of cyclosporine, danazol, or gemfibrozil with VYTORIN. Gemfibrozil may cause myopathy when given alone. |
| Intervention: | Concomitant use of cyclosporine, danazol, or gemfibrozil with VYTORIN is contraindicated [see Contraindications (4)]. |
| Amiodarone, Dronedarone, Ranolazine, or Calcium Channel Blockers | |
| Clinical Impact: | The risk of myopathy and rhabdomyolysis is increased by concomitant use of amiodarone, dronedarone, ranolazine, or calcium channel blockers with VYTORIN. |
| Intervention: | For patients taking verapamil, diltiazem, or dronedarone, do not exceed VYTORIN 10/10 mg daily. For patients taking amiodarone, amlodipine, or ranolazine, do not exceed VYTORIN 10/20 mg daily [see Dosage and Administration (2.3)]. |
| Lomitapide | |
| Clinical Impact: | Simvastatin exposure is approximately doubled with concomitant use of lomitapide and the risk of myopathy and rhabdomyolysis is increased. |
| Intervention: | Reduce the dose of VYTORIN by 50% if initiating lomitapide. Do not exceed VYTORIN 10/20 mg daily (or VYTORIN 10/40 mg daily for patients who have previously taken VYTORIN 10/80 mg daily chronically) while taking lomitapide [see Dosage and Administration (2.1, 2.3)]. |
| Daptomycin | |
| Clinical Impact: | Cases of rhabdomyolysis have been reported with simvastatin administered with daptomycin. Both VYTORIN and daptomycin can cause myopathy and rhabdomyolysis when given alone and the risk of myopathy and rhabdomyolysis may be increased by coadministration. |
| Intervention: | If treatment with daptomycin is required, consider temporarily suspending VYTORIN during the course of daptomycin treatment. |
| Niacin | |
| Clinical Impact: | Cases of myopathy and rhabdomyolysis have been observed with concomitant use of lipid modifying dosages of niacin-containing products (≥1 gram/day niacin) with VYTORIN. The risk of myopathy is greater in Chinese patients. In a clinical trial (median follow-up 3.9 years) of patients at high risk of CVD and with well-controlled LDL-C levels on simvastatin 40 mg/day with or without ezetimibe 10 mg/day, there was no incremental benefit on cardiovascular outcomes with the addition of lipid-modifying doses of niacin |
| Intervention: | Concomitant use of VYTORIN with lipid-modifying dosages of niacin is not recommended in Chinese patients [see Use in Specific Populations (8.8)]. For non-Chinese patients, consider if the benefit of using lipid-modifying doses of niacin concomitantly with VYTORIN outweighs the increased risk of myopathy and rhabdomyolysis. If concomitant use is decided, monitor patients for signs and symptoms of myopathy, particularly during initiation of therapy and during upward dose titration of either drug. |
| Fibrates (other than Gemfibrozil) | |
| Clinical Impact: | Fibrates may cause myopathy when given alone. The risk of myopathy and rhabdomyolysis is increased with concomitant use of fibrates with VYTORIN. |
| Intervention: | Consider if the benefit of using fibrates concomitantly with VYTORIN outweighs the increased risk of myopathy and rhabdomyolysis. If concomitant use is decided, monitor patients for signs and symptoms of myopathy, particularly during initiation of therapy and during upward dose titration of either drug. |
| Colchicine | |
| Clinical Impact: | Cases of myopathy and rhabdomyolysis have been reported with concomitant use of colchicine with VYTORIN. |
| Intervention: | Consider if the benefit of using colchicine concomitantly with VYTORIN outweighs the increased risk of myopathy and rhabdomyolysis. If concomitant use is decided, monitor patients for signs and symptoms of myopathy, particularly during initiation of therapy and during upward dose titration of either drug. |
| Grapefruit Juice | |
| Clinical Impact: | Grapefruit juice can raise the plasma levels of simvastatin and may increase the risk of myopathy and rhabdomyolysis. |
| Intervention: | Avoid grapefruit juice when taking VYTORIN. |
Structured Label Content
Section 42229-5 (42229-5)
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
VYTORIN
In the VYTORIN (ezetimibe and simvastatin) placebo-controlled clinical trials database of 1420 patients (age range 20-83 years, 52% female, 87% White, 3% Black or African American, 3% Asians, 5% other races identified as Hispanic or Latino ethnicity) with a median treatment duration of 27 weeks, 5% of patients on VYTORIN and 2.2% of patients on placebo discontinued due to adverse reactions.
The most commonly reported adverse reactions (incidence ≥2% and greater than placebo) in controlled clinical trials were: headache (5.8%), increased ALT (3.7%), myalgia (3.6%), upper respiratory tract infection (3.6%), and diarrhea (2.8%). The most common adverse reactions in the group treated with VYTORIN that led to treatment discontinuation and occurred at a rate greater than placebo were: increased ALT (0.9%), myalgia (0.6%), increased AST (0.4%), and back pain (0.4%).
VYTORIN has been evaluated for safety in more than 10,189 patients in clinical trials.
Table 1 summarizes the frequency of clinical adverse reactions reported in ≥2% of patients treated with VYTORIN (n=1420) and at an incidence greater than placebo from four placebo-controlled trials.
| % Placebo N = 371 |
% Ezetimibe 10 mg N = 302 |
% Simvastatin All doses.
N = 1234 |
% VYTORIN
N = 1420 |
|
|---|---|---|---|---|
| Headache | 5.4 | 6.0 | 5.9 | 5.8 |
| Upper respiratory tract infection | 2.7 | 5.0 | 5.0 | 3.6 |
| Myalgia | 2.4 | 2.3 | 2.6 | 3.6 |
| Diarrhea | 2.2 | 5.0 | 3.7 | 2.8 |
| Pain in extremity | 1.3 | 3.0 | 2.0 | 2.3 |
| Influenza | 0.8 | 1.0 | 1.9 | 2.3 |
Section 42230-3 (42230-3)
| This Patient Information has been approved by the U.S. Food and Drug Administration. | Revised: 2/2024 |
|
PATIENT INFORMATION VYTORIN® [VI-tor-in] (ezetimibe and simvastatin) tablets, for oral use |
|
| Read this Information carefully before you start taking VYTORIN® and each time you get a VYTORIN. There may be new information. This information does not take the place of talking with your healthcare provider about your medical condition or your treatment. If you have any questions about VYTORIN, ask your healthcare provider. Only your healthcare provider can determine if VYTORIN is right for you. | |
|
What is VYTORIN? VYTORIN is a prescription medicine that contains the cholesterol lowering medicines, simvastatin and ezetimibe:
The safety and effectiveness of VYTORIN has not been established in children younger than 10 years of age with inherited heterozygous familial hypercholesterolemia (HeFH) or other types of hyperlipidemia. |
|
Do not take VYTORIN if you:
Ask your healthcare provider or pharmacist if you are not sure if your medicine is listed above. |
|
Before you take VYTORIN, tell your healthcare provider about all of your medical conditions, including if you:
|
|
|
Tell your healthcare provider about all the medicines you take, including prescription and over-the-counter medicines, vitamins, and herbal supplements. Talk to your healthcare provider before you start taking any new medicines. Tell your healthcare provider who prescribes VYTORIN if another healthcare provider increases the dose of another medicine you are taking. VYTORIN may affect the way other medicines work, and other medicines may affect how VYTORIN works. Especially tell your healthcare provider if you take:
Taking VYTORIN with certain substances can also increase the risk of muscle problems. Especially tell your healthcare provider if you take:
Ask your healthcare provider or pharmacist for a list of medicines if you are not sure. Know the medicines you take. Keep a list of them to show your healthcare provider and pharmacist when you get a new medicine. |
|
How should I take VYTORIN?
If you take too much VYTORIN, call your healthcare provider or Poison Help Line at 1-800-222-1222 or go to the nearest hospital emergency room right away. |
|
|
What are the possible side effects of VYTORIN? VYTORIN may cause serious side effects including: |
|
The most common side effects of VYTORIN include:
Tell your healthcare provider if you have any side effect that bothers you or does not go away. These are not all the possible side effects of VYTORIN. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. |
|
How should I store VYTORIN?
Keep VYTORIN and all medicines out of the reach of children. |
|
| General information about safe and effective use of VYTORIN. | |
| Medicines are sometimes prescribed for purposes other than those listed in a Patient Information leaflet. Do not use VYTORIN for a condition for which it was not prescribed. Do not give VYTORIN to other people, even if they have the same symptoms that you have. It may harm them. | |
| You can ask your pharmacist or healthcare provider for information about VYTORIN that is written for health professionals. | |
| What are the ingredients in VYTORIN? | |
| Active Ingredients: ezetimibe and simvastatin. | |
| Inactive Ingredients: butylated hydroxyanisole, citric acid monohydrate, croscarmellose sodium, hypromellose, lactose monohydrate, magnesium stearate, microcrystalline cellulose, and propyl gallate. | |
|
Distributed by: Organon LLC, a subsidiary of For patent information: www.organon.com/our-solutions/patent/ © 2024 Organon group of companies. All rights reserved. For more information, go to www.organon.com/our-focus/products-list/ or call 1-844-674-3200. usppi-og0653a-t-2402r001 |
Section 43683-2 (43683-2)
Section 44425-7 (44425-7)
Storage
Store at 68°F to 77°F (20°C to 25°C). [See USP Controlled Room Temperature.] Keep container tightly closed.
10 Overdosage (10 OVERDOSAGE)
No specific antidotes for VYTORIN are known. In the event of an overdose with VYTORIN, consider contacting the Poison Help Line (1-800-222-1222) or a medical toxicologist for overdosage management recommendations.
8.2 Lactation
Risk Summary
There is no information about the presence of ezetimibe or simvastatin in human breast milk, the effects of the drug on the breastfed infant or the effect of the drug on milk production. However, it has been shown that other statins pass into human milk. Statins, including VYTORIN, decrease cholesterol synthesis and possibly the synthesis of other biologically active substances derived from cholesterol and may cause harm to the breast fed infant.
Because of the potential for serious adverse reactions in a breastfed infant, based on the mechanism of action, advise patients that breastfeeding is not recommended during treatment with VYTORIN [see Use in Specific Populations (8.2) and Clinical Pharmacology (12.1)].
Data
Animal Data
Ezetimibe was present in the milk of lactating rats. The pup to maternal plasma ratio for total ezetimibe was 0.5 on lactation day 12.
11 Description (11 DESCRIPTION)
VYTORIN contains ezetimibe, a dietary cholesterol absorption inhibitor, and simvastatin, an HMG CoA reductase inhibitor.
The chemical name of ezetimibe is 1-(4-fluorophenyl)-3(R)-[3-(4-fluorophenyl)-3(S)-hydroxypropyl]-4(S)-(4-hydroxyphenyl)-2-azetidinone. The empirical formula is C24H21F2NO3 and its molecular weight is 409.4.
Ezetimibe is a white, crystalline powder that is freely to very soluble in ethanol, methanol, and acetone and practically insoluble in water. Its structural formula is:
Simvastatin, an inactive lactone, is hydrolyzed to the corresponding β-hydroxyacid form, which is an inhibitor of HMG-CoA reductase. Simvastatin is butanoic acid, 2,2-dimethyl-,1,2,3,7,8,8a-hexahydro-3,7-dimethyl-8-[2-(tetrahydro-4-hydroxy-6-oxo-2H-pyran-2-yl)-ethyl]-1-naphthalenyl ester, [1S-[1α,3α,7β,8β(2S*,4S*),-8aβ]]. The empirical formula of simvastatin is C25H38O5 and its molecular weight is 418.57.
Simvastatin is a white to off-white, nonhygroscopic, crystalline powder that is practically insoluble in water and freely soluble in chloroform, methanol and ethanol. Its structural formula is:
VYTORIN is available for oral use as tablets containing 10 mg of ezetimibe, and 10 mg of simvastatin (VYTORIN 10/10), 20 mg of simvastatin (VYTORIN 10/20), 40 mg of simvastatin (VYTORIN 10/40), or 80 mg of simvastatin (VYTORIN 10/80). Each tablet contains the following inactive ingredients: butylated hydroxyanisole NF, citric acid monohydrate USP, croscarmellose sodium NF, hypromellose USP, lactose monohydrate NF, magnesium stearate NF, microcrystalline cellulose NF, and propyl gallate NF.
8.4 Pediatric Use
The safety and effectiveness of ezetimibe in combination with a statin as an adjunct to diet to reduce LDL-C have been established in pediatric patients 10 years of age and older with HeFH. Use of VYTORIN for this indication is based on a double-blind, placebo-controlled clinical trial in 248 pediatric patients (142 males and 106 postmenarchal females) 10 years of age and older with HeFH [see Clinical Studies (14)]. In this limited controlled trial, there was no significant effect on growth or sexual maturation in the adolescent males or females, or on menstrual cycle length in females.
The safety and effectiveness of VYTORIN have not been established in pediatric patients younger than 10 years of age with HeFH, or in pediatric patients with other types of hyperlipidemia.
8.5 Geriatric Use
Advanced age (≥65 years) is a risk factor for VYTORIN-associated myopathy and rhabdomyolysis. Dose selection for an elderly patient should be cautious, recognizing the greater frequency of decreased hepatic, renal, or cardiac function, and of concomitant disease or other drug therapy and the higher risk of myopathy. Monitor geriatric patients receiving VYTORIN for the increased risk of myopathy [see Warnings and Precautions (5.1)].
Of the 10,189 patients who received VYTORIN in clinical studies, 3242 (32%) were 65 and older (this included 844 (8%) who were 75 and older). No overall differences in safety or effectiveness were observed between these subjects and younger subjects, and other reported clinical experience has not identified differences in responses between the elderly and younger patients but greater sensitivity of some older individuals cannot be ruled out.
14 Clinical Studies (14 CLINICAL STUDIES)
Primary Hyperlipidemia in Adults
VYTORIN
VYTORIN reduces LDL-C in adult patients with primary hyperlipidemia. Maximal to near maximal response is generally achieved within 2 weeks and maintained during chronic therapy.
VYTORIN is effective in males and females with primary hyperlipidemia. There were insufficient numbers of patients who self-identified as Black or African American, Asian, or other races to determine if these patients responded differently than White patients.
Five multicenter, double-blind trials conducted with either VYTORIN or coadministered ezetimibe and simvastatin equivalent to VYTORIN in patients with primary hyperlipidemia are reported: two were comparisons with simvastatin, two were comparisons with atorvastatin, and one was a comparison with rosuvastatin.
In a multicenter, double-blind, placebo-controlled, 12-week trial, 1528 patients with primary hyperlipidemia were randomized to one of ten treatment groups: placebo, ezetimibe (10 mg), simvastatin (10 mg, 20 mg, 40 mg, or 80 mg), or VYTORIN (10/10, 10/20, 10/40, or 10/80).
When patients receiving VYTORIN were compared to those receiving all doses of simvastatin, VYTORIN significantly lowered total-C, LDL-C, Apo B, TG, and non-HDL-C. The effects of VYTORIN on HDL-C were similar to the effects seen with simvastatin. Further analysis showed VYTORIN significantly increased HDL-C compared with placebo. (See Table 8.) The lipid response to VYTORIN was similar in patients with TG levels greater than or less than 200 mg/dL.
| Treatment | |||||||
|---|---|---|---|---|---|---|---|
| (Daily Dose) | N | Total-C | LDL-C | Apo B | HDL-C | TG | Non-HDL-C |
| Pooled data (All VYTORIN doses) VYTORIN doses pooled (10/10-10/80) significantly reduced total-C, LDL-C, Apo B, TG, and non-HDL-C compared to simvastatin and significantly increased HDL-C compared to placebo.
|
609 | -38 | -53 | -42 | +7 | -24 | -49 |
| Pooled data (All simvastatin doses) | 622 | -28 | -39 | -32 | +7 | -21 | -36 |
| Ezetimibe 10 mg | 149 | -13 | -19 | -15 | +5 | -11 | -18 |
| Placebo | 148 | -1 | -2 | 0 | 0 | -2 | -2 |
| VYTORIN by dose | |||||||
| 10/10 | 152 | -31 | -45 | -35 | +8 | -23 | -41 |
| 10/20 | 156 | -36 | -52 | -41 | +10 | -24 | -47 |
| 10/40 | 147 | -39 | -55 | -44 | +6 | -23 | -51 |
| 10/80 | 154 | -43 | -60 | -49 | +6 | -31 | -56 |
| Simvastatin by dose | |||||||
| 10 mg | 158 | -23 | -33 | -26 | +5 | -17 | -30 |
| 20 mg | 150 | -24 | -34 | -28 | +7 | -18 | -32 |
| 40 mg | 156 | -29 | -41 | -33 | +8 | -21 | -38 |
| 80 mg | 158 | -35 | -49 | -39 | +7 | -27 | -45 |
In a multicenter, double-blind, controlled, 23-week trial, 710 patients with known CHD or CHD risk equivalents, as defined by the NCEP ATP III guidelines, and an LDL-C ≥130 mg/dL were randomized to one of four treatment groups: coadministered ezetimibe and simvastatin equivalent to VYTORIN (10/10, 10/20, and 10/40) or simvastatin 20 mg. Patients not reaching an LDL-C <100 mg/dL had their simvastatin dose titrated at 6-week intervals to a maximal dose of 80 mg. At Week 5, the LDL-C reductions with VYTORIN 10/10, 10/20, or 10/40 were significantly larger than with simvastatin 20 mg (see Table 9).
| Simvastatin 20 mg |
VYTORIN 10/10 |
VYTORIN 10/20 |
VYTORIN 10/40 |
|
|---|---|---|---|---|
| N | 253 | 251 | 109 | 97 |
| Mean baseline LDL-C | 174 | 165 | 167 | 171 |
| Percent change LDL-C | -38 | -47 | -53 | -59 |
In a multicenter, double-blind, 6-week trial, 1902 patients with primary hyperlipidemia were randomized to one of eight treatment groups: VYTORIN (10/10, 10/20, 10/40, or 10/80) or atorvastatin (10 mg, 20 mg, 40 mg, or 80 mg).
Across the dosage range, when patients receiving VYTORIN were compared to those receiving milligram-equivalent statin doses of atorvastatin, VYTORIN lowered total-C, LDL-C, Apo B, and non-HDL-C significantly more than atorvastatin. Only the 10/40 mg and 10/80 mg VYTORIN doses increased HDL-C significantly more than the corresponding milligram-equivalent statin dose of atorvastatin. The effects of VYTORIN on TG were similar to the effects seen with atorvastatin. (See Table 10.)
| Treatment | |||||||
|---|---|---|---|---|---|---|---|
| (Daily Dose) | N | Total-C VYTORIN doses pooled (10/10-10/80) provided significantly greater reductions in total-C, LDL-C, Apo B, and non-HDL-C compared to atorvastatin doses pooled (10-80).
|
LDL-C | Apo B | HDL-C | TG | Non-HDL-C |
| VYTORIN by dose | |||||||
| 10/10 | 230 | -34 p<0.05 for difference with atorvastatin at equal mg doses of the simvastatin component.
|
-47 | -37 | +8 | -26 | -43 |
| 10/20 | 233 | -37 | -51 | -40 | +7 | -25 | -46 |
| 10/40 | 236 | -41 | -57 | -46 | +9 | -27 | -52 |
| 10/80 | 224 | -43 | -59 | -48 | +8 | -31 | -54 |
| Atorvastatin by dose | |||||||
| 10 mg | 235 | -27 | -36 | -31 | +7 | -21 | -34 |
| 20 mg | 230 | -32 | -44 | -37 | +5 | -25 | -41 |
| 40 mg | 232 | -36 | -48 | -40 | +4 | -24 | -45 |
| 80 mg | 230 | -40 | -53 | -44 | +1 | -32 | -50 |
In a multicenter, double-blind, 24-week, forced-titration trial, 788 patients with primary hyperlipidemia were randomized to receive coadministered ezetimibe and simvastatin equivalent to VYTORIN (10/10 and 10/20) or atorvastatin 10 mg. For all three treatment groups, the dose of the statin was titrated at 6-week intervals to 80 mg. At each pre-specified dose comparison, VYTORIN lowered LDL-C to a greater degree than atorvastatin (see Table 11).
| Treatment | N | Total-C | LDL-C | Apo B | HDL-C | TG | Non-HDL-C |
|---|---|---|---|---|---|---|---|
| Week 6 | |||||||
| Atorvastatin 10 mg Atorvastatin: 10 mg start dose titrated to 20 mg, 40 mg, and 80 mg through Weeks 6, 12, 18, and 24.
|
262 | -28 | -37 | -32 | +5 | -23 | -35 |
| VYTORIN 10/10 VYTORIN: 10/10 start dose titrated to 10/20, 10/40, and 10/80 through Weeks 6, 12, 18, and 24.
|
263 | -34 p≤0.05 for difference with atorvastatin in the specified week.
|
-46 | -38 | +8 | -26 | -43 |
| VYTORIN 10/20 VYTORIN: 10/20 start dose titrated to 10/40, 10/40, and 10/80 through Weeks 6, 12, 18, and 24.
|
263 | -36 | -50 | -41 | +10 | -25 | -46 |
| Week 12 | |||||||
| Atorvastatin 20 mg | 246 | -33 | -44 | -38 | +7 | -28 | -42 |
| VYTORIN 10/20 | 250 | -37 | -50 | -41 | +9 | -28 | -46 |
| VYTORIN 10/40 | 252 | -39 | -54 | -45 | +12 | -31 | -50 |
| Week 18 | |||||||
| Atorvastatin 40 mg | 237 | -37 | -49 | -42 | +8 | -31 | -47 |
| VYTORIN 10/40 Data pooled for common doses of VYTORIN at Weeks 18 and 24.
|
482 | -40 | -56 | -45 | +11 | -32 | -52 |
| Week 24 | |||||||
| Atorvastatin 80 mg | 228 | -40 | -53 | -45 | +6 | -35 | -50 |
| VYTORIN 10/80 | 459 | -43 | -59 | -49 | +12 | -35 | -55 |
In a multicenter, double-blind, 6-week trial, 2959 patients with primary hyperlipidemia, were randomized to one of six treatment groups: VYTORIN (10/20, 10/40, or 10/80) or rosuvastatin (10 mg, 20 mg, or 40 mg).
The effects of VYTORIN and rosuvastatin on total-C, LDL-C, Apo B, TG, non-HDL-C and HDL-C are shown in Table 12.
| Treatment | |||||||
|---|---|---|---|---|---|---|---|
| (Daily Dose) | N | Total-C VYTORIN doses pooled (10/20-10/80) provided significantly greater reductions in total-C, LDL-C, Apo B, and non-HDL-C compared to rosuvastatin doses pooled (10-40 mg).
|
LDL-C | Apo B | HDL-C | TG | Non-HDL-C |
| VYTORIN by dose | |||||||
| 10/20 | 476 | -37 p<0.05 vs. rosuvastatin 10 mg.
|
-52 | -42 | +7 | -23 | -47 |
| 10/40 | 477 | -39 p<0.05 vs. rosuvastatin 20 mg.
|
-55 | -44 | +8 | -27 | -50 |
| 10/80 | 474 | -44 p<0.05 vs. rosuvastatin 40 mg.
|
-61 | -50 | +8 | -30 | -56 |
| Rosuvastatin by dose | |||||||
| 10 mg | 475 | -32 | -46 | -37 | +7 | -20 | -42 |
| 20 mg | 478 | -37 | -52 | -43 | +8 | -26 | -48 |
| 40 mg | 475 | -41 | -57 | -47 | +8 | -28 | -52 |
In a multicenter, double-blind, 24-week trial, 214 patients with type 2 diabetes mellitus treated with thiazolidinediones (rosiglitazone or pioglitazone) for a minimum of 3 months and simvastatin 20 mg for a minimum of 6 weeks were randomized to receive either simvastatin 40 mg or the coadministered active ingredients equivalent to VYTORIN 10/20. The median LDL-C and HbA1c levels at baseline were 89 mg/dL and 7.1%, respectively.
VYTORIN 10/20 was significantly more effective than doubling the dose of simvastatin to 40 mg. The median percent changes from baseline for VYTORIN vs. simvastatin were: LDL-C -25% and -5%; total-C -16% and -5%; Apo B -19% and -5%; and non-HDL-C -23% and -5%. Results for HDL-C and TG between the two treatment groups were not significantly different.
Ezetimibe
In two multicenter, double-blind, placebo-controlled, 12-week trials in 1719 patients with primary hyperlipidemia, ezetimibe significantly lowered total-C (-13%), LDL-C (-19%), Apo B (-14%), and TG (-8%), and increased HDL-C (+3%) compared to placebo. Reduction in LDL-C was consistent across age, sex, and baseline LDL-C.
Simvastatin
In two large, placebo-controlled clinical trials, the Scandinavian Simvastatin Survival Trial (N=4,444 patients) and the Heart Protection Trial (N=20,536 patients), the effects of treatment with simvastatin were assessed in patients at high risk of coronary events because of existing coronary heart disease, diabetes, peripheral vessel disease, history of stroke or other cerebrovascular disease. Simvastatin was proven to reduce: the risk of total mortality by reducing CHD deaths; the risk of non-fatal myocardial infarction and stroke; and the need for coronary and non-coronary revascularization procedures.
No incremental benefit of VYTORIN on cardiovascular morbidity and mortality over and above that demonstrated for simvastatin has been established.
Heterozygous Familial Hypercholesterolemia (HeFH) in Pediatric Patients
The effects of ezetimibe coadministered with simvastatin (n=126) compared to simvastatin monotherapy (n=122) have been evaluated in males and females with HeFH. In a multicenter, double-blind, controlled trial followed by an open-label phase, 142 males and 106 postmenarchal females, 10 to 17 years of age (mean age 14.2 years, 43% females, 82% White, 4% Asian, 2% Black or African American, 13% multi- racial; 14% identified as Hispanic or Latino ethnicity) with HeFH were randomized to receive either ezetimibe coadministered with simvastatin or simvastatin monotherapy. Inclusion in the trial required 1) a baseline LDL-C level between 160 and 400 mg/dL and 2) a medical history and clinical presentation consistent with HeFH. The mean baseline LDL-C value was 225 mg/dL (range: 161 to 351 mg/dL) in the ezetimibe coadministered with simvastatin group compared to 219 mg/dL (range: 149 to 336 mg/dL) in the simvastatin monotherapy group. The patients received coadministered ezetimibe and simvastatin (10 mg, 20 mg, or 40 mg) or simvastatin monotherapy (10 mg, 20 mg, or 40 mg) for 6 weeks, coadministered ezetimibe and 40- mg simvastatin or 40-mg simvastatin monotherapy for the next 27 weeks, and open-label coadministered ezetimibe and simvastatin (10 mg, 20 mg, or 40 mg) for 20 weeks thereafter.
The results of the trial at Week 6 are summarized in Table 13. Results at Week 33 were consistent with those at Week 6.
| Total-C | LDL-C | Apo B | Non-HDL-C | |
|---|---|---|---|---|
| Mean percent difference between treatment groups | -12% | -15% | -12% | -14% |
| 95% Confidence Interval | (-15%,-9%) | (-18%,-12%) | (-15%,-9%) | (-17%,-11%) |
Homozygous Familial Hypercholesterolemia (HoFH) in Adults
A double-blind, randomized, 12-week trial was performed in patients with a clinical and/or genotypic diagnosis of HoFH. Data were analyzed from a subgroup of patients (n=14) receiving simvastatin 40 mg at baseline. Increasing the dose of simvastatin from 40 to 80 mg (n=5) produced a reduction of LDL-C of 13% from baseline on simvastatin 40 mg. Coadministered ezetimibe and simvastatin equivalent to VYTORIN (10/40 and 10/80 pooled, n=9), produced a reduction of LDL-C of 23% from baseline on simvastatin 40 mg. In those patients coadministered ezetimibe and simvastatin equivalent to VYTORIN (10/80, n=5), a reduction of LDL-C of 29% from baseline on simvastatin 40 mg was produced.
Chronic Kidney Disease (CKD) in Adults
The Trial of Heart and Renal Protection (SHARP) was a multinational, randomized, placebo-controlled, double-blind trial that investigated the effect of VYTORIN on the time to a first major vascular event (MVE) among 9438 patients with moderate to severe chronic kidney disease (approximately one-third on dialysis at baseline) who did not have a history of myocardial infarction or coronary revascularization. An MVE was defined as nonfatal MI, cardiac death, stroke, or any revascularization procedure. Patients were allocated to treatment using a method that took into account the distribution of 8 important baseline characteristics of patients already enrolled and minimized the imbalance of those characteristics across the groups.
For the first year, 9438 patients were allocated 4:4:1, to VYTORIN 10/20, placebo, or simvastatin 20 mg daily, respectively. The 1-year simvastatin arm enabled the comparison of VYTORIN to simvastatin with regard to safety and effect on lipid levels. At 1 year the simvastatin-only arm was re-allocated 1:1 to VYTORIN 10/20 or placebo. A total of 9270 patients were ever allocated to VYTORIN 10/20 (n=4650) or placebo (n=4620) during the trial. The median follow-up duration was 4.9 years. Patients had a mean age of 61 years; 63% were male, 72% were White, and 23% were diabetic; and, for those not on dialysis at baseline, the median serum creatinine was 2.5 mg/dL and the median estimated glomerular filtration rate (eGFR) was 25.6 mL/min/1.73 m2, with 94% of patients having an eGFR < 45 mL/min/1.73m2. Eligibility did not depend on lipid levels. Mean LDL-C at baseline was 108 mg/dL. At 1 year, the mean LDL-C was 26% lower in the simvastatin arm and 38% lower in the VYTORIN arm relative to placebo. At the midpoint of the trial (2.5 years), the mean LDL-C was 32% lower for VYTORIN relative to placebo. Patients no longer taking trial medication were included in all lipid measurements.
In the primary intent-to-treat analysis, 639 (15.2%) of 4193 patients initially allocated to VYTORIN and 749 (17.9%) of 4191 patients initially allocated to placebo experienced an MVE. This corresponded to a relative risk reduction of 16% (p=0.001) (see Figure 1). Similarly, 526 (11.3%) of 4650 patients ever allocated to VYTORIN and 619 (13.4%) of 4620 patients ever allocated to placebo experienced a major atherosclerotic event (MAE; a subset of the MVE composite that excluded non-coronary cardiac deaths and hemorrhagic stroke), corresponding to a relative risk reduction of 17% (p=0.002). The trial demonstrated that treatment with VYTORIN 10/20 mg versus placebo reduced the risk for MVE and MAE in this CKD population. The trial design precluded drawing conclusions regarding the independent contribution of either ezetimibe or simvastatin to the observed effect.
The treatment effect of VYTORIN on MVE was attenuated among patients on dialysis at baseline compared with those not on dialysis at baseline. Among 3023 patients on dialysis at baseline, VYTORIN reduced the risk of MVE by 6% (RR 0.94: 95% CI 0.80-1.09) compared with 22% (RR 0.78: 95% CI 0.69-0.89) among 6247 patients not on dialysis at baseline (interaction P=0.08).
| Figure 1: Effect of VYTORIN on the Primary Endpoint of Risk of Major Vascular Events |
The individual components of MVE in all patients ever allocated to VYTORIN or placebo are presented in Table 14.
| Outcome | VYTORIN 10/20 (N=4650) |
Placebo (N=4620) |
Risk Ratio (95% CI) |
P-value |
|---|---|---|---|---|
| Major Vascular Events | 701 (15.1%) | 814 (17.6%) | 0.85 (0.77-0.94) | 0.001 |
| Nonfatal MI | 134 (2.9%) | 159 (3.4%) | 0.84 (0.66-1.05) | 0.12 |
| Cardiac Death | 253 (5.4%) | 272 (5.9%) | 0.93 (0.78-1.10) | 0.38 |
| Any Stroke | 171 (3.7%) | 210 (4.5%) | 0.81 (0.66-0.99) | 0.038 |
| Non-hemorrhagic Stroke | 131 (2.8%) | 174 (3.8%) | 0.75 (0.60-0.94) | 0.011 |
| Hemorrhagic Stroke | 45 (1.0%) | 37 (0.8%) | 1.21 (0.78-1.86) | 0.40 |
| Any Revascularization | 284 (6.1%) | 352 (7.6%) | 0.79 (0.68-0.93) | 0.004 |
Among patients not on dialysis at baseline, VYTORIN did not reduce the risk of progressing to end-stage renal disease compared with placebo (RR 0.97: 95% CI 0.89-1.05).
Simvastatin Cardiovascular Outcome Trials in Adults at High Risk of Coronary Heart Disease Events
In a randomized, double-blind, placebo-controlled, multi-centered trial [the Scandinavian Simvastatin Survival Trial (Trial 4S)], the effect of therapy with simvastatin on total mortality was assessed in 4,444 adult patients with CHD (history of angina and/or a previous myocardial infarction) and baseline total cholesterol (total-C) between 212 and 309 mg/dL who were on a lipid-lowering diet. In Trial 4S, patients were treated with standard care, including lipid-lowering diet, and randomized to either simvastatin 20-40 mg/day (n=2,221) or placebo (n=2,223) for a median duration of 5.4 years.
- Simvastatin significantly reduced the risk of mortality by 30% (p=0.0003, 182 deaths in the simvastatin group vs 256 deaths in the placebo group). The risk of CHD mortality was significantly reduced by 42% (p=0.00001, 111 deaths in the simvastatin group vs 189 deaths in the placebo group). There was no statistically significant difference between groups in non-cardiovascular mortality.
- Simvastatin significantly reduced the risk for the secondary composite endpoint (time to first occurrence of CHD death, definite or probable hospital verified non-fatal MI, silent MI verified by ECG, or resuscitated cardiac arrest) by 34% (p<0.00001, 431 vs 622 patients with one or more events). Simvastatin reduced the risk of major coronary events to a similar extent across the range of baseline total and LDL cholesterol levels. The risk of having a hospital-verified non-fatal MI was reduced by 37%.
- Simvastatin significantly reduced the risk for undergoing myocardial revascularization procedures (coronary artery bypass grafting or percutaneous transluminal coronary angioplasty) by 37% (p<0.00001, 252 vs 383 patients).
- Simvastatin significantly reduced the risk of fatal plus non-fatal cerebrovascular events (combined stroke and transient ischemic attacks) by 28% (p=0.033, 75 vs 102 patients).
- Over the course of the trial, treatment with simvastatin led to mean reductions in total-C, LDL-C and triglycerides (TG) of 25%, 35%, and 10%, respectively, and a mean increase in high-density lipoprotein cholesterol (HDL-C) of 8%. In contrast, treatment with placebo led to increases in total- C, LDL-C and TG of 1%, 1%, and 7%, respectively.
- Because there were only 53 female deaths (approximately 18% of the trial population was female), the effect of simvastatin on mortality in females could not be adequately assessed. However, simvastatin significantly reduced the risk of having major coronary events in females by 34% (60 vs 91 women with one or more event).
- Simvastatin resulted in similar decreases in relative risk for total mortality, CHD mortality, and major coronary events in geriatric patients (≥65 years) compared with younger adults.
The Heart Protection Trial (Trial HPS) was a randomized, placebo-controlled, double-blind, multi- centered trial with a mean duration of 5 years conducted in 10,269 patients on simvastatin 40 mg and 10,267 on placebo. Patients had a mean age of 64 years (range 40-80 years old), 97% were White, and were at high risk of developing a major coronary event because of existing CHD (65%), diabetes (Type 2, 26%; Type 1, 3%), history of stroke or other cerebrovascular disease (16%), peripheral vascular disease (33%), or they were males ≥65 years with hypertension in (6%). At baseline:
- 3,421 patients (17%) had LDL-C levels below 100 mg/dL, including 953 (5%) below 80 mg/dL; and
- 10,047 patients (49%) had levels greater than 130 mg/dL.
Patients were randomized to simvastatin or placebo using a covariate adaptive method which considered the distribution of 10 important baseline characteristics of patients already enrolled.
The Trial HPS results showed that simvastatin 40 mg/day significantly reduced: total and CHD mortality; and non-fatal MI, stroke, and revascularization procedures (coronary and non-coronary) (see Table 15).
| Endpoint | Simvastatin (N=10,269) n (%) n = number of patients with indicated event
|
Placebo (N=10,267) n (%) |
Risk Reduction (%) (95% CI) |
p-Value |
|---|---|---|---|---|
| Primary | ||||
| Mortality | 1,328 (12.9%) |
1,507 (14.7%) |
13% (6-19%) | p=0.0003 |
| CHD mortality | 587 (5.7%) | 707 (6.9%) | 18% (8-26%) | p=0.0005 |
| Secondary | ||||
| Non-fatal MI | 357 (3.5%) | 574 (5.6%) | 38% (30-46%) | p<0.0001 |
| Stroke | 444 (4.3%) | 585 (5.7%) | 25% (15-34%) | p<0.0001 |
| Tertiary | ||||
| Coronary revascularization | 513 (5%) | 725 (7.1%) | 30% (22-38%) | p<0.0001 |
| Peripheral and other non-coronary revascularization | 450 (4.4%) | 532 (5.2%) | 16% (5-26%) | p=0.006 |
Two composite endpoints were defined to have enough events to assess relative risk reductions across a range of baseline characteristics:
- Major coronary events (MCE) was comprised of CHD mortality and non-fatal MI. Analyzed by time-to-first event; 898 patients (8.7%) treated with simvastatin had events and 1,212 patients (11.8%) treated with placebo had events.
- Major vascular events (MVE) was comprised of MCE, stroke, and revascularization procedures including coronary, peripheral and other non-coronary procedures. Analyzed by time-to-first event; 2,033 patients (19.8%) treated with simvastatin had events and 2,585 patients (25.2%) on placebo had events.
Simvastatin use led to significant relative risk reductions for both composite endpoints (27% for MCE and 24% for MVE, p<0.0001) and for all components of the composite endpoints. The risk reductions produced by simvastatin in both MCE and MVE were evident and consistent regardless of cardiovascular disease related medical history at trial entry (i.e., CHD alone; or peripheral vascular disease, cerebrovascular disease, diabetes or treated hypertension, with or without CHD), gender, age, baseline levels of LDL-C, baseline concomitant cardiovascular medications (i.e., aspirin, beta blockers, or calcium channel blockers), smoking status, or obesity. Patients with diabetes showed risk reductions for MCE and MVE due to simvastatin treatment regardless of baseline HbA1c levels or obesity.
4 Contraindications (4 CONTRAINDICATIONS)
VYTORIN is contraindicated in the following conditions:
- Concomitant use of strong CYP3A4 inhibitors (select azole anti-fungals, macrolide antibiotics, anti-viral medications, and nefazodone) [see Drug Interactions (7.1)].
- Concomitant use of cyclosporine, danazol, or danazol [see Drug Interactions (7.1)].
- Acute liver failure or decompensated cirrhosis [see Warnings and Precautions (5.3)].
- Hypersensitivity to simvastatin, ezetimibe, or any excipients in VYTORIN. Hypersensitivity reactions, including anaphylaxis, angioedema, and Stevens-Johnson syndrome, have been reported [see Adverse Reactions (6.2)].
6 Adverse Reactions (6 ADVERSE REACTIONS)
The following serious adverse reactions are discussed in greater detail in other sections of the label:
- Myopathy and Rhabdomyolysis [see Warnings and Precautions (5.1)]
- Immune-Mediated Necrotizing Myopathy [see Warnings and Precautions (5.2)]
- Hepatic Dysfunction [see Warnings and Precautions (5.3)]
- Increases in HbA1c and Fasting Serum Glucose Levels [see Warnings and Precautions (5.4)]
7 Drug Interactions (7 DRUG INTERACTIONS)
VYTORIN
8.6 Renal Impairment
Renal impairment is a risk factor for myopathy and rhabdomyolysis. Monitor all patients with renal impairment for development of myopathy. Doses of VYTORIN exceeding 10/20 mg should be used with caution and close monitoring in patients with moderate to severe renal impairment [see Dosage and Administration (2.4) and Warnings and Precautions (5.1)].
In the SHARP trial of 9270 patients with moderate to severe renal impairment (6247 non-dialysis patients with median serum creatinine 2.5 mg/dL and median estimated glomerular filtration rate 25.6 mL/min/1.73 m2, and 3023 dialysis patients), the incidence of serious adverse events, adverse events leading to discontinuation of trial treatment, or adverse events of special interest (musculoskeletal adverse events, liver enzyme abnormalities, incident cancer) was similar between patients ever assigned to VYTORIN 10/20 mg (n=4650) or placebo (n=4620) during a median follow-up of 4.9 years.
8.8 Chinese Patients
In a clinical trial in which patients at high risk of CVD were treated with simvastatin 40 mg/day (median follow-up 3.9 years), the incidence of myopathy was approximately 0.05% for non-Chinese patients (n=7367) compared with 0.24% for Chinese patients (n=5468). In this trial the incidence of myopathy for Chinese patients on simvastatin 40 mg/day or ezetimibe and simvastatin 10/40 mg/day coadministered with extended-release niacin 2 g/day was 1.24%.
Chinese patients may be at higher risk for myopathy, monitor these patients appropriately. Coadministration of VYTORIN with lipid-modifying doses of niacin-containing products (≥1 g/day niacin) is not recommended in Chinese patients [see Warnings and Precautions (5.1) and Drug Interactions (7.1)].
12.2 Pharmacodynamics
VYTORIN reduces total cholesterol (total-C), LDL-C, apolipoprotein (Apo) B, and non-high-density lipoprotein cholesterol (non-HDL-C) in patients with hyperlipidemia.
Ezetimibe
In a 2-week clinical trial in 18 hypercholesterolemic patients, ezetimibe inhibited intestinal cholesterol absorption by 54%, compared with placebo. Ezetimibe had no clinically meaningful effect on the plasma concentrations of the fat-soluble vitamins A, D, and E and did not impair adrenocortical steroid hormone production.
Simvastatin
Inhibition of HMG-CoA reductase by simvastatin acid accelerates the expression of LDL-receptors, followed by the uptake of LDL-C from blood to the liver, leading to a decrease in plasma LDL-C and total cholesterol. Sustained inhibition of cholesterol synthesis in the liver also decreases levels of very-low density lipoproteins. The maximum LDL-C reduction of ZOCOR is usually achieved by 4 weeks and is maintained after that.
12.3 Pharmacokinetics
The results of a bioequivalence trial in healthy subjects demonstrated that the VYTORIN (ezetimibe and simvastatin) 10 mg/10 mg to 10 mg/80 mg combination tablets are bioequivalent to coadministration of corresponding doses of ezetimibe (ZETIA®) and simvastatin (ZOCOR®) as individual tablets.
8.7 Hepatic Impairment
VYTORIN is contraindicated in patients with acute liver failure or decompensated cirrhosis. [See Contraindications (4) and Warnings and Precautions (5.3).]
1 Indications and Usage (1 INDICATIONS AND USAGE)
VYTORIN
VYTORIN® is a combination of simvastatin and ezetimibe indicated:
-
As an adjunct to diet to reduce elevated low density lipoprotein cholesterol (LDL-C):
- In adults with primary hyperlipidemia.
- In adults and pediatric patients aged 10 years and older with heterozygous familial hypercholesterolemia (HeFH).
- As an adjunct to other LDL-C-lowering therapies to reduce elevated LDL-C in adults with homozygous familial hypercholesterolemia (HoFH).
Simvastatin
Simvastatin, when used as a component of VYTORIN, is indicated to reduce the risk of total mortality by reducing risk of coronary heart disease death, non-fatal myocardial infarction and stroke, and the need for coronary and non-coronary revascularization procedures in adults with established coronary heart disease, cerebrovascular disease, peripheral vascular disease, and/or diabetes, who are at high risk of coronary heart disease events.
5.3 Hepatic Dysfunction
Increases in serum transaminases have been reported with use of VYTORIN [see Adverse Reactions (6.1)]. In most cases, these changes appeared soon after initiation, were transient, were not accompanied by symptoms, and resolved or improved on continued therapy or after a brief interruption in therapy. Marked persistent increases of hepatic transaminases have also occurred with VYTORIN. There have been rare postmarketing reports of fatal and non-fatal hepatic failure in patients taking statins, including VYTORIN.
In three placebo-controlled, 12-week trials, the incidence of consecutive elevations (≥3 X ULN) in serum transaminases was 1.7% overall for patients treated with VYTORIN and appeared to be dose-related with an incidence of 2.6% for patients treated with VYTORIN 10/80. In controlled long-term (48-week) extensions, which included both newly-treated and previously-treated patients, the incidence of consecutive elevations (≥3 X ULN) in serum transaminases was 1.8% overall and 3.6% for patients treated with VYTORIN 10/80. These elevations in transaminases were generally asymptomatic, not associated with cholestasis, and returned to baseline after discontinuation of therapy or with continued treatment.
In SHARP, 9270 patients with chronic kidney disease were allocated to receive VYTORIN 10/20 mg daily (n=4650), or placebo (n=4620). During a median follow-up period of 4.9 years, the incidence of consecutive elevations of transaminases (>3 X ULN) was 0.7% for VYTORIN and 0.6% for placebo.
Patients who consume substantial quantities of alcohol and/or have a history of liver disease may be at increased risk for hepatic injury.
Consider liver enzyme testing before VYTORIN initiation and when clinically indicated thereafter. VYTORIN is contraindicated in patients with acute liver failure or decompensated cirrhosis [see Contraindications (4)]. If serious hepatic injury with clinical symptoms and/or hyperbilirubinemia or jaundice occurs, promptly discontinue VYTORIN.
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
- Myopathy and Rhabdomyolysis: Risk factors include age 65 years or greater, uncontrolled hypothyroidism, renal impairment, concomitant use with certain other drugs, and higher VYTORIN dosage. Chinese patients may be at higher risk for myopathy. Discontinue VYTORIN if markedly elevated CK levels occur or myopathy is diagnosed or suspected. Temporarily discontinue VYTORIN in patients experiencing an acute or serious condition at high risk of developing renal failure secondary to rhabdomyolysis. Inform patients of the risk of myopathy and rhabdomyolysis when starting or increasing VYTORIN dosage. Instruct patients to promptly report unexplained muscle pain, tenderness, or weakness, particularly if accompanied by malaise or fever. (5.1)
- Immune-Mediated Necrotizing Myopathy (IMNM): Rare reports of IMNM, an autoimmune myopathy, have been reported. Discontinue VYTORIN if IMNM is suspected. (5.2)
- Hepatic Dysfunction: Increases in serum transaminases have occurred, some persistent. Rare reports of fatal and non-fatal hepatic failure have occurred. Consider testing liver enzyme before initiating therapy and as clinically indicated thereafter. If serious hepatic injury with clinical symptoms and/or hyperbilirubinemia or jaundice occurs, promptly discontinue VYTORIN. (5.3)
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
-
Important Dosage and Administration Information: (2.1)
- Take VYTORIN orally once daily in the evening with or without food.
- Maximum recommended dosage is VYTORIN 10/40 mg once daily. VYTORIN 10/80 mg daily dosage is restricted to patients who have been taking VYTORIN 10/80 mg daily chronically (e.g., for 12 months or more) without evidence of muscle toxicity.
- For patients that require a high-intensity statin or are unable to achieve their LDL-C goal receiving VYTORIN 10/40 mg daily, prescribe alternative LDL-C-lowering treatment.
- If as dose is missed, take the missed dose as soon as possible. Do not double the next dose.
- Assess LDL-C when clinically appropriate, as early as 2 weeks after initiating VYTORIN, and adjust the dosage if necessary.
- Adults: Recommended dosage range of 10/10 mg to 10/40 mg once daily. (2.2)
- See full prescribing information for VYTORIN dosage modifications due to drug interactions. (2.3)
- Patients with Renal Impairment: Doses exceeding 10/20 mg should be used with caution and close monitoring in patients with moderate to severe renal impairment. (2.4)
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
VYTORIN tablets:
- 10/10, (ezetimibe 10 mg and simvastatin 10 mg tablets) are white to off-white capsule-shaped and debossed with “311” on one side.
- 10/20, (ezetimibe 10 mg and simvastatin 20 mg tablets) are white to off-white capsule-shaped and debossed with “312” on one side.
- 10/40, (ezetimibe 10 mg and simvastatin 40 mg tablets) are white to off-white capsule-shaped and debossed with “313” on one side.
- 10/80, (ezetimibe 10 mg and simvastatin 80 mg tablets) are white to off-white capsule-shaped and debossed with “315” on one side.
6.2 Postmarketing Experience
The following adverse reactions have been identified during post-approval use of VYTORIN. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Body as Whole: fever, chills, malaise, asthenia
Blood and Lymphatic System Disorders: anemia, thrombocytopenia, leukopenia, hemolytic anemia, positive ANA, ESR increase, eosinophilia
Gastrointestinal Disorders: pancreatitis, nausea, vomiting
Hepatobiliary Disorders: cholelithiasis, cholecystitis, elevations in liver transaminases including elevations more than 5 X ULN, hepatitis/jaundice, fatal and non-fatal hepatic failure
Immune System Disorders: hypersensitivity syndrome including: anaphylaxis, angioedema, lupus erythematous-like syndrome, dermatomyositis, vasculitis
Musculoskeletal and Connective Tissue Disorders: muscle cramps, immune-mediated necrotizing myopathy, rhabdomyolysis, myalgia, arthralgia, polymyalgia rheumatica, arthritis, elevated creatine phosphokinase
Nervous System Disorders: dizziness, depression, paresthesia, peripheral neuropathy, rare reports of cognitive impairment (e.g., memory loss, forgetfulness, amnesia, memory impairment, confusion) associated with statin use. Cognitive impairment was generally nonserious, and reversible upon statin discontinuation, with variable times to symptom onset (1 day to years) and symptom resolution (median of 3 weeks). There have been rare reports of new-onset or exacerbation of myasthenia gravis, including ocular myasthenia, and reports of recurrence when the same or a different statin was administered.
Skin and Subcutaneous Tissue Disorders: rash, pruritus, alopecia, a variety of skin changes (e.g., nodules, discoloration, dryness of skin/mucous membranes, changes to hair/nails), purpura, lichen planus, urticaria, photosensitivity, flushing, toxic epidermal necrolysis, erythema multiforme, including Stevens-Johnson syndrome.
Respiratory and Thoracic: interstitial lung disease, dyspnea
Reproductive System Disorders: erectile dysfunction
8 Use in Specific Populations (8 USE IN SPECIFIC POPULATIONS)
5.1 Myopathy and Rhabdomyolysis
VYTORIN may cause myopathy and rhabdomyolysis. Acute kidney injury secondary to myoglobinuria and rare fatalities have occurred as a result of rhabdomyolysis in patients treated with statins, including VYTORIN.
In clinical trials of 24,747 simvastatin-treated patients with a median follow-up of 4 years, the incidence of myopathy, defined as unexplained muscle weakness, pain, or tenderness accompanied by creatinine kinase (CK) increases greater than ten times the upper limit of normal (10 X ULN), were approximately 0.03%, 0.08%, and 0.61% in patients treated with simvastatin 20 mg, 40 mg, and 80 mg daily, respectively. In another clinical trial of 12,064 simvastatin-treated patients (with a history of myocardial infarction) with a mean follow-up of 6.7 years, the incidences of myopathy in patients taking simvastatin 20 mg and 80 mg daily were approximately 0.02% and 0.9%, respectively. The incidences of rhabdomyolysis (defined as myopathy with a CK >40 X ULN) in patients taking simvastatin 20 mg and 80 mg daily were approximately 0% and 0.4%, respectively [see Adverse Reactions (6.1)].
In the Trial of Heart and Renal Protection (SHARP), 9270 patients with chronic kidney disease were allocated to receive VYTORIN 10/20 mg daily (n=4650) or placebo (n=4620). During a median follow-up period of 4.9 years, the incidence of myopathy (defined as unexplained muscle weakness or pain with a serum creatine kinase [CK] >10 times upper limit of normal [ULN]) was 0.2% for VYTORIN and 0.1% for placebo: the incidence of rhabdomyolysis (defined as myopathy with a CK > 40 times ULN) was 0.09% for VYTORIN and 0.02% for placebo.
In postmarketing experience with ezetimibe, cases of myopathy and rhabdomyolysis have been reported. Most patients who developed rhabdomyolysis were taking a statin prior to initiating ezetimibe. However, rhabdomyolysis has been reported with ezetimibe monotherapy and with the addition of ezetimibe to agents known to be associated with increased risk of rhabdomyolysis, such as fibric acid derivatives. VYTORIN and a fenofibrate, if taking concomitantly, should both be immediately discontinued if myopathy is diagnosed or suspected.
Risk Factors for Myopathy
Risk factors for myopathy include age 65 years or greater, uncontrolled hypothyroidism, renal impairment, concomitant use with certain other drugs (including other lipid-lowering therapies), and higher VYTORIN dosage; Chinese patients on VYTORIN may be at higher risk for myopathy [see Contraindications (4), Drug Interactions (7.1), and Use in Specific Populations (8.8)]. The risk of myopathy is increased by elevated plasma levels of simvastatin and simvastatin acid. The risk is also greater in patients taking VYTORIN 80 mg daily compared with patients taking lower VYTORIN dosages and compared with patients using other statins with similar or greater LDL-C-lowering efficacy [see Adverse Reactions (6.1)].
Steps to Prevent or Reduce the Risk of Myopathy and Rhabdomyolysis
The concomitant use of strong CYP3A4 inhibitors with VYTORIN is contraindicated. If short-term treatment with strong CYP3A4 inhibitors is required, temporarily suspend VYTORIN during the duration of strong CYP3A4 inhibitor treatment. The concomitant use of VYTORIN with gemfibrozil, cyclosporine, or danazol is also contraindicated [see Contraindications (4) and Drug Interactions (7.1)].
VYTORIN dosage modifications are recommended for patients taking lomitapide, verapamil, diltiazem, dronedarone, amiodarone, amlodipine or ranolazine [see Dosage and Administration (2.5)]. VYTORIN use should be temporarily suspended in patients taking daptomycin. Lipid modifying doses (≥1 gram/day) of niacin, fibrates, colchicine, and grapefruit juice may also increase the risk of myopathy and rhabdomyolysis [see Drug Interactions (7.1)].
Use the 80 mg daily dosage of VYTORIN only in patients who have been taking simvastatin 80 mg daily chronically without evidence of muscle toxicity [see Dosage and Administration (2.1)]. If patients treated with VYTORIN 80 mg are prescribed an interacting drug that increases the risk for myopathy and rhabdomyolysis, switch to an alternate statin [see Drug Interactions (7.1)].
Discontinue VYTORIN if markedly elevated CK levels occur or if myopathy is either diagnosed or suspected. Muscle symptoms and CK increases may resolve if VYTORIN is discontinued. Temporarily discontinue VYTORIN in patients experiencing an acute or serious condition at high risk of developing renal failure secondary to rhabdomyolysis, e.g., sepsis; shock; severe hypovolemia; major surgery; trauma; severe metabolic, endocrine, or electrolyte disorders; or uncontrolled epilepsy.
Inform patients of the risk of myopathy and rhabdomyolysis when starting or increasing the VYTORIN dosage and advise patients receiving VYTORIN 80 mg of the increased risk of myopathy and rhabdomyolysis. Instruct patients to promptly report any unexplained muscle pain, tenderness or weakness, particularly if accompanied by malaise or fever.
17 Patient Counseling Information (17 PATIENT COUNSELING INFORMATION)
Advise the patient to read the FDA-approved patient labeling (Patient Information).
Myopathy and Rhabdomyolysis
Advise patients that VYTORIN may cause myopathy and rhabdomyolysis. Inform patients taking the 80 mg daily dose of simvastatin that they are at an increased risk. Inform patients that the risk is also increased when taking certain types of medication or consuming grapefruit juice and they should discuss all medication, both prescription and over the counter, with their healthcare provider. Instruct patients to inform other healthcare providers prescribing a new medication or increasing the dose of an existing medication that they are taking VYTORIN. Instruct patients to promptly report any unexplained muscle pain, tenderness or weakness particularly if accompanied by malaise or fever [see Contraindications (4), Warnings and Precautions (5.1), and Drug Interactions (7.1)].
Hepatic Dysfunction
Inform patients that VYTORIN may cause liver enzyme elevations and possibly liver failure. Advise patients to promptly report fatigue, anorexia, right upper abdominal discomfort, dark urine or jaundice [see Warnings and Precautions (5.3)].
Increases in HbA1c and Fasting Serum Glucose Levels
Inform patients that increases in HbA1c and fasting serum glucose levels may occur with VYTORIN. Encourage patients to optimize lifestyle measures, including regular exercise, maintaining a healthy body weight, and making healthy food choices [see Warnings and Precautions (5.4)].
Pregnancy
Advise pregnant patients and patients who can become pregnant of the potential risk to a fetus. Advise patients to inform their healthcare provider of a known or suspected pregnancy to discuss if VYTORIN should be discontinued [see Use in Specific Populations (8.1)].
Lactation
Advise patients that breastfeeding is not recommended during treatment with VYTORIN [see Use in Specific Populations (8.2)].
Missed Dose
Instruct patients to take VYTORIN only as prescribed. If a dose is missed, it should be taken as soon as possible. Advise patients not to double their next dose.
16 How Supplied/storage and Handling (16 HOW SUPPLIED/STORAGE AND HANDLING)
VYTORIN tablets are supplied as follows:
| Strength | How Supplied | NDC | Tablet Description |
|---|---|---|---|
| 10/10 mg | unit of use bottles of 30 | 78206-174-01 | white to off-white capsule-shaped tablets with code “311” on one side |
| unit of use bottles of 90 | 78206-174-02 | ||
| 10/20 mg | unit of use bottles of 30 | 78206-175-01 | white to off-white capsule-shaped tablets with code “312” on one side |
| unit of use bottles of 90 | 78206-175-02 | ||
| 10/40 mg | unit of use bottles of 30 | 78206-176-01 | white to off-white capsule-shaped tablets with code “313” on one side |
| unit of use bottles of 90 | 78206-176-02 | ||
| 10/80 mg | unit of use bottles of 30 | 78206-177-01 | white to off-white capsule-shaped tablets with code “315” on one side |
| unit of use bottles of 90 | 78206-177-02 |
7.3 Vytorin’s Effect On Other Drugs (7.3 VYTORIN’s Effect on Other Drugs)
Table 4 presents VYTORIN’s effect on other drugs and instructions for preventing or managing them.
| Coumarin Anticoagulants | |
|---|---|
| Clinical Impact: | VYTORIN may potentiate the effect of coumarin anticoagulants and increase the INR. The concomitant use of simvastatin (20 to 40 mg) and coumarin anticoagulants increased the INR from a baseline of 1.7 to 1.8 in healthy subjects and from 2.6 to 3.4 in patients with hyperlipidemia. There are postmarketing reports of clinically evident bleeding and/or increased INR in patients taking concomitant statins (with or without ezetimibe) and coumarin anticoagulants. |
| Intervention: | In patients taking coumarin anticoagulants, obtain an INR before starting VYTORIN and frequently enough after initiation, dose titration, or discontinuation to ensure that no significant alteration in INR occurs. Once the INR is stable, monitor INR at regularly recommended intervals. |
| Digoxin | |
| Clinical Impact: | Concomitant use of digoxin with VYTORIN may result in elevated plasma digoxin concentrations [see Clinical Pharmacology (12.3)]. |
| Intervention: | Monitor digoxin levels in patients taking digoxin when VYTORIN is initiated. |
| Fenofibrates | |
| Clinical Impact: | Both ezetimibe and fenofibrates may increase cholesterol excretion into the bile, leading to cholelithiasis. |
| Intervention: | If cholelithiasis is suspected in a patient receiving VYTORIN and a fenofibrate, gallbladder studies are indicated and alternative lipid-lowering therapy should be considered [see the product labeling for fenofibrate and fenofibric acid]. |
2.2 Recommended Dosage in Adult Patients
The recommended dosage range of VYTORIN 10/10 mg to 10/40 mg once a day.
5.2 Immune Mediated Necrotizing Myopathy (5.2 Immune-Mediated Necrotizing Myopathy)
There have been rare reports of immune-mediated necrotizing myopathy (IMNM), an autoimmune myopathy, associated with statin use, including reports of recurrence when the same or a different statin was administered. IMNM is characterized by proximal muscle weakness and elevated serum creatine kinase that persist despite discontinuation of statin treatment; positive anti-HMG CoA reductase antibody; muscle biopsy showing necrotizing myopathy without significant inflammation; and improvement with immunosuppressive agents. Additional neuromuscular and serologic testing may be necessary. Treatment with immunosuppressive agents may be required. Discontinue VYTORIN if IMNM is suspected.
2.5 Dosage Modifications Due to Drug Interactions
Concomitant use of VYTORIN with the following drugs requires dosage modification of VYTORIN [see Warnings and Precautions (5.1) and Drug Interactions (7.1)].
Patients taking Lomitapide
Reduce the dosage of VYTORIN by 50%. Do not exceed VYTORIN 10/20 mg once daily (or 10/40 mg once daily for patients who have previously taken VYTORIN 10/80 mg daily chronically while taking lomitapide) [see Dosage and Administration (2.1)].
Patients taking Verapamil, Diltiazem, or Dronedarone
Do not exceed VYTORIN 10/10 mg once daily.
Patients taking Amiodarone, Amlodipine, or Ranolazine
Do not exceed VYTORIN 10/20 mg once daily.
Patients taking Bile Acid Sequestrants
In patients taking a bile acid sequestrant, administer VYTORIN at least 2 hours before or 4 hours after the bile acid sequestrant.
2.1 Important Dosage and Administration Information
- Take VYTORIN orally once daily in the evening with or without food.
- The maximum recommended dosage is VYTORIN 10/40 mg once daily. The VYTORIN 10/80 mg daily dosage is restricted to adult patients who have been taking VYTORIN 10/80 mg daily chronically (e.g., for 12 months or more) without evidence of muscle toxicity [see Warnings and Precautions (5.1)].
- For patients that require a high-intensity statin or are unable to achieve their LDL-C goal receiving VYTORIN 10/40 mg daily, prescribe alternative LDL-C-lowering treatment.
- If as dose is missed, take the missed dose as soon as possible. Do not double the next dose.
- Assess LDL-C when clinically appropriate, as early as 4 weeks after initiating VYTORIN, and adjust the dosage if necessary.
5.4 Increases in Hba1c and Fasting Serum Glucose Levels (5.4 Increases in HbA1c and Fasting Serum Glucose Levels)
Increases in HbA1c and fasting serum glucose levels have been reported with statins, including VYTORIN. Optimize lifestyle measures, including regular exercise, maintaining a healthy body weight, and making healthy food choices.
2.4 Recommended Dosage in Patients With Renal Impairment (2.4 Recommended Dosage in Patients with Renal Impairment)
Renal impairment is a risk factor for statin-associated myopathy. Doses of VYTORIN exceeding 10/20 mg should be used with caution and close monitoring in patients with moderate to severe renal impairment [see Warnings and Precautions (5.1) and Use in Specific Populations (8.6)].
There are no dosage adjustment recommendations for patients with mild renal impairment.
Principal Display Panel 10 Mg /10 Mg Tablet Bottle Label (PRINCIPAL DISPLAY PANEL - 10 mg /10 mg Tablet Bottle Label)
NDC 78206-174-01
Vytorin
®
(ezetimibe and
simvastatin) tablets
10 mg /10 mg
Each tablet contains 10 mg ezetimibe and
10 mg simvastatin.
Rx only
30 Tablets
Principal Display Panel 10 Mg /20 Mg Tablet Bottle Label (PRINCIPAL DISPLAY PANEL - 10 mg /20 mg Tablet Bottle Label)
NDC 78206-175-01
Vytorin
®
(ezetimibe and
simvastatin) tablets
10 mg /20 mg
Each tablet contains 10 mg ezetimibe and
20 mg simvastatin.
Rx only
30 Tablets
Principal Display Panel 10 Mg /40 Mg Tablet Bottle Label (PRINCIPAL DISPLAY PANEL - 10 mg /40 mg Tablet Bottle Label)
NDC 78206-176-01
Vytorin
®
(ezetimibe and
simvastatin) tablets
10 mg /40 mg
Each tablet contains 10 mg ezetimibe and
40 mg simvastatin.
Rx only
30 Tablets
Principal Display Panel 10 Mg /80 Mg Tablet Bottle Label (PRINCIPAL DISPLAY PANEL - 10 mg /80 mg Tablet Bottle Label)
NDC 78206-177-01
Vytorin
®
(ezetimibe and
simvastatin) tablets
10 mg /80 mg
Each tablet contains 10 mg ezetimibe and
80 mg simvastatin.
Rx only
30 Tablets
7.2 Drug Interactions That Decrease the Efficacy of Vytorin (7.2 Drug Interactions that Decrease the Efficacy of VYTORIN)
Table 3 presents drug interactions that may decrease the efficacy of VYTORIN and instructions for preventing or managing them.
| Bile Acid Sequestrants | |
|---|---|
| Clinical Impact: | Concomitant cholestyramine administration decreased the mean exposure of total ezetimibe approximately 55%. The incremental LDL-C reduction due to adding VYTORIN to cholestyramine may be reduced by this interaction [see Clinical Pharmacology (12.3)]. |
| Intervention: | In patients taking a bile acid sequestrant, administer VYTORIN at least 2 hours before or at least 4 hours after cholestyramine [see Dosage and Administration (2.3)]. |
2.3 Recommended Dosage in Pediatric Patients 10 Years of Age and Older With Hefh (2.3 Recommended Dosage in Pediatric Patients 10 Years of Age and Older with HeFH)
The recommended dosage range of VYTORIN 10/10 mg to 10/40 mg once a day.
7.1 Drug Interactions That Increase the Risk of Myopathy and Rhabdomyolysis With Vytorin (7.1 Drug Interactions that Increase the Risk of Myopathy and Rhabdomyolysis with VYTORIN)
VYTORIN is a substrate of CYP3A4 and of the transport protein OATP1B1. VYTORIN plasma levels can be significantly increased with concomitant administration of inhibitors of CYP3A4 and OATP1B1.
Table 2 includes a list of drugs that increase the risk of myopathy and rhabdomyolysis when used concomitantly with VYTORIN and instructions for preventing or managing them [see Warnings and Precautions (5.1) and Clinical Pharmacology (12.3)].
| Strong CYP3A4 inhibitors | |
|---|---|
| Clinical Impact: | Simvastatin is a substrate of CYP3A4. Concomitant use of strong CYP3A4 inhibitors with VYTORIN increases simvastatin exposure and increases the risk of myopathy and rhabdomyolysis, particularly with higher VYTORIN dosages. |
| Intervention: | Concomitant use of strong CYP3A4 inhibitors with VYTORIN is contraindicated [see Contraindications (4)]. If treatment with a CYP3A4 inhibitor is unavoidable, suspend VYTORIN during the course of strong CYP3A4 inhibitor treatment. |
| Examples: | Select azole anti-fungals (e.g., itraconazole, ketoconazole, posaconazole, and voriconazole), select macrolide antibiotics (e.g., erythromycin and clarithromycin, telithromycin), select HIV protease inhibitors (e.g., nelfinavir, ritonavir, and darunavir/ritonavir), select HCV protease inhibitors (e.g., boceprevir and telaprevir), cobicistat-containing products, and nefazodone. |
| Cyclosporine, Danazol, or Gemfibrozil | |
| Clinical Impact: | The risk of myopathy and rhabdomyolysis is increased with concomitant use of cyclosporine, danazol, or gemfibrozil with VYTORIN. Gemfibrozil may cause myopathy when given alone. |
| Intervention: | Concomitant use of cyclosporine, danazol, or gemfibrozil with VYTORIN is contraindicated [see Contraindications (4)]. |
| Amiodarone, Dronedarone, Ranolazine, or Calcium Channel Blockers | |
| Clinical Impact: | The risk of myopathy and rhabdomyolysis is increased by concomitant use of amiodarone, dronedarone, ranolazine, or calcium channel blockers with VYTORIN. |
| Intervention: | For patients taking verapamil, diltiazem, or dronedarone, do not exceed VYTORIN 10/10 mg daily. For patients taking amiodarone, amlodipine, or ranolazine, do not exceed VYTORIN 10/20 mg daily [see Dosage and Administration (2.3)]. |
| Lomitapide | |
| Clinical Impact: | Simvastatin exposure is approximately doubled with concomitant use of lomitapide and the risk of myopathy and rhabdomyolysis is increased. |
| Intervention: | Reduce the dose of VYTORIN by 50% if initiating lomitapide. Do not exceed VYTORIN 10/20 mg daily (or VYTORIN 10/40 mg daily for patients who have previously taken VYTORIN 10/80 mg daily chronically) while taking lomitapide [see Dosage and Administration (2.1, 2.3)]. |
| Daptomycin | |
| Clinical Impact: | Cases of rhabdomyolysis have been reported with simvastatin administered with daptomycin. Both VYTORIN and daptomycin can cause myopathy and rhabdomyolysis when given alone and the risk of myopathy and rhabdomyolysis may be increased by coadministration. |
| Intervention: | If treatment with daptomycin is required, consider temporarily suspending VYTORIN during the course of daptomycin treatment. |
| Niacin | |
| Clinical Impact: | Cases of myopathy and rhabdomyolysis have been observed with concomitant use of lipid modifying dosages of niacin-containing products (≥1 gram/day niacin) with VYTORIN. The risk of myopathy is greater in Chinese patients. In a clinical trial (median follow-up 3.9 years) of patients at high risk of CVD and with well-controlled LDL-C levels on simvastatin 40 mg/day with or without ezetimibe 10 mg/day, there was no incremental benefit on cardiovascular outcomes with the addition of lipid-modifying doses of niacin |
| Intervention: | Concomitant use of VYTORIN with lipid-modifying dosages of niacin is not recommended in Chinese patients [see Use in Specific Populations (8.8)]. For non-Chinese patients, consider if the benefit of using lipid-modifying doses of niacin concomitantly with VYTORIN outweighs the increased risk of myopathy and rhabdomyolysis. If concomitant use is decided, monitor patients for signs and symptoms of myopathy, particularly during initiation of therapy and during upward dose titration of either drug. |
| Fibrates (other than Gemfibrozil) | |
| Clinical Impact: | Fibrates may cause myopathy when given alone. The risk of myopathy and rhabdomyolysis is increased with concomitant use of fibrates with VYTORIN. |
| Intervention: | Consider if the benefit of using fibrates concomitantly with VYTORIN outweighs the increased risk of myopathy and rhabdomyolysis. If concomitant use is decided, monitor patients for signs and symptoms of myopathy, particularly during initiation of therapy and during upward dose titration of either drug. |
| Colchicine | |
| Clinical Impact: | Cases of myopathy and rhabdomyolysis have been reported with concomitant use of colchicine with VYTORIN. |
| Intervention: | Consider if the benefit of using colchicine concomitantly with VYTORIN outweighs the increased risk of myopathy and rhabdomyolysis. If concomitant use is decided, monitor patients for signs and symptoms of myopathy, particularly during initiation of therapy and during upward dose titration of either drug. |
| Grapefruit Juice | |
| Clinical Impact: | Grapefruit juice can raise the plasma levels of simvastatin and may increase the risk of myopathy and rhabdomyolysis. |
| Intervention: | Avoid grapefruit juice when taking VYTORIN. |
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:52:35.074549 · Updated: 2026-03-14T22:44:06.575433