These Highlights Do Not Include All The Information Needed To Use Contepo Safely And Effectively. See Full Prescribing Information For Contepo.
855574f2-39f8-43bc-a3d2-79dbb578cb94
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
CONTEPO is an epoxide antibacterial indicated for the treatment of patients 18 years of age and older with complicated urinary tract infections (cUTI) including acute pyelonephritis caused by susceptible isolates of Escherichia coli and Klebsiella pneumoniae . ( 1.1 ) Usage to Reduce Development of Drug-Resistant Bacteria To reduce the development of drug-resistant bacteria and maintain the effectiveness of CONTEPO and other antibacterial drugs, CONTEPO should be used only to treat infections that are proven or strongly suspected to be caused by bacteria. ( 1.2 )
Indications and Usage
CONTEPO is an epoxide antibacterial indicated for the treatment of patients 18 years of age and older with complicated urinary tract infections (cUTI) including acute pyelonephritis caused by susceptible isolates of Escherichia coli and Klebsiella pneumoniae . ( 1.1 ) Usage to Reduce Development of Drug-Resistant Bacteria To reduce the development of drug-resistant bacteria and maintain the effectiveness of CONTEPO and other antibacterial drugs, CONTEPO should be used only to treat infections that are proven or strongly suspected to be caused by bacteria. ( 1.2 )
Dosage and Administration
Administer CONTEPO, 6 grams every 8 hours by intravenous (IV) infusion over 1 hour for up to 14 days, in patients 18 years of age or older with an estimated creatinine clearance (CLcr) greater than 50 mL/min. ( 2.1 ) The recommended dosage in patients 18 years of age and older with an estimated CLcr of 50 mL/min or less is presented in the table below. ( 2.2 ) a CLcr estimated using Cockcroft-Gault Equation. b All doses of CONTEPO are administered by intravenous infusion over 1 hour. Estimated CLcr (mL/min) a Loading Dose b Maintenance Dosage b Dose Frequency 41-50 6 grams 4 grams Every 8 hours 31-40 6 grams 3 grams Every 8 hours 21-30 6 grams 5 grams Every 24 hours 11-20 6 grams 3 grams Every 24 hours Approximately 60% to 80% of the fosfomycin dose is cleared from the body by hemodialysis. Administer CONTEPO after hemodialysis on hemodialysis days. ( 2.2 )
Warnings and Precautions
Serum Electrolyte Abnormalities : CONTEPO contains 1980 mg sodium in each vial. The high sodium load associated with the use of CONTEPO may result in changes in serum electrolytes, such as increased levels of sodium and decreased levels of potassium, calcium and phosphorus. A low-sodium diet is recommended during CONTEPO treatment. Monitor serum electrolyte levels and fluid status during CONTEPO treatment. Monitor signs and symptoms of edema, particularly in patients with cardiac insufficiency, renal impairment, cirrhosis, hypertension, hyperaldosteronism, hypernatremia or pulmonary edema. ( 5.1 ) QT Prolongation: CONTEPO has been shown to prolong the QT interval in some patients in the clinical trial. Avoid CONTEPO in patients with known prolongation of the QT interval or ventricular arrhythmias, including a history of torsade de pointes. ( 5.2 , 7.1 ) Increased Transaminase Levels : Increase in alanine aminotransferase (ALT) and aspartate aminotransferase (AST) were reported in the clinical trial. Monitor hepatic enzymes during CONTEPO treatment. ( 5.3 ) Hypersensitivity Reactions : Reactions such as rash, urticaria and anaphylaxis were reported with the use of CONTEPO. Before initiating therapy with CONTEPO, it is important to inquire about previous hypersensitivity reactions to oral or parenteral fosfomycin. If an allergic reaction occurs, discontinue CONTEPO immediately. ( 5.4 ) Neutropenia Including Agranulocytosis : Neutropenia, including agranulocytosis, has occurred in patients receiving IV fosfomycin treatment. Monitor complete blood count during CONTEPO therapy. If such reactions occur, discontinue CONTEPO and institute appropriate treatment ( 5.5 ). Clostridioides difficile -Associated Diarrhea (CDAD) : This has been reported with nearly all systemic antibacterial agents, including CONTEPO. Evaluate patients if diarrhea occurs. ( 5.6 )
Contraindications
CONTEPO is contraindicated in patients with known serious hypersensitivity to fosfomycin, or any of the excipients [ see Warnings and Precautions ( 5.2 ) ] .
Adverse Reactions
The following adverse reactions are discussed in greater detail in the Warnings and Precautions section: Serum Electrolyte Abnormalities [see Warnings and Precautions ( 5.1 )] QT Prolongation [see Warnings and Precautions ( 5.2 )] Increased Transaminase Levels [see Warnings and Precautions ( 5.3 )] Hypersensitivity Reactions [see Warnings and Precautions ( 5.4 )] Neutropenia Including Agranulocytosis [see Warnings and Precautions ( 5.5 )] Clostridioides difficile -Associated Diarrhea [see Warnings and Precautions ( 5.6 )] Development of Drug-Resistant Bacteria [see Warnings and Precautions ( 5.7 )]
Drug Interactions
Avoid co-administration of CONTEPO with drugs known to prolong the QT interval. ( 5.2 , 7.1 )
Medication Information
Warnings and Precautions
Serum Electrolyte Abnormalities : CONTEPO contains 1980 mg sodium in each vial. The high sodium load associated with the use of CONTEPO may result in changes in serum electrolytes, such as increased levels of sodium and decreased levels of potassium, calcium and phosphorus. A low-sodium diet is recommended during CONTEPO treatment. Monitor serum electrolyte levels and fluid status during CONTEPO treatment. Monitor signs and symptoms of edema, particularly in patients with cardiac insufficiency, renal impairment, cirrhosis, hypertension, hyperaldosteronism, hypernatremia or pulmonary edema. ( 5.1 ) QT Prolongation: CONTEPO has been shown to prolong the QT interval in some patients in the clinical trial. Avoid CONTEPO in patients with known prolongation of the QT interval or ventricular arrhythmias, including a history of torsade de pointes. ( 5.2 , 7.1 ) Increased Transaminase Levels : Increase in alanine aminotransferase (ALT) and aspartate aminotransferase (AST) were reported in the clinical trial. Monitor hepatic enzymes during CONTEPO treatment. ( 5.3 ) Hypersensitivity Reactions : Reactions such as rash, urticaria and anaphylaxis were reported with the use of CONTEPO. Before initiating therapy with CONTEPO, it is important to inquire about previous hypersensitivity reactions to oral or parenteral fosfomycin. If an allergic reaction occurs, discontinue CONTEPO immediately. ( 5.4 ) Neutropenia Including Agranulocytosis : Neutropenia, including agranulocytosis, has occurred in patients receiving IV fosfomycin treatment. Monitor complete blood count during CONTEPO therapy. If such reactions occur, discontinue CONTEPO and institute appropriate treatment ( 5.5 ). Clostridioides difficile -Associated Diarrhea (CDAD) : This has been reported with nearly all systemic antibacterial agents, including CONTEPO. Evaluate patients if diarrhea occurs. ( 5.6 )
Indications and Usage
CONTEPO is an epoxide antibacterial indicated for the treatment of patients 18 years of age and older with complicated urinary tract infections (cUTI) including acute pyelonephritis caused by susceptible isolates of Escherichia coli and Klebsiella pneumoniae . ( 1.1 ) Usage to Reduce Development of Drug-Resistant Bacteria To reduce the development of drug-resistant bacteria and maintain the effectiveness of CONTEPO and other antibacterial drugs, CONTEPO should be used only to treat infections that are proven or strongly suspected to be caused by bacteria. ( 1.2 )
Dosage and Administration
Administer CONTEPO, 6 grams every 8 hours by intravenous (IV) infusion over 1 hour for up to 14 days, in patients 18 years of age or older with an estimated creatinine clearance (CLcr) greater than 50 mL/min. ( 2.1 ) The recommended dosage in patients 18 years of age and older with an estimated CLcr of 50 mL/min or less is presented in the table below. ( 2.2 ) a CLcr estimated using Cockcroft-Gault Equation. b All doses of CONTEPO are administered by intravenous infusion over 1 hour. Estimated CLcr (mL/min) a Loading Dose b Maintenance Dosage b Dose Frequency 41-50 6 grams 4 grams Every 8 hours 31-40 6 grams 3 grams Every 8 hours 21-30 6 grams 5 grams Every 24 hours 11-20 6 grams 3 grams Every 24 hours Approximately 60% to 80% of the fosfomycin dose is cleared from the body by hemodialysis. Administer CONTEPO after hemodialysis on hemodialysis days. ( 2.2 )
Contraindications
CONTEPO is contraindicated in patients with known serious hypersensitivity to fosfomycin, or any of the excipients [ see Warnings and Precautions ( 5.2 ) ] .
Adverse Reactions
The following adverse reactions are discussed in greater detail in the Warnings and Precautions section: Serum Electrolyte Abnormalities [see Warnings and Precautions ( 5.1 )] QT Prolongation [see Warnings and Precautions ( 5.2 )] Increased Transaminase Levels [see Warnings and Precautions ( 5.3 )] Hypersensitivity Reactions [see Warnings and Precautions ( 5.4 )] Neutropenia Including Agranulocytosis [see Warnings and Precautions ( 5.5 )] Clostridioides difficile -Associated Diarrhea [see Warnings and Precautions ( 5.6 )] Development of Drug-Resistant Bacteria [see Warnings and Precautions ( 5.7 )]
Drug Interactions
Avoid co-administration of CONTEPO with drugs known to prolong the QT interval. ( 5.2 , 7.1 )
Description
CONTEPO is an epoxide antibacterial indicated for the treatment of patients 18 years of age and older with complicated urinary tract infections (cUTI) including acute pyelonephritis caused by susceptible isolates of Escherichia coli and Klebsiella pneumoniae . ( 1.1 ) Usage to Reduce Development of Drug-Resistant Bacteria To reduce the development of drug-resistant bacteria and maintain the effectiveness of CONTEPO and other antibacterial drugs, CONTEPO should be used only to treat infections that are proven or strongly suspected to be caused by bacteria. ( 1.2 )
Section 42229-5
Preparation
CONTEPO is supplied as a dry powder in a single-dose vial that must be constituted and further diluted prior to intravenous infusion as described below. CONTEPO does not contain preservatives. Aseptic technique must be used for constitution and dilution prior to IV infusion.
- Constitute the vial with 30 mL of Sterile Water for Injection, USP and gently mix to completely dissolve contents. A slight degree of warming occurs when the powder is dissolved. The constituted solution should appear clear and colorless. Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration, whenever solution and container permit. The constituted solution is not for direct injection and must be further diluted immediately with Sterile Water for Injection, USP [see Dosage and Administration (2.4)] before intravenous infusion.
- To prepare the infusion solution, first remove 80 mL from a 250 mL intravenous bag of Sterile Water for Injection, USP for infusion so that it contains approximately 170 mL.
- Then add the required volume of constituted solution to the infusion bag according to Table 2. Discard unused portion. The constituted and further diluted solution of CONTEPO has a pH of 7.4 to 7.8.
| CONTEPO Dose | Volume to Withdraw from Constituted Vial |
Volume of Final Infusion Bag
(Approximate) |
Final Infusion Concentration of CONTEPO
(Approximate) |
| 6 grams | 32.6 mL (Entire Contents) |
202 mL | 30 mg/mL |
| 5 grams | 27 mL | 197 mL | 25 mg/mL |
| 4 grams | 21.5 mL | 192 mL | 20 mg/mL |
| 3 grams | 16 mL | 186 mL | 15 mg/mL |
10 Overdosage
To date, no cases of accidental overdose with clinically relevant intolerances have been reported. In the event of an overdose, the patient must be monitored and treated symptomatically. Fosfomycin is cleared from the body by hemodialysis, during which patients with end stage renal disease have an increased mean fosfomycin elimination half-life to approximately 4 hours.
8.2 Lactation
Risk Summary
Fosfomycin is present in human milk. There are no data on the effects of fosfomycin on the breastfed child or on milk production. Because of the potential for adverse reactions in a breastfed infant, advise patients not to breastfeed during treatment with CONTEPO and for 24 hours after the last dose.
11 Description
CONTEPO (fosfomycin) for injection, for intravenous use, contains fosfomycin disodium, an epoxide antibacterial drug.
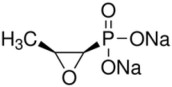
Fosfomycin disodium is a powder with the chemical name of disodium [(2R,3S)-3-methyloxiran-2-yl]-dioxido-oxophosphorane, an empirical formula of C3H5Na2O4P and molecular weight of 182.
Figure 1 Chemical Structure of Fosfomycin Disodium
Each CONTEPO for Injection single-dose vial contains white to almost white sterile powder with 6 grams of fosfomycin (equivalent to 7.9 grams fosfomycin disodium) and the inactive ingredient succinic acid (150 mg) for pH adjustment. It is intended for constitution and further dilution prior to intravenous infusion . Each gram of fosfomycin disodium contains 330 mg of sodium (i.e., each vial contains 1,980 mg of sodium).
8.4 Pediatric Use
Safety and effectiveness of CONTEPO in patients less than 18 years of age has not been established.
8.5 Geriatric Use
Of the 233 patients treated with CONTEPO in Trial 1, 32% (74/233) were 65 years of age and older, including 11.2% (26/233) who were 75 years of age and older. For patients included in the microbiological modified intent-to-treat (mMITT) population, lower overall success rates were observed for CONTEPO-treated and piperacillin/tazobactam-treated patients ≥ 65 years of age (53.6% and 43.9%, respectively) as compared to patients < 65 years (68.4% and 61.6%, respectively).
For patients ≥ 65 years of age, the incidence rate of adverse reactions was 39.2% (29/74) in CONTEPO-treated patients and 28.6% (22/77) in the piperacillin/tazobactam-treated patients. For patients <65 years of age, the incidence rate of adverse reactions was 43.4% (69/159) in CONTEPO-treated patients and 33.8% (52/154) in the piperacillin/tazobactam-treated patients.
Because elderly patients are more likely to have decreased cardiac and renal function, care should be taken in dose selection, and electrolytes, fluid status, and renal function should be monitored. Dosage adjustment in elderly patients should take into account renal function [ see Dosage and Administration (2.2, 2.3, 2.4) and Clinical Pharmacology (12.3) ].
4 Contraindications
CONTEPO is contraindicated in patients with known serious hypersensitivity to fosfomycin, or any of the excipients [ see Warnings and Precautions (5.2) ].
5.2 Qt Prolongation
CONTEPO has been shown to prolong the QT interval in some patients. QT prolongation can lead to development of torsade de pointes-type ventricular tachycardia with the risk increasing as the degree of prolongation increases. In Trial 1, 3.6% of patients treated with CONTEPO had > 60 msec increase in QTcF interval from baseline and 1% of patients had QTcF > 480 msec. Torsade de pointes has been reported during postmarketing experience with fosfomycin [see Adverse Reactions (6.2)]. The risk of QT prolongation may increase in patients with electrolyte abnormalities (such as hypokalemia and hypocalcemia), patients with conditions that have potential to cause electrolyte imbalance (such as renal impairment), or patients taking other drugs affecting electrolyte balance or QT prolongation. Avoid CONTEPO in patients with known QT prolongation or ventricular arrhythmias, including a history of torsade de pointes. Monitor electrolytes during treatment with CONTEPO [see Warnings and Precautions (5.1), Drug Interactions (7.1) and Clinical Pharmacology (12.2)].
6 Adverse Reactions
The following adverse reactions are discussed in greater detail in the Warnings and Precautions section:
- Serum Electrolyte Abnormalities [see Warnings and Precautions (5.1)]
- QT Prolongation [see Warnings and Precautions (5.2)]
- Increased Transaminase Levels [see Warnings and Precautions (5.3)]
- Hypersensitivity Reactions [see Warnings and Precautions (5.4)]
- Neutropenia Including Agranulocytosis [see Warnings and Precautions (5.5)]
- Clostridioides difficile-Associated Diarrhea [see Warnings and Precautions (5.6)]
- Development of Drug-Resistant Bacteria [see Warnings and Precautions (5.7)]
7 Drug Interactions
8.6 Renal Impairment
Dosage adjustment is required for patients with estimated CLcr 50 mL/min or less. Monitor estimated CLcr and adjust the dosage of CONTEPO accordingly [ see Dosage and Administration (2.2) ].
In patients requiring hemodialysis, CONTEPO should be administered after hemodialysis on hemodialysis days [see Dosage and Administration (2.2), Clinical Pharmacology (12.3)].
12.2 Pharmacodynamics
The ratio of the unbound plasma fosfomycin AUC to MIC against the infecting organism has been shown to correlate with activity in animal models of infection.
12.3 Pharmacokinetics
The mean pharmacokinetic parameters of fosfomycin in healthy adults with normal renal function after single doses of 6 grams administered as 1-hour IV infusion are summarized along with additional pharmacokinetic information in Table 4.
|
a Based on non-compartmental analysis of PK data |
|
| C max (mcg/mL) | 228 ± 43 |
| AUC 0-inf (mcg∙hr/mL) | 734 ± 134 |
| Dose Proportionality | Fosfomycin Cmax and AUC0-inf increase proportionally with dose |
| Distribution | |
| Volume of Distribution (L) | 27 ± 5.2 |
| Protein Binding | Fosfomycin is not bound to plasma proteins |
| Elimination | |
| Half-Life (h) | 2.8 ± 0.6 |
| Total Clearance (L/h) | 8.5 ± 1.7 |
| Metabolism | Fosfomycin is not metabolized. |
| Excretion | Urine: 70% of dose is excreted unchanged at 12 hours; 74-80% of dose is excreted unchanged at 48 hours |
2.1 Recommended Dosage
The recommended dosage of CONTEPO is 6 grams administered every 8 hours by intravenous (IV) infusion over 1 hour in patients 18 years of age or older with an estimated creatinine clearance (CLcr) greater than 50 mL/min. The duration of therapy is up to 14 days and should be guided by the severity of infection and the patient's clinical status. During treatment, different dosage recommendations may be required based on change in estimated CLcr [ see Dosage and Administration (2.2) ].
8.7 Hepatic Impairment
1 Indications and Usage
CONTEPO is an epoxide antibacterial indicated for the treatment of patients 18 years of age and older with complicated urinary tract infections (cUTI) including acute pyelonephritis caused by susceptible isolates of Escherichia coli and Klebsiella pneumoniae. (1.1)
Usage to Reduce Development of Drug-Resistant Bacteria
To reduce the development of drug-resistant bacteria and maintain the effectiveness of CONTEPO and other antibacterial drugs, CONTEPO should be used only to treat infections that are proven or strongly suspected to be caused by bacteria. (1.2)
12.1 Mechanism of Action
CONTEPO is an antibacterial drug [ see Microbiology (12.4) ].
2.5 Drug Incompatibility
The compatibility of CONTEPO with other drugs and infusion solutions has not been established. CONTEPO should not be mixed or co-administered with solutions containing other drugs.
5 Warnings and Precautions
- Serum Electrolyte Abnormalities: CONTEPO contains 1980 mg sodium in each vial. The high sodium load associated with the use of CONTEPO may result in changes in serum electrolytes, such as increased levels of sodium and decreased levels of potassium, calcium and phosphorus. A low-sodium diet is recommended during CONTEPO treatment. Monitor serum electrolyte levels and fluid status during CONTEPO treatment. Monitor signs and symptoms of edema, particularly in patients with cardiac insufficiency, renal impairment, cirrhosis, hypertension, hyperaldosteronism, hypernatremia or pulmonary edema. (5.1)
- QT Prolongation: CONTEPO has been shown to prolong the QT interval in some patients in the clinical trial. Avoid CONTEPO in patients with known prolongation of the QT interval or ventricular arrhythmias, including a history of torsade de pointes. (5.2, 7.1)
- Increased Transaminase Levels: Increase in alanine aminotransferase (ALT) and aspartate aminotransferase (AST) were reported in the clinical trial. Monitor hepatic enzymes during CONTEPO treatment. (5.3)
- Hypersensitivity Reactions: Reactions such as rash, urticaria and anaphylaxis were reported with the use of CONTEPO. Before initiating therapy with CONTEPO, it is important to inquire about previous hypersensitivity reactions to oral or parenteral fosfomycin. If an allergic reaction occurs, discontinue CONTEPO immediately. (5.4)
- Neutropenia Including Agranulocytosis: Neutropenia, including agranulocytosis, has occurred in patients receiving IV fosfomycin treatment. Monitor complete blood count during CONTEPO therapy. If such reactions occur, discontinue CONTEPO and institute appropriate treatment (5.5).
- Clostridioides difficile -Associated Diarrhea (CDAD): This has been reported with nearly all systemic antibacterial agents, including CONTEPO. Evaluate patients if diarrhea occurs. (5.6)
2 Dosage and Administration
- Administer CONTEPO, 6 grams every 8 hours by intravenous (IV) infusion over 1 hour for up to 14 days, in patients 18 years of age or older with an estimated creatinine clearance (CLcr) greater than 50 mL/min. (2.1)
- The recommended dosage in patients 18 years of age and older with an estimated CLcr of 50 mL/min or less is presented in the table below. (2.2)
|
aCLcr estimated using Cockcroft-Gault Equation. |
|||
|
bAll doses of CONTEPO are administered by intravenous infusion over 1 hour. |
|||
| Estimated CLcr (mL/min) a | Loading Dose b | Maintenance Dosage b | |
| Dose | Frequency | ||
| 41-50 | 6 grams | 4 grams | Every 8 hours |
| 31-40 | 6 grams | 3 grams | Every 8 hours |
| 21-30 | 6 grams | 5 grams | Every 24 hours |
| 11-20 | 6 grams | 3 grams | Every 24 hours |
- Approximately 60% to 80% of the fosfomycin dose is cleared from the body by hemodialysis. Administer CONTEPO after hemodialysis on hemodialysis days. (2.2)
3 Dosage Forms and Strengths
CONTEPO for Injection contains 6 grams of fosfomycin, and is supplied as a white or almost white, sterile powder in single-dose vials, for constitution and further dilution.
6.2 Postmarketing Experience
The following additional adverse reactions were not reported with CONTEPO-treated patients in Trial 1 but have been identified with the use of oral fosfomycin tromethamine or during use of intravenous fosfomycin sodium outside of the United States for various indications and dosing regimens. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure:
Blood and lymphatic system disorders: aplastic anemia, eosinophilia, agranulocytosis, leukopenia, pancytopenia
Cardiac disorders: torsade de pointes
Ear and labyrinth disorders: vertigo
Eye disorders: visual impairment
Gastrointestinal disorders: dyspepsia, C. difficile-associated diarrhea and colitis, toxic megacolon
Hepatobiliary disorders: alkaline phosphatase increased, cholestatic hepatitis, icterus, hepatic necrosis
Immune system disorders: anaphylaxis
Metabolism and nutrition disorders: decreased appetite
Nervous system disorders: cerebral edema, dizziness, optic neuritis
Psychiatric disorders: confusion
Respiratory, thoracic, and mediastinal disorders: asthma attack, pulmonary edema
Skin and subcutaneous tissue disorders: angioedema, facial edema
Vascular disorders: hypertension
5.6 clostridioides Difficile
Clostridioides difficile-associated diarrhea (CDAD) has been reported with use of nearly all systemic antibacterial agents, including CONTEPO, and may range in severity from mild to fatal colitis. Treatment with antibacterial agents alters the normal flora of the colon and may permit overgrowth of C. difficile.
C. difficile produces toxins A and B which contribute to the development of CDAD. CDAD must be considered in all patients who present with diarrhea following antibacterial use. Careful medical history is necessary because CDAD has been reported to occur more than 2 months after administration of antibacterial agents.
If CDAD is confirmed, discontinue antibacterials not directed against C. difficile, if possible. Manage fluid and electrolyte levels as appropriate, supplement protein intake, monitor antibacterial treatment of C. difficile, and institute surgical evaluation as clinically indicated.
8 Use in Specific Populations
Lactation: Breastfeeding not recommended during treatment and 24 hours after the last dose (8.2).
5.4 Hypersensitivity Reactions
CONTEPO is contraindicated in patients with known serious hypersensitivity to fosfomycin, or any of the excipients [see Contraindications (4)]. Hypersensitivity reactions, such as rash and urticaria, were reported in patients treated with CONTEPO in Trial 1. Anaphylaxis has been reported postmarketing [see Adverse Reactions (6.2)]. Before initiating therapy with CONTEPO, it is important to inquire about previous hypersensitivity reactions to oral or parenteral fosfomycin. If an allergic reaction to CONTEPO occurs, discontinue the drug immediately.
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
CONTEPO was evaluated in a comparator-controlled clinical trial (Trial 1) in patients with cUTI, including acute pyelonephritis, which included 233 patients treated with CONTEPO and 231 treated with comparator (piperacillin/tazobactam 4.5 g every 8 hours) for 7 days, allowing bacteremic patients to receive up to 14 days. No switch to oral antibacterial drugs was allowed. The median age of treated patients was 54 years (range 18-89 years) and 64% were female. All patients were white (100%). Patients (99%) were predominantly enrolled in Eastern Europe. Concomitant bacteremia was identified in 9% of patients at baseline.
5.3 Increased Transaminase Levels
In Trial 1, increases in transaminases occurred more frequently in CONTEPO-treated patients compared to piperacillin/tazobactam-treated patients. Transaminases (Alanine Aminotransferase (ALT) or Aspartate Aminotransferase (AST) were elevated ≥ 3x upper limit of normal (ULN) in 10.3% of patients receiving CONTEPO and 4.8% of patients receiving piperacillin/tazobactam. Transaminase elevations were asymptomatic and reversible. No concurrent increases in serum bilirubin or alkaline phosphatase were observed. No patients met Hy's Law criteria, and no patients discontinued CONTEPO therapy because of treatment-related transaminase elevation [see Adverse Reactions (6.1)]. Monitor hepatic enzymes during CONTEPO treatment.
7.1 Drugs That Prolong Qt Interval
Co-administration of CONTEPO with other drugs known to prolong the QT interval may increase the risk for ventricular arrhythmia. Avoid co-administration of CONTEPO with drugs known to prolong the QT interval, such as class IA or class III antiarrhythmic medications, tricyclic antidepressants, macrolides, and antipsychotics [see Warnings and Precautions (5.2)].
5.1 Serum Electrolyte Abnormalities
CONTEPO contains 1,980 mg of sodium in each vial. The high sodium load associated with the use of CONTEPO may result in changes in serum electrolytes, such as increased levels of serum sodium and decreased levels of potassium, calcium, and phosphorous. Electrolyte disturbances, such as hypokalemia and hypocalcemia, may potentiate cardiac effects, including QT prolongation [ see Warnings and Precautions (5.2) and Clinical Pharmacology (12.2) ].
In Trial 1, a comparator-controlled clinical trial in patients with cUTI, hypokalemia, hypernatremia, hypophosphatemia, and hypocalcemia occurred more frequently in CONTEPO-treated patients compared with piperacillin/tazobactam-treated patients [ see Adverse Reactions (6.1) ]. Hypokalemia with serum potassium less than 3.0 mEq/L and/or requiring potassium supplementation occurred in 9.9% of patients receiving CONTEPO and 1.7% of patients receiving piperacillin/tazobactam. Hypophosphatemia with serum phosphate concentrations less than 1.0 mg/dL occurred in 2.1% of patients receiving CONTEPO and none of the patients receiving piperacillin/tazobactam. Hypernatremia with serum sodium greater than 150 mEq/L occurred in 3.4% of patients receiving CONTEPO and 0.9% of patients receiving piperacillin/tazobactam. Hypocalcemia with corrected serum calcium less than 8.0 mg/dL occurred in 3.9% of patients receiving CONTEPO and 2.6% of patients receiving piperacillin/tazobactam.
A low-sodium diet is recommended during CONTEPO treatment. Minimize administration of drugs containing sodium. Monitor serum electrolyte levels (sodium, potassium, calcium, magnesium, and phosphorus) and fluid status during treatment with CONTEPO. Electrolyte supplementation may be necessary in some cases. Monitor for signs of edema, particularly in patients who should restrict their sodium intake or are prone to fluid overload (e.g., cardiac insufficiency, renal impairment, cirrhosis, hypertension, hyperaldosteronism, hypernatremia or pulmonary edema) [ see Adverse Reactions (6.1) ].
5.5 neutropenia Including Agranulocytosis
Neutropenia has been reported in patients receiving IV fosfomycin therapy. In Trial 1, 6.4% of patients in the CONTEPO arm developed neutropenia (absolute neutrophil count less than 1500 cells/mm3) as compared to 3.9% in the piperacillin/tazobactam comparator arm. In the post marketing setting, neutropenia cases progressing to agranulocytosis have been reported with IV fosfomycin therapy. Monitor complete blood counts during CONTEPO therapy particularly in patients with pre-existing conditions or patients receiving concomitant drugs that may predispose to bone marrow suppression. Discontinue CONTEPO if neutropenia occurs and consider alternative therapies.
5.7 Development of Drug Resistant Bacteria
Prescribing CONTEPO in the absence of a proven or strongly suspected bacterial infection indication is unlikely to provide benefit to the patient and increases the risk of the development of drug resistant bacteria [ see Indications and Usage (1.2) ].
2.4 Stability of Contepo Solution in Intravenous Fluids
Because CONTEPO contains a high sodium content (1,980 mg per vial) [see Warnings and Precautions (5.2)], the infusion solution for dilution is Sterile Water for Injection, USP. After dilution, CONTEPO solution for administration is stable for 16 hours at room temperature (20°C to 25°C) at a concentration of 15 mg/mL to 30 mg/mL in Sterile Water for Injection, USP.
1.2 Usage to Reduce Development of Drug Resistant Bacteria
To reduce the development of drug-resistant bacteria and maintain the effectiveness of CONTEPO and other antibacterial drugs, CONTEPO should be used only to treat infections that are proven or strongly suspected to be caused by susceptible bacteria. When culture and susceptibility information are available, they should be considered in selecting or modifying antibacterial therapy. In the absence of such data, local epidemiology and susceptibility patterns may contribute to the empiric selection of therapy.
Principal Display Panel Contepo 6 Grams Per Vial Carton Label
NDC 71288-035-52
Rx Only
Contepo
(fosfomycin) for injection
6 grams per vial
For Intravenous Infusion only
Must be constituted and further diluted.
12 Single-Dose Vials -
Discard Unused Portion
Principal Display Panel Contepo 6 Grams Per Vial Container Label
NDC 71288-035-51
Rx Only
Contepo
(fosfomycin) for injection
6 grams per vial
For Intravenous Infusion only
Must be constituted and further diluted.
Single-Dose Vial - Discard Unused Portion
14.1 Complicated Urinary Tract Infections, Including Acute Pyelonephritis
A total of 464 adults hospitalized with cUTI (including acute pyelonephritis) were randomized and received study medications in a multinational, double-blind study (Trial 1, NCT02753946) comparing CONTEPO 6 g intravenously every 8 hours to piperacillin/tazobactam 4.5 g intravenously every 8 hours for 7 days of therapy. Treatment was allowed for up to 14 days in bacteremic patients. The study did not include a switch to oral antibacterial drugs.
The microbiological modified intent-to-treat (mMITT) population included all patients who received study medication and had at least 1 baseline uropathogen, excluding patients with organisms resistant to study drugs at baseline. This population consisted of 339 patients with cUTI, including 184 patients (54%) with acute pyelonephritis. The median age was 53 years and 64% were female. Concomitant bacteremia was identified in 9% of patients at baseline, and 32% of patients met 2 or more systemic inflammatory response syndrome (SIRS) criteria at baseline.
Overall success was defined as clinical cure plus microbiological eradication (baseline uropathogens with growth in urine ≥105 CFU/mL were reduced to <104 CFU/mL) at the test-of-cure (TOC) visit, 19 (+2) days after randomization. CONTEPO demonstrated efficacy with regard to the overall response at the TOC visit in the mMITT population (Table 5). A sensitivity analysis for overall success at the TOC visit using a threshold of 103 CFU/ml for microbiological eradication demonstrated similar efficacy results.
In the mMITT population, the overall success rates at TOC in patients with concurrent bacteremia were 9/19 (47.4%) for CONTEPO-treated patients and 5/13 (38.5%) in the piperacillin/tazobactam-treated patients.
Overall response rates at the TOC visit by pathogen in the mMITT population is presented in Table 6.
|
1 Patients with an organism resistant to study drugs at baseline were to be excluded. All of the patients excluded |
|||
|
(14 in CONTEPO arm, 9 in piperacillin/tazobactam arm) had an organism resistant to piperacillin/tazobactam. |
|||
|
2 CONTEPO 6 g intravenously every 8 hours |
|||
|
3 Piperacillin/tazobactam 4.5 g every 8 hours |
|||
| Response 1 |
CONTEPO
2
n/N (%) |
Piperacillin/ Tazobactam 3 n/N (%) |
Treatment Difference
(95% CI) |
| Overall success | 108/170 (63.5) | 94/169 (55.6) | 7.9 (-3.1, 18.9) |
| Clinical cure | 154/170 (90.6) | 155/169 (91.7) | -1.1 (-7.8, 5.5) |
| Microbiological eradication | 110/170 (64.7) | 97/169 (57.4) | 7.3 (-3.6, 18.3) |
|
1 Patients with an organism resistant to piperacillin/tazobactam at baseline were excluded |
||
| Pathogen 1 |
CONTEPO n/N (%) |
Piperacillin/ Tazobactam n/N (%) |
| Escherichia coli | 87/130 (66.9) | 75/130 (57.7) |
| Klebsiella pneumoniae | 8/18 (44.4) | 11/20 (55.0) |
1.1 Complicated Urinary Tract Infections (cuti), Including Acute Pyelonephritis
CONTEPO is indicated for the treatment of patients 18 years and older with complicated urinary tract infections (cUTI), including acute pyelonephritis, caused by susceptible isolates of Escherichia coli and Klebsiella pneumoniae.
2.2 recommended Dosage in Patients (18 Years of Age and Older) With Renal Impairment
The recommended dosage of CONTEPO in patients 18 years of age and older with an estimated CLcr of 50 mL/min or less is presented in Table 1. Monitor estimated CLcr and adjust the dosage of CONTEPO accordingly [ see Warnings and Precautions (5.1), Use in Specific Populations (8.6) and Clinical Pharmacology (12.3) ].
|
a CLcr estimated by Cockcroft-Gault Equation. |
|||
|
bAll doses of CONTEPO are administered by IV infusion over 1 hour. |
|||
| Estimated CLcr (mL/min) a | Loading Dose b | Maintenance Dosage b | |
| Dose | Frequency | ||
| 41-50 | 6 grams | 4 grams | Every 8 hours |
| 31-40 | 6 grams | 3 grams | Every 8 hours |
| 21-30 | 6 grams | 5 grams | Every 24 hours |
| 11-20 | 6 grams | 3 grams | Every 24 hours |
Approximately 60 to 80 % of the fosfomycin dose is cleared from the body by hemodialysis. Administer CONTEPO after hemodialysis on hemodialysis days.
Structured Label Content
Section 42229-5 (42229-5)
Preparation
CONTEPO is supplied as a dry powder in a single-dose vial that must be constituted and further diluted prior to intravenous infusion as described below. CONTEPO does not contain preservatives. Aseptic technique must be used for constitution and dilution prior to IV infusion.
- Constitute the vial with 30 mL of Sterile Water for Injection, USP and gently mix to completely dissolve contents. A slight degree of warming occurs when the powder is dissolved. The constituted solution should appear clear and colorless. Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration, whenever solution and container permit. The constituted solution is not for direct injection and must be further diluted immediately with Sterile Water for Injection, USP [see Dosage and Administration (2.4)] before intravenous infusion.
- To prepare the infusion solution, first remove 80 mL from a 250 mL intravenous bag of Sterile Water for Injection, USP for infusion so that it contains approximately 170 mL.
- Then add the required volume of constituted solution to the infusion bag according to Table 2. Discard unused portion. The constituted and further diluted solution of CONTEPO has a pH of 7.4 to 7.8.
| CONTEPO Dose | Volume to Withdraw from Constituted Vial |
Volume of Final Infusion Bag
(Approximate) |
Final Infusion Concentration of CONTEPO
(Approximate) |
| 6 grams | 32.6 mL (Entire Contents) |
202 mL | 30 mg/mL |
| 5 grams | 27 mL | 197 mL | 25 mg/mL |
| 4 grams | 21.5 mL | 192 mL | 20 mg/mL |
| 3 grams | 16 mL | 186 mL | 15 mg/mL |
10 Overdosage (10 OVERDOSAGE)
To date, no cases of accidental overdose with clinically relevant intolerances have been reported. In the event of an overdose, the patient must be monitored and treated symptomatically. Fosfomycin is cleared from the body by hemodialysis, during which patients with end stage renal disease have an increased mean fosfomycin elimination half-life to approximately 4 hours.
8.2 Lactation
Risk Summary
Fosfomycin is present in human milk. There are no data on the effects of fosfomycin on the breastfed child or on milk production. Because of the potential for adverse reactions in a breastfed infant, advise patients not to breastfeed during treatment with CONTEPO and for 24 hours after the last dose.
11 Description (11 DESCRIPTION)
CONTEPO (fosfomycin) for injection, for intravenous use, contains fosfomycin disodium, an epoxide antibacterial drug.
Fosfomycin disodium is a powder with the chemical name of disodium [(2R,3S)-3-methyloxiran-2-yl]-dioxido-oxophosphorane, an empirical formula of C3H5Na2O4P and molecular weight of 182.
Figure 1 Chemical Structure of Fosfomycin Disodium
Each CONTEPO for Injection single-dose vial contains white to almost white sterile powder with 6 grams of fosfomycin (equivalent to 7.9 grams fosfomycin disodium) and the inactive ingredient succinic acid (150 mg) for pH adjustment. It is intended for constitution and further dilution prior to intravenous infusion . Each gram of fosfomycin disodium contains 330 mg of sodium (i.e., each vial contains 1,980 mg of sodium).
8.4 Pediatric Use
Safety and effectiveness of CONTEPO in patients less than 18 years of age has not been established.
8.5 Geriatric Use
Of the 233 patients treated with CONTEPO in Trial 1, 32% (74/233) were 65 years of age and older, including 11.2% (26/233) who were 75 years of age and older. For patients included in the microbiological modified intent-to-treat (mMITT) population, lower overall success rates were observed for CONTEPO-treated and piperacillin/tazobactam-treated patients ≥ 65 years of age (53.6% and 43.9%, respectively) as compared to patients < 65 years (68.4% and 61.6%, respectively).
For patients ≥ 65 years of age, the incidence rate of adverse reactions was 39.2% (29/74) in CONTEPO-treated patients and 28.6% (22/77) in the piperacillin/tazobactam-treated patients. For patients <65 years of age, the incidence rate of adverse reactions was 43.4% (69/159) in CONTEPO-treated patients and 33.8% (52/154) in the piperacillin/tazobactam-treated patients.
Because elderly patients are more likely to have decreased cardiac and renal function, care should be taken in dose selection, and electrolytes, fluid status, and renal function should be monitored. Dosage adjustment in elderly patients should take into account renal function [ see Dosage and Administration (2.2, 2.3, 2.4) and Clinical Pharmacology (12.3) ].
4 Contraindications (4 CONTRAINDICATIONS)
CONTEPO is contraindicated in patients with known serious hypersensitivity to fosfomycin, or any of the excipients [ see Warnings and Precautions (5.2) ].
5.2 Qt Prolongation (5.2 QT Prolongation)
CONTEPO has been shown to prolong the QT interval in some patients. QT prolongation can lead to development of torsade de pointes-type ventricular tachycardia with the risk increasing as the degree of prolongation increases. In Trial 1, 3.6% of patients treated with CONTEPO had > 60 msec increase in QTcF interval from baseline and 1% of patients had QTcF > 480 msec. Torsade de pointes has been reported during postmarketing experience with fosfomycin [see Adverse Reactions (6.2)]. The risk of QT prolongation may increase in patients with electrolyte abnormalities (such as hypokalemia and hypocalcemia), patients with conditions that have potential to cause electrolyte imbalance (such as renal impairment), or patients taking other drugs affecting electrolyte balance or QT prolongation. Avoid CONTEPO in patients with known QT prolongation or ventricular arrhythmias, including a history of torsade de pointes. Monitor electrolytes during treatment with CONTEPO [see Warnings and Precautions (5.1), Drug Interactions (7.1) and Clinical Pharmacology (12.2)].
6 Adverse Reactions (6 ADVERSE REACTIONS)
The following adverse reactions are discussed in greater detail in the Warnings and Precautions section:
- Serum Electrolyte Abnormalities [see Warnings and Precautions (5.1)]
- QT Prolongation [see Warnings and Precautions (5.2)]
- Increased Transaminase Levels [see Warnings and Precautions (5.3)]
- Hypersensitivity Reactions [see Warnings and Precautions (5.4)]
- Neutropenia Including Agranulocytosis [see Warnings and Precautions (5.5)]
- Clostridioides difficile-Associated Diarrhea [see Warnings and Precautions (5.6)]
- Development of Drug-Resistant Bacteria [see Warnings and Precautions (5.7)]
7 Drug Interactions (7 DRUG INTERACTIONS)
8.6 Renal Impairment
Dosage adjustment is required for patients with estimated CLcr 50 mL/min or less. Monitor estimated CLcr and adjust the dosage of CONTEPO accordingly [ see Dosage and Administration (2.2) ].
In patients requiring hemodialysis, CONTEPO should be administered after hemodialysis on hemodialysis days [see Dosage and Administration (2.2), Clinical Pharmacology (12.3)].
12.2 Pharmacodynamics
The ratio of the unbound plasma fosfomycin AUC to MIC against the infecting organism has been shown to correlate with activity in animal models of infection.
12.3 Pharmacokinetics
The mean pharmacokinetic parameters of fosfomycin in healthy adults with normal renal function after single doses of 6 grams administered as 1-hour IV infusion are summarized along with additional pharmacokinetic information in Table 4.
|
a Based on non-compartmental analysis of PK data |
|
| C max (mcg/mL) | 228 ± 43 |
| AUC 0-inf (mcg∙hr/mL) | 734 ± 134 |
| Dose Proportionality | Fosfomycin Cmax and AUC0-inf increase proportionally with dose |
| Distribution | |
| Volume of Distribution (L) | 27 ± 5.2 |
| Protein Binding | Fosfomycin is not bound to plasma proteins |
| Elimination | |
| Half-Life (h) | 2.8 ± 0.6 |
| Total Clearance (L/h) | 8.5 ± 1.7 |
| Metabolism | Fosfomycin is not metabolized. |
| Excretion | Urine: 70% of dose is excreted unchanged at 12 hours; 74-80% of dose is excreted unchanged at 48 hours |
2.1 Recommended Dosage
The recommended dosage of CONTEPO is 6 grams administered every 8 hours by intravenous (IV) infusion over 1 hour in patients 18 years of age or older with an estimated creatinine clearance (CLcr) greater than 50 mL/min. The duration of therapy is up to 14 days and should be guided by the severity of infection and the patient's clinical status. During treatment, different dosage recommendations may be required based on change in estimated CLcr [ see Dosage and Administration (2.2) ].
8.7 Hepatic Impairment
1 Indications and Usage (1 INDICATIONS AND USAGE)
CONTEPO is an epoxide antibacterial indicated for the treatment of patients 18 years of age and older with complicated urinary tract infections (cUTI) including acute pyelonephritis caused by susceptible isolates of Escherichia coli and Klebsiella pneumoniae. (1.1)
Usage to Reduce Development of Drug-Resistant Bacteria
To reduce the development of drug-resistant bacteria and maintain the effectiveness of CONTEPO and other antibacterial drugs, CONTEPO should be used only to treat infections that are proven or strongly suspected to be caused by bacteria. (1.2)
12.1 Mechanism of Action
CONTEPO is an antibacterial drug [ see Microbiology (12.4) ].
2.5 Drug Incompatibility
The compatibility of CONTEPO with other drugs and infusion solutions has not been established. CONTEPO should not be mixed or co-administered with solutions containing other drugs.
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
- Serum Electrolyte Abnormalities: CONTEPO contains 1980 mg sodium in each vial. The high sodium load associated with the use of CONTEPO may result in changes in serum electrolytes, such as increased levels of sodium and decreased levels of potassium, calcium and phosphorus. A low-sodium diet is recommended during CONTEPO treatment. Monitor serum electrolyte levels and fluid status during CONTEPO treatment. Monitor signs and symptoms of edema, particularly in patients with cardiac insufficiency, renal impairment, cirrhosis, hypertension, hyperaldosteronism, hypernatremia or pulmonary edema. (5.1)
- QT Prolongation: CONTEPO has been shown to prolong the QT interval in some patients in the clinical trial. Avoid CONTEPO in patients with known prolongation of the QT interval or ventricular arrhythmias, including a history of torsade de pointes. (5.2, 7.1)
- Increased Transaminase Levels: Increase in alanine aminotransferase (ALT) and aspartate aminotransferase (AST) were reported in the clinical trial. Monitor hepatic enzymes during CONTEPO treatment. (5.3)
- Hypersensitivity Reactions: Reactions such as rash, urticaria and anaphylaxis were reported with the use of CONTEPO. Before initiating therapy with CONTEPO, it is important to inquire about previous hypersensitivity reactions to oral or parenteral fosfomycin. If an allergic reaction occurs, discontinue CONTEPO immediately. (5.4)
- Neutropenia Including Agranulocytosis: Neutropenia, including agranulocytosis, has occurred in patients receiving IV fosfomycin treatment. Monitor complete blood count during CONTEPO therapy. If such reactions occur, discontinue CONTEPO and institute appropriate treatment (5.5).
- Clostridioides difficile -Associated Diarrhea (CDAD): This has been reported with nearly all systemic antibacterial agents, including CONTEPO. Evaluate patients if diarrhea occurs. (5.6)
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
- Administer CONTEPO, 6 grams every 8 hours by intravenous (IV) infusion over 1 hour for up to 14 days, in patients 18 years of age or older with an estimated creatinine clearance (CLcr) greater than 50 mL/min. (2.1)
- The recommended dosage in patients 18 years of age and older with an estimated CLcr of 50 mL/min or less is presented in the table below. (2.2)
|
aCLcr estimated using Cockcroft-Gault Equation. |
|||
|
bAll doses of CONTEPO are administered by intravenous infusion over 1 hour. |
|||
| Estimated CLcr (mL/min) a | Loading Dose b | Maintenance Dosage b | |
| Dose | Frequency | ||
| 41-50 | 6 grams | 4 grams | Every 8 hours |
| 31-40 | 6 grams | 3 grams | Every 8 hours |
| 21-30 | 6 grams | 5 grams | Every 24 hours |
| 11-20 | 6 grams | 3 grams | Every 24 hours |
- Approximately 60% to 80% of the fosfomycin dose is cleared from the body by hemodialysis. Administer CONTEPO after hemodialysis on hemodialysis days. (2.2)
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
CONTEPO for Injection contains 6 grams of fosfomycin, and is supplied as a white or almost white, sterile powder in single-dose vials, for constitution and further dilution.
6.2 Postmarketing Experience
The following additional adverse reactions were not reported with CONTEPO-treated patients in Trial 1 but have been identified with the use of oral fosfomycin tromethamine or during use of intravenous fosfomycin sodium outside of the United States for various indications and dosing regimens. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure:
Blood and lymphatic system disorders: aplastic anemia, eosinophilia, agranulocytosis, leukopenia, pancytopenia
Cardiac disorders: torsade de pointes
Ear and labyrinth disorders: vertigo
Eye disorders: visual impairment
Gastrointestinal disorders: dyspepsia, C. difficile-associated diarrhea and colitis, toxic megacolon
Hepatobiliary disorders: alkaline phosphatase increased, cholestatic hepatitis, icterus, hepatic necrosis
Immune system disorders: anaphylaxis
Metabolism and nutrition disorders: decreased appetite
Nervous system disorders: cerebral edema, dizziness, optic neuritis
Psychiatric disorders: confusion
Respiratory, thoracic, and mediastinal disorders: asthma attack, pulmonary edema
Skin and subcutaneous tissue disorders: angioedema, facial edema
Vascular disorders: hypertension
5.6 clostridioides Difficile (5.6 Clostridioides difficile)
Clostridioides difficile-associated diarrhea (CDAD) has been reported with use of nearly all systemic antibacterial agents, including CONTEPO, and may range in severity from mild to fatal colitis. Treatment with antibacterial agents alters the normal flora of the colon and may permit overgrowth of C. difficile.
C. difficile produces toxins A and B which contribute to the development of CDAD. CDAD must be considered in all patients who present with diarrhea following antibacterial use. Careful medical history is necessary because CDAD has been reported to occur more than 2 months after administration of antibacterial agents.
If CDAD is confirmed, discontinue antibacterials not directed against C. difficile, if possible. Manage fluid and electrolyte levels as appropriate, supplement protein intake, monitor antibacterial treatment of C. difficile, and institute surgical evaluation as clinically indicated.
8 Use in Specific Populations (8 USE IN SPECIFIC POPULATIONS)
Lactation: Breastfeeding not recommended during treatment and 24 hours after the last dose (8.2).
5.4 Hypersensitivity Reactions
CONTEPO is contraindicated in patients with known serious hypersensitivity to fosfomycin, or any of the excipients [see Contraindications (4)]. Hypersensitivity reactions, such as rash and urticaria, were reported in patients treated with CONTEPO in Trial 1. Anaphylaxis has been reported postmarketing [see Adverse Reactions (6.2)]. Before initiating therapy with CONTEPO, it is important to inquire about previous hypersensitivity reactions to oral or parenteral fosfomycin. If an allergic reaction to CONTEPO occurs, discontinue the drug immediately.
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
CONTEPO was evaluated in a comparator-controlled clinical trial (Trial 1) in patients with cUTI, including acute pyelonephritis, which included 233 patients treated with CONTEPO and 231 treated with comparator (piperacillin/tazobactam 4.5 g every 8 hours) for 7 days, allowing bacteremic patients to receive up to 14 days. No switch to oral antibacterial drugs was allowed. The median age of treated patients was 54 years (range 18-89 years) and 64% were female. All patients were white (100%). Patients (99%) were predominantly enrolled in Eastern Europe. Concomitant bacteremia was identified in 9% of patients at baseline.
5.3 Increased Transaminase Levels
In Trial 1, increases in transaminases occurred more frequently in CONTEPO-treated patients compared to piperacillin/tazobactam-treated patients. Transaminases (Alanine Aminotransferase (ALT) or Aspartate Aminotransferase (AST) were elevated ≥ 3x upper limit of normal (ULN) in 10.3% of patients receiving CONTEPO and 4.8% of patients receiving piperacillin/tazobactam. Transaminase elevations were asymptomatic and reversible. No concurrent increases in serum bilirubin or alkaline phosphatase were observed. No patients met Hy's Law criteria, and no patients discontinued CONTEPO therapy because of treatment-related transaminase elevation [see Adverse Reactions (6.1)]. Monitor hepatic enzymes during CONTEPO treatment.
7.1 Drugs That Prolong Qt Interval (7.1 Drugs that prolong QT interval)
Co-administration of CONTEPO with other drugs known to prolong the QT interval may increase the risk for ventricular arrhythmia. Avoid co-administration of CONTEPO with drugs known to prolong the QT interval, such as class IA or class III antiarrhythmic medications, tricyclic antidepressants, macrolides, and antipsychotics [see Warnings and Precautions (5.2)].
5.1 Serum Electrolyte Abnormalities
CONTEPO contains 1,980 mg of sodium in each vial. The high sodium load associated with the use of CONTEPO may result in changes in serum electrolytes, such as increased levels of serum sodium and decreased levels of potassium, calcium, and phosphorous. Electrolyte disturbances, such as hypokalemia and hypocalcemia, may potentiate cardiac effects, including QT prolongation [ see Warnings and Precautions (5.2) and Clinical Pharmacology (12.2) ].
In Trial 1, a comparator-controlled clinical trial in patients with cUTI, hypokalemia, hypernatremia, hypophosphatemia, and hypocalcemia occurred more frequently in CONTEPO-treated patients compared with piperacillin/tazobactam-treated patients [ see Adverse Reactions (6.1) ]. Hypokalemia with serum potassium less than 3.0 mEq/L and/or requiring potassium supplementation occurred in 9.9% of patients receiving CONTEPO and 1.7% of patients receiving piperacillin/tazobactam. Hypophosphatemia with serum phosphate concentrations less than 1.0 mg/dL occurred in 2.1% of patients receiving CONTEPO and none of the patients receiving piperacillin/tazobactam. Hypernatremia with serum sodium greater than 150 mEq/L occurred in 3.4% of patients receiving CONTEPO and 0.9% of patients receiving piperacillin/tazobactam. Hypocalcemia with corrected serum calcium less than 8.0 mg/dL occurred in 3.9% of patients receiving CONTEPO and 2.6% of patients receiving piperacillin/tazobactam.
A low-sodium diet is recommended during CONTEPO treatment. Minimize administration of drugs containing sodium. Monitor serum electrolyte levels (sodium, potassium, calcium, magnesium, and phosphorus) and fluid status during treatment with CONTEPO. Electrolyte supplementation may be necessary in some cases. Monitor for signs of edema, particularly in patients who should restrict their sodium intake or are prone to fluid overload (e.g., cardiac insufficiency, renal impairment, cirrhosis, hypertension, hyperaldosteronism, hypernatremia or pulmonary edema) [ see Adverse Reactions (6.1) ].
5.5 neutropenia Including Agranulocytosis (5.5 Neutropenia Including Agranulocytosis)
Neutropenia has been reported in patients receiving IV fosfomycin therapy. In Trial 1, 6.4% of patients in the CONTEPO arm developed neutropenia (absolute neutrophil count less than 1500 cells/mm3) as compared to 3.9% in the piperacillin/tazobactam comparator arm. In the post marketing setting, neutropenia cases progressing to agranulocytosis have been reported with IV fosfomycin therapy. Monitor complete blood counts during CONTEPO therapy particularly in patients with pre-existing conditions or patients receiving concomitant drugs that may predispose to bone marrow suppression. Discontinue CONTEPO if neutropenia occurs and consider alternative therapies.
5.7 Development of Drug Resistant Bacteria (5.7 Development of Drug-resistant Bacteria)
Prescribing CONTEPO in the absence of a proven or strongly suspected bacterial infection indication is unlikely to provide benefit to the patient and increases the risk of the development of drug resistant bacteria [ see Indications and Usage (1.2) ].
2.4 Stability of Contepo Solution in Intravenous Fluids (2.4 Stability of CONTEPO Solution in Intravenous Fluids)
Because CONTEPO contains a high sodium content (1,980 mg per vial) [see Warnings and Precautions (5.2)], the infusion solution for dilution is Sterile Water for Injection, USP. After dilution, CONTEPO solution for administration is stable for 16 hours at room temperature (20°C to 25°C) at a concentration of 15 mg/mL to 30 mg/mL in Sterile Water for Injection, USP.
1.2 Usage to Reduce Development of Drug Resistant Bacteria (1.2 Usage to Reduce Development of Drug-Resistant Bacteria)
To reduce the development of drug-resistant bacteria and maintain the effectiveness of CONTEPO and other antibacterial drugs, CONTEPO should be used only to treat infections that are proven or strongly suspected to be caused by susceptible bacteria. When culture and susceptibility information are available, they should be considered in selecting or modifying antibacterial therapy. In the absence of such data, local epidemiology and susceptibility patterns may contribute to the empiric selection of therapy.
Principal Display Panel Contepo 6 Grams Per Vial Carton Label (PRINCIPAL DISPLAY PANEL - CONTEPO 6 grams per vial Carton Label)
NDC 71288-035-52
Rx Only
Contepo
(fosfomycin) for injection
6 grams per vial
For Intravenous Infusion only
Must be constituted and further diluted.
12 Single-Dose Vials -
Discard Unused Portion
Principal Display Panel Contepo 6 Grams Per Vial Container Label (PRINCIPAL DISPLAY PANEL - CONTEPO 6 grams per vial Container Label)
NDC 71288-035-51
Rx Only
Contepo
(fosfomycin) for injection
6 grams per vial
For Intravenous Infusion only
Must be constituted and further diluted.
Single-Dose Vial - Discard Unused Portion
14.1 Complicated Urinary Tract Infections, Including Acute Pyelonephritis
A total of 464 adults hospitalized with cUTI (including acute pyelonephritis) were randomized and received study medications in a multinational, double-blind study (Trial 1, NCT02753946) comparing CONTEPO 6 g intravenously every 8 hours to piperacillin/tazobactam 4.5 g intravenously every 8 hours for 7 days of therapy. Treatment was allowed for up to 14 days in bacteremic patients. The study did not include a switch to oral antibacterial drugs.
The microbiological modified intent-to-treat (mMITT) population included all patients who received study medication and had at least 1 baseline uropathogen, excluding patients with organisms resistant to study drugs at baseline. This population consisted of 339 patients with cUTI, including 184 patients (54%) with acute pyelonephritis. The median age was 53 years and 64% were female. Concomitant bacteremia was identified in 9% of patients at baseline, and 32% of patients met 2 or more systemic inflammatory response syndrome (SIRS) criteria at baseline.
Overall success was defined as clinical cure plus microbiological eradication (baseline uropathogens with growth in urine ≥105 CFU/mL were reduced to <104 CFU/mL) at the test-of-cure (TOC) visit, 19 (+2) days after randomization. CONTEPO demonstrated efficacy with regard to the overall response at the TOC visit in the mMITT population (Table 5). A sensitivity analysis for overall success at the TOC visit using a threshold of 103 CFU/ml for microbiological eradication demonstrated similar efficacy results.
In the mMITT population, the overall success rates at TOC in patients with concurrent bacteremia were 9/19 (47.4%) for CONTEPO-treated patients and 5/13 (38.5%) in the piperacillin/tazobactam-treated patients.
Overall response rates at the TOC visit by pathogen in the mMITT population is presented in Table 6.
|
1 Patients with an organism resistant to study drugs at baseline were to be excluded. All of the patients excluded |
|||
|
(14 in CONTEPO arm, 9 in piperacillin/tazobactam arm) had an organism resistant to piperacillin/tazobactam. |
|||
|
2 CONTEPO 6 g intravenously every 8 hours |
|||
|
3 Piperacillin/tazobactam 4.5 g every 8 hours |
|||
| Response 1 |
CONTEPO
2
n/N (%) |
Piperacillin/ Tazobactam 3 n/N (%) |
Treatment Difference
(95% CI) |
| Overall success | 108/170 (63.5) | 94/169 (55.6) | 7.9 (-3.1, 18.9) |
| Clinical cure | 154/170 (90.6) | 155/169 (91.7) | -1.1 (-7.8, 5.5) |
| Microbiological eradication | 110/170 (64.7) | 97/169 (57.4) | 7.3 (-3.6, 18.3) |
|
1 Patients with an organism resistant to piperacillin/tazobactam at baseline were excluded |
||
| Pathogen 1 |
CONTEPO n/N (%) |
Piperacillin/ Tazobactam n/N (%) |
| Escherichia coli | 87/130 (66.9) | 75/130 (57.7) |
| Klebsiella pneumoniae | 8/18 (44.4) | 11/20 (55.0) |
1.1 Complicated Urinary Tract Infections (cuti), Including Acute Pyelonephritis (1.1 Complicated Urinary Tract Infections (cUTI), including Acute Pyelonephritis)
CONTEPO is indicated for the treatment of patients 18 years and older with complicated urinary tract infections (cUTI), including acute pyelonephritis, caused by susceptible isolates of Escherichia coli and Klebsiella pneumoniae.
2.2 recommended Dosage in Patients (18 Years of Age and Older) With Renal Impairment (2.2 Recommended Dosage in Patients (18 Years of Age and Older) with Renal Impairment)
The recommended dosage of CONTEPO in patients 18 years of age and older with an estimated CLcr of 50 mL/min or less is presented in Table 1. Monitor estimated CLcr and adjust the dosage of CONTEPO accordingly [ see Warnings and Precautions (5.1), Use in Specific Populations (8.6) and Clinical Pharmacology (12.3) ].
|
a CLcr estimated by Cockcroft-Gault Equation. |
|||
|
bAll doses of CONTEPO are administered by IV infusion over 1 hour. |
|||
| Estimated CLcr (mL/min) a | Loading Dose b | Maintenance Dosage b | |
| Dose | Frequency | ||
| 41-50 | 6 grams | 4 grams | Every 8 hours |
| 31-40 | 6 grams | 3 grams | Every 8 hours |
| 21-30 | 6 grams | 5 grams | Every 24 hours |
| 11-20 | 6 grams | 3 grams | Every 24 hours |
Approximately 60 to 80 % of the fosfomycin dose is cleared from the body by hemodialysis. Administer CONTEPO after hemodialysis on hemodialysis days.
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:54:28.258381 · Updated: 2026-03-14T22:48:57.475644