Lidocaine And Prilocaine Cream, 2.5%/2.5%
833cd52c-6470-49c4-937f-1393971f4db9
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
Rx only
Indications and Usage
Lidocaine and prilocaine cream, 2.5%/2.5% (a eutectic mixture of lidocaine 2.5% and prilocaine 2.5%) is indicated as a topical anesthetic for use on: - normal intact skin for local analgesia. - genital mucous membranes for superficial minor surgery and as pretreatment for infiltration anesthesia. Lidocaine and prilocaine cream, 2.5%/2.5% is not recommended in any clinical situation when penetration or migration beyond the tympanic membrane into the middle ear is possible because of the ototoxic effects observed in animal studies (see WARNINGS ).
Contraindications
Lidocaine and prilocaine cream, 2.5%/2.5% is contraindicated in patients with a known history of sensitivity to local anesthetics of the amide type or to any other component of the product.
How Supplied
Lidocaine and prilocaine cream, 2.5%/2.5% is supplied as follows: NDC 0168-0357-30 30 gram tube, with a child-resistant cap NDC 0168-0357-55 5 gram tube, FOR HOSPITAL USE ONLY NDC 0168-0357-56 5 gram tube, with 12 dressings, FOR HOSPITAL USE ONLY NOT FOR OPHTHALMIC USE. KEEP CONTAINER TIGHTLY CLOSED AT ALL TIMES WHEN NOT IN USE. KEEP OUT OF THE REACH OF CHILDREN. Store at 20°C to 25°C (68°F to 77°F); excursions permitted to 15°C to 30°C (59°F to 86°F) [See USP Controlled Room Temperature]. E. FOUGERA & CO. A division of Fougera PHARMACEUTICALS INC. Melville, New York 11747 Revised: 01/2024
Medication Information
Indications and Usage
Lidocaine and prilocaine cream, 2.5%/2.5% (a eutectic mixture of lidocaine 2.5% and prilocaine 2.5%) is indicated as a topical anesthetic for use on:
- normal intact skin for local analgesia.
- genital mucous membranes for superficial minor surgery and as pretreatment for infiltration anesthesia.
Lidocaine and prilocaine cream, 2.5%/2.5% is not recommended in any clinical situation when penetration or migration beyond the tympanic membrane into the middle ear is possible because of the ototoxic effects observed in animal studies (see WARNINGS ).
Contraindications
Lidocaine and prilocaine cream, 2.5%/2.5% is contraindicated in patients with a known history of sensitivity to local anesthetics of the amide type or to any other component of the product.
How Supplied
Lidocaine and prilocaine cream, 2.5%/2.5% is supplied as follows:
NDC 0168-0357-30 30 gram tube, with a child-resistant cap
NDC 0168-0357-55 5 gram tube, FOR HOSPITAL USE ONLY
NDC 0168-0357-56 5 gram tube, with 12 dressings, FOR HOSPITAL USE ONLY
NOT FOR OPHTHALMIC USE.
KEEP CONTAINER TIGHTLY CLOSED AT ALL TIMES WHEN NOT IN USE.
KEEP OUT OF THE REACH OF CHILDREN.
Store at 20°C to 25°C (68°F to 77°F); excursions permitted to 15°C to 30°C (59°F to 86°F) [See USP Controlled Room Temperature].
E. FOUGERA & CO.
A division of
Fougera
PHARMACEUTICALS INC.
Melville, New York 11747
Revised: 01/2024
Description
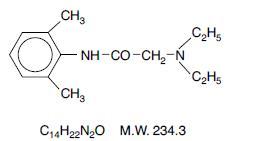
Lidocaine and prilocaine cream, 2.5%/2.5% is an emulsion in which the oil phase is a eutectic mixture of lidocaine and prilocaine in a ratio of 1:1 by weight. This eutectic mixture has a melting point below room temperature and therefore both local anesthetics exist as a liquid oil rather than as crystals. It is packaged in 30 gram tubes and 5 gram tubes for hospital use. Lidocaine is chemically designated as acetamide, 2-(diethylamino)-N-(2,6-dimethylphenyl), has an octanol: water partition ratio of 43 at pH 7.4, and has the following structure:
Prilocaine is chemically designated as propanamide, N-(2-methylphenyl)-2-(propylamino), has an octanol: water partition ratio of 25 at pH 7.4, and has the following structure:
Each gram of lidocaine and prilocaine cream, 2.5%/2.5% contains lidocaine 25 mg, prilocaine 25 mg, polyoxyethylene fatty acid esters (as emulsifiers), carbomer 934P (as a thickening agent), sodium hydroxide to adjust to a pH approximating 9, and purified water. Lidocaine and prilocaine cream, 2.5%/2.5% contains no preservative, however it passes the USP antimicrobial effectiveness test due to the pH. The specific gravity of lidocaine and prilocaine cream, 2.5%/2.5% is approximately 1.00.
Section 34072-9
General: Repeated doses of lidocaine and prilocaine cream, 2.5%/2.5% may increase blood levels of lidocaine and prilocaine. Lidocaine and prilocaine cream, 2.5%/2.5% should be used with caution in patients who may be more sensitive to the systemic effects of lidocaine and prilocaine including acutely ill, debilitated, or elderly patients.
Lidocaine and prilocaine cream, 2.5%/2.5% should not be applied to open wounds.
Care should be taken not to allow lidocaine and prilocaine cream, 2.5%/2.5% to come in contact with the eye because animal studies have demonstrated severe eye irritation. Also the loss of protective reflexes can permit corneal irritation and potential abrasion. Absorption of lidocaine and prilocaine cream, 2.5%/2.5% in conjunctival tissues has not been determined. If eye contact occurs, immediately wash out the eye with water or saline and protect the eye until sensation returns.
Patients allergic to para-aminobenzoic acid derivatives (procaine, tetracaine, benzocaine, etc.) have not shown cross sensitivity to lidocaine and/or prilocaine, however, lidocaine and prilocaine cream, 2.5%/2.5% should be used with caution in patients with a history of drug sensitivities, especially if the etiologic agent is uncertain.
Patients with severe hepatic disease, because of their inability to metabolize local anesthetics normally, are at greater risk of developing toxic plasma concentrations of lidocaine and prilocaine.
Lidocaine and prilocaine have been shown to inhibit viral and bacterial growth. The effect of lidocaine and prilocaine cream, 2.5%/2.5% on intradermal injections of live vaccines has not been determined.
Section 34073-7
Drug Interactions: Lidocaine and prilocaine cream, 2.5%/2.5% should be used with caution in patients receiving Class I antiarrhythmic drugs (such as tocainide and mexiletine) since the toxic effects are additive and potentially synergistic.
Patients who are administered local anesthetics are at increased risk of developing methemoglobinemia when concurrently exposed to the following drugs, which could include other local anesthetics:
Examples of Drugs Associated with Methemoglobinemia:
|
Class |
Examples |
|
Nitrates/Nitrites |
nitric oxide, nitroglycerin, nitroprusside, nitrous oxide |
|
Local anesthetics |
articaine, benzocaine, bupivacaine, lidocaine, mepivacaine, prilocaine, procaine, ropivacaine, tetracaine |
|
Antineoplastic agents |
cyclophosphamide, flutamide, hydroxyurea, ifosfamide, rasburicase |
|
Antibiotics |
dapsone, nitrofurantoin, para-aminosalicylic acid, sulfonamides |
|
Antimalarials |
chloroquine, primaquine |
|
Anticonvulsants |
Phenobarbital, phenytoin, sodium valproate |
|
Other drugs |
acetaminophen, metoclopramide, quinine, sulfasalazine |
Specific interaction studies with lidocaine/prilocaine and class III anti-arrhythmic drugs (e.g., amiodarone, bretylium, sotalol, dofetilide) have not been performed, but caution is advised (see WARNINGS ).
Should lidocaine and prilocaine cream, 2.5%/2.5% be used concomitantly with other products containing lidocaine and/or prilocaine, cumulative doses from all formulations must be considered.
Section 34076-0
Information for Patients: Inform patients that use of local anesthetics may cause methemoglobinemia, a serious condition that must be treated promptly. Advise patients or caregivers to stop use and seek immediate medical attention if they or someone in their care experience the following signs or symptoms: pale, gray, or blue colored skin (cyanosis); headache; rapid heart rate; shortness of breath; lightheadedness; or fatigue.
When lidocaine and prilocaine cream, 2.5%/2.5% is used, the patient should be aware that the production of dermal analgesia may be accompanied by the block of all sensations in the treated skin. For this reason, the patient should avoid inadvertent trauma to the treated area by scratching, rubbing, or exposure to extreme hot or cold temperatures until complete sensation has returned.
Lidocaine and prilocaine cream, 2.5%/2.5% should not be applied near the eyes or on open wounds.
Section 34079-4
Labor and Delivery: Neither lidocaine nor prilocaine are contraindicated in labor and delivery. Should lidocaine and prilocaine cream, 2.5%/2.5% be used concomitantly with other products containing lidocaine and/or prilocaine, cumulative doses from all formulations must be considered.
Section 34080-2
Nursing Mothers: Lidocaine, and probably prilocaine, are excreted in human milk. Therefore, caution should be exercised when lidocaine and prilocaine cream, 2.5%/2.5% is administered to a nursing mother since the milk:plasma ratio of lidocaine is 0.4 and is not determined for prilocaine.
Section 34081-0
Pediatric Use: Controlled studies of lidocaine and prilocaine cream, 2.5%/2.5% in children under the age of seven years have shown less overall benefit than in older children or adults. These results illustrate the importance of emotional and psychological support of younger children undergoing medical or surgical procedures.
Lidocaine and prilocaine cream, 2.5%/2.5% should be used with care in patients with conditions or therapy associated with methemoglobinemia (see Methemoglobinemia subsection of WARNINGS).
When using lidocaine and prilocaine cream, 2.5%/2.5% in young children, especially infants under the age of 3 months, care must be taken to insure that the caregiver understands the need to limit the dose and area of application, and to prevent accidental ingestion (see DOSAGE AND ADMINISTRATION and Methemoglobinemia ).
In neonates (minimum gestation age: 37 weeks) and children weighing less than 20 kg, the area and duration of application should be limited (see TABLE 2 in Individualization of Dose). Studies have not demonstrated the efficacy of lidocaine and prilocaine cream, 2.5%/2.5% for heel lancing in neonates.
Section 42229-5
Rx only
Section 43679-0
Mechanism of Action: Lidocaine and prilocaine cream, 2.5%/2.5%, applied to intact skin under occlusive dressing, provides dermal analgesia by the release of lidocaine and prilocaine from the cream into the epidermal and dermal layers of the skin and by the accumulation of lidocaine and prilocaine in the vicinity of dermal pain receptors and nerve endings. Lidocaine and prilocaine are amide-type local anesthetic agents. Both lidocaine and prilocaine stabilize neuronal membranes by inhibiting the ionic fluxes required for the initiation and conduction of impulses, thereby effecting local anesthetic action.
The onset, depth and duration of dermal analgesia on intact skin provided by lidocaine and prilocaine cream, 2.5%/2.5% depends primarily on the duration of application. To provide sufficient analgesia for clinical procedures such as intravenous catheter placement and venipuncture, lidocaine and prilocaine cream, 2.5%/2.5% should be applied under an occlusive dressing for at least 1 hour. To provide dermal analgesia for clinical procedures such as split skin graft harvesting, lidocaine and prilocaine cream, 2.5%/2.5% should be applied under occlusive dressing for at least 2 hours. Satisfactory dermal analgesia is achieved 1 hour after application, reaches maximum at 2 to 3 hours, and persists for 1 to 2 hours after removal. Absorption from the genital mucosa is more rapid and onset time is shorter (5 to 10 minutes) than after application to intact skin. After a 5 to 10 minute application of lidocaine and prilocaine cream, 2.5%/2.5% to female genital mucosa, the average duration of effective analgesia to an argon laser stimulus (which produced a sharp, pricking pain) was 15 to 20 minutes (individual variations in the range of 5 to 45 minutes).
Dermal application of lidocaine and prilocaine cream, 2.5%/2.5% may cause a transient, local blanching followed by a transient, local redness or erythema.
Section 43682-4
Pharmacokinetics: Lidocaine and prilocaine cream, 2.5%/2.5% is a eutectic mixture of lidocaine 2.5% and prilocaine 2.5% formulated as an oil in water emulsion. In this eutectic mixture, both anesthetics are liquid at room temperature (see DESCRIPTION ) and the penetration and subsequent systemic absorption of both prilocaine and lidocaine are enhanced over that which would be seen if each component in crystalline form was applied separately as a 2.5% topical cream.
Warnings
Application of lidocaine and prilocaine cream, 2.5%/2.5% to larger areas or for longer times than those recommended could result in sufficient absorption of lidocaine and prilocaine resulting in serious adverse effects (see Individualization of Dose ).
Patients treated with class III anti-arrhythmic drugs (e.g., amiodarone, bretylium, sotalol, dofetilide) should be under close surveillance and ECG monitoring considered, because cardiac effects may be additive.
Studies in laboratory animals (guinea pigs) have shown that lidocaine and prilocaine cream, 2.5%/2.5% has an ototoxic effect when instilled into the middle ear. In these same studies, animals exposed to lidocaine and prilocaine cream, 2.5%/2.5% only in the external auditory canal, showed no abnormality. Lidocaine and prilocaine cream, 2.5%/2.5% should not be used in any clinical situation when its penetration or migration beyond the tympanic membrane into the middle ear is possible.
Overdosage
Peak blood levels following a 60 g application to 400 cm2 of intact skin for 3 hours are 0.05 to 0.16 mcg/mL for lidocaine and 0.02 to 0.10 mcg/mL for prilocaine. Toxic levels of lidocaine (>5 mcg/mL) and/or prilocaine (>6 mcg/mL) cause decreases in cardiac output, total peripheral resistance and mean arterial pressure. These changes may be attributable to direct depressant effects of these local anesthetic agents on the cardiovascular system. In the absence of massive topical overdose or oral ingestion, evaluation should include evaluation of other etiologies for the clinical effects or overdosage from other sources of lidocaine, prilocaine or other local anesthetics. Consult the package inserts for parenteral Xylocaine (lidocaine HCl) or Citanest (prilocaine HCl) for further information for the management of overdose.
Geriatric Use
Of the total number of patients in clinical studies of lidocaine and prilocaine cream, 2.5%/2.5%, 180 were age 65 to 74 and 138 were 75 and over. No overall differences in safety or efficacy were observed between these patients and younger patients. Other reported clinical experience has not identified differences in responses between the elderly and younger patients, but greater sensitivity of some older individuals cannot be ruled out.
Plasma levels of lidocaine and prilocaine in geriatric and non-geriatric patients following application of a thick layer of lidocaine and prilocaine cream, 2.5%/2.5% are very low and well below potentially toxic levels. However, there are no sufficient data to evaluate quantitative differences in systemic plasma levels of lidocaine and prilocaine between geriatric and non-geriatric patients following application of lidocaine and prilocaine cream, 2.5%/2.5%.
Consideration should be given for those elderly patients who have enhanced sensitivity to systemic absorption (see PRECAUTIONS ).
After intravenous dosing, the elimination half-life of lidocaine is significantly longer in elderly patients (2.5 hours) than in younger patients (1.5 hours). (See CLINICAL PHARMACOLOGY ).
Clinical Studies
Lidocaine and prilocaine cream, 2.5%/2.5% application in adults prior to IV cannulation or venipuncture was studied in 200 patients in four clinical studies in Europe. Application for at least 1 hour provided significantly more dermal analgesia than placebo cream or ethyl chloride. Lidocaine and prilocaine cream, 2.5%/2.5% was comparable to subcutaneous lidocaine, but was less efficacious than intradermal lidocaine. Most patients found lidocaine and prilocaine cream, 2.5%/2.5% treatment preferable to lidocaine infiltration or ethyl chloride spray.
Lidocaine and prilocaine cream, 2.5%/2.5% was compared with 0.5% lidocaine infiltration prior to skin graft harvesting in one open label study in 80 adult patients in England. Application of lidocaine and prilocaine cream, 2.5%/2.5% for 2 to 5 hours provided dermal analgesia comparable to lidocaine infiltration.
Lidocaine and prilocaine cream, 2.5%/2.5% application in children was studied in seven non-US studies (320 patients) and one US study (100 patients). In controlled studies, application of lidocaine and prilocaine cream, 2.5%/2.5% for at least 1 hour with or without presurgical medication prior to needle insertion provided significantly more pain reduction than placebo. In children under the age of seven years, lidocaine and prilocaine cream, 2.5%/2.5% was less effective than in older children or adults.
Lidocaine and prilocaine cream, 2.5%/2.5% was compared with placebo in the laser treatment of facial port-wine stains in 72 pediatric patients (ages 5 to 16). Lidocaine and prilocaine cream, 2.5%/2.5% was effective in providing pain relief during laser treatment.
Lidocaine and prilocaine cream, 2.5%/2.5% alone was compared with lidocaine and prilocaine cream, 2.5%/2.5% followed by lidocaine infiltration and lidocaine infiltration alone prior to cryotherapy for the removal of male genital warts. The data from 121 patients demonstrated that lidocaine and prilocaine cream, 2.5%/2.5% was not effective as a sole anesthetic agent in managing the pain from the surgical procedure. The administration of lidocaine and prilocaine cream, 2.5%/2.5% prior to lidocaine infiltration provided significant relief of discomfort associated with local anesthetic infiltration and thus was effective in the overall reduction of pain from the procedure only when used in conjunction with local anesthetic infiltration of lidocaine.
Lidocaine and prilocaine cream, 2.5%/2.5% was studied in 105 full term neonates (gestational age: 37 weeks) for blood drawing and circumcision procedures. When considering the use of lidocaine and prilocaine cream, 2.5%/2.5% in neonates, the primary concerns are the systemic absorption of the active ingredients and the subsequent formation of methemoglobin. In clinical studies performed in neonates, the plasma levels of lidocaine, prilocaine, and methemoglobin were not reported in a range expected to cause clinical symptoms.
Local dermal effects associated with lidocaine and prilocaine cream, 2.5%/2.5% application in these studies on intact skin included paleness, redness and edema and were transient in nature (see ADVERSE REACTIONS ).
The application of lidocaine and prilocaine cream, 2.5%/2.5% on genital mucous membranes for minor, superficial surgical procedures (e.g., removal of condylomata acuminata) was studied in 80 patients in a placebo-controlled clinical trial (60 patients received lidocaine and prilocaine cream, 2.5%/2.5% and 20 patients received placebo). Lidocaine and prilocaine cream, 2.5%/2.5% (5 to 10 g) applied between 1 and 75 minutes before surgery, with a median time of 15 minutes, provided effective local anesthesia for minor superficial surgical procedures. The greatest extent of analgesia, as measured by VAS scores, was attained after 5 to 15 minutes’ application. The application of lidocaine and prilocaine cream, 2.5%/2.5% to genital mucous membranes as pretreatment for local anesthetic infiltration was studied in a double-blind, placebo-controlled study in 44 female patients (21 patients received lidocaine and prilocaine cream, 2.5%/2.5% and 23 patients received placebo) scheduled for infiltration prior to a surgical procedure of the external vulva or genital mucosa. Lidocaine and prilocaine cream, 2.5%/2.5% applied to the genital mucous membranes for 5 to 10 minutes resulted in adequate topical anesthesia for local anesthetic injection.
Adult Patients Intact Skin
A thick layer of lidocaine and prilocaine cream, 2.5%/2.5% is applied to intact skin and covered with an occlusive dressing (see INSTRUCTIONS FOR APPLICATION ).
Instructions for Application
Lidocaine and Prilocaine Cream, 2.5%/2.5%
-
1.In adults, apply 2.5 g of cream per 20 to 25 cm2 (approx. 2 in. by 2 in.) of skin in a thick layer at the site of the procedure. For adult and pediatric patients, apply ONLY as prescribed by your physician. If your child is below the age of 3 months or small for their age, please inform your doctor before applying lidocaine and prilocaine cream, 2.5%/2.5%, which can be harmful, if applied over too much skin at one time in young children. If your child becomes very dizzy, excessively sleepy, or develops duskiness of the face or lips after applying lidocaine and prilocaine cream, 2.5%/2.5%, remove the cream and contact your physician at once.
-
-
2.Take the dressing (may be supplied in this package) or other occlusive dressing and remove the center cut-out piece.
-
3.Peel the paper liner from the dressing. (Instructions continued on reverse side.)
-
4.Cover the lidocaine and prilocaine cream, 2.5%/2.5% so that you get a thick layer underneath. Do not spread out the cream. Smooth down the dressing edges carefully and ensure it is secure to avoid leakage. (This is especially important when the patient is a child.)
-
5.The time of application can be marked directly on the occlusive dressing. Lidocaine and prilocaine cream, 2.5%/2.5% must be applied at least 1 hour before the start of a routine procedure and for 2 hours before the start of a painful procedure.
-
6.Remove the occlusive dressing, wipe off the lidocaine and prilocaine cream, 2.5%/2.5%, clean the entire area with an antiseptic solution and prepare the patient for the procedure. The duration of effective skin anesthesia will be at least 1 hour after removal of the occlusive dressing.
PRECAUTIONS
-
1.Do not apply near eyes or open wounds.
-
2.Keep out of the reach of children.
-
3.If your child becomes very dizzy, excessively sleepy, or develops duskiness of the face or lips after applying lidocaine and prilocaine cream. 2.5%/2.5%, remove the cream and contact the child’s physician at once.
Pediatric Patients Intact Skin
The following are the maximum recommended doses, application areas and application times for lidocaine and prilocaine cream, 2.5%/2.5% based on a child's age and weight:
|
Age and Body Weight Requirements |
Maximum Total Dose of |
Maximum |
Maximum |
|
0 up to 3 months or < 5 kg |
1g |
10 cm2 |
1 hour |
|
3 up to 12 months and >5 kg |
2g |
20 cm2 |
4 hours |
|
1 to 6 years and >10 kg |
10g |
100 cm2 |
4 hours |
|
7 to 12 years and >20 kg |
20g |
200 cm2 |
4 hours |
Please note: If a patient greater than 3 months old does not meet the minimum weight requirement, the maximum total dose of lidocaine and prilocaine cream, 2.5%/2.5% should be restricted to that which corresponds to the patient's weight (see INSTRUCTIONS FOR APPLICATION ).
Practitioners should carefully instruct caregivers to avoid application of excessive amounts of lidocaine and prilocaine cream, 2.5%/2.5% (see PRECAUTIONS ).
When applying lidocaine and prilocaine cream, 2.5%/2.5% to the skin of young children, care must be taken to maintain careful observation of the child to prevent accidental ingestion of lidocaine and prilocaine cream, 2.5%/2.5% or the occlusive dressing. A secondary protective covering to prevent inadvertent disruption of the application site may be useful.
Lidocaine and prilocaine cream, 2.5%/2.5% should not be used in neonates with a gestational age less than 37 weeks nor in infants under the age of 12 months who are receiving treatment with methemoglobin-inducing agents (see Methemoglobinemia subsection of WARNINGS).
When lidocaine and prilocaine cream, 2.5%/2.5% is used concomitantly with other products containing local anesthetic agents, the amount absorbed from all formulations must be considered (see Individualization of Dose ). The amount absorbed in the case of lidocaine and prilocaine cream, 2.5%/2.5% is determined by the area over which it is applied and the duration of application under occlusion (see Table 2 , ** footnote, in Individualization of Dose).
Although the incidence of systemic adverse reactions with lidocaine and prilocaine cream, 2.5%/2.5% is very low, caution should be exercised, particularly when applying it over large areas and leaving it on for longer than 2 hours. The incidence of systemic adverse reactions can be expected to be directly proportional to the area and time of exposure (see Individualization of Dose ).
Use in Pregnancy: Teratogenic Effects:
Reproduction studies with lidocaine have been performed in rats and have revealed no evidence of harm to the fetus (30 mg/kg subcutaneously; 22 times SDA). Reproduction studies with prilocaine have been performed in rats and have revealed no evidence of impaired fertility or harm to the fetus (300 mg/kg intramuscularly; 188 times SDA). There are, however, no adequate and well-controlled studies in pregnant women. Because animal reproduction studies are not always predictive of human response, lidocaine and prilocaine cream, 2.5%/2.5% should be used during pregnancy only if clearly needed.
Reproduction studies have been performed in rats receiving subcutaneous administration of an aqueous mixture containing lidocaine HCl and prilocaine HCl at 1:1 (w/w). At 40 mg/kg each, a dose equivalent to 29 times SDA lidocaine and 25 times SDA prilocaine, no teratogenic, embryotoxic or fetotoxic effects were observed.
Adult Female Patients Genital Mucous Membranes
For minor procedures on the female external genitalia, such as removal of condylomata acuminata, as well as for use as pretreatment for anesthetic infiltration, apply a thick layer (5 to 10 grams) of lidocaine and prilocaine cream, 2.5%/2.5% for 5 to 10 minutes.
Occlusion is not necessary for absorption, but may be helpful to keep the cream in place. Patients should be lying down during the lidocaine and prilocaine cream, 2.5%/2.5% application, especially if no occlusion is used. The procedure or the local anesthetic infiltration should be performed immediately after the removal of lidocaine and prilocaine cream, 2.5%/2.5%.
Package Label – Principal Display Panel – 30 G Carton
NDC 0168-0357-30
Rx only
Lidocaine and
Prilocaine Cream, 2.5%/2.5%
FOUGERA®
NOT FOR OPHTHALMIC USE
FOR EXTERNAL USE ONLY
NET WT 30 grams
Package Label – Principal Display Panel – 30 G Container
NDC 0168-0357-30
Rx only
Lidocaine and
Prilocaine Cream, 2.5%/2.5%
CHILD-RESISTANT PACKAGE
FOUGERA®
NOT FOR OPHTHALMIC USE
FOR EXTERNAL USE ONLY
NET WT 30 grams
Structured Label Content
Section 34072-9 (34072-9)
General: Repeated doses of lidocaine and prilocaine cream, 2.5%/2.5% may increase blood levels of lidocaine and prilocaine. Lidocaine and prilocaine cream, 2.5%/2.5% should be used with caution in patients who may be more sensitive to the systemic effects of lidocaine and prilocaine including acutely ill, debilitated, or elderly patients.
Lidocaine and prilocaine cream, 2.5%/2.5% should not be applied to open wounds.
Care should be taken not to allow lidocaine and prilocaine cream, 2.5%/2.5% to come in contact with the eye because animal studies have demonstrated severe eye irritation. Also the loss of protective reflexes can permit corneal irritation and potential abrasion. Absorption of lidocaine and prilocaine cream, 2.5%/2.5% in conjunctival tissues has not been determined. If eye contact occurs, immediately wash out the eye with water or saline and protect the eye until sensation returns.
Patients allergic to para-aminobenzoic acid derivatives (procaine, tetracaine, benzocaine, etc.) have not shown cross sensitivity to lidocaine and/or prilocaine, however, lidocaine and prilocaine cream, 2.5%/2.5% should be used with caution in patients with a history of drug sensitivities, especially if the etiologic agent is uncertain.
Patients with severe hepatic disease, because of their inability to metabolize local anesthetics normally, are at greater risk of developing toxic plasma concentrations of lidocaine and prilocaine.
Lidocaine and prilocaine have been shown to inhibit viral and bacterial growth. The effect of lidocaine and prilocaine cream, 2.5%/2.5% on intradermal injections of live vaccines has not been determined.
Section 34073-7 (34073-7)
Drug Interactions: Lidocaine and prilocaine cream, 2.5%/2.5% should be used with caution in patients receiving Class I antiarrhythmic drugs (such as tocainide and mexiletine) since the toxic effects are additive and potentially synergistic.
Patients who are administered local anesthetics are at increased risk of developing methemoglobinemia when concurrently exposed to the following drugs, which could include other local anesthetics:
Examples of Drugs Associated with Methemoglobinemia:
|
Class |
Examples |
|
Nitrates/Nitrites |
nitric oxide, nitroglycerin, nitroprusside, nitrous oxide |
|
Local anesthetics |
articaine, benzocaine, bupivacaine, lidocaine, mepivacaine, prilocaine, procaine, ropivacaine, tetracaine |
|
Antineoplastic agents |
cyclophosphamide, flutamide, hydroxyurea, ifosfamide, rasburicase |
|
Antibiotics |
dapsone, nitrofurantoin, para-aminosalicylic acid, sulfonamides |
|
Antimalarials |
chloroquine, primaquine |
|
Anticonvulsants |
Phenobarbital, phenytoin, sodium valproate |
|
Other drugs |
acetaminophen, metoclopramide, quinine, sulfasalazine |
Specific interaction studies with lidocaine/prilocaine and class III anti-arrhythmic drugs (e.g., amiodarone, bretylium, sotalol, dofetilide) have not been performed, but caution is advised (see WARNINGS ).
Should lidocaine and prilocaine cream, 2.5%/2.5% be used concomitantly with other products containing lidocaine and/or prilocaine, cumulative doses from all formulations must be considered.
Section 34076-0 (34076-0)
Information for Patients: Inform patients that use of local anesthetics may cause methemoglobinemia, a serious condition that must be treated promptly. Advise patients or caregivers to stop use and seek immediate medical attention if they or someone in their care experience the following signs or symptoms: pale, gray, or blue colored skin (cyanosis); headache; rapid heart rate; shortness of breath; lightheadedness; or fatigue.
When lidocaine and prilocaine cream, 2.5%/2.5% is used, the patient should be aware that the production of dermal analgesia may be accompanied by the block of all sensations in the treated skin. For this reason, the patient should avoid inadvertent trauma to the treated area by scratching, rubbing, or exposure to extreme hot or cold temperatures until complete sensation has returned.
Lidocaine and prilocaine cream, 2.5%/2.5% should not be applied near the eyes or on open wounds.
Section 34079-4 (34079-4)
Labor and Delivery: Neither lidocaine nor prilocaine are contraindicated in labor and delivery. Should lidocaine and prilocaine cream, 2.5%/2.5% be used concomitantly with other products containing lidocaine and/or prilocaine, cumulative doses from all formulations must be considered.
Section 34080-2 (34080-2)
Nursing Mothers: Lidocaine, and probably prilocaine, are excreted in human milk. Therefore, caution should be exercised when lidocaine and prilocaine cream, 2.5%/2.5% is administered to a nursing mother since the milk:plasma ratio of lidocaine is 0.4 and is not determined for prilocaine.
Section 34081-0 (34081-0)
Pediatric Use: Controlled studies of lidocaine and prilocaine cream, 2.5%/2.5% in children under the age of seven years have shown less overall benefit than in older children or adults. These results illustrate the importance of emotional and psychological support of younger children undergoing medical or surgical procedures.
Lidocaine and prilocaine cream, 2.5%/2.5% should be used with care in patients with conditions or therapy associated with methemoglobinemia (see Methemoglobinemia subsection of WARNINGS).
When using lidocaine and prilocaine cream, 2.5%/2.5% in young children, especially infants under the age of 3 months, care must be taken to insure that the caregiver understands the need to limit the dose and area of application, and to prevent accidental ingestion (see DOSAGE AND ADMINISTRATION and Methemoglobinemia ).
In neonates (minimum gestation age: 37 weeks) and children weighing less than 20 kg, the area and duration of application should be limited (see TABLE 2 in Individualization of Dose). Studies have not demonstrated the efficacy of lidocaine and prilocaine cream, 2.5%/2.5% for heel lancing in neonates.
Section 42229-5 (42229-5)
Rx only
Section 43679-0 (43679-0)
Mechanism of Action: Lidocaine and prilocaine cream, 2.5%/2.5%, applied to intact skin under occlusive dressing, provides dermal analgesia by the release of lidocaine and prilocaine from the cream into the epidermal and dermal layers of the skin and by the accumulation of lidocaine and prilocaine in the vicinity of dermal pain receptors and nerve endings. Lidocaine and prilocaine are amide-type local anesthetic agents. Both lidocaine and prilocaine stabilize neuronal membranes by inhibiting the ionic fluxes required for the initiation and conduction of impulses, thereby effecting local anesthetic action.
The onset, depth and duration of dermal analgesia on intact skin provided by lidocaine and prilocaine cream, 2.5%/2.5% depends primarily on the duration of application. To provide sufficient analgesia for clinical procedures such as intravenous catheter placement and venipuncture, lidocaine and prilocaine cream, 2.5%/2.5% should be applied under an occlusive dressing for at least 1 hour. To provide dermal analgesia for clinical procedures such as split skin graft harvesting, lidocaine and prilocaine cream, 2.5%/2.5% should be applied under occlusive dressing for at least 2 hours. Satisfactory dermal analgesia is achieved 1 hour after application, reaches maximum at 2 to 3 hours, and persists for 1 to 2 hours after removal. Absorption from the genital mucosa is more rapid and onset time is shorter (5 to 10 minutes) than after application to intact skin. After a 5 to 10 minute application of lidocaine and prilocaine cream, 2.5%/2.5% to female genital mucosa, the average duration of effective analgesia to an argon laser stimulus (which produced a sharp, pricking pain) was 15 to 20 minutes (individual variations in the range of 5 to 45 minutes).
Dermal application of lidocaine and prilocaine cream, 2.5%/2.5% may cause a transient, local blanching followed by a transient, local redness or erythema.
Section 43682-4 (43682-4)
Pharmacokinetics: Lidocaine and prilocaine cream, 2.5%/2.5% is a eutectic mixture of lidocaine 2.5% and prilocaine 2.5% formulated as an oil in water emulsion. In this eutectic mixture, both anesthetics are liquid at room temperature (see DESCRIPTION ) and the penetration and subsequent systemic absorption of both prilocaine and lidocaine are enhanced over that which would be seen if each component in crystalline form was applied separately as a 2.5% topical cream.
Warnings (WARNINGS)
Application of lidocaine and prilocaine cream, 2.5%/2.5% to larger areas or for longer times than those recommended could result in sufficient absorption of lidocaine and prilocaine resulting in serious adverse effects (see Individualization of Dose ).
Patients treated with class III anti-arrhythmic drugs (e.g., amiodarone, bretylium, sotalol, dofetilide) should be under close surveillance and ECG monitoring considered, because cardiac effects may be additive.
Studies in laboratory animals (guinea pigs) have shown that lidocaine and prilocaine cream, 2.5%/2.5% has an ototoxic effect when instilled into the middle ear. In these same studies, animals exposed to lidocaine and prilocaine cream, 2.5%/2.5% only in the external auditory canal, showed no abnormality. Lidocaine and prilocaine cream, 2.5%/2.5% should not be used in any clinical situation when its penetration or migration beyond the tympanic membrane into the middle ear is possible.
Overdosage (OVERDOSAGE)
Peak blood levels following a 60 g application to 400 cm2 of intact skin for 3 hours are 0.05 to 0.16 mcg/mL for lidocaine and 0.02 to 0.10 mcg/mL for prilocaine. Toxic levels of lidocaine (>5 mcg/mL) and/or prilocaine (>6 mcg/mL) cause decreases in cardiac output, total peripheral resistance and mean arterial pressure. These changes may be attributable to direct depressant effects of these local anesthetic agents on the cardiovascular system. In the absence of massive topical overdose or oral ingestion, evaluation should include evaluation of other etiologies for the clinical effects or overdosage from other sources of lidocaine, prilocaine or other local anesthetics. Consult the package inserts for parenteral Xylocaine (lidocaine HCl) or Citanest (prilocaine HCl) for further information for the management of overdose.
Description (DESCRIPTION)
Lidocaine and prilocaine cream, 2.5%/2.5% is an emulsion in which the oil phase is a eutectic mixture of lidocaine and prilocaine in a ratio of 1:1 by weight. This eutectic mixture has a melting point below room temperature and therefore both local anesthetics exist as a liquid oil rather than as crystals. It is packaged in 30 gram tubes and 5 gram tubes for hospital use. Lidocaine is chemically designated as acetamide, 2-(diethylamino)-N-(2,6-dimethylphenyl), has an octanol: water partition ratio of 43 at pH 7.4, and has the following structure:
Prilocaine is chemically designated as propanamide, N-(2-methylphenyl)-2-(propylamino), has an octanol: water partition ratio of 25 at pH 7.4, and has the following structure:
Each gram of lidocaine and prilocaine cream, 2.5%/2.5% contains lidocaine 25 mg, prilocaine 25 mg, polyoxyethylene fatty acid esters (as emulsifiers), carbomer 934P (as a thickening agent), sodium hydroxide to adjust to a pH approximating 9, and purified water. Lidocaine and prilocaine cream, 2.5%/2.5% contains no preservative, however it passes the USP antimicrobial effectiveness test due to the pH. The specific gravity of lidocaine and prilocaine cream, 2.5%/2.5% is approximately 1.00.
How Supplied (HOW SUPPLIED)
Lidocaine and prilocaine cream, 2.5%/2.5% is supplied as follows:
NDC 0168-0357-30 30 gram tube, with a child-resistant cap
NDC 0168-0357-55 5 gram tube, FOR HOSPITAL USE ONLY
NDC 0168-0357-56 5 gram tube, with 12 dressings, FOR HOSPITAL USE ONLY
NOT FOR OPHTHALMIC USE.
KEEP CONTAINER TIGHTLY CLOSED AT ALL TIMES WHEN NOT IN USE.
KEEP OUT OF THE REACH OF CHILDREN.
Store at 20°C to 25°C (68°F to 77°F); excursions permitted to 15°C to 30°C (59°F to 86°F) [See USP Controlled Room Temperature].
E. FOUGERA & CO.
A division of
Fougera
PHARMACEUTICALS INC.
Melville, New York 11747
Revised: 01/2024
Geriatric Use
Of the total number of patients in clinical studies of lidocaine and prilocaine cream, 2.5%/2.5%, 180 were age 65 to 74 and 138 were 75 and over. No overall differences in safety or efficacy were observed between these patients and younger patients. Other reported clinical experience has not identified differences in responses between the elderly and younger patients, but greater sensitivity of some older individuals cannot be ruled out.
Plasma levels of lidocaine and prilocaine in geriatric and non-geriatric patients following application of a thick layer of lidocaine and prilocaine cream, 2.5%/2.5% are very low and well below potentially toxic levels. However, there are no sufficient data to evaluate quantitative differences in systemic plasma levels of lidocaine and prilocaine between geriatric and non-geriatric patients following application of lidocaine and prilocaine cream, 2.5%/2.5%.
Consideration should be given for those elderly patients who have enhanced sensitivity to systemic absorption (see PRECAUTIONS ).
After intravenous dosing, the elimination half-life of lidocaine is significantly longer in elderly patients (2.5 hours) than in younger patients (1.5 hours). (See CLINICAL PHARMACOLOGY ).
Clinical Studies (CLINICAL STUDIES)
Lidocaine and prilocaine cream, 2.5%/2.5% application in adults prior to IV cannulation or venipuncture was studied in 200 patients in four clinical studies in Europe. Application for at least 1 hour provided significantly more dermal analgesia than placebo cream or ethyl chloride. Lidocaine and prilocaine cream, 2.5%/2.5% was comparable to subcutaneous lidocaine, but was less efficacious than intradermal lidocaine. Most patients found lidocaine and prilocaine cream, 2.5%/2.5% treatment preferable to lidocaine infiltration or ethyl chloride spray.
Lidocaine and prilocaine cream, 2.5%/2.5% was compared with 0.5% lidocaine infiltration prior to skin graft harvesting in one open label study in 80 adult patients in England. Application of lidocaine and prilocaine cream, 2.5%/2.5% for 2 to 5 hours provided dermal analgesia comparable to lidocaine infiltration.
Lidocaine and prilocaine cream, 2.5%/2.5% application in children was studied in seven non-US studies (320 patients) and one US study (100 patients). In controlled studies, application of lidocaine and prilocaine cream, 2.5%/2.5% for at least 1 hour with or without presurgical medication prior to needle insertion provided significantly more pain reduction than placebo. In children under the age of seven years, lidocaine and prilocaine cream, 2.5%/2.5% was less effective than in older children or adults.
Lidocaine and prilocaine cream, 2.5%/2.5% was compared with placebo in the laser treatment of facial port-wine stains in 72 pediatric patients (ages 5 to 16). Lidocaine and prilocaine cream, 2.5%/2.5% was effective in providing pain relief during laser treatment.
Lidocaine and prilocaine cream, 2.5%/2.5% alone was compared with lidocaine and prilocaine cream, 2.5%/2.5% followed by lidocaine infiltration and lidocaine infiltration alone prior to cryotherapy for the removal of male genital warts. The data from 121 patients demonstrated that lidocaine and prilocaine cream, 2.5%/2.5% was not effective as a sole anesthetic agent in managing the pain from the surgical procedure. The administration of lidocaine and prilocaine cream, 2.5%/2.5% prior to lidocaine infiltration provided significant relief of discomfort associated with local anesthetic infiltration and thus was effective in the overall reduction of pain from the procedure only when used in conjunction with local anesthetic infiltration of lidocaine.
Lidocaine and prilocaine cream, 2.5%/2.5% was studied in 105 full term neonates (gestational age: 37 weeks) for blood drawing and circumcision procedures. When considering the use of lidocaine and prilocaine cream, 2.5%/2.5% in neonates, the primary concerns are the systemic absorption of the active ingredients and the subsequent formation of methemoglobin. In clinical studies performed in neonates, the plasma levels of lidocaine, prilocaine, and methemoglobin were not reported in a range expected to cause clinical symptoms.
Local dermal effects associated with lidocaine and prilocaine cream, 2.5%/2.5% application in these studies on intact skin included paleness, redness and edema and were transient in nature (see ADVERSE REACTIONS ).
The application of lidocaine and prilocaine cream, 2.5%/2.5% on genital mucous membranes for minor, superficial surgical procedures (e.g., removal of condylomata acuminata) was studied in 80 patients in a placebo-controlled clinical trial (60 patients received lidocaine and prilocaine cream, 2.5%/2.5% and 20 patients received placebo). Lidocaine and prilocaine cream, 2.5%/2.5% (5 to 10 g) applied between 1 and 75 minutes before surgery, with a median time of 15 minutes, provided effective local anesthesia for minor superficial surgical procedures. The greatest extent of analgesia, as measured by VAS scores, was attained after 5 to 15 minutes’ application. The application of lidocaine and prilocaine cream, 2.5%/2.5% to genital mucous membranes as pretreatment for local anesthetic infiltration was studied in a double-blind, placebo-controlled study in 44 female patients (21 patients received lidocaine and prilocaine cream, 2.5%/2.5% and 23 patients received placebo) scheduled for infiltration prior to a surgical procedure of the external vulva or genital mucosa. Lidocaine and prilocaine cream, 2.5%/2.5% applied to the genital mucous membranes for 5 to 10 minutes resulted in adequate topical anesthesia for local anesthetic injection.
Contraindications (CONTRAINDICATIONS)
Lidocaine and prilocaine cream, 2.5%/2.5% is contraindicated in patients with a known history of sensitivity to local anesthetics of the amide type or to any other component of the product.
Indications and Usage (INDICATIONS AND USAGE)
Lidocaine and prilocaine cream, 2.5%/2.5% (a eutectic mixture of lidocaine 2.5% and prilocaine 2.5%) is indicated as a topical anesthetic for use on:
- normal intact skin for local analgesia.
- genital mucous membranes for superficial minor surgery and as pretreatment for infiltration anesthesia.
Lidocaine and prilocaine cream, 2.5%/2.5% is not recommended in any clinical situation when penetration or migration beyond the tympanic membrane into the middle ear is possible because of the ototoxic effects observed in animal studies (see WARNINGS ).
Adult Patients Intact Skin (Adult Patients-Intact Skin)
A thick layer of lidocaine and prilocaine cream, 2.5%/2.5% is applied to intact skin and covered with an occlusive dressing (see INSTRUCTIONS FOR APPLICATION ).
Instructions for Application (INSTRUCTIONS FOR APPLICATION)
Lidocaine and Prilocaine Cream, 2.5%/2.5%
-
1.In adults, apply 2.5 g of cream per 20 to 25 cm2 (approx. 2 in. by 2 in.) of skin in a thick layer at the site of the procedure. For adult and pediatric patients, apply ONLY as prescribed by your physician. If your child is below the age of 3 months or small for their age, please inform your doctor before applying lidocaine and prilocaine cream, 2.5%/2.5%, which can be harmful, if applied over too much skin at one time in young children. If your child becomes very dizzy, excessively sleepy, or develops duskiness of the face or lips after applying lidocaine and prilocaine cream, 2.5%/2.5%, remove the cream and contact your physician at once.
-
-
2.Take the dressing (may be supplied in this package) or other occlusive dressing and remove the center cut-out piece.
-
3.Peel the paper liner from the dressing. (Instructions continued on reverse side.)
-
4.Cover the lidocaine and prilocaine cream, 2.5%/2.5% so that you get a thick layer underneath. Do not spread out the cream. Smooth down the dressing edges carefully and ensure it is secure to avoid leakage. (This is especially important when the patient is a child.)
-
5.The time of application can be marked directly on the occlusive dressing. Lidocaine and prilocaine cream, 2.5%/2.5% must be applied at least 1 hour before the start of a routine procedure and for 2 hours before the start of a painful procedure.
-
6.Remove the occlusive dressing, wipe off the lidocaine and prilocaine cream, 2.5%/2.5%, clean the entire area with an antiseptic solution and prepare the patient for the procedure. The duration of effective skin anesthesia will be at least 1 hour after removal of the occlusive dressing.
PRECAUTIONS
-
1.Do not apply near eyes or open wounds.
-
2.Keep out of the reach of children.
-
3.If your child becomes very dizzy, excessively sleepy, or develops duskiness of the face or lips after applying lidocaine and prilocaine cream. 2.5%/2.5%, remove the cream and contact the child’s physician at once.
Pediatric Patients Intact Skin (Pediatric Patients-Intact Skin)
The following are the maximum recommended doses, application areas and application times for lidocaine and prilocaine cream, 2.5%/2.5% based on a child's age and weight:
|
Age and Body Weight Requirements |
Maximum Total Dose of |
Maximum |
Maximum |
|
0 up to 3 months or < 5 kg |
1g |
10 cm2 |
1 hour |
|
3 up to 12 months and >5 kg |
2g |
20 cm2 |
4 hours |
|
1 to 6 years and >10 kg |
10g |
100 cm2 |
4 hours |
|
7 to 12 years and >20 kg |
20g |
200 cm2 |
4 hours |
Please note: If a patient greater than 3 months old does not meet the minimum weight requirement, the maximum total dose of lidocaine and prilocaine cream, 2.5%/2.5% should be restricted to that which corresponds to the patient's weight (see INSTRUCTIONS FOR APPLICATION ).
Practitioners should carefully instruct caregivers to avoid application of excessive amounts of lidocaine and prilocaine cream, 2.5%/2.5% (see PRECAUTIONS ).
When applying lidocaine and prilocaine cream, 2.5%/2.5% to the skin of young children, care must be taken to maintain careful observation of the child to prevent accidental ingestion of lidocaine and prilocaine cream, 2.5%/2.5% or the occlusive dressing. A secondary protective covering to prevent inadvertent disruption of the application site may be useful.
Lidocaine and prilocaine cream, 2.5%/2.5% should not be used in neonates with a gestational age less than 37 weeks nor in infants under the age of 12 months who are receiving treatment with methemoglobin-inducing agents (see Methemoglobinemia subsection of WARNINGS).
When lidocaine and prilocaine cream, 2.5%/2.5% is used concomitantly with other products containing local anesthetic agents, the amount absorbed from all formulations must be considered (see Individualization of Dose ). The amount absorbed in the case of lidocaine and prilocaine cream, 2.5%/2.5% is determined by the area over which it is applied and the duration of application under occlusion (see Table 2 , ** footnote, in Individualization of Dose).
Although the incidence of systemic adverse reactions with lidocaine and prilocaine cream, 2.5%/2.5% is very low, caution should be exercised, particularly when applying it over large areas and leaving it on for longer than 2 hours. The incidence of systemic adverse reactions can be expected to be directly proportional to the area and time of exposure (see Individualization of Dose ).
Use in Pregnancy: Teratogenic Effects:
Reproduction studies with lidocaine have been performed in rats and have revealed no evidence of harm to the fetus (30 mg/kg subcutaneously; 22 times SDA). Reproduction studies with prilocaine have been performed in rats and have revealed no evidence of impaired fertility or harm to the fetus (300 mg/kg intramuscularly; 188 times SDA). There are, however, no adequate and well-controlled studies in pregnant women. Because animal reproduction studies are not always predictive of human response, lidocaine and prilocaine cream, 2.5%/2.5% should be used during pregnancy only if clearly needed.
Reproduction studies have been performed in rats receiving subcutaneous administration of an aqueous mixture containing lidocaine HCl and prilocaine HCl at 1:1 (w/w). At 40 mg/kg each, a dose equivalent to 29 times SDA lidocaine and 25 times SDA prilocaine, no teratogenic, embryotoxic or fetotoxic effects were observed.
Adult Female Patients Genital Mucous Membranes (Adult Female Patients-Genital Mucous Membranes)
For minor procedures on the female external genitalia, such as removal of condylomata acuminata, as well as for use as pretreatment for anesthetic infiltration, apply a thick layer (5 to 10 grams) of lidocaine and prilocaine cream, 2.5%/2.5% for 5 to 10 minutes.
Occlusion is not necessary for absorption, but may be helpful to keep the cream in place. Patients should be lying down during the lidocaine and prilocaine cream, 2.5%/2.5% application, especially if no occlusion is used. The procedure or the local anesthetic infiltration should be performed immediately after the removal of lidocaine and prilocaine cream, 2.5%/2.5%.
Package Label – Principal Display Panel – 30 G Carton (PACKAGE LABEL – PRINCIPAL DISPLAY PANEL – 30 G CARTON)
NDC 0168-0357-30
Rx only
Lidocaine and
Prilocaine Cream, 2.5%/2.5%
FOUGERA®
NOT FOR OPHTHALMIC USE
FOR EXTERNAL USE ONLY
NET WT 30 grams
Package Label – Principal Display Panel – 30 G Container (PACKAGE LABEL – PRINCIPAL DISPLAY PANEL – 30 G CONTAINER)
NDC 0168-0357-30
Rx only
Lidocaine and
Prilocaine Cream, 2.5%/2.5%
CHILD-RESISTANT PACKAGE
FOUGERA®
NOT FOR OPHTHALMIC USE
FOR EXTERNAL USE ONLY
NET WT 30 grams
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:50:19.851328 · Updated: 2026-03-14T22:37:11.582303