These Highlights Do Not Include All The Information Needed To Use Symfi
81a55dd9-78a8-49c3-88ab-8f5bffafa359
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Indications and Usage
SYMFI ® (efavirenz, lamivudine and tenofovir disoproxil fumarate) is indicated as a complete regimen for the treatment of human immunodeficiency virus type 1 (HIV-1) infection in adult and pediatric patients weighing at least 40 kg.
Dosage and Administration
• Testing: Prior to initiation and during treatment with SYMFI, patients should be tested for hepatitis B virus infection, and estimated creatinine clearance, urine glucose, and urine protein should be obtained. ( 2.1 ) • Recommended dose: One tablet taken orally once daily on an empty stomach, preferably at bedtime. ( 2.2 ) • Renal Impairment: Not recommended in patients with CrCL less than 50 mL/min or patients with end-stage renal disease requiring hemodialysis. ( 2.3 ) • Hepatic Impairment: Not recommended for patients with moderate or severe hepatic impairment. Use caution in patients with mild hepatic impairment. ( 2.4 )
Contraindications
SYMFI is contraindicated: • in patients with a previous hypersensitivity reaction (e.g., Stevens-Johnson syndrome, erythema multiforme, or toxic skin eruptions) to any of the components contained in the formulation [see Warnings and Precautions (5.8) ] . • when coadministered with elbasvir and grazoprevir [see Warnings and Precautions (5.3) and Drug Interactions (7.5) ].
Warnings and Precautions
• Lactic Acidosis/Severe Hepatomegaly with Steatosis: Discontinue treatment in patients who develop symptoms or laboratory findings suggestive of lactic acidosis or pronounced hepatotoxicity. ( 5.2 ) • New Onset or Worsening Renal Impairment: Can include acute renal failure and Fanconi syndrome. Avoid administering SYMFI with concurrent or recent use of nephrotoxic drugs. ( 5.4 ) • Serious Psychiatric Symptoms: Immediate medical evaluation is recommended for serious psychiatric symptoms such as severe depression or suicidal ideation. ( 5.5 ) • Nervous System Symptoms (NSS): NSS are frequent, usually begin 1 to 2 days after initiating therapy and resolve in 2 to 4 weeks. Dosing at bedtime may improve tolerability. NSS are not predictive of onset of psychiatric symptoms. ( 5.6 ) • Rash: Rash usually begins within 1 to 2 weeks after initiating therapy and resolves within 4 weeks. Discontinue if severe rash develops. ( 5.8 ) • Hepatotoxicity: Monitor liver function tests before and during treatment in patients with underlying hepatic disease, including hepatitis B or C coinfection, marked transaminase elevations, or who are taking medications associated with liver toxicity. Among reported cases of hepatic failure, a few occurred in patients with no pre-existing hepatic disease. ( 5.9 , 8.7 ) • Pancreatitis: Use with caution in pediatric patients with a history of pancreatitis or other significant risk factors for pancreatitis. Discontinue SYMFI as clinically appropriate. ( 5.10 ) • Convulsions: Use caution in patients with a history of seizures. ( 5.11 ) • Lipids: Total cholesterol and triglyceride elevations. Monitor before therapy and periodically thereafter. ( 5.12 ) • Decreases in Bone Mineral Density (BMD): Observed in HIV-infected patients. Consider assessment of BMD in patients with a history of pathologic fracture or other risk factors for osteoporosis or bone loss. ( 5.13 ) • Immune Reconstitution Syndrome: Observed in HIV-infected patients. May necessitate further evaluation and treatment. ( 5.14 ) • Redistribution/Accumulation of Body Fat: Observed in HIV-infected patients receiving antiretroviral combination therapy. ( 5.15 )
Adverse Reactions
The following adverse reactions are discussed in other sections of the labeling: • Exacerbations of Hepatitis B [see Boxed Warning , Warnings and Precautions (5.1) ] . • Lactic Acidosis/Severe Hepatomegaly with Steatosis [see Warnings and Precautions (5.2) ] . • New Onset or Worsening Renal Impairment [see Warnings and Precautions (5.4) ] . • Psychiatric Symptoms [see Warnings and Precautions (5.5) ] . • Nervous System Symptoms [see Warnings and Precautions (5.6) ] . • Skin and Systemic Hypersensitivity Reaction [see Warnings and Precautions (5.8) ] . • Hepatotoxicity [see Warnings and Precautions (5.9) ]. • Pancreatitis [see Warnings and Precautions (5.10) ] . • Bone Loss and Mineralization Effects [see Warnings and Precautions (5.13) ] . • Immune Reconstitution Syndrome [see Warnings and Precautions (5.14) ] . • Fat Redistribution [see Warnings and Precautions (5.15) ] .
Drug Interactions
• SYMFI should not be administered with other antiretroviral medications for the treatment of HIV-1 infection. ( 7.1 ) • Coadministration of SYMFI can alter the concentrations of other drugs and other drugs may alter the concentration of SYMFI. The potential for drug-drug interactions should be considered before and during therapy. ( 5.3 , 7 )
How Supplied
SYMFI (efavirenz, lamivudine and tenofovir disoproxil fumarate) Tablets 600 mg/300 mg/300 mg are white, film-coated, capsule shaped, debossed with M 152 on one side of the tablet and plain on the other side. They are available as follows: NDC 49502-475-93 cartons containing bottles of 30 tablets with desiccant, induction seal and child-resistant cap NDC 49502-475-77 cartons containing bottles of 90 tablets with desiccant, induction seal and child-resistant cap Store below 30°C (86°F). Keep the bottle tightly closed. Dispense in original container. Do not use if seal over bottle opening is broken or missing.
Storage and Handling
SYMFI (efavirenz, lamivudine and tenofovir disoproxil fumarate) Tablets 600 mg/300 mg/300 mg are white, film-coated, capsule shaped, debossed with M 152 on one side of the tablet and plain on the other side. They are available as follows: NDC 49502-475-93 cartons containing bottles of 30 tablets with desiccant, induction seal and child-resistant cap NDC 49502-475-77 cartons containing bottles of 90 tablets with desiccant, induction seal and child-resistant cap Store below 30°C (86°F). Keep the bottle tightly closed. Dispense in original container. Do not use if seal over bottle opening is broken or missing.
Patient Information
SYMFI ® (SIM-fee) (efavirenz, lamivudine and tenofovir disoproxil fumarate) tablets What is the most important information I should know about SYMFI? SYMFI can cause serious side effects, including: • Worsening of Hepatitis B virus infection. If you have Human Immunodeficiency Virus type 1 (HIV-1) and Hepatitis B Virus (HBV) infection, your HBV may get worse (flare-up) if you stop taking SYMFI. A “flare-up” is when your HBV infection suddenly returns in a worse way than before. Your healthcare provider will test you for HBV infection before you start treatment with SYMFI. o It is not known if SYMFI is safe and effective in people who have both HIV-1 and HBV infection. o Do not run out of SYMFI. Refill your prescription or talk to your healthcare provider before your SYMFI is all gone. o Do not stop SYMFI without first talking to your healthcare provider. If you stop taking SYMFI, your healthcare provider will need to check your health often and do blood tests regularly for several months to check your liver. For more information about side effects, see “What are the possible side effects of SYMFI?” What is SYMFI? SYMFI is a prescription medicine that is used without other antiretroviral medicines to treat Human Immunodeficiency Virus-1 (HIV-1) in adults and children weighing at least 88 pounds (40 kg). HIV-1 is the virus that causes AIDS (Acquired Immune Deficiency Syndrome). SYMFI contains the prescription medicines efavirenz, lamivudine and tenofovir disoproxil fumarate. Do not take SYMFI if you: • are allergic to efavirenz, lamivudine, tenofovir disoproxil fumarate, or any of the ingredients in SYMFI. See the end of this Patient Information leaflet for a complete list of ingredients in SYMFI. • are currently taking elbasvir and grazoprevir. Before you take SYMFI, tell your healthcare provider about all of your medical conditions, including if you: • have liver problems, including hepatitis B or C infection • have kidney problems, including end-stage renal disease (ESRD) that requires dialysis • have a history of mental health problems • have a history of drug or alcohol abuse • have a heart problem, including QT prolongation • have bone problems, including a history of bone fractures • have a history of seizures • are pregnant or plan to become pregnant. SYMFI may harm your unborn baby. o You should not become pregnant during treatment with SYMFI. Tell your healthcare provider right away if you think you may be pregnant or become pregnant during treatment with SYMFI. o Females who are able to become pregnant should use effective birth control during treatment with SYMFI and for 12 weeks after stopping treatment. A barrier form of birth control should always be used along with another type of birth control. o If you are able to become pregnant, your healthcare provider should do a pregnancy test before you start SYMFI. Pregnancy Registry. There is a pregnancy registry for women who take SYMFI during pregnancy. The purpose of this registry is to collect information about the health of you and your baby. Talk to your healthcare provider about how you can take part in this registry. • are breastfeeding or plan to breastfeed. Do not breastfeed if you take SYMFI. o You should not breastfeed if you have HIV-1 because of the risk of passing HIV-1 to your baby. o Talk to your healthcare provider about the best way to feed your baby. Tell your healthcare provider about all the medicines you take, including prescription and over-the-counter medicines, vitamins and herbal supplements. Some medicines interact with SYMFI. SYMFI may affect the way other medicines work, and other medicines may affect how SYMFI works. Keep a list of your medicines and show it to your healthcare provider and pharmacist when you get a new medicine. • You can ask your healthcare provider or pharmacist for a list of medicines that interact with SYMFI. • Do not start taking a new medicine without telling your healthcare provider. Your healthcare provider can tell you if it is safe to take SYMFI with other medicines. How should I take SYMFI? • Take SYMFI exactly as your healthcare provider tells you to take it. • Take SYMFI 1 time each day, preferably at bedtime. Taking SYMFI at bedtime might help to make some of the side effects less bothersome. • Take SYMFI on an empty stomach. • Do not miss a dose of SYMFI. If you miss a dose, take the missed dose as soon as you remember. If it is almost time for your next dose of SYMFI, do not take the missed dose. Take the next dose at your regular time. • Stay under the care of your healthcare provider during treatment with SYMFI. • Do not run out of SYMFI. The virus in your blood may increase and the virus may become harder to treat. When your supply starts to run low, get more from your healthcare provider or pharmacy. • If you take too much SYMFI, go to the nearest hospital emergency room right away. What should I avoid while taking SYMFI? You should avoid taking medicines that contain sorbitol during treatment with SYMFI. What are the possible side effects of SYMFI? SYMFI may cause serious side effects, including: • See “What is the most important information I should know about SYMFI?” • Build-up of an acid in your blood (lactic acidosis). Lactic acidosis can happen in some people who take SYMFI. Lactic acidosis is a serious medical emergency that can lead to death. Call your healthcare provider right away if you get any of the following symptoms that could be signs of lactic acidosis: o feel very weak or tired o unusual (not normal) muscle pain o trouble breathing o stomach pain with nausea or vomiting o feel cold, especially in your arms and legs o feel dizzy or lightheaded o have a fast or irregular heartbeat • Severe liver problems can happen in people who take SYMFI. In some cases, these severe liver problems can lead to death. Your liver may become large (hepatomegaly) and you may develop fat in your liver (steatosis). Inflammation of your liver (hepatitis) that can lead to liver failure requiring a liver transplant has been reported in some people treated with SYMFI. Your healthcare provider may do blood tests to check your liver before and during treatment with SYMFI. Call your healthcare provider right away if you get any of the following signs or symptoms of liver problems: o your skin or the white part of your eyes turns yellow (jaundice) o dark or “tea-colored” urine o light-colored stools (bowel movements) o confusion o tiredness o loss of appetite for several days or longer o nausea and vomiting o pain, aching, or tenderness on the right side of your stomach-area o weakness o stomach (abdomen) swelling You may be more likely to get lactic acidosis or serious liver problems if you are female or very overweight (obese). • New or worse kidney problems, including kidney failure. Your healthcare provider may do blood and urine tests to check your kidneys before and during treatment with SYMFI. Tell your healthcare provider if you get signs and symptoms of kidney problems, including bone pain that does not go away or worsening bone pain, pain in your arms, hands, legs or feet, broken (fractured) bones, muscle pain or weakness. • Serious mental health problems. Get medical help right away if you get any of the following symptoms: o feel sad or hopeless o feel anxious or restless o do not trust other people o hear or see things that are not real o are not able to move or speak normally o have thoughts of hurting yourself (suicide) or have tried to hurt yourself or others o are not able to tell the difference between what is true or real and what is false or unreal • Nervous system symptoms are common in people who take SYMFI and can be severe. These symptoms usually begin during the first or second day of treatment with SYMFI and usually go away after 2 to 4 weeks of treatment. Some symptoms may occur months to years after beginning SYMFI therapy. These symptoms may become worse if you drink alcohol, take a medicine for mental health problems, or use certain street drugs during treatment with SYMFI. Symptoms may include: o dizziness o trouble sleeping o unusual dreams o trouble concentrating o drowsiness o lack of coordination or balance If you have dizziness, trouble concentrating or drowsiness, do not drive a car, use machinery, or do anything that needs you to be alert. Some nervous system symptoms (e.g., confusion, slow thoughts and physical movement, and delusions [false beliefs] or hallucinations [seeing or hearing things that others do not see or hear]) may occur months to years after beginning SYMFI therapy. Promptly contact your health care provider should any of these symptoms occur. • Skin reactions and allergic reactions. Skin reactions or rash can happen and can sometimes be severe. Skin rash usually goes away without any change in treatment. If you develop a rash or a rash with any of the following symptoms, call your healthcare provider right away: o itching o fever o swelling of your face o blisters or skin lesions o peeling skin o mouth sores o red or inflamed eyes • Risk of inflammation of the pancreas (pancreatitis). Children may be at risk for developing pancreatitis during treatment with SYMFI if they: o have taken nucleoside analogue medicines in the past o have a history of pancreatitis o have other risk factors for pancreatitis Call your healthcare provider right away if your child develops signs and symptoms of pancreatitis including severe upper stomach-area pain, with or without nausea and vomiting. Your healthcare provider may tell you to stop giving SYMFI to your child if their symptoms and blood test results show that your child may have pancreatitis. • Seizures. Seizures are more likely to happen if you have had seizures in the past. • Increases in blood fat levels (cholesterol and triglycerides). Your healthcare provider will check your blood fat levels before and during treatment with SYMFI. • Bone problems can happen in some people who take SYMFI. Bone problems include bone pain, softening or thinning (which may lead to fractures). Your healthcare provider may need to do tests to check your bones. Tell your healthcare provider if you have any bone pain, pain in your hands or feet, or muscle pain or weakness during treatment with SYMFI. • Changes in your immune system (Immune Reconstitution Syndrome) can happen when you start taking HIV-1 medicines. Your immune system may get stronger and begin to fight infections that have been hidden in your body for a long time. Tell your healthcare provider if you start having new symptoms after starting your HIV-1 medicine. • Changes in body fat can happen in some people who take HIV-1 medicines. These changes may include increased amount of fat in the upper back and neck (“buffalo hump”), breast, and around the main part of your body (trunk). Loss of fat from the legs, arms, and face may also happen. The cause and long-term health effects of these conditions are not known. • Changes in the electrical activity of your heart called QT prolongation. QT prolongation can cause irregular heartbeats that can be life-threatening. Tell your healthcare provider if you feel faint, lightheaded, dizzy, or feel your heart beating irregularly or fast during treatment with SYMFI. The most common side effects of SYMFI are: • trouble concentrating • headache • not feeling well • nasal signs and symptoms • rash • trouble sleeping • depression • cough • abnormal dreams • nausea • tiredness • diarrhea • dizziness • pain • weakness Tell your healthcare provider if you have any side effect that bothers you or that does not go away. These are not all the possible side effects of SYMFI. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. How should I store SYMFI? • Store SYMFI tablets below 86°F (30°C). • Keep SYMFI tablets in the original container. Keep SYMFI and all medicines out of the reach of children. General information about the safe and effective use of SYMFI. Medicines are sometimes prescribed for purposes other than those listed in a Patient Information leaflet. Do not use SYMFI for a condition for which it was not prescribed. Do not give SYMFI to other people, even if they have the same symptoms that you have. It may harm them. If you would like more information, talk with your healthcare provider. You can ask your pharmacist or healthcare provider for information about SYMFI that is written for health professionals. What are the ingredients in SYMFI? Active ingredient: efavirenz, lamivudine, and tenofovir disoproxil fumarate Inactive ingredients: croscarmellose sodium, hydroxypropyl cellulose, lactose monohydrate, magnesium stearate, microcrystalline cellulose, polyethylene glycol, polyvinyl alcohol, sodium chloride, sodium lauryl sulfate, talc and titanium dioxide. SYMFI ® is a registered trademark of Mylan Pharmaceuticals Inc. Other brands listed are the registered trademarks of their respective owners and are not trademarks of Mylan Laboratories Limited or Mylan Pharmaceuticals Inc. Manufactured for: Mylan Specialty L.P. Morgantown, WV 26505 U.S.A. Manufactured by: Mylan Laboratories Limited Hyderabad — 500 096, India 75075345 MS:TLET:R2 For more information, call Mylan at 1-877-446-3679 (1-877-4-INFO-RX). This Patient Information has been approved by the U.S. Food and Drug Administration. Revised: 10/2019
Description
Warnings and Precautions ( 5.1 , 5.2 , 5.3 , 5.4 , 5.6 , 5.13 , 5.14 ) 10/2019 Warnings and Precautions, Use with Interferon- and Ribavirin-Based Regimens (previous 5.10) Removed 10/2019
Medication Information
Warnings and Precautions
• Lactic Acidosis/Severe Hepatomegaly with Steatosis: Discontinue treatment in patients who develop symptoms or laboratory findings suggestive of lactic acidosis or pronounced hepatotoxicity. ( 5.2 ) • New Onset or Worsening Renal Impairment: Can include acute renal failure and Fanconi syndrome. Avoid administering SYMFI with concurrent or recent use of nephrotoxic drugs. ( 5.4 ) • Serious Psychiatric Symptoms: Immediate medical evaluation is recommended for serious psychiatric symptoms such as severe depression or suicidal ideation. ( 5.5 ) • Nervous System Symptoms (NSS): NSS are frequent, usually begin 1 to 2 days after initiating therapy and resolve in 2 to 4 weeks. Dosing at bedtime may improve tolerability. NSS are not predictive of onset of psychiatric symptoms. ( 5.6 ) • Rash: Rash usually begins within 1 to 2 weeks after initiating therapy and resolves within 4 weeks. Discontinue if severe rash develops. ( 5.8 ) • Hepatotoxicity: Monitor liver function tests before and during treatment in patients with underlying hepatic disease, including hepatitis B or C coinfection, marked transaminase elevations, or who are taking medications associated with liver toxicity. Among reported cases of hepatic failure, a few occurred in patients with no pre-existing hepatic disease. ( 5.9 , 8.7 ) • Pancreatitis: Use with caution in pediatric patients with a history of pancreatitis or other significant risk factors for pancreatitis. Discontinue SYMFI as clinically appropriate. ( 5.10 ) • Convulsions: Use caution in patients with a history of seizures. ( 5.11 ) • Lipids: Total cholesterol and triglyceride elevations. Monitor before therapy and periodically thereafter. ( 5.12 ) • Decreases in Bone Mineral Density (BMD): Observed in HIV-infected patients. Consider assessment of BMD in patients with a history of pathologic fracture or other risk factors for osteoporosis or bone loss. ( 5.13 ) • Immune Reconstitution Syndrome: Observed in HIV-infected patients. May necessitate further evaluation and treatment. ( 5.14 ) • Redistribution/Accumulation of Body Fat: Observed in HIV-infected patients receiving antiretroviral combination therapy. ( 5.15 )
Indications and Usage
SYMFI ® (efavirenz, lamivudine and tenofovir disoproxil fumarate) is indicated as a complete regimen for the treatment of human immunodeficiency virus type 1 (HIV-1) infection in adult and pediatric patients weighing at least 40 kg.
Dosage and Administration
• Testing: Prior to initiation and during treatment with SYMFI, patients should be tested for hepatitis B virus infection, and estimated creatinine clearance, urine glucose, and urine protein should be obtained. ( 2.1 ) • Recommended dose: One tablet taken orally once daily on an empty stomach, preferably at bedtime. ( 2.2 ) • Renal Impairment: Not recommended in patients with CrCL less than 50 mL/min or patients with end-stage renal disease requiring hemodialysis. ( 2.3 ) • Hepatic Impairment: Not recommended for patients with moderate or severe hepatic impairment. Use caution in patients with mild hepatic impairment. ( 2.4 )
Contraindications
SYMFI is contraindicated: • in patients with a previous hypersensitivity reaction (e.g., Stevens-Johnson syndrome, erythema multiforme, or toxic skin eruptions) to any of the components contained in the formulation [see Warnings and Precautions (5.8) ] . • when coadministered with elbasvir and grazoprevir [see Warnings and Precautions (5.3) and Drug Interactions (7.5) ].
Adverse Reactions
The following adverse reactions are discussed in other sections of the labeling: • Exacerbations of Hepatitis B [see Boxed Warning , Warnings and Precautions (5.1) ] . • Lactic Acidosis/Severe Hepatomegaly with Steatosis [see Warnings and Precautions (5.2) ] . • New Onset or Worsening Renal Impairment [see Warnings and Precautions (5.4) ] . • Psychiatric Symptoms [see Warnings and Precautions (5.5) ] . • Nervous System Symptoms [see Warnings and Precautions (5.6) ] . • Skin and Systemic Hypersensitivity Reaction [see Warnings and Precautions (5.8) ] . • Hepatotoxicity [see Warnings and Precautions (5.9) ]. • Pancreatitis [see Warnings and Precautions (5.10) ] . • Bone Loss and Mineralization Effects [see Warnings and Precautions (5.13) ] . • Immune Reconstitution Syndrome [see Warnings and Precautions (5.14) ] . • Fat Redistribution [see Warnings and Precautions (5.15) ] .
Drug Interactions
• SYMFI should not be administered with other antiretroviral medications for the treatment of HIV-1 infection. ( 7.1 ) • Coadministration of SYMFI can alter the concentrations of other drugs and other drugs may alter the concentration of SYMFI. The potential for drug-drug interactions should be considered before and during therapy. ( 5.3 , 7 )
Storage and Handling
SYMFI (efavirenz, lamivudine and tenofovir disoproxil fumarate) Tablets 600 mg/300 mg/300 mg are white, film-coated, capsule shaped, debossed with M 152 on one side of the tablet and plain on the other side. They are available as follows: NDC 49502-475-93 cartons containing bottles of 30 tablets with desiccant, induction seal and child-resistant cap NDC 49502-475-77 cartons containing bottles of 90 tablets with desiccant, induction seal and child-resistant cap Store below 30°C (86°F). Keep the bottle tightly closed. Dispense in original container. Do not use if seal over bottle opening is broken or missing.
How Supplied
SYMFI (efavirenz, lamivudine and tenofovir disoproxil fumarate) Tablets 600 mg/300 mg/300 mg are white, film-coated, capsule shaped, debossed with M 152 on one side of the tablet and plain on the other side. They are available as follows: NDC 49502-475-93 cartons containing bottles of 30 tablets with desiccant, induction seal and child-resistant cap NDC 49502-475-77 cartons containing bottles of 90 tablets with desiccant, induction seal and child-resistant cap Store below 30°C (86°F). Keep the bottle tightly closed. Dispense in original container. Do not use if seal over bottle opening is broken or missing.
Patient Information
|
SYMFI® (SIM-fee) |
|
|
What is the most important information I should know about SYMFI? SYMFI can cause serious side effects, including: |
|
|
|
|
For more information about side effects, see “What are the possible side effects of SYMFI?” |
|
|
What is SYMFI? SYMFI is a prescription medicine that is used without other antiretroviral medicines to treat Human Immunodeficiency Virus-1 (HIV-1) in adults and children weighing at least 88 pounds (40 kg). HIV-1 is the virus that causes AIDS (Acquired Immune Deficiency Syndrome). SYMFI contains the prescription medicines efavirenz, lamivudine and tenofovir disoproxil fumarate. |
|
|
Do not take SYMFI if you:
|
|
|
Before you take SYMFI, tell your healthcare provider about all of your medical conditions, including if you:
Tell your healthcare provider about all the medicines you take, including prescription and over-the-counter medicines, vitamins and herbal supplements. Some medicines interact with SYMFI. SYMFI may affect the way other medicines work, and other medicines may affect how SYMFI works. Keep a list of your medicines and show it to your healthcare provider and pharmacist when you get a new medicine.
|
|
|
How should I take SYMFI?
|
|
|
What should I avoid while taking SYMFI? You should avoid taking medicines that contain sorbitol during treatment with SYMFI. |
|
|
What are the possible side effects of SYMFI? SYMFI may cause serious side effects, including:
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
The most common side effects of SYMFI are: |
|
|
|
|
Tell your healthcare provider if you have any side effect that bothers you or that does not go away. These are not all the possible side effects of SYMFI. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. |
|
|
How should I store SYMFI?
Keep SYMFI and all medicines out of the reach of children. |
|
|
General information about the safe and effective use of SYMFI. Medicines are sometimes prescribed for purposes other than those listed in a Patient Information leaflet. Do not use SYMFI for a condition for which it was not prescribed. Do not give SYMFI to other people, even if they have the same symptoms that you have. It may harm them. If you would like more information, talk with your healthcare provider. You can ask your pharmacist or healthcare provider for information about SYMFI that is written for health professionals. |
|
|
What are the ingredients in SYMFI? Active ingredient: efavirenz, lamivudine, and tenofovir disoproxil fumarate Inactive ingredients: croscarmellose sodium, hydroxypropyl cellulose, lactose monohydrate, magnesium stearate, microcrystalline cellulose, polyethylene glycol, polyvinyl alcohol, sodium chloride, sodium lauryl sulfate, talc and titanium dioxide. SYMFI® is a registered trademark of Mylan Pharmaceuticals Inc. Other brands listed are the registered trademarks of their respective owners and are not trademarks of Mylan Laboratories Limited or Mylan Pharmaceuticals Inc. Manufactured for: Manufactured by: 75075345 For more information, call Mylan at 1-877-446-3679 (1-877-4-INFO-RX). |
This Patient Information has been approved by the U.S. Food and Drug Administration. Revised: 10/2019
Description
Warnings and Precautions ( 5.1 , 5.2 , 5.3 , 5.4 , 5.6 , 5.13 , 5.14 ) 10/2019 Warnings and Precautions, Use with Interferon- and Ribavirin-Based Regimens (previous 5.10) Removed 10/2019
Gender
There are no significant or clinically relevant gender differences in the pharmacokinetics of EFV, 3TC, and TDF.
Section 43683-2
Efavirenz
Body as a Whole: allergic reactions, asthenia, redistribution/accumulation of body fat [see Warnings and Precautions (5.15) ].
Central and Peripheral Nervous System: abnormal coordination, ataxia, encephalopathy, cerebellar coordination and balance disturbances, convulsions, hypoesthesia, paresthesia, neuropathy, tremor, vertigo.
Endocrine: gynecomastia.
Gastrointestinal: constipation, malabsorption.
Cardiovascular: flushing, palpitations.
Liver and Biliary System: hepatic enzyme increase, hepatic failure, hepatitis.
Metabolic and Nutritional: hypercholesterolemia, hypertriglyceridemia.
Musculoskeletal: arthralgia, myalgia, myopathy.
Psychiatric: aggressive reactions, agitation, delusions, emotional lability, mania, neurosis, paranoia, psychosis, suicide, catatonia.
Respiratory: dyspnea.
Skin and Appendages: erythema multiforme, photoallergic dermatitis, Stevens-Johnson syndrome.
Special Senses: abnormal vision, tinnitus.
Ribavirin
In vitro data indicate ribavirin reduces phosphorylation of 3TC, stavudine, and zidovudine. However, no pharmacokinetic (e.g., plasma concentrations or intracellular triphosphorylated active metabolite concentrations) or pharmacodynamic (e.g., loss of HIV-1/HCV virologic suppression) interaction was observed when ribavirin and 3TC (n = 18), stavudine (n = 10), or zidovudine (n = 6) were coadministered as part of a multi-drug regimen to HIV-1/HCV co-infected subjects.
Trial 903
Data through 144 weeks are reported for Trial 903, a double-blind, active-controlled multicenter trial comparing EFV 600 mg + 3TC 300 mg + TDF 300 mg vs. EFV 600 mg + 3TC 300 mg + stavudine (d4T) 40 mg in 600 antiretroviral-naïve subjects. Subjects had a mean age of 36 years (range 18-64); 74% were male, 64% were Caucasian, and 20% were Black. The mean baseline CD4+ cell count was 279 cells/mm3 (range 3-956) and median baseline plasma HIV-1 RNA was 77,600 copies/mL (range 417−5,130,000). Subjects were stratified by baseline HIV-1 RNA and CD4+ cell count. Forty-three percent of subjects had baseline viral loads > 100,000 copies/mL and 39% had CD4+ cell counts < 200 cells/mm3. Table 9 provides treatment outcomes through 48 and 144 weeks.
|
Outcomes |
At Week 48 |
At Week 144 |
||
|
EFV + 3TC + TDF (N = 299) |
EFV + 3TC + d4T (N = 301) |
EFV + 3TC + TDF (N = 299) |
EFV + 3TC + d4T (N = 301) |
|
|
Responder Subjects achieved and maintained confirmed HIV-1 RNA < 400 copies/mL through Week 48 and 144.
|
79% |
82% |
68% |
62% |
|
Virologic failure Includes confirmed viral rebound and failure to achieve confirmed < 400 copies/mL through Week 48 and 144.
|
6% |
4% |
10% |
8% |
|
Rebound |
5% |
3% |
8% |
7% |
|
Never suppressed |
0% |
1% |
0% |
0% |
|
Added an antiretroviral agent |
1% |
1% |
2% |
1% |
|
Death |
< 1% |
1% |
< 1% |
2% |
|
Discontinued due to adverse event |
6% |
6% |
8% |
13% |
|
Discontinued for other reasons Includes lost to follow-up, subject’s withdrawal, noncompliance, protocol violation and other reasons.
|
8% |
7% |
14% |
15% |
Achievement of plasma HIV-1 RNA concentrations of < 400 copies/mL at Week 144 was similar between the two treatment groups for the population stratified at baseline on the basis of HIV-1 RNA concentration (> or ≤ 100,000 copies/mL) and CD4+ cell count (< or ≥ 200 cells/mm3). Through 144 weeks of therapy, 62% and 58% of subjects in the TDF and d4T arms, respectively, achieved and maintained confirmed HIV-1 RNA < 50 copies/mL. The mean increase from baseline in CD4+ cell count was 263 cells/mm3 for the TDF arm and 283 cells/mm3 for the d4T arm.
Through 144 weeks, 11 subjects in the TDF group and 9 subjects in the d4T group experienced a new CDC Class C event.
Lamivudine
Body as a Whole: redistribution/accumulation of body fat [see Warnings and Precautions (5.15) ].
Endocrine and Metabolic: hyperglycemia.
General: weakness.
Hemic and Lymphatic: anemia (including pure red cell aplasia and severe anemias progressing on therapy).
Hepatic and Pancreatic: lactic acidosis and hepatic steatosis, posttreatment exacerbation of hepatitis B [see Boxed Warning, Warnings and Precautions (5.1, 5.2)].
Hypersensitivity: anaphylaxis, urticaria.
Musculoskeletal: muscle weakness, CPK elevation, rhabdomyolysis.
Skin: Alopecia, pruritus.
7.8 Sorbitol
Coadministration of single doses of 3TC and sorbitol resulted in a sorbitol dose-dependent reduction in 3TC exposures. When possible, avoid use of sorbitol-containing medicines with 3TC [see Clinical Pharmacology (12.3)].
Pancreatitis
Pancreatitis, which has been fatal in some cases, has been observed in antiretroviral nucleoside-experienced pediatric subjects receiving 3TC alone or in combination with other antiretroviral agents [see Warnings and Precautions (5.10) ].
Risk Summary
There are retrospective case reports of neural tube defects in infants whose mothers were exposed to EFV-containing regimens in the first trimester of pregnancy.
Although a causal relationship has not been established between exposure to EFV in the first trimester and neural tube defects, similar malformations have been observed in studies conducted in monkeys at doses similar to the human dose. In addition, fetal and embryonic toxicities occurred in rats, at a dose ten times less than the human exposure at recommended clinical dose. Because of the potential risk of neural tube defects, EFV should not be used in the first trimester of pregnancy. Advise pregnant women of the potential risk to a fetus.
Prospective pregnancy data from the APR are not sufficient to adequately assess this risk of birth defects or miscarriage. EFV and 3TC have been evaluated in a limited number of women as reported to the APR. Available data from the APR show no difference in the risk of major birth defects for EFV and 3TC compared to the background rate for major birth defects of 2.7% in the U.S. reference population of the Metropolitan Atlanta Congenital Defects Program (MACDP).
Available data from the APR also show no increase in the overall risk of major birth defects with first trimester exposure for TDF (2.1%) compared with the background rate for major birth defects of 2.7% in a U.S. reference population of the MACDP (see Data).
3TC produced embryonic toxicity in rabbits at a dose that produced similar human exposures as the recommended clinical dose. The relevance of animal findings to human pregnancy registry data is not known.
The rate of miscarriage is not reported in the APR. The estimated background rate of miscarriage in clinically recognized pregnancies in the U.S. general population is 15% to 20%. The background risk for major birth defects and miscarriage for the indicated population is unknown. The APR uses the MACDP as the U.S. reference population for birth defects in the general population. The MACDP evaluates women and infants from a limited geographic area and does not include outcomes for births that occurred at less than 20 weeks’ gestation.
10 Overdosage
If overdose occurs, the patient must be monitored for evidence of toxicity, and standard supportive treatment applied as necessary.
Efavirenz: Some patients accidentally taking 600 mg twice daily have reported increased nervous system symptoms. One patient experienced involuntary muscle contractions.
Treatment of overdose with EFV should consist of general supportive measures, including monitoring of vital signs and observation of the patient’s clinical status. Administration of activated charcoal may be used to aid removal of unabsorbed drug. There is no specific antidote for overdose with efavirenz. Since efavirenz is highly protein bound, dialysis is unlikely to significantly remove the drug from blood.
Lamivudine: There is no known specific treatment for overdose with 3TC. If overdose occurs, the patient should be monitored and standard supportive treatment applied as required because a negligible amount of 3TC was removed via (4-hour) hemodialysis, continuous ambulatory peritoneal dialysis, and automated peritoneal dialysis, it is not known if continuous hemodialysis would provide clinical benefit in a 3TC overdose event.
Tenofovir Disoproxil Fumarate: Limited clinical experience at doses higher than the therapeutic dose of TDF 300 mg is available.
Tenofovir is efficiently removed by hemodialysis with an extraction coefficient of approximately 54%. Following a single 300 mg dose of tenofovir disoproxil fumarate, a 4-hour hemodialysis session removed approximately 10% of the administered tenofovir dose.
Contraception
Females of reproductive potential should use effective contraception during treatment with SYMFI and for 12 weeks after discontinuing SYMFI due to the long half-life of EFV. Barrier contraception should always be used in combination with other methods of contraception. Hormonal methods that contain progesterone may have decreased effectiveness [see Drug Interactions (7.5)].
11 Description
SYMFI tablets contain efavirenz (EFV), an HIV-1 specific, non-nucleoside, reverse transcriptase inhibitor (NNRTI), lamivudine (also known as 3TC), a synthetic nucleoside analogue with activity against HIV-1 and tenofovir disoproxil fumarate (TDF) (a prodrug of tenofovir), a fumaric acid salt of bis-isopropoxycarbonyloxymethyl ester derivative of tenofovir. TDF is converted in vivo to tenofovir, an acyclic nucleoside phosphonate (nucleotide) analog of adenosine 5’-monophosphate. Tenofovir exhibits activity against HIV-1 reverse transcriptase.
SYMFI tablets are for oral administration. Each film-coated tablet contains 600 mg of efavirenz, 300 mg of lamivudine and 300 mg of tenofovir disoproxil fumarate, which is equivalent to 245 mg of tenofovir disoproxil, and the following inactive ingredients: croscarmellose sodium, hydroxypropyl cellulose, lactose monohydrate, magnesium stearate, microcrystalline cellulose, polyethylene glycol, polyvinyl alcohol, sodium chloride, sodium lauryl sulfate, talc and titanium dioxide.
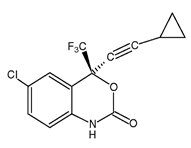
Efavirenz: The chemical name of efavirenz is (4S)-6-chloro-4-(cyclopropylethynyl)-1,4-dihydro-4-(trifluoromethyl)-2H-3,1-benzoxazin-2-one. Its molecular formula is C14H9ClF3NO2 and its structural formula is:
Efavirenz is a white to slightly pink crystalline powder with a molecular mass of 315.68. It is soluble in methanol and practically insoluble in water (< 10 microgram/mL).
Lamivudine: The chemical name of lamivudine is (-)-1-[(2R,5S)-2-(Hydroxymethyl)-1,3-oxathiolan-5-yl]cytosine. Lamivudine is the (-)enantiomer of a dideoxy analogue of cytidine. Lamivudine has also been referred to as (-)2′,3′-dideoxy, 3′-thiacytidine. It has a molecular formula of C8H11N3O3S and a molecular weight of 229.26 g per mol. It has the following structural formula:
Lamivudine is a white to off-white solid with a solubility of approximately 70 mg per mL in water at 20°C.
Tenofovir Disoproxil Fumarate: The chemical name of tenofovir DF is 9-[(R)-2-[[Bis[[(isopropoxycarbonyl)oxy]methoxy]phosphinyl]methoxy]propyl]adenine fumarate (1:1). It has a molecular formula of C19H30N5O10P•C4H4O4 and a molecular weight of 635.51. It has the following structural formula:
Tenofovir DF is a white to off-white powder with a solubility of 13.4 mg/mL in distilled water at 25°C. It has an octanol/phosphate buffer (pH 6.5) partition coefficient (log p) of 1.25 at 25°C.
Interferon Alfa
There was no significant pharmacokinetic interaction between 3TC and interferon alfa in a trial of 19 healthy male subjects.
5.11 Convulsions
Convulsions have been observed in patients receiving EFV, generally in the presence of known medical history of seizures [see Nonclinical Toxicology (13.2)]. Caution should be taken in any patient with a history of seizures. Patients who are receiving concomitant anticonvulsant medications primarily metabolized by the liver, such as phenytoin and phenobarbital, may require periodic monitoring of plasma levels [see Drug Interactions (7.5)].
5.10 Pancreatitis
In pediatric patients with a history of prior antiretroviral nucleoside exposure, a history of pancreatitis, or other significant risk factors for the development of pancreatitis, 3TC, a component of SYMFI, should be used with caution. Treatment with SYMFI should be stopped immediately if clinical signs, symptoms, or laboratory abnormalities suggestive of pancreatitis occur [see Adverse Reactions (6.1)].
8.4 Pediatric Use
The safety and effectiveness of SYMFI as a fixed-dose tablet in pediatric patients infected with HIV-1 and weighing at least 40 kg have been established based on clinical studies using the individual components (efavirenz, lamivudine, and tenofovir disoproxil fumarate).
8.5 Geriatric Use
Clinical studies of SYMFI did not include sufficient numbers of subjects aged 65 and over to determine whether they respond differently from younger subjects. In general, caution should be exercised in the administration of 3TC in elderly patients reflecting the greater frequency of decreased hepatic, renal, or cardiac function, and of concomitant disease or other drug therapy.
Pregnancy Testing
Females of reproductive potential should undergo pregnancy testing before initiation of SYMFI.
5.9 Hepatotoxicity
Postmarketing cases of hepatitis, including fulminant hepatitis progressing to liver failure requiring transplantation or resulting in death, have been reported in patients treated with EFV. Reports have included patients with underlying hepatic disease, including coinfection with hepatitis B or C, and patients without pre-existing hepatic disease or other identifiable risk factors.
EFV, a component of SYMFI, is not recommended for patients with moderate or severe hepatic impairment. Careful monitoring is recommended for patients with mild hepatic impairment receiving EFV [see Adverse Reactions (6.1) and Use in Specific Populations (8.7)].
Monitoring of liver enzymes before and during treatment is recommended for all patients [see Dosage and Administration (2.1)]. Consider discontinuing SYMFI in patients with persistent elevations of serum transaminases to greater than five times the upper limit of the normal range.
Discontinue SYMFI if elevation of serum transaminases is accompanied by clinical signs or symptoms of hepatitis or hepatic decompensation.
Geriatric Patients
The pharmacokinetics of 3TC and TDF have not been studied in patients over 65 years of age.
4 Contraindications
SYMFI is contraindicated:
-
•in patients with a previous hypersensitivity reaction (e.g., Stevens-Johnson syndrome, erythema multiforme, or toxic skin eruptions) to any of the components contained in the formulation [see Warnings and Precautions (5.8)].
-
•when coadministered with elbasvir and grazoprevir [see Warnings and Precautions (5.3) and Drug Interactions (7.5)].
6 Adverse Reactions
The following adverse reactions are discussed in other sections of the labeling:
-
•Exacerbations of Hepatitis B [see Boxed Warning, Warnings and Precautions (5.1)].
-
•Lactic Acidosis/Severe Hepatomegaly with Steatosis [see Warnings and Precautions (5.2) ].
-
•New Onset or Worsening Renal Impairment [see Warnings and Precautions (5.4)].
-
•Psychiatric Symptoms [see Warnings and Precautions (5.5)].
-
•Nervous System Symptoms [see Warnings and Precautions (5.6)].
-
•Skin and Systemic Hypersensitivity Reaction [see Warnings and Precautions (5.8)].
-
•Hepatotoxicity [see Warnings and Precautions (5.9)].
-
•Pancreatitis [see Warnings and Precautions (5.10) ].
-
•Bone Loss and Mineralization Effects [see Warnings and Precautions (5.13) ].
-
•Immune Reconstitution Syndrome [see Warnings and Precautions (5.14) ].
-
•Fat Redistribution [see Warnings and Precautions (5.15) ].
7 Drug Interactions
-
•SYMFI should not be administered with other antiretroviral medications for the treatment of HIV-1 infection. (7.1)
-
•Coadministration of SYMFI can alter the concentrations of other drugs and other drugs may alter the concentration of SYMFI. The potential for drug-drug interactions should be considered before and during therapy. (5.3, 7)
8.6 Renal Impairment
SYMFI is not recommended for patients with impaired renal function (i.e., creatinine clearance less than 50 mL/min) or patients with end-stage renal disease (ESRD) requiring hemodialysis because it is a fixed-dose combination formulation that cannot be adjusted [see Dosage and Administration (2.3)].
Sorbitol (excipient)
3TC and sorbitol solutions were coadministered to 16 healthy adult subjects in an open-label, randomized-sequence, 4-period, crossover trial. Each subject received a single 300-mg dose of 3TC oral solution alone or coadministered with a single dose of 3.2 grams, 10.2 grams, or 13.4 grams of sorbitol in solution. Coadministration of 3TC with sorbitol resulted in dose-dependent decreases of 20%, 39%, and 44% in the AUC(0-24), 14%, 32%, and 36% in the AUC(∞), and 28%, 52%, and 55% in the Cmax of lamivudine, respectively.
12.3 Pharmacokinetics
The effect of food on SYMFI has not been evaluated.
5.12 Lipid Elevations
Treatment with EFV has resulted in increases in the concentration of total cholesterol and triglycerides. Cholesterol and triglyceride testing should be performed before initiating EFV therapy and at periodic intervals during therapy.
5.16 Qtc Prolongation
QTc prolongation has been observed with the use of EFV [see Drug Interactions (7.2, 7.5) and Clinical Pharmacology (12.2)]. Consider alternatives to products containing EFV when coadministered with a drug with a known risk of Torsade de Pointes or when administered to patients at higher risk of Torsade de Pointes.
8.7 Hepatic Impairment
SYMFI is not recommended for patients with moderate or severe hepatic impairment because there are insufficient data to determine whether dose adjustment is necessary. Patients with mild hepatic impairment may be treated with SYMFI without any adjustment in dose [see Dosage and Administration (2.4), Warnings and Precautions (5.9) and Clinical Pharmacology (12.3) ].
Mineralization Defects
Cases of osteomalacia associated with proximal renal tubulopathy, manifested as bone pain or pain in extremities and which may contribute to fractures, have been reported in association with TDF use [see Adverse Reactions (6.2)]. Arthralgia and muscle pain or weakness have also been reported in cases of proximal renal tubulopathy. Hypophosphatemia and osteomalacia secondary to proximal renal tubulopathy should be considered in patients at risk of renal dysfunction who present with persistent or worsening bone or muscle symptoms while receiving TDF-containing products [see Warnings and Precautions (5.4)].
1 Indications and Usage
SYMFI® (efavirenz, lamivudine and tenofovir disoproxil fumarate) is indicated as a complete regimen for the treatment of human immunodeficiency virus type 1 (HIV-1) infection in adult and pediatric patients weighing at least 40 kg.
5.15 Fat Redistribution
In HIV-infected patients, redistribution/accumulation of body fat including central obesity, dorsocervical fat enlargement (buffalo hump), peripheral wasting, facial wasting, breast enlargement, and “cushingoid appearance” have been observed in patients receiving combination antiretroviral therapy. The mechanism and long-term consequences of these events are currently unknown. A causal relationship has not been established.
7.2 Qt Prolonging Drugs
There is limited information available on the potential for a pharmacodynamic interaction between EFV and drugs that prolong the QTc interval. QTc prolongation has been observed with the use of EFV [see Clinical Pharmacology (12.2)]. Consider alternatives to EFV when coadministered with a drug with a known risk of Torsade de Pointes.
12.1 Mechanism of Action
SYMFI is a fixed-dose combination of antiviral drugs EFV, 3TC, and TDF with antiviral activity against HIV-1 [see Microbiology (12.4)].
5.5 Psychiatric Symptoms
Serious psychiatric adverse experiences have been reported in patients treated with EFV, a component of SYMFI. In controlled trials of 1008 patients treated with regimens containing EFV for a mean of 2.1 years and 635 patients treated with control regimens for a mean of 1.5 years, the frequency (regardless of causality) of specific serious psychiatric events among patients who received EFV or control regimens, respectively, were severe depression (2.4%, 0.9%), suicidal ideation (0.7%, 0.3%), nonfatal suicide attempts (0.5%, 0), aggressive behavior (0.4%, 0.5%), paranoid reactions (0.4%, 0.3%), and manic reactions (0.2%, 0.3%). When psychiatric symptoms similar to those noted above were combined and evaluated as a group in a multifactorial analysis of data from a study using EFV 600 mg, treatment with EFV was associated with an increase in the occurrence of these selected psychiatric symptoms. Other factors associated with an increase in the occurrence of these psychiatric symptoms were history of injection drug use, psychiatric history, and receipt of psychiatric medication at study entry; similar associations were observed in both the EFV and control treatment groups. In a study using EFV 600 mg, onset of new serious psychiatric symptoms occurred throughout the study for both EFV-treated and control-treated patients. One percent of EFV-treated patients discontinued or interrupted treatment because of one or more of these selected psychiatric symptoms.
There have also been occasional postmarketing reports of death by suicide, delusions, psychosis-like behavior, although a causal relationship to the use of EFV cannot be determined from these reports [see Adverse Reactions (6.2)]. Postmarketing cases of catatonia have also been reported and may be associated with increased efavirenz exposure. Patients with serious psychiatric adverse experiences should seek immediate medical evaluation to assess the possibility that the symptoms may be related to the use of EFV, and if so, to determine whether the risks of continued therapy outweigh the benefits.
Efavirenz and Lamivudine
There are no significant or clinically relevant racial differences in EFV and 3TC pharmacokinetics.
Laboratory Abnormalities
Table 2 provides a list of laboratory abnormalities (Grades 3-4) observed in Trial 903. With the exception of fasting cholesterol and fasting triglyceride elevations that were more common in the d4T group (40% and 9%) compared with the TDF group (19% and 1%) respectively, laboratory abnormalities observed in this trial occurred with similar frequency in the TDF and d4T treatment arms.
|
TDF + 3TC + EFV |
d4T + 3TC + EFV |
|
|
N = 299 |
N = 301 |
|
|
Any ≥ Grade 3 Laboratory Abnormality |
36% |
42% |
|
Fasting Cholesterol (> 240 mg/dL) |
19% |
40% |
|
Creatine Kinase (M: > 990 U/L; F: > 845 U/L) |
12% |
12% |
|
Serum Amylase (> 175 U/L) |
9% |
8% |
|
AST (M: > 180 U/L; F: > 170 U/L) |
5% |
7% |
|
ALT (M: > 215 U/L; F: > 170 U/L) |
4% |
5% |
|
Hematuria (> 100 RBC/HPF) |
7% |
7% |
|
Neutrophils (< 750/mm3) |
3% |
1% |
|
Fasting Triglycerides (> 750 mg/dL) |
1% |
9% |
5.7 Embryo Fetal Toxicity
EFV, a component of SYMFI, may cause fetal harm when administered during the first trimester to a pregnant woman. Advise females of reproductive potential who are receiving EFV to avoid pregnancy [see Use in Specific Populations (8.1, 8.3)].
Cardiac Electrophysiology
The effect of EFV on the QTc interval was evaluated in an open-label, positive and placebo-controlled, fixed single sequence 3-period, 3-treatment crossover QT study in 58 healthy subjects enriched for CYP2B6 polymorphisms. The mean Cmax of EFV in subjects with CYP2B6 *6/*6 genotype following the administration of 600 mg daily dose for 14 days was 2.25-fold the mean Cmax observed in subjects with CYP2B6 *1/*1 genotype. A positive relationship between EFV concentration and QTc prolongation was observed. Based on the concentration-QTc relationship, the mean QTc prolongation and its upper bound 90% confidence interval are 8.7 ms and 11.3 ms in subjects with CYP2B6*6/*6 genotype following the administration of 600 mg daily dose for 14 days [see Warnings and Precautions (5.16) ].
5 Warnings and Precautions
-
•Lactic Acidosis/Severe Hepatomegaly with Steatosis: Discontinue treatment in patients who develop symptoms or laboratory findings suggestive of lactic acidosis or pronounced hepatotoxicity. (5.2)
-
•New Onset or Worsening Renal Impairment: Can include acute renal failure and Fanconi syndrome. Avoid administering SYMFI with concurrent or recent use of nephrotoxic drugs. (5.4)
-
•Serious Psychiatric Symptoms:Immediate medical evaluation is recommended for serious psychiatric symptoms such as severe depression or suicidal ideation. (5.5)
-
•Nervous System Symptoms (NSS): NSS are frequent, usually begin 1 to 2 days after initiating therapy and resolve in 2 to 4 weeks. Dosing at bedtime may improve tolerability. NSS are not predictive of onset of psychiatric symptoms. (5.6)
-
•Rash: Rash usually begins within 1 to 2 weeks after initiating therapy and resolves within 4 weeks. Discontinue if severe rash develops. (5.8)
-
•Hepatotoxicity: Monitor liver function tests before and during treatment in patients with underlying hepatic disease, including hepatitis B or C coinfection, marked transaminase elevations, or who are taking medications associated with liver toxicity. Among reported cases of hepatic failure, a few occurred in patients with no pre-existing hepatic disease. (5.9, 8.7)
-
•Pancreatitis: Use with caution in pediatric patients with a history of pancreatitis or other significant risk factors for pancreatitis. Discontinue SYMFI as clinically appropriate. (5.10)
-
•Convulsions: Use caution in patients with a history of seizures. (5.11)
-
•Lipids: Total cholesterol and triglyceride elevations. Monitor before therapy and periodically thereafter. (5.12)
-
•Decreases in Bone Mineral Density (BMD): Observed in HIV-infected patients. Consider assessment of BMD in patients with a history of pathologic fracture or other risk factors for osteoporosis or bone loss. (5.13)
-
•Immune Reconstitution Syndrome: Observed in HIV-infected patients. May necessitate further evaluation and treatment. (5.14)
-
•Redistribution/Accumulation of Body Fat: Observed in HIV-infected patients receiving antiretroviral combination therapy. (5.15)
Bone Mineral Density (bmd)
In clinical trials in HIV-1-infected adults, TDF was associated with slightly greater decreases in BMD and increases in biochemical markers of bone metabolism, suggesting increased bone turnover relative to comparators [see Adverse Reactions (6.1)]. Serum parathyroid hormone levels and 1,25 Vitamin D levels were also higher in subjects receiving TDF.
The effects of TDF-associated changes in BMD and biochemical markers on long-term bone health and future fracture risk in adults and pediatric subjects 2 years and older are unknown. The long-term effect of lower spine and total body BMD on skeletal growth in pediatric patients, and in particular, the effects of long-duration exposuire in younger children is unknown.
Although the effect of supplementation with calcium and vitamin D was not studied, such supplementation may be beneficial. Assessment of BMD should be considered for adult and pediatric patients who have a history of pathologic bone fracture or other risk factors for osteoporosis or bone loss. If bone abnormalities are suspected then appropriate consultation should be obtained.
2 Dosage and Administration
-
•Testing: Prior to initiation and during treatment with SYMFI, patients should be tested for hepatitis B virus infection, and estimated creatinine clearance, urine glucose, and urine protein should be obtained. (2.1)
-
•Recommended dose: One tablet taken orally once daily on an empty stomach, preferably at bedtime. (2.2)
-
•Renal Impairment: Not recommended in patients with CrCL less than 50 mL/min or patients with end-stage renal disease requiring hemodialysis. (2.3)
-
•Hepatic Impairment: Not recommended for patients with moderate or severe hepatic impairment. Use caution in patients with mild hepatic impairment. (2.4)
5.6 Nervous System Symptoms
Fifty-three percent (531/1008) of patients receiving EFV, a component of SYMFI, in controlled trials reported central nervous system symptoms (any grade, regardless of causality) compared to 25% (156/635) of patients receiving control regimens. These symptoms included, but were not limited to, dizziness (28.1% of the 1008 patients), insomnia (16.3%), impaired concentration (8.3%), somnolence (7.0%), abnormal dreams (6.2%), and hallucinations (1.2%). These symptoms were severe in 2.0% of patients and 2.1% of patients discontinued therapy as a result. These symptoms usually begin during the first or second day of therapy and generally resolve after the first 2 to 4 weeks of therapy. After 4 weeks of therapy, the prevalence of nervous system symptoms of at least moderate severity ranged from 5% to 9% in patients treated with regimens containing EFV and from 3% to 5% in patients treated with a control regimen. Inform patients that these common symptoms were likely to improve with continued therapy and were not predictive of subsequent onset of the less frequent psychiatric symptoms [see Warnings and Precautions (5.5)]. Dosing at bedtime may improve the tolerability of these nervous system symptoms [see Dosage and Administration (2.2)].
Late-onset neurotoxicity, including ataxia and encephalopathy (impaired consciousness, confusion, psychomotor slowing, psychosis, delirium), may occur months to years after beginning efavirenz therapy. Some events of late-onset neurotoxicity have occurred in patients with CYP2B6 genetic polymorphisms which are associated with increased efavirenz levels despite daily dosages of 600 mg of efavirenz. Patients presenting with signs and symptoms of serious neurologic adverse experiences should be evaluated promptly to assess the possibility that these events may be related to efavirenz use, and whether discontinuation of SYMFI is warranted.
Pregnancy Exposure Registry
There is a pregnancy exposure registry that monitors pregnancy outcomes in women exposed to SYMFI during pregnancy. Healthcare providers are encouraged to register patients by calling the Antiretroviral Pregnancy Registry (APR) at 1-800-258-4263.
3 Dosage Forms and Strengths
Tablets: 600 mg of efavirenz, 300 mg of lamivudine, and 300 mg of tenofovir disoproxil fumarate (equivalent to 245 mg of tenofovir disoproxil).
The tablets are white, film-coated, capsule shaped, debossed with M 152 on one side of the tablet and plain on the other side.
6.2 Postmarketing Experience
The following adverse reactions have been identified during post-approval use for each of the individual components of SYMFI (EFV, 3TC, and TDF). Because these reactions are reported voluntarily from a population of unknown size, it is not always possible to reliably estimate their frequency or establish causal relationship to drug exposure. These reactions have been chosen for inclusion due to a combination of their seriousness, frequency of reporting, or potential causal connection to EFV, 3TC, and TDF.
8 Use in Specific Populations
-
•Pregnancy: Women should avoid pregnancy during EFV therapy, a component of SYMFI, and for 12 weeks after discontinuation. (5.7, 8.1, 8.3)
-
•Lactation: Breastfeeding not recommended due to potential for HIV transmission. (8.2)
-
•Females and Males of Reproductive Potential: Pregnancy testing and contraception are recommended. (8.3)
Tenofovir Disoproxil Fumarate
Immune System Disorders: allergic reaction, including angioedema.
Metabolism and Nutrition Disorders: lactic acidosis, hypokalemia, hypophosphatemia.
Respiratory, Thoracic, and Mediastinal Disorders: dyspnea.
Gastrointestinal Disorders: pancreatitis, increased amylase, abdominal pain.
Renal and Urinary Disorders: renal insufficiency, acute renal failure, renal failure, acute tubular necrosis, Fanconi syndrome, proximal renal tubulopathy, interstitial nephritis (including acute cases), nephrogenic diabetes insipidus, renal insufficiency, increased creatinine, proteinuria, polyuria [see Warnings and Precautions (5.4)].
Hepatobiliary Disorders: hepatic steatosis, hepatitis, increased liver enzymes (most commonly AST, ALT gamma GT).
Skin and Subcutaneous Tissue Disorders: rash.
Musculoskeletal and Connective Tissue Disorders: rhabdomyolysis, osteomalacia (manifested as bone pain and which may contribute to fractures), muscular weakness, myopathy.
General Disorders and Administration Site Conditions: asthenia.
The following adverse reactions, listed under the body system headings above, may occur as a consequence of proximal renal tubulopathy: rhabdomyolysis, osteomalacia, hypokalemia, muscular weakness, myopathy, hypophosphatemia.
Trimethoprim/sulfamethoxazole
3TC and TMP/SMX were coadministered to 14 HIV-1-positive subjects in a single-center, open-label, randomized, crossover trial. Each subject received treatment with a single 300-mg dose of 3TC and TMP 160 mg/SMX 800 mg once a day for 5 days with concomitant administration of 3TC 300 mg with the fifth dose in a crossover design. Coadministration of TMP/SMX with 3TC resulted in an increase of 43% ± 23% (mean ± SD) in 3TC AUC∞, a decrease of 29% ± 13% in 3TC oral clearance, and a decrease of 30% ± 36% in 3TC renal clearance. The pharmacokinetic properties of TMP and SMX were not altered by coadministration with 3TC. There is no information regarding the effect on 3TC pharmacokinetics of higher doses of TMP/SMX such as those used in treating PCP.
6.1 Clinical Trials Experience
Because clinical studies are conducted under widely varying conditions, the adverse reaction rates observed in clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
Patients With Renal Impairment
Assessment of Drug Interactions
[See Drug Interactions (7).]
Changes in Bone Mineral Density
In HIV-1-infected adult subjects in Trial 903, there was a significantly greater mean percentage decrease from baseline in BMD at the lumbar spine in subjects receiving TDF + 3TC + EFV (-2.2% ± 3.9) compared with subjects receiving d4T + 3TC + EFV (-1.0% ± 4.6) through 144 weeks. Changes in BMD at the hip were similar between the two treatment groups (-2.8% ± 3.5 in the TDF group vs. -2.4% ± 4.5 in the d4T group). In both groups, the majority of the reduction in BMD occurred in the first 24-48 weeks of the trial and this reduction was sustained through Week 144. Twenty-eight percent of TDF-treated subjects vs. 21% of the d4T-treated subjects lost at least 5% of BMD at the spine or 7% of BMD at the hip. Clinically relevant fractures (excluding fingers and toes) were reported in 4 subjects in the TDF group and 6 subjects in the d4T group. In addition, there were significant increases in biochemical markers of bone metabolism (serum bone-specific alkaline phosphatase, serum osteocalcin, serum C telopeptide, and urinary N telopeptide) and higher serum parathyroid hormone levels and 1,25 Vitamin D levels in the TDF group relative to the d4T group; however, except for bone-specific alkaline phosphatase, these changes resulted in values that remained within the normal range [see Warnings and Precautions (5.13) ].
Treatment Naïve Adult Patients
The efficacy of EFV 600 mg, 3TC 300 mg, and TDF 300 mg in the treatment of HIV-1 infection in adults with no antiretroviral treatment history was established in Trial 903.
7.4 Cannabinoid Test Interaction
EFV does not bind to cannabinoid receptors. False-positive urine cannabinoid test results have been reported with some screening assays in uninfected and HIV-infected subjects receiving EFV. Confirmation of positive screening tests for cannabinoids by a more specific method is recommended.
17 Patient Counseling Information
Advise the patient to read the FDA-approved patient labeling (Patient Information).
Drug Interactions: SYMFI may interact with many drugs; therefore, advise patients to report to their healthcare provider the use of any other prescription, nonprescription medication, or herbal products, particularly St. John’s wort [see Contraindications (4) and Drug Interactions (7)].
Post Treatment Acute Exacerbation of Hepatitis B in Patients with HBV Co-Infection: Inform patients that severe acute exacerbations of hepatitis have been reported in patients who are infected with HBV or coinfected with HBV and HIV-1 and have discontinued 3TC and TDF, components of SYMFI. Test patients with HIV-1 for hepatitis B virus (HBV) before initiating antiretroviral therapy. In patients with chronic hepatitis B, it is important to obtain HIV antibody testing prior to initiating 3TC and TDF, components of SYMFI [see Warnings and Precautions (5.1) ].
Lactic Acidosis and Severe Hepatomegaly: Inform patients that lactic acidosis and severe hepatomegaly with steatosis, including fatal cases, have been reported. Treatment with SYMFI should be suspended in any patient who develops clinical symptoms suggestive of lactic acidosis or pronounced hepatotoxicity (including nausea, vomiting, unusual or unexpected stomach discomfort, and weakness) [see Warnings and Precautions (5.2)].
New Onset or Worsening Renal Impairment: Inform patients that renal impairment, including cases of acute renal failure and Fanconi syndrome, has been reported. Advise patients with impaired renal function (i.e., creatinine clearance less than 50 mL/min) or patients with end-stage renal disease (ESRD) requiring hemodialysis to avoid SYMFI with concurrent or recent use of a nephrotoxic agent (e.g., high-dose or multiple NSAIDs) for patients [see Dosage and Administration (2.3), Warnings and Precautions (5.4)].
Psychiatric Symptoms: Inform patients that serious psychiatric symptoms including severe depression, suicide attempts, aggressive behavior, delusions, paranoia, psychosis-like symptoms and catatonia have been reported in patients receiving EFV [see Warnings and Precautions (5.5)]. Advise patients to seek immediate medical evaluation if they experience severe psychiatric adverse experiences. Advise patients to inform their physician of any history of mental illness or substance abuse.
Nervous System Symptoms: Inform patients that central nervous system symptoms (NSS) including dizziness, insomnia, impaired concentration, drowsiness, and abnormal dreams are commonly reported during the first weeks of therapy with EFV, a component of SYMFI [see Warnings and Precautions (5.6)]. Dosing at bedtime may improve the tolerability of these symptoms, which are likely to improve with continued therapy. Alert patients to the potential for additive effects when used concomitantly with alcohol or psychoactive drugs. Instruct patients that if they experience NSS they should avoid potentially hazardous tasks such as driving or operating machinery.
Inform patients that there is a risk of developing late-onset neurotoxicity, including ataxia and encephalopathy, which may occur months to years after beginning efavirenz therapy [see Warnings and Precautions (5.6)].
Embryo-Fetal Toxicity: Advise female patients that EFV, a component of SYMFI may cause fetal harm when administered during the first trimester to a pregnant woman. Advise females of reproductive potential to use effective contraception as well as a barrier method during treatment with SYMFI and for 12 weeks after discontinuation of use. Advise patients to contact their healthcare provider if they plan to become pregnant, become pregnant, or if pregnancy is suspected during treatment with SYMFI [see Warnings and Precautions (5.7), Use in Specific Populations (8.1, 8.3)].
Rash: Inform patients that rash is a common side effect of EFV [see Warnings and Precautions (5.8)]. Rashes usually go away without any change in treatment. However, since rash may be serious, patients should be advised to contact their physician promptly if rash occurs.
Hepatotoxicity: Inform patients to watch for early warning signs of liver inflammation or failure, such as fatigue, weakness, lack of appetite, nausea and vomiting, as well as later signs such as jaundice, confusion, abdominal swelling, and discolored feces and to consult their healthcare provider promptly if such symptoms occur [see Warnings and Precautions (5.9)].
Pancreatitis: Advise patients or guardians to monitor pediatric patients for signs and symptoms of pancreatitis [see Warnings and Precautions (5.10) ].
Convulsions: Advise patients that convulsions have been observed in patients receiving EFV, a component of SYMFI, generally in patients with known medical history of seizures [see Warnings and Precautions (5.11) ].
Lipid Elevations: Advise patients treatment with EFV, a component of SYMFI has resulted in increases in the concentration of total cholesterol and triglycerides [see Warnings and Precautions (5.12) ].
Bone Loss and Mineralization Effects: Inform patients that decreases in bone mineral density have been observed with the use of 3TC and TDF, components of SYMFI, in patients with HIV [see Warnings and Precautions (5.13) ].
Immune Reconstitution Syndrome: Advise patients to inform their healthcare provider immediately of any symptoms of infection, as in some patients with advanced HIV infection, signs and symptoms of inflammation from previous infections may occur soon after anti-HIV treatment is started [see Warnings and Precautions (5.14) ].
Fat Redistribution: Inform patients that redistribution or accumulation of body fat may occur in patients receiving antiretroviral therapy, including SYMFI, and that the cause and long‑term health effects of these conditions are not known at this time [see Warnings and Precautions (5.15) ].
Administration Instructions: Inform patients that it is important to take SYMFI once daily on a regular dosing schedule on an empty stomach, preferably at bedtime, and to avoid missing doses as it can result in development of resistance. Advise patients if a dose is missed, take it as soon as possible unless it is almost time for the next dose. Also advise patients that dosing at bedtime may improve the tolerability of nervous system symptoms [see Dosage and Administration (2.2)].
Pregnancy Registry: Advise patients that there is an antiretroviral pregnancy registry to monitor fetal outcomes in women exposed to SYMFI [see Use in Specific Populations (8.1)].
Lactation: Instruct women with HIV-1 infection not to breastfeed because HIV-1 can be passed to the baby in breast milk [see Use in Specific Populations (8.2)].
SYMFI® is a registered trademark of Mylan Pharmaceuticals Inc.
Other brands listed are the registered trademarks of their respective owners and are not trademarks of Mylan Laboratories Limited or Mylan Pharmaceuticals Inc.
Rx only
Manufactured for:
Mylan Specialty L.P.
Morgantown, WV 26505 U.S.A.
Manufactured by:
Mylan Laboratories Limited
Hyderabad — 500 096, India
7.3 Drugs Affecting Renal Function
Tenofovir is primarily eliminated by the kidneys [see Clinical Pharmacology (12.3)]. Coadministration of EFV/3TC/TDF with drugs that are eliminated by active tubular secretion may increase concentrations of tenofovir and/or the coadministered drug. Some examples include, but are not limited to, acyclovir, cidofovir, ganciclovir, valacyclovir, valganciclovir, aminoglycosides (e.g., gentamicin), and high-dose or multiple NSAIDs [see Warnings and Precautions (5.4)]. Drugs that decrease renal function may increase concentrations of tenofovir.
5.14 Immune Reconstitution Syndrome
Immune reconstitution syndrome has been reported in HIV-infected patients treated with combination antiretroviral therapy, including EFV, 3TC, and TDF. During the initial phase of combination antiretroviral treatment, patients whose immune system responds may develop an inflammatory response to indolent or residual opportunistic infections (such as Mycobacterium avium infection, cytomegalovirus, Pneumocystis jirovecii pneumonia [PCP], or tuberculosis), which may necessitate further evaluation and treatment.
Autoimmune disorders (such as Graves’ disease, polymyositis, Guillain-Barre syndrome, and autoimmune hepatitis) have also been reported to occur in the setting of immune reconstitution; however, the time to onset is more variable, and can occur many months after initiation of treatment.
16 How Supplied/storage and Handling
SYMFI (efavirenz, lamivudine and tenofovir disoproxil fumarate) Tablets 600 mg/300 mg/300 mg are white, film-coated, capsule shaped, debossed with M 152 on one side of the tablet and plain on the other side. They are available as follows:
NDC 49502-475-93
cartons containing bottles of 30 tablets with desiccant, induction seal and child-resistant cap
NDC 49502-475-77
cartons containing bottles of 90 tablets with desiccant, induction seal and child-resistant cap
Store below 30°C (86°F).
Keep the bottle tightly closed.
Dispense in original container.
Do not use if seal over bottle opening is broken or missing.
2.3 Not Recommended in Renal Impairment
Because SYMFI is a fixed-dose combination tablet and cannot be dose adjusted, it is not recommended for patients with impaired renal function (creatinine clearance less than 50 mL/min) or patients with end-stage renal disease (ESRD) requiring hemodialysis [see Use in Specific Populations (8.6)].
Posttreatment Exacerbations of Hepatitis
All patients with HIV-1 should be tested for the presence of chronic hepatitis B virus (HBV) before initiating antiretroviral therapy [see Dosage and Administration (2.1)]. Discontinuation of anti-HBV therapy, including 3TC and TDF, may be associated with severe acute exacerbations of hepatitis B. Patients infected with HBV who discontinue SYMFI should be closely monitored with both clinical and laboratory follow-up for at least several months after stopping treatment. If appropriate, resumption of anti-hepatitis B therapy may be warranted.
5.4 New Onset Or Worsening Renal Impairment
TDF, a component of SYMFI is principally eliminated by the kidney. Renal impairment, including cases of acute renal failure and Fanconi syndrome (renal tubular injury with severe hypophosphatemia), has been reported with the use of TDF [see Adverse Reactions (6.2)].
Prior to initiation and during use of SYMFI, on a clinically appropriate schedule, assess serum creatinine, estimated creatinine clearance, urine glucose, and urine protein in all patients.
Avoid SYMFI with concurrent or recent use of a nephrotoxic agent (e.g., high-dose or multiple non-steroidal anti-inflammatory drugs [NSAIDs]) [see Drug Interactions (7.3)]. Cases of acute renal failure after initiation of high-dose or multiple NSAIDs have been reported in HIV-infected patients with risk factors for renal dysfunction who appeared stable on TDF. Some patients required hospitalization and renal replacement therapy. Alternatives to NSAIDs should be considered, if needed, in patients at risk for renal dysfunction.
Persistent or worsening bone pain, pain in extremities, fractures and/or muscular pain or weakness may be manifestations of proximal renal tubulopathy and should prompt an evaluation of renal function in patients at risk of renal dysfunction.
Principal Display Panel 600 Mg/300 Mg/300 Mg
NDC 49502-475-93 Rx only
SYMFI®
(efavirenz, lamivudine,
and tenofovir disoproxil
fumarate) tablets
600 mg/300 mg/300 mg*
Note to pharmacist: Do not cover
ALERT box with pharmacy label.
ALERT: Find out about
medicines that should NOT
be taken with SYMFI®.
30 tablets
*Each film-coated tablet contains:
Efavirenz, USP 600 mg
Lamivudine, USP 300 mg
Tenofovir Disoproxil Fumarate 300 mg
(equivalent to 245 mg of tenofovir
disoproxil)
Usual Dosage: See accompanying
prescribing information.
Keep this and all medication
out of the reach of children.
Store below 30°C (86°F).
Dispense only in original container.
Keep container tightly closed.
Manufactured for:
Mylan Specialty L.P.
Morgantown, WV 26505 U.S.A.
Made in India
Code No.: MP/DRUGS/25/1/2014
MS:MXI:47593:1C:R3
Mylan.com
SYMFI® is a registered
trademark of Mylan
Pharmaceuticals Inc.
5.8 Skin and Systemic Hypersensitivity Reaction
In controlled clinical trials, 26% (266/1008) of patients treated with 600 mg EFV experienced new-onset skin rash compared with 17% (111/635) of patients treated in control groups. Rash associated with blistering, moist desquamation, or ulceration occurred in 0.9% (9/1008) of patients treated with EFV. The incidence of Grade 4 rash (e.g., erythema multiforme, Stevens-Johnson syndrome) in patients treated with EFV in all studies and expanded access was 0.1%. Rashes are usually mild-to-moderate maculopapular skin eruptions that occur within the first 2 weeks of initiating therapy with EFV (median time to onset of rash in adults was 11 days) and, in most patients continuing therapy with EFV, rash resolves within 1 month (median duration, 16 days). The discontinuation rate for rash in clinical trials was 1.7% (17/1008).
EFV can generally be reinitiated in patients interrupting therapy because of rash. EFV should be discontinued in patients developing severe rash associated with blistering, desquamation, mucosal involvement, or fever. Appropriate antihistamines and/or corticosteroids may improve the tolerability and hasten the resolution of rash. For patients who have had a life-threatening cutaneous reaction (e.g., Stevens-Johnson syndrome), alternate therapy should be considered [see Contraindications (4)].
8.3 Females and Males of Reproductive Potential
Because of potential teratogenic effects, pregnancy should be avoided in women receiving SYMFI [see Warnings and Precautions (5.7), Use in Specific Populations (8.1)].
7.7 Drugs Inhibiting Organic Cation Transporters
3TC, a component of SYMFI, is predominantly eliminated in the urine by active organic cationic secretion. The possibility of interactions with other drugs administered concurrently should be considered, particularly when their main route of elimination is active renal secretion via the organic cationic transport system (e.g., trimethoprim) [see Clinical Pharmacology (12.3)]. No data are available regarding interactions with other drugs that have renal clearance mechanisms similar to that of 3TC.
7.6 Drugs Without Clinically Significant Interactions
No dosage adjustment is recommended when SYMFI is administered with the following: aluminum/magnesium hydroxide antacids, azithromycin, cetirizine, famotidine, fluconazole, and lorazepam.
Effect of 3tc On the Pharmacokinetics of Other Agents
Based on in vitro study results, 3TC at therapeutic drug exposures is not expected to affect the pharmacokinetics of drugs that are substrates of the following transporters: organic anion transporter polypeptide 1B1/3 (OATP1B1/3), breast cancer resistance protein (BCRP), P-glycoprotein (P-gp), multidrug and toxin extrusion protein 1 (MATE1), MATE2-K, organic cation transporter 1 (OCT1), OCT2, or OCT3.
Effect of Other Agents On the Pharmacokinetics of 3tc
3TC is a substrate of MATE1, MATE2-K, and OCT2 in vitro. Trimethoprim (an inhibitor of these drug transporters) has been shown to increase 3TC plasma concentrations. This interaction is not considered clinically significant as no dose adjustment of 3TC is needed.
3TC is a substrate of P-gp and BCRP; however, considering its absolute bioavailability (87%), it is unlikely that these transporters play a significant role in the absorption of 3TC. Therefore, coadministration of drugs that are inhibitors of these efflux transporters is unlikely to affect the disposition and elimination of 3TC.
7.1 Not Recommended With Other Antiretroviral Medications
SYMFI is a complete regimen for the treatment of HIV-1 infection; therefore, it should not be administered with other antiretroviral medications for treatment of HIV-1 infection.
5.2 Lactic Acidosis and Severe Hepatomegaly With Steatosis
Lactic acidosis and severe hepatomegaly with steatosis, including fatal cases, have been reported with the use of nucleoside analogs and other antiretrovirals. Female sex and obesity may be risk factors for the development of lactic acidosis and severe hepatomegaly with steatosis in patients treated with antiretroviral nucleoside analogues. Treatment should be suspended in any patient who develops clinical or laboratory findings suggestive of lactic acidosis or pronounced hepatotoxicity, which may include hepatomegaly and steatosis even in the absence of marked transaminase elevations.
Important Differences Among Lamivudine Containing Products
SYMFI tablets contain a higher dose of the same active ingredient, 3TC, than EPIVIR-HBV® tablets. EPIVIR-HBV was developed for patients with chronic hepatitis B. The formulation and dosage of 3TC in EPIVIR-HBV are not appropriate for patients co-infected with HIV-1 and HBV. Safety and efficacy of 3TC have not been established for treatment of chronic hepatitis B in patients co-infected with HIV-1 and HBV.
If treatment with EPIVIR-HBV, TDF, or a tenofovir alafenamide (TAF)-containing product is prescribed for chronic hepatitis B for a patient with unrecognized or untreated HIV-1 infection, rapid emergence of HIV-1 resistance is likely to result because of the subtherapeutic dose and the inappropriateness of monotherapy HIV-1 treatment.
Warning: Post Treatment Acute Exacerbations of Hepatitis B
Severe acute exacerbations of hepatitis B have been reported in patients who are co-infected with hepatitis B virus (HBV) and human immunodeficiency virus (HIV-1) and have discontinued lamivudine or tenofovir disoproxil fumarate, two components of SYMFI. Monitor hepatic function closely in these patients and, if appropriate, initiate anti-hepatitis B treatment [see Warnings and Precautions (5.1) ].
2.4 Not Recommended in Moderate to Severe Hepatic Impairment
SYMFI is not recommended in patients with moderate or severe hepatic impairment (Child-Pugh B or C) [see Warnings and Precautions (5.9) and Use in Specific Populations (8.7)].
7.5 Established and Other Potentially Significant Interactions
EFV has been shown in vivo to induce CYP3A and CYP2B6. Other compounds that are substrates of CYP3A or CYP2B6 may have decreased plasma concentrations when coadministered with EFV.
Drugs that induce CYP3A activity (e.g., phenobarbital, rifampin, rifabutin) would be expected to increase the clearance of EFV resulting in lowered plasma concentrations.
No drug interaction studies have been conducted using SYMFI. However, drug interaction studies have been conducted with the individual components of SYMFI (EFV, 3TC, and TDF) [see Clinical Pharmacology (12.3)].
Drug interactions with EFV are summarized in Table 3 [for pharmacokinetics data see Clinical Pharmacology (12.3, Tables 6 and 7)]. This table includes potentially significant interactions, but is not all inclusive.
| This table is not all-inclusive. | ||
|
Concomitant Drug Class: Drug Name |
Effect |
Clinical Comment |
|
Anticoagulant: Warfarin |
↑ or ↓ warfarin |
Monitor INR and adjust warfarin dosage if necessary. |
|
Anticonvulsants: Carbamazepine |
↓ carbamazepine The interaction between EFV and the drug was evaluated in a clinical study. All other drug interactions shown are predicted.
↓ EFV* |
There are insufficient data to make a dose recommendation for EFV. Alternative anticonvulsant treatment should be used. |
|
Phenytoin Phenobarbital |
↓ anticonvulsant ↓ EFV |
Monitor anticonvulsant plasma levels periodically because of potential for reduction in anticonvulsant and/or EFV plasma levels. |
|
Antidepressants: Bupropion |
↓ bupropion |
Increases in bupropion dosage should be guided by clinical response. Bupropion dose should not exceed the maximum recommended dose.
|
|
Sertraline |
↓ sertraline |
Increases in sertraline dosage should be guided by clinical response. |
|
Antifungals: Itraconazole
Ketoconazole |
↓ itraconazole ↓ hydroxyitraconazole ↓ ketoconazole |
Consider alternative antifungal treatment because no dose recommendation for itraconazole or ketoconazole can be made.
|
|
Posaconazole |
↓ posaconazole |
Avoid concomitant use unless the benefit outweighs the risks. |
|
Anti-infective: Clarithromycin |
↓ clarithromycin ↑ 14-OH metabolite |
Consider alternatives to macrolide antibiotics because of the risk of QT interval prolongation. |
|
Antimycobacterial: Rifabutin |
↓ rifabutin |
Increase daily dose of rifabutin by 50%. Consider doubling the rifabutin dose in regimens where rifabutin is given 2 or 3 times a week.
|
|
Rifampin |
↓ EFV |
Increase EFV total daily dose to 800 mg once daily when coadministered with rifampin to patients weighing 50 kg or more. |
|
Antimalarials: Artemether/lumefantrine |
↓ artemether ↓ dihydroartemisinin ↓ lumefantrine |
Consider alternatives to artemether/lumefantrine because of the risk of QT interval prolongation [see Warnings and Precautions (5.16) ].
|
|
Atovaquone/ proguanil |
↓ atovaquone ↓ proguanil |
Concomitant administration is not recommended. |
|
Calcium channel blockers: Diltiazem |
↓ diltiazem ↓ desacetyl diltiazem ↓ N-monodesmethyldiltiazem |
Diltiazem dose adjustments should be guided by clinical response (refer to the full prescribing information for diltiazem).
|
|
Others (e.g., felodipine, nicardipine, nifedipine, verapamil) |
↓ calcium channel blocker |
When coadministered with EFV, dosage adjustment of calcium channel blocker may be needed and should be guided by clinical response (refer to the full prescribing information for the calcium channel blocker). |
|
HMG-CoA reductase inhibitors: Atorvastatin Pravastatin Simvastatin |
↓ atorvastatin ↓ pravastatin ↓ simvastatin |
Plasma concentrations of atorvastatin, pravastatin, and simvastatin decreased. Consult the full prescribing information for the HMG-CoA reductase inhibitor for guidance on individualizing the dose. |
|
Hepatitis C antiviral agents: Boceprevir |
↓ boceprevir |
Concomitant administration of boceprevir is not recommended. |
|
Elbasvir/Grazoprevir |
↓ elbasvir ↓ grazoprevir |
Coadministration of EFV with elbasvir/grazoprevir is contraindicated [see Contraindications (4)] because it may lead to loss of virologic response to elbasvir/grazoprevir.
|
|
Pibrentasvir/Glecaprevir |
↓ pibrentasvir ↓ glecaprevir |
Coadministration of EFV is not recommended because it may lead to reduced therapeutic effect of pibrentasvir/glecaprevir.
|
|
Simeprevir |
↓ simeprevir ↔ EFV |
Concomitant administration of simeprevir is not recommended.
|
|
Velpatasvir/Sofosbuvir |
↓ velpatasvir |
Coadministration of EFV and sofosbuvir/velpatasvir is not recommended because it may result in loss of therapeutic effect of sofosbuvir/velpatasvir.
|
|
Velpatasvir/Sofosbuvir/ |
↓ velpatasvir ↓ voxilaprevir |
Coadministration of EFV and sofosbuvir/velpatasvir/voxilaprevir is not recommended because it may result in loss of therapeutic effect of sofosbuvir/velpatasvir/voxilaprevir.
|
|
Ledipasvir/Sofosbuvir |
↑ TDF |
Monitor for adverse reactions associated with TDF. |
|
Hepatitis B antiviral agents Adefovir dipivoxil |
Concomitant administration of adefovir dipivoxil is not recommended. |
|
|
Hormonal contraceptives: Oral Ethinyl estradiol/ Norgestimate |
↓ active metabolites of norgestimate |
A reliable method of barrier contraception should be used in addition to hormonal contraceptives.
|
|
Implant Etonogestrel |
↓ etonogestrel |
A reliable method of barrier contraception should be used in addition to hormonal contraceptives. Decreased exposure of etonogestrel may be expected. There have been postmarketing reports of contraceptive failure with etonogestrel in EFV-exposed patients. |
|
Immunosuppressants: sirolimus, and others metabolized by CYP3A |
↓ immunosuppressant |
Dose adjustments of the immunosuppressant may be required. Close monitoring of immunosuppressant concentrations for at least 2 weeks (until stable concentrations are reached) is recommended when starting or stopping treatment with EFV. |
|
Narcotic analgesic: Methadone |
↓ methadone |
Monitor for signs of methadone withdrawal and increase methadone dose if required to alleviate withdrawal symptoms. |
2.1 Testing Prior to Initiation and During Treatment With Symfi
Prior to initiation of SYMFI, test patients for hepatitis B virus infection [see Warnings and Precautions (5.1) ].
It is recommended that serum creatinine, serum phosphorus, estimated creatinine clearance, urine glucose, and urine protein be assessed before initiating SYMFI and during therapy in all patients as clinically appropriate [see Warnings and Precautions (5.4)].
Monitor hepatic function prior to and during treatment with SYMFI [see Warnings and Precautions (5.9)].
Clinical Trials in Treatment Naïve Hiv 1 Infected Adult Subjects
In Trial 903, 600 antiretroviral-naïve subjects received TDF (N = 299) or stavudine (d4T) (N = 301) administered in combination with 3TC and EFV for 144 weeks. The most common adverse reactions were mild to moderate gastrointestinal events and dizziness. Mild adverse reactions (Grade 1) were common with a similar incidence in both arms and included dizziness, diarrhea, and nausea. Table 1 provides the treatment-emergent adverse reactions (Grades 2-4) occurring in greater than or equal to 5% of subjects treated in any treatment group.
|
TDF + 3TC + EFV |
d4T + 3TC + EFV |
|
|
N = 299 |
N = 301 |
|
|
Rash event Rash event includes rash, pruritus, maculopapular rash, urticaria, vesiculobullous rash, and pustular rash.
|
18% |
12% |
|
Headache |
14% |
17% |
|
Pain |
13% |
12% |
|
Diarrhea |
11% |
13% |
|
Depression |
11% |
10% |
|
Back pain |
9% |
8% |
|
Nausea |
8% |
9% |
|
Fever |
8% |
7% |
|
Abdominal pain |
7% |
12% |
|
Asthenia |
6% |
7% |
|
Anxiety |
6% |
6% |
|
Vomiting |
5% |
9% |
|
Insomnia |
5% |
8% |
|
Arthralgia |
5% |
7% |
|
Pneumonia |
5% |
5% |
|
Dyspepsia |
4% |
5% |
|
Dizziness |
3% |
6% |
|
Myalgia |
3% |
5% |
|
Lipodystrophy Lipodystrophy represents a variety of investigator-described adverse events not a protocol-defined syndrome.
|
1% |
8% |
|
Peripheral neuropathy Peripheral neuropathy includes peripheral neuritis and neuropathy.
|
1% |
5% |
2.2 Recommended Dosage for Adult and Pediatric Patients Weighing At Least 40 Kg
SYMFI is a three-drug fixed-dose combination product containing 600 mg of efavirenz (EFV), 300 mg of lamivudine (3TC), and 300 mg of tenofovir disoproxil fumarate (TDF). The recommended dosage of SYMFI in HIV-1-infected adults and pediatric patients who weigh at least 40 kg, and can swallow a solid tablet, is one tablet taken orally once daily. SYMFI tablets should be taken on an empty stomach, preferably at bedtime. Dosing at bedtime may improve the tolerability of nervous system symptoms [see Warnings and Precautions (5.6) and Adverse Reactions (6.1)].
5.3 Risk of Adverse Reactions Or Loss of Virologic Response Due to Drug Interactions
The concomitant use of SYMFI and other drugs may result in known or potentially significant drug interactions, some of which may lead to [see Contraindications (4) and Drug Interactions (7.5)]:
-
•Loss of therapeutic effect of SYMFI and possible development of resistance.
-
•Possible clinically significant adverse reactions from greater exposures of concomitant drugs.
See Table 3 for steps to prevent or manage these possible and known significant drug interactions, including dosing recommendations. Consider the potential for drug interactions prior to and during therapy with SYMFI; review concomitant medications during therapy with SYMFI; and monitor for the adverse reactions associated with the concomitant drugs.
Structured Label Content
Patient Information
|
SYMFI® (SIM-fee) |
|
|
What is the most important information I should know about SYMFI? SYMFI can cause serious side effects, including: |
|
|
|
|
For more information about side effects, see “What are the possible side effects of SYMFI?” |
|
|
What is SYMFI? SYMFI is a prescription medicine that is used without other antiretroviral medicines to treat Human Immunodeficiency Virus-1 (HIV-1) in adults and children weighing at least 88 pounds (40 kg). HIV-1 is the virus that causes AIDS (Acquired Immune Deficiency Syndrome). SYMFI contains the prescription medicines efavirenz, lamivudine and tenofovir disoproxil fumarate. |
|
|
Do not take SYMFI if you:
|
|
|
Before you take SYMFI, tell your healthcare provider about all of your medical conditions, including if you:
Tell your healthcare provider about all the medicines you take, including prescription and over-the-counter medicines, vitamins and herbal supplements. Some medicines interact with SYMFI. SYMFI may affect the way other medicines work, and other medicines may affect how SYMFI works. Keep a list of your medicines and show it to your healthcare provider and pharmacist when you get a new medicine.
|
|
|
How should I take SYMFI?
|
|
|
What should I avoid while taking SYMFI? You should avoid taking medicines that contain sorbitol during treatment with SYMFI. |
|
|
What are the possible side effects of SYMFI? SYMFI may cause serious side effects, including:
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
The most common side effects of SYMFI are: |
|
|
|
|
Tell your healthcare provider if you have any side effect that bothers you or that does not go away. These are not all the possible side effects of SYMFI. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. |
|
|
How should I store SYMFI?
Keep SYMFI and all medicines out of the reach of children. |
|
|
General information about the safe and effective use of SYMFI. Medicines are sometimes prescribed for purposes other than those listed in a Patient Information leaflet. Do not use SYMFI for a condition for which it was not prescribed. Do not give SYMFI to other people, even if they have the same symptoms that you have. It may harm them. If you would like more information, talk with your healthcare provider. You can ask your pharmacist or healthcare provider for information about SYMFI that is written for health professionals. |
|
|
What are the ingredients in SYMFI? Active ingredient: efavirenz, lamivudine, and tenofovir disoproxil fumarate Inactive ingredients: croscarmellose sodium, hydroxypropyl cellulose, lactose monohydrate, magnesium stearate, microcrystalline cellulose, polyethylene glycol, polyvinyl alcohol, sodium chloride, sodium lauryl sulfate, talc and titanium dioxide. SYMFI® is a registered trademark of Mylan Pharmaceuticals Inc. Other brands listed are the registered trademarks of their respective owners and are not trademarks of Mylan Laboratories Limited or Mylan Pharmaceuticals Inc. Manufactured for: Manufactured by: 75075345 For more information, call Mylan at 1-877-446-3679 (1-877-4-INFO-RX). |
This Patient Information has been approved by the U.S. Food and Drug Administration. Revised: 10/2019
Gender
There are no significant or clinically relevant gender differences in the pharmacokinetics of EFV, 3TC, and TDF.
Section 43683-2 (43683-2)
Efavirenz
Body as a Whole: allergic reactions, asthenia, redistribution/accumulation of body fat [see Warnings and Precautions (5.15) ].
Central and Peripheral Nervous System: abnormal coordination, ataxia, encephalopathy, cerebellar coordination and balance disturbances, convulsions, hypoesthesia, paresthesia, neuropathy, tremor, vertigo.
Endocrine: gynecomastia.
Gastrointestinal: constipation, malabsorption.
Cardiovascular: flushing, palpitations.
Liver and Biliary System: hepatic enzyme increase, hepatic failure, hepatitis.
Metabolic and Nutritional: hypercholesterolemia, hypertriglyceridemia.
Musculoskeletal: arthralgia, myalgia, myopathy.
Psychiatric: aggressive reactions, agitation, delusions, emotional lability, mania, neurosis, paranoia, psychosis, suicide, catatonia.
Respiratory: dyspnea.
Skin and Appendages: erythema multiforme, photoallergic dermatitis, Stevens-Johnson syndrome.
Special Senses: abnormal vision, tinnitus.
Ribavirin
In vitro data indicate ribavirin reduces phosphorylation of 3TC, stavudine, and zidovudine. However, no pharmacokinetic (e.g., plasma concentrations or intracellular triphosphorylated active metabolite concentrations) or pharmacodynamic (e.g., loss of HIV-1/HCV virologic suppression) interaction was observed when ribavirin and 3TC (n = 18), stavudine (n = 10), or zidovudine (n = 6) were coadministered as part of a multi-drug regimen to HIV-1/HCV co-infected subjects.
Trial 903
Data through 144 weeks are reported for Trial 903, a double-blind, active-controlled multicenter trial comparing EFV 600 mg + 3TC 300 mg + TDF 300 mg vs. EFV 600 mg + 3TC 300 mg + stavudine (d4T) 40 mg in 600 antiretroviral-naïve subjects. Subjects had a mean age of 36 years (range 18-64); 74% were male, 64% were Caucasian, and 20% were Black. The mean baseline CD4+ cell count was 279 cells/mm3 (range 3-956) and median baseline plasma HIV-1 RNA was 77,600 copies/mL (range 417−5,130,000). Subjects were stratified by baseline HIV-1 RNA and CD4+ cell count. Forty-three percent of subjects had baseline viral loads > 100,000 copies/mL and 39% had CD4+ cell counts < 200 cells/mm3. Table 9 provides treatment outcomes through 48 and 144 weeks.
|
Outcomes |
At Week 48 |
At Week 144 |
||
|
EFV + 3TC + TDF (N = 299) |
EFV + 3TC + d4T (N = 301) |
EFV + 3TC + TDF (N = 299) |
EFV + 3TC + d4T (N = 301) |
|
|
Responder Subjects achieved and maintained confirmed HIV-1 RNA < 400 copies/mL through Week 48 and 144.
|
79% |
82% |
68% |
62% |
|
Virologic failure Includes confirmed viral rebound and failure to achieve confirmed < 400 copies/mL through Week 48 and 144.
|
6% |
4% |
10% |
8% |
|
Rebound |
5% |
3% |
8% |
7% |
|
Never suppressed |
0% |
1% |
0% |
0% |
|
Added an antiretroviral agent |
1% |
1% |
2% |
1% |
|
Death |
< 1% |
1% |
< 1% |
2% |
|
Discontinued due to adverse event |
6% |
6% |
8% |
13% |
|
Discontinued for other reasons Includes lost to follow-up, subject’s withdrawal, noncompliance, protocol violation and other reasons.
|
8% |
7% |
14% |
15% |
Achievement of plasma HIV-1 RNA concentrations of < 400 copies/mL at Week 144 was similar between the two treatment groups for the population stratified at baseline on the basis of HIV-1 RNA concentration (> or ≤ 100,000 copies/mL) and CD4+ cell count (< or ≥ 200 cells/mm3). Through 144 weeks of therapy, 62% and 58% of subjects in the TDF and d4T arms, respectively, achieved and maintained confirmed HIV-1 RNA < 50 copies/mL. The mean increase from baseline in CD4+ cell count was 263 cells/mm3 for the TDF arm and 283 cells/mm3 for the d4T arm.
Through 144 weeks, 11 subjects in the TDF group and 9 subjects in the d4T group experienced a new CDC Class C event.
Lamivudine
Body as a Whole: redistribution/accumulation of body fat [see Warnings and Precautions (5.15) ].
Endocrine and Metabolic: hyperglycemia.
General: weakness.
Hemic and Lymphatic: anemia (including pure red cell aplasia and severe anemias progressing on therapy).
Hepatic and Pancreatic: lactic acidosis and hepatic steatosis, posttreatment exacerbation of hepatitis B [see Boxed Warning, Warnings and Precautions (5.1, 5.2)].
Hypersensitivity: anaphylaxis, urticaria.
Musculoskeletal: muscle weakness, CPK elevation, rhabdomyolysis.
Skin: Alopecia, pruritus.
7.8 Sorbitol
Coadministration of single doses of 3TC and sorbitol resulted in a sorbitol dose-dependent reduction in 3TC exposures. When possible, avoid use of sorbitol-containing medicines with 3TC [see Clinical Pharmacology (12.3)].
Pancreatitis
Pancreatitis, which has been fatal in some cases, has been observed in antiretroviral nucleoside-experienced pediatric subjects receiving 3TC alone or in combination with other antiretroviral agents [see Warnings and Precautions (5.10) ].
Risk Summary
There are retrospective case reports of neural tube defects in infants whose mothers were exposed to EFV-containing regimens in the first trimester of pregnancy.
Although a causal relationship has not been established between exposure to EFV in the first trimester and neural tube defects, similar malformations have been observed in studies conducted in monkeys at doses similar to the human dose. In addition, fetal and embryonic toxicities occurred in rats, at a dose ten times less than the human exposure at recommended clinical dose. Because of the potential risk of neural tube defects, EFV should not be used in the first trimester of pregnancy. Advise pregnant women of the potential risk to a fetus.
Prospective pregnancy data from the APR are not sufficient to adequately assess this risk of birth defects or miscarriage. EFV and 3TC have been evaluated in a limited number of women as reported to the APR. Available data from the APR show no difference in the risk of major birth defects for EFV and 3TC compared to the background rate for major birth defects of 2.7% in the U.S. reference population of the Metropolitan Atlanta Congenital Defects Program (MACDP).
Available data from the APR also show no increase in the overall risk of major birth defects with first trimester exposure for TDF (2.1%) compared with the background rate for major birth defects of 2.7% in a U.S. reference population of the MACDP (see Data).
3TC produced embryonic toxicity in rabbits at a dose that produced similar human exposures as the recommended clinical dose. The relevance of animal findings to human pregnancy registry data is not known.
The rate of miscarriage is not reported in the APR. The estimated background rate of miscarriage in clinically recognized pregnancies in the U.S. general population is 15% to 20%. The background risk for major birth defects and miscarriage for the indicated population is unknown. The APR uses the MACDP as the U.S. reference population for birth defects in the general population. The MACDP evaluates women and infants from a limited geographic area and does not include outcomes for births that occurred at less than 20 weeks’ gestation.
10 Overdosage (10 OVERDOSAGE)
If overdose occurs, the patient must be monitored for evidence of toxicity, and standard supportive treatment applied as necessary.
Efavirenz: Some patients accidentally taking 600 mg twice daily have reported increased nervous system symptoms. One patient experienced involuntary muscle contractions.
Treatment of overdose with EFV should consist of general supportive measures, including monitoring of vital signs and observation of the patient’s clinical status. Administration of activated charcoal may be used to aid removal of unabsorbed drug. There is no specific antidote for overdose with efavirenz. Since efavirenz is highly protein bound, dialysis is unlikely to significantly remove the drug from blood.
Lamivudine: There is no known specific treatment for overdose with 3TC. If overdose occurs, the patient should be monitored and standard supportive treatment applied as required because a negligible amount of 3TC was removed via (4-hour) hemodialysis, continuous ambulatory peritoneal dialysis, and automated peritoneal dialysis, it is not known if continuous hemodialysis would provide clinical benefit in a 3TC overdose event.
Tenofovir Disoproxil Fumarate: Limited clinical experience at doses higher than the therapeutic dose of TDF 300 mg is available.
Tenofovir is efficiently removed by hemodialysis with an extraction coefficient of approximately 54%. Following a single 300 mg dose of tenofovir disoproxil fumarate, a 4-hour hemodialysis session removed approximately 10% of the administered tenofovir dose.
Contraception
Females of reproductive potential should use effective contraception during treatment with SYMFI and for 12 weeks after discontinuing SYMFI due to the long half-life of EFV. Barrier contraception should always be used in combination with other methods of contraception. Hormonal methods that contain progesterone may have decreased effectiveness [see Drug Interactions (7.5)].
11 Description (11 DESCRIPTION)
SYMFI tablets contain efavirenz (EFV), an HIV-1 specific, non-nucleoside, reverse transcriptase inhibitor (NNRTI), lamivudine (also known as 3TC), a synthetic nucleoside analogue with activity against HIV-1 and tenofovir disoproxil fumarate (TDF) (a prodrug of tenofovir), a fumaric acid salt of bis-isopropoxycarbonyloxymethyl ester derivative of tenofovir. TDF is converted in vivo to tenofovir, an acyclic nucleoside phosphonate (nucleotide) analog of adenosine 5’-monophosphate. Tenofovir exhibits activity against HIV-1 reverse transcriptase.
SYMFI tablets are for oral administration. Each film-coated tablet contains 600 mg of efavirenz, 300 mg of lamivudine and 300 mg of tenofovir disoproxil fumarate, which is equivalent to 245 mg of tenofovir disoproxil, and the following inactive ingredients: croscarmellose sodium, hydroxypropyl cellulose, lactose monohydrate, magnesium stearate, microcrystalline cellulose, polyethylene glycol, polyvinyl alcohol, sodium chloride, sodium lauryl sulfate, talc and titanium dioxide.
Efavirenz: The chemical name of efavirenz is (4S)-6-chloro-4-(cyclopropylethynyl)-1,4-dihydro-4-(trifluoromethyl)-2H-3,1-benzoxazin-2-one. Its molecular formula is C14H9ClF3NO2 and its structural formula is:
Efavirenz is a white to slightly pink crystalline powder with a molecular mass of 315.68. It is soluble in methanol and practically insoluble in water (< 10 microgram/mL).
Lamivudine: The chemical name of lamivudine is (-)-1-[(2R,5S)-2-(Hydroxymethyl)-1,3-oxathiolan-5-yl]cytosine. Lamivudine is the (-)enantiomer of a dideoxy analogue of cytidine. Lamivudine has also been referred to as (-)2′,3′-dideoxy, 3′-thiacytidine. It has a molecular formula of C8H11N3O3S and a molecular weight of 229.26 g per mol. It has the following structural formula:
Lamivudine is a white to off-white solid with a solubility of approximately 70 mg per mL in water at 20°C.
Tenofovir Disoproxil Fumarate: The chemical name of tenofovir DF is 9-[(R)-2-[[Bis[[(isopropoxycarbonyl)oxy]methoxy]phosphinyl]methoxy]propyl]adenine fumarate (1:1). It has a molecular formula of C19H30N5O10P•C4H4O4 and a molecular weight of 635.51. It has the following structural formula:
Tenofovir DF is a white to off-white powder with a solubility of 13.4 mg/mL in distilled water at 25°C. It has an octanol/phosphate buffer (pH 6.5) partition coefficient (log p) of 1.25 at 25°C.
Interferon Alfa
There was no significant pharmacokinetic interaction between 3TC and interferon alfa in a trial of 19 healthy male subjects.
5.11 Convulsions
Convulsions have been observed in patients receiving EFV, generally in the presence of known medical history of seizures [see Nonclinical Toxicology (13.2)]. Caution should be taken in any patient with a history of seizures. Patients who are receiving concomitant anticonvulsant medications primarily metabolized by the liver, such as phenytoin and phenobarbital, may require periodic monitoring of plasma levels [see Drug Interactions (7.5)].
5.10 Pancreatitis
In pediatric patients with a history of prior antiretroviral nucleoside exposure, a history of pancreatitis, or other significant risk factors for the development of pancreatitis, 3TC, a component of SYMFI, should be used with caution. Treatment with SYMFI should be stopped immediately if clinical signs, symptoms, or laboratory abnormalities suggestive of pancreatitis occur [see Adverse Reactions (6.1)].
8.4 Pediatric Use
The safety and effectiveness of SYMFI as a fixed-dose tablet in pediatric patients infected with HIV-1 and weighing at least 40 kg have been established based on clinical studies using the individual components (efavirenz, lamivudine, and tenofovir disoproxil fumarate).
8.5 Geriatric Use
Clinical studies of SYMFI did not include sufficient numbers of subjects aged 65 and over to determine whether they respond differently from younger subjects. In general, caution should be exercised in the administration of 3TC in elderly patients reflecting the greater frequency of decreased hepatic, renal, or cardiac function, and of concomitant disease or other drug therapy.
Pregnancy Testing
Females of reproductive potential should undergo pregnancy testing before initiation of SYMFI.
5.9 Hepatotoxicity
Postmarketing cases of hepatitis, including fulminant hepatitis progressing to liver failure requiring transplantation or resulting in death, have been reported in patients treated with EFV. Reports have included patients with underlying hepatic disease, including coinfection with hepatitis B or C, and patients without pre-existing hepatic disease or other identifiable risk factors.
EFV, a component of SYMFI, is not recommended for patients with moderate or severe hepatic impairment. Careful monitoring is recommended for patients with mild hepatic impairment receiving EFV [see Adverse Reactions (6.1) and Use in Specific Populations (8.7)].
Monitoring of liver enzymes before and during treatment is recommended for all patients [see Dosage and Administration (2.1)]. Consider discontinuing SYMFI in patients with persistent elevations of serum transaminases to greater than five times the upper limit of the normal range.
Discontinue SYMFI if elevation of serum transaminases is accompanied by clinical signs or symptoms of hepatitis or hepatic decompensation.
Geriatric Patients
The pharmacokinetics of 3TC and TDF have not been studied in patients over 65 years of age.
4 Contraindications (4 CONTRAINDICATIONS)
SYMFI is contraindicated:
-
•in patients with a previous hypersensitivity reaction (e.g., Stevens-Johnson syndrome, erythema multiforme, or toxic skin eruptions) to any of the components contained in the formulation [see Warnings and Precautions (5.8)].
-
•when coadministered with elbasvir and grazoprevir [see Warnings and Precautions (5.3) and Drug Interactions (7.5)].
6 Adverse Reactions (6 ADVERSE REACTIONS)
The following adverse reactions are discussed in other sections of the labeling:
-
•Exacerbations of Hepatitis B [see Boxed Warning, Warnings and Precautions (5.1)].
-
•Lactic Acidosis/Severe Hepatomegaly with Steatosis [see Warnings and Precautions (5.2) ].
-
•New Onset or Worsening Renal Impairment [see Warnings and Precautions (5.4)].
-
•Psychiatric Symptoms [see Warnings and Precautions (5.5)].
-
•Nervous System Symptoms [see Warnings and Precautions (5.6)].
-
•Skin and Systemic Hypersensitivity Reaction [see Warnings and Precautions (5.8)].
-
•Hepatotoxicity [see Warnings and Precautions (5.9)].
-
•Pancreatitis [see Warnings and Precautions (5.10) ].
-
•Bone Loss and Mineralization Effects [see Warnings and Precautions (5.13) ].
-
•Immune Reconstitution Syndrome [see Warnings and Precautions (5.14) ].
-
•Fat Redistribution [see Warnings and Precautions (5.15) ].
7 Drug Interactions (7 DRUG INTERACTIONS)
-
•SYMFI should not be administered with other antiretroviral medications for the treatment of HIV-1 infection. (7.1)
-
•Coadministration of SYMFI can alter the concentrations of other drugs and other drugs may alter the concentration of SYMFI. The potential for drug-drug interactions should be considered before and during therapy. (5.3, 7)
8.6 Renal Impairment
SYMFI is not recommended for patients with impaired renal function (i.e., creatinine clearance less than 50 mL/min) or patients with end-stage renal disease (ESRD) requiring hemodialysis because it is a fixed-dose combination formulation that cannot be adjusted [see Dosage and Administration (2.3)].
Sorbitol (excipient) (Sorbitol (Excipient))
3TC and sorbitol solutions were coadministered to 16 healthy adult subjects in an open-label, randomized-sequence, 4-period, crossover trial. Each subject received a single 300-mg dose of 3TC oral solution alone or coadministered with a single dose of 3.2 grams, 10.2 grams, or 13.4 grams of sorbitol in solution. Coadministration of 3TC with sorbitol resulted in dose-dependent decreases of 20%, 39%, and 44% in the AUC(0-24), 14%, 32%, and 36% in the AUC(∞), and 28%, 52%, and 55% in the Cmax of lamivudine, respectively.
12.3 Pharmacokinetics
The effect of food on SYMFI has not been evaluated.
5.12 Lipid Elevations
Treatment with EFV has resulted in increases in the concentration of total cholesterol and triglycerides. Cholesterol and triglyceride testing should be performed before initiating EFV therapy and at periodic intervals during therapy.
5.16 Qtc Prolongation (5.16 QTc Prolongation)
QTc prolongation has been observed with the use of EFV [see Drug Interactions (7.2, 7.5) and Clinical Pharmacology (12.2)]. Consider alternatives to products containing EFV when coadministered with a drug with a known risk of Torsade de Pointes or when administered to patients at higher risk of Torsade de Pointes.
8.7 Hepatic Impairment
SYMFI is not recommended for patients with moderate or severe hepatic impairment because there are insufficient data to determine whether dose adjustment is necessary. Patients with mild hepatic impairment may be treated with SYMFI without any adjustment in dose [see Dosage and Administration (2.4), Warnings and Precautions (5.9) and Clinical Pharmacology (12.3) ].
Mineralization Defects
Cases of osteomalacia associated with proximal renal tubulopathy, manifested as bone pain or pain in extremities and which may contribute to fractures, have been reported in association with TDF use [see Adverse Reactions (6.2)]. Arthralgia and muscle pain or weakness have also been reported in cases of proximal renal tubulopathy. Hypophosphatemia and osteomalacia secondary to proximal renal tubulopathy should be considered in patients at risk of renal dysfunction who present with persistent or worsening bone or muscle symptoms while receiving TDF-containing products [see Warnings and Precautions (5.4)].
1 Indications and Usage (1 INDICATIONS AND USAGE)
SYMFI® (efavirenz, lamivudine and tenofovir disoproxil fumarate) is indicated as a complete regimen for the treatment of human immunodeficiency virus type 1 (HIV-1) infection in adult and pediatric patients weighing at least 40 kg.
5.15 Fat Redistribution
In HIV-infected patients, redistribution/accumulation of body fat including central obesity, dorsocervical fat enlargement (buffalo hump), peripheral wasting, facial wasting, breast enlargement, and “cushingoid appearance” have been observed in patients receiving combination antiretroviral therapy. The mechanism and long-term consequences of these events are currently unknown. A causal relationship has not been established.
7.2 Qt Prolonging Drugs (7.2 QT Prolonging Drugs)
There is limited information available on the potential for a pharmacodynamic interaction between EFV and drugs that prolong the QTc interval. QTc prolongation has been observed with the use of EFV [see Clinical Pharmacology (12.2)]. Consider alternatives to EFV when coadministered with a drug with a known risk of Torsade de Pointes.
12.1 Mechanism of Action
SYMFI is a fixed-dose combination of antiviral drugs EFV, 3TC, and TDF with antiviral activity against HIV-1 [see Microbiology (12.4)].
5.5 Psychiatric Symptoms
Serious psychiatric adverse experiences have been reported in patients treated with EFV, a component of SYMFI. In controlled trials of 1008 patients treated with regimens containing EFV for a mean of 2.1 years and 635 patients treated with control regimens for a mean of 1.5 years, the frequency (regardless of causality) of specific serious psychiatric events among patients who received EFV or control regimens, respectively, were severe depression (2.4%, 0.9%), suicidal ideation (0.7%, 0.3%), nonfatal suicide attempts (0.5%, 0), aggressive behavior (0.4%, 0.5%), paranoid reactions (0.4%, 0.3%), and manic reactions (0.2%, 0.3%). When psychiatric symptoms similar to those noted above were combined and evaluated as a group in a multifactorial analysis of data from a study using EFV 600 mg, treatment with EFV was associated with an increase in the occurrence of these selected psychiatric symptoms. Other factors associated with an increase in the occurrence of these psychiatric symptoms were history of injection drug use, psychiatric history, and receipt of psychiatric medication at study entry; similar associations were observed in both the EFV and control treatment groups. In a study using EFV 600 mg, onset of new serious psychiatric symptoms occurred throughout the study for both EFV-treated and control-treated patients. One percent of EFV-treated patients discontinued or interrupted treatment because of one or more of these selected psychiatric symptoms.
There have also been occasional postmarketing reports of death by suicide, delusions, psychosis-like behavior, although a causal relationship to the use of EFV cannot be determined from these reports [see Adverse Reactions (6.2)]. Postmarketing cases of catatonia have also been reported and may be associated with increased efavirenz exposure. Patients with serious psychiatric adverse experiences should seek immediate medical evaluation to assess the possibility that the symptoms may be related to the use of EFV, and if so, to determine whether the risks of continued therapy outweigh the benefits.
Efavirenz and Lamivudine
There are no significant or clinically relevant racial differences in EFV and 3TC pharmacokinetics.
Laboratory Abnormalities
Table 2 provides a list of laboratory abnormalities (Grades 3-4) observed in Trial 903. With the exception of fasting cholesterol and fasting triglyceride elevations that were more common in the d4T group (40% and 9%) compared with the TDF group (19% and 1%) respectively, laboratory abnormalities observed in this trial occurred with similar frequency in the TDF and d4T treatment arms.
|
TDF + 3TC + EFV |
d4T + 3TC + EFV |
|
|
N = 299 |
N = 301 |
|
|
Any ≥ Grade 3 Laboratory Abnormality |
36% |
42% |
|
Fasting Cholesterol (> 240 mg/dL) |
19% |
40% |
|
Creatine Kinase (M: > 990 U/L; F: > 845 U/L) |
12% |
12% |
|
Serum Amylase (> 175 U/L) |
9% |
8% |
|
AST (M: > 180 U/L; F: > 170 U/L) |
5% |
7% |
|
ALT (M: > 215 U/L; F: > 170 U/L) |
4% |
5% |
|
Hematuria (> 100 RBC/HPF) |
7% |
7% |
|
Neutrophils (< 750/mm3) |
3% |
1% |
|
Fasting Triglycerides (> 750 mg/dL) |
1% |
9% |
5.7 Embryo Fetal Toxicity (5.7 Embryo-Fetal Toxicity)
EFV, a component of SYMFI, may cause fetal harm when administered during the first trimester to a pregnant woman. Advise females of reproductive potential who are receiving EFV to avoid pregnancy [see Use in Specific Populations (8.1, 8.3)].
Cardiac Electrophysiology
The effect of EFV on the QTc interval was evaluated in an open-label, positive and placebo-controlled, fixed single sequence 3-period, 3-treatment crossover QT study in 58 healthy subjects enriched for CYP2B6 polymorphisms. The mean Cmax of EFV in subjects with CYP2B6 *6/*6 genotype following the administration of 600 mg daily dose for 14 days was 2.25-fold the mean Cmax observed in subjects with CYP2B6 *1/*1 genotype. A positive relationship between EFV concentration and QTc prolongation was observed. Based on the concentration-QTc relationship, the mean QTc prolongation and its upper bound 90% confidence interval are 8.7 ms and 11.3 ms in subjects with CYP2B6*6/*6 genotype following the administration of 600 mg daily dose for 14 days [see Warnings and Precautions (5.16) ].
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
-
•Lactic Acidosis/Severe Hepatomegaly with Steatosis: Discontinue treatment in patients who develop symptoms or laboratory findings suggestive of lactic acidosis or pronounced hepatotoxicity. (5.2)
-
•New Onset or Worsening Renal Impairment: Can include acute renal failure and Fanconi syndrome. Avoid administering SYMFI with concurrent or recent use of nephrotoxic drugs. (5.4)
-
•Serious Psychiatric Symptoms:Immediate medical evaluation is recommended for serious psychiatric symptoms such as severe depression or suicidal ideation. (5.5)
-
•Nervous System Symptoms (NSS): NSS are frequent, usually begin 1 to 2 days after initiating therapy and resolve in 2 to 4 weeks. Dosing at bedtime may improve tolerability. NSS are not predictive of onset of psychiatric symptoms. (5.6)
-
•Rash: Rash usually begins within 1 to 2 weeks after initiating therapy and resolves within 4 weeks. Discontinue if severe rash develops. (5.8)
-
•Hepatotoxicity: Monitor liver function tests before and during treatment in patients with underlying hepatic disease, including hepatitis B or C coinfection, marked transaminase elevations, or who are taking medications associated with liver toxicity. Among reported cases of hepatic failure, a few occurred in patients with no pre-existing hepatic disease. (5.9, 8.7)
-
•Pancreatitis: Use with caution in pediatric patients with a history of pancreatitis or other significant risk factors for pancreatitis. Discontinue SYMFI as clinically appropriate. (5.10)
-
•Convulsions: Use caution in patients with a history of seizures. (5.11)
-
•Lipids: Total cholesterol and triglyceride elevations. Monitor before therapy and periodically thereafter. (5.12)
-
•Decreases in Bone Mineral Density (BMD): Observed in HIV-infected patients. Consider assessment of BMD in patients with a history of pathologic fracture or other risk factors for osteoporosis or bone loss. (5.13)
-
•Immune Reconstitution Syndrome: Observed in HIV-infected patients. May necessitate further evaluation and treatment. (5.14)
-
•Redistribution/Accumulation of Body Fat: Observed in HIV-infected patients receiving antiretroviral combination therapy. (5.15)
Bone Mineral Density (bmd) (Bone Mineral Density (BMD))
In clinical trials in HIV-1-infected adults, TDF was associated with slightly greater decreases in BMD and increases in biochemical markers of bone metabolism, suggesting increased bone turnover relative to comparators [see Adverse Reactions (6.1)]. Serum parathyroid hormone levels and 1,25 Vitamin D levels were also higher in subjects receiving TDF.
The effects of TDF-associated changes in BMD and biochemical markers on long-term bone health and future fracture risk in adults and pediatric subjects 2 years and older are unknown. The long-term effect of lower spine and total body BMD on skeletal growth in pediatric patients, and in particular, the effects of long-duration exposuire in younger children is unknown.
Although the effect of supplementation with calcium and vitamin D was not studied, such supplementation may be beneficial. Assessment of BMD should be considered for adult and pediatric patients who have a history of pathologic bone fracture or other risk factors for osteoporosis or bone loss. If bone abnormalities are suspected then appropriate consultation should be obtained.
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
-
•Testing: Prior to initiation and during treatment with SYMFI, patients should be tested for hepatitis B virus infection, and estimated creatinine clearance, urine glucose, and urine protein should be obtained. (2.1)
-
•Recommended dose: One tablet taken orally once daily on an empty stomach, preferably at bedtime. (2.2)
-
•Renal Impairment: Not recommended in patients with CrCL less than 50 mL/min or patients with end-stage renal disease requiring hemodialysis. (2.3)
-
•Hepatic Impairment: Not recommended for patients with moderate or severe hepatic impairment. Use caution in patients with mild hepatic impairment. (2.4)
5.6 Nervous System Symptoms
Fifty-three percent (531/1008) of patients receiving EFV, a component of SYMFI, in controlled trials reported central nervous system symptoms (any grade, regardless of causality) compared to 25% (156/635) of patients receiving control regimens. These symptoms included, but were not limited to, dizziness (28.1% of the 1008 patients), insomnia (16.3%), impaired concentration (8.3%), somnolence (7.0%), abnormal dreams (6.2%), and hallucinations (1.2%). These symptoms were severe in 2.0% of patients and 2.1% of patients discontinued therapy as a result. These symptoms usually begin during the first or second day of therapy and generally resolve after the first 2 to 4 weeks of therapy. After 4 weeks of therapy, the prevalence of nervous system symptoms of at least moderate severity ranged from 5% to 9% in patients treated with regimens containing EFV and from 3% to 5% in patients treated with a control regimen. Inform patients that these common symptoms were likely to improve with continued therapy and were not predictive of subsequent onset of the less frequent psychiatric symptoms [see Warnings and Precautions (5.5)]. Dosing at bedtime may improve the tolerability of these nervous system symptoms [see Dosage and Administration (2.2)].
Late-onset neurotoxicity, including ataxia and encephalopathy (impaired consciousness, confusion, psychomotor slowing, psychosis, delirium), may occur months to years after beginning efavirenz therapy. Some events of late-onset neurotoxicity have occurred in patients with CYP2B6 genetic polymorphisms which are associated with increased efavirenz levels despite daily dosages of 600 mg of efavirenz. Patients presenting with signs and symptoms of serious neurologic adverse experiences should be evaluated promptly to assess the possibility that these events may be related to efavirenz use, and whether discontinuation of SYMFI is warranted.
Pregnancy Exposure Registry
There is a pregnancy exposure registry that monitors pregnancy outcomes in women exposed to SYMFI during pregnancy. Healthcare providers are encouraged to register patients by calling the Antiretroviral Pregnancy Registry (APR) at 1-800-258-4263.
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
Tablets: 600 mg of efavirenz, 300 mg of lamivudine, and 300 mg of tenofovir disoproxil fumarate (equivalent to 245 mg of tenofovir disoproxil).
The tablets are white, film-coated, capsule shaped, debossed with M 152 on one side of the tablet and plain on the other side.
6.2 Postmarketing Experience
The following adverse reactions have been identified during post-approval use for each of the individual components of SYMFI (EFV, 3TC, and TDF). Because these reactions are reported voluntarily from a population of unknown size, it is not always possible to reliably estimate their frequency or establish causal relationship to drug exposure. These reactions have been chosen for inclusion due to a combination of their seriousness, frequency of reporting, or potential causal connection to EFV, 3TC, and TDF.
8 Use in Specific Populations (8 USE IN SPECIFIC POPULATIONS)
-
•Pregnancy: Women should avoid pregnancy during EFV therapy, a component of SYMFI, and for 12 weeks after discontinuation. (5.7, 8.1, 8.3)
-
•Lactation: Breastfeeding not recommended due to potential for HIV transmission. (8.2)
-
•Females and Males of Reproductive Potential: Pregnancy testing and contraception are recommended. (8.3)
Tenofovir Disoproxil Fumarate
Immune System Disorders: allergic reaction, including angioedema.
Metabolism and Nutrition Disorders: lactic acidosis, hypokalemia, hypophosphatemia.
Respiratory, Thoracic, and Mediastinal Disorders: dyspnea.
Gastrointestinal Disorders: pancreatitis, increased amylase, abdominal pain.
Renal and Urinary Disorders: renal insufficiency, acute renal failure, renal failure, acute tubular necrosis, Fanconi syndrome, proximal renal tubulopathy, interstitial nephritis (including acute cases), nephrogenic diabetes insipidus, renal insufficiency, increased creatinine, proteinuria, polyuria [see Warnings and Precautions (5.4)].
Hepatobiliary Disorders: hepatic steatosis, hepatitis, increased liver enzymes (most commonly AST, ALT gamma GT).
Skin and Subcutaneous Tissue Disorders: rash.
Musculoskeletal and Connective Tissue Disorders: rhabdomyolysis, osteomalacia (manifested as bone pain and which may contribute to fractures), muscular weakness, myopathy.
General Disorders and Administration Site Conditions: asthenia.
The following adverse reactions, listed under the body system headings above, may occur as a consequence of proximal renal tubulopathy: rhabdomyolysis, osteomalacia, hypokalemia, muscular weakness, myopathy, hypophosphatemia.
Trimethoprim/sulfamethoxazole (Trimethoprim/Sulfamethoxazole)
3TC and TMP/SMX were coadministered to 14 HIV-1-positive subjects in a single-center, open-label, randomized, crossover trial. Each subject received treatment with a single 300-mg dose of 3TC and TMP 160 mg/SMX 800 mg once a day for 5 days with concomitant administration of 3TC 300 mg with the fifth dose in a crossover design. Coadministration of TMP/SMX with 3TC resulted in an increase of 43% ± 23% (mean ± SD) in 3TC AUC∞, a decrease of 29% ± 13% in 3TC oral clearance, and a decrease of 30% ± 36% in 3TC renal clearance. The pharmacokinetic properties of TMP and SMX were not altered by coadministration with 3TC. There is no information regarding the effect on 3TC pharmacokinetics of higher doses of TMP/SMX such as those used in treating PCP.
6.1 Clinical Trials Experience
Because clinical studies are conducted under widely varying conditions, the adverse reaction rates observed in clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
Patients With Renal Impairment (Patients with Renal Impairment)
Assessment of Drug Interactions
[See Drug Interactions (7).]
Changes in Bone Mineral Density
In HIV-1-infected adult subjects in Trial 903, there was a significantly greater mean percentage decrease from baseline in BMD at the lumbar spine in subjects receiving TDF + 3TC + EFV (-2.2% ± 3.9) compared with subjects receiving d4T + 3TC + EFV (-1.0% ± 4.6) through 144 weeks. Changes in BMD at the hip were similar between the two treatment groups (-2.8% ± 3.5 in the TDF group vs. -2.4% ± 4.5 in the d4T group). In both groups, the majority of the reduction in BMD occurred in the first 24-48 weeks of the trial and this reduction was sustained through Week 144. Twenty-eight percent of TDF-treated subjects vs. 21% of the d4T-treated subjects lost at least 5% of BMD at the spine or 7% of BMD at the hip. Clinically relevant fractures (excluding fingers and toes) were reported in 4 subjects in the TDF group and 6 subjects in the d4T group. In addition, there were significant increases in biochemical markers of bone metabolism (serum bone-specific alkaline phosphatase, serum osteocalcin, serum C telopeptide, and urinary N telopeptide) and higher serum parathyroid hormone levels and 1,25 Vitamin D levels in the TDF group relative to the d4T group; however, except for bone-specific alkaline phosphatase, these changes resulted in values that remained within the normal range [see Warnings and Precautions (5.13) ].
Treatment Naïve Adult Patients (Treatment-Naïve Adult Patients)
The efficacy of EFV 600 mg, 3TC 300 mg, and TDF 300 mg in the treatment of HIV-1 infection in adults with no antiretroviral treatment history was established in Trial 903.
7.4 Cannabinoid Test Interaction
EFV does not bind to cannabinoid receptors. False-positive urine cannabinoid test results have been reported with some screening assays in uninfected and HIV-infected subjects receiving EFV. Confirmation of positive screening tests for cannabinoids by a more specific method is recommended.
17 Patient Counseling Information (17 PATIENT COUNSELING INFORMATION)
Advise the patient to read the FDA-approved patient labeling (Patient Information).
Drug Interactions: SYMFI may interact with many drugs; therefore, advise patients to report to their healthcare provider the use of any other prescription, nonprescription medication, or herbal products, particularly St. John’s wort [see Contraindications (4) and Drug Interactions (7)].
Post Treatment Acute Exacerbation of Hepatitis B in Patients with HBV Co-Infection: Inform patients that severe acute exacerbations of hepatitis have been reported in patients who are infected with HBV or coinfected with HBV and HIV-1 and have discontinued 3TC and TDF, components of SYMFI. Test patients with HIV-1 for hepatitis B virus (HBV) before initiating antiretroviral therapy. In patients with chronic hepatitis B, it is important to obtain HIV antibody testing prior to initiating 3TC and TDF, components of SYMFI [see Warnings and Precautions (5.1) ].
Lactic Acidosis and Severe Hepatomegaly: Inform patients that lactic acidosis and severe hepatomegaly with steatosis, including fatal cases, have been reported. Treatment with SYMFI should be suspended in any patient who develops clinical symptoms suggestive of lactic acidosis or pronounced hepatotoxicity (including nausea, vomiting, unusual or unexpected stomach discomfort, and weakness) [see Warnings and Precautions (5.2)].
New Onset or Worsening Renal Impairment: Inform patients that renal impairment, including cases of acute renal failure and Fanconi syndrome, has been reported. Advise patients with impaired renal function (i.e., creatinine clearance less than 50 mL/min) or patients with end-stage renal disease (ESRD) requiring hemodialysis to avoid SYMFI with concurrent or recent use of a nephrotoxic agent (e.g., high-dose or multiple NSAIDs) for patients [see Dosage and Administration (2.3), Warnings and Precautions (5.4)].
Psychiatric Symptoms: Inform patients that serious psychiatric symptoms including severe depression, suicide attempts, aggressive behavior, delusions, paranoia, psychosis-like symptoms and catatonia have been reported in patients receiving EFV [see Warnings and Precautions (5.5)]. Advise patients to seek immediate medical evaluation if they experience severe psychiatric adverse experiences. Advise patients to inform their physician of any history of mental illness or substance abuse.
Nervous System Symptoms: Inform patients that central nervous system symptoms (NSS) including dizziness, insomnia, impaired concentration, drowsiness, and abnormal dreams are commonly reported during the first weeks of therapy with EFV, a component of SYMFI [see Warnings and Precautions (5.6)]. Dosing at bedtime may improve the tolerability of these symptoms, which are likely to improve with continued therapy. Alert patients to the potential for additive effects when used concomitantly with alcohol or psychoactive drugs. Instruct patients that if they experience NSS they should avoid potentially hazardous tasks such as driving or operating machinery.
Inform patients that there is a risk of developing late-onset neurotoxicity, including ataxia and encephalopathy, which may occur months to years after beginning efavirenz therapy [see Warnings and Precautions (5.6)].
Embryo-Fetal Toxicity: Advise female patients that EFV, a component of SYMFI may cause fetal harm when administered during the first trimester to a pregnant woman. Advise females of reproductive potential to use effective contraception as well as a barrier method during treatment with SYMFI and for 12 weeks after discontinuation of use. Advise patients to contact their healthcare provider if they plan to become pregnant, become pregnant, or if pregnancy is suspected during treatment with SYMFI [see Warnings and Precautions (5.7), Use in Specific Populations (8.1, 8.3)].
Rash: Inform patients that rash is a common side effect of EFV [see Warnings and Precautions (5.8)]. Rashes usually go away without any change in treatment. However, since rash may be serious, patients should be advised to contact their physician promptly if rash occurs.
Hepatotoxicity: Inform patients to watch for early warning signs of liver inflammation or failure, such as fatigue, weakness, lack of appetite, nausea and vomiting, as well as later signs such as jaundice, confusion, abdominal swelling, and discolored feces and to consult their healthcare provider promptly if such symptoms occur [see Warnings and Precautions (5.9)].
Pancreatitis: Advise patients or guardians to monitor pediatric patients for signs and symptoms of pancreatitis [see Warnings and Precautions (5.10) ].
Convulsions: Advise patients that convulsions have been observed in patients receiving EFV, a component of SYMFI, generally in patients with known medical history of seizures [see Warnings and Precautions (5.11) ].
Lipid Elevations: Advise patients treatment with EFV, a component of SYMFI has resulted in increases in the concentration of total cholesterol and triglycerides [see Warnings and Precautions (5.12) ].
Bone Loss and Mineralization Effects: Inform patients that decreases in bone mineral density have been observed with the use of 3TC and TDF, components of SYMFI, in patients with HIV [see Warnings and Precautions (5.13) ].
Immune Reconstitution Syndrome: Advise patients to inform their healthcare provider immediately of any symptoms of infection, as in some patients with advanced HIV infection, signs and symptoms of inflammation from previous infections may occur soon after anti-HIV treatment is started [see Warnings and Precautions (5.14) ].
Fat Redistribution: Inform patients that redistribution or accumulation of body fat may occur in patients receiving antiretroviral therapy, including SYMFI, and that the cause and long‑term health effects of these conditions are not known at this time [see Warnings and Precautions (5.15) ].
Administration Instructions: Inform patients that it is important to take SYMFI once daily on a regular dosing schedule on an empty stomach, preferably at bedtime, and to avoid missing doses as it can result in development of resistance. Advise patients if a dose is missed, take it as soon as possible unless it is almost time for the next dose. Also advise patients that dosing at bedtime may improve the tolerability of nervous system symptoms [see Dosage and Administration (2.2)].
Pregnancy Registry: Advise patients that there is an antiretroviral pregnancy registry to monitor fetal outcomes in women exposed to SYMFI [see Use in Specific Populations (8.1)].
Lactation: Instruct women with HIV-1 infection not to breastfeed because HIV-1 can be passed to the baby in breast milk [see Use in Specific Populations (8.2)].
SYMFI® is a registered trademark of Mylan Pharmaceuticals Inc.
Other brands listed are the registered trademarks of their respective owners and are not trademarks of Mylan Laboratories Limited or Mylan Pharmaceuticals Inc.
Rx only
Manufactured for:
Mylan Specialty L.P.
Morgantown, WV 26505 U.S.A.
Manufactured by:
Mylan Laboratories Limited
Hyderabad — 500 096, India
7.3 Drugs Affecting Renal Function
Tenofovir is primarily eliminated by the kidneys [see Clinical Pharmacology (12.3)]. Coadministration of EFV/3TC/TDF with drugs that are eliminated by active tubular secretion may increase concentrations of tenofovir and/or the coadministered drug. Some examples include, but are not limited to, acyclovir, cidofovir, ganciclovir, valacyclovir, valganciclovir, aminoglycosides (e.g., gentamicin), and high-dose or multiple NSAIDs [see Warnings and Precautions (5.4)]. Drugs that decrease renal function may increase concentrations of tenofovir.
5.14 Immune Reconstitution Syndrome
Immune reconstitution syndrome has been reported in HIV-infected patients treated with combination antiretroviral therapy, including EFV, 3TC, and TDF. During the initial phase of combination antiretroviral treatment, patients whose immune system responds may develop an inflammatory response to indolent or residual opportunistic infections (such as Mycobacterium avium infection, cytomegalovirus, Pneumocystis jirovecii pneumonia [PCP], or tuberculosis), which may necessitate further evaluation and treatment.
Autoimmune disorders (such as Graves’ disease, polymyositis, Guillain-Barre syndrome, and autoimmune hepatitis) have also been reported to occur in the setting of immune reconstitution; however, the time to onset is more variable, and can occur many months after initiation of treatment.
16 How Supplied/storage and Handling (16 HOW SUPPLIED/STORAGE AND HANDLING)
SYMFI (efavirenz, lamivudine and tenofovir disoproxil fumarate) Tablets 600 mg/300 mg/300 mg are white, film-coated, capsule shaped, debossed with M 152 on one side of the tablet and plain on the other side. They are available as follows:
NDC 49502-475-93
cartons containing bottles of 30 tablets with desiccant, induction seal and child-resistant cap
NDC 49502-475-77
cartons containing bottles of 90 tablets with desiccant, induction seal and child-resistant cap
Store below 30°C (86°F).
Keep the bottle tightly closed.
Dispense in original container.
Do not use if seal over bottle opening is broken or missing.
2.3 Not Recommended in Renal Impairment
Because SYMFI is a fixed-dose combination tablet and cannot be dose adjusted, it is not recommended for patients with impaired renal function (creatinine clearance less than 50 mL/min) or patients with end-stage renal disease (ESRD) requiring hemodialysis [see Use in Specific Populations (8.6)].
Posttreatment Exacerbations of Hepatitis
All patients with HIV-1 should be tested for the presence of chronic hepatitis B virus (HBV) before initiating antiretroviral therapy [see Dosage and Administration (2.1)]. Discontinuation of anti-HBV therapy, including 3TC and TDF, may be associated with severe acute exacerbations of hepatitis B. Patients infected with HBV who discontinue SYMFI should be closely monitored with both clinical and laboratory follow-up for at least several months after stopping treatment. If appropriate, resumption of anti-hepatitis B therapy may be warranted.
5.4 New Onset Or Worsening Renal Impairment (5.4 New Onset or Worsening Renal Impairment)
TDF, a component of SYMFI is principally eliminated by the kidney. Renal impairment, including cases of acute renal failure and Fanconi syndrome (renal tubular injury with severe hypophosphatemia), has been reported with the use of TDF [see Adverse Reactions (6.2)].
Prior to initiation and during use of SYMFI, on a clinically appropriate schedule, assess serum creatinine, estimated creatinine clearance, urine glucose, and urine protein in all patients.
Avoid SYMFI with concurrent or recent use of a nephrotoxic agent (e.g., high-dose or multiple non-steroidal anti-inflammatory drugs [NSAIDs]) [see Drug Interactions (7.3)]. Cases of acute renal failure after initiation of high-dose or multiple NSAIDs have been reported in HIV-infected patients with risk factors for renal dysfunction who appeared stable on TDF. Some patients required hospitalization and renal replacement therapy. Alternatives to NSAIDs should be considered, if needed, in patients at risk for renal dysfunction.
Persistent or worsening bone pain, pain in extremities, fractures and/or muscular pain or weakness may be manifestations of proximal renal tubulopathy and should prompt an evaluation of renal function in patients at risk of renal dysfunction.
Principal Display Panel 600 Mg/300 Mg/300 Mg (PRINCIPAL DISPLAY PANEL - 600 mg/300 mg/300 mg)
NDC 49502-475-93 Rx only
SYMFI®
(efavirenz, lamivudine,
and tenofovir disoproxil
fumarate) tablets
600 mg/300 mg/300 mg*
Note to pharmacist: Do not cover
ALERT box with pharmacy label.
ALERT: Find out about
medicines that should NOT
be taken with SYMFI®.
30 tablets
*Each film-coated tablet contains:
Efavirenz, USP 600 mg
Lamivudine, USP 300 mg
Tenofovir Disoproxil Fumarate 300 mg
(equivalent to 245 mg of tenofovir
disoproxil)
Usual Dosage: See accompanying
prescribing information.
Keep this and all medication
out of the reach of children.
Store below 30°C (86°F).
Dispense only in original container.
Keep container tightly closed.
Manufactured for:
Mylan Specialty L.P.
Morgantown, WV 26505 U.S.A.
Made in India
Code No.: MP/DRUGS/25/1/2014
MS:MXI:47593:1C:R3
Mylan.com
SYMFI® is a registered
trademark of Mylan
Pharmaceuticals Inc.
5.8 Skin and Systemic Hypersensitivity Reaction
In controlled clinical trials, 26% (266/1008) of patients treated with 600 mg EFV experienced new-onset skin rash compared with 17% (111/635) of patients treated in control groups. Rash associated with blistering, moist desquamation, or ulceration occurred in 0.9% (9/1008) of patients treated with EFV. The incidence of Grade 4 rash (e.g., erythema multiforme, Stevens-Johnson syndrome) in patients treated with EFV in all studies and expanded access was 0.1%. Rashes are usually mild-to-moderate maculopapular skin eruptions that occur within the first 2 weeks of initiating therapy with EFV (median time to onset of rash in adults was 11 days) and, in most patients continuing therapy with EFV, rash resolves within 1 month (median duration, 16 days). The discontinuation rate for rash in clinical trials was 1.7% (17/1008).
EFV can generally be reinitiated in patients interrupting therapy because of rash. EFV should be discontinued in patients developing severe rash associated with blistering, desquamation, mucosal involvement, or fever. Appropriate antihistamines and/or corticosteroids may improve the tolerability and hasten the resolution of rash. For patients who have had a life-threatening cutaneous reaction (e.g., Stevens-Johnson syndrome), alternate therapy should be considered [see Contraindications (4)].
8.3 Females and Males of Reproductive Potential
Because of potential teratogenic effects, pregnancy should be avoided in women receiving SYMFI [see Warnings and Precautions (5.7), Use in Specific Populations (8.1)].
7.7 Drugs Inhibiting Organic Cation Transporters
3TC, a component of SYMFI, is predominantly eliminated in the urine by active organic cationic secretion. The possibility of interactions with other drugs administered concurrently should be considered, particularly when their main route of elimination is active renal secretion via the organic cationic transport system (e.g., trimethoprim) [see Clinical Pharmacology (12.3)]. No data are available regarding interactions with other drugs that have renal clearance mechanisms similar to that of 3TC.
7.6 Drugs Without Clinically Significant Interactions (7.6 Drugs without Clinically Significant Interactions)
No dosage adjustment is recommended when SYMFI is administered with the following: aluminum/magnesium hydroxide antacids, azithromycin, cetirizine, famotidine, fluconazole, and lorazepam.
Effect of 3tc On the Pharmacokinetics of Other Agents (Effect of 3TC on the Pharmacokinetics of Other Agents)
Based on in vitro study results, 3TC at therapeutic drug exposures is not expected to affect the pharmacokinetics of drugs that are substrates of the following transporters: organic anion transporter polypeptide 1B1/3 (OATP1B1/3), breast cancer resistance protein (BCRP), P-glycoprotein (P-gp), multidrug and toxin extrusion protein 1 (MATE1), MATE2-K, organic cation transporter 1 (OCT1), OCT2, or OCT3.
Effect of Other Agents On the Pharmacokinetics of 3tc (Effect of Other Agents on the Pharmacokinetics of 3TC)
3TC is a substrate of MATE1, MATE2-K, and OCT2 in vitro. Trimethoprim (an inhibitor of these drug transporters) has been shown to increase 3TC plasma concentrations. This interaction is not considered clinically significant as no dose adjustment of 3TC is needed.
3TC is a substrate of P-gp and BCRP; however, considering its absolute bioavailability (87%), it is unlikely that these transporters play a significant role in the absorption of 3TC. Therefore, coadministration of drugs that are inhibitors of these efflux transporters is unlikely to affect the disposition and elimination of 3TC.
7.1 Not Recommended With Other Antiretroviral Medications (7.1 Not Recommended with Other Antiretroviral Medications)
SYMFI is a complete regimen for the treatment of HIV-1 infection; therefore, it should not be administered with other antiretroviral medications for treatment of HIV-1 infection.
5.2 Lactic Acidosis and Severe Hepatomegaly With Steatosis (5.2 Lactic Acidosis and Severe Hepatomegaly with Steatosis)
Lactic acidosis and severe hepatomegaly with steatosis, including fatal cases, have been reported with the use of nucleoside analogs and other antiretrovirals. Female sex and obesity may be risk factors for the development of lactic acidosis and severe hepatomegaly with steatosis in patients treated with antiretroviral nucleoside analogues. Treatment should be suspended in any patient who develops clinical or laboratory findings suggestive of lactic acidosis or pronounced hepatotoxicity, which may include hepatomegaly and steatosis even in the absence of marked transaminase elevations.
Important Differences Among Lamivudine Containing Products (Important Differences Among Lamivudine-Containing Products)
SYMFI tablets contain a higher dose of the same active ingredient, 3TC, than EPIVIR-HBV® tablets. EPIVIR-HBV was developed for patients with chronic hepatitis B. The formulation and dosage of 3TC in EPIVIR-HBV are not appropriate for patients co-infected with HIV-1 and HBV. Safety and efficacy of 3TC have not been established for treatment of chronic hepatitis B in patients co-infected with HIV-1 and HBV.
If treatment with EPIVIR-HBV, TDF, or a tenofovir alafenamide (TAF)-containing product is prescribed for chronic hepatitis B for a patient with unrecognized or untreated HIV-1 infection, rapid emergence of HIV-1 resistance is likely to result because of the subtherapeutic dose and the inappropriateness of monotherapy HIV-1 treatment.
Warning: Post Treatment Acute Exacerbations of Hepatitis B (WARNING: POST TREATMENT ACUTE EXACERBATIONS OF HEPATITIS B)
Severe acute exacerbations of hepatitis B have been reported in patients who are co-infected with hepatitis B virus (HBV) and human immunodeficiency virus (HIV-1) and have discontinued lamivudine or tenofovir disoproxil fumarate, two components of SYMFI. Monitor hepatic function closely in these patients and, if appropriate, initiate anti-hepatitis B treatment [see Warnings and Precautions (5.1) ].
2.4 Not Recommended in Moderate to Severe Hepatic Impairment
SYMFI is not recommended in patients with moderate or severe hepatic impairment (Child-Pugh B or C) [see Warnings and Precautions (5.9) and Use in Specific Populations (8.7)].
7.5 Established and Other Potentially Significant Interactions
EFV has been shown in vivo to induce CYP3A and CYP2B6. Other compounds that are substrates of CYP3A or CYP2B6 may have decreased plasma concentrations when coadministered with EFV.
Drugs that induce CYP3A activity (e.g., phenobarbital, rifampin, rifabutin) would be expected to increase the clearance of EFV resulting in lowered plasma concentrations.
No drug interaction studies have been conducted using SYMFI. However, drug interaction studies have been conducted with the individual components of SYMFI (EFV, 3TC, and TDF) [see Clinical Pharmacology (12.3)].
Drug interactions with EFV are summarized in Table 3 [for pharmacokinetics data see Clinical Pharmacology (12.3, Tables 6 and 7)]. This table includes potentially significant interactions, but is not all inclusive.
| This table is not all-inclusive. | ||
|
Concomitant Drug Class: Drug Name |
Effect |
Clinical Comment |
|
Anticoagulant: Warfarin |
↑ or ↓ warfarin |
Monitor INR and adjust warfarin dosage if necessary. |
|
Anticonvulsants: Carbamazepine |
↓ carbamazepine The interaction between EFV and the drug was evaluated in a clinical study. All other drug interactions shown are predicted.
↓ EFV* |
There are insufficient data to make a dose recommendation for EFV. Alternative anticonvulsant treatment should be used. |
|
Phenytoin Phenobarbital |
↓ anticonvulsant ↓ EFV |
Monitor anticonvulsant plasma levels periodically because of potential for reduction in anticonvulsant and/or EFV plasma levels. |
|
Antidepressants: Bupropion |
↓ bupropion |
Increases in bupropion dosage should be guided by clinical response. Bupropion dose should not exceed the maximum recommended dose.
|
|
Sertraline |
↓ sertraline |
Increases in sertraline dosage should be guided by clinical response. |
|
Antifungals: Itraconazole
Ketoconazole |
↓ itraconazole ↓ hydroxyitraconazole ↓ ketoconazole |
Consider alternative antifungal treatment because no dose recommendation for itraconazole or ketoconazole can be made.
|
|
Posaconazole |
↓ posaconazole |
Avoid concomitant use unless the benefit outweighs the risks. |
|
Anti-infective: Clarithromycin |
↓ clarithromycin ↑ 14-OH metabolite |
Consider alternatives to macrolide antibiotics because of the risk of QT interval prolongation. |
|
Antimycobacterial: Rifabutin |
↓ rifabutin |
Increase daily dose of rifabutin by 50%. Consider doubling the rifabutin dose in regimens where rifabutin is given 2 or 3 times a week.
|
|
Rifampin |
↓ EFV |
Increase EFV total daily dose to 800 mg once daily when coadministered with rifampin to patients weighing 50 kg or more. |
|
Antimalarials: Artemether/lumefantrine |
↓ artemether ↓ dihydroartemisinin ↓ lumefantrine |
Consider alternatives to artemether/lumefantrine because of the risk of QT interval prolongation [see Warnings and Precautions (5.16) ].
|
|
Atovaquone/ proguanil |
↓ atovaquone ↓ proguanil |
Concomitant administration is not recommended. |
|
Calcium channel blockers: Diltiazem |
↓ diltiazem ↓ desacetyl diltiazem ↓ N-monodesmethyldiltiazem |
Diltiazem dose adjustments should be guided by clinical response (refer to the full prescribing information for diltiazem).
|
|
Others (e.g., felodipine, nicardipine, nifedipine, verapamil) |
↓ calcium channel blocker |
When coadministered with EFV, dosage adjustment of calcium channel blocker may be needed and should be guided by clinical response (refer to the full prescribing information for the calcium channel blocker). |
|
HMG-CoA reductase inhibitors: Atorvastatin Pravastatin Simvastatin |
↓ atorvastatin ↓ pravastatin ↓ simvastatin |
Plasma concentrations of atorvastatin, pravastatin, and simvastatin decreased. Consult the full prescribing information for the HMG-CoA reductase inhibitor for guidance on individualizing the dose. |
|
Hepatitis C antiviral agents: Boceprevir |
↓ boceprevir |
Concomitant administration of boceprevir is not recommended. |
|
Elbasvir/Grazoprevir |
↓ elbasvir ↓ grazoprevir |
Coadministration of EFV with elbasvir/grazoprevir is contraindicated [see Contraindications (4)] because it may lead to loss of virologic response to elbasvir/grazoprevir.
|
|
Pibrentasvir/Glecaprevir |
↓ pibrentasvir ↓ glecaprevir |
Coadministration of EFV is not recommended because it may lead to reduced therapeutic effect of pibrentasvir/glecaprevir.
|
|
Simeprevir |
↓ simeprevir ↔ EFV |
Concomitant administration of simeprevir is not recommended.
|
|
Velpatasvir/Sofosbuvir |
↓ velpatasvir |
Coadministration of EFV and sofosbuvir/velpatasvir is not recommended because it may result in loss of therapeutic effect of sofosbuvir/velpatasvir.
|
|
Velpatasvir/Sofosbuvir/ |
↓ velpatasvir ↓ voxilaprevir |
Coadministration of EFV and sofosbuvir/velpatasvir/voxilaprevir is not recommended because it may result in loss of therapeutic effect of sofosbuvir/velpatasvir/voxilaprevir.
|
|
Ledipasvir/Sofosbuvir |
↑ TDF |
Monitor for adverse reactions associated with TDF. |
|
Hepatitis B antiviral agents Adefovir dipivoxil |
Concomitant administration of adefovir dipivoxil is not recommended. |
|
|
Hormonal contraceptives: Oral Ethinyl estradiol/ Norgestimate |
↓ active metabolites of norgestimate |
A reliable method of barrier contraception should be used in addition to hormonal contraceptives.
|
|
Implant Etonogestrel |
↓ etonogestrel |
A reliable method of barrier contraception should be used in addition to hormonal contraceptives. Decreased exposure of etonogestrel may be expected. There have been postmarketing reports of contraceptive failure with etonogestrel in EFV-exposed patients. |
|
Immunosuppressants: sirolimus, and others metabolized by CYP3A |
↓ immunosuppressant |
Dose adjustments of the immunosuppressant may be required. Close monitoring of immunosuppressant concentrations for at least 2 weeks (until stable concentrations are reached) is recommended when starting or stopping treatment with EFV. |
|
Narcotic analgesic: Methadone |
↓ methadone |
Monitor for signs of methadone withdrawal and increase methadone dose if required to alleviate withdrawal symptoms. |
2.1 Testing Prior to Initiation and During Treatment With Symfi (2.1 Testing Prior to Initiation and During Treatment with SYMFI)
Prior to initiation of SYMFI, test patients for hepatitis B virus infection [see Warnings and Precautions (5.1) ].
It is recommended that serum creatinine, serum phosphorus, estimated creatinine clearance, urine glucose, and urine protein be assessed before initiating SYMFI and during therapy in all patients as clinically appropriate [see Warnings and Precautions (5.4)].
Monitor hepatic function prior to and during treatment with SYMFI [see Warnings and Precautions (5.9)].
Clinical Trials in Treatment Naïve Hiv 1 Infected Adult Subjects (Clinical Trials in Treatment-Naïve HIV-1 Infected Adult Subjects)
In Trial 903, 600 antiretroviral-naïve subjects received TDF (N = 299) or stavudine (d4T) (N = 301) administered in combination with 3TC and EFV for 144 weeks. The most common adverse reactions were mild to moderate gastrointestinal events and dizziness. Mild adverse reactions (Grade 1) were common with a similar incidence in both arms and included dizziness, diarrhea, and nausea. Table 1 provides the treatment-emergent adverse reactions (Grades 2-4) occurring in greater than or equal to 5% of subjects treated in any treatment group.
|
TDF + 3TC + EFV |
d4T + 3TC + EFV |
|
|
N = 299 |
N = 301 |
|
|
Rash event Rash event includes rash, pruritus, maculopapular rash, urticaria, vesiculobullous rash, and pustular rash.
|
18% |
12% |
|
Headache |
14% |
17% |
|
Pain |
13% |
12% |
|
Diarrhea |
11% |
13% |
|
Depression |
11% |
10% |
|
Back pain |
9% |
8% |
|
Nausea |
8% |
9% |
|
Fever |
8% |
7% |
|
Abdominal pain |
7% |
12% |
|
Asthenia |
6% |
7% |
|
Anxiety |
6% |
6% |
|
Vomiting |
5% |
9% |
|
Insomnia |
5% |
8% |
|
Arthralgia |
5% |
7% |
|
Pneumonia |
5% |
5% |
|
Dyspepsia |
4% |
5% |
|
Dizziness |
3% |
6% |
|
Myalgia |
3% |
5% |
|
Lipodystrophy Lipodystrophy represents a variety of investigator-described adverse events not a protocol-defined syndrome.
|
1% |
8% |
|
Peripheral neuropathy Peripheral neuropathy includes peripheral neuritis and neuropathy.
|
1% |
5% |
2.2 Recommended Dosage for Adult and Pediatric Patients Weighing At Least 40 Kg (2.2 Recommended Dosage for Adult and Pediatric Patients Weighing at Least 40 kg)
SYMFI is a three-drug fixed-dose combination product containing 600 mg of efavirenz (EFV), 300 mg of lamivudine (3TC), and 300 mg of tenofovir disoproxil fumarate (TDF). The recommended dosage of SYMFI in HIV-1-infected adults and pediatric patients who weigh at least 40 kg, and can swallow a solid tablet, is one tablet taken orally once daily. SYMFI tablets should be taken on an empty stomach, preferably at bedtime. Dosing at bedtime may improve the tolerability of nervous system symptoms [see Warnings and Precautions (5.6) and Adverse Reactions (6.1)].
5.3 Risk of Adverse Reactions Or Loss of Virologic Response Due to Drug Interactions (5.3 Risk of Adverse Reactions or Loss of Virologic Response Due to Drug Interactions)
The concomitant use of SYMFI and other drugs may result in known or potentially significant drug interactions, some of which may lead to [see Contraindications (4) and Drug Interactions (7.5)]:
-
•Loss of therapeutic effect of SYMFI and possible development of resistance.
-
•Possible clinically significant adverse reactions from greater exposures of concomitant drugs.
See Table 3 for steps to prevent or manage these possible and known significant drug interactions, including dosing recommendations. Consider the potential for drug interactions prior to and during therapy with SYMFI; review concomitant medications during therapy with SYMFI; and monitor for the adverse reactions associated with the concomitant drugs.
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:45:39.142302 · Updated: 2026-03-14T22:22:55.765381