Acetylcysteine Solution, Usp
8165ad85-98e7-438f-9567-5cfda88d0ebf
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
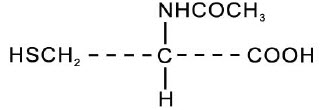
Acetylcysteine solution is for inhalation (mucolytic agent) or oral administration (acetaminophen antidote), available as a sterile, unpreserved solutions (not for injection). The solutions contain 20% (Acetylcysteine Solution 20%) or 10% (Acetylcysteine Solution 10%) acetylcysteine, with disodium edetate in water for injection. Sodium hydroxide and/or hydrochloric acid is added to adjust to pH (range 6.0 - 7.5). Acetylcysteine is the N-acetyl derivative of the naturally-occurring amino acid, L-cysteine. The compound is a white crystalline powder with the molecular formula C 5 H 9 NO 3 S, a molecular weight of 163.2, and chemical name of N-acetyl-L-cysteine. Acetylcysteine has the following structural formula: This product contains the following inactive ingredients: edetate disodium, sodium hydroxide and water for injection.
Indications and Usage
Acetylcysteine solution is indicated as adjuvant therapy for patients with abnormal, viscid, or inspissated mucous secretions in such conditions as: Chronic bronchopulmonary disease (chronic emphysema, emphysema with bronchitis, chronic asthmatic bronchitis, tuberculosis, bronchiectasis and primary amyloidosis of the lung) Acute bronchopulmonary disease (pneumonia, bronchitis, tracheobronchitis) Pulmonary complications of cystic fibrosis Tracheostomy care Pulmonary complications associated with surgery Use during anesthesia Post-traumatic chest conditions Atelectasis due to mucous obstruction Diagnostic bronchial studies (bronchograms, bronchospirometry, and bronchial wedge catheterization)
Contraindications
Acetylcysteine solution is contraindicated in those patients who are sensitive to it.
Adverse Reactions
Adverse effects have included stomatitis, nausea, vomiting, fever, rhinorrhea, drowsiness, clamminess, chest tightness, and bronchoconstriction. Clinically overt acetylcysteine induced bronchospasm occurs infrequently and unpredictably even in patients with asthmatic bronchitis or bronchitis complicating bronchial asthma. Acquired sensitization to acetylcysteine has been reported rarely. Reports of sensitization in patients have not been confirmed by patch testing. Sensitization has been confirmed in several inhalation therapists who reported a history of dermal eruptions after frequent and extended exposure to acetylcysteine. Reports of irritation to the tracheal and bronchial tracts have been received and although hemoptysis has occurred in patients receiving acetylcysteine such findings are not uncommon in patients with bronchopulmonary disease and a causal relationship has not been established.
Drug Interactions
Drug stability and safety of acetylcysteine when mixed with other drugs in a nebulizer have not been established.
How Supplied
Acetylcysteine solution is supplied as a clear, colorless liquid in a clear glass vial with an elastomeric stopper and an aluminum seal with a plastic flip-off dust cover containing 4 to 10 mL. The 20% solution may be diluted to a lesser concentration with either Sodium Chloride for Injection, Sodium Chloride for Inhalation, Sterile Water for Injection, or Sterile Water for Inhalation. The 10% solution may be used undiluted. Acetylcysteine solution is sterile and can be used for inhalation (mucolytic agent) or oral administration (acetaminophen antidote). Acetylcysteine solution is not for parenteral injection. It is available as: Acetylcysteine solution 10% (100 mg acetylcysteine per mL). Sterile, not for injection. NDC 42494-435-25 Cartons of twenty-five 4 mL vials NDC 42494-439-03 Cartons of three 10 mL vials, 1 plastic dropper Acetylcysteine solution 20% (200 mg acetylcysteine per mL). Sterile, not for injection. NDC 42494-436-25 Cartons of twenty-five 4 mL vials NDC 42494-440-03 Cartons of three 10 mL vials, 1 plastic dropper
Medication Information
Indications and Usage
Acetylcysteine solution is indicated as adjuvant therapy for patients with abnormal, viscid, or inspissated mucous secretions in such conditions as:
-
Chronic bronchopulmonary disease (chronic emphysema, emphysema with bronchitis, chronic asthmatic bronchitis, tuberculosis, bronchiectasis and primary amyloidosis of the lung)
-
Acute bronchopulmonary disease (pneumonia, bronchitis, tracheobronchitis)
-
Pulmonary complications of cystic fibrosis
-
Tracheostomy care
-
Pulmonary complications associated with surgery
-
Use during anesthesia
-
Post-traumatic chest conditions
-
Atelectasis due to mucous obstruction
-
Diagnostic bronchial studies (bronchograms, bronchospirometry, and bronchial wedge catheterization)
Contraindications
Acetylcysteine solution is contraindicated in those patients who are sensitive to it.
Adverse Reactions
Adverse effects have included stomatitis, nausea, vomiting, fever, rhinorrhea, drowsiness, clamminess, chest tightness, and bronchoconstriction. Clinically overt acetylcysteine induced bronchospasm occurs infrequently and unpredictably even in patients with asthmatic bronchitis or bronchitis complicating bronchial asthma.
Acquired sensitization to acetylcysteine has been reported rarely. Reports of sensitization in patients have not been confirmed by patch testing. Sensitization has been confirmed in several inhalation therapists who reported a history of dermal eruptions after frequent and extended exposure to acetylcysteine.
Reports of irritation to the tracheal and bronchial tracts have been received and although hemoptysis has occurred in patients receiving acetylcysteine such findings are not uncommon in patients with bronchopulmonary disease and a causal relationship has not been established.
Drug Interactions
Drug stability and safety of acetylcysteine when mixed with other drugs in a nebulizer have not been established.
How Supplied
Acetylcysteine solution is supplied as a clear, colorless liquid in a clear glass vial with an elastomeric stopper and an aluminum seal with a plastic flip-off dust cover containing 4 to 10 mL. The 20% solution may be diluted to a lesser concentration with either Sodium Chloride for Injection, Sodium Chloride for Inhalation, Sterile Water for Injection, or Sterile Water for Inhalation. The 10% solution may be used undiluted.
Acetylcysteine solution is sterile and can be used for inhalation (mucolytic agent) or oral administration (acetaminophen antidote).
Acetylcysteine solution is not for parenteral injection. It is available as:
Acetylcysteine solution 10% (100 mg acetylcysteine per mL). Sterile, not for injection.
| NDC 42494-435-25 | Cartons of twenty-five 4 mL vials |
| NDC 42494-439-03 | Cartons of three 10 mL vials, 1 plastic dropper |
Acetylcysteine solution 20% (200 mg acetylcysteine per mL). Sterile, not for injection.
| NDC 42494-436-25 | Cartons of twenty-five 4 mL vials |
| NDC 42494-440-03 | Cartons of three 10 mL vials, 1 plastic dropper |
Description
Acetylcysteine solution is for inhalation (mucolytic agent) or oral administration (acetaminophen antidote), available as a sterile, unpreserved solutions (not for injection). The solutions contain 20% (Acetylcysteine Solution 20%) or 10% (Acetylcysteine Solution 10%) acetylcysteine, with disodium edetate in water for injection. Sodium hydroxide and/or hydrochloric acid is added to adjust to pH (range 6.0 - 7.5). Acetylcysteine is the N-acetyl derivative of the naturally-occurring amino acid, L-cysteine. The compound is a white crystalline powder with the molecular formula C5H9NO3S, a molecular weight of 163.2, and chemical name of N-acetyl-L-cysteine. Acetylcysteine has the following structural formula:
This product contains the following inactive ingredients: edetate disodium, sodium hydroxide and water for injection.
Section 42229-5
Rx only
Manufactured for:
Cameron Pharmaceuticals
Louisville, Kentucky 40245, USA
Made in China
Revised April 2025
SG250500
General
With the administration of acetylcysteine solution, the patient may observe initially a slight disagreeable odor that is soon not noticeable. With a face mask there may be stickiness on the face after nebulization. This is easily removed by washing with water.
Under certain conditions, a color change may occur in acetylcysteine solution in the opened bottle. The light purple color is the result of a chemical reaction which does not significantly affect safety or mucolytic effectiveness of acetylcysteine solution.
Continued nebulization of acetylcysteine solution with a dry gas will result in an increased concentration of the drug in the nebulizer because of evaporation of the solvent. Extreme concentration may impede nebulization and efficient delivery of the drug. Dilution of the nebulizing solution with appropriate amounts of Sterile Water for Injection, USP, as concentration occurs, will obviate this problem.
Storage
Store unopened vials at 20 ° - 25 °C (68 ° - 77 °F); excursions permitted to 15 °- 30 °C (59 ° – 86 °F) (see USP Controlled Room Temperature).
Acetylcysteine solution does not contain an antimicrobial agent, and care must be taken to minimize contamination of the sterile solution. Dilutions of acetylcysteine should be used freshly prepared and utilized within one hour. If only a portion of the solution in a vial is used, store the remaining undiluted portion in a refrigerator and use within 96 hours. A change in color may occur after opening. This does change the efficacy of the drug.
Warnings
After proper administration of acetylcysteine solution, an increased volume of liquified bronchial secretions may occur. When cough is inadequate, the airway must be maintained open by mechanical suction if necessary. Where there is a mechanical block due to foreign body or local accumulation, the airway should be cleared by endotracheal aspiration, with or without bronchoscopy. Asthmatics under treatment with acetylcysteine solution should be watched carefully. Most patients with bronchospasm are quickly relieved by the use of a bronchodilator given by nebulization. If bronchospasm progresses, the medication should be discontinued immediately.
Apparatus
Acetylcysteine solution is usually administered as fine nebulae and the nebulizer used should be capable of providing optimal quantities of a suitable range of particle sizes.
Commercially available nebulizers will produce nebulae of acetylcysteine solution satisfactory for retention in the respiratory tract. Most of the nebulizers tested will supply a high proportion of the drug solution as particles of less than 10 microns in diameter. Mitchell2 has shown that particles less than 10 microns should be retained in the respiratory tract satisfactorily.
Various intermittent positive pressure breathing devices nebulized acetylcysteine solution with a satisfactory efficiency including: No. 40 De Vilbiss (The De Vilbiss Co., Somerset, Pennsylvania) and the Bennett Twin-Jet Nebulizer (Puritan Bennett Corp., Oak at 13th, Kansas City, Missouri).
The nebulized solution may be inhaled directly from the nebulizer. Nebulizers may also be attached to plastic face masks or plastic mouthpieces. Suitable nebulizers may also be fitted for use with the various intermittent positive pressure breathing (IPPB) machines. The nebulizing equipment should be cleaned immediately after use because the residues may clog the smaller orifices or corrode metal parts.
Hand bulbs are not recommended for routine use for nebulizing acetylcysteine solution because their output is generally too small. Also, some hand-operated nebulizers deliver particles that are larger than optimum for inhalation therapy.
Acetylcysteine solution should not be placed directly into the chamber of a heated (hot pot) nebulizer. A heated nebulizer may be part of the nebulization assembly to provide a warm saturated atmosphere if the acetylcysteine solution aerosol is introduced by means of a separate unheated nebulizer. Usual precautions for administration of warm saturated nebulae should be observed.
The nebulized solution may be breathed directly from the nebulizer. Nebulizers may also be attached to plastic face masks, plastic face tents, plastic mouth pieces, conventional plastic oxygen tents, or head tents. Suitable nebulizers may also be fitted for use with the various intermittent positive pressure breathing (IPPB) machines.
The nebulizing equipment should be cleaned immediately after use, otherwise the residues may occlude the fine orifices or corrode metal parts.
Lactation
It is not known whether this drug is excreted in human milk. Because many drugs are excreted in human milk, caution should be exercised when acetylcysteine solution is administered to a nursing woman.
Materials
Acetylcysteine solution may be administered using conventional nebulizers made of plastic or glass. Certain materials used in nebulization equipment react with acetylcysteine solution. The most reactive of these are certain metals (notably iron and copper) and rubber. Where materials may come into contact with acetylcysteine solution, parts made of the following acceptable materials should be used: glass, plastic, aluminum, anodized aluminum, chromed metal, tantalum, sterling silver, or stainless steel. Silver may become tarnished after exposure, but this is not harmful to the drug action or to the patient.
References
-
1.Bonanomi L, Gazzaniga A. Toxicological, pharmacokinetic and metabolic studies on acetylcysteine. Eur J Respir Dis 1981; 61 (suppl III): 45-51.
-
2.Am Rev Respir Dis 1960; 82:627-639.
Mutagenesis
Published data1 indicate that acetylcysteine is not mutagenic in the Ames test, both with and without metabolic activation.
Precautions
Occasionally severe and persistent vomiting occurs as a symptom of acute acetaminophen overdose. Treatment with oral acetylcysteine may aggravate the vomiting. Patients at risk of gastric hemorrhage (eg, esophageal varices, peptic ulcers, etc.) should be evaluated concerning the risk of upper gastrointestinal hemorrhage versus the risk of developing hepatic toxicity, and treatment with acetylcysteine given accordingly.
Dilution of the acetylcysteine (see Preparation of Acetylcysteine Solution for Oral Administration ) minimizes the propensity of oral acetylcysteine to aggravate vomiting.
Compatibility
The physical and chemical compatibility of acetylcysteine solutions with certain other drugs that might be concomitantly administered by nebulization, direct instillation, or topical application has been studied.
Acetylcysteine solution should not be mixed with certain antibiotics. For example, the antibiotics tetracycline hydrochloride, oxytetracycline hydrochloride, and erythromycin lactobionate were found to be incompatible when mixed in the same solution. These agents may be administered from separate solutions if administration of these agents is desirable.
The supplying of these data should not be interpreted as a recommendation for combining acetylcysteine solution with other drugs. The table is not presented as positive assurance that no incompatibility will be present, since these data are based only on short-term compatibility studies done in the Mead Johnson Research Center. Manufacturers may change their formulations, and this could alter compatibilities. These data are intended to serve only as a guide for predicting compounding problems.
If it is deemed advisable to prepare an admixture, it should be administered as soon as possible after preparation. Do not store unused mixtures.
| RATIO TESTED Entries are final concentrations. Values in parentheses relate volumes of acetylcysteine solutions to volume of test solutions.
|
|||
|---|---|---|---|
| PRODUCT AND/OR AGENT | COMPATIBILITY RATING | ACETYL-CYSTEINE | PRODUCT OR AGENT |
| 4. The admixture was a slightly darker shade of yellow than a control solution of the PRODUCT AND/OR AGENT. | |||
| ANESTHETIC, GAS | |||
| Halothane | Compatible | 20% | Infinite |
| Nitrous Oxide | Compatible | 20% | Infinite |
| ANESTHETIC, LOCAL | |||
| Cocaine HCl | Compatible | 10% | 5% |
| Lidocaine HCl | Compatible | 10% | 2% |
| Tetracaine HCl | Compatible | 10% | 1% |
| ANTIBACTERIALS (A parenteral form of each antibiotic was used) | |||
| Bacitracin The active ingredient in the PRODUCT AND/OR AGENT was also assayed after mixing. Some of the admixtures developed minor physical changes which were considered to be insufficient to rate the admixture Incompatible. These are listed in footnotes 3, 4, and 5.
,
A strong odor developed after storage for 24 hours at room temperature. (mix and use at once) |
Compatible | 10% | 5,000 U/mL |
| Chloramphenicol Sodium Succinate | Compatible | 20% | 20 mg/mL |
| Carbenicillin Disodium (mix and use at once) | Compatible | 10% | 125 mg/mL |
| Gentamicin Sulfate | Compatible | 10% | 20 mg/mL |
| Kanamycin Sulfate (mix and use at once) | Compatible | 10% | 167 mg/mL |
| Compatible | 17% | 85 mg/mL | |
| Lincomycin HCl | Compatible | 10% | 150 mg/mL |
| Neomycin Sulfate | Compatible | 10% | 100 mg/mL |
| Novobiocin Sodium | Compatible | 10% | 25 mg/mL |
| Penicillin G Potassium (mix and use at once) | Compatible | 10% | 25,000 U/mL |
| Compatible | 10% | 100,000 U/mL | |
| Polymyxin B Sulfate | Compatible | 10% | 50,000 U/mL |
| Cephalothin Sodium | Compatible | 10% | 110 mg/mL |
| Colistimethate Sodium (mix and use at once) | Compatible | 10% | 37.5 mg/mL |
| Vancomycin HCl | Compatible | 10% | 25 mg/mL |
| Amphotericin B | Incompatible | 4% - 15% | 1 – 4 mg/mL |
| Chlortetracycline HCl | Incompatible | 10% | 12.5 mg/mL |
| Erythromycin Lactobionate | Incompatible | 10% | 15 mg/mL |
| Oxytetracycline HCl | Incompatible | 10% | 12.5 mg/mL |
| Ampicillin Sodium | Incompatible | 10% | 50 mg/mL |
| Tetracycline HCl | Incompatible | 10% | 12.5 mg/mL |
| BRONCHODILATORS | |||
| Isoproterenol HCl | Compatible | 3.0% | 0.5% |
| Isoproterenol HCl | Compatible | 10% | 0.05% |
| Isoproterenol HCl | Compatible | 20% | 0.05% |
| Isoproterenol HCl | Compatible | 13.3% (2 parts) | 0.33% (1 part) |
| Isoetharine HCl | Compatible | 13.3% (2 parts) | (1 part) |
| Epinephrine HCl | Compatible | 13.3% (2 parts) | 0.33% (1 part) |
| CONTRAST MEDIA | |||
| Iodized Oil | Incompatible | 20%/20 mL | 40%/10 mL |
| DECONGESTANTS | |||
| Phenylephrine HCl | Compatible | 3.0% | 0.25% |
| Phenylephrine HCl | Compatible | 13.3% (2 parts) | 0.17% (1 part) |
| ENZYMES | |||
| Chymotrypsin | Incompatible | 5% | 400 γ/mL |
| Trypsin | Incompatible | 5% | 400 γ/mL |
| SOLVENTS | |||
| Alcohol | Compatible | 12% | 10% - 20% |
| Propylene Glycol | Compatible | 3% | 10% |
| STEROIDS | |||
| Dexamethasone Sodium Phosphate | Compatible | 16% | 0.8 mg/mL |
| Prednisolone Sodium Phosphate A light tan color developed after storage for 24 hours at room temperature.
|
Compatible | 16.7% | 3.3 mg/mL |
| OTHER AGENTS | |||
| Hydrogen Peroxide | Incompatible | (All ratios) | |
| Sodium Bicarbonate | Compatible | 20% (1 part) | 4.2% (1 part) |
Carcinogenesis
Carcinogenicity studies in laboratory animals have not been performed with acetylcysteine alone, nor with acetylcysteine in combination with isoproterenol.
Long-term oral studies of acetylcysteine alone in rats (12 months of treatment followed by 6 months of observation) at doses up to 1,000 mg/kg/day (5.2 times the human mucolytic dose) provided no evidence of oncogenic activity.
Nebulizing Gases
Compressed tank gas (air) or an air compressor should be used to provide pressure for nebulizing the solution. Oxygen may also be used but should be used with the usual precautions in patients with severe respiratory disease and CO2 retention.
Direct Instillation
When used by direct instillation, 1 to 2 mL of a 10% to 20% solution may be given as often as every hour.
When used for the routine nursing care of patients with tracheostomy, 1 to 2 mL of a 10% to 20% solution may be given every 1 to 4 hours by instillation into the tracheostomy.
Acetylcysteine solution may be introduced directly into a particular segment of the bronchopulmonary tree by inserting (under local anesthesia and direct vision) a small plastic catheter into the trachea. Two to 5 mL of the 20% solution may then be instilled by means of a syringe connected to the catheter.
Acetylcysteine solution may also be given through a percutaneous intratracheal catheter. One to 2 mL of the 20% or 2 to 4 mL of the 10% solution every 1 to 4 hours may then be given by a syringe attached to the catheter.
Teratogenic Effects
In a teratology study of acetylcysteine in the rabbit, oral doses of 500 mg/kg/day (2.6 times the human mucolytic dose) were administered to pregnant does by intubation on days 6 through 16 of gestation. Acetylcysteine was found to be nonteratogenic under the conditions of the study.
In the rabbit, two groups (one of 14 and one of 16 pregnant females) were exposed to an aerosol of 10% acetylcysteine and 0.05% isoproterenol hydrochloride for 30 or 35 minutes twice a day from the 6th through the 18th day of pregnancy. No teratogenic effects were observed among the offspring.
Teratology and a perinatal and postnatal toxicity study in rats were performed with a combination of acetylcysteine and isoproterenol administered by the inhalation route. In the rat, two groups of 25 pregnant females each were exposed to the aerosol for 30 and 35 minutes, respectively, twice a day from the 6th through the 15th day of gestation. No teratogenic effects were observed among the offspring.
In the pregnant rat (30 rats per group), twice-daily exposure to an aerosol of acetylcysteine and isoproterenol for 30 or 35 minutes from the 15th day of gestation through the 21st day postpartum was without adverse effect on dams or newborns.
Reproduction studies of acetylcysteine solution with isoproterenol have been performed in rats and of acetylcysteine alone in rabbits at doses up to 2.6 times the human dose. These have revealed no evidence of impaired fertility or harm to the fetus due to acetylcysteine. There are, however, no adequate and well-controlled studies in pregnant women. Because animal reproduction studies may not always be predictive of human responses, this drug should be used during pregnancy only if clearly needed.
Clinical Pharmacology
The viscosity of pulmonary mucous secretions depends on the concentrations of mucoprotein and, to a lesser extent, deoxyribonucleic acid (DNA). The latter increases with increasing purulence owing to the presence of cellular debris. The mucolytic action of acetylcysteine is related to the sulfhydryl group in the molecule. This group probably "opens" disulfide linkages in mucus thereby lowering the viscosity. The mucolytic activity of acetylcysteine is unaltered by the presence of DNA, and increases with increasing pH. Significant mucolysis occurs between pH 7 and 9.
Acetylcysteine undergoes rapid deacetylation in vivo to yield cysteine or oxidation to yield diacetylcystine.
Occasionally, patients exposed to the inhalation of an acetylcysteine aerosol respond with the development of increased airways obstruction of varying and unpredictable severity. Those patients who are reactors cannot be identified a priori from a random patient population. Even when patients are known to have reacted previously to the inhalation of an acetylcysteine aerosol, they may not react during a subsequent treatment. The converse is also true; patients who have had inhalation treatments of acetylcysteine without incident may still react to subsequent inhalation with increased airways obstruction. Most patients with bronchospasm are quickly relieved by the use of a bronchodilator given by nebulization. If bronchospasm progresses, the medication should be discontinued immediately.
Prolonged Nebulization
When three fourths of the initial volume of acetylcysteine solution has been nebulized, a quantity of Sterile Water for Injection, USP (approximately equal to the volume of solution remaining) should be added to the nebulizer. This obviates any concentration of the agent in the residual solvent remaining after prolonged nebulization.
Diagnostic Bronchograms
For diagnostic bronchial studies, two to three administrations of 1 to 2 mL of the 20% solution or 2 to 4 mL of the 10% solution should be given by nebulization or by instillation intratracheally, prior to the procedure.
Impairment of Fertility
A reproductive toxicity test to assess potential impairment of fertility was performed with acetylcysteine (10%) combined with isoproterenol (0.05%) and administered as an aerosol into a chamber of 12.43 cubic meters. The combination was administered for 25, 30, or 35 minutes twice a day for 68 days before mating, to 200 male and 150 female rats; no adverse effects were noted in dams or pups. Females after mating were continued on treatment for the next 42 days.
Reproductive toxicity studies of acetylcysteine in the rat given oral doses of acetylcysteine up to 1,000 mg/kg (5.2 times the human mucolytic dose) have also been reported in the literature.1 The only adverse effect observed was a slight non-dose-related reduction in fertility at dose levels of 500 or 1,000 mg/kg/day (2.6 or 5.2 times the human mucolytic dose) in the Segment I study.
Dosage Guide and Preparation
Doses in relation to body weight are:
| Body Weight | grams Acetylcysteine | mL of 20% Acetylcysteine solution | mL of Diluent | Total mL of 5% Solution | |
|---|---|---|---|---|---|
| (kg) | (lb) | ||||
| 100-109 | 220-240 | 15 | 75 | 225 | 300 |
| 90-99 | 198-218 | 14 | 70 | 210 | 280 |
| 80-89 | 176-196 | 13 | 65 | 195 | 260 |
| 70-79 | 154-174 | 11 | 55 | 165 | 220 |
| 60-69 | 132-152 | 10 | 50 | 150 | 200 |
| 50-59 | 110-130 | 8 | 40 | 120 | 160 |
| 40-49 | 88-108 | 7 | 35 | 105 | 140 |
| 30-39 | 66-86 | 6 | 30 | 90 | 120 |
| 20-29 | 44-64 | 4 | 20 | 60 | 80 |
| Maintenance Dose | |||||
| (kg) | (lb) | ||||
| 100-109 | 220-240 | 7.5 | 37 | 113 | 150 |
| 90-99 | 198-218 | 7 | 35 | 105 | 140 |
| 80-89 | 176-196 | 6.5 | 33 | 97 | 130 |
| 70-79 | 154-174 | 5.5 | 28 | 82 | 110 |
| 60-69 | 132-152 | 5 | 25 | 75 | 100 |
| 50-59 | 110-130 | 4 | 20 | 60 | 80 |
| 40-49 | 88-108 | 3.5 | 18 | 52 | 70 |
| 30-39 | 66-86 | 3 | 15 | 45 | 60 |
| 20-29 | 44-64 | 2 | 10 | 30 | 40 |
Nebulization Tent, Croupette
In special circumstances it may be necessary to nebulize into a tent or Croupette, and this method of use must be individualized to take into account the available equipment and the patient's particular needs. This form of administration requires very large volumes of the solution, occasionally as much as 300 mL during a single treatment period.
If a tent or Croupette must be used, the recommended dose is the volume of acetylcysteine solution (using 10% or 20%) that will maintain a very heavy mist in the tent or Croupette for the desired period. Administration for intermittent or continuous prolonged periods, including overnight, may be desirable.
Acetaminophen Assay Methodology
Assay procedures most suitable for determining acetaminophen concentrations utilize high pressure liquid chromatography (HPLC) or gas liquid chromatography (GLC). The assay should measure only parent acetaminophen and not conjugated. The assay procedures listed below fulfill this requirement:
Selected Techniques (non Inclusive)
HPLC:
-
1.Blair D, Rumack BH. Clin Chem. 1977; 23(4): 743-745.
-
2.Howie D, Andriaenssens Pl, Prescott LF. J Pharm Pharmacol 1977; 29(4):235-237.
GLC
-
3.Prescott LF. J Pharm Pharmacol 1971; 23(10):807-808.
Colorimetric
-
4.Glynn JP, Kendal SE. Lancet 1975; 1(May 17):1147-1148.
Interpretation of Acetaminophen Assays
-
1.When results of the plasma acetaminophen assay are available refer to the nomogram below to determine if plasma concentration is in the potentially toxic range. Values above the solid line connecting 200 mcg/mL at least 4 hours with 50 mcg/mL at 12 hours are associated with a possibility of hepatic toxicity if an antidote is not administered. (Do not wait for assay results to begin acetylcysteine treatment.)
-
2.If the predetoxification plasma level is above the broken line continue with maintenance doses of acetylcysteine. It is better to err on the safe side and thus the broken line is placed 25% below the solid line which defines possible toxicity.
-
3.If the predetoxification plasma level is below the broken line described above, there is minimal risk of hepatic toxicity and acetylcysteine treatment can be discontinued.
Estimating Potential for Hepatotoxicity
The following nomogram has been developed to estimate the probability that plasma levels in relation to intervals post ingestion will result in hepatotoxicity.
Supportive Treatment of Acetaminophen Overdose
-
1.Maintain fluid and electrolyte balance based on clinical evaluation of state of hydration and serum electrolytes.
-
2.Treat as necessary for hypoglycemia.
-
3.Administer vitamin K1 if prothrombin time ratio exceeds 1.5 or fresh frozen plasma if the prothrombin time ratio exceeds 3.0.
-
4.Diuretics and forced diuresis should be avoided.
Principal Display Panel 100 Mg/ml Vial Carton
NDC 42494-435-25
Rx Only
Acetylcysteine Solution, USP
10% (100 mg/mL)
For Inhalation (Mucolytic Agent) or Oral Administration (Acetaminophen Antidote)
NOT FOR INJECTION
PRESERVATIVE FREE
25 x 4 mL Vials
Principal Display Panel 200 Mg/ml Vial Carton
NDC 42494-436-25
Rx Only
Acetylcysteine Solution, USP
20% (200 mg/mL)
For Inhalation (Mucolytic Agent) or Oral Administration (Acetaminophen Antidote)
NOT FOR INJECTION
PRESERVATIVE FREE
25 x 4 mL Vials
Nebulization Face Mask, Mouth Piece, Tracheostomy
When nebulized into a face mask, mouth piece, or tracheostomy, 1 to 10 mL of the 20% solution or 2 to 20 mL of the 10% solution may be given every 2 to 6 hours; the recommended dose for most patients is 3 to 5 mL of the 20% solution or 6 to 10 mL of the 10% solution 3 to 4 times a day.
Acetaminophen Assays Interpretation and Methodology
The acute ingestion of acetaminophen in quantities of 150 mg/kg or greater may result in hepatic toxicity. However, the reported history of the quantity of a drug ingested as an overdose is often inaccurate and is not a reliable guide to therapy of the overdose. THEREFORE, PLASMA OR SERUM ACETAMINOPHEN CONCENTRATIONS, DETERMINED AS EARLY AS POSSIBLE, BUT NO SOONER THAN 4 HOURS FOLLOWING AN ACUTE OVERDOSE, ARE ESSENTIAL IN ASSESSING THE POTENTIAL RISK OF HEPATOTOXICITY. IF AN ASSAY FOR ACETAMINOPHEN CANNOT BE OBTAINED, IT IS NECESSARY TO ASSUME THAT THE OVERDOSE IS POTENTIALLY TOXIC.
Preparation of Acetylcysteine for Oral Administration
Oral administration requires dilution of the 20% solution with diet cola or other diet soft drinks, to a final concentration of 5% (see Dosage Guide and Preparation table). If administered via gastric tube or Miller-Abbott tube, water may be used as the diluent. The dilutions should be freshly prepared and utilized within one hour. Remaining undiluted solutions in opened vials can be stored in the refrigerator up to 96 hours. ACETYLCYSTEINE IS NOT APPROVED FOR PARENTERAL INJECTION.
Structured Label Content
Section 42229-5 (42229-5)
Rx only
Manufactured for:
Cameron Pharmaceuticals
Louisville, Kentucky 40245, USA
Made in China
Revised April 2025
SG250500
General
With the administration of acetylcysteine solution, the patient may observe initially a slight disagreeable odor that is soon not noticeable. With a face mask there may be stickiness on the face after nebulization. This is easily removed by washing with water.
Under certain conditions, a color change may occur in acetylcysteine solution in the opened bottle. The light purple color is the result of a chemical reaction which does not significantly affect safety or mucolytic effectiveness of acetylcysteine solution.
Continued nebulization of acetylcysteine solution with a dry gas will result in an increased concentration of the drug in the nebulizer because of evaporation of the solvent. Extreme concentration may impede nebulization and efficient delivery of the drug. Dilution of the nebulizing solution with appropriate amounts of Sterile Water for Injection, USP, as concentration occurs, will obviate this problem.
Storage (STORAGE)
Store unopened vials at 20 ° - 25 °C (68 ° - 77 °F); excursions permitted to 15 °- 30 °C (59 ° – 86 °F) (see USP Controlled Room Temperature).
Acetylcysteine solution does not contain an antimicrobial agent, and care must be taken to minimize contamination of the sterile solution. Dilutions of acetylcysteine should be used freshly prepared and utilized within one hour. If only a portion of the solution in a vial is used, store the remaining undiluted portion in a refrigerator and use within 96 hours. A change in color may occur after opening. This does change the efficacy of the drug.
Warnings (WARNINGS)
After proper administration of acetylcysteine solution, an increased volume of liquified bronchial secretions may occur. When cough is inadequate, the airway must be maintained open by mechanical suction if necessary. Where there is a mechanical block due to foreign body or local accumulation, the airway should be cleared by endotracheal aspiration, with or without bronchoscopy. Asthmatics under treatment with acetylcysteine solution should be watched carefully. Most patients with bronchospasm are quickly relieved by the use of a bronchodilator given by nebulization. If bronchospasm progresses, the medication should be discontinued immediately.
Apparatus (APPARATUS)
Acetylcysteine solution is usually administered as fine nebulae and the nebulizer used should be capable of providing optimal quantities of a suitable range of particle sizes.
Commercially available nebulizers will produce nebulae of acetylcysteine solution satisfactory for retention in the respiratory tract. Most of the nebulizers tested will supply a high proportion of the drug solution as particles of less than 10 microns in diameter. Mitchell2 has shown that particles less than 10 microns should be retained in the respiratory tract satisfactorily.
Various intermittent positive pressure breathing devices nebulized acetylcysteine solution with a satisfactory efficiency including: No. 40 De Vilbiss (The De Vilbiss Co., Somerset, Pennsylvania) and the Bennett Twin-Jet Nebulizer (Puritan Bennett Corp., Oak at 13th, Kansas City, Missouri).
The nebulized solution may be inhaled directly from the nebulizer. Nebulizers may also be attached to plastic face masks or plastic mouthpieces. Suitable nebulizers may also be fitted for use with the various intermittent positive pressure breathing (IPPB) machines. The nebulizing equipment should be cleaned immediately after use because the residues may clog the smaller orifices or corrode metal parts.
Hand bulbs are not recommended for routine use for nebulizing acetylcysteine solution because their output is generally too small. Also, some hand-operated nebulizers deliver particles that are larger than optimum for inhalation therapy.
Acetylcysteine solution should not be placed directly into the chamber of a heated (hot pot) nebulizer. A heated nebulizer may be part of the nebulization assembly to provide a warm saturated atmosphere if the acetylcysteine solution aerosol is introduced by means of a separate unheated nebulizer. Usual precautions for administration of warm saturated nebulae should be observed.
The nebulized solution may be breathed directly from the nebulizer. Nebulizers may also be attached to plastic face masks, plastic face tents, plastic mouth pieces, conventional plastic oxygen tents, or head tents. Suitable nebulizers may also be fitted for use with the various intermittent positive pressure breathing (IPPB) machines.
The nebulizing equipment should be cleaned immediately after use, otherwise the residues may occlude the fine orifices or corrode metal parts.
Lactation
It is not known whether this drug is excreted in human milk. Because many drugs are excreted in human milk, caution should be exercised when acetylcysteine solution is administered to a nursing woman.
Materials (MATERIALS)
Acetylcysteine solution may be administered using conventional nebulizers made of plastic or glass. Certain materials used in nebulization equipment react with acetylcysteine solution. The most reactive of these are certain metals (notably iron and copper) and rubber. Where materials may come into contact with acetylcysteine solution, parts made of the following acceptable materials should be used: glass, plastic, aluminum, anodized aluminum, chromed metal, tantalum, sterling silver, or stainless steel. Silver may become tarnished after exposure, but this is not harmful to the drug action or to the patient.
References (REFERENCES)
-
1.Bonanomi L, Gazzaniga A. Toxicological, pharmacokinetic and metabolic studies on acetylcysteine. Eur J Respir Dis 1981; 61 (suppl III): 45-51.
-
2.Am Rev Respir Dis 1960; 82:627-639.
Description (DESCRIPTION)
Acetylcysteine solution is for inhalation (mucolytic agent) or oral administration (acetaminophen antidote), available as a sterile, unpreserved solutions (not for injection). The solutions contain 20% (Acetylcysteine Solution 20%) or 10% (Acetylcysteine Solution 10%) acetylcysteine, with disodium edetate in water for injection. Sodium hydroxide and/or hydrochloric acid is added to adjust to pH (range 6.0 - 7.5). Acetylcysteine is the N-acetyl derivative of the naturally-occurring amino acid, L-cysteine. The compound is a white crystalline powder with the molecular formula C5H9NO3S, a molecular weight of 163.2, and chemical name of N-acetyl-L-cysteine. Acetylcysteine has the following structural formula:
This product contains the following inactive ingredients: edetate disodium, sodium hydroxide and water for injection.
Mutagenesis
Published data1 indicate that acetylcysteine is not mutagenic in the Ames test, both with and without metabolic activation.
Precautions (PRECAUTIONS)
Occasionally severe and persistent vomiting occurs as a symptom of acute acetaminophen overdose. Treatment with oral acetylcysteine may aggravate the vomiting. Patients at risk of gastric hemorrhage (eg, esophageal varices, peptic ulcers, etc.) should be evaluated concerning the risk of upper gastrointestinal hemorrhage versus the risk of developing hepatic toxicity, and treatment with acetylcysteine given accordingly.
Dilution of the acetylcysteine (see Preparation of Acetylcysteine Solution for Oral Administration ) minimizes the propensity of oral acetylcysteine to aggravate vomiting.
How Supplied (HOW SUPPLIED)
Acetylcysteine solution is supplied as a clear, colorless liquid in a clear glass vial with an elastomeric stopper and an aluminum seal with a plastic flip-off dust cover containing 4 to 10 mL. The 20% solution may be diluted to a lesser concentration with either Sodium Chloride for Injection, Sodium Chloride for Inhalation, Sterile Water for Injection, or Sterile Water for Inhalation. The 10% solution may be used undiluted.
Acetylcysteine solution is sterile and can be used for inhalation (mucolytic agent) or oral administration (acetaminophen antidote).
Acetylcysteine solution is not for parenteral injection. It is available as:
Acetylcysteine solution 10% (100 mg acetylcysteine per mL). Sterile, not for injection.
| NDC 42494-435-25 | Cartons of twenty-five 4 mL vials |
| NDC 42494-439-03 | Cartons of three 10 mL vials, 1 plastic dropper |
Acetylcysteine solution 20% (200 mg acetylcysteine per mL). Sterile, not for injection.
| NDC 42494-436-25 | Cartons of twenty-five 4 mL vials |
| NDC 42494-440-03 | Cartons of three 10 mL vials, 1 plastic dropper |
Compatibility
The physical and chemical compatibility of acetylcysteine solutions with certain other drugs that might be concomitantly administered by nebulization, direct instillation, or topical application has been studied.
Acetylcysteine solution should not be mixed with certain antibiotics. For example, the antibiotics tetracycline hydrochloride, oxytetracycline hydrochloride, and erythromycin lactobionate were found to be incompatible when mixed in the same solution. These agents may be administered from separate solutions if administration of these agents is desirable.
The supplying of these data should not be interpreted as a recommendation for combining acetylcysteine solution with other drugs. The table is not presented as positive assurance that no incompatibility will be present, since these data are based only on short-term compatibility studies done in the Mead Johnson Research Center. Manufacturers may change their formulations, and this could alter compatibilities. These data are intended to serve only as a guide for predicting compounding problems.
If it is deemed advisable to prepare an admixture, it should be administered as soon as possible after preparation. Do not store unused mixtures.
| RATIO TESTED Entries are final concentrations. Values in parentheses relate volumes of acetylcysteine solutions to volume of test solutions.
|
|||
|---|---|---|---|
| PRODUCT AND/OR AGENT | COMPATIBILITY RATING | ACETYL-CYSTEINE | PRODUCT OR AGENT |
| 4. The admixture was a slightly darker shade of yellow than a control solution of the PRODUCT AND/OR AGENT. | |||
| ANESTHETIC, GAS | |||
| Halothane | Compatible | 20% | Infinite |
| Nitrous Oxide | Compatible | 20% | Infinite |
| ANESTHETIC, LOCAL | |||
| Cocaine HCl | Compatible | 10% | 5% |
| Lidocaine HCl | Compatible | 10% | 2% |
| Tetracaine HCl | Compatible | 10% | 1% |
| ANTIBACTERIALS (A parenteral form of each antibiotic was used) | |||
| Bacitracin The active ingredient in the PRODUCT AND/OR AGENT was also assayed after mixing. Some of the admixtures developed minor physical changes which were considered to be insufficient to rate the admixture Incompatible. These are listed in footnotes 3, 4, and 5.
,
A strong odor developed after storage for 24 hours at room temperature. (mix and use at once) |
Compatible | 10% | 5,000 U/mL |
| Chloramphenicol Sodium Succinate | Compatible | 20% | 20 mg/mL |
| Carbenicillin Disodium (mix and use at once) | Compatible | 10% | 125 mg/mL |
| Gentamicin Sulfate | Compatible | 10% | 20 mg/mL |
| Kanamycin Sulfate (mix and use at once) | Compatible | 10% | 167 mg/mL |
| Compatible | 17% | 85 mg/mL | |
| Lincomycin HCl | Compatible | 10% | 150 mg/mL |
| Neomycin Sulfate | Compatible | 10% | 100 mg/mL |
| Novobiocin Sodium | Compatible | 10% | 25 mg/mL |
| Penicillin G Potassium (mix and use at once) | Compatible | 10% | 25,000 U/mL |
| Compatible | 10% | 100,000 U/mL | |
| Polymyxin B Sulfate | Compatible | 10% | 50,000 U/mL |
| Cephalothin Sodium | Compatible | 10% | 110 mg/mL |
| Colistimethate Sodium (mix and use at once) | Compatible | 10% | 37.5 mg/mL |
| Vancomycin HCl | Compatible | 10% | 25 mg/mL |
| Amphotericin B | Incompatible | 4% - 15% | 1 – 4 mg/mL |
| Chlortetracycline HCl | Incompatible | 10% | 12.5 mg/mL |
| Erythromycin Lactobionate | Incompatible | 10% | 15 mg/mL |
| Oxytetracycline HCl | Incompatible | 10% | 12.5 mg/mL |
| Ampicillin Sodium | Incompatible | 10% | 50 mg/mL |
| Tetracycline HCl | Incompatible | 10% | 12.5 mg/mL |
| BRONCHODILATORS | |||
| Isoproterenol HCl | Compatible | 3.0% | 0.5% |
| Isoproterenol HCl | Compatible | 10% | 0.05% |
| Isoproterenol HCl | Compatible | 20% | 0.05% |
| Isoproterenol HCl | Compatible | 13.3% (2 parts) | 0.33% (1 part) |
| Isoetharine HCl | Compatible | 13.3% (2 parts) | (1 part) |
| Epinephrine HCl | Compatible | 13.3% (2 parts) | 0.33% (1 part) |
| CONTRAST MEDIA | |||
| Iodized Oil | Incompatible | 20%/20 mL | 40%/10 mL |
| DECONGESTANTS | |||
| Phenylephrine HCl | Compatible | 3.0% | 0.25% |
| Phenylephrine HCl | Compatible | 13.3% (2 parts) | 0.17% (1 part) |
| ENZYMES | |||
| Chymotrypsin | Incompatible | 5% | 400 γ/mL |
| Trypsin | Incompatible | 5% | 400 γ/mL |
| SOLVENTS | |||
| Alcohol | Compatible | 12% | 10% - 20% |
| Propylene Glycol | Compatible | 3% | 10% |
| STEROIDS | |||
| Dexamethasone Sodium Phosphate | Compatible | 16% | 0.8 mg/mL |
| Prednisolone Sodium Phosphate A light tan color developed after storage for 24 hours at room temperature.
|
Compatible | 16.7% | 3.3 mg/mL |
| OTHER AGENTS | |||
| Hydrogen Peroxide | Incompatible | (All ratios) | |
| Sodium Bicarbonate | Compatible | 20% (1 part) | 4.2% (1 part) |
Carcinogenesis
Carcinogenicity studies in laboratory animals have not been performed with acetylcysteine alone, nor with acetylcysteine in combination with isoproterenol.
Long-term oral studies of acetylcysteine alone in rats (12 months of treatment followed by 6 months of observation) at doses up to 1,000 mg/kg/day (5.2 times the human mucolytic dose) provided no evidence of oncogenic activity.
Nebulizing Gases (NEBULIZING GASES)
Compressed tank gas (air) or an air compressor should be used to provide pressure for nebulizing the solution. Oxygen may also be used but should be used with the usual precautions in patients with severe respiratory disease and CO2 retention.
Adverse Reactions (ADVERSE REACTIONS)
Adverse effects have included stomatitis, nausea, vomiting, fever, rhinorrhea, drowsiness, clamminess, chest tightness, and bronchoconstriction. Clinically overt acetylcysteine induced bronchospasm occurs infrequently and unpredictably even in patients with asthmatic bronchitis or bronchitis complicating bronchial asthma.
Acquired sensitization to acetylcysteine has been reported rarely. Reports of sensitization in patients have not been confirmed by patch testing. Sensitization has been confirmed in several inhalation therapists who reported a history of dermal eruptions after frequent and extended exposure to acetylcysteine.
Reports of irritation to the tracheal and bronchial tracts have been received and although hemoptysis has occurred in patients receiving acetylcysteine such findings are not uncommon in patients with bronchopulmonary disease and a causal relationship has not been established.
Contraindications (CONTRAINDICATIONS)
Acetylcysteine solution is contraindicated in those patients who are sensitive to it.
Drug Interactions
Drug stability and safety of acetylcysteine when mixed with other drugs in a nebulizer have not been established.
Direct Instillation (DIRECT INSTILLATION)
When used by direct instillation, 1 to 2 mL of a 10% to 20% solution may be given as often as every hour.
When used for the routine nursing care of patients with tracheostomy, 1 to 2 mL of a 10% to 20% solution may be given every 1 to 4 hours by instillation into the tracheostomy.
Acetylcysteine solution may be introduced directly into a particular segment of the bronchopulmonary tree by inserting (under local anesthesia and direct vision) a small plastic catheter into the trachea. Two to 5 mL of the 20% solution may then be instilled by means of a syringe connected to the catheter.
Acetylcysteine solution may also be given through a percutaneous intratracheal catheter. One to 2 mL of the 20% or 2 to 4 mL of the 10% solution every 1 to 4 hours may then be given by a syringe attached to the catheter.
Teratogenic Effects
In a teratology study of acetylcysteine in the rabbit, oral doses of 500 mg/kg/day (2.6 times the human mucolytic dose) were administered to pregnant does by intubation on days 6 through 16 of gestation. Acetylcysteine was found to be nonteratogenic under the conditions of the study.
In the rabbit, two groups (one of 14 and one of 16 pregnant females) were exposed to an aerosol of 10% acetylcysteine and 0.05% isoproterenol hydrochloride for 30 or 35 minutes twice a day from the 6th through the 18th day of pregnancy. No teratogenic effects were observed among the offspring.
Teratology and a perinatal and postnatal toxicity study in rats were performed with a combination of acetylcysteine and isoproterenol administered by the inhalation route. In the rat, two groups of 25 pregnant females each were exposed to the aerosol for 30 and 35 minutes, respectively, twice a day from the 6th through the 15th day of gestation. No teratogenic effects were observed among the offspring.
In the pregnant rat (30 rats per group), twice-daily exposure to an aerosol of acetylcysteine and isoproterenol for 30 or 35 minutes from the 15th day of gestation through the 21st day postpartum was without adverse effect on dams or newborns.
Reproduction studies of acetylcysteine solution with isoproterenol have been performed in rats and of acetylcysteine alone in rabbits at doses up to 2.6 times the human dose. These have revealed no evidence of impaired fertility or harm to the fetus due to acetylcysteine. There are, however, no adequate and well-controlled studies in pregnant women. Because animal reproduction studies may not always be predictive of human responses, this drug should be used during pregnancy only if clearly needed.
Clinical Pharmacology (CLINICAL PHARMACOLOGY)
The viscosity of pulmonary mucous secretions depends on the concentrations of mucoprotein and, to a lesser extent, deoxyribonucleic acid (DNA). The latter increases with increasing purulence owing to the presence of cellular debris. The mucolytic action of acetylcysteine is related to the sulfhydryl group in the molecule. This group probably "opens" disulfide linkages in mucus thereby lowering the viscosity. The mucolytic activity of acetylcysteine is unaltered by the presence of DNA, and increases with increasing pH. Significant mucolysis occurs between pH 7 and 9.
Acetylcysteine undergoes rapid deacetylation in vivo to yield cysteine or oxidation to yield diacetylcystine.
Occasionally, patients exposed to the inhalation of an acetylcysteine aerosol respond with the development of increased airways obstruction of varying and unpredictable severity. Those patients who are reactors cannot be identified a priori from a random patient population. Even when patients are known to have reacted previously to the inhalation of an acetylcysteine aerosol, they may not react during a subsequent treatment. The converse is also true; patients who have had inhalation treatments of acetylcysteine without incident may still react to subsequent inhalation with increased airways obstruction. Most patients with bronchospasm are quickly relieved by the use of a bronchodilator given by nebulization. If bronchospasm progresses, the medication should be discontinued immediately.
Indications and Usage (INDICATIONS AND USAGE)
Acetylcysteine solution is indicated as adjuvant therapy for patients with abnormal, viscid, or inspissated mucous secretions in such conditions as:
-
Chronic bronchopulmonary disease (chronic emphysema, emphysema with bronchitis, chronic asthmatic bronchitis, tuberculosis, bronchiectasis and primary amyloidosis of the lung)
-
Acute bronchopulmonary disease (pneumonia, bronchitis, tracheobronchitis)
-
Pulmonary complications of cystic fibrosis
-
Tracheostomy care
-
Pulmonary complications associated with surgery
-
Use during anesthesia
-
Post-traumatic chest conditions
-
Atelectasis due to mucous obstruction
-
Diagnostic bronchial studies (bronchograms, bronchospirometry, and bronchial wedge catheterization)
Prolonged Nebulization (PROLONGED NEBULIZATION)
When three fourths of the initial volume of acetylcysteine solution has been nebulized, a quantity of Sterile Water for Injection, USP (approximately equal to the volume of solution remaining) should be added to the nebulizer. This obviates any concentration of the agent in the residual solvent remaining after prolonged nebulization.
Diagnostic Bronchograms (DIAGNOSTIC BRONCHOGRAMS)
For diagnostic bronchial studies, two to three administrations of 1 to 2 mL of the 20% solution or 2 to 4 mL of the 10% solution should be given by nebulization or by instillation intratracheally, prior to the procedure.
Impairment of Fertility
A reproductive toxicity test to assess potential impairment of fertility was performed with acetylcysteine (10%) combined with isoproterenol (0.05%) and administered as an aerosol into a chamber of 12.43 cubic meters. The combination was administered for 25, 30, or 35 minutes twice a day for 68 days before mating, to 200 male and 150 female rats; no adverse effects were noted in dams or pups. Females after mating were continued on treatment for the next 42 days.
Reproductive toxicity studies of acetylcysteine in the rat given oral doses of acetylcysteine up to 1,000 mg/kg (5.2 times the human mucolytic dose) have also been reported in the literature.1 The only adverse effect observed was a slight non-dose-related reduction in fertility at dose levels of 500 or 1,000 mg/kg/day (2.6 or 5.2 times the human mucolytic dose) in the Segment I study.
Dosage Guide and Preparation (DOSAGE GUIDE AND PREPARATION)
Doses in relation to body weight are:
| Body Weight | grams Acetylcysteine | mL of 20% Acetylcysteine solution | mL of Diluent | Total mL of 5% Solution | |
|---|---|---|---|---|---|
| (kg) | (lb) | ||||
| 100-109 | 220-240 | 15 | 75 | 225 | 300 |
| 90-99 | 198-218 | 14 | 70 | 210 | 280 |
| 80-89 | 176-196 | 13 | 65 | 195 | 260 |
| 70-79 | 154-174 | 11 | 55 | 165 | 220 |
| 60-69 | 132-152 | 10 | 50 | 150 | 200 |
| 50-59 | 110-130 | 8 | 40 | 120 | 160 |
| 40-49 | 88-108 | 7 | 35 | 105 | 140 |
| 30-39 | 66-86 | 6 | 30 | 90 | 120 |
| 20-29 | 44-64 | 4 | 20 | 60 | 80 |
| Maintenance Dose | |||||
| (kg) | (lb) | ||||
| 100-109 | 220-240 | 7.5 | 37 | 113 | 150 |
| 90-99 | 198-218 | 7 | 35 | 105 | 140 |
| 80-89 | 176-196 | 6.5 | 33 | 97 | 130 |
| 70-79 | 154-174 | 5.5 | 28 | 82 | 110 |
| 60-69 | 132-152 | 5 | 25 | 75 | 100 |
| 50-59 | 110-130 | 4 | 20 | 60 | 80 |
| 40-49 | 88-108 | 3.5 | 18 | 52 | 70 |
| 30-39 | 66-86 | 3 | 15 | 45 | 60 |
| 20-29 | 44-64 | 2 | 10 | 30 | 40 |
Nebulization Tent, Croupette (NEBULIZATION TENT, CROUPETTE)
In special circumstances it may be necessary to nebulize into a tent or Croupette, and this method of use must be individualized to take into account the available equipment and the patient's particular needs. This form of administration requires very large volumes of the solution, occasionally as much as 300 mL during a single treatment period.
If a tent or Croupette must be used, the recommended dose is the volume of acetylcysteine solution (using 10% or 20%) that will maintain a very heavy mist in the tent or Croupette for the desired period. Administration for intermittent or continuous prolonged periods, including overnight, may be desirable.
Acetaminophen Assay Methodology (ACETAMINOPHEN ASSAY METHODOLOGY)
Assay procedures most suitable for determining acetaminophen concentrations utilize high pressure liquid chromatography (HPLC) or gas liquid chromatography (GLC). The assay should measure only parent acetaminophen and not conjugated. The assay procedures listed below fulfill this requirement:
Selected Techniques (non Inclusive) (SELECTED TECHNIQUES (NON INCLUSIVE))
HPLC:
-
1.Blair D, Rumack BH. Clin Chem. 1977; 23(4): 743-745.
-
2.Howie D, Andriaenssens Pl, Prescott LF. J Pharm Pharmacol 1977; 29(4):235-237.
GLC
-
3.Prescott LF. J Pharm Pharmacol 1971; 23(10):807-808.
Colorimetric
-
4.Glynn JP, Kendal SE. Lancet 1975; 1(May 17):1147-1148.
Interpretation of Acetaminophen Assays (INTERPRETATION OF ACETAMINOPHEN ASSAYS)
-
1.When results of the plasma acetaminophen assay are available refer to the nomogram below to determine if plasma concentration is in the potentially toxic range. Values above the solid line connecting 200 mcg/mL at least 4 hours with 50 mcg/mL at 12 hours are associated with a possibility of hepatic toxicity if an antidote is not administered. (Do not wait for assay results to begin acetylcysteine treatment.)
-
2.If the predetoxification plasma level is above the broken line continue with maintenance doses of acetylcysteine. It is better to err on the safe side and thus the broken line is placed 25% below the solid line which defines possible toxicity.
-
3.If the predetoxification plasma level is below the broken line described above, there is minimal risk of hepatic toxicity and acetylcysteine treatment can be discontinued.
Estimating Potential for Hepatotoxicity
The following nomogram has been developed to estimate the probability that plasma levels in relation to intervals post ingestion will result in hepatotoxicity.
Supportive Treatment of Acetaminophen Overdose
-
1.Maintain fluid and electrolyte balance based on clinical evaluation of state of hydration and serum electrolytes.
-
2.Treat as necessary for hypoglycemia.
-
3.Administer vitamin K1 if prothrombin time ratio exceeds 1.5 or fresh frozen plasma if the prothrombin time ratio exceeds 3.0.
-
4.Diuretics and forced diuresis should be avoided.
Principal Display Panel 100 Mg/ml Vial Carton (PRINCIPAL DISPLAY PANEL - 100 mg/mL Vial Carton)
NDC 42494-435-25
Rx Only
Acetylcysteine Solution, USP
10% (100 mg/mL)
For Inhalation (Mucolytic Agent) or Oral Administration (Acetaminophen Antidote)
NOT FOR INJECTION
PRESERVATIVE FREE
25 x 4 mL Vials
Principal Display Panel 200 Mg/ml Vial Carton (PRINCIPAL DISPLAY PANEL - 200 mg/mL Vial Carton)
NDC 42494-436-25
Rx Only
Acetylcysteine Solution, USP
20% (200 mg/mL)
For Inhalation (Mucolytic Agent) or Oral Administration (Acetaminophen Antidote)
NOT FOR INJECTION
PRESERVATIVE FREE
25 x 4 mL Vials
Nebulization Face Mask, Mouth Piece, Tracheostomy (NEBULIZATION-FACE MASK, MOUTH PIECE, TRACHEOSTOMY)
When nebulized into a face mask, mouth piece, or tracheostomy, 1 to 10 mL of the 20% solution or 2 to 20 mL of the 10% solution may be given every 2 to 6 hours; the recommended dose for most patients is 3 to 5 mL of the 20% solution or 6 to 10 mL of the 10% solution 3 to 4 times a day.
Acetaminophen Assays Interpretation and Methodology (Acetaminophen Assays - Interpretation and Methodology)
The acute ingestion of acetaminophen in quantities of 150 mg/kg or greater may result in hepatic toxicity. However, the reported history of the quantity of a drug ingested as an overdose is often inaccurate and is not a reliable guide to therapy of the overdose. THEREFORE, PLASMA OR SERUM ACETAMINOPHEN CONCENTRATIONS, DETERMINED AS EARLY AS POSSIBLE, BUT NO SOONER THAN 4 HOURS FOLLOWING AN ACUTE OVERDOSE, ARE ESSENTIAL IN ASSESSING THE POTENTIAL RISK OF HEPATOTOXICITY. IF AN ASSAY FOR ACETAMINOPHEN CANNOT BE OBTAINED, IT IS NECESSARY TO ASSUME THAT THE OVERDOSE IS POTENTIALLY TOXIC.
Preparation of Acetylcysteine for Oral Administration
Oral administration requires dilution of the 20% solution with diet cola or other diet soft drinks, to a final concentration of 5% (see Dosage Guide and Preparation table). If administered via gastric tube or Miller-Abbott tube, water may be used as the diluent. The dilutions should be freshly prepared and utilized within one hour. Remaining undiluted solutions in opened vials can be stored in the refrigerator up to 96 hours. ACETYLCYSTEINE IS NOT APPROVED FOR PARENTERAL INJECTION.
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:49:08.915938 · Updated: 2026-03-14T22:32:10.275892