These Highlights Do Not Include All The Information Needed To Use Vancomycin Hydrochloride Capsules Safely And Effectively. See Full Prescribing Information For Vancomycin Hydrochloride Capsules.
7bbd2c81-33d9-4397-8795-8b9fa28cb5cf
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
Vancomycin Hydrochloride Capsules are indicated for the treatment of C. difficile -associated diarrhea. Vancomycin Hydrochloride Capsules are also used for the treatment of enterocolitis caused by Staphylococcus aureus (including methicillin-resistant strains) in adult and pediatric patients less than 18 years of age.
Indications and Usage
Vancomycin Hydrochloride Capsules are indicated for the treatment of C. difficile -associated diarrhea. Vancomycin Hydrochloride Capsules are also used for the treatment of enterocolitis caused by Staphylococcus aureus (including methicillin-resistant strains) in adult and pediatric patients less than 18 years of age.
Dosage and Administration
C. difficile -associated diarrhea: Adult Patients (18 years of age or greater): 125 mg orally 4 times daily for 10 days. ( 2.1 ) Pediatric Patients (less than 18 years of age): 40 mg/kg in 3 or 4 divided doses for 7 to 10 days. The total daily dosage should not exceed 2 g. ( 2.2 ) Staphylococcal enterocolitis: Adult Patients (18 years of age or greater): 500 mg to 2 g orally in 3 or 4 divided doses for 7 to 10 days. ( 2.1 ) Pediatric Patients (less than 18 years of age): 40 mg/kg in 3 or 4 divided doses for 7 to 10 days. The total daily dosage should not exceed 2 g. ( 2.2 )
Warnings and Precautions
Vancomycin hydrochloride capsules must be given orally for treatment of staphylococcal enterocolitis and C. difficile -associated diarrhea. Orally administered vancomycin hydrochloride capsules are not effective for other types of infections. ( 5.1 ) Clinically significant serum concentrations have been reported in some patients who have taken multiple oral doses of vancomycin hydrochloride capsules for active C. difficile -associated diarrhea. Monitoring of serum concentrations may be appropriate in some instances. ( 5.2 ) Nephrotoxicity has occurred following oral vancomycin hydrochloride capsule therapy and can occur either during or after completion of therapy. The risk is increased in geriatric patients. ( 5.3 ) Monitor renal function. Ototoxicity has occurred in patients receiving vancomycin hydrochloride capsules. ( 5.4 ) Assessment of auditory function may be appropriate in some instances. Severe Dermatologic Reactions: Discontinue vancomycin hydrochloride capsules at the first appearance of skin rashes, mucosal lesions, or blisters. ( 5.5 ) Prescribing vancomycin hydrochloride capsules in the absence of a proven or strongly suspected bacterial infection is unlikely to provide benefit to the patient and increases the risk of the development of drug resistant bacteria. ( 5.6 ) The 125 mg strength capsules contains FD&C Yellow No. 5 (tartrazine) which may cause allergic-type reactions (including bronchial asthma) in certain susceptible persons. ( 5.7 )
Contraindications
Vancomycin Hydrochloride Capsules are contraindicated in patients with known hypersensitivity to vancomycin.
Adverse Reactions
The most common adverse reactions (≥ 10%) were nausea (17%), abdominal pain (15%), and hypokalemia (13%). ( 6.1 ) To report SUSPECTED ADVERSE REACTIONS, contact Cameron Pharmaceuticals, LLC 1-888-296-9383 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
Drug Interactions
No drug interaction studies have been conducted.
Storage and Handling
Vancomycin Hydrochloride Capsules, USP are available in: The 250 mg Capsules have a blue cap and dark-yellow body imprinted with "OP65" on both cap and body in white ink. NDC: 72162-2306-4: 50 Capsules in a Bottle Store at 20° to 25°C (68° to 77°F); excursions permitted to 15° to 30°C (59° to 86°F). [See USP Controlled Room Temperature] Repackaged/Relabeled by: Bryant Ranch Prepack, Inc. Burbank, CA 91504
How Supplied
Vancomycin Hydrochloride Capsules, USP are available in: The 250 mg Capsules have a blue cap and dark-yellow body imprinted with "OP65" on both cap and body in white ink. NDC: 72162-2306-4: 50 Capsules in a Bottle Store at 20° to 25°C (68° to 77°F); excursions permitted to 15° to 30°C (59° to 86°F). [See USP Controlled Room Temperature] Repackaged/Relabeled by: Bryant Ranch Prepack, Inc. Burbank, CA 91504
Medication Information
Warnings and Precautions
Vancomycin hydrochloride capsules must be given orally for treatment of staphylococcal enterocolitis and C. difficile -associated diarrhea. Orally administered vancomycin hydrochloride capsules are not effective for other types of infections. ( 5.1 ) Clinically significant serum concentrations have been reported in some patients who have taken multiple oral doses of vancomycin hydrochloride capsules for active C. difficile -associated diarrhea. Monitoring of serum concentrations may be appropriate in some instances. ( 5.2 ) Nephrotoxicity has occurred following oral vancomycin hydrochloride capsule therapy and can occur either during or after completion of therapy. The risk is increased in geriatric patients. ( 5.3 ) Monitor renal function. Ototoxicity has occurred in patients receiving vancomycin hydrochloride capsules. ( 5.4 ) Assessment of auditory function may be appropriate in some instances. Severe Dermatologic Reactions: Discontinue vancomycin hydrochloride capsules at the first appearance of skin rashes, mucosal lesions, or blisters. ( 5.5 ) Prescribing vancomycin hydrochloride capsules in the absence of a proven or strongly suspected bacterial infection is unlikely to provide benefit to the patient and increases the risk of the development of drug resistant bacteria. ( 5.6 ) The 125 mg strength capsules contains FD&C Yellow No. 5 (tartrazine) which may cause allergic-type reactions (including bronchial asthma) in certain susceptible persons. ( 5.7 )
Indications and Usage
Vancomycin Hydrochloride Capsules are indicated for the treatment of C. difficile -associated diarrhea. Vancomycin Hydrochloride Capsules are also used for the treatment of enterocolitis caused by Staphylococcus aureus (including methicillin-resistant strains) in adult and pediatric patients less than 18 years of age.
Dosage and Administration
C. difficile -associated diarrhea: Adult Patients (18 years of age or greater): 125 mg orally 4 times daily for 10 days. ( 2.1 ) Pediatric Patients (less than 18 years of age): 40 mg/kg in 3 or 4 divided doses for 7 to 10 days. The total daily dosage should not exceed 2 g. ( 2.2 ) Staphylococcal enterocolitis: Adult Patients (18 years of age or greater): 500 mg to 2 g orally in 3 or 4 divided doses for 7 to 10 days. ( 2.1 ) Pediatric Patients (less than 18 years of age): 40 mg/kg in 3 or 4 divided doses for 7 to 10 days. The total daily dosage should not exceed 2 g. ( 2.2 )
Contraindications
Vancomycin Hydrochloride Capsules are contraindicated in patients with known hypersensitivity to vancomycin.
Adverse Reactions
The most common adverse reactions (≥ 10%) were nausea (17%), abdominal pain (15%), and hypokalemia (13%). ( 6.1 ) To report SUSPECTED ADVERSE REACTIONS, contact Cameron Pharmaceuticals, LLC 1-888-296-9383 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
Drug Interactions
No drug interaction studies have been conducted.
Storage and Handling
Vancomycin Hydrochloride Capsules, USP are available in: The 250 mg Capsules have a blue cap and dark-yellow body imprinted with "OP65" on both cap and body in white ink. NDC: 72162-2306-4: 50 Capsules in a Bottle Store at 20° to 25°C (68° to 77°F); excursions permitted to 15° to 30°C (59° to 86°F). [See USP Controlled Room Temperature] Repackaged/Relabeled by: Bryant Ranch Prepack, Inc. Burbank, CA 91504
How Supplied
Vancomycin Hydrochloride Capsules, USP are available in: The 250 mg Capsules have a blue cap and dark-yellow body imprinted with "OP65" on both cap and body in white ink. NDC: 72162-2306-4: 50 Capsules in a Bottle Store at 20° to 25°C (68° to 77°F); excursions permitted to 15° to 30°C (59° to 86°F). [See USP Controlled Room Temperature] Repackaged/Relabeled by: Bryant Ranch Prepack, Inc. Burbank, CA 91504
Description
Vancomycin Hydrochloride Capsules are indicated for the treatment of C. difficile -associated diarrhea. Vancomycin Hydrochloride Capsules are also used for the treatment of enterocolitis caused by Staphylococcus aureus (including methicillin-resistant strains) in adult and pediatric patients less than 18 years of age.
Section 42229-5
Limitations of Use
- Parenteral administration of vancomycin is not effective for the above infections; therefore, Vancomycin Hydrochloride Capsules must be given orally for these infections.
- Orally administered Vancomycin Hydrochloride Capsules is not effective for other types of infections.
To reduce the development of drug-resistant bacteria and maintain the effectiveness of Vancomycin Hydrochloride Capsules and other antibacterial drugs, Vancomycin Hydrochloride Capsules should be used only to treat or prevent infections that are proven or strongly suspected to be caused by susceptible bacteria. When culture and susceptibility information are available, they should be considered in selecting or modifying antibacterial therapy. In the absence of such data, local epidemiology and susceptibility patterns may contribute to the empiric selection of therapy.
Section 51945-4
Vancomycin HCl 250mg Capsules #50
2.1 Adults
Vancomycin Hydrochloride Capsules are used in treating C. difficile-associated diarrhea and staphylococcal enterocolitis.
- C. difficile-associated diarrhea: The recommended dose is 125 mg administered orally 4 times daily for 10 days.
- Staphylococcal enterocolitis: Total daily dosage is 500 mg to 2 g administered orally in 3 or 4 divided doses for 7 to 10 days.
10 Overdosage
Supportive care is advised, with maintenance of glomerular filtration. Vancomycin is poorly removed by dialysis. Hemofiltration and hemoperfusion with polysulfone resin have been reported to result in increased vancomycin clearance.
To obtain current information about the treatment of overdose, contact a certified Poison Control Center (1-800-222-1222 or www.poison.org). In managing overdosage, consider the possibility of multiple drug overdoses, interaction among drugs, and unusual drug kinetics.
15 References
1. Byrd RA., Gries CL, Buening M.: Developmental Toxicology Studies of Vancomycin Hydrochloride Administered Intravenously to Rats and Rabbits. Fundam Appl Toxicol 1994; 23: 590-597.
11 Description
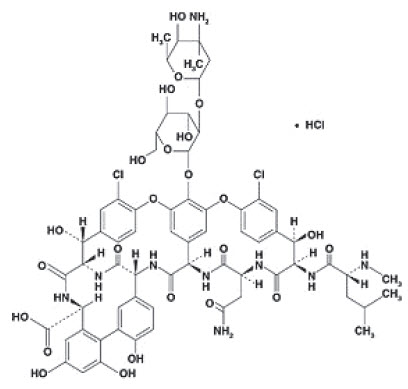
Vancomycin Hydrochloride Capsules USP for oral administration contain chromatographically purified vancomycin hydrochloride, a tricyclic glycopeptide antibiotic derived from Amycolatopsis orientalis (formerly Nocardia orientalis), which has the chemical formula C66H75Cl2N9O24∙HCl. The molecular weight of vancomycin hydrochloride is 1485.73; 500 mg of the base is equivalent to 0.34 mmol.
The capsules contain 125 mg vancomycin (equivalent to 128 mg vancomycin hydrochloride). These capsules also contain polyethylene glycol 6000, FD&C Yellow No. 5, titanium dioxide, FD&C Blue No. 1, sodium lauryl sulfate and gelatin.
The capsules contain 250 mg vancomycin (equivalent to 256 mg vancomycin hydrochloride). These capsules also contain polyethylene glycol 6000, yellow iron oxide, titanium dioxide, FD&C Blue No. 1, sodium lauryl sulfate, gelatin.
Both 125 mg and 250 mg capsules are imprinted with ink which may contain titanium dioxide, carnauba wax, white shellac, glyceryl monooleate.
Vancomycin hydrochloride has the structural formula:
5.4 Ototoxicity
Ototoxicity has occurred in patients receiving vancomycin. It may be transient or permanent. It has been reported mostly in patients who have been given excessive intravenous doses, who have an underlying hearing loss, or who are receiving concomitant therapy with another ototoxic agent, such as an aminoglycoside. Serial tests of auditory function may be helpful in order to minimize the risk of ototoxicity (see ADVERSE REACTIONS, Postmarketing Experience [6.2] ).
5.1 Oral Use Only
Vancomycin Hydrochloride Capsules for the treatment of colitis are for oral use only and are not systemically absorbed.
Vancomycin Hydrochloride Capsules must be given orally for treatment of staphylococcal enterocolitis and Clostridium difficile-associated diarrhea. Orally administered Vancomycin Hydrochloride Capsules are not effective for other types of infections.
Parenteral administration of vancomycin is not effective for treatment of staphylococcal enterocolitis and C. difficile-associated diarrhea. If parenteral vancomycin therapy is desired, use an intravenous preparation of vancomycin and consult the package insert accompanying that preparation.
8.4 Pediatric Use
Vancomycin Hydrochloride Capsules are indicated in pediatric patients less than 18 years of age for the treatment of C. difficile associated diarrhea and enterocolitis caused by S. aureus (including methicillin-resistant strains) [see Indications and Usage (1) and Dosage and Administration (2.2) ].
8.5 Geriatric Use
In clinical trials, 54% of vancomycin hydrochloride-treated subjects were >65 years of age. Of these, 40% were between the ages of >65 and 75, and 60% were >75 years of age.
Clinical studies with vancomycin hydrochloride in diarrhea associated with Clostridium difficile have demonstrated that geriatric subjects are at increased risk of developing nephrotoxicity following treatment with oral vancomycin hydrochloride, which may occur during or after completion of therapy. In patients >65 years of age, including those with normal renal function prior to treatment, renal function should be monitored during and following treatment with vancomycin hydrochloride to detect potential vancomycin induced nephrotoxicity (see WARNINGS AND PRECAUTIONS, Nephrotoxicity [5.3]; ADVERSE REACTIONS, Clinical Trials Experience [6.1] and CLINICAL STUDIES, Diarrhea Associated with Clostridium difficile [14.1] ). Patients >65 years of age may take longer to respond to therapy compared to patients ≤65 years of age (see CLINICAL STUDIES, Diarrhea Associated with Clostridium difficile [14.1] ). Clinicians should be aware of the importance of appropriate duration of vancomycin hydrochloride treatment in patients >65 years of age and not discontinue or switch to alternative treatment prematurely.
5.3 Nephrotoxicity
Nephrotoxicity (e.g., reports of renal failure, renal impairment, blood creatinine increased) has occurred following oral Vancomycin Hydrochloride Capsules therapy in randomized controlled clinical studies, and can occur either during or after completion of therapy. The risk of nephrotoxicity is increased in patients >65 years of age (see ADVERSE REACTIONS, Clinical Trial Experience [6.1] and USE IN SPECIFIC POPULATIONS, Geriatric Use [8.5] ).
In patients >65 years of age, including those with normal renal function prior to treatment, renal function should be monitored during and following treatment with Vancomycin Hydrochloride Capsules to detect potential vancomycin induced nephrotoxicity.
4 Contraindications
Vancomycin Hydrochloride Capsules are contraindicated in patients with known hypersensitivity to vancomycin.
6 Adverse Reactions
The most common adverse reactions (≥ 10%) were nausea (17%), abdominal pain (15%), and hypokalemia (13%). (6.1)
To report SUSPECTED ADVERSE REACTIONS, contact Cameron Pharmaceuticals, LLC 1-888-296-9383 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
7 Drug Interactions
No drug interaction studies have been conducted.
12.3 Pharmacokinetics
Vancomycin is poorly absorbed after oral administration. During multiple dosing of 250 mg every 8 hours for 7 doses, fecal concentrations of vancomycin in volunteers exceeded 100 mg/kg in the majority of samples. No blood concentrations were detected and urinary recovery did not exceed 0.76%. In anephric subjects with no inflammatory bowel disease who received vancomycin oral solution 2 g for 16 days, blood concentrations of vancomycin were less than or equal to 0.66 µg/mL in 2 of 5 subjects.
No measurable blood concentrations were attained in the other 3 subjects. Following doses of 2 g daily, concentrations of drug were >3100 mg/kg in the feces and <1 mcg/mL in the serum of subjects with normal renal function who had C. difficile-associated diarrhea. After multiple-dose oral administration of vancomycin, measurable serum concentrations may occur in patients with active C. difficile associated diarrhea, and, in the presence of renal impairment, the possibility of accumulation exists. It should be noted that the total systemic and renal clearances of vancomycin are reduced in the elderly (see Use in Specific Population [8.5] ).
1 Indications and Usage
Vancomycin Hydrochloride Capsules are indicated for the treatment of C. difficile-associated diarrhea. Vancomycin Hydrochloride Capsules are also used for the treatment of enterocolitis caused by Staphylococcus aureus (including methicillin-resistant strains) in adult and pediatric patients less than 18 years of age.
12.1 Mechanism of Action
Vancomycin is an antibacterial drug (see Microbiology [12.4] ).
5 Warnings and Precautions
- Vancomycin hydrochloride capsules must be given orally for treatment of staphylococcal enterocolitis and C. difficile-associated diarrhea. Orally administered vancomycin hydrochloride capsules are not effective for other types of infections. (5.1)
- Clinically significant serum concentrations have been reported in some patients who have taken multiple oral doses of vancomycin hydrochloride capsules for active C. difficile-associated diarrhea. Monitoring of serum concentrations may be appropriate in some instances. (5.2)
- Nephrotoxicity has occurred following oral vancomycin hydrochloride capsule therapy and can occur either during or after completion of therapy. The risk is increased in geriatric patients. (5.3) Monitor renal function.
- Ototoxicity has occurred in patients receiving vancomycin hydrochloride capsules. (5.4) Assessment of auditory function may be appropriate in some instances.
- Severe Dermatologic Reactions: Discontinue vancomycin hydrochloride capsules at the first appearance of skin rashes, mucosal lesions, or blisters. (5.5)
- Prescribing vancomycin hydrochloride capsules in the absence of a proven or strongly suspected bacterial infection is unlikely to provide benefit to the patient and increases the risk of the development of drug resistant bacteria. (5.6)
- The 125 mg strength capsules contains FD&C Yellow No. 5 (tartrazine) which may cause allergic-type reactions (including bronchial asthma) in certain susceptible persons. (5.7)
2 Dosage and Administration
- C. difficile-associated diarrhea:
- Adult Patients (18 years of age or greater): 125 mg orally 4 times daily for 10 days. (2.1)
- Pediatric Patients (less than 18 years of age): 40 mg/kg in 3 or 4 divided doses for 7 to 10 days. The total daily dosage should not exceed 2 g. (2.2)
- Staphylococcal enterocolitis:
- Adult Patients (18 years of age or greater): 500 mg to 2 g orally in 3 or 4 divided doses for 7 to 10 days. (2.1)
- Pediatric Patients (less than 18 years of age): 40 mg/kg in 3 or 4 divided doses for 7 to 10 days. The total daily dosage should not exceed 2 g. (2.2)
3 Dosage Forms and Strengths
Vancomycin Hydrochloride Capsules USP 125 mg
Vancomycin Hydrochloride Capsules USP 250 mg
CAPSULES have a blue cap and dark-yellow body imprinted with "OP65" on both cap and body in white ink.6.2 Postmarketing Experience
The following adverse reactions have been identified during post-approval use of vancomycin hydrochloride. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
8 Use in Specific Populations
6.1 Clinical Trials Experience
Because clinical studies are conducted under widely varying conditions, adverse reaction rates observed in the clinical studies of a drug cannot be directly compared to rates in the clinical studies of another drug and may not reflect the rates observed in practice.
The data described below reflect exposure to vancomycin hydrochloride in 260 adult subjects in two Phase 3 clinical trials for the treatment of diarrhea associated with C. difficile. In both trials, subjects received vancomycin hydrochloride capsules 125 mg orally four times daily. The mean duration of treatment was 9.4 days. The median age of patients was 67, ranging between 19 and 96 years of age. Patients were predominantly Caucasian (93%) and 52% were male.
Adverse reactions occurring in ≥ 5% of vancomycin hydrochloride-treated subjects are shown in Table 1. The most common adverse reactions associated with vancomycin hydrochloride (≥ 10%) were nausea, abdominal pain, and hypokalemia.
| System/Organ Class | Adverse Reaction | Vancomycin Hydrochloride % (N=260) |
|---|---|---|
| Gastrointestinal disorders | Nausea | 17 |
| Abdominal pain | 15 | |
| Vomiting | 9 | |
| Diarrhea | 9 | |
| Flatulence | 8 | |
| General disorders and administration site conditions | Pyrexia | 9 |
| Edema peripheral | 6 | |
| Fatigue | 5 | |
| Infections and infestations | Urinary tract infection | 8 |
| Metabolism and nutrition disorders | Hypokalemia | 13 |
| Musculoskeletal and connective tissue disorders | Back pain | 6 |
| Nervous system disorders | Headache | 7 |
Nephrotoxicity (e.g., reports of renal failure, renal impairment, blood creatinine increased) occurred in 5% of subjects treated with vancomycin hydrochloride. Nephrotoxicity following vancomycin hydrochloride typically first occurred within one week after completion of treatment (median day of onset was Day 16). Nephrotoxicity following vancomycin hydrochloride occurred in 6% of subjects >65 years of age and 3% of subjects ≤65 years of age (see WARNINGS AND PRECAUTIONS, Nephrotoxicity [5.3] ).
The incidences of hypokalemia, urinary tract infection, peripheral edema, insomnia, constipation, anemia, depression, vomiting, and hypotension were higher among subjects >65 years of age than in subjects ≤65 years of age (see USE IN SPECIFIC POPULATIONS, Geriatric Use [8.5] ).
Discontinuation of study drug due to adverse events occurred in 7% of subjects treated with vancomycin hydrochloride. The most common adverse events leading to discontinuation of vancomycin hydrochloride were C. difficile colitis (<1%), nausea (<1%), and vomiting (<1%).
5.5 Severe Dermatologic Reactions
Severe dermatologic reactions such as toxic epidermal necrolysis (TEN), Stevens-Johnson syndrome (SJS), drug reaction with eosinophilia and systemic symptoms (DRESS), acute generalized exanthematous pustulosis (AGEP), and linear IgA bullous dermatosis (LABD) have been reported in association with the use of vancomycin. Cutaneous signs or symptoms reported include skin rashes, mucosal lesions, and blisters.
Discontinue Vancomycin Hydrochloride Capsules at the first appearance of signs and symptoms of TEN, SJS, DRESS,AGEP, or LABD.
16 How Supplied/storage and Handling
Vancomycin Hydrochloride Capsules, USP are available in:
The 250 mg Capsules have a blue cap and dark-yellow body imprinted with "OP65" on both cap and body in white ink.
NDC: 72162-2306-4: 50 Capsules in a Bottle
Store at 20° to 25°C (68° to 77°F); excursions permitted to 15° to 30°C (59° to 86°F). [See USP Controlled Room Temperature]
Repackaged/Relabeled by:
Bryant Ranch Prepack, Inc.
Burbank, CA 91504
5.2 Potential for Systemic Absorption
Clinically significant serum concentrations have been reported in some patients who have taken multiple oral doses of Vancomycin Hydrochloride Capsules for active C. difficile-associated diarrhea. Some patients with inflammatory disorders of the intestinal mucosa also may have significant systemic absorption of vancomycin. These patients may be at risk for the development of adverse reactions associated with higher doses of Vancomycin Hydrochloride Capsules; therefore, monitoring of serum concentrations of vancomycin may be appropriate in some instances, e.g., in patients with renal insufficiency and/or colitis or in those receiving concomitant therapy with an aminoglycoside antibiotic.
5.6 Development of Drug Resistant Bacteria
Prescribing Vancomycin Hydrochloride Capsules in the absence of a proven or strongly suspected bacterial infection or a prophylactic indication is unlikely to provide benefit to the patient and increases the risk of the development of drug resistant bacteria.
5.7 Risk of Allergic Reactions Due to Tartrazine
The 125 mg strength capsules contains FD&C Yellow No. 5 (tartrazine) which may cause allergic-type reactions (including bronchial asthma) in certain susceptible persons. Although the overall incidence of FD&C Yellow No. 5 (tartrazine) sensitivity in the general population is low, it is frequently seen in patients who also have aspirin hypersensitivity.
2.2 Pediatric Patients (less Than 18 Years of Age)
For both C. difficile-associated diarrhea and staphylococcal enterocolitis, the usual daily dosage is 40 mg/kg in 3 or 4 divided doses for 7 to 10 days. The total daily dosage should not exceed 2 g.
14.1 Diarrhea Associated With Clostridium Difficile
In two trials, Vancomycin Hydrochloride Capsules 125 mg orally four times daily for 10 days was evaluated in 266 adult subjects with C. difficile-associated diarrhea (CDAD). Enrolled subjects were 18 years of age or older and received no more than 48 hours of treatment with oral vancomycin hydrochloride or oral/intravenous metronidazole in the 5 days preceding enrollment. CDAD was definite as ≥3 loose or watery bowel movements within the 24 hours preceding enrollment, and the presence of either C. difficile toxin A or B, or pseudomembranes on endoscopy within the 72 hours preceding enrollment. Subjects with fulminant C. difficile disease, sepsis with hypotension, ileus, peritoneal signs or severe hepatic disease were excluded.
Efficacy analyses were performed on the Full Analysis Set (FAS), which included randomized subjects who received at least one dose of vancomycin hydrochloride and had any post-dosing investigator evaluation data (N=259; 134 in Trial 1 and 125 in Trial 2).
The demographic profile and baseline CDAD characteristics of enrolled subjects were similar in the two trials. Vancomycin Hydrochloride-treated subjects had a median age of 67 years, were mainly white (93%), and male (52%). CDAD was classified as severe (defined as 10 or more unformed bowel movements per day or WBC ≥15000/mm3) in 25% of subjects, and 47% were previously treated for CDAD.
Efficacy was assessed by using clinical success, defined as diarrhea resolution and the absence of severe abdominal discomfort due to CDAD, on Day 10. An additional efficacy endpoint was the time to resolution of diarrhea, defined as the beginning of diarrhea resolution that was sustained through the end of the prescribed active treatment period.
The results for clinical success for vancomycin hydrochloride-treated subjects in both trials are shown in Table 2.
| Clinical Success Rate | 95% Confidence Interval | |
|---|---|---|
| Vancomycin Hydrochloride % (N) |
||
| Trial 1 | 81.3 (134) | (74.4, 88.3) |
| Trial 2 | 80.8 (125) | (73.5, 88.1) |
The median time to resolution of diarrhea was 5 days and 4 days in Trial 1 and Trial 2, respectively. For subjects older than 65 years of age, the median time to resolution was 6 days and 4 days in Trial 1 and Trial 2, respectively. In subjects with diarrhea resolution at end-of-treatment with Vancomycin Hydrochloride Capsules, recurrence of CDAD during the following four weeks occurred in 25 of 107 (23%) and 18 of 102 (18%) in Trial 1 and Trial 2, respectively.
Restriction Endonuclease Analysis (REA) was used to identify C. difficile baseline isolates in the BI group. In Trial 1, the Vancomycin Hydrochloride-treated subjects were classified at baseline as follows 31 (23%) with BI strain, 69 (52%) with non-BI strain, and 34 (25%) with unknown strain. Clinical success rates were 87% for BI strain, 81% for non-BI strain, and 76% for unknown strain. In subjects with diarrhea resolution at end-of-treatment with vancomycin hydrochloride, recurrence of CDAD during the following four weeks occurred in 7 of 26 subjects with BI strain, 12 of 56 subjects with non-BI strain, and 6 of 25 subjects with unknown strain.
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
No long-term carcinogenesis studies in animals have been conducted.
At concentrations up to 1000 mcg/mL, vancomycin had no mutagenic effect in vitro in the mouse lymphoma forward mutation assay or the primary rat hepatocyte unscheduled DNA synthesis assay. The concentrations tested in vitro were above the peak plasma vancomycin concentrations of 20 to 40 mcg/mL usually achieved in humans after slow infusion of the maximum recommended dose of 1 g. Vancomycin had no mutagenic effect in vivo in the Chinese hamster sister chromatid exchange assay (400 mg/kg IP) or the mouse micronucleus assay (800 mg/kg IP).
No definitive fertility studies have been conducted.
Structured Label Content
Section 42229-5 (42229-5)
Limitations of Use
- Parenteral administration of vancomycin is not effective for the above infections; therefore, Vancomycin Hydrochloride Capsules must be given orally for these infections.
- Orally administered Vancomycin Hydrochloride Capsules is not effective for other types of infections.
To reduce the development of drug-resistant bacteria and maintain the effectiveness of Vancomycin Hydrochloride Capsules and other antibacterial drugs, Vancomycin Hydrochloride Capsules should be used only to treat or prevent infections that are proven or strongly suspected to be caused by susceptible bacteria. When culture and susceptibility information are available, they should be considered in selecting or modifying antibacterial therapy. In the absence of such data, local epidemiology and susceptibility patterns may contribute to the empiric selection of therapy.
Section 51945-4 (51945-4)
Vancomycin HCl 250mg Capsules #50
2.1 Adults
Vancomycin Hydrochloride Capsules are used in treating C. difficile-associated diarrhea and staphylococcal enterocolitis.
- C. difficile-associated diarrhea: The recommended dose is 125 mg administered orally 4 times daily for 10 days.
- Staphylococcal enterocolitis: Total daily dosage is 500 mg to 2 g administered orally in 3 or 4 divided doses for 7 to 10 days.
10 Overdosage (10 OVERDOSAGE)
Supportive care is advised, with maintenance of glomerular filtration. Vancomycin is poorly removed by dialysis. Hemofiltration and hemoperfusion with polysulfone resin have been reported to result in increased vancomycin clearance.
To obtain current information about the treatment of overdose, contact a certified Poison Control Center (1-800-222-1222 or www.poison.org). In managing overdosage, consider the possibility of multiple drug overdoses, interaction among drugs, and unusual drug kinetics.
15 References (15 REFERENCES)
1. Byrd RA., Gries CL, Buening M.: Developmental Toxicology Studies of Vancomycin Hydrochloride Administered Intravenously to Rats and Rabbits. Fundam Appl Toxicol 1994; 23: 590-597.
11 Description (11 DESCRIPTION)
Vancomycin Hydrochloride Capsules USP for oral administration contain chromatographically purified vancomycin hydrochloride, a tricyclic glycopeptide antibiotic derived from Amycolatopsis orientalis (formerly Nocardia orientalis), which has the chemical formula C66H75Cl2N9O24∙HCl. The molecular weight of vancomycin hydrochloride is 1485.73; 500 mg of the base is equivalent to 0.34 mmol.
The capsules contain 125 mg vancomycin (equivalent to 128 mg vancomycin hydrochloride). These capsules also contain polyethylene glycol 6000, FD&C Yellow No. 5, titanium dioxide, FD&C Blue No. 1, sodium lauryl sulfate and gelatin.
The capsules contain 250 mg vancomycin (equivalent to 256 mg vancomycin hydrochloride). These capsules also contain polyethylene glycol 6000, yellow iron oxide, titanium dioxide, FD&C Blue No. 1, sodium lauryl sulfate, gelatin.
Both 125 mg and 250 mg capsules are imprinted with ink which may contain titanium dioxide, carnauba wax, white shellac, glyceryl monooleate.
Vancomycin hydrochloride has the structural formula:
5.4 Ototoxicity
Ototoxicity has occurred in patients receiving vancomycin. It may be transient or permanent. It has been reported mostly in patients who have been given excessive intravenous doses, who have an underlying hearing loss, or who are receiving concomitant therapy with another ototoxic agent, such as an aminoglycoside. Serial tests of auditory function may be helpful in order to minimize the risk of ototoxicity (see ADVERSE REACTIONS, Postmarketing Experience [6.2] ).
5.1 Oral Use Only
Vancomycin Hydrochloride Capsules for the treatment of colitis are for oral use only and are not systemically absorbed.
Vancomycin Hydrochloride Capsules must be given orally for treatment of staphylococcal enterocolitis and Clostridium difficile-associated diarrhea. Orally administered Vancomycin Hydrochloride Capsules are not effective for other types of infections.
Parenteral administration of vancomycin is not effective for treatment of staphylococcal enterocolitis and C. difficile-associated diarrhea. If parenteral vancomycin therapy is desired, use an intravenous preparation of vancomycin and consult the package insert accompanying that preparation.
8.4 Pediatric Use
Vancomycin Hydrochloride Capsules are indicated in pediatric patients less than 18 years of age for the treatment of C. difficile associated diarrhea and enterocolitis caused by S. aureus (including methicillin-resistant strains) [see Indications and Usage (1) and Dosage and Administration (2.2) ].
8.5 Geriatric Use
In clinical trials, 54% of vancomycin hydrochloride-treated subjects were >65 years of age. Of these, 40% were between the ages of >65 and 75, and 60% were >75 years of age.
Clinical studies with vancomycin hydrochloride in diarrhea associated with Clostridium difficile have demonstrated that geriatric subjects are at increased risk of developing nephrotoxicity following treatment with oral vancomycin hydrochloride, which may occur during or after completion of therapy. In patients >65 years of age, including those with normal renal function prior to treatment, renal function should be monitored during and following treatment with vancomycin hydrochloride to detect potential vancomycin induced nephrotoxicity (see WARNINGS AND PRECAUTIONS, Nephrotoxicity [5.3]; ADVERSE REACTIONS, Clinical Trials Experience [6.1] and CLINICAL STUDIES, Diarrhea Associated with Clostridium difficile [14.1] ). Patients >65 years of age may take longer to respond to therapy compared to patients ≤65 years of age (see CLINICAL STUDIES, Diarrhea Associated with Clostridium difficile [14.1] ). Clinicians should be aware of the importance of appropriate duration of vancomycin hydrochloride treatment in patients >65 years of age and not discontinue or switch to alternative treatment prematurely.
5.3 Nephrotoxicity
Nephrotoxicity (e.g., reports of renal failure, renal impairment, blood creatinine increased) has occurred following oral Vancomycin Hydrochloride Capsules therapy in randomized controlled clinical studies, and can occur either during or after completion of therapy. The risk of nephrotoxicity is increased in patients >65 years of age (see ADVERSE REACTIONS, Clinical Trial Experience [6.1] and USE IN SPECIFIC POPULATIONS, Geriatric Use [8.5] ).
In patients >65 years of age, including those with normal renal function prior to treatment, renal function should be monitored during and following treatment with Vancomycin Hydrochloride Capsules to detect potential vancomycin induced nephrotoxicity.
4 Contraindications (4 CONTRAINDICATIONS)
Vancomycin Hydrochloride Capsules are contraindicated in patients with known hypersensitivity to vancomycin.
6 Adverse Reactions (6 ADVERSE REACTIONS)
The most common adverse reactions (≥ 10%) were nausea (17%), abdominal pain (15%), and hypokalemia (13%). (6.1)
To report SUSPECTED ADVERSE REACTIONS, contact Cameron Pharmaceuticals, LLC 1-888-296-9383 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
7 Drug Interactions (7 DRUG INTERACTIONS)
No drug interaction studies have been conducted.
12.3 Pharmacokinetics
Vancomycin is poorly absorbed after oral administration. During multiple dosing of 250 mg every 8 hours for 7 doses, fecal concentrations of vancomycin in volunteers exceeded 100 mg/kg in the majority of samples. No blood concentrations were detected and urinary recovery did not exceed 0.76%. In anephric subjects with no inflammatory bowel disease who received vancomycin oral solution 2 g for 16 days, blood concentrations of vancomycin were less than or equal to 0.66 µg/mL in 2 of 5 subjects.
No measurable blood concentrations were attained in the other 3 subjects. Following doses of 2 g daily, concentrations of drug were >3100 mg/kg in the feces and <1 mcg/mL in the serum of subjects with normal renal function who had C. difficile-associated diarrhea. After multiple-dose oral administration of vancomycin, measurable serum concentrations may occur in patients with active C. difficile associated diarrhea, and, in the presence of renal impairment, the possibility of accumulation exists. It should be noted that the total systemic and renal clearances of vancomycin are reduced in the elderly (see Use in Specific Population [8.5] ).
1 Indications and Usage (1 INDICATIONS AND USAGE)
Vancomycin Hydrochloride Capsules are indicated for the treatment of C. difficile-associated diarrhea. Vancomycin Hydrochloride Capsules are also used for the treatment of enterocolitis caused by Staphylococcus aureus (including methicillin-resistant strains) in adult and pediatric patients less than 18 years of age.
12.1 Mechanism of Action
Vancomycin is an antibacterial drug (see Microbiology [12.4] ).
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
- Vancomycin hydrochloride capsules must be given orally for treatment of staphylococcal enterocolitis and C. difficile-associated diarrhea. Orally administered vancomycin hydrochloride capsules are not effective for other types of infections. (5.1)
- Clinically significant serum concentrations have been reported in some patients who have taken multiple oral doses of vancomycin hydrochloride capsules for active C. difficile-associated diarrhea. Monitoring of serum concentrations may be appropriate in some instances. (5.2)
- Nephrotoxicity has occurred following oral vancomycin hydrochloride capsule therapy and can occur either during or after completion of therapy. The risk is increased in geriatric patients. (5.3) Monitor renal function.
- Ototoxicity has occurred in patients receiving vancomycin hydrochloride capsules. (5.4) Assessment of auditory function may be appropriate in some instances.
- Severe Dermatologic Reactions: Discontinue vancomycin hydrochloride capsules at the first appearance of skin rashes, mucosal lesions, or blisters. (5.5)
- Prescribing vancomycin hydrochloride capsules in the absence of a proven or strongly suspected bacterial infection is unlikely to provide benefit to the patient and increases the risk of the development of drug resistant bacteria. (5.6)
- The 125 mg strength capsules contains FD&C Yellow No. 5 (tartrazine) which may cause allergic-type reactions (including bronchial asthma) in certain susceptible persons. (5.7)
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
- C. difficile-associated diarrhea:
- Adult Patients (18 years of age or greater): 125 mg orally 4 times daily for 10 days. (2.1)
- Pediatric Patients (less than 18 years of age): 40 mg/kg in 3 or 4 divided doses for 7 to 10 days. The total daily dosage should not exceed 2 g. (2.2)
- Staphylococcal enterocolitis:
- Adult Patients (18 years of age or greater): 500 mg to 2 g orally in 3 or 4 divided doses for 7 to 10 days. (2.1)
- Pediatric Patients (less than 18 years of age): 40 mg/kg in 3 or 4 divided doses for 7 to 10 days. The total daily dosage should not exceed 2 g. (2.2)
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
Vancomycin Hydrochloride Capsules USP 125 mg
Vancomycin Hydrochloride Capsules USP 250 mg
CAPSULES have a blue cap and dark-yellow body imprinted with "OP65" on both cap and body in white ink.6.2 Postmarketing Experience
The following adverse reactions have been identified during post-approval use of vancomycin hydrochloride. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
8 Use in Specific Populations (8 USE IN SPECIFIC POPULATIONS)
6.1 Clinical Trials Experience
Because clinical studies are conducted under widely varying conditions, adverse reaction rates observed in the clinical studies of a drug cannot be directly compared to rates in the clinical studies of another drug and may not reflect the rates observed in practice.
The data described below reflect exposure to vancomycin hydrochloride in 260 adult subjects in two Phase 3 clinical trials for the treatment of diarrhea associated with C. difficile. In both trials, subjects received vancomycin hydrochloride capsules 125 mg orally four times daily. The mean duration of treatment was 9.4 days. The median age of patients was 67, ranging between 19 and 96 years of age. Patients were predominantly Caucasian (93%) and 52% were male.
Adverse reactions occurring in ≥ 5% of vancomycin hydrochloride-treated subjects are shown in Table 1. The most common adverse reactions associated with vancomycin hydrochloride (≥ 10%) were nausea, abdominal pain, and hypokalemia.
| System/Organ Class | Adverse Reaction | Vancomycin Hydrochloride % (N=260) |
|---|---|---|
| Gastrointestinal disorders | Nausea | 17 |
| Abdominal pain | 15 | |
| Vomiting | 9 | |
| Diarrhea | 9 | |
| Flatulence | 8 | |
| General disorders and administration site conditions | Pyrexia | 9 |
| Edema peripheral | 6 | |
| Fatigue | 5 | |
| Infections and infestations | Urinary tract infection | 8 |
| Metabolism and nutrition disorders | Hypokalemia | 13 |
| Musculoskeletal and connective tissue disorders | Back pain | 6 |
| Nervous system disorders | Headache | 7 |
Nephrotoxicity (e.g., reports of renal failure, renal impairment, blood creatinine increased) occurred in 5% of subjects treated with vancomycin hydrochloride. Nephrotoxicity following vancomycin hydrochloride typically first occurred within one week after completion of treatment (median day of onset was Day 16). Nephrotoxicity following vancomycin hydrochloride occurred in 6% of subjects >65 years of age and 3% of subjects ≤65 years of age (see WARNINGS AND PRECAUTIONS, Nephrotoxicity [5.3] ).
The incidences of hypokalemia, urinary tract infection, peripheral edema, insomnia, constipation, anemia, depression, vomiting, and hypotension were higher among subjects >65 years of age than in subjects ≤65 years of age (see USE IN SPECIFIC POPULATIONS, Geriatric Use [8.5] ).
Discontinuation of study drug due to adverse events occurred in 7% of subjects treated with vancomycin hydrochloride. The most common adverse events leading to discontinuation of vancomycin hydrochloride were C. difficile colitis (<1%), nausea (<1%), and vomiting (<1%).
5.5 Severe Dermatologic Reactions
Severe dermatologic reactions such as toxic epidermal necrolysis (TEN), Stevens-Johnson syndrome (SJS), drug reaction with eosinophilia and systemic symptoms (DRESS), acute generalized exanthematous pustulosis (AGEP), and linear IgA bullous dermatosis (LABD) have been reported in association with the use of vancomycin. Cutaneous signs or symptoms reported include skin rashes, mucosal lesions, and blisters.
Discontinue Vancomycin Hydrochloride Capsules at the first appearance of signs and symptoms of TEN, SJS, DRESS,AGEP, or LABD.
16 How Supplied/storage and Handling (16 HOW SUPPLIED/STORAGE AND HANDLING)
Vancomycin Hydrochloride Capsules, USP are available in:
The 250 mg Capsules have a blue cap and dark-yellow body imprinted with "OP65" on both cap and body in white ink.
NDC: 72162-2306-4: 50 Capsules in a Bottle
Store at 20° to 25°C (68° to 77°F); excursions permitted to 15° to 30°C (59° to 86°F). [See USP Controlled Room Temperature]
Repackaged/Relabeled by:
Bryant Ranch Prepack, Inc.
Burbank, CA 91504
5.2 Potential for Systemic Absorption
Clinically significant serum concentrations have been reported in some patients who have taken multiple oral doses of Vancomycin Hydrochloride Capsules for active C. difficile-associated diarrhea. Some patients with inflammatory disorders of the intestinal mucosa also may have significant systemic absorption of vancomycin. These patients may be at risk for the development of adverse reactions associated with higher doses of Vancomycin Hydrochloride Capsules; therefore, monitoring of serum concentrations of vancomycin may be appropriate in some instances, e.g., in patients with renal insufficiency and/or colitis or in those receiving concomitant therapy with an aminoglycoside antibiotic.
5.6 Development of Drug Resistant Bacteria (5.6 Development of Drug-Resistant Bacteria)
Prescribing Vancomycin Hydrochloride Capsules in the absence of a proven or strongly suspected bacterial infection or a prophylactic indication is unlikely to provide benefit to the patient and increases the risk of the development of drug resistant bacteria.
5.7 Risk of Allergic Reactions Due to Tartrazine (5.7 Risk of Allergic Reactions due to Tartrazine)
The 125 mg strength capsules contains FD&C Yellow No. 5 (tartrazine) which may cause allergic-type reactions (including bronchial asthma) in certain susceptible persons. Although the overall incidence of FD&C Yellow No. 5 (tartrazine) sensitivity in the general population is low, it is frequently seen in patients who also have aspirin hypersensitivity.
2.2 Pediatric Patients (less Than 18 Years of Age) (2.2 Pediatric Patients (less than 18 years of age))
For both C. difficile-associated diarrhea and staphylococcal enterocolitis, the usual daily dosage is 40 mg/kg in 3 or 4 divided doses for 7 to 10 days. The total daily dosage should not exceed 2 g.
14.1 Diarrhea Associated With Clostridium Difficile (14.1 Diarrhea Associated with Clostridium difficile)
In two trials, Vancomycin Hydrochloride Capsules 125 mg orally four times daily for 10 days was evaluated in 266 adult subjects with C. difficile-associated diarrhea (CDAD). Enrolled subjects were 18 years of age or older and received no more than 48 hours of treatment with oral vancomycin hydrochloride or oral/intravenous metronidazole in the 5 days preceding enrollment. CDAD was definite as ≥3 loose or watery bowel movements within the 24 hours preceding enrollment, and the presence of either C. difficile toxin A or B, or pseudomembranes on endoscopy within the 72 hours preceding enrollment. Subjects with fulminant C. difficile disease, sepsis with hypotension, ileus, peritoneal signs or severe hepatic disease were excluded.
Efficacy analyses were performed on the Full Analysis Set (FAS), which included randomized subjects who received at least one dose of vancomycin hydrochloride and had any post-dosing investigator evaluation data (N=259; 134 in Trial 1 and 125 in Trial 2).
The demographic profile and baseline CDAD characteristics of enrolled subjects were similar in the two trials. Vancomycin Hydrochloride-treated subjects had a median age of 67 years, were mainly white (93%), and male (52%). CDAD was classified as severe (defined as 10 or more unformed bowel movements per day or WBC ≥15000/mm3) in 25% of subjects, and 47% were previously treated for CDAD.
Efficacy was assessed by using clinical success, defined as diarrhea resolution and the absence of severe abdominal discomfort due to CDAD, on Day 10. An additional efficacy endpoint was the time to resolution of diarrhea, defined as the beginning of diarrhea resolution that was sustained through the end of the prescribed active treatment period.
The results for clinical success for vancomycin hydrochloride-treated subjects in both trials are shown in Table 2.
| Clinical Success Rate | 95% Confidence Interval | |
|---|---|---|
| Vancomycin Hydrochloride % (N) |
||
| Trial 1 | 81.3 (134) | (74.4, 88.3) |
| Trial 2 | 80.8 (125) | (73.5, 88.1) |
The median time to resolution of diarrhea was 5 days and 4 days in Trial 1 and Trial 2, respectively. For subjects older than 65 years of age, the median time to resolution was 6 days and 4 days in Trial 1 and Trial 2, respectively. In subjects with diarrhea resolution at end-of-treatment with Vancomycin Hydrochloride Capsules, recurrence of CDAD during the following four weeks occurred in 25 of 107 (23%) and 18 of 102 (18%) in Trial 1 and Trial 2, respectively.
Restriction Endonuclease Analysis (REA) was used to identify C. difficile baseline isolates in the BI group. In Trial 1, the Vancomycin Hydrochloride-treated subjects were classified at baseline as follows 31 (23%) with BI strain, 69 (52%) with non-BI strain, and 34 (25%) with unknown strain. Clinical success rates were 87% for BI strain, 81% for non-BI strain, and 76% for unknown strain. In subjects with diarrhea resolution at end-of-treatment with vancomycin hydrochloride, recurrence of CDAD during the following four weeks occurred in 7 of 26 subjects with BI strain, 12 of 56 subjects with non-BI strain, and 6 of 25 subjects with unknown strain.
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
No long-term carcinogenesis studies in animals have been conducted.
At concentrations up to 1000 mcg/mL, vancomycin had no mutagenic effect in vitro in the mouse lymphoma forward mutation assay or the primary rat hepatocyte unscheduled DNA synthesis assay. The concentrations tested in vitro were above the peak plasma vancomycin concentrations of 20 to 40 mcg/mL usually achieved in humans after slow infusion of the maximum recommended dose of 1 g. Vancomycin had no mutagenic effect in vivo in the Chinese hamster sister chromatid exchange assay (400 mg/kg IP) or the mouse micronucleus assay (800 mg/kg IP).
No definitive fertility studies have been conducted.
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:41:03.115271 · Updated: 2026-03-14T22:04:55.765860