These Highlights Do Not Include All The Information Needed To Use Tiglutik® Safely And Effectively. See Full Prescribing Information For Tiglutik.
75d68f19-4208-109e-e053-2991aa0ac857
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
Dosage and Administration ( 2.1 , 2.3 ) 12/2019
Indications and Usage
TIGLUTIK is indicated for the treatment of amyotrophic lateral sclerosis (ALS).
Dosage and Administration
Recommended dosage: 50 mg (10 mL), twice daily, taken orally or via percutaneous endoscopic gastrostomy tubes (PEG-tubes), every 12 hours ( 2.1 ) Measure serum aminotransferases before and during treatment ( 2.2 , 5.1 ) Take at least 1 hour before or 2 hours after a meal ( 2.3 )
Warnings and Precautions
Hepatic injury: Use of TIGLUTIK is not recommended in patients with baseline elevations of serum aminotransferases greater than 5 times the upper limit of normal; discontinue TIGLUTIK if there is evidence of liver dysfunction ( 5.1 ) Neutropenia: Advise patients to report any febrile illness ( 5.2 ) Interstitial lung disease: Discontinue TIGLUTIK if interstitial lung disease develops ( 5.3 )
Contraindications
TIGLUTIK is contraindicated in patients with a history of severe hypersensitivity reactions to riluzole or to any of its components (anaphylaxis has occurred) [see Adverse Reactions (6.1) ].
Adverse Reactions
The following adverse reactions are described below and elsewhere in the labeling: Hepatic Injury [see Warnings and Precautions (5.1) ] Neutropenia [see Warnings and Precautions (5.2) ] Interstitial Lung Disease [see Warnings and Precautions (5.3) ]
Drug Interactions
Strong to moderate CYP1A2 inhibitors: Co-administration may increase TIGLUTIK-associated adverse reactions ( 7.1 ) Strong to moderate CYP1A2 inducers: Co-administration may result in decreased efficacy ( 7.2 ) Hepatotoxic drugs: TIGLUTIK-treated patients that take other hepatotoxic drugs may be at increased risk for hepatotoxicity ( 7.3 )
Storage and Handling
Store at 20-25°C (68-77°F), excursions permitted to 15-30°C (59-86°F) [see USP Controlled Room Temperature], and protect from bright light. Do not freeze. Store upright. Use within 15 days after initially opening of each bottle. Discard any unused TIGLUTIK remaining after 15 days of first opening of the bottle.
How Supplied
TIGLUTIK (50 mg/10 mL) oral suspension is supplied in amber glass bottles closed with child-resistant tamper evident screw caps. Each bottle contains 300 mL of oral suspension and is intended for multi-dose use, NDC 70726-0303-2. TIGLUTIK is supplied in a carton, NDC 70726-0303-1, containing: Two bottles, each containing 300 mL oral suspension Two 10 mL oral syringes Two syringe bottle adapters Two syringe tip caps Prescribing Information, including Instructions for Use
Medication Information
Warnings and Precautions
Hepatic injury: Use of TIGLUTIK is not recommended in patients with baseline elevations of serum aminotransferases greater than 5 times the upper limit of normal; discontinue TIGLUTIK if there is evidence of liver dysfunction ( 5.1 ) Neutropenia: Advise patients to report any febrile illness ( 5.2 ) Interstitial lung disease: Discontinue TIGLUTIK if interstitial lung disease develops ( 5.3 )
Indications and Usage
TIGLUTIK is indicated for the treatment of amyotrophic lateral sclerosis (ALS).
Dosage and Administration
Recommended dosage: 50 mg (10 mL), twice daily, taken orally or via percutaneous endoscopic gastrostomy tubes (PEG-tubes), every 12 hours ( 2.1 ) Measure serum aminotransferases before and during treatment ( 2.2 , 5.1 ) Take at least 1 hour before or 2 hours after a meal ( 2.3 )
Contraindications
TIGLUTIK is contraindicated in patients with a history of severe hypersensitivity reactions to riluzole or to any of its components (anaphylaxis has occurred) [see Adverse Reactions (6.1) ].
Adverse Reactions
The following adverse reactions are described below and elsewhere in the labeling: Hepatic Injury [see Warnings and Precautions (5.1) ] Neutropenia [see Warnings and Precautions (5.2) ] Interstitial Lung Disease [see Warnings and Precautions (5.3) ]
Drug Interactions
Strong to moderate CYP1A2 inhibitors: Co-administration may increase TIGLUTIK-associated adverse reactions ( 7.1 ) Strong to moderate CYP1A2 inducers: Co-administration may result in decreased efficacy ( 7.2 ) Hepatotoxic drugs: TIGLUTIK-treated patients that take other hepatotoxic drugs may be at increased risk for hepatotoxicity ( 7.3 )
Storage and Handling
Store at 20-25°C (68-77°F), excursions permitted to 15-30°C (59-86°F) [see USP Controlled Room Temperature], and protect from bright light. Do not freeze. Store upright. Use within 15 days after initially opening of each bottle. Discard any unused TIGLUTIK remaining after 15 days of first opening of the bottle.
How Supplied
TIGLUTIK (50 mg/10 mL) oral suspension is supplied in amber glass bottles closed with child-resistant tamper evident screw caps. Each bottle contains 300 mL of oral suspension and is intended for multi-dose use, NDC 70726-0303-2. TIGLUTIK is supplied in a carton, NDC 70726-0303-1, containing: Two bottles, each containing 300 mL oral suspension Two 10 mL oral syringes Two syringe bottle adapters Two syringe tip caps Prescribing Information, including Instructions for Use
Description
Dosage and Administration ( 2.1 , 2.3 ) 12/2019
Section 42229-5
Adverse Reactions in Controlled Clinical Trials of Riluzole Tablets
In the placebo-controlled clinical trials in patients with ALS (Study 1 and 2), a total of 313 patients received riluzole 50 mg twice daily [see Clinical Studies (14)]. The most common adverse reactions in riluzole-treated patients (in at least 5% of patients and more frequently than on placebo) were asthenia, nausea, decreased lung function, hypertension, and abdominal pain. The most common adverse reactions leading to discontinuation in the riluzole group were nausea, abdominal pain, constipation, and elevated ALT.
There was no difference in the rate of adverse reactions leading to discontinuation between females and males. However, the incidence of dizziness was higher in females (11%) than in males (4%). The adverse reaction profile was similar in older and younger patients. There are insufficient data to assess racial differences in the adverse reaction profile.
Table 1 lists adverse reactions that occurred in at least 2% of riluzole-treated patients (50 mg twice daily) in pooled Study 1 and 2, and at a higher rate than on placebo.
| Adverse Reaction | Riluzole Tablets
50 mg twice daily (N=313) % |
Placebo
(N=320) % |
|---|---|---|
| Asthenia | 19 | 12 |
| Nausea | 16 | 11 |
| Decreased lung function | 10 | 9 |
| Hypertension | 5 | 4 |
| Abdominal pain | 5 | 4 |
| Vomiting | 4 | 2 |
| Arthralgia | 4 | 3 |
| Dizziness | 4 | 3 |
| Dry mouth | 4 | 3 |
| Insomnia | 4 | 3 |
| Pruritus | 4 | 3 |
| Tachycardia | 3 | 1 |
| Flatulence | 3 | 2 |
| Increased cough | 3 | 2 |
| Peripheral edema | 3 | 2 |
| Urinary Tract Infection | 3 | 2 |
| Circumoral paresthesia | 2 | 0 |
| Somnolence | 2 | 1 |
| Vertigo | 2 | 1 |
| Eczema | 2 | 1 |
10 Overdosage
Reported symptoms of overdose following ingestion of riluzole ranging from 1.5 to 3 grams (30 to 60 times the recommended dose) included acute toxic encephalopathy, coma, drowsiness, memory loss, and methemoglobinemia.
No specific antidote for the treatment of TIGLUTIK overdose is available. For current information on the management of poisoning or overdosage, contact a certified poison control center.
11 Description
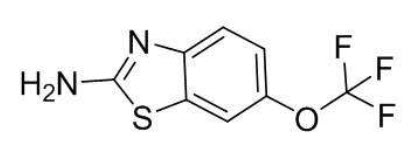
Riluzole is a member of the benzothiazole class. The chemical designation for riluzole is 2-amino-6-(trifluoromethoxy)benzothiazole. Its molecular formula is C 8H 5F 3N 2OS, and its molecular weight is 234.2. The chemical structure is:
Riluzole is a white to slightly yellow powder that is very soluble in dimethylformamide, dimethylsulfoxide, and methanol; freely soluble in dichloromethane; sparingly soluble in 0.1 N HCl; and very slightly soluble in water and in 0.1 N NaOH.
TIGLUTIK (50 mg/10mL) oral suspension is a slightly brown, opaque, homogeneous suspension containing 50 mg of riluzole per 10 mL of suspension.
TIGLUTIK also contains the following inactive ingredients: magnesium aluminum silicate, noncrystallizing sorbitol solution, polyoxyl 20 cetostearyl ether, purified water, saccharin sodium, simethicone emulsion, sodium lauryl sulfate, and xanthan gum.
5.2 Neutropenia
TIGLUTIK can cause neutropenia. Cases of severe neutropenia (absolute neutrophil count less than 500 per mm 3) within the first 2 months of riluzole treatment have been reported. Advise patients to report febrile illnesses.
16.1 How Supplied
TIGLUTIK (50 mg/10 mL) oral suspension is supplied in amber glass bottles closed with child-resistant tamper evident screw caps. Each bottle contains 300 mL of oral suspension and is intended for multi-dose use, NDC 70726-0303-2.
TIGLUTIK is supplied in a carton, NDC 70726-0303-1, containing:
- Two bottles, each containing 300 mL oral suspension
- Two 10 mL oral syringes
- Two syringe bottle adapters
- Two syringe tip caps
- Prescribing Information, including Instructions for Use
8.4 Pediatric Use
Safety and effectiveness in pediatric patients have not been established.
8.5 Geriatric Use
In clinical studies of riluzole, 30% of patients were 65 years and over. No overall differences in safety or effectiveness were observed between these patients and younger patients, and other reported clinical experience has not identified differences in responses between the elderly and younger patients, but greater sensitivity of some older individuals cannot be ruled out.
5.1 Hepatic Injury
TIGLUTIK can cause liver injury. Cases of drug-induced liver injury, some of which were fatal, have been reported in patients taking riluzole. Asymptomatic elevations of hepatic transaminases have also been reported, and in some patients have recurred upon re-challenge with riluzole.
In clinical studies, the incidence of elevations in hepatic transaminases was greater in riluzole-treated patients than placebo-treated patients. The incidence of elevations of ALT above 5 times the upper limit of normal (ULN) was 2% in riluzole-treated patients. Maximum increases in ALT occurred within 3 months after starting riluzole. About 50% and 8% of riluzole-treated patients in pooled controlled efficacy studies (Studies 1 and 2) had at least one elevated ALT level above ULN and above 3 times ULN, respectively [see Clinical Studies (14)].
Monitor patients for signs and symptoms of hepatic injury, every month for the first 3 months of treatment, and periodically thereafter. The use of TIGLUTIK is not recommended if patients develop hepatic transaminases levels greater than 5 times the ULN. Discontinue TIGLUTIK if there is evidence of liver dysfunction (e.g., elevated bilirubin). Concomitant use with other hepatotoxic drugs may increase the risk for hepatotoxicity [see Drug Interactions (7.3)] .
14 Clinical Studies
The efficacy of TIGLUTIK is based upon bioavailability studies comparing oral riluzole tablets to TIGLUTIK oral suspension [see Clinical Pharmacology (12.3)].
The efficacy of riluzole was demonstrated in two studies (Study 1 and 2) that evaluated 50 mg riluzole oral tablets twice daily in patients with amyotrophic lateral sclerosis (ALS). Both studies included patients with either familial or sporadic ALS, disease duration of less than 5 years, and baseline forced vital capacity greater than or equal to 60% of normal.
Study 1 was a randomized, double-blind, placebo-controlled clinical study that enrolled 155 patients with ALS. Patients were randomized to receive riluzole 50 mg twice daily (n=77) or placebo (n=78) and were followed for at least 13 months (up to a maximum duration of 18 months). The clinical outcome measure was time to tracheostomy or death.
The time to tracheostomy or death was longer for patients receiving riluzole compared to placebo. There was an early increase in survival in patients receiving riluzole compared to placebo. Figure 1 displays the survival curves for time to death or tracheostomy. The vertical axis represents the proportion of individuals alive without tracheostomy at various times following treatment initiation (horizontal axis). Although these survival curves were not statistically significantly different when evaluated by the analysis specified in the study protocol (Logrank test p=0.12), the difference was found to be significant by another appropriate analysis (Wilcoxon test p=0.05). As seen in Figure 1, the study showed an early increase in survival in patients given riluzole. Among the patients in whom the endpoint of tracheostomy or death was reached during the study, the difference in median survival between the riluzole 50 mg twice daily and placebo groups was approximately 90 days.
Figure 1. Time to Tracheostomy or Death in ALS Patients in Study 1 (Kaplan-Meier Curves)
Study 2 was a randomized, double-blind, placebo-controlled clinical study that enrolled 959 patients with ALS. Patients were randomized to riluzole 50 mg twice daily (n=236) or placebo (n=242) and were followed for at least 12 months (up to a maximum duration of 18 months). The clinical outcome measure was time to tracheostomy or death.
The time to tracheostomy or death was longer for patients receiving riluzole compared to placebo. Figure 2 displays the survival curves for time to death or tracheostomy for patients randomized to either riluzole 100 mg per day or placebo. Although these survival curves were not statistically significantly different when evaluated by the analysis specified in the study protocol (Logrank test p=0.076), the difference was found to be significant by another appropriate analysis (Wilcoxon test p=0.05). Not displayed in Figure 2 are the results of riluzole 50 mg per day (one-half of the recommended daily dose), which could not be statistically distinguished from placebo, or the results of riluzole 200 mg per day (two times the recommended daily dose), which were not distinguishable from the 100 mg per day results. Among the patients in whom the endpoint of tracheostomy or death was reached during the study, the difference in median survival between riluzole and placebo was approximately 60 days.
Although riluzole improved survival in both studies, measures of muscle strength and neurological function did not show a benefit.
Figure 2. Time to Tracheostomy or Death in ALS Patients in Study 2 (Kaplan-Meier Curves)
4 Contraindications
TIGLUTIK is contraindicated in patients with a history of severe hypersensitivity reactions to riluzole or to any of its components (anaphylaxis has occurred) [see Adverse Reactions (6.1)].
6 Adverse Reactions
The following adverse reactions are described below and elsewhere in the labeling:
- Hepatic Injury [see Warnings and Precautions (5.1)]
- Neutropenia [see Warnings and Precautions (5.2)]
- Interstitial Lung Disease [see Warnings and Precautions (5.3)]
7 Drug Interactions
- Strong to moderate CYP1A2 inhibitors: Co-administration may increase TIGLUTIK-associated adverse reactions ( 7.1)
- Strong to moderate CYP1A2 inducers: Co-administration may result in decreased efficacy ( 7.2)
- Hepatotoxic drugs: TIGLUTIK-treated patients that take other hepatotoxic drugs may be at increased risk for hepatotoxicity ( 7.3)
12.2 Pharmacodynamics
The clinical pharmacodynamics of riluzole has not been determined in humans.
12.3 Pharmacokinetics
A pharmacokinetic study in healthy adult subjects who received riluzole suspension 50 mg under fasting conditions demonstrated similar pharmacokinetics following intragastric administration via feeding tubes and oral administration.
Table 2 displays the pharmacokinetic parameters of riluzole.
| Absorption | |
| Bioavailability (oral) | Approximately 60% |
| Dose Proportionality | Linear over a dose range of 25 mg to 100 mg every 12 hours (1/2 to 2 times the recommended dosage) |
| Food effect
Information specific to TIGLUTIK
|
AUC ↓ 9% and Cmax ↓ 55% (high fat meal) |
| Time to peak plasma concentration (median) | 0.8 hours |
| Distribution | |
| Plasma Protein Binding | 96% (Mainly to albumin and lipoproteins) |
| Elimination | |
| Elimination half-life |
|
| Accumulation | Approximately 2-fold |
| Metabolism | |
| Fraction metabolized (% dose) | At least 88% |
| Primary metabolic pathway(s) [in vitro] |
|
| Active Metabolites | Some metabolites appear pharmacologically active in vitro, but the clinical implications are not known. |
| Excretion | |
| Primary elimination pathways (% dose) |
|
7.3 Hepatotoxic Drugs
Clinical trials in ALS patients excluded patients on concomitant medications which were potentially hepatotoxic (e.g., allopurinol, methyldopa, sulfasalazine). TIGLUTIK-treated patients who take other hepatotoxic drugs may be at an increased risk for hepatotoxicity [see Warnings and Precautions (5.1)].
8.7 Japanese Patients
Japanese patients are more likely to have higher riluzole concentrations. Consequently, the risk of adverse reactions may be greater in Japanese patients [see Clinical Pharmacology (12.3)].
2.1 Dosage Information
The recommended dosage for TIGLUTIK is 50 mg (10 mL) taken orally or via Percutaneous Endoscopic Gastrostomy tubes (PEG-tubes) twice daily, every 12 hours. TIGLUTIK should be taken at least 1 hour before or 2 hours after a meal [see Clinical Pharmacology (12.3)].
8.6 Hepatic Impairment
Patients with mild [Child-Pugh's (CP) score A] or moderate (CP score B) hepatic impairment had increases in AUC, compared to patients with normal hepatic function. Thus, patients with mild or moderate hepatic impairment may be at increased risk of adverse reactions. The impact of severe hepatic impairment on riluzole exposure is unknown.
Use of TIGLUTIK is not recommended in patients with baseline elevations of serum aminotransferases greater than 5 times upper limit of normal or evidence of liver dysfunction (e.g., elevated bilirubin) [see Clinical Pharmacology (12.3)].
1 Indications and Usage
TIGLUTIK is indicated for the treatment of amyotrophic lateral sclerosis (ALS).
12.1 Mechanism of Action
The mechanism by which riluzole exerts its therapeutic effects in patients with ALS is unknown.
16.2 Storage and Handling
Store at 20-25°C (68-77°F), excursions permitted to 15-30°C (59-86°F) [see USP Controlled Room Temperature], and protect from bright light. Do not freeze. Store upright.
Use within 15 days after initially opening of each bottle. Discard any unused TIGLUTIK remaining after 15 days of first opening of the bottle.
5 Warnings and Precautions
- Hepatic injury: Use of TIGLUTIK is not recommended in patients with baseline elevations of serum aminotransferases greater than 5 times the upper limit of normal; discontinue TIGLUTIK if there is evidence of liver dysfunction ( 5.1)
- Neutropenia: Advise patients to report any febrile illness ( 5.2)
- Interstitial lung disease: Discontinue TIGLUTIK if interstitial lung disease develops ( 5.3)
2 Dosage and Administration
3 Dosage Forms and Strengths
Oral suspension: 50 mg/10 mL (5 mg/mL) slightly brown, opaque, homogeneous suspension in a 300-mL multiple-dose amber bottle.
6.2 Postmarketing Experience
The following adverse reactions have been identified during post-approval use of riluzole. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
- Acute hepatitis and icteric toxic hepatitis [see Warnings and Precautions (5.1)]
- Renal tubular impairment
- Pancreatitis
5.3 Interstitial Lung Disease
TIGLUTIK can cause interstitial lung disease, including hypersensitivity pneumonitis. Discontinue TIGLUTIK immediately if interstitial lung disease develops.
8 Use in Specific Populations
- Pregnancy: Based on animal data, may cause fetal harm ( 8.1)
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
2.2 Monitoring to Assess Safety
Measure serum aminotransferases before and during treatment with TIGLUTIK [see Warnings and Precautions (5.1)].
17 Patient Counseling Information
Advise the patient to read the FDA-approved patient labeling (Instructions for Use).
2.3 Important Administration Instructions
Gently shake the TIGLUTIK bottle for at least 30 seconds before administration.Gently shake the TIGLUTIK bottle for at least 30 seconds before administration.
TIGLUTIK can be administered by mouth or via percutaneous endoscopic gastrostomy tubes (PEG-tubes). Both silicone and polyurethane PEG tubes can be used.
See the Instructions for Use for further administration details.See the Instructions for Use for further administration details.
Principal Display Panel 300 Ml Bottle Carton
NDC 70726-0303-1
R xonly
Tiglutik
®
riluzole
oral suspension
50 mg/10 mL (5 mg/mL)
For Oral Administration
Shake gently before use
Contents of this package:
- Two bottles, each containing 300 mL
- Two 10 mL oral syringes
- Two syringe bottle adapters
- Two syringe tip caps
- One Prescribing Information, including
Instructions for Use
This product is a liquid suspension and is
supplied with syringes for oral administration.
Before use, please read the enclosed
Prescribing Information.
600 mL (two bottles/300 mL each)
Not To Be Dispensed Separately
8.3 Females and Males of Reproductive Potential
In rats, oral administration of riluzole resulted in decreased fertility indices and increases in embryolethality [see Nonclinical Toxicology (13.1)].
Structured Label Content
Section 42229-5 (42229-5)
Adverse Reactions in Controlled Clinical Trials of Riluzole Tablets
In the placebo-controlled clinical trials in patients with ALS (Study 1 and 2), a total of 313 patients received riluzole 50 mg twice daily [see Clinical Studies (14)]. The most common adverse reactions in riluzole-treated patients (in at least 5% of patients and more frequently than on placebo) were asthenia, nausea, decreased lung function, hypertension, and abdominal pain. The most common adverse reactions leading to discontinuation in the riluzole group were nausea, abdominal pain, constipation, and elevated ALT.
There was no difference in the rate of adverse reactions leading to discontinuation between females and males. However, the incidence of dizziness was higher in females (11%) than in males (4%). The adverse reaction profile was similar in older and younger patients. There are insufficient data to assess racial differences in the adverse reaction profile.
Table 1 lists adverse reactions that occurred in at least 2% of riluzole-treated patients (50 mg twice daily) in pooled Study 1 and 2, and at a higher rate than on placebo.
| Adverse Reaction | Riluzole Tablets
50 mg twice daily (N=313) % |
Placebo
(N=320) % |
|---|---|---|
| Asthenia | 19 | 12 |
| Nausea | 16 | 11 |
| Decreased lung function | 10 | 9 |
| Hypertension | 5 | 4 |
| Abdominal pain | 5 | 4 |
| Vomiting | 4 | 2 |
| Arthralgia | 4 | 3 |
| Dizziness | 4 | 3 |
| Dry mouth | 4 | 3 |
| Insomnia | 4 | 3 |
| Pruritus | 4 | 3 |
| Tachycardia | 3 | 1 |
| Flatulence | 3 | 2 |
| Increased cough | 3 | 2 |
| Peripheral edema | 3 | 2 |
| Urinary Tract Infection | 3 | 2 |
| Circumoral paresthesia | 2 | 0 |
| Somnolence | 2 | 1 |
| Vertigo | 2 | 1 |
| Eczema | 2 | 1 |
10 Overdosage (10 OVERDOSAGE)
Reported symptoms of overdose following ingestion of riluzole ranging from 1.5 to 3 grams (30 to 60 times the recommended dose) included acute toxic encephalopathy, coma, drowsiness, memory loss, and methemoglobinemia.
No specific antidote for the treatment of TIGLUTIK overdose is available. For current information on the management of poisoning or overdosage, contact a certified poison control center.
11 Description (11 DESCRIPTION)
Riluzole is a member of the benzothiazole class. The chemical designation for riluzole is 2-amino-6-(trifluoromethoxy)benzothiazole. Its molecular formula is C 8H 5F 3N 2OS, and its molecular weight is 234.2. The chemical structure is:
Riluzole is a white to slightly yellow powder that is very soluble in dimethylformamide, dimethylsulfoxide, and methanol; freely soluble in dichloromethane; sparingly soluble in 0.1 N HCl; and very slightly soluble in water and in 0.1 N NaOH.
TIGLUTIK (50 mg/10mL) oral suspension is a slightly brown, opaque, homogeneous suspension containing 50 mg of riluzole per 10 mL of suspension.
TIGLUTIK also contains the following inactive ingredients: magnesium aluminum silicate, noncrystallizing sorbitol solution, polyoxyl 20 cetostearyl ether, purified water, saccharin sodium, simethicone emulsion, sodium lauryl sulfate, and xanthan gum.
5.2 Neutropenia
TIGLUTIK can cause neutropenia. Cases of severe neutropenia (absolute neutrophil count less than 500 per mm 3) within the first 2 months of riluzole treatment have been reported. Advise patients to report febrile illnesses.
16.1 How Supplied
TIGLUTIK (50 mg/10 mL) oral suspension is supplied in amber glass bottles closed with child-resistant tamper evident screw caps. Each bottle contains 300 mL of oral suspension and is intended for multi-dose use, NDC 70726-0303-2.
TIGLUTIK is supplied in a carton, NDC 70726-0303-1, containing:
- Two bottles, each containing 300 mL oral suspension
- Two 10 mL oral syringes
- Two syringe bottle adapters
- Two syringe tip caps
- Prescribing Information, including Instructions for Use
8.4 Pediatric Use
Safety and effectiveness in pediatric patients have not been established.
8.5 Geriatric Use
In clinical studies of riluzole, 30% of patients were 65 years and over. No overall differences in safety or effectiveness were observed between these patients and younger patients, and other reported clinical experience has not identified differences in responses between the elderly and younger patients, but greater sensitivity of some older individuals cannot be ruled out.
5.1 Hepatic Injury
TIGLUTIK can cause liver injury. Cases of drug-induced liver injury, some of which were fatal, have been reported in patients taking riluzole. Asymptomatic elevations of hepatic transaminases have also been reported, and in some patients have recurred upon re-challenge with riluzole.
In clinical studies, the incidence of elevations in hepatic transaminases was greater in riluzole-treated patients than placebo-treated patients. The incidence of elevations of ALT above 5 times the upper limit of normal (ULN) was 2% in riluzole-treated patients. Maximum increases in ALT occurred within 3 months after starting riluzole. About 50% and 8% of riluzole-treated patients in pooled controlled efficacy studies (Studies 1 and 2) had at least one elevated ALT level above ULN and above 3 times ULN, respectively [see Clinical Studies (14)].
Monitor patients for signs and symptoms of hepatic injury, every month for the first 3 months of treatment, and periodically thereafter. The use of TIGLUTIK is not recommended if patients develop hepatic transaminases levels greater than 5 times the ULN. Discontinue TIGLUTIK if there is evidence of liver dysfunction (e.g., elevated bilirubin). Concomitant use with other hepatotoxic drugs may increase the risk for hepatotoxicity [see Drug Interactions (7.3)] .
14 Clinical Studies (14 CLINICAL STUDIES)
The efficacy of TIGLUTIK is based upon bioavailability studies comparing oral riluzole tablets to TIGLUTIK oral suspension [see Clinical Pharmacology (12.3)].
The efficacy of riluzole was demonstrated in two studies (Study 1 and 2) that evaluated 50 mg riluzole oral tablets twice daily in patients with amyotrophic lateral sclerosis (ALS). Both studies included patients with either familial or sporadic ALS, disease duration of less than 5 years, and baseline forced vital capacity greater than or equal to 60% of normal.
Study 1 was a randomized, double-blind, placebo-controlled clinical study that enrolled 155 patients with ALS. Patients were randomized to receive riluzole 50 mg twice daily (n=77) or placebo (n=78) and were followed for at least 13 months (up to a maximum duration of 18 months). The clinical outcome measure was time to tracheostomy or death.
The time to tracheostomy or death was longer for patients receiving riluzole compared to placebo. There was an early increase in survival in patients receiving riluzole compared to placebo. Figure 1 displays the survival curves for time to death or tracheostomy. The vertical axis represents the proportion of individuals alive without tracheostomy at various times following treatment initiation (horizontal axis). Although these survival curves were not statistically significantly different when evaluated by the analysis specified in the study protocol (Logrank test p=0.12), the difference was found to be significant by another appropriate analysis (Wilcoxon test p=0.05). As seen in Figure 1, the study showed an early increase in survival in patients given riluzole. Among the patients in whom the endpoint of tracheostomy or death was reached during the study, the difference in median survival between the riluzole 50 mg twice daily and placebo groups was approximately 90 days.
Figure 1. Time to Tracheostomy or Death in ALS Patients in Study 1 (Kaplan-Meier Curves)
Study 2 was a randomized, double-blind, placebo-controlled clinical study that enrolled 959 patients with ALS. Patients were randomized to riluzole 50 mg twice daily (n=236) or placebo (n=242) and were followed for at least 12 months (up to a maximum duration of 18 months). The clinical outcome measure was time to tracheostomy or death.
The time to tracheostomy or death was longer for patients receiving riluzole compared to placebo. Figure 2 displays the survival curves for time to death or tracheostomy for patients randomized to either riluzole 100 mg per day or placebo. Although these survival curves were not statistically significantly different when evaluated by the analysis specified in the study protocol (Logrank test p=0.076), the difference was found to be significant by another appropriate analysis (Wilcoxon test p=0.05). Not displayed in Figure 2 are the results of riluzole 50 mg per day (one-half of the recommended daily dose), which could not be statistically distinguished from placebo, or the results of riluzole 200 mg per day (two times the recommended daily dose), which were not distinguishable from the 100 mg per day results. Among the patients in whom the endpoint of tracheostomy or death was reached during the study, the difference in median survival between riluzole and placebo was approximately 60 days.
Although riluzole improved survival in both studies, measures of muscle strength and neurological function did not show a benefit.
Figure 2. Time to Tracheostomy or Death in ALS Patients in Study 2 (Kaplan-Meier Curves)
4 Contraindications (4 CONTRAINDICATIONS)
TIGLUTIK is contraindicated in patients with a history of severe hypersensitivity reactions to riluzole or to any of its components (anaphylaxis has occurred) [see Adverse Reactions (6.1)].
6 Adverse Reactions (6 ADVERSE REACTIONS)
The following adverse reactions are described below and elsewhere in the labeling:
- Hepatic Injury [see Warnings and Precautions (5.1)]
- Neutropenia [see Warnings and Precautions (5.2)]
- Interstitial Lung Disease [see Warnings and Precautions (5.3)]
7 Drug Interactions (7 DRUG INTERACTIONS)
- Strong to moderate CYP1A2 inhibitors: Co-administration may increase TIGLUTIK-associated adverse reactions ( 7.1)
- Strong to moderate CYP1A2 inducers: Co-administration may result in decreased efficacy ( 7.2)
- Hepatotoxic drugs: TIGLUTIK-treated patients that take other hepatotoxic drugs may be at increased risk for hepatotoxicity ( 7.3)
12.2 Pharmacodynamics
The clinical pharmacodynamics of riluzole has not been determined in humans.
12.3 Pharmacokinetics
A pharmacokinetic study in healthy adult subjects who received riluzole suspension 50 mg under fasting conditions demonstrated similar pharmacokinetics following intragastric administration via feeding tubes and oral administration.
Table 2 displays the pharmacokinetic parameters of riluzole.
| Absorption | |
| Bioavailability (oral) | Approximately 60% |
| Dose Proportionality | Linear over a dose range of 25 mg to 100 mg every 12 hours (1/2 to 2 times the recommended dosage) |
| Food effect
Information specific to TIGLUTIK
|
AUC ↓ 9% and Cmax ↓ 55% (high fat meal) |
| Time to peak plasma concentration (median) | 0.8 hours |
| Distribution | |
| Plasma Protein Binding | 96% (Mainly to albumin and lipoproteins) |
| Elimination | |
| Elimination half-life |
|
| Accumulation | Approximately 2-fold |
| Metabolism | |
| Fraction metabolized (% dose) | At least 88% |
| Primary metabolic pathway(s) [in vitro] |
|
| Active Metabolites | Some metabolites appear pharmacologically active in vitro, but the clinical implications are not known. |
| Excretion | |
| Primary elimination pathways (% dose) |
|
7.3 Hepatotoxic Drugs
Clinical trials in ALS patients excluded patients on concomitant medications which were potentially hepatotoxic (e.g., allopurinol, methyldopa, sulfasalazine). TIGLUTIK-treated patients who take other hepatotoxic drugs may be at an increased risk for hepatotoxicity [see Warnings and Precautions (5.1)].
8.7 Japanese Patients
Japanese patients are more likely to have higher riluzole concentrations. Consequently, the risk of adverse reactions may be greater in Japanese patients [see Clinical Pharmacology (12.3)].
2.1 Dosage Information
The recommended dosage for TIGLUTIK is 50 mg (10 mL) taken orally or via Percutaneous Endoscopic Gastrostomy tubes (PEG-tubes) twice daily, every 12 hours. TIGLUTIK should be taken at least 1 hour before or 2 hours after a meal [see Clinical Pharmacology (12.3)].
8.6 Hepatic Impairment
Patients with mild [Child-Pugh's (CP) score A] or moderate (CP score B) hepatic impairment had increases in AUC, compared to patients with normal hepatic function. Thus, patients with mild or moderate hepatic impairment may be at increased risk of adverse reactions. The impact of severe hepatic impairment on riluzole exposure is unknown.
Use of TIGLUTIK is not recommended in patients with baseline elevations of serum aminotransferases greater than 5 times upper limit of normal or evidence of liver dysfunction (e.g., elevated bilirubin) [see Clinical Pharmacology (12.3)].
1 Indications and Usage (1 INDICATIONS AND USAGE)
TIGLUTIK is indicated for the treatment of amyotrophic lateral sclerosis (ALS).
12.1 Mechanism of Action
The mechanism by which riluzole exerts its therapeutic effects in patients with ALS is unknown.
16.2 Storage and Handling
Store at 20-25°C (68-77°F), excursions permitted to 15-30°C (59-86°F) [see USP Controlled Room Temperature], and protect from bright light. Do not freeze. Store upright.
Use within 15 days after initially opening of each bottle. Discard any unused TIGLUTIK remaining after 15 days of first opening of the bottle.
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
- Hepatic injury: Use of TIGLUTIK is not recommended in patients with baseline elevations of serum aminotransferases greater than 5 times the upper limit of normal; discontinue TIGLUTIK if there is evidence of liver dysfunction ( 5.1)
- Neutropenia: Advise patients to report any febrile illness ( 5.2)
- Interstitial lung disease: Discontinue TIGLUTIK if interstitial lung disease develops ( 5.3)
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
Oral suspension: 50 mg/10 mL (5 mg/mL) slightly brown, opaque, homogeneous suspension in a 300-mL multiple-dose amber bottle.
6.2 Postmarketing Experience
The following adverse reactions have been identified during post-approval use of riluzole. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
- Acute hepatitis and icteric toxic hepatitis [see Warnings and Precautions (5.1)]
- Renal tubular impairment
- Pancreatitis
5.3 Interstitial Lung Disease
TIGLUTIK can cause interstitial lung disease, including hypersensitivity pneumonitis. Discontinue TIGLUTIK immediately if interstitial lung disease develops.
8 Use in Specific Populations (8 USE IN SPECIFIC POPULATIONS)
- Pregnancy: Based on animal data, may cause fetal harm ( 8.1)
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
2.2 Monitoring to Assess Safety
Measure serum aminotransferases before and during treatment with TIGLUTIK [see Warnings and Precautions (5.1)].
17 Patient Counseling Information (17 PATIENT COUNSELING INFORMATION)
Advise the patient to read the FDA-approved patient labeling (Instructions for Use).
2.3 Important Administration Instructions
Gently shake the TIGLUTIK bottle for at least 30 seconds before administration.Gently shake the TIGLUTIK bottle for at least 30 seconds before administration.
TIGLUTIK can be administered by mouth or via percutaneous endoscopic gastrostomy tubes (PEG-tubes). Both silicone and polyurethane PEG tubes can be used.
See the Instructions for Use for further administration details.See the Instructions for Use for further administration details.
Principal Display Panel 300 Ml Bottle Carton (PRINCIPAL DISPLAY PANEL - 300 mL Bottle Carton)
NDC 70726-0303-1
R xonly
Tiglutik
®
riluzole
oral suspension
50 mg/10 mL (5 mg/mL)
For Oral Administration
Shake gently before use
Contents of this package:
- Two bottles, each containing 300 mL
- Two 10 mL oral syringes
- Two syringe bottle adapters
- Two syringe tip caps
- One Prescribing Information, including
Instructions for Use
This product is a liquid suspension and is
supplied with syringes for oral administration.
Before use, please read the enclosed
Prescribing Information.
600 mL (two bottles/300 mL each)
Not To Be Dispensed Separately
8.3 Females and Males of Reproductive Potential
In rats, oral administration of riluzole resulted in decreased fertility indices and increases in embryolethality [see Nonclinical Toxicology (13.1)].
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:51:55.808967 · Updated: 2026-03-14T22:42:19.657154