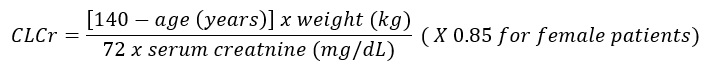These Highlights Do Not Include All The Information Needed To Use Pregabalin Capsules Safely And Effectively. See Full Prescribing Information For Pregabalin Capsules.
65d9e751-61c2-4741-85c0-2526cfdc765c
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
Warnings and Precautions ( 5.3 , 5.4 ) 04/2025
Indications and Usage
Pregabalin Capsules are indicated for: Management of neuropathic pain associated with diabetic peripheral neuropathy Management of postherpetic neuralgia Adjunctive therapy for the treatment of partial-onset seizures in patients 1 month of age and older Management of fibromyalgia Management of neuropathic pain associated with spinal cord injury
Dosage and Administration
For adult indications, begin dosing at 150 mg/day. For partial-onset seizure dosing in pediatric patients 1 month of age and older, refer to section 2.4. ( 2.2 , 2.3 , 2.4 , 2.5 , 2.6 ) Dosing recommendations: INDICATION Dosing Regimen Maximum Dose DPN Pain ( 2.2 ) 3 divided doses per day 300 mg/day within 1 week PHN ( 2.3 ) 2 or 3 divided doses per day 300 mg/day within 1 week. Maximum dose of 600 mg/day. Adjunctive Therapy for Partial-Onset Seizures in Pediatric and Adult Patients Weighing 30 kg or More ( 2.4 ) 2 or 3 divided doses per day Maximum dose of 600 mg/day. Adjunctive Therapy for Partial-Onset Seizures in Pediatric Patients Weighing Less than 30 kg ( 2.4 ) 1 month to less than 4 years: 3 divided doses per day 4 years and older: 2 or 3 divided doses per day 14 mg/kg/day. Fibromyalgia ( 2.5 ) 2 divided doses per day 300 mg/day within 1 week. Maximum dose of 450 mg/day. Neuropathic Pain Associated with Spinal Cord Injury ( 2.6 ) 2 divided doses per day 300 mg/day within 1 week. Maximum dose of 600 mg/day. Dose should be adjusted in adult patients with reduced renal function. ( 2.7 )
Warnings and Precautions
Angioedema (e.g., swelling of the throat, head, and neck) can occur, and may be associated with life-threatening respiratory compromise requiring emergency treatment. Discontinue Pregabalin Capsules immediately in these cases. ( 5.1 ) Hypersensitivity reactions (e.g., hives, dyspnea, and wheezing) can occur. Discontinue Pregabalin Capsules immediately in these patients. ( 5.2 ) Antiepileptic drugs, including pregabalin, the active ingredient in Pregabalin Capsules, increase the risk of suicidal thoughts or behavior. ( 5.3 ) Abrupt or rapid discontinuation may increase the risk for seizures. Withdrawal symptoms or suicidal behavior and ideation have been observed after discontinuation. Taper Pregabalin Capsules gradually over a minimum of 1 week. (5.4) Respiratory depression: May occur with Pregabalin Capsules, when used with concomitant CNS depressants or in the setting of underlying respiratory impairment. Monitor patients and adjust dosage as appropriate. ( 5.5 ) Pregabalin Capsules may cause dizziness and somnolence and impair patients’ ability to drive or operate machinery. ( 5.6 ) Pregabalin Capsules may cause peripheral edema. Exercise caution when co-administering Pregabalin Capsules and thiazolidinedione antidiabetic agents. ( 5.7 )
Contraindications
Pregabalin Capsules are contraindicated in patients with known hypersensitivity to pregabalin or any of its components. Angioedema and hypersensitivity reactions have occurred in patients receiving pregabalin therapy [see Warnings and Precautions (5.2) ].
Adverse Reactions
Following is a list of treatment-emergent adverse reactions reported by patients treated with Pregabalin Capsules during all clinical trials. The listing does not include those events already listed in the previous tables or elsewhere in labeling, those events for which a drug cause was remote, those events which were so general as to be uninformative, and those events reported only once which did not have a substantial probability of being acutely life-threatening. Events are categorized by body system and listed in order of decreasing frequency according to the following definitions: frequent adverse reactions are those occurring on one or more occasions in at least 1/100 patients; infrequent adverse reactions are those occurring in 1/100 to 1/1000 patients; rare reactions are those occurring in fewer than 1/1000 patients. Events of major clinical importance are described in the Warnings and Precautions section (5). Body as a Whole – Frequent : Abdominal pain, Allergic reaction, Fever, Infrequent : Abscess, Cellulitis, Chills, Malaise, Neck rigidity, Overdose, Pelvic pain, Photosensitivity reaction, Rare : Anaphylactoid reaction, Ascites, Granuloma, Hangover effect, Intentional Injury, Retroperitoneal Fibrosis, Shock Cardiovascular System – Infrequent : Deep thrombophlebitis, Heart failure, Hypotension, Postural hypotension, Retinal vascular disorder, Syncope; Rare : ST Depressed, Ventricular Fibrillation Digestive System – Frequent : Gastroenteritis, Increased appetite; Infrequent : Cholecystitis, Cholelithiasis, Colitis, Dysphagia, Esophagitis, Gastritis, Gastrointestinal hemorrhage, Melena, Mouth ulceration, Pancreatitis, Rectal hemorrhage, Tongue edema; Rare : Aphthous stomatitis, Esophageal Ulcer, Periodontal abscess Hemic and Lymphatic System – Frequent : Ecchymosis; Infrequent : Anemia, Eosinophilia, Hypochromic anemia, Leukocytosis, Leukopenia, Lymphadenopathy, Thrombocytopenia; Rare : Myelofibrosis, Polycythemia, Prothrombin decreased, Purpura, Thrombocythemia, Alanine aminotransferase increased, Aspartate aminotransferase increased Metabolic and Nutritional Disorders – Rare : Glucose Tolerance Decreased, Urate Crystalluria Musculoskeletal System – Frequent : Arthralgia, Leg cramps, Myalgia, Myasthenia; Infrequent : Arthrosis; Rare : Chondrodystrophy, Generalized Spasm Nervous System – Frequent : Anxiety, Depersonalization, Hypertonia, Hypoesthesia, Libido decreased, Nystagmus, Paresthesia, Sedation, Stupor, Twitching; Infrequent : Abnormal dreams, Agitation, Apathy, Aphasia, Circumoral paresthesia, Dysarthria, Hallucinations, Hostility, Hyperalgesia, Hyperesthesia, Hyperkinesia, Hypokinesia, Hypotonia, Libido increased, Myoclonus, Neuralgia; Rare : Addiction, Cerebellar syndrome, Cogwheel rigidity, Coma, Delirium, Delusions, Dysautonomia, Dyskinesia, Dystonia, Encephalopathy, Extrapyramidal syndrome, Guillain-Barré syndrome, Hypalgesia, Intracranial hypertension, Manic reaction, Paranoid reaction, Peripheral neuritis, Personality disorder, Psychotic depression, Schizophrenic reaction, Sleep disorder, Torticollis, Trismus Respiratory System – Rare : Apnea, Atelectasis, Bronchiolitis, Hiccup, Laryngismus, Lung edema, Lung fibrosis, Yawn Skin and Appendages – Frequent : Pruritus, Infrequent : Alopecia, Dry skin, Eczema, Hirsutism, Skin ulcer, Urticaria, Vesiculobullous rash; Rare : Angioedema, Exfoliative dermatitis, Lichenoid dermatitis, Melanosis, Nail Disorder, Petechial rash, Purpuric rash, Pustular rash, Skin atrophy, Skin necrosis, Skin nodule, Stevens-Johnson syndrome, Subcutaneous nodule Special senses – Frequent : Conjunctivitis, Diplopia, Otitis media, Tinnitus; Infrequent : Abnormality of accommodation, Blepharitis, Dry eyes, Eye hemorrhage, Hyperacusis, Photophobia, Retinal edema, Taste loss, Taste perversion; Rare : Anisocoria, Blindness, Corneal ulcer, Exophthalmos, Extraocular palsy, Iritis, Keratitis, Keratoconjunctivitis, Miosis, Mydriasis, Night blindness, Ophthalmoplegia, Optic atrophy, Papilledema, Parosmia, Ptosis, Uveitis Urogenital System – Frequent : Anorgasmia, Impotence, Urinary frequency, Urinary incontinence; Infrequent : Abnormal ejaculation, Albuminuria, Amenorrhea, Dysmenorrhea, Dysuria, Hematuria, Kidney calculus, Leukorrhea, Menorrhagia, Metrorrhagia, Nephritis, Oliguria, Urinary retention, Urine abnormality; Rare : Acute kidney failure, Balanitis, Bladder Neoplasm, Cervicitis, Dyspareunia, Epididymitis, Female lactation, Glomerulitis, Ovarian disorder, Pyelonephritis
Drug Interactions
Since Pregabalin Capsules are predominantly excreted unchanged in the urine, undergoes negligible metabolism in humans (less than 2% of a dose recovered in urine as metabolites), and does not bind to plasma proteins, its pharmacokinetics are unlikely to be affected by other agents through metabolic interactions or protein binding displacement. In vitro and in vivo studies showed that Pregabalin Capsules are unlikely to be involved in significant pharmacokinetic drug interactions. Specifically, there are no pharmacokinetic interactions between pregabalin and the following antiepileptic drugs: carbamazepine, valproic acid, lamotrigine, phenytoin, phenobarbital, and topiramate. Important pharmacokinetic interactions would also not be expected to occur between Pregabalin Capsules and commonly used antiepileptic drugs [see Clinical Pharmacology (12) ] .
Medication Information
Warnings and Precautions
Angioedema (e.g., swelling of the throat, head, and neck) can occur, and may be associated with life-threatening respiratory compromise requiring emergency treatment. Discontinue Pregabalin Capsules immediately in these cases. ( 5.1 ) Hypersensitivity reactions (e.g., hives, dyspnea, and wheezing) can occur. Discontinue Pregabalin Capsules immediately in these patients. ( 5.2 ) Antiepileptic drugs, including pregabalin, the active ingredient in Pregabalin Capsules, increase the risk of suicidal thoughts or behavior. ( 5.3 ) Abrupt or rapid discontinuation may increase the risk for seizures. Withdrawal symptoms or suicidal behavior and ideation have been observed after discontinuation. Taper Pregabalin Capsules gradually over a minimum of 1 week. (5.4) Respiratory depression: May occur with Pregabalin Capsules, when used with concomitant CNS depressants or in the setting of underlying respiratory impairment. Monitor patients and adjust dosage as appropriate. ( 5.5 ) Pregabalin Capsules may cause dizziness and somnolence and impair patients’ ability to drive or operate machinery. ( 5.6 ) Pregabalin Capsules may cause peripheral edema. Exercise caution when co-administering Pregabalin Capsules and thiazolidinedione antidiabetic agents. ( 5.7 )
Indications and Usage
Pregabalin Capsules are indicated for: Management of neuropathic pain associated with diabetic peripheral neuropathy Management of postherpetic neuralgia Adjunctive therapy for the treatment of partial-onset seizures in patients 1 month of age and older Management of fibromyalgia Management of neuropathic pain associated with spinal cord injury
Dosage and Administration
For adult indications, begin dosing at 150 mg/day. For partial-onset seizure dosing in pediatric patients 1 month of age and older, refer to section 2.4. ( 2.2 , 2.3 , 2.4 , 2.5 , 2.6 ) Dosing recommendations: INDICATION Dosing Regimen Maximum Dose DPN Pain ( 2.2 ) 3 divided doses per day 300 mg/day within 1 week PHN ( 2.3 ) 2 or 3 divided doses per day 300 mg/day within 1 week. Maximum dose of 600 mg/day. Adjunctive Therapy for Partial-Onset Seizures in Pediatric and Adult Patients Weighing 30 kg or More ( 2.4 ) 2 or 3 divided doses per day Maximum dose of 600 mg/day. Adjunctive Therapy for Partial-Onset Seizures in Pediatric Patients Weighing Less than 30 kg ( 2.4 ) 1 month to less than 4 years: 3 divided doses per day 4 years and older: 2 or 3 divided doses per day 14 mg/kg/day. Fibromyalgia ( 2.5 ) 2 divided doses per day 300 mg/day within 1 week. Maximum dose of 450 mg/day. Neuropathic Pain Associated with Spinal Cord Injury ( 2.6 ) 2 divided doses per day 300 mg/day within 1 week. Maximum dose of 600 mg/day. Dose should be adjusted in adult patients with reduced renal function. ( 2.7 )
Contraindications
Pregabalin Capsules are contraindicated in patients with known hypersensitivity to pregabalin or any of its components. Angioedema and hypersensitivity reactions have occurred in patients receiving pregabalin therapy [see Warnings and Precautions (5.2) ].
Adverse Reactions
Following is a list of treatment-emergent adverse reactions reported by patients treated with Pregabalin Capsules during all clinical trials. The listing does not include those events already listed in the previous tables or elsewhere in labeling, those events for which a drug cause was remote, those events which were so general as to be uninformative, and those events reported only once which did not have a substantial probability of being acutely life-threatening. Events are categorized by body system and listed in order of decreasing frequency according to the following definitions: frequent adverse reactions are those occurring on one or more occasions in at least 1/100 patients; infrequent adverse reactions are those occurring in 1/100 to 1/1000 patients; rare reactions are those occurring in fewer than 1/1000 patients. Events of major clinical importance are described in the Warnings and Precautions section (5). Body as a Whole – Frequent : Abdominal pain, Allergic reaction, Fever, Infrequent : Abscess, Cellulitis, Chills, Malaise, Neck rigidity, Overdose, Pelvic pain, Photosensitivity reaction, Rare : Anaphylactoid reaction, Ascites, Granuloma, Hangover effect, Intentional Injury, Retroperitoneal Fibrosis, Shock Cardiovascular System – Infrequent : Deep thrombophlebitis, Heart failure, Hypotension, Postural hypotension, Retinal vascular disorder, Syncope; Rare : ST Depressed, Ventricular Fibrillation Digestive System – Frequent : Gastroenteritis, Increased appetite; Infrequent : Cholecystitis, Cholelithiasis, Colitis, Dysphagia, Esophagitis, Gastritis, Gastrointestinal hemorrhage, Melena, Mouth ulceration, Pancreatitis, Rectal hemorrhage, Tongue edema; Rare : Aphthous stomatitis, Esophageal Ulcer, Periodontal abscess Hemic and Lymphatic System – Frequent : Ecchymosis; Infrequent : Anemia, Eosinophilia, Hypochromic anemia, Leukocytosis, Leukopenia, Lymphadenopathy, Thrombocytopenia; Rare : Myelofibrosis, Polycythemia, Prothrombin decreased, Purpura, Thrombocythemia, Alanine aminotransferase increased, Aspartate aminotransferase increased Metabolic and Nutritional Disorders – Rare : Glucose Tolerance Decreased, Urate Crystalluria Musculoskeletal System – Frequent : Arthralgia, Leg cramps, Myalgia, Myasthenia; Infrequent : Arthrosis; Rare : Chondrodystrophy, Generalized Spasm Nervous System – Frequent : Anxiety, Depersonalization, Hypertonia, Hypoesthesia, Libido decreased, Nystagmus, Paresthesia, Sedation, Stupor, Twitching; Infrequent : Abnormal dreams, Agitation, Apathy, Aphasia, Circumoral paresthesia, Dysarthria, Hallucinations, Hostility, Hyperalgesia, Hyperesthesia, Hyperkinesia, Hypokinesia, Hypotonia, Libido increased, Myoclonus, Neuralgia; Rare : Addiction, Cerebellar syndrome, Cogwheel rigidity, Coma, Delirium, Delusions, Dysautonomia, Dyskinesia, Dystonia, Encephalopathy, Extrapyramidal syndrome, Guillain-Barré syndrome, Hypalgesia, Intracranial hypertension, Manic reaction, Paranoid reaction, Peripheral neuritis, Personality disorder, Psychotic depression, Schizophrenic reaction, Sleep disorder, Torticollis, Trismus Respiratory System – Rare : Apnea, Atelectasis, Bronchiolitis, Hiccup, Laryngismus, Lung edema, Lung fibrosis, Yawn Skin and Appendages – Frequent : Pruritus, Infrequent : Alopecia, Dry skin, Eczema, Hirsutism, Skin ulcer, Urticaria, Vesiculobullous rash; Rare : Angioedema, Exfoliative dermatitis, Lichenoid dermatitis, Melanosis, Nail Disorder, Petechial rash, Purpuric rash, Pustular rash, Skin atrophy, Skin necrosis, Skin nodule, Stevens-Johnson syndrome, Subcutaneous nodule Special senses – Frequent : Conjunctivitis, Diplopia, Otitis media, Tinnitus; Infrequent : Abnormality of accommodation, Blepharitis, Dry eyes, Eye hemorrhage, Hyperacusis, Photophobia, Retinal edema, Taste loss, Taste perversion; Rare : Anisocoria, Blindness, Corneal ulcer, Exophthalmos, Extraocular palsy, Iritis, Keratitis, Keratoconjunctivitis, Miosis, Mydriasis, Night blindness, Ophthalmoplegia, Optic atrophy, Papilledema, Parosmia, Ptosis, Uveitis Urogenital System – Frequent : Anorgasmia, Impotence, Urinary frequency, Urinary incontinence; Infrequent : Abnormal ejaculation, Albuminuria, Amenorrhea, Dysmenorrhea, Dysuria, Hematuria, Kidney calculus, Leukorrhea, Menorrhagia, Metrorrhagia, Nephritis, Oliguria, Urinary retention, Urine abnormality; Rare : Acute kidney failure, Balanitis, Bladder Neoplasm, Cervicitis, Dyspareunia, Epididymitis, Female lactation, Glomerulitis, Ovarian disorder, Pyelonephritis
Drug Interactions
Since Pregabalin Capsules are predominantly excreted unchanged in the urine, undergoes negligible metabolism in humans (less than 2% of a dose recovered in urine as metabolites), and does not bind to plasma proteins, its pharmacokinetics are unlikely to be affected by other agents through metabolic interactions or protein binding displacement. In vitro and in vivo studies showed that Pregabalin Capsules are unlikely to be involved in significant pharmacokinetic drug interactions. Specifically, there are no pharmacokinetic interactions between pregabalin and the following antiepileptic drugs: carbamazepine, valproic acid, lamotrigine, phenytoin, phenobarbital, and topiramate. Important pharmacokinetic interactions would also not be expected to occur between Pregabalin Capsules and commonly used antiepileptic drugs [see Clinical Pharmacology (12) ] .
Description
Warnings and Precautions ( 5.3 , 5.4 ) 04/2025
Section 42229-5
Pharmacodynamics
Multiple oral doses of Pregabalin Capsules were co-administered with oxycodone, lorazepam, or ethanol. Although no pharmacokinetic interactions were seen, additive effects on cognitive and gross motor functioning were seen when Pregabalin Capsules were co-administered with these drugs. No clinically important effects on respiration were seen.
Section 42231-1
|
MEDICATION GUIDE Pregabalin (pree gab' a lin) Capsules, CV |
||
| This Medication Guide has been approved by the U.S. Food and Drug Administration. | Revised: 10/2025 | |
|
Read this Medication Guide before you start taking Pregabalin Capsules and each time you get a refill. There may be new information. This information does not take the place of talking to your healthcare provider about your medical condition or treatment. If you have any questions about Pregabalin Capsules, ask your healthcare provider or pharmacist. |
||
|
What is the most important information I should know about Pregabalin Capsules? Pregabalin Capsules may cause serious side effects including: |
||
|
|
|
|
These serious side effects are described below:
|
||
|
|
|
|
If you have suicidal thoughts or actions, do not stop Pregabalin Capsules without first talking to a healthcare provider.
How can I watch for early symptoms of suicidal thoughts and actions?
|
||
|
||
|
What is Pregabalin Capsules? Pregabalin Capsules are a prescription medicine used in adults, 18 years of age and older to treat:
It is not known if Pregabalin Capsules are safe and effective in people under 18 years of age for the treatment of fibromyalgia and neuropathic pain with diabetes, shingles, or spinal cord injury. Pregabalin Capsules is a prescription medicine used in people 1 month of age and older to treat:
For the treatment of partial-onset seizures when taken together with other seizure medicines, it is not known if Pregabalin Capsules are safe and effective in children under 1 month of age. |
||
|
Who should not take Pregabalin Capsules? Do not take Pregabalin Capsules if you are allergic to pregabalin or any of the ingredients in Pregabalin Capsules. See “ What is the most important information I should know about Pregabalin Capsules?” for the signs of an allergic reaction. See the end of this Medication Guide for a complete list of ingredients in Pregabalin Capsules. |
||
|
What should I tell my healthcare provider before taking Pregabalin Capsules? Before taking Pregabalin Capsules, tell your healthcare provider about all your medical conditions, including if you:
Tell your healthcare provider about all the medicines you take, including prescription and over-the-counter medicines, vitamins or herbal supplements. Pregabalin Capsules and other medicines may affect each other causing side effects. Especially tell your healthcare provider if you take:
Know the medicines you take. Keep a list of them with you to show your healthcare provider and pharmacist each time you get a new medicine. Do not start a new medicine without talking with your healthcare provider. |
||
|
How should I take Pregabalin Capsules?
|
||
|
What should I avoid while taking Pregabalin Capsules?
|
||
|
What are the possible side effects of Pregabalin Capsules? Pregabalin Capsules may cause serious side effects, including:
The most common side effects of Pregabalin Capsules in adults are: |
||
|
|
|
|
The most common side effects of Pregabalin Capsules in childrenare weight gain, increase in appetite, and sleepiness. Pregabalin Capsules caused skin sores in animal studies. Skin sores did not happen in studies in people. If you have diabetes, you should pay attention to your skin while taking Pregabalin Capsules and tell your healthcare provider about any sores or skin problems. Tell your healthcare provider about any side effect that bothers you or that does not go away. These are not all the possible side effects of Pregabalin Capsules. For more information, ask your healthcare provider or pharmacist. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. |
||
|
How should I store Pregabalin Capsules?
Keep Pregabalin Capsules and all medicines out of the reach of children. |
||
|
General information about the safe and effective use of Pregabalin Capsules Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not use Pregabalin Capsules for a condition for which it was not prescribed. Do not give Pregabalin Capsules to other people, even if they have the same symptoms you have. It may harm them. You can ask your healthcare provider or pharmacist for information about Pregabalin Capsules that is written for health professionals. |
||
|
What are the ingredients in Pregabalin Capsules? Active ingredient: pregabalin Inactive ingredients: Pregabalin Capsules: pregelatinized starch, talc Capsule shell: gelatin, titanium dioxide, sodium lauryl sulfate and water; Orange capsule shell (75 mg, 100 mg, 200 mg, 225 mg and 300 mg strengths) also contains red iron oxide. Colloidal silicon dioxide is used as processing aid. Imprinting ink: shellac, black iron oxide, propylene glycol, potassium hydroxide.
Manufactured by:
All brand names listed are the registered trademarks of their respective owners and are not trademarks of Eskayef Pharmaceuticals Limited. |
PM06168 V09
Section 44425-7
Storage and Handling
Store at 20° to 25° C (68° to 77° F), excursions permitted between 15° to 30° C (59° to 86° F) [see USP Controlled Room Temperature].
Section 51945-4
NDC 72658-0808-1
Pregabalin Capsules CV
25 mg
PHARMACIST: Dispense the accompanying Medication Guide to each patient.
60 Capsules
Rx only
SK+F
9.2 Abuse
In a study of recreational users (N=15) of sedative/hypnotic drugs, including alcohol, Pregabalin Capsules (450 mg, single dose) received subjective ratings of “good drug effect,” “high” and “liking” to a degree that was similar to diazepam (30 mg, single dose). In controlled clinical studies in over 5500 patients, 4 % of Pregabalin Capsules-treated patients and 1 % of placebo-treated patients overall reported euphoria as an adverse reaction, though in some patient populations studied, this reporting rate was higher and ranged from 1 to 12%.
11 Description
Pregabalin is described chemically as ( S)-3-(aminomethyl)-5-methylhexanoic acid. The molecular formula is C 8H 17NO 2 and the molecular weight is 159.23. The chemical structure of pregabalin is:
Pregabalin is a white to off-white, crystalline solid with a pK a1 of 4.2 and a pK a2 of 10.6. It is freely soluble in 1N Hydrochloric acid and sparingly soluble in water. The log of the partition coefficient (n-octanol/0.05M phosphate buffer) at pH 7.4 is – 1.35.
Pregabalin Capsules are administered orally and are supplied as imprinted hard-shell capsules containing 25, 50, 75, 100, 150, 200, 225, and 300 mg of pregabalin, along with pregelatinized starch and talc as inactive ingredients. The capsule shells contain gelatin, titanium dioxide, sodium lauryl sulfate and water. In addition, the orange capsule shells (75 mg, 100 mg, 200 mg, 225 mg and 300 mg strengths) contain red iron oxide. Colloidal silicon dioxide is used as processing aid. The imprinting ink contains shellac, black iron oxide, propylene glycol, potassium hydroxide.
5.1 Angioedema
There have been postmarketing reports of angioedema in patients during initial and chronic treatment with Pregabalin Capsules. Specific symptoms included swelling of the face, mouth (tongue, lips, and gums), and neck (throat and larynx). There were reports of life-threatening angioedema with respiratory compromise requiring emergency treatment. Discontinue Pregabalin Capsules immediately in patients with these symptoms.
Exercise caution when prescribing Pregabalin Capsules to patients who have had a previous episode of angioedema. In addition, patients who are taking other drugs associated with angioedema (e.g., angiotensin converting enzyme inhibitors [ACE-inhibitors]) may be at increased risk of developing angioedema.
9.3 Dependence
In clinical studies, following abrupt or rapid discontinuation of Pregabalin Capsules, some patients reported symptoms including insomnia, nausea, headache or diarrhea [see Warnings and Precautions (5.4)] , consistent with physical dependence. In the postmarketing setting, in addition to these reported symptoms, other reported adverse reactions include, but are not limited to, seizures, depression, suicidal ideation and behavior, agitation, confusion, disorientation, psychotic symptoms, pain, sweating, tremor, dizziness, and malaise.
5.8 Weight Gain
Pregabalin Capsules treatment may cause weight gain. In Pregabalin Capsules controlled clinical trials in adult patients of up to 14 weeks, a gain of 7% or more over baseline weight was observed in 9% of Pregabalin Capsules-treated patients and 2% of placebo-treated patients. Few patients treated with Pregabalin Capsules (0.3%) withdrew from controlled trials due to weight gain. Pregabalin Capsules associated weight gain was related to dose and duration of exposure but did not appear to be associated with baseline BMI, gender, or age. Weight gain was not limited to patients with edema [see Warnings and Precautions (5.7)] .
Although weight gain was not associated with clinically important changes in blood pressure in short-term controlled studies, the long-term cardiovascular effects of Pregabalin Capsules-associated weight gain are unknown.
Among diabetic patients, Pregabalin Capsules-treated patients gained an average of 1.6 kg (range: -16 to 16 kg), compared to an average 0.3 kg (range: -10 to 9 kg) weight gain in placebo patients. In a cohort of 333 diabetic patients who received Pregabalin Capsules for at least 2 years, the average weight gain was 5.2 kg.
While the effects of Pregabalin Capsules-associated weight gain on glycemic control have not been systematically assessed, in controlled and longer-term open label clinical trials with diabetic patients, Pregabalin Capsules treatment did not appear to be associated with loss of glycemic control (as measured by HbA 1C).
8.5 Geriatric Use
In controlled clinical studies of Pregabalin Capsules in neuropathic pain associated with diabetic peripheral neuropathy, 246 patients were 65 to 74 years of age, and 73 patients were 75 years of age or older.
In controlled clinical studies of Pregabalin Capsules in neuropathic pain associated with postherpetic neuralgia, 282 patients were 65 to 74 years of age, and 379 patients were 75 years of age or older.
In controlled clinical studies of Pregabalin Capsules in epilepsy, there were only 10 patients 65 to 74 years of age, and 2 patients who were 75 years of age or older.
No overall differences in safety and efficacy were observed between these patients and younger patients.
In controlled clinical studies of Pregabalin Capsules in fibromyalgia, 106 patients were 65 years of age or older. Although the adverse reaction profile was similar between the two age groups, the following neurological adverse reactions were more frequent in patients 65 years of age or older: dizziness, vision blurred, balance disorder, tremor, confusional state, coordination abnormal, and lethargy.
Pregabalin Capsules are known to be substantially excreted by the kidney, and the risk of toxic reactions to Pregabalin Capsules may be greater in patients with impaired renal function. Because Pregabalin Capsules are eliminated primarily by renal excretion, adjust the dose for elderly patients with renal impairment [see Dosage and Administration (2.7)] .
4 Contraindications
Pregabalin Capsules are contraindicated in patients with known hypersensitivity to pregabalin or any of its components. Angioedema and hypersensitivity reactions have occurred in patients receiving pregabalin therapy [see Warnings and Precautions (5.2)].
6 Adverse Reactions
The following serious adverse reactions are described elsewhere in the labeling:
- Angioedema [see Warnings and Precautions (5.1)]
- Hypersensitivity [see Warnings and Precautions (5.2)]
- Suicidal Behavior and Ideation [see Warnings and Precautions (5.3)]
- Increased Risk of Adverse Reactions with Abrupt or Rapid Discontinuation [see Warnings and Precautions (5.4)]
- Respiratory Depression [see Warnings and Precautions (5.5)]
- Dizziness and Somnolence [see Warnings and Precautions (5.6)]
- Peripheral Edema [see Warnings and Precautions (5.7)]
- Weight Gain [see Warnings and Precautions (5.8)]
- Tumorigenic Potential [see Warnings and Precautions (5.9)]
- Ophthalmological Effects [see Warnings and Precautions (5.10)]
- Creatine Kinase Elevations [see Warnings and Precautions (5.11)]
- Decreased Platelet Count [see Warnings and Precautions (5.12)]
- PR Interval Prolongation [see Warnings and Precautions (5.13)]
7 Drug Interactions
Since Pregabalin Capsules are predominantly excreted unchanged in the urine, undergoes negligible metabolism in humans (less than 2% of a dose recovered in urine as metabolites), and does not bind to plasma proteins, its pharmacokinetics are unlikely to be affected by other agents through metabolic interactions or protein binding displacement. In vitro and in vivo studies showed that Pregabalin Capsules are unlikely to be involved in significant pharmacokinetic drug interactions. Specifically, there are no pharmacokinetic interactions between pregabalin and the following antiepileptic drugs: carbamazepine, valproic acid, lamotrigine, phenytoin, phenobarbital, and topiramate. Important pharmacokinetic interactions would also not be expected to occur between Pregabalin Capsules and commonly used antiepileptic drugs [see Clinical Pharmacology (12)] .
5.2 Hypersensitivity
There have been postmarketing reports of hypersensitivity in patients shortly after initiation of treatment with Pregabalin Capsules. Adverse reactions included skin redness, blisters, hives, rash, dyspnea, and wheezing. Discontinue Pregabalin Capsules immediately in patients with these symptoms.
5.7 Peripheral Edema
Pregabalin Capsules treatment may cause peripheral edema. In short-term trials of patients without clinically significant heart or peripheral vascular disease, there was no apparent association between peripheral edema and cardiovascular complications such as hypertension or congestive heart failure. Peripheral edema was not associated with laboratory changes suggestive of deterioration in renal or hepatic function.
In controlled clinical trials in adult patients, the incidence of peripheral edema was 6% in the Pregabalin Capsules group compared with 2% in the placebo group. In controlled clinical trials, 0.5% of Pregabalin Capsules patients and 0.2% placebo patients withdrew due to peripheral edema.
Higher frequencies of weight gain and peripheral edema were observed in patients taking both Pregabalin Capsules and a thiazolidinedione antidiabetic agent compared to patients taking either drug alone. The majority of patients using thiazolidinedione antidiabetic agents in the overall safety database were participants in studies of pain associated with diabetic peripheral neuropathy. In this population, peripheral edema was reported in 3% (2/60) of patients who were using thiazolidinedione antidiabetic agents only, 8% (69/859) of patients who were treated with Pregabalin Capsules only, and 19% (23/120) of patients who were on both Pregabalin Capsules and thiazolidinedione antidiabetic agents. Similarly, weight gain was reported in 0% (0/60) of patients on thiazolidinediones only; 4% (35/859) of patients on Pregabalin Capsules only; and 7.5% (9/120) of patients on both drugs.
As the thiazolidinedione class of antidiabetic drugs can cause weight gain and/or fluid retention, possibly exacerbating or leading to heart failure, exercise caution when co-administering Pregabalin Capsules and these agents.
Because there are limited data on congestive heart failure patients with New York Heart Association (NYHA) Class III or IV cardiac status, exercise caution when using Pregabalin Capsules in these patients.
8.6 Renal Impairment
Pregabalin Capsules are eliminated primarily by renal excretion and dose adjustment is recommended for adult patients with renal impairment [see Dosage and Administration (2.7) and Clinical Pharmacology (12.3)]. The use of Pregabalin Capsules in pediatric patients with compromised renal function has not been studied.
12.3 Pharmacokinetics
Pregabalin is well absorbed after oral administration, is eliminated largely by renal excretion, and has an elimination half-life of about 6 hours.
1 Indications and Usage
Pregabalin Capsules are indicated for:
- Management of neuropathic pain associated with diabetic peripheral neuropathy
- Management of postherpetic neuralgia
- Adjunctive therapy for the treatment of partial-onset seizures in patients 1 month of age and older
- Management of fibromyalgia
- Management of neuropathic pain associated with spinal cord injury
12.1 Mechanism of Action
Pregabalin Capsules (pregabalin) binds with high affinity to the alpha 2-delta site (an auxiliary subunit of voltage-gated calcium channels) in central nervous system tissues. Although the mechanism of action of pregabalin has not been fully elucidated, results with genetically modified mice and with compounds structurally related to pregabalin (such as gabapentin) suggest that binding to the alpha 2-delta subunit may be involved in pregabalin's anti-nociceptive and antiseizure effects in animals. In animal models of nerve damage, pregabalin has been shown to reduce calcium-dependent release of pro-nociceptive neurotransmitters in the spinal cord, possibly by disrupting alpha 2-delta containing-calcium channel trafficking and/or reducing calcium currents. Evidence from other animal models of nerve damage and persistent pain suggest the anti-nociceptive activities of pregabalin may also be mediated through interactions with descending noradrenergic and serotonergic pathways originating from the brainstem that modulate pain transmission in the spinal cord.
While pregabalin is a structural derivative of the inhibitory neurotransmitter gamma-aminobutyric acid (GABA), it does not bind directly to GABA A, GABA B, or benzodiazepine receptors, does not augment GABA A responses in cultured neurons, does not alter rat brain GABA concentration or have acute effects on GABA uptake or degradation. However, in cultured neurons prolonged application of pregabalin increases the density of GABA transporter protein and increases the rate of functional GABA transport. Pregabalin does not block sodium channels, is not active at opiate receptors, and does not alter cyclooxygenase enzyme activity. It is inactive at serotonin and dopamine receptors and does not inhibit dopamine, serotonin, or noradrenaline reuptake.
9.1 Controlled Substance
Pregabalin is a Schedule V controlled substance.
Pregabalin Capsules are not known to be active at receptor sites associated with drugs of abuse. As with any CNS active drug, carefully evaluate patients for history of drug abuse and observe them for signs of Pregabalin Capsules misuse or abuse (e.g., development of tolerance, dose escalation, drug-seeking behavior).
5.9 Tumorigenic Potential
In standard preclinical in vivo lifetime carcinogenicity studies of Pregabalin Capsules, an unexpectedly high incidence of hemangiosarcoma was identified in two different strains of mice [ see Nonclinical Toxicology (13.1) ]. The clinical significance of this finding is unknown. Clinical experience during Pregabalin Capsules premarketing development provides no direct means to assess its potential for inducing tumors in humans.
In clinical studies across various patient populations, comprising 6396 patient-years of exposure in patients greater than 12 years of age, new or worsening-preexisting tumors were reported in 57 patients. Without knowledge of the background incidence and recurrence in similar populations not treated with Pregabalin Capsules, it is impossible to know whether the incidence seen in these cohorts is or is not affected by treatment.
5 Warnings and Precautions
- Angioedema (e.g., swelling of the throat, head, and neck) can occur, and may be associated with life-threatening respiratory compromise requiring emergency treatment. Discontinue Pregabalin Capsules immediately in these cases. ( 5.1)
- Hypersensitivity reactions (e.g., hives, dyspnea, and wheezing) can occur. Discontinue Pregabalin Capsules immediately in these patients. ( 5.2)
- Antiepileptic drugs, including pregabalin, the active ingredient in Pregabalin Capsules, increase the risk of suicidal thoughts or behavior. ( 5.3)
- Abrupt or rapid discontinuation may increase the risk for seizures. Withdrawal symptoms or suicidal behavior and ideation have been observed after discontinuation. Taper Pregabalin Capsules gradually over a minimum of 1 week. (5.4)
- Respiratory depression: May occur with Pregabalin Capsules, when used with concomitant CNS depressants or in the setting of underlying respiratory impairment. Monitor patients and adjust dosage as appropriate. ( 5.5)
- Pregabalin Capsules may cause dizziness and somnolence and impair patients’ ability to drive or operate machinery. ( 5.6)
- Pregabalin Capsules may cause peripheral edema. Exercise caution when co-administering Pregabalin Capsules and thiazolidinedione antidiabetic agents. ( 5.7)
14.2 Postherpetic Neuralgia
The efficacy of Pregabalin Capsules for the management of postherpetic neuralgia was established in three double-blind, placebo-controlled, multicenter studies. These studies enrolled patients with neuralgia persisting for at least 3 months following healing of herpes zoster rash and a minimum baseline score of greater than or equal to 4 on an 11-point numerical pain rating scale ranging from 0 (no pain) to 10 (worst possible pain). Seventy-three percent of patients completed the studies. The baseline mean pain scores across the 3 studies ranged from 6 to 7. Patients were permitted up to 4 grams of acetaminophen per day as needed for pain, in addition to pregabalin. Patients recorded their pain daily in a diary.
2 Dosage and Administration
- For adult indications, begin dosing at 150 mg/day. For partial-onset seizure dosing in pediatric patients 1 month of age and older, refer to section 2.4. ( 2.2, 2.3, 2.4, 2.5, 2.6)
- Dosing recommendations:
| INDICATION | Dosing Regimen | Maximum Dose |
|---|---|---|
| DPN Pain ( 2.2) | 3 divided doses per day | 300 mg/day within 1 week |
| PHN ( 2.3) | 2 or 3 divided doses per day | 300 mg/day within 1 week. Maximum dose of 600 mg/day. |
| Adjunctive Therapy for Partial-Onset Seizures in Pediatric and Adult Patients Weighing 30 kg or More ( 2.4) | 2 or 3 divided doses per day | Maximum dose of 600 mg/day. |
| Adjunctive Therapy for Partial-Onset Seizures in Pediatric Patients Weighing Less than 30 kg ( 2.4) |
1 month to less than 4 years: 3 divided doses per day 4 years and older: 2 or 3 divided doses per day |
14 mg/kg/day. |
| Fibromyalgia ( 2.5) | 2 divided doses per day | 300 mg/day within 1 week. Maximum dose of 450 mg/day. |
| Neuropathic Pain Associated with Spinal Cord Injury ( 2.6) | 2 divided doses per day | 300 mg/day within 1 week. Maximum dose of 600 mg/day. |
- Dose should be adjusted in adult patients with reduced renal function. ( 2.7)
5.5 respiratory Depression
There is evidence from case reports, human studies, and animal studies associating Pregabalin Capsules with serious, life-threatening, or fatal respiratory depression when co-administered with central nervous system (CNS) depressants, including opioids, or in the setting of underlying respiratory impairment. When the decision is made to co-prescribe Pregabalin Capsules with another CNS depressant, particularly an opioid, or to prescribe Pregabalin Capsules to patients with underlying respiratory impairment, monitor patients for symptoms of respiratory depression and sedation, and consider initiating Pregabalin Capsules at a low dose. The management of respiratory depression may include close observation, supportive measures, and reduction or withdrawal of CNS depressants (including Pregabalin Capsules).
There is more limited evidence from case reports, animal studies, and human studies associating Pregabalin Capsules with serious respiratory depression, without co-administered CNS depressants or without underlying respiratory impairment.
3 Dosage Forms and Strengths
Capsules: 25 mg, 50 mg, 75 mg, 100 mg, 150 mg, 200 mg, 225 mg, and 300 mg
[see Description (11) a nd How Supplied/Storage and Handling (16) ]
5.6 Dizziness and Somnolence
Pregabalin Capsules may cause dizziness and somnolence. Inform patients that Pregabalin Capsules-related dizziness and somnolence may impair their ability to perform tasks such as driving or operating machinery [see Patient Counseling Information (17)] .
In the Pregabalin Capsules controlled trials in adult patients, dizziness was experienced by 30% of Pregabalin Capsules-treated patients compared to 8% of placebo-treated patients; somnolence was experienced by 23% of Pregabalin Capsules-treated patients compared to 8% of placebo-treated patients. Dizziness and somnolence generally began shortly after the initiation of Pregabalin Capsules therapy and occurred more frequently at higher doses. Dizziness and somnolence were the adverse reactions most frequently leading to withdrawal (4% each) from controlled studies. In Pregabalin Capsules-treated patients reporting these adverse reactions in short-term, controlled studies, dizziness persisted until the last dose in 30% and somnolence persisted until the last dose in 42% of patients [see Drug Interactions (7)].
In the pregabalin controlled trials in pediatric patients 4 to less than 17 years of age and 1 month to less than 4 years of age for the treatment of partial-onset seizures, somnolence was reported in 21% and 15% of pregabalin-treated patients compared to 14% and 9% of placebo-treated patients, respectively, and occurred more frequently at higher doses. For patients 1 month to less than 4 years of age, somnolence includes related terms lethargy, sluggishness, and hypersomnia.
6.2 Postmarketing Experience
The following adverse reactions have been identified during postapproval use of Pregabalin Capsules. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Nervous System Disorders – Headache
Gastrointestinal Disorders – Nausea, Diarrhea
Reproductive System and Breast Disorders – Gynecomastia, Breast Enlargement
Skin and subcutaneous tissue disorders – Bullous pemphigoid
There are postmarketing reports of life-threatening or fatal respiratory depression in patients taking Pregabalin Capsules with opioids or other CNS depressants, or in the setting of underlying respiratory impairment.
In addition, there are postmarketing reports of events related to reduced lower gastrointestinal tract function (e.g., intestinal obstruction, paralytic ileus, constipation) when Pregabalin Capsules were co-administered with medications that have the potential to produce constipation, such as opioid analgesics.
There are postmarketing reports of withdrawal symptoms after discontinuation of pregabalin. Reported adverse reactions include, but are not limited to, seizures, depression, suicidal ideation and behavior, agitation, confusion, disorientation, psychotic symptoms, anxiety, insomnia, nausea, pain, sweating, tremor, headache, dizziness, malaise, and diarrhea.
5.10 Ophthalmological Effects
In controlled studies in adult patients, a higher proportion of patients treated with Pregabalin Capsules reported blurred vision (7%) than did patients treated with placebo (2%), which resolved in a majority of cases with continued dosing. Less than 1% of patients discontinued Pregabalin Capsules treatment due to vision-related events (primarily blurred vision).
Prospectively planned ophthalmologic testing, including visual acuity testing, formal visual field testing and dilated funduscopic examination, was performed in over 3600 patients. In these patients, visual acuity was reduced in 7% of patients treated with Pregabalin Capsules, and 5% of placebo-treated patients. Visual field changes were detected in 13% of Pregabalin Capsules-treated, and 12% of placebo-treated patients. Funduscopic changes were observed in 2% of Pregabalin Capsules-treated and 2% of placebo-treated patients.
Although the clinical significance of the ophthalmologic findings is unknown, inform patients to notify their physician if changes in vision occur. If visual disturbance persists, consider further assessment. Consider more frequent assessment for patients who are already routinely monitored for ocular conditions [ see Patient Counseling Information (17 )] .
5.12 Decreased Platelet Count
Pregabalin Capsules treatment was associated with a decrease in platelet count. Pregabalin Capsules-treated subjects experienced a mean maximal decrease in platelet count of 20 × 10 3/µL, compared to 11 × 10 3/µL in placebo patients. In the overall database of controlled trials in adult patients, 2% of placebo patients and 3% of Pregabalin Capsules patients experienced a potentially clinically significant decrease in platelets, defined as 20% below baseline value and less than 150 × 10 3/µL. A single Pregabalin Capsules-treated subject developed severe thrombocytopenia with a platelet count less than 20 × 10 3/µL. In randomized controlled trials, Pregabalin Capsules were not associated with an increase in bleeding-related adverse reactions.
5.13 Pr Interval Prolongation
Pregabalin Capsules treatment was associated with PR interval prolongation. In analyses of clinical trial ECG data in adult patients, the mean PR interval increase was 3–6 msec at Pregabalin Capsules doses greater than or equal to 300 mg/day. This mean change difference was not associated with an increased risk of PR increase greater than or equal to 25% from baseline, an increased percentage of subjects with on-treatment PR greater than 200 msec, or an increased risk of adverse reactions of second or third degree AV block.
Subgroup analyses did not identify an increased risk of PR prolongation in patients with baseline PR prolongation or in patients taking other PR prolonging medications. However, these analyses cannot be considered definitive because of the limited number of patients in these categories.
8 Use in Specific Populations
- Lactation: Breastfeeding is not recommended. ( 8.2)
Comparison of Gender and Race
The overall adverse event profile of pregabalin was similar between women and men. There are insufficient data to support a statement regarding the distribution of adverse experience reports by race.
Most Common Adverse Reactions
Table 4 lists all adverse reactions, regardless of causality, occurring in greater than or equal to 1% of patients with neuropathic pain associated with diabetic neuropathy in the combined Pregabalin Capsules group for which the incidence was greater in this combined Pregabalin Capsules group than in the placebo group. A majority of pregabalin-treated patients in clinical studies had adverse reactions with a maximum intensity of “mild” or “moderate”.
|
Body system
Preferred term |
75 mg/day
[N=77] % |
150 mg/day
[N=212] % |
300 mg/day
[N=321] % |
600 mg/day
[N=369] % |
All PGB
PGB: pregabalin
[N=979] % |
Placebo
[N=459] % |
|---|---|---|---|---|---|---|
|
Body as a whole |
||||||
|
Asthenia |
4 |
2 |
4 |
7 |
5 |
2 |
|
Accidental injury |
5 |
2 |
2 |
6 |
4 |
3 |
|
Back pain |
0 |
2 |
1 |
2 |
2 |
0 |
|
Chest pain |
4 |
1 |
1 |
2 |
2 |
1 |
|
Face edema |
0 |
1 |
1 |
2 |
1 |
0 |
|
Digestive system |
||||||
|
Dry mouth |
3 |
2 |
5 |
7 |
5 |
1 |
|
Constipation |
0 |
2 |
4 |
6 |
4 |
2 |
|
Flatulence |
3 |
0 |
2 |
3 |
2 |
1 |
|
Metabolic and nutritional disorders |
||||||
|
Peripheral edema |
4 |
6 |
9 |
12 |
9 |
2 |
|
Weight gain |
0 |
4 |
4 |
6 |
4 |
0 |
|
Edema |
0 |
2 |
4 |
2 |
2 |
0 |
|
Hypoglycemia |
1 |
3 |
2 |
1 |
2 |
1 |
|
Nervous system |
||||||
|
Dizziness |
8 |
9 |
23 |
29 |
21 |
5 |
|
Somnolence |
4 |
6 |
13 |
16 |
12 |
3 |
|
Neuropathy |
9 |
2 |
2 |
5 |
4 |
3 |
|
Ataxia |
6 |
1 |
2 |
4 |
3 |
1 |
|
Vertigo |
1 |
2 |
2 |
4 |
3 |
1 |
|
Confusion |
0 |
1 |
2 |
3 |
2 |
1 |
|
Euphoria |
0 |
0 |
3 |
2 |
2 |
0 |
|
Incoordination |
1 |
0 |
2 |
2 |
2 |
0 |
|
Thinking abnormal Thinking abnormal primarily consists of events related to difficulty with concentration/attention but also includes events related to cognition and language problems and slowed thinking.
|
1 |
0 |
1 |
3 |
2 |
0 |
|
Tremor |
1 |
1 |
1 |
2 |
1 |
0 |
|
Abnormal gait |
1 |
0 |
1 |
3 |
1 |
0 |
|
Amnesia |
3 |
1 |
0 |
2 |
1 |
0 |
|
Nervousness |
0 |
1 |
1 |
1 |
1 |
0 |
|
Respiratory system |
||||||
|
Dyspnea |
3 |
0 |
2 |
2 |
2 |
1 |
|
Special senses |
||||||
|
Blurry vision Investigator term; summary level term is amblyopia
|
3 |
1 |
3 |
6 |
4 |
2 |
|
Abnormal vision |
1 |
0 |
1 |
1 |
1 |
0 |
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
In all controlled and uncontrolled trials across various patient populations during the premarketing development of Pregabalin Capsules, more than 10,000 patients have received Pregabalin Capsules. Approximately 5000 patients were treated for 6 months or more, over 3100 patients were treated for 1 year or longer, and over 1400 patients were treated for at least 2 years.
14.4 Management of Fibromyalgia
The efficacy of Pregabalin Capsules for management of fibromyalgia was established in one 14-week, double-blind, placebo-controlled, multicenter study (F1) and one six-month, randomized withdrawal study (F2). Studies F1 and F2 enrolled patients with a diagnosis of fibromyalgia using the American College of Rheumatology (ACR) criteria (history of widespread pain for 3 months, and pain present at 11 or more of the 18 specific tender point sites). The studies showed a reduction in pain by visual analog scale. In addition, improvement was demonstrated based on a patient global assessment (PGIC), and on the Fibromyalgia Impact Questionnaire (FIQ).
5.11 Creatine Kinase Elevations
Pregabalin Capsules treatment was associated with creatine kinase elevations. Mean changes in creatine kinase from baseline to the maximum value were 60 U/L for Pregabalin Capsules-treated patients and 28 U/L for the placebo patients. In all controlled trials in adult patients across multiple patient populations, 1.5% of patients on Pregabalin Capsules and 0.7% of placebo patients had a value of creatine kinase at least three times the upper limit of normal. Three Pregabalin Capsules-treated subjects had events reported as rhabdomyolysis in premarketing clinical trials. The relationship between these myopathy events and Pregabalin Capsules is not completely understood because the cases had documented factors that may have caused or contributed to these events. Instruct patients to promptly report unexplained muscle pain, tenderness, or weakness, particularly if these muscle symptoms are accompanied by malaise or fever. Discontinue treatment with Pregabalin Capsules if myopathy is diagnosed or suspected or if markedly elevated creatine kinase levels occur.
17 Patient Counseling Information
Advise the patient to read the FDA-approved patient labeling (Medication Guide).
5.3 Suicidal Behavior and Ideation
Antiepileptic drugs (AEDs), including pregabalin, the active ingredient in Pregabalin Capsules, increase the risk of suicidal thoughts or behavior in patients taking these drugs for any indication. Suicidal behavior and ideation have also been reported in patients after discontinuation of pregabalin [see Warnings and Precautions (5.4)] . Monitor patients treated with any AED for any indication for the emergence or worsening of depression, suicidal thoughts or behavior, and/or any unusual changes in mood or behavior.
Pooled analyses of 199 placebo-controlled clinical trials (mono- and adjunctive therapy) of 11 different AEDs showed that patients randomized to one of the AEDs had approximately twice the risk (adjusted Relative Risk 1.8, 95% CI:1.2, 2.7) of suicidal thinking or behavior compared to patients randomized to placebo. In these trials, which had a median treatment duration of 12 weeks, the estimated incidence rate of suicidal behavior or ideation among 27,863 AED-treated patients was 0.43%, compared to 0.24% among 16,029 placebo-treated patients, representing an increase of approximately one case of suicidal thinking or behavior for every 530 patients treated. There were four suicides in drug-treated patients in the trials and none in placebo-treated patients, but the number is too small to allow any conclusion about drug effect on suicide.
The increased risk of suicidal thoughts or behavior with AEDs was observed as early as one week after starting drug treatment with AEDs and persisted for the duration of treatment assessed. Because most trials included in the analysis did not extend beyond 24 weeks, the risk of suicidal thoughts or behavior beyond 24 weeks could not be assessed.
The risk of suicidal thoughts or behavior was generally consistent among drugs in the data analyzed. The finding of increased risk with AEDs of varying mechanisms of action and across a range of indications suggests that the risk applies to all AEDs used for any indication. The risk did not vary substantially by age (5–100 years) in the clinical trials analyzed.
Table 3 shows absolute and relative risk by indication for all evaluated AEDs.
|
Indication |
Placebo
|
Drug Patients
|
Relative Risk:
|
Risk Difference: Additional Drug Patients with
|
|
Epilepsy |
1.0 |
3.4 |
3.5 |
2.4 |
|
Psychiatric |
5.7 |
8.5 |
1.5 |
2.9 |
|
Other |
1.0 |
1.8 |
1.9 |
0.9 |
|
Total |
2.4 |
4.3 |
1.8 |
1.9 |
The relative risk for suicidal thoughts or behavior was higher in clinical trials for epilepsy than in clinical trials for psychiatric or other conditions, but the absolute risk differences were similar for the epilepsy and psychiatric indications.
Anyone considering prescribing Pregabalin Capsules or any other AED must balance the risk of suicidal thoughts or behavior with the risk of untreated illness. Epilepsy and many other illnesses for which AEDs are prescribed are themselves associated with morbidity and mortality and an increased risk of suicidal thoughts and behavior. Should suicidal thoughts and behavior emerge during treatment, the prescriber needs to consider whether the emergence of these symptoms in any given patient may be related to the illness being treated.
2.3 Postherpetic Neuralgia in Adults
The recommended dose of Pregabalin Capsules is 75 to 150 mg two times a day, or 50 to 100 mg three times a day (150 to 300 mg/day) in patients with creatinine clearance of at least 60 mL/min. Begin dosing at 75 mg two times a day, or 50 mg three times a day (150 mg/day). The dose may be increased to 300 mg/day within 1 week based on efficacy and tolerability.
Patients who do not experience sufficient pain relief following 2 to 4 weeks of treatment with 300 mg/day, and who are able to tolerate Pregabalin Capsules, may be treated with up to 300 mg two times a day, or 200 mg three times a day (600 mg/day). In view of the dose-dependent adverse reactions and the higher rate of treatment discontinuation due to adverse reactions, reserve dosing above 300 mg/day for those patients who have on-going pain and are tolerating 300 mg daily [see Adverse Reactions (6.1)] .
2.1 Important Administration Instructions
Pregabalin Capsules are given orally with or without food.
When discontinuing Pregabalin Capsules, taper gradually over a minimum of 1 week [see Warnings and Precautions (5.4)] .
Because Pregabalin Capsules are eliminated primarily by renal excretion, adjust the dose in adult patients with reduced renal function [see Dosage and Administration (2.7)].
2.5 Management of Fibromyalgia in Adults
The recommended dose of Pregabalin Capsules for fibromyalgia is 300 to 450 mg/day. Begin dosing at 75 mg two times a day (150 mg/day). The dose may be increased to 150 mg two times a day (300 mg/day) within 1 week based on efficacy and tolerability. Patients who do not experience sufficient benefit with 300 mg/day may be further increased to 225 mg two times a day (450 mg/day). Although Pregabalin Capsules were also studied at 600 mg/day, there is no evidence that this dose confers additional benefit and this dose was less well tolerated. In view of the dose-dependent adverse reactions, treatment with doses above 450 mg/day is not recommended [see Adverse Reactions (6.1)] .
Adverse Reactions Leading to Discontinuation
In clinical trials in adults with neuropathic pain associated with diabetic peripheral neuropathy, 9% of patients treated with Pregabalin Capsules and 4% of patients treated with placebo discontinued prematurely due to adverse reactions. In the Pregabalin Capsules treatment group, the most common reasons for discontinuation due to adverse reactions were dizziness (3%) and somnolence (2%). In comparison, less than 1% of placebo patients withdrew due to dizziness and somnolence. Other reasons for discontinuation from the trials, occurring with greater frequency in the Pregabalin Capsules group than in the placebo group, were asthenia, confusion, and peripheral edema. Each of these events led to withdrawal in approximately 1% of patients.
2.7 Dosing for Adult Patients With Renal Impairment
In view of dose-dependent adverse reactions and since pregabalin is eliminated primarily by renal excretion, adjust the dose in adult patients with reduced renal function. The use of Pregabalin Capsules in pediatric patients with compromised renal function has not been studied.
Base the dose adjustment in patients with renal impairment on creatinine clearance (CLcr), as indicated in Table 2. To use this dosing table, an estimate of the patient's CLcr in mL/min is needed. CLcr in mL/min may be estimated from serum creatinine (mg/dL) determination using the Cockcroft and Gault equation:
Next, refer to the Dosage and Administration section to determine the recommended total daily dose based on indication, for a patient with normal renal function (CLcr greater than or equal to 60 mL/min). Then refer to Table 2 to determine the corresponding renal adjusted dose.
(For example: A patient initiating Pregabalin Capsules therapy for postherpetic neuralgia with normal renal function (CLcr greater than or equal to 60 mL/min), receives a total daily dose of 150 mg/day pregabalin. Therefore, a renal impaired patient with a CLcr of 50 mL/min would receive a total daily dose of 75 mg/day pregabalin administered in two or three divided doses.)
For patients undergoing hemodialysis, adjust the pregabalin daily dose based on renal function. In addition to the daily dose adjustment, administer a supplemental dose immediately following every 4-hour hemodialysis treatment (see Table 2).
| TID = Three divided doses; BID = Two divided doses; QD = Single daily dose. | |||||
|
Creatinine Clearance (CLcr)
|
Total Pregabalin Daily Dose (mg/day) Total daily dose (mg/day) should be divided as indicated by dose regimen to provide mg/dose.
|
Dose Regimen |
|||
|
Greater than or equal to 60 |
150 |
300 |
450 |
600 |
BID or TID |
|
30-60 |
75 |
150 |
225 |
300 |
BID or TID |
|
15-30 |
25-50 |
75 |
100-150 |
150 |
QD or BID |
|
Less than 15 |
25 |
25-50 |
50-75 |
75 |
QD |
|
Supplementary dosage following hemodialysis (mg) Supplementary dose is a single additional dose.
|
|||||
|
Patients on the 25 mg QD regimen: take one supplemental dose of 25 mg or 50 mg Patients on the 25-50 mg QD regimen: take one supplemental dose of 50 mg or 75 mg Patients on the 50-75 mg QD regimen: take one supplemental dose of 75 mg or 100 mg Patients on the 75 mg QD regimen: take one supplemental dose of 100 mg or 150 mg |
2.6 Neuropathic Pain Associated With Spinal Cord Injury in Adults
The recommended dose range of Pregabalin Capsules for the treatment of neuropathic pain associated with spinal cord injury is 150 to 600 mg/day. The recommended starting dose is 75 mg two times a day (150 mg/day). The dose may be increased to 150 mg two times a day (300 mg/day) within 1 week based on efficacy and tolerability. Patients who do not experience sufficient pain relief after 2 to 3 weeks of treatment with 150 mg two times a day and who tolerate Pregabalin Capsules may be treated with up to 300 mg two times a day [see Clinical Studies (14.5)] .
14.1 Neuropathic Pain Associated With Diabetic Peripheral Neuropathy
The efficacy of the maximum recommended dose of Pregabalin Capsules for the management of neuropathic pain associated with diabetic peripheral neuropathy was established in three double-blind, placebo-controlled, multicenter studies with three times a day dosing, two of which studied the maximum recommended dose. Patients were enrolled with either Type 1 or Type 2 diabetes mellitus and a diagnosis of painful distal symmetrical sensorimotor polyneuropathy for 1 to 5 years. A total of 89% of patients completed Studies DPN 1 and DPN 2. The patients had a minimum mean baseline pain score of greater than or equal to 4 on an 11-point numerical pain rating scale ranging from 0 (no pain) to 10 (worst possible pain). The baseline mean pain scores across the two studies ranged from 6.1 to 6.7. Patients were permitted up to 4 grams of acetaminophen per day as needed for pain, in addition to pregabalin. Patients recorded their pain daily in a diary.
14.5 Management of Neuropathic Pain Associated With Spinal Cord Injury
The efficacy of Pregabalin Capsules for the management of neuropathic pain associated with spinal cord injury was established in two double-blind, placebo-controlled, multicenter studies. Patients were enrolled with neuropathic pain associated with spinal cord injury that persisted continuously for at least three months or with relapses and remissions for at least six months. A total of 63% of patients completed study 1 and 84% completed study 2. The patients had a minimum mean baseline pain score of greater than or equal to 4 on an 11-point numerical pain rating scale ranging from 0 (no pain) to 10 (worst possible pain). The baseline mean pain scores across the two studies ranged from 6.5 to 6.7.
Patients were allowed to take opioids, non-opioid analgesics, antiepileptic drugs, muscle relaxants, and antidepressant drugs if the dose was stable for 30 days prior to screening. Patients were allowed to take acetaminophen and nonsteroidal anti-inflammatory drugs during the studies.
Study SCI 1: This 12-week, randomized, double-blind, parallel-group, multicenter, flexible dose (150-600 mg/day) study compared pregabalin with placebo. The 12-week study consisted of a 3-week dose adjustment phase and a 9-week dose maintenance phase. Treatment with Pregabalin Capsules 150-600 mg/day statistically significantly improved the endpoint weekly mean pain score, and increased the proportion of patients with at least a 30% and 50% reduction in pain score from baseline. The fraction of patients achieving various levels of improvement in pain intensity from baseline to Week 12 is presented in Figure 11. Some patients experienced a decrease in pain as early as week 1, which persisted throughout the study.
Figure 11: Patients Achieving Various Levels of Improvement in Pain Intensity – Study SCI 1
Study SCI 2: This 16-week, randomized, double-blind, placebo-controlled, parallel-group, multicenter, flexible dose (150-600 mg/day, in increments of 150 mg) study compared the efficacy, safety and tolerability of pregabalin with placebo. The 16-week study consisted of a 4-week dose adjustment phase and a 12-week dose maintenance phase. Treatment with Pregabalin Capsules statistically significantly improved the endpoint weekly mean pain score, and increased the proportion of patients with at least a 30% and 50% reduction in pain score from baseline. The fraction of patients achieving various levels of improvement in pain intensity from baseline to Week 16 is presented in Figure 12. Some patients experienced a decrease in pain as early as week 1, which persisted throughout the study.
Figure 12: Patients Achieving Various Levels of Improvement in Pain Intensity – Study SCI 2
Most Common Adverse Reactions in All Controlled Clinical Studies in Adults
In premarketing controlled trials of all adult patient populations combined (including DPN, PHN, and adult patients with partial-onset seizures), dizziness, somnolence, dry mouth, edema, blurred vision, weight gain, and “thinking abnormal” (primarily difficulty with concentration/attention) were more commonly reported by subjects treated with Pregabalin Capsules than by subjects treated with placebo (greater than or equal to 5% and twice the rate of that seen in placebo).
5.4 Increased Risk of Adverse Reactions With Abrupt Or Rapid Discontinuation
As with all antiepileptic drugs (AEDs), withdraw Pregabalin Capsules gradually to minimize the potential of increased seizure frequency in patients with seizure disorders.
Following abrupt or rapid discontinuation of Pregabalin Capsules, some patients reported symptoms including insomnia, nausea, headache, anxiety, hyperhidrosis, and diarrhea [see Adverse Reactions (6.2), Drug Abuse and Dependence (9.3)] . Suicidal behavior and ideation have also been reported in patients after discontinuation of pregabalin [see Warnings and Precautions (5.3)] .
If Pregabalin Capsules are discontinued, taper the drug gradually over a minimum of 1 week rather than discontinue the drug abruptly.
2.2 Neuropathic Pain Associated With Diabetic Peripheral Neuropathy in Adults
The maximum recommended dose of Pregabalin Capsules is 100 mg three times a day (300 mg/day) in patients with creatinine clearance of at least 60 mL/min. Begin dosing at 50 mg three times a day (150 mg/day). The dose may be increased to 300 mg/day within 1 week based on efficacy and tolerability.
Although Pregabalin Capsules were also studied at 600 mg/day, there is no evidence that this dose confers additional significant benefit and this dose was less well tolerated. In view of the dose-dependent adverse reactions, treatment with doses above 300 mg/day is not recommended [see Adverse Reactions (6.1)] .
Other Adverse Reactions Observed During the Clinical Studies of Pregabalin Capsules
Following is a list of treatment-emergent adverse reactions reported by patients treated with Pregabalin Capsules during all clinical trials. The listing does not include those events already listed in the previous tables or elsewhere in labeling, those events for which a drug cause was remote, those events which were so general as to be uninformative, and those events reported only once which did not have a substantial probability of being acutely life-threatening.
Events are categorized by body system and listed in order of decreasing frequency according to the following definitions: frequentadverse reactions are those occurring on one or more occasions in at least 1/100 patients; infrequentadverse reactions are those occurring in 1/100 to 1/1000 patients; rarereactions are those occurring in fewer than 1/1000 patients. Events of major clinical importance are described in the Warnings and Precautionssection (5).
Body as a Whole – Frequent: Abdominal pain, Allergic reaction, Fever, Infrequent: Abscess, Cellulitis, Chills, Malaise, Neck rigidity, Overdose, Pelvic pain, Photosensitivity reaction, Rare: Anaphylactoid reaction, Ascites, Granuloma, Hangover effect, Intentional Injury, Retroperitoneal Fibrosis, Shock
Cardiovascular System – Infrequent: Deep thrombophlebitis, Heart failure, Hypotension, Postural hypotension, Retinal vascular disorder, Syncope; Rare: ST Depressed, Ventricular Fibrillation
Digestive System – Frequent: Gastroenteritis, Increased appetite; Infrequent: Cholecystitis, Cholelithiasis, Colitis, Dysphagia, Esophagitis, Gastritis, Gastrointestinal hemorrhage, Melena, Mouth ulceration, Pancreatitis, Rectal hemorrhage, Tongue edema; Rare: Aphthous stomatitis, Esophageal Ulcer, Periodontal abscess
Hemic and Lymphatic System – Frequent: Ecchymosis; Infrequent: Anemia, Eosinophilia, Hypochromic anemia, Leukocytosis, Leukopenia, Lymphadenopathy, Thrombocytopenia; Rare: Myelofibrosis, Polycythemia, Prothrombin decreased, Purpura, Thrombocythemia, Alanine aminotransferase increased, Aspartate aminotransferase increased
Metabolic and Nutritional Disorders – Rare: Glucose Tolerance Decreased, Urate Crystalluria
Musculoskeletal System – Frequent: Arthralgia, Leg cramps, Myalgia, Myasthenia; Infrequent: Arthrosis; Rare: Chondrodystrophy, Generalized Spasm
Nervous System – Frequent: Anxiety, Depersonalization, Hypertonia, Hypoesthesia, Libido decreased, Nystagmus, Paresthesia, Sedation, Stupor, Twitching; Infrequent: Abnormal dreams, Agitation, Apathy, Aphasia, Circumoral paresthesia, Dysarthria, Hallucinations, Hostility, Hyperalgesia, Hyperesthesia, Hyperkinesia, Hypokinesia, Hypotonia, Libido increased, Myoclonus, Neuralgia; Rare: Addiction, Cerebellar syndrome, Cogwheel rigidity, Coma, Delirium, Delusions, Dysautonomia, Dyskinesia, Dystonia, Encephalopathy, Extrapyramidal syndrome, Guillain-Barré syndrome, Hypalgesia, Intracranial hypertension, Manic reaction, Paranoid reaction, Peripheral neuritis, Personality disorder, Psychotic depression, Schizophrenic reaction, Sleep disorder, Torticollis, Trismus
Respiratory System – Rare: Apnea, Atelectasis, Bronchiolitis, Hiccup, Laryngismus, Lung edema, Lung fibrosis, Yawn
Skin and Appendages – Frequent: Pruritus, Infrequent: Alopecia, Dry skin, Eczema, Hirsutism, Skin ulcer, Urticaria, Vesiculobullous rash; Rare: Angioedema, Exfoliative dermatitis, Lichenoid dermatitis, Melanosis, Nail Disorder, Petechial rash, Purpuric rash, Pustular rash, Skin atrophy, Skin necrosis, Skin nodule, Stevens-Johnson syndrome, Subcutaneous nodule
Special senses – Frequent: Conjunctivitis, Diplopia, Otitis media, Tinnitus; Infrequent: Abnormality of accommodation, Blepharitis, Dry eyes, Eye hemorrhage, Hyperacusis, Photophobia, Retinal edema, Taste loss, Taste perversion; Rare: Anisocoria, Blindness, Corneal ulcer, Exophthalmos, Extraocular palsy, Iritis, Keratitis, Keratoconjunctivitis, Miosis, Mydriasis, Night blindness, Ophthalmoplegia, Optic atrophy, Papilledema, Parosmia, Ptosis, Uveitis
Urogenital System – Frequent: Anorgasmia, Impotence, Urinary frequency, Urinary incontinence; Infrequent: Abnormal ejaculation, Albuminuria, Amenorrhea, Dysmenorrhea, Dysuria, Hematuria, Kidney calculus, Leukorrhea, Menorrhagia, Metrorrhagia, Nephritis, Oliguria, Urinary retention, Urine abnormality; Rare: Acute kidney failure, Balanitis, Bladder Neoplasm, Cervicitis, Dyspareunia, Epididymitis, Female lactation, Glomerulitis, Ovarian disorder, Pyelonephritis
2.4 adjunctive Therapy for Partial Onset Seizures in Patients 1 Month of Age and Older
The recommended dosages for adults and pediatric patients 1 month of age and older are included in Table 1. Administer the total daily dosage orally in two or three divided doses as indicated in Table 1. In pediatric patients, the recommended dosing regimen is dependent upon body weight. Based on clinical response and tolerability, dosage may be increased, approximately weekly.
|
Age and Body Weight |
Recommended Initial Dosage |
Recommended Maximum Dosage |
Frequency of Administration |
|
Adults (17 years and older) |
150 mg/day |
600 mg/day |
2 or 3 divided doses |
|
Pediatric patients weighing 30 kg or more |
2.5 mg/kg/day |
10 mg/kg/day (not to exceed 600 mg/day) |
2 or 3 divided doses |
|
Pediatric patients weighing less than 30 kg |
3.5 mg/kg/day |
14 mg/kg/day |
1 month to less than 4 years of age:
4 years of age and older:
|
Both the efficacy and adverse event profiles of Pregabalin Capsules have been shown to be dose‑related.
The effect of dose escalation rate on the tolerability of Pregabalin Capsules has not been formally studied.
The efficacy of adjunctive Pregabalin Capsules in patients taking gabapentin has not been evaluated in controlled trials. Consequently, dosing recommendations for the use of Pregabalin Capsules with gabapentin cannot be offered.
Adverse Reactions Most Commonly Leading to Discontinuation in All Premarketing Controlled Clinical Studies
In premarketing controlled trials of all adult populations combined, 14% of patients treated with Pregabalin Capsules and 7% of patients treated with placebo discontinued prematurely due to adverse reactions. In the Pregabalin Capsules treatment group, the adverse reactions most frequently leading to discontinuation were dizziness (4%) and somnolence (4%). In the placebo group, 1% of patients withdrew due to dizziness and less than 1% withdrew due to somnolence. Other adverse reactions that led to discontinuation from controlled trials more frequently in the Pregabalin Capsules group compared to the placebo group were ataxia, confusion, asthenia, thinking abnormal, blurred vision, incoordination, and peripheral edema (1% each).
Structured Label Content
Section 42229-5 (42229-5)
Pharmacodynamics
Multiple oral doses of Pregabalin Capsules were co-administered with oxycodone, lorazepam, or ethanol. Although no pharmacokinetic interactions were seen, additive effects on cognitive and gross motor functioning were seen when Pregabalin Capsules were co-administered with these drugs. No clinically important effects on respiration were seen.
Section 42231-1 (42231-1)
|
MEDICATION GUIDE Pregabalin (pree gab' a lin) Capsules, CV |
||
| This Medication Guide has been approved by the U.S. Food and Drug Administration. | Revised: 10/2025 | |
|
Read this Medication Guide before you start taking Pregabalin Capsules and each time you get a refill. There may be new information. This information does not take the place of talking to your healthcare provider about your medical condition or treatment. If you have any questions about Pregabalin Capsules, ask your healthcare provider or pharmacist. |
||
|
What is the most important information I should know about Pregabalin Capsules? Pregabalin Capsules may cause serious side effects including: |
||
|
|
|
|
These serious side effects are described below:
|
||
|
|
|
|
If you have suicidal thoughts or actions, do not stop Pregabalin Capsules without first talking to a healthcare provider.
How can I watch for early symptoms of suicidal thoughts and actions?
|
||
|
||
|
What is Pregabalin Capsules? Pregabalin Capsules are a prescription medicine used in adults, 18 years of age and older to treat:
It is not known if Pregabalin Capsules are safe and effective in people under 18 years of age for the treatment of fibromyalgia and neuropathic pain with diabetes, shingles, or spinal cord injury. Pregabalin Capsules is a prescription medicine used in people 1 month of age and older to treat:
For the treatment of partial-onset seizures when taken together with other seizure medicines, it is not known if Pregabalin Capsules are safe and effective in children under 1 month of age. |
||
|
Who should not take Pregabalin Capsules? Do not take Pregabalin Capsules if you are allergic to pregabalin or any of the ingredients in Pregabalin Capsules. See “ What is the most important information I should know about Pregabalin Capsules?” for the signs of an allergic reaction. See the end of this Medication Guide for a complete list of ingredients in Pregabalin Capsules. |
||
|
What should I tell my healthcare provider before taking Pregabalin Capsules? Before taking Pregabalin Capsules, tell your healthcare provider about all your medical conditions, including if you:
Tell your healthcare provider about all the medicines you take, including prescription and over-the-counter medicines, vitamins or herbal supplements. Pregabalin Capsules and other medicines may affect each other causing side effects. Especially tell your healthcare provider if you take:
Know the medicines you take. Keep a list of them with you to show your healthcare provider and pharmacist each time you get a new medicine. Do not start a new medicine without talking with your healthcare provider. |
||
|
How should I take Pregabalin Capsules?
|
||
|
What should I avoid while taking Pregabalin Capsules?
|
||
|
What are the possible side effects of Pregabalin Capsules? Pregabalin Capsules may cause serious side effects, including:
The most common side effects of Pregabalin Capsules in adults are: |
||
|
|
|
|
The most common side effects of Pregabalin Capsules in childrenare weight gain, increase in appetite, and sleepiness. Pregabalin Capsules caused skin sores in animal studies. Skin sores did not happen in studies in people. If you have diabetes, you should pay attention to your skin while taking Pregabalin Capsules and tell your healthcare provider about any sores or skin problems. Tell your healthcare provider about any side effect that bothers you or that does not go away. These are not all the possible side effects of Pregabalin Capsules. For more information, ask your healthcare provider or pharmacist. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. |
||
|
How should I store Pregabalin Capsules?
Keep Pregabalin Capsules and all medicines out of the reach of children. |
||
|
General information about the safe and effective use of Pregabalin Capsules Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not use Pregabalin Capsules for a condition for which it was not prescribed. Do not give Pregabalin Capsules to other people, even if they have the same symptoms you have. It may harm them. You can ask your healthcare provider or pharmacist for information about Pregabalin Capsules that is written for health professionals. |
||
|
What are the ingredients in Pregabalin Capsules? Active ingredient: pregabalin Inactive ingredients: Pregabalin Capsules: pregelatinized starch, talc Capsule shell: gelatin, titanium dioxide, sodium lauryl sulfate and water; Orange capsule shell (75 mg, 100 mg, 200 mg, 225 mg and 300 mg strengths) also contains red iron oxide. Colloidal silicon dioxide is used as processing aid. Imprinting ink: shellac, black iron oxide, propylene glycol, potassium hydroxide.
Manufactured by:
All brand names listed are the registered trademarks of their respective owners and are not trademarks of Eskayef Pharmaceuticals Limited. |
PM06168 V09
Section 44425-7 (44425-7)
Storage and Handling
Store at 20° to 25° C (68° to 77° F), excursions permitted between 15° to 30° C (59° to 86° F) [see USP Controlled Room Temperature].
Section 51945-4 (51945-4)
NDC 72658-0808-1
Pregabalin Capsules CV
25 mg
PHARMACIST: Dispense the accompanying Medication Guide to each patient.
60 Capsules
Rx only
SK+F
9.2 Abuse
In a study of recreational users (N=15) of sedative/hypnotic drugs, including alcohol, Pregabalin Capsules (450 mg, single dose) received subjective ratings of “good drug effect,” “high” and “liking” to a degree that was similar to diazepam (30 mg, single dose). In controlled clinical studies in over 5500 patients, 4 % of Pregabalin Capsules-treated patients and 1 % of placebo-treated patients overall reported euphoria as an adverse reaction, though in some patient populations studied, this reporting rate was higher and ranged from 1 to 12%.
11 Description (11 DESCRIPTION)
Pregabalin is described chemically as ( S)-3-(aminomethyl)-5-methylhexanoic acid. The molecular formula is C 8H 17NO 2 and the molecular weight is 159.23. The chemical structure of pregabalin is:
Pregabalin is a white to off-white, crystalline solid with a pK a1 of 4.2 and a pK a2 of 10.6. It is freely soluble in 1N Hydrochloric acid and sparingly soluble in water. The log of the partition coefficient (n-octanol/0.05M phosphate buffer) at pH 7.4 is – 1.35.
Pregabalin Capsules are administered orally and are supplied as imprinted hard-shell capsules containing 25, 50, 75, 100, 150, 200, 225, and 300 mg of pregabalin, along with pregelatinized starch and talc as inactive ingredients. The capsule shells contain gelatin, titanium dioxide, sodium lauryl sulfate and water. In addition, the orange capsule shells (75 mg, 100 mg, 200 mg, 225 mg and 300 mg strengths) contain red iron oxide. Colloidal silicon dioxide is used as processing aid. The imprinting ink contains shellac, black iron oxide, propylene glycol, potassium hydroxide.
5.1 Angioedema
There have been postmarketing reports of angioedema in patients during initial and chronic treatment with Pregabalin Capsules. Specific symptoms included swelling of the face, mouth (tongue, lips, and gums), and neck (throat and larynx). There were reports of life-threatening angioedema with respiratory compromise requiring emergency treatment. Discontinue Pregabalin Capsules immediately in patients with these symptoms.
Exercise caution when prescribing Pregabalin Capsules to patients who have had a previous episode of angioedema. In addition, patients who are taking other drugs associated with angioedema (e.g., angiotensin converting enzyme inhibitors [ACE-inhibitors]) may be at increased risk of developing angioedema.
9.3 Dependence
In clinical studies, following abrupt or rapid discontinuation of Pregabalin Capsules, some patients reported symptoms including insomnia, nausea, headache or diarrhea [see Warnings and Precautions (5.4)] , consistent with physical dependence. In the postmarketing setting, in addition to these reported symptoms, other reported adverse reactions include, but are not limited to, seizures, depression, suicidal ideation and behavior, agitation, confusion, disorientation, psychotic symptoms, pain, sweating, tremor, dizziness, and malaise.
5.8 Weight Gain
Pregabalin Capsules treatment may cause weight gain. In Pregabalin Capsules controlled clinical trials in adult patients of up to 14 weeks, a gain of 7% or more over baseline weight was observed in 9% of Pregabalin Capsules-treated patients and 2% of placebo-treated patients. Few patients treated with Pregabalin Capsules (0.3%) withdrew from controlled trials due to weight gain. Pregabalin Capsules associated weight gain was related to dose and duration of exposure but did not appear to be associated with baseline BMI, gender, or age. Weight gain was not limited to patients with edema [see Warnings and Precautions (5.7)] .
Although weight gain was not associated with clinically important changes in blood pressure in short-term controlled studies, the long-term cardiovascular effects of Pregabalin Capsules-associated weight gain are unknown.
Among diabetic patients, Pregabalin Capsules-treated patients gained an average of 1.6 kg (range: -16 to 16 kg), compared to an average 0.3 kg (range: -10 to 9 kg) weight gain in placebo patients. In a cohort of 333 diabetic patients who received Pregabalin Capsules for at least 2 years, the average weight gain was 5.2 kg.
While the effects of Pregabalin Capsules-associated weight gain on glycemic control have not been systematically assessed, in controlled and longer-term open label clinical trials with diabetic patients, Pregabalin Capsules treatment did not appear to be associated with loss of glycemic control (as measured by HbA 1C).
8.5 Geriatric Use
In controlled clinical studies of Pregabalin Capsules in neuropathic pain associated with diabetic peripheral neuropathy, 246 patients were 65 to 74 years of age, and 73 patients were 75 years of age or older.
In controlled clinical studies of Pregabalin Capsules in neuropathic pain associated with postherpetic neuralgia, 282 patients were 65 to 74 years of age, and 379 patients were 75 years of age or older.
In controlled clinical studies of Pregabalin Capsules in epilepsy, there were only 10 patients 65 to 74 years of age, and 2 patients who were 75 years of age or older.
No overall differences in safety and efficacy were observed between these patients and younger patients.
In controlled clinical studies of Pregabalin Capsules in fibromyalgia, 106 patients were 65 years of age or older. Although the adverse reaction profile was similar between the two age groups, the following neurological adverse reactions were more frequent in patients 65 years of age or older: dizziness, vision blurred, balance disorder, tremor, confusional state, coordination abnormal, and lethargy.
Pregabalin Capsules are known to be substantially excreted by the kidney, and the risk of toxic reactions to Pregabalin Capsules may be greater in patients with impaired renal function. Because Pregabalin Capsules are eliminated primarily by renal excretion, adjust the dose for elderly patients with renal impairment [see Dosage and Administration (2.7)] .
4 Contraindications (4 CONTRAINDICATIONS)
Pregabalin Capsules are contraindicated in patients with known hypersensitivity to pregabalin or any of its components. Angioedema and hypersensitivity reactions have occurred in patients receiving pregabalin therapy [see Warnings and Precautions (5.2)].
6 Adverse Reactions (6 ADVERSE REACTIONS)
The following serious adverse reactions are described elsewhere in the labeling:
- Angioedema [see Warnings and Precautions (5.1)]
- Hypersensitivity [see Warnings and Precautions (5.2)]
- Suicidal Behavior and Ideation [see Warnings and Precautions (5.3)]
- Increased Risk of Adverse Reactions with Abrupt or Rapid Discontinuation [see Warnings and Precautions (5.4)]
- Respiratory Depression [see Warnings and Precautions (5.5)]
- Dizziness and Somnolence [see Warnings and Precautions (5.6)]
- Peripheral Edema [see Warnings and Precautions (5.7)]
- Weight Gain [see Warnings and Precautions (5.8)]
- Tumorigenic Potential [see Warnings and Precautions (5.9)]
- Ophthalmological Effects [see Warnings and Precautions (5.10)]
- Creatine Kinase Elevations [see Warnings and Precautions (5.11)]
- Decreased Platelet Count [see Warnings and Precautions (5.12)]
- PR Interval Prolongation [see Warnings and Precautions (5.13)]
7 Drug Interactions (7 DRUG INTERACTIONS)
Since Pregabalin Capsules are predominantly excreted unchanged in the urine, undergoes negligible metabolism in humans (less than 2% of a dose recovered in urine as metabolites), and does not bind to plasma proteins, its pharmacokinetics are unlikely to be affected by other agents through metabolic interactions or protein binding displacement. In vitro and in vivo studies showed that Pregabalin Capsules are unlikely to be involved in significant pharmacokinetic drug interactions. Specifically, there are no pharmacokinetic interactions between pregabalin and the following antiepileptic drugs: carbamazepine, valproic acid, lamotrigine, phenytoin, phenobarbital, and topiramate. Important pharmacokinetic interactions would also not be expected to occur between Pregabalin Capsules and commonly used antiepileptic drugs [see Clinical Pharmacology (12)] .
5.2 Hypersensitivity
There have been postmarketing reports of hypersensitivity in patients shortly after initiation of treatment with Pregabalin Capsules. Adverse reactions included skin redness, blisters, hives, rash, dyspnea, and wheezing. Discontinue Pregabalin Capsules immediately in patients with these symptoms.
5.7 Peripheral Edema
Pregabalin Capsules treatment may cause peripheral edema. In short-term trials of patients without clinically significant heart or peripheral vascular disease, there was no apparent association between peripheral edema and cardiovascular complications such as hypertension or congestive heart failure. Peripheral edema was not associated with laboratory changes suggestive of deterioration in renal or hepatic function.
In controlled clinical trials in adult patients, the incidence of peripheral edema was 6% in the Pregabalin Capsules group compared with 2% in the placebo group. In controlled clinical trials, 0.5% of Pregabalin Capsules patients and 0.2% placebo patients withdrew due to peripheral edema.
Higher frequencies of weight gain and peripheral edema were observed in patients taking both Pregabalin Capsules and a thiazolidinedione antidiabetic agent compared to patients taking either drug alone. The majority of patients using thiazolidinedione antidiabetic agents in the overall safety database were participants in studies of pain associated with diabetic peripheral neuropathy. In this population, peripheral edema was reported in 3% (2/60) of patients who were using thiazolidinedione antidiabetic agents only, 8% (69/859) of patients who were treated with Pregabalin Capsules only, and 19% (23/120) of patients who were on both Pregabalin Capsules and thiazolidinedione antidiabetic agents. Similarly, weight gain was reported in 0% (0/60) of patients on thiazolidinediones only; 4% (35/859) of patients on Pregabalin Capsules only; and 7.5% (9/120) of patients on both drugs.
As the thiazolidinedione class of antidiabetic drugs can cause weight gain and/or fluid retention, possibly exacerbating or leading to heart failure, exercise caution when co-administering Pregabalin Capsules and these agents.
Because there are limited data on congestive heart failure patients with New York Heart Association (NYHA) Class III or IV cardiac status, exercise caution when using Pregabalin Capsules in these patients.
8.6 Renal Impairment
Pregabalin Capsules are eliminated primarily by renal excretion and dose adjustment is recommended for adult patients with renal impairment [see Dosage and Administration (2.7) and Clinical Pharmacology (12.3)]. The use of Pregabalin Capsules in pediatric patients with compromised renal function has not been studied.
12.3 Pharmacokinetics
Pregabalin is well absorbed after oral administration, is eliminated largely by renal excretion, and has an elimination half-life of about 6 hours.
1 Indications and Usage (1 INDICATIONS AND USAGE)
Pregabalin Capsules are indicated for:
- Management of neuropathic pain associated with diabetic peripheral neuropathy
- Management of postherpetic neuralgia
- Adjunctive therapy for the treatment of partial-onset seizures in patients 1 month of age and older
- Management of fibromyalgia
- Management of neuropathic pain associated with spinal cord injury
12.1 Mechanism of Action
Pregabalin Capsules (pregabalin) binds with high affinity to the alpha 2-delta site (an auxiliary subunit of voltage-gated calcium channels) in central nervous system tissues. Although the mechanism of action of pregabalin has not been fully elucidated, results with genetically modified mice and with compounds structurally related to pregabalin (such as gabapentin) suggest that binding to the alpha 2-delta subunit may be involved in pregabalin's anti-nociceptive and antiseizure effects in animals. In animal models of nerve damage, pregabalin has been shown to reduce calcium-dependent release of pro-nociceptive neurotransmitters in the spinal cord, possibly by disrupting alpha 2-delta containing-calcium channel trafficking and/or reducing calcium currents. Evidence from other animal models of nerve damage and persistent pain suggest the anti-nociceptive activities of pregabalin may also be mediated through interactions with descending noradrenergic and serotonergic pathways originating from the brainstem that modulate pain transmission in the spinal cord.
While pregabalin is a structural derivative of the inhibitory neurotransmitter gamma-aminobutyric acid (GABA), it does not bind directly to GABA A, GABA B, or benzodiazepine receptors, does not augment GABA A responses in cultured neurons, does not alter rat brain GABA concentration or have acute effects on GABA uptake or degradation. However, in cultured neurons prolonged application of pregabalin increases the density of GABA transporter protein and increases the rate of functional GABA transport. Pregabalin does not block sodium channels, is not active at opiate receptors, and does not alter cyclooxygenase enzyme activity. It is inactive at serotonin and dopamine receptors and does not inhibit dopamine, serotonin, or noradrenaline reuptake.
9.1 Controlled Substance
Pregabalin is a Schedule V controlled substance.
Pregabalin Capsules are not known to be active at receptor sites associated with drugs of abuse. As with any CNS active drug, carefully evaluate patients for history of drug abuse and observe them for signs of Pregabalin Capsules misuse or abuse (e.g., development of tolerance, dose escalation, drug-seeking behavior).
5.9 Tumorigenic Potential
In standard preclinical in vivo lifetime carcinogenicity studies of Pregabalin Capsules, an unexpectedly high incidence of hemangiosarcoma was identified in two different strains of mice [ see Nonclinical Toxicology (13.1) ]. The clinical significance of this finding is unknown. Clinical experience during Pregabalin Capsules premarketing development provides no direct means to assess its potential for inducing tumors in humans.
In clinical studies across various patient populations, comprising 6396 patient-years of exposure in patients greater than 12 years of age, new or worsening-preexisting tumors were reported in 57 patients. Without knowledge of the background incidence and recurrence in similar populations not treated with Pregabalin Capsules, it is impossible to know whether the incidence seen in these cohorts is or is not affected by treatment.
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
- Angioedema (e.g., swelling of the throat, head, and neck) can occur, and may be associated with life-threatening respiratory compromise requiring emergency treatment. Discontinue Pregabalin Capsules immediately in these cases. ( 5.1)
- Hypersensitivity reactions (e.g., hives, dyspnea, and wheezing) can occur. Discontinue Pregabalin Capsules immediately in these patients. ( 5.2)
- Antiepileptic drugs, including pregabalin, the active ingredient in Pregabalin Capsules, increase the risk of suicidal thoughts or behavior. ( 5.3)
- Abrupt or rapid discontinuation may increase the risk for seizures. Withdrawal symptoms or suicidal behavior and ideation have been observed after discontinuation. Taper Pregabalin Capsules gradually over a minimum of 1 week. (5.4)
- Respiratory depression: May occur with Pregabalin Capsules, when used with concomitant CNS depressants or in the setting of underlying respiratory impairment. Monitor patients and adjust dosage as appropriate. ( 5.5)
- Pregabalin Capsules may cause dizziness and somnolence and impair patients’ ability to drive or operate machinery. ( 5.6)
- Pregabalin Capsules may cause peripheral edema. Exercise caution when co-administering Pregabalin Capsules and thiazolidinedione antidiabetic agents. ( 5.7)
14.2 Postherpetic Neuralgia
The efficacy of Pregabalin Capsules for the management of postherpetic neuralgia was established in three double-blind, placebo-controlled, multicenter studies. These studies enrolled patients with neuralgia persisting for at least 3 months following healing of herpes zoster rash and a minimum baseline score of greater than or equal to 4 on an 11-point numerical pain rating scale ranging from 0 (no pain) to 10 (worst possible pain). Seventy-three percent of patients completed the studies. The baseline mean pain scores across the 3 studies ranged from 6 to 7. Patients were permitted up to 4 grams of acetaminophen per day as needed for pain, in addition to pregabalin. Patients recorded their pain daily in a diary.
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
- For adult indications, begin dosing at 150 mg/day. For partial-onset seizure dosing in pediatric patients 1 month of age and older, refer to section 2.4. ( 2.2, 2.3, 2.4, 2.5, 2.6)
- Dosing recommendations:
| INDICATION | Dosing Regimen | Maximum Dose |
|---|---|---|
| DPN Pain ( 2.2) | 3 divided doses per day | 300 mg/day within 1 week |
| PHN ( 2.3) | 2 or 3 divided doses per day | 300 mg/day within 1 week. Maximum dose of 600 mg/day. |
| Adjunctive Therapy for Partial-Onset Seizures in Pediatric and Adult Patients Weighing 30 kg or More ( 2.4) | 2 or 3 divided doses per day | Maximum dose of 600 mg/day. |
| Adjunctive Therapy for Partial-Onset Seizures in Pediatric Patients Weighing Less than 30 kg ( 2.4) |
1 month to less than 4 years: 3 divided doses per day 4 years and older: 2 or 3 divided doses per day |
14 mg/kg/day. |
| Fibromyalgia ( 2.5) | 2 divided doses per day | 300 mg/day within 1 week. Maximum dose of 450 mg/day. |
| Neuropathic Pain Associated with Spinal Cord Injury ( 2.6) | 2 divided doses per day | 300 mg/day within 1 week. Maximum dose of 600 mg/day. |
- Dose should be adjusted in adult patients with reduced renal function. ( 2.7)
5.5 respiratory Depression (5.5 Respiratory Depression)
There is evidence from case reports, human studies, and animal studies associating Pregabalin Capsules with serious, life-threatening, or fatal respiratory depression when co-administered with central nervous system (CNS) depressants, including opioids, or in the setting of underlying respiratory impairment. When the decision is made to co-prescribe Pregabalin Capsules with another CNS depressant, particularly an opioid, or to prescribe Pregabalin Capsules to patients with underlying respiratory impairment, monitor patients for symptoms of respiratory depression and sedation, and consider initiating Pregabalin Capsules at a low dose. The management of respiratory depression may include close observation, supportive measures, and reduction or withdrawal of CNS depressants (including Pregabalin Capsules).
There is more limited evidence from case reports, animal studies, and human studies associating Pregabalin Capsules with serious respiratory depression, without co-administered CNS depressants or without underlying respiratory impairment.
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
Capsules: 25 mg, 50 mg, 75 mg, 100 mg, 150 mg, 200 mg, 225 mg, and 300 mg
[see Description (11) a nd How Supplied/Storage and Handling (16) ]
5.6 Dizziness and Somnolence
Pregabalin Capsules may cause dizziness and somnolence. Inform patients that Pregabalin Capsules-related dizziness and somnolence may impair their ability to perform tasks such as driving or operating machinery [see Patient Counseling Information (17)] .
In the Pregabalin Capsules controlled trials in adult patients, dizziness was experienced by 30% of Pregabalin Capsules-treated patients compared to 8% of placebo-treated patients; somnolence was experienced by 23% of Pregabalin Capsules-treated patients compared to 8% of placebo-treated patients. Dizziness and somnolence generally began shortly after the initiation of Pregabalin Capsules therapy and occurred more frequently at higher doses. Dizziness and somnolence were the adverse reactions most frequently leading to withdrawal (4% each) from controlled studies. In Pregabalin Capsules-treated patients reporting these adverse reactions in short-term, controlled studies, dizziness persisted until the last dose in 30% and somnolence persisted until the last dose in 42% of patients [see Drug Interactions (7)].
In the pregabalin controlled trials in pediatric patients 4 to less than 17 years of age and 1 month to less than 4 years of age for the treatment of partial-onset seizures, somnolence was reported in 21% and 15% of pregabalin-treated patients compared to 14% and 9% of placebo-treated patients, respectively, and occurred more frequently at higher doses. For patients 1 month to less than 4 years of age, somnolence includes related terms lethargy, sluggishness, and hypersomnia.
6.2 Postmarketing Experience
The following adverse reactions have been identified during postapproval use of Pregabalin Capsules. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Nervous System Disorders – Headache
Gastrointestinal Disorders – Nausea, Diarrhea
Reproductive System and Breast Disorders – Gynecomastia, Breast Enlargement
Skin and subcutaneous tissue disorders – Bullous pemphigoid
There are postmarketing reports of life-threatening or fatal respiratory depression in patients taking Pregabalin Capsules with opioids or other CNS depressants, or in the setting of underlying respiratory impairment.
In addition, there are postmarketing reports of events related to reduced lower gastrointestinal tract function (e.g., intestinal obstruction, paralytic ileus, constipation) when Pregabalin Capsules were co-administered with medications that have the potential to produce constipation, such as opioid analgesics.
There are postmarketing reports of withdrawal symptoms after discontinuation of pregabalin. Reported adverse reactions include, but are not limited to, seizures, depression, suicidal ideation and behavior, agitation, confusion, disorientation, psychotic symptoms, anxiety, insomnia, nausea, pain, sweating, tremor, headache, dizziness, malaise, and diarrhea.
5.10 Ophthalmological Effects
In controlled studies in adult patients, a higher proportion of patients treated with Pregabalin Capsules reported blurred vision (7%) than did patients treated with placebo (2%), which resolved in a majority of cases with continued dosing. Less than 1% of patients discontinued Pregabalin Capsules treatment due to vision-related events (primarily blurred vision).
Prospectively planned ophthalmologic testing, including visual acuity testing, formal visual field testing and dilated funduscopic examination, was performed in over 3600 patients. In these patients, visual acuity was reduced in 7% of patients treated with Pregabalin Capsules, and 5% of placebo-treated patients. Visual field changes were detected in 13% of Pregabalin Capsules-treated, and 12% of placebo-treated patients. Funduscopic changes were observed in 2% of Pregabalin Capsules-treated and 2% of placebo-treated patients.
Although the clinical significance of the ophthalmologic findings is unknown, inform patients to notify their physician if changes in vision occur. If visual disturbance persists, consider further assessment. Consider more frequent assessment for patients who are already routinely monitored for ocular conditions [ see Patient Counseling Information (17 )] .
5.12 Decreased Platelet Count
Pregabalin Capsules treatment was associated with a decrease in platelet count. Pregabalin Capsules-treated subjects experienced a mean maximal decrease in platelet count of 20 × 10 3/µL, compared to 11 × 10 3/µL in placebo patients. In the overall database of controlled trials in adult patients, 2% of placebo patients and 3% of Pregabalin Capsules patients experienced a potentially clinically significant decrease in platelets, defined as 20% below baseline value and less than 150 × 10 3/µL. A single Pregabalin Capsules-treated subject developed severe thrombocytopenia with a platelet count less than 20 × 10 3/µL. In randomized controlled trials, Pregabalin Capsules were not associated with an increase in bleeding-related adverse reactions.
5.13 Pr Interval Prolongation (5.13 PR Interval Prolongation)
Pregabalin Capsules treatment was associated with PR interval prolongation. In analyses of clinical trial ECG data in adult patients, the mean PR interval increase was 3–6 msec at Pregabalin Capsules doses greater than or equal to 300 mg/day. This mean change difference was not associated with an increased risk of PR increase greater than or equal to 25% from baseline, an increased percentage of subjects with on-treatment PR greater than 200 msec, or an increased risk of adverse reactions of second or third degree AV block.
Subgroup analyses did not identify an increased risk of PR prolongation in patients with baseline PR prolongation or in patients taking other PR prolonging medications. However, these analyses cannot be considered definitive because of the limited number of patients in these categories.
8 Use in Specific Populations (8 USE IN SPECIFIC POPULATIONS)
- Lactation: Breastfeeding is not recommended. ( 8.2)
Comparison of Gender and Race
The overall adverse event profile of pregabalin was similar between women and men. There are insufficient data to support a statement regarding the distribution of adverse experience reports by race.
Most Common Adverse Reactions
Table 4 lists all adverse reactions, regardless of causality, occurring in greater than or equal to 1% of patients with neuropathic pain associated with diabetic neuropathy in the combined Pregabalin Capsules group for which the incidence was greater in this combined Pregabalin Capsules group than in the placebo group. A majority of pregabalin-treated patients in clinical studies had adverse reactions with a maximum intensity of “mild” or “moderate”.
|
Body system
Preferred term |
75 mg/day
[N=77] % |
150 mg/day
[N=212] % |
300 mg/day
[N=321] % |
600 mg/day
[N=369] % |
All PGB
PGB: pregabalin
[N=979] % |
Placebo
[N=459] % |
|---|---|---|---|---|---|---|
|
Body as a whole |
||||||
|
Asthenia |
4 |
2 |
4 |
7 |
5 |
2 |
|
Accidental injury |
5 |
2 |
2 |
6 |
4 |
3 |
|
Back pain |
0 |
2 |
1 |
2 |
2 |
0 |
|
Chest pain |
4 |
1 |
1 |
2 |
2 |
1 |
|
Face edema |
0 |
1 |
1 |
2 |
1 |
0 |
|
Digestive system |
||||||
|
Dry mouth |
3 |
2 |
5 |
7 |
5 |
1 |
|
Constipation |
0 |
2 |
4 |
6 |
4 |
2 |
|
Flatulence |
3 |
0 |
2 |
3 |
2 |
1 |
|
Metabolic and nutritional disorders |
||||||
|
Peripheral edema |
4 |
6 |
9 |
12 |
9 |
2 |
|
Weight gain |
0 |
4 |
4 |
6 |
4 |
0 |
|
Edema |
0 |
2 |
4 |
2 |
2 |
0 |
|
Hypoglycemia |
1 |
3 |
2 |
1 |
2 |
1 |
|
Nervous system |
||||||
|
Dizziness |
8 |
9 |
23 |
29 |
21 |
5 |
|
Somnolence |
4 |
6 |
13 |
16 |
12 |
3 |
|
Neuropathy |
9 |
2 |
2 |
5 |
4 |
3 |
|
Ataxia |
6 |
1 |
2 |
4 |
3 |
1 |
|
Vertigo |
1 |
2 |
2 |
4 |
3 |
1 |
|
Confusion |
0 |
1 |
2 |
3 |
2 |
1 |
|
Euphoria |
0 |
0 |
3 |
2 |
2 |
0 |
|
Incoordination |
1 |
0 |
2 |
2 |
2 |
0 |
|
Thinking abnormal Thinking abnormal primarily consists of events related to difficulty with concentration/attention but also includes events related to cognition and language problems and slowed thinking.
|
1 |
0 |
1 |
3 |
2 |
0 |
|
Tremor |
1 |
1 |
1 |
2 |
1 |
0 |
|
Abnormal gait |
1 |
0 |
1 |
3 |
1 |
0 |
|
Amnesia |
3 |
1 |
0 |
2 |
1 |
0 |
|
Nervousness |
0 |
1 |
1 |
1 |
1 |
0 |
|
Respiratory system |
||||||
|
Dyspnea |
3 |
0 |
2 |
2 |
2 |
1 |
|
Special senses |
||||||
|
Blurry vision Investigator term; summary level term is amblyopia
|
3 |
1 |
3 |
6 |
4 |
2 |
|
Abnormal vision |
1 |
0 |
1 |
1 |
1 |
0 |
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
In all controlled and uncontrolled trials across various patient populations during the premarketing development of Pregabalin Capsules, more than 10,000 patients have received Pregabalin Capsules. Approximately 5000 patients were treated for 6 months or more, over 3100 patients were treated for 1 year or longer, and over 1400 patients were treated for at least 2 years.
14.4 Management of Fibromyalgia
The efficacy of Pregabalin Capsules for management of fibromyalgia was established in one 14-week, double-blind, placebo-controlled, multicenter study (F1) and one six-month, randomized withdrawal study (F2). Studies F1 and F2 enrolled patients with a diagnosis of fibromyalgia using the American College of Rheumatology (ACR) criteria (history of widespread pain for 3 months, and pain present at 11 or more of the 18 specific tender point sites). The studies showed a reduction in pain by visual analog scale. In addition, improvement was demonstrated based on a patient global assessment (PGIC), and on the Fibromyalgia Impact Questionnaire (FIQ).
5.11 Creatine Kinase Elevations
Pregabalin Capsules treatment was associated with creatine kinase elevations. Mean changes in creatine kinase from baseline to the maximum value were 60 U/L for Pregabalin Capsules-treated patients and 28 U/L for the placebo patients. In all controlled trials in adult patients across multiple patient populations, 1.5% of patients on Pregabalin Capsules and 0.7% of placebo patients had a value of creatine kinase at least three times the upper limit of normal. Three Pregabalin Capsules-treated subjects had events reported as rhabdomyolysis in premarketing clinical trials. The relationship between these myopathy events and Pregabalin Capsules is not completely understood because the cases had documented factors that may have caused or contributed to these events. Instruct patients to promptly report unexplained muscle pain, tenderness, or weakness, particularly if these muscle symptoms are accompanied by malaise or fever. Discontinue treatment with Pregabalin Capsules if myopathy is diagnosed or suspected or if markedly elevated creatine kinase levels occur.
17 Patient Counseling Information (17 PATIENT COUNSELING INFORMATION)
Advise the patient to read the FDA-approved patient labeling (Medication Guide).
5.3 Suicidal Behavior and Ideation
Antiepileptic drugs (AEDs), including pregabalin, the active ingredient in Pregabalin Capsules, increase the risk of suicidal thoughts or behavior in patients taking these drugs for any indication. Suicidal behavior and ideation have also been reported in patients after discontinuation of pregabalin [see Warnings and Precautions (5.4)] . Monitor patients treated with any AED for any indication for the emergence or worsening of depression, suicidal thoughts or behavior, and/or any unusual changes in mood or behavior.
Pooled analyses of 199 placebo-controlled clinical trials (mono- and adjunctive therapy) of 11 different AEDs showed that patients randomized to one of the AEDs had approximately twice the risk (adjusted Relative Risk 1.8, 95% CI:1.2, 2.7) of suicidal thinking or behavior compared to patients randomized to placebo. In these trials, which had a median treatment duration of 12 weeks, the estimated incidence rate of suicidal behavior or ideation among 27,863 AED-treated patients was 0.43%, compared to 0.24% among 16,029 placebo-treated patients, representing an increase of approximately one case of suicidal thinking or behavior for every 530 patients treated. There were four suicides in drug-treated patients in the trials and none in placebo-treated patients, but the number is too small to allow any conclusion about drug effect on suicide.
The increased risk of suicidal thoughts or behavior with AEDs was observed as early as one week after starting drug treatment with AEDs and persisted for the duration of treatment assessed. Because most trials included in the analysis did not extend beyond 24 weeks, the risk of suicidal thoughts or behavior beyond 24 weeks could not be assessed.
The risk of suicidal thoughts or behavior was generally consistent among drugs in the data analyzed. The finding of increased risk with AEDs of varying mechanisms of action and across a range of indications suggests that the risk applies to all AEDs used for any indication. The risk did not vary substantially by age (5–100 years) in the clinical trials analyzed.
Table 3 shows absolute and relative risk by indication for all evaluated AEDs.
|
Indication |
Placebo
|
Drug Patients
|
Relative Risk:
|
Risk Difference: Additional Drug Patients with
|
|
Epilepsy |
1.0 |
3.4 |
3.5 |
2.4 |
|
Psychiatric |
5.7 |
8.5 |
1.5 |
2.9 |
|
Other |
1.0 |
1.8 |
1.9 |
0.9 |
|
Total |
2.4 |
4.3 |
1.8 |
1.9 |
The relative risk for suicidal thoughts or behavior was higher in clinical trials for epilepsy than in clinical trials for psychiatric or other conditions, but the absolute risk differences were similar for the epilepsy and psychiatric indications.
Anyone considering prescribing Pregabalin Capsules or any other AED must balance the risk of suicidal thoughts or behavior with the risk of untreated illness. Epilepsy and many other illnesses for which AEDs are prescribed are themselves associated with morbidity and mortality and an increased risk of suicidal thoughts and behavior. Should suicidal thoughts and behavior emerge during treatment, the prescriber needs to consider whether the emergence of these symptoms in any given patient may be related to the illness being treated.
2.3 Postherpetic Neuralgia in Adults
The recommended dose of Pregabalin Capsules is 75 to 150 mg two times a day, or 50 to 100 mg three times a day (150 to 300 mg/day) in patients with creatinine clearance of at least 60 mL/min. Begin dosing at 75 mg two times a day, or 50 mg three times a day (150 mg/day). The dose may be increased to 300 mg/day within 1 week based on efficacy and tolerability.
Patients who do not experience sufficient pain relief following 2 to 4 weeks of treatment with 300 mg/day, and who are able to tolerate Pregabalin Capsules, may be treated with up to 300 mg two times a day, or 200 mg three times a day (600 mg/day). In view of the dose-dependent adverse reactions and the higher rate of treatment discontinuation due to adverse reactions, reserve dosing above 300 mg/day for those patients who have on-going pain and are tolerating 300 mg daily [see Adverse Reactions (6.1)] .
2.1 Important Administration Instructions
Pregabalin Capsules are given orally with or without food.
When discontinuing Pregabalin Capsules, taper gradually over a minimum of 1 week [see Warnings and Precautions (5.4)] .
Because Pregabalin Capsules are eliminated primarily by renal excretion, adjust the dose in adult patients with reduced renal function [see Dosage and Administration (2.7)].
2.5 Management of Fibromyalgia in Adults
The recommended dose of Pregabalin Capsules for fibromyalgia is 300 to 450 mg/day. Begin dosing at 75 mg two times a day (150 mg/day). The dose may be increased to 150 mg two times a day (300 mg/day) within 1 week based on efficacy and tolerability. Patients who do not experience sufficient benefit with 300 mg/day may be further increased to 225 mg two times a day (450 mg/day). Although Pregabalin Capsules were also studied at 600 mg/day, there is no evidence that this dose confers additional benefit and this dose was less well tolerated. In view of the dose-dependent adverse reactions, treatment with doses above 450 mg/day is not recommended [see Adverse Reactions (6.1)] .
Adverse Reactions Leading to Discontinuation
In clinical trials in adults with neuropathic pain associated with diabetic peripheral neuropathy, 9% of patients treated with Pregabalin Capsules and 4% of patients treated with placebo discontinued prematurely due to adverse reactions. In the Pregabalin Capsules treatment group, the most common reasons for discontinuation due to adverse reactions were dizziness (3%) and somnolence (2%). In comparison, less than 1% of placebo patients withdrew due to dizziness and somnolence. Other reasons for discontinuation from the trials, occurring with greater frequency in the Pregabalin Capsules group than in the placebo group, were asthenia, confusion, and peripheral edema. Each of these events led to withdrawal in approximately 1% of patients.
2.7 Dosing for Adult Patients With Renal Impairment (2.7 Dosing for Adult Patients with Renal Impairment)
In view of dose-dependent adverse reactions and since pregabalin is eliminated primarily by renal excretion, adjust the dose in adult patients with reduced renal function. The use of Pregabalin Capsules in pediatric patients with compromised renal function has not been studied.
Base the dose adjustment in patients with renal impairment on creatinine clearance (CLcr), as indicated in Table 2. To use this dosing table, an estimate of the patient's CLcr in mL/min is needed. CLcr in mL/min may be estimated from serum creatinine (mg/dL) determination using the Cockcroft and Gault equation:
Next, refer to the Dosage and Administration section to determine the recommended total daily dose based on indication, for a patient with normal renal function (CLcr greater than or equal to 60 mL/min). Then refer to Table 2 to determine the corresponding renal adjusted dose.
(For example: A patient initiating Pregabalin Capsules therapy for postherpetic neuralgia with normal renal function (CLcr greater than or equal to 60 mL/min), receives a total daily dose of 150 mg/day pregabalin. Therefore, a renal impaired patient with a CLcr of 50 mL/min would receive a total daily dose of 75 mg/day pregabalin administered in two or three divided doses.)
For patients undergoing hemodialysis, adjust the pregabalin daily dose based on renal function. In addition to the daily dose adjustment, administer a supplemental dose immediately following every 4-hour hemodialysis treatment (see Table 2).
| TID = Three divided doses; BID = Two divided doses; QD = Single daily dose. | |||||
|
Creatinine Clearance (CLcr)
|
Total Pregabalin Daily Dose (mg/day) Total daily dose (mg/day) should be divided as indicated by dose regimen to provide mg/dose.
|
Dose Regimen |
|||
|
Greater than or equal to 60 |
150 |
300 |
450 |
600 |
BID or TID |
|
30-60 |
75 |
150 |
225 |
300 |
BID or TID |
|
15-30 |
25-50 |
75 |
100-150 |
150 |
QD or BID |
|
Less than 15 |
25 |
25-50 |
50-75 |
75 |
QD |
|
Supplementary dosage following hemodialysis (mg) Supplementary dose is a single additional dose.
|
|||||
|
Patients on the 25 mg QD regimen: take one supplemental dose of 25 mg or 50 mg Patients on the 25-50 mg QD regimen: take one supplemental dose of 50 mg or 75 mg Patients on the 50-75 mg QD regimen: take one supplemental dose of 75 mg or 100 mg Patients on the 75 mg QD regimen: take one supplemental dose of 100 mg or 150 mg |
2.6 Neuropathic Pain Associated With Spinal Cord Injury in Adults (2.6 Neuropathic Pain Associated with Spinal Cord Injury in Adults)
The recommended dose range of Pregabalin Capsules for the treatment of neuropathic pain associated with spinal cord injury is 150 to 600 mg/day. The recommended starting dose is 75 mg two times a day (150 mg/day). The dose may be increased to 150 mg two times a day (300 mg/day) within 1 week based on efficacy and tolerability. Patients who do not experience sufficient pain relief after 2 to 3 weeks of treatment with 150 mg two times a day and who tolerate Pregabalin Capsules may be treated with up to 300 mg two times a day [see Clinical Studies (14.5)] .
14.1 Neuropathic Pain Associated With Diabetic Peripheral Neuropathy (14.1 Neuropathic Pain Associated with Diabetic Peripheral Neuropathy)
The efficacy of the maximum recommended dose of Pregabalin Capsules for the management of neuropathic pain associated with diabetic peripheral neuropathy was established in three double-blind, placebo-controlled, multicenter studies with three times a day dosing, two of which studied the maximum recommended dose. Patients were enrolled with either Type 1 or Type 2 diabetes mellitus and a diagnosis of painful distal symmetrical sensorimotor polyneuropathy for 1 to 5 years. A total of 89% of patients completed Studies DPN 1 and DPN 2. The patients had a minimum mean baseline pain score of greater than or equal to 4 on an 11-point numerical pain rating scale ranging from 0 (no pain) to 10 (worst possible pain). The baseline mean pain scores across the two studies ranged from 6.1 to 6.7. Patients were permitted up to 4 grams of acetaminophen per day as needed for pain, in addition to pregabalin. Patients recorded their pain daily in a diary.
14.5 Management of Neuropathic Pain Associated With Spinal Cord Injury (14.5 Management of Neuropathic Pain Associated with Spinal Cord Injury)
The efficacy of Pregabalin Capsules for the management of neuropathic pain associated with spinal cord injury was established in two double-blind, placebo-controlled, multicenter studies. Patients were enrolled with neuropathic pain associated with spinal cord injury that persisted continuously for at least three months or with relapses and remissions for at least six months. A total of 63% of patients completed study 1 and 84% completed study 2. The patients had a minimum mean baseline pain score of greater than or equal to 4 on an 11-point numerical pain rating scale ranging from 0 (no pain) to 10 (worst possible pain). The baseline mean pain scores across the two studies ranged from 6.5 to 6.7.
Patients were allowed to take opioids, non-opioid analgesics, antiepileptic drugs, muscle relaxants, and antidepressant drugs if the dose was stable for 30 days prior to screening. Patients were allowed to take acetaminophen and nonsteroidal anti-inflammatory drugs during the studies.
Study SCI 1: This 12-week, randomized, double-blind, parallel-group, multicenter, flexible dose (150-600 mg/day) study compared pregabalin with placebo. The 12-week study consisted of a 3-week dose adjustment phase and a 9-week dose maintenance phase. Treatment with Pregabalin Capsules 150-600 mg/day statistically significantly improved the endpoint weekly mean pain score, and increased the proportion of patients with at least a 30% and 50% reduction in pain score from baseline. The fraction of patients achieving various levels of improvement in pain intensity from baseline to Week 12 is presented in Figure 11. Some patients experienced a decrease in pain as early as week 1, which persisted throughout the study.
Figure 11: Patients Achieving Various Levels of Improvement in Pain Intensity – Study SCI 1
Study SCI 2: This 16-week, randomized, double-blind, placebo-controlled, parallel-group, multicenter, flexible dose (150-600 mg/day, in increments of 150 mg) study compared the efficacy, safety and tolerability of pregabalin with placebo. The 16-week study consisted of a 4-week dose adjustment phase and a 12-week dose maintenance phase. Treatment with Pregabalin Capsules statistically significantly improved the endpoint weekly mean pain score, and increased the proportion of patients with at least a 30% and 50% reduction in pain score from baseline. The fraction of patients achieving various levels of improvement in pain intensity from baseline to Week 16 is presented in Figure 12. Some patients experienced a decrease in pain as early as week 1, which persisted throughout the study.
Figure 12: Patients Achieving Various Levels of Improvement in Pain Intensity – Study SCI 2
Most Common Adverse Reactions in All Controlled Clinical Studies in Adults
In premarketing controlled trials of all adult patient populations combined (including DPN, PHN, and adult patients with partial-onset seizures), dizziness, somnolence, dry mouth, edema, blurred vision, weight gain, and “thinking abnormal” (primarily difficulty with concentration/attention) were more commonly reported by subjects treated with Pregabalin Capsules than by subjects treated with placebo (greater than or equal to 5% and twice the rate of that seen in placebo).
5.4 Increased Risk of Adverse Reactions With Abrupt Or Rapid Discontinuation (5.4 Increased Risk of Adverse Reactions with Abrupt or Rapid Discontinuation)
As with all antiepileptic drugs (AEDs), withdraw Pregabalin Capsules gradually to minimize the potential of increased seizure frequency in patients with seizure disorders.
Following abrupt or rapid discontinuation of Pregabalin Capsules, some patients reported symptoms including insomnia, nausea, headache, anxiety, hyperhidrosis, and diarrhea [see Adverse Reactions (6.2), Drug Abuse and Dependence (9.3)] . Suicidal behavior and ideation have also been reported in patients after discontinuation of pregabalin [see Warnings and Precautions (5.3)] .
If Pregabalin Capsules are discontinued, taper the drug gradually over a minimum of 1 week rather than discontinue the drug abruptly.
2.2 Neuropathic Pain Associated With Diabetic Peripheral Neuropathy in Adults (2.2 Neuropathic Pain Associated with Diabetic Peripheral Neuropathy in Adults)
The maximum recommended dose of Pregabalin Capsules is 100 mg three times a day (300 mg/day) in patients with creatinine clearance of at least 60 mL/min. Begin dosing at 50 mg three times a day (150 mg/day). The dose may be increased to 300 mg/day within 1 week based on efficacy and tolerability.
Although Pregabalin Capsules were also studied at 600 mg/day, there is no evidence that this dose confers additional significant benefit and this dose was less well tolerated. In view of the dose-dependent adverse reactions, treatment with doses above 300 mg/day is not recommended [see Adverse Reactions (6.1)] .
Other Adverse Reactions Observed During the Clinical Studies of Pregabalin Capsules
Following is a list of treatment-emergent adverse reactions reported by patients treated with Pregabalin Capsules during all clinical trials. The listing does not include those events already listed in the previous tables or elsewhere in labeling, those events for which a drug cause was remote, those events which were so general as to be uninformative, and those events reported only once which did not have a substantial probability of being acutely life-threatening.
Events are categorized by body system and listed in order of decreasing frequency according to the following definitions: frequentadverse reactions are those occurring on one or more occasions in at least 1/100 patients; infrequentadverse reactions are those occurring in 1/100 to 1/1000 patients; rarereactions are those occurring in fewer than 1/1000 patients. Events of major clinical importance are described in the Warnings and Precautionssection (5).
Body as a Whole – Frequent: Abdominal pain, Allergic reaction, Fever, Infrequent: Abscess, Cellulitis, Chills, Malaise, Neck rigidity, Overdose, Pelvic pain, Photosensitivity reaction, Rare: Anaphylactoid reaction, Ascites, Granuloma, Hangover effect, Intentional Injury, Retroperitoneal Fibrosis, Shock
Cardiovascular System – Infrequent: Deep thrombophlebitis, Heart failure, Hypotension, Postural hypotension, Retinal vascular disorder, Syncope; Rare: ST Depressed, Ventricular Fibrillation
Digestive System – Frequent: Gastroenteritis, Increased appetite; Infrequent: Cholecystitis, Cholelithiasis, Colitis, Dysphagia, Esophagitis, Gastritis, Gastrointestinal hemorrhage, Melena, Mouth ulceration, Pancreatitis, Rectal hemorrhage, Tongue edema; Rare: Aphthous stomatitis, Esophageal Ulcer, Periodontal abscess
Hemic and Lymphatic System – Frequent: Ecchymosis; Infrequent: Anemia, Eosinophilia, Hypochromic anemia, Leukocytosis, Leukopenia, Lymphadenopathy, Thrombocytopenia; Rare: Myelofibrosis, Polycythemia, Prothrombin decreased, Purpura, Thrombocythemia, Alanine aminotransferase increased, Aspartate aminotransferase increased
Metabolic and Nutritional Disorders – Rare: Glucose Tolerance Decreased, Urate Crystalluria
Musculoskeletal System – Frequent: Arthralgia, Leg cramps, Myalgia, Myasthenia; Infrequent: Arthrosis; Rare: Chondrodystrophy, Generalized Spasm
Nervous System – Frequent: Anxiety, Depersonalization, Hypertonia, Hypoesthesia, Libido decreased, Nystagmus, Paresthesia, Sedation, Stupor, Twitching; Infrequent: Abnormal dreams, Agitation, Apathy, Aphasia, Circumoral paresthesia, Dysarthria, Hallucinations, Hostility, Hyperalgesia, Hyperesthesia, Hyperkinesia, Hypokinesia, Hypotonia, Libido increased, Myoclonus, Neuralgia; Rare: Addiction, Cerebellar syndrome, Cogwheel rigidity, Coma, Delirium, Delusions, Dysautonomia, Dyskinesia, Dystonia, Encephalopathy, Extrapyramidal syndrome, Guillain-Barré syndrome, Hypalgesia, Intracranial hypertension, Manic reaction, Paranoid reaction, Peripheral neuritis, Personality disorder, Psychotic depression, Schizophrenic reaction, Sleep disorder, Torticollis, Trismus
Respiratory System – Rare: Apnea, Atelectasis, Bronchiolitis, Hiccup, Laryngismus, Lung edema, Lung fibrosis, Yawn
Skin and Appendages – Frequent: Pruritus, Infrequent: Alopecia, Dry skin, Eczema, Hirsutism, Skin ulcer, Urticaria, Vesiculobullous rash; Rare: Angioedema, Exfoliative dermatitis, Lichenoid dermatitis, Melanosis, Nail Disorder, Petechial rash, Purpuric rash, Pustular rash, Skin atrophy, Skin necrosis, Skin nodule, Stevens-Johnson syndrome, Subcutaneous nodule
Special senses – Frequent: Conjunctivitis, Diplopia, Otitis media, Tinnitus; Infrequent: Abnormality of accommodation, Blepharitis, Dry eyes, Eye hemorrhage, Hyperacusis, Photophobia, Retinal edema, Taste loss, Taste perversion; Rare: Anisocoria, Blindness, Corneal ulcer, Exophthalmos, Extraocular palsy, Iritis, Keratitis, Keratoconjunctivitis, Miosis, Mydriasis, Night blindness, Ophthalmoplegia, Optic atrophy, Papilledema, Parosmia, Ptosis, Uveitis
Urogenital System – Frequent: Anorgasmia, Impotence, Urinary frequency, Urinary incontinence; Infrequent: Abnormal ejaculation, Albuminuria, Amenorrhea, Dysmenorrhea, Dysuria, Hematuria, Kidney calculus, Leukorrhea, Menorrhagia, Metrorrhagia, Nephritis, Oliguria, Urinary retention, Urine abnormality; Rare: Acute kidney failure, Balanitis, Bladder Neoplasm, Cervicitis, Dyspareunia, Epididymitis, Female lactation, Glomerulitis, Ovarian disorder, Pyelonephritis
2.4 adjunctive Therapy for Partial Onset Seizures in Patients 1 Month of Age and Older (2.4 Adjunctive Therapy for Partial-Onset Seizures in Patients 1 Month of Age and Older)
The recommended dosages for adults and pediatric patients 1 month of age and older are included in Table 1. Administer the total daily dosage orally in two or three divided doses as indicated in Table 1. In pediatric patients, the recommended dosing regimen is dependent upon body weight. Based on clinical response and tolerability, dosage may be increased, approximately weekly.
|
Age and Body Weight |
Recommended Initial Dosage |
Recommended Maximum Dosage |
Frequency of Administration |
|
Adults (17 years and older) |
150 mg/day |
600 mg/day |
2 or 3 divided doses |
|
Pediatric patients weighing 30 kg or more |
2.5 mg/kg/day |
10 mg/kg/day (not to exceed 600 mg/day) |
2 or 3 divided doses |
|
Pediatric patients weighing less than 30 kg |
3.5 mg/kg/day |
14 mg/kg/day |
1 month to less than 4 years of age:
4 years of age and older:
|
Both the efficacy and adverse event profiles of Pregabalin Capsules have been shown to be dose‑related.
The effect of dose escalation rate on the tolerability of Pregabalin Capsules has not been formally studied.
The efficacy of adjunctive Pregabalin Capsules in patients taking gabapentin has not been evaluated in controlled trials. Consequently, dosing recommendations for the use of Pregabalin Capsules with gabapentin cannot be offered.
Adverse Reactions Most Commonly Leading to Discontinuation in All Premarketing Controlled Clinical Studies
In premarketing controlled trials of all adult populations combined, 14% of patients treated with Pregabalin Capsules and 7% of patients treated with placebo discontinued prematurely due to adverse reactions. In the Pregabalin Capsules treatment group, the adverse reactions most frequently leading to discontinuation were dizziness (4%) and somnolence (4%). In the placebo group, 1% of patients withdrew due to dizziness and less than 1% withdrew due to somnolence. Other adverse reactions that led to discontinuation from controlled trials more frequently in the Pregabalin Capsules group compared to the placebo group were ataxia, confusion, asthenia, thinking abnormal, blurred vision, incoordination, and peripheral edema (1% each).
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:51:49.198931 · Updated: 2026-03-14T22:41:48.077270