These Highlights Do Not Include All The Information Needed To Use Valproic Acid Safely And Effectively. See Full Prescribing Information For Valproic Acid Oral Solution Usp.
65c1589e-c591-4b79-b75e-884c0d609ae8
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
WARNING: LIFE THREATENING ADVERSE REACTIONS See full prescribing information for complete boxed warning. Hepatotoxicity, including fatalities, usually during the first 6 months of treatment. Children under the age of two years and patients with mitochondrial disorders are at higher risk. Monitor patients closely, and perform serum liver testing prior to therapy and at frequent intervals thereafter ( 5.1 ) Fetal Risk, particularly neural tube defects, other major malformations, and decreased IQ ( 5.2 , 5.3 , 5.4 ) Pancreatitis, including fatal hemorrhagic cases ( 5.5 )
Indications and Usage
Valproic acid is indicated for: Monotherapy and adjunctive therapy of complex partial seizures; sole and adjunctive therapy of simple and complex absence seizures; adjunctive therapy in patients with multiple seizure types that include absence seizures ( 1 )
Dosage and Administration
Valproic acid is intended for oral administration. ( 2.1 ) Simple and Complex Absence Seizures: Start at 10 to 15 mg/kg/day, increasing at 1 week intervals by 5 to 10 mg/kg/week until seizure control or limiting side effects ( 2.1 ) Safety of doses above 60 mg/kg/day is not established ( 2.1 , 2.2 )
Warnings and Precautions
Hepatotoxicity; evaluate high risk populations and monitor serum liver tests ( 5.1 ) Birth defects, decreased IQ, and neurodevelopmental disorders following in utero exposure; should not be used to treat women with epilepsy or bipolar disorder who are pregnant or who plan to become pregnant or to treat a woman of childbearing potential unless other medications have failed to provide adequate symptom control or are otherwise unacceptable ( 5.2 , 5.3 , 5.4 ) Pancreatitis; Valproic acid should ordinarily be discontinued ( 5.5 ) Suicidal behavior or ideation; Antiepileptic drugs, including valproic acid, increase the risk of suicidal thoughts or behavior ( 5.7 ) Bleeding and other hematopoietic disorders; monitor platelet counts and coagulation tests ( 5.8 ) Hyperammonemia and hyperammonemic encephalopathy; measure ammonia level if unexplained lethargy and vomiting or changes in mental status, and also with concomitant topiramate use; consider discontinuation of valproate therapy ( 5.6 , 5.9 , 5.10 ) Hypothermia; Hypothermia has been reported during valproate therapy with or without associated hyperammonemia. This adverse reaction can also occur in patients using concomitant topiramate ( 5.11 ) Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS)/Multiorgan hypersensitivity reaction; discontinue valproic acid ( 5.12 ) Somnolence in the elderly can occur. Valproic acid dosage should be increased slowly and with regular monitoring for fluid and nutritional intake ( 5.14 )
Contraindications
Valproic acid should not be administered to patients with hepatic disease or significant hepatic dysfunction [see Warnings and Precautions (5.1) ] . Valproic acid is contraindicated in patients known to have mitochondrial disorders caused by mutations in mitochondrial DNA polymerase γ (POLG; e.g., Alpers-Huttenlocher Syndrome) and children under two years of age who are suspected of having a POLG-related disorder [see Warnings and Precautions (5.1) ] . Valproic acid is contraindicated in patients with known hypersensitivity to the drug [see Warnings and Precautions (5.12) ] . Valproic acid is contraindicated in patients with known urea cycle disorders [see Warnings and Precautions (5.6) ] . For use in prophylaxis of migraine headaches: Valproic acid is contraindicated in women who are pregnant and in women of childbearing potential who are not using effective contraception [see Warnings and Precautions (5.2 , 5.3 , 5.4) and Use in Specific Populations (8.1) ] .
Adverse Reactions
The following serious adverse reactions are described below and elsewhere in the labeling: Hepatic failure [see Warnings and Precautions (5.1) ] Birth defects [see Warnings and Precautions (5.2) ] Decreased IQ following in utero exposure [see Warnings and Precautions (5.3) ] Pancreatitis [see Warnings and Precautions (5.5) ] Hyperammonemic encephalopathy [see Warnings and Precautions (5.6 , 5.9 , 5.10) ] Suicidal behavior and ideation [see Warnings and Precautions (5.7) ] Bleeding and other hematopoietic disorders [see Warnings and Precautions (5.8) ] Hypothermia [see Warnings and Precautions (5.11) ] Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS)/Multiorgan hypersensitivity reactions [see Warnings and Precautions (5.12) ] Somnolence in the elderly [see Warnings and Precautions (5.14) ] Because clinical studies are conducted under widely varying conditions, adverse reaction rates observed in the clinical studies of a drug cannot be directly compared to rates in the clinical studies of another drug and may not reflect the rates observed in practice.
Drug Interactions
Hepatic enzyme-inducing drugs (e.g., phenytoin, carbamazepine, phenobarbital, primidone, rifampin) can increase valproate clearance, while enzyme inhibitors (e.g., felbamate) can decrease valproate clearance. Therefore increased monitoring of valproate and concomitant drug concentrations and dosage adjustment are indicated whenever enzyme-inducing or inhibiting drugs are introduced or withdrawn ( 7.1 ) Aspirin, carbapenem antibiotics, estrogen-containing hormonal contraceptives: Monitoring of valproate concentrations is recommended ( 7.1 ) Co-administration of valproate can affect the pharmacokinetics of other drugs (e.g., diazepam, ethosuximide, lamotrigine, phenytoin) by inhibiting their metabolism or protein binding displacement ( 7.2 ) Patients stabilized on rufinamide should begin valproate therapy at a low dose, and titrate to clinically effective dose ( 7.2 ) Dosage adjustment of amitriptyline/nortriptyline, propofol, warfarin, and zidovudine may be necessary if used concomitantly with Valproic acid ( 7.2 ) Topiramate: Hyperammonemia and encephalopathy ( 5.10 , 7.3 )
Medication Information
Warnings and Precautions
Hepatotoxicity; evaluate high risk populations and monitor serum liver tests ( 5.1 ) Birth defects, decreased IQ, and neurodevelopmental disorders following in utero exposure; should not be used to treat women with epilepsy or bipolar disorder who are pregnant or who plan to become pregnant or to treat a woman of childbearing potential unless other medications have failed to provide adequate symptom control or are otherwise unacceptable ( 5.2 , 5.3 , 5.4 ) Pancreatitis; Valproic acid should ordinarily be discontinued ( 5.5 ) Suicidal behavior or ideation; Antiepileptic drugs, including valproic acid, increase the risk of suicidal thoughts or behavior ( 5.7 ) Bleeding and other hematopoietic disorders; monitor platelet counts and coagulation tests ( 5.8 ) Hyperammonemia and hyperammonemic encephalopathy; measure ammonia level if unexplained lethargy and vomiting or changes in mental status, and also with concomitant topiramate use; consider discontinuation of valproate therapy ( 5.6 , 5.9 , 5.10 ) Hypothermia; Hypothermia has been reported during valproate therapy with or without associated hyperammonemia. This adverse reaction can also occur in patients using concomitant topiramate ( 5.11 ) Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS)/Multiorgan hypersensitivity reaction; discontinue valproic acid ( 5.12 ) Somnolence in the elderly can occur. Valproic acid dosage should be increased slowly and with regular monitoring for fluid and nutritional intake ( 5.14 )
Indications and Usage
Valproic acid is indicated for: Monotherapy and adjunctive therapy of complex partial seizures; sole and adjunctive therapy of simple and complex absence seizures; adjunctive therapy in patients with multiple seizure types that include absence seizures ( 1 )
Dosage and Administration
Valproic acid is intended for oral administration. ( 2.1 ) Simple and Complex Absence Seizures: Start at 10 to 15 mg/kg/day, increasing at 1 week intervals by 5 to 10 mg/kg/week until seizure control or limiting side effects ( 2.1 ) Safety of doses above 60 mg/kg/day is not established ( 2.1 , 2.2 )
Dosage Forms and Strengths
Valproic Acid Oral Solution USP is available as a red, cherry flavored oral solution containing the equivalent of 250 mg valproic acid per 5 mL as the sodium salt and supplied in the following oral dosage forms:
NDC: 70518-3805-00
NDC: 70518-3805-01
NDC: 70518-3805-02
NDC: 70518-3805-03
PACKAGING: 10 in 1 BOX
PACKAGING: 5 mL in 1 CUP, UNIT DOSE
PACKAGING: 10 in 1 BOX
PACKAGING: 10 mL in 1 CUP, UNIT DOSE
STORAGE
Store at 20° to 25°C (68° to 77°F). [See USP Controlled Room Temperature].
Repackaged and Distributed By:
Remedy Repack, Inc.
625 Kolter Dr. Suite #4 Indiana, PA 1-724-465-8762
Contraindications
Valproic acid should not be administered to patients with hepatic disease or significant hepatic dysfunction [see Warnings and Precautions (5.1) ] . Valproic acid is contraindicated in patients known to have mitochondrial disorders caused by mutations in mitochondrial DNA polymerase γ (POLG; e.g., Alpers-Huttenlocher Syndrome) and children under two years of age who are suspected of having a POLG-related disorder [see Warnings and Precautions (5.1) ] . Valproic acid is contraindicated in patients with known hypersensitivity to the drug [see Warnings and Precautions (5.12) ] . Valproic acid is contraindicated in patients with known urea cycle disorders [see Warnings and Precautions (5.6) ] . For use in prophylaxis of migraine headaches: Valproic acid is contraindicated in women who are pregnant and in women of childbearing potential who are not using effective contraception [see Warnings and Precautions (5.2 , 5.3 , 5.4) and Use in Specific Populations (8.1) ] .
Adverse Reactions
The following serious adverse reactions are described below and elsewhere in the labeling: Hepatic failure [see Warnings and Precautions (5.1) ] Birth defects [see Warnings and Precautions (5.2) ] Decreased IQ following in utero exposure [see Warnings and Precautions (5.3) ] Pancreatitis [see Warnings and Precautions (5.5) ] Hyperammonemic encephalopathy [see Warnings and Precautions (5.6 , 5.9 , 5.10) ] Suicidal behavior and ideation [see Warnings and Precautions (5.7) ] Bleeding and other hematopoietic disorders [see Warnings and Precautions (5.8) ] Hypothermia [see Warnings and Precautions (5.11) ] Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS)/Multiorgan hypersensitivity reactions [see Warnings and Precautions (5.12) ] Somnolence in the elderly [see Warnings and Precautions (5.14) ] Because clinical studies are conducted under widely varying conditions, adverse reaction rates observed in the clinical studies of a drug cannot be directly compared to rates in the clinical studies of another drug and may not reflect the rates observed in practice.
Drug Interactions
Hepatic enzyme-inducing drugs (e.g., phenytoin, carbamazepine, phenobarbital, primidone, rifampin) can increase valproate clearance, while enzyme inhibitors (e.g., felbamate) can decrease valproate clearance. Therefore increased monitoring of valproate and concomitant drug concentrations and dosage adjustment are indicated whenever enzyme-inducing or inhibiting drugs are introduced or withdrawn ( 7.1 ) Aspirin, carbapenem antibiotics, estrogen-containing hormonal contraceptives: Monitoring of valproate concentrations is recommended ( 7.1 ) Co-administration of valproate can affect the pharmacokinetics of other drugs (e.g., diazepam, ethosuximide, lamotrigine, phenytoin) by inhibiting their metabolism or protein binding displacement ( 7.2 ) Patients stabilized on rufinamide should begin valproate therapy at a low dose, and titrate to clinically effective dose ( 7.2 ) Dosage adjustment of amitriptyline/nortriptyline, propofol, warfarin, and zidovudine may be necessary if used concomitantly with Valproic acid ( 7.2 ) Topiramate: Hyperammonemia and encephalopathy ( 5.10 , 7.3 )
Description
WARNING: LIFE THREATENING ADVERSE REACTIONS See full prescribing information for complete boxed warning. Hepatotoxicity, including fatalities, usually during the first 6 months of treatment. Children under the age of two years and patients with mitochondrial disorders are at higher risk. Monitor patients closely, and perform serum liver testing prior to therapy and at frequent intervals thereafter ( 5.1 ) Fetal Risk, particularly neural tube defects, other major malformations, and decreased IQ ( 5.2 , 5.3 , 5.4 ) Pancreatitis, including fatal hemorrhagic cases ( 5.5 )
Section 42229-5
Hepatotoxicity
Section 51945-4
DRUG: VALPROIC ACID
GENERIC: VALPROIC ACID
DOSAGE: SOLUTION
ADMINSTRATION: ORAL
NDC: 70518-3805-0
NDC: 70518-3805-1
NDC: 70518-3805-2
NDC: 70518-3805-3
COLOR: red
FLAVOR: CHERRY
OUTER PACKAGING: 10 in 1 BOX
PACKAGING: 5 mL in 1 CUP, UNIT-DOSE
OUTER PACKAGING: 10 in 1 BOX
PACKAGING: 10 mL in 1 CUP, UNIT DOSE
ACTIVE INGREDIENT(S):
- VALPROIC ACID 250mg in 5mL
INACTIVE INGREDIENT(S):
- FD&C RED NO. 40
- METHYLPARABEN
- GLYCERIN
- SODIUM HYDROXIDE
- SORBITOL
- SUCROSE
- ANHYDROUS CITRIC ACID
- WATER
6.2 Mania
Although valproic acid has not been evaluated for safety and efficacy in the treatment of manic episodes associated with bipolar disorder, the following adverse reactions not listed above were reported by 1% or more of patients from two placebo-controlled clinical trials of divalproex sodium tablets.
Body as a Whole: Chills, neck pain, neck rigidity.
Cardiovascular System: Hypotension, postural hypotension, vasodilation.
Digestive System: Fecal incontinence, gastroenteritis, glossitis.
Musculoskeletal System: Arthrosis.
Nervous System: Agitation, catatonic reaction, hypokinesia, reflexes increased, tardive dyskinesia, vertigo.
Skin and Appendages: Furunculosis, maculopapular rash, seborrhea.
Special Senses: Conjunctivitis, dry eyes, eye pain.
Urogenital System: Dysuria.
1.1 Epilepsy
Valproic acid is indicated as monotherapy and adjunctive therapy in the treatment of patients with complex partial seizures that occur either in isolation or in association with other types of seizures. Valproic acid is indicated for use as sole and adjunctive therapy in the treatment of simple and complex absence seizures, and adjunctively in patients with multiple seizure types which include absence seizures.
Simple absence is defined as very brief clouding of the sensorium or loss of consciousness accompanied by certain generalized epileptic discharges without other detectable clinical signs. Complex absence is the term used when other signs are also present.
See Warnings and Precautions (5.1) for statement regarding fatal hepatic dysfunction.
2.1 Epilepsy
Valproic acid is intended for oral administration.
Patients should be informed to take valproic acid every day as prescribed. If a dose is missed it should be taken as soon as possible, unless it is almost time for the next dose. If a dose is skipped, the patient should not double the next dose.
Valproic acid is indicated as monotherapy and adjunctive therapy in complex partial seizures in adults and pediatric patients down to the age of 10 years, and in simple and complex absence seizures. As the valproic acid dosage is titrated upward, concentrations of clonazepam, diazepam, ethosuximide, lamotrigine, tolbutamide, phenobarbital, carbamazepine, and/or phenytoin may be affected [see Drug Interactions (7.2)] .
6.1 Epilepsy
The data described in the following section were obtained using divalproex sodium tablets.
Based on a placebo-controlled trial of adjunctive therapy for treatment of complex partial seizures, divalproex sodium was generally well tolerated with most adverse reactions rated as mild to moderate in severity. Intolerance was the primary reason for discontinuation in the divalproex sodium treated patients (6%), compared to 1% of placebo-treated patients.
Table 3 lists treatment-emergent adverse reactions which were reported by ≥ 5% of divalproex sodium-treated patients and for which the incidence was greater than in the placebo group, in a placebo-controlled trial of adjunctive therapy for treatment of complex partial seizures. Since patients were also treated with other antiepilepsy drugs, it is not possible, in most cases, to determine whether the following adverse reactions can be ascribed to divalproex sodium alone, or the combination of divalproex sodium and other antiepilepsy drugs.
| Body System/Reaction | Divalproex Sodium
(n = 77) % |
Placebo
(n = 70) % |
|---|---|---|
| Body as a Whole | ||
| Headache | 31 | 21 |
| Asthenia | 27 | 7 |
| Fever | 6 | 4 |
| Gastrointestinal System | ||
| Nausea | 48 | 14 |
| Vomiting | 27 | 7 |
| Abdominal Pain | 23 | 6 |
| Diarrhea | 13 | 6 |
| Anorexia | 12 | 0 |
| Dyspepsia | 8 | 4 |
| Constipation | 5 | 1 |
| Nervous System | ||
| Somnolence | 27 | 11 |
| Tremor | 25 | 6 |
| Dizziness | 25 | 13 |
| Diplopia | 16 | 9 |
| Amblyopia/Blurred Vision | 12 | 9 |
| Ataxia | 8 | 1 |
| Nystagmus | 8 | 1 |
| Emotional Lability | 6 | 4 |
| Thinking Abnormal | 6 | 0 |
| Amnesia | 5 | 1 |
| Respiratory System | ||
| Flu Syndrome | 12 | 9 |
| Infection | 12 | 6 |
| Bronchitis | 5 | 1 |
| Rhinitis | 5 | 4 |
| Other | ||
| Alopecia | 6 | 1 |
| Weight Loss | 6 | 0 |
Table 4 lists treatment-emergent adverse reactions which were reported by ≥ 5% of patients in the high dose divalproex sodium group, and for which the incidence was greater than in the low dose group, in a controlled trial of divalproex sodium monotherapy treatment of complex partial seizures. Since patients were being titrated off another antiepilepsy drug during the first portion of the trial, it is not possible, in many cases, to determine whether the following adverse reactions can be ascribed to divalproex sodium alone, or the combination of divalproex sodium and other antiepilepsy drugs.
| Body System/Reaction | High Dose
(n = 131) % |
Low Dose
(n = 134) % |
|---|---|---|
| Body as a Whole | ||
| Asthenia | 21 | 10 |
| Digestive System | ||
| Nausea | 34 | 26 |
| Diarrhea | 23 | 19 |
| Vomiting | 23 | 15 |
| Abdominal Pain | 12 | 9 |
| Anorexia | 11 | 4 |
| Dyspepsia | 11 | 10 |
| Hemic/Lymphatic System | ||
| Thrombocytopenia | 24 | 1 |
| Ecchymosis | 5 | 4 |
| Metabolic/Nutritional | ||
| Weight Gain | 9 | 4 |
| Peripheral Edema | 8 | 3 |
| Nervous System | ||
| Tremor | 57 | 19 |
| Somnolence | 30 | 18 |
| Dizziness | 18 | 13 |
| Insomnia | 15 | 9 |
| Nervousness | 11 | 7 |
| Amnesia | 7 | 4 |
| Nystagmus | 7 | 1 |
| Depression | 5 | 4 |
| Respiratory System | ||
| Infection | 20 | 13 |
| Pharyngitis | 8 | 2 |
| Dyspnea | 5 | 1 |
| Skin and Appendages | ||
| Alopecia | 24 | 13 |
| Special Senses | ||
| Amblyopia/Blurred Vision | 8 | 4 |
| Tinnitus | 7 | 1 |
| 1 Headache was the only adverse reaction that occurred in ≥ 5% of patients in the high dose group and at an equal or greater incidence in the low dose group. |
The following additional adverse reactions were reported by greater than 1% but less than 5% of the 358 patients treated with divalproex sodium in the controlled trials of complex partial seizures:
Body as a Whole: Back pain, chest pain, malaise.
Cardiovascular System: Tachycardia, hypertension, palpitation.
Digestive System: Increased appetite, flatulence, hematemesis, eructation, pancreatitis, periodontal abscess.
Hemic and Lymphatic System: Petechia.
Metabolic and Nutritional Disorders: SGOT increased, SGPT increased.
Musculoskeletal System: Myalgia, twitching, arthralgia, leg cramps, myasthenia.
Nervous System: Anxiety, confusion, abnormal gait, paresthesia, hypertonia, incoordination, abnormal dreams, personality disorder.
Respiratory System: Sinusitis, cough increased, pneumonia, epistaxis.
Skin and Appendages: Rash, pruritus, dry skin.
Special Senses: Taste perversion, abnormal vision, deafness, otitis media.
Urogenital System: Urinary incontinence, vaginitis, dysmenorrhea, amenorrhea, urinary frequency.
6.3 Migraine
Although valproic acid has not been evaluated for safety and efficacy in the prophylactic treatment of migraine headaches, the following adverse reactions not listed above were reported by 1% or more of patients from two placebo-controlled clinical trials of divalproex sodium tablets.
Body as a Whole: Face edema.
Digestive System: Dry mouth, stomatitis.
Urogenital System: Cystitis, metrorrhagia, and vaginal hemorrhage.
10 Overdosage
Overdosage with valproate may result in somnolence, heart block, deep coma, and hypernatremia. Fatalities have been reported; however, patients have recovered from valproate levels as high as 2,120 mcg/mL.
In overdose situations, the fraction of drug not bound to protein is high and hemodialysis or tandem hemodialysis plus hemoperfusion may result in significant removal of drug. The benefit of gastric lavage or emesis will vary with the time since ingestion. General supportive measures should be applied with particular attention to the maintenance of adequate urinary output.
Naloxone has been reported to reverse the CNS depressant effects of valproate overdosage. Because naloxone could theoretically also reverse the antiepileptic effects of valproate, it should be used with caution in patients with epilepsy.
14.1 Epilepsy
The efficacy of divalproex sodium in reducing the incidence of complex partial seizures (CPS) that occur in isolation or in association with other seizure types was established in two controlled trials.
In one, multi-clinic, placebo-controlled study employing an add-on design (adjunctive therapy), 144 patients who continued to suffer eight or more CPS per 8 weeks during an 8 week period of monotherapy with doses of either carbamazepine or phenytoin sufficient to assure plasma concentrations within the "therapeutic range" were randomized to receive, in addition to their original antiepilepsy drug (AED), either divalproex sodium or placebo. Randomized patients were to be followed for a total of 16 weeks. The following table presents the findings.
| Add-on Treatment | Number of Patients | Baseline Incidence | Experimental Incidence |
|---|---|---|---|
| Divalproex sodium | 75 | 16.0 | 8.9 * |
| Placebo | 69 | 14.5 | 11.5 |
Figure 1 presents the proportion of patients (X axis) whose percentage reduction from baseline in complex partial seizure rates was at least as great as that indicated on the Y axis in the adjunctive therapy study. A positive percent reduction indicates an improvement (i.e., a decrease in seizure frequency), while a negative percent reduction indicates worsening. Thus, in a display of this type, the curve for an effective treatment is shifted to the left of the curve for placebo. This figure shows that the proportion of patients achieving any particular level of improvement was consistently higher for divalproex sodium than for placebo. For example, 45% of patients treated with divalproex sodium had a ≥ 50% reduction in complex partial seizure rate compared to 23% of patients treated with placebo.
Figure 1
The second study assessed the capacity of divalproex sodium to reduce the incidence of CPS when administered as the sole AED. The study compared the incidence of CPS among patients randomized to either a high or low dose treatment arm. Patients qualified for entry into the randomized comparison phase of this study only if 1) they continued to experience 2 or more CPS per 4 weeks during an 8 to 12 week long period of monotherapy with adequate doses of an AED (i.e., phenytoin, carbamazepine, phenobarbital, or primidone) and 2) they made a successful transition over a two week interval to divalproex sodium. Patients entering the randomized phase were then brought to their assigned target dose, gradually tapered off their concomitant AED and followed for an interval as long as 22 weeks. Less than 50% of the patients randomized, however, completed the study. In patients converted to divalproex sodium monotherapy, the mean total valproate concentrations during monotherapy were 71 and 123 mcg/mL in the low dose and high dose groups, respectively.
The following table presents the findings for all patients randomized who had at least one post-randomization assessment.
| Treatment | Number of Patients | Baseline Incidence | Randomized Phase Incidence |
|---|---|---|---|
| High dose divalproex sodium | 131 | 13.2 | 10.7 * |
| Low dose divalproex sodium | 134 | 14.2 | 13.8 |
Figure 2 presents the proportion of patients (X axis) whose percentage reduction from baseline in complex partial seizure rates was at least as great as that indicated on the Y axis in the monotherapy study. A positive percent reduction indicates an improvement (i.e., a decrease in seizure frequency), while a negative percent reduction indicates worsening. Thus, in a display of this type, the curve for a more effective treatment is shifted to the left of the curve for a less effective treatment. This figure shows that the proportion of patients achieving any particular level of reduction was consistently higher for high dose divalproex sodium than for low dose divalproex sodium. For example, when switching from carbamazepine, phenytoin, phenobarbital or primidone monotherapy to high dose divalproex sodium monotherapy, 63% of patients experienced no change or a reduction in complex partial seizure rates compared to 54% of patients receiving low dose divalproex sodium.
Figure 2
Information on pediatric studies is presented in section 8.
15 References
1. Meador KJ, Baker GA, Browning N, et al. Fetal antiepileptic drug exposure and cognitive outcomes at age 6 years (NEAD study): a prospective observational study. Lancet Neurology 2013; 12 (3):244-252.
11 Description
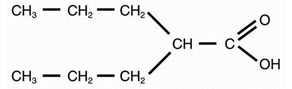
Valproic acid is a carboxylic acid designated as 2-propylpentanoic acid. It is also known as dipropylacetic acid. Valproic acid has the following structure:
Valproic acid (pKa 4.8) has a molecular weight of 144 and occurs as a colorless liquid with a characteristic odor. It is slightly soluble in water (1.3 mg/mL) and very soluble in organic solvents.
Valproic Acid Oral Solution USP is an antiepileptic for oral administration and contains the equivalent of 250 mg valproic acid per 5 mL as the sodium salt.
7.3 Topiramate
Concomitant administration of valproate and topiramate has been associated with hyperammonemia with and without encephalopathy [see Contraindications (4)and Warnings and Precautions (5.6, 5.9, 5.10)] . Concomitant administration of topiramate with valproate has also been associated with hypothermia in patients who have tolerated either drug alone. It may be prudent to examine blood ammonia levels in patients in whom the onset of hypothermia has been reported [see Warnings and Precautions (5.9, 5.11)] .
5.11 Hypothermia
Hypothermia, defined as an unintentional drop in body core temperature to <35°C (95°F), has been reported in association with valproate therapy both in conjunction with and in the absence of hyperammonemia. This adverse reaction can also occur in patients using concomitant topiramate with valproate after starting topiramate treatment or after increasing the daily dose of topiramate [see Drug Interactions (7.3)] . Consideration should be given to stopping valproate in patients who develop hypothermia, which may be manifested by a variety of clinical abnormalities including lethargy, confusion, coma, and significant alterations in other major organ systems such as the cardiovascular and respiratory systems. Clinical management and assessment should include examination of blood ammonia levels.
5.5 Pancreatitis
Cases of life-threatening pancreatitis have been reported in both children and adults receiving valproate. Some of the cases have been described as hemorrhagic with rapid progression from initial symptoms to death. Some cases have occurred shortly after initial use as well as after several years of use. The rate based upon the reported cases exceeds that expected in the general population and there have been cases in which pancreatitis recurred after rechallenge with valproate. In clinical trials, there were 2 cases of pancreatitis without alternative etiology in 2,416 patients, representing 1,044 patient-years experience. Patients and guardians should be warned that abdominal pain, nausea, vomiting, and/or anorexia can be symptoms of pancreatitis that require prompt medical evaluation. If pancreatitis is diagnosed, valproic acid should ordinarily be discontinued. Alternative treatment for the underlying medical condition should be initiated as clinically indicated [see Boxed Warning] .
Medication Guide
VALPROIC ACID ORAL SOLUTION USP
(VAL-pro-IC)
Read this Medication Guide before you start taking valproic acid and each time you get a refill. There may be new information. This information does not take the place of talking to your healthcare provider about your medical condition or treatment.
What is the most important information I should know about valproic acid?
Do not stop taking valproic acid without first talking to your healthcare provider.
Stopping valproic acid suddenly can cause serious problems.
Valproic acid can cause serious side effects, including:
1. Serious liver damage that can cause death, especially in children younger than 2 years old.
The risk of getting this serious liver damage is more likely to happen within the first 6 months of treatment.
Call your healthcare provider right away if you get any of the following symptoms: In some cases, liver damage may continue despite stopping the drug.
- nausea or vomiting that does not go away
- loss of appetite
- pain on the right side of your stomach (abdomen)
- dark urine
- swelling of your face
- yellowing of your skin or the whites of your eyes
2. Valproic acid may harm your unborn baby.
- If you take valproic acid during pregnancy for any medical condition, your baby is at risk for serious birth defects that affect the brain and spinal cord and are called spina bifida or neural tube defects. These defects occur in 1 to 2 out of every 100 babies born to mothers who use this medicine during pregnancy. These defects can begin in the first month, even before you know you are pregnant. Other birth defects that affect the structures of the heart, head, arms, legs, and the opening where the urine comes out (urethra) on the bottom of the penis can also happen. Decreased hearing or hearing loss can also happen.
- Birth defects may occur even in children born to women who are not taking any medicines and do not have other risk factors.
- Taking folic acid supplements before getting pregnant and during early pregnancy can lower the chance of having a baby with a neural tube defect.
- If you take valproic acid during pregnancy for any medical condition, your child is at risk for having lower IQ and may be at risk for developing autism or attention deficit/hyperactivity disorder.
- There may be other medicines to treat your condition that have a lower chance of causing birth defects, decreased IQ, or other disorders in your child.
- Women who are pregnant must not take valproic acid to prevent migraine headaches.
- All women of childbearing age (including girls from the start of puberty) should talk to their healthcare provider about using other possible treatments instead of valproic acid. If the decision is made to use valproic acid, you should use effective birth control (contraception).
- Tell your healthcare provider right away if you become pregnant while taking valproic acid. You and your healthcare provider should decide if you will continue to take valproic acid while you are pregnant.
- Pregnancy Registry: If you become pregnant while taking valproic acid, talk to your healthcare provider about registering with the North American Antiepileptic Drug Pregnancy Registry. You can enroll in this registry by calling toll-free 1-888-233-2334 or by visiting the website, http://www.aedpregnancyregistry.org/. The purpose of this registry is to collect information about the safety of antiepileptic drugs during pregnancy.
3. Inflammation of your pancreas that can cause death.
Call your healthcare provider right away if you have any of these symptoms:
- severe stomach pain that you may also feel in your back
- nausea or vomiting that does not go away
4. Like other antiepileptic drugs, valproic acid may cause suicidal thoughts or actions in a very small number of people, about 1 in 500.
Call a healthcare provider right away if you have any of these symptoms, especially if they are new, worse, or worry you:
- thoughts about suicide or dying
- attempts to commit suicide
- new or worse depression
- new or worse anxiety
- feeling agitated or restless
- panic attacks
- trouble sleeping (insomnia)
- new or worse irritability
- acting aggressive, being angry, or violent
- acting on dangerous impulses
- an extreme increase in activity and talking (mania)
- other unusual changes in behavior or mood
How can I watch for early symptoms of suicidal thoughts and actions?
- Pay attention to any changes, especially sudden changes in mood, behaviors, thoughts, or feelings.
- Keep all follow-up visits with your healthcare provider as scheduled.
Call your healthcare provider between visits as needed, especially if you are worried about symptoms.
Do not stop valproic acid without first talking to a healthcare provider.Stopping valproic acid suddenly can cause serious problems. Stopping a seizure medicine suddenly in a patient who has epilepsy can cause seizures that will not stop (status epilepticus).
Suicidal thoughts or actions can be caused by things other than medicines. If you have suicidal thoughts or actions, your healthcare provider may check for other causes.
What is valproic acid?
Valproic acid is a prescription medicine used alone or with other medicines, to treat:
- complex partial seizures in adults and children 10 years of age and older
- simple and complex absence seizures, with or without other seizure types
Who should not take valproic acid?
Do not take valproic acid if you:
- have liver problems
- have or think you have a genetic liver problem caused by a mitochondrial disorder (e.g., Alpers-Huttenlocher syndrome)
- are allergic to divalproex sodium, valproic acid, sodium valproate, or any of the ingredients in valproic acid. See the end of this leaflet for a complete list of ingredients in valproic acid.
- have a genetic problem called urea cycle disorder
- are taking it to prevent migraine headaches and are either pregnant or may become pregnant because you are not using effective birth control (contraception)
What should I tell my healthcare provider before taking valproic acid?
Before you take valproic acid, tell your healthcare provider if you:
- have a genetic liver problem caused by a mitochondrial disorder (e.g., Alpers-Huttenlocher syndrome)
- drink alcohol
- are pregnant or breastfeeding. Valproic acid can pass into breast milk. Talk to your healthcare provider about the best way to feed your baby if you take valproic acid.
- have or have had depression, mood problems, or suicidal thoughts or behavior
- have any other medical conditions
Tell your healthcare provider about all the medicines you take,including prescription and non-prescription medicines, vitamins, herbal supplements and medicines that you take for a short period of time.
Taking valproic acid with certain other medicines can cause side effects or affect how well they work. Do not start or stop other medicines without talking to your healthcare provider.
Know the medicines you take. Keep a list of them and show it to your healthcare provider and pharmacist each time you get a new medicine.
How should I take valproic acid?
- Take valproic acid exactly as your healthcare provider tells you. Your healthcare provider will tell you how much valproic acid to take and when to take it.
- Your healthcare provider may change your dose.
- Do not change your dose of valproic acid without talking to your healthcare provider.
- Do not stop taking valproic acid without first talking to your healthcare provider. Stopping valproic acid suddenly can cause serious problems.
- If you take too much valproic acid, call your healthcare provider or local Poison Control Center right away.
What should I avoid while taking valproic acid?
- Valproic acid can cause drowsiness and dizziness. Do not drink alcohol or take other medicines that make you sleepy or dizzy while taking valproic acid, until you talk with your doctor. Taking valproic acid with alcohol or drugs that cause sleepiness or dizziness may make your sleepiness or dizziness worse.
- Do not drive a car or operate dangerous machinery until you know how valproic acid affects you. Valproic acid can slow your thinking and motor skills.
What are the possible side effects of valproic acid?
- See "What is the most important information I should know about valproic acid?"
Valproic acid can cause serious side effects including:
- Bleeding problems:red or purple spots on your skin, bruising, pain and swelling into your joints due to bleeding or bleeding from your mouth or nose.
- High ammonia levels in your blood:feeling tired, vomiting, changes in mental status.
- Low body temperature (hypothermia):drop in your body temperature to less than 95°F, feeling tired, confusion, coma.
- Allergic (hypersensitivity) reactions:fever, skin rash, hives, sores in your mouth, blistering and peeling of your skin, swelling of your lymph nodes, swelling of your face, eyes, lips, tongue, or throat, trouble swallowing or breathing.
- Drowsiness or sleepiness in the elderly.This extreme drowsiness may cause you to eat or drink less than you normally would. Tell your doctor if you are not able to eat or drink as you normally do. Your doctor may start you at a lower dose of valproic acid.
Call your healthcare provider right away, if you have any of the symptoms listed above.
The common side effects of valproic acid include:
- nausea
- headache
- sleepiness
- vomiting
- weakness
- tremor
- dizziness
- stomach pain
- blurry vision
- double vision
- diarrhea
- increased appetite
- weight gain
- hair loss
- loss of appetite
- problems with walking or coordination
These are not all of the possible side effects of valproic acid. For more information, ask your healthcare provider or pharmacist.
Tell your healthcare provider if you have any side effect that bothers you or that does not go away.
Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.
How should I store Valproic Acid Oral Solution USP?
- Store at 20° to 25°C (68° to 77°F). [See USP Controlled Room Temperature].
Keep valproic acid and all medicines out of the reach of children.
General information about the safe and effective use of valproic acid.
Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not use valproic acid for a condition for which it was not prescribed. Do not give valproic acid to other people, even if they have the same symptoms that you have. It may harm them.
This Medication Guide summarizes the most important information about valproic acid. If you would like more information, talk with your healthcare provider. You can ask your pharmacist or healthcare provider for information about valproic acid that is written for health professionals.
For more information, call Pharmaceutical Associates, Inc. at 1-800-845-8210 or visit www.paipharma.com.
What are the ingredients in Valproic Acid Oral Solution USP?
Active ingredient: valproic acid
Inactive ingredients: cherry flavor, FD&C Red No. 40, glycerin, methylparaben, purified water, sodium hydroxide, sorbitol and sucrose. May also contain citric acid and sodium hydroxide to adjust pH.
This Medication Guide has been approved by the U.S. Food and Drug Administration.
Repackaged By / Distributed By: RemedyRepack Inc.
625 Kolter Drive, Indiana, PA 15701
(724) 465-8762
8.4 Pediatric Use
Experience has indicated that pediatric patients under the age of two years are at a considerably increased risk of developing fatal hepatotoxicity, especially those with the aforementioned conditions [see Boxed Warning] . When valproic acid is used in this patient group, it should be used with extreme caution and as a sole agent. The benefits of therapy should be weighed against the risks. Above the age of 2 years, experience in epilepsy has indicated that the incidence of fatal hepatotoxicity decreases considerably in progressively older patient groups.
Younger children, especially those receiving enzyme-inducing drugs, will require larger maintenance doses to attain targeted total and unbound valproate concentrations. Pediatric patients (i.e., between 3 months and 10 years) have 50% higher clearances expressed on weight (i.e., mL/min/kg) than do adults. Over the age of 10 years, children have pharmacokinetic parameters that approximate those of adults.
The variability in free fraction limits the clinical usefulness of monitoring total serum valproic acid concentrations. Interpretation of valproic acid concentrations in children should include consideration of factors that affect hepatic metabolism and protein binding.
8.5 Geriatric Use
No patients above the age of 65 years were enrolled in double-blind prospective clinical trials of mania associated with bipolar illness. In a case review study of 583 patients, 72 patients (12%) were greater than 65 years of age. A higher percentage of patients above 65 years of age reported accidental injury, infection, pain, somnolence, and tremor.
Discontinuation of valproate was occasionally associated with the latter two events. It is not clear whether these events indicate additional risk or whether they result from preexisting medical illness and concomitant medication use among these patients.
A study of elderly patients with dementia revealed drug related somnolence and discontinuation for somnolence [see Warnings and Precautions (5.14)] . The starting dose should be reduced in these patients, and dosage reductions or discontinuation should be considered in patients with excessive somnolence [see Dosage and Administration (2.2)] .
5.9 Hyperammonemia
Hyperammonemia has been reported in association with valproate therapy and may be present despite normal liver function tests. In patients who develop unexplained lethargy and vomiting or changes in mental status, hyperammonemic encephalopathy should be considered and an ammonia level should be measured. Hyperammonemia should also be considered in patients who present with hypothermia [see Warnings and Precautions (5.11)] . If ammonia is increased, valproate therapy should be discontinued. Appropriate interventions for treatment of hyperammonemia should be initiated, and such patients should undergo investigation for underlying urea cycle disorders [see Contraindications (4)and Warnings and Precautions (5.6, 5.10)] .
Asymptomatic elevations of ammonia are more common and when present, require close monitoring of plasma ammonia levels. If the elevation persists, discontinuation of valproate therapy should be considered.
14 Clinical Studies
The studies described in the following section were conducted using divalproex sodium tablets.
4 Contraindications
- Valproic acid should not be administered to patients with hepatic disease or significant hepatic dysfunction [see Warnings and Precautions (5.1)] .
- Valproic acid is contraindicated in patients known to have mitochondrial disorders caused by mutations in mitochondrial DNA polymerase γ (POLG; e.g., Alpers-Huttenlocher Syndrome) and children under two years of age who are suspected of having a POLG-related disorder [see Warnings and Precautions (5.1)] .
- Valproic acid is contraindicated in patients with known hypersensitivity to the drug [see Warnings and Precautions (5.12)] .
- Valproic acid is contraindicated in patients with known urea cycle disorders [see Warnings and Precautions (5.6)] .
- For use in prophylaxis of migraine headaches: Valproic acid is contraindicated in women who are pregnant and in women of childbearing potential who are not using effective contraception [see Warnings and Precautions (5.2, 5.3, 5.4)and Use in Specific Populations (8.1)] .
6 Adverse Reactions
The following serious adverse reactions are described below and elsewhere in the labeling:
- Hepatic failure [see Warnings and Precautions (5.1)]
- Birth defects [see Warnings and Precautions (5.2)]
- Decreased IQ following in uteroexposure [see Warnings and Precautions (5.3)]
- Pancreatitis [see Warnings and Precautions (5.5)]
- Hyperammonemic encephalopathy [see Warnings and Precautions (5.6, 5.9, 5.10)]
- Suicidal behavior and ideation [see Warnings and Precautions (5.7)]
- Bleeding and other hematopoietic disorders [see Warnings and Precautions (5.8)]
- Hypothermia [see Warnings and Precautions (5.11)]
- Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS)/Multiorgan hypersensitivity reactions [see Warnings and Precautions (5.12)]
- Somnolence in the elderly [see Warnings and Precautions (5.14)]
Because clinical studies are conducted under widely varying conditions, adverse reaction rates observed in the clinical studies of a drug cannot be directly compared to rates in the clinical studies of another drug and may not reflect the rates observed in practice.
7 Drug Interactions
- Hepatic enzyme-inducing drugs (e.g., phenytoin, carbamazepine, phenobarbital, primidone, rifampin) can increase valproate clearance, while enzyme inhibitors (e.g., felbamate) can decrease valproate clearance. Therefore increased monitoring of valproate and concomitant drug concentrations and dosage adjustment are indicated whenever enzyme-inducing or inhibiting drugs are introduced or withdrawn ( 7.1)
- Aspirin, carbapenem antibiotics, estrogen-containing hormonal contraceptives: Monitoring of valproate concentrations is recommended ( 7.1)
- Co-administration of valproate can affect the pharmacokinetics of other drugs (e.g., diazepam, ethosuximide, lamotrigine, phenytoin) by inhibiting their metabolism or protein binding displacement ( 7.2)
- Patients stabilized on rufinamide should begin valproate therapy at a low dose, and titrate to clinically effective dose ( 7.2)
- Dosage adjustment of amitriptyline/nortriptyline, propofol, warfarin, and zidovudine may be necessary if used concomitantly with Valproic acid ( 7.2)
- Topiramate: Hyperammonemia and encephalopathy ( 5.10, 7.3)
12.2 Pharmacodynamics
The relationship between plasma concentration and clinical response is not well documented. One contributing factor is the nonlinear, concentration dependent protein binding of valproate which affects the clearance of the drug. Thus, monitoring of total serum valproate cannot provide a reliable index of the bioactive valproate species.
For example, because the plasma protein binding of valproate is concentration dependent, the free fraction increases from approximately 10% at 40 mcg/mL to 18.5% at 130 mcg/mL. Higher than expected free fractions occur in the elderly, in hyperlipidemic patients, and in patients with hepatic and renal diseases.
1 Indications and Usage
Valproic acid is indicated for:
- Monotherapy and adjunctive therapy of complex partial seizures; sole and adjunctive therapy of simple and complex absence seizures; adjunctive therapy in patients with multiple seizure types that include absence seizures ( 1)
12.1 Mechanism of Action
Valproic acid dissociates to the valproate ion in the gastrointestinal tract. The mechanisms by which valproate exerts its therapeutic effects have not been established. It has been suggested that its activity in epilepsy is related to increased brain concentrations of gamma-aminobutyric acid (GABA).
5.6 Urea Cycle Disorders
Valproic acid is contraindicated in patients with known urea cycle disorders (UCD).
Hyperammonemic encephalopathy, sometimes fatal, has been reported following initiation of valproate therapy in patients with urea cycle disorders, a group of uncommon genetic abnormalities, particularly ornithine transcarbamylase deficiency. Prior to the initiation of valproic acid therapy, evaluation for UCD should be considered in the following patients: 1) those with a history of unexplained encephalopathy or coma, encephalopathy associated with a protein load, pregnancy-related or postpartum encephalopathy, unexplained mental retardation, or history of elevated plasma ammonia or glutamine; 2) those with cyclical vomiting and lethargy, episodic extreme irritability, ataxia, low BUN, or protein avoidance; 3) those with a family history of UCD or a family history of unexplained infant deaths (particularly males); 4) those with other signs or symptoms of UCD. Patients who develop symptoms of unexplained hyperammonemic encephalopathy while receiving valproate therapy should receive prompt treatment (including discontinuation of valproate therapy) and be evaluated for underlying urea cycle disorders [see Contraindications (4)and Warnings and Precautions (5.10)] .
1.2 Important Limitations
Because of the risk to the fetus of decreased IQ, neurodevelopmental disorders, neural tube defects, and other major congenital malformations, which may occur very early in pregnancy, valproate should not be used to treat women with epilepsy or bipolar disorder who are pregnant or who plan to become pregnant unless other medications have failed to provide adequate symptom control or are otherwise unacceptable. Valproate should not be administered to a woman of childbearing potential unless other medications have failed to provide adequate symptom control or are otherwise unacceptable [see Warnings and Precautions (5.2, 5.3, 5.4), Use in Specific Populations (8.1), and Patient Counseling Information (17)] .
For prophylaxis of migraine headaches, valproate is contraindicated in women who are pregnant and in women of childbearing potential who are not using effective contraception [see Contraindications (4)].
5 Warnings and Precautions
- Hepatotoxicity; evaluate high risk populations and monitor serum liver tests ( 5.1)
- Birth defects, decreased IQ, and neurodevelopmental disorders following in uteroexposure; should not be used to treat women with epilepsy or bipolar disorder who are pregnant or who plan to become pregnant or to treat a woman of childbearing potential unless other medications have failed to provide adequate symptom control or are otherwise unacceptable ( 5.2, 5.3, 5.4)
- Pancreatitis; Valproic acid should ordinarily be discontinued ( 5.5)
- Suicidal behavior or ideation; Antiepileptic drugs, including valproic acid, increase the risk of suicidal thoughts or behavior ( 5.7)
- Bleeding and other hematopoietic disorders; monitor platelet counts and coagulation tests ( 5.8)
- Hyperammonemia and hyperammonemic encephalopathy; measure ammonia level if unexplained lethargy and vomiting or changes in mental status, and also with concomitant topiramate use; consider discontinuation of valproate therapy ( 5.6, 5.9, 5.10)
- Hypothermia; Hypothermia has been reported during valproate therapy with or without associated hyperammonemia. This adverse reaction can also occur in patients using concomitant topiramate ( 5.11)
- Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS)/Multiorgan hypersensitivity reaction; discontinue valproic acid ( 5.12)
- Somnolence in the elderly can occur. Valproic acid dosage should be increased slowly and with regular monitoring for fluid and nutritional intake ( 5.14)
2 Dosage and Administration
3 Dosage Forms and Strengths
Valproic Acid Oral Solution USP is available as a red, cherry flavored Oral Solution containing the equivalent of 250 mg valproic acid per 5 mL as the sodium salt.
5.2 Structural Birth Defects
Valproate can cause fetal harm when administered to a pregnant woman. Pregnancy registry data show that maternal valproate use can cause neural tube defects and other structural abnormalities (e.g., craniofacial defects, cardiovascular malformations, hypospadias, limb malformations). The rate of congenital malformations among babies born to mothers using valproate is about four times higher than the rate among babies born to epileptic mothers using other anti-seizure monotherapies. Evidence suggests that folic acid supplementation prior to conception and during the first trimester of pregnancy decreases the risk for congenital neural tube defects in the general population [see Use in Specific Populations (8.1)] .
6.4 Postmarketing Experience
The following adverse reactions have been identified during post approval use of divalproex sodium. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Dermatologic: Hair texture changes, hair color changes, photosensitivity, erythema multiforme, toxic epidermal necrolysis, nail and nail bed disorders, and Stevens-Johnson syndrome.
Psychiatric: Emotional upset, psychosis, aggression, psychomotor hyperactivity, hostility, disturbance in attention, learning disorder, and behavioral deterioration.
Neurologic: Paradoxical convulsion, parkinsonism
There have been several reports of acute or subacute cognitive decline and behavioral changes (apathy or irritability) with cerebral pseudoatrophy on imaging associated with valproate therapy; both the cognitive/behavioral changes and cerebral pseudoatrophy reversed partially or fully after valproate discontinuation.
There have been reports of acute or subacute encephalopathy in the absence of elevated ammonia levels, elevated valproate levels, or neuroimaging changes. The encephalopathy reversed partially or fully after valproate discontinuation.
Musculoskeletal: Fractures, decreased bone mineral density, osteopenia, osteoporosis, and weakness.
Hematologic: Relative lymphocytosis, macrocytosis, leukopenia, anemia including macrocytic with or without folate deficiency, bone marrow suppression, pancytopenia, aplastic anemia, agranulocytosis, and acute intermittent porphyria.
Endocrine: Irregular menses, secondary amenorrhea, hyperandrogenism, hirsutism, elevated testosterone level, breast enlargement, galactorrhea, parotid gland swelling, polycystic ovary disease, decreased carnitine concentrations, hyponatremia, hyperglycinemia, and inappropriate ADH secretion.
There have been rare reports of Fanconi's syndrome occurring chiefly in children.
Metabolism and nutrition: Weight gain.
Reproductive: Aspermia, azoospermia, decreased sperm count, decreased spermatozoa motility, male infertility, and abnormal spermatozoa morphology.
Genitourinary: Enuresis and urinary tract infection.
Special Senses: Hearing loss.
Other: Allergic reaction, anaphylaxis, developmental delay, bone pain, bradycardia, and cutaneous vasculitis.
8 Use in Specific Populations
- Pregnancy: Valproic acid can cause congenital malformations including neural tube defects, decreased IQ, and neurodevelopmental disorders ( 5.2, 5.3, 8.1)
- Pediatric: Children under the age of two years are at considerably higher risk of fatal hepatotoxicity ( 5.1, 8.4)
- Geriatric: Reduce starting dose; increase dosage more slowly; monitor fluid and nutritional intake, and somnolence ( 5.14, 8.5)
5.14 Somnolence in the Elderly
In a double-blind, multicenter trial of valproate in elderly patients with dementia (mean age = 83 years), doses were increased by 125 mg/day to a target dose of 20 mg/kg/day. A significantly higher proportion of valproate patients had somnolence compared to placebo, and although not statistically significant, there was a higher proportion of patients with dehydration. Discontinuations for somnolence were also significantly higher than with placebo. In some patients with somnolence (approximately one-half), there was associated reduced nutritional intake and weight loss. There was a trend for the patients who experienced these events to have a lower baseline albumin concentration, lower valproate clearance, and a higher BUN. In elderly patients, dosage should be increased more slowly and with regular monitoring for fluid and nutritional intake, dehydration, somnolence, and other adverse reactions. Dose reductions or discontinuation of valproate should be considered in patients with decreased food or fluid intake and in patients with excessive somnolence [see Dosage and Administration (2.2)] .
17 Patient Counseling Information
Advise the patient to read the FDA-approved patient labeling (Medication Guide).
Repackaged By / Distributed By: RemedyRepack Inc.
625 Kolter Drive, Indiana, PA 15701
(724) 465-8762
5.7 Suicidal Behavior and Ideation
Antiepileptic drugs (AEDs), including valproic acid, increase the risk of suicidal thoughts or behavior in patients taking these drugs for any indication. Patients treated with any AED for any indication should be monitored for the emergence or worsening of depression, suicidal thoughts or behavior, and/or any unusual changes in mood or behavior.
Pooled analyses of 199 placebo-controlled clinical trials (mono- and adjunctive therapy) of 11 different AEDs showed that patients randomized to one of the AEDs had approximately twice the risk (adjusted Relative Risk 1.8, 95% CI:1.2, 2.7) of suicidal thinking or behavior compared to patients randomized to placebo. In these trials, which had a median treatment duration of 12 weeks, the estimated incidence rate of suicidal behavior or ideation among 27,863 AED-treated patients was 0.43%, compared to 0.24% among 16,029 placebo-treated patients, representing an increase of approximately one case of suicidal thinking or behavior for every 530 patients treated. There were four suicides in drug-treated patients in the trials and none in placebo-treated patients, but the number is too small to allow any conclusion about drug effect on suicide.
The increased risk of suicidal thoughts or behavior with AEDs was observed as early as one week after starting drug treatment with AEDs and persisted for the duration of treatment assessed. Because most trials included in the analysis did not extend beyond 24 weeks, the risk of suicidal thoughts or behavior beyond 24 weeks could not be assessed.
The risk of suicidal thoughts or behavior was generally consistent among drugs in the data analyzed. The finding of increased risk with AEDs of varying mechanisms of action and across a range of indications suggests that the risk applies to all AEDs used for any indication. The risk did not vary substantially by age (5-100 years) in the clinical trials analyzed.
Table 2 shows absolute and relative risk by indication for all evaluated AEDs.
| Indication | Placebo Patients with Events Per 1,000 Patients | Drug Patients with Events Per 1,000 Patients | Relative Risk: Incidence of Events in Drug Patients/Incidence in Placebo Patients | Risk Difference: Additional Drug Patients with Events Per 1,000 Patients |
|---|---|---|---|---|
| Epilepsy | 1.0 | 3.4 | 3.5 | 2.4 |
| Psychiatric | 5.7 | 8.5 | 1.5 | 2.9 |
| Other | 1.0 | 1.8 | 1.9 | 0.9 |
| Total | 2.4 | 4.3 | 1.8 | 1.9 |
The relative risk for suicidal thoughts or behavior was higher in clinical trials for epilepsy than in clinical trials for psychiatric or other conditions, but the absolute risk differences were similar for the epilepsy and psychiatric indications.
Anyone considering prescribing valproic acid or any other AED must balance the risk of suicidal thoughts or behavior with the risk of untreated illness. Epilepsy and many other illnesses for which AEDs are prescribed are themselves associated with morbidity and mortality and an increased risk of suicidal thoughts and behavior. Should suicidal thoughts and behavior emerge during treatment, the prescriber needs to consider whether the emergence of these symptoms in any given patient may be related to the illness being treated.
5.3 Decreased Iq Following in Utero
Valproate can cause decreased IQ scores following in uteroexposure. Published epidemiological studies have indicated that children exposed to valproate in uterohave lower cognitive test scores than children exposed in uteroto either another antiepileptic drug or to no antiepileptic drugs. The largest of these studies 1is a prospective cohort study conducted in the United States and United Kingdom that found that children with prenatal exposure to valproate (n=62) had lower IQ scores at age 6 (97 [95% C.I. 94-101]) than children with prenatal exposure to the other antiepileptic drug monotherapy treatments evaluated: lamotrigine (108 [95% C.I. 105-110]), carbamazepine (105 [95% C.I. 102-108]), and phenytoin (108 [95% C.I. 104-112]). It is not known when during pregnancy cognitive effects in valproate-exposed children occur. Because the women in this study were exposed to antiepileptic drugs throughout pregnancy, whether the risk for decreased IQ was related to a particular time period during pregnancy could not be assessed.
Although all of the available studies have methodological limitations, the weight of the evidence supports the conclusion that valproate exposure in uterocan cause decreased IQ in children.
In animal studies, offspring with prenatal exposure to valproate had malformations similar to those seen in humans and demonstrated neurobehavioral deficits [see Use in Specific Populations (8.1)] .
7.2 Effects of Valproate On Other Drugs
Valproate has been found to be a weak inhibitor of some P450 isozymes, epoxide hydrase, and glucuronosyltransferases.
The following list provides information about the potential for an influence of valproate co-administration on the pharmacokinetics or pharmacodynamics of several commonly prescribed medications. The list is not exhaustive, since new interactions are continuously being reported.
2.3 Dosing in Patients Taking Rufinamide
Patients stabilized on rufinamide before being prescribed valproate should begin valproate therapy at a low dose and titrate to a clinically effective dose [see Drug Interactions (7.2)] .
5.15 Monitoring: Drug Plasma Concentration
Since valproate may interact with concurrently administered drugs which are capable of enzyme induction, periodic plasma concentration determinations of valproate and concomitant drugs are recommended during the early course of therapy [see Drug Interactions (7)] .
5.4 Use in Women of Childbearing Potential
Because of the risk to the fetus of decreased IQ, neurodevelopmental disorders, and major congenital malformations (including neural tube defects), which may occur very early in pregnancy, valproate should not be administered to a woman of childbearing potential unless other medications have failed to provide adequate symptom control or are otherwise unacceptable. This is especially important when valproate use is considered for a condition not usually associated with permanent injury or death such as prophylaxis of migraine headaches [see Contraindications (4)] . Women should use effective contraception while using valproate.
Women of childbearing potential should be counseled regularly regarding the relative risks and benefits of valproate use during pregnancy. This is especially important for women planning a pregnancy and for girls at the onset of puberty; alternative therapeutic options should be considered for these patients [see Boxed Warningand Use in Specific Populations (8.1)].
To prevent major seizures, valproate should not be discontinued abruptly, as this can precipitate status epilepticus with resulting maternal and fetal hypoxia and threat to life.
Evidence suggests that folic acid supplementation prior to conception and during the first trimester of pregnancy decreases the risk for congenital neural tube defects in the general population. It is not known whether the risk of neural tube defects or decreased IQ in the offspring of women receiving valproate is reduced by folic acid supplementation. Dietary folic acid supplementation both prior to conception and during pregnancy should be routinely recommended for patients using valproate.
Warning: Life Threatening Adverse Reactions
WARNING: LIFE THREATENING ADVERSE REACTIONS
See full prescribing information for complete boxed warning.
- Hepatotoxicity, including fatalities, usually during the first 6 months of treatment. Children under the age of two years and patients with mitochondrial disorders are at higher risk. Monitor patients closely, and perform serum liver testing prior to therapy and at frequent intervals thereafter ( 5.1)
- Fetal Risk, particularly neural tube defects, other major malformations, and decreased IQ ( 5.2, 5.3, 5.4)
- Pancreatitis, including fatal hemorrhagic cases ( 5.5)
5.13 Interaction With Carbapenem Antibiotics
Carbapenem antibiotics (for example, ertapenem, imipenem, meropenem; this is not a complete list) may reduce serum valproate concentrations to subtherapeutic levels, resulting in loss of seizure control. Serum valproate concentrations should be monitored frequently after initiating carbapenem therapy. Alternative antibacterial or anticonvulsant therapy should be considered if serum valproate concentrations drop significantly or seizure control deteriorates [see Drug Interactions (7.1)] .
5.17 Effect On Hiv and Cmv Viruses Replication
There are in vitrostudies that suggest valproate stimulates the replication of the HIV and CMV viruses under certain experimental conditions. The clinical consequence, if any, is not known. Additionally, the relevance of these in vitrofindings is uncertain for patients receiving maximally suppressive antiretroviral therapy. Nevertheless, these data should be borne in mind when interpreting the results from regular monitoring of the viral load in HIV infected patients receiving valproate or when following CMV infected patients clinically.
5.8 Bleeding and Other Hematopoietic Disorders
Valproate is associated with dose-related thrombocytopenia. In a clinical trial of divalproex sodium as monotherapy in patients with epilepsy, 34/126 patients (27%) receiving approximately 50 mg/kg/day on average, had at least one value of platelets ≤ 75 × 10 9/L. Approximately half of these patients had treatment discontinued, with return of platelet counts to normal. In the remaining patients, platelet counts normalized with continued treatment. In this study, the probability of thrombocytopenia appeared to increase significantly at total valproate concentrations of ≥110 mcg/mL (females) or ≥ 135 mcg/mL (males). The therapeutic benefit which may accompany the higher doses should therefore be weighed against the possibility of a greater incidence of adverse effects. Valproate use has also been associated with decreases in other cell lines and myelodysplasia.
Because of reports of cytopenias, inhibition of the secondary phase of platelet aggregation, and abnormal coagulation parameters, (e.g., low fibrinogen, coagulation factor deficiencies, acquired von Willebrand's disease), measurements of complete blood counts and coagulation tests are recommended before initiating therapy and at periodic intervals. It is recommended that patients receiving valproic acid be monitored for blood counts and coagulation parameters prior to planned surgery and during pregnancy [see Use in Specific Populations (8.1)] . Evidence of hemorrhage, bruising, or a disorder of hemostasis/coagulation is an indication for reduction of the dosage or withdrawal of therapy.
5.16 Effect On Ketone and Thyroid Function Tests
Valproate is partially eliminated in the urine as a keto-metabolite which may lead to a false interpretation of the urine ketone test.
There have been reports of altered thyroid function tests associated with valproate. The clinical significance of these is unknown.
7.1 Effects of Co Administered Drugs On Valproate Clearance
Drugs that affect the level of expression of hepatic enzymes, particularly those that elevate levels of glucuronosyltransferases (such as ritonavir), may increase the clearance of valproate. For example, phenytoin, carbamazepine, and phenobarbital (or primidone) can double the clearance of valproate. Thus, patients on monotherapy will generally have longer half-lives and higher concentrations than patients receiving polytherapy with antiepilepsy drugs.
In contrast, drugs that are inhibitors of cytochrome P450 isozymes, e.g., antidepressants, may be expected to have little effect on valproate clearance because cytochrome P450 microsomal mediated oxidation is a relatively minor secondary metabolic pathway compared to glucuronidation and beta-oxidation.
Because of these changes in valproate clearance, monitoring of valproate and concomitant drug concentrations should be increased whenever enzyme inducing drugs are introduced or withdrawn.
The following list provides information about the potential for an influence of several commonly prescribed medications on valproate pharmacokinetics. The list is not exhaustive nor could it be, since new interactions are continuously being reported.
5.10 Hyperammonemia and Encephalopathy Associated With Concomitant Topiramate Use
Concomitant administration of topiramate and valproate has been associated with hyperammonemia with or without encephalopathy in patients who have tolerated either drug alone. Clinical symptoms of hyperammonemic encephalopathy often include acute alterations in level of consciousness and/or cognitive function with lethargy or vomiting. Hypothermia can also be a manifestation of hyperammonemia [see Warnings and Precautions (5.11)] . In most cases, symptoms and signs abated with discontinuation of either drug. This adverse reaction is not due to a pharmacokinetic interaction. Patients with inborn errors of metabolism or reduced hepatic mitochondrial activity may be at an increased risk for hyperammonemia with or without encephalopathy. Although not studied, an interaction of topiramate and valproate may exacerbate existing defects or unmask deficiencies in susceptible persons. In patients who develop unexplained lethargy, vomiting, or changes in mental status, hyperammonemic encephalopathy should be considered and an ammonia level should be measured [see Contraindications (4)and Warnings and Precautions (5.6, 5.9)] .
5.12 Drug Reaction With Eosinophilia and Systemic Symptoms (dress)/multiorgan Hypersensitivity Reactions
Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS), also known as Multiorgan Hypersensitivity, has been reported in patients taking valproate. DRESS may be fatal or life-threatening. DRESS typically, although not exclusively, presents with fever, rash, lymphadenopathy, and/or facial swelling, in association with other organ system involvement, such as hepatitis, nephritis, hematological abnormalities, myocarditis, or myositis sometimes resembling an acute viral infection. Eosinophilia is often present. Because this disorder is variable in its expression, other organ systems not noted here may be involved. It is important to note that early manifestations of hypersensitivity, such as fever or lymphadenopathy, may be present even though rash is not evident. If such signs or symptoms are present, the patient should be evaluated immediately. Valproate should be discontinued and not be resumed if an alternative etiology for the signs or symptoms cannot be established.
Structured Label Content
Dosage Forms and Strengths (34069-5)
Valproic Acid Oral Solution USP is available as a red, cherry flavored oral solution containing the equivalent of 250 mg valproic acid per 5 mL as the sodium salt and supplied in the following oral dosage forms:
NDC: 70518-3805-00
NDC: 70518-3805-01
NDC: 70518-3805-02
NDC: 70518-3805-03
PACKAGING: 10 in 1 BOX
PACKAGING: 5 mL in 1 CUP, UNIT DOSE
PACKAGING: 10 in 1 BOX
PACKAGING: 10 mL in 1 CUP, UNIT DOSE
STORAGE
Store at 20° to 25°C (68° to 77°F). [See USP Controlled Room Temperature].
Repackaged and Distributed By:
Remedy Repack, Inc.
625 Kolter Dr. Suite #4 Indiana, PA 1-724-465-8762
Section 42229-5 (42229-5)
Hepatotoxicity
Section 51945-4 (51945-4)
DRUG: VALPROIC ACID
GENERIC: VALPROIC ACID
DOSAGE: SOLUTION
ADMINSTRATION: ORAL
NDC: 70518-3805-0
NDC: 70518-3805-1
NDC: 70518-3805-2
NDC: 70518-3805-3
COLOR: red
FLAVOR: CHERRY
OUTER PACKAGING: 10 in 1 BOX
PACKAGING: 5 mL in 1 CUP, UNIT-DOSE
OUTER PACKAGING: 10 in 1 BOX
PACKAGING: 10 mL in 1 CUP, UNIT DOSE
ACTIVE INGREDIENT(S):
- VALPROIC ACID 250mg in 5mL
INACTIVE INGREDIENT(S):
- FD&C RED NO. 40
- METHYLPARABEN
- GLYCERIN
- SODIUM HYDROXIDE
- SORBITOL
- SUCROSE
- ANHYDROUS CITRIC ACID
- WATER
6.2 Mania
Although valproic acid has not been evaluated for safety and efficacy in the treatment of manic episodes associated with bipolar disorder, the following adverse reactions not listed above were reported by 1% or more of patients from two placebo-controlled clinical trials of divalproex sodium tablets.
Body as a Whole: Chills, neck pain, neck rigidity.
Cardiovascular System: Hypotension, postural hypotension, vasodilation.
Digestive System: Fecal incontinence, gastroenteritis, glossitis.
Musculoskeletal System: Arthrosis.
Nervous System: Agitation, catatonic reaction, hypokinesia, reflexes increased, tardive dyskinesia, vertigo.
Skin and Appendages: Furunculosis, maculopapular rash, seborrhea.
Special Senses: Conjunctivitis, dry eyes, eye pain.
Urogenital System: Dysuria.
1.1 Epilepsy
Valproic acid is indicated as monotherapy and adjunctive therapy in the treatment of patients with complex partial seizures that occur either in isolation or in association with other types of seizures. Valproic acid is indicated for use as sole and adjunctive therapy in the treatment of simple and complex absence seizures, and adjunctively in patients with multiple seizure types which include absence seizures.
Simple absence is defined as very brief clouding of the sensorium or loss of consciousness accompanied by certain generalized epileptic discharges without other detectable clinical signs. Complex absence is the term used when other signs are also present.
See Warnings and Precautions (5.1) for statement regarding fatal hepatic dysfunction.
2.1 Epilepsy
Valproic acid is intended for oral administration.
Patients should be informed to take valproic acid every day as prescribed. If a dose is missed it should be taken as soon as possible, unless it is almost time for the next dose. If a dose is skipped, the patient should not double the next dose.
Valproic acid is indicated as monotherapy and adjunctive therapy in complex partial seizures in adults and pediatric patients down to the age of 10 years, and in simple and complex absence seizures. As the valproic acid dosage is titrated upward, concentrations of clonazepam, diazepam, ethosuximide, lamotrigine, tolbutamide, phenobarbital, carbamazepine, and/or phenytoin may be affected [see Drug Interactions (7.2)] .
6.1 Epilepsy
The data described in the following section were obtained using divalproex sodium tablets.
Based on a placebo-controlled trial of adjunctive therapy for treatment of complex partial seizures, divalproex sodium was generally well tolerated with most adverse reactions rated as mild to moderate in severity. Intolerance was the primary reason for discontinuation in the divalproex sodium treated patients (6%), compared to 1% of placebo-treated patients.
Table 3 lists treatment-emergent adverse reactions which were reported by ≥ 5% of divalproex sodium-treated patients and for which the incidence was greater than in the placebo group, in a placebo-controlled trial of adjunctive therapy for treatment of complex partial seizures. Since patients were also treated with other antiepilepsy drugs, it is not possible, in most cases, to determine whether the following adverse reactions can be ascribed to divalproex sodium alone, or the combination of divalproex sodium and other antiepilepsy drugs.
| Body System/Reaction | Divalproex Sodium
(n = 77) % |
Placebo
(n = 70) % |
|---|---|---|
| Body as a Whole | ||
| Headache | 31 | 21 |
| Asthenia | 27 | 7 |
| Fever | 6 | 4 |
| Gastrointestinal System | ||
| Nausea | 48 | 14 |
| Vomiting | 27 | 7 |
| Abdominal Pain | 23 | 6 |
| Diarrhea | 13 | 6 |
| Anorexia | 12 | 0 |
| Dyspepsia | 8 | 4 |
| Constipation | 5 | 1 |
| Nervous System | ||
| Somnolence | 27 | 11 |
| Tremor | 25 | 6 |
| Dizziness | 25 | 13 |
| Diplopia | 16 | 9 |
| Amblyopia/Blurred Vision | 12 | 9 |
| Ataxia | 8 | 1 |
| Nystagmus | 8 | 1 |
| Emotional Lability | 6 | 4 |
| Thinking Abnormal | 6 | 0 |
| Amnesia | 5 | 1 |
| Respiratory System | ||
| Flu Syndrome | 12 | 9 |
| Infection | 12 | 6 |
| Bronchitis | 5 | 1 |
| Rhinitis | 5 | 4 |
| Other | ||
| Alopecia | 6 | 1 |
| Weight Loss | 6 | 0 |
Table 4 lists treatment-emergent adverse reactions which were reported by ≥ 5% of patients in the high dose divalproex sodium group, and for which the incidence was greater than in the low dose group, in a controlled trial of divalproex sodium monotherapy treatment of complex partial seizures. Since patients were being titrated off another antiepilepsy drug during the first portion of the trial, it is not possible, in many cases, to determine whether the following adverse reactions can be ascribed to divalproex sodium alone, or the combination of divalproex sodium and other antiepilepsy drugs.
| Body System/Reaction | High Dose
(n = 131) % |
Low Dose
(n = 134) % |
|---|---|---|
| Body as a Whole | ||
| Asthenia | 21 | 10 |
| Digestive System | ||
| Nausea | 34 | 26 |
| Diarrhea | 23 | 19 |
| Vomiting | 23 | 15 |
| Abdominal Pain | 12 | 9 |
| Anorexia | 11 | 4 |
| Dyspepsia | 11 | 10 |
| Hemic/Lymphatic System | ||
| Thrombocytopenia | 24 | 1 |
| Ecchymosis | 5 | 4 |
| Metabolic/Nutritional | ||
| Weight Gain | 9 | 4 |
| Peripheral Edema | 8 | 3 |
| Nervous System | ||
| Tremor | 57 | 19 |
| Somnolence | 30 | 18 |
| Dizziness | 18 | 13 |
| Insomnia | 15 | 9 |
| Nervousness | 11 | 7 |
| Amnesia | 7 | 4 |
| Nystagmus | 7 | 1 |
| Depression | 5 | 4 |
| Respiratory System | ||
| Infection | 20 | 13 |
| Pharyngitis | 8 | 2 |
| Dyspnea | 5 | 1 |
| Skin and Appendages | ||
| Alopecia | 24 | 13 |
| Special Senses | ||
| Amblyopia/Blurred Vision | 8 | 4 |
| Tinnitus | 7 | 1 |
| 1 Headache was the only adverse reaction that occurred in ≥ 5% of patients in the high dose group and at an equal or greater incidence in the low dose group. |
The following additional adverse reactions were reported by greater than 1% but less than 5% of the 358 patients treated with divalproex sodium in the controlled trials of complex partial seizures:
Body as a Whole: Back pain, chest pain, malaise.
Cardiovascular System: Tachycardia, hypertension, palpitation.
Digestive System: Increased appetite, flatulence, hematemesis, eructation, pancreatitis, periodontal abscess.
Hemic and Lymphatic System: Petechia.
Metabolic and Nutritional Disorders: SGOT increased, SGPT increased.
Musculoskeletal System: Myalgia, twitching, arthralgia, leg cramps, myasthenia.
Nervous System: Anxiety, confusion, abnormal gait, paresthesia, hypertonia, incoordination, abnormal dreams, personality disorder.
Respiratory System: Sinusitis, cough increased, pneumonia, epistaxis.
Skin and Appendages: Rash, pruritus, dry skin.
Special Senses: Taste perversion, abnormal vision, deafness, otitis media.
Urogenital System: Urinary incontinence, vaginitis, dysmenorrhea, amenorrhea, urinary frequency.
6.3 Migraine
Although valproic acid has not been evaluated for safety and efficacy in the prophylactic treatment of migraine headaches, the following adverse reactions not listed above were reported by 1% or more of patients from two placebo-controlled clinical trials of divalproex sodium tablets.
Body as a Whole: Face edema.
Digestive System: Dry mouth, stomatitis.
Urogenital System: Cystitis, metrorrhagia, and vaginal hemorrhage.
10 Overdosage (10 OVERDOSAGE)
Overdosage with valproate may result in somnolence, heart block, deep coma, and hypernatremia. Fatalities have been reported; however, patients have recovered from valproate levels as high as 2,120 mcg/mL.
In overdose situations, the fraction of drug not bound to protein is high and hemodialysis or tandem hemodialysis plus hemoperfusion may result in significant removal of drug. The benefit of gastric lavage or emesis will vary with the time since ingestion. General supportive measures should be applied with particular attention to the maintenance of adequate urinary output.
Naloxone has been reported to reverse the CNS depressant effects of valproate overdosage. Because naloxone could theoretically also reverse the antiepileptic effects of valproate, it should be used with caution in patients with epilepsy.
14.1 Epilepsy
The efficacy of divalproex sodium in reducing the incidence of complex partial seizures (CPS) that occur in isolation or in association with other seizure types was established in two controlled trials.
In one, multi-clinic, placebo-controlled study employing an add-on design (adjunctive therapy), 144 patients who continued to suffer eight or more CPS per 8 weeks during an 8 week period of monotherapy with doses of either carbamazepine or phenytoin sufficient to assure plasma concentrations within the "therapeutic range" were randomized to receive, in addition to their original antiepilepsy drug (AED), either divalproex sodium or placebo. Randomized patients were to be followed for a total of 16 weeks. The following table presents the findings.
| Add-on Treatment | Number of Patients | Baseline Incidence | Experimental Incidence |
|---|---|---|---|
| Divalproex sodium | 75 | 16.0 | 8.9 * |
| Placebo | 69 | 14.5 | 11.5 |
Figure 1 presents the proportion of patients (X axis) whose percentage reduction from baseline in complex partial seizure rates was at least as great as that indicated on the Y axis in the adjunctive therapy study. A positive percent reduction indicates an improvement (i.e., a decrease in seizure frequency), while a negative percent reduction indicates worsening. Thus, in a display of this type, the curve for an effective treatment is shifted to the left of the curve for placebo. This figure shows that the proportion of patients achieving any particular level of improvement was consistently higher for divalproex sodium than for placebo. For example, 45% of patients treated with divalproex sodium had a ≥ 50% reduction in complex partial seizure rate compared to 23% of patients treated with placebo.
Figure 1
The second study assessed the capacity of divalproex sodium to reduce the incidence of CPS when administered as the sole AED. The study compared the incidence of CPS among patients randomized to either a high or low dose treatment arm. Patients qualified for entry into the randomized comparison phase of this study only if 1) they continued to experience 2 or more CPS per 4 weeks during an 8 to 12 week long period of monotherapy with adequate doses of an AED (i.e., phenytoin, carbamazepine, phenobarbital, or primidone) and 2) they made a successful transition over a two week interval to divalproex sodium. Patients entering the randomized phase were then brought to their assigned target dose, gradually tapered off their concomitant AED and followed for an interval as long as 22 weeks. Less than 50% of the patients randomized, however, completed the study. In patients converted to divalproex sodium monotherapy, the mean total valproate concentrations during monotherapy were 71 and 123 mcg/mL in the low dose and high dose groups, respectively.
The following table presents the findings for all patients randomized who had at least one post-randomization assessment.
| Treatment | Number of Patients | Baseline Incidence | Randomized Phase Incidence |
|---|---|---|---|
| High dose divalproex sodium | 131 | 13.2 | 10.7 * |
| Low dose divalproex sodium | 134 | 14.2 | 13.8 |
Figure 2 presents the proportion of patients (X axis) whose percentage reduction from baseline in complex partial seizure rates was at least as great as that indicated on the Y axis in the monotherapy study. A positive percent reduction indicates an improvement (i.e., a decrease in seizure frequency), while a negative percent reduction indicates worsening. Thus, in a display of this type, the curve for a more effective treatment is shifted to the left of the curve for a less effective treatment. This figure shows that the proportion of patients achieving any particular level of reduction was consistently higher for high dose divalproex sodium than for low dose divalproex sodium. For example, when switching from carbamazepine, phenytoin, phenobarbital or primidone monotherapy to high dose divalproex sodium monotherapy, 63% of patients experienced no change or a reduction in complex partial seizure rates compared to 54% of patients receiving low dose divalproex sodium.
Figure 2
Information on pediatric studies is presented in section 8.
15 References (15 REFERENCES)
1. Meador KJ, Baker GA, Browning N, et al. Fetal antiepileptic drug exposure and cognitive outcomes at age 6 years (NEAD study): a prospective observational study. Lancet Neurology 2013; 12 (3):244-252.
11 Description (11 DESCRIPTION)
Valproic acid is a carboxylic acid designated as 2-propylpentanoic acid. It is also known as dipropylacetic acid. Valproic acid has the following structure:
Valproic acid (pKa 4.8) has a molecular weight of 144 and occurs as a colorless liquid with a characteristic odor. It is slightly soluble in water (1.3 mg/mL) and very soluble in organic solvents.
Valproic Acid Oral Solution USP is an antiepileptic for oral administration and contains the equivalent of 250 mg valproic acid per 5 mL as the sodium salt.
7.3 Topiramate
Concomitant administration of valproate and topiramate has been associated with hyperammonemia with and without encephalopathy [see Contraindications (4)and Warnings and Precautions (5.6, 5.9, 5.10)] . Concomitant administration of topiramate with valproate has also been associated with hypothermia in patients who have tolerated either drug alone. It may be prudent to examine blood ammonia levels in patients in whom the onset of hypothermia has been reported [see Warnings and Precautions (5.9, 5.11)] .
5.11 Hypothermia
Hypothermia, defined as an unintentional drop in body core temperature to <35°C (95°F), has been reported in association with valproate therapy both in conjunction with and in the absence of hyperammonemia. This adverse reaction can also occur in patients using concomitant topiramate with valproate after starting topiramate treatment or after increasing the daily dose of topiramate [see Drug Interactions (7.3)] . Consideration should be given to stopping valproate in patients who develop hypothermia, which may be manifested by a variety of clinical abnormalities including lethargy, confusion, coma, and significant alterations in other major organ systems such as the cardiovascular and respiratory systems. Clinical management and assessment should include examination of blood ammonia levels.
5.5 Pancreatitis
Cases of life-threatening pancreatitis have been reported in both children and adults receiving valproate. Some of the cases have been described as hemorrhagic with rapid progression from initial symptoms to death. Some cases have occurred shortly after initial use as well as after several years of use. The rate based upon the reported cases exceeds that expected in the general population and there have been cases in which pancreatitis recurred after rechallenge with valproate. In clinical trials, there were 2 cases of pancreatitis without alternative etiology in 2,416 patients, representing 1,044 patient-years experience. Patients and guardians should be warned that abdominal pain, nausea, vomiting, and/or anorexia can be symptoms of pancreatitis that require prompt medical evaluation. If pancreatitis is diagnosed, valproic acid should ordinarily be discontinued. Alternative treatment for the underlying medical condition should be initiated as clinically indicated [see Boxed Warning] .
Medication Guide (MEDICATION GUIDE)
VALPROIC ACID ORAL SOLUTION USP
(VAL-pro-IC)
Read this Medication Guide before you start taking valproic acid and each time you get a refill. There may be new information. This information does not take the place of talking to your healthcare provider about your medical condition or treatment.
What is the most important information I should know about valproic acid?
Do not stop taking valproic acid without first talking to your healthcare provider.
Stopping valproic acid suddenly can cause serious problems.
Valproic acid can cause serious side effects, including:
1. Serious liver damage that can cause death, especially in children younger than 2 years old.
The risk of getting this serious liver damage is more likely to happen within the first 6 months of treatment.
Call your healthcare provider right away if you get any of the following symptoms: In some cases, liver damage may continue despite stopping the drug.
- nausea or vomiting that does not go away
- loss of appetite
- pain on the right side of your stomach (abdomen)
- dark urine
- swelling of your face
- yellowing of your skin or the whites of your eyes
2. Valproic acid may harm your unborn baby.
- If you take valproic acid during pregnancy for any medical condition, your baby is at risk for serious birth defects that affect the brain and spinal cord and are called spina bifida or neural tube defects. These defects occur in 1 to 2 out of every 100 babies born to mothers who use this medicine during pregnancy. These defects can begin in the first month, even before you know you are pregnant. Other birth defects that affect the structures of the heart, head, arms, legs, and the opening where the urine comes out (urethra) on the bottom of the penis can also happen. Decreased hearing or hearing loss can also happen.
- Birth defects may occur even in children born to women who are not taking any medicines and do not have other risk factors.
- Taking folic acid supplements before getting pregnant and during early pregnancy can lower the chance of having a baby with a neural tube defect.
- If you take valproic acid during pregnancy for any medical condition, your child is at risk for having lower IQ and may be at risk for developing autism or attention deficit/hyperactivity disorder.
- There may be other medicines to treat your condition that have a lower chance of causing birth defects, decreased IQ, or other disorders in your child.
- Women who are pregnant must not take valproic acid to prevent migraine headaches.
- All women of childbearing age (including girls from the start of puberty) should talk to their healthcare provider about using other possible treatments instead of valproic acid. If the decision is made to use valproic acid, you should use effective birth control (contraception).
- Tell your healthcare provider right away if you become pregnant while taking valproic acid. You and your healthcare provider should decide if you will continue to take valproic acid while you are pregnant.
- Pregnancy Registry: If you become pregnant while taking valproic acid, talk to your healthcare provider about registering with the North American Antiepileptic Drug Pregnancy Registry. You can enroll in this registry by calling toll-free 1-888-233-2334 or by visiting the website, http://www.aedpregnancyregistry.org/. The purpose of this registry is to collect information about the safety of antiepileptic drugs during pregnancy.
3. Inflammation of your pancreas that can cause death.
Call your healthcare provider right away if you have any of these symptoms:
- severe stomach pain that you may also feel in your back
- nausea or vomiting that does not go away
4. Like other antiepileptic drugs, valproic acid may cause suicidal thoughts or actions in a very small number of people, about 1 in 500.
Call a healthcare provider right away if you have any of these symptoms, especially if they are new, worse, or worry you:
- thoughts about suicide or dying
- attempts to commit suicide
- new or worse depression
- new or worse anxiety
- feeling agitated or restless
- panic attacks
- trouble sleeping (insomnia)
- new or worse irritability
- acting aggressive, being angry, or violent
- acting on dangerous impulses
- an extreme increase in activity and talking (mania)
- other unusual changes in behavior or mood
How can I watch for early symptoms of suicidal thoughts and actions?
- Pay attention to any changes, especially sudden changes in mood, behaviors, thoughts, or feelings.
- Keep all follow-up visits with your healthcare provider as scheduled.
Call your healthcare provider between visits as needed, especially if you are worried about symptoms.
Do not stop valproic acid without first talking to a healthcare provider.Stopping valproic acid suddenly can cause serious problems. Stopping a seizure medicine suddenly in a patient who has epilepsy can cause seizures that will not stop (status epilepticus).
Suicidal thoughts or actions can be caused by things other than medicines. If you have suicidal thoughts or actions, your healthcare provider may check for other causes.
What is valproic acid?
Valproic acid is a prescription medicine used alone or with other medicines, to treat:
- complex partial seizures in adults and children 10 years of age and older
- simple and complex absence seizures, with or without other seizure types
Who should not take valproic acid?
Do not take valproic acid if you:
- have liver problems
- have or think you have a genetic liver problem caused by a mitochondrial disorder (e.g., Alpers-Huttenlocher syndrome)
- are allergic to divalproex sodium, valproic acid, sodium valproate, or any of the ingredients in valproic acid. See the end of this leaflet for a complete list of ingredients in valproic acid.
- have a genetic problem called urea cycle disorder
- are taking it to prevent migraine headaches and are either pregnant or may become pregnant because you are not using effective birth control (contraception)
What should I tell my healthcare provider before taking valproic acid?
Before you take valproic acid, tell your healthcare provider if you:
- have a genetic liver problem caused by a mitochondrial disorder (e.g., Alpers-Huttenlocher syndrome)
- drink alcohol
- are pregnant or breastfeeding. Valproic acid can pass into breast milk. Talk to your healthcare provider about the best way to feed your baby if you take valproic acid.
- have or have had depression, mood problems, or suicidal thoughts or behavior
- have any other medical conditions
Tell your healthcare provider about all the medicines you take,including prescription and non-prescription medicines, vitamins, herbal supplements and medicines that you take for a short period of time.
Taking valproic acid with certain other medicines can cause side effects or affect how well they work. Do not start or stop other medicines without talking to your healthcare provider.
Know the medicines you take. Keep a list of them and show it to your healthcare provider and pharmacist each time you get a new medicine.
How should I take valproic acid?
- Take valproic acid exactly as your healthcare provider tells you. Your healthcare provider will tell you how much valproic acid to take and when to take it.
- Your healthcare provider may change your dose.
- Do not change your dose of valproic acid without talking to your healthcare provider.
- Do not stop taking valproic acid without first talking to your healthcare provider. Stopping valproic acid suddenly can cause serious problems.
- If you take too much valproic acid, call your healthcare provider or local Poison Control Center right away.
What should I avoid while taking valproic acid?
- Valproic acid can cause drowsiness and dizziness. Do not drink alcohol or take other medicines that make you sleepy or dizzy while taking valproic acid, until you talk with your doctor. Taking valproic acid with alcohol or drugs that cause sleepiness or dizziness may make your sleepiness or dizziness worse.
- Do not drive a car or operate dangerous machinery until you know how valproic acid affects you. Valproic acid can slow your thinking and motor skills.
What are the possible side effects of valproic acid?
- See "What is the most important information I should know about valproic acid?"
Valproic acid can cause serious side effects including:
- Bleeding problems:red or purple spots on your skin, bruising, pain and swelling into your joints due to bleeding or bleeding from your mouth or nose.
- High ammonia levels in your blood:feeling tired, vomiting, changes in mental status.
- Low body temperature (hypothermia):drop in your body temperature to less than 95°F, feeling tired, confusion, coma.
- Allergic (hypersensitivity) reactions:fever, skin rash, hives, sores in your mouth, blistering and peeling of your skin, swelling of your lymph nodes, swelling of your face, eyes, lips, tongue, or throat, trouble swallowing or breathing.
- Drowsiness or sleepiness in the elderly.This extreme drowsiness may cause you to eat or drink less than you normally would. Tell your doctor if you are not able to eat or drink as you normally do. Your doctor may start you at a lower dose of valproic acid.
Call your healthcare provider right away, if you have any of the symptoms listed above.
The common side effects of valproic acid include:
- nausea
- headache
- sleepiness
- vomiting
- weakness
- tremor
- dizziness
- stomach pain
- blurry vision
- double vision
- diarrhea
- increased appetite
- weight gain
- hair loss
- loss of appetite
- problems with walking or coordination
These are not all of the possible side effects of valproic acid. For more information, ask your healthcare provider or pharmacist.
Tell your healthcare provider if you have any side effect that bothers you or that does not go away.
Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.
How should I store Valproic Acid Oral Solution USP?
- Store at 20° to 25°C (68° to 77°F). [See USP Controlled Room Temperature].
Keep valproic acid and all medicines out of the reach of children.
General information about the safe and effective use of valproic acid.
Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not use valproic acid for a condition for which it was not prescribed. Do not give valproic acid to other people, even if they have the same symptoms that you have. It may harm them.
This Medication Guide summarizes the most important information about valproic acid. If you would like more information, talk with your healthcare provider. You can ask your pharmacist or healthcare provider for information about valproic acid that is written for health professionals.
For more information, call Pharmaceutical Associates, Inc. at 1-800-845-8210 or visit www.paipharma.com.
What are the ingredients in Valproic Acid Oral Solution USP?
Active ingredient: valproic acid
Inactive ingredients: cherry flavor, FD&C Red No. 40, glycerin, methylparaben, purified water, sodium hydroxide, sorbitol and sucrose. May also contain citric acid and sodium hydroxide to adjust pH.
This Medication Guide has been approved by the U.S. Food and Drug Administration.
Repackaged By / Distributed By: RemedyRepack Inc.
625 Kolter Drive, Indiana, PA 15701
(724) 465-8762
8.4 Pediatric Use
Experience has indicated that pediatric patients under the age of two years are at a considerably increased risk of developing fatal hepatotoxicity, especially those with the aforementioned conditions [see Boxed Warning] . When valproic acid is used in this patient group, it should be used with extreme caution and as a sole agent. The benefits of therapy should be weighed against the risks. Above the age of 2 years, experience in epilepsy has indicated that the incidence of fatal hepatotoxicity decreases considerably in progressively older patient groups.
Younger children, especially those receiving enzyme-inducing drugs, will require larger maintenance doses to attain targeted total and unbound valproate concentrations. Pediatric patients (i.e., between 3 months and 10 years) have 50% higher clearances expressed on weight (i.e., mL/min/kg) than do adults. Over the age of 10 years, children have pharmacokinetic parameters that approximate those of adults.
The variability in free fraction limits the clinical usefulness of monitoring total serum valproic acid concentrations. Interpretation of valproic acid concentrations in children should include consideration of factors that affect hepatic metabolism and protein binding.
8.5 Geriatric Use
No patients above the age of 65 years were enrolled in double-blind prospective clinical trials of mania associated with bipolar illness. In a case review study of 583 patients, 72 patients (12%) were greater than 65 years of age. A higher percentage of patients above 65 years of age reported accidental injury, infection, pain, somnolence, and tremor.
Discontinuation of valproate was occasionally associated with the latter two events. It is not clear whether these events indicate additional risk or whether they result from preexisting medical illness and concomitant medication use among these patients.
A study of elderly patients with dementia revealed drug related somnolence and discontinuation for somnolence [see Warnings and Precautions (5.14)] . The starting dose should be reduced in these patients, and dosage reductions or discontinuation should be considered in patients with excessive somnolence [see Dosage and Administration (2.2)] .
5.9 Hyperammonemia
Hyperammonemia has been reported in association with valproate therapy and may be present despite normal liver function tests. In patients who develop unexplained lethargy and vomiting or changes in mental status, hyperammonemic encephalopathy should be considered and an ammonia level should be measured. Hyperammonemia should also be considered in patients who present with hypothermia [see Warnings and Precautions (5.11)] . If ammonia is increased, valproate therapy should be discontinued. Appropriate interventions for treatment of hyperammonemia should be initiated, and such patients should undergo investigation for underlying urea cycle disorders [see Contraindications (4)and Warnings and Precautions (5.6, 5.10)] .
Asymptomatic elevations of ammonia are more common and when present, require close monitoring of plasma ammonia levels. If the elevation persists, discontinuation of valproate therapy should be considered.
14 Clinical Studies (14 CLINICAL STUDIES)
The studies described in the following section were conducted using divalproex sodium tablets.
4 Contraindications (4 CONTRAINDICATIONS)
- Valproic acid should not be administered to patients with hepatic disease or significant hepatic dysfunction [see Warnings and Precautions (5.1)] .
- Valproic acid is contraindicated in patients known to have mitochondrial disorders caused by mutations in mitochondrial DNA polymerase γ (POLG; e.g., Alpers-Huttenlocher Syndrome) and children under two years of age who are suspected of having a POLG-related disorder [see Warnings and Precautions (5.1)] .
- Valproic acid is contraindicated in patients with known hypersensitivity to the drug [see Warnings and Precautions (5.12)] .
- Valproic acid is contraindicated in patients with known urea cycle disorders [see Warnings and Precautions (5.6)] .
- For use in prophylaxis of migraine headaches: Valproic acid is contraindicated in women who are pregnant and in women of childbearing potential who are not using effective contraception [see Warnings and Precautions (5.2, 5.3, 5.4)and Use in Specific Populations (8.1)] .
6 Adverse Reactions (6 ADVERSE REACTIONS)
The following serious adverse reactions are described below and elsewhere in the labeling:
- Hepatic failure [see Warnings and Precautions (5.1)]
- Birth defects [see Warnings and Precautions (5.2)]
- Decreased IQ following in uteroexposure [see Warnings and Precautions (5.3)]
- Pancreatitis [see Warnings and Precautions (5.5)]
- Hyperammonemic encephalopathy [see Warnings and Precautions (5.6, 5.9, 5.10)]
- Suicidal behavior and ideation [see Warnings and Precautions (5.7)]
- Bleeding and other hematopoietic disorders [see Warnings and Precautions (5.8)]
- Hypothermia [see Warnings and Precautions (5.11)]
- Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS)/Multiorgan hypersensitivity reactions [see Warnings and Precautions (5.12)]
- Somnolence in the elderly [see Warnings and Precautions (5.14)]
Because clinical studies are conducted under widely varying conditions, adverse reaction rates observed in the clinical studies of a drug cannot be directly compared to rates in the clinical studies of another drug and may not reflect the rates observed in practice.
7 Drug Interactions (7 DRUG INTERACTIONS)
- Hepatic enzyme-inducing drugs (e.g., phenytoin, carbamazepine, phenobarbital, primidone, rifampin) can increase valproate clearance, while enzyme inhibitors (e.g., felbamate) can decrease valproate clearance. Therefore increased monitoring of valproate and concomitant drug concentrations and dosage adjustment are indicated whenever enzyme-inducing or inhibiting drugs are introduced or withdrawn ( 7.1)
- Aspirin, carbapenem antibiotics, estrogen-containing hormonal contraceptives: Monitoring of valproate concentrations is recommended ( 7.1)
- Co-administration of valproate can affect the pharmacokinetics of other drugs (e.g., diazepam, ethosuximide, lamotrigine, phenytoin) by inhibiting their metabolism or protein binding displacement ( 7.2)
- Patients stabilized on rufinamide should begin valproate therapy at a low dose, and titrate to clinically effective dose ( 7.2)
- Dosage adjustment of amitriptyline/nortriptyline, propofol, warfarin, and zidovudine may be necessary if used concomitantly with Valproic acid ( 7.2)
- Topiramate: Hyperammonemia and encephalopathy ( 5.10, 7.3)
12.2 Pharmacodynamics
The relationship between plasma concentration and clinical response is not well documented. One contributing factor is the nonlinear, concentration dependent protein binding of valproate which affects the clearance of the drug. Thus, monitoring of total serum valproate cannot provide a reliable index of the bioactive valproate species.
For example, because the plasma protein binding of valproate is concentration dependent, the free fraction increases from approximately 10% at 40 mcg/mL to 18.5% at 130 mcg/mL. Higher than expected free fractions occur in the elderly, in hyperlipidemic patients, and in patients with hepatic and renal diseases.
1 Indications and Usage (1 INDICATIONS AND USAGE)
Valproic acid is indicated for:
- Monotherapy and adjunctive therapy of complex partial seizures; sole and adjunctive therapy of simple and complex absence seizures; adjunctive therapy in patients with multiple seizure types that include absence seizures ( 1)
12.1 Mechanism of Action
Valproic acid dissociates to the valproate ion in the gastrointestinal tract. The mechanisms by which valproate exerts its therapeutic effects have not been established. It has been suggested that its activity in epilepsy is related to increased brain concentrations of gamma-aminobutyric acid (GABA).
5.6 Urea Cycle Disorders
Valproic acid is contraindicated in patients with known urea cycle disorders (UCD).
Hyperammonemic encephalopathy, sometimes fatal, has been reported following initiation of valproate therapy in patients with urea cycle disorders, a group of uncommon genetic abnormalities, particularly ornithine transcarbamylase deficiency. Prior to the initiation of valproic acid therapy, evaluation for UCD should be considered in the following patients: 1) those with a history of unexplained encephalopathy or coma, encephalopathy associated with a protein load, pregnancy-related or postpartum encephalopathy, unexplained mental retardation, or history of elevated plasma ammonia or glutamine; 2) those with cyclical vomiting and lethargy, episodic extreme irritability, ataxia, low BUN, or protein avoidance; 3) those with a family history of UCD or a family history of unexplained infant deaths (particularly males); 4) those with other signs or symptoms of UCD. Patients who develop symptoms of unexplained hyperammonemic encephalopathy while receiving valproate therapy should receive prompt treatment (including discontinuation of valproate therapy) and be evaluated for underlying urea cycle disorders [see Contraindications (4)and Warnings and Precautions (5.10)] .
1.2 Important Limitations
Because of the risk to the fetus of decreased IQ, neurodevelopmental disorders, neural tube defects, and other major congenital malformations, which may occur very early in pregnancy, valproate should not be used to treat women with epilepsy or bipolar disorder who are pregnant or who plan to become pregnant unless other medications have failed to provide adequate symptom control or are otherwise unacceptable. Valproate should not be administered to a woman of childbearing potential unless other medications have failed to provide adequate symptom control or are otherwise unacceptable [see Warnings and Precautions (5.2, 5.3, 5.4), Use in Specific Populations (8.1), and Patient Counseling Information (17)] .
For prophylaxis of migraine headaches, valproate is contraindicated in women who are pregnant and in women of childbearing potential who are not using effective contraception [see Contraindications (4)].
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
- Hepatotoxicity; evaluate high risk populations and monitor serum liver tests ( 5.1)
- Birth defects, decreased IQ, and neurodevelopmental disorders following in uteroexposure; should not be used to treat women with epilepsy or bipolar disorder who are pregnant or who plan to become pregnant or to treat a woman of childbearing potential unless other medications have failed to provide adequate symptom control or are otherwise unacceptable ( 5.2, 5.3, 5.4)
- Pancreatitis; Valproic acid should ordinarily be discontinued ( 5.5)
- Suicidal behavior or ideation; Antiepileptic drugs, including valproic acid, increase the risk of suicidal thoughts or behavior ( 5.7)
- Bleeding and other hematopoietic disorders; monitor platelet counts and coagulation tests ( 5.8)
- Hyperammonemia and hyperammonemic encephalopathy; measure ammonia level if unexplained lethargy and vomiting or changes in mental status, and also with concomitant topiramate use; consider discontinuation of valproate therapy ( 5.6, 5.9, 5.10)
- Hypothermia; Hypothermia has been reported during valproate therapy with or without associated hyperammonemia. This adverse reaction can also occur in patients using concomitant topiramate ( 5.11)
- Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS)/Multiorgan hypersensitivity reaction; discontinue valproic acid ( 5.12)
- Somnolence in the elderly can occur. Valproic acid dosage should be increased slowly and with regular monitoring for fluid and nutritional intake ( 5.14)
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
Valproic Acid Oral Solution USP is available as a red, cherry flavored Oral Solution containing the equivalent of 250 mg valproic acid per 5 mL as the sodium salt.
5.2 Structural Birth Defects
Valproate can cause fetal harm when administered to a pregnant woman. Pregnancy registry data show that maternal valproate use can cause neural tube defects and other structural abnormalities (e.g., craniofacial defects, cardiovascular malformations, hypospadias, limb malformations). The rate of congenital malformations among babies born to mothers using valproate is about four times higher than the rate among babies born to epileptic mothers using other anti-seizure monotherapies. Evidence suggests that folic acid supplementation prior to conception and during the first trimester of pregnancy decreases the risk for congenital neural tube defects in the general population [see Use in Specific Populations (8.1)] .
6.4 Postmarketing Experience
The following adverse reactions have been identified during post approval use of divalproex sodium. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Dermatologic: Hair texture changes, hair color changes, photosensitivity, erythema multiforme, toxic epidermal necrolysis, nail and nail bed disorders, and Stevens-Johnson syndrome.
Psychiatric: Emotional upset, psychosis, aggression, psychomotor hyperactivity, hostility, disturbance in attention, learning disorder, and behavioral deterioration.
Neurologic: Paradoxical convulsion, parkinsonism
There have been several reports of acute or subacute cognitive decline and behavioral changes (apathy or irritability) with cerebral pseudoatrophy on imaging associated with valproate therapy; both the cognitive/behavioral changes and cerebral pseudoatrophy reversed partially or fully after valproate discontinuation.
There have been reports of acute or subacute encephalopathy in the absence of elevated ammonia levels, elevated valproate levels, or neuroimaging changes. The encephalopathy reversed partially or fully after valproate discontinuation.
Musculoskeletal: Fractures, decreased bone mineral density, osteopenia, osteoporosis, and weakness.
Hematologic: Relative lymphocytosis, macrocytosis, leukopenia, anemia including macrocytic with or without folate deficiency, bone marrow suppression, pancytopenia, aplastic anemia, agranulocytosis, and acute intermittent porphyria.
Endocrine: Irregular menses, secondary amenorrhea, hyperandrogenism, hirsutism, elevated testosterone level, breast enlargement, galactorrhea, parotid gland swelling, polycystic ovary disease, decreased carnitine concentrations, hyponatremia, hyperglycinemia, and inappropriate ADH secretion.
There have been rare reports of Fanconi's syndrome occurring chiefly in children.
Metabolism and nutrition: Weight gain.
Reproductive: Aspermia, azoospermia, decreased sperm count, decreased spermatozoa motility, male infertility, and abnormal spermatozoa morphology.
Genitourinary: Enuresis and urinary tract infection.
Special Senses: Hearing loss.
Other: Allergic reaction, anaphylaxis, developmental delay, bone pain, bradycardia, and cutaneous vasculitis.
8 Use in Specific Populations (8 USE IN SPECIFIC POPULATIONS)
- Pregnancy: Valproic acid can cause congenital malformations including neural tube defects, decreased IQ, and neurodevelopmental disorders ( 5.2, 5.3, 8.1)
- Pediatric: Children under the age of two years are at considerably higher risk of fatal hepatotoxicity ( 5.1, 8.4)
- Geriatric: Reduce starting dose; increase dosage more slowly; monitor fluid and nutritional intake, and somnolence ( 5.14, 8.5)
5.14 Somnolence in the Elderly
In a double-blind, multicenter trial of valproate in elderly patients with dementia (mean age = 83 years), doses were increased by 125 mg/day to a target dose of 20 mg/kg/day. A significantly higher proportion of valproate patients had somnolence compared to placebo, and although not statistically significant, there was a higher proportion of patients with dehydration. Discontinuations for somnolence were also significantly higher than with placebo. In some patients with somnolence (approximately one-half), there was associated reduced nutritional intake and weight loss. There was a trend for the patients who experienced these events to have a lower baseline albumin concentration, lower valproate clearance, and a higher BUN. In elderly patients, dosage should be increased more slowly and with regular monitoring for fluid and nutritional intake, dehydration, somnolence, and other adverse reactions. Dose reductions or discontinuation of valproate should be considered in patients with decreased food or fluid intake and in patients with excessive somnolence [see Dosage and Administration (2.2)] .
17 Patient Counseling Information (17 PATIENT COUNSELING INFORMATION)
Advise the patient to read the FDA-approved patient labeling (Medication Guide).
Repackaged By / Distributed By: RemedyRepack Inc.
625 Kolter Drive, Indiana, PA 15701
(724) 465-8762
5.7 Suicidal Behavior and Ideation
Antiepileptic drugs (AEDs), including valproic acid, increase the risk of suicidal thoughts or behavior in patients taking these drugs for any indication. Patients treated with any AED for any indication should be monitored for the emergence or worsening of depression, suicidal thoughts or behavior, and/or any unusual changes in mood or behavior.
Pooled analyses of 199 placebo-controlled clinical trials (mono- and adjunctive therapy) of 11 different AEDs showed that patients randomized to one of the AEDs had approximately twice the risk (adjusted Relative Risk 1.8, 95% CI:1.2, 2.7) of suicidal thinking or behavior compared to patients randomized to placebo. In these trials, which had a median treatment duration of 12 weeks, the estimated incidence rate of suicidal behavior or ideation among 27,863 AED-treated patients was 0.43%, compared to 0.24% among 16,029 placebo-treated patients, representing an increase of approximately one case of suicidal thinking or behavior for every 530 patients treated. There were four suicides in drug-treated patients in the trials and none in placebo-treated patients, but the number is too small to allow any conclusion about drug effect on suicide.
The increased risk of suicidal thoughts or behavior with AEDs was observed as early as one week after starting drug treatment with AEDs and persisted for the duration of treatment assessed. Because most trials included in the analysis did not extend beyond 24 weeks, the risk of suicidal thoughts or behavior beyond 24 weeks could not be assessed.
The risk of suicidal thoughts or behavior was generally consistent among drugs in the data analyzed. The finding of increased risk with AEDs of varying mechanisms of action and across a range of indications suggests that the risk applies to all AEDs used for any indication. The risk did not vary substantially by age (5-100 years) in the clinical trials analyzed.
Table 2 shows absolute and relative risk by indication for all evaluated AEDs.
| Indication | Placebo Patients with Events Per 1,000 Patients | Drug Patients with Events Per 1,000 Patients | Relative Risk: Incidence of Events in Drug Patients/Incidence in Placebo Patients | Risk Difference: Additional Drug Patients with Events Per 1,000 Patients |
|---|---|---|---|---|
| Epilepsy | 1.0 | 3.4 | 3.5 | 2.4 |
| Psychiatric | 5.7 | 8.5 | 1.5 | 2.9 |
| Other | 1.0 | 1.8 | 1.9 | 0.9 |
| Total | 2.4 | 4.3 | 1.8 | 1.9 |
The relative risk for suicidal thoughts or behavior was higher in clinical trials for epilepsy than in clinical trials for psychiatric or other conditions, but the absolute risk differences were similar for the epilepsy and psychiatric indications.
Anyone considering prescribing valproic acid or any other AED must balance the risk of suicidal thoughts or behavior with the risk of untreated illness. Epilepsy and many other illnesses for which AEDs are prescribed are themselves associated with morbidity and mortality and an increased risk of suicidal thoughts and behavior. Should suicidal thoughts and behavior emerge during treatment, the prescriber needs to consider whether the emergence of these symptoms in any given patient may be related to the illness being treated.
5.3 Decreased Iq Following in Utero (5.3 Decreased IQ Following in utero)
Valproate can cause decreased IQ scores following in uteroexposure. Published epidemiological studies have indicated that children exposed to valproate in uterohave lower cognitive test scores than children exposed in uteroto either another antiepileptic drug or to no antiepileptic drugs. The largest of these studies 1is a prospective cohort study conducted in the United States and United Kingdom that found that children with prenatal exposure to valproate (n=62) had lower IQ scores at age 6 (97 [95% C.I. 94-101]) than children with prenatal exposure to the other antiepileptic drug monotherapy treatments evaluated: lamotrigine (108 [95% C.I. 105-110]), carbamazepine (105 [95% C.I. 102-108]), and phenytoin (108 [95% C.I. 104-112]). It is not known when during pregnancy cognitive effects in valproate-exposed children occur. Because the women in this study were exposed to antiepileptic drugs throughout pregnancy, whether the risk for decreased IQ was related to a particular time period during pregnancy could not be assessed.
Although all of the available studies have methodological limitations, the weight of the evidence supports the conclusion that valproate exposure in uterocan cause decreased IQ in children.
In animal studies, offspring with prenatal exposure to valproate had malformations similar to those seen in humans and demonstrated neurobehavioral deficits [see Use in Specific Populations (8.1)] .
7.2 Effects of Valproate On Other Drugs (7.2 Effects of Valproate on Other Drugs)
Valproate has been found to be a weak inhibitor of some P450 isozymes, epoxide hydrase, and glucuronosyltransferases.
The following list provides information about the potential for an influence of valproate co-administration on the pharmacokinetics or pharmacodynamics of several commonly prescribed medications. The list is not exhaustive, since new interactions are continuously being reported.
2.3 Dosing in Patients Taking Rufinamide
Patients stabilized on rufinamide before being prescribed valproate should begin valproate therapy at a low dose and titrate to a clinically effective dose [see Drug Interactions (7.2)] .
5.15 Monitoring: Drug Plasma Concentration
Since valproate may interact with concurrently administered drugs which are capable of enzyme induction, periodic plasma concentration determinations of valproate and concomitant drugs are recommended during the early course of therapy [see Drug Interactions (7)] .
5.4 Use in Women of Childbearing Potential
Because of the risk to the fetus of decreased IQ, neurodevelopmental disorders, and major congenital malformations (including neural tube defects), which may occur very early in pregnancy, valproate should not be administered to a woman of childbearing potential unless other medications have failed to provide adequate symptom control or are otherwise unacceptable. This is especially important when valproate use is considered for a condition not usually associated with permanent injury or death such as prophylaxis of migraine headaches [see Contraindications (4)] . Women should use effective contraception while using valproate.
Women of childbearing potential should be counseled regularly regarding the relative risks and benefits of valproate use during pregnancy. This is especially important for women planning a pregnancy and for girls at the onset of puberty; alternative therapeutic options should be considered for these patients [see Boxed Warningand Use in Specific Populations (8.1)].
To prevent major seizures, valproate should not be discontinued abruptly, as this can precipitate status epilepticus with resulting maternal and fetal hypoxia and threat to life.
Evidence suggests that folic acid supplementation prior to conception and during the first trimester of pregnancy decreases the risk for congenital neural tube defects in the general population. It is not known whether the risk of neural tube defects or decreased IQ in the offspring of women receiving valproate is reduced by folic acid supplementation. Dietary folic acid supplementation both prior to conception and during pregnancy should be routinely recommended for patients using valproate.
Warning: Life Threatening Adverse Reactions (WARNING: LIFE THREATENING ADVERSE REACTIONS)
WARNING: LIFE THREATENING ADVERSE REACTIONS
See full prescribing information for complete boxed warning.
- Hepatotoxicity, including fatalities, usually during the first 6 months of treatment. Children under the age of two years and patients with mitochondrial disorders are at higher risk. Monitor patients closely, and perform serum liver testing prior to therapy and at frequent intervals thereafter ( 5.1)
- Fetal Risk, particularly neural tube defects, other major malformations, and decreased IQ ( 5.2, 5.3, 5.4)
- Pancreatitis, including fatal hemorrhagic cases ( 5.5)
5.13 Interaction With Carbapenem Antibiotics (5.13 Interaction with Carbapenem Antibiotics)
Carbapenem antibiotics (for example, ertapenem, imipenem, meropenem; this is not a complete list) may reduce serum valproate concentrations to subtherapeutic levels, resulting in loss of seizure control. Serum valproate concentrations should be monitored frequently after initiating carbapenem therapy. Alternative antibacterial or anticonvulsant therapy should be considered if serum valproate concentrations drop significantly or seizure control deteriorates [see Drug Interactions (7.1)] .
5.17 Effect On Hiv and Cmv Viruses Replication (5.17 Effect on HIV and CMV Viruses Replication)
There are in vitrostudies that suggest valproate stimulates the replication of the HIV and CMV viruses under certain experimental conditions. The clinical consequence, if any, is not known. Additionally, the relevance of these in vitrofindings is uncertain for patients receiving maximally suppressive antiretroviral therapy. Nevertheless, these data should be borne in mind when interpreting the results from regular monitoring of the viral load in HIV infected patients receiving valproate or when following CMV infected patients clinically.
5.8 Bleeding and Other Hematopoietic Disorders
Valproate is associated with dose-related thrombocytopenia. In a clinical trial of divalproex sodium as monotherapy in patients with epilepsy, 34/126 patients (27%) receiving approximately 50 mg/kg/day on average, had at least one value of platelets ≤ 75 × 10 9/L. Approximately half of these patients had treatment discontinued, with return of platelet counts to normal. In the remaining patients, platelet counts normalized with continued treatment. In this study, the probability of thrombocytopenia appeared to increase significantly at total valproate concentrations of ≥110 mcg/mL (females) or ≥ 135 mcg/mL (males). The therapeutic benefit which may accompany the higher doses should therefore be weighed against the possibility of a greater incidence of adverse effects. Valproate use has also been associated with decreases in other cell lines and myelodysplasia.
Because of reports of cytopenias, inhibition of the secondary phase of platelet aggregation, and abnormal coagulation parameters, (e.g., low fibrinogen, coagulation factor deficiencies, acquired von Willebrand's disease), measurements of complete blood counts and coagulation tests are recommended before initiating therapy and at periodic intervals. It is recommended that patients receiving valproic acid be monitored for blood counts and coagulation parameters prior to planned surgery and during pregnancy [see Use in Specific Populations (8.1)] . Evidence of hemorrhage, bruising, or a disorder of hemostasis/coagulation is an indication for reduction of the dosage or withdrawal of therapy.
5.16 Effect On Ketone and Thyroid Function Tests (5.16 Effect on Ketone and Thyroid Function Tests)
Valproate is partially eliminated in the urine as a keto-metabolite which may lead to a false interpretation of the urine ketone test.
There have been reports of altered thyroid function tests associated with valproate. The clinical significance of these is unknown.
7.1 Effects of Co Administered Drugs On Valproate Clearance (7.1 Effects of Co-Administered Drugs on Valproate Clearance)
Drugs that affect the level of expression of hepatic enzymes, particularly those that elevate levels of glucuronosyltransferases (such as ritonavir), may increase the clearance of valproate. For example, phenytoin, carbamazepine, and phenobarbital (or primidone) can double the clearance of valproate. Thus, patients on monotherapy will generally have longer half-lives and higher concentrations than patients receiving polytherapy with antiepilepsy drugs.
In contrast, drugs that are inhibitors of cytochrome P450 isozymes, e.g., antidepressants, may be expected to have little effect on valproate clearance because cytochrome P450 microsomal mediated oxidation is a relatively minor secondary metabolic pathway compared to glucuronidation and beta-oxidation.
Because of these changes in valproate clearance, monitoring of valproate and concomitant drug concentrations should be increased whenever enzyme inducing drugs are introduced or withdrawn.
The following list provides information about the potential for an influence of several commonly prescribed medications on valproate pharmacokinetics. The list is not exhaustive nor could it be, since new interactions are continuously being reported.
5.10 Hyperammonemia and Encephalopathy Associated With Concomitant Topiramate Use (5.10 Hyperammonemia and Encephalopathy Associated with Concomitant Topiramate Use)
Concomitant administration of topiramate and valproate has been associated with hyperammonemia with or without encephalopathy in patients who have tolerated either drug alone. Clinical symptoms of hyperammonemic encephalopathy often include acute alterations in level of consciousness and/or cognitive function with lethargy or vomiting. Hypothermia can also be a manifestation of hyperammonemia [see Warnings and Precautions (5.11)] . In most cases, symptoms and signs abated with discontinuation of either drug. This adverse reaction is not due to a pharmacokinetic interaction. Patients with inborn errors of metabolism or reduced hepatic mitochondrial activity may be at an increased risk for hyperammonemia with or without encephalopathy. Although not studied, an interaction of topiramate and valproate may exacerbate existing defects or unmask deficiencies in susceptible persons. In patients who develop unexplained lethargy, vomiting, or changes in mental status, hyperammonemic encephalopathy should be considered and an ammonia level should be measured [see Contraindications (4)and Warnings and Precautions (5.6, 5.9)] .
5.12 Drug Reaction With Eosinophilia and Systemic Symptoms (dress)/multiorgan Hypersensitivity Reactions (5.12 Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS)/Multiorgan Hypersensitivity Reactions)
Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS), also known as Multiorgan Hypersensitivity, has been reported in patients taking valproate. DRESS may be fatal or life-threatening. DRESS typically, although not exclusively, presents with fever, rash, lymphadenopathy, and/or facial swelling, in association with other organ system involvement, such as hepatitis, nephritis, hematological abnormalities, myocarditis, or myositis sometimes resembling an acute viral infection. Eosinophilia is often present. Because this disorder is variable in its expression, other organ systems not noted here may be involved. It is important to note that early manifestations of hypersensitivity, such as fever or lymphadenopathy, may be present even though rash is not evident. If such signs or symptoms are present, the patient should be evaluated immediately. Valproate should be discontinued and not be resumed if an alternative etiology for the signs or symptoms cannot be established.
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:48:34.215291 · Updated: 2026-03-14T22:30:18.174146