These Highlights Do Not Include All The Information Needed To Use Tirosint ®
5d378add-f13d-40f2-99dc-0f2340ab44b7
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
Thyroid hormones, including TIROSINT-SOL, either alone or with other therapeutic agents, should not be used for the treatment of obesity or for weight loss. In euthyroid patients, doses within the range of daily hormonal requirements are ineffective for weight reduction. Larger doses may produce serious or even life threatening manifestations of toxicity, particularly when given in association with sympathomimetic amines such as those used for their anorectic effects [see Adverse Reactions (6) , Drug Interactions (7.7) , and Overdosage (10) ].
Dosage and Administration
Administer once daily, on an empty stomach, 15 minutes before breakfast ( 2.1 ) Administer at least 4 hours before or after drugs that are known to interfere with absorption ( 2.1 ) Evaluate the need for dose adjustments when regularly administering within an hour of certain foods that may affect TIROSINT-SOL absorption ( 2.1 ) To administer TIROSINT-SOL in water, squeeze the contents of one single unit-dose ampule into a glass or cup containing water ( 2.1 ) To administer TIROSINT-SOL directly, either squeeze it into the mouth OR onto a spoon and immediately consume ( 2.1 ) Starting dose depends on a variety of factors, including age, body weight, cardiovascular status, and concomitant medications, co-administered food, and the specific nature of the condition being treated. Peak therapeutic effect may not be attained for 4-6 weeks ( 2.2 ) See full prescribing information for dosing in specific patient populations ( 2.3 ) Adequacy of therapy determined with periodic monitoring of TSH and/or T4 as well as clinical status ( 2.4 )
Warnings and Precautions
Serious risks related to overtreatment or undertreatment with TIROSINT-SOL: Titrate the dose of TIROSINT-SOL carefully and monitor response to titration. ( 5.1 ) Cardiac adverse reactions in the elderly and in patients with underlying cardiovascular disease : Initiate TIROSINT-SOL at less than the full replacement dose because of the increased risk of cardiac adverse reactions, including atrial fibrillation. ( 2.3 , 5.2 , 8.5 ) Myxedema coma: Do not use oral thyroid hormone drug products to treat myxedema coma. ( 5.3 ) Acute adrenal crisis in patients with concomitant adrenal insufficiency: Treat with replacement glucocorticoids prior to initiation of TIROSINT‑SOL treatment. ( 5.4 ) Worsening of diabetic control: therapy in patients with diabetes mellitus may worsen glycemic control and result in increased antidiabetic agent or insulin requirements. Carefully monitor glycemic control after starting, changing, or discontinuing thyroid hormone therapy. ( 5.5 ) Decreased bone mineral density associated with thyroid hormone over-replacement: Over-replacement can increase bone resorption and decrease bone mineral density. Give the lowest effective dose. 5.6 )
Contraindications
TIROSINT-SOL is contraindicated in patients with: Hypersensitivity to glycerol, the inactive ingredient in TIROSINT-SOL [see Adverse Events (6) ]. Uncorrected adrenal insufficiency [see Warnings and Precautions (5.4) ]
Adverse Reactions
Adverse reactions associated with TIROSINT-SOL therapy are primarily those of hyperthyroidism due to therapeutic overdosage [see Warnings and Precautions (5) and Overdosage (10) ]. They include the following: General: fatigue, increased appetite, weight loss, heat intolerance, fever, excessive sweating Central nervous system: headache, hyperactivity, nervousness, anxiety, irritability, emotional lability, insomnia Musculoskeletal: tremors, muscle weakness, muscle spasm Cardiovascular: palpitations, tachycardia, arrhythmias, increased pulse and blood pressure, heart failure, angina, myocardial infarction, cardiac arrest Respiratory : dyspnea Gastrointestinal (GI): diarrhea, vomiting, abdominal cramps, elevations in liver function tests Dermatologic: hair loss, flushing, rash Endocrine: decreased bone mineral density Reproductive: menstrual irregularities, impaired fertility Seizures have been reported rarely with the institution of levothyroxine therapy.
Drug Interactions
See full prescribing information for drugs that affect thyroid hormone pharmacokinetics and metabolism (e.g., absorption, synthesis, secretion, catabolism, protein binding, and target tissue response) and may alter the therapeutic response to TIROSINT-SOL ( 7 )
Storage and Handling
Store TIROSINT-SOL in the original container (closed pouch) at 20°C to 25°C (68°F to 77°F); excursions permitted to 15° to 30°C (59°F to 86°F) [See USP Controlled Room Temperature]. Use TIROSINT-SOL oral solution within three (3) months after opening the pouch. Keep the ampules in the pouch until ready to use as important information may be lost (i.e., manufacturer/distributor names and distributor contact phone number).
How Supplied
TIROSINT-SOL (levothyroxine sodium) oral solution is a clear, colorless to slightly yellow solution supplied in a 1 mL white, non-transparent, unit-dose ampule. The dosage strength is identified on the box and the pouch, and is associated with a distinct color. Each ampule bears a colored label with the dosage strength and the product name (TIROSINT-SOL) (Table 10). Table 10. TIROSINT-SOL Solution Strengths and Packaging Description Strength (mcg/mL) Color a Box NDC (30 Unit-Dose Ampules) Pouch NDC (5 Unit-Dose Ampules) 13 Green 71858-0105-5 71858-0105-4 25 Orange 71858-0110-5 71858-0110-4 37.5 Dark Blue 71858-0112-5 71858-0112-4 44 Red 71858-0113-5 71858-0113-4 50 White 71858-0115-5 71858-0115-4 62.5 Grey 71858-0117-5 71858-0117-4 75 Purple 71858-0120-5 71858-0120-4 88 Olive 71858-0125-5 71858-0125-4 100 Yellow 71858-0130-5 71858-0130-4 112 Rose 71858-0135-5 71858-0135-4 125 Brown 71858-0140-5 71858-0140-4 137 Turquoise 71858-0145-5 71858-0145-4 150 Blue 71858-0150-5 71858-0150-4 175 Lilac 71858-0155-5 71858-0155-4 200 Pink 71858-0160-5 71858-0160-4
Medication Information
Recent Major Changes
Warnings and Precautions
Serious risks related to overtreatment or undertreatment with TIROSINT-SOL: Titrate the dose of TIROSINT-SOL carefully and monitor response to titration. ( 5.1 ) Cardiac adverse reactions in the elderly and in patients with underlying cardiovascular disease : Initiate TIROSINT-SOL at less than the full replacement dose because of the increased risk of cardiac adverse reactions, including atrial fibrillation. ( 2.3 , 5.2 , 8.5 ) Myxedema coma: Do not use oral thyroid hormone drug products to treat myxedema coma. ( 5.3 ) Acute adrenal crisis in patients with concomitant adrenal insufficiency: Treat with replacement glucocorticoids prior to initiation of TIROSINT‑SOL treatment. ( 5.4 ) Worsening of diabetic control: therapy in patients with diabetes mellitus may worsen glycemic control and result in increased antidiabetic agent or insulin requirements. Carefully monitor glycemic control after starting, changing, or discontinuing thyroid hormone therapy. ( 5.5 ) Decreased bone mineral density associated with thyroid hormone over-replacement: Over-replacement can increase bone resorption and decrease bone mineral density. Give the lowest effective dose. 5.6 )
Dosage and Administration
Administer once daily, on an empty stomach, 15 minutes before breakfast ( 2.1 ) Administer at least 4 hours before or after drugs that are known to interfere with absorption ( 2.1 ) Evaluate the need for dose adjustments when regularly administering within an hour of certain foods that may affect TIROSINT-SOL absorption ( 2.1 ) To administer TIROSINT-SOL in water, squeeze the contents of one single unit-dose ampule into a glass or cup containing water ( 2.1 ) To administer TIROSINT-SOL directly, either squeeze it into the mouth OR onto a spoon and immediately consume ( 2.1 ) Starting dose depends on a variety of factors, including age, body weight, cardiovascular status, and concomitant medications, co-administered food, and the specific nature of the condition being treated. Peak therapeutic effect may not be attained for 4-6 weeks ( 2.2 ) See full prescribing information for dosing in specific patient populations ( 2.3 ) Adequacy of therapy determined with periodic monitoring of TSH and/or T4 as well as clinical status ( 2.4 )
Contraindications
TIROSINT-SOL is contraindicated in patients with: Hypersensitivity to glycerol, the inactive ingredient in TIROSINT-SOL [see Adverse Events (6) ]. Uncorrected adrenal insufficiency [see Warnings and Precautions (5.4) ]
Adverse Reactions
Adverse reactions associated with TIROSINT-SOL therapy are primarily those of hyperthyroidism due to therapeutic overdosage [see Warnings and Precautions (5) and Overdosage (10) ]. They include the following: General: fatigue, increased appetite, weight loss, heat intolerance, fever, excessive sweating Central nervous system: headache, hyperactivity, nervousness, anxiety, irritability, emotional lability, insomnia Musculoskeletal: tremors, muscle weakness, muscle spasm Cardiovascular: palpitations, tachycardia, arrhythmias, increased pulse and blood pressure, heart failure, angina, myocardial infarction, cardiac arrest Respiratory : dyspnea Gastrointestinal (GI): diarrhea, vomiting, abdominal cramps, elevations in liver function tests Dermatologic: hair loss, flushing, rash Endocrine: decreased bone mineral density Reproductive: menstrual irregularities, impaired fertility Seizures have been reported rarely with the institution of levothyroxine therapy.
Drug Interactions
See full prescribing information for drugs that affect thyroid hormone pharmacokinetics and metabolism (e.g., absorption, synthesis, secretion, catabolism, protein binding, and target tissue response) and may alter the therapeutic response to TIROSINT-SOL ( 7 )
Storage and Handling
Store TIROSINT-SOL in the original container (closed pouch) at 20°C to 25°C (68°F to 77°F); excursions permitted to 15° to 30°C (59°F to 86°F) [See USP Controlled Room Temperature].
Use TIROSINT-SOL oral solution within three (3) months after opening the pouch. Keep the ampules in the pouch until ready to use as important information may be lost (i.e., manufacturer/distributor names and distributor contact phone number).
How Supplied
TIROSINT-SOL (levothyroxine sodium) oral solution is a clear, colorless to slightly yellow solution supplied in a 1 mL white, non-transparent, unit-dose ampule. The dosage strength is identified on the box and the pouch, and is associated with a distinct color. Each ampule bears a colored label with the dosage strength and the product name (TIROSINT-SOL) (Table 10).
| Strength (mcg/mL) | Color a | Box NDC
(30 Unit-Dose Ampules) |
Pouch NDC
(5 Unit-Dose Ampules) |
|---|---|---|---|
| 13 | Green | 71858-0105-5 | 71858-0105-4 |
| 25 | Orange | 71858-0110-5 | 71858-0110-4 |
| 37.5 | Dark Blue | 71858-0112-5 | 71858-0112-4 |
| 44 | Red | 71858-0113-5 | 71858-0113-4 |
| 50 | White | 71858-0115-5 | 71858-0115-4 |
| 62.5 | Grey | 71858-0117-5 | 71858-0117-4 |
| 75 | Purple | 71858-0120-5 | 71858-0120-4 |
| 88 | Olive | 71858-0125-5 | 71858-0125-4 |
| 100 | Yellow | 71858-0130-5 | 71858-0130-4 |
| 112 | Rose | 71858-0135-5 | 71858-0135-4 |
| 125 | Brown | 71858-0140-5 | 71858-0140-4 |
| 137 | Turquoise | 71858-0145-5 | 71858-0145-4 |
| 150 | Blue | 71858-0150-5 | 71858-0150-4 |
| 175 | Lilac | 71858-0155-5 | 71858-0155-4 |
| 200 | Pink | 71858-0160-5 | 71858-0160-4 |
Description
Thyroid hormones, including TIROSINT-SOL, either alone or with other therapeutic agents, should not be used for the treatment of obesity or for weight loss. In euthyroid patients, doses within the range of daily hormonal requirements are ineffective for weight reduction. Larger doses may produce serious or even life threatening manifestations of toxicity, particularly when given in association with sympathomimetic amines such as those used for their anorectic effects [see Adverse Reactions (6) , Drug Interactions (7.7) , and Overdosage (10) ].
Section 42229-5
Hypothyroidism
TIROSINT-SOL is indicated in adult and pediatric patients, including neonates, as a replacement therapy in primary (thyroidal), secondary (pituitary), and tertiary (hypothalamic) congenital or acquired hypothyroidism.
Section 42230-3
| This Patient Information has been approved by the U.S. Food and Drug Administration | Issued: 07/2024 | ||
| PATIENT INFORMATION | |||
|
TIROSINT
®
-SOL [tee-row-sent-sōl]
(levothyroxine sodium) oral solution |
|||
|
What is the most important information I should know about TIROSINT-SOL?
Do not use TIROSINT-SOL to treat weight problems or weight loss. |
|||
| What is TIROSINT-SOL? | |||
TIROSINT-SOL is a prescription medicine that contains a hormone called levothyroxine which is normally produced by the thyroid gland. TIROSINT-SOL is used:
|
|||
| TIROSINT-SOL should not be used to treat people who are recovering from swelling of the thyroid gland (thyroiditis) and whose bodies do not produce enough levothyroxine for a short time. | |||
Do not take TIROSINT-SOL:
|
|||
Before you take TIROSINT-SOL, tell your doctor about all of your medical conditions, including if you:
|
|||
| Tell your doctor about all the medicines you are taking including prescription and over-the-counter medicines, vitamins and herbal supplements. TIROSINT-SOL may affect the way other medicines work, and other medicines may affect how TIROSINT-SOL works so your doctor may have to adjust the amount of medicines you take. You can ask your doctor or pharmacist for a list of medicines that interact with TIROSINT-SOL. | |||
How should I take TIROSINT-SOL?
|
|||
|
What are the possible side effects of TIROSINT-SOL?
TIROSINT-SOL may cause serious side effects, including: |
|||
|
|||
|
|
|
|
| Other side effects may include partial hair loss during the first months of treatment with TIROSINT-SOL. This usually lasts a short period of time (temporary). | |||
| These are not all the possible side effects of TIROSINT-SOL. Call your doctor for medical advice about side effects. You may report side effects to IBSA Pharma Inc. at 1-800-587-3513 or FDA at 1-800-FDA-1088. | |||
How should I store TIROSINT-SOL?
|
|||
| Keep TIROSINT-SOL and all medicines out of the reach of children. | |||
| General information about the safe and effective use of TIROSINT-SOL | |||
| Medicines are sometimes prescribed for purposes other than those listed in a Patient Information leaflet. Do not use TIROSINT-SOL for a condition for which it was not prescribed. Do not give TIROSINT-SOL to other people, even if they have the same symptoms as you. It may harm them. You can ask your pharmacist or doctor for information about TIROSINT-SOL that is written for health professionals. | |||
|
What are the ingredients in TIROSINT- SOL oral solution?
Active ingredient: levothyroxine sodium Inactive ingredients: glycerol, and water Manufactured by: IBSA Institut Biochimique SA, 6912 Pazzallo, Switzerland Marketed and distributed by: IBSA Pharma Inc, Parsippany, NJ 07054 USA For more information, go to www.tirosintsol.com or call 1-800-587-3513. |
|||
Section 59845-8
Instructions for Use
TIROSINT
®-SOL (tee-row-sent-sōl)
(levothyroxine sodium)
oral solution
Read this Instructions for Use before you start taking TIROSINT-SOL and each time you get a refill. There may be new information. This leaflet does not take the place of talking to your healthcare provider about your medical condition or treatment.
Important Information:
- TIROSINT-SOL is for oral use only. Do not inhale, inject, or place TIROSINT-SOL in the eyes.
- TIROSINT-SOL can be taken:
- by diluting or mixing in water first or
- by directly squeezing into the mouth or onto a spoon.
- Do not dilute or mix TIROSINT-SOL with any liquid other than water.
- Open the ampule and prepare the solution right before you take TIROSINT-SOL.
- After you have diluted or mixed TIROSINT-SOL it must be taken or thrown away.
Step 1. Using scissors, open the aluminum pouch by cutting the edge along the dotted line (See Figure A) .
Figure A
Step 2. Remove 1 ampule from the strip to be used right away (See Figure B) . Return the unused ampules back into the pouch before storing.
Figure B
Step 3. Hold the TIROSINT-SOL ampule upright (cap on top) between the first finger and thumb without squeezing the ampule. Open the ampule by twisting off the top (See Figure C) .
Figure C
Step 4.
Taking TIROSINT-SOL by diluting or mixing:
- Turn the ampule upside down.
- Squeeze the middle, softer part of the ampule between the first finger and thumb slowly to release the liquid medicine into a glass or cup containing water, then release the pressure and wait a few seconds (See Figure D).
- Keeping the ampule upside down, repeat this step for a minimum of 5 times, until no more liquid medicine comes out of the ampule.
- Stir the solution.
- Drink all the liquid medicine right away.
- Rinse the glass or cup with more water and drink to make sure all the medicine has been taken.
Figure D
Taking TIROSINT-SOL directly into the mouth or by spoon:
- Turn the ampule upside down.
- Squeeze the middle, softer part of the ampule between the first finger and thumb slowly to release the liquid medicine into the mouth or onto a spoon, then release the pressure and wait a few seconds (See Figure E).
- Keeping the ampule upside down, repeat this step for a minimum of 5 times, until no more liquid medicine comes out of the ampule.
Figure E
Step 5. Throw away (discard) the empty ampule.
How should I store TIROSINT-SOL?
- Store TIROSINT-SOL at room temperature between 68°F to 77°F (20°C to 25°C).
- Use TIROSINT-SOL within three (3) months after opening the pouch. Keep TIROSINT-SOL in the original closed pouch until you are ready to use it as important information may be lost (i.e., manufacturer/distributor names and distributor contact phone number.
- Do not store the diluted or mixed TIROSINT-SOL solution.
Keep TIROSINT-SOL and all medicines out of the reach of children.
This Instructions for Use has been approved by the U.S. Food and Drug Administration.
Manufacturer: IBSA Institut Biochimique SA, 6912 Pazzallo, Switzerland
Marketed and Distributed by: IBSA Pharma Inc., Parsippany, NJ 07054 USA
Issued: July 2024
FI/169 (USA) 5000003397 Rev. 06 06.24
7.6 Ketamine
Concurrent use of ketamine and TIROSINT-SOL may produce marked hypertension and tachycardia. Closely monitor blood pressure and heart rate in these patients.
10 Overdosage
The signs and symptoms of overdosage are those of hyperthyroidism [see Warnings and Precautions (5) and Adverse Reactions (6)]. In addition, confusion and disorientation may occur. Cerebral embolism, shock, coma, and death have been reported. Seizures occurred in a 3-year-old child ingesting 3.6 mg of levothyroxine. Symptoms may not necessarily be evident or may not appear until several days after ingestion of levothyroxine sodium.
Reduce the TIROSINT-SOL dose or discontinue temporarily if signs or symptoms of overdosage occur. Initiate appropriate supportive treatment as dictated by the patient's medical status.
For current information on the management of poisoning or overdosage, contact the National Poison Control Center at 1-800-222-1222 or www.poison.org.
11 Description
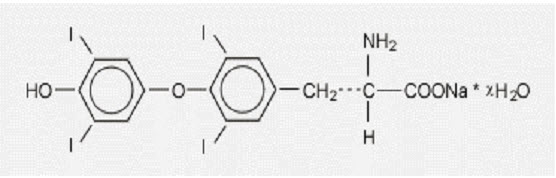
TIROSINT-SOL (levothyroxine sodium) oral solution contains synthetic L-3,3',5,5'-tetraiodothyronine sodium salt [levothyroxine (T4) sodium]. Synthetic T4 is chemically identical to that produced in the human thyroid gland. Levothyroxine (T4) sodium has an empirical formula of C 15H 10I 4NNaO 4 ∙ x H 2O (where x = 5), molecular weight of 798.86 g/mol (anhydrous), and structural formula as shown:
TIROSINT-SOL oral solution is a clear, colorless to slightly yellow solution supplied in a 1 mL white, non-transparent, unit-dose ampule and is available in the following strengths (mcg/mL): 13, 25, 37.5, 44, 50, 62.5, 75, 88, 100, 112, 125, 137, 150, 175, 200.
The inactive ingredients in TIROSINT-SOL are glycerol and water.
5.3 Myxedema Coma
Myxedema coma is a life-threatening emergency characterized by poor circulation and hypometabolism, and may result in unpredictable absorption of levothyroxine sodium from the gastrointestinal tract. Use of oral thyroid hormone drug products is not recommended to treat myxedema coma. Administer thyroid hormone products formulated for intravenous administration to treat myxedema coma.
8.4 Pediatric Use
TIROSINT-SOL is indicated in patients from birth to less than 17 years of age:
- As a replacement therapy in primary (thyroidal), secondary (pituitary), and tertiary (hypothalamic) congenital or acquired hypothyroidism
- As an adjunct to surgery and radioiodine therapy in the management of thyrotropin-dependent well-differentiated thyroid cancer
Rapid restoration of normal serum T4 concentrations is essential for preventing the adverse effects of congenital hypothyroidism on cognitive development as well as on overall physical growth and maturation. Therefore, initiate TIROSINT-SOL therapy immediately upon diagnosis. Levothyroxine is generally continued for life in these patients [see Warnings and Precautions (5.1)].
Closely monitor infants during the first two weeks of TIROSINT-SOL therapy for cardiac overload and arrhythmias.
8.5 Geriatric Use
Because of the increased prevalence of cardiovascular disease among the elderly, initiate TIROSINT-SOL at less than the full replacement dose [ see Dosage and Administration (2.3) and Warnings and Precautions (5.1) ]. Atrial arrhythmias can occur in elderly patients. Atrial fibrillation is the most common of the arrhythmias observed with levothyroxine overtreatment in the elderly .
4 Contraindications
TIROSINT-SOL is contraindicated in patients with:
- Hypersensitivity to glycerol, the inactive ingredient in TIROSINT-SOL [see Adverse Events (6)].
- Uncorrected adrenal insufficiency [see Warnings and Precautions (5.4)]
6 Adverse Reactions
Adverse reactions associated with TIROSINT-SOL therapy are primarily those of hyperthyroidism due to therapeutic overdosage [see Warnings and Precautions (5) and Overdosage (10)]. They include the following:
- General: fatigue, increased appetite, weight loss, heat intolerance, fever, excessive sweating
- Central nervous system: headache, hyperactivity, nervousness, anxiety, irritability, emotional lability, insomnia
- Musculoskeletal: tremors, muscle weakness, muscle spasm
- Cardiovascular: palpitations, tachycardia, arrhythmias, increased pulse and blood pressure, heart failure, angina, myocardial infarction, cardiac arrest
- Respiratory: dyspnea
- Gastrointestinal (GI): diarrhea, vomiting, abdominal cramps, elevations in liver function tests
- Dermatologic: hair loss, flushing, rash
- Endocrine: decreased bone mineral density
- Reproductive: menstrual irregularities, impaired fertility
Seizures have been reported rarely with the institution of levothyroxine therapy.
7 Drug Interactions
See full prescribing information for drugs that affect thyroid hormone pharmacokinetics and metabolism (e.g., absorption, synthesis, secretion, catabolism, protein binding, and target tissue response) and may alter the therapeutic response to TIROSINT-SOL ( 7)
7.7 Sympathomimetics
Concurrent use of sympathomimetics and TIROSINT-SOL may increase the effects of sympathomimetics or thyroid hormone. Thyroid hormones may increase the risk of coronary insufficiency when sympathomimetic agents are administered to patients with coronary artery disease.
12.2 Pharmacodynamics
Oral levothyroxine sodium is a synthetic T4 hormone that exerts the same physiologic effect as endogenous T4, thereby maintaining normal T4 levels when a deficiency is present.
1 Indication and Usage
TIROSINT-SOL is L-thyroxine (T4) indicated in adult and pediatric patients, including neonates, for:
- Hypothyroidism - As replacement therapy in primary (thyroidal), secondary (pituitary), and tertiary (hypothalamic) congenital or acquired hypothyroidism ( 1)
- Pituitary Thyrotropin (Thyroid-Stimulating Hormone, TSH) Suppression - As an adjunct to surgery and radioiodine therapy in the management of thyrotropin-dependent well-differentiated thyroid cancer ( 1)
Limitations of Use
7.3 Oral Anticoagulants
TIROSINT-SOL increases the response to oral anticoagulant therapy. Therefore, a decrease in the dose of anticoagulant may be warranted with correction of the hypothyroid state or when the TIROSINT-SOL dose is increased. Closely monitor coagulation tests to permit appropriate and timely dosage adjustments.
12.1 Mechanism of Action
Thyroid hormones exert their physiologic actions through control of DNA transcription and protein synthesis. Triiodothyronine (T3) and L-thyroxine (T4) diffuse into the cell nucleus and bind to thyroid receptor proteins attached to DNA. This hormone nuclear receptor complex activates gene transcription and synthesis of messenger RNA and cytoplasmic proteins.
The physiological actions of thyroid hormones are produced predominantly by T3, the majority of which (approximately 80%) is derived from T4 by deiodination in peripheral tissues.
7.2 Antidiabetic Therapy
Addition of TIROSINT-SOL therapy in patients with diabetes mellitus may worsen glycemic control and result in increased antidiabetic agent or insulin requirements. Carefully monitor glycemic control, especially when thyroid therapy is started, changed, or discontinued [see Warnings and Precautions (5.5)] .
7.4 Digitalis Glycosides
TIROSINT-SOL may reduce the therapeutic effects of digitalis glycosides. Serum digitalis glycoside levels may decrease when a hypothyroid patient becomes euthyroid, necessitating an increase in the dose of digitalis glycosides.
5 Warnings and Precautions
- Serious risks related to overtreatment or undertreatment with TIROSINT-SOL: Titrate the dose of TIROSINT-SOL carefully and monitor response to titration. ( 5.1)
- Cardiac adverse reactions in the elderly and in patients with underlying cardiovascular disease: Initiate TIROSINT-SOL at less than the full replacement dose because of the increased risk of cardiac adverse reactions, including atrial fibrillation. ( 2.3, 5.2, 8.5)
- Myxedema coma: Do not use oral thyroid hormone drug products to treat myxedema coma. ( 5.3)
- Acute adrenal crisis in patients with concomitant adrenal insufficiency: Treat with replacement glucocorticoids prior to initiation of TIROSINT‑SOL treatment. ( 5.4)
- Worsening of diabetic control: therapy in patients with diabetes mellitus may worsen glycemic control and result in increased antidiabetic agent or insulin requirements. Carefully monitor glycemic control after starting, changing, or discontinuing thyroid hormone therapy. ( 5.5)
- Decreased bone mineral density associated with thyroid hormone over-replacement: Over-replacement can increase bone resorption and decrease bone mineral density. Give the lowest effective dose. 5.6)
7.5 Antidepressant Therapy
Concurrent use of tricyclic (e.g., amitriptyline) or tetracyclic (e.g., maprotiline) antidepressants and TIROSINT-SOL may increase the therapeutic and toxic effects of both drugs, possibly due to increased receptor sensitivity to catecholamines. Toxic effects may include increased risk of cardiac arrhythmias and central nervous system stimulation. TIROSINT-SOL may accelerate the onset of action of tricyclics. Administration of sertraline in patients stabilized on TIROSINT-SOL may result in increased TIROSINT-SOL requirements.
7.9 Drug Food Interactions
Consumption of certain foods may affect TIROSINT-SOL absorption thereby necessitating adjustments in dosing [see Dosage and Administration (2.1)] . Soybean flour (infant formula), cottonseed meal, walnuts, and dietary fiber may bind and decrease the absorption of TIROSINT-SOL from the gastrointestinal tract. Grapefruit juice may delay the absorption of levothyroxine and reduce its bioavailability.
2 Dosage and Administration
- Administer once daily, on an empty stomach, 15 minutes before breakfast ( 2.1)
- Administer at least 4 hours before or after drugs that are known to interfere with absorption ( 2.1)
- Evaluate the need for dose adjustments when regularly administering within an hour of certain foods that may affect TIROSINT-SOL absorption ( 2.1)
- To administer TIROSINT-SOL in water, squeeze the contents of one single unit-dose ampule into a glass or cup containing water ( 2.1)
- To administer TIROSINT-SOL directly, either squeeze it into the mouth OR onto a spoon and immediately consume ( 2.1)
- Starting dose depends on a variety of factors, including age, body weight, cardiovascular status, and concomitant medications, co-administered food, and the specific nature of the condition being treated. Peak therapeutic effect may not be attained for 4-6 weeks ( 2.2)
- See full prescribing information for dosing in specific patient populations ( 2.3)
- Adequacy of therapy determined with periodic monitoring of TSH and/or T4 as well as clinical status ( 2.4)
3 Dosage Forms and Strengths
TIROSINT-SOL oral solution is a clear, colorless to slightly yellow solution supplied in a 1 mL white, non-transparent, unit-dose ampule. Each ampule bears a colored label with the dosage strength and the product name (TIROSINT-SOL) (Table 4).
Table 4. TIROSINT-SOL Solution Strengths and Identifying Features
| Strength (mcg/mL) | Color |
|---|---|
| 13 | Green |
| 25 | Orange |
| 37.5 | Dark Blue |
| 44 | Red |
| 50 | White |
| 75 | Purple |
| 62.5 | Grey |
| 88 | Olive |
| 100 | Yellow |
| 112 | Rose |
| 125 | Brown |
| 137 | Turquoise |
| 150 | Blue |
| 175 | Lilac |
| 200 | Pink |
8 Use in Specific Populations
7.8 Tyrosine Kinase Inhibitors
Concurrent use of tyrosine-kinase inhibitors such as imatinib may cause hypothyroidism. Closely monitor TSH levels in such patients.
17 Patient Counseling Information
Advise the patient and/or caregiver to read the FDA-approved patient labeling (Patient Information and Instructions for Use).
5.5 Worsening of Diabetic Control
Addition of levothyroxine therapy in patients with diabetes mellitus may worsen glycemic control and result in increased antidiabetic agent or insulin requirements. Carefully monitor glycemic control after starting, changing, or discontinuing TIROSINT-SOL [see Drug Interactions (7.2)] .
2.3 Recommended Dosage and Titration
Primary, Secondary, and Tertiary Hypothyroidism in Adults
2.1 General Administration Information
Administer TIROSINT-SOL as a single daily oral dose, on an empty stomach,15 minutes before breakfast.
Administer TIROSINT-SOL at least 4 hours before or after drugs known to interfere with TIROSINT-SOL absorption [see Drug Interactions (7.1)] .
Evaluate the need for dose adjustments when regularly administering within an hour of certain foods that may affect TIROSINT-SOL absorption [see Dosage and Administration (2.2 and 2.3) , Drug Interactions (7.9) and Clinical Pharmacology (12.3)] .
TIROSINT-SOL may be administered in water or directly into the mouth:
- To administer TIROSINT-SOL in water, squeeze the contents of one single unit-dose ampule into a glass or cup containing water. Stir the diluted TIROSINT-SOL and drink all of it immediately. Rinse the glass or cup with additional water and drink the contents to ensure that the total dose is taken. Do not dilute TIROSINT-SOL in a medium other than water. Open the ampule and prepare the solution immediately before intake.
- To administer TIROSINT-SOL directly (without water), either squeeze it into the mouth OR onto a spoon and immediately consume.
7.10 Drug Laboratory Test Interactions
Consider changes in TBG concentration when interpreting T4 and T3 values. Measure and evaluate unbound (free) hormone and/or determine the free-T4 index (FT4I) in this circumstance. Pregnancy, infectious hepatitis, estrogens, estrogen-containing oral contraceptives, and acute intermittent porphyria increase TBG concentrations. Nephrosis, severe hypoproteinemia, severe liver disease, acromegaly, androgens and corticosteroids decrease TBG concentration. Familial hyper- or hypo-thyroxine binding globulinemias have been described, with the incidence of TBG deficiency approximating 1 in 9000.
2.2 Important Considerations for Dosing
The dosage of TIROSINT-SOL for hypothyroidism or pituitary TSH suppression depends on a variety of factors including: the patient's age, body weight, cardiovascular status, concomitant medical conditions (including pregnancy), concomitant medications, co-administered food, and the specific nature of the condition being treated [see Dosage and Administration (2.3), Warnings and Precautions (5), and Drug Interactions (7)] . Dosing must be individualized to account for these factors and dosage adjustments made based on periodic assessment of the patient's clinical response and laboratory parameters [see Dosage and Administration (2.4)] .
For adult patients with primary hypothyroidism, titrate until the patient is clinically euthyroid and the serum TSH returns to normal [see Dosage and Administration (2.3)].
For secondary or tertiary hypothyroidism, serum TSH is not a reliable measure of TIROSINT-SOL dosage adequacy and should not be used to monitor therapy. Use the serum free-T4 level to titrate TIROSINT-SOL dosing until the patient is clinically euthyroid and the serum free-T4 level is restored to the upper half of the normal range [see Dosage and Administration (2.3)].
The peak therapeutic effect of a given dose of TIROSINT-SOL may not be attained for 4 to 6 weeks.
2.4 Monitoring Tsh And/or Thyroxine (t4) Levels
Assess the adequacy of therapy by periodic assessment of laboratory tests and clinical evaluation. Persistent clinical and laboratory evidence of hypothyroidism, despite an apparent adequate replacement dose of TIROSINT-SOL, may be evidence of inadequate absorption, poor compliance, drug interactions, or a combination of these factors.
Warning: Not for Treatment of Obesity Or for Weight Loss
- Thyroid hormones, including TIROSINT-SOL, either alone or with other therapeutic agents, should not be used for the treatment of obesity or for weight loss.
- In euthyroid patients, doses within the range of daily hormonal requirements are ineffective for weight reduction.
- Larger doses may produce serious or even life threatening manifestations of toxicity, particularly when given in association with sympathomimetic amines such as those used for their anorectic effects [see Adverse Reactions (6), Drug Interactions (7.7), and Overdosage (10)].
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Long-term carcinogenicity studies in animals to evaluate the carcinogenic potential of levothyroxine have not been performed. Studies to evaluate mutagenic potential and animal fertility have not been performed.
7.1 Drugs Known to Affect Thyroid Hormone Pharmacokinetics
Many drugs can exert effects on thyroid hormone pharmacokinetics and metabolism (e.g., absorption, synthesis, secretion, catabolism, protein binding, and target tissue response) and may alter the therapeutic response to TIROSINT-SOL (Tables 5 to 8).
Table 5. Drugs That May Decrease T4 Absorption (Hypothyroidism)
|
Potential impact: Concurrent use may reduce the efficacy of TIROSINT-SOL by binding and delaying or preventing absorption, potentially resulting in hypothyroidism. |
|
|
Drug or Drug Class |
Effect |
|
Phosphate Binders (e.g., calcium carbonate, ferrous sulfate, sevelamer, lanthanum) |
Phosphate binders may bind to levothyroxine. Administer TIROSINT-SOL at least 4 hours apart from these agents. |
|
Orlistat |
Monitor patients treated concomitantly with orlistat and TIROSINT‑SOL for changes in thyroid function. |
|
Bile Acid Sequestrants (e.g., colesevelam, cholestyramine, colestipol Ion Exchange Resins (e.g., Kayexalate) |
Bile acid sequestrants and ion exchange resins are known to decrease levothyroxine absorption. Administer TIROSINT-SOL at least 4 hours prior to these drugs or monitor TSH levels. |
|
Sucralfate Antacids (e.g., aluminum & magnesium hydroxides, simethicone) |
Gastric acidity is an essential requirement for adequate absorption of levothyroxine. However, gastric acidity may not be as essential for the absorption of TIROSINT-SOL. Sucralfate and antacids may cause hypochlorhydria, affect gastric pH, and reduce levothyroxine absorption. Monitor patients appropriately. |
Table 6. Drugs That May Alter T4 and Triiodothyronine (T3) Serum Transport Without Affecting Free Thyroxine (FT4) Concentration (Euthyroidism)
|
Drug or Drug Class |
Effect |
|
Clofibrate Estrogen-containing oral contraceptives Estrogens (oral) Heroin / Methadone 5-Fluorouracil Mitotane Tamoxifen |
These drugs may increase serum thyroxine-binding globulin (TBG) concentration. |
|
Androgens / Anabolic Steroids
|
These drugs may decrease serum TBG concentration. |
|
Potential impact (below): Administration of these agents with TIROSINT-SOL results in an initial transient increase in FT4. Continued administration results in a decrease in serum T4 and normal FT4 and TSH concentrations. |
|
|
Salicylates (> 2 g/day) |
Salicylates inhibit binding of T4 and T3 to TBG and transthyretin. An initial increase in serum FT4 is followed by return of FT4 to normal levels with sustained therapeutic serum salicylate concentrations, although total T4 levels may decrease by as much as 30%. |
|
Other drugs: Carbamazepine Furosemide (> 80 mg IV) Heparin Hydantoins Non-Steroidal Anti-inflammatory Drugs: Fenamates |
These drugs may cause protein-binding site displacement. Furosemide has been shown to inhibit the protein binding of T4 to TBG and albumin, causing an increase free‑T4 fraction in serum. Furosemide competes for T4-binding sites on TBG, prealbumin, and albumin, so that a single high dose can acutely lower the total T4 level. Phenytoin and carbamazepine reduce serum protein binding of levothyroxine, and total and free‑T4 may be reduced by 20% to 40%, but most patients have normal serum TSH levels and are clinically euthyroid. Closely monitor thyroid hormone parameters. |
Table 7. Drugs That May Alter Hepatic Metabolism of T4 (Hypothyroidism)
|
Potential impact: Stimulation of hepatic microsomal drug-metabolizing enzyme activity may cause increased hepatic degradation of levothyroxine, resulting in increased TIROSINT-SOL requirements. |
|
|
Drug or Drug Class |
Effect |
|
Phenobarbital Rifampin |
Phenobarbital has been shown to reduce the response to thyroxine. Phenobarbital increases L-thyroxine metabolism by inducing uridine 5’ diphospho-glucuronosyltransferase (UGT) and leads to a lower T4 serum levels. Changes in thyroid status may occur if barbiturates are added or withdrawn from patients being treated for hypothyroidism. Rifampin has been shown to accelerate the metabolism of levothyroxine. |
Table 8. Drugs That May Decrease Conversion of T4 to T3
|
Potential impact: Administration of these enzyme inhibitors decreases the peripheral conversion of T4 to T3, leading to decreased T3 levels. However, serum T4 levels are usually normal but may occasionally be slightly increased. |
|
|
Drug or Drug Class |
Effect |
|
Beta-adrenergic antagonists (e.g., Propranolol > 160 mg/day) |
In patients treated with large doses of propranolol (> 160 mg/day), T3 and T4 levels change, TSH levels remain normal, and patients are clinically euthyroid. Actions of particular beta-adrenergic antagonists may be impaired when a hypothyroid patient is converted to the euthyroid state. |
|
Glucocorticoids (e.g., Dexamethasone > 4 mg/day) |
Short-term administration of large doses of glucocorticoids may decrease serum T3 concentrations by 30% with minimal change in serum T4 levels. However, long-term glucocorticoid therapy may result in slightly decreased T3 and T4 levels due to decreased TBG production (See above). |
|
Other drugs: Amiodarone |
Amiodarone inhibits peripheral conversion of T4 to T3 and may cause isolated biochemical changes (increase in serum free-T4, and decrease or normal free-T3) in clinically euthyroid patients. |
Principal Display Panel 13 Microgram/ml Ampule Pouch Carton
NDC 71858-0105-5
TIROSINT
® - SOL
(levothyroxine sodium) Oral Solution
13 microgram/mL
For Oral Use Only – NOT for Inhalation, Injection or Ophthalmic Use
R x Only
6 pouches x 5 ampules
IBSA
Principal Display Panel 25 Microgram/ml Ampule Pouch Carton
NDC 71858-0110-5
TIROSINT
® - SOL
(levothyroxine sodium) Oral Solution
25 microgram/mL
For Oral Use Only – NOT for Inhalation, Injection or Ophthalmic Use
R x Only
6 pouches x 5 ampules
IBSA
Principal Display Panel 44 Microgram/ml Ampule Pouch Carton
NDC 71858-0113-5
TIROSINT
® - SOL
(levothyroxine sodium) Oral Solution
44 microgram/mL
For Oral Use Only – NOT for Inhalation, Injection or Ophthalmic Use
R x Only
6 pouches x 5 ampules
IBSA
Principal Display Panel 50 Microgram/ml Ampule Pouch Carton
NDC 71858-0115-5
TIROSINT
® - SOL
(levothyroxine sodium) Oral Solution
50 microgram/mL
For Oral Use Only – NOT for Inhalation, Injection or Ophthalmic Use
R x Only
6 pouches x 5 ampules
IBSA
Principal Display Panel 75 Microgram/ml Ampule Pouch Carton
NDC 71858-0120-5
TIROSINT
® - SOL
(levothyroxine sodium) Oral Solution
75 microgram/mL
For Oral Use Only – NOT for Inhalation, Injection or Ophthalmic Use
R x Only
6 pouches x 5 ampules
IBSA
Principal Display Panel 88 Microgram/ml Ampule Pouch Carton
NDC 71858-0125-5
TIROSINT
® - SOL
(levothyroxine sodium) Oral Solution
88 microgram/mL
For Oral Use Only – NOT for Inhalation, Injection or Ophthalmic Use
R x Only
6 pouches x 5 ampules
IBSA
Principal Display Panel 100 Microgram/ml Ampule Pouch Carton
NDC 71858-0130-5
TIROSINT
® - SOL
(levothyroxine sodium) Oral Solution
100 microgram/mL
For Oral Use Only – NOT for Inhalation, Injection or Ophthalmic Use
R x Only
6 pouches x 5 ampules
IBSA
Principal Display Panel 112 Microgram/ml Ampule Pouch Carton
NDC 71858-0135-5
TIROSINT
® - SOL
(levothyroxine sodium) Oral Solution
112 microgram/mL
For Oral Use Only – NOT for Inhalation, Injection or Ophthalmic Use
R x Only
6 pouches x 5 ampules
IBSA
Principal Display Panel 125 Microgram/ml Ampule Pouch Carton
NDC 71858-0140-5
TIROSINT
® - SOL
(levothyroxine sodium) Oral Solution
125 microgram/mL
For Oral Use Only – NOT for Inhalation, Injection or Ophthalmic Use
R x Only
6 pouches x 5 ampules
IBSA
Principal Display Panel 137 Microgram/ml Ampule Pouch Carton
NDC 71858-0145-5
TIROSINT
® - SOL
(levothyroxine sodium) Oral Solution
137 microgram/mL
For Oral Use Only – NOT for Inhalation, Injection or Ophthalmic Use
R x Only
6 pouches x 5 ampules
IBSA
Principal Display Panel 150 Microgram/ml Ampule Pouch Carton
NDC 71858-0150-5
TIROSINT
® - SOL
(levothyroxine sodium) Oral Solution
150 microgram/mL
For Oral Use Only – NOT for Inhalation, Injection or Ophthalmic Use
R x Only
6 pouches x 5 ampules
IBSA
Principal Display Panel 175 Microgram/ml Ampule Pouch Carton
NDC 71858-0155-5
TIROSINT
® - SOL
(levothyroxine sodium) Oral Solution
175 microgram/mL
For Oral Use Only – NOT for Inhalation, Injection or Ophthalmic Use
R x Only
6 pouches x 5 ampules
IBSA
Principal Display Panel 200 Microgram/ml Ampule Pouch Carton
NDC 71858-0160-5
TIROSINT
® - SOL
(levothyroxine sodium) Oral Solution
200 microgram/mL
For Oral Use Only – NOT for Inhalation, Injection or Ophthalmic Use
R x Only
6 pouches x 5 ampules
IBSA
Principal Display Panel 37.5 Microgram/ml Ampule Pouch Carton
NDC 71858-0112-5
TIROSINT
® - SOL
(levothyroxine sodium) Oral Solution
37.5 microgram/mL
For Oral Use Only – NOT for Inhalation, Injection or Ophthalmic Use
R x Only
6 pouches x 5 ampules
IBSA
Principal Display Panel 62.5 Microgram/ml Ampule Pouch Carton
NDC 71858-0117-5
TIROSINT
® - SOL
(levothyroxine sodium) Oral Solution
62.5 microgram/mL
For Oral Use Only – NOT for Inhalation, Injection or Ophthalmic Use
R x Only
6 pouches x 5 ampules
IBSA
5.4 Acute Adrenal Crisis in Patients With Concomitant Adrenal Insufficiency
Thyroid hormone increases metabolic clearance of glucocorticoids. Initiation of thyroid hormone therapy prior to initiating glucocorticoid therapy may precipitate an acute adrenal crisis in patients with adrenal insufficiency. Treat patients with adrenal insufficiency with replacement glucocorticoids prior to initiating treatment with TIROSINT-SOL [see Contraindications (4)].
5.1 Serious Risks Related to Overtreatment Or Undertreatment With Tirosint Sol
TIROSINT-SOL has a narrow therapeutic index. Overtreatment or undertreatment with TIROSINT-SOL may have negative effects on growth and development, cardiovascular function, bone metabolism, reproductive function, cognitive function, gastrointestinal function, and glucose and lipid metabolism in adult or pediatric patients.
In pediatric patients with congenital and acquired hypothyroidism, undertreatment may adversely affect cognitive development and linear growth, and overtreatment is associated with craniosynostosis and acceleration of bone age [see Use in Specific Populations (8.4)].
Titrate the dose of TIROSINT-SOL carefully and monitor response to titration to avoid these effects [see Dosage and Administration (2.4)]. Consider the potential for food or drug interactions and adjust the administration or dosage of TIROSINT-SOL as needed [see Dosage and Administration (2.4), Drug Interactions (7.1), and Clinical Pharmacology (12.3)].
5.6 Decreased Bone Mineral Density Associated With Thyroid Hormone Over Replacement
Increased bone resorption and decreased bone mineral density may occur as a result of levothyroxine over-replacement, particularly in post-menopausal women. The increased bone resorption may be associated with increased serum levels and urinary excretion of calcium and phosphorous, elevations in bone alkaline phosphatase, and suppressed serum parathyroid hormone levels. Administer the minimum dose of TIROSINT-SOL that achieves the desired clinical and biochemical response to mitigate this risk.
5.2 Cardiac Adverse Reactions in the Elderly and in Patients With Underlying Cardiovascular Disease
Overtreatment with levothyroxine may cause an increase in heart rate, cardiac wall thickness, and cardiac contractility, and may precipitate angina or arrhythmias, particularly in patients with cardiovascular disease and in elderly patients. Initiate TIROSINT-SOL therapy in this population at lower doses than those recommended in younger individuals or in patients without cardiac disease [see Dosage and Administration (2.3) and Use in Specific Populations (8.5)].
Monitor for cardiac arrhythmias during surgical procedures in patients with coronary artery disease receiving suppressive TIROSINT-SOL therapy. Monitor patients receiving concomitant TIROSINT-SOL and sympathomimetic agents for signs and symptoms of coronary insufficiency . If cardiac symptoms develop or worsen, reduce the TIROSINT-SOL dose or withhold it for one week and restart at a lower dose.
Structured Label Content
Section 42229-5 (42229-5)
Hypothyroidism
TIROSINT-SOL is indicated in adult and pediatric patients, including neonates, as a replacement therapy in primary (thyroidal), secondary (pituitary), and tertiary (hypothalamic) congenital or acquired hypothyroidism.
Section 42230-3 (42230-3)
| This Patient Information has been approved by the U.S. Food and Drug Administration | Issued: 07/2024 | ||
| PATIENT INFORMATION | |||
|
TIROSINT
®
-SOL [tee-row-sent-sōl]
(levothyroxine sodium) oral solution |
|||
|
What is the most important information I should know about TIROSINT-SOL?
Do not use TIROSINT-SOL to treat weight problems or weight loss. |
|||
| What is TIROSINT-SOL? | |||
TIROSINT-SOL is a prescription medicine that contains a hormone called levothyroxine which is normally produced by the thyroid gland. TIROSINT-SOL is used:
|
|||
| TIROSINT-SOL should not be used to treat people who are recovering from swelling of the thyroid gland (thyroiditis) and whose bodies do not produce enough levothyroxine for a short time. | |||
Do not take TIROSINT-SOL:
|
|||
Before you take TIROSINT-SOL, tell your doctor about all of your medical conditions, including if you:
|
|||
| Tell your doctor about all the medicines you are taking including prescription and over-the-counter medicines, vitamins and herbal supplements. TIROSINT-SOL may affect the way other medicines work, and other medicines may affect how TIROSINT-SOL works so your doctor may have to adjust the amount of medicines you take. You can ask your doctor or pharmacist for a list of medicines that interact with TIROSINT-SOL. | |||
How should I take TIROSINT-SOL?
|
|||
|
What are the possible side effects of TIROSINT-SOL?
TIROSINT-SOL may cause serious side effects, including: |
|||
|
|||
|
|
|
|
| Other side effects may include partial hair loss during the first months of treatment with TIROSINT-SOL. This usually lasts a short period of time (temporary). | |||
| These are not all the possible side effects of TIROSINT-SOL. Call your doctor for medical advice about side effects. You may report side effects to IBSA Pharma Inc. at 1-800-587-3513 or FDA at 1-800-FDA-1088. | |||
How should I store TIROSINT-SOL?
|
|||
| Keep TIROSINT-SOL and all medicines out of the reach of children. | |||
| General information about the safe and effective use of TIROSINT-SOL | |||
| Medicines are sometimes prescribed for purposes other than those listed in a Patient Information leaflet. Do not use TIROSINT-SOL for a condition for which it was not prescribed. Do not give TIROSINT-SOL to other people, even if they have the same symptoms as you. It may harm them. You can ask your pharmacist or doctor for information about TIROSINT-SOL that is written for health professionals. | |||
|
What are the ingredients in TIROSINT- SOL oral solution?
Active ingredient: levothyroxine sodium Inactive ingredients: glycerol, and water Manufactured by: IBSA Institut Biochimique SA, 6912 Pazzallo, Switzerland Marketed and distributed by: IBSA Pharma Inc, Parsippany, NJ 07054 USA For more information, go to www.tirosintsol.com or call 1-800-587-3513. |
|||
Section 59845-8 (59845-8)
Instructions for Use
TIROSINT
®-SOL (tee-row-sent-sōl)
(levothyroxine sodium)
oral solution
Read this Instructions for Use before you start taking TIROSINT-SOL and each time you get a refill. There may be new information. This leaflet does not take the place of talking to your healthcare provider about your medical condition or treatment.
Important Information:
- TIROSINT-SOL is for oral use only. Do not inhale, inject, or place TIROSINT-SOL in the eyes.
- TIROSINT-SOL can be taken:
- by diluting or mixing in water first or
- by directly squeezing into the mouth or onto a spoon.
- Do not dilute or mix TIROSINT-SOL with any liquid other than water.
- Open the ampule and prepare the solution right before you take TIROSINT-SOL.
- After you have diluted or mixed TIROSINT-SOL it must be taken or thrown away.
Step 1. Using scissors, open the aluminum pouch by cutting the edge along the dotted line (See Figure A) .
Figure A
Step 2. Remove 1 ampule from the strip to be used right away (See Figure B) . Return the unused ampules back into the pouch before storing.
Figure B
Step 3. Hold the TIROSINT-SOL ampule upright (cap on top) between the first finger and thumb without squeezing the ampule. Open the ampule by twisting off the top (See Figure C) .
Figure C
Step 4.
Taking TIROSINT-SOL by diluting or mixing:
- Turn the ampule upside down.
- Squeeze the middle, softer part of the ampule between the first finger and thumb slowly to release the liquid medicine into a glass or cup containing water, then release the pressure and wait a few seconds (See Figure D).
- Keeping the ampule upside down, repeat this step for a minimum of 5 times, until no more liquid medicine comes out of the ampule.
- Stir the solution.
- Drink all the liquid medicine right away.
- Rinse the glass or cup with more water and drink to make sure all the medicine has been taken.
Figure D
Taking TIROSINT-SOL directly into the mouth or by spoon:
- Turn the ampule upside down.
- Squeeze the middle, softer part of the ampule between the first finger and thumb slowly to release the liquid medicine into the mouth or onto a spoon, then release the pressure and wait a few seconds (See Figure E).
- Keeping the ampule upside down, repeat this step for a minimum of 5 times, until no more liquid medicine comes out of the ampule.
Figure E
Step 5. Throw away (discard) the empty ampule.
How should I store TIROSINT-SOL?
- Store TIROSINT-SOL at room temperature between 68°F to 77°F (20°C to 25°C).
- Use TIROSINT-SOL within three (3) months after opening the pouch. Keep TIROSINT-SOL in the original closed pouch until you are ready to use it as important information may be lost (i.e., manufacturer/distributor names and distributor contact phone number.
- Do not store the diluted or mixed TIROSINT-SOL solution.
Keep TIROSINT-SOL and all medicines out of the reach of children.
This Instructions for Use has been approved by the U.S. Food and Drug Administration.
Manufacturer: IBSA Institut Biochimique SA, 6912 Pazzallo, Switzerland
Marketed and Distributed by: IBSA Pharma Inc., Parsippany, NJ 07054 USA
Issued: July 2024
FI/169 (USA) 5000003397 Rev. 06 06.24
7.6 Ketamine
Concurrent use of ketamine and TIROSINT-SOL may produce marked hypertension and tachycardia. Closely monitor blood pressure and heart rate in these patients.
How Supplied
TIROSINT-SOL (levothyroxine sodium) oral solution is a clear, colorless to slightly yellow solution supplied in a 1 mL white, non-transparent, unit-dose ampule. The dosage strength is identified on the box and the pouch, and is associated with a distinct color. Each ampule bears a colored label with the dosage strength and the product name (TIROSINT-SOL) (Table 10).
| Strength (mcg/mL) | Color a | Box NDC
(30 Unit-Dose Ampules) |
Pouch NDC
(5 Unit-Dose Ampules) |
|---|---|---|---|
| 13 | Green | 71858-0105-5 | 71858-0105-4 |
| 25 | Orange | 71858-0110-5 | 71858-0110-4 |
| 37.5 | Dark Blue | 71858-0112-5 | 71858-0112-4 |
| 44 | Red | 71858-0113-5 | 71858-0113-4 |
| 50 | White | 71858-0115-5 | 71858-0115-4 |
| 62.5 | Grey | 71858-0117-5 | 71858-0117-4 |
| 75 | Purple | 71858-0120-5 | 71858-0120-4 |
| 88 | Olive | 71858-0125-5 | 71858-0125-4 |
| 100 | Yellow | 71858-0130-5 | 71858-0130-4 |
| 112 | Rose | 71858-0135-5 | 71858-0135-4 |
| 125 | Brown | 71858-0140-5 | 71858-0140-4 |
| 137 | Turquoise | 71858-0145-5 | 71858-0145-4 |
| 150 | Blue | 71858-0150-5 | 71858-0150-4 |
| 175 | Lilac | 71858-0155-5 | 71858-0155-4 |
| 200 | Pink | 71858-0160-5 | 71858-0160-4 |
10 Overdosage (10 OVERDOSAGE)
The signs and symptoms of overdosage are those of hyperthyroidism [see Warnings and Precautions (5) and Adverse Reactions (6)]. In addition, confusion and disorientation may occur. Cerebral embolism, shock, coma, and death have been reported. Seizures occurred in a 3-year-old child ingesting 3.6 mg of levothyroxine. Symptoms may not necessarily be evident or may not appear until several days after ingestion of levothyroxine sodium.
Reduce the TIROSINT-SOL dose or discontinue temporarily if signs or symptoms of overdosage occur. Initiate appropriate supportive treatment as dictated by the patient's medical status.
For current information on the management of poisoning or overdosage, contact the National Poison Control Center at 1-800-222-1222 or www.poison.org.
11 Description (11 DESCRIPTION)
TIROSINT-SOL (levothyroxine sodium) oral solution contains synthetic L-3,3',5,5'-tetraiodothyronine sodium salt [levothyroxine (T4) sodium]. Synthetic T4 is chemically identical to that produced in the human thyroid gland. Levothyroxine (T4) sodium has an empirical formula of C 15H 10I 4NNaO 4 ∙ x H 2O (where x = 5), molecular weight of 798.86 g/mol (anhydrous), and structural formula as shown:
TIROSINT-SOL oral solution is a clear, colorless to slightly yellow solution supplied in a 1 mL white, non-transparent, unit-dose ampule and is available in the following strengths (mcg/mL): 13, 25, 37.5, 44, 50, 62.5, 75, 88, 100, 112, 125, 137, 150, 175, 200.
The inactive ingredients in TIROSINT-SOL are glycerol and water.
5.3 Myxedema Coma
Myxedema coma is a life-threatening emergency characterized by poor circulation and hypometabolism, and may result in unpredictable absorption of levothyroxine sodium from the gastrointestinal tract. Use of oral thyroid hormone drug products is not recommended to treat myxedema coma. Administer thyroid hormone products formulated for intravenous administration to treat myxedema coma.
8.4 Pediatric Use
TIROSINT-SOL is indicated in patients from birth to less than 17 years of age:
- As a replacement therapy in primary (thyroidal), secondary (pituitary), and tertiary (hypothalamic) congenital or acquired hypothyroidism
- As an adjunct to surgery and radioiodine therapy in the management of thyrotropin-dependent well-differentiated thyroid cancer
Rapid restoration of normal serum T4 concentrations is essential for preventing the adverse effects of congenital hypothyroidism on cognitive development as well as on overall physical growth and maturation. Therefore, initiate TIROSINT-SOL therapy immediately upon diagnosis. Levothyroxine is generally continued for life in these patients [see Warnings and Precautions (5.1)].
Closely monitor infants during the first two weeks of TIROSINT-SOL therapy for cardiac overload and arrhythmias.
8.5 Geriatric Use
Because of the increased prevalence of cardiovascular disease among the elderly, initiate TIROSINT-SOL at less than the full replacement dose [ see Dosage and Administration (2.3) and Warnings and Precautions (5.1) ]. Atrial arrhythmias can occur in elderly patients. Atrial fibrillation is the most common of the arrhythmias observed with levothyroxine overtreatment in the elderly .
4 Contraindications (4 CONTRAINDICATIONS)
TIROSINT-SOL is contraindicated in patients with:
- Hypersensitivity to glycerol, the inactive ingredient in TIROSINT-SOL [see Adverse Events (6)].
- Uncorrected adrenal insufficiency [see Warnings and Precautions (5.4)]
6 Adverse Reactions (6 ADVERSE REACTIONS)
Adverse reactions associated with TIROSINT-SOL therapy are primarily those of hyperthyroidism due to therapeutic overdosage [see Warnings and Precautions (5) and Overdosage (10)]. They include the following:
- General: fatigue, increased appetite, weight loss, heat intolerance, fever, excessive sweating
- Central nervous system: headache, hyperactivity, nervousness, anxiety, irritability, emotional lability, insomnia
- Musculoskeletal: tremors, muscle weakness, muscle spasm
- Cardiovascular: palpitations, tachycardia, arrhythmias, increased pulse and blood pressure, heart failure, angina, myocardial infarction, cardiac arrest
- Respiratory: dyspnea
- Gastrointestinal (GI): diarrhea, vomiting, abdominal cramps, elevations in liver function tests
- Dermatologic: hair loss, flushing, rash
- Endocrine: decreased bone mineral density
- Reproductive: menstrual irregularities, impaired fertility
Seizures have been reported rarely with the institution of levothyroxine therapy.
7 Drug Interactions (7 DRUG INTERACTIONS)
See full prescribing information for drugs that affect thyroid hormone pharmacokinetics and metabolism (e.g., absorption, synthesis, secretion, catabolism, protein binding, and target tissue response) and may alter the therapeutic response to TIROSINT-SOL ( 7)
7.7 Sympathomimetics
Concurrent use of sympathomimetics and TIROSINT-SOL may increase the effects of sympathomimetics or thyroid hormone. Thyroid hormones may increase the risk of coronary insufficiency when sympathomimetic agents are administered to patients with coronary artery disease.
Recent Major Changes (RECENT MAJOR CHANGES)
Storage and Handling
Store TIROSINT-SOL in the original container (closed pouch) at 20°C to 25°C (68°F to 77°F); excursions permitted to 15° to 30°C (59°F to 86°F) [See USP Controlled Room Temperature].
Use TIROSINT-SOL oral solution within three (3) months after opening the pouch. Keep the ampules in the pouch until ready to use as important information may be lost (i.e., manufacturer/distributor names and distributor contact phone number).
12.2 Pharmacodynamics
Oral levothyroxine sodium is a synthetic T4 hormone that exerts the same physiologic effect as endogenous T4, thereby maintaining normal T4 levels when a deficiency is present.
1 Indication and Usage (1 INDICATION AND USAGE)
TIROSINT-SOL is L-thyroxine (T4) indicated in adult and pediatric patients, including neonates, for:
- Hypothyroidism - As replacement therapy in primary (thyroidal), secondary (pituitary), and tertiary (hypothalamic) congenital or acquired hypothyroidism ( 1)
- Pituitary Thyrotropin (Thyroid-Stimulating Hormone, TSH) Suppression - As an adjunct to surgery and radioiodine therapy in the management of thyrotropin-dependent well-differentiated thyroid cancer ( 1)
Limitations of Use
7.3 Oral Anticoagulants
TIROSINT-SOL increases the response to oral anticoagulant therapy. Therefore, a decrease in the dose of anticoagulant may be warranted with correction of the hypothyroid state or when the TIROSINT-SOL dose is increased. Closely monitor coagulation tests to permit appropriate and timely dosage adjustments.
12.1 Mechanism of Action
Thyroid hormones exert their physiologic actions through control of DNA transcription and protein synthesis. Triiodothyronine (T3) and L-thyroxine (T4) diffuse into the cell nucleus and bind to thyroid receptor proteins attached to DNA. This hormone nuclear receptor complex activates gene transcription and synthesis of messenger RNA and cytoplasmic proteins.
The physiological actions of thyroid hormones are produced predominantly by T3, the majority of which (approximately 80%) is derived from T4 by deiodination in peripheral tissues.
7.2 Antidiabetic Therapy
Addition of TIROSINT-SOL therapy in patients with diabetes mellitus may worsen glycemic control and result in increased antidiabetic agent or insulin requirements. Carefully monitor glycemic control, especially when thyroid therapy is started, changed, or discontinued [see Warnings and Precautions (5.5)] .
7.4 Digitalis Glycosides
TIROSINT-SOL may reduce the therapeutic effects of digitalis glycosides. Serum digitalis glycoside levels may decrease when a hypothyroid patient becomes euthyroid, necessitating an increase in the dose of digitalis glycosides.
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
- Serious risks related to overtreatment or undertreatment with TIROSINT-SOL: Titrate the dose of TIROSINT-SOL carefully and monitor response to titration. ( 5.1)
- Cardiac adverse reactions in the elderly and in patients with underlying cardiovascular disease: Initiate TIROSINT-SOL at less than the full replacement dose because of the increased risk of cardiac adverse reactions, including atrial fibrillation. ( 2.3, 5.2, 8.5)
- Myxedema coma: Do not use oral thyroid hormone drug products to treat myxedema coma. ( 5.3)
- Acute adrenal crisis in patients with concomitant adrenal insufficiency: Treat with replacement glucocorticoids prior to initiation of TIROSINT‑SOL treatment. ( 5.4)
- Worsening of diabetic control: therapy in patients with diabetes mellitus may worsen glycemic control and result in increased antidiabetic agent or insulin requirements. Carefully monitor glycemic control after starting, changing, or discontinuing thyroid hormone therapy. ( 5.5)
- Decreased bone mineral density associated with thyroid hormone over-replacement: Over-replacement can increase bone resorption and decrease bone mineral density. Give the lowest effective dose. 5.6)
7.5 Antidepressant Therapy
Concurrent use of tricyclic (e.g., amitriptyline) or tetracyclic (e.g., maprotiline) antidepressants and TIROSINT-SOL may increase the therapeutic and toxic effects of both drugs, possibly due to increased receptor sensitivity to catecholamines. Toxic effects may include increased risk of cardiac arrhythmias and central nervous system stimulation. TIROSINT-SOL may accelerate the onset of action of tricyclics. Administration of sertraline in patients stabilized on TIROSINT-SOL may result in increased TIROSINT-SOL requirements.
7.9 Drug Food Interactions (7.9 Drug-Food Interactions)
Consumption of certain foods may affect TIROSINT-SOL absorption thereby necessitating adjustments in dosing [see Dosage and Administration (2.1)] . Soybean flour (infant formula), cottonseed meal, walnuts, and dietary fiber may bind and decrease the absorption of TIROSINT-SOL from the gastrointestinal tract. Grapefruit juice may delay the absorption of levothyroxine and reduce its bioavailability.
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
- Administer once daily, on an empty stomach, 15 minutes before breakfast ( 2.1)
- Administer at least 4 hours before or after drugs that are known to interfere with absorption ( 2.1)
- Evaluate the need for dose adjustments when regularly administering within an hour of certain foods that may affect TIROSINT-SOL absorption ( 2.1)
- To administer TIROSINT-SOL in water, squeeze the contents of one single unit-dose ampule into a glass or cup containing water ( 2.1)
- To administer TIROSINT-SOL directly, either squeeze it into the mouth OR onto a spoon and immediately consume ( 2.1)
- Starting dose depends on a variety of factors, including age, body weight, cardiovascular status, and concomitant medications, co-administered food, and the specific nature of the condition being treated. Peak therapeutic effect may not be attained for 4-6 weeks ( 2.2)
- See full prescribing information for dosing in specific patient populations ( 2.3)
- Adequacy of therapy determined with periodic monitoring of TSH and/or T4 as well as clinical status ( 2.4)
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
TIROSINT-SOL oral solution is a clear, colorless to slightly yellow solution supplied in a 1 mL white, non-transparent, unit-dose ampule. Each ampule bears a colored label with the dosage strength and the product name (TIROSINT-SOL) (Table 4).
Table 4. TIROSINT-SOL Solution Strengths and Identifying Features
| Strength (mcg/mL) | Color |
|---|---|
| 13 | Green |
| 25 | Orange |
| 37.5 | Dark Blue |
| 44 | Red |
| 50 | White |
| 75 | Purple |
| 62.5 | Grey |
| 88 | Olive |
| 100 | Yellow |
| 112 | Rose |
| 125 | Brown |
| 137 | Turquoise |
| 150 | Blue |
| 175 | Lilac |
| 200 | Pink |
8 Use in Specific Populations (8 USE IN SPECIFIC POPULATIONS)
7.8 Tyrosine Kinase Inhibitors (7.8 Tyrosine-Kinase Inhibitors)
Concurrent use of tyrosine-kinase inhibitors such as imatinib may cause hypothyroidism. Closely monitor TSH levels in such patients.
17 Patient Counseling Information (17 PATIENT COUNSELING INFORMATION)
Advise the patient and/or caregiver to read the FDA-approved patient labeling (Patient Information and Instructions for Use).
5.5 Worsening of Diabetic Control
Addition of levothyroxine therapy in patients with diabetes mellitus may worsen glycemic control and result in increased antidiabetic agent or insulin requirements. Carefully monitor glycemic control after starting, changing, or discontinuing TIROSINT-SOL [see Drug Interactions (7.2)] .
2.3 Recommended Dosage and Titration
Primary, Secondary, and Tertiary Hypothyroidism in Adults
2.1 General Administration Information
Administer TIROSINT-SOL as a single daily oral dose, on an empty stomach,15 minutes before breakfast.
Administer TIROSINT-SOL at least 4 hours before or after drugs known to interfere with TIROSINT-SOL absorption [see Drug Interactions (7.1)] .
Evaluate the need for dose adjustments when regularly administering within an hour of certain foods that may affect TIROSINT-SOL absorption [see Dosage and Administration (2.2 and 2.3) , Drug Interactions (7.9) and Clinical Pharmacology (12.3)] .
TIROSINT-SOL may be administered in water or directly into the mouth:
- To administer TIROSINT-SOL in water, squeeze the contents of one single unit-dose ampule into a glass or cup containing water. Stir the diluted TIROSINT-SOL and drink all of it immediately. Rinse the glass or cup with additional water and drink the contents to ensure that the total dose is taken. Do not dilute TIROSINT-SOL in a medium other than water. Open the ampule and prepare the solution immediately before intake.
- To administer TIROSINT-SOL directly (without water), either squeeze it into the mouth OR onto a spoon and immediately consume.
7.10 Drug Laboratory Test Interactions (7.10 Drug-Laboratory Test Interactions)
Consider changes in TBG concentration when interpreting T4 and T3 values. Measure and evaluate unbound (free) hormone and/or determine the free-T4 index (FT4I) in this circumstance. Pregnancy, infectious hepatitis, estrogens, estrogen-containing oral contraceptives, and acute intermittent porphyria increase TBG concentrations. Nephrosis, severe hypoproteinemia, severe liver disease, acromegaly, androgens and corticosteroids decrease TBG concentration. Familial hyper- or hypo-thyroxine binding globulinemias have been described, with the incidence of TBG deficiency approximating 1 in 9000.
2.2 Important Considerations for Dosing
The dosage of TIROSINT-SOL for hypothyroidism or pituitary TSH suppression depends on a variety of factors including: the patient's age, body weight, cardiovascular status, concomitant medical conditions (including pregnancy), concomitant medications, co-administered food, and the specific nature of the condition being treated [see Dosage and Administration (2.3), Warnings and Precautions (5), and Drug Interactions (7)] . Dosing must be individualized to account for these factors and dosage adjustments made based on periodic assessment of the patient's clinical response and laboratory parameters [see Dosage and Administration (2.4)] .
For adult patients with primary hypothyroidism, titrate until the patient is clinically euthyroid and the serum TSH returns to normal [see Dosage and Administration (2.3)].
For secondary or tertiary hypothyroidism, serum TSH is not a reliable measure of TIROSINT-SOL dosage adequacy and should not be used to monitor therapy. Use the serum free-T4 level to titrate TIROSINT-SOL dosing until the patient is clinically euthyroid and the serum free-T4 level is restored to the upper half of the normal range [see Dosage and Administration (2.3)].
The peak therapeutic effect of a given dose of TIROSINT-SOL may not be attained for 4 to 6 weeks.
2.4 Monitoring Tsh And/or Thyroxine (t4) Levels (2.4 Monitoring TSH and/or Thyroxine (T4) Levels)
Assess the adequacy of therapy by periodic assessment of laboratory tests and clinical evaluation. Persistent clinical and laboratory evidence of hypothyroidism, despite an apparent adequate replacement dose of TIROSINT-SOL, may be evidence of inadequate absorption, poor compliance, drug interactions, or a combination of these factors.
Warning: Not for Treatment of Obesity Or for Weight Loss (WARNING: NOT FOR TREATMENT OF OBESITY OR FOR WEIGHT LOSS)
- Thyroid hormones, including TIROSINT-SOL, either alone or with other therapeutic agents, should not be used for the treatment of obesity or for weight loss.
- In euthyroid patients, doses within the range of daily hormonal requirements are ineffective for weight reduction.
- Larger doses may produce serious or even life threatening manifestations of toxicity, particularly when given in association with sympathomimetic amines such as those used for their anorectic effects [see Adverse Reactions (6), Drug Interactions (7.7), and Overdosage (10)].
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Long-term carcinogenicity studies in animals to evaluate the carcinogenic potential of levothyroxine have not been performed. Studies to evaluate mutagenic potential and animal fertility have not been performed.
7.1 Drugs Known to Affect Thyroid Hormone Pharmacokinetics
Many drugs can exert effects on thyroid hormone pharmacokinetics and metabolism (e.g., absorption, synthesis, secretion, catabolism, protein binding, and target tissue response) and may alter the therapeutic response to TIROSINT-SOL (Tables 5 to 8).
Table 5. Drugs That May Decrease T4 Absorption (Hypothyroidism)
|
Potential impact: Concurrent use may reduce the efficacy of TIROSINT-SOL by binding and delaying or preventing absorption, potentially resulting in hypothyroidism. |
|
|
Drug or Drug Class |
Effect |
|
Phosphate Binders (e.g., calcium carbonate, ferrous sulfate, sevelamer, lanthanum) |
Phosphate binders may bind to levothyroxine. Administer TIROSINT-SOL at least 4 hours apart from these agents. |
|
Orlistat |
Monitor patients treated concomitantly with orlistat and TIROSINT‑SOL for changes in thyroid function. |
|
Bile Acid Sequestrants (e.g., colesevelam, cholestyramine, colestipol Ion Exchange Resins (e.g., Kayexalate) |
Bile acid sequestrants and ion exchange resins are known to decrease levothyroxine absorption. Administer TIROSINT-SOL at least 4 hours prior to these drugs or monitor TSH levels. |
|
Sucralfate Antacids (e.g., aluminum & magnesium hydroxides, simethicone) |
Gastric acidity is an essential requirement for adequate absorption of levothyroxine. However, gastric acidity may not be as essential for the absorption of TIROSINT-SOL. Sucralfate and antacids may cause hypochlorhydria, affect gastric pH, and reduce levothyroxine absorption. Monitor patients appropriately. |
Table 6. Drugs That May Alter T4 and Triiodothyronine (T3) Serum Transport Without Affecting Free Thyroxine (FT4) Concentration (Euthyroidism)
|
Drug or Drug Class |
Effect |
|
Clofibrate Estrogen-containing oral contraceptives Estrogens (oral) Heroin / Methadone 5-Fluorouracil Mitotane Tamoxifen |
These drugs may increase serum thyroxine-binding globulin (TBG) concentration. |
|
Androgens / Anabolic Steroids
|
These drugs may decrease serum TBG concentration. |
|
Potential impact (below): Administration of these agents with TIROSINT-SOL results in an initial transient increase in FT4. Continued administration results in a decrease in serum T4 and normal FT4 and TSH concentrations. |
|
|
Salicylates (> 2 g/day) |
Salicylates inhibit binding of T4 and T3 to TBG and transthyretin. An initial increase in serum FT4 is followed by return of FT4 to normal levels with sustained therapeutic serum salicylate concentrations, although total T4 levels may decrease by as much as 30%. |
|
Other drugs: Carbamazepine Furosemide (> 80 mg IV) Heparin Hydantoins Non-Steroidal Anti-inflammatory Drugs: Fenamates |
These drugs may cause protein-binding site displacement. Furosemide has been shown to inhibit the protein binding of T4 to TBG and albumin, causing an increase free‑T4 fraction in serum. Furosemide competes for T4-binding sites on TBG, prealbumin, and albumin, so that a single high dose can acutely lower the total T4 level. Phenytoin and carbamazepine reduce serum protein binding of levothyroxine, and total and free‑T4 may be reduced by 20% to 40%, but most patients have normal serum TSH levels and are clinically euthyroid. Closely monitor thyroid hormone parameters. |
Table 7. Drugs That May Alter Hepatic Metabolism of T4 (Hypothyroidism)
|
Potential impact: Stimulation of hepatic microsomal drug-metabolizing enzyme activity may cause increased hepatic degradation of levothyroxine, resulting in increased TIROSINT-SOL requirements. |
|
|
Drug or Drug Class |
Effect |
|
Phenobarbital Rifampin |
Phenobarbital has been shown to reduce the response to thyroxine. Phenobarbital increases L-thyroxine metabolism by inducing uridine 5’ diphospho-glucuronosyltransferase (UGT) and leads to a lower T4 serum levels. Changes in thyroid status may occur if barbiturates are added or withdrawn from patients being treated for hypothyroidism. Rifampin has been shown to accelerate the metabolism of levothyroxine. |
Table 8. Drugs That May Decrease Conversion of T4 to T3
|
Potential impact: Administration of these enzyme inhibitors decreases the peripheral conversion of T4 to T3, leading to decreased T3 levels. However, serum T4 levels are usually normal but may occasionally be slightly increased. |
|
|
Drug or Drug Class |
Effect |
|
Beta-adrenergic antagonists (e.g., Propranolol > 160 mg/day) |
In patients treated with large doses of propranolol (> 160 mg/day), T3 and T4 levels change, TSH levels remain normal, and patients are clinically euthyroid. Actions of particular beta-adrenergic antagonists may be impaired when a hypothyroid patient is converted to the euthyroid state. |
|
Glucocorticoids (e.g., Dexamethasone > 4 mg/day) |
Short-term administration of large doses of glucocorticoids may decrease serum T3 concentrations by 30% with minimal change in serum T4 levels. However, long-term glucocorticoid therapy may result in slightly decreased T3 and T4 levels due to decreased TBG production (See above). |
|
Other drugs: Amiodarone |
Amiodarone inhibits peripheral conversion of T4 to T3 and may cause isolated biochemical changes (increase in serum free-T4, and decrease or normal free-T3) in clinically euthyroid patients. |
Principal Display Panel 13 Microgram/ml Ampule Pouch Carton (PRINCIPAL DISPLAY PANEL - 13 microgram/mL Ampule Pouch Carton)
NDC 71858-0105-5
TIROSINT
® - SOL
(levothyroxine sodium) Oral Solution
13 microgram/mL
For Oral Use Only – NOT for Inhalation, Injection or Ophthalmic Use
R x Only
6 pouches x 5 ampules
IBSA
Principal Display Panel 25 Microgram/ml Ampule Pouch Carton (PRINCIPAL DISPLAY PANEL - 25 microgram/mL Ampule Pouch Carton)
NDC 71858-0110-5
TIROSINT
® - SOL
(levothyroxine sodium) Oral Solution
25 microgram/mL
For Oral Use Only – NOT for Inhalation, Injection or Ophthalmic Use
R x Only
6 pouches x 5 ampules
IBSA
Principal Display Panel 44 Microgram/ml Ampule Pouch Carton (PRINCIPAL DISPLAY PANEL - 44 microgram/mL Ampule Pouch Carton)
NDC 71858-0113-5
TIROSINT
® - SOL
(levothyroxine sodium) Oral Solution
44 microgram/mL
For Oral Use Only – NOT for Inhalation, Injection or Ophthalmic Use
R x Only
6 pouches x 5 ampules
IBSA
Principal Display Panel 50 Microgram/ml Ampule Pouch Carton (PRINCIPAL DISPLAY PANEL - 50 microgram/mL Ampule Pouch Carton)
NDC 71858-0115-5
TIROSINT
® - SOL
(levothyroxine sodium) Oral Solution
50 microgram/mL
For Oral Use Only – NOT for Inhalation, Injection or Ophthalmic Use
R x Only
6 pouches x 5 ampules
IBSA
Principal Display Panel 75 Microgram/ml Ampule Pouch Carton (PRINCIPAL DISPLAY PANEL - 75 microgram/mL Ampule Pouch Carton)
NDC 71858-0120-5
TIROSINT
® - SOL
(levothyroxine sodium) Oral Solution
75 microgram/mL
For Oral Use Only – NOT for Inhalation, Injection or Ophthalmic Use
R x Only
6 pouches x 5 ampules
IBSA
Principal Display Panel 88 Microgram/ml Ampule Pouch Carton (PRINCIPAL DISPLAY PANEL - 88 microgram/mL Ampule Pouch Carton)
NDC 71858-0125-5
TIROSINT
® - SOL
(levothyroxine sodium) Oral Solution
88 microgram/mL
For Oral Use Only – NOT for Inhalation, Injection or Ophthalmic Use
R x Only
6 pouches x 5 ampules
IBSA
Principal Display Panel 100 Microgram/ml Ampule Pouch Carton (PRINCIPAL DISPLAY PANEL - 100 microgram/mL Ampule Pouch Carton)
NDC 71858-0130-5
TIROSINT
® - SOL
(levothyroxine sodium) Oral Solution
100 microgram/mL
For Oral Use Only – NOT for Inhalation, Injection or Ophthalmic Use
R x Only
6 pouches x 5 ampules
IBSA
Principal Display Panel 112 Microgram/ml Ampule Pouch Carton (PRINCIPAL DISPLAY PANEL - 112 microgram/mL Ampule Pouch Carton)
NDC 71858-0135-5
TIROSINT
® - SOL
(levothyroxine sodium) Oral Solution
112 microgram/mL
For Oral Use Only – NOT for Inhalation, Injection or Ophthalmic Use
R x Only
6 pouches x 5 ampules
IBSA
Principal Display Panel 125 Microgram/ml Ampule Pouch Carton (PRINCIPAL DISPLAY PANEL - 125 microgram/mL Ampule Pouch Carton)
NDC 71858-0140-5
TIROSINT
® - SOL
(levothyroxine sodium) Oral Solution
125 microgram/mL
For Oral Use Only – NOT for Inhalation, Injection or Ophthalmic Use
R x Only
6 pouches x 5 ampules
IBSA
Principal Display Panel 137 Microgram/ml Ampule Pouch Carton (PRINCIPAL DISPLAY PANEL - 137 microgram/mL Ampule Pouch Carton)
NDC 71858-0145-5
TIROSINT
® - SOL
(levothyroxine sodium) Oral Solution
137 microgram/mL
For Oral Use Only – NOT for Inhalation, Injection or Ophthalmic Use
R x Only
6 pouches x 5 ampules
IBSA
Principal Display Panel 150 Microgram/ml Ampule Pouch Carton (PRINCIPAL DISPLAY PANEL - 150 microgram/mL Ampule Pouch Carton)
NDC 71858-0150-5
TIROSINT
® - SOL
(levothyroxine sodium) Oral Solution
150 microgram/mL
For Oral Use Only – NOT for Inhalation, Injection or Ophthalmic Use
R x Only
6 pouches x 5 ampules
IBSA
Principal Display Panel 175 Microgram/ml Ampule Pouch Carton (PRINCIPAL DISPLAY PANEL - 175 microgram/mL Ampule Pouch Carton)
NDC 71858-0155-5
TIROSINT
® - SOL
(levothyroxine sodium) Oral Solution
175 microgram/mL
For Oral Use Only – NOT for Inhalation, Injection or Ophthalmic Use
R x Only
6 pouches x 5 ampules
IBSA
Principal Display Panel 200 Microgram/ml Ampule Pouch Carton (PRINCIPAL DISPLAY PANEL - 200 microgram/mL Ampule Pouch Carton)
NDC 71858-0160-5
TIROSINT
® - SOL
(levothyroxine sodium) Oral Solution
200 microgram/mL
For Oral Use Only – NOT for Inhalation, Injection or Ophthalmic Use
R x Only
6 pouches x 5 ampules
IBSA
Principal Display Panel 37.5 Microgram/ml Ampule Pouch Carton (PRINCIPAL DISPLAY PANEL - 37.5 microgram/mL Ampule Pouch Carton)
NDC 71858-0112-5
TIROSINT
® - SOL
(levothyroxine sodium) Oral Solution
37.5 microgram/mL
For Oral Use Only – NOT for Inhalation, Injection or Ophthalmic Use
R x Only
6 pouches x 5 ampules
IBSA
Principal Display Panel 62.5 Microgram/ml Ampule Pouch Carton (PRINCIPAL DISPLAY PANEL - 62.5 microgram/mL Ampule Pouch Carton)
NDC 71858-0117-5
TIROSINT
® - SOL
(levothyroxine sodium) Oral Solution
62.5 microgram/mL
For Oral Use Only – NOT for Inhalation, Injection or Ophthalmic Use
R x Only
6 pouches x 5 ampules
IBSA
5.4 Acute Adrenal Crisis in Patients With Concomitant Adrenal Insufficiency (5.4 Acute Adrenal Crisis in Patients with Concomitant Adrenal Insufficiency)
Thyroid hormone increases metabolic clearance of glucocorticoids. Initiation of thyroid hormone therapy prior to initiating glucocorticoid therapy may precipitate an acute adrenal crisis in patients with adrenal insufficiency. Treat patients with adrenal insufficiency with replacement glucocorticoids prior to initiating treatment with TIROSINT-SOL [see Contraindications (4)].
5.1 Serious Risks Related to Overtreatment Or Undertreatment With Tirosint Sol (5.1 Serious Risks Related to Overtreatment or Undertreatment with TIROSINT-SOL)
TIROSINT-SOL has a narrow therapeutic index. Overtreatment or undertreatment with TIROSINT-SOL may have negative effects on growth and development, cardiovascular function, bone metabolism, reproductive function, cognitive function, gastrointestinal function, and glucose and lipid metabolism in adult or pediatric patients.
In pediatric patients with congenital and acquired hypothyroidism, undertreatment may adversely affect cognitive development and linear growth, and overtreatment is associated with craniosynostosis and acceleration of bone age [see Use in Specific Populations (8.4)].
Titrate the dose of TIROSINT-SOL carefully and monitor response to titration to avoid these effects [see Dosage and Administration (2.4)]. Consider the potential for food or drug interactions and adjust the administration or dosage of TIROSINT-SOL as needed [see Dosage and Administration (2.4), Drug Interactions (7.1), and Clinical Pharmacology (12.3)].
5.6 Decreased Bone Mineral Density Associated With Thyroid Hormone Over Replacement (5.6 Decreased Bone Mineral Density Associated with Thyroid Hormone Over-Replacement)
Increased bone resorption and decreased bone mineral density may occur as a result of levothyroxine over-replacement, particularly in post-menopausal women. The increased bone resorption may be associated with increased serum levels and urinary excretion of calcium and phosphorous, elevations in bone alkaline phosphatase, and suppressed serum parathyroid hormone levels. Administer the minimum dose of TIROSINT-SOL that achieves the desired clinical and biochemical response to mitigate this risk.
5.2 Cardiac Adverse Reactions in the Elderly and in Patients With Underlying Cardiovascular Disease (5.2 Cardiac Adverse Reactions in the Elderly and in Patients with Underlying Cardiovascular Disease)
Overtreatment with levothyroxine may cause an increase in heart rate, cardiac wall thickness, and cardiac contractility, and may precipitate angina or arrhythmias, particularly in patients with cardiovascular disease and in elderly patients. Initiate TIROSINT-SOL therapy in this population at lower doses than those recommended in younger individuals or in patients without cardiac disease [see Dosage and Administration (2.3) and Use in Specific Populations (8.5)].
Monitor for cardiac arrhythmias during surgical procedures in patients with coronary artery disease receiving suppressive TIROSINT-SOL therapy. Monitor patients receiving concomitant TIROSINT-SOL and sympathomimetic agents for signs and symptoms of coronary insufficiency . If cardiac symptoms develop or worsen, reduce the TIROSINT-SOL dose or withhold it for one week and restart at a lower dose.
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:48:25.193745 · Updated: 2026-03-14T22:29:49.659194