These Highlights Do Not Include All The Information Needed To Use Precedex Safely And Effectively. See Full Prescribing Information For Precedex.
548a88c0-afda-427e-75ac-5af0cfa2224c
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
Dosage and Administration, Preparation of Solution ( 2.4 ) 10/2024
Indications and Usage
PRECEDEX is a alpha 2 -adrenergic receptor agonist indicated for: • Sedation of initially intubated and mechanically ventilated adult patients during treatment in an intensive care setting. Administer PRECEDEX by continuous infusion not to exceed 24 hours. ( 1.1 ) • Sedation of non-intubated adult patients prior to and/or during surgical and other procedures. ( 1.2 ) • Sedation of non-intubated pediatric patients aged 1 month to less than 18 years prior to and during non-invasive procedures. ( 1.2 )
Dosage and Administration
• Individualize and titrate PRECEDEX dosing to desired clinical effect. ( 2.1 ) • Administer PRECEDEX using a controlled infusion device. ( 2.1 ) • Dilute the 200 mcg/2 mL (100 mcg/mL) vial contents in 0.9% sodium chloride solution to achieve required concentration (4 mcg/mL) prior to administration. ( 2.4 ) • The 80 mcg/20 mL single-dose vial, and 200 mcg/50 mL, 400 mcg/100 mL, and 1,000 mcg/250 mL single-dose bottles and single-dose flexible containers do not require further dilution prior to administration. ( 2.4 ) • For Adult Intensive Care Unit Sedation : Initiate at one mcg/kg over 10 minutes , followed by a maintenance infusion of 0.2 mcg/kg/ hour to 0.7 mcg/kg/ hour . ( 2.2 ) • For Adult Procedural Sedation : Initiate at one mcg/kg over 10 minutes , followed by a maintenance infusion initiated at 0.6 mcg/kg/ hour and titrated to achieve desired clinical effect with doses ranging from 0.2 mcg/kg/ hour to 1 mcg/kg/ hour . ( 2.2 ) • For Sedation of Pediatric Patients During Non-invasive Procedures : Patients 1 month to less than 2 years old initiate at 1.5 mcg/kg over 10 minutes followed by a maintenance infusion of 1.5 mcg/kg/ hour and titrated to achieve desired clinical effect with dosage ranging from 0.5 mcg/kg/ hour to 1.5 mcg/kg/ hour ; patients 2 to less than 18 years old initiate at 2 mcg/kg over 10 minutes followed by a maintenance infusion of 1.5 mcg/kg/ hour and titrated to achieve desired clinical effect with dosage ranging from 0.5 mcg/kg/ hour to 1.5 mcg/kg/ hour . ( 2.2 ) • Alternative Doses : Recommended for patients over 65 years of age and awake fiberoptic intubation patients. ( 2.2 )
Warnings and Precautions
• Monitoring : Continuously monitor patients while receiving PRECEDEX. ( 5.1 ) • Bradycardia and Sinus Arrest : Have occurred in young healthy volunteers with high vagal tone or with different routes of administration, e.g., rapid intravenous or bolus administration. ( 5.2 ) • Hypotension and Bradycardia : May necessitate medical intervention. May be more pronounced in patients with hypovolemia, diabetes mellitus, or chronic hypertension, and in the elderly. Use with caution in patients with advanced heart block or severe ventricular dysfunction. ( 5.2 ) • Co-administration with Other Vasodilators or Negative Chronotropic Agents : Use with caution due to additive pharmacodynamic effects. ( 5.2 ) • Transient Hypertension : Observed primarily during the loading dose. Consider reduction in loading infusion rate. ( 5.3 ) • Arousability : Patients can become aroused/alert with stimulation; this alone should not be considered as lack of efficacy. ( 5.4 ) • Tolerance and Tachyphylaxis : Prolonged exposure to dexmedetomidine beyond 24 hours may be associated with tolerance and tachyphylaxis and a dose-related increase in adverse events. ( 5.6 )
Contraindications
None.
Adverse Reactions
The following clinically significant adverse reactions are described elsewhere in the labeling: • Hypotension, bradycardia and sinus arrest [see Warnings and Precautions (5.2) ] • Transient hypertension [see Warnings and Precautions (5.3) ]
Drug Interactions
Anesthetics, Sedatives, Hypnotics, Opioids: Enhancement of pharmacodynamic effects. Reduction in dosage of PRECEDEX or the concomitant medication may be required. ( 7.1 )
Medication Information
Warnings and Precautions
• Monitoring : Continuously monitor patients while receiving PRECEDEX. ( 5.1 ) • Bradycardia and Sinus Arrest : Have occurred in young healthy volunteers with high vagal tone or with different routes of administration, e.g., rapid intravenous or bolus administration. ( 5.2 ) • Hypotension and Bradycardia : May necessitate medical intervention. May be more pronounced in patients with hypovolemia, diabetes mellitus, or chronic hypertension, and in the elderly. Use with caution in patients with advanced heart block or severe ventricular dysfunction. ( 5.2 ) • Co-administration with Other Vasodilators or Negative Chronotropic Agents : Use with caution due to additive pharmacodynamic effects. ( 5.2 ) • Transient Hypertension : Observed primarily during the loading dose. Consider reduction in loading infusion rate. ( 5.3 ) • Arousability : Patients can become aroused/alert with stimulation; this alone should not be considered as lack of efficacy. ( 5.4 ) • Tolerance and Tachyphylaxis : Prolonged exposure to dexmedetomidine beyond 24 hours may be associated with tolerance and tachyphylaxis and a dose-related increase in adverse events. ( 5.6 )
Indications and Usage
PRECEDEX is a alpha 2 -adrenergic receptor agonist indicated for: • Sedation of initially intubated and mechanically ventilated adult patients during treatment in an intensive care setting. Administer PRECEDEX by continuous infusion not to exceed 24 hours. ( 1.1 ) • Sedation of non-intubated adult patients prior to and/or during surgical and other procedures. ( 1.2 ) • Sedation of non-intubated pediatric patients aged 1 month to less than 18 years prior to and during non-invasive procedures. ( 1.2 )
Dosage and Administration
• Individualize and titrate PRECEDEX dosing to desired clinical effect. ( 2.1 ) • Administer PRECEDEX using a controlled infusion device. ( 2.1 ) • Dilute the 200 mcg/2 mL (100 mcg/mL) vial contents in 0.9% sodium chloride solution to achieve required concentration (4 mcg/mL) prior to administration. ( 2.4 ) • The 80 mcg/20 mL single-dose vial, and 200 mcg/50 mL, 400 mcg/100 mL, and 1,000 mcg/250 mL single-dose bottles and single-dose flexible containers do not require further dilution prior to administration. ( 2.4 ) • For Adult Intensive Care Unit Sedation : Initiate at one mcg/kg over 10 minutes , followed by a maintenance infusion of 0.2 mcg/kg/ hour to 0.7 mcg/kg/ hour . ( 2.2 ) • For Adult Procedural Sedation : Initiate at one mcg/kg over 10 minutes , followed by a maintenance infusion initiated at 0.6 mcg/kg/ hour and titrated to achieve desired clinical effect with doses ranging from 0.2 mcg/kg/ hour to 1 mcg/kg/ hour . ( 2.2 ) • For Sedation of Pediatric Patients During Non-invasive Procedures : Patients 1 month to less than 2 years old initiate at 1.5 mcg/kg over 10 minutes followed by a maintenance infusion of 1.5 mcg/kg/ hour and titrated to achieve desired clinical effect with dosage ranging from 0.5 mcg/kg/ hour to 1.5 mcg/kg/ hour ; patients 2 to less than 18 years old initiate at 2 mcg/kg over 10 minutes followed by a maintenance infusion of 1.5 mcg/kg/ hour and titrated to achieve desired clinical effect with dosage ranging from 0.5 mcg/kg/ hour to 1.5 mcg/kg/ hour . ( 2.2 ) • Alternative Doses : Recommended for patients over 65 years of age and awake fiberoptic intubation patients. ( 2.2 )
Contraindications
None.
Adverse Reactions
The following clinically significant adverse reactions are described elsewhere in the labeling: • Hypotension, bradycardia and sinus arrest [see Warnings and Precautions (5.2) ] • Transient hypertension [see Warnings and Precautions (5.3) ]
Drug Interactions
Anesthetics, Sedatives, Hypnotics, Opioids: Enhancement of pharmacodynamic effects. Reduction in dosage of PRECEDEX or the concomitant medication may be required. ( 7.1 )
Description
Dosage and Administration, Preparation of Solution ( 2.4 ) 10/2024
Section 42229-5
PRECEDEX Presentations Requiring Dilution:
-
•PRECEDEX Injection, 200 mcg/2 mL (100 mcg/mL)
PRECEDEX must be diluted with 0.9% sodium chloride injection to achieve required concentration (4 mcg/mL) prior to administration. Preparation of solutions is the same, whether for the loading dose or maintenance infusion.
To prepare the infusion, withdraw 2 mL of PRECEDEX Injection, and add to 48 mL of 0.9% sodium chloride injection to a total of 50 mL. Shake gently to mix well.
Section 43683-2
|
Dosage and Administration, Preparation of Solution (2.4) |
10/2024 |
Section 44425-7
Store at 20°C to 25°C (68°F to 77°F); excursions permitted between 15°C to 30°C (59°F to 86°F). [See USP Controlled Room Temperature.]
Do not use if product is discolored or if precipitate matter is present.
PRECEDEX (dexmedetomidine hydrochloride) injection 200 mcg/2 mL (100 mcg/mL) is clear and colorless. The strength is based on the dexmedetomidine base. Discard unused portion.
|
Unit of Sale |
Concentration |
|
NDC 0409-1638-02 Tray of 25 single-dose clear glass vials |
200 mcg/2 mL (100 mcg/mL) |
PRECEDEX (dexmedetomidine hydrochloride in 0.9% Sodium Chloride) injection (4 mcg/mL) is clear and colorless. The strength is based on the dexmedetomidine base. Discard unused portion.
|
Unit of Sale |
Concentration |
|
NDC 0409-1660-20 Carton of 10 single-dose clear glass vials |
80 mcg/20 mL (4 mcg/mL) |
|
NDC 0409-1660-50 Tray of 20 single-dose clear glass bottles |
200 mcg/50 mL (4 mcg/mL) |
|
NDC 0409-1660-10 Tray of 10 single-dose clear glass bottles |
400 mcg/100 mL (4 mcg/mL) |
|
NDC 0409-1596-10 Case of 10 cartons containing 1 single-dose clear glass bottle |
400 mcg/100 mL (4 mcg/mL) |
|
NDC 0409-1434-01 Carton containing 1 single-dose clear glass bottle |
1,000 mcg/250 mL (4 mcg/mL) |
|
NDC 0409-7838-24 Case of 24 single-dose flexible containers |
200 mcg/50 mL (4 mcg/mL) |
|
NDC 0409-7853-24 Case of 24 single-dose flexible containers |
400 mcg/100 mL (4 mcg/mL) |
|
NDC 0409-7875-12 Case of 12 single-dose flexible containers |
1,000 mcg/250 mL (4 mcg/mL) |
10 Overdosage
The tolerability of PRECEDEX was studied in one study in which healthy adult subjects were administered doses at and above the recommended dose of 0.2 mcg/kg/hr to 0.7 mcg/kg/hr. The maximum blood concentration achieved in this study was approximately 13 times the upper boundary of the therapeutic range. The most notable effects observed in two subjects who achieved the highest doses were first degree atrioventricular block and second-degree heart block. No hemodynamic compromise was noted with the atrioventricular block and the heart block resolved spontaneously within one minute.
Five adult patients received an overdose of PRECEDEX in the intensive care unit sedation studies. Two of these patients had no symptoms reported; one patient received a 2 mcg/kg loading dose over 10 minutes (twice the recommended loading dose) and one patient received a maintenance infusion of 0.8 mcg/kg/hr. Two other patients who received a 2 mcg/kg loading dose over 10 minutes, experienced bradycardia and/or hypotension. One patient who received a loading bolus dose of undiluted PRECEDEX (19.4 mcg/kg), had cardiac arrest from which he was successfully resuscitated.
11 Description
PRECEDEX (dexmedetomidine hydrochloride) injection (100 mcg/mL) is a sterile, nonpyrogenic solution suitable for intravenous infusion following dilution. PRECEDEX (dexmedetomidine hydrochloride) in 0.9% Sodium Chloride Injection (4 mcg/mL) is a sterile, nonpyrogenic ready to use solution suitable for intravenous infusion.
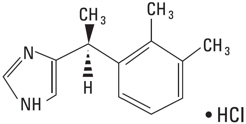
PRECEDEX contains dexmedetomidine hydrochloride as the active pharmaceutical ingredient. Dexmedetomidine hydrochloride is a central alpha2-adrenergic agonist. Dexmedetomidine hydrochloride is the S-enantiomer of medetomidine. Dexmedetomidine hydrochloride chemical name is 1H-Imidazole, 4-[1-(2,3-dimethylphenyl)ethyl]-, monohydrochloride, (S). Dexmedetomidine hydrochloride has a molecular weight of 236.7 and the empirical formula is C13H16N2•HCl and the structural formula is:
Dexmedetomidine hydrochloride is a white or almost white powder that is freely soluble in water and has a pKa of 7.1. Its partition coefficient in-octanol: water at pH 7.4 is 2.89.
PRECEDEX Injection is intended to be used after dilution. It is supplied as a clear, colorless, isotonic solution with a pH between 4.5 to 7.0. Each mL contains 118 mcg of dexmedetomidine hydrochloride (equivalent to 100 mcg or 0.1 mg of dexmedetomidine) and 9 mg of sodium chloride in water for injection. The solution is preservative-free and contains no additives or chemical stabilizers.
PRECEDEX in 0.9% Sodium Chloride Injection is ready to be used. It is supplied as a clear, colorless, isotonic solution with a pH between 4.5 to 8.0. Each mL contains 4.72 mcg of dexmedetomidine hydrochloride (equivalent to 4 mcg or 0.004 mg of dexmedetomidine) and 9 mg sodium chloride in water for injection. The solution is preservative-free and contains no additives or chemical stabilizers.
5.5 Withdrawal
9.3 Dependence
The dependence potential of PRECEDEX has not been studied in humans. However, since studies in rodents and primates have demonstrated that PRECEDEX exhibits pharmacologic actions similar to those of clonidine, it is possible that PRECEDEX may produce a clonidine-like withdrawal syndrome upon abrupt discontinuation [see Warnings and Precautions (5.5)].
5.4 Arousability
Some patients receiving PRECEDEX have been observed to be arousable and alert when stimulated. This alone should not be considered as evidence of lack of efficacy in the absence of other clinical signs and symptoms.
8.4 Pediatric Use
Sedation for Non-Invasive Procedures
The safety and efficacy of PRECEDEX have been established in pediatric patients 1 month to less than 18 years of age for sedation during non-invasive procedures. Use in this age group is based on one randomized double-blind, dose-ranging safety and efficacy trial in non-intubated pediatric patients 1 month to less than 17 years of age who required sedation prior to undergoing MRI scans [see Clinical Studies (14.2)]. An increase in frequency of bradypnea, bradycardia, hypertension and hypotension was observed in pediatric patients treated with PRECEDEX [see Adverse Reactions (6.1)]. The overall safety profile of PRECEDEX in pediatric patients was consistent with the known safety profile in adults [see Adverse Reactions (6.1)].
The safety and effectiveness of PRECEDEX have not been established in pediatric patients less than 1 month of age.
ICU Sedation
The safety and efficacy of PRECEDEX have not been established in pediatric patients for ICU sedation. One assessor-blinded trial in pediatric patients and two open label studies in neonates were conducted to assess efficacy for ICU sedation. These studies did not meet their primary efficacy endpoints and the safety data submitted were insufficient to fully characterize the safety profile of PRECEDEX for these patient populations.
14 Clinical Studies
The safety and efficacy of PRECEDEX has been evaluated in four randomized, double-blind, placebo-controlled multicenter clinical trials in 1,185 adult patients.
4 Contraindications
None.
6 Adverse Reactions
The following clinically significant adverse reactions are described elsewhere in the labeling:
-
•Hypotension, bradycardia and sinus arrest [see Warnings and Precautions (5.2)]
-
•Transient hypertension [see Warnings and Precautions (5.3)]
7 Drug Interactions
Anesthetics, Sedatives, Hypnotics, Opioids: Enhancement of pharmacodynamic effects. Reduction in dosage of PRECEDEX or the concomitant medication may be required. (7.1)
12.2 Pharmacodynamics
In a study in healthy adult volunteers (N = 10), respiratory rate and oxygen saturation remained within normal limits and there was no evidence of respiratory depression when PRECEDEX was administered by intravenous infusion at doses within the recommended dose range (0.2 mcg/kg/hr to 0.7 mcg/kg/hr).
12.3 Pharmacokinetics
Following intravenous administration to adults, dexmedetomidine exhibits the following pharmacokinetic parameters: a rapid distribution phase with a distribution half-life (t1/2) of approximately 6 minutes; a terminal elimination half-life (t1/2) of approximately 2 hours; and steady-state volume of distribution (Vss) of approximately 118 liters. Clearance is estimated to be approximately 39 L/h. The mean body weight associated with this clearance estimate was 72 kg.
Dexmedetomidine exhibits linear pharmacokinetics in the dosage range of 0.2 mcg/kg/hr to 0.7 mcg/kg/hr when administered to adults by intravenous infusion for up to 24 hours. Table 10 shows the main pharmacokinetic parameters when PRECEDEX was infused (after appropriate loading doses) at maintenance infusion rates of 0.17 mcg/kg/hr (target plasma concentration of 0.3 ng/mL) for 12 and 24 hours, 0.33 mcg/kg/hr (target plasma concentration of 0.6 ng/mL) for 24 hours, and 0.70 mcg/kg/hr (target plasma concentration of 1.25 ng/mL) for 24 hours.
| Parameter | Loading Infusion (min)/Total Infusion Duration (hrs) | |||
|---|---|---|---|---|
| 10 min/12 hrs | 10 min/24 hrs | 10 min/24 hrs | 35 min/24 hrs | |
| Dexmedetomidine Target Plasma Concentration (ng/mL) and Dose (mcg/kg/hr) | ||||
| 0.3/0.17 | 0.3/0.17 | 0.6/0.33 | 1.25/0.70 | |
| Abbreviations: t1/2 = half‑life, CL = clearance, Vss = steady‑state volume of distribution. | ||||
|
t1/2 Presented as harmonic mean and pseudo standard deviation.
, hour
|
1.78 ± 0.30 |
2.22 ± 0.59 |
2.23 ± 0.21 |
2.50 ± 0.61 |
|
CL, liter/hour |
46.3 ± 8.3 |
43.1 ± 6.5 |
35.3 ± 6.8 |
36.5 ± 7.5 |
|
Vss, liter |
88.7 ± 22.9 |
102.4 ± 20.3 |
93.6 ± 17.0 |
99.6 ± 17.8 |
|
Avg Css Mean Css = Average steady-state concentration of dexmedetomidine. The mean Css was calculated based on post-dose sampling from 2.5 to 9 hours samples for 12 hour infusion and post-dose sampling from 2.5 to 18 hours for 24 hour infusions.
, ng/mL
|
0.27 ± 0.05 |
0.27 ± 0.05 |
0.67 ± 0.10 |
1.37 ± 0.20 |
The loading doses for each of the above indicated groups were 0.5, 0.5, 1 and 2.2 mcg/kg, respectively.
Dexmedetomidine pharmacokinetic parameters in adults after PRECEDEX maintenance doses of 0.2 mcg/kg/hr to 1.4 mcg/kg/hr for >24 hours were similar to the pharmacokinetic (PK) parameters after PRECEDEX maintenance dosing for <24 hours in other studies. The values for clearance (CL), volume of distribution (V), and t1/2 were 39.4 L/hr, 152 L, and 2.67 hours, respectively.
2.3 Dosage Adjustment
Due to possible pharmacodynamic interactions, a reduction in dosage of PRECEDEX or other concomitant anesthetics, sedatives, hypnotics or opioids may be required when co-administered [see Drug Interactions (7.1)].
Dosage reductions may need to be considered for adult patients with hepatic impairment, and geriatric patients [see Warnings and Precautions (5.8), Use in Specific Populations (8.6), Clinical Pharmacology (12.3)].
2.2 Recommended Dosage
| INDICATION | DOSAGE AND ADMINISTRATION |
|---|---|
|
Initiation of Intensive Care Unit Sedation |
For adult patients: a loading infusion of one mcg/kg over 10 minutes . For adult patients being converted from alternate sedative therapy: a loading dose may not be required. For patients over 65 years of age: Consider a dose reduction [see Use in Specific Populations (8.5)]. For adult patients with impaired hepatic function: Consider a dose reduction [see Use in Specific Populations (8.6), Clinical Pharmacology (12.3)]. |
|
Maintenance of Intensive Care Unit Sedation |
For adult patients: a maintenance infusion of 0.2 mcg/kg/ hour to 0.7 mcg/kg/ hour . The rate of the maintenance infusion should be adjusted to achieve the desired level of sedation. For patients over 65 years of age: Consider a dose reduction [see Use in Specific Populations (8.5)]. For adult patients with impaired hepatic function: Consider a dose reduction [see Use in Specific Populations (8.6), Clinical Pharmacology (12.3)] |
|
Initiation of Procedural Sedation |
For adult patients: a loading infusion of one mcg/kg over 10 minutes . For less invasive procedures such as ophthalmic surgery, a loading infusion of 0.5 mcg/kg given over 10 minutes may be suitable. For awake fiberoptic intubation in adult patients: a loading infusion of one mcg/kg over 10 minutes . For patients over 65 years of age: a loading infusion of 0.5 mcg/kg over 10 minutes [see Use in Specific Populations (8.5)]. For adult patients with impaired hepatic function: Consider a dose reduction [see Use in Specific Populations (8.6), Clinical Pharmacology (12.3)]. |
|
Maintenance of Procedural Sedation |
For adult patients: the maintenance infusion is generally initiated at 0.6 mcg/kg/ hour and titrated to achieve desired clinical effect with doses ranging from 0.2 mcg/kg/ hour to 1 mcg/kg/ hour . Adjust the rate of the maintenance infusion to achieve the targeted level of sedation. For awake fiberoptic intubation in adult patients: a maintenance infusion of 0.7 mcg/kg/ hour is recommended until the endotracheal tube is secured. For patients over 65 years of age: Consider a dose reduction [see Use in Specific Populations (8.5)]. For adult patients with impaired hepatic function: Consider a dose reduction [see Use in Specific Populations (8.6), Clinical Pharmacology (12.3)]. |
|
INDICATION |
DOSAGE AND ADMINISTRATION |
|
Initiation of Sedation During Non‑invasive Procedures |
For pediatric patients:
Consider a reduction in dosage if clinically indicated. |
|
Maintenance of Sedation During Non-invasive Procedures |
For pediatric patients:
As clinically warranted, titrate the maintenance dose to individual patient clinical response. |
5.8 Hepatic Impairment
Since PRECEDEX clearance decreases with severity of hepatic impairment, dose reduction should be considered in patients with impaired hepatic function [see Dosage and Administration (2.2, 2.3)].
8.6 Hepatic Impairment
Since PRECEDEX clearance decreases with increasing severity of hepatic impairment, dose reduction should be considered in patients with impaired hepatic function [see Dosage and Administration (2.2, 2.3), Clinical Pharmacology (12.3)].
1 Indications and Usage
PRECEDEX is a alpha2-adrenergic receptor agonist indicated for:
-
•Sedation of initially intubated and mechanically ventilated adult patients during treatment in an intensive care setting. Administer PRECEDEX by continuous infusion not to exceed 24 hours. (1.1)
-
•Sedation of non-intubated adult patients prior to and/or during surgical and other procedures. (1.2)
-
•Sedation of non-intubated pediatric patients aged 1 month to less than 18 years prior to and during non-invasive procedures. (1.2)
1.2 Procedural Sedation
PRECEDEX is indicated for sedation of non-intubated adult patients prior to and/or during surgical and other procedures.
PRECEDEX is indicated for sedation of non-intubated pediatric patients aged 1 month to less than 18 years prior to and during non-invasive procedures.
5.1 Drug Administration
PRECEDEX should be administered only by persons skilled in the management of patients in the intensive care or operating room setting. Due to the known pharmacological effects of PRECEDEX, patients should be continuously monitored while receiving PRECEDEX.
12.1 Mechanism of Action
PRECEDEX is a relatively selective centrally acting alpha2-adrenergic agonist with sedative properties. Alpha2 selectivity is observed in animals following slow intravenous infusion of low and medium doses (10–300 mcg/kg). Both alpha1 and alpha2 activity is observed following slow intravenous infusion of high doses (≥1,000 mcg/kg) or with rapid intravenous administration.
14.2 Procedural Sedation
Adult Patients
The safety and efficacy of PRECEDEX for sedation of non-intubated adult patients prior to and/or during surgical and other procedures was evaluated in two randomized, double-blind, placebo-controlled multicenter clinical trials. Study 1 evaluated the sedative properties of PRECEDEX in adult patients having a variety of elective surgeries/procedures performed under monitored anesthesia care. Study 2 evaluated PRECEDEX in adult patients undergoing awake fiberoptic intubation prior to a surgical or diagnostic procedure.
In Study 1, the sedative properties of PRECEDEX were evaluated by comparing the percent of adult patients not requiring rescue midazolam to achieve a specified level of sedation using the standardized Observer's Assessment of Alertness/Sedation Scale (see Table 15).
|
Assessment Categories |
||||
|
Responsiveness |
Speech |
Facial Expression |
Eyes |
Composite Score |
|
Responds readily to name spoken in normal tone |
Normal |
Normal |
Clear, no ptosis |
5 (alert) |
|
Lethargic response to name spoken in normal tone |
Mild slowing or thickening |
Mild relaxation |
Glazed or mild ptosis (less than half the eye) |
4 |
|
Responds only after name is called loudly and/or repeatedly |
Slurring or prominent slowing |
Marked relaxation |
Glazed and marked ptosis (half the eye or more) |
3 |
|
Responds only after mild prodding or shaking |
Few recognizable words |
– |
– |
2 |
|
Does not respond to mild prodding or shaking |
– |
– |
– |
1 (deep sleep) |
Adult patients were randomized to receive a loading infusion of either PRECEDEX 1 mcg/kg, PRECEDEX 0.5 mcg/kg, or placebo (normal saline) given over 10 minutes and followed by a maintenance infusion started at 0.6 mcg/kg/hr. The maintenance infusion of study drug could be titrated from 0.2 mcg/kg/hr to 1 mcg/kg/hr to achieve the targeted sedation score (Observer's Assessment of Alertness/Sedation Scale ≤4). Adult patients were allowed to receive rescue midazolam as needed to achieve and/or maintain an Observer's Assessment of Alertness/Sedation Scale ≤4. After achieving the desired level of sedation, a local or regional anesthetic block was performed. Demographic characteristics were similar between the PRECEDEX and comparator groups. Efficacy results showed that PRECEDEX was more effective than the comparator group when used to sedate non‑intubated patients requiring monitored anesthesia care during surgical and other procedures (see Table 15).
In Study 2, the sedative properties of PRECEDEX were evaluated by comparing the percent of adult patients requiring rescue midazolam to achieve or maintain a specified level of sedation using the Ramsay Sedation Scale score ≥2 (see Table 12). Adult patients were randomized to receive a loading infusion of PRECEDEX 1 mcg/kg or placebo (normal saline) given over 10 minutes and followed by a fixed maintenance infusion of 0.7 mcg/kg/hr. After achieving the desired level of sedation, topicalization of the airway occurred. Adult patients were allowed to receive rescue midazolam as needed to achieve and/or maintain a Ramsay Sedation Scale ≥2. Demographic characteristics were similar between the PRECEDEX and comparator groups. For efficacy results see Table 16.
|
Study |
Loading Infusion Treatment Arm |
Number of Patients Enrolled Based on ITT population defined as all randomized and treated patients.
|
% Not Requiring Midazolam Rescue |
Confidence Normal approximation to the binomial with continuity correction.
Interval on the Difference vs. Placebo
|
Mean (SD) Total Dose (mg) of Rescue Midazolam Required |
Confidence Intervals of the Mean Rescue Dose |
|
Study 1 |
Dexmedetomidine |
134 |
40 |
37 (27, 48) |
1.4 (1.7) |
-2.7 |
|
Dexmedetomidine |
129 |
54 |
51 (40, 62) |
0.9 (1.5) |
-3.1 |
|
|
Placebo |
63 |
3 |
– |
4.1 (3.0) |
– |
|
|
Study 2 |
Dexmedetomidine |
55 |
53 |
39 (20, 57) |
1.1 (1.5) |
-1.8 |
|
Placebo |
50 |
14 |
– |
2.9 (3.0) |
– |
Pediatric Patients
The safety and efficacy of PRECEDEX for sedation of non-intubated pediatric patients aged 1 month to less than 17 years undergoing MRI scans was evaluated in one randomized, double-blind, dose-ranging, dose‑controlled multicenter clinical trial utilizing 3 different PRECEDEX dosages. The sedative properties of PRECEDEX were evaluated by age group and by the percent of pediatric patients at the high dose level versus the low dose level who did not require concomitant propofol to complete the MRI scan.
A total of 122 pediatric patients were randomized to the PRECEDEX low dose group (42 of 122), the middle dose group (42 of 122) or the high dose treatment group (38 of 122). All patients received a PRECEDEX loading dose infusion over 10 minutes followed by a maintenance infusion for the duration of the MRI scan (Table 17). If an adequate level of sedation was not achieved within 5 minutes after the start of the PRECEDEX maintenance infusion, patients could receive concomitant propofol as needed based on clinical judgment to achieve and/or maintain adequate sedation.
|
High Dose |
Middle Dose |
Low Dose |
||||
|
Age |
Loading Dose (10 min) |
Maintenance Dose |
Loading Dose (10 min) |
Maintenance Dose |
Loading Dose (10 min) |
Maintenance Dose |
|
1 month to less than 2 years |
1.5 mcg/kg |
1.5 mcg/kg/h |
1 mcg/kg |
1 mcg/kg/h |
0.5 mcg/kg |
0.5 mcg/kg/h |
|
2 to less than 17 years |
2 mcg/kg |
1.5 mcg/kg/h |
1.2 mcg /kg |
1 mcg/kg/h |
0.5 mcg/kg |
0.5 mcg kg/h |
The primary efficacy results from this pediatric procedural sedation study are summarized in Table 18. In the combined age group, the percent of pediatric patients not requiring concomitant propofol was 14.3% (6/42) in the low dose group and 63.2% (24/38) in the high dose group. The percentage of patients at the PRECEDEX high dose who completed the MRI without concomitant propofol was statistically greater than the percentage in the PRECEDEX low dose group (p<0.001).
|
Age Group |
High Dose |
Middle Dose |
Low Dose |
High Dose vs Low Dose |
||
|
n (%) 95% CI Exact 95% CI of proportion of subjects not requiring propofol in each dose level.
|
n (%) 95% CI |
n (%) 95% CI |
Odds Ratio 95% CI p-values; CI is confidence interval of odds ratio.
|
p-value |
||
|
1 month to less than 2 years |
N=59 |
9/18 (50.0%) (0.26, 0.74) |
2/21 (9.5%) (0.01, 0.30) |
2/20 (15.0%) (0.03, 0.38) |
0.18 (0.04, 0.82) |
0.022 |
|
2 to less than 17 years |
N=63 |
15/20 (75.0%) (0.51, 0.91) |
13/21 (61.9%) (0.38, 0.82) |
3/22 (13.6%) (0.03, 0.35) |
0.05 (0.01, 0.26) |
<0.001 |
|
Overall |
N=122 |
24/38 (63.2%) (0.46, 0.78) |
15/42 (35.7%) (0.22, 0.52) |
6/42 (14.3%) (0.05, 0.29) |
0.10 (0.03, 0.29) |
<0.001 |
Secondarily, the sedative properties were also evaluated by examining the percent of time at a target sedation score using the Pediatric Sedation State Scale (PSSS). The PSSS is a validated 6-point scale specifically designed for evaluating pediatric patients undergoing sedation for diagnostic and therapeutic procedures. The PSSS measures the effectiveness and quality of procedural sedation in children. The target sedation level was indicated by a PSSS score of 2 (i.e., patient is quiet [asleep or awake], not moving during procedure, has no frown [or brow furrow] indicating pain or anxiety and no verbalization of any complaint).
In the PRECEDEX high dose group, pediatric patients in both the combined and individual age group were at the target sedation rating scale score (PSSS of 2) for a mean >87% of the time during the PRECEDEX maintenance infusion. In both the combined and individual age group, an increase in the percentage of time at the target sedation rating scale score (PSSS of 2) was observed with increasing PRECEDEX dosage.
9.1 Controlled Substance
PRECEDEX (dexmedetomidine hydrochloride) is not a controlled substance.
5 Warnings and Precautions
-
•Monitoring: Continuously monitor patients while receiving PRECEDEX. (5.1)
-
•Bradycardia and Sinus Arrest: Have occurred in young healthy volunteers with high vagal tone or with different routes of administration, e.g., rapid intravenous or bolus administration. (5.2)
-
•Hypotension and Bradycardia: May necessitate medical intervention. May be more pronounced in patients with hypovolemia, diabetes mellitus, or chronic hypertension, and in the elderly. Use with caution in patients with advanced heart block or severe ventricular dysfunction. (5.2)
-
•Co-administration with Other Vasodilators or Negative Chronotropic Agents: Use with caution due to additive pharmacodynamic effects. (5.2)
-
•Transient Hypertension: Observed primarily during the loading dose. Consider reduction in loading infusion rate. (5.3)
-
•Arousability: Patients can become aroused/alert with stimulation; this alone should not be considered as lack of efficacy. (5.4)
-
•Tolerance and Tachyphylaxis: Prolonged exposure to dexmedetomidine beyond 24 hours may be associated with tolerance and tachyphylaxis and a dose-related increase in adverse events. (5.6)
5.3 Transient Hypertension
Transient hypertension has been observed primarily during the loading dose in association with the initial peripheral vasoconstrictive effects of PRECEDEX. Treatment of the transient hypertension has generally not been necessary, although reduction of the loading infusion rate may be desirable.
7.2 Neuromuscular Blockers
In one study of 10 healthy adult volunteers, administration of PRECEDEX for 45 minutes at a plasma concentration of one ng/mL resulted in no clinically meaningful increases in the magnitude of neuromuscular blockade associated with rocuronium administration.
2 Dosage and Administration
-
•Individualize and titrate PRECEDEX dosing to desired clinical effect. (2.1)
-
•Administer PRECEDEX using a controlled infusion device. (2.1)
-
•Dilute the 200 mcg/2 mL (100 mcg/mL) vial contents in 0.9% sodium chloride solution to achieve required concentration (4 mcg/mL) prior to administration. (2.4)
-
•The 80 mcg/20 mL single-dose vial, and 200 mcg/50 mL, 400 mcg/100 mL, and 1,000 mcg/250 mL single-dose bottles and single-dose flexible containers do not require further dilution prior to administration. (2.4)
-
•For Adult Intensive Care Unit Sedation: Initiate at one mcg/kg over 10 minutes , followed by a maintenance infusion of 0.2 mcg/kg/ hour to 0.7 mcg/kg/ hour . (2.2)
-
•For Adult Procedural Sedation: Initiate at one mcg/kg over 10 minutes , followed by a maintenance infusion initiated at 0.6 mcg/kg/ hour and titrated to achieve desired clinical effect with doses ranging from 0.2 mcg/kg/ hour to 1 mcg/kg/ hour . (2.2)
-
•For Sedation of Pediatric Patients During Non-invasive Procedures: Patients 1 month to less than 2 years old initiate at 1.5 mcg/kg over 10 minutes followed by a maintenance infusion of 1.5 mcg/kg/ hour and titrated to achieve desired clinical effect with dosage ranging from 0.5 mcg/kg/ hour to 1.5 mcg/kg/ hour ; patients 2 to less than 18 years old initiate at 2 mcg/kg over 10 minutes followed by a maintenance infusion of 1.5 mcg/kg/ hour and titrated to achieve desired clinical effect with dosage ranging from 0.5 mcg/kg/ hour to 1.5 mcg/kg/ hour . (2.2)
-
•Alternative Doses: Recommended for patients over 65 years of age and awake fiberoptic intubation patients. (2.2)
2.4 Preparation of Solution
Strict aseptic technique must always be maintained during handling of PRECEDEX.
Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration, whenever solution and container permit. Do not use if product is discolored or if precipitate matter is present.
5.7 Hyperthermia Or Pyrexia
PRECEDEX may induce hyperthermia or pyrexia, which may be resistant to traditional cooling methods, such as administration of cooled intravenous fluids and antipyretic medications. Discontinue PRECEDEX if drug‑related hyperthermia or pyrexia is suspected and monitor patients until body temperature normalizes.
3 Dosage Forms and Strengths
PRECEDEX Presentations Requiring Dilution:
PRECEDEX (dexmedetomidine hydrochloride) injection is a clear and colorless solution, to be used after dilution. It is available as:
-
•200 mcg/2 mL (100 mcg/mL) single-dose vial.
PRECEDEX Presentations that are Ready To Use:
PRECEDEX (dexmedetomidine hydrochloride) in 0.9% sodium chloride injection is a clear and colorless solution, ready to use. It is available as:
-
•PRECEDEX 80 mcg/20 mL (4 mcg/mL) single-dose vial.
-
•PRECEDEX 200 mcg/50 mL (4 mcg/mL) single-dose glass bottle.
-
•PRECEDEX 400 mcg/100 mL (4 mcg/mL) single-dose glass bottle.
-
•PRECEDEX 1,000 mcg/250 mL (4 mcg/mL) single-dose glass bottle.
-
•PRECEDEX 200 mcg/50 mL (4 mcg/mL) single-dose flexible container.
-
•PRECEDEX 400 mcg/100 mL (4 mcg/mL) single-dose flexible container.
-
•PRECEDEX 1,000 mcg/250 mL (4 mcg/mL) single-dose flexible container.
6.2 Postmarketing Experience
The following adverse reactions have been identified during post‑approval use of PRECEDEX. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Hypotension and bradycardia were the most common adverse reactions associated with the use of PRECEDEX during post‑approval use of the drug.
| System Organ Class | Preferred Term |
|---|---|
|
Blood and Lymphatic System Disorders |
Anemia |
|
Cardiac Disorders |
Arrhythmia, atrial fibrillation, atrioventricular block, bradycardia, cardiac arrest, cardiac disorder, extrasystoles, myocardial infarction, supraventricular tachycardia, tachycardia, ventricular arrhythmia, ventricular tachycardia |
|
Eye Disorders |
Photopsia, visual impairment |
|
Gastrointestinal Disorders |
Abdominal pain, diarrhea, nausea, vomiting |
|
General Disorders and Administration Site Conditions |
Chills, hyperpyrexia, pain, pyrexia, thirst |
|
Hepatobiliary Disorders |
Hepatic function abnormal, hyperbilirubinemia |
|
Investigations |
Alanine aminotransferase increased, aspartate aminotransferase increased, blood alkaline phosphatase increased, blood urea increased, electrocardiogram T wave inversion, gammaglutamyltransferase increased, electrocardiogram QT prolonged |
|
Metabolism and Nutrition Disorders |
Acidosis, hyperkalemia, hypoglycemia, hypovolemia, hypernatremia |
|
Nervous System Disorders |
Convulsion, dizziness, headache, neuralgia, neuritis, speech disorder |
|
Psychiatric Disorders |
Agitation, confusional state, delirium, hallucination, illusion |
|
Renal and Urinary Disorders |
Oliguria, polyuria |
|
Respiratory, Thoracic and Mediastinal Disorders |
Apnea, bronchospasm, dyspnea, hypercapnia, hypoventilation, hypoxia, pulmonary congestion, respiratory acidosis |
|
Skin and Subcutaneous Tissue Disorders |
Hyperhidrosis, pruritus, rash, urticaria |
|
Surgical and Medical Procedures |
Light anesthesia |
|
Vascular Disorders |
Blood pressure fluctuation, hemorrhage, hypertension, hypotension |
8 Use in Specific Populations
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reactions rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
Most common treatment-emergent adverse reactions, occurring in greater than 2% of adult patients in both Intensive Care Unit and procedural sedation studies include hypotension, bradycardia and dry mouth.
2.1 Administration Instructions
-
•PRECEDEX dosing should be individualized and titrated to desired clinical response.
-
•PRECEDEX is not indicated for infusions lasting longer than 24 hours.
-
•PRECEDEX should be administered using a controlled infusion device.
5.6 Tolerance and Tachyphylaxis
Use of dexmedetomidine beyond 24 hours has been associated with tolerance and tachyphylaxis and a dose‑related increase in adverse reactions [see Adverse Reactions (6.1)].
1.1 Intensive Care Unit Sedation
PRECEDEX is indicated for sedation of initially intubated and mechanically ventilated adult patients during treatment in an intensive care setting. PRECEDEX should be administered by continuous infusion not to exceed 24 hours.
PRECEDEX has been continuously infused in mechanically ventilated adult patients prior to extubation, during extubation, and post-extubation. It is not necessary to discontinue PRECEDEX prior to extubation.
14.1 Intensive Care Unit Sedation
Two randomized, double-blind, parallel-group, placebo-controlled multicenter clinical trials included 754 adult patients being treated in a surgical intensive care unit. All patients were initially intubated and received mechanical ventilation. These trials evaluated the sedative properties of PRECEDEX by comparing the amount of rescue medication (midazolam in one trial and propofol in the second) required to achieve a specified level of sedation (using the standardized Ramsay Sedation Scale) between PRECEDEX and placebo from onset of treatment to extubation or to a total treatment duration of 24 hours. The Ramsay Level of Sedation Scale is displayed in Table 12.
|
Clinical Score |
Level of Sedation Achieved |
|
6 |
Asleep, no response |
|
5 |
Asleep, sluggish response to light glabellar tap or loud auditory stimulus |
|
4 |
Asleep, but with brisk response to light glabellar tap or loud auditory stimulus |
|
3 |
Patient responds to commands |
|
2 |
Patient cooperative, oriented, and tranquil |
|
1 |
Patient anxious, agitated, or restless |
In the first study, 175 adult patients were randomized to receive placebo and 178 to receive PRECEDEX by intravenous infusion at a dose of 0.4 mcg/kg/hr (with allowed adjustment between 0.2 mcg/kg/hr and 0.7 mcg/kg/hr) following an initial loading infusion of one mcg/kg intravenous over 10 minutes. The study drug infusion rate was adjusted to maintain a Ramsay sedation score of ≥3. Patients were allowed to receive "rescue" midazolam as needed to augment the study drug infusion. In addition, morphine sulfate was administered for pain as needed. The primary outcome measure for this study was the total amount of rescue medication (midazolam) needed to maintain sedation as specified while intubated. Patients randomized to placebo received significantly more midazolam than patients randomized to PRECEDEX (see Table 13).
A second prospective primary analysis assessed the sedative effects of PRECEDEX by comparing the percentage of adult patients who achieved a Ramsay sedation score of ≥3 during intubation without the use of additional rescue medication. A significantly greater percentage of adult patients in the PRECEDEX group maintained a Ramsay sedation score of ≥3 without receiving any midazolam rescue compared to the placebo group (see Table 13).
| ITT (intent-to-treat) population includes all randomized patients. | |||
|
Placebo
|
PRECEDEX
|
p-value |
|
|
Mean Total Dose (mg) of Midazolam |
19 mg |
5 mg |
0.0011 ANOVA model with treatment center.
|
|
Standard deviation |
53 mg |
19 mg |
|
|
Categorized Midazolam Use |
|||
|
0 mg |
43 (25%) |
108 (61%) |
<0.001 Chi-square.
|
|
0–4 mg |
34 (19%) |
36 (20%) |
|
|
>4 mg |
98 (56%) |
34 (19%) |
A prospective secondary analysis assessed the dose of morphine sulfate administered to adult patients in the PRECEDEX and placebo groups. On average, PRECEDEX-treated patients received less morphine sulfate for pain than placebo‑treated patients (0.47 versus 0.83 mg/h). In addition, 44% (79 of 178 patients) of PRECEDEX patients received no morphine sulfate for pain versus 19% (33 of 175 patients) in the placebo group.
In a second study, 198 adult patients were randomized to receive placebo and 203 to receive PRECEDEX by intravenous infusion at a dose of 0.4 mcg/kg/hr (with allowed adjustment between 0.2 mcg/kg/hr and 0.7 mcg/kg/hr) following an initial loading infusion of one mcg/kg intravenous over 10 minutes. The study drug infusion was adjusted to maintain a Ramsay sedation score of ≥3. Patients were allowed to receive "rescue" propofol as needed to augment the study drug infusion. In addition, morphine sulfate was administered as needed for pain. The primary outcome measure for this study was the total amount of rescue medication (propofol) needed to maintain sedation as specified while intubated.
Adult patients randomized to placebo received significantly more propofol than adult patients randomized to PRECEDEX (see Table 14).
A significantly greater percentage of adult patients in the PRECEDEX group compared to the placebo group maintained a Ramsay sedation score of ≥3 without receiving any propofol rescue (see Table 14).
|
Placebo
|
PRECEDEX
|
p-value |
|
|
Mean Total Dose (mg) of Propofol |
513 mg |
72 mg |
<0.0001 ANOVA model with treatment center.
|
|
Standard deviation |
782 mg |
249 mg |
|
|
Categorized Propofol Use |
|||
|
0 mg |
47 (24%) |
122 (60%) |
<0.001 Chi-square.
|
|
0–50 mg |
30 (15%) |
43 (21%) |
|
|
>50 mg |
121 (61%) |
38 (19%) |
A prospective secondary analysis assessed the dose of morphine sulfate administered to adult patients in the PRECEDEX and placebo groups. On average, PRECEDEX-treated patients received less morphine sulfate for pain than placebo-treated patients (0.43 versus 0.89 mg/h). In addition, 41% (83 of 203 patients) of PRECEDEX patients received no morphine sulfate for pain versus 15% (30 of 198 patients) in the placebo group.
In a controlled clinical trial, PRECEDEX was compared to midazolam for ICU sedation exceeding 24 hours duration. PRECEDEX was not shown to be superior to midazolam for the primary efficacy endpoint, the percent of time patients were adequately sedated (81% versus 81%). In addition, administration of PRECEDEX for longer than 24 hours was associated with tolerance, tachyphylaxis, and a dose-related increase in adverse events [see Adverse Reactions (6.1)].
17 Patient Counseling Information
PRECEDEX is indicated for short-term intravenous sedation. Dosage must be individualized and titrated to the desired clinical effect. Blood pressure, heart rate and oxygen levels will be monitored both continuously during the infusion of PRECEDEX and as clinically appropriate after discontinuation.
-
•When PRECEDEX is infused for more than 6 hours, patients should be informed to report nervousness, agitation, and headaches that may occur for up to 48 hours.
-
•Additionally, patients should be informed to report symptoms that may occur within 48 hours after the administration of PRECEDEX such as: weakness, confusion, excessive sweating, weight loss, abdominal pain, salt cravings, diarrhea, constipation, dizziness or light-headedness.
-
•Advise breastfeeding mothers who were exposed to PRECEDEX to monitor breastfed neonates for irritability [see Use in Specific Populations (8.2)].
2.5 Administration With Other Fluids
PRECEDEX infusion should not be co-administered through the same intravenous catheter with blood or plasma because physical compatibility has not been established.
PRECEDEX has been shown to be incompatible when administered with the following drugs: amphotericin B, diazepam.
PRECEDEX has been shown to be compatible when administered with the following intravenous fluids:
-
•0.9% sodium chloride in water
-
•5% dextrose in water
-
•20% mannitol
-
•Lactated Ringer's solution
-
•100 mg/mL magnesium sulfate solution
-
•0.3% potassium chloride solution
2.6 Compatibility With Natural Rubber
Compatibility studies have demonstrated the potential for absorption of PRECEDEX to some types of natural rubber. Although PRECEDEX is dosed to effect, it is advisable to use administration components made with synthetic or coated natural rubber gaskets.
Principal Display Panel 2 Ml Vial Tray
2 mL Single-dose Fliptop Vials
Preservative-Free
NDC 0409-1638-02
Contains 25 of NDC 0409-1638-32
Precedex™
DEXMEDETOMIDINE HCl INJECTION
Rx only
200 mcg/2 mL
(100 mcg/mL)
For Intravenous use.
MUST BE DILUTED
Hospira
Principal Display Panel 2 Ml Vial Label
2 mL NDC 0409-1638-32
Precedex™
DEXMEDETOMIDINE
HCl INJECTION
Rx only
200 mcg/2 mL
(100 mcg/mL)
For Intravenous use.
MUST BE DILUTED
Dist. by Hospira, Inc.,
Lake Forest, IL 60045 USA
RL–7616
##–###–AA
DMMMYYYY
13.2 Animal Toxicology And/or Pharmacology
There were no differences in the adrenocorticotropic hormone (ACTH)-stimulated cortisol response in dogs following a single-dose of dexmedetomidine compared to saline control. However, after continuous subcutaneous infusions of dexmedetomidine at 3 mcg/kg/hr and 10 mcg/kg/hr for one week in dogs (exposures estimated to be within the clinical range), the ACTH-stimulated cortisol response was diminished by approximately 27% and 40%, respectively, compared to saline-treated control animals indicating a dose‑dependent adrenal suppression.
Principal Display Panel 20 Ml Vial Label
20 mL
NDC 0409-1660-22
Single-dose vial. Discard unused portion.
Precedex™
Dexmedetomidine HCl
in 0.9% Sodium Chloride Injection
80 mcg/20 mL
(4 mcg/mL)
Distributed by Hospira, Inc., Lake Forest, IL 60045 USA
Principal Display Panel 20 Ml Vial Carton
10 units x 20 mL
Rx only
NDC 0409-1660-20
Contains 10 of NDC 0409-1660-22
Single-dose vial. Discard unused portion.
Precedex™
Dexmedetomidine HCl in 0.9% Sodium Chloride Injection
80 mcg/20 mL
(4 mcg/mL)
Hospira
For Intravenous Use
Principal Display Panel 50 Ml Bottle Tray
20 Units X 50 mL
Rx only
NDC 0409-1660-50
Contains 20 of NDC 0409-1660-55
Single-dose bottle. Discard unused portion.
Precedex™
Dexmedetomidine HCl
in 0.9% Sodium Chloride Injection
200 mcg/50 mL
(4 mcg/mL)
For Intravenous Use
Hospira
Principal Display Panel 100 Ml Bottle Tray
10 Units X 100 mL
Rx only
NDC 0409-1660-10
Contains 10 of NDC 0409-1660-35
Single-dose bottle. Discard unused portion.
Precedex™
Dexmedetomidine HCl in 0.9% Sodium Chloride Injection
400 mcg/100 mL
(4 mcg/mL)
For Intravenous Use
Hospira
Principal Display Panel 50 Ml Bottle Label
50 mL
Rx only
NDC 0409-1660-55
Single-dose bottle. Discard unused portion.
Precedex™
Dexmedetomidine HCl
in 0.9% Sodium Chloride
Injection
200 mcg/50 mL
(4 mcg/mL)
For Intravenous Use
Principal Display Panel – 50 Ml Bag 7838
50 mL Single-dose. Discard unused portion.
NDC 0409-7838-01
PrecedexTM
Dexmedetomidine HCl
in 0.9% Sodium Chloride
Injection
Rx only
200 mcg/50 mL (4mcg/mL)
For Intravenous Infusion Each mL contains 4 mcg of dexmedetomidine
provided as 4.72 mcg dexmedetomidine HCl and 9 mg of sodium chloride in
water for injection.
Recommended Dosage: See prescribing information. Store at 20˚C to 25˚C
(68˚F to 77˚F). [See USP Controlled Room Temperature.] Do not freeze.
This product is not made with natural rubber latex.
Preservative-Free.
1000072255
Distributed by Hospira, Inc.
Lake Forest, IL 60045 USA
Hospira
Principal Display Panel 100 Ml Bottle Label
100 mL
Rx only
NDC 0409-1660-35
Single-dose bottle. Discard unused portion.
Precedex™
Dexmedetomidine HCl
in 0.9% Sodium Chloride
Injection
400 mcg/100 mL
(4 mcg/mL)
For Intravenous Use
Principal Display Panel 250 Ml Bottle Label
250 mL
Rx only
NDC 0409-1434-01
Single-dose bottle. Discard unused portion.
Precedex™
Dexmedetomidine HCl
in 0.9% Sodium
Chloride Injection
1,000 mcg/250 mL
(4 mcg/mL)
For Intravenous Use
Principal Display Panel – 100 Ml Bag 7853
100 mL Single-dose. Discard unused portion.
NDC 0409-7853-01
PrecedexTM
Dexmedetomidine HCl
in 0.9% Sodium Chloride
Injection
Rx only
400 mcg/100 mL (4 mcg/mL)
For Intravenous Infusion Each mL contains 4 mcg of dexmedetomidine provided
as 4.72 mcg dexmedetomidine HCl and 9 mg of sodium chloride in water for
injection.
Recommended Dosage: See prescribing information. Storage at 20ºC to 25ºC
(68ºF to 77ºF).[See USP Controlled Room Temperature.] Do not Freeze.
This product is not made with natural rubber latex.
Preservative-Free.
1000072256
Distributed by Hospira, Inc.
Lake Forest, IL 60045 USA
Hospira
Principal Display Panel – 250 Ml Bag 7875
250 mL Single-dose. Discard unused portion.
NDC 0409-7875-01
PrecedexTM
Dexmedetomidine HCl
in 0.9% Sodium Chloride
Injection
1,000 mcg/250 mL (4 mcg/mL)
For Intravenous Infusion Each mL contains 4 mcg of dexmedetomidine provided
as 4.72 mcg dexmedetomidine HCl and 9 mg of sodium chloride in water for
injection.
Recommended Dosage: See prescribing information. Store at
20˚C to 25˚C (68˚F to 77˚F). [See USP Controlled Room
Temperature.] Do not freeze.
This product is not made with natural
rubber latex.
Preservative-Free.
Rx only
1000072257
Distributed by Hospira, Inc.
Lake Forest, IL 60045 USA
Hospira
5.2 Hypotension, Bradycardia, and Sinus Arrest
Clinically significant episodes of bradycardia and sinus arrest have been reported with PRECEDEX administration in young, healthy adult volunteers with high vagal tone or with different routes of administration including rapid intravenous or bolus administration.
Reports of hypotension and bradycardia have been associated with PRECEDEX infusion. Some of these cases have resulted in fatalities. If medical intervention is required, treatment may include decreasing or stopping the infusion of PRECEDEX, increasing the rate of intravenous fluid administration, elevation of the lower extremities, and use of pressor agents. Because PRECEDEX has the potential to augment bradycardia induced by vagal stimuli, clinicians should be prepared to intervene. The intravenous administration of anticholinergic agents (e.g., glycopyrrolate, atropine) should be considered to modify vagal tone. In clinical trials, glycopyrrolate or atropine were effective in the treatment of most episodes of PRECEDEX-induced bradycardia. However, in some patients with significant cardiovascular dysfunction, more advanced resuscitative measures were required.
Caution should be exercised when administering PRECEDEX to patients with advanced heart block and/or severe ventricular dysfunction. Because PRECEDEX decreases sympathetic nervous system activity, hypotension and/or bradycardia may be expected to be more pronounced in patients with hypovolemia, diabetes mellitus, or chronic hypertension and in elderly patients.
In clinical trials where other vasodilators or negative chronotropic agents were co-administered with PRECEDEX an additive pharmacodynamic effect was not observed. Nonetheless, caution should be used when such agents are administered concomitantly with PRECEDEX.
7.1 Anesthetics, Sedatives, Hypnotics, Opioids
Co-administration of PRECEDEX with anesthetics, sedatives, hypnotics, and opioids is likely to lead to an enhancement of effects. Specific studies have confirmed these effects with sevoflurane, isoflurane, propofol, alfentanil, and midazolam. No pharmacokinetic interactions between PRECEDEX and isoflurane, propofol, alfentanil and midazolam have been demonstrated. However, due to possible pharmacodynamic interactions, when co-administered with PRECEDEX, a reduction in dosage of PRECEDEX or the concomitant anesthetic, sedative, hypnotic or opioid may be required.
Principal Display Panel 250 Ml Bottle Carton
NDC 0409-1434-01
1 Unit X 250 mL
Rx only
Single-dose bottle.
Discard unused portion.
Precedex™
Dexmedetomidine HCl
in 0.9% Sodium Chloride
Injection
1,000 mcg/250 mL
(4 mcg/mL)
For Intravenous Use
Hospira
Principal Display Panel – 100 Ml Bottle Label 1596
100 mL
Rx only
NDC 0409-1596-01
Single-dose bottle. Discard unused portion.
PrecedexTM
Dexmedetomidine HCl
in 0.9% Sodium Chloride
Injection
400 mcg/100 mL
(4 mcg/mL)
For Intravenous Use
Principal Display Panel – 100 Ml Bottle Carton 1596
NDC 0409-1596-01
Rx only
100 mL Single-dose bottle.
Discard unused portion.
PrecedexTM
Dexmedetomidine HCl
in 0.9% Sodium Chloride
Injection
400 mcg/100 mL
(4 mcg/mL)
For Intravenous Use
Hospira
Structured Label Content
Section 42229-5 (42229-5)
PRECEDEX Presentations Requiring Dilution:
-
•PRECEDEX Injection, 200 mcg/2 mL (100 mcg/mL)
PRECEDEX must be diluted with 0.9% sodium chloride injection to achieve required concentration (4 mcg/mL) prior to administration. Preparation of solutions is the same, whether for the loading dose or maintenance infusion.
To prepare the infusion, withdraw 2 mL of PRECEDEX Injection, and add to 48 mL of 0.9% sodium chloride injection to a total of 50 mL. Shake gently to mix well.
Section 43683-2 (43683-2)
|
Dosage and Administration, Preparation of Solution (2.4) |
10/2024 |
Section 44425-7 (44425-7)
Store at 20°C to 25°C (68°F to 77°F); excursions permitted between 15°C to 30°C (59°F to 86°F). [See USP Controlled Room Temperature.]
Do not use if product is discolored or if precipitate matter is present.
PRECEDEX (dexmedetomidine hydrochloride) injection 200 mcg/2 mL (100 mcg/mL) is clear and colorless. The strength is based on the dexmedetomidine base. Discard unused portion.
|
Unit of Sale |
Concentration |
|
NDC 0409-1638-02 Tray of 25 single-dose clear glass vials |
200 mcg/2 mL (100 mcg/mL) |
PRECEDEX (dexmedetomidine hydrochloride in 0.9% Sodium Chloride) injection (4 mcg/mL) is clear and colorless. The strength is based on the dexmedetomidine base. Discard unused portion.
|
Unit of Sale |
Concentration |
|
NDC 0409-1660-20 Carton of 10 single-dose clear glass vials |
80 mcg/20 mL (4 mcg/mL) |
|
NDC 0409-1660-50 Tray of 20 single-dose clear glass bottles |
200 mcg/50 mL (4 mcg/mL) |
|
NDC 0409-1660-10 Tray of 10 single-dose clear glass bottles |
400 mcg/100 mL (4 mcg/mL) |
|
NDC 0409-1596-10 Case of 10 cartons containing 1 single-dose clear glass bottle |
400 mcg/100 mL (4 mcg/mL) |
|
NDC 0409-1434-01 Carton containing 1 single-dose clear glass bottle |
1,000 mcg/250 mL (4 mcg/mL) |
|
NDC 0409-7838-24 Case of 24 single-dose flexible containers |
200 mcg/50 mL (4 mcg/mL) |
|
NDC 0409-7853-24 Case of 24 single-dose flexible containers |
400 mcg/100 mL (4 mcg/mL) |
|
NDC 0409-7875-12 Case of 12 single-dose flexible containers |
1,000 mcg/250 mL (4 mcg/mL) |
10 Overdosage (10 OVERDOSAGE)
The tolerability of PRECEDEX was studied in one study in which healthy adult subjects were administered doses at and above the recommended dose of 0.2 mcg/kg/hr to 0.7 mcg/kg/hr. The maximum blood concentration achieved in this study was approximately 13 times the upper boundary of the therapeutic range. The most notable effects observed in two subjects who achieved the highest doses were first degree atrioventricular block and second-degree heart block. No hemodynamic compromise was noted with the atrioventricular block and the heart block resolved spontaneously within one minute.
Five adult patients received an overdose of PRECEDEX in the intensive care unit sedation studies. Two of these patients had no symptoms reported; one patient received a 2 mcg/kg loading dose over 10 minutes (twice the recommended loading dose) and one patient received a maintenance infusion of 0.8 mcg/kg/hr. Two other patients who received a 2 mcg/kg loading dose over 10 minutes, experienced bradycardia and/or hypotension. One patient who received a loading bolus dose of undiluted PRECEDEX (19.4 mcg/kg), had cardiac arrest from which he was successfully resuscitated.
11 Description (11 DESCRIPTION)
PRECEDEX (dexmedetomidine hydrochloride) injection (100 mcg/mL) is a sterile, nonpyrogenic solution suitable for intravenous infusion following dilution. PRECEDEX (dexmedetomidine hydrochloride) in 0.9% Sodium Chloride Injection (4 mcg/mL) is a sterile, nonpyrogenic ready to use solution suitable for intravenous infusion.
PRECEDEX contains dexmedetomidine hydrochloride as the active pharmaceutical ingredient. Dexmedetomidine hydrochloride is a central alpha2-adrenergic agonist. Dexmedetomidine hydrochloride is the S-enantiomer of medetomidine. Dexmedetomidine hydrochloride chemical name is 1H-Imidazole, 4-[1-(2,3-dimethylphenyl)ethyl]-, monohydrochloride, (S). Dexmedetomidine hydrochloride has a molecular weight of 236.7 and the empirical formula is C13H16N2•HCl and the structural formula is:
Dexmedetomidine hydrochloride is a white or almost white powder that is freely soluble in water and has a pKa of 7.1. Its partition coefficient in-octanol: water at pH 7.4 is 2.89.
PRECEDEX Injection is intended to be used after dilution. It is supplied as a clear, colorless, isotonic solution with a pH between 4.5 to 7.0. Each mL contains 118 mcg of dexmedetomidine hydrochloride (equivalent to 100 mcg or 0.1 mg of dexmedetomidine) and 9 mg of sodium chloride in water for injection. The solution is preservative-free and contains no additives or chemical stabilizers.
PRECEDEX in 0.9% Sodium Chloride Injection is ready to be used. It is supplied as a clear, colorless, isotonic solution with a pH between 4.5 to 8.0. Each mL contains 4.72 mcg of dexmedetomidine hydrochloride (equivalent to 4 mcg or 0.004 mg of dexmedetomidine) and 9 mg sodium chloride in water for injection. The solution is preservative-free and contains no additives or chemical stabilizers.
5.5 Withdrawal
9.3 Dependence
The dependence potential of PRECEDEX has not been studied in humans. However, since studies in rodents and primates have demonstrated that PRECEDEX exhibits pharmacologic actions similar to those of clonidine, it is possible that PRECEDEX may produce a clonidine-like withdrawal syndrome upon abrupt discontinuation [see Warnings and Precautions (5.5)].
5.4 Arousability
Some patients receiving PRECEDEX have been observed to be arousable and alert when stimulated. This alone should not be considered as evidence of lack of efficacy in the absence of other clinical signs and symptoms.
8.4 Pediatric Use
Sedation for Non-Invasive Procedures
The safety and efficacy of PRECEDEX have been established in pediatric patients 1 month to less than 18 years of age for sedation during non-invasive procedures. Use in this age group is based on one randomized double-blind, dose-ranging safety and efficacy trial in non-intubated pediatric patients 1 month to less than 17 years of age who required sedation prior to undergoing MRI scans [see Clinical Studies (14.2)]. An increase in frequency of bradypnea, bradycardia, hypertension and hypotension was observed in pediatric patients treated with PRECEDEX [see Adverse Reactions (6.1)]. The overall safety profile of PRECEDEX in pediatric patients was consistent with the known safety profile in adults [see Adverse Reactions (6.1)].
The safety and effectiveness of PRECEDEX have not been established in pediatric patients less than 1 month of age.
ICU Sedation
The safety and efficacy of PRECEDEX have not been established in pediatric patients for ICU sedation. One assessor-blinded trial in pediatric patients and two open label studies in neonates were conducted to assess efficacy for ICU sedation. These studies did not meet their primary efficacy endpoints and the safety data submitted were insufficient to fully characterize the safety profile of PRECEDEX for these patient populations.
14 Clinical Studies (14 CLINICAL STUDIES)
The safety and efficacy of PRECEDEX has been evaluated in four randomized, double-blind, placebo-controlled multicenter clinical trials in 1,185 adult patients.
4 Contraindications (4 CONTRAINDICATIONS)
None.
6 Adverse Reactions (6 ADVERSE REACTIONS)
The following clinically significant adverse reactions are described elsewhere in the labeling:
-
•Hypotension, bradycardia and sinus arrest [see Warnings and Precautions (5.2)]
-
•Transient hypertension [see Warnings and Precautions (5.3)]
7 Drug Interactions (7 DRUG INTERACTIONS)
Anesthetics, Sedatives, Hypnotics, Opioids: Enhancement of pharmacodynamic effects. Reduction in dosage of PRECEDEX or the concomitant medication may be required. (7.1)
12.2 Pharmacodynamics
In a study in healthy adult volunteers (N = 10), respiratory rate and oxygen saturation remained within normal limits and there was no evidence of respiratory depression when PRECEDEX was administered by intravenous infusion at doses within the recommended dose range (0.2 mcg/kg/hr to 0.7 mcg/kg/hr).
12.3 Pharmacokinetics
Following intravenous administration to adults, dexmedetomidine exhibits the following pharmacokinetic parameters: a rapid distribution phase with a distribution half-life (t1/2) of approximately 6 minutes; a terminal elimination half-life (t1/2) of approximately 2 hours; and steady-state volume of distribution (Vss) of approximately 118 liters. Clearance is estimated to be approximately 39 L/h. The mean body weight associated with this clearance estimate was 72 kg.
Dexmedetomidine exhibits linear pharmacokinetics in the dosage range of 0.2 mcg/kg/hr to 0.7 mcg/kg/hr when administered to adults by intravenous infusion for up to 24 hours. Table 10 shows the main pharmacokinetic parameters when PRECEDEX was infused (after appropriate loading doses) at maintenance infusion rates of 0.17 mcg/kg/hr (target plasma concentration of 0.3 ng/mL) for 12 and 24 hours, 0.33 mcg/kg/hr (target plasma concentration of 0.6 ng/mL) for 24 hours, and 0.70 mcg/kg/hr (target plasma concentration of 1.25 ng/mL) for 24 hours.
| Parameter | Loading Infusion (min)/Total Infusion Duration (hrs) | |||
|---|---|---|---|---|
| 10 min/12 hrs | 10 min/24 hrs | 10 min/24 hrs | 35 min/24 hrs | |
| Dexmedetomidine Target Plasma Concentration (ng/mL) and Dose (mcg/kg/hr) | ||||
| 0.3/0.17 | 0.3/0.17 | 0.6/0.33 | 1.25/0.70 | |
| Abbreviations: t1/2 = half‑life, CL = clearance, Vss = steady‑state volume of distribution. | ||||
|
t1/2 Presented as harmonic mean and pseudo standard deviation.
, hour
|
1.78 ± 0.30 |
2.22 ± 0.59 |
2.23 ± 0.21 |
2.50 ± 0.61 |
|
CL, liter/hour |
46.3 ± 8.3 |
43.1 ± 6.5 |
35.3 ± 6.8 |
36.5 ± 7.5 |
|
Vss, liter |
88.7 ± 22.9 |
102.4 ± 20.3 |
93.6 ± 17.0 |
99.6 ± 17.8 |
|
Avg Css Mean Css = Average steady-state concentration of dexmedetomidine. The mean Css was calculated based on post-dose sampling from 2.5 to 9 hours samples for 12 hour infusion and post-dose sampling from 2.5 to 18 hours for 24 hour infusions.
, ng/mL
|
0.27 ± 0.05 |
0.27 ± 0.05 |
0.67 ± 0.10 |
1.37 ± 0.20 |
The loading doses for each of the above indicated groups were 0.5, 0.5, 1 and 2.2 mcg/kg, respectively.
Dexmedetomidine pharmacokinetic parameters in adults after PRECEDEX maintenance doses of 0.2 mcg/kg/hr to 1.4 mcg/kg/hr for >24 hours were similar to the pharmacokinetic (PK) parameters after PRECEDEX maintenance dosing for <24 hours in other studies. The values for clearance (CL), volume of distribution (V), and t1/2 were 39.4 L/hr, 152 L, and 2.67 hours, respectively.
2.3 Dosage Adjustment
Due to possible pharmacodynamic interactions, a reduction in dosage of PRECEDEX or other concomitant anesthetics, sedatives, hypnotics or opioids may be required when co-administered [see Drug Interactions (7.1)].
Dosage reductions may need to be considered for adult patients with hepatic impairment, and geriatric patients [see Warnings and Precautions (5.8), Use in Specific Populations (8.6), Clinical Pharmacology (12.3)].
2.2 Recommended Dosage
| INDICATION | DOSAGE AND ADMINISTRATION |
|---|---|
|
Initiation of Intensive Care Unit Sedation |
For adult patients: a loading infusion of one mcg/kg over 10 minutes . For adult patients being converted from alternate sedative therapy: a loading dose may not be required. For patients over 65 years of age: Consider a dose reduction [see Use in Specific Populations (8.5)]. For adult patients with impaired hepatic function: Consider a dose reduction [see Use in Specific Populations (8.6), Clinical Pharmacology (12.3)]. |
|
Maintenance of Intensive Care Unit Sedation |
For adult patients: a maintenance infusion of 0.2 mcg/kg/ hour to 0.7 mcg/kg/ hour . The rate of the maintenance infusion should be adjusted to achieve the desired level of sedation. For patients over 65 years of age: Consider a dose reduction [see Use in Specific Populations (8.5)]. For adult patients with impaired hepatic function: Consider a dose reduction [see Use in Specific Populations (8.6), Clinical Pharmacology (12.3)] |
|
Initiation of Procedural Sedation |
For adult patients: a loading infusion of one mcg/kg over 10 minutes . For less invasive procedures such as ophthalmic surgery, a loading infusion of 0.5 mcg/kg given over 10 minutes may be suitable. For awake fiberoptic intubation in adult patients: a loading infusion of one mcg/kg over 10 minutes . For patients over 65 years of age: a loading infusion of 0.5 mcg/kg over 10 minutes [see Use in Specific Populations (8.5)]. For adult patients with impaired hepatic function: Consider a dose reduction [see Use in Specific Populations (8.6), Clinical Pharmacology (12.3)]. |
|
Maintenance of Procedural Sedation |
For adult patients: the maintenance infusion is generally initiated at 0.6 mcg/kg/ hour and titrated to achieve desired clinical effect with doses ranging from 0.2 mcg/kg/ hour to 1 mcg/kg/ hour . Adjust the rate of the maintenance infusion to achieve the targeted level of sedation. For awake fiberoptic intubation in adult patients: a maintenance infusion of 0.7 mcg/kg/ hour is recommended until the endotracheal tube is secured. For patients over 65 years of age: Consider a dose reduction [see Use in Specific Populations (8.5)]. For adult patients with impaired hepatic function: Consider a dose reduction [see Use in Specific Populations (8.6), Clinical Pharmacology (12.3)]. |
|
INDICATION |
DOSAGE AND ADMINISTRATION |
|
Initiation of Sedation During Non‑invasive Procedures |
For pediatric patients:
Consider a reduction in dosage if clinically indicated. |
|
Maintenance of Sedation During Non-invasive Procedures |
For pediatric patients:
As clinically warranted, titrate the maintenance dose to individual patient clinical response. |
5.8 Hepatic Impairment
Since PRECEDEX clearance decreases with severity of hepatic impairment, dose reduction should be considered in patients with impaired hepatic function [see Dosage and Administration (2.2, 2.3)].
8.6 Hepatic Impairment
Since PRECEDEX clearance decreases with increasing severity of hepatic impairment, dose reduction should be considered in patients with impaired hepatic function [see Dosage and Administration (2.2, 2.3), Clinical Pharmacology (12.3)].
1 Indications and Usage (1 INDICATIONS AND USAGE)
PRECEDEX is a alpha2-adrenergic receptor agonist indicated for:
-
•Sedation of initially intubated and mechanically ventilated adult patients during treatment in an intensive care setting. Administer PRECEDEX by continuous infusion not to exceed 24 hours. (1.1)
-
•Sedation of non-intubated adult patients prior to and/or during surgical and other procedures. (1.2)
-
•Sedation of non-intubated pediatric patients aged 1 month to less than 18 years prior to and during non-invasive procedures. (1.2)
1.2 Procedural Sedation
PRECEDEX is indicated for sedation of non-intubated adult patients prior to and/or during surgical and other procedures.
PRECEDEX is indicated for sedation of non-intubated pediatric patients aged 1 month to less than 18 years prior to and during non-invasive procedures.
5.1 Drug Administration
PRECEDEX should be administered only by persons skilled in the management of patients in the intensive care or operating room setting. Due to the known pharmacological effects of PRECEDEX, patients should be continuously monitored while receiving PRECEDEX.
12.1 Mechanism of Action
PRECEDEX is a relatively selective centrally acting alpha2-adrenergic agonist with sedative properties. Alpha2 selectivity is observed in animals following slow intravenous infusion of low and medium doses (10–300 mcg/kg). Both alpha1 and alpha2 activity is observed following slow intravenous infusion of high doses (≥1,000 mcg/kg) or with rapid intravenous administration.
14.2 Procedural Sedation
Adult Patients
The safety and efficacy of PRECEDEX for sedation of non-intubated adult patients prior to and/or during surgical and other procedures was evaluated in two randomized, double-blind, placebo-controlled multicenter clinical trials. Study 1 evaluated the sedative properties of PRECEDEX in adult patients having a variety of elective surgeries/procedures performed under monitored anesthesia care. Study 2 evaluated PRECEDEX in adult patients undergoing awake fiberoptic intubation prior to a surgical or diagnostic procedure.
In Study 1, the sedative properties of PRECEDEX were evaluated by comparing the percent of adult patients not requiring rescue midazolam to achieve a specified level of sedation using the standardized Observer's Assessment of Alertness/Sedation Scale (see Table 15).
|
Assessment Categories |
||||
|
Responsiveness |
Speech |
Facial Expression |
Eyes |
Composite Score |
|
Responds readily to name spoken in normal tone |
Normal |
Normal |
Clear, no ptosis |
5 (alert) |
|
Lethargic response to name spoken in normal tone |
Mild slowing or thickening |
Mild relaxation |
Glazed or mild ptosis (less than half the eye) |
4 |
|
Responds only after name is called loudly and/or repeatedly |
Slurring or prominent slowing |
Marked relaxation |
Glazed and marked ptosis (half the eye or more) |
3 |
|
Responds only after mild prodding or shaking |
Few recognizable words |
– |
– |
2 |
|
Does not respond to mild prodding or shaking |
– |
– |
– |
1 (deep sleep) |
Adult patients were randomized to receive a loading infusion of either PRECEDEX 1 mcg/kg, PRECEDEX 0.5 mcg/kg, or placebo (normal saline) given over 10 minutes and followed by a maintenance infusion started at 0.6 mcg/kg/hr. The maintenance infusion of study drug could be titrated from 0.2 mcg/kg/hr to 1 mcg/kg/hr to achieve the targeted sedation score (Observer's Assessment of Alertness/Sedation Scale ≤4). Adult patients were allowed to receive rescue midazolam as needed to achieve and/or maintain an Observer's Assessment of Alertness/Sedation Scale ≤4. After achieving the desired level of sedation, a local or regional anesthetic block was performed. Demographic characteristics were similar between the PRECEDEX and comparator groups. Efficacy results showed that PRECEDEX was more effective than the comparator group when used to sedate non‑intubated patients requiring monitored anesthesia care during surgical and other procedures (see Table 15).
In Study 2, the sedative properties of PRECEDEX were evaluated by comparing the percent of adult patients requiring rescue midazolam to achieve or maintain a specified level of sedation using the Ramsay Sedation Scale score ≥2 (see Table 12). Adult patients were randomized to receive a loading infusion of PRECEDEX 1 mcg/kg or placebo (normal saline) given over 10 minutes and followed by a fixed maintenance infusion of 0.7 mcg/kg/hr. After achieving the desired level of sedation, topicalization of the airway occurred. Adult patients were allowed to receive rescue midazolam as needed to achieve and/or maintain a Ramsay Sedation Scale ≥2. Demographic characteristics were similar between the PRECEDEX and comparator groups. For efficacy results see Table 16.
|
Study |
Loading Infusion Treatment Arm |
Number of Patients Enrolled Based on ITT population defined as all randomized and treated patients.
|
% Not Requiring Midazolam Rescue |
Confidence Normal approximation to the binomial with continuity correction.
Interval on the Difference vs. Placebo
|
Mean (SD) Total Dose (mg) of Rescue Midazolam Required |
Confidence Intervals of the Mean Rescue Dose |
|
Study 1 |
Dexmedetomidine |
134 |
40 |
37 (27, 48) |
1.4 (1.7) |
-2.7 |
|
Dexmedetomidine |
129 |
54 |
51 (40, 62) |
0.9 (1.5) |
-3.1 |
|
|
Placebo |
63 |
3 |
– |
4.1 (3.0) |
– |
|
|
Study 2 |
Dexmedetomidine |
55 |
53 |
39 (20, 57) |
1.1 (1.5) |
-1.8 |
|
Placebo |
50 |
14 |
– |
2.9 (3.0) |
– |
Pediatric Patients
The safety and efficacy of PRECEDEX for sedation of non-intubated pediatric patients aged 1 month to less than 17 years undergoing MRI scans was evaluated in one randomized, double-blind, dose-ranging, dose‑controlled multicenter clinical trial utilizing 3 different PRECEDEX dosages. The sedative properties of PRECEDEX were evaluated by age group and by the percent of pediatric patients at the high dose level versus the low dose level who did not require concomitant propofol to complete the MRI scan.
A total of 122 pediatric patients were randomized to the PRECEDEX low dose group (42 of 122), the middle dose group (42 of 122) or the high dose treatment group (38 of 122). All patients received a PRECEDEX loading dose infusion over 10 minutes followed by a maintenance infusion for the duration of the MRI scan (Table 17). If an adequate level of sedation was not achieved within 5 minutes after the start of the PRECEDEX maintenance infusion, patients could receive concomitant propofol as needed based on clinical judgment to achieve and/or maintain adequate sedation.
|
High Dose |
Middle Dose |
Low Dose |
||||
|
Age |
Loading Dose (10 min) |
Maintenance Dose |
Loading Dose (10 min) |
Maintenance Dose |
Loading Dose (10 min) |
Maintenance Dose |
|
1 month to less than 2 years |
1.5 mcg/kg |
1.5 mcg/kg/h |
1 mcg/kg |
1 mcg/kg/h |
0.5 mcg/kg |
0.5 mcg/kg/h |
|
2 to less than 17 years |
2 mcg/kg |
1.5 mcg/kg/h |
1.2 mcg /kg |
1 mcg/kg/h |
0.5 mcg/kg |
0.5 mcg kg/h |
The primary efficacy results from this pediatric procedural sedation study are summarized in Table 18. In the combined age group, the percent of pediatric patients not requiring concomitant propofol was 14.3% (6/42) in the low dose group and 63.2% (24/38) in the high dose group. The percentage of patients at the PRECEDEX high dose who completed the MRI without concomitant propofol was statistically greater than the percentage in the PRECEDEX low dose group (p<0.001).
|
Age Group |
High Dose |
Middle Dose |
Low Dose |
High Dose vs Low Dose |
||
|
n (%) 95% CI Exact 95% CI of proportion of subjects not requiring propofol in each dose level.
|
n (%) 95% CI |
n (%) 95% CI |
Odds Ratio 95% CI p-values; CI is confidence interval of odds ratio.
|
p-value |
||
|
1 month to less than 2 years |
N=59 |
9/18 (50.0%) (0.26, 0.74) |
2/21 (9.5%) (0.01, 0.30) |
2/20 (15.0%) (0.03, 0.38) |
0.18 (0.04, 0.82) |
0.022 |
|
2 to less than 17 years |
N=63 |
15/20 (75.0%) (0.51, 0.91) |
13/21 (61.9%) (0.38, 0.82) |
3/22 (13.6%) (0.03, 0.35) |
0.05 (0.01, 0.26) |
<0.001 |
|
Overall |
N=122 |
24/38 (63.2%) (0.46, 0.78) |
15/42 (35.7%) (0.22, 0.52) |
6/42 (14.3%) (0.05, 0.29) |
0.10 (0.03, 0.29) |
<0.001 |
Secondarily, the sedative properties were also evaluated by examining the percent of time at a target sedation score using the Pediatric Sedation State Scale (PSSS). The PSSS is a validated 6-point scale specifically designed for evaluating pediatric patients undergoing sedation for diagnostic and therapeutic procedures. The PSSS measures the effectiveness and quality of procedural sedation in children. The target sedation level was indicated by a PSSS score of 2 (i.e., patient is quiet [asleep or awake], not moving during procedure, has no frown [or brow furrow] indicating pain or anxiety and no verbalization of any complaint).
In the PRECEDEX high dose group, pediatric patients in both the combined and individual age group were at the target sedation rating scale score (PSSS of 2) for a mean >87% of the time during the PRECEDEX maintenance infusion. In both the combined and individual age group, an increase in the percentage of time at the target sedation rating scale score (PSSS of 2) was observed with increasing PRECEDEX dosage.
9.1 Controlled Substance
PRECEDEX (dexmedetomidine hydrochloride) is not a controlled substance.
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
-
•Monitoring: Continuously monitor patients while receiving PRECEDEX. (5.1)
-
•Bradycardia and Sinus Arrest: Have occurred in young healthy volunteers with high vagal tone or with different routes of administration, e.g., rapid intravenous or bolus administration. (5.2)
-
•Hypotension and Bradycardia: May necessitate medical intervention. May be more pronounced in patients with hypovolemia, diabetes mellitus, or chronic hypertension, and in the elderly. Use with caution in patients with advanced heart block or severe ventricular dysfunction. (5.2)
-
•Co-administration with Other Vasodilators or Negative Chronotropic Agents: Use with caution due to additive pharmacodynamic effects. (5.2)
-
•Transient Hypertension: Observed primarily during the loading dose. Consider reduction in loading infusion rate. (5.3)
-
•Arousability: Patients can become aroused/alert with stimulation; this alone should not be considered as lack of efficacy. (5.4)
-
•Tolerance and Tachyphylaxis: Prolonged exposure to dexmedetomidine beyond 24 hours may be associated with tolerance and tachyphylaxis and a dose-related increase in adverse events. (5.6)
5.3 Transient Hypertension
Transient hypertension has been observed primarily during the loading dose in association with the initial peripheral vasoconstrictive effects of PRECEDEX. Treatment of the transient hypertension has generally not been necessary, although reduction of the loading infusion rate may be desirable.
7.2 Neuromuscular Blockers
In one study of 10 healthy adult volunteers, administration of PRECEDEX for 45 minutes at a plasma concentration of one ng/mL resulted in no clinically meaningful increases in the magnitude of neuromuscular blockade associated with rocuronium administration.
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
-
•Individualize and titrate PRECEDEX dosing to desired clinical effect. (2.1)
-
•Administer PRECEDEX using a controlled infusion device. (2.1)
-
•Dilute the 200 mcg/2 mL (100 mcg/mL) vial contents in 0.9% sodium chloride solution to achieve required concentration (4 mcg/mL) prior to administration. (2.4)
-
•The 80 mcg/20 mL single-dose vial, and 200 mcg/50 mL, 400 mcg/100 mL, and 1,000 mcg/250 mL single-dose bottles and single-dose flexible containers do not require further dilution prior to administration. (2.4)
-
•For Adult Intensive Care Unit Sedation: Initiate at one mcg/kg over 10 minutes , followed by a maintenance infusion of 0.2 mcg/kg/ hour to 0.7 mcg/kg/ hour . (2.2)
-
•For Adult Procedural Sedation: Initiate at one mcg/kg over 10 minutes , followed by a maintenance infusion initiated at 0.6 mcg/kg/ hour and titrated to achieve desired clinical effect with doses ranging from 0.2 mcg/kg/ hour to 1 mcg/kg/ hour . (2.2)
-
•For Sedation of Pediatric Patients During Non-invasive Procedures: Patients 1 month to less than 2 years old initiate at 1.5 mcg/kg over 10 minutes followed by a maintenance infusion of 1.5 mcg/kg/ hour and titrated to achieve desired clinical effect with dosage ranging from 0.5 mcg/kg/ hour to 1.5 mcg/kg/ hour ; patients 2 to less than 18 years old initiate at 2 mcg/kg over 10 minutes followed by a maintenance infusion of 1.5 mcg/kg/ hour and titrated to achieve desired clinical effect with dosage ranging from 0.5 mcg/kg/ hour to 1.5 mcg/kg/ hour . (2.2)
-
•Alternative Doses: Recommended for patients over 65 years of age and awake fiberoptic intubation patients. (2.2)
2.4 Preparation of Solution
Strict aseptic technique must always be maintained during handling of PRECEDEX.
Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration, whenever solution and container permit. Do not use if product is discolored or if precipitate matter is present.
5.7 Hyperthermia Or Pyrexia (5.7 Hyperthermia or Pyrexia)
PRECEDEX may induce hyperthermia or pyrexia, which may be resistant to traditional cooling methods, such as administration of cooled intravenous fluids and antipyretic medications. Discontinue PRECEDEX if drug‑related hyperthermia or pyrexia is suspected and monitor patients until body temperature normalizes.
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
PRECEDEX Presentations Requiring Dilution:
PRECEDEX (dexmedetomidine hydrochloride) injection is a clear and colorless solution, to be used after dilution. It is available as:
-
•200 mcg/2 mL (100 mcg/mL) single-dose vial.
PRECEDEX Presentations that are Ready To Use:
PRECEDEX (dexmedetomidine hydrochloride) in 0.9% sodium chloride injection is a clear and colorless solution, ready to use. It is available as:
-
•PRECEDEX 80 mcg/20 mL (4 mcg/mL) single-dose vial.
-
•PRECEDEX 200 mcg/50 mL (4 mcg/mL) single-dose glass bottle.
-
•PRECEDEX 400 mcg/100 mL (4 mcg/mL) single-dose glass bottle.
-
•PRECEDEX 1,000 mcg/250 mL (4 mcg/mL) single-dose glass bottle.
-
•PRECEDEX 200 mcg/50 mL (4 mcg/mL) single-dose flexible container.
-
•PRECEDEX 400 mcg/100 mL (4 mcg/mL) single-dose flexible container.
-
•PRECEDEX 1,000 mcg/250 mL (4 mcg/mL) single-dose flexible container.
6.2 Postmarketing Experience
The following adverse reactions have been identified during post‑approval use of PRECEDEX. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Hypotension and bradycardia were the most common adverse reactions associated with the use of PRECEDEX during post‑approval use of the drug.
| System Organ Class | Preferred Term |
|---|---|
|
Blood and Lymphatic System Disorders |
Anemia |
|
Cardiac Disorders |
Arrhythmia, atrial fibrillation, atrioventricular block, bradycardia, cardiac arrest, cardiac disorder, extrasystoles, myocardial infarction, supraventricular tachycardia, tachycardia, ventricular arrhythmia, ventricular tachycardia |
|
Eye Disorders |
Photopsia, visual impairment |
|
Gastrointestinal Disorders |
Abdominal pain, diarrhea, nausea, vomiting |
|
General Disorders and Administration Site Conditions |
Chills, hyperpyrexia, pain, pyrexia, thirst |
|
Hepatobiliary Disorders |
Hepatic function abnormal, hyperbilirubinemia |
|
Investigations |
Alanine aminotransferase increased, aspartate aminotransferase increased, blood alkaline phosphatase increased, blood urea increased, electrocardiogram T wave inversion, gammaglutamyltransferase increased, electrocardiogram QT prolonged |
|
Metabolism and Nutrition Disorders |
Acidosis, hyperkalemia, hypoglycemia, hypovolemia, hypernatremia |
|
Nervous System Disorders |
Convulsion, dizziness, headache, neuralgia, neuritis, speech disorder |
|
Psychiatric Disorders |
Agitation, confusional state, delirium, hallucination, illusion |
|
Renal and Urinary Disorders |
Oliguria, polyuria |
|
Respiratory, Thoracic and Mediastinal Disorders |
Apnea, bronchospasm, dyspnea, hypercapnia, hypoventilation, hypoxia, pulmonary congestion, respiratory acidosis |
|
Skin and Subcutaneous Tissue Disorders |
Hyperhidrosis, pruritus, rash, urticaria |
|
Surgical and Medical Procedures |
Light anesthesia |
|
Vascular Disorders |
Blood pressure fluctuation, hemorrhage, hypertension, hypotension |
8 Use in Specific Populations (8 USE IN SPECIFIC POPULATIONS)
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reactions rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
Most common treatment-emergent adverse reactions, occurring in greater than 2% of adult patients in both Intensive Care Unit and procedural sedation studies include hypotension, bradycardia and dry mouth.
2.1 Administration Instructions
-
•PRECEDEX dosing should be individualized and titrated to desired clinical response.
-
•PRECEDEX is not indicated for infusions lasting longer than 24 hours.
-
•PRECEDEX should be administered using a controlled infusion device.
5.6 Tolerance and Tachyphylaxis
Use of dexmedetomidine beyond 24 hours has been associated with tolerance and tachyphylaxis and a dose‑related increase in adverse reactions [see Adverse Reactions (6.1)].
1.1 Intensive Care Unit Sedation
PRECEDEX is indicated for sedation of initially intubated and mechanically ventilated adult patients during treatment in an intensive care setting. PRECEDEX should be administered by continuous infusion not to exceed 24 hours.
PRECEDEX has been continuously infused in mechanically ventilated adult patients prior to extubation, during extubation, and post-extubation. It is not necessary to discontinue PRECEDEX prior to extubation.
14.1 Intensive Care Unit Sedation
Two randomized, double-blind, parallel-group, placebo-controlled multicenter clinical trials included 754 adult patients being treated in a surgical intensive care unit. All patients were initially intubated and received mechanical ventilation. These trials evaluated the sedative properties of PRECEDEX by comparing the amount of rescue medication (midazolam in one trial and propofol in the second) required to achieve a specified level of sedation (using the standardized Ramsay Sedation Scale) between PRECEDEX and placebo from onset of treatment to extubation or to a total treatment duration of 24 hours. The Ramsay Level of Sedation Scale is displayed in Table 12.
|
Clinical Score |
Level of Sedation Achieved |
|
6 |
Asleep, no response |
|
5 |
Asleep, sluggish response to light glabellar tap or loud auditory stimulus |
|
4 |
Asleep, but with brisk response to light glabellar tap or loud auditory stimulus |
|
3 |
Patient responds to commands |
|
2 |
Patient cooperative, oriented, and tranquil |
|
1 |
Patient anxious, agitated, or restless |
In the first study, 175 adult patients were randomized to receive placebo and 178 to receive PRECEDEX by intravenous infusion at a dose of 0.4 mcg/kg/hr (with allowed adjustment between 0.2 mcg/kg/hr and 0.7 mcg/kg/hr) following an initial loading infusion of one mcg/kg intravenous over 10 minutes. The study drug infusion rate was adjusted to maintain a Ramsay sedation score of ≥3. Patients were allowed to receive "rescue" midazolam as needed to augment the study drug infusion. In addition, morphine sulfate was administered for pain as needed. The primary outcome measure for this study was the total amount of rescue medication (midazolam) needed to maintain sedation as specified while intubated. Patients randomized to placebo received significantly more midazolam than patients randomized to PRECEDEX (see Table 13).
A second prospective primary analysis assessed the sedative effects of PRECEDEX by comparing the percentage of adult patients who achieved a Ramsay sedation score of ≥3 during intubation without the use of additional rescue medication. A significantly greater percentage of adult patients in the PRECEDEX group maintained a Ramsay sedation score of ≥3 without receiving any midazolam rescue compared to the placebo group (see Table 13).
| ITT (intent-to-treat) population includes all randomized patients. | |||
|
Placebo
|
PRECEDEX
|
p-value |
|
|
Mean Total Dose (mg) of Midazolam |
19 mg |
5 mg |
0.0011 ANOVA model with treatment center.
|
|
Standard deviation |
53 mg |
19 mg |
|
|
Categorized Midazolam Use |
|||
|
0 mg |
43 (25%) |
108 (61%) |
<0.001 Chi-square.
|
|
0–4 mg |
34 (19%) |
36 (20%) |
|
|
>4 mg |
98 (56%) |
34 (19%) |
A prospective secondary analysis assessed the dose of morphine sulfate administered to adult patients in the PRECEDEX and placebo groups. On average, PRECEDEX-treated patients received less morphine sulfate for pain than placebo‑treated patients (0.47 versus 0.83 mg/h). In addition, 44% (79 of 178 patients) of PRECEDEX patients received no morphine sulfate for pain versus 19% (33 of 175 patients) in the placebo group.
In a second study, 198 adult patients were randomized to receive placebo and 203 to receive PRECEDEX by intravenous infusion at a dose of 0.4 mcg/kg/hr (with allowed adjustment between 0.2 mcg/kg/hr and 0.7 mcg/kg/hr) following an initial loading infusion of one mcg/kg intravenous over 10 minutes. The study drug infusion was adjusted to maintain a Ramsay sedation score of ≥3. Patients were allowed to receive "rescue" propofol as needed to augment the study drug infusion. In addition, morphine sulfate was administered as needed for pain. The primary outcome measure for this study was the total amount of rescue medication (propofol) needed to maintain sedation as specified while intubated.
Adult patients randomized to placebo received significantly more propofol than adult patients randomized to PRECEDEX (see Table 14).
A significantly greater percentage of adult patients in the PRECEDEX group compared to the placebo group maintained a Ramsay sedation score of ≥3 without receiving any propofol rescue (see Table 14).
|
Placebo
|
PRECEDEX
|
p-value |
|
|
Mean Total Dose (mg) of Propofol |
513 mg |
72 mg |
<0.0001 ANOVA model with treatment center.
|
|
Standard deviation |
782 mg |
249 mg |
|
|
Categorized Propofol Use |
|||
|
0 mg |
47 (24%) |
122 (60%) |
<0.001 Chi-square.
|
|
0–50 mg |
30 (15%) |
43 (21%) |
|
|
>50 mg |
121 (61%) |
38 (19%) |
A prospective secondary analysis assessed the dose of morphine sulfate administered to adult patients in the PRECEDEX and placebo groups. On average, PRECEDEX-treated patients received less morphine sulfate for pain than placebo-treated patients (0.43 versus 0.89 mg/h). In addition, 41% (83 of 203 patients) of PRECEDEX patients received no morphine sulfate for pain versus 15% (30 of 198 patients) in the placebo group.
In a controlled clinical trial, PRECEDEX was compared to midazolam for ICU sedation exceeding 24 hours duration. PRECEDEX was not shown to be superior to midazolam for the primary efficacy endpoint, the percent of time patients were adequately sedated (81% versus 81%). In addition, administration of PRECEDEX for longer than 24 hours was associated with tolerance, tachyphylaxis, and a dose-related increase in adverse events [see Adverse Reactions (6.1)].
17 Patient Counseling Information (17 PATIENT COUNSELING INFORMATION)
PRECEDEX is indicated for short-term intravenous sedation. Dosage must be individualized and titrated to the desired clinical effect. Blood pressure, heart rate and oxygen levels will be monitored both continuously during the infusion of PRECEDEX and as clinically appropriate after discontinuation.
-
•When PRECEDEX is infused for more than 6 hours, patients should be informed to report nervousness, agitation, and headaches that may occur for up to 48 hours.
-
•Additionally, patients should be informed to report symptoms that may occur within 48 hours after the administration of PRECEDEX such as: weakness, confusion, excessive sweating, weight loss, abdominal pain, salt cravings, diarrhea, constipation, dizziness or light-headedness.
-
•Advise breastfeeding mothers who were exposed to PRECEDEX to monitor breastfed neonates for irritability [see Use in Specific Populations (8.2)].
2.5 Administration With Other Fluids (2.5 Administration with Other Fluids)
PRECEDEX infusion should not be co-administered through the same intravenous catheter with blood or plasma because physical compatibility has not been established.
PRECEDEX has been shown to be incompatible when administered with the following drugs: amphotericin B, diazepam.
PRECEDEX has been shown to be compatible when administered with the following intravenous fluids:
-
•0.9% sodium chloride in water
-
•5% dextrose in water
-
•20% mannitol
-
•Lactated Ringer's solution
-
•100 mg/mL magnesium sulfate solution
-
•0.3% potassium chloride solution
2.6 Compatibility With Natural Rubber (2.6 Compatibility with Natural Rubber)
Compatibility studies have demonstrated the potential for absorption of PRECEDEX to some types of natural rubber. Although PRECEDEX is dosed to effect, it is advisable to use administration components made with synthetic or coated natural rubber gaskets.
Principal Display Panel 2 Ml Vial Tray (PRINCIPAL DISPLAY PANEL - 2 mL Vial Tray)
2 mL Single-dose Fliptop Vials
Preservative-Free
NDC 0409-1638-02
Contains 25 of NDC 0409-1638-32
Precedex™
DEXMEDETOMIDINE HCl INJECTION
Rx only
200 mcg/2 mL
(100 mcg/mL)
For Intravenous use.
MUST BE DILUTED
Hospira
Principal Display Panel 2 Ml Vial Label (PRINCIPAL DISPLAY PANEL - 2 mL Vial Label)
2 mL NDC 0409-1638-32
Precedex™
DEXMEDETOMIDINE
HCl INJECTION
Rx only
200 mcg/2 mL
(100 mcg/mL)
For Intravenous use.
MUST BE DILUTED
Dist. by Hospira, Inc.,
Lake Forest, IL 60045 USA
RL–7616
##–###–AA
DMMMYYYY
13.2 Animal Toxicology And/or Pharmacology (13.2 Animal Toxicology and/or Pharmacology)
There were no differences in the adrenocorticotropic hormone (ACTH)-stimulated cortisol response in dogs following a single-dose of dexmedetomidine compared to saline control. However, after continuous subcutaneous infusions of dexmedetomidine at 3 mcg/kg/hr and 10 mcg/kg/hr for one week in dogs (exposures estimated to be within the clinical range), the ACTH-stimulated cortisol response was diminished by approximately 27% and 40%, respectively, compared to saline-treated control animals indicating a dose‑dependent adrenal suppression.
Principal Display Panel 20 Ml Vial Label (PRINCIPAL DISPLAY PANEL - 20 mL Vial Label)
20 mL
NDC 0409-1660-22
Single-dose vial. Discard unused portion.
Precedex™
Dexmedetomidine HCl
in 0.9% Sodium Chloride Injection
80 mcg/20 mL
(4 mcg/mL)
Distributed by Hospira, Inc., Lake Forest, IL 60045 USA
Principal Display Panel 20 Ml Vial Carton (PRINCIPAL DISPLAY PANEL - 20 mL Vial Carton)
10 units x 20 mL
Rx only
NDC 0409-1660-20
Contains 10 of NDC 0409-1660-22
Single-dose vial. Discard unused portion.
Precedex™
Dexmedetomidine HCl in 0.9% Sodium Chloride Injection
80 mcg/20 mL
(4 mcg/mL)
Hospira
For Intravenous Use
Principal Display Panel 50 Ml Bottle Tray (PRINCIPAL DISPLAY PANEL - 50 mL Bottle Tray)
20 Units X 50 mL
Rx only
NDC 0409-1660-50
Contains 20 of NDC 0409-1660-55
Single-dose bottle. Discard unused portion.
Precedex™
Dexmedetomidine HCl
in 0.9% Sodium Chloride Injection
200 mcg/50 mL
(4 mcg/mL)
For Intravenous Use
Hospira
Principal Display Panel 100 Ml Bottle Tray (PRINCIPAL DISPLAY PANEL - 100 mL Bottle Tray)
10 Units X 100 mL
Rx only
NDC 0409-1660-10
Contains 10 of NDC 0409-1660-35
Single-dose bottle. Discard unused portion.
Precedex™
Dexmedetomidine HCl in 0.9% Sodium Chloride Injection
400 mcg/100 mL
(4 mcg/mL)
For Intravenous Use
Hospira
Principal Display Panel 50 Ml Bottle Label (PRINCIPAL DISPLAY PANEL - 50 mL Bottle Label)
50 mL
Rx only
NDC 0409-1660-55
Single-dose bottle. Discard unused portion.
Precedex™
Dexmedetomidine HCl
in 0.9% Sodium Chloride
Injection
200 mcg/50 mL
(4 mcg/mL)
For Intravenous Use
Principal Display Panel – 50 Ml Bag 7838 (PRINCIPAL DISPLAY PANEL – 50 mL Bag - 7838)
50 mL Single-dose. Discard unused portion.
NDC 0409-7838-01
PrecedexTM
Dexmedetomidine HCl
in 0.9% Sodium Chloride
Injection
Rx only
200 mcg/50 mL (4mcg/mL)
For Intravenous Infusion Each mL contains 4 mcg of dexmedetomidine
provided as 4.72 mcg dexmedetomidine HCl and 9 mg of sodium chloride in
water for injection.
Recommended Dosage: See prescribing information. Store at 20˚C to 25˚C
(68˚F to 77˚F). [See USP Controlled Room Temperature.] Do not freeze.
This product is not made with natural rubber latex.
Preservative-Free.
1000072255
Distributed by Hospira, Inc.
Lake Forest, IL 60045 USA
Hospira
Principal Display Panel 100 Ml Bottle Label (PRINCIPAL DISPLAY PANEL - 100 mL Bottle Label)
100 mL
Rx only
NDC 0409-1660-35
Single-dose bottle. Discard unused portion.
Precedex™
Dexmedetomidine HCl
in 0.9% Sodium Chloride
Injection
400 mcg/100 mL
(4 mcg/mL)
For Intravenous Use
Principal Display Panel 250 Ml Bottle Label (PRINCIPAL DISPLAY PANEL - 250 mL Bottle Label)
250 mL
Rx only
NDC 0409-1434-01
Single-dose bottle. Discard unused portion.
Precedex™
Dexmedetomidine HCl
in 0.9% Sodium
Chloride Injection
1,000 mcg/250 mL
(4 mcg/mL)
For Intravenous Use
Principal Display Panel – 100 Ml Bag 7853 (PRINCIPAL DISPLAY PANEL – 100 mL Bag - 7853)
100 mL Single-dose. Discard unused portion.
NDC 0409-7853-01
PrecedexTM
Dexmedetomidine HCl
in 0.9% Sodium Chloride
Injection
Rx only
400 mcg/100 mL (4 mcg/mL)
For Intravenous Infusion Each mL contains 4 mcg of dexmedetomidine provided
as 4.72 mcg dexmedetomidine HCl and 9 mg of sodium chloride in water for
injection.
Recommended Dosage: See prescribing information. Storage at 20ºC to 25ºC
(68ºF to 77ºF).[See USP Controlled Room Temperature.] Do not Freeze.
This product is not made with natural rubber latex.
Preservative-Free.
1000072256
Distributed by Hospira, Inc.
Lake Forest, IL 60045 USA
Hospira
Principal Display Panel – 250 Ml Bag 7875 (PRINCIPAL DISPLAY PANEL – 250 mL Bag - 7875)
250 mL Single-dose. Discard unused portion.
NDC 0409-7875-01
PrecedexTM
Dexmedetomidine HCl
in 0.9% Sodium Chloride
Injection
1,000 mcg/250 mL (4 mcg/mL)
For Intravenous Infusion Each mL contains 4 mcg of dexmedetomidine provided
as 4.72 mcg dexmedetomidine HCl and 9 mg of sodium chloride in water for
injection.
Recommended Dosage: See prescribing information. Store at
20˚C to 25˚C (68˚F to 77˚F). [See USP Controlled Room
Temperature.] Do not freeze.
This product is not made with natural
rubber latex.
Preservative-Free.
Rx only
1000072257
Distributed by Hospira, Inc.
Lake Forest, IL 60045 USA
Hospira
5.2 Hypotension, Bradycardia, and Sinus Arrest
Clinically significant episodes of bradycardia and sinus arrest have been reported with PRECEDEX administration in young, healthy adult volunteers with high vagal tone or with different routes of administration including rapid intravenous or bolus administration.
Reports of hypotension and bradycardia have been associated with PRECEDEX infusion. Some of these cases have resulted in fatalities. If medical intervention is required, treatment may include decreasing or stopping the infusion of PRECEDEX, increasing the rate of intravenous fluid administration, elevation of the lower extremities, and use of pressor agents. Because PRECEDEX has the potential to augment bradycardia induced by vagal stimuli, clinicians should be prepared to intervene. The intravenous administration of anticholinergic agents (e.g., glycopyrrolate, atropine) should be considered to modify vagal tone. In clinical trials, glycopyrrolate or atropine were effective in the treatment of most episodes of PRECEDEX-induced bradycardia. However, in some patients with significant cardiovascular dysfunction, more advanced resuscitative measures were required.
Caution should be exercised when administering PRECEDEX to patients with advanced heart block and/or severe ventricular dysfunction. Because PRECEDEX decreases sympathetic nervous system activity, hypotension and/or bradycardia may be expected to be more pronounced in patients with hypovolemia, diabetes mellitus, or chronic hypertension and in elderly patients.
In clinical trials where other vasodilators or negative chronotropic agents were co-administered with PRECEDEX an additive pharmacodynamic effect was not observed. Nonetheless, caution should be used when such agents are administered concomitantly with PRECEDEX.
7.1 Anesthetics, Sedatives, Hypnotics, Opioids
Co-administration of PRECEDEX with anesthetics, sedatives, hypnotics, and opioids is likely to lead to an enhancement of effects. Specific studies have confirmed these effects with sevoflurane, isoflurane, propofol, alfentanil, and midazolam. No pharmacokinetic interactions between PRECEDEX and isoflurane, propofol, alfentanil and midazolam have been demonstrated. However, due to possible pharmacodynamic interactions, when co-administered with PRECEDEX, a reduction in dosage of PRECEDEX or the concomitant anesthetic, sedative, hypnotic or opioid may be required.
Principal Display Panel 250 Ml Bottle Carton (PRINCIPAL DISPLAY PANEL - 250 mL Bottle Carton)
NDC 0409-1434-01
1 Unit X 250 mL
Rx only
Single-dose bottle.
Discard unused portion.
Precedex™
Dexmedetomidine HCl
in 0.9% Sodium Chloride
Injection
1,000 mcg/250 mL
(4 mcg/mL)
For Intravenous Use
Hospira
Principal Display Panel – 100 Ml Bottle Label 1596 (PRINCIPAL DISPLAY PANEL – 100 mL Bottle Label - 1596)
100 mL
Rx only
NDC 0409-1596-01
Single-dose bottle. Discard unused portion.
PrecedexTM
Dexmedetomidine HCl
in 0.9% Sodium Chloride
Injection
400 mcg/100 mL
(4 mcg/mL)
For Intravenous Use
Principal Display Panel – 100 Ml Bottle Carton 1596 (PRINCIPAL DISPLAY PANEL – 100 mL Bottle Carton - 1596)
NDC 0409-1596-01
Rx only
100 mL Single-dose bottle.
Discard unused portion.
PrecedexTM
Dexmedetomidine HCl
in 0.9% Sodium Chloride
Injection
400 mcg/100 mL
(4 mcg/mL)
For Intravenous Use
Hospira
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:52:06.471450 · Updated: 2026-03-14T22:42:47.502846