Amantadine Hydrochloride Capsules, Usp
5232b933-1df9-43b4-8ac2-61bfa4855e68
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
Rx only
Indications and Usage
Amantadine hydrochloride capsules are indicated for the prophylaxis and treatment of signs and symptoms of infection caused by various strains of influenza A virus. Amantadine hydrochloride capsules are also indicated in the treatment of parkinsonism and drug-induced extrapyramidal reactions.
Dosage and Administration
The dose of amantadine hydrochloride capsules may need reduction in patients with congestive heart failure, peripheral edema, orthostatic hypotension, or impaired renal function (see Dosage for Impaired Renal Function ).
Contraindications
Amantadine hydrochloride is contraindicated in patients with known hypersensitivity to amantadine hydrochloride or to any of the other ingredients in Amantadine hydrochloride.
Adverse Reactions
The adverse reactions reported most frequently at the recommended dose of amantadine hydrochloride (5% to 10%) are: nausea, dizziness (lightheadedness), and insomnia. Less frequently (1% to 5%) reported adverse reactions are: depression, anxiety and irritability, hallucinations, confusion, anorexia, dry mouth, constipation, ataxia, livedo reticularis, peripheral edema, orthostatic hypotension, headache, somnolence, nervousness, dream abnormality, agitation, dry nose, diarrhea and fatigue. Infrequently (0.1% to 1%) occurring adverse reactions are: congestive heart failure, psychosis, urinary retention, dyspnea, skin rash, vomiting, weakness, slurred speech, euphoria, thinking abnormality, amnesia, hyperkinesia, hypertension, decreased libido, and visual disturbance, including punctate subepithelial or other corneal opacity, corneal edema, decreased visual acuity, sensitivity to light, and optic nerve palsy. Rare (less than 0.1%) occurring adverse reactions are: instances of convulsion, leukopenia, neutropenia, eczematoid dermatitis, oculogyric episodes, suicidal attempt, suicide, and suicidal ideation (see WARNINGS ). Other adverse reactions reported during postmarketing experience with amantadine hydrochloride usage include: Nervous System/Psychiatric – coma, stupor, delirium, hypokinesia, hypertonia, delusions, aggressive behavior, paranoid reaction, manic reaction, involuntary muscle contractions, gait abnormalities, paresthesia, EEG changes, and tremor. Abrupt discontinuation may also precipitate delirium, agitation, delusions, hallucinations, paranoid reaction, stupor, anxiety, depression and slurred speech; Cardiovascular – cardiac arrest, arrhythmias including malignant arrhythmias, hypotension, and tachycardia; Respiratory – acute respiratory failure, pulmonary edema, and tachypnea; Gastrointestinal – dysphagia; Hematologic – leukocytosis, agranulocytosis; Special Senses – keratitis and mydriasis; Skin and Appendages – pruritus and diaphoresis; Miscellaneous - neuroleptic malignant syndrome (see WARNINGS ), allergic reactions including anaphylactic reactions, edema and fever. Laboratory Test – elevated: CPK, BUN, serum creatinine, alkaline phosphatase, LDH, bilirubin, GGT, SGOT, and SGPT.
How Supplied
Amantadine hydrochloride capsules, USP are available as yellow, soft gelatin capsules containing 100 mg of amantadine hydrochloride and imprinted C-122 Bottles of 100 with child-resistant closure, NDC 0832-1015-00 Bottles of 500, NDC 0832-1015-50
Medication Information
Indications and Usage
Amantadine hydrochloride capsules are indicated for the prophylaxis and treatment of signs and symptoms of infection caused by various strains of influenza A virus. Amantadine hydrochloride capsules are also indicated in the treatment of parkinsonism and drug-induced extrapyramidal reactions.
Dosage and Administration
The dose of amantadine hydrochloride capsules may need reduction in patients with congestive heart failure, peripheral edema, orthostatic hypotension, or impaired renal function (see Dosage for Impaired Renal Function).
Contraindications
Amantadine hydrochloride is contraindicated in patients with known hypersensitivity to amantadine hydrochloride or to any of the other ingredients in Amantadine hydrochloride.
Adverse Reactions
The adverse reactions reported most frequently at the recommended dose of amantadine hydrochloride (5% to 10%) are: nausea, dizziness (lightheadedness), and insomnia.
Less frequently (1% to 5%) reported adverse reactions are: depression, anxiety and irritability, hallucinations, confusion, anorexia, dry mouth, constipation, ataxia, livedo reticularis, peripheral edema, orthostatic hypotension, headache, somnolence, nervousness, dream abnormality, agitation, dry nose, diarrhea and fatigue.
Infrequently (0.1% to 1%) occurring adverse reactions are: congestive heart failure, psychosis, urinary retention, dyspnea, skin rash, vomiting, weakness, slurred speech, euphoria, thinking abnormality, amnesia, hyperkinesia, hypertension, decreased libido, and visual disturbance, including punctate subepithelial or other corneal opacity, corneal edema, decreased visual acuity, sensitivity to light, and optic nerve palsy.
Rare (less than 0.1%) occurring adverse reactions are: instances of convulsion, leukopenia, neutropenia, eczematoid dermatitis, oculogyric episodes, suicidal attempt, suicide, and suicidal ideation (see WARNINGS).
Other adverse reactions reported during postmarketing experience with amantadine hydrochloride usage include:
Nervous System/Psychiatric –coma, stupor, delirium, hypokinesia, hypertonia, delusions, aggressive behavior, paranoid reaction, manic reaction, involuntary muscle contractions, gait abnormalities, paresthesia, EEG changes, and tremor. Abrupt discontinuation may also precipitate delirium, agitation, delusions, hallucinations, paranoid reaction, stupor, anxiety, depression and slurred speech;
Cardiovascular –cardiac arrest, arrhythmias including malignant arrhythmias, hypotension, and tachycardia;
Respiratory –acute respiratory failure, pulmonary edema, and tachypnea;
Gastrointestinal –dysphagia;
Hematologic –leukocytosis, agranulocytosis;
Special Senses –keratitis and mydriasis;
Skin and Appendages –pruritus and diaphoresis;
Miscellaneous -neuroleptic malignant syndrome (see WARNINGS), allergic reactions including anaphylactic reactions, edema and fever.
Laboratory Test –elevated: CPK, BUN, serum creatinine, alkaline phosphatase, LDH, bilirubin, GGT, SGOT, and SGPT.
How Supplied
Amantadine hydrochloride capsules, USP are available as yellow, soft gelatin capsules containing 100 mg of amantadine hydrochloride and imprinted C-122
| Bottles of 100 with child-resistant closure, | NDC 0832-1015-00 | |
| Bottles of 500, | NDC 0832-1015-50 |
Description
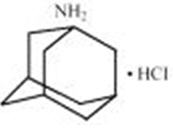
Amantadine hydrochloride, USP is designated chemically as 1 adamantanamine hydrochloride. Its molecular weight is 187.71 with a molecular formula C 10H 18NCl. It has the following structural formula.
|
|
C 10H 18NCl |
Amantadine hydrochloride, USP is a stable white or nearly white crystalline powder, freely soluble in water and soluble in alcohol and in chloroform.
Amantadine hydrochloride, USP has pharmacological actions as both an anti-Parkinson and an antiviral drug.
Each capsule intended for oral administration contains 100 mg amantadine hydrochloride and has the following inactive ingredients: D&C Yellow No. 10, gelatin, glycerin, hydrogenated vegetable oil, lecithin, simethicone, soybean oil, titanium dioxide and white wax. The black imprint ink ingredients are hypromellose, iron oxide black, propylene glycol and purified water.
Section 34073-7
Drug Interactions
Careful observation is required when amantadine hydrochloride is administered concurrently with central nervous system stimulants. Agents with anticholinergic properties may potentiate the anticholinergic-like side effects of amantadine.
Coadministration of thioridazine has been reported to worsen the tremor in elderly patients with Parkinson's disease, however, it is not known if other phenothiazines produce a similar response. Coadministration of triamterene and hydrochlorothiazide capsules resulted in a higher plasma amantadine concentration in a 61 year-old man receiving amantadine (hydrochloride capsules) 100 mg t.i.d. for Parkinson's disease. 1It is not known which of the components of triamterene and hydrochlorothiazide capsules contributed to the observation or if related drugs produce a similar response.
Coadministration of quinine or quinidine with amantadine was shown to reduce the renal clearance of amantadine by about 30%.
The concurrent use of amantadine hydrochloride with live attenuated influenza vaccine (LAIV) intranasal has not been evaluated. However, because of the potential for interference between these products, LAIV should not be administered within 2 weeks before or 48 hours after administration of amantadine hydrochloride, unless medically indicated. The concern about possible interference arises from the potential for antiviral drugs to inhibit replication of live vaccine virus. Trivalent inactivated influenza vaccine can be administered at any time relative to use of amantadine hydrochloride.
Section 34080-2
Nursing Mothers
Amantadine hydrochloride is excreted in human milk. Use is not recommended in nursing mothers.
Section 34081-0
Pediatric Use
The safety and efficacy of amantadine hydrochloride in newborn infants and infants below the age of 1 year have not been established.
Section 34082-8
Usage in the Elderly
Because amantadine hydrochloride is primarily excreted in the urine, it accumulates in the plasma and in the body when renal function declines. Thus, the dose of amantadine hydrochloride should be reduced in patients with renal impairment and in individuals who are 65 years of age or older. The dose of amantadine hydrochloride may need reduction in patients with congestive heart failure, peripheral edema, or orthostatic hypotension (see DOSAGE AND ADMINISTRATION).
Section 34083-6
Carcinogenesis and Mutagenesis
Long-term in vivoanimal studies designed to evaluate the carcinogenic potential of amantadine have not been performed. In several in vitroassays for gene mutation, amantadine hydrochloride did not increase the number of spontaneously observed mutations in four strains of Salmonella typhimurium(Ames Test) or in a mammalian cell line (Chinese Hamster Ovary cells) when incubations were performed either with or without a liver metabolic activation extract. Further, there was no evidence of chromosome damage observed in an in vitrotest using freshly derived and stimulated human peripheral blood lymphocytes (with and without metabolic activation) or in an in vivomouse bone marrow micronucleus test (140 to 550 mg/kg; estimated human equivalent doses of 11.7 to 45.8 mg/kg based on body surface area conversion).
Section 42228-7
Pregnancy
The effect of amantadine on embryofetal and peri-postnatal development has not been adequately tested, that is, in studies conducted under Good Laboratory Practice (GLP) and according to current recommended methodology. However, in two non-GLP studies in rats in which females were dosed from 5 days prior to mating to Day 6 of gestation or on Days 7 to 14 of gestation, amantadine hydrochloride produced increases in embryonic death at an oral dose of 100 mg/kg (or 3 times the maximum recommended human dose on a mg/m 2basis). In the non-GLP rat study in which females were dosed on Days 7 to 14 of gestation, there was a marked increase in severe visceral and skeletal malformations at oral doses of 50 and 100 mg/kg (or 1.5 and 3 times, respectively, the maximum recommended human dose on a mg/m 2basis). The no-effect dose for teratogenicity was 37 mg/kg (equal to the maximum recommended human dose on a mg/m 2basis). The safety margins reported may not accurately reflect the risk considering the questionable quality of the study on which they are based. There are no adequate and well-controlled studies in pregnant women. Human data regarding teratogenicity after maternal use of amantadine is scarce. Tetralogy of Fallot and tibial hemimelia (normal karyotype) occurred in an infant exposed to amantadine during the first trimester of pregnancy (100 mg P.O. for 7 days during the 6 thand 7 thweek of gestation). Cardiovascular maldevelopment (single ventricle with pulmonary atresia) was associated with maternal exposure to amantadine (100 mg/d) administered during the first 2 weeks of pregnancy.
Amantadine hydrochloride should be used during pregnancy only if the potential benefit justifies the potential risk to the embryo or fetus.
Section 42229-5
Rx only
Section 43679-0
Mechanism of Action
Section 44425-7
Store at 20° to 25°C (68° to 77°F); excursions permitted to 15° to 30°C (59° to 86°F) [See USP Controlled Room Temperature].
Pharmacist: Dispense in a tight, light-resistant container as defined in the USP with a child-resistant closure.
Keep out of reach of children.
Overdosage
Deaths have been reported from overdose with amantadine hydrochloride. The lowest reported acute lethal dose was 1 gram. Because some patients have attempted suicide by overdosing with amantadine, prescriptions should be written for the smallest quantity consistent with good patient management.
Acute toxicity may be attributable to the anticholinergic effects of amantadine. Drug overdose has resulted in cardiac, respiratory, renal or central nervous system toxicity. Cardiac dysfunction includes arrhythmia, tachycardia and hypertension. Pulmonary edema and respiratory distress (including adult respiratory distress syndrome – ARDS) have been reported; renal dysfunction including increased BUN, decreased creatinine clearance and renal insufficiency can occur. Central nervous system effects that have been reported include insomnia, anxiety, agitation, aggressive behavior, hypertonia, hyperkinesia, ataxia, gait abnormality, tremor, confusion, disorientation, depersonalization, fear, delirium, hallucinations, psychotic reactions, lethargy, somnolence and coma. Seizures may be exacerbated in patients with prior history of seizure disorders. Hyperthermia has also been observed in cases where a drug overdose has occurred.
There is no specific antidote for an overdose of amantadine hydrochloride. However, slowly administered intravenous physostigmine in 1 and 2 mg doses in an adult 2at 1- to 2-hour intervals and 0.5 mg doses in a child 3at 5- to 10-minute intervals up to a maximum of 2 mg/hour have been reported to be effective in the control of central nervous system toxicity caused by amantadine hydrochloride. For acute overdosing, general supportive measures should be employed along with immediate gastric lavage or induction of emesis. Fluids should be forced, and if necessary, given intravenously. The pH of the urine has been reported to influence the excretion rate of amantadine hydrochloride. Since the excretion rate of amantadine hydrochloride increases rapidly when the urine is acidic, the administration of urine acidifying drugs may increase the elimination of the drug from the body. The blood pressure, pulse, respiration and temperature should be monitored. The patient should be observed for hyperactivity and convulsions; if required, sedation, and anticonvulsant therapy should be administered. The patient should be observed for the possible development of arrhythmias and hypotension; if required, appropriate antiarrhythmic and antihypotensive therapy should be given. Electrocardiographic monitoring may be required after ingestion, since malignant tachyarrhythmias can appear after overdose.
Care should be exercised when administering adrenergic agents, such as isoproterenol, to patients with an amantadine hydrochloride overdose, since the dopaminergic activity of amantadine hydrochloride has been reported to induce malignant arrhythmias.
The blood electrolytes, urine pH and urinary output should be monitored. If there is no record of recent voiding, catheterization should be done.
References
1.W.W. Wilson and A.H. Rajput, Amantadine-Dyazide Interaction, Can. Med. Assoc. J.129:974-975, 1983.
2. D.F. Casey, N. Engl. J. Med.298:516, 1978.
3. C.D. Berkowitz, J. Pediatr. 95:144, 1979.
Manufactured for
UPSHER-SMITH LABORATORIES, LLC
Maple Grove, MN 55369
MADE IN CANADA
Revised 1019
Precautions
Amantadine hydrochloride should not be discontinued abruptly in patients with Parkinson's disease since a few patients have experienced a parkinsonian crisis, i.e., a sudden marked clinical deterioration, when this medication was suddenly stopped. The dose of anticholinergic drugs or of amantadine hydrochloride should be reduced if atropine-like effects appear when these drugs are used concurrently. Abrupt discontinuation may also precipitate delirium, agitation, delusions, hallucinations, paranoid reaction, stupor, anxiety, depression and slurred speech.
Pharmacokinetics
Amantadine hydrochloride is well absorbed orally. Maximum plasma concentrations are directly related to dose for doses up to 200 mg/day. Doses above 200 mg/day may result in a greater than proportional increase in maximum plasma concentrations. It is primarily excreted unchanged in the urine by glomerular filtration and tubular secretion. Eight metabolites of amantadine have been identified in human urine. One metabolite, an N-acetylated compound, was quantified in human urine and accounted for 5% to 15% of the administered dose. Plasma acetylamantadine accounted for up to 80% of the concurrent amantadine plasma concentration in 5 of 12 healthy volunteers following the ingestion of a 200 mg dose of amantadine. Acetylamantadine was not detected in the plasma of the remaining seven volunteers. The contribution of this metabolite to efficacy or toxicity is not known.
There appears to be a relationship between plasma amantadine concentrations and toxicity. As concentration increases, toxicity seems to be more prevalent, however, absolute values of amantadine concentrations associated with adverse effects have not been fully defined.
Amantadine pharmacokinetics were determined in 24 normal adult male volunteers after the oral administration of a single amantadine hydrochloride 100 mg soft gel capsule. The mean ± SD maximum plasma concentration was 0.22 ± 0.03 mcg/mL (range: 0.18 to 0.32 mcg/mL). The time to peak concentration was 3.3 ± 1.5 hours (range: 1.5 to 8 hours). The apparent oral clearance was 0.28 ± 0.11 L/hr/kg (range: 0.14 to 0.62 L/hr/kg). The half-life was 17 ± 4 hours (range: 10 to 25 hours). Across other studies, amantadine plasma half-life has averaged 16 ± 6 hours (range: 9 to 31 hours) in 19 healthy volunteers.
After oral administration of a single dose of 100 mg amantadine syrup to five healthy volunteers, the mean ± SD maximum plasma concentration C maxwas 0.24 ± 0.04 mcg/mL and ranged from 0.18 to 0.28 mcg/mL. After 15 days of amantadine 100 mg b.i.d., the C maxwas 0.47 ± 0.11 mcg/mL in four of the five volunteers. The administration of amantadine tablets as a 200 mg single dose to 6 healthy subjects resulted in a C maxof 0.51 ± 0.14 mcg/mL. Across studies, the time to C max(T max) averaged about 2 to 4 hours.
Plasma amantadine clearance ranged from 0.2 to 0.3 L/hr/kg after the administration of 5 mg to 25 mg intravenous doses of amantadine to 15 healthy volunteers.
In six healthy volunteers, the ratio of amantadine renal clearance to apparent oral plasma clearance was 0.79 ± 0.17 (mean ± SD).
The volume of distribution determined after the intravenous administration of amantadine to 15 healthy subjects was 3 to 8 L/kg, suggesting tissue binding. Amantadine, after single oral 200 mg doses to 6 healthy young subjects and to 6 healthy elderly subjects has been found in nasal mucus at mean ± SD concentrations of 0.15 ± 0.16, 0.28 ± 0.26, and 0.39 ± 0.34 mcg/g at 1, 4 and 8 hours after dosing, respectively. These concentrations represented 31 ± 33%, 59 ± 61% and 95 ± 86% of the corresponding plasma amantadine concentrations. Amantadine is approximately 67% bound to plasma proteins over a concentration range of 0.1 to 2 mcg/mL. Following the administration of amantadine 100 mg as a single dose, the mean ± SD red blood cell to plasma ratio ranged from 2.7 ± 0.5 in 6 healthy subjects to 1.4 ± 0.2 in 8 patients with renal insufficiency.
The apparent oral plasma clearance of amantadine is reduced and the plasma half-life and plasma concentrations are increased in healthy elderly individuals age 60 and older. After single dose administration of 25 to 75 mg to 7 healthy, elderly male volunteers, the apparent plasma clearance of amantadine was 0.10 ± 0.04 L/hr/kg (range 0.06 to 0.17 L/hr/kg) and the half-life was 29 ± 7 hours (range 20 to 41 hours). Whether these changes are due to decline in renal function or other age-related factors is not known.
In a study of young healthy subjects (n=20), mean renal clearance of amantadine, normalized for body mass index, was 1.5-fold higher in males compared to females (p<0.032).
Compared with otherwise healthy adult individuals, the clearance of amantadine is significantly reduced in adult patients with renal insufficiency. The elimination half-life increases two to three-fold or greater when creatinine clearance is less than 40 mL/min/1.73 m 2and averages eight days in patients on chronic maintenance hemodialysis. Amantadine is removed in negligible amounts by hemodialysis.
The pH of the urine has been reported to influence the excretion rate of amantadine hydrochloride. Since the excretion rate of amantadine hydrochloride increases rapidly when the urine is acidic, the administration of urine acidifying drugs may increase the elimination of the drug from the body.
Information for Patients:
Patients should be advised of the following information:
Blurry vision and/or impaired mental acuity may occur.
Gradually increase physical activity as the symptoms of Parkinson's disease improve.
Avoid excessive alcohol usage, since it may increase the potential for CNS effects such as dizziness, confusion, light-headedness and orthostatic hypotension.
Avoid getting up suddenly from a sitting or lying position. If dizziness or lightheadedness occurs, notify physician.
Notify physician if mood/mental changes, swelling of extremities, difficulty urinating and/or shortness of breath occur.
Do not take more medication than prescribed because of the risk of overdose. If there is no improvement in a few days, or if medication appears less effective after a few weeks, discuss with a physician.
Consult physician before discontinuing medication.
Seek medical attention immediately if it is suspected that an overdose of medication has been taken.
Dosage for Impaired Renal Function:
Depending upon creatinine clearance, the following dosage adjustments are recommended:
| CREATININE CLEARANCE
(mL/min/1.73 m 2) |
AMANTADINE HYDROCHLORIDE
CAPSULES DOSAGE |
|---|---|
| 30 to 50 | 200 mg 1 stday and 100 mg each day thereafter |
| 15 to 29 | 200 mg 1 stday followed by 100 mg on alternate days |
| <15 | 200 mg every 7 days |
The recommended dosage for patients on hemodialysis is 200 mg every 7 days.
Principal Display Panel 100 Mg Capsule Bottle Label
NDC 0832-1015-00
Amantadine
Hydrochloride
Capsules, USP
100 mg
100 Capsules
Rx only
UPSHER-SMITH
Structured Label Content
Section 34073-7 (34073-7)
Drug Interactions
Careful observation is required when amantadine hydrochloride is administered concurrently with central nervous system stimulants. Agents with anticholinergic properties may potentiate the anticholinergic-like side effects of amantadine.
Coadministration of thioridazine has been reported to worsen the tremor in elderly patients with Parkinson's disease, however, it is not known if other phenothiazines produce a similar response. Coadministration of triamterene and hydrochlorothiazide capsules resulted in a higher plasma amantadine concentration in a 61 year-old man receiving amantadine (hydrochloride capsules) 100 mg t.i.d. for Parkinson's disease. 1It is not known which of the components of triamterene and hydrochlorothiazide capsules contributed to the observation or if related drugs produce a similar response.
Coadministration of quinine or quinidine with amantadine was shown to reduce the renal clearance of amantadine by about 30%.
The concurrent use of amantadine hydrochloride with live attenuated influenza vaccine (LAIV) intranasal has not been evaluated. However, because of the potential for interference between these products, LAIV should not be administered within 2 weeks before or 48 hours after administration of amantadine hydrochloride, unless medically indicated. The concern about possible interference arises from the potential for antiviral drugs to inhibit replication of live vaccine virus. Trivalent inactivated influenza vaccine can be administered at any time relative to use of amantadine hydrochloride.
Section 34080-2 (34080-2)
Nursing Mothers
Amantadine hydrochloride is excreted in human milk. Use is not recommended in nursing mothers.
Section 34081-0 (34081-0)
Pediatric Use
The safety and efficacy of amantadine hydrochloride in newborn infants and infants below the age of 1 year have not been established.
Section 34082-8 (34082-8)
Usage in the Elderly
Because amantadine hydrochloride is primarily excreted in the urine, it accumulates in the plasma and in the body when renal function declines. Thus, the dose of amantadine hydrochloride should be reduced in patients with renal impairment and in individuals who are 65 years of age or older. The dose of amantadine hydrochloride may need reduction in patients with congestive heart failure, peripheral edema, or orthostatic hypotension (see DOSAGE AND ADMINISTRATION).
Section 34083-6 (34083-6)
Carcinogenesis and Mutagenesis
Long-term in vivoanimal studies designed to evaluate the carcinogenic potential of amantadine have not been performed. In several in vitroassays for gene mutation, amantadine hydrochloride did not increase the number of spontaneously observed mutations in four strains of Salmonella typhimurium(Ames Test) or in a mammalian cell line (Chinese Hamster Ovary cells) when incubations were performed either with or without a liver metabolic activation extract. Further, there was no evidence of chromosome damage observed in an in vitrotest using freshly derived and stimulated human peripheral blood lymphocytes (with and without metabolic activation) or in an in vivomouse bone marrow micronucleus test (140 to 550 mg/kg; estimated human equivalent doses of 11.7 to 45.8 mg/kg based on body surface area conversion).
Section 42228-7 (42228-7)
Pregnancy
The effect of amantadine on embryofetal and peri-postnatal development has not been adequately tested, that is, in studies conducted under Good Laboratory Practice (GLP) and according to current recommended methodology. However, in two non-GLP studies in rats in which females were dosed from 5 days prior to mating to Day 6 of gestation or on Days 7 to 14 of gestation, amantadine hydrochloride produced increases in embryonic death at an oral dose of 100 mg/kg (or 3 times the maximum recommended human dose on a mg/m 2basis). In the non-GLP rat study in which females were dosed on Days 7 to 14 of gestation, there was a marked increase in severe visceral and skeletal malformations at oral doses of 50 and 100 mg/kg (or 1.5 and 3 times, respectively, the maximum recommended human dose on a mg/m 2basis). The no-effect dose for teratogenicity was 37 mg/kg (equal to the maximum recommended human dose on a mg/m 2basis). The safety margins reported may not accurately reflect the risk considering the questionable quality of the study on which they are based. There are no adequate and well-controlled studies in pregnant women. Human data regarding teratogenicity after maternal use of amantadine is scarce. Tetralogy of Fallot and tibial hemimelia (normal karyotype) occurred in an infant exposed to amantadine during the first trimester of pregnancy (100 mg P.O. for 7 days during the 6 thand 7 thweek of gestation). Cardiovascular maldevelopment (single ventricle with pulmonary atresia) was associated with maternal exposure to amantadine (100 mg/d) administered during the first 2 weeks of pregnancy.
Amantadine hydrochloride should be used during pregnancy only if the potential benefit justifies the potential risk to the embryo or fetus.
Section 42229-5 (42229-5)
Rx only
Section 43679-0 (43679-0)
Mechanism of Action
Section 44425-7 (44425-7)
Store at 20° to 25°C (68° to 77°F); excursions permitted to 15° to 30°C (59° to 86°F) [See USP Controlled Room Temperature].
Pharmacist: Dispense in a tight, light-resistant container as defined in the USP with a child-resistant closure.
Keep out of reach of children.
Overdosage (OVERDOSAGE)
Deaths have been reported from overdose with amantadine hydrochloride. The lowest reported acute lethal dose was 1 gram. Because some patients have attempted suicide by overdosing with amantadine, prescriptions should be written for the smallest quantity consistent with good patient management.
Acute toxicity may be attributable to the anticholinergic effects of amantadine. Drug overdose has resulted in cardiac, respiratory, renal or central nervous system toxicity. Cardiac dysfunction includes arrhythmia, tachycardia and hypertension. Pulmonary edema and respiratory distress (including adult respiratory distress syndrome – ARDS) have been reported; renal dysfunction including increased BUN, decreased creatinine clearance and renal insufficiency can occur. Central nervous system effects that have been reported include insomnia, anxiety, agitation, aggressive behavior, hypertonia, hyperkinesia, ataxia, gait abnormality, tremor, confusion, disorientation, depersonalization, fear, delirium, hallucinations, psychotic reactions, lethargy, somnolence and coma. Seizures may be exacerbated in patients with prior history of seizure disorders. Hyperthermia has also been observed in cases where a drug overdose has occurred.
There is no specific antidote for an overdose of amantadine hydrochloride. However, slowly administered intravenous physostigmine in 1 and 2 mg doses in an adult 2at 1- to 2-hour intervals and 0.5 mg doses in a child 3at 5- to 10-minute intervals up to a maximum of 2 mg/hour have been reported to be effective in the control of central nervous system toxicity caused by amantadine hydrochloride. For acute overdosing, general supportive measures should be employed along with immediate gastric lavage or induction of emesis. Fluids should be forced, and if necessary, given intravenously. The pH of the urine has been reported to influence the excretion rate of amantadine hydrochloride. Since the excretion rate of amantadine hydrochloride increases rapidly when the urine is acidic, the administration of urine acidifying drugs may increase the elimination of the drug from the body. The blood pressure, pulse, respiration and temperature should be monitored. The patient should be observed for hyperactivity and convulsions; if required, sedation, and anticonvulsant therapy should be administered. The patient should be observed for the possible development of arrhythmias and hypotension; if required, appropriate antiarrhythmic and antihypotensive therapy should be given. Electrocardiographic monitoring may be required after ingestion, since malignant tachyarrhythmias can appear after overdose.
Care should be exercised when administering adrenergic agents, such as isoproterenol, to patients with an amantadine hydrochloride overdose, since the dopaminergic activity of amantadine hydrochloride has been reported to induce malignant arrhythmias.
The blood electrolytes, urine pH and urinary output should be monitored. If there is no record of recent voiding, catheterization should be done.
References (REFERENCES)
1.W.W. Wilson and A.H. Rajput, Amantadine-Dyazide Interaction, Can. Med. Assoc. J.129:974-975, 1983.
2. D.F. Casey, N. Engl. J. Med.298:516, 1978.
3. C.D. Berkowitz, J. Pediatr. 95:144, 1979.
Manufactured for
UPSHER-SMITH LABORATORIES, LLC
Maple Grove, MN 55369
MADE IN CANADA
Revised 1019
Description (DESCRIPTION)
Amantadine hydrochloride, USP is designated chemically as 1 adamantanamine hydrochloride. Its molecular weight is 187.71 with a molecular formula C 10H 18NCl. It has the following structural formula.
|
|
C 10H 18NCl |
Amantadine hydrochloride, USP is a stable white or nearly white crystalline powder, freely soluble in water and soluble in alcohol and in chloroform.
Amantadine hydrochloride, USP has pharmacological actions as both an anti-Parkinson and an antiviral drug.
Each capsule intended for oral administration contains 100 mg amantadine hydrochloride and has the following inactive ingredients: D&C Yellow No. 10, gelatin, glycerin, hydrogenated vegetable oil, lecithin, simethicone, soybean oil, titanium dioxide and white wax. The black imprint ink ingredients are hypromellose, iron oxide black, propylene glycol and purified water.
Precautions (PRECAUTIONS)
Amantadine hydrochloride should not be discontinued abruptly in patients with Parkinson's disease since a few patients have experienced a parkinsonian crisis, i.e., a sudden marked clinical deterioration, when this medication was suddenly stopped. The dose of anticholinergic drugs or of amantadine hydrochloride should be reduced if atropine-like effects appear when these drugs are used concurrently. Abrupt discontinuation may also precipitate delirium, agitation, delusions, hallucinations, paranoid reaction, stupor, anxiety, depression and slurred speech.
How Supplied (HOW SUPPLIED)
Amantadine hydrochloride capsules, USP are available as yellow, soft gelatin capsules containing 100 mg of amantadine hydrochloride and imprinted C-122
| Bottles of 100 with child-resistant closure, | NDC 0832-1015-00 | |
| Bottles of 500, | NDC 0832-1015-50 |
Pharmacokinetics
Amantadine hydrochloride is well absorbed orally. Maximum plasma concentrations are directly related to dose for doses up to 200 mg/day. Doses above 200 mg/day may result in a greater than proportional increase in maximum plasma concentrations. It is primarily excreted unchanged in the urine by glomerular filtration and tubular secretion. Eight metabolites of amantadine have been identified in human urine. One metabolite, an N-acetylated compound, was quantified in human urine and accounted for 5% to 15% of the administered dose. Plasma acetylamantadine accounted for up to 80% of the concurrent amantadine plasma concentration in 5 of 12 healthy volunteers following the ingestion of a 200 mg dose of amantadine. Acetylamantadine was not detected in the plasma of the remaining seven volunteers. The contribution of this metabolite to efficacy or toxicity is not known.
There appears to be a relationship between plasma amantadine concentrations and toxicity. As concentration increases, toxicity seems to be more prevalent, however, absolute values of amantadine concentrations associated with adverse effects have not been fully defined.
Amantadine pharmacokinetics were determined in 24 normal adult male volunteers after the oral administration of a single amantadine hydrochloride 100 mg soft gel capsule. The mean ± SD maximum plasma concentration was 0.22 ± 0.03 mcg/mL (range: 0.18 to 0.32 mcg/mL). The time to peak concentration was 3.3 ± 1.5 hours (range: 1.5 to 8 hours). The apparent oral clearance was 0.28 ± 0.11 L/hr/kg (range: 0.14 to 0.62 L/hr/kg). The half-life was 17 ± 4 hours (range: 10 to 25 hours). Across other studies, amantadine plasma half-life has averaged 16 ± 6 hours (range: 9 to 31 hours) in 19 healthy volunteers.
After oral administration of a single dose of 100 mg amantadine syrup to five healthy volunteers, the mean ± SD maximum plasma concentration C maxwas 0.24 ± 0.04 mcg/mL and ranged from 0.18 to 0.28 mcg/mL. After 15 days of amantadine 100 mg b.i.d., the C maxwas 0.47 ± 0.11 mcg/mL in four of the five volunteers. The administration of amantadine tablets as a 200 mg single dose to 6 healthy subjects resulted in a C maxof 0.51 ± 0.14 mcg/mL. Across studies, the time to C max(T max) averaged about 2 to 4 hours.
Plasma amantadine clearance ranged from 0.2 to 0.3 L/hr/kg after the administration of 5 mg to 25 mg intravenous doses of amantadine to 15 healthy volunteers.
In six healthy volunteers, the ratio of amantadine renal clearance to apparent oral plasma clearance was 0.79 ± 0.17 (mean ± SD).
The volume of distribution determined after the intravenous administration of amantadine to 15 healthy subjects was 3 to 8 L/kg, suggesting tissue binding. Amantadine, after single oral 200 mg doses to 6 healthy young subjects and to 6 healthy elderly subjects has been found in nasal mucus at mean ± SD concentrations of 0.15 ± 0.16, 0.28 ± 0.26, and 0.39 ± 0.34 mcg/g at 1, 4 and 8 hours after dosing, respectively. These concentrations represented 31 ± 33%, 59 ± 61% and 95 ± 86% of the corresponding plasma amantadine concentrations. Amantadine is approximately 67% bound to plasma proteins over a concentration range of 0.1 to 2 mcg/mL. Following the administration of amantadine 100 mg as a single dose, the mean ± SD red blood cell to plasma ratio ranged from 2.7 ± 0.5 in 6 healthy subjects to 1.4 ± 0.2 in 8 patients with renal insufficiency.
The apparent oral plasma clearance of amantadine is reduced and the plasma half-life and plasma concentrations are increased in healthy elderly individuals age 60 and older. After single dose administration of 25 to 75 mg to 7 healthy, elderly male volunteers, the apparent plasma clearance of amantadine was 0.10 ± 0.04 L/hr/kg (range 0.06 to 0.17 L/hr/kg) and the half-life was 29 ± 7 hours (range 20 to 41 hours). Whether these changes are due to decline in renal function or other age-related factors is not known.
In a study of young healthy subjects (n=20), mean renal clearance of amantadine, normalized for body mass index, was 1.5-fold higher in males compared to females (p<0.032).
Compared with otherwise healthy adult individuals, the clearance of amantadine is significantly reduced in adult patients with renal insufficiency. The elimination half-life increases two to three-fold or greater when creatinine clearance is less than 40 mL/min/1.73 m 2and averages eight days in patients on chronic maintenance hemodialysis. Amantadine is removed in negligible amounts by hemodialysis.
The pH of the urine has been reported to influence the excretion rate of amantadine hydrochloride. Since the excretion rate of amantadine hydrochloride increases rapidly when the urine is acidic, the administration of urine acidifying drugs may increase the elimination of the drug from the body.
Adverse Reactions (ADVERSE REACTIONS)
The adverse reactions reported most frequently at the recommended dose of amantadine hydrochloride (5% to 10%) are: nausea, dizziness (lightheadedness), and insomnia.
Less frequently (1% to 5%) reported adverse reactions are: depression, anxiety and irritability, hallucinations, confusion, anorexia, dry mouth, constipation, ataxia, livedo reticularis, peripheral edema, orthostatic hypotension, headache, somnolence, nervousness, dream abnormality, agitation, dry nose, diarrhea and fatigue.
Infrequently (0.1% to 1%) occurring adverse reactions are: congestive heart failure, psychosis, urinary retention, dyspnea, skin rash, vomiting, weakness, slurred speech, euphoria, thinking abnormality, amnesia, hyperkinesia, hypertension, decreased libido, and visual disturbance, including punctate subepithelial or other corneal opacity, corneal edema, decreased visual acuity, sensitivity to light, and optic nerve palsy.
Rare (less than 0.1%) occurring adverse reactions are: instances of convulsion, leukopenia, neutropenia, eczematoid dermatitis, oculogyric episodes, suicidal attempt, suicide, and suicidal ideation (see WARNINGS).
Other adverse reactions reported during postmarketing experience with amantadine hydrochloride usage include:
Nervous System/Psychiatric –coma, stupor, delirium, hypokinesia, hypertonia, delusions, aggressive behavior, paranoid reaction, manic reaction, involuntary muscle contractions, gait abnormalities, paresthesia, EEG changes, and tremor. Abrupt discontinuation may also precipitate delirium, agitation, delusions, hallucinations, paranoid reaction, stupor, anxiety, depression and slurred speech;
Cardiovascular –cardiac arrest, arrhythmias including malignant arrhythmias, hypotension, and tachycardia;
Respiratory –acute respiratory failure, pulmonary edema, and tachypnea;
Gastrointestinal –dysphagia;
Hematologic –leukocytosis, agranulocytosis;
Special Senses –keratitis and mydriasis;
Skin and Appendages –pruritus and diaphoresis;
Miscellaneous -neuroleptic malignant syndrome (see WARNINGS), allergic reactions including anaphylactic reactions, edema and fever.
Laboratory Test –elevated: CPK, BUN, serum creatinine, alkaline phosphatase, LDH, bilirubin, GGT, SGOT, and SGPT.
Contraindications (CONTRAINDICATIONS)
Amantadine hydrochloride is contraindicated in patients with known hypersensitivity to amantadine hydrochloride or to any of the other ingredients in Amantadine hydrochloride.
Indications and Usage (INDICATIONS AND USAGE)
Amantadine hydrochloride capsules are indicated for the prophylaxis and treatment of signs and symptoms of infection caused by various strains of influenza A virus. Amantadine hydrochloride capsules are also indicated in the treatment of parkinsonism and drug-induced extrapyramidal reactions.
Dosage and Administration (DOSAGE AND ADMINISTRATION)
The dose of amantadine hydrochloride capsules may need reduction in patients with congestive heart failure, peripheral edema, orthostatic hypotension, or impaired renal function (see Dosage for Impaired Renal Function).
Information for Patients:
Patients should be advised of the following information:
Blurry vision and/or impaired mental acuity may occur.
Gradually increase physical activity as the symptoms of Parkinson's disease improve.
Avoid excessive alcohol usage, since it may increase the potential for CNS effects such as dizziness, confusion, light-headedness and orthostatic hypotension.
Avoid getting up suddenly from a sitting or lying position. If dizziness or lightheadedness occurs, notify physician.
Notify physician if mood/mental changes, swelling of extremities, difficulty urinating and/or shortness of breath occur.
Do not take more medication than prescribed because of the risk of overdose. If there is no improvement in a few days, or if medication appears less effective after a few weeks, discuss with a physician.
Consult physician before discontinuing medication.
Seek medical attention immediately if it is suspected that an overdose of medication has been taken.
Dosage for Impaired Renal Function:
Depending upon creatinine clearance, the following dosage adjustments are recommended:
| CREATININE CLEARANCE
(mL/min/1.73 m 2) |
AMANTADINE HYDROCHLORIDE
CAPSULES DOSAGE |
|---|---|
| 30 to 50 | 200 mg 1 stday and 100 mg each day thereafter |
| 15 to 29 | 200 mg 1 stday followed by 100 mg on alternate days |
| <15 | 200 mg every 7 days |
The recommended dosage for patients on hemodialysis is 200 mg every 7 days.
Principal Display Panel 100 Mg Capsule Bottle Label (PRINCIPAL DISPLAY PANEL - 100 mg Capsule Bottle Label)
NDC 0832-1015-00
Amantadine
Hydrochloride
Capsules, USP
100 mg
100 Capsules
Rx only
UPSHER-SMITH
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:48:08.318148 · Updated: 2026-03-14T22:29:06.951873