These Highlights Do Not Include All The Information Needed To Use Paroxetine Extended-release Tablets, Usp Safely And Effectively. See Full Prescribing Information For Paroxetine Extended-release Tablets, Usp.
51189cf4-4122-48d4-b47f-4f98a8dfb8e0
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
Antidepressants increased the risk of suicidal thoughts and behaviors in pediatric and young adult patients in short-term studies. Closely monitor all antidepressant-treated patients for clinical worsening, and for emergence of suicidal thoughts and behaviors [see Warnings and Precautions (5.1) ] . Paroxetine Extended-Release Tablets are not approved for use in pediatric patients [see Use in Specific Populations (8.4) ] .
Indications and Usage
Paroxetine Extended-Release Tablets, USP are indicated in adults for the treatment of: Major depressive disorder (MDD) Panic disorder (PD) Social anxiety disorder (SAD) Premenstrual dysphoric disorder (PMDD)
Dosage and Administration
Swallow tablet whole; do not chew or crush. ( 2.1 ) Recommended starting and maximum daily dosage: ( 2.2 , 2.3 ) Indication Starting Dose Maximum Dose MDD 25 mg/day 62.5 mg/day PD 12.5 mg/day 75 mg/day SAD 12.5 mg/day 37.5 mg/day PMDD 12.5 mg/day 25 mg/day For PMDD, dose continuously or intermittently (luteal phase only). ( 2.3 ) If inadequate response to starting dosage, titrate in 12.5 mg per day increments once weekly. ( 2.2 , 2.3 ) Elderly patients, patients with severe renal impairment, or severe hepatic impairment: Starting dose is 12.5 mg per day. Do not exceed 50 mg per day for treatment of MDD and PD and 37.5 mg per day for treatment of SAD. ( 2.5 ) When discontinuing Paroxetine Extended-Release Tablets, reduce dose gradually. ( 2.7 )
Warnings and Precautions
Serotonin Syndrome: Increased risk when co-administered with other serotonergic agents, but also when taken alone. If serotonin syndrome occurs, discontinue Paroxetine Extended-Release Tablets and serotonergic agents and initiate supportive measures. ( 5.2 ) Embryofetal Toxicity: May cause fetal harm. Meta-analysis of epidemiological studies has shown increased risk (less than 2-fold) of cardiovascular malformations with exposure during the first trimester. ( 5.4 , 8.1 ) Increased Risk of Bleeding : Concomitant use of aspirin, nonsteroidal anti-inflammatory drugs, other antiplatelet drugs, warfarin, and other anticoagulant drugs may increase risk. ( 5.5 ) Activation of Mania/Hypomania : Screen patients for bipolar disorder. ( 5.6 ) Seizures : Use with caution in patients with seizure disorders. ( 5.8 ) Angle-Closure Glaucoma : Angle-closure glaucoma has occurred in patients with untreated anatomically narrow angles treated with antidepressants. ( 5.9 ) Sexual Dysfunction : Paroxetine Extended-Release Tablets may cause symptoms of sexual dysfunction. ( 5.13 )
Contraindications
Paroxetine Extended-Release Tablets are contraindicated in patients: Taking, or within 14 days of stopping, MAOIs (including the MAOIs linezolid and intravenous methylene blue) because of an increased risk of serotonin syndrome [see Warnings and Precautions (5.2) , Drug Interactions (7) ]. Taking thioridazine because of risk of QT prolongation [see Warnings and Precautions (5.3) , Drug Interactions (7) ] . Taking pimozide because of risk of QT prolongation [see Warnings and Precautions (5.3) , Drug Interactions (7) ] . With known hypersensitivity (e.g., anaphylaxis, angioedema, Stevens-Johnson syndrome) to paroxetine or to any of the inactive ingredients in Paroxetine Extended-Release Tablets [see Adverse Reactions (6.1 , 6.2) ] .
Adverse Reactions
The following adverse reactions are included in more detail in other sections of the prescribing information: Hypersensitivity reactions to paroxetine [see Contraindications (4) ] Suicidal Thoughts and Behaviors [see Warnings and Precautions (5.1) ] Serotonin Syndrome [see Warnings and Precautions (5.2) ] Embryofetal Toxicity [see Warnings and Precautions (5.4) ] Increased Risk of Bleeding [see Warnings and Precautions (5.5) ] Activation of Mania/Hypomania [see Warnings and Precautions (5.6) ] Discontinuation Syndrome [see Warnings and Precautions (5.7) ] Seizures [see Warnings and Precautions (5.8) ] Angle-closure Glaucoma [see Warnings and Precautions (5.9) ] Hyponatremia [see Warnings and Precautions (5.10) ] Bone Fracture [see Warnings and Precautions (5.12) ] Sexual Dysfunction [see Warnings and Precautions (5.13) ]
Drug Interactions
Drugs Highly Bound to Plasma Protein : Monitor for adverse reactions and reduce dosage of Paroxetine Extended-Release Tablets or other protein-bound drugs (e.g., warfarin) as warranted. ( 7 ) Drugs Metabolized by CYP2D6 : Reduce dosage of drugs metabolized by CYP2D6 as warranted. ( 7 ) Concomitant use with Tamoxifen : Consider use of an alternative antidepressant with little or no CYP2D6 inhibition. ( 5.11 , 7 )
Storage and Handling
Paroxetine Extended-Release Tablets, USP are supplied as: a round, extended-release tablet as follows: 25 mg Brown enteric coated, round, bi-convex tablets, with one side debossed 2272 and the other side blank: NDC 63629-9499-01 Bottles of 30 Store at 20°C to 25°C (68°F to 77°F) [see USP Controlled Room Temperature]. Repackaged/Relabeled by: Bryant Ranch Prepack, Inc. Burbank, CA 91504
How Supplied
Paroxetine Extended-Release Tablets, USP are supplied as: a round, extended-release tablet as follows: 25 mg Brown enteric coated, round, bi-convex tablets, with one side debossed 2272 and the other side blank: NDC 63629-9499-01 Bottles of 30 Store at 20°C to 25°C (68°F to 77°F) [see USP Controlled Room Temperature]. Repackaged/Relabeled by: Bryant Ranch Prepack, Inc. Burbank, CA 91504
Medication Information
Warnings and Precautions
Serotonin Syndrome: Increased risk when co-administered with other serotonergic agents, but also when taken alone. If serotonin syndrome occurs, discontinue Paroxetine Extended-Release Tablets and serotonergic agents and initiate supportive measures. ( 5.2 ) Embryofetal Toxicity: May cause fetal harm. Meta-analysis of epidemiological studies has shown increased risk (less than 2-fold) of cardiovascular malformations with exposure during the first trimester. ( 5.4 , 8.1 ) Increased Risk of Bleeding : Concomitant use of aspirin, nonsteroidal anti-inflammatory drugs, other antiplatelet drugs, warfarin, and other anticoagulant drugs may increase risk. ( 5.5 ) Activation of Mania/Hypomania : Screen patients for bipolar disorder. ( 5.6 ) Seizures : Use with caution in patients with seizure disorders. ( 5.8 ) Angle-Closure Glaucoma : Angle-closure glaucoma has occurred in patients with untreated anatomically narrow angles treated with antidepressants. ( 5.9 ) Sexual Dysfunction : Paroxetine Extended-Release Tablets may cause symptoms of sexual dysfunction. ( 5.13 )
Indications and Usage
Paroxetine Extended-Release Tablets, USP are indicated in adults for the treatment of: Major depressive disorder (MDD) Panic disorder (PD) Social anxiety disorder (SAD) Premenstrual dysphoric disorder (PMDD)
Dosage and Administration
Swallow tablet whole; do not chew or crush. ( 2.1 ) Recommended starting and maximum daily dosage: ( 2.2 , 2.3 ) Indication Starting Dose Maximum Dose MDD 25 mg/day 62.5 mg/day PD 12.5 mg/day 75 mg/day SAD 12.5 mg/day 37.5 mg/day PMDD 12.5 mg/day 25 mg/day For PMDD, dose continuously or intermittently (luteal phase only). ( 2.3 ) If inadequate response to starting dosage, titrate in 12.5 mg per day increments once weekly. ( 2.2 , 2.3 ) Elderly patients, patients with severe renal impairment, or severe hepatic impairment: Starting dose is 12.5 mg per day. Do not exceed 50 mg per day for treatment of MDD and PD and 37.5 mg per day for treatment of SAD. ( 2.5 ) When discontinuing Paroxetine Extended-Release Tablets, reduce dose gradually. ( 2.7 )
Contraindications
Paroxetine Extended-Release Tablets are contraindicated in patients: Taking, or within 14 days of stopping, MAOIs (including the MAOIs linezolid and intravenous methylene blue) because of an increased risk of serotonin syndrome [see Warnings and Precautions (5.2) , Drug Interactions (7) ]. Taking thioridazine because of risk of QT prolongation [see Warnings and Precautions (5.3) , Drug Interactions (7) ] . Taking pimozide because of risk of QT prolongation [see Warnings and Precautions (5.3) , Drug Interactions (7) ] . With known hypersensitivity (e.g., anaphylaxis, angioedema, Stevens-Johnson syndrome) to paroxetine or to any of the inactive ingredients in Paroxetine Extended-Release Tablets [see Adverse Reactions (6.1 , 6.2) ] .
Adverse Reactions
The following adverse reactions are included in more detail in other sections of the prescribing information: Hypersensitivity reactions to paroxetine [see Contraindications (4) ] Suicidal Thoughts and Behaviors [see Warnings and Precautions (5.1) ] Serotonin Syndrome [see Warnings and Precautions (5.2) ] Embryofetal Toxicity [see Warnings and Precautions (5.4) ] Increased Risk of Bleeding [see Warnings and Precautions (5.5) ] Activation of Mania/Hypomania [see Warnings and Precautions (5.6) ] Discontinuation Syndrome [see Warnings and Precautions (5.7) ] Seizures [see Warnings and Precautions (5.8) ] Angle-closure Glaucoma [see Warnings and Precautions (5.9) ] Hyponatremia [see Warnings and Precautions (5.10) ] Bone Fracture [see Warnings and Precautions (5.12) ] Sexual Dysfunction [see Warnings and Precautions (5.13) ]
Drug Interactions
Drugs Highly Bound to Plasma Protein : Monitor for adverse reactions and reduce dosage of Paroxetine Extended-Release Tablets or other protein-bound drugs (e.g., warfarin) as warranted. ( 7 ) Drugs Metabolized by CYP2D6 : Reduce dosage of drugs metabolized by CYP2D6 as warranted. ( 7 ) Concomitant use with Tamoxifen : Consider use of an alternative antidepressant with little or no CYP2D6 inhibition. ( 5.11 , 7 )
Storage and Handling
Paroxetine Extended-Release Tablets, USP are supplied as: a round, extended-release tablet as follows: 25 mg Brown enteric coated, round, bi-convex tablets, with one side debossed 2272 and the other side blank: NDC 63629-9499-01 Bottles of 30 Store at 20°C to 25°C (68°F to 77°F) [see USP Controlled Room Temperature]. Repackaged/Relabeled by: Bryant Ranch Prepack, Inc. Burbank, CA 91504
How Supplied
Paroxetine Extended-Release Tablets, USP are supplied as: a round, extended-release tablet as follows: 25 mg Brown enteric coated, round, bi-convex tablets, with one side debossed 2272 and the other side blank: NDC 63629-9499-01 Bottles of 30 Store at 20°C to 25°C (68°F to 77°F) [see USP Controlled Room Temperature]. Repackaged/Relabeled by: Bryant Ranch Prepack, Inc. Burbank, CA 91504
Description
Antidepressants increased the risk of suicidal thoughts and behaviors in pediatric and young adult patients in short-term studies. Closely monitor all antidepressant-treated patients for clinical worsening, and for emergence of suicidal thoughts and behaviors [see Warnings and Precautions (5.1) ] . Paroxetine Extended-Release Tablets are not approved for use in pediatric patients [see Use in Specific Populations (8.4) ] .
Section 42229-5
Adverse Reactions Leading to Discontinuation in Patients with MDD, PD, SAD, and PMDD
In pooled studies in patients with MDD, PD and SAD, the most common adverse reactions leading to study withdrawal were: nausea (up to 4% of patients), asthenia, headache, depression, insomnia, and abnormal liver function tests (each occurring in up to 2% of patients), and dizziness, somnolence, and diarrhea (each occurring in up to 1% of patients).
In pooled studies for PMDD, the most common adverse reactions leading to study withdrawal were: nausea (occurring in up to 6% of patients), asthenia (occurring in up to 5% of patients), somnolence (occurring in up to 4% of patients), insomnia (occurring in approximately 2% of patients); and impaired concentration, dry mouth, dizziness, decreased appetite, sweating, tremor, yawn, and diarrhea (occurring in less than or equal to 2% of patients).
Section 42231-1
| Medication Guide Paroxetine (par ox' e teen) Extended-Release Tablets, USP |
|||
|---|---|---|---|
| This Medication Guide has been approved by the U.S. Food and Drug Administration. | Revised: 4/2024 | ||
|
What is the most important information I should know about Paroxetine Extended-Release Tablets? Paroxetine Extended-Release Tablets can cause serious side effects, including:
|
|||
|
|
||
|
What are Paroxetine Extended-Release Tablets?
Paroxetine Extended-Release Tablets are a prescription medicine used in adults to treat:
|
|||
Do not take Paroxetine Extended-Release Tablets if you:
Do not start taking an MAOI for at least 14 days after you stop treatment with Paroxetine Extended-Release Tablets. |
|||
Before taking Paroxetine Extended-Release Tablets, tell your healthcare provider about all your medical conditions, including if you:
Paroxetine Extended-Release Tablets and some other medicines may affect each other causing possible serious side effects. Paroxetine Extended-Release Tablets may affect the way other medicines work and other medicines may affect the way Paroxetine Extended-Release Tablets work. Especially tell your healthcare provider if you take:
Do not start or stop any other medicines during treatment with Paroxetine Extended-Release Tablets without talking to your healthcare provider first. Stopping Paroxetine Extended-Release Tablets suddenly may cause you to have serious side effects. See, "What are the possible side effects of Paroxetine Extended-Release Tablets?" Know the medicines you take. Keep a list of them to show to your healthcare provider and pharmacist when you get a new medicine. |
|||
How should I take Paroxetine Extended-Release Tablets?
|
|||
|
What are possible side effects of Paroxetine Extended-Release Tablets? Paroxetine Extended-Release Tablets can cause serious side effects, including:
|
|||
|
|
||
|
|||
|
|
||
|
|||
|
|
|
|
The most common side effects Paroxetine Extended-Release Tablets include: |
|||
|
|
||
| These are not all the possible side effects of Paroxetine Extended-Release Tablets. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. |
|||
| How should I store Paroxetine Extended-Release Tablets? | |||
|
|||
| Keep Paroxetine Extended-Release Tablets and all medicines out of the reach of children. | |||
|
General information about the safe and effective use of Paroxetine Extended-Release Tablets.
Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not take Paroxetine Extended-Release Tablets for a condition for which it was not prescribed. Do not give Paroxetine Extended-Release Tablets to other people, even if they have the same symptoms that you have. It may harm them. You may ask your healthcare provider or pharmacist for information about Paroxetine Extended-Release Tablets that is written for healthcare professionals. |
|||
|
What are the ingredients in Paroxetine Extended-Release Tablets?
Active ingredient: paroxetine hydrochloride Inactive ingredients: carboxymethylcellulose sodium, copovidone, glyceryl monostearate, hypromellose, lactose monohydrate, magnesium stearate, methacrylic acid – ethyl acrylate copolymer (1:1), polysorbate 80, silicon dioxide, sodium lauryl sulfate, talcum, titanium dioxide, and triethyl citrate. In addition, the 25 mg tablets also contain the following coloring agents: iron oxide black and iron oxide red and the 37.5 mg tablets contain iron oxide red and iron oxide yellow. |
|||
| Manufactured by: Beijing Sciecure Pharmaceutical Co., Ltd. Shunyi District, Beijing 101301, China Manufactured for: Sciecure Pharma Inc. Monmouth Junction, NJ 08852 USA Marketed by: Rhodes Pharmaceuticals Wilson, NC 27893 USA For more information about Paroxetine Extended-Release Tablets, call Rhodes Pharmaceuticals at 1-888-827-0616. |
Section 51945-4
Paroxetine Extended-ReleaseTablets 25 mg
5.8 Seizures
Paroxetine Extended-Release Tablets have not been systematically evaluated in patients with seizure disorders. Patients with history of seizures were excluded from clinical studies. Paroxetine Extended-Release Tablets should be prescribed with caution in patients with a seizure disorder and should be discontinued in any patient who develops seizures.
10 Overdosage
The following have been reported with paroxetine tablet overdosage:
- Seizures, which may be delayed, and altered mental status including coma.
- Cardiovascular toxicity, which may be delayed, including QRS and QTc interval prolongation. Hypertension most commonly seen, but rarely can see hypotension alone or with co-ingestants including alcohol.
- Serotonin syndrome (patients with a multiple drug overdosage with other proserotonergic drugs may have a higher risk).
Gastrointestinal decontamination with activated charcoal should be considered in patients who present early after a paroxetine overdose.
Consider contacting a Poison Center (1-800-222-1222) or a medical toxicologist for additional overdosage management recommendations.
11 Description
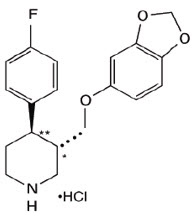
Paroxetine Extended-Release Tablets, USP contain paroxetine hydrochloride, an SSRI. It is the hydrochloride salt of a phenylpiperidine compound identified chemically as (-)-trans-4R-(4'-fluorophenyl)-3S-[(3',4'-methylenedioxyphenoxy) methyl] piperidine hydrochloride hemihydrate and has the empirical formula of C19H20FNO3∙HCl∙1/2H2O. The molecular weight is 374.8 g/mol (329.4 g/mol as free base). The structural formula of paroxetine hydrochloride is:
Paroxetine hydrochloride is an odorless, off-white powder, having a melting point range of 120°C to 138°C and a solubility of 5.4 mg/mL in water.
Each enteric coated, extended-release tablet contains paroxetine base of 12.5 mg (white tablet), 25 mg (brown tablet), 37.5 mg (orange tablet), which is equivalent to 14.25 mg, 28.51 mg, or 42.76 mg of paroxetine hydrochloride, respectively. Each tablet consists of a hydrophilic matrix that contains the active material.
Inactive ingredients consist of carboxymethylcellulose sodium, copovidone, glyceryl monostearate, hypromellose, lactose monohydrate, magnesium stearate, methacrylic acid – ethyl acrylate copolymer (1:1), polysorbate 80, silicon dioxide, sodium lauryl sulfate, talcum, titanium dioxide, and triethyl citrate. In addition, the 25 mg tablets also contain the following coloring agents: iron oxide black and iron oxide red and the 37.5 mg tablets contain iron oxide red and iron oxide yellow.
USP dissolution test is pending.
5.10 Hyponatremia
Hyponatremia may occur as a result of treatment with SNRIs and SSRIs, including Paroxetine Extended-Release Tablets. Cases with serum sodium lower than 110 mmol/L have been reported. Signs and symptoms of hyponatremia include headache, difficulty concentrating, memory impairment, confusion, weakness, and unsteadiness, which may lead to falls. Signs and symptoms associated with more severe and/or acute cases have included hallucination, syncope, seizure, coma, respiratory arrest, and death. In many cases, this hyponatremia appears to be the result of the syndrome of inappropriate antidiuretic hormone secretion (SIADH).
In patients with symptomatic hyponatremia, discontinue Paroxetine Extended-Release Tablets and institute appropriate medical intervention. Elderly patients, patients taking diuretics, and those who are volume-depleted may be at greater risk of developing hyponatremia with SNRIs and SSRIs [see Use in Specific Populations (8.5)].
8.4 Pediatric Use
The safety and effectiveness of Paroxetine Extended-Release Tablets in pediatric patients have not been established [see Boxed Warning, Warnings and Precautions (5.1)].
Three placebo-controlled trials in 752 pediatric patients with MDD have been conducted with immediate-release paroxetine, and effectiveness was not established in pediatric patients.
Decreased appetite and weight loss have been observed in association with the use of SSRIs.
In placebo-controlled clinical trials conducted with pediatric patients, the following adverse reactions were reported in at least 2% of pediatric patients treated with immediate-release paroxetine hydrochloride and at a rate at least twice that for pediatric patients receiving placebo: emotional lability (including self-harm, suicidal thoughts, attempted suicide, crying, and mood fluctuations), hostility, decreased appetite, tremor, sweating, hyperkinesia, and agitation.
Adverse reactions upon discontinuation of treatment with immediate-release paroxetine hydrochloride in the pediatric clinical trials that included a taper phase regimen, which occurred in at least 2% of patients and at a rate at least twice that of placebo, were: emotional lability (including suicidal ideation, suicide attempt, mood changes, and tearfulness), nervousness, dizziness, nausea, and abdominal pain.
8.5 Geriatric Use
SSRIs and SNRIs, including Paroxetine Extended-Release Tablets, have been associated with cases of clinically significant hyponatremia in elderly patients, who may be at greater risk for this adverse reaction [see Warnings and Precautions (5.9)].
In premarketing clinical trials with immediate-release paroxetine hydrochloride, 17% of paroxetine treated patients (approximately 700) were 65 years or older. Pharmacokinetic studies revealed a decreased clearance in the elderly, and a lower starting dose is recommended; however, no overall differences in safety or effectiveness were observed between these subjects and younger subjects [see Dosage and Administration (2.5), Clinical Pharmacology (12.3)].
5.12 Bone Fracture
Epidemiological studies on bone fracture risk during exposure to some antidepressants, including SSRIs, have reported an association between antidepressant treatment and fractures. There are multiple possible causes for this observation, and it is unknown to what extent fracture risk is directly attributable to SSRI treatment.
14.2 Panic Disorder
The effectiveness of Paroxetine Extended-Release Tablets in the treatment of panic disorder (PD) was evaluated in three 10-week, multicenter, flexible-dose studies (Studies 4, 5, and 6) comparing Paroxetine Extended-Release Tablets (12.5 to 75 mg daily) to placebo in adult outpatients 19 to 72 years of age who met panic disorder (with or without agoraphobia) criteria according to DSM-IV. These trials were assessed on the basis of their outcomes on 3 variables: (1) the proportions of patients free of full panic attacks at Week 10; (2) change from baseline to Week 10 in the median number of full panic attacks; and (3) change from baseline to Week 10 in the median Clinical Global Impression Severity score. For Studies 4 and 5, Paroxetine Extended-Release Tablets were superior to placebo on 2 of these 3 variables. Study 6 failed to consistently demonstrate a statistically significant difference between Paroxetine Extended-Release Tablets and placebo on any of these variables.
For all 3 studies, the mean dose of Paroxetine Extended-Release Tablets for completers at Week 10 was approximately 50 mg/day. Subgroup analyses did not indicate that there were any differences in treatment outcomes as a function of age or gender.
Long-term maintenance effects of paroxetine in patients with PD were demonstrated in a randomized-withdrawal study using immediate-release paroxetine. Patients who were responders during a 10-week, double-blind trial (followed by a 3-month double-blind maintenance phase) of immediate-release paroxetine were re-randomized to continue immediate-release paroxetine or placebo in a 3-month, double-blind withdrawal phase. Patients randomized to immediate-release paroxetine were statistically significantly less likely to relapse than placebo-treated patients.
4 Contraindications
Paroxetine Extended-Release Tablets are contraindicated in patients:
- Taking, or within 14 days of stopping, MAOIs (including the MAOIs linezolid and intravenous methylene blue) because of an increased risk of serotonin syndrome [see Warnings and Precautions (5.2), Drug Interactions (7)].
- Taking thioridazine because of risk of QT prolongation [see Warnings and Precautions (5.3), Drug Interactions (7)].
- Taking pimozide because of risk of QT prolongation [see Warnings and Precautions (5.3), Drug Interactions (7)].
- With known hypersensitivity (e.g., anaphylaxis, angioedema, Stevens-Johnson syndrome) to paroxetine or to any of the inactive ingredients in Paroxetine Extended-Release Tablets [see Adverse Reactions (6.1, 6.2)].
6 Adverse Reactions
The following adverse reactions are included in more detail in other sections of the prescribing information:
- Hypersensitivity reactions to paroxetine [see Contraindications (4)]
- Suicidal Thoughts and Behaviors [see Warnings and Precautions (5.1)]
- Serotonin Syndrome [see Warnings and Precautions (5.2)]
- Embryofetal Toxicity [see Warnings and Precautions (5.4)]
- Increased Risk of Bleeding [see Warnings and Precautions (5.5)]
- Activation of Mania/Hypomania [see Warnings and Precautions (5.6)]
- Discontinuation Syndrome [see Warnings and Precautions (5.7)]
- Seizures [see Warnings and Precautions (5.8)]
- Angle-closure Glaucoma [see Warnings and Precautions (5.9)]
- Hyponatremia [see Warnings and Precautions (5.10)]
- Bone Fracture [see Warnings and Precautions (5.12)]
- Sexual Dysfunction [see Warnings and Precautions (5.13)]
7 Drug Interactions
- Drugs Highly Bound to Plasma Protein: Monitor for adverse reactions and reduce dosage of Paroxetine Extended-Release Tablets or other protein-bound drugs (e.g., warfarin) as warranted. (7)
- Drugs Metabolized by CYP2D6: Reduce dosage of drugs metabolized by CYP2D6 as warranted. (7)
- Concomitant use with Tamoxifen: Consider use of an alternative antidepressant with little or no CYP2D6 inhibition. (5.11, 7)
12.2 Pharmacodynamics
Studies at clinically relevant doses in humans have demonstrated that paroxetine blocks the uptake of serotonin into human platelets. In vitro studies in animals also suggest that paroxetine is a potent and highly selective inhibitor of neuronal serotonin reuptake (SSRI) and has only very weak effects on norepinephrine and dopamine neuronal reuptake.
5.2 Serotonin Syndrome
Serotonin-norepinephrine reuptake inhibitors (SNRIs) and SSRIs, including Paroxetine Extended-Release Tablets, can precipitate serotonin syndrome, a potentially life-threatening condition. The risk is increased with concomitant use of other serotonergic drugs (including triptans, tricyclic antidepressants, fentanyl, lithium, tramadol, meperidine, methadone, tryptophan, buspirone, amphetamines, and St. John's Wort) and with drugs that impair metabolism of serotonin, i.e., MAOIs [see Contraindications (4), Drug Interactions (7.1)]. Serotonin syndrome can also occur when these drugs are used alone.
Serotonin syndrome signs and symptoms may include mental status changes (e.g., agitation, hallucinations, delirium, and coma), autonomic instability (e.g., tachycardia, labile blood pressure, dizziness, diaphoresis, flushing, hyperthermia), neuromuscular symptoms (e.g., tremor, rigidity, myoclonus, hyperreflexia, incoordination), seizures, and gastrointestinal symptoms (e.g., nausea, vomiting, diarrhea).
The concomitant use of Paroxetine Extended-Release Tablets with MAOIs is contraindicated. In addition, do not initiate Paroxetine Extended-Release Tablets in a patient being treated with MAOIs such as linezolid or intravenous methylene blue. No reports involved the administration of methylene blue by other routes (such as oral tablets or local tissue injection). If it is necessary to initiate treatment with an MAOI such as linezolid or intravenous methylene blue in a patient taking Paroxetine Extended-Release Tablets, discontinue Paroxetine Extended-Release Tablets before initiating treatment with the MAOI [see Contraindications (4), Drug Interactions (7.1)].
Monitor all patients taking Paroxetine Extended-Release Tablets for the emergence of serotonin syndrome. Discontinue treatment with Paroxetine Extended-Release Tablets and any concomitant serotonergic agents immediately if the above symptoms occur, and initiate supportive symptomatic treatment. If concomitant use of Paroxetine Extended-Release Tablets with other serotonergic drugs is clinically warranted, inform patients of the increased risk for serotonin syndrome and monitor for symptoms.
1 Indications and Usage
Paroxetine Extended-Release Tablets, USP are indicated in adults for the treatment of:
- Major depressive disorder (MDD)
- Panic disorder (PD)
- Social anxiety disorder (SAD)
- Premenstrual dysphoric disorder (PMDD)
5.13 Sexual Dysfunction
Use of SSRIs, including Paroxetine Extended-Release Tablets, may cause symptoms of sexual dysfunction [see Adverse Reactions (6.1)]. In male patients, SSRI use may result in ejaculatory delay or failure, decreased libido, and erectile dysfunction. In female patients, SSRI use may result in decreased libido and delayed or absent orgasm.
It is important for prescribers to inquire about sexual function prior to initiation of Paroxetine Extended-Release Tablets and to inquire specifically about changes in sexual function during treatment, because sexual function may not be spontaneously reported. When evaluating changes in sexual function, obtaining a detailed history (including timing of symptom onset) is important because sexual symptoms may have other causes, including the underlying psychiatric disorder. Discuss potential management strategies to support patients in making informed decisions about treatment.
12.1 Mechanism of Action
The mechanism of action of paroxetine in the treatment of major depressive disorder (MDD), panic disorder (PD), social anxiety disorder (SAD), and premenstrual dysphoric disorder (PMDD) is unknown, but is presumed to be linked to potentiation of serotonergic activity in the central nervous system resulting from inhibition of neuronal reuptake of serotonin (5-HT).
5.4 Embryofetal Toxicity
Based on meta-analyses of epidemiological studies, exposure to paroxetine in the first trimester of pregnancy is associated with a less than 2-fold increase in the rate of cardiovascular malformations among infants. For women who intend to become pregnant or who are in their first trimester of pregnancy, Paroxetine Extended-Release Tablets should be initiated only after consideration of the other available treatment options [see Use in Specific Populations (8.1)].
5 Warnings and Precautions
- Serotonin Syndrome: Increased risk when co-administered with other serotonergic agents, but also when taken alone. If serotonin syndrome occurs, discontinue Paroxetine Extended-Release Tablets and serotonergic agents and initiate supportive measures. (5.2)
- Embryofetal Toxicity: May cause fetal harm. Meta-analysis of epidemiological studies has shown increased risk (less than 2-fold) of cardiovascular malformations with exposure during the first trimester. (5.4, 8.1)
- Increased Risk of Bleeding: Concomitant use of aspirin, nonsteroidal anti-inflammatory drugs, other antiplatelet drugs, warfarin, and other anticoagulant drugs may increase risk. (5.5)
- Activation of Mania/Hypomania: Screen patients for bipolar disorder. (5.6)
- Seizures: Use with caution in patients with seizure disorders. (5.8)
- Angle-Closure Glaucoma: Angle-closure glaucoma has occurred in patients with untreated anatomically narrow angles treated with antidepressants. (5.9)
- Sexual Dysfunction: Paroxetine Extended-Release Tablets may cause symptoms of sexual dysfunction. (5.13)
5.9 Angle Closure Glaucoma
The pupillary dilation that occurs following use of many antidepressant drugs including Paroxetine Extended-Release Tablets may trigger an angle closure attack in a patient with anatomically narrow angles who does not have a patent iridectomy. Cases of angle-closure glaucoma associated with use of paroxetine hydrochloride tablets have been reported. Avoid use of antidepressants, including Paroxetine Extended-Release Tablets, in patients with untreated anatomically narrow angles.
2 Dosage and Administration
- Swallow tablet whole; do not chew or crush. (2.1)
- Recommended starting and maximum daily dosage: (2.2, 2.3)
Indication Starting Dose Maximum Dose MDD 25 mg/day 62.5 mg/day PD 12.5 mg/day 75 mg/day SAD 12.5 mg/day 37.5 mg/day PMDD 12.5 mg/day 25 mg/day - For PMDD, dose continuously or intermittently (luteal phase only). (2.3)
- If inadequate response to starting dosage, titrate in 12.5 mg per day increments once weekly. (2.2, 2.3)
- Elderly patients, patients with severe renal impairment, or severe hepatic impairment: Starting dose is 12.5 mg per day. Do not exceed 50 mg per day for treatment of MDD and PD and 37.5 mg per day for treatment of SAD. (2.5)
- When discontinuing Paroxetine Extended-Release Tablets, reduce dose gradually. (2.7)
14.3 Social Anxiety Disorder
The efficacy of Paroxetine Extended-Release Tablets as a treatment for social anxiety disorder (SAD) was established, in part, on the basis of extrapolation from the established effectiveness of immediate-release paroxetine in the treatment of SAD. In addition, the effectiveness of Paroxetine Extended-Release Tablets in the treatment of SAD was demonstrated in one 12-week, multicenter, double-blind, flexible-dose, placebo-controlled study of adult outpatients with a primary diagnosis of SAD by DSM-IV criteria (Study 7). In Study 7, the effectiveness of Paroxetine Extended-Release Tablets (12.5 to 37.5 mg daily) compared to placebo was evaluated on the basis of (1) change from baseline in the Liebowitz Social Anxiety Scale (LSAS) total score at Week 12 and (2) the proportion of responders who scored 1 or 2 (very much improved or much improved) on the CGI Global Improvement score at Week 12.
In Study 7, Paroxetine Extended-Release Tablets demonstrated statistically significant superiority over placebo on both the change on LSAS total score at Week 12 and the CGI Improvement responder criterion at Week 12. For patients who completed the trial, 64% of patients treated with Paroxetine Extended-Release Tablets compared to 35% of patients treated with placebo were CGI Improvement responders at Week 12.
Subgroup analyses did not indicate that there were any differences in treatment outcomes as a function of gender. Subgroup analyses of studies utilizing the immediate-release formulation of paroxetine generally did not indicate differences in treatment outcomes as a function of age, race, or gender.
3 Dosage Forms and Strengths
Paroxetine Extended-Release Tablets are available as:
- 12.5 mg: White enteric coated, round, bi-convex tablets, with one side debossed 2271 and the other side blank.
- 25 mg: Brown enteric coated, round, bi-convex tablets, with one side debossed 2272 and the other side blank.
- 37.5 mg: Orange enteric coated, round, bi-convex tablets, with one side debossed 2273 and the other side blank.
5.7 Discontinuation Syndrome
Adverse reactions after discontinuation of serotonergic antidepressants, particularly after abrupt discontinuation, include: nausea, sweating, dysphoric mood, irritability, agitation, dizziness, sensory disturbances (e.g., paresthesia, such as electric shock sensations), tremor, anxiety, confusion, headache, lethargy, emotional lability, insomnia, hypomania, tinnitus, and seizures. A gradual reduction in dosage rather than abrupt cessation is recommended whenever possible [see Dosage and Administration (2.7)].
Adverse reactions have been reported upon discontinuation of treatment with paroxetine in pediatric patients. The safety and effectiveness of Paroxetine Extended-Release Tablets in pediatric patients have not been established [see Boxed Warning, Warnings and Precautions (5.1), Use in Specific Populations (8.4)].
6.2 Postmarketing Experience
The following reactions have been identified during post approval use of paroxetine. Because these reactions are reported voluntarily from a population of unknown size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Acute pancreatitis, elevated liver function tests (the most severe cases were deaths due to liver necrosis, and grossly elevated transaminases associated with severe liver dysfunction), Guillain-Barré syndrome, Stevens-Johnson syndrome, toxic epidermal necrolysis, drug reaction with eosinophilia and systemic symptoms (DRESS), priapism, syndrome of inappropriate ADH secretion (SIADH), prolactinemia and galactorrhea; extrapyramidal symptoms which have included akathisia, bradykinesia, cogwheel rigidity, dystonia, hypertonia, trismus; status epilepticus, acute renal failure, pulmonary hypertension, allergic alveolitis, anosmia, hyposmia, anaphylaxis, eclampsia, laryngismus, optic neuritis, porphyria, restless legs syndrome (RLS), ventricular fibrillation, ventricular tachycardia (including torsade de pointes), hemolytic anemia, events related to impaired hematopoiesis (including aplastic anemia, pancytopenia, bone marrow aplasia, and agranulocytosis), and vasculitic syndromes (such as Henoch-Schönlein purpura).
8 Use in Specific Populations
- Pregnancy: SSRI use, particularly later in pregnancy, may increase the risk of persistent pulmonary hypertension and symptoms of poor adaptation (respiratory distress, temperature instability, feeding difficulty, hypotonia, irritability) in the neonate. (5.4, 8.1)
- Nursing Mothers: Discontinue drug or nursing taking into consideration importance of drug to mother. (8.3)
14.1 Major Depressive Disorder
The efficacy of Paroxetine Extended-Release Tablets as a treatment for major depressive disorder (MDD) was established in two 12-week, multicenter, randomized, double-blind, placebo-controlled, flexible dose studies with Paroxetine Extended-Release Tablets (Study 1 and Study 2) in adult patients who met Diagnostic and Statistical Manual of Mental Disorders (DSM)-IV criteria for MDD. Study 1 and 2 included patients 18 to 65 years old who received Paroxetine Extended-Release Tablets doses of 25 to 62.5 mg/day (N= 212) or placebo (N= 211) once daily compared to immediate-release paroxetine 20 to 50 mg (N=217). A third 12-week, multicenter, randomized, double-blind, placebo-controlled, flexible dose study with Paroxetine Extended-Release Tablets (Study 3) included elderly patients, ranging in age from 60 to 88 years old and used Paroxetine Extended-Release Tablets doses of 12.5 to 50 mg/day (N=104) or placebo (N=109) once daily compared to immediate-release paroxetine 10 to 40 mg (N=106). In all three studies, Paroxetine Extended-Release Tablets were statistically superior to placebo in improving depressive symptoms as measured by the following: the mean change from baseline in the Hamilton Depression Rating Scale (HDRS) total score at Week 12, the mean change from baseline in the Hamilton Depressed Mood item score at Week 12, and the mean change from baseline in the Clinical Global Impression (CGI)–Severity of Illness score.
Long-term efficacy of paroxetine for treatment of MDD in outpatients was established with one randomized withdrawal study with immediate-release paroxetine. Patients who responded to immediate-release paroxetine (HDRS total score <8) during an initial 8-week open-label treatment phase were then randomized to continue immediate-release paroxetine or placebo, for up to 1 year. Patients treated with immediate-release paroxetine demonstrated a statistically significant lower relapse rate during the withdrawal phase (15%) compared to those on placebo (39%). Effectiveness was similar for male and female patients.
5.5 Increased Risk of Bleeding
Drugs that interfere with serotonin reuptake inhibition, including Paroxetine Extended-Release Tablets, increase the risk of bleeding events. Concomitant use of aspirin, nonsteroidal anti-inflammatory drugs (NSAIDS), other antiplatelet drugs, warfarin, and other anticoagulants may add to this risk. Case reports and epidemiological studies (case-control and cohort design) have demonstrated an association between use of drugs that interfere with serotonin reuptake and the occurrence of gastrointestinal bleeding. Based on data from the published observational studies, exposure to SSRIs, particularly in the month before delivery, has been associated with a less than 2-fold increase in the risk of postpartum hemorrhage [see Use in Specific Populations (8.1)]. Bleeding events related to drugs that interfere with serotonin reuptake have ranged from ecchymoses, hematomas, epistaxis, and petechiae to life-threatening hemorrhages.
Inform patients about the increased risk of bleeding associated with the concomitant use of Paroxetine Extended-Release Tablets and antiplatelet agents or anticoagulants. For patients taking warfarin, carefully monitor the international normalized ratio.
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
Safety data for Paroxetine Extended-Release Tablets is from 11 short-term, placebo-controlled clinical trials including 3 studies in patients with major depressive disorder (MDD) (Studies 1, 2, and 3), 3 studies in patients with panic disorder (PD) (Studies 4, 5, and 6), 1 study in patients with social anxiety disorder (SAD) (Study 7), and 4 studies in female patients with premenstrual dysphoric disorder (PMDD) (Studies 8, 9, 10, and 11) [see Clinical Studies (14)]. These 11 trials included 1627 patients treated with Paroxetine Extended-Release Tablets.
- Studies 1 and 2 were 12-week studies that enrolled patients 18 to 65 years old who received Paroxetine Extended-Release Tablets at doses ranging from 25 mg to 62.5 mg once daily. Study 3 was a 12-week study in patients 60 to 88 years old who received Paroxetine Extended-Release Tablets at doses ranging from 12.5 mg to 50 mg once daily.
- Studies 4, 5, and 6 were 10-week studies in patients 19 to 72 years old who received Paroxetine Extended-Release Tablets at doses ranging from 12.5 mg to 75 mg once daily.
- Study 7 was a 12-week study that enrolled adult patients who received Paroxetine Extended-Release Tablets at doses ranging from 12.5 mg to 37.5 mg once daily.
- Studies 8, 9, and 10 were 12-week, placebo-controlled trials in female patients 18 to 46 years old who received Paroxetine Extended-Release Tablets at doses of 12.5 mg or 25 mg once daily. Study 11 was a 12-week placebo-controlled trial in patients 18 to 46 years old who received Paroxetine Extended-Release Tablets 2 weeks prior to the onset of menses (luteal phase dosing) at doses of 12.5 mg or 25 mg once daily.
17 Patient Counseling Information
Advise the patient to read the FDA-approved patient labeling (Medication Guide).
8.6 Renal And/or Hepatic Impairment
Increased plasma concentrations of paroxetine occur in patients with renal and hepatic impairment. The initial dosage of Paroxetine Extended-Release Tablets should be reduced in patients with severe renal impairment and patients with severe hepatic impairment [see Dosage and Administration (2.5) and Clinical Pharmacology (12.3)].
14.4 Premenstrual Dysphoric Disorder
The effectiveness of Paroxetine Extended-Release Tablets for the treatment of Premenstrual Dysphoric Disorder (PMDD) utilizing a continuous dosing regimen has been established in 2 placebo-controlled trials in female patients ages 18 to 46 (Studies 8 and 9 [N=672]). Patients in these trials met DSM-IV criteria for PMDD. Of 1,030 patients including Study 10, who were treated with daily doses of Paroxetine Extended-Release Tablets 12.5 or 25 mg/day, or placebo continuously throughout the menstrual cycle for a period of 3 menstrual cycles, the mean duration of the PMDD symptoms was approximately 11 ± 7 years. Patients on systemic hormonal contraceptives were excluded from these trials. Therefore, the efficacy of Paroxetine Extended-Release Tablets in combination with systemic (including oral) hormonal contraceptives for the continuous daily treatment of PMDD is unknown.
The VAS score is a patient-rated instrument that mirrors the diagnostic criteria of PMDD as identified in the DSM-IV, and includes assessments for mood, physical symptoms, and other symptoms associated with PMDD. In Studies 8 and 9, 12.5 mg/day and 25 mg/day of Paroxetine Extended-Release Tablets were statistically significantly more effective than placebo as measured by change from baseline to Month 3 on the luteal phase VAS score.
In an additional study employing luteal phase dosing (Study 11), patients (N = 366) were treated for the 2 weeks prior to the onset of menses with 12.5 or 25 mg/day of Paroxetine Extended-Release Tablets or placebo for a period of 3 months. In this trial,12.5 mg/day and 25 mg/day of Paroxetine Extended-Release Tablets, as luteal phase dosing, was statistically significantly more effective than placebo as measured by change from baseline to luteal phase VAS score at Month 3.
There is insufficient information to determine the effect of race or age on outcome in Studies 8, 9, 10, and 11.
16 How Supplied/storage and Handling
Paroxetine Extended-Release Tablets, USP are supplied as: a round, extended-release tablet as follows:
25 mg Brown enteric coated, round, bi-convex tablets, with one side debossed 2272 and the other side blank:
- NDC 63629-9499-01 Bottles of 30
Store at 20°C to 25°C (68°F to 77°F) [see USP Controlled Room Temperature].
Repackaged/Relabeled by:
Bryant Ranch Prepack, Inc.
Burbank, CA 91504
5.6 Activation of Mania Or Hypomania
In patients with bipolar disorder, treating a depressive episode with Paroxetine Extended-Release Tablets or another antidepressant may precipitate a mixed/manic episode. During controlled clinical trials of immediate-release paroxetine hydrochloride, hypomania or mania occurred in approximately 1% of paroxetine-treated unipolar patients compared to 1.1% of active-control and 0.3% of placebo-treated unipolar patients. Prior to initiating treatment with Paroxetine Extended-Release Tablets, screen patients for any personal or family history of bipolar disorder, mania, or hypomania.
5.11 Reduction of Efficacy of Tamoxifen
Some studies have shown that the efficacy of tamoxifen, as measured by the risk of breast cancer relapse/mortality, may be reduced with concomitant use of paroxetine as a result of paroxetine's irreversible inhibition of CYP2D6 and lower blood levels of tamoxifen [see Drug Interactions (7.1)]. One study suggests that the risk may increase with longer duration of coadministration. However, other studies have failed to demonstrate such a risk. When tamoxifen is used for the treatment or prevention of breast cancer, prescribers should consider using an alternative antidepressant with little or no CYP2D6 inhibition.
Warning: Suicidal Thoughts and Behaviors
Antidepressants increased the risk of suicidal thoughts and behaviors in pediatric and young adult patients in short-term studies. Closely monitor all antidepressant-treated patients for clinical worsening, and for emergence of suicidal thoughts and behaviors [see Warnings and Precautions (5.1)]. Paroxetine Extended-Release Tablets are not approved for use in pediatric patients [see Use in Specific Populations (8.4)].
2.1 Important Administration Instructions
Administer Paroxetine Extended-Release Tablets as a single daily dose in the morning, with or without food. Swallow tablets whole and do not chew or crush.
5.3 Drug Interactions Leading to Qt Prolongation
The CYP2D6 inhibitory properties of paroxetine can elevate plasma levels of thioridazine and pimozide. Since thioridazine and pimozide given alone produce prolongation of the QTc interval and increase the risk of serious ventricular arrhythmias, the use of Paroxetine Extended-Release Tablets is contraindicated in combination with thioridazine and pimozide [see Contraindications (4), Drug Interactions (7), Clinical Pharmacology (12.3)].
2.3 Dosage in Patients With Premenstrual Dysphoric Disorder
The recommended starting dosage in women with PMDD is 12.5 mg per day. Paroxetine Extended-Release Tablets may be administered either continuously (every day throughout the menstrual cycle) or intermittently (only during the luteal phase of the menstrual cycle, i.e., starting the daily dosage 14 days prior to the anticipated onset of menstruation and continuing through the onset of menses). Intermittent dosing is repeated with each new cycle.
In patients with an inadequate response, the dosage may be increased to the maximum recommended dosage of 25 mg per day, depending on tolerability. Institute dosage adjustments at intervals of at least 1 week.
5.1 Suicidal Thoughts and Behaviors in Adolescents and Young Adults
In pooled analyses of placebo-controlled trials of antidepressant drugs (SSRIs and other antidepressant classes) that included approximately 77,000 adult patients and 4,500 pediatric patients, the incidence of suicidal thoughts and behaviors in antidepressant-treated patients age 24 years and younger was greater than in placebo-treated patients. There was considerable variation in risk of suicidal thoughts and behaviors among drugs, but there was an increased risk identified in young patients for most drugs studied. There were differences in absolute risk of suicidal thoughts and behaviors across the different indications, with the highest incidence in patients with MDD. The drug-placebo differences in the number of cases of suicidal thoughts and behaviors per 1000 patients treated are provided in Table 2.
| Age Range | Drug-Placebo Difference in Number of Patients of Suicidal Thoughts and Behaviors per 1,000 Patients Treated |
|---|---|
| Increases Compared to Placebo | |
| <18 years old | 14 additional patients |
| 18 to 24 years old | 5 additional patients |
| Decreases Compared to Placebo | |
| 25 to 64 years old | 1 fewer patient |
| ≥65 years old | 6 fewer patients |
It is unknown whether the risk of suicidal thoughts and behaviors in children, adolescents, and young adults extends to longer-term use, i.e., beyond four months. However, there is substantial evidence from placebo-controlled maintenance trials in adults with MDD that antidepressants delay the recurrence of depression and that depression itself is a risk factor for suicidal thoughts and behaviors.
Monitor all antidepressant-treated patients for any indication for clinical worsening and emergence of suicidal thoughts and behaviors, especially during the initial few months of drug therapy, and at times of dosage changes. Counsel family members or caregivers of patients to monitor for changes in behavior and to alert the healthcare provider. Consider changing the therapeutic regimen, including possibly discontinuing Paroxetine Extended-Release Tablets, in patients whose depression is persistently worse, or who are experiencing emergent suicidal thoughts or behaviors.
2.7 Discontinuation of Treatment With Paroxetine Extended Release Tablets
Adverse reactions may occur upon discontinuation of Paroxetine Extended-Release Tablets [see Warnings and Precautions (5.7)]. Gradually reduce the dosage rather than stopping Paroxetine Extended-Release Tablets abruptly whenever possible.
2.6 Switching Patients to Or From A Monoamine Oxidase Inhibitor Antidepressant
At least 14 days must elapse between discontinuation of a monoamine oxidase inhibitor (MAOI) antidepressant and initiation of Paroxetine Extended-Release Tablets. In addition, at least 14 days must elapse after stopping Paroxetine Extended-Release Tablets before starting an MAOI antidepressant [see Contraindications (4), Warnings and Precautions (5.2)].
2.4 Screen for Bipolar Disorder Prior to Starting Paroxetine Extended Release Tablets
Prior to initiating treatment with Paroxetine Extended-Release Tablets or another antidepressant, screen patients for a personal or family history of bipolar disorder, mania, or hypomania [see Warnings and Precautions (5.6)].
7.1 Clinically Significant Drug Interactions With Paroxetine Extended Release Tablets
Table 6 includes clinically significant drug interactions with Paroxetine Extended-Release Tablets
| Monoamine Oxidase Inhibitors (MAOIs) | |
| Clinical Impact | The concomitant use of SSRIs, including Paroxetine Extended-Release Tablets, and MAOIs increases the risk of serotonin syndrome. |
| Intervention | Paroxetine Extended-Release Tablets are contraindicated in patients taking MAOIs, including MAOIs such as linezolid or intravenous methylene blue [see Dosage and Administration (2.6), Contraindications (4), Warnings and Precautions (5.2)]. |
| Examples | selegiline, tranylcypromine, isocarboxazid, phenelzine, linezolid, methylene blue |
| Pimozide and Thioridazine | |
| Clinical Impact | Increased plasma concentrations of pimozide and thioridazine, drugs with a narrow therapeutic index, may increase the risk of QTc prolongation and ventricular arrhythmias. |
| Intervention | Paroxetine Extended-Release Tablets are contraindicated in patients taking pimozide or thioridazine [see Contraindications (4)]. |
| Other Serotonergic Drugs | |
| Clinical Impact | The concomitant use of serotonergic drugs with Paroxetine Extended-Release Tablets increases the risk of serotonin syndrome. |
| Intervention | Monitor patients for signs and symptoms of serotonin syndrome, particularly during treatment initiation and dosage increases. If serotonin syndrome occurs, consider discontinuation of Paroxetine Extended-Release Tablets and/or concomitant serotonergic drugs [see Warnings and Precautions (5.2)]. |
| Examples | Other SSRIs, SNRIs, triptans, tricyclic antidepressants, opioids, lithium, tryptophan, buspirone, St. John's Wort |
| Drugs that Interfere with Hemostasis (antiplatelet agents and anticoagulants) | |
| Clinical Impact | The concurrent use of an antiplatelet agent or anticoagulant with Paroxetine Extended-Release Tablets may potentiate the risk of bleeding. |
| Intervention | Inform patients of the increased risk of bleeding associated with the concomitant use of Paroxetine Extended-Release Tablets and antiplatelet agents and anticoagulants. For patients taking warfarin, carefully monitor the international normalized ratio [see Warnings and Precautions (5.5)]. |
| Examples | aspirin, clopidogrel, heparin, warfarin |
| Drugs Highly Bound to Plasma Protein | |
| Clinical Impact | Paroxetine Extended-Release Tablets are highly bound to plasma protein. The concomitant use of Paroxetine Extended-Release Tablets with another drug that is highly bound to plasma protein may increase free concentrations of Paroxetine Extended-Release Tablets or other tightly-bound drugs in plasma. |
| Intervention | Monitor for adverse reactions and reduce dosage of Paroxetine Extended-Release Tablets or other protein-bound drugs as warranted. |
| Examples | warfarin |
| Drugs Metabolized by CYP2D6 | |
| Clinical Impact | Paroxetine Extended-Release Tablets are a CYP2D6 inhibitor [see Clinical Pharmacology (12.3)]. The concomitant use of Paroxetine Extended-Release Tablets with a CYP2D6 substrate may increase the exposure of the CYP2D6 substrate. |
| Intervention | Decrease the dosage of a CYP2D6 substrate if needed with concomitant Paroxetine Extended-Release Tablets use. Conversely, an increase in dosage of a CYP2D6 substrate may be needed if Paroxetine Extended-Release Tablets are discontinued. |
| Examples | propafenone, flecainide, atomoxetine, desipramine, dextromethorphan, metoprolol, nebivolol, perphenazine, tolterodine, venlafaxine, risperidone. |
| Tamoxifen | |
| Clinical Impact | Concomitant use of tamoxifen with Paroxetine Extended-Release Tablets may lead to reduced plasma concentrations of the active metabolite (endoxifen) and reduced efficacy of tamoxifen. |
| Intervention | Consider use of an alternative antidepressant little or no CYP2D6 inhibition [see Warnings and Precautions (5.11)]. |
| Fosamprenavir/Ritonavir | |
| Clinical Impact | Co-administration of fosamprenavir/ritonavir with paroxetine significantly decreased plasma levels of paroxetine. |
| Intervention | Any dose adjustment should be guided by clinical effect (tolerability and efficacy). |
2.2 Dosage in Patients With Major Depressive Disorder, Panic Disorder, and Social Anxiety Disorder
The recommended initial dosage and maximum dosage of Paroxetine Extended-Release Tablets in patients with MDD, PD, and SAD are presented in Table 1.
In patients with an inadequate response, dosage may be increased in increments of 12.5 mg per day at intervals of at least 1 week, depending on tolerability.
| Indication | Starting Dose | Maximum Dose |
|---|---|---|
| MDD | 25 mg | 62.5 mg |
| PD | 12.5 mg | 75 mg |
| SAD | 12.5 mg | 37.5 mg |
2.5 Dosage Modifications for Elderly Patients, Patients With Severe Renal Impairment, and Patients With Severe Hepatic Impairment
The recommended initial dose of Paroxetine Extended-Release Tablets is 12.5 mg per day for elderly patients, patients with severe renal impairment, and patients with severe hepatic impairment. Reduce initial dose and increase up-titration intervals if necessary. Dosage should not exceed 50 mg per day for MDD or PD and should not exceed 37.5 mg per day for SAD [see Use in Specific Populations (8.5, 8.6)].
Structured Label Content
Section 42229-5 (42229-5)
Adverse Reactions Leading to Discontinuation in Patients with MDD, PD, SAD, and PMDD
In pooled studies in patients with MDD, PD and SAD, the most common adverse reactions leading to study withdrawal were: nausea (up to 4% of patients), asthenia, headache, depression, insomnia, and abnormal liver function tests (each occurring in up to 2% of patients), and dizziness, somnolence, and diarrhea (each occurring in up to 1% of patients).
In pooled studies for PMDD, the most common adverse reactions leading to study withdrawal were: nausea (occurring in up to 6% of patients), asthenia (occurring in up to 5% of patients), somnolence (occurring in up to 4% of patients), insomnia (occurring in approximately 2% of patients); and impaired concentration, dry mouth, dizziness, decreased appetite, sweating, tremor, yawn, and diarrhea (occurring in less than or equal to 2% of patients).
Section 42231-1 (42231-1)
| Medication Guide Paroxetine (par ox' e teen) Extended-Release Tablets, USP |
|||
|---|---|---|---|
| This Medication Guide has been approved by the U.S. Food and Drug Administration. | Revised: 4/2024 | ||
|
What is the most important information I should know about Paroxetine Extended-Release Tablets? Paroxetine Extended-Release Tablets can cause serious side effects, including:
|
|||
|
|
||
|
What are Paroxetine Extended-Release Tablets?
Paroxetine Extended-Release Tablets are a prescription medicine used in adults to treat:
|
|||
Do not take Paroxetine Extended-Release Tablets if you:
Do not start taking an MAOI for at least 14 days after you stop treatment with Paroxetine Extended-Release Tablets. |
|||
Before taking Paroxetine Extended-Release Tablets, tell your healthcare provider about all your medical conditions, including if you:
Paroxetine Extended-Release Tablets and some other medicines may affect each other causing possible serious side effects. Paroxetine Extended-Release Tablets may affect the way other medicines work and other medicines may affect the way Paroxetine Extended-Release Tablets work. Especially tell your healthcare provider if you take:
Do not start or stop any other medicines during treatment with Paroxetine Extended-Release Tablets without talking to your healthcare provider first. Stopping Paroxetine Extended-Release Tablets suddenly may cause you to have serious side effects. See, "What are the possible side effects of Paroxetine Extended-Release Tablets?" Know the medicines you take. Keep a list of them to show to your healthcare provider and pharmacist when you get a new medicine. |
|||
How should I take Paroxetine Extended-Release Tablets?
|
|||
|
What are possible side effects of Paroxetine Extended-Release Tablets? Paroxetine Extended-Release Tablets can cause serious side effects, including:
|
|||
|
|
||
|
|||
|
|
||
|
|||
|
|
|
|
The most common side effects Paroxetine Extended-Release Tablets include: |
|||
|
|
||
| These are not all the possible side effects of Paroxetine Extended-Release Tablets. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. |
|||
| How should I store Paroxetine Extended-Release Tablets? | |||
|
|||
| Keep Paroxetine Extended-Release Tablets and all medicines out of the reach of children. | |||
|
General information about the safe and effective use of Paroxetine Extended-Release Tablets.
Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not take Paroxetine Extended-Release Tablets for a condition for which it was not prescribed. Do not give Paroxetine Extended-Release Tablets to other people, even if they have the same symptoms that you have. It may harm them. You may ask your healthcare provider or pharmacist for information about Paroxetine Extended-Release Tablets that is written for healthcare professionals. |
|||
|
What are the ingredients in Paroxetine Extended-Release Tablets?
Active ingredient: paroxetine hydrochloride Inactive ingredients: carboxymethylcellulose sodium, copovidone, glyceryl monostearate, hypromellose, lactose monohydrate, magnesium stearate, methacrylic acid – ethyl acrylate copolymer (1:1), polysorbate 80, silicon dioxide, sodium lauryl sulfate, talcum, titanium dioxide, and triethyl citrate. In addition, the 25 mg tablets also contain the following coloring agents: iron oxide black and iron oxide red and the 37.5 mg tablets contain iron oxide red and iron oxide yellow. |
|||
| Manufactured by: Beijing Sciecure Pharmaceutical Co., Ltd. Shunyi District, Beijing 101301, China Manufactured for: Sciecure Pharma Inc. Monmouth Junction, NJ 08852 USA Marketed by: Rhodes Pharmaceuticals Wilson, NC 27893 USA For more information about Paroxetine Extended-Release Tablets, call Rhodes Pharmaceuticals at 1-888-827-0616. |
Section 51945-4 (51945-4)
Paroxetine Extended-ReleaseTablets 25 mg
5.8 Seizures
Paroxetine Extended-Release Tablets have not been systematically evaluated in patients with seizure disorders. Patients with history of seizures were excluded from clinical studies. Paroxetine Extended-Release Tablets should be prescribed with caution in patients with a seizure disorder and should be discontinued in any patient who develops seizures.
10 Overdosage (10 OVERDOSAGE)
The following have been reported with paroxetine tablet overdosage:
- Seizures, which may be delayed, and altered mental status including coma.
- Cardiovascular toxicity, which may be delayed, including QRS and QTc interval prolongation. Hypertension most commonly seen, but rarely can see hypotension alone or with co-ingestants including alcohol.
- Serotonin syndrome (patients with a multiple drug overdosage with other proserotonergic drugs may have a higher risk).
Gastrointestinal decontamination with activated charcoal should be considered in patients who present early after a paroxetine overdose.
Consider contacting a Poison Center (1-800-222-1222) or a medical toxicologist for additional overdosage management recommendations.
11 Description (11 DESCRIPTION)
Paroxetine Extended-Release Tablets, USP contain paroxetine hydrochloride, an SSRI. It is the hydrochloride salt of a phenylpiperidine compound identified chemically as (-)-trans-4R-(4'-fluorophenyl)-3S-[(3',4'-methylenedioxyphenoxy) methyl] piperidine hydrochloride hemihydrate and has the empirical formula of C19H20FNO3∙HCl∙1/2H2O. The molecular weight is 374.8 g/mol (329.4 g/mol as free base). The structural formula of paroxetine hydrochloride is:
Paroxetine hydrochloride is an odorless, off-white powder, having a melting point range of 120°C to 138°C and a solubility of 5.4 mg/mL in water.
Each enteric coated, extended-release tablet contains paroxetine base of 12.5 mg (white tablet), 25 mg (brown tablet), 37.5 mg (orange tablet), which is equivalent to 14.25 mg, 28.51 mg, or 42.76 mg of paroxetine hydrochloride, respectively. Each tablet consists of a hydrophilic matrix that contains the active material.
Inactive ingredients consist of carboxymethylcellulose sodium, copovidone, glyceryl monostearate, hypromellose, lactose monohydrate, magnesium stearate, methacrylic acid – ethyl acrylate copolymer (1:1), polysorbate 80, silicon dioxide, sodium lauryl sulfate, talcum, titanium dioxide, and triethyl citrate. In addition, the 25 mg tablets also contain the following coloring agents: iron oxide black and iron oxide red and the 37.5 mg tablets contain iron oxide red and iron oxide yellow.
USP dissolution test is pending.
5.10 Hyponatremia
Hyponatremia may occur as a result of treatment with SNRIs and SSRIs, including Paroxetine Extended-Release Tablets. Cases with serum sodium lower than 110 mmol/L have been reported. Signs and symptoms of hyponatremia include headache, difficulty concentrating, memory impairment, confusion, weakness, and unsteadiness, which may lead to falls. Signs and symptoms associated with more severe and/or acute cases have included hallucination, syncope, seizure, coma, respiratory arrest, and death. In many cases, this hyponatremia appears to be the result of the syndrome of inappropriate antidiuretic hormone secretion (SIADH).
In patients with symptomatic hyponatremia, discontinue Paroxetine Extended-Release Tablets and institute appropriate medical intervention. Elderly patients, patients taking diuretics, and those who are volume-depleted may be at greater risk of developing hyponatremia with SNRIs and SSRIs [see Use in Specific Populations (8.5)].
8.4 Pediatric Use
The safety and effectiveness of Paroxetine Extended-Release Tablets in pediatric patients have not been established [see Boxed Warning, Warnings and Precautions (5.1)].
Three placebo-controlled trials in 752 pediatric patients with MDD have been conducted with immediate-release paroxetine, and effectiveness was not established in pediatric patients.
Decreased appetite and weight loss have been observed in association with the use of SSRIs.
In placebo-controlled clinical trials conducted with pediatric patients, the following adverse reactions were reported in at least 2% of pediatric patients treated with immediate-release paroxetine hydrochloride and at a rate at least twice that for pediatric patients receiving placebo: emotional lability (including self-harm, suicidal thoughts, attempted suicide, crying, and mood fluctuations), hostility, decreased appetite, tremor, sweating, hyperkinesia, and agitation.
Adverse reactions upon discontinuation of treatment with immediate-release paroxetine hydrochloride in the pediatric clinical trials that included a taper phase regimen, which occurred in at least 2% of patients and at a rate at least twice that of placebo, were: emotional lability (including suicidal ideation, suicide attempt, mood changes, and tearfulness), nervousness, dizziness, nausea, and abdominal pain.
8.5 Geriatric Use
SSRIs and SNRIs, including Paroxetine Extended-Release Tablets, have been associated with cases of clinically significant hyponatremia in elderly patients, who may be at greater risk for this adverse reaction [see Warnings and Precautions (5.9)].
In premarketing clinical trials with immediate-release paroxetine hydrochloride, 17% of paroxetine treated patients (approximately 700) were 65 years or older. Pharmacokinetic studies revealed a decreased clearance in the elderly, and a lower starting dose is recommended; however, no overall differences in safety or effectiveness were observed between these subjects and younger subjects [see Dosage and Administration (2.5), Clinical Pharmacology (12.3)].
5.12 Bone Fracture
Epidemiological studies on bone fracture risk during exposure to some antidepressants, including SSRIs, have reported an association between antidepressant treatment and fractures. There are multiple possible causes for this observation, and it is unknown to what extent fracture risk is directly attributable to SSRI treatment.
14.2 Panic Disorder
The effectiveness of Paroxetine Extended-Release Tablets in the treatment of panic disorder (PD) was evaluated in three 10-week, multicenter, flexible-dose studies (Studies 4, 5, and 6) comparing Paroxetine Extended-Release Tablets (12.5 to 75 mg daily) to placebo in adult outpatients 19 to 72 years of age who met panic disorder (with or without agoraphobia) criteria according to DSM-IV. These trials were assessed on the basis of their outcomes on 3 variables: (1) the proportions of patients free of full panic attacks at Week 10; (2) change from baseline to Week 10 in the median number of full panic attacks; and (3) change from baseline to Week 10 in the median Clinical Global Impression Severity score. For Studies 4 and 5, Paroxetine Extended-Release Tablets were superior to placebo on 2 of these 3 variables. Study 6 failed to consistently demonstrate a statistically significant difference between Paroxetine Extended-Release Tablets and placebo on any of these variables.
For all 3 studies, the mean dose of Paroxetine Extended-Release Tablets for completers at Week 10 was approximately 50 mg/day. Subgroup analyses did not indicate that there were any differences in treatment outcomes as a function of age or gender.
Long-term maintenance effects of paroxetine in patients with PD were demonstrated in a randomized-withdrawal study using immediate-release paroxetine. Patients who were responders during a 10-week, double-blind trial (followed by a 3-month double-blind maintenance phase) of immediate-release paroxetine were re-randomized to continue immediate-release paroxetine or placebo in a 3-month, double-blind withdrawal phase. Patients randomized to immediate-release paroxetine were statistically significantly less likely to relapse than placebo-treated patients.
4 Contraindications (4 CONTRAINDICATIONS)
Paroxetine Extended-Release Tablets are contraindicated in patients:
- Taking, or within 14 days of stopping, MAOIs (including the MAOIs linezolid and intravenous methylene blue) because of an increased risk of serotonin syndrome [see Warnings and Precautions (5.2), Drug Interactions (7)].
- Taking thioridazine because of risk of QT prolongation [see Warnings and Precautions (5.3), Drug Interactions (7)].
- Taking pimozide because of risk of QT prolongation [see Warnings and Precautions (5.3), Drug Interactions (7)].
- With known hypersensitivity (e.g., anaphylaxis, angioedema, Stevens-Johnson syndrome) to paroxetine or to any of the inactive ingredients in Paroxetine Extended-Release Tablets [see Adverse Reactions (6.1, 6.2)].
6 Adverse Reactions (6 ADVERSE REACTIONS)
The following adverse reactions are included in more detail in other sections of the prescribing information:
- Hypersensitivity reactions to paroxetine [see Contraindications (4)]
- Suicidal Thoughts and Behaviors [see Warnings and Precautions (5.1)]
- Serotonin Syndrome [see Warnings and Precautions (5.2)]
- Embryofetal Toxicity [see Warnings and Precautions (5.4)]
- Increased Risk of Bleeding [see Warnings and Precautions (5.5)]
- Activation of Mania/Hypomania [see Warnings and Precautions (5.6)]
- Discontinuation Syndrome [see Warnings and Precautions (5.7)]
- Seizures [see Warnings and Precautions (5.8)]
- Angle-closure Glaucoma [see Warnings and Precautions (5.9)]
- Hyponatremia [see Warnings and Precautions (5.10)]
- Bone Fracture [see Warnings and Precautions (5.12)]
- Sexual Dysfunction [see Warnings and Precautions (5.13)]
7 Drug Interactions (7 DRUG INTERACTIONS)
- Drugs Highly Bound to Plasma Protein: Monitor for adverse reactions and reduce dosage of Paroxetine Extended-Release Tablets or other protein-bound drugs (e.g., warfarin) as warranted. (7)
- Drugs Metabolized by CYP2D6: Reduce dosage of drugs metabolized by CYP2D6 as warranted. (7)
- Concomitant use with Tamoxifen: Consider use of an alternative antidepressant with little or no CYP2D6 inhibition. (5.11, 7)
12.2 Pharmacodynamics
Studies at clinically relevant doses in humans have demonstrated that paroxetine blocks the uptake of serotonin into human platelets. In vitro studies in animals also suggest that paroxetine is a potent and highly selective inhibitor of neuronal serotonin reuptake (SSRI) and has only very weak effects on norepinephrine and dopamine neuronal reuptake.
5.2 Serotonin Syndrome
Serotonin-norepinephrine reuptake inhibitors (SNRIs) and SSRIs, including Paroxetine Extended-Release Tablets, can precipitate serotonin syndrome, a potentially life-threatening condition. The risk is increased with concomitant use of other serotonergic drugs (including triptans, tricyclic antidepressants, fentanyl, lithium, tramadol, meperidine, methadone, tryptophan, buspirone, amphetamines, and St. John's Wort) and with drugs that impair metabolism of serotonin, i.e., MAOIs [see Contraindications (4), Drug Interactions (7.1)]. Serotonin syndrome can also occur when these drugs are used alone.
Serotonin syndrome signs and symptoms may include mental status changes (e.g., agitation, hallucinations, delirium, and coma), autonomic instability (e.g., tachycardia, labile blood pressure, dizziness, diaphoresis, flushing, hyperthermia), neuromuscular symptoms (e.g., tremor, rigidity, myoclonus, hyperreflexia, incoordination), seizures, and gastrointestinal symptoms (e.g., nausea, vomiting, diarrhea).
The concomitant use of Paroxetine Extended-Release Tablets with MAOIs is contraindicated. In addition, do not initiate Paroxetine Extended-Release Tablets in a patient being treated with MAOIs such as linezolid or intravenous methylene blue. No reports involved the administration of methylene blue by other routes (such as oral tablets or local tissue injection). If it is necessary to initiate treatment with an MAOI such as linezolid or intravenous methylene blue in a patient taking Paroxetine Extended-Release Tablets, discontinue Paroxetine Extended-Release Tablets before initiating treatment with the MAOI [see Contraindications (4), Drug Interactions (7.1)].
Monitor all patients taking Paroxetine Extended-Release Tablets for the emergence of serotonin syndrome. Discontinue treatment with Paroxetine Extended-Release Tablets and any concomitant serotonergic agents immediately if the above symptoms occur, and initiate supportive symptomatic treatment. If concomitant use of Paroxetine Extended-Release Tablets with other serotonergic drugs is clinically warranted, inform patients of the increased risk for serotonin syndrome and monitor for symptoms.
1 Indications and Usage (1 INDICATIONS AND USAGE)
Paroxetine Extended-Release Tablets, USP are indicated in adults for the treatment of:
- Major depressive disorder (MDD)
- Panic disorder (PD)
- Social anxiety disorder (SAD)
- Premenstrual dysphoric disorder (PMDD)
5.13 Sexual Dysfunction
Use of SSRIs, including Paroxetine Extended-Release Tablets, may cause symptoms of sexual dysfunction [see Adverse Reactions (6.1)]. In male patients, SSRI use may result in ejaculatory delay or failure, decreased libido, and erectile dysfunction. In female patients, SSRI use may result in decreased libido and delayed or absent orgasm.
It is important for prescribers to inquire about sexual function prior to initiation of Paroxetine Extended-Release Tablets and to inquire specifically about changes in sexual function during treatment, because sexual function may not be spontaneously reported. When evaluating changes in sexual function, obtaining a detailed history (including timing of symptom onset) is important because sexual symptoms may have other causes, including the underlying psychiatric disorder. Discuss potential management strategies to support patients in making informed decisions about treatment.
12.1 Mechanism of Action
The mechanism of action of paroxetine in the treatment of major depressive disorder (MDD), panic disorder (PD), social anxiety disorder (SAD), and premenstrual dysphoric disorder (PMDD) is unknown, but is presumed to be linked to potentiation of serotonergic activity in the central nervous system resulting from inhibition of neuronal reuptake of serotonin (5-HT).
5.4 Embryofetal Toxicity
Based on meta-analyses of epidemiological studies, exposure to paroxetine in the first trimester of pregnancy is associated with a less than 2-fold increase in the rate of cardiovascular malformations among infants. For women who intend to become pregnant or who are in their first trimester of pregnancy, Paroxetine Extended-Release Tablets should be initiated only after consideration of the other available treatment options [see Use in Specific Populations (8.1)].
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
- Serotonin Syndrome: Increased risk when co-administered with other serotonergic agents, but also when taken alone. If serotonin syndrome occurs, discontinue Paroxetine Extended-Release Tablets and serotonergic agents and initiate supportive measures. (5.2)
- Embryofetal Toxicity: May cause fetal harm. Meta-analysis of epidemiological studies has shown increased risk (less than 2-fold) of cardiovascular malformations with exposure during the first trimester. (5.4, 8.1)
- Increased Risk of Bleeding: Concomitant use of aspirin, nonsteroidal anti-inflammatory drugs, other antiplatelet drugs, warfarin, and other anticoagulant drugs may increase risk. (5.5)
- Activation of Mania/Hypomania: Screen patients for bipolar disorder. (5.6)
- Seizures: Use with caution in patients with seizure disorders. (5.8)
- Angle-Closure Glaucoma: Angle-closure glaucoma has occurred in patients with untreated anatomically narrow angles treated with antidepressants. (5.9)
- Sexual Dysfunction: Paroxetine Extended-Release Tablets may cause symptoms of sexual dysfunction. (5.13)
5.9 Angle Closure Glaucoma (5.9 Angle-Closure Glaucoma)
The pupillary dilation that occurs following use of many antidepressant drugs including Paroxetine Extended-Release Tablets may trigger an angle closure attack in a patient with anatomically narrow angles who does not have a patent iridectomy. Cases of angle-closure glaucoma associated with use of paroxetine hydrochloride tablets have been reported. Avoid use of antidepressants, including Paroxetine Extended-Release Tablets, in patients with untreated anatomically narrow angles.
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
- Swallow tablet whole; do not chew or crush. (2.1)
- Recommended starting and maximum daily dosage: (2.2, 2.3)
Indication Starting Dose Maximum Dose MDD 25 mg/day 62.5 mg/day PD 12.5 mg/day 75 mg/day SAD 12.5 mg/day 37.5 mg/day PMDD 12.5 mg/day 25 mg/day - For PMDD, dose continuously or intermittently (luteal phase only). (2.3)
- If inadequate response to starting dosage, titrate in 12.5 mg per day increments once weekly. (2.2, 2.3)
- Elderly patients, patients with severe renal impairment, or severe hepatic impairment: Starting dose is 12.5 mg per day. Do not exceed 50 mg per day for treatment of MDD and PD and 37.5 mg per day for treatment of SAD. (2.5)
- When discontinuing Paroxetine Extended-Release Tablets, reduce dose gradually. (2.7)
14.3 Social Anxiety Disorder
The efficacy of Paroxetine Extended-Release Tablets as a treatment for social anxiety disorder (SAD) was established, in part, on the basis of extrapolation from the established effectiveness of immediate-release paroxetine in the treatment of SAD. In addition, the effectiveness of Paroxetine Extended-Release Tablets in the treatment of SAD was demonstrated in one 12-week, multicenter, double-blind, flexible-dose, placebo-controlled study of adult outpatients with a primary diagnosis of SAD by DSM-IV criteria (Study 7). In Study 7, the effectiveness of Paroxetine Extended-Release Tablets (12.5 to 37.5 mg daily) compared to placebo was evaluated on the basis of (1) change from baseline in the Liebowitz Social Anxiety Scale (LSAS) total score at Week 12 and (2) the proportion of responders who scored 1 or 2 (very much improved or much improved) on the CGI Global Improvement score at Week 12.
In Study 7, Paroxetine Extended-Release Tablets demonstrated statistically significant superiority over placebo on both the change on LSAS total score at Week 12 and the CGI Improvement responder criterion at Week 12. For patients who completed the trial, 64% of patients treated with Paroxetine Extended-Release Tablets compared to 35% of patients treated with placebo were CGI Improvement responders at Week 12.
Subgroup analyses did not indicate that there were any differences in treatment outcomes as a function of gender. Subgroup analyses of studies utilizing the immediate-release formulation of paroxetine generally did not indicate differences in treatment outcomes as a function of age, race, or gender.
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
Paroxetine Extended-Release Tablets are available as:
- 12.5 mg: White enteric coated, round, bi-convex tablets, with one side debossed 2271 and the other side blank.
- 25 mg: Brown enteric coated, round, bi-convex tablets, with one side debossed 2272 and the other side blank.
- 37.5 mg: Orange enteric coated, round, bi-convex tablets, with one side debossed 2273 and the other side blank.
5.7 Discontinuation Syndrome
Adverse reactions after discontinuation of serotonergic antidepressants, particularly after abrupt discontinuation, include: nausea, sweating, dysphoric mood, irritability, agitation, dizziness, sensory disturbances (e.g., paresthesia, such as electric shock sensations), tremor, anxiety, confusion, headache, lethargy, emotional lability, insomnia, hypomania, tinnitus, and seizures. A gradual reduction in dosage rather than abrupt cessation is recommended whenever possible [see Dosage and Administration (2.7)].
Adverse reactions have been reported upon discontinuation of treatment with paroxetine in pediatric patients. The safety and effectiveness of Paroxetine Extended-Release Tablets in pediatric patients have not been established [see Boxed Warning, Warnings and Precautions (5.1), Use in Specific Populations (8.4)].
6.2 Postmarketing Experience
The following reactions have been identified during post approval use of paroxetine. Because these reactions are reported voluntarily from a population of unknown size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Acute pancreatitis, elevated liver function tests (the most severe cases were deaths due to liver necrosis, and grossly elevated transaminases associated with severe liver dysfunction), Guillain-Barré syndrome, Stevens-Johnson syndrome, toxic epidermal necrolysis, drug reaction with eosinophilia and systemic symptoms (DRESS), priapism, syndrome of inappropriate ADH secretion (SIADH), prolactinemia and galactorrhea; extrapyramidal symptoms which have included akathisia, bradykinesia, cogwheel rigidity, dystonia, hypertonia, trismus; status epilepticus, acute renal failure, pulmonary hypertension, allergic alveolitis, anosmia, hyposmia, anaphylaxis, eclampsia, laryngismus, optic neuritis, porphyria, restless legs syndrome (RLS), ventricular fibrillation, ventricular tachycardia (including torsade de pointes), hemolytic anemia, events related to impaired hematopoiesis (including aplastic anemia, pancytopenia, bone marrow aplasia, and agranulocytosis), and vasculitic syndromes (such as Henoch-Schönlein purpura).
8 Use in Specific Populations (8 USE IN SPECIFIC POPULATIONS)
- Pregnancy: SSRI use, particularly later in pregnancy, may increase the risk of persistent pulmonary hypertension and symptoms of poor adaptation (respiratory distress, temperature instability, feeding difficulty, hypotonia, irritability) in the neonate. (5.4, 8.1)
- Nursing Mothers: Discontinue drug or nursing taking into consideration importance of drug to mother. (8.3)
14.1 Major Depressive Disorder
The efficacy of Paroxetine Extended-Release Tablets as a treatment for major depressive disorder (MDD) was established in two 12-week, multicenter, randomized, double-blind, placebo-controlled, flexible dose studies with Paroxetine Extended-Release Tablets (Study 1 and Study 2) in adult patients who met Diagnostic and Statistical Manual of Mental Disorders (DSM)-IV criteria for MDD. Study 1 and 2 included patients 18 to 65 years old who received Paroxetine Extended-Release Tablets doses of 25 to 62.5 mg/day (N= 212) or placebo (N= 211) once daily compared to immediate-release paroxetine 20 to 50 mg (N=217). A third 12-week, multicenter, randomized, double-blind, placebo-controlled, flexible dose study with Paroxetine Extended-Release Tablets (Study 3) included elderly patients, ranging in age from 60 to 88 years old and used Paroxetine Extended-Release Tablets doses of 12.5 to 50 mg/day (N=104) or placebo (N=109) once daily compared to immediate-release paroxetine 10 to 40 mg (N=106). In all three studies, Paroxetine Extended-Release Tablets were statistically superior to placebo in improving depressive symptoms as measured by the following: the mean change from baseline in the Hamilton Depression Rating Scale (HDRS) total score at Week 12, the mean change from baseline in the Hamilton Depressed Mood item score at Week 12, and the mean change from baseline in the Clinical Global Impression (CGI)–Severity of Illness score.
Long-term efficacy of paroxetine for treatment of MDD in outpatients was established with one randomized withdrawal study with immediate-release paroxetine. Patients who responded to immediate-release paroxetine (HDRS total score <8) during an initial 8-week open-label treatment phase were then randomized to continue immediate-release paroxetine or placebo, for up to 1 year. Patients treated with immediate-release paroxetine demonstrated a statistically significant lower relapse rate during the withdrawal phase (15%) compared to those on placebo (39%). Effectiveness was similar for male and female patients.
5.5 Increased Risk of Bleeding
Drugs that interfere with serotonin reuptake inhibition, including Paroxetine Extended-Release Tablets, increase the risk of bleeding events. Concomitant use of aspirin, nonsteroidal anti-inflammatory drugs (NSAIDS), other antiplatelet drugs, warfarin, and other anticoagulants may add to this risk. Case reports and epidemiological studies (case-control and cohort design) have demonstrated an association between use of drugs that interfere with serotonin reuptake and the occurrence of gastrointestinal bleeding. Based on data from the published observational studies, exposure to SSRIs, particularly in the month before delivery, has been associated with a less than 2-fold increase in the risk of postpartum hemorrhage [see Use in Specific Populations (8.1)]. Bleeding events related to drugs that interfere with serotonin reuptake have ranged from ecchymoses, hematomas, epistaxis, and petechiae to life-threatening hemorrhages.
Inform patients about the increased risk of bleeding associated with the concomitant use of Paroxetine Extended-Release Tablets and antiplatelet agents or anticoagulants. For patients taking warfarin, carefully monitor the international normalized ratio.
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
Safety data for Paroxetine Extended-Release Tablets is from 11 short-term, placebo-controlled clinical trials including 3 studies in patients with major depressive disorder (MDD) (Studies 1, 2, and 3), 3 studies in patients with panic disorder (PD) (Studies 4, 5, and 6), 1 study in patients with social anxiety disorder (SAD) (Study 7), and 4 studies in female patients with premenstrual dysphoric disorder (PMDD) (Studies 8, 9, 10, and 11) [see Clinical Studies (14)]. These 11 trials included 1627 patients treated with Paroxetine Extended-Release Tablets.
- Studies 1 and 2 were 12-week studies that enrolled patients 18 to 65 years old who received Paroxetine Extended-Release Tablets at doses ranging from 25 mg to 62.5 mg once daily. Study 3 was a 12-week study in patients 60 to 88 years old who received Paroxetine Extended-Release Tablets at doses ranging from 12.5 mg to 50 mg once daily.
- Studies 4, 5, and 6 were 10-week studies in patients 19 to 72 years old who received Paroxetine Extended-Release Tablets at doses ranging from 12.5 mg to 75 mg once daily.
- Study 7 was a 12-week study that enrolled adult patients who received Paroxetine Extended-Release Tablets at doses ranging from 12.5 mg to 37.5 mg once daily.
- Studies 8, 9, and 10 were 12-week, placebo-controlled trials in female patients 18 to 46 years old who received Paroxetine Extended-Release Tablets at doses of 12.5 mg or 25 mg once daily. Study 11 was a 12-week placebo-controlled trial in patients 18 to 46 years old who received Paroxetine Extended-Release Tablets 2 weeks prior to the onset of menses (luteal phase dosing) at doses of 12.5 mg or 25 mg once daily.
17 Patient Counseling Information (17 PATIENT COUNSELING INFORMATION)
Advise the patient to read the FDA-approved patient labeling (Medication Guide).
8.6 Renal And/or Hepatic Impairment (8.6 Renal and/or Hepatic Impairment)
Increased plasma concentrations of paroxetine occur in patients with renal and hepatic impairment. The initial dosage of Paroxetine Extended-Release Tablets should be reduced in patients with severe renal impairment and patients with severe hepatic impairment [see Dosage and Administration (2.5) and Clinical Pharmacology (12.3)].
14.4 Premenstrual Dysphoric Disorder
The effectiveness of Paroxetine Extended-Release Tablets for the treatment of Premenstrual Dysphoric Disorder (PMDD) utilizing a continuous dosing regimen has been established in 2 placebo-controlled trials in female patients ages 18 to 46 (Studies 8 and 9 [N=672]). Patients in these trials met DSM-IV criteria for PMDD. Of 1,030 patients including Study 10, who were treated with daily doses of Paroxetine Extended-Release Tablets 12.5 or 25 mg/day, or placebo continuously throughout the menstrual cycle for a period of 3 menstrual cycles, the mean duration of the PMDD symptoms was approximately 11 ± 7 years. Patients on systemic hormonal contraceptives were excluded from these trials. Therefore, the efficacy of Paroxetine Extended-Release Tablets in combination with systemic (including oral) hormonal contraceptives for the continuous daily treatment of PMDD is unknown.
The VAS score is a patient-rated instrument that mirrors the diagnostic criteria of PMDD as identified in the DSM-IV, and includes assessments for mood, physical symptoms, and other symptoms associated with PMDD. In Studies 8 and 9, 12.5 mg/day and 25 mg/day of Paroxetine Extended-Release Tablets were statistically significantly more effective than placebo as measured by change from baseline to Month 3 on the luteal phase VAS score.
In an additional study employing luteal phase dosing (Study 11), patients (N = 366) were treated for the 2 weeks prior to the onset of menses with 12.5 or 25 mg/day of Paroxetine Extended-Release Tablets or placebo for a period of 3 months. In this trial,12.5 mg/day and 25 mg/day of Paroxetine Extended-Release Tablets, as luteal phase dosing, was statistically significantly more effective than placebo as measured by change from baseline to luteal phase VAS score at Month 3.
There is insufficient information to determine the effect of race or age on outcome in Studies 8, 9, 10, and 11.
16 How Supplied/storage and Handling (16 HOW SUPPLIED/STORAGE AND HANDLING)
Paroxetine Extended-Release Tablets, USP are supplied as: a round, extended-release tablet as follows:
25 mg Brown enteric coated, round, bi-convex tablets, with one side debossed 2272 and the other side blank:
- NDC 63629-9499-01 Bottles of 30
Store at 20°C to 25°C (68°F to 77°F) [see USP Controlled Room Temperature].
Repackaged/Relabeled by:
Bryant Ranch Prepack, Inc.
Burbank, CA 91504
5.6 Activation of Mania Or Hypomania (5.6 Activation of Mania or Hypomania)
In patients with bipolar disorder, treating a depressive episode with Paroxetine Extended-Release Tablets or another antidepressant may precipitate a mixed/manic episode. During controlled clinical trials of immediate-release paroxetine hydrochloride, hypomania or mania occurred in approximately 1% of paroxetine-treated unipolar patients compared to 1.1% of active-control and 0.3% of placebo-treated unipolar patients. Prior to initiating treatment with Paroxetine Extended-Release Tablets, screen patients for any personal or family history of bipolar disorder, mania, or hypomania.
5.11 Reduction of Efficacy of Tamoxifen
Some studies have shown that the efficacy of tamoxifen, as measured by the risk of breast cancer relapse/mortality, may be reduced with concomitant use of paroxetine as a result of paroxetine's irreversible inhibition of CYP2D6 and lower blood levels of tamoxifen [see Drug Interactions (7.1)]. One study suggests that the risk may increase with longer duration of coadministration. However, other studies have failed to demonstrate such a risk. When tamoxifen is used for the treatment or prevention of breast cancer, prescribers should consider using an alternative antidepressant with little or no CYP2D6 inhibition.
Warning: Suicidal Thoughts and Behaviors (WARNING: SUICIDAL THOUGHTS AND BEHAVIORS)
Antidepressants increased the risk of suicidal thoughts and behaviors in pediatric and young adult patients in short-term studies. Closely monitor all antidepressant-treated patients for clinical worsening, and for emergence of suicidal thoughts and behaviors [see Warnings and Precautions (5.1)]. Paroxetine Extended-Release Tablets are not approved for use in pediatric patients [see Use in Specific Populations (8.4)].
2.1 Important Administration Instructions
Administer Paroxetine Extended-Release Tablets as a single daily dose in the morning, with or without food. Swallow tablets whole and do not chew or crush.
5.3 Drug Interactions Leading to Qt Prolongation (5.3 Drug Interactions Leading to QT Prolongation)
The CYP2D6 inhibitory properties of paroxetine can elevate plasma levels of thioridazine and pimozide. Since thioridazine and pimozide given alone produce prolongation of the QTc interval and increase the risk of serious ventricular arrhythmias, the use of Paroxetine Extended-Release Tablets is contraindicated in combination with thioridazine and pimozide [see Contraindications (4), Drug Interactions (7), Clinical Pharmacology (12.3)].
2.3 Dosage in Patients With Premenstrual Dysphoric Disorder (2.3 Dosage in Patients with Premenstrual Dysphoric Disorder)
The recommended starting dosage in women with PMDD is 12.5 mg per day. Paroxetine Extended-Release Tablets may be administered either continuously (every day throughout the menstrual cycle) or intermittently (only during the luteal phase of the menstrual cycle, i.e., starting the daily dosage 14 days prior to the anticipated onset of menstruation and continuing through the onset of menses). Intermittent dosing is repeated with each new cycle.
In patients with an inadequate response, the dosage may be increased to the maximum recommended dosage of 25 mg per day, depending on tolerability. Institute dosage adjustments at intervals of at least 1 week.
5.1 Suicidal Thoughts and Behaviors in Adolescents and Young Adults
In pooled analyses of placebo-controlled trials of antidepressant drugs (SSRIs and other antidepressant classes) that included approximately 77,000 adult patients and 4,500 pediatric patients, the incidence of suicidal thoughts and behaviors in antidepressant-treated patients age 24 years and younger was greater than in placebo-treated patients. There was considerable variation in risk of suicidal thoughts and behaviors among drugs, but there was an increased risk identified in young patients for most drugs studied. There were differences in absolute risk of suicidal thoughts and behaviors across the different indications, with the highest incidence in patients with MDD. The drug-placebo differences in the number of cases of suicidal thoughts and behaviors per 1000 patients treated are provided in Table 2.
| Age Range | Drug-Placebo Difference in Number of Patients of Suicidal Thoughts and Behaviors per 1,000 Patients Treated |
|---|---|
| Increases Compared to Placebo | |
| <18 years old | 14 additional patients |
| 18 to 24 years old | 5 additional patients |
| Decreases Compared to Placebo | |
| 25 to 64 years old | 1 fewer patient |
| ≥65 years old | 6 fewer patients |
It is unknown whether the risk of suicidal thoughts and behaviors in children, adolescents, and young adults extends to longer-term use, i.e., beyond four months. However, there is substantial evidence from placebo-controlled maintenance trials in adults with MDD that antidepressants delay the recurrence of depression and that depression itself is a risk factor for suicidal thoughts and behaviors.
Monitor all antidepressant-treated patients for any indication for clinical worsening and emergence of suicidal thoughts and behaviors, especially during the initial few months of drug therapy, and at times of dosage changes. Counsel family members or caregivers of patients to monitor for changes in behavior and to alert the healthcare provider. Consider changing the therapeutic regimen, including possibly discontinuing Paroxetine Extended-Release Tablets, in patients whose depression is persistently worse, or who are experiencing emergent suicidal thoughts or behaviors.
2.7 Discontinuation of Treatment With Paroxetine Extended Release Tablets (2.7 Discontinuation of Treatment with Paroxetine Extended-Release Tablets)
Adverse reactions may occur upon discontinuation of Paroxetine Extended-Release Tablets [see Warnings and Precautions (5.7)]. Gradually reduce the dosage rather than stopping Paroxetine Extended-Release Tablets abruptly whenever possible.
2.6 Switching Patients to Or From A Monoamine Oxidase Inhibitor Antidepressant (2.6 Switching Patients to or from a Monoamine Oxidase Inhibitor Antidepressant)
At least 14 days must elapse between discontinuation of a monoamine oxidase inhibitor (MAOI) antidepressant and initiation of Paroxetine Extended-Release Tablets. In addition, at least 14 days must elapse after stopping Paroxetine Extended-Release Tablets before starting an MAOI antidepressant [see Contraindications (4), Warnings and Precautions (5.2)].
2.4 Screen for Bipolar Disorder Prior to Starting Paroxetine Extended Release Tablets (2.4 Screen for Bipolar Disorder Prior to Starting Paroxetine Extended-Release Tablets)
Prior to initiating treatment with Paroxetine Extended-Release Tablets or another antidepressant, screen patients for a personal or family history of bipolar disorder, mania, or hypomania [see Warnings and Precautions (5.6)].
7.1 Clinically Significant Drug Interactions With Paroxetine Extended Release Tablets (7.1 Clinically Significant Drug Interactions with Paroxetine Extended-Release Tablets)
Table 6 includes clinically significant drug interactions with Paroxetine Extended-Release Tablets
| Monoamine Oxidase Inhibitors (MAOIs) | |
| Clinical Impact | The concomitant use of SSRIs, including Paroxetine Extended-Release Tablets, and MAOIs increases the risk of serotonin syndrome. |
| Intervention | Paroxetine Extended-Release Tablets are contraindicated in patients taking MAOIs, including MAOIs such as linezolid or intravenous methylene blue [see Dosage and Administration (2.6), Contraindications (4), Warnings and Precautions (5.2)]. |
| Examples | selegiline, tranylcypromine, isocarboxazid, phenelzine, linezolid, methylene blue |
| Pimozide and Thioridazine | |
| Clinical Impact | Increased plasma concentrations of pimozide and thioridazine, drugs with a narrow therapeutic index, may increase the risk of QTc prolongation and ventricular arrhythmias. |
| Intervention | Paroxetine Extended-Release Tablets are contraindicated in patients taking pimozide or thioridazine [see Contraindications (4)]. |
| Other Serotonergic Drugs | |
| Clinical Impact | The concomitant use of serotonergic drugs with Paroxetine Extended-Release Tablets increases the risk of serotonin syndrome. |
| Intervention | Monitor patients for signs and symptoms of serotonin syndrome, particularly during treatment initiation and dosage increases. If serotonin syndrome occurs, consider discontinuation of Paroxetine Extended-Release Tablets and/or concomitant serotonergic drugs [see Warnings and Precautions (5.2)]. |
| Examples | Other SSRIs, SNRIs, triptans, tricyclic antidepressants, opioids, lithium, tryptophan, buspirone, St. John's Wort |
| Drugs that Interfere with Hemostasis (antiplatelet agents and anticoagulants) | |
| Clinical Impact | The concurrent use of an antiplatelet agent or anticoagulant with Paroxetine Extended-Release Tablets may potentiate the risk of bleeding. |
| Intervention | Inform patients of the increased risk of bleeding associated with the concomitant use of Paroxetine Extended-Release Tablets and antiplatelet agents and anticoagulants. For patients taking warfarin, carefully monitor the international normalized ratio [see Warnings and Precautions (5.5)]. |
| Examples | aspirin, clopidogrel, heparin, warfarin |
| Drugs Highly Bound to Plasma Protein | |
| Clinical Impact | Paroxetine Extended-Release Tablets are highly bound to plasma protein. The concomitant use of Paroxetine Extended-Release Tablets with another drug that is highly bound to plasma protein may increase free concentrations of Paroxetine Extended-Release Tablets or other tightly-bound drugs in plasma. |
| Intervention | Monitor for adverse reactions and reduce dosage of Paroxetine Extended-Release Tablets or other protein-bound drugs as warranted. |
| Examples | warfarin |
| Drugs Metabolized by CYP2D6 | |
| Clinical Impact | Paroxetine Extended-Release Tablets are a CYP2D6 inhibitor [see Clinical Pharmacology (12.3)]. The concomitant use of Paroxetine Extended-Release Tablets with a CYP2D6 substrate may increase the exposure of the CYP2D6 substrate. |
| Intervention | Decrease the dosage of a CYP2D6 substrate if needed with concomitant Paroxetine Extended-Release Tablets use. Conversely, an increase in dosage of a CYP2D6 substrate may be needed if Paroxetine Extended-Release Tablets are discontinued. |
| Examples | propafenone, flecainide, atomoxetine, desipramine, dextromethorphan, metoprolol, nebivolol, perphenazine, tolterodine, venlafaxine, risperidone. |
| Tamoxifen | |
| Clinical Impact | Concomitant use of tamoxifen with Paroxetine Extended-Release Tablets may lead to reduced plasma concentrations of the active metabolite (endoxifen) and reduced efficacy of tamoxifen. |
| Intervention | Consider use of an alternative antidepressant little or no CYP2D6 inhibition [see Warnings and Precautions (5.11)]. |
| Fosamprenavir/Ritonavir | |
| Clinical Impact | Co-administration of fosamprenavir/ritonavir with paroxetine significantly decreased plasma levels of paroxetine. |
| Intervention | Any dose adjustment should be guided by clinical effect (tolerability and efficacy). |
2.2 Dosage in Patients With Major Depressive Disorder, Panic Disorder, and Social Anxiety Disorder (2.2 Dosage in Patients with Major Depressive Disorder, Panic Disorder, and Social Anxiety Disorder)
The recommended initial dosage and maximum dosage of Paroxetine Extended-Release Tablets in patients with MDD, PD, and SAD are presented in Table 1.
In patients with an inadequate response, dosage may be increased in increments of 12.5 mg per day at intervals of at least 1 week, depending on tolerability.
| Indication | Starting Dose | Maximum Dose |
|---|---|---|
| MDD | 25 mg | 62.5 mg |
| PD | 12.5 mg | 75 mg |
| SAD | 12.5 mg | 37.5 mg |
2.5 Dosage Modifications for Elderly Patients, Patients With Severe Renal Impairment, and Patients With Severe Hepatic Impairment (2.5 Dosage Modifications for Elderly Patients, Patients with Severe Renal Impairment, and Patients with Severe Hepatic Impairment)
The recommended initial dose of Paroxetine Extended-Release Tablets is 12.5 mg per day for elderly patients, patients with severe renal impairment, and patients with severe hepatic impairment. Reduce initial dose and increase up-titration intervals if necessary. Dosage should not exceed 50 mg per day for MDD or PD and should not exceed 37.5 mg per day for SAD [see Use in Specific Populations (8.5, 8.6)].
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:48:09.135106 · Updated: 2026-03-14T22:29:06.951873