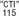glimepiride tablets, usp. these highlights do not include all the information needed to use glimepiride safely and effectively. see full pr…
4f83e203-c102-47fa-bb8e-4fc5541e0d6f
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Indications and Usage
Glimepiride Tablet are indicated as an adjunct to diet and exercise to improve glycemic control in adults with type 2 diabetes mellitus [see Clinical Studies ( 14.1 ) ]. Limitations of Use Glimepiride should not be used for the treatment of type 1 diabetes mellitus or diabetic ketoacidosis, as it would not be effective in these settings.
Dosage and Administration
Recommended starting dose is 1 or 2 mg once daily. Increase in 1 or 2 mg increments no more frequently than every 1-2 weeks based on glycemic response. Maximum recommended dose is 8 mg once daily ( 2.1 ). Administer with breakfast or first meal of the day ( 2.1 ). Use 1 mg starting dose and titrate slowly in patients at increased risk for hypoglycemia (e.g., elderly, patients with renal impairment) ( 2.1 ).
Contraindications
Glimepiride Tablets USP are contraindicated in patients with a history of a hypersensitivity reaction to: Glimepiride or any of the product's ingredients [ see Warnings and Precautions ( 5.2 ) ]. Sulfonamide derivatives: Patients who have developed an allergic reaction to sulfonamide derivatives may develop an allergic reaction to glimepiride. Do not use glimepiride in patients who have a history of an allergic reaction to sulfonamide derivatives.
Warnings and Precautions
Hypoglycemia: May be severe. Ensure proper patient selection, dosing, and instructions, particularly in at-risk populations (e.g., elderly, renally impaired) and when used with other anti-diabetic medications ( 5.1 ). Hypersensitivity Reactions: Postmarketing reports include anaphylaxis, angioedema and Stevens-Johnson Syndrome. Promptly discontinue glimepiride, assess for other causes, institute appropriate monitoring and treatment, and initiate alternative treatment for diabetes ( 5.2 ). Hemolytic Anemia: Can occur if glucose 6-phosphate dehydrogenase (G6PD) deficient. Consider a non-sulfonylurea alternative. ( 5.3 ). Potential Increased Risk of Cardiovascular Mortality with Sulfonylureas: Inform patient of risks, benefits and treatment alternatives ( 5.4 ). Macrovascular Outcomes: No clinical studies establishing conclusive evidence of macrovascular risk reduction with glimepiride or any other anti-diabetic drug ( 5.5 ).
Adverse Reactions
The following serious adverse reactions are discussed in more detail below and elsewhere in the labeling: Hypoglycemia [see Warnings and Precautions ( 5.1 ) ] Hemolytic anemia [see Warnings and Precautions ( 5.3 ) ]
Drug Interactions
Certain medications may affect glucose metabolism, requiring glimepiride dose adjustment and close monitoring of blood glucose ( 7.1 ). Miconazole: Severe hypoglycemia can occur when glimepiride and oral miconazole are used concomitantly. ( 7.2 ). Cytochrome P450 2C9 interactions: Inhibitors and inducers of cytochrome P450 2C9 may affect glycemic control by altering glimepiride plasma concentrations ( 7.3 ). Colesevelam: Coadministration may reduce glimepiride absorption. Glimepiride should be administered at least 4 hours prior to colesevelam ( 2.1 , 7.4 ).
How Supplied
Glimepiride Tablets are available in the following strengths and package sizes: 1 mg (Scored white to off-white, round imprinted with "CTI 115" on one side) are supplied in: Bottles of 100 . . . . . . . . .(NDC 60429-918-01) 2 mg (Scored white to off-white, round imprinted with "CTI 116" on one side) are supplied in: Bottles of 100 . . . . . . . . .(NDC 60429-919-01) 4 mg (Scored white to off-white, round imprinted with "CTI 117" on one side) are supplied in: Bottles of 100 . . . . . . . . .(NDC 60429-920-01) Store at 25ºC (77ºF); excursions permitted to 20ºC to 25ºC (68º to 77ºF) (See USP Controlled Room Temperature). Dispense in well-closed containers with safety closures.
Storage and Handling
Glimepiride Tablets are available in the following strengths and package sizes: 1 mg (Scored white to off-white, round imprinted with "CTI 115" on one side) are supplied in: Bottles of 100 . . . . . . . . .(NDC 60429-918-01) 2 mg (Scored white to off-white, round imprinted with "CTI 116" on one side) are supplied in: Bottles of 100 . . . . . . . . .(NDC 60429-919-01) 4 mg (Scored white to off-white, round imprinted with "CTI 117" on one side) are supplied in: Bottles of 100 . . . . . . . . .(NDC 60429-920-01) Store at 25ºC (77ºF); excursions permitted to 20ºC to 25ºC (68º to 77ºF) (See USP Controlled Room Temperature). Dispense in well-closed containers with safety closures.
Description
Glimepiride Tablet are indicated as an adjunct to diet and exercise to improve glycemic control in adults with type 2 diabetes mellitus [see Clinical Studies ( 14.1 ) ]. Limitations of Use Glimepiride should not be used for the treatment of type 1 diabetes mellitus or diabetic ketoacidosis, as it would not be effective in these settings.
Medication Information
Warnings and Precautions
Hypoglycemia: May be severe. Ensure proper patient selection, dosing, and instructions, particularly in at-risk populations (e.g., elderly, renally impaired) and when used with other anti-diabetic medications ( 5.1 ). Hypersensitivity Reactions: Postmarketing reports include anaphylaxis, angioedema and Stevens-Johnson Syndrome. Promptly discontinue glimepiride, assess for other causes, institute appropriate monitoring and treatment, and initiate alternative treatment for diabetes ( 5.2 ). Hemolytic Anemia: Can occur if glucose 6-phosphate dehydrogenase (G6PD) deficient. Consider a non-sulfonylurea alternative. ( 5.3 ). Potential Increased Risk of Cardiovascular Mortality with Sulfonylureas: Inform patient of risks, benefits and treatment alternatives ( 5.4 ). Macrovascular Outcomes: No clinical studies establishing conclusive evidence of macrovascular risk reduction with glimepiride or any other anti-diabetic drug ( 5.5 ).
Indications and Usage
Glimepiride Tablet are indicated as an adjunct to diet and exercise to improve glycemic control in adults with type 2 diabetes mellitus [see Clinical Studies ( 14.1 ) ]. Limitations of Use Glimepiride should not be used for the treatment of type 1 diabetes mellitus or diabetic ketoacidosis, as it would not be effective in these settings.
Dosage and Administration
Recommended starting dose is 1 or 2 mg once daily. Increase in 1 or 2 mg increments no more frequently than every 1-2 weeks based on glycemic response. Maximum recommended dose is 8 mg once daily ( 2.1 ). Administer with breakfast or first meal of the day ( 2.1 ). Use 1 mg starting dose and titrate slowly in patients at increased risk for hypoglycemia (e.g., elderly, patients with renal impairment) ( 2.1 ).
Contraindications
Glimepiride Tablets USP are contraindicated in patients with a history of a hypersensitivity reaction to: Glimepiride or any of the product's ingredients [ see Warnings and Precautions ( 5.2 ) ]. Sulfonamide derivatives: Patients who have developed an allergic reaction to sulfonamide derivatives may develop an allergic reaction to glimepiride. Do not use glimepiride in patients who have a history of an allergic reaction to sulfonamide derivatives.
Adverse Reactions
The following serious adverse reactions are discussed in more detail below and elsewhere in the labeling: Hypoglycemia [see Warnings and Precautions ( 5.1 ) ] Hemolytic anemia [see Warnings and Precautions ( 5.3 ) ]
Drug Interactions
Certain medications may affect glucose metabolism, requiring glimepiride dose adjustment and close monitoring of blood glucose ( 7.1 ). Miconazole: Severe hypoglycemia can occur when glimepiride and oral miconazole are used concomitantly. ( 7.2 ). Cytochrome P450 2C9 interactions: Inhibitors and inducers of cytochrome P450 2C9 may affect glycemic control by altering glimepiride plasma concentrations ( 7.3 ). Colesevelam: Coadministration may reduce glimepiride absorption. Glimepiride should be administered at least 4 hours prior to colesevelam ( 2.1 , 7.4 ).
Storage and Handling
Glimepiride Tablets are available in the following strengths and package sizes: 1 mg (Scored white to off-white, round imprinted with "CTI 115" on one side) are supplied in: Bottles of 100 . . . . . . . . .(NDC 60429-918-01) 2 mg (Scored white to off-white, round imprinted with "CTI 116" on one side) are supplied in: Bottles of 100 . . . . . . . . .(NDC 60429-919-01) 4 mg (Scored white to off-white, round imprinted with "CTI 117" on one side) are supplied in: Bottles of 100 . . . . . . . . .(NDC 60429-920-01) Store at 25ºC (77ºF); excursions permitted to 20ºC to 25ºC (68º to 77ºF) (See USP Controlled Room Temperature). Dispense in well-closed containers with safety closures.
How Supplied
Glimepiride Tablets are available in the following strengths and package sizes: 1 mg (Scored white to off-white, round imprinted with "CTI 115" on one side) are supplied in: Bottles of 100 . . . . . . . . .(NDC 60429-918-01) 2 mg (Scored white to off-white, round imprinted with "CTI 116" on one side) are supplied in: Bottles of 100 . . . . . . . . .(NDC 60429-919-01) 4 mg (Scored white to off-white, round imprinted with "CTI 117" on one side) are supplied in: Bottles of 100 . . . . . . . . .(NDC 60429-920-01) Store at 25ºC (77ºF); excursions permitted to 20ºC to 25ºC (68º to 77ºF) (See USP Controlled Room Temperature). Dispense in well-closed containers with safety closures.
Description
Glimepiride Tablet are indicated as an adjunct to diet and exercise to improve glycemic control in adults with type 2 diabetes mellitus [see Clinical Studies ( 14.1 ) ]. Limitations of Use Glimepiride should not be used for the treatment of type 1 diabetes mellitus or diabetic ketoacidosis, as it would not be effective in these settings.
Section 42229-5
All sulfonylureas, including glimepiride, can cause severe hypoglycemia [see Adverse Reactions ( 6.1) ]. The patient's ability to concentrate and react may be impaired as a result of hypoglycemia. These impairments may present a risk in situations where these abilities are especially important, such as driving or operating other machinery. Severe hypoglycemia can lead to unconsciousness or convulsions and may result in temporary or permanent impairment of brain function or death.
Patients must be educated to recognize and manage hypoglycemia. Use caution when initiating and increasing glimepiride doses in patients who may be predisposed to hypoglycemia (e.g., the elderly, patients with renal impairment, patients on other anti- diabetic medications). Debilitated or malnourished patients, and those with adrenal, pituitary, or hepatic impairment are particularly susceptible to the hypoglycemic action of glucose-lowering medications. Hypoglycemia is also more likely to occur when caloric intake is deficient, after severe or prolonged exercise, or when alcohol is ingested.
Early warning symptoms of hypoglycemia may be different or less pronounced in patients with autonomic neuropathy, the elderly, and in patients who are taking beta-adrenergic blocking medications or other sympatholytic agents. These situations may result in severe hypoglycemia before the patient is aware of the hypoglycemia.
Section 51945-4
Principal Display Panel – 1 mg Bottle Label
NDC 60429-918-01
Glimepiride
Tablets USP
1 mg
Once a day
Rx only
100 Tablets
10 Overdosage
An overdosage of glimepiride, as with other sulfonylureas, can produce severe hypoglycemia. Mild episodes of hypoglycemia can be treated with oral glucose. Severe hypoglycemic reactions constitute medical emergencies requiring immediate treatment. Severe hypoglycemia with coma, seizure, or neurological impairment can be treated with glucagon or intravenous glucose. Continued observation and additional carbohydrate intake may be necessary because hypoglycemia may recur after apparent clinical recovery [see Warnings and Precautions ( 5.1) ].
8.2 Lactation
Risk Summary
Breastfed infants of lactating women using Glimepiride should be monitored for symptoms of hypoglycemia (see Clinical Considerations). It is not known whether Glimepiride is excreted in human milk and there are no data on the effects of Glimepiride on milk production. Glimepiride is present in rat milk [see Data]. The developmental and health benefits of breastfeeding should be considered along with the mother's clinical need for Glimepiride and any potential adverse effects on the breastfed child from Glimepiride or from the underlying maternal condition.
Clinical Considerations
Monitoring for adverse reactions
Monitor breastfed infants for signs of hypoglycemia (e.g., jitters, cyanosis, apnea, hypothermia, excessive sleepiness, poor feeding, seizures).
Data
During prenatal and postnatal studies in rats, significant concentrations of glimepiride were present in breast milk and the serum of the pups.
Offspring of rats exposed to high levels of glimepiride during pregnancy and lactation developed skeletal deformities consisting of shortening, thickening and bending of the humerus during the postnatal period. These skeletal deformations were determined to be the result of nursing from mothers exposed to glimepiride.
11 Description
Glimepiride Tablets are an oral sulfonylurea that contains the active ingredient glimepiride. Chemically, glimepiride is identified as 1-[[p-[2-(3-ethyl-4-methyl-2-oxo-3-pyrroline-1-carboxamido) ethyl]phenyl]sulfonyl]-3-(trans-4-methylcyclohexyl)urea (C 24H 34N 4O 5S) with a molecular weight of 490.62. Glimepiride is a white to yellowish-white, crystalline, odorless to practically odorless powder and is practically insoluble in water.
The structural formula is:
Glimepiride Tablets contain the active ingredient glimepiride and the following inactive ingredients: lactose monohydrate, magnesium stearate, microcrystalline cellulose, poloxamer, povidone, and sodium starch glycolate.
7.2 Miconazole
A potential interaction between oral miconazole and sulfonylureas leading to severe hypoglycemia has been reported. Whether this interaction also occurs with other dosage forms of miconazole is not known.
14.1 Monotherapy
A total of 304 patients with type 2 diabetes already treated with sulfonylurea therapy participated in a 14-week, multicenter, randomized, double-blind, placebo-controlled trial evaluating the safety and efficacy of Glimepiride monotherapy. Patients discontinued their sulfonylurea therapy then entered a 3-week placebo washout period followed by randomization into 1 of 4 treatment groups: placebo (n=74), glimepiride 1 mg (n=78), glimepiride 4 mg (n=76) and glimepiride 8 mg (n=76). All patients randomized to glimepiride started 1 mg daily. Patients randomized to glimepiride 4 mg or 8 mg had blinded, forced titration of the glimepiride dose at weekly intervals, first to 4 mg and then to 8 mg, as long as the dose was tolerated, until the randomized dose was reached. Patients randomized to the 4 mg dose reached the assigned dose at Week 2. Patients randomized to the 8 mg dose reached the assigned dose at Week 3. Once the randomized dose level was reached, patients were to be maintained at that dose until Week 14. Approximately 66% of the placebo-treated patients completed the trial compared to 81% of patients treated with glimepiride 1 mg and 92% of patients treated with glimepiride 4 mg or 8 mg. Compared to placebo, treatment with glimepiride 1 mg, 4 mg and 8 mg daily provided statistically significant improvements in HbA 1Ccompared to placebo (Table 3)
|
Placebo (N=74) |
Glimepiride | |||
|
1 mg (N=78) |
4 mg (N=76) |
8 mg (N=76) |
||
| HbA 1C(%) | ||||
| n=59 | n=65 | n=65 | n=68 | |
| Baseline (mean) | 8.0 | 7.9 | 7.9 | 8.0 |
|
Change from Baseline (adjusted mean b) |
1.5 | 0.3 | -0.3 | -0.4 |
|
Difference from Placebo (adjusted mean b) 95% confidence interval |
-1.2* (-1.5, -0.8) |
-1.8* (-2.1, -1.4) |
-1.8* (-2.2, -1.5) |
|
| Mean Baseline Weight (kg) | ||||
| n=67 | n=76 | n=57 | n=73 | |
| Baseline (mean) | 85.7 | 84.3 | 86.1 | 85.5 |
|
Change from Baseline (adjusted mean b) |
-2.3 | -0.2 | 0.5 | 1.0 |
|
Difference from Placebo (adjusted mean b) 95% confidence interval |
2.0* (1.4, 2.7) |
2.8* (2.1, 3.5) |
3.2* (2.5, 4.0) |
|
|
aIntent-to-treat population using last observation on study bLeast squares mean adjusted for baseline value * p≤0.001 |
A total of 249 patients who were treatment-naïve or who had received limited treatment with antidiabetic therapy in the past were randomized to receive 22 weeks of treatment with either Glimepiride (n=123) or placebo (n=126) in a multicenter, randomized, double-blind, placebo-controlled, dose-titration trial. The starting dose of Glimepiride was 1 mg daily and was titrated upward or downward at 2-week intervals to a goal FPG of 90-150 mg/dL. Blood glucose levels for both FPG and PPG were analyzed in the laboratory. Following 10 weeks of dose adjustment, patients were maintained at their optimal dose (1, 2, 3, 4, 6 or 8 mg) for the remaining 12 weeks of the trial.
Treatment with Glimepiride provided statistically significant improvements in HbA
1Cand FPG compared to placebo (Table 4).
|
Placebo (N=126) |
Glimepiride (N=123) |
|
| HbA 1C(%) | n=97 | n=106 |
| Baseline (mean) | 9.1 | 9.3 |
|
Change from Baseline (adjust mean b) |
-1.1* | -2.2* |
|
Difference from Placebo (adjusted mean b) 95% confidence interval |
-1.1* (-1.5, -0.8) |
|
| Body Weight (kg) | n=122 | n=119 |
| Baseline (mean) | 86.5 | 87.1 |
|
Change from Baseline (adjust mean b) |
-0.9 | 1.8 |
|
Difference from Placebo (adjust mean b) 95% confidence interval |
2.7 (1.9, 3.6) |
|
|
aIntent to treat population using last observation on study bLeast squares mean adjusted for baseline value *p≤0.001 |
8.4 Pediatric Use
The pharmacokinetics, efficacy and safety of glimepiride have been evaluated in pediatric patients with type 2 diabetes as described below. Glimepiride is not recommended in pediatric patients because of its adverse effects on body weight and hypoglycemia.
The pharmacokinetics of a 1 mg single dose of glimepiride was evaluated in 30 patients with type 2 diabetes (male = 7; female = 23) between ages 10 and 17 years. The mean (± SD) AUC (0-last)(339±203 ng•hr/mL), Cmax (102±48 ng/mL) and t1/2 (3.1±1.7 hours) for glimepiride were comparable to historical data from adults (AUC ( 0-last) 315±96 ng•hr/mL, Cmax 103±34 ng/mL and t1/2 5.3±4.1 hours).
The safety and efficacy of glimepiride in pediatric patients was evaluated in a single-blind, 24-week trial that randomized 272 patients (8-17 years of age) with type 2 diabetes to glimepiride (n=135) or metformin (n=137). Both treatment-naïve patients (those treated with only diet and exercise for at least 2 weeks prior to randomization) and previously treated patients (those previously treated or currently treated with other oral antidiabetic medications for at least 3 months) were eligible to participate. Patients who were receiving oral antidiabetic agents at the time of study entry discontinued these medications before randomization without a washout period. Glimepiride was initiated at 1 mg, and then titrated up to 2, 4 or 8 mg (mean last dose 4 mg) through Week 12, targeting a self-monitored fasting fingerstick blood glucose < 126 mg/dL. Metformin was initiated at 500 mg twice daily and titrated at Week 12 up to 1000 mg twice daily (mean last dose 1365 mg).
After 24 weeks, the overall mean treatment difference in HbA 1cbetween glimepiride and metformin was 0.2%, favoring metformin (95% confidence interval -0.3% to +0.6%).
Based on these results, the trial did not meet its primary objective of showing a similar reduction in HbA 1cwith glimepiride compared to metformin.
|
* Intent-to-treat population using last-observation-carried-forward for missing data (Glimepiride, n=127; metformin, n=126) |
||
|
+ adjusted for baseline HbA 1Cand Tanner Stage |
||
|
** Difference is Glimepiride – metformin with positive differences favoring metformin |
||
| Metformin | Glimepiride | |
| Treatment-Naïve Patients* | N=69 | N=72 |
| HbA 1C (%) | ||
| Baseline (mean) | 8.2 | 8.3 |
| Change from baseline (adjusted LS mean) + | -1.2 | -1.0 |
| Adjusted Treatment Difference** (95%CI) | 0.2 (-0.3; 0.6) | |
| Previously Treated Patients* | N=57 | N=55 |
| HbA 1C (%) | ||
| Baseline (mean) | 9.0 | 8.7 |
| Change from baseline (adjusted LS mean) + | -0.2 | 0.2 |
| Adjusted Treatment Difference** (95%CI) | 0.4 (-0.4; 1.2) | |
| Body Weight (kg)* | N=126 | N=129 |
| Baseline (mean) | 67.3 | 66.5 |
| Change from baseline (adjusted LS mean)+ | 0.7 | 2.0 |
| Adjusted Treatment Difference** (95% CI) | 1.3 (0.3; 2.3) |
The profile of adverse reactions in pediatric patients treated with glimepiride was similar to that observed in adults [see Adverse Reactions( 6)].
Hypoglycemic events documented by blood glucose values <36 mg/dL were observed in 4% of pediatric patients treated with glimepiride and in 1% of pediatric patients treated with metformin. One patient in each treatment group experienced a severe hypoglycemic episode (severity was determined by the investigator based on observed signs and symptoms).
8.5 Geriatric Use
In clinical trials of glimepiride, 1053 of 3491 patients (30%) were >65 years of age. No overall differences in safety or effectiveness were observed between these patients and younger patients, but greater sensitivity of some older individuals cannot be ruled out.
There were no significant differences in glimepiride pharmacokinetics between patients with type 2 diabetes ≤65 years (n=49) and those >65 years (n=42) [see Clinical Pharmacology ( 12.3) ].
Glimepiride is substantially excreted by the kidney. Elderly patients are more likely to have renal impairment. In addition, hypoglycemia may be difficult to recognize in the elderly [see Dosage and Administration ( 2.1) and Warnings and Precautions ( 5.1) ]. Use caution when initiating glimepiride and increasing the dose of glimepiride in this patient population.
4 Contraindications
Glimepiride Tablets USP are contraindicated in patients with a history of a hypersensitivity reaction to:
- Glimepiride or any of the product's ingredients [ see Warnings and Precautions ( 5.2) ].
- Sulfonamide derivatives: Patients who have developed an allergic reaction to sulfonamide derivatives may develop an allergic reaction to glimepiride. Do not use glimepiride in patients who have a history of an allergic reaction to sulfonamide derivatives.
6 Adverse Reactions
7 Drug Interactions
- Certain medications may affect glucose metabolism, requiring glimepiride dose adjustment and close monitoring of blood glucose ( 7.1).
- Miconazole: Severe hypoglycemia can occur when glimepiride and oral miconazole are used concomitantly. ( 7.2).
- Cytochrome P450 2C9 interactions: Inhibitors and inducers of cytochrome P450 2C9 may affect glycemic control by altering glimepiride plasma concentrations ( 7.3).
- Colesevelam: Coadministration may reduce glimepiride absorption. Glimepiride should be administered at least 4 hours prior to colesevelam ( 2.1, 7.4).
5.3 Hemolytic Anemia
Sulfonylureas can cause hemolytic anemia in patients with glucose 6-phosphate dehydrogenase (G6PD) deficiency. Because glimepiride is a sulfonylurea, use caution in patients with G6PD deficiency and consider the use of a non-sulfonylurea alternative.
There are also postmarketing reports of hemolytic anemia in patients receiving glimepiride who did not have known G6PD deficiency [see Adverse Reactions ( 6.2) ].
8.6 Renal Impairment
To minimize the risk of hypoglycemia, the recommended starting dose of glimepiride is 1 mg daily for all patients with type 2 diabetes and renal impairment [see Dosage and Administration ( 2.1) and Warnings and Precautions ( 5.1) ].
A multiple-dose titration study was conducted in 16 patients with type 2 diabetes and renal impairment using doses ranging from 1 mg to 8 mg daily for 3 months. Baseline creatinine clearance ranged from 10-60 mL/min. The pharmacokinetics of glimepiride were evaluated in the multiple-dose titration study and the results were consistent with those observed in patients enrolled in a single-dose study. In both studies, the relative total clearance of glimepiride increased when kidney function was impaired. Both studies also demonstrated that the elimination of the two major metabolites was reduced in patients with renal impairment [see Clinical Pharmacology ( 12.3) ].
12.2 Pharmacodynamics
In healthy subjects, the time to reach maximal effect (minimum blood glucose concentrations) was approximately 2-3 hours after single oral doses of glimepiride. The effects of glimepiride on HbA 1c, fasting plasma glucose, and post-prandial glucose have been assessed in clinical trials [ see Clinical Studies ( 14) ].
2.1 Recommended Dosing
Glimepiride should be administered with breakfast or the first main meal of the day.
The recommended starting dose of glimepiride is 1 mg or 2 mg once daily. Patients at increased risk for hypoglycemia (e.g., the elderly or patients with renal impairment) should be started on 1 mg once daily [see Warnings and Precautions ( 5.1) and Use in Specific Populations ( 8.5, 8.6) ].
After reaching a daily dose of 2 mg, further dose increases can be made in increments of 1 mg or 2 mg based upon the patient's glycemic response. Uptitration should not occur more frequently than every 1-2 weeks. A conservative titration scheme is recommended for patients at increased risk for hypoglycemia [see Warnings and Precautions ( 5.1) and Use in Specific Populations ( 8.5, 8.6) ].
The maximum recommended dose is 8 mg once daily.
Patients being transferred to glimepiride from longer half-life sulfonylureas (e.g., chlorpropamide) may have overlapping drug effect for 1-2 weeks and should be appropriately monitored for hypoglycemia.
When colesevelam is coadministered with glimepiride, maximum plasma concentration and total exposure to glimepiride is reduced. Therefore, glimepiride should be administered at least 4 hours prior to colesevelam.
1 Indications and Usage
Glimepiride Tablet are indicated as an adjunct to diet and exercise to improve glycemic control in adults with type 2 diabetes mellitus [see Clinical Studies ( 14.1) ].
Limitations of Use
Glimepiride should not be used for the treatment of type 1 diabetes mellitus or diabetic ketoacidosis, as it would not be effective in these settings.
12.1 Mechanism of Action
Glimepiride primarily lowers blood glucose by stimulating the release of insulin from pancreatic beta cells. Sulfonylureas bind to the sulfonylurea receptor in the pancreatic beta-cell plasma membrane, leading to closure of the ATP-sensitive potassium channel, thereby stimulating the release of insulin.
5 Warnings and Precautions
- Hypoglycemia: May be severe. Ensure proper patient selection, dosing, and instructions, particularly in at-risk populations (e.g., elderly, renally impaired) and when used with other anti-diabetic medications ( 5.1).
- Hypersensitivity Reactions: Postmarketing reports include anaphylaxis, angioedema and Stevens-Johnson Syndrome. Promptly discontinue glimepiride, assess for other causes, institute appropriate monitoring and treatment, and initiate alternative treatment for diabetes ( 5.2).
- Hemolytic Anemia: Can occur if glucose 6-phosphate dehydrogenase (G6PD) deficient. Consider a non-sulfonylurea alternative. ( 5.3).
- Potential Increased Risk of Cardiovascular Mortality with Sulfonylureas: Inform patient of risks, benefits and treatment alternatives ( 5.4).
- Macrovascular Outcomes: No clinical studies establishing conclusive evidence of macrovascular risk reduction with glimepiride or any other anti-diabetic drug ( 5.5).
5.5 Macrovascular Outcomes
There have been no clinical studies establishing conclusive evidence of macrovascular risk reduction with glimepiride or any other anti-diabetic drug.
2 Dosage and Administration
- Recommended starting dose is 1 or 2 mg once daily. Increase in 1 or 2 mg increments no more frequently than every 1-2 weeks based on glycemic response. Maximum recommended dose is 8 mg once daily ( 2.1).
- Administer with breakfast or first meal of the day ( 2.1).
- Use 1 mg starting dose and titrate slowly in patients at increased risk for hypoglycemia (e.g., elderly, patients with renal impairment) ( 2.1).
3 Dosage Forms and Strengths
Glimepiride Tablets USP are formulated as tablets of:
-
1 mg (Scored white to off-white, round imprinted with
on one side) -
2 mg (Scored white to off-white, round imprinted with
on one side) -
4 mg (Scored white to off-white, round imprinted with
on one side)
6.2 Postmarketing Experience
The following adverse reactions have been identified during post-approval use of glimepiride. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
- Serious hypersensitivity reactions, including anaphylaxis, angioedema, and Stevens-Johnson Syndrome [see Warnings and Precautions ( 5.2) ]
- Hemolytic anemia in patients with and without G6PD deficiency [see Warnings and Precautions ( 5.3) ]
- Impairment of liver function (e.g. with cholestasis and jaundice), as well as hepatitis, which may progress to liver failure.
- Porphyria cutanea tarda, photosensitivity reactions and allergic vasculitis
- Leukopenia, agranulocytosis, aplastic anemia, and pancytopenia
- Thrombocytopenia (including severe cases with platelet count less than 10,000/μL) and thrombocytopenic purpura
- Hepatic porphyria reactions and disulfiram-like reactions
- Hyponatremia and syndrome of inappropriate antidiuretic hormone secretion (SIADH), most often in patients who are on other medications or who have medical conditions known to cause hyponatremia or increase release of antidiuretic hormone
- Dysgeusia
- Alopecia
8 Use in Specific Populations
5.2 Hypersensitivity Reactions
There have been postmarketing reports of hypersensitivity reactions in patients treated with glimepiride, including serious reactions such as anaphylaxis, angioedema, and Stevens-Johnson Syndrome. If a hypersensitivity reaction is suspected, promptly discontinue glimepiride, assess for other potential causes for the reaction, and institute alternative treatment for diabetes.
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
Approximately 2,800 patients with type 2 diabetes have been treated with glimepiride in the controlled clinical trials. In these trials, approximately 1,700 patients were treated with glimepiride for at least 1 year.
Table 1summarizes adverse events, other than hypoglycemia, that were reported in 11 pooled placebo-controlled trials, whether or not considered to be possibly or probably related to study medication. Treatment duration ranged from 13 weeks to 12 months. Terms that are reported represent those that occurred at an incidence of ≥5% among glimepiride -treated patients and more commonly than in patients who received placebo.
|
*Glimepiride doses ranged from 1-16 mg administered daily |
||
|
†Insufficient information to determine whether any of the accidental injury events were associated with hypoglycemia |
||
|
Glimepiride
N=745 % |
Placebo
N=294 % |
|
| Headache | 8.2 | 7.8 |
| Accidental Injury † | 5.8 | 3.4 |
| Flu Syndrome | 5.4 | 4.4 |
| Nausea | 5.0 | 3.4 |
| Dizziness | 5.0 | 2.4 |
16 How Supplied/storage and Handling
Glimepiride Tablets are available in the following strengths and package sizes:
- 1 mg (Scored white to off-white, round imprinted with "CTI 115" on one side) are supplied in:
Bottles of 100 . . . . . . . . .(NDC 60429-918-01)
- 2 mg (Scored white to off-white, round imprinted with "CTI 116" on one side) are supplied in:
Bottles of 100 . . . . . . . . .(NDC 60429-919-01)
- 4 mg (Scored white to off-white, round imprinted with "CTI 117" on one side) are supplied in:
Bottles of 100 . . . . . . . . .(NDC 60429-920-01)
Store at 25ºC (77ºF); excursions permitted to 20ºC to 25ºC (68º to 77ºF) (See USP Controlled Room Temperature).
Dispense in well-closed containers with safety closures.
7.3 Cytochrome P450 2c9 Interactions
There may be an interaction between glimepiride and inhibitors (e.g., fluconazole) and inducers (e.g., rifampin) of cytochrome P450 2C9. Fluconazole may inhibit the metabolism of glimepiride, causing increased plasma concentrations of glimepiride which may lead to hypoglycemia. Rifampin may induce the metabolism of glimepiride, causing decreased plasma concentrations of glimepiride which may lead to worsening glycemic control.
7.1 Drugs Affecting Glucose Metabolism
A number of medications affect glucose metabolism and may require glimepiride dose adjustment and particularly close monitoring for hypoglycemia or worsening glycemic control.
The following are examples of medications that may increase the glucose-lowering effect of sulfonylureas including glimepiride, increasing the susceptibility to and/or intensity of hypoglycemia: oral anti-diabetic medications, pramlintide acetate, insulin, angiotensin converting enzyme (ACE) inhibitors, H2 receptor antagonists, fibrates, propoxyphene, pentoxifylline, somatostatin analogs, anabolic steroids and androgens, cyclophosphamide, phenyramidol, guanethidine, fluconazole, sulfinpyrazone, tetracyclines, clarithromycin, disopyramide, quinolones, and those drugs that are highly protein-bound, such as fluoxetine, nonsteroidal anti-inflammatory drugs, salicylates, sulfonamides, chloramphenicol, coumarins, probenecid and monoamine oxidase inhibitors. When these medications are administered to a patient receiving glimepiride, monitor the patient closely for hypoglycemia. When these medications are withdrawn from a patient receiving glimepiride, monitor the patient closely for worsening glycemic control.
The following are examples of medications that may reduce the glucose-lowering effect of sulfonylureas including glimepiride, leading to worsening glycemic control: danazol, glucagon, somatropin, protease inhibitors, atypical antipsychotic medications (e.g., olanzapine and clozapine), barbiturates, diazoxide, laxatives, rifampin, thiazides and other diuretics, corticosteroids, phenothiazines, thyroid hormones, estrogens, oral contraceptives, phenytoin, nicotinic acid, sympathomimetics (e.g., epinephrine, albuterol, terbutaline), and isoniazid. When these medications are administered to a patient receiving glimepiride, monitor the patient closely for worsening glycemic control. When these medications are withdrawn from a patient receiving glimepiride, monitor the patient closely for hypoglycemia.
Beta-blockers, clonidine, and reserpine may lead to either potentiation or weakening of glimepiride's glucose-lowering effect.
Both acute and chronic alcohol intake may potentiate or weaken the glucose-lowering action of glimepiride in an unpredictable fashion.
The signs of hypoglycemia may be reduced or absent in patients taking sympatholytic drugs such as beta-blockers, clonidine, guanethidine, and reserpine.
7.4 Concomitant Administration of Colesevelam
Colesevelam can reduce the maximum plasma concentration and total exposure of glimepiride when the two are coadministered. However, absorption is not reduced when glimepiride is administered 4 hours prior to colesevelam. Therefore, glimepiride should be administered at least 4 hours prior to colesevelam.
13.1 Carcinogenesis, Mutagenesis, and Impairment of Fertility
Studies in rats at doses of up to 5000 parts per million (ppm) in complete feed (approximately 340 times the maximum recommended human dose, based on surface area) for 30 months showed no evidence of carcinogenesis. In mice, administration of glimepiride for 24 months resulted in an increase in benign pancreatic adenoma formation that was dose-related and was thought to be the result of chronic pancreatic stimulation. No adenoma formation in mice was observed at a dose of 320 ppm in complete feed, or 46-54 mg/kg body weight/day. This is about 35 times the maximum human recommended dose of 8 mg once daily based on surface area. Glimepiride was non-mutagenic in a battery of in vitro and in vivomutagenicity studies (Ames test, somatic cell mutation, chromosomal aberration, unscheduled DNA synthesis, and mouse micronucleus test).
There was no effect of glimepiride on male mouse fertility in animals exposed up to 2500 mg/kg body weight (>1,700 times the maximum recommended human dose based on surface area). Glimepiride had no effect on the fertility of male and female rats administered up to 4000 mg/kg body weight (approximately 4,000 times the maximum recommended human dose based on surface area).
5.4 Increased Risk of Cardiovascular Mortality With Sulfonylureas
The administration of oral hypoglycemic drugs has been reported to be associated with increased cardiovascular mortality as compared to treatment with diet alone or diet plus insulin. This warning is based on the study conducted by the University Group Diabetes Program (UGDP), a long-term, prospective clinical trial designed to evaluate the effectiveness of glucose-lowering drugs in preventing or delaying vascular complications in patients with non-insulin-dependent diabetes. The study involved 823 patients who were randomly assigned to one of four treatment groups.
UGDP reported that patients treated for 5 to 8 years with diet plus a fixed dose of tolbutamide (1.5 grams per day) had a rate of cardiovascular mortality approximately 2-1/2 times that of patients treated with diet alone. A significant increase in total mortality was not observed, but the use of tolbutamide was discontinued based on the increase in cardiovascular mortality, thus limiting the opportunity for the study to show an increase in overall mortality. Despite controversy regarding the interpretation of these results, the findings of the UGDP study provide an adequate basis for this warning. The patient should be informed of the potential risks and advantages of glimepiride and of alternative modes of therapy.
Although only one drug in the sulfonylurea class (tolbutamide) was included in this study, it is prudent from a safety standpoint to consider that this warning may also apply to other oral hypoglycemic drugs in this class, in view of their close similarities in mode of action and chemical structure.
Structured Label Content
Section 42229-5 (42229-5)
All sulfonylureas, including glimepiride, can cause severe hypoglycemia [see Adverse Reactions ( 6.1) ]. The patient's ability to concentrate and react may be impaired as a result of hypoglycemia. These impairments may present a risk in situations where these abilities are especially important, such as driving or operating other machinery. Severe hypoglycemia can lead to unconsciousness or convulsions and may result in temporary or permanent impairment of brain function or death.
Patients must be educated to recognize and manage hypoglycemia. Use caution when initiating and increasing glimepiride doses in patients who may be predisposed to hypoglycemia (e.g., the elderly, patients with renal impairment, patients on other anti- diabetic medications). Debilitated or malnourished patients, and those with adrenal, pituitary, or hepatic impairment are particularly susceptible to the hypoglycemic action of glucose-lowering medications. Hypoglycemia is also more likely to occur when caloric intake is deficient, after severe or prolonged exercise, or when alcohol is ingested.
Early warning symptoms of hypoglycemia may be different or less pronounced in patients with autonomic neuropathy, the elderly, and in patients who are taking beta-adrenergic blocking medications or other sympatholytic agents. These situations may result in severe hypoglycemia before the patient is aware of the hypoglycemia.
Section 51945-4 (51945-4)
Principal Display Panel – 1 mg Bottle Label
NDC 60429-918-01
Glimepiride
Tablets USP
1 mg
Once a day
Rx only
100 Tablets
10 Overdosage (10 OVERDOSAGE)
An overdosage of glimepiride, as with other sulfonylureas, can produce severe hypoglycemia. Mild episodes of hypoglycemia can be treated with oral glucose. Severe hypoglycemic reactions constitute medical emergencies requiring immediate treatment. Severe hypoglycemia with coma, seizure, or neurological impairment can be treated with glucagon or intravenous glucose. Continued observation and additional carbohydrate intake may be necessary because hypoglycemia may recur after apparent clinical recovery [see Warnings and Precautions ( 5.1) ].
8.2 Lactation
Risk Summary
Breastfed infants of lactating women using Glimepiride should be monitored for symptoms of hypoglycemia (see Clinical Considerations). It is not known whether Glimepiride is excreted in human milk and there are no data on the effects of Glimepiride on milk production. Glimepiride is present in rat milk [see Data]. The developmental and health benefits of breastfeeding should be considered along with the mother's clinical need for Glimepiride and any potential adverse effects on the breastfed child from Glimepiride or from the underlying maternal condition.
Clinical Considerations
Monitoring for adverse reactions
Monitor breastfed infants for signs of hypoglycemia (e.g., jitters, cyanosis, apnea, hypothermia, excessive sleepiness, poor feeding, seizures).
Data
During prenatal and postnatal studies in rats, significant concentrations of glimepiride were present in breast milk and the serum of the pups.
Offspring of rats exposed to high levels of glimepiride during pregnancy and lactation developed skeletal deformities consisting of shortening, thickening and bending of the humerus during the postnatal period. These skeletal deformations were determined to be the result of nursing from mothers exposed to glimepiride.
11 Description (11 DESCRIPTION)
Glimepiride Tablets are an oral sulfonylurea that contains the active ingredient glimepiride. Chemically, glimepiride is identified as 1-[[p-[2-(3-ethyl-4-methyl-2-oxo-3-pyrroline-1-carboxamido) ethyl]phenyl]sulfonyl]-3-(trans-4-methylcyclohexyl)urea (C 24H 34N 4O 5S) with a molecular weight of 490.62. Glimepiride is a white to yellowish-white, crystalline, odorless to practically odorless powder and is practically insoluble in water.
The structural formula is:
Glimepiride Tablets contain the active ingredient glimepiride and the following inactive ingredients: lactose monohydrate, magnesium stearate, microcrystalline cellulose, poloxamer, povidone, and sodium starch glycolate.
7.2 Miconazole
A potential interaction between oral miconazole and sulfonylureas leading to severe hypoglycemia has been reported. Whether this interaction also occurs with other dosage forms of miconazole is not known.
14.1 Monotherapy
A total of 304 patients with type 2 diabetes already treated with sulfonylurea therapy participated in a 14-week, multicenter, randomized, double-blind, placebo-controlled trial evaluating the safety and efficacy of Glimepiride monotherapy. Patients discontinued their sulfonylurea therapy then entered a 3-week placebo washout period followed by randomization into 1 of 4 treatment groups: placebo (n=74), glimepiride 1 mg (n=78), glimepiride 4 mg (n=76) and glimepiride 8 mg (n=76). All patients randomized to glimepiride started 1 mg daily. Patients randomized to glimepiride 4 mg or 8 mg had blinded, forced titration of the glimepiride dose at weekly intervals, first to 4 mg and then to 8 mg, as long as the dose was tolerated, until the randomized dose was reached. Patients randomized to the 4 mg dose reached the assigned dose at Week 2. Patients randomized to the 8 mg dose reached the assigned dose at Week 3. Once the randomized dose level was reached, patients were to be maintained at that dose until Week 14. Approximately 66% of the placebo-treated patients completed the trial compared to 81% of patients treated with glimepiride 1 mg and 92% of patients treated with glimepiride 4 mg or 8 mg. Compared to placebo, treatment with glimepiride 1 mg, 4 mg and 8 mg daily provided statistically significant improvements in HbA 1Ccompared to placebo (Table 3)
|
Placebo (N=74) |
Glimepiride | |||
|
1 mg (N=78) |
4 mg (N=76) |
8 mg (N=76) |
||
| HbA 1C(%) | ||||
| n=59 | n=65 | n=65 | n=68 | |
| Baseline (mean) | 8.0 | 7.9 | 7.9 | 8.0 |
|
Change from Baseline (adjusted mean b) |
1.5 | 0.3 | -0.3 | -0.4 |
|
Difference from Placebo (adjusted mean b) 95% confidence interval |
-1.2* (-1.5, -0.8) |
-1.8* (-2.1, -1.4) |
-1.8* (-2.2, -1.5) |
|
| Mean Baseline Weight (kg) | ||||
| n=67 | n=76 | n=57 | n=73 | |
| Baseline (mean) | 85.7 | 84.3 | 86.1 | 85.5 |
|
Change from Baseline (adjusted mean b) |
-2.3 | -0.2 | 0.5 | 1.0 |
|
Difference from Placebo (adjusted mean b) 95% confidence interval |
2.0* (1.4, 2.7) |
2.8* (2.1, 3.5) |
3.2* (2.5, 4.0) |
|
|
aIntent-to-treat population using last observation on study bLeast squares mean adjusted for baseline value * p≤0.001 |
A total of 249 patients who were treatment-naïve or who had received limited treatment with antidiabetic therapy in the past were randomized to receive 22 weeks of treatment with either Glimepiride (n=123) or placebo (n=126) in a multicenter, randomized, double-blind, placebo-controlled, dose-titration trial. The starting dose of Glimepiride was 1 mg daily and was titrated upward or downward at 2-week intervals to a goal FPG of 90-150 mg/dL. Blood glucose levels for both FPG and PPG were analyzed in the laboratory. Following 10 weeks of dose adjustment, patients were maintained at their optimal dose (1, 2, 3, 4, 6 or 8 mg) for the remaining 12 weeks of the trial.
Treatment with Glimepiride provided statistically significant improvements in HbA
1Cand FPG compared to placebo (Table 4).
|
Placebo (N=126) |
Glimepiride (N=123) |
|
| HbA 1C(%) | n=97 | n=106 |
| Baseline (mean) | 9.1 | 9.3 |
|
Change from Baseline (adjust mean b) |
-1.1* | -2.2* |
|
Difference from Placebo (adjusted mean b) 95% confidence interval |
-1.1* (-1.5, -0.8) |
|
| Body Weight (kg) | n=122 | n=119 |
| Baseline (mean) | 86.5 | 87.1 |
|
Change from Baseline (adjust mean b) |
-0.9 | 1.8 |
|
Difference from Placebo (adjust mean b) 95% confidence interval |
2.7 (1.9, 3.6) |
|
|
aIntent to treat population using last observation on study bLeast squares mean adjusted for baseline value *p≤0.001 |
8.4 Pediatric Use
The pharmacokinetics, efficacy and safety of glimepiride have been evaluated in pediatric patients with type 2 diabetes as described below. Glimepiride is not recommended in pediatric patients because of its adverse effects on body weight and hypoglycemia.
The pharmacokinetics of a 1 mg single dose of glimepiride was evaluated in 30 patients with type 2 diabetes (male = 7; female = 23) between ages 10 and 17 years. The mean (± SD) AUC (0-last)(339±203 ng•hr/mL), Cmax (102±48 ng/mL) and t1/2 (3.1±1.7 hours) for glimepiride were comparable to historical data from adults (AUC ( 0-last) 315±96 ng•hr/mL, Cmax 103±34 ng/mL and t1/2 5.3±4.1 hours).
The safety and efficacy of glimepiride in pediatric patients was evaluated in a single-blind, 24-week trial that randomized 272 patients (8-17 years of age) with type 2 diabetes to glimepiride (n=135) or metformin (n=137). Both treatment-naïve patients (those treated with only diet and exercise for at least 2 weeks prior to randomization) and previously treated patients (those previously treated or currently treated with other oral antidiabetic medications for at least 3 months) were eligible to participate. Patients who were receiving oral antidiabetic agents at the time of study entry discontinued these medications before randomization without a washout period. Glimepiride was initiated at 1 mg, and then titrated up to 2, 4 or 8 mg (mean last dose 4 mg) through Week 12, targeting a self-monitored fasting fingerstick blood glucose < 126 mg/dL. Metformin was initiated at 500 mg twice daily and titrated at Week 12 up to 1000 mg twice daily (mean last dose 1365 mg).
After 24 weeks, the overall mean treatment difference in HbA 1cbetween glimepiride and metformin was 0.2%, favoring metformin (95% confidence interval -0.3% to +0.6%).
Based on these results, the trial did not meet its primary objective of showing a similar reduction in HbA 1cwith glimepiride compared to metformin.
|
* Intent-to-treat population using last-observation-carried-forward for missing data (Glimepiride, n=127; metformin, n=126) |
||
|
+ adjusted for baseline HbA 1Cand Tanner Stage |
||
|
** Difference is Glimepiride – metformin with positive differences favoring metformin |
||
| Metformin | Glimepiride | |
| Treatment-Naïve Patients* | N=69 | N=72 |
| HbA 1C (%) | ||
| Baseline (mean) | 8.2 | 8.3 |
| Change from baseline (adjusted LS mean) + | -1.2 | -1.0 |
| Adjusted Treatment Difference** (95%CI) | 0.2 (-0.3; 0.6) | |
| Previously Treated Patients* | N=57 | N=55 |
| HbA 1C (%) | ||
| Baseline (mean) | 9.0 | 8.7 |
| Change from baseline (adjusted LS mean) + | -0.2 | 0.2 |
| Adjusted Treatment Difference** (95%CI) | 0.4 (-0.4; 1.2) | |
| Body Weight (kg)* | N=126 | N=129 |
| Baseline (mean) | 67.3 | 66.5 |
| Change from baseline (adjusted LS mean)+ | 0.7 | 2.0 |
| Adjusted Treatment Difference** (95% CI) | 1.3 (0.3; 2.3) |
The profile of adverse reactions in pediatric patients treated with glimepiride was similar to that observed in adults [see Adverse Reactions( 6)].
Hypoglycemic events documented by blood glucose values <36 mg/dL were observed in 4% of pediatric patients treated with glimepiride and in 1% of pediatric patients treated with metformin. One patient in each treatment group experienced a severe hypoglycemic episode (severity was determined by the investigator based on observed signs and symptoms).
8.5 Geriatric Use
In clinical trials of glimepiride, 1053 of 3491 patients (30%) were >65 years of age. No overall differences in safety or effectiveness were observed between these patients and younger patients, but greater sensitivity of some older individuals cannot be ruled out.
There were no significant differences in glimepiride pharmacokinetics between patients with type 2 diabetes ≤65 years (n=49) and those >65 years (n=42) [see Clinical Pharmacology ( 12.3) ].
Glimepiride is substantially excreted by the kidney. Elderly patients are more likely to have renal impairment. In addition, hypoglycemia may be difficult to recognize in the elderly [see Dosage and Administration ( 2.1) and Warnings and Precautions ( 5.1) ]. Use caution when initiating glimepiride and increasing the dose of glimepiride in this patient population.
4 Contraindications (4 CONTRAINDICATIONS)
Glimepiride Tablets USP are contraindicated in patients with a history of a hypersensitivity reaction to:
- Glimepiride or any of the product's ingredients [ see Warnings and Precautions ( 5.2) ].
- Sulfonamide derivatives: Patients who have developed an allergic reaction to sulfonamide derivatives may develop an allergic reaction to glimepiride. Do not use glimepiride in patients who have a history of an allergic reaction to sulfonamide derivatives.
6 Adverse Reactions (6 ADVERSE REACTIONS)
7 Drug Interactions (7 DRUG INTERACTIONS)
- Certain medications may affect glucose metabolism, requiring glimepiride dose adjustment and close monitoring of blood glucose ( 7.1).
- Miconazole: Severe hypoglycemia can occur when glimepiride and oral miconazole are used concomitantly. ( 7.2).
- Cytochrome P450 2C9 interactions: Inhibitors and inducers of cytochrome P450 2C9 may affect glycemic control by altering glimepiride plasma concentrations ( 7.3).
- Colesevelam: Coadministration may reduce glimepiride absorption. Glimepiride should be administered at least 4 hours prior to colesevelam ( 2.1, 7.4).
5.3 Hemolytic Anemia
Sulfonylureas can cause hemolytic anemia in patients with glucose 6-phosphate dehydrogenase (G6PD) deficiency. Because glimepiride is a sulfonylurea, use caution in patients with G6PD deficiency and consider the use of a non-sulfonylurea alternative.
There are also postmarketing reports of hemolytic anemia in patients receiving glimepiride who did not have known G6PD deficiency [see Adverse Reactions ( 6.2) ].
8.6 Renal Impairment
To minimize the risk of hypoglycemia, the recommended starting dose of glimepiride is 1 mg daily for all patients with type 2 diabetes and renal impairment [see Dosage and Administration ( 2.1) and Warnings and Precautions ( 5.1) ].
A multiple-dose titration study was conducted in 16 patients with type 2 diabetes and renal impairment using doses ranging from 1 mg to 8 mg daily for 3 months. Baseline creatinine clearance ranged from 10-60 mL/min. The pharmacokinetics of glimepiride were evaluated in the multiple-dose titration study and the results were consistent with those observed in patients enrolled in a single-dose study. In both studies, the relative total clearance of glimepiride increased when kidney function was impaired. Both studies also demonstrated that the elimination of the two major metabolites was reduced in patients with renal impairment [see Clinical Pharmacology ( 12.3) ].
12.2 Pharmacodynamics
In healthy subjects, the time to reach maximal effect (minimum blood glucose concentrations) was approximately 2-3 hours after single oral doses of glimepiride. The effects of glimepiride on HbA 1c, fasting plasma glucose, and post-prandial glucose have been assessed in clinical trials [ see Clinical Studies ( 14) ].
2.1 Recommended Dosing
Glimepiride should be administered with breakfast or the first main meal of the day.
The recommended starting dose of glimepiride is 1 mg or 2 mg once daily. Patients at increased risk for hypoglycemia (e.g., the elderly or patients with renal impairment) should be started on 1 mg once daily [see Warnings and Precautions ( 5.1) and Use in Specific Populations ( 8.5, 8.6) ].
After reaching a daily dose of 2 mg, further dose increases can be made in increments of 1 mg or 2 mg based upon the patient's glycemic response. Uptitration should not occur more frequently than every 1-2 weeks. A conservative titration scheme is recommended for patients at increased risk for hypoglycemia [see Warnings and Precautions ( 5.1) and Use in Specific Populations ( 8.5, 8.6) ].
The maximum recommended dose is 8 mg once daily.
Patients being transferred to glimepiride from longer half-life sulfonylureas (e.g., chlorpropamide) may have overlapping drug effect for 1-2 weeks and should be appropriately monitored for hypoglycemia.
When colesevelam is coadministered with glimepiride, maximum plasma concentration and total exposure to glimepiride is reduced. Therefore, glimepiride should be administered at least 4 hours prior to colesevelam.
1 Indications and Usage (1 INDICATIONS AND USAGE)
Glimepiride Tablet are indicated as an adjunct to diet and exercise to improve glycemic control in adults with type 2 diabetes mellitus [see Clinical Studies ( 14.1) ].
Limitations of Use
Glimepiride should not be used for the treatment of type 1 diabetes mellitus or diabetic ketoacidosis, as it would not be effective in these settings.
12.1 Mechanism of Action
Glimepiride primarily lowers blood glucose by stimulating the release of insulin from pancreatic beta cells. Sulfonylureas bind to the sulfonylurea receptor in the pancreatic beta-cell plasma membrane, leading to closure of the ATP-sensitive potassium channel, thereby stimulating the release of insulin.
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
- Hypoglycemia: May be severe. Ensure proper patient selection, dosing, and instructions, particularly in at-risk populations (e.g., elderly, renally impaired) and when used with other anti-diabetic medications ( 5.1).
- Hypersensitivity Reactions: Postmarketing reports include anaphylaxis, angioedema and Stevens-Johnson Syndrome. Promptly discontinue glimepiride, assess for other causes, institute appropriate monitoring and treatment, and initiate alternative treatment for diabetes ( 5.2).
- Hemolytic Anemia: Can occur if glucose 6-phosphate dehydrogenase (G6PD) deficient. Consider a non-sulfonylurea alternative. ( 5.3).
- Potential Increased Risk of Cardiovascular Mortality with Sulfonylureas: Inform patient of risks, benefits and treatment alternatives ( 5.4).
- Macrovascular Outcomes: No clinical studies establishing conclusive evidence of macrovascular risk reduction with glimepiride or any other anti-diabetic drug ( 5.5).
5.5 Macrovascular Outcomes
There have been no clinical studies establishing conclusive evidence of macrovascular risk reduction with glimepiride or any other anti-diabetic drug.
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
- Recommended starting dose is 1 or 2 mg once daily. Increase in 1 or 2 mg increments no more frequently than every 1-2 weeks based on glycemic response. Maximum recommended dose is 8 mg once daily ( 2.1).
- Administer with breakfast or first meal of the day ( 2.1).
- Use 1 mg starting dose and titrate slowly in patients at increased risk for hypoglycemia (e.g., elderly, patients with renal impairment) ( 2.1).
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
Glimepiride Tablets USP are formulated as tablets of:
-
1 mg (Scored white to off-white, round imprinted with
on one side) -
2 mg (Scored white to off-white, round imprinted with
on one side) -
4 mg (Scored white to off-white, round imprinted with
on one side)
6.2 Postmarketing Experience
The following adverse reactions have been identified during post-approval use of glimepiride. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
- Serious hypersensitivity reactions, including anaphylaxis, angioedema, and Stevens-Johnson Syndrome [see Warnings and Precautions ( 5.2) ]
- Hemolytic anemia in patients with and without G6PD deficiency [see Warnings and Precautions ( 5.3) ]
- Impairment of liver function (e.g. with cholestasis and jaundice), as well as hepatitis, which may progress to liver failure.
- Porphyria cutanea tarda, photosensitivity reactions and allergic vasculitis
- Leukopenia, agranulocytosis, aplastic anemia, and pancytopenia
- Thrombocytopenia (including severe cases with platelet count less than 10,000/μL) and thrombocytopenic purpura
- Hepatic porphyria reactions and disulfiram-like reactions
- Hyponatremia and syndrome of inappropriate antidiuretic hormone secretion (SIADH), most often in patients who are on other medications or who have medical conditions known to cause hyponatremia or increase release of antidiuretic hormone
- Dysgeusia
- Alopecia
8 Use in Specific Populations (8 USE IN SPECIFIC POPULATIONS)
5.2 Hypersensitivity Reactions
There have been postmarketing reports of hypersensitivity reactions in patients treated with glimepiride, including serious reactions such as anaphylaxis, angioedema, and Stevens-Johnson Syndrome. If a hypersensitivity reaction is suspected, promptly discontinue glimepiride, assess for other potential causes for the reaction, and institute alternative treatment for diabetes.
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
Approximately 2,800 patients with type 2 diabetes have been treated with glimepiride in the controlled clinical trials. In these trials, approximately 1,700 patients were treated with glimepiride for at least 1 year.
Table 1summarizes adverse events, other than hypoglycemia, that were reported in 11 pooled placebo-controlled trials, whether or not considered to be possibly or probably related to study medication. Treatment duration ranged from 13 weeks to 12 months. Terms that are reported represent those that occurred at an incidence of ≥5% among glimepiride -treated patients and more commonly than in patients who received placebo.
|
*Glimepiride doses ranged from 1-16 mg administered daily |
||
|
†Insufficient information to determine whether any of the accidental injury events were associated with hypoglycemia |
||
|
Glimepiride
N=745 % |
Placebo
N=294 % |
|
| Headache | 8.2 | 7.8 |
| Accidental Injury † | 5.8 | 3.4 |
| Flu Syndrome | 5.4 | 4.4 |
| Nausea | 5.0 | 3.4 |
| Dizziness | 5.0 | 2.4 |
16 How Supplied/storage and Handling (16 HOW SUPPLIED/STORAGE AND HANDLING)
Glimepiride Tablets are available in the following strengths and package sizes:
- 1 mg (Scored white to off-white, round imprinted with "CTI 115" on one side) are supplied in:
Bottles of 100 . . . . . . . . .(NDC 60429-918-01)
- 2 mg (Scored white to off-white, round imprinted with "CTI 116" on one side) are supplied in:
Bottles of 100 . . . . . . . . .(NDC 60429-919-01)
- 4 mg (Scored white to off-white, round imprinted with "CTI 117" on one side) are supplied in:
Bottles of 100 . . . . . . . . .(NDC 60429-920-01)
Store at 25ºC (77ºF); excursions permitted to 20ºC to 25ºC (68º to 77ºF) (See USP Controlled Room Temperature).
Dispense in well-closed containers with safety closures.
7.3 Cytochrome P450 2c9 Interactions (7.3 Cytochrome P450 2C9 Interactions)
There may be an interaction between glimepiride and inhibitors (e.g., fluconazole) and inducers (e.g., rifampin) of cytochrome P450 2C9. Fluconazole may inhibit the metabolism of glimepiride, causing increased plasma concentrations of glimepiride which may lead to hypoglycemia. Rifampin may induce the metabolism of glimepiride, causing decreased plasma concentrations of glimepiride which may lead to worsening glycemic control.
7.1 Drugs Affecting Glucose Metabolism
A number of medications affect glucose metabolism and may require glimepiride dose adjustment and particularly close monitoring for hypoglycemia or worsening glycemic control.
The following are examples of medications that may increase the glucose-lowering effect of sulfonylureas including glimepiride, increasing the susceptibility to and/or intensity of hypoglycemia: oral anti-diabetic medications, pramlintide acetate, insulin, angiotensin converting enzyme (ACE) inhibitors, H2 receptor antagonists, fibrates, propoxyphene, pentoxifylline, somatostatin analogs, anabolic steroids and androgens, cyclophosphamide, phenyramidol, guanethidine, fluconazole, sulfinpyrazone, tetracyclines, clarithromycin, disopyramide, quinolones, and those drugs that are highly protein-bound, such as fluoxetine, nonsteroidal anti-inflammatory drugs, salicylates, sulfonamides, chloramphenicol, coumarins, probenecid and monoamine oxidase inhibitors. When these medications are administered to a patient receiving glimepiride, monitor the patient closely for hypoglycemia. When these medications are withdrawn from a patient receiving glimepiride, monitor the patient closely for worsening glycemic control.
The following are examples of medications that may reduce the glucose-lowering effect of sulfonylureas including glimepiride, leading to worsening glycemic control: danazol, glucagon, somatropin, protease inhibitors, atypical antipsychotic medications (e.g., olanzapine and clozapine), barbiturates, diazoxide, laxatives, rifampin, thiazides and other diuretics, corticosteroids, phenothiazines, thyroid hormones, estrogens, oral contraceptives, phenytoin, nicotinic acid, sympathomimetics (e.g., epinephrine, albuterol, terbutaline), and isoniazid. When these medications are administered to a patient receiving glimepiride, monitor the patient closely for worsening glycemic control. When these medications are withdrawn from a patient receiving glimepiride, monitor the patient closely for hypoglycemia.
Beta-blockers, clonidine, and reserpine may lead to either potentiation or weakening of glimepiride's glucose-lowering effect.
Both acute and chronic alcohol intake may potentiate or weaken the glucose-lowering action of glimepiride in an unpredictable fashion.
The signs of hypoglycemia may be reduced or absent in patients taking sympatholytic drugs such as beta-blockers, clonidine, guanethidine, and reserpine.
7.4 Concomitant Administration of Colesevelam
Colesevelam can reduce the maximum plasma concentration and total exposure of glimepiride when the two are coadministered. However, absorption is not reduced when glimepiride is administered 4 hours prior to colesevelam. Therefore, glimepiride should be administered at least 4 hours prior to colesevelam.
13.1 Carcinogenesis, Mutagenesis, and Impairment of Fertility
Studies in rats at doses of up to 5000 parts per million (ppm) in complete feed (approximately 340 times the maximum recommended human dose, based on surface area) for 30 months showed no evidence of carcinogenesis. In mice, administration of glimepiride for 24 months resulted in an increase in benign pancreatic adenoma formation that was dose-related and was thought to be the result of chronic pancreatic stimulation. No adenoma formation in mice was observed at a dose of 320 ppm in complete feed, or 46-54 mg/kg body weight/day. This is about 35 times the maximum human recommended dose of 8 mg once daily based on surface area. Glimepiride was non-mutagenic in a battery of in vitro and in vivomutagenicity studies (Ames test, somatic cell mutation, chromosomal aberration, unscheduled DNA synthesis, and mouse micronucleus test).
There was no effect of glimepiride on male mouse fertility in animals exposed up to 2500 mg/kg body weight (>1,700 times the maximum recommended human dose based on surface area). Glimepiride had no effect on the fertility of male and female rats administered up to 4000 mg/kg body weight (approximately 4,000 times the maximum recommended human dose based on surface area).
5.4 Increased Risk of Cardiovascular Mortality With Sulfonylureas (5.4 Increased Risk of Cardiovascular Mortality with Sulfonylureas)
The administration of oral hypoglycemic drugs has been reported to be associated with increased cardiovascular mortality as compared to treatment with diet alone or diet plus insulin. This warning is based on the study conducted by the University Group Diabetes Program (UGDP), a long-term, prospective clinical trial designed to evaluate the effectiveness of glucose-lowering drugs in preventing or delaying vascular complications in patients with non-insulin-dependent diabetes. The study involved 823 patients who were randomly assigned to one of four treatment groups.
UGDP reported that patients treated for 5 to 8 years with diet plus a fixed dose of tolbutamide (1.5 grams per day) had a rate of cardiovascular mortality approximately 2-1/2 times that of patients treated with diet alone. A significant increase in total mortality was not observed, but the use of tolbutamide was discontinued based on the increase in cardiovascular mortality, thus limiting the opportunity for the study to show an increase in overall mortality. Despite controversy regarding the interpretation of these results, the findings of the UGDP study provide an adequate basis for this warning. The patient should be informed of the potential risks and advantages of glimepiride and of alternative modes of therapy.
Although only one drug in the sulfonylurea class (tolbutamide) was included in this study, it is prudent from a safety standpoint to consider that this warning may also apply to other oral hypoglycemic drugs in this class, in view of their close similarities in mode of action and chemical structure.
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:44:08.750840 · Updated: 2026-03-14T22:18:52.014204