These Highlights Do Not Include All The Information Needed To Use Soliqua 100/33 Safely And Effectively.
4bba538b-cf7c-4310-ae8f-cb711ed21bcc
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
Warnings and Precautions, Severe Gastrointestinal Adverse Reactions ( 5.8 ) 5/2025 Warnings and Precautions, Pulmonary Aspiration During General Anesthesia or Deep Sedation ( 5.13 ) 11/2024
Indications and Usage
SOLIQUA 100/33 is a combination of insulin glargine and lixisenatide and is indicated as an adjunct to diet and exercise to improve glycemic control in adults with type 2 diabetes mellitus.
Dosage and Administration
Inject subcutaneously once a day within the hour prior to the first meal of the day. ( 2.1 ) SOLIQUA 100/33 pen delivers 15 units to 60 units per injection. ( 2.1 , 2.2 ) Maximum daily dosage is 60 units (60 units of insulin glargine and 20 mcg of lixisenatide). ( 2.1 ) Discontinue basal insulin or GLP-1 receptor agonist prior to initiation. ( 2.2 ) In patients naive to basal insulin or to a GLP-1 receptor agonist, currently on less than 30 units of basal insulin, or on a GLP-1 receptor agonist, the recommended starting dosage is 15 units subcutaneously once daily. ( 2.2 ) In patients inadequately controlled on 30 to 60 units of basal insulin, the starting dosage is 30 units subcutaneously once daily. ( 2.2 ) See Full Prescribing Information for titration recommendations. ( 2.3 ) Inject subcutaneously in abdominal area, thigh, or upper arm and rotate injection sites within the same region from one injection to the next to reduce risk of lipodystrophy and localized cutaneous amyloidosis. ( 2.5 ) Do not administer intravenously, or via an infusion pump. ( 2.5 ) Do not dilute or mix with any other insulin products or solutions. ( 2.5 )
Warnings and Precautions
Anaphylaxis and Serious Hypersensitivity Reactions : Severe, life-threatening, and generalized allergic reactions can occur. Instruct patients to discontinue use if a reaction occurs and promptly seek medical attention. ( 5.1 ) Acute Pancreatitis : Has been observed in patients treated with GLP-1 receptor agonists, including SOLIQUA 100/33. Discontinue if pancreatitis is suspected. ( 5.2 ) Never share a SOLIQUA 100/33 prefilled pen between patients, even if the needle is changed. ( 5.3 ) Hyperglycemia or Hypoglycemia with Changes in Insulin Regimen : Make changes to a patient's insulin regimen (e.g., insulin strength, manufacturer, type, injection site or method of administration) under close medical supervision with increased frequency of blood glucose monitoring. ( 5.4 ) Overdose Due to Medication Errors : SOLIQUA 100/33 contains two drugs. Instruct patients to always check the label before each injection since accidental mix-ups with insulin products can occur. Do not exceed the maximum dose or use with other GLP-1 receptor agonists. ( 5.5 ) Hypoglycemia : May be life-threatening. Increase frequency of glucose monitoring with changes to insulin dosage, coadministered glucose lowering medications, meal pattern, physical activity; and in patients with renal or hepatic impairment and hypoglycemia unawareness. ( 5.6 ) Acute kidney injury Due to Volume Depletion : Monitor renal function in patients reporting adverse reactions that could lead to volume depletion. SOLIQUA 100/33 is not recommended in patients with end-stage renal disease. ( 5.7 ) Severe Gastrointestinal Adverse Reactions: Use has been associated with gastrointestinal adverse reactions, sometimes severe. SOLIQUA 100/33 is not recommended in patients with severe gastroparesis ( 5.8 ). Immunogenicity : Patients may develop antibodies to insulin glargine and lixisenatide. If there is worsening glycemic control or failure to achieve targeted glycemic control, significant injection-site reactions or allergic reactions, alternative antidiabetic therapy should be considered. ( 5.9 ) Hypokalemia : May be life-threatening. Monitor potassium levels in patients at risk of hypokalemia and treat if indicated. ( 5.10 ) Fluid Retention and Heart Failure with Use of PPAR-gamma agonists ) : Observe for signs and symptoms of heart failure; consider dosage reduction or discontinuation if heart failure occurs. ( 5.11 ) Acute Gallbladder Disease : If cholelithiasis or cholecystitis are suspected, gallbladder studies are indicated. ( 5.12 ) Pulmonary Aspiration During General Anesthesia or Deep Sedation: Has been reported in patients receiving GLP-1 receptor agonists undergoing elective surgeries or procedures. Instruct patients to inform healthcare providers of any planned surgeries or procedures . ( 5.13 )
Contraindications
SOLIQUA 100/33 is contraindicated: During episodes of hypoglycemia [see Warnings and Precautions (5.6) ] . In patients with serious hypersensitivity to insulin glargine, lixisenatide, or any of the excipients in SOLIQUA 100/33. Hypersensitivity reactions including anaphylaxis have occurred with both lixisenatide and insulin glargine [see Warnings and Precautions (5.1) and Adverse Reactions (6.1) ] .
Adverse Reactions
Use of GLP-1 receptor agonists, including SOLIQUA 100/33, has been associated with gastrointestinal adverse reactions, sometimes severe [see Adverse Reactions (6.) ] . SOLIQUA 100/33 is not recommended in patients with severe gastroparesis.
Drug Interactions
Drugs that affect glucose metabolism : Adjustment of SOLIQUA 100/33 dosage may be needed; closely monitor blood glucose. ( 7.1 ) Antiadrenergic Drugs (e.g., beta-blockers, clonidine, guanethidine, and reserpine): Hypoglycemia signs and symptoms may be reduced. ( 7.1 ) Effects of delayed gastric emptying on oral medications : Lixisenatide delays gastric emptying which may impact absorption of concomitantly administered oral medications. Oral contraceptives and other medications such as antibiotics and acetaminophen should be taken at least 1 hour prior to SOLIQUA 100/33 administration or 11 hours after. ( 7.2 )
How Supplied
SOLIQUA 100/33 (insulin glargine and lixisenatide) injection is a clear, colorless to almost colorless solution in a 3 mL prefilled, disposable, single-patient-use pen: Dosage Unit/Strength Package size NDC # 3 mL SOLIQUA 100/33 single-patient-use pen 100 units/mL insulin glargine and 33 mcg/mL lixisenatide Package of 5 0024-5761-05 Needles are not included. Only use needles that are compatible for use with SOLIQUA 100/33 prefilled pen.
Medication Information
Warnings and Precautions
Anaphylaxis and Serious Hypersensitivity Reactions : Severe, life-threatening, and generalized allergic reactions can occur. Instruct patients to discontinue use if a reaction occurs and promptly seek medical attention. ( 5.1 ) Acute Pancreatitis : Has been observed in patients treated with GLP-1 receptor agonists, including SOLIQUA 100/33. Discontinue if pancreatitis is suspected. ( 5.2 ) Never share a SOLIQUA 100/33 prefilled pen between patients, even if the needle is changed. ( 5.3 ) Hyperglycemia or Hypoglycemia with Changes in Insulin Regimen : Make changes to a patient's insulin regimen (e.g., insulin strength, manufacturer, type, injection site or method of administration) under close medical supervision with increased frequency of blood glucose monitoring. ( 5.4 ) Overdose Due to Medication Errors : SOLIQUA 100/33 contains two drugs. Instruct patients to always check the label before each injection since accidental mix-ups with insulin products can occur. Do not exceed the maximum dose or use with other GLP-1 receptor agonists. ( 5.5 ) Hypoglycemia : May be life-threatening. Increase frequency of glucose monitoring with changes to insulin dosage, coadministered glucose lowering medications, meal pattern, physical activity; and in patients with renal or hepatic impairment and hypoglycemia unawareness. ( 5.6 ) Acute kidney injury Due to Volume Depletion : Monitor renal function in patients reporting adverse reactions that could lead to volume depletion. SOLIQUA 100/33 is not recommended in patients with end-stage renal disease. ( 5.7 ) Severe Gastrointestinal Adverse Reactions: Use has been associated with gastrointestinal adverse reactions, sometimes severe. SOLIQUA 100/33 is not recommended in patients with severe gastroparesis ( 5.8 ). Immunogenicity : Patients may develop antibodies to insulin glargine and lixisenatide. If there is worsening glycemic control or failure to achieve targeted glycemic control, significant injection-site reactions or allergic reactions, alternative antidiabetic therapy should be considered. ( 5.9 ) Hypokalemia : May be life-threatening. Monitor potassium levels in patients at risk of hypokalemia and treat if indicated. ( 5.10 ) Fluid Retention and Heart Failure with Use of PPAR-gamma agonists ) : Observe for signs and symptoms of heart failure; consider dosage reduction or discontinuation if heart failure occurs. ( 5.11 ) Acute Gallbladder Disease : If cholelithiasis or cholecystitis are suspected, gallbladder studies are indicated. ( 5.12 ) Pulmonary Aspiration During General Anesthesia or Deep Sedation: Has been reported in patients receiving GLP-1 receptor agonists undergoing elective surgeries or procedures. Instruct patients to inform healthcare providers of any planned surgeries or procedures . ( 5.13 )
Indications and Usage
SOLIQUA 100/33 is a combination of insulin glargine and lixisenatide and is indicated as an adjunct to diet and exercise to improve glycemic control in adults with type 2 diabetes mellitus.
Dosage and Administration
Inject subcutaneously once a day within the hour prior to the first meal of the day. ( 2.1 ) SOLIQUA 100/33 pen delivers 15 units to 60 units per injection. ( 2.1 , 2.2 ) Maximum daily dosage is 60 units (60 units of insulin glargine and 20 mcg of lixisenatide). ( 2.1 ) Discontinue basal insulin or GLP-1 receptor agonist prior to initiation. ( 2.2 ) In patients naive to basal insulin or to a GLP-1 receptor agonist, currently on less than 30 units of basal insulin, or on a GLP-1 receptor agonist, the recommended starting dosage is 15 units subcutaneously once daily. ( 2.2 ) In patients inadequately controlled on 30 to 60 units of basal insulin, the starting dosage is 30 units subcutaneously once daily. ( 2.2 ) See Full Prescribing Information for titration recommendations. ( 2.3 ) Inject subcutaneously in abdominal area, thigh, or upper arm and rotate injection sites within the same region from one injection to the next to reduce risk of lipodystrophy and localized cutaneous amyloidosis. ( 2.5 ) Do not administer intravenously, or via an infusion pump. ( 2.5 ) Do not dilute or mix with any other insulin products or solutions. ( 2.5 )
Contraindications
SOLIQUA 100/33 is contraindicated: During episodes of hypoglycemia [see Warnings and Precautions (5.6) ] . In patients with serious hypersensitivity to insulin glargine, lixisenatide, or any of the excipients in SOLIQUA 100/33. Hypersensitivity reactions including anaphylaxis have occurred with both lixisenatide and insulin glargine [see Warnings and Precautions (5.1) and Adverse Reactions (6.1) ] .
Adverse Reactions
Use of GLP-1 receptor agonists, including SOLIQUA 100/33, has been associated with gastrointestinal adverse reactions, sometimes severe [see Adverse Reactions (6.) ] . SOLIQUA 100/33 is not recommended in patients with severe gastroparesis.
Drug Interactions
Drugs that affect glucose metabolism : Adjustment of SOLIQUA 100/33 dosage may be needed; closely monitor blood glucose. ( 7.1 ) Antiadrenergic Drugs (e.g., beta-blockers, clonidine, guanethidine, and reserpine): Hypoglycemia signs and symptoms may be reduced. ( 7.1 ) Effects of delayed gastric emptying on oral medications : Lixisenatide delays gastric emptying which may impact absorption of concomitantly administered oral medications. Oral contraceptives and other medications such as antibiotics and acetaminophen should be taken at least 1 hour prior to SOLIQUA 100/33 administration or 11 hours after. ( 7.2 )
How Supplied
SOLIQUA 100/33 (insulin glargine and lixisenatide) injection is a clear, colorless to almost colorless solution in a 3 mL prefilled, disposable, single-patient-use pen: Dosage Unit/Strength Package size NDC # 3 mL SOLIQUA 100/33 single-patient-use pen 100 units/mL insulin glargine and 33 mcg/mL lixisenatide Package of 5 0024-5761-05 Needles are not included. Only use needles that are compatible for use with SOLIQUA 100/33 prefilled pen.
Description
Warnings and Precautions, Severe Gastrointestinal Adverse Reactions ( 5.8 ) 5/2025 Warnings and Precautions, Pulmonary Aspiration During General Anesthesia or Deep Sedation ( 5.13 ) 11/2024
Section 42229-5
Limitations of Use:
- SOLIQUA 100/33 contains lixisenatide. Coadministration with any other product containing lixisenatide or another glucagon-like peptide-1 (GLP-1) receptor agonist is not recommended [see Warnings and Precautions (5.5)].
- SOLIQUA 100/33 is not recommended for the treatment of diabetic ketoacidosis.
- SOLIQUA 100/33 has not been studied in combination with prandial insulin.
Section 42231-1
| This Medication Guide has been approved by the U.S. Food and Drug Administration. | Revised: July 2025 | ||
|
Medication Guide SOLIQUA® 100/33 (So - lee - kwa) (insulin glargine and lixisenatide) injection, for subcutaneous use |
|||
|
What is the most important information I should know about SOLIQUA 100/33? SOLIQUA 100/33 can cause serious side effects including inflammation of the pancreas (pancreatitis). Stop using SOLIQUA 100/33 and call your healthcare provider right away if you have severe pain in your stomach area (abdomen) that will not go away, with or without vomiting. You may feel the pain from your abdomen to your back. |
|||
|
What is SOLIQUA 100/33?
SOLIQUA 100/33 is an injectable prescription medicine that contains 2 diabetes medicines, insulin glargine and lixisenatide, that is used along with diet and exercise to improve blood sugar (glucose) in adults with type 2 diabetes.
|
|||
|
Who should not use SOLIQUA 100/33? Do not use SOLIQUA 100/33 if you:
|
|||
Before using SOLIQUA 100/33, tell your healthcare provider about all your medical conditions including if you:
Before using SOLIQUA 100/33, talk to your healthcare provider about low blood sugar and how to manage it. Especially tell your healthcare provider if you take:
|
|||
How should I use SOLIQUA 100/33?
|
|||
|
What should I avoid while taking SOLIQUA 100/33? While taking SOLIQUA 100/33 do not:
|
|||
|
What are the possible side effects of SOLIQUA 100/33? SOLIQUA 100/33 can cause serious side effects including:
|
|||
|
|
||
|
|||
|
|
|
|
|
|||
|
|
||
|
|||
|
|
||
| Talk to your healthcare provider about any side effect that bothers you or does not go away. These are not all the possible side effects of SOLIQUA 100/33 Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. |
|||
How should I store SOLIQUA 100/33?
|
|||
|
General information about the safe and effective use of SOLIQUA 100/33.
Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not use SOLIQUA 100/33 for a condition for which it was not prescribed. Do not give SOLIQUA 100/33 to other people, even if they have the same symptoms that you have. It may harm them. You can ask your pharmacist or healthcare provider for information about SOLIQUA 100/33 that is written for health professionals. |
|||
|
What are the ingredients in SOLIQUA 100/33?
Active ingredients: insulin glargine and lixisenatide Inactive ingredients: glycerol (20 mg), metacresol (2.7 mg), methionine (3 mg), zinc (30 mcg) and Water for Injection, USP. Hydrochloric acid and/or sodium hydroxide are added as needed to adjust the pH. |
|||
| Manufactured by: sanofi-aventis U.S. LLC, Morristown, NJ 07960 A SANOFI COMPANY U.S. License No. 1752 For more information, go to www.soliqua100-33.com or call sanofi-aventis at 1-800-633-1610. |
Section 43683-2
16.2 Storage
Dispense in the original sealed carton with the enclosed Instructions for Use.
Prior to first use, SOLIQUA 100/33 pen should be stored in a refrigerator, 36°F–46°F (2°C–8°C). Do not freeze. Discard SOLIQUA 100/33 if it has been frozen. Protect from light.
After first use, store at room temperature up to 77°F (25°C). Replace the pen cap after each use to protect from light.
Discard pen 28 days after first use.
Remove the needle after each injection and store the SOLIQUA 100/33 pen without a needle attached.
11 Description
SOLIQUA 100/33 is a combination of insulin glargine, an insulin analog, and lixisenatide, a GLP-1 receptor agonist.
Insulin glargine is a human insulin analog produced by recombinant DNA technology utilizing a nonpathogenic laboratory strain of Escherichia coli (K12) as the production organism. The minimum potency of insulin glargine is NLT 15 units/mg. Insulin glargine differs from human insulin in that the amino acid asparagine at position A21 is replaced by glycine and two arginines are added at the C-terminus of the B-chain. Insulin glargine has low aqueous solubility at neutral pH. At pH 4 insulin glargine is completely soluble. It has a molecular weight of 6.063 kDa.
Lixisenatide is a synthetic analogue of human GLP-1, which acts as a GLP-1 receptor agonist. Lixisenatide is a protein containing 44 amino acids, which is amidated at the C-terminal amino acid (position 44) and has a molecular weight of 4.8585 kDa.
SOLIQUA 100/33 (insulin glargine and lixisenatide) injection is a sterile, colorless to almost colorless solution for subcutaneous use. SOLIQUA 100/33 is supplied as a prefilled single-patient-use disposable pen contain 300 units of insulin glargine and 100 mcg of lixisenatide in 3 mL of a clear, colorless to almost colorless, sterile, and aqueous solution. Each mL contains 100 units of insulin glargine and 33 mcg of lixisenatide and the inactive ingredients: glycerol (20 mg), metacresol (2.7 mg), methionine (3 mg), zinc (30 mcg), and Water for Injection, USP. Hydrochloric acid and/or sodium hydroxide may be added to adjust the pH. The approximate pH is 4.5.
2.4 Missed Doses
Instruct patients who miss a dose of SOLIQUA 100/33 to resume the once-daily regimen as prescribed with the next scheduled dose. Do not administer an extra dose or increase the dose to make up for the missed dose.
5.10 Hypokalemia
All insulin-containing products, including SOLIQUA 100/33, cause a shift in potassium from the extracellular to intracellular space, possibly leading to hypokalemia. Untreated hypokalemia may cause respiratory paralysis, ventricular arrhythmia, and death. Monitor potassium levels in patients at risk for hypokalemia if indicated (e.g., patients using potassium-lowering medications, patients taking medications sensitive to serum potassium concentrations).
5.6 Hypoglycemia
Hypoglycemia is the most common adverse reaction associated with insulin-containing products, including SOLIQUA 100/33 [see Adverse Reactions (6.1)]. Severe hypoglycemia can cause seizures, may be life-threatening or cause death. Hypoglycemia can impair concentration ability and reaction time; this may place an individual and others at risk in situations where these abilities are important (e.g., driving or operating other machinery). SOLIQUA 100/33 (an insulin-containing product), or any insulin, should not be used during episodes of hypoglycemia [see Contraindications (4)].
Hypoglycemia can happen suddenly, and symptoms may differ in each individual and change over time in the same individual. Symptomatic awareness of hypoglycemia may be less pronounced in patients with longstanding diabetes, in patients with diabetic nerve disease, in patients using medications that block the sympathetic nervous system (e.g., beta-blockers) [see Drug Interactions (7.1)], or in patients who experience recurrent hypoglycemia.
16.1 How Supplied
SOLIQUA 100/33 (insulin glargine and lixisenatide) injection is a clear, colorless to almost colorless solution in a 3 mL prefilled, disposable, single-patient-use pen:
| Dosage Unit/Strength | Package size | NDC # |
|---|---|---|
| 3 mL SOLIQUA 100/33 single-patient-use pen 100 units/mL insulin glargine and 33 mcg/mL lixisenatide |
Package of 5 | 0024-5761-05 |
Needles are not included. Only use needles that are compatible for use with SOLIQUA 100/33 prefilled pen.
8.4 Pediatric Use
Safety and effectiveness of SOLIQUA 100/33 have not been established in pediatric patients.
8.5 Geriatric Use
Of the total number of subjects (n=834) in controlled clinical studies of patients with type 2 diabetes, who were treated with SOLIQUA 100/33, 25.2% (n=210) were ≥65 years of age and 4% (n=33) were ≥75 years of age. No overall differences in effectiveness and safety were observed in the subgroup analyses across the age groups.
Nevertheless, caution should be exercised when SOLIQUA 100/33 is administered to geriatric patients. In elderly patients with diabetes, the initial dosing, dose increments, and maintenance dosage should be conservative to avoid hypoglycemic reactions. Hypoglycemia may be difficult to recognize in the elderly.
5.9 Immunogenicity
Patients may develop antibodies to insulin and lixisenatide following treatment. A pooled analysis of studies of lixisenatide-treated patients showed that 70% were antibody positive at Week 24. In the subset of patients (2.4%) with the highest antibody concentrations (>100 nmol/L), an attenuated glycemic response was observed. A higher incidence of allergic reactions and injection-site reactions occurred in antibody positive patients [see Warnings and Precautions (5.1), Adverse Reactions (6.2)].
If there is worsening glycemic control or failure to achieve targeted glycemic control, significant injection-site reactions or allergic reactions, alternative antidiabetic therapy should be considered.
4 Contraindications
SOLIQUA 100/33 is contraindicated:
- During episodes of hypoglycemia [see Warnings and Precautions (5.6)].
- In patients with serious hypersensitivity to insulin glargine, lixisenatide, or any of the excipients in SOLIQUA 100/33. Hypersensitivity reactions including anaphylaxis have occurred with both lixisenatide and insulin glargine [see Warnings and Precautions (5.1) and Adverse Reactions (6.1)].
6 Adverse Reactions
The following adverse reactions are discussed elsewhere:
- Anaphylaxis and Serious Hypersensitivity Reactions [see Warnings and Precautions (5.1)]
- Acute Pancreatitis [see Warnings and Precautions (5.2)]
- Hypoglycemia [see Warnings and Precautions (5.6)]
- Acute Kidney Injury Due to Volume Depletion [see Warnings and Precautions (5.7)]
- Severe Gastrointestinal Adverse Reactions [see Warnings and Precautions (5.8)]
- Hypokalemia [see Warnings and Precautions (5.10)]
- Acute Gallbladder Disease [see Warnings and Precautions (5.12)]
- Pulmonary Aspiration During General Anesthesia or Deep Sedation [see Warnings and Precautions (5.13)]
7 Drug Interactions
- Drugs that affect glucose metabolism: Adjustment of SOLIQUA 100/33 dosage may be needed; closely monitor blood glucose. (7.1)
- Antiadrenergic Drugs (e.g., beta-blockers, clonidine, guanethidine, and reserpine): Hypoglycemia signs and symptoms may be reduced. (7.1)
- Effects of delayed gastric emptying on oral medications: Lixisenatide delays gastric emptying which may impact absorption of concomitantly administered oral medications. Oral contraceptives and other medications such as antibiotics and acetaminophen should be taken at least 1 hour prior to SOLIQUA 100/33 administration or 11 hours after. (7.2)
8.6 Renal Impairment
Frequent glucose monitoring and dose adjustment may be necessary for SOLIQUA 100/33 in patients with renal impairment [see Warnings and Precautions (5.7)].
Instructions for Use
Read these instructions carefully before using your SOLIQUA 100/33 pen.
Do not share your SOLIQUA 100/33 pen with other people, even if the needle has been changed. You may give other people a serious infection, or get a serious infection from them.
SOLIQUA 100/33 is an injectable prescription medicine that contains 2 diabetes medicines, insulin glargine and lixisenatide in a SoloStar pen. The drug combination in this pen is only for the daily injection of 15 to 60 units of SOLIQUA 100/33. Each unit dialed contains 1 unit insulin glargine and 0.33 mcg lixisenatide.
People who are blind or have other vision problems should not use the SOLIQUA 100/33 pen without help from a person trained to use the pen.
Important information
- Check the label on the SOLIQUA 100/33 pen each time you give your injection to make sure you are using the correct medicine.
- Do not use your pen if it is damaged or if you are not sure that it is working correctly.
- Perform a safety test before each injection (see "Step 3: Do a safety test").
- Always carry a spare pen and spare needles in case they are lost or stop working.
- Do not reuse needles. Always use a new sterile needle for each injection. This helps stop blocked needles, contamination, and infection. If you reuse needles, you might not get your dose (underdosing) or get too much (overdosing).
- Do not use SOLIQUA 100/33 in an insulin pump or inject SOLIQUA 100/33 into your vein (intravenously).
- Do not mix SOLIQUA 100/33 in any other type of insulin or liquid medicine prior to injection.
- Change (rotate) your injection sites within the area you chose with each dose (see "Places to inject").
Learn to inject
- Talk with your healthcare provider about how to use the SOLIQUA 100/33 pen and how to inject correctly before using your pen.
- Ask for help if you have problems handling the pen.
- Read all of these instructions before using your pen. You may get too much or too little medicine if you do not follow the instructions correctly.
Need help?
If you have any questions about your pen or about diabetes, ask your healthcare provider, go to www.soliqua100-33.com or call sanofi-aventis at 1-800-633-1610.
Supplies you will need:
- 1 SOLIQUA 100/33 pen
- 1 new sterile needle (see Step 2 "Attach a new needle" )
- 1 alcohol swab
- a puncture-resistant container for used needles and pens (see "Throwing your pen away" at the end of this Instructions for Use)
Places to inject
- Inject your SOLIQUA 100/33 dose exactly as your healthcare provider has shown you.
- Inject your SOLIQUA 100/33 dose under the skin (subcutaneously) of your upper legs (thighs), upper arms, or stomach area (abdomen).
- Change (rotate) your injection sites within the area you choose for each dose to reduce your risk of getting pits in skin or thickened skin (lipodystrophy) and skin with lumps (localized cutaneous amyloidosis) at the injection sites.
- Do not inject where the skin has pits, is thickened, or has lumps.
- Do not inject where the skin is tender, bruised, scaly or hard, or into scars or damaged skin.
Get to know your pen
Step 1: Check your pen
Take a new pen out of the refrigerator at least 1 hour before you inject. Cold medicine is more painful to inject.
-
1ACheck the name and expiration date on the label of your pen.
- Make sure you have the correct medicine. This pen is colored light green with an orange injection button (see the "Get to know your pen" diagram).
- Do not use your pen after the expiration date on the pen label.
-
1BPull off the pen cap.
-
1CCheck that the medicine is clear and colorless to almost colorless.
- If you see small particles, return it to your pharmacy for a replacement.
-
1DWipe the rubber seal with an alcohol swab.
If you have other injector pens
- Making sure you have the correct medicine is especially important if you have other injector pens.
Step 2: Attach a new needle
- Do not reuse needles. Always use a new sterile needle for each injection. This helps stop blocked needles, contamination and infection.
- Only use needles that are meant to be used with SOLIQUA 100/33. Needles are supplied separately. If you do not know what needles to use, ask your healthcare provider or pharmacist.
-
2ATake a new needle and peel off the protective seal.
-
2BKeep the needle straight and screw it onto the pen until fixed. Do not over-tighten.
-
2CPull off the outer needle cap. Keep this for later.
-
2DPull off the inner needle cap and throw it away.
Handling needles
- Take care when handling needles to prevent needle-stick injury and cross-infection.
Step 3: Do a safety test
Perform a safety test before each injection to:
- Check your pen and the needle to make sure they are working properly.
- Make sure that you get the correct dose.
-
3ASelect 2 units by turning the dose selector until the dose pointer is at the 2 mark.
-
3BPress the injection button all the way in.
- When the medicine comes out of the needle tip, your pen is working correctly.
If no liquid appears:
- You may need to repeat this step up to 3 times before seeing the medicine.
- If no medicine comes out after the third time, the needle may be blocked. If this happens:
- Do not use your pen if still no medicine comes out of the needle tip. Use a new pen.
- Do not use a syringe to remove medicine from your pen.
If you see air bubbles
- You may see air bubbles in the medicine. This is normal, they will not harm you.
Step 4: Select the dose
- Do not select a dose or press the injection button without a needle attached. This may damage your pen.
- Only use this pen to inject your daily dose from 15 to 60 units. Do not change your dose unless your healthcare provider has told you to change your dose.
- Do not use this pen if you need a single daily dose that is more than 60 units.
- Do not use the pen if your single daily dose is less than 15 units, the black area in dose window as shown in the picture.
-
4AMake sure a needle is attached and the dose is set to "0".
-
4BTurn the dose selector until the dose pointer lines up with your dose.
- Do not dial your dose by counting the clicks, because you might dial the wrong dose. Always check the number in the dose window to make sure you dialed the correct dose.
- If you turn past your dose, you can turn back down.
- If there are not enough units left in your pen for your dose, the dose selector will stop at the number of units left.
- If you cannot select your full prescribed dose, use a new pen.
How to read the dose window
- Each line in the dose window equals 1 unit of SOLIQUA 100/33.
- Even numbers are shown in line with the dose pointer, as shown in picture.
30 units selected
- Odd numbers are shown as a line between even numbers, as shown in picture.
29 units selected
Units of medicine in your pen
- This pen contains 300 units of SOLIQUA 100/33 and it is intended to be used for more than one dose.
Step 5: Inject your dose
If you find it hard to press the injection button in, do not force it as this may break your pen. See the section after Step 5E below for help.
-
5AChoose a place to inject as shown in the picture labeled "Places to inject."
-
5BPush the needle into your skin as shown by your healthcare provider.
- Do not touch the injection button yet.
-
5CPlace your thumb on the injection button. Then press all the way in and hold.
- Do not press injection button at an angle. Your thumb could block the dose selector from turning.
-
5DKeep the injection button held in and when you see "0" in the dose window, slowly count to 10.
- This will make sure you get your full dose.
-
5EAfter holding and slowly counting to 10, release the injection button. Then remove the needle from your skin.
If you find it hard to press the injection button in:
- Change the needle (see Step 6 to remove the needle and Step 2 to attach a new needle) then do a safety test (see Step 3 ).
- If you still find it hard to press in, get a new pen.
- Do not use a syringe to remove medicine from your pen.
Step 6: Remove the needle
- Take care when handling needles to prevent needle-stick injury and cross-infection.
- Do not put the inner needle cap back on.
-
6AGrip the widest part of the outer needle cap. Keep the needle straight and guide it into the outer needle cap back. Then push firmly on.
- The needle can puncture the cap if it is recapped at an angle.
-
6BGrip and squeeze the widest part of the outer needle cap. Turn your pen several times with your other hand to remove the needle.
- Try again if the needle does not come off the first time.
-
6CThrow away the used needle in a puncture-resistant container (see "Throwing your pen away" at the end of this Instructions for Use).
-
6DPut your pen cap back on.
- Do not put the pen back in the refrigerator.
Use by
- Only use your pen for up to 28 days after its first use.
How to store your pen
Before first use
- Keep new pens in the refrigerator between 36°F to 46°F (2°C to 8°C).
- Do not freeze. If you accidentally freeze your pen, throw it away.
After first use
- Keep your pen at room temperature, up to 77°F (25°C).
- Do not put your pen back in the refrigerator.
- Do not store your pen with the needle attached.
- Store the pen with your pen cap on.
Keep this pen out of the sight and reach of children.
How to care for your pen
Handle your pen with care
- Do not drop your pen or knock it against hard surfaces.
- If you think that your pen may be damaged, do not try to fix it. Use a new one.
Protect your pen from dust and dirt
- You can clean the outside of your pen by wiping it with a damp cloth (water only). Do not soak, wash or lubricate the pen. This may damage it.
Throwing your pen away
- Put the used SOLIQUA 100/33 pen in a FDA-cleared sharps disposal container right away after use. Do not throw away (dispose of) the SOLIQUA 100/33 pen in your household trash.
- If you do not have a FDA-cleared sharps disposal container, you may use a household container that is:
- made of a heavy-duty plastic,
- can be closed with a tight-fitting, puncture-resistant lid, without sharps being able to come out,
- upright and stable during use,
- leak-resistant, and
- properly labeled to warn of hazardous waste inside the container.
- When your sharps disposal container is almost full, you will need to follow your community guidelines for the right way to dispose of your sharps disposal container. There may be state or local laws about how you should throw away used needles and syringes. For more information about safe sharps disposal, and for specific information about sharps disposal in the state that you live in, go to the FDA's website at: http://www.fda.gov/safesharpsdisposal.
Manufactured by:
sanofi-aventis U.S. LLC
Morristown, NJ 07960 A SANOFI COMPANY
U.S. License No. 1752
©2025 sanofi-aventis U.S. LLC
SOLIQUA and SoloStar are registered trademarks of sanofi-aventis U.S. LLC.
This Instructions for Use has been approved by the U.S. Food and Drug Administration.
Revised: July 2025
5.2 Acute Pancreatitis
Acute pancreatitis, including fatal and non-fatal hemorrhagic or necrotizing pancreatitis, has been observed in patients treated with GLP-1 receptor agonists [see Adverse Reactions (6)].
After initiation of SOLIQUA 100/33, observe patients carefully for signs and symptoms of pancreatitis (including persistent severe abdominal pain, sometimes radiating to the back and which may or may not be accompanied by vomiting). If pancreatitis is suspected, discontinue SOLIQUA 100/33 and initiate appropriate management.
8.7 Hepatic Impairment
The effect of hepatic impairment on the pharmacokinetics of SOLIQUA 100/33 has not been studied. Frequent glucose monitoring and dose adjustment may be necessary for SOLIQUA 100/33 in patients with hepatic impairment [see Warnings and Precautions (5.6)].
1 Indications and Usage
SOLIQUA 100/33 is a combination of insulin glargine and lixisenatide and is indicated as an adjunct to diet and exercise to improve glycemic control in adults with type 2 diabetes mellitus.
5 Warnings and Precautions
- Anaphylaxis and Serious Hypersensitivity Reactions: Severe, life-threatening, and generalized allergic reactions can occur. Instruct patients to discontinue use if a reaction occurs and promptly seek medical attention. (5.1)
- Acute Pancreatitis: Has been observed in patients treated with GLP-1 receptor agonists, including SOLIQUA 100/33. Discontinue if pancreatitis is suspected. (5.2)
- Never share a SOLIQUA 100/33 prefilled pen between patients, even if the needle is changed. (5.3)
- Hyperglycemia or Hypoglycemia with Changes in Insulin Regimen: Make changes to a patient's insulin regimen (e.g., insulin strength, manufacturer, type, injection site or method of administration) under close medical supervision with increased frequency of blood glucose monitoring. (5.4)
- Overdose Due to Medication Errors: SOLIQUA 100/33 contains two drugs. Instruct patients to always check the label before each injection since accidental mix-ups with insulin products can occur. Do not exceed the maximum dose or use with other GLP-1 receptor agonists. (5.5)
- Hypoglycemia: May be life-threatening. Increase frequency of glucose monitoring with changes to insulin dosage, coadministered glucose lowering medications, meal pattern, physical activity; and in patients with renal or hepatic impairment and hypoglycemia unawareness. (5.6)
- Acute kidney injury Due to Volume Depletion: Monitor renal function in patients reporting adverse reactions that could lead to volume depletion. SOLIQUA 100/33 is not recommended in patients with end-stage renal disease. (5.7)
- Severe Gastrointestinal Adverse Reactions: Use has been associated with gastrointestinal adverse reactions, sometimes severe. SOLIQUA 100/33 is not recommended in patients with severe gastroparesis (5.8).
- Immunogenicity: Patients may develop antibodies to insulin glargine and lixisenatide. If there is worsening glycemic control or failure to achieve targeted glycemic control, significant injection-site reactions or allergic reactions, alternative antidiabetic therapy should be considered. (5.9)
- Hypokalemia: May be life-threatening. Monitor potassium levels in patients at risk of hypokalemia and treat if indicated. (5.10)
- Fluid Retention and Heart Failure with Use of PPAR-gamma agonists ): Observe for signs and symptoms of heart failure; consider dosage reduction or discontinuation if heart failure occurs. (5.11)
- Acute Gallbladder Disease: If cholelithiasis or cholecystitis are suspected, gallbladder studies are indicated. (5.12)
- Pulmonary Aspiration During General Anesthesia or Deep Sedation: Has been reported in patients receiving GLP-1 receptor agonists undergoing elective surgeries or procedures. Instruct patients to inform healthcare providers of any planned surgeries or procedures.(5.13)
2 Dosage and Administration
- Inject subcutaneously once a day within the hour prior to the first meal of the day. (2.1)
- SOLIQUA 100/33 pen delivers 15 units to 60 units per injection. (2.1, 2.2)
- Maximum daily dosage is 60 units (60 units of insulin glargine and 20 mcg of lixisenatide). (2.1)
- Discontinue basal insulin or GLP-1 receptor agonist prior to initiation. (2.2)
- In patients naive to basal insulin or to a GLP-1 receptor agonist, currently on less than 30 units of basal insulin, or on a GLP-1 receptor agonist, the recommended starting dosage is 15 units subcutaneously once daily. (2.2)
- In patients inadequately controlled on 30 to 60 units of basal insulin, the starting dosage is 30 units subcutaneously once daily. (2.2)
- See Full Prescribing Information for titration recommendations. (2.3)
- Inject subcutaneously in abdominal area, thigh, or upper arm and rotate injection sites within the same region from one injection to the next to reduce risk of lipodystrophy and localized cutaneous amyloidosis. (2.5)
- Do not administer intravenously, or via an infusion pump. (2.5)
- Do not dilute or mix with any other insulin products or solutions. (2.5)
3 Dosage Forms and Strengths
SOLIQUA 100/33 is a clear, colorless to almost colorless solution available as:
Injection: 100 units of insulin glargine and 33 mcg of lixisenatide per mL in a 3 mL prefilled, disposable, single-patient-use SoloStar® pen.
6.3 Postmarketing Experience
The following additional adverse reactions have been identified during post approval use. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
2.2 Recommended Starting Dose
In patients naive to basal insulin or to a GLP-1 receptor agonist, currently on a GLP-1 receptor agonist or currently on less than 30 units of basal insulin daily:
- Discontinue therapy with basal insulin or a GLP-1 receptor agonist prior to initiation of SOLIQUA 100/33.
- The recommended starting dosage of SOLIQUA 100/33 is 15 units (15 units insulin glargine and 5 mcg lixisenatide) given subcutaneously once daily.
In patients currently on 30 to 60 units of basal insulin daily, with or without a GLP-1 receptor agonist:
- Discontinue therapy with basal insulin or GLP-1 receptor agonist prior to initiation of SOLIQUA 100/33.
- The recommended starting dosage of SOLIQUA 100/33 is 30 units (30 units insulin glargine and 10 mcg lixisenatide) given subcutaneously once daily.
| SOLIQUA 100/33 (dose window display) The dose window on the SOLIQUA 100/33 pen displays numbers for the even units and displays lines for the odd units.
|
Insulin glargine component dose | Lixisenatide component dose | Comment |
|---|---|---|---|
| 2 | --- | --- | Safety test dose – not for injection |
| 15 | 15 units | 5 mcg | Recommended starting dosage for patients naive to basal insulin or GLP-1 receptor agonist, currently on GLP-1 receptor agonist, or currently on less than 30 units of basal insulin daily |
| 16 | 16 units | 5.3 mcg | |
| 17 | 17 units | 5.7 mcg | |
| 18 | 18 units | 6 mcg | |
| 19 | 19 units | 6.3 mcg | |
| 20 | 20 units | 6.7 mcg | |
| 21 | 21 units | 7 mcg | |
| 22 | 22 units | 7.3 mcg | |
| 23 | 23 units | 7.7 mcg | |
| 24 | 24 units | 8 mcg | |
| 25 | 25 units | 8.3 mcg | |
| 26 | 26 units | 8.7 mcg | |
| 27 | 27 units | 9 mcg | |
| 28 | 28 units | 9.3 mcg | |
| 29 | 29 units | 9.7 mcg | |
| 30 | 30 units | 10 mcg | Recommended starting dosage for patients currently on 30 to 60 units of basal insulin daily, with or without a GLP-1 receptor agonist: |
| 31 | 31 units | 10.3 mcg | |
| 32 | 32 units | 10.7 mcg | |
| 33 | 33 units | 11 mcg | |
| 34 | 34 units | 11.3 mcg | |
| 35 | 35 units | 11.7 mcg | |
| 36 | 36 units | 12 mcg | |
| 37 | 37 units | 12.3 mcg | |
| 38 | 38 units | 12.7 mcg | |
| 39 | 39 units | 13 mcg | |
| 40 | 40 units | 13.3 mcg | |
| 41 | 41 units | 13.7 mcg | |
| 42 | 42 units | 14 mcg | |
| 43 | 43 units | 14.3 mcg | |
| 44 | 44 units | 14.7 mcg | |
| 45 | 45 units | 15 mcg | |
| 46 | 46 units | 15.3 mcg | |
| 47 | 47 units | 15.7 mcg | |
| 48 | 48 units | 16 mcg | |
| 49 | 49 units | 16.3 mcg | |
| 50 | 50 units | 16.7 mcg | |
| 51 | 51 units | 17 mcg | |
| 52 | 52 units | 17.3 mcg | |
| 53 | 53 units | 17.7 mcg | |
| 54 | 54 units | 18 mcg | |
| 55 | 55 units | 18.3 mcg | |
| 56 | 56 units | 18.7 mcg | |
| 57 | 57 units | 19 mcg | |
| 58 | 58 units | 19.3 mcg | |
| 59 | 59 units | 19.7 mcg | |
| 60 | 60 units | 20 mcg | Maximum daily dosage [see Warnings and Precautions (5.5)] |
8 Use in Specific Populations
- Pregnancy: SOLIQUA 100/33 should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus. (8.1)
5.12 Acute Gallbladder Disease
Acute events of gallbladder disease such as cholelithiasis or cholecystitis have been reported in GLP-1 receptor agonist trials and postmarketing. In a cardiovascular outcomes trial, cholelithiasis occurred in 0.4% of lixisenatide-treated patients versus 0.2% in placebo-treated patients and acute cholecystitis in 0.3% of lixisenatide-treated patients versus 0.2% in placebo-treated patients. If cholelithiasis is suspected, gallbladder studies and appropriate clinical follow-up are indicated.
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in clinical trials of a drug cannot be directly compared to rates in the clinical trial of another drug and may not reflect the rates observed in practice.
The safety of SOLIQUA 100/33 (n=834, with a mean treatment duration of 203 days) has been evaluated in two clinical studies (30 weeks duration) in type 2 diabetes patients. The studies, Study A and B [see Clinical Studies (14)], had the following characteristics: mean age was approximately 59 years; approximately 50% were male, 90% were Caucasian, 6% were Black or African American, and 18% were Hispanic. The mean duration of diabetes was 10.3 years, mean HbA1c at screening for Study A was 8.2 and Study B was 8.5. The mean BMI at baseline was 32 kg/m2. Baseline eGFR was ≥60 mL/min in 87.2% of the pooled study population and mean baseline eGFR was 83.0 mL/min/1.73 m2.
| SOLIQUA 100/33, % (n=834) |
|
|---|---|
| Nausea | 10.0 |
| Nasopharyngitis | 7.0 |
| Diarrhea | 7.0 |
| Upper respiratory tract infection | 5.5 |
| Headache | 5.4 |
2.3 Titration of Soliqua 100/33
- After starting with the recommended dosage of SOLIQUA 100/33, [see Dosage and Administration (2.2)], titrate the dosage upwards or downwards by two to four units (see Table 2) every week based on the patient's metabolic needs, blood glucose monitoring results, and glycemic control goal until the desired fasting plasma glucose is achieved.
- To minimize the risk of hypoglycemia or hyperglycemia, additional titration may be needed with changes in physical activity, meal patterns (i.e., macronutrient content or timing of food intake), or renal or hepatic function; during acute illness; or when used with other medications [see Warnings and Precautions (5.4) and Drug Interactions (7)].
| Self-Monitored Fasting Plasma Glucose | SOLIQUA 100/33 Dosage Adjustment |
|---|---|
| Above target range | +2 units (2 units of insulin glargine and 0.66 mcg of lixisenatide) to +4 units (4 units of insulin glargine and 1.32 mcg of lixisenatide) |
| Within target range | 0 units |
| Below target range | -2 units (2 units of insulin glargine and 0.66 mcg of lixisenatide) to -4 units (4 units of insulin glargine and 1.32 mcg of lixisenatide) |
2.1 Important Dosage Information
- SOLIQUA 100/33 is a combination of insulin glargine and lixisenatide.
- Administer SOLIQUA 100/33 subcutaneously once a day within the hour prior to the first meal of the day.
- The SOLIQUA 100/33 pen delivers doses from 15 to 60 units in a single injection. Table 1 presents the units of insulin glargine and the micrograms of lixisenatide in each dosage of SOLIQUA 100/33 [see Dosage and Administration (2.2)].
- The maximum dose of SOLIQUA 100/33 is 60 units daily (60 units insulin glargine and 20 mcg lixisenatide) [see Warnings and Precautions (5.5)].
14.1 Overview of Clinical Studies
SOLIQUA 100/33 was evaluated in two randomized clinical studies in patients with type 2 diabetes mellitus. In each of the active-controlled trials, treatment with SOLIQUA 100/33 produced statistically significant improvements in HbA1c.
17 Patient Counseling Information
Advise the patient to read the FDA-approved patient labeling (Medication Guide and Instructions for Use).
5.5 Overdose Due to Medication Errors
SOLIQUA 100/33 contains two drugs: insulin glargine and lixisenatide. Administration of more than 60 units of SOLIQUA 100/33 daily can result in overdose of the lixisenatide component. Do not exceed the 20-mcg maximum recommended dose of lixisenatide or use with other GLP-1 receptor agonists.
Accidental mix-ups between insulin products have been reported. To avoid medication errors between SOLIQUA 100/33 and other insulins, instruct patients to always check the insulin label before each injection.
2.5 Important Administration Instructions
- The SOLIQUA 100/33 prefilled pen is for single-patient-use only [see Warnings and Precautions (5.3)].
- Train patients on proper use and injection technique before initiating SOLIQUA 100/33.
- Always check the SOLIQUA 100/33 label before administration [see Warnings and Precautions (5.5)].
- Visually inspect for particulate matter and discoloration prior to administration. Only use SOLIQUA 100/33 if the solution is clear and colorless to almost colorless.
- Inject SOLIQUA 100/33 subcutaneously into the abdominal area, thigh, or upper arm.
- Rotate injection sites within the same region from one injection to the next to reduce the risk of lipodystrophy and localized cutaneous amyloidosis. Do not inject into areas of lipodystrophy or localized cutaneous amyloidosis [see Warnings and Precautions (5.2), Adverse Reactions (6)].
- During changes to a patient's insulin regimen, increase the frequency of blood glucose monitoring [see Warnings and Precautions (5.4)].
- Do not administer intravenously or via an insulin pump.
- Use SOLIQUA 100/33 with caution in patients with visual impairment who may rely on audible clicks to dial their dose.
- The SOLIQUA 100/33 pen dials in 1-unit increments.
- Do not dilute or mix SOLIQUA 100/33 with any other insulin or solution.
- Do not split the dose of SOLIQUA 100/33.
Principal Display Panel 3 Ml Pen Carton
NDC 0024-5761-05
Rx only
SOLIQUA® 100/33
(insulin glargine and lixisenatide) injection
For Single Patient Use Only
100 units/mL and 33 mcg/mL
With each unit of insulin glargine,
the pen also delivers 0.33 mcg of lixisenatide
Only for Doses from 15 to 60 Units
For subcutaneous injection only
Dispense with the medication guide
Solution for injection in a SoloStar® disposable insulin delivery device
Never remove medication using a syringe
Do not mix with other insulins
Use only if solution is clear and colorless with no particles visible
Five 3 mL prefilled pens (15 mL total) – Dispense in this sealed carton
*Needles not included (see back panel)
SANOFI
5.8 Severe Gastrointestinal Adverse Reactions
Use of GLP-1 receptor agonists, including SOLIQUA 100/33, has been associated with gastrointestinal adverse reactions, sometimes severe [see Adverse Reactions (6.)]. SOLIQUA 100/33 is not recommended in patients with severe gastroparesis.
5.7 Acute Kidney Injury Due to Volume Depletion
There have been postmarketing reports of acute kidney injury, in some cases requiring hemodialysis, in patients treated with GLP-1 receptor agonists [see Adverse Reactions (6.3)]. The majority of the reported events occurred in patients who experienced gastrointestinal reactions leading to dehydration such as nausea, vomiting, or diarrhea [see Adverse Reactions (6.1)]. Monitor renal function in patients reporting adverse reactions to SOLIQUA 100/33 that could lead to volume depletion, especially during dosage initiation and escalation of SOLIQUA 100/33.SOLIQUA 100/33 is not recommended in patients with end-stage renal disease [see Use in Specific Populations (8.6)].
7.1 Medications That Can Affect Glucose Metabolism
A number of medications affect glucose metabolism and may require dose adjustment of SOLIQUA 100/33 and particularly close monitoring.
| Drugs That May Increase the Risk of Hypoglycemia | |
| Drugs: | Antidiabetic agents, ACE inhibitors, angiotensin II receptor blocking agents, disopyramide, fibrates, fluoxetine, monoamine oxidase inhibitors, pentoxifylline, pramlintide, salicylates, somatostatin analogs (e.g., octreotide), and sulfonamide antibiotics. |
| Intervention: | Dose reductions and increased frequency of glucose monitoring may be required when SOLIQUA 100/33 is coadministered with these drugs. |
| Drugs That May Decrease the Blood Glucose Lowering Effect of SOLIQUA 100/33 | |
| Drugs: | Atypical antipsychotics (e.g., olanzapine and clozapine), corticosteroids, danazol, diuretics, estrogens, glucagon, isoniazid, niacin, oral contraceptives, phenothiazines, progestogens (e.g., in oral contraceptives), protease inhibitors, somatropin, sympathomimetic agents (e.g., albuterol, epinephrine, terbutaline), and thyroid hormones. |
| Intervention: | Dose increases and increased frequency of glucose monitoring may be required when SOLIQUA 100/33 is coadministered with these drugs. |
| Drugs That May Increase or Decrease the Blood Glucose Lowering Effect of SOLIQUA 100/33 | |
| Drugs: | Alcohol, beta-blockers, clonidine, and lithium salts. Pentamidine may cause hypoglycemia, which may sometimes be followed by hyperglycemia. |
| Intervention: | Dose adjustment and increased frequency of glucose monitoring may be required when SOLIQUA 100/33 is coadministered with these drugs. |
| Drugs That May Blunt Signs and Symptoms of Hypoglycemia | |
| Drugs: | Beta-blockers, clonidine, guanethidine, and reserpine. |
| Intervention: | Increased frequency of glucose monitoring may be required when SOLIQUA 100/33 is coadministered with these drugs. |
5.1 Anaphylaxis and Serious Hypersensitivity Reactions
In clinical trials of lixisenatide there have been cases of anaphylaxis (frequency of 0.1% or 10 cases per 10,000 patient-years) and other serious hypersensitivity reactions including angioedema. Severe, life-threatening, generalized allergic reactions, including anaphylaxis, generalized skin reactions, angioedema, bronchospasm, hypotension, and shock can occur with insulins, including insulin glargine. There have been postmarketing reports of serious hypersensitivity reactions, including anaphylactic reactions and angioedema, in patients treated with SOLIQUA 100/33 [see Adverse Reactions (6.1)].
Inform and closely monitor patients with a history of anaphylaxis or angioedema with another GLP-1 receptor agonist for allergic reactions, because it is unknown whether such patients will be predisposed to anaphylaxis with SOLIQUA 100/33. SOLIQUA 100/33 is contraindicated in patients with known serious hypersensitivity to lixisenatide or insulin glargine [see Contraindications (4)]. If a hypersensitivity reaction occurs, the patient should discontinue SOLIQUA 100/33 and promptly seek medical attention.
7.2 Effects of Delayed Gastric Emptying On Oral Medications
Lixisenatide-containing products, including SOLIQUA 100/33, delay gastric emptying which may reduce the rate of absorption of orally administered medications. Use caution when coadministering oral medications that have a narrow therapeutic ratio or that require careful clinical monitoring. These medications should be adequately monitored when concomitantly administered with lixisenatide. If such medications are to be administered with food, patients should be advised to take them with a meal or snack when lixisenatide is not administered.
- Antibiotics, acetaminophen, or other medications that are particularly dependent on threshold concentrations for efficacy or for which a delay in effect is undesirable should be administered at least 1 hour before SOLIQUA 100/33 injection [see Clinical Pharmacology (12.3)].
- Oral contraceptives should be taken at least 1 hour before SOLIQUA 100/33 administration or 11 hours after [see Clinical Pharmacology (12.3)].
5.3 Never Share A Soliqua 100/33 Prefilled Pen Between Patients
SOLIQUA 100/33 prefilled pens must never be shared between patients, even if the needle is changed. Sharing of the pen poses a risk for transmission of blood-borne pathogens.
5.4 Hyperglycemia Or Hypoglycemia With Changes in Insulin Regimen
Changes in insulin regimen (e.g., insulin strength, manufacturer, type, injection site or method of administration) may affect glycemic control and predispose to hypoglycemia [see Warnings and Precautions (5.6)] or hyperglycemia. Repeated insulin injections into areas of lipodystrophy or localized cutaneous amyloidosis have been reported to result in hyperglycemia; and a sudden change in the injection site (to unaffected area) has been reported to result in hypoglycemia [see Adverse Reactions (6)].
Make any changes to a patient's insulin regimen under close medical supervision with increased frequency of blood glucose monitoring. Advise patients who have repeatedly injected into areas of lipodystrophy or localized cutaneous amyloidosis to change the injection site to unaffected areas and closely monitor for hypoglycemia. Adjustments in concomitant oral antidiabetic treatment may be needed. When converting from basal insulin therapy or a GLP-1 receptor agonist to SOLIQUA 100/33 follow dosing recommendations [see Dosage and Administration (2.2, 2.3)].
5.13 Pulmonary Aspiration During General Anesthesia Or Deep Sedation
SOLIQUA 100/33 delays gastric emptying [see Clinical Pharmacology (12.1)]. There have been rare postmarketing reports of pulmonary aspiration in patients receiving GLP-1 receptor agonists undergoing elective surgeries or procedures requiring general anesthesia or deep sedation who had residual gastric contents despite reported adherence to preoperative fasting recommendations.
Available data are insufficient to inform recommendations to mitigate the risk of pulmonary aspiration during general anesthesia or deep sedation in patients taking SOLIQUA 100/33, including whether modifying preoperative fasting recommendations or temporarily discontinuing SOLIQUA 100/33 could reduce the incidence of retained gastric contents. Instruct patients to inform healthcare providers prior to any planned surgeries or procedures if they are taking SOLIQUA 100/33.
14.2 Clinical Study in Patients With Type 2 Diabetes Uncontrolled On Oad Treatment
A total of 1170 patients with type 2 diabetes were randomized in an open-label, 30-week, active-controlled study (Study A: NCT05058147) to evaluate the efficacy and safety of SOLIQUA 100/33 compared to the individual components, insulin glargine 100 units/mL and lixisenatide.
Patients with type 2 diabetes, treated with metformin alone or treated with metformin and a second OAD treatment that could be a sulfonylurea or a glinide or a sodium-glucose cotransporter-2 (SGLT-2) inhibitor or a dipeptidyl peptidase-4 (DPP-4) inhibitor, and who were not adequately controlled with this treatment (HbA1c range 7.5% to 10% for patients previously treated with metformin alone and 7% to 9% for patients previously treated with metformin and a second OAD treatment) entered a run-in period for 4 weeks. During this run-in period, metformin treatment was optimized and all other OADs were discontinued. At the end of the run-in period, patients who remained inadequately controlled (HbA1c between 7% and 10%) were randomized to either SOLIQUA 100/33 (n=469), insulin glargine 100 units/mL (n=467), or lixisenatide (n=234).
The type 2 diabetes population had the following characteristics: mean age was 58.4 years, 50.6% were male, 90.1% were Caucasian, 6.7% were Black or African American, and 19.1% were Hispanic. At screening, the mean duration of diabetes was approximately 9 years, the mean BMI was approximately 31.7 kg/m2, and mean eGFR was 84.8 mL/min/1.73 m2.
SOLIQUA 100/33 and insulin glargine were to be titrated weekly to target a fasting plasma glucose goal of <100 mg/dL. Patients could not increase their dose by more than 4 units per week and the prespecified maximum dose of insulin glargine was limited to 60 units. The targeted fasting plasma glucose goal was achieved in 35% of patients in both groups at 30 weeks.
At Week 30, SOLIQUA 100/33 provided statistically significant improvement in HbA1c (p-value <0.0001) compared to insulin glargine 100 units/mL and lixisenatide-treated patients (-1.6%, -1.3%, and -0.9%). In a prespecified analysis of this primary endpoint, the differences observed were consistent with regard to baseline OAD use (metformin alone or metformin plus second OAD).
The mean difference (95% CI) in HbA1c reduction between SOLIQUA 100/33 and insulin glargine was -0.3% (-0.4, -0.2) and -0.7% (-0.8, -0.6) compared to lixisenatide.
See Table 5 for the other endpoints in the study. The difference in the glucose lowering effect observed in the trial may not necessarily reflect the effect that will be observed in the care setting where insulin glargine dosage can be different than that used in the trial.
| SOLIQUA 100/33 | Insulin Glargine 100 units/mL | Lixisenatide | |
|---|---|---|---|
| Number of subjects (randomized and treated) | 469 | 467 | 233 |
| HbA1c (%) | |||
| Baseline (mean; post run-in phase) | 8.1 | 8.1 | 8.1 |
| End of study (mean) | 6.5 | 6.8 | 7.3 |
| LS change from baseline (mean) Estimated using an ANCOVA with treatment, randomization strata, and country as fixed factors and baseline HbA1c as covariate. Twenty-six (5.5%) patients in the SOLIQUA 100/33 arm and 21 (4.5%) patients in the insulin glargine 100 units/mL arm, and 13 (5.6%) patients in the lixisenatide arm had missing HbA1c measurement at Week 30. Missing measurements were imputed using multiple imputations with respect to the baseline value of the subject.
|
-1.6 | -1.3 | -0.9 |
| LS mean difference vs insulin glargine | -0.3 | ||
| [95% confidence interval] | [-0.4, -0.2] The trial was designed to show the contribution of the GLP-1 component to glycemic lowering, and the insulin glargine dose and the dosing algorithm were selected to isolate the effect of the GLP-1 component. At the end of the trial, the doses of insulin glargine were equivalent between treatment groups. The mean final dose of SOLIQUA 100/33 at week 30 was 39.8 units (for SOLIQUA 100/33: 39.8 units insulin glargine/13.1 mcg lixisenatide) and 40.5 units in the insulin glargine–treated patients. The difference in effect observed in the trial may not necessarily reflect the effect that will be observed in the care setting where alternative insulin glargine dosage can be used.
|
– | |
| (p-value) | (<0.0001) | ||
| LS mean difference vs lixisenatide | -0.7 | ||
| [95% confidence interval] | – | – | [-0.8, -0.6] Lixisenatide was given at the maintenance dose of 20 mcg.
|
| (p-value) | (<0.0001) | ||
| Number of Patients (%) reaching HbA1c <7% at week 30 | 345 (74%) | 277 (59%) | 76 (33%) |
| Fasting plasma glucose (mg/dL) | |||
| Baseline (mean) | 177.9 | 175.7 | 175.8 |
| End of study (mean) | 113.9 | 117.6 | 149.0 |
| LS change from baseline (mean) | -59.1 | -55.8 | -27.2 |
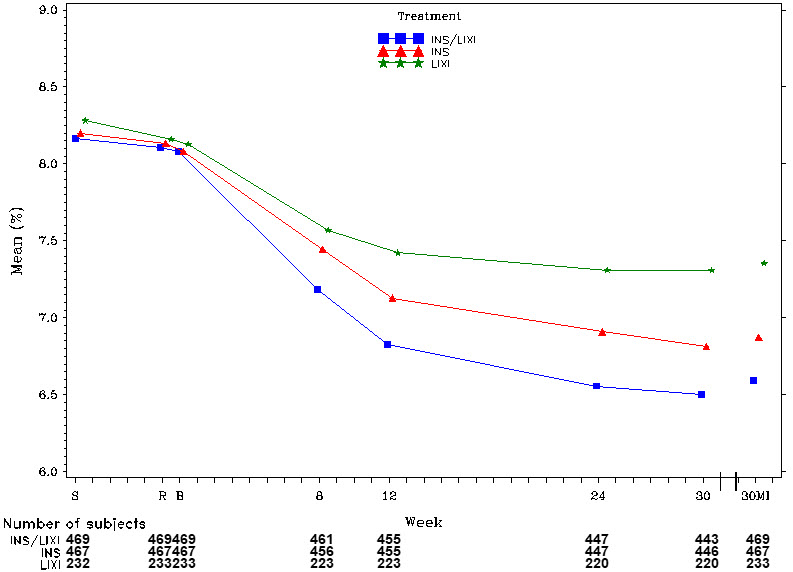
Figure 1: Mean HbA1c (%) Over Time – Randomized and Treated Population
S = Screening (Week 6), R = Run-in (Week 1), B = Baseline, MI = Multiple imputation.
INS/LIXI = fixed ratio combination, INS = Insulin Glargine, LIXI = Lixisenatide
Note: The plot included all scheduled measurements obtained during the study, including those obtained after IMP discontinuation or introduction of rescue medication.
30MI: Missing HbA1c values at Week 30 in each group were imputed using their baseline HbA1c values plus an error. The error is normally distributed with mean zero and a standard deviation set equal to the estimated pooled standard deviation.
5.11 Fluid Retention and Heart Failure With Concomitant Use of Ppar Gamma Agonists
Thiazolidinediones (TZDs), which are peroxisome proliferator-activated receptor (PPAR)-gamma agonists, can cause dose-related fluid retention, particularly when used in combination with insulin-containing products, including SOLIQUA 100/33. Fluid retention may lead to or exacerbate heart failure. Patients treated with SOLIQUA 100/33 and a PPAR-gamma agonist should be observed for signs and symptoms of heart failure. If heart failure develops, it should be managed according to current standards of care, and discontinuation or dose reduction of the PPAR-gamma agonist must be considered.
14.3 Clinical Studies in Patients With Type 2 Diabetes Uncontrolled On Basal Insulin
A total of 736 patients with type 2 diabetes participated in a randomized, 30-week, active-controlled, open-label, 2-treatment arm, parallel-group, multicenter study (Study B: NCT02058160) to evaluate the efficacy and safety of SOLIQUA 100/33 compared to insulin glargine 100 units/mL.
Patients screened had type 2 diabetes were treated with basal insulin for at least 6 months, receiving a stable daily dose of between 15 and 40 units alone or combined with 1 or 2 OADs (metformin, sulfonylurea, glinide, SGLT-2 inhibitor or a DPP-4 inhibitor), had an HbA1c between 7.5% and 10% and a FPG less than or equal to 180 mg/dL or 200 mg/dL depending on their previous antidiabetic treatment.
This type 2 diabetes population had the following characteristics: Mean age was 60 years, 46.7% were male, 91.7% were Caucasian, 5.2% were Black or African American and 17.9% were Hispanic. At screening, the mean duration of diabetes was approximately 12 years, the mean BMI was approximately 31 kg/m2, mean eGFR was 80.6 mL/min/1.73 m2 and 86.1% of patients had an eGFR ≥60 mL/min.
After screening, eligible patients (n=1018) entered a 6-week run-in phase where patients remained on or were switched to insulin glargine 100 units/mL, if they were treated with another basal insulin, and had their insulin glargine dose titrated/stabilized while continuing metformin (if previously taken). The mean HbA1c decreased during run-in period from 8.5% to 8.1%. Any other OADs were discontinued.
At the end of the run-in period, patients with an HbA1c between 7% and 10%, FPG ≤140 mg/dL and insulin glargine daily dose of 20 to 50 units (mean of 35 units), were randomized to either SOLIQUA 100/33 (n=367) or insulin glargine 100 units/mL (n=369).
SOLIQUA 100/33 and insulin glargine were to be titrated weekly to target a fasting plasma glucose goal of <100 mg/dL. The mean dose of insulin glargine at baseline was 35 units. The maximum dose of insulin glargine allowed in the trial was 60 units (insulin dose cap) in both groups. The targeted fasting plasma glucose goal was achieved in 33% of patients in both groups at 30 weeks.
At Week 30, there was a reduction in HbA1c from baseline of -1.1% for SOLIQUA 100/33 and -0.6% for insulin glargine 100 units/mL. The mean difference (95% CI) in HbA1c reduction between SOLIQUA 100/33 and insulin glargine was -0.5 [-0.6, -0.4] and statistically significant. The trial was designed to show the contribution of the GLP-1 component to glycemic lowering and the insulin glargine dose and the dosing algorithm was selected to isolate the effect of the GLP-1 component. At the end of the trial, the doses of insulin glargine were equivalent between treatment groups. The mean final dose of SOLIQUA 100/33 and insulin glargine at week 30 was 46.7 units (for SOLIQUA 100/33: 46.7 units insulin glargine/15.6 mcg lixisenatide). The difference in effect observed in the trial may not necessarily reflect the effect that will be observed in the care setting where alternative insulin glargine dosage can be used. See Table 6 for the other endpoints in the study.
| SOLIQUA 100/33 | Insulin Glargine 100 units/mL | |
|---|---|---|
| Number of Subjects (randomized and treated) | 365 | 365 |
| HbA1c (%) | ||
| Baseline (mean; post run-in phase) | 8.1 | 8.1 |
| End of study (mean) | 6.9 | 7.5 |
| LS change from baseline (mean) Estimated using an ANCOVA with treatment, randomization strata, and country as fixed factors and baseline HbA1c as covariate. Twenty (5.5%) patients in the SOLIQUA 100/33 arm and 10 (2.7%) patients in the insulin glargine 100 units/mL arm had missing HbA1c measurement at Week 30. Missing measurements were imputed using multiple imputations with respect to the baseline value of the subject.
|
-1.1 | -0.6 |
| Difference vs insulin glargine | -0.5 | |
| [95% confidence interval] | [-0.6, -0.4] p<0.01; The trial was designed to show the contribution of the GLP-1 component to glucose lowering. The insulin glargine dose in this trial was capped at a maximum dose of 60 units and the dosing algorithm was selected to isolate the effect of the GLP-1 component. At the end of the trial, the doses of insulin glargine were equivalent between treatment groups. The mean final dose of SOLIQUA 100/33 and insulin glargine at week 30 was 46.7 units (for SOLIQUA 100/33: 46.7 units insulin glargine/15.6 mcg lixisenatide). The difference in effect observed in the trial may not necessarily reflect the effect that will be observed in the care setting where alternative insulin glargine dosage can be used.
|
|
| Patients [n (%)] reaching HbA1c <7% at week 30 Patients with missing HbA1c measurement at Week 30 were considered non-responders.
|
201 (55.1%) | 108 (29.6%) |
| Fasting plasma glucose (mg/dL) | ||
| Baseline (mean) | 132.3 | 132.0 |
| End of study (mean) | 121.9 | 120.5 |
| LS change from baseline (mean) | -5.7 | -7.0 |
Structured Label Content
Section 42229-5 (42229-5)
Limitations of Use:
- SOLIQUA 100/33 contains lixisenatide. Coadministration with any other product containing lixisenatide or another glucagon-like peptide-1 (GLP-1) receptor agonist is not recommended [see Warnings and Precautions (5.5)].
- SOLIQUA 100/33 is not recommended for the treatment of diabetic ketoacidosis.
- SOLIQUA 100/33 has not been studied in combination with prandial insulin.
Section 42231-1 (42231-1)
| This Medication Guide has been approved by the U.S. Food and Drug Administration. | Revised: July 2025 | ||
|
Medication Guide SOLIQUA® 100/33 (So - lee - kwa) (insulin glargine and lixisenatide) injection, for subcutaneous use |
|||
|
What is the most important information I should know about SOLIQUA 100/33? SOLIQUA 100/33 can cause serious side effects including inflammation of the pancreas (pancreatitis). Stop using SOLIQUA 100/33 and call your healthcare provider right away if you have severe pain in your stomach area (abdomen) that will not go away, with or without vomiting. You may feel the pain from your abdomen to your back. |
|||
|
What is SOLIQUA 100/33?
SOLIQUA 100/33 is an injectable prescription medicine that contains 2 diabetes medicines, insulin glargine and lixisenatide, that is used along with diet and exercise to improve blood sugar (glucose) in adults with type 2 diabetes.
|
|||
|
Who should not use SOLIQUA 100/33? Do not use SOLIQUA 100/33 if you:
|
|||
Before using SOLIQUA 100/33, tell your healthcare provider about all your medical conditions including if you:
Before using SOLIQUA 100/33, talk to your healthcare provider about low blood sugar and how to manage it. Especially tell your healthcare provider if you take:
|
|||
How should I use SOLIQUA 100/33?
|
|||
|
What should I avoid while taking SOLIQUA 100/33? While taking SOLIQUA 100/33 do not:
|
|||
|
What are the possible side effects of SOLIQUA 100/33? SOLIQUA 100/33 can cause serious side effects including:
|
|||
|
|
||
|
|||
|
|
|
|
|
|||
|
|
||
|
|||
|
|
||
| Talk to your healthcare provider about any side effect that bothers you or does not go away. These are not all the possible side effects of SOLIQUA 100/33 Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. |
|||
How should I store SOLIQUA 100/33?
|
|||
|
General information about the safe and effective use of SOLIQUA 100/33.
Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not use SOLIQUA 100/33 for a condition for which it was not prescribed. Do not give SOLIQUA 100/33 to other people, even if they have the same symptoms that you have. It may harm them. You can ask your pharmacist or healthcare provider for information about SOLIQUA 100/33 that is written for health professionals. |
|||
|
What are the ingredients in SOLIQUA 100/33?
Active ingredients: insulin glargine and lixisenatide Inactive ingredients: glycerol (20 mg), metacresol (2.7 mg), methionine (3 mg), zinc (30 mcg) and Water for Injection, USP. Hydrochloric acid and/or sodium hydroxide are added as needed to adjust the pH. |
|||
| Manufactured by: sanofi-aventis U.S. LLC, Morristown, NJ 07960 A SANOFI COMPANY U.S. License No. 1752 For more information, go to www.soliqua100-33.com or call sanofi-aventis at 1-800-633-1610. |
Section 43683-2 (43683-2)
16.2 Storage
Dispense in the original sealed carton with the enclosed Instructions for Use.
Prior to first use, SOLIQUA 100/33 pen should be stored in a refrigerator, 36°F–46°F (2°C–8°C). Do not freeze. Discard SOLIQUA 100/33 if it has been frozen. Protect from light.
After first use, store at room temperature up to 77°F (25°C). Replace the pen cap after each use to protect from light.
Discard pen 28 days after first use.
Remove the needle after each injection and store the SOLIQUA 100/33 pen without a needle attached.
11 Description (11 DESCRIPTION)
SOLIQUA 100/33 is a combination of insulin glargine, an insulin analog, and lixisenatide, a GLP-1 receptor agonist.
Insulin glargine is a human insulin analog produced by recombinant DNA technology utilizing a nonpathogenic laboratory strain of Escherichia coli (K12) as the production organism. The minimum potency of insulin glargine is NLT 15 units/mg. Insulin glargine differs from human insulin in that the amino acid asparagine at position A21 is replaced by glycine and two arginines are added at the C-terminus of the B-chain. Insulin glargine has low aqueous solubility at neutral pH. At pH 4 insulin glargine is completely soluble. It has a molecular weight of 6.063 kDa.
Lixisenatide is a synthetic analogue of human GLP-1, which acts as a GLP-1 receptor agonist. Lixisenatide is a protein containing 44 amino acids, which is amidated at the C-terminal amino acid (position 44) and has a molecular weight of 4.8585 kDa.
SOLIQUA 100/33 (insulin glargine and lixisenatide) injection is a sterile, colorless to almost colorless solution for subcutaneous use. SOLIQUA 100/33 is supplied as a prefilled single-patient-use disposable pen contain 300 units of insulin glargine and 100 mcg of lixisenatide in 3 mL of a clear, colorless to almost colorless, sterile, and aqueous solution. Each mL contains 100 units of insulin glargine and 33 mcg of lixisenatide and the inactive ingredients: glycerol (20 mg), metacresol (2.7 mg), methionine (3 mg), zinc (30 mcg), and Water for Injection, USP. Hydrochloric acid and/or sodium hydroxide may be added to adjust the pH. The approximate pH is 4.5.
2.4 Missed Doses
Instruct patients who miss a dose of SOLIQUA 100/33 to resume the once-daily regimen as prescribed with the next scheduled dose. Do not administer an extra dose or increase the dose to make up for the missed dose.
5.10 Hypokalemia
All insulin-containing products, including SOLIQUA 100/33, cause a shift in potassium from the extracellular to intracellular space, possibly leading to hypokalemia. Untreated hypokalemia may cause respiratory paralysis, ventricular arrhythmia, and death. Monitor potassium levels in patients at risk for hypokalemia if indicated (e.g., patients using potassium-lowering medications, patients taking medications sensitive to serum potassium concentrations).
5.6 Hypoglycemia
Hypoglycemia is the most common adverse reaction associated with insulin-containing products, including SOLIQUA 100/33 [see Adverse Reactions (6.1)]. Severe hypoglycemia can cause seizures, may be life-threatening or cause death. Hypoglycemia can impair concentration ability and reaction time; this may place an individual and others at risk in situations where these abilities are important (e.g., driving or operating other machinery). SOLIQUA 100/33 (an insulin-containing product), or any insulin, should not be used during episodes of hypoglycemia [see Contraindications (4)].
Hypoglycemia can happen suddenly, and symptoms may differ in each individual and change over time in the same individual. Symptomatic awareness of hypoglycemia may be less pronounced in patients with longstanding diabetes, in patients with diabetic nerve disease, in patients using medications that block the sympathetic nervous system (e.g., beta-blockers) [see Drug Interactions (7.1)], or in patients who experience recurrent hypoglycemia.
16.1 How Supplied
SOLIQUA 100/33 (insulin glargine and lixisenatide) injection is a clear, colorless to almost colorless solution in a 3 mL prefilled, disposable, single-patient-use pen:
| Dosage Unit/Strength | Package size | NDC # |
|---|---|---|
| 3 mL SOLIQUA 100/33 single-patient-use pen 100 units/mL insulin glargine and 33 mcg/mL lixisenatide |
Package of 5 | 0024-5761-05 |
Needles are not included. Only use needles that are compatible for use with SOLIQUA 100/33 prefilled pen.
8.4 Pediatric Use
Safety and effectiveness of SOLIQUA 100/33 have not been established in pediatric patients.
8.5 Geriatric Use
Of the total number of subjects (n=834) in controlled clinical studies of patients with type 2 diabetes, who were treated with SOLIQUA 100/33, 25.2% (n=210) were ≥65 years of age and 4% (n=33) were ≥75 years of age. No overall differences in effectiveness and safety were observed in the subgroup analyses across the age groups.
Nevertheless, caution should be exercised when SOLIQUA 100/33 is administered to geriatric patients. In elderly patients with diabetes, the initial dosing, dose increments, and maintenance dosage should be conservative to avoid hypoglycemic reactions. Hypoglycemia may be difficult to recognize in the elderly.
5.9 Immunogenicity
Patients may develop antibodies to insulin and lixisenatide following treatment. A pooled analysis of studies of lixisenatide-treated patients showed that 70% were antibody positive at Week 24. In the subset of patients (2.4%) with the highest antibody concentrations (>100 nmol/L), an attenuated glycemic response was observed. A higher incidence of allergic reactions and injection-site reactions occurred in antibody positive patients [see Warnings and Precautions (5.1), Adverse Reactions (6.2)].
If there is worsening glycemic control or failure to achieve targeted glycemic control, significant injection-site reactions or allergic reactions, alternative antidiabetic therapy should be considered.
4 Contraindications (4 CONTRAINDICATIONS)
SOLIQUA 100/33 is contraindicated:
- During episodes of hypoglycemia [see Warnings and Precautions (5.6)].
- In patients with serious hypersensitivity to insulin glargine, lixisenatide, or any of the excipients in SOLIQUA 100/33. Hypersensitivity reactions including anaphylaxis have occurred with both lixisenatide and insulin glargine [see Warnings and Precautions (5.1) and Adverse Reactions (6.1)].
6 Adverse Reactions (6 ADVERSE REACTIONS)
The following adverse reactions are discussed elsewhere:
- Anaphylaxis and Serious Hypersensitivity Reactions [see Warnings and Precautions (5.1)]
- Acute Pancreatitis [see Warnings and Precautions (5.2)]
- Hypoglycemia [see Warnings and Precautions (5.6)]
- Acute Kidney Injury Due to Volume Depletion [see Warnings and Precautions (5.7)]
- Severe Gastrointestinal Adverse Reactions [see Warnings and Precautions (5.8)]
- Hypokalemia [see Warnings and Precautions (5.10)]
- Acute Gallbladder Disease [see Warnings and Precautions (5.12)]
- Pulmonary Aspiration During General Anesthesia or Deep Sedation [see Warnings and Precautions (5.13)]
7 Drug Interactions (7 DRUG INTERACTIONS)
- Drugs that affect glucose metabolism: Adjustment of SOLIQUA 100/33 dosage may be needed; closely monitor blood glucose. (7.1)
- Antiadrenergic Drugs (e.g., beta-blockers, clonidine, guanethidine, and reserpine): Hypoglycemia signs and symptoms may be reduced. (7.1)
- Effects of delayed gastric emptying on oral medications: Lixisenatide delays gastric emptying which may impact absorption of concomitantly administered oral medications. Oral contraceptives and other medications such as antibiotics and acetaminophen should be taken at least 1 hour prior to SOLIQUA 100/33 administration or 11 hours after. (7.2)
8.6 Renal Impairment
Frequent glucose monitoring and dose adjustment may be necessary for SOLIQUA 100/33 in patients with renal impairment [see Warnings and Precautions (5.7)].
Instructions for Use (INSTRUCTIONS FOR USE)
Read these instructions carefully before using your SOLIQUA 100/33 pen.
Do not share your SOLIQUA 100/33 pen with other people, even if the needle has been changed. You may give other people a serious infection, or get a serious infection from them.
SOLIQUA 100/33 is an injectable prescription medicine that contains 2 diabetes medicines, insulin glargine and lixisenatide in a SoloStar pen. The drug combination in this pen is only for the daily injection of 15 to 60 units of SOLIQUA 100/33. Each unit dialed contains 1 unit insulin glargine and 0.33 mcg lixisenatide.
People who are blind or have other vision problems should not use the SOLIQUA 100/33 pen without help from a person trained to use the pen.
Important information
- Check the label on the SOLIQUA 100/33 pen each time you give your injection to make sure you are using the correct medicine.
- Do not use your pen if it is damaged or if you are not sure that it is working correctly.
- Perform a safety test before each injection (see "Step 3: Do a safety test").
- Always carry a spare pen and spare needles in case they are lost or stop working.
- Do not reuse needles. Always use a new sterile needle for each injection. This helps stop blocked needles, contamination, and infection. If you reuse needles, you might not get your dose (underdosing) or get too much (overdosing).
- Do not use SOLIQUA 100/33 in an insulin pump or inject SOLIQUA 100/33 into your vein (intravenously).
- Do not mix SOLIQUA 100/33 in any other type of insulin or liquid medicine prior to injection.
- Change (rotate) your injection sites within the area you chose with each dose (see "Places to inject").
Learn to inject
- Talk with your healthcare provider about how to use the SOLIQUA 100/33 pen and how to inject correctly before using your pen.
- Ask for help if you have problems handling the pen.
- Read all of these instructions before using your pen. You may get too much or too little medicine if you do not follow the instructions correctly.
Need help?
If you have any questions about your pen or about diabetes, ask your healthcare provider, go to www.soliqua100-33.com or call sanofi-aventis at 1-800-633-1610.
Supplies you will need:
- 1 SOLIQUA 100/33 pen
- 1 new sterile needle (see Step 2 "Attach a new needle" )
- 1 alcohol swab
- a puncture-resistant container for used needles and pens (see "Throwing your pen away" at the end of this Instructions for Use)
Places to inject
- Inject your SOLIQUA 100/33 dose exactly as your healthcare provider has shown you.
- Inject your SOLIQUA 100/33 dose under the skin (subcutaneously) of your upper legs (thighs), upper arms, or stomach area (abdomen).
- Change (rotate) your injection sites within the area you choose for each dose to reduce your risk of getting pits in skin or thickened skin (lipodystrophy) and skin with lumps (localized cutaneous amyloidosis) at the injection sites.
- Do not inject where the skin has pits, is thickened, or has lumps.
- Do not inject where the skin is tender, bruised, scaly or hard, or into scars or damaged skin.
Get to know your pen
Step 1: Check your pen
Take a new pen out of the refrigerator at least 1 hour before you inject. Cold medicine is more painful to inject.
-
1ACheck the name and expiration date on the label of your pen.
- Make sure you have the correct medicine. This pen is colored light green with an orange injection button (see the "Get to know your pen" diagram).
- Do not use your pen after the expiration date on the pen label.
-
1BPull off the pen cap.
-
1CCheck that the medicine is clear and colorless to almost colorless.
- If you see small particles, return it to your pharmacy for a replacement.
-
1DWipe the rubber seal with an alcohol swab.
If you have other injector pens
- Making sure you have the correct medicine is especially important if you have other injector pens.
Step 2: Attach a new needle
- Do not reuse needles. Always use a new sterile needle for each injection. This helps stop blocked needles, contamination and infection.
- Only use needles that are meant to be used with SOLIQUA 100/33. Needles are supplied separately. If you do not know what needles to use, ask your healthcare provider or pharmacist.
-
2ATake a new needle and peel off the protective seal.
-
2BKeep the needle straight and screw it onto the pen until fixed. Do not over-tighten.
-
2CPull off the outer needle cap. Keep this for later.
-
2DPull off the inner needle cap and throw it away.
Handling needles
- Take care when handling needles to prevent needle-stick injury and cross-infection.
Step 3: Do a safety test
Perform a safety test before each injection to:
- Check your pen and the needle to make sure they are working properly.
- Make sure that you get the correct dose.
-
3ASelect 2 units by turning the dose selector until the dose pointer is at the 2 mark.
-
3BPress the injection button all the way in.
- When the medicine comes out of the needle tip, your pen is working correctly.
If no liquid appears:
- You may need to repeat this step up to 3 times before seeing the medicine.
- If no medicine comes out after the third time, the needle may be blocked. If this happens:
- Do not use your pen if still no medicine comes out of the needle tip. Use a new pen.
- Do not use a syringe to remove medicine from your pen.
If you see air bubbles
- You may see air bubbles in the medicine. This is normal, they will not harm you.
Step 4: Select the dose
- Do not select a dose or press the injection button without a needle attached. This may damage your pen.
- Only use this pen to inject your daily dose from 15 to 60 units. Do not change your dose unless your healthcare provider has told you to change your dose.
- Do not use this pen if you need a single daily dose that is more than 60 units.
- Do not use the pen if your single daily dose is less than 15 units, the black area in dose window as shown in the picture.
-
4AMake sure a needle is attached and the dose is set to "0".
-
4BTurn the dose selector until the dose pointer lines up with your dose.
- Do not dial your dose by counting the clicks, because you might dial the wrong dose. Always check the number in the dose window to make sure you dialed the correct dose.
- If you turn past your dose, you can turn back down.
- If there are not enough units left in your pen for your dose, the dose selector will stop at the number of units left.
- If you cannot select your full prescribed dose, use a new pen.
How to read the dose window
- Each line in the dose window equals 1 unit of SOLIQUA 100/33.
- Even numbers are shown in line with the dose pointer, as shown in picture.
30 units selected
- Odd numbers are shown as a line between even numbers, as shown in picture.
29 units selected
Units of medicine in your pen
- This pen contains 300 units of SOLIQUA 100/33 and it is intended to be used for more than one dose.
Step 5: Inject your dose
If you find it hard to press the injection button in, do not force it as this may break your pen. See the section after Step 5E below for help.
-
5AChoose a place to inject as shown in the picture labeled "Places to inject."
-
5BPush the needle into your skin as shown by your healthcare provider.
- Do not touch the injection button yet.
-
5CPlace your thumb on the injection button. Then press all the way in and hold.
- Do not press injection button at an angle. Your thumb could block the dose selector from turning.
-
5DKeep the injection button held in and when you see "0" in the dose window, slowly count to 10.
- This will make sure you get your full dose.
-
5EAfter holding and slowly counting to 10, release the injection button. Then remove the needle from your skin.
If you find it hard to press the injection button in:
- Change the needle (see Step 6 to remove the needle and Step 2 to attach a new needle) then do a safety test (see Step 3 ).
- If you still find it hard to press in, get a new pen.
- Do not use a syringe to remove medicine from your pen.
Step 6: Remove the needle
- Take care when handling needles to prevent needle-stick injury and cross-infection.
- Do not put the inner needle cap back on.
-
6AGrip the widest part of the outer needle cap. Keep the needle straight and guide it into the outer needle cap back. Then push firmly on.
- The needle can puncture the cap if it is recapped at an angle.
-
6BGrip and squeeze the widest part of the outer needle cap. Turn your pen several times with your other hand to remove the needle.
- Try again if the needle does not come off the first time.
-
6CThrow away the used needle in a puncture-resistant container (see "Throwing your pen away" at the end of this Instructions for Use).
-
6DPut your pen cap back on.
- Do not put the pen back in the refrigerator.
Use by
- Only use your pen for up to 28 days after its first use.
How to store your pen
Before first use
- Keep new pens in the refrigerator between 36°F to 46°F (2°C to 8°C).
- Do not freeze. If you accidentally freeze your pen, throw it away.
After first use
- Keep your pen at room temperature, up to 77°F (25°C).
- Do not put your pen back in the refrigerator.
- Do not store your pen with the needle attached.
- Store the pen with your pen cap on.
Keep this pen out of the sight and reach of children.
How to care for your pen
Handle your pen with care
- Do not drop your pen or knock it against hard surfaces.
- If you think that your pen may be damaged, do not try to fix it. Use a new one.
Protect your pen from dust and dirt
- You can clean the outside of your pen by wiping it with a damp cloth (water only). Do not soak, wash or lubricate the pen. This may damage it.
Throwing your pen away
- Put the used SOLIQUA 100/33 pen in a FDA-cleared sharps disposal container right away after use. Do not throw away (dispose of) the SOLIQUA 100/33 pen in your household trash.
- If you do not have a FDA-cleared sharps disposal container, you may use a household container that is:
- made of a heavy-duty plastic,
- can be closed with a tight-fitting, puncture-resistant lid, without sharps being able to come out,
- upright and stable during use,
- leak-resistant, and
- properly labeled to warn of hazardous waste inside the container.
- When your sharps disposal container is almost full, you will need to follow your community guidelines for the right way to dispose of your sharps disposal container. There may be state or local laws about how you should throw away used needles and syringes. For more information about safe sharps disposal, and for specific information about sharps disposal in the state that you live in, go to the FDA's website at: http://www.fda.gov/safesharpsdisposal.
Manufactured by:
sanofi-aventis U.S. LLC
Morristown, NJ 07960 A SANOFI COMPANY
U.S. License No. 1752
©2025 sanofi-aventis U.S. LLC
SOLIQUA and SoloStar are registered trademarks of sanofi-aventis U.S. LLC.
This Instructions for Use has been approved by the U.S. Food and Drug Administration.
Revised: July 2025
5.2 Acute Pancreatitis
Acute pancreatitis, including fatal and non-fatal hemorrhagic or necrotizing pancreatitis, has been observed in patients treated with GLP-1 receptor agonists [see Adverse Reactions (6)].
After initiation of SOLIQUA 100/33, observe patients carefully for signs and symptoms of pancreatitis (including persistent severe abdominal pain, sometimes radiating to the back and which may or may not be accompanied by vomiting). If pancreatitis is suspected, discontinue SOLIQUA 100/33 and initiate appropriate management.
8.7 Hepatic Impairment
The effect of hepatic impairment on the pharmacokinetics of SOLIQUA 100/33 has not been studied. Frequent glucose monitoring and dose adjustment may be necessary for SOLIQUA 100/33 in patients with hepatic impairment [see Warnings and Precautions (5.6)].
1 Indications and Usage (1 INDICATIONS AND USAGE)
SOLIQUA 100/33 is a combination of insulin glargine and lixisenatide and is indicated as an adjunct to diet and exercise to improve glycemic control in adults with type 2 diabetes mellitus.
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
- Anaphylaxis and Serious Hypersensitivity Reactions: Severe, life-threatening, and generalized allergic reactions can occur. Instruct patients to discontinue use if a reaction occurs and promptly seek medical attention. (5.1)
- Acute Pancreatitis: Has been observed in patients treated with GLP-1 receptor agonists, including SOLIQUA 100/33. Discontinue if pancreatitis is suspected. (5.2)
- Never share a SOLIQUA 100/33 prefilled pen between patients, even if the needle is changed. (5.3)
- Hyperglycemia or Hypoglycemia with Changes in Insulin Regimen: Make changes to a patient's insulin regimen (e.g., insulin strength, manufacturer, type, injection site or method of administration) under close medical supervision with increased frequency of blood glucose monitoring. (5.4)
- Overdose Due to Medication Errors: SOLIQUA 100/33 contains two drugs. Instruct patients to always check the label before each injection since accidental mix-ups with insulin products can occur. Do not exceed the maximum dose or use with other GLP-1 receptor agonists. (5.5)
- Hypoglycemia: May be life-threatening. Increase frequency of glucose monitoring with changes to insulin dosage, coadministered glucose lowering medications, meal pattern, physical activity; and in patients with renal or hepatic impairment and hypoglycemia unawareness. (5.6)
- Acute kidney injury Due to Volume Depletion: Monitor renal function in patients reporting adverse reactions that could lead to volume depletion. SOLIQUA 100/33 is not recommended in patients with end-stage renal disease. (5.7)
- Severe Gastrointestinal Adverse Reactions: Use has been associated with gastrointestinal adverse reactions, sometimes severe. SOLIQUA 100/33 is not recommended in patients with severe gastroparesis (5.8).
- Immunogenicity: Patients may develop antibodies to insulin glargine and lixisenatide. If there is worsening glycemic control or failure to achieve targeted glycemic control, significant injection-site reactions or allergic reactions, alternative antidiabetic therapy should be considered. (5.9)
- Hypokalemia: May be life-threatening. Monitor potassium levels in patients at risk of hypokalemia and treat if indicated. (5.10)
- Fluid Retention and Heart Failure with Use of PPAR-gamma agonists ): Observe for signs and symptoms of heart failure; consider dosage reduction or discontinuation if heart failure occurs. (5.11)
- Acute Gallbladder Disease: If cholelithiasis or cholecystitis are suspected, gallbladder studies are indicated. (5.12)
- Pulmonary Aspiration During General Anesthesia or Deep Sedation: Has been reported in patients receiving GLP-1 receptor agonists undergoing elective surgeries or procedures. Instruct patients to inform healthcare providers of any planned surgeries or procedures.(5.13)
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
- Inject subcutaneously once a day within the hour prior to the first meal of the day. (2.1)
- SOLIQUA 100/33 pen delivers 15 units to 60 units per injection. (2.1, 2.2)
- Maximum daily dosage is 60 units (60 units of insulin glargine and 20 mcg of lixisenatide). (2.1)
- Discontinue basal insulin or GLP-1 receptor agonist prior to initiation. (2.2)
- In patients naive to basal insulin or to a GLP-1 receptor agonist, currently on less than 30 units of basal insulin, or on a GLP-1 receptor agonist, the recommended starting dosage is 15 units subcutaneously once daily. (2.2)
- In patients inadequately controlled on 30 to 60 units of basal insulin, the starting dosage is 30 units subcutaneously once daily. (2.2)
- See Full Prescribing Information for titration recommendations. (2.3)
- Inject subcutaneously in abdominal area, thigh, or upper arm and rotate injection sites within the same region from one injection to the next to reduce risk of lipodystrophy and localized cutaneous amyloidosis. (2.5)
- Do not administer intravenously, or via an infusion pump. (2.5)
- Do not dilute or mix with any other insulin products or solutions. (2.5)
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
SOLIQUA 100/33 is a clear, colorless to almost colorless solution available as:
Injection: 100 units of insulin glargine and 33 mcg of lixisenatide per mL in a 3 mL prefilled, disposable, single-patient-use SoloStar® pen.
6.3 Postmarketing Experience
The following additional adverse reactions have been identified during post approval use. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
2.2 Recommended Starting Dose
In patients naive to basal insulin or to a GLP-1 receptor agonist, currently on a GLP-1 receptor agonist or currently on less than 30 units of basal insulin daily:
- Discontinue therapy with basal insulin or a GLP-1 receptor agonist prior to initiation of SOLIQUA 100/33.
- The recommended starting dosage of SOLIQUA 100/33 is 15 units (15 units insulin glargine and 5 mcg lixisenatide) given subcutaneously once daily.
In patients currently on 30 to 60 units of basal insulin daily, with or without a GLP-1 receptor agonist:
- Discontinue therapy with basal insulin or GLP-1 receptor agonist prior to initiation of SOLIQUA 100/33.
- The recommended starting dosage of SOLIQUA 100/33 is 30 units (30 units insulin glargine and 10 mcg lixisenatide) given subcutaneously once daily.
| SOLIQUA 100/33 (dose window display) The dose window on the SOLIQUA 100/33 pen displays numbers for the even units and displays lines for the odd units.
|
Insulin glargine component dose | Lixisenatide component dose | Comment |
|---|---|---|---|
| 2 | --- | --- | Safety test dose – not for injection |
| 15 | 15 units | 5 mcg | Recommended starting dosage for patients naive to basal insulin or GLP-1 receptor agonist, currently on GLP-1 receptor agonist, or currently on less than 30 units of basal insulin daily |
| 16 | 16 units | 5.3 mcg | |
| 17 | 17 units | 5.7 mcg | |
| 18 | 18 units | 6 mcg | |
| 19 | 19 units | 6.3 mcg | |
| 20 | 20 units | 6.7 mcg | |
| 21 | 21 units | 7 mcg | |
| 22 | 22 units | 7.3 mcg | |
| 23 | 23 units | 7.7 mcg | |
| 24 | 24 units | 8 mcg | |
| 25 | 25 units | 8.3 mcg | |
| 26 | 26 units | 8.7 mcg | |
| 27 | 27 units | 9 mcg | |
| 28 | 28 units | 9.3 mcg | |
| 29 | 29 units | 9.7 mcg | |
| 30 | 30 units | 10 mcg | Recommended starting dosage for patients currently on 30 to 60 units of basal insulin daily, with or without a GLP-1 receptor agonist: |
| 31 | 31 units | 10.3 mcg | |
| 32 | 32 units | 10.7 mcg | |
| 33 | 33 units | 11 mcg | |
| 34 | 34 units | 11.3 mcg | |
| 35 | 35 units | 11.7 mcg | |
| 36 | 36 units | 12 mcg | |
| 37 | 37 units | 12.3 mcg | |
| 38 | 38 units | 12.7 mcg | |
| 39 | 39 units | 13 mcg | |
| 40 | 40 units | 13.3 mcg | |
| 41 | 41 units | 13.7 mcg | |
| 42 | 42 units | 14 mcg | |
| 43 | 43 units | 14.3 mcg | |
| 44 | 44 units | 14.7 mcg | |
| 45 | 45 units | 15 mcg | |
| 46 | 46 units | 15.3 mcg | |
| 47 | 47 units | 15.7 mcg | |
| 48 | 48 units | 16 mcg | |
| 49 | 49 units | 16.3 mcg | |
| 50 | 50 units | 16.7 mcg | |
| 51 | 51 units | 17 mcg | |
| 52 | 52 units | 17.3 mcg | |
| 53 | 53 units | 17.7 mcg | |
| 54 | 54 units | 18 mcg | |
| 55 | 55 units | 18.3 mcg | |
| 56 | 56 units | 18.7 mcg | |
| 57 | 57 units | 19 mcg | |
| 58 | 58 units | 19.3 mcg | |
| 59 | 59 units | 19.7 mcg | |
| 60 | 60 units | 20 mcg | Maximum daily dosage [see Warnings and Precautions (5.5)] |
8 Use in Specific Populations (8 USE IN SPECIFIC POPULATIONS)
- Pregnancy: SOLIQUA 100/33 should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus. (8.1)
5.12 Acute Gallbladder Disease
Acute events of gallbladder disease such as cholelithiasis or cholecystitis have been reported in GLP-1 receptor agonist trials and postmarketing. In a cardiovascular outcomes trial, cholelithiasis occurred in 0.4% of lixisenatide-treated patients versus 0.2% in placebo-treated patients and acute cholecystitis in 0.3% of lixisenatide-treated patients versus 0.2% in placebo-treated patients. If cholelithiasis is suspected, gallbladder studies and appropriate clinical follow-up are indicated.
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in clinical trials of a drug cannot be directly compared to rates in the clinical trial of another drug and may not reflect the rates observed in practice.
The safety of SOLIQUA 100/33 (n=834, with a mean treatment duration of 203 days) has been evaluated in two clinical studies (30 weeks duration) in type 2 diabetes patients. The studies, Study A and B [see Clinical Studies (14)], had the following characteristics: mean age was approximately 59 years; approximately 50% were male, 90% were Caucasian, 6% were Black or African American, and 18% were Hispanic. The mean duration of diabetes was 10.3 years, mean HbA1c at screening for Study A was 8.2 and Study B was 8.5. The mean BMI at baseline was 32 kg/m2. Baseline eGFR was ≥60 mL/min in 87.2% of the pooled study population and mean baseline eGFR was 83.0 mL/min/1.73 m2.
| SOLIQUA 100/33, % (n=834) |
|
|---|---|
| Nausea | 10.0 |
| Nasopharyngitis | 7.0 |
| Diarrhea | 7.0 |
| Upper respiratory tract infection | 5.5 |
| Headache | 5.4 |
2.3 Titration of Soliqua 100/33 (2.3 Titration of SOLIQUA 100/33)
- After starting with the recommended dosage of SOLIQUA 100/33, [see Dosage and Administration (2.2)], titrate the dosage upwards or downwards by two to four units (see Table 2) every week based on the patient's metabolic needs, blood glucose monitoring results, and glycemic control goal until the desired fasting plasma glucose is achieved.
- To minimize the risk of hypoglycemia or hyperglycemia, additional titration may be needed with changes in physical activity, meal patterns (i.e., macronutrient content or timing of food intake), or renal or hepatic function; during acute illness; or when used with other medications [see Warnings and Precautions (5.4) and Drug Interactions (7)].
| Self-Monitored Fasting Plasma Glucose | SOLIQUA 100/33 Dosage Adjustment |
|---|---|
| Above target range | +2 units (2 units of insulin glargine and 0.66 mcg of lixisenatide) to +4 units (4 units of insulin glargine and 1.32 mcg of lixisenatide) |
| Within target range | 0 units |
| Below target range | -2 units (2 units of insulin glargine and 0.66 mcg of lixisenatide) to -4 units (4 units of insulin glargine and 1.32 mcg of lixisenatide) |
2.1 Important Dosage Information
- SOLIQUA 100/33 is a combination of insulin glargine and lixisenatide.
- Administer SOLIQUA 100/33 subcutaneously once a day within the hour prior to the first meal of the day.
- The SOLIQUA 100/33 pen delivers doses from 15 to 60 units in a single injection. Table 1 presents the units of insulin glargine and the micrograms of lixisenatide in each dosage of SOLIQUA 100/33 [see Dosage and Administration (2.2)].
- The maximum dose of SOLIQUA 100/33 is 60 units daily (60 units insulin glargine and 20 mcg lixisenatide) [see Warnings and Precautions (5.5)].
14.1 Overview of Clinical Studies
SOLIQUA 100/33 was evaluated in two randomized clinical studies in patients with type 2 diabetes mellitus. In each of the active-controlled trials, treatment with SOLIQUA 100/33 produced statistically significant improvements in HbA1c.
17 Patient Counseling Information (17 PATIENT COUNSELING INFORMATION)
Advise the patient to read the FDA-approved patient labeling (Medication Guide and Instructions for Use).
5.5 Overdose Due to Medication Errors
SOLIQUA 100/33 contains two drugs: insulin glargine and lixisenatide. Administration of more than 60 units of SOLIQUA 100/33 daily can result in overdose of the lixisenatide component. Do not exceed the 20-mcg maximum recommended dose of lixisenatide or use with other GLP-1 receptor agonists.
Accidental mix-ups between insulin products have been reported. To avoid medication errors between SOLIQUA 100/33 and other insulins, instruct patients to always check the insulin label before each injection.
2.5 Important Administration Instructions
- The SOLIQUA 100/33 prefilled pen is for single-patient-use only [see Warnings and Precautions (5.3)].
- Train patients on proper use and injection technique before initiating SOLIQUA 100/33.
- Always check the SOLIQUA 100/33 label before administration [see Warnings and Precautions (5.5)].
- Visually inspect for particulate matter and discoloration prior to administration. Only use SOLIQUA 100/33 if the solution is clear and colorless to almost colorless.
- Inject SOLIQUA 100/33 subcutaneously into the abdominal area, thigh, or upper arm.
- Rotate injection sites within the same region from one injection to the next to reduce the risk of lipodystrophy and localized cutaneous amyloidosis. Do not inject into areas of lipodystrophy or localized cutaneous amyloidosis [see Warnings and Precautions (5.2), Adverse Reactions (6)].
- During changes to a patient's insulin regimen, increase the frequency of blood glucose monitoring [see Warnings and Precautions (5.4)].
- Do not administer intravenously or via an insulin pump.
- Use SOLIQUA 100/33 with caution in patients with visual impairment who may rely on audible clicks to dial their dose.
- The SOLIQUA 100/33 pen dials in 1-unit increments.
- Do not dilute or mix SOLIQUA 100/33 with any other insulin or solution.
- Do not split the dose of SOLIQUA 100/33.
Principal Display Panel 3 Ml Pen Carton (PRINCIPAL DISPLAY PANEL - 3 mL Pen Carton)
NDC 0024-5761-05
Rx only
SOLIQUA® 100/33
(insulin glargine and lixisenatide) injection
For Single Patient Use Only
100 units/mL and 33 mcg/mL
With each unit of insulin glargine,
the pen also delivers 0.33 mcg of lixisenatide
Only for Doses from 15 to 60 Units
For subcutaneous injection only
Dispense with the medication guide
Solution for injection in a SoloStar® disposable insulin delivery device
Never remove medication using a syringe
Do not mix with other insulins
Use only if solution is clear and colorless with no particles visible
Five 3 mL prefilled pens (15 mL total) – Dispense in this sealed carton
*Needles not included (see back panel)
SANOFI
5.8 Severe Gastrointestinal Adverse Reactions
Use of GLP-1 receptor agonists, including SOLIQUA 100/33, has been associated with gastrointestinal adverse reactions, sometimes severe [see Adverse Reactions (6.)]. SOLIQUA 100/33 is not recommended in patients with severe gastroparesis.
5.7 Acute Kidney Injury Due to Volume Depletion
There have been postmarketing reports of acute kidney injury, in some cases requiring hemodialysis, in patients treated with GLP-1 receptor agonists [see Adverse Reactions (6.3)]. The majority of the reported events occurred in patients who experienced gastrointestinal reactions leading to dehydration such as nausea, vomiting, or diarrhea [see Adverse Reactions (6.1)]. Monitor renal function in patients reporting adverse reactions to SOLIQUA 100/33 that could lead to volume depletion, especially during dosage initiation and escalation of SOLIQUA 100/33.SOLIQUA 100/33 is not recommended in patients with end-stage renal disease [see Use in Specific Populations (8.6)].
7.1 Medications That Can Affect Glucose Metabolism (7.1 Medications that Can Affect Glucose Metabolism)
A number of medications affect glucose metabolism and may require dose adjustment of SOLIQUA 100/33 and particularly close monitoring.
| Drugs That May Increase the Risk of Hypoglycemia | |
| Drugs: | Antidiabetic agents, ACE inhibitors, angiotensin II receptor blocking agents, disopyramide, fibrates, fluoxetine, monoamine oxidase inhibitors, pentoxifylline, pramlintide, salicylates, somatostatin analogs (e.g., octreotide), and sulfonamide antibiotics. |
| Intervention: | Dose reductions and increased frequency of glucose monitoring may be required when SOLIQUA 100/33 is coadministered with these drugs. |
| Drugs That May Decrease the Blood Glucose Lowering Effect of SOLIQUA 100/33 | |
| Drugs: | Atypical antipsychotics (e.g., olanzapine and clozapine), corticosteroids, danazol, diuretics, estrogens, glucagon, isoniazid, niacin, oral contraceptives, phenothiazines, progestogens (e.g., in oral contraceptives), protease inhibitors, somatropin, sympathomimetic agents (e.g., albuterol, epinephrine, terbutaline), and thyroid hormones. |
| Intervention: | Dose increases and increased frequency of glucose monitoring may be required when SOLIQUA 100/33 is coadministered with these drugs. |
| Drugs That May Increase or Decrease the Blood Glucose Lowering Effect of SOLIQUA 100/33 | |
| Drugs: | Alcohol, beta-blockers, clonidine, and lithium salts. Pentamidine may cause hypoglycemia, which may sometimes be followed by hyperglycemia. |
| Intervention: | Dose adjustment and increased frequency of glucose monitoring may be required when SOLIQUA 100/33 is coadministered with these drugs. |
| Drugs That May Blunt Signs and Symptoms of Hypoglycemia | |
| Drugs: | Beta-blockers, clonidine, guanethidine, and reserpine. |
| Intervention: | Increased frequency of glucose monitoring may be required when SOLIQUA 100/33 is coadministered with these drugs. |
5.1 Anaphylaxis and Serious Hypersensitivity Reactions
In clinical trials of lixisenatide there have been cases of anaphylaxis (frequency of 0.1% or 10 cases per 10,000 patient-years) and other serious hypersensitivity reactions including angioedema. Severe, life-threatening, generalized allergic reactions, including anaphylaxis, generalized skin reactions, angioedema, bronchospasm, hypotension, and shock can occur with insulins, including insulin glargine. There have been postmarketing reports of serious hypersensitivity reactions, including anaphylactic reactions and angioedema, in patients treated with SOLIQUA 100/33 [see Adverse Reactions (6.1)].
Inform and closely monitor patients with a history of anaphylaxis or angioedema with another GLP-1 receptor agonist for allergic reactions, because it is unknown whether such patients will be predisposed to anaphylaxis with SOLIQUA 100/33. SOLIQUA 100/33 is contraindicated in patients with known serious hypersensitivity to lixisenatide or insulin glargine [see Contraindications (4)]. If a hypersensitivity reaction occurs, the patient should discontinue SOLIQUA 100/33 and promptly seek medical attention.
7.2 Effects of Delayed Gastric Emptying On Oral Medications (7.2 Effects of Delayed Gastric Emptying on Oral Medications)
Lixisenatide-containing products, including SOLIQUA 100/33, delay gastric emptying which may reduce the rate of absorption of orally administered medications. Use caution when coadministering oral medications that have a narrow therapeutic ratio or that require careful clinical monitoring. These medications should be adequately monitored when concomitantly administered with lixisenatide. If such medications are to be administered with food, patients should be advised to take them with a meal or snack when lixisenatide is not administered.
- Antibiotics, acetaminophen, or other medications that are particularly dependent on threshold concentrations for efficacy or for which a delay in effect is undesirable should be administered at least 1 hour before SOLIQUA 100/33 injection [see Clinical Pharmacology (12.3)].
- Oral contraceptives should be taken at least 1 hour before SOLIQUA 100/33 administration or 11 hours after [see Clinical Pharmacology (12.3)].
5.3 Never Share A Soliqua 100/33 Prefilled Pen Between Patients (5.3 Never Share a SOLIQUA 100/33 Prefilled Pen Between Patients)
SOLIQUA 100/33 prefilled pens must never be shared between patients, even if the needle is changed. Sharing of the pen poses a risk for transmission of blood-borne pathogens.
5.4 Hyperglycemia Or Hypoglycemia With Changes in Insulin Regimen (5.4 Hyperglycemia or Hypoglycemia with Changes in Insulin Regimen)
Changes in insulin regimen (e.g., insulin strength, manufacturer, type, injection site or method of administration) may affect glycemic control and predispose to hypoglycemia [see Warnings and Precautions (5.6)] or hyperglycemia. Repeated insulin injections into areas of lipodystrophy or localized cutaneous amyloidosis have been reported to result in hyperglycemia; and a sudden change in the injection site (to unaffected area) has been reported to result in hypoglycemia [see Adverse Reactions (6)].
Make any changes to a patient's insulin regimen under close medical supervision with increased frequency of blood glucose monitoring. Advise patients who have repeatedly injected into areas of lipodystrophy or localized cutaneous amyloidosis to change the injection site to unaffected areas and closely monitor for hypoglycemia. Adjustments in concomitant oral antidiabetic treatment may be needed. When converting from basal insulin therapy or a GLP-1 receptor agonist to SOLIQUA 100/33 follow dosing recommendations [see Dosage and Administration (2.2, 2.3)].
5.13 Pulmonary Aspiration During General Anesthesia Or Deep Sedation (5.13 Pulmonary Aspiration During General Anesthesia or Deep Sedation)
SOLIQUA 100/33 delays gastric emptying [see Clinical Pharmacology (12.1)]. There have been rare postmarketing reports of pulmonary aspiration in patients receiving GLP-1 receptor agonists undergoing elective surgeries or procedures requiring general anesthesia or deep sedation who had residual gastric contents despite reported adherence to preoperative fasting recommendations.
Available data are insufficient to inform recommendations to mitigate the risk of pulmonary aspiration during general anesthesia or deep sedation in patients taking SOLIQUA 100/33, including whether modifying preoperative fasting recommendations or temporarily discontinuing SOLIQUA 100/33 could reduce the incidence of retained gastric contents. Instruct patients to inform healthcare providers prior to any planned surgeries or procedures if they are taking SOLIQUA 100/33.
14.2 Clinical Study in Patients With Type 2 Diabetes Uncontrolled On Oad Treatment (14.2 Clinical Study in Patients with Type 2 Diabetes Uncontrolled on OAD Treatment)
A total of 1170 patients with type 2 diabetes were randomized in an open-label, 30-week, active-controlled study (Study A: NCT05058147) to evaluate the efficacy and safety of SOLIQUA 100/33 compared to the individual components, insulin glargine 100 units/mL and lixisenatide.
Patients with type 2 diabetes, treated with metformin alone or treated with metformin and a second OAD treatment that could be a sulfonylurea or a glinide or a sodium-glucose cotransporter-2 (SGLT-2) inhibitor or a dipeptidyl peptidase-4 (DPP-4) inhibitor, and who were not adequately controlled with this treatment (HbA1c range 7.5% to 10% for patients previously treated with metformin alone and 7% to 9% for patients previously treated with metformin and a second OAD treatment) entered a run-in period for 4 weeks. During this run-in period, metformin treatment was optimized and all other OADs were discontinued. At the end of the run-in period, patients who remained inadequately controlled (HbA1c between 7% and 10%) were randomized to either SOLIQUA 100/33 (n=469), insulin glargine 100 units/mL (n=467), or lixisenatide (n=234).
The type 2 diabetes population had the following characteristics: mean age was 58.4 years, 50.6% were male, 90.1% were Caucasian, 6.7% were Black or African American, and 19.1% were Hispanic. At screening, the mean duration of diabetes was approximately 9 years, the mean BMI was approximately 31.7 kg/m2, and mean eGFR was 84.8 mL/min/1.73 m2.
SOLIQUA 100/33 and insulin glargine were to be titrated weekly to target a fasting plasma glucose goal of <100 mg/dL. Patients could not increase their dose by more than 4 units per week and the prespecified maximum dose of insulin glargine was limited to 60 units. The targeted fasting plasma glucose goal was achieved in 35% of patients in both groups at 30 weeks.
At Week 30, SOLIQUA 100/33 provided statistically significant improvement in HbA1c (p-value <0.0001) compared to insulin glargine 100 units/mL and lixisenatide-treated patients (-1.6%, -1.3%, and -0.9%). In a prespecified analysis of this primary endpoint, the differences observed were consistent with regard to baseline OAD use (metformin alone or metformin plus second OAD).
The mean difference (95% CI) in HbA1c reduction between SOLIQUA 100/33 and insulin glargine was -0.3% (-0.4, -0.2) and -0.7% (-0.8, -0.6) compared to lixisenatide.
See Table 5 for the other endpoints in the study. The difference in the glucose lowering effect observed in the trial may not necessarily reflect the effect that will be observed in the care setting where insulin glargine dosage can be different than that used in the trial.
| SOLIQUA 100/33 | Insulin Glargine 100 units/mL | Lixisenatide | |
|---|---|---|---|
| Number of subjects (randomized and treated) | 469 | 467 | 233 |
| HbA1c (%) | |||
| Baseline (mean; post run-in phase) | 8.1 | 8.1 | 8.1 |
| End of study (mean) | 6.5 | 6.8 | 7.3 |
| LS change from baseline (mean) Estimated using an ANCOVA with treatment, randomization strata, and country as fixed factors and baseline HbA1c as covariate. Twenty-six (5.5%) patients in the SOLIQUA 100/33 arm and 21 (4.5%) patients in the insulin glargine 100 units/mL arm, and 13 (5.6%) patients in the lixisenatide arm had missing HbA1c measurement at Week 30. Missing measurements were imputed using multiple imputations with respect to the baseline value of the subject.
|
-1.6 | -1.3 | -0.9 |
| LS mean difference vs insulin glargine | -0.3 | ||
| [95% confidence interval] | [-0.4, -0.2] The trial was designed to show the contribution of the GLP-1 component to glycemic lowering, and the insulin glargine dose and the dosing algorithm were selected to isolate the effect of the GLP-1 component. At the end of the trial, the doses of insulin glargine were equivalent between treatment groups. The mean final dose of SOLIQUA 100/33 at week 30 was 39.8 units (for SOLIQUA 100/33: 39.8 units insulin glargine/13.1 mcg lixisenatide) and 40.5 units in the insulin glargine–treated patients. The difference in effect observed in the trial may not necessarily reflect the effect that will be observed in the care setting where alternative insulin glargine dosage can be used.
|
– | |
| (p-value) | (<0.0001) | ||
| LS mean difference vs lixisenatide | -0.7 | ||
| [95% confidence interval] | – | – | [-0.8, -0.6] Lixisenatide was given at the maintenance dose of 20 mcg.
|
| (p-value) | (<0.0001) | ||
| Number of Patients (%) reaching HbA1c <7% at week 30 | 345 (74%) | 277 (59%) | 76 (33%) |
| Fasting plasma glucose (mg/dL) | |||
| Baseline (mean) | 177.9 | 175.7 | 175.8 |
| End of study (mean) | 113.9 | 117.6 | 149.0 |
| LS change from baseline (mean) | -59.1 | -55.8 | -27.2 |
Figure 1: Mean HbA1c (%) Over Time – Randomized and Treated Population
S = Screening (Week 6), R = Run-in (Week 1), B = Baseline, MI = Multiple imputation.
INS/LIXI = fixed ratio combination, INS = Insulin Glargine, LIXI = Lixisenatide
Note: The plot included all scheduled measurements obtained during the study, including those obtained after IMP discontinuation or introduction of rescue medication.
30MI: Missing HbA1c values at Week 30 in each group were imputed using their baseline HbA1c values plus an error. The error is normally distributed with mean zero and a standard deviation set equal to the estimated pooled standard deviation.
5.11 Fluid Retention and Heart Failure With Concomitant Use of Ppar Gamma Agonists (5.11 Fluid Retention and Heart Failure with Concomitant Use of PPAR-gamma Agonists)
Thiazolidinediones (TZDs), which are peroxisome proliferator-activated receptor (PPAR)-gamma agonists, can cause dose-related fluid retention, particularly when used in combination with insulin-containing products, including SOLIQUA 100/33. Fluid retention may lead to or exacerbate heart failure. Patients treated with SOLIQUA 100/33 and a PPAR-gamma agonist should be observed for signs and symptoms of heart failure. If heart failure develops, it should be managed according to current standards of care, and discontinuation or dose reduction of the PPAR-gamma agonist must be considered.
14.3 Clinical Studies in Patients With Type 2 Diabetes Uncontrolled On Basal Insulin (14.3 Clinical Studies in Patients with Type 2 Diabetes Uncontrolled on Basal Insulin)
A total of 736 patients with type 2 diabetes participated in a randomized, 30-week, active-controlled, open-label, 2-treatment arm, parallel-group, multicenter study (Study B: NCT02058160) to evaluate the efficacy and safety of SOLIQUA 100/33 compared to insulin glargine 100 units/mL.
Patients screened had type 2 diabetes were treated with basal insulin for at least 6 months, receiving a stable daily dose of between 15 and 40 units alone or combined with 1 or 2 OADs (metformin, sulfonylurea, glinide, SGLT-2 inhibitor or a DPP-4 inhibitor), had an HbA1c between 7.5% and 10% and a FPG less than or equal to 180 mg/dL or 200 mg/dL depending on their previous antidiabetic treatment.
This type 2 diabetes population had the following characteristics: Mean age was 60 years, 46.7% were male, 91.7% were Caucasian, 5.2% were Black or African American and 17.9% were Hispanic. At screening, the mean duration of diabetes was approximately 12 years, the mean BMI was approximately 31 kg/m2, mean eGFR was 80.6 mL/min/1.73 m2 and 86.1% of patients had an eGFR ≥60 mL/min.
After screening, eligible patients (n=1018) entered a 6-week run-in phase where patients remained on or were switched to insulin glargine 100 units/mL, if they were treated with another basal insulin, and had their insulin glargine dose titrated/stabilized while continuing metformin (if previously taken). The mean HbA1c decreased during run-in period from 8.5% to 8.1%. Any other OADs were discontinued.
At the end of the run-in period, patients with an HbA1c between 7% and 10%, FPG ≤140 mg/dL and insulin glargine daily dose of 20 to 50 units (mean of 35 units), were randomized to either SOLIQUA 100/33 (n=367) or insulin glargine 100 units/mL (n=369).
SOLIQUA 100/33 and insulin glargine were to be titrated weekly to target a fasting plasma glucose goal of <100 mg/dL. The mean dose of insulin glargine at baseline was 35 units. The maximum dose of insulin glargine allowed in the trial was 60 units (insulin dose cap) in both groups. The targeted fasting plasma glucose goal was achieved in 33% of patients in both groups at 30 weeks.
At Week 30, there was a reduction in HbA1c from baseline of -1.1% for SOLIQUA 100/33 and -0.6% for insulin glargine 100 units/mL. The mean difference (95% CI) in HbA1c reduction between SOLIQUA 100/33 and insulin glargine was -0.5 [-0.6, -0.4] and statistically significant. The trial was designed to show the contribution of the GLP-1 component to glycemic lowering and the insulin glargine dose and the dosing algorithm was selected to isolate the effect of the GLP-1 component. At the end of the trial, the doses of insulin glargine were equivalent between treatment groups. The mean final dose of SOLIQUA 100/33 and insulin glargine at week 30 was 46.7 units (for SOLIQUA 100/33: 46.7 units insulin glargine/15.6 mcg lixisenatide). The difference in effect observed in the trial may not necessarily reflect the effect that will be observed in the care setting where alternative insulin glargine dosage can be used. See Table 6 for the other endpoints in the study.
| SOLIQUA 100/33 | Insulin Glargine 100 units/mL | |
|---|---|---|
| Number of Subjects (randomized and treated) | 365 | 365 |
| HbA1c (%) | ||
| Baseline (mean; post run-in phase) | 8.1 | 8.1 |
| End of study (mean) | 6.9 | 7.5 |
| LS change from baseline (mean) Estimated using an ANCOVA with treatment, randomization strata, and country as fixed factors and baseline HbA1c as covariate. Twenty (5.5%) patients in the SOLIQUA 100/33 arm and 10 (2.7%) patients in the insulin glargine 100 units/mL arm had missing HbA1c measurement at Week 30. Missing measurements were imputed using multiple imputations with respect to the baseline value of the subject.
|
-1.1 | -0.6 |
| Difference vs insulin glargine | -0.5 | |
| [95% confidence interval] | [-0.6, -0.4] p<0.01; The trial was designed to show the contribution of the GLP-1 component to glucose lowering. The insulin glargine dose in this trial was capped at a maximum dose of 60 units and the dosing algorithm was selected to isolate the effect of the GLP-1 component. At the end of the trial, the doses of insulin glargine were equivalent between treatment groups. The mean final dose of SOLIQUA 100/33 and insulin glargine at week 30 was 46.7 units (for SOLIQUA 100/33: 46.7 units insulin glargine/15.6 mcg lixisenatide). The difference in effect observed in the trial may not necessarily reflect the effect that will be observed in the care setting where alternative insulin glargine dosage can be used.
|
|
| Patients [n (%)] reaching HbA1c <7% at week 30 Patients with missing HbA1c measurement at Week 30 were considered non-responders.
|
201 (55.1%) | 108 (29.6%) |
| Fasting plasma glucose (mg/dL) | ||
| Baseline (mean) | 132.3 | 132.0 |
| End of study (mean) | 121.9 | 120.5 |
| LS change from baseline (mean) | -5.7 | -7.0 |
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:48:34.113685 · Updated: 2026-03-14T22:30:18.174146