These Highlights Do Not Include All The Information Needed To Use Erzofri ®
492bf9dd-868e-421a-92db-8cca8973aac1
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
Elderly patients with dementia-related psychosis treated with antipsychotic drugs are at an increased risk of death. ERZOFRI is not approved for use in patients with dementia-related psychosis. [see Warnings and Precautions (5.1) ] .
Indications and Usage
ERZOFRI is indicated for the treatment of: Schizophrenia in adults . Schizoaffective disorder in adults as monotherapy and as an adjunct to mood stabilizers or antidepressants .
Dosage and Administration
For patients naïve to oral or injectable paliperidone, or oral or injectable risperidone, establish tolerability with oral paliperidone or oral risperidone prior to initiating treatment with ERZOFRI. ( 2.1 ) Each injection must be administered by a healthcare professional. ( 2.1 ) Initiate ERZOFRI by intramuscular injection in the deltoid muscle. Following the initial dose, monthly doses can be administered in either the gluteal or deltoid muscle. Do not administer by any other route. ( 2.1 ) Dosage recommendations: Indication Initial Dose (deltoid) Day 1 Monthly Dosage Administered 4 weeks after the first injection. (deltoid or gluteal) Maximum Monthly Dosage Schizophrenia ( 2.1 ) 351 mg 39 mg to 234 mg Recommended monthly dosage for treatment of schizophrenia is 117 mg. Some patients may benefit from lower or higher monthly doses within the additional available strengths (39 mg, 78 mg, 156 mg, and 234 mg). 234 mg Schizoaffective disorder ( 2.1 ) 351 mg 78 mg to 234 mg Adjust dose based on tolerability and/or efficacy using available strengths. The 39 mg strength was not studied in the long-term schizoaffective disorder study. 234 mg Missed dose: Refer to the Full Prescribing Information. ( 2.2 ) Mild renal impairment: Administer 234 mg on treatment Day 1 in the deltoid muscle. Follow with the recommended monthly maintenance dose of 78 mg, administered in the deltoid or gluteal muscle. Adjust monthly maintenance dose based on tolerability and/or efficacy within the strengths of 39 mg, 78 mg, 117 mg, or 156 mg. The maximum monthly dosage is 156 mg for patients with mild renal impairment. ( 2.4 ) See Full Prescribing Information for important preparation and administration information. ( 2.7 )
Warnings and Precautions
Cerebrovascular Adverse Reactions, in Elderly Patients with Dementia-Related Psychosis: Increased incidence of cerebrovascular adverse reactions (e.g., stroke, transient ischemic attack, including fatalities). ( 5.2 ) Neuroleptic Malignant Syndrome: Manage with immediate discontinuation of drug and close monitoring. ( 5.3 ) QT Prolongation: Avoid use with drugs that also increase QT interval and in patients with risk factors for prolonged QT interval. ( 5.4 ) Tardive Dyskinesia: Discontinue drug if clinically appropriate. ( 5.5 ) Metabolic Changes: Monitor for hyperglycemia/diabetes mellitus, dyslipidemia, and weight gain. ( 5.6 ) Orthostatic Hypotension and Syncope: Use with caution in patients with known cardiovascular or cerebrovascular disease and patients predisposed to hypotension. ( 5.7 ) Leukopenia, Neutropenia, and Agranulocytosis: Perform complete blood counts (CBC) in patients with history of clinically significant low white blood cell count (WBC) or history of leukopenia or neutropenia. Consider discontinuing ERZOFRI if clinically significant decline in WBC in the absence of other causative factors. ( 5.9 ) Hyperprolactinemia: Prolactin elevations occur and persist during chronic administration. ( 5.10 ) Potential for Cognitive and Motor Impairment: Use caution when operating machinery. ( 5.11 ) Seizures: Use cautiously in patients with a history of seizures or with conditions that lower the seizure threshold. ( 5.12 )
Contraindications
ERZOFRI is contraindicated in patients with a known hypersensitivity to either paliperidone or risperidone, or to any of the excipients in the ERZOFRI formulation. Hypersensitivity reactions, including anaphylactic reactions and angioedema, have been reported in patients treated with risperidone and in patients treated with paliperidone [see Adverse Reactions (6.1 , 6.2) ] .
Adverse Reactions
In placebo-controlled trials with risperidone, aripiprazole, and olanzapine in elderly subjects with dementia, there was a higher incidence of cerebrovascular adverse reactions (cerebrovascular accidents and transient ischemic attacks) including fatalities compared to placebo-treated subjects. No studies have been conducted with oral paliperidone, 1-month or 3-month paliperidone palmitate extended-release injectable suspensions, or ERZOFRI, in elderly patients with dementia. ERZOFRI is not approved for the treatment of patients with dementia-related psychosis [see Boxed Warning and Warnings and Precautions (5.1) ] .
Drug Interactions
Drugs that may cause orthostatic hypotension: An additive effect may occur when co-administered with ERZOFRI. ( 7.1 ) Strong CYP3A4 and P-glycoprotein (P-gp) inducers : Avoid using a strong inducer of CYP3A4 and/or P-gp during a dosing interval for ERZOFRI. If concomitant use is necessary, consider using paliperidone extended-release tablets. ( 2.5 , 7.1 , 12.3 )
Medication Information
Warnings and Precautions
Cerebrovascular Adverse Reactions, in Elderly Patients with Dementia-Related Psychosis: Increased incidence of cerebrovascular adverse reactions (e.g., stroke, transient ischemic attack, including fatalities). ( 5.2 ) Neuroleptic Malignant Syndrome: Manage with immediate discontinuation of drug and close monitoring. ( 5.3 ) QT Prolongation: Avoid use with drugs that also increase QT interval and in patients with risk factors for prolonged QT interval. ( 5.4 ) Tardive Dyskinesia: Discontinue drug if clinically appropriate. ( 5.5 ) Metabolic Changes: Monitor for hyperglycemia/diabetes mellitus, dyslipidemia, and weight gain. ( 5.6 ) Orthostatic Hypotension and Syncope: Use with caution in patients with known cardiovascular or cerebrovascular disease and patients predisposed to hypotension. ( 5.7 ) Leukopenia, Neutropenia, and Agranulocytosis: Perform complete blood counts (CBC) in patients with history of clinically significant low white blood cell count (WBC) or history of leukopenia or neutropenia. Consider discontinuing ERZOFRI if clinically significant decline in WBC in the absence of other causative factors. ( 5.9 ) Hyperprolactinemia: Prolactin elevations occur and persist during chronic administration. ( 5.10 ) Potential for Cognitive and Motor Impairment: Use caution when operating machinery. ( 5.11 ) Seizures: Use cautiously in patients with a history of seizures or with conditions that lower the seizure threshold. ( 5.12 )
Indications and Usage
ERZOFRI is indicated for the treatment of: Schizophrenia in adults . Schizoaffective disorder in adults as monotherapy and as an adjunct to mood stabilizers or antidepressants .
Dosage and Administration
For patients naïve to oral or injectable paliperidone, or oral or injectable risperidone, establish tolerability with oral paliperidone or oral risperidone prior to initiating treatment with ERZOFRI. ( 2.1 ) Each injection must be administered by a healthcare professional. ( 2.1 ) Initiate ERZOFRI by intramuscular injection in the deltoid muscle. Following the initial dose, monthly doses can be administered in either the gluteal or deltoid muscle. Do not administer by any other route. ( 2.1 ) Dosage recommendations: Indication Initial Dose (deltoid) Day 1 Monthly Dosage Administered 4 weeks after the first injection. (deltoid or gluteal) Maximum Monthly Dosage Schizophrenia ( 2.1 ) 351 mg 39 mg to 234 mg Recommended monthly dosage for treatment of schizophrenia is 117 mg. Some patients may benefit from lower or higher monthly doses within the additional available strengths (39 mg, 78 mg, 156 mg, and 234 mg). 234 mg Schizoaffective disorder ( 2.1 ) 351 mg 78 mg to 234 mg Adjust dose based on tolerability and/or efficacy using available strengths. The 39 mg strength was not studied in the long-term schizoaffective disorder study. 234 mg Missed dose: Refer to the Full Prescribing Information. ( 2.2 ) Mild renal impairment: Administer 234 mg on treatment Day 1 in the deltoid muscle. Follow with the recommended monthly maintenance dose of 78 mg, administered in the deltoid or gluteal muscle. Adjust monthly maintenance dose based on tolerability and/or efficacy within the strengths of 39 mg, 78 mg, 117 mg, or 156 mg. The maximum monthly dosage is 156 mg for patients with mild renal impairment. ( 2.4 ) See Full Prescribing Information for important preparation and administration information. ( 2.7 )
Contraindications
ERZOFRI is contraindicated in patients with a known hypersensitivity to either paliperidone or risperidone, or to any of the excipients in the ERZOFRI formulation. Hypersensitivity reactions, including anaphylactic reactions and angioedema, have been reported in patients treated with risperidone and in patients treated with paliperidone [see Adverse Reactions (6.1 , 6.2) ] .
Adverse Reactions
In placebo-controlled trials with risperidone, aripiprazole, and olanzapine in elderly subjects with dementia, there was a higher incidence of cerebrovascular adverse reactions (cerebrovascular accidents and transient ischemic attacks) including fatalities compared to placebo-treated subjects. No studies have been conducted with oral paliperidone, 1-month or 3-month paliperidone palmitate extended-release injectable suspensions, or ERZOFRI, in elderly patients with dementia. ERZOFRI is not approved for the treatment of patients with dementia-related psychosis [see Boxed Warning and Warnings and Precautions (5.1) ] .
Drug Interactions
Drugs that may cause orthostatic hypotension: An additive effect may occur when co-administered with ERZOFRI. ( 7.1 ) Strong CYP3A4 and P-glycoprotein (P-gp) inducers : Avoid using a strong inducer of CYP3A4 and/or P-gp during a dosing interval for ERZOFRI. If concomitant use is necessary, consider using paliperidone extended-release tablets. ( 2.5 , 7.1 , 12.3 )
Description
Elderly patients with dementia-related psychosis treated with antipsychotic drugs are at an increased risk of death. ERZOFRI is not approved for use in patients with dementia-related psychosis. [see Warnings and Precautions (5.1) ] .
Section 42229-5
Dosing Window
To avoid a missed monthly dose, patients may be given the injection up to 7 days before or after the monthly time point.
Section 42230-3
| PATIENT INFORMATION
ERZOFRI ®(er-ZOH-free) (paliperidone palmitate) extended-release injectable suspension |
||
|---|---|---|
| This Patient Information has been approved by the U.S. Food and Drug Administration. | Revised: 3/2025 | |
| What is the most important information I should know about ERZOFRI? | ||
ERZOFRI may cause serious side effects, including:
|
||
| What is ERZOFRI? | ||
| ERZOFRI is a prescription medicine given by injection by a healthcare provider and used to treat: | ||
|
||
| It is not known if ERZOFRI is safe and effective in children. | ||
| Who should not receive ERZOFRI? | ||
| Do not receive ERZOFRI if youare allergic to paliperidone, risperidone, or any of the ingredients in ERZOFRI. See the end of this Patient Information leaflet for a complete list of ingredients in ERZOFRI. | ||
Before receiving ERZOFRI, tell your healthcare provider about all your medical conditions, including if you:
|
||
| Tell your healthcare provider about all the medicines you take,including prescription and over-the-counter medicines, vitamins, and herbal supplements. ERZOFRI and certain other medicines may affect each other causing possible serious side effects or affect the way each other works. Know the medicines you take. Keep a list of them to show to your healthcare provider or pharmacist when you get a new medicine. | ||
How will I receive ERZOFRI?
|
||
What should I avoid while receiving ERZOFRI?
|
||
|
|
|
|
||
| What are the possible side effects of ERZOFRI? | ||
ERZOFRI may cause serious side effects, including:
|
||
|
|
|
|
||
|
|
|
|
||
|
||
| The most common side effects of ERZOFRI include: | ||
|
|
|
| Tell your healthcare provider if you have any side effect that bothers you or does not go away. | ||
| These are not all of the possible side effects of ERZOFRI. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. | ||
| General information about the safe and effective use of ERZOFRI. | ||
| Medicines are sometimes prescribed for purposes other than those listed in a Patient Information leaflet. You can ask your pharmacist or healthcare provider for information about ERZOFRI that is written for health professionals. | ||
| What are the ingredients in ERZOFRI? | ||
| Active ingredient: paliperidone palmitate | ||
| Inactive ingredients:citric acid monohydrate, dibasic sodium phosphate anhydrous, monobasic sodium phosphate monohydrate, polyethylene glycol 4000, polysorbate 20, sodium hydroxide, and water for injection. | ||
| Manufactured by: Shandong Luye Pharmaceutical Co., Ltd., No.15 Chuangye Road, Yantai, Shandong Province, China 264003 | ||
| Manufactured for: Luye Innomind Pharma Shijiazhuang Co., Ltd., Shijiazhuang, Hebei Province, China 050000
For more information call 1-800-548-9765. |
Section 43683-2
| Warnings and Precautions ( 5.10) | 1/2025 |
Section 44425-7
Storage and Handling
Store at 20°C to 25°C (68°F to 77°F); excursions permitted between 15°C and 30°C (59°F to 86°F) [see USP Controlled Room Temperature]. Do not mix with any other product or diluent.
5.8 Falls
Somnolence, postural hypotension, motor and sensory instability have been reported with the use of antipsychotics, including paliperidone palmitate, which may lead to falls and, consequently, fractures or other fall-related injuries. For patients, particularly the elderly, with diseases, conditions, or medications that could exacerbate these effects, assess the risk of falls when initiating antipsychotic treatment and recurrently for patients on long-term antipsychotic therapy.
5.12 Seizures
In the four fixed-dose double-blind placebo-controlled studies in subjects with schizophrenia, <1% (1 out of 1,293) of subjects treated with another once-a-month paliperidone palmitate extended-release injectable suspension (PP1M) in the recommended dose range of 39 mg to 234 mg experienced a convulsion compared with <1% (1 out of 510) of placebo-treated subjects who experienced a grand mal convulsion.
Like other antipsychotic drugs, ERZOFRI should be used cautiously in patients with a history of seizures or other conditions that potentially lower the seizure threshold. Conditions that lower the seizure threshold may be more prevalent in patients 65 years or older.
5.14 Priapism
Drugs with alpha-adrenergic blocking effects have been reported to induce priapism. Although no cases of priapism have been reported in clinical trials with another once-a-month paliperidone palmitate extended-release injectable suspension (PP1M), priapism has been reported with oral paliperidone during postmarketing surveillance. Severe priapism may require surgical intervention.
11 Description
ERZOFRI (paliperidone palmitate) extended-release injectable suspension contains a racemic mixture of (+)- and (-)- paliperidone palmitate. Paliperidone palmitate, is an atypical antipsychotic belonging to the chemical class of benzisoxazole derivatives. The chemical name is (9 RS)-3-[2-[4-(6-Fluoro-1,2-benzisoxazol-3-yl)piperidin-1-yl]ethyl]-2-methyl-4-oxo-6,7,8,9-tetrahydro-4 H-pyrido[1,2- a]pyrimadin-9-yl hexadecanoate. Its molecular formula is C 39H 57FN 4O 4and its molecular weight is 664.89. The structural formula is:
Paliperidone palmitate is very slightly soluble in ethanol and methanol, practically insoluble in water, and slightly soluble in ethyl acetate.
ERZOFRI is available as a white to off-white sterile aqueous extended-release suspension for intramuscular injection in the following dose strengths of paliperidone palmitate (deliverable volume) in single-dose prefilled syringes: 39 mg (0.25 mL), 78 mg (0.5 mL), 117 mg (0.75 mL), 156 mg (1 mL), 234 mg (1.5 mL), and 351 mg (2.25 mL). The drug product hydrolyzes in vivo to the active moiety, paliperidone, resulting in dose strengths of 25 mg, 50 mg, 75 mg, 100 mg, 150 mg, and 225 mg of paliperidone, respectively.
The inactive ingredients are citric acid monohydrate (5 mg/mL), dibasic sodium phosphate anhydrous (5 mg/mL), monobasic sodium phosphate monohydrate (2.5 mg/mL), polyethylene glycol 4000 (30 mg/mL), polysorbate 20 (12 mg/mL), sodium hydroxide to adjust pH, and water for injection. The drug product pH is 6.5 to 7.5.
5.13 Dysphagia
Esophageal dysmotility and aspiration have been associated with antipsychotic drug use. ERZOFRI and other antipsychotic drugs should be used cautiously in patients at risk for aspiration.
8.4 Pediatric Use
Safety and effectiveness of ERZOFRI in pediatric patients have not been established.
8.5 Geriatric Use
Clinical studies of ERZOFRI did not include sufficient numbers of subjects aged 65 and over to determine whether they respond differently from younger subjects. Other reported clinical experience has not identified differences in responses between the elderly and younger patients.
Paliperidone palmitate is substantially excreted by the kidney and clearance is decreased in patients with renal impairment [see Clinical Pharmacology (12.3)] , who should be given reduced doses. Because geriatric patients are more likely to have decreased renal function, adjust dose based on renal function [see Dosage and Administration (2.4)].
14.1 Schizophrenia
The efficacy of ERZOFRI for the treatment of schizophrenia in adults is based upon adequate and well-controlled studies of another once-a-month paliperidone palmitate extended-release injectable suspension (also referred to as "PP1M" in this section). The results of these adequate and well-controlled studies of another PP1M are presented below.
4 Contraindications
ERZOFRI is contraindicated in patients with a known hypersensitivity to either paliperidone or risperidone, or to any of the excipients in the ERZOFRI formulation. Hypersensitivity reactions, including anaphylactic reactions and angioedema, have been reported in patients treated with risperidone and in patients treated with paliperidone [see Adverse Reactions (6.1, 6.2)] .
5.4 Qt Prolongation
Paliperidone causes a modest increase in the corrected QT (QTc) interval. The use of paliperidone should be avoided in combination with other drugs that are known to prolong QTc including Class 1A (e.g., quinidine, procainamide) or Class III (e.g., amiodarone, sotalol) antiarrhythmic medications, antipsychotic medications (e.g., chlorpromazine, thioridazine), antibiotics (e.g., gatifloxacin, moxifloxacin), or any other class of medications known to prolong the QTc interval. Paliperidone should also be avoided in patients with congenital long QT syndrome and in patients with a history of cardiac arrhythmias.
Certain circumstances may increase the risk of the occurrence of Torsades de pointes and/or sudden death in association with the use of drugs that prolong the QTc interval, including (1) bradycardia; (2) hypokalemia or hypomagnesemia; (3) concomitant use of other drugs that prolong the QTc interval; and (4) presence of congenital prolongation of the QT interval.
The effects of oral paliperidone on the QT interval were evaluated in a double-blind, active-controlled (moxifloxacin 400 mg single dose), multicenter QT study in adults with schizophrenia and schizoaffective disorder, and in three placebo- and active-controlled 6-week, fixed-dose efficacy trials in adults with schizophrenia.
In the QT study (n=141) of oral paliperidone, the 8 mg dose of immediate-release oral paliperidone (n=50) showed a mean placebo-subtracted increase from baseline in QTcLD (QT interval corrected for heart rate using the population specified linear derived method) of 12.3 msec (90% CI: 8.9; 15.6) on Day 8 at 1.5 hours post-dose. The mean steady-state peak plasma concentration for this 8 mg oral dose of immediate release paliperidone (C max ss= 113 ng/mL) was more than 2-fold the exposure observed with the maximum recommended 234 mg maintenance dose of another once-a-month paliperidone extended-release injectable suspension administered in the deltoid muscle (predicted median C max-ss= 50 ng/mL). In this same study, a 4 mg dose of the immediate-release oral formulation of paliperidone, for which C max-ss= 35 ng/mL, showed an increased placebo-subtracted QTcLD of 6.8 msec (90% CI: 3.6; 10.1) on Day 2 at 1.5 hours post-dose.
In the three fixed-dose efficacy studies of oral paliperidone extended release in subjects with schizophrenia, electrocardiogram (ECG) measurements taken at various time points showed only one subject in the oral paliperidone 12 mg group had a change exceeding 60 msec at one time- point on Day 6 (increase of 62 msec).
In the four fixed-dose efficacy studies of another once-a-month paliperidone palmitate extended-release injectable suspension in subjects with schizophrenia and in the long-term study in subjects with schizoaffective disorder, no subject experienced a change in QTcLD exceeding 60 msec and no subject had a QTcLD value of > 500 msec at any time point. In the maintenance study in subjects with schizophrenia, no subject had a QTcLD change > 60 msec, and one subject had a QTcLD value of 507 msec (Bazett's QT corrected interval [QTcB] value of 483 msec); this latter subject also had a heart rate of 45 beats per minute.
6 Adverse Reactions
The following are discussed in more detail in other sections of the labeling:
- Increased mortality in elderly patients with dementia-related psychosis [see Boxed Warningand Warnings and Precautions (5.1)]
- Cerebrovascular adverse reactions, including stroke, in elderly patients with dementia-related psychosis [see Warnings and Precautions (5.2)]
- Neuroleptic malignant syndrome [see Warnings and Precautions (5.3)]
- QT prolongation [see Warnings and Precautions (5.4)]
- Tardive dyskinesia [see Warnings and Precautions (5.5)]
- Metabolic changes [see Warnings and Precautions (5.6)]
- Orthostatic hypotension and syncope [see Warnings and Precautions (5.7)]
- Falls [see Warnings and Precautions (5.8)]
- Leukopenia, neutropenia, and agranulocytosis [see Warnings and Precautions (5.9)]
- Hyperprolactinemia [see Warnings and Precautions (5.10)]
- Potential for cognitive and motor impairment [see Warnings and Precautions (5.11)]
- Seizures [see Warnings and Precautions (5.12)]
- Dysphagia [see Warnings and Precautions (5.13)]
- Priapism [see Warnings and Precautions (5.14)]
- Disruption of body temperature regulation [see Warnings and Precautions (5.15)]
7 Drug Interactions
- Drugs that may cause orthostatic hypotension:An additive effect may occur when co-administered with ERZOFRI. ( 7.1)
- Strong CYP3A4 and P-glycoprotein (P-gp) inducers: Avoid using a strong inducer of CYP3A4 and/or P-gp during a dosing interval for ERZOFRI. If concomitant use is necessary, consider using paliperidone extended-release tablets. ( 2.5, 7.1, 12.3)
8.6 Renal Impairment
Use of ERZOFRI is not recommended in patients with moderate or severe renal impairment (creatinine clearance < 50 mL/min). Dose reduction is recommended for patients with mild renal impairment (creatinine clearance ≥ 50 mL/min to < 80 mL/min) [see Dosage and Administration (2.4)and Clinical Pharmacology (12.3)] .
12.2 Pharmacodynamics
Paliperidone is an antagonist at the central dopamine Type 2 (D 2) and serotonin Type 2 (5HT 2A) receptors with binding affinities (Ki values) of 1.6-2.8 nM for D 2and 0.8-1.2 nM for 5HT 2Areceptors. Paliperidone also acts as an antagonist at the α 1and α 2adrenergic receptors and H 1histaminergic receptors. Paliperidone has no affinity for cholinergic muscarinic or β 1- and β 2-adrenergic receptors. The pharmacological activity of the (+)- and (-)- paliperidone enantiomers is qualitatively and quantitatively similar .
12.3 Pharmacokinetics
The overall exposures (AUC) of paliperidone following another once-a-month paliperidone palmitate extended-release injectable suspension (also referred to as "PP1M" in this section) administration was dose-proportional over a dose range of 39 mg to 234 mg, and peak plasma concentrations (C max) were less than dose-proportional for doses exceeding 78 mg. Steady state plasma exposures of ERZOFRI are reached 7 days after the first injection.
5.6 Metabolic Changes
Atypical antipsychotic drugs have been associated with metabolic changes that may increase cardiovascular/cerebrovascular risk. These metabolic changes include hyperglycemia, dyslipidemia, and body weight gain. While all of the drugs in the class have been shown to produce some metabolic changes, each drug has its own specific risk profile.
2.1 Recommended Dosage
For patients who have never taken oral or injectable paliperidone, or oral or injectable risperidone, establish tolerability with oral paliperidone or oral risperidone prior to initiating treatment with ERZOFRI.
ERZOFRI must be administered by a healthcare professional as an intramuscular injection. Do not administer ERZOFRI by any other route. For detailed preparation and administration instructions, see Dosage and Administration (2.7) .
See Table 1for dosage recommendations for ERZOFRI in the treatment of schizophrenia in adults or the treatment of schizoaffective disorder in adults as monotherapy and as an adjunct to mood stabilizers or antidepressants.
The initial dosage of ERZOFRI is 351 mg on treatment Day 1 administered in the deltoid muscle. Following the initial dose, monthly doses can be administered in either the deltoid or gluteal muscle [see Clinical Pharmacology (12.3)] .
| Indication | Initial Dose
(deltoid) Day 1 |
Monthly Dosage
Administered 4 weeks after the first injection.
(deltoid or gluteal) |
Maximum Monthly Dosage |
|---|---|---|---|
| Schizophrenia | 351 mg | 39 mg to 234 mg
The recommended monthly dosage for treatment of schizophrenia is 117 mg. Some patients may benefit from lower or higher monthly doses within the additional available strengths (39 mg, 78 mg, 156 mg, and 234 mg).
|
234 mg |
| Schizoaffective disorder | 351 mg | 78 mg to 234 mg
Adjust dose based on tolerability and/or efficacy using available strengths. The 39 mg strength was not studied in the long-term schizoaffective disorder study.
|
234 mg |
Adjust dosage monthly depending on clinical response and tolerability. When making dose adjustments, the pharmacokinetic profile of ERZOFRI should be considered [see Clinical Pharmacology (12.3)] , as the full effect of the dose adjustment may not be apparent for several months.
5.5 Tardive Dyskinesia
Tardive dyskinesia, a syndrome consisting of potentially irreversible, involuntary, dyskinetic movements, may develop in patients treated with antipsychotic drugs. Although the prevalence of the syndrome appears to be highest among the elderly, especially elderly women, it is impossible to predict which patients will develop the syndrome. Whether antipsychotic drug products differ in their potential to cause tardive dyskinesia is unknown.
The risk of developing tardive dyskinesia and the likelihood that it will become irreversible appear to increase with the duration of treatment and the cumulative dose. The syndrome can develop after relatively brief treatment periods, even at low doses. It may also occur after discontinuation of treatment.
Tardive dyskinesia may remit, partially or completely, if antipsychotic treatment is discontinued. Antipsychotic treatment itself may suppress (or partially suppress) the signs and symptoms of the syndrome and may thus mask the underlying process. The effect that symptomatic suppression has upon the long-term course of the syndrome is unknown.
Given these considerations, ERZOFRI should be prescribed in a manner that is most likely to minimize the occurrence of tardive dyskinesia. Chronic antipsychotic treatment should generally be reserved for patients: (1) who suffer from a chronic illness that is known to respond to antipsychotic drugs and (2) for whom alternative, equally effective, but potentially less harmful treatments are not available or appropriate. In patients who do require chronic treatment, use the lowest dose and the shortest duration of treatment producing a satisfactory clinical response. Periodically reassess the need for continued treatment.
If signs and symptoms of tardive dyskinesia appear in a patient on ERZOFRI, drug discontinuation should be considered. However, some patients may require treatment with ERZOFRI despite the presence of the syndrome.
8.7 Hepatic Impairment
ERZOFRI has not been studied in patients with hepatic impairment. Based on a study with oral paliperidone, no dose adjustment is required in patients with mild or moderate hepatic impairment. Paliperidone has not been studied in patients with severe hepatic impairment [see Clinical Pharmacology (12.3)] .
1 Indications and Usage
ERZOFRI is indicated for the treatment of:
- Schizophrenia in adults .
- Schizoaffective disorder in adults as monotherapy and as an adjunct to mood stabilizers or antidepressants .
5.10 Hyperprolactinemia
Like other drugs that antagonize dopamine D 2receptors, paliperidone elevates prolactin levels and the elevation persists during chronic administration. Paliperidone has a prolactin-elevating effect similar to that seen with risperidone, a drug that is associated with higher levels of prolactin than other antipsychotic drugs.
Hyperprolactinemia, regardless of etiology, may suppress hypothalamic GnRH, resulting in reduced pituitary gonadotrophin secretion. This, in turn, may inhibit reproductive function by impairing gonadal steroidogenesis in both female and male patients. Galactorrhea, amenorrhea, gynecomastia, and impotence have been reported in patients receiving prolactin-elevating compounds. Long-standing hyperprolactinemia when associated with hypogonadism may lead to decreased bone density in both female and male subjects.
Tissue culture experiments indicate that approximately one-third of human breast cancers are prolactin dependent in vitro, a factor of potential importance if the prescription of these drugs is considered in a patient with previously detected breast cancer. An increase in the incidence of pituitary gland, mammary gland, and pancreatic islet cell neoplasia (mammary adenocarcinomas, pituitary and pancreatic adenomas) was observed in the risperidone carcinogenicity studies conducted in mice and rats [see Nonclinical Toxicology (13.1)] . Published epidemiologic studies have shown inconsistent results when exploring the potential association between hyperprolactinemia and breast cancer.
Prolactin data from two long-term, double-blind, placebo-controlled studies with another PP1M are presented below; one study was in a population of patients with schizophrenia; the second study was in patients with schizoaffective disorder.
12.1 Mechanism of Action
Paliperidone palmitate is hydrolyzed to paliperidone [see Clinical Pharmacology (12.3)] . Paliperidone is the major active metabolite of risperidone. The mechanism of action of paliperidone in the listed indications is unclear. However, the drug's effect in schizophrenia could be mediated through a combination of central dopamine Type 2 (D 2)and serotonin Type 2 (5HT 2A) receptor antagonism.
5 Warnings and Precautions
- Cerebrovascular Adverse Reactions, in Elderly Patients with Dementia-Related Psychosis:Increased incidence of cerebrovascular adverse reactions (e.g., stroke, transient ischemic attack, including fatalities). ( 5.2)
- Neuroleptic Malignant Syndrome:Manage with immediate discontinuation of drug and close monitoring. ( 5.3)
- QT Prolongation:Avoid use with drugs that also increase QT interval and in patients with risk factors for prolonged QT interval. ( 5.4)
- Tardive Dyskinesia:Discontinue drug if clinically appropriate. ( 5.5)
- Metabolic Changes:Monitor for hyperglycemia/diabetes mellitus, dyslipidemia, and weight gain. ( 5.6)
- Orthostatic Hypotension and Syncope:Use with caution in patients with known cardiovascular or cerebrovascular disease and patients predisposed to hypotension. ( 5.7)
- Leukopenia, Neutropenia, and Agranulocytosis:Perform complete blood counts (CBC) in patients with history of clinically significant low white blood cell count (WBC) or history of leukopenia or neutropenia. Consider discontinuing ERZOFRI if clinically significant decline in WBC in the absence of other causative factors. ( 5.9)
- Hyperprolactinemia:Prolactin elevations occur and persist during chronic administration. ( 5.10)
- Potential for Cognitive and Motor Impairment:Use caution when operating machinery. ( 5.11)
- Seizures:Use cautiously in patients with a history of seizures or with conditions that lower the seizure threshold. ( 5.12)
2 Dosage and Administration
- For patients naïve to oral or injectable paliperidone, or oral or injectable risperidone, establish tolerability with oral paliperidone or oral risperidone prior to initiating treatment with ERZOFRI. ( 2.1)
- Each injection must be administered by a healthcare professional. ( 2.1)
- Initiate ERZOFRI by intramuscular injection in the deltoid muscle. Following the initial dose, monthly doses can be administered in either the gluteal or deltoid muscle. Do not administer by any other route. ( 2.1)
- Dosage recommendations:
| Indication | Initial Dose
(deltoid) Day 1 |
Monthly Dosage
Administered 4 weeks after the first injection. (deltoid or gluteal)
|
Maximum Monthly Dosage |
|---|---|---|---|
| Schizophrenia ( 2.1) | 351 mg | 39 mg to 234 mg
Recommended monthly dosage for treatment of schizophrenia is 117 mg. Some patients may benefit from lower or higher monthly doses within the additional available strengths (39 mg, 78 mg, 156 mg, and 234 mg).
|
234 mg |
| Schizoaffective disorder ( 2.1) | 351 mg | 78 mg to 234 mg
Adjust dose based on tolerability and/or efficacy using available strengths. The 39 mg strength was not studied in the long-term schizoaffective disorder study.
|
234 mg |
- Missed dose: Refer to the Full Prescribing Information. ( 2.2)
- Mild renal impairment: Administer 234 mg on treatment Day 1 in the deltoid muscle. Follow with the recommended monthly maintenance dose of 78 mg, administered in the deltoid or gluteal muscle. Adjust monthly maintenance dose based on tolerability and/or efficacy within the strengths of 39 mg, 78 mg, 117 mg, or 156 mg. The maximum monthly dosage is 156 mg for patients with mild renal impairment. ( 2.4)
- See Full Prescribing Information for important preparation and administration information. ( 2.7)
3 Dosage Forms and Strengths
Extended-release injectable suspension: white to off-white aqueous suspension available in dose strengths of 39 mg/0.25 mL, 78 mg/0.5 mL, 117 mg/0.75 mL, 156 mg/mL, 234 mg/1.5 mL, and 351 mg/2.25 mL paliperidone palmitate.
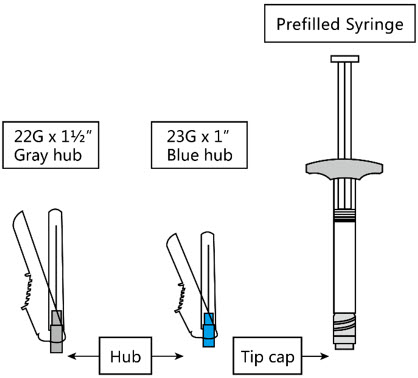
Each strength is provided as a kit, which includes: one single-dose prefilled syringe and 2 safety needles (a 1 ½-inch 22 gauge needle and a 1-inch 23 gauge needle).
6.2 Postmarketing Experience
The following adverse reactions have been identified during post-approval use of paliperidone; because these reactions were reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure: angioedema, catatonia, ileus, somnambulism, swollen tongue, thrombotic thrombocytopenic purpura, urinary incontinence, and urinary retention.
Cases of anaphylactic reaction after injection with another once-a-month paliperidone palmitate extended-release injectable suspension product have been reported during postmarketing experience in patients who have previously tolerated oral risperidone or oral paliperidone.
Paliperidone is the major active metabolite of risperidone. Adverse reactions reported with oral risperidone and risperidone long-acting injection can be found in the Adverse Reactions (6)sections of the package inserts for those products.
14.2 Schizoaffective Disorder
The efficacy of ERZOFRI for the treatment of schizoaffective disorder in adults as monotherapy and as an adjunct to mood stabilizers or antidepressants is based upon an adequate and well-controlled study of another PP1M. The results of the adequate and well-controlled study is presented below.
8 Use in Specific Populations
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in clinical practice.
The safety of ERZOFRI for the treatment of schizophrenia in adults and schizoaffective disorder in adults as monotherapy and as an adjunct to mood stabilizers or antidepressants is based upon adequate and well-controlled studies of another once-a-month paliperidone palmitate extended-release injectable suspension (also referred to as "PP1M" in this section). Below is a display of adverse reactions with another PP1M from those adequate and well-controlled studies.
Injection site reactions for ERZOFRI presented in this section (see " Pain and Injection Site Reactions with ERZOFRI " below) are based on pharmacokinetic studies.
17 Patient Counseling Information
Advise the patient to read the FDA-approved patient labeling (Patient Information).
5.3 Neuroleptic Malignant Syndrome
Neuroleptic Malignant Syndrome (NMS), a potentially fatal symptom complex, has been reported in association with antipsychotic drugs, including paliperidone.
Clinical manifestations of NMS are hyperpyrexia, muscle rigidity, altered mental status including delirium, and autonomic instability (irregular pulse or blood pressure, tachycardia, diaphoresis, and cardiac dysrhythmia). Additional signs may include elevated creatine phosphokinase, myoglobinuria (rhabdomyolysis), and acute renal failure.
If NMS is suspected, immediately discontinue ERZOFRI and provide symptomatic treatment and monitoring.
2.6 Switching From Other Antipsychotics
There are no systematically collected data to specifically address switching patients with schizophrenia or schizoaffective disorder from other antipsychotics to ERZOFRI or concerning concomitant administration with other antipsychotics.
5.7 Orthostatic Hypotension and Syncope
Paliperidone can induce orthostatic hypotension and syncope in some patients because of its alpha- adrenergic blocking activity. Syncope was reported in < 1% (4/1293) of subjects treated with another once-a-month paliperidone palmitate extended-release injectable suspension (PP1M) in the recommended maintenance dose range of 39 mg to 234 mg in the four fixed- dose, double-blind, placebo-controlled trials compared with 0% (0/510) of subjects treated with placebo. In the four fixed-dose efficacy studies in subjects with schizophrenia, orthostatic hypotension was reported as an adverse event by < 1% (2/1293) of the PP1M-treated subjects compared to 0% (0/510) with placebo. Incidences of orthostatic hypotension and syncope in the long-term studies in subjects with schizophrenia and schizoaffective disorder were similar to those observed in the short-term studies.
Use ERZOFRI with caution in patients with known cardiovascular disease (e.g., heart failure, history of myocardial infarction or ischemia, conduction abnormalities), cerebrovascular disease, or conditions that predispose the patient to hypotension (e.g., dehydration, hypovolemia, and treatment with antihypertensive medications). Monitoring of orthostatic vital signs should be considered in patients who are vulnerable to hypotension.
5.15 Disruption of Body Temperature Regulation
Disruption of the body's ability to reduce core body temperature has been attributed to antipsychotic agents. Appropriate care is advised when prescribing ERZOFRI to patients who will be experiencing conditions which may contribute to an elevation in core body temperature, e.g., exercising strenuously, exposure to extreme heat, receiving concomitant medication with anticholinergic activity, or being subject to dehydration.
2.7 Preparation and Administration Instructions
- To be prepared and administered by a healthcare professional only.
- Read the instructions for preparation and administration below for preparation and administration considerations.
- For deltoid or gluteal intramuscular injection only. Do not inject by any other route.
- Administer the initial dosage of ERZOFRI in the deltoid muscle. Subsequent monthly dosages may be administered in the deltoid or gluteal muscle.
- As a universal precaution, always wear gloves.
- Do not substitute any component of the drug kit.
The kit contains a prefilled syringe and 2 safety needles (a 1 ½-inch 22 gauge needle and a 1-inch 23 gauge needle).
ERZOFRI is for single use only.
Step 1. Select Needle
| For Deltoid injection | For Gluteal injection |
|---|---|
| If the patient weighs less than 90 kg, use the 1-inch 23gauge needle (needle with bluecolored hub) | Use the 1 ½-inch 22gauge needle (needle with graycolored hub) regardless of patient's weight |
| If the patient weighs 90 kg or more, use the 1 ½-inch 22gauge needle (needle with graycolored hub) |
Step 2. Prepare for Injection
| a. Open needle pouch | b. Shake vigorously for at least 10 seconds | c. Remove cap |
| First, peel the safety needle pouch half way open. Place on a clean surface. | Shake the syringe vigorously for a minimum of 10 seconds to ensure a homogeneous suspension. | While holding the syringe upright, remove the rubber tip cap with an easy counterclockwise twisting motion. Do not touch syringe tip. |
| d. Attach needle | e. Remove needle sheath | f. Remove air bubbles |
| Grasp the needle sheath using the plastic peel pouch. Attach the safety needle to the luer connection of the syringe with an easy clockwise twisting motion.
Do notremove the pouch until the syringe and needle are securely attached. |
Pull the needle sheath away from the needle with a straight pull. Do not twist the sheath as the needle may be loosened from the syringe. | Bring the syringe with the attached needle in upright position to de-aerate. De-aerate the syringe by moving the plunger rod carefully forward. |
Step 3. Inject
| Inject the entire contents intramuscularly slowly, deep into the selected deltoid or gluteal muscle of the patient. Do not administer by any other route. | ||
|
|
|
Step 4. After Injection
| Secure Needle | Dispose properly |
| a |
Dispose of the syringe and unused needle in an approved sharps container. |
| b | |
| c | |
| After the injection is complete, use either thumb or finger of one hand (a, b) or a flat surface (c) to activate the needle protection system. The needle protection system is fully activated when a 'click' is heard. |
Principal Display Panel 156 Mg/ml Syringe Kit
NDC 72526-108-11
Rx Only
Erzofri
®
(paliperidone palmitate)
extended-release injectable suspension
156 mg/mL
For Single Use Only.
Use entire contents of syringe.
FOR INTRAMUSCULAR INJECTION ONLY.
Shake before using. Each injection must be administered by a healthcare professional.
5.9 Leukopenia, Neutropenia, and Agranulocytosis
In clinical trial and/or postmarketing experience, events of leukopenia and neutropenia have been reported temporally related to antipsychotic agents, including once-a-month paliperidone palmitate extended-release injectable suspension (PP1M). Agranulocytosis has also been reported.
Possible risk factors for leukopenia/neutropenia include pre-existing low white blood cell count (WBC)/absolute neutrophil count (ANC) and history of drug-induced leukopenia/neutropenia. In patients with a history of a clinically significant low WBC/ANC or a drug-induced leukopenia/neutropenia, perform a complete blood count (CBC) frequently during the first few months of therapy. In such patients, consider discontinuation of ERZOFRI at the first sign of a clinically significant decline in WBC in the absence of other causative factors.
Monitor patients with clinically significant neutropenia for fever or other symptoms or signs of infection and treat promptly if such symptoms or signs occur. Discontinue ERZOFRI in patients with severe neutropenia (absolute neutrophil count < 1000/mm 3) and follow their WBC until recovery.
5.11 Potential for Cognitive and Motor Impairment
Somnolence, sedation, and dizziness were reported as adverse reactions in subjects treated with another once-a-month paliperidone palmitate extended-release injectable suspension (PP1M) [see Adverse Reactions (6.1)] . Antipsychotics, including ERZOFRI, have the potential to impair judgment, thinking, or motor skills. Patients should be cautioned about performing activities requiring mental alertness, such as operating hazardous machinery or operating a motor vehicle, until they are reasonably certain that paliperidone therapy does not adversely affect them.
2.3 Use With Risperidone Or With Oral Paliperidone
Paliperidone is the major active metabolite of risperidone. Exercise caution if ERZOFRI is co-administered with risperidone or with oral paliperidone for extended periods of time. Safety data involving concomitant use of ERZOFRI with other antipsychotics is limited.
Principal Display Panel 78 Mg/0.5 Ml Syringe Kit
NDC 72526-106-11
Rx Only
Erzofri
®
(paliperidone palmitate)
extended-release injectable suspension
78 mg/0.5 mL
For Single Use Only.
Use entire contents of syringe.
FOR INTRAMUSCULAR INJECTION ONLY.
Shake before using. Each injection must be administered by a healthcare professional.
Principal Display Panel 234 Mg/1.5 Ml Syringe Kit
NDC 72526-109-11
Rx Only
Erzofri
®
(paliperidone palmitate)
extended-release injectable suspension
234 mg/1.5 mL
For Single Use Only.
Use entire contents of syringe.
FOR INTRAMUSCULAR INJECTION ONLY.
Shake before using. Each injection must be administered by a healthcare professional.
Principal Display Panel 39 Mg/0.25 Ml Syringe Kit
NDC 72526-105-11
Rx Only
Erzofri
®
(paliperidone palmitate)
extended-release injectable suspension
39 mg/0.25 mL
For Single Use Only.
Use entire contents of syringe.
FOR INTRAMUSCULAR INJECTION ONLY.
Shake before using. Each injection must be administered by a healthcare professional.
Principal Display Panel 117 Mg/0.75 Ml Syringe Kit
NDC 72526-107-11
Rx Only
Erzofri
®
(paliperidone palmitate)
extended-release injectable suspension
117 mg/0.75 mL
For Single Use Only.
Use entire contents of syringe.
FOR INTRAMUSCULAR INJECTION ONLY.
Shake before using. Each injection must be administered by a healthcare professional.
Principal Display Panel 351 Mg/2.25 Ml Syringe Kit
NDC 72526-110-11
Rx Only
Erzofri
®
(paliperidone palmitate)
extended-release injectable suspension
351 mg/2.25 mL
For Single Use Only.
Use entire contents of syringe.
FOR INTRAMUSCULAR INJECTION ONLY.
Shake before using. Each injection must be administered by a healthcare professional.
8.8 Patients With Parkinson's Disease Or Lewy Body Dementia
Patients with Parkinson's Disease or Dementia with Lewy Bodies can experience increased sensitivity to ERZOFRI. Manifestations can include confusion, obtundation, postural instability with frequent falls, extrapyramidal symptoms, and clinical features consistent with neuroleptic malignant syndrome.
2.4 Dosage Recommendations for Patients With Renal Impairment
For patients with mild renal impairment (creatinine clearance ≥ 50 mL/min to < 80 mL/min [Cockcroft-Gault Formula]), initiate ERZOFRI with a dose of 234 mg on treatment Day 1 in the deltoid muscle. Follow with the recommended monthly dosage of 78 mg, administered in either the deltoid or gluteal muscle. Adjust monthly dosage based on tolerability and/or response within the strengths of 39 mg, 78 mg, 117 mg, or 156 mg. The maximum monthly dosage is 156 mg for patients with mild renal impairment [see Use in Specific Populations (8.6)and Clinical Pharmacology (12.3)] .
ERZOFRI is not recommended in patients with moderate or severe renal impairment (creatinine clearance < 50 mL/min) [see Use in Specific Populations (8.6)and Clinical Pharmacology (12.3)].
7.1 Drugs Having Clinically Important Interactions With Erzofri
Because paliperidone palmitate is hydrolyzed to paliperidone [see Clinical Pharmacology (12.3)] , results from studies with oral paliperidone should be taken into consideration when assessing drug-drug interaction potential.
Table 12 presents clinically significant drug interactions with ERZOFRI.
| Centrally Acting Drugs and Alcohol | |
| Clinical Rationale: | Given the primary CNS effects of paliperidone, concomitant use of centrally acting drugs and alcohol may modulate the CNS effects of ERZOFRI. |
| Clinical Recommendation: | ERZOFRI should be used with caution in combination with other centrally acting drugs and alcohol [see Adverse Reactions (6.1, 6.2)] . |
| Drugs with Potential for Inducing Orthostatic Hypotension | |
| Clinical Rationale: | Because ERZOFRI has the potential for inducing orthostatic hypotension, an additive effect may occur when ERZOFRI is administered with other therapeutic agents that have this potential [see Warnings and Precautions (5.7)] . |
| Clinical Recommendation: | Monitor orthostatic vital signs in patients who are vulnerable to hypotension [see Warnings and Precautions (5.7)] . |
| Strong Inducers of CYP3A4 and P-gp | |
| Clinical Rationale: | The concomitant use of paliperidone and strong inducers of CYP3A4 and P-gp may decrease the exposure of paliperidone [see Clinical Pharmacology (12.3)] . |
| Clinical Recommendation: | Avoid using CYP3A4 and/or P-gp inducers with ERZOFRI during the 1-month dosing interval, if possible. If administering a strong inducer is necessary, consider managing the patient using paliperidone extended-release tablets [see Dosage and Administration (2.5)] . |
| Levodopa and Other Dopamine Agonists | |
| Clinical Rationale: | Paliperidone may antagonize the effect of levodopa and other dopamine agonists. |
| Clinical Recommendation: | Monitor and manage patient as clinically appropriate. |
7.2 Drugs Having No Clinically Important Interactions With Erzofri
Based on pharmacokinetic studies with oral paliperidone, no dosage adjustment of ERZOFRI is required when administered with valproate [see Clinical Pharmacology (12.3)]. Additionally, no dosage adjustment is necessary for valproate when co-administered with ERZOFRI [See Clinical Pharmacology (12.3)].
Pharmacokinetic interaction between lithium and ERZOFRI is also unlikely.
Paliperidone is not expected to cause clinically important pharmacokinetic interactions with drugs that are metabolized by cytochrome P450 isozymes. In vitrostudies indicate that CYP2D6 and CYP3A4 may be involved in paliperidone metabolism; however, there is no evidence in vivothat inhibitors of these enzymes significantly affect the metabolism of paliperidone. Paliperidone is not a substrate of CYP1A2, CYP2A6, CYP2C9, and CYP2C19; an interaction with inhibitors or inducers of these isozymes is unlikely. [see Clinical Pharmacology (12.3)]
5.1 Increased Mortality in Elderly Patients With Dementia Related Psychosis
Elderly patients with dementia-related psychosis treated with antipsychotic drugs are at an increased risk of death. Analyses of 17 placebo-controlled trials (modal duration of 10 weeks), largely in patients taking atypical antipsychotic drugs, revealed a risk of death in drug-treated patients of between 1.6 to 1.7 times the risk of death in placebo-treated patients. Over the course of a typical 10-week controlled trial, the rate of death in drug-treated patients was about 4.5%, compared to a rate of about 2.6% in the placebo group.
Although the causes of death were varied, most of the deaths appeared to be either cardiovascular (e.g., heart failure, sudden death) or infectious (e.g., pneumonia) in nature. Observational studies suggest that, similar to atypical antipsychotic drugs, treatment with conventional antipsychotic drugs may increase mortality. The extent to which the findings of increased mortality in observational studies may be attributed to the antipsychotic drug as opposed to some characteristic(s) of the patients is not clear.
ERZOFRI is not approved for the treatment of patients with dementia-related psychosis [see Boxed Warningand Warnings and Precautions (5.2)] .
Warning: Increased Mortality in Elderly Patients With Dementia Related Psychosis
Elderly patients with dementia-related psychosis treated with antipsychotic drugs are at an increased risk of death. ERZOFRI is not approved for use in patients with dementia-related psychosis. [see Warnings and Precautions (5.1)] .
2.5 Dosage Modifications for Concomitant Use With Strong Cyp3a4 Inducers And/or P Gp Inducers
Avoid using a strong inducer of CYP3A4 and/or P-gp during the one-month dosing interval for ERZOFRI, if possible. If administering a strong inducer is necessary, consider managing the patient using paliperidone extended-release tablets [see Drug Interactions (7.1)and Clinical Pharmacology (12.3)] .
5.2 Cerebrovascular Adverse Reactions, Including Stroke, in Elderly Patients With Dementia Related Psychosis
In placebo-controlled trials with risperidone, aripiprazole, and olanzapine in elderly subjects with dementia, there was a higher incidence of cerebrovascular adverse reactions (cerebrovascular accidents and transient ischemic attacks) including fatalities compared to placebo-treated subjects. No studies have been conducted with oral paliperidone, 1-month or 3-month paliperidone palmitate extended-release injectable suspensions, or ERZOFRI, in elderly patients with dementia. ERZOFRI is not approved for the treatment of patients with dementia-related psychosis [see Boxed Warningand Warnings and Precautions (5.1)] .
Structured Label Content
Section 42229-5 (42229-5)
Dosing Window
To avoid a missed monthly dose, patients may be given the injection up to 7 days before or after the monthly time point.
Section 42230-3 (42230-3)
| PATIENT INFORMATION
ERZOFRI ®(er-ZOH-free) (paliperidone palmitate) extended-release injectable suspension |
||
|---|---|---|
| This Patient Information has been approved by the U.S. Food and Drug Administration. | Revised: 3/2025 | |
| What is the most important information I should know about ERZOFRI? | ||
ERZOFRI may cause serious side effects, including:
|
||
| What is ERZOFRI? | ||
| ERZOFRI is a prescription medicine given by injection by a healthcare provider and used to treat: | ||
|
||
| It is not known if ERZOFRI is safe and effective in children. | ||
| Who should not receive ERZOFRI? | ||
| Do not receive ERZOFRI if youare allergic to paliperidone, risperidone, or any of the ingredients in ERZOFRI. See the end of this Patient Information leaflet for a complete list of ingredients in ERZOFRI. | ||
Before receiving ERZOFRI, tell your healthcare provider about all your medical conditions, including if you:
|
||
| Tell your healthcare provider about all the medicines you take,including prescription and over-the-counter medicines, vitamins, and herbal supplements. ERZOFRI and certain other medicines may affect each other causing possible serious side effects or affect the way each other works. Know the medicines you take. Keep a list of them to show to your healthcare provider or pharmacist when you get a new medicine. | ||
How will I receive ERZOFRI?
|
||
What should I avoid while receiving ERZOFRI?
|
||
|
|
|
|
||
| What are the possible side effects of ERZOFRI? | ||
ERZOFRI may cause serious side effects, including:
|
||
|
|
|
|
||
|
|
|
|
||
|
||
| The most common side effects of ERZOFRI include: | ||
|
|
|
| Tell your healthcare provider if you have any side effect that bothers you or does not go away. | ||
| These are not all of the possible side effects of ERZOFRI. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. | ||
| General information about the safe and effective use of ERZOFRI. | ||
| Medicines are sometimes prescribed for purposes other than those listed in a Patient Information leaflet. You can ask your pharmacist or healthcare provider for information about ERZOFRI that is written for health professionals. | ||
| What are the ingredients in ERZOFRI? | ||
| Active ingredient: paliperidone palmitate | ||
| Inactive ingredients:citric acid monohydrate, dibasic sodium phosphate anhydrous, monobasic sodium phosphate monohydrate, polyethylene glycol 4000, polysorbate 20, sodium hydroxide, and water for injection. | ||
| Manufactured by: Shandong Luye Pharmaceutical Co., Ltd., No.15 Chuangye Road, Yantai, Shandong Province, China 264003 | ||
| Manufactured for: Luye Innomind Pharma Shijiazhuang Co., Ltd., Shijiazhuang, Hebei Province, China 050000
For more information call 1-800-548-9765. |
Section 43683-2 (43683-2)
| Warnings and Precautions ( 5.10) | 1/2025 |
Section 44425-7 (44425-7)
Storage and Handling
Store at 20°C to 25°C (68°F to 77°F); excursions permitted between 15°C and 30°C (59°F to 86°F) [see USP Controlled Room Temperature]. Do not mix with any other product or diluent.
5.8 Falls
Somnolence, postural hypotension, motor and sensory instability have been reported with the use of antipsychotics, including paliperidone palmitate, which may lead to falls and, consequently, fractures or other fall-related injuries. For patients, particularly the elderly, with diseases, conditions, or medications that could exacerbate these effects, assess the risk of falls when initiating antipsychotic treatment and recurrently for patients on long-term antipsychotic therapy.
5.12 Seizures
In the four fixed-dose double-blind placebo-controlled studies in subjects with schizophrenia, <1% (1 out of 1,293) of subjects treated with another once-a-month paliperidone palmitate extended-release injectable suspension (PP1M) in the recommended dose range of 39 mg to 234 mg experienced a convulsion compared with <1% (1 out of 510) of placebo-treated subjects who experienced a grand mal convulsion.
Like other antipsychotic drugs, ERZOFRI should be used cautiously in patients with a history of seizures or other conditions that potentially lower the seizure threshold. Conditions that lower the seizure threshold may be more prevalent in patients 65 years or older.
5.14 Priapism
Drugs with alpha-adrenergic blocking effects have been reported to induce priapism. Although no cases of priapism have been reported in clinical trials with another once-a-month paliperidone palmitate extended-release injectable suspension (PP1M), priapism has been reported with oral paliperidone during postmarketing surveillance. Severe priapism may require surgical intervention.
11 Description (11 DESCRIPTION)
ERZOFRI (paliperidone palmitate) extended-release injectable suspension contains a racemic mixture of (+)- and (-)- paliperidone palmitate. Paliperidone palmitate, is an atypical antipsychotic belonging to the chemical class of benzisoxazole derivatives. The chemical name is (9 RS)-3-[2-[4-(6-Fluoro-1,2-benzisoxazol-3-yl)piperidin-1-yl]ethyl]-2-methyl-4-oxo-6,7,8,9-tetrahydro-4 H-pyrido[1,2- a]pyrimadin-9-yl hexadecanoate. Its molecular formula is C 39H 57FN 4O 4and its molecular weight is 664.89. The structural formula is:
Paliperidone palmitate is very slightly soluble in ethanol and methanol, practically insoluble in water, and slightly soluble in ethyl acetate.
ERZOFRI is available as a white to off-white sterile aqueous extended-release suspension for intramuscular injection in the following dose strengths of paliperidone palmitate (deliverable volume) in single-dose prefilled syringes: 39 mg (0.25 mL), 78 mg (0.5 mL), 117 mg (0.75 mL), 156 mg (1 mL), 234 mg (1.5 mL), and 351 mg (2.25 mL). The drug product hydrolyzes in vivo to the active moiety, paliperidone, resulting in dose strengths of 25 mg, 50 mg, 75 mg, 100 mg, 150 mg, and 225 mg of paliperidone, respectively.
The inactive ingredients are citric acid monohydrate (5 mg/mL), dibasic sodium phosphate anhydrous (5 mg/mL), monobasic sodium phosphate monohydrate (2.5 mg/mL), polyethylene glycol 4000 (30 mg/mL), polysorbate 20 (12 mg/mL), sodium hydroxide to adjust pH, and water for injection. The drug product pH is 6.5 to 7.5.
5.13 Dysphagia
Esophageal dysmotility and aspiration have been associated with antipsychotic drug use. ERZOFRI and other antipsychotic drugs should be used cautiously in patients at risk for aspiration.
8.4 Pediatric Use
Safety and effectiveness of ERZOFRI in pediatric patients have not been established.
8.5 Geriatric Use
Clinical studies of ERZOFRI did not include sufficient numbers of subjects aged 65 and over to determine whether they respond differently from younger subjects. Other reported clinical experience has not identified differences in responses between the elderly and younger patients.
Paliperidone palmitate is substantially excreted by the kidney and clearance is decreased in patients with renal impairment [see Clinical Pharmacology (12.3)] , who should be given reduced doses. Because geriatric patients are more likely to have decreased renal function, adjust dose based on renal function [see Dosage and Administration (2.4)].
14.1 Schizophrenia
The efficacy of ERZOFRI for the treatment of schizophrenia in adults is based upon adequate and well-controlled studies of another once-a-month paliperidone palmitate extended-release injectable suspension (also referred to as "PP1M" in this section). The results of these adequate and well-controlled studies of another PP1M are presented below.
4 Contraindications (4 CONTRAINDICATIONS)
ERZOFRI is contraindicated in patients with a known hypersensitivity to either paliperidone or risperidone, or to any of the excipients in the ERZOFRI formulation. Hypersensitivity reactions, including anaphylactic reactions and angioedema, have been reported in patients treated with risperidone and in patients treated with paliperidone [see Adverse Reactions (6.1, 6.2)] .
5.4 Qt Prolongation (5.4 QT Prolongation)
Paliperidone causes a modest increase in the corrected QT (QTc) interval. The use of paliperidone should be avoided in combination with other drugs that are known to prolong QTc including Class 1A (e.g., quinidine, procainamide) or Class III (e.g., amiodarone, sotalol) antiarrhythmic medications, antipsychotic medications (e.g., chlorpromazine, thioridazine), antibiotics (e.g., gatifloxacin, moxifloxacin), or any other class of medications known to prolong the QTc interval. Paliperidone should also be avoided in patients with congenital long QT syndrome and in patients with a history of cardiac arrhythmias.
Certain circumstances may increase the risk of the occurrence of Torsades de pointes and/or sudden death in association with the use of drugs that prolong the QTc interval, including (1) bradycardia; (2) hypokalemia or hypomagnesemia; (3) concomitant use of other drugs that prolong the QTc interval; and (4) presence of congenital prolongation of the QT interval.
The effects of oral paliperidone on the QT interval were evaluated in a double-blind, active-controlled (moxifloxacin 400 mg single dose), multicenter QT study in adults with schizophrenia and schizoaffective disorder, and in three placebo- and active-controlled 6-week, fixed-dose efficacy trials in adults with schizophrenia.
In the QT study (n=141) of oral paliperidone, the 8 mg dose of immediate-release oral paliperidone (n=50) showed a mean placebo-subtracted increase from baseline in QTcLD (QT interval corrected for heart rate using the population specified linear derived method) of 12.3 msec (90% CI: 8.9; 15.6) on Day 8 at 1.5 hours post-dose. The mean steady-state peak plasma concentration for this 8 mg oral dose of immediate release paliperidone (C max ss= 113 ng/mL) was more than 2-fold the exposure observed with the maximum recommended 234 mg maintenance dose of another once-a-month paliperidone extended-release injectable suspension administered in the deltoid muscle (predicted median C max-ss= 50 ng/mL). In this same study, a 4 mg dose of the immediate-release oral formulation of paliperidone, for which C max-ss= 35 ng/mL, showed an increased placebo-subtracted QTcLD of 6.8 msec (90% CI: 3.6; 10.1) on Day 2 at 1.5 hours post-dose.
In the three fixed-dose efficacy studies of oral paliperidone extended release in subjects with schizophrenia, electrocardiogram (ECG) measurements taken at various time points showed only one subject in the oral paliperidone 12 mg group had a change exceeding 60 msec at one time- point on Day 6 (increase of 62 msec).
In the four fixed-dose efficacy studies of another once-a-month paliperidone palmitate extended-release injectable suspension in subjects with schizophrenia and in the long-term study in subjects with schizoaffective disorder, no subject experienced a change in QTcLD exceeding 60 msec and no subject had a QTcLD value of > 500 msec at any time point. In the maintenance study in subjects with schizophrenia, no subject had a QTcLD change > 60 msec, and one subject had a QTcLD value of 507 msec (Bazett's QT corrected interval [QTcB] value of 483 msec); this latter subject also had a heart rate of 45 beats per minute.
6 Adverse Reactions (6 ADVERSE REACTIONS)
The following are discussed in more detail in other sections of the labeling:
- Increased mortality in elderly patients with dementia-related psychosis [see Boxed Warningand Warnings and Precautions (5.1)]
- Cerebrovascular adverse reactions, including stroke, in elderly patients with dementia-related psychosis [see Warnings and Precautions (5.2)]
- Neuroleptic malignant syndrome [see Warnings and Precautions (5.3)]
- QT prolongation [see Warnings and Precautions (5.4)]
- Tardive dyskinesia [see Warnings and Precautions (5.5)]
- Metabolic changes [see Warnings and Precautions (5.6)]
- Orthostatic hypotension and syncope [see Warnings and Precautions (5.7)]
- Falls [see Warnings and Precautions (5.8)]
- Leukopenia, neutropenia, and agranulocytosis [see Warnings and Precautions (5.9)]
- Hyperprolactinemia [see Warnings and Precautions (5.10)]
- Potential for cognitive and motor impairment [see Warnings and Precautions (5.11)]
- Seizures [see Warnings and Precautions (5.12)]
- Dysphagia [see Warnings and Precautions (5.13)]
- Priapism [see Warnings and Precautions (5.14)]
- Disruption of body temperature regulation [see Warnings and Precautions (5.15)]
7 Drug Interactions (7 DRUG INTERACTIONS)
- Drugs that may cause orthostatic hypotension:An additive effect may occur when co-administered with ERZOFRI. ( 7.1)
- Strong CYP3A4 and P-glycoprotein (P-gp) inducers: Avoid using a strong inducer of CYP3A4 and/or P-gp during a dosing interval for ERZOFRI. If concomitant use is necessary, consider using paliperidone extended-release tablets. ( 2.5, 7.1, 12.3)
8.6 Renal Impairment
Use of ERZOFRI is not recommended in patients with moderate or severe renal impairment (creatinine clearance < 50 mL/min). Dose reduction is recommended for patients with mild renal impairment (creatinine clearance ≥ 50 mL/min to < 80 mL/min) [see Dosage and Administration (2.4)and Clinical Pharmacology (12.3)] .
12.2 Pharmacodynamics
Paliperidone is an antagonist at the central dopamine Type 2 (D 2) and serotonin Type 2 (5HT 2A) receptors with binding affinities (Ki values) of 1.6-2.8 nM for D 2and 0.8-1.2 nM for 5HT 2Areceptors. Paliperidone also acts as an antagonist at the α 1and α 2adrenergic receptors and H 1histaminergic receptors. Paliperidone has no affinity for cholinergic muscarinic or β 1- and β 2-adrenergic receptors. The pharmacological activity of the (+)- and (-)- paliperidone enantiomers is qualitatively and quantitatively similar .
12.3 Pharmacokinetics
The overall exposures (AUC) of paliperidone following another once-a-month paliperidone palmitate extended-release injectable suspension (also referred to as "PP1M" in this section) administration was dose-proportional over a dose range of 39 mg to 234 mg, and peak plasma concentrations (C max) were less than dose-proportional for doses exceeding 78 mg. Steady state plasma exposures of ERZOFRI are reached 7 days after the first injection.
5.6 Metabolic Changes
Atypical antipsychotic drugs have been associated with metabolic changes that may increase cardiovascular/cerebrovascular risk. These metabolic changes include hyperglycemia, dyslipidemia, and body weight gain. While all of the drugs in the class have been shown to produce some metabolic changes, each drug has its own specific risk profile.
2.1 Recommended Dosage
For patients who have never taken oral or injectable paliperidone, or oral or injectable risperidone, establish tolerability with oral paliperidone or oral risperidone prior to initiating treatment with ERZOFRI.
ERZOFRI must be administered by a healthcare professional as an intramuscular injection. Do not administer ERZOFRI by any other route. For detailed preparation and administration instructions, see Dosage and Administration (2.7) .
See Table 1for dosage recommendations for ERZOFRI in the treatment of schizophrenia in adults or the treatment of schizoaffective disorder in adults as monotherapy and as an adjunct to mood stabilizers or antidepressants.
The initial dosage of ERZOFRI is 351 mg on treatment Day 1 administered in the deltoid muscle. Following the initial dose, monthly doses can be administered in either the deltoid or gluteal muscle [see Clinical Pharmacology (12.3)] .
| Indication | Initial Dose
(deltoid) Day 1 |
Monthly Dosage
Administered 4 weeks after the first injection.
(deltoid or gluteal) |
Maximum Monthly Dosage |
|---|---|---|---|
| Schizophrenia | 351 mg | 39 mg to 234 mg
The recommended monthly dosage for treatment of schizophrenia is 117 mg. Some patients may benefit from lower or higher monthly doses within the additional available strengths (39 mg, 78 mg, 156 mg, and 234 mg).
|
234 mg |
| Schizoaffective disorder | 351 mg | 78 mg to 234 mg
Adjust dose based on tolerability and/or efficacy using available strengths. The 39 mg strength was not studied in the long-term schizoaffective disorder study.
|
234 mg |
Adjust dosage monthly depending on clinical response and tolerability. When making dose adjustments, the pharmacokinetic profile of ERZOFRI should be considered [see Clinical Pharmacology (12.3)] , as the full effect of the dose adjustment may not be apparent for several months.
5.5 Tardive Dyskinesia
Tardive dyskinesia, a syndrome consisting of potentially irreversible, involuntary, dyskinetic movements, may develop in patients treated with antipsychotic drugs. Although the prevalence of the syndrome appears to be highest among the elderly, especially elderly women, it is impossible to predict which patients will develop the syndrome. Whether antipsychotic drug products differ in their potential to cause tardive dyskinesia is unknown.
The risk of developing tardive dyskinesia and the likelihood that it will become irreversible appear to increase with the duration of treatment and the cumulative dose. The syndrome can develop after relatively brief treatment periods, even at low doses. It may also occur after discontinuation of treatment.
Tardive dyskinesia may remit, partially or completely, if antipsychotic treatment is discontinued. Antipsychotic treatment itself may suppress (or partially suppress) the signs and symptoms of the syndrome and may thus mask the underlying process. The effect that symptomatic suppression has upon the long-term course of the syndrome is unknown.
Given these considerations, ERZOFRI should be prescribed in a manner that is most likely to minimize the occurrence of tardive dyskinesia. Chronic antipsychotic treatment should generally be reserved for patients: (1) who suffer from a chronic illness that is known to respond to antipsychotic drugs and (2) for whom alternative, equally effective, but potentially less harmful treatments are not available or appropriate. In patients who do require chronic treatment, use the lowest dose and the shortest duration of treatment producing a satisfactory clinical response. Periodically reassess the need for continued treatment.
If signs and symptoms of tardive dyskinesia appear in a patient on ERZOFRI, drug discontinuation should be considered. However, some patients may require treatment with ERZOFRI despite the presence of the syndrome.
8.7 Hepatic Impairment
ERZOFRI has not been studied in patients with hepatic impairment. Based on a study with oral paliperidone, no dose adjustment is required in patients with mild or moderate hepatic impairment. Paliperidone has not been studied in patients with severe hepatic impairment [see Clinical Pharmacology (12.3)] .
1 Indications and Usage (1 INDICATIONS AND USAGE)
ERZOFRI is indicated for the treatment of:
- Schizophrenia in adults .
- Schizoaffective disorder in adults as monotherapy and as an adjunct to mood stabilizers or antidepressants .
5.10 Hyperprolactinemia
Like other drugs that antagonize dopamine D 2receptors, paliperidone elevates prolactin levels and the elevation persists during chronic administration. Paliperidone has a prolactin-elevating effect similar to that seen with risperidone, a drug that is associated with higher levels of prolactin than other antipsychotic drugs.
Hyperprolactinemia, regardless of etiology, may suppress hypothalamic GnRH, resulting in reduced pituitary gonadotrophin secretion. This, in turn, may inhibit reproductive function by impairing gonadal steroidogenesis in both female and male patients. Galactorrhea, amenorrhea, gynecomastia, and impotence have been reported in patients receiving prolactin-elevating compounds. Long-standing hyperprolactinemia when associated with hypogonadism may lead to decreased bone density in both female and male subjects.
Tissue culture experiments indicate that approximately one-third of human breast cancers are prolactin dependent in vitro, a factor of potential importance if the prescription of these drugs is considered in a patient with previously detected breast cancer. An increase in the incidence of pituitary gland, mammary gland, and pancreatic islet cell neoplasia (mammary adenocarcinomas, pituitary and pancreatic adenomas) was observed in the risperidone carcinogenicity studies conducted in mice and rats [see Nonclinical Toxicology (13.1)] . Published epidemiologic studies have shown inconsistent results when exploring the potential association between hyperprolactinemia and breast cancer.
Prolactin data from two long-term, double-blind, placebo-controlled studies with another PP1M are presented below; one study was in a population of patients with schizophrenia; the second study was in patients with schizoaffective disorder.
12.1 Mechanism of Action
Paliperidone palmitate is hydrolyzed to paliperidone [see Clinical Pharmacology (12.3)] . Paliperidone is the major active metabolite of risperidone. The mechanism of action of paliperidone in the listed indications is unclear. However, the drug's effect in schizophrenia could be mediated through a combination of central dopamine Type 2 (D 2)and serotonin Type 2 (5HT 2A) receptor antagonism.
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
- Cerebrovascular Adverse Reactions, in Elderly Patients with Dementia-Related Psychosis:Increased incidence of cerebrovascular adverse reactions (e.g., stroke, transient ischemic attack, including fatalities). ( 5.2)
- Neuroleptic Malignant Syndrome:Manage with immediate discontinuation of drug and close monitoring. ( 5.3)
- QT Prolongation:Avoid use with drugs that also increase QT interval and in patients with risk factors for prolonged QT interval. ( 5.4)
- Tardive Dyskinesia:Discontinue drug if clinically appropriate. ( 5.5)
- Metabolic Changes:Monitor for hyperglycemia/diabetes mellitus, dyslipidemia, and weight gain. ( 5.6)
- Orthostatic Hypotension and Syncope:Use with caution in patients with known cardiovascular or cerebrovascular disease and patients predisposed to hypotension. ( 5.7)
- Leukopenia, Neutropenia, and Agranulocytosis:Perform complete blood counts (CBC) in patients with history of clinically significant low white blood cell count (WBC) or history of leukopenia or neutropenia. Consider discontinuing ERZOFRI if clinically significant decline in WBC in the absence of other causative factors. ( 5.9)
- Hyperprolactinemia:Prolactin elevations occur and persist during chronic administration. ( 5.10)
- Potential for Cognitive and Motor Impairment:Use caution when operating machinery. ( 5.11)
- Seizures:Use cautiously in patients with a history of seizures or with conditions that lower the seizure threshold. ( 5.12)
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
- For patients naïve to oral or injectable paliperidone, or oral or injectable risperidone, establish tolerability with oral paliperidone or oral risperidone prior to initiating treatment with ERZOFRI. ( 2.1)
- Each injection must be administered by a healthcare professional. ( 2.1)
- Initiate ERZOFRI by intramuscular injection in the deltoid muscle. Following the initial dose, monthly doses can be administered in either the gluteal or deltoid muscle. Do not administer by any other route. ( 2.1)
- Dosage recommendations:
| Indication | Initial Dose
(deltoid) Day 1 |
Monthly Dosage
Administered 4 weeks after the first injection. (deltoid or gluteal)
|
Maximum Monthly Dosage |
|---|---|---|---|
| Schizophrenia ( 2.1) | 351 mg | 39 mg to 234 mg
Recommended monthly dosage for treatment of schizophrenia is 117 mg. Some patients may benefit from lower or higher monthly doses within the additional available strengths (39 mg, 78 mg, 156 mg, and 234 mg).
|
234 mg |
| Schizoaffective disorder ( 2.1) | 351 mg | 78 mg to 234 mg
Adjust dose based on tolerability and/or efficacy using available strengths. The 39 mg strength was not studied in the long-term schizoaffective disorder study.
|
234 mg |
- Missed dose: Refer to the Full Prescribing Information. ( 2.2)
- Mild renal impairment: Administer 234 mg on treatment Day 1 in the deltoid muscle. Follow with the recommended monthly maintenance dose of 78 mg, administered in the deltoid or gluteal muscle. Adjust monthly maintenance dose based on tolerability and/or efficacy within the strengths of 39 mg, 78 mg, 117 mg, or 156 mg. The maximum monthly dosage is 156 mg for patients with mild renal impairment. ( 2.4)
- See Full Prescribing Information for important preparation and administration information. ( 2.7)
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
Extended-release injectable suspension: white to off-white aqueous suspension available in dose strengths of 39 mg/0.25 mL, 78 mg/0.5 mL, 117 mg/0.75 mL, 156 mg/mL, 234 mg/1.5 mL, and 351 mg/2.25 mL paliperidone palmitate.
Each strength is provided as a kit, which includes: one single-dose prefilled syringe and 2 safety needles (a 1 ½-inch 22 gauge needle and a 1-inch 23 gauge needle).
6.2 Postmarketing Experience
The following adverse reactions have been identified during post-approval use of paliperidone; because these reactions were reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure: angioedema, catatonia, ileus, somnambulism, swollen tongue, thrombotic thrombocytopenic purpura, urinary incontinence, and urinary retention.
Cases of anaphylactic reaction after injection with another once-a-month paliperidone palmitate extended-release injectable suspension product have been reported during postmarketing experience in patients who have previously tolerated oral risperidone or oral paliperidone.
Paliperidone is the major active metabolite of risperidone. Adverse reactions reported with oral risperidone and risperidone long-acting injection can be found in the Adverse Reactions (6)sections of the package inserts for those products.
14.2 Schizoaffective Disorder
The efficacy of ERZOFRI for the treatment of schizoaffective disorder in adults as monotherapy and as an adjunct to mood stabilizers or antidepressants is based upon an adequate and well-controlled study of another PP1M. The results of the adequate and well-controlled study is presented below.
8 Use in Specific Populations (8 USE IN SPECIFIC POPULATIONS)
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in clinical practice.
The safety of ERZOFRI for the treatment of schizophrenia in adults and schizoaffective disorder in adults as monotherapy and as an adjunct to mood stabilizers or antidepressants is based upon adequate and well-controlled studies of another once-a-month paliperidone palmitate extended-release injectable suspension (also referred to as "PP1M" in this section). Below is a display of adverse reactions with another PP1M from those adequate and well-controlled studies.
Injection site reactions for ERZOFRI presented in this section (see " Pain and Injection Site Reactions with ERZOFRI " below) are based on pharmacokinetic studies.
17 Patient Counseling Information (17 PATIENT COUNSELING INFORMATION)
Advise the patient to read the FDA-approved patient labeling (Patient Information).
5.3 Neuroleptic Malignant Syndrome
Neuroleptic Malignant Syndrome (NMS), a potentially fatal symptom complex, has been reported in association with antipsychotic drugs, including paliperidone.
Clinical manifestations of NMS are hyperpyrexia, muscle rigidity, altered mental status including delirium, and autonomic instability (irregular pulse or blood pressure, tachycardia, diaphoresis, and cardiac dysrhythmia). Additional signs may include elevated creatine phosphokinase, myoglobinuria (rhabdomyolysis), and acute renal failure.
If NMS is suspected, immediately discontinue ERZOFRI and provide symptomatic treatment and monitoring.
2.6 Switching From Other Antipsychotics (2.6 Switching from Other Antipsychotics)
There are no systematically collected data to specifically address switching patients with schizophrenia or schizoaffective disorder from other antipsychotics to ERZOFRI or concerning concomitant administration with other antipsychotics.
5.7 Orthostatic Hypotension and Syncope
Paliperidone can induce orthostatic hypotension and syncope in some patients because of its alpha- adrenergic blocking activity. Syncope was reported in < 1% (4/1293) of subjects treated with another once-a-month paliperidone palmitate extended-release injectable suspension (PP1M) in the recommended maintenance dose range of 39 mg to 234 mg in the four fixed- dose, double-blind, placebo-controlled trials compared with 0% (0/510) of subjects treated with placebo. In the four fixed-dose efficacy studies in subjects with schizophrenia, orthostatic hypotension was reported as an adverse event by < 1% (2/1293) of the PP1M-treated subjects compared to 0% (0/510) with placebo. Incidences of orthostatic hypotension and syncope in the long-term studies in subjects with schizophrenia and schizoaffective disorder were similar to those observed in the short-term studies.
Use ERZOFRI with caution in patients with known cardiovascular disease (e.g., heart failure, history of myocardial infarction or ischemia, conduction abnormalities), cerebrovascular disease, or conditions that predispose the patient to hypotension (e.g., dehydration, hypovolemia, and treatment with antihypertensive medications). Monitoring of orthostatic vital signs should be considered in patients who are vulnerable to hypotension.
5.15 Disruption of Body Temperature Regulation
Disruption of the body's ability to reduce core body temperature has been attributed to antipsychotic agents. Appropriate care is advised when prescribing ERZOFRI to patients who will be experiencing conditions which may contribute to an elevation in core body temperature, e.g., exercising strenuously, exposure to extreme heat, receiving concomitant medication with anticholinergic activity, or being subject to dehydration.
2.7 Preparation and Administration Instructions
- To be prepared and administered by a healthcare professional only.
- Read the instructions for preparation and administration below for preparation and administration considerations.
- For deltoid or gluteal intramuscular injection only. Do not inject by any other route.
- Administer the initial dosage of ERZOFRI in the deltoid muscle. Subsequent monthly dosages may be administered in the deltoid or gluteal muscle.
- As a universal precaution, always wear gloves.
- Do not substitute any component of the drug kit.
The kit contains a prefilled syringe and 2 safety needles (a 1 ½-inch 22 gauge needle and a 1-inch 23 gauge needle).
ERZOFRI is for single use only.
Step 1. Select Needle
| For Deltoid injection | For Gluteal injection |
|---|---|
| If the patient weighs less than 90 kg, use the 1-inch 23gauge needle (needle with bluecolored hub) | Use the 1 ½-inch 22gauge needle (needle with graycolored hub) regardless of patient's weight |
| If the patient weighs 90 kg or more, use the 1 ½-inch 22gauge needle (needle with graycolored hub) |
Step 2. Prepare for Injection
| a. Open needle pouch | b. Shake vigorously for at least 10 seconds | c. Remove cap |
| First, peel the safety needle pouch half way open. Place on a clean surface. | Shake the syringe vigorously for a minimum of 10 seconds to ensure a homogeneous suspension. | While holding the syringe upright, remove the rubber tip cap with an easy counterclockwise twisting motion. Do not touch syringe tip. |
| d. Attach needle | e. Remove needle sheath | f. Remove air bubbles |
| Grasp the needle sheath using the plastic peel pouch. Attach the safety needle to the luer connection of the syringe with an easy clockwise twisting motion.
Do notremove the pouch until the syringe and needle are securely attached. |
Pull the needle sheath away from the needle with a straight pull. Do not twist the sheath as the needle may be loosened from the syringe. | Bring the syringe with the attached needle in upright position to de-aerate. De-aerate the syringe by moving the plunger rod carefully forward. |
Step 3. Inject
| Inject the entire contents intramuscularly slowly, deep into the selected deltoid or gluteal muscle of the patient. Do not administer by any other route. | ||
|
|
|
Step 4. After Injection
| Secure Needle | Dispose properly |
| a |
Dispose of the syringe and unused needle in an approved sharps container. |
| b | |
| c | |
| After the injection is complete, use either thumb or finger of one hand (a, b) or a flat surface (c) to activate the needle protection system. The needle protection system is fully activated when a 'click' is heard. |
Principal Display Panel 156 Mg/ml Syringe Kit (PRINCIPAL DISPLAY PANEL - 156 mg/mL Syringe Kit)
NDC 72526-108-11
Rx Only
Erzofri
®
(paliperidone palmitate)
extended-release injectable suspension
156 mg/mL
For Single Use Only.
Use entire contents of syringe.
FOR INTRAMUSCULAR INJECTION ONLY.
Shake before using. Each injection must be administered by a healthcare professional.
5.9 Leukopenia, Neutropenia, and Agranulocytosis
In clinical trial and/or postmarketing experience, events of leukopenia and neutropenia have been reported temporally related to antipsychotic agents, including once-a-month paliperidone palmitate extended-release injectable suspension (PP1M). Agranulocytosis has also been reported.
Possible risk factors for leukopenia/neutropenia include pre-existing low white blood cell count (WBC)/absolute neutrophil count (ANC) and history of drug-induced leukopenia/neutropenia. In patients with a history of a clinically significant low WBC/ANC or a drug-induced leukopenia/neutropenia, perform a complete blood count (CBC) frequently during the first few months of therapy. In such patients, consider discontinuation of ERZOFRI at the first sign of a clinically significant decline in WBC in the absence of other causative factors.
Monitor patients with clinically significant neutropenia for fever or other symptoms or signs of infection and treat promptly if such symptoms or signs occur. Discontinue ERZOFRI in patients with severe neutropenia (absolute neutrophil count < 1000/mm 3) and follow their WBC until recovery.
5.11 Potential for Cognitive and Motor Impairment
Somnolence, sedation, and dizziness were reported as adverse reactions in subjects treated with another once-a-month paliperidone palmitate extended-release injectable suspension (PP1M) [see Adverse Reactions (6.1)] . Antipsychotics, including ERZOFRI, have the potential to impair judgment, thinking, or motor skills. Patients should be cautioned about performing activities requiring mental alertness, such as operating hazardous machinery or operating a motor vehicle, until they are reasonably certain that paliperidone therapy does not adversely affect them.
2.3 Use With Risperidone Or With Oral Paliperidone (2.3 Use with Risperidone or with Oral Paliperidone)
Paliperidone is the major active metabolite of risperidone. Exercise caution if ERZOFRI is co-administered with risperidone or with oral paliperidone for extended periods of time. Safety data involving concomitant use of ERZOFRI with other antipsychotics is limited.
Principal Display Panel 78 Mg/0.5 Ml Syringe Kit (PRINCIPAL DISPLAY PANEL - 78 mg/0.5 mL Syringe Kit)
NDC 72526-106-11
Rx Only
Erzofri
®
(paliperidone palmitate)
extended-release injectable suspension
78 mg/0.5 mL
For Single Use Only.
Use entire contents of syringe.
FOR INTRAMUSCULAR INJECTION ONLY.
Shake before using. Each injection must be administered by a healthcare professional.
Principal Display Panel 234 Mg/1.5 Ml Syringe Kit (PRINCIPAL DISPLAY PANEL - 234 mg/1.5 mL Syringe Kit)
NDC 72526-109-11
Rx Only
Erzofri
®
(paliperidone palmitate)
extended-release injectable suspension
234 mg/1.5 mL
For Single Use Only.
Use entire contents of syringe.
FOR INTRAMUSCULAR INJECTION ONLY.
Shake before using. Each injection must be administered by a healthcare professional.
Principal Display Panel 39 Mg/0.25 Ml Syringe Kit (PRINCIPAL DISPLAY PANEL - 39 mg/0.25 mL Syringe Kit)
NDC 72526-105-11
Rx Only
Erzofri
®
(paliperidone palmitate)
extended-release injectable suspension
39 mg/0.25 mL
For Single Use Only.
Use entire contents of syringe.
FOR INTRAMUSCULAR INJECTION ONLY.
Shake before using. Each injection must be administered by a healthcare professional.
Principal Display Panel 117 Mg/0.75 Ml Syringe Kit (PRINCIPAL DISPLAY PANEL - 117 mg/0.75 mL Syringe Kit)
NDC 72526-107-11
Rx Only
Erzofri
®
(paliperidone palmitate)
extended-release injectable suspension
117 mg/0.75 mL
For Single Use Only.
Use entire contents of syringe.
FOR INTRAMUSCULAR INJECTION ONLY.
Shake before using. Each injection must be administered by a healthcare professional.
Principal Display Panel 351 Mg/2.25 Ml Syringe Kit (PRINCIPAL DISPLAY PANEL - 351 mg/2.25 mL Syringe Kit)
NDC 72526-110-11
Rx Only
Erzofri
®
(paliperidone palmitate)
extended-release injectable suspension
351 mg/2.25 mL
For Single Use Only.
Use entire contents of syringe.
FOR INTRAMUSCULAR INJECTION ONLY.
Shake before using. Each injection must be administered by a healthcare professional.
8.8 Patients With Parkinson's Disease Or Lewy Body Dementia (8.8 Patients with Parkinson's Disease or Lewy Body Dementia)
Patients with Parkinson's Disease or Dementia with Lewy Bodies can experience increased sensitivity to ERZOFRI. Manifestations can include confusion, obtundation, postural instability with frequent falls, extrapyramidal symptoms, and clinical features consistent with neuroleptic malignant syndrome.
2.4 Dosage Recommendations for Patients With Renal Impairment (2.4 Dosage Recommendations for Patients with Renal Impairment)
For patients with mild renal impairment (creatinine clearance ≥ 50 mL/min to < 80 mL/min [Cockcroft-Gault Formula]), initiate ERZOFRI with a dose of 234 mg on treatment Day 1 in the deltoid muscle. Follow with the recommended monthly dosage of 78 mg, administered in either the deltoid or gluteal muscle. Adjust monthly dosage based on tolerability and/or response within the strengths of 39 mg, 78 mg, 117 mg, or 156 mg. The maximum monthly dosage is 156 mg for patients with mild renal impairment [see Use in Specific Populations (8.6)and Clinical Pharmacology (12.3)] .
ERZOFRI is not recommended in patients with moderate or severe renal impairment (creatinine clearance < 50 mL/min) [see Use in Specific Populations (8.6)and Clinical Pharmacology (12.3)].
7.1 Drugs Having Clinically Important Interactions With Erzofri (7.1 Drugs Having Clinically Important Interactions with ERZOFRI)
Because paliperidone palmitate is hydrolyzed to paliperidone [see Clinical Pharmacology (12.3)] , results from studies with oral paliperidone should be taken into consideration when assessing drug-drug interaction potential.
Table 12 presents clinically significant drug interactions with ERZOFRI.
| Centrally Acting Drugs and Alcohol | |
| Clinical Rationale: | Given the primary CNS effects of paliperidone, concomitant use of centrally acting drugs and alcohol may modulate the CNS effects of ERZOFRI. |
| Clinical Recommendation: | ERZOFRI should be used with caution in combination with other centrally acting drugs and alcohol [see Adverse Reactions (6.1, 6.2)] . |
| Drugs with Potential for Inducing Orthostatic Hypotension | |
| Clinical Rationale: | Because ERZOFRI has the potential for inducing orthostatic hypotension, an additive effect may occur when ERZOFRI is administered with other therapeutic agents that have this potential [see Warnings and Precautions (5.7)] . |
| Clinical Recommendation: | Monitor orthostatic vital signs in patients who are vulnerable to hypotension [see Warnings and Precautions (5.7)] . |
| Strong Inducers of CYP3A4 and P-gp | |
| Clinical Rationale: | The concomitant use of paliperidone and strong inducers of CYP3A4 and P-gp may decrease the exposure of paliperidone [see Clinical Pharmacology (12.3)] . |
| Clinical Recommendation: | Avoid using CYP3A4 and/or P-gp inducers with ERZOFRI during the 1-month dosing interval, if possible. If administering a strong inducer is necessary, consider managing the patient using paliperidone extended-release tablets [see Dosage and Administration (2.5)] . |
| Levodopa and Other Dopamine Agonists | |
| Clinical Rationale: | Paliperidone may antagonize the effect of levodopa and other dopamine agonists. |
| Clinical Recommendation: | Monitor and manage patient as clinically appropriate. |
7.2 Drugs Having No Clinically Important Interactions With Erzofri (7.2 Drugs Having No Clinically Important Interactions with ERZOFRI)
Based on pharmacokinetic studies with oral paliperidone, no dosage adjustment of ERZOFRI is required when administered with valproate [see Clinical Pharmacology (12.3)]. Additionally, no dosage adjustment is necessary for valproate when co-administered with ERZOFRI [See Clinical Pharmacology (12.3)].
Pharmacokinetic interaction between lithium and ERZOFRI is also unlikely.
Paliperidone is not expected to cause clinically important pharmacokinetic interactions with drugs that are metabolized by cytochrome P450 isozymes. In vitrostudies indicate that CYP2D6 and CYP3A4 may be involved in paliperidone metabolism; however, there is no evidence in vivothat inhibitors of these enzymes significantly affect the metabolism of paliperidone. Paliperidone is not a substrate of CYP1A2, CYP2A6, CYP2C9, and CYP2C19; an interaction with inhibitors or inducers of these isozymes is unlikely. [see Clinical Pharmacology (12.3)]
5.1 Increased Mortality in Elderly Patients With Dementia Related Psychosis (5.1 Increased Mortality in Elderly Patients with Dementia-Related Psychosis)
Elderly patients with dementia-related psychosis treated with antipsychotic drugs are at an increased risk of death. Analyses of 17 placebo-controlled trials (modal duration of 10 weeks), largely in patients taking atypical antipsychotic drugs, revealed a risk of death in drug-treated patients of between 1.6 to 1.7 times the risk of death in placebo-treated patients. Over the course of a typical 10-week controlled trial, the rate of death in drug-treated patients was about 4.5%, compared to a rate of about 2.6% in the placebo group.
Although the causes of death were varied, most of the deaths appeared to be either cardiovascular (e.g., heart failure, sudden death) or infectious (e.g., pneumonia) in nature. Observational studies suggest that, similar to atypical antipsychotic drugs, treatment with conventional antipsychotic drugs may increase mortality. The extent to which the findings of increased mortality in observational studies may be attributed to the antipsychotic drug as opposed to some characteristic(s) of the patients is not clear.
ERZOFRI is not approved for the treatment of patients with dementia-related psychosis [see Boxed Warningand Warnings and Precautions (5.2)] .
Warning: Increased Mortality in Elderly Patients With Dementia Related Psychosis (WARNING: INCREASED MORTALITY IN ELDERLY PATIENTS WITH DEMENTIA- RELATED PSYCHOSIS)
Elderly patients with dementia-related psychosis treated with antipsychotic drugs are at an increased risk of death. ERZOFRI is not approved for use in patients with dementia-related psychosis. [see Warnings and Precautions (5.1)] .
2.5 Dosage Modifications for Concomitant Use With Strong Cyp3a4 Inducers And/or P Gp Inducers (2.5 Dosage Modifications for Concomitant Use with Strong CYP3A4 Inducers and/or P-gp Inducers)
Avoid using a strong inducer of CYP3A4 and/or P-gp during the one-month dosing interval for ERZOFRI, if possible. If administering a strong inducer is necessary, consider managing the patient using paliperidone extended-release tablets [see Drug Interactions (7.1)and Clinical Pharmacology (12.3)] .
5.2 Cerebrovascular Adverse Reactions, Including Stroke, in Elderly Patients With Dementia Related Psychosis (5.2 Cerebrovascular Adverse Reactions, Including Stroke, in Elderly Patients with Dementia-Related Psychosis)
In placebo-controlled trials with risperidone, aripiprazole, and olanzapine in elderly subjects with dementia, there was a higher incidence of cerebrovascular adverse reactions (cerebrovascular accidents and transient ischemic attacks) including fatalities compared to placebo-treated subjects. No studies have been conducted with oral paliperidone, 1-month or 3-month paliperidone palmitate extended-release injectable suspensions, or ERZOFRI, in elderly patients with dementia. ERZOFRI is not approved for the treatment of patients with dementia-related psychosis [see Boxed Warningand Warnings and Precautions (5.1)] .
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:47:22.619244 · Updated: 2026-03-14T22:51:48.679170