These Highlights Do Not Include All The Information Needed To Use Qsymia ®
40dd5602-53da-45ac-bb4b-15789aba40f9
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
QSYMIA is indicated in combination with a reduced-calorie diet and increased physical activity to reduce excess body weight and maintain weight reduction long term in: Adults and pediatric patients aged 12 years and older with obesity Adults with overweight in the presence of at least one weight-related comorbid condition
Indications and Usage
QSYMIA is indicated in combination with a reduced-calorie diet and increased physical activity to reduce excess body weight and maintain weight reduction long term in: Adults and pediatric patients aged 12 years and older with obesity Adults with overweight in the presence of at least one weight-related comorbid condition
Dosage and Administration
The recommended dosage, titration, and administration of QSYMIA are as follows: Take QSYMIA orally once daily in the morning with or without food. Avoid administration of QSYMIA in the evening due to the possibility of insomnia. The recommended starting dosage of QSYMIA is one capsule (containing 3.75 mg of phentermine and 23 mg of topiramate) (3.75 mg/23 mg) taken orally once daily for 14 days; after 14 days increase to the recommended dosage of QSYMIA 7.5 mg/46 mg orally once daily. After 12 weeks of treatment with QSYMIA 7.5 mg/46 mg, evaluate weight loss for adults or BMI reduction for pediatric patients aged 12 years and older. If an adult patient has not lost at least 3% of baseline body weight or a pediatric patient has not experienced a reduction of at least 3% of baseline BMI, increase the dosage to QSYMIA 11.25 mg/69 mg orally once daily for 14 days; followed by an increase in the dosage to QSYMIA 15 mg/92 mg orally once daily. After 12 weeks of treatment with QSYMIA 15 mg/92 mg, evaluate weight loss for adults or BMI reduction for pediatric patients aged 12 years and older. If an adult patient has not lost at least 5% of baseline body weight or a pediatric patient has not experienced a reduction of at least 5% of baseline BMI, discontinue QSYMIA [see Dosage and Administration (2.3) ] , as it is unlikely that the patient will achieve and sustain clinically meaningful weight loss with continued treatment. Monitor the rate of weight loss in pediatric patients. If weight loss exceeds 2 lbs (0.9 kg)/week, consider dosage reduction.
Warnings and Precautions
Embryo-Fetal Toxicity : Can cause fetal harm. In patients who can become pregnant, a negative pregnancy test is recommended before initiating QSYMIA and monthly during therapy; advise use of effective contraception. QSYMIA is available through a limited program under a Risk Evaluation and Mitigation Strategy (REMS) ( 5.1 ). Suicidal Behavior and Ideation : Monitor for depression or suicidal thoughts. Discontinue QSYMIA if symptoms develop ( 5.2 ). Risk of Ophthalmologic Adverse Reactions : Acute myopia and secondary angle closure glaucoma have been reported. Immediately discontinue QSYMIA if symptoms develop. Consider QSYMIA discontinuation if visual field defects occur ( 5.3 ). Mood and Sleep Disorders : Consider dosage reduction or discontinuation for clinically significant or persistent mood or sleep disorder symptoms ( 5.4 ). Cognitive Impairment : May cause disturbances in attention or memory, or speech/language problems. Caution patients about operating automobiles or hazardous machinery when starting treatment ( 5.5 ). Slowing of Linear Growth : Consider dosage reduction or discontinuation if pediatric patients are not growing or gaining height as expected ( 5.6 ). Metabolic Acidosis : Measure electrolytes before and during treatment. If persistent metabolic acidosis develops, reduce dosage or discontinue QSYMIA ( 5.7 ). Decrease in Renal Function : Measure creatinine before and during treatment. For persistent creatinine elevations, reduce dosage or discontinue QSYMIA ( 5.8 ). Serious Skin Reactions: QSYMIA should be discontinued at the first sign of a rash, unless the rash is clearly not drug-related ( 5.13 ).
Contraindications
QSYMIA is contraindicated in patients: Who are pregnant [see Warnings and Precautions (5.1) and Use in Specific Populations (8.1) ] With glaucoma [see Warnings and Precautions (5.3) ] With hyperthyroidism Taking or within 14 days of stopping a monoamine oxidase inhibitors [see Drug Interactions (7) ] With known hypersensitivity to phentermine, topiramate or any of the excipients in QSYMIA, or idiosyncrasy to the sympathomimetic amines [see Adverse Reactions (6.2) ] .
Adverse Reactions
The following clinically significant adverse reactions are described elsewhere in the labeling: Embryo-Fetal Toxicity [see Warnings and Precautions (5.1) and Use in Specific Populations (8.1 , 8.6) ] Suicidal Behavior and Ideation [see Warnings and Precautions (5.2) ] Risk of Ophthalmologic Adverse Reactions [see Warnings and Precautions (5.3) ] Mood and Sleep Disorders [see Warnings and Precautions (5.4) ] Cognitive Impairment [see Warnings and Precautions (5.5) ] Slowing of Linear Growth [see Warnings and Precautions (5.6) ] Metabolic Acidosis [see Warnings and Precautions (5.7) ] Decrease in Renal Function [see Warnings and Precautions (5.8) ] Risk of Seizures with Abrupt Withdrawal of QSYMIA [see Warnings and Precautions (5.9) ] Kidney Stones [see Warnings and Precautions (5.10) ] Oligohydrosis and Hyperthermia [see Warnings and Precautions (5.11) ] Hypokalemia [see Warnings and Precautions (5.12) ] Serious Skin Reactions [see Warnings and Precautions (5.13) ]
Drug Interactions
Table 5 displays clinically significant drug interactions with QSYMIA. Table 5. Clinically Significant Drug Interactions with QSYMIA Monoamine Oxidase Inhibitors Clinical Impact Concomitant use of phentermine with monoamine oxidase inhibitors (MAOIs) increases the risk of hypertensive crisis. Intervention Concomitant use of QSYMIA is contraindicated during MAOI treatment and within 14 days of stopping an MAOI. Oral Contraceptives Clinical Impact Co-administration of multiple-dose QSYMIA 15 mg/92 mg once daily with a single dose of oral contraceptive containing 35 µg ethinyl estradiol (estrogen component) and 1 mg norethindrone (progestin component), in obese otherwise healthy volunteers, decreased the exposure of ethinyl estradiol by 16% and increased the exposure of norethindrone by 22% [see Clinical Pharmacology (12.3) ] . Although this interaction is not anticipated to increase the risk of pregnancy, irregular bleeding (spotting) may occur more frequently due to both the increased exposure to the progestin and lower exposure to the estrogen, which tends to stabilize the endometrium. Intervention Inform patients not to discontinue their combination oral contraceptive if spotting occurs, but to notify their health care provider if the spotting is troubling to them. CNS Depressants Including Alcohol Clinical Impact The concomitant use of alcohol or CNS depressant drugs (e.g., barbiturates, benzodiazepines, and sleep medications) with phentermine or topiramate may potentiate CNS depression such as dizziness or cognitive adverse reactions, or other centrally mediated effects of these agents. Intervention Advise patients not to drive or operate machinery until they have gained sufficient experience on QSYMIA to gauge whether it adversely affects their mental performance, motor performance, and/or vision. Caution patients against excessive alcohol intake when taking QSYMIA. Consider QSYMIA dosage reduction or discontinuation if cognitive dysfunction persists [see Warnings and Precautions (5.5) ]. Non-Potassium Sparing Diuretics Clinical Impact Concurrent use of QSYMIA with non-potassium sparing diuretics may potentiate the potassium-wasting action of these diuretics. Concomitant administration of hydrochlorothiazide alone with topiramate alone has been shown to increase the C max and AUC of topiramate by 27% and 29%, respectively. Intervention When QSYMIA is used concomitantly with non-potassium-sparing diuretics, measure potassium before and during QSYMIA treatment [see Warnings and Precautions (5.12) and Clinical Pharmacology (12.3) ] . Antiepileptic Drugs Clinical Impact Concomitant administration of phenytoin or carbamazepine with topiramate in patients with epilepsy, decreased plasma concentrations of topiramate by 48% and 40%, respectively, when compared to topiramate given alone [see Clinical Pharmacology (12.3) ] . Concomitant administration of valproic acid and topiramate has been associated with hyperammonemia with and without encephalopathy. Concomitant administration of topiramate with valproic acid in patients has also been associated with hypothermia (with and without hyperammonemia). Intervention Consider measuring blood ammonia in patients in whom the onset of hypothermia or encephalopathy has been reported [see Clinical Pharmacology (12.3) ] . Carbonic Anhydrase Inhibitors Clinical Impact Concomitant use of topiramate with any other carbonic anhydrase inhibitor may increase the severity of metabolic acidosis and may also increase the risk of kidney stone formation. Intervention Avoid the use of QSYMIA with other drugs that inhibit carbonic anhydrase. If concomitant use of QSYMIA with another carbonic anhydrase inhibitor is unavoidable, monitor patient for the appearance or worsening of metabolic acidosis [see Warnings and Precautions (5.7 , 5.10) ] . Pioglitazone Clinical Impact A decrease in the exposure of pioglitazone and its active metabolites were noted with the concurrent use of pioglitazone and topiramate in a clinical trial. The clinical relevance of these observations is unknown. Intervention Consider increased glycemic monitoring when using pioglitazone and QSYMIA concomitantly [see Clinical Pharmacology (12.3) ] . Amitriptyline Clinical Impact Some patients may experience a large increase in amitriptyline concentration in the presence of topiramate. Intervention Any adjustments in amitriptyline dose when used with QSYMIA should be made according to the patient's clinical response and not on the basis of amitriptyline levels [see Clinical Pharmacology (12.3) ] .
Storage and Handling
QSYMIA (phentermine and topiramate extended-release capsules) are available as follows (see Table 15 ): Table 15. QSYMIA Presentations Strength (phentermine mg/topiramate mg) Description How Supplied NDC 3.75 mg/23 mg extended-release capsules Purple cap imprinted with VIVUS, Purple body imprinted with 3.75/23 Unit of Use Bottle (14 capsules) 62541-201-14 Pharmacy Bottle (30 capsules) 62541-201-30 7.5 mg/46 mg extended-release capsules Purple cap imprinted with VIVUS, Yellow body imprinted with 7.5/46 Unit of Use Bottle (30 capsules) 62541-202-30 11.25 mg/69 mg extended-release capsules Yellow cap imprinted with VIVUS, Yellow body imprinted with 11.25/69 Pharmacy Bottle (30 capsules) 62541-203-30 15 mg/92 mg extended-release capsules Yellow cap imprinted with VIVUS, White body imprinted with 15/92 Unit of Use Bottle (30 capsules) 62541-204-30 3.75 mg/23 mg and 7.5 mg/46 mg extended-release capsules Purple cap imprinted with VIVUS, Purple body imprinted with 3.75/23 and Purple cap imprinted with VIVUS, Yellow body imprinted with 7.5/46 Starter Pack - Blister Configuration (28 Capsules) 62541-210-28 11.25 mg/69 mg and 15 mg/92 mg extended-release capsules Yellow cap imprinted with VIVUS, Yellow body imprinted with 11.25/69 Dose Escalation Pack – Blister Configuration (28 Capsules) 62541-220-28
How Supplied
QSYMIA (phentermine and topiramate extended-release capsules) are available as follows (see Table 15 ): Table 15. QSYMIA Presentations Strength (phentermine mg/topiramate mg) Description How Supplied NDC 3.75 mg/23 mg extended-release capsules Purple cap imprinted with VIVUS, Purple body imprinted with 3.75/23 Unit of Use Bottle (14 capsules) 62541-201-14 Pharmacy Bottle (30 capsules) 62541-201-30 7.5 mg/46 mg extended-release capsules Purple cap imprinted with VIVUS, Yellow body imprinted with 7.5/46 Unit of Use Bottle (30 capsules) 62541-202-30 11.25 mg/69 mg extended-release capsules Yellow cap imprinted with VIVUS, Yellow body imprinted with 11.25/69 Pharmacy Bottle (30 capsules) 62541-203-30 15 mg/92 mg extended-release capsules Yellow cap imprinted with VIVUS, White body imprinted with 15/92 Unit of Use Bottle (30 capsules) 62541-204-30 3.75 mg/23 mg and 7.5 mg/46 mg extended-release capsules Purple cap imprinted with VIVUS, Purple body imprinted with 3.75/23 and Purple cap imprinted with VIVUS, Yellow body imprinted with 7.5/46 Starter Pack - Blister Configuration (28 Capsules) 62541-210-28 11.25 mg/69 mg and 15 mg/92 mg extended-release capsules Yellow cap imprinted with VIVUS, Yellow body imprinted with 11.25/69 Dose Escalation Pack – Blister Configuration (28 Capsules) 62541-220-28
Medication Information
Warnings and Precautions
Embryo-Fetal Toxicity : Can cause fetal harm. In patients who can become pregnant, a negative pregnancy test is recommended before initiating QSYMIA and monthly during therapy; advise use of effective contraception. QSYMIA is available through a limited program under a Risk Evaluation and Mitigation Strategy (REMS) ( 5.1 ). Suicidal Behavior and Ideation : Monitor for depression or suicidal thoughts. Discontinue QSYMIA if symptoms develop ( 5.2 ). Risk of Ophthalmologic Adverse Reactions : Acute myopia and secondary angle closure glaucoma have been reported. Immediately discontinue QSYMIA if symptoms develop. Consider QSYMIA discontinuation if visual field defects occur ( 5.3 ). Mood and Sleep Disorders : Consider dosage reduction or discontinuation for clinically significant or persistent mood or sleep disorder symptoms ( 5.4 ). Cognitive Impairment : May cause disturbances in attention or memory, or speech/language problems. Caution patients about operating automobiles or hazardous machinery when starting treatment ( 5.5 ). Slowing of Linear Growth : Consider dosage reduction or discontinuation if pediatric patients are not growing or gaining height as expected ( 5.6 ). Metabolic Acidosis : Measure electrolytes before and during treatment. If persistent metabolic acidosis develops, reduce dosage or discontinue QSYMIA ( 5.7 ). Decrease in Renal Function : Measure creatinine before and during treatment. For persistent creatinine elevations, reduce dosage or discontinue QSYMIA ( 5.8 ). Serious Skin Reactions: QSYMIA should be discontinued at the first sign of a rash, unless the rash is clearly not drug-related ( 5.13 ).
Indications and Usage
QSYMIA is indicated in combination with a reduced-calorie diet and increased physical activity to reduce excess body weight and maintain weight reduction long term in: Adults and pediatric patients aged 12 years and older with obesity Adults with overweight in the presence of at least one weight-related comorbid condition
Dosage and Administration
The recommended dosage, titration, and administration of QSYMIA are as follows: Take QSYMIA orally once daily in the morning with or without food. Avoid administration of QSYMIA in the evening due to the possibility of insomnia. The recommended starting dosage of QSYMIA is one capsule (containing 3.75 mg of phentermine and 23 mg of topiramate) (3.75 mg/23 mg) taken orally once daily for 14 days; after 14 days increase to the recommended dosage of QSYMIA 7.5 mg/46 mg orally once daily. After 12 weeks of treatment with QSYMIA 7.5 mg/46 mg, evaluate weight loss for adults or BMI reduction for pediatric patients aged 12 years and older. If an adult patient has not lost at least 3% of baseline body weight or a pediatric patient has not experienced a reduction of at least 3% of baseline BMI, increase the dosage to QSYMIA 11.25 mg/69 mg orally once daily for 14 days; followed by an increase in the dosage to QSYMIA 15 mg/92 mg orally once daily. After 12 weeks of treatment with QSYMIA 15 mg/92 mg, evaluate weight loss for adults or BMI reduction for pediatric patients aged 12 years and older. If an adult patient has not lost at least 5% of baseline body weight or a pediatric patient has not experienced a reduction of at least 5% of baseline BMI, discontinue QSYMIA [see Dosage and Administration (2.3) ] , as it is unlikely that the patient will achieve and sustain clinically meaningful weight loss with continued treatment. Monitor the rate of weight loss in pediatric patients. If weight loss exceeds 2 lbs (0.9 kg)/week, consider dosage reduction.
Contraindications
QSYMIA is contraindicated in patients: Who are pregnant [see Warnings and Precautions (5.1) and Use in Specific Populations (8.1) ] With glaucoma [see Warnings and Precautions (5.3) ] With hyperthyroidism Taking or within 14 days of stopping a monoamine oxidase inhibitors [see Drug Interactions (7) ] With known hypersensitivity to phentermine, topiramate or any of the excipients in QSYMIA, or idiosyncrasy to the sympathomimetic amines [see Adverse Reactions (6.2) ] .
Adverse Reactions
The following clinically significant adverse reactions are described elsewhere in the labeling: Embryo-Fetal Toxicity [see Warnings and Precautions (5.1) and Use in Specific Populations (8.1 , 8.6) ] Suicidal Behavior and Ideation [see Warnings and Precautions (5.2) ] Risk of Ophthalmologic Adverse Reactions [see Warnings and Precautions (5.3) ] Mood and Sleep Disorders [see Warnings and Precautions (5.4) ] Cognitive Impairment [see Warnings and Precautions (5.5) ] Slowing of Linear Growth [see Warnings and Precautions (5.6) ] Metabolic Acidosis [see Warnings and Precautions (5.7) ] Decrease in Renal Function [see Warnings and Precautions (5.8) ] Risk of Seizures with Abrupt Withdrawal of QSYMIA [see Warnings and Precautions (5.9) ] Kidney Stones [see Warnings and Precautions (5.10) ] Oligohydrosis and Hyperthermia [see Warnings and Precautions (5.11) ] Hypokalemia [see Warnings and Precautions (5.12) ] Serious Skin Reactions [see Warnings and Precautions (5.13) ]
Drug Interactions
Table 5 displays clinically significant drug interactions with QSYMIA. Table 5. Clinically Significant Drug Interactions with QSYMIA Monoamine Oxidase Inhibitors Clinical Impact Concomitant use of phentermine with monoamine oxidase inhibitors (MAOIs) increases the risk of hypertensive crisis. Intervention Concomitant use of QSYMIA is contraindicated during MAOI treatment and within 14 days of stopping an MAOI. Oral Contraceptives Clinical Impact Co-administration of multiple-dose QSYMIA 15 mg/92 mg once daily with a single dose of oral contraceptive containing 35 µg ethinyl estradiol (estrogen component) and 1 mg norethindrone (progestin component), in obese otherwise healthy volunteers, decreased the exposure of ethinyl estradiol by 16% and increased the exposure of norethindrone by 22% [see Clinical Pharmacology (12.3) ] . Although this interaction is not anticipated to increase the risk of pregnancy, irregular bleeding (spotting) may occur more frequently due to both the increased exposure to the progestin and lower exposure to the estrogen, which tends to stabilize the endometrium. Intervention Inform patients not to discontinue their combination oral contraceptive if spotting occurs, but to notify their health care provider if the spotting is troubling to them. CNS Depressants Including Alcohol Clinical Impact The concomitant use of alcohol or CNS depressant drugs (e.g., barbiturates, benzodiazepines, and sleep medications) with phentermine or topiramate may potentiate CNS depression such as dizziness or cognitive adverse reactions, or other centrally mediated effects of these agents. Intervention Advise patients not to drive or operate machinery until they have gained sufficient experience on QSYMIA to gauge whether it adversely affects their mental performance, motor performance, and/or vision. Caution patients against excessive alcohol intake when taking QSYMIA. Consider QSYMIA dosage reduction or discontinuation if cognitive dysfunction persists [see Warnings and Precautions (5.5) ]. Non-Potassium Sparing Diuretics Clinical Impact Concurrent use of QSYMIA with non-potassium sparing diuretics may potentiate the potassium-wasting action of these diuretics. Concomitant administration of hydrochlorothiazide alone with topiramate alone has been shown to increase the C max and AUC of topiramate by 27% and 29%, respectively. Intervention When QSYMIA is used concomitantly with non-potassium-sparing diuretics, measure potassium before and during QSYMIA treatment [see Warnings and Precautions (5.12) and Clinical Pharmacology (12.3) ] . Antiepileptic Drugs Clinical Impact Concomitant administration of phenytoin or carbamazepine with topiramate in patients with epilepsy, decreased plasma concentrations of topiramate by 48% and 40%, respectively, when compared to topiramate given alone [see Clinical Pharmacology (12.3) ] . Concomitant administration of valproic acid and topiramate has been associated with hyperammonemia with and without encephalopathy. Concomitant administration of topiramate with valproic acid in patients has also been associated with hypothermia (with and without hyperammonemia). Intervention Consider measuring blood ammonia in patients in whom the onset of hypothermia or encephalopathy has been reported [see Clinical Pharmacology (12.3) ] . Carbonic Anhydrase Inhibitors Clinical Impact Concomitant use of topiramate with any other carbonic anhydrase inhibitor may increase the severity of metabolic acidosis and may also increase the risk of kidney stone formation. Intervention Avoid the use of QSYMIA with other drugs that inhibit carbonic anhydrase. If concomitant use of QSYMIA with another carbonic anhydrase inhibitor is unavoidable, monitor patient for the appearance or worsening of metabolic acidosis [see Warnings and Precautions (5.7 , 5.10) ] . Pioglitazone Clinical Impact A decrease in the exposure of pioglitazone and its active metabolites were noted with the concurrent use of pioglitazone and topiramate in a clinical trial. The clinical relevance of these observations is unknown. Intervention Consider increased glycemic monitoring when using pioglitazone and QSYMIA concomitantly [see Clinical Pharmacology (12.3) ] . Amitriptyline Clinical Impact Some patients may experience a large increase in amitriptyline concentration in the presence of topiramate. Intervention Any adjustments in amitriptyline dose when used with QSYMIA should be made according to the patient's clinical response and not on the basis of amitriptyline levels [see Clinical Pharmacology (12.3) ] .
Storage and Handling
QSYMIA (phentermine and topiramate extended-release capsules) are available as follows (see Table 15 ): Table 15. QSYMIA Presentations Strength (phentermine mg/topiramate mg) Description How Supplied NDC 3.75 mg/23 mg extended-release capsules Purple cap imprinted with VIVUS, Purple body imprinted with 3.75/23 Unit of Use Bottle (14 capsules) 62541-201-14 Pharmacy Bottle (30 capsules) 62541-201-30 7.5 mg/46 mg extended-release capsules Purple cap imprinted with VIVUS, Yellow body imprinted with 7.5/46 Unit of Use Bottle (30 capsules) 62541-202-30 11.25 mg/69 mg extended-release capsules Yellow cap imprinted with VIVUS, Yellow body imprinted with 11.25/69 Pharmacy Bottle (30 capsules) 62541-203-30 15 mg/92 mg extended-release capsules Yellow cap imprinted with VIVUS, White body imprinted with 15/92 Unit of Use Bottle (30 capsules) 62541-204-30 3.75 mg/23 mg and 7.5 mg/46 mg extended-release capsules Purple cap imprinted with VIVUS, Purple body imprinted with 3.75/23 and Purple cap imprinted with VIVUS, Yellow body imprinted with 7.5/46 Starter Pack - Blister Configuration (28 Capsules) 62541-210-28 11.25 mg/69 mg and 15 mg/92 mg extended-release capsules Yellow cap imprinted with VIVUS, Yellow body imprinted with 11.25/69 Dose Escalation Pack – Blister Configuration (28 Capsules) 62541-220-28
How Supplied
QSYMIA (phentermine and topiramate extended-release capsules) are available as follows (see Table 15 ): Table 15. QSYMIA Presentations Strength (phentermine mg/topiramate mg) Description How Supplied NDC 3.75 mg/23 mg extended-release capsules Purple cap imprinted with VIVUS, Purple body imprinted with 3.75/23 Unit of Use Bottle (14 capsules) 62541-201-14 Pharmacy Bottle (30 capsules) 62541-201-30 7.5 mg/46 mg extended-release capsules Purple cap imprinted with VIVUS, Yellow body imprinted with 7.5/46 Unit of Use Bottle (30 capsules) 62541-202-30 11.25 mg/69 mg extended-release capsules Yellow cap imprinted with VIVUS, Yellow body imprinted with 11.25/69 Pharmacy Bottle (30 capsules) 62541-203-30 15 mg/92 mg extended-release capsules Yellow cap imprinted with VIVUS, White body imprinted with 15/92 Unit of Use Bottle (30 capsules) 62541-204-30 3.75 mg/23 mg and 7.5 mg/46 mg extended-release capsules Purple cap imprinted with VIVUS, Purple body imprinted with 3.75/23 and Purple cap imprinted with VIVUS, Yellow body imprinted with 7.5/46 Starter Pack - Blister Configuration (28 Capsules) 62541-210-28 11.25 mg/69 mg and 15 mg/92 mg extended-release capsules Yellow cap imprinted with VIVUS, Yellow body imprinted with 11.25/69 Dose Escalation Pack – Blister Configuration (28 Capsules) 62541-220-28
Description
QSYMIA is indicated in combination with a reduced-calorie diet and increased physical activity to reduce excess body weight and maintain weight reduction long term in: Adults and pediatric patients aged 12 years and older with obesity Adults with overweight in the presence of at least one weight-related comorbid condition
Section 42229-5
Limitations of Use
- The effect of QSYMIA on cardiovascular morbidity and mortality has not been established.
- The safety and effectiveness of QSYMIA in combination with other products intended for weight loss, including prescription drugs, over-the-counter drugs, and herbal preparations, have not been established.
Section 42231-1
| MEDICATION GUIDE
QSYMIA ®(Kyoo sim ee uh) (phentermine and topiramate extended-release capsules) for oral use, CIV |
|
|---|---|
| This Medication Guide has been approved by the U.S. Food and Drug Administration.
PH-03-002-16 |
Revised: 09/2024 |
|
What is the most important information I should know about QSYMIA?
QSYMIA can cause serious side effects, including :
|
|
What is QSYMIA?
|
|
Who should not take QSYMIA? Do not take QSYMIA if you:
|
|
Before taking QSYMIA, tell your health care provider about all of your medical conditions, including if you:
Especially tell your health care provider if you take:
Know the medicines you take. Keep a list of them to show your health care provider and pharmacist each time you get a new medicine. Do not start a new medicine without talking to your health care provider. |
|
How should I take QSYMIA?
|
|
What should I avoid while taking QSYMIA?
|
|
|
What are the possible side effects of QSYMIA?
QSYMIA can cause serious side effects, including:
These are not all of the possible side effects of QSYMIA. For more information, ask your health care provider or pharmacist. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. You can also report side effects to VIVUS at 1-888-998-4887. |
|
How should I store QSYMIA?
|
|
|
General Information about the safe and effective use of QSYMIA.
Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not use QSYMIA for a condition for which it was not prescribed. Do not give QSYMIA to other people, even if they have the same symptoms you have. It may harm them. You can ask your pharmacist or health care provider for information about QSYMIA that is written for health professionals. |
|
|
What are the ingredients in QSYMIA?
Active Ingredient: phentermine hydrochloride and topiramate extended-release. Inactive Ingredients: FD&C Blue #1, FD&C Red #3, FD&C Yellow #5 and #6, ethylcellulose, gelatin, methylcellulose, microcrystalline cellulose, povidone, starch, sucrose, talc, titanium dioxide, and pharmaceutical black and white inks. Copyright © 2012 - 2025 VIVUS LLC All rights reserved. VIVUS LLC 900 E. Hamilton Ave., Suite 550 Campbell, CA 95008 USA US Patent Numbers: 7,056,890; 7,553,818; 7,659,256; 7,674,776; 8,580,298; 8,580,299; 8,895,057; 8,895,058; 9,011,905; and 9,011,906. QSYMIA is a registered trademark of VIVUS LLC. |
Section 44425-7
Store at 20°C to 25°C (68°F to 77°F), excursions permitted between 15°C and 30°C (59°F and 86°F) [see USP Controlled Room Temperature]. Keep container tightly closed and protect from moisture.
9.2 Abuse
Phentermine has a known potential for abuse. Abuse is the intentional, non-therapeutic use of a drug, even once, for its desirable psychological or physiological effects.
Phentermine is related chemically and pharmacologically to amphetamines. Amphetamines and other stimulant drugs have been extensively abused. Abuse of amphetamines and related drugs (e.g., phentermine) may be associated with impaired control over drug use and severe social dysfunction. There are reports of patients who have increased the dosage of these drugs to many times higher than recommended. Assess the risk of abuse prior to prescribing QSYMIA as part of a weight reduction and long-term maintenance of body weight program.
10 Overdosage
In the event of a significant overdose with QSYMIA, if the ingestion is recent, the stomach should be emptied immediately by gastric lavage or by induction of emesis. Appropriate supportive treatment should be provided according to the patient's clinical signs and symptoms. In the event of an overdose of QSYMIA, consider contacting the Poison Help line (1-800-222-1222) or a medical toxicologist for additional overdosage management recommendations.
Acute overdose of phentermine may be associated with restlessness, tremor, hyperreflexia, rapid respiration, confusion, aggressiveness, hallucinations, and panic states. Fatigue and depression usually follow the central stimulation. Cardiovascular effects include arrhythmia, hypertension or hypotension, and circulatory collapse. Gastrointestinal symptoms include nausea, vomiting, diarrhea, and abdominal cramps. Fatal poisoning usually terminates in convulsions and coma. Manifestations of chronic intoxication with anorectic drugs include severe dermatoses, marked insomnia, irritability, hyperactivity, and personality changes. A severe manifestation of chronic intoxication is psychosis, often clinically indistinguishable from schizophrenia.
Management of acute phentermine intoxication is largely symptomatic and includes lavage and sedation with a barbiturate. Acidification of the urine increases phentermine excretion. Intravenous phentolamine has been suggested for possible acute, severe hypertension, if this complicates phentermine overdosage.
Topiramate overdose has resulted in severe metabolic acidosis. Other signs and symptoms include convulsions, drowsiness, speech disturbance, blurred vision, diplopia, impaired mentation, lethargy, abnormal coordination, stupor, hypotension, abdominal pain, agitation, dizziness, and depression. The clinical consequences were not severe in most cases, but deaths have been reported after overdoses involving topiramate. A patient who ingested a dose between 96 and 110 gm topiramate was admitted to hospital with coma lasting 20 to 24 hours followed by full recovery after 3 to 4 days.
Hemodialysis is an effective means of removing topiramate from the body.
11 Description
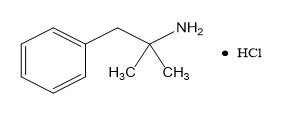
QSYMIA extended-release capsules are comprised of immediate-release phentermine hydrochloride (expressed as the weight of the free base) and extended-release topiramate. QSYMIA contains phentermine hydrochloride, a sympathomimetic amine anorectic, and topiramate, a sulfamate-substituted monosaccharide.
9.3 Dependence
Physical dependence may occur in patients treated with QSYMIA. Physical dependence is a state that develops as a result of physiological adaptation in response to repeated drug use, manifested by withdrawal signs and symptoms after abrupt discontinuation or a significant dose reduction of a drug.
The following adverse reactions have been associated with the abrupt discontinuation of the individual components of QSYMIA:
- For topiramate, abrupt discontinuation has been associated with seizures in patients without a history of seizures or epilepsy [see Warnings and Precautions (5.9)] .
- For phentermine, abrupt discontinuation following prolonged high dosage administration results in extreme fatigue and mental depression; changes are also noted on a sleep electroencephalogram.
Thus, in situations where rapid withdrawal of QSYMIA is required, appropriate medical monitoring is recommended. Patients discontinuing QSYMIA 15 mg/92 mg should be gradually tapered to reduce the possibility of precipitating a seizure [see Dosage and Administration (2.3)] .
5.12 Hypokalemia
QSYMIA can increase the risk of hypokalemia through its inhibition of carbonic anhydrase activity. In addition, when QSYMIA is used in conjunction with non-potassium sparing diuretics this may further potentiate potassium-wasting. Measure potassium before and during treatment with QSYMIA [see Adverse Reactions (6.1), Drug Interactions (7), and Clinical Pharmacology (12.3)] .
8.4 Pediatric Use
The safety and effectiveness of QSYMIA as an adjunct to a reduced-calorie diet and increased physical activity for weight reduction and long-term maintenance of body weight have been established in pediatric patients aged 12 years and older with obesity. Use of QSYMIA for this indication is supported by a 56-week, double-blind, placebo-controlled study in 223 pediatric patients aged 12 years and above, a pharmacokinetic study in pediatric patients, and studies in adults with obesity [see Clinical Pharmacology (12.3)and Clinical Studies (14)] .
In a pediatric clinical trial, there was one episode of serious suicidal ideation in a QSYMIA-treated patient requiring hospitalization and pharmacologic treatment [see Warnings and Precautions (5.2)] more patients treated with QSYMIA versus placebo reported adverse reactions related to mood (e.g., depression, anxiety) and sleep disorders (e.g., insomnia) [see Warnings and Precautions (5.4)] . Increases in bone mineral density and linear growth were attenuated in QSYMIA- versus placebo-treated patients [see Warnings and Precautions (5.6)] . Serious adverse reactions seen in pediatric patients using topiramate include acute angle glaucoma, oligohidrosis and hyperthermia, metabolic acidosis, cognitive and neuropsychiatric reactions, hyperammonemia and encephalopathy, and kidney stones.
The safety and effectiveness of QSYMIA in pediatric patients below the age of 12 years have not been established.
8.5 Geriatric Use
In the QSYMIA clinical trials, a total of 254 (7%) of the patients were 65 to 69 years of age; no patients 70 years of age or older were enrolled.
Clinical studies of QSYMIA did not include sufficient numbers of patients aged 65 and over to determine whether they respond differently from younger patients. In general, dose selection for an elderly patient should be cautious, usually starting at the low end of the dosing range, reflecting the greater frequency of decreased hepatic, renal, or cardiac function, and of concomitant disease or other drug therapy.
5.10 Kidney Stones
QSYMIA has been associated with kidney stone formation [see Adverse Reactions (6.1)] . Topiramate inhibits carbonic anhydrase activity and promotes kidney stone formation by reducing urinary citrate excretion and increasing urine pH. Patients on a ketogenic diet may be at increased risk for kidney stone formation. An increase in urinary calcium and a marked decrease in urinary citrate was observed in topiramate-treated pediatric patients in a one-year, active-controlled study. Increased ratio of urinary calcium/citrate increases the risk of kidney stones and/or nephrocalcinosis.
Avoid the use of QSYMIA with other drugs that inhibit carbonic anhydrase [see Drug Interactions (7)] . Advise patients to increase fluid intake (to increase urinary output), which may decrease the concentration of substances involved in kidney stone formation.
4 Contraindications
QSYMIA is contraindicated in patients:
- Who are pregnant [see Warnings and Precautions (5.1)and Use in Specific Populations (8.1)]
- With glaucoma [see Warnings and Precautions (5.3)]
- With hyperthyroidism
- Taking or within 14 days of stopping a monoamine oxidase inhibitors [see Drug Interactions (7)]
- With known hypersensitivity to phentermine, topiramate or any of the excipients in QSYMIA, or idiosyncrasy to the sympathomimetic amines [see Adverse Reactions (6.2)] .
6 Adverse Reactions
The following clinically significant adverse reactions are described elsewhere in the labeling:
- Embryo-Fetal Toxicity [see Warnings and Precautions (5.1) and Use in Specific Populations (8.1, 8.6)]
- Suicidal Behavior and Ideation [see Warnings and Precautions (5.2)]
- Risk of Ophthalmologic Adverse Reactions [see Warnings and Precautions (5.3)]
- Mood and Sleep Disorders [see Warnings and Precautions (5.4)]
- Cognitive Impairment [see Warnings and Precautions (5.5)]
- Slowing of Linear Growth [see Warnings and Precautions (5.6)]
- Metabolic Acidosis [see Warnings and Precautions (5.7)]
- Decrease in Renal Function [see Warnings and Precautions (5.8)]
- Risk of Seizures with Abrupt Withdrawal of QSYMIA [see Warnings and Precautions (5.9)]
- Kidney Stones [see Warnings and Precautions (5.10)]
- Oligohydrosis and Hyperthermia [see Warnings and Precautions (5.11)]
- Hypokalemia [see Warnings and Precautions (5.12)]
- Serious Skin Reactions [see Warnings and Precautions (5.13)]
7 Drug Interactions
Table 5 displays clinically significant drug interactions with QSYMIA.
| Monoamine Oxidase Inhibitors | |
| Clinical Impact | Concomitant use of phentermine with monoamine oxidase inhibitors (MAOIs) increases the risk of hypertensive crisis. |
| Intervention | Concomitant use of QSYMIA is contraindicated during MAOI treatment and within 14 days of stopping an MAOI. |
| Oral Contraceptives | |
| Clinical Impact | Co-administration of multiple-dose QSYMIA 15 mg/92 mg once daily with a single dose of oral contraceptive containing 35 µg ethinyl estradiol (estrogen component) and 1 mg norethindrone (progestin component), in obese otherwise healthy volunteers, decreased the exposure of ethinyl estradiol by 16% and increased the exposure of norethindrone by 22% [see Clinical Pharmacology (12.3)] . Although this interaction is not anticipated to increase the risk of pregnancy, irregular bleeding (spotting) may occur more frequently due to both the increased exposure to the progestin and lower exposure to the estrogen, which tends to stabilize the endometrium. |
| Intervention | Inform patients not to discontinue their combination oral contraceptive if spotting occurs, but to notify their health care provider if the spotting is troubling to them. |
| CNS Depressants Including Alcohol | |
| Clinical Impact | The concomitant use of alcohol or CNS depressant drugs (e.g., barbiturates, benzodiazepines, and sleep medications) with phentermine or topiramate may potentiate CNS depression such as dizziness or cognitive adverse reactions, or other centrally mediated effects of these agents. |
| Intervention | Advise patients not to drive or operate machinery until they have gained sufficient experience on QSYMIA to gauge whether it adversely affects their mental performance, motor performance, and/or vision. Caution patients against excessive alcohol intake when taking QSYMIA. Consider QSYMIA dosage reduction or discontinuation if cognitive dysfunction persists [see Warnings and Precautions (5.5)]. |
| Non-Potassium Sparing Diuretics | |
| Clinical Impact | Concurrent use of QSYMIA with non-potassium sparing diuretics may potentiate the potassium-wasting action of these diuretics. Concomitant administration of hydrochlorothiazide alone with topiramate alone has been shown to increase the C max and AUC of topiramate by 27% and 29%, respectively. |
| Intervention | When QSYMIA is used concomitantly with non-potassium-sparing diuretics, measure potassium before and during QSYMIA treatment [see Warnings and Precautions (5.12) and Clinical Pharmacology (12.3)] . |
| Antiepileptic Drugs | |
| Clinical Impact | Concomitant administration of phenytoin or carbamazepine with topiramate in patients with epilepsy, decreased plasma concentrations of topiramate by 48% and 40%, respectively, when compared to topiramate given alone [see Clinical Pharmacology (12.3)] . Concomitant administration of valproic acid and topiramate has been associated with hyperammonemia with and without encephalopathy. Concomitant administration of topiramate with valproic acid in patients has also been associated with hypothermia (with and without hyperammonemia). |
| Intervention | Consider measuring blood ammonia in patients in whom the onset of hypothermia or encephalopathy has been reported [see Clinical Pharmacology (12.3)] . |
| Carbonic Anhydrase Inhibitors | |
| Clinical Impact | Concomitant use of topiramate with any other carbonic anhydrase inhibitor may increase the severity of metabolic acidosis and may also increase the risk of kidney stone formation. |
| Intervention | Avoid the use of QSYMIA with other drugs that inhibit carbonic anhydrase. If concomitant use of QSYMIA with another carbonic anhydrase inhibitor is unavoidable, monitor patient for the appearance or worsening of metabolic acidosis [see Warnings and Precautions (5.7, 5.10)] . |
| Pioglitazone | |
| Clinical Impact | A decrease in the exposure of pioglitazone and its active metabolites were noted with the concurrent use of pioglitazone and topiramate in a clinical trial. The clinical relevance of these observations is unknown. |
| Intervention | Consider increased glycemic monitoring when using pioglitazone and QSYMIA concomitantly [see Clinical Pharmacology (12.3)] . |
| Amitriptyline | |
| Clinical Impact | Some patients may experience a large increase in amitriptyline concentration in the presence of topiramate. |
| Intervention | Any adjustments in amitriptyline dose when used with QSYMIA should be made according to the patient's clinical response and not on the basis of amitriptyline levels [see Clinical Pharmacology (12.3)] . |
8.6 Renal Impairment
Compared to healthy volunteers with normal renal function, patients with moderate and severe renal impairment as estimated by the Cockcroft-Gault equation had higher exposures to phentermine and topiramate.
The recommended dosage of QSYMIA in patients with mild renal impairment (CrCl greater or equal to 50 and less than 80 mL/min) is the same as the recommended dosage for patients with normal renal function.
In patients with moderate (CrCl greater than or equal to 30 to less than 50 mL/min) and severe (CrCl less than 30 mL/min) renal impairment, the maximum recommended dosage is QSYMIA 7.5 mg/46 mg once daily.
QSYMIA has not been studied in patients with end-stage renal disease on dialysis. Avoid QSYMIA in this patient population [see Dosage and Administration (2.4) and Clinical Pharmacology (12.3)] .
12.2 Pharmacodynamics
Typical actions of amphetamines include central nervous system stimulation and elevation of blood pressure. Tachyphylaxis and tolerance have been demonstrated with drugs in this class.
5.7 Metabolic Acidosis
Hyperchloremic, non-anion gap, metabolic acidosis (decreased serum bicarbonate below the normal reference range in the absence of chronic respiratory alkalosis) has been reported in patients treated with QSYMIA [see Adverse Reactions (6.1)] . Manifestations of acute or chronic metabolic acidosis may include hyperventilation, nonspecific symptoms such as fatigue and anorexia, or more severe sequelae including cardiac arrhythmias or stupor. Chronic, untreated metabolic acidosis may increase the risk for nephrolithiasis or nephrocalcinosis and may also result in osteomalacia (referred to as rickets in pediatric patients) and/or osteoporosis with an increased risk for fractures. Chronic metabolic acidosis in pediatric patients may also reduce growth rates, which may decrease the maximal height achieved.
Conditions or therapies that predispose to acidosis (i.e., renal disease, severe respiratory disorders, status epilepticus, diarrhea, surgery, or ketogenic diet) may be additive to the bicarbonate lowering effects of QSYMIA. Concomitant use of QSYMIA and a carbonic anhydrase inhibitor may increase the severity of metabolic acidosis and may also increase the risk of kidney stone formation [see Warnings and Precautions (5.10)] . Avoid use of QSYMIA with other carbonic anhydrase inhibitors. If concomitant use of QSYMIA with another carbonic anhydrase inhibitor is unavoidable, the patient should be monitored for the appearance or worsening of metabolic acidosis.
Measure electrolytes including serum bicarbonate prior to starting QSYMIA and during QSYMIA treatment. In QSYMIA clinical trials, the peak reduction in serum bicarbonate typically occurred within 4 weeks of titration to the assigned dose, and in most patients, there was a correction of bicarbonate by week 56, without any dosage reduction. However, if persistent metabolic acidosis develops while taking QSYMIA, reduce the dosage or discontinue QSYMIA [see Warnings and Precautions (5.9)] .
8.7 Hepatic Impairment
In patients with mild (Child-Pugh 5 - 6) and moderate (Child-Pugh 7 - 9) hepatic impairment, exposure to phentermine was higher compared to healthy volunteers with normal hepatic function. Exposure to topiramate was similar among patients with mild and moderate hepatic impairment and healthy volunteers.
The recommended dosage of QSYMIA in patients with mild hepatic impairment (Child-Pugh 5 - 6) is the same as the recommended dosage in patients with normal hepatic function.
In patients with moderate hepatic impairment, the maximum recommended dosage is QSYMIA 7.5 mg/46 mg once daily.
QSYMIA has not been studied in patients with severe hepatic impairment (Child-Pugh score 10 - 15). Avoid QSYMIA in this patient population [see Dosage and Administration (2.5) and Clinical Pharmacology (12.3)] .
1 Indications and Usage
QSYMIA is indicated in combination with a reduced-calorie diet and increased physical activity to reduce excess body weight and maintain weight reduction long term in:
- Adults and pediatric patients aged 12 years and older with obesity
- Adults with overweight in the presence of at least one weight-related comorbid condition
12.1 Mechanism of Action
Phentermine is a sympathomimetic amine with pharmacologic activity similar to the prototype drugs of this class used in obesity, amphetamine (d- and d/l-amphetamine). Drugs of this class used in obesity are commonly known as "anorectics" or "anorexigenics." The effect of phentermine on weight reduction and long-term maintenance of body weight is likely mediated by release of catecholamines in the hypothalamus, resulting in reduced appetite and decreased food consumption, but other metabolic effects may also be involved. The exact mechanism of action is not known.
The precise mechanism of action of topiramate on weight reduction and long-term maintenance of body weight is not known. Topiramate's effect on weight reduction and long-term maintenance of body weight may be due to its effects on both appetite suppression and satiety enhancement, induced by a combination of pharmacologic effects including augmenting the activity of the neurotransmitter gamma-aminobutyrate, modulation of voltage-gated ion channels, inhibition of AMPA/kainite excitatory glutamate receptors, or inhibition of carbonic anhydrase.
5.5 Cognitive Impairment
QSYMIA can cause cognitive dysfunction (e.g., impairment of concentration/attention, difficulty with memory, and speech or language problems, particularly word-finding difficulties). Rapid titration or high initial doses of QSYMIA may be associated with higher rates of cognitive events such as attention, memory, and language/word-finding difficulties [see Adverse Reactions (6.1)] . The concomitant use of alcohol or central nervous system (CNS) depressant drugs with QSYMIA may potentiate CNS depression or other centrally mediated effects of these agents, such as dizziness, cognitive adverse reactions, drowsiness, light-headedness, impaired coordination, and somnolence.
Caution patients about operating hazardous machinery, including automobiles, until they are reasonably certain QSYMIA therapy does not affect them adversely. Caution patients against excessive alcohol intake while receiving QSYMIA.
If cognitive dysfunction persists, consider dosage reduction or discontinuation of QSYMIA [see Warnings and Precautions (5.9)] .
9.1 Controlled Substance
QSYMIA contains phentermine, a Schedule IV controlled substance, and topiramate, which is not a controlled substance.
5.1 Embryo Fetal Toxicity
QSYMIA can cause fetal harm. Data from pregnancy registries and epidemiologic studies indicate that a fetus exposed to topiramate in the first trimester of pregnancy has an increased risk of major congenital malformations, including but not limited to cleft lip and/or cleft palate (oral clefts), and of being small for gestational age (SGA). When multiple species of pregnant animals received topiramate at clinically relevant doses, structural malformations, including craniofacial defects, and reduced fetal weights occurred in offspring. A negative pregnancy test is recommended before initiating QSYMIA treatment in patients who can become pregnant and monthly during QSYMIA therapy. Advise patients who can become pregnant of the potential risk to a fetus and to use effective contraception during QSYMIA therapy [see Use in Specific Populations (8.1, 8.3)] .
5 Warnings and Precautions
- Embryo-Fetal Toxicity: Can cause fetal harm. In patients who can become pregnant, a negative pregnancy test is recommended before initiating QSYMIA and monthly during therapy; advise use of effective contraception. QSYMIA is available through a limited program under a Risk Evaluation and Mitigation Strategy (REMS) ( 5.1).
- Suicidal Behavior and Ideation: Monitor for depression or suicidal thoughts. Discontinue QSYMIA if symptoms develop ( 5.2).
- Risk of Ophthalmologic Adverse Reactions: Acute myopia and secondary angle closure glaucoma have been reported. Immediately discontinue QSYMIA if symptoms develop. Consider QSYMIA discontinuation if visual field defects occur ( 5.3).
- Mood and Sleep Disorders: Consider dosage reduction or discontinuation for clinically significant or persistent mood or sleep disorder symptoms ( 5.4).
- Cognitive Impairment: May cause disturbances in attention or memory, or speech/language problems. Caution patients about operating automobiles or hazardous machinery when starting treatment ( 5.5).
- Slowing of Linear Growth: Consider dosage reduction or discontinuation if pediatric patients are not growing or gaining height as expected ( 5.6).
- Metabolic Acidosis: Measure electrolytes before and during treatment. If persistent metabolic acidosis develops, reduce dosage or discontinue QSYMIA ( 5.7).
- Decrease in Renal Function: Measure creatinine before and during treatment. For persistent creatinine elevations, reduce dosage or discontinue QSYMIA ( 5.8).
- Serious Skin Reactions:QSYMIA should be discontinued at the first sign of a rash, unless the rash is clearly not drug-related ( 5.13).
2 Dosage and Administration
- Take orally once daily in morning. Avoid administration in evening to prevent insomnia ( 2.2).
- Recommended starting dosage is 3.75 mg/23 mg (phentermine mg/topiramate mg) daily for 14 days; then increase to 7.5 mg/46 mg daily ( 2.2).
- Escalate dosage based on weight loss in adults or BMI reduction in pediatric patients. See the Full Prescribing Information for details regarding discontinuation or dosage escalation ( 2.2).
- Gradually discontinue 15 mg/92 mg dosage to prevent possible seizure ( 2.3).
- Do not exceed 7.5 mg/46 mg dosage for patients with moderate or severe renal impairment or patients with moderate hepatic impairment ( 2.4, 2.5).
5.13 Serious Skin Reactions
Serious skin reactions (Stevens-Johnson Syndrome [SJS] and Toxic Epidermal Necrolysis [TEN]) have been reported in patients receiving topiramate. QSYMIA should be discontinued at the first sign of a rash, unless the rash is clearly not drug-related. If signs or symptoms suggest SJS/TEN, use of this drug should not be resumed, and alternative therapy should be considered. Inform patients about the signs of serious skin reactions.
3 Dosage Forms and Strengths
QSYMIA extended-release capsules are available in four strengths (phentermine mg/topiramate mg):
- 3.75 mg/23 mg - purple cap imprinted with VIVUS and purple body imprinted with 3.75/23
- 7.5 mg/46 mg - purple cap imprinted with VIVUS and yellow body imprinted with 7.5/46
- 11.25 mg/69 mg - yellow cap imprinted with VIVUS and yellow body imprinted with 11.25/69
- 15 mg/92 mg - yellow cap imprinted with VIVUS and white body imprinted with 15/92
5.4 Mood and Sleep Disorders
QSYMIA can cause mood disorders, including depression and anxiety, as well as insomnia. Patients with a history of depression may be at increased risk of recurrent depression or other mood disorders while taking QSYMIA [see Adverse Reactions (6.1)] .
Consider dosage reduction or discontinuation of QSYMIA if clinically significant or persistent symptoms occur. Discontinue QSYMIA if patients have symptoms of suicidal ideation or behavior [see Warnings and Precautions (5.2)] .
5.6 Slowing of Linear Growth
QSYMIA is associated with a reduction in height velocity (centimeters of height gained per year) in obese pediatric patients 12 to 17 years of age. In a 56-week study, average height increased from baseline in both QSYMIA- and placebo-treated patients; however, a lower height velocity of -1.3 to -1.4 cm/year was observed in QSYMIA-treated compared to placebo-treated patients. Monitor height velocity in pediatric patients treated with QSYMIA. Consider dosage reduction or discontinuation of QSYMIA if pediatric patients are not growing or gaining height as expected [see Warnings and Precautions (5.9)] .
6.2 Postmarketing Experience
The following adverse reactions have been reported during post approval use of QSYMIA, phentermine, and topiramate. Because these reactions are reported voluntarily from a population of uncertain size it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
8 Use in Specific Populations
- Lactation: Breastfeeding not recommended ( 8.2).
5.8 Decrease in Renal Function
QSYMIA can cause an increase in serum creatinine that reflects a decrease in renal function (glomerular filtration rate). In clinical trials, peak increases in serum creatinine were observed after 4 to 8 weeks of treatment. On average, serum creatinine gradually declined but remained elevated over baseline creatinine values. The changes in serum creatinine (and measured GFR) with short-term (4-weeks) QSYMIA treatment appear reversible with treatment discontinuation, but the effect of chronic treatment on renal function is not known.
Measure serum creatinine prior to starting QSYMIA and during QSYMIA treatment. If persistent elevations in creatinine occur, reduce the dosage or discontinue QSYMIA [see Warnings and Precautions (5.9), Adverse Reactions (6.1), and Clinical Pharmacology (12.2)] .
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical studies of another drug and may not reflect the rates observed in practice.
The data described herein reflect exposure to QSYMIA in two 1-year, randomized, double-blind, placebo-controlled, multicenter clinical trials and two supportive trials in 2,318 adult patients with overweight or obesity [936 (40%) patients with hypertension, 309 (13%) patients with type 2 diabetes mellitus, 808 (35%) patients with BMI greater than 40 kg/m 2] exposed for a mean duration of 298 days. Data in this section also describe adverse reactions from a 1-year, randomized, double-blind, placebo-controlled multicenter clinical trial that evaluated 223 pediatric patients (12 to 17 years old) with obesity [see Clinical Studies (14)] .
17 Patient Counseling Information
Advise the patient to read the FDA-approved patient labeling (Medication Guide).
5.2 Suicidal Behavior and Ideation
Antiepileptic drugs (AEDs), including topiramate, increase the risk of suicidal thoughts or behavior in patients taking these drugs for any indication. Pooled analyses of 199 placebo-controlled clinical studies (monotherapy and adjunctive therapy, median treatment duration 12 weeks) of 11 different AEDs across several indications showed that patients randomized to one of the AEDs had approximately twice the risk (adjusted Relative Risk 1.8, 95% CI 1.2, 2.7) of suicidal thinking or behavior compared to patients randomized to placebo. The estimated incidence rate of suicidal behavior or ideation among 27,863 AED-treated patients was 0.43%, compared to 0.24% among 16,029 placebo-treated patients, representing an increase of approximately one case of suicidal thinking or behavior for every 530 patients treated. There were four suicides in AED-treated patients in the trials and none in placebo-treated patients, but the number is too small to allow any conclusion about AED effect on suicide. The increased risk of suicidal thoughts or behavior with AEDs was observed as early as 1 week after starting drug treatment with AEDs and persisted for the duration of treatment assessed. Because most trials included in the analysis did not extend beyond 24 weeks, the risk of suicidal thoughts or behavior beyond 24 weeks could not be assessed. The risk of suicidal thoughts or behavior was generally consistent among drugs in the data analyzed. The finding of increased risk with AEDs of varying mechanisms of action and across a range of indications suggests that the risk applies to all AEDs used for any indication. The risk did not vary substantially by age in the clinical trials analyzed.
In a QSYMIA clinical trial of pediatric patients aged 12 years and older, 1 (0.6%) of the 167 QSYMIA-treated patients reported suicidal ideation and behavior which required hospitalization. No placebo-treated patients reported suicidal behavior or ideation.
Monitor all patients for the emergence or worsening of depression, suicidal thoughts or behavior, and/or any unusual changes in mood or behavior. Discontinue QSYMIA in patients who experience suicidal thoughts or behaviors [see Warnings and Precautions (5.9)] . Avoid QSYMIA in patients with a history of suicidal attempts or active suicidal ideation.
5.11 Oligohidrosis and Hyperthermia
Oligohidrosis (decreased sweating), infrequently resulting in hospitalization, has been reported in association with the use of topiramate. Decreased sweating and an elevation in body temperature above normal characterized these cases. Some of the cases have been reported with topiramate after exposure to elevated environmental temperatures.
The majority of the reports associated with topiramate have been in pediatric patients. Advise all patients and caregivers to monitor for decreased sweating and increased body temperature during physical activity, especially in hot weather. Patients on concomitant medications that predispose them to heat-related disorders may be at increased risk.
16 How Supplied/storage and Handling
QSYMIA (phentermine and topiramate extended-release capsules) are available as follows (see Table 15):
| Strength
(phentermine mg/topiramate mg) |
Description | How Supplied | NDC |
|---|---|---|---|
| 3.75 mg/23 mg extended-release capsules | Purple cap imprinted with VIVUS, Purple body imprinted with 3.75/23 | Unit of Use Bottle (14 capsules) | 62541-201-14 |
| Pharmacy Bottle (30 capsules) | 62541-201-30 | ||
| 7.5 mg/46 mg extended-release capsules | Purple cap imprinted with VIVUS, Yellow body imprinted with 7.5/46 | Unit of Use Bottle (30 capsules) | 62541-202-30 |
| 11.25 mg/69 mg extended-release capsules | Yellow cap imprinted with VIVUS, Yellow body imprinted with 11.25/69 | Pharmacy Bottle (30 capsules) | 62541-203-30 |
| 15 mg/92 mg extended-release capsules | Yellow cap imprinted with VIVUS, White body imprinted with 15/92 | Unit of Use Bottle (30 capsules) | 62541-204-30 |
| 3.75 mg/23 mg and 7.5 mg/46 mg extended-release capsules | Purple cap imprinted with VIVUS, Purple body imprinted with 3.75/23 and Purple cap imprinted with VIVUS, Yellow body imprinted with 7.5/46 | Starter Pack - Blister Configuration (28 Capsules) | 62541-210-28 |
| 11.25 mg/69 mg and 15 mg/92 mg extended-release capsules | Yellow cap imprinted with VIVUS, Yellow body imprinted with 11.25/69 | Dose Escalation Pack – Blister Configuration (28 Capsules) | 62541-220-28 |
2.2 Recommended Dosage and Administration
The recommended dosage, titration, and administration of QSYMIA are as follows:
- Take QSYMIA orally once daily in the morning with or without food. Avoid administration of QSYMIA in the evening due to the possibility of insomnia.
- The recommended starting dosage of QSYMIA is one capsule (containing 3.75 mg of phentermine and 23 mg of topiramate) (3.75 mg/23 mg) taken orally once daily for 14 days; after 14 days increase to the recommended dosage of QSYMIA 7.5 mg/46 mg orally once daily.
- After 12 weeks of treatment with QSYMIA 7.5 mg/46 mg, evaluate weight loss for adults or BMI reduction for pediatric patients aged 12 years and older. If an adult patient has not lost at least 3% of baseline body weight or a pediatric patient has not experienced a reduction of at least 3% of baseline BMI, increase the dosage to QSYMIA 11.25 mg/69 mg orally once daily for 14 days; followed by an increase in the dosage to QSYMIA 15 mg/92 mg orally once daily.
- After 12 weeks of treatment with QSYMIA 15 mg/92 mg, evaluate weight loss for adults or BMI reduction for pediatric patients aged 12 years and older. If an adult patient has not lost at least 5% of baseline body weight or a pediatric patient has not experienced a reduction of at least 5% of baseline BMI, discontinue QSYMIA [see Dosage and Administration (2.3)] , as it is unlikely that the patient will achieve and sustain clinically meaningful weight loss with continued treatment.
- Monitor the rate of weight loss in pediatric patients. If weight loss exceeds 2 lbs (0.9 kg)/week, consider dosage reduction.
2.3 Discontinuation of Qsymia 15 Mg/92 Mg
Discontinue QSYMIA 15 mg/92 mg gradually by taking QSYMIA 15 mg/92 mg orally once daily every other day for at least 1 week prior to stopping treatment altogether, due to the possibility of precipitating a seizure [see Warnings and Precautions (5.9) and Drug Abuse and Dependence (9.3)] .
5.9 Risk of Seizures With Abrupt Withdrawal of Qsymia
Abrupt withdrawal of topiramate has been associated with seizures in individuals without a history of seizures or epilepsy. In situations where immediate termination of QSYMIA is medically required, appropriate monitoring is recommended. Patients discontinuing QSYMIA 15 mg/92 mg should be gradually tapered to reduce the possibility of precipitating a seizure [see Dosage and Administration (2.3) and Drug Abuse and Dependence (9.3)] .
2.4 Recommended Dosage in Patients With Renal Impairment
- The recommended dosage in patients with mild (CrCl greater or equal to 50 and less than 80 mL/min) renal impairment is the same as the recommended dosage for patients with normal renal function [see Warnings and Precautions (5.9), Use in Specific Populations (8.6), and Clinical Pharmacology (12.3)] .
- In patients with severe [creatinine clearance (CrCl) less than 30 mL/min] or moderate (CrCl greater than or equal to 30 and less than 50 mL/min) renal impairment (CrCl calculated using the Cockcroft-Gault equation with actual body weight), the maximum recommended dosage is QSYMIA 7.5 mg/46 mg once daily.
- Avoid use of QSYMIA in patients with end-stage renal disease on dialysis.
2.5 Recommended Dosage in Patients With Hepatic Impairment
- The recommended dosage of QSYMIA in patients with mild hepatic impairment (Child-Pugh 5 - 6) is the same as the recommended dosage in patients with normal hepatic function [see Use in Specific Populations (8.7) and Clinical Pharmacology (12.3)] .
- In patients with moderate hepatic impairment (Child-Pugh score 7 - 9), the maximum recommended dosage is QSYMIA 7.5 mg/46 mg orally once daily.
- Avoid use of QSYMIA in patients with severe hepatic impairment (Child-Pugh score 10 - 15).
Principal Display Panel 15 Mg/92 Mg Capsule Bottle Label
NDC NUMBER 62541-204-30
QSYMIA
®
(phentermine and topiramate
extended-release capsules) CIV
15 mg/92 mg
30 Capsules
Rx only
DISPENSE WITH MEDICATION GUIDE
Principal Display Panel 7.5 Mg/46 Mg Capsule Bottle Label
NDC NUMBER 62541-202-30
QSYMIA
®
(phentermine and topiramate
extended-release capsules) CIV
7.5 mg/46 mg
30 Capsules
Rx only
DISPENSE WITH MEDICATION GUIDE
Principal Display Panel 3.75 Mg/23 Mg Capsule Bottle Label
NDC NUMBER 62541-201-30
QSYMIA
®
(phentermine and topiramate
extended-release capsules) CIV
3.75 mg/23 mg
30 Capsules
Rx only
DISPENSE WITH MEDICATION GUIDE
Principal Display Panel 11.25 Mg/69 Mg Capsule Bottle Label
NDC NUMBER 62541-203-30
QSYMIA
®
(phentermine and topiramate
extended-release capsules) CIV
11.25 mg/69 mg
30 Capsules
Rx only
DISPENSE WITH MEDICATION GUIDE
2.1 Recommended Testing Prior to and During Treatment With Qsymia
Prior to QSYMIA initiation and during treatment with QSYMIA, the following is recommended:
- Obtain a negative pregnancy test before initiating QSYMIA in patients who can become pregnant and monthly during QSYMIA therapy. QSYMIA is contraindicated during pregnancy [see Contraindications (4), Warnings and Precautions (5.1), and Use in Specific Populations (8.3)] .
- Obtain a blood chemistry profile that includes bicarbonate, creatinine, and potassium in all patients, and glucose in patients with type 2 diabetes mellitus on antidiabetic medication prior to initiating QSYMIA treatment and periodically during treatment [see Warnings and Precautions (5.7, 5.8, 5.12)] .
5.14 Allergic Reactions Due to Inactive Ingredient Fd&c Yellow No. 5
This product contains FD&C Yellow No. 5 (tartrazine) which may cause allergic-type reactions (including bronchial asthma) in certain susceptible persons. Although the overall incidence of FD&C Yellow No. 5 (tartrazine) sensitivity in the general population is low, it is frequently seen in patients who also have aspirin hypersensitivity.
Structured Label Content
Section 42229-5 (42229-5)
Limitations of Use
- The effect of QSYMIA on cardiovascular morbidity and mortality has not been established.
- The safety and effectiveness of QSYMIA in combination with other products intended for weight loss, including prescription drugs, over-the-counter drugs, and herbal preparations, have not been established.
Section 42231-1 (42231-1)
| MEDICATION GUIDE
QSYMIA ®(Kyoo sim ee uh) (phentermine and topiramate extended-release capsules) for oral use, CIV |
|
|---|---|
| This Medication Guide has been approved by the U.S. Food and Drug Administration.
PH-03-002-16 |
Revised: 09/2024 |
|
What is the most important information I should know about QSYMIA?
QSYMIA can cause serious side effects, including :
|
|
What is QSYMIA?
|
|
Who should not take QSYMIA? Do not take QSYMIA if you:
|
|
Before taking QSYMIA, tell your health care provider about all of your medical conditions, including if you:
Especially tell your health care provider if you take:
Know the medicines you take. Keep a list of them to show your health care provider and pharmacist each time you get a new medicine. Do not start a new medicine without talking to your health care provider. |
|
How should I take QSYMIA?
|
|
What should I avoid while taking QSYMIA?
|
|
|
What are the possible side effects of QSYMIA?
QSYMIA can cause serious side effects, including:
These are not all of the possible side effects of QSYMIA. For more information, ask your health care provider or pharmacist. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. You can also report side effects to VIVUS at 1-888-998-4887. |
|
How should I store QSYMIA?
|
|
|
General Information about the safe and effective use of QSYMIA.
Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not use QSYMIA for a condition for which it was not prescribed. Do not give QSYMIA to other people, even if they have the same symptoms you have. It may harm them. You can ask your pharmacist or health care provider for information about QSYMIA that is written for health professionals. |
|
|
What are the ingredients in QSYMIA?
Active Ingredient: phentermine hydrochloride and topiramate extended-release. Inactive Ingredients: FD&C Blue #1, FD&C Red #3, FD&C Yellow #5 and #6, ethylcellulose, gelatin, methylcellulose, microcrystalline cellulose, povidone, starch, sucrose, talc, titanium dioxide, and pharmaceutical black and white inks. Copyright © 2012 - 2025 VIVUS LLC All rights reserved. VIVUS LLC 900 E. Hamilton Ave., Suite 550 Campbell, CA 95008 USA US Patent Numbers: 7,056,890; 7,553,818; 7,659,256; 7,674,776; 8,580,298; 8,580,299; 8,895,057; 8,895,058; 9,011,905; and 9,011,906. QSYMIA is a registered trademark of VIVUS LLC. |
Section 44425-7 (44425-7)
Store at 20°C to 25°C (68°F to 77°F), excursions permitted between 15°C and 30°C (59°F and 86°F) [see USP Controlled Room Temperature]. Keep container tightly closed and protect from moisture.
9.2 Abuse
Phentermine has a known potential for abuse. Abuse is the intentional, non-therapeutic use of a drug, even once, for its desirable psychological or physiological effects.
Phentermine is related chemically and pharmacologically to amphetamines. Amphetamines and other stimulant drugs have been extensively abused. Abuse of amphetamines and related drugs (e.g., phentermine) may be associated with impaired control over drug use and severe social dysfunction. There are reports of patients who have increased the dosage of these drugs to many times higher than recommended. Assess the risk of abuse prior to prescribing QSYMIA as part of a weight reduction and long-term maintenance of body weight program.
10 Overdosage (10 OVERDOSAGE)
In the event of a significant overdose with QSYMIA, if the ingestion is recent, the stomach should be emptied immediately by gastric lavage or by induction of emesis. Appropriate supportive treatment should be provided according to the patient's clinical signs and symptoms. In the event of an overdose of QSYMIA, consider contacting the Poison Help line (1-800-222-1222) or a medical toxicologist for additional overdosage management recommendations.
Acute overdose of phentermine may be associated with restlessness, tremor, hyperreflexia, rapid respiration, confusion, aggressiveness, hallucinations, and panic states. Fatigue and depression usually follow the central stimulation. Cardiovascular effects include arrhythmia, hypertension or hypotension, and circulatory collapse. Gastrointestinal symptoms include nausea, vomiting, diarrhea, and abdominal cramps. Fatal poisoning usually terminates in convulsions and coma. Manifestations of chronic intoxication with anorectic drugs include severe dermatoses, marked insomnia, irritability, hyperactivity, and personality changes. A severe manifestation of chronic intoxication is psychosis, often clinically indistinguishable from schizophrenia.
Management of acute phentermine intoxication is largely symptomatic and includes lavage and sedation with a barbiturate. Acidification of the urine increases phentermine excretion. Intravenous phentolamine has been suggested for possible acute, severe hypertension, if this complicates phentermine overdosage.
Topiramate overdose has resulted in severe metabolic acidosis. Other signs and symptoms include convulsions, drowsiness, speech disturbance, blurred vision, diplopia, impaired mentation, lethargy, abnormal coordination, stupor, hypotension, abdominal pain, agitation, dizziness, and depression. The clinical consequences were not severe in most cases, but deaths have been reported after overdoses involving topiramate. A patient who ingested a dose between 96 and 110 gm topiramate was admitted to hospital with coma lasting 20 to 24 hours followed by full recovery after 3 to 4 days.
Hemodialysis is an effective means of removing topiramate from the body.
11 Description (11 DESCRIPTION)
QSYMIA extended-release capsules are comprised of immediate-release phentermine hydrochloride (expressed as the weight of the free base) and extended-release topiramate. QSYMIA contains phentermine hydrochloride, a sympathomimetic amine anorectic, and topiramate, a sulfamate-substituted monosaccharide.
9.3 Dependence
Physical dependence may occur in patients treated with QSYMIA. Physical dependence is a state that develops as a result of physiological adaptation in response to repeated drug use, manifested by withdrawal signs and symptoms after abrupt discontinuation or a significant dose reduction of a drug.
The following adverse reactions have been associated with the abrupt discontinuation of the individual components of QSYMIA:
- For topiramate, abrupt discontinuation has been associated with seizures in patients without a history of seizures or epilepsy [see Warnings and Precautions (5.9)] .
- For phentermine, abrupt discontinuation following prolonged high dosage administration results in extreme fatigue and mental depression; changes are also noted on a sleep electroencephalogram.
Thus, in situations where rapid withdrawal of QSYMIA is required, appropriate medical monitoring is recommended. Patients discontinuing QSYMIA 15 mg/92 mg should be gradually tapered to reduce the possibility of precipitating a seizure [see Dosage and Administration (2.3)] .
5.12 Hypokalemia
QSYMIA can increase the risk of hypokalemia through its inhibition of carbonic anhydrase activity. In addition, when QSYMIA is used in conjunction with non-potassium sparing diuretics this may further potentiate potassium-wasting. Measure potassium before and during treatment with QSYMIA [see Adverse Reactions (6.1), Drug Interactions (7), and Clinical Pharmacology (12.3)] .
8.4 Pediatric Use
The safety and effectiveness of QSYMIA as an adjunct to a reduced-calorie diet and increased physical activity for weight reduction and long-term maintenance of body weight have been established in pediatric patients aged 12 years and older with obesity. Use of QSYMIA for this indication is supported by a 56-week, double-blind, placebo-controlled study in 223 pediatric patients aged 12 years and above, a pharmacokinetic study in pediatric patients, and studies in adults with obesity [see Clinical Pharmacology (12.3)and Clinical Studies (14)] .
In a pediatric clinical trial, there was one episode of serious suicidal ideation in a QSYMIA-treated patient requiring hospitalization and pharmacologic treatment [see Warnings and Precautions (5.2)] more patients treated with QSYMIA versus placebo reported adverse reactions related to mood (e.g., depression, anxiety) and sleep disorders (e.g., insomnia) [see Warnings and Precautions (5.4)] . Increases in bone mineral density and linear growth were attenuated in QSYMIA- versus placebo-treated patients [see Warnings and Precautions (5.6)] . Serious adverse reactions seen in pediatric patients using topiramate include acute angle glaucoma, oligohidrosis and hyperthermia, metabolic acidosis, cognitive and neuropsychiatric reactions, hyperammonemia and encephalopathy, and kidney stones.
The safety and effectiveness of QSYMIA in pediatric patients below the age of 12 years have not been established.
8.5 Geriatric Use
In the QSYMIA clinical trials, a total of 254 (7%) of the patients were 65 to 69 years of age; no patients 70 years of age or older were enrolled.
Clinical studies of QSYMIA did not include sufficient numbers of patients aged 65 and over to determine whether they respond differently from younger patients. In general, dose selection for an elderly patient should be cautious, usually starting at the low end of the dosing range, reflecting the greater frequency of decreased hepatic, renal, or cardiac function, and of concomitant disease or other drug therapy.
5.10 Kidney Stones
QSYMIA has been associated with kidney stone formation [see Adverse Reactions (6.1)] . Topiramate inhibits carbonic anhydrase activity and promotes kidney stone formation by reducing urinary citrate excretion and increasing urine pH. Patients on a ketogenic diet may be at increased risk for kidney stone formation. An increase in urinary calcium and a marked decrease in urinary citrate was observed in topiramate-treated pediatric patients in a one-year, active-controlled study. Increased ratio of urinary calcium/citrate increases the risk of kidney stones and/or nephrocalcinosis.
Avoid the use of QSYMIA with other drugs that inhibit carbonic anhydrase [see Drug Interactions (7)] . Advise patients to increase fluid intake (to increase urinary output), which may decrease the concentration of substances involved in kidney stone formation.
4 Contraindications (4 CONTRAINDICATIONS)
QSYMIA is contraindicated in patients:
- Who are pregnant [see Warnings and Precautions (5.1)and Use in Specific Populations (8.1)]
- With glaucoma [see Warnings and Precautions (5.3)]
- With hyperthyroidism
- Taking or within 14 days of stopping a monoamine oxidase inhibitors [see Drug Interactions (7)]
- With known hypersensitivity to phentermine, topiramate or any of the excipients in QSYMIA, or idiosyncrasy to the sympathomimetic amines [see Adverse Reactions (6.2)] .
6 Adverse Reactions (6 ADVERSE REACTIONS)
The following clinically significant adverse reactions are described elsewhere in the labeling:
- Embryo-Fetal Toxicity [see Warnings and Precautions (5.1) and Use in Specific Populations (8.1, 8.6)]
- Suicidal Behavior and Ideation [see Warnings and Precautions (5.2)]
- Risk of Ophthalmologic Adverse Reactions [see Warnings and Precautions (5.3)]
- Mood and Sleep Disorders [see Warnings and Precautions (5.4)]
- Cognitive Impairment [see Warnings and Precautions (5.5)]
- Slowing of Linear Growth [see Warnings and Precautions (5.6)]
- Metabolic Acidosis [see Warnings and Precautions (5.7)]
- Decrease in Renal Function [see Warnings and Precautions (5.8)]
- Risk of Seizures with Abrupt Withdrawal of QSYMIA [see Warnings and Precautions (5.9)]
- Kidney Stones [see Warnings and Precautions (5.10)]
- Oligohydrosis and Hyperthermia [see Warnings and Precautions (5.11)]
- Hypokalemia [see Warnings and Precautions (5.12)]
- Serious Skin Reactions [see Warnings and Precautions (5.13)]
7 Drug Interactions (7 DRUG INTERACTIONS)
Table 5 displays clinically significant drug interactions with QSYMIA.
| Monoamine Oxidase Inhibitors | |
| Clinical Impact | Concomitant use of phentermine with monoamine oxidase inhibitors (MAOIs) increases the risk of hypertensive crisis. |
| Intervention | Concomitant use of QSYMIA is contraindicated during MAOI treatment and within 14 days of stopping an MAOI. |
| Oral Contraceptives | |
| Clinical Impact | Co-administration of multiple-dose QSYMIA 15 mg/92 mg once daily with a single dose of oral contraceptive containing 35 µg ethinyl estradiol (estrogen component) and 1 mg norethindrone (progestin component), in obese otherwise healthy volunteers, decreased the exposure of ethinyl estradiol by 16% and increased the exposure of norethindrone by 22% [see Clinical Pharmacology (12.3)] . Although this interaction is not anticipated to increase the risk of pregnancy, irregular bleeding (spotting) may occur more frequently due to both the increased exposure to the progestin and lower exposure to the estrogen, which tends to stabilize the endometrium. |
| Intervention | Inform patients not to discontinue their combination oral contraceptive if spotting occurs, but to notify their health care provider if the spotting is troubling to them. |
| CNS Depressants Including Alcohol | |
| Clinical Impact | The concomitant use of alcohol or CNS depressant drugs (e.g., barbiturates, benzodiazepines, and sleep medications) with phentermine or topiramate may potentiate CNS depression such as dizziness or cognitive adverse reactions, or other centrally mediated effects of these agents. |
| Intervention | Advise patients not to drive or operate machinery until they have gained sufficient experience on QSYMIA to gauge whether it adversely affects their mental performance, motor performance, and/or vision. Caution patients against excessive alcohol intake when taking QSYMIA. Consider QSYMIA dosage reduction or discontinuation if cognitive dysfunction persists [see Warnings and Precautions (5.5)]. |
| Non-Potassium Sparing Diuretics | |
| Clinical Impact | Concurrent use of QSYMIA with non-potassium sparing diuretics may potentiate the potassium-wasting action of these diuretics. Concomitant administration of hydrochlorothiazide alone with topiramate alone has been shown to increase the C max and AUC of topiramate by 27% and 29%, respectively. |
| Intervention | When QSYMIA is used concomitantly with non-potassium-sparing diuretics, measure potassium before and during QSYMIA treatment [see Warnings and Precautions (5.12) and Clinical Pharmacology (12.3)] . |
| Antiepileptic Drugs | |
| Clinical Impact | Concomitant administration of phenytoin or carbamazepine with topiramate in patients with epilepsy, decreased plasma concentrations of topiramate by 48% and 40%, respectively, when compared to topiramate given alone [see Clinical Pharmacology (12.3)] . Concomitant administration of valproic acid and topiramate has been associated with hyperammonemia with and without encephalopathy. Concomitant administration of topiramate with valproic acid in patients has also been associated with hypothermia (with and without hyperammonemia). |
| Intervention | Consider measuring blood ammonia in patients in whom the onset of hypothermia or encephalopathy has been reported [see Clinical Pharmacology (12.3)] . |
| Carbonic Anhydrase Inhibitors | |
| Clinical Impact | Concomitant use of topiramate with any other carbonic anhydrase inhibitor may increase the severity of metabolic acidosis and may also increase the risk of kidney stone formation. |
| Intervention | Avoid the use of QSYMIA with other drugs that inhibit carbonic anhydrase. If concomitant use of QSYMIA with another carbonic anhydrase inhibitor is unavoidable, monitor patient for the appearance or worsening of metabolic acidosis [see Warnings and Precautions (5.7, 5.10)] . |
| Pioglitazone | |
| Clinical Impact | A decrease in the exposure of pioglitazone and its active metabolites were noted with the concurrent use of pioglitazone and topiramate in a clinical trial. The clinical relevance of these observations is unknown. |
| Intervention | Consider increased glycemic monitoring when using pioglitazone and QSYMIA concomitantly [see Clinical Pharmacology (12.3)] . |
| Amitriptyline | |
| Clinical Impact | Some patients may experience a large increase in amitriptyline concentration in the presence of topiramate. |
| Intervention | Any adjustments in amitriptyline dose when used with QSYMIA should be made according to the patient's clinical response and not on the basis of amitriptyline levels [see Clinical Pharmacology (12.3)] . |
8.6 Renal Impairment
Compared to healthy volunteers with normal renal function, patients with moderate and severe renal impairment as estimated by the Cockcroft-Gault equation had higher exposures to phentermine and topiramate.
The recommended dosage of QSYMIA in patients with mild renal impairment (CrCl greater or equal to 50 and less than 80 mL/min) is the same as the recommended dosage for patients with normal renal function.
In patients with moderate (CrCl greater than or equal to 30 to less than 50 mL/min) and severe (CrCl less than 30 mL/min) renal impairment, the maximum recommended dosage is QSYMIA 7.5 mg/46 mg once daily.
QSYMIA has not been studied in patients with end-stage renal disease on dialysis. Avoid QSYMIA in this patient population [see Dosage and Administration (2.4) and Clinical Pharmacology (12.3)] .
12.2 Pharmacodynamics
Typical actions of amphetamines include central nervous system stimulation and elevation of blood pressure. Tachyphylaxis and tolerance have been demonstrated with drugs in this class.
5.7 Metabolic Acidosis
Hyperchloremic, non-anion gap, metabolic acidosis (decreased serum bicarbonate below the normal reference range in the absence of chronic respiratory alkalosis) has been reported in patients treated with QSYMIA [see Adverse Reactions (6.1)] . Manifestations of acute or chronic metabolic acidosis may include hyperventilation, nonspecific symptoms such as fatigue and anorexia, or more severe sequelae including cardiac arrhythmias or stupor. Chronic, untreated metabolic acidosis may increase the risk for nephrolithiasis or nephrocalcinosis and may also result in osteomalacia (referred to as rickets in pediatric patients) and/or osteoporosis with an increased risk for fractures. Chronic metabolic acidosis in pediatric patients may also reduce growth rates, which may decrease the maximal height achieved.
Conditions or therapies that predispose to acidosis (i.e., renal disease, severe respiratory disorders, status epilepticus, diarrhea, surgery, or ketogenic diet) may be additive to the bicarbonate lowering effects of QSYMIA. Concomitant use of QSYMIA and a carbonic anhydrase inhibitor may increase the severity of metabolic acidosis and may also increase the risk of kidney stone formation [see Warnings and Precautions (5.10)] . Avoid use of QSYMIA with other carbonic anhydrase inhibitors. If concomitant use of QSYMIA with another carbonic anhydrase inhibitor is unavoidable, the patient should be monitored for the appearance or worsening of metabolic acidosis.
Measure electrolytes including serum bicarbonate prior to starting QSYMIA and during QSYMIA treatment. In QSYMIA clinical trials, the peak reduction in serum bicarbonate typically occurred within 4 weeks of titration to the assigned dose, and in most patients, there was a correction of bicarbonate by week 56, without any dosage reduction. However, if persistent metabolic acidosis develops while taking QSYMIA, reduce the dosage or discontinue QSYMIA [see Warnings and Precautions (5.9)] .
8.7 Hepatic Impairment
In patients with mild (Child-Pugh 5 - 6) and moderate (Child-Pugh 7 - 9) hepatic impairment, exposure to phentermine was higher compared to healthy volunteers with normal hepatic function. Exposure to topiramate was similar among patients with mild and moderate hepatic impairment and healthy volunteers.
The recommended dosage of QSYMIA in patients with mild hepatic impairment (Child-Pugh 5 - 6) is the same as the recommended dosage in patients with normal hepatic function.
In patients with moderate hepatic impairment, the maximum recommended dosage is QSYMIA 7.5 mg/46 mg once daily.
QSYMIA has not been studied in patients with severe hepatic impairment (Child-Pugh score 10 - 15). Avoid QSYMIA in this patient population [see Dosage and Administration (2.5) and Clinical Pharmacology (12.3)] .
1 Indications and Usage (1 INDICATIONS AND USAGE)
QSYMIA is indicated in combination with a reduced-calorie diet and increased physical activity to reduce excess body weight and maintain weight reduction long term in:
- Adults and pediatric patients aged 12 years and older with obesity
- Adults with overweight in the presence of at least one weight-related comorbid condition
12.1 Mechanism of Action
Phentermine is a sympathomimetic amine with pharmacologic activity similar to the prototype drugs of this class used in obesity, amphetamine (d- and d/l-amphetamine). Drugs of this class used in obesity are commonly known as "anorectics" or "anorexigenics." The effect of phentermine on weight reduction and long-term maintenance of body weight is likely mediated by release of catecholamines in the hypothalamus, resulting in reduced appetite and decreased food consumption, but other metabolic effects may also be involved. The exact mechanism of action is not known.
The precise mechanism of action of topiramate on weight reduction and long-term maintenance of body weight is not known. Topiramate's effect on weight reduction and long-term maintenance of body weight may be due to its effects on both appetite suppression and satiety enhancement, induced by a combination of pharmacologic effects including augmenting the activity of the neurotransmitter gamma-aminobutyrate, modulation of voltage-gated ion channels, inhibition of AMPA/kainite excitatory glutamate receptors, or inhibition of carbonic anhydrase.
5.5 Cognitive Impairment
QSYMIA can cause cognitive dysfunction (e.g., impairment of concentration/attention, difficulty with memory, and speech or language problems, particularly word-finding difficulties). Rapid titration or high initial doses of QSYMIA may be associated with higher rates of cognitive events such as attention, memory, and language/word-finding difficulties [see Adverse Reactions (6.1)] . The concomitant use of alcohol or central nervous system (CNS) depressant drugs with QSYMIA may potentiate CNS depression or other centrally mediated effects of these agents, such as dizziness, cognitive adverse reactions, drowsiness, light-headedness, impaired coordination, and somnolence.
Caution patients about operating hazardous machinery, including automobiles, until they are reasonably certain QSYMIA therapy does not affect them adversely. Caution patients against excessive alcohol intake while receiving QSYMIA.
If cognitive dysfunction persists, consider dosage reduction or discontinuation of QSYMIA [see Warnings and Precautions (5.9)] .
9.1 Controlled Substance
QSYMIA contains phentermine, a Schedule IV controlled substance, and topiramate, which is not a controlled substance.
5.1 Embryo Fetal Toxicity (5.1 Embryo-Fetal Toxicity)
QSYMIA can cause fetal harm. Data from pregnancy registries and epidemiologic studies indicate that a fetus exposed to topiramate in the first trimester of pregnancy has an increased risk of major congenital malformations, including but not limited to cleft lip and/or cleft palate (oral clefts), and of being small for gestational age (SGA). When multiple species of pregnant animals received topiramate at clinically relevant doses, structural malformations, including craniofacial defects, and reduced fetal weights occurred in offspring. A negative pregnancy test is recommended before initiating QSYMIA treatment in patients who can become pregnant and monthly during QSYMIA therapy. Advise patients who can become pregnant of the potential risk to a fetus and to use effective contraception during QSYMIA therapy [see Use in Specific Populations (8.1, 8.3)] .
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
- Embryo-Fetal Toxicity: Can cause fetal harm. In patients who can become pregnant, a negative pregnancy test is recommended before initiating QSYMIA and monthly during therapy; advise use of effective contraception. QSYMIA is available through a limited program under a Risk Evaluation and Mitigation Strategy (REMS) ( 5.1).
- Suicidal Behavior and Ideation: Monitor for depression or suicidal thoughts. Discontinue QSYMIA if symptoms develop ( 5.2).
- Risk of Ophthalmologic Adverse Reactions: Acute myopia and secondary angle closure glaucoma have been reported. Immediately discontinue QSYMIA if symptoms develop. Consider QSYMIA discontinuation if visual field defects occur ( 5.3).
- Mood and Sleep Disorders: Consider dosage reduction or discontinuation for clinically significant or persistent mood or sleep disorder symptoms ( 5.4).
- Cognitive Impairment: May cause disturbances in attention or memory, or speech/language problems. Caution patients about operating automobiles or hazardous machinery when starting treatment ( 5.5).
- Slowing of Linear Growth: Consider dosage reduction or discontinuation if pediatric patients are not growing or gaining height as expected ( 5.6).
- Metabolic Acidosis: Measure electrolytes before and during treatment. If persistent metabolic acidosis develops, reduce dosage or discontinue QSYMIA ( 5.7).
- Decrease in Renal Function: Measure creatinine before and during treatment. For persistent creatinine elevations, reduce dosage or discontinue QSYMIA ( 5.8).
- Serious Skin Reactions:QSYMIA should be discontinued at the first sign of a rash, unless the rash is clearly not drug-related ( 5.13).
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
- Take orally once daily in morning. Avoid administration in evening to prevent insomnia ( 2.2).
- Recommended starting dosage is 3.75 mg/23 mg (phentermine mg/topiramate mg) daily for 14 days; then increase to 7.5 mg/46 mg daily ( 2.2).
- Escalate dosage based on weight loss in adults or BMI reduction in pediatric patients. See the Full Prescribing Information for details regarding discontinuation or dosage escalation ( 2.2).
- Gradually discontinue 15 mg/92 mg dosage to prevent possible seizure ( 2.3).
- Do not exceed 7.5 mg/46 mg dosage for patients with moderate or severe renal impairment or patients with moderate hepatic impairment ( 2.4, 2.5).
5.13 Serious Skin Reactions
Serious skin reactions (Stevens-Johnson Syndrome [SJS] and Toxic Epidermal Necrolysis [TEN]) have been reported in patients receiving topiramate. QSYMIA should be discontinued at the first sign of a rash, unless the rash is clearly not drug-related. If signs or symptoms suggest SJS/TEN, use of this drug should not be resumed, and alternative therapy should be considered. Inform patients about the signs of serious skin reactions.
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
QSYMIA extended-release capsules are available in four strengths (phentermine mg/topiramate mg):
- 3.75 mg/23 mg - purple cap imprinted with VIVUS and purple body imprinted with 3.75/23
- 7.5 mg/46 mg - purple cap imprinted with VIVUS and yellow body imprinted with 7.5/46
- 11.25 mg/69 mg - yellow cap imprinted with VIVUS and yellow body imprinted with 11.25/69
- 15 mg/92 mg - yellow cap imprinted with VIVUS and white body imprinted with 15/92
5.4 Mood and Sleep Disorders
QSYMIA can cause mood disorders, including depression and anxiety, as well as insomnia. Patients with a history of depression may be at increased risk of recurrent depression or other mood disorders while taking QSYMIA [see Adverse Reactions (6.1)] .
Consider dosage reduction or discontinuation of QSYMIA if clinically significant or persistent symptoms occur. Discontinue QSYMIA if patients have symptoms of suicidal ideation or behavior [see Warnings and Precautions (5.2)] .
5.6 Slowing of Linear Growth
QSYMIA is associated with a reduction in height velocity (centimeters of height gained per year) in obese pediatric patients 12 to 17 years of age. In a 56-week study, average height increased from baseline in both QSYMIA- and placebo-treated patients; however, a lower height velocity of -1.3 to -1.4 cm/year was observed in QSYMIA-treated compared to placebo-treated patients. Monitor height velocity in pediatric patients treated with QSYMIA. Consider dosage reduction or discontinuation of QSYMIA if pediatric patients are not growing or gaining height as expected [see Warnings and Precautions (5.9)] .
6.2 Postmarketing Experience
The following adverse reactions have been reported during post approval use of QSYMIA, phentermine, and topiramate. Because these reactions are reported voluntarily from a population of uncertain size it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
8 Use in Specific Populations (8 USE IN SPECIFIC POPULATIONS)
- Lactation: Breastfeeding not recommended ( 8.2).
5.8 Decrease in Renal Function
QSYMIA can cause an increase in serum creatinine that reflects a decrease in renal function (glomerular filtration rate). In clinical trials, peak increases in serum creatinine were observed after 4 to 8 weeks of treatment. On average, serum creatinine gradually declined but remained elevated over baseline creatinine values. The changes in serum creatinine (and measured GFR) with short-term (4-weeks) QSYMIA treatment appear reversible with treatment discontinuation, but the effect of chronic treatment on renal function is not known.
Measure serum creatinine prior to starting QSYMIA and during QSYMIA treatment. If persistent elevations in creatinine occur, reduce the dosage or discontinue QSYMIA [see Warnings and Precautions (5.9), Adverse Reactions (6.1), and Clinical Pharmacology (12.2)] .
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical studies of another drug and may not reflect the rates observed in practice.
The data described herein reflect exposure to QSYMIA in two 1-year, randomized, double-blind, placebo-controlled, multicenter clinical trials and two supportive trials in 2,318 adult patients with overweight or obesity [936 (40%) patients with hypertension, 309 (13%) patients with type 2 diabetes mellitus, 808 (35%) patients with BMI greater than 40 kg/m 2] exposed for a mean duration of 298 days. Data in this section also describe adverse reactions from a 1-year, randomized, double-blind, placebo-controlled multicenter clinical trial that evaluated 223 pediatric patients (12 to 17 years old) with obesity [see Clinical Studies (14)] .
17 Patient Counseling Information (17 PATIENT COUNSELING INFORMATION)
Advise the patient to read the FDA-approved patient labeling (Medication Guide).
5.2 Suicidal Behavior and Ideation
Antiepileptic drugs (AEDs), including topiramate, increase the risk of suicidal thoughts or behavior in patients taking these drugs for any indication. Pooled analyses of 199 placebo-controlled clinical studies (monotherapy and adjunctive therapy, median treatment duration 12 weeks) of 11 different AEDs across several indications showed that patients randomized to one of the AEDs had approximately twice the risk (adjusted Relative Risk 1.8, 95% CI 1.2, 2.7) of suicidal thinking or behavior compared to patients randomized to placebo. The estimated incidence rate of suicidal behavior or ideation among 27,863 AED-treated patients was 0.43%, compared to 0.24% among 16,029 placebo-treated patients, representing an increase of approximately one case of suicidal thinking or behavior for every 530 patients treated. There were four suicides in AED-treated patients in the trials and none in placebo-treated patients, but the number is too small to allow any conclusion about AED effect on suicide. The increased risk of suicidal thoughts or behavior with AEDs was observed as early as 1 week after starting drug treatment with AEDs and persisted for the duration of treatment assessed. Because most trials included in the analysis did not extend beyond 24 weeks, the risk of suicidal thoughts or behavior beyond 24 weeks could not be assessed. The risk of suicidal thoughts or behavior was generally consistent among drugs in the data analyzed. The finding of increased risk with AEDs of varying mechanisms of action and across a range of indications suggests that the risk applies to all AEDs used for any indication. The risk did not vary substantially by age in the clinical trials analyzed.
In a QSYMIA clinical trial of pediatric patients aged 12 years and older, 1 (0.6%) of the 167 QSYMIA-treated patients reported suicidal ideation and behavior which required hospitalization. No placebo-treated patients reported suicidal behavior or ideation.
Monitor all patients for the emergence or worsening of depression, suicidal thoughts or behavior, and/or any unusual changes in mood or behavior. Discontinue QSYMIA in patients who experience suicidal thoughts or behaviors [see Warnings and Precautions (5.9)] . Avoid QSYMIA in patients with a history of suicidal attempts or active suicidal ideation.
5.11 Oligohidrosis and Hyperthermia
Oligohidrosis (decreased sweating), infrequently resulting in hospitalization, has been reported in association with the use of topiramate. Decreased sweating and an elevation in body temperature above normal characterized these cases. Some of the cases have been reported with topiramate after exposure to elevated environmental temperatures.
The majority of the reports associated with topiramate have been in pediatric patients. Advise all patients and caregivers to monitor for decreased sweating and increased body temperature during physical activity, especially in hot weather. Patients on concomitant medications that predispose them to heat-related disorders may be at increased risk.
16 How Supplied/storage and Handling (16 HOW SUPPLIED/STORAGE AND HANDLING)
QSYMIA (phentermine and topiramate extended-release capsules) are available as follows (see Table 15):
| Strength
(phentermine mg/topiramate mg) |
Description | How Supplied | NDC |
|---|---|---|---|
| 3.75 mg/23 mg extended-release capsules | Purple cap imprinted with VIVUS, Purple body imprinted with 3.75/23 | Unit of Use Bottle (14 capsules) | 62541-201-14 |
| Pharmacy Bottle (30 capsules) | 62541-201-30 | ||
| 7.5 mg/46 mg extended-release capsules | Purple cap imprinted with VIVUS, Yellow body imprinted with 7.5/46 | Unit of Use Bottle (30 capsules) | 62541-202-30 |
| 11.25 mg/69 mg extended-release capsules | Yellow cap imprinted with VIVUS, Yellow body imprinted with 11.25/69 | Pharmacy Bottle (30 capsules) | 62541-203-30 |
| 15 mg/92 mg extended-release capsules | Yellow cap imprinted with VIVUS, White body imprinted with 15/92 | Unit of Use Bottle (30 capsules) | 62541-204-30 |
| 3.75 mg/23 mg and 7.5 mg/46 mg extended-release capsules | Purple cap imprinted with VIVUS, Purple body imprinted with 3.75/23 and Purple cap imprinted with VIVUS, Yellow body imprinted with 7.5/46 | Starter Pack - Blister Configuration (28 Capsules) | 62541-210-28 |
| 11.25 mg/69 mg and 15 mg/92 mg extended-release capsules | Yellow cap imprinted with VIVUS, Yellow body imprinted with 11.25/69 | Dose Escalation Pack – Blister Configuration (28 Capsules) | 62541-220-28 |
2.2 Recommended Dosage and Administration
The recommended dosage, titration, and administration of QSYMIA are as follows:
- Take QSYMIA orally once daily in the morning with or without food. Avoid administration of QSYMIA in the evening due to the possibility of insomnia.
- The recommended starting dosage of QSYMIA is one capsule (containing 3.75 mg of phentermine and 23 mg of topiramate) (3.75 mg/23 mg) taken orally once daily for 14 days; after 14 days increase to the recommended dosage of QSYMIA 7.5 mg/46 mg orally once daily.
- After 12 weeks of treatment with QSYMIA 7.5 mg/46 mg, evaluate weight loss for adults or BMI reduction for pediatric patients aged 12 years and older. If an adult patient has not lost at least 3% of baseline body weight or a pediatric patient has not experienced a reduction of at least 3% of baseline BMI, increase the dosage to QSYMIA 11.25 mg/69 mg orally once daily for 14 days; followed by an increase in the dosage to QSYMIA 15 mg/92 mg orally once daily.
- After 12 weeks of treatment with QSYMIA 15 mg/92 mg, evaluate weight loss for adults or BMI reduction for pediatric patients aged 12 years and older. If an adult patient has not lost at least 5% of baseline body weight or a pediatric patient has not experienced a reduction of at least 5% of baseline BMI, discontinue QSYMIA [see Dosage and Administration (2.3)] , as it is unlikely that the patient will achieve and sustain clinically meaningful weight loss with continued treatment.
- Monitor the rate of weight loss in pediatric patients. If weight loss exceeds 2 lbs (0.9 kg)/week, consider dosage reduction.
2.3 Discontinuation of Qsymia 15 Mg/92 Mg (2.3 Discontinuation of QSYMIA 15 mg/92 mg)
Discontinue QSYMIA 15 mg/92 mg gradually by taking QSYMIA 15 mg/92 mg orally once daily every other day for at least 1 week prior to stopping treatment altogether, due to the possibility of precipitating a seizure [see Warnings and Precautions (5.9) and Drug Abuse and Dependence (9.3)] .
5.9 Risk of Seizures With Abrupt Withdrawal of Qsymia (5.9 Risk of Seizures with Abrupt Withdrawal of QSYMIA)
Abrupt withdrawal of topiramate has been associated with seizures in individuals without a history of seizures or epilepsy. In situations where immediate termination of QSYMIA is medically required, appropriate monitoring is recommended. Patients discontinuing QSYMIA 15 mg/92 mg should be gradually tapered to reduce the possibility of precipitating a seizure [see Dosage and Administration (2.3) and Drug Abuse and Dependence (9.3)] .
2.4 Recommended Dosage in Patients With Renal Impairment (2.4 Recommended Dosage in Patients with Renal Impairment)
- The recommended dosage in patients with mild (CrCl greater or equal to 50 and less than 80 mL/min) renal impairment is the same as the recommended dosage for patients with normal renal function [see Warnings and Precautions (5.9), Use in Specific Populations (8.6), and Clinical Pharmacology (12.3)] .
- In patients with severe [creatinine clearance (CrCl) less than 30 mL/min] or moderate (CrCl greater than or equal to 30 and less than 50 mL/min) renal impairment (CrCl calculated using the Cockcroft-Gault equation with actual body weight), the maximum recommended dosage is QSYMIA 7.5 mg/46 mg once daily.
- Avoid use of QSYMIA in patients with end-stage renal disease on dialysis.
2.5 Recommended Dosage in Patients With Hepatic Impairment (2.5 Recommended Dosage in Patients with Hepatic Impairment)
- The recommended dosage of QSYMIA in patients with mild hepatic impairment (Child-Pugh 5 - 6) is the same as the recommended dosage in patients with normal hepatic function [see Use in Specific Populations (8.7) and Clinical Pharmacology (12.3)] .
- In patients with moderate hepatic impairment (Child-Pugh score 7 - 9), the maximum recommended dosage is QSYMIA 7.5 mg/46 mg orally once daily.
- Avoid use of QSYMIA in patients with severe hepatic impairment (Child-Pugh score 10 - 15).
Principal Display Panel 15 Mg/92 Mg Capsule Bottle Label (PRINCIPAL DISPLAY PANEL - 15 mg/92 mg Capsule Bottle Label)
NDC NUMBER 62541-204-30
QSYMIA
®
(phentermine and topiramate
extended-release capsules) CIV
15 mg/92 mg
30 Capsules
Rx only
DISPENSE WITH MEDICATION GUIDE
Principal Display Panel 7.5 Mg/46 Mg Capsule Bottle Label (PRINCIPAL DISPLAY PANEL - 7.5 mg/46 mg Capsule Bottle Label)
NDC NUMBER 62541-202-30
QSYMIA
®
(phentermine and topiramate
extended-release capsules) CIV
7.5 mg/46 mg
30 Capsules
Rx only
DISPENSE WITH MEDICATION GUIDE
Principal Display Panel 3.75 Mg/23 Mg Capsule Bottle Label (PRINCIPAL DISPLAY PANEL - 3.75 mg/23 mg Capsule Bottle Label)
NDC NUMBER 62541-201-30
QSYMIA
®
(phentermine and topiramate
extended-release capsules) CIV
3.75 mg/23 mg
30 Capsules
Rx only
DISPENSE WITH MEDICATION GUIDE
Principal Display Panel 11.25 Mg/69 Mg Capsule Bottle Label (PRINCIPAL DISPLAY PANEL - 11.25 mg/69 mg Capsule Bottle Label)
NDC NUMBER 62541-203-30
QSYMIA
®
(phentermine and topiramate
extended-release capsules) CIV
11.25 mg/69 mg
30 Capsules
Rx only
DISPENSE WITH MEDICATION GUIDE
2.1 Recommended Testing Prior to and During Treatment With Qsymia (2.1 Recommended Testing Prior to and During Treatment with QSYMIA)
Prior to QSYMIA initiation and during treatment with QSYMIA, the following is recommended:
- Obtain a negative pregnancy test before initiating QSYMIA in patients who can become pregnant and monthly during QSYMIA therapy. QSYMIA is contraindicated during pregnancy [see Contraindications (4), Warnings and Precautions (5.1), and Use in Specific Populations (8.3)] .
- Obtain a blood chemistry profile that includes bicarbonate, creatinine, and potassium in all patients, and glucose in patients with type 2 diabetes mellitus on antidiabetic medication prior to initiating QSYMIA treatment and periodically during treatment [see Warnings and Precautions (5.7, 5.8, 5.12)] .
5.14 Allergic Reactions Due to Inactive Ingredient Fd&c Yellow No. 5 (5.14 Allergic Reactions Due to Inactive Ingredient FD&C Yellow No. 5)
This product contains FD&C Yellow No. 5 (tartrazine) which may cause allergic-type reactions (including bronchial asthma) in certain susceptible persons. Although the overall incidence of FD&C Yellow No. 5 (tartrazine) sensitivity in the general population is low, it is frequently seen in patients who also have aspirin hypersensitivity.
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:49:20.952591 · Updated: 2026-03-14T22:32:57.903315