These Highlights Do Not Include All The Information Needed To Use Diclofenac Epolamine Topical System 1.3 % Safely And Effectively. See Full Prescribing Information For Diclofenac Epolamine Topical System 1.3%.
3fa49554-d85f-a1d5-e063-6294a90a8baf
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
WARNING: RISK OF SERIOUS CARDIOVASCULAR and GASTROINTESTINAL EVENTS See full prescribing information for complete boxed warning. Nonsteroidal anti-inflammatory drugs (NSAIDs) cause an increased risk of serious cardiovascular thrombotic events, including myocardial infarction and stroke, which can be fatal. This risk may occur early in treatment and may increase with duration of use ( 5.1 ) DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is contraindicated in the setting of coronary artery bypass graft (CABG) surgery ( 4 , 5.1 ) NSAIDs cause an increased risk of serious gastrointestinal (GI) adverse events including bleeding, ulceration, and perforation of the stomach or intestines, which can be fatal. These events can occur at any time during use and without warning symptoms. Elderly patients and patients with a prior history of peptic ulcer disease and/or GI bleeding are at greater risk for serious GI events ( 5.2 )
Indications and Usage
DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is indicated for the topical treatment of acute pain due to minor strains, sprains, and contusions in adults and pediatric patients 6 years and older.
Dosage and Administration
Use the lowest effective dosage for shortest duration consist with the individual patient treatment goals ( 2.1 ) The recommended dose of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% for adults and pediatric patients 6 years and older is one (1) topical system to the most painful area twice a day. ( 2 ) DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% should not be applied to damaged or non-intact skin. ( 2 )
Warnings and Precautions
Hepatotoxicity : Inform patients of warning signs and symptoms of hepatotoxicity. Discontinue if abnormal liver tests persist or worsen or if clinical signs and symptoms of liver disease develop ( 5.3 ) Hypertension : Patients taking some antihypertensive medications may have impaired response to these therapies when taking NSAIDs. Monitor blood pressure ( 5.4 , 7 ) Heart Failure and Edema: Avoid use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% in patients with severe heart failure unless benefits are expected to outweigh risk of worsening heart failure ( 5.5 ) Renal Toxicity: Monitor renal function in patients with renal or hepatic impairment, heart failure, dehydration, or hypovolemia. Avoid use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% in patients with advanced renal disease unless benefits are expected to outweigh risk of worsening renal function ( 5.6 ) Anaphylactic Reactions : Seek emergency help if an anaphylactic reaction occurs ( 5.7 ) Exacerbation of Asthma Related to Aspirin Sensitivity : DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is contraindicated in patients with aspirin-sensitive asthma. Monitor patients with preexisting asthma (without aspirin sensitivity) ( 5.8 ) Serious Skin Reactions: Discontinue DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% at first appearance of skin rash or other signs of hypersensitivity ( 5.9 ) Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS) : Discontinue and evaluate clinically ( 5.10 ). Fetal Toxicity : Limit use of NSAIDs, including DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3 % between about 20 to 30 weeks in pregnancy due to the risk of oligohydramnios/fetal renal dysfunction. Avoid use of NSAIDs in women at about 30 weeks gestation and later in pregnancy due to the risks of oligohydramnios/fetal renal dysfunction and premature closure of the fetal ductus arteriosus ( 5.11 , 8.1 ). Hematologic Toxicity : Monitor hemoglobin or hematocrit in patients with any signs or symptoms of anemia ( 5.12 , 7 )
Contraindications
DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is contraindicated in the following patients: Known hypersensitivity (e.g., anaphylactic reactions and serious skin reactions) to diclofenac or any components of the drug product [ see Warnings and Precautions (5.7 , 5.9 ) ] History of asthma, urticaria, or other allergic-type reactions after taking aspirin or other NSAIDs. Severe, sometimes fatal, anaphylactic reactions to NSAIDs have been reported in such patients [ see Warnings and Precautions (5.7 , 5.8 ) ] In the setting of coronary artery bypass graft (CABG) surgery [ see Warnings and Precautions (5.1) ] DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is contraindicated for use on non-intact or damaged skin resulting from any etiology, including exudative dermatitis, eczema, infection lesions, burns or wounds.
Adverse Reactions
The following adverse reactions are discussed in greater detail in other sections of the labeling: Cardiovascular Thrombotic Events [ see Warnings and Precautions (5.1) ] GI Bleeding, Ulceration and Perforation [ see Warnings and Precautions (5.2) ] Hepatotoxicity [ see Warnings and Precautions (5.3) ] Hypertension [ see Warnings and Precautions (5.4) ] Heart Failure and Edema [ see Warnings and Precautions (5.5) ] Renal Toxicity and Hyperkalemia [ see Warnings and Precautions (5.6) ] Anaphylactic Reactions [ see Warnings and Precautions (5.7) ] Serious Skin Reactions [ see Warnings and Precautions (5.9) ] Hematologic Toxicity [ see Warnings and Precautions (5.12) ]
Drug Interactions
See Table 2 for clinically significant drug interactions with diclofenac. Table 2: Clinically Significant Drug Interactions with Diclofenac Drugs That Interfere with Hemostasis Clinical Impact: Diclofenac and anticoagulants such as warfarin have a synergistic effect on bleeding. The concomitant use of diclofenac and anticoagulants have an increased risk of serious bleeding compared to the use of either drug alone. Serotonin release by platelets plays an important role in hemostasis. Case-control and cohort epidemiological studies showed that concomitant use of drugs that interfere with serotonin reuptake and an NSAID may potentiate the risk of bleeding more than an NSAID alone. Intervention: Monitor patients with concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% with anticoagulants (e.g., warfarin), antiplatelet agents (e.g., aspirin), selective serotonin reuptake inhibitors (SSRIs), and serotonin norepinephrine reuptake inhibitors (SNRIs) for signs of bleeding [ see Warnings and Precautions (5.12) ]. Aspirin Clinical Impact: Controlled clinical studies showed that the concomitant use of NSAIDs and analgesic doses of aspirin does not produce any greater therapeutic effect than the use of NSAIDs alone. In a clinical study, the concomitant use of an NSAID and aspirin was associated with a significantly increased incidence of GI adverse reactions as compared to use of the NSAID alone [ see Warnings and Precautions (5.2) ]. Intervention: Concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and analgesic doses of aspirin is not generally recommended because of the increased risk of bleeding [ see Warnings and Precautions (5.12) ]. DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is not a substitute for low dose aspirin for cardiovascular protection. ACE Inhibitors, Angiotensin Receptor Blockers, and Beta-Blockers Clinical Impact: NSAIDs may diminish the antihypertensive effect of angiotensin converting enzyme (ACE) inhibitors, angiotensin receptor blockers (ARBs), or beta-blockers (including propranolol). In patients who are elderly, volume-depleted (including those on diuretic therapy), or have renal impairment, co-administration of an NSAID with ACE inhibitors or ARBs may result in deterioration of renal function, including possible acute renal failure. These effects are usually reversible. Intervention: During concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and ACE-inhibitors, ARBs, or beta-blockers, monitor blood pressure to ensure that the desired blood pressure is obtained. During concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and ACE-inhibitors or ARBs in patients who are elderly, volume-depleted, or have impaired renal function, monitor for signs of worsening renal function [ see Warnings and Precautions (5.6) ] . When these drugs are administered concomitantly, patients should be adequately hydrated. Assess renal function at the beginning of the concomitant treatment and periodically thereafter. Diuretics Clinical Impact: Clinical studies, as well as post-marketing observations, showed that NSAIDs reduced the natriuretic effect of loop diuretics (e.g., furosemide) and thiazide diuretics in some patients. This effect has been attributed to the NSAID inhibition of renal prostaglandin synthesis. Intervention: During concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% with diuretics, observe patients for signs of worsening renal function, in addition to assuring diuretic efficacy including antihypertensive effects [ see Warnings and Precautions (5.6) ]. Digoxin Clinical Impact: The concomitant use of diclofenac with digoxin has been reported to increase the serum concentration and prolong the half-life of digoxin. Intervention: During concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and digoxin, monitor serum digoxin levels. Lithium Clinical Impact: NSAIDs have produced elevations in plasma lithium levels and reductions in renal lithium clearance . The mean minimum lithium concentration increased 15%, and the renal clearance decreased by approximately 20%. This effect has been attributed to NSAID inhibition of renal prostaglandin synthesis. Intervention: During concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and lithium, monitor patients for signs of lithium toxicity. Methotrexate Clinical Impact: Concomitant use of NSAIDs and methotrexate may increase the risk for methotrexate toxicity (e.g., neutropenia, thrombocytopenia, renal dysfunction). Intervention: During concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and methotrexate, monitor patients for methotrexate toxicity. Cyclosporine Clinical Impact: Concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and cyclosporine may increase cyclosporine's nephrotoxicity. Intervention: During concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and cyclosporine, monitor patients for signs of worsening renal function. NSAIDs and Salicylates Clinical Impact: Concomitant use of diclofenac with other NSAIDs or salicylates (e.g., diflunisal, salsalate) increases the risk of GI toxicity, with little or no increase in efficacy [ see Warnings and Precautions (5.2) ] . Intervention: The concomitant use of diclofenac with other NSAIDs or salicylates is not recommended. Pemetrexed Clinical Impact: Concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and pemetrexed may increase the risk of pemetrexed-associated myelosuppression, renal, and GI toxicity (see the pemetrexed prescribing information). Intervention: During concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and pemetrexed, in patients with renal impairment whose creatinine clearance ranges from 45 to 79 mL/min, monitor for myelosuppression, renal and GI toxicity. NSAIDs with short elimination half-lives (e.g., diclofenac, indomethacin) should be avoided for a period of two days before, the day of, and two days following administration of pemetrexed. In the absence of data regarding potential interaction between pemetrexed and NSAIDs with longer half-lives (e.g., meloxicam, nabumetone), patients taking these NSAIDs should interrupt dosing for at least five days before, the day of, and two days following pemetrexed administration.
Storage and Handling
The DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is supplied in resealable envelopes, each containing 5 topical systems (10 cm × 14 cm), with 6 envelopes per box (NDC 85509-1405-3). Each individual topical system is debossed with "YARAL < DICLOFENAC EPOLAMINE TOPICAL SYSTEM > 1.3%". The product is intended for topical use only. Keep out of reach of children and pets. Envelopes should be sealed at all times when not in use. Curad® Hold Tite™ is a trademark of Medline Industries, Inc., and Surgilast® Tubular Elastic Dressing is a trademark of Derma Sciences, Inc. Repackaged/Relabeled by: PHOENIX RX LLC Hatboro, PA 19040
How Supplied
The DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is supplied in resealable envelopes, each containing 5 topical systems (10 cm × 14 cm), with 6 envelopes per box (NDC 85509-1405-3). Each individual topical system is debossed with "YARAL < DICLOFENAC EPOLAMINE TOPICAL SYSTEM > 1.3%". The product is intended for topical use only. Keep out of reach of children and pets. Envelopes should be sealed at all times when not in use. Curad® Hold Tite™ is a trademark of Medline Industries, Inc., and Surgilast® Tubular Elastic Dressing is a trademark of Derma Sciences, Inc. Repackaged/Relabeled by: PHOENIX RX LLC Hatboro, PA 19040
Medication Information
Warnings and Precautions
Hepatotoxicity : Inform patients of warning signs and symptoms of hepatotoxicity. Discontinue if abnormal liver tests persist or worsen or if clinical signs and symptoms of liver disease develop ( 5.3 ) Hypertension : Patients taking some antihypertensive medications may have impaired response to these therapies when taking NSAIDs. Monitor blood pressure ( 5.4 , 7 ) Heart Failure and Edema: Avoid use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% in patients with severe heart failure unless benefits are expected to outweigh risk of worsening heart failure ( 5.5 ) Renal Toxicity: Monitor renal function in patients with renal or hepatic impairment, heart failure, dehydration, or hypovolemia. Avoid use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% in patients with advanced renal disease unless benefits are expected to outweigh risk of worsening renal function ( 5.6 ) Anaphylactic Reactions : Seek emergency help if an anaphylactic reaction occurs ( 5.7 ) Exacerbation of Asthma Related to Aspirin Sensitivity : DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is contraindicated in patients with aspirin-sensitive asthma. Monitor patients with preexisting asthma (without aspirin sensitivity) ( 5.8 ) Serious Skin Reactions: Discontinue DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% at first appearance of skin rash or other signs of hypersensitivity ( 5.9 ) Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS) : Discontinue and evaluate clinically ( 5.10 ). Fetal Toxicity : Limit use of NSAIDs, including DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3 % between about 20 to 30 weeks in pregnancy due to the risk of oligohydramnios/fetal renal dysfunction. Avoid use of NSAIDs in women at about 30 weeks gestation and later in pregnancy due to the risks of oligohydramnios/fetal renal dysfunction and premature closure of the fetal ductus arteriosus ( 5.11 , 8.1 ). Hematologic Toxicity : Monitor hemoglobin or hematocrit in patients with any signs or symptoms of anemia ( 5.12 , 7 )
Indications and Usage
DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is indicated for the topical treatment of acute pain due to minor strains, sprains, and contusions in adults and pediatric patients 6 years and older.
Dosage and Administration
Use the lowest effective dosage for shortest duration consist with the individual patient treatment goals ( 2.1 ) The recommended dose of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% for adults and pediatric patients 6 years and older is one (1) topical system to the most painful area twice a day. ( 2 ) DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% should not be applied to damaged or non-intact skin. ( 2 )
Contraindications
DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is contraindicated in the following patients: Known hypersensitivity (e.g., anaphylactic reactions and serious skin reactions) to diclofenac or any components of the drug product [ see Warnings and Precautions (5.7 , 5.9 ) ] History of asthma, urticaria, or other allergic-type reactions after taking aspirin or other NSAIDs. Severe, sometimes fatal, anaphylactic reactions to NSAIDs have been reported in such patients [ see Warnings and Precautions (5.7 , 5.8 ) ] In the setting of coronary artery bypass graft (CABG) surgery [ see Warnings and Precautions (5.1) ] DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is contraindicated for use on non-intact or damaged skin resulting from any etiology, including exudative dermatitis, eczema, infection lesions, burns or wounds.
Adverse Reactions
The following adverse reactions are discussed in greater detail in other sections of the labeling: Cardiovascular Thrombotic Events [ see Warnings and Precautions (5.1) ] GI Bleeding, Ulceration and Perforation [ see Warnings and Precautions (5.2) ] Hepatotoxicity [ see Warnings and Precautions (5.3) ] Hypertension [ see Warnings and Precautions (5.4) ] Heart Failure and Edema [ see Warnings and Precautions (5.5) ] Renal Toxicity and Hyperkalemia [ see Warnings and Precautions (5.6) ] Anaphylactic Reactions [ see Warnings and Precautions (5.7) ] Serious Skin Reactions [ see Warnings and Precautions (5.9) ] Hematologic Toxicity [ see Warnings and Precautions (5.12) ]
Drug Interactions
See Table 2 for clinically significant drug interactions with diclofenac. Table 2: Clinically Significant Drug Interactions with Diclofenac Drugs That Interfere with Hemostasis Clinical Impact: Diclofenac and anticoagulants such as warfarin have a synergistic effect on bleeding. The concomitant use of diclofenac and anticoagulants have an increased risk of serious bleeding compared to the use of either drug alone. Serotonin release by platelets plays an important role in hemostasis. Case-control and cohort epidemiological studies showed that concomitant use of drugs that interfere with serotonin reuptake and an NSAID may potentiate the risk of bleeding more than an NSAID alone. Intervention: Monitor patients with concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% with anticoagulants (e.g., warfarin), antiplatelet agents (e.g., aspirin), selective serotonin reuptake inhibitors (SSRIs), and serotonin norepinephrine reuptake inhibitors (SNRIs) for signs of bleeding [ see Warnings and Precautions (5.12) ]. Aspirin Clinical Impact: Controlled clinical studies showed that the concomitant use of NSAIDs and analgesic doses of aspirin does not produce any greater therapeutic effect than the use of NSAIDs alone. In a clinical study, the concomitant use of an NSAID and aspirin was associated with a significantly increased incidence of GI adverse reactions as compared to use of the NSAID alone [ see Warnings and Precautions (5.2) ]. Intervention: Concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and analgesic doses of aspirin is not generally recommended because of the increased risk of bleeding [ see Warnings and Precautions (5.12) ]. DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is not a substitute for low dose aspirin for cardiovascular protection. ACE Inhibitors, Angiotensin Receptor Blockers, and Beta-Blockers Clinical Impact: NSAIDs may diminish the antihypertensive effect of angiotensin converting enzyme (ACE) inhibitors, angiotensin receptor blockers (ARBs), or beta-blockers (including propranolol). In patients who are elderly, volume-depleted (including those on diuretic therapy), or have renal impairment, co-administration of an NSAID with ACE inhibitors or ARBs may result in deterioration of renal function, including possible acute renal failure. These effects are usually reversible. Intervention: During concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and ACE-inhibitors, ARBs, or beta-blockers, monitor blood pressure to ensure that the desired blood pressure is obtained. During concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and ACE-inhibitors or ARBs in patients who are elderly, volume-depleted, or have impaired renal function, monitor for signs of worsening renal function [ see Warnings and Precautions (5.6) ] . When these drugs are administered concomitantly, patients should be adequately hydrated. Assess renal function at the beginning of the concomitant treatment and periodically thereafter. Diuretics Clinical Impact: Clinical studies, as well as post-marketing observations, showed that NSAIDs reduced the natriuretic effect of loop diuretics (e.g., furosemide) and thiazide diuretics in some patients. This effect has been attributed to the NSAID inhibition of renal prostaglandin synthesis. Intervention: During concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% with diuretics, observe patients for signs of worsening renal function, in addition to assuring diuretic efficacy including antihypertensive effects [ see Warnings and Precautions (5.6) ]. Digoxin Clinical Impact: The concomitant use of diclofenac with digoxin has been reported to increase the serum concentration and prolong the half-life of digoxin. Intervention: During concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and digoxin, monitor serum digoxin levels. Lithium Clinical Impact: NSAIDs have produced elevations in plasma lithium levels and reductions in renal lithium clearance . The mean minimum lithium concentration increased 15%, and the renal clearance decreased by approximately 20%. This effect has been attributed to NSAID inhibition of renal prostaglandin synthesis. Intervention: During concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and lithium, monitor patients for signs of lithium toxicity. Methotrexate Clinical Impact: Concomitant use of NSAIDs and methotrexate may increase the risk for methotrexate toxicity (e.g., neutropenia, thrombocytopenia, renal dysfunction). Intervention: During concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and methotrexate, monitor patients for methotrexate toxicity. Cyclosporine Clinical Impact: Concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and cyclosporine may increase cyclosporine's nephrotoxicity. Intervention: During concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and cyclosporine, monitor patients for signs of worsening renal function. NSAIDs and Salicylates Clinical Impact: Concomitant use of diclofenac with other NSAIDs or salicylates (e.g., diflunisal, salsalate) increases the risk of GI toxicity, with little or no increase in efficacy [ see Warnings and Precautions (5.2) ] . Intervention: The concomitant use of diclofenac with other NSAIDs or salicylates is not recommended. Pemetrexed Clinical Impact: Concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and pemetrexed may increase the risk of pemetrexed-associated myelosuppression, renal, and GI toxicity (see the pemetrexed prescribing information). Intervention: During concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and pemetrexed, in patients with renal impairment whose creatinine clearance ranges from 45 to 79 mL/min, monitor for myelosuppression, renal and GI toxicity. NSAIDs with short elimination half-lives (e.g., diclofenac, indomethacin) should be avoided for a period of two days before, the day of, and two days following administration of pemetrexed. In the absence of data regarding potential interaction between pemetrexed and NSAIDs with longer half-lives (e.g., meloxicam, nabumetone), patients taking these NSAIDs should interrupt dosing for at least five days before, the day of, and two days following pemetrexed administration.
Storage and Handling
The DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is supplied in resealable envelopes, each containing 5 topical systems (10 cm × 14 cm), with 6 envelopes per box (NDC 85509-1405-3). Each individual topical system is debossed with "YARAL < DICLOFENAC EPOLAMINE TOPICAL SYSTEM > 1.3%". The product is intended for topical use only. Keep out of reach of children and pets. Envelopes should be sealed at all times when not in use. Curad® Hold Tite™ is a trademark of Medline Industries, Inc., and Surgilast® Tubular Elastic Dressing is a trademark of Derma Sciences, Inc. Repackaged/Relabeled by: PHOENIX RX LLC Hatboro, PA 19040
How Supplied
The DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is supplied in resealable envelopes, each containing 5 topical systems (10 cm × 14 cm), with 6 envelopes per box (NDC 85509-1405-3). Each individual topical system is debossed with "YARAL < DICLOFENAC EPOLAMINE TOPICAL SYSTEM > 1.3%". The product is intended for topical use only. Keep out of reach of children and pets. Envelopes should be sealed at all times when not in use. Curad® Hold Tite™ is a trademark of Medline Industries, Inc., and Surgilast® Tubular Elastic Dressing is a trademark of Derma Sciences, Inc. Repackaged/Relabeled by: PHOENIX RX LLC Hatboro, PA 19040
Description
WARNING: RISK OF SERIOUS CARDIOVASCULAR and GASTROINTESTINAL EVENTS See full prescribing information for complete boxed warning. Nonsteroidal anti-inflammatory drugs (NSAIDs) cause an increased risk of serious cardiovascular thrombotic events, including myocardial infarction and stroke, which can be fatal. This risk may occur early in treatment and may increase with duration of use ( 5.1 ) DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is contraindicated in the setting of coronary artery bypass graft (CABG) surgery ( 4 , 5.1 ) NSAIDs cause an increased risk of serious gastrointestinal (GI) adverse events including bleeding, ulceration, and perforation of the stomach or intestines, which can be fatal. These events can occur at any time during use and without warning symptoms. Elderly patients and patients with a prior history of peptic ulcer disease and/or GI bleeding are at greater risk for serious GI events ( 5.2 )
Section 42229-5
Cardiovascular Thrombotic Events
- Nonsteroidal anti-inflammatory drugs (NSAIDs) cause an increased risk of serious cardiovascular thrombotic events, including myocardial infarction and stroke, which can be fatal. This risk may occur early in treatment and may increase with duration of use [ see Warnings and Precautions (5.1) ].
- DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is contraindicated in the setting of coronary artery bypass graft (CABG) surgery [ see Contraindications (4)and Warnings and Precautions (5.1) ] .
Section 42231-1
| Medication Guide for Nonsteroidal Anti-inflammatory Drugs (NSAIDs) | ||
|---|---|---|
|
What is the most important information I should know about medicines called Nonsteroidal Anti-inflammatory Drugs (NSAIDs)?
NSAIDs can cause serious side effects, including:
|
||
|
|
|
| NSAIDs should only be used: | ||
|
||
|
What are NSAIDs?
NSAIDs are used to treat pain and redness, swelling, and heat (inflammation) from medical conditions such as different types of arthritis, menstrual cramps, and other types of short-term pain. |
||
|
Who should not take NSAIDs?
Do not take NSAIDs:
|
||
Before taking NSAIDS, tell your healthcare provider about all of your medical conditions, including if you:
|
||
|
What are the possible side effects of NSAIDs?
NSAIDs can cause serious side effects, including: See " What is the most important information I should know about medicines called Nonsteroidal Anti-inflammatory Drugs (NSAIDs)?
|
||
|
|
|
| Stop taking your NSAID and call your healthcare provider right away if you get any of the following symptoms: | ||
|
|
|
|
If you take too much of your NSAID, call your healthcare provider or get medical help right away.These are not all the possible side effects of NSAIDs. For more information, ask your healthcare provider or pharmacist about NSAIDs.
Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. |
||
Other information about NSAIDs
|
||
|
General information about the safe and effective use of NSAIDs
Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not use NSAIDs for a condition for which it was not prescribed. Do not give NSAIDs to other people, even if they have the same symptoms that you have. It may harm them. If you would like more information about NSAIDs, talk with your healthcare provider. You can ask your pharmacist or healthcare provider for information about NSAIDs that is written for health professionals. |
Manufactured for:IBSA Institut Biochimique SA, 6912 Pazzallo, Switzerland
Distributed by:YARAL Pharma, Inc., Parsippany, NJ 07054 USA
For more information, call 1-866-218-9009
This Medication Guide has been approved by the U.S. Food and Drug Administration.
Revised: 07-2023
1320 edition VII
Section 43683-2
| Warning and Precautions ( 5.9) | 11/2024 |
Section 44425-7
Storage
Store at 20°C to 25°C (68°F to 77°F); excursions permitted between 15°C to 30°C (59°F to 86°F) [see USP Controlled Room Temperature].
10 Overdosage
Symptoms following acute NSAID overdosages have been typically limited to lethargy, drowsiness, nausea, vomiting, and epigastric pain, which have been generally reversible with supportive care. Gastrointestinal bleeding has occurred. Hypertension, acute renal failure, respiratory depression, and coma have occurred, but were rare [ see Warnings and Precautions (5.1, 5.2, 5.4, 5.6) ].
Manage patients with symptomatic and supportive care following an NSAID overdosage. There are no specific antidotes. Forced diuresis, alkalinization of urine, hemodialysis, or hemoperfusion may not be useful due to high protein binding.
For additional information about overdosage treatment contact a poison control center (1-800-222-1222).
11 Description
DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is a nonsteroidal anti-inflammatory drug for topical application. DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is a 10 cm × 14 cm topical system comprised of an adhesive material containing 1.3% diclofenac epolamine which is applied to a non-woven polyester felt backing and covered with a polypropylene film release liner. The release liner is removed prior to topical application to the skin.
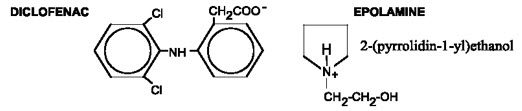
The chemical name of diclofenac epolamine is 2-[(2,6-dichlorophenyl) amino] benzeneacetic acid, (2-(pyrrolidin-1-yl) ethanol salt, with a molecular formula of C 20H 24Cl 2N 2O 3,and molecular weight 411.3, an n-octanol/water partition coefficient of 8 at pH 8.5, and the following chemical structure:
Each adhesive topical system contains 180 mg of diclofenac epolamine (13 mg per gram adhesive) in an aqueous base. It also contains the following inactive ingredients: butylene glycol, carboxymethylcellulose sodium, dihydroxyaluminum aminoacetate, edetate disodium, fragrance (Dalin PH), gelatin, kaolin, methylparaben, polysorbate 80, povidone, propylene glycol, propylparaben, sodium polyacrylate, sorbitol solution, tartaric acid, titanium dioxide, and purified water.
5.4 Hypertension
NSAIDs, including DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3%, can lead to new onset of hypertension or worsening of preexisting hypertension, either of which may contribute to the increased incidence of CV events. Patients taking angiotensin converting enzyme (ACE) inhibitors, thiazide diuretics, or loop diuretics may have impaired response to these therapies when taking NSAIDs [ see Drug Interactions (7) ].
Monitor blood pressure (BP) during the initiation of NSAID treatment and throughout the course of therapy.
5.16 Eye Exposure
Avoid contact of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% with eyes and mucosa. Advise patients that if eye contact occurs, immediately wash out the eye with water or saline and consult a physician if irritation persists for more than an hour.
8.4 Pediatric Use
The safety and effectiveness of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% have been established in pediatric patients 6 years and older based on evidence from adequate and well-controlled studies with DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3 % in adults, as well as an open-label study in pediatric patients 6 years and older. The pediatric study enrolled 104 patients, 6 years of age and older with minor soft tissue injuries. One DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3 % was applied to the injury site twice daily for a maximum of 14 days or until treatment was no longer required for pain management, whichever occurred first. Based on the available data from the pediatric study, the safety profile of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3 % topical system in pediatric patients is similar to that in adults. The safety and effectiveness of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3 % has not been investigated in pediatric patients less than 6 years old. [ see Clinical Trials Experience (6.1), Clinical Pharmacology (12.3) ].
8.5 Geriatric Use
Elderly patients, compared to younger patients, are at greater risk for NSAID-associated serious cardiovascular, gastrointestinal, and/or renal adverse reactions. If the anticipated benefit for the elderly patient outweighs these potential risks, start dosing at the low end of the dosing range, and monitor patients for adverse effects [ see Warnings and Precautions (5.1, 5.2, 5.3, 5.6, 5.14)].
Clinical studies of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% did not include sufficient numbers of subjects aged 65 and over to determine whether they respond differently from younger subjects. Other reported clinical experience has not identified differences in responses between the elderly and younger patients.
5.3 Hepatotoxicity
In clinical trials of oral diclofenac containing products, meaningful elevations (i.e., more than 3 times the ULN) of AST (SGOT) were observed in about 2% of approximately 5,700 patients at some time during diclofenac treatment (ALT was not measured in all studies).
In a large open-label, controlled trial of 3,700 patients treated with oral diclofenac sodium for 2-6 months, patients were monitored first at 8 weeks and 1,200 patients were monitored again at 24 weeks. Meaningful elevations of ALT and/or AST occurred in about 4% of the 3,700 patients and included marked elevations (greater than 8 times the ULN) in about 1% of the 3,700 patients. In that open-label study, a higher incidence of borderline (less than 3 times the ULN), moderate (3-8 times the ULN), and marked (greater than 8 times the ULN) elevations of ALT or AST was observed in patients receiving diclofenac when compared to other NSAIDs. Elevations in transaminases were seen more frequently in patients with osteoarthritis than in those with rheumatoid arthritis.
Almost all meaningful elevations in transaminases were detected before patients became symptomatic. Abnormal tests occurred during the first 2 months of therapy with diclofenac in 42 of the 51 patients in all trials who developed marked transaminase elevations.
In postmarketing reports, cases of drug-induced hepatotoxicity have been reported in the first month, and in some cases, the first 2 months of therapy, but can occur at any time during treatment with diclofenac. Postmarketing surveillance has reported cases of severe hepatic reactions, including liver necrosis, jaundice, fulminant hepatitis with and without jaundice, and liver failure. Some of these reported cases resulted in fatalities or liver transplantation.
In a European retrospective population-based, case-controlled study, 10 cases of diclofenac associated drug-induced liver injury with current use compared with non-use of diclofenac were associated with a statistically significant 4-fold adjusted odds ratio of liver injury. In this particular study, based on an overall number of 10 cases of liver injury associated with diclofenac, the adjusted odds ratio increased further with female gender, doses of 150 mg or more, and duration of use for more than 90 days.
Physicians should measure transaminases at baseline and periodically in patients receiving long-term therapy with diclofenac, because severe hepatotoxicity may develop without a prodrome of distinguishing symptoms. The optimum times for making the first and subsequent transaminase measurements are not known. Based on clinical trial data and postmarketing experiences, transaminases should be monitored within 4 to 8 weeks after initiating treatment with diclofenac. However, severe hepatic reactions can occur at any time during treatment with diclofenac.
If abnormal liver tests persist or worsen, if clinical signs and/or symptoms consistent with liver disease develop, or if systemic manifestations occur (e.g., eosinophilia, rash, abdominal pain, diarrhea, dark urine, etc.), DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% should be discontinued immediately.
Inform patients of the warning signs and symptoms of hepatotoxicity (e.g., nausea, fatigue, lethargy, diarrhea, pruritus, jaundice, right upper quadrant tenderness, and "flu-like" symptoms). If clinical signs and symptoms consistent with liver disease develop, or if systemic manifestations occur (e.g., eosinophilia, rash, etc.), discontinue DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% immediately, and perform a clinical evaluation of the patient.
To minimize the potential risk for an adverse liver related event in patients treated with DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3%, use the lowest effective dose for the shortest duration possible. Exercise caution when prescribing DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% with concomitant drugs that are known to be potentially hepatotoxic (e.g., acetaminophen, antibiotics, anti-epileptics).
4 Contraindications
DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is contraindicated in the following patients:
- Known hypersensitivity (e.g., anaphylactic reactions and serious skin reactions) to diclofenac or any components of the drug product [ see Warnings and Precautions (5.7, 5.9) ]
- History of asthma, urticaria, or other allergic-type reactions after taking aspirin or other NSAIDs. Severe, sometimes fatal, anaphylactic reactions to NSAIDs have been reported in such patients [ see Warnings and Precautions (5.7, 5.8) ]
- In the setting of coronary artery bypass graft (CABG) surgery [ see Warnings and Precautions (5.1) ]
- DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is contraindicated for use on non-intact or damaged skin resulting from any etiology, including exudative dermatitis, eczema, infection lesions, burns or wounds.
6 Adverse Reactions
The following adverse reactions are discussed in greater detail in other sections of the labeling:
- Cardiovascular Thrombotic Events [ see Warnings and Precautions (5.1) ]
- GI Bleeding, Ulceration and Perforation [ see Warnings and Precautions (5.2) ]
- Hepatotoxicity [ see Warnings and Precautions (5.3) ]
- Hypertension [ see Warnings and Precautions (5.4) ]
- Heart Failure and Edema [ see Warnings and Precautions (5.5) ]
- Renal Toxicity and Hyperkalemia [ see Warnings and Precautions (5.6) ]
- Anaphylactic Reactions [ see Warnings and Precautions (5.7) ]
- Serious Skin Reactions [ see Warnings and Precautions (5.9) ]
- Hematologic Toxicity [ see Warnings and Precautions (5.12) ]
7 Drug Interactions
See Table 2 for clinically significant drug interactions with diclofenac.
| Drugs That Interfere with Hemostasis | |
| Clinical Impact: |
|
| Intervention: | Monitor patients with concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% with anticoagulants (e.g., warfarin), antiplatelet agents (e.g., aspirin), selective serotonin reuptake inhibitors (SSRIs), and serotonin norepinephrine reuptake inhibitors (SNRIs) for signs of bleeding [ see Warnings and Precautions (5.12) ]. |
| Aspirin | |
| Clinical Impact: | Controlled clinical studies showed that the concomitant use of NSAIDs and analgesic doses of aspirin does not produce any greater therapeutic effect than the use of NSAIDs alone. In a clinical study, the concomitant use of an NSAID and aspirin was associated with a significantly increased incidence of GI adverse reactions as compared to use of the NSAID alone [ see Warnings and Precautions (5.2) ]. |
| Intervention: | Concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and analgesic doses of aspirin is not generally recommended because of the increased risk of bleeding [
see
Warnings and Precautions (5.12)
].
DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is not a substitute for low dose aspirin for cardiovascular protection. |
| ACE Inhibitors, Angiotensin Receptor Blockers, and Beta-Blockers | |
| Clinical Impact: |
|
| Intervention: |
|
| Diuretics | |
| Clinical Impact: | Clinical studies, as well as post-marketing observations, showed that NSAIDs reduced the natriuretic effect of loop diuretics (e.g., furosemide) and thiazide diuretics in some patients. This effect has been attributed to the NSAID inhibition of renal prostaglandin synthesis. |
| Intervention: | During concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% with diuretics, observe patients for signs of worsening renal function, in addition to assuring diuretic efficacy including antihypertensive effects [ see Warnings and Precautions (5.6) ]. |
| Digoxin | |
| Clinical Impact: | The concomitant use of diclofenac with digoxin has been reported to increase the serum concentration and prolong the half-life of digoxin. |
| Intervention: | During concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and digoxin, monitor serum digoxin levels. |
| Lithium | |
| Clinical Impact: | NSAIDs have produced elevations in plasma lithium levels and reductions in renal lithium clearance .The mean minimum lithium concentration increased 15%, and the renal clearance decreased by approximately 20%. This effect has been attributed to NSAID inhibition of renal prostaglandin synthesis. |
| Intervention: | During concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and lithium, monitor patients for signs of lithium toxicity. |
| Methotrexate | |
| Clinical Impact: | Concomitant use of NSAIDs and methotrexate may increase the risk for methotrexate toxicity (e.g., neutropenia, thrombocytopenia, renal dysfunction). |
| Intervention: | During concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and methotrexate, monitor patients for methotrexate toxicity. |
| Cyclosporine | |
| Clinical Impact: | Concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and cyclosporine may increase cyclosporine's nephrotoxicity. |
| Intervention: | During concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and cyclosporine, monitor patients for signs of worsening renal function. |
| NSAIDs and Salicylates | |
| Clinical Impact: | Concomitant use of diclofenac with other NSAIDs or salicylates (e.g., diflunisal, salsalate) increases the risk of GI toxicity, with little or no increase in efficacy [ see Warnings and Precautions (5.2) ] . |
| Intervention: | The concomitant use of diclofenac with other NSAIDs or salicylates is not recommended. |
| Pemetrexed | |
| Clinical Impact: | Concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and pemetrexed may increase the risk of pemetrexed-associated myelosuppression, renal, and GI toxicity (see the pemetrexed prescribing information). |
| Intervention: | During concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and pemetrexed, in patients with renal impairment whose creatinine clearance ranges from 45 to 79 mL/min, monitor for myelosuppression, renal and GI toxicity.
NSAIDs with short elimination half-lives (e.g., diclofenac, indomethacin) should be avoided for a period of two days before, the day of, and two days following administration of pemetrexed. In the absence of data regarding potential interaction between pemetrexed and NSAIDs with longer half-lives (e.g., meloxicam, nabumetone), patients taking these NSAIDs should interrupt dosing for at least five days before, the day of, and two days following pemetrexed administration. |
12.2 Pharmacodynamics
DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% applied to intact skin provides local analgesia by releasing diclofenac epolamine from the topical system into the skin.
1 Indications and Usage
DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is indicated for the topical treatment of acute pain due to minor strains, sprains, and contusions in adults and pediatric patients 6 years and older.
2.2 Special Precautions
- Inform patients that, if DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% begins to peel-off, the edges of the topical system may be taped down. If problems with adhesion persist, patients may overlay the topical system with a mesh netting sleeve, where appropriate (e.g. to secure topical systems applied to ankles, knees, or elbows). The mesh netting sleeve (e.g. Curad® Hold Tite™, Surgilast® Tubular Elastic Dressing) must allow air to pass through and not be occlusive (non-breathable).
- Do not apply DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% to non-intact or damaged skin resulting from any etiology e.g. exudative dermatitis, eczema, infected lesion, burns or wounds.
- Do not wear a DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% when bathing or showering.
- Wash your hands after applying, handling or removing the topical system.
- Avoid eye contact.
- Do not use combination therapy with DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and an oral NSAID unless the benefit outweighs the risk and conduct periodic laboratory evaluations.
12.1 Mechanism of Action
Diclofenac has analgesic, anti-inflammatory, and antipyretic properties.
The mechanism of action of diclofenac, like that of other NSAIDs, is not completely understood but involves inhibition of cyclooxygenase (COX-1 and COX-2).
Diclofenac is a potent inhibitor of prostaglandin synthesis in vitro. Diclofenac concentrations reached during therapy have produced in vivo effects. Prostaglandins sensitize afferent nerves and potentiate the action of bradykinin in inducing pain in animal models. Prostaglandins are mediators of inflammation. Because diclofenac is an inhibitor of prostaglandin synthesis, its mode of action may be due to a decrease of prostaglandins in peripheral tissues.
5.12 Hematologic Toxicity
Anemia has occurred in NSAID-treated patients. This may be due to occult or gross blood loss, fluid retention, or an incompletely described effect on erythropoiesis. If a patient treated with DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% has any signs or symptoms of anemia, monitor hemoglobin or hematocrit.
NSAIDs, including DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3%, may increase the risk of bleeding events. Co-morbid conditions such as coagulation disorders, concomitant use of warfarin, other anticoagulants, antiplatelet agents (e.g., aspirin), serotonin reuptake inhibitors (SSRIs) and serotonin norepinephrine reuptake inhibitors (SNRIs) may increase this risk. Monitor these patients for signs of bleeding [ see Drug Interactions (7) ].
5 Warnings and Precautions
- Hepatotoxicity: Inform patients of warning signs and symptoms of hepatotoxicity. Discontinue if abnormal liver tests persist or worsen or if clinical signs and symptoms of liver disease develop ( 5.3)
- Hypertension: Patients taking some antihypertensive medications may have impaired response to these therapies when taking NSAIDs. Monitor blood pressure ( 5.4, 7)
- Heart Failure and Edema:Avoid use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% in patients with severe heart failure unless benefits are expected to outweigh risk of worsening heart failure ( 5.5)
- Renal Toxicity:Monitor renal function in patients with renal or hepatic impairment, heart failure, dehydration, or hypovolemia. Avoid use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% in patients with advanced renal disease unless benefits are expected to outweigh risk of worsening renal function ( 5.6)
- Anaphylactic Reactions: Seek emergency help if an anaphylactic reaction occurs ( 5.7)
- Exacerbation of Asthma Related to Aspirin Sensitivity: DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is contraindicated in patients with aspirin-sensitive asthma. Monitor patients with preexisting asthma (without aspirin sensitivity) ( 5.8)
- Serious Skin Reactions:Discontinue DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% at first appearance of skin rash or other signs of hypersensitivity ( 5.9)
- Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS): Discontinue and evaluate clinically ( 5.10).
- Fetal Toxicity: Limit use of NSAIDs, including DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3 % between about 20 to 30 weeks in pregnancy due to the risk of oligohydramnios/fetal renal dysfunction. Avoid use of NSAIDs in women at about 30 weeks gestation and later in pregnancy due to the risks of oligohydramnios/fetal renal dysfunction and premature closure of the fetal ductus arteriosus ( 5.11, 8.1).
- Hematologic Toxicity: Monitor hemoglobin or hematocrit in patients with any signs or symptoms of anemia ( 5.12, 7)
5.14 Laboratory Monitoring
Because serious GI bleeding, hepatotoxicity, and renal injury can occur without warning symptoms or signs, consider monitoring patients on long-term NSAID treatment with a CBC and a chemistry profile periodically [ see Warnings and Precautions (5.2, 5.3, 5.6) ].
5.7 Anaphylactic Reactions
Diclofenac has been associated with anaphylactic reactions in patients with and without known hypersensitivity to diclofenac and in patients with aspirin-sensitive asthma [see Contraindications (4)and Warnings and Precautions (5.8) ]. Seek emergency help if an anaphylactic reaction occurs.
5.9 Serious Skin Reactions
NSAIDs, including diclofenac, can cause serious skin adverse reactions such as exfoliative dermatitis, Stevens-Johnson Syndrome (SJS), and toxic epidermal necrolysis (TEN), which can be fatal.NSAIDs can also cause fixed drug eruption (FDE). FDE may present as a more severe variant known as generalized bullous fixed drug eruption (GBFDE), which can be life-threatening. These serious events may occur without warning. Inform patients about the signs and symptoms of serious skin reactions, and to discontinue the use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% at the first appearance of skin rash or any other sign of hypersensitivity. DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is contraindicated in patients with previous serious skin reactions to NSAIDs [ see Contraindications (4) ].
2 Dosage and Administration
- Use the lowest effective dosage for shortest duration consist with the individual patient treatment goals ( 2.1)
- The recommended dose of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% for adults and pediatric patients 6 years and older is one (1) topical system to the most painful area twice a day. ( 2)
- DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% should not be applied to damaged or non-intact skin. ( 2)
5.5 Heart Failure and Edema
The Coxib and traditional NSAID Trialists' Collaboration meta-analysis of randomized controlled trials demonstrated an approximately two-fold increase in hospitalizations for heart failure in COX-2 selective-treated patients and nonselective NSAID-treated patients compared to placebo-treated patients. In a Danish National Registry study of patients with heart failure, NSAID use increased the risk of MI, hospitalization for heart failure, and death.
Additionally, fluid retention and edema have been observed in some patients treated with NSAIDs. Use of diclofenac may blunt the CV effects of several therapeutic agents used to treat these medical conditions (e.g., diuretics, ACE inhibitors, or angiotensin receptor blockers [ARBs]) [ see Drug Interactions (7) ].
Avoid the use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% in patients with severe heart failure unless the benefits are expected to outweigh the risk of worsening heart failure. If DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is used in patients with severe heart failure, monitor patients for signs of worsening heart failure.
3 Dosage Forms and Strengths
Diclofenac Epolamine Topical System is a 10 cm × 14 cm topical system that contains 1.3% diclofenac epolamine, and is debossed with YARAL <DICLOFENAC EPOLAMINE TOPICAL SYSTEM> 1.3%.
6.2 Postmarketing Experience
The following adverse reactions have been identified during post-approval use of diclofenac.
Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Skin and Appendages: Exfoliative dermatitis, Stevens-Johnson Syndrome (SJS), toxic epidermal necrolysis (TEN), and fixed drug eruption (FDE).
8 Use in Specific Populations
- Infertility: NSAIDs are associated with reversible infertility. Consider withdrawal of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% in women who have difficulties conceiving ( 8.3)
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared with rates in the clinical trials of another drug and may not reflect the rates observed in practice.
2.1 General Dosing Instructions
Use the lowest effective dosage for the shortest duration consistent with individual patient treatment goals [ see Warnings and Precautions (5) ].
The recommended dose of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is one (1) topical system to the most painful area twice a day both in adults and pediatric patients 6 years of age and older.
17 Patient Counseling Information
Advise the patient to read the FDA-approved patient labeling (Medication Guide) that accompanies each prescription dispensed, as well as the Directions for Use on the product packaging. Inform patients, families, or their caregivers of the following information before initiating therapy with DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and periodically during the course of ongoing therapy.
16 How Supplied/storage and Handling
The DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is supplied in resealable envelopes, each containing 5 topical systems (10 cm × 14 cm), with 6 envelopes per box (NDC 85509-1405-3). Each individual topical system is debossed with "YARAL < DICLOFENAC EPOLAMINE TOPICAL SYSTEM > 1.3%".
- The product is intended for topical use only.
- Keep out of reach of children and pets.
- Envelopes should be sealed at all times when not in use.
- Curad® Hold Tite™ is a trademark of Medline Industries, Inc., and Surgilast® Tubular Elastic Dressing is a trademark of Derma Sciences, Inc.
Repackaged/Relabeled by:
PHOENIX RX LLC
Hatboro, PA 19040
5.1 Cardiovascular Thrombotic Events
Clinical trials of several COX-2 selective and nonselective NSAIDs of up to three years duration have shown an increased risk of serious cardiovascular (CV) thrombotic events, including myocardial infarction (MI) and stroke, which can be fatal. Based on available data, it is unclear that the risk for CV thrombotic events is similar for all NSAIDs. The relative increase in serious CV thrombotic events over baseline conferred by NSAID use appears to be similar in those with and without known CV disease or risk factors for CV disease. However, patients with known CV disease or risk factors had a higher absolute incidence of excess serious CV thrombotic events, due to their increased baseline rate. Some observational studies found that this increased risk of serious CV thrombotic events began as early as the first weeks of treatment. The increase in CV thrombotic risk has been observed most consistently at higher doses.
To minimize the potential risk for an adverse CV event in NSAID-treated patients, use the lowest effective dose for the shortest duration possible. Physicians and patients should remain alert for the development of such events, throughout the entire treatment course, even in the absence of previous CV symptoms. Patients should be informed about the symptoms of serious CV events and the steps to take if they occur.
There is no consistent evidence that concurrent use of aspirin mitigates the increased risk of serious CV thrombotic events associated with NSAID use. The concurrent use of aspirin and an NSAID, such as diclofenac, increases the risk of serious gastrointestinal (GI) events [ see Warnings and Precautions (5.2) ].
5.15 Accidental Exposure in Children
Even a used DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% contains a large amount of diclofenac epolamine (as much as 170 mg). The potential therefore exists for a small child or pet to suffer serious adverse effects from chewing or ingesting a new or used DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3%. It is important for patients to store and dispose of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% out of the reach of children and pets.
14.1 Strains, Sprains, and Contusions
Efficacy of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% was demonstrated in two of four studies of patients with minor strains, sprains, and contusions. Patients were randomly assigned to treatment with the DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3%, or a placebo identical to the DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% minus the active ingredient. In the first of these two studies, patients with ankle sprains were treated once daily for a week. In the second study, patients with strains, sprains and contusions were treated twice daily for up to two weeks. Pain was assessed over the period of treatment. Patients treated with the DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% experienced a greater reduction in pain as compared to patients randomized to placebo as evidenced by the responder curves presented below ( Figures 1-4).
Figure 1: Patients Achieving Various Levels of Pain Relief at Day 3; 14-Day Study
Figure 2: Patients Achieving Various Levels of Pain Relief at End of Study; 14-Day Study
Figure 3: Patients Achieving Various Levels of Pain Relief at Day 3; 7-Day Study
Figure 4: Patients Achieving Various Levels of Pain Relief at End of Study; 7-Day Study
5.13 Masking of Inflammation and Fever
The pharmacological activity of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% in reducing inflammation, and possibly fever, may diminish the utility of diagnostic signs in detecting infections.
5.17 Oral Nonsteroidal Anti Inflammatory Drugs
Concomitant use of oral and topical NSAIDs may result in a higher rate of hemorrhage, more frequent abnormal creatinine, urea and hemoglobin. Do not use combination therapy with DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and an oral NSAID unless the benefit outweighs the risk.
Principal Display Panel 30 Topical System Pouch Carton
NDC 85509-1405-3
diclofenac epolamine
topical system 1.3%
30 TOPICAL SYSTEMS (10 CM X 14 CM EACH)
Dispense with enclosed Medication Guide
Change diclofenac epolamine topical system once every 12 hours
Fold used topical systems so that the adhesive side sticks to itself and
safely discard used topical systems where children and pets cannot get them.
Rx only
5.8 Exacerbation of Asthma Related to Aspirin Sensitivity
A subpopulation of patients with asthma may have aspirin-sensitive asthma which may include chronic rhinosinusitis complicated by nasal polyps; severe, potentially fatal bronchospasm; and/or intolerance to aspirin and other NSAIDs. Because cross-reactivity between aspirin and other NSAIDs has been reported in such aspirin-sensitive patients, DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is contraindicated in patients with this form of aspirin sensitivity [ see Contraindications (4) ]. When DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is used in patients with preexisting asthma (without known aspirin sensitivity), monitor patients for changes in the signs and symptoms of asthma.
5.2 Gastrointestinal Bleeding, Ulceration, and Perforation
NSAIDs, including diclofenac, cause serious gastrointestinal (GI) adverse events including inflammation, bleeding, ulceration, and perforation of the esophagus, stomach, small intestine, or large intestine, which can be fatal. These serious adverse events can occur at any time, with or without warning symptoms, in patients treated with NSAIDs.
Only one in five patients who develop a serious upper GI adverse event on NSAID therapy is symptomatic. Upper GI ulcers, gross bleeding, or perforation caused by NSAIDs occurred in approximately 1% of patients treated for 3-6 months, and in about 2%-4% of patients treated for one year. However, even short-term NSAID therapy is not without risk.
5.10 Drug Reaction With Eosinophilia and Systemic Symptoms (dress)
Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS) has been reported in patients taking NSAIDs such as DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% . Some of these events have been fatal or life-threatening. DRESS typically, although not exclusively, presents with fever, rash, lymphadenopathy, and/or facial swelling. Other clinical manifestations may include hepatitis, nephritis, hematological abnormalities, myocarditis, or myositis. Sometimes symptoms of DRESS may resemble an acute viral infection. Eosinophilia is often present. Because this disorder is variable in its presentation, other organ systems not noted here may be involved.
It is important to note that early manifestations of hypersensitivity, such as fever or lymphadenopathy, may be present even though rash is not evident. If such signs or symptoms are present, discontinue DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and evaluate the patient immediately
Warning: Risk of Serious Cardiovascular and Gastrointestinal Events
WARNING: RISK OF SERIOUS CARDIOVASCULAR and GASTROINTESTINAL EVENTS
See full prescribing information for complete boxed warning.
- Nonsteroidal anti-inflammatory drugs (NSAIDs) cause an increased risk of serious cardiovascular thrombotic events, including myocardial infarction and stroke, which can be fatal. This risk may occur early in treatment and may increase with duration of use ( 5.1)
- DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is contraindicated in the setting of coronary artery bypass graft (CABG) surgery ( 4, 5.1)
- NSAIDs cause an increased risk of serious gastrointestinal (GI) adverse events including bleeding, ulceration, and perforation of the stomach or intestines, which can be fatal. These events can occur at any time during use and without warning symptoms. Elderly patients and patients with a prior history of peptic ulcer disease and/or GI bleeding are at greater risk for serious GI events ( 5.2)
Structured Label Content
Section 42229-5 (42229-5)
Cardiovascular Thrombotic Events
- Nonsteroidal anti-inflammatory drugs (NSAIDs) cause an increased risk of serious cardiovascular thrombotic events, including myocardial infarction and stroke, which can be fatal. This risk may occur early in treatment and may increase with duration of use [ see Warnings and Precautions (5.1) ].
- DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is contraindicated in the setting of coronary artery bypass graft (CABG) surgery [ see Contraindications (4)and Warnings and Precautions (5.1) ] .
Section 42231-1 (42231-1)
| Medication Guide for Nonsteroidal Anti-inflammatory Drugs (NSAIDs) | ||
|---|---|---|
|
What is the most important information I should know about medicines called Nonsteroidal Anti-inflammatory Drugs (NSAIDs)?
NSAIDs can cause serious side effects, including:
|
||
|
|
|
| NSAIDs should only be used: | ||
|
||
|
What are NSAIDs?
NSAIDs are used to treat pain and redness, swelling, and heat (inflammation) from medical conditions such as different types of arthritis, menstrual cramps, and other types of short-term pain. |
||
|
Who should not take NSAIDs?
Do not take NSAIDs:
|
||
Before taking NSAIDS, tell your healthcare provider about all of your medical conditions, including if you:
|
||
|
What are the possible side effects of NSAIDs?
NSAIDs can cause serious side effects, including: See " What is the most important information I should know about medicines called Nonsteroidal Anti-inflammatory Drugs (NSAIDs)?
|
||
|
|
|
| Stop taking your NSAID and call your healthcare provider right away if you get any of the following symptoms: | ||
|
|
|
|
If you take too much of your NSAID, call your healthcare provider or get medical help right away.These are not all the possible side effects of NSAIDs. For more information, ask your healthcare provider or pharmacist about NSAIDs.
Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. |
||
Other information about NSAIDs
|
||
|
General information about the safe and effective use of NSAIDs
Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not use NSAIDs for a condition for which it was not prescribed. Do not give NSAIDs to other people, even if they have the same symptoms that you have. It may harm them. If you would like more information about NSAIDs, talk with your healthcare provider. You can ask your pharmacist or healthcare provider for information about NSAIDs that is written for health professionals. |
Manufactured for:IBSA Institut Biochimique SA, 6912 Pazzallo, Switzerland
Distributed by:YARAL Pharma, Inc., Parsippany, NJ 07054 USA
For more information, call 1-866-218-9009
This Medication Guide has been approved by the U.S. Food and Drug Administration.
Revised: 07-2023
1320 edition VII
Section 43683-2 (43683-2)
| Warning and Precautions ( 5.9) | 11/2024 |
Section 44425-7 (44425-7)
Storage
Store at 20°C to 25°C (68°F to 77°F); excursions permitted between 15°C to 30°C (59°F to 86°F) [see USP Controlled Room Temperature].
10 Overdosage (10 OVERDOSAGE)
Symptoms following acute NSAID overdosages have been typically limited to lethargy, drowsiness, nausea, vomiting, and epigastric pain, which have been generally reversible with supportive care. Gastrointestinal bleeding has occurred. Hypertension, acute renal failure, respiratory depression, and coma have occurred, but were rare [ see Warnings and Precautions (5.1, 5.2, 5.4, 5.6) ].
Manage patients with symptomatic and supportive care following an NSAID overdosage. There are no specific antidotes. Forced diuresis, alkalinization of urine, hemodialysis, or hemoperfusion may not be useful due to high protein binding.
For additional information about overdosage treatment contact a poison control center (1-800-222-1222).
11 Description (11 DESCRIPTION)
DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is a nonsteroidal anti-inflammatory drug for topical application. DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is a 10 cm × 14 cm topical system comprised of an adhesive material containing 1.3% diclofenac epolamine which is applied to a non-woven polyester felt backing and covered with a polypropylene film release liner. The release liner is removed prior to topical application to the skin.
The chemical name of diclofenac epolamine is 2-[(2,6-dichlorophenyl) amino] benzeneacetic acid, (2-(pyrrolidin-1-yl) ethanol salt, with a molecular formula of C 20H 24Cl 2N 2O 3,and molecular weight 411.3, an n-octanol/water partition coefficient of 8 at pH 8.5, and the following chemical structure:
Each adhesive topical system contains 180 mg of diclofenac epolamine (13 mg per gram adhesive) in an aqueous base. It also contains the following inactive ingredients: butylene glycol, carboxymethylcellulose sodium, dihydroxyaluminum aminoacetate, edetate disodium, fragrance (Dalin PH), gelatin, kaolin, methylparaben, polysorbate 80, povidone, propylene glycol, propylparaben, sodium polyacrylate, sorbitol solution, tartaric acid, titanium dioxide, and purified water.
5.4 Hypertension
NSAIDs, including DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3%, can lead to new onset of hypertension or worsening of preexisting hypertension, either of which may contribute to the increased incidence of CV events. Patients taking angiotensin converting enzyme (ACE) inhibitors, thiazide diuretics, or loop diuretics may have impaired response to these therapies when taking NSAIDs [ see Drug Interactions (7) ].
Monitor blood pressure (BP) during the initiation of NSAID treatment and throughout the course of therapy.
5.16 Eye Exposure
Avoid contact of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% with eyes and mucosa. Advise patients that if eye contact occurs, immediately wash out the eye with water or saline and consult a physician if irritation persists for more than an hour.
8.4 Pediatric Use
The safety and effectiveness of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% have been established in pediatric patients 6 years and older based on evidence from adequate and well-controlled studies with DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3 % in adults, as well as an open-label study in pediatric patients 6 years and older. The pediatric study enrolled 104 patients, 6 years of age and older with minor soft tissue injuries. One DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3 % was applied to the injury site twice daily for a maximum of 14 days or until treatment was no longer required for pain management, whichever occurred first. Based on the available data from the pediatric study, the safety profile of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3 % topical system in pediatric patients is similar to that in adults. The safety and effectiveness of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3 % has not been investigated in pediatric patients less than 6 years old. [ see Clinical Trials Experience (6.1), Clinical Pharmacology (12.3) ].
8.5 Geriatric Use
Elderly patients, compared to younger patients, are at greater risk for NSAID-associated serious cardiovascular, gastrointestinal, and/or renal adverse reactions. If the anticipated benefit for the elderly patient outweighs these potential risks, start dosing at the low end of the dosing range, and monitor patients for adverse effects [ see Warnings and Precautions (5.1, 5.2, 5.3, 5.6, 5.14)].
Clinical studies of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% did not include sufficient numbers of subjects aged 65 and over to determine whether they respond differently from younger subjects. Other reported clinical experience has not identified differences in responses between the elderly and younger patients.
5.3 Hepatotoxicity
In clinical trials of oral diclofenac containing products, meaningful elevations (i.e., more than 3 times the ULN) of AST (SGOT) were observed in about 2% of approximately 5,700 patients at some time during diclofenac treatment (ALT was not measured in all studies).
In a large open-label, controlled trial of 3,700 patients treated with oral diclofenac sodium for 2-6 months, patients were monitored first at 8 weeks and 1,200 patients were monitored again at 24 weeks. Meaningful elevations of ALT and/or AST occurred in about 4% of the 3,700 patients and included marked elevations (greater than 8 times the ULN) in about 1% of the 3,700 patients. In that open-label study, a higher incidence of borderline (less than 3 times the ULN), moderate (3-8 times the ULN), and marked (greater than 8 times the ULN) elevations of ALT or AST was observed in patients receiving diclofenac when compared to other NSAIDs. Elevations in transaminases were seen more frequently in patients with osteoarthritis than in those with rheumatoid arthritis.
Almost all meaningful elevations in transaminases were detected before patients became symptomatic. Abnormal tests occurred during the first 2 months of therapy with diclofenac in 42 of the 51 patients in all trials who developed marked transaminase elevations.
In postmarketing reports, cases of drug-induced hepatotoxicity have been reported in the first month, and in some cases, the first 2 months of therapy, but can occur at any time during treatment with diclofenac. Postmarketing surveillance has reported cases of severe hepatic reactions, including liver necrosis, jaundice, fulminant hepatitis with and without jaundice, and liver failure. Some of these reported cases resulted in fatalities or liver transplantation.
In a European retrospective population-based, case-controlled study, 10 cases of diclofenac associated drug-induced liver injury with current use compared with non-use of diclofenac were associated with a statistically significant 4-fold adjusted odds ratio of liver injury. In this particular study, based on an overall number of 10 cases of liver injury associated with diclofenac, the adjusted odds ratio increased further with female gender, doses of 150 mg or more, and duration of use for more than 90 days.
Physicians should measure transaminases at baseline and periodically in patients receiving long-term therapy with diclofenac, because severe hepatotoxicity may develop without a prodrome of distinguishing symptoms. The optimum times for making the first and subsequent transaminase measurements are not known. Based on clinical trial data and postmarketing experiences, transaminases should be monitored within 4 to 8 weeks after initiating treatment with diclofenac. However, severe hepatic reactions can occur at any time during treatment with diclofenac.
If abnormal liver tests persist or worsen, if clinical signs and/or symptoms consistent with liver disease develop, or if systemic manifestations occur (e.g., eosinophilia, rash, abdominal pain, diarrhea, dark urine, etc.), DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% should be discontinued immediately.
Inform patients of the warning signs and symptoms of hepatotoxicity (e.g., nausea, fatigue, lethargy, diarrhea, pruritus, jaundice, right upper quadrant tenderness, and "flu-like" symptoms). If clinical signs and symptoms consistent with liver disease develop, or if systemic manifestations occur (e.g., eosinophilia, rash, etc.), discontinue DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% immediately, and perform a clinical evaluation of the patient.
To minimize the potential risk for an adverse liver related event in patients treated with DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3%, use the lowest effective dose for the shortest duration possible. Exercise caution when prescribing DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% with concomitant drugs that are known to be potentially hepatotoxic (e.g., acetaminophen, antibiotics, anti-epileptics).
4 Contraindications (4 CONTRAINDICATIONS)
DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is contraindicated in the following patients:
- Known hypersensitivity (e.g., anaphylactic reactions and serious skin reactions) to diclofenac or any components of the drug product [ see Warnings and Precautions (5.7, 5.9) ]
- History of asthma, urticaria, or other allergic-type reactions after taking aspirin or other NSAIDs. Severe, sometimes fatal, anaphylactic reactions to NSAIDs have been reported in such patients [ see Warnings and Precautions (5.7, 5.8) ]
- In the setting of coronary artery bypass graft (CABG) surgery [ see Warnings and Precautions (5.1) ]
- DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is contraindicated for use on non-intact or damaged skin resulting from any etiology, including exudative dermatitis, eczema, infection lesions, burns or wounds.
6 Adverse Reactions (6 ADVERSE REACTIONS)
The following adverse reactions are discussed in greater detail in other sections of the labeling:
- Cardiovascular Thrombotic Events [ see Warnings and Precautions (5.1) ]
- GI Bleeding, Ulceration and Perforation [ see Warnings and Precautions (5.2) ]
- Hepatotoxicity [ see Warnings and Precautions (5.3) ]
- Hypertension [ see Warnings and Precautions (5.4) ]
- Heart Failure and Edema [ see Warnings and Precautions (5.5) ]
- Renal Toxicity and Hyperkalemia [ see Warnings and Precautions (5.6) ]
- Anaphylactic Reactions [ see Warnings and Precautions (5.7) ]
- Serious Skin Reactions [ see Warnings and Precautions (5.9) ]
- Hematologic Toxicity [ see Warnings and Precautions (5.12) ]
7 Drug Interactions (7 DRUG INTERACTIONS)
See Table 2 for clinically significant drug interactions with diclofenac.
| Drugs That Interfere with Hemostasis | |
| Clinical Impact: |
|
| Intervention: | Monitor patients with concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% with anticoagulants (e.g., warfarin), antiplatelet agents (e.g., aspirin), selective serotonin reuptake inhibitors (SSRIs), and serotonin norepinephrine reuptake inhibitors (SNRIs) for signs of bleeding [ see Warnings and Precautions (5.12) ]. |
| Aspirin | |
| Clinical Impact: | Controlled clinical studies showed that the concomitant use of NSAIDs and analgesic doses of aspirin does not produce any greater therapeutic effect than the use of NSAIDs alone. In a clinical study, the concomitant use of an NSAID and aspirin was associated with a significantly increased incidence of GI adverse reactions as compared to use of the NSAID alone [ see Warnings and Precautions (5.2) ]. |
| Intervention: | Concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and analgesic doses of aspirin is not generally recommended because of the increased risk of bleeding [
see
Warnings and Precautions (5.12)
].
DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is not a substitute for low dose aspirin for cardiovascular protection. |
| ACE Inhibitors, Angiotensin Receptor Blockers, and Beta-Blockers | |
| Clinical Impact: |
|
| Intervention: |
|
| Diuretics | |
| Clinical Impact: | Clinical studies, as well as post-marketing observations, showed that NSAIDs reduced the natriuretic effect of loop diuretics (e.g., furosemide) and thiazide diuretics in some patients. This effect has been attributed to the NSAID inhibition of renal prostaglandin synthesis. |
| Intervention: | During concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% with diuretics, observe patients for signs of worsening renal function, in addition to assuring diuretic efficacy including antihypertensive effects [ see Warnings and Precautions (5.6) ]. |
| Digoxin | |
| Clinical Impact: | The concomitant use of diclofenac with digoxin has been reported to increase the serum concentration and prolong the half-life of digoxin. |
| Intervention: | During concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and digoxin, monitor serum digoxin levels. |
| Lithium | |
| Clinical Impact: | NSAIDs have produced elevations in plasma lithium levels and reductions in renal lithium clearance .The mean minimum lithium concentration increased 15%, and the renal clearance decreased by approximately 20%. This effect has been attributed to NSAID inhibition of renal prostaglandin synthesis. |
| Intervention: | During concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and lithium, monitor patients for signs of lithium toxicity. |
| Methotrexate | |
| Clinical Impact: | Concomitant use of NSAIDs and methotrexate may increase the risk for methotrexate toxicity (e.g., neutropenia, thrombocytopenia, renal dysfunction). |
| Intervention: | During concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and methotrexate, monitor patients for methotrexate toxicity. |
| Cyclosporine | |
| Clinical Impact: | Concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and cyclosporine may increase cyclosporine's nephrotoxicity. |
| Intervention: | During concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and cyclosporine, monitor patients for signs of worsening renal function. |
| NSAIDs and Salicylates | |
| Clinical Impact: | Concomitant use of diclofenac with other NSAIDs or salicylates (e.g., diflunisal, salsalate) increases the risk of GI toxicity, with little or no increase in efficacy [ see Warnings and Precautions (5.2) ] . |
| Intervention: | The concomitant use of diclofenac with other NSAIDs or salicylates is not recommended. |
| Pemetrexed | |
| Clinical Impact: | Concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and pemetrexed may increase the risk of pemetrexed-associated myelosuppression, renal, and GI toxicity (see the pemetrexed prescribing information). |
| Intervention: | During concomitant use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and pemetrexed, in patients with renal impairment whose creatinine clearance ranges from 45 to 79 mL/min, monitor for myelosuppression, renal and GI toxicity.
NSAIDs with short elimination half-lives (e.g., diclofenac, indomethacin) should be avoided for a period of two days before, the day of, and two days following administration of pemetrexed. In the absence of data regarding potential interaction between pemetrexed and NSAIDs with longer half-lives (e.g., meloxicam, nabumetone), patients taking these NSAIDs should interrupt dosing for at least five days before, the day of, and two days following pemetrexed administration. |
12.2 Pharmacodynamics
DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% applied to intact skin provides local analgesia by releasing diclofenac epolamine from the topical system into the skin.
1 Indications and Usage (1 INDICATIONS AND USAGE)
DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is indicated for the topical treatment of acute pain due to minor strains, sprains, and contusions in adults and pediatric patients 6 years and older.
2.2 Special Precautions
- Inform patients that, if DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% begins to peel-off, the edges of the topical system may be taped down. If problems with adhesion persist, patients may overlay the topical system with a mesh netting sleeve, where appropriate (e.g. to secure topical systems applied to ankles, knees, or elbows). The mesh netting sleeve (e.g. Curad® Hold Tite™, Surgilast® Tubular Elastic Dressing) must allow air to pass through and not be occlusive (non-breathable).
- Do not apply DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% to non-intact or damaged skin resulting from any etiology e.g. exudative dermatitis, eczema, infected lesion, burns or wounds.
- Do not wear a DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% when bathing or showering.
- Wash your hands after applying, handling or removing the topical system.
- Avoid eye contact.
- Do not use combination therapy with DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and an oral NSAID unless the benefit outweighs the risk and conduct periodic laboratory evaluations.
12.1 Mechanism of Action
Diclofenac has analgesic, anti-inflammatory, and antipyretic properties.
The mechanism of action of diclofenac, like that of other NSAIDs, is not completely understood but involves inhibition of cyclooxygenase (COX-1 and COX-2).
Diclofenac is a potent inhibitor of prostaglandin synthesis in vitro. Diclofenac concentrations reached during therapy have produced in vivo effects. Prostaglandins sensitize afferent nerves and potentiate the action of bradykinin in inducing pain in animal models. Prostaglandins are mediators of inflammation. Because diclofenac is an inhibitor of prostaglandin synthesis, its mode of action may be due to a decrease of prostaglandins in peripheral tissues.
5.12 Hematologic Toxicity
Anemia has occurred in NSAID-treated patients. This may be due to occult or gross blood loss, fluid retention, or an incompletely described effect on erythropoiesis. If a patient treated with DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% has any signs or symptoms of anemia, monitor hemoglobin or hematocrit.
NSAIDs, including DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3%, may increase the risk of bleeding events. Co-morbid conditions such as coagulation disorders, concomitant use of warfarin, other anticoagulants, antiplatelet agents (e.g., aspirin), serotonin reuptake inhibitors (SSRIs) and serotonin norepinephrine reuptake inhibitors (SNRIs) may increase this risk. Monitor these patients for signs of bleeding [ see Drug Interactions (7) ].
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
- Hepatotoxicity: Inform patients of warning signs and symptoms of hepatotoxicity. Discontinue if abnormal liver tests persist or worsen or if clinical signs and symptoms of liver disease develop ( 5.3)
- Hypertension: Patients taking some antihypertensive medications may have impaired response to these therapies when taking NSAIDs. Monitor blood pressure ( 5.4, 7)
- Heart Failure and Edema:Avoid use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% in patients with severe heart failure unless benefits are expected to outweigh risk of worsening heart failure ( 5.5)
- Renal Toxicity:Monitor renal function in patients with renal or hepatic impairment, heart failure, dehydration, or hypovolemia. Avoid use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% in patients with advanced renal disease unless benefits are expected to outweigh risk of worsening renal function ( 5.6)
- Anaphylactic Reactions: Seek emergency help if an anaphylactic reaction occurs ( 5.7)
- Exacerbation of Asthma Related to Aspirin Sensitivity: DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is contraindicated in patients with aspirin-sensitive asthma. Monitor patients with preexisting asthma (without aspirin sensitivity) ( 5.8)
- Serious Skin Reactions:Discontinue DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% at first appearance of skin rash or other signs of hypersensitivity ( 5.9)
- Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS): Discontinue and evaluate clinically ( 5.10).
- Fetal Toxicity: Limit use of NSAIDs, including DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3 % between about 20 to 30 weeks in pregnancy due to the risk of oligohydramnios/fetal renal dysfunction. Avoid use of NSAIDs in women at about 30 weeks gestation and later in pregnancy due to the risks of oligohydramnios/fetal renal dysfunction and premature closure of the fetal ductus arteriosus ( 5.11, 8.1).
- Hematologic Toxicity: Monitor hemoglobin or hematocrit in patients with any signs or symptoms of anemia ( 5.12, 7)
5.14 Laboratory Monitoring
Because serious GI bleeding, hepatotoxicity, and renal injury can occur without warning symptoms or signs, consider monitoring patients on long-term NSAID treatment with a CBC and a chemistry profile periodically [ see Warnings and Precautions (5.2, 5.3, 5.6) ].
5.7 Anaphylactic Reactions
Diclofenac has been associated with anaphylactic reactions in patients with and without known hypersensitivity to diclofenac and in patients with aspirin-sensitive asthma [see Contraindications (4)and Warnings and Precautions (5.8) ]. Seek emergency help if an anaphylactic reaction occurs.
5.9 Serious Skin Reactions
NSAIDs, including diclofenac, can cause serious skin adverse reactions such as exfoliative dermatitis, Stevens-Johnson Syndrome (SJS), and toxic epidermal necrolysis (TEN), which can be fatal.NSAIDs can also cause fixed drug eruption (FDE). FDE may present as a more severe variant known as generalized bullous fixed drug eruption (GBFDE), which can be life-threatening. These serious events may occur without warning. Inform patients about the signs and symptoms of serious skin reactions, and to discontinue the use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% at the first appearance of skin rash or any other sign of hypersensitivity. DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is contraindicated in patients with previous serious skin reactions to NSAIDs [ see Contraindications (4) ].
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
- Use the lowest effective dosage for shortest duration consist with the individual patient treatment goals ( 2.1)
- The recommended dose of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% for adults and pediatric patients 6 years and older is one (1) topical system to the most painful area twice a day. ( 2)
- DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% should not be applied to damaged or non-intact skin. ( 2)
5.5 Heart Failure and Edema
The Coxib and traditional NSAID Trialists' Collaboration meta-analysis of randomized controlled trials demonstrated an approximately two-fold increase in hospitalizations for heart failure in COX-2 selective-treated patients and nonselective NSAID-treated patients compared to placebo-treated patients. In a Danish National Registry study of patients with heart failure, NSAID use increased the risk of MI, hospitalization for heart failure, and death.
Additionally, fluid retention and edema have been observed in some patients treated with NSAIDs. Use of diclofenac may blunt the CV effects of several therapeutic agents used to treat these medical conditions (e.g., diuretics, ACE inhibitors, or angiotensin receptor blockers [ARBs]) [ see Drug Interactions (7) ].
Avoid the use of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% in patients with severe heart failure unless the benefits are expected to outweigh the risk of worsening heart failure. If DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is used in patients with severe heart failure, monitor patients for signs of worsening heart failure.
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
Diclofenac Epolamine Topical System is a 10 cm × 14 cm topical system that contains 1.3% diclofenac epolamine, and is debossed with YARAL <DICLOFENAC EPOLAMINE TOPICAL SYSTEM> 1.3%.
6.2 Postmarketing Experience
The following adverse reactions have been identified during post-approval use of diclofenac.
Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Skin and Appendages: Exfoliative dermatitis, Stevens-Johnson Syndrome (SJS), toxic epidermal necrolysis (TEN), and fixed drug eruption (FDE).
8 Use in Specific Populations (8 USE IN SPECIFIC POPULATIONS)
- Infertility: NSAIDs are associated with reversible infertility. Consider withdrawal of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% in women who have difficulties conceiving ( 8.3)
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared with rates in the clinical trials of another drug and may not reflect the rates observed in practice.
2.1 General Dosing Instructions
Use the lowest effective dosage for the shortest duration consistent with individual patient treatment goals [ see Warnings and Precautions (5) ].
The recommended dose of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is one (1) topical system to the most painful area twice a day both in adults and pediatric patients 6 years of age and older.
17 Patient Counseling Information (17 PATIENT COUNSELING INFORMATION)
Advise the patient to read the FDA-approved patient labeling (Medication Guide) that accompanies each prescription dispensed, as well as the Directions for Use on the product packaging. Inform patients, families, or their caregivers of the following information before initiating therapy with DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and periodically during the course of ongoing therapy.
16 How Supplied/storage and Handling (16 HOW SUPPLIED/STORAGE AND HANDLING)
The DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is supplied in resealable envelopes, each containing 5 topical systems (10 cm × 14 cm), with 6 envelopes per box (NDC 85509-1405-3). Each individual topical system is debossed with "YARAL < DICLOFENAC EPOLAMINE TOPICAL SYSTEM > 1.3%".
- The product is intended for topical use only.
- Keep out of reach of children and pets.
- Envelopes should be sealed at all times when not in use.
- Curad® Hold Tite™ is a trademark of Medline Industries, Inc., and Surgilast® Tubular Elastic Dressing is a trademark of Derma Sciences, Inc.
Repackaged/Relabeled by:
PHOENIX RX LLC
Hatboro, PA 19040
5.1 Cardiovascular Thrombotic Events
Clinical trials of several COX-2 selective and nonselective NSAIDs of up to three years duration have shown an increased risk of serious cardiovascular (CV) thrombotic events, including myocardial infarction (MI) and stroke, which can be fatal. Based on available data, it is unclear that the risk for CV thrombotic events is similar for all NSAIDs. The relative increase in serious CV thrombotic events over baseline conferred by NSAID use appears to be similar in those with and without known CV disease or risk factors for CV disease. However, patients with known CV disease or risk factors had a higher absolute incidence of excess serious CV thrombotic events, due to their increased baseline rate. Some observational studies found that this increased risk of serious CV thrombotic events began as early as the first weeks of treatment. The increase in CV thrombotic risk has been observed most consistently at higher doses.
To minimize the potential risk for an adverse CV event in NSAID-treated patients, use the lowest effective dose for the shortest duration possible. Physicians and patients should remain alert for the development of such events, throughout the entire treatment course, even in the absence of previous CV symptoms. Patients should be informed about the symptoms of serious CV events and the steps to take if they occur.
There is no consistent evidence that concurrent use of aspirin mitigates the increased risk of serious CV thrombotic events associated with NSAID use. The concurrent use of aspirin and an NSAID, such as diclofenac, increases the risk of serious gastrointestinal (GI) events [ see Warnings and Precautions (5.2) ].
5.15 Accidental Exposure in Children
Even a used DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% contains a large amount of diclofenac epolamine (as much as 170 mg). The potential therefore exists for a small child or pet to suffer serious adverse effects from chewing or ingesting a new or used DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3%. It is important for patients to store and dispose of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% out of the reach of children and pets.
14.1 Strains, Sprains, and Contusions
Efficacy of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% was demonstrated in two of four studies of patients with minor strains, sprains, and contusions. Patients were randomly assigned to treatment with the DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3%, or a placebo identical to the DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% minus the active ingredient. In the first of these two studies, patients with ankle sprains were treated once daily for a week. In the second study, patients with strains, sprains and contusions were treated twice daily for up to two weeks. Pain was assessed over the period of treatment. Patients treated with the DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% experienced a greater reduction in pain as compared to patients randomized to placebo as evidenced by the responder curves presented below ( Figures 1-4).
Figure 1: Patients Achieving Various Levels of Pain Relief at Day 3; 14-Day Study
Figure 2: Patients Achieving Various Levels of Pain Relief at End of Study; 14-Day Study
Figure 3: Patients Achieving Various Levels of Pain Relief at Day 3; 7-Day Study
Figure 4: Patients Achieving Various Levels of Pain Relief at End of Study; 7-Day Study
5.13 Masking of Inflammation and Fever
The pharmacological activity of DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% in reducing inflammation, and possibly fever, may diminish the utility of diagnostic signs in detecting infections.
5.17 Oral Nonsteroidal Anti Inflammatory Drugs (5.17 Oral Nonsteroidal Anti-inflammatory Drugs)
Concomitant use of oral and topical NSAIDs may result in a higher rate of hemorrhage, more frequent abnormal creatinine, urea and hemoglobin. Do not use combination therapy with DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and an oral NSAID unless the benefit outweighs the risk.
Principal Display Panel 30 Topical System Pouch Carton (PRINCIPAL DISPLAY PANEL - 30 Topical System Pouch Carton)
NDC 85509-1405-3
diclofenac epolamine
topical system 1.3%
30 TOPICAL SYSTEMS (10 CM X 14 CM EACH)
Dispense with enclosed Medication Guide
Change diclofenac epolamine topical system once every 12 hours
Fold used topical systems so that the adhesive side sticks to itself and
safely discard used topical systems where children and pets cannot get them.
Rx only
5.8 Exacerbation of Asthma Related to Aspirin Sensitivity
A subpopulation of patients with asthma may have aspirin-sensitive asthma which may include chronic rhinosinusitis complicated by nasal polyps; severe, potentially fatal bronchospasm; and/or intolerance to aspirin and other NSAIDs. Because cross-reactivity between aspirin and other NSAIDs has been reported in such aspirin-sensitive patients, DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is contraindicated in patients with this form of aspirin sensitivity [ see Contraindications (4) ]. When DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is used in patients with preexisting asthma (without known aspirin sensitivity), monitor patients for changes in the signs and symptoms of asthma.
5.2 Gastrointestinal Bleeding, Ulceration, and Perforation
NSAIDs, including diclofenac, cause serious gastrointestinal (GI) adverse events including inflammation, bleeding, ulceration, and perforation of the esophagus, stomach, small intestine, or large intestine, which can be fatal. These serious adverse events can occur at any time, with or without warning symptoms, in patients treated with NSAIDs.
Only one in five patients who develop a serious upper GI adverse event on NSAID therapy is symptomatic. Upper GI ulcers, gross bleeding, or perforation caused by NSAIDs occurred in approximately 1% of patients treated for 3-6 months, and in about 2%-4% of patients treated for one year. However, even short-term NSAID therapy is not without risk.
5.10 Drug Reaction With Eosinophilia and Systemic Symptoms (dress) (5.10 Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS))
Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS) has been reported in patients taking NSAIDs such as DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% . Some of these events have been fatal or life-threatening. DRESS typically, although not exclusively, presents with fever, rash, lymphadenopathy, and/or facial swelling. Other clinical manifestations may include hepatitis, nephritis, hematological abnormalities, myocarditis, or myositis. Sometimes symptoms of DRESS may resemble an acute viral infection. Eosinophilia is often present. Because this disorder is variable in its presentation, other organ systems not noted here may be involved.
It is important to note that early manifestations of hypersensitivity, such as fever or lymphadenopathy, may be present even though rash is not evident. If such signs or symptoms are present, discontinue DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% and evaluate the patient immediately
Warning: Risk of Serious Cardiovascular and Gastrointestinal Events (WARNING: RISK OF SERIOUS CARDIOVASCULAR and GASTROINTESTINAL EVENTS)
WARNING: RISK OF SERIOUS CARDIOVASCULAR and GASTROINTESTINAL EVENTS
See full prescribing information for complete boxed warning.
- Nonsteroidal anti-inflammatory drugs (NSAIDs) cause an increased risk of serious cardiovascular thrombotic events, including myocardial infarction and stroke, which can be fatal. This risk may occur early in treatment and may increase with duration of use ( 5.1)
- DICLOFENAC EPOLAMINE TOPICAL SYSTEM 1.3% is contraindicated in the setting of coronary artery bypass graft (CABG) surgery ( 4, 5.1)
- NSAIDs cause an increased risk of serious gastrointestinal (GI) adverse events including bleeding, ulceration, and perforation of the stomach or intestines, which can be fatal. These events can occur at any time during use and without warning symptoms. Elderly patients and patients with a prior history of peptic ulcer disease and/or GI bleeding are at greater risk for serious GI events ( 5.2)
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:49:55.892010 · Updated: 2026-03-14T22:35:08.076257