Ndc 59088-247-07
3f2f0f2b-2759-c010-e063-6394a90a8e5e
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
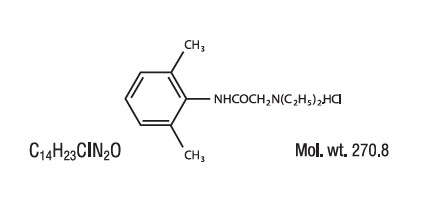
Lidocaine 5% Gel contains 50 mg of Lidocaine HCI per gram in a mild acidic vehicle with Aqua (Purified Water), Aloe Barbadensis (Aloe Vera) Leaf Juice, Caprylyl Glycol, Carbomer, Chlorphenesin, Cucumis Sativus (Cucumber) Fruit Extract, Dimethicone, Glycerin, Phenoxyethanol, Propanediol, Propylene Glycol, Sodium Hydroxide. Lidocaine HCl is chemically designated as acetamide, 2-(diethylamino)-N-(2,6 dimethylphenyl), and has the following structure:
Contraindications
Tuberculous or fungal lesions of skin vaccinia, varicella and acute herpes simplex and in persons who have shown hypersensitivity to any of its components. Lidocaine is contraindicated in patients with a known history of hypersensitivity to local anesthetics of the amide type.
Adverse Reactions
During or immediately after treatment, the skin at the site of treatment may develop erythema or edema or may be the locus of abnormal sensation.
How Supplied
Lidocaine 5% Gel is supplied in a 3 oz. (85 g) tube with CRC cap (NDC 59088-247-07). KEEP THIS AND ALL MEDICATIONS OUT OF THE REACH OF CHILDREN. Store at 20º-25ºC (68º-77º F) [see USP Controlled Room Temperature]. Protect from freezing.
Medication Information
Contraindications
Tuberculous or fungal lesions of skin vaccinia, varicella and acute herpes simplex and in persons who have shown hypersensitivity to any of its components. Lidocaine is contraindicated in patients with a known history of hypersensitivity to local anesthetics of the amide type.
Adverse Reactions
During or immediately after treatment, the skin at the site of treatment may develop erythema or edema or may be the locus of abnormal sensation.
How Supplied
Lidocaine 5% Gel is supplied in a 3 oz. (85 g) tube with CRC cap (NDC 59088-247-07). KEEP THIS AND ALL MEDICATIONS OUT OF THE REACH OF CHILDREN. Store at 20º-25ºC (68º-77º F) [see USP Controlled Room Temperature]. Protect from freezing.
Description
Lidocaine 5% Gel contains 50 mg of Lidocaine HCI per gram in a mild acidic vehicle with Aqua (Purified Water), Aloe Barbadensis (Aloe Vera) Leaf Juice, Caprylyl Glycol, Carbomer, Chlorphenesin, Cucumis Sativus (Cucumber) Fruit Extract, Dimethicone, Glycerin, Phenoxyethanol, Propanediol, Propylene Glycol, Sodium Hydroxide.
Lidocaine HCl is chemically designated as acetamide, 2-(diethylamino)-N-(2,6 dimethylphenyl), and has the following structure:
Label
Manufactured by:
PureTek Corporation
Panorama City, CA 91402
For questions or information call toll-free:
877-921-7873
Dosage:
Adults and children 12 years of age and older: apply a thin film to the affected areas(s) two or three times per day or as directed by a licensed healthcare practitioner.
Warnings:
For external use only. Not for ophthalmic use.
Indications:
For the temporary relief of pain.
Precautions:
If irritation or sensitivity occurs or infection appears, discontinue use and institute appropriate therapy. Lidocaine 5% Gel should be used with caution in ill, elderly, debilitated patients and children who may be more sensitive to the systemic effects of lidocaine.
How Supplied:
Lidocaine 5% Gel is supplied in a 3 oz. (85 g) tube with CRC cap (NDC 59088-247-07).
KEEP THIS AND ALL MEDICATIONS OUT OF THE REACH OF CHILDREN.
Store at 20º-25ºC (68º-77º F) [see USP Controlled Room Temperature]. Protect from freezing.
Pediatric Use:
Dosage in pediatric patients would be reduced commensurate with age, body weight and physical condition.
Nursing Mothers:
It is not known whether this drug is excreted in human milk. Because many drugs are excreted in human milk, caution should be exercised when this drug is administered to a nursing mother.
Pharmacokinetics:
Lidocaine may be absorbed following topical administration to mucous membranes, its rate and extent of absorption depending upon the specific site of application, duration of exposure, concentration and total dosage. In general, the rate of absorption of local anesthetic agents following topical application occurs most rapidly after intratracheal administration. Lidocaine is also well-absorbed from the gastrointestinal tract, but little intact drug appears in the circulation because of biotransformation in the liver. Lidocaine is metabolized rapidly by the liver and metabolites and unchanged drug are excreted by the kidneys. Biotransformation includes oxidative N-dealkylation, ring hydroxylation, cleavage of the amide linkage and conjugation. N-dealkylation, a major pathway of biotransformation, yields the metabolites monoethylglycinexylidide and glycinexylidide. The pharmacological/ toxicological actions of these metabolites are similar to, but less potent than, those of lidocaine. Approximately 90% of lidocaine administered is excreted in the form of various metabolites and less than 10% is excreted unchanged. The primary metabolite in urine is a conjugate of 4-hydroxy-2, 6-dimethylaniline. The plasma binding of lidocaine is dependent on drug concentration and the fraction bound decreases with increasing concentration. At concentrations of 1 to 4 g of free base per mL, 60 to 80 percent of lidocaine is protein bound. Binding is also dependent on the plasma concentration of the alpha-1-acid glycoprotein. Lidocaine crosses the blood-brain and placental barriers, presumably by passive diffusion. Studies of lidocaine metabolism following intravenous bolus injections have shown that the elimination half-life of this agent is typically 1.5 to 2 hours. Because of the rapid rate at which lidocaine is metabolized, any condition that affects liver function may alter lidocaine kinetics. The half-life may be prolonged two-fold or more in patients with liver dysfunction. Renal dysfunction does not affect lidocaine kinetics, but may increase the accumulation of metabolites. Factors such as acidosis and the use of CNS stimulants and depressants affect the CNS levels of lidocaine required to produce overt systemic effects. Objective adverse manifestations become increasingly apparent with increasing venous plasma levels above 6 g free base per mL. In the rhesus monkey, arterial blood levels of 18-21 g/mL have been shown to be threshold for convulsive activity.
Use in Pregnancy:
Teratogenic Effects; Pregnancy Category B. Reproduction studies have been performed for lidocaine in rats at doses up to 6.6 times the human dose and have revealed no evidence of harm to the fetus caused by lidocaine. There are, however, no adequate and well-controlled studies in pregnant women. Animal reproduction studies are not always predictive of human response. General consideration should be given to this fact before administering lidocaine to women of childbearing potential, especially during early pregnancy when maximum organogenesis takes place.
Adverse Reactions:
During or immediately after treatment, the skin at the site of treatment may develop erythema or edema or may be the locus of abnormal sensation.
Contraindications:
Tuberculous or fungal lesions of skin vaccinia, varicella and acute herpes simplex and in persons who have shown hypersensitivity to any of its components. Lidocaine is contraindicated in patients with a known history of hypersensitivity to local anesthetics of the amide type.
Clinical Pharmacology:
Mechanism of Action: Lidocaine 5% Gel releases lidocaine from a mild acidic vehicle to stabilize the neuronal membrane by inhibiting the ionic fluxes required for initiation and conduction of impulses, thereby effecting local anesthetic action. A mild acidic vehicle lowers pH to increase protection against alkaline irritants and to provide a favorable environment for healing.
Carcinogenesis, Mutagenesis and Impairment of Fertility:
Studies of lidocaine in animals to evaluate the carcinogenic and mutagenic potential of the effect on fertility have not been conducted.
Structured Label Content
Label (LABEL)
Manufactured by:
PureTek Corporation
Panorama City, CA 91402
For questions or information call toll-free:
877-921-7873
Dosage: (DOSAGE:)
Adults and children 12 years of age and older: apply a thin film to the affected areas(s) two or three times per day or as directed by a licensed healthcare practitioner.
Warnings: (WARNINGS:)
For external use only. Not for ophthalmic use.
Description (DESCRIPTION)
Lidocaine 5% Gel contains 50 mg of Lidocaine HCI per gram in a mild acidic vehicle with Aqua (Purified Water), Aloe Barbadensis (Aloe Vera) Leaf Juice, Caprylyl Glycol, Carbomer, Chlorphenesin, Cucumis Sativus (Cucumber) Fruit Extract, Dimethicone, Glycerin, Phenoxyethanol, Propanediol, Propylene Glycol, Sodium Hydroxide.
Lidocaine HCl is chemically designated as acetamide, 2-(diethylamino)-N-(2,6 dimethylphenyl), and has the following structure:
Indications: (INDICATIONS:)
For the temporary relief of pain.
Precautions: (PRECAUTIONS:)
If irritation or sensitivity occurs or infection appears, discontinue use and institute appropriate therapy. Lidocaine 5% Gel should be used with caution in ill, elderly, debilitated patients and children who may be more sensitive to the systemic effects of lidocaine.
How Supplied: (HOW SUPPLIED:)
Lidocaine 5% Gel is supplied in a 3 oz. (85 g) tube with CRC cap (NDC 59088-247-07).
KEEP THIS AND ALL MEDICATIONS OUT OF THE REACH OF CHILDREN.
Store at 20º-25ºC (68º-77º F) [see USP Controlled Room Temperature]. Protect from freezing.
Pediatric Use:
Dosage in pediatric patients would be reduced commensurate with age, body weight and physical condition.
Nursing Mothers:
It is not known whether this drug is excreted in human milk. Because many drugs are excreted in human milk, caution should be exercised when this drug is administered to a nursing mother.
Pharmacokinetics:
Lidocaine may be absorbed following topical administration to mucous membranes, its rate and extent of absorption depending upon the specific site of application, duration of exposure, concentration and total dosage. In general, the rate of absorption of local anesthetic agents following topical application occurs most rapidly after intratracheal administration. Lidocaine is also well-absorbed from the gastrointestinal tract, but little intact drug appears in the circulation because of biotransformation in the liver. Lidocaine is metabolized rapidly by the liver and metabolites and unchanged drug are excreted by the kidneys. Biotransformation includes oxidative N-dealkylation, ring hydroxylation, cleavage of the amide linkage and conjugation. N-dealkylation, a major pathway of biotransformation, yields the metabolites monoethylglycinexylidide and glycinexylidide. The pharmacological/ toxicological actions of these metabolites are similar to, but less potent than, those of lidocaine. Approximately 90% of lidocaine administered is excreted in the form of various metabolites and less than 10% is excreted unchanged. The primary metabolite in urine is a conjugate of 4-hydroxy-2, 6-dimethylaniline. The plasma binding of lidocaine is dependent on drug concentration and the fraction bound decreases with increasing concentration. At concentrations of 1 to 4 g of free base per mL, 60 to 80 percent of lidocaine is protein bound. Binding is also dependent on the plasma concentration of the alpha-1-acid glycoprotein. Lidocaine crosses the blood-brain and placental barriers, presumably by passive diffusion. Studies of lidocaine metabolism following intravenous bolus injections have shown that the elimination half-life of this agent is typically 1.5 to 2 hours. Because of the rapid rate at which lidocaine is metabolized, any condition that affects liver function may alter lidocaine kinetics. The half-life may be prolonged two-fold or more in patients with liver dysfunction. Renal dysfunction does not affect lidocaine kinetics, but may increase the accumulation of metabolites. Factors such as acidosis and the use of CNS stimulants and depressants affect the CNS levels of lidocaine required to produce overt systemic effects. Objective adverse manifestations become increasingly apparent with increasing venous plasma levels above 6 g free base per mL. In the rhesus monkey, arterial blood levels of 18-21 g/mL have been shown to be threshold for convulsive activity.
Use in Pregnancy:
Teratogenic Effects; Pregnancy Category B. Reproduction studies have been performed for lidocaine in rats at doses up to 6.6 times the human dose and have revealed no evidence of harm to the fetus caused by lidocaine. There are, however, no adequate and well-controlled studies in pregnant women. Animal reproduction studies are not always predictive of human response. General consideration should be given to this fact before administering lidocaine to women of childbearing potential, especially during early pregnancy when maximum organogenesis takes place.
Adverse Reactions: (ADVERSE REACTIONS:)
During or immediately after treatment, the skin at the site of treatment may develop erythema or edema or may be the locus of abnormal sensation.
Contraindications: (CONTRAINDICATIONS:)
Tuberculous or fungal lesions of skin vaccinia, varicella and acute herpes simplex and in persons who have shown hypersensitivity to any of its components. Lidocaine is contraindicated in patients with a known history of hypersensitivity to local anesthetics of the amide type.
Clinical Pharmacology: (CLINICAL PHARMACOLOGY:)
Mechanism of Action: Lidocaine 5% Gel releases lidocaine from a mild acidic vehicle to stabilize the neuronal membrane by inhibiting the ionic fluxes required for initiation and conduction of impulses, thereby effecting local anesthetic action. A mild acidic vehicle lowers pH to increase protection against alkaline irritants and to provide a favorable environment for healing.
Carcinogenesis, Mutagenesis and Impairment of Fertility:
Studies of lidocaine in animals to evaluate the carcinogenic and mutagenic potential of the effect on fertility have not been conducted.
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:49:43.475561 · Updated: 2026-03-14T22:34:21.968394