Risperidone Tablets, Usp
3d4c51e2-b09b-9fd0-e063-6294a90ae699
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
Elderly patients with dementia-related psychosis treated with antipsychotic drugs are at an increased risk of death. Risperidone is not approved for the treatment of patients with dementia-related psychosis. [see Warnings and Precautions (5.1) ]
Indications and Usage
Risperidone is an atypical antipsychotic indicated for: Treatment of schizophrenia ( 1.1 ) As monotherapy or adjunctive therapy with lithium or valproate, for the treatment of acute manic or mixed episodes associated with Bipolar I Disorder ( 1.2 ) Treatment of irritability associated with autistic disorder ( 1.3 )
Dosage and Administration
Table 1. Recommended Daily Dosage by Indication Initial Dose Titration (Increments) Target Dose Effective Dose Range Schizophrenia: adults ( 2.1 ) 2 mg 1 to 2 mg 4 to 8 mg 4 to 16 mg Schizophrenia: adolescents ( 2.2 ) 0.5 mg 0.5 to 1 mg 3 mg 1 to 6 mg Bipolar mania: adults ( 2.2 ) 2 to 3 mg 1 mg 1 to 6 mg 1 to 6 mg Bipolar mania: children and adolescents ( 2.2 ) 0.5 mg 0.5 to 1 mg 1 to 2.5 mg 1 to 6 mg Irritability in autistic disorder ( 2.3 ) 0.25 mg Can increase to 0.5 mg by Day 4: (body weight less than 20 kg) After Day 4, at intervals of > 2 weeks: 0.25 mg (body weight less than 20 kg) 0.5 mg: (body weight less than 20 kg) 0.5 to 3 mg 0.5 mg Can increase to 1 mg by Day 4: (body weight greater than or equal to 20 kg) 0.5 mg (body weight greater than or equal to 20 kg) 1 mg: (body weight greater than or equal to 20 kg) Severe Renal and Hepatic Impairment in Adults: use a lower starting dose of 0.5 mg twice daily. May increase to dosages above 1.5 mg twice daily at intervals of one week or longer.
Warnings and Precautions
Cerebrovascular events, including stroke, in elderly patients with dementia-related psychosis: risperidone is not approved for use in patients with dementia-related psychosis. ( 5.2 ) Neuroleptic Malignant Syndrome: Manage with immediate discontinuation of risperidone and close monitoring. ( 5.3 ) Tardive dyskinesia: Consider discontinuing risperidone if clinically indicated. ( 5.4 ) Metabolic Changes: Atypical antipsychotic drugs have been associated with metabolic changes that may increase cardiovascular/ cerebrovascular risk. These metabolic changes include hyperglycemia, dyslipidemia, and weight gain. ( 5.5 ) Hyperglycemia and Diabetes Mellitus: Monitor patients for symptoms of hyperglycemia including polydipsia, polyuria, polyphagia, and weakness. Monitor glucose regularly in patients with diabetes or at risk for diabetes. ( 5.5 ) Dyslipidemia: Undesirable alterations have been observed in patients treated with atypical antipsychotics. ( 5.5 ) Weight Gain: Significant weight gain has been reported. Monitor weight gain. ( 5.5 ) Hyperprolactinemia: Prolactin elevations occur and persist during chronic administration. ( 5.6 ) Orthostatic hypotension: For patients at risk, consider a lower starting dose and slower titration. ( 5.7 ) Leukopenia, Neutropenia, and Agranulocytosis: Perform complete blood counts in patients with a history of clinically significant low white blood cell count (WBC). Consider discontinuing risperidone if a clinically significant decline in WBC occurs in the absence of other causative factors. ( 5.9 ) Potential for cognitive and motor impairment: Use caution when operating machinery. ( 5.10 ) Seizures: Use cautiously in patients with a history of seizures or with conditions that lower the seizure threshold. ( 5.11 )
Contraindications
Risperidone is contraindicated in patients with a known hypersensitivity to either risperidone or paliperidone, or to any of the excipients in the risperidone formulation. Hypersensitivity reactions, including anaphylactic reactions and angioedema, have been reported in patients treated with risperidone and in patients treated with paliperidone. Paliperidone is a metabolite of risperidone.
Adverse Reactions
Cerebrovascular adverse reactions (e.g., stroke, transient ischemic attack), including fatalities, were reported in patients (mean age 85 years; range 73- 97) in trials of risperidone in elderly patients with dementia-related psychosis. In placebo-controlled trials, there was a significantly higher incidence of cerebrovascular adverse events in patients treated with risperidone compared to patients treated with placebo. Risperidone is not approved for the treatment of patients with dementia-related psychosis [see Boxed Warning and Warnings and Precautions (5.1) ] .
Drug Interactions
When risperidone is co-administered with enzyme inducers (e.g., carbamazepine), the dose of risperidone should be increased up to double the patient's usual dose. It may be necessary to decrease the risperidone dose when enzyme inducers such as carbamazepine are discontinued [see Drug Interactions (7.1) ] . Similar effect may be expected with co-administration of risperidone with other enzyme inducers (e.g., phenytoin, rifampin, and phenobarbital). When fluoxetine or paroxetine is co-administered with risperidone, the dose of risperidone should be reduced. The risperidone dose should not exceed 8 mg per day in adults when co-administered with these drugs. When initiating therapy, risperidone should be titrated slowly. It may be necessary to increase the risperidone dose when enzyme inhibitors such as fluoxetine or paroxetine are discontinued [see Drug Interactions (7.1) ] .
Storage and Handling
Store at 20-25°C (68-77°F); excursions permitted to 15°-30°C (59°-86°F) [see USP Controlled Room Temperature]. Protect from light and moisture. Keep out of reach of children.
How Supplied
Risperidone Tablets, USP 0.25 mg are available as dark yellow, film-coated, capsule-shaped, convex tablet, debossed "R1" on one side and "R" on the other side, packaged as follows: Risperidone Tablets, USP 0.5 mg are available as reddish brown, film-coated, capsule-shaped, convex tablet, debossed "R2" on one side and "R" on the other side, packaged as follows: Risperidone Tablets, USP 1 mg are available as white, film-coated, capsule-shaped, convex tablet, debossed "R3" on one side and "R" on the other side, packaged as follows: Risperidone Tablets, USP 2 mg are available as pink, film-coated, capsule-shaped, convex tablet, debossed "R4" on one side and "R" on the other side, packaged as follows: Bottles of 60 : (NDC 42291-977-60) Bottles of 500 : (NDC 42291-977-50) Risperidone Tablets, USP 3 mg are available as yellow, film-coated, capsule-shaped, convex tablet, debossed "R5" on one side and "R" on the other side, packaged as follows: Bottles of 60 : (NDC 42291-978-60) Bottles of 500 : (NDC 42291-978-50) Risperidone Tablets, USP 4 mg are available as green, film-coated, capsule-shaped, convex tablet, debossed "R6" on one side and "R" on the other side, packaged as follows: Bottles of 60 : (NDC 42291-979-60) Bottles of 500 : (NDC 42291-979-50)
Medication Information
Warnings and Precautions
Cerebrovascular events, including stroke, in elderly patients with dementia-related psychosis: risperidone is not approved for use in patients with dementia-related psychosis. ( 5.2 ) Neuroleptic Malignant Syndrome: Manage with immediate discontinuation of risperidone and close monitoring. ( 5.3 ) Tardive dyskinesia: Consider discontinuing risperidone if clinically indicated. ( 5.4 ) Metabolic Changes: Atypical antipsychotic drugs have been associated with metabolic changes that may increase cardiovascular/ cerebrovascular risk. These metabolic changes include hyperglycemia, dyslipidemia, and weight gain. ( 5.5 ) Hyperglycemia and Diabetes Mellitus: Monitor patients for symptoms of hyperglycemia including polydipsia, polyuria, polyphagia, and weakness. Monitor glucose regularly in patients with diabetes or at risk for diabetes. ( 5.5 ) Dyslipidemia: Undesirable alterations have been observed in patients treated with atypical antipsychotics. ( 5.5 ) Weight Gain: Significant weight gain has been reported. Monitor weight gain. ( 5.5 ) Hyperprolactinemia: Prolactin elevations occur and persist during chronic administration. ( 5.6 ) Orthostatic hypotension: For patients at risk, consider a lower starting dose and slower titration. ( 5.7 ) Leukopenia, Neutropenia, and Agranulocytosis: Perform complete blood counts in patients with a history of clinically significant low white blood cell count (WBC). Consider discontinuing risperidone if a clinically significant decline in WBC occurs in the absence of other causative factors. ( 5.9 ) Potential for cognitive and motor impairment: Use caution when operating machinery. ( 5.10 ) Seizures: Use cautiously in patients with a history of seizures or with conditions that lower the seizure threshold. ( 5.11 )
Indications and Usage
Risperidone is an atypical antipsychotic indicated for: Treatment of schizophrenia ( 1.1 ) As monotherapy or adjunctive therapy with lithium or valproate, for the treatment of acute manic or mixed episodes associated with Bipolar I Disorder ( 1.2 ) Treatment of irritability associated with autistic disorder ( 1.3 )
Dosage and Administration
Table 1. Recommended Daily Dosage by Indication Initial Dose Titration (Increments) Target Dose Effective Dose Range Schizophrenia: adults ( 2.1 ) 2 mg 1 to 2 mg 4 to 8 mg 4 to 16 mg Schizophrenia: adolescents ( 2.2 ) 0.5 mg 0.5 to 1 mg 3 mg 1 to 6 mg Bipolar mania: adults ( 2.2 ) 2 to 3 mg 1 mg 1 to 6 mg 1 to 6 mg Bipolar mania: children and adolescents ( 2.2 ) 0.5 mg 0.5 to 1 mg 1 to 2.5 mg 1 to 6 mg Irritability in autistic disorder ( 2.3 ) 0.25 mg Can increase to 0.5 mg by Day 4: (body weight less than 20 kg) After Day 4, at intervals of > 2 weeks: 0.25 mg (body weight less than 20 kg) 0.5 mg: (body weight less than 20 kg) 0.5 to 3 mg 0.5 mg Can increase to 1 mg by Day 4: (body weight greater than or equal to 20 kg) 0.5 mg (body weight greater than or equal to 20 kg) 1 mg: (body weight greater than or equal to 20 kg) Severe Renal and Hepatic Impairment in Adults: use a lower starting dose of 0.5 mg twice daily. May increase to dosages above 1.5 mg twice daily at intervals of one week or longer.
Contraindications
Risperidone is contraindicated in patients with a known hypersensitivity to either risperidone or paliperidone, or to any of the excipients in the risperidone formulation. Hypersensitivity reactions, including anaphylactic reactions and angioedema, have been reported in patients treated with risperidone and in patients treated with paliperidone. Paliperidone is a metabolite of risperidone.
Adverse Reactions
Cerebrovascular adverse reactions (e.g., stroke, transient ischemic attack), including fatalities, were reported in patients (mean age 85 years; range 73- 97) in trials of risperidone in elderly patients with dementia-related psychosis. In placebo-controlled trials, there was a significantly higher incidence of cerebrovascular adverse events in patients treated with risperidone compared to patients treated with placebo. Risperidone is not approved for the treatment of patients with dementia-related psychosis [see Boxed Warning and Warnings and Precautions (5.1) ] .
Drug Interactions
When risperidone is co-administered with enzyme inducers (e.g., carbamazepine), the dose of risperidone should be increased up to double the patient's usual dose. It may be necessary to decrease the risperidone dose when enzyme inducers such as carbamazepine are discontinued [see Drug Interactions (7.1) ] . Similar effect may be expected with co-administration of risperidone with other enzyme inducers (e.g., phenytoin, rifampin, and phenobarbital). When fluoxetine or paroxetine is co-administered with risperidone, the dose of risperidone should be reduced. The risperidone dose should not exceed 8 mg per day in adults when co-administered with these drugs. When initiating therapy, risperidone should be titrated slowly. It may be necessary to increase the risperidone dose when enzyme inhibitors such as fluoxetine or paroxetine are discontinued [see Drug Interactions (7.1) ] .
Storage and Handling
Store at 20-25°C (68-77°F); excursions permitted to 15°-30°C (59°-86°F) [see USP Controlled Room Temperature]. Protect from light and moisture. Keep out of reach of children.
How Supplied
Risperidone Tablets, USP 0.25 mg are available as dark yellow, film-coated, capsule-shaped, convex tablet, debossed "R1" on one side and "R" on the other side, packaged as follows: Risperidone Tablets, USP 0.5 mg are available as reddish brown, film-coated, capsule-shaped, convex tablet, debossed "R2" on one side and "R" on the other side, packaged as follows: Risperidone Tablets, USP 1 mg are available as white, film-coated, capsule-shaped, convex tablet, debossed "R3" on one side and "R" on the other side, packaged as follows: Risperidone Tablets, USP 2 mg are available as pink, film-coated, capsule-shaped, convex tablet, debossed "R4" on one side and "R" on the other side, packaged as follows: Bottles of 60 : (NDC 42291-977-60) Bottles of 500 : (NDC 42291-977-50) Risperidone Tablets, USP 3 mg are available as yellow, film-coated, capsule-shaped, convex tablet, debossed "R5" on one side and "R" on the other side, packaged as follows: Bottles of 60 : (NDC 42291-978-60) Bottles of 500 : (NDC 42291-978-50) Risperidone Tablets, USP 4 mg are available as green, film-coated, capsule-shaped, convex tablet, debossed "R6" on one side and "R" on the other side, packaged as follows: Bottles of 60 : (NDC 42291-979-60) Bottles of 500 : (NDC 42291-979-50)
Description
Elderly patients with dementia-related psychosis treated with antipsychotic drugs are at an increased risk of death. Risperidone is not approved for the treatment of patients with dementia-related psychosis. [see Warnings and Precautions (5.1) ]
Section 42229-5
Monotherapy
Risperidone tablets are indicated for the treatment of acute manic or mixed episodes associated with Bipolar I Disorder. Efficacy was established in 2 short-term trials in adults and one short-term trial in children and adolescents (ages 10 to 17 years) [see Clinical Studies (14.2)] .
Section 43683-2
| Warnings and Precautions ( 5.6) | 1/2025 |
5.8 Falls
Somnolence, postural hypotension, motor and sensory instability have been reported with the use of antipsychotics, including risperidone, which may lead to falls and, consequently, fractures or other fall-related injuries. For patients, particularly the elderly, with diseases, conditions, or medications that could exacerbate these effects, assess the risk of falls when initiating antipsychotic treatment and recurrently for patients on long-term antipsychotic therapy.
9.2 Abuse
Risperidone has not been systematically studied in animals or humans for its potential for abuse. While the clinical trials did not reveal any tendency for any drug-seeking behavior, these observations were not systematic and it is not possible to predict on the basis of this limited experience the extent to which a CNS-active drug will be misused, diverted, and/or abused once marketed. Consequently, patients should be evaluated carefully for a history of drug abuse, and such patients should be observed closely for signs of risperidone misuse or abuse (e.g., development of tolerance, increases in dose, drug-seeking behavior).
5.11 Seizures
During premarketing testing in adult patients with schizophrenia, seizures occurred in 0.3% (9/2607) of risperidonetreated patients, two in association with hyponatremia. Risperidone should be used cautiously in patients with a history of seizures.
5.13 Priapism
Priapism has been reported during postmarketing surveillance. Severe priapism may require surgical intervention.
11 Description
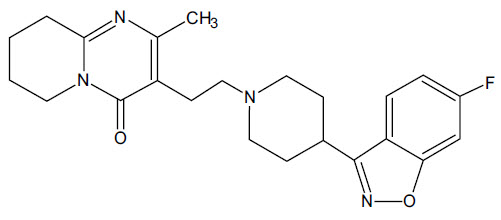
Risperidone Tablets, USP contains risperidone, an atypical antipsychotic belonging to the chemical class of benzisoxazole derivatives. The chemical designation is 3-[2-[4-(6-fluoro-1,2-benzisoxazol-3-yl)-1-piperidinyl] ethyl]-6,7,8,9-tetrahydro-2-methyl-4H-pyrido[1,2-a]pyrimidin-4-one. Its molecular formula is C 23H 27FN 4O 2and its molecular weight is 410.49. The structural formula is:
Risperidone is a white or almost white powder. It is practically insoluble in water, freely soluble in methylene chloride, sparingly soluble in alcohol. It dissolves in dilute acid solutions. Risperidone Tablets, USP are available in 0.25 mg (dark yellow), 0.5 mg (Reddish brown), 1 mg (white) strengths, 2 mg (pink), 3 mg (yellow) and 4 mg (green) strengths.
Each tablet for oral administration contains the following inactive ingredients: Anhydrous Lactose, Sodium Lauryl Sulfate, Microcrystalline Cellulose (101), Colloidal Silicon Dioxide, Sodium Starch Glycolate (Type A), Magnesium Stearate, HPMC 2910/ Hypromellose, Macrogol/ PEG (MW 400), Macrogol/ PEG (MW 8000), Titanium Dioxide. Also, the tablet contains Polyvinyl Alcohol Part Hydrolyzed (used for 0.25, 0.5, 2, 3, 4 mg tablets), Macrogol/ PEG (MW 3350) (used for 0.25, 0.5, 2, 3, 4 mg tablets), Talc (used for 0.25, 0.5, 2, 3, 4 mg tablets), D&C Yellow #10 Aluminium Lake (used for 0.25, 4 mg tablets), FD&C Yellow #6/ Sunset Yellow FCF Aluminium Lake (used for 0.25, 2, 4 mg tablets), Iron Oxide Red (used for 0.5 mg tablets), Lactose Monohydrate, Triacetin & Stearic Acid (used for 1 mg tablets), FD&C Red #40/Allura Red AC Aluminum Lake (used for 2 mg tablets) ,Iron Oxide Yellow (used for 3 mg tablets) and FD&C Blue #1/ Brilliant Blue FCF Aluminium Lake (used for 4 mg tablets).
5.12 Dysphagia
Esophageal dysmotility and aspiration have been associated with antipsychotic drug use. Aspiration pneumonia is a common cause of morbidity and mortality in patients with advanced Alzheimer's dementia. Risperidone and other antipsychotic drugs should be used cautiously in patients at risk for aspiration pneumonia [see Boxed Warningand Warnings and Precautions (5.1)] .
9.3 Dependence
Risperidone has not been systematically studied in animals or humans for its potential for tolerance or physical dependence.
1.1 Schizophrenia
Risperidone tablets are indicated for the treatment of schizophrenia. Efficacy was established in 4 short-term trials in adults, 2 short-term trials in adolescents (ages 13 to 17 years), and one long-term maintenance trial in adults [see Clinical Studies (14.1)] .
16.1 How Supplied
Risperidone Tablets, USP 0.25 mg are available as dark yellow, film-coated, capsule-shaped, convex tablet, debossed "R1" on one side and "R" on the other side, packaged as follows:
Risperidone Tablets, USP 0.5 mg are available as reddish brown, film-coated, capsule-shaped, convex tablet, debossed "R2" on one side and "R" on the other side, packaged as follows:
Risperidone Tablets, USP 1 mg are available as white, film-coated, capsule-shaped, convex tablet, debossed "R3" on one side and "R" on the other side, packaged as follows:
Risperidone Tablets, USP 2 mg are available as pink, film-coated, capsule-shaped, convex tablet, debossed "R4" on one side and "R" on the other side, packaged as follows:
| Bottles of 60 | : (NDC 42291-977-60) |
| Bottles of 500 | : (NDC 42291-977-50) |
Risperidone Tablets, USP 3 mg are available as yellow, film-coated, capsule-shaped, convex tablet, debossed "R5" on one side and "R" on the other side, packaged as follows:
| Bottles of 60 | : (NDC 42291-978-60) |
| Bottles of 500 | : (NDC 42291-978-50) |
Risperidone Tablets, USP 4 mg are available as green, film-coated, capsule-shaped, convex tablet, debossed "R6" on one side and "R" on the other side, packaged as follows:
| Bottles of 60 | : (NDC 42291-979-60) |
| Bottles of 500 | : (NDC 42291-979-50) |
8.5 Geriatric Use
Clinical studies of risperidone in the treatment of schizophrenia did not include sufficient numbers of patients aged 65 and over to determine whether or not they respond differently than younger patients. Other reported clinical experience has not identified differences in responses between elderly and younger patients. In general, a lower starting dose is recommended for an elderly patient, reflecting a decreased pharmacokinetic clearance in the elderly, as well as a greater frequency of decreased hepatic, renal, or cardiac function, and of concomitant disease or other drug therapy [see Clinical Pharmacology (12.3)and Dosage and Administration (2.4, 2.5)] . While elderly patients exhibit a greater tendency to orthostatic hypotension, its risk in the elderly may be minimized by limiting the initial dose to 0.5 mg twice daily followed by careful titration [see Warnings and Precautions (5.7)] . Monitoring of orthostatic vital signs should be considered in patients for whom this is of concern.
This drug is substantially excreted by the kidneys, and the risk of toxic reactions to this drug may be greater in patients with impaired renal function. Because elderly patients are more likely to have decreased renal function, care should be taken in dose selection, and it may be useful to monitor renal function [see Dosage and Administration (2.4)] .
4 Contraindications
Risperidone is contraindicated in patients with a known hypersensitivity to either risperidone or paliperidone, or to any of the excipients in the risperidone formulation. Hypersensitivity reactions, including anaphylactic reactions and angioedema, have been reported in patients treated with risperidone and in patients treated with paliperidone. Paliperidone is a metabolite of risperidone.
6 Adverse Reactions
The following are discussed in more detail in other sections of the labeling:
- Increased mortality in elderly patients with dementia-related psychosis [see Boxed Warningand Warnings and Precautions (5.1)]
- Cerebrovascular adverse events, including stroke, in elderly patients with dementia-related psychosis [see Warnings and Precautions (5.2)]
- Neuroleptic malignant syndrome [see Warnings and Precautions (5.3)]
- Tardive dyskinesia [see Warnings and Precautions (5.4)]
- Metabolic Changes (Hyperglycemia and diabetes mellitus, Dyslipidemia, and Weight Gain) [see Warnings and Precautions (5.5)]
- Hyperprolactinemia [see Warnings and Precautions (5.6)]
- Orthostatic hypotension [see Warnings and Precautions (5.7)]
- Falls [see Warnings and Precautions (5.8)]
- Leukopenia, neutropenia, and agranulocytosis [see Warnings and Precautions (5.9)]
- Potential for cognitive and motor impairment [see Warnings and Precautions (5.10)]
- Seizures [see Warnings and Precautions (5.11)]
- Dysphagia [see Warnings and Precautions (5.12)]
- Priapism [see Warnings and Precautions (5.13)]
- Disruption of body temperature regulation [see Warnings and Precautions (5.14)]
The most common adverse reactions in clinical trials (>5% and twice placebo) were parkinsonism, akathisia, dystonia, tremor, sedation, dizziness, anxiety, blurred vision, nausea, vomiting, upper abdominal pain, stomach discomfort, dyspepsia, diarrhea, salivary hypersecretion, constipation, dry mouth, increased appetite, increased weight, fatigue, rash, nasal congestion, upper respiratory tract infection, nasopharyngitis, and pharyngolaryngeal pain.
The most common adverse reactions that were associated with discontinuation from clinical trials (causing discontinuation in >1% of adults and/or > 2% of pediatrics) were nausea, somnolence, sedation, vomiting, dizziness, and akathisia [see Adverse Reactions, Discontinuations Due to Adverse Reactions (6.1)].
The data described in this section are derived from a clinical trial database consisting of 9803 adult and pediatric patients exposed to one or more doses of Risperidone for the treatment of schizophrenia, bipolar mania, autistic disorder, and other psychiatric disorders in pediatrics and elderly patients with dementia. Of these 9803 patients, 2687 were patients who received risperidone while participating in double-blind, placebo-controlled trials. The conditions and duration of treatment with risperidone varied greatly and included (in overlapping categories) doubleblind, fixed- and flexible-dose, placebo- or active-controlled studies and open-label phases of studies, inpatients and outpatients, and short-term (up to 12 weeks) and longer-term (up to 3 years) exposures. Safety was assessed by collecting adverse events and performing physical examinations, vital signs, body weights, laboratory analyses, and ECGs.
7 Drug Interactions
- Carbamazepine and other enzyme inducers decrease plasma concentrations of risperidone. Increase the risperidone dose up to double the patient's usual dose. Titrate slowly. ( 7.1)
- Fluoxetine, paroxetine, and other CYP 2D6 enzyme inhibitors increase plasma concentrations of risperidone. Reduce the initial dose. Do not exceed a final dose of 8 mg per day of risperidone. ( 7.1)
8.6 Renal Impairment
In patients with moderate to severe (Cl cr59 to 15 mL/min) renal disease, clearance of the sum of risperidone and its active metabolite decreased by 60%, compared to young healthy subjects. Risperidone doses should be reduced in patients with renal disease [see Dosage and Administration (2.4)] .
10.1 Human Experience
Premarketing experience included eight reports of acute risperidone overdosage with estimated doses ranging from 20 to 300 mg and no fatalities. In general, reported signs and symptoms were those resulting from an exaggeration of the drug's known pharmacological effects, i.e., drowsiness and sedation, tachycardia and hypotension, and extrapyramidal symptoms. One case, involving an estimated overdose of 240 mg, was associated with hyponatremia, hypokalemia, prolonged QT, and widened QRS. Another case, involving an estimated overdose of 36 mg, was associated with a seizure.
Postmarketing experience includes reports of acute risperidone overdosage, with estimated doses of up to 360 mg. In general, the most frequently reported signs and symptoms are those resulting from an exaggeration of the drug's known pharmacological effects, i.e., drowsiness, sedation, tachycardia, hypotension, and extrapyramidal symptoms. Other adverse reactions reported since market introduction related to risperidone overdose include prolonged QT interval and convulsions. Torsade de pointes has been reported in association with combined overdose of risperidone and paroxetine.
12.2 Pharmacodynamics
Risperidone is a monoaminergic antagonist with high affinity (Ki of 0.12 to 7.3 nM) for the serotonin Type 2 (5HT 2), dopamine Type 2 (D 2), α 1and α 2adrenergic, and H 1histaminergic receptors. Risperidone showed low to moderate affinity (Ki of 47 to 253 nM) for the serotonin 5HT 1c, 5HT 1D, and 5HT 1Areceptors, weak affinity (Ki of 620 to 800 nM) for the dopamine D 1and haloperidol-sensitive sigma site, and no affinity (when tested at concentrations > 10 -5M) for cholinergic muscarinic or β 1and β 2adrenergic receptors.
5.5 Metabolic Changes
Atypical antipsychotic drugs have been associated with metabolic changes that may increase cardiovascular/ cerebrovascular risk. These metabolic changes include hyperglycemia, dyslipidemia, and body weight gain. While all of the drugs in the class have been shown to produce some metabolic changes, each drug has its own specific risk profile.
5.4 Tardive Dyskinesia
Tardive dyskinesia, a syndrome consisting of potentially irreversible, involuntary, dyskinetic movements, may develop in patients treated with antipsychotic drugs. Although the prevalence of the syndrome appears to be highest among the elderly, especially elderly women, it is impossible to predict which patients will develop the syndrome. Whether antipsychotic drug products differ in their potential to cause tardive dyskinesia is unknown.
The risk of developing tardive dyskinesia and the likelihood that it will become irreversible increase with the duration of treatment and the cumulative dose. The syndrome can develop after relatively brief treatment periods, even at low doses. It may also occur after discontinuation of treatment.
Tardive dyskinesia may remit, partially or completely, if antipsychotic treatment is discontinued. Antipsychotic treatment, itself, however, may suppress (or partially suppress) the signs and symptoms of the syndrome, possibly masking the underlying process. The effect that symptomatic suppression has upon the long-term course of the syndrome is unknown.
Given these considerations, risperidone should be prescribed in a manner that is most likely to minimize the occurrence of tardive dyskinesia. Chronic antipsychotic treatment should generally be reserved for patients: (1) who suffer from a chronic illness that is known to respond to antipsychotic drugs, and (2) for whom alternative, equally effective, but potentially less harmful treatments are not available or appropriate. In patients who do require chronic treatment, use the lowest dose and the shortest duration of treatment producing a satisfactory clinical response. Periodically reassess the need for continued treatment.
If signs and symptoms of tardive dyskinesia appear in a patient on risperidone, drug discontinuation should be considered. However, some patients may require treatment with risperidone despite the presence of the syndrome.
5.6 Hyperprolactinemia
As with other drugs that antagonize dopamine D 2receptors, risperidone elevates prolactin levels and the elevation persists during chronic administration. Risperidone is associated with higher levels of prolactin elevation than other antipsychotic agents.
Hyperprolactinemia may suppress hypothalamic GnRH, resulting in reduced pituitary gonadotropin secretion. This, in turn, may inhibit reproductive function by impairing gonadal steroidogenesis in both female and male patients. Galactorrhea, amenorrhea, gynecomastia, and impotence have been reported in patients receiving prolactin-elevating compounds. Long-standing hyperprolactinemia when associated with hypogonadism may lead to decreased bone density in both female and male subjects.
Tissue culture experiments indicate that approximately one-third of human breast cancers are prolactin dependent in vitro, a factor of potential importance if the prescription of these drugs is contemplated in a patient with previously detected breast cancer. An increase in pituitary gland, mammary gland, and pancreatic islet cell neoplasia (mammary adenocarcinomas, pituitary and pancreatic adenomas) was observed in the risperidone carcinogenicity studies conducted in mice and rats [see Nonclinical Toxicology (13.1)] . Published epidemiologic studies have shown inconsistent results when exploring the potential association between hyperprolactinemia and breast cancer.
8.7 Hepatic Impairment
While the pharmacokinetics of risperidone in subjects with liver disease were comparable to those in young healthy subjects, the mean free fraction of risperidone in plasma was increased by about 35% because of the diminished concentration of both albumin and α 1-acid glycoprotein. Risperidone doses should be reduced in patients with liver disease [see Dosage and Administration (2.4)] .
1 Indications and Usage
Risperidone is an atypical antipsychotic indicated for:
12.1 Mechanism of Action
The mechanism of action of risperidone in schizophrenia is unclear. The drug's therapeutic activity in schizophrenia could be mediated through a combination of dopamine Type 2 (D 2) and serotonin Type 2 (5HT 2) receptor antagonism. The clinical effect from risperidone results from the combined concentrations of risperidone and its major metabolite, 9-hydroxyrisperidone (paliperidone) [see Clinical Pharmacology (12.3)] . Antagonism at receptors other than D 2and 5HT 2may explain some of the other effects of risperidone [see Clinical Pharmacology (12.1)] .
9.1 Controlled Substance
Risperidone is not a controlled substance.
16.2 Storage and Handling
Store at 20-25°C (68-77°F); excursions permitted to 15°-30°C (59°-86°F) [see USP Controlled Room Temperature]. Protect from light and moisture. Keep out of reach of children.
5 Warnings and Precautions
- Cerebrovascular events, including stroke, in elderly patients with dementia-related psychosis: risperidone is not approved for use in patients with dementia-related psychosis. ( 5.2)
- Neuroleptic Malignant Syndrome: Manage with immediate discontinuation of risperidone and close monitoring. ( 5.3)
- Tardive dyskinesia: Consider discontinuing risperidone if clinically indicated. ( 5.4)
- Metabolic Changes: Atypical antipsychotic drugs have been associated with metabolic changes that may increase cardiovascular/ cerebrovascular risk. These metabolic changes include hyperglycemia, dyslipidemia, and weight gain. (
5.5)
- Hyperglycemia and Diabetes Mellitus:Monitor patients for symptoms of hyperglycemia including polydipsia, polyuria, polyphagia, and weakness. Monitor glucose regularly in patients with diabetes or at risk for diabetes. ( 5.5)
- Dyslipidemia:Undesirable alterations have been observed in patients treated with atypical antipsychotics. ( 5.5)
- Weight Gain:Significant weight gain has been reported. Monitor weight gain. ( 5.5)
- Hyperprolactinemia: Prolactin elevations occur and persist during chronic administration. ( 5.6)
- Orthostatic hypotension: For patients at risk, consider a lower starting dose and slower titration. ( 5.7)
- Leukopenia, Neutropenia, and Agranulocytosis: Perform complete blood counts in patients with a history of clinically significant low white blood cell count (WBC). Consider discontinuing risperidone if a clinically significant decline in WBC occurs in the absence of other causative factors. ( 5.9)
- Potential for cognitive and motor impairment: Use caution when operating machinery. ( 5.10)
- Seizures: Use cautiously in patients with a history of seizures or with conditions that lower the seizure threshold. ( 5.11)
2 Dosage and Administration
| Initial Dose | Titration
(Increments) |
Target Dose | Effective Dose Range | |
|---|---|---|---|---|
| Schizophrenia: adults ( 2.1) | 2 mg | 1 to 2 mg | 4 to 8 mg | 4 to 16 mg |
| Schizophrenia: adolescents ( 2.2) | 0.5 mg | 0.5 to 1 mg | 3 mg | 1 to 6 mg |
| Bipolar mania: adults ( 2.2) | 2 to 3 mg | 1 mg | 1 to 6 mg | 1 to 6 mg |
| Bipolar mania: children and adolescents ( 2.2) | 0.5 mg | 0.5 to 1 mg | 1 to 2.5 mg | 1 to 6 mg |
| Irritability in autistic disorder ( 2.3) | 0.25 mg Can increase to 0.5 mg by Day 4: (body weight less than 20 kg) | After Day 4, at intervals of > 2 weeks: 0.25 mg (body weight less than 20 kg) | 0.5 mg: (body weight less than 20 kg) | 0.5 to 3 mg |
| 0.5 mg Can increase to 1 mg by Day 4: (body weight greater than or equal to 20 kg) | 0.5 mg (body weight greater than or equal to 20 kg) | 1 mg: (body weight greater than or equal to 20 kg) |
Severe Renal and Hepatic Impairment in Adults: use a lower starting dose of 0.5 mg twice daily. May increase to dosages above 1.5 mg twice daily at intervals of one week or longer.
5.7 Orthostatic Hypotension
Risperidone may induce orthostatic hypotension associated with dizziness, tachycardia, and in some patients, syncope, especially during the initial dose-titration period, probably reflecting its alpha-adrenergic antagonistic properties. Syncope was reported in 0.2% (6/2607) of risperidone-treated patients in Phase 2 and 3 studies in adults with schizophrenia. The risk of orthostatic hypotension and syncope may be minimized by limiting the initial dose to 2 mg total (either once daily or 1 mg twice daily) in normal adults and 0.5 mg twice daily in the elderly and patients with renal or hepatic impairment [see Dosage and Administration (2.1, 2.4)] .
Monitoring of orthostatic vital signs should be considered in patients for whom this is of concern. A dose reduction should be considered if hypotension occurs. Risperidone should be used with particular caution in patients with known cardiovascular disease (history of myocardial infarction or ischemia, heart failure, or conduction abnormalities), cerebrovascular disease, and conditions which would predispose patients to hypotension, e.g., dehydration and hypovolemia, and in the elderly and patients with renal or hepatic impairment. Monitoring of orthostatic vital signs should be considered if hypotension occurs. Clinically significant hypotension has been observed with concomitant use of risperidone and antihypertensive medication.
3 Dosage Forms and Strengths
Risperidone Tablets, USP 0.25 mg:
Dark yellow, film-coated, capsule-shaped, convex tablet, debossed "R1" on one side and "R" on the other side.
Risperidone Tablets, USP 0.5 mg:
Reddish brown, film-coated, capsule-shaped, convex tablet, debossed "R2" on one side and "R" on the other side.
Risperidone Tablets, USP 1 mg:
White, film-coated, capsule-shaped, convex tablet, debossed "R3" on one side and "R" on the other side.
Risperidone Tablets, USP 2 mg:
Pink, film-coated, capsule-shaped, convex tablet, debossed "R4" on one side and "R" on the other side.
Risperidone Tablets, USP 3 mg:
Yellow, film-coated, capsule-shaped, convex tablet, debossed "R5" on one side and "R" on the other side.
Risperidone Tablets, USP 4 mg:
Green, film-coated, capsule-shaped, convex tablet, debossed "R6" on one side and "R" on the other side.
6.2 Postmarketing Experience
The following adverse reactions have been identified during postapproval use of risperidone. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure. These adverse reactions include: alopecia, anaphylactic reaction, angioedema, atrial fibrillation, cardiopulmonary arrest, catatonia, diabetic ketoacidosis in patients with impaired glucose metabolism, dysgeusia, hypoglycemia, hypothermia, ileus, inappropriate antidiuretic hormone secretion, intestinal obstruction, jaundice, mania, pancreatitis, pituitary adenoma, precocious puberty, pulmonary embolism, QT prolongation, sleep apnea syndrome, somnambulism, Stevens-Johnson syndrome and toxic epidermal necrolysis (SJS/TEN), sudden death, thrombocytopenia, thrombotic thrombocytopenic purpura, urinary retention, and water intoxication.
Postmarketing cases of extrapyramidal symptoms (dystonia and dyskinesia) have been reported in patients concomitantly taking methylphenidate and risperidone when there was an increase or decrease in dosage, initiation, or discontinuation of either or both medications.
To report SUSPECTED ADVERSE REACTIONS, contact AvKARE at 1-855-361-3993; email [email protected] or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
10.2 Management of Overdosage
For the most up to date information on the management of risperidone overdosage, contact a certified poison control center (1-800-222-1222 or www.poison.org). Provide supportive care including close medical supervision and monitoring. Treatment should consist of general measures employed in the management of overdosage with any drug. Consider the possibility of multiple drug overdosage. Ensure an adequate airway, oxygenation, and ventilation. Monitor cardiac rhythm and vital signs. Use supportive and symptomatic measures. There is no specific antidote to risperidone.
8 Use in Specific Populations
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in clinical practice.
5.14 Body Temperature Regulation
Disruption of body temperature regulation has been attributed to antipsychotic agents. Both hyperthermia and hypothermia have been reported in association with oral risperidone use. Caution is advised when prescribing for patients who will be exposed to temperature extremes.
17 Patient Counseling Information
Physicians are advised to discuss the following issues with patients for whom they prescribe risperidone.
5.3 Neuroleptic Malignant Syndrome
Neuroleptic Malignant Syndrome (NMS), a potentially fatal symptom complex, has been reported in association with antipsychotic drugs. Clinical manifestations of NMS are hyperpyrexia, muscle rigidity, altered mental status including delirium, and autonomic instability (irregular pulse or blood pressure, tachycardia, diaphoresis, and cardiac dysrhythmia). Additional signs may include elevated creatine phosphokinase, myoglobinuria (rhabdomyolysis), and acute renal failure.
If NMS is suspected, immediately discontinue risperidone and provide symptomatic treatment and monitoring.
7.1 Pharmacokinetic Related Interactions
The dose of risperidone should be adjusted when used in combination with CYP2D6 enzyme inhibitors (e.g., fluoxetine, and paroxetine) and enzyme inducers (e.g., carbamazepine) [see Table 18and Dosage and Administration (2.5)]. Dose adjustment is not recommended for risperidone when co-administered with ranitidine, cimetidine, amitriptyline, or erythromycin [see Table 18] .
| Coadministered Drug | Dosing Schedule | Effect on Active Moiety (Risperidone + 9-Hydroxy-Risperidone (Ratio
Change relative to reference )
|
Risperidone Dose Recommendation | ||
|---|---|---|---|---|---|
| Coadministered Drug | Risperidone | AUC | C max | ||
| Enzyme (CYP2D6) Inhibitors | |||||
| Fluoxetine | 20 mg/day | 2 or 3 mg twice daily | 1.4 | 1.5 | Re-evaluate dosing. Do not exceed 8 mg/day |
| Paroxetine | 10 mg/day | 4 mg/day | 1.3 | - | Re-evaluate dosing. Do not exceed 8 mg/day |
| 20 mg/day | 4 mg/day | 1.6 | - | ||
| 40 mg/day | 4 mg/day | 1.8 | - | ||
| Enzyme (CYP3A/ PgP inducers) Inducers | |||||
| Carbamazepine | 573 ± 168 mg/day | 3 mg twice daily | 0.51 | 0.55 | Titrate dose upwards. Do not exceed twice the patient's usual dose |
| Enzyme (CYP3A) Inhibitors | |||||
| Ranitidine | 150 mg twice daily | 1 mg single dose | 1.2 | 1.4 | Dose adjustment not needed |
| Cimetidine | 400 mg twice daily | 1 mg single dose | 1.1 | 1.3 | Dose adjustment not needed |
| Erythromycin | 500 mg four times daily | 1 mg single dose | 1.1 | 0.94 | Dose adjustment not needed |
| Other Drugs | |||||
| Amitriptyline | 50 mg twice daily | 3 mg twice daily | 1.2 | 1.1 | Dose adjustment not needed |
5.9 Leukopenia, Neutropenia, and Agranulocytosis
Class Effect:In clinical trial and/or postmarketing experience, events of leukopenia/neutropenia have been reported temporally related to antipsychotic agents, including risperidone. Agranulocytosis has also been reported.
Possible risk factors for leukopenia/neutropenia include pre-existing low white blood cell count (WBC) and history of drug-induced leukopenia/neutropenia. Patients with a history of a clinically significant low WBC or a drug-induced leukopenia/neutropenia should have their complete blood count (CBC) monitored frequently during the first few months of therapy and discontinuation of risperidone should be considered at the first sign of a clinically significant decline in WBC in the absence of other causative factors.
Patients with clinically significant neutropenia should be carefully monitored for fever or other symptoms or signs of infection and treated promptly if such symptoms or signs occur. Patients with severe neutropenia (absolute neutrophil count <1000/mm 3) should discontinue risperidone and have their WBC followed until recovery.
5.10 Potential for Cognitive and Motor Impairment
Somnolence was a commonly reported adverse reaction associated with risperidone treatment, especially when ascertained by direct questioning of patients. This adverse reaction is dose-related, and in a study utilizing a checklist to detect adverse events, 41% of the high-dose patients (risperidone 16 mg/day) reported somnolence compared to 16% of placebo patients. Direct questioning is more sensitive for detecting adverse events than spontaneous reporting, by which 8% of risperidone 16 mg/day patients and 1% of placebo patients reported somnolence as an adverse reaction. Since risperidone has the potential to impair judgment, thinking, or motor skills, patients should be cautioned about operating hazardous machinery, including automobiles, until they are reasonably certain that risperidone therapy does not affect them adversely.
1.3 Irritability Associated With Autistic Disorder
Risperidone tablets are indicated for the treatment of irritability associated with autistic disorder, including symptoms of aggression towards others, deliberate self-injuriousness, temper tantrums, and quickly changing moods. Efficacy was established in 3 short-term trials in children and adolescents (ages 5 to 17 years) [see Clinical Studies (14.4)] .
Principal Display Panel 2 Mg Tablet Bottle Label
Principal Display Panel 3 Mg Tablet Bottle Label
Principal Display Panel 4 Mg Tablet Bottle Label
2.5 Dose Adjustments for Specific Drug Interactions
When risperidone is co-administered with enzyme inducers (e.g., carbamazepine), the dose of risperidone should be increased up to double the patient's usual dose. It may be necessary to decrease the risperidone dose when enzyme inducers such as carbamazepine are discontinued [see Drug Interactions (7.1)] . Similar effect may be expected with co-administration of risperidone with other enzyme inducers (e.g., phenytoin, rifampin, and phenobarbital).
When fluoxetine or paroxetine is co-administered with risperidone, the dose of risperidone should be reduced. The risperidone dose should not exceed 8 mg per day in adults when co-administered with these drugs. When initiating therapy, risperidone should be titrated slowly. It may be necessary to increase the risperidone dose when enzyme inhibitors such as fluoxetine or paroxetine are discontinued [see Drug Interactions (7.1)] .
8.8 Patients With Parkinson's Disease Or Lewy Body Dementia
Patients with Parkinson's Disease or Dementia with Lewy Bodies can experience increased sensitivity to risperidone. Manifestations can include confusion, obtundation, postural instability with frequent falls, extrapyramidal symptoms, and clinical features consistent with neuroleptic malignant syndrome.
2.4 Dosing in Patients With Severe Renal Or Hepatic Impairment
For patients with severe renal impairment (Cl cr< 30 mL/min) or hepatic impairment (10-15 points on Child Pugh System), the initial starting dose is 0.5 mg twice daily. The dose may be increased in increments of 0.5 mg or less, administered twice daily. For doses above 1.5 mg twice daily, increase in intervals of one week or greater [see Use in Specific Populations (8.6and 8.7)] .
14.3 Bipolar Mania Adjunctive Therapy With Lithium Or Valproate
The efficacy of risperidone with concomitant lithium or valproate in the treatment of acute manic or mixed episodes was established in one controlled trial in adult patients who met the DSM-IV criteria for Bipolar I Disorder. This trial included patients with or without psychotic features and with or without a rapid-cycling course.
- In this 3-week placebo-controlled combination trial, 148 in- or outpatients on lithium or valproate therapy with inadequately controlled manic or mixed symptoms were randomized to receive risperidone, placebo, or an active comparator, in combination with their original therapy. Risperidone, in a dose range of 1-6 mg/day, once daily, starting at 2 mg/day (mean modal dose of 3.8 mg/day), combined with lithium or valproate (in a therapeutic range of 0.6 mEq/L to 1.4 mEq/L or 50 mcg/mL to 120 mcg/mL, respectively) was superior to lithium or valproate alone in the reduction of YMRS total score.
- In a second 3-week placebo-controlled combination trial, 142 in- or outpatients on lithium, valproate, or carbamazepine therapy with inadequately controlled manic or mixed symptoms were randomized to receive risperidone or placebo, in combination with their original therapy. Risperidone, in a dose range of 1-6 mg/ day, once daily, starting at 2 mg/day (mean modal dose of 3.7 mg/day), combined with lithium, valproate, or carbamazepine (in therapeutic ranges of 0.6 mEq/L to 1.4 mEq/L for lithium, 50 mcg/mL to 125 mcg/mL for valproate, or 4-12 mcg/mL for carbamazepine, respectively) was not superior to lithium, valproate, or carbamazepine alone in the reduction of YMRS total score. A possible explanation for the failure of this trial was induction of risperidone and 9-hydroxyrisperidone clearance by carbamazepine, leading to subtherapeutic levels of risperidone and 9-hydroxyrisperidone.
5.1 Increased Mortality in Elderly Patients With Dementia Related Psychosis
Elderly patients with dementia-related psychosis treated with antipsychotic drugs are at an increased risk of death.
Analyses of 17 placebo-controlled trials (modal duration of 10 weeks), largely in patients taking atypical antipsychotic drugs, revealed a risk of death in drug-treated patients of between 1.6 to 1.7 times the risk of death in placebo-treated patients. Over the course of a typical 10-week controlled trial, the rate of death in drug-treated patients was about 4.5%, compared to a rate of about 2.6% in the placebo group. Although the causes of death were varied, most of the deaths appeared to be either cardiovascular (e.g., heart failure, sudden death) or infectious (e.g., pneumonia) in nature. Observational studies suggest that, similar to atypical antipsychotic drugs, treatment with conventional antipsychotic drugs may increase mortality. The extent to which the findings of increased mortality in observational studies may be attributed to the antipsychotic drug as opposed to some characteristic(s) of the patients is not clear.
In two of four placebo-controlled trials in elderly patients with dementia-related psychosis, a higher incidence of mortality was observed in patients treated with furosemide plus risperidone when compared to patients treated with risperidone alone or with placebo plus furosemide. No pathological mechanism has been identified to explain this finding, and no consistent pattern for cause of death was observed.
Risperidone is not approved for the treatment of dementia-related psychosis [see Boxed Warning] .
Warning: Increased Mortality in Elderly Patients With Dementia Related Psychosis
Elderly patients with dementia-related psychosis treated with antipsychotic drugs are at an increased risk of death. Risperidone is not approved for the treatment of patients with dementia-related psychosis. [see Warnings and Precautions (5.1)]
2.3 Irritability Associated With Autistic Disorder Pediatrics (children and Adolescents)
The dosage of risperidone should be individualized according to the response and tolerability of the patient. The total daily dose of risperidone can be administered once daily, or half the total daily dose can be administered twice daily.
For patients with body weight less than 20 kg, initiate dosing at 0.25 mg per day. For patients with body weight greater than or equal to 20 kg, initiate dosing at 0.5 mg per day. After a minimum of four days, the dose may be increased to the recommended dose of 0.5 mg per day for patients less than 20 kg and 1.0 mg per day for patients greater than or equal to 20 kg. Maintain this dose for a minimum of 14 days. In patients not achieving sufficient clinical response, the dose may be increased at intervals of 2 weeks or greater, in increments of 0.25 mg per day for patients less than 20 kg, or increments of 0.5 mg per day for patients greater than or equal to 20 kg. The effective dose range is 0.5 mg to 3 mg per day. No dosing data are available for children who weigh less than 15 kg.
Once sufficient clinical response has been achieved and maintained, consider gradually lowering the dose to achieve the optimal balance of efficacy and safety. The physician who elects to use risperidone for extended periods should periodically re-evaluate the long-term risks and benefits of the drug for the individual patient.
Patients experiencing persistent somnolence may benefit from a once-daily dose administered at bedtime or administering half the daily dose twice daily, or a reduction of the dose.
5.2 Cerebrovascular Adverse Reactions, Including Stroke, in Elderly Patients With Dementia Related Psychosis
Cerebrovascular adverse reactions (e.g., stroke, transient ischemic attack), including fatalities, were reported in patients (mean age 85 years; range 73- 97) in trials of risperidone in elderly patients with dementia-related psychosis. In placebo-controlled trials, there was a significantly higher incidence of cerebrovascular adverse events in patients treated with risperidone compared to patients treated with placebo. Risperidone is not approved for the treatment of patients with dementia-related psychosis [see Boxed Warningand Warnings and Precautions (5.1)] .
Structured Label Content
Section 42229-5 (42229-5)
Monotherapy
Risperidone tablets are indicated for the treatment of acute manic or mixed episodes associated with Bipolar I Disorder. Efficacy was established in 2 short-term trials in adults and one short-term trial in children and adolescents (ages 10 to 17 years) [see Clinical Studies (14.2)] .
Section 43683-2 (43683-2)
| Warnings and Precautions ( 5.6) | 1/2025 |
5.8 Falls
Somnolence, postural hypotension, motor and sensory instability have been reported with the use of antipsychotics, including risperidone, which may lead to falls and, consequently, fractures or other fall-related injuries. For patients, particularly the elderly, with diseases, conditions, or medications that could exacerbate these effects, assess the risk of falls when initiating antipsychotic treatment and recurrently for patients on long-term antipsychotic therapy.
9.2 Abuse
Risperidone has not been systematically studied in animals or humans for its potential for abuse. While the clinical trials did not reveal any tendency for any drug-seeking behavior, these observations were not systematic and it is not possible to predict on the basis of this limited experience the extent to which a CNS-active drug will be misused, diverted, and/or abused once marketed. Consequently, patients should be evaluated carefully for a history of drug abuse, and such patients should be observed closely for signs of risperidone misuse or abuse (e.g., development of tolerance, increases in dose, drug-seeking behavior).
5.11 Seizures
During premarketing testing in adult patients with schizophrenia, seizures occurred in 0.3% (9/2607) of risperidonetreated patients, two in association with hyponatremia. Risperidone should be used cautiously in patients with a history of seizures.
5.13 Priapism
Priapism has been reported during postmarketing surveillance. Severe priapism may require surgical intervention.
11 Description (11 DESCRIPTION)
Risperidone Tablets, USP contains risperidone, an atypical antipsychotic belonging to the chemical class of benzisoxazole derivatives. The chemical designation is 3-[2-[4-(6-fluoro-1,2-benzisoxazol-3-yl)-1-piperidinyl] ethyl]-6,7,8,9-tetrahydro-2-methyl-4H-pyrido[1,2-a]pyrimidin-4-one. Its molecular formula is C 23H 27FN 4O 2and its molecular weight is 410.49. The structural formula is:
Risperidone is a white or almost white powder. It is practically insoluble in water, freely soluble in methylene chloride, sparingly soluble in alcohol. It dissolves in dilute acid solutions. Risperidone Tablets, USP are available in 0.25 mg (dark yellow), 0.5 mg (Reddish brown), 1 mg (white) strengths, 2 mg (pink), 3 mg (yellow) and 4 mg (green) strengths.
Each tablet for oral administration contains the following inactive ingredients: Anhydrous Lactose, Sodium Lauryl Sulfate, Microcrystalline Cellulose (101), Colloidal Silicon Dioxide, Sodium Starch Glycolate (Type A), Magnesium Stearate, HPMC 2910/ Hypromellose, Macrogol/ PEG (MW 400), Macrogol/ PEG (MW 8000), Titanium Dioxide. Also, the tablet contains Polyvinyl Alcohol Part Hydrolyzed (used for 0.25, 0.5, 2, 3, 4 mg tablets), Macrogol/ PEG (MW 3350) (used for 0.25, 0.5, 2, 3, 4 mg tablets), Talc (used for 0.25, 0.5, 2, 3, 4 mg tablets), D&C Yellow #10 Aluminium Lake (used for 0.25, 4 mg tablets), FD&C Yellow #6/ Sunset Yellow FCF Aluminium Lake (used for 0.25, 2, 4 mg tablets), Iron Oxide Red (used for 0.5 mg tablets), Lactose Monohydrate, Triacetin & Stearic Acid (used for 1 mg tablets), FD&C Red #40/Allura Red AC Aluminum Lake (used for 2 mg tablets) ,Iron Oxide Yellow (used for 3 mg tablets) and FD&C Blue #1/ Brilliant Blue FCF Aluminium Lake (used for 4 mg tablets).
5.12 Dysphagia
Esophageal dysmotility and aspiration have been associated with antipsychotic drug use. Aspiration pneumonia is a common cause of morbidity and mortality in patients with advanced Alzheimer's dementia. Risperidone and other antipsychotic drugs should be used cautiously in patients at risk for aspiration pneumonia [see Boxed Warningand Warnings and Precautions (5.1)] .
9.3 Dependence
Risperidone has not been systematically studied in animals or humans for its potential for tolerance or physical dependence.
1.1 Schizophrenia
Risperidone tablets are indicated for the treatment of schizophrenia. Efficacy was established in 4 short-term trials in adults, 2 short-term trials in adolescents (ages 13 to 17 years), and one long-term maintenance trial in adults [see Clinical Studies (14.1)] .
16.1 How Supplied
Risperidone Tablets, USP 0.25 mg are available as dark yellow, film-coated, capsule-shaped, convex tablet, debossed "R1" on one side and "R" on the other side, packaged as follows:
Risperidone Tablets, USP 0.5 mg are available as reddish brown, film-coated, capsule-shaped, convex tablet, debossed "R2" on one side and "R" on the other side, packaged as follows:
Risperidone Tablets, USP 1 mg are available as white, film-coated, capsule-shaped, convex tablet, debossed "R3" on one side and "R" on the other side, packaged as follows:
Risperidone Tablets, USP 2 mg are available as pink, film-coated, capsule-shaped, convex tablet, debossed "R4" on one side and "R" on the other side, packaged as follows:
| Bottles of 60 | : (NDC 42291-977-60) |
| Bottles of 500 | : (NDC 42291-977-50) |
Risperidone Tablets, USP 3 mg are available as yellow, film-coated, capsule-shaped, convex tablet, debossed "R5" on one side and "R" on the other side, packaged as follows:
| Bottles of 60 | : (NDC 42291-978-60) |
| Bottles of 500 | : (NDC 42291-978-50) |
Risperidone Tablets, USP 4 mg are available as green, film-coated, capsule-shaped, convex tablet, debossed "R6" on one side and "R" on the other side, packaged as follows:
| Bottles of 60 | : (NDC 42291-979-60) |
| Bottles of 500 | : (NDC 42291-979-50) |
8.5 Geriatric Use
Clinical studies of risperidone in the treatment of schizophrenia did not include sufficient numbers of patients aged 65 and over to determine whether or not they respond differently than younger patients. Other reported clinical experience has not identified differences in responses between elderly and younger patients. In general, a lower starting dose is recommended for an elderly patient, reflecting a decreased pharmacokinetic clearance in the elderly, as well as a greater frequency of decreased hepatic, renal, or cardiac function, and of concomitant disease or other drug therapy [see Clinical Pharmacology (12.3)and Dosage and Administration (2.4, 2.5)] . While elderly patients exhibit a greater tendency to orthostatic hypotension, its risk in the elderly may be minimized by limiting the initial dose to 0.5 mg twice daily followed by careful titration [see Warnings and Precautions (5.7)] . Monitoring of orthostatic vital signs should be considered in patients for whom this is of concern.
This drug is substantially excreted by the kidneys, and the risk of toxic reactions to this drug may be greater in patients with impaired renal function. Because elderly patients are more likely to have decreased renal function, care should be taken in dose selection, and it may be useful to monitor renal function [see Dosage and Administration (2.4)] .
4 Contraindications (4 CONTRAINDICATIONS)
Risperidone is contraindicated in patients with a known hypersensitivity to either risperidone or paliperidone, or to any of the excipients in the risperidone formulation. Hypersensitivity reactions, including anaphylactic reactions and angioedema, have been reported in patients treated with risperidone and in patients treated with paliperidone. Paliperidone is a metabolite of risperidone.
6 Adverse Reactions (6 ADVERSE REACTIONS)
The following are discussed in more detail in other sections of the labeling:
- Increased mortality in elderly patients with dementia-related psychosis [see Boxed Warningand Warnings and Precautions (5.1)]
- Cerebrovascular adverse events, including stroke, in elderly patients with dementia-related psychosis [see Warnings and Precautions (5.2)]
- Neuroleptic malignant syndrome [see Warnings and Precautions (5.3)]
- Tardive dyskinesia [see Warnings and Precautions (5.4)]
- Metabolic Changes (Hyperglycemia and diabetes mellitus, Dyslipidemia, and Weight Gain) [see Warnings and Precautions (5.5)]
- Hyperprolactinemia [see Warnings and Precautions (5.6)]
- Orthostatic hypotension [see Warnings and Precautions (5.7)]
- Falls [see Warnings and Precautions (5.8)]
- Leukopenia, neutropenia, and agranulocytosis [see Warnings and Precautions (5.9)]
- Potential for cognitive and motor impairment [see Warnings and Precautions (5.10)]
- Seizures [see Warnings and Precautions (5.11)]
- Dysphagia [see Warnings and Precautions (5.12)]
- Priapism [see Warnings and Precautions (5.13)]
- Disruption of body temperature regulation [see Warnings and Precautions (5.14)]
The most common adverse reactions in clinical trials (>5% and twice placebo) were parkinsonism, akathisia, dystonia, tremor, sedation, dizziness, anxiety, blurred vision, nausea, vomiting, upper abdominal pain, stomach discomfort, dyspepsia, diarrhea, salivary hypersecretion, constipation, dry mouth, increased appetite, increased weight, fatigue, rash, nasal congestion, upper respiratory tract infection, nasopharyngitis, and pharyngolaryngeal pain.
The most common adverse reactions that were associated with discontinuation from clinical trials (causing discontinuation in >1% of adults and/or > 2% of pediatrics) were nausea, somnolence, sedation, vomiting, dizziness, and akathisia [see Adverse Reactions, Discontinuations Due to Adverse Reactions (6.1)].
The data described in this section are derived from a clinical trial database consisting of 9803 adult and pediatric patients exposed to one or more doses of Risperidone for the treatment of schizophrenia, bipolar mania, autistic disorder, and other psychiatric disorders in pediatrics and elderly patients with dementia. Of these 9803 patients, 2687 were patients who received risperidone while participating in double-blind, placebo-controlled trials. The conditions and duration of treatment with risperidone varied greatly and included (in overlapping categories) doubleblind, fixed- and flexible-dose, placebo- or active-controlled studies and open-label phases of studies, inpatients and outpatients, and short-term (up to 12 weeks) and longer-term (up to 3 years) exposures. Safety was assessed by collecting adverse events and performing physical examinations, vital signs, body weights, laboratory analyses, and ECGs.
7 Drug Interactions (7 DRUG INTERACTIONS)
- Carbamazepine and other enzyme inducers decrease plasma concentrations of risperidone. Increase the risperidone dose up to double the patient's usual dose. Titrate slowly. ( 7.1)
- Fluoxetine, paroxetine, and other CYP 2D6 enzyme inhibitors increase plasma concentrations of risperidone. Reduce the initial dose. Do not exceed a final dose of 8 mg per day of risperidone. ( 7.1)
8.6 Renal Impairment
In patients with moderate to severe (Cl cr59 to 15 mL/min) renal disease, clearance of the sum of risperidone and its active metabolite decreased by 60%, compared to young healthy subjects. Risperidone doses should be reduced in patients with renal disease [see Dosage and Administration (2.4)] .
10.1 Human Experience
Premarketing experience included eight reports of acute risperidone overdosage with estimated doses ranging from 20 to 300 mg and no fatalities. In general, reported signs and symptoms were those resulting from an exaggeration of the drug's known pharmacological effects, i.e., drowsiness and sedation, tachycardia and hypotension, and extrapyramidal symptoms. One case, involving an estimated overdose of 240 mg, was associated with hyponatremia, hypokalemia, prolonged QT, and widened QRS. Another case, involving an estimated overdose of 36 mg, was associated with a seizure.
Postmarketing experience includes reports of acute risperidone overdosage, with estimated doses of up to 360 mg. In general, the most frequently reported signs and symptoms are those resulting from an exaggeration of the drug's known pharmacological effects, i.e., drowsiness, sedation, tachycardia, hypotension, and extrapyramidal symptoms. Other adverse reactions reported since market introduction related to risperidone overdose include prolonged QT interval and convulsions. Torsade de pointes has been reported in association with combined overdose of risperidone and paroxetine.
12.2 Pharmacodynamics
Risperidone is a monoaminergic antagonist with high affinity (Ki of 0.12 to 7.3 nM) for the serotonin Type 2 (5HT 2), dopamine Type 2 (D 2), α 1and α 2adrenergic, and H 1histaminergic receptors. Risperidone showed low to moderate affinity (Ki of 47 to 253 nM) for the serotonin 5HT 1c, 5HT 1D, and 5HT 1Areceptors, weak affinity (Ki of 620 to 800 nM) for the dopamine D 1and haloperidol-sensitive sigma site, and no affinity (when tested at concentrations > 10 -5M) for cholinergic muscarinic or β 1and β 2adrenergic receptors.
5.5 Metabolic Changes
Atypical antipsychotic drugs have been associated with metabolic changes that may increase cardiovascular/ cerebrovascular risk. These metabolic changes include hyperglycemia, dyslipidemia, and body weight gain. While all of the drugs in the class have been shown to produce some metabolic changes, each drug has its own specific risk profile.
5.4 Tardive Dyskinesia
Tardive dyskinesia, a syndrome consisting of potentially irreversible, involuntary, dyskinetic movements, may develop in patients treated with antipsychotic drugs. Although the prevalence of the syndrome appears to be highest among the elderly, especially elderly women, it is impossible to predict which patients will develop the syndrome. Whether antipsychotic drug products differ in their potential to cause tardive dyskinesia is unknown.
The risk of developing tardive dyskinesia and the likelihood that it will become irreversible increase with the duration of treatment and the cumulative dose. The syndrome can develop after relatively brief treatment periods, even at low doses. It may also occur after discontinuation of treatment.
Tardive dyskinesia may remit, partially or completely, if antipsychotic treatment is discontinued. Antipsychotic treatment, itself, however, may suppress (or partially suppress) the signs and symptoms of the syndrome, possibly masking the underlying process. The effect that symptomatic suppression has upon the long-term course of the syndrome is unknown.
Given these considerations, risperidone should be prescribed in a manner that is most likely to minimize the occurrence of tardive dyskinesia. Chronic antipsychotic treatment should generally be reserved for patients: (1) who suffer from a chronic illness that is known to respond to antipsychotic drugs, and (2) for whom alternative, equally effective, but potentially less harmful treatments are not available or appropriate. In patients who do require chronic treatment, use the lowest dose and the shortest duration of treatment producing a satisfactory clinical response. Periodically reassess the need for continued treatment.
If signs and symptoms of tardive dyskinesia appear in a patient on risperidone, drug discontinuation should be considered. However, some patients may require treatment with risperidone despite the presence of the syndrome.
5.6 Hyperprolactinemia
As with other drugs that antagonize dopamine D 2receptors, risperidone elevates prolactin levels and the elevation persists during chronic administration. Risperidone is associated with higher levels of prolactin elevation than other antipsychotic agents.
Hyperprolactinemia may suppress hypothalamic GnRH, resulting in reduced pituitary gonadotropin secretion. This, in turn, may inhibit reproductive function by impairing gonadal steroidogenesis in both female and male patients. Galactorrhea, amenorrhea, gynecomastia, and impotence have been reported in patients receiving prolactin-elevating compounds. Long-standing hyperprolactinemia when associated with hypogonadism may lead to decreased bone density in both female and male subjects.
Tissue culture experiments indicate that approximately one-third of human breast cancers are prolactin dependent in vitro, a factor of potential importance if the prescription of these drugs is contemplated in a patient with previously detected breast cancer. An increase in pituitary gland, mammary gland, and pancreatic islet cell neoplasia (mammary adenocarcinomas, pituitary and pancreatic adenomas) was observed in the risperidone carcinogenicity studies conducted in mice and rats [see Nonclinical Toxicology (13.1)] . Published epidemiologic studies have shown inconsistent results when exploring the potential association between hyperprolactinemia and breast cancer.
8.7 Hepatic Impairment
While the pharmacokinetics of risperidone in subjects with liver disease were comparable to those in young healthy subjects, the mean free fraction of risperidone in plasma was increased by about 35% because of the diminished concentration of both albumin and α 1-acid glycoprotein. Risperidone doses should be reduced in patients with liver disease [see Dosage and Administration (2.4)] .
1 Indications and Usage (1 INDICATIONS AND USAGE)
Risperidone is an atypical antipsychotic indicated for:
12.1 Mechanism of Action
The mechanism of action of risperidone in schizophrenia is unclear. The drug's therapeutic activity in schizophrenia could be mediated through a combination of dopamine Type 2 (D 2) and serotonin Type 2 (5HT 2) receptor antagonism. The clinical effect from risperidone results from the combined concentrations of risperidone and its major metabolite, 9-hydroxyrisperidone (paliperidone) [see Clinical Pharmacology (12.3)] . Antagonism at receptors other than D 2and 5HT 2may explain some of the other effects of risperidone [see Clinical Pharmacology (12.1)] .
9.1 Controlled Substance
Risperidone is not a controlled substance.
16.2 Storage and Handling
Store at 20-25°C (68-77°F); excursions permitted to 15°-30°C (59°-86°F) [see USP Controlled Room Temperature]. Protect from light and moisture. Keep out of reach of children.
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
- Cerebrovascular events, including stroke, in elderly patients with dementia-related psychosis: risperidone is not approved for use in patients with dementia-related psychosis. ( 5.2)
- Neuroleptic Malignant Syndrome: Manage with immediate discontinuation of risperidone and close monitoring. ( 5.3)
- Tardive dyskinesia: Consider discontinuing risperidone if clinically indicated. ( 5.4)
- Metabolic Changes: Atypical antipsychotic drugs have been associated with metabolic changes that may increase cardiovascular/ cerebrovascular risk. These metabolic changes include hyperglycemia, dyslipidemia, and weight gain. (
5.5)
- Hyperglycemia and Diabetes Mellitus:Monitor patients for symptoms of hyperglycemia including polydipsia, polyuria, polyphagia, and weakness. Monitor glucose regularly in patients with diabetes or at risk for diabetes. ( 5.5)
- Dyslipidemia:Undesirable alterations have been observed in patients treated with atypical antipsychotics. ( 5.5)
- Weight Gain:Significant weight gain has been reported. Monitor weight gain. ( 5.5)
- Hyperprolactinemia: Prolactin elevations occur and persist during chronic administration. ( 5.6)
- Orthostatic hypotension: For patients at risk, consider a lower starting dose and slower titration. ( 5.7)
- Leukopenia, Neutropenia, and Agranulocytosis: Perform complete blood counts in patients with a history of clinically significant low white blood cell count (WBC). Consider discontinuing risperidone if a clinically significant decline in WBC occurs in the absence of other causative factors. ( 5.9)
- Potential for cognitive and motor impairment: Use caution when operating machinery. ( 5.10)
- Seizures: Use cautiously in patients with a history of seizures or with conditions that lower the seizure threshold. ( 5.11)
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
| Initial Dose | Titration
(Increments) |
Target Dose | Effective Dose Range | |
|---|---|---|---|---|
| Schizophrenia: adults ( 2.1) | 2 mg | 1 to 2 mg | 4 to 8 mg | 4 to 16 mg |
| Schizophrenia: adolescents ( 2.2) | 0.5 mg | 0.5 to 1 mg | 3 mg | 1 to 6 mg |
| Bipolar mania: adults ( 2.2) | 2 to 3 mg | 1 mg | 1 to 6 mg | 1 to 6 mg |
| Bipolar mania: children and adolescents ( 2.2) | 0.5 mg | 0.5 to 1 mg | 1 to 2.5 mg | 1 to 6 mg |
| Irritability in autistic disorder ( 2.3) | 0.25 mg Can increase to 0.5 mg by Day 4: (body weight less than 20 kg) | After Day 4, at intervals of > 2 weeks: 0.25 mg (body weight less than 20 kg) | 0.5 mg: (body weight less than 20 kg) | 0.5 to 3 mg |
| 0.5 mg Can increase to 1 mg by Day 4: (body weight greater than or equal to 20 kg) | 0.5 mg (body weight greater than or equal to 20 kg) | 1 mg: (body weight greater than or equal to 20 kg) |
Severe Renal and Hepatic Impairment in Adults: use a lower starting dose of 0.5 mg twice daily. May increase to dosages above 1.5 mg twice daily at intervals of one week or longer.
5.7 Orthostatic Hypotension
Risperidone may induce orthostatic hypotension associated with dizziness, tachycardia, and in some patients, syncope, especially during the initial dose-titration period, probably reflecting its alpha-adrenergic antagonistic properties. Syncope was reported in 0.2% (6/2607) of risperidone-treated patients in Phase 2 and 3 studies in adults with schizophrenia. The risk of orthostatic hypotension and syncope may be minimized by limiting the initial dose to 2 mg total (either once daily or 1 mg twice daily) in normal adults and 0.5 mg twice daily in the elderly and patients with renal or hepatic impairment [see Dosage and Administration (2.1, 2.4)] .
Monitoring of orthostatic vital signs should be considered in patients for whom this is of concern. A dose reduction should be considered if hypotension occurs. Risperidone should be used with particular caution in patients with known cardiovascular disease (history of myocardial infarction or ischemia, heart failure, or conduction abnormalities), cerebrovascular disease, and conditions which would predispose patients to hypotension, e.g., dehydration and hypovolemia, and in the elderly and patients with renal or hepatic impairment. Monitoring of orthostatic vital signs should be considered if hypotension occurs. Clinically significant hypotension has been observed with concomitant use of risperidone and antihypertensive medication.
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
Risperidone Tablets, USP 0.25 mg:
Dark yellow, film-coated, capsule-shaped, convex tablet, debossed "R1" on one side and "R" on the other side.
Risperidone Tablets, USP 0.5 mg:
Reddish brown, film-coated, capsule-shaped, convex tablet, debossed "R2" on one side and "R" on the other side.
Risperidone Tablets, USP 1 mg:
White, film-coated, capsule-shaped, convex tablet, debossed "R3" on one side and "R" on the other side.
Risperidone Tablets, USP 2 mg:
Pink, film-coated, capsule-shaped, convex tablet, debossed "R4" on one side and "R" on the other side.
Risperidone Tablets, USP 3 mg:
Yellow, film-coated, capsule-shaped, convex tablet, debossed "R5" on one side and "R" on the other side.
Risperidone Tablets, USP 4 mg:
Green, film-coated, capsule-shaped, convex tablet, debossed "R6" on one side and "R" on the other side.
6.2 Postmarketing Experience
The following adverse reactions have been identified during postapproval use of risperidone. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure. These adverse reactions include: alopecia, anaphylactic reaction, angioedema, atrial fibrillation, cardiopulmonary arrest, catatonia, diabetic ketoacidosis in patients with impaired glucose metabolism, dysgeusia, hypoglycemia, hypothermia, ileus, inappropriate antidiuretic hormone secretion, intestinal obstruction, jaundice, mania, pancreatitis, pituitary adenoma, precocious puberty, pulmonary embolism, QT prolongation, sleep apnea syndrome, somnambulism, Stevens-Johnson syndrome and toxic epidermal necrolysis (SJS/TEN), sudden death, thrombocytopenia, thrombotic thrombocytopenic purpura, urinary retention, and water intoxication.
Postmarketing cases of extrapyramidal symptoms (dystonia and dyskinesia) have been reported in patients concomitantly taking methylphenidate and risperidone when there was an increase or decrease in dosage, initiation, or discontinuation of either or both medications.
To report SUSPECTED ADVERSE REACTIONS, contact AvKARE at 1-855-361-3993; email [email protected] or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
10.2 Management of Overdosage
For the most up to date information on the management of risperidone overdosage, contact a certified poison control center (1-800-222-1222 or www.poison.org). Provide supportive care including close medical supervision and monitoring. Treatment should consist of general measures employed in the management of overdosage with any drug. Consider the possibility of multiple drug overdosage. Ensure an adequate airway, oxygenation, and ventilation. Monitor cardiac rhythm and vital signs. Use supportive and symptomatic measures. There is no specific antidote to risperidone.
8 Use in Specific Populations (8 USE IN SPECIFIC POPULATIONS)
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in clinical practice.
5.14 Body Temperature Regulation
Disruption of body temperature regulation has been attributed to antipsychotic agents. Both hyperthermia and hypothermia have been reported in association with oral risperidone use. Caution is advised when prescribing for patients who will be exposed to temperature extremes.
17 Patient Counseling Information (17 PATIENT COUNSELING INFORMATION)
Physicians are advised to discuss the following issues with patients for whom they prescribe risperidone.
5.3 Neuroleptic Malignant Syndrome
Neuroleptic Malignant Syndrome (NMS), a potentially fatal symptom complex, has been reported in association with antipsychotic drugs. Clinical manifestations of NMS are hyperpyrexia, muscle rigidity, altered mental status including delirium, and autonomic instability (irregular pulse or blood pressure, tachycardia, diaphoresis, and cardiac dysrhythmia). Additional signs may include elevated creatine phosphokinase, myoglobinuria (rhabdomyolysis), and acute renal failure.
If NMS is suspected, immediately discontinue risperidone and provide symptomatic treatment and monitoring.
7.1 Pharmacokinetic Related Interactions (7.1 Pharmacokinetic-related Interactions)
The dose of risperidone should be adjusted when used in combination with CYP2D6 enzyme inhibitors (e.g., fluoxetine, and paroxetine) and enzyme inducers (e.g., carbamazepine) [see Table 18and Dosage and Administration (2.5)]. Dose adjustment is not recommended for risperidone when co-administered with ranitidine, cimetidine, amitriptyline, or erythromycin [see Table 18] .
| Coadministered Drug | Dosing Schedule | Effect on Active Moiety (Risperidone + 9-Hydroxy-Risperidone (Ratio
Change relative to reference )
|
Risperidone Dose Recommendation | ||
|---|---|---|---|---|---|
| Coadministered Drug | Risperidone | AUC | C max | ||
| Enzyme (CYP2D6) Inhibitors | |||||
| Fluoxetine | 20 mg/day | 2 or 3 mg twice daily | 1.4 | 1.5 | Re-evaluate dosing. Do not exceed 8 mg/day |
| Paroxetine | 10 mg/day | 4 mg/day | 1.3 | - | Re-evaluate dosing. Do not exceed 8 mg/day |
| 20 mg/day | 4 mg/day | 1.6 | - | ||
| 40 mg/day | 4 mg/day | 1.8 | - | ||
| Enzyme (CYP3A/ PgP inducers) Inducers | |||||
| Carbamazepine | 573 ± 168 mg/day | 3 mg twice daily | 0.51 | 0.55 | Titrate dose upwards. Do not exceed twice the patient's usual dose |
| Enzyme (CYP3A) Inhibitors | |||||
| Ranitidine | 150 mg twice daily | 1 mg single dose | 1.2 | 1.4 | Dose adjustment not needed |
| Cimetidine | 400 mg twice daily | 1 mg single dose | 1.1 | 1.3 | Dose adjustment not needed |
| Erythromycin | 500 mg four times daily | 1 mg single dose | 1.1 | 0.94 | Dose adjustment not needed |
| Other Drugs | |||||
| Amitriptyline | 50 mg twice daily | 3 mg twice daily | 1.2 | 1.1 | Dose adjustment not needed |
5.9 Leukopenia, Neutropenia, and Agranulocytosis
Class Effect:In clinical trial and/or postmarketing experience, events of leukopenia/neutropenia have been reported temporally related to antipsychotic agents, including risperidone. Agranulocytosis has also been reported.
Possible risk factors for leukopenia/neutropenia include pre-existing low white blood cell count (WBC) and history of drug-induced leukopenia/neutropenia. Patients with a history of a clinically significant low WBC or a drug-induced leukopenia/neutropenia should have their complete blood count (CBC) monitored frequently during the first few months of therapy and discontinuation of risperidone should be considered at the first sign of a clinically significant decline in WBC in the absence of other causative factors.
Patients with clinically significant neutropenia should be carefully monitored for fever or other symptoms or signs of infection and treated promptly if such symptoms or signs occur. Patients with severe neutropenia (absolute neutrophil count <1000/mm 3) should discontinue risperidone and have their WBC followed until recovery.
5.10 Potential for Cognitive and Motor Impairment
Somnolence was a commonly reported adverse reaction associated with risperidone treatment, especially when ascertained by direct questioning of patients. This adverse reaction is dose-related, and in a study utilizing a checklist to detect adverse events, 41% of the high-dose patients (risperidone 16 mg/day) reported somnolence compared to 16% of placebo patients. Direct questioning is more sensitive for detecting adverse events than spontaneous reporting, by which 8% of risperidone 16 mg/day patients and 1% of placebo patients reported somnolence as an adverse reaction. Since risperidone has the potential to impair judgment, thinking, or motor skills, patients should be cautioned about operating hazardous machinery, including automobiles, until they are reasonably certain that risperidone therapy does not affect them adversely.
1.3 Irritability Associated With Autistic Disorder (1.3 Irritability Associated with Autistic Disorder)
Risperidone tablets are indicated for the treatment of irritability associated with autistic disorder, including symptoms of aggression towards others, deliberate self-injuriousness, temper tantrums, and quickly changing moods. Efficacy was established in 3 short-term trials in children and adolescents (ages 5 to 17 years) [see Clinical Studies (14.4)] .
Principal Display Panel 2 Mg Tablet Bottle Label (PRINCIPAL DISPLAY PANEL - 2 mg Tablet Bottle Label)
Principal Display Panel 3 Mg Tablet Bottle Label (PRINCIPAL DISPLAY PANEL - 3 mg Tablet Bottle Label)
Principal Display Panel 4 Mg Tablet Bottle Label (PRINCIPAL DISPLAY PANEL - 4 mg Tablet Bottle Label)
2.5 Dose Adjustments for Specific Drug Interactions
When risperidone is co-administered with enzyme inducers (e.g., carbamazepine), the dose of risperidone should be increased up to double the patient's usual dose. It may be necessary to decrease the risperidone dose when enzyme inducers such as carbamazepine are discontinued [see Drug Interactions (7.1)] . Similar effect may be expected with co-administration of risperidone with other enzyme inducers (e.g., phenytoin, rifampin, and phenobarbital).
When fluoxetine or paroxetine is co-administered with risperidone, the dose of risperidone should be reduced. The risperidone dose should not exceed 8 mg per day in adults when co-administered with these drugs. When initiating therapy, risperidone should be titrated slowly. It may be necessary to increase the risperidone dose when enzyme inhibitors such as fluoxetine or paroxetine are discontinued [see Drug Interactions (7.1)] .
8.8 Patients With Parkinson's Disease Or Lewy Body Dementia (8.8 Patients with Parkinson's Disease or Lewy Body Dementia)
Patients with Parkinson's Disease or Dementia with Lewy Bodies can experience increased sensitivity to risperidone. Manifestations can include confusion, obtundation, postural instability with frequent falls, extrapyramidal symptoms, and clinical features consistent with neuroleptic malignant syndrome.
2.4 Dosing in Patients With Severe Renal Or Hepatic Impairment (2.4 Dosing in Patients with Severe Renal or Hepatic Impairment)
For patients with severe renal impairment (Cl cr< 30 mL/min) or hepatic impairment (10-15 points on Child Pugh System), the initial starting dose is 0.5 mg twice daily. The dose may be increased in increments of 0.5 mg or less, administered twice daily. For doses above 1.5 mg twice daily, increase in intervals of one week or greater [see Use in Specific Populations (8.6and 8.7)] .
14.3 Bipolar Mania Adjunctive Therapy With Lithium Or Valproate (14.3 Bipolar Mania- Adjunctive Therapy with Lithium or Valproate)
The efficacy of risperidone with concomitant lithium or valproate in the treatment of acute manic or mixed episodes was established in one controlled trial in adult patients who met the DSM-IV criteria for Bipolar I Disorder. This trial included patients with or without psychotic features and with or without a rapid-cycling course.
- In this 3-week placebo-controlled combination trial, 148 in- or outpatients on lithium or valproate therapy with inadequately controlled manic or mixed symptoms were randomized to receive risperidone, placebo, or an active comparator, in combination with their original therapy. Risperidone, in a dose range of 1-6 mg/day, once daily, starting at 2 mg/day (mean modal dose of 3.8 mg/day), combined with lithium or valproate (in a therapeutic range of 0.6 mEq/L to 1.4 mEq/L or 50 mcg/mL to 120 mcg/mL, respectively) was superior to lithium or valproate alone in the reduction of YMRS total score.
- In a second 3-week placebo-controlled combination trial, 142 in- or outpatients on lithium, valproate, or carbamazepine therapy with inadequately controlled manic or mixed symptoms were randomized to receive risperidone or placebo, in combination with their original therapy. Risperidone, in a dose range of 1-6 mg/ day, once daily, starting at 2 mg/day (mean modal dose of 3.7 mg/day), combined with lithium, valproate, or carbamazepine (in therapeutic ranges of 0.6 mEq/L to 1.4 mEq/L for lithium, 50 mcg/mL to 125 mcg/mL for valproate, or 4-12 mcg/mL for carbamazepine, respectively) was not superior to lithium, valproate, or carbamazepine alone in the reduction of YMRS total score. A possible explanation for the failure of this trial was induction of risperidone and 9-hydroxyrisperidone clearance by carbamazepine, leading to subtherapeutic levels of risperidone and 9-hydroxyrisperidone.
5.1 Increased Mortality in Elderly Patients With Dementia Related Psychosis (5.1 Increased Mortality in Elderly Patients with Dementia-Related Psychosis)
Elderly patients with dementia-related psychosis treated with antipsychotic drugs are at an increased risk of death.
Analyses of 17 placebo-controlled trials (modal duration of 10 weeks), largely in patients taking atypical antipsychotic drugs, revealed a risk of death in drug-treated patients of between 1.6 to 1.7 times the risk of death in placebo-treated patients. Over the course of a typical 10-week controlled trial, the rate of death in drug-treated patients was about 4.5%, compared to a rate of about 2.6% in the placebo group. Although the causes of death were varied, most of the deaths appeared to be either cardiovascular (e.g., heart failure, sudden death) or infectious (e.g., pneumonia) in nature. Observational studies suggest that, similar to atypical antipsychotic drugs, treatment with conventional antipsychotic drugs may increase mortality. The extent to which the findings of increased mortality in observational studies may be attributed to the antipsychotic drug as opposed to some characteristic(s) of the patients is not clear.
In two of four placebo-controlled trials in elderly patients with dementia-related psychosis, a higher incidence of mortality was observed in patients treated with furosemide plus risperidone when compared to patients treated with risperidone alone or with placebo plus furosemide. No pathological mechanism has been identified to explain this finding, and no consistent pattern for cause of death was observed.
Risperidone is not approved for the treatment of dementia-related psychosis [see Boxed Warning] .
Warning: Increased Mortality in Elderly Patients With Dementia Related Psychosis (WARNING: INCREASED MORTALITY IN ELDERLY PATIENTS WITH DEMENTIA-RELATED PSYCHOSIS)
Elderly patients with dementia-related psychosis treated with antipsychotic drugs are at an increased risk of death. Risperidone is not approved for the treatment of patients with dementia-related psychosis. [see Warnings and Precautions (5.1)]
2.3 Irritability Associated With Autistic Disorder Pediatrics (children and Adolescents) (2.3 Irritability Associated with Autistic Disorder- Pediatrics (Children and Adolescents))
The dosage of risperidone should be individualized according to the response and tolerability of the patient. The total daily dose of risperidone can be administered once daily, or half the total daily dose can be administered twice daily.
For patients with body weight less than 20 kg, initiate dosing at 0.25 mg per day. For patients with body weight greater than or equal to 20 kg, initiate dosing at 0.5 mg per day. After a minimum of four days, the dose may be increased to the recommended dose of 0.5 mg per day for patients less than 20 kg and 1.0 mg per day for patients greater than or equal to 20 kg. Maintain this dose for a minimum of 14 days. In patients not achieving sufficient clinical response, the dose may be increased at intervals of 2 weeks or greater, in increments of 0.25 mg per day for patients less than 20 kg, or increments of 0.5 mg per day for patients greater than or equal to 20 kg. The effective dose range is 0.5 mg to 3 mg per day. No dosing data are available for children who weigh less than 15 kg.
Once sufficient clinical response has been achieved and maintained, consider gradually lowering the dose to achieve the optimal balance of efficacy and safety. The physician who elects to use risperidone for extended periods should periodically re-evaluate the long-term risks and benefits of the drug for the individual patient.
Patients experiencing persistent somnolence may benefit from a once-daily dose administered at bedtime or administering half the daily dose twice daily, or a reduction of the dose.
5.2 Cerebrovascular Adverse Reactions, Including Stroke, in Elderly Patients With Dementia Related Psychosis (5.2 Cerebrovascular Adverse Reactions, Including Stroke, in Elderly Patients with Dementia-Related Psychosis)
Cerebrovascular adverse reactions (e.g., stroke, transient ischemic attack), including fatalities, were reported in patients (mean age 85 years; range 73- 97) in trials of risperidone in elderly patients with dementia-related psychosis. In placebo-controlled trials, there was a significantly higher incidence of cerebrovascular adverse events in patients treated with risperidone compared to patients treated with placebo. Risperidone is not approved for the treatment of patients with dementia-related psychosis [see Boxed Warningand Warnings and Precautions (5.1)] .
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:49:06.817894 · Updated: 2026-03-14T22:31:57.634451