Linezolid
374af2a7-d994-40bd-a86a-cd9038d0b72c
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Indications and Usage
Linezolid is an oxazolidinone-class antibacterial indicated in adults and children for the treatment of the following infections caused by susceptible Gram-positive bacteria: Nosocomial pneumonia ( 1.1 ); Community-acquired pneumonia ( 1.2 ); Complicated skin and skin structure infections, including diabetic foot infections, without concomitant osteomyelitis ( 1.3 ); Uncomplicated skin and skin structure infections ( 1.4 ); Vancomycin-resistant Enterococcus faecium infections. ( 1.5 ) Limitations of Use ( 1.6 ): • Linezolid is not indicated for the treatment of Gram-negative infections. • The safety and efficacy of linezolid formulations given for longer than 28 days have not been evaluated in controlled clinical trials. To reduce the development of drug-resistant bacteria and maintain the effectiveness of linezolid formulations and other antibacterial drugs, linezolid should be used only to treat or prevent infections that are proven or strongly suspected to be caused by bacteria. ( 1.7 )
Dosage and Administration
Dosage, Route, and Frequency of Administration Infection Pediatric Patients (Birth through 11 years of Age) Adults and Adolescents (12 years and Older) Duration (days) Nosocomial pneumonia 10 mg/kg intravenous or oral every 8 hours 600 mg intravenous or oral every 12 hours 10 to 14 Community-acquired pneumonia, including concurrent bacteremia Complicated skin and skin structure infections Vancomycin-resistant Enterococcus faecium infections , including concurrent bacteremia 10 mg/kg intravenous or oral every 8 hours 600 mg intravenous or oral every 12 hours 14 to 28 Uncomplicated skin and skin structure infections less than 5 yrs: 10 mg/kg oral every 8 hours 5–11 yrs: 10 mg/kg oral every 12 hours Adults: 400 mg oral every 12 hours Adolescents: 600 mg oral every 12 hours 10 to 14
Contraindications
• Known hypersensitivity to linezolid or any of the other product components. ( 4.1 ) • Patients taking any monoamine oxidase inhibitors (MAOI) or within two weeks of taking an MAOI. ( 4.2 )
Warnings and Precautions
• Myelosuppression: Monitor complete blood counts weekly. Thrombocytopenia has been reported more often in patients with severe renal and in patients with moderate to severe hepatic impairment. Consider discontinuation in patients who develop or have worsening myelosuppression. ( 5.1 ) • Peripheral and Optic Neuropathy: Reported primarily in patients treated for longer than 28 days. If patients experience symptoms of visual impairment, prompt ophthalmic evaluation is recommended. ( 5.2 ) • Serotonin Syndrome: Monitor patients taking serotonergic agents, including antidepressants and opioids, for signs of serotonin syndrome. Patients taking serotonergic antidepressants should receive linezolid only if no other therapies are available. Discontinue serotonergic antidepressants and monitor patients for signs and symptoms of both serotonin syndrome and antidepressant discontinuation. ( 5.3 ) • A mortality imbalance was seen in an investigational study in linezolid-treated patients with catheter-related bloodstream infections. ( 5.4 ) • Clostridioides difficile- Associated Diarrhea: Evaluate if diarrhea occurs. ( 5.5 ) • Potential interactions producing elevation of blood pressure: monitor blood pressure. ( 5.6 ) • Rhabdomyolysis: If signs or symptoms of rhabdomyolysis are observed, discontinue Linezolid Tablets and initiate appropriate therapy. ( 5.9 ) • Hypoglycemia: Postmarketing cases of symptomatic hypoglycemia have been reported in patients with diabetes mellitus receiving insulin or oral hypoglycemic agents. ( 5.10 ) • Hyponatremia and/or Syndrome of Inappropriate Antidiuretic Hormone Secretion (SIADH): Monitor serum sodium levels regularly in patients at risk of hyponatremia and/or SIADH. ( 5.11 )
Adverse Reactions
The following clinically significant adverse reactions are described elsewhere in the labeling: • Myelosuppression [ see Warnings and Precautions (5.1) ] • Peripheral and Optic Neuropathy [ see Warnings and Precautions (5.2) ] • Serotonin Syndrome [ see Warnings and Precautions (5.3) ] • Clostridioides difficile -Associated Diarrhea [ see Warnings and Precautions (5.5) ] • Lactic Acidosis [ see Warnings and Precautions (5.7) ] • Convulsions [ see Warnings and Precautions (5.8) ] • Rhabdomyolysis [ see Warnings and Precautions (5.9) ] • Hypoglycemia [ see Warnings and Precautions (5.10) ] • Hyponatremia and/or Syndrome of Inappropriate Antidiuretic Hormone Secretion (SIADH) [ see Warnings and Precautions (5.11) ]
Drug Interactions
Monoamine oxidase inhibitors and potential for interaction with adrenergic and serotonergic agents. ( 4.2 , 5.3 , 5.6 , 7 , 12.3 )
How Supplied
Linezolid Tablets are available as follows: 600 mg (white, capsule-shaped, film-coated tablet debossed with "ZYV" on one side and "600" on the other) 20 tablets in HDPE bottle NDC 59762-1307-1 Unit dose packages of 20 tablets NDC 59762-1307-2
Storage and Handling
Linezolid Tablets are available as follows: 600 mg (white, capsule-shaped, film-coated tablet debossed with "ZYV" on one side and "600" on the other) 20 tablets in HDPE bottle NDC 59762-1307-1 Unit dose packages of 20 tablets NDC 59762-1307-2
Description
Warnings and Precautions, Myelosuppression ( 5.1 ) 7/2023 Warnings and Precautions, Rhabdomyolysis ( 5.9 ) 6/2024
Medication Information
Warnings and Precautions
• Myelosuppression: Monitor complete blood counts weekly. Thrombocytopenia has been reported more often in patients with severe renal and in patients with moderate to severe hepatic impairment. Consider discontinuation in patients who develop or have worsening myelosuppression. ( 5.1 ) • Peripheral and Optic Neuropathy: Reported primarily in patients treated for longer than 28 days. If patients experience symptoms of visual impairment, prompt ophthalmic evaluation is recommended. ( 5.2 ) • Serotonin Syndrome: Monitor patients taking serotonergic agents, including antidepressants and opioids, for signs of serotonin syndrome. Patients taking serotonergic antidepressants should receive linezolid only if no other therapies are available. Discontinue serotonergic antidepressants and monitor patients for signs and symptoms of both serotonin syndrome and antidepressant discontinuation. ( 5.3 ) • A mortality imbalance was seen in an investigational study in linezolid-treated patients with catheter-related bloodstream infections. ( 5.4 ) • Clostridioides difficile- Associated Diarrhea: Evaluate if diarrhea occurs. ( 5.5 ) • Potential interactions producing elevation of blood pressure: monitor blood pressure. ( 5.6 ) • Rhabdomyolysis: If signs or symptoms of rhabdomyolysis are observed, discontinue Linezolid Tablets and initiate appropriate therapy. ( 5.9 ) • Hypoglycemia: Postmarketing cases of symptomatic hypoglycemia have been reported in patients with diabetes mellitus receiving insulin or oral hypoglycemic agents. ( 5.10 ) • Hyponatremia and/or Syndrome of Inappropriate Antidiuretic Hormone Secretion (SIADH): Monitor serum sodium levels regularly in patients at risk of hyponatremia and/or SIADH. ( 5.11 )
Indications and Usage
Linezolid is an oxazolidinone-class antibacterial indicated in adults and children for the treatment of the following infections caused by susceptible Gram-positive bacteria: Nosocomial pneumonia ( 1.1 ); Community-acquired pneumonia ( 1.2 ); Complicated skin and skin structure infections, including diabetic foot infections, without concomitant osteomyelitis ( 1.3 ); Uncomplicated skin and skin structure infections ( 1.4 ); Vancomycin-resistant Enterococcus faecium infections. ( 1.5 ) Limitations of Use ( 1.6 ): • Linezolid is not indicated for the treatment of Gram-negative infections. • The safety and efficacy of linezolid formulations given for longer than 28 days have not been evaluated in controlled clinical trials. To reduce the development of drug-resistant bacteria and maintain the effectiveness of linezolid formulations and other antibacterial drugs, linezolid should be used only to treat or prevent infections that are proven or strongly suspected to be caused by bacteria. ( 1.7 )
Dosage and Administration
Dosage, Route, and Frequency of Administration Infection Pediatric Patients (Birth through 11 years of Age) Adults and Adolescents (12 years and Older) Duration (days) Nosocomial pneumonia 10 mg/kg intravenous or oral every 8 hours 600 mg intravenous or oral every 12 hours 10 to 14 Community-acquired pneumonia, including concurrent bacteremia Complicated skin and skin structure infections Vancomycin-resistant Enterococcus faecium infections , including concurrent bacteremia 10 mg/kg intravenous or oral every 8 hours 600 mg intravenous or oral every 12 hours 14 to 28 Uncomplicated skin and skin structure infections less than 5 yrs: 10 mg/kg oral every 8 hours 5–11 yrs: 10 mg/kg oral every 12 hours Adults: 400 mg oral every 12 hours Adolescents: 600 mg oral every 12 hours 10 to 14
Contraindications
• Known hypersensitivity to linezolid or any of the other product components. ( 4.1 ) • Patients taking any monoamine oxidase inhibitors (MAOI) or within two weeks of taking an MAOI. ( 4.2 )
Adverse Reactions
The following clinically significant adverse reactions are described elsewhere in the labeling: • Myelosuppression [ see Warnings and Precautions (5.1) ] • Peripheral and Optic Neuropathy [ see Warnings and Precautions (5.2) ] • Serotonin Syndrome [ see Warnings and Precautions (5.3) ] • Clostridioides difficile -Associated Diarrhea [ see Warnings and Precautions (5.5) ] • Lactic Acidosis [ see Warnings and Precautions (5.7) ] • Convulsions [ see Warnings and Precautions (5.8) ] • Rhabdomyolysis [ see Warnings and Precautions (5.9) ] • Hypoglycemia [ see Warnings and Precautions (5.10) ] • Hyponatremia and/or Syndrome of Inappropriate Antidiuretic Hormone Secretion (SIADH) [ see Warnings and Precautions (5.11) ]
Drug Interactions
Monoamine oxidase inhibitors and potential for interaction with adrenergic and serotonergic agents. ( 4.2 , 5.3 , 5.6 , 7 , 12.3 )
Storage and Handling
Linezolid Tablets are available as follows: 600 mg (white, capsule-shaped, film-coated tablet debossed with "ZYV" on one side and "600" on the other) 20 tablets in HDPE bottle NDC 59762-1307-1 Unit dose packages of 20 tablets NDC 59762-1307-2
How Supplied
Linezolid Tablets are available as follows: 600 mg (white, capsule-shaped, film-coated tablet debossed with "ZYV" on one side and "600" on the other) 20 tablets in HDPE bottle NDC 59762-1307-1 Unit dose packages of 20 tablets NDC 59762-1307-2
Description
Warnings and Precautions, Myelosuppression ( 5.1 ) 7/2023 Warnings and Precautions, Rhabdomyolysis ( 5.9 ) 6/2024
Section 34073-7
Drug Interactions
Section 42229-5
Adults
The safety of linezolid formulations was evaluated in 2,046 adult patients enrolled in seven Phase 3 comparator-controlled clinical trials, who were treated for up to 28 days.
Of the patients treated for uncomplicated skin and skin structure infections (uSSSIs), 25.4% of linezolid-treated and 19.6% of comparator-treated patients experienced at least one drug-related adverse event. For all other indications, 20.4% of linezolid -treated and 14.3% of comparator-treated patients experienced at least one drug-related adverse event.
Table 2 shows the incidence of all-causality, treatment-emergent adverse reactions reported in at least 1% of adult patients in these trials by dose of linezolid.
| ADVERSE REACTIONS | Uncomplicated Skin and Skin Structure Infections | All Other Indications | ||
|---|---|---|---|---|
|
Linezolid
400 mg by mouth every 12 hours (n=548) |
Clarithromycin
250 mg by mouth every 12 hours (n=537) |
Linezolid
600 mg every 12 hours (n=1498) |
All Other Comparators
Comparators included cefpodoxime proxetil 200 mg by mouth every 12 hours; ceftriaxone 1 g intravenously every 12 hours; dicloxacillin 500 mg by mouth every 6 hours; oxacillin 2 g intravenously every 6 hours; vancomycin 1 g intravenously every 12 hours.
(n=1464) |
|
|
Headache |
8.8 |
8.4 |
5.7 |
4.4 |
|
Diarrhea |
8.2 |
6.1 |
8.3 |
6.4 |
|
Nausea |
5.1 |
4.5 |
6.6 |
4.6 |
|
Vomiting |
2.0 |
1.5 |
4.3 |
2.3 |
|
Dizziness |
2.6 |
3.0 |
1.8 |
1.5 |
|
Rash |
1.1 |
1.1 |
2.3 |
2.6 |
|
Anemia |
0.4 |
0 |
2.1 |
1.4 |
|
Taste alteration |
1.8 |
2.0 |
1.0 |
0.3 |
|
Vaginal moniliasis |
1.8 |
1.3 |
1.1 |
0.5 |
|
Oral moniliasis |
0.5 |
0 |
1.7 |
1.0 |
|
Abnormal liver function tests |
0.4 |
0.2 |
1.6 |
0.8 |
|
Fungal infection |
1.5 |
0.2 |
0.3 |
0.2 |
|
Tongue discoloration |
1.3 |
0 |
0.3 |
0 |
|
Localized abdominal pain |
1.3 |
0.6 |
1.2 |
0.8 |
|
Generalized abdominal pain |
0.9 |
0.4 |
1.2 |
1.0 |
Of the patients treated for uSSSIs, 3.5% of linezolid-treated and 2.4% of comparator-treated patients discontinued treatment due to drug-related adverse events. For all other indications, discontinuations due to drug-related adverse events occurred in 2.1% of linezolid-treated and 1.7% of comparator-treated patients. The most common reported drug-related adverse events leading to discontinuation of treatment were nausea, headache, diarrhea, and vomiting.
Section 43679-0
Mechanism of Action
Linezolid is a synthetic antibacterial agent of the oxazolidinone class, which has clinical utility in the treatment of infections caused by aerobic Gram-positive bacteria. The in vitro spectrum of activity of linezolid also includes certain Gram-negative bacteria and anaerobic bacteria. Linezolid binds to a site on the bacterial 23S ribosomal RNA of the 50S subunit and prevents the formation of a functional 70S initiation complex, which is essential for bacterial reproduction. The results of time-kill studies have shown linezolid to be bacteriostatic against enterococci and staphylococci. For streptococci, linezolid was found to be bactericidal for the majority of isolates.
Section 43683-2
Section 44425-7
Store at 25ºC (77ºF). Protect from light. Keep bottles tightly closed to protect from moisture.
1.7 Usage
To reduce the development of drug-resistant bacteria and maintain the effectiveness of linezolid and other antibacterial drugs, linezolid should be used only to treat or prevent infections that are proven or strongly suspected to be caused by susceptible bacteria. When culture and susceptibility information are available, they should be considered in selecting or modifying antibacterial therapy. In the absence of such data, local epidemiology and susceptibility patterns may contribute to the empiric selection of therapy.
10 Overdosage
In the event of overdosage, supportive care is advised, with maintenance of glomerular filtration. Hemodialysis may facilitate more rapid elimination of linezolid. In a Phase 1 clinical trial, approximately 30% of a dose of linezolid was removed during a 3-hour hemodialysis session beginning 3 hours after the dose of linezolid was administered. Data are not available for removal of linezolid with peritoneal dialysis or hemoperfusion. Clinical signs of acute toxicity in animals were decreased activity and ataxia in rats and vomiting and tremors in dogs treated with 3,000 mg/kg/day and 2,000 mg/kg/day, respectively.
11 Description
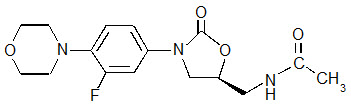
Linezolid Tablets contain linezolid, which is a synthetic antibacterial agent of the oxazolidinone class. The chemical name for linezolid is (S)-N-[[3-[3-Fluoro-4-(4-morpholinyl)phenyl]-2-oxo-5-oxazolidinyl] methyl]-acetamide.
The empirical formula is C16H20FN3O4. Its molecular weight is 337.35, and its chemical structure is represented below:
Linezolid Tablet for oral administration contains 600 mg linezolid as a film-coated compressed tablet. Inactive ingredients are carnauba wax, corn starch, hydroxypropylcellulose, hypromellose, magnesium stearate, microcrystalline cellulose, polyethylene glycol, sodium starch glycolate, and titanium dioxide. The sodium (Na+) content is 2.92 mg per 600 mg tablet (0.1 mEq/tablet).
5.8 Convulsions
Convulsions have been reported in patients when treated with linezolid. In some of these cases, a history of seizures or risk factors for seizures was reported.
5.10 Hypoglycemia
Postmarketing cases of symptomatic hypoglycemia have been reported in patients with diabetes mellitus receiving insulin or oral hypoglycemic agents when treated with linezolid, a reversible, nonselective MAO inhibitor. Some MAO inhibitors have been associated with hypoglycemic episodes in diabetic patients receiving insulin or hypoglycemic agents. While a causal relationship between linezolid and hypoglycemia has not been established, diabetic patients should be cautioned of potential hypoglycemic reactions when treated with linezolid.
If hypoglycemia occurs, a decrease in the dose of insulin or oral hypoglycemic agent, or discontinuation of oral hypoglycemic agent, insulin, or Linezolid Tablets may be required.
8.4 Pediatric Use
The safety and effectiveness of linezolid for the treatment of pediatric patients with the following infections are supported by evidence from adequate and well-controlled studies in adults, pharmacokinetic data in pediatric patients, and additional data from a comparator-controlled study of Gram-positive infections in pediatric patients ranging in age from birth through 11 years [see Indications and Usage (1), Clinical Pharmacology (12.3) and Clinical Studies (14) ]:
-
•nosocomial pneumonia
-
•complicated skin and skin structure infections
-
•community-acquired pneumonia (also supported by evidence from an uncontrolled study in patients ranging in age from 8 months through 12 years)
-
•vancomycin-resistant Enterococcus faecium infections
The safety and effectiveness of linezolid for the treatment of pediatric patients with the following infection have been established in a comparator-controlled study in pediatric patients ranging in age from 5 through 17 years [see Clinical Studies (14) ]:
-
•uncomplicated skin and skin structure infections caused by Staphylococcus aureus (methicillin-susceptible strains only) or Streptococcus pyogenes
Pharmacokinetic information generated in pediatric patients with ventriculoperitoneal shunts showed variable cerebrospinal fluid (CSF) linezolid concentrations following single and multiple dosing of linezolid; therapeutic concentrations were not consistently achieved or maintained in the CSF. Therefore, the use of linezolid for the empiric treatment of pediatric patients with central nervous system infections is not recommended.
The pharmacokinetics of linezolid have been evaluated in pediatric patients from birth to 17 years of age. In general, weight-based clearance of linezolid gradually decreases with increasing age of pediatric patients. However, in preterm (gestational age < 34 weeks) neonates < 7 days of age, linezolid clearance is often lower than in full-term neonates < 7 days of age. Consequently, preterm neonates < 7 days of age may need an alternative linezolid dosing regimen of 10 mg/kg every 12 hours [see Dosage and Administration (2.1) and Clinical Pharmacology (12.3) ].
In limited clinical experience, 5 out of 6 (83%) pediatric patients with infections due to Gram-positive pathogens with minimum inhibitory concentrations (MICs) of 4 mcg/mL treated with linezolid had clinical cures. However, pediatric patients exhibit wider variability in linezolid clearance and systemic exposure (AUC) compared with adults. In pediatric patients with a sub-optimal clinical response, particularly those with pathogens with MIC of 4 mcg/mL, lower systemic exposure, site and severity of infection, and the underlying medical condition should be considered when assessing clinical response [see Clinical Pharmacology (12.3) and Dosage and Administration (2) ].
8.5 Geriatric Use
Of the 2,046 patients treated with linezolid in Phase 3 comparator-controlled clinical trials, 589 (29%) were 65 years or older and 253 (12%) were 75 years or older. No overall differences in safety or effectiveness were observed between these patients and younger patients, and other reported clinical experience has not identified differences in responses between the elderly and younger patients, but greater sensitivity of some older individuals cannot be ruled out.
5.9 Rhabdomyolysis
Rhabdomyolysis has been reported with the use of linezolid, including Linezolid Tablets [see Adverse Reactions (6.2) ]. If signs or symptoms of rhabdomyolysis such as muscle pain, tenderness or weakness, dark urine or elevated creatine phosphokinase are observed, discontinue Linezolid Tablets and initiate appropriate therapy.
4 Contraindications
5.7 Lactic Acidosis
Lactic acidosis has been reported with the use of linezolid. In reported cases, patients experienced repeated episodes of nausea and vomiting. Patients who develop recurrent nausea or vomiting, unexplained acidosis, or a low bicarbonate level while receiving linezolid should receive immediate medical evaluation.
6 Adverse Reactions
The following clinically significant adverse reactions are described elsewhere in the labeling:
-
•Myelosuppression [see Warnings and Precautions (5.1) ]
-
•Peripheral and Optic Neuropathy [see Warnings and Precautions (5.2) ]
-
•Serotonin Syndrome [see Warnings and Precautions (5.3) ]
-
•Clostridioides difficile-Associated Diarrhea [see Warnings and Precautions (5.5) ]
-
•Lactic Acidosis [see Warnings and Precautions (5.7) ]
-
•Convulsions [see Warnings and Precautions (5.8) ]
-
•Rhabdomyolysis [see Warnings and Precautions (5.9) ]
-
•Hypoglycemia [see Warnings and Precautions (5.10) ]
-
•Hyponatremia and/or Syndrome of Inappropriate Antidiuretic Hormone Secretion (SIADH) [see Warnings and Precautions (5.11) ]
7 Drug Interactions
4.1 Hypersensitivity
Linezolid formulations are contraindicated for use in patients who have known hypersensitivity to linezolid or any of the other product components.
5.1 Myelosuppression
Myelosuppression (including anemia, leukopenia, pancytopenia, and thrombocytopenia) has been reported in patients receiving linezolid. In cases where the outcome is known, when linezolid was discontinued, the affected hematologic parameters have risen toward pretreatment levels. Thrombocytopenia has been reported more often in patients with severe renal impairment, whether or not on dialysis, and in patients with moderate to severe hepatic impairment. Complete blood counts should be monitored weekly in patients who receive linezolid, particularly in those who receive linezolid for longer than two weeks, those with pre-existing myelosuppression, those with severe renal impairment or moderate to severe hepatic impairment, those receiving concomitant drugs that produce bone marrow suppression, or those with a chronic infection who have received previous or concomitant antibacterial drug therapy. Discontinuation of therapy with linezolid should be considered in patients who develop or have worsening myelosuppression [see Adverse Reactions (6.2)] .
12.2 Pharmacodynamics
In a randomized, positive- and placebo-controlled crossover thorough QT study, 40 healthy subjects were administered a single linezolid 600 mg dose via a 1 hour IV infusion, a single linezolid 1,200 mg dose via a 1 hour IV infusion, placebo, and a single oral dose of positive control. At both the 600 mg and 1,200 mg linezolid doses, no significant effect on QTc interval was detected at peak plasma concentration or at any other time.
12.3 Pharmacokinetics
The mean pharmacokinetic parameters of linezolid in adults after single and multiple oral and intravenous doses are summarized in Table 8. Plasma concentrations of linezolid at steady-state after oral doses of 600 mg given every 12 hours are shown in Figure 1.
| Dose of Linezolid |
Cmax
mcg/mL |
Cmin
mcg/mL |
Tmax
hrs |
AUC
AUC for single dose = AUC0–∞; for multiple dose = AUC0–τ
mcg∙h/mL |
t1/2
hrs |
CL
mL/min |
|---|---|---|---|---|---|---|
| Cmax = Maximum plasma concentration; Cmin = Minimum plasma concentration; Tmax = Time to Cmax; AUC = Area under concentration-time curve; t1/2 = Elimination half-life; CL = Systemic clearance | ||||||
|
400 mg tablet |
||||||
|
single dose Data dose-normalized from 375 mg
|
8.10 |
--- |
1.52 |
55.10 |
5.20 |
146 |
|
every 12 hours |
11.00 |
3.08 |
1.12 |
73.40 |
4.69 |
110 |
|
600 mg tablet |
||||||
|
single dose |
12.70 |
--- |
1.28 |
91.40 |
4.26 |
127 |
|
every 12 hours |
21.20 |
6.15 |
1.03 |
138.00 |
5.40 |
80 |
|
600 mg IV injection Data dose-normalized from 625 mg, intravenous dose was given as 0.5-hour infusion.
|
||||||
|
single dose |
12.90 |
--- |
0.50 |
80.20 |
4.40 |
138 |
|
every 12 hours |
15.10 |
3.68 |
0.51 |
89.70 |
4.80 |
123 |
|
600 mg oral suspension |
||||||
|
single dose |
11.00 |
--- |
0.97 |
80.80 |
4.60 |
141 |
Figure 1. Plasma Concentrations of Linezolid in Adults at Steady-State Following Oral Dosing Every 12 Hours (Mean ± Standard Deviation, n=16)
1.6 Limitations of Use
-
•Linezolid is not indicated for the treatment of Gram-negative infections. It is critical that specific Gram-negative therapy be initiated immediately if a concomitant Gram-negative pathogen is documented or suspected [see Warnings and Precautions (5.4) ].
-
•The safety and efficacy of linezolid formulations given for longer than 28 days have not been evaluated in controlled clinical trials [see Clinical Studies (14) ].
5.3 Serotonin Syndrome
Spontaneous reports of serotonin syndrome including fatal cases associated with the co-administration of linezolid and serotonergic agents, including antidepressants such as selective serotonin reuptake inhibitors (SSRIs), have been reported.
Unless clinically appropriate and patients are carefully observed for signs and/or symptoms of serotonin syndrome or neuroleptic malignant syndrome-like (NMS-like) reactions, linezolid should not be administered to patients with carcinoid syndrome and/or patients taking any of the following medications: serotonin re-uptake inhibitors, tricyclic antidepressants, bupropion, buspirone, serotonin 5-HT1 receptor agonists (triptans), and opioids, including meperidine [see Drug Interactions (7) and Clinical Pharmacology (12.3) ].
In some cases, a patient already receiving a serotonergic antidepressant or buspirone may require urgent treatment with linezolid. If alternatives to linezolid are not available and the potential benefits of linezolid outweigh the risks of serotonin syndrome or NMS-like reactions, the serotonergic antidepressant should be stopped promptly and linezolid administered. The patient should be monitored for two weeks (five weeks if fluoxetine was taken) or until 24 hours after the last dose of linezolid, whichever comes first. Symptoms of serotonin syndrome or NMS-like reactions include hyperthermia, rigidity, myoclonus, autonomic instability, and mental status changes that include extreme agitation progressing to delirium and coma. The patient should also be monitored for discontinuation symptoms of the antidepressant (see package insert of the specified agent(s) for a description of the associated discontinuation symptoms).
1 Indications and Usage
Linezolid is an oxazolidinone-class antibacterial indicated in adults and children for the treatment of the following infections caused by susceptible Gram-positive bacteria: Nosocomial pneumonia (1.1); Community-acquired pneumonia (1.2); Complicated skin and skin structure infections, including diabetic foot infections, without concomitant osteomyelitis (1.3); Uncomplicated skin and skin structure infections (1.4); Vancomycin-resistant Enterococcus faecium infections. (1.5)
Limitations of Use (
1.6
):
-
•Linezolid is not indicated for the treatment of Gram-negative infections.
-
•The safety and efficacy of linezolid formulations given for longer than 28 days have not been evaluated in controlled clinical trials.
To reduce the development of drug-resistant bacteria and maintain the effectiveness of linezolid formulations and other antibacterial drugs, linezolid should be used only to treat or prevent infections that are proven or strongly suspected to be caused by bacteria. (1.7)
1.1 Nosocomial Pneumonia
Linezolid is indicated for the treatment of nosocomial pneumonia caused by Staphylococcus aureus (methicillin-susceptible and -resistant isolates) or Streptococcus pneumoniae [see Clinical Studies (14) ].
12.1 Mechanism of Action
Linezolid is an antibacterial drug [see Microbiology (12.4) ].
5 Warnings and Precautions
-
•Myelosuppression: Monitor complete blood counts weekly. Thrombocytopenia has been reported more often in patients with severe renal and in patients with moderate to severe hepatic impairment. Consider discontinuation in patients who develop or have worsening myelosuppression. (5.1)
-
•Peripheral and Optic Neuropathy: Reported primarily in patients treated for longer than 28 days. If patients experience symptoms of visual impairment, prompt ophthalmic evaluation is recommended. (5.2)
-
•Serotonin Syndrome: Monitor patients taking serotonergic agents, including antidepressants and opioids, for signs of serotonin syndrome. Patients taking serotonergic antidepressants should receive linezolid only if no other therapies are available. Discontinue serotonergic antidepressants and monitor patients for signs and symptoms of both serotonin syndrome and antidepressant discontinuation. (5.3)
-
•A mortality imbalance was seen in an investigational study in linezolid-treated patients with catheter-related bloodstream infections. (5.4)
-
•Clostridioides difficile-Associated Diarrhea: Evaluate if diarrhea occurs. (5.5)
-
•Potential interactions producing elevation of blood pressure: monitor blood pressure. (5.6)
-
•Rhabdomyolysis: If signs or symptoms of rhabdomyolysis are observed, discontinue LinezolidTablets and initiate appropriate therapy. (5.9)
-
•Hypoglycemia: Postmarketing cases of symptomatic hypoglycemia have been reported in patients with diabetes mellitus receiving insulin or oral hypoglycemic agents. (5.10)
-
•Hyponatremia and/or Syndrome of Inappropriate Antidiuretic Hormone Secretion (SIADH): Monitor serum sodium levels regularly in patients at risk of hyponatremia and/or SIADH. (5.11)
2 Dosage and Administration
| Dosage, Route, and Frequency of Administration | |||
|---|---|---|---|
| Infection |
Pediatric Patients
(Birth through 11 years of Age) |
Adults and Adolescents
(12 years and Older) |
Duration
(days) |
|
Nosocomial pneumonia |
10 mg/kg intravenous or oral every 8 hours |
600 mg intravenous or oral every 12 hours |
10 to 14 |
|
Community-acquired pneumonia, including concurrent bacteremia |
|||
|
Complicated skin and skin structure infections |
|||
|
Vancomycin-resistant Enterococcus faecium infections, including concurrent bacteremia |
10 mg/kg intravenous or oral every 8 hours |
600 mg intravenous or oral every 12 hours |
14 to 28 |
|
Uncomplicated skin and skin structure infections |
less than 5 yrs: 10 mg/kg oral every 8 hours |
Adults: 400 mg oral every 12 hours |
10 to 14 |
3 Dosage Forms and Strengths
LINEZOLID 600 mg Tablet:
white, capsule-shaped, film-coated tablet debossed with "ZYV" on one side and "600" on the other.
5.5 Clostridioides Difficile
Clostridioides difficile-Associated Diarrhea (CDAD) has been reported with use of nearly all antibacterial agents, including linezolid, and may range in severity from mild diarrhea to fatal colitis. Treatment with antibacterial agents alters the normal flora of the colon leading to overgrowth of C. difficile.
C. difficile produces toxins A and B which contribute to the development of CDAD. Hypertoxin producing strains of C. difficile cause increased morbidity and mortality, as these infections can be refractory to antimicrobial therapy and may require colectomy. CDAD must be considered in all patients who present with diarrhea following antibacterial drug use.
Careful medical history is necessary since CDAD has been reported to occur over two months after the administration of antibacterial agents.
If CDAD is suspected or confirmed, ongoing antibacterial drug use not directed against C. difficile may need to be discontinued. Appropriate fluid and electrolyte management, protein supplementation, antibacterial drug treatment of C. difficile, and surgical evaluation should be instituted as clinically indicated.
6.2 Postmarketing Experience
The following adverse reactions have been identified during post-approval use of linezolid. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure;
-
•Anaphylaxis, angioedema, bullous skin disorders including severe cutaneous adverse reactions (SCAR) such as toxic epidermal necrolysis and Stevens-Johnson syndrome, and hypersensitivity vasculitis.
-
•Myelosuppression (including anemia, leukopenia, pancytopenia, and thrombocytopenia). Thrombocytopenia has been reported more often in patients with severe renal impairment and in patients with moderate to severe hepatic impairment [see Warnings and Precautions (5.1) ]; sideroblastic anemia.
-
•Peripheral neuropathy, and optic neuropathy sometimes progressing to loss of vision [see Warnings and Precautions (5.2) ].
-
•Serotonin syndrome has been reported in patients receiving concomitant serotonergic agents, including antidepressants such as selective serotonin reuptake inhibitors (SSRIs) and opioids, and linezolid [see Warnings and Precautions (5.3) ].
-
•Lactic acidosis [see Warnings and Precautions (5.7) ]. Although these reports have primarily been in patients treated for longer than the maximum recommended duration of 28 days, these events have also been reported in patients receiving shorter courses of therapy.
-
•Convulsions [see Warnings and Precautions (5.8) ].
-
•Rhabdomyolysis [see Warnings and Precautions (5.9) ].
-
•Hypoglycemia, including symptomatic episodes [see Warnings and Precautions (5.10) ].
-
•Hyponatremia and/or Syndrome of Inappropriate Antidiuretic Hormone Secretion (SIADH) [see Warnings and Precautions (5.11) ].
-
•Superficial tooth discoloration and tongue discoloration have been reported with the use of linezolid. The tooth discoloration was removable with professional dental cleaning (manual descaling) in cases with known outcome.
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
1.2 Community Acquired Pneumonia
Linezolid is indicated for the treatment of community-acquired pneumonia caused by Streptococcus pneumoniae, including cases with concurrent bacteremia, or Staphylococcus aureus (methicillin-susceptible isolates only) [see Clinical Studies (14) ].
4.2 Monoamine Oxidase Inhibitors
Linezolid should not be used in patients taking any medicinal product which inhibits monoamine oxidases A or B (e.g., phenelzine, isocarboxazid) or within two weeks of taking any such medicinal product.
7.1 Monoamine Oxidase Inhibitors
Linezolid is a reversible, nonselective inhibitor of monoamine oxidase [see Contraindications (4.2) and Clinical Pharmacology (12.3) ].
5.2 Peripheral and Optic Neuropathy
Peripheral and optic neuropathies have been reported in patients treated with linezolid, primarily in those patients treated for longer than the maximum recommended duration of 28 days. In cases of optic neuropathy that progressed to loss of vision, patients were treated for extended periods beyond the maximum recommended duration. Visual blurring has been reported in some patients treated with linezolid for less than 28 days. Peripheral and optic neuropathy has also been reported in children.
If patients experience symptoms of visual impairment, such as changes in visual acuity, changes in color vision, blurred vision, or visual field defect, prompt ophthalmic evaluation is recommended. Visual function should be monitored in all patients taking linezolid for extended periods (≥ 3 months) and in all patients reporting new visual symptoms regardless of length of therapy with linezolid. If peripheral or optic neuropathy occurs, the continued use of linezolid in these patients should be weighed against the potential risks.
16 How Supplied/storage and Handling
Linezolid Tablets are available as follows:
600 mg (white, capsule-shaped, film-coated tablet debossed with "ZYV" on one side and "600" on the other)
|
20 tablets in HDPE bottle |
NDC 59762-1307-1 |
|
Unit dose packages of 20 tablets |
NDC 59762-1307-2 |
2.1 General Dosage and Administration
The recommended dosage for linezolid formulations for the treatment of infections is described in Table 1.
| Dosage, Route and Frequency of Administration | Recommended Duration of Treatment (consecutive days) | ||
|---|---|---|---|
|
Infection
Due to the designated pathogens [see Indications and Usage (1)
]
|
Pediatric Patients
Neonates less than 7 days: Most pre-term neonates less than 7 days of age (gestational age less than 34 weeks) have lower systemic linezolid clearance values and larger AUC values than many full-term neonates and older infants. These neonates should be initiated with a dosing regimen of 10 mg/kg every 12 hours. Consideration may be given to the use of 10 mg/kg every 8 hours regimen in neonates with a sub-optimal clinical response. All neonatal patients should receive 10 mg/kg every 8 hours by 7 days of life [see Use in Specific Populations (8.4) and Clinical Pharmacology (12.3)
].
(Birth through 11 Years of Age)
|
Adults and Adolescents
(12 Years and Older) |
|
|
Nosocomial pneumonia |
10 mg/kg intravenously or oral Oral dosing using either linezolid Tablets or linezolid for Oral Suspension [see How Supplied/Storage and Handling (16)
]. every 8 hours
|
600 mg intravenously or oral every 12 hours |
10 to 14 |
|
Community-acquired pneumonia, including concurrent bacteremia |
|||
|
Complicated skin and skin structure infections |
|||
|
Vancomycin-resistant Enterococcus faecium infections, including concurrent bacteremia |
10 mg/kg intravenously or oral every 8 hours |
600 mg intravenously or oral every 12 hours |
14 to 28 |
|
Uncomplicated skin and skin structure infections |
less than 5 yrs: 10 mg/kg oral every 8 hours5–11 yrs: 10 mg/kg oral every 12 hours |
Adults: 400 mg oral every 12 hoursAdolescents: 600 mg oral every 12 hours |
10 to 14 |
No dose adjustment is necessary when switching from intravenous to oral administration.
7.2 Adrenergic and Serotonergic Agents
Linezolid has the potential for interaction with adrenergic and serotonergic agents [see Warnings and Precautions (5.3, 5.6) and Clinical Pharmacology (12.3) ].
13.2 Animal Toxicology And/or Pharmacology
Target organs of linezolid toxicity were similar in juvenile and adult rats and dogs. Dose- and time-dependent myelosuppression, as evidenced by bone marrow hypocellularity/decreased hematopoiesis, decreased extramedullary hematopoiesis in spleen and liver, and decreased levels of circulating erythrocytes, leukocytes, and platelets have been seen in animal studies. Lymphoid depletion occurred in thymus, lymph nodes, and spleen. Generally, the lymphoid findings were associated with anorexia, weight loss, and suppression of body weight gain, which may have contributed to the observed effects.
In rats administered linezolid orally for 6 months, non-reversible, minimal to mild axonal degeneration of sciatic nerves was observed at 80 mg/kg/day; minimal degeneration of the sciatic nerve was also observed in 1 male at this dose level at a 3-month interim necropsy. Sensitive morphologic evaluation of perfusion-fixed tissues was conducted to investigate evidence of optic nerve degeneration. Minimal to moderate optic nerve degeneration was evident in 2 male rats after 6 months of dosing, but the direct relationship to drug was equivocal because of the acute nature of the finding and its asymmetrical distribution. The nerve degeneration observed was microscopically comparable to spontaneous unilateral optic nerve degeneration reported in aging rats and may be an exacerbation of common background change.
These effects were observed at exposure levels that are comparable to those observed in some human subjects. The hematopoietic and lymphoid effects were reversible, although in some studies, reversal was incomplete within the duration of the recovery period.
5.12 Development of Drug Resistant Bacteria
Prescribing linezolid in the absence of a proven or strongly suspected bacterial infection or a prophylactic indication is unlikely to provide benefit to the patient and increases the risk of the development of drug-resistant bacteria.
1.5 Vancomycin Resistant Enterococcus Faecium
Linezolid is indicated for the treatment of vancomycin-resistant Enterococcus faecium infections, including cases with concurrent bacteremia [see Clinical Studies (14) ].
1.3 Complicated Skin and Skin Structure Infections
Linezolid is indicated for the treatment of complicated skin and skin structure infections, including diabetic foot infections, without concomitant osteomyelitis, caused by Staphylococcus aureus (methicillin-susceptible and -resistant isolates), Streptococcus pyogenes, or Streptococcus agalactiae. Linezolid has not been studied in the treatment of decubitus ulcers [see Clinical Studies (14) ].
1.4 Uncomplicated Skin and Skin Structure Infections
Linezolid is indicated for the treatment of uncomplicated skin and skin structure infections caused by Staphylococcus aureus (methicillin-susceptible isolates only) or Streptococcus pyogenes [see Clinical Studies (14) ].
Principal Display Panel 600 Mg Tablet Bottle Label
NDC 59762-1307-1
20 Tablets
GREENSTONE® BRAND
linezolid
tablets
600 mg
Rx only
Principal Display Panel 600 Mg Tablet Blister Pack Box
NDC 59762-1307-2
20 Tablets
GREENSTONE® BRAND
linezolid tablets
600 mg
For in-institution use only
Rx only
UNIT DOSE
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Lifetime studies in animals have not been conducted to evaluate the carcinogenic potential of linezolid. Neither mutagenic nor clastogenic potential was found in a battery of tests including: assays for mutagenicity (Ames bacterial reversion and CHO cell mutation), an in vitro unscheduled DNA synthesis (UDS) assay, an in vitro chromosome aberration assay in human lymphocytes, and an in vivo mouse micronucleus assay.
Linezolid did not affect the fertility or reproductive performance of adult female rats given oral doses of up to 100 mg/kg/day for 14 days prior to mating through Gestation Day 7. It reversibly decreased fertility and reproductive performance in adult male rats when given at doses ≥ 50 mg/kg/day, with exposures approximately equal to or greater than the expected human exposure level (exposure comparisons are based on AUCs). The reversible fertility effects were mediated through altered spermatogenesis. Affected spermatids contained abnormally formed and oriented mitochondria and were non-viable. Epithelial cell hypertrophy and hyperplasia in the epididymis was observed in conjunction with decreased fertility. Similar epididymal changes were not seen in dogs.
In sexually mature male rats exposed to drug as juveniles, mildly decreased fertility was observed following treatment with linezolid through most of their period of sexual development (50 mg/kg/day from days 7 to 36 of age, and 100 mg/kg/day from days 37 to 55 of age), with exposures up to 1.7 times greater than mean AUCs observed in pediatric patients aged 3 months to 11 years. Decreased fertility was not observed with shorter treatment periods, corresponding to exposure in utero through the early neonatal period (gestation day 6 through postnatal day 5), neonatal exposure (postnatal days 5 to 21), or to juvenile exposure (postnatal days 22 to 35). Reversible reductions in sperm motility and altered sperm morphology were observed in rats treated from postnatal day 22 to 35.
Principal Display Panel 600 Mg Tablet Blister Pack Label
linezolid tablets
600 mg
Distributed by:
Greenstone LLC
Morgantown, WV 26505 U.S.A.
MADE IN SINGAPORE
5.6 Potential Interactions Producing Elevation of Blood Pressure
Unless patients are monitored for potential increases in blood pressure, linezolid should not be administered to patients with uncontrolled hypertension, pheochromocytoma, thyrotoxicosis and/or patients taking any of the following types of medications: directly and indirectly acting sympathomimetic agents (e.g., pseudoephedrine), vasopressive agents (e.g., epinephrine, norepinephrine), dopaminergic agents (e.g., dopamine, dobutamine) [see Drug Interactions (7) and Clinical Pharmacology (12.3) ].
5.11 Hyponatremia And/or Syndrome of Inappropriate Antidiuretic Hormone Secretion (siadh)
Postmarketing cases of hyponatremia and/or Syndrome of Inappropriate Antidiuretic Hormone Secretion (SIADH) have been observed in patients treated with linezolid. In reported cases, the signs and symptoms included confusion, somnolence, generalized weakness, and in severe cases led to respiratory failure and even death. Monitor serum sodium levels regularly in the elderly, in patients taking diuretics, and in other patients at risk of hyponatremia and/or SIADH while taking linezolid. If signs and symptoms of hyponatremia and/or SIADH occur, discontinue linezolid, and institute appropriate supportive measures.
5.4 Mortality Imbalance in An Investigational Study in Patients With Catheter Related Bloodstream Infections, Including Those With Catheter Site Infections
An imbalance in mortality was seen in patients treated with linezolid relative to vancomycin/dicloxacillin/oxacillin in an open-label study in seriously ill patients with intravascular catheter-related infections [78/363 (21.5%) vs. 58/363 (16.0%); odds ratio 1.426, 95% CI 0.970, 2.098]. While causality has not been established, this observed imbalance occurred primarily in linezolid-treated patients in whom either Gram-negative pathogens, mixed Gram-negative and Gram-positive pathogens, or no pathogen were identified at baseline, but was not seen in patients with Gram-positive infections only.
Linezolid is not approved and should not be used for the treatment of patients with catheter-related bloodstream infections or catheter-site infections.
Linezolid has no clinical activity against Gram-negative pathogens and is not indicated for the treatment of Gram-negative infections. It is critical that specific Gram-negative therapy be initiated immediately if a concomitant Gram-negative pathogen is documented or suspected [see Indications and Usage (1) ].
Structured Label Content
Section 34073-7 (34073-7)
Drug Interactions
Section 42229-5 (42229-5)
Adults
The safety of linezolid formulations was evaluated in 2,046 adult patients enrolled in seven Phase 3 comparator-controlled clinical trials, who were treated for up to 28 days.
Of the patients treated for uncomplicated skin and skin structure infections (uSSSIs), 25.4% of linezolid-treated and 19.6% of comparator-treated patients experienced at least one drug-related adverse event. For all other indications, 20.4% of linezolid -treated and 14.3% of comparator-treated patients experienced at least one drug-related adverse event.
Table 2 shows the incidence of all-causality, treatment-emergent adverse reactions reported in at least 1% of adult patients in these trials by dose of linezolid.
| ADVERSE REACTIONS | Uncomplicated Skin and Skin Structure Infections | All Other Indications | ||
|---|---|---|---|---|
|
Linezolid
400 mg by mouth every 12 hours (n=548) |
Clarithromycin
250 mg by mouth every 12 hours (n=537) |
Linezolid
600 mg every 12 hours (n=1498) |
All Other Comparators
Comparators included cefpodoxime proxetil 200 mg by mouth every 12 hours; ceftriaxone 1 g intravenously every 12 hours; dicloxacillin 500 mg by mouth every 6 hours; oxacillin 2 g intravenously every 6 hours; vancomycin 1 g intravenously every 12 hours.
(n=1464) |
|
|
Headache |
8.8 |
8.4 |
5.7 |
4.4 |
|
Diarrhea |
8.2 |
6.1 |
8.3 |
6.4 |
|
Nausea |
5.1 |
4.5 |
6.6 |
4.6 |
|
Vomiting |
2.0 |
1.5 |
4.3 |
2.3 |
|
Dizziness |
2.6 |
3.0 |
1.8 |
1.5 |
|
Rash |
1.1 |
1.1 |
2.3 |
2.6 |
|
Anemia |
0.4 |
0 |
2.1 |
1.4 |
|
Taste alteration |
1.8 |
2.0 |
1.0 |
0.3 |
|
Vaginal moniliasis |
1.8 |
1.3 |
1.1 |
0.5 |
|
Oral moniliasis |
0.5 |
0 |
1.7 |
1.0 |
|
Abnormal liver function tests |
0.4 |
0.2 |
1.6 |
0.8 |
|
Fungal infection |
1.5 |
0.2 |
0.3 |
0.2 |
|
Tongue discoloration |
1.3 |
0 |
0.3 |
0 |
|
Localized abdominal pain |
1.3 |
0.6 |
1.2 |
0.8 |
|
Generalized abdominal pain |
0.9 |
0.4 |
1.2 |
1.0 |
Of the patients treated for uSSSIs, 3.5% of linezolid-treated and 2.4% of comparator-treated patients discontinued treatment due to drug-related adverse events. For all other indications, discontinuations due to drug-related adverse events occurred in 2.1% of linezolid-treated and 1.7% of comparator-treated patients. The most common reported drug-related adverse events leading to discontinuation of treatment were nausea, headache, diarrhea, and vomiting.
Section 43679-0 (43679-0)
Mechanism of Action
Linezolid is a synthetic antibacterial agent of the oxazolidinone class, which has clinical utility in the treatment of infections caused by aerobic Gram-positive bacteria. The in vitro spectrum of activity of linezolid also includes certain Gram-negative bacteria and anaerobic bacteria. Linezolid binds to a site on the bacterial 23S ribosomal RNA of the 50S subunit and prevents the formation of a functional 70S initiation complex, which is essential for bacterial reproduction. The results of time-kill studies have shown linezolid to be bacteriostatic against enterococci and staphylococci. For streptococci, linezolid was found to be bactericidal for the majority of isolates.
Section 43683-2 (43683-2)
Section 44425-7 (44425-7)
Store at 25ºC (77ºF). Protect from light. Keep bottles tightly closed to protect from moisture.
1.7 Usage
To reduce the development of drug-resistant bacteria and maintain the effectiveness of linezolid and other antibacterial drugs, linezolid should be used only to treat or prevent infections that are proven or strongly suspected to be caused by susceptible bacteria. When culture and susceptibility information are available, they should be considered in selecting or modifying antibacterial therapy. In the absence of such data, local epidemiology and susceptibility patterns may contribute to the empiric selection of therapy.
10 Overdosage (10 OVERDOSAGE)
In the event of overdosage, supportive care is advised, with maintenance of glomerular filtration. Hemodialysis may facilitate more rapid elimination of linezolid. In a Phase 1 clinical trial, approximately 30% of a dose of linezolid was removed during a 3-hour hemodialysis session beginning 3 hours after the dose of linezolid was administered. Data are not available for removal of linezolid with peritoneal dialysis or hemoperfusion. Clinical signs of acute toxicity in animals were decreased activity and ataxia in rats and vomiting and tremors in dogs treated with 3,000 mg/kg/day and 2,000 mg/kg/day, respectively.
11 Description (11 DESCRIPTION)
Linezolid Tablets contain linezolid, which is a synthetic antibacterial agent of the oxazolidinone class. The chemical name for linezolid is (S)-N-[[3-[3-Fluoro-4-(4-morpholinyl)phenyl]-2-oxo-5-oxazolidinyl] methyl]-acetamide.
The empirical formula is C16H20FN3O4. Its molecular weight is 337.35, and its chemical structure is represented below:
Linezolid Tablet for oral administration contains 600 mg linezolid as a film-coated compressed tablet. Inactive ingredients are carnauba wax, corn starch, hydroxypropylcellulose, hypromellose, magnesium stearate, microcrystalline cellulose, polyethylene glycol, sodium starch glycolate, and titanium dioxide. The sodium (Na+) content is 2.92 mg per 600 mg tablet (0.1 mEq/tablet).
5.8 Convulsions
Convulsions have been reported in patients when treated with linezolid. In some of these cases, a history of seizures or risk factors for seizures was reported.
5.10 Hypoglycemia
Postmarketing cases of symptomatic hypoglycemia have been reported in patients with diabetes mellitus receiving insulin or oral hypoglycemic agents when treated with linezolid, a reversible, nonselective MAO inhibitor. Some MAO inhibitors have been associated with hypoglycemic episodes in diabetic patients receiving insulin or hypoglycemic agents. While a causal relationship between linezolid and hypoglycemia has not been established, diabetic patients should be cautioned of potential hypoglycemic reactions when treated with linezolid.
If hypoglycemia occurs, a decrease in the dose of insulin or oral hypoglycemic agent, or discontinuation of oral hypoglycemic agent, insulin, or Linezolid Tablets may be required.
8.4 Pediatric Use
The safety and effectiveness of linezolid for the treatment of pediatric patients with the following infections are supported by evidence from adequate and well-controlled studies in adults, pharmacokinetic data in pediatric patients, and additional data from a comparator-controlled study of Gram-positive infections in pediatric patients ranging in age from birth through 11 years [see Indications and Usage (1), Clinical Pharmacology (12.3) and Clinical Studies (14) ]:
-
•nosocomial pneumonia
-
•complicated skin and skin structure infections
-
•community-acquired pneumonia (also supported by evidence from an uncontrolled study in patients ranging in age from 8 months through 12 years)
-
•vancomycin-resistant Enterococcus faecium infections
The safety and effectiveness of linezolid for the treatment of pediatric patients with the following infection have been established in a comparator-controlled study in pediatric patients ranging in age from 5 through 17 years [see Clinical Studies (14) ]:
-
•uncomplicated skin and skin structure infections caused by Staphylococcus aureus (methicillin-susceptible strains only) or Streptococcus pyogenes
Pharmacokinetic information generated in pediatric patients with ventriculoperitoneal shunts showed variable cerebrospinal fluid (CSF) linezolid concentrations following single and multiple dosing of linezolid; therapeutic concentrations were not consistently achieved or maintained in the CSF. Therefore, the use of linezolid for the empiric treatment of pediatric patients with central nervous system infections is not recommended.
The pharmacokinetics of linezolid have been evaluated in pediatric patients from birth to 17 years of age. In general, weight-based clearance of linezolid gradually decreases with increasing age of pediatric patients. However, in preterm (gestational age < 34 weeks) neonates < 7 days of age, linezolid clearance is often lower than in full-term neonates < 7 days of age. Consequently, preterm neonates < 7 days of age may need an alternative linezolid dosing regimen of 10 mg/kg every 12 hours [see Dosage and Administration (2.1) and Clinical Pharmacology (12.3) ].
In limited clinical experience, 5 out of 6 (83%) pediatric patients with infections due to Gram-positive pathogens with minimum inhibitory concentrations (MICs) of 4 mcg/mL treated with linezolid had clinical cures. However, pediatric patients exhibit wider variability in linezolid clearance and systemic exposure (AUC) compared with adults. In pediatric patients with a sub-optimal clinical response, particularly those with pathogens with MIC of 4 mcg/mL, lower systemic exposure, site and severity of infection, and the underlying medical condition should be considered when assessing clinical response [see Clinical Pharmacology (12.3) and Dosage and Administration (2) ].
8.5 Geriatric Use
Of the 2,046 patients treated with linezolid in Phase 3 comparator-controlled clinical trials, 589 (29%) were 65 years or older and 253 (12%) were 75 years or older. No overall differences in safety or effectiveness were observed between these patients and younger patients, and other reported clinical experience has not identified differences in responses between the elderly and younger patients, but greater sensitivity of some older individuals cannot be ruled out.
5.9 Rhabdomyolysis
Rhabdomyolysis has been reported with the use of linezolid, including Linezolid Tablets [see Adverse Reactions (6.2) ]. If signs or symptoms of rhabdomyolysis such as muscle pain, tenderness or weakness, dark urine or elevated creatine phosphokinase are observed, discontinue Linezolid Tablets and initiate appropriate therapy.
4 Contraindications (4 CONTRAINDICATIONS)
5.7 Lactic Acidosis
Lactic acidosis has been reported with the use of linezolid. In reported cases, patients experienced repeated episodes of nausea and vomiting. Patients who develop recurrent nausea or vomiting, unexplained acidosis, or a low bicarbonate level while receiving linezolid should receive immediate medical evaluation.
6 Adverse Reactions (6 ADVERSE REACTIONS)
The following clinically significant adverse reactions are described elsewhere in the labeling:
-
•Myelosuppression [see Warnings and Precautions (5.1) ]
-
•Peripheral and Optic Neuropathy [see Warnings and Precautions (5.2) ]
-
•Serotonin Syndrome [see Warnings and Precautions (5.3) ]
-
•Clostridioides difficile-Associated Diarrhea [see Warnings and Precautions (5.5) ]
-
•Lactic Acidosis [see Warnings and Precautions (5.7) ]
-
•Convulsions [see Warnings and Precautions (5.8) ]
-
•Rhabdomyolysis [see Warnings and Precautions (5.9) ]
-
•Hypoglycemia [see Warnings and Precautions (5.10) ]
-
•Hyponatremia and/or Syndrome of Inappropriate Antidiuretic Hormone Secretion (SIADH) [see Warnings and Precautions (5.11) ]
7 Drug Interactions (7 DRUG INTERACTIONS)
4.1 Hypersensitivity
Linezolid formulations are contraindicated for use in patients who have known hypersensitivity to linezolid or any of the other product components.
5.1 Myelosuppression
Myelosuppression (including anemia, leukopenia, pancytopenia, and thrombocytopenia) has been reported in patients receiving linezolid. In cases where the outcome is known, when linezolid was discontinued, the affected hematologic parameters have risen toward pretreatment levels. Thrombocytopenia has been reported more often in patients with severe renal impairment, whether or not on dialysis, and in patients with moderate to severe hepatic impairment. Complete blood counts should be monitored weekly in patients who receive linezolid, particularly in those who receive linezolid for longer than two weeks, those with pre-existing myelosuppression, those with severe renal impairment or moderate to severe hepatic impairment, those receiving concomitant drugs that produce bone marrow suppression, or those with a chronic infection who have received previous or concomitant antibacterial drug therapy. Discontinuation of therapy with linezolid should be considered in patients who develop or have worsening myelosuppression [see Adverse Reactions (6.2)] .
12.2 Pharmacodynamics
In a randomized, positive- and placebo-controlled crossover thorough QT study, 40 healthy subjects were administered a single linezolid 600 mg dose via a 1 hour IV infusion, a single linezolid 1,200 mg dose via a 1 hour IV infusion, placebo, and a single oral dose of positive control. At both the 600 mg and 1,200 mg linezolid doses, no significant effect on QTc interval was detected at peak plasma concentration or at any other time.
12.3 Pharmacokinetics
The mean pharmacokinetic parameters of linezolid in adults after single and multiple oral and intravenous doses are summarized in Table 8. Plasma concentrations of linezolid at steady-state after oral doses of 600 mg given every 12 hours are shown in Figure 1.
| Dose of Linezolid |
Cmax
mcg/mL |
Cmin
mcg/mL |
Tmax
hrs |
AUC
AUC for single dose = AUC0–∞; for multiple dose = AUC0–τ
mcg∙h/mL |
t1/2
hrs |
CL
mL/min |
|---|---|---|---|---|---|---|
| Cmax = Maximum plasma concentration; Cmin = Minimum plasma concentration; Tmax = Time to Cmax; AUC = Area under concentration-time curve; t1/2 = Elimination half-life; CL = Systemic clearance | ||||||
|
400 mg tablet |
||||||
|
single dose Data dose-normalized from 375 mg
|
8.10 |
--- |
1.52 |
55.10 |
5.20 |
146 |
|
every 12 hours |
11.00 |
3.08 |
1.12 |
73.40 |
4.69 |
110 |
|
600 mg tablet |
||||||
|
single dose |
12.70 |
--- |
1.28 |
91.40 |
4.26 |
127 |
|
every 12 hours |
21.20 |
6.15 |
1.03 |
138.00 |
5.40 |
80 |
|
600 mg IV injection Data dose-normalized from 625 mg, intravenous dose was given as 0.5-hour infusion.
|
||||||
|
single dose |
12.90 |
--- |
0.50 |
80.20 |
4.40 |
138 |
|
every 12 hours |
15.10 |
3.68 |
0.51 |
89.70 |
4.80 |
123 |
|
600 mg oral suspension |
||||||
|
single dose |
11.00 |
--- |
0.97 |
80.80 |
4.60 |
141 |
Figure 1. Plasma Concentrations of Linezolid in Adults at Steady-State Following Oral Dosing Every 12 Hours (Mean ± Standard Deviation, n=16)
1.6 Limitations of Use
-
•Linezolid is not indicated for the treatment of Gram-negative infections. It is critical that specific Gram-negative therapy be initiated immediately if a concomitant Gram-negative pathogen is documented or suspected [see Warnings and Precautions (5.4) ].
-
•The safety and efficacy of linezolid formulations given for longer than 28 days have not been evaluated in controlled clinical trials [see Clinical Studies (14) ].
5.3 Serotonin Syndrome
Spontaneous reports of serotonin syndrome including fatal cases associated with the co-administration of linezolid and serotonergic agents, including antidepressants such as selective serotonin reuptake inhibitors (SSRIs), have been reported.
Unless clinically appropriate and patients are carefully observed for signs and/or symptoms of serotonin syndrome or neuroleptic malignant syndrome-like (NMS-like) reactions, linezolid should not be administered to patients with carcinoid syndrome and/or patients taking any of the following medications: serotonin re-uptake inhibitors, tricyclic antidepressants, bupropion, buspirone, serotonin 5-HT1 receptor agonists (triptans), and opioids, including meperidine [see Drug Interactions (7) and Clinical Pharmacology (12.3) ].
In some cases, a patient already receiving a serotonergic antidepressant or buspirone may require urgent treatment with linezolid. If alternatives to linezolid are not available and the potential benefits of linezolid outweigh the risks of serotonin syndrome or NMS-like reactions, the serotonergic antidepressant should be stopped promptly and linezolid administered. The patient should be monitored for two weeks (five weeks if fluoxetine was taken) or until 24 hours after the last dose of linezolid, whichever comes first. Symptoms of serotonin syndrome or NMS-like reactions include hyperthermia, rigidity, myoclonus, autonomic instability, and mental status changes that include extreme agitation progressing to delirium and coma. The patient should also be monitored for discontinuation symptoms of the antidepressant (see package insert of the specified agent(s) for a description of the associated discontinuation symptoms).
1 Indications and Usage (1 INDICATIONS AND USAGE)
Linezolid is an oxazolidinone-class antibacterial indicated in adults and children for the treatment of the following infections caused by susceptible Gram-positive bacteria: Nosocomial pneumonia (1.1); Community-acquired pneumonia (1.2); Complicated skin and skin structure infections, including diabetic foot infections, without concomitant osteomyelitis (1.3); Uncomplicated skin and skin structure infections (1.4); Vancomycin-resistant Enterococcus faecium infections. (1.5)
Limitations of Use (
1.6
):
-
•Linezolid is not indicated for the treatment of Gram-negative infections.
-
•The safety and efficacy of linezolid formulations given for longer than 28 days have not been evaluated in controlled clinical trials.
To reduce the development of drug-resistant bacteria and maintain the effectiveness of linezolid formulations and other antibacterial drugs, linezolid should be used only to treat or prevent infections that are proven or strongly suspected to be caused by bacteria. (1.7)
1.1 Nosocomial Pneumonia
Linezolid is indicated for the treatment of nosocomial pneumonia caused by Staphylococcus aureus (methicillin-susceptible and -resistant isolates) or Streptococcus pneumoniae [see Clinical Studies (14) ].
12.1 Mechanism of Action
Linezolid is an antibacterial drug [see Microbiology (12.4) ].
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
-
•Myelosuppression: Monitor complete blood counts weekly. Thrombocytopenia has been reported more often in patients with severe renal and in patients with moderate to severe hepatic impairment. Consider discontinuation in patients who develop or have worsening myelosuppression. (5.1)
-
•Peripheral and Optic Neuropathy: Reported primarily in patients treated for longer than 28 days. If patients experience symptoms of visual impairment, prompt ophthalmic evaluation is recommended. (5.2)
-
•Serotonin Syndrome: Monitor patients taking serotonergic agents, including antidepressants and opioids, for signs of serotonin syndrome. Patients taking serotonergic antidepressants should receive linezolid only if no other therapies are available. Discontinue serotonergic antidepressants and monitor patients for signs and symptoms of both serotonin syndrome and antidepressant discontinuation. (5.3)
-
•A mortality imbalance was seen in an investigational study in linezolid-treated patients with catheter-related bloodstream infections. (5.4)
-
•Clostridioides difficile-Associated Diarrhea: Evaluate if diarrhea occurs. (5.5)
-
•Potential interactions producing elevation of blood pressure: monitor blood pressure. (5.6)
-
•Rhabdomyolysis: If signs or symptoms of rhabdomyolysis are observed, discontinue LinezolidTablets and initiate appropriate therapy. (5.9)
-
•Hypoglycemia: Postmarketing cases of symptomatic hypoglycemia have been reported in patients with diabetes mellitus receiving insulin or oral hypoglycemic agents. (5.10)
-
•Hyponatremia and/or Syndrome of Inappropriate Antidiuretic Hormone Secretion (SIADH): Monitor serum sodium levels regularly in patients at risk of hyponatremia and/or SIADH. (5.11)
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
| Dosage, Route, and Frequency of Administration | |||
|---|---|---|---|
| Infection |
Pediatric Patients
(Birth through 11 years of Age) |
Adults and Adolescents
(12 years and Older) |
Duration
(days) |
|
Nosocomial pneumonia |
10 mg/kg intravenous or oral every 8 hours |
600 mg intravenous or oral every 12 hours |
10 to 14 |
|
Community-acquired pneumonia, including concurrent bacteremia |
|||
|
Complicated skin and skin structure infections |
|||
|
Vancomycin-resistant Enterococcus faecium infections, including concurrent bacteremia |
10 mg/kg intravenous or oral every 8 hours |
600 mg intravenous or oral every 12 hours |
14 to 28 |
|
Uncomplicated skin and skin structure infections |
less than 5 yrs: 10 mg/kg oral every 8 hours |
Adults: 400 mg oral every 12 hours |
10 to 14 |
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
LINEZOLID 600 mg Tablet:
white, capsule-shaped, film-coated tablet debossed with "ZYV" on one side and "600" on the other.
5.5 Clostridioides Difficile (5.5 Clostridioides difficile)
Clostridioides difficile-Associated Diarrhea (CDAD) has been reported with use of nearly all antibacterial agents, including linezolid, and may range in severity from mild diarrhea to fatal colitis. Treatment with antibacterial agents alters the normal flora of the colon leading to overgrowth of C. difficile.
C. difficile produces toxins A and B which contribute to the development of CDAD. Hypertoxin producing strains of C. difficile cause increased morbidity and mortality, as these infections can be refractory to antimicrobial therapy and may require colectomy. CDAD must be considered in all patients who present with diarrhea following antibacterial drug use.
Careful medical history is necessary since CDAD has been reported to occur over two months after the administration of antibacterial agents.
If CDAD is suspected or confirmed, ongoing antibacterial drug use not directed against C. difficile may need to be discontinued. Appropriate fluid and electrolyte management, protein supplementation, antibacterial drug treatment of C. difficile, and surgical evaluation should be instituted as clinically indicated.
6.2 Postmarketing Experience
The following adverse reactions have been identified during post-approval use of linezolid. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure;
-
•Anaphylaxis, angioedema, bullous skin disorders including severe cutaneous adverse reactions (SCAR) such as toxic epidermal necrolysis and Stevens-Johnson syndrome, and hypersensitivity vasculitis.
-
•Myelosuppression (including anemia, leukopenia, pancytopenia, and thrombocytopenia). Thrombocytopenia has been reported more often in patients with severe renal impairment and in patients with moderate to severe hepatic impairment [see Warnings and Precautions (5.1) ]; sideroblastic anemia.
-
•Peripheral neuropathy, and optic neuropathy sometimes progressing to loss of vision [see Warnings and Precautions (5.2) ].
-
•Serotonin syndrome has been reported in patients receiving concomitant serotonergic agents, including antidepressants such as selective serotonin reuptake inhibitors (SSRIs) and opioids, and linezolid [see Warnings and Precautions (5.3) ].
-
•Lactic acidosis [see Warnings and Precautions (5.7) ]. Although these reports have primarily been in patients treated for longer than the maximum recommended duration of 28 days, these events have also been reported in patients receiving shorter courses of therapy.
-
•Convulsions [see Warnings and Precautions (5.8) ].
-
•Rhabdomyolysis [see Warnings and Precautions (5.9) ].
-
•Hypoglycemia, including symptomatic episodes [see Warnings and Precautions (5.10) ].
-
•Hyponatremia and/or Syndrome of Inappropriate Antidiuretic Hormone Secretion (SIADH) [see Warnings and Precautions (5.11) ].
-
•Superficial tooth discoloration and tongue discoloration have been reported with the use of linezolid. The tooth discoloration was removable with professional dental cleaning (manual descaling) in cases with known outcome.
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
1.2 Community Acquired Pneumonia (1.2 Community-acquired Pneumonia)
Linezolid is indicated for the treatment of community-acquired pneumonia caused by Streptococcus pneumoniae, including cases with concurrent bacteremia, or Staphylococcus aureus (methicillin-susceptible isolates only) [see Clinical Studies (14) ].
4.2 Monoamine Oxidase Inhibitors
Linezolid should not be used in patients taking any medicinal product which inhibits monoamine oxidases A or B (e.g., phenelzine, isocarboxazid) or within two weeks of taking any such medicinal product.
7.1 Monoamine Oxidase Inhibitors
Linezolid is a reversible, nonselective inhibitor of monoamine oxidase [see Contraindications (4.2) and Clinical Pharmacology (12.3) ].
5.2 Peripheral and Optic Neuropathy
Peripheral and optic neuropathies have been reported in patients treated with linezolid, primarily in those patients treated for longer than the maximum recommended duration of 28 days. In cases of optic neuropathy that progressed to loss of vision, patients were treated for extended periods beyond the maximum recommended duration. Visual blurring has been reported in some patients treated with linezolid for less than 28 days. Peripheral and optic neuropathy has also been reported in children.
If patients experience symptoms of visual impairment, such as changes in visual acuity, changes in color vision, blurred vision, or visual field defect, prompt ophthalmic evaluation is recommended. Visual function should be monitored in all patients taking linezolid for extended periods (≥ 3 months) and in all patients reporting new visual symptoms regardless of length of therapy with linezolid. If peripheral or optic neuropathy occurs, the continued use of linezolid in these patients should be weighed against the potential risks.
16 How Supplied/storage and Handling (16 HOW SUPPLIED/STORAGE AND HANDLING)
Linezolid Tablets are available as follows:
600 mg (white, capsule-shaped, film-coated tablet debossed with "ZYV" on one side and "600" on the other)
|
20 tablets in HDPE bottle |
NDC 59762-1307-1 |
|
Unit dose packages of 20 tablets |
NDC 59762-1307-2 |
2.1 General Dosage and Administration
The recommended dosage for linezolid formulations for the treatment of infections is described in Table 1.
| Dosage, Route and Frequency of Administration | Recommended Duration of Treatment (consecutive days) | ||
|---|---|---|---|
|
Infection
Due to the designated pathogens [see Indications and Usage (1)
]
|
Pediatric Patients
Neonates less than 7 days: Most pre-term neonates less than 7 days of age (gestational age less than 34 weeks) have lower systemic linezolid clearance values and larger AUC values than many full-term neonates and older infants. These neonates should be initiated with a dosing regimen of 10 mg/kg every 12 hours. Consideration may be given to the use of 10 mg/kg every 8 hours regimen in neonates with a sub-optimal clinical response. All neonatal patients should receive 10 mg/kg every 8 hours by 7 days of life [see Use in Specific Populations (8.4) and Clinical Pharmacology (12.3)
].
(Birth through 11 Years of Age)
|
Adults and Adolescents
(12 Years and Older) |
|
|
Nosocomial pneumonia |
10 mg/kg intravenously or oral Oral dosing using either linezolid Tablets or linezolid for Oral Suspension [see How Supplied/Storage and Handling (16)
]. every 8 hours
|
600 mg intravenously or oral every 12 hours |
10 to 14 |
|
Community-acquired pneumonia, including concurrent bacteremia |
|||
|
Complicated skin and skin structure infections |
|||
|
Vancomycin-resistant Enterococcus faecium infections, including concurrent bacteremia |
10 mg/kg intravenously or oral every 8 hours |
600 mg intravenously or oral every 12 hours |
14 to 28 |
|
Uncomplicated skin and skin structure infections |
less than 5 yrs: 10 mg/kg oral every 8 hours5–11 yrs: 10 mg/kg oral every 12 hours |
Adults: 400 mg oral every 12 hoursAdolescents: 600 mg oral every 12 hours |
10 to 14 |
No dose adjustment is necessary when switching from intravenous to oral administration.
7.2 Adrenergic and Serotonergic Agents
Linezolid has the potential for interaction with adrenergic and serotonergic agents [see Warnings and Precautions (5.3, 5.6) and Clinical Pharmacology (12.3) ].
13.2 Animal Toxicology And/or Pharmacology (13.2 Animal Toxicology and/or Pharmacology)
Target organs of linezolid toxicity were similar in juvenile and adult rats and dogs. Dose- and time-dependent myelosuppression, as evidenced by bone marrow hypocellularity/decreased hematopoiesis, decreased extramedullary hematopoiesis in spleen and liver, and decreased levels of circulating erythrocytes, leukocytes, and platelets have been seen in animal studies. Lymphoid depletion occurred in thymus, lymph nodes, and spleen. Generally, the lymphoid findings were associated with anorexia, weight loss, and suppression of body weight gain, which may have contributed to the observed effects.
In rats administered linezolid orally for 6 months, non-reversible, minimal to mild axonal degeneration of sciatic nerves was observed at 80 mg/kg/day; minimal degeneration of the sciatic nerve was also observed in 1 male at this dose level at a 3-month interim necropsy. Sensitive morphologic evaluation of perfusion-fixed tissues was conducted to investigate evidence of optic nerve degeneration. Minimal to moderate optic nerve degeneration was evident in 2 male rats after 6 months of dosing, but the direct relationship to drug was equivocal because of the acute nature of the finding and its asymmetrical distribution. The nerve degeneration observed was microscopically comparable to spontaneous unilateral optic nerve degeneration reported in aging rats and may be an exacerbation of common background change.
These effects were observed at exposure levels that are comparable to those observed in some human subjects. The hematopoietic and lymphoid effects were reversible, although in some studies, reversal was incomplete within the duration of the recovery period.
5.12 Development of Drug Resistant Bacteria (5.12 Development of Drug-Resistant Bacteria)
Prescribing linezolid in the absence of a proven or strongly suspected bacterial infection or a prophylactic indication is unlikely to provide benefit to the patient and increases the risk of the development of drug-resistant bacteria.
1.5 Vancomycin Resistant Enterococcus Faecium (1.5 Vancomycin-resistant Enterococcus faecium)
Linezolid is indicated for the treatment of vancomycin-resistant Enterococcus faecium infections, including cases with concurrent bacteremia [see Clinical Studies (14) ].
1.3 Complicated Skin and Skin Structure Infections
Linezolid is indicated for the treatment of complicated skin and skin structure infections, including diabetic foot infections, without concomitant osteomyelitis, caused by Staphylococcus aureus (methicillin-susceptible and -resistant isolates), Streptococcus pyogenes, or Streptococcus agalactiae. Linezolid has not been studied in the treatment of decubitus ulcers [see Clinical Studies (14) ].
1.4 Uncomplicated Skin and Skin Structure Infections
Linezolid is indicated for the treatment of uncomplicated skin and skin structure infections caused by Staphylococcus aureus (methicillin-susceptible isolates only) or Streptococcus pyogenes [see Clinical Studies (14) ].
Principal Display Panel 600 Mg Tablet Bottle Label (PRINCIPAL DISPLAY PANEL - 600 mg Tablet Bottle Label)
NDC 59762-1307-1
20 Tablets
GREENSTONE® BRAND
linezolid
tablets
600 mg
Rx only
Principal Display Panel 600 Mg Tablet Blister Pack Box (PRINCIPAL DISPLAY PANEL - 600 mg Tablet Blister Pack Box)
NDC 59762-1307-2
20 Tablets
GREENSTONE® BRAND
linezolid tablets
600 mg
For in-institution use only
Rx only
UNIT DOSE
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Lifetime studies in animals have not been conducted to evaluate the carcinogenic potential of linezolid. Neither mutagenic nor clastogenic potential was found in a battery of tests including: assays for mutagenicity (Ames bacterial reversion and CHO cell mutation), an in vitro unscheduled DNA synthesis (UDS) assay, an in vitro chromosome aberration assay in human lymphocytes, and an in vivo mouse micronucleus assay.
Linezolid did not affect the fertility or reproductive performance of adult female rats given oral doses of up to 100 mg/kg/day for 14 days prior to mating through Gestation Day 7. It reversibly decreased fertility and reproductive performance in adult male rats when given at doses ≥ 50 mg/kg/day, with exposures approximately equal to or greater than the expected human exposure level (exposure comparisons are based on AUCs). The reversible fertility effects were mediated through altered spermatogenesis. Affected spermatids contained abnormally formed and oriented mitochondria and were non-viable. Epithelial cell hypertrophy and hyperplasia in the epididymis was observed in conjunction with decreased fertility. Similar epididymal changes were not seen in dogs.
In sexually mature male rats exposed to drug as juveniles, mildly decreased fertility was observed following treatment with linezolid through most of their period of sexual development (50 mg/kg/day from days 7 to 36 of age, and 100 mg/kg/day from days 37 to 55 of age), with exposures up to 1.7 times greater than mean AUCs observed in pediatric patients aged 3 months to 11 years. Decreased fertility was not observed with shorter treatment periods, corresponding to exposure in utero through the early neonatal period (gestation day 6 through postnatal day 5), neonatal exposure (postnatal days 5 to 21), or to juvenile exposure (postnatal days 22 to 35). Reversible reductions in sperm motility and altered sperm morphology were observed in rats treated from postnatal day 22 to 35.
Principal Display Panel 600 Mg Tablet Blister Pack Label (PRINCIPAL DISPLAY PANEL - 600 mg Tablet Blister Pack Label)
linezolid tablets
600 mg
Distributed by:
Greenstone LLC
Morgantown, WV 26505 U.S.A.
MADE IN SINGAPORE
5.6 Potential Interactions Producing Elevation of Blood Pressure
Unless patients are monitored for potential increases in blood pressure, linezolid should not be administered to patients with uncontrolled hypertension, pheochromocytoma, thyrotoxicosis and/or patients taking any of the following types of medications: directly and indirectly acting sympathomimetic agents (e.g., pseudoephedrine), vasopressive agents (e.g., epinephrine, norepinephrine), dopaminergic agents (e.g., dopamine, dobutamine) [see Drug Interactions (7) and Clinical Pharmacology (12.3) ].
5.11 Hyponatremia And/or Syndrome of Inappropriate Antidiuretic Hormone Secretion (siadh) (5.11 Hyponatremia and/or Syndrome of Inappropriate Antidiuretic Hormone Secretion (SIADH))
Postmarketing cases of hyponatremia and/or Syndrome of Inappropriate Antidiuretic Hormone Secretion (SIADH) have been observed in patients treated with linezolid. In reported cases, the signs and symptoms included confusion, somnolence, generalized weakness, and in severe cases led to respiratory failure and even death. Monitor serum sodium levels regularly in the elderly, in patients taking diuretics, and in other patients at risk of hyponatremia and/or SIADH while taking linezolid. If signs and symptoms of hyponatremia and/or SIADH occur, discontinue linezolid, and institute appropriate supportive measures.
5.4 Mortality Imbalance in An Investigational Study in Patients With Catheter Related Bloodstream Infections, Including Those With Catheter Site Infections (5.4 Mortality Imbalance in an Investigational Study in Patients with Catheter-Related Bloodstream Infections, Including Those with Catheter-site Infections)
An imbalance in mortality was seen in patients treated with linezolid relative to vancomycin/dicloxacillin/oxacillin in an open-label study in seriously ill patients with intravascular catheter-related infections [78/363 (21.5%) vs. 58/363 (16.0%); odds ratio 1.426, 95% CI 0.970, 2.098]. While causality has not been established, this observed imbalance occurred primarily in linezolid-treated patients in whom either Gram-negative pathogens, mixed Gram-negative and Gram-positive pathogens, or no pathogen were identified at baseline, but was not seen in patients with Gram-positive infections only.
Linezolid is not approved and should not be used for the treatment of patients with catheter-related bloodstream infections or catheter-site infections.
Linezolid has no clinical activity against Gram-negative pathogens and is not indicated for the treatment of Gram-negative infections. It is critical that specific Gram-negative therapy be initiated immediately if a concomitant Gram-negative pathogen is documented or suspected [see Indications and Usage (1) ].
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:47:18.770445 · Updated: 2026-03-14T22:26:48.659833