These Highlights Do Not Include All The Information Needed To Use Bridion Safely And Effectively. See Full Prescribing Information For Bridion.
37276948-ff0f-e0ab-e063-6394a90a0973
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
Indication and Usage ( 1 ) 12/2024
Indications and Usage
BRIDION ® is indicated for the reversal of neuromuscular blockade induced by rocuronium bromide and vecuronium bromide in adult and pediatric patients undergoing surgery.
Dosage and Administration
Dosing is based on actual body weight ( 2.1 ) Monitor for twitch responses to determine the timing and dose for BRIDION administration. ( 2.1 ) Administer as a single bolus injection. ( 2.1 ) For rocuronium and vecuronium: 4 mg/kg is recommended if spontaneous recovery of the twitch response has reached 1 to 2 post-tetanic counts (PTC) and there are no twitch responses to train-of-four (TOF) stimulation. ( 2.2 ) 2 mg/kg is recommended if spontaneous recovery has reached the reappearance of the second twitch in response to TOF stimulation. ( 2.2 ) For rocuronium only: 16 mg/kg is recommended if there is a clinical need to reverse neuromuscular blockade soon (approximately 3 minutes) after administration of a single dose of 1.2 mg/kg of rocuronium. Immediate reversal in pediatric patients has not been studied. ( 2.2 )
Warnings and Precautions
Anaphylaxis : Be prepared for hypersensitivity reactions (including anaphylactic reactions) and take necessary precautions. ( 5.1 ) Marked Bradycardia : Cases of marked bradycardia, some of which have resulted in cardiac arrest, have been observed within minutes after administration. Monitor for hemodynamic changes and administer anticholinergic agents such as atropine if clinically significant bradycardia is observed. ( 5.2 ) Respiratory Function Monitoring : Ventilatory support is mandatory until adequate spontaneous respiration is restored and the ability to maintain a patent airway is assured. Provide adequate ventilation if neuromuscular blockade persists after BRIDION or recurs following extubation. ( 5.3 , 5.4 ) Waiting Times for Re-Administration of Neuromuscular Blocking Agents : If re-administration of a neuromuscular blocking agent is required after reversal with BRIDION, waiting times should be based on the dose of BRIDION and the renal function of the patient. Consider use of a nonsteroidal neuromuscular blocking agent. ( 5.5 )
Contraindications
BRIDION is contraindicated in patients with known hypersensitivity to sugammadex or any of its components. Hypersensitivity reactions that occurred varied from isolated skin reactions to serious systemic reactions (i.e., anaphylaxis, anaphylactic shock) and have occurred in patients with no prior exposure to sugammadex [see Warnings and Precautions (5.1) , Adverse Reactions (6) ] .
Adverse Reactions
The following serious adverse reactions are described elsewhere in the labeling: Anaphylaxis and Hypersensitivity [see Contraindications (4) , Warnings and Precautions (5.1) ] Marked Bradycardia [see Warnings and Precautions (5.2) ]
Drug Interactions
Toremifene : Concomitant use can delay recovery. ( 7.2 ) Hormonal contraceptives : Patients must use an additional, non-hormonal method of contraception for 7 days following BRIDION administration. ( 5.6 , 7.3 )
Storage and Handling
BRIDION (sugammadex) injection is a clear, colorless to slightly yellow-brown, non-pyrogenic aqueous solution intended for intravenous infusion. BRIDION is available in the following presentations: BRIDION 2-mL single-dose vial containing 200 mg sugammadex (100 mg/mL) NDC 84549-423-12 The packaging of this product is not made with natural rubber latex.
How Supplied
BRIDION (sugammadex) injection is a clear, colorless to slightly yellow-brown, non-pyrogenic aqueous solution intended for intravenous infusion. BRIDION is available in the following presentations: BRIDION 2-mL single-dose vial containing 200 mg sugammadex (100 mg/mL) NDC 84549-423-12 The packaging of this product is not made with natural rubber latex.
Medication Information
Warnings and Precautions
Anaphylaxis : Be prepared for hypersensitivity reactions (including anaphylactic reactions) and take necessary precautions. ( 5.1 ) Marked Bradycardia : Cases of marked bradycardia, some of which have resulted in cardiac arrest, have been observed within minutes after administration. Monitor for hemodynamic changes and administer anticholinergic agents such as atropine if clinically significant bradycardia is observed. ( 5.2 ) Respiratory Function Monitoring : Ventilatory support is mandatory until adequate spontaneous respiration is restored and the ability to maintain a patent airway is assured. Provide adequate ventilation if neuromuscular blockade persists after BRIDION or recurs following extubation. ( 5.3 , 5.4 ) Waiting Times for Re-Administration of Neuromuscular Blocking Agents : If re-administration of a neuromuscular blocking agent is required after reversal with BRIDION, waiting times should be based on the dose of BRIDION and the renal function of the patient. Consider use of a nonsteroidal neuromuscular blocking agent. ( 5.5 )
Indications and Usage
BRIDION ® is indicated for the reversal of neuromuscular blockade induced by rocuronium bromide and vecuronium bromide in adult and pediatric patients undergoing surgery.
Dosage and Administration
Dosing is based on actual body weight ( 2.1 ) Monitor for twitch responses to determine the timing and dose for BRIDION administration. ( 2.1 ) Administer as a single bolus injection. ( 2.1 ) For rocuronium and vecuronium: 4 mg/kg is recommended if spontaneous recovery of the twitch response has reached 1 to 2 post-tetanic counts (PTC) and there are no twitch responses to train-of-four (TOF) stimulation. ( 2.2 ) 2 mg/kg is recommended if spontaneous recovery has reached the reappearance of the second twitch in response to TOF stimulation. ( 2.2 ) For rocuronium only: 16 mg/kg is recommended if there is a clinical need to reverse neuromuscular blockade soon (approximately 3 minutes) after administration of a single dose of 1.2 mg/kg of rocuronium. Immediate reversal in pediatric patients has not been studied. ( 2.2 )
Contraindications
BRIDION is contraindicated in patients with known hypersensitivity to sugammadex or any of its components. Hypersensitivity reactions that occurred varied from isolated skin reactions to serious systemic reactions (i.e., anaphylaxis, anaphylactic shock) and have occurred in patients with no prior exposure to sugammadex [see Warnings and Precautions (5.1) , Adverse Reactions (6) ] .
Adverse Reactions
The following serious adverse reactions are described elsewhere in the labeling: Anaphylaxis and Hypersensitivity [see Contraindications (4) , Warnings and Precautions (5.1) ] Marked Bradycardia [see Warnings and Precautions (5.2) ]
Drug Interactions
Toremifene : Concomitant use can delay recovery. ( 7.2 ) Hormonal contraceptives : Patients must use an additional, non-hormonal method of contraception for 7 days following BRIDION administration. ( 5.6 , 7.3 )
Storage and Handling
BRIDION (sugammadex) injection is a clear, colorless to slightly yellow-brown, non-pyrogenic aqueous solution intended for intravenous infusion. BRIDION is available in the following presentations: BRIDION 2-mL single-dose vial containing 200 mg sugammadex (100 mg/mL) NDC 84549-423-12 The packaging of this product is not made with natural rubber latex.
How Supplied
BRIDION (sugammadex) injection is a clear, colorless to slightly yellow-brown, non-pyrogenic aqueous solution intended for intravenous infusion. BRIDION is available in the following presentations: BRIDION 2-mL single-dose vial containing 200 mg sugammadex (100 mg/mL) NDC 84549-423-12 The packaging of this product is not made with natural rubber latex.
Description
Indication and Usage ( 1 ) 12/2024
Section 42229-5
For rocuronium and vecuronium:
- A dose of 4 mg/kg BRIDION is recommended if spontaneous recovery of the twitch response has reached 1 to 2 post-tetanic counts (PTC) and there are no twitch responses to train-of-four (TOF) stimulation following rocuronium- or vecuronium-induced neuromuscular blockade [see Warnings and Precautions (5.8)].
- A dose of 2 mg/kg BRIDION is recommended if spontaneous recovery has reached the reappearance of the second twitch (T 2) in response to TOF stimulation following rocuronium- or vecuronium-induced neuromuscular blockade [see Warnings and Precautions (5.8)].
Section 43683-2
| Indication and Usage ( 1) | 12/2024 |
Section 44425-7
Store at 25°C (77°F); excursions permitted to 15°C to 30°C (59°F to 86°F) (see USP Controlled Room Temperature). Protect from light. When not protected from light, the vial should be used within 5 days.
Discard unused portion.
7.1 Summary
The information reported in sections 7.2– 7.4is based on binding affinity between BRIDION and other drugs, preclinical experiments, clinical studies and simulations of a pharmacokinetic-pharmacodynamic (PK-PD) model. Based on these considerations, no clinically significant pharmacodynamic interactions with other drugs are expected, with the exception of toremifene and hormonal contraceptives.
10 Overdosage
In premarketing clinical trials, one case of accidental overdose with 40 mg/kg BRIDION was reported without significant effects.
BRIDION can be removed using hemodialysis with a high-flux filter, but not with a low-flux filter. Based upon clinical studies, BRIDION concentrations in plasma are reduced with a high-flux filter by about 70% after a 3- to 6-hour dialysis session.
11 Description
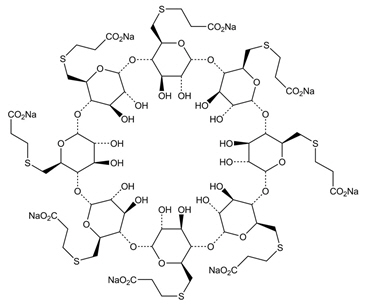
BRIDION (sugammadex) injection, for intravenous use, contains sugammadex sodium, a modified gamma cyclodextrin chemically designated as 6 A,6 B,6 C,6 D,6 E,6 F,6 G,6 H-Octakis-S-(2-carboxyethyl)-6 A,6 B,6 C,6 D,6 E,6 F,6 G,6 H-octathio- γ -cyclodextrin sodium salt(1:8) with a molecular weight of 2178.01. The structural formula is:
BRIDION is supplied as a sterile, non-pyrogenic aqueous solution that is clear, colorless to slightly yellow-brown for intravenous injection only. Each mL contains 100 mg sugammadex, which is equivalent to 108.8 mg sugammadex sodium. The aqueous solution is adjusted to a pH of between 7 and 8 with hydrochloric acid and/or sodium hydroxide. The osmolality of the product is between 300 and 500 mOsmol/kg.
BRIDION may contain up to 7 mg/mL of the mono OH-derivative of sugammadex [see Clinical Pharmacology (12.2)] . This derivative is chemically designated as 6 A,6 B,6 C,6 D,6 E,6 F,6 G-Heptakis-S-(2-carboxyethyl)-6 A,6 B,6 C,6 D,6 E,6 F,6 G-heptathio- γ -cyclodextrin sodiumsalt (1:7) with a molecular weight of 2067.90. The structural formula is:
8.4 Pediatric Use
The safety and effectiveness of BRIDION for reversal of neuromuscular blockade induced by rocuronium bromide or vecuronium bromide have been established in pediatric patients from birth and older. Use of BRIDION in these age groups is supported by evidence from adequate and well-controlled studies of BRIDION [see Clinical Pharmacology (12.3)and Clinical Studies (14.1)]. In pediatric patients, the safety profile is generally consistent with that observed in adults [see Adverse Reactions (6.1)] .
8.5 Geriatric Use
BRIDION has been administered in a dedicated clinical study to a total 102 geriatric patients that compared the time to recovery from neuromuscular blockade induced by rocuronium (0.6 mg/kg) following administration of 2 mg/kg BRIDION given at the reappearance of T 2in 65-74 year-olds (N=62) and ≥75 year-olds (N=40) compared with 18-64 year-olds (N=48). The median time to recovery of the TOF (T 4/T 1) ratio to 0.9 in 18-64 year-olds was 2.2 minutes; in 65-74 year-olds it was 2.5 minutes, and in ≥75 year-olds it was 3.6 minutes. For time to recovery from neuromuscular blockade induced by rocuronium following administration of 4 mg/kg BRIDION given at 1-2 PTCs, results across clinical trials revealed a median recovery of 2.5 minutes for geriatric patients (≥65 years, N=63) versus 2.0 minutes, for adults aged 18-64 years (N=359). Hence no dose adjustment is necessary in geriatric patients with normal organ function [see Dosage and Administration (2.2)] .
This drug is known to be substantially excreted by the kidney, and the risk of adverse reactions to this drug may be greater in patients with impaired renal function. Because elderly patients are more likely to have decreased renal function, care should be taken in dose selection, and it may be useful to monitor renal function [see Use in Specific Populations (8.6), Clinical Pharmacology (12.3)] .
4 Contraindications
BRIDION is contraindicated in patients with known hypersensitivity to sugammadex or any of its components. Hypersensitivity reactions that occurred varied from isolated skin reactions to serious systemic reactions (i.e., anaphylaxis, anaphylactic shock) and have occurred in patients with no prior exposure to sugammadex [see Warnings and Precautions (5.1), Adverse Reactions (6)] .
6 Adverse Reactions
The following serious adverse reactions are described elsewhere in the labeling:
- Anaphylaxis and Hypersensitivity [see Contraindications (4), Warnings and Precautions (5.1)]
- Marked Bradycardia [see Warnings and Precautions (5.2)]
7 Drug Interactions
8.6 Renal Impairment
This drug is known to be substantially excreted by the kidney. Effect of mild or moderate renal impairment (creatinine clearance ≥30 and ≤80 mL/min) on sugammadex PK and PD was obtained from a study in elderly patients [see Use in Specific Populations (8.5)] . Although clearance of drug decreased in elderly subjects with mild and moderate renal impairment, there was no significant difference in the ability of sugammadex to reverse the pharmacodynamic effect of rocuronium. Hence, no dosage adjustment is necessary for mild and moderate renal impairment. BRIDION is not recommended for use in patients with severe renal impairment (creatinine clearance <30 mL/min) due to insufficient safety information combined with the prolonged and increased overall exposure in these patients [see Warnings and Precautions (5.11), Clinical Pharmacology (12.3)] .
8.8 Cardiac Patients
One trial of 76 patients who were diagnosed with or have a history of cardiac disease (e.g., patients with ischemic heart disease, chronic heart failure, or arrhythmia) of primarily NYHA (New York Heart Association) Class II investigated time to recovery from neuromuscular blockade induced by rocuronium 0.6 mg/kg following administration of 2 mg/kg or 4 mg/kg BRIDION given at the reappearance of T 2. The trial showed that the median time to recovery of the T 4/T 1ratio to 0.9 was 1.7 minutes and 1.3 minutes, respectively, in the 2 mg/kg and 4 mg/kg BRIDION dose groups. This is similar to the median values observed in the other trials; therefore, no dosage adjustment is necessary [see Dosage and Administration (2.2)] .
12.2 Pharmacodynamics
BRIDION has been administered in doses ranging from 0.5 mg/kg to 16 mg/kg in dose response trials of rocuronium-induced blockade (0.6, 0.9, 1 and 1.2 mg/kg with and without maintenance doses) and vecuronium-induced blockade (0.1 mg/kg with or without maintenance doses) at different time points/depths of block. In these trials a clear dose-response relationship was observed.
BRIDION may contain up to 7% of the mono OH-derivative of sugammadex. In preclinical pharmacology studies, the mono OH-derivative was demonstrated to have ~50% of the affinity as sugammadex for rocuronium and vecuronium and that product with up to 7% of the mono OH-derivative has nearly similar efficacy in reversing rocuronium- or vecuronium-induced blockade.
Although sugammadex has greatest affinity for aminosteroid neuromuscular blocking agents such as rocuronium and vecuronium, plasma levels of endogenous or exogenous compounds with a similar steroidal structure, such as some hormones, hormonal contraceptives, and pheromones may also be reduced following administration of sugammadex [see Drug Interactions (7.3)] .
12.3 Pharmacokinetics
The sugammadex pharmacokinetic parameters were calculated from the total sum of non-complex-bound and complex-bound concentrations of sugammadex. Pharmacokinetic parameters as clearance and volume of distribution are assumed to be the same for non-complex-bound and complex-bound sugammadex in anesthetized patients.
5.11 Renal Impairment
BRIDION is not recommended for use in patients with severe renal impairment, including those requiring dialysis [see Use in Specific Populations (8.6)] . With regard to the recommended waiting time for re-administration in patients with mild or moderate renal impairment, see Waiting Times for Re-Administration of Neuromuscular Blocking Agents for Intubation Following Reversal with BRIDION [see Warnings and Precautions (5.5)] .
5.12 Light Anesthesia
When neuromuscular blockade was reversed intentionally in the middle of anesthesia in clinical trials, e.g., when investigating urgent reversal, signs of light anesthesia were noted occasionally (movement, coughing, grimacing and suckling of the tracheal tube).
2.2 Recommended Dosing
BRIDION can be used to reverse different levels of rocuronium- or vecuronium-induced neuromuscular blockade.
2.3 Drug Compatibility
May inject BRIDION into the intravenous line of a running infusion with the following intravenous solutions:
- 0.9% sodium chloride
- 5% dextrose
- 0.45% sodium chloride and 2.5% dextrose
- 5% dextrose in 0.9% sodium chloride
- isolyte P with 5% dextrose
- Ringer's lactate solution
- Ringer's solution
Ensure the infusion line is adequately flushed (e.g., with 0.9% sodium chloride) between administration of BRIDION and other drugs.
Do not mix BRIDION with other products except those listed above.
BRIDION is physically incompatible with verapamil, ondansetron, and ranitidine.
Visually inspect parenteral drug products for particulate matter and discoloration prior to administration, whenever the solution and container permit.
5.2 Marked Bradycardia
Cases of marked bradycardia, some of which have resulted in cardiac arrest, have been observed within minutes after the administration of BRIDION [see Adverse Reactions (6.2)] . Patients should be closely monitored for hemodynamic changes during and after reversal of neuromuscular blockade. Treatment with anticholinergic agents, such as atropine, should be administered if clinically significant bradycardia is observed.
8.7 Hepatic Impairment
BRIDION is not metabolized nor excreted by the liver; therefore, dedicated trials in patients with hepatic impairment have not been conducted. Exercise caution when administering BRIDION to patients with hepatic impairment accompanied by coagulopathy or severe edema [see Warnings and Precautions (5.10, 5.14)] .
8.9 Pulmonary Patients
One trial of 77 patients who were diagnosed with or have a history of pulmonary complications investigated the time to recovery from neuromuscular blockade induced by rocuronium (0.6 mg/kg) following administration of 2 mg/kg or 4 mg/kg BRIDION given at the first signs of recovery (reappearance of T 2). The trial showed that for these patients the median time to recovery of the T 4/T 1ratio to 0.9 was 2.1 minutes after a dose of 2 mg/kg BRIDION and 1.9 minutes after a dose of 4 mg/kg BRIDION. This is similar to the median values observed in the other trials; therefore, no dosage adjustment is necessary. [See Dosage and Administration (2.2), Adverse Reactions (6.1).]
1 Indications and Usage
BRIDION ®is indicated for the reversal of neuromuscular blockade induced by rocuronium bromide and vecuronium bromide in adult and pediatric patients undergoing surgery.
12.1 Mechanism of Action
BRIDION is a modified gamma cyclodextrin. It forms a complex with the neuromuscular blocking agents rocuronium and vecuronium, and it reduces the amount of neuromuscular blocking agent available to bind to nicotinic cholinergic receptors in the neuromuscular junction. This results in the reversal of neuromuscular blockade induced by rocuronium and vecuronium.
5 Warnings and Precautions
Anaphylaxis: Be prepared for hypersensitivity reactions (including anaphylactic reactions) and take necessary precautions. ( 5.1)
Marked Bradycardia: Cases of marked bradycardia, some of which have resulted in cardiac arrest, have been observed within minutes after administration. Monitor for hemodynamic changes and administer anticholinergic agents such as atropine if clinically significant bradycardia is observed. ( 5.2)
Respiratory Function Monitoring: Ventilatory support is mandatory until adequate spontaneous respiration is restored and the ability to maintain a patent airway is assured. Provide adequate ventilation if neuromuscular blockade persists after BRIDION or recurs following extubation. ( 5.3, 5.4)
Waiting Times for Re-Administration of Neuromuscular Blocking Agents: If re-administration of a neuromuscular blocking agent is required after reversal with BRIDION, waiting times should be based on the dose of BRIDION and the renal function of the patient. Consider use of a nonsteroidal neuromuscular blocking agent. ( 5.5)
2 Dosage and Administration
- Dosing is based on actual body weight ( 2.1)
- Monitor for twitch responses to determine the timing and dose for BRIDION administration. ( 2.1)
- Administer as a single bolus injection. ( 2.1)
For rocuronium and vecuronium:
- 4 mg/kg is recommended if spontaneous recovery of the twitch response has reached 1 to 2 post-tetanic counts (PTC) and there are no twitch responses to train-of-four (TOF) stimulation. ( 2.2)
- 2 mg/kg is recommended if spontaneous recovery has reached the reappearance of the second twitch in response to TOF stimulation. ( 2.2)
For rocuronium only:
- 16 mg/kg is recommended if there is a clinical need to reverse neuromuscular blockade soon (approximately 3 minutes) after administration of a single dose of 1.2 mg/kg of rocuronium. Immediate reversal in pediatric patients has not been studied. ( 2.2)
3 Dosage Forms and Strengths
BRIDION (sugammadex) injection is a sterile, clear, colorless to slightly yellow-brown, non-pyrogenic aqueous solution intended for intravenous infusion. BRIDION is available as follows:
- 200 mg/2 mL (100 mg/mL) in a single-dose vial for bolus injection
- 500 mg/5 mL (100 mg/mL), in a single-dose vial for bolus injection
6.2 Post Marketing Experience
The following adverse reactions have been identified during post-approval use of BRIDION. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
8 Use in Specific Populations
Severe Renal Impairment: Not recommended. ( 8.6)
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
Adult Patients
The data described below reflect 2914 subjects exposed to 2, 4, or 16 mg/kg BRIDION and 544 to placebo in pooled Phase 1-3 studies. The population was 18 to 92 years old, 47% male and 53% female, 34% ASA (American Society of Anesthesiologists) Class 1, 51% ASA Class 2, and 14% ASA Class 3, and 82% Caucasian. Most subjects received a single dose of BRIDION 2 mg/kg or 4 mg/kg.
Adverse reactions reported in ≥10% of patients at a 2, 4, or 16 mg/kg BRIDION dose with a rate higher than the placebo rate are: vomiting, pain, nausea, hypotension, and headache.
All adverse reactions occurring in ≥2% of subjects treated with BRIDION and more often than placebo for adult subjects who received anesthesia and/or neuromuscular blocking agent in pooled Phase 1 to 3 studies are presented in Table 2.
| Sugammadex | Placebo | |||
|---|---|---|---|---|
| Body System
Preferred Term |
2 mg/kg
(N=895) n (%) |
4 mg/kg
(N=1921) n (%) |
16 mg/kg
(N=98) n (%) |
(N=544)
n (%) |
| Injury, poisoning and procedural complications | ||||
| Incision site pain | 58 (6) | 106 (6) | 4 (4) | 6 (1) |
| Procedural complication | 13 (1) | 27 (1) | 8 (8) | 3 (1) |
| Airway complication of anesthesia | 11 (1) | 13 (1) | 9 (9) | 0 |
| Anesthetic complication | 8 (1) | 14 (1) | 9 (9) | 1 (<1) |
| Wound hemorrhage | 5 (1) | 38 (2) | 0 | 8 (1) |
| Recurrence of neuromuscular blockade | 0 | 1 (<1) | 2 (2) | 0 |
| Gastrointestinal disorders | ||||
| Nausea
Combinations of preferred terms are as follows:
Nausea includes preferred terms nausea and procedural nausea
Vomiting includes preferred terms vomiting and procedural vomiting
Abdominal pain includes preferred terms abdominal pain, abdominal pain upper, abdominal discomfort, abdominal pain lower, and epigastric discomfort
Pain includes preferred terms pain and procedural pain
Red blood cell count decreased includes preferred terms red blood cell count decreased, hemoglobin decreased, and hematocrit decreased
Electrocardiogram QT interval abnormal includes preferred terms electrocardiogram QT interval abnormal and electrocardiogram QT interval prolonged
Hypertension includes preferred terms hypertension, procedural hypertension, and blood pressure increased
Hypotension includes preferred terms hypotension, procedural hypotension, and blood pressure decreased
Tachycardia includes preferred terms tachycardia and heart rate increased
Bradycardia includes preferred terms bradycardia and heart rate decreased
|
208 (23) | 503 (26) | 23 (23) | 127 (23) |
| Vomiting | 98 (11) | 236 (12) | 15 (15) | 57 (10) |
| Abdominal pain | 48 (5) | 68 (4) | 6 (6) | 17 (3) |
| Flatulence | 17 (2) | 51 (3) | 1 (1) | 10 (2) |
| Dry mouth | 9 (1) | 5 (<1) | 2 (2) | 0 |
| General disorders and administration site conditions | ||||
| Pain | 434 (48) | 993 (52) | 35 (36) | 207 (38) |
| Pyrexia | 77 (9) | 109 (6) | 5 (5) | 17 (3) |
| Chills | 30 (3) | 61 (3) | 7 (7) | 27 (5) |
| Nervous system disorders | ||||
| Headache | 61 (7) | 99 (5) | 10 (10) | 42 (8) |
| Dizziness | 44 (5) | 67 (3) | 6 (6) | 13 (2) |
| Hypoesthesia | 12 (1) | 24 (1) | 3 (3) | 9 (2) |
| Respiratory, thoracic and mediastinal disorders | ||||
| Oropharyngeal pain | 42 (5) | 66 (3) | 5 (5) | 27 (5) |
| Cough | 13 (1) | 49 (3) | 8 (8) | 11 (2) |
| Musculoskeletal and connective tissue disorders | ||||
| Pain in extremity | 13 (1) | 35 (2) | 6 (6) | 15 (3) |
| Musculoskeletal pain | 16 (2) | 33 (2) | 1 (1) | 6 (1) |
| Myalgia | 5 (1) | 17 (1) | 2 (2) | 3 (1) |
| Psychiatric disorders | ||||
| Insomnia | 20 (2) | 103 (5) | 5 (5) | 22 (4) |
| Anxiety | 14 (2) | 19 (1) | 3 (3) | 1 (<1) |
| Restlessness | 3 (<1) | 17 (1) | 2 (2) | 2 (<1) |
| Depression | 2 (<1) | 5 (<1) | 2 (2) | 0 |
| Investigations | ||||
| Red blood cell count decreased | 13 (1) | 34 (2) | 1 (1) | 2 (<1) |
| Electrocardiogram QT interval abnormal | 13 (1) | 7 (<1) | 6 (6) | 4 (1) |
| Blood creatine phosphokinase increased | 9 (1) | 14 (1) | 2 (2) | 1 (<1) |
| Vascular disorders | ||||
| Hypertension | 48 (5) | 96 (5) | 9 (9) | 38 (7) |
| Hypotension | 33 (4) | 102 (5) | 13 (13) | 20 (4) |
| Skin and subcutaneous tissue disorders | ||||
| Pruritus | 17 (2) | 50 (3) | 2 (2) | 9 (2) |
| Erythema | 5 (1) | 31 (2) | 0 | 6 (1) |
| Metabolism and nutrition disorders | ||||
| Hypocalcemia | 15 (2) | 12 (1) | 0 | 4 (1) |
| Cardiac disorders | ||||
| Tachycardia | 17 (2) | 29 (2) | 5 (5) | 4 (1) |
| Bradycardia | 9 (1) | 21 (1) | 5 (5) | 6 (1) |
| Surgical and medical procedures | ||||
| Hysterectomy | 0 | 0 | 2 (2) | 0 |
17 Patient Counseling Information
- Advise females of reproductive potential using hormonal contraceptives that BRIDION may reduce the contraceptive effect .Instruct females to use an additional, non-hormonal method of contraception for the next 7 days following BRIDION administration [see Drug Interactions (7.3)].
16 How Supplied/storage and Handling
BRIDION (sugammadex) injection is a clear, colorless to slightly yellow-brown, non-pyrogenic aqueous solution intended for intravenous infusion. BRIDION is available in the following presentations:
- BRIDION 2-mL single-dose vial containing 200 mg sugammadex (100 mg/mL)
NDC 84549-423-12
The packaging of this product is not made with natural rubber latex.
5.1 Anaphylaxis and Hypersensitivity
Clinicians should be prepared for the possibility of drug hypersensitivity reactions (including anaphylactic reactions) and take the necessary precautions [see Contraindications (4), Adverse Reactions (6.1)] .
Potentially serious hypersensitivity reactions, including anaphylaxis, have occurred in patients treated with BRIDION. The nature and frequency of anaphylaxis and hypersensitivity associated with BRIDION administration were evaluated in a randomized, double-blind, placebo-controlled, parallel-group, repeat-dose study in which 375 subjects were randomized to receive 3 doses of BRIDION IV with a 5-week washout period: 151 subjects received 4 mg/kg, 148 received 16 mg/kg and 76 received placebo. The frequency of anaphylaxis for the 299 healthy volunteers treated with intravenous BRIDION was 0.3% (n=1 in the BRIDION 16 mg/kg group on the first dose). Signs and symptoms included conjunctival edema, urticaria, erythema, swelling of the uvula and reduction in peak expiratory flow within 5 minutes of dose administration. The most common hypersensitivity adverse reactions reported were nausea, pruritus and urticaria and showed a dose response relationship, occurring more frequently in the 16 mg/kg group compared to the 4 mg/kg and placebo groups.
Anaphylaxis has also been reported in the post-marketing setting, including at doses less than 16 mg/kg. The most commonly described clinical features in reports of anaphylaxis were dermatologic symptoms (including urticaria, rash, erythema, flushing and skin eruption); and clinically important hypotension often requiring the use of vasopressors for circulatory support. In addition, prolonged hospitalization and/or the use of additional respiratory support until full recovery (re-intubation, prolonged intubation, manual or mechanical ventilation) have been noted in a number of the anaphylaxis reports.
5.10 Risk of Coagulopathy and Bleeding
BRIDION doses up to 16 mg/kg were associated with increases in the coagulation parameters activated partial thromboplastin time (aPTT) and prothrombin time/international normalized ratio [PT(INR)] of up to 25% for up to 1 hour in healthy volunteers.
In patients undergoing major orthopedic surgery of the lower extremity who were concomitantly treated with heparin or low molecular weight heparin for thromboprophylaxis, increases in aPTT and PT(INR) of 5.5% and 3.0%, respectively, were observed in the hour following BRIDION 4 mg/kg administration. This clinical trial did not demonstrate an increased blood loss or anemia incidence with BRIDION compared with usual treatment. The rate of adjudicated bleeding events within 24 hours was 2.9% for sugammadex and 4.1% for usual care. The rate of post-operative anemia was 21% for sugammadex and 22% for usual care. The mean 24-hour drainage volume was 0.46 L for sugammadex and 0.48 L for usual care. The need for any post-operative transfusion was 37% for sugammadex and 39% for usual care.
In vitroexperiments demonstrated additional aPTT and PT(INR) prolongations for sugammadex in combination with vitamin K antagonists, unfractionated heparin, low molecular weight heparinoids, rivaroxaban, and dabigatran up to ~25% and ~50% at C maxlevels of sugammadex corresponding to 4 mg/kg and 16 mg/kg doses, respectively.
Since bleeding risk has been studied systematically with only heparin and low molecular weight heparin thromboprophylaxis and 4 mg/kg doses of sugammadex coagulation parameters should be carefully monitored in patients with known coagulopathies, being treated with therapeutic anticoagulation, receiving thromboprophylaxis drugs other than heparin and low molecular weight heparin, or receiving thromboprophylaxis drugs and who then receive a dose of 16 mg/kg sugammadex.
7.4 Interference With Laboratory Tests
BRIDION may interfere with the serum progesterone assay. Interference with this test was observed at sugammadex plasma concentrations of 100 mcg/mL, which may be observed for up to 30 minutes after a 16 mg/kg dose.
13.2 Animal Toxicology And/or Pharmacology
Bone and teeth retention of sugammadex occurred in rats after intravenous injection, with mean half-lives of 172 and 8 days, respectively. Sugammadex bound to hydroxyapatite in an in vitrostudy and distributed in the bone formation area where hydroxyapatite is present for mineralization in vivo.
In adult rat bone toxicity studies, a single dose of sugammadex at 2000 mg/kg (approximately 24 times the maximum recommended human dose (MRHD) of 16 mg/kg by AUC comparison) administered to adult rats caused a slight increase in bone resorption, but had no effect on teeth color. No adverse bone effects were seen following a single dose of sugammadex at 500 mg/kg (4 times the MRHD dose of 16 mg/kg based on plasma AUC comparison).
In a bone repair study, adult rats were treated with intravenous sugammadex weekly for 6 weeks at 0, 30, 120, and 500 mg/kg (approximately 0.4, 1, and 6 times the MRHD, respectively, by AUC comparison). Based on histological data, high dose animals with post-fracture treatment, showed a statistically significant increase in callus formation and decrease in bone formation, suggesting a potential for a slight delay in the bone healing process. However, there were no statistically significant effects on bone volume or bone mineral density.
In juvenile animal studies, bone and teeth deposition was significantly higher in juvenile rats compared to adults. In addition, sugammadex administered to juvenile rats daily for 4 weeks caused slight bone length decrease (approximately 3%), which did not recover after an 8-week treatment-free period, and reversible whitish discoloration of the teeth at a dose approximately 0.6 times the MRHD, while weekly administration for 8 weeks did not produce similar changes in bone and teeth at doses up to 1.2 times the MRHD [see Use in Specific Populations (8.4)] .
Principal Display Panel 2 Ml Vial Carton
8.10 Obese Patients With A Bmi ≥40 Kg/m 2
A trial of 188 obese patients, with a body mass index ≥40 kg/m 2, investigated the time to recovery from moderate or deep neuromuscular blockade induced by rocuronium or vecuronium. Patients received 2 mg/kg or 4 mg/kg BRIDION, as appropriate for level of block, dosed according to either actual body weight (ABW) or ideal body weight (IBW) in random, double-blinded fashion. Pooled across depth of block and neuromuscular blocking agent, the median time to recover to a train-of-four (TOF) ratio ≥0.9 in patients dosed by ABW (1.8 minutes) was statistically significantly faster compared to patients dosed by IBW (3.3 minutes).
The adverse reaction profile was generally similar to the profile in adult patients in pooled Phase 1 to 3 studies [see Adverse Reactions (6.1)] . No dosage adjustment is necessary [see Dosage and Administration (2.2)] .
5.4 Risk of Prolonged Neuromuscular Blockade
In clinical trials, a small number of patients experienced a delayed or minimal response to the administration of BRIDION [see Clinical Studies (14.1)] . Thus, it is important to monitor ventilation until recovery occurs.
2.1 Important Dosing and Administration Information
BRIDION dosing is based on actual body weight.
BRIDION (sugammadex) injection, for intravenous use, should be administered by trained healthcare providers familiar with the use, actions, characteristics, and complications of neuromuscular blocking agents (NMBA) and neuromuscular block reversal agents.
Doses and timing of BRIDION administration should be based on monitoring for twitch responses and the extent of spontaneous recovery that has occurred.
Administer BRIDION intravenously as a single bolus injection. The bolus injection may be given over 10 seconds, into an existing intravenous line. BRIDION has only been administered as a single bolus injection in clinical trials.
From the time of BRIDION administration until complete recovery of neuromuscular function, monitor the patient to assure adequate ventilation and maintenance of a patent airway. Satisfactory recovery should be determined through assessment of skeletal muscle tone and respiratory measurements in addition to the response to peripheral nerve stimulation.
The recommended dose of BRIDION does not depend on the anesthetic regimen.
Preparation of dilution for pediatric use:
BRIDION 100 mg/mL may be diluted to a concentration of 10 mg/mL, using 0.9% sodium chloride injection, USP, to increase the accuracy of dosing in the pediatric population.
- To prepare the required dose, aseptically transfer all the contents of the 2 mL vial of BRIDION 2-mL single-dose vials containing 200 mg sugammadex (100 mg/mL) to a bottle (or intravenous bag) containing 18 mL of 0.9% sodium chloride injection, to achieve a final concentration of 10 mg/mL sugammadex. The diluted solution should be used immediately.
- BRIDION injection is a single-dose sterile solution without preservatives. Discard any unused portion from the vial.
5.3 Respiratory Function Monitoring During Recovery
Ventilatory support is mandatory for patients until adequate spontaneous respiration is restored and the ability to maintain a patent airway is assured. Even if recovery from neuromuscular blockade is complete, other drugs used in the peri- and post-operative period could depress respiratory function and therefore ventilatory support might still be required.
Should neuromuscular blockade persist after BRIDION administration or recur following extubation, take appropriate steps to provide adequate ventilation.
8.11 American Society of Anesthesiologists Class 3 Or 4 Patients
One trial of 331 patients who were assessed as ASA Class 3 or 4 investigated the incidence of treatment-emergent arrhythmias (sinus bradycardia, sinus tachycardia, or other cardiac arrhythmias) after administration of sugammadex.
In patients receiving sugammadex (2 mg/kg, 4 mg/kg, or 16 mg/kg), the number (%) of patients with treatment-emergent sinus bradycardia (up to 35 minutes post-administration of sugammadex) was 1/105 (1.0%) in the 2 mg/kg sugammadex treatment group, 2/107 (1.9%) in the 4 mg/kg sugammadex treatment group, and 5/68 (7.4%) in the 16 mg/kg sugammadex treatment group, compared to 4/51 (7.8%) in the neostigmine (50 µg/kg up to 5 mg maximum dose) + glycopyrrolate (10 µg/kg up to 1 mg maximum dose) treatment group. The number of patients with treatment-emergent sinus tachycardia (up to 35 minutes post-administration of sugammadex) was 7/105 (6.7%) in the 2 mg/kg sugammadex treatment group, 10/107 (9.3%) in the 4 mg/kg sugammadex treatment group, and 6/68 (8.8%) in the 16 mg/kg sugammadex treatment group, compared to 11/51 (21.6%) in the neostigmine + glycopyrrolate treatment group. The number of other treatment-emergent arrhythmias (up to 35 minutes post administration of sugammadex) was 1/105 (1.0%) in the 2 mg/kg sugammadex treatment group, 0/107 (0%) in the 4 mg/kg sugammadex treatment group, and 1/68 (1.5%) in the 16 mg/kg sugammadex treatment group, compared to 1/51 (2.0%) in the neostigmine + glycopyrrolate treatment group. The adverse reaction profiles in ASA Class 3 and 4 patients were generally similar to those in adult patients in pooled Phase 1 to 3 studies; therefore, no dosage adjustment is necessary [see Dosage and Administration (2.1), Adverse Reactions (6.1)] .
5.6 Interactions Potentially Affecting the Efficacy of Other Drugs
Due to the administration of BRIDION, certain drugs, including hormonal contraceptives, could become less effective due to a lowering of the (free) plasma concentrations. In this situation, consider the re-administration of the other drug, the administration of a therapeutically equivalent drug (preferably from a different chemical class), and/or non-pharmacological interventions as appropriate [see Drug Interactions (7.3)] .
5.13 Reversal After Rocuronium Or Vecuronium Administration in the Icu
BRIDION has not been studied for reversal following rocuronium or vecuronium administration in the ICU.
7.3 Interaction Potentially Affecting the Efficacy of Hormonal Contraceptives
In vitrobinding studies indicate that BRIDION may bind to progestogen, thereby decreasing progestogen exposure. Therefore, the administration of a bolus dose of BRIDION is considered to be equivalent to missing dose(s) of oralcontraceptives containing an estrogen or progestogen. If an oral contraceptive is taken on the same day that BRIDION is administered, the patient must use an additional, non-hormonal contraceptive method or back-up method of contraception (such as condoms and spermicides) for the next 7 days.
In the case of non-oralhormonal contraceptives, the patient must use an additional, non-hormonal contraceptive method or back-up method of contraception (such as condoms and spermicides) for the next 7 days.
5.7 Risk of Recurrence of Neuromuscular Blockade Due to Displacement Interactions
Recurrence of neuromuscular blockade may occur due to displacement of rocuronium or vecuronium from BRIDION by other drugs [see Drug Interactions (7.2)] . In this situation the patient may require mechanical ventilation. Administration of the drug which caused displacement should be stopped in case of an infusion. The risk of displacement reactions will be the highest in the time period equivalent to 3 times the half-life of BRIDION [see Clinical Pharmacology (12.3)] .
5.14 Reversal of Neuromuscular Blocking Agents Other Than Rocuronium Or Vecuronium
Do not use BRIDION to reverse blockade induced by nonsteroidalneuromuscular blocking agents such as succinylcholine or benzylisoquinolinium compounds.
Do not use BRIDION to reverse neuromuscular blockade induced by steroidalneuromuscular blocking agents other than rocuronium or vecuronium.
5.8 Risk of Recurrence of Neuromuscular Blockade With Lower Than Recommended Dosing
The use of lower than recommended doses of BRIDION may lead to an increased risk of recurrence of neuromuscular blockade after initial reversal and is not recommended [see Dosage and Administration (2.2), Adverse Reactions (6.1)] .
5.5 Waiting Times for Re Administration of Neuromuscular Blocking Agents for Intubation Following Reversal With Bridion
A minimum waiting time is necessary before administration of a steroidal neuromuscular blocking agent after administration of BRIDION.
| Minimum Waiting Time | NMBA and Dose to be Administered |
|---|---|
| 5 minutes | 1.2 mg/kg rocuronium |
| 4 hours | 0.6 mg/kg rocuronium or
0.1 mg/kg vecuronium |
When rocuronium 1.2 mg/kg is administered within 30 minutes after reversal with BRIDION, the onset of neuromuscular blockade may be delayed up to approximately 4 minutes and the duration of neuromuscular blockade may be shortened up to approximately 15 minutes.
The recommended waiting time in patients with mild or moderate renal impairment for re-use of 0.6 mg/kg rocuronium or 0.1 mg/kg vecuronium after reversal with up to 4 mg/kg BRIDION should be 24 hours. If a shorter waiting time is required, the rocuronium dose for a new neuromuscular blockade should be 1.2 mg/kg.
For re-administration of rocuronium or administration of vecuronium after reversal of rocuronium with 16 mg/kg BRIDION, a waiting time of 24 hours is suggested.
If neuromuscular blockade is required before the recommended waiting time has elapsed, use a nonsteroidal neuromuscular blocking agent. The onset of a depolarizing neuromuscular blocking agent might be slower than expected, because a substantial fraction of postjunctional nicotinic receptors can still be occupied by the neuromuscular blocking agent.
5.9 Risk of Recurrence of Neuromuscular Blockade Due to the Administration of Drugs That Potentiate Neuromuscular Blockade
When drugs which potentiate neuromuscular blockade are used in the post-operative phase, special attention should be paid to the possibility of recurrence of neuromuscular blockade. Refer to the package insert for rocuronium or vecuronium for a list of the specific drugs which potentiate neuromuscular blockade. In case recurrence of neuromuscular blockade is observed, the patient may require mechanical ventilation.
Structured Label Content
Section 42229-5 (42229-5)
For rocuronium and vecuronium:
- A dose of 4 mg/kg BRIDION is recommended if spontaneous recovery of the twitch response has reached 1 to 2 post-tetanic counts (PTC) and there are no twitch responses to train-of-four (TOF) stimulation following rocuronium- or vecuronium-induced neuromuscular blockade [see Warnings and Precautions (5.8)].
- A dose of 2 mg/kg BRIDION is recommended if spontaneous recovery has reached the reappearance of the second twitch (T 2) in response to TOF stimulation following rocuronium- or vecuronium-induced neuromuscular blockade [see Warnings and Precautions (5.8)].
Section 43683-2 (43683-2)
| Indication and Usage ( 1) | 12/2024 |
Section 44425-7 (44425-7)
Store at 25°C (77°F); excursions permitted to 15°C to 30°C (59°F to 86°F) (see USP Controlled Room Temperature). Protect from light. When not protected from light, the vial should be used within 5 days.
Discard unused portion.
7.1 Summary
The information reported in sections 7.2– 7.4is based on binding affinity between BRIDION and other drugs, preclinical experiments, clinical studies and simulations of a pharmacokinetic-pharmacodynamic (PK-PD) model. Based on these considerations, no clinically significant pharmacodynamic interactions with other drugs are expected, with the exception of toremifene and hormonal contraceptives.
10 Overdosage (10 OVERDOSAGE)
In premarketing clinical trials, one case of accidental overdose with 40 mg/kg BRIDION was reported without significant effects.
BRIDION can be removed using hemodialysis with a high-flux filter, but not with a low-flux filter. Based upon clinical studies, BRIDION concentrations in plasma are reduced with a high-flux filter by about 70% after a 3- to 6-hour dialysis session.
11 Description (11 DESCRIPTION)
BRIDION (sugammadex) injection, for intravenous use, contains sugammadex sodium, a modified gamma cyclodextrin chemically designated as 6 A,6 B,6 C,6 D,6 E,6 F,6 G,6 H-Octakis-S-(2-carboxyethyl)-6 A,6 B,6 C,6 D,6 E,6 F,6 G,6 H-octathio- γ -cyclodextrin sodium salt(1:8) with a molecular weight of 2178.01. The structural formula is:
BRIDION is supplied as a sterile, non-pyrogenic aqueous solution that is clear, colorless to slightly yellow-brown for intravenous injection only. Each mL contains 100 mg sugammadex, which is equivalent to 108.8 mg sugammadex sodium. The aqueous solution is adjusted to a pH of between 7 and 8 with hydrochloric acid and/or sodium hydroxide. The osmolality of the product is between 300 and 500 mOsmol/kg.
BRIDION may contain up to 7 mg/mL of the mono OH-derivative of sugammadex [see Clinical Pharmacology (12.2)] . This derivative is chemically designated as 6 A,6 B,6 C,6 D,6 E,6 F,6 G-Heptakis-S-(2-carboxyethyl)-6 A,6 B,6 C,6 D,6 E,6 F,6 G-heptathio- γ -cyclodextrin sodiumsalt (1:7) with a molecular weight of 2067.90. The structural formula is:
8.4 Pediatric Use
The safety and effectiveness of BRIDION for reversal of neuromuscular blockade induced by rocuronium bromide or vecuronium bromide have been established in pediatric patients from birth and older. Use of BRIDION in these age groups is supported by evidence from adequate and well-controlled studies of BRIDION [see Clinical Pharmacology (12.3)and Clinical Studies (14.1)]. In pediatric patients, the safety profile is generally consistent with that observed in adults [see Adverse Reactions (6.1)] .
8.5 Geriatric Use
BRIDION has been administered in a dedicated clinical study to a total 102 geriatric patients that compared the time to recovery from neuromuscular blockade induced by rocuronium (0.6 mg/kg) following administration of 2 mg/kg BRIDION given at the reappearance of T 2in 65-74 year-olds (N=62) and ≥75 year-olds (N=40) compared with 18-64 year-olds (N=48). The median time to recovery of the TOF (T 4/T 1) ratio to 0.9 in 18-64 year-olds was 2.2 minutes; in 65-74 year-olds it was 2.5 minutes, and in ≥75 year-olds it was 3.6 minutes. For time to recovery from neuromuscular blockade induced by rocuronium following administration of 4 mg/kg BRIDION given at 1-2 PTCs, results across clinical trials revealed a median recovery of 2.5 minutes for geriatric patients (≥65 years, N=63) versus 2.0 minutes, for adults aged 18-64 years (N=359). Hence no dose adjustment is necessary in geriatric patients with normal organ function [see Dosage and Administration (2.2)] .
This drug is known to be substantially excreted by the kidney, and the risk of adverse reactions to this drug may be greater in patients with impaired renal function. Because elderly patients are more likely to have decreased renal function, care should be taken in dose selection, and it may be useful to monitor renal function [see Use in Specific Populations (8.6), Clinical Pharmacology (12.3)] .
4 Contraindications (4 CONTRAINDICATIONS)
BRIDION is contraindicated in patients with known hypersensitivity to sugammadex or any of its components. Hypersensitivity reactions that occurred varied from isolated skin reactions to serious systemic reactions (i.e., anaphylaxis, anaphylactic shock) and have occurred in patients with no prior exposure to sugammadex [see Warnings and Precautions (5.1), Adverse Reactions (6)] .
6 Adverse Reactions (6 ADVERSE REACTIONS)
The following serious adverse reactions are described elsewhere in the labeling:
- Anaphylaxis and Hypersensitivity [see Contraindications (4), Warnings and Precautions (5.1)]
- Marked Bradycardia [see Warnings and Precautions (5.2)]
7 Drug Interactions (7 DRUG INTERACTIONS)
8.6 Renal Impairment
This drug is known to be substantially excreted by the kidney. Effect of mild or moderate renal impairment (creatinine clearance ≥30 and ≤80 mL/min) on sugammadex PK and PD was obtained from a study in elderly patients [see Use in Specific Populations (8.5)] . Although clearance of drug decreased in elderly subjects with mild and moderate renal impairment, there was no significant difference in the ability of sugammadex to reverse the pharmacodynamic effect of rocuronium. Hence, no dosage adjustment is necessary for mild and moderate renal impairment. BRIDION is not recommended for use in patients with severe renal impairment (creatinine clearance <30 mL/min) due to insufficient safety information combined with the prolonged and increased overall exposure in these patients [see Warnings and Precautions (5.11), Clinical Pharmacology (12.3)] .
8.8 Cardiac Patients
One trial of 76 patients who were diagnosed with or have a history of cardiac disease (e.g., patients with ischemic heart disease, chronic heart failure, or arrhythmia) of primarily NYHA (New York Heart Association) Class II investigated time to recovery from neuromuscular blockade induced by rocuronium 0.6 mg/kg following administration of 2 mg/kg or 4 mg/kg BRIDION given at the reappearance of T 2. The trial showed that the median time to recovery of the T 4/T 1ratio to 0.9 was 1.7 minutes and 1.3 minutes, respectively, in the 2 mg/kg and 4 mg/kg BRIDION dose groups. This is similar to the median values observed in the other trials; therefore, no dosage adjustment is necessary [see Dosage and Administration (2.2)] .
12.2 Pharmacodynamics
BRIDION has been administered in doses ranging from 0.5 mg/kg to 16 mg/kg in dose response trials of rocuronium-induced blockade (0.6, 0.9, 1 and 1.2 mg/kg with and without maintenance doses) and vecuronium-induced blockade (0.1 mg/kg with or without maintenance doses) at different time points/depths of block. In these trials a clear dose-response relationship was observed.
BRIDION may contain up to 7% of the mono OH-derivative of sugammadex. In preclinical pharmacology studies, the mono OH-derivative was demonstrated to have ~50% of the affinity as sugammadex for rocuronium and vecuronium and that product with up to 7% of the mono OH-derivative has nearly similar efficacy in reversing rocuronium- or vecuronium-induced blockade.
Although sugammadex has greatest affinity for aminosteroid neuromuscular blocking agents such as rocuronium and vecuronium, plasma levels of endogenous or exogenous compounds with a similar steroidal structure, such as some hormones, hormonal contraceptives, and pheromones may also be reduced following administration of sugammadex [see Drug Interactions (7.3)] .
12.3 Pharmacokinetics
The sugammadex pharmacokinetic parameters were calculated from the total sum of non-complex-bound and complex-bound concentrations of sugammadex. Pharmacokinetic parameters as clearance and volume of distribution are assumed to be the same for non-complex-bound and complex-bound sugammadex in anesthetized patients.
5.11 Renal Impairment
BRIDION is not recommended for use in patients with severe renal impairment, including those requiring dialysis [see Use in Specific Populations (8.6)] . With regard to the recommended waiting time for re-administration in patients with mild or moderate renal impairment, see Waiting Times for Re-Administration of Neuromuscular Blocking Agents for Intubation Following Reversal with BRIDION [see Warnings and Precautions (5.5)] .
5.12 Light Anesthesia
When neuromuscular blockade was reversed intentionally in the middle of anesthesia in clinical trials, e.g., when investigating urgent reversal, signs of light anesthesia were noted occasionally (movement, coughing, grimacing and suckling of the tracheal tube).
2.2 Recommended Dosing
BRIDION can be used to reverse different levels of rocuronium- or vecuronium-induced neuromuscular blockade.
2.3 Drug Compatibility
May inject BRIDION into the intravenous line of a running infusion with the following intravenous solutions:
- 0.9% sodium chloride
- 5% dextrose
- 0.45% sodium chloride and 2.5% dextrose
- 5% dextrose in 0.9% sodium chloride
- isolyte P with 5% dextrose
- Ringer's lactate solution
- Ringer's solution
Ensure the infusion line is adequately flushed (e.g., with 0.9% sodium chloride) between administration of BRIDION and other drugs.
Do not mix BRIDION with other products except those listed above.
BRIDION is physically incompatible with verapamil, ondansetron, and ranitidine.
Visually inspect parenteral drug products for particulate matter and discoloration prior to administration, whenever the solution and container permit.
5.2 Marked Bradycardia
Cases of marked bradycardia, some of which have resulted in cardiac arrest, have been observed within minutes after the administration of BRIDION [see Adverse Reactions (6.2)] . Patients should be closely monitored for hemodynamic changes during and after reversal of neuromuscular blockade. Treatment with anticholinergic agents, such as atropine, should be administered if clinically significant bradycardia is observed.
8.7 Hepatic Impairment
BRIDION is not metabolized nor excreted by the liver; therefore, dedicated trials in patients with hepatic impairment have not been conducted. Exercise caution when administering BRIDION to patients with hepatic impairment accompanied by coagulopathy or severe edema [see Warnings and Precautions (5.10, 5.14)] .
8.9 Pulmonary Patients
One trial of 77 patients who were diagnosed with or have a history of pulmonary complications investigated the time to recovery from neuromuscular blockade induced by rocuronium (0.6 mg/kg) following administration of 2 mg/kg or 4 mg/kg BRIDION given at the first signs of recovery (reappearance of T 2). The trial showed that for these patients the median time to recovery of the T 4/T 1ratio to 0.9 was 2.1 minutes after a dose of 2 mg/kg BRIDION and 1.9 minutes after a dose of 4 mg/kg BRIDION. This is similar to the median values observed in the other trials; therefore, no dosage adjustment is necessary. [See Dosage and Administration (2.2), Adverse Reactions (6.1).]
1 Indications and Usage (1 INDICATIONS AND USAGE)
BRIDION ®is indicated for the reversal of neuromuscular blockade induced by rocuronium bromide and vecuronium bromide in adult and pediatric patients undergoing surgery.
12.1 Mechanism of Action
BRIDION is a modified gamma cyclodextrin. It forms a complex with the neuromuscular blocking agents rocuronium and vecuronium, and it reduces the amount of neuromuscular blocking agent available to bind to nicotinic cholinergic receptors in the neuromuscular junction. This results in the reversal of neuromuscular blockade induced by rocuronium and vecuronium.
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
Anaphylaxis: Be prepared for hypersensitivity reactions (including anaphylactic reactions) and take necessary precautions. ( 5.1)
Marked Bradycardia: Cases of marked bradycardia, some of which have resulted in cardiac arrest, have been observed within minutes after administration. Monitor for hemodynamic changes and administer anticholinergic agents such as atropine if clinically significant bradycardia is observed. ( 5.2)
Respiratory Function Monitoring: Ventilatory support is mandatory until adequate spontaneous respiration is restored and the ability to maintain a patent airway is assured. Provide adequate ventilation if neuromuscular blockade persists after BRIDION or recurs following extubation. ( 5.3, 5.4)
Waiting Times for Re-Administration of Neuromuscular Blocking Agents: If re-administration of a neuromuscular blocking agent is required after reversal with BRIDION, waiting times should be based on the dose of BRIDION and the renal function of the patient. Consider use of a nonsteroidal neuromuscular blocking agent. ( 5.5)
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
- Dosing is based on actual body weight ( 2.1)
- Monitor for twitch responses to determine the timing and dose for BRIDION administration. ( 2.1)
- Administer as a single bolus injection. ( 2.1)
For rocuronium and vecuronium:
- 4 mg/kg is recommended if spontaneous recovery of the twitch response has reached 1 to 2 post-tetanic counts (PTC) and there are no twitch responses to train-of-four (TOF) stimulation. ( 2.2)
- 2 mg/kg is recommended if spontaneous recovery has reached the reappearance of the second twitch in response to TOF stimulation. ( 2.2)
For rocuronium only:
- 16 mg/kg is recommended if there is a clinical need to reverse neuromuscular blockade soon (approximately 3 minutes) after administration of a single dose of 1.2 mg/kg of rocuronium. Immediate reversal in pediatric patients has not been studied. ( 2.2)
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
BRIDION (sugammadex) injection is a sterile, clear, colorless to slightly yellow-brown, non-pyrogenic aqueous solution intended for intravenous infusion. BRIDION is available as follows:
- 200 mg/2 mL (100 mg/mL) in a single-dose vial for bolus injection
- 500 mg/5 mL (100 mg/mL), in a single-dose vial for bolus injection
6.2 Post Marketing Experience (6.2 Post-Marketing Experience)
The following adverse reactions have been identified during post-approval use of BRIDION. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
8 Use in Specific Populations (8 USE IN SPECIFIC POPULATIONS)
Severe Renal Impairment: Not recommended. ( 8.6)
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
Adult Patients
The data described below reflect 2914 subjects exposed to 2, 4, or 16 mg/kg BRIDION and 544 to placebo in pooled Phase 1-3 studies. The population was 18 to 92 years old, 47% male and 53% female, 34% ASA (American Society of Anesthesiologists) Class 1, 51% ASA Class 2, and 14% ASA Class 3, and 82% Caucasian. Most subjects received a single dose of BRIDION 2 mg/kg or 4 mg/kg.
Adverse reactions reported in ≥10% of patients at a 2, 4, or 16 mg/kg BRIDION dose with a rate higher than the placebo rate are: vomiting, pain, nausea, hypotension, and headache.
All adverse reactions occurring in ≥2% of subjects treated with BRIDION and more often than placebo for adult subjects who received anesthesia and/or neuromuscular blocking agent in pooled Phase 1 to 3 studies are presented in Table 2.
| Sugammadex | Placebo | |||
|---|---|---|---|---|
| Body System
Preferred Term |
2 mg/kg
(N=895) n (%) |
4 mg/kg
(N=1921) n (%) |
16 mg/kg
(N=98) n (%) |
(N=544)
n (%) |
| Injury, poisoning and procedural complications | ||||
| Incision site pain | 58 (6) | 106 (6) | 4 (4) | 6 (1) |
| Procedural complication | 13 (1) | 27 (1) | 8 (8) | 3 (1) |
| Airway complication of anesthesia | 11 (1) | 13 (1) | 9 (9) | 0 |
| Anesthetic complication | 8 (1) | 14 (1) | 9 (9) | 1 (<1) |
| Wound hemorrhage | 5 (1) | 38 (2) | 0 | 8 (1) |
| Recurrence of neuromuscular blockade | 0 | 1 (<1) | 2 (2) | 0 |
| Gastrointestinal disorders | ||||
| Nausea
Combinations of preferred terms are as follows:
Nausea includes preferred terms nausea and procedural nausea
Vomiting includes preferred terms vomiting and procedural vomiting
Abdominal pain includes preferred terms abdominal pain, abdominal pain upper, abdominal discomfort, abdominal pain lower, and epigastric discomfort
Pain includes preferred terms pain and procedural pain
Red blood cell count decreased includes preferred terms red blood cell count decreased, hemoglobin decreased, and hematocrit decreased
Electrocardiogram QT interval abnormal includes preferred terms electrocardiogram QT interval abnormal and electrocardiogram QT interval prolonged
Hypertension includes preferred terms hypertension, procedural hypertension, and blood pressure increased
Hypotension includes preferred terms hypotension, procedural hypotension, and blood pressure decreased
Tachycardia includes preferred terms tachycardia and heart rate increased
Bradycardia includes preferred terms bradycardia and heart rate decreased
|
208 (23) | 503 (26) | 23 (23) | 127 (23) |
| Vomiting | 98 (11) | 236 (12) | 15 (15) | 57 (10) |
| Abdominal pain | 48 (5) | 68 (4) | 6 (6) | 17 (3) |
| Flatulence | 17 (2) | 51 (3) | 1 (1) | 10 (2) |
| Dry mouth | 9 (1) | 5 (<1) | 2 (2) | 0 |
| General disorders and administration site conditions | ||||
| Pain | 434 (48) | 993 (52) | 35 (36) | 207 (38) |
| Pyrexia | 77 (9) | 109 (6) | 5 (5) | 17 (3) |
| Chills | 30 (3) | 61 (3) | 7 (7) | 27 (5) |
| Nervous system disorders | ||||
| Headache | 61 (7) | 99 (5) | 10 (10) | 42 (8) |
| Dizziness | 44 (5) | 67 (3) | 6 (6) | 13 (2) |
| Hypoesthesia | 12 (1) | 24 (1) | 3 (3) | 9 (2) |
| Respiratory, thoracic and mediastinal disorders | ||||
| Oropharyngeal pain | 42 (5) | 66 (3) | 5 (5) | 27 (5) |
| Cough | 13 (1) | 49 (3) | 8 (8) | 11 (2) |
| Musculoskeletal and connective tissue disorders | ||||
| Pain in extremity | 13 (1) | 35 (2) | 6 (6) | 15 (3) |
| Musculoskeletal pain | 16 (2) | 33 (2) | 1 (1) | 6 (1) |
| Myalgia | 5 (1) | 17 (1) | 2 (2) | 3 (1) |
| Psychiatric disorders | ||||
| Insomnia | 20 (2) | 103 (5) | 5 (5) | 22 (4) |
| Anxiety | 14 (2) | 19 (1) | 3 (3) | 1 (<1) |
| Restlessness | 3 (<1) | 17 (1) | 2 (2) | 2 (<1) |
| Depression | 2 (<1) | 5 (<1) | 2 (2) | 0 |
| Investigations | ||||
| Red blood cell count decreased | 13 (1) | 34 (2) | 1 (1) | 2 (<1) |
| Electrocardiogram QT interval abnormal | 13 (1) | 7 (<1) | 6 (6) | 4 (1) |
| Blood creatine phosphokinase increased | 9 (1) | 14 (1) | 2 (2) | 1 (<1) |
| Vascular disorders | ||||
| Hypertension | 48 (5) | 96 (5) | 9 (9) | 38 (7) |
| Hypotension | 33 (4) | 102 (5) | 13 (13) | 20 (4) |
| Skin and subcutaneous tissue disorders | ||||
| Pruritus | 17 (2) | 50 (3) | 2 (2) | 9 (2) |
| Erythema | 5 (1) | 31 (2) | 0 | 6 (1) |
| Metabolism and nutrition disorders | ||||
| Hypocalcemia | 15 (2) | 12 (1) | 0 | 4 (1) |
| Cardiac disorders | ||||
| Tachycardia | 17 (2) | 29 (2) | 5 (5) | 4 (1) |
| Bradycardia | 9 (1) | 21 (1) | 5 (5) | 6 (1) |
| Surgical and medical procedures | ||||
| Hysterectomy | 0 | 0 | 2 (2) | 0 |
17 Patient Counseling Information (17 PATIENT COUNSELING INFORMATION)
- Advise females of reproductive potential using hormonal contraceptives that BRIDION may reduce the contraceptive effect .Instruct females to use an additional, non-hormonal method of contraception for the next 7 days following BRIDION administration [see Drug Interactions (7.3)].
16 How Supplied/storage and Handling (16 HOW SUPPLIED/STORAGE AND HANDLING)
BRIDION (sugammadex) injection is a clear, colorless to slightly yellow-brown, non-pyrogenic aqueous solution intended for intravenous infusion. BRIDION is available in the following presentations:
- BRIDION 2-mL single-dose vial containing 200 mg sugammadex (100 mg/mL)
NDC 84549-423-12
The packaging of this product is not made with natural rubber latex.
5.1 Anaphylaxis and Hypersensitivity
Clinicians should be prepared for the possibility of drug hypersensitivity reactions (including anaphylactic reactions) and take the necessary precautions [see Contraindications (4), Adverse Reactions (6.1)] .
Potentially serious hypersensitivity reactions, including anaphylaxis, have occurred in patients treated with BRIDION. The nature and frequency of anaphylaxis and hypersensitivity associated with BRIDION administration were evaluated in a randomized, double-blind, placebo-controlled, parallel-group, repeat-dose study in which 375 subjects were randomized to receive 3 doses of BRIDION IV with a 5-week washout period: 151 subjects received 4 mg/kg, 148 received 16 mg/kg and 76 received placebo. The frequency of anaphylaxis for the 299 healthy volunteers treated with intravenous BRIDION was 0.3% (n=1 in the BRIDION 16 mg/kg group on the first dose). Signs and symptoms included conjunctival edema, urticaria, erythema, swelling of the uvula and reduction in peak expiratory flow within 5 minutes of dose administration. The most common hypersensitivity adverse reactions reported were nausea, pruritus and urticaria and showed a dose response relationship, occurring more frequently in the 16 mg/kg group compared to the 4 mg/kg and placebo groups.
Anaphylaxis has also been reported in the post-marketing setting, including at doses less than 16 mg/kg. The most commonly described clinical features in reports of anaphylaxis were dermatologic symptoms (including urticaria, rash, erythema, flushing and skin eruption); and clinically important hypotension often requiring the use of vasopressors for circulatory support. In addition, prolonged hospitalization and/or the use of additional respiratory support until full recovery (re-intubation, prolonged intubation, manual or mechanical ventilation) have been noted in a number of the anaphylaxis reports.
5.10 Risk of Coagulopathy and Bleeding
BRIDION doses up to 16 mg/kg were associated with increases in the coagulation parameters activated partial thromboplastin time (aPTT) and prothrombin time/international normalized ratio [PT(INR)] of up to 25% for up to 1 hour in healthy volunteers.
In patients undergoing major orthopedic surgery of the lower extremity who were concomitantly treated with heparin or low molecular weight heparin for thromboprophylaxis, increases in aPTT and PT(INR) of 5.5% and 3.0%, respectively, were observed in the hour following BRIDION 4 mg/kg administration. This clinical trial did not demonstrate an increased blood loss or anemia incidence with BRIDION compared with usual treatment. The rate of adjudicated bleeding events within 24 hours was 2.9% for sugammadex and 4.1% for usual care. The rate of post-operative anemia was 21% for sugammadex and 22% for usual care. The mean 24-hour drainage volume was 0.46 L for sugammadex and 0.48 L for usual care. The need for any post-operative transfusion was 37% for sugammadex and 39% for usual care.
In vitroexperiments demonstrated additional aPTT and PT(INR) prolongations for sugammadex in combination with vitamin K antagonists, unfractionated heparin, low molecular weight heparinoids, rivaroxaban, and dabigatran up to ~25% and ~50% at C maxlevels of sugammadex corresponding to 4 mg/kg and 16 mg/kg doses, respectively.
Since bleeding risk has been studied systematically with only heparin and low molecular weight heparin thromboprophylaxis and 4 mg/kg doses of sugammadex coagulation parameters should be carefully monitored in patients with known coagulopathies, being treated with therapeutic anticoagulation, receiving thromboprophylaxis drugs other than heparin and low molecular weight heparin, or receiving thromboprophylaxis drugs and who then receive a dose of 16 mg/kg sugammadex.
7.4 Interference With Laboratory Tests (7.4 Interference with Laboratory Tests)
BRIDION may interfere with the serum progesterone assay. Interference with this test was observed at sugammadex plasma concentrations of 100 mcg/mL, which may be observed for up to 30 minutes after a 16 mg/kg dose.
13.2 Animal Toxicology And/or Pharmacology (13.2 Animal Toxicology and/or Pharmacology)
Bone and teeth retention of sugammadex occurred in rats after intravenous injection, with mean half-lives of 172 and 8 days, respectively. Sugammadex bound to hydroxyapatite in an in vitrostudy and distributed in the bone formation area where hydroxyapatite is present for mineralization in vivo.
In adult rat bone toxicity studies, a single dose of sugammadex at 2000 mg/kg (approximately 24 times the maximum recommended human dose (MRHD) of 16 mg/kg by AUC comparison) administered to adult rats caused a slight increase in bone resorption, but had no effect on teeth color. No adverse bone effects were seen following a single dose of sugammadex at 500 mg/kg (4 times the MRHD dose of 16 mg/kg based on plasma AUC comparison).
In a bone repair study, adult rats were treated with intravenous sugammadex weekly for 6 weeks at 0, 30, 120, and 500 mg/kg (approximately 0.4, 1, and 6 times the MRHD, respectively, by AUC comparison). Based on histological data, high dose animals with post-fracture treatment, showed a statistically significant increase in callus formation and decrease in bone formation, suggesting a potential for a slight delay in the bone healing process. However, there were no statistically significant effects on bone volume or bone mineral density.
In juvenile animal studies, bone and teeth deposition was significantly higher in juvenile rats compared to adults. In addition, sugammadex administered to juvenile rats daily for 4 weeks caused slight bone length decrease (approximately 3%), which did not recover after an 8-week treatment-free period, and reversible whitish discoloration of the teeth at a dose approximately 0.6 times the MRHD, while weekly administration for 8 weeks did not produce similar changes in bone and teeth at doses up to 1.2 times the MRHD [see Use in Specific Populations (8.4)] .
Principal Display Panel 2 Ml Vial Carton (PRINCIPAL DISPLAY PANEL - 2 mL Vial Carton)
8.10 Obese Patients With A Bmi ≥40 Kg/m 2 (8.10 Obese Patients with a BMI ≥40 kg/m 2)
A trial of 188 obese patients, with a body mass index ≥40 kg/m 2, investigated the time to recovery from moderate or deep neuromuscular blockade induced by rocuronium or vecuronium. Patients received 2 mg/kg or 4 mg/kg BRIDION, as appropriate for level of block, dosed according to either actual body weight (ABW) or ideal body weight (IBW) in random, double-blinded fashion. Pooled across depth of block and neuromuscular blocking agent, the median time to recover to a train-of-four (TOF) ratio ≥0.9 in patients dosed by ABW (1.8 minutes) was statistically significantly faster compared to patients dosed by IBW (3.3 minutes).
The adverse reaction profile was generally similar to the profile in adult patients in pooled Phase 1 to 3 studies [see Adverse Reactions (6.1)] . No dosage adjustment is necessary [see Dosage and Administration (2.2)] .
5.4 Risk of Prolonged Neuromuscular Blockade
In clinical trials, a small number of patients experienced a delayed or minimal response to the administration of BRIDION [see Clinical Studies (14.1)] . Thus, it is important to monitor ventilation until recovery occurs.
2.1 Important Dosing and Administration Information
BRIDION dosing is based on actual body weight.
BRIDION (sugammadex) injection, for intravenous use, should be administered by trained healthcare providers familiar with the use, actions, characteristics, and complications of neuromuscular blocking agents (NMBA) and neuromuscular block reversal agents.
Doses and timing of BRIDION administration should be based on monitoring for twitch responses and the extent of spontaneous recovery that has occurred.
Administer BRIDION intravenously as a single bolus injection. The bolus injection may be given over 10 seconds, into an existing intravenous line. BRIDION has only been administered as a single bolus injection in clinical trials.
From the time of BRIDION administration until complete recovery of neuromuscular function, monitor the patient to assure adequate ventilation and maintenance of a patent airway. Satisfactory recovery should be determined through assessment of skeletal muscle tone and respiratory measurements in addition to the response to peripheral nerve stimulation.
The recommended dose of BRIDION does not depend on the anesthetic regimen.
Preparation of dilution for pediatric use:
BRIDION 100 mg/mL may be diluted to a concentration of 10 mg/mL, using 0.9% sodium chloride injection, USP, to increase the accuracy of dosing in the pediatric population.
- To prepare the required dose, aseptically transfer all the contents of the 2 mL vial of BRIDION 2-mL single-dose vials containing 200 mg sugammadex (100 mg/mL) to a bottle (or intravenous bag) containing 18 mL of 0.9% sodium chloride injection, to achieve a final concentration of 10 mg/mL sugammadex. The diluted solution should be used immediately.
- BRIDION injection is a single-dose sterile solution without preservatives. Discard any unused portion from the vial.
5.3 Respiratory Function Monitoring During Recovery
Ventilatory support is mandatory for patients until adequate spontaneous respiration is restored and the ability to maintain a patent airway is assured. Even if recovery from neuromuscular blockade is complete, other drugs used in the peri- and post-operative period could depress respiratory function and therefore ventilatory support might still be required.
Should neuromuscular blockade persist after BRIDION administration or recur following extubation, take appropriate steps to provide adequate ventilation.
8.11 American Society of Anesthesiologists Class 3 Or 4 Patients (8.11 American Society of Anesthesiologists Class 3 or 4 Patients)
One trial of 331 patients who were assessed as ASA Class 3 or 4 investigated the incidence of treatment-emergent arrhythmias (sinus bradycardia, sinus tachycardia, or other cardiac arrhythmias) after administration of sugammadex.
In patients receiving sugammadex (2 mg/kg, 4 mg/kg, or 16 mg/kg), the number (%) of patients with treatment-emergent sinus bradycardia (up to 35 minutes post-administration of sugammadex) was 1/105 (1.0%) in the 2 mg/kg sugammadex treatment group, 2/107 (1.9%) in the 4 mg/kg sugammadex treatment group, and 5/68 (7.4%) in the 16 mg/kg sugammadex treatment group, compared to 4/51 (7.8%) in the neostigmine (50 µg/kg up to 5 mg maximum dose) + glycopyrrolate (10 µg/kg up to 1 mg maximum dose) treatment group. The number of patients with treatment-emergent sinus tachycardia (up to 35 minutes post-administration of sugammadex) was 7/105 (6.7%) in the 2 mg/kg sugammadex treatment group, 10/107 (9.3%) in the 4 mg/kg sugammadex treatment group, and 6/68 (8.8%) in the 16 mg/kg sugammadex treatment group, compared to 11/51 (21.6%) in the neostigmine + glycopyrrolate treatment group. The number of other treatment-emergent arrhythmias (up to 35 minutes post administration of sugammadex) was 1/105 (1.0%) in the 2 mg/kg sugammadex treatment group, 0/107 (0%) in the 4 mg/kg sugammadex treatment group, and 1/68 (1.5%) in the 16 mg/kg sugammadex treatment group, compared to 1/51 (2.0%) in the neostigmine + glycopyrrolate treatment group. The adverse reaction profiles in ASA Class 3 and 4 patients were generally similar to those in adult patients in pooled Phase 1 to 3 studies; therefore, no dosage adjustment is necessary [see Dosage and Administration (2.1), Adverse Reactions (6.1)] .
5.6 Interactions Potentially Affecting the Efficacy of Other Drugs
Due to the administration of BRIDION, certain drugs, including hormonal contraceptives, could become less effective due to a lowering of the (free) plasma concentrations. In this situation, consider the re-administration of the other drug, the administration of a therapeutically equivalent drug (preferably from a different chemical class), and/or non-pharmacological interventions as appropriate [see Drug Interactions (7.3)] .
5.13 Reversal After Rocuronium Or Vecuronium Administration in the Icu (5.13 Reversal after Rocuronium or Vecuronium Administration in the ICU)
BRIDION has not been studied for reversal following rocuronium or vecuronium administration in the ICU.
7.3 Interaction Potentially Affecting the Efficacy of Hormonal Contraceptives
In vitrobinding studies indicate that BRIDION may bind to progestogen, thereby decreasing progestogen exposure. Therefore, the administration of a bolus dose of BRIDION is considered to be equivalent to missing dose(s) of oralcontraceptives containing an estrogen or progestogen. If an oral contraceptive is taken on the same day that BRIDION is administered, the patient must use an additional, non-hormonal contraceptive method or back-up method of contraception (such as condoms and spermicides) for the next 7 days.
In the case of non-oralhormonal contraceptives, the patient must use an additional, non-hormonal contraceptive method or back-up method of contraception (such as condoms and spermicides) for the next 7 days.
5.7 Risk of Recurrence of Neuromuscular Blockade Due to Displacement Interactions
Recurrence of neuromuscular blockade may occur due to displacement of rocuronium or vecuronium from BRIDION by other drugs [see Drug Interactions (7.2)] . In this situation the patient may require mechanical ventilation. Administration of the drug which caused displacement should be stopped in case of an infusion. The risk of displacement reactions will be the highest in the time period equivalent to 3 times the half-life of BRIDION [see Clinical Pharmacology (12.3)] .
5.14 Reversal of Neuromuscular Blocking Agents Other Than Rocuronium Or Vecuronium (5.14 Reversal of Neuromuscular Blocking Agents Other Than Rocuronium or Vecuronium)
Do not use BRIDION to reverse blockade induced by nonsteroidalneuromuscular blocking agents such as succinylcholine or benzylisoquinolinium compounds.
Do not use BRIDION to reverse neuromuscular blockade induced by steroidalneuromuscular blocking agents other than rocuronium or vecuronium.
5.8 Risk of Recurrence of Neuromuscular Blockade With Lower Than Recommended Dosing (5.8 Risk of Recurrence of Neuromuscular Blockade with Lower Than Recommended Dosing)
The use of lower than recommended doses of BRIDION may lead to an increased risk of recurrence of neuromuscular blockade after initial reversal and is not recommended [see Dosage and Administration (2.2), Adverse Reactions (6.1)] .
5.5 Waiting Times for Re Administration of Neuromuscular Blocking Agents for Intubation Following Reversal With Bridion (5.5 Waiting Times for Re-Administration of Neuromuscular Blocking Agents for Intubation Following Reversal with BRIDION)
A minimum waiting time is necessary before administration of a steroidal neuromuscular blocking agent after administration of BRIDION.
| Minimum Waiting Time | NMBA and Dose to be Administered |
|---|---|
| 5 minutes | 1.2 mg/kg rocuronium |
| 4 hours | 0.6 mg/kg rocuronium or
0.1 mg/kg vecuronium |
When rocuronium 1.2 mg/kg is administered within 30 minutes after reversal with BRIDION, the onset of neuromuscular blockade may be delayed up to approximately 4 minutes and the duration of neuromuscular blockade may be shortened up to approximately 15 minutes.
The recommended waiting time in patients with mild or moderate renal impairment for re-use of 0.6 mg/kg rocuronium or 0.1 mg/kg vecuronium after reversal with up to 4 mg/kg BRIDION should be 24 hours. If a shorter waiting time is required, the rocuronium dose for a new neuromuscular blockade should be 1.2 mg/kg.
For re-administration of rocuronium or administration of vecuronium after reversal of rocuronium with 16 mg/kg BRIDION, a waiting time of 24 hours is suggested.
If neuromuscular blockade is required before the recommended waiting time has elapsed, use a nonsteroidal neuromuscular blocking agent. The onset of a depolarizing neuromuscular blocking agent might be slower than expected, because a substantial fraction of postjunctional nicotinic receptors can still be occupied by the neuromuscular blocking agent.
5.9 Risk of Recurrence of Neuromuscular Blockade Due to the Administration of Drugs That Potentiate Neuromuscular Blockade (5.9 Risk of Recurrence of Neuromuscular Blockade Due to the Administration of Drugs that Potentiate Neuromuscular Blockade)
When drugs which potentiate neuromuscular blockade are used in the post-operative phase, special attention should be paid to the possibility of recurrence of neuromuscular blockade. Refer to the package insert for rocuronium or vecuronium for a list of the specific drugs which potentiate neuromuscular blockade. In case recurrence of neuromuscular blockade is observed, the patient may require mechanical ventilation.
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:51:19.497757 · Updated: 2026-03-14T22:40:03.259578