These Highlights Do Not Include All The Information Needed To Use Azithromycin For Injection Safely And Effectively. See Full Prescribing Information For Azithromycin For Injection.
324330c5-20fe-4b22-adf2-14a6e91e71ef
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
Warnings and Precautions, Cardiovascular Death ( 5.5 ) 11/2021
Indications and Usage
Azithromycin for injection is a macrolide antibacterial drug indicated for the treatment of patients with infections caused by susceptible strains of the designated microorganisms in the conditions listed below.
Dosage and Administration
[See Indications and Usage ( 1 ) and Clinical Pharmacology ( 12.3 )]
Warnings and Precautions
Serious (including fatal) allergic and skin reactions. Discontinue azithromycin and initiate appropriate therapy if reaction occurs. ( 5.1 ) Hepatotoxicity: Severe and sometimes fatal, hepatoxicity has been reported. Discontinue azithromycin immediately if signs and symptoms of hepatitis occur. ( 5.2 ) Infantile Hypertrophic Pyloric Stenosis (IHPS): Following the use of azithromycin in neonates (treatment up to 42 days of life), IHPS has been reported. Direct parents and caregivers to contact their physician if vomiting or irritability with feeding occurs. ( 5.3 ) Prolongation of QT interval and cases of torsades de pointes have been reported. This risk which can be fatal should be considered in patients with certain cardiovascular disorders including known QT prolongation or history torsades de pointes, those with proarrhythmic conditions, and with other drugs that prolong the QT interval. ( 5.4 ) Cardiovascular Death: Some observational studies have shown an approximately two-fold increased short-term potential risk of acute cardiovascular death in adults exposed to azithromycin relative to other antibacterial drugs, including amoxicillin. Consider balancing this potential risk with treatment benefits when prescribing azithromycin. ( 5.5 ) Clostridioides difficile -Associated Diarrhea: Evaluate patients if diarrhea occurs. ( 5.6 ) Azithromycin may exacerbate muscle weakness in persons with myasthenia gravis. ( 5.7 )
Contraindications
Patients with known hypersensitivity to azithromycin, erythromycin, any macrolide, or ketolide antibacterial drug. ( 4.1 ) Patients with a history of cholestatic jaundice/hepatic dysfunction associated with prior use of azithromycin. ( 4.2 )
Adverse Reactions
The following clinically significant adverse reactions are described elsewhere in labeling: Hypersensitivity [see Warnings and Precautions ( 5.1 )] Hepatotoxicity [see Warnings and Precautions ( 5.2 )] Infantile Hypertrophic Pyloric Stenosis (IHPS) [see Warnings and Precautions ( 5.3 )] QT Prolongation [see Warnings and Precautions ( 5.4 )] Cardiovascular Death [see Warnings and Precautions ( 5.5 )] Clostridioides difficile- Associated Diarrhea (CDAD) [see Warnings and Precautions ( 5.6 )] Exacerbation of Myasthenia Gravis [see Warnings and Precautions ( 5.7 )]
Drug Interactions
Nelfinavir: Close monitoring for known adverse reactions of azithromycin, such as liver enzyme abnormalities and hearing impairment, is warranted. ( 7.1 ) Warfarin: Use with azithromycin may increase coagulation times; monitor prothrombin time. ( 7.2 )
Storage and Handling
Azithromycin for Injection, USP is supplied as follows: NDC Azithromycin for Injection, USP Package Factor 70860-100-10 500 mg Single-Dose Vial 10 vials per carton Azithromycin for Injection, USP is supplied in lyophilized form under a vacuum in a 10 mL single-dose vial equivalent to 500 mg of azithromycin for intravenous administration. Each vial also contains sodium hydroxide and 384.5 mg citric acid.
How Supplied
Azithromycin for Injection, USP is supplied as follows: NDC Azithromycin for Injection, USP Package Factor 70860-100-10 500 mg Single-Dose Vial 10 vials per carton Azithromycin for Injection, USP is supplied in lyophilized form under a vacuum in a 10 mL single-dose vial equivalent to 500 mg of azithromycin for intravenous administration. Each vial also contains sodium hydroxide and 384.5 mg citric acid.
Medication Information
Warnings and Precautions
Serious (including fatal) allergic and skin reactions. Discontinue azithromycin and initiate appropriate therapy if reaction occurs. ( 5.1 ) Hepatotoxicity: Severe and sometimes fatal, hepatoxicity has been reported. Discontinue azithromycin immediately if signs and symptoms of hepatitis occur. ( 5.2 ) Infantile Hypertrophic Pyloric Stenosis (IHPS): Following the use of azithromycin in neonates (treatment up to 42 days of life), IHPS has been reported. Direct parents and caregivers to contact their physician if vomiting or irritability with feeding occurs. ( 5.3 ) Prolongation of QT interval and cases of torsades de pointes have been reported. This risk which can be fatal should be considered in patients with certain cardiovascular disorders including known QT prolongation or history torsades de pointes, those with proarrhythmic conditions, and with other drugs that prolong the QT interval. ( 5.4 ) Cardiovascular Death: Some observational studies have shown an approximately two-fold increased short-term potential risk of acute cardiovascular death in adults exposed to azithromycin relative to other antibacterial drugs, including amoxicillin. Consider balancing this potential risk with treatment benefits when prescribing azithromycin. ( 5.5 ) Clostridioides difficile -Associated Diarrhea: Evaluate patients if diarrhea occurs. ( 5.6 ) Azithromycin may exacerbate muscle weakness in persons with myasthenia gravis. ( 5.7 )
Indications and Usage
Azithromycin for injection is a macrolide antibacterial drug indicated for the treatment of patients with infections caused by susceptible strains of the designated microorganisms in the conditions listed below.
Dosage and Administration
[See Indications and Usage ( 1 ) and Clinical Pharmacology ( 12.3 )]
Contraindications
Patients with known hypersensitivity to azithromycin, erythromycin, any macrolide, or ketolide antibacterial drug. ( 4.1 ) Patients with a history of cholestatic jaundice/hepatic dysfunction associated with prior use of azithromycin. ( 4.2 )
Adverse Reactions
The following clinically significant adverse reactions are described elsewhere in labeling: Hypersensitivity [see Warnings and Precautions ( 5.1 )] Hepatotoxicity [see Warnings and Precautions ( 5.2 )] Infantile Hypertrophic Pyloric Stenosis (IHPS) [see Warnings and Precautions ( 5.3 )] QT Prolongation [see Warnings and Precautions ( 5.4 )] Cardiovascular Death [see Warnings and Precautions ( 5.5 )] Clostridioides difficile- Associated Diarrhea (CDAD) [see Warnings and Precautions ( 5.6 )] Exacerbation of Myasthenia Gravis [see Warnings and Precautions ( 5.7 )]
Drug Interactions
Nelfinavir: Close monitoring for known adverse reactions of azithromycin, such as liver enzyme abnormalities and hearing impairment, is warranted. ( 7.1 ) Warfarin: Use with azithromycin may increase coagulation times; monitor prothrombin time. ( 7.2 )
Storage and Handling
Azithromycin for Injection, USP is supplied as follows: NDC Azithromycin for Injection, USP Package Factor 70860-100-10 500 mg Single-Dose Vial 10 vials per carton Azithromycin for Injection, USP is supplied in lyophilized form under a vacuum in a 10 mL single-dose vial equivalent to 500 mg of azithromycin for intravenous administration. Each vial also contains sodium hydroxide and 384.5 mg citric acid.
How Supplied
Azithromycin for Injection, USP is supplied as follows: NDC Azithromycin for Injection, USP Package Factor 70860-100-10 500 mg Single-Dose Vial 10 vials per carton Azithromycin for Injection, USP is supplied in lyophilized form under a vacuum in a 10 mL single-dose vial equivalent to 500 mg of azithromycin for intravenous administration. Each vial also contains sodium hydroxide and 384.5 mg citric acid.
Description
Warnings and Precautions, Cardiovascular Death ( 5.5 ) 11/2021
Section 42229-5
Reconstitution
Prepare the initial solution of azithromycin for injection by adding 4.8 mL of Sterile Water for Injection to the 500 mg vial, and shaking the vial until all of the drug is dissolved. Since azithromycin for injection is supplied under vacuum, it is recommended that a standard 5 mL (non-automated) syringe be used to ensure that the exact amount of 4.8 mL of Sterile Water is dispensed. Each mL of reconstituted solution contains 100 mg azithromycin. Reconstituted solution is stable for 24 hr when stored below 30°C (86°F).
Parenteral drug products should be inspected visually for particulate matter prior to administration. If particulate matter is evident in reconstituted fluids, the drug solution should be discarded.
Dilute this solution further prior to administration as instructed below.
Section 43683-2
| Warnings and Precautions, Cardiovascular Death ( 5.5) | 11/2021 |
Section 44425-7
Storage Conditions
Store at 20° to 25°C (68° to 77°F). [See USP Controlled Room Temperature.]
Sterile, Nonpyrogenic, Preservative-free.
The container closure is not made with natural rubber latex.
*Normosol ®-M in 5% dextrose and Normosol ®-R in 5% dextrose are the trademarks of Hospira.
Section 51945-4
PACKAGE LABEL – PRINCIPAL DISPLAY PANEL – Vial Label
NDC 70860-100-41
Azithromycin for Injection, USP
500 mg per vial (equivalent to azithromycin)
Rx only
FOR INTRAVENOUS INFUSION ONLY
Single-Dose Vial
1.3 Usage
To reduce the development of drug-resistant bacteria and maintain the effectiveness of azithromycin and other antibacterial drugs, azithromycin should be used only to treat infections that are proven or strongly suspected to be caused by susceptible bacteria. When culture and susceptibility information are available, they should be considered in selecting or modifying antibacterial therapy. In the absence of such data, local epidemiology and susceptibility patterns may contribute to the empiric selection of therapy.
7.2 Warfarin
Spontaneous postmarketing reports suggest that concomitant administration of azithromycin may potentiate the effects of oral anticoagulants such as warfarin, although the prothrombin time was not affected in the dedicated drug interaction study with azithromycin and warfarin. Prothrombin times should be carefully monitored while patients are receiving azithromycin and oral anticoagulants concomitantly.
10 Overdosage
Adverse reactions experienced in higher than recommended doses were similar to those seen at normal doses particularly nausea, diarrhea, and vomiting. In the event of overdosage, general symptomatic and supportive measures are indicated as required.
11 Description
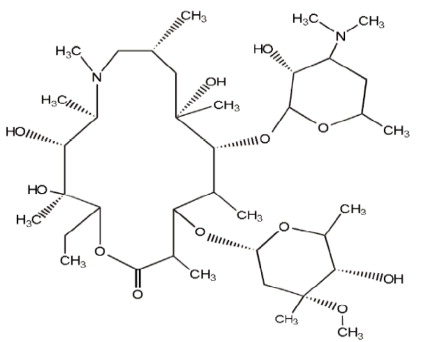
Azithromycin for Injection, USP contains the active ingredient azithromycin, an azalide, a subclass of macrolide antibacterial drug, for intravenous injection. Azithromycin has the chemical name (2R,3S,4R,5R,8R,10R,11R,12S,13S,14R)-13-[(2,6-dideoxy-3- C-methyl-3- O-methyl-α- L-ribo-hexopyranosyl)oxy]-2-ethyl-3,4,10-trihydroxy-3,5,6,8,10,12,14-hepta-methyl-11-[[3,4,6-trideoxy-3-(dimethylamino)-β- D- xylo-hexopyranosyl]oxy]-1-oxa-6-azacyclopentadecan-15-one. Azithromycin is derived from erythromycin; however, it differs chemically from erythromycin in that a methyl-substituted nitrogen atom is incorporated into the lactone ring. Its molecular formula is C 38H 72N 2O 12, and its molecular weight is 749.00. Azithromycin has the following structural formula:
Azithromycin, as the monohydrate, is a white crystalline powder with a molecular formula of C 38H 72N 2O 12· H 2O and a molecular weight of 767.0.
Azithromycin for Injection, USP consists of azithromycin monohydrate and the following inactive ingredients: citric acid and sodium hydroxide. Azithromycin for Injection, USP is supplied in lyophilized form in a 10 mL single-dose vial equivalent to 500 mg of azithromycin for intravenous administration. Reconstitution, according to label directions, results in approximately 5 mL of azithromycin for intravenous injection with each mL containing azithromycin monohydrate equivalent to 100 mg of azithromycin.
7.1 Nelfinavir
Co-administration of nelfinavir at steady-state with a single oral dose of azithromycin resulted in increased azithromycin serum concentrations. Although a dose adjustment of azithromycin is not recommended when administered in combination with nelfinavir, close monitoring for known adverse reactions of azithromycin, such as liver enzyme abnormalities and hearing impairment, is warranted [see Adverse Reactions ( 6)] .
8.4 Pediatric Use
Safety and effectiveness of azithromycin for injection in children or adolescents under 16 years have not been established. In controlled clinical studies, azithromycin has been administered to pediatric patients (age 6 months to 16 years) by the oral route. For information regarding the use of azithromycin for oral suspension in the treatment of pediatric patients, [see Indications and Usage ( 1), and Dosage and Administration ( 2)] of the prescribing information for azithromycin for oral suspension 100 mg/5 mL and 200 mg/5 mL bottles.
8.5 Geriatric Use
Pharmacokinetic studies with intravenous azithromycin have not been performed in older volunteers. Pharmacokinetics of azithromycin following oral administration in older volunteers (65 to 85 years old) were similar to those in younger volunteers (18 to 40 years old) for the 5-day therapeutic regimen.
In multiple-dose clinical trials of intravenous azithromycin in the treatment of community-acquired pneumonia, 45% of patients (188/414) were at least 65 years of age and 22% of patients (91/414) were at least 75 years of age. No overall differences in safety were observed between these subjects and younger subjects in terms of adverse reactions, laboratory abnormalities, and discontinuations. Similar decreases in clinical response were noted in azithromycin- and comparator-treated patients with increasing age.
Azithromycin for injection contains 114 mg (4.96 mEq) of sodium per vial. At the usual recommended doses, patients would receive 114 mg (4.96 mEq) of sodium. The geriatric population may respond with a blunted natriuresis to salt loading. The total sodium content from dietary and non-dietary sources may be clinically important with regard to such diseases as congestive heart failure.
Elderly patients may be more susceptible to development of torsades de pointes arrhythmias than younger patients [see Warnings and Precautions ( 5.4)] .
5.2 Hepatotoxicity
Abnormal liver function, hepatitis, cholestatic jaundice, hepatic necrosis, and hepatic failure have been reported, some of which have resulted in death. Discontinue azithromycin immediately if signs and symptoms of hepatitis occur.
4 Contraindications
5.4 Qt Prolongation
Prolonged cardiac repolarization and QT interval, imparting a risk of developing cardiac arrhythmia and torsades de pointes, have been seen with treatment with macrolides, including azithromycin. Cases of torsades de pointes have been spontaneously reported during postmarketing surveillance in patients receiving azithromycin. Providers should consider the risk of QT prolongation, which can be fatal when weighing the risks and benefits of azithromycin for at-risk groups including:
- patients with known prolongation of the QT interval, a history of torsades de pointes, congenital long QT syndrome, bradyarrhythmias or uncompensated heart failure
- patients on drugs known to prolong the QT interval
- patients with ongoing proarrhythmic conditions such as uncorrected hypokalemia or hypomagnesemia, clinically significant bradycardia, and in patients receiving Class IA (quinidine, procainamide) or Class III (dofetilide, amiodarone, sotalol) antiarrhythmic agents.
Elderly patients may be more susceptible to drug-associated effects on the QT interval.
6 Adverse Reactions
The following clinically significant adverse reactions are described elsewhere in labeling:
- Hypersensitivity [see Warnings and Precautions ( 5.1)]
- Hepatotoxicity [see Warnings and Precautions ( 5.2)]
- Infantile Hypertrophic Pyloric Stenosis (IHPS) [see Warnings and Precautions ( 5.3)]
- QT Prolongation [see Warnings and Precautions ( 5.4)]
- Cardiovascular Death [see Warnings and Precautions ( 5.5)]
- Clostridioides difficile-Associated Diarrhea (CDAD) [see Warnings and Precautions ( 5.6)]
- Exacerbation of Myasthenia Gravis [see Warnings and Precautions ( 5.7)]
7 Drug Interactions
4.1 Hypersensitivity
Azithromycin is contraindicated in patients with known hypersensitivity to azithromycin, erythromycin, any macrolide or ketolide drugs.
5.1 Hypersensitivity
Serious allergic reactions, including angioedema, anaphylaxis, and dermatologic reactions including Acute Generalized Exanthematous Pustulosis (AGEP), Stevens-Johnson Syndrome, and toxic epidermal necrolysis have been reported in patients on azithromycin therapy
[see Contraindications (
4.1)]
.
Fatalities have been reported. Cases of Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS) have also been reported. Despite initially successful symptomatic treatment of the allergic symptoms, when symptomatic therapy was discontinued, the allergic symptoms recurred soon thereafter in some patients without further azithromycin exposure. These patients required prolonged periods of observation and symptomatic treatment. The relationship of these episodes to the long tissue half-life of azithromycin and subsequent prolonged exposure to antigen is unknown at present.
If an allergic reaction occurs, the drug should be discontinued and appropriate therapy should be instituted. Physicians should be aware that the allergic symptoms may reappear after symptomatic therapy has been discontinued.
12.2 Pharmacodynamics
Based on animal models of infection, the antibacterial activity of azithromycin appears to correlate with the ratio of area under the concentration-time curve to minimum inhibitory concentration (AUC/MIC) for certain pathogens (
S. pneumoniae and S. aureus). The principal pharmacokinetic/pharmacodynamic parameter best associated with clinical and microbiological cure has not been elucidated in clinical trials with azithromycin.
12.3 Pharmacokinetics
In patients hospitalized with community-acquired pneumonia receiving single daily one-hour intravenous infusions for 2 to 5 days of 500 mg azithromycin at a concentration of 2 mg/mL, the mean C
max± S.D. achieved was 3.63 ± 1.60 mcg/mL, while the 24-hour trough level was 0.20 ± 0.15 mcg/mL, and the AUC
24was 9.60 ± 4.80 mcg·hr/mL.
The mean C
max, 24-hour trough and AUC
24values were 1.14 ± 0.14 mcg/mL, 0.18 ± 0.02 mcg/mL, and 8.03 ± 0.86 mcg·hr/mL, respectively, in normal volunteers receiving a 3-hour intravenous infusion of 500 mg azithromycin at a concentration of 1 mg/mL. Similar pharmacokinetic values were obtained in patients hospitalized with community-acquired pneumonia who received the same 3-hour dosage regimen for 2 to 5 days.
|
a500 mg (2 mg/mL) for 2 to 5 days in community-acquired pneumonia patients. |
|||||||||
|
b500 mg (1 mg/mL) for 5 days in healthy subjects. |
|||||||||
|
Infusion
Concentration, Duration |
Time after starting the infusion (hr) | ||||||||
| 0.5 | 1 | 2 | 3 | 4 | 6 | 8 | 12 | 24 | |
|
2 mg/mL,
1 hr a |
2.98 ± 1.12 | 3.63 ± 1.73 | 0.60 ± 0.31 | 0.40 ± 0.23 | 0.33 ± 0.16 | 0.26 ± 0.14 | 0.27 ± 0.15 | 0.20 ± 0.12 | 0.20 ± 0.15 |
|
1 mg/mL,
3 hr b |
0.91 ± 0.13 | 1.02 ± 0.11 | 1.14 ± 0.13 | 1.13 ± 0.16 | 0.32 ± 0.05 | 0.28 ± 0.04 | 0.27 ± 0.03 | 0.22 ± 0.02 | 0.18 ± 0.02 |
Comparison of the plasma pharmacokinetic parameters following the 1st and 5th daily doses of 500 mg intravenous azithromycin showed only an 8% increase in C maxbut a 61% increase in AUC 24reflecting a threefold rise in C 24trough levels.
Following single-oral doses of 500 mg azithromycin (two 250 mg capsules) to 12 healthy volunteers, C max, trough level, and AUC 24were reported to be 0.41 mcg/mL, 0.05 mcg/mL, and 2.6 mcg·hr/mL, respectively. These oral values are approximately 38%, 83%, and 52% of the values observed following a single 500-mg I.V. 3-hour infusion (C max: 1.08 mcg/mL, trough: 0.06 mcg/mL, and AUC 24: 5.0 mcg·hr/mL). Thus, plasma concentrations are higher following the intravenous regimen throughout the 24-hour interval.
1 Indications and Usage
Azithromycin for injection is a macrolide antibacterial drug indicated for the treatment of patients with infections caused by susceptible strains of the designated microorganisms in the conditions listed below.
4.2 Hepatic Dysfunction
Azithromycin is contraindicated in patients with a history of cholestatic jaundice/hepatic dysfunction associated with prior use of azithromycin.
12.1 Mechanism of Action
Azithromycin is a macrolide antibacterial drug [see Microbiology ( 12.4)] .
5.5 Cardiovascular Death
Some observational studies have shown an approximately two-fold increased short-term potential risk of acute cardiovascular death in adults exposed to azithromycin relative to other antibacterial drugs, including amoxicillin. The five-day cardiovascular mortality observed in these studies ranged from 20 to 400 per million azithromycin treatment courses. This potential risk was noted to be greater during the first five days of azithromycin use and does not appear to be limited to those patients with preexisting cardiovascular diseases. The data in these observational studies are insufficient to establish or exclude a causal relationship between acute cardiovascular death and azithromycin use. Consider balancing this potential risk with treatment benefits when prescribing azithromycin.
5 Warnings and Precautions
- Serious (including fatal) allergic and skin reactions. Discontinue azithromycin and initiate appropriate therapy if reaction occurs. ( 5.1)
- Hepatotoxicity: Severe and sometimes fatal, hepatoxicity has been reported. Discontinue azithromycin immediately if signs and symptoms of hepatitis occur. ( 5.2)
- Infantile Hypertrophic Pyloric Stenosis (IHPS): Following the use of azithromycin in neonates (treatment up to 42 days of life), IHPS has been reported. Direct parents and caregivers to contact their physician if vomiting or irritability with feeding occurs. ( 5.3)
- Prolongation of QT interval and cases of torsades de pointes have been reported. This risk which can be fatal should be considered in patients with certain cardiovascular disorders including known QT prolongation or history torsades de pointes, those with proarrhythmic conditions, and with other drugs that prolong the QT interval. ( 5.4)
- Cardiovascular Death: Some observational studies have shown an approximately two-fold increased short-term potential risk of acute cardiovascular death in adults exposed to azithromycin relative to other antibacterial drugs, including amoxicillin. Consider balancing this potential risk with treatment benefits when prescribing azithromycin. ( 5.5)
- Clostridioides difficile-Associated Diarrhea: Evaluate patients if diarrhea occurs. ( 5.6)
- Azithromycin may exacerbate muscle weakness in persons with myasthenia gravis. ( 5.7)
5.8 Infusion Site Reactions
Azithromycin for injection should be reconstituted and diluted as directed and administered as an intravenous infusion over not less than 60 minutes
[see Dosage and Administration (
2)].
Local IV site reactions have been reported with the intravenous administration of azithromycin. The incidence and severity of these reactions were the same when 500 mg azithromycin was given over 1 hour (2 mg/mL as 250 mL infusion) or over 3 hr (1 mg/mL as 500 mL infusion) [see Adverse Reactions ( 6)] . All volunteers who received infusate concentrations above 2.0 mg/mL experienced local IV site reactions and, therefore, higher concentrations should be avoided.
3 Dosage Forms and Strengths
Azithromycin for Injection, USP is supplied in lyophilized form in a 10 mL single-dose vial equivalent to 500 mg of azithromycin for intravenous administration.
5.6 Clostridioides Difficile
Clostridioides difficileassociated diarrhea (CDAD) has been reported with use of nearly all antibacterial agents, including azithromycin for injection, and may range in severity from mild diarrhea to fatal colitis. Treatment with antibacterial agents alters the normal flora of the colon leading to overgrowth of C. difficile.
C. difficileproduces toxins A and B which contribute to the development of CDAD. Hypertoxin producing strains of C. difficilecause increased morbidity and mortality, as these infections can be refractory to antibacterial therapy and may require colectomy. CDAD must be considered in all patients who present with diarrhea following antibacterial use. Careful medical history is necessary since CDAD has been reported to occur over two months after the administration of antibacterial agents.
If CDAD is suspected or confirmed, ongoing antibacterial use not directed against C. difficilemay need to be discontinued. Appropriate fluid and electrolyte management, protein supplementation, antibacterial treatment of C. difficile, and surgical evaluation should be instituted as clinically indicated.
6.2 Postmarketing Experience
The following adverse reactions have been identified during post-approval use of azithromycin. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Adverse reactions reported with azithromycin during the postmarketing period in adult and/or pediatric patients for which a causal relationship may not be established include:
Allergic:Arthralgia, edema, urticaria and angioedema.
Cardiovascular:Arrhythmias including ventricular tachycardia and hypotension. There have been reports of QT prolongation, torsades de pointes, and cardiovascular death.
Gastrointestinal:Anorexia, constipation, dyspepsia, flatulence, vomiting/diarrhea, pseudomembranous colitis, pancreatitis, oral candidiasis, pyloric stenosis, and reports of tongue discoloration.
General:Asthenia, paresthesia, fatigue, malaise and anaphylaxis (including fatalities).
Genitourinary:Interstitial nephritis and acute renal failure and vaginitis.
Hematopoietic:Thrombocytopenia.
Liver/biliary:Abnormal liver function, hepatitis, cholestatic jaundice, hepatic necrosis, and hepatic failure [see Warnings and Precautions ( 5.2)] .
Nervous system:Convulsions, dizziness/vertigo, headache, somnolence, hyperactivity, nervousness, agitation and syncope.
Psychiatric:Aggressive reaction and anxiety.
Skin/appendages:Pruritus, serious skin reactions including, erythema multiforme, AGEP, Stevens-Johnson syndrome, toxic epidermal necrolysis, and DRESS.
Special senses:Hearing disturbances including hearing loss, deafness and/or tinnitus and reports of taste/smell perversion and/or loss.
6.3 Laboratory Abnormalities
Significant abnormalities (irrespective of drug relationship) occurring during the clinical trials were reported as follows:
- elevated ALT (SGPT), AST (SGOT), creatinine (4 to 6%)
- elevated LDH, bilirubin (1 to 3%)
- leukopenia, neutropenia, decreased platelet count, and elevated serum alkaline phosphatase (less than 1%)
When follow-up was provided, changes in laboratory tests appeared to be reversible.
In multiple-dose clinical trials involving more than 750 patients treated with azithromycin (IV/Oral), less than 2% of patients discontinued azithromycin therapy because of treatment-related liver enzyme abnormalities.
8 Use in Specific Populations
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
In clinical trials of intravenous azithromycin for community-acquired pneumonia, in which 2 to 5 IV doses were given, the reported adverse reactions were mild to moderate in severity and were reversible upon discontinuation of the drug. The majority of patients in these trials had one or more co-morbid diseases and were receiving concomitant medications. Approximately 1.2% of the patients discontinued intravenous azithromycin therapy, and a total of 2.4% discontinued azithromycin therapy by either the intravenous or oral route because of clinical or laboratory side effects.
In clinical trials conducted in patients with pelvic inflammatory disease, in which 1 to 2 IV doses were given, 2% of women who received monotherapy with azithromycin and 4% who received azithromycin plus metronidazole discontinued therapy due to clinical side effects.
Clinical adverse reactions leading to discontinuations from these studies were gastrointestinal (abdominal pain, nausea, vomiting, diarrhea), and rashes; laboratory side effects leading to discontinuation were increases in transaminase levels and/or alkaline phosphatase levels.
Overall, the most common adverse reactions associated with treatment in adult patients who received IV/Oral azithromycin in studies of community-acquired pneumonia were related to the gastrointestinal system with diarrhea/loose stools (4.3%), nausea (3.9%), abdominal pain (2.7%), and vomiting (1.4%) being the most frequently reported. Approximately 12% of patients experienced a side effect related to the intravenous infusion; most common were pain at the injection site (6.5%) and local inflammation (3.1%).
The most common adverse reactions associated with treatment in adult women who received IV/Oral azithromycin in trials of pelvic inflammatory disease were related to the gastrointestinal system. Diarrhea (8.5%) and nausea (6.6%) were most commonly reported, followed by vaginitis (2.8%), abdominal pain (1.9%), anorexia (1.9%), rash and pruritus (1.9%). When azithromycin was co-administered with metronidazole in these trials, a higher proportion of women experienced adverse reactions of nausea (10.3%), abdominal pain (3.7%), vomiting (2.8%), infusion site reaction, stomatitis, dizziness, or dyspnea (all at 1.9%).
Adverse reactions that occurred with a frequency of 1% or less included the following:
Gastrointestinal:Dyspepsia, flatulence, mucositis, oral moniliasis, and gastritis.
Nervous system:Headache, somnolence.
Allergic:Bronchospasm.
Special senses:Taste perversion.
1.2 Pelvic Inflammatory Disease
due to
Chlamydia trachomatis,
Neisseria gonorrhoeae, or
Mycoplasma hominisin patients who require initial intravenous therapy. If anaerobic microorganisms are suspected of contributing to the infection, an antimicrobial agent with anaerobic activity should be administered in combination with azithromycin for injection.
Azithromycin for injection should be followed by azithromycin by the oral route as required [see Dosage and Administration ( 2)] .
2.2 Pelvic Inflammatory Disease
The recommended dose of azithromycin for injection for the treatment of adult patients with pelvic inflammatory disease due to the indicated organisms is 500 mg as a single daily dose by the intravenous route for one or two days. Intravenous therapy should be followed by azithromycin by the oral route at a single, daily dose of 250 mg to complete a 7-day course of therapy. The timing of the switch to oral therapy should be done at the discretion of the physician and in accordance with clinical response.
1.1 Community Acquired Pneumonia
due to Chlamydophila pneumoniae, Haemophilus influenzae, Legionella pneumophila, Moraxella catarrhalis, Mycoplasma pneumoniae, Staphylococcus aureus,or Streptococcus pneumoniaein patients who require initial intravenous therapy.
2.1 Community Acquired Pneumonia
The recommended dose of azithromycin for injection for the treatment of adult patients with community-acquired pneumonia due to the indicated organisms is 500 mg as a single daily dose by the intravenous route for at least two days. Intravenous therapy should be followed by azithromycin by the oral route at a single, daily dose of 500 mg, administered as two 250 mg tablets to complete a 7- to 10-day course of therapy. The timing of the switch to oral therapy should be done at the discretion of the physician and in accordance with clinical response.
14.1 Community Acquired Pneumonia
In a controlled trial of community-acquired pneumonia performed in the U.S., azithromycin (500 mg as a single daily dose by the intravenous route for 2 to 5 days, followed by 500 mg/day by the oral route to complete 7 to 10 days therapy) was compared to cefuroxime (2,250 mg/day in three divided doses by the intravenous route for 2 to 5 days followed by 1,000 mg/day in two divided doses by the oral route to complete 7 to 10 days therapy), with or without erythromycin. For the 291 patients who were evaluable for clinical efficacy, the clinical outcome rates, i.e., cure, improved, and success (cure + improved) among the 277 patients seen at 10 to 14 days post-therapy were as follows:
| Clinical Outcome | Azithromycin | Comparator |
| Cure | 46% | 44% |
| Improved | 32% | 30% |
| Success (Cure + Improved) | 78% | 74% |
In a separate, uncontrolled clinical and microbiological trial performed in the U.S., 94 patients with community-acquired pneumonia who received azithromycin in the same regimen were evaluable for clinical efficacy. The clinical outcome rates, i.e., cure, improved, and success (cure + improved) among the 84 patients seen at 10 to 14 days post-therapy were as follows:
| Clinical Outcome | Azithromycin |
| Cure | 60% |
| Improved | 29% |
| Success (Cure + Improved) | 89% |
Microbiological determinations in both trials were made at the pre-treatment visit and, where applicable, were reassessed at later visits. Serological testing was done on baseline and final visit specimens. The following combined presumptive bacteriological eradication rates were obtained from the evaluable groups:
Combined Bacteriological Eradication Rates for Azithromycin:
|
aNineteen of twenty-four patients (79%) with positive blood cultures for S. pneumoniaewere cured (intent-to-treat analysis) with eradication of the pathogen. |
|
| (at last completed visit) | Azithromycin |
| S. pneumoniae | 64/67 (96%) a |
| H. influenzae | 41/43 (95%) |
| M. catarrhalis | 9/10 (90%) |
| S. aureus | 9/10 (90%) |
The presumed bacteriological outcomes at 10 to 14 days post-therapy for patients treated with azithromycin with evidence (serology and/or culture) of atypical pathogens for both trials were as follows:
| Evidence of Infection | Total | Cure | Improved | Cure + Improved |
| Mycoplasma pneumoniae | 18 | 11 (61%) | 5 (28%) | 16 (89%) |
| Chlamydia pneumoniae | 34 | 15 (44%) | 13 (38%) | 28 (82%) |
| Legionella pneumophila | 16 | 5 (31%) | 8 (50%) | 13 (81%) |
17 Patient Counseling Information
Patients should be informed of the following serious and potentially serious adverse reactions that have been associated with azithromycin for injection.
16 How Supplied/storage and Handling
Azithromycin for Injection, USP is supplied as follows:
| NDC | Azithromycin for Injection, USP | Package Factor |
| 70860-100-10 | 500 mg Single-Dose Vial | 10 vials per carton |
Azithromycin for Injection, USP is supplied in lyophilized form under a vacuum in a 10 mL single-dose vial equivalent to 500 mg of azithromycin for intravenous administration. Each vial also contains sodium hydroxide and 384.5 mg citric acid.
5.7 Exacerbation of Myasthenia Gravis
Exacerbations of symptoms of myasthenia gravis and new onset of myasthenic syndrome have been reported in patients receiving azithromycin therapy.
13.2 Animal Toxicology And/or Pharmacology
Phospholipidosis (intracellular phospholipid accumulation) has been observed in some tissues of mice, rats, and dogs given multiple oral doses of azithromycin. It has been demonstrated in numerous organ systems (e.g., eye, dorsal root ganglia, liver, gallbladder, kidney, spleen, and/or pancreas) in dogs and rats treated with azithromycin at doses which, expressed on the basis of body surface area, are similar to or less than the highest recommended adult human dose. This effect has been shown to be reversible after cessation of azithromycin treatment. Based on the pharmacokinetic data, phospholipidosis has been seen in the rat (50 mg/kg/day dose) at the observed maximal plasma concentration of 1.3 mcg/mL (1.6 times the observed C maxof 0.821 mcg/mL at the adult dose of 2 g). Similarly, it has been shown in the dog (10 mg/kg/day dose) at the observed maximal serum concentration of 1 mcg/mL (1.2 times the observed C maxof 0.821 mcg/mL at the adult dose of 2 g).
Phospholipidosis was also observed in neonatal rats dosed for 18 days at 30 mg/kg/day, which is less than the pediatric dose of 60 mg/kg based on body surface area. It was not observed in neonatal rats treated for 10 days at 40 mg/kg/day with mean maximal serum concentrations of 1.86 mcg/mL, approximately 1.5 times the C maxof 1.27 mcg/mL at the pediatric dose. Phospholipidosis has been observed in neonatal dogs (10 mg/kg/day) at maximum mean whole blood concentrations of 3.54 mcg/mL, approximately 3 times the pediatric dose C max. The significance of the findings for animals and for humans is unknown.
5.9 Development of Drug Resistant Bacteria
Prescribing azithromycin in the absence of a proven or strongly suspected bacterial infection is unlikely to provide benefit to the patient and increases the risk of the development of drug-resistant bacteria.
5.3 Infantile Hypertrophic Pyloric Stenosis (ihps)
Following the use of azithromycin in neonates (treatment up to 42 days of life), IHPS has been reported. Direct parents and caregivers to contact their physician if vomiting or irritability with feeding occurs.
7.3 Potential Drug Drug Interaction With Macrolides
Interactions with digoxin, colchicine or phenytoin have not been reported in clinical trials with azithromycin. No specific drug interaction studies have been performed to evaluate potential drug-drug interaction. However, drug interactions have been observed with other macrolide products. Until further data are developed regarding drug interactions when digoxin, colchicine or phenytoin are used with azithromycin careful monitoring of patients is advised.
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Long-term studies in animals have not been performed to evaluate carcinogenic potential. Azithromycin has shown no mutagenic potential in standard laboratory tests: mouse lymphoma assay, human lymphocyte clastogenic assay, and mouse bone marrow clastogenic assay. In fertility studies conducted in male and female rats, oral administration of azithromycin for 64 to 66 days (males) or 15 days (females) prior to and during cohabitation resulted in decreased pregnancy rate at 20 and 30 mg/kg/day when both males and females were treated with azithromycin. This minimal effect on pregnancy rate (approximately 12% reduction compared to concurrent controls) did not become more pronounced when the dose was increased from 20 to 30 mg/kg/day (approximately 0.4 to 0.6 times the adult daily dose of 500 mg based on body surface area) and it was not observed when only one animal in the mated pair was treated. There were no effects on any other reproductive parameters, and there were no effects on fertility at 10 mg/kg/day. The relevance of these findings to patients being treated with azithromycin at the doses and durations recommended in the prescribing information is uncertain.
2.3 Preparation of the Solution for Intravenous Administration
The infusate concentration and rate of infusion for azithromycin for injection should be either 1 mg/mL over 3 hr or 2 mg/mL over 1 hr. Azithromycin for injection should not be given as a bolus or as an intramuscular injection.
Structured Label Content
Section 42229-5 (42229-5)
Reconstitution
Prepare the initial solution of azithromycin for injection by adding 4.8 mL of Sterile Water for Injection to the 500 mg vial, and shaking the vial until all of the drug is dissolved. Since azithromycin for injection is supplied under vacuum, it is recommended that a standard 5 mL (non-automated) syringe be used to ensure that the exact amount of 4.8 mL of Sterile Water is dispensed. Each mL of reconstituted solution contains 100 mg azithromycin. Reconstituted solution is stable for 24 hr when stored below 30°C (86°F).
Parenteral drug products should be inspected visually for particulate matter prior to administration. If particulate matter is evident in reconstituted fluids, the drug solution should be discarded.
Dilute this solution further prior to administration as instructed below.
Section 43683-2 (43683-2)
| Warnings and Precautions, Cardiovascular Death ( 5.5) | 11/2021 |
Section 44425-7 (44425-7)
Storage Conditions
Store at 20° to 25°C (68° to 77°F). [See USP Controlled Room Temperature.]
Sterile, Nonpyrogenic, Preservative-free.
The container closure is not made with natural rubber latex.
*Normosol ®-M in 5% dextrose and Normosol ®-R in 5% dextrose are the trademarks of Hospira.
Section 51945-4 (51945-4)
PACKAGE LABEL – PRINCIPAL DISPLAY PANEL – Vial Label
NDC 70860-100-41
Azithromycin for Injection, USP
500 mg per vial (equivalent to azithromycin)
Rx only
FOR INTRAVENOUS INFUSION ONLY
Single-Dose Vial
1.3 Usage
To reduce the development of drug-resistant bacteria and maintain the effectiveness of azithromycin and other antibacterial drugs, azithromycin should be used only to treat infections that are proven or strongly suspected to be caused by susceptible bacteria. When culture and susceptibility information are available, they should be considered in selecting or modifying antibacterial therapy. In the absence of such data, local epidemiology and susceptibility patterns may contribute to the empiric selection of therapy.
7.2 Warfarin
Spontaneous postmarketing reports suggest that concomitant administration of azithromycin may potentiate the effects of oral anticoagulants such as warfarin, although the prothrombin time was not affected in the dedicated drug interaction study with azithromycin and warfarin. Prothrombin times should be carefully monitored while patients are receiving azithromycin and oral anticoagulants concomitantly.
10 Overdosage (10 OVERDOSAGE)
Adverse reactions experienced in higher than recommended doses were similar to those seen at normal doses particularly nausea, diarrhea, and vomiting. In the event of overdosage, general symptomatic and supportive measures are indicated as required.
11 Description (11 DESCRIPTION)
Azithromycin for Injection, USP contains the active ingredient azithromycin, an azalide, a subclass of macrolide antibacterial drug, for intravenous injection. Azithromycin has the chemical name (2R,3S,4R,5R,8R,10R,11R,12S,13S,14R)-13-[(2,6-dideoxy-3- C-methyl-3- O-methyl-α- L-ribo-hexopyranosyl)oxy]-2-ethyl-3,4,10-trihydroxy-3,5,6,8,10,12,14-hepta-methyl-11-[[3,4,6-trideoxy-3-(dimethylamino)-β- D- xylo-hexopyranosyl]oxy]-1-oxa-6-azacyclopentadecan-15-one. Azithromycin is derived from erythromycin; however, it differs chemically from erythromycin in that a methyl-substituted nitrogen atom is incorporated into the lactone ring. Its molecular formula is C 38H 72N 2O 12, and its molecular weight is 749.00. Azithromycin has the following structural formula:
Azithromycin, as the monohydrate, is a white crystalline powder with a molecular formula of C 38H 72N 2O 12· H 2O and a molecular weight of 767.0.
Azithromycin for Injection, USP consists of azithromycin monohydrate and the following inactive ingredients: citric acid and sodium hydroxide. Azithromycin for Injection, USP is supplied in lyophilized form in a 10 mL single-dose vial equivalent to 500 mg of azithromycin for intravenous administration. Reconstitution, according to label directions, results in approximately 5 mL of azithromycin for intravenous injection with each mL containing azithromycin monohydrate equivalent to 100 mg of azithromycin.
7.1 Nelfinavir
Co-administration of nelfinavir at steady-state with a single oral dose of azithromycin resulted in increased azithromycin serum concentrations. Although a dose adjustment of azithromycin is not recommended when administered in combination with nelfinavir, close monitoring for known adverse reactions of azithromycin, such as liver enzyme abnormalities and hearing impairment, is warranted [see Adverse Reactions ( 6)] .
8.4 Pediatric Use
Safety and effectiveness of azithromycin for injection in children or adolescents under 16 years have not been established. In controlled clinical studies, azithromycin has been administered to pediatric patients (age 6 months to 16 years) by the oral route. For information regarding the use of azithromycin for oral suspension in the treatment of pediatric patients, [see Indications and Usage ( 1), and Dosage and Administration ( 2)] of the prescribing information for azithromycin for oral suspension 100 mg/5 mL and 200 mg/5 mL bottles.
8.5 Geriatric Use
Pharmacokinetic studies with intravenous azithromycin have not been performed in older volunteers. Pharmacokinetics of azithromycin following oral administration in older volunteers (65 to 85 years old) were similar to those in younger volunteers (18 to 40 years old) for the 5-day therapeutic regimen.
In multiple-dose clinical trials of intravenous azithromycin in the treatment of community-acquired pneumonia, 45% of patients (188/414) were at least 65 years of age and 22% of patients (91/414) were at least 75 years of age. No overall differences in safety were observed between these subjects and younger subjects in terms of adverse reactions, laboratory abnormalities, and discontinuations. Similar decreases in clinical response were noted in azithromycin- and comparator-treated patients with increasing age.
Azithromycin for injection contains 114 mg (4.96 mEq) of sodium per vial. At the usual recommended doses, patients would receive 114 mg (4.96 mEq) of sodium. The geriatric population may respond with a blunted natriuresis to salt loading. The total sodium content from dietary and non-dietary sources may be clinically important with regard to such diseases as congestive heart failure.
Elderly patients may be more susceptible to development of torsades de pointes arrhythmias than younger patients [see Warnings and Precautions ( 5.4)] .
5.2 Hepatotoxicity
Abnormal liver function, hepatitis, cholestatic jaundice, hepatic necrosis, and hepatic failure have been reported, some of which have resulted in death. Discontinue azithromycin immediately if signs and symptoms of hepatitis occur.
4 Contraindications (4 CONTRAINDICATIONS)
5.4 Qt Prolongation (5.4 QT Prolongation)
Prolonged cardiac repolarization and QT interval, imparting a risk of developing cardiac arrhythmia and torsades de pointes, have been seen with treatment with macrolides, including azithromycin. Cases of torsades de pointes have been spontaneously reported during postmarketing surveillance in patients receiving azithromycin. Providers should consider the risk of QT prolongation, which can be fatal when weighing the risks and benefits of azithromycin for at-risk groups including:
- patients with known prolongation of the QT interval, a history of torsades de pointes, congenital long QT syndrome, bradyarrhythmias or uncompensated heart failure
- patients on drugs known to prolong the QT interval
- patients with ongoing proarrhythmic conditions such as uncorrected hypokalemia or hypomagnesemia, clinically significant bradycardia, and in patients receiving Class IA (quinidine, procainamide) or Class III (dofetilide, amiodarone, sotalol) antiarrhythmic agents.
Elderly patients may be more susceptible to drug-associated effects on the QT interval.
6 Adverse Reactions (6 ADVERSE REACTIONS)
The following clinically significant adverse reactions are described elsewhere in labeling:
- Hypersensitivity [see Warnings and Precautions ( 5.1)]
- Hepatotoxicity [see Warnings and Precautions ( 5.2)]
- Infantile Hypertrophic Pyloric Stenosis (IHPS) [see Warnings and Precautions ( 5.3)]
- QT Prolongation [see Warnings and Precautions ( 5.4)]
- Cardiovascular Death [see Warnings and Precautions ( 5.5)]
- Clostridioides difficile-Associated Diarrhea (CDAD) [see Warnings and Precautions ( 5.6)]
- Exacerbation of Myasthenia Gravis [see Warnings and Precautions ( 5.7)]
7 Drug Interactions (7 DRUG INTERACTIONS)
4.1 Hypersensitivity
Azithromycin is contraindicated in patients with known hypersensitivity to azithromycin, erythromycin, any macrolide or ketolide drugs.
5.1 Hypersensitivity
Serious allergic reactions, including angioedema, anaphylaxis, and dermatologic reactions including Acute Generalized Exanthematous Pustulosis (AGEP), Stevens-Johnson Syndrome, and toxic epidermal necrolysis have been reported in patients on azithromycin therapy
[see Contraindications (
4.1)]
.
Fatalities have been reported. Cases of Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS) have also been reported. Despite initially successful symptomatic treatment of the allergic symptoms, when symptomatic therapy was discontinued, the allergic symptoms recurred soon thereafter in some patients without further azithromycin exposure. These patients required prolonged periods of observation and symptomatic treatment. The relationship of these episodes to the long tissue half-life of azithromycin and subsequent prolonged exposure to antigen is unknown at present.
If an allergic reaction occurs, the drug should be discontinued and appropriate therapy should be instituted. Physicians should be aware that the allergic symptoms may reappear after symptomatic therapy has been discontinued.
12.2 Pharmacodynamics
Based on animal models of infection, the antibacterial activity of azithromycin appears to correlate with the ratio of area under the concentration-time curve to minimum inhibitory concentration (AUC/MIC) for certain pathogens (
S. pneumoniae and S. aureus). The principal pharmacokinetic/pharmacodynamic parameter best associated with clinical and microbiological cure has not been elucidated in clinical trials with azithromycin.
12.3 Pharmacokinetics
In patients hospitalized with community-acquired pneumonia receiving single daily one-hour intravenous infusions for 2 to 5 days of 500 mg azithromycin at a concentration of 2 mg/mL, the mean C
max± S.D. achieved was 3.63 ± 1.60 mcg/mL, while the 24-hour trough level was 0.20 ± 0.15 mcg/mL, and the AUC
24was 9.60 ± 4.80 mcg·hr/mL.
The mean C
max, 24-hour trough and AUC
24values were 1.14 ± 0.14 mcg/mL, 0.18 ± 0.02 mcg/mL, and 8.03 ± 0.86 mcg·hr/mL, respectively, in normal volunteers receiving a 3-hour intravenous infusion of 500 mg azithromycin at a concentration of 1 mg/mL. Similar pharmacokinetic values were obtained in patients hospitalized with community-acquired pneumonia who received the same 3-hour dosage regimen for 2 to 5 days.
|
a500 mg (2 mg/mL) for 2 to 5 days in community-acquired pneumonia patients. |
|||||||||
|
b500 mg (1 mg/mL) for 5 days in healthy subjects. |
|||||||||
|
Infusion
Concentration, Duration |
Time after starting the infusion (hr) | ||||||||
| 0.5 | 1 | 2 | 3 | 4 | 6 | 8 | 12 | 24 | |
|
2 mg/mL,
1 hr a |
2.98 ± 1.12 | 3.63 ± 1.73 | 0.60 ± 0.31 | 0.40 ± 0.23 | 0.33 ± 0.16 | 0.26 ± 0.14 | 0.27 ± 0.15 | 0.20 ± 0.12 | 0.20 ± 0.15 |
|
1 mg/mL,
3 hr b |
0.91 ± 0.13 | 1.02 ± 0.11 | 1.14 ± 0.13 | 1.13 ± 0.16 | 0.32 ± 0.05 | 0.28 ± 0.04 | 0.27 ± 0.03 | 0.22 ± 0.02 | 0.18 ± 0.02 |
Comparison of the plasma pharmacokinetic parameters following the 1st and 5th daily doses of 500 mg intravenous azithromycin showed only an 8% increase in C maxbut a 61% increase in AUC 24reflecting a threefold rise in C 24trough levels.
Following single-oral doses of 500 mg azithromycin (two 250 mg capsules) to 12 healthy volunteers, C max, trough level, and AUC 24were reported to be 0.41 mcg/mL, 0.05 mcg/mL, and 2.6 mcg·hr/mL, respectively. These oral values are approximately 38%, 83%, and 52% of the values observed following a single 500-mg I.V. 3-hour infusion (C max: 1.08 mcg/mL, trough: 0.06 mcg/mL, and AUC 24: 5.0 mcg·hr/mL). Thus, plasma concentrations are higher following the intravenous regimen throughout the 24-hour interval.
1 Indications and Usage (1 INDICATIONS AND USAGE)
Azithromycin for injection is a macrolide antibacterial drug indicated for the treatment of patients with infections caused by susceptible strains of the designated microorganisms in the conditions listed below.
4.2 Hepatic Dysfunction
Azithromycin is contraindicated in patients with a history of cholestatic jaundice/hepatic dysfunction associated with prior use of azithromycin.
12.1 Mechanism of Action
Azithromycin is a macrolide antibacterial drug [see Microbiology ( 12.4)] .
5.5 Cardiovascular Death
Some observational studies have shown an approximately two-fold increased short-term potential risk of acute cardiovascular death in adults exposed to azithromycin relative to other antibacterial drugs, including amoxicillin. The five-day cardiovascular mortality observed in these studies ranged from 20 to 400 per million azithromycin treatment courses. This potential risk was noted to be greater during the first five days of azithromycin use and does not appear to be limited to those patients with preexisting cardiovascular diseases. The data in these observational studies are insufficient to establish or exclude a causal relationship between acute cardiovascular death and azithromycin use. Consider balancing this potential risk with treatment benefits when prescribing azithromycin.
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
- Serious (including fatal) allergic and skin reactions. Discontinue azithromycin and initiate appropriate therapy if reaction occurs. ( 5.1)
- Hepatotoxicity: Severe and sometimes fatal, hepatoxicity has been reported. Discontinue azithromycin immediately if signs and symptoms of hepatitis occur. ( 5.2)
- Infantile Hypertrophic Pyloric Stenosis (IHPS): Following the use of azithromycin in neonates (treatment up to 42 days of life), IHPS has been reported. Direct parents and caregivers to contact their physician if vomiting or irritability with feeding occurs. ( 5.3)
- Prolongation of QT interval and cases of torsades de pointes have been reported. This risk which can be fatal should be considered in patients with certain cardiovascular disorders including known QT prolongation or history torsades de pointes, those with proarrhythmic conditions, and with other drugs that prolong the QT interval. ( 5.4)
- Cardiovascular Death: Some observational studies have shown an approximately two-fold increased short-term potential risk of acute cardiovascular death in adults exposed to azithromycin relative to other antibacterial drugs, including amoxicillin. Consider balancing this potential risk with treatment benefits when prescribing azithromycin. ( 5.5)
- Clostridioides difficile-Associated Diarrhea: Evaluate patients if diarrhea occurs. ( 5.6)
- Azithromycin may exacerbate muscle weakness in persons with myasthenia gravis. ( 5.7)
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
5.8 Infusion Site Reactions
Azithromycin for injection should be reconstituted and diluted as directed and administered as an intravenous infusion over not less than 60 minutes
[see Dosage and Administration (
2)].
Local IV site reactions have been reported with the intravenous administration of azithromycin. The incidence and severity of these reactions were the same when 500 mg azithromycin was given over 1 hour (2 mg/mL as 250 mL infusion) or over 3 hr (1 mg/mL as 500 mL infusion) [see Adverse Reactions ( 6)] . All volunteers who received infusate concentrations above 2.0 mg/mL experienced local IV site reactions and, therefore, higher concentrations should be avoided.
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
Azithromycin for Injection, USP is supplied in lyophilized form in a 10 mL single-dose vial equivalent to 500 mg of azithromycin for intravenous administration.
5.6 Clostridioides Difficile (5.6 Clostridioides difficile)
Clostridioides difficileassociated diarrhea (CDAD) has been reported with use of nearly all antibacterial agents, including azithromycin for injection, and may range in severity from mild diarrhea to fatal colitis. Treatment with antibacterial agents alters the normal flora of the colon leading to overgrowth of C. difficile.
C. difficileproduces toxins A and B which contribute to the development of CDAD. Hypertoxin producing strains of C. difficilecause increased morbidity and mortality, as these infections can be refractory to antibacterial therapy and may require colectomy. CDAD must be considered in all patients who present with diarrhea following antibacterial use. Careful medical history is necessary since CDAD has been reported to occur over two months after the administration of antibacterial agents.
If CDAD is suspected or confirmed, ongoing antibacterial use not directed against C. difficilemay need to be discontinued. Appropriate fluid and electrolyte management, protein supplementation, antibacterial treatment of C. difficile, and surgical evaluation should be instituted as clinically indicated.
6.2 Postmarketing Experience
The following adverse reactions have been identified during post-approval use of azithromycin. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Adverse reactions reported with azithromycin during the postmarketing period in adult and/or pediatric patients for which a causal relationship may not be established include:
Allergic:Arthralgia, edema, urticaria and angioedema.
Cardiovascular:Arrhythmias including ventricular tachycardia and hypotension. There have been reports of QT prolongation, torsades de pointes, and cardiovascular death.
Gastrointestinal:Anorexia, constipation, dyspepsia, flatulence, vomiting/diarrhea, pseudomembranous colitis, pancreatitis, oral candidiasis, pyloric stenosis, and reports of tongue discoloration.
General:Asthenia, paresthesia, fatigue, malaise and anaphylaxis (including fatalities).
Genitourinary:Interstitial nephritis and acute renal failure and vaginitis.
Hematopoietic:Thrombocytopenia.
Liver/biliary:Abnormal liver function, hepatitis, cholestatic jaundice, hepatic necrosis, and hepatic failure [see Warnings and Precautions ( 5.2)] .
Nervous system:Convulsions, dizziness/vertigo, headache, somnolence, hyperactivity, nervousness, agitation and syncope.
Psychiatric:Aggressive reaction and anxiety.
Skin/appendages:Pruritus, serious skin reactions including, erythema multiforme, AGEP, Stevens-Johnson syndrome, toxic epidermal necrolysis, and DRESS.
Special senses:Hearing disturbances including hearing loss, deafness and/or tinnitus and reports of taste/smell perversion and/or loss.
6.3 Laboratory Abnormalities
Significant abnormalities (irrespective of drug relationship) occurring during the clinical trials were reported as follows:
- elevated ALT (SGPT), AST (SGOT), creatinine (4 to 6%)
- elevated LDH, bilirubin (1 to 3%)
- leukopenia, neutropenia, decreased platelet count, and elevated serum alkaline phosphatase (less than 1%)
When follow-up was provided, changes in laboratory tests appeared to be reversible.
In multiple-dose clinical trials involving more than 750 patients treated with azithromycin (IV/Oral), less than 2% of patients discontinued azithromycin therapy because of treatment-related liver enzyme abnormalities.
8 Use in Specific Populations (8 USE IN SPECIFIC POPULATIONS)
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
In clinical trials of intravenous azithromycin for community-acquired pneumonia, in which 2 to 5 IV doses were given, the reported adverse reactions were mild to moderate in severity and were reversible upon discontinuation of the drug. The majority of patients in these trials had one or more co-morbid diseases and were receiving concomitant medications. Approximately 1.2% of the patients discontinued intravenous azithromycin therapy, and a total of 2.4% discontinued azithromycin therapy by either the intravenous or oral route because of clinical or laboratory side effects.
In clinical trials conducted in patients with pelvic inflammatory disease, in which 1 to 2 IV doses were given, 2% of women who received monotherapy with azithromycin and 4% who received azithromycin plus metronidazole discontinued therapy due to clinical side effects.
Clinical adverse reactions leading to discontinuations from these studies were gastrointestinal (abdominal pain, nausea, vomiting, diarrhea), and rashes; laboratory side effects leading to discontinuation were increases in transaminase levels and/or alkaline phosphatase levels.
Overall, the most common adverse reactions associated with treatment in adult patients who received IV/Oral azithromycin in studies of community-acquired pneumonia were related to the gastrointestinal system with diarrhea/loose stools (4.3%), nausea (3.9%), abdominal pain (2.7%), and vomiting (1.4%) being the most frequently reported. Approximately 12% of patients experienced a side effect related to the intravenous infusion; most common were pain at the injection site (6.5%) and local inflammation (3.1%).
The most common adverse reactions associated with treatment in adult women who received IV/Oral azithromycin in trials of pelvic inflammatory disease were related to the gastrointestinal system. Diarrhea (8.5%) and nausea (6.6%) were most commonly reported, followed by vaginitis (2.8%), abdominal pain (1.9%), anorexia (1.9%), rash and pruritus (1.9%). When azithromycin was co-administered with metronidazole in these trials, a higher proportion of women experienced adverse reactions of nausea (10.3%), abdominal pain (3.7%), vomiting (2.8%), infusion site reaction, stomatitis, dizziness, or dyspnea (all at 1.9%).
Adverse reactions that occurred with a frequency of 1% or less included the following:
Gastrointestinal:Dyspepsia, flatulence, mucositis, oral moniliasis, and gastritis.
Nervous system:Headache, somnolence.
Allergic:Bronchospasm.
Special senses:Taste perversion.
1.2 Pelvic Inflammatory Disease
due to
Chlamydia trachomatis,
Neisseria gonorrhoeae, or
Mycoplasma hominisin patients who require initial intravenous therapy. If anaerobic microorganisms are suspected of contributing to the infection, an antimicrobial agent with anaerobic activity should be administered in combination with azithromycin for injection.
Azithromycin for injection should be followed by azithromycin by the oral route as required [see Dosage and Administration ( 2)] .
2.2 Pelvic Inflammatory Disease
The recommended dose of azithromycin for injection for the treatment of adult patients with pelvic inflammatory disease due to the indicated organisms is 500 mg as a single daily dose by the intravenous route for one or two days. Intravenous therapy should be followed by azithromycin by the oral route at a single, daily dose of 250 mg to complete a 7-day course of therapy. The timing of the switch to oral therapy should be done at the discretion of the physician and in accordance with clinical response.
1.1 Community Acquired Pneumonia (1.1 Community-Acquired Pneumonia)
due to Chlamydophila pneumoniae, Haemophilus influenzae, Legionella pneumophila, Moraxella catarrhalis, Mycoplasma pneumoniae, Staphylococcus aureus,or Streptococcus pneumoniaein patients who require initial intravenous therapy.
2.1 Community Acquired Pneumonia (2.1 Community-Acquired Pneumonia)
The recommended dose of azithromycin for injection for the treatment of adult patients with community-acquired pneumonia due to the indicated organisms is 500 mg as a single daily dose by the intravenous route for at least two days. Intravenous therapy should be followed by azithromycin by the oral route at a single, daily dose of 500 mg, administered as two 250 mg tablets to complete a 7- to 10-day course of therapy. The timing of the switch to oral therapy should be done at the discretion of the physician and in accordance with clinical response.
14.1 Community Acquired Pneumonia (14.1 Community-Acquired Pneumonia)
In a controlled trial of community-acquired pneumonia performed in the U.S., azithromycin (500 mg as a single daily dose by the intravenous route for 2 to 5 days, followed by 500 mg/day by the oral route to complete 7 to 10 days therapy) was compared to cefuroxime (2,250 mg/day in three divided doses by the intravenous route for 2 to 5 days followed by 1,000 mg/day in two divided doses by the oral route to complete 7 to 10 days therapy), with or without erythromycin. For the 291 patients who were evaluable for clinical efficacy, the clinical outcome rates, i.e., cure, improved, and success (cure + improved) among the 277 patients seen at 10 to 14 days post-therapy were as follows:
| Clinical Outcome | Azithromycin | Comparator |
| Cure | 46% | 44% |
| Improved | 32% | 30% |
| Success (Cure + Improved) | 78% | 74% |
In a separate, uncontrolled clinical and microbiological trial performed in the U.S., 94 patients with community-acquired pneumonia who received azithromycin in the same regimen were evaluable for clinical efficacy. The clinical outcome rates, i.e., cure, improved, and success (cure + improved) among the 84 patients seen at 10 to 14 days post-therapy were as follows:
| Clinical Outcome | Azithromycin |
| Cure | 60% |
| Improved | 29% |
| Success (Cure + Improved) | 89% |
Microbiological determinations in both trials were made at the pre-treatment visit and, where applicable, were reassessed at later visits. Serological testing was done on baseline and final visit specimens. The following combined presumptive bacteriological eradication rates were obtained from the evaluable groups:
Combined Bacteriological Eradication Rates for Azithromycin:
|
aNineteen of twenty-four patients (79%) with positive blood cultures for S. pneumoniaewere cured (intent-to-treat analysis) with eradication of the pathogen. |
|
| (at last completed visit) | Azithromycin |
| S. pneumoniae | 64/67 (96%) a |
| H. influenzae | 41/43 (95%) |
| M. catarrhalis | 9/10 (90%) |
| S. aureus | 9/10 (90%) |
The presumed bacteriological outcomes at 10 to 14 days post-therapy for patients treated with azithromycin with evidence (serology and/or culture) of atypical pathogens for both trials were as follows:
| Evidence of Infection | Total | Cure | Improved | Cure + Improved |
| Mycoplasma pneumoniae | 18 | 11 (61%) | 5 (28%) | 16 (89%) |
| Chlamydia pneumoniae | 34 | 15 (44%) | 13 (38%) | 28 (82%) |
| Legionella pneumophila | 16 | 5 (31%) | 8 (50%) | 13 (81%) |
17 Patient Counseling Information (17 PATIENT COUNSELING INFORMATION)
Patients should be informed of the following serious and potentially serious adverse reactions that have been associated with azithromycin for injection.
16 How Supplied/storage and Handling (16 HOW SUPPLIED/STORAGE AND HANDLING)
Azithromycin for Injection, USP is supplied as follows:
| NDC | Azithromycin for Injection, USP | Package Factor |
| 70860-100-10 | 500 mg Single-Dose Vial | 10 vials per carton |
Azithromycin for Injection, USP is supplied in lyophilized form under a vacuum in a 10 mL single-dose vial equivalent to 500 mg of azithromycin for intravenous administration. Each vial also contains sodium hydroxide and 384.5 mg citric acid.
5.7 Exacerbation of Myasthenia Gravis
Exacerbations of symptoms of myasthenia gravis and new onset of myasthenic syndrome have been reported in patients receiving azithromycin therapy.
13.2 Animal Toxicology And/or Pharmacology (13.2 Animal Toxicology and/or Pharmacology)
Phospholipidosis (intracellular phospholipid accumulation) has been observed in some tissues of mice, rats, and dogs given multiple oral doses of azithromycin. It has been demonstrated in numerous organ systems (e.g., eye, dorsal root ganglia, liver, gallbladder, kidney, spleen, and/or pancreas) in dogs and rats treated with azithromycin at doses which, expressed on the basis of body surface area, are similar to or less than the highest recommended adult human dose. This effect has been shown to be reversible after cessation of azithromycin treatment. Based on the pharmacokinetic data, phospholipidosis has been seen in the rat (50 mg/kg/day dose) at the observed maximal plasma concentration of 1.3 mcg/mL (1.6 times the observed C maxof 0.821 mcg/mL at the adult dose of 2 g). Similarly, it has been shown in the dog (10 mg/kg/day dose) at the observed maximal serum concentration of 1 mcg/mL (1.2 times the observed C maxof 0.821 mcg/mL at the adult dose of 2 g).
Phospholipidosis was also observed in neonatal rats dosed for 18 days at 30 mg/kg/day, which is less than the pediatric dose of 60 mg/kg based on body surface area. It was not observed in neonatal rats treated for 10 days at 40 mg/kg/day with mean maximal serum concentrations of 1.86 mcg/mL, approximately 1.5 times the C maxof 1.27 mcg/mL at the pediatric dose. Phospholipidosis has been observed in neonatal dogs (10 mg/kg/day) at maximum mean whole blood concentrations of 3.54 mcg/mL, approximately 3 times the pediatric dose C max. The significance of the findings for animals and for humans is unknown.
5.9 Development of Drug Resistant Bacteria (5.9 Development of Drug-Resistant Bacteria)
Prescribing azithromycin in the absence of a proven or strongly suspected bacterial infection is unlikely to provide benefit to the patient and increases the risk of the development of drug-resistant bacteria.
5.3 Infantile Hypertrophic Pyloric Stenosis (ihps) (5.3 Infantile Hypertrophic Pyloric Stenosis (IHPS))
Following the use of azithromycin in neonates (treatment up to 42 days of life), IHPS has been reported. Direct parents and caregivers to contact their physician if vomiting or irritability with feeding occurs.
7.3 Potential Drug Drug Interaction With Macrolides (7.3 Potential Drug-Drug Interaction with Macrolides)
Interactions with digoxin, colchicine or phenytoin have not been reported in clinical trials with azithromycin. No specific drug interaction studies have been performed to evaluate potential drug-drug interaction. However, drug interactions have been observed with other macrolide products. Until further data are developed regarding drug interactions when digoxin, colchicine or phenytoin are used with azithromycin careful monitoring of patients is advised.
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Long-term studies in animals have not been performed to evaluate carcinogenic potential. Azithromycin has shown no mutagenic potential in standard laboratory tests: mouse lymphoma assay, human lymphocyte clastogenic assay, and mouse bone marrow clastogenic assay. In fertility studies conducted in male and female rats, oral administration of azithromycin for 64 to 66 days (males) or 15 days (females) prior to and during cohabitation resulted in decreased pregnancy rate at 20 and 30 mg/kg/day when both males and females were treated with azithromycin. This minimal effect on pregnancy rate (approximately 12% reduction compared to concurrent controls) did not become more pronounced when the dose was increased from 20 to 30 mg/kg/day (approximately 0.4 to 0.6 times the adult daily dose of 500 mg based on body surface area) and it was not observed when only one animal in the mated pair was treated. There were no effects on any other reproductive parameters, and there were no effects on fertility at 10 mg/kg/day. The relevance of these findings to patients being treated with azithromycin at the doses and durations recommended in the prescribing information is uncertain.
2.3 Preparation of the Solution for Intravenous Administration
The infusate concentration and rate of infusion for azithromycin for injection should be either 1 mg/mL over 3 hr or 2 mg/mL over 1 hr. Azithromycin for injection should not be given as a bolus or as an intramuscular injection.
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:45:21.491205 · Updated: 2026-03-14T22:22:13.322156