These Highlights Do Not Include All The Information Needed To Use Ondansetron Injection Safely And Effectively. See Full Prescribing Information For Ondansetron Injection.
30107d6f-5128-484f-b713-65244a98dc67
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
Ondansetron injection is a 5-HT 3 receptor antagonist indicated for the prevention of: • nausea and vomiting associated with initial and repeat courses of emetogenic cancer chemotherapy. ( 1.1 ) • postoperative nausea and/or vomiting. ( 1.2 )
Indications and Usage
Ondansetron injection is a 5-HT 3 receptor antagonist indicated for the prevention of: • nausea and vomiting associated with initial and repeat courses of emetogenic cancer chemotherapy. ( 1.1 ) • postoperative nausea and/or vomiting. ( 1.2 )
Dosage and Administration
Prevention of Nausea and Vomiting Associated With Initial and Repeat Courses of Emetogenic Cancer Chemotherapy ( 2.1 ): • Dilution of ondansetron injection in 50 mL of 5% Dextrose Injection or 0.9% Sodium Chloride Injection is required before administration to adult and pediatric patients. • Adults and pediatric patients 6 months of age and older: The recommended dosage is 0.15 mg/kg per dose for 3 doses (maximum of 16 mg per dose), infused intravenously over 15 minutes. • Administer the first dose 30 minutes before the start of chemotherapy and subsequent doses 4 and 8 hours after the first dose. Prevention of Postoperative Nausea and/or Vomiting ( 2.2 ): • Dilution of ondansetron injection is not required before administration to adult and pediatric patients. • See full prescribing information for the recommended dosage and administration instructions for adult and pediatric patients 1 month of age and older. Patients With Severe Hepatic Impairment ( 2.3 ): • Do not exceed a total daily dose of 8 mg.
Warnings and Precautions
• Hypersensitivity Reactions: Hypersensitivity reactions, including anaphylaxis and bronchospasm have been reported in patients who have exhibited hypersensitivity to other selective 5-HT 3 receptor antagonists. ( 5.1 ) • QT Prolongation and Torsade de Pointes: QT prolongation occurs in a dose-dependent manner. Cases of Torsade de Pointes have been reported. Avoid ondansetron injection in patients with congenital long QT syndrome. ( 5.2 ) • Serotonin Syndrome : Serotonin syndrome has been reported with 5-HT 3 receptor agonists alone but particularly with concomitant use of serotonergic drugs. ( 5.3 ) • Myocardial Ischemia: Do not exceed the recommended infusion rate and monitor patients during and after administration. ( 2.1 , 2.2 , 5.4 ) • Masking of Progressive Ileus and/or Gastric Distension Following Abdominal Surgery or Chemotherapy-Induced Nausea and Vomiting: Monitor for decreased bowel activity, particularly in patients with risk factors for gastrointestinal obstruction. ( 5.5 )
Contraindications
Ondansetron injection is contraindicated for patients known to have hypersensitivity (e.g., anaphylaxis) to this product or any of its components. Anaphylactic reactions have been reported in patients taking ondansetron [see Adverse Reactions ( 6.2 )]. The concomitant use of apomorphine with ondansetron is contraindicated based on reports of profound hypotension and loss of consciousness when apomorphine was administered with ondansetron.
Adverse Reactions
The following clinically significant adverse reactions are described elsewhere in the labeling: • Hypersensitivity Reactions [see Warnings and Precautions (5.1) ] • QT Prolongation [see Warnings and Precautions (5.2) ] • Serotonin Syndrome [see Warnings and Precautions (5.3) ] • Myocardial Ischemia [see Warnings and Precautions (5.4) ] • Masking of Progressive Ileus and Gastric Distension [see Warnings and Precautions (5.5) ]
Storage and Handling
Ondansetron Injection USP, 4 mg/2 mL (2 mg/mL), is supplied as follows: Overbagged with 5 x 2 mL single-dose vials in each bag, NDC 55154-4453-5 WARNING: This Unit Dose package is not child resistant and is Intended for Institutional Use Only. Keep this and all drugs out of the reach of children.
How Supplied
Ondansetron Injection USP, 4 mg/2 mL (2 mg/mL), is supplied as follows: Overbagged with 5 x 2 mL single-dose vials in each bag, NDC 55154-4453-5 WARNING: This Unit Dose package is not child resistant and is Intended for Institutional Use Only. Keep this and all drugs out of the reach of children.
Medication Information
Warnings and Precautions
• Hypersensitivity Reactions: Hypersensitivity reactions, including anaphylaxis and bronchospasm have been reported in patients who have exhibited hypersensitivity to other selective 5-HT 3 receptor antagonists. ( 5.1 ) • QT Prolongation and Torsade de Pointes: QT prolongation occurs in a dose-dependent manner. Cases of Torsade de Pointes have been reported. Avoid ondansetron injection in patients with congenital long QT syndrome. ( 5.2 ) • Serotonin Syndrome : Serotonin syndrome has been reported with 5-HT 3 receptor agonists alone but particularly with concomitant use of serotonergic drugs. ( 5.3 ) • Myocardial Ischemia: Do not exceed the recommended infusion rate and monitor patients during and after administration. ( 2.1 , 2.2 , 5.4 ) • Masking of Progressive Ileus and/or Gastric Distension Following Abdominal Surgery or Chemotherapy-Induced Nausea and Vomiting: Monitor for decreased bowel activity, particularly in patients with risk factors for gastrointestinal obstruction. ( 5.5 )
Indications and Usage
Ondansetron injection is a 5-HT 3 receptor antagonist indicated for the prevention of: • nausea and vomiting associated with initial and repeat courses of emetogenic cancer chemotherapy. ( 1.1 ) • postoperative nausea and/or vomiting. ( 1.2 )
Dosage and Administration
Prevention of Nausea and Vomiting Associated With Initial and Repeat Courses of Emetogenic Cancer Chemotherapy ( 2.1 ): • Dilution of ondansetron injection in 50 mL of 5% Dextrose Injection or 0.9% Sodium Chloride Injection is required before administration to adult and pediatric patients. • Adults and pediatric patients 6 months of age and older: The recommended dosage is 0.15 mg/kg per dose for 3 doses (maximum of 16 mg per dose), infused intravenously over 15 minutes. • Administer the first dose 30 minutes before the start of chemotherapy and subsequent doses 4 and 8 hours after the first dose. Prevention of Postoperative Nausea and/or Vomiting ( 2.2 ): • Dilution of ondansetron injection is not required before administration to adult and pediatric patients. • See full prescribing information for the recommended dosage and administration instructions for adult and pediatric patients 1 month of age and older. Patients With Severe Hepatic Impairment ( 2.3 ): • Do not exceed a total daily dose of 8 mg.
Contraindications
Ondansetron injection is contraindicated for patients known to have hypersensitivity (e.g., anaphylaxis) to this product or any of its components. Anaphylactic reactions have been reported in patients taking ondansetron [see Adverse Reactions ( 6.2 )]. The concomitant use of apomorphine with ondansetron is contraindicated based on reports of profound hypotension and loss of consciousness when apomorphine was administered with ondansetron.
Adverse Reactions
The following clinically significant adverse reactions are described elsewhere in the labeling: • Hypersensitivity Reactions [see Warnings and Precautions (5.1) ] • QT Prolongation [see Warnings and Precautions (5.2) ] • Serotonin Syndrome [see Warnings and Precautions (5.3) ] • Myocardial Ischemia [see Warnings and Precautions (5.4) ] • Masking of Progressive Ileus and Gastric Distension [see Warnings and Precautions (5.5) ]
Storage and Handling
Ondansetron Injection USP, 4 mg/2 mL (2 mg/mL), is supplied as follows: Overbagged with 5 x 2 mL single-dose vials in each bag, NDC 55154-4453-5 WARNING: This Unit Dose package is not child resistant and is Intended for Institutional Use Only. Keep this and all drugs out of the reach of children.
How Supplied
Ondansetron Injection USP, 4 mg/2 mL (2 mg/mL), is supplied as follows: Overbagged with 5 x 2 mL single-dose vials in each bag, NDC 55154-4453-5 WARNING: This Unit Dose package is not child resistant and is Intended for Institutional Use Only. Keep this and all drugs out of the reach of children.
Description
Ondansetron injection is a 5-HT 3 receptor antagonist indicated for the prevention of: • nausea and vomiting associated with initial and repeat courses of emetogenic cancer chemotherapy. ( 1.1 ) • postoperative nausea and/or vomiting. ( 1.2 )
Data
Human Data
Available data on ondansetron use in pregnant women from several published epidemiological studies preclude an assessment of a drug-associated risk of adverse fetal outcomes due to important methodological limitations, including the uncertainty of whether women who filled a prescription actually took the medication, the concomitant use of other medications or treatments, recall bias, and other unadjusted confounders.
Ondansetron exposure in utero has not been associated with overall major congenital malformations in aggregate analyses. One large retrospective cohort study examined 1970 women who received a prescription for ondansetron during pregnancy and reported no association between ondansetron exposure and major congenital malformations, miscarriage, stillbirth, preterm delivery, infants of low birth weight, or infants small for gestational age.
Two large retrospective cohort studies and one case-control study have assessed ondansetron exposure in the first trimester and risk of cardiovascular defects with inconsistent findings. Relative risks (RR) ranged from 0.97 (95% CI 0.86 to 1.10) to 1.62 (95% CI 1.04, 2.54). A subset analysis in one of the cohort studies observed that ondansetron was specifically associated with cardiac septal defects (RR 2.05, 95% CI 1.19, 3.28); however this association was not confirmed in other studies.
Several studies have assessed ondansetron and the risk of oral clefts with inconsistent findings. A retrospective cohort study of 1.8 million pregnancies in the US Medicaid Database showed an increased risk of oral clefts among 88,467 pregnancies in which oral ondansetron was prescribed in the first trimester (RR 1.24, 95% CI 1.03, 1.48), but no such association was reported with intravenous ondansetron in 23,866 pregnancies (RR 0.95, 95% CI 0.63, 1.43). In the subgroup of women who received both forms of administration, the RR was 1.07 (95% CI 0.59, 1.93). Two case-control studies, using data from birth defects surveillance programs, reported conflicting associations between maternal use of ondansetron and isolated cleft palate (OR 1.6 [95% CI 1.1, 2.3] and 0.5 [95% CI 0.3, 1.0]). It is unknown whether ondansetron exposure in utero in the cases of cleft palate occurred during the time of palate formation (the palate is formed between the 6th and 9th weeks of pregnancy).
Animal Data
In embryo-fetal development studies in rats and rabbits, pregnant animals received intravenous doses of ondansetron up to 10 mg/kg/day and 4 mg/kg/day, respectively, during the period of organogenesis. With the exception of short periods of maternal weight loss and a slight increase in the incidence of early uterine deaths at the high dose level in rabbits, there were no significant effects of ondansetron on the maternal animals or the development of the offspring. At doses of 10 mg/kg/day in rats and 4 mg/kg/day in rabbits, the maternal exposure margin was approximately 3.6 and 2.9 times the maximum recommended human oral dose of 0.15 mg/kg given three times a day, respectively, based on BSA.
No intravenous pre- and post-natal developmental toxicity study was performed with ondansetron. In an oral pre- and post-natal development study pregnant rats received oral doses of ondansetron up to 15 mg/kg/day from Day 17 of pregnancy to litter Day 21. With the exception of a slight reduction in maternal body weight gain, there were no effects upon the pregnant rats and the pre- and postnatal development of their offspring, including reproductive performance of the mated F1 generation.
Section 42229-5
Dosage and Administration
The recommended dosage for adult and pediatric patients 6 months of age and older for prevention of nausea and vomiting associated with emetogenic chemotherapy is 0.15‑mg/kg per dose for 3 doses (maximum of 16 mg per dose).
Caution: Dilution of ondansetron injection is required in adult and pediatric patients prior to administration.
Infuse intravenously over 15 minutes beginning 30 minutes before the start of emetogenic chemotherapy and then repeat 4 and 8 hours after the first dose.
Section 44425-7
Storage: Store between 20°C to 25°C (68°F to 77°F) [see USP controlled room temperature]. Protect from light.
7.4 Tramadol
Although there are no data on pharmacokinetic drug interactions between ondansetron and tramadol, data from two small trials indicate that concomitant use of ondansetron may result in reduced analgesic activity of tramadol. Patients on concomitant ondansetron self-administered tramadol more frequently in these trials, leading to an increased cumulative dose in patient-controlled administration of tramadol.
Risk Summary
Published epidemiological studies on the association between ondansetron use and major birth defects have reported inconsistent findings and have important methodological limitations that preclude conclusions about the safety of ondansetron use in pregnancy (see Data). Available postmarketing data have not identified a drug-associated risk of miscarriage or adverse maternal outcomes. Reproductive studies in rats and rabbits did not show evidence of harm to the fetus when ondansetron was administered intravenously during organogenesis at approximately 3.6 and 2.9 times the maximum recommended human intravenous dose of 0.15 mg/kg given three times a day, based on body surface area (BSA), respectively (see Data).
The background risk of major birth defects and miscarriage for the indicated population is unknown. All pregnancies have a background risk of birth defect, miscarriages, or other adverse outcomes. In the US general population, the estimated background risk of major birth defects and miscarriages in clinically recognized pregnancies is 2% to 4% and 15% to 20%, respectively.
10 Overdosage
There is no specific antidote for ondansetron overdose. Patients should be managed with appropriate supportive therapy. Individual intravenous doses as large as 150 mg and total daily intravenous doses as large as 252 mg have been inadvertently administered without significant adverse events. These doses are more than 10 times the recommended daily dose.
In addition to the adverse reactions listed above, the following events have been described in the setting of ondansetron overdose: “Sudden blindness” (amaurosis) of 2 to 3 minutes' duration plus severe constipation occurred in one patient that was administered 72 mg of ondansetron intravenously as a single dose. Hypotension (and faintness) occurred in another patient that took 48 mg of ondansetron hydrochloride tablets. Following infusion of 32 mg over only a 4-minute period, a vasovagal episode with transient second-degree heart block was observed. In all instances, the events resolved completely.
Pediatric cases consistent with serotonin syndrome have been reported after inadvertent oral overdoses of ondansetron (exceeding estimated ingestion of 5 mg/kg) in young children. Reported symptoms included somnolence, agitation, tachycardia, tachypnea, hypertension, flushing, mydriasis, diaphoresis, myoclonic movements, horizontal nystagmus, hyperreflexia, and seizure. Patients required supportive care, including intubation in some cases, with complete recovery without sequelae within 1 to 2 days.
7.7 Temazepam
The co-administration of ondansetron had no effect on the pharmacokinetics and pharmacodynamics of temazepam.
11 Description
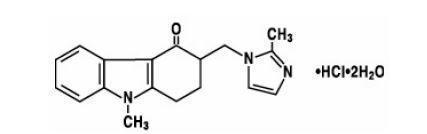
The active ingredient of ondansetron injection, USP is ondansetron hydrochloride, a selective blocking agent of the serotonin 5-HT3 receptor type. Its chemical name is (±) 1, 2, 3, 9-tetrahydro-9- methyl-3-[(2-methyl-1H-imidazol-1-yl)methyl]-4H-carbazol-4-one, monohydrochloride, dihydrate. It has the following structural formula:
-
The empirical formula is C18H19N3O•HCl•2H2O, representing a molecular weight of 365.9 g/mol.
Ondansetron HCl is a white to off-white powder that is soluble in water and normal saline.
Each 1 mL of aqueous solution in the 2 mL single-dose vial contains 2 mg of ondansetron as the hydrochloride dihydrate; 9 mg of sodium chloride, USP; and 0.5 mg of citric acid monohydrate, USP and 0.25 mg of sodium citrate dihydrate, USP as buffers in Water for Injection, USP.
-
Ondansetron injection, USP is a clear, colorless, nonpyrogenic, sterile solution for intravenous use. The pH of the injection solution is 3.3 to 4.0.
7.2 Apomorphine
Based on reports of profound hypotension and loss of consciousness when apomorphine was administered with ondansetron, the concomitant use of apomorphine with ondansetron is contraindicated [see Contraindications (4)].
7.6 Chemotherapy
In humans, carmustine, etoposide, and cisplatin do not affect the pharmacokinetics of ondansetron.
In a crossover trial in 76 pediatric patients, intravenous ondansetron did not increase blood levels of high-dose methotrexate.
8.4 Pediatric Use
Little information is available about the use of ondansetron in pediatric surgical patients younger than 1 month [see Clinical Studies (14.2)]. Little information is available about the use of ondansetron in pediatric cancer patients younger than 6 months [see Clinical Studies (14.1), Dosage and Administration (2)].
The clearance of ondansetron in pediatric patients aged 1 month to 4 months is slower and the half-life is ~2.5-fold longer than patients who are aged > 4 to 24 months. As a precaution, it is recommended that patients younger than 4 months receiving this drug be closely monitored [see Clinical Pharmacology (12.3)].
8.5 Geriatric Use
Of the total number of subjects enrolled in cancer chemotherapy-induced and postoperative nausea and vomiting US- and foreign-controlled clinical trials, 862 were aged 65 years and older. No overall differences in safety or effectiveness were observed between subjects 65 years and older and younger subjects. A reduction in clearance and increase in elimination half-life were seen in patients older than 75 years compared with younger subjects [see Clinical Pharmacology (12.3)]. There were an insufficient number of patients older than 75 years of age and older in the clinical trials to permit safety or efficacy conclusions in this age-group. Other reported clinical experience has not identified differences in responses between the elderly and younger patients, but greater sensitivity of some older individuals cannot be ruled out. Dosage adjustment is not needed in patients over the age of 65.
14 Clinical Studies
-
The clinical efficacy of ondansetron hydrochloride, the active ingredient of ondansetron injection, was assessed in clinical trials as described below.
4 Contraindications
Ondansetron injection is contraindicated for patients known to have hypersensitivity (e.g., anaphylaxis) to this product or any of its components. Anaphylactic reactions have been reported in patients taking ondansetron [see Adverse Reactions (6.2)].
The concomitant use of apomorphine with ondansetron is contraindicated based on reports of profound hypotension and loss of consciousness when apomorphine was administered with ondansetron.
5.2 Qt Prolongation
Ondansetron prolongs the QT interval in a dose-dependent manner [see Clinical Pharmacology (12.2)]. In addition, postmarketing cases of Torsade de Pointes have been reported in patients using ondansetron. Avoid ondansetron injection in patients with congenital long QT syndrome. Electrocardiogram (ECG) monitoring is recommended in patients with electrolyte abnormalities (e.g., hypokalemia or hypomagnesemia), congestive heart failure, bradyarrhythmias, or patients taking other medicinal products that lead to QT prolongation.
6 Adverse Reactions
The following clinically significant adverse reactions are described elsewhere in the labeling:
-
•Hypersensitivity Reactions [see Warnings and Precautions (5.1)]
-
•QT Prolongation [see Warnings and Precautions (5.2)]
-
•Serotonin Syndrome [see Warnings and Precautions (5.3)]
-
•Myocardial Ischemia [see Warnings and Precautions (5.4)]
-
•Masking of Progressive Ileus and Gastric Distension [see Warnings and Precautions (5.5)]
8.7 Renal Impairment
Although plasma clearance is reduced in patients with severe renal impairment (creatinine clearance < 30 mL/min), no dosage adjustment is recommended [see Clinical Pharmacology (12.3)].
12.2 Pharmacodynamics
In normal volunteers, single intravenous doses of 0.15 mg/kg of ondansetron had no effect on esophageal motility, gastric motility, lower esophageal sphincter pressure, or small intestinal transit time. In another trial in 6 normal male volunteers, a 16 mg dose infused over 5 minutes showed no effect of the drug on cardiac output, heart rate, stroke volume, blood pressure, or ECG. Multiday administration of ondansetron has been shown to slow colonic transit in normal volunteers. Ondansetron has no effect on plasma prolactin concentrations. In a gender balanced pharmacodynamic trial (n = 56), ondansetron 4 mg administered intravenously or intramuscularly was dynamically similar in the prevention of nausea and vomiting using the ipecacuanha model of emesis.
Cardiac Electrophysiology
QTc interval prolongation was studied in a double-blind, single intravenous dose, placebo- and positive-controlled, crossover trial in 58 healthy subjects. The maximum mean (95% upper confidence bound) difference in QTcF from placebo after baseline correction was 19.5 (21.8) ms and 5.6 (7.4) ms after 15-minute intravenous infusions of 32 mg and 8 mg ondansetron injection, respectively. A significant exposure-response relationship was identified between ondansetron concentration and ΔΔQTcF. Using the established exposure-response relationship, 24 mg infused intravenously over 15 minutes had a mean predicted (95% upper prediction interval) ΔΔQTcF of 14.0 (16.3) ms. In contrast, 16 mg infused intravenously over 15 minutes using the same model had a mean predicted (95% upper prediction interval) ΔΔQTcF of 9.1 (11.2) ms. In this study, the 8-mg dose infused over 15 minutes did not prolong the QT interval to any clinically relevant extent.
12.3 Pharmacokinetics
In normal adult volunteers, the following mean pharmacokinetic data have been determined following a single 0.15-mg/kg intravenous dose.
|
Age-group
(years)
|
n
|
Peak Plasma
|
Mean Elimination
Half-life (h)
|
Plasma Clearance
(L/h/kg)
|
|
19 to 40 |
11 |
102 |
3.5 |
0.381 |
|
61 to 74 |
12 |
106 |
4.7 |
0.319 |
|
≥ 75 |
11 |
170 |
5.5 |
0.262 |
5.3 Serotonin Syndrome
The development of serotonin syndrome has been reported with 5-HT3 receptor antagonists. Most reports have been associated with concomitant use of serotonergic drugs (e.g., selective serotonin reuptake inhibitors (SSRIs), serotonin and norepinephrine reuptake inhibitors (SNRIs), monoamine oxidase inhibitors, mirtazapine, fentanyl, lithium, tramadol, and intravenous methylene blue). Some of the reported cases were fatal. Serotonin syndrome occurring with overdose of ondansetron injection alone has also been reported. The majority of reports of serotonin syndrome related to 5-HT3 receptor antagonist use occurred in a post-anesthesia care unit or an infusion center.
Symptoms associated with serotonin syndrome may include the following combination of signs and symptoms: mental status changes (e.g., agitation, hallucinations, delirium, and coma), autonomic instability (e.g., tachycardia, labile blood pressure, dizziness, diaphoresis, flushing, hyperthermia), neuromuscular symptoms (e.g., tremor, rigidity, myoclonus, hyperreflexia, incoordination), seizures, with or without gastrointestinal symptoms (e.g., nausea, vomiting, diarrhea). Patients should be monitored for the emergence of serotonin syndrome, especially with concomitant use of ondansetron injection and other serotonergic drugs. If symptoms of serotonin syndrome occur, discontinue ondansetron injection and initiate supportive treatment. Patients should be informed of the increased risk of serotonin syndrome, especially if ondansetron injection is used concomitantly with other serotonergic drugs [see Drug Interactions (7.5), Overdosage (10)].
7.5 Serotonergic Drugs
Serotonin syndrome (including altered mental status, autonomic instability, and neuromuscular symptoms) has been described following the concomitant use of 5-HT3 receptor antagonists and other serotonergic drugs, including SSRIs and SNRIs [see Warnings and Precautions (5.3)].
8.6 Hepatic Impairment
In patients with severe hepatic impairment (Child-Pugh score of 10 or greater), clearance is reduced and apparent volume of distribution is increased with a resultant increase in plasma half-life [see Clinical Pharmacology (12.3)] . In such patients, a total daily dose of 8 mg should not be exceeded [see Dosage and Administration (2.3)].
1 Indications and Usage
5.4 Myocardial Ischemia
Myocardial ischemia has been reported in patients treated with ondansetron. In some cases, predominantly during intravenous administration, the symptoms appeared immediately after administration but resolved with prompt treatment. Coronary artery spasm appears to be the most common underlying cause. Therefore, do not exceed the recommended infusion rate of ondansetron injection and monitor patients for signs and symptoms of myocardial ischemia during and after administration [see Dosage and Administration (2.1, 2.2) and Adverse Reactions (6.2)].
12.1 Mechanism of Action
Ondansetron is a selective 5-HT3 receptor antagonist. While ondansetron's mechanism of action has not been fully characterized, it is not a dopamine-receptor antagonist.
5 Warnings and Precautions
-
•Hypersensitivity Reactions: Hypersensitivity reactions, including anaphylaxis and bronchospasm have been reported in patients who have exhibited hypersensitivity to other selective 5-HT3 receptor antagonists. (5.1)
-
•QT Prolongation and Torsade de Pointes: QT prolongation occurs in a dose-dependent manner. Cases of Torsade de Pointes have been reported. Avoid ondansetron injection in patients with congenital long QT syndrome. (5.2)
-
•Serotonin Syndrome: Serotonin syndrome has been reported with 5-HT3 receptor agonists alone but particularly with concomitant use of serotonergic drugs. (5.3)
-
•Myocardial Ischemia: Do not exceed the recommended infusion rate and monitor patients during and after administration. (2.1, 2.2, 5.4)
-
•Masking of Progressive Ileus and/or Gastric Distension Following Abdominal Surgery or Chemotherapy-Induced Nausea and Vomiting: Monitor for decreased bowel activity, particularly in patients with risk factors for gastrointestinal obstruction. (5.5)
2 Dosage and Administration
Prevention of Nausea and Vomiting Associated With Initial and Repeat Courses of Emetogenic Cancer Chemotherapy ( 2.1 ):
-
•Dilution of ondansetron injection in 50 mL of 5% Dextrose Injection or 0.9% Sodium Chloride Injection is required before administration to adult and pediatric patients.
-
•Adults and pediatric patients 6 months of age and older: The recommended dosage is 0.15 mg/kg per dose for 3 doses (maximum of 16 mg per dose), infused intravenously over 15 minutes.
-
•Administer the first dose 30 minutes before the start of chemotherapy and subsequent doses 4 and 8 hours after the first dose.
Prevention of Postoperative Nausea and/or Vomiting (
2.2
):
-
•Dilution of ondansetron injection is not required before administration to adult and pediatric patients.
-
•See full prescribing information for the recommended dosage and administration instructions for adult and pediatric patients 1 month of age and older.
Patients With Severe Hepatic Impairment (
2.3
):
-
•Do not exceed a total daily dose of 8 mg.
9 Drug Abuse and Dependence
Animal studies have shown that ondansetron is not discriminated as a benzodiazepine nor does it substitute for benzodiazepines in direct addiction studies.
Package/label Display Panel
NDC 55154-4453-5
ONDANSETRON INJECTION, USP
4 mg/2 mL (2 mg/mL)
5 X 2 mL SINGLE-USE VIALS
3 Dosage Forms and Strengths
Ondansetron injection USP, 4 mg/2 mL (2 mg/mL) is a clear, colorless, nonpyrogenic, sterile solution available in a 2 mL single-dose vial.
6.2 Postmarketing Experience
The following adverse reactions have been identified during postapproval use of ondansetron. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure. The reactions have been chosen for inclusion due to a combination of their seriousness, frequency of reporting, or potential causal connection to ondansetron.
Cardiovascular
Arrhythmias (including ventricular and supraventricular tachycardia, premature ventricular contractions, and atrial fibrillation), bradycardia, electrocardiographic alterations (including second-degree heart block, QT/QTc interval prolongation, and ST segment depression), palpitations, and syncope. Rarely and predominantly with intravenous ondansetron, transient ECG changes, including QT/QTc interval prolongation have been reported [see Warnings and Precautions (5.2)].
Myocardial ischemia was reported predominately with intravenous administration [see Warnings and Precautions (5.4)].
General
Flushing: Rare cases of hypersensitivity reactions, sometimes severe (e.g., anaphylactic reactions, angioedema, bronchospasm, cardiopulmonary arrest, hypotension, laryngeal edema, laryngospasm, shock, shortness of breath, stridor) have also been reported. A positive lymphocyte transformation test to ondansetron has been reported, which suggests immunologic sensitivity to ondansetron.
Hepatobiliary
Liver enzyme abnormalities have been reported. Liver failure and death have been reported in patients with cancer receiving concurrent medications, including potentially hepatotoxic cytotoxic chemotherapy and antibiotics.
Local Reactions
Pain, redness, and burning at site of injection.
Lower Respiratory
Hiccups.
Neurological
Oculogyric crisis, appearing alone, as well as with other dystonic reactions. Transient dizziness during or shortly after intravenous infusion.
Skin
Urticaria, Stevens-Johnson syndrome, and toxic epidermal necrolysis.
Eye Disorders
Cases of transient blindness, predominantly during intravenous administration, have been reported. These cases of transient blindness were reported to resolve within a few minutes up to 48 hours. Transient blurred vision, in some cases associated with abnormalities of accommodation, has also been reported.
7.8 Alfentanil and Atracurium
Ondansetron does not alter the respiratory depressant effects produced by alfentanil or the degree of neuromuscular blockade produced by atracurium. Interactions with general or local anesthetics have not been studied.
5.1 Hypersensitivity Reactions
Hypersensitivity reactions, including anaphylaxis and bronchospasm, have been reported in patients who have exhibited hypersensitivity to other selective 5-HT3 receptor antagonists.
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared with rates in the clinical trials of another drug and may not reflect the rates observed in clinical practice.
The following adverse reactions have been reported in clinical trials of adult patients treated with ondansetron, the active ingredient of intravenous ondansetron injection across a range of dosages. A causal relationship to therapy with ondansetron injection (ondansetron) was unclear in many cases.
17 Patient Counseling Information
Hypersensitivity Reactions
Inform patients that ondansetron injection may cause hypersensitivity reactions, some as severe as anaphylaxis and bronchospasm. The patient should report any signs and symptoms of hypersensitivity reactions, including fever, chills, rash, or breathing problems [see Warnings and Precautions (5.1)].
QT Prolongation
Patients should be informed that ondansetron injection may cause serious cardiac arrhythmias, such as QT prolongation. Patients should be instructed to tell their healthcare provider right away if they perceive a change in their heart rate, if they feel lightheaded, or if they have a syncopal episode.
Patients should be informed that the chances of developing severe cardiac arrhythmias, such as QT prolongation and Torsade de Pointes are higher in the following people:
-
•Patients with a personal or family history of abnormal heart rhythms, such as congenital long QT syndrome;
-
•Patients who take medications, such as diuretics, which may cause electrolyte abnormalities;
-
•Patients with hypokalemia or hypomagnesemia.
Ondansetron injection should be avoided in these patients, since they may be more at risk for cardiac arrhythmias, such as QT prolongation and Torsade de Pointes [see Warnings and Precautions (5.2)].
Drug Interactions
-
•Instruct the patient to report the use of all medications, especially apomorphine, to their healthcare provider. Concomitant use of apomorphine and ondansetron injection may cause a significant drop in blood pressure and loss of consciousness.
-
•Advise patients of the possibility of serotonin syndrome with concomitant use of ondansetron injection and another serotonergic agent, such as medications to treat depression and migraines. Advise patients to seek immediate medical attention if the following symptoms occur: changes in mental status, autonomic instability, neuromuscular symptoms with or without gastrointestinal symptoms [see Warnings and Precautions (5.3)].
Myocardial Ischemia
Inform patients that ondansetron injection may cause myocardial ischemia during or after the administration. Advise patients to seek immediate medical help if any symptoms suggestive of a myocardial ischemia occur, such as sudden chest pain or chest tightness [see Warnings and Precautions (5.4)].
Masking of Progressive Ileus and Gastric Distension
Inform patients following abdominal surgery or those with chemotherapy-induced nausea and vomiting that ondansetron injection may mask signs and symptoms of bowel obstruction. Instruct patients to immediately report any signs or symptoms consistent with a potential bowel obstruction to their healthcare provider [see Warnings and Precautions (5.5)].
Manufactured for:
Baxter Healthcare Corporation
Deerfield, IL 60015 USA
Manufactured by:
Baxter Pharmaceuticals India Private Ltd
Ahmedabad 382213, India
Distributed By:
Cardinal Health
Dublin, OH 43017
L55233370124
1400008740
16 How Supplied/storage and Handling
Ondansetron Injection USP, 4 mg/2 mL (2 mg/mL), is supplied as follows:
Overbagged with 5 x 2 mL single-dose vials in each bag, NDC 55154-4453-5
WARNING: This Unit Dose package is not child resistant and is Intended for Institutional Use Only. Keep this and all drugs out of the reach of children.
7.3 Phenytoin, Carbamazepine, and Rifampin
In patients treated with potent inducers of CYP3A4 (i.e., phenytoin, carbamazepine, and rifampin), the clearance of ondansetron was significantly increased and ondansetron blood concentrations were decreased. However, on the basis of available data, no dosage adjustment for ondansetron is recommended for patients on these drugs [see Clinical Pharmacology (12.3)].
7.1 Drugs Affecting Cytochrome P 450 Enzymes
Ondansetron does not appear to induce or inhibit the cytochrome P-450 drug-metabolizing enzyme system of the liver. Because ondansetron is metabolized by hepatic cytochrome P-450 drug-metabolizing enzymes (CYP3A4, CYP2D6, CYP1A2), inducers or inhibitors of these enzymes may change the clearance and, hence, the half-life of ondansetron [see Clinical Pharmacology (12.3)]. On the basis of limited available data, no dosage adjustment is recommended for patients on these drugs.
14.1 Chemotherapy Induced Nausea and Vomiting
Adults
In a double-blind trial of three different dosing regimens of ondansetron injection, 0.015 mg/kg, 0.15 mg/kg, and 0.30 mg/kg, each given three times during the course of cancer chemotherapy, the 0.15-mg/kg dosing regimen was more effective than the 0.015-mg/kg dosing regimen. The 0.30-mg/kg dosing regimen was not shown to be more effective than the 0.15-mg/kg dosing regimen.
1.2 Prevention of Postoperative Nausea And/or Vomiting
Ondansetron injection is indicated for the prevention of postoperative nausea and/or vomiting. As with other antiemetics, routine prophylaxis is not recommended for patients in whom there is little expectation that nausea and/or vomiting will occur postoperatively. In patients in whom nausea and/or vomiting must be avoided postoperatively, ondansetron injection is recommended even when the incidence of postoperative nausea and/or vomiting is low. For patients who do not receive prophylactic ondansetron injection and experience nausea and/or vomiting postoperatively, ondansetron injection may be given to prevent further episodes.
Ondansetron injection is approved for patients aged 1 month and older.
2.2 Prevention of Postoperative Nausea And/or Vomiting
Important Preparation Instructions
-
•Dilution of ondansetron injection is not required before administration to adult and pediatric patients.
-
•Inspect ondansetron injection visually for particulate matter and discoloration before administration; discard if present.
5.5 Masking of Progressive Ileus and Gastric Distension
The use of ondansetron injection in patients following abdominal surgery or in patients with chemotherapy-induced nausea and vomiting may mask a progressive ileus and gastric distension. Monitor for decreased bowel activity, particularly in patients with risk factors for gastrointestinal obstruction.
Ondansetron injection is not a drug that stimulates gastric or intestinal peristalsis. It should not be used instead of nasogastric suction.
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenic effects were not seen in 2-year studies in rats and mice with oral ondansetron doses up to 10 and 30 mg/kg per day, respectively (approximately 3.6 and 5.4 times the recommended human intravenous dose of 0.15 mg/kg given three times a day, based on BSA).
Ondansetron was not mutagenic in standard tests for mutagenicity.
Oral administration of ondansetron up to 15 mg/kg per day (approximately 3.8 times the recommended human intravenous dose, based on BSA) did not affect fertility or general reproductive performance of male and female rats.
2.3 Dosage Adjustment for Patients With hepatic Impairment
In patients with severe hepatic impairment (Child-Pugh score of 10 or greater), a single maximal daily dose of 8 mg infused over 15 minutes beginning 30 minutes before the start of the emetogenic chemotherapy is recommended. There is no experience beyond first-day administration of ondansetron in these patients [see Use in Specific Populations (8.6)].
2.1 Prevention of Nausea and Vomiting Associated With Initial and Repeat Courses of Emetogenic Chemotherapy
Important Preparation Instructions
-
•Dilution of ondansetron injection in 50 mL of 5% Dextrose Injection or 0.9% Sodium Chloride Injection is required before administration to adult and pediatric patients for the prevention of nausea and vomiting associated with emetogenic chemotherapy.
For pediatric patients between 6 months and 1 year of age and/or 10 kg or less: Depending on the fluid needs of the patient, ondansetron injection may be diluted in 10 to 50 mL of 5% Dextrose Injection or 0.9% Sodium Chloride Injection.
-
•Occasionally, ondansetron precipitates at the stopper/vial interface in vials stored upright. Potency and safety are not affected. If a precipitate is observed, resolubilize by shaking the vial vigorously.
-
•Do not mix ondansetron injection with solutions for which physical and chemical compatibility has not been established. In particular, this applies to alkaline solutions as a precipitate may form.
-
•Inspect the diluted ondansetron injection solution for particulate matter and discoloration before administration; discard if present.
-
•Storage: After dilution, do not use beyond 24 hours. Although ondansetron injection is chemically and physically stable when diluted as recommended, sterile precautions should be observed because diluents generally do not contain preservative.
-
•Compatibility: Ondansetron injection is compatible and stable at room temperature under normal lighting conditions for 48 hours after dilution with the following intravenous fluids: 0.9% Sodium Chloride Injection, 5% Dextrose Injection, 5% Dextrose and 0.9% Sodium Chloride Injection, 5% Dextrose and 0.45% Sodium Chloride Injection, and 3% Sodium Chloride Injection.
1.1 Prevention of Nausea and Vomiting Associated With Initial and Repeat Courses of Emetogenic Cancer Chemotherapy
Ondansetron injection is indicated for the prevention of nausea and vomiting associated with initial and repeat courses of emetogenic cancer chemotherapy, including high-dose cisplatin.
Ondansetron injection is approved for patients aged 6 months and older.
Structured Label Content
Data
Human Data
Available data on ondansetron use in pregnant women from several published epidemiological studies preclude an assessment of a drug-associated risk of adverse fetal outcomes due to important methodological limitations, including the uncertainty of whether women who filled a prescription actually took the medication, the concomitant use of other medications or treatments, recall bias, and other unadjusted confounders.
Ondansetron exposure in utero has not been associated with overall major congenital malformations in aggregate analyses. One large retrospective cohort study examined 1970 women who received a prescription for ondansetron during pregnancy and reported no association between ondansetron exposure and major congenital malformations, miscarriage, stillbirth, preterm delivery, infants of low birth weight, or infants small for gestational age.
Two large retrospective cohort studies and one case-control study have assessed ondansetron exposure in the first trimester and risk of cardiovascular defects with inconsistent findings. Relative risks (RR) ranged from 0.97 (95% CI 0.86 to 1.10) to 1.62 (95% CI 1.04, 2.54). A subset analysis in one of the cohort studies observed that ondansetron was specifically associated with cardiac septal defects (RR 2.05, 95% CI 1.19, 3.28); however this association was not confirmed in other studies.
Several studies have assessed ondansetron and the risk of oral clefts with inconsistent findings. A retrospective cohort study of 1.8 million pregnancies in the US Medicaid Database showed an increased risk of oral clefts among 88,467 pregnancies in which oral ondansetron was prescribed in the first trimester (RR 1.24, 95% CI 1.03, 1.48), but no such association was reported with intravenous ondansetron in 23,866 pregnancies (RR 0.95, 95% CI 0.63, 1.43). In the subgroup of women who received both forms of administration, the RR was 1.07 (95% CI 0.59, 1.93). Two case-control studies, using data from birth defects surveillance programs, reported conflicting associations between maternal use of ondansetron and isolated cleft palate (OR 1.6 [95% CI 1.1, 2.3] and 0.5 [95% CI 0.3, 1.0]). It is unknown whether ondansetron exposure in utero in the cases of cleft palate occurred during the time of palate formation (the palate is formed between the 6th and 9th weeks of pregnancy).
Animal Data
In embryo-fetal development studies in rats and rabbits, pregnant animals received intravenous doses of ondansetron up to 10 mg/kg/day and 4 mg/kg/day, respectively, during the period of organogenesis. With the exception of short periods of maternal weight loss and a slight increase in the incidence of early uterine deaths at the high dose level in rabbits, there were no significant effects of ondansetron on the maternal animals or the development of the offspring. At doses of 10 mg/kg/day in rats and 4 mg/kg/day in rabbits, the maternal exposure margin was approximately 3.6 and 2.9 times the maximum recommended human oral dose of 0.15 mg/kg given three times a day, respectively, based on BSA.
No intravenous pre- and post-natal developmental toxicity study was performed with ondansetron. In an oral pre- and post-natal development study pregnant rats received oral doses of ondansetron up to 15 mg/kg/day from Day 17 of pregnancy to litter Day 21. With the exception of a slight reduction in maternal body weight gain, there were no effects upon the pregnant rats and the pre- and postnatal development of their offspring, including reproductive performance of the mated F1 generation.
Section 42229-5 (42229-5)
Dosage and Administration
The recommended dosage for adult and pediatric patients 6 months of age and older for prevention of nausea and vomiting associated with emetogenic chemotherapy is 0.15‑mg/kg per dose for 3 doses (maximum of 16 mg per dose).
Caution: Dilution of ondansetron injection is required in adult and pediatric patients prior to administration.
Infuse intravenously over 15 minutes beginning 30 minutes before the start of emetogenic chemotherapy and then repeat 4 and 8 hours after the first dose.
Section 44425-7 (44425-7)
Storage: Store between 20°C to 25°C (68°F to 77°F) [see USP controlled room temperature]. Protect from light.
7.4 Tramadol
Although there are no data on pharmacokinetic drug interactions between ondansetron and tramadol, data from two small trials indicate that concomitant use of ondansetron may result in reduced analgesic activity of tramadol. Patients on concomitant ondansetron self-administered tramadol more frequently in these trials, leading to an increased cumulative dose in patient-controlled administration of tramadol.
Risk Summary
Published epidemiological studies on the association between ondansetron use and major birth defects have reported inconsistent findings and have important methodological limitations that preclude conclusions about the safety of ondansetron use in pregnancy (see Data). Available postmarketing data have not identified a drug-associated risk of miscarriage or adverse maternal outcomes. Reproductive studies in rats and rabbits did not show evidence of harm to the fetus when ondansetron was administered intravenously during organogenesis at approximately 3.6 and 2.9 times the maximum recommended human intravenous dose of 0.15 mg/kg given three times a day, based on body surface area (BSA), respectively (see Data).
The background risk of major birth defects and miscarriage for the indicated population is unknown. All pregnancies have a background risk of birth defect, miscarriages, or other adverse outcomes. In the US general population, the estimated background risk of major birth defects and miscarriages in clinically recognized pregnancies is 2% to 4% and 15% to 20%, respectively.
10 Overdosage (10 OVERDOSAGE)
There is no specific antidote for ondansetron overdose. Patients should be managed with appropriate supportive therapy. Individual intravenous doses as large as 150 mg and total daily intravenous doses as large as 252 mg have been inadvertently administered without significant adverse events. These doses are more than 10 times the recommended daily dose.
In addition to the adverse reactions listed above, the following events have been described in the setting of ondansetron overdose: “Sudden blindness” (amaurosis) of 2 to 3 minutes' duration plus severe constipation occurred in one patient that was administered 72 mg of ondansetron intravenously as a single dose. Hypotension (and faintness) occurred in another patient that took 48 mg of ondansetron hydrochloride tablets. Following infusion of 32 mg over only a 4-minute period, a vasovagal episode with transient second-degree heart block was observed. In all instances, the events resolved completely.
Pediatric cases consistent with serotonin syndrome have been reported after inadvertent oral overdoses of ondansetron (exceeding estimated ingestion of 5 mg/kg) in young children. Reported symptoms included somnolence, agitation, tachycardia, tachypnea, hypertension, flushing, mydriasis, diaphoresis, myoclonic movements, horizontal nystagmus, hyperreflexia, and seizure. Patients required supportive care, including intubation in some cases, with complete recovery without sequelae within 1 to 2 days.
7.7 Temazepam
The co-administration of ondansetron had no effect on the pharmacokinetics and pharmacodynamics of temazepam.
11 Description (11 DESCRIPTION)
The active ingredient of ondansetron injection, USP is ondansetron hydrochloride, a selective blocking agent of the serotonin 5-HT3 receptor type. Its chemical name is (±) 1, 2, 3, 9-tetrahydro-9- methyl-3-[(2-methyl-1H-imidazol-1-yl)methyl]-4H-carbazol-4-one, monohydrochloride, dihydrate. It has the following structural formula:
-
The empirical formula is C18H19N3O•HCl•2H2O, representing a molecular weight of 365.9 g/mol.
Ondansetron HCl is a white to off-white powder that is soluble in water and normal saline.
Each 1 mL of aqueous solution in the 2 mL single-dose vial contains 2 mg of ondansetron as the hydrochloride dihydrate; 9 mg of sodium chloride, USP; and 0.5 mg of citric acid monohydrate, USP and 0.25 mg of sodium citrate dihydrate, USP as buffers in Water for Injection, USP.
-
Ondansetron injection, USP is a clear, colorless, nonpyrogenic, sterile solution for intravenous use. The pH of the injection solution is 3.3 to 4.0.
7.2 Apomorphine
Based on reports of profound hypotension and loss of consciousness when apomorphine was administered with ondansetron, the concomitant use of apomorphine with ondansetron is contraindicated [see Contraindications (4)].
7.6 Chemotherapy
In humans, carmustine, etoposide, and cisplatin do not affect the pharmacokinetics of ondansetron.
In a crossover trial in 76 pediatric patients, intravenous ondansetron did not increase blood levels of high-dose methotrexate.
8.4 Pediatric Use
Little information is available about the use of ondansetron in pediatric surgical patients younger than 1 month [see Clinical Studies (14.2)]. Little information is available about the use of ondansetron in pediatric cancer patients younger than 6 months [see Clinical Studies (14.1), Dosage and Administration (2)].
The clearance of ondansetron in pediatric patients aged 1 month to 4 months is slower and the half-life is ~2.5-fold longer than patients who are aged > 4 to 24 months. As a precaution, it is recommended that patients younger than 4 months receiving this drug be closely monitored [see Clinical Pharmacology (12.3)].
8.5 Geriatric Use
Of the total number of subjects enrolled in cancer chemotherapy-induced and postoperative nausea and vomiting US- and foreign-controlled clinical trials, 862 were aged 65 years and older. No overall differences in safety or effectiveness were observed between subjects 65 years and older and younger subjects. A reduction in clearance and increase in elimination half-life were seen in patients older than 75 years compared with younger subjects [see Clinical Pharmacology (12.3)]. There were an insufficient number of patients older than 75 years of age and older in the clinical trials to permit safety or efficacy conclusions in this age-group. Other reported clinical experience has not identified differences in responses between the elderly and younger patients, but greater sensitivity of some older individuals cannot be ruled out. Dosage adjustment is not needed in patients over the age of 65.
14 Clinical Studies (14 CLINICAL STUDIES)
-
The clinical efficacy of ondansetron hydrochloride, the active ingredient of ondansetron injection, was assessed in clinical trials as described below.
4 Contraindications (4 CONTRAINDICATIONS)
Ondansetron injection is contraindicated for patients known to have hypersensitivity (e.g., anaphylaxis) to this product or any of its components. Anaphylactic reactions have been reported in patients taking ondansetron [see Adverse Reactions (6.2)].
The concomitant use of apomorphine with ondansetron is contraindicated based on reports of profound hypotension and loss of consciousness when apomorphine was administered with ondansetron.
5.2 Qt Prolongation (5.2 QT Prolongation)
Ondansetron prolongs the QT interval in a dose-dependent manner [see Clinical Pharmacology (12.2)]. In addition, postmarketing cases of Torsade de Pointes have been reported in patients using ondansetron. Avoid ondansetron injection in patients with congenital long QT syndrome. Electrocardiogram (ECG) monitoring is recommended in patients with electrolyte abnormalities (e.g., hypokalemia or hypomagnesemia), congestive heart failure, bradyarrhythmias, or patients taking other medicinal products that lead to QT prolongation.
6 Adverse Reactions (6 ADVERSE REACTIONS)
The following clinically significant adverse reactions are described elsewhere in the labeling:
-
•Hypersensitivity Reactions [see Warnings and Precautions (5.1)]
-
•QT Prolongation [see Warnings and Precautions (5.2)]
-
•Serotonin Syndrome [see Warnings and Precautions (5.3)]
-
•Myocardial Ischemia [see Warnings and Precautions (5.4)]
-
•Masking of Progressive Ileus and Gastric Distension [see Warnings and Precautions (5.5)]
8.7 Renal Impairment
Although plasma clearance is reduced in patients with severe renal impairment (creatinine clearance < 30 mL/min), no dosage adjustment is recommended [see Clinical Pharmacology (12.3)].
12.2 Pharmacodynamics
In normal volunteers, single intravenous doses of 0.15 mg/kg of ondansetron had no effect on esophageal motility, gastric motility, lower esophageal sphincter pressure, or small intestinal transit time. In another trial in 6 normal male volunteers, a 16 mg dose infused over 5 minutes showed no effect of the drug on cardiac output, heart rate, stroke volume, blood pressure, or ECG. Multiday administration of ondansetron has been shown to slow colonic transit in normal volunteers. Ondansetron has no effect on plasma prolactin concentrations. In a gender balanced pharmacodynamic trial (n = 56), ondansetron 4 mg administered intravenously or intramuscularly was dynamically similar in the prevention of nausea and vomiting using the ipecacuanha model of emesis.
Cardiac Electrophysiology
QTc interval prolongation was studied in a double-blind, single intravenous dose, placebo- and positive-controlled, crossover trial in 58 healthy subjects. The maximum mean (95% upper confidence bound) difference in QTcF from placebo after baseline correction was 19.5 (21.8) ms and 5.6 (7.4) ms after 15-minute intravenous infusions of 32 mg and 8 mg ondansetron injection, respectively. A significant exposure-response relationship was identified between ondansetron concentration and ΔΔQTcF. Using the established exposure-response relationship, 24 mg infused intravenously over 15 minutes had a mean predicted (95% upper prediction interval) ΔΔQTcF of 14.0 (16.3) ms. In contrast, 16 mg infused intravenously over 15 minutes using the same model had a mean predicted (95% upper prediction interval) ΔΔQTcF of 9.1 (11.2) ms. In this study, the 8-mg dose infused over 15 minutes did not prolong the QT interval to any clinically relevant extent.
12.3 Pharmacokinetics
In normal adult volunteers, the following mean pharmacokinetic data have been determined following a single 0.15-mg/kg intravenous dose.
|
Age-group
(years)
|
n
|
Peak Plasma
|
Mean Elimination
Half-life (h)
|
Plasma Clearance
(L/h/kg)
|
|
19 to 40 |
11 |
102 |
3.5 |
0.381 |
|
61 to 74 |
12 |
106 |
4.7 |
0.319 |
|
≥ 75 |
11 |
170 |
5.5 |
0.262 |
5.3 Serotonin Syndrome
The development of serotonin syndrome has been reported with 5-HT3 receptor antagonists. Most reports have been associated with concomitant use of serotonergic drugs (e.g., selective serotonin reuptake inhibitors (SSRIs), serotonin and norepinephrine reuptake inhibitors (SNRIs), monoamine oxidase inhibitors, mirtazapine, fentanyl, lithium, tramadol, and intravenous methylene blue). Some of the reported cases were fatal. Serotonin syndrome occurring with overdose of ondansetron injection alone has also been reported. The majority of reports of serotonin syndrome related to 5-HT3 receptor antagonist use occurred in a post-anesthesia care unit or an infusion center.
Symptoms associated with serotonin syndrome may include the following combination of signs and symptoms: mental status changes (e.g., agitation, hallucinations, delirium, and coma), autonomic instability (e.g., tachycardia, labile blood pressure, dizziness, diaphoresis, flushing, hyperthermia), neuromuscular symptoms (e.g., tremor, rigidity, myoclonus, hyperreflexia, incoordination), seizures, with or without gastrointestinal symptoms (e.g., nausea, vomiting, diarrhea). Patients should be monitored for the emergence of serotonin syndrome, especially with concomitant use of ondansetron injection and other serotonergic drugs. If symptoms of serotonin syndrome occur, discontinue ondansetron injection and initiate supportive treatment. Patients should be informed of the increased risk of serotonin syndrome, especially if ondansetron injection is used concomitantly with other serotonergic drugs [see Drug Interactions (7.5), Overdosage (10)].
7.5 Serotonergic Drugs
Serotonin syndrome (including altered mental status, autonomic instability, and neuromuscular symptoms) has been described following the concomitant use of 5-HT3 receptor antagonists and other serotonergic drugs, including SSRIs and SNRIs [see Warnings and Precautions (5.3)].
8.6 Hepatic Impairment
In patients with severe hepatic impairment (Child-Pugh score of 10 or greater), clearance is reduced and apparent volume of distribution is increased with a resultant increase in plasma half-life [see Clinical Pharmacology (12.3)] . In such patients, a total daily dose of 8 mg should not be exceeded [see Dosage and Administration (2.3)].
1 Indications and Usage (1 INDICATIONS AND USAGE)
5.4 Myocardial Ischemia
Myocardial ischemia has been reported in patients treated with ondansetron. In some cases, predominantly during intravenous administration, the symptoms appeared immediately after administration but resolved with prompt treatment. Coronary artery spasm appears to be the most common underlying cause. Therefore, do not exceed the recommended infusion rate of ondansetron injection and monitor patients for signs and symptoms of myocardial ischemia during and after administration [see Dosage and Administration (2.1, 2.2) and Adverse Reactions (6.2)].
12.1 Mechanism of Action
Ondansetron is a selective 5-HT3 receptor antagonist. While ondansetron's mechanism of action has not been fully characterized, it is not a dopamine-receptor antagonist.
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
-
•Hypersensitivity Reactions: Hypersensitivity reactions, including anaphylaxis and bronchospasm have been reported in patients who have exhibited hypersensitivity to other selective 5-HT3 receptor antagonists. (5.1)
-
•QT Prolongation and Torsade de Pointes: QT prolongation occurs in a dose-dependent manner. Cases of Torsade de Pointes have been reported. Avoid ondansetron injection in patients with congenital long QT syndrome. (5.2)
-
•Serotonin Syndrome: Serotonin syndrome has been reported with 5-HT3 receptor agonists alone but particularly with concomitant use of serotonergic drugs. (5.3)
-
•Myocardial Ischemia: Do not exceed the recommended infusion rate and monitor patients during and after administration. (2.1, 2.2, 5.4)
-
•Masking of Progressive Ileus and/or Gastric Distension Following Abdominal Surgery or Chemotherapy-Induced Nausea and Vomiting: Monitor for decreased bowel activity, particularly in patients with risk factors for gastrointestinal obstruction. (5.5)
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
Prevention of Nausea and Vomiting Associated With Initial and Repeat Courses of Emetogenic Cancer Chemotherapy ( 2.1 ):
-
•Dilution of ondansetron injection in 50 mL of 5% Dextrose Injection or 0.9% Sodium Chloride Injection is required before administration to adult and pediatric patients.
-
•Adults and pediatric patients 6 months of age and older: The recommended dosage is 0.15 mg/kg per dose for 3 doses (maximum of 16 mg per dose), infused intravenously over 15 minutes.
-
•Administer the first dose 30 minutes before the start of chemotherapy and subsequent doses 4 and 8 hours after the first dose.
Prevention of Postoperative Nausea and/or Vomiting (
2.2
):
-
•Dilution of ondansetron injection is not required before administration to adult and pediatric patients.
-
•See full prescribing information for the recommended dosage and administration instructions for adult and pediatric patients 1 month of age and older.
Patients With Severe Hepatic Impairment (
2.3
):
-
•Do not exceed a total daily dose of 8 mg.
9 Drug Abuse and Dependence (9 DRUG ABUSE AND DEPENDENCE)
Animal studies have shown that ondansetron is not discriminated as a benzodiazepine nor does it substitute for benzodiazepines in direct addiction studies.
Package/label Display Panel (Package/Label Display Panel)
NDC 55154-4453-5
ONDANSETRON INJECTION, USP
4 mg/2 mL (2 mg/mL)
5 X 2 mL SINGLE-USE VIALS
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
Ondansetron injection USP, 4 mg/2 mL (2 mg/mL) is a clear, colorless, nonpyrogenic, sterile solution available in a 2 mL single-dose vial.
6.2 Postmarketing Experience
The following adverse reactions have been identified during postapproval use of ondansetron. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure. The reactions have been chosen for inclusion due to a combination of their seriousness, frequency of reporting, or potential causal connection to ondansetron.
Cardiovascular
Arrhythmias (including ventricular and supraventricular tachycardia, premature ventricular contractions, and atrial fibrillation), bradycardia, electrocardiographic alterations (including second-degree heart block, QT/QTc interval prolongation, and ST segment depression), palpitations, and syncope. Rarely and predominantly with intravenous ondansetron, transient ECG changes, including QT/QTc interval prolongation have been reported [see Warnings and Precautions (5.2)].
Myocardial ischemia was reported predominately with intravenous administration [see Warnings and Precautions (5.4)].
General
Flushing: Rare cases of hypersensitivity reactions, sometimes severe (e.g., anaphylactic reactions, angioedema, bronchospasm, cardiopulmonary arrest, hypotension, laryngeal edema, laryngospasm, shock, shortness of breath, stridor) have also been reported. A positive lymphocyte transformation test to ondansetron has been reported, which suggests immunologic sensitivity to ondansetron.
Hepatobiliary
Liver enzyme abnormalities have been reported. Liver failure and death have been reported in patients with cancer receiving concurrent medications, including potentially hepatotoxic cytotoxic chemotherapy and antibiotics.
Local Reactions
Pain, redness, and burning at site of injection.
Lower Respiratory
Hiccups.
Neurological
Oculogyric crisis, appearing alone, as well as with other dystonic reactions. Transient dizziness during or shortly after intravenous infusion.
Skin
Urticaria, Stevens-Johnson syndrome, and toxic epidermal necrolysis.
Eye Disorders
Cases of transient blindness, predominantly during intravenous administration, have been reported. These cases of transient blindness were reported to resolve within a few minutes up to 48 hours. Transient blurred vision, in some cases associated with abnormalities of accommodation, has also been reported.
7.8 Alfentanil and Atracurium
Ondansetron does not alter the respiratory depressant effects produced by alfentanil or the degree of neuromuscular blockade produced by atracurium. Interactions with general or local anesthetics have not been studied.
5.1 Hypersensitivity Reactions
Hypersensitivity reactions, including anaphylaxis and bronchospasm, have been reported in patients who have exhibited hypersensitivity to other selective 5-HT3 receptor antagonists.
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared with rates in the clinical trials of another drug and may not reflect the rates observed in clinical practice.
The following adverse reactions have been reported in clinical trials of adult patients treated with ondansetron, the active ingredient of intravenous ondansetron injection across a range of dosages. A causal relationship to therapy with ondansetron injection (ondansetron) was unclear in many cases.
17 Patient Counseling Information (17 PATIENT COUNSELING INFORMATION)
Hypersensitivity Reactions
Inform patients that ondansetron injection may cause hypersensitivity reactions, some as severe as anaphylaxis and bronchospasm. The patient should report any signs and symptoms of hypersensitivity reactions, including fever, chills, rash, or breathing problems [see Warnings and Precautions (5.1)].
QT Prolongation
Patients should be informed that ondansetron injection may cause serious cardiac arrhythmias, such as QT prolongation. Patients should be instructed to tell their healthcare provider right away if they perceive a change in their heart rate, if they feel lightheaded, or if they have a syncopal episode.
Patients should be informed that the chances of developing severe cardiac arrhythmias, such as QT prolongation and Torsade de Pointes are higher in the following people:
-
•Patients with a personal or family history of abnormal heart rhythms, such as congenital long QT syndrome;
-
•Patients who take medications, such as diuretics, which may cause electrolyte abnormalities;
-
•Patients with hypokalemia or hypomagnesemia.
Ondansetron injection should be avoided in these patients, since they may be more at risk for cardiac arrhythmias, such as QT prolongation and Torsade de Pointes [see Warnings and Precautions (5.2)].
Drug Interactions
-
•Instruct the patient to report the use of all medications, especially apomorphine, to their healthcare provider. Concomitant use of apomorphine and ondansetron injection may cause a significant drop in blood pressure and loss of consciousness.
-
•Advise patients of the possibility of serotonin syndrome with concomitant use of ondansetron injection and another serotonergic agent, such as medications to treat depression and migraines. Advise patients to seek immediate medical attention if the following symptoms occur: changes in mental status, autonomic instability, neuromuscular symptoms with or without gastrointestinal symptoms [see Warnings and Precautions (5.3)].
Myocardial Ischemia
Inform patients that ondansetron injection may cause myocardial ischemia during or after the administration. Advise patients to seek immediate medical help if any symptoms suggestive of a myocardial ischemia occur, such as sudden chest pain or chest tightness [see Warnings and Precautions (5.4)].
Masking of Progressive Ileus and Gastric Distension
Inform patients following abdominal surgery or those with chemotherapy-induced nausea and vomiting that ondansetron injection may mask signs and symptoms of bowel obstruction. Instruct patients to immediately report any signs or symptoms consistent with a potential bowel obstruction to their healthcare provider [see Warnings and Precautions (5.5)].
Manufactured for:
Baxter Healthcare Corporation
Deerfield, IL 60015 USA
Manufactured by:
Baxter Pharmaceuticals India Private Ltd
Ahmedabad 382213, India
Distributed By:
Cardinal Health
Dublin, OH 43017
L55233370124
1400008740
16 How Supplied/storage and Handling (16 HOW SUPPLIED/STORAGE AND HANDLING)
Ondansetron Injection USP, 4 mg/2 mL (2 mg/mL), is supplied as follows:
Overbagged with 5 x 2 mL single-dose vials in each bag, NDC 55154-4453-5
WARNING: This Unit Dose package is not child resistant and is Intended for Institutional Use Only. Keep this and all drugs out of the reach of children.
7.3 Phenytoin, Carbamazepine, and Rifampin
In patients treated with potent inducers of CYP3A4 (i.e., phenytoin, carbamazepine, and rifampin), the clearance of ondansetron was significantly increased and ondansetron blood concentrations were decreased. However, on the basis of available data, no dosage adjustment for ondansetron is recommended for patients on these drugs [see Clinical Pharmacology (12.3)].
7.1 Drugs Affecting Cytochrome P 450 Enzymes (7.1 Drugs Affecting Cytochrome P-450 Enzymes)
Ondansetron does not appear to induce or inhibit the cytochrome P-450 drug-metabolizing enzyme system of the liver. Because ondansetron is metabolized by hepatic cytochrome P-450 drug-metabolizing enzymes (CYP3A4, CYP2D6, CYP1A2), inducers or inhibitors of these enzymes may change the clearance and, hence, the half-life of ondansetron [see Clinical Pharmacology (12.3)]. On the basis of limited available data, no dosage adjustment is recommended for patients on these drugs.
14.1 Chemotherapy Induced Nausea and Vomiting (14.1 Chemotherapy-Induced Nausea and Vomiting)
Adults
In a double-blind trial of three different dosing regimens of ondansetron injection, 0.015 mg/kg, 0.15 mg/kg, and 0.30 mg/kg, each given three times during the course of cancer chemotherapy, the 0.15-mg/kg dosing regimen was more effective than the 0.015-mg/kg dosing regimen. The 0.30-mg/kg dosing regimen was not shown to be more effective than the 0.15-mg/kg dosing regimen.
1.2 Prevention of Postoperative Nausea And/or Vomiting (1.2 Prevention of Postoperative Nausea and/or Vomiting)
Ondansetron injection is indicated for the prevention of postoperative nausea and/or vomiting. As with other antiemetics, routine prophylaxis is not recommended for patients in whom there is little expectation that nausea and/or vomiting will occur postoperatively. In patients in whom nausea and/or vomiting must be avoided postoperatively, ondansetron injection is recommended even when the incidence of postoperative nausea and/or vomiting is low. For patients who do not receive prophylactic ondansetron injection and experience nausea and/or vomiting postoperatively, ondansetron injection may be given to prevent further episodes.
Ondansetron injection is approved for patients aged 1 month and older.
2.2 Prevention of Postoperative Nausea And/or Vomiting (2.2 Prevention of Postoperative Nausea and/or Vomiting)
Important Preparation Instructions
-
•Dilution of ondansetron injection is not required before administration to adult and pediatric patients.
-
•Inspect ondansetron injection visually for particulate matter and discoloration before administration; discard if present.
5.5 Masking of Progressive Ileus and Gastric Distension
The use of ondansetron injection in patients following abdominal surgery or in patients with chemotherapy-induced nausea and vomiting may mask a progressive ileus and gastric distension. Monitor for decreased bowel activity, particularly in patients with risk factors for gastrointestinal obstruction.
Ondansetron injection is not a drug that stimulates gastric or intestinal peristalsis. It should not be used instead of nasogastric suction.
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenic effects were not seen in 2-year studies in rats and mice with oral ondansetron doses up to 10 and 30 mg/kg per day, respectively (approximately 3.6 and 5.4 times the recommended human intravenous dose of 0.15 mg/kg given three times a day, based on BSA).
Ondansetron was not mutagenic in standard tests for mutagenicity.
Oral administration of ondansetron up to 15 mg/kg per day (approximately 3.8 times the recommended human intravenous dose, based on BSA) did not affect fertility or general reproductive performance of male and female rats.
2.3 Dosage Adjustment for Patients With hepatic Impairment (2.3 Dosage Adjustment for Patients With Hepatic Impairment)
In patients with severe hepatic impairment (Child-Pugh score of 10 or greater), a single maximal daily dose of 8 mg infused over 15 minutes beginning 30 minutes before the start of the emetogenic chemotherapy is recommended. There is no experience beyond first-day administration of ondansetron in these patients [see Use in Specific Populations (8.6)].
2.1 Prevention of Nausea and Vomiting Associated With Initial and Repeat Courses of Emetogenic Chemotherapy
Important Preparation Instructions
-
•Dilution of ondansetron injection in 50 mL of 5% Dextrose Injection or 0.9% Sodium Chloride Injection is required before administration to adult and pediatric patients for the prevention of nausea and vomiting associated with emetogenic chemotherapy.
For pediatric patients between 6 months and 1 year of age and/or 10 kg or less: Depending on the fluid needs of the patient, ondansetron injection may be diluted in 10 to 50 mL of 5% Dextrose Injection or 0.9% Sodium Chloride Injection.
-
•Occasionally, ondansetron precipitates at the stopper/vial interface in vials stored upright. Potency and safety are not affected. If a precipitate is observed, resolubilize by shaking the vial vigorously.
-
•Do not mix ondansetron injection with solutions for which physical and chemical compatibility has not been established. In particular, this applies to alkaline solutions as a precipitate may form.
-
•Inspect the diluted ondansetron injection solution for particulate matter and discoloration before administration; discard if present.
-
•Storage: After dilution, do not use beyond 24 hours. Although ondansetron injection is chemically and physically stable when diluted as recommended, sterile precautions should be observed because diluents generally do not contain preservative.
-
•Compatibility: Ondansetron injection is compatible and stable at room temperature under normal lighting conditions for 48 hours after dilution with the following intravenous fluids: 0.9% Sodium Chloride Injection, 5% Dextrose Injection, 5% Dextrose and 0.9% Sodium Chloride Injection, 5% Dextrose and 0.45% Sodium Chloride Injection, and 3% Sodium Chloride Injection.
1.1 Prevention of Nausea and Vomiting Associated With Initial and Repeat Courses of Emetogenic Cancer Chemotherapy
Ondansetron injection is indicated for the prevention of nausea and vomiting associated with initial and repeat courses of emetogenic cancer chemotherapy, including high-dose cisplatin.
Ondansetron injection is approved for patients aged 6 months and older.
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:52:34.011449 · Updated: 2026-03-14T22:44:06.575433