These Highlights Do Not Include All The Information Needed To Use Oxaliplatin Injection Safely And Effectively. See Full Prescribing Information For Oxaliplatin Injection.
29a5d098-bfa7-4a65-bb4f-5daa1fef1c2f
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
Serious and fatal hypersensitivity adverse reactions, including anaphylaxis, can occur with Oxaliplatin Injection within minutes of administration and during any cycle. Oxaliplatin Injection is contraindicated in patients with hypersensitivity reactions to oxaliplatin and other platinum-based drugs [see Contraindications ( 4 )] . Immediately and permanently discontinue Oxaliplatin Injection for hypersensitivity reactions and administer appropriate treatment for management of the hypersensitivity reaction [see Warnings and Precautions ( 5.1 )] .
Indications and Usage
Oxaliplatin Injection, in combination with infusional fluorouracil and leucovorin, is indicated for: adjuvant treatment of stage III colon cancer in patients who have undergone complete resection of the primary tumor. treatment of advanced colorectal cancer.
Dosage and Administration
Administer oxaliplatin injection 85 mg/m 2 as an intravenous infusion over 120 minutes concurrently with leucovorin over 120 minutes in separate bags, followed by fluorouracil on Day 1 of each 14-day cycle. Administer fluorouracil and leucovorin on Day 2 as recommended. ( 2.1 ) Adjuvant Treatment : Continue treatment for up to 12 cycles or unacceptable toxicity. ( 2.1 ) Advanced Colorectal Cancer : Continue treatment until disease progression or unacceptable toxicity. ( 2.1 )
Warnings and Precautions
Peripheral Sensory Neuropathy : Acute and delayed neuropathy can occur. Avoid topical application of ice. Reduce the dose or permanently discontinue oxaliplatin as recommended. ( 5.2 ) Severe Myelosuppression : Delay oxaliplatin until neutrophils are greater than or equal to 1.5 x 10 9 /L and platelets are greater than or equal to 75 x 10 9 /L. Withhold oxaliplatin for sepsis or septic shock. Dose reduce after recovery from grade 4 neutropenia, febrile neutropenia, or grade 3-4 thrombocytopenia as recommended. ( 5.3 ) Posterior Reversible Encephalopathy Syndrome (PRES) : Permanently discontinue oxaliplatin in patients who develop PRES. ( 5.4 ) Pulmonary Toxicity : Withhold oxaliplatin until investigation excludes interstitial lung disease or pulmonary fibrosis. ( 5.5 ) Hepatotoxicity : Monitor liver function tests at baseline, before each subsequent cycle, and as clinically indicated. ( 5.6 ) QT Interval Prolongation : Avoid in patients with congenital long QT syndrome. Monitor electrocardiograms in patients with congestive heart failure, bradyarrhythmias, and electrolyte abnormalities, and in patients taking drugs known to prolong the QT interval. Correct electrolyte abnormalities prior to initiating oxaliplatin and periodically during treatment. ( 5.7 ) Rhabdomyolysis : Permanently discontinue oxaliplatin if rhabdomyolysis occurs. ( 5.8 ) Hemorrhage : Increase frequency of monitoring in patients who are receiving oxaliplatin with fluorouracil/leucovorin and oral anticoagulants. ( 5.9 ) Embryo-Fetal Toxicity : Can cause fetal harm. Advise pregnant women of the potential risk to a fetus. Advise males and females of reproductive potential to use an effective method of contraception. ( 5.10 , 8.1 , 8.3 )
Contraindications
Oxaliplatin injection is contraindicated in patients with a history of a hypersensitivity reaction to oxaliplatin or other platinum-based drugs. Reactions have included anaphylaxis [see Warnings and Precautions ( 5.1 )] .
Adverse Reactions
The following clinically significant adverse reactions are described elsewhere in labeling: Hypersensitivity Reactions [see Warnings and Precautions ( 5.1 )] Peripheral Sensory Neuropathy [see Warnings and Precautions ( 5.2 )] Severe Myelosuppression [see Warnings and Precautions ( 5.3 )] Posterior Reversible Encephalopathy Syndrome [see Warnings and Precautions ( 5.4 )] Pulmonary Toxicity [see Warnings and Precautions ( 5.5 )] Hepatotoxicity [see Warnings and Precautions ( 5.6 )] QT Interval Prolongation and Ventricular Arrhythmias [see Warnings and Precautions ( 5.7 )] Rhabdomyolysis [see Warnings and Precautions ( 5.8 )] Hemorrhage [see Warnings and Precautions ( 5.9 )]
Storage and Handling
Oxaliplatin Injection, USP is supplied as follows: NDC Oxaliplatin Injection, USP (5 mg per mL) Package Factor 25021-233-10 50 mg per 10 mL Single-Dose Vial 1 vial per carton 25021-233-20 100 mg per 20 mL Single-Dose Vial 1 vial per carton Water for Injection, USP is present as an inactive ingredient. Tartaric Acid, NF and Sodium Hydroxide, NF are used in combination as a buffering system. Store at 20° to 25°C (68° to 77°F); excursions permitted between 15° and 30°C (59° and 86°F). [See USP Controlled Room Temperature.] Do not freeze. Protect from light. Retain in carton until time of use. Discard unused portion. Oxaliplatin Injection, USP is a cytotoxic drug. Follow applicable special handling and disposal procedures. 1 The use of gloves is recommended. If a solution of Oxaliplatin Injection, USP contacts the skin, wash the skin immediately and thoroughly with soap and water. If Oxaliplatin Injection, USP contacts the mucous membranes, flush thoroughly with water. Sterile, Nonpyrogenic, Preservative-free. The container closure is not made with natural rubber latex.
How Supplied
Oxaliplatin Injection, USP is supplied as follows: NDC Oxaliplatin Injection, USP (5 mg per mL) Package Factor 25021-233-10 50 mg per 10 mL Single-Dose Vial 1 vial per carton 25021-233-20 100 mg per 20 mL Single-Dose Vial 1 vial per carton Water for Injection, USP is present as an inactive ingredient. Tartaric Acid, NF and Sodium Hydroxide, NF are used in combination as a buffering system. Store at 20° to 25°C (68° to 77°F); excursions permitted between 15° and 30°C (59° and 86°F). [See USP Controlled Room Temperature.] Do not freeze. Protect from light. Retain in carton until time of use. Discard unused portion. Oxaliplatin Injection, USP is a cytotoxic drug. Follow applicable special handling and disposal procedures. 1 The use of gloves is recommended. If a solution of Oxaliplatin Injection, USP contacts the skin, wash the skin immediately and thoroughly with soap and water. If Oxaliplatin Injection, USP contacts the mucous membranes, flush thoroughly with water. Sterile, Nonpyrogenic, Preservative-free. The container closure is not made with natural rubber latex.
Medication Information
Warnings and Precautions
Peripheral Sensory Neuropathy : Acute and delayed neuropathy can occur. Avoid topical application of ice. Reduce the dose or permanently discontinue oxaliplatin as recommended. ( 5.2 ) Severe Myelosuppression : Delay oxaliplatin until neutrophils are greater than or equal to 1.5 x 10 9 /L and platelets are greater than or equal to 75 x 10 9 /L. Withhold oxaliplatin for sepsis or septic shock. Dose reduce after recovery from grade 4 neutropenia, febrile neutropenia, or grade 3-4 thrombocytopenia as recommended. ( 5.3 ) Posterior Reversible Encephalopathy Syndrome (PRES) : Permanently discontinue oxaliplatin in patients who develop PRES. ( 5.4 ) Pulmonary Toxicity : Withhold oxaliplatin until investigation excludes interstitial lung disease or pulmonary fibrosis. ( 5.5 ) Hepatotoxicity : Monitor liver function tests at baseline, before each subsequent cycle, and as clinically indicated. ( 5.6 ) QT Interval Prolongation : Avoid in patients with congenital long QT syndrome. Monitor electrocardiograms in patients with congestive heart failure, bradyarrhythmias, and electrolyte abnormalities, and in patients taking drugs known to prolong the QT interval. Correct electrolyte abnormalities prior to initiating oxaliplatin and periodically during treatment. ( 5.7 ) Rhabdomyolysis : Permanently discontinue oxaliplatin if rhabdomyolysis occurs. ( 5.8 ) Hemorrhage : Increase frequency of monitoring in patients who are receiving oxaliplatin with fluorouracil/leucovorin and oral anticoagulants. ( 5.9 ) Embryo-Fetal Toxicity : Can cause fetal harm. Advise pregnant women of the potential risk to a fetus. Advise males and females of reproductive potential to use an effective method of contraception. ( 5.10 , 8.1 , 8.3 )
Indications and Usage
Oxaliplatin Injection, in combination with infusional fluorouracil and leucovorin, is indicated for: adjuvant treatment of stage III colon cancer in patients who have undergone complete resection of the primary tumor. treatment of advanced colorectal cancer.
Dosage and Administration
Administer oxaliplatin injection 85 mg/m 2 as an intravenous infusion over 120 minutes concurrently with leucovorin over 120 minutes in separate bags, followed by fluorouracil on Day 1 of each 14-day cycle. Administer fluorouracil and leucovorin on Day 2 as recommended. ( 2.1 ) Adjuvant Treatment : Continue treatment for up to 12 cycles or unacceptable toxicity. ( 2.1 ) Advanced Colorectal Cancer : Continue treatment until disease progression or unacceptable toxicity. ( 2.1 )
Contraindications
Oxaliplatin injection is contraindicated in patients with a history of a hypersensitivity reaction to oxaliplatin or other platinum-based drugs. Reactions have included anaphylaxis [see Warnings and Precautions ( 5.1 )] .
Adverse Reactions
The following clinically significant adverse reactions are described elsewhere in labeling: Hypersensitivity Reactions [see Warnings and Precautions ( 5.1 )] Peripheral Sensory Neuropathy [see Warnings and Precautions ( 5.2 )] Severe Myelosuppression [see Warnings and Precautions ( 5.3 )] Posterior Reversible Encephalopathy Syndrome [see Warnings and Precautions ( 5.4 )] Pulmonary Toxicity [see Warnings and Precautions ( 5.5 )] Hepatotoxicity [see Warnings and Precautions ( 5.6 )] QT Interval Prolongation and Ventricular Arrhythmias [see Warnings and Precautions ( 5.7 )] Rhabdomyolysis [see Warnings and Precautions ( 5.8 )] Hemorrhage [see Warnings and Precautions ( 5.9 )]
Storage and Handling
Oxaliplatin Injection, USP is supplied as follows: NDC Oxaliplatin Injection, USP (5 mg per mL) Package Factor 25021-233-10 50 mg per 10 mL Single-Dose Vial 1 vial per carton 25021-233-20 100 mg per 20 mL Single-Dose Vial 1 vial per carton Water for Injection, USP is present as an inactive ingredient. Tartaric Acid, NF and Sodium Hydroxide, NF are used in combination as a buffering system. Store at 20° to 25°C (68° to 77°F); excursions permitted between 15° and 30°C (59° and 86°F). [See USP Controlled Room Temperature.] Do not freeze. Protect from light. Retain in carton until time of use. Discard unused portion. Oxaliplatin Injection, USP is a cytotoxic drug. Follow applicable special handling and disposal procedures. 1 The use of gloves is recommended. If a solution of Oxaliplatin Injection, USP contacts the skin, wash the skin immediately and thoroughly with soap and water. If Oxaliplatin Injection, USP contacts the mucous membranes, flush thoroughly with water. Sterile, Nonpyrogenic, Preservative-free. The container closure is not made with natural rubber latex.
How Supplied
Oxaliplatin Injection, USP is supplied as follows: NDC Oxaliplatin Injection, USP (5 mg per mL) Package Factor 25021-233-10 50 mg per 10 mL Single-Dose Vial 1 vial per carton 25021-233-20 100 mg per 20 mL Single-Dose Vial 1 vial per carton Water for Injection, USP is present as an inactive ingredient. Tartaric Acid, NF and Sodium Hydroxide, NF are used in combination as a buffering system. Store at 20° to 25°C (68° to 77°F); excursions permitted between 15° and 30°C (59° and 86°F). [See USP Controlled Room Temperature.] Do not freeze. Protect from light. Retain in carton until time of use. Discard unused portion. Oxaliplatin Injection, USP is a cytotoxic drug. Follow applicable special handling and disposal procedures. 1 The use of gloves is recommended. If a solution of Oxaliplatin Injection, USP contacts the skin, wash the skin immediately and thoroughly with soap and water. If Oxaliplatin Injection, USP contacts the mucous membranes, flush thoroughly with water. Sterile, Nonpyrogenic, Preservative-free. The container closure is not made with natural rubber latex.
Description
Serious and fatal hypersensitivity adverse reactions, including anaphylaxis, can occur with Oxaliplatin Injection within minutes of administration and during any cycle. Oxaliplatin Injection is contraindicated in patients with hypersensitivity reactions to oxaliplatin and other platinum-based drugs [see Contraindications ( 4 )] . Immediately and permanently discontinue Oxaliplatin Injection for hypersensitivity reactions and administer appropriate treatment for management of the hypersensitivity reaction [see Warnings and Precautions ( 5.1 )] .
Section 42229-5
Day 1
Administer oxaliplatin injection 85 mg/m2 as an intravenous infusion over 120 minutes and leucovorin 200 mg/m2 as an intravenous infusion over 120 minutes at the same time in separate bags, followed by fluorouracil 400 mg/m2 as intravenous bolus over 2 to 4 minutes, followed by fluorouracil 600 mg/m2 as a 22-hour continuous infusion.
Section 42230-3
FDA-Approved Patient Labeling
|
This Patient Information has been approved by the U.S. Food and Drug Administration. |
|
|
Patient Information
Oxaliplatin (ox-AL-i-PLA-tin) Injection injection, for intravenous use |
|
|
What is the most important information I should know about Oxaliplatin Injection? Oxaliplatin Injection can cause serious allergic reactions, including allergic reactions that can lead to death. Oxaliplatin Injection is a platinum-based medicine. Serious allergic reactions including death can happen in people who take Oxaliplatin Injection and who have had previous allergic reactions to platinum-based medicines. Serious allergic reactions can happen within a few minutes of your Oxaliplatin Injection infusion or any time during your treatment with Oxaliplatin Injection. Get emergency help right away if you:
|
|
|
|
| See “What are the possible side effects of Oxaliplatin Injection?” for information about other serious side effects. |
|
|
What is Oxaliplatin Injection?
Oxaliplatin Injection is an anti-cancer (chemotherapy) medicine that is used with other anti-cancer medicines called fluorouracil and leucovorin to treat people with:
|
|
|
Do not receive Oxaliplatin Injection if you are allergic to oxaliplatin or any of the ingredients in Oxaliplatin Injection or if you are allergic to other platinum-based medicines. See the end of this leaflet for a complete list of the ingredients in Oxaliplatin Injection. Ask your doctor if you are not sure if you have taken a platinum-based medicine. |
|
Before receiving Oxaliplatin Injection, tell your doctor about all of your medical conditions, including if you:
Know the medicines you take. Keep a list of them and show it to your doctor and pharmacist when you get a new medicine. |
|
How will I receive Oxaliplatin Injection?
You will not get Oxaliplatin Injection on Day 2. Leucovorin and fluorouracil will be given the same way as on Day 1. The fluorouracil will be given through your IV with a pump. If you have any problems with the pump or the tube, call your doctor, your nurse, or the person who is responsible for your pump. Do not let anyone other than a healthcare provider touch your infusion pump or tubing. |
|
What should I avoid while receiving Oxaliplatin Injection?
Talk with your doctor and nurse about your level of activity during treatment with Oxaliplatin Injection. Follow their instructions. |
|
|
What are the possible side effects of Oxaliplatin Injection? Oxaliplatin Injection can cause serious side effects, including:
|
|
|
|
|
|
|
|
| The most common side effects of Oxaliplatin Injection include: | |
|
|
|
Oxaliplatin Injection may cause fertility problems in males and females. Talk to your doctor if this is a concern for you. Tell your doctor if you have any side effect that bothers you or that does not go away. These are not all the possible side effects of Oxaliplatin Injection. For more information, ask your doctor or pharmacist. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. |
|
|
How can I reduce the side effects caused by cold temperatures?
|
|
|
General information about the safe and effective use of Oxaliplatin Injection.
Medicines are sometimes prescribed for purposes other than those listed in the Patient Information leaflet. You can ask your doctor or pharmacist for information about Oxaliplatin Injection that is written for health professionals. |
|
|
What are the ingredients in Oxaliplatin Injection?
Active ingredient: Oxaliplatin Inactive ingredient: Water for Injection, USP, Tartaric Acid, NF and Sodium Hydroxide, NF are used as inactive ingredients and/or in combination as a buffering system. sagent ® Mfd. for SAGENT Pharmaceuticals Schaumburg, IL 60173 (USA) Made in China ©2025 Sagent Pharmaceuticals Revised: May 2025 |
Section 51945-4
PACKAGE LABEL – PRINCIPAL DISPLAY PANEL – Vial Label
NDC 25021-233-10
Rx only
OXALIPLATIN Injection, USP
50 mg per 10 mL (5 mg per mL)
For Intravenous Use Only
10 mL Single-Dose Vial
See package insert for further required dilution
DO NOT MIX OR ADD TO SODIUM CHLORIDE/
CHLORIDE-CONTAINING SOLUTIONS
Caution: Cytotoxic Agent
10 Overdosage
The maximum dose of oxaliplatin that has been administered in a single infusion is 825 mg. Several cases of overdoses have been reported with oxaliplatin. Adverse reactions observed following an overdosage were grade 4 thrombocytopenia (less than 25,000/mm3) without bleeding, anemia, sensory neuropathy (including paresthesia, dysesthesia, laryngospasm and facial muscle spasms), gastrointestinal disorders (including nausea, vomiting, stomatitis, flatulence, abdomen enlarged and grade 4 intestinal obstruction), grade 4 dehydration, dyspnea, wheezing, chest pain, respiratory failure, severe bradycardia, and death.
Closely monitor patients suspected of receiving an overdose, including for the adverse reactions described above and administer appropriate supportive treatment.
15 References
- “OSHA Hazardous Drugs.” OSHA. http://www.osha.gov/SLTC/hazardousdrugs/index.html
11 Description
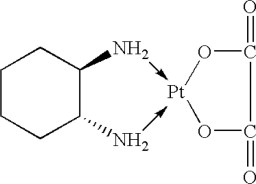
Oxaliplatin is a platinum-based drug with the molecular formula C8H14N2O4Pt and the chemical name of cis-[(1 R,2 R)-1,2-cyclohexanediamine-N,N′] [oxalato(2-)- O,O′] platinum. Oxaliplatin is an organoplatinum complex in which the platinum atom is complexed with 1,2-diaminocyclohexane (DACH) and with an oxalate ligand as a leaving group.
The molecular weight is 397.3. Oxaliplatin is slightly soluble in water at 6 mg/mL, very slightly soluble in methanol, and practically insoluble in ethanol and acetone.
Oxaliplatin Injection, USP, for intravenous use, is supplied in vials containing 50 mg or 100 mg of oxaliplatin as a sterile, preservative-free, aqueous solution at a concentration of 5 mg/mL. Water for Injection, USP is present as an inactive ingredient. Tartaric Acid, NF and Sodium Hydroxide, NF are used in combination as a buffering system.
5.9 Hemorrhage
The incidence of hemorrhage in clinical trials was higher on the oxaliplatin combination arm compared to the fluorouracil/leucovorin arm. These reactions included gastrointestinal bleeding, hematuria, and epistaxis. In the adjuvant treatment trial, 2 patients died from intracerebral hemorrhage [see Adverse Reactions (6.1)].
Prolonged prothrombin time and INR occasionally associated with hemorrhage have been reported in patients who received oxaliplatin with fluorouracil/leucovorin while on anticoagulants [see Adverse Reactions (6.2)]. Increase frequency of monitoring in patients who are receiving oxaliplatin with fluorouracil/leucovorin and oral anticoagulants [see Drug Interactions (7.3)].
Thrombocytopenia and immune-mediated thrombocytopenia have been observed with oxaliplatin. Rapid onset of thrombocytopenia and greater risk of bleeding have been observed in immune-mediated thrombocytopenia. In this case, consider discontinuing oxaliplatin.
8.4 Pediatric Use
The safety and effectiveness of oxaliplatin in pediatrics have not been established. Safety and effectiveness were assessed across 4 open-label studies in 235 patients aged 7 months to 22 years with solid tumors.
In a multicenter, open-label, non-comparative, non-randomized study (ARD5531), oxaliplatin was administered to 43 patients with refractory or relapsed malignant solid tumors, mainly neuroblastoma and osteosarcoma. The dose limiting toxicity (DLT) was sensory neuropathy at a dose of 110 mg/m2. The main adverse reactions were: paresthesia (60%, grade 3-4: 7%), fever (40%, grade 3-4: 7%), and thrombocytopenia (40%, grade 3-4: 27%). No responses were observed.
In an open-label non-randomized study (DFI7434), oxaliplatin was administered to 26 pediatric patients with metastatic or unresectable solid tumors, mainly neuroblastoma and ganglioneuroblastoma. The DLT was sensory neuropathy at a dose of 160 mg/m2. No responses were observed.
In an open-label, single-agent study (ARD5021), oxaliplatin was administered to 43 pediatric patients with recurrent or refractory embryonal CNS tumors. The most common adverse reactions reported were: leukopenia (67%, grade 3-4: 12%), anemia (65%, grade 3-4: 5%), thrombocytopenia (65%, grade 3-4: 26%), vomiting (65%, grade 3-4: 7%), neutropenia (58%, grade 3-4: 16%), and sensory neuropathy (40%, grade 3-4: 5%).
In an open-label single-agent study (ARD5530), oxaliplatin was administered to 123 pediatric patients with recurrent solid tumors, including neuroblastoma, osteosarcoma, Ewing sarcoma or peripheral PNET, ependymoma, rhabdomyosarcoma, hepatoblastoma, high grade astrocytoma, brain stem glioma, low grade astrocytoma, malignant germ cell tumor and other tumors. The most common adverse reactions reported were: sensory neuropathy (52%, grade 3-4: 12%), thrombocytopenia (37%, grade 3-4: 17%), anemia (37%, grade 3-4: 9%), vomiting (26%, grade 3-4: 4%), increased ALT (24%, grade 3-4: 6%), increased AST (24%, grade 3-4: 2%), and nausea (23%, grade 3-4: 3%).
The pharmacokinetic parameters of ultrafiltrable platinum were evaluated in 105 pediatric patients during the first cycle. The mean clearance in pediatric patients estimated by the population pharmacokinetic analysis was 4.7 L/h (%CV, 41%). Mean platinum pharmacokinetic parameters in ultrafiltrate were Cmax of 0.75 ± 0.24 mcg/mL, AUC0-48h of 7.52 ± 5.07 mcg•h/mL and AUCinf of 8.83 ± 1.57 mcg•h/mL at 85 mg/m2 of oxaliplatin and Cmax of 1.10 ± 0.43 mcg/mL, AUC0-48h of 9.74 ± 2.52 mcg•h/mL and AUCinf of 17.3 ± 5.34 mcg•h/mL at 130 mg/m2 of oxaliplatin.
8.5 Geriatric Use
In the adjuvant treatment trial [see Clinical Studies (14.1)], 400 patients who received oxaliplatin with fluorouracil/leucovorin were greater than or equal to 65 years. The effect of oxaliplatin in patients greater than or equal to 65 years was not conclusive. Patients greater than or equal to 65 years receiving oxaliplatin experienced more diarrhea and grade 3-4 neutropenia (45% vs 39%) compared to patients less than 65 years.
In the previously untreated advanced colorectal cancer trial [see Clinical Studies (14.2)], 99 patients who received oxaliplatin with fluorouracil and leucovorin were greater than or equal to 65 years. The same efficacy improvements in response rate, time to tumor progression, and overall survival were observed in the greater than or equal to 65 years patients as in the overall study population. Adverse reactions were similar in patients less than 65 and greater than or equal to 65 years, but older patients may have been more susceptible to diarrhea, dehydration, hypokalemia, leukopenia, fatigue, and syncope.
In the previously treated advanced colorectal cancer trial [see Clinical Studies (14.3)], 55 patients who received oxaliplatin with fluorouracil and leucovorin were greater than or equal to 65 years. No overall differences in effectiveness were observed between these patients and younger adults. Adverse reactions were similar in patients less than 65 and greater than or equal to 65 years, but older patients may have been more susceptible to diarrhea, dehydration, hypokalemia, and fatigue.
No significant effect of age on the clearance of ultrafiltrable platinum has been observed [see Clinical Pharmacology (12.3)].
5.6 Hepatotoxicity
In the adjuvant treatment trial, increased transaminases (57% vs 34%) and alkaline phosphatase (42% vs 20%) occurred more commonly in the oxaliplatin arm than in the fluorouracil/leucovorin arm [see Adverse Reactions (6.1)]. The incidence of increased bilirubin was similar on both arms. Changes noted on liver biopsies include: peliosis, nodular regenerative hyperplasia or sinusoidal alterations, perisinusoidal fibrosis, and veno-occlusive lesions.
Consider evaluating patients who develop abnormal liver tests or portal hypertension, which cannot be explained by liver metastases, for hepatic vascular disorders. Monitor liver function tests at baseline, before each subsequent cycle, and as clinically indicated.
5.8 Rhabdomyolysis
Rhabdomyolysis, including fatal cases, has been reported with oxaliplatin [see Adverse Reactions (6.2)]. Permanently discontinue oxaliplatin for any signs or symptoms of rhabdomyolysis.
4 Contraindications
Oxaliplatin injection is contraindicated in patients with a history of a hypersensitivity reaction to oxaliplatin or other platinum-based drugs. Reactions have included anaphylaxis [see Warnings and Precautions (5.1)].
6 Adverse Reactions
The following clinically significant adverse reactions are described elsewhere in labeling:
- Hypersensitivity Reactions [see Warnings and Precautions (5.1)]
- Peripheral Sensory Neuropathy [see Warnings and Precautions (5.2)]
- Severe Myelosuppression [see Warnings and Precautions (5.3)]
- Posterior Reversible Encephalopathy Syndrome [see Warnings and Precautions (5.4)]
- Pulmonary Toxicity [see Warnings and Precautions (5.5)]
- Hepatotoxicity [see Warnings and Precautions (5.6)]
- QT Interval Prolongation and Ventricular Arrhythmias [see Warnings and Precautions (5.7)]
- Rhabdomyolysis [see Warnings and Precautions (5.8)]
- Hemorrhage [see Warnings and Precautions (5.9)]
12.2 Pharmacodynamics
A pharmacodynamic relationship between platinum ultrafiltrate levels and clinical safety and effectiveness has not been established.
12.3 Pharmacokinetics
The reactive oxaliplatin derivatives are present as a fraction of the unbound platinum in plasma ultrafiltrate. After a single 2-hour intravenous infusion of oxaliplatin at a dose of 85 mg/m2, pharmacokinetic parameters expressed as ultrafiltrable platinum were Cmax of 0.814 mcg/mL and volume of distribution of 440 L.
Interpatient and intrapatient variability in ultrafiltrable platinum exposure (AUC0-48hr) assessed over 3 cycles was 23% and 6%, respectively.
2.1 Recommended Dosage
Administer oxaliplatin injection in combination with fluorouracil and leucovorin every 2 weeks.
- For adjuvant treatment, continue treatment for up to 12 cycles or unacceptable toxicity.
- For advanced colorectal cancer, continue treatment until disease progression or unacceptable toxicity.
5.5 Pulmonary Toxicity
Oxaliplatin has been associated with pulmonary fibrosis (less than 1% of patients), which may be fatal [see Adverse Reactions (6.1)].
In the adjuvant treatment trial, the combined incidence of cough and dyspnea was 7.4% (any grade), including less than 1% (grade 3) in the oxaliplatin arm. One patient died from eosinophilic pneumonia in the oxaliplatin arm.
In the previously untreated advanced colorectal cancer trial, the combined incidence of cough, dyspnea, and hypoxia was 43% (any grade), including 7% (grade 3-4) in the oxaliplatin with fluorouracil/leucovorin arm.
In case of unexplained respiratory symptoms, such as non-productive cough, dyspnea, crackles, or radiological pulmonary infiltrates, withhold oxaliplatin until further pulmonary investigation excludes interstitial lung disease or pulmonary fibrosis. Permanently discontinue oxaliplatin for confirmed interstitial lung disease or pulmonary fibrosis.
1 Indications and Usage
Oxaliplatin Injection, in combination with infusional fluorouracil and leucovorin, is indicated for:
- adjuvant treatment of stage III colon cancer in patients who have undergone complete resection of the primary tumor.
- treatment of advanced colorectal cancer.
12.1 Mechanism of Action
Oxaliplatin undergoes nonenzymatic conversion in physiologic solutions to active derivatives via displacement of the labile oxalate ligand. Several transient reactive species are formed, including monoaquo and diaquo DACH platinum, which covalently bind with macromolecules. Both inter-and intrastrand Pt-DNA crosslinks are formed. Crosslinks are formed between the N7 positions of two adjacent guanines (GG), adjacent adenine-guanines (AG), and guanines separated by an intervening nucleotide (GNG). These crosslinks inhibit DNA replication and transcription. Cytotoxicity is cell-cycle nonspecific.
In vivo studies have shown antitumor activity of oxaliplatin against colon carcinoma. In combination with fluorouracil, oxaliplatin exhibits in vitro and in vivo antiproliferative activity greater than either compound alone in several tumor models (HT29 [colon], GR [mammary], and L1210 [leukemia]).
5 Warnings and Precautions
- Peripheral Sensory Neuropathy: Acute and delayed neuropathy can occur. Avoid topical application of ice. Reduce the dose or permanently discontinue oxaliplatin as recommended. (5.2)
- Severe Myelosuppression: Delay oxaliplatin until neutrophils are greater than or equal to 1.5 x 109/L and platelets are greater than or equal to 75 x 109/L. Withhold oxaliplatin for sepsis or septic shock. Dose reduce after recovery from grade 4 neutropenia, febrile neutropenia, or grade 3-4 thrombocytopenia as recommended. (5.3)
- Posterior Reversible Encephalopathy Syndrome (PRES): Permanently discontinue oxaliplatin in patients who develop PRES. (5.4)
- Pulmonary Toxicity: Withhold oxaliplatin until investigation excludes interstitial lung disease or pulmonary fibrosis. (5.5)
- Hepatotoxicity: Monitor liver function tests at baseline, before each subsequent cycle, and as clinically indicated. (5.6)
- QT Interval Prolongation: Avoid in patients with congenital long QT syndrome. Monitor electrocardiograms in patients with congestive heart failure, bradyarrhythmias, and electrolyte abnormalities, and in patients taking drugs known to prolong the QT interval. Correct electrolyte abnormalities prior to initiating oxaliplatin and periodically during treatment. (5.7)
- Rhabdomyolysis: Permanently discontinue oxaliplatin if rhabdomyolysis occurs. (5.8)
- Hemorrhage: Increase frequency of monitoring in patients who are receiving oxaliplatin with fluorouracil/leucovorin and oral anticoagulants. (5.9)
- Embryo-Fetal Toxicity: Can cause fetal harm. Advise pregnant women of the potential risk to a fetus. Advise males and females of reproductive potential to use an effective method of contraception. (5.10, 8.1, 8.3)
5.10 Embryo Fetal Toxicity
Based on findings from animal studies and its mechanism of action, oxaliplatin can cause fetal harm when administered to a pregnant woman. The available human data do not establish the presence or absence of major birth defects or miscarriage related to the use of oxaliplatin. Reproductive toxicity studies demonstrated adverse effects on embryo-fetal development in rats at maternal doses that were below the recommended human dose based on body surface area. Advise pregnant women of the potential risk to a fetus. Advise females of reproductive potential to use effective contraception during treatment with oxaliplatin and for 9 months after the final dose. Advise males with female partners of reproductive potential to use effective contraception during treatment with oxaliplatin and for 6 months after the final dose [see Use in Specific Populations (8.1, 8.3)].
2 Dosage and Administration
- Administer oxaliplatin injection 85 mg/m2 as an intravenous infusion over 120 minutes concurrently with leucovorin over 120 minutes in separate bags, followed by fluorouracil on Day 1 of each 14-day cycle. Administer fluorouracil and leucovorin on Day 2 as recommended. (2.1)
- Adjuvant Treatment: Continue treatment for up to 12 cycles or unacceptable toxicity. (2.1)
- Advanced Colorectal Cancer: Continue treatment until disease progression or unacceptable toxicity. (2.1)
5.3 Severe Myelosuppression
Grade 3 or 4 neutropenia occurred in 41% to 44% of patients with colorectal cancer who received oxaliplatin with fluorouracil/leucovorin. Sepsis, neutropenic sepsis and septic shock, including fatal outcomes, occurred in patients who received oxaliplatin [see Adverse Reactions (6.1, 6.2)].
Grade 3 or 4 thrombocytopenia occurred in 2% to 5% of patients with colorectal cancer who received oxaliplatin with fluorouracil/leucovorin.
Monitor complete blood cell count at baseline, before each subsequent cycle and as clinically indicated. Delay oxaliplatin until neutrophils are greater than or equal to 1.5 x 109/L and platelets are greater than or equal to 75 x 109/L. Withhold oxaliplatin for sepsis or septic shock. Dose reduce oxaliplatin after recovery from grade 4 neutropenia, febrile neutropenia or grade 3-4 thrombocytopenia as recommended [see Dosage and Administration (2.2)].
7.3 Use With Anticoagulants
Prolonged prothrombin time and INR occasionally associated with hemorrhage have been reported in patients who received oxaliplatin with fluorouracil/leucovorin while on anticoagulants [see Warnings and Precautions (5.9), Adverse Reactions (6.2)]. Increase frequency of monitoring in patients who are receiving oxaliplatin with fluorouracil/leucovorin and oral anticoagulants.
3 Dosage Forms and Strengths
Oxaliplatin Injection, USP: 50 mg (5 mg per mL) or 100 mg (5 mg per mL) clear, colorless solution in a single-dose vial.
6.2 Postmarketing Experience
The following adverse reactions have been identified during postapproval use of oxaliplatin. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
- General: angioedema, anaphylactic shock
- Cardiovascular: QT prolongation leading to ventricular arrhythmias, including fatal torsade de pointes; bradyarrhythmia
- Neurological: loss of deep tendon reflexes, dysarthria, Lhermitte's sign, cranial nerve palsies, fasciculations, convulsion
- Hearing and vestibular system: deafness
- Infections: septic shock, including fatal outcomes
- Infusion-related reactions and hypersensitivity reactions: laryngospasm
- Hepatic and gastrointestinal: severe diarrhea/vomiting resulting in hypokalemia, colitis (including Clostridium difficile diarrhea), metabolic acidosis, ileus, intestinal obstruction, pancreatitis, sinusoidal obstruction syndrome, perisinusoidal fibrosis which rarely may progress, focal nodular hyperplasia, esophagitis
- Musculoskeletal and connective tissue: rhabdomyolysis, including fatal outcomes
- Platelet, bleeding, and clotting disorders: immuno-allergic thrombocytopenia, prolonged prothrombin time and INR in patients receiving anticoagulants
- Blood disorders: secondary leukemia
- Red blood cell: hemolytic uremic syndrome, immuno-allergic hemolytic anemia
- Renal: acute tubular necrosis, acute interstitial nephritis, acute renal failure
- Respiratory: interstitial lung diseases (sometimes fatal) and pneumonia (including fatal outcomes)
- Vision: decrease of visual acuity, visual field disturbance, optic neuritis and transient vision loss (reversible following treatment discontinuation)
- Injury, poisoning, and procedural complications: fall-related injuries
8 Use in Specific Populations
- Females: Advise female patients of reproductive potential to use effective contraception while receiving oxaliplatin injection and for 9 months after the final dose. (8.3)
- Males: Based on its mechanism action as a genotoxic drug, advise males with female partners of reproductive potential to use effective contraception while receiving oxaliplatin injection and for 6 months after the final dose [see Nonclinical Toxicology (13.1)].
5.1 Hypersensitivity Reactions
Serious and fatal hypersensitivity reactions, including anaphylaxis, can occur with oxaliplatin within minutes of administration and during any cycle. Grade 3-4 hypersensitivity reactions, including anaphylaxis, occurred in 2% to 3% of patients with colon cancer who received oxaliplatin. Hypersensitivity reactions, including rash, urticaria, erythema, pruritus, and rarely, bronchospasm and hypotension, were similar in nature and severity to those reported with other platinum-based drugs.
Oxaliplatin is contraindicated in patients with hypersensitivity reactions to platinum-based drugs [see Contraindications (4)]. Immediately and permanently discontinue oxaliplatin for hypersensitivity reactions and administer appropriate treatment for management of hypersensitivity reactions.
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
More than 1100 patients with stage II or III colon cancer and more than 4,000 patients with advanced colorectal cancer were treated in trials with oxaliplatin. The most common adverse reactions in patients with stage II or III colon cancer receiving adjuvant treatment were peripheral sensory neuropathy, neutropenia, thrombocytopenia, anemia, nausea, increase in transaminases and alkaline phosphatase, diarrhea, emesis, fatigue and stomatitis. The most common adverse reactions in previously untreated and treated patients with advanced colorectal cancer were peripheral sensory neuropathies, fatigue, neutropenia, nausea, emesis, and diarrhea.
17 Patient Counseling Information
5.2 Peripheral Sensory Neuropathy
Oxaliplatin can cause acute and delayed neuropathy. Reduce the dose or permanently discontinue oxaliplatin for persistent neurosensory reactions based on the severity of the adverse reaction [see Dosage and Administration (2.2)].
7.2 Use With Nephrotoxic Products
Because platinum-containing species are eliminated primarily through the kidney, clearance of these products may be decreased by coadministration of potentially nephrotoxic compounds [see Clinical Pharmacology (12.3)]. Avoid coadministration of oxaliplatin with medicinal products known to cause nephrotoxicity.
2.4 Preparation and Administration
- Oxaliplatin injection is a cytotoxic drug. Follow applicable special handling and disposal procedures.1
- Do not freeze.
- Protect the concentrated solution from light.
- Dilute concentrated solution with 250 to 500 mL of 5% Dextrose Injection, USP. Do not dilute with sodium chloride solution or other chloride-containing solutions.
- Store diluted solution for no more than 6 hours at room temperature (20°C to 25°C [68°F to 77°F]) or 24 hours under refrigeration (2°C to 8°C [36°F to 46°F]). Protection from light is not required.
- Visually inspect for particulate matter and discoloration prior to administration and discard if present.
- Do not mix oxaliplatin injection or administer oxaliplatin injection through the same infusion line concurrently with alkaline medications or media (such as basic solutions of fluorouracil).
- Flush the infusion line with 5% Dextrose Injection, USP prior to administration of any concomitant medication.
- Do not use needles or intravenous administration sets containing aluminum parts for the preparation or mixing of oxaliplatin injection. Aluminum has been reported to cause degradation of platinum compounds.
- Administer oxaliplatin injection as an intravenous infusion over 120 minutes concurrently with leucovorin over 120 minutes in separate bags.
8.6 Patients With Renal Impairment
The AUC of unbound platinum in plasma ultrafiltrate was increased in patients with renal impairment [see Clinical Pharmacology (12.3)]. No dose reduction is recommended for patients with mild (creatinine clearance 50 to 79 mL/min) or moderate (creatinine clearance 30 to 49 mL/min) renal impairment, calculated by Cockcroft-Gault equation. Reduce the dose of oxaliplatin in patients with severe renal impairment (creatinine clearance less than 30 mL/min) [see Dosage and Administration (2.3)].
16 How Supplied/storage and Handling
Oxaliplatin Injection, USP is supplied as follows:
| NDC | Oxaliplatin Injection, USP (5 mg per mL) | Package Factor |
| 25021-233-10 | 50 mg per 10 mL Single-Dose Vial | 1 vial per carton |
| 25021-233-20 | 100 mg per 20 mL Single-Dose Vial | 1 vial per carton |
Water for Injection, USP is present as an inactive ingredient. Tartaric Acid, NF and Sodium Hydroxide, NF are used in combination as a buffering system.
Store at 20° to 25°C (68° to 77°F); excursions permitted between 15° and 30°C (59° and 86°F). [See USP Controlled Room Temperature.]
Do not freeze.
Protect from light. Retain in carton until time of use.
Discard unused portion.
Oxaliplatin Injection, USP is a cytotoxic drug. Follow applicable special handling and disposal procedures.1 The use of gloves is recommended. If a solution of Oxaliplatin Injection, USP contacts the skin, wash the skin immediately and thoroughly with soap and water. If Oxaliplatin Injection, USP contacts the mucous membranes, flush thoroughly with water.
Sterile, Nonpyrogenic, Preservative-free.
The container closure is not made with natural rubber latex.
7.1 Drugs That Prolong the Qt Interval
QT interval prolongation and ventricular arrhythmias can occur with oxaliplatin [see Warnings and Precautions (5.7)]. Avoid coadministration of oxaliplatin with medicinal products with a known potential to prolong the QT interval.
2.2 Dose Modifications for Adverse Reactions
Prolongation of infusion time for oxaliplatin injection from 2 hours to 6 hours may mitigate acute toxicities, such as non-life-threatening infusion-related reactions.
Permanently discontinue oxaliplatin injection for any of the following:
- Hypersensitivity Reactions [see Warnings and Precautions (5.1)]
- Posterior reversible encephalopathy syndrome (PRES) [see Warnings and Precautions (5.4)]
- Confirmed interstitial lung disease or pulmonary fibrosis [see Warnings and Precautions (5.5)]
- Rhabdomyolysis [see Warnings and Precautions (5.8)]
Refer to the fluorouracil and leucovorin prescribing information for dosage modifications for adverse reactions.
5.4 Posterior Reversible Encephalopathy Syndrome
PRES occurred in less than 0.1% of patients across clinical trials [see Adverse Reactions (6.1)]. Signs and symptoms of PRES can include headache, altered mental functioning, seizures, abnormal vision from blurriness to blindness, associated or not with hypertension. Confirm the diagnosis of PRES with magnetic resonance imaging. Permanently discontinue oxaliplatin in patients who develop PRES.
14.3 Previously Treated Advanced Colorectal Cancer
The efficacy of oxaliplatin in combination with fluorouracil (FU)/leucovorin (LV) was evaluated in a multicenter, open-label, randomized, three-arm controlled trial was conducted in the US and Canada in patients with advanced colorectal cancer who had relapsed/progressed during or within 6 months of first-line treatment with bolus fluorouracil/leucovorin and irinotecan (A multicenter, open-label, randomized, three-arm study of 5-fluorouracil (5-FU) + leucovorin (LV) or oxaliplatin or a combination of 5-FU/LV + oxaliplatin as second-line treatment of metastatic colorectal carcinoma: NCT00008281). Patients were randomized to one of three regimens; the dosing regimens are presented in Table 22. Eligible patients were at least 18 years of age, had unresectable, measurable, histologically proven colorectal adenocarcinoma, with a Karnofsky performance status (KPS) greater than 50%. Patients had to have aspartate transaminase (AST), alanine transaminase (ALT) and alkaline phosphatase less than or equal to 2x upper limit of normal (ULN), unless liver metastases were present and documented at baseline by CT or MRI scan, in which case less than or equal to 5 x ULN was permitted. Prior radiotherapy was permitted if it had been completed at least 3 weeks before randomization. The main efficacy outcome measure was 3-year disease-free survival (DFS) and an additional outcome measure was overall survival (OS).
| Treatment Arm | Dose | Regimen |
| Oxaliplatin + FU/LV (N=152) |
Day 1:
Oxaliplatin: 85 mg/m2 (2-hour infusion) + LV 200 mg/m2 (2-hour infusion), followed by FU: 400 mg/m2 (bolus), 600 mg/m2 (22-hour infusion) Day 2: LV 200 mg/m2 (2-hour infusion), followed by FU: 400 mg/m2 (bolus), 600 mg/m2 (22-hour infusion) |
every 2 weeks |
| FU/LV (N=151) |
Day 1: LV 200 mg/m2 (2-hour infusion), followed by FU: 400 mg/m2 (bolus), 600 mg/m2 (22-hour infusion) Day 2: LV 200 mg/m2 (2-hour infusion), followed by FU: 400 mg/m2 (bolus), 600 mg/m2 (22-hour infusion) |
every 2 weeks |
| Oxaliplatin (N=156) |
Day 1: Oxaliplatin 85 mg/m2 (2-hour infusion) | every 2 weeks |
Patients must have had at least one unidimensional lesion measuring greater than or equal to 20 mm using conventional CT or MRI scans or greater than or equal to 10 mm using a spiral CT scan. Tumor response and progression were assessed every 3 cycles (6 weeks) using the Response Evaluation Criteria in Solid Tumors (RECIST) until radiological documentation of progression or for 13 months following the first dose of study drug(s), whichever came first. Confirmed responses were based on two tumor assessments separated by at least 4 weeks. Baseline characteristics are shown in Table 23.
| Oxaliplatin + | Oxaliplatin | FU/LV | |
| FU/LV | N=156 | N=151 | |
| N=152 | |||
| Sex: Male (%) | 57.2 | 60.9 | 54.3 |
| Female (%) | 42.8 | 39.1 | 45.7 |
| Median age (years) | 59.0 | 61.0 | 60.0 |
| Range | 22 to 88 | 27 to 79 | 21 to 80 |
| Race (%) | |||
| Caucasian | 88.8 | 84.6 | 87.4 |
| Black | 5.9 | 7.1 | 7.9 |
| Asian | 2.6 | 2.6 | 1.3 |
| Other | 2.6 | 5.8 | 3.3 |
| KPS (%) | |||
| 70 to 100 | 95.4 | 92.3 | 94.7 |
| 50 to 60 | 2.0 | 4.5 | 2.6 |
| Not reported | 2.6 | 3.2 | 2.6 |
| Prior radiotherapy (%) | 25.0 | 19.2 | 25.2 |
| Prior pelvic radiation (%) | 21.1 | 13.5 | 18.5 |
| Number of metastatic sites (%) | |||
| 1 | 25.7 | 31.4 | 27.2 |
| ≥2 | 74.3 | 67.9 | 72.2 |
| Liver involvement (%) | |||
| Liver only | 18.4 | 25.6 | 22.5 |
| Liver + other | 53.3 | 59.0 | 60.3 |
The median number of cycles administered per patient was 6 for the oxaliplatin and fluorouracil/leucovorin combination and 3 each for fluorouracil/leucovorin alone and oxaliplatin alone. Patients treated with the combination of oxaliplatin and fluorouracil/leucovorin had an increased response rate compared to patients given fluorouracil/leucovorin or oxaliplatin alone. Efficacy results are summarized in Tables 24 and 25.
| Best Response | Oxaliplatin + | Oxaliplatin | FU/LV |
| FU/LV | N=156 | N=151 | |
| N=152 | |||
| Complete Response | 0 | 0 | 0 |
| Partial Response | 13 (9%) | 2 (1%) | 0 |
| P-value | 0.0002 FU/LV vs Oxaliplatin + FU/LV | ||
| 95% CI | 4.6%, 14.2% | 0.2%, 4.6% | 0, 2.4% |
|
*This is not an ITT analysis. Events were limited to radiographic disease progression documented by independent review of radiographs. Clinical progression was not included in this analysis, and 18% of patients were excluded from the analysis based on unavailability of the radiographs for independent review. |
|||
| Arm | Oxaliplatin + | Oxaliplatin | FU/LV |
| FU/LV | N=156 | N=151 | |
| N=152 | |||
| Number of progressors | 50 | 101 | 74 |
| Number of patients with no radiological evaluation beyond baseline | 17 (11%) | 16 (10%) | 22 (15%) |
| Median TTP (months) | 4.6 | 1.6 | 2.7 |
| 95% CI | 4.2, 6.1 | 1.4, 2.7 | 1.8, 3.0 |
At the time of the interim analysis 49% of the radiographic progression events had occurred. In this interim analysis an estimated 2-month increase in median time to radiographic progression was observed compared to fluorouracil/leucovorin alone.
14.2 Previously Untreated Advanced Colorectal Cancer
The efficacy of oxaliplatin in combination with fluorouracil (FU)/leucovorin (LV) was evaluated in a North American, multicenter, open-label, randomized, active-controlled trial (A Randomized Phase III Trial of Three Different Regimens of CPT-11 Plus 5-Fluorouracil and Leucovorin Compared to 5-Fluorouracil and Leucovorin in Patients with Advanced Adenocarcinoma of the Colon and Rectum; NCT00003594). The trial included 7 arms at different times during its conduct, four of which were closed due to either changes in the standard of care, toxicity, or simplification. During the trial, the control arm was changed to irinotecan with fluorouracil/leucovorin.
The results reported below compared the efficacy of oxaliplatin with fluorouracil/leucovorin and oxaliplatin with irinotecan to an approved control regimen of irinotecan with fluorouracil/leucovorin in 795 concurrently randomized patients previously untreated for locally advanced or metastatic colorectal cancer. Table 19 presents the dosing regimens for the three arms. After completion of enrollment, the dose of irinotecan with fluorouracil/leucovorin was decreased due to toxicity.
Eligible patients were at least 18 years of age; had known locally advanced, locally recurrent, or metastatic colorectal adenocarcinoma not curable by surgery or amenable to radiation therapy; with an Eastern Cooperative Oncology Group (ECOG) performance status ≤0, 1, or 2. Patients had to have absolute neutrophil count (ANC) greater than or equal to 1.5 x 109/L, platelets greater than or equal to 100 x 109/L, hemoglobin greater than or equal to 9.0 g/dL, creatinine less than or equal to 1.5 x upper limit of normal (ULN), total bilirubin less than or equal to 1.5 mg/dL, aspartate transaminase (AST) less than or equal to 5 x ULN, and alkaline phosphatase less than or equal to 5 x ULN. Patients may have received adjuvant treatment for resected Stage II or III disease without recurrence within 12 months. Randomization was stratified by ECOG performance status (0, 1 vs 2), prior adjuvant chemotherapy (yes vs no), prior immunotherapy (yes vs no), and age (less than 65 vs greater than or equal to 65 years). Although no post study treatment was specified in the protocol, 65% to 72% of patients received additional post study chemotherapy after study treatment discontinuation on all arms. Fifty-eight percent of patients on the oxaliplatin with fluorouracil/leucovorin arm received an irinotecan-containing regimen and 23% of patients on the irinotecan with fluorouracil/leucovorin arm received an oxaliplatin-containing regimen.
The main efficacy outcome measure was 3-year disease-free survival (DFS) and additional efficacy outcome measures were overall survival (OS).
| Treatment Arm | Dose | Regimen |
| Oxaliplatin + FU/LV (FOLFOX4) (N=267) |
Day 1:
Oxaliplatin: 85 mg/m2 (2-hour infusion) + LV 200 mg/m2 (2-hour infusion), followed by FU: 400 mg/m2 (bolus), 600 mg/m2 (22-hour infusion) Day 2: LV 200 mg/m2 (2-hour infusion), followed by FU: 400 mg/m2 (bolus), 600 mg/m2 (22-hour infusion) |
every 2 weeks |
| Irinotecan + FU/LV (IFL) (N=264) |
Day 1: Irinotecan 125 mg/m2 as a 90–min infusion + LV 20 mg/m2 | every 6 weeks |
| as a 15-min infusion or intravenous push, followed by | ||
| FU 500 mg/m2 intravenous bolus weekly x 4 | ||
| Oxaliplatin + Irinotecan (IROX) (N=264) |
Day 1: Oxaliplatin: 85 mg/m2 intravenous (2-hour infusion) + irinotecan 200 mg/m2 intravenous over 30 minutes | every 3 weeks |
Table 20 presents the baseline characteristics.
| Oxaliplatin + | Irinotecan + | Oxaliplatin + | |
| FU/LV | FU/LV | Irinotecan | |
| N=267 | N=264 | N=264 | |
| Sex: Male (%) | 58.8 | 65.2 | 61.0 |
| Female (%) | 41.2 | 34.8 | 39.0 |
| Median age (years) | 61.0 | 61.0 | 61.0 |
| <65 years of age (%) | 61 | 62 | 63 |
| ≥65 years of age (%) | 39 | 38 | 37 |
| ECOG (%) | |||
| 0-1 | 94.4 | 95.5 | 94.7 |
| 2 | 5.6 | 4.5 | 5.3 |
| Involved organs (%) | |||
| Colon only | 0.7 | 0.8 | 0.4 |
| Liver only | 39.3 | 44.3 | 39.0 |
| Liver + other | 41.2 | 38.6 | 40.9 |
| Lung only | 6.4 | 3.8 | 5.3 |
| Other (including lymph nodes) | 11.6 | 11.0 | 12.9 |
| Not reported | 0.7 | 1.5 | 1.5 |
| Prior radiation (%) | 3.0 | 1.5 | 3.0 |
| Prior surgery (%) | 74.5 | 79.2 | 81.8 |
| Prior adjuvant (%) | 15.7 | 14.8 | 15.2 |
The median number of cycles administered per patient was 10 (23.9 weeks) for the oxaliplatin plus fluorouracil/leucovorin regimen, 4 (23.6 weeks) for the irinotecan plus fluorouracil/leucovorin regimen, and 7 (21.0 weeks) for the oxaliplatin plus irinotecan regimen.
Patients who received oxaliplatin with fluorouracil/leucovorin had a significantly longer time to tumor progression based on investigator assessment, longer OS, and a significantly higher confirmed response rate based on investigator assessment compared to patients who received irinotecan with fluorouracil/leucovorin. Efficacy results are summarized in Table 21 and Figure 3.
|
*A hazard ratio of less than 1 favors Oxaliplatin + Infusional fluorouracil/leucovorin |
|||
|
†Compared to irinotecan plus fluorouracil/leucovorin (IFL) arm |
|||
|
‡ Based on all patients with measurable disease at baseline |
|||
|
The numbers in the response rate and TTP analysis are based on unblinded investigator assessment. |
|||
|
Oxaliplatin +
FU/LV N=267 |
Irinotecan + | Oxaliplatin + | |
| FU/LV | Irinotecan | ||
| N=264 | N=264 | ||
| Survival (ITT) | |||
| Number of deaths (%) | 155 (58.1) | 192 (72.7) | 175 (66.3) |
| Median survival (months) | 19.4 | 14.6 | 17.6 |
| Hazard ratio (95% CI)* | 0.65 (0.53, 0.80)† | - | |
| P-value | <0.0001† | - | |
| TTP (ITT, investigator assessment) | |||
| Percentage of progressors | 82.8 | 81.8 | 89.4 |
| Median TTP (months) | 8.7 | 6.9 | 6.5 |
| Hazard ratio (95% CI)* | 0.74 (0.61, 0.89)† | - | |
| P-value | 0.0014† | - | |
| Response Rate (investigator assessment) ‡ | |||
| Patients with measurable disease | 210 | 212 | 215 |
| Complete response, N (%) | 13 (6.2) | 5 (2.4) | 7 (3.3) |
| Partial response, N (%) | 82 (39.0) | 64 (30.2) | 67 (31.2) |
| Complete and partial response, N (%) | 95 (45.2) | 69 (32.5) | 74 (34.4) |
| 95% CI | (38.5, 52.0) | (26.2, 38.9) | (28.1, 40.8) |
| P-value | 0.0080† | - |
Figure 3: Kaplan-Meier Curves for Overall Survival in Previously Untreated Advanced Colorectal Cancer Trial
* Log rank test comparing oxaliplatin plus FU/LV to irinotecan plus FU/LV.
In descriptive subgroup analyses, the improvement in overall survival (OS) for oxaliplatin with fluorouracil/leucovorin compared to irinotecan with fluorouracil/leucovorin appeared to be maintained across age groups, prior adjuvant treatment, number of organs involved and both sexes; however, the effect appeared larger among women than men.
5.7 Qt Interval Prolongation and Ventricular Arrhythmias
QT prolongation and ventricular arrhythmias, including fatal torsade de pointes, have been reported with oxaliplatin [see Adverse Reactions (6.2)].
Avoid oxaliplatin in patients with congenital long QT syndrome. Monitor electrocardiograms (ECG) in patients with congestive heart failure, bradyarrhythmias, and electrolyte abnormalities and in patients taking drugs known to prolong the QT interval, including Class Ia and III antiarrhythmics [see Drug Interactions (7.1)]. Monitor and correct electrolyte abnormalities prior to initiating oxaliplatin and periodically during treatment.
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Long-term animal studies have not been performed to evaluate the carcinogenic potential of oxaliplatin. Oxaliplatin was not mutagenic to bacteria (Ames test) but was mutagenic to mammalian cells in vitro (L5178Y mouse lymphoma assay). Oxaliplatin was clastogenic both in vitro (chromosome aberration in human lymphocytes) and in vivo (mouse bone marrow micronucleus assay).
In a fertility study, male rats were given oxaliplatin at 0, 0.5, 1, or 2 mg/kg/day for five days every 21 days for a total of three cycles prior to mating with females that received two cycles of oxaliplatin on the same schedule. A dose of 2 mg/kg/day (less than one-seventh the recommended human dose on a body surface area basis) did not affect pregnancy rate, but resulted in 97% postimplantation loss (increased early resorptions, decreased live fetuses, decreased live births), and delayed growth (decreased fetal weight).
Testicular damage, characterized by degeneration, hypoplasia, and atrophy, was observed in dogs administered oxaliplatin at 0.75 mg/kg/day (approximately one-sixth of the recommended human dose on a body surface area basis) x 5 days every 28 days for three cycles. A no effect level was not identified.
2.3 Dose Modifications for Patients With Renal Impairment
Warning: Hypersensitivity Reactions, Including Anaphylaxis
Serious and fatal hypersensitivity adverse reactions, including anaphylaxis, can occur with Oxaliplatin Injection within minutes of administration and during any cycle. Oxaliplatin Injection is contraindicated in patients with hypersensitivity reactions to oxaliplatin and other platinum-based drugs [see Contraindications (4)] . Immediately and permanently discontinue Oxaliplatin Injection for hypersensitivity reactions and administer appropriate treatment for management of the hypersensitivity reaction [see Warnings and Precautions (5.1)] .
14.1 Adjuvant Treatment With Oxaliplatin in Combination With Fluorouracil and Leucovorin
The efficacy of oxaliplatin in combination with fluorouracil (FU)/leucovorin (LV) was evaluated in an international, multicenter, randomized (1:1) trial (The Multicenter International Study of Oxaliplatin/5-Fluorouracil/Leucovorin in the Adjuvant Treatment of Colon Cancer [MOSAIC], NCT00275210) in patients with stage II (Dukes' B2) or III (Dukes' C) colon cancer who had undergone complete resection of the primary tumor. Patients were randomized to receive oxaliplatin with fluorouracil/leucovorin or fluorouracil/leucovorin alone for a total of 6 months (i.e., 12 cycles). Table 14 shows the dosing regimens for the two arms.
Eligible patients were between 18 and 75 years of age, had histologically proven stage II (T3-T4 N0 M0; Dukes' B2) or III (any T N1-2 M0; Dukes' C) colon carcinoma (with the inferior pole of the tumor above the peritoneal reflection, i.e., greater than or equal to 15 cm from the anal margin) and had undergone (within 7 weeks prior to randomization) complete resection of the primary tumor without gross or microscopic evidence of residual disease and carcino-embryogenic antigen (CEA) less than 10 ng/mL. Additional eligibility criteria were no prior chemotherapy, immunotherapy or radiotherapy; Eastern Cooperative Oncology Group performance status of 0, 1, or 2 (Karnofsky Performance Status greater than or equal to 60%); no pre-existing neuropathy; and absolute neutrophil count (ANC) greater than or equal to 1.5 x 109/L, platelets greater than or equal to 100 x 109/L, serum creatinine less than or equal to 1.25 x upper limit normal (ULN), total bilirubin less than 2 x ULN, and aspartate transaminase (AST)/alanine transaminase (ALT) less than 2 x ULN. The major efficacy outcome was 3-year disease-free survival (DFS).
| Treatment Arm | Dose | Regimen |
| Oxaliplatin + | Day 1: Oxaliplatin: 85 mg/m2 (2-hour infusion) + LV: 200 mg/m2 (2-hour infusion), followed by FU: 400 mg/m2 (bolus), 600 mg/m2 (22-hour infusion) |
every 2 weeks 12 cycles |
| FU/LV | ||
| (FOLFOX4) | ||
| (N =1123) | Day 2: LV: 200 mg/m2 (2-hour infusion), followed by FU: 400 mg/m2 (bolus), 600 mg/m2 (22-hour infusion) |
|
| Day 1: LV: 200 mg/m2 (2-hour infusion), followed by FU: 400 mg/m2 (bolus), 600 mg/m2 (22-hour infusion) |
every 2 weeks 12 cycles |
|
| FU/LV | ||
| (N=1123) | ||
| Day 2: LV: 200 mg/m2 (2-hour infusion), followed by FU: 400 mg/m2 (bolus), 600 mg/m2 (22-hour infusion) |
||
There were 2246 patients enrolled, of whom 1347 (60%) had Stage III disease. Tables 15 and 16 show the baseline characteristics and exposure to oxaliplatin.
|
Oxaliplatin + Infusional FU/LV |
Infusional FU/LV | |
| N=1123 | N=1123 | |
| Sex: Male (%) | 56.1 | 52.4 |
| Female (%) | 43.9 | 47.6 |
| Median age (years) | 61.0 | 60.0 |
| <65 years of age (%) | 64.4 | 66.2 |
| ≥65 years of age (%) | 35.6 | 33.8 |
| KPS (%) | ||
| 100 | 29.7 | 30.5 |
| 90 | 52.2 | 53.9 |
| 80 | 4.4 | 3.3 |
| 70 | 13.2 | 11.9 |
| ≤60 | 0.6 | 0.4 |
| Primary site (%) | ||
| Colon including cecum | 54.6 | 54.4 |
| Sigmoid | 31.9 | 33.8 |
| Recto sigmoid | 12.9 | 10.9 |
| Other including rectum | 0.6 | 0.9 |
| Bowel obstruction (%) | ||
| Yes | 17.9 | 19.3 |
| Perforation (%) | ||
| Yes | 6.9 | 6.9 |
| Stage at Randomization (%) | ||
| II (T=3,4 N=0, M=0) | 40.1 | 39.9 |
| III (T=any, N=1,2, M=0) | 59.6 | 59.3 |
| IV (T=any, N=any, M=1) | 0.4 | 0.8 |
| Staging - T (%) | ||
| T1 | 0.5 | 0.7 |
| T2 | 4.5 | 4.8 |
| T3 | 76.0 | 75.9 |
| T4 | 19.0 | 18.5 |
| Staging - N (%) | ||
| N0 | 40.2 | 39.9 |
| N1 | 39.4 | 39.4 |
| N2 | 20.4 | 20.7 |
| Staging - M (%) | ||
| M1 | 0.4 | 0.8 |
|
Oxaliplatin + Infusional FU/LV N=1108 |
Infusional FU/LV N=1111 |
|
| Median Relative Dose Intensity (%) | ||
| FU | 84.4 | 97.7 |
| Oxaliplatin | 80.5 | N/A |
| Median Number of Cycles | 12 | 12 |
| Median Number of Cycles with Oxaliplatin | 11 | N/A |
The median duration of follow-up was approximately 77 months. In the overall and the stage III colon cancer populations, DFS was statistically significantly improved in the oxaliplatin-containing arm compared to fluorouracil/leucovorin alone; however, a statistically significant improvement in DFS was not observed in Stage II patients. No significant differences in overall survival (OS) were detected in the overall population or those with Stage III disease. Table 17 and Figures 1 and 2 summarize the 5-year DFS rates in the overall randomized population and in patients with stage II and III disease based on an intention-to-treat (ITT) analysis.
|
A hazard ratio of less than 1 favors Oxaliplatin + Infusional FU/LV |
||
|
Data cut off for disease-free survival June 1, 2006 |
||
| Parameter |
Oxaliplatin + Infusional FU/LV |
Infusional FU/LV |
| Overall | ||
| Number of patients | 1123 | 1123 |
| Number of events - relapse or death (%) | 304 (27.1) | 360 (32.1) |
| 5-yr Disease-free survival % (95% CI) | 73.3 (70.7, 76.0) | 67.4 (64.6, 70.2) |
| Hazard ratio (95% CI) | 0.80 (0.68, 0.93) | |
| Stratified Log rank test | p=0.003 | |
| Stage III (Dukes' C) | ||
| Number of patients | 672 | 675 |
| Number of events - relapse or death (%) | 226 (33.6) | 271 (40.1) |
| 5-yr Disease-free survival % (95% CI) | 66.4 (62.7, 70.0) | 58.9 (55.2, 62.7) |
| Hazard ratio (95% CI) | 0.78 (0.65, 0.93) | |
| Log rank test | p=0.005 | |
| Stage II (Dukes' B2) | ||
| Number of patients | 451 | 448 |
| Number of events - relapse or death (%) | 78 (17.3) | 89 (19.9) |
| 5-yr Disease-free survival % (95% CI) | 83.7 (80.2, 87.1) | 79.9 (76.2, 83.7) |
| Hazard ratio (95% CI) | 0.84 (0.62, 1.14) | |
| Log rank test | p=0.258 |
Figure 1: Kaplan-Meier Curves of Disease-Free Survival (cutoff: 1 June 2006) in Adjuvant Treatment Trial – ITT Population
Figure 2: Kaplan-Meier Curves of Disease-Free Survival in Stage III Patients (cutoff: 1 June 2006) in Adjuvant Treatment Trial – ITT Population
Table 18 summarizes the OS results in the overall randomized population and in patients with stage II and III disease, based on the ITT analysis.
|
A hazard ratio of less than 1 favors oxaliplatin + Infusional FU/LV |
||
|
Data cut off for overall survival January 16, 2007 |
||
| Parameter | Oxaliplatin + | Infusional FU/LV |
| Infusional FU/LV | ||
| Overall | ||
| Number of patients | 1123 | 1123 |
| Number of death events (%) | 245 (21.8) | 283 (25.2) |
| Hazard ratio (95% CI) | 0.84 (0.71, 1.00) | |
| Stage III (Dukes' C) | ||
| Number of patients | 672 | 675 |
| Number of death events (%) | 182 (27.1) | 220 (32.6) |
| Hazard ratio (95% CI) | 0.80 (0.65, 0.97) | |
| Stage II (Dukes' B2) | ||
| Number of patients | 451 | 448 |
| Number of death events (%) | 63 (14.0) | 63 (14.1) |
| Hazard ratio (95% CI) | 1.00 (0.70, 1.41) |
Structured Label Content
Section 42229-5 (42229-5)
Day 1
Administer oxaliplatin injection 85 mg/m2 as an intravenous infusion over 120 minutes and leucovorin 200 mg/m2 as an intravenous infusion over 120 minutes at the same time in separate bags, followed by fluorouracil 400 mg/m2 as intravenous bolus over 2 to 4 minutes, followed by fluorouracil 600 mg/m2 as a 22-hour continuous infusion.
Section 42230-3 (42230-3)
FDA-Approved Patient Labeling
|
This Patient Information has been approved by the U.S. Food and Drug Administration. |
|
|
Patient Information
Oxaliplatin (ox-AL-i-PLA-tin) Injection injection, for intravenous use |
|
|
What is the most important information I should know about Oxaliplatin Injection? Oxaliplatin Injection can cause serious allergic reactions, including allergic reactions that can lead to death. Oxaliplatin Injection is a platinum-based medicine. Serious allergic reactions including death can happen in people who take Oxaliplatin Injection and who have had previous allergic reactions to platinum-based medicines. Serious allergic reactions can happen within a few minutes of your Oxaliplatin Injection infusion or any time during your treatment with Oxaliplatin Injection. Get emergency help right away if you:
|
|
|
|
| See “What are the possible side effects of Oxaliplatin Injection?” for information about other serious side effects. |
|
|
What is Oxaliplatin Injection?
Oxaliplatin Injection is an anti-cancer (chemotherapy) medicine that is used with other anti-cancer medicines called fluorouracil and leucovorin to treat people with:
|
|
|
Do not receive Oxaliplatin Injection if you are allergic to oxaliplatin or any of the ingredients in Oxaliplatin Injection or if you are allergic to other platinum-based medicines. See the end of this leaflet for a complete list of the ingredients in Oxaliplatin Injection. Ask your doctor if you are not sure if you have taken a platinum-based medicine. |
|
Before receiving Oxaliplatin Injection, tell your doctor about all of your medical conditions, including if you:
Know the medicines you take. Keep a list of them and show it to your doctor and pharmacist when you get a new medicine. |
|
How will I receive Oxaliplatin Injection?
You will not get Oxaliplatin Injection on Day 2. Leucovorin and fluorouracil will be given the same way as on Day 1. The fluorouracil will be given through your IV with a pump. If you have any problems with the pump or the tube, call your doctor, your nurse, or the person who is responsible for your pump. Do not let anyone other than a healthcare provider touch your infusion pump or tubing. |
|
What should I avoid while receiving Oxaliplatin Injection?
Talk with your doctor and nurse about your level of activity during treatment with Oxaliplatin Injection. Follow their instructions. |
|
|
What are the possible side effects of Oxaliplatin Injection? Oxaliplatin Injection can cause serious side effects, including:
|
|
|
|
|
|
|
|
| The most common side effects of Oxaliplatin Injection include: | |
|
|
|
Oxaliplatin Injection may cause fertility problems in males and females. Talk to your doctor if this is a concern for you. Tell your doctor if you have any side effect that bothers you or that does not go away. These are not all the possible side effects of Oxaliplatin Injection. For more information, ask your doctor or pharmacist. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. |
|
|
How can I reduce the side effects caused by cold temperatures?
|
|
|
General information about the safe and effective use of Oxaliplatin Injection.
Medicines are sometimes prescribed for purposes other than those listed in the Patient Information leaflet. You can ask your doctor or pharmacist for information about Oxaliplatin Injection that is written for health professionals. |
|
|
What are the ingredients in Oxaliplatin Injection?
Active ingredient: Oxaliplatin Inactive ingredient: Water for Injection, USP, Tartaric Acid, NF and Sodium Hydroxide, NF are used as inactive ingredients and/or in combination as a buffering system. sagent ® Mfd. for SAGENT Pharmaceuticals Schaumburg, IL 60173 (USA) Made in China ©2025 Sagent Pharmaceuticals Revised: May 2025 |
Section 51945-4 (51945-4)
PACKAGE LABEL – PRINCIPAL DISPLAY PANEL – Vial Label
NDC 25021-233-10
Rx only
OXALIPLATIN Injection, USP
50 mg per 10 mL (5 mg per mL)
For Intravenous Use Only
10 mL Single-Dose Vial
See package insert for further required dilution
DO NOT MIX OR ADD TO SODIUM CHLORIDE/
CHLORIDE-CONTAINING SOLUTIONS
Caution: Cytotoxic Agent
10 Overdosage (10 OVERDOSAGE)
The maximum dose of oxaliplatin that has been administered in a single infusion is 825 mg. Several cases of overdoses have been reported with oxaliplatin. Adverse reactions observed following an overdosage were grade 4 thrombocytopenia (less than 25,000/mm3) without bleeding, anemia, sensory neuropathy (including paresthesia, dysesthesia, laryngospasm and facial muscle spasms), gastrointestinal disorders (including nausea, vomiting, stomatitis, flatulence, abdomen enlarged and grade 4 intestinal obstruction), grade 4 dehydration, dyspnea, wheezing, chest pain, respiratory failure, severe bradycardia, and death.
Closely monitor patients suspected of receiving an overdose, including for the adverse reactions described above and administer appropriate supportive treatment.
15 References (15 REFERENCES)
- “OSHA Hazardous Drugs.” OSHA. http://www.osha.gov/SLTC/hazardousdrugs/index.html
11 Description (11 DESCRIPTION)
Oxaliplatin is a platinum-based drug with the molecular formula C8H14N2O4Pt and the chemical name of cis-[(1 R,2 R)-1,2-cyclohexanediamine-N,N′] [oxalato(2-)- O,O′] platinum. Oxaliplatin is an organoplatinum complex in which the platinum atom is complexed with 1,2-diaminocyclohexane (DACH) and with an oxalate ligand as a leaving group.
The molecular weight is 397.3. Oxaliplatin is slightly soluble in water at 6 mg/mL, very slightly soluble in methanol, and practically insoluble in ethanol and acetone.
Oxaliplatin Injection, USP, for intravenous use, is supplied in vials containing 50 mg or 100 mg of oxaliplatin as a sterile, preservative-free, aqueous solution at a concentration of 5 mg/mL. Water for Injection, USP is present as an inactive ingredient. Tartaric Acid, NF and Sodium Hydroxide, NF are used in combination as a buffering system.
5.9 Hemorrhage
The incidence of hemorrhage in clinical trials was higher on the oxaliplatin combination arm compared to the fluorouracil/leucovorin arm. These reactions included gastrointestinal bleeding, hematuria, and epistaxis. In the adjuvant treatment trial, 2 patients died from intracerebral hemorrhage [see Adverse Reactions (6.1)].
Prolonged prothrombin time and INR occasionally associated with hemorrhage have been reported in patients who received oxaliplatin with fluorouracil/leucovorin while on anticoagulants [see Adverse Reactions (6.2)]. Increase frequency of monitoring in patients who are receiving oxaliplatin with fluorouracil/leucovorin and oral anticoagulants [see Drug Interactions (7.3)].
Thrombocytopenia and immune-mediated thrombocytopenia have been observed with oxaliplatin. Rapid onset of thrombocytopenia and greater risk of bleeding have been observed in immune-mediated thrombocytopenia. In this case, consider discontinuing oxaliplatin.
8.4 Pediatric Use
The safety and effectiveness of oxaliplatin in pediatrics have not been established. Safety and effectiveness were assessed across 4 open-label studies in 235 patients aged 7 months to 22 years with solid tumors.
In a multicenter, open-label, non-comparative, non-randomized study (ARD5531), oxaliplatin was administered to 43 patients with refractory or relapsed malignant solid tumors, mainly neuroblastoma and osteosarcoma. The dose limiting toxicity (DLT) was sensory neuropathy at a dose of 110 mg/m2. The main adverse reactions were: paresthesia (60%, grade 3-4: 7%), fever (40%, grade 3-4: 7%), and thrombocytopenia (40%, grade 3-4: 27%). No responses were observed.
In an open-label non-randomized study (DFI7434), oxaliplatin was administered to 26 pediatric patients with metastatic or unresectable solid tumors, mainly neuroblastoma and ganglioneuroblastoma. The DLT was sensory neuropathy at a dose of 160 mg/m2. No responses were observed.
In an open-label, single-agent study (ARD5021), oxaliplatin was administered to 43 pediatric patients with recurrent or refractory embryonal CNS tumors. The most common adverse reactions reported were: leukopenia (67%, grade 3-4: 12%), anemia (65%, grade 3-4: 5%), thrombocytopenia (65%, grade 3-4: 26%), vomiting (65%, grade 3-4: 7%), neutropenia (58%, grade 3-4: 16%), and sensory neuropathy (40%, grade 3-4: 5%).
In an open-label single-agent study (ARD5530), oxaliplatin was administered to 123 pediatric patients with recurrent solid tumors, including neuroblastoma, osteosarcoma, Ewing sarcoma or peripheral PNET, ependymoma, rhabdomyosarcoma, hepatoblastoma, high grade astrocytoma, brain stem glioma, low grade astrocytoma, malignant germ cell tumor and other tumors. The most common adverse reactions reported were: sensory neuropathy (52%, grade 3-4: 12%), thrombocytopenia (37%, grade 3-4: 17%), anemia (37%, grade 3-4: 9%), vomiting (26%, grade 3-4: 4%), increased ALT (24%, grade 3-4: 6%), increased AST (24%, grade 3-4: 2%), and nausea (23%, grade 3-4: 3%).
The pharmacokinetic parameters of ultrafiltrable platinum were evaluated in 105 pediatric patients during the first cycle. The mean clearance in pediatric patients estimated by the population pharmacokinetic analysis was 4.7 L/h (%CV, 41%). Mean platinum pharmacokinetic parameters in ultrafiltrate were Cmax of 0.75 ± 0.24 mcg/mL, AUC0-48h of 7.52 ± 5.07 mcg•h/mL and AUCinf of 8.83 ± 1.57 mcg•h/mL at 85 mg/m2 of oxaliplatin and Cmax of 1.10 ± 0.43 mcg/mL, AUC0-48h of 9.74 ± 2.52 mcg•h/mL and AUCinf of 17.3 ± 5.34 mcg•h/mL at 130 mg/m2 of oxaliplatin.
8.5 Geriatric Use
In the adjuvant treatment trial [see Clinical Studies (14.1)], 400 patients who received oxaliplatin with fluorouracil/leucovorin were greater than or equal to 65 years. The effect of oxaliplatin in patients greater than or equal to 65 years was not conclusive. Patients greater than or equal to 65 years receiving oxaliplatin experienced more diarrhea and grade 3-4 neutropenia (45% vs 39%) compared to patients less than 65 years.
In the previously untreated advanced colorectal cancer trial [see Clinical Studies (14.2)], 99 patients who received oxaliplatin with fluorouracil and leucovorin were greater than or equal to 65 years. The same efficacy improvements in response rate, time to tumor progression, and overall survival were observed in the greater than or equal to 65 years patients as in the overall study population. Adverse reactions were similar in patients less than 65 and greater than or equal to 65 years, but older patients may have been more susceptible to diarrhea, dehydration, hypokalemia, leukopenia, fatigue, and syncope.
In the previously treated advanced colorectal cancer trial [see Clinical Studies (14.3)], 55 patients who received oxaliplatin with fluorouracil and leucovorin were greater than or equal to 65 years. No overall differences in effectiveness were observed between these patients and younger adults. Adverse reactions were similar in patients less than 65 and greater than or equal to 65 years, but older patients may have been more susceptible to diarrhea, dehydration, hypokalemia, and fatigue.
No significant effect of age on the clearance of ultrafiltrable platinum has been observed [see Clinical Pharmacology (12.3)].
5.6 Hepatotoxicity
In the adjuvant treatment trial, increased transaminases (57% vs 34%) and alkaline phosphatase (42% vs 20%) occurred more commonly in the oxaliplatin arm than in the fluorouracil/leucovorin arm [see Adverse Reactions (6.1)]. The incidence of increased bilirubin was similar on both arms. Changes noted on liver biopsies include: peliosis, nodular regenerative hyperplasia or sinusoidal alterations, perisinusoidal fibrosis, and veno-occlusive lesions.
Consider evaluating patients who develop abnormal liver tests or portal hypertension, which cannot be explained by liver metastases, for hepatic vascular disorders. Monitor liver function tests at baseline, before each subsequent cycle, and as clinically indicated.
5.8 Rhabdomyolysis
Rhabdomyolysis, including fatal cases, has been reported with oxaliplatin [see Adverse Reactions (6.2)]. Permanently discontinue oxaliplatin for any signs or symptoms of rhabdomyolysis.
4 Contraindications (4 CONTRAINDICATIONS)
Oxaliplatin injection is contraindicated in patients with a history of a hypersensitivity reaction to oxaliplatin or other platinum-based drugs. Reactions have included anaphylaxis [see Warnings and Precautions (5.1)].
6 Adverse Reactions (6 ADVERSE REACTIONS)
The following clinically significant adverse reactions are described elsewhere in labeling:
- Hypersensitivity Reactions [see Warnings and Precautions (5.1)]
- Peripheral Sensory Neuropathy [see Warnings and Precautions (5.2)]
- Severe Myelosuppression [see Warnings and Precautions (5.3)]
- Posterior Reversible Encephalopathy Syndrome [see Warnings and Precautions (5.4)]
- Pulmonary Toxicity [see Warnings and Precautions (5.5)]
- Hepatotoxicity [see Warnings and Precautions (5.6)]
- QT Interval Prolongation and Ventricular Arrhythmias [see Warnings and Precautions (5.7)]
- Rhabdomyolysis [see Warnings and Precautions (5.8)]
- Hemorrhage [see Warnings and Precautions (5.9)]
12.2 Pharmacodynamics
A pharmacodynamic relationship between platinum ultrafiltrate levels and clinical safety and effectiveness has not been established.
12.3 Pharmacokinetics
The reactive oxaliplatin derivatives are present as a fraction of the unbound platinum in plasma ultrafiltrate. After a single 2-hour intravenous infusion of oxaliplatin at a dose of 85 mg/m2, pharmacokinetic parameters expressed as ultrafiltrable platinum were Cmax of 0.814 mcg/mL and volume of distribution of 440 L.
Interpatient and intrapatient variability in ultrafiltrable platinum exposure (AUC0-48hr) assessed over 3 cycles was 23% and 6%, respectively.
2.1 Recommended Dosage
Administer oxaliplatin injection in combination with fluorouracil and leucovorin every 2 weeks.
- For adjuvant treatment, continue treatment for up to 12 cycles or unacceptable toxicity.
- For advanced colorectal cancer, continue treatment until disease progression or unacceptable toxicity.
5.5 Pulmonary Toxicity
Oxaliplatin has been associated with pulmonary fibrosis (less than 1% of patients), which may be fatal [see Adverse Reactions (6.1)].
In the adjuvant treatment trial, the combined incidence of cough and dyspnea was 7.4% (any grade), including less than 1% (grade 3) in the oxaliplatin arm. One patient died from eosinophilic pneumonia in the oxaliplatin arm.
In the previously untreated advanced colorectal cancer trial, the combined incidence of cough, dyspnea, and hypoxia was 43% (any grade), including 7% (grade 3-4) in the oxaliplatin with fluorouracil/leucovorin arm.
In case of unexplained respiratory symptoms, such as non-productive cough, dyspnea, crackles, or radiological pulmonary infiltrates, withhold oxaliplatin until further pulmonary investigation excludes interstitial lung disease or pulmonary fibrosis. Permanently discontinue oxaliplatin for confirmed interstitial lung disease or pulmonary fibrosis.
1 Indications and Usage (1 INDICATIONS AND USAGE)
Oxaliplatin Injection, in combination with infusional fluorouracil and leucovorin, is indicated for:
- adjuvant treatment of stage III colon cancer in patients who have undergone complete resection of the primary tumor.
- treatment of advanced colorectal cancer.
12.1 Mechanism of Action
Oxaliplatin undergoes nonenzymatic conversion in physiologic solutions to active derivatives via displacement of the labile oxalate ligand. Several transient reactive species are formed, including monoaquo and diaquo DACH platinum, which covalently bind with macromolecules. Both inter-and intrastrand Pt-DNA crosslinks are formed. Crosslinks are formed between the N7 positions of two adjacent guanines (GG), adjacent adenine-guanines (AG), and guanines separated by an intervening nucleotide (GNG). These crosslinks inhibit DNA replication and transcription. Cytotoxicity is cell-cycle nonspecific.
In vivo studies have shown antitumor activity of oxaliplatin against colon carcinoma. In combination with fluorouracil, oxaliplatin exhibits in vitro and in vivo antiproliferative activity greater than either compound alone in several tumor models (HT29 [colon], GR [mammary], and L1210 [leukemia]).
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
- Peripheral Sensory Neuropathy: Acute and delayed neuropathy can occur. Avoid topical application of ice. Reduce the dose or permanently discontinue oxaliplatin as recommended. (5.2)
- Severe Myelosuppression: Delay oxaliplatin until neutrophils are greater than or equal to 1.5 x 109/L and platelets are greater than or equal to 75 x 109/L. Withhold oxaliplatin for sepsis or septic shock. Dose reduce after recovery from grade 4 neutropenia, febrile neutropenia, or grade 3-4 thrombocytopenia as recommended. (5.3)
- Posterior Reversible Encephalopathy Syndrome (PRES): Permanently discontinue oxaliplatin in patients who develop PRES. (5.4)
- Pulmonary Toxicity: Withhold oxaliplatin until investigation excludes interstitial lung disease or pulmonary fibrosis. (5.5)
- Hepatotoxicity: Monitor liver function tests at baseline, before each subsequent cycle, and as clinically indicated. (5.6)
- QT Interval Prolongation: Avoid in patients with congenital long QT syndrome. Monitor electrocardiograms in patients with congestive heart failure, bradyarrhythmias, and electrolyte abnormalities, and in patients taking drugs known to prolong the QT interval. Correct electrolyte abnormalities prior to initiating oxaliplatin and periodically during treatment. (5.7)
- Rhabdomyolysis: Permanently discontinue oxaliplatin if rhabdomyolysis occurs. (5.8)
- Hemorrhage: Increase frequency of monitoring in patients who are receiving oxaliplatin with fluorouracil/leucovorin and oral anticoagulants. (5.9)
- Embryo-Fetal Toxicity: Can cause fetal harm. Advise pregnant women of the potential risk to a fetus. Advise males and females of reproductive potential to use an effective method of contraception. (5.10, 8.1, 8.3)
5.10 Embryo Fetal Toxicity (5.10 Embryo-Fetal Toxicity)
Based on findings from animal studies and its mechanism of action, oxaliplatin can cause fetal harm when administered to a pregnant woman. The available human data do not establish the presence or absence of major birth defects or miscarriage related to the use of oxaliplatin. Reproductive toxicity studies demonstrated adverse effects on embryo-fetal development in rats at maternal doses that were below the recommended human dose based on body surface area. Advise pregnant women of the potential risk to a fetus. Advise females of reproductive potential to use effective contraception during treatment with oxaliplatin and for 9 months after the final dose. Advise males with female partners of reproductive potential to use effective contraception during treatment with oxaliplatin and for 6 months after the final dose [see Use in Specific Populations (8.1, 8.3)].
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
- Administer oxaliplatin injection 85 mg/m2 as an intravenous infusion over 120 minutes concurrently with leucovorin over 120 minutes in separate bags, followed by fluorouracil on Day 1 of each 14-day cycle. Administer fluorouracil and leucovorin on Day 2 as recommended. (2.1)
- Adjuvant Treatment: Continue treatment for up to 12 cycles or unacceptable toxicity. (2.1)
- Advanced Colorectal Cancer: Continue treatment until disease progression or unacceptable toxicity. (2.1)
5.3 Severe Myelosuppression
Grade 3 or 4 neutropenia occurred in 41% to 44% of patients with colorectal cancer who received oxaliplatin with fluorouracil/leucovorin. Sepsis, neutropenic sepsis and septic shock, including fatal outcomes, occurred in patients who received oxaliplatin [see Adverse Reactions (6.1, 6.2)].
Grade 3 or 4 thrombocytopenia occurred in 2% to 5% of patients with colorectal cancer who received oxaliplatin with fluorouracil/leucovorin.
Monitor complete blood cell count at baseline, before each subsequent cycle and as clinically indicated. Delay oxaliplatin until neutrophils are greater than or equal to 1.5 x 109/L and platelets are greater than or equal to 75 x 109/L. Withhold oxaliplatin for sepsis or septic shock. Dose reduce oxaliplatin after recovery from grade 4 neutropenia, febrile neutropenia or grade 3-4 thrombocytopenia as recommended [see Dosage and Administration (2.2)].
7.3 Use With Anticoagulants (7.3 Use with Anticoagulants)
Prolonged prothrombin time and INR occasionally associated with hemorrhage have been reported in patients who received oxaliplatin with fluorouracil/leucovorin while on anticoagulants [see Warnings and Precautions (5.9), Adverse Reactions (6.2)]. Increase frequency of monitoring in patients who are receiving oxaliplatin with fluorouracil/leucovorin and oral anticoagulants.
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
Oxaliplatin Injection, USP: 50 mg (5 mg per mL) or 100 mg (5 mg per mL) clear, colorless solution in a single-dose vial.
6.2 Postmarketing Experience
The following adverse reactions have been identified during postapproval use of oxaliplatin. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
- General: angioedema, anaphylactic shock
- Cardiovascular: QT prolongation leading to ventricular arrhythmias, including fatal torsade de pointes; bradyarrhythmia
- Neurological: loss of deep tendon reflexes, dysarthria, Lhermitte's sign, cranial nerve palsies, fasciculations, convulsion
- Hearing and vestibular system: deafness
- Infections: septic shock, including fatal outcomes
- Infusion-related reactions and hypersensitivity reactions: laryngospasm
- Hepatic and gastrointestinal: severe diarrhea/vomiting resulting in hypokalemia, colitis (including Clostridium difficile diarrhea), metabolic acidosis, ileus, intestinal obstruction, pancreatitis, sinusoidal obstruction syndrome, perisinusoidal fibrosis which rarely may progress, focal nodular hyperplasia, esophagitis
- Musculoskeletal and connective tissue: rhabdomyolysis, including fatal outcomes
- Platelet, bleeding, and clotting disorders: immuno-allergic thrombocytopenia, prolonged prothrombin time and INR in patients receiving anticoagulants
- Blood disorders: secondary leukemia
- Red blood cell: hemolytic uremic syndrome, immuno-allergic hemolytic anemia
- Renal: acute tubular necrosis, acute interstitial nephritis, acute renal failure
- Respiratory: interstitial lung diseases (sometimes fatal) and pneumonia (including fatal outcomes)
- Vision: decrease of visual acuity, visual field disturbance, optic neuritis and transient vision loss (reversible following treatment discontinuation)
- Injury, poisoning, and procedural complications: fall-related injuries
8 Use in Specific Populations (8 USE IN SPECIFIC POPULATIONS)
- Females: Advise female patients of reproductive potential to use effective contraception while receiving oxaliplatin injection and for 9 months after the final dose. (8.3)
- Males: Based on its mechanism action as a genotoxic drug, advise males with female partners of reproductive potential to use effective contraception while receiving oxaliplatin injection and for 6 months after the final dose [see Nonclinical Toxicology (13.1)].
5.1 Hypersensitivity Reactions
Serious and fatal hypersensitivity reactions, including anaphylaxis, can occur with oxaliplatin within minutes of administration and during any cycle. Grade 3-4 hypersensitivity reactions, including anaphylaxis, occurred in 2% to 3% of patients with colon cancer who received oxaliplatin. Hypersensitivity reactions, including rash, urticaria, erythema, pruritus, and rarely, bronchospasm and hypotension, were similar in nature and severity to those reported with other platinum-based drugs.
Oxaliplatin is contraindicated in patients with hypersensitivity reactions to platinum-based drugs [see Contraindications (4)]. Immediately and permanently discontinue oxaliplatin for hypersensitivity reactions and administer appropriate treatment for management of hypersensitivity reactions.
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
More than 1100 patients with stage II or III colon cancer and more than 4,000 patients with advanced colorectal cancer were treated in trials with oxaliplatin. The most common adverse reactions in patients with stage II or III colon cancer receiving adjuvant treatment were peripheral sensory neuropathy, neutropenia, thrombocytopenia, anemia, nausea, increase in transaminases and alkaline phosphatase, diarrhea, emesis, fatigue and stomatitis. The most common adverse reactions in previously untreated and treated patients with advanced colorectal cancer were peripheral sensory neuropathies, fatigue, neutropenia, nausea, emesis, and diarrhea.
17 Patient Counseling Information (17 PATIENT COUNSELING INFORMATION)
5.2 Peripheral Sensory Neuropathy
Oxaliplatin can cause acute and delayed neuropathy. Reduce the dose or permanently discontinue oxaliplatin for persistent neurosensory reactions based on the severity of the adverse reaction [see Dosage and Administration (2.2)].
7.2 Use With Nephrotoxic Products (7.2 Use with Nephrotoxic Products)
Because platinum-containing species are eliminated primarily through the kidney, clearance of these products may be decreased by coadministration of potentially nephrotoxic compounds [see Clinical Pharmacology (12.3)]. Avoid coadministration of oxaliplatin with medicinal products known to cause nephrotoxicity.
2.4 Preparation and Administration
- Oxaliplatin injection is a cytotoxic drug. Follow applicable special handling and disposal procedures.1
- Do not freeze.
- Protect the concentrated solution from light.
- Dilute concentrated solution with 250 to 500 mL of 5% Dextrose Injection, USP. Do not dilute with sodium chloride solution or other chloride-containing solutions.
- Store diluted solution for no more than 6 hours at room temperature (20°C to 25°C [68°F to 77°F]) or 24 hours under refrigeration (2°C to 8°C [36°F to 46°F]). Protection from light is not required.
- Visually inspect for particulate matter and discoloration prior to administration and discard if present.
- Do not mix oxaliplatin injection or administer oxaliplatin injection through the same infusion line concurrently with alkaline medications or media (such as basic solutions of fluorouracil).
- Flush the infusion line with 5% Dextrose Injection, USP prior to administration of any concomitant medication.
- Do not use needles or intravenous administration sets containing aluminum parts for the preparation or mixing of oxaliplatin injection. Aluminum has been reported to cause degradation of platinum compounds.
- Administer oxaliplatin injection as an intravenous infusion over 120 minutes concurrently with leucovorin over 120 minutes in separate bags.
8.6 Patients With Renal Impairment (8.6 Patients with Renal Impairment)
The AUC of unbound platinum in plasma ultrafiltrate was increased in patients with renal impairment [see Clinical Pharmacology (12.3)]. No dose reduction is recommended for patients with mild (creatinine clearance 50 to 79 mL/min) or moderate (creatinine clearance 30 to 49 mL/min) renal impairment, calculated by Cockcroft-Gault equation. Reduce the dose of oxaliplatin in patients with severe renal impairment (creatinine clearance less than 30 mL/min) [see Dosage and Administration (2.3)].
16 How Supplied/storage and Handling (16 HOW SUPPLIED/STORAGE AND HANDLING)
Oxaliplatin Injection, USP is supplied as follows:
| NDC | Oxaliplatin Injection, USP (5 mg per mL) | Package Factor |
| 25021-233-10 | 50 mg per 10 mL Single-Dose Vial | 1 vial per carton |
| 25021-233-20 | 100 mg per 20 mL Single-Dose Vial | 1 vial per carton |
Water for Injection, USP is present as an inactive ingredient. Tartaric Acid, NF and Sodium Hydroxide, NF are used in combination as a buffering system.
Store at 20° to 25°C (68° to 77°F); excursions permitted between 15° and 30°C (59° and 86°F). [See USP Controlled Room Temperature.]
Do not freeze.
Protect from light. Retain in carton until time of use.
Discard unused portion.
Oxaliplatin Injection, USP is a cytotoxic drug. Follow applicable special handling and disposal procedures.1 The use of gloves is recommended. If a solution of Oxaliplatin Injection, USP contacts the skin, wash the skin immediately and thoroughly with soap and water. If Oxaliplatin Injection, USP contacts the mucous membranes, flush thoroughly with water.
Sterile, Nonpyrogenic, Preservative-free.
The container closure is not made with natural rubber latex.
7.1 Drugs That Prolong the Qt Interval (7.1 Drugs that Prolong the QT Interval)
QT interval prolongation and ventricular arrhythmias can occur with oxaliplatin [see Warnings and Precautions (5.7)]. Avoid coadministration of oxaliplatin with medicinal products with a known potential to prolong the QT interval.
2.2 Dose Modifications for Adverse Reactions
Prolongation of infusion time for oxaliplatin injection from 2 hours to 6 hours may mitigate acute toxicities, such as non-life-threatening infusion-related reactions.
Permanently discontinue oxaliplatin injection for any of the following:
- Hypersensitivity Reactions [see Warnings and Precautions (5.1)]
- Posterior reversible encephalopathy syndrome (PRES) [see Warnings and Precautions (5.4)]
- Confirmed interstitial lung disease or pulmonary fibrosis [see Warnings and Precautions (5.5)]
- Rhabdomyolysis [see Warnings and Precautions (5.8)]
Refer to the fluorouracil and leucovorin prescribing information for dosage modifications for adverse reactions.
5.4 Posterior Reversible Encephalopathy Syndrome
PRES occurred in less than 0.1% of patients across clinical trials [see Adverse Reactions (6.1)]. Signs and symptoms of PRES can include headache, altered mental functioning, seizures, abnormal vision from blurriness to blindness, associated or not with hypertension. Confirm the diagnosis of PRES with magnetic resonance imaging. Permanently discontinue oxaliplatin in patients who develop PRES.
14.3 Previously Treated Advanced Colorectal Cancer
The efficacy of oxaliplatin in combination with fluorouracil (FU)/leucovorin (LV) was evaluated in a multicenter, open-label, randomized, three-arm controlled trial was conducted in the US and Canada in patients with advanced colorectal cancer who had relapsed/progressed during or within 6 months of first-line treatment with bolus fluorouracil/leucovorin and irinotecan (A multicenter, open-label, randomized, three-arm study of 5-fluorouracil (5-FU) + leucovorin (LV) or oxaliplatin or a combination of 5-FU/LV + oxaliplatin as second-line treatment of metastatic colorectal carcinoma: NCT00008281). Patients were randomized to one of three regimens; the dosing regimens are presented in Table 22. Eligible patients were at least 18 years of age, had unresectable, measurable, histologically proven colorectal adenocarcinoma, with a Karnofsky performance status (KPS) greater than 50%. Patients had to have aspartate transaminase (AST), alanine transaminase (ALT) and alkaline phosphatase less than or equal to 2x upper limit of normal (ULN), unless liver metastases were present and documented at baseline by CT or MRI scan, in which case less than or equal to 5 x ULN was permitted. Prior radiotherapy was permitted if it had been completed at least 3 weeks before randomization. The main efficacy outcome measure was 3-year disease-free survival (DFS) and an additional outcome measure was overall survival (OS).
| Treatment Arm | Dose | Regimen |
| Oxaliplatin + FU/LV (N=152) |
Day 1:
Oxaliplatin: 85 mg/m2 (2-hour infusion) + LV 200 mg/m2 (2-hour infusion), followed by FU: 400 mg/m2 (bolus), 600 mg/m2 (22-hour infusion) Day 2: LV 200 mg/m2 (2-hour infusion), followed by FU: 400 mg/m2 (bolus), 600 mg/m2 (22-hour infusion) |
every 2 weeks |
| FU/LV (N=151) |
Day 1: LV 200 mg/m2 (2-hour infusion), followed by FU: 400 mg/m2 (bolus), 600 mg/m2 (22-hour infusion) Day 2: LV 200 mg/m2 (2-hour infusion), followed by FU: 400 mg/m2 (bolus), 600 mg/m2 (22-hour infusion) |
every 2 weeks |
| Oxaliplatin (N=156) |
Day 1: Oxaliplatin 85 mg/m2 (2-hour infusion) | every 2 weeks |
Patients must have had at least one unidimensional lesion measuring greater than or equal to 20 mm using conventional CT or MRI scans or greater than or equal to 10 mm using a spiral CT scan. Tumor response and progression were assessed every 3 cycles (6 weeks) using the Response Evaluation Criteria in Solid Tumors (RECIST) until radiological documentation of progression or for 13 months following the first dose of study drug(s), whichever came first. Confirmed responses were based on two tumor assessments separated by at least 4 weeks. Baseline characteristics are shown in Table 23.
| Oxaliplatin + | Oxaliplatin | FU/LV | |
| FU/LV | N=156 | N=151 | |
| N=152 | |||
| Sex: Male (%) | 57.2 | 60.9 | 54.3 |
| Female (%) | 42.8 | 39.1 | 45.7 |
| Median age (years) | 59.0 | 61.0 | 60.0 |
| Range | 22 to 88 | 27 to 79 | 21 to 80 |
| Race (%) | |||
| Caucasian | 88.8 | 84.6 | 87.4 |
| Black | 5.9 | 7.1 | 7.9 |
| Asian | 2.6 | 2.6 | 1.3 |
| Other | 2.6 | 5.8 | 3.3 |
| KPS (%) | |||
| 70 to 100 | 95.4 | 92.3 | 94.7 |
| 50 to 60 | 2.0 | 4.5 | 2.6 |
| Not reported | 2.6 | 3.2 | 2.6 |
| Prior radiotherapy (%) | 25.0 | 19.2 | 25.2 |
| Prior pelvic radiation (%) | 21.1 | 13.5 | 18.5 |
| Number of metastatic sites (%) | |||
| 1 | 25.7 | 31.4 | 27.2 |
| ≥2 | 74.3 | 67.9 | 72.2 |
| Liver involvement (%) | |||
| Liver only | 18.4 | 25.6 | 22.5 |
| Liver + other | 53.3 | 59.0 | 60.3 |
The median number of cycles administered per patient was 6 for the oxaliplatin and fluorouracil/leucovorin combination and 3 each for fluorouracil/leucovorin alone and oxaliplatin alone. Patients treated with the combination of oxaliplatin and fluorouracil/leucovorin had an increased response rate compared to patients given fluorouracil/leucovorin or oxaliplatin alone. Efficacy results are summarized in Tables 24 and 25.
| Best Response | Oxaliplatin + | Oxaliplatin | FU/LV |
| FU/LV | N=156 | N=151 | |
| N=152 | |||
| Complete Response | 0 | 0 | 0 |
| Partial Response | 13 (9%) | 2 (1%) | 0 |
| P-value | 0.0002 FU/LV vs Oxaliplatin + FU/LV | ||
| 95% CI | 4.6%, 14.2% | 0.2%, 4.6% | 0, 2.4% |
|
*This is not an ITT analysis. Events were limited to radiographic disease progression documented by independent review of radiographs. Clinical progression was not included in this analysis, and 18% of patients were excluded from the analysis based on unavailability of the radiographs for independent review. |
|||
| Arm | Oxaliplatin + | Oxaliplatin | FU/LV |
| FU/LV | N=156 | N=151 | |
| N=152 | |||
| Number of progressors | 50 | 101 | 74 |
| Number of patients with no radiological evaluation beyond baseline | 17 (11%) | 16 (10%) | 22 (15%) |
| Median TTP (months) | 4.6 | 1.6 | 2.7 |
| 95% CI | 4.2, 6.1 | 1.4, 2.7 | 1.8, 3.0 |
At the time of the interim analysis 49% of the radiographic progression events had occurred. In this interim analysis an estimated 2-month increase in median time to radiographic progression was observed compared to fluorouracil/leucovorin alone.
14.2 Previously Untreated Advanced Colorectal Cancer
The efficacy of oxaliplatin in combination with fluorouracil (FU)/leucovorin (LV) was evaluated in a North American, multicenter, open-label, randomized, active-controlled trial (A Randomized Phase III Trial of Three Different Regimens of CPT-11 Plus 5-Fluorouracil and Leucovorin Compared to 5-Fluorouracil and Leucovorin in Patients with Advanced Adenocarcinoma of the Colon and Rectum; NCT00003594). The trial included 7 arms at different times during its conduct, four of which were closed due to either changes in the standard of care, toxicity, or simplification. During the trial, the control arm was changed to irinotecan with fluorouracil/leucovorin.
The results reported below compared the efficacy of oxaliplatin with fluorouracil/leucovorin and oxaliplatin with irinotecan to an approved control regimen of irinotecan with fluorouracil/leucovorin in 795 concurrently randomized patients previously untreated for locally advanced or metastatic colorectal cancer. Table 19 presents the dosing regimens for the three arms. After completion of enrollment, the dose of irinotecan with fluorouracil/leucovorin was decreased due to toxicity.
Eligible patients were at least 18 years of age; had known locally advanced, locally recurrent, or metastatic colorectal adenocarcinoma not curable by surgery or amenable to radiation therapy; with an Eastern Cooperative Oncology Group (ECOG) performance status ≤0, 1, or 2. Patients had to have absolute neutrophil count (ANC) greater than or equal to 1.5 x 109/L, platelets greater than or equal to 100 x 109/L, hemoglobin greater than or equal to 9.0 g/dL, creatinine less than or equal to 1.5 x upper limit of normal (ULN), total bilirubin less than or equal to 1.5 mg/dL, aspartate transaminase (AST) less than or equal to 5 x ULN, and alkaline phosphatase less than or equal to 5 x ULN. Patients may have received adjuvant treatment for resected Stage II or III disease without recurrence within 12 months. Randomization was stratified by ECOG performance status (0, 1 vs 2), prior adjuvant chemotherapy (yes vs no), prior immunotherapy (yes vs no), and age (less than 65 vs greater than or equal to 65 years). Although no post study treatment was specified in the protocol, 65% to 72% of patients received additional post study chemotherapy after study treatment discontinuation on all arms. Fifty-eight percent of patients on the oxaliplatin with fluorouracil/leucovorin arm received an irinotecan-containing regimen and 23% of patients on the irinotecan with fluorouracil/leucovorin arm received an oxaliplatin-containing regimen.
The main efficacy outcome measure was 3-year disease-free survival (DFS) and additional efficacy outcome measures were overall survival (OS).
| Treatment Arm | Dose | Regimen |
| Oxaliplatin + FU/LV (FOLFOX4) (N=267) |
Day 1:
Oxaliplatin: 85 mg/m2 (2-hour infusion) + LV 200 mg/m2 (2-hour infusion), followed by FU: 400 mg/m2 (bolus), 600 mg/m2 (22-hour infusion) Day 2: LV 200 mg/m2 (2-hour infusion), followed by FU: 400 mg/m2 (bolus), 600 mg/m2 (22-hour infusion) |
every 2 weeks |
| Irinotecan + FU/LV (IFL) (N=264) |
Day 1: Irinotecan 125 mg/m2 as a 90–min infusion + LV 20 mg/m2 | every 6 weeks |
| as a 15-min infusion or intravenous push, followed by | ||
| FU 500 mg/m2 intravenous bolus weekly x 4 | ||
| Oxaliplatin + Irinotecan (IROX) (N=264) |
Day 1: Oxaliplatin: 85 mg/m2 intravenous (2-hour infusion) + irinotecan 200 mg/m2 intravenous over 30 minutes | every 3 weeks |
Table 20 presents the baseline characteristics.
| Oxaliplatin + | Irinotecan + | Oxaliplatin + | |
| FU/LV | FU/LV | Irinotecan | |
| N=267 | N=264 | N=264 | |
| Sex: Male (%) | 58.8 | 65.2 | 61.0 |
| Female (%) | 41.2 | 34.8 | 39.0 |
| Median age (years) | 61.0 | 61.0 | 61.0 |
| <65 years of age (%) | 61 | 62 | 63 |
| ≥65 years of age (%) | 39 | 38 | 37 |
| ECOG (%) | |||
| 0-1 | 94.4 | 95.5 | 94.7 |
| 2 | 5.6 | 4.5 | 5.3 |
| Involved organs (%) | |||
| Colon only | 0.7 | 0.8 | 0.4 |
| Liver only | 39.3 | 44.3 | 39.0 |
| Liver + other | 41.2 | 38.6 | 40.9 |
| Lung only | 6.4 | 3.8 | 5.3 |
| Other (including lymph nodes) | 11.6 | 11.0 | 12.9 |
| Not reported | 0.7 | 1.5 | 1.5 |
| Prior radiation (%) | 3.0 | 1.5 | 3.0 |
| Prior surgery (%) | 74.5 | 79.2 | 81.8 |
| Prior adjuvant (%) | 15.7 | 14.8 | 15.2 |
The median number of cycles administered per patient was 10 (23.9 weeks) for the oxaliplatin plus fluorouracil/leucovorin regimen, 4 (23.6 weeks) for the irinotecan plus fluorouracil/leucovorin regimen, and 7 (21.0 weeks) for the oxaliplatin plus irinotecan regimen.
Patients who received oxaliplatin with fluorouracil/leucovorin had a significantly longer time to tumor progression based on investigator assessment, longer OS, and a significantly higher confirmed response rate based on investigator assessment compared to patients who received irinotecan with fluorouracil/leucovorin. Efficacy results are summarized in Table 21 and Figure 3.
|
*A hazard ratio of less than 1 favors Oxaliplatin + Infusional fluorouracil/leucovorin |
|||
|
†Compared to irinotecan plus fluorouracil/leucovorin (IFL) arm |
|||
|
‡ Based on all patients with measurable disease at baseline |
|||
|
The numbers in the response rate and TTP analysis are based on unblinded investigator assessment. |
|||
|
Oxaliplatin +
FU/LV N=267 |
Irinotecan + | Oxaliplatin + | |
| FU/LV | Irinotecan | ||
| N=264 | N=264 | ||
| Survival (ITT) | |||
| Number of deaths (%) | 155 (58.1) | 192 (72.7) | 175 (66.3) |
| Median survival (months) | 19.4 | 14.6 | 17.6 |
| Hazard ratio (95% CI)* | 0.65 (0.53, 0.80)† | - | |
| P-value | <0.0001† | - | |
| TTP (ITT, investigator assessment) | |||
| Percentage of progressors | 82.8 | 81.8 | 89.4 |
| Median TTP (months) | 8.7 | 6.9 | 6.5 |
| Hazard ratio (95% CI)* | 0.74 (0.61, 0.89)† | - | |
| P-value | 0.0014† | - | |
| Response Rate (investigator assessment) ‡ | |||
| Patients with measurable disease | 210 | 212 | 215 |
| Complete response, N (%) | 13 (6.2) | 5 (2.4) | 7 (3.3) |
| Partial response, N (%) | 82 (39.0) | 64 (30.2) | 67 (31.2) |
| Complete and partial response, N (%) | 95 (45.2) | 69 (32.5) | 74 (34.4) |
| 95% CI | (38.5, 52.0) | (26.2, 38.9) | (28.1, 40.8) |
| P-value | 0.0080† | - |
Figure 3: Kaplan-Meier Curves for Overall Survival in Previously Untreated Advanced Colorectal Cancer Trial
* Log rank test comparing oxaliplatin plus FU/LV to irinotecan plus FU/LV.
In descriptive subgroup analyses, the improvement in overall survival (OS) for oxaliplatin with fluorouracil/leucovorin compared to irinotecan with fluorouracil/leucovorin appeared to be maintained across age groups, prior adjuvant treatment, number of organs involved and both sexes; however, the effect appeared larger among women than men.
5.7 Qt Interval Prolongation and Ventricular Arrhythmias (5.7 QT Interval Prolongation and Ventricular Arrhythmias)
QT prolongation and ventricular arrhythmias, including fatal torsade de pointes, have been reported with oxaliplatin [see Adverse Reactions (6.2)].
Avoid oxaliplatin in patients with congenital long QT syndrome. Monitor electrocardiograms (ECG) in patients with congestive heart failure, bradyarrhythmias, and electrolyte abnormalities and in patients taking drugs known to prolong the QT interval, including Class Ia and III antiarrhythmics [see Drug Interactions (7.1)]. Monitor and correct electrolyte abnormalities prior to initiating oxaliplatin and periodically during treatment.
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Long-term animal studies have not been performed to evaluate the carcinogenic potential of oxaliplatin. Oxaliplatin was not mutagenic to bacteria (Ames test) but was mutagenic to mammalian cells in vitro (L5178Y mouse lymphoma assay). Oxaliplatin was clastogenic both in vitro (chromosome aberration in human lymphocytes) and in vivo (mouse bone marrow micronucleus assay).
In a fertility study, male rats were given oxaliplatin at 0, 0.5, 1, or 2 mg/kg/day for five days every 21 days for a total of three cycles prior to mating with females that received two cycles of oxaliplatin on the same schedule. A dose of 2 mg/kg/day (less than one-seventh the recommended human dose on a body surface area basis) did not affect pregnancy rate, but resulted in 97% postimplantation loss (increased early resorptions, decreased live fetuses, decreased live births), and delayed growth (decreased fetal weight).
Testicular damage, characterized by degeneration, hypoplasia, and atrophy, was observed in dogs administered oxaliplatin at 0.75 mg/kg/day (approximately one-sixth of the recommended human dose on a body surface area basis) x 5 days every 28 days for three cycles. A no effect level was not identified.
2.3 Dose Modifications for Patients With Renal Impairment (2.3 Dose Modifications for Patients with Renal Impairment)
Warning: Hypersensitivity Reactions, Including Anaphylaxis (WARNING: HYPERSENSITIVITY REACTIONS, INCLUDING ANAPHYLAXIS)
Serious and fatal hypersensitivity adverse reactions, including anaphylaxis, can occur with Oxaliplatin Injection within minutes of administration and during any cycle. Oxaliplatin Injection is contraindicated in patients with hypersensitivity reactions to oxaliplatin and other platinum-based drugs [see Contraindications (4)] . Immediately and permanently discontinue Oxaliplatin Injection for hypersensitivity reactions and administer appropriate treatment for management of the hypersensitivity reaction [see Warnings and Precautions (5.1)] .
14.1 Adjuvant Treatment With Oxaliplatin in Combination With Fluorouracil and Leucovorin (14.1 Adjuvant Treatment with Oxaliplatin in Combination with Fluorouracil and Leucovorin)
The efficacy of oxaliplatin in combination with fluorouracil (FU)/leucovorin (LV) was evaluated in an international, multicenter, randomized (1:1) trial (The Multicenter International Study of Oxaliplatin/5-Fluorouracil/Leucovorin in the Adjuvant Treatment of Colon Cancer [MOSAIC], NCT00275210) in patients with stage II (Dukes' B2) or III (Dukes' C) colon cancer who had undergone complete resection of the primary tumor. Patients were randomized to receive oxaliplatin with fluorouracil/leucovorin or fluorouracil/leucovorin alone for a total of 6 months (i.e., 12 cycles). Table 14 shows the dosing regimens for the two arms.
Eligible patients were between 18 and 75 years of age, had histologically proven stage II (T3-T4 N0 M0; Dukes' B2) or III (any T N1-2 M0; Dukes' C) colon carcinoma (with the inferior pole of the tumor above the peritoneal reflection, i.e., greater than or equal to 15 cm from the anal margin) and had undergone (within 7 weeks prior to randomization) complete resection of the primary tumor without gross or microscopic evidence of residual disease and carcino-embryogenic antigen (CEA) less than 10 ng/mL. Additional eligibility criteria were no prior chemotherapy, immunotherapy or radiotherapy; Eastern Cooperative Oncology Group performance status of 0, 1, or 2 (Karnofsky Performance Status greater than or equal to 60%); no pre-existing neuropathy; and absolute neutrophil count (ANC) greater than or equal to 1.5 x 109/L, platelets greater than or equal to 100 x 109/L, serum creatinine less than or equal to 1.25 x upper limit normal (ULN), total bilirubin less than 2 x ULN, and aspartate transaminase (AST)/alanine transaminase (ALT) less than 2 x ULN. The major efficacy outcome was 3-year disease-free survival (DFS).
| Treatment Arm | Dose | Regimen |
| Oxaliplatin + | Day 1: Oxaliplatin: 85 mg/m2 (2-hour infusion) + LV: 200 mg/m2 (2-hour infusion), followed by FU: 400 mg/m2 (bolus), 600 mg/m2 (22-hour infusion) |
every 2 weeks 12 cycles |
| FU/LV | ||
| (FOLFOX4) | ||
| (N =1123) | Day 2: LV: 200 mg/m2 (2-hour infusion), followed by FU: 400 mg/m2 (bolus), 600 mg/m2 (22-hour infusion) |
|
| Day 1: LV: 200 mg/m2 (2-hour infusion), followed by FU: 400 mg/m2 (bolus), 600 mg/m2 (22-hour infusion) |
every 2 weeks 12 cycles |
|
| FU/LV | ||
| (N=1123) | ||
| Day 2: LV: 200 mg/m2 (2-hour infusion), followed by FU: 400 mg/m2 (bolus), 600 mg/m2 (22-hour infusion) |
||
There were 2246 patients enrolled, of whom 1347 (60%) had Stage III disease. Tables 15 and 16 show the baseline characteristics and exposure to oxaliplatin.
|
Oxaliplatin + Infusional FU/LV |
Infusional FU/LV | |
| N=1123 | N=1123 | |
| Sex: Male (%) | 56.1 | 52.4 |
| Female (%) | 43.9 | 47.6 |
| Median age (years) | 61.0 | 60.0 |
| <65 years of age (%) | 64.4 | 66.2 |
| ≥65 years of age (%) | 35.6 | 33.8 |
| KPS (%) | ||
| 100 | 29.7 | 30.5 |
| 90 | 52.2 | 53.9 |
| 80 | 4.4 | 3.3 |
| 70 | 13.2 | 11.9 |
| ≤60 | 0.6 | 0.4 |
| Primary site (%) | ||
| Colon including cecum | 54.6 | 54.4 |
| Sigmoid | 31.9 | 33.8 |
| Recto sigmoid | 12.9 | 10.9 |
| Other including rectum | 0.6 | 0.9 |
| Bowel obstruction (%) | ||
| Yes | 17.9 | 19.3 |
| Perforation (%) | ||
| Yes | 6.9 | 6.9 |
| Stage at Randomization (%) | ||
| II (T=3,4 N=0, M=0) | 40.1 | 39.9 |
| III (T=any, N=1,2, M=0) | 59.6 | 59.3 |
| IV (T=any, N=any, M=1) | 0.4 | 0.8 |
| Staging - T (%) | ||
| T1 | 0.5 | 0.7 |
| T2 | 4.5 | 4.8 |
| T3 | 76.0 | 75.9 |
| T4 | 19.0 | 18.5 |
| Staging - N (%) | ||
| N0 | 40.2 | 39.9 |
| N1 | 39.4 | 39.4 |
| N2 | 20.4 | 20.7 |
| Staging - M (%) | ||
| M1 | 0.4 | 0.8 |
|
Oxaliplatin + Infusional FU/LV N=1108 |
Infusional FU/LV N=1111 |
|
| Median Relative Dose Intensity (%) | ||
| FU | 84.4 | 97.7 |
| Oxaliplatin | 80.5 | N/A |
| Median Number of Cycles | 12 | 12 |
| Median Number of Cycles with Oxaliplatin | 11 | N/A |
The median duration of follow-up was approximately 77 months. In the overall and the stage III colon cancer populations, DFS was statistically significantly improved in the oxaliplatin-containing arm compared to fluorouracil/leucovorin alone; however, a statistically significant improvement in DFS was not observed in Stage II patients. No significant differences in overall survival (OS) were detected in the overall population or those with Stage III disease. Table 17 and Figures 1 and 2 summarize the 5-year DFS rates in the overall randomized population and in patients with stage II and III disease based on an intention-to-treat (ITT) analysis.
|
A hazard ratio of less than 1 favors Oxaliplatin + Infusional FU/LV |
||
|
Data cut off for disease-free survival June 1, 2006 |
||
| Parameter |
Oxaliplatin + Infusional FU/LV |
Infusional FU/LV |
| Overall | ||
| Number of patients | 1123 | 1123 |
| Number of events - relapse or death (%) | 304 (27.1) | 360 (32.1) |
| 5-yr Disease-free survival % (95% CI) | 73.3 (70.7, 76.0) | 67.4 (64.6, 70.2) |
| Hazard ratio (95% CI) | 0.80 (0.68, 0.93) | |
| Stratified Log rank test | p=0.003 | |
| Stage III (Dukes' C) | ||
| Number of patients | 672 | 675 |
| Number of events - relapse or death (%) | 226 (33.6) | 271 (40.1) |
| 5-yr Disease-free survival % (95% CI) | 66.4 (62.7, 70.0) | 58.9 (55.2, 62.7) |
| Hazard ratio (95% CI) | 0.78 (0.65, 0.93) | |
| Log rank test | p=0.005 | |
| Stage II (Dukes' B2) | ||
| Number of patients | 451 | 448 |
| Number of events - relapse or death (%) | 78 (17.3) | 89 (19.9) |
| 5-yr Disease-free survival % (95% CI) | 83.7 (80.2, 87.1) | 79.9 (76.2, 83.7) |
| Hazard ratio (95% CI) | 0.84 (0.62, 1.14) | |
| Log rank test | p=0.258 |
Figure 1: Kaplan-Meier Curves of Disease-Free Survival (cutoff: 1 June 2006) in Adjuvant Treatment Trial – ITT Population
Figure 2: Kaplan-Meier Curves of Disease-Free Survival in Stage III Patients (cutoff: 1 June 2006) in Adjuvant Treatment Trial – ITT Population
Table 18 summarizes the OS results in the overall randomized population and in patients with stage II and III disease, based on the ITT analysis.
|
A hazard ratio of less than 1 favors oxaliplatin + Infusional FU/LV |
||
|
Data cut off for overall survival January 16, 2007 |
||
| Parameter | Oxaliplatin + | Infusional FU/LV |
| Infusional FU/LV | ||
| Overall | ||
| Number of patients | 1123 | 1123 |
| Number of death events (%) | 245 (21.8) | 283 (25.2) |
| Hazard ratio (95% CI) | 0.84 (0.71, 1.00) | |
| Stage III (Dukes' C) | ||
| Number of patients | 672 | 675 |
| Number of death events (%) | 182 (27.1) | 220 (32.6) |
| Hazard ratio (95% CI) | 0.80 (0.65, 0.97) | |
| Stage II (Dukes' B2) | ||
| Number of patients | 451 | 448 |
| Number of death events (%) | 63 (14.0) | 63 (14.1) |
| Hazard ratio (95% CI) | 1.00 (0.70, 1.41) |
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:49:38.068958 · Updated: 2026-03-14T22:33:53.508557