These Highlights Do Not Include All The Information Needed To Use Nateglinide Tablets Safely And Effectively. See Full Prescribing Information For Nateglinide Tablets.
21b211b5-cc92-490f-9903-42fff6a946cd
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
Nateglinide tablets are indicated as an adjunct to diet and exercise to improve glycemic control in adults with type 2 diabetes mellitus.
Indications and Usage
Nateglinide tablets are indicated as an adjunct to diet and exercise to improve glycemic control in adults with type 2 diabetes mellitus.
Dosage and Administration
The recommended dose of nateglinide tablets is 120 mg orally three times daily before meals. The recommended dose of nateglinide tablets is 60 mg orally three times daily before meals in patients who are near glycemic goal when treatment is initiated. Instruct patients to take nateglinide tablets 1 to 30 minutes before meals. In patients who skip meals, instruct patients to skip the scheduled dose of nateglinide tablets to reduce the risk of hypoglycemia {see Warnings and Precautions (5.1) ].
Warnings and Precautions
Hypoglycemia: Nateglinide may cause hypoglycemia. Administer before meals to reduce the risk of hypoglycemia. Skip the scheduled dose of nateglinide if a meal is skipped to reduce the risk of hypoglycemia. ( 5.1 ) Macrovascular outcomes: There have been no clinical studies establishing conclusive evidence of macrovascular risk reduction with nateglinide. ( 5.2 )
Contraindications
Nateglinide is contraindicated in patients with a history of hypersensitivity to nateglinide or its inactive ingredients.
Adverse Reactions
The following serious adverse reaction is also described elsewhere in the labeling: Hypoglycemia [see Warnings and Precautions (5. 1) ]
Drug Interactions
Table 2 includes a list of drugs with clinically important drug interactions when concomitantly administered or withdrawn with nateglinide tablets and instructions for managing or preventing them. Table 2: Clinically Significant Drug Interactions with Nateglinide Drugs That May Increase the Blood-Glucose-Lowering Effect of Nateglinide and Susceptibility to Hypoglycemia Drugs: Nonsteroidal anti-inflammatory drugs (NSAIDs), salicylates, monoamine oxidase inhibitors, non-selective beta-adrenergic-blocking agents, anabolic hormones (e.g. methandrostenolone), guanethidine, gymnema sylvestre, glucomannan, thioctic acid, and inhibitors of CYP2C9 (e.g. amiodarone, fluconazole, voriconazole, sulfinpyrazone) or in patients known to be poor metabolizers of CYP2C9 substrates, alcohol. Intervention: Dose increases and increased frequency of glucose monitoring may be required when nateglinide tablets are coadministered with these drugs. Drugs and Herbals That May Reduce the Blood-Glucose-Lowering Effect of Nateglinide and Increase Susceptibility to Hyperglycemia Drugs: Thiazides, corticosteroids, thyroid products, sympathomimetics, somatropin, somatostatin analogues (e.g. lanreotide, octreotide), and CYP inducers (e.g. rifampin, phenytoin and St John's Wort). Intervention: Dose increases and increased frequency of glucose monitoring may be required when nateglinide tablets are coadministered with these drugs. Drugs That May Blunt Signs and Symptoms of Hypoglycemia Drugs: beta-blockers, clonidine, guanethidine, and reserpine Intervention: Increased frequency of glucose monitoring may be required when nateglinide tablets are coadministered with these drugs.
Medication Information
Warnings and Precautions
Hypoglycemia: Nateglinide may cause hypoglycemia. Administer before meals to reduce the risk of hypoglycemia. Skip the scheduled dose of nateglinide if a meal is skipped to reduce the risk of hypoglycemia. ( 5.1 ) Macrovascular outcomes: There have been no clinical studies establishing conclusive evidence of macrovascular risk reduction with nateglinide. ( 5.2 )
Indications and Usage
Nateglinide tablets are indicated as an adjunct to diet and exercise to improve glycemic control in adults with type 2 diabetes mellitus.
Dosage and Administration
The recommended dose of nateglinide tablets is 120 mg orally three times daily before meals. The recommended dose of nateglinide tablets is 60 mg orally three times daily before meals in patients who are near glycemic goal when treatment is initiated. Instruct patients to take nateglinide tablets 1 to 30 minutes before meals. In patients who skip meals, instruct patients to skip the scheduled dose of nateglinide tablets to reduce the risk of hypoglycemia {see Warnings and Precautions (5.1) ].
Contraindications
Nateglinide is contraindicated in patients with a history of hypersensitivity to nateglinide or its inactive ingredients.
Adverse Reactions
The following serious adverse reaction is also described elsewhere in the labeling: Hypoglycemia [see Warnings and Precautions (5. 1) ]
Drug Interactions
Table 2 includes a list of drugs with clinically important drug interactions when concomitantly administered or withdrawn with nateglinide tablets and instructions for managing or preventing them. Table 2: Clinically Significant Drug Interactions with Nateglinide Drugs That May Increase the Blood-Glucose-Lowering Effect of Nateglinide and Susceptibility to Hypoglycemia Drugs: Nonsteroidal anti-inflammatory drugs (NSAIDs), salicylates, monoamine oxidase inhibitors, non-selective beta-adrenergic-blocking agents, anabolic hormones (e.g. methandrostenolone), guanethidine, gymnema sylvestre, glucomannan, thioctic acid, and inhibitors of CYP2C9 (e.g. amiodarone, fluconazole, voriconazole, sulfinpyrazone) or in patients known to be poor metabolizers of CYP2C9 substrates, alcohol. Intervention: Dose increases and increased frequency of glucose monitoring may be required when nateglinide tablets are coadministered with these drugs. Drugs and Herbals That May Reduce the Blood-Glucose-Lowering Effect of Nateglinide and Increase Susceptibility to Hyperglycemia Drugs: Thiazides, corticosteroids, thyroid products, sympathomimetics, somatropin, somatostatin analogues (e.g. lanreotide, octreotide), and CYP inducers (e.g. rifampin, phenytoin and St John's Wort). Intervention: Dose increases and increased frequency of glucose monitoring may be required when nateglinide tablets are coadministered with these drugs. Drugs That May Blunt Signs and Symptoms of Hypoglycemia Drugs: beta-blockers, clonidine, guanethidine, and reserpine Intervention: Increased frequency of glucose monitoring may be required when nateglinide tablets are coadministered with these drugs.
Description
Nateglinide tablets are indicated as an adjunct to diet and exercise to improve glycemic control in adults with type 2 diabetes mellitus.
Section 42229-5
Limitations of Use:
Nateglinide tablets should not be used in patients with type 1 diabetes mellitus or for the treatment of diabetic ketoacidosis.
Section 44425-7
Storage and Handling
Store at 20° to 25°C (68° to 77°F); excursions permitted between 15° to 30°C (59° to 86°F) [see USP Controlled Room Temperature.] Dispense in a tight container (USP).
10 Overdosage
There have been no instances of overdose with nateglinide in clinical trials. However, an overdose may result in an exaggerated glucose-lowering effect with the development of hypoglycemic symptoms. Hypoglycemic symptoms without loss of consciousness or neurological findings should be treated with oral glucose and adjustments in dosage and/or meal patterns. Severe hypoglycemic reactions with coma, seizure, or other neurological symptoms should be treated with intravenous glucose. As nateglinide are highly protein bound, dialysis is not an efficient means of removing it from the blood.
8.1 Pregnancy
There are no adequate and well-controlled studies of nateglinide in pregnant women. It is unknown whether nateglinide can cause fetal harm when administered to a pregnant woman. Nateglinide tablets should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus.
In the rabbit, embryonic development was adversely affected and the incidence of gall bladder agenesis or small gallbladder was increased at a dose of 500 mg/kg (approximately 27 times the human therapeutic exposure of 120 mg three times daily, based on body surface area). Nateglinide was not teratogenic in rats at doses up to 1,000 mg/kg (approximately 27 times the human therapeutic exposure based on body surface area).
11 Description
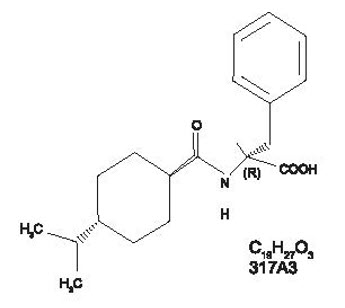
Nateglinide, USP is an oral blood glucose-lowering drug of the glinide class. Nateglinide, USP (-)-N-[(trans-4-isopropylcyclohexane)carbonyl]-D-phenylalanine, is structurally unrelated to the oral sulfonylurea insulin secretagogues.
The structural formula is as shown:
Nateglinide is a white or almost white powder with a molecular weight of 317.42. It is freely soluble in methanol, methylene chloride and in alcohol, soluble in ether, sparingly soluble in acetonitrile and in octanol, practically insoluble in water. Nateglinide tablets contain 60 mg, or 120mg, of nateglinide for oral administration.
Inactive ingredients: colloidal silicon dioxide, corn starch, croscarmellose sodium, hypromellose, mannitol, iron oxide (yellow and red), polyethylene glycol, povidone, pre-gelatinized starch, sodium lauryl sulphate, sodium starch glycolate, sodium stearyl fumarate, talc and titanium dioxide.
Film-coating material contains opadry pink and opadry yellow for the 60 mg and 120 mg. Opadry pink contains hypromellose, iron oxide red, macrogol and titanium dioxide. Opadry yellow contains hypromellose, iron oxides (yellow and red), macrogol, titanium dioxide, and talc.
14.1 Monotherapy
In a 24-week, double-blind, placebo-controlled study, patients with type 2 diabetes were randomized to receive either nateglinide tablets (60 mg or 120 mg three times daily before meals) or placebo. Patients previously treated with antidiabetic medications were required to discontinue that medication for at least 2 months before randomization.
At Week 24, treatment with nateglinide tablets before meals resulted in statistically significant reductions in mean HbA1C and mean fasting plasma glucose (FPG) compared to placebo (see Table 5). The reductions in HbA1C and FPG were similar for patient's naive to, and those previously exposed to, antidiabetic medications.
| Placebo | Nateglinide Tablets 60 mg three times daily before meals |
Nateglinide Tablets 120 mg three times daily before meals |
|
|---|---|---|---|
| HbA1C (%) | N=168 | N=167 | N=168 |
| Baseline (mean) | 8.0 | 7.9 | 8.1 |
| Change from baseline (mean) | +0.2 | -0.3 | -0.5 |
| Difference from placebo (mean) | -0.5 p-value≤0.004
|
-0.7 | |
| FPG (mg/dL) | N=172 | N=171 | N=169 |
| Baseline (mean) | 167.9 | 161.0 | 166.5 |
| Change from baseline (mean) | +9.1 | +0.4 | -4.5 |
| Difference from placebo (mean) | -8.7 | -13.6 |
5.1 Hypoglycemia
All glinides, including nateglinide can cause hypoglycemia [see Adverse Reactions (6.1)]. Severe hypoglycemia can cause seizures, may be life-threatening, or cause death. Hypoglycemia can impair concentration ability and reaction time; this may place an individual and others at risk in situations where these abilities are important (e.g., driving or operating other machinery).
Hypoglycemia can happen suddenly and symptoms may differ in each individual and change over time in the same individual. Symptomatic awareness of hypoglycemia may be less pronounced in patients with longstanding diabetes, in patients with diabetic neuropathy (nerve disease), in patients using medications that block the sympathetic nervous system (e.g., beta-blockers) {see Drug Interactions (7)), or in patients who experience recurrent hypoglycemia.
Factors which may increase the risk of hypoglycemia include changes in meal pattern (e.g., macronutrient content), changes in level of physical activity, changes to coadministered medication {see Drug Interactions (7)], and concomitant use with other antidiabetic agents. Patients with renal or hepatic impairment may be at higher risk of hypoglycemia [see Use in Specific Populations (8.6, 8.7), Clinical Pharmacology (12.3)].
Patients should take nateglinide before meals and be instructed to skip the dose of nateglinide if a meal is skipped [see Dosage and Administration (2)1. Patients and caregivers must be educated to recognize and manage hypoglycemia. Self-monitoring of blood glucose plays an essential role in the prevention and management of hypoglycemia. In patients at higher risk for hypoglycemia and patients who have reduced symptomatic awareness of hypoglycemia, increased frequency of blood glucose monitoring is recommended.
8.4 Pediatric Use
The safety and effectiveness of nateglinide have not been established in pediatric patients.
8.5 Geriatric Use
436 patients 65 years and older, and 80 patients 75 years and older were exposed to nateglinide in clinical studies. No differences were observed in safety or efficacy of nateglinide tablets between patients age 65 and over, and those under age 65. However, greater sensitivity of some older individuals to nateglinide tablets therapy cannot be ruled out.
4 Contraindications
Nateglinide is contraindicated in patients with a history of hypersensitivity to nateglinide or its inactive ingredients.
6 Adverse Reactions
The following serious adverse reaction is also described elsewhere in the labeling:
Hypoglycemia [see Warnings and Precautions (5. 1)]
7 Drug Interactions
Table 2 includes a list of drugs with clinically important drug interactions when concomitantly administered or withdrawn with nateglinide tablets and instructions for managing or preventing them.
| Drugs That May Increase the Blood-Glucose-Lowering Effect of Nateglinide and Susceptibility to Hypoglycemia | |
| Drugs: | Nonsteroidal anti-inflammatory drugs (NSAIDs), salicylates, monoamine oxidase inhibitors, non-selective beta-adrenergic-blocking agents, anabolic hormones (e.g. methandrostenolone), guanethidine, gymnema sylvestre, glucomannan, thioctic acid, and inhibitors of CYP2C9 (e.g. amiodarone, fluconazole, voriconazole, sulfinpyrazone) or in patients known to be poor metabolizers of CYP2C9 substrates, alcohol. |
| Intervention: | Dose increases and increased frequency of glucose monitoring may be required when nateglinide tablets are coadministered with these drugs. |
| Drugs and Herbals That May Reduce the Blood-Glucose-Lowering Effect of Nateglinide and Increase Susceptibility to Hyperglycemia | |
| Drugs: | Thiazides, corticosteroids, thyroid products, sympathomimetics, somatropin, somatostatin analogues (e.g. lanreotide, octreotide), and CYP inducers (e.g. rifampin, phenytoin and St John's Wort). |
| Intervention: | Dose increases and increased frequency of glucose monitoring may be required when nateglinide tablets are coadministered with these drugs. |
| Drugs That May Blunt Signs and Symptoms of Hypoglycemia | |
| Drugs: | beta-blockers, clonidine, guanethidine, and reserpine |
| Intervention: | Increased frequency of glucose monitoring may be required when nateglinide tablets are coadministered with these drugs. |
8.3 Nursing Mothers
It is not known whether nateglinide is excreted in human milk. Nateglinide is excreted in rat milk. Offspring of rats exposed to 1,000 mg/kg nateglinide (approximately 27 times the human therapeutic exposure of 120 mg three times daily, based on body surface area) had lower body weight. Because the potential for hypoglycemia in nursing infants may exist, a decision should be made as to whether nateglinide should be discontinued in nursing mothers, or if mothers should discontinue nursing.
8.6 Renal Impairment
No dosage adjustment is recommended in patients with mild to severe renal impairment [see Clinical Pharmacology (12.3)].
12.2 Pharmacodynamics
Nateglinide tablets stimulates pancreatic insulin secretion within 20 minutes of oral administration. When nateglinide tablets are dosed before meals, the peak rise in plasma insulin occurs approximately 1 hour after dosing and falls to baseline by 4 hours after dosing.
12.3 Pharmacokinetics
In patients with Type 2 diabetes, multiple dose administration of nateglinide over the dosage range of 60 mg to 240 mg shows linear pharmacokinetics for both AUC and C MAX. In patients with Type 2 diabetes, there is no apparent accumulation of nateglinide upon multiple dosing of up to 240 mg three times daily for 7 days.
1 Indications and Usage
Nateglinide tablets are indicated as an adjunct to diet and exercise to improve glycemic control in adults with type 2 diabetes mellitus.
8. 7 Hepatic Impairment
No dose adjustment is recommended for patients with mild hepatic impairment. Use of nateglinide in patients with moderate-to-severe hepatic impairment has not been studied and therefore, should be used with caution in these patients [see Clinical Pharmacology (12.3)].
12.1 Mechanism of Action
Nateglinide lowers blood glucose levels by stimulating insulin secretion from the pancreas. This action is dependent upon functioning beta-cells in the pancreatic islets. Nateglinide interacts with the ATP-sensitive potassium (K +ATP) channel on pancreatic beta-cells. The subsequent depolarization of the beta cell opens the calcium channel, producing calcium influx and insulin secretion. The extent of insulin release is glucose dependent and diminishes at low glucose levels. Nateglinide is highly tissue selective with low affinity for heart and skeletal muscle.
5 Warnings and Precautions
- Hypoglycemia: Nateglinide may cause hypoglycemia. Administer before meals to reduce the risk of hypoglycemia. Skip the scheduled dose of nateglinide if a meal is skipped to reduce the risk of hypoglycemia. (5.1)
- Macrovascular outcomes: There have been no clinical studies establishing conclusive evidence of macrovascular risk reduction with nateglinide. (5.2)
5.2 Macrovascular Outcomes
There have been no clinical studies establishing conclusive evidence of macrovascular risk reduction with nateglinide.
2 Dosage and Administration
The recommended dose of nateglinide tablets is 120 mg orally three times daily before meals.
The recommended dose of nateglinide tablets is 60 mg orally three times daily before meals in patients who are near glycemic goal when treatment is initiated.
Instruct patients to take nateglinide tablets 1 to 30 minutes before meals.
In patients who skip meals, instruct patients to skip the scheduled dose of nateglinide tablets to reduce the risk of hypoglycemia {see Warnings and Precautions (5.1)].
3 Dosage Forms and Strengths
- 60 mg tablets: Pink, round, beveled edge tablet with "C" debossed on one side and "123" on the other side
- 120 mg tablets: Yellow, ovaloid tablet with "C" debossed on one side and "125" on the other side
6.2 Postmarketing Experience
The following adverse reactions have been identified during post-approval use of nateglinide tablets. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
- Hypersensitivity reactions: Rash, itching, and urticaria
- Hepatobiliary Disorders: Jaundice, cholestatic hepatitis, and elevated liver enzymes
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
In clinical trials, approximately 2,600 patients with type 2 diabetes mellitus were treated with nateglinide. Of these, approximately 1,335 patients were treated for 6 months or longer and approximately 190 patients for one year or longer. Table 1 shows the most common adverse reactions associated with nateglinide.
| Placebo N=458 |
Nateglinide N=1,441 |
|
|---|---|---|
| Preferred Term | ||
| Upper Respiratory Infection | 8.1 | 10.5 |
| Back Pain | 3.7 | 4.0 |
| Flu Symptoms | 2.6 | 3.6 |
| Dizziness | 2.2 | 3.6 |
| Arthropathy | 2.2 | 3.3 |
| Diarrhea | 3.1 | 3.2 |
| Accidental Trauma | 1.7 | 2.9 |
| Bronchitis | 2.6 | 2.7 |
| Coughing | 2.2 | 2.4 |
14.2 Monotherapy Compared to Glyburide
In a 24-week, double-blind, active-controlled trial, patients with type 2 diabetes who had been on a sulfonylurea for 3 or more months and who had a baseline HbA 1 C greater than or equal to 6.5% were randomized to receive nateglinide tablets (60 mg or 120 mg three times daily before meals) or glyburide 10 mg once daily. Patients randomized to nateglinide tablets had statistically significant increases in mean HbA1C and mean FPG at endpoint compared to patients randomized to glyburide.
| Glyburide 10 mg Once daily | Nateglinide 60 mg three times daily before meals | Nateglinide 120 mg three times daily before meals | |
|---|---|---|---|
| HbA1C (%) | N=183 | N=178 | N=179 |
| Baseline (mean) | 7.8 | 8.0 | 7.9 |
| Change from baseline (mean) | 0.3 | 1.3 | 1.1 |
| Difference from glyburide | 1.0 p-value <0.001
|
0.9 | |
| FPG(mmol/L) | N=184 | N=182 | N=180 |
| Baseline (mean) | 9.44 | 9.67 | 9.61 |
| Change from baseline (mean) | 0.19 | 3.06 | 2.84 |
| Difference from glyburide | 2.87 | 2.66 |
14.5 Add On Combination Therapy With Glyburide
In a 12-week study of patients with type 2 diabetes inadequately controlled on glyburide 10 mg once daily, the addition of nateglinide (60 mg or 120 mg three times daily before meals) did not produce any additional benefit.
| Placebo + roalglitazone 8 mg once daily | Nateglinide 120 mg before meals + rosiglitazone 8 mg once daily | |
|---|---|---|
| HbA1C (%) | N=191 | N=194 |
| Baseline (mean) | 8.4 | 8.3 |
| Change from baseline (mean) | 0.03 | -0.7 |
| Difference from rosiglitazone (mean) | -0.7 p-value≤0.0001
|
14.3 Monotherapy and in Combination With Metformin
In a 24-week, double-blind, active- and placebo-controlled study, patients with type 2 diabetes were randomized to receive either nateglinide alone (120 mg three times daily before meals), metformin alone (500 mg three times daily), a combination of nateglinide tablets 120 mg (three times daily before meals) and metformin (500 mg three times daily), or placebo. Fifty-seven percent of patients were previously untreated with oral antidiabetic therapy. Patients previously treated with antidiabetic medications were required to discontinue medication for at least 2 months before randomization.
At Week 24, statistically significant reductions in mean HbA1c and FPG were observed with metformin monotherapy compared to nateglinide tablets monotherapy, and the combination of nateglinide tablets and metformin compared to either nateglinide tablets or metformin monotherapy (see Table 7).
Compared to placebo, nateglinide monotherapy was associated with a statistically significant increase in mean body weight, while no significant change in body weight was observed with metformin monotherapy or combination of nateglinide and metformin therapy (see Table 7). Among the subset of patients previously treated with other antidiabetic agents, primarily glyburide, HbA1C in the nateglinide monotherapy group increased slightly from baseline, whereas HbA1C was reduced in the metformin monotherapy group (see Table 7).
| Placebo | Nateglinide 120 mg three times daily | Metformin 500 mg three times daily | Nateglinide 120 mg before meals plus Metformin Metformin was administered three times daily
|
|
|---|---|---|---|---|
| HbA1C(%) All | N=160 | N=171 | N=172 | N=162 |
| Baseline (mean) | 8.3 | 8.3 | 8.4 | 8.4 |
| Change from baseline (mean) | +0.4 | -0.4 p-value≤0.03 vs. metformin
p-value≤0.05 vs. combination
|
-0.8 | -1.5 |
| Difference from placebo | -0.8 p-value≤0.05 vs. placebo
|
-1.2 | -1.9 | |
| Naïve | N=98 | N=99 | N=98 | N=81 |
| Baseline (mean) | 8.2 | 8.1 | 8.3 | 8.2 |
| Change from baseline (mean) | +0.3 | -0.7 | -0.8 | -1.6 |
| Difference from placebo | -1.0 | -1.1 | -1.9 | |
| Non-Naïve | N=62 | N=72 | N=74 | N=81 |
| Baseline (mean) | 8.3 | 8.5 | 8.7 | 8.7 |
| Change from baseline (mean) | +0.6 | +0.004 | -0.8 | -1.4 |
| Difference from placebo | -0.6 | -1.4a | -2.0 | |
| FPG (mg/dL) | ||||
| All | N=166 | N=173 | N=174 | N=167 |
| Baseline (mean) | 194.0 | 196.5 | 196.0 | 197.7 |
| Change from baseline (mean) | +8.0 | -13.1 | -30.0 | -44.9 |
| Difference from placebo | -21.1 | -38.0 | -52.9 |
In another 24-week, double-blind, placebo-controlled trial, patients with type 2 diabetes with HbA1C greater than or equal to 6.8% after treatment with metformin (greater than or equal to 1,500 mg daily for at least 1 month) were first entered into a four week run-in period of metformin monotherapy (2,000 mg daily) and then randomized to receive either nateglinide tablets (60 mg or 120 mg three limes daily before meals) or placebo as add-on to metformin. At the end of treatment, nateglinide tablets 60 mg and 120 mg three times daily resulted in a statistically significantly greater reductions in HbA1C compared to placebo when added to metformin (-0.4% and -0.6% for nateglinide tablets 60 mg and nateglinide tablets 120 mg plus metformin, respectively).
| Placebo + 006Detformin | Nateglinide 60 mg + metformin | Nateglinide 120 mg + metformin | |
|---|---|---|---|
| HbA1C (%) | N=150 | N=152 | N=154 |
| Baseline (mean) | 8.2 | 8.0 | 8.2 |
| Change from baseline (mean) | 0.01 | -0.4 | -0.6 |
| Difference from metformin | -0.4 p-value 0.003 vs. metformin
|
-0.6 p-value < 0.001 vs. metformin
All nateglinide /placebo taken three times daily before meals; all metformin 1,000 mg twice daily. |
14.4 Add On Combination Therapy With Rosiglitazone
A 24-week, double blind, multicenter, placebo-controlled trial was performed in patients with type 2 diabetes not adequately controlled on rosiglitazone 8 mg daily. The addition of nateglinide (120 mg three times per day with meals) was associated with statistically significantly greater reductions in HbA1C compared to placebo as add-on to rosiglitazone. The mean change in weight from baseline was +3 kg for patients treated with nateglinide tablets compared to +1 kg for patients treated with placebo when added to rosiglitazone.
| Placebo + roalglitazone 8 mg once daily | Nateglinide 120 mg before meals + rosiglitazone 8 mg once daily | |
|---|---|---|
| HbA1C (%) | N=191 | N=194 |
| Baseline (mean) | 8.4 | 8.3 |
| Change from baseline (mean) | 0.03 | -0.7 |
| Difference from rosiglitazone (mean) | -0.7 p-value≤0.0001
|
Principal Display Panel 60 Mg Tablet Bottle Label
NDC 75834-205-01
NATEGLINIDE
TABLETS, USP
60 mg
100 Tablets
NIVAGEN
Rx only
Principal Display Panel 120 Mg Tablet Bottle Label
NDC 75834-206-01
NATEGLINIDE
TABLETS, USP
120 mg
100 Tablets
NIVAGEN
Rx only
Structured Label Content
Section 42229-5 (42229-5)
Limitations of Use:
Nateglinide tablets should not be used in patients with type 1 diabetes mellitus or for the treatment of diabetic ketoacidosis.
Section 44425-7 (44425-7)
Storage and Handling
Store at 20° to 25°C (68° to 77°F); excursions permitted between 15° to 30°C (59° to 86°F) [see USP Controlled Room Temperature.] Dispense in a tight container (USP).
10 Overdosage (10 OVERDOSAGE)
There have been no instances of overdose with nateglinide in clinical trials. However, an overdose may result in an exaggerated glucose-lowering effect with the development of hypoglycemic symptoms. Hypoglycemic symptoms without loss of consciousness or neurological findings should be treated with oral glucose and adjustments in dosage and/or meal patterns. Severe hypoglycemic reactions with coma, seizure, or other neurological symptoms should be treated with intravenous glucose. As nateglinide are highly protein bound, dialysis is not an efficient means of removing it from the blood.
8.1 Pregnancy
There are no adequate and well-controlled studies of nateglinide in pregnant women. It is unknown whether nateglinide can cause fetal harm when administered to a pregnant woman. Nateglinide tablets should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus.
In the rabbit, embryonic development was adversely affected and the incidence of gall bladder agenesis or small gallbladder was increased at a dose of 500 mg/kg (approximately 27 times the human therapeutic exposure of 120 mg three times daily, based on body surface area). Nateglinide was not teratogenic in rats at doses up to 1,000 mg/kg (approximately 27 times the human therapeutic exposure based on body surface area).
11 Description (11 DESCRIPTION)
Nateglinide, USP is an oral blood glucose-lowering drug of the glinide class. Nateglinide, USP (-)-N-[(trans-4-isopropylcyclohexane)carbonyl]-D-phenylalanine, is structurally unrelated to the oral sulfonylurea insulin secretagogues.
The structural formula is as shown:
Nateglinide is a white or almost white powder with a molecular weight of 317.42. It is freely soluble in methanol, methylene chloride and in alcohol, soluble in ether, sparingly soluble in acetonitrile and in octanol, practically insoluble in water. Nateglinide tablets contain 60 mg, or 120mg, of nateglinide for oral administration.
Inactive ingredients: colloidal silicon dioxide, corn starch, croscarmellose sodium, hypromellose, mannitol, iron oxide (yellow and red), polyethylene glycol, povidone, pre-gelatinized starch, sodium lauryl sulphate, sodium starch glycolate, sodium stearyl fumarate, talc and titanium dioxide.
Film-coating material contains opadry pink and opadry yellow for the 60 mg and 120 mg. Opadry pink contains hypromellose, iron oxide red, macrogol and titanium dioxide. Opadry yellow contains hypromellose, iron oxides (yellow and red), macrogol, titanium dioxide, and talc.
14.1 Monotherapy
In a 24-week, double-blind, placebo-controlled study, patients with type 2 diabetes were randomized to receive either nateglinide tablets (60 mg or 120 mg three times daily before meals) or placebo. Patients previously treated with antidiabetic medications were required to discontinue that medication for at least 2 months before randomization.
At Week 24, treatment with nateglinide tablets before meals resulted in statistically significant reductions in mean HbA1C and mean fasting plasma glucose (FPG) compared to placebo (see Table 5). The reductions in HbA1C and FPG were similar for patient's naive to, and those previously exposed to, antidiabetic medications.
| Placebo | Nateglinide Tablets 60 mg three times daily before meals |
Nateglinide Tablets 120 mg three times daily before meals |
|
|---|---|---|---|
| HbA1C (%) | N=168 | N=167 | N=168 |
| Baseline (mean) | 8.0 | 7.9 | 8.1 |
| Change from baseline (mean) | +0.2 | -0.3 | -0.5 |
| Difference from placebo (mean) | -0.5 p-value≤0.004
|
-0.7 | |
| FPG (mg/dL) | N=172 | N=171 | N=169 |
| Baseline (mean) | 167.9 | 161.0 | 166.5 |
| Change from baseline (mean) | +9.1 | +0.4 | -4.5 |
| Difference from placebo (mean) | -8.7 | -13.6 |
5.1 Hypoglycemia
All glinides, including nateglinide can cause hypoglycemia [see Adverse Reactions (6.1)]. Severe hypoglycemia can cause seizures, may be life-threatening, or cause death. Hypoglycemia can impair concentration ability and reaction time; this may place an individual and others at risk in situations where these abilities are important (e.g., driving or operating other machinery).
Hypoglycemia can happen suddenly and symptoms may differ in each individual and change over time in the same individual. Symptomatic awareness of hypoglycemia may be less pronounced in patients with longstanding diabetes, in patients with diabetic neuropathy (nerve disease), in patients using medications that block the sympathetic nervous system (e.g., beta-blockers) {see Drug Interactions (7)), or in patients who experience recurrent hypoglycemia.
Factors which may increase the risk of hypoglycemia include changes in meal pattern (e.g., macronutrient content), changes in level of physical activity, changes to coadministered medication {see Drug Interactions (7)], and concomitant use with other antidiabetic agents. Patients with renal or hepatic impairment may be at higher risk of hypoglycemia [see Use in Specific Populations (8.6, 8.7), Clinical Pharmacology (12.3)].
Patients should take nateglinide before meals and be instructed to skip the dose of nateglinide if a meal is skipped [see Dosage and Administration (2)1. Patients and caregivers must be educated to recognize and manage hypoglycemia. Self-monitoring of blood glucose plays an essential role in the prevention and management of hypoglycemia. In patients at higher risk for hypoglycemia and patients who have reduced symptomatic awareness of hypoglycemia, increased frequency of blood glucose monitoring is recommended.
8.4 Pediatric Use
The safety and effectiveness of nateglinide have not been established in pediatric patients.
8.5 Geriatric Use
436 patients 65 years and older, and 80 patients 75 years and older were exposed to nateglinide in clinical studies. No differences were observed in safety or efficacy of nateglinide tablets between patients age 65 and over, and those under age 65. However, greater sensitivity of some older individuals to nateglinide tablets therapy cannot be ruled out.
4 Contraindications (4 CONTRAINDICATIONS)
Nateglinide is contraindicated in patients with a history of hypersensitivity to nateglinide or its inactive ingredients.
6 Adverse Reactions (6 ADVERSE REACTIONS)
The following serious adverse reaction is also described elsewhere in the labeling:
Hypoglycemia [see Warnings and Precautions (5. 1)]
7 Drug Interactions (7 DRUG INTERACTIONS)
Table 2 includes a list of drugs with clinically important drug interactions when concomitantly administered or withdrawn with nateglinide tablets and instructions for managing or preventing them.
| Drugs That May Increase the Blood-Glucose-Lowering Effect of Nateglinide and Susceptibility to Hypoglycemia | |
| Drugs: | Nonsteroidal anti-inflammatory drugs (NSAIDs), salicylates, monoamine oxidase inhibitors, non-selective beta-adrenergic-blocking agents, anabolic hormones (e.g. methandrostenolone), guanethidine, gymnema sylvestre, glucomannan, thioctic acid, and inhibitors of CYP2C9 (e.g. amiodarone, fluconazole, voriconazole, sulfinpyrazone) or in patients known to be poor metabolizers of CYP2C9 substrates, alcohol. |
| Intervention: | Dose increases and increased frequency of glucose monitoring may be required when nateglinide tablets are coadministered with these drugs. |
| Drugs and Herbals That May Reduce the Blood-Glucose-Lowering Effect of Nateglinide and Increase Susceptibility to Hyperglycemia | |
| Drugs: | Thiazides, corticosteroids, thyroid products, sympathomimetics, somatropin, somatostatin analogues (e.g. lanreotide, octreotide), and CYP inducers (e.g. rifampin, phenytoin and St John's Wort). |
| Intervention: | Dose increases and increased frequency of glucose monitoring may be required when nateglinide tablets are coadministered with these drugs. |
| Drugs That May Blunt Signs and Symptoms of Hypoglycemia | |
| Drugs: | beta-blockers, clonidine, guanethidine, and reserpine |
| Intervention: | Increased frequency of glucose monitoring may be required when nateglinide tablets are coadministered with these drugs. |
8.3 Nursing Mothers
It is not known whether nateglinide is excreted in human milk. Nateglinide is excreted in rat milk. Offspring of rats exposed to 1,000 mg/kg nateglinide (approximately 27 times the human therapeutic exposure of 120 mg three times daily, based on body surface area) had lower body weight. Because the potential for hypoglycemia in nursing infants may exist, a decision should be made as to whether nateglinide should be discontinued in nursing mothers, or if mothers should discontinue nursing.
8.6 Renal Impairment
No dosage adjustment is recommended in patients with mild to severe renal impairment [see Clinical Pharmacology (12.3)].
12.2 Pharmacodynamics
Nateglinide tablets stimulates pancreatic insulin secretion within 20 minutes of oral administration. When nateglinide tablets are dosed before meals, the peak rise in plasma insulin occurs approximately 1 hour after dosing and falls to baseline by 4 hours after dosing.
12.3 Pharmacokinetics
In patients with Type 2 diabetes, multiple dose administration of nateglinide over the dosage range of 60 mg to 240 mg shows linear pharmacokinetics for both AUC and C MAX. In patients with Type 2 diabetes, there is no apparent accumulation of nateglinide upon multiple dosing of up to 240 mg three times daily for 7 days.
1 Indications and Usage (1 INDICATIONS AND USAGE)
Nateglinide tablets are indicated as an adjunct to diet and exercise to improve glycemic control in adults with type 2 diabetes mellitus.
8. 7 Hepatic Impairment
No dose adjustment is recommended for patients with mild hepatic impairment. Use of nateglinide in patients with moderate-to-severe hepatic impairment has not been studied and therefore, should be used with caution in these patients [see Clinical Pharmacology (12.3)].
12.1 Mechanism of Action
Nateglinide lowers blood glucose levels by stimulating insulin secretion from the pancreas. This action is dependent upon functioning beta-cells in the pancreatic islets. Nateglinide interacts with the ATP-sensitive potassium (K +ATP) channel on pancreatic beta-cells. The subsequent depolarization of the beta cell opens the calcium channel, producing calcium influx and insulin secretion. The extent of insulin release is glucose dependent and diminishes at low glucose levels. Nateglinide is highly tissue selective with low affinity for heart and skeletal muscle.
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
- Hypoglycemia: Nateglinide may cause hypoglycemia. Administer before meals to reduce the risk of hypoglycemia. Skip the scheduled dose of nateglinide if a meal is skipped to reduce the risk of hypoglycemia. (5.1)
- Macrovascular outcomes: There have been no clinical studies establishing conclusive evidence of macrovascular risk reduction with nateglinide. (5.2)
5.2 Macrovascular Outcomes
There have been no clinical studies establishing conclusive evidence of macrovascular risk reduction with nateglinide.
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
The recommended dose of nateglinide tablets is 120 mg orally three times daily before meals.
The recommended dose of nateglinide tablets is 60 mg orally three times daily before meals in patients who are near glycemic goal when treatment is initiated.
Instruct patients to take nateglinide tablets 1 to 30 minutes before meals.
In patients who skip meals, instruct patients to skip the scheduled dose of nateglinide tablets to reduce the risk of hypoglycemia {see Warnings and Precautions (5.1)].
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
- 60 mg tablets: Pink, round, beveled edge tablet with "C" debossed on one side and "123" on the other side
- 120 mg tablets: Yellow, ovaloid tablet with "C" debossed on one side and "125" on the other side
6.2 Postmarketing Experience
The following adverse reactions have been identified during post-approval use of nateglinide tablets. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
- Hypersensitivity reactions: Rash, itching, and urticaria
- Hepatobiliary Disorders: Jaundice, cholestatic hepatitis, and elevated liver enzymes
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
In clinical trials, approximately 2,600 patients with type 2 diabetes mellitus were treated with nateglinide. Of these, approximately 1,335 patients were treated for 6 months or longer and approximately 190 patients for one year or longer. Table 1 shows the most common adverse reactions associated with nateglinide.
| Placebo N=458 |
Nateglinide N=1,441 |
|
|---|---|---|
| Preferred Term | ||
| Upper Respiratory Infection | 8.1 | 10.5 |
| Back Pain | 3.7 | 4.0 |
| Flu Symptoms | 2.6 | 3.6 |
| Dizziness | 2.2 | 3.6 |
| Arthropathy | 2.2 | 3.3 |
| Diarrhea | 3.1 | 3.2 |
| Accidental Trauma | 1.7 | 2.9 |
| Bronchitis | 2.6 | 2.7 |
| Coughing | 2.2 | 2.4 |
14.2 Monotherapy Compared to Glyburide
In a 24-week, double-blind, active-controlled trial, patients with type 2 diabetes who had been on a sulfonylurea for 3 or more months and who had a baseline HbA 1 C greater than or equal to 6.5% were randomized to receive nateglinide tablets (60 mg or 120 mg three times daily before meals) or glyburide 10 mg once daily. Patients randomized to nateglinide tablets had statistically significant increases in mean HbA1C and mean FPG at endpoint compared to patients randomized to glyburide.
| Glyburide 10 mg Once daily | Nateglinide 60 mg three times daily before meals | Nateglinide 120 mg three times daily before meals | |
|---|---|---|---|
| HbA1C (%) | N=183 | N=178 | N=179 |
| Baseline (mean) | 7.8 | 8.0 | 7.9 |
| Change from baseline (mean) | 0.3 | 1.3 | 1.1 |
| Difference from glyburide | 1.0 p-value <0.001
|
0.9 | |
| FPG(mmol/L) | N=184 | N=182 | N=180 |
| Baseline (mean) | 9.44 | 9.67 | 9.61 |
| Change from baseline (mean) | 0.19 | 3.06 | 2.84 |
| Difference from glyburide | 2.87 | 2.66 |
14.5 Add On Combination Therapy With Glyburide (14.5 Add-On Combination Therapy With Glyburide)
In a 12-week study of patients with type 2 diabetes inadequately controlled on glyburide 10 mg once daily, the addition of nateglinide (60 mg or 120 mg three times daily before meals) did not produce any additional benefit.
| Placebo + roalglitazone 8 mg once daily | Nateglinide 120 mg before meals + rosiglitazone 8 mg once daily | |
|---|---|---|
| HbA1C (%) | N=191 | N=194 |
| Baseline (mean) | 8.4 | 8.3 |
| Change from baseline (mean) | 0.03 | -0.7 |
| Difference from rosiglitazone (mean) | -0.7 p-value≤0.0001
|
14.3 Monotherapy and in Combination With Metformin (14.3 Monotherapy and In Combination With Metformin)
In a 24-week, double-blind, active- and placebo-controlled study, patients with type 2 diabetes were randomized to receive either nateglinide alone (120 mg three times daily before meals), metformin alone (500 mg three times daily), a combination of nateglinide tablets 120 mg (three times daily before meals) and metformin (500 mg three times daily), or placebo. Fifty-seven percent of patients were previously untreated with oral antidiabetic therapy. Patients previously treated with antidiabetic medications were required to discontinue medication for at least 2 months before randomization.
At Week 24, statistically significant reductions in mean HbA1c and FPG were observed with metformin monotherapy compared to nateglinide tablets monotherapy, and the combination of nateglinide tablets and metformin compared to either nateglinide tablets or metformin monotherapy (see Table 7).
Compared to placebo, nateglinide monotherapy was associated with a statistically significant increase in mean body weight, while no significant change in body weight was observed with metformin monotherapy or combination of nateglinide and metformin therapy (see Table 7). Among the subset of patients previously treated with other antidiabetic agents, primarily glyburide, HbA1C in the nateglinide monotherapy group increased slightly from baseline, whereas HbA1C was reduced in the metformin monotherapy group (see Table 7).
| Placebo | Nateglinide 120 mg three times daily | Metformin 500 mg three times daily | Nateglinide 120 mg before meals plus Metformin Metformin was administered three times daily
|
|
|---|---|---|---|---|
| HbA1C(%) All | N=160 | N=171 | N=172 | N=162 |
| Baseline (mean) | 8.3 | 8.3 | 8.4 | 8.4 |
| Change from baseline (mean) | +0.4 | -0.4 p-value≤0.03 vs. metformin
p-value≤0.05 vs. combination
|
-0.8 | -1.5 |
| Difference from placebo | -0.8 p-value≤0.05 vs. placebo
|
-1.2 | -1.9 | |
| Naïve | N=98 | N=99 | N=98 | N=81 |
| Baseline (mean) | 8.2 | 8.1 | 8.3 | 8.2 |
| Change from baseline (mean) | +0.3 | -0.7 | -0.8 | -1.6 |
| Difference from placebo | -1.0 | -1.1 | -1.9 | |
| Non-Naïve | N=62 | N=72 | N=74 | N=81 |
| Baseline (mean) | 8.3 | 8.5 | 8.7 | 8.7 |
| Change from baseline (mean) | +0.6 | +0.004 | -0.8 | -1.4 |
| Difference from placebo | -0.6 | -1.4a | -2.0 | |
| FPG (mg/dL) | ||||
| All | N=166 | N=173 | N=174 | N=167 |
| Baseline (mean) | 194.0 | 196.5 | 196.0 | 197.7 |
| Change from baseline (mean) | +8.0 | -13.1 | -30.0 | -44.9 |
| Difference from placebo | -21.1 | -38.0 | -52.9 |
In another 24-week, double-blind, placebo-controlled trial, patients with type 2 diabetes with HbA1C greater than or equal to 6.8% after treatment with metformin (greater than or equal to 1,500 mg daily for at least 1 month) were first entered into a four week run-in period of metformin monotherapy (2,000 mg daily) and then randomized to receive either nateglinide tablets (60 mg or 120 mg three limes daily before meals) or placebo as add-on to metformin. At the end of treatment, nateglinide tablets 60 mg and 120 mg three times daily resulted in a statistically significantly greater reductions in HbA1C compared to placebo when added to metformin (-0.4% and -0.6% for nateglinide tablets 60 mg and nateglinide tablets 120 mg plus metformin, respectively).
| Placebo + 006Detformin | Nateglinide 60 mg + metformin | Nateglinide 120 mg + metformin | |
|---|---|---|---|
| HbA1C (%) | N=150 | N=152 | N=154 |
| Baseline (mean) | 8.2 | 8.0 | 8.2 |
| Change from baseline (mean) | 0.01 | -0.4 | -0.6 |
| Difference from metformin | -0.4 p-value 0.003 vs. metformin
|
-0.6 p-value < 0.001 vs. metformin
All nateglinide /placebo taken three times daily before meals; all metformin 1,000 mg twice daily. |
14.4 Add On Combination Therapy With Rosiglitazone (14.4 Add-On Combination Therapy With Rosiglitazone)
A 24-week, double blind, multicenter, placebo-controlled trial was performed in patients with type 2 diabetes not adequately controlled on rosiglitazone 8 mg daily. The addition of nateglinide (120 mg three times per day with meals) was associated with statistically significantly greater reductions in HbA1C compared to placebo as add-on to rosiglitazone. The mean change in weight from baseline was +3 kg for patients treated with nateglinide tablets compared to +1 kg for patients treated with placebo when added to rosiglitazone.
| Placebo + roalglitazone 8 mg once daily | Nateglinide 120 mg before meals + rosiglitazone 8 mg once daily | |
|---|---|---|
| HbA1C (%) | N=191 | N=194 |
| Baseline (mean) | 8.4 | 8.3 |
| Change from baseline (mean) | 0.03 | -0.7 |
| Difference from rosiglitazone (mean) | -0.7 p-value≤0.0001
|
Principal Display Panel 60 Mg Tablet Bottle Label (PRINCIPAL DISPLAY PANEL - 60 mg Tablet Bottle Label)
NDC 75834-205-01
NATEGLINIDE
TABLETS, USP
60 mg
100 Tablets
NIVAGEN
Rx only
Principal Display Panel 120 Mg Tablet Bottle Label (PRINCIPAL DISPLAY PANEL - 120 mg Tablet Bottle Label)
NDC 75834-206-01
NATEGLINIDE
TABLETS, USP
120 mg
100 Tablets
NIVAGEN
Rx only
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:35:47.999591 · Updated: 2026-03-14T21:44:26.969907