These Highlights Do Not Include All The Information Needed To Use Meropenem For Injection Safely And Effectively. See Full Prescribing Information For meropenem For Injection
1f9591ed-3a6c-422e-b1be-7b3e4fe5bf3c
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
Warnings and Precautions, Rhabdomyolysis ( 5.3 ) 12/2024
Indications and Usage
Meropenen for injection is a penem antibacterial indicated for the treatment of: •Complicated skin and skin structure infections (adult patients and pediatric patients 3 months of age and older only). ( 1.1 ) •Complicated intra-abdominal infections (adult and pediatric patients). ( 1.2 ) •Bacterial meningitis (pediatric patients 3 months of age and older only). ( 1.3 ) To reduce the development of drug-resistant bacteria and maintain the effectiveness of meropenen for injection and other antibacterial drugs, meropenen for injection should only be used to treat or prevent infections that are proven or strongly suspected to be caused by susceptible bacteria.
Dosage and Administration
•500 mg every 8 hours by intravenous infusion over 15 to 30 minutes for complicated skin and skin structure infections (cSSSI) for adult patients. When treating infections caused by Pseudomonas aeruginosa , a dose of 1 gram every 8 hours is recommended. ( 2.1 ) •1 gram every 8 hours by intravenous infusion over 15 minutes to 30 minutes for intra-abdominal infections for adult patients. ( 2.1 ) •1 gram every 8 hours by intravenous bolus injection (5 mL to 20 mL) over 3 minutes to 5 minutes for adult patients. ( 2.1 ) •Dosage should be reduced in adult patients with renal impairment. ( 2.2 ) Recommended Meropenen for Injection Dosage Schedule for Adult Patients with Renal Impairment Creatinine Clearance (mL/min) Dose (dependent on type of infection) Dosing Interval Greater than 50 Recommended dose (500 mg cSSSI and 1 gram Intra-abdominal) Every 8 hours 26-50 Recommended dose Every 12 hours 10-25 One-half recommended dose Every 12 hours Less than 10 One-half recommended dose Every 24 hours Pediatric patients 3 months of age and older Recommended Meropenen for Injection Dosage Schedule for Pediatric Patients 3 Months of Age and Older with Normal Renal Function ( 2.3 ) Type of Infection Dose (mg/kg) Up to a Maximum Dose Dosing Interval Complicated skin and skin structure 20 mg/kg (or 1 gram for pediatric patients weighing over 50 kg) every 8 hours is recommended when treating complicated skin and skin structure infections caused by P. aeruginosa. ( 2.3 ) 10 500 mg Every 8 hours Intra-abdominal 20 1 gram Every 8 hours Meningitis 40 2 gram Every 8 hours -Intravenous infusion is to be given over approximately 15 minutes to 30 minutes.-Intravenous bolus injection (5 mL to 20 mL) is to be given over approximately 3 minutes-5 minutes.-There is no experience in pediatric patients with renal impairment. Pediatric patients less than 3 months of age Recommended Meropenen for Injection Dosage Schedule for Pediatric Patients Less than 3 Months of Age with Complicated Intra-Abdominal Infections and Normal Renal Function ( 2.3 ) Age Group Dose (mg/kg) Dose Interval Infants less than 32 weeks GA and PNA less than 2 weeks 20 Every 12 hours Infants less than 32 weeks GA and PNA 2 weeks and older 20 Every 8 hours Infants 32 weeks and older GA and PNA less than 2 weeks 20 Every 8 hours Infants 32 weeks and older GA and PNA 2 weeks and older 30 Every 8 hours - Intravenous infusion is to be given over 30 minutes. - There is no experience in pediatric patients with renal impairment. GA: gestational age and PNA: postnatal age
Warnings and Precautions
•Serious and occasionally fatal hypersensitivity (anaphylactic) reactions have been reported in patients receiving β-lactams. ( 5.1 ) •Severe cutaneous adverse reactions have been reported in patients receiving meropenen. ( 5.2 ) •Rhabdomyolysis: If signs or symptoms of rhabdomyolysis are observed, discontinue meropenem for injection and initiate appropriate therapy. ( 5.3 ) •Seizures and other adverse CNS experiences have been reported during treatment. ( 5.4 ) •Co-administration of meropenen with valproic acid or divalproex sodium reduces the serum concentration of valproic acid potentially increasing the risk of breakthrough seizures. ( 5.5 , 7.2 ) • Clostridioides difficile- associated diarrhea (ranging from mild diarrhea to fatal colitis) has been reported. Evaluate if diarrhea occurs. ( 5.6 ) •In patients with renal dysfunction, thrombocytopenia has been observed. ( 5.9 )
Contraindications
Meropenen for injection is contraindicated in patients with known hypersensitivity to any component of this product or to other drugs in the same class or in patients who have demonstrated anaphylactic reactions to beta (β)-lactams.
Adverse Reactions
Severe cutaneous adverse reactions (SCAR) such as Stevens-Johnson syndrome (SJS), toxic epidermal necrolysis (TEN), drug reaction with eosinophilia and systemic symptoms (DRESS), erythema multiforme (EM) and acute generalized exanthematous pustulosis (AGEP) have been reported in patients receiving meropenen [see Adverse Reactions (6.2) ] . If signs and symptoms suggestive of these reactions appear, meropenem should be withdrawn immediately and an alternative treatment should be considered.
Drug Interactions
•Co-administration of meropenen with probenecid inhibits renal excretion of meropenem and is therefore not recommended. ( 7.1 ) •The concomitant use of meropenen and valproic acid or divalproex sodium is generally not recommended. Antibacterial drugs other than carbapenems should be considered to treat infections in patients whose seizures are well controlled on valproic acid or divalproex sodium. ( 5.5 , 7.2 )
Medication Information
Warnings and Precautions
•Serious and occasionally fatal hypersensitivity (anaphylactic) reactions have been reported in patients receiving β-lactams. ( 5.1 ) •Severe cutaneous adverse reactions have been reported in patients receiving meropenen. ( 5.2 ) •Rhabdomyolysis: If signs or symptoms of rhabdomyolysis are observed, discontinue meropenem for injection and initiate appropriate therapy. ( 5.3 ) •Seizures and other adverse CNS experiences have been reported during treatment. ( 5.4 ) •Co-administration of meropenen with valproic acid or divalproex sodium reduces the serum concentration of valproic acid potentially increasing the risk of breakthrough seizures. ( 5.5 , 7.2 ) • Clostridioides difficile- associated diarrhea (ranging from mild diarrhea to fatal colitis) has been reported. Evaluate if diarrhea occurs. ( 5.6 ) •In patients with renal dysfunction, thrombocytopenia has been observed. ( 5.9 )
Indications and Usage
Meropenen for injection is a penem antibacterial indicated for the treatment of: •Complicated skin and skin structure infections (adult patients and pediatric patients 3 months of age and older only). ( 1.1 ) •Complicated intra-abdominal infections (adult and pediatric patients). ( 1.2 ) •Bacterial meningitis (pediatric patients 3 months of age and older only). ( 1.3 ) To reduce the development of drug-resistant bacteria and maintain the effectiveness of meropenen for injection and other antibacterial drugs, meropenen for injection should only be used to treat or prevent infections that are proven or strongly suspected to be caused by susceptible bacteria.
Dosage and Administration
•500 mg every 8 hours by intravenous infusion over 15 to 30 minutes for complicated skin and skin structure infections (cSSSI) for adult patients. When treating infections caused by Pseudomonas aeruginosa , a dose of 1 gram every 8 hours is recommended. ( 2.1 ) •1 gram every 8 hours by intravenous infusion over 15 minutes to 30 minutes for intra-abdominal infections for adult patients. ( 2.1 ) •1 gram every 8 hours by intravenous bolus injection (5 mL to 20 mL) over 3 minutes to 5 minutes for adult patients. ( 2.1 ) •Dosage should be reduced in adult patients with renal impairment. ( 2.2 ) Recommended Meropenen for Injection Dosage Schedule for Adult Patients with Renal Impairment Creatinine Clearance (mL/min) Dose (dependent on type of infection) Dosing Interval Greater than 50 Recommended dose (500 mg cSSSI and 1 gram Intra-abdominal) Every 8 hours 26-50 Recommended dose Every 12 hours 10-25 One-half recommended dose Every 12 hours Less than 10 One-half recommended dose Every 24 hours Pediatric patients 3 months of age and older Recommended Meropenen for Injection Dosage Schedule for Pediatric Patients 3 Months of Age and Older with Normal Renal Function ( 2.3 ) Type of Infection Dose (mg/kg) Up to a Maximum Dose Dosing Interval Complicated skin and skin structure 20 mg/kg (or 1 gram for pediatric patients weighing over 50 kg) every 8 hours is recommended when treating complicated skin and skin structure infections caused by P. aeruginosa. ( 2.3 ) 10 500 mg Every 8 hours Intra-abdominal 20 1 gram Every 8 hours Meningitis 40 2 gram Every 8 hours -Intravenous infusion is to be given over approximately 15 minutes to 30 minutes.-Intravenous bolus injection (5 mL to 20 mL) is to be given over approximately 3 minutes-5 minutes.-There is no experience in pediatric patients with renal impairment. Pediatric patients less than 3 months of age Recommended Meropenen for Injection Dosage Schedule for Pediatric Patients Less than 3 Months of Age with Complicated Intra-Abdominal Infections and Normal Renal Function ( 2.3 ) Age Group Dose (mg/kg) Dose Interval Infants less than 32 weeks GA and PNA less than 2 weeks 20 Every 12 hours Infants less than 32 weeks GA and PNA 2 weeks and older 20 Every 8 hours Infants 32 weeks and older GA and PNA less than 2 weeks 20 Every 8 hours Infants 32 weeks and older GA and PNA 2 weeks and older 30 Every 8 hours - Intravenous infusion is to be given over 30 minutes. - There is no experience in pediatric patients with renal impairment. GA: gestational age and PNA: postnatal age
Contraindications
Meropenen for injection is contraindicated in patients with known hypersensitivity to any component of this product or to other drugs in the same class or in patients who have demonstrated anaphylactic reactions to beta (β)-lactams.
Adverse Reactions
Severe cutaneous adverse reactions (SCAR) such as Stevens-Johnson syndrome (SJS), toxic epidermal necrolysis (TEN), drug reaction with eosinophilia and systemic symptoms (DRESS), erythema multiforme (EM) and acute generalized exanthematous pustulosis (AGEP) have been reported in patients receiving meropenen [see Adverse Reactions (6.2) ] . If signs and symptoms suggestive of these reactions appear, meropenem should be withdrawn immediately and an alternative treatment should be considered.
Drug Interactions
•Co-administration of meropenen with probenecid inhibits renal excretion of meropenem and is therefore not recommended. ( 7.1 ) •The concomitant use of meropenen and valproic acid or divalproex sodium is generally not recommended. Antibacterial drugs other than carbapenems should be considered to treat infections in patients whose seizures are well controlled on valproic acid or divalproex sodium. ( 5.5 , 7.2 )
Description
Warnings and Precautions, Rhabdomyolysis ( 5.3 ) 12/2024
Section 42229-5
Pediatric Patients 3 Months of Age and Older•For pediatric patients 3 months of age and older, the meropenen for injection dose is 10 mg/kg, 20 mg/kg or 40 mg/kg every 8 hours (maximum dose is 2 grams every 8 hours), depending on the type of infection (cSSSI, cIAI, intra-abdominal infection or meningitis). Seedosing table 2below.•For pediatric patients weighing over 50 kg administer meropenen for injection at a dose of 500 mg every 8 hours for cSSSI, 1 gram every 8 hours for cIAI and 2 grams every 8 hours for meningitis.•Administer meropenen for injection as an intravenous infusion over approximately 15 minutes to 30 minutes or as an intravenous bolus injection (5 mL to 20 mL) over approximately 3 minutes to 5 minutes.•There is limited safety data available to support the administration of a 40 mg/kg (up to a maximum of 2 grams) bolus dose.
| Type of Infection | Dose (mg/kg) | Up to a Maximum Dose | Dosing Interval |
|---|---|---|---|
| There is no experience in pediatric patients with renal impairment. When treating cSSSI caused byP. aeruginosa, a dose of 20 mg/kg (or 1 gram for pediatric patients weighing over 50 kg) every 8 hours is recommended. |
|||
| Complicated skin and skin structure infections | 10 | 500 mg | Every 8 hours |
| Complicated intra-abdominal infections | 20 | 1 gram | Every 8 hours |
| Meningitis | 40 | 2 grams | Every 8 hours |
Section 43683-2
|
Warnings and Precautions, Rhabdomyolysis (5.3) |
12/2024 |
Section 44425-7
Meropenem for Injection, USP is supplied in 20 mL and 30 mL injection vials containing sufficient meropenem to deliver 500 mg or 1 gram for intravenous administration, respectively. The dry powder should be stored at 20°–25°C (68°–77°F) [see USP Controlled Room Temperature].
500 mg Injection Vial (NDC 51810-502-01) in a pack of 10 x 500 mg Injection Vials (NDC 51810-502-02)
1 gram Injection Vial (NDC 51810-503-01) in a pack of 10 x 1 g Injection Vials (NDC 51810-503-02)
1.4 Usage
To reduce the development of drug-resistant bacteria and maintain the effectiveness of meropenen for injection and other antibacterial drugs, meropenen for injection should only be used to treat or prevent infections that are proven or strongly suspected to be caused by susceptible bacteria. When culture and susceptibility information are available, they should be considered in selecting or modifying antibacterial therapy. In the absence of such data, local epidemiology and susceptibility patterns may contribute to the empiric selection of therapy.
10 Overdosage
In mice and rats, large intravenous doses of meropenem (2200 mg/kg to 4000 mg/kg) have been associated with ataxia, dyspnea, convulsions, and mortalities.
Intentional overdosing of meropenem is unlikely, although accidental overdosing might occur if large doses are given to patients with reduced renal function. The largest dose of meropenem administered in clinical trials has been 2 grams given intravenously every 8 hours. At this dosage, no adverse pharmacological effects or increased safety risks have been observed.
Limited postmarketing experience indicates that if adverse events occur following overdosage, they are consistent with the adverse event profile described in the Adverse Reactions section and are generally mild in severity and resolve on withdrawal or dose reduction. Consider symptomatic treatments. In individuals with normal renal function, rapid renal elimination takes place. Meropenem and its metabolite are readily dialyzable and effectively removed by hemodialysis; however, no information is available on the use of hemodialysis to treat overdosage.
15 References
-
1.Cockcroft DW, MH Gault, 1976, Prediction of creatinine clearance from serum creatinine, Nephron, 16:31–41.
-
2.Kawamura S, AW Russell, SJ Freeman, and RA Siddall, 1992, Reproductive and Developmental Toxicity of Meropenem in Rats, Chemotherapy, 40:S238–250.
11 Description
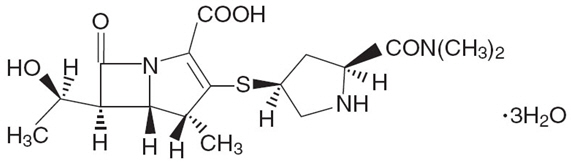
Meropenem for Injection, USP (meropenem for injection) is a sterile, pyrogen-free, synthetic, carbapenem antibacterial for intravenous administration. It is (4R,5S,6S)-3- [[(3S,5S)-5-(Dimethylcarbamoyl)-3-pyrrolidinyl]thio]-6- [(1R)-1-hydroxyethyl]-4-methyl-7-oxo-1-azabicyclo[3.2.0]hept-2-ene-2-carboxylic acid trihydrate. Its empirical formula is C17H25N3O5S∙3H2O with a molecular weight of 437.52. Its structural formula is:
Meropenem for Injection, USP is a white to pale yellow crystalline powder. The solution varies from colorless to yellow depending on the concentration. The pH of freshly constituted solutions is between 7.3 and 8.3. Meropenem is soluble in 5% monobasic potassium phosphate solution, sparingly soluble in water, very slightly soluble in hydrated ethanol, and practically insoluble in acetone or ether.
When re-constituted as instructed, each 1 gram Meropenem for Injection, USP vial will deliver 1 gram of meropenem and 90.2 mg of sodium as sodium carbonate (3.92 mEq). Each 500 mg Meropenem for Injection, USP vial will deliver 500 mg meropenem and 45.1 mg of sodium as sodium carbonate (1.96 mEq) [ see Dosage and Administration (2.4) ].
7.1 Probenecid
Probenecid competes with meropenem for active tubular secretion, resulting in increased plasma concentrations of meropenem. Co-administration of probenecid with meropenem is not recommended.
2.5 Compatibility
Compatibility of meropenen for injection with other drugs has not been established. Meropenen for injection should not be mixed with or physically added to solutions containing other drugs.
7.2 Valproic Acid
Case reports in the literature have shown that co-administration of carbapenems, including meropenem, to patients receiving valproic acid or divalproex sodium results in a reduction in valproic acid concentrations. The valproic acid concentrations may drop below the therapeutic range as a result of this interaction, therefore increasing the risk of breakthrough seizures. Although the mechanism of this interaction is unknown, data from in vitro and animal studies suggest that carbapenems may inhibit the hydrolysis of valproic acid's glucuronide metabolite (VPA-g) back to valproic acid, thus decreasing the serum concentrations of valproic acid. If administration of meropenem is necessary, then supplemental anti-convulsant therapy should be considered [see Warnings and Precautions (5.5) ].
8.4 Pediatric Use
The safety and effectiveness of meropenem have been established for pediatric patients 3 months of age and older with complicated skin and skin structure infections and bacterial meningitis, and for pediatric patients of all ages with complicated intra-abdominal infections.
8.5 Geriatric Use
Of the total number of subjects in clinical studies of meropenem, approximately 1100 (30%) were 65 years of age and older, while 400 (11%) were 75 years and older. Additionally, in a study of 511 patients with complicated skin and skin structure infections, 93 (18%) were 65 years of age and older, while 38 (7%) were 75 years and older. No overall differences in safety or effectiveness were observed between these subjects and younger subjects; spontaneous reports and other reported clinical experience have not identified differences in responses between the elderly and younger patients, but greater sensitivity of some older individuals cannot be ruled out.
Meropenem is known to be substantially excreted by the kidney, and the risk of adverse reactions to this drug may be greater in patients with renal impairment. Because elderly patients are more likely to have decreased renal function, care should be taken in dose selection, and it may be useful to monitor renal function.
A pharmacokinetic study with meropenem in elderly patients has shown a reduction in the plasma clearance of meropenem that correlates with age-associated reduction in creatinine clearance [see Clinical Pharmacology (12.3) ].
2.1 Adult Patients
The recommended dose of meropenen for injection is 500 mg given every 8 hours for skin and skin structure infections and 1 gram given every 8 hours for intra-abdominal infections. When treating complicated skin and skin structure infections caused by P. aeruginosa, a dose of 1 gram every 8 hours is recommended.
Meropenen for injection should be administered by intravenous infusion over approximately 15 minutes to 30 minutes. Doses of 1 gram may also be administered as an intravenous bolus injection (5 mL to 20 mL) over approximately 3 minutes to 5 minutes.
5.3 Rhabdomyolysis
Rhabdomyolysis has been reported with the use of meropenem [see Adverse Reactions (6.2)]. If signs or symptoms of rhabdomyolysis such as muscle pain, tenderness or weakness, dark urine or elevated creatine phosphokinase are observed, discontinue meropenen and initiate appropriate therapy.
4 Contraindications
Meropenen for injection is contraindicated in patients with known hypersensitivity to any component of this product or to other drugs in the same class or in patients who have demonstrated anaphylactic reactions to beta (β)-lactams.
6 Adverse Reactions
The following are discussed in greater detail in other sections of labeling:
-
•Hypersensitivity Reactions [see Warnings and Precautions (5.1)]
-
•Severe Cutaneous Adverse Reactions [see Warnings and Precautions (5.2)]
-
•Rhabdomyolysis [see Warnings and Precautions (5.3)]
-
•Seizure Potential [see Warnings and Precautions (5.4) ]
-
•Risk of Breakthrough Seizures Due to Drug Interaction with Valproic Acid [see Warnings and Precautions (5.5) ]
-
•Clostridioides difficile – associated Diarrhea [see Warnings and Precautions (5.6) ]
-
•Development of Drug-Resistant Bacteria [see Warnings and Precautions (5.7) ]
-
•Overgrowth of Nonsusceptible Organisms [see Warnings and Precautions (5.8) ]
-
•Thrombocytopenia [see Warnings and Precautions (5.9) ]
-
•Potential for Neuromotor Impairment [see Warnings and Precautions (5.10) ]
7 Drug Interactions
•Co-administration of meropenen with probenecid inhibits renal excretion of meropenem and is therefore not recommended. (7.1)
•The concomitant use of meropenen and valproic acid or divalproex sodium is generally not recommended. Antibacterial drugs other than carbapenems should be considered to treat infections in patients whose seizures are well controlled on valproic acid or divalproex sodium. (5.5, 7.2)
5.9 Thrombocytopenia
In patients with renal impairment, thrombocytopenia has been observed but no clinical bleeding reported [see Dosage and Administration (2.2), Adverse Reactions (6.1), Use in Specific Populations (8.5) and (8.6), and Clinical Pharmacology (12.3) ].
12.2 Pharmacodynamics
The percentage of time of a dosing interval that unbound plasma concentration of meropenem exceeds the meropenem minimum inhibitory concentration (MIC) against the infecting organism has been shown to best correlate with efficacy in animal and in vitro models of infection.
5.4 Seizure Potential
Seizures and other adverse CNS experiences have been reported during treatment with meropenen. These experiences have occurred most commonly in patients with CNS disorders (e.g., brain lesions or history of seizures) or with bacterial meningitis and/or compromised renal function [see Adverse Reactions (6.1) and Drug Interactions (7.2)]. During clinical investigations, 2904 immunocompetent adult patients were treated for non-CNS infections with the overall seizure rate being 0.7% (based on 20 patients with this adverse event). All meropenem-treated patients with seizures had pre-existing contributing factors. Among these are included prior history of seizures or CNS abnormality and concomitant medications with seizure potential. Dosage adjustment is recommended in patients with advanced age and/or adult patients with creatinine clearance of 50 mL/min or less [see Dosage and Administration (2.2)]. Close adherence to the recommended dosage regimens is urged, especially in patients with known factors that predispose to convulsive activity. Continue anti-convulsant therapy in patients with known seizure disorders. If focal tremors, myoclonus, or seizures occur, evaluate neurologically, placed on anti-convulsant therapy if not already instituted, and re-examine the dosage of meropenen to determine whether it should be decreased or discontinued.
1 Indications and Usage
Meropenen for injection is a penem antibacterial indicated for the treatment of:
•Complicated skin and skin structure infections (adult patients and pediatric patients 3 months of age and older only). (1.1)
•Complicated intra-abdominal infections (adult and pediatric patients). (1.2)
•Bacterial meningitis (pediatric patients 3 months of age and older only). (1.3)
To reduce the development of drug-resistant bacteria and maintain the effectiveness of meropenen for injection and other antibacterial drugs, meropenen for injection should only be used to treat or prevent infections that are proven or strongly suspected to be caused by susceptible bacteria.
12.1 Mechanism of Action
Meropenem is an antibacterial drug [see Microbiology (12.4) ].
14.3 Bacterial Meningitis
Four hundred forty-six patients (397 pediatric patients 3 months to less than 17 years of age) were enrolled in 4 separate clinical trials and randomized to treatment with meropenem (n=225) at a dose of 40 mg/kg every 8 hours or a comparator drug, i.e., cefotaxime (n=187) or ceftriaxone (n=34), at the approved dosing regimens. A comparable number of patients were found to be clinically evaluable (ranging from 61–68%) and with a similar distribution of pathogens isolated on initial CSF culture.
Patients were defined as clinically not cured if any one of the following three criteria were met:
1.At the 5–7 week post-completion of therapy visit, the patient had any one of the following: moderate to severe motor, behavior or development deficits, hearing loss of greater than 60 decibels in one or both ears, or blindness.2.During therapy the patient's clinical status necessitated the addition of other antibacterial drugs.3.Either during or post-therapy, the patient developed a large subdural effusion needing surgical drainage, or a cerebral abscess, or a bacteriologic relapse.
Using the definition, the following efficacy rates were obtained, per organism (noted in Table 10). The values represent the number of patients clinically cured/number of clinically evaluable patients, with the percent cure in parentheses.
| MICROORGANISMS | MEROPENEM | COMPARATOR |
|---|---|---|
|
S. pneumoniae |
17/24 (71) |
19/30 (63) |
|
H. influenzae (+) (+) β-lactamase-producing
|
8/10 (80) |
6/6 (100) |
|
H. influenzae (-/NT) (-/NT) non-β-lactamase-producing or not tested
|
44/59 (75) |
44/60 (73) |
|
N. meningitidis |
30/35 (86) |
35/39 (90) |
|
Total (including others) |
102/131 (78) |
108/140 (77) |
Sequelae were the most common reason patients were assessed as clinically not cured.
Five patients were found to be bacteriologically not cured, 3 in the comparator group (1 relapse and 2 patients with cerebral abscesses) and 2 in the meropenem group (1 relapse and 1 with continued growth of Pseudomonas aeruginosa).
With respect to hearing loss, 263 of the 271 evaluable patients had at least one hearing test performed post-therapy. The following table shows the degree of hearing loss between the meropenem-treated patients and the comparator-treated patients.
| Degree of Hearing Loss (in one or both ears) |
Meropenem
n = 128 |
Comparator
n = 135 |
|---|---|---|
|
No loss |
61% |
56% |
|
20–40 decibels |
20% |
24% |
|
Greater than 40–60 decibels |
8% |
7% |
|
Greater than 60 decibels |
9% |
10% |
2.6 Stability and Storage
Freshly prepared solutions of meropenen for injection should be used. However, re-constituted solutions of meropenen for injection maintain satisfactory potency under the conditions described below. Solutions of intravenous meropenen for injection should not be frozen.
5 Warnings and Precautions
•Serious and occasionally fatal hypersensitivity (anaphylactic) reactions have been reported in patients receiving β-lactams. (5.1)
•Severe cutaneous adverse reactions have been reported in patients receiving meropenen. (5.2)
•Rhabdomyolysis: If signs or symptoms of rhabdomyolysis are observed, discontinue meropenem for injection and initiate appropriate therapy. (5.3)
•Seizures and other adverse CNS experiences have been reported during treatment. (5.4)
•Co-administration of meropenen with valproic acid or divalproex sodium reduces the serum concentration of valproic acid potentially increasing the risk of breakthrough seizures. (5.5, 7.2)
•Clostridioides difficile-associated diarrhea (ranging from mild diarrhea to fatal colitis) has been reported. Evaluate if diarrhea occurs. (5.6)
•In patients with renal dysfunction, thrombocytopenia has been observed. (5.9)
2 Dosage and Administration
•500 mg every 8 hours by intravenous infusion over 15 to 30 minutes for complicated skin and skin structure infections (cSSSI) for adult patients. When treating infections caused by Pseudomonas aeruginosa, a dose of 1 gram every 8 hours is recommended. (2.1)
•1 gram every 8 hours by intravenous infusion over 15 minutes to 30 minutes for intra-abdominal infections for adult patients. (2.1)
•1 gram every 8 hours by intravenous bolus injection (5 mL to 20 mL) over 3 minutes to 5 minutes for adult patients. (2.1)
•Dosage should be reduced in adult patients with renal impairment. (2.2)
|
Recommended Meropenen for Injection Dosage Schedule for Adult Patients with Renal Impairment |
||
|
Creatinine Clearance (mL/min) |
Dose (dependent on type of infection) |
Dosing Interval |
|
Greater than 50 |
Recommended dose (500 mg cSSSI and 1 gram Intra-abdominal) |
Every 8 hours |
|
26-50 |
Recommended dose |
Every 12 hours |
|
10-25 |
One-half recommended dose |
Every 12 hours |
|
Less than 10 |
One-half recommended dose |
Every 24 hours |
Pediatric patients 3 months of age and older
|
Recommended Meropenen for Injection Dosage Schedule for Pediatric Patients 3 Months of Age and Older with Normal Renal Function (2.3) |
|||
|
Type of Infection |
Dose (mg/kg) |
Up to a Maximum Dose |
Dosing Interval |
|
Complicated skin and skin structure 20 mg/kg (or 1 gram for pediatric patients weighing over 50 kg) every 8 hours is recommended when treating complicated skin and skin structure infections caused by P. aeruginosa. (2.3)
|
10 |
500 mg |
Every 8 hours |
|
Intra-abdominal |
20 |
1 gram |
Every 8 hours |
|
Meningitis |
40 |
2 gram |
Every 8 hours |
| -Intravenous infusion is to be given over approximately 15 minutes to 30 minutes.-Intravenous bolus injection (5 mL to 20 mL) is to be given over approximately 3 minutes-5 minutes.-There is no experience in pediatric patients with renal impairment. |
Pediatric patients less than 3 months of age
|
Recommended Meropenen for Injection Dosage Schedule for Pediatric Patients Less than 3 Months of Age with Complicated Intra-Abdominal Infections and Normal Renal Function (2.3) |
||
|
Age Group |
Dose (mg/kg) |
Dose Interval |
|
Infants less than 32 weeks GA and PNA less than 2 weeks |
20 |
Every 12 hours |
|
Infants less than 32 weeks GA and PNA 2 weeks and older |
20 |
Every 8 hours |
|
Infants 32 weeks and older GA and PNA less than 2 weeks |
20 |
Every 8 hours |
|
Infants 32 weeks and older GA and PNA 2 weeks and older |
30 |
Every 8 hours |
|
- Intravenous infusion is to be given over 30 minutes. - There is no experience in pediatric patients with renal impairment. GA: gestational age and PNA: postnatal age |
3 Dosage Forms and Strengths
Single dose clear glass vials of Meropenen for Injection, USP containing 500 mg or 1 gram (as the trihydrate blended with anhydrous sodium carbonate for re-constitution) of sterile meropenem powder.
5.6 Clostridioides Difficile
Clostridioides difficile-associated diarrhea (CDAD) has been reported with use of nearly all antibacterial agents, including meropenen, and may range in severity from mild diarrhea to fatal colitis. Treatment with antibacterial agents alters the normal flora of the colon leading to overgrowth of C. difficile.
C. difficile produces toxins A and B which contribute to the development of CDAD. Hypertoxin producing isolates of C. difficile cause increased morbidity and mortality, as these infections can be refractory to antimicrobial therapy and may require colectomy. CDAD must be considered in all patients who present with diarrhea following antibacterial drug use. Careful medical history is necessary since CDAD has been reported to occur over two months after the administration of antibacterial agents.
If CDAD is suspected or confirmed, ongoing antibacterial drug use not directed against C. difficile may need to be discontinued. Appropriate fluid and electrolyte management, protein supplementation, antibacterial drug treatment of C. difficile, and surgical evaluation should be instituted as clinically indicated.
6.2 Post Marketing Experience
The following adverse reactions have been identified during post-approval use of meropenem, including meropenem. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Worldwide post-marketing adverse reactions not otherwise listed in the Adverse Reactions from Clinical Trials section of this prescribing information and reported as possibly, probably, or definitely drug related are listed within each body system in order of decreasing severity.
Blood and Lymphatic System Disorders: agranulocytosis, neutropenia, and leukopenia; a positive direct or indirect Coombs test, and hemolytic anemia.
Immune System Disorders: angioedema.
Skin and Subcutaneous Disorders: Stevens-Johnson syndrome, toxic epidermal necrolysis, drug reaction with eosinophilia and systemic symptoms (DRESS), erythema multiforme and acute generalized exanthematous pustulosis.
Musculoskeletal Disorders: rhabdomyolysis.
Hepatic Disorders: drug-induced liver injury.
8 Use in Specific Populations
5.1 Hypersensitivity Reactions
Serious and occasionally fatal hypersensitivity (anaphylactic) reactions have been reported in patients receiving therapy with β-lactams. These reactions are more likely to occur in individuals with a history of sensitivity to multiple allergens.
There have been reports of individuals with a history of penicillin hypersensitivity who have experienced severe hypersensitivity reactions when treated with another β-lactam. Before initiating therapy with meropenen, it is important to inquire about previous hypersensitivity reactions to penicillins, cephalosporins, other β-lactams, and other allergens. If an allergic reaction to meropenen occurs, discontinue the drug immediately.
17 Patient Counseling Information
•Counsel patients that antibacterial drugs including meropenem for injection should only be used to treat bacterial infections. They do not treat viral infections (e.g., the common cold). When meropenem for injection is prescribed to treat a bacterial infection, tell patients that although it is common to feel better early in the course of therapy, take the medication exactly as directed. Skipping doses or not completing the full course of therapy may (1) decrease the effectiveness of the immediate treatment and (2) increase the likelihood that bacteria will develop resistance and will not be treatable by meropenem for injection or other antibacterial drugs in the future.•Counsel patients that diarrhea is a common problem caused by antibacterial drugs which usually ends when the antibacterial drug is discontinued. Sometimes after starting treatment with antibacterial drugs, patients can develop watery and bloody stools (with or without stomach cramps and fever) even as late as two or more months after having taken the last dose of the antibacterial drug. If this occurs, patients should contact their physician as soon as possible [seeWarnings and Precautions (5.6)].•Counsel patients to inform their physician if they are taking valproic acid or divalproex sodium. Valproic acid concentrations in the blood may drop below the therapeutic range upon co-administration with meropenem for injection. If treatment with meropenem for injection is necessary and continued, alternative or supplemental anti-convulsant medication to prevent and/or treat seizures may be needed [seeWarnings and Precautions (5.5)].•Patients receiving meropenem for injection on an outpatient basis must be alerted of adverse events such as seizures, delirium, headaches and/or paresthesias that could interfere with mental alertness and/or cause motor impairment. Until it is reasonably well established that meropenem for injection is well tolerated, patients should not operate machinery or motorized vehicles [see Warnings and Precautions (5.10) ].
8.6 Patients With Renal Impairment
Dosage adjustment is necessary in patients with creatinine clearance 50 mL/min or less [see Dosage and Administration (2.2) , Warnings and Precautions (5.9) , and Clinical Pharmacology (12.3) ].
5.2 Severe Cutaneous Adverse Reactions
Severe cutaneous adverse reactions (SCAR) such as Stevens-Johnson syndrome (SJS), toxic epidermal necrolysis (TEN), drug reaction with eosinophilia and systemic symptoms (DRESS), erythema multiforme (EM) and acute generalized exanthematous pustulosis (AGEP) have been reported in patients receiving meropenen [see Adverse Reactions (6.2)]. If signs and symptoms suggestive of these reactions appear, meropenem should be withdrawn immediately and an alternative treatment should be considered.
5.10 Potential for Neuromotor Impairment
Alert patients receiving meropenen on an outpatient basis regarding adverse events such as seizures, delirium, headaches and/or paresthesias that could interfere with mental alertness and/or cause motor impairment. Until it is reasonably well established that meropenen is well tolerated, advise patients not to operate machinery or motorized vehicles [see Adverse Reactions (6.1)].
Principal Display Panel 1 G Vial Label
NDC 51810-503-01
Meropenem for Injection, USP
1 g/vial meropenem equivalent
For Intravenous Use only
Contents are Sterile Single-Dose Vial
Rx Only
Principal Display Panel 1 G Vial Carton
DC 51810-503-02
Meropenem for Injection, USP
1 g/vial meropenem equivalent
For Intravenous Use only
10 × 1 g Single-Dose Vials
Rx Only
5.7 Development of Drug Resistant Bacteria
Prescribing meropenen in the absence of a proven or strongly suspected bacterial infection or a prophylactic indication is unlikely to provide benefit to the patient and increases the risk of the development of drug-resistant bacteria.
5.8 Overgrowth of Nonsusceptible Organisms
As with other broad-spectrum antibacterial drugs, prolonged use of meropenem may result in overgrowth of nonsusceptible organisms. Repeated evaluation of the patient is essential. If superinfection does occur during therapy, appropriate measures should be taken.
6.1 Adverse Reactions From Clinical Trials
Because clinical trials are conducted under widely varying conditions, adverse reactions rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
14.2 Complicated Intra Abdominal Infections
One controlled clinical study of complicated intra-abdominal infection was performed in the United States where meropenem was compared with clindamycin/tobramycin. Three controlled clinical studies of complicated intra-abdominal infections were performed in Europe; meropenem was compared with imipenem (two trials) and cefotaxime/metronidazole (one trial).
Using strict evaluability criteria and microbiologic eradication and clinical cures at follow-up which occurred 7 or more days after completion of therapy, the presumptive microbiologic eradication/clinical cure rates and statistical findings are provided in Table 9:
| Treatment Arm | No. evaluable/ No. enrolled (%) | Microbiologic Eradication Rate | Clinical Cure Rate | Outcome |
|---|---|---|---|---|
|
meropenem |
146/516 (28%) |
98/146 (67%) |
101/146 (69%) |
|
|
imipenem |
65/220 (30%) |
40/65 (62%) |
42/65 (65%) |
meropenem equivalent to control |
|
cefotaxime/metronidazole |
26/85 (30%) |
22/26 (85%) |
22/26 (85%) |
meropenem not equivalent to control |
|
clindamycin/tobramycin |
50/212 (24%) |
38/50 (76%) |
38/50 (76%) |
meropenem equivalent to control |
The finding that meropenem was not statistically equivalent to cefotaxime/metronidazole may have been due to uneven assignment of more seriously ill patients to the meropenem arm. Currently there is no additional information available to further interpret this observation.
Principal Display Panel 500 Mg Vial Label
NDC 51810-502-01
Meropenem for Injection, USP
500 mg/vial meropenem equivalent
For Intravenous Use only
Contents are Sterile Single-Dose Vial
Rx Only
Principal Display Panel 500 Mg Vial Carton
DC 51810-502-02
Meropenem for Injection, USP
500 mg/vial meropenem equivalent
For Intravenous Use only
10 × 500 mg Single-Dose Vials
Rx Only
2.2 Use in Adult Patients With Renal Impairment
Dosage should be reduced in patients with creatinine clearance of 50 mL/min or less. (See dosing table below.)
When only serum creatinine is available, the following formula (Cockcroft and Gault equation)1 may be used to estimate creatinine clearance.
Males: Creatinine Clearance (mL/min) =
Weight (kg) × (140 - age)
72 × serum creatinine (mg/dL)
Females: 0.85 × above value
| Creatinine Clearance (mL/min) | Dose (dependent on type of infection) | Dosing Interval |
|---|---|---|
|
Greater than 50 |
Recommended dose (500 mg cSSSI and 1 gram Intra-abdominal) |
Every 8 hours |
|
26–50 |
Recommended dose |
Every 12 hours |
|
10–25 |
One-half recommended dose |
Every 12 hours |
|
Less than 10 |
One-half recommended dose |
Every 24 hours |
There is inadequate information regarding the use of meropenen for injection in patients on hemodialysis or peritoneal dialysis.
14.1 Complicated Skin and Skin Structure Infections
Adult patients with complicated skin and skin structure infections including complicated cellulitis, complex abscesses, perirectal abscesses, and skin infections requiring intravenous antimicrobials, hospitalization, and surgical intervention were enrolled in a randomized, multi-center, international, double-blind trial. The study evaluated meropenem at doses of 500 mg administered intravenously every 8 hours and imipenem-cilastatin at doses of 500 mg administered intravenously every 8 hours. The study compared the clinical response between treatment groups in the clinically evaluable population at the follow-up visit (test-of-cure). The trial was conducted in the United States, South Africa, Canada, and Brazil. At enrollment, approximately 37% of the patients had underlying diabetes, 12% had underlying peripheral vascular disease and 67% had a surgical intervention. The study included 510 patients randomized to meropenem and 527 patients randomized to imipenem-cilastatin. Two hundred and sixty one (261) patients randomized to meropenem and 287 patients randomized to imipenem-cilastatin were clinically evaluable. The success rates in the clinically evaluable patients at the follow-up visit were 86% (225/261) in the meropenem arm and 83% (238/287) in imipenem-cilastatin arm.
The success rates for the clinically evaluable population are provided in Table 7.
| Population | Meropenem n n=number of patients with satisfactory response.
/N
N=number of patients in the clinically evaluable population or respective subgroup within treatment groups.
(%)
|
Imipenem-cilastatin
n /N (%) |
|---|---|---|
|
Total |
225/261 (86) |
238/287 (83) |
|
Diabetes mellitus |
83/97 (86) |
76/105 (72) |
|
No diabetes mellitus |
142/164 (87) |
162/182 (89) |
|
Less than 65 years of age |
190/218 (87) |
205/241 (85) |
|
65 years of age or older |
35/43 (81) |
33/46 (72) |
|
Men |
130/148 (88) |
137/172 (80) |
|
Women |
95/113 (84) |
101/115 (88) |
The clinical efficacy rates by pathogen are provided in Table 8. The values represent the number of patients clinically cured/number of clinically evaluable patients at the post-treatment follow-up visit, with the percent cure in parentheses (Fully Evaluable analysis set).
|
MICROORGANISMS
Patients may have more than one pretreatment pathogen.
|
Meropenem n n=number of patients with satisfactory response.
/N
N=number of patients in the clinically evaluable population or subgroup within treatment groups.
(%)
%= Percent of satisfactory clinical response at follow-up evaluation.
|
Imipenem-cilastatin
n /N (%) |
|---|---|---|
|
Gram-positive aerobes |
||
|
Staphylococcus aureus, methicillin susceptible |
82/88 (93) |
84/100 (84) |
|
Streptococcus pyogenes (Group A) |
26/29 (90) |
28/32 (88) |
|
Streptococcus agalactiae (Group B) |
12/17 (71) |
16/19 (84) |
|
Enterococcus faecalis |
9/12 (75) |
14/20 (70) |
|
Viridans group streptococci |
11/12 (92) |
5/6 (83) |
|
Gram-negative aerobes |
||
|
Escherichia coli |
12/15 (80) |
15/21 (71) |
|
Pseudomonas aeruginosa |
11/15 (73) |
13/15 (87) |
|
Proteus mirabilis |
11/13 (85) |
6/7 (86) |
|
Anaerobes |
||
|
Bacteroides fragilis |
10/11 (91) |
9/10 (90) |
|
Peptostreptococcus Species |
10/13 (77) |
14/16 (88) |
The proportion of patients who discontinued study treatment due to an adverse event was similar for both treatment groups (meropenem, 2.5% and imipenem-cilastatin, 2.7%).
1.2 Complicated Intra Abdominal Infections (adult and Pediatric Patients)
Meropenen for injection is indicated for the treatment of complicated appendicitis and peritonitis caused by viridans group streptococci, Escherichia coli, Klebsiella pneumoniae, Pseudomonas aeruginosa, Bacteroides fragilis, B. thetaiotaomicron, and Peptostreptococcus species.
1.3 Bacterial Meningitis (pediatric Patients 3 Months of Age and Older Only)
Meropenen for injection is indicated for the treatment of bacterial meningitis caused by Haemophilus influenzae, Neisseria meningitidis and penicillin-susceptible isolates of Streptococcus pneumoniae.
Meropenen for injection has been found to be effective in eliminating concurrent bacteremia in association with bacterial meningitis.
5.5 Risk of Breakthrough Seizures Due to Drug Interaction With Valproic Acid
The concomitant use of meropenem and valproic acid or divalproex sodium is generally not recommended. Case reports in the literature have shown that co-administration of carbapenems, including meropenem, to patients receiving valproic acid or divalproex sodium results in a reduction in valproic acid concentrations. The valproic acid concentrations may drop below the therapeutic range as a result of this interaction, therefore increasing the risk of breakthrough seizures. Increasing the dose of valproic acid or divalproex sodium may not be sufficient to overcome this interaction. Consider administration of antibacterial drugs other than carbapenems to treat infections in patients whose seizures are well controlled on valproic acid or divalproex sodium. If administration of meropenen is necessary, consider supplemental anti-convulsant therapy [see Drug Interactions (7.2)].
1.1 Complicated Skin and Skin Structure Infections (adult Patients and Pediatric Patients 3 Months of Age and Older Only)
Meropenen for injection is indicated for the treatment of complicated skin and skin structure infections (cSSSI) due to Staphylococcus aureus (methicillin-susceptible isolates only), Streptococcus pyogenes, Streptococcus agalactiae, viridans group streptococci, Enterococcus faecalis (vancomycin-susceptible isolates only), Pseudomonas aeruginosa, Escherichia coli, Proteus mirabilis, Bacteroides fragilis, and Peptostreptococcus species.
Structured Label Content
Section 42229-5 (42229-5)
Pediatric Patients 3 Months of Age and Older•For pediatric patients 3 months of age and older, the meropenen for injection dose is 10 mg/kg, 20 mg/kg or 40 mg/kg every 8 hours (maximum dose is 2 grams every 8 hours), depending on the type of infection (cSSSI, cIAI, intra-abdominal infection or meningitis). Seedosing table 2below.•For pediatric patients weighing over 50 kg administer meropenen for injection at a dose of 500 mg every 8 hours for cSSSI, 1 gram every 8 hours for cIAI and 2 grams every 8 hours for meningitis.•Administer meropenen for injection as an intravenous infusion over approximately 15 minutes to 30 minutes or as an intravenous bolus injection (5 mL to 20 mL) over approximately 3 minutes to 5 minutes.•There is limited safety data available to support the administration of a 40 mg/kg (up to a maximum of 2 grams) bolus dose.
| Type of Infection | Dose (mg/kg) | Up to a Maximum Dose | Dosing Interval |
|---|---|---|---|
| There is no experience in pediatric patients with renal impairment. When treating cSSSI caused byP. aeruginosa, a dose of 20 mg/kg (or 1 gram for pediatric patients weighing over 50 kg) every 8 hours is recommended. |
|||
| Complicated skin and skin structure infections | 10 | 500 mg | Every 8 hours |
| Complicated intra-abdominal infections | 20 | 1 gram | Every 8 hours |
| Meningitis | 40 | 2 grams | Every 8 hours |
Section 43683-2 (43683-2)
|
Warnings and Precautions, Rhabdomyolysis (5.3) |
12/2024 |
Section 44425-7 (44425-7)
Meropenem for Injection, USP is supplied in 20 mL and 30 mL injection vials containing sufficient meropenem to deliver 500 mg or 1 gram for intravenous administration, respectively. The dry powder should be stored at 20°–25°C (68°–77°F) [see USP Controlled Room Temperature].
500 mg Injection Vial (NDC 51810-502-01) in a pack of 10 x 500 mg Injection Vials (NDC 51810-502-02)
1 gram Injection Vial (NDC 51810-503-01) in a pack of 10 x 1 g Injection Vials (NDC 51810-503-02)
1.4 Usage
To reduce the development of drug-resistant bacteria and maintain the effectiveness of meropenen for injection and other antibacterial drugs, meropenen for injection should only be used to treat or prevent infections that are proven or strongly suspected to be caused by susceptible bacteria. When culture and susceptibility information are available, they should be considered in selecting or modifying antibacterial therapy. In the absence of such data, local epidemiology and susceptibility patterns may contribute to the empiric selection of therapy.
10 Overdosage (10 OVERDOSAGE)
In mice and rats, large intravenous doses of meropenem (2200 mg/kg to 4000 mg/kg) have been associated with ataxia, dyspnea, convulsions, and mortalities.
Intentional overdosing of meropenem is unlikely, although accidental overdosing might occur if large doses are given to patients with reduced renal function. The largest dose of meropenem administered in clinical trials has been 2 grams given intravenously every 8 hours. At this dosage, no adverse pharmacological effects or increased safety risks have been observed.
Limited postmarketing experience indicates that if adverse events occur following overdosage, they are consistent with the adverse event profile described in the Adverse Reactions section and are generally mild in severity and resolve on withdrawal or dose reduction. Consider symptomatic treatments. In individuals with normal renal function, rapid renal elimination takes place. Meropenem and its metabolite are readily dialyzable and effectively removed by hemodialysis; however, no information is available on the use of hemodialysis to treat overdosage.
15 References (15 REFERENCES)
-
1.Cockcroft DW, MH Gault, 1976, Prediction of creatinine clearance from serum creatinine, Nephron, 16:31–41.
-
2.Kawamura S, AW Russell, SJ Freeman, and RA Siddall, 1992, Reproductive and Developmental Toxicity of Meropenem in Rats, Chemotherapy, 40:S238–250.
11 Description (11 DESCRIPTION)
Meropenem for Injection, USP (meropenem for injection) is a sterile, pyrogen-free, synthetic, carbapenem antibacterial for intravenous administration. It is (4R,5S,6S)-3- [[(3S,5S)-5-(Dimethylcarbamoyl)-3-pyrrolidinyl]thio]-6- [(1R)-1-hydroxyethyl]-4-methyl-7-oxo-1-azabicyclo[3.2.0]hept-2-ene-2-carboxylic acid trihydrate. Its empirical formula is C17H25N3O5S∙3H2O with a molecular weight of 437.52. Its structural formula is:
Meropenem for Injection, USP is a white to pale yellow crystalline powder. The solution varies from colorless to yellow depending on the concentration. The pH of freshly constituted solutions is between 7.3 and 8.3. Meropenem is soluble in 5% monobasic potassium phosphate solution, sparingly soluble in water, very slightly soluble in hydrated ethanol, and practically insoluble in acetone or ether.
When re-constituted as instructed, each 1 gram Meropenem for Injection, USP vial will deliver 1 gram of meropenem and 90.2 mg of sodium as sodium carbonate (3.92 mEq). Each 500 mg Meropenem for Injection, USP vial will deliver 500 mg meropenem and 45.1 mg of sodium as sodium carbonate (1.96 mEq) [ see Dosage and Administration (2.4) ].
7.1 Probenecid
Probenecid competes with meropenem for active tubular secretion, resulting in increased plasma concentrations of meropenem. Co-administration of probenecid with meropenem is not recommended.
2.5 Compatibility
Compatibility of meropenen for injection with other drugs has not been established. Meropenen for injection should not be mixed with or physically added to solutions containing other drugs.
7.2 Valproic Acid
Case reports in the literature have shown that co-administration of carbapenems, including meropenem, to patients receiving valproic acid or divalproex sodium results in a reduction in valproic acid concentrations. The valproic acid concentrations may drop below the therapeutic range as a result of this interaction, therefore increasing the risk of breakthrough seizures. Although the mechanism of this interaction is unknown, data from in vitro and animal studies suggest that carbapenems may inhibit the hydrolysis of valproic acid's glucuronide metabolite (VPA-g) back to valproic acid, thus decreasing the serum concentrations of valproic acid. If administration of meropenem is necessary, then supplemental anti-convulsant therapy should be considered [see Warnings and Precautions (5.5) ].
8.4 Pediatric Use
The safety and effectiveness of meropenem have been established for pediatric patients 3 months of age and older with complicated skin and skin structure infections and bacterial meningitis, and for pediatric patients of all ages with complicated intra-abdominal infections.
8.5 Geriatric Use
Of the total number of subjects in clinical studies of meropenem, approximately 1100 (30%) were 65 years of age and older, while 400 (11%) were 75 years and older. Additionally, in a study of 511 patients with complicated skin and skin structure infections, 93 (18%) were 65 years of age and older, while 38 (7%) were 75 years and older. No overall differences in safety or effectiveness were observed between these subjects and younger subjects; spontaneous reports and other reported clinical experience have not identified differences in responses between the elderly and younger patients, but greater sensitivity of some older individuals cannot be ruled out.
Meropenem is known to be substantially excreted by the kidney, and the risk of adverse reactions to this drug may be greater in patients with renal impairment. Because elderly patients are more likely to have decreased renal function, care should be taken in dose selection, and it may be useful to monitor renal function.
A pharmacokinetic study with meropenem in elderly patients has shown a reduction in the plasma clearance of meropenem that correlates with age-associated reduction in creatinine clearance [see Clinical Pharmacology (12.3) ].
2.1 Adult Patients
The recommended dose of meropenen for injection is 500 mg given every 8 hours for skin and skin structure infections and 1 gram given every 8 hours for intra-abdominal infections. When treating complicated skin and skin structure infections caused by P. aeruginosa, a dose of 1 gram every 8 hours is recommended.
Meropenen for injection should be administered by intravenous infusion over approximately 15 minutes to 30 minutes. Doses of 1 gram may also be administered as an intravenous bolus injection (5 mL to 20 mL) over approximately 3 minutes to 5 minutes.
5.3 Rhabdomyolysis
Rhabdomyolysis has been reported with the use of meropenem [see Adverse Reactions (6.2)]. If signs or symptoms of rhabdomyolysis such as muscle pain, tenderness or weakness, dark urine or elevated creatine phosphokinase are observed, discontinue meropenen and initiate appropriate therapy.
4 Contraindications (4 CONTRAINDICATIONS)
Meropenen for injection is contraindicated in patients with known hypersensitivity to any component of this product or to other drugs in the same class or in patients who have demonstrated anaphylactic reactions to beta (β)-lactams.
6 Adverse Reactions (6 ADVERSE REACTIONS)
The following are discussed in greater detail in other sections of labeling:
-
•Hypersensitivity Reactions [see Warnings and Precautions (5.1)]
-
•Severe Cutaneous Adverse Reactions [see Warnings and Precautions (5.2)]
-
•Rhabdomyolysis [see Warnings and Precautions (5.3)]
-
•Seizure Potential [see Warnings and Precautions (5.4) ]
-
•Risk of Breakthrough Seizures Due to Drug Interaction with Valproic Acid [see Warnings and Precautions (5.5) ]
-
•Clostridioides difficile – associated Diarrhea [see Warnings and Precautions (5.6) ]
-
•Development of Drug-Resistant Bacteria [see Warnings and Precautions (5.7) ]
-
•Overgrowth of Nonsusceptible Organisms [see Warnings and Precautions (5.8) ]
-
•Thrombocytopenia [see Warnings and Precautions (5.9) ]
-
•Potential for Neuromotor Impairment [see Warnings and Precautions (5.10) ]
7 Drug Interactions (7 DRUG INTERACTIONS)
•Co-administration of meropenen with probenecid inhibits renal excretion of meropenem and is therefore not recommended. (7.1)
•The concomitant use of meropenen and valproic acid or divalproex sodium is generally not recommended. Antibacterial drugs other than carbapenems should be considered to treat infections in patients whose seizures are well controlled on valproic acid or divalproex sodium. (5.5, 7.2)
5.9 Thrombocytopenia
In patients with renal impairment, thrombocytopenia has been observed but no clinical bleeding reported [see Dosage and Administration (2.2), Adverse Reactions (6.1), Use in Specific Populations (8.5) and (8.6), and Clinical Pharmacology (12.3) ].
12.2 Pharmacodynamics
The percentage of time of a dosing interval that unbound plasma concentration of meropenem exceeds the meropenem minimum inhibitory concentration (MIC) against the infecting organism has been shown to best correlate with efficacy in animal and in vitro models of infection.
5.4 Seizure Potential
Seizures and other adverse CNS experiences have been reported during treatment with meropenen. These experiences have occurred most commonly in patients with CNS disorders (e.g., brain lesions or history of seizures) or with bacterial meningitis and/or compromised renal function [see Adverse Reactions (6.1) and Drug Interactions (7.2)]. During clinical investigations, 2904 immunocompetent adult patients were treated for non-CNS infections with the overall seizure rate being 0.7% (based on 20 patients with this adverse event). All meropenem-treated patients with seizures had pre-existing contributing factors. Among these are included prior history of seizures or CNS abnormality and concomitant medications with seizure potential. Dosage adjustment is recommended in patients with advanced age and/or adult patients with creatinine clearance of 50 mL/min or less [see Dosage and Administration (2.2)]. Close adherence to the recommended dosage regimens is urged, especially in patients with known factors that predispose to convulsive activity. Continue anti-convulsant therapy in patients with known seizure disorders. If focal tremors, myoclonus, or seizures occur, evaluate neurologically, placed on anti-convulsant therapy if not already instituted, and re-examine the dosage of meropenen to determine whether it should be decreased or discontinued.
1 Indications and Usage (1 INDICATIONS AND USAGE)
Meropenen for injection is a penem antibacterial indicated for the treatment of:
•Complicated skin and skin structure infections (adult patients and pediatric patients 3 months of age and older only). (1.1)
•Complicated intra-abdominal infections (adult and pediatric patients). (1.2)
•Bacterial meningitis (pediatric patients 3 months of age and older only). (1.3)
To reduce the development of drug-resistant bacteria and maintain the effectiveness of meropenen for injection and other antibacterial drugs, meropenen for injection should only be used to treat or prevent infections that are proven or strongly suspected to be caused by susceptible bacteria.
12.1 Mechanism of Action
Meropenem is an antibacterial drug [see Microbiology (12.4) ].
14.3 Bacterial Meningitis
Four hundred forty-six patients (397 pediatric patients 3 months to less than 17 years of age) were enrolled in 4 separate clinical trials and randomized to treatment with meropenem (n=225) at a dose of 40 mg/kg every 8 hours or a comparator drug, i.e., cefotaxime (n=187) or ceftriaxone (n=34), at the approved dosing regimens. A comparable number of patients were found to be clinically evaluable (ranging from 61–68%) and with a similar distribution of pathogens isolated on initial CSF culture.
Patients were defined as clinically not cured if any one of the following three criteria were met:
1.At the 5–7 week post-completion of therapy visit, the patient had any one of the following: moderate to severe motor, behavior or development deficits, hearing loss of greater than 60 decibels in one or both ears, or blindness.2.During therapy the patient's clinical status necessitated the addition of other antibacterial drugs.3.Either during or post-therapy, the patient developed a large subdural effusion needing surgical drainage, or a cerebral abscess, or a bacteriologic relapse.
Using the definition, the following efficacy rates were obtained, per organism (noted in Table 10). The values represent the number of patients clinically cured/number of clinically evaluable patients, with the percent cure in parentheses.
| MICROORGANISMS | MEROPENEM | COMPARATOR |
|---|---|---|
|
S. pneumoniae |
17/24 (71) |
19/30 (63) |
|
H. influenzae (+) (+) β-lactamase-producing
|
8/10 (80) |
6/6 (100) |
|
H. influenzae (-/NT) (-/NT) non-β-lactamase-producing or not tested
|
44/59 (75) |
44/60 (73) |
|
N. meningitidis |
30/35 (86) |
35/39 (90) |
|
Total (including others) |
102/131 (78) |
108/140 (77) |
Sequelae were the most common reason patients were assessed as clinically not cured.
Five patients were found to be bacteriologically not cured, 3 in the comparator group (1 relapse and 2 patients with cerebral abscesses) and 2 in the meropenem group (1 relapse and 1 with continued growth of Pseudomonas aeruginosa).
With respect to hearing loss, 263 of the 271 evaluable patients had at least one hearing test performed post-therapy. The following table shows the degree of hearing loss between the meropenem-treated patients and the comparator-treated patients.
| Degree of Hearing Loss (in one or both ears) |
Meropenem
n = 128 |
Comparator
n = 135 |
|---|---|---|
|
No loss |
61% |
56% |
|
20–40 decibels |
20% |
24% |
|
Greater than 40–60 decibels |
8% |
7% |
|
Greater than 60 decibels |
9% |
10% |
2.6 Stability and Storage
Freshly prepared solutions of meropenen for injection should be used. However, re-constituted solutions of meropenen for injection maintain satisfactory potency under the conditions described below. Solutions of intravenous meropenen for injection should not be frozen.
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
•Serious and occasionally fatal hypersensitivity (anaphylactic) reactions have been reported in patients receiving β-lactams. (5.1)
•Severe cutaneous adverse reactions have been reported in patients receiving meropenen. (5.2)
•Rhabdomyolysis: If signs or symptoms of rhabdomyolysis are observed, discontinue meropenem for injection and initiate appropriate therapy. (5.3)
•Seizures and other adverse CNS experiences have been reported during treatment. (5.4)
•Co-administration of meropenen with valproic acid or divalproex sodium reduces the serum concentration of valproic acid potentially increasing the risk of breakthrough seizures. (5.5, 7.2)
•Clostridioides difficile-associated diarrhea (ranging from mild diarrhea to fatal colitis) has been reported. Evaluate if diarrhea occurs. (5.6)
•In patients with renal dysfunction, thrombocytopenia has been observed. (5.9)
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
•500 mg every 8 hours by intravenous infusion over 15 to 30 minutes for complicated skin and skin structure infections (cSSSI) for adult patients. When treating infections caused by Pseudomonas aeruginosa, a dose of 1 gram every 8 hours is recommended. (2.1)
•1 gram every 8 hours by intravenous infusion over 15 minutes to 30 minutes for intra-abdominal infections for adult patients. (2.1)
•1 gram every 8 hours by intravenous bolus injection (5 mL to 20 mL) over 3 minutes to 5 minutes for adult patients. (2.1)
•Dosage should be reduced in adult patients with renal impairment. (2.2)
|
Recommended Meropenen for Injection Dosage Schedule for Adult Patients with Renal Impairment |
||
|
Creatinine Clearance (mL/min) |
Dose (dependent on type of infection) |
Dosing Interval |
|
Greater than 50 |
Recommended dose (500 mg cSSSI and 1 gram Intra-abdominal) |
Every 8 hours |
|
26-50 |
Recommended dose |
Every 12 hours |
|
10-25 |
One-half recommended dose |
Every 12 hours |
|
Less than 10 |
One-half recommended dose |
Every 24 hours |
Pediatric patients 3 months of age and older
|
Recommended Meropenen for Injection Dosage Schedule for Pediatric Patients 3 Months of Age and Older with Normal Renal Function (2.3) |
|||
|
Type of Infection |
Dose (mg/kg) |
Up to a Maximum Dose |
Dosing Interval |
|
Complicated skin and skin structure 20 mg/kg (or 1 gram for pediatric patients weighing over 50 kg) every 8 hours is recommended when treating complicated skin and skin structure infections caused by P. aeruginosa. (2.3)
|
10 |
500 mg |
Every 8 hours |
|
Intra-abdominal |
20 |
1 gram |
Every 8 hours |
|
Meningitis |
40 |
2 gram |
Every 8 hours |
| -Intravenous infusion is to be given over approximately 15 minutes to 30 minutes.-Intravenous bolus injection (5 mL to 20 mL) is to be given over approximately 3 minutes-5 minutes.-There is no experience in pediatric patients with renal impairment. |
Pediatric patients less than 3 months of age
|
Recommended Meropenen for Injection Dosage Schedule for Pediatric Patients Less than 3 Months of Age with Complicated Intra-Abdominal Infections and Normal Renal Function (2.3) |
||
|
Age Group |
Dose (mg/kg) |
Dose Interval |
|
Infants less than 32 weeks GA and PNA less than 2 weeks |
20 |
Every 12 hours |
|
Infants less than 32 weeks GA and PNA 2 weeks and older |
20 |
Every 8 hours |
|
Infants 32 weeks and older GA and PNA less than 2 weeks |
20 |
Every 8 hours |
|
Infants 32 weeks and older GA and PNA 2 weeks and older |
30 |
Every 8 hours |
|
- Intravenous infusion is to be given over 30 minutes. - There is no experience in pediatric patients with renal impairment. GA: gestational age and PNA: postnatal age |
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
Single dose clear glass vials of Meropenen for Injection, USP containing 500 mg or 1 gram (as the trihydrate blended with anhydrous sodium carbonate for re-constitution) of sterile meropenem powder.
5.6 Clostridioides Difficile (5.6 Clostridioides difficile)
Clostridioides difficile-associated diarrhea (CDAD) has been reported with use of nearly all antibacterial agents, including meropenen, and may range in severity from mild diarrhea to fatal colitis. Treatment with antibacterial agents alters the normal flora of the colon leading to overgrowth of C. difficile.
C. difficile produces toxins A and B which contribute to the development of CDAD. Hypertoxin producing isolates of C. difficile cause increased morbidity and mortality, as these infections can be refractory to antimicrobial therapy and may require colectomy. CDAD must be considered in all patients who present with diarrhea following antibacterial drug use. Careful medical history is necessary since CDAD has been reported to occur over two months after the administration of antibacterial agents.
If CDAD is suspected or confirmed, ongoing antibacterial drug use not directed against C. difficile may need to be discontinued. Appropriate fluid and electrolyte management, protein supplementation, antibacterial drug treatment of C. difficile, and surgical evaluation should be instituted as clinically indicated.
6.2 Post Marketing Experience (6.2 Post marketing Experience)
The following adverse reactions have been identified during post-approval use of meropenem, including meropenem. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Worldwide post-marketing adverse reactions not otherwise listed in the Adverse Reactions from Clinical Trials section of this prescribing information and reported as possibly, probably, or definitely drug related are listed within each body system in order of decreasing severity.
Blood and Lymphatic System Disorders: agranulocytosis, neutropenia, and leukopenia; a positive direct or indirect Coombs test, and hemolytic anemia.
Immune System Disorders: angioedema.
Skin and Subcutaneous Disorders: Stevens-Johnson syndrome, toxic epidermal necrolysis, drug reaction with eosinophilia and systemic symptoms (DRESS), erythema multiforme and acute generalized exanthematous pustulosis.
Musculoskeletal Disorders: rhabdomyolysis.
Hepatic Disorders: drug-induced liver injury.
8 Use in Specific Populations (8 USE IN SPECIFIC POPULATIONS)
5.1 Hypersensitivity Reactions
Serious and occasionally fatal hypersensitivity (anaphylactic) reactions have been reported in patients receiving therapy with β-lactams. These reactions are more likely to occur in individuals with a history of sensitivity to multiple allergens.
There have been reports of individuals with a history of penicillin hypersensitivity who have experienced severe hypersensitivity reactions when treated with another β-lactam. Before initiating therapy with meropenen, it is important to inquire about previous hypersensitivity reactions to penicillins, cephalosporins, other β-lactams, and other allergens. If an allergic reaction to meropenen occurs, discontinue the drug immediately.
17 Patient Counseling Information (17 PATIENT COUNSELING INFORMATION)
•Counsel patients that antibacterial drugs including meropenem for injection should only be used to treat bacterial infections. They do not treat viral infections (e.g., the common cold). When meropenem for injection is prescribed to treat a bacterial infection, tell patients that although it is common to feel better early in the course of therapy, take the medication exactly as directed. Skipping doses or not completing the full course of therapy may (1) decrease the effectiveness of the immediate treatment and (2) increase the likelihood that bacteria will develop resistance and will not be treatable by meropenem for injection or other antibacterial drugs in the future.•Counsel patients that diarrhea is a common problem caused by antibacterial drugs which usually ends when the antibacterial drug is discontinued. Sometimes after starting treatment with antibacterial drugs, patients can develop watery and bloody stools (with or without stomach cramps and fever) even as late as two or more months after having taken the last dose of the antibacterial drug. If this occurs, patients should contact their physician as soon as possible [seeWarnings and Precautions (5.6)].•Counsel patients to inform their physician if they are taking valproic acid or divalproex sodium. Valproic acid concentrations in the blood may drop below the therapeutic range upon co-administration with meropenem for injection. If treatment with meropenem for injection is necessary and continued, alternative or supplemental anti-convulsant medication to prevent and/or treat seizures may be needed [seeWarnings and Precautions (5.5)].•Patients receiving meropenem for injection on an outpatient basis must be alerted of adverse events such as seizures, delirium, headaches and/or paresthesias that could interfere with mental alertness and/or cause motor impairment. Until it is reasonably well established that meropenem for injection is well tolerated, patients should not operate machinery or motorized vehicles [see Warnings and Precautions (5.10) ].
8.6 Patients With Renal Impairment (8.6 Patients with Renal Impairment)
Dosage adjustment is necessary in patients with creatinine clearance 50 mL/min or less [see Dosage and Administration (2.2) , Warnings and Precautions (5.9) , and Clinical Pharmacology (12.3) ].
5.2 Severe Cutaneous Adverse Reactions
Severe cutaneous adverse reactions (SCAR) such as Stevens-Johnson syndrome (SJS), toxic epidermal necrolysis (TEN), drug reaction with eosinophilia and systemic symptoms (DRESS), erythema multiforme (EM) and acute generalized exanthematous pustulosis (AGEP) have been reported in patients receiving meropenen [see Adverse Reactions (6.2)]. If signs and symptoms suggestive of these reactions appear, meropenem should be withdrawn immediately and an alternative treatment should be considered.
5.10 Potential for Neuromotor Impairment
Alert patients receiving meropenen on an outpatient basis regarding adverse events such as seizures, delirium, headaches and/or paresthesias that could interfere with mental alertness and/or cause motor impairment. Until it is reasonably well established that meropenen is well tolerated, advise patients not to operate machinery or motorized vehicles [see Adverse Reactions (6.1)].
Principal Display Panel 1 G Vial Label (PRINCIPAL DISPLAY PANEL - 1 g Vial Label)
NDC 51810-503-01
Meropenem for Injection, USP
1 g/vial meropenem equivalent
For Intravenous Use only
Contents are Sterile Single-Dose Vial
Rx Only
Principal Display Panel 1 G Vial Carton (PRINCIPAL DISPLAY PANEL - 1 g Vial Carton)
DC 51810-503-02
Meropenem for Injection, USP
1 g/vial meropenem equivalent
For Intravenous Use only
10 × 1 g Single-Dose Vials
Rx Only
5.7 Development of Drug Resistant Bacteria (5.7 Development of Drug-Resistant Bacteria)
Prescribing meropenen in the absence of a proven or strongly suspected bacterial infection or a prophylactic indication is unlikely to provide benefit to the patient and increases the risk of the development of drug-resistant bacteria.
5.8 Overgrowth of Nonsusceptible Organisms
As with other broad-spectrum antibacterial drugs, prolonged use of meropenem may result in overgrowth of nonsusceptible organisms. Repeated evaluation of the patient is essential. If superinfection does occur during therapy, appropriate measures should be taken.
6.1 Adverse Reactions From Clinical Trials (6.1 Adverse Reactions from Clinical Trials)
Because clinical trials are conducted under widely varying conditions, adverse reactions rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
14.2 Complicated Intra Abdominal Infections (14.2 Complicated Intra-Abdominal Infections)
One controlled clinical study of complicated intra-abdominal infection was performed in the United States where meropenem was compared with clindamycin/tobramycin. Three controlled clinical studies of complicated intra-abdominal infections were performed in Europe; meropenem was compared with imipenem (two trials) and cefotaxime/metronidazole (one trial).
Using strict evaluability criteria and microbiologic eradication and clinical cures at follow-up which occurred 7 or more days after completion of therapy, the presumptive microbiologic eradication/clinical cure rates and statistical findings are provided in Table 9:
| Treatment Arm | No. evaluable/ No. enrolled (%) | Microbiologic Eradication Rate | Clinical Cure Rate | Outcome |
|---|---|---|---|---|
|
meropenem |
146/516 (28%) |
98/146 (67%) |
101/146 (69%) |
|
|
imipenem |
65/220 (30%) |
40/65 (62%) |
42/65 (65%) |
meropenem equivalent to control |
|
cefotaxime/metronidazole |
26/85 (30%) |
22/26 (85%) |
22/26 (85%) |
meropenem not equivalent to control |
|
clindamycin/tobramycin |
50/212 (24%) |
38/50 (76%) |
38/50 (76%) |
meropenem equivalent to control |
The finding that meropenem was not statistically equivalent to cefotaxime/metronidazole may have been due to uneven assignment of more seriously ill patients to the meropenem arm. Currently there is no additional information available to further interpret this observation.
Principal Display Panel 500 Mg Vial Label (PRINCIPAL DISPLAY PANEL - 500 mg Vial Label)
NDC 51810-502-01
Meropenem for Injection, USP
500 mg/vial meropenem equivalent
For Intravenous Use only
Contents are Sterile Single-Dose Vial
Rx Only
Principal Display Panel 500 Mg Vial Carton (PRINCIPAL DISPLAY PANEL - 500 mg Vial Carton)
DC 51810-502-02
Meropenem for Injection, USP
500 mg/vial meropenem equivalent
For Intravenous Use only
10 × 500 mg Single-Dose Vials
Rx Only
2.2 Use in Adult Patients With Renal Impairment (2.2 Use in Adult Patients with Renal Impairment)
Dosage should be reduced in patients with creatinine clearance of 50 mL/min or less. (See dosing table below.)
When only serum creatinine is available, the following formula (Cockcroft and Gault equation)1 may be used to estimate creatinine clearance.
Males: Creatinine Clearance (mL/min) =
Weight (kg) × (140 - age)
72 × serum creatinine (mg/dL)
Females: 0.85 × above value
| Creatinine Clearance (mL/min) | Dose (dependent on type of infection) | Dosing Interval |
|---|---|---|
|
Greater than 50 |
Recommended dose (500 mg cSSSI and 1 gram Intra-abdominal) |
Every 8 hours |
|
26–50 |
Recommended dose |
Every 12 hours |
|
10–25 |
One-half recommended dose |
Every 12 hours |
|
Less than 10 |
One-half recommended dose |
Every 24 hours |
There is inadequate information regarding the use of meropenen for injection in patients on hemodialysis or peritoneal dialysis.
14.1 Complicated Skin and Skin Structure Infections
Adult patients with complicated skin and skin structure infections including complicated cellulitis, complex abscesses, perirectal abscesses, and skin infections requiring intravenous antimicrobials, hospitalization, and surgical intervention were enrolled in a randomized, multi-center, international, double-blind trial. The study evaluated meropenem at doses of 500 mg administered intravenously every 8 hours and imipenem-cilastatin at doses of 500 mg administered intravenously every 8 hours. The study compared the clinical response between treatment groups in the clinically evaluable population at the follow-up visit (test-of-cure). The trial was conducted in the United States, South Africa, Canada, and Brazil. At enrollment, approximately 37% of the patients had underlying diabetes, 12% had underlying peripheral vascular disease and 67% had a surgical intervention. The study included 510 patients randomized to meropenem and 527 patients randomized to imipenem-cilastatin. Two hundred and sixty one (261) patients randomized to meropenem and 287 patients randomized to imipenem-cilastatin were clinically evaluable. The success rates in the clinically evaluable patients at the follow-up visit were 86% (225/261) in the meropenem arm and 83% (238/287) in imipenem-cilastatin arm.
The success rates for the clinically evaluable population are provided in Table 7.
| Population | Meropenem n n=number of patients with satisfactory response.
/N
N=number of patients in the clinically evaluable population or respective subgroup within treatment groups.
(%)
|
Imipenem-cilastatin
n /N (%) |
|---|---|---|
|
Total |
225/261 (86) |
238/287 (83) |
|
Diabetes mellitus |
83/97 (86) |
76/105 (72) |
|
No diabetes mellitus |
142/164 (87) |
162/182 (89) |
|
Less than 65 years of age |
190/218 (87) |
205/241 (85) |
|
65 years of age or older |
35/43 (81) |
33/46 (72) |
|
Men |
130/148 (88) |
137/172 (80) |
|
Women |
95/113 (84) |
101/115 (88) |
The clinical efficacy rates by pathogen are provided in Table 8. The values represent the number of patients clinically cured/number of clinically evaluable patients at the post-treatment follow-up visit, with the percent cure in parentheses (Fully Evaluable analysis set).
|
MICROORGANISMS
Patients may have more than one pretreatment pathogen.
|
Meropenem n n=number of patients with satisfactory response.
/N
N=number of patients in the clinically evaluable population or subgroup within treatment groups.
(%)
%= Percent of satisfactory clinical response at follow-up evaluation.
|
Imipenem-cilastatin
n /N (%) |
|---|---|---|
|
Gram-positive aerobes |
||
|
Staphylococcus aureus, methicillin susceptible |
82/88 (93) |
84/100 (84) |
|
Streptococcus pyogenes (Group A) |
26/29 (90) |
28/32 (88) |
|
Streptococcus agalactiae (Group B) |
12/17 (71) |
16/19 (84) |
|
Enterococcus faecalis |
9/12 (75) |
14/20 (70) |
|
Viridans group streptococci |
11/12 (92) |
5/6 (83) |
|
Gram-negative aerobes |
||
|
Escherichia coli |
12/15 (80) |
15/21 (71) |
|
Pseudomonas aeruginosa |
11/15 (73) |
13/15 (87) |
|
Proteus mirabilis |
11/13 (85) |
6/7 (86) |
|
Anaerobes |
||
|
Bacteroides fragilis |
10/11 (91) |
9/10 (90) |
|
Peptostreptococcus Species |
10/13 (77) |
14/16 (88) |
The proportion of patients who discontinued study treatment due to an adverse event was similar for both treatment groups (meropenem, 2.5% and imipenem-cilastatin, 2.7%).
1.2 Complicated Intra Abdominal Infections (adult and Pediatric Patients) (1.2 Complicated Intra-abdominal Infections (Adult and Pediatric Patients))
Meropenen for injection is indicated for the treatment of complicated appendicitis and peritonitis caused by viridans group streptococci, Escherichia coli, Klebsiella pneumoniae, Pseudomonas aeruginosa, Bacteroides fragilis, B. thetaiotaomicron, and Peptostreptococcus species.
1.3 Bacterial Meningitis (pediatric Patients 3 Months of Age and Older Only) (1.3 Bacterial Meningitis (Pediatric Patients 3 Months of Age and Older Only))
Meropenen for injection is indicated for the treatment of bacterial meningitis caused by Haemophilus influenzae, Neisseria meningitidis and penicillin-susceptible isolates of Streptococcus pneumoniae.
Meropenen for injection has been found to be effective in eliminating concurrent bacteremia in association with bacterial meningitis.
5.5 Risk of Breakthrough Seizures Due to Drug Interaction With Valproic Acid (5.5 Risk of Breakthrough Seizures Due to Drug Interaction with Valproic Acid)
The concomitant use of meropenem and valproic acid or divalproex sodium is generally not recommended. Case reports in the literature have shown that co-administration of carbapenems, including meropenem, to patients receiving valproic acid or divalproex sodium results in a reduction in valproic acid concentrations. The valproic acid concentrations may drop below the therapeutic range as a result of this interaction, therefore increasing the risk of breakthrough seizures. Increasing the dose of valproic acid or divalproex sodium may not be sufficient to overcome this interaction. Consider administration of antibacterial drugs other than carbapenems to treat infections in patients whose seizures are well controlled on valproic acid or divalproex sodium. If administration of meropenen is necessary, consider supplemental anti-convulsant therapy [see Drug Interactions (7.2)].
1.1 Complicated Skin and Skin Structure Infections (adult Patients and Pediatric Patients 3 Months of Age and Older Only) (1.1 Complicated Skin and Skin Structure Infections (Adult Patients and Pediatric Patients 3 Months of Age and Older Only))
Meropenen for injection is indicated for the treatment of complicated skin and skin structure infections (cSSSI) due to Staphylococcus aureus (methicillin-susceptible isolates only), Streptococcus pyogenes, Streptococcus agalactiae, viridans group streptococci, Enterococcus faecalis (vancomycin-susceptible isolates only), Pseudomonas aeruginosa, Escherichia coli, Proteus mirabilis, Bacteroides fragilis, and Peptostreptococcus species.
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:49:33.024505 · Updated: 2026-03-14T22:33:41.553358