These Highlights Do Not Include All The Information Needed To Use Vinorelbine Injection Safely And Effectively. See Full Prescribing Information For Vinorelbine Injection.
10a70995-e04d-4044-b1dc-c9aa27460397
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
Severe myelosuppression resulting in serious infection, septic shock, hospitalization and death can occur [see Warnings and Precautions ( 5.1 )]. Decrease the dose or withhold vinorelbine in accord with recommended dose modifications [see Dosage and Administration ( 2.2 )].
Indications and Usage
Vinorelbine Injection is indicated: In combination with cisplatin for first-line treatment of patients with locally advanced or metastatic non-small cell lung cancer (NSCLC) As a single agent for the treatment of patients with metastatic NSCLC
Dosage and Administration
In combination with cisplatin: 25 to 30 mg/m 2 as an intravenous injection or infusion once weekly ( 2.1 ) Single agent: 30 mg/m 2 as intravenously once a week ( 2.1 ) Adjust dose in patients with decreased neutrophil counts or elevated serum total bilirubin ( 2.2 )
Warnings and Precautions
Hepatic Toxicity: Monitor hepatic function prior to initiation and during treatment ( 5.2 ) Severe constipation and bowel obstruction, including necrosis and perforation, occur. Institute a prophylactic bowel regimen to mitigate potential constipation, bowel obstruction and/or paralytic ileus ( 5.3 ) Extravasation can result in severe tissue injury, local tissue necrosis and/or thrombophlebitis. Immediately stop vinorelbine and institute recommended management procedures ( 5.4 ) Neurologic Toxicity: Severe sensory and motor neuropathies occur. Monitor patients for new or worsening signs and symptoms of neuropathy. Discontinue for Grade 2 or greater neuropathy ( 5.5 ) Pulmonary toxicity and respiratory failure occur. Interrupt vinorelbine in patients who develop unexplained dyspnea or have any evidence of pulmonary toxicity. Permanently discontinue for confirmed interstitial pneumonitis or ARDS ( 5.6 ) Embryo-Fetal Toxicity: Can cause fetal harm. Advise females of reproductive potential of potential risk to the fetus and to use effective contraception ( 5.7 , 8.1 , 8.3 )
Contraindications
None
Adverse Reactions
The following clinically significant adverse reactions are described elsewhere in the labeling: Myelosuppression [see Warnings and Precautions ( 5.1 )] Hepatic Toxicity [see Warnings and Precautions ( 5.2 )] Severe Constipation and Bowel Obstruction [see Warnings and Precautions ( 5.3 )] Extravasation and Tissue Injury [see Warnings and Precautions ( 5.4 )] Neurologic Toxicity [see Warnings and Precautions ( 5.5 )] Pulmonary Toxicity and Respiratory Failure [see Warnings and Precautions ( 5.6 )]
Drug Interactions
Inhibitors of CYP3A4: May cause earlier onset and/or increased severity of adverse reactions ( 7.1 )
Storage and Handling
Vinorelbine Injection, USP is supplied as follows: Vinorelbine Injection, USP NDC (10 mg per mL) Package Factor 25021-204-01 10 mg per mL Single-Dose Vial 1 vial per carton 25021-204-05 50 mg per 5 mL Single-Dose Vial 1 vial per carton Vinorelbine Injection, USP is a clear, colorless to pale yellow aqueous solution.
How Supplied
Vinorelbine Injection, USP is supplied as follows: Vinorelbine Injection, USP NDC (10 mg per mL) Package Factor 25021-204-01 10 mg per mL Single-Dose Vial 1 vial per carton 25021-204-05 50 mg per 5 mL Single-Dose Vial 1 vial per carton Vinorelbine Injection, USP is a clear, colorless to pale yellow aqueous solution.
Medication Information
Warnings and Precautions
Hepatic Toxicity: Monitor hepatic function prior to initiation and during treatment ( 5.2 ) Severe constipation and bowel obstruction, including necrosis and perforation, occur. Institute a prophylactic bowel regimen to mitigate potential constipation, bowel obstruction and/or paralytic ileus ( 5.3 ) Extravasation can result in severe tissue injury, local tissue necrosis and/or thrombophlebitis. Immediately stop vinorelbine and institute recommended management procedures ( 5.4 ) Neurologic Toxicity: Severe sensory and motor neuropathies occur. Monitor patients for new or worsening signs and symptoms of neuropathy. Discontinue for Grade 2 or greater neuropathy ( 5.5 ) Pulmonary toxicity and respiratory failure occur. Interrupt vinorelbine in patients who develop unexplained dyspnea or have any evidence of pulmonary toxicity. Permanently discontinue for confirmed interstitial pneumonitis or ARDS ( 5.6 ) Embryo-Fetal Toxicity: Can cause fetal harm. Advise females of reproductive potential of potential risk to the fetus and to use effective contraception ( 5.7 , 8.1 , 8.3 )
Indications and Usage
Vinorelbine Injection is indicated: In combination with cisplatin for first-line treatment of patients with locally advanced or metastatic non-small cell lung cancer (NSCLC) As a single agent for the treatment of patients with metastatic NSCLC
Dosage and Administration
In combination with cisplatin: 25 to 30 mg/m 2 as an intravenous injection or infusion once weekly ( 2.1 ) Single agent: 30 mg/m 2 as intravenously once a week ( 2.1 ) Adjust dose in patients with decreased neutrophil counts or elevated serum total bilirubin ( 2.2 )
Contraindications
None
Adverse Reactions
The following clinically significant adverse reactions are described elsewhere in the labeling: Myelosuppression [see Warnings and Precautions ( 5.1 )] Hepatic Toxicity [see Warnings and Precautions ( 5.2 )] Severe Constipation and Bowel Obstruction [see Warnings and Precautions ( 5.3 )] Extravasation and Tissue Injury [see Warnings and Precautions ( 5.4 )] Neurologic Toxicity [see Warnings and Precautions ( 5.5 )] Pulmonary Toxicity and Respiratory Failure [see Warnings and Precautions ( 5.6 )]
Drug Interactions
Inhibitors of CYP3A4: May cause earlier onset and/or increased severity of adverse reactions ( 7.1 )
Storage and Handling
Vinorelbine Injection, USP is supplied as follows: Vinorelbine Injection, USP NDC (10 mg per mL) Package Factor 25021-204-01 10 mg per mL Single-Dose Vial 1 vial per carton 25021-204-05 50 mg per 5 mL Single-Dose Vial 1 vial per carton Vinorelbine Injection, USP is a clear, colorless to pale yellow aqueous solution.
How Supplied
Vinorelbine Injection, USP is supplied as follows: Vinorelbine Injection, USP NDC (10 mg per mL) Package Factor 25021-204-01 10 mg per mL Single-Dose Vial 1 vial per carton 25021-204-05 50 mg per 5 mL Single-Dose Vial 1 vial per carton Vinorelbine Injection, USP is a clear, colorless to pale yellow aqueous solution.
Description
Severe myelosuppression resulting in serious infection, septic shock, hospitalization and death can occur [see Warnings and Precautions ( 5.1 )]. Decrease the dose or withhold vinorelbine in accord with recommended dose modifications [see Dosage and Administration ( 2.2 )].
Section 42229-5
In Combination with Cisplatin 100 mg/m 2
- The recommended dosage of Vinorelbine Injection is 25 mg/m2 administered as an intravenous injection or infusion over 6 to 10 minutes on Days 1, 8, 15 and 22 of a 28-day cycle in combination with cisplatin 100 mg/m2 on Day 1 only of each 28-day cycle.
Section 44425-7
Storage Conditions
Store refrigerated between 2° and 8°C (36° and 46°F).
Do not freeze.
Protect from light. Retain in carton until time of use.
Discard unused portion.
Unopened vials of Vinorelbine Injection, USP are stable at 25°C (77°F) for up to 72 hours. Store diluted solutions of Vinorelbine Injection, USP at 5° to 30°C (41° to 86°F) [see Dosage and Administration (2.3)].
Vinorelbine Injection, USP is a cytotoxic drug. Follow applicable special handling and disposal procedures.1
Sterile, Nonpyrogenic, Preservative-free.
The container closure is not made with natural rubber latex.
Section 51945-4
PACKAGE LABEL – PRINCIPAL DISPLAY PANEL – Vial Label
NDC 25021-204-01
VINORELBINE INJECTION, USP
10 mg per mL
Rx only
1 mL Single-Dose Vial
Must Be Diluted
For Intravenous Use Only
Caution: Cytotoxic Agent
10 Overdosage
There is no known antidote for overdoses of vinorelbine. Overdoses involving quantities up to 10 times the recommended dose (30 mg/m2) have been reported. The adverse reactions described were consistent with those listed in the ADVERSE REACTIONS section, including paralytic ileus, stomatitis and esophagitis. Bone marrow aplasia, sepsis and paresis have also been reported. Fatalities have occurred following overdose of vinorelbine. If overdosage occurs, general supportive measures together with appropriate blood transfusions, growth factors and antibiotics should be instituted as deemed necessary by the physician.
15 References
- OSHA. http://www.osha.gov/SLTC/hazardousdrugs/index.html
11 Description
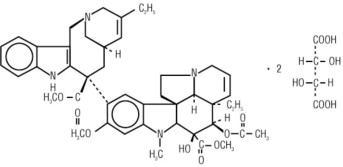
Vinorelbine Injection, USP contains vinorelbine, a semi-synthetic vinca alkaloid. The molecular formula for vinorelbine tartrate is C45H54N4O8•2C4H6O6. It has a molecular weight of 1079.11. The structural formula is as follows:
Vinorelbine tartrate is a white to light yellow amorphous powder. It is easily soluble in water, very soluble in methanol and practically insoluble in hexane.
Vinorelbine Injection, USP is a sterile nonpyrogenic aqueous solution for intravenous use. Each milliliter of solution contains 10 mg vinorelbine (equivalent to 13.85 mg vinorelbine tartrate) in Water for Injection, USP. The pH of Vinorelbine Injection, USP is approximately 3.5.
14.2 Single Agent
The safety and efficacy of vinorelbine as a single agent was evaluated in one randomized multicenter trial. Study 3 was a randomized, open-label clinical trial of vinorelbine or fluorouracil (FU) plus leucovorin (LV) in patients with Stage IV NSCLC who had not received prior chemotherapy. A total of 211 patients were randomized 2:1 to receive vinorelbine 30 mg/m2 weekly of an 8-week cycle (N=143) or FU 425 mg/m2 bolus intravenously plus LV 20 mg/m2 bolus intravenously daily for 5 days of a 4-weeks cycle (N=68).
Patient demographics and disease characteristics were in general similar between arms. In the overall population, the median age was 61 years (range 32 to 83), 74% were male, 88% were White, 46% had adenocarcinoma histology. Fifty percent of the patients had Karnofsky performance status ≥ 90 in the vinorelbine arm compared to 38% in the FU/LV arm.
The primary efficacy outcome of the study was overall survival. The median survival time was 30 weeks versus 22 weeks for patients receiving vinorelbine versus FU/LV, respectively (p=0.06). Partial objective responses were observed in 11.1% (95% CI=6.2%, 17.9%) and 3.5% (95% CI=0.4%, 11.9%) of patients who received vinorelbine and FU/LV, respectively.
8.4 Pediatric Use
The safety and effectiveness of vinorelbine in pediatric patients have not been established.
Results from a single-arm study of vinorelbine administered at the dose of 33.75 mg/m2 (for 35 patients) or at the dose of 30 mg/m2 (for 11 patients) every week for 6 weeks followed by 2 weeks of rest were evaluated (courses of 8 weeks). Forty-six patients age 1 to 25 (median 11 years) with recurrent solid malignant tumors, including rhabdomyosarcoma or undifferentiated sarcoma (N=21 patients), neuroblastoma (N= 4 patients) and central nervous system (CNS) tumors (N=21 patients), were enrolled. The most significant grade 3 or 4 hematological adverse reactions were neutropenia (70%) and anemia (33%). The most significant grade 3 or 4 non-hematological adverse reactions were motor (15%) or cranial (13%) neuropathy, hypoxia (13%) and dyspnea (11%). Objective tumor response was observed in 2 out of 21 patients with rhabdomyosarcoma or undifferentiated sarcoma. No objective tumor response was observed in patients with CNS tumors (N=21) or neuroblastoma (N=4).
8.5 Geriatric Use
Of the 769 number of patients who received vinorelbine as a single agent and in combination with cisplatin in studies 1, 2 and 3, 247 patients were 65 years of age or older. No overall differences in safety, efficacy and pharmacokinetic parameters were observed between these patients and younger patients [see Clinical Pharmacology (12.3)].
4 Contraindications
None
6 Adverse Reactions
The following clinically significant adverse reactions are described elsewhere in the labeling:
- Myelosuppression [see Warnings and Precautions (5.1)]
- Hepatic Toxicity [see Warnings and Precautions (5.2)]
- Severe Constipation and Bowel Obstruction [see Warnings and Precautions (5.3)]
- Extravasation and Tissue Injury [see Warnings and Precautions (5.4)]
- Neurologic Toxicity [see Warnings and Precautions (5.5)]
- Pulmonary Toxicity and Respiratory Failure [see Warnings and Precautions (5.6)]
7 Drug Interactions
- Inhibitors of CYP3A4: May cause earlier onset and/or increased severity of adverse reactions (7.1)
5.1 Myelosuppression
Myelosuppression, manifested by neutropenia, anemia and thrombocytopenia, occur in patients receiving vinorelbine as a single agent and in combination with cisplatin [see Adverse Reactions (6.1, 6.2)]. Neutropenia is the major dose-limiting toxicity with vinorelbine. Grade 3-4 neutropenia occurred in 53% of patients treated with vinorelbine at 30 mg/m2 per week. Dose adjustment due to myelosuppression occurred in 51% of patients (Study 2). In clinical trials with vinorelbine administered at 30 mg/m2 per week, neutropenia resulted in hospitalizations for pyrexia and/or sepsis in 8% of patients. Death due to sepsis occurred in 1% of patients. Neutropenia nadirs occur between 7 and 10 days after dosing with neutropenia count recovery usually occurring within the following 7 to 14 days.
Monitor complete blood counts prior to each dose of vinorelbine. Do not administer vinorelbine to patients with neutrophil counts <1,000 cells/mm3. Adjustments in the dosage of vinorelbine should be based on neutrophil counts obtained on the day of treatment [see Dosage and Administration (2.2)].
5.2 Hepatic Toxicity
Drug-induced liver injury manifest by elevated aspartate aminotransferase (AST) and bilirubin occur in patients receiving vinorelbine as a single agent and in combination with cytotoxic agents. Assess hepatic function prior to initiation of vinorelbine and periodically during treatment. Reduce the dose of vinorelbine for patients who develop elevations in total bilirubin ≥ 2 times upper limit of normal [see Dosage and Administration (2.2) and Use in Specific Populations (8.6)].
7.1 Cyp3a Inhibitors
Exercise caution in patients concurrently taking drugs known to inhibit CYP3A. Concurrent administration of vinorelbine with a CYP3A inhibitor may cause an earlier onset and/or an increased severity of adverse reactions.
12.3 Pharmacokinetics
The pharmacokinetics of vinorelbine were studied in 49 patients who received doses of 30 mg/m2 administered as 15- to 20-minute constant-rate infusions. Vinorelbine concentrations in plasma decay in a triphasic manner.
8.6 Hepatic Impairment
The influence of hepatic impairment on the pharmacokinetics of vinorelbine has not been evaluated, but the liver plays an important role in the metabolism of vinorelbine. Elevated AST occurs in >60% of the patients receiving vinorelbine as a single agent (6% Grade 3-4). Therefore, exercise caution in patients with hepatic impairment. Reduce the dose of vinorelbine for patients with elevated serum total bilirubin concentrations [see Dosage and Administration (2.2) and Warnings and Precautions (5.2)].
1 Indications and Usage
Vinorelbine Injection is indicated:
- In combination with cisplatin for first-line treatment of patients with locally advanced or metastatic non-small cell lung cancer (NSCLC)
- As a single agent for the treatment of patients with metastatic NSCLC
5.5 Neurologic Toxicity
Sensory and motor neuropathies, including severe neuropathies, occur in patients receiving vinorelbine. Monitor patients for new or worsening signs and symptoms of neuropathy, such as paresthesia, hyperesthesia, hyporeflexia and muscle weakness while receiving vinorelbine. Discontinue vinorelbine for CTCAE Grade 2 or greater neuropathy [see Dosage and Administration (2.2) and Adverse Reactions (6.1)].
12.1 Mechanism of Action
Vinorelbine is a vinca alkaloid that interferes with microtubule assembly. The antitumor activity of vinorelbine is thought to be due primarily to inhibition of mitosis at metaphase through its interaction with tubulin. Vinorelbine may also interfere with: 1) amino acid, cyclic AMP and glutathione metabolism, 2) calmodulin-dependent Ca++-transport ATPase activity, 3) cellular respiration, and 4) nucleic acid and lipid biosynthesis. Vinorelbine inhibited mitotic microtubule formation in intact mouse embryo tectal plates at a concentration of 2 μM inducing a blockade of cells at metaphase, but produced depolymerization of axonal microtubules at a concentration 40 μM, suggesting a modest selectivity of vinorelbine for mitotic microtubules.
5.7 Embryo Fetal Toxicity
Based on findings from animal studies and its mechanism of action, vinorelbine can cause fetal harm when administered to a pregnant woman. In animal reproduction studies in mice and rabbits, embryo and fetal toxicity were observed with administration of vinorelbine at doses approximately 0.33 and 0.18 times the human therapeutic dose, respectively.
Advise pregnant women of the potential risk to a fetus. Advise females of reproductive potential to use effective contraception during treatment with vinorelbine and for 6 months after the final dose. Advise males with female partners of reproductive potential to use effective contraception during treatment with vinorelbine and for 3 months after the final dose [see Use in Specific Populations (8.1, 8.3)].
Warning: Myelosuppression
5 Warnings and Precautions
- Hepatic Toxicity: Monitor hepatic function prior to initiation and during treatment (5.2)
- Severe constipation and bowel obstruction, including necrosis and perforation, occur. Institute a prophylactic bowel regimen to mitigate potential constipation, bowel obstruction and/or paralytic ileus (5.3)
- Extravasation can result in severe tissue injury, local tissue necrosis and/or thrombophlebitis. Immediately stop vinorelbine and institute recommended management procedures (5.4)
- Neurologic Toxicity: Severe sensory and motor neuropathies occur. Monitor patients for new or worsening signs and symptoms of neuropathy. Discontinue for Grade 2 or greater neuropathy (5.5)
- Pulmonary toxicity and respiratory failure occur. Interrupt vinorelbine in patients who develop unexplained dyspnea or have any evidence of pulmonary toxicity. Permanently discontinue for confirmed interstitial pneumonitis or ARDS (5.6)
- Embryo-Fetal Toxicity: Can cause fetal harm. Advise females of reproductive potential of potential risk to the fetus and to use effective contraception (5.7, 8.1, 8.3)
2 Dosage and Administration
3 Dosage Forms and Strengths
Vinorelbine Injection, USP: 1 mL (10 mg per 1 mL) and 5 mL (50 mg per 5 mL) clear colorless to pale yellow solution in single-dose vial.
6.2 Postmarketing Experience
The following adverse reactions have been identified during postapproval use of vinorelbine. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Infections: pneumonia
Immune system disorders: anaphylactic reaction, pruritus, urticaria, angioedema
Nervous system disorders: loss of deep tendon reflexes, muscular weakness, gait disturbance, headache
Ear and labyrinth disorders: vestibular disorder, hearing impaired
Cardiac disorders: tachycardia
Respiratory disorders: pulmonary edema
Vascular disorders: pulmonary embolism, deep vein thrombosis, hypertension, hypotension, flushing, vasodilatation
Gastrointestinal disorders: mucosal inflammation, dysphagia, pancreatitis
Skin disorders: generalized cutaneous reactions (rash), palmar-plantar erythrodysesthesia syndrome
Musculoskeletal and connective tissue disorders: jaw pain, myalgia, arthralgia
General disorders and administration site conditions: injection site rash, urticaria, blistering, sloughing of skin
Injury, poisoning and procedural complications: radiation recall phenomenon, dermatitis, esophagitis
Laboratory abnormalities: electrolyte imbalance including hyponatremia
Other: tumor pain, back pain, abdominal pain
8 Use in Specific Populations
- Lactation: Advise not to breastfeed (8.2)
6.1 Clinical Trials Experience
Because clinical trials are conducted under varying designs and in different patient populations, the adverse reaction rates reported in one clinical trial may not be easily compared to those rates reported in another clinical trial and may not reflect the rates actually observed in clinical practice.
14.1 Combination Use With Cisplatin
The safety and efficacy of vinorelbine in combination with cisplatin was evaluated in two randomized, multicenter trials.
5.4 Extravasation and Tissue Injury
Extravasation of vinorelbine can result in severe irritation, local tissue necrosis and/or thrombophlebitis. If signs or symptoms of extravasation occur, immediately stop administration of vinorelbine and institute recommended management procedures [see Dosage and Administration (2.2) and Adverse Reactions (6.1)].
16 How Supplied/storage and Handling
Vinorelbine Injection, USP is supplied as follows:
| Vinorelbine Injection, USP | ||
| NDC | (10 mg per mL) | Package Factor |
| 25021-204-01 | 10 mg per mL Single-Dose Vial | 1 vial per carton |
| 25021-204-05 | 50 mg per 5 mL Single-Dose Vial | 1 vial per carton |
Vinorelbine Injection, USP is a clear, colorless to pale yellow aqueous solution.
5.3 Severe Constipation and Bowel Obstruction
Severe and fatal paralytic ileus, constipation, intestinal obstruction, necrosis, and perforation occur in patients receiving vinorelbine. Institute a prophylactic bowel regimen to mitigate potential constipation, bowel obstruction and/or paralytic ileus, considering adequate dietary fiber intake, hydration and routine use of stool softeners.
5.6 Pulmonary Toxicity and Respiratory Failure
Pulmonary toxicity, including severe acute bronchospasm, interstitial pneumonitis, acute respiratory distress syndrome (ARDS) occur in patients receiving vinorelbine. Interstitial pneumonitis and ARDS included fatalities. The mean time to onset of interstitial pneumonitis and ARDS after vinorelbine administration was one week (range 3 to 8 days) [see Adverse Reactions (6.1)]. Interrupt vinorelbine in patients who develop unexplained dyspnea or have any evidence of pulmonary toxicity. Permanently discontinue vinorelbine for confirmed interstitial pneumonitis or ARDS.
2.4 Procedures for Proper Handling and Disposal
Vinorelbine Injection is a cytotoxic drug. Follow applicable special handling and disposal procedures1.
Exercise caution in handling and preparing the solution of Vinorelbine Injection. The use of gloves is recommended. If the solution of Vinorelbine Injection contacts the skin or mucosa, immediately wash the skin or mucosa thoroughly with soap and water.
Avoid contamination of the eye with Vinorelbine Injection. If exposure occurs, flush the eyes with water immediately and thoroughly.
Discard unused portion.
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
The carcinogenic potential of vinorelbine has not been studied. Vinorelbine has been shown to affect chromosome number and possibly structure in vivo (polyploidy in bone marrow cells from Chinese hamsters and a positive micronucleus test in mice). It was not mutagenic in the Ames test and gave inconclusive results in the mouse lymphoma TK Locus assay.
Vinorelbine did not affect fertility to a statistically significant extent when administered to rats on either a once-weekly (9 mg/m2, approximately one third the human dose) or alternate-day schedule (4.2 mg/m2, approximately 0.14 times the human recommended dose) prior to and during mating. In male rats, administration of vinorelbine twice weekly for 13 or 26 weeks at dose levels of 2.1 and 7.2 mg/m2 (approximately 0.07 and 0.24 times the recommended human dose), respectively, resulted in decreased spermatogenesis and prostate/seminal vesicle secretion.
Structured Label Content
Section 42229-5 (42229-5)
In Combination with Cisplatin 100 mg/m 2
- The recommended dosage of Vinorelbine Injection is 25 mg/m2 administered as an intravenous injection or infusion over 6 to 10 minutes on Days 1, 8, 15 and 22 of a 28-day cycle in combination with cisplatin 100 mg/m2 on Day 1 only of each 28-day cycle.
Section 44425-7 (44425-7)
Storage Conditions
Store refrigerated between 2° and 8°C (36° and 46°F).
Do not freeze.
Protect from light. Retain in carton until time of use.
Discard unused portion.
Unopened vials of Vinorelbine Injection, USP are stable at 25°C (77°F) for up to 72 hours. Store diluted solutions of Vinorelbine Injection, USP at 5° to 30°C (41° to 86°F) [see Dosage and Administration (2.3)].
Vinorelbine Injection, USP is a cytotoxic drug. Follow applicable special handling and disposal procedures.1
Sterile, Nonpyrogenic, Preservative-free.
The container closure is not made with natural rubber latex.
Section 51945-4 (51945-4)
PACKAGE LABEL – PRINCIPAL DISPLAY PANEL – Vial Label
NDC 25021-204-01
VINORELBINE INJECTION, USP
10 mg per mL
Rx only
1 mL Single-Dose Vial
Must Be Diluted
For Intravenous Use Only
Caution: Cytotoxic Agent
10 Overdosage (10 OVERDOSAGE)
There is no known antidote for overdoses of vinorelbine. Overdoses involving quantities up to 10 times the recommended dose (30 mg/m2) have been reported. The adverse reactions described were consistent with those listed in the ADVERSE REACTIONS section, including paralytic ileus, stomatitis and esophagitis. Bone marrow aplasia, sepsis and paresis have also been reported. Fatalities have occurred following overdose of vinorelbine. If overdosage occurs, general supportive measures together with appropriate blood transfusions, growth factors and antibiotics should be instituted as deemed necessary by the physician.
15 References (15 REFERENCES)
- OSHA. http://www.osha.gov/SLTC/hazardousdrugs/index.html
11 Description (11 DESCRIPTION)
Vinorelbine Injection, USP contains vinorelbine, a semi-synthetic vinca alkaloid. The molecular formula for vinorelbine tartrate is C45H54N4O8•2C4H6O6. It has a molecular weight of 1079.11. The structural formula is as follows:
Vinorelbine tartrate is a white to light yellow amorphous powder. It is easily soluble in water, very soluble in methanol and practically insoluble in hexane.
Vinorelbine Injection, USP is a sterile nonpyrogenic aqueous solution for intravenous use. Each milliliter of solution contains 10 mg vinorelbine (equivalent to 13.85 mg vinorelbine tartrate) in Water for Injection, USP. The pH of Vinorelbine Injection, USP is approximately 3.5.
14.2 Single Agent
The safety and efficacy of vinorelbine as a single agent was evaluated in one randomized multicenter trial. Study 3 was a randomized, open-label clinical trial of vinorelbine or fluorouracil (FU) plus leucovorin (LV) in patients with Stage IV NSCLC who had not received prior chemotherapy. A total of 211 patients were randomized 2:1 to receive vinorelbine 30 mg/m2 weekly of an 8-week cycle (N=143) or FU 425 mg/m2 bolus intravenously plus LV 20 mg/m2 bolus intravenously daily for 5 days of a 4-weeks cycle (N=68).
Patient demographics and disease characteristics were in general similar between arms. In the overall population, the median age was 61 years (range 32 to 83), 74% were male, 88% were White, 46% had adenocarcinoma histology. Fifty percent of the patients had Karnofsky performance status ≥ 90 in the vinorelbine arm compared to 38% in the FU/LV arm.
The primary efficacy outcome of the study was overall survival. The median survival time was 30 weeks versus 22 weeks for patients receiving vinorelbine versus FU/LV, respectively (p=0.06). Partial objective responses were observed in 11.1% (95% CI=6.2%, 17.9%) and 3.5% (95% CI=0.4%, 11.9%) of patients who received vinorelbine and FU/LV, respectively.
8.4 Pediatric Use
The safety and effectiveness of vinorelbine in pediatric patients have not been established.
Results from a single-arm study of vinorelbine administered at the dose of 33.75 mg/m2 (for 35 patients) or at the dose of 30 mg/m2 (for 11 patients) every week for 6 weeks followed by 2 weeks of rest were evaluated (courses of 8 weeks). Forty-six patients age 1 to 25 (median 11 years) with recurrent solid malignant tumors, including rhabdomyosarcoma or undifferentiated sarcoma (N=21 patients), neuroblastoma (N= 4 patients) and central nervous system (CNS) tumors (N=21 patients), were enrolled. The most significant grade 3 or 4 hematological adverse reactions were neutropenia (70%) and anemia (33%). The most significant grade 3 or 4 non-hematological adverse reactions were motor (15%) or cranial (13%) neuropathy, hypoxia (13%) and dyspnea (11%). Objective tumor response was observed in 2 out of 21 patients with rhabdomyosarcoma or undifferentiated sarcoma. No objective tumor response was observed in patients with CNS tumors (N=21) or neuroblastoma (N=4).
8.5 Geriatric Use
Of the 769 number of patients who received vinorelbine as a single agent and in combination with cisplatin in studies 1, 2 and 3, 247 patients were 65 years of age or older. No overall differences in safety, efficacy and pharmacokinetic parameters were observed between these patients and younger patients [see Clinical Pharmacology (12.3)].
4 Contraindications (4 CONTRAINDICATIONS)
None
6 Adverse Reactions (6 ADVERSE REACTIONS)
The following clinically significant adverse reactions are described elsewhere in the labeling:
- Myelosuppression [see Warnings and Precautions (5.1)]
- Hepatic Toxicity [see Warnings and Precautions (5.2)]
- Severe Constipation and Bowel Obstruction [see Warnings and Precautions (5.3)]
- Extravasation and Tissue Injury [see Warnings and Precautions (5.4)]
- Neurologic Toxicity [see Warnings and Precautions (5.5)]
- Pulmonary Toxicity and Respiratory Failure [see Warnings and Precautions (5.6)]
7 Drug Interactions (7 DRUG INTERACTIONS)
- Inhibitors of CYP3A4: May cause earlier onset and/or increased severity of adverse reactions (7.1)
5.1 Myelosuppression
Myelosuppression, manifested by neutropenia, anemia and thrombocytopenia, occur in patients receiving vinorelbine as a single agent and in combination with cisplatin [see Adverse Reactions (6.1, 6.2)]. Neutropenia is the major dose-limiting toxicity with vinorelbine. Grade 3-4 neutropenia occurred in 53% of patients treated with vinorelbine at 30 mg/m2 per week. Dose adjustment due to myelosuppression occurred in 51% of patients (Study 2). In clinical trials with vinorelbine administered at 30 mg/m2 per week, neutropenia resulted in hospitalizations for pyrexia and/or sepsis in 8% of patients. Death due to sepsis occurred in 1% of patients. Neutropenia nadirs occur between 7 and 10 days after dosing with neutropenia count recovery usually occurring within the following 7 to 14 days.
Monitor complete blood counts prior to each dose of vinorelbine. Do not administer vinorelbine to patients with neutrophil counts <1,000 cells/mm3. Adjustments in the dosage of vinorelbine should be based on neutrophil counts obtained on the day of treatment [see Dosage and Administration (2.2)].
5.2 Hepatic Toxicity
Drug-induced liver injury manifest by elevated aspartate aminotransferase (AST) and bilirubin occur in patients receiving vinorelbine as a single agent and in combination with cytotoxic agents. Assess hepatic function prior to initiation of vinorelbine and periodically during treatment. Reduce the dose of vinorelbine for patients who develop elevations in total bilirubin ≥ 2 times upper limit of normal [see Dosage and Administration (2.2) and Use in Specific Populations (8.6)].
7.1 Cyp3a Inhibitors (7.1 CYP3A Inhibitors)
Exercise caution in patients concurrently taking drugs known to inhibit CYP3A. Concurrent administration of vinorelbine with a CYP3A inhibitor may cause an earlier onset and/or an increased severity of adverse reactions.
12.3 Pharmacokinetics
The pharmacokinetics of vinorelbine were studied in 49 patients who received doses of 30 mg/m2 administered as 15- to 20-minute constant-rate infusions. Vinorelbine concentrations in plasma decay in a triphasic manner.
8.6 Hepatic Impairment
The influence of hepatic impairment on the pharmacokinetics of vinorelbine has not been evaluated, but the liver plays an important role in the metabolism of vinorelbine. Elevated AST occurs in >60% of the patients receiving vinorelbine as a single agent (6% Grade 3-4). Therefore, exercise caution in patients with hepatic impairment. Reduce the dose of vinorelbine for patients with elevated serum total bilirubin concentrations [see Dosage and Administration (2.2) and Warnings and Precautions (5.2)].
1 Indications and Usage (1 INDICATIONS AND USAGE)
Vinorelbine Injection is indicated:
- In combination with cisplatin for first-line treatment of patients with locally advanced or metastatic non-small cell lung cancer (NSCLC)
- As a single agent for the treatment of patients with metastatic NSCLC
5.5 Neurologic Toxicity
Sensory and motor neuropathies, including severe neuropathies, occur in patients receiving vinorelbine. Monitor patients for new or worsening signs and symptoms of neuropathy, such as paresthesia, hyperesthesia, hyporeflexia and muscle weakness while receiving vinorelbine. Discontinue vinorelbine for CTCAE Grade 2 or greater neuropathy [see Dosage and Administration (2.2) and Adverse Reactions (6.1)].
12.1 Mechanism of Action
Vinorelbine is a vinca alkaloid that interferes with microtubule assembly. The antitumor activity of vinorelbine is thought to be due primarily to inhibition of mitosis at metaphase through its interaction with tubulin. Vinorelbine may also interfere with: 1) amino acid, cyclic AMP and glutathione metabolism, 2) calmodulin-dependent Ca++-transport ATPase activity, 3) cellular respiration, and 4) nucleic acid and lipid biosynthesis. Vinorelbine inhibited mitotic microtubule formation in intact mouse embryo tectal plates at a concentration of 2 μM inducing a blockade of cells at metaphase, but produced depolymerization of axonal microtubules at a concentration 40 μM, suggesting a modest selectivity of vinorelbine for mitotic microtubules.
5.7 Embryo Fetal Toxicity (5.7 Embryo-Fetal Toxicity)
Based on findings from animal studies and its mechanism of action, vinorelbine can cause fetal harm when administered to a pregnant woman. In animal reproduction studies in mice and rabbits, embryo and fetal toxicity were observed with administration of vinorelbine at doses approximately 0.33 and 0.18 times the human therapeutic dose, respectively.
Advise pregnant women of the potential risk to a fetus. Advise females of reproductive potential to use effective contraception during treatment with vinorelbine and for 6 months after the final dose. Advise males with female partners of reproductive potential to use effective contraception during treatment with vinorelbine and for 3 months after the final dose [see Use in Specific Populations (8.1, 8.3)].
Warning: Myelosuppression (WARNING: MYELOSUPPRESSION)
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
- Hepatic Toxicity: Monitor hepatic function prior to initiation and during treatment (5.2)
- Severe constipation and bowel obstruction, including necrosis and perforation, occur. Institute a prophylactic bowel regimen to mitigate potential constipation, bowel obstruction and/or paralytic ileus (5.3)
- Extravasation can result in severe tissue injury, local tissue necrosis and/or thrombophlebitis. Immediately stop vinorelbine and institute recommended management procedures (5.4)
- Neurologic Toxicity: Severe sensory and motor neuropathies occur. Monitor patients for new or worsening signs and symptoms of neuropathy. Discontinue for Grade 2 or greater neuropathy (5.5)
- Pulmonary toxicity and respiratory failure occur. Interrupt vinorelbine in patients who develop unexplained dyspnea or have any evidence of pulmonary toxicity. Permanently discontinue for confirmed interstitial pneumonitis or ARDS (5.6)
- Embryo-Fetal Toxicity: Can cause fetal harm. Advise females of reproductive potential of potential risk to the fetus and to use effective contraception (5.7, 8.1, 8.3)
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
Vinorelbine Injection, USP: 1 mL (10 mg per 1 mL) and 5 mL (50 mg per 5 mL) clear colorless to pale yellow solution in single-dose vial.
6.2 Postmarketing Experience
The following adverse reactions have been identified during postapproval use of vinorelbine. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Infections: pneumonia
Immune system disorders: anaphylactic reaction, pruritus, urticaria, angioedema
Nervous system disorders: loss of deep tendon reflexes, muscular weakness, gait disturbance, headache
Ear and labyrinth disorders: vestibular disorder, hearing impaired
Cardiac disorders: tachycardia
Respiratory disorders: pulmonary edema
Vascular disorders: pulmonary embolism, deep vein thrombosis, hypertension, hypotension, flushing, vasodilatation
Gastrointestinal disorders: mucosal inflammation, dysphagia, pancreatitis
Skin disorders: generalized cutaneous reactions (rash), palmar-plantar erythrodysesthesia syndrome
Musculoskeletal and connective tissue disorders: jaw pain, myalgia, arthralgia
General disorders and administration site conditions: injection site rash, urticaria, blistering, sloughing of skin
Injury, poisoning and procedural complications: radiation recall phenomenon, dermatitis, esophagitis
Laboratory abnormalities: electrolyte imbalance including hyponatremia
Other: tumor pain, back pain, abdominal pain
8 Use in Specific Populations (8 USE IN SPECIFIC POPULATIONS)
- Lactation: Advise not to breastfeed (8.2)
6.1 Clinical Trials Experience
Because clinical trials are conducted under varying designs and in different patient populations, the adverse reaction rates reported in one clinical trial may not be easily compared to those rates reported in another clinical trial and may not reflect the rates actually observed in clinical practice.
14.1 Combination Use With Cisplatin (14.1 Combination Use with Cisplatin)
The safety and efficacy of vinorelbine in combination with cisplatin was evaluated in two randomized, multicenter trials.
5.4 Extravasation and Tissue Injury
Extravasation of vinorelbine can result in severe irritation, local tissue necrosis and/or thrombophlebitis. If signs or symptoms of extravasation occur, immediately stop administration of vinorelbine and institute recommended management procedures [see Dosage and Administration (2.2) and Adverse Reactions (6.1)].
16 How Supplied/storage and Handling (16 HOW SUPPLIED/STORAGE AND HANDLING)
Vinorelbine Injection, USP is supplied as follows:
| Vinorelbine Injection, USP | ||
| NDC | (10 mg per mL) | Package Factor |
| 25021-204-01 | 10 mg per mL Single-Dose Vial | 1 vial per carton |
| 25021-204-05 | 50 mg per 5 mL Single-Dose Vial | 1 vial per carton |
Vinorelbine Injection, USP is a clear, colorless to pale yellow aqueous solution.
5.3 Severe Constipation and Bowel Obstruction
Severe and fatal paralytic ileus, constipation, intestinal obstruction, necrosis, and perforation occur in patients receiving vinorelbine. Institute a prophylactic bowel regimen to mitigate potential constipation, bowel obstruction and/or paralytic ileus, considering adequate dietary fiber intake, hydration and routine use of stool softeners.
5.6 Pulmonary Toxicity and Respiratory Failure
Pulmonary toxicity, including severe acute bronchospasm, interstitial pneumonitis, acute respiratory distress syndrome (ARDS) occur in patients receiving vinorelbine. Interstitial pneumonitis and ARDS included fatalities. The mean time to onset of interstitial pneumonitis and ARDS after vinorelbine administration was one week (range 3 to 8 days) [see Adverse Reactions (6.1)]. Interrupt vinorelbine in patients who develop unexplained dyspnea or have any evidence of pulmonary toxicity. Permanently discontinue vinorelbine for confirmed interstitial pneumonitis or ARDS.
2.4 Procedures for Proper Handling and Disposal
Vinorelbine Injection is a cytotoxic drug. Follow applicable special handling and disposal procedures1.
Exercise caution in handling and preparing the solution of Vinorelbine Injection. The use of gloves is recommended. If the solution of Vinorelbine Injection contacts the skin or mucosa, immediately wash the skin or mucosa thoroughly with soap and water.
Avoid contamination of the eye with Vinorelbine Injection. If exposure occurs, flush the eyes with water immediately and thoroughly.
Discard unused portion.
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
The carcinogenic potential of vinorelbine has not been studied. Vinorelbine has been shown to affect chromosome number and possibly structure in vivo (polyploidy in bone marrow cells from Chinese hamsters and a positive micronucleus test in mice). It was not mutagenic in the Ames test and gave inconclusive results in the mouse lymphoma TK Locus assay.
Vinorelbine did not affect fertility to a statistically significant extent when administered to rats on either a once-weekly (9 mg/m2, approximately one third the human dose) or alternate-day schedule (4.2 mg/m2, approximately 0.14 times the human recommended dose) prior to and during mating. In male rats, administration of vinorelbine twice weekly for 13 or 26 weeks at dose levels of 2.1 and 7.2 mg/m2 (approximately 0.07 and 0.24 times the recommended human dose), respectively, resulted in decreased spermatogenesis and prostate/seminal vesicle secretion.
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:42:54.053121 · Updated: 2026-03-14T22:11:32.415850