0d3a966f-f937-05a8-a90f-5aa52ebbd613
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
See full prescribing information for complete boxed warning. When pregnancy is detected, discontinue ZESTORETIC as soon as possible. Drugs that act directly on the renin-angiotensin system can cause injury and death to the developing fetus. See Warnings: Fetal Toxicity.
Indications and Usage
ZESTORETIC is indicated for the treatment of hypertension, to lower blood pressure. Lowering blood pressure lowers the risk of fatal and non-fatal cardiovascular events, primarily strokes and myocardial infarctions. These benefits have been seen in controlled trials of antihypertensive drugs from a wide variety of pharmacologic classes including lisinopril and hydrochlorothiazide. Control of high blood pressure should be part of comprehensive cardiovascular risk management, including, as appropriate, lipid control, diabetes management, antithrombotic therapy, smoking cessation, exercise, and limited sodium intake. Many patients will require more than 1 drug to achieve blood pressure goals. For specific advice on goals and management, see published guidelines, such as those of the National High Blood Pressure Education Program’s Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure (JNC). Numerous antihypertensive drugs, from a variety of pharmacologic classes and with different mechanisms of action, have been shown in randomized controlled trials to reduce cardiovascular morbidity and mortality, and it can be concluded that it is blood pressure reduction, and not some other pharmacologic property of the drugs, that is largely responsible for those benefits. The largest and most consistent cardiovascular outcome benefit has been a reduction in the risk of stroke, but reductions in myocardial infarction and cardiovascular mortality also have been seen regularly. Elevated systolic or diastolic pressure causes increased cardiovascular risk, and the absolute risk increase per mmHg is greater at higher blood pressures, so that even modest reductions of severe hypertension can provide substantial benefit. Relative risk reduction from blood pressure reduction is similar across populations with varying absolute risk, so the absolute benefit is greater in patients who are at higher risk independent of their hypertension (for example, patients with diabetes or hyperlipidemia), and such patients would be expected to benefit from more aggressive treatment to a lower blood pressure goal. Some antihypertensive drugs have smaller blood pressure effects (as monotherapy) in black patients, and many antihypertensive drugs have additional approved indications and effects (e.g., on angina, heart failure, or diabetic kidney disease). These considerations may guide selection of therapy. These fixed-dose combinations are not indicated for initial therapy (see DOSAGE AND ADMINISTRATION ). In using ZESTORETIC, consideration should be given to the fact that an angiotensin-converting enzyme inhibitor, captopril, has caused agranulocytosis, particularly in patients with renal impairment or collagen vascular disease, and that available data are insufficient to show that lisinopril does not have a similar risk (see WARNINGS ). In considering the use of ZESTORETIC, it should be noted that ACE inhibitors have been associated with a higher rate of angioedema in black than in nonblack patients (see WARNINGS, Lisinopril ).
Dosage and Administration
Lisinopril monotherapy is an effective treatment of hypertension in once-daily doses of 10 mg to 80 mg, while hydrochlorothiazide monotherapy is effective in doses of 12.5 mg per day to 50 mg per day. In clinical trials of lisinopril/hydrochlorothiazide combination therapy using lisinopril doses of 10 mg to 80 mg and hydrochlorothiazide doses of 6.25 mg to 50 mg, the antihypertensive response rates generally increased with increasing dose of either component. The side effects (see WARNINGS ) of lisinopril are generally rare and apparently independent of dose; those of hydrochlorothiazide are a mixture of dose-dependent phenomena (primarily hypokalemia) and dose-independent phenomena (e.g., pancreatitis), the former much more common than the latter. Therapy with any combination of lisinopril and hydrochlorothiazide may be associated with either or both dose-independent or dose-dependent side effects, but addition of lisinopril in clinical trials blunted the hypokalemia normally seen with diuretics. To minimize dose-dependent side effects, it is usually appropriate to begin combination therapy only after a patient has failed to achieve the desired effect with monotherapy. Dose Titration Guided by Clinical Effect: A patient whose blood pressure is not adequately controlled with either lisinopril or hydrochlorothiazide monotherapy may be switched to lisinopril/HCTZ 10/12.5 or lisinopril/HCTZ 20/12.5, depending on current monotherapy dose. Further increases of either or both components should depend on clinical response with blood pressure measured at the interdosing interval to ensure that there is an adequate antihypertensive effect at that time. The hydrochlorothiazide dose should generally not be increased until 2 to 3 weeks have elapsed. After addition of the diuretic it may be possible to reduce the dose of lisinopril. Patients whose blood pressures are adequately controlled with 25 mg of daily hydrochlorothiazide, but who experience significant potassium loss with this regimen may achieve similar or greater blood-pressure control without electrolyte disturbance if they are switched to lisinopril/HCTZ 10/12.5. In patients who are currently being treated with a diuretic, symptomatic hypotension occasionally may occur following the initial dose of lisinopril. The diuretic should, if possible, be discontinued for two to three days before beginning therapy with lisinopril to reduce the likelihood of hypotension (see WARNINGS ). If the patient's blood pressure is not controlled with lisinopril alone, diuretic therapy may be resumed. If the diuretic cannot be discontinued, an initial dose of 5 mg of lisinopril should be used under medical supervision for at least two hours and until blood pressure has stabilized for at least an additional hour (see WARNINGS and PRECAUTIONS, Drug Interactions ). Concomitant administration of ZESTORETIC with potassium supplements, potassium salt substitutes or potassium-sparing diuretics may lead to increases of serum potassium (see PRECAUTIONS ). Replacement Therapy: The combination may be substituted for the titrated individual components. Use in Renal Impairment: Regimens of therapy with lisinopril/HCTZ need not take account of renal function as long as the patient's creatinine clearance is >30 mL/min/1.7m 2 (serum creatinine roughly ≤3 mg/dL or 265 μmol/L). In patients with more severe renal impairment, loop diuretics are preferred to thiazides, so lisinopril/HCTZ is not recommended (see WARNINGS , Anaphylactoid Reactions During Membrane Exposure ).
Contraindications
ZESTORETIC is contraindicated in patients who are hypersensitive to this product and in patients with a history of angioedema related to previous treatment with an angiotensin-converting enzyme inhibitor and in patients with hereditary or idiopathic angioedema. Because of the hydrochlorothiazide component, this product is contraindicated in patients with anuria or hypersensitivity to other sulfonamide-derived drugs. ZESTORETIC is contraindicated in combination with a neprilysin inhibitor (e.g., sacubitril). Do not administer ZESTORETIC within 36 hours of switching to or from sacubitril/valsartan, a neprilysin inhibitor (see WARNINGS ). Do not co-administer aliskiren with ZESTORETIC in patients with diabetes (see PRECAUTIONS, Drug Interactions ).
Adverse Reactions
ZESTORETIC has been evaluated for safety in 930 patients including 100 patients treated for 50 weeks or more. In clinical trials with ZESTORETIC no adverse experiences peculiar to this combination drug have been observed. Adverse experiences that have occurred have been limited to those that have been previously reported with lisinopril or hydrochlorothiazide. The most frequent clinical adverse experiences in controlled trials (including open label extensions) with any combination of lisinopril and hydrochlorothiazide were: dizziness (7.5%), headache (5.2%), cough (3.9%), fatigue (3.7%) and orthostatic effects (3.2%) all of which were more common than in placebo-treated patients. Generally, adverse experiences were mild and transient in nature, but see WARNINGS regarding angioedema and excessive hypotension or syncope. Discontinuation of therapy due to adverse effects was required in 4.4% of patients principally because of dizziness, cough, fatigue and muscle cramps. Adverse experiences occurring in greater than one percent of patients treated with lisinopril plus hydrochlorothiazide in controlled clinical trials are shown below. Percent of Patients in Controlled Studies Lisinopril and Hydrochlorothiazide (n=930) Incidence (discontinuation) Placebo (n=207) Incidence Dizziness 7.5 (0.8) 1.9 Headache 5.2 (0.3) 1.9 Cough 3.9 (0.6) 1.0 Fatigue 3.7 (0.4) 1.0 Orthostatic Effects 3.2 (0.1) 1.0 Diarrhea 2.5 (0.2) 2.4 Nausea 2.2 (0.1) 2.4 Upper Respiratory Infection 2.2 (0.0) 0.0 Muscle Cramps 2.0 (0.4) 0.5 Asthenia 1.8 (0.2) 1.0 Paresthesia 1.5 (0.1) 0.0 Hypotension 1.4 (0.3) 0.5 Vomiting 1.4 (0.1) 0.5 Dyspepsia 1.3 (0.0) 0.0 Rash 1.2 (0.1) 0.5 Impotence 1.2 (0.3) 0.0 Clinical adverse experiences occurring in 0.3% to 1.0% of patients in controlled trials and rarer, serious, possibly drug-related events reported in marketing experience are listed below: Body as a Whole: Chest pain, abdominal pain, syncope, chest discomfort, fever, trauma, virus infection. Cardiovascular: Palpitation, orthostatic hypotension. Digestive: Gastrointestinal cramps, dry mouth, constipation, heartburn. Musculoskeletal: Back pain, shoulder pain, knee pain, back strain, myalgia, foot pain. Nervous/Psychiatric: Decreased libido, vertigo, depression, somnolence. Respiratory: Common cold, nasal congestion, influenza, bronchitis, pharyngeal pain, dyspnea, pulmonary congestion, chronic sinusitis, allergic rhinitis, pharyngeal discomfort. Skin: Flushing, pruritus, skin inflammation, diaphoresis, cutaneous pseudolymphoma. Special Senses: Blurred vision, tinnitus, otalgia. Urogenital: Urinary tract infection. Angioedema: Angioedema of the face, extremities, lips, tongue, glottis and/or larynx has been reported (see WARNINGS ). In rare cases, intestinal angioedema has been reported in post marketing experience. Hypotension: In clinical trials, adverse effects relating to hypotension occurred as follows: hypotension (1.4%), orthostatic hypotension (0.5%), other orthostatic effects (3.2%). In addition syncope occurred in 0.8% of patients (see WARNINGS ). Cough: See PRECAUTIONS - Cough .
How Supplied
ZESTORETIC 10-12.5 Tablets: Peach, round, biconvex, uncoated tablets identified with "141" debossed on one side and "ZESTORETIC" on the other side are supplied in bottles of 90 tablets (NDC 52427-435-90). ZESTORETIC 20-12.5 Tablets: White, round, biconvex, uncoated tablets identified with "142" debossed on one side and "ZESTORETIC" on the other side are supplied in bottles of 90 tablets (NDC 52427-436-90). ZESTORETIC 20-25 Tablets: Peach, round, biconvex, uncoated tablets identified with “145” debossed on one side and "ZESTORETIC" on the other side are supplied in bottles of 90 tablets (NDC 52427-437-90). Storage Store at controlled room temperature, 20°C to 25°C (68°F to 77°F) [see USP]. Protect from excessive light and humidity.
Medication Information
Indications and Usage
ZESTORETIC is indicated for the treatment of hypertension, to lower blood pressure. Lowering blood pressure lowers the risk of fatal and non-fatal cardiovascular events, primarily strokes and myocardial infarctions. These benefits have been seen in controlled trials of antihypertensive drugs from a wide variety of pharmacologic classes including lisinopril and hydrochlorothiazide.
Control of high blood pressure should be part of comprehensive cardiovascular risk management, including, as appropriate, lipid control, diabetes management, antithrombotic therapy, smoking cessation, exercise, and limited sodium intake. Many patients will require more than 1 drug to achieve blood pressure goals. For specific advice on goals and management, see published guidelines, such as those of the National High Blood Pressure Education Program’s Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure (JNC).
Numerous antihypertensive drugs, from a variety of pharmacologic classes and with different mechanisms of action, have been shown in randomized controlled trials to reduce cardiovascular morbidity and mortality, and it can be concluded that it is blood pressure reduction, and not some other pharmacologic property of the drugs, that is largely responsible for those benefits. The largest and most consistent cardiovascular outcome benefit has been a reduction in the risk of stroke, but reductions in myocardial infarction and cardiovascular mortality also have been seen regularly.
Elevated systolic or diastolic pressure causes increased cardiovascular risk, and the absolute risk increase per mmHg is greater at higher blood pressures, so that even modest reductions of severe hypertension can provide substantial benefit. Relative risk reduction from blood pressure reduction is similar across populations with varying absolute risk, so the absolute benefit is greater in patients who are at higher risk independent of their hypertension (for example, patients with diabetes or hyperlipidemia), and such patients would be expected to benefit from more aggressive treatment to a lower blood pressure goal.
Some antihypertensive drugs have smaller blood pressure effects (as monotherapy) in black patients, and many antihypertensive drugs have additional approved indications and effects (e.g., on angina, heart failure, or diabetic kidney disease). These considerations may guide selection of therapy.
These fixed-dose combinations are not indicated for initial therapy (see DOSAGE AND ADMINISTRATION ).
In using ZESTORETIC, consideration should be given to the fact that an angiotensin-converting enzyme inhibitor, captopril, has caused agranulocytosis, particularly in patients with renal impairment or collagen vascular disease, and that available data are insufficient to show that lisinopril does not have a similar risk (see WARNINGS ).
In considering the use of ZESTORETIC, it should be noted that ACE inhibitors have been associated with a higher rate of angioedema in black than in nonblack patients (see WARNINGS, Lisinopril ).
Dosage and Administration
Lisinopril monotherapy is an effective treatment of hypertension in once-daily doses of 10 mg to 80 mg, while hydrochlorothiazide monotherapy is effective in doses of 12.5 mg per day to 50 mg per day. In clinical trials of lisinopril/hydrochlorothiazide combination therapy using lisinopril doses of 10 mg to 80 mg and hydrochlorothiazide doses of 6.25 mg to 50 mg, the antihypertensive response rates generally increased with increasing dose of either component.
The side effects (see WARNINGS ) of lisinopril are generally rare and apparently independent of dose; those of hydrochlorothiazide are a mixture of dose-dependent phenomena (primarily hypokalemia) and dose-independent phenomena (e.g., pancreatitis), the former much more common than the latter. Therapy with any combination of lisinopril and hydrochlorothiazide may be associated with either or both dose-independent or dose-dependent side effects, but addition of lisinopril in clinical trials blunted the hypokalemia normally seen with diuretics.
To minimize dose-dependent side effects, it is usually appropriate to begin combination therapy only after a patient has failed to achieve the desired effect with monotherapy.
Dose Titration Guided by Clinical Effect: A patient whose blood pressure is not adequately controlled with either lisinopril or hydrochlorothiazide monotherapy may be switched to lisinopril/HCTZ 10/12.5 or lisinopril/HCTZ 20/12.5, depending on current monotherapy dose. Further increases of either or both components should depend on clinical response with blood pressure measured at the interdosing interval to ensure that there is an adequate antihypertensive effect at that time. The hydrochlorothiazide dose should generally not be increased until 2 to 3 weeks have elapsed. After addition of the diuretic it may be possible to reduce the dose of lisinopril. Patients whose blood pressures are adequately controlled with 25 mg of daily hydrochlorothiazide, but who experience significant potassium loss with this regimen may achieve similar or greater blood-pressure control without electrolyte disturbance if they are switched to lisinopril/HCTZ 10/12.5.
In patients who are currently being treated with a diuretic, symptomatic hypotension occasionally may occur following the initial dose of lisinopril. The diuretic should, if possible, be discontinued for two to three days before beginning therapy with lisinopril to reduce the likelihood of hypotension (see WARNINGS ). If the patient's blood pressure is not controlled with lisinopril alone, diuretic therapy may be resumed.
If the diuretic cannot be discontinued, an initial dose of 5 mg of lisinopril should be used under medical supervision for at least two hours and until blood pressure has stabilized for at least an additional hour (see WARNINGS and PRECAUTIONS, Drug Interactions ).
Concomitant administration of ZESTORETIC with potassium supplements, potassium salt substitutes or potassium-sparing diuretics may lead to increases of serum potassium (see PRECAUTIONS ).
Replacement Therapy: The combination may be substituted for the titrated individual components.
Use in Renal Impairment: Regimens of therapy with lisinopril/HCTZ need not take account of renal function as long as the patient's creatinine clearance is >30 mL/min/1.7m2 (serum creatinine roughly ≤3 mg/dL or 265 μmol/L). In patients with more severe renal impairment, loop diuretics are preferred to thiazides, so lisinopril/HCTZ is not recommended (see WARNINGS , Anaphylactoid Reactions During Membrane Exposure).
Contraindications
ZESTORETIC is contraindicated in patients who are hypersensitive to this product and in patients with a history of angioedema related to previous treatment with an angiotensin-converting enzyme inhibitor and in patients with hereditary or idiopathic angioedema. Because of the hydrochlorothiazide component, this product is contraindicated in patients with anuria or hypersensitivity to other sulfonamide-derived drugs.
ZESTORETIC is contraindicated in combination with a neprilysin inhibitor (e.g., sacubitril). Do not administer ZESTORETIC within 36 hours of switching to or from sacubitril/valsartan, a neprilysin inhibitor (see
WARNINGS
).
Do not co-administer aliskiren with ZESTORETIC in patients with diabetes (see
PRECAUTIONS, Drug Interactions
).
Adverse Reactions
ZESTORETIC has been evaluated for safety in 930 patients including 100 patients treated for 50 weeks or more.
In clinical trials with ZESTORETIC no adverse experiences peculiar to this combination drug have been observed. Adverse experiences that have occurred have been limited to those that have been previously reported with lisinopril or hydrochlorothiazide.
The most frequent clinical adverse experiences in controlled trials (including open label extensions) with any combination of lisinopril and hydrochlorothiazide were: dizziness (7.5%), headache (5.2%), cough (3.9%), fatigue (3.7%) and orthostatic effects (3.2%) all of which were more common than in placebo-treated patients. Generally, adverse experiences were mild and transient in nature, but see WARNINGS regarding angioedema and excessive hypotension or syncope. Discontinuation of therapy due to adverse effects was required in 4.4% of patients principally because of dizziness, cough, fatigue and muscle cramps.
Adverse experiences occurring in greater than one percent of patients treated with lisinopril plus hydrochlorothiazide in controlled clinical trials are shown below.
Percent of Patients in Controlled Studies
|
Lisinopril and Hydrochlorothiazide (n=930)
Incidence (discontinuation) |
Placebo (n=207)
Incidence |
||
| Dizziness | 7.5 | (0.8) | 1.9 |
| Headache | 5.2 | (0.3) | 1.9 |
| Cough | 3.9 | (0.6) | 1.0 |
| Fatigue | 3.7 | (0.4) | 1.0 |
| Orthostatic Effects | 3.2 | (0.1) | 1.0 |
| Diarrhea | 2.5 | (0.2) | 2.4 |
| Nausea | 2.2 | (0.1) | 2.4 |
| Upper Respiratory Infection |
2.2 | (0.0) | 0.0 |
| Muscle Cramps | 2.0 | (0.4) | 0.5 |
| Asthenia | 1.8 | (0.2) | 1.0 |
| Paresthesia | 1.5 | (0.1) | 0.0 |
| Hypotension | 1.4 | (0.3) | 0.5 |
| Vomiting | 1.4 | (0.1) | 0.5 |
| Dyspepsia | 1.3 | (0.0) | 0.0 |
| Rash | 1.2 | (0.1) | 0.5 |
| Impotence | 1.2 | (0.3) | 0.0 |
Clinical adverse experiences occurring in 0.3% to 1.0% of patients in controlled trials and rarer, serious, possibly drug-related events reported in marketing experience are listed below:
Body as a Whole: Chest pain, abdominal pain, syncope, chest discomfort, fever, trauma, virus infection. Cardiovascular: Palpitation, orthostatic hypotension. Digestive: Gastrointestinal cramps, dry mouth, constipation, heartburn. Musculoskeletal: Back pain, shoulder pain, knee pain, back strain, myalgia, foot pain. Nervous/Psychiatric: Decreased libido, vertigo, depression, somnolence. Respiratory: Common cold, nasal congestion, influenza, bronchitis, pharyngeal pain, dyspnea, pulmonary congestion, chronic sinusitis, allergic rhinitis, pharyngeal discomfort. Skin: Flushing, pruritus, skin inflammation, diaphoresis, cutaneous pseudolymphoma. Special Senses: Blurred vision, tinnitus, otalgia. Urogenital: Urinary tract infection.
Angioedema: Angioedema of the face, extremities, lips, tongue, glottis and/or larynx has been reported (see WARNINGS ).
In rare cases, intestinal angioedema has been reported in post marketing experience.
Hypotension: In clinical trials, adverse effects relating to hypotension occurred as follows: hypotension (1.4%), orthostatic hypotension (0.5%), other orthostatic effects (3.2%). In addition syncope occurred in 0.8% of patients (see WARNINGS ).
Cough: See PRECAUTIONS - Cough.
How Supplied
ZESTORETIC 10-12.5 Tablets: Peach, round, biconvex, uncoated tablets identified with "141" debossed on one side and "ZESTORETIC" on the other side are supplied in bottles of 90 tablets (NDC 52427-435-90).
ZESTORETIC 20-12.5 Tablets: White, round, biconvex, uncoated tablets identified with "142" debossed on one side and "ZESTORETIC" on the other side are supplied in bottles of 90 tablets (NDC 52427-436-90).
ZESTORETIC 20-25 Tablets: Peach, round, biconvex, uncoated tablets identified with “145” debossed on one side and "ZESTORETIC" on the other side are supplied in bottles of 90 tablets (NDC 52427-437-90).
Storage
Store at controlled room temperature, 20°C to 25°C (68°F to 77°F) [see USP]. Protect from excessive light and humidity.
Description
ZESTORETIC® (Lisinopril and Hydrochlorothiazide) combines an angiotensin converting enzyme inhibitor, lisinopril, and a diuretic, hydrochlorothiazide.
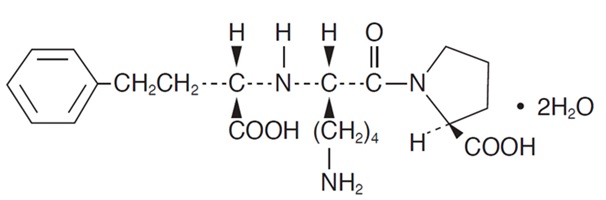
Lisinopril, USP a synthetic peptide derivative, is an oral long-acting angiotensin converting enzyme inhibitor. It is chemically described as (S)-1-[N2-(1-carboxy-3-phenylpropyl)-L-lysyl]-L-proline dihydrate. Its empirical formula is C21H31N3O5 . 2H2O and its structural formula is:
Lisinopril, USP is a white to off-white, crystalline powder, with a molecular weight of 441.53. It is soluble in water, sparingly soluble in methanol, and practically insoluble in ethanol.
Hydrochlorothiazide, USP is 6-chloro-3,4-dihydro-2H-1,2,4-benzothiadiazine-7-sulfonamide 1,1-dioxide. Its empirical formula is C7H8ClN3O4S2 and its structural formula is:
Hydrochlorothiazide, USP is a white, or practically white, crystalline powder with a molecular weight of 297.72, which is slightly soluble in water, but freely soluble in sodium hydroxide solution.
ZESTORETIC is available for oral use in three tablet combinations of lisinopril, USP with hydrochlorothiazide, USP: ZESTORETIC 10-12.5 containing 10 mg lisinopril, USP and 12.5 mg hydrochlorothiazide, USP; ZESTORETIC 20-12.5 containing 20 mg lisinopril, USP and 12.5 mg hydrochlorothiazide, USP; and, ZESTORETIC 20-25 containing 20 mg lisinopril, USP and 25 mg hydrochlorothiazide, USP.
Inactive Ingredients:
10-12.5 Tablets - calcium phosphate, magnesium stearate, mannitol, red ferric oxide, corn starch, yellow ferric oxide.
20-12.5 Tablets - calcium phosphate, magnesium stearate, mannitol, corn starch.
20-25 Tablets - calcium phosphate, magnesium stearate, mannitol, red ferric oxide, corn starch, yellow ferric oxide.
F
Pregnancy category D
Use of drugs that act on the renin-angiotensin system during the second and third trimesters of pregnancy reduces fetal renal function and increases fetal and neonatal morbidity and death. Resulting oligohydramnios can be associated with fetal lung hypoplasia and skeletal deformations. Potential neonatal adverse effects include skull hypoplasia, anuria, hypotension, renal failure, and death. When pregnancy is detected, discontinue ZESTORETIC as soon as possible. These adverse outcomes are usually associated with use of these drugs in the second and third trimester of pregnancy. Most epidemiologic studies examining fetal abnormalities after exposure to antihypertensive use in the first trimester have not distinguished drugs affecting the renin-angiotensin system from other antihypertensive agents. Appropriate management of maternal hypertension during pregnancy is important to optimize outcomes for both mother and fetus.
In the unusual case that there is no appropriate alternative to therapy with drugs affecting the renin-angiotensin system for a particular patient, apprise the mother of the potential risk to the fetus. Perform serial ultrasound examinations to assess the intra-amniotic environment. If oligohydramnios is observed, discontinue ZESTORETIC, unless it is considered lifesaving for the mother. Fetal testing may be appropriate, based on the week of pregnancy. Patients and physicians should be aware, however, that oligohydramnios may not appear until after the fetus has sustained irreversible injury. Closely observe infants with histories of in utero exposure to ZESTORETIC for hypotension, oliguria, and hyperkalemia. (See Precautions, Pediatric Use ).
No teratogenic effects of lisinopril were seen in studies of pregnant rats, mice, and rabbits. On a mg/kg basis, the doses used were up to 625 times (in mice), 188 times (in rats), and 0.6 times (in rabbits) the maximum recommended human dose.
Lisinopril and Hydrochlorothiazide
Teratogenicity studies were conducted in mice and rats with up to 90 mg/kg/day of lisinopril (56 times the maximum recommended human dose) in combination with 10 mg/kg/day of hydrochlorothiazide (2.5 times the maximum recommended human dose). Maternal or fetotoxic effects were not seen in mice with the combination. In rats decreased maternal weight gain and decreased fetal weight occurred down to 3/10 mg/kg/day (the lowest dose tested). Associated with the decreased fetal weight was a delay in fetal ossification. The decreased fetal weight and delay in fetal ossification were not seen in saline-supplemented animals given 90/10 mg/kg/day.
When used in pregnancy, during the second and third trimesters, ACE inhibitors can cause injury and even death to the developing fetus. When pregnancy is detected, discontinue ZESTORETIC as soon as possible (see Lisinopril, Fetal Toxicity ).
H
Two-year feeding studies in mice and rats conducted under the auspices of the National Toxicology Program (NTP) uncovered no evidence of a carcinogenic potential of hydrochlorothiazide in female mice (at doses of up to approximately 600 mg/kg/day) or in male and female rats (at doses of up to approximately 100 mg/kg/day). These doses are 150 times and 12 times for mice and 25 times and 4 times for rats the maximum human daily dose based on mg/kg and mg/m2, respectively. The NTP, however, found equivocal evidence for hepatocarcinogenicity in male mice.
Hydrochlorothiazide was not genotoxic in vitro in the Ames mutagenicity assay of Salmonella typhimurium strains TA 98, TA 100, TA 1535, TA 1537, and TA 1538 and in the Chinese Hamster Ovary (CHO) test for chromosomal aberrations, or in vivo in assays using mouse germinal cell chromosomes, Chinese hamster bone marrow chromosomes, and the Drosophila sex-linked recessive lethal trait gene. Positive test results were obtained only in the in vitro CHO Sister Chromatid Exchange (clastogenicity) and in the Mouse Lymphoma Cell (mutagenicity) assays, using concentrations of hydrochlorothiazide from 43 mcg/mL to 1300 mcg/mL, and in the Aspergillus nidulans nondisjunction assay at an unspecified concentration.
Hydrochlorothiazide had no adverse effects on the fertility of mice and rats of either sex in studies wherein these species were exposed, via their diet, to doses of up to 100 mg/kg and 4 mg/kg, respectively, prior to conception and throughout gestation. In mice this dose is 25 times and 2 times the maximum daily human dose based on mg/kg and mg/m2, respectively. In rats this dose is 1 times and 0.2 times the maximum daily human dose based on mg/kg and mg/m2, respectively.
L
There was no evidence of a tumorigenic effect when lisinopril was administered for 105 weeks to male and female rats at doses up to 90 mg/kg/day (about 56 or 9 times* the maximum daily human dose, based on body weight and body surface area, respectively). There was no evidence of carcinogenicity when lisinopril was administered for 92 weeks to (male and female) mice at doses up to 135 mg/kg/day (about 84 times* the maximum recommended daily human dose). This dose was 6.8 times the maximum human dose based on body surface area in mice.
*Calculations assume a human weight of 50 kg and human body surface area of 1.62m2.
Lisinopril was not mutagenic in the Ames microbial mutagen test with or without metabolic activation. It was also negative in a forward mutation assay using Chinese hamster lung cells. Lisinopril did not produce single strand DNA breaks in an in vitro alkaline elution rat hepatocyte assay. In addition, lisinopril did not produce increases in chromosomal aberrations in an in vitro test in Chinese hamster ovary cells or in an in vivo study in mouse bone marrow.
There were no adverse effects on reproductive performance in male and female rats treated with up to 300 mg/kg/day of lisinopril. This dose is 188 times and 30 times the maximum daily human dose based on mg/kg and mg/m2, respectively.
Section 42229-5
*AN69 is a registered trademark of Hospal Ltd.
ZESTORETIC is a trademark of Alvogen AZ IP Holdings LLC.
Product of USA
Distributed by:
Almatica Pharma LLC
Morristown, NJ 07960 USA
PI435-10
Rev. 03/2025
Section 51945-4
NDC 52427-435-90
Rx only
ZESTORETIC®
10/12.5
(lisinopril/hydrochlorothiazide)
Each tablet contains:
10 mg lisinopril, USP and
12.5 mg hydrochlorothiazide
, USP
90 tablets
General
Warnings
Lisinopril
Mechanism of Action
Lisinopril inhibits angiotensin-converting enzyme (ACE) in human subjects and animals. ACE is a peptidyl dipeptidase that catalyzes the conversion of angiotensin I to the vasoconstrictor substance, angiotensin II. Angiotensin II also stimulates aldosterone secretion by the adrenal cortex. Inhibition of ACE results in decreased plasma angiotensin II which leads to decreased vasopressor activity and to decreased aldosterone secretion. The latter decrease may result in a small increase of serum potassium. Removal of angiotensin II negative feedback on renin secretion leads to increased plasma renin activity. In hypertensive patients with normal renal function treated with lisinopril alone for up to 24 weeks, the mean increase in serum potassium was less than 0.1 mEq/L; however, approximately 15 percent of patients had increases greater than 0.5 mEq/L and approximately six percent had a decrease greater than 0.5 mEq/L. In the same study, patients treated with lisinopril plus a thiazide diuretic showed essentially no change in serum potassium (see PRECAUTIONS ).
ACE is identical to kininase, an enzyme that degrades bradykinin. Whether increased levels of bradykinin, a potent vasodepressor peptide, play a role in the therapeutic effects of lisinopril remains to be elucidated.
While the mechanism through which lisinopril lowers blood pressure is believed to be primarily suppression of the renin-angiotensin-aldosterone system, lisinopril is antihypertensive even in patients with low-renin hypertension. Although lisinopril was antihypertensive in all races studied, black hypertensive patients (usually a low-renin hypertensive population) had a smaller average response to lisinopril monotherapy than nonblack patients.
Pharmacokinetics and Metabolism
Following oral administration of lisinopril, peak serum concentrations occur within about 7 hours. Declining serum concentrations exhibit a prolonged terminal phase which does not contribute to drug accumulation. This terminal phase probably represents saturable binding to ACE and is not proportional to dose. Lisinopril does not appear to be bound to other serum proteins.
Lisinopril does not undergo metabolism and is excreted unchanged entirely in the urine. Based on urinary recovery, the mean extent of absorption of lisinopril is approximately 25 percent, with large intersubject variability (6% to 60%) at all doses tested (5 mg to 80 mg). Lisinopril absorption is not influenced by the presence of food in the gastrointestinal tract.
Upon multiple dosing, lisinopril exhibits an effective half-life of accumulation of 12 hours.
Impaired renal function decreases elimination of lisinopril, which is excreted principally through the kidneys, but this decrease becomes clinically important only when the glomerular filtration rate is below 30 mL/min. Above this glomerular filtration rate, the elimination half-life is little changed. With greater impairment, however, peak and trough lisinopril levels increase, time to peak concentration increases and time to attain steady state is prolonged. Older patients, on average, have (approximately doubled) higher blood levels and area under the plasma concentration time curve (AUC) than younger patients (see DOSAGE AND ADMINISTRATION ). In a multiple dose pharmacokinetic study in elderly versus young hypertensive patients using the lisinopril/hydrochlorothiazide combination, the AUC increased approximately 120% for lisinopril and approximately 80% for hydrochlorothiazide in older patients. Lisinopril can be removed by hemodialysis.
Studies in rats indicate that lisinopril crosses the blood-brain barrier poorly. Multiple doses of lisinopril in rats do not result in accumulation in any tissues; however, milk of lactating rats contains radioactivity following administration of 14C lisinopril. By whole body autoradiography, radioactivity was found in the placenta following administration of labeled drug to pregnant rats, but none was found in the fetuses.
Pharmacodynamics
Administration of lisinopril to patients with hypertension results in a reduction of supine and standing blood pressure to about the same extent with no compensatory tachycardia. Symptomatic postural hypotension is usually not observed although it can occur and should be anticipated in volume and/or salt-depleted patients (see WARNINGS ).
In most patients studied, onset of antihypertensive activity was seen at one hour after oral administration of an individual dose of lisinopril, with peak reduction of blood pressure achieved by six hours.
In some patients achievement of optimal blood pressure reduction may require two to four weeks of therapy.
At recommended single daily doses, antihypertensive effects have been maintained for at least 24 hours, after dosing, although the effect at 24 hours was substantially smaller than the effect six hours after dosing.
The antihypertensive effects of lisinopril have continued during long-term therapy. Abrupt withdrawal of lisinopril has not been associated with a rapid increase in blood pressure; nor with a significant overshoot of pretreatment blood pressure.
In hemodynamic studies in patients with essential hypertension, blood pressure reduction was accompanied by a reduction in peripheral arterial resistance with little or no change in cardiac output and in heart rate. In a study in nine hypertensive patients, following administration of lisinopril, there was an increase in mean renal blood flow that was not significant. Data from several small studies are inconsistent with respect to the effect of lisinopril on glomerular filtration rate in hypertensive patients with normal renal function, but suggest that changes, if any, are not large.
In patients with renovascular hypertension lisinopril has been shown to be well tolerated and effective in controlling blood pressure (see PRECAUTIONS ).
Overdosage
No specific information is available on the treatment of overdosage with ZESTORETIC. Treatment is symptomatic and supportive. Therapy with ZESTORETIC should be discontinued and the patient observed closely. Suggested measures include induction of emesis and/or gastric lavage, and correction of dehydration, electrolyte imbalance and hypotension by established procedures.
Geriatric Use
Clinical studies of ZESTORETIC did not include sufficient numbers of subjects aged 65 and over to determine whether they respond differently from younger subjects. Other reported clinical experience has not identified differences in responses between the elderly and younger patients. In general, dose selection for an elderly patient should be cautious, usually starting at the low end of the dosing range, reflecting the greater frequency of decreased hepatic, renal, or cardiac function, and of concomitant disease or other drug therapy.
This drug is known to be substantially excreted by the kidney, and the risk of toxic reactions to this drug may be greater in patients with impaired renal function. Because elderly patients are more likely to have decreased renal function, care should be taken in dose selection. Evaluation of the hypertensive patient should always include assessment of renal function.
Pediatric Use
Neonates with a history of in utero exposure to ZESTORETIC:
If oliguria or hypotension occurs, direct attention toward support of blood pressure and renal perfusion. Exchange transfusions or dialysis may be required as a means of reversing hypotension and/or substituting for disordered renal function. Lisinopril, which crosses the placenta, has been removed from neonatal circulation by peritoneal dialysis with some clinical benefit, and theoretically may be removed by exchange transfusion, although there is no experience with the latter procedure.
Safety and effectiveness in pediatric patients have not been established.
Nursing Mothers
It is not known whether lisinopril is excreted in human milk. However, milk of lactating rats contains radioactivity following administration of 14C lisinopril. In another study, lisinopril was present in rat milk at levels similar to plasma levels in the dams. Thiazides do appear in human milk. Because of the potential for serious adverse reactions in nursing infants from ACE inhibitors and hydrochlorothiazide, a decision should be made whether to discontinue nursing and/or discontinue ZESTORETIC, taking into account the importance of the drug to the mother.
Hydrochlorothiazide
The mechanism of the antihypertensive effect of thiazides is unknown. Thiazides do not usually affect normal blood pressure.
Hydrochlorothiazide is a diuretic and antihypertensive. It affects the distal renal tubular mechanism of electrolyte reabsorption. Hydrochlorothiazide increases excretion of sodium and chloride in approximately equivalent amounts. Natriuresis may be accompanied by some loss of potassium and bicarbonate.
After oral use diuresis begins within two hours, peaks in about four hours and lasts about 6 to 12 hours.
Hydrochlorothiazide is not metabolized but is eliminated rapidly by the kidney. When plasma levels have been followed for at least 24 hours, the plasma half-life has been observed to vary between 5.6 and 14.8 hours. At least 61 percent of the oral dose is eliminated unchanged within 24 hours. Hydrochlorothiazide crosses the placental but not the blood-brain barrier.
Clinical Pharmacology
Warning: Fetal Toxicity
See full prescribing information for complete boxed warning.
- When pregnancy is detected, discontinue ZESTORETIC as soon as possible.
- Drugs that act directly on the renin-angiotensin system can cause injury and death to the developing fetus. See Warnings: Fetal Toxicity.
Information for Patients
Angioedema: Angioedema, including laryngeal edema may occur at any time during treatment with angiotensin-converting enzyme inhibitors, including ZESTORETIC. Patients should be so advised and told to report immediately any signs or symptoms suggesting angioedema (swelling of face, extremities, eyes, lips, tongue, difficulty in swallowing or breathing) and to take no more drug until they have consulted with the prescribing physician.
Symptomatic Hypotension: Patients should be cautioned to report lightheadedness especially during the first few days of therapy. If actual syncope occurs, the patients should be told to discontinue the drug until they have consulted with the prescribing physician.
All patients should be cautioned that excessive perspiration and dehydration may lead to an excessive fall in blood pressure because of reduction in fluid volume. Other causes of volume depletion such as vomiting or diarrhea may also lead to a fall in blood pressure; patients should be advised to consult with their physician.
Hyperkalemia: Patients should be told not to use salt substitutes containing potassium without consulting their physician.
Leukopenia/Neutropenia: Patients should be told to report promptly any indication of infection (e.g., sore throat, fever) which may be a sign of leukopenia/neutropenia.
Pregnancy: Female patients of childbearing age should be told about the consequences of exposure to ZESTORETIC during pregnancy. Discuss treatment options with women planning to become pregnant. Patients should be asked to report pregnancies to their physicians as soon as possible.
Non-melanoma Skin Cancer: Instruct patients taking hydrochlorothiazide to protect skin from the sun and undergo regular skin cancer screening.
NOTE: As with many other drugs, certain advice to patients being treated with ZESTORETIC is warranted. This information is intended to aid in the safe and effective use of this medication. It is not a disclosure of all possible adverse or intended effects.
Clinical Laboratory Test Findings
Serum Electrolytes: (See PRECAUTIONS ).
Creatinine, Blood Urea Nitrogen: Minor reversible increases in blood urea nitrogen and serum creatinine were observed in patients with essential hypertension treated with ZESTORETIC. More marked increases have also been reported and were more likely to occur in patients with renal artery stenosis (see PRECAUTIONS ).
Serum Uric Acid, Glucose, Magnesium, Cholesterol, Triglycerides and Calcium: (See PRECAUTIONS ).
Hemoglobin and Hematocrit: Small decreases in hemoglobin and hematocrit (mean decreases of approximately 0.5 g% and 1.5 vol%, respectively) occurred frequently in hypertensive patients treated with ZESTORETIC but were rarely of clinical importance unless another cause of anemia coexisted. In clinical trials, 0.4% of patients discontinued therapy due to anemia.
Liver Function Tests: Rarely, elevations of liver enzymes and/or serum bilirubin have occurred. (See WARNINGS, Hepatic Failure).
Other adverse reactions that have been reported with the individual components are listed below:
Lisinopril - In clinical trials adverse reactions which occurred with lisinopril were also seen with ZESTORETIC. In addition, and since lisinopril has been marketed, the following adverse reactions have been reported with lisinopril and should be considered potential adverse reactions for ZESTORETIC: Body as a Whole: Anaphylactoid reactions (see WARNINGS, Anaphylactoid Reactions During Membrane Exposure), malaise, edema, facial edema, pain, pelvic pain, flank pain, chills; Cardiovascular: Cardiac arrest, myocardial infarction or cerebrovascular accident, possibly secondary to excessive hypotension in high risk patients (see WARNINGS, Hypotension), pulmonary embolism and infarction, worsening of heart failure, arrhythmias (including tachycardia, ventricular tachycardia, atrial tachycardia, atrial fibrillation, bradycardia, and premature ventricular contractions), angina pectoris, transient ischemic attacks, paroxysmal nocturnal dyspnea, decreased blood pressure, peripheral edema, vasculitis; Digestive: Pancreatitis, hepatitis (hepatocellular or cholestatic jaundice) (see WARNINGS, Hepatic Failure), gastritis, anorexia, flatulence, increased salivation; Endocrine: Diabetes mellitus, inappropriate antidiuretic hormone secretion; Hematologic: Rare cases of bone marrow depression, hemolytic anemia, leukopenia/neutropenia, and thrombocytopenia have been reported in which a causal relationship to lisinopril can not be excluded; Metabolic: Gout, weight loss, dehydration, fluid overload, weight gain; Musculoskeletal: Arthritis, arthralgia, neck pain, hip pain, joint pain, leg pain, arm pain, lumbago; Nervous System/Psychiatric: Ataxia, memory impairment, tremor, insomnia, stroke, nervousness, confusion, peripheral neuropathy (e.g., paresthesia, dysesthesia), spasm, hypersomnia, irritability; mood alterations (including depressive symptoms); hallucinations; Respiratory: Malignant lung neoplasms, hemoptysis, pulmonary edema, pulmonary infiltrates, bronchospasm, asthma, pleural effusion, pneumonia, eosinophilic pneumonitis, wheezing, orthopnea, painful respiration, epistaxis, laryngitis, sinusitis, pharyngitis, rhinitis, rhinorrhea, chest sound abnormalities; Skin: Urticaria, alopecia, herpes zoster, photosensitivity, skin lesions, skin infections, pemphigus, erythema, psoriasis, rare cases of other severe skin reactions, including toxic epidermal necrolysis and Stevens-Johnson Syndrome (causal relationship has not been established); Special Senses: Visual loss, diplopia, photophobia, taste alteration, olfactory disturbance; Urogenital: Acute renal failure, oliguria, anuria, uremia, progressive azotemia, renal dysfunction (see PRECAUTIONS and DOSAGE AND ADMINISTRATION ), pyelonephritis, dysuria, breast pain.
Miscellaneous: A symptom complex has been reported which may include a positive ANA, an elevated erythrocyte sedimentation rate, arthralgia/arthritis, myalgia, fever, vasculitis, eosinophilia and leukocytosis. Rash, photosensitivity or other dermatological manifestations may occur alone or in combination with these symptoms.
Hydrochlorothiazide - Body as a Whole: Weakness; Digestive: Anorexia, gastric irritation, cramping, jaundice (intrahepatic cholestatic jaundice) (see WARNINGS, Hepatic Failure), pancreatitis, sialoadenitis, constipation; Hematologic: Leukopenia, agranulocytosis, thrombocytopenia, aplastic anemia, hemolytic anemia; Musculoskeletal: Muscle spasm; Nervous System/Psychiatric: Restlessness; Renal: Renal failure, renal dysfunction, interstitial nephritis (see WARNINGS); Skin: Erythema multiforme including Stevens-Johnson Syndrome, exfoliative dermatitis including toxic epidermal necrolysis, alopecia; Special Senses: Xanthopsia; Hypersensitivity: Purpura, photosensitivity, urticaria, necrotizing angiitis (vasculitis and cutaneous vasculitis), respiratory distress including pneumonitis and pulmonary edema, anaphylactic reactions.
Postmarketing Experience
Non-melanoma Skin Cancer
Hydrochlorothiazide is associated with an increased risk of non-melanoma skin cancer. In a study conducted in the Sentinel System, increased risk was predominantly for squamous cell carcinoma (SCC) and in white patients taking large cumulative doses. The increased risk for SCC in the overall population was approximately 1 additional case per 16,000 patients per year, and for white patients taking a cumulative dose of ≥50,000mg the risk increase was approximately 1 additional SCC case for every 6,700 patients per year.
To report SUSPECTED ADVERSE REACTIONS, contact Almatica Pharma LLC at 1-877-447-7979 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch for voluntary reporting of adverse reactions.
Lisinopril and Hydrochlorothiazide
As a result of its diuretic effects, hydrochlorothiazide increases plasma renin activity, increases aldosterone secretion, and decreases serum potassium. Administration of lisinopril blocks the renin-angiotensin aldosterone axis and tends to reverse the potassium loss associated with the diuretic.
In clinical studies, the extent of blood pressure reduction seen with the combination of lisinopril and hydrochlorothiazide was approximately additive. The ZESTORETIC 10-12.5 combination worked equally well in black and white patients. The ZESTORETIC 20-12.5 and ZESTORETIC 20-25 combinations appeared somewhat less effective in black patients, but relatively few black patients were studied. In most patients, the antihypertensive effect of ZESTORETIC was sustained for at least 24 hours.
In a randomized, controlled comparison, the mean antihypertensive effects of ZESTORETIC 20-12.5 and ZESTORETIC 20-25 were similar, suggesting that many patients who respond adequately to the latter combination may be controlled with ZESTORETIC 20-12.5 (see DOSAGE AND ADMINISTRATION ).
Concomitant administration of lisinopril and hydrochlorothiazide has little or no effect on the bioavailability of either drug. The combination tablet is bioequivalent to concomitant administration of the separate entities.
Structured Label Content
F
Pregnancy category D
Use of drugs that act on the renin-angiotensin system during the second and third trimesters of pregnancy reduces fetal renal function and increases fetal and neonatal morbidity and death. Resulting oligohydramnios can be associated with fetal lung hypoplasia and skeletal deformations. Potential neonatal adverse effects include skull hypoplasia, anuria, hypotension, renal failure, and death. When pregnancy is detected, discontinue ZESTORETIC as soon as possible. These adverse outcomes are usually associated with use of these drugs in the second and third trimester of pregnancy. Most epidemiologic studies examining fetal abnormalities after exposure to antihypertensive use in the first trimester have not distinguished drugs affecting the renin-angiotensin system from other antihypertensive agents. Appropriate management of maternal hypertension during pregnancy is important to optimize outcomes for both mother and fetus.
In the unusual case that there is no appropriate alternative to therapy with drugs affecting the renin-angiotensin system for a particular patient, apprise the mother of the potential risk to the fetus. Perform serial ultrasound examinations to assess the intra-amniotic environment. If oligohydramnios is observed, discontinue ZESTORETIC, unless it is considered lifesaving for the mother. Fetal testing may be appropriate, based on the week of pregnancy. Patients and physicians should be aware, however, that oligohydramnios may not appear until after the fetus has sustained irreversible injury. Closely observe infants with histories of in utero exposure to ZESTORETIC for hypotension, oliguria, and hyperkalemia. (See Precautions, Pediatric Use ).
No teratogenic effects of lisinopril were seen in studies of pregnant rats, mice, and rabbits. On a mg/kg basis, the doses used were up to 625 times (in mice), 188 times (in rats), and 0.6 times (in rabbits) the maximum recommended human dose.
Lisinopril and Hydrochlorothiazide
Teratogenicity studies were conducted in mice and rats with up to 90 mg/kg/day of lisinopril (56 times the maximum recommended human dose) in combination with 10 mg/kg/day of hydrochlorothiazide (2.5 times the maximum recommended human dose). Maternal or fetotoxic effects were not seen in mice with the combination. In rats decreased maternal weight gain and decreased fetal weight occurred down to 3/10 mg/kg/day (the lowest dose tested). Associated with the decreased fetal weight was a delay in fetal ossification. The decreased fetal weight and delay in fetal ossification were not seen in saline-supplemented animals given 90/10 mg/kg/day.
When used in pregnancy, during the second and third trimesters, ACE inhibitors can cause injury and even death to the developing fetus. When pregnancy is detected, discontinue ZESTORETIC as soon as possible (see Lisinopril, Fetal Toxicity ).
H
Two-year feeding studies in mice and rats conducted under the auspices of the National Toxicology Program (NTP) uncovered no evidence of a carcinogenic potential of hydrochlorothiazide in female mice (at doses of up to approximately 600 mg/kg/day) or in male and female rats (at doses of up to approximately 100 mg/kg/day). These doses are 150 times and 12 times for mice and 25 times and 4 times for rats the maximum human daily dose based on mg/kg and mg/m2, respectively. The NTP, however, found equivocal evidence for hepatocarcinogenicity in male mice.
Hydrochlorothiazide was not genotoxic in vitro in the Ames mutagenicity assay of Salmonella typhimurium strains TA 98, TA 100, TA 1535, TA 1537, and TA 1538 and in the Chinese Hamster Ovary (CHO) test for chromosomal aberrations, or in vivo in assays using mouse germinal cell chromosomes, Chinese hamster bone marrow chromosomes, and the Drosophila sex-linked recessive lethal trait gene. Positive test results were obtained only in the in vitro CHO Sister Chromatid Exchange (clastogenicity) and in the Mouse Lymphoma Cell (mutagenicity) assays, using concentrations of hydrochlorothiazide from 43 mcg/mL to 1300 mcg/mL, and in the Aspergillus nidulans nondisjunction assay at an unspecified concentration.
Hydrochlorothiazide had no adverse effects on the fertility of mice and rats of either sex in studies wherein these species were exposed, via their diet, to doses of up to 100 mg/kg and 4 mg/kg, respectively, prior to conception and throughout gestation. In mice this dose is 25 times and 2 times the maximum daily human dose based on mg/kg and mg/m2, respectively. In rats this dose is 1 times and 0.2 times the maximum daily human dose based on mg/kg and mg/m2, respectively.
L
There was no evidence of a tumorigenic effect when lisinopril was administered for 105 weeks to male and female rats at doses up to 90 mg/kg/day (about 56 or 9 times* the maximum daily human dose, based on body weight and body surface area, respectively). There was no evidence of carcinogenicity when lisinopril was administered for 92 weeks to (male and female) mice at doses up to 135 mg/kg/day (about 84 times* the maximum recommended daily human dose). This dose was 6.8 times the maximum human dose based on body surface area in mice.
*Calculations assume a human weight of 50 kg and human body surface area of 1.62m2.
Lisinopril was not mutagenic in the Ames microbial mutagen test with or without metabolic activation. It was also negative in a forward mutation assay using Chinese hamster lung cells. Lisinopril did not produce single strand DNA breaks in an in vitro alkaline elution rat hepatocyte assay. In addition, lisinopril did not produce increases in chromosomal aberrations in an in vitro test in Chinese hamster ovary cells or in an in vivo study in mouse bone marrow.
There were no adverse effects on reproductive performance in male and female rats treated with up to 300 mg/kg/day of lisinopril. This dose is 188 times and 30 times the maximum daily human dose based on mg/kg and mg/m2, respectively.
Section 42229-5 (42229-5)
*AN69 is a registered trademark of Hospal Ltd.
ZESTORETIC is a trademark of Alvogen AZ IP Holdings LLC.
Product of USA
Distributed by:
Almatica Pharma LLC
Morristown, NJ 07960 USA
PI435-10
Rev. 03/2025
Section 51945-4 (51945-4)
NDC 52427-435-90
Rx only
ZESTORETIC®
10/12.5
(lisinopril/hydrochlorothiazide)
Each tablet contains:
10 mg lisinopril, USP and
12.5 mg hydrochlorothiazide
, USP
90 tablets
General
Warnings (WARNINGS)
Lisinopril
Mechanism of Action
Lisinopril inhibits angiotensin-converting enzyme (ACE) in human subjects and animals. ACE is a peptidyl dipeptidase that catalyzes the conversion of angiotensin I to the vasoconstrictor substance, angiotensin II. Angiotensin II also stimulates aldosterone secretion by the adrenal cortex. Inhibition of ACE results in decreased plasma angiotensin II which leads to decreased vasopressor activity and to decreased aldosterone secretion. The latter decrease may result in a small increase of serum potassium. Removal of angiotensin II negative feedback on renin secretion leads to increased plasma renin activity. In hypertensive patients with normal renal function treated with lisinopril alone for up to 24 weeks, the mean increase in serum potassium was less than 0.1 mEq/L; however, approximately 15 percent of patients had increases greater than 0.5 mEq/L and approximately six percent had a decrease greater than 0.5 mEq/L. In the same study, patients treated with lisinopril plus a thiazide diuretic showed essentially no change in serum potassium (see PRECAUTIONS ).
ACE is identical to kininase, an enzyme that degrades bradykinin. Whether increased levels of bradykinin, a potent vasodepressor peptide, play a role in the therapeutic effects of lisinopril remains to be elucidated.
While the mechanism through which lisinopril lowers blood pressure is believed to be primarily suppression of the renin-angiotensin-aldosterone system, lisinopril is antihypertensive even in patients with low-renin hypertension. Although lisinopril was antihypertensive in all races studied, black hypertensive patients (usually a low-renin hypertensive population) had a smaller average response to lisinopril monotherapy than nonblack patients.
Pharmacokinetics and Metabolism
Following oral administration of lisinopril, peak serum concentrations occur within about 7 hours. Declining serum concentrations exhibit a prolonged terminal phase which does not contribute to drug accumulation. This terminal phase probably represents saturable binding to ACE and is not proportional to dose. Lisinopril does not appear to be bound to other serum proteins.
Lisinopril does not undergo metabolism and is excreted unchanged entirely in the urine. Based on urinary recovery, the mean extent of absorption of lisinopril is approximately 25 percent, with large intersubject variability (6% to 60%) at all doses tested (5 mg to 80 mg). Lisinopril absorption is not influenced by the presence of food in the gastrointestinal tract.
Upon multiple dosing, lisinopril exhibits an effective half-life of accumulation of 12 hours.
Impaired renal function decreases elimination of lisinopril, which is excreted principally through the kidneys, but this decrease becomes clinically important only when the glomerular filtration rate is below 30 mL/min. Above this glomerular filtration rate, the elimination half-life is little changed. With greater impairment, however, peak and trough lisinopril levels increase, time to peak concentration increases and time to attain steady state is prolonged. Older patients, on average, have (approximately doubled) higher blood levels and area under the plasma concentration time curve (AUC) than younger patients (see DOSAGE AND ADMINISTRATION ). In a multiple dose pharmacokinetic study in elderly versus young hypertensive patients using the lisinopril/hydrochlorothiazide combination, the AUC increased approximately 120% for lisinopril and approximately 80% for hydrochlorothiazide in older patients. Lisinopril can be removed by hemodialysis.
Studies in rats indicate that lisinopril crosses the blood-brain barrier poorly. Multiple doses of lisinopril in rats do not result in accumulation in any tissues; however, milk of lactating rats contains radioactivity following administration of 14C lisinopril. By whole body autoradiography, radioactivity was found in the placenta following administration of labeled drug to pregnant rats, but none was found in the fetuses.
Pharmacodynamics
Administration of lisinopril to patients with hypertension results in a reduction of supine and standing blood pressure to about the same extent with no compensatory tachycardia. Symptomatic postural hypotension is usually not observed although it can occur and should be anticipated in volume and/or salt-depleted patients (see WARNINGS ).
In most patients studied, onset of antihypertensive activity was seen at one hour after oral administration of an individual dose of lisinopril, with peak reduction of blood pressure achieved by six hours.
In some patients achievement of optimal blood pressure reduction may require two to four weeks of therapy.
At recommended single daily doses, antihypertensive effects have been maintained for at least 24 hours, after dosing, although the effect at 24 hours was substantially smaller than the effect six hours after dosing.
The antihypertensive effects of lisinopril have continued during long-term therapy. Abrupt withdrawal of lisinopril has not been associated with a rapid increase in blood pressure; nor with a significant overshoot of pretreatment blood pressure.
In hemodynamic studies in patients with essential hypertension, blood pressure reduction was accompanied by a reduction in peripheral arterial resistance with little or no change in cardiac output and in heart rate. In a study in nine hypertensive patients, following administration of lisinopril, there was an increase in mean renal blood flow that was not significant. Data from several small studies are inconsistent with respect to the effect of lisinopril on glomerular filtration rate in hypertensive patients with normal renal function, but suggest that changes, if any, are not large.
In patients with renovascular hypertension lisinopril has been shown to be well tolerated and effective in controlling blood pressure (see PRECAUTIONS ).
Overdosage (OVERDOSAGE)
No specific information is available on the treatment of overdosage with ZESTORETIC. Treatment is symptomatic and supportive. Therapy with ZESTORETIC should be discontinued and the patient observed closely. Suggested measures include induction of emesis and/or gastric lavage, and correction of dehydration, electrolyte imbalance and hypotension by established procedures.
Description (DESCRIPTION)
ZESTORETIC® (Lisinopril and Hydrochlorothiazide) combines an angiotensin converting enzyme inhibitor, lisinopril, and a diuretic, hydrochlorothiazide.
Lisinopril, USP a synthetic peptide derivative, is an oral long-acting angiotensin converting enzyme inhibitor. It is chemically described as (S)-1-[N2-(1-carboxy-3-phenylpropyl)-L-lysyl]-L-proline dihydrate. Its empirical formula is C21H31N3O5 . 2H2O and its structural formula is:
Lisinopril, USP is a white to off-white, crystalline powder, with a molecular weight of 441.53. It is soluble in water, sparingly soluble in methanol, and practically insoluble in ethanol.
Hydrochlorothiazide, USP is 6-chloro-3,4-dihydro-2H-1,2,4-benzothiadiazine-7-sulfonamide 1,1-dioxide. Its empirical formula is C7H8ClN3O4S2 and its structural formula is:
Hydrochlorothiazide, USP is a white, or practically white, crystalline powder with a molecular weight of 297.72, which is slightly soluble in water, but freely soluble in sodium hydroxide solution.
ZESTORETIC is available for oral use in three tablet combinations of lisinopril, USP with hydrochlorothiazide, USP: ZESTORETIC 10-12.5 containing 10 mg lisinopril, USP and 12.5 mg hydrochlorothiazide, USP; ZESTORETIC 20-12.5 containing 20 mg lisinopril, USP and 12.5 mg hydrochlorothiazide, USP; and, ZESTORETIC 20-25 containing 20 mg lisinopril, USP and 25 mg hydrochlorothiazide, USP.
Inactive Ingredients:
10-12.5 Tablets - calcium phosphate, magnesium stearate, mannitol, red ferric oxide, corn starch, yellow ferric oxide.
20-12.5 Tablets - calcium phosphate, magnesium stearate, mannitol, corn starch.
20-25 Tablets - calcium phosphate, magnesium stearate, mannitol, red ferric oxide, corn starch, yellow ferric oxide.
How Supplied (HOW SUPPLIED)
ZESTORETIC 10-12.5 Tablets: Peach, round, biconvex, uncoated tablets identified with "141" debossed on one side and "ZESTORETIC" on the other side are supplied in bottles of 90 tablets (NDC 52427-435-90).
ZESTORETIC 20-12.5 Tablets: White, round, biconvex, uncoated tablets identified with "142" debossed on one side and "ZESTORETIC" on the other side are supplied in bottles of 90 tablets (NDC 52427-436-90).
ZESTORETIC 20-25 Tablets: Peach, round, biconvex, uncoated tablets identified with “145” debossed on one side and "ZESTORETIC" on the other side are supplied in bottles of 90 tablets (NDC 52427-437-90).
Storage
Store at controlled room temperature, 20°C to 25°C (68°F to 77°F) [see USP]. Protect from excessive light and humidity.
Geriatric Use
Clinical studies of ZESTORETIC did not include sufficient numbers of subjects aged 65 and over to determine whether they respond differently from younger subjects. Other reported clinical experience has not identified differences in responses between the elderly and younger patients. In general, dose selection for an elderly patient should be cautious, usually starting at the low end of the dosing range, reflecting the greater frequency of decreased hepatic, renal, or cardiac function, and of concomitant disease or other drug therapy.
This drug is known to be substantially excreted by the kidney, and the risk of toxic reactions to this drug may be greater in patients with impaired renal function. Because elderly patients are more likely to have decreased renal function, care should be taken in dose selection. Evaluation of the hypertensive patient should always include assessment of renal function.
Pediatric Use
Neonates with a history of in utero exposure to ZESTORETIC:
If oliguria or hypotension occurs, direct attention toward support of blood pressure and renal perfusion. Exchange transfusions or dialysis may be required as a means of reversing hypotension and/or substituting for disordered renal function. Lisinopril, which crosses the placenta, has been removed from neonatal circulation by peritoneal dialysis with some clinical benefit, and theoretically may be removed by exchange transfusion, although there is no experience with the latter procedure.
Safety and effectiveness in pediatric patients have not been established.
Nursing Mothers
It is not known whether lisinopril is excreted in human milk. However, milk of lactating rats contains radioactivity following administration of 14C lisinopril. In another study, lisinopril was present in rat milk at levels similar to plasma levels in the dams. Thiazides do appear in human milk. Because of the potential for serious adverse reactions in nursing infants from ACE inhibitors and hydrochlorothiazide, a decision should be made whether to discontinue nursing and/or discontinue ZESTORETIC, taking into account the importance of the drug to the mother.
Adverse Reactions (ADVERSE REACTIONS)
ZESTORETIC has been evaluated for safety in 930 patients including 100 patients treated for 50 weeks or more.
In clinical trials with ZESTORETIC no adverse experiences peculiar to this combination drug have been observed. Adverse experiences that have occurred have been limited to those that have been previously reported with lisinopril or hydrochlorothiazide.
The most frequent clinical adverse experiences in controlled trials (including open label extensions) with any combination of lisinopril and hydrochlorothiazide were: dizziness (7.5%), headache (5.2%), cough (3.9%), fatigue (3.7%) and orthostatic effects (3.2%) all of which were more common than in placebo-treated patients. Generally, adverse experiences were mild and transient in nature, but see WARNINGS regarding angioedema and excessive hypotension or syncope. Discontinuation of therapy due to adverse effects was required in 4.4% of patients principally because of dizziness, cough, fatigue and muscle cramps.
Adverse experiences occurring in greater than one percent of patients treated with lisinopril plus hydrochlorothiazide in controlled clinical trials are shown below.
Percent of Patients in Controlled Studies
|
Lisinopril and Hydrochlorothiazide (n=930)
Incidence (discontinuation) |
Placebo (n=207)
Incidence |
||
| Dizziness | 7.5 | (0.8) | 1.9 |
| Headache | 5.2 | (0.3) | 1.9 |
| Cough | 3.9 | (0.6) | 1.0 |
| Fatigue | 3.7 | (0.4) | 1.0 |
| Orthostatic Effects | 3.2 | (0.1) | 1.0 |
| Diarrhea | 2.5 | (0.2) | 2.4 |
| Nausea | 2.2 | (0.1) | 2.4 |
| Upper Respiratory Infection |
2.2 | (0.0) | 0.0 |
| Muscle Cramps | 2.0 | (0.4) | 0.5 |
| Asthenia | 1.8 | (0.2) | 1.0 |
| Paresthesia | 1.5 | (0.1) | 0.0 |
| Hypotension | 1.4 | (0.3) | 0.5 |
| Vomiting | 1.4 | (0.1) | 0.5 |
| Dyspepsia | 1.3 | (0.0) | 0.0 |
| Rash | 1.2 | (0.1) | 0.5 |
| Impotence | 1.2 | (0.3) | 0.0 |
Clinical adverse experiences occurring in 0.3% to 1.0% of patients in controlled trials and rarer, serious, possibly drug-related events reported in marketing experience are listed below:
Body as a Whole: Chest pain, abdominal pain, syncope, chest discomfort, fever, trauma, virus infection. Cardiovascular: Palpitation, orthostatic hypotension. Digestive: Gastrointestinal cramps, dry mouth, constipation, heartburn. Musculoskeletal: Back pain, shoulder pain, knee pain, back strain, myalgia, foot pain. Nervous/Psychiatric: Decreased libido, vertigo, depression, somnolence. Respiratory: Common cold, nasal congestion, influenza, bronchitis, pharyngeal pain, dyspnea, pulmonary congestion, chronic sinusitis, allergic rhinitis, pharyngeal discomfort. Skin: Flushing, pruritus, skin inflammation, diaphoresis, cutaneous pseudolymphoma. Special Senses: Blurred vision, tinnitus, otalgia. Urogenital: Urinary tract infection.
Angioedema: Angioedema of the face, extremities, lips, tongue, glottis and/or larynx has been reported (see WARNINGS ).
In rare cases, intestinal angioedema has been reported in post marketing experience.
Hypotension: In clinical trials, adverse effects relating to hypotension occurred as follows: hypotension (1.4%), orthostatic hypotension (0.5%), other orthostatic effects (3.2%). In addition syncope occurred in 0.8% of patients (see WARNINGS ).
Cough: See PRECAUTIONS - Cough.
Contraindications (CONTRAINDICATIONS)
ZESTORETIC is contraindicated in patients who are hypersensitive to this product and in patients with a history of angioedema related to previous treatment with an angiotensin-converting enzyme inhibitor and in patients with hereditary or idiopathic angioedema. Because of the hydrochlorothiazide component, this product is contraindicated in patients with anuria or hypersensitivity to other sulfonamide-derived drugs.
ZESTORETIC is contraindicated in combination with a neprilysin inhibitor (e.g., sacubitril). Do not administer ZESTORETIC within 36 hours of switching to or from sacubitril/valsartan, a neprilysin inhibitor (see
WARNINGS
).
Do not co-administer aliskiren with ZESTORETIC in patients with diabetes (see
PRECAUTIONS, Drug Interactions
).
Hydrochlorothiazide
The mechanism of the antihypertensive effect of thiazides is unknown. Thiazides do not usually affect normal blood pressure.
Hydrochlorothiazide is a diuretic and antihypertensive. It affects the distal renal tubular mechanism of electrolyte reabsorption. Hydrochlorothiazide increases excretion of sodium and chloride in approximately equivalent amounts. Natriuresis may be accompanied by some loss of potassium and bicarbonate.
After oral use diuresis begins within two hours, peaks in about four hours and lasts about 6 to 12 hours.
Hydrochlorothiazide is not metabolized but is eliminated rapidly by the kidney. When plasma levels have been followed for at least 24 hours, the plasma half-life has been observed to vary between 5.6 and 14.8 hours. At least 61 percent of the oral dose is eliminated unchanged within 24 hours. Hydrochlorothiazide crosses the placental but not the blood-brain barrier.
Clinical Pharmacology (CLINICAL PHARMACOLOGY)
Indications and Usage (INDICATIONS AND USAGE)
ZESTORETIC is indicated for the treatment of hypertension, to lower blood pressure. Lowering blood pressure lowers the risk of fatal and non-fatal cardiovascular events, primarily strokes and myocardial infarctions. These benefits have been seen in controlled trials of antihypertensive drugs from a wide variety of pharmacologic classes including lisinopril and hydrochlorothiazide.
Control of high blood pressure should be part of comprehensive cardiovascular risk management, including, as appropriate, lipid control, diabetes management, antithrombotic therapy, smoking cessation, exercise, and limited sodium intake. Many patients will require more than 1 drug to achieve blood pressure goals. For specific advice on goals and management, see published guidelines, such as those of the National High Blood Pressure Education Program’s Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure (JNC).
Numerous antihypertensive drugs, from a variety of pharmacologic classes and with different mechanisms of action, have been shown in randomized controlled trials to reduce cardiovascular morbidity and mortality, and it can be concluded that it is blood pressure reduction, and not some other pharmacologic property of the drugs, that is largely responsible for those benefits. The largest and most consistent cardiovascular outcome benefit has been a reduction in the risk of stroke, but reductions in myocardial infarction and cardiovascular mortality also have been seen regularly.
Elevated systolic or diastolic pressure causes increased cardiovascular risk, and the absolute risk increase per mmHg is greater at higher blood pressures, so that even modest reductions of severe hypertension can provide substantial benefit. Relative risk reduction from blood pressure reduction is similar across populations with varying absolute risk, so the absolute benefit is greater in patients who are at higher risk independent of their hypertension (for example, patients with diabetes or hyperlipidemia), and such patients would be expected to benefit from more aggressive treatment to a lower blood pressure goal.
Some antihypertensive drugs have smaller blood pressure effects (as monotherapy) in black patients, and many antihypertensive drugs have additional approved indications and effects (e.g., on angina, heart failure, or diabetic kidney disease). These considerations may guide selection of therapy.
These fixed-dose combinations are not indicated for initial therapy (see DOSAGE AND ADMINISTRATION ).
In using ZESTORETIC, consideration should be given to the fact that an angiotensin-converting enzyme inhibitor, captopril, has caused agranulocytosis, particularly in patients with renal impairment or collagen vascular disease, and that available data are insufficient to show that lisinopril does not have a similar risk (see WARNINGS ).
In considering the use of ZESTORETIC, it should be noted that ACE inhibitors have been associated with a higher rate of angioedema in black than in nonblack patients (see WARNINGS, Lisinopril ).
Warning: Fetal Toxicity (WARNING: FETAL TOXICITY)
See full prescribing information for complete boxed warning.
- When pregnancy is detected, discontinue ZESTORETIC as soon as possible.
- Drugs that act directly on the renin-angiotensin system can cause injury and death to the developing fetus. See Warnings: Fetal Toxicity.
Information for Patients
Angioedema: Angioedema, including laryngeal edema may occur at any time during treatment with angiotensin-converting enzyme inhibitors, including ZESTORETIC. Patients should be so advised and told to report immediately any signs or symptoms suggesting angioedema (swelling of face, extremities, eyes, lips, tongue, difficulty in swallowing or breathing) and to take no more drug until they have consulted with the prescribing physician.
Symptomatic Hypotension: Patients should be cautioned to report lightheadedness especially during the first few days of therapy. If actual syncope occurs, the patients should be told to discontinue the drug until they have consulted with the prescribing physician.
All patients should be cautioned that excessive perspiration and dehydration may lead to an excessive fall in blood pressure because of reduction in fluid volume. Other causes of volume depletion such as vomiting or diarrhea may also lead to a fall in blood pressure; patients should be advised to consult with their physician.
Hyperkalemia: Patients should be told not to use salt substitutes containing potassium without consulting their physician.
Leukopenia/Neutropenia: Patients should be told to report promptly any indication of infection (e.g., sore throat, fever) which may be a sign of leukopenia/neutropenia.
Pregnancy: Female patients of childbearing age should be told about the consequences of exposure to ZESTORETIC during pregnancy. Discuss treatment options with women planning to become pregnant. Patients should be asked to report pregnancies to their physicians as soon as possible.
Non-melanoma Skin Cancer: Instruct patients taking hydrochlorothiazide to protect skin from the sun and undergo regular skin cancer screening.
NOTE: As with many other drugs, certain advice to patients being treated with ZESTORETIC is warranted. This information is intended to aid in the safe and effective use of this medication. It is not a disclosure of all possible adverse or intended effects.
Dosage and Administration (DOSAGE AND ADMINISTRATION)
Lisinopril monotherapy is an effective treatment of hypertension in once-daily doses of 10 mg to 80 mg, while hydrochlorothiazide monotherapy is effective in doses of 12.5 mg per day to 50 mg per day. In clinical trials of lisinopril/hydrochlorothiazide combination therapy using lisinopril doses of 10 mg to 80 mg and hydrochlorothiazide doses of 6.25 mg to 50 mg, the antihypertensive response rates generally increased with increasing dose of either component.
The side effects (see WARNINGS ) of lisinopril are generally rare and apparently independent of dose; those of hydrochlorothiazide are a mixture of dose-dependent phenomena (primarily hypokalemia) and dose-independent phenomena (e.g., pancreatitis), the former much more common than the latter. Therapy with any combination of lisinopril and hydrochlorothiazide may be associated with either or both dose-independent or dose-dependent side effects, but addition of lisinopril in clinical trials blunted the hypokalemia normally seen with diuretics.
To minimize dose-dependent side effects, it is usually appropriate to begin combination therapy only after a patient has failed to achieve the desired effect with monotherapy.
Dose Titration Guided by Clinical Effect: A patient whose blood pressure is not adequately controlled with either lisinopril or hydrochlorothiazide monotherapy may be switched to lisinopril/HCTZ 10/12.5 or lisinopril/HCTZ 20/12.5, depending on current monotherapy dose. Further increases of either or both components should depend on clinical response with blood pressure measured at the interdosing interval to ensure that there is an adequate antihypertensive effect at that time. The hydrochlorothiazide dose should generally not be increased until 2 to 3 weeks have elapsed. After addition of the diuretic it may be possible to reduce the dose of lisinopril. Patients whose blood pressures are adequately controlled with 25 mg of daily hydrochlorothiazide, but who experience significant potassium loss with this regimen may achieve similar or greater blood-pressure control without electrolyte disturbance if they are switched to lisinopril/HCTZ 10/12.5.
In patients who are currently being treated with a diuretic, symptomatic hypotension occasionally may occur following the initial dose of lisinopril. The diuretic should, if possible, be discontinued for two to three days before beginning therapy with lisinopril to reduce the likelihood of hypotension (see WARNINGS ). If the patient's blood pressure is not controlled with lisinopril alone, diuretic therapy may be resumed.
If the diuretic cannot be discontinued, an initial dose of 5 mg of lisinopril should be used under medical supervision for at least two hours and until blood pressure has stabilized for at least an additional hour (see WARNINGS and PRECAUTIONS, Drug Interactions ).
Concomitant administration of ZESTORETIC with potassium supplements, potassium salt substitutes or potassium-sparing diuretics may lead to increases of serum potassium (see PRECAUTIONS ).
Replacement Therapy: The combination may be substituted for the titrated individual components.
Use in Renal Impairment: Regimens of therapy with lisinopril/HCTZ need not take account of renal function as long as the patient's creatinine clearance is >30 mL/min/1.7m2 (serum creatinine roughly ≤3 mg/dL or 265 μmol/L). In patients with more severe renal impairment, loop diuretics are preferred to thiazides, so lisinopril/HCTZ is not recommended (see WARNINGS , Anaphylactoid Reactions During Membrane Exposure).
Clinical Laboratory Test Findings
Serum Electrolytes: (See PRECAUTIONS ).
Creatinine, Blood Urea Nitrogen: Minor reversible increases in blood urea nitrogen and serum creatinine were observed in patients with essential hypertension treated with ZESTORETIC. More marked increases have also been reported and were more likely to occur in patients with renal artery stenosis (see PRECAUTIONS ).
Serum Uric Acid, Glucose, Magnesium, Cholesterol, Triglycerides and Calcium: (See PRECAUTIONS ).
Hemoglobin and Hematocrit: Small decreases in hemoglobin and hematocrit (mean decreases of approximately 0.5 g% and 1.5 vol%, respectively) occurred frequently in hypertensive patients treated with ZESTORETIC but were rarely of clinical importance unless another cause of anemia coexisted. In clinical trials, 0.4% of patients discontinued therapy due to anemia.
Liver Function Tests: Rarely, elevations of liver enzymes and/or serum bilirubin have occurred. (See WARNINGS, Hepatic Failure).
Other adverse reactions that have been reported with the individual components are listed below:
Lisinopril - In clinical trials adverse reactions which occurred with lisinopril were also seen with ZESTORETIC. In addition, and since lisinopril has been marketed, the following adverse reactions have been reported with lisinopril and should be considered potential adverse reactions for ZESTORETIC: Body as a Whole: Anaphylactoid reactions (see WARNINGS, Anaphylactoid Reactions During Membrane Exposure), malaise, edema, facial edema, pain, pelvic pain, flank pain, chills; Cardiovascular: Cardiac arrest, myocardial infarction or cerebrovascular accident, possibly secondary to excessive hypotension in high risk patients (see WARNINGS, Hypotension), pulmonary embolism and infarction, worsening of heart failure, arrhythmias (including tachycardia, ventricular tachycardia, atrial tachycardia, atrial fibrillation, bradycardia, and premature ventricular contractions), angina pectoris, transient ischemic attacks, paroxysmal nocturnal dyspnea, decreased blood pressure, peripheral edema, vasculitis; Digestive: Pancreatitis, hepatitis (hepatocellular or cholestatic jaundice) (see WARNINGS, Hepatic Failure), gastritis, anorexia, flatulence, increased salivation; Endocrine: Diabetes mellitus, inappropriate antidiuretic hormone secretion; Hematologic: Rare cases of bone marrow depression, hemolytic anemia, leukopenia/neutropenia, and thrombocytopenia have been reported in which a causal relationship to lisinopril can not be excluded; Metabolic: Gout, weight loss, dehydration, fluid overload, weight gain; Musculoskeletal: Arthritis, arthralgia, neck pain, hip pain, joint pain, leg pain, arm pain, lumbago; Nervous System/Psychiatric: Ataxia, memory impairment, tremor, insomnia, stroke, nervousness, confusion, peripheral neuropathy (e.g., paresthesia, dysesthesia), spasm, hypersomnia, irritability; mood alterations (including depressive symptoms); hallucinations; Respiratory: Malignant lung neoplasms, hemoptysis, pulmonary edema, pulmonary infiltrates, bronchospasm, asthma, pleural effusion, pneumonia, eosinophilic pneumonitis, wheezing, orthopnea, painful respiration, epistaxis, laryngitis, sinusitis, pharyngitis, rhinitis, rhinorrhea, chest sound abnormalities; Skin: Urticaria, alopecia, herpes zoster, photosensitivity, skin lesions, skin infections, pemphigus, erythema, psoriasis, rare cases of other severe skin reactions, including toxic epidermal necrolysis and Stevens-Johnson Syndrome (causal relationship has not been established); Special Senses: Visual loss, diplopia, photophobia, taste alteration, olfactory disturbance; Urogenital: Acute renal failure, oliguria, anuria, uremia, progressive azotemia, renal dysfunction (see PRECAUTIONS and DOSAGE AND ADMINISTRATION ), pyelonephritis, dysuria, breast pain.
Miscellaneous: A symptom complex has been reported which may include a positive ANA, an elevated erythrocyte sedimentation rate, arthralgia/arthritis, myalgia, fever, vasculitis, eosinophilia and leukocytosis. Rash, photosensitivity or other dermatological manifestations may occur alone or in combination with these symptoms.
Hydrochlorothiazide - Body as a Whole: Weakness; Digestive: Anorexia, gastric irritation, cramping, jaundice (intrahepatic cholestatic jaundice) (see WARNINGS, Hepatic Failure), pancreatitis, sialoadenitis, constipation; Hematologic: Leukopenia, agranulocytosis, thrombocytopenia, aplastic anemia, hemolytic anemia; Musculoskeletal: Muscle spasm; Nervous System/Psychiatric: Restlessness; Renal: Renal failure, renal dysfunction, interstitial nephritis (see WARNINGS); Skin: Erythema multiforme including Stevens-Johnson Syndrome, exfoliative dermatitis including toxic epidermal necrolysis, alopecia; Special Senses: Xanthopsia; Hypersensitivity: Purpura, photosensitivity, urticaria, necrotizing angiitis (vasculitis and cutaneous vasculitis), respiratory distress including pneumonitis and pulmonary edema, anaphylactic reactions.
Postmarketing Experience
Non-melanoma Skin Cancer
Hydrochlorothiazide is associated with an increased risk of non-melanoma skin cancer. In a study conducted in the Sentinel System, increased risk was predominantly for squamous cell carcinoma (SCC) and in white patients taking large cumulative doses. The increased risk for SCC in the overall population was approximately 1 additional case per 16,000 patients per year, and for white patients taking a cumulative dose of ≥50,000mg the risk increase was approximately 1 additional SCC case for every 6,700 patients per year.
To report SUSPECTED ADVERSE REACTIONS, contact Almatica Pharma LLC at 1-877-447-7979 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch for voluntary reporting of adverse reactions.
Lisinopril and Hydrochlorothiazide
As a result of its diuretic effects, hydrochlorothiazide increases plasma renin activity, increases aldosterone secretion, and decreases serum potassium. Administration of lisinopril blocks the renin-angiotensin aldosterone axis and tends to reverse the potassium loss associated with the diuretic.
In clinical studies, the extent of blood pressure reduction seen with the combination of lisinopril and hydrochlorothiazide was approximately additive. The ZESTORETIC 10-12.5 combination worked equally well in black and white patients. The ZESTORETIC 20-12.5 and ZESTORETIC 20-25 combinations appeared somewhat less effective in black patients, but relatively few black patients were studied. In most patients, the antihypertensive effect of ZESTORETIC was sustained for at least 24 hours.
In a randomized, controlled comparison, the mean antihypertensive effects of ZESTORETIC 20-12.5 and ZESTORETIC 20-25 were similar, suggesting that many patients who respond adequately to the latter combination may be controlled with ZESTORETIC 20-12.5 (see DOSAGE AND ADMINISTRATION ).
Concomitant administration of lisinopril and hydrochlorothiazide has little or no effect on the bioavailability of either drug. The combination tablet is bioequivalent to concomitant administration of the separate entities.
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:47:21.553227 · Updated: 2026-03-14T22:26:55.770037