These Highlights Do Not Include All The Information Needed To Use Procrit Safely And Effectively. See Full Prescribing Information For Procrit.
0c721ba4-ae19-417f-aae1-221ed1a0866a
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
WARNING: ESAs INCREASE THE RISK OF DEATH, MYOCARDIAL INFARCTION, STROKE, VENOUS THROMBOEMBOLISM, THROMBOSIS OF VASCULAR ACCESS AND TUMOR PROGRESSION OR RECURRENCE See full prescribing information for complete boxed warning. Chronic Kidney Disease: In controlled trials, patients experienced greater risks for death, serious adverse cardiovascular reactions, and stroke when administered erythropoiesis-stimulating agents (ESAs) to target a hemoglobin level of greater than 11 g/dL ( 5.1 ). No trial has identified a hemoglobin target level, ESA dose, or dosing strategy that does not increase these risks ( 2.2 ). Use the lowest PROCRIT dose sufficient to reduce the need for red blood cell (RBC) transfusions ( 5.1 ). Cancer: ESAs shortened overall survival and/or increased the risk of tumor progression or recurrence in clinical studies of patients with breast, non-small cell lung, head and neck, lymphoid, and cervical cancers ( 5.2 ). Use the lowest dose to avoid RBC transfusions ( 2.4 ). Use ESAs only for anemia from myelosuppressive chemotherapy ( 1.3 ). ESAs are not indicated for patients receiving myelosuppressive chemotherapy when the anticipated outcome is cure ( 1.5 ). Discontinue following the completion of a chemotherapy course ( 2.4 ). Perisurgery: Due to increased risk of deep venous thrombosis (DVT), DVT prophylaxis is recommended ( 5.1 ).
Indications and Usage
PROCRIT is an erythropoiesis-stimulating agent (ESA) indicated for: Treatment of anemia due to Chronic Kidney Disease (CKD) in patients on dialysis and not on dialysis ( 1.1 ). Zidovudine in patients with Human Immunodeficiency Virus (HIV) infection ( 1.2 ). The effects of concomitant myelosuppressive chemotherapy, and upon initiation, there is a minimum of two additional months of planned chemotherapy ( 1.3 ). Reduction of allogeneic red blood cell (RBC) transfusions in patients undergoing elective, noncardiac, nonvascular surgery ( 1.4 ). Limitations of Use PROCRIT has not been shown to improve quality of life, fatigue, or patient well-being ( 1.5 ). PROCRIT is not indicated for use: In patients with cancer receiving hormonal agents, biologic products, or radiotherapy, unless also receiving concomitant myelosuppressive chemotherapy ( 1.5 ). In patients with cancer receiving myelosuppressive chemotherapy when the anticipated outcome is cure ( 1.5 ). In patients with cancer receiving myelosuppressive chemotherapy in whom the anemia can be managed by transfusion ( 1.5 ). In patients scheduled for surgery who are willing to donate autologous blood ( 1.5 ). In patients undergoing cardiac or vascular surgery ( 1.5 ). As a substitute for RBC transfusions in patients who require immediate correction of anemia ( 1.5 ).
Dosage and Administration
Evaluate iron status before and during treatment and maintain iron repletion. Correct or exclude other causes of anemia before initiating treatment ( 2.1 ). In pregnant women, lactating women, neonates, infants: Use only single-dose vials ( 2.1 ). Patients with CKD: Initial dose: 50 to 100 Units/kg 3 times weekly (adults) and 50 Units/kg 3 times weekly (pediatric patients). Individualize maintenance dose. Intravenous route recommended for patients on hemodialysis ( 2.2 ). Patients on Zidovudine due to HIV Infection: 100 Units/kg 3 times weekly ( 2.3 ). Patients with Cancer on Chemotherapy: 40,000 Units weekly or 150 Units/kg 3 times weekly (adults); 600 Units/kg intravenously weekly (pediatric patients ≥ 5 years) ( 2.4 ). Surgery Patients: 300 Units/kg per day daily for 15 days or 600 Units/kg weekly ( 2.5 ).
Warnings and Precautions
Increased Mortality, Myocardial Infarction, Stroke, and Thromboembolism: Using ESAs to target a hemoglobin level of greater than 11 g/dL increases the risk of serious adverse cardiovascular reactions and has not been shown to provide additional benefit ( 5.1 and 14.1 ). Use caution in patients with coexistent cardiovascular disease and stroke ( 5.1 ). Increased Mortality and/or Increased Risk of Tumor Progression or Recurrence in Patients with Cancer ( 5.2 ). Hypertension: Control hypertension prior to initiating and during treatment with PROCRIT ( 5.3 ). Seizures: PROCRIT increases the risk for seizures in patients with CKD ( 5.4 ). Increase monitoring of these patients for changes in seizure frequency or premonitory symptoms ( 5.4 ). PRCA: If severe anemia and low reticulocyte count develop during PROCRIT treatment, withhold PROCRIT and evaluate for PRCA ( 5.6 ). Serious Allergic Reactions: Discontinue PROCRIT and manage reactions ( 5.7 ). Severe Cutaneous Reactions: Discontinue PROCRIT ( 5.8 ).
Contraindications
PROCRIT is contraindicated in patients with: Uncontrolled hypertension [see Warnings and Precautions (5.3) ] Pure red cell aplasia (PRCA) that begins after treatment with PROCRIT or other erythropoietin protein drugs [see Warnings and Precautions (5.6) ] Serious allergic reactions to PROCRIT [see Warnings and Precautions (5.7) ] PROCRIT from multiple-dose vials contains benzyl alcohol and is contraindicated in: Neonates, infants, pregnant women, and lactating women [see Warnings and Precautions (5.9) , Use in Specific Populations (8.1 , 8.2 , 8.4) ].
Adverse Reactions
The following serious adverse reactions are discussed in greater detail in other sections of the label: Increased Mortality, Myocardial Infarction, Stroke, and Thromboembolism [see Warnings and Precautions (5.1) ] Increased Mortality and/or Increased Risk of Tumor Progression or Recurrence in Patients with Cancer [see Warnings and Precautions (5.2) ] Hypertension [see Warnings and Precautions (5.3) ] Seizures [see Warnings and Precautions (5.4) ] PRCA [see Warnings and Precautions (5.6) ] Serious Allergic Reactions [see Warnings and Precautions (5.7) ] Severe Cutaneous Reactions [see Warnings and Precautions (5.8) ]
Storage and Handling
PROCRIT (epoetin alfa) injection is a sterile, clear, and colorless solution available as: Preservative-free, single-dose vials (in citrate-buffered formulation) : 2,000 Units/mL (NDC 59676-302-01), 3,000 Units/mL (NDC 59676-303-01), 4,000 Units/mL (NDC 59676-304-01), or 10,000 Units/mL (NDC 59676-310-01) supplied in cartons, each carton containing six 1 mL single-dose vials. Preservative-free, single-dose vials (in citrate-buffered formulation) : 10,000 Units/mL (NDC 59676-310-02) supplied in dispensing packs (tray) containing 25 single-dose 1 mL vials. Preservative-free, single-dose vials (in phosphate-buffered formulation) : 40,000 Units/mL (NDC 59676-340-01) supplied in dispensing packs containing four 1 mL single-dose vials. Preserved, multiple-dose vials : 20,000 Units/2mL (10,000 Units/mL) (NDC 59676-312-04) supplied in dispensing packs containing four 2 mL multiple-dose vials. Preserved, multiple-dose vials : 20,000 Units/mL (NDC 59676-320-04) supplied in dispensing packs containing four 1 mL multiple-dose vials.
How Supplied
PROCRIT (epoetin alfa) injection is a sterile, clear, and colorless solution available as: Preservative-free, single-dose vials (in citrate-buffered formulation) : 2,000 Units/mL (NDC 59676-302-01), 3,000 Units/mL (NDC 59676-303-01), 4,000 Units/mL (NDC 59676-304-01), or 10,000 Units/mL (NDC 59676-310-01) supplied in cartons, each carton containing six 1 mL single-dose vials. Preservative-free, single-dose vials (in citrate-buffered formulation) : 10,000 Units/mL (NDC 59676-310-02) supplied in dispensing packs (tray) containing 25 single-dose 1 mL vials. Preservative-free, single-dose vials (in phosphate-buffered formulation) : 40,000 Units/mL (NDC 59676-340-01) supplied in dispensing packs containing four 1 mL single-dose vials. Preserved, multiple-dose vials : 20,000 Units/2mL (10,000 Units/mL) (NDC 59676-312-04) supplied in dispensing packs containing four 2 mL multiple-dose vials. Preserved, multiple-dose vials : 20,000 Units/mL (NDC 59676-320-04) supplied in dispensing packs containing four 1 mL multiple-dose vials.
Medication Information
Warnings and Precautions
Increased Mortality, Myocardial Infarction, Stroke, and Thromboembolism: Using ESAs to target a hemoglobin level of greater than 11 g/dL increases the risk of serious adverse cardiovascular reactions and has not been shown to provide additional benefit ( 5.1 and 14.1 ). Use caution in patients with coexistent cardiovascular disease and stroke ( 5.1 ). Increased Mortality and/or Increased Risk of Tumor Progression or Recurrence in Patients with Cancer ( 5.2 ). Hypertension: Control hypertension prior to initiating and during treatment with PROCRIT ( 5.3 ). Seizures: PROCRIT increases the risk for seizures in patients with CKD ( 5.4 ). Increase monitoring of these patients for changes in seizure frequency or premonitory symptoms ( 5.4 ). PRCA: If severe anemia and low reticulocyte count develop during PROCRIT treatment, withhold PROCRIT and evaluate for PRCA ( 5.6 ). Serious Allergic Reactions: Discontinue PROCRIT and manage reactions ( 5.7 ). Severe Cutaneous Reactions: Discontinue PROCRIT ( 5.8 ).
Indications and Usage
PROCRIT is an erythropoiesis-stimulating agent (ESA) indicated for: Treatment of anemia due to Chronic Kidney Disease (CKD) in patients on dialysis and not on dialysis ( 1.1 ). Zidovudine in patients with Human Immunodeficiency Virus (HIV) infection ( 1.2 ). The effects of concomitant myelosuppressive chemotherapy, and upon initiation, there is a minimum of two additional months of planned chemotherapy ( 1.3 ). Reduction of allogeneic red blood cell (RBC) transfusions in patients undergoing elective, noncardiac, nonvascular surgery ( 1.4 ). Limitations of Use PROCRIT has not been shown to improve quality of life, fatigue, or patient well-being ( 1.5 ). PROCRIT is not indicated for use: In patients with cancer receiving hormonal agents, biologic products, or radiotherapy, unless also receiving concomitant myelosuppressive chemotherapy ( 1.5 ). In patients with cancer receiving myelosuppressive chemotherapy when the anticipated outcome is cure ( 1.5 ). In patients with cancer receiving myelosuppressive chemotherapy in whom the anemia can be managed by transfusion ( 1.5 ). In patients scheduled for surgery who are willing to donate autologous blood ( 1.5 ). In patients undergoing cardiac or vascular surgery ( 1.5 ). As a substitute for RBC transfusions in patients who require immediate correction of anemia ( 1.5 ).
Dosage and Administration
Evaluate iron status before and during treatment and maintain iron repletion. Correct or exclude other causes of anemia before initiating treatment ( 2.1 ). In pregnant women, lactating women, neonates, infants: Use only single-dose vials ( 2.1 ). Patients with CKD: Initial dose: 50 to 100 Units/kg 3 times weekly (adults) and 50 Units/kg 3 times weekly (pediatric patients). Individualize maintenance dose. Intravenous route recommended for patients on hemodialysis ( 2.2 ). Patients on Zidovudine due to HIV Infection: 100 Units/kg 3 times weekly ( 2.3 ). Patients with Cancer on Chemotherapy: 40,000 Units weekly or 150 Units/kg 3 times weekly (adults); 600 Units/kg intravenously weekly (pediatric patients ≥ 5 years) ( 2.4 ). Surgery Patients: 300 Units/kg per day daily for 15 days or 600 Units/kg weekly ( 2.5 ).
Contraindications
PROCRIT is contraindicated in patients with: Uncontrolled hypertension [see Warnings and Precautions (5.3) ] Pure red cell aplasia (PRCA) that begins after treatment with PROCRIT or other erythropoietin protein drugs [see Warnings and Precautions (5.6) ] Serious allergic reactions to PROCRIT [see Warnings and Precautions (5.7) ] PROCRIT from multiple-dose vials contains benzyl alcohol and is contraindicated in: Neonates, infants, pregnant women, and lactating women [see Warnings and Precautions (5.9) , Use in Specific Populations (8.1 , 8.2 , 8.4) ].
Adverse Reactions
The following serious adverse reactions are discussed in greater detail in other sections of the label: Increased Mortality, Myocardial Infarction, Stroke, and Thromboembolism [see Warnings and Precautions (5.1) ] Increased Mortality and/or Increased Risk of Tumor Progression or Recurrence in Patients with Cancer [see Warnings and Precautions (5.2) ] Hypertension [see Warnings and Precautions (5.3) ] Seizures [see Warnings and Precautions (5.4) ] PRCA [see Warnings and Precautions (5.6) ] Serious Allergic Reactions [see Warnings and Precautions (5.7) ] Severe Cutaneous Reactions [see Warnings and Precautions (5.8) ]
Storage and Handling
PROCRIT (epoetin alfa) injection is a sterile, clear, and colorless solution available as: Preservative-free, single-dose vials (in citrate-buffered formulation) : 2,000 Units/mL (NDC 59676-302-01), 3,000 Units/mL (NDC 59676-303-01), 4,000 Units/mL (NDC 59676-304-01), or 10,000 Units/mL (NDC 59676-310-01) supplied in cartons, each carton containing six 1 mL single-dose vials. Preservative-free, single-dose vials (in citrate-buffered formulation) : 10,000 Units/mL (NDC 59676-310-02) supplied in dispensing packs (tray) containing 25 single-dose 1 mL vials. Preservative-free, single-dose vials (in phosphate-buffered formulation) : 40,000 Units/mL (NDC 59676-340-01) supplied in dispensing packs containing four 1 mL single-dose vials. Preserved, multiple-dose vials : 20,000 Units/2mL (10,000 Units/mL) (NDC 59676-312-04) supplied in dispensing packs containing four 2 mL multiple-dose vials. Preserved, multiple-dose vials : 20,000 Units/mL (NDC 59676-320-04) supplied in dispensing packs containing four 1 mL multiple-dose vials.
How Supplied
PROCRIT (epoetin alfa) injection is a sterile, clear, and colorless solution available as: Preservative-free, single-dose vials (in citrate-buffered formulation) : 2,000 Units/mL (NDC 59676-302-01), 3,000 Units/mL (NDC 59676-303-01), 4,000 Units/mL (NDC 59676-304-01), or 10,000 Units/mL (NDC 59676-310-01) supplied in cartons, each carton containing six 1 mL single-dose vials. Preservative-free, single-dose vials (in citrate-buffered formulation) : 10,000 Units/mL (NDC 59676-310-02) supplied in dispensing packs (tray) containing 25 single-dose 1 mL vials. Preservative-free, single-dose vials (in phosphate-buffered formulation) : 40,000 Units/mL (NDC 59676-340-01) supplied in dispensing packs containing four 1 mL single-dose vials. Preserved, multiple-dose vials : 20,000 Units/2mL (10,000 Units/mL) (NDC 59676-312-04) supplied in dispensing packs containing four 2 mL multiple-dose vials. Preserved, multiple-dose vials : 20,000 Units/mL (NDC 59676-320-04) supplied in dispensing packs containing four 1 mL multiple-dose vials.
Description
WARNING: ESAs INCREASE THE RISK OF DEATH, MYOCARDIAL INFARCTION, STROKE, VENOUS THROMBOEMBOLISM, THROMBOSIS OF VASCULAR ACCESS AND TUMOR PROGRESSION OR RECURRENCE See full prescribing information for complete boxed warning. Chronic Kidney Disease: In controlled trials, patients experienced greater risks for death, serious adverse cardiovascular reactions, and stroke when administered erythropoiesis-stimulating agents (ESAs) to target a hemoglobin level of greater than 11 g/dL ( 5.1 ). No trial has identified a hemoglobin target level, ESA dose, or dosing strategy that does not increase these risks ( 2.2 ). Use the lowest PROCRIT dose sufficient to reduce the need for red blood cell (RBC) transfusions ( 5.1 ). Cancer: ESAs shortened overall survival and/or increased the risk of tumor progression or recurrence in clinical studies of patients with breast, non-small cell lung, head and neck, lymphoid, and cervical cancers ( 5.2 ). Use the lowest dose to avoid RBC transfusions ( 2.4 ). Use ESAs only for anemia from myelosuppressive chemotherapy ( 1.3 ). ESAs are not indicated for patients receiving myelosuppressive chemotherapy when the anticipated outcome is cure ( 1.5 ). Discontinue following the completion of a chemotherapy course ( 2.4 ). Perisurgery: Due to increased risk of deep venous thrombosis (DVT), DVT prophylaxis is recommended ( 5.1 ).
Section 42229-5
Chronic Kidney Disease:
- In controlled trials, patients with chronic kidney disease (CKD) experienced greater risks for death, serious adverse cardiovascular reactions, and stroke when administered erythropoiesis-stimulating agents (ESAs) to target a hemoglobin level of greater than 11 g/dL [see Warnings and Precautions (5.1)] .
- No trial has identified a hemoglobin target level, ESA dose, or dosing strategy that does not increase these risks [see Dosage and Administration (2.2)] .
- Use the lowest PROCRIT dose sufficient to reduce the need for red blood cell (RBC) transfusions [see Warnings and Precautions (5.1)] .
Section 42231-1
| This Medication Guide has been approved by the U.S. Food and Drug Administration. | Revised 04/2024 | |
|
MEDICATION GUIDE
PROCRIT ®(PRO'–KRIT) (epoetin alfa) |
||
|
Read this Medication Guide:
This Medication Guide does not take the place of talking to your healthcare provider about your medical condition or your treatment. Talk with your healthcare provider regularly about the use of PROCRIT and ask if there is new information about PROCRIT. |
||
|
What is the most important information I should know about PROCRIT? PROCRIT may cause serious side effects that can lead to death, including: For people with cancer:
For all people who take PROCRIT, including people with cancer or chronic kidney disease:
See " What are the possible side effects of PROCRIT?" below for more information. If you decide to take PROCRIT, your healthcare provider should prescribe the smallest dose of PROCRIT that is necessary to reduce your chance of needing RBC transfusions. |
||
|
What is PROCRIT? PROCRIT is a prescription medicine used to treat anemia. People with anemia have a lower-than-normal number of RBCs. PROCRIT works like the human protein called erythropoietin to help your body make more RBCs. PROCRIT is used to reduce or avoid the need for RBC transfusions. PROCRIT may be used to treat anemia if it is caused by:
PROCRIT may also be used to reduce the chance you will need RBC transfusions if you are scheduled for certain surgeries where a lot of blood loss is expected. If your hemoglobin level stays too high or if your hemoglobin goes up too quickly, this may lead to serious health problems which may result in death. These serious health problems may happen if you take PROCRIT, even if you do not have an increase in your hemoglobin level. PROCRIT has not been proven to improve quality of life, fatigue, or well-being. PROCRIT should not be usedfor treatment of anemia:
PROCRIT should not be used to reduce the chance you will need RBC transfusions if:
It is not known if PROCRIT is safe and effective in treating anemia in children less than 1 month old who have chronic kidney disease and in children less than 5 years old who have anemia caused by chemotherapy. |
||
|
Who should not take PROCRIT? Do not take PROCRIT if you:
Do notgive PROCRIT from multiple-dose vials to:
|
||
|
Before taking PROCRIT, tell your healthcare provider about all of your medical conditions,including if you:
Tell your healthcare provider about all the medicines you take, including prescription and over-the-counter medicines, vitamins, and herbal supplements. |
||
|
How should I take PROCRIT?
|
||
|
What are the possible side effects of PROCRIT? PROCRIT may cause serious side effects, including:
Common side effects of PROCRIT include: |
||
|
|
|
These are not all of the possible side effects of PROCRIT. Your healthcare provider can give you a more complete list. Tell your healthcare provider about any side effects that bother you or that do not go away. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. |
||
|
How should I store PROCRIT?
Keep PROCRIT and all medicines out of the reach of children. |
||
|
General information about the safe and effective use of PROCRIT Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not use PROCRIT for a condition for which it was not prescribed. Do not give PROCRIT to other people even if they have the same symptoms that you have. It may harm them. You can ask your healthcare provider or pharmacist for information about PROCRIT that is written for healthcare professionals. |
||
|
What are the ingredients in PROCRIT? Active ingredient:epoetin alfa Inactive ingredients:
Manufactured by:
Manufactured for:
For more information, go to the following website: www.PROCRIT.com or call 1-800-JANSSEN (1-800-526-7736). |
Section 44425-7
Store at 36°F to 46°F (2°C to 8°C). Do not freeze.
Do not shake. Do not use PROCRIT that has been shaken or frozen.
Store PROCRIT vials in the original carton until use to protect from light.
Section 59845-8
Instructions for Use
PROCRIT
®(PRO'–KRIT)
(epoetin alfa)
Use these Instructions for Use if you or your caregiver has been trained to give PROCRIT injections at home. Do not give yourself the injection unless you have received training from your healthcare provider. If you are not sure about giving the injection or you have questions, ask your healthcare provider for help.
Before reading these Instructions for Use, read the Medication Guide that comes with PROCRIT for the most important information you need to know.
When you receive your PROCRIT vial and syringes make sure that:
- The name PROCRIT appears on the carton and vial label.
- The expiration date on the vial label has not passed. Do not use a vial of PROCRIT after the expiration date on the label.
- The dose strength of the PROCRIT vial (number of Units per mL on the vial label) is the same as your healthcare provider prescribed.
- You understand what the dose strength of PROCRIT means. PROCRIT vials come in several dose strengths. For example, the dose strength may be described as 10,000 Units/mL on the vial label. This strength means that 10,000 Units of medicine are contained in each 1 mL (milliliter) of liquid. Your healthcare provider may also refer to a mL as a "cc." One mL is the same as one "cc."
- The PROCRIT liquid in the vial is clear and colorless. Do not use PROCRIT if the liquid in the vial looks discolored or cloudy, or if the liquid has lumps, flakes, or particles.
- The PROCRIT vial has a color cap on the top of the vial. Do not use a vial of PROCRIT if the color cap on the top of the vial has been removed or is missing.
- Use only the type of disposable syringe and needle that your healthcare provider has prescribed.
- Do not shake PROCRIT. Shaking could cause PROCRIT not to work. If you shake PROCRIT, the solution in the vial may look foamy and should not be used.
- Do not freeze PROCRIT. Do not use a vial of PROCRIT that has been frozen.
- Store PROCRIT in the refrigerator between 36°F to 46°F (2°C to 8°C).
- Keep PROCRIT away from light.
- Single-dose vials of PROCRIT should be used only one time. Throw the vial away after use even if there is medicine left in the vial.
- After removing a dose from the multidose vial, store the vial in the refrigerator (but not the freezer). Do not store the vial for more than 21 days.
- Throw away the multidose vial as directed by your healthcare provider:
- if there is not enough medicine left in the multidose vial for another dose, or
- if it has been more than 21 days since you first put a needle into the multidose vial.
How should I prepare for an injection of PROCRIT?
- Always keep an extra syringe and needle on hand.
- Follow your healthcare provider's instructions on how to measure your dose of PROCRIT. This dose will be measured in Units per mL or cc (1 mL is the same as 1 cc). Use a syringe that is marked in tenths of mL (for example, 0.2 mL or 0.2 cc). Using the wrong syringe can lead to a mistake in your dose and you could inject too much or too little PROCRIT.
Only use disposable syringes and needles. Use the syringes and needles only one time and then throw them away as instructed by your healthcare provider .
What do I need to know about the different types of PROCRIT vials?
PROCRIT comes in two different types of vials.
- Single-dose Vials
- Multidose Vials
The multidose vial of PROCRIT contains the preservative benzyl alcohol. Benzyl alcohol has been shown to cause brain damage, other serious side effects, and death in newborn and premature babies.PROCRIT that comes in single-dose vials does not contain benzyl alcohol.
Important: Follow these instructions exactly to help avoid infections.
Preparing the dose:
- Remove the vial of PROCRIT from the refrigerator. During this time, protect the solution from light.
- Do not use a single-dose vial of PROCRIT more than one time.
- Do not shake PROCRIT.
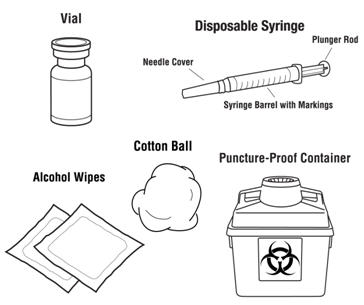
- Gather the other supplies you will need for your injection (vial, syringe, alcohol wipes, cotton ball, and a puncture-proof container for throwing away the syringe and needle). See Figure 1.
- Check the date on the PROCRIT vial to be sure that the drug has not expired.
- Wash your hands well with soap and water before preparing the medicine. See Figure 2.
- Flip off the protective color cap on the top of the vial. Do not remove the grey rubber stopper. Wipe the top of the grey rubber stopper with an alcohol wipe. See Figures 3and 4.
| Figure 3 | Figure 4 |
- Check the package containing the syringe. If the package has been opened or damaged, do not use that syringe. Throw away the syringe in the puncture-proof disposable container. If the syringe package is undamaged, open the package and remove the syringe.
- Using a syringe and needle that has been recommended by your healthcare provider, carefully remove the needle cover. See Figure 5. Then draw air into the syringe by pulling back on the plunger. The amount of air drawn into the syringe should be equal to the amount (mL or cc) of the PROCRIT dose prescribed by your healthcare provider. See Figure 6.
| Figure 5 | Figure 6 |
- With the vial on a flat work surface, insert the needle straight down through the grey rubber stopper of the PROCRIT vial. See Figure 7.
- Push the plunger of the syringe down to inject the air from the syringe into the vial of PROCRIT. The air injected into the vial will allow PROCRIT to be easily withdrawn into the syringe. See Figure 7.
- Keep the needle inside the vial. Turn the vial and syringe upside down. Be sure the tip of the needle is in the PROCRIT liquid. Keep the vial upside down. Slowly pull back on the plunger to fill the syringe with PROCRIT liquid to the number (mL or cc) that matches the dose your healthcare provider prescribed. See Figure 8.
- Keep the needle in the vial. Check for air bubbles in the syringe. A small amount of air is harmless. Too large an air bubble will give you the wrong PROCRIT dose. To remove air bubbles, gently tap the syringe with your fingers until the air bubbles rise to the top of the syringe. Slowly push the plunger up to force the air bubbles out of the syringe. Keep the tip of the needle in the PROCRIT liquid. Pull the plunger back to the number on the syringe that matches your dose. Check again for air bubbles. If there are still air bubbles, repeat the steps above to remove them. See Figures 9and 10.
| Figure 9 | Figure 10 |
- Double-check that you have the correct dose in the syringe. Lay the vial down on its side with the needle still in it until after you have selected and prepared your site for injection.
Selecting and preparing the injection site:
PROCRIT can be injected into your body using two different ways (routes) as described below. Follow your healthcare provider's instructions about how you should inject PROCRIT. In patients on hemodialysis, the intravenous (IV) route is recommended.
-
Subcutaneous Route:
- PROCRIT can be injected directly into a layer of fat under your skin. This is called a subcutaneous injection. When giving subcutaneous injections, follow your healthcare provider's instructions about changing the site for each injection. You may wish to write down the site where you have injected.
- Do not inject PROCRIT into an area that is tender, red, bruised, hard, or has scars or stretch marks. Recommended sites for injection are shown in Figure 11 below, including:
- The outer area of the upper arms
- The abdomen (except for the 2-inch area around the navel)
- The front of the middle thighs
- The upper outer area of the buttocks
- Clean the skin with an alcohol wipe where the injection is to be made. Be careful not to touch the skin that has been wiped clean. See
Figure 12.
- Double-check that the correct amount of PROCRIT is in the syringe.
- Remove the prepared syringe and needle from the vial of PROCRIT and hold it in the hand that you will use to inject the medicine.
- Use the other hand to pinch a fold of skin at the cleaned injection site. Do not touch the cleaned area of skin. See
Figure 13.
- Hold the syringe like you would hold a pencil. Use a quick "dart-like" motion to insert the needle either straight up and down (90-degree angle) or at a slight angle (45 degrees) into the skin. Inject the prescribed dose subcutaneously as directed by your doctor, nurse or pharmacist. See
Figure 14.
- Pull the needle out of the skin and press a cotton ball or gauze over the injection site and hold it there for several seconds. Do not recap the needle.
- Dispose of the used syringe and needle as described below. Do not reuse syringes and needles.
-
Intravenous Route:
- PROCRIT can be injected in your vein through a special access port placed by your healthcare provider. This type of PROCRIT injection is called an intravenous (IV) injection. This route is usually for hemodialysis patients.
- If you have a dialysis vascular access, make sure it is working by checking it as your healthcare provider has shown you. Be sure to let your healthcare provider know right away if you are having any problems, or if you have any questions.
- Wipe off the venous port of the hemodialysis tubing with an alcohol wipe. See
Figure 15.
- Insert the needle of the syringe into the cleaned venous port and push the plunger all the way down to inject all the PROCRIT. See
Figure 16.
- Remove the syringe from the venous port. Do not recap the needle.
- Dispose of the used syringe and needle as described below.
How should I dispose of the vials, syringes, and needles?
Do not reuse the single-dose vials, syringes, or needles. Throw away the vials, syringes, and needles as instructed by your healthcare provider or by following these steps:
- Do not throw the vials, syringes, or needles in the household trash or recycle.
- Do not put the needle cover back on the needle.
- Place all used needles and syringes in a puncture-proof disposable container with a lid. Do not use glass or clear plastic containers, or any container that will be recycled or returned to a store.
- Keep the puncture-proof disposable container out of the reach of children.
- When the puncture-proof disposable container is full, tape around the cap or lid to make sure the cap or lid does not come off. Throw away the puncture-proof disposable container as instructed by your healthcare provider. There may be special state and local laws for disposing of used needles and syringes. Do not throw the puncture-proof disposable container in the household trash. Do not recycle.
Keep PROCRIT and all medicines out of reach of children.
These Instructions for Use have been approved by the U.S. Food and Drug Administration.
Manufactured by:
Amgen Inc.
One Amgen Center Drive
Thousand Oaks, CA 91320-1799 U.S.A.
Manufactured for:
Janssen Products, LP
Horsham, Pennsylvania 19044
© Janssen Products, LP 2000
Printed in U. S. A.
Revised: 05/2012
9.2 Abuse
Abuse is the intentional, non-therapeutic use of a drug, even once, for its desirable psychological or physiological effects. Abuse of PROCRIT may be seen in athletes for the effects on erythropoiesis. Abuse of drugs that increase erythropoiesis, such as PROCRIT, by healthy persons may lead to life-threatening cardiovascular complications (e.g., stroke, myocardial infarction, or thromboembolism) [see Warnings and Precautions (5.1)].
In animal studies, epoetin alfa did not distribute to the CNS nor produce behavioral effects that are consistent with CNS activity.
5.4 Seizures
PROCRIT increases the risk of seizures in patients with CKD. During the first several months following initiation of PROCRIT, monitor patients closely for premonitory neurologic symptoms. Advise patients to contact their healthcare practitioner for new-onset seizures, premonitory symptoms or change in seizure frequency.
10 Overdosage
PROCRIT overdosage can cause hemoglobin levels above the desired level, which should be managed with discontinuation or reduction of PROCRIT dosage and/or with phlebotomy, as clinically indicated [see Clinical Pharmacology (12.2)] . Cases of severe hypertension have been observed following overdose with ESAs [see Warnings and Precautions (5.3)].
11 Description
Epoetin alfa is a 165-amino acid erythropoiesis-stimulating glycoprotein manufactured by recombinant DNA technology. It has a molecular weight of approximately 30,400 daltons and is produced by mammalian cells into which the human erythropoietin gene has been introduced. The product contains the identical amino acid sequence of isolated natural erythropoietin.
PROCRIT (epoetin alfa) injection for intravenous or subcutaneous administration is formulated as a sterile, clear, colorless liquid in vials in multiple formulations. Single-dose vials, formulated with an isotonic sodium chloride/sodium citrate-buffered solution, are supplied in multiple strengths. Each single-dose 1 mL vial contains 2,000, 3,000, 4,000, or 10,000 Units of epoetin alfa, Albumin (Human) (2.5 mg), citric acid (0.06 mg), sodium chloride (5.9 mg), and sodium citrate (5.8 mg) in Water for Injection, USP (pH 6.9 ± 0.3). Single-dose 1 mL vials formulated with an isotonic sodium chloride/sodium phosphate buffer contain 40,000 Units of epoetin alfa albumin (human) (2.5 mg), citric acid (0.0068 mg), sodium chloride (5.8 mg), sodium citrate (0.7 mg), sodium phosphate dibasic anhydrate (1.8 mg), and sodium phosphate monobasic monohydrate (1.2 mg) in Water for Injection, USP (pH 6.9 ± 0.3). Multiple-dose, 2 mL vials contain 10,000 Units epoetin alfa, albumin (human) (2.5 mg), benzyl alcohol (1%), sodium chloride (8.2 mg), citric acid (0.11 mg), and sodium citrate (1.3 mg) per 1 mL Water for Injection, USP (pH 6.1 ± 0.3). Multiple-dose 1 mL vials contain 20,000 Units epoetin alfa, albumin (human) (2.5 mg), benzyl alcohol (1%), sodium chloride (8.2 mg), citric acid (0.11 mg), and sodium citrate (1.3 mg), per 1 mL in Water for Injection, USP (pH 6.1 ± 0.3).
5.3 Hypertension
PROCRIT is contraindicated in patients with uncontrolled hypertension. Following initiation and titration of PROCRIT, approximately 25% of patients on dialysis required initiation of or increases in antihypertensive therapy; hypertensive encephalopathy and seizures have been reported in patients with CKD receiving PROCRIT.
Appropriately control hypertension prior to initiation of and during treatment with PROCRIT. Reduce or withhold PROCRIT if blood pressure becomes difficult to control. Advise patients of the importance of compliance with antihypertensive therapy and dietary restrictions [see Patient Counseling Information (17)] .
8.4 Pediatric Use
The multiple-dose vials are formulated with benzyl alcohol and are contraindicated for use in neonates and infants [see Contraindications (4), Warnings and Precautions (5.9)] . When therapy with PROCRIT is needed in neonates and infants, use the single-dose vial, which is a benzyl alcohol-free formulation. Do not mix the single-dose vials with bacteriostatic saline when administering PROCRIT to neonates or infants because it contains benzyl alcohol [see Dosage and Administration (2.6)] .
Serious adverse reactions including fatal reactions and the "gasping syndrome" occurred in premature neonates and infants in the neonatal intensive care unit who received drugs containing benzyl alcohol as a preservative. In these cases, benzyl alcohol dosages of 99 to 234 mg/kg/day produced high levels of benzyl alcohol and its metabolites in the blood and urine (blood levels of benzyl alcohol were 0.61 to 1.378 mmol/L). Additional adverse reactions included gradual neurological deterioration, seizures, intracranial hemorrhage, hematologic abnormalities, skin breakdown, hepatic and renal failure, hypotension, bradycardia, and cardiovascular collapse. Preterm, low birth weight infants may be more likely to develop these reactions because they may be less able to metabolize benzyl alcohol. The minimum amount of benzyl alcohol at which serious adverse reactions may occur is not known [see Warnings and Precautions (5.9)] .
8.5 Geriatric Use
Of the 4553 patients who received PROCRIT in the 6 studies for treatment of anemia due to CKD not receiving dialysis, 2726 (60%) were age 65 years and over, while 1418 (31%) were 75 years and over. Of the 757 patients who received PROCRIT in the 3 studies of CKD patients on dialysis, 361 (47%) were age 65 years and over, while 100 (13%) were 75 years and over. No differences in safety or effectiveness were observed between geriatric and younger patients. Dose selection and adjustment for an elderly patient should be individualized to achieve and maintain the target hemoglobin [see Dosage and Administration (2)] .
Among 778 patients enrolled in the 3 clinical studies of PROCRIT for the treatment of anemia due to concomitant chemotherapy, 419 received PROCRIT and 359 received placebo. Of the 419 who received PROCRIT, 247 (59%) were age 65 years and over, while 78 (19%) were 75 years and over. No overall differences in safety or effectiveness were observed between geriatric and younger patients. The dose requirements for PROCRIT in geriatric and younger patients within the 3 studies were similar.
Among 1731 patients enrolled in the 6 clinical studies of PROCRIT for reduction of allogeneic RBC transfusions in patients undergoing elective surgery, 1085 received PROCRIT and 646 received placebo or standard of care treatment. Of the 1085 patients who received PROCRIT, 582 (54%) were age 65 years and over, while 245 (23%) were 75 years and over. No overall differences in safety or effectiveness were observed between geriatric and younger patients. The dose requirements for PROCRIT in geriatric and younger patients within the 4 studies using the 3 times weekly schedule and 2 studies using the weekly schedule were similar.
Insufficient numbers of patients age 65 years or older were enrolled in clinical studies of PROCRIT for the treatment of patients treated with zidovudine for HIV Infection to determine whether they respond differently from younger patients .
6.3 Immunogenicity
As with all therapeutic proteins, there is a potential for immunogenicity. The detection of antibody formation is highly dependent on the sensitivity and specificity of the assay. Additionally, the observed incidence of antibody (including neutralizing antibody) positivity in an assay may be influenced by several factors, including assay methodology, sample handling, timing of sample collection, concomitant medications, and underlying disease. For these reasons, comparison of the incidence of antibodies to epoetin alfa with the incidence of antibodies to other products may be misleading.
Neutralizing antibodies to epoetin alfa that cross-react with endogenous erythropoietin and other ESAs can result in PRCA or severe anemia (with or without other cytopenias) [see Warnings and Precautions (5.6)] .
4 Contraindications
PROCRIT is contraindicated in patients with:
- Uncontrolled hypertension [see Warnings and Precautions (5.3)]
- Pure red cell aplasia (PRCA) that begins after treatment with PROCRIT or other erythropoietin protein drugs [see Warnings and Precautions (5.6)]
- Serious allergic reactions to PROCRIT [see Warnings and Precautions (5.7)]
PROCRIT from multiple-dose vials contains benzyl alcohol and is contraindicated in:
- Neonates, infants, pregnant women, and lactating women [see Warnings and Precautions (5.9), Use in Specific Populations (8.1, 8.2, 8.4)].
6 Adverse Reactions
The following serious adverse reactions are discussed in greater detail in other sections of the label:
- Increased Mortality, Myocardial Infarction, Stroke, and Thromboembolism [see Warnings and Precautions (5.1)]
- Increased Mortality and/or Increased Risk of Tumor Progression or Recurrence in Patients with Cancer [see Warnings and Precautions (5.2)]
- Hypertension [see Warnings and Precautions (5.3)]
- Seizures [see Warnings and Precautions (5.4)]
- PRCA [see Warnings and Precautions (5.6)]
- Serious Allergic Reactions [see Warnings and Precautions (5.7)]
- Severe Cutaneous Reactions [see Warnings and Precautions (5.8)]
2.5 Surgery Patients
The recommended PROCRIT regimens are:
- 300 Units/kg per day subcutaneously for 15 days total: administered daily for 10 days before surgery, on the day of surgery, and for 4 days after surgery.
- 600 Units/kg subcutaneously in 4 doses administered 21, 14, and 7 days before surgery and on the day of surgery.
Deep venous thrombosis prophylaxis is recommended during PROCRIT therapy [see Warnings and Precautions (5.1)] .
12.2 Pharmacodynamics
PROCRIT increases the reticulocyte count within 10 days of initiation, followed by increases in the RBC count, hemoglobin, and hematocrit, usually within 2 to 6 weeks. The rate of hemoglobin increase varies among patients and is dependent upon the dose of PROCRIT administered. For correction of anemia in hemodialysis patients, a greater biologic response is not observed at doses exceeding 300 Units/kg 3 times weekly.
12.3 Pharmacokinetics
In adult and pediatric patients with CKD, the elimination half-life (t 1/2) of plasma erythropoietin after intravenous administration of PROCRIT ranged from 4 to 13 hours. After subcutaneous administration, C maxwas achieved within 5 to 24 hours. The t 1/2in adult patients with serum creatinine greater than 3 mg/dL was similar between those not on dialysis and those maintained on dialysis. The pharmacokinetic data indicate no apparent difference in PROCRIT t 1/2among adult patients above or below 65 years of age.
A pharmacokinetic study comparing 150 Units/kg subcutaneous 3 times weekly to 40,000 Units subcutaneous weekly dosing regimen was conducted for 4 weeks in healthy subjects (n=12) and for 6 weeks in anemic cancer patients (n=32) receiving cyclic chemotherapy. There was no accumulation of serum erythropoietin after the 2 dosing regimens during the study period. The 40,000 Units weekly regimen had a higher C max(3- to 7-fold), longer T max(2- to 3-fold), higher AUC 0–168 h(2- to 3-fold) of erythropoietin and lower clearance (CL) (50%) than the 150 Units/kg 3 times weekly regimen. In anemic cancer patients, the average t 1/2was similar (40 hours with range of 16 to 67 hours) after both dosing regimens. After the 150 Units/kg 3 times weekly dosing, the values of T maxand CL were similar (13.3 ± 12.4 vs. 14.2 ± 6.7 hours, and 20.2 ± 15.9 vs. 23.6 ± 9.5 mL/hr/kg) between week 1 when patients were receiving chemotherapy (n=14) and week 3 when patients were not receiving chemotherapy (n=4). Differences were observed after the 40,000 Units weekly dosing with longer T max(38 ± 18 hours) and lower CL (9.2 ± 4.7 mL/hr/kg) during week 1 when patients were receiving chemotherapy (n=18) compared with those (22 ± 4.5 hours, 13.9 ± 7.6 mL/hr/kg, respectively) during week 3 when patients were not receiving chemotherapy (n=7).
The pharmacokinetic profile of PROCRIT in pediatric patients appeared similar to that of adults.
The pharmacokinetics of PROCRIT has not been studied in patients with HIV Infection.
14.4 Surgery Patients
The safety and efficacy of PROCRIT were evaluated in a placebo-controlled, double-blind study (S1) enrolling 316 patients scheduled for major, elective orthopedic hip or knee surgery who were expected to require ≥ 2 units of blood and who were not able or willing to participate in an autologous blood donation program. Patients were stratified into 1 of 3 groups based on their pretreatment hemoglobin [≤ 10 g/dL (n=2), > 10 to ≤ 13 g/dL (n=96), and > 13 to ≤ 15 g/dL (n=218)] and then randomly assigned to receive 300 Units/kg PROCRIT, 100 Units/kg PROCRIT, or placebo by subcutaneous injection for 10 days before surgery, on the day of surgery, and for 4 days after surgery. All patients received oral iron and a low-dose, postoperative warfarin regimen.
Treatment with PROCRIT 300 Units/kg significantly (p=0.024) reduced the risk of allogeneic RBC transfusion in patients with a pretreatment hemoglobin of > 10 to ≤ 13 g/dL; 5/31 (16%) of patients treated with PROCRIT 300 Units/kg, 6/26 (23%) of patients treated with PROCRIT 100 Units/kg, and 13/29 (45%) of placebo-treated patients were transfused. There was no significant difference in the number of patients transfused between PROCRIT (9% 300 Units/kg, 6% 100 Units/kg) and placebo (13%) in the > 13 to ≤ 15 g/dL hemoglobin stratum. There were too few patients in the ≤ 10 g/dL group to determine if PROCRIT is useful in this hemoglobin strata. In the > 10 to ≤ 13 g/dL pretreatment stratum, the mean number of units transfused per PROCRIT-treated patient (0.45 units blood for 300 Units/kg, 0.42 units blood for 100 Units/kg) was less than the mean transfused per placebo-treated patient (1.14 units) (overall p=0.028). In addition, mean hemoglobin, hematocrit, and reticulocyte counts increased significantly during the presurgery period in patients treated with PROCRIT.
PROCRIT was also evaluated in an open-label, parallel-group study (S2) enrolling 145 patients with a pretreatment hemoglobin level of ≥ 10 to ≤ 13 g/dL who were scheduled for major orthopedic hip or knee surgery and who were not participating in an autologous program. Patients were randomly assigned to receive 1 of 2 subcutaneous dosing regimens of PROCRIT (600 Units/kg once weekly for 3 weeks prior to surgery and on the day of surgery, or 300 Units/kg once daily for 10 days prior to surgery, on the day of surgery, and for 4 days after surgery). All patients received oral iron and appropriate pharmacologic anticoagulation therapy.
From pretreatment to presurgery, the mean increase in hemoglobin in the 600 Units/kg weekly group (1.44 g/dL) was greater than that observed in the 300 Units/kg daily group. The mean increase in absolute reticulocyte count was smaller in the weekly group (0.11 × 10 6/mm 3) compared to the daily group (0.17 × 10 6/mm 3). Mean hemoglobin levels were similar for the 2 treatment groups throughout the postsurgical period.
The erythropoietic response observed in both treatment groups resulted in similar RBC transfusion rates [11/69 (16%) in the 600 Units/kg weekly group and 14/71 (20%) in the 300 Units/kg daily group]. The mean number of units transfused per patient was approximately 0.3 units in both treatment groups.
1.5 Limitations of Use
PROCRIT has not been shown to improve quality of life, fatigue, or patient well-being.
PROCRIT is not indicated for use:
- In patients with cancer receiving hormonal agents, biologic products, or radiotherapy, unless also receiving concomitant myelosuppressive chemotherapy.
- In patients with cancer receiving myelosuppressive chemotherapy when the anticipated outcome is cure.
- In patients with cancer receiving myelosuppressive chemotherapy in whom the anemia can be managed by transfusion.
- In patients scheduled for surgery who are willing to donate autologous blood.
- In patients undergoing cardiac or vascular surgery.
- As a substitute for RBC transfusions in patients who require immediate correction of anemia.
1 Indications and Usage
PROCRIT is an erythropoiesis-stimulating agent (ESA) indicated for:
- Treatment of anemia due to
- Chronic Kidney Disease (CKD) in patients on dialysis and not on dialysis ( 1.1).
- Zidovudine in patients with Human Immunodeficiency Virus (HIV) infection ( 1.2).
- The effects of concomitant myelosuppressive chemotherapy, and upon initiation, there is a minimum of two additional months of planned chemotherapy ( 1.3).
- Reduction of allogeneic red blood cell (RBC) transfusions in patients undergoing elective, noncardiac, nonvascular surgery ( 1.4).
Limitations of Use
PROCRIT has not been shown to improve quality of life, fatigue, or patient well-being ( 1.5).
PROCRIT is not indicated for use:
- In patients with cancer receiving hormonal agents, biologic products, or radiotherapy, unless also receiving concomitant myelosuppressive chemotherapy ( 1.5).
- In patients with cancer receiving myelosuppressive chemotherapy when the anticipated outcome is cure ( 1.5).
- In patients with cancer receiving myelosuppressive chemotherapy in whom the anemia can be managed by transfusion ( 1.5).
- In patients scheduled for surgery who are willing to donate autologous blood ( 1.5).
- In patients undergoing cardiac or vascular surgery ( 1.5).
- As a substitute for RBC transfusions in patients who require immediate correction of anemia ( 1.5).
12.1 Mechanism of Action
PROCRIT stimulates erythropoiesis by the same mechanism as endogenous erythropoietin.
5.11 Dialysis Management
Patients may require adjustments in their dialysis prescriptions after initiation of PROCRIT. Patients receiving PROCRIT may require increased anticoagulation with heparin to prevent clotting of the extracorporeal circuit during hemodialysis.
9.1 Controlled Substance
PROCRIT contains epoetin alfa, which is not a controlled substance.
5.6 Pure Red Cell Aplasia
Cases of PRCA and of severe anemia, with or without other cytopenias that arise following the development of neutralizing antibodies to erythropoietin have been reported in patients treated with PROCRIT. This has been reported predominantly in patients with CKD receiving ESAs by subcutaneous administration. PRCA has also been reported in patients receiving ESAs for anemia related to hepatitis C treatment (an indication for which PROCRIT is not approved).
If severe anemia and low reticulocyte count develop during treatment with PROCRIT, withhold PROCRIT and evaluate patients for neutralizing antibodies to erythropoietin. Contact Janssen Products, LP at 1-800-JANSSEN (1-800-526-7736) to perform assays for binding and neutralizing antibodies. Permanently discontinue PROCRIT in patients who develop PRCA following treatment with PROCRIT or other erythropoietin protein drugs. Do not switch patients to other ESAs.
5 Warnings and Precautions
- Increased Mortality, Myocardial Infarction, Stroke, and Thromboembolism: Using ESAs to target a hemoglobin level of greater than 11 g/dL increases the risk of serious adverse cardiovascular reactions and has not been shown to provide additional benefit ( 5.1and 14.1). Use caution in patients with coexistent cardiovascular disease and stroke ( 5.1).
- Increased Mortality and/or Increased Risk of Tumor Progression or Recurrence in Patients with Cancer ( 5.2).
- Hypertension: Control hypertension prior to initiating and during treatment with PROCRIT ( 5.3).
- Seizures: PROCRIT increases the risk for seizures in patients with CKD ( 5.4). Increase monitoring of these patients for changes in seizure frequency or premonitory symptoms ( 5.4).
- PRCA: If severe anemia and low reticulocyte count develop during PROCRIT treatment, withhold PROCRIT and evaluate for PRCA ( 5.6).
- Serious Allergic Reactions: Discontinue PROCRIT and manage reactions ( 5.7).
- Severe Cutaneous Reactions: Discontinue PROCRIT ( 5.8).
2 Dosage and Administration
- Evaluate iron status before and during treatment and maintain iron repletion. Correct or exclude other causes of anemia before initiating treatment ( 2.1).
- In pregnant women, lactating women, neonates, infants: Use only single-dose vials ( 2.1).
- Patients with CKD: Initial dose: 50 to 100 Units/kg 3 times weekly (adults) and 50 Units/kg 3 times weekly (pediatric patients). Individualize maintenance dose. Intravenous route recommended for patients on hemodialysis ( 2.2).
- Patients on Zidovudine due to HIV Infection: 100 Units/kg 3 times weekly ( 2.3).
- Patients with Cancer on Chemotherapy: 40,000 Units weekly or 150 Units/kg 3 times weekly (adults); 600 Units/kg intravenously weekly (pediatric patients ≥ 5 years) ( 2.4).
- Surgery Patients: 300 Units/kg per day daily for 15 days or 600 Units/kg weekly ( 2.5).
3 Dosage Forms and Strengths
Injection:
- 2,000 Units/mL, 3,000 Units/mL, 4,000 Units/mL, 10,000 Units/mL, and 40,000 Units/mL of PROCRIT as a clear and colorless liquid in single-dose vials
- 20,000 Units/2 mL (10,000 Units/mL) and 20,000 Units/mL of PROCRIT as a clear and colorless liquid in multiple-dose vials (contains benzyl alcohol)
6.2 Postmarketing Experience
The following adverse reactions have been identified during post-approval use of PROCRIT.
Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
- Seizures [see Warnings and Precautions (5.4)]
- PRCA [see Warnings and Precautions (5.6)]
- Serious Allergic Reactions [see Warnings and Precautions (5.7)]
- Injection Site Reactions, including irritation and pain
- Porphyria
- Severe Cutaneous Reactions [see Warnings and Precautions (5.8)]
6.1 Clinical Trial Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of other drugs and may not reflect the rates observed in practice.
5.7 Serious Allergic Reactions
Serious allergic reactions, including anaphylactic reactions, angioedema, bronchospasm, skin rash, and urticaria may occur with PROCRIT. Immediately and permanently discontinue PROCRIT and administer appropriate therapy if a serious allergic or anaphylactic reaction occurs.
5.8 Severe Cutaneous Reactions
Blistering and skin exfoliation reactions including Erythema multiforme and Stevens-Johnson Syndrome (SJS)/Toxic Epidermal Necrolysis (TEN), have been reported in patients treated with ESAs (including PROCRIT) in the postmarketing setting. Discontinue PROCRIT therapy immediately if a severe cutaneous reaction, such as SJS/TEN, is suspected.
17 Patient Counseling Information
Advise the patient to read the FDA-approved patient labeling (Medication Guide and Instructions for Use).
Inform patients:
- Of the increased risks of mortality, serious cardiovascular reactions, thromboembolic reactions, stroke, and tumor progression [see Warnings and Precautions (5.1, 5.2)] .
- To undergo regular blood pressure monitoring, adhere to prescribed anti-hypertensive regimen and follow recommended dietary restrictions.
- To contact their healthcare provider for new-onset neurologic symptoms or change in seizure frequency.
- Of the need to have regular laboratory tests for hemoglobin.
- Risks are associated with benzyl alcohol in neonates, infants, pregnant women, and lactating women [see Use in Specific Populations (8.1, 8.2, 8.4)].
Instruct patients who self-administer PROCRIT of the:
- Importance of following the Instructions for Use.
- Dangers of reusing needles, syringes, or unused portions of single-dose vials.
- Proper disposal of used syringes, needles, and unused vials, and of the full container.
2.6 Preparation and Administration
- Do not shake. Do not use PROCRIT that has been shaken or frozen.
- Protect vials from light.
- Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration. Do not use any vials exhibiting particulate matter or discoloration.
- Discard unused portions of PROCRIT in preservative-free vials. Do not re-enter preservative-free vials.
- Store unused portions of PROCRIT in multiple-dose vials at 36°F to 46°F (2°C to 8°C). Discard 21 days after initial entry.
- Do not dilute. Do not mix with other drug solutions except for admixing as described below:
Preservative-free PROCRIT from single-dose vials may be admixed in a syringe with bacteriostatic 0.9% sodium chloride injection, USP, with benzyl alcohol 0.9% (bacteriostatic saline) in a 1:1 ratio using aseptic technique at the time of administration. Do not mix PROCRIT with bacteriostatic saline when administering to pregnant women, lactating women, neonates, and infants [see Use in Specific Populations (8.1, 8.2, 8.4)].
2.4 Patients On Cancer Chemotherapy
Initiate PROCRIT in patients on cancer chemotherapy only if the hemoglobin is less than 10 g/dL, and if there is a minimum of two additional months of planned chemotherapy.
Use the lowest dose of PROCRIT necessary to avoid RBC transfusions.
16 How Supplied/storage and Handling
PROCRIT (epoetin alfa) injection is a sterile, clear, and colorless solution available as:
Preservative-free, single-dose vials (in citrate-buffered formulation): 2,000 Units/mL (NDC 59676-302-01), 3,000 Units/mL (NDC 59676-303-01), 4,000 Units/mL (NDC 59676-304-01), or 10,000 Units/mL (NDC 59676-310-01) supplied in cartons, each carton containing six 1 mL single-dose vials.
Preservative-free, single-dose vials (in citrate-buffered formulation): 10,000 Units/mL (NDC 59676-310-02) supplied in dispensing packs (tray) containing 25 single-dose 1 mL vials.
Preservative-free, single-dose vials (in phosphate-buffered formulation): 40,000 Units/mL (NDC 59676-340-01) supplied in dispensing packs containing four 1 mL single-dose vials.
Preserved, multiple-dose vials: 20,000 Units/2mL (10,000 Units/mL) (NDC 59676-312-04) supplied in dispensing packs containing four 2 mL multiple-dose vials.
Preserved, multiple-dose vials: 20,000 Units/mL (NDC 59676-320-04) supplied in dispensing packs containing four 1 mL multiple-dose vials.
1.1 Anemia Due to Chronic Kidney Disease
PROCRIT is indicated for the treatment of anemia due to chronic kidney disease (CKD), including patients on dialysis and not on dialysis to decrease the need for red blood cell (RBC) transfusion.
2.2 Patients With Chronic Kidney Disease
In controlled trials, patients experienced greater risks for death, serious adverse cardiovascular reactions, and stroke when administered ESAs to target a hemoglobin level of greater than 11 g/dL. No trial has identified a hemoglobin target level, ESA dose, or dosing strategy that does not increase these risks. Individualize dosing and use the lowest dose of PROCRIT sufficient to reduce the need for RBC transfusions [see Warnings and Precautions (5.1)] . Physicians and patients should weigh the possible benefits of decreasing transfusions against the increased risks of death and other serious cardiovascular adverse reactions [see Boxed Warningand Clinical Studies (14)].
14.3 Patients With Cancer On Chemotherapy
The safety and effectiveness of PROCRIT was assessed in two multicenter, randomized (1:1), placebo-controlled, double-blind studies (Study C1 and Study C2) and a pooled analysis of six additional randomized (1:1), multicenter, placebo-controlled, double-blind studies. All studies were conducted in patients with anemia due to concomitantly administered cancer chemotherapy. Study C1 enrolled 344 adult patients, Study C2 enrolled 222 pediatric patients, and the pooled analysis contained 131 patients randomized to epoetin alfa or placebo. In Studies C1 and C2, efficacy was demonstrated by a reduction in the proportion of patients who received an RBC transfusion, from week 5 through end of the study, with the last-known RBC transfusion status carried forward for patients who discontinued treatment. In the pooled analysis, efficacy was demonstrated by a reduction in the proportion of patients who received an RBC transfusion from week 5 through end of the study in the subset of patients who were remaining on therapy for 6 or more weeks.
Principal Display Panel 2,000 Unit Vial Carton
2,000 Units/mL
NDC 59676
-302-01
6-1 mL Single-dose vials
Discard unused portion.
PROCRIT
®
EPOETIN ALFA
2,000 Units/mL
For Intravenous or Subcutaneous Use Only
Sterile Solution — No Preservative
Attention: Dispense the enclosed Medication Guide to each patient.
For more copies see Procrit.com or call 1-800-526-7736.
Each 1 mL vial contains: 2,000 units of recombinant epoetin alfa and
2.5 mg Albumin (Human) in a sterile, buffered solution (pH 6.9 ± 0.3)
of sodium citrate (5.8 mg), sodium chloride (5.9 mg) and citric acid
(0.06 mg) in Water for Injection, USP. No U.S. standard of potency.
Rx only
Principal Display Panel 3,000 Unit Vial Carton
3,000 Units/mL
NDC59676
-303-01
6-1 mL Single-dose vials
Discard unused portion.
PROCRIT
®
EPOETIN ALFA
3,000 Units/mL
For Intravenous or Subcutaneous Use Only
Sterile Solution — No Preservative
Attention: Dispense the enclosed Medication Guide to each patient.
For more copies see Procrit.com or call 1-800-526-7736.
Each 1 mL vial contains: 3,000 units of recombinant epoetin alfa and
2.5 mg Albumin (Human) in a sterile, buffered solution (pH 6.9 ± 0.3)
of sodium citrate (5.8 mg), sodium chloride (5.9 mg) and citric acid
(0.06 mg) in Water for Injection, USP. No U.S. standard of potency.
Rx only
Principal Display Panel 4,000 Unit Vial Carton
4,000 Units/mL
NDC59676
-304-01
6-1 mL Single-dose vials
Discard unused portion.
PROCRIT
®
EPOETIN ALFA
4,000 Units/mL
For Intravenous or Subcutaneous Use Only
Sterile Solution — No Preservative
Attention: Dispense the enclosed Medication Guide to each patient.
For more copies see Procrit.com or call 1-800-526-7736.
Each 1 mL vial contains: 4,000 units of recombinant epoetin alfa and
2.5 mg Albumin (Human) in a sterile, buffered solution (pH 6.9 ± 0.3)
of sodium citrate (5.8 mg), sodium chloride (5.9 mg) and citric acid
(0.06 mg) in Water for Injection, USP. No U.S. standard of potency.
Rx only
Principal Display Panel 10,000 Unit Vial Carton
10,000 Units/mL
NDC59676
-310-01
6-1 mL Single-dose vials
Discard unused portion.
PROCRIT
®
EPOETIN ALFA
10,000 Units/mL
For Intravenous or Subcutaneous Use Only
Sterile Solution — No Preservative
Attention: Dispense the enclosed Medication Guide to each patient.
For more copies see Procrit.com or call 1-800-526-7736.
Each 1 mL vial contains: 10,000 units of recombinant epoetin alfa and
2.5 mg Albumin (Human) in a sterile, buffered solution (pH 6.9 ± 0.3)
of sodium citrate (5.8 mg), sodium chloride (5.9 mg) and citric acid
(0.06 mg) in Water for Injection, USP. No U.S. standard of potency.
Rx only
Principal Display Panel 40,000 Unit Vial Carton
40,000 Units/mL
NDC59676
-340-01
4-1 mL Single-dose vials
Discard unused portion.
PROCRIT
®
EPOETIN ALFA
40,000 Units/mL
For Intravenous or Subcutaneous Use Only
Sterile Solution — No Preservative
Attention: Dispense the enclosed Medication Guide to each patient.
For more copies see Procrit.com or call 1-800-526-7736.
Each 1 mL vial contains: 40,000 units of recombinant
epoetin alfa and 2.5 mg Albumin (Human) in a sterile,
buffered solution (pH 6.9 ± 0.3) of sodium phosphate
monobasic monohydrate (1.2 mg), sodium phosphate
dibasic anhydrate (1.8 mg), sodium citrate (0.7 mg),
sodium chloride (5.8 mg), and citric acid (6.8 mcg) in
Water for Injection, USP. No U.S. standard of potency.
Rx only
5.5 Lack Or Loss of Hemoglobin Response to Procrit
For lack or loss of hemoglobin response to PROCRIT, initiate a search for causative factors (e.g., iron deficiency, infection, inflammation, bleeding). If typical causes of lack or loss of hemoglobin response are excluded, evaluate for PRCA [see Warnings and Precautions (5.6)] . In the absence of PRCA, follow dosing recommendations for management of patients with an insufficient hemoglobin response to PROCRIT therapy [see Dosage and Administration (2.2)] .
14.2 Zidovudine Treated Patients With Hiv Infection
The safety and efficacy of PROCRIT were evaluated in 4 placebo-controlled studies enrolling 297 anemic patients (hemoglobin < 10 g/dL) with HIV Infection receiving concomitant therapy with zidovudine. In the subgroup of patients (89/125 PROCRIT and 88/130 placebo) with pre-study endogenous serum erythropoietin levels ≤ 500 mUnits/mL, PROCRIT reduced the mean cumulative number of units of blood transfused per patient by approximately 40% as compared to the placebo group. Among those patients who required RBC transfusions at baseline, 43% of patients treated with PROCRIT versus 18% of placebo-treated patients were RBC transfusion-independent during the second and third months of therapy. PROCRIT therapy also resulted in significant increases in hemoglobin in comparison to placebo. When examining the results according to the weekly dose of zidovudine received during month 3 of therapy, there was a statistically significant reduction (p < 0.003) in RBC transfusion requirements in patients treated with PROCRIT (n=51) compared to placebo-treated patients (n=54) whose mean weekly zidovudine dose was ≤ 4200 mg/week.
Approximately 17% of the patients with endogenous serum erythropoietin levels ≤ 500 mUnits/mL receiving PROCRIT in doses from 100 to 200 Units/kg 3 times weekly achieved a hemoglobin of 12.7 g/dL without administration of RBC transfusions or significant reduction in zidovudine dose. In the subgroup of patients whose pre-study endogenous serum erythropoietin levels were > 500 mUnits/mL, PROCRIT therapy did not reduce RBC transfusion requirements or increase hemoglobin compared to the corresponding responses in placebo-treated patients.
1.3 Anemia Due to Chemotherapy in Patients With Cancer
PROCRIT is indicated for the treatment of anemia in patients with non-myeloid malignancies where anemia is due to the effect of concomitant myelosuppressive chemotherapy, and upon initiation, there is a minimum of two additional months of planned chemotherapy.
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
The carcinogenic potential of PROCRIT has not been evaluated.
PROCRIT was not mutagenic or clastogenic under the conditions tested: PROCRIT was negative in the in vitrobacterial reverse mutation assay (Ames test), in the in vitromammalian cell gene mutation assay (the hypoxanthine-guanine phosphoribosyl transferase [HGPRT] locus), in an in vitrochromosomal aberration assay in mammalian cells, and in the in vivomouse micronucleus assay.
When administered intravenously to male and female rats prior to and during mating, and to females through the beginning of implantation (up to gestational day 7; dosing stopped prior to the beginning of organogenesis), doses of 100 and 500 Units/kg/day of PROCRIT caused slight increases in pre-implantation loss, post-implantation loss and decreases in the incidence of live fetuses. It is not clear whether these effects reflect a drug effect on the uterine environment or on the conceptus. This animal dose level of 100 Units/kg/day approximates the clinical recommended starting dose, depending on the patient's treatment indication, but may be lower than the clinical dose in patients whose doses have been adjusted.
1.2 Anemia Due to Zidovudine in Patients With Hiv Infection
PROCRIT is indicated for the treatment of anemia due to zidovudine administered at ≤ 4200 mg/week in patients with HIV Infection with endogenous serum erythropoietin levels of ≤ 500 mUnits/mL.
5.10 Risk of Infectious Diseases Due to Albumin (human) Content
PROCRIT contains albumin, a derivative of human blood [see Description (11)] . Based on effective donor screening and product manufacturing processes, it carries an extremely remote risk for transmission of viral diseases. A theoretical risk for transmission of Creutzfeldt-Jakob disease (CJD) also is considered extremely remote. No cases of transmission of viral diseases or CJD have ever been identified for albumin.
Principal Display Panel 20,000 Units/ml Multiple Dose Vial Carton
PRINCIPAL DISPLAY PANEL - 20,000 Unit Vial Carton
20,000 Units/mL
NDC59676-
320-04
4-1 mL Multiple-dose Vials
PROCRIT
®
EPOETIN ALFA
20,000 Units/mL
Multiple-dose Vials
Sterile solution — Preserved. 20,000 Units/mL
For Intravenous or Subcutaneous Use Only
Attention: Dispense the enclosed Medication Guide to each patient.
For more copies see Procrit.com or call 1-800-526-7736.
1 mL
Rx only
Principal Display Panel 20,000 Units/2 Ml Multiple Dose Vial Carton
PRINCIPAL DISPLAY PANEL - 20,000 Units/2 mL Vial Carton
20,000 Units/2 mL
(10,000 Units/mL)
NDC59676-
312-04
4-2 mL Multiple-dose Vials
PROCRIT
®
EPOETIN ALFA
20,000 Units/2 mL (10,000 Units/mL)
Multiple-dose Vials
Sterile solution — Preserved. 10,000 Units/mL
For Intravenous or Subcutaneous Use Only.
Attention: Dispense the enclosed Medication Guide to each patient.
For more copies see Procrit.com or call 1-800-526-7736.
2 mL
Rx only
5.9 Risk of Serious Adverse Reactions Due to Benzyl Alcohol Preservative
PROCRIT from multiple-dose vials contains benzyl alcohol and is contraindicated for use in neonates, infants, pregnant women, and lactating women [see Contraindications (4)] . In addition, do not mix PROCRIT with bacteriostatic saline (which also contains benzyl alcohol) when administering PROCRIT to these patient populations [see Dosage and Administration (2)].
Serious and fatal reactions including "gasping syndrome" can occur in neonates and infants treated with benzyl alcohol-preserved drugs, including PROCRIT multiple-dose vials. The "gasping syndrome" is characterized by central nervous system (CNS) depression, metabolic acidosis, and gasping respirations. There is a potential for similar risks to fetuses and infants exposed to benzyl alcohol in uteroor in breast-fed milk, respectively. PROCRIT multiple-dose vials contain 11 mg of benzyl alcohol per mL. The minimum amount of benzyl alcohol at which serious adverse reactions may occur is not known [see Use in Specific Populations (8.1, 8.2, and 8.4)] .
5.1 Increased Mortality, Myocardial Infarction, Stroke, and Thromboembolism
- In controlled clinical trials of patients with CKD comparing higher hemoglobin targets (13 – 14 g/dL) to lower targets (9 – 11.3 g/dL), PROCRIT and other ESAs increased the risk of death, myocardial infarction, stroke, congestive heart failure, thrombosis of hemodialysis vascular access, and other thromboembolic events in the higher target groups.
- Using ESAs to target a hemoglobin level of greater than 11 g/dL increases the risk of serious adverse cardiovascular reactions and has not been shown to provide additional benefit [see Clinical Studies (14.1)] . Use caution in patients with coexistent cardiovascular disease and stroke [see Dosage and Administration (2.2)] . Patients with CKD and an insufficient hemoglobin response to ESA therapy may be at even greater risk for cardiovascular reactions and mortality than other patients. A rate of hemoglobin rise of greater than 1 g/dL over 2 weeks may contribute to these risks.
- In controlled clinical trials of patients with cancer, PROCRIT and other ESAs increased the risks for death and serious adverse cardiovascular reactions. These adverse reactions included myocardial infarction and stroke.
- In controlled clinical trials, ESAs increased the risk of death in patients undergoing coronary artery bypass graft surgery (CABG) and the risk of deep venous thrombosis (DVT) in patients undergoing orthopedic procedures.
The design and overall results of the 3 large trials comparing higher and lower hemoglobin targets are shown in Table 1.
| Normal Hematocrit Study (NHS)
(N=1265) |
CHOIR
(N=1432) |
TREAT
(N=4038) |
|
|---|---|---|---|
| Time Period of Trial | 1993 to 1996 | 2003 to 2006 | 2004 to 2009 |
| Population | CKD patients on hemodialysis with coexisting CHF or CAD, hematocrit 30 ± 3% on epoetin alfa | CKD patients not on dialysis with hemoglobin < 11 g/dL not previously administered epoetin alfa | CKD patients not on dialysis with type II diabetes, hemoglobin ≤ 11 g/dL |
|
Hemoglobin Target;
Higher vs. Lower (g/dL) |
14.0 vs. 10.0 | 13.5 vs. 11.3 | 13.0 vs. ≥ 9.0 |
|
Median (Q1, Q3)
Achieved Hemoglobin level (g/dL) |
12.6 (11.6, 13.3) vs. 10.3 (10.0, 10.7) | 13.0 (12.2, 13.4) vs. 11.4 (11.1, 11.6) | 12.5 (12.0, 12.8) vs. 10.6 (9.9, 11.3) |
| Primary Endpoint | All-cause mortality or non-fatal MI | All-cause mortality, MI, hospitalization for CHF, or stroke | All-cause mortality, MI, myocardial ischemia, heart failure, and stroke |
| Hazard Ratio or Relative Risk (95% CI) | 1.28 (1.06 – 1.56) | 1.34 (1.03 – 1.74) | 1.05 (0.94 – 1.17) |
| Adverse Outcome for Higher Target Group | All-cause mortality | All-cause mortality | Stroke |
| Hazard Ratio or Relative Risk (95% CI) | 1.27 (1.04 – 1.54) | 1.48 (0.97 – 2.27) | 1.92 (1.38 – 2.68) |
5.2 Increased Mortality And/or Increased Risk of Tumor Progression Or Recurrence in Patients With Cancer
ESAs resulted in decreased locoregional control/progression-free survival (PFS) and/or overall survival (OS) (see Table 2).
Adverse effects on PFS and/or OS were observed in studies of patients receiving chemotherapy for breast cancer (Studies 1, 2, and 4), lymphoid malignancy (Study 3), and cervical cancer (Study 5); in patients with advanced head and neck cancer receiving radiation therapy (Studies 6 and 7); and in patients with non-small cell lung cancer or various malignancies who were not receiving chemotherapy or radiotherapy (Studies 8 and 9).
| Study/Tumor/(n) | Hemoglobin Target | Achieved Hemoglobin
(Median; Q1, Q3 Q1=25
th percentile, Q3=75
th percentile
)
|
Primary Efficacy Outcome | Adverse Outcome for ESA- containing Arm |
|---|---|---|---|---|
| Chemotherapy | ||||
|
Study 1
Metastatic breast cancer (n=2098) |
≤12 g/dL
This study did not include a defined hemoglobin target. Doses were titrated to achieve and maintain the lowest hemoglobin level sufficient to avoid transfusion and not to exceed 12 g/dL.
|
11.6 g/dL
10.7, 12.1 g/dL |
Progression-free survival (PFS) | Decreased progression-free and overall survival |
|
Study 2
Metastatic breast cancer (n=939) |
12–14 g/dL | 12.9 g/dL;
12.2, 13.3 g/dL |
12-month overall survival | Decreased 12-month survival |
|
Study 3
Lymphoid malignancy (n=344) |
13–15 g/dL (M)
13–14 g/dL (F) |
11 g/dL;
9.8, 12.1 g/dL |
Proportion of patients achieving a hemoglobin response | Decreased overall survival |
|
Study 4
Early breast cancer (n=733) |
12.5–13 g/dL | 13.1 g/dL;
12.5, 13.7 g/dL |
Relapse-free and overall survival | Decreased 3-year relapse-free and overall survival |
|
Study 5
Cervical cancer (n=114) |
12–14 g/dL | 12.7 g/dL;
12.1, 13.3 g/dL |
Progression-free and overall survival and locoregional control | Decreased 3-year progression-free and overall survival and locoregional control |
| Radiotherapy Alone | ||||
|
Study 6
Head and neck cancer (n=351) |
≥ 15 g/dL (M)
≥ 14 g/dL (F) |
Not available | Locoregional progression-free survival | Decreased 5-year locoregional progression-free and overall survival |
|
Study 7
Head and neck cancer (n=522) |
14–15.5 g/dL | Not available | Locoregional disease control | Decreased locoregional disease control |
| No Chemotherapy or Radiotherapy | ||||
|
Study 8
Non-small cell lung cancer (n=70) |
12–14 g/dL | Not available | Quality of life | Decreased overall survival |
|
Study 9
Non-myeloid malignancy (n=989) |
12–13 g/dL | 10.6 g/dL;
9.4, 11.8 g/dL |
RBC transfusions | Decreased overall survival |
1.4 Reduction of Allogeneic Red Blood Cell Transfusions in Patients Undergoing Elective, Noncardiac, Nonvascular Surgery
PROCRIT is indicated to reduce the need for allogeneic RBC transfusions among patients with perioperative hemoglobin > 10 to ≤ 13 g/dL who are at high risk for perioperative blood loss from elective, noncardiac, nonvascular surgery. PROCRIT is not indicated for patients who are willing to donate autologous blood pre-operatively.
Warning: Esas Increase the Risk of Death, Myocardial Infarction, Stroke, Venous Thromboembolism, Thrombosis of Vascular Access and Tumor Progression Or Recurrence
WARNING: ESAs INCREASE THE RISK OF DEATH, MYOCARDIAL INFARCTION, STROKE, VENOUS THROMBOEMBOLISM, THROMBOSIS OF VASCULAR ACCESS AND TUMOR PROGRESSION OR RECURRENCE
See full prescribing information for complete boxed warning.
Chronic Kidney Disease:
- In controlled trials, patients experienced greater risks for death, serious adverse cardiovascular reactions, and stroke when administered erythropoiesis-stimulating agents (ESAs) to target a hemoglobin level of greater than 11 g/dL ( 5.1).
- No trial has identified a hemoglobin target level, ESA dose, or dosing strategy that does not increase these risks ( 2.2).
- Use the lowest PROCRIT dose sufficient to reduce the need for red blood cell (RBC) transfusions ( 5.1).
Cancer:
- ESAs shortened overall survival and/or increased the risk of tumor progression or recurrence in clinical studies of patients with breast, non-small cell lung, head and neck, lymphoid, and cervical cancers ( 5.2).
- Use the lowest dose to avoid RBC transfusions ( 2.4).
- Use ESAs only for anemia from myelosuppressive chemotherapy ( 1.3).
- ESAs are not indicated for patients receiving myelosuppressive chemotherapy when the anticipated outcome is cure ( 1.5).
- Discontinue following the completion of a chemotherapy course ( 2.4).
Perisurgery:
- Due to increased risk of deep venous thrombosis (DVT), DVT prophylaxis is recommended ( 5.1).
Structured Label Content
Section 42229-5 (42229-5)
Chronic Kidney Disease:
- In controlled trials, patients with chronic kidney disease (CKD) experienced greater risks for death, serious adverse cardiovascular reactions, and stroke when administered erythropoiesis-stimulating agents (ESAs) to target a hemoglobin level of greater than 11 g/dL [see Warnings and Precautions (5.1)] .
- No trial has identified a hemoglobin target level, ESA dose, or dosing strategy that does not increase these risks [see Dosage and Administration (2.2)] .
- Use the lowest PROCRIT dose sufficient to reduce the need for red blood cell (RBC) transfusions [see Warnings and Precautions (5.1)] .
Section 42231-1 (42231-1)
| This Medication Guide has been approved by the U.S. Food and Drug Administration. | Revised 04/2024 | |
|
MEDICATION GUIDE
PROCRIT ®(PRO'–KRIT) (epoetin alfa) |
||
|
Read this Medication Guide:
This Medication Guide does not take the place of talking to your healthcare provider about your medical condition or your treatment. Talk with your healthcare provider regularly about the use of PROCRIT and ask if there is new information about PROCRIT. |
||
|
What is the most important information I should know about PROCRIT? PROCRIT may cause serious side effects that can lead to death, including: For people with cancer:
For all people who take PROCRIT, including people with cancer or chronic kidney disease:
See " What are the possible side effects of PROCRIT?" below for more information. If you decide to take PROCRIT, your healthcare provider should prescribe the smallest dose of PROCRIT that is necessary to reduce your chance of needing RBC transfusions. |
||
|
What is PROCRIT? PROCRIT is a prescription medicine used to treat anemia. People with anemia have a lower-than-normal number of RBCs. PROCRIT works like the human protein called erythropoietin to help your body make more RBCs. PROCRIT is used to reduce or avoid the need for RBC transfusions. PROCRIT may be used to treat anemia if it is caused by:
PROCRIT may also be used to reduce the chance you will need RBC transfusions if you are scheduled for certain surgeries where a lot of blood loss is expected. If your hemoglobin level stays too high or if your hemoglobin goes up too quickly, this may lead to serious health problems which may result in death. These serious health problems may happen if you take PROCRIT, even if you do not have an increase in your hemoglobin level. PROCRIT has not been proven to improve quality of life, fatigue, or well-being. PROCRIT should not be usedfor treatment of anemia:
PROCRIT should not be used to reduce the chance you will need RBC transfusions if:
It is not known if PROCRIT is safe and effective in treating anemia in children less than 1 month old who have chronic kidney disease and in children less than 5 years old who have anemia caused by chemotherapy. |
||
|
Who should not take PROCRIT? Do not take PROCRIT if you:
Do notgive PROCRIT from multiple-dose vials to:
|
||
|
Before taking PROCRIT, tell your healthcare provider about all of your medical conditions,including if you:
Tell your healthcare provider about all the medicines you take, including prescription and over-the-counter medicines, vitamins, and herbal supplements. |
||
|
How should I take PROCRIT?
|
||
|
What are the possible side effects of PROCRIT? PROCRIT may cause serious side effects, including:
Common side effects of PROCRIT include: |
||
|
|
|
These are not all of the possible side effects of PROCRIT. Your healthcare provider can give you a more complete list. Tell your healthcare provider about any side effects that bother you or that do not go away. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. |
||
|
How should I store PROCRIT?
Keep PROCRIT and all medicines out of the reach of children. |
||
|
General information about the safe and effective use of PROCRIT Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not use PROCRIT for a condition for which it was not prescribed. Do not give PROCRIT to other people even if they have the same symptoms that you have. It may harm them. You can ask your healthcare provider or pharmacist for information about PROCRIT that is written for healthcare professionals. |
||
|
What are the ingredients in PROCRIT? Active ingredient:epoetin alfa Inactive ingredients:
Manufactured by:
Manufactured for:
For more information, go to the following website: www.PROCRIT.com or call 1-800-JANSSEN (1-800-526-7736). |
Section 44425-7 (44425-7)
Store at 36°F to 46°F (2°C to 8°C). Do not freeze.
Do not shake. Do not use PROCRIT that has been shaken or frozen.
Store PROCRIT vials in the original carton until use to protect from light.
Section 59845-8 (59845-8)
Instructions for Use
PROCRIT
®(PRO'–KRIT)
(epoetin alfa)
Use these Instructions for Use if you or your caregiver has been trained to give PROCRIT injections at home. Do not give yourself the injection unless you have received training from your healthcare provider. If you are not sure about giving the injection or you have questions, ask your healthcare provider for help.
Before reading these Instructions for Use, read the Medication Guide that comes with PROCRIT for the most important information you need to know.
When you receive your PROCRIT vial and syringes make sure that:
- The name PROCRIT appears on the carton and vial label.
- The expiration date on the vial label has not passed. Do not use a vial of PROCRIT after the expiration date on the label.
- The dose strength of the PROCRIT vial (number of Units per mL on the vial label) is the same as your healthcare provider prescribed.
- You understand what the dose strength of PROCRIT means. PROCRIT vials come in several dose strengths. For example, the dose strength may be described as 10,000 Units/mL on the vial label. This strength means that 10,000 Units of medicine are contained in each 1 mL (milliliter) of liquid. Your healthcare provider may also refer to a mL as a "cc." One mL is the same as one "cc."
- The PROCRIT liquid in the vial is clear and colorless. Do not use PROCRIT if the liquid in the vial looks discolored or cloudy, or if the liquid has lumps, flakes, or particles.
- The PROCRIT vial has a color cap on the top of the vial. Do not use a vial of PROCRIT if the color cap on the top of the vial has been removed or is missing.
- Use only the type of disposable syringe and needle that your healthcare provider has prescribed.
- Do not shake PROCRIT. Shaking could cause PROCRIT not to work. If you shake PROCRIT, the solution in the vial may look foamy and should not be used.
- Do not freeze PROCRIT. Do not use a vial of PROCRIT that has been frozen.
- Store PROCRIT in the refrigerator between 36°F to 46°F (2°C to 8°C).
- Keep PROCRIT away from light.
- Single-dose vials of PROCRIT should be used only one time. Throw the vial away after use even if there is medicine left in the vial.
- After removing a dose from the multidose vial, store the vial in the refrigerator (but not the freezer). Do not store the vial for more than 21 days.
- Throw away the multidose vial as directed by your healthcare provider:
- if there is not enough medicine left in the multidose vial for another dose, or
- if it has been more than 21 days since you first put a needle into the multidose vial.
How should I prepare for an injection of PROCRIT?
- Always keep an extra syringe and needle on hand.
- Follow your healthcare provider's instructions on how to measure your dose of PROCRIT. This dose will be measured in Units per mL or cc (1 mL is the same as 1 cc). Use a syringe that is marked in tenths of mL (for example, 0.2 mL or 0.2 cc). Using the wrong syringe can lead to a mistake in your dose and you could inject too much or too little PROCRIT.
Only use disposable syringes and needles. Use the syringes and needles only one time and then throw them away as instructed by your healthcare provider .
What do I need to know about the different types of PROCRIT vials?
PROCRIT comes in two different types of vials.
- Single-dose Vials
- Multidose Vials
The multidose vial of PROCRIT contains the preservative benzyl alcohol. Benzyl alcohol has been shown to cause brain damage, other serious side effects, and death in newborn and premature babies.PROCRIT that comes in single-dose vials does not contain benzyl alcohol.
Important: Follow these instructions exactly to help avoid infections.
Preparing the dose:
- Remove the vial of PROCRIT from the refrigerator. During this time, protect the solution from light.
- Do not use a single-dose vial of PROCRIT more than one time.
- Do not shake PROCRIT.
- Gather the other supplies you will need for your injection (vial, syringe, alcohol wipes, cotton ball, and a puncture-proof container for throwing away the syringe and needle). See Figure 1.
- Check the date on the PROCRIT vial to be sure that the drug has not expired.
- Wash your hands well with soap and water before preparing the medicine. See Figure 2.
- Flip off the protective color cap on the top of the vial. Do not remove the grey rubber stopper. Wipe the top of the grey rubber stopper with an alcohol wipe. See Figures 3and 4.
| Figure 3 | Figure 4 |
- Check the package containing the syringe. If the package has been opened or damaged, do not use that syringe. Throw away the syringe in the puncture-proof disposable container. If the syringe package is undamaged, open the package and remove the syringe.
- Using a syringe and needle that has been recommended by your healthcare provider, carefully remove the needle cover. See Figure 5. Then draw air into the syringe by pulling back on the plunger. The amount of air drawn into the syringe should be equal to the amount (mL or cc) of the PROCRIT dose prescribed by your healthcare provider. See Figure 6.
| Figure 5 | Figure 6 |
- With the vial on a flat work surface, insert the needle straight down through the grey rubber stopper of the PROCRIT vial. See Figure 7.
- Push the plunger of the syringe down to inject the air from the syringe into the vial of PROCRIT. The air injected into the vial will allow PROCRIT to be easily withdrawn into the syringe. See Figure 7.
- Keep the needle inside the vial. Turn the vial and syringe upside down. Be sure the tip of the needle is in the PROCRIT liquid. Keep the vial upside down. Slowly pull back on the plunger to fill the syringe with PROCRIT liquid to the number (mL or cc) that matches the dose your healthcare provider prescribed. See Figure 8.
- Keep the needle in the vial. Check for air bubbles in the syringe. A small amount of air is harmless. Too large an air bubble will give you the wrong PROCRIT dose. To remove air bubbles, gently tap the syringe with your fingers until the air bubbles rise to the top of the syringe. Slowly push the plunger up to force the air bubbles out of the syringe. Keep the tip of the needle in the PROCRIT liquid. Pull the plunger back to the number on the syringe that matches your dose. Check again for air bubbles. If there are still air bubbles, repeat the steps above to remove them. See Figures 9and 10.
| Figure 9 | Figure 10 |
- Double-check that you have the correct dose in the syringe. Lay the vial down on its side with the needle still in it until after you have selected and prepared your site for injection.
Selecting and preparing the injection site:
PROCRIT can be injected into your body using two different ways (routes) as described below. Follow your healthcare provider's instructions about how you should inject PROCRIT. In patients on hemodialysis, the intravenous (IV) route is recommended.
-
Subcutaneous Route:
- PROCRIT can be injected directly into a layer of fat under your skin. This is called a subcutaneous injection. When giving subcutaneous injections, follow your healthcare provider's instructions about changing the site for each injection. You may wish to write down the site where you have injected.
- Do not inject PROCRIT into an area that is tender, red, bruised, hard, or has scars or stretch marks. Recommended sites for injection are shown in Figure 11 below, including:
- The outer area of the upper arms
- The abdomen (except for the 2-inch area around the navel)
- The front of the middle thighs
- The upper outer area of the buttocks
- Clean the skin with an alcohol wipe where the injection is to be made. Be careful not to touch the skin that has been wiped clean. See
Figure 12.
- Double-check that the correct amount of PROCRIT is in the syringe.
- Remove the prepared syringe and needle from the vial of PROCRIT and hold it in the hand that you will use to inject the medicine.
- Use the other hand to pinch a fold of skin at the cleaned injection site. Do not touch the cleaned area of skin. See
Figure 13.
- Hold the syringe like you would hold a pencil. Use a quick "dart-like" motion to insert the needle either straight up and down (90-degree angle) or at a slight angle (45 degrees) into the skin. Inject the prescribed dose subcutaneously as directed by your doctor, nurse or pharmacist. See
Figure 14.
- Pull the needle out of the skin and press a cotton ball or gauze over the injection site and hold it there for several seconds. Do not recap the needle.
- Dispose of the used syringe and needle as described below. Do not reuse syringes and needles.
-
Intravenous Route:
- PROCRIT can be injected in your vein through a special access port placed by your healthcare provider. This type of PROCRIT injection is called an intravenous (IV) injection. This route is usually for hemodialysis patients.
- If you have a dialysis vascular access, make sure it is working by checking it as your healthcare provider has shown you. Be sure to let your healthcare provider know right away if you are having any problems, or if you have any questions.
- Wipe off the venous port of the hemodialysis tubing with an alcohol wipe. See
Figure 15.
- Insert the needle of the syringe into the cleaned venous port and push the plunger all the way down to inject all the PROCRIT. See
Figure 16.
- Remove the syringe from the venous port. Do not recap the needle.
- Dispose of the used syringe and needle as described below.
How should I dispose of the vials, syringes, and needles?
Do not reuse the single-dose vials, syringes, or needles. Throw away the vials, syringes, and needles as instructed by your healthcare provider or by following these steps:
- Do not throw the vials, syringes, or needles in the household trash or recycle.
- Do not put the needle cover back on the needle.
- Place all used needles and syringes in a puncture-proof disposable container with a lid. Do not use glass or clear plastic containers, or any container that will be recycled or returned to a store.
- Keep the puncture-proof disposable container out of the reach of children.
- When the puncture-proof disposable container is full, tape around the cap or lid to make sure the cap or lid does not come off. Throw away the puncture-proof disposable container as instructed by your healthcare provider. There may be special state and local laws for disposing of used needles and syringes. Do not throw the puncture-proof disposable container in the household trash. Do not recycle.
Keep PROCRIT and all medicines out of reach of children.
These Instructions for Use have been approved by the U.S. Food and Drug Administration.
Manufactured by:
Amgen Inc.
One Amgen Center Drive
Thousand Oaks, CA 91320-1799 U.S.A.
Manufactured for:
Janssen Products, LP
Horsham, Pennsylvania 19044
© Janssen Products, LP 2000
Printed in U. S. A.
Revised: 05/2012
9.2 Abuse
Abuse is the intentional, non-therapeutic use of a drug, even once, for its desirable psychological or physiological effects. Abuse of PROCRIT may be seen in athletes for the effects on erythropoiesis. Abuse of drugs that increase erythropoiesis, such as PROCRIT, by healthy persons may lead to life-threatening cardiovascular complications (e.g., stroke, myocardial infarction, or thromboembolism) [see Warnings and Precautions (5.1)].
In animal studies, epoetin alfa did not distribute to the CNS nor produce behavioral effects that are consistent with CNS activity.
5.4 Seizures
PROCRIT increases the risk of seizures in patients with CKD. During the first several months following initiation of PROCRIT, monitor patients closely for premonitory neurologic symptoms. Advise patients to contact their healthcare practitioner for new-onset seizures, premonitory symptoms or change in seizure frequency.
10 Overdosage (10 OVERDOSAGE)
PROCRIT overdosage can cause hemoglobin levels above the desired level, which should be managed with discontinuation or reduction of PROCRIT dosage and/or with phlebotomy, as clinically indicated [see Clinical Pharmacology (12.2)] . Cases of severe hypertension have been observed following overdose with ESAs [see Warnings and Precautions (5.3)].
11 Description (11 DESCRIPTION)
Epoetin alfa is a 165-amino acid erythropoiesis-stimulating glycoprotein manufactured by recombinant DNA technology. It has a molecular weight of approximately 30,400 daltons and is produced by mammalian cells into which the human erythropoietin gene has been introduced. The product contains the identical amino acid sequence of isolated natural erythropoietin.
PROCRIT (epoetin alfa) injection for intravenous or subcutaneous administration is formulated as a sterile, clear, colorless liquid in vials in multiple formulations. Single-dose vials, formulated with an isotonic sodium chloride/sodium citrate-buffered solution, are supplied in multiple strengths. Each single-dose 1 mL vial contains 2,000, 3,000, 4,000, or 10,000 Units of epoetin alfa, Albumin (Human) (2.5 mg), citric acid (0.06 mg), sodium chloride (5.9 mg), and sodium citrate (5.8 mg) in Water for Injection, USP (pH 6.9 ± 0.3). Single-dose 1 mL vials formulated with an isotonic sodium chloride/sodium phosphate buffer contain 40,000 Units of epoetin alfa albumin (human) (2.5 mg), citric acid (0.0068 mg), sodium chloride (5.8 mg), sodium citrate (0.7 mg), sodium phosphate dibasic anhydrate (1.8 mg), and sodium phosphate monobasic monohydrate (1.2 mg) in Water for Injection, USP (pH 6.9 ± 0.3). Multiple-dose, 2 mL vials contain 10,000 Units epoetin alfa, albumin (human) (2.5 mg), benzyl alcohol (1%), sodium chloride (8.2 mg), citric acid (0.11 mg), and sodium citrate (1.3 mg) per 1 mL Water for Injection, USP (pH 6.1 ± 0.3). Multiple-dose 1 mL vials contain 20,000 Units epoetin alfa, albumin (human) (2.5 mg), benzyl alcohol (1%), sodium chloride (8.2 mg), citric acid (0.11 mg), and sodium citrate (1.3 mg), per 1 mL in Water for Injection, USP (pH 6.1 ± 0.3).
5.3 Hypertension
PROCRIT is contraindicated in patients with uncontrolled hypertension. Following initiation and titration of PROCRIT, approximately 25% of patients on dialysis required initiation of or increases in antihypertensive therapy; hypertensive encephalopathy and seizures have been reported in patients with CKD receiving PROCRIT.
Appropriately control hypertension prior to initiation of and during treatment with PROCRIT. Reduce or withhold PROCRIT if blood pressure becomes difficult to control. Advise patients of the importance of compliance with antihypertensive therapy and dietary restrictions [see Patient Counseling Information (17)] .
8.4 Pediatric Use
The multiple-dose vials are formulated with benzyl alcohol and are contraindicated for use in neonates and infants [see Contraindications (4), Warnings and Precautions (5.9)] . When therapy with PROCRIT is needed in neonates and infants, use the single-dose vial, which is a benzyl alcohol-free formulation. Do not mix the single-dose vials with bacteriostatic saline when administering PROCRIT to neonates or infants because it contains benzyl alcohol [see Dosage and Administration (2.6)] .
Serious adverse reactions including fatal reactions and the "gasping syndrome" occurred in premature neonates and infants in the neonatal intensive care unit who received drugs containing benzyl alcohol as a preservative. In these cases, benzyl alcohol dosages of 99 to 234 mg/kg/day produced high levels of benzyl alcohol and its metabolites in the blood and urine (blood levels of benzyl alcohol were 0.61 to 1.378 mmol/L). Additional adverse reactions included gradual neurological deterioration, seizures, intracranial hemorrhage, hematologic abnormalities, skin breakdown, hepatic and renal failure, hypotension, bradycardia, and cardiovascular collapse. Preterm, low birth weight infants may be more likely to develop these reactions because they may be less able to metabolize benzyl alcohol. The minimum amount of benzyl alcohol at which serious adverse reactions may occur is not known [see Warnings and Precautions (5.9)] .
8.5 Geriatric Use
Of the 4553 patients who received PROCRIT in the 6 studies for treatment of anemia due to CKD not receiving dialysis, 2726 (60%) were age 65 years and over, while 1418 (31%) were 75 years and over. Of the 757 patients who received PROCRIT in the 3 studies of CKD patients on dialysis, 361 (47%) were age 65 years and over, while 100 (13%) were 75 years and over. No differences in safety or effectiveness were observed between geriatric and younger patients. Dose selection and adjustment for an elderly patient should be individualized to achieve and maintain the target hemoglobin [see Dosage and Administration (2)] .
Among 778 patients enrolled in the 3 clinical studies of PROCRIT for the treatment of anemia due to concomitant chemotherapy, 419 received PROCRIT and 359 received placebo. Of the 419 who received PROCRIT, 247 (59%) were age 65 years and over, while 78 (19%) were 75 years and over. No overall differences in safety or effectiveness were observed between geriatric and younger patients. The dose requirements for PROCRIT in geriatric and younger patients within the 3 studies were similar.
Among 1731 patients enrolled in the 6 clinical studies of PROCRIT for reduction of allogeneic RBC transfusions in patients undergoing elective surgery, 1085 received PROCRIT and 646 received placebo or standard of care treatment. Of the 1085 patients who received PROCRIT, 582 (54%) were age 65 years and over, while 245 (23%) were 75 years and over. No overall differences in safety or effectiveness were observed between geriatric and younger patients. The dose requirements for PROCRIT in geriatric and younger patients within the 4 studies using the 3 times weekly schedule and 2 studies using the weekly schedule were similar.
Insufficient numbers of patients age 65 years or older were enrolled in clinical studies of PROCRIT for the treatment of patients treated with zidovudine for HIV Infection to determine whether they respond differently from younger patients .
6.3 Immunogenicity
As with all therapeutic proteins, there is a potential for immunogenicity. The detection of antibody formation is highly dependent on the sensitivity and specificity of the assay. Additionally, the observed incidence of antibody (including neutralizing antibody) positivity in an assay may be influenced by several factors, including assay methodology, sample handling, timing of sample collection, concomitant medications, and underlying disease. For these reasons, comparison of the incidence of antibodies to epoetin alfa with the incidence of antibodies to other products may be misleading.
Neutralizing antibodies to epoetin alfa that cross-react with endogenous erythropoietin and other ESAs can result in PRCA or severe anemia (with or without other cytopenias) [see Warnings and Precautions (5.6)] .
4 Contraindications (4 CONTRAINDICATIONS)
PROCRIT is contraindicated in patients with:
- Uncontrolled hypertension [see Warnings and Precautions (5.3)]
- Pure red cell aplasia (PRCA) that begins after treatment with PROCRIT or other erythropoietin protein drugs [see Warnings and Precautions (5.6)]
- Serious allergic reactions to PROCRIT [see Warnings and Precautions (5.7)]
PROCRIT from multiple-dose vials contains benzyl alcohol and is contraindicated in:
- Neonates, infants, pregnant women, and lactating women [see Warnings and Precautions (5.9), Use in Specific Populations (8.1, 8.2, 8.4)].
6 Adverse Reactions (6 ADVERSE REACTIONS)
The following serious adverse reactions are discussed in greater detail in other sections of the label:
- Increased Mortality, Myocardial Infarction, Stroke, and Thromboembolism [see Warnings and Precautions (5.1)]
- Increased Mortality and/or Increased Risk of Tumor Progression or Recurrence in Patients with Cancer [see Warnings and Precautions (5.2)]
- Hypertension [see Warnings and Precautions (5.3)]
- Seizures [see Warnings and Precautions (5.4)]
- PRCA [see Warnings and Precautions (5.6)]
- Serious Allergic Reactions [see Warnings and Precautions (5.7)]
- Severe Cutaneous Reactions [see Warnings and Precautions (5.8)]
2.5 Surgery Patients
The recommended PROCRIT regimens are:
- 300 Units/kg per day subcutaneously for 15 days total: administered daily for 10 days before surgery, on the day of surgery, and for 4 days after surgery.
- 600 Units/kg subcutaneously in 4 doses administered 21, 14, and 7 days before surgery and on the day of surgery.
Deep venous thrombosis prophylaxis is recommended during PROCRIT therapy [see Warnings and Precautions (5.1)] .
12.2 Pharmacodynamics
PROCRIT increases the reticulocyte count within 10 days of initiation, followed by increases in the RBC count, hemoglobin, and hematocrit, usually within 2 to 6 weeks. The rate of hemoglobin increase varies among patients and is dependent upon the dose of PROCRIT administered. For correction of anemia in hemodialysis patients, a greater biologic response is not observed at doses exceeding 300 Units/kg 3 times weekly.
12.3 Pharmacokinetics
In adult and pediatric patients with CKD, the elimination half-life (t 1/2) of plasma erythropoietin after intravenous administration of PROCRIT ranged from 4 to 13 hours. After subcutaneous administration, C maxwas achieved within 5 to 24 hours. The t 1/2in adult patients with serum creatinine greater than 3 mg/dL was similar between those not on dialysis and those maintained on dialysis. The pharmacokinetic data indicate no apparent difference in PROCRIT t 1/2among adult patients above or below 65 years of age.
A pharmacokinetic study comparing 150 Units/kg subcutaneous 3 times weekly to 40,000 Units subcutaneous weekly dosing regimen was conducted for 4 weeks in healthy subjects (n=12) and for 6 weeks in anemic cancer patients (n=32) receiving cyclic chemotherapy. There was no accumulation of serum erythropoietin after the 2 dosing regimens during the study period. The 40,000 Units weekly regimen had a higher C max(3- to 7-fold), longer T max(2- to 3-fold), higher AUC 0–168 h(2- to 3-fold) of erythropoietin and lower clearance (CL) (50%) than the 150 Units/kg 3 times weekly regimen. In anemic cancer patients, the average t 1/2was similar (40 hours with range of 16 to 67 hours) after both dosing regimens. After the 150 Units/kg 3 times weekly dosing, the values of T maxand CL were similar (13.3 ± 12.4 vs. 14.2 ± 6.7 hours, and 20.2 ± 15.9 vs. 23.6 ± 9.5 mL/hr/kg) between week 1 when patients were receiving chemotherapy (n=14) and week 3 when patients were not receiving chemotherapy (n=4). Differences were observed after the 40,000 Units weekly dosing with longer T max(38 ± 18 hours) and lower CL (9.2 ± 4.7 mL/hr/kg) during week 1 when patients were receiving chemotherapy (n=18) compared with those (22 ± 4.5 hours, 13.9 ± 7.6 mL/hr/kg, respectively) during week 3 when patients were not receiving chemotherapy (n=7).
The pharmacokinetic profile of PROCRIT in pediatric patients appeared similar to that of adults.
The pharmacokinetics of PROCRIT has not been studied in patients with HIV Infection.
14.4 Surgery Patients
The safety and efficacy of PROCRIT were evaluated in a placebo-controlled, double-blind study (S1) enrolling 316 patients scheduled for major, elective orthopedic hip or knee surgery who were expected to require ≥ 2 units of blood and who were not able or willing to participate in an autologous blood donation program. Patients were stratified into 1 of 3 groups based on their pretreatment hemoglobin [≤ 10 g/dL (n=2), > 10 to ≤ 13 g/dL (n=96), and > 13 to ≤ 15 g/dL (n=218)] and then randomly assigned to receive 300 Units/kg PROCRIT, 100 Units/kg PROCRIT, or placebo by subcutaneous injection for 10 days before surgery, on the day of surgery, and for 4 days after surgery. All patients received oral iron and a low-dose, postoperative warfarin regimen.
Treatment with PROCRIT 300 Units/kg significantly (p=0.024) reduced the risk of allogeneic RBC transfusion in patients with a pretreatment hemoglobin of > 10 to ≤ 13 g/dL; 5/31 (16%) of patients treated with PROCRIT 300 Units/kg, 6/26 (23%) of patients treated with PROCRIT 100 Units/kg, and 13/29 (45%) of placebo-treated patients were transfused. There was no significant difference in the number of patients transfused between PROCRIT (9% 300 Units/kg, 6% 100 Units/kg) and placebo (13%) in the > 13 to ≤ 15 g/dL hemoglobin stratum. There were too few patients in the ≤ 10 g/dL group to determine if PROCRIT is useful in this hemoglobin strata. In the > 10 to ≤ 13 g/dL pretreatment stratum, the mean number of units transfused per PROCRIT-treated patient (0.45 units blood for 300 Units/kg, 0.42 units blood for 100 Units/kg) was less than the mean transfused per placebo-treated patient (1.14 units) (overall p=0.028). In addition, mean hemoglobin, hematocrit, and reticulocyte counts increased significantly during the presurgery period in patients treated with PROCRIT.
PROCRIT was also evaluated in an open-label, parallel-group study (S2) enrolling 145 patients with a pretreatment hemoglobin level of ≥ 10 to ≤ 13 g/dL who were scheduled for major orthopedic hip or knee surgery and who were not participating in an autologous program. Patients were randomly assigned to receive 1 of 2 subcutaneous dosing regimens of PROCRIT (600 Units/kg once weekly for 3 weeks prior to surgery and on the day of surgery, or 300 Units/kg once daily for 10 days prior to surgery, on the day of surgery, and for 4 days after surgery). All patients received oral iron and appropriate pharmacologic anticoagulation therapy.
From pretreatment to presurgery, the mean increase in hemoglobin in the 600 Units/kg weekly group (1.44 g/dL) was greater than that observed in the 300 Units/kg daily group. The mean increase in absolute reticulocyte count was smaller in the weekly group (0.11 × 10 6/mm 3) compared to the daily group (0.17 × 10 6/mm 3). Mean hemoglobin levels were similar for the 2 treatment groups throughout the postsurgical period.
The erythropoietic response observed in both treatment groups resulted in similar RBC transfusion rates [11/69 (16%) in the 600 Units/kg weekly group and 14/71 (20%) in the 300 Units/kg daily group]. The mean number of units transfused per patient was approximately 0.3 units in both treatment groups.
1.5 Limitations of Use
PROCRIT has not been shown to improve quality of life, fatigue, or patient well-being.
PROCRIT is not indicated for use:
- In patients with cancer receiving hormonal agents, biologic products, or radiotherapy, unless also receiving concomitant myelosuppressive chemotherapy.
- In patients with cancer receiving myelosuppressive chemotherapy when the anticipated outcome is cure.
- In patients with cancer receiving myelosuppressive chemotherapy in whom the anemia can be managed by transfusion.
- In patients scheduled for surgery who are willing to donate autologous blood.
- In patients undergoing cardiac or vascular surgery.
- As a substitute for RBC transfusions in patients who require immediate correction of anemia.
1 Indications and Usage (1 INDICATIONS AND USAGE)
PROCRIT is an erythropoiesis-stimulating agent (ESA) indicated for:
- Treatment of anemia due to
- Chronic Kidney Disease (CKD) in patients on dialysis and not on dialysis ( 1.1).
- Zidovudine in patients with Human Immunodeficiency Virus (HIV) infection ( 1.2).
- The effects of concomitant myelosuppressive chemotherapy, and upon initiation, there is a minimum of two additional months of planned chemotherapy ( 1.3).
- Reduction of allogeneic red blood cell (RBC) transfusions in patients undergoing elective, noncardiac, nonvascular surgery ( 1.4).
Limitations of Use
PROCRIT has not been shown to improve quality of life, fatigue, or patient well-being ( 1.5).
PROCRIT is not indicated for use:
- In patients with cancer receiving hormonal agents, biologic products, or radiotherapy, unless also receiving concomitant myelosuppressive chemotherapy ( 1.5).
- In patients with cancer receiving myelosuppressive chemotherapy when the anticipated outcome is cure ( 1.5).
- In patients with cancer receiving myelosuppressive chemotherapy in whom the anemia can be managed by transfusion ( 1.5).
- In patients scheduled for surgery who are willing to donate autologous blood ( 1.5).
- In patients undergoing cardiac or vascular surgery ( 1.5).
- As a substitute for RBC transfusions in patients who require immediate correction of anemia ( 1.5).
12.1 Mechanism of Action
PROCRIT stimulates erythropoiesis by the same mechanism as endogenous erythropoietin.
5.11 Dialysis Management
Patients may require adjustments in their dialysis prescriptions after initiation of PROCRIT. Patients receiving PROCRIT may require increased anticoagulation with heparin to prevent clotting of the extracorporeal circuit during hemodialysis.
9.1 Controlled Substance
PROCRIT contains epoetin alfa, which is not a controlled substance.
5.6 Pure Red Cell Aplasia
Cases of PRCA and of severe anemia, with or without other cytopenias that arise following the development of neutralizing antibodies to erythropoietin have been reported in patients treated with PROCRIT. This has been reported predominantly in patients with CKD receiving ESAs by subcutaneous administration. PRCA has also been reported in patients receiving ESAs for anemia related to hepatitis C treatment (an indication for which PROCRIT is not approved).
If severe anemia and low reticulocyte count develop during treatment with PROCRIT, withhold PROCRIT and evaluate patients for neutralizing antibodies to erythropoietin. Contact Janssen Products, LP at 1-800-JANSSEN (1-800-526-7736) to perform assays for binding and neutralizing antibodies. Permanently discontinue PROCRIT in patients who develop PRCA following treatment with PROCRIT or other erythropoietin protein drugs. Do not switch patients to other ESAs.
5 Warnings and Precautions (5 WARNINGS AND PRECAUTIONS)
- Increased Mortality, Myocardial Infarction, Stroke, and Thromboembolism: Using ESAs to target a hemoglobin level of greater than 11 g/dL increases the risk of serious adverse cardiovascular reactions and has not been shown to provide additional benefit ( 5.1and 14.1). Use caution in patients with coexistent cardiovascular disease and stroke ( 5.1).
- Increased Mortality and/or Increased Risk of Tumor Progression or Recurrence in Patients with Cancer ( 5.2).
- Hypertension: Control hypertension prior to initiating and during treatment with PROCRIT ( 5.3).
- Seizures: PROCRIT increases the risk for seizures in patients with CKD ( 5.4). Increase monitoring of these patients for changes in seizure frequency or premonitory symptoms ( 5.4).
- PRCA: If severe anemia and low reticulocyte count develop during PROCRIT treatment, withhold PROCRIT and evaluate for PRCA ( 5.6).
- Serious Allergic Reactions: Discontinue PROCRIT and manage reactions ( 5.7).
- Severe Cutaneous Reactions: Discontinue PROCRIT ( 5.8).
2 Dosage and Administration (2 DOSAGE AND ADMINISTRATION)
- Evaluate iron status before and during treatment and maintain iron repletion. Correct or exclude other causes of anemia before initiating treatment ( 2.1).
- In pregnant women, lactating women, neonates, infants: Use only single-dose vials ( 2.1).
- Patients with CKD: Initial dose: 50 to 100 Units/kg 3 times weekly (adults) and 50 Units/kg 3 times weekly (pediatric patients). Individualize maintenance dose. Intravenous route recommended for patients on hemodialysis ( 2.2).
- Patients on Zidovudine due to HIV Infection: 100 Units/kg 3 times weekly ( 2.3).
- Patients with Cancer on Chemotherapy: 40,000 Units weekly or 150 Units/kg 3 times weekly (adults); 600 Units/kg intravenously weekly (pediatric patients ≥ 5 years) ( 2.4).
- Surgery Patients: 300 Units/kg per day daily for 15 days or 600 Units/kg weekly ( 2.5).
3 Dosage Forms and Strengths (3 DOSAGE FORMS AND STRENGTHS)
Injection:
- 2,000 Units/mL, 3,000 Units/mL, 4,000 Units/mL, 10,000 Units/mL, and 40,000 Units/mL of PROCRIT as a clear and colorless liquid in single-dose vials
- 20,000 Units/2 mL (10,000 Units/mL) and 20,000 Units/mL of PROCRIT as a clear and colorless liquid in multiple-dose vials (contains benzyl alcohol)
6.2 Postmarketing Experience
The following adverse reactions have been identified during post-approval use of PROCRIT.
Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
- Seizures [see Warnings and Precautions (5.4)]
- PRCA [see Warnings and Precautions (5.6)]
- Serious Allergic Reactions [see Warnings and Precautions (5.7)]
- Injection Site Reactions, including irritation and pain
- Porphyria
- Severe Cutaneous Reactions [see Warnings and Precautions (5.8)]
6.1 Clinical Trial Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of other drugs and may not reflect the rates observed in practice.
5.7 Serious Allergic Reactions
Serious allergic reactions, including anaphylactic reactions, angioedema, bronchospasm, skin rash, and urticaria may occur with PROCRIT. Immediately and permanently discontinue PROCRIT and administer appropriate therapy if a serious allergic or anaphylactic reaction occurs.
5.8 Severe Cutaneous Reactions
Blistering and skin exfoliation reactions including Erythema multiforme and Stevens-Johnson Syndrome (SJS)/Toxic Epidermal Necrolysis (TEN), have been reported in patients treated with ESAs (including PROCRIT) in the postmarketing setting. Discontinue PROCRIT therapy immediately if a severe cutaneous reaction, such as SJS/TEN, is suspected.
17 Patient Counseling Information (17 PATIENT COUNSELING INFORMATION)
Advise the patient to read the FDA-approved patient labeling (Medication Guide and Instructions for Use).
Inform patients:
- Of the increased risks of mortality, serious cardiovascular reactions, thromboembolic reactions, stroke, and tumor progression [see Warnings and Precautions (5.1, 5.2)] .
- To undergo regular blood pressure monitoring, adhere to prescribed anti-hypertensive regimen and follow recommended dietary restrictions.
- To contact their healthcare provider for new-onset neurologic symptoms or change in seizure frequency.
- Of the need to have regular laboratory tests for hemoglobin.
- Risks are associated with benzyl alcohol in neonates, infants, pregnant women, and lactating women [see Use in Specific Populations (8.1, 8.2, 8.4)].
Instruct patients who self-administer PROCRIT of the:
- Importance of following the Instructions for Use.
- Dangers of reusing needles, syringes, or unused portions of single-dose vials.
- Proper disposal of used syringes, needles, and unused vials, and of the full container.
2.6 Preparation and Administration
- Do not shake. Do not use PROCRIT that has been shaken or frozen.
- Protect vials from light.
- Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration. Do not use any vials exhibiting particulate matter or discoloration.
- Discard unused portions of PROCRIT in preservative-free vials. Do not re-enter preservative-free vials.
- Store unused portions of PROCRIT in multiple-dose vials at 36°F to 46°F (2°C to 8°C). Discard 21 days after initial entry.
- Do not dilute. Do not mix with other drug solutions except for admixing as described below:
Preservative-free PROCRIT from single-dose vials may be admixed in a syringe with bacteriostatic 0.9% sodium chloride injection, USP, with benzyl alcohol 0.9% (bacteriostatic saline) in a 1:1 ratio using aseptic technique at the time of administration. Do not mix PROCRIT with bacteriostatic saline when administering to pregnant women, lactating women, neonates, and infants [see Use in Specific Populations (8.1, 8.2, 8.4)].
2.4 Patients On Cancer Chemotherapy (2.4 Patients on Cancer Chemotherapy)
Initiate PROCRIT in patients on cancer chemotherapy only if the hemoglobin is less than 10 g/dL, and if there is a minimum of two additional months of planned chemotherapy.
Use the lowest dose of PROCRIT necessary to avoid RBC transfusions.
16 How Supplied/storage and Handling (16 HOW SUPPLIED/STORAGE AND HANDLING)
PROCRIT (epoetin alfa) injection is a sterile, clear, and colorless solution available as:
Preservative-free, single-dose vials (in citrate-buffered formulation): 2,000 Units/mL (NDC 59676-302-01), 3,000 Units/mL (NDC 59676-303-01), 4,000 Units/mL (NDC 59676-304-01), or 10,000 Units/mL (NDC 59676-310-01) supplied in cartons, each carton containing six 1 mL single-dose vials.
Preservative-free, single-dose vials (in citrate-buffered formulation): 10,000 Units/mL (NDC 59676-310-02) supplied in dispensing packs (tray) containing 25 single-dose 1 mL vials.
Preservative-free, single-dose vials (in phosphate-buffered formulation): 40,000 Units/mL (NDC 59676-340-01) supplied in dispensing packs containing four 1 mL single-dose vials.
Preserved, multiple-dose vials: 20,000 Units/2mL (10,000 Units/mL) (NDC 59676-312-04) supplied in dispensing packs containing four 2 mL multiple-dose vials.
Preserved, multiple-dose vials: 20,000 Units/mL (NDC 59676-320-04) supplied in dispensing packs containing four 1 mL multiple-dose vials.
1.1 Anemia Due to Chronic Kidney Disease
PROCRIT is indicated for the treatment of anemia due to chronic kidney disease (CKD), including patients on dialysis and not on dialysis to decrease the need for red blood cell (RBC) transfusion.
2.2 Patients With Chronic Kidney Disease (2.2 Patients with Chronic Kidney Disease)
In controlled trials, patients experienced greater risks for death, serious adverse cardiovascular reactions, and stroke when administered ESAs to target a hemoglobin level of greater than 11 g/dL. No trial has identified a hemoglobin target level, ESA dose, or dosing strategy that does not increase these risks. Individualize dosing and use the lowest dose of PROCRIT sufficient to reduce the need for RBC transfusions [see Warnings and Precautions (5.1)] . Physicians and patients should weigh the possible benefits of decreasing transfusions against the increased risks of death and other serious cardiovascular adverse reactions [see Boxed Warningand Clinical Studies (14)].
14.3 Patients With Cancer On Chemotherapy (14.3 Patients with Cancer on Chemotherapy)
The safety and effectiveness of PROCRIT was assessed in two multicenter, randomized (1:1), placebo-controlled, double-blind studies (Study C1 and Study C2) and a pooled analysis of six additional randomized (1:1), multicenter, placebo-controlled, double-blind studies. All studies were conducted in patients with anemia due to concomitantly administered cancer chemotherapy. Study C1 enrolled 344 adult patients, Study C2 enrolled 222 pediatric patients, and the pooled analysis contained 131 patients randomized to epoetin alfa or placebo. In Studies C1 and C2, efficacy was demonstrated by a reduction in the proportion of patients who received an RBC transfusion, from week 5 through end of the study, with the last-known RBC transfusion status carried forward for patients who discontinued treatment. In the pooled analysis, efficacy was demonstrated by a reduction in the proportion of patients who received an RBC transfusion from week 5 through end of the study in the subset of patients who were remaining on therapy for 6 or more weeks.
Principal Display Panel 2,000 Unit Vial Carton (PRINCIPAL DISPLAY PANEL - 2,000 Unit Vial Carton)
2,000 Units/mL
NDC 59676
-302-01
6-1 mL Single-dose vials
Discard unused portion.
PROCRIT
®
EPOETIN ALFA
2,000 Units/mL
For Intravenous or Subcutaneous Use Only
Sterile Solution — No Preservative
Attention: Dispense the enclosed Medication Guide to each patient.
For more copies see Procrit.com or call 1-800-526-7736.
Each 1 mL vial contains: 2,000 units of recombinant epoetin alfa and
2.5 mg Albumin (Human) in a sterile, buffered solution (pH 6.9 ± 0.3)
of sodium citrate (5.8 mg), sodium chloride (5.9 mg) and citric acid
(0.06 mg) in Water for Injection, USP. No U.S. standard of potency.
Rx only
Principal Display Panel 3,000 Unit Vial Carton (PRINCIPAL DISPLAY PANEL - 3,000 Unit Vial Carton)
3,000 Units/mL
NDC59676
-303-01
6-1 mL Single-dose vials
Discard unused portion.
PROCRIT
®
EPOETIN ALFA
3,000 Units/mL
For Intravenous or Subcutaneous Use Only
Sterile Solution — No Preservative
Attention: Dispense the enclosed Medication Guide to each patient.
For more copies see Procrit.com or call 1-800-526-7736.
Each 1 mL vial contains: 3,000 units of recombinant epoetin alfa and
2.5 mg Albumin (Human) in a sterile, buffered solution (pH 6.9 ± 0.3)
of sodium citrate (5.8 mg), sodium chloride (5.9 mg) and citric acid
(0.06 mg) in Water for Injection, USP. No U.S. standard of potency.
Rx only
Principal Display Panel 4,000 Unit Vial Carton (PRINCIPAL DISPLAY PANEL - 4,000 Unit Vial Carton)
4,000 Units/mL
NDC59676
-304-01
6-1 mL Single-dose vials
Discard unused portion.
PROCRIT
®
EPOETIN ALFA
4,000 Units/mL
For Intravenous or Subcutaneous Use Only
Sterile Solution — No Preservative
Attention: Dispense the enclosed Medication Guide to each patient.
For more copies see Procrit.com or call 1-800-526-7736.
Each 1 mL vial contains: 4,000 units of recombinant epoetin alfa and
2.5 mg Albumin (Human) in a sterile, buffered solution (pH 6.9 ± 0.3)
of sodium citrate (5.8 mg), sodium chloride (5.9 mg) and citric acid
(0.06 mg) in Water for Injection, USP. No U.S. standard of potency.
Rx only
Principal Display Panel 10,000 Unit Vial Carton (PRINCIPAL DISPLAY PANEL - 10,000 Unit Vial Carton)
10,000 Units/mL
NDC59676
-310-01
6-1 mL Single-dose vials
Discard unused portion.
PROCRIT
®
EPOETIN ALFA
10,000 Units/mL
For Intravenous or Subcutaneous Use Only
Sterile Solution — No Preservative
Attention: Dispense the enclosed Medication Guide to each patient.
For more copies see Procrit.com or call 1-800-526-7736.
Each 1 mL vial contains: 10,000 units of recombinant epoetin alfa and
2.5 mg Albumin (Human) in a sterile, buffered solution (pH 6.9 ± 0.3)
of sodium citrate (5.8 mg), sodium chloride (5.9 mg) and citric acid
(0.06 mg) in Water for Injection, USP. No U.S. standard of potency.
Rx only
Principal Display Panel 40,000 Unit Vial Carton (PRINCIPAL DISPLAY PANEL - 40,000 Unit Vial Carton)
40,000 Units/mL
NDC59676
-340-01
4-1 mL Single-dose vials
Discard unused portion.
PROCRIT
®
EPOETIN ALFA
40,000 Units/mL
For Intravenous or Subcutaneous Use Only
Sterile Solution — No Preservative
Attention: Dispense the enclosed Medication Guide to each patient.
For more copies see Procrit.com or call 1-800-526-7736.
Each 1 mL vial contains: 40,000 units of recombinant
epoetin alfa and 2.5 mg Albumin (Human) in a sterile,
buffered solution (pH 6.9 ± 0.3) of sodium phosphate
monobasic monohydrate (1.2 mg), sodium phosphate
dibasic anhydrate (1.8 mg), sodium citrate (0.7 mg),
sodium chloride (5.8 mg), and citric acid (6.8 mcg) in
Water for Injection, USP. No U.S. standard of potency.
Rx only
5.5 Lack Or Loss of Hemoglobin Response to Procrit (5.5 Lack or Loss of Hemoglobin Response to PROCRIT)
For lack or loss of hemoglobin response to PROCRIT, initiate a search for causative factors (e.g., iron deficiency, infection, inflammation, bleeding). If typical causes of lack or loss of hemoglobin response are excluded, evaluate for PRCA [see Warnings and Precautions (5.6)] . In the absence of PRCA, follow dosing recommendations for management of patients with an insufficient hemoglobin response to PROCRIT therapy [see Dosage and Administration (2.2)] .
14.2 Zidovudine Treated Patients With Hiv Infection (14.2 Zidovudine-treated Patients with HIV Infection)
The safety and efficacy of PROCRIT were evaluated in 4 placebo-controlled studies enrolling 297 anemic patients (hemoglobin < 10 g/dL) with HIV Infection receiving concomitant therapy with zidovudine. In the subgroup of patients (89/125 PROCRIT and 88/130 placebo) with pre-study endogenous serum erythropoietin levels ≤ 500 mUnits/mL, PROCRIT reduced the mean cumulative number of units of blood transfused per patient by approximately 40% as compared to the placebo group. Among those patients who required RBC transfusions at baseline, 43% of patients treated with PROCRIT versus 18% of placebo-treated patients were RBC transfusion-independent during the second and third months of therapy. PROCRIT therapy also resulted in significant increases in hemoglobin in comparison to placebo. When examining the results according to the weekly dose of zidovudine received during month 3 of therapy, there was a statistically significant reduction (p < 0.003) in RBC transfusion requirements in patients treated with PROCRIT (n=51) compared to placebo-treated patients (n=54) whose mean weekly zidovudine dose was ≤ 4200 mg/week.
Approximately 17% of the patients with endogenous serum erythropoietin levels ≤ 500 mUnits/mL receiving PROCRIT in doses from 100 to 200 Units/kg 3 times weekly achieved a hemoglobin of 12.7 g/dL without administration of RBC transfusions or significant reduction in zidovudine dose. In the subgroup of patients whose pre-study endogenous serum erythropoietin levels were > 500 mUnits/mL, PROCRIT therapy did not reduce RBC transfusion requirements or increase hemoglobin compared to the corresponding responses in placebo-treated patients.
1.3 Anemia Due to Chemotherapy in Patients With Cancer (1.3 Anemia Due to Chemotherapy in Patients with Cancer)
PROCRIT is indicated for the treatment of anemia in patients with non-myeloid malignancies where anemia is due to the effect of concomitant myelosuppressive chemotherapy, and upon initiation, there is a minimum of two additional months of planned chemotherapy.
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
The carcinogenic potential of PROCRIT has not been evaluated.
PROCRIT was not mutagenic or clastogenic under the conditions tested: PROCRIT was negative in the in vitrobacterial reverse mutation assay (Ames test), in the in vitromammalian cell gene mutation assay (the hypoxanthine-guanine phosphoribosyl transferase [HGPRT] locus), in an in vitrochromosomal aberration assay in mammalian cells, and in the in vivomouse micronucleus assay.
When administered intravenously to male and female rats prior to and during mating, and to females through the beginning of implantation (up to gestational day 7; dosing stopped prior to the beginning of organogenesis), doses of 100 and 500 Units/kg/day of PROCRIT caused slight increases in pre-implantation loss, post-implantation loss and decreases in the incidence of live fetuses. It is not clear whether these effects reflect a drug effect on the uterine environment or on the conceptus. This animal dose level of 100 Units/kg/day approximates the clinical recommended starting dose, depending on the patient's treatment indication, but may be lower than the clinical dose in patients whose doses have been adjusted.
1.2 Anemia Due to Zidovudine in Patients With Hiv Infection (1.2 Anemia Due to Zidovudine in Patients with HIV Infection)
PROCRIT is indicated for the treatment of anemia due to zidovudine administered at ≤ 4200 mg/week in patients with HIV Infection with endogenous serum erythropoietin levels of ≤ 500 mUnits/mL.
5.10 Risk of Infectious Diseases Due to Albumin (human) Content (5.10 Risk of Infectious Diseases Due to Albumin (Human) Content)
PROCRIT contains albumin, a derivative of human blood [see Description (11)] . Based on effective donor screening and product manufacturing processes, it carries an extremely remote risk for transmission of viral diseases. A theoretical risk for transmission of Creutzfeldt-Jakob disease (CJD) also is considered extremely remote. No cases of transmission of viral diseases or CJD have ever been identified for albumin.
Principal Display Panel 20,000 Units/ml Multiple Dose Vial Carton (PRINCIPAL DISPLAY PANEL - 20,000 Units/mL Multiple-dose Vial Carton)
PRINCIPAL DISPLAY PANEL - 20,000 Unit Vial Carton
20,000 Units/mL
NDC59676-
320-04
4-1 mL Multiple-dose Vials
PROCRIT
®
EPOETIN ALFA
20,000 Units/mL
Multiple-dose Vials
Sterile solution — Preserved. 20,000 Units/mL
For Intravenous or Subcutaneous Use Only
Attention: Dispense the enclosed Medication Guide to each patient.
For more copies see Procrit.com or call 1-800-526-7736.
1 mL
Rx only
Principal Display Panel 20,000 Units/2 Ml Multiple Dose Vial Carton (PRINCIPAL DISPLAY PANEL - 20,000 Units/2 mL Multiple-dose Vial Carton)
PRINCIPAL DISPLAY PANEL - 20,000 Units/2 mL Vial Carton
20,000 Units/2 mL
(10,000 Units/mL)
NDC59676-
312-04
4-2 mL Multiple-dose Vials
PROCRIT
®
EPOETIN ALFA
20,000 Units/2 mL (10,000 Units/mL)
Multiple-dose Vials
Sterile solution — Preserved. 10,000 Units/mL
For Intravenous or Subcutaneous Use Only.
Attention: Dispense the enclosed Medication Guide to each patient.
For more copies see Procrit.com or call 1-800-526-7736.
2 mL
Rx only
5.9 Risk of Serious Adverse Reactions Due to Benzyl Alcohol Preservative
PROCRIT from multiple-dose vials contains benzyl alcohol and is contraindicated for use in neonates, infants, pregnant women, and lactating women [see Contraindications (4)] . In addition, do not mix PROCRIT with bacteriostatic saline (which also contains benzyl alcohol) when administering PROCRIT to these patient populations [see Dosage and Administration (2)].
Serious and fatal reactions including "gasping syndrome" can occur in neonates and infants treated with benzyl alcohol-preserved drugs, including PROCRIT multiple-dose vials. The "gasping syndrome" is characterized by central nervous system (CNS) depression, metabolic acidosis, and gasping respirations. There is a potential for similar risks to fetuses and infants exposed to benzyl alcohol in uteroor in breast-fed milk, respectively. PROCRIT multiple-dose vials contain 11 mg of benzyl alcohol per mL. The minimum amount of benzyl alcohol at which serious adverse reactions may occur is not known [see Use in Specific Populations (8.1, 8.2, and 8.4)] .
5.1 Increased Mortality, Myocardial Infarction, Stroke, and Thromboembolism
- In controlled clinical trials of patients with CKD comparing higher hemoglobin targets (13 – 14 g/dL) to lower targets (9 – 11.3 g/dL), PROCRIT and other ESAs increased the risk of death, myocardial infarction, stroke, congestive heart failure, thrombosis of hemodialysis vascular access, and other thromboembolic events in the higher target groups.
- Using ESAs to target a hemoglobin level of greater than 11 g/dL increases the risk of serious adverse cardiovascular reactions and has not been shown to provide additional benefit [see Clinical Studies (14.1)] . Use caution in patients with coexistent cardiovascular disease and stroke [see Dosage and Administration (2.2)] . Patients with CKD and an insufficient hemoglobin response to ESA therapy may be at even greater risk for cardiovascular reactions and mortality than other patients. A rate of hemoglobin rise of greater than 1 g/dL over 2 weeks may contribute to these risks.
- In controlled clinical trials of patients with cancer, PROCRIT and other ESAs increased the risks for death and serious adverse cardiovascular reactions. These adverse reactions included myocardial infarction and stroke.
- In controlled clinical trials, ESAs increased the risk of death in patients undergoing coronary artery bypass graft surgery (CABG) and the risk of deep venous thrombosis (DVT) in patients undergoing orthopedic procedures.
The design and overall results of the 3 large trials comparing higher and lower hemoglobin targets are shown in Table 1.
| Normal Hematocrit Study (NHS)
(N=1265) |
CHOIR
(N=1432) |
TREAT
(N=4038) |
|
|---|---|---|---|
| Time Period of Trial | 1993 to 1996 | 2003 to 2006 | 2004 to 2009 |
| Population | CKD patients on hemodialysis with coexisting CHF or CAD, hematocrit 30 ± 3% on epoetin alfa | CKD patients not on dialysis with hemoglobin < 11 g/dL not previously administered epoetin alfa | CKD patients not on dialysis with type II diabetes, hemoglobin ≤ 11 g/dL |
|
Hemoglobin Target;
Higher vs. Lower (g/dL) |
14.0 vs. 10.0 | 13.5 vs. 11.3 | 13.0 vs. ≥ 9.0 |
|
Median (Q1, Q3)
Achieved Hemoglobin level (g/dL) |
12.6 (11.6, 13.3) vs. 10.3 (10.0, 10.7) | 13.0 (12.2, 13.4) vs. 11.4 (11.1, 11.6) | 12.5 (12.0, 12.8) vs. 10.6 (9.9, 11.3) |
| Primary Endpoint | All-cause mortality or non-fatal MI | All-cause mortality, MI, hospitalization for CHF, or stroke | All-cause mortality, MI, myocardial ischemia, heart failure, and stroke |
| Hazard Ratio or Relative Risk (95% CI) | 1.28 (1.06 – 1.56) | 1.34 (1.03 – 1.74) | 1.05 (0.94 – 1.17) |
| Adverse Outcome for Higher Target Group | All-cause mortality | All-cause mortality | Stroke |
| Hazard Ratio or Relative Risk (95% CI) | 1.27 (1.04 – 1.54) | 1.48 (0.97 – 2.27) | 1.92 (1.38 – 2.68) |
5.2 Increased Mortality And/or Increased Risk of Tumor Progression Or Recurrence in Patients With Cancer (5.2 Increased Mortality and/or Increased Risk of Tumor Progression or Recurrence in Patients with Cancer)
ESAs resulted in decreased locoregional control/progression-free survival (PFS) and/or overall survival (OS) (see Table 2).
Adverse effects on PFS and/or OS were observed in studies of patients receiving chemotherapy for breast cancer (Studies 1, 2, and 4), lymphoid malignancy (Study 3), and cervical cancer (Study 5); in patients with advanced head and neck cancer receiving radiation therapy (Studies 6 and 7); and in patients with non-small cell lung cancer or various malignancies who were not receiving chemotherapy or radiotherapy (Studies 8 and 9).
| Study/Tumor/(n) | Hemoglobin Target | Achieved Hemoglobin
(Median; Q1, Q3 Q1=25
th percentile, Q3=75
th percentile
)
|
Primary Efficacy Outcome | Adverse Outcome for ESA- containing Arm |
|---|---|---|---|---|
| Chemotherapy | ||||
|
Study 1
Metastatic breast cancer (n=2098) |
≤12 g/dL
This study did not include a defined hemoglobin target. Doses were titrated to achieve and maintain the lowest hemoglobin level sufficient to avoid transfusion and not to exceed 12 g/dL.
|
11.6 g/dL
10.7, 12.1 g/dL |
Progression-free survival (PFS) | Decreased progression-free and overall survival |
|
Study 2
Metastatic breast cancer (n=939) |
12–14 g/dL | 12.9 g/dL;
12.2, 13.3 g/dL |
12-month overall survival | Decreased 12-month survival |
|
Study 3
Lymphoid malignancy (n=344) |
13–15 g/dL (M)
13–14 g/dL (F) |
11 g/dL;
9.8, 12.1 g/dL |
Proportion of patients achieving a hemoglobin response | Decreased overall survival |
|
Study 4
Early breast cancer (n=733) |
12.5–13 g/dL | 13.1 g/dL;
12.5, 13.7 g/dL |
Relapse-free and overall survival | Decreased 3-year relapse-free and overall survival |
|
Study 5
Cervical cancer (n=114) |
12–14 g/dL | 12.7 g/dL;
12.1, 13.3 g/dL |
Progression-free and overall survival and locoregional control | Decreased 3-year progression-free and overall survival and locoregional control |
| Radiotherapy Alone | ||||
|
Study 6
Head and neck cancer (n=351) |
≥ 15 g/dL (M)
≥ 14 g/dL (F) |
Not available | Locoregional progression-free survival | Decreased 5-year locoregional progression-free and overall survival |
|
Study 7
Head and neck cancer (n=522) |
14–15.5 g/dL | Not available | Locoregional disease control | Decreased locoregional disease control |
| No Chemotherapy or Radiotherapy | ||||
|
Study 8
Non-small cell lung cancer (n=70) |
12–14 g/dL | Not available | Quality of life | Decreased overall survival |
|
Study 9
Non-myeloid malignancy (n=989) |
12–13 g/dL | 10.6 g/dL;
9.4, 11.8 g/dL |
RBC transfusions | Decreased overall survival |
1.4 Reduction of Allogeneic Red Blood Cell Transfusions in Patients Undergoing Elective, Noncardiac, Nonvascular Surgery
PROCRIT is indicated to reduce the need for allogeneic RBC transfusions among patients with perioperative hemoglobin > 10 to ≤ 13 g/dL who are at high risk for perioperative blood loss from elective, noncardiac, nonvascular surgery. PROCRIT is not indicated for patients who are willing to donate autologous blood pre-operatively.
Warning: Esas Increase the Risk of Death, Myocardial Infarction, Stroke, Venous Thromboembolism, Thrombosis of Vascular Access and Tumor Progression Or Recurrence (WARNING: ESAs INCREASE THE RISK OF DEATH, MYOCARDIAL INFARCTION, STROKE, VENOUS THROMBOEMBOLISM, THROMBOSIS OF VASCULAR ACCESS AND TUMOR PROGRESSION OR RECURRENCE)
WARNING: ESAs INCREASE THE RISK OF DEATH, MYOCARDIAL INFARCTION, STROKE, VENOUS THROMBOEMBOLISM, THROMBOSIS OF VASCULAR ACCESS AND TUMOR PROGRESSION OR RECURRENCE
See full prescribing information for complete boxed warning.
Chronic Kidney Disease:
- In controlled trials, patients experienced greater risks for death, serious adverse cardiovascular reactions, and stroke when administered erythropoiesis-stimulating agents (ESAs) to target a hemoglobin level of greater than 11 g/dL ( 5.1).
- No trial has identified a hemoglobin target level, ESA dose, or dosing strategy that does not increase these risks ( 2.2).
- Use the lowest PROCRIT dose sufficient to reduce the need for red blood cell (RBC) transfusions ( 5.1).
Cancer:
- ESAs shortened overall survival and/or increased the risk of tumor progression or recurrence in clinical studies of patients with breast, non-small cell lung, head and neck, lymphoid, and cervical cancers ( 5.2).
- Use the lowest dose to avoid RBC transfusions ( 2.4).
- Use ESAs only for anemia from myelosuppressive chemotherapy ( 1.3).
- ESAs are not indicated for patients receiving myelosuppressive chemotherapy when the anticipated outcome is cure ( 1.5).
- Discontinue following the completion of a chemotherapy course ( 2.4).
Perisurgery:
- Due to increased risk of deep venous thrombosis (DVT), DVT prophylaxis is recommended ( 5.1).
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:46:33.657595 · Updated: 2026-03-14T22:25:04.498043