Dolishaletm
036a15be-8c2e-4f65-b5dc-f333e2994d4a
34391-3
HUMAN PRESCRIPTION DRUG LABEL
Drug Facts
Composition & Product
Identifiers & Packaging
Description
Patients should be counseled that oral contraceptives do not protect against transmission of HIV (AIDS) and other sexually transmitted diseases (STDs) such as chlamydia, genital herpes, genital warts, gonorrhea, hepatitis B, and syphilis.
Indications and Usage
DOLISHALE is indicated for the prevention of pregnancy in women who elect to use oral contraceptives as a method of contraception. Oral contraceptives are highly effective for pregnancy prevention. Table 2 lists the typical unintended pregnancy rates for users of combination oral contraceptives and other methods of contraception. The efficacy of these contraceptive methods, except sterilization, the IUD, and implants, depend upon the reliability with which they are used. Correct and consistent use of methods can result in lower failure rates. Table 2: Percentage of Women Experiencing an Unintended Pregnancy During The First Year of Typical Use and The First Year of Perfect Use of Contraception and The Percentage Continuing Use at The End of the First Year. United States. % of Women Experiencing an Unintended Pregnancy within the First Year of Use % of Women Continuing Use at One Year 3 Method (1) Typical Use 1 (2) Perfect Use 2 (3) (4) Chance 4 85 85 Spermicides 5 26 6 40 Periodic abstinence 25 63 Calendar 9 Ovulation Method 3 Sympto-Thermal 6 2 Post-Ovulation 1 Cap 7 Parous Women 40 26 42 Nulliparous Women 20 9 56 Sponge Parous Women 40 20 42 Nulliparous Women 20 9 56 Diaphragm 7 20 6 56 Withdrawal 19 4 Condom 8 Female (Reality™) 21 5 56 Male 14 3 61 Pill 5 71 Progestin only 0.5 Combined 0.1 IUD Progesterone T 2.0 1.5 81 Copper T380A 0.8 0.6 78 LNg 20 0.1 0.1 81 Depo-Provera ® 0.3 0.3 70 Levonorgestrel Implants (Norplant ® ) 0.05 0.05 88 Female Sterilization 0.5 0.5 100 Male Sterilization 0.15 0.10 100 Emergency Contraceptive Pills: The FDA has concluded that certain combined oral contraceptives containing ethinyl estradiol and norgestrel or levonorgestrel are safe and effective for use as postcoital emergency contraception. Treatment initiated within 72 hours after unprotected intercourse reduces the risk of pregnancy by at least 75%. 9 Lactation Amenorrhea Method: LAM is a highly effective, temporary method of contraception. 10 Source: Trussell J. Contraceptive efficacy. In: Hatcher RA, Trussell J, Stewart F, Cates W, Stewart GK, Kowel D, Guest F. Contraceptive Technology: Seventeenth Revised Edition. New York NY: Irvington Publishers; 1998. 1. Among typical couples who initiate use of a method (not necessarily for the first time), the percentage who experience an accidental pregnancy during the first year if they do not stop use for any other reason. 2. Among couples who initiate use of a method (not necessarily for the first time) and who use it perfectly (both consistently and correctly), the percentage who experience an accidental pregnancy during the first year if they do not stop use for any other reason. 3. Among couples attempting to avoid pregnancy, the percentage who continue to use a method for one year. 4. The percents becoming pregnant in columns (2) and (3) are based on data from populations where contraception is not used and from women who cease using contraception in order to become pregnant. Among such populations, about 89% become pregnant within one year. This estimate was lowered slightly (to 85%) to represent the percent who would become pregnant within one year among women now relying on reversible methods of contraception if they abandoned contraception altogether. 5. Foams, creams, gels, vaginal suppositories, and vaginal film. 6. Cervical mucus (ovulation) method supplemented by calendar in the pre-ovulatory and basal body temperature in the post-ovulatory phases. 7. With spermicidal cream or jelly. 8. Without spermicides. 9. The treatment schedule is one dose within 72 hours after unprotected intercourse, and a second dose 12 hours after the first dose. The FDA has declared the following dosage regimens of oral contraceptives to be safe and effective for emergency contraception: for tablets containing 50 mcg of ethinyl estradiol and 500 mcg of norgestrel 1 dose is 2 tablets; for tablets containing 20 mcg of ethinyl estradiol and 100 mcg of levonorgestrel 1 dose is 5 tablets; for tablets containing 30 mcg of ethinyl estradiol and 150 mcg of levonorgestrel 1 dose is 4 tablets. 10. However, to maintain effective protection against pregnancy, another method of contraception must be used as soon as menstruation resumes, the frequency or duration of breastfeeds is reduced, bottle feeds are introduced, or the baby reaches 6 months of age.
Dosage and Administration
To achieve maximum contraceptive effectiveness, DOLISHALE (levonorgestrel and ethinyl estradiol tablets) must be taken exactly as directed and at intervals not exceeding 24 hours. The possibility of ovulation and conception prior to initiation of medication should be considered. Women who do not wish to become pregnant after discontinuation should be advised to immediately use another method of birth control. The dosage of DOLISHALE is one green tablet daily without any tablet-free interval. It is recommended that DOLISHALE tablets be taken at the same time each day. Initiation of Therapy Instructions for beginning DOLISHALE are provided in Table 4 below. Table 4 Current contraceptive therapy DOLISHALE start day Nonhormonal back-up method of birth control needed when correctly starting DOLISHALE? None Day 1 of patient's menstrual cycle (during the first 24 hours of her period) No 21-day COC regimen OR 28-day COC regimen Day 1 of patient's withdrawal bleed, at the latest 7 days after her last active tablet. No Progestin-only pill Day after taking a progestin-only pill Yes, for the first 7 days of DOLISHALE tablet taking Implant Day of implant removal Yes, for the first 7 days of DOLISHALE tablet taking Injection Day the next injection is due Yes, for the first 7 days of DOLISHALE tablet taking If spotting or unscheduled bleeding occurs, the patient is instructed to continue on the same regimen. This type of bleeding is usually transient and without significance; however, if the bleeding is persistent or prolonged, the patient is advised to consult her health care professional. The possibility of ovulation increases with each successive day that scheduled green tablets are missed. If the patient has not adhered to the prescribed schedule (missed one or more tablets or started taking them on a day later than she should have), the probability of pregnancy should be considered. Hormonal contraception must be discontinued if pregnancy is confirmed. The risk of pregnancy increases with each tablet missed. For additional patient instructions regarding missed tablets, see the WHAT TO DO IF YOU MISS PILLS section in the DETAILED PATIENT LABELING below. DOLISHALE may be initiated no earlier than day 28 postpartum in the nonlactating mother or after a second-trimester abortion due to the increased risk for thromboembolism (see CONTRAINDICATIONS , WARNINGS , and PRECAUTIONS concerning thromboembolic disease). The patient should be advised to use a nonhormonal back-up method for the first 7 days of tablet-taking. However, if intercourse has already occurred, pregnancy should be excluded before the start of combined oral contraceptive use or the patient must wait for her first menstrual period. In the case of first-trimester abortion, if the patient starts DOLISHALE immediately, additional contraceptive measures are not needed.
Contraindications
Combination oral contraceptives should not be used in women with any of the following conditions: • Thrombophlebitis or thromboembolic disorders • History of deep-vein thrombophlebitis or thromboembolic disorders • Cerebrovascular or coronary artery disease (current or past history) • Valvular heart disease with thrombogenic complications • Thrombogenic rhythm disorders • Hereditary or acquired thrombophilias • Major surgery with prolonged immobilization • Diabetes with vascular involvement • Headaches with focal neurological symptoms such as aura • Uncontrolled hypertension • Current diagnosis of, or history of, breast cancer, which may be hormone-sensitive • Carcinoma of the endometrium or other known or suspected estrogen-dependent neoplasia Undiagnosed abnormal genital bleeding • Cholestatic jaundice of pregnancy or jaundice with prior pill use • Hepatic adenomas or carcinomas, or active liver disease • Known or suspected pregnancy • Hypersensitivity to any of the components of DOLISHALE • Are receiving Hepatitis C drug combinations containing ombitasvir/paritaprevir/ritonavir, with or without dasabuvir, due to the potential for ALT elevations (see Warnings, RISK OF LIVER ENZYME ELEVATIONS WITH CONCOMITANT HEPATITIS C TREATMENT ).
Adverse Reactions
Post Marketing Experience Five studies that compared breast cancer risk between ever-users (current or past use) of COCs and never-users of COCs reported no association between ever use of COCs and breast cancer risk, with effect estimates ranging from 0.90 - 1.12 (Figure 6). Three studies compared breast cancer risk between current or recent COC users (<6 months since last use) and never users of COCs (Figure 6). One of these studies reported no association between breast cancer risk and COC use. The other two studies found an increased relative risk of 1.19 - 1.33 with current or recent use. Both of these studies found an increased risk of breast cancer with current use of longer duration, with relative risks ranging from 1.03 with less than one year of COC use to approximately 1.4 with more than 8-10 years of COC use. Figure 6. Risk of Breast Cancer with Combined Oral Contraceptive Use RR = relative risk; OR = odds ratio; HR = hazard ratio. “ever COC” are females with current or past COC use; “never COC use” are females that never used COCs. An increased risk of the following serious adverse reactions (see WARNINGS section for additional information) has been associated with the use of oral contraceptives: Thromboembolic and thrombotic disorders and other vascular problems (including thrombophlebitis and venous thrombosis with or without pulmonary embolism, mesenteric thrombosis, arterial thromboembolism, myocardial infarction, cerebral hemorrhage, cerebral thrombosis, transient ischemic attack), carcinoma of the reproductive organs and breasts, hepatic neoplasia/liver disease (including hepatic adenomas or benign liver tumors), ocular lesions (including retinal vascular thrombosis), gallbladder disease, carbohydrate and lipid effects, elevated blood pressure, and headache including migraine. The following adverse reactions have been reported in patients receiving oral contraceptives and are believed to be drug related (alphabetically listed): • Acne • Amenorrhea • Anaphylactic/anaphylactoid reactions, including urticaria, angioedema, and severe reactions with respiratory and circulatory symptoms • Breast changes: tenderness, pain, enlargement, secretion • Budd-Chiari syndrome • Cervical erosion and secretion, change in • Cholestatic jaundice • Chorea, exacerbation of • Colitis • Contact lenses, intolerance to • Corneal curvature (steepening), change in • Dizziness • Edema/fluid retention • Erythema multiforme • Erythema nodosum • Focal nodular hyperplasia • Gastrointestinal symptoms (such as abdominal pain, cramps, and bloating) • Hirsutism • Infertility after discontinuation of treatment, temporary • Lactation, diminution in, when given immediately postpartum • Libido, change in • Melasma/chloasma which may persist • Menstrual flow, change in • Mood changes, including depression • Nausea • Nervousness • Pancreatitis • Porphyria, exacerbation of • Rash (allergic) • Scalp hair, loss of • Serum folate levels, decrease in • Spotting • Systemic lupus erythematosus, exacerbation of • Unscheduled bleeding • Vaginitis, including candidiasis • Varicose veins, aggravation of • Vomiting • Weight or appetite (increase or decrease), change in The following adverse reactions have been reported in users of oral contraceptives: • Cataracts • Cystitis-like syndrome • Dysmenorrhea • Hemolytic uremic syndrome • Hemorrhagic eruption • Optic neuritis, which may lead to partial or complete loss of vision • Premenstrual syndrome • Renal function, impaired To report SUSPECTED ADVERSE REACTIONS, contact Ingenus Pharmaceuticals, LLC Toll-Free at 1-877-748-1970 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch .
Drug Interactions
Changes in Contraceptive Effectiveness Associated with Coadministration of Other Products: Contraceptive effectiveness may be reduced when hormonal contraceptives are coadministered with antibiotics, anticonvulsants, and other drugs that increase the metabolism of contraceptive steroids. This could result in unintended pregnancy or unscheduled bleeding. Examples include rifampin, rifabutin, barbiturates, primidone, phenylbutazone, phenytoin, dexamethasone, carbamazepine, felbamate, oxcarbazepine, topiramate, griseofulvin, and modafinil. In such cases a nonhormonal back-up method of birth control should be considered. Several cases of contraceptive failure and unscheduled bleeding have been reported in the literature with concomitant administration of antibiotics such as ampicillin and other penicillins, and tetracyclines. However, clinical pharmacology studies investigating drug interactions between combined oral contraceptives and these antibiotics have reported inconsistent results. Enterohepatic recirculation of estrogens may also be decreased by substances that reduce gut transit time. Several of the anti-HIV protease inhibitors have been studied with coadministration of oral combination hormonal contraceptives; significant changes (increase and decrease) in the plasma levels of the estrogen and progestin have been noted in some cases. The safety and efficacy of oral contraceptive products may be affected with coadministration of anti-HIV protease inhibitors. Health care professionals should refer to the label of the individual anti-HIV protease inhibitors for further drug-drug interaction information. Concomitant Use with HCV Combination Therapy – Liver Enzyme Elevation Do not co-administer DOLISHALE with HCV drug combinations containing ombitasvir/paritaprevir/ritonavir, with or without dasabuvir, due to potential for ALT elevations (see Warnings, RISK OF LIVER ENZYME ELEVATIONS WITH CONCOMITANT HEPATITIS C TREATMENT ). Herbal products containing St. John's Wort (Hypericum perforatum) may induce hepatic enzymes (cytochrome P 450) and p-glycoprotein transporter and may reduce the effectiveness of contraceptive steroids. This may also result in unscheduled bleeding. Increase in Plasma Levels Associated with Coadministered Drugs: Coadministration of atorvastatin and certain oral contraceptives containing ethinyl estradiol increases AUC values for ethinyl estradiol by approximately 20%. Ascorbic acid and acetaminophen increase the bioavailability of ethinyl estradiol since these drugs act as competitive inhibitors for sulfation of ethinyl estradiol in the gastrointestinal wall, a known pathway of elimination for ethinyl estradiol. CYP 3A4 inhibitors such as indinavir, itraconazole, ketoconazole, fluconazole, and troleandomycin may increase plasma hormone levels. Troleandomycin may also increase the risk of intrahepatic cholestasis during coadministration with combination oral contraceptives. Changes in Plasma Levels of Coadministered Drugs: Combination hormonal contraceptives containing some synthetic estrogens (eg, ethinyl estradiol) may inhibit the metabolism of other compounds. Increased plasma concentrations of cyclosporine, prednisolone and other corticosteroids, and theophylline have been reported with concomitant administration of oral contraceptives. Decreased plasma concentrations of acetaminophen and lamotrigine, and increased clearance of temazepam, salicylic acid, morphine, and clofibric acid, due to induction of conjugation (particularly glucuronidation), have been noted when these drugs were administered with oral contraceptives. The prescribing information of concomitant medications should be consulted to identify potential interactions.
How Supplied
DOLISHALE(90 mcg levonorgestrel and 20 mcg ethinyl estradiol) tablets are available in a blister pack, arranged in 4 rows of 7 active tablets as follows: 28 round, green biconvex tablets debossed with "H1" on one side. DOLISHALE Tablets are available in the following packaging configurations: Carton of 1 Blister Card of 28 Tablets NDC 50742-659-28 Carton of 3 Blister Cards of 28 Tablets Each NDC 50742-659-84 Carton of 6 Blister Cards of 28 Tablets Each NDC 50742-659-68 Store at 20° to 25°C (68° to 77°F). [See USP Controlled Room Temperature]. References available upon request. Rx Only Iss: 12/2024 I0154 Rev B Manufactured for: Ingenus Pharmaceuticals, LLC Orlando, FL 32839-6408 Product of China
Medication Information
Recent Major Changes
Cigarette smoking increases the risk of serious cardiovascular side effects from oral contraceptive use. This risk increases with age and with the extent of smoking (in epidemiologic studies, 15 or more cigarettes per day was associated with a significantly increased risk) and is quite marked in women over 35 years of age. Women who use oral contraceptives should be strongly advised not to smoke.
Indications and Usage
DOLISHALE is indicated for the prevention of pregnancy in women who elect to use oral contraceptives as a method of contraception.
Oral contraceptives are highly effective for pregnancy prevention. Table 2 lists the typical unintended pregnancy rates for users of combination oral contraceptives and other methods of contraception. The efficacy of these contraceptive methods, except sterilization, the IUD, and implants, depend upon the reliability with which they are used. Correct and consistent use of methods can result in lower failure rates.
Table 2: Percentage of Women Experiencing an Unintended Pregnancy During The First Year of Typical Use and The First Year of Perfect Use of Contraception and The Percentage Continuing Use at The End of the First Year. United States.
| % of Women Experiencing an Unintended Pregnancy within the First Year of Use | % of Women Continuing Use at One Year3 | ||
| Method (1) | Typical Use1 (2) | Perfect Use2 (3) | (4) |
| Chance4 | 85 | 85 | |
| Spermicides5 | 26 | 6 | 40 |
| Periodic abstinence | 25 | 63 | |
| Calendar | 9 | ||
| Ovulation Method | 3 | ||
| Sympto-Thermal6 | 2 | ||
| Post-Ovulation | 1 | ||
| Cap7 | |||
| Parous Women | 40 | 26 | 42 |
| Nulliparous Women | 20 | 9 | 56 |
| Sponge | |||
| Parous Women | 40 | 20 | 42 |
| Nulliparous Women | 20 | 9 | 56 |
| Diaphragm7 | 20 | 6 | 56 |
| Withdrawal | 19 | 4 | |
| Condom8 | |||
| Female (Reality™) | 21 | 5 | 56 |
| Male | 14 | 3 | 61 |
| Pill | 5 | 71 | |
| Progestin only | 0.5 | ||
| Combined | 0.1 | ||
| IUD | |||
| Progesterone T | 2.0 | 1.5 | 81 |
| Copper T380A | 0.8 | 0.6 | 78 |
| LNg 20 | 0.1 | 0.1 | 81 |
| Depo-Provera® | 0.3 | 0.3 | 70 |
| Levonorgestrel Implants (Norplant®) |
0.05 | 0.05 | 88 |
| Female Sterilization | 0.5 | 0.5 | 100 |
| Male Sterilization | 0.15 | 0.10 | 100 |
Emergency Contraceptive Pills: The FDA has concluded that certain combined oral contraceptives containing ethinyl estradiol and norgestrel or levonorgestrel are safe and effective for use as postcoital emergency contraception. Treatment initiated within 72 hours after unprotected intercourse reduces the risk of pregnancy by at least 75%.9
Lactation Amenorrhea Method: LAM is a highly effective, temporary method of contraception.10
Source: Trussell J. Contraceptive efficacy. In: Hatcher RA, Trussell J, Stewart F, Cates W, Stewart GK, Kowel D, Guest F. Contraceptive Technology: Seventeenth Revised Edition. New York NY: Irvington Publishers; 1998.
1. Among typical couples who initiate use of a method (not necessarily for the first time), the percentage who experience an accidental pregnancy during the first year if they do not stop use for any other reason.
2. Among couples who initiate use of a method (not necessarily for the first time) and who use it perfectly (both consistently and correctly), the percentage who experience an accidental pregnancy during the first year if they do not stop use for any other reason.
3. Among couples attempting to avoid pregnancy, the percentage who continue to use a method for one year.
4. The percents becoming pregnant in columns (2) and (3) are based on data from populations where contraception is not used and from women who cease using contraception in order to become pregnant. Among such populations, about 89% become pregnant within one year. This estimate was lowered slightly (to 85%) to represent the percent who would become pregnant within one year among women now relying on reversible methods of contraception if they abandoned contraception altogether.
5. Foams, creams, gels, vaginal suppositories, and vaginal film.
6. Cervical mucus (ovulation) method supplemented by calendar in the pre-ovulatory and basal body temperature in the post-ovulatory phases.
7. With spermicidal cream or jelly.
8. Without spermicides.
9. The treatment schedule is one dose within 72 hours after unprotected intercourse, and a second dose 12 hours after the first dose. The FDA has declared the following dosage regimens of oral contraceptives to be safe and effective for emergency contraception: for tablets containing 50 mcg of ethinyl estradiol and 500 mcg of norgestrel 1 dose is 2 tablets; for tablets containing 20 mcg of ethinyl estradiol and 100 mcg of levonorgestrel 1 dose is 5 tablets; for tablets containing 30 mcg of ethinyl estradiol and 150 mcg of levonorgestrel 1 dose is 4 tablets.
10. However, to maintain effective protection against pregnancy, another method of contraception must be used as soon as menstruation resumes, the frequency or duration of breastfeeds is reduced, bottle feeds are introduced, or the baby reaches 6 months of age.
Dosage and Administration
To achieve maximum contraceptive effectiveness, DOLISHALE (levonorgestrel and ethinyl estradiol tablets) must be taken exactly as directed and at intervals not exceeding 24 hours. The possibility of ovulation and conception prior to initiation of medication should be considered. Women who do not wish to become pregnant after discontinuation should be advised to immediately use another method of birth control. The dosage of DOLISHALE is one green tablet daily without any tablet-free interval.
It is recommended that DOLISHALE tablets be taken at the same time each day.
Initiation of Therapy
Instructions for beginning DOLISHALE are provided in Table 4 below.
Table 4
|
Current
contraceptive therapy |
DOLISHALE start day |
Nonhormonal back-up method of birth control needed when correctly starting DOLISHALE? |
| None | Day 1 of patient's menstrual cycle (during the first 24 hours of her period) | No |
| 21-day COC regimen OR 28-day COC regimen |
Day 1 of patient's withdrawal bleed, at the latest 7 days after her last active tablet. | No |
| Progestin-only pill | Day after taking a progestin-only pill | Yes, for the first 7 days of DOLISHALE tablet taking |
| Implant | Day of implant removal | Yes, for the first 7 days of DOLISHALE tablet taking |
| Injection | Day the next injection is due | Yes, for the first 7 days of DOLISHALE tablet taking |
If spotting or unscheduled bleeding occurs, the patient is instructed to continue on the same regimen. This type of bleeding is usually transient and without significance; however, if the bleeding is persistent or prolonged, the patient is advised to consult her health care professional. The possibility of ovulation increases with each successive day that scheduled green tablets are missed. If the patient has not adhered to the prescribed schedule (missed one or more tablets or started taking them on a day later than she should have), the probability of pregnancy should be considered. Hormonal contraception must be discontinued if pregnancy is confirmed.
The risk of pregnancy increases with each tablet missed. For additional patient instructions regarding missed tablets, see the WHAT TO DO IF YOU MISS PILLS section in the DETAILED PATIENT LABELING below.
DOLISHALE may be initiated no earlier than day 28 postpartum in the nonlactating mother or after a second-trimester abortion due to the increased risk for thromboembolism (see CONTRAINDICATIONS , WARNINGS , and PRECAUTIONS concerning thromboembolic disease). The patient should be advised to use a nonhormonal back-up method for the first 7 days of tablet-taking. However, if intercourse has already occurred, pregnancy should be excluded before the start of combined oral contraceptive use or the patient must wait for her first menstrual period.
In the case of first-trimester abortion, if the patient starts DOLISHALE immediately, additional contraceptive measures are not needed.
Contraindications
Combination oral contraceptives should not be used in women with any of the following conditions:
• Thrombophlebitis or thromboembolic disorders
• History of deep-vein thrombophlebitis or thromboembolic disorders
• Cerebrovascular or coronary artery disease (current or past history)
• Valvular heart disease with thrombogenic complications
• Thrombogenic rhythm disorders
• Hereditary or acquired thrombophilias
• Major surgery with prolonged immobilization
• Diabetes with vascular involvement
• Headaches with focal neurological symptoms such as aura
• Uncontrolled hypertension
• Current diagnosis of, or history of, breast cancer, which may be hormone-sensitive
• Carcinoma of the endometrium or other known or suspected estrogen-dependent neoplasia Undiagnosed abnormal genital bleeding
• Cholestatic jaundice of pregnancy or jaundice with prior pill use
• Hepatic adenomas or carcinomas, or active liver disease
• Known or suspected pregnancy
• Hypersensitivity to any of the components of DOLISHALE
• Are receiving Hepatitis C drug combinations containing ombitasvir/paritaprevir/ritonavir, with or without dasabuvir, due to the potential for ALT elevations (see Warnings, RISK OF LIVER ENZYME ELEVATIONS WITH CONCOMITANT HEPATITIS C TREATMENT ).
Adverse Reactions
Post Marketing Experience
Five studies that compared breast cancer risk between ever-users (current or past use) of COCs and never-users of COCs reported no association between ever use of COCs and breast cancer risk, with effect estimates ranging from 0.90 - 1.12 (Figure 6).
Three studies compared breast cancer risk between current or recent COC users (<6 months since last use) and never users of COCs (Figure 6). One of these studies reported no association between breast cancer risk and COC use. The other two studies found an increased relative risk of 1.19 - 1.33 with current or recent use. Both of these studies found an increased risk of breast cancer with current use of longer duration, with relative risks ranging from 1.03 with less than one year of COC use to approximately 1.4 with more than 8-10 years of COC use.
Figure 6. Risk of Breast Cancer with Combined Oral Contraceptive Use
RR = relative risk; OR = odds ratio; HR = hazard ratio. “ever COC” are females with current or past COC use; “never COC use” are females that never used COCs.
An increased risk of the following serious adverse reactions (see WARNINGS section for additional information) has been associated with the use of oral contraceptives:
Thromboembolic and thrombotic disorders and other vascular problems (including thrombophlebitis and venous thrombosis with or without pulmonary embolism, mesenteric thrombosis, arterial thromboembolism, myocardial infarction, cerebral hemorrhage, cerebral thrombosis, transient ischemic attack), carcinoma of the reproductive organs and breasts, hepatic neoplasia/liver disease (including hepatic adenomas or benign liver tumors), ocular lesions (including retinal vascular thrombosis), gallbladder disease, carbohydrate and lipid effects, elevated blood pressure, and headache including migraine.
The following adverse reactions have been reported in patients receiving oral contraceptives and are believed to be drug related (alphabetically listed):
• Acne
• Amenorrhea
• Anaphylactic/anaphylactoid reactions, including urticaria, angioedema, and severe reactions with respiratory and circulatory symptoms
• Breast changes: tenderness, pain, enlargement, secretion
• Budd-Chiari syndrome
• Cervical erosion and secretion, change in
• Cholestatic jaundice
• Chorea, exacerbation of
• Colitis
• Contact lenses, intolerance to
• Corneal curvature (steepening), change in
• Dizziness
• Edema/fluid retention
• Erythema multiforme
• Erythema nodosum
• Focal nodular hyperplasia
• Gastrointestinal symptoms (such as abdominal pain, cramps, and bloating)
• Hirsutism
• Infertility after discontinuation of treatment, temporary
• Lactation, diminution in, when given immediately postpartum
• Libido, change in
• Melasma/chloasma which may persist
• Menstrual flow, change in
• Mood changes, including depression
• Nausea
• Nervousness
• Pancreatitis
• Porphyria, exacerbation of
• Rash (allergic)
• Scalp hair, loss of
• Serum folate levels, decrease in
• Spotting
• Systemic lupus erythematosus, exacerbation of
• Unscheduled bleeding
• Vaginitis, including candidiasis
• Varicose veins, aggravation of
• Vomiting
• Weight or appetite (increase or decrease), change in
The following adverse reactions have been reported in users of oral contraceptives:
• Cataracts
• Cystitis-like syndrome
• Dysmenorrhea
• Hemolytic uremic syndrome
• Hemorrhagic eruption
• Optic neuritis, which may lead to partial or complete loss of vision
• Premenstrual syndrome
• Renal function, impaired
To report SUSPECTED ADVERSE REACTIONS, contact Ingenus Pharmaceuticals, LLC Toll-Free at 1-877-748-1970 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch .
Drug Interactions
Changes in Contraceptive Effectiveness Associated with Coadministration of Other Products: Contraceptive effectiveness may be reduced when hormonal contraceptives are coadministered with antibiotics, anticonvulsants, and other drugs that increase the metabolism of contraceptive steroids. This could result in unintended pregnancy or unscheduled bleeding. Examples include rifampin, rifabutin, barbiturates, primidone, phenylbutazone, phenytoin, dexamethasone, carbamazepine, felbamate, oxcarbazepine, topiramate, griseofulvin, and modafinil. In such cases a nonhormonal back-up method of birth control should be considered. Several cases of contraceptive failure and unscheduled bleeding have been reported in the literature with concomitant administration of antibiotics such as ampicillin and other penicillins, and tetracyclines. However, clinical pharmacology studies investigating drug interactions between combined oral contraceptives and these antibiotics have reported inconsistent results. Enterohepatic recirculation of estrogens may also be decreased by substances that reduce gut transit time. Several of the anti-HIV protease inhibitors have been studied with coadministration of oral combination hormonal contraceptives; significant changes (increase and decrease) in the plasma levels of the estrogen and progestin have been noted in some cases. The safety and efficacy of oral contraceptive products may be affected with coadministration of anti-HIV protease inhibitors. Health care professionals should refer to the label of the individual anti-HIV protease inhibitors for further drug-drug interaction information. Concomitant Use with HCV Combination Therapy – Liver Enzyme Elevation Do not co-administer DOLISHALE with HCV drug combinations containing ombitasvir/paritaprevir/ritonavir, with or without dasabuvir, due to potential for ALT elevations (see Warnings, RISK OF LIVER ENZYME ELEVATIONS WITH CONCOMITANT HEPATITIS C TREATMENT ). Herbal products containing St. John's Wort (Hypericum perforatum) may induce hepatic enzymes (cytochrome P 450) and p-glycoprotein transporter and may reduce the effectiveness of contraceptive steroids. This may also result in unscheduled bleeding. Increase in Plasma Levels Associated with Coadministered Drugs: Coadministration of atorvastatin and certain oral contraceptives containing ethinyl estradiol increases AUC values for ethinyl estradiol by approximately 20%. Ascorbic acid and acetaminophen increase the bioavailability of ethinyl estradiol since these drugs act as competitive inhibitors for sulfation of ethinyl estradiol in the gastrointestinal wall, a known pathway of elimination for ethinyl estradiol. CYP 3A4 inhibitors such as indinavir, itraconazole, ketoconazole, fluconazole, and troleandomycin may increase plasma hormone levels. Troleandomycin may also increase the risk of intrahepatic cholestasis during coadministration with combination oral contraceptives. Changes in Plasma Levels of Coadministered Drugs: Combination hormonal contraceptives containing some synthetic estrogens (eg, ethinyl estradiol) may inhibit the metabolism of other compounds. Increased plasma concentrations of cyclosporine, prednisolone and other corticosteroids, and theophylline have been reported with concomitant administration of oral contraceptives. Decreased plasma concentrations of acetaminophen and lamotrigine, and increased clearance of temazepam, salicylic acid, morphine, and clofibric acid, due to induction of conjugation (particularly glucuronidation), have been noted when these drugs were administered with oral contraceptives. The prescribing information of concomitant medications should be consulted to identify potential interactions.
How Supplied
DOLISHALE(90 mcg levonorgestrel and 20 mcg ethinyl estradiol) tablets are available in a blister pack, arranged in 4 rows of 7 active tablets as follows:
28 round, green biconvex tablets debossed with "H1" on one side.
DOLISHALE Tablets are available in the following packaging configurations:
Carton of 1 Blister Card of 28 Tablets NDC 50742-659-28
Carton of 3 Blister Cards of 28 Tablets Each NDC 50742-659-84
Carton of 6 Blister Cards of 28 Tablets Each NDC 50742-659-68
Store at 20° to 25°C (68° to 77°F). [See USP Controlled Room Temperature].
References available upon request.
Rx Only
Iss: 12/2024
I0154
Rev B
Manufactured for:
Ingenus Pharmaceuticals, LLC
Orlando, FL 32839-6408
Product of China
Description
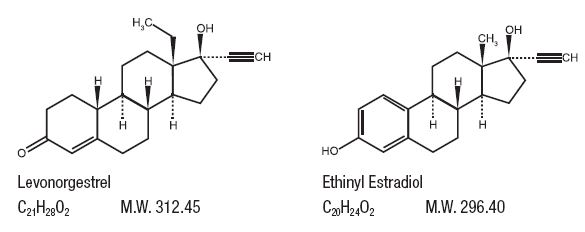
Twenty-eight (28) green tablets each containing 90 mcg of levonorgestrel (17α)-(–)13-ethyl-17-hydroxy-18, 19-dinorpregn-4-en-20-yn-3-one, a totally synthetic progestogen, and 20 mcg of ethinyl estradiol, (17α)-19-norpregna-1,3,5(10)-trien-20-yne-3,17-diol. The inactive ingredients present are titanium dioxide, macrogol/PEG 3000 NF, talc, polyvinyl alcohol, lecithin (soya), FD&C Blue #2 Aluminum Lake, FD&C Yellow #5 Aluminum Lake, FD&C Red #40 Aluminum Lake, lactose monohydrate, magnesium stearate and pregelatinized starch.
Section 42229-5
Patients should be counseled that oral contraceptives do not protect against transmission of HIV (AIDS) and other sexually transmitted diseases (STDs) such as chlamydia, genital herpes, genital warts, gonorrhea, hepatitis B, and syphilis.
1. General
Patients should be counseled that oral contraceptives do not protect against transmission of HIV (AIDS) and other sexually transmitted diseases (STDs) such as chlamydia, genital herpes, genital warts, gonorrhea, hepatitis B, and syphilis.
Scheduled withdrawal bleeding does not occur with the use of DOLISHALE, therefore, the absence of withdrawal bleeding cannot be used as a sign of an unexpected pregnancy and as such, unexpected pregnancy may be difficult to recognize. Although pregnancy is unlikely if DOLISHALE is taken as directed, if for any reason, pregnancy is suspected in a woman using DOLISHALE, a pregnancy test should be performed.
Overdosage
Symptoms of oral contraceptive overdosage in adults and children may include nausea, vomiting, breast tenderness, dizziness, abdominal pain, drowsiness/fatigue; withdrawal bleeding may occur in females. There is no specific antidote and further treatment of overdose, if necessary, is directed to the symptoms.
Precautions
This product contains FD&C Yellow No. 5 (tartrazine) which may cause allergic-type reactions (including bronchial asthma) in certain susceptible persons. Although the overall incidence of FD&C Yellow No. 5 (tartrazine) sensitivity in the general population is low, it is frequently seen in patients who also have aspirin hypersensitivity.
12. Pregnancy
Pregnancy Category X. See CONTRAINDICATIONS and WARNINGS sections.
Mode of Action
Combination oral contraceptives act by suppression of gonadotropins. Although the primary mechanism of this action is inhibition of ovulation, other alterations include changes in the cervical mucus (which increase the difficulty of sperm entry into the uterus) and the endometrium (which reduce the likelihood of implantation).
Clinical Studies
The efficacy and safety of levonorgestrel and ethinyl estradiol tablets were studied in 2 one-year clinical trials of subjects age 18 to 49. There were no exclusions for body mass index (BMI), weight, or bleeding history.
The primary efficacy and safety study (313-NA) was a one-year open-label clinical trial that treated 2,134 subjects in North America. Of these subjects 1,213 (56.8%) discontinued prematurely, including 102 (4.8%) discontinued by the Sponsor for early study closure. The mean weight of subjects in this study was 70.38 kg. The efficacy of levonorgestrel and ethinyl estradiol tablets was assessed by the number of pregnancies that occurred after the onset of treatment and within 14 days of the last dose. Among subjects 35 years or less, there were 23 pregnancies (4 of these occurred during the interval 1 to 14 days after the last day of pill use) during 12,572 28-day pill packs of use. The resulting total Pearl Index was 2.38 (95% CI: 1.51, 3.57) and the one-year life table pregnancy rate was 2.39 (95% CI: 1.57, 3.62). Pill pack cycles during which subjects used back-up contraception or were not sexually active were not included in these calculations. Among women 35 years or less who took the pills completely as directed, there were 15 pregnancies (method failures) resulting in a Pearl Index of 1.55 (95% CI: 0.87, 2.56) and the one-year life table pregnancy rate was 1.59 (95% CI: 0.95 to 2.67).
In a second supportive study conducted in Europe (315-EU), 641 subjects were randomized to levonorgestrel and ethinyl estradiol tablets (n=323) or the cyclic comparator of 100 mcg levonorgestrel and 20 mcg ethinyl estradiol (n=318). The mean weight of subjects in this study was 63.86 kg. The efficacy analysis among women 35 years or less included 2,756 levonorgestrel and ethinyl estradiol tablet pill packs and 2,886 cyclic comparator pill packs. There was one pregnancy in the levonorgestrel and ethinyl estradiol group that occurred within 14 days following the last dose. There were three pregnancies in the cyclic comparator group.
Pharmacokinetics
Absorption
No specific investigation of the absolute bioavailability of levonorgestrel and ethinyl estradiol tablets in humans has been conducted. However, literature indicates that levonorgestrel is rapidly and completely absorbed after oral administration (bioavailability about 100%) and is not subject to first-pass metabolism. Ethinyl estradiol is rapidly and almost completely absorbed from the gastrointestinal tract but, due to first-pass metabolism in gut mucosa and liver, the bioavailability of ethinyl estradiol is between 38% and 48%.
A summary of the single dose and multiple dose levonorgestrel and ethinyl estradiol pharmacokinetic parameters for 18 women under fasting conditions is provided in Table 1. The plasma concentrations of levonorgestrel and ethinyl estradiol reached steady-state by approximately day 14. Levonorgestrel and ethinyl estradiol concentrations did not increase from days 14 to 28, but did increase from days 1 to 28.
Table 1: Mean (SD) Pharmacokinetic Parameters of Levonorgestrel and Ethinyl Estradiol Tablets Over a 28-Day Dosing Period
| LNG | ||||
|
Day |
Cmax
(ng/mL) |
Tmax
(h) |
t1/2
(h) |
AUC0-24
(ng•h/mL) |
| 1 | 2.4 (0.9) | 1.2 (0.4) | - | 16 (8) |
| 14 | 5.4 (2.1) | 1.7 (1.4) | - | 68 (36) |
| 28 | 5.7 (2.1) | 1.3 (0.8) | 36 (19) | 74 (41) |
| EE | ||||
| Day | (pg/mL) | (h) | (h) | (pg h/mL) |
| 1 | 47.7 (20.1) | 1.3 (0.5) | - | 378 (140) |
| 14 | 72.7 (37.2) | 1.4 (0.5) | - | 695 (361) |
| 28 | 74.4 (29.7) | 1.4 (0.5) | 21 (7) | 717 (351) |
The mean plasma concentrations of levonorgestrel and ethinyl estradiol following single (day 1) and multiple (days 14 and 28) oral administrations of levonorgestrel 90 mcg in combination with ethinyl estradiol 20 mcg to 18 healthy women is provided in Figure 1.
Figure 1: Mean Plasma ± SD†Concentrations of Levonorgestrel and Ethinyl Estradiol Following Single (Day 1) and Multiple (Days 14 and 28) Oral Administrations of Levonorgestrel 90 mcg in Combination with Ethinyl Estradiol 20 mcg to Healthy Women
The effect of food on the rate and the extent of levonorgestrel and ethinyl estradiol absorption following oral administration of DOLISHALE has not been evaluated.
Distribution
Levonorgestrel in serum is primarily bound to sex hormone-binding globulin (SHBG). Ethinyl estradiol is about 97% bound to serum albumin. Ethinyl estradiol does not bind to SHBG, but induces SHBG synthesis.
Metabolism
Levonorgestrel: The most important metabolic pathways are reduction of the Δ4-3-oxo group and hydroxylation at positions 2α, 1β, and 16β, followed by conjugation. Most of the circulating metabolites are sulfates of 3α, 5β-tetrahydro-levonorgestrel, while excretion occurs predominantly in the form of glucuronides. Some of the parent levonorgestrel also circulates as 17β-sulfate. Metabolic clearance rates may differ among individuals by several-fold, and this may account in part for the wide variation observed in levonorgestrel concentrations among users.
Ethinyl estradiol: Cytochrome P450 enzymes (CYP3A4) in the liver are responsible for the 2-hydroxylation that is the major oxidative reaction. The 2-hydroxy metabolite is further transformed by methylation, sulfation, and glucuronidation prior to urinary and fecal excretion. Levels of CYP3A4 vary widely among individuals and can explain the variation in rates of ethinyl estradiol 2-hydroxylation.
Excretion
The terminal elimination half-life for levonorgestrel in levonorgestrel and ethinyl estradiol tablets is about 36 hours. Levonorgestrel and its metabolites are excreted in the urine (40% to 68%) and in feces (16% to 48%). The terminal elimination half-life of ethinyl estradiol in levonorgestrel and ethinyl estradiol tablets is about 21 hours.
Ethinyl estradiol is excreted in the urine and feces as glucuronide and sulfate conjugates and undergoes enterohepatic recirculation.
14. Pediatric Use
Safety and efficacy of levonorgestrel and ethinyl estradiol tablets have been established in women of reproductive age. Safety and efficacy are expected to be the same for postpubertal adolescents under the age of 16 and for users 16 years and older. Use of this product before menarche is not indicated.
15. Geriatric Use
This product has not been studied in women over 65 years of age and is not indicated in this population.
4. Liver Function
If jaundice develops in any woman receiving such drugs, the medication should be discontinued. Steroid hormones may be poorly metabolized in patients with impaired liver function.
7. Contact Lenses
Contact-lens wearers who develop visual changes or changes in lens tolerance should be assessed by an ophthalmologist.
11. Carcinogenesis
See WARNINGS section.
3. Lipid Disorders
Women who are being treated for hyperlipidemias should be followed closely if they elect to use oral contraceptives. Some progestogens may elevate LDL levels and may render the control of hyperlipidemias more difficult. (See WARNINGS , 1a., 1d., and 9.)
A small proportion of women will have adverse lipid changes while taking oral contraceptives. Nonhormonal contraception should be considered in women with uncontrolled dyslipidemias. Persistent hypertriglyceridemia may occur in a small population of combination oral contraceptive users. Elevations of plasma triglycerides may lead to pancreatitis and other complications.
5. Fluid Retention
Oral contraceptives may cause some degree of fluid retention. They should be prescribed with caution, and only with careful monitoring, in patients with conditions which might be aggravated by fluid retention.
13. Nursing Mothers
Small amounts of oral contraceptive steroids and/or metabolites have been identified in the milk of nursing mothers, and a few adverse effects on the child have been reported, including jaundice and breast enlargement. In addition, combination oral contraceptives given in the postpartum period may interfere with lactation by decreasing the quantity and quality of breast milk. If possible, the nursing mother should be advised not to use combination oral contraceptives, but to use other forms of contraception until she has completely weaned her child.
8. Gastrointestinal
Diarrhea and/or vomiting may reduce hormone absorption resulting in decreased serum concentrations.
Special Populations
Race
No formal studies on the effect of race on the pharmacokinetic parameters of levonorgestrel and ethinyl estradiol tablets were conducted.
Hepatic Insufficiency
No formal studies have evaluated the effect of hepatic disease on the disposition of levonorgestrel and ethinyl estradiol tablets. However, steroid hormones may be poorly metabolized in patients with impaired liver function.
Renal Insufficiency
No formal studies have evaluated the effect of renal disease on the disposition of levonorgestrel and ethinyl estradiol tablets.
Drug-Drug Interactions
See PRECAUTIONS section - Drug Interactions.
9. Drug Interactions
Changes in Contraceptive Effectiveness Associated with Coadministration of Other Products: Contraceptive effectiveness may be reduced when hormonal contraceptives are coadministered with antibiotics, anticonvulsants, and other drugs that increase the metabolism of contraceptive steroids. This could result in unintended pregnancy or unscheduled bleeding. Examples include rifampin, rifabutin, barbiturates, primidone, phenylbutazone, phenytoin, dexamethasone, carbamazepine, felbamate, oxcarbazepine, topiramate, griseofulvin, and modafinil. In such cases a nonhormonal back-up method of birth control should be considered.
Several cases of contraceptive failure and unscheduled bleeding have been reported in the literature with concomitant administration of antibiotics such as ampicillin and other penicillins, and tetracyclines. However, clinical pharmacology studies investigating drug interactions between combined oral contraceptives and these antibiotics have reported inconsistent results. Enterohepatic recirculation of estrogens may also be decreased by substances that reduce gut transit time.
Several of the anti-HIV protease inhibitors have been studied with coadministration of oral combination hormonal contraceptives; significant changes (increase and decrease) in the plasma levels of the estrogen and progestin have been noted in some cases. The safety and efficacy of oral contraceptive products may be affected with coadministration of anti-HIV protease inhibitors. Health care professionals should refer to the label of the individual anti-HIV protease inhibitors for further drug-drug interaction information.
Concomitant Use with HCV Combination Therapy – Liver Enzyme Elevation Do not co-administer DOLISHALE with HCV drug combinations containing ombitasvir/paritaprevir/ritonavir, with or without dasabuvir, due to potential for ALT elevations (see Warnings, RISK OF LIVER ENZYME ELEVATIONS WITH CONCOMITANT HEPATITIS C TREATMENT ).
Herbal products containing St. John's Wort (Hypericum perforatum) may induce hepatic enzymes (cytochrome P 450) and p-glycoprotein transporter and may reduce the effectiveness of contraceptive steroids. This may also result in unscheduled bleeding.
Increase in Plasma Levels Associated with Coadministered Drugs:
Coadministration of atorvastatin and certain oral contraceptives containing ethinyl estradiol increases AUC values for ethinyl estradiol by approximately 20%. Ascorbic acid and acetaminophen increase the bioavailability of ethinyl estradiol since these drugs act as competitive inhibitors for sulfation of ethinyl estradiol in the gastrointestinal wall, a known pathway of elimination for ethinyl estradiol. CYP 3A4 inhibitors such as indinavir, itraconazole, ketoconazole, fluconazole, and troleandomycin may increase plasma hormone levels. Troleandomycin may also increase the risk of intrahepatic cholestasis during coadministration with combination oral contraceptives.
Changes in Plasma Levels of Coadministered Drugs:
Combination hormonal contraceptives containing some synthetic estrogens (eg, ethinyl estradiol) may inhibit the metabolism of other compounds. Increased plasma concentrations of cyclosporine, prednisolone and other corticosteroids, and theophylline have been reported with concomitant administration of oral contraceptives. Decreased plasma concentrations of acetaminophen and lamotrigine, and increased clearance of temazepam, salicylic acid, morphine, and clofibric acid, due to induction of conjugation (particularly glucuronidation), have been noted when these drugs were administered with oral contraceptives.
The prescribing information of concomitant medications should be consulted to identify potential interactions.
6. Emotional Disorders
Patients becoming significantly depressed while taking oral contraceptives should stop the medication and use an alternate method of contraception in an attempt to determine whether the symptom is drug related. Women with a history of depression should be carefully observed and the drug discontinued if depression recurs to a serious degree.
Detailed Patient Labeling
This product (like all oral contraceptives) is intended to prevent pregnancy. Oral contraceptives do not protect against transmission of HIV (AIDS) and other sexually transmitted diseases (STDs) such as chlamydia, genital herpes, genital warts, gonorrhea, hepatitis B, and syphilis.
INTRODUCTION
Any woman who considers using oral contraceptives (the "birth-control pill" or "the pill") should understand the benefits and risks of using this form of birth control. This leaflet will give you much of the information you will need to make this decision and will also help you determine if you are at risk of developing any of the serious side effects of the pill. It will tell you how to use the pill properly so that it will be as effective as possible. However, this leaflet is not a replacement for a careful discussion between you and your health care professional. You should discuss the information provided in this leaflet with him or her, both when you first start taking the pill and during your revisits. You should also follow your health care professional's advice with regard to regular check-ups while you are on the pill.
DOLISHALE is a birth-control pill that is taken every day. When you take DOLISHALE, the lining of your uterus does not undergo the changes needed for menstruation, and therefore you do not have regular menstrual periods. You are likely to have unscheduled or unplanned bleeding or spotting when you start to use DOLISHALE. The number of days each month with unscheduled bleeding and spotting usually decreases over time for the majority of women. When using DOLISHALE, the convenience of having no regular menstrual periods should be weighed against the inconvenience of unscheduled or unplanned breakthrough bleeding and spotting.
EFFECTIVENESS OF ORAL CONTRACEPTIVES
Oral contraceptives or "birth-control pills" or "the pill" are used to prevent pregnancy and are more effective than other nonsurgical methods of birth control. When they are taken correctly, without missing any pills the chance of becoming pregnant is approximately 1 to 2% per year (1 to 2 pregnancies per 100 women per year of use). Average failure rates are approximately 5% per year (5 pregnancies per 100 women per year of use) when women who miss pills are included. The chance of becoming pregnant increases with each missed pill.
In comparison, average failure rates for other methods of birth control during the first year of use are as follows:
| IUD: 0.1 to 2% |
Female condom alone: 21% |
| Depo-Provera® (injectable progestogen): 0.3% |
Cervical cap |
| Norplant® System (levonorgestrel implants): 0.05% |
Never given birth: 20% |
| Diaphragm with spermicides: 20% |
Given birth: 40% |
| Spermicides alone: 26% |
Periodic abstinence: 25% |
| Male condom alone: 14% |
No methods: 85% |
WHO SHOULD NOT TAKE ORAL CONTRACEPTIVES
Although cardiovascular disease risks may be increased with oral contraceptive use in healthy, non-smoking women over 40 (even with the newer low-dose formulations), there are also greater potential health risks associated with pregnancy in older women.
Instructions for the Patient
HOW TO TAKE DOLISHALE
Important Points to Remember
Before You Start Taking DOLISHALE:
1. BE SURE TO READ THESE DIRECTIONS:
Before you start taking DOLISHALE.
And
Anytime you are not sure what to do.
2. THE RIGHT WAY TO TAKE DOLISHALE IS TO TAKE ONE PILL EVERY DAY AT THE SAME TIME.
If you miss pills, you could get pregnant. This includes starting the pack late. The more pills you miss, the more likely you are to get pregnant. See "WHAT TO DO IF YOU MISS PILLS" below.
3. MANY WOMEN HAVE SPOTTING OR LIGHT BLEEDING, OR MAY FEEL SICK TO THEIR STOMACH DURING THE FIRST 1 to 3 PACKS OF PILLS.
If you feel sick to your stomach, do not stop taking DOLISHALE. This will usually go away. If it doesn't go away, check with your health care professional.
4. MOST WOMEN HAVE SPOTTING OR BLEEDING DURING THE FIRST FEW MONTHS OF TAKING DOLISHALE. Do not stop taking your pills even if you are having bleeding or spotting. If the bleeding or spotting lasts for more than 7 consecutive days, talk to your health care provider.
5. MISSING PILLS CAN ALSO CAUSE SPOTTING OR LIGHT BLEEDING, even when you make up these missed pills.
On the days you take 2 pills to make up for missed pills, you could also feel a little sick to your stomach.
6. IF YOU VOMIT (within 4 hours after you take your pill), you should follow the instructions for WHAT TO DO IF YOU MISS PILLS. IF YOU HAVE DIARRHEA or IF YOU TAKE SOME MEDICINES, including some antibiotics, your pills may not work as well.
Use a back-up nonhormonal method (such as condoms and/or spermicide) until you check with your health care professional.
7. IF YOU HAVE TROUBLE REMEMBERING TO TAKE DOLISHALE, talk to your health care professional about how to make pill-taking easier or about using another method of birth control.
8. IF YOU HAVE ANY QUESTIONS OR ARE UNSURE ABOUT THE INFORMATION IN THIS LEAFLET, call your health care professional.
BEFORE YOU START TAKING DOLISHALE
1. DECIDE WHAT TIME OF DAY YOU WANT TO TAKE YOUR PILL. It is important to take your pill at the SAME TIME every day.
2. LOOK AT YOUR DOLISHALE BLISTER CARD. The pill pack has 28 "active" green pills (with hormones).
3. ALSO FIND:
1) where on the pack to start taking pills,
2) in what order to take the pills (follow the arrows),
3) check picture of pill pack and additional instructions for using this package below.
4. BE SURE YOU HAVE READY AT ALL TIMES:
ANOTHER KIND OF NONHORMONAL BIRTH CONTROL (such as condoms and/or spermicide) to use as a back-up in case you miss pills.
AN EXTRA, FULL PILL PACK.
WHEN TO START THE FIRST PACK OF DOLISHALE
Day 1 Start
1. If the first day of your period (this is the day you start bleeding or spotting, even if it is almost midnight when the bleeding begins) is Sunday, then follow the days of the week imprinted on the plastic compact. You do not need to use the Day Label Stickers.
2. If the first day of your period (this is the day you start bleeding or spotting, even if it is almost midnight when the bleeding begins) is on a day other than Sunday, then pick the day label sticker that starts with that day of the week.
3. Place this chosen day label sticker over the area that has the days of the week (starting with Sunday) imprinted on the plastic compact as shown in the graphic above.
4. Take the first "active" green pill of the first pack during the first 24 hours of your period.
5. You will not need to use a back-up nonhormonal method of birth control, since you are starting the pill at the beginning of your period.
WHAT TO DO DURING THE MONTH
1. TAKE ONE PILL AT THE SAME TIME EVERY DAY UNTIL THE PACK IS EMPTY.
Do not skip pills even if you are spotting or bleeding or feel sick to your stomach (nausea).
Do not skip pills even if you do not have sex very often.
2. WHEN YOU FINISH A PACK
Start the next pack on the day after your last pill. Do not wait any days between packs.
IF YOU SWITCH FROM ANOTHER BRAND OF COMBINATION PILLS:
When switching from a 21 pill pack: Start DOLISHALE on the first day of your period (withdrawal bleed). Be sure that no more than 7 days pass between the last day of your 21-day pack and your first DOLISHALE pill.
When switching from a 28 pill pack (21 active and 7 inactive pills, or 24 active and 4 inactive pills): Start DOLISHALE on the first day of your period (withdrawal bleed). Be sure that no more than 7 days pass after the last active pill and your first DOLISHALE pill.
IF YOU SWITCH FROM ANOTHER TYPE OF BIRTH CONTROL
When switching from other types of birth control such as pills containing only a progestin (progestin only pill or POP), an injection, or an implant, your health care professional will provide you with instructions for when to start DOLISHALE.
WHAT TO DO IF YOU MISS PILLS
Combination oral contraceptives may not be as effective if you miss pills. Instructions for what to do if you miss pills are provided in the following table.
| # of pills missed in a row | What to do when you miss a pill(s) |
| 1 missed pill | • Take the missed pill as soon as you remember. THEN • Take the next pill at your regular time. This means you may take 2 pills in 1 day. • You COULD BECOME PREGNANT if you have sex during the 7 days after you restart your pills. You MUST use a nonhormonal birth-control method (such as condoms and/or spermicide) as a back-up for those 7 days. |
| 2 missed pills and remembered on the day of the second missed pill |
• Take 2 missed pills on the day you remember. The following day you are back on schedule to take 1 pill a day. For example, you take your pills in the morning and you missed 1 pill on Monday and 1 on Tuesday. On Tuesday evening you remembered that you missed your Monday and Tuesday pills. You take the 2 missed pills on Tuesday evening and on Wednesday morning you're back on schedule and you take 1 pill. • You COULD BECOME PREGNANT if you have sex during the 7 days after you restart your pills. You MUST use a nonhormonal birth-control method (such as condoms and/or spermicide) as a back-up for those 7 days. |
| 2 missed pills and remembered on the day after the second pill is missed |
• Take 2 missed pills on the day you remember. The next day you take 2 pills. The following day you are back on schedule to take your pills. For example, you take your pills in the morning and you missed 1 pill on Monday and 1 on Tuesday. On Wednesday morning you remembered that you missed your Monday and Tuesday pills. You take the 2 missed pills on Wednesday morning and 2 pills on Thursday morning. On Friday morning you're back on schedule and you take 1 pill. • You COULD BECOME PREGNANT if you have sex during the 7 days after you restart your pills. You MUST use a nonhormonal birth-control method (such as condoms and/or spermicide) as a back-up for those 7 days. |
| 3 or more missed pills | • Contact your health care professional for further advice. Keep taking one pill every day until you reach your health care professional. Do not take the missed pills. • You COULD BECOME PREGNANT if you have sex during the 7 days after you restart your pills. You MUST use a nonhormonal birth-control method (such as condoms and/or spermicide) as a back-up for those 7 days. |
FINALLY, IF YOU ARE STILL NOT SURE WHAT TO DO ABOUT THE PILLS YOU HAVE MISSED
Use a BACK-UP NONHORMONAL BIRTH-CONTROL METHOD anytime you have sex.
PREGNANCY AFTER STOPPING THE PILL
If you do not desire pregnancy, you should use another method of birth-control immediately after stopping DOLISHALE. You can get pregnant within days after stopping DOLISHALE.
For additional information see "Detailed Patient Labeling."
16. Information for the Patient
See DETAILED PATIENT LABELING printed below.
Noncontraceptive Health Benefits
The following noncontraceptive health benefits related to the use of oral contraceptives are supported by epidemiological studies which largely utilized oral contraceptive formulations containing doses exceeding 0.035 mg of ethinyl estradiol or 0.05 mg of mestranol.
Effects on menses:
May decrease blood loss and may decrease the incidence of iron-deficiency anemia
May decrease incidence of dysmenorrhea
Effects related to inhibition of ovulation:
May decrease incidence of functional ovarian cysts
May decrease incidence of ectopic pregnancies
Effects from long-term use:
May decrease incidence of fibroadenomas and fibrocystic disease of the breast
May decrease incidence of acute pelvic inflammatory disease
May decrease incidence of endometrial cancer
May decrease incidence of ovarian cancer
Brief Summary Patient Package Insert
This product (like all oral contraceptives) is intended to prevent pregnancy. Oral contraceptives do not protect against transmission of HIV (AIDS) and other sexually transmitted diseases (STDs) such as chlamydia, genital herpes, genital warts, gonorrhea, hepatitis B, and syphilis.
Oral contraceptives, also known as "birth-control pills" or "the pill," are taken to prevent pregnancy, and when taken correctly, have a failure rate of approximately 1 to 2% per year (1 to 2 pregnancies per 100 women per year of use) when used without missing any pills. The average failure rate of large numbers of pill users is approximately 5% per year (5 pregnancies per 100 women per year of use) when women who miss pills are included. However, forgetting to take pills considerably increases the chances of pregnancy.
DOLISHALE is a birth-control pill that is taken every day. When you take DOLISHALE, the lining of your uterus does not undergo the changes needed for menstruation, and therefore you do not have regular menstrual periods. You are likely to have unscheduled or unplanned bleeding or spotting when you start to use DOLISHALE. The number of days each month with unscheduled bleeding and spotting usually decreases over time for the majority of women. When using DOLISHALE , the convenience of having no regular menstrual periods should be weighed against the inconvenience of unscheduled or unplanned breakthrough bleeding and spotting.
For the majority of women, oral contraceptives can be taken safely. However, there are some women who are at high risk of developing certain serious diseases that can be life-threatening or may cause temporary or permanent disability or death. The risks associated with taking oral contraceptives increase significantly if you:
• smoke
• have high blood pressure, diabetes, high cholesterol, or a tendency to form blood clots, or are obese
• have or have had clotting disorders, heart attack, stroke, angina pectoris, cancer of the breast or sex organs, jaundice, malignant or benign liver tumors, or major surgery with prolonged immobilization
• have headaches with neurological symptoms
You should not take the pill if you suspect you are pregnant or have unexplained vaginal bleeding.
Although cardiovascular disease risks may be increased with oral contraceptive use in healthy, non-smoking women over 40 (even with the newer low-dose formulations), there are also greater potential health risks associated with pregnancy in older women.
2. Physical Examination and Follow Up
A periodic personal and family medical history and complete physical examination are appropriate for all women, including women using oral contraceptives. The physical examination, however, may be deferred until after initiation of oral contraceptives if requested by the woman and judged appropriate by the clinician. The physical examination should include special reference to blood pressure, breasts, abdomen, and pelvic organs, including cervical cytology, and relevant laboratory tests. In case of undiagnosed, persistent, or recurrent abnormal vaginal bleeding, appropriate diagnostic measures should be conducted to rule out malignancy. Women with a strong family history of breast cancer or who have breast nodules should be monitored with particular care.
10. Interactions With Laboratory Tests
Certain endocrine- and liver-function tests and blood components may be affected by oral contraceptives:
a. Increased prothrombin and factors VII, VIII, IX, and X; decreased antithrombin 3; increased norepinephrine-induced platelet aggregability.
b. Increased thyroid-binding globulin (TBG) leading to increased circulating total thyroid hormone, as measured by protein-bound iodine (PBI), T4 by column or by radioimmunoassay. Free T3 resin uptake is decreased, reflecting the elevated TBG; free T4 concentration is unaltered.
c. Other binding proteins may be elevated in serum ie, corticosteroid binding globulin (CBG), sex hormone-binding globulins (SHBG) leading to increased levels of total circulating corticosteroids and sex steroids, respectively. Free or biologically active hormone concentrations are unchanged.
d. Triglycerides may be increased and levels of various other lipids and lipoproteins may be affected.
e. Glucose tolerance may be decreased.
f. Serum folate levels may be depressed by oral contraceptive therapy. This may be of clinical significance if a woman becomes pregnant shortly after discontinuing oral contraceptives.
Principal Display Panel 1 Cycle Carton
Principal Display Panel 3 Cycle Carton
Inhibition of Menses (bleeding Profile)
The bleeding profile for subjects in Study 313-NA also was assessed. Women with a history of unscheduled bleeding and/or spotting were not excluded from the study.
In those subjects who provided complete bleeding data, the percentage of patients who were amenorrheic in a given cycle and remained amenorrheic through cycle 13 (cumulative amenorrhea rate) was determined (Figure 2).
Figure 2: Percentage of Subjects with Cumulative Amenorrhea for Each Pill Pack through Pill Pack 13
When prescribing DOLISHALE, the convenience of having no scheduled menstrual bleeding should be weighed against the inconvenience of unscheduled bleeding and spotting (see WARNINGS, 12 ).
Structured Label Content
Recent Major Changes (34066-1)
Cigarette smoking increases the risk of serious cardiovascular side effects from oral contraceptive use. This risk increases with age and with the extent of smoking (in epidemiologic studies, 15 or more cigarettes per day was associated with a significantly increased risk) and is quite marked in women over 35 years of age. Women who use oral contraceptives should be strongly advised not to smoke.
Section 42229-5 (42229-5)
Patients should be counseled that oral contraceptives do not protect against transmission of HIV (AIDS) and other sexually transmitted diseases (STDs) such as chlamydia, genital herpes, genital warts, gonorrhea, hepatitis B, and syphilis.
1. General
Patients should be counseled that oral contraceptives do not protect against transmission of HIV (AIDS) and other sexually transmitted diseases (STDs) such as chlamydia, genital herpes, genital warts, gonorrhea, hepatitis B, and syphilis.
Scheduled withdrawal bleeding does not occur with the use of DOLISHALE, therefore, the absence of withdrawal bleeding cannot be used as a sign of an unexpected pregnancy and as such, unexpected pregnancy may be difficult to recognize. Although pregnancy is unlikely if DOLISHALE is taken as directed, if for any reason, pregnancy is suspected in a woman using DOLISHALE, a pregnancy test should be performed.
Overdosage (OVERDOSAGE)
Symptoms of oral contraceptive overdosage in adults and children may include nausea, vomiting, breast tenderness, dizziness, abdominal pain, drowsiness/fatigue; withdrawal bleeding may occur in females. There is no specific antidote and further treatment of overdose, if necessary, is directed to the symptoms.
Description (DESCRIPTION)
Twenty-eight (28) green tablets each containing 90 mcg of levonorgestrel (17α)-(–)13-ethyl-17-hydroxy-18, 19-dinorpregn-4-en-20-yn-3-one, a totally synthetic progestogen, and 20 mcg of ethinyl estradiol, (17α)-19-norpregna-1,3,5(10)-trien-20-yne-3,17-diol. The inactive ingredients present are titanium dioxide, macrogol/PEG 3000 NF, talc, polyvinyl alcohol, lecithin (soya), FD&C Blue #2 Aluminum Lake, FD&C Yellow #5 Aluminum Lake, FD&C Red #40 Aluminum Lake, lactose monohydrate, magnesium stearate and pregelatinized starch.
Precautions (PRECAUTIONS)
This product contains FD&C Yellow No. 5 (tartrazine) which may cause allergic-type reactions (including bronchial asthma) in certain susceptible persons. Although the overall incidence of FD&C Yellow No. 5 (tartrazine) sensitivity in the general population is low, it is frequently seen in patients who also have aspirin hypersensitivity.
How Supplied (HOW SUPPLIED)
DOLISHALE(90 mcg levonorgestrel and 20 mcg ethinyl estradiol) tablets are available in a blister pack, arranged in 4 rows of 7 active tablets as follows:
28 round, green biconvex tablets debossed with "H1" on one side.
DOLISHALE Tablets are available in the following packaging configurations:
Carton of 1 Blister Card of 28 Tablets NDC 50742-659-28
Carton of 3 Blister Cards of 28 Tablets Each NDC 50742-659-84
Carton of 6 Blister Cards of 28 Tablets Each NDC 50742-659-68
Store at 20° to 25°C (68° to 77°F). [See USP Controlled Room Temperature].
References available upon request.
Rx Only
Iss: 12/2024
I0154
Rev B
Manufactured for:
Ingenus Pharmaceuticals, LLC
Orlando, FL 32839-6408
Product of China
12. Pregnancy
Pregnancy Category X. See CONTRAINDICATIONS and WARNINGS sections.
Mode of Action
Combination oral contraceptives act by suppression of gonadotropins. Although the primary mechanism of this action is inhibition of ovulation, other alterations include changes in the cervical mucus (which increase the difficulty of sperm entry into the uterus) and the endometrium (which reduce the likelihood of implantation).
Clinical Studies
The efficacy and safety of levonorgestrel and ethinyl estradiol tablets were studied in 2 one-year clinical trials of subjects age 18 to 49. There were no exclusions for body mass index (BMI), weight, or bleeding history.
The primary efficacy and safety study (313-NA) was a one-year open-label clinical trial that treated 2,134 subjects in North America. Of these subjects 1,213 (56.8%) discontinued prematurely, including 102 (4.8%) discontinued by the Sponsor for early study closure. The mean weight of subjects in this study was 70.38 kg. The efficacy of levonorgestrel and ethinyl estradiol tablets was assessed by the number of pregnancies that occurred after the onset of treatment and within 14 days of the last dose. Among subjects 35 years or less, there were 23 pregnancies (4 of these occurred during the interval 1 to 14 days after the last day of pill use) during 12,572 28-day pill packs of use. The resulting total Pearl Index was 2.38 (95% CI: 1.51, 3.57) and the one-year life table pregnancy rate was 2.39 (95% CI: 1.57, 3.62). Pill pack cycles during which subjects used back-up contraception or were not sexually active were not included in these calculations. Among women 35 years or less who took the pills completely as directed, there were 15 pregnancies (method failures) resulting in a Pearl Index of 1.55 (95% CI: 0.87, 2.56) and the one-year life table pregnancy rate was 1.59 (95% CI: 0.95 to 2.67).
In a second supportive study conducted in Europe (315-EU), 641 subjects were randomized to levonorgestrel and ethinyl estradiol tablets (n=323) or the cyclic comparator of 100 mcg levonorgestrel and 20 mcg ethinyl estradiol (n=318). The mean weight of subjects in this study was 63.86 kg. The efficacy analysis among women 35 years or less included 2,756 levonorgestrel and ethinyl estradiol tablet pill packs and 2,886 cyclic comparator pill packs. There was one pregnancy in the levonorgestrel and ethinyl estradiol group that occurred within 14 days following the last dose. There were three pregnancies in the cyclic comparator group.
Pharmacokinetics
Absorption
No specific investigation of the absolute bioavailability of levonorgestrel and ethinyl estradiol tablets in humans has been conducted. However, literature indicates that levonorgestrel is rapidly and completely absorbed after oral administration (bioavailability about 100%) and is not subject to first-pass metabolism. Ethinyl estradiol is rapidly and almost completely absorbed from the gastrointestinal tract but, due to first-pass metabolism in gut mucosa and liver, the bioavailability of ethinyl estradiol is between 38% and 48%.
A summary of the single dose and multiple dose levonorgestrel and ethinyl estradiol pharmacokinetic parameters for 18 women under fasting conditions is provided in Table 1. The plasma concentrations of levonorgestrel and ethinyl estradiol reached steady-state by approximately day 14. Levonorgestrel and ethinyl estradiol concentrations did not increase from days 14 to 28, but did increase from days 1 to 28.
Table 1: Mean (SD) Pharmacokinetic Parameters of Levonorgestrel and Ethinyl Estradiol Tablets Over a 28-Day Dosing Period
| LNG | ||||
|
Day |
Cmax
(ng/mL) |
Tmax
(h) |
t1/2
(h) |
AUC0-24
(ng•h/mL) |
| 1 | 2.4 (0.9) | 1.2 (0.4) | - | 16 (8) |
| 14 | 5.4 (2.1) | 1.7 (1.4) | - | 68 (36) |
| 28 | 5.7 (2.1) | 1.3 (0.8) | 36 (19) | 74 (41) |
| EE | ||||
| Day | (pg/mL) | (h) | (h) | (pg h/mL) |
| 1 | 47.7 (20.1) | 1.3 (0.5) | - | 378 (140) |
| 14 | 72.7 (37.2) | 1.4 (0.5) | - | 695 (361) |
| 28 | 74.4 (29.7) | 1.4 (0.5) | 21 (7) | 717 (351) |
The mean plasma concentrations of levonorgestrel and ethinyl estradiol following single (day 1) and multiple (days 14 and 28) oral administrations of levonorgestrel 90 mcg in combination with ethinyl estradiol 20 mcg to 18 healthy women is provided in Figure 1.
Figure 1: Mean Plasma ± SD†Concentrations of Levonorgestrel and Ethinyl Estradiol Following Single (Day 1) and Multiple (Days 14 and 28) Oral Administrations of Levonorgestrel 90 mcg in Combination with Ethinyl Estradiol 20 mcg to Healthy Women
The effect of food on the rate and the extent of levonorgestrel and ethinyl estradiol absorption following oral administration of DOLISHALE has not been evaluated.
Distribution
Levonorgestrel in serum is primarily bound to sex hormone-binding globulin (SHBG). Ethinyl estradiol is about 97% bound to serum albumin. Ethinyl estradiol does not bind to SHBG, but induces SHBG synthesis.
Metabolism
Levonorgestrel: The most important metabolic pathways are reduction of the Δ4-3-oxo group and hydroxylation at positions 2α, 1β, and 16β, followed by conjugation. Most of the circulating metabolites are sulfates of 3α, 5β-tetrahydro-levonorgestrel, while excretion occurs predominantly in the form of glucuronides. Some of the parent levonorgestrel also circulates as 17β-sulfate. Metabolic clearance rates may differ among individuals by several-fold, and this may account in part for the wide variation observed in levonorgestrel concentrations among users.
Ethinyl estradiol: Cytochrome P450 enzymes (CYP3A4) in the liver are responsible for the 2-hydroxylation that is the major oxidative reaction. The 2-hydroxy metabolite is further transformed by methylation, sulfation, and glucuronidation prior to urinary and fecal excretion. Levels of CYP3A4 vary widely among individuals and can explain the variation in rates of ethinyl estradiol 2-hydroxylation.
Excretion
The terminal elimination half-life for levonorgestrel in levonorgestrel and ethinyl estradiol tablets is about 36 hours. Levonorgestrel and its metabolites are excreted in the urine (40% to 68%) and in feces (16% to 48%). The terminal elimination half-life of ethinyl estradiol in levonorgestrel and ethinyl estradiol tablets is about 21 hours.
Ethinyl estradiol is excreted in the urine and feces as glucuronide and sulfate conjugates and undergoes enterohepatic recirculation.
14. Pediatric Use
Safety and efficacy of levonorgestrel and ethinyl estradiol tablets have been established in women of reproductive age. Safety and efficacy are expected to be the same for postpubertal adolescents under the age of 16 and for users 16 years and older. Use of this product before menarche is not indicated.
15. Geriatric Use
This product has not been studied in women over 65 years of age and is not indicated in this population.
4. Liver Function
If jaundice develops in any woman receiving such drugs, the medication should be discontinued. Steroid hormones may be poorly metabolized in patients with impaired liver function.
7. Contact Lenses
Contact-lens wearers who develop visual changes or changes in lens tolerance should be assessed by an ophthalmologist.
Adverse Reactions (ADVERSE REACTIONS)
Post Marketing Experience
Five studies that compared breast cancer risk between ever-users (current or past use) of COCs and never-users of COCs reported no association between ever use of COCs and breast cancer risk, with effect estimates ranging from 0.90 - 1.12 (Figure 6).
Three studies compared breast cancer risk between current or recent COC users (<6 months since last use) and never users of COCs (Figure 6). One of these studies reported no association between breast cancer risk and COC use. The other two studies found an increased relative risk of 1.19 - 1.33 with current or recent use. Both of these studies found an increased risk of breast cancer with current use of longer duration, with relative risks ranging from 1.03 with less than one year of COC use to approximately 1.4 with more than 8-10 years of COC use.
Figure 6. Risk of Breast Cancer with Combined Oral Contraceptive Use
RR = relative risk; OR = odds ratio; HR = hazard ratio. “ever COC” are females with current or past COC use; “never COC use” are females that never used COCs.
An increased risk of the following serious adverse reactions (see WARNINGS section for additional information) has been associated with the use of oral contraceptives:
Thromboembolic and thrombotic disorders and other vascular problems (including thrombophlebitis and venous thrombosis with or without pulmonary embolism, mesenteric thrombosis, arterial thromboembolism, myocardial infarction, cerebral hemorrhage, cerebral thrombosis, transient ischemic attack), carcinoma of the reproductive organs and breasts, hepatic neoplasia/liver disease (including hepatic adenomas or benign liver tumors), ocular lesions (including retinal vascular thrombosis), gallbladder disease, carbohydrate and lipid effects, elevated blood pressure, and headache including migraine.
The following adverse reactions have been reported in patients receiving oral contraceptives and are believed to be drug related (alphabetically listed):
• Acne
• Amenorrhea
• Anaphylactic/anaphylactoid reactions, including urticaria, angioedema, and severe reactions with respiratory and circulatory symptoms
• Breast changes: tenderness, pain, enlargement, secretion
• Budd-Chiari syndrome
• Cervical erosion and secretion, change in
• Cholestatic jaundice
• Chorea, exacerbation of
• Colitis
• Contact lenses, intolerance to
• Corneal curvature (steepening), change in
• Dizziness
• Edema/fluid retention
• Erythema multiforme
• Erythema nodosum
• Focal nodular hyperplasia
• Gastrointestinal symptoms (such as abdominal pain, cramps, and bloating)
• Hirsutism
• Infertility after discontinuation of treatment, temporary
• Lactation, diminution in, when given immediately postpartum
• Libido, change in
• Melasma/chloasma which may persist
• Menstrual flow, change in
• Mood changes, including depression
• Nausea
• Nervousness
• Pancreatitis
• Porphyria, exacerbation of
• Rash (allergic)
• Scalp hair, loss of
• Serum folate levels, decrease in
• Spotting
• Systemic lupus erythematosus, exacerbation of
• Unscheduled bleeding
• Vaginitis, including candidiasis
• Varicose veins, aggravation of
• Vomiting
• Weight or appetite (increase or decrease), change in
The following adverse reactions have been reported in users of oral contraceptives:
• Cataracts
• Cystitis-like syndrome
• Dysmenorrhea
• Hemolytic uremic syndrome
• Hemorrhagic eruption
• Optic neuritis, which may lead to partial or complete loss of vision
• Premenstrual syndrome
• Renal function, impaired
To report SUSPECTED ADVERSE REACTIONS, contact Ingenus Pharmaceuticals, LLC Toll-Free at 1-877-748-1970 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch .
Contraindications (CONTRAINDICATIONS)
Combination oral contraceptives should not be used in women with any of the following conditions:
• Thrombophlebitis or thromboembolic disorders
• History of deep-vein thrombophlebitis or thromboembolic disorders
• Cerebrovascular or coronary artery disease (current or past history)
• Valvular heart disease with thrombogenic complications
• Thrombogenic rhythm disorders
• Hereditary or acquired thrombophilias
• Major surgery with prolonged immobilization
• Diabetes with vascular involvement
• Headaches with focal neurological symptoms such as aura
• Uncontrolled hypertension
• Current diagnosis of, or history of, breast cancer, which may be hormone-sensitive
• Carcinoma of the endometrium or other known or suspected estrogen-dependent neoplasia Undiagnosed abnormal genital bleeding
• Cholestatic jaundice of pregnancy or jaundice with prior pill use
• Hepatic adenomas or carcinomas, or active liver disease
• Known or suspected pregnancy
• Hypersensitivity to any of the components of DOLISHALE
• Are receiving Hepatitis C drug combinations containing ombitasvir/paritaprevir/ritonavir, with or without dasabuvir, due to the potential for ALT elevations (see Warnings, RISK OF LIVER ENZYME ELEVATIONS WITH CONCOMITANT HEPATITIS C TREATMENT ).
11. Carcinogenesis
See WARNINGS section.
3. Lipid Disorders
Women who are being treated for hyperlipidemias should be followed closely if they elect to use oral contraceptives. Some progestogens may elevate LDL levels and may render the control of hyperlipidemias more difficult. (See WARNINGS , 1a., 1d., and 9.)
A small proportion of women will have adverse lipid changes while taking oral contraceptives. Nonhormonal contraception should be considered in women with uncontrolled dyslipidemias. Persistent hypertriglyceridemia may occur in a small population of combination oral contraceptive users. Elevations of plasma triglycerides may lead to pancreatitis and other complications.
5. Fluid Retention
Oral contraceptives may cause some degree of fluid retention. They should be prescribed with caution, and only with careful monitoring, in patients with conditions which might be aggravated by fluid retention.
13. Nursing Mothers
Small amounts of oral contraceptive steroids and/or metabolites have been identified in the milk of nursing mothers, and a few adverse effects on the child have been reported, including jaundice and breast enlargement. In addition, combination oral contraceptives given in the postpartum period may interfere with lactation by decreasing the quantity and quality of breast milk. If possible, the nursing mother should be advised not to use combination oral contraceptives, but to use other forms of contraception until she has completely weaned her child.
8. Gastrointestinal
Diarrhea and/or vomiting may reduce hormone absorption resulting in decreased serum concentrations.
Special Populations
Race
No formal studies on the effect of race on the pharmacokinetic parameters of levonorgestrel and ethinyl estradiol tablets were conducted.
Hepatic Insufficiency
No formal studies have evaluated the effect of hepatic disease on the disposition of levonorgestrel and ethinyl estradiol tablets. However, steroid hormones may be poorly metabolized in patients with impaired liver function.
Renal Insufficiency
No formal studies have evaluated the effect of renal disease on the disposition of levonorgestrel and ethinyl estradiol tablets.
Drug-Drug Interactions
See PRECAUTIONS section - Drug Interactions.
9. Drug Interactions
Changes in Contraceptive Effectiveness Associated with Coadministration of Other Products: Contraceptive effectiveness may be reduced when hormonal contraceptives are coadministered with antibiotics, anticonvulsants, and other drugs that increase the metabolism of contraceptive steroids. This could result in unintended pregnancy or unscheduled bleeding. Examples include rifampin, rifabutin, barbiturates, primidone, phenylbutazone, phenytoin, dexamethasone, carbamazepine, felbamate, oxcarbazepine, topiramate, griseofulvin, and modafinil. In such cases a nonhormonal back-up method of birth control should be considered.
Several cases of contraceptive failure and unscheduled bleeding have been reported in the literature with concomitant administration of antibiotics such as ampicillin and other penicillins, and tetracyclines. However, clinical pharmacology studies investigating drug interactions between combined oral contraceptives and these antibiotics have reported inconsistent results. Enterohepatic recirculation of estrogens may also be decreased by substances that reduce gut transit time.
Several of the anti-HIV protease inhibitors have been studied with coadministration of oral combination hormonal contraceptives; significant changes (increase and decrease) in the plasma levels of the estrogen and progestin have been noted in some cases. The safety and efficacy of oral contraceptive products may be affected with coadministration of anti-HIV protease inhibitors. Health care professionals should refer to the label of the individual anti-HIV protease inhibitors for further drug-drug interaction information.
Concomitant Use with HCV Combination Therapy – Liver Enzyme Elevation Do not co-administer DOLISHALE with HCV drug combinations containing ombitasvir/paritaprevir/ritonavir, with or without dasabuvir, due to potential for ALT elevations (see Warnings, RISK OF LIVER ENZYME ELEVATIONS WITH CONCOMITANT HEPATITIS C TREATMENT ).
Herbal products containing St. John's Wort (Hypericum perforatum) may induce hepatic enzymes (cytochrome P 450) and p-glycoprotein transporter and may reduce the effectiveness of contraceptive steroids. This may also result in unscheduled bleeding.
Increase in Plasma Levels Associated with Coadministered Drugs:
Coadministration of atorvastatin and certain oral contraceptives containing ethinyl estradiol increases AUC values for ethinyl estradiol by approximately 20%. Ascorbic acid and acetaminophen increase the bioavailability of ethinyl estradiol since these drugs act as competitive inhibitors for sulfation of ethinyl estradiol in the gastrointestinal wall, a known pathway of elimination for ethinyl estradiol. CYP 3A4 inhibitors such as indinavir, itraconazole, ketoconazole, fluconazole, and troleandomycin may increase plasma hormone levels. Troleandomycin may also increase the risk of intrahepatic cholestasis during coadministration with combination oral contraceptives.
Changes in Plasma Levels of Coadministered Drugs:
Combination hormonal contraceptives containing some synthetic estrogens (eg, ethinyl estradiol) may inhibit the metabolism of other compounds. Increased plasma concentrations of cyclosporine, prednisolone and other corticosteroids, and theophylline have been reported with concomitant administration of oral contraceptives. Decreased plasma concentrations of acetaminophen and lamotrigine, and increased clearance of temazepam, salicylic acid, morphine, and clofibric acid, due to induction of conjugation (particularly glucuronidation), have been noted when these drugs were administered with oral contraceptives.
The prescribing information of concomitant medications should be consulted to identify potential interactions.
Indications and Usage (INDICATIONS AND USAGE)
DOLISHALE is indicated for the prevention of pregnancy in women who elect to use oral contraceptives as a method of contraception.
Oral contraceptives are highly effective for pregnancy prevention. Table 2 lists the typical unintended pregnancy rates for users of combination oral contraceptives and other methods of contraception. The efficacy of these contraceptive methods, except sterilization, the IUD, and implants, depend upon the reliability with which they are used. Correct and consistent use of methods can result in lower failure rates.
Table 2: Percentage of Women Experiencing an Unintended Pregnancy During The First Year of Typical Use and The First Year of Perfect Use of Contraception and The Percentage Continuing Use at The End of the First Year. United States.
| % of Women Experiencing an Unintended Pregnancy within the First Year of Use | % of Women Continuing Use at One Year3 | ||
| Method (1) | Typical Use1 (2) | Perfect Use2 (3) | (4) |
| Chance4 | 85 | 85 | |
| Spermicides5 | 26 | 6 | 40 |
| Periodic abstinence | 25 | 63 | |
| Calendar | 9 | ||
| Ovulation Method | 3 | ||
| Sympto-Thermal6 | 2 | ||
| Post-Ovulation | 1 | ||
| Cap7 | |||
| Parous Women | 40 | 26 | 42 |
| Nulliparous Women | 20 | 9 | 56 |
| Sponge | |||
| Parous Women | 40 | 20 | 42 |
| Nulliparous Women | 20 | 9 | 56 |
| Diaphragm7 | 20 | 6 | 56 |
| Withdrawal | 19 | 4 | |
| Condom8 | |||
| Female (Reality™) | 21 | 5 | 56 |
| Male | 14 | 3 | 61 |
| Pill | 5 | 71 | |
| Progestin only | 0.5 | ||
| Combined | 0.1 | ||
| IUD | |||
| Progesterone T | 2.0 | 1.5 | 81 |
| Copper T380A | 0.8 | 0.6 | 78 |
| LNg 20 | 0.1 | 0.1 | 81 |
| Depo-Provera® | 0.3 | 0.3 | 70 |
| Levonorgestrel Implants (Norplant®) |
0.05 | 0.05 | 88 |
| Female Sterilization | 0.5 | 0.5 | 100 |
| Male Sterilization | 0.15 | 0.10 | 100 |
Emergency Contraceptive Pills: The FDA has concluded that certain combined oral contraceptives containing ethinyl estradiol and norgestrel or levonorgestrel are safe and effective for use as postcoital emergency contraception. Treatment initiated within 72 hours after unprotected intercourse reduces the risk of pregnancy by at least 75%.9
Lactation Amenorrhea Method: LAM is a highly effective, temporary method of contraception.10
Source: Trussell J. Contraceptive efficacy. In: Hatcher RA, Trussell J, Stewart F, Cates W, Stewart GK, Kowel D, Guest F. Contraceptive Technology: Seventeenth Revised Edition. New York NY: Irvington Publishers; 1998.
1. Among typical couples who initiate use of a method (not necessarily for the first time), the percentage who experience an accidental pregnancy during the first year if they do not stop use for any other reason.
2. Among couples who initiate use of a method (not necessarily for the first time) and who use it perfectly (both consistently and correctly), the percentage who experience an accidental pregnancy during the first year if they do not stop use for any other reason.
3. Among couples attempting to avoid pregnancy, the percentage who continue to use a method for one year.
4. The percents becoming pregnant in columns (2) and (3) are based on data from populations where contraception is not used and from women who cease using contraception in order to become pregnant. Among such populations, about 89% become pregnant within one year. This estimate was lowered slightly (to 85%) to represent the percent who would become pregnant within one year among women now relying on reversible methods of contraception if they abandoned contraception altogether.
5. Foams, creams, gels, vaginal suppositories, and vaginal film.
6. Cervical mucus (ovulation) method supplemented by calendar in the pre-ovulatory and basal body temperature in the post-ovulatory phases.
7. With spermicidal cream or jelly.
8. Without spermicides.
9. The treatment schedule is one dose within 72 hours after unprotected intercourse, and a second dose 12 hours after the first dose. The FDA has declared the following dosage regimens of oral contraceptives to be safe and effective for emergency contraception: for tablets containing 50 mcg of ethinyl estradiol and 500 mcg of norgestrel 1 dose is 2 tablets; for tablets containing 20 mcg of ethinyl estradiol and 100 mcg of levonorgestrel 1 dose is 5 tablets; for tablets containing 30 mcg of ethinyl estradiol and 150 mcg of levonorgestrel 1 dose is 4 tablets.
10. However, to maintain effective protection against pregnancy, another method of contraception must be used as soon as menstruation resumes, the frequency or duration of breastfeeds is reduced, bottle feeds are introduced, or the baby reaches 6 months of age.
6. Emotional Disorders
Patients becoming significantly depressed while taking oral contraceptives should stop the medication and use an alternate method of contraception in an attempt to determine whether the symptom is drug related. Women with a history of depression should be carefully observed and the drug discontinued if depression recurs to a serious degree.
Detailed Patient Labeling (DETAILED PATIENT LABELING)
This product (like all oral contraceptives) is intended to prevent pregnancy. Oral contraceptives do not protect against transmission of HIV (AIDS) and other sexually transmitted diseases (STDs) such as chlamydia, genital herpes, genital warts, gonorrhea, hepatitis B, and syphilis.
INTRODUCTION
Any woman who considers using oral contraceptives (the "birth-control pill" or "the pill") should understand the benefits and risks of using this form of birth control. This leaflet will give you much of the information you will need to make this decision and will also help you determine if you are at risk of developing any of the serious side effects of the pill. It will tell you how to use the pill properly so that it will be as effective as possible. However, this leaflet is not a replacement for a careful discussion between you and your health care professional. You should discuss the information provided in this leaflet with him or her, both when you first start taking the pill and during your revisits. You should also follow your health care professional's advice with regard to regular check-ups while you are on the pill.
DOLISHALE is a birth-control pill that is taken every day. When you take DOLISHALE, the lining of your uterus does not undergo the changes needed for menstruation, and therefore you do not have regular menstrual periods. You are likely to have unscheduled or unplanned bleeding or spotting when you start to use DOLISHALE. The number of days each month with unscheduled bleeding and spotting usually decreases over time for the majority of women. When using DOLISHALE, the convenience of having no regular menstrual periods should be weighed against the inconvenience of unscheduled or unplanned breakthrough bleeding and spotting.
EFFECTIVENESS OF ORAL CONTRACEPTIVES
Oral contraceptives or "birth-control pills" or "the pill" are used to prevent pregnancy and are more effective than other nonsurgical methods of birth control. When they are taken correctly, without missing any pills the chance of becoming pregnant is approximately 1 to 2% per year (1 to 2 pregnancies per 100 women per year of use). Average failure rates are approximately 5% per year (5 pregnancies per 100 women per year of use) when women who miss pills are included. The chance of becoming pregnant increases with each missed pill.
In comparison, average failure rates for other methods of birth control during the first year of use are as follows:
| IUD: 0.1 to 2% |
Female condom alone: 21% |
| Depo-Provera® (injectable progestogen): 0.3% |
Cervical cap |
| Norplant® System (levonorgestrel implants): 0.05% |
Never given birth: 20% |
| Diaphragm with spermicides: 20% |
Given birth: 40% |
| Spermicides alone: 26% |
Periodic abstinence: 25% |
| Male condom alone: 14% |
No methods: 85% |
WHO SHOULD NOT TAKE ORAL CONTRACEPTIVES
Although cardiovascular disease risks may be increased with oral contraceptive use in healthy, non-smoking women over 40 (even with the newer low-dose formulations), there are also greater potential health risks associated with pregnancy in older women.
Dosage and Administration (DOSAGE AND ADMINISTRATION)
To achieve maximum contraceptive effectiveness, DOLISHALE (levonorgestrel and ethinyl estradiol tablets) must be taken exactly as directed and at intervals not exceeding 24 hours. The possibility of ovulation and conception prior to initiation of medication should be considered. Women who do not wish to become pregnant after discontinuation should be advised to immediately use another method of birth control. The dosage of DOLISHALE is one green tablet daily without any tablet-free interval.
It is recommended that DOLISHALE tablets be taken at the same time each day.
Initiation of Therapy
Instructions for beginning DOLISHALE are provided in Table 4 below.
Table 4
|
Current
contraceptive therapy |
DOLISHALE start day |
Nonhormonal back-up method of birth control needed when correctly starting DOLISHALE? |
| None | Day 1 of patient's menstrual cycle (during the first 24 hours of her period) | No |
| 21-day COC regimen OR 28-day COC regimen |
Day 1 of patient's withdrawal bleed, at the latest 7 days after her last active tablet. | No |
| Progestin-only pill | Day after taking a progestin-only pill | Yes, for the first 7 days of DOLISHALE tablet taking |
| Implant | Day of implant removal | Yes, for the first 7 days of DOLISHALE tablet taking |
| Injection | Day the next injection is due | Yes, for the first 7 days of DOLISHALE tablet taking |
If spotting or unscheduled bleeding occurs, the patient is instructed to continue on the same regimen. This type of bleeding is usually transient and without significance; however, if the bleeding is persistent or prolonged, the patient is advised to consult her health care professional. The possibility of ovulation increases with each successive day that scheduled green tablets are missed. If the patient has not adhered to the prescribed schedule (missed one or more tablets or started taking them on a day later than she should have), the probability of pregnancy should be considered. Hormonal contraception must be discontinued if pregnancy is confirmed.
The risk of pregnancy increases with each tablet missed. For additional patient instructions regarding missed tablets, see the WHAT TO DO IF YOU MISS PILLS section in the DETAILED PATIENT LABELING below.
DOLISHALE may be initiated no earlier than day 28 postpartum in the nonlactating mother or after a second-trimester abortion due to the increased risk for thromboembolism (see CONTRAINDICATIONS , WARNINGS , and PRECAUTIONS concerning thromboembolic disease). The patient should be advised to use a nonhormonal back-up method for the first 7 days of tablet-taking. However, if intercourse has already occurred, pregnancy should be excluded before the start of combined oral contraceptive use or the patient must wait for her first menstrual period.
In the case of first-trimester abortion, if the patient starts DOLISHALE immediately, additional contraceptive measures are not needed.
Instructions for the Patient
HOW TO TAKE DOLISHALE
Important Points to Remember
Before You Start Taking DOLISHALE:
1. BE SURE TO READ THESE DIRECTIONS:
Before you start taking DOLISHALE.
And
Anytime you are not sure what to do.
2. THE RIGHT WAY TO TAKE DOLISHALE IS TO TAKE ONE PILL EVERY DAY AT THE SAME TIME.
If you miss pills, you could get pregnant. This includes starting the pack late. The more pills you miss, the more likely you are to get pregnant. See "WHAT TO DO IF YOU MISS PILLS" below.
3. MANY WOMEN HAVE SPOTTING OR LIGHT BLEEDING, OR MAY FEEL SICK TO THEIR STOMACH DURING THE FIRST 1 to 3 PACKS OF PILLS.
If you feel sick to your stomach, do not stop taking DOLISHALE. This will usually go away. If it doesn't go away, check with your health care professional.
4. MOST WOMEN HAVE SPOTTING OR BLEEDING DURING THE FIRST FEW MONTHS OF TAKING DOLISHALE. Do not stop taking your pills even if you are having bleeding or spotting. If the bleeding or spotting lasts for more than 7 consecutive days, talk to your health care provider.
5. MISSING PILLS CAN ALSO CAUSE SPOTTING OR LIGHT BLEEDING, even when you make up these missed pills.
On the days you take 2 pills to make up for missed pills, you could also feel a little sick to your stomach.
6. IF YOU VOMIT (within 4 hours after you take your pill), you should follow the instructions for WHAT TO DO IF YOU MISS PILLS. IF YOU HAVE DIARRHEA or IF YOU TAKE SOME MEDICINES, including some antibiotics, your pills may not work as well.
Use a back-up nonhormonal method (such as condoms and/or spermicide) until you check with your health care professional.
7. IF YOU HAVE TROUBLE REMEMBERING TO TAKE DOLISHALE, talk to your health care professional about how to make pill-taking easier or about using another method of birth control.
8. IF YOU HAVE ANY QUESTIONS OR ARE UNSURE ABOUT THE INFORMATION IN THIS LEAFLET, call your health care professional.
BEFORE YOU START TAKING DOLISHALE
1. DECIDE WHAT TIME OF DAY YOU WANT TO TAKE YOUR PILL. It is important to take your pill at the SAME TIME every day.
2. LOOK AT YOUR DOLISHALE BLISTER CARD. The pill pack has 28 "active" green pills (with hormones).
3. ALSO FIND:
1) where on the pack to start taking pills,
2) in what order to take the pills (follow the arrows),
3) check picture of pill pack and additional instructions for using this package below.
4. BE SURE YOU HAVE READY AT ALL TIMES:
ANOTHER KIND OF NONHORMONAL BIRTH CONTROL (such as condoms and/or spermicide) to use as a back-up in case you miss pills.
AN EXTRA, FULL PILL PACK.
WHEN TO START THE FIRST PACK OF DOLISHALE
Day 1 Start
1. If the first day of your period (this is the day you start bleeding or spotting, even if it is almost midnight when the bleeding begins) is Sunday, then follow the days of the week imprinted on the plastic compact. You do not need to use the Day Label Stickers.
2. If the first day of your period (this is the day you start bleeding or spotting, even if it is almost midnight when the bleeding begins) is on a day other than Sunday, then pick the day label sticker that starts with that day of the week.
3. Place this chosen day label sticker over the area that has the days of the week (starting with Sunday) imprinted on the plastic compact as shown in the graphic above.
4. Take the first "active" green pill of the first pack during the first 24 hours of your period.
5. You will not need to use a back-up nonhormonal method of birth control, since you are starting the pill at the beginning of your period.
WHAT TO DO DURING THE MONTH
1. TAKE ONE PILL AT THE SAME TIME EVERY DAY UNTIL THE PACK IS EMPTY.
Do not skip pills even if you are spotting or bleeding or feel sick to your stomach (nausea).
Do not skip pills even if you do not have sex very often.
2. WHEN YOU FINISH A PACK
Start the next pack on the day after your last pill. Do not wait any days between packs.
IF YOU SWITCH FROM ANOTHER BRAND OF COMBINATION PILLS:
When switching from a 21 pill pack: Start DOLISHALE on the first day of your period (withdrawal bleed). Be sure that no more than 7 days pass between the last day of your 21-day pack and your first DOLISHALE pill.
When switching from a 28 pill pack (21 active and 7 inactive pills, or 24 active and 4 inactive pills): Start DOLISHALE on the first day of your period (withdrawal bleed). Be sure that no more than 7 days pass after the last active pill and your first DOLISHALE pill.
IF YOU SWITCH FROM ANOTHER TYPE OF BIRTH CONTROL
When switching from other types of birth control such as pills containing only a progestin (progestin only pill or POP), an injection, or an implant, your health care professional will provide you with instructions for when to start DOLISHALE.
WHAT TO DO IF YOU MISS PILLS
Combination oral contraceptives may not be as effective if you miss pills. Instructions for what to do if you miss pills are provided in the following table.
| # of pills missed in a row | What to do when you miss a pill(s) |
| 1 missed pill | • Take the missed pill as soon as you remember. THEN • Take the next pill at your regular time. This means you may take 2 pills in 1 day. • You COULD BECOME PREGNANT if you have sex during the 7 days after you restart your pills. You MUST use a nonhormonal birth-control method (such as condoms and/or spermicide) as a back-up for those 7 days. |
| 2 missed pills and remembered on the day of the second missed pill |
• Take 2 missed pills on the day you remember. The following day you are back on schedule to take 1 pill a day. For example, you take your pills in the morning and you missed 1 pill on Monday and 1 on Tuesday. On Tuesday evening you remembered that you missed your Monday and Tuesday pills. You take the 2 missed pills on Tuesday evening and on Wednesday morning you're back on schedule and you take 1 pill. • You COULD BECOME PREGNANT if you have sex during the 7 days after you restart your pills. You MUST use a nonhormonal birth-control method (such as condoms and/or spermicide) as a back-up for those 7 days. |
| 2 missed pills and remembered on the day after the second pill is missed |
• Take 2 missed pills on the day you remember. The next day you take 2 pills. The following day you are back on schedule to take your pills. For example, you take your pills in the morning and you missed 1 pill on Monday and 1 on Tuesday. On Wednesday morning you remembered that you missed your Monday and Tuesday pills. You take the 2 missed pills on Wednesday morning and 2 pills on Thursday morning. On Friday morning you're back on schedule and you take 1 pill. • You COULD BECOME PREGNANT if you have sex during the 7 days after you restart your pills. You MUST use a nonhormonal birth-control method (such as condoms and/or spermicide) as a back-up for those 7 days. |
| 3 or more missed pills | • Contact your health care professional for further advice. Keep taking one pill every day until you reach your health care professional. Do not take the missed pills. • You COULD BECOME PREGNANT if you have sex during the 7 days after you restart your pills. You MUST use a nonhormonal birth-control method (such as condoms and/or spermicide) as a back-up for those 7 days. |
FINALLY, IF YOU ARE STILL NOT SURE WHAT TO DO ABOUT THE PILLS YOU HAVE MISSED
Use a BACK-UP NONHORMONAL BIRTH-CONTROL METHOD anytime you have sex.
PREGNANCY AFTER STOPPING THE PILL
If you do not desire pregnancy, you should use another method of birth-control immediately after stopping DOLISHALE. You can get pregnant within days after stopping DOLISHALE.
For additional information see "Detailed Patient Labeling."
16. Information for the Patient
See DETAILED PATIENT LABELING printed below.
Noncontraceptive Health Benefits (NONCONTRACEPTIVE HEALTH BENEFITS)
The following noncontraceptive health benefits related to the use of oral contraceptives are supported by epidemiological studies which largely utilized oral contraceptive formulations containing doses exceeding 0.035 mg of ethinyl estradiol or 0.05 mg of mestranol.
Effects on menses:
May decrease blood loss and may decrease the incidence of iron-deficiency anemia
May decrease incidence of dysmenorrhea
Effects related to inhibition of ovulation:
May decrease incidence of functional ovarian cysts
May decrease incidence of ectopic pregnancies
Effects from long-term use:
May decrease incidence of fibroadenomas and fibrocystic disease of the breast
May decrease incidence of acute pelvic inflammatory disease
May decrease incidence of endometrial cancer
May decrease incidence of ovarian cancer
Brief Summary Patient Package Insert
This product (like all oral contraceptives) is intended to prevent pregnancy. Oral contraceptives do not protect against transmission of HIV (AIDS) and other sexually transmitted diseases (STDs) such as chlamydia, genital herpes, genital warts, gonorrhea, hepatitis B, and syphilis.
Oral contraceptives, also known as "birth-control pills" or "the pill," are taken to prevent pregnancy, and when taken correctly, have a failure rate of approximately 1 to 2% per year (1 to 2 pregnancies per 100 women per year of use) when used without missing any pills. The average failure rate of large numbers of pill users is approximately 5% per year (5 pregnancies per 100 women per year of use) when women who miss pills are included. However, forgetting to take pills considerably increases the chances of pregnancy.
DOLISHALE is a birth-control pill that is taken every day. When you take DOLISHALE, the lining of your uterus does not undergo the changes needed for menstruation, and therefore you do not have regular menstrual periods. You are likely to have unscheduled or unplanned bleeding or spotting when you start to use DOLISHALE. The number of days each month with unscheduled bleeding and spotting usually decreases over time for the majority of women. When using DOLISHALE , the convenience of having no regular menstrual periods should be weighed against the inconvenience of unscheduled or unplanned breakthrough bleeding and spotting.
For the majority of women, oral contraceptives can be taken safely. However, there are some women who are at high risk of developing certain serious diseases that can be life-threatening or may cause temporary or permanent disability or death. The risks associated with taking oral contraceptives increase significantly if you:
• smoke
• have high blood pressure, diabetes, high cholesterol, or a tendency to form blood clots, or are obese
• have or have had clotting disorders, heart attack, stroke, angina pectoris, cancer of the breast or sex organs, jaundice, malignant or benign liver tumors, or major surgery with prolonged immobilization
• have headaches with neurological symptoms
You should not take the pill if you suspect you are pregnant or have unexplained vaginal bleeding.
Although cardiovascular disease risks may be increased with oral contraceptive use in healthy, non-smoking women over 40 (even with the newer low-dose formulations), there are also greater potential health risks associated with pregnancy in older women.
2. Physical Examination and Follow Up (2. Physical Examination and Follow-Up)
A periodic personal and family medical history and complete physical examination are appropriate for all women, including women using oral contraceptives. The physical examination, however, may be deferred until after initiation of oral contraceptives if requested by the woman and judged appropriate by the clinician. The physical examination should include special reference to blood pressure, breasts, abdomen, and pelvic organs, including cervical cytology, and relevant laboratory tests. In case of undiagnosed, persistent, or recurrent abnormal vaginal bleeding, appropriate diagnostic measures should be conducted to rule out malignancy. Women with a strong family history of breast cancer or who have breast nodules should be monitored with particular care.
10. Interactions With Laboratory Tests (10. Interactions with Laboratory Tests)
Certain endocrine- and liver-function tests and blood components may be affected by oral contraceptives:
a. Increased prothrombin and factors VII, VIII, IX, and X; decreased antithrombin 3; increased norepinephrine-induced platelet aggregability.
b. Increased thyroid-binding globulin (TBG) leading to increased circulating total thyroid hormone, as measured by protein-bound iodine (PBI), T4 by column or by radioimmunoassay. Free T3 resin uptake is decreased, reflecting the elevated TBG; free T4 concentration is unaltered.
c. Other binding proteins may be elevated in serum ie, corticosteroid binding globulin (CBG), sex hormone-binding globulins (SHBG) leading to increased levels of total circulating corticosteroids and sex steroids, respectively. Free or biologically active hormone concentrations are unchanged.
d. Triglycerides may be increased and levels of various other lipids and lipoproteins may be affected.
e. Glucose tolerance may be decreased.
f. Serum folate levels may be depressed by oral contraceptive therapy. This may be of clinical significance if a woman becomes pregnant shortly after discontinuing oral contraceptives.
Principal Display Panel 1 Cycle Carton (PRINCIPAL DISPLAY PANEL 1-cycle carton)
Principal Display Panel 3 Cycle Carton (PRINCIPAL DISPLAY PANEL 3-cycle carton)
Inhibition of Menses (bleeding Profile) (Inhibition of Menses (Bleeding Profile))
The bleeding profile for subjects in Study 313-NA also was assessed. Women with a history of unscheduled bleeding and/or spotting were not excluded from the study.
In those subjects who provided complete bleeding data, the percentage of patients who were amenorrheic in a given cycle and remained amenorrheic through cycle 13 (cumulative amenorrhea rate) was determined (Figure 2).
Figure 2: Percentage of Subjects with Cumulative Amenorrhea for Each Pill Pack through Pill Pack 13
When prescribing DOLISHALE, the convenience of having no scheduled menstrual bleeding should be weighed against the inconvenience of unscheduled bleeding and spotting (see WARNINGS, 12 ).
Advanced Ingredient Data
Raw Label Data
All Sections (JSON)
Additional Information
Back to search View SPL set listing Open on DailyMed ↗
Source: dailymed · Ingested: 2026-02-15T11:46:31.817430 · Updated: 2026-03-14T22:25:04.498043